The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Study Questions and Answers
|
|
|
- Ellen Martha O’Brien’
- 5 years ago
- Views:
Transcription
1 The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Study Questions and Answers About the ECHO Study Background and Implications for the Field How the Study Works About the Products About the ECHO Study 1. What is the ECHO Study? The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Study is an open-label randomised clinical trial comparing three highly effective, reversible methods of contraception the progestogen-only injectable depot medroxyprogesterone acetate (DMPA), a progestogen implant called Jadelle and the copper IUD to evaluate whether there is any difference in the risk of HIV acquisition among women using these methods. The study will also compare side effects, pregnancy rates and women s patterns of use for the three contraceptive methods. 2. Why is the ECHO Study needed? More than 150 million women worldwide use various hormonal contraceptives, including progestogen-only contraceptives such as injectables, for family planning. In sub-saharan Africa, progestogen-only injectable contraceptives are the most commonly used method. Over the past 25 years, as the HIV epidemic took hold in many countries, a number of observational studies explored whether or not hormonal methods increase the risk of HIV acquisition. No association between combined hormonal contraceptive methods which include the use of two hormones (estrogen and progestogen) to prevent pregnancy from occurring and HIV acquisition has been shown. For women using progestogen-only injectables, the cumulative evidence from observational studies indicates a possible increased risk of HIV acquisition (particularly with DMPA), but it is uncertain whether there is a causal relationship, as opposed to just an observed association, due to the methodological limitations of these studies. Few studies have examined whether hormonal implants or intrauterine devices (IUDs) affect users risk of HIV acquisition. (See Background for additional information.) ECHO Study Q&A Revised 10 November
2 Given the widespread use of DMPA in areas of high HIV incidence, the question of whether DMPA increases women s risk of HIV is a critical public health issue requiring the strongest evidence possible. Women need to know whether the use of DMPA or highly effective alternatives to DMPA affects their risk of acquiring HIV so they can make informed choices about contraception. ECHO will provide high-quality information about contraceptive risks and benefits that women can use in making contraceptive decisions, that healthcare providers will use for contraceptive counselling, and to inform policy-makers decisions for programmes. 3. What is the status of the ECHO Study? The ECHO Study began enrolling participants in December 2015, with a plan to enrol women. The study reached this target on 29 August 2017 and officially closed enrolment on 12 September 2017 with a total of participants at 12 sites in South Africa, Kenya, Swaziland and Zambia. Results are expected in The trial s independent Data and Safety Monitoring Board (DSMB) has met five times, most recently in March 2017, to conduct planned periodic reviews of data from the study and performance metrics such as enrolment, retention and method refusal rates. After each review, the DSMB reaffirmed the continued need for ECHO and its ongoing equipoise and recommended that the study continue. (See question #11 for further details.) 4. How do the latest changes to the WHO guidelines on the use of hormonal contraception for women at high HIV risk affect the ECHO Study? Based on a December 2016 expert consultation to review the latest evidence on hormonal contraception and HIV, in March 2017 the WHO changed its recommendation for progestogenonly injectables for women at high risk of HIV from can use without restriction (Medical Eligibility Criteria category 1) to can use because the advantages of these methods generally outweigh the possible increased risk of HIV acquisition (MEC category 2). The ECHO team informed all study participants of this updated WHO guidance, which says that women at high risk of acquiring HIV can use progestogen-only injectables but should be advised about: 1) concerns that these methods may increase their risk of HIV acquisition; 2) continued uncertainty over whether the use of these methods causes increased risk; and 3) how to minimise their risk of acquiring HIV. 5. What does the WHO guidance say about the ECHO Study? The WHO recommendations reaffirm the need for randomised clinical trials, such as ECHO, to determine whether there is a causal relationship between hormonal contraceptive use and the risk of HIV acquisition. ECHO Study Q&A Revised 10 November
3 6. How was the change in the WHO guidance communicated to ECHO Study participants? The ECHO team is fully committed to ensuring all study participants are kept informed about any updates in the science and guidelines. All study materials, including outreach and recruitment materials and the informed consent form, were updated to reflect the change in the WHO guidelines on DMPA. These revisions were reviewed by local ethics committees (institutional review boards). All women interested in joining ECHO were informed about the new WHO guidance by trained staff as part of the recruitment and informed consent process. Women already enrolled in the ECHO Study were also informed about the new guidance, and counsellors were equipped to answer any questions they had. (See How the Study Works, questions #14 15) 7. What data will the ECHO Study produce, and how will the data be used? The primary findings will be the comparative risk of HIV acquisition among the three contraceptive methods studied. This information will be published and submitted to WHO for review of its contraceptive guidance. WHO's contraceptive guidance is used worldwide by programme managers, policy-makers and clinicians. The study team is committed to ensuring that study participants and other women at high risk of HIV, as well as other stakeholders, have timely access to the information provided by the study. Results will also be presented to national and international policy-makers, scientists and advocates. Background of the ECHO Study and Implications for the Field 8. What are the origins of the ECHO Study? In February 2012, a World Health Organization expert group met to review all the available data on hormonal contraception and HIV risk. The group found that the information on combined oral contraceptive pills was reassuring, but the data on the safety of progestogen-only injectables were inconclusive, with some but not all studies showing an increased risk of HIV acquisition. These data came from observational studies and secondary analyses that are subject to bias and other limitations, making it difficult to interpret the data. The group concluded that there was an urgent need for further research carefully designed to show whether or not use of progestogenonly injectables increases the risk of HIV acquisition a conclusion that was reaffirmed in 2014 and ECHO Study Q&A Revised 23 March
4 9. What are the current data available? What does the evidence say? Research on hormonal contraceptive (HC) use and risk of HIV acquisition has yielded mixed results. The most recent data are from a systematic review 1 commissioned by the World Health Organization to analyse studies published from 15 January 2014 to 15 January 2016 and to synthesise the results with those from a previous systematic review. 2 The updated systematic review found that most of the data for oral contraceptive pills, injectable norethisterone enanthate (NET-EN) and levonorgestrel implants do not suggest an association with HIV acquisition, though data for NET-EN and especially implants are very limited. Data are also very limited on the copper intrauterine device (IUD), and no data are available on whether contraceptive rings or patches, combined injectables or levonorgestrel IUDs affect the risk of HIV acquisition. Some studies suggest increased risk of HIV acquisition among users of DMPA. Data from recent studies included in the latest systematic review strengthen concerns about a possible increased risk of HIV acquisition associated with DMPA use. 1 After reviewing the evidence, a WHO technical consultation concluded that the available evidence continues to indicate an association between use of progestogen injectables and an increased risk of acquiring HIV; however, it is unknown whether the associations seen in these observational studies were due to a true biological effect or the limitations of such studies. 10. What are the limitations of the studies on the potential link between DMPA use and HIV risk? All the studies have been observational studies, in which women choose which contraceptive methods they use. Women who choose to use DMPA may be different from women who do not use DMPA particularly those who do not use contraception at all in important ways that affect their risk of HIV and are difficult to measure. (See #12.) The WHO statement notes that data from observational studies come with a high level of uncertainty and calls for randomised clinical trials to provide better information about possible causality. 11. What are the implications of these findings for the ECHO Study? ECHO is a randomised controlled trial (RCT) designed to address the long-standing concern in the public health community of a possible association between hormonal contraception (especially 1 Polis CB, Curtis KM, Hannaford PC, et al. An updated systematic review of the epidemiological evidence on hormonal contraceptive methods and HIV acquisition in women. AIDS 2016; 30(17): Polis CB, Phillips SJ, Curtis KM, et al. Hormonal contraceptive methods and risk of HIV acquisition in women: a systematic review of epidemiological evidence. Contraception 2014; 90: ; Polis CB, Curtis KM. Use of hormonal contraceptives and HIV acquisition in women: a systematic review of the epidemiological evidence. Lancet Inf Dis 2013; 13: ECHO Study Q&A Revised 23 March
5 DMPA) and the risk of HIV acquisition. On 2 March 2017, the ECHO Study s DSMB met and agreed that the results of the updated systematic review and the new WHO guidance underscore the need for an RCT that will yield higher-quality evidence than the available data from observational studies. The DSMB members also weighed the data and potential risk with the benefits of injectable contraception, along with the ease and acceptability of use, and concluded that the ECHO trial is in equipoise. This means there is scientific uncertainty about methods. Importantly, ECHO is designed to assess the relative risks and benefits of alternative contraceptive methods the levonorgestrel implant and the copper IUD compared to DMPA and to each other. The recent systematic review includes very little data to weigh whether implants and IUDs are better alternatives to DMPA with respect to HIV or other risks and benefits. 12. Why is a randomised study needed? Randomised clinical trials are considered the gold standard in producing reliable scientific evidence about the effect of a medical intervention. When women have an equal chance of using any of the contraceptive methods under study, sexual behaviours and other factors that might influence HIV risk are equally likely to occur across the groups of women who are randomly allocated by computer to use one of the study methods. As a result, with a randomised trial there is more certainty that a true difference in HIV acquisition is being measured and that any differences measured can be more certainly attributed to the contraceptive method used. How the Study Works 13. How many women enrolled in the ECHO Study? And who was eligible to join the study? A total of sexually active HIV-negative women ages 16 to 35 years enrolled in the ECHO Study. Women were eligible to join the study if they were seeking effective contraception, were willing to be randomly assigned to any of the study groups and did not want to become pregnant for the duration of the study. Women who had recently given birth also had to be at least six weeks postpartum to be eligible to enrol. Another eligibility requirement was that participants intended to stay in the area for the duration of their participation in the study. Young women ages 16 and 17 years were eligible to join the study upon approval based on local and national regulations and the relevant ethics committee s guidance. Where required, as in South Africa, the study sought the informed consent of a parent or legal guardian in addition to that of the minor participant. In other countries, such as Kenya, a previously pregnant 16- to 17- year-old is considered a legally emancipated minor ; in these instances, informed consent was sought directly from the young woman. ECHO Study Q&A Revised 23 March
6 14. How were participants recruited for the study? Recruitment teams partnered with local organisations and conducted community outreach events to introduce the study to potential participants. They handed out flyers, gave health talks and encouraged women who were interested in the study to visit the local study site for further information. At the sites, educational sessions were held, and women received additional information that they could take home to learn more about the study before deciding whether to participate. After a woman decided that she wanted to participate, she engaged in an informed consent process. Each potential participant sat with a counsellor, and together they went through the informed consent form, discussing why the study was being conducted, the aims of the study, the study procedures, and the risks and benefits of participating. After the potential participant understood and had signed the informed consent form, screening tests and counselling were carried out. If the tests confirmed that the woman was eligible and if she still wanted to participate in the study, only then could she be enrolled. 15. How does the ECHO Study work? Women interested in joining the study learned about the study procedures and the risks and benefits of participation through an informed consent process. Counsellors carefully explained how the study randomly assigned participants to receive one of three contraceptives: DMPA, a hormonal implant containing levonorgestrel or the copper IUD. They counselled each woman to ensure she would be happy with any of the three study methods. Screening and enrolment occurred during separate visits to ensure that each woman had time to consider her options and did not feel pressured to take part in the study or to start a method she did not want. Women who enrolled in the study and were randomly assigned to a method are asked to visit the study clinic every three months. During these regular visits, they receive counselling on contraception and HIV risk reduction and are assessed for pregnancy, HIV and other sexually transmitted infections (STIs), and side effects from the contraception. They are also asked limited questions about sexual behaviour (for example, about condom use and number of partners) and their experiences with the contraceptive method they are using. Women assigned to receive injectable contraception are given injections according to the product s dosing schedule. To analyse the study results, the researchers will compare the number of women in each group who acquired HIV, became pregnant or experienced side effects that led them to stop using the contraceptive method to which they were randomly assigned. ECHO Study Q&A Revised 23 March
7 16. Do the study participants benefit directly from the study? All participants receive contraceptives and ongoing health services and care throughout the study. All participants also receive counselling on HIV prevention and care, as well as screening and treatment for sexually transmitted infections, and are offered pre-exposure prophylaxis (PrEP) either at the study site or through referrals. 17. Do participants have the option to receive antiretroviral pre-exposure prophylaxis (PrEP)? The ECHO Study is committed to providing the highest standards of HIV prevention services to participants as recommended by Good Participatory Practice guidelines. Participants interested in antiretroviral pre-exposure prophylaxis (PrEP) have been referred to services as programmes became available in each study community. In response to the South African Medical Research Council s recommendation in November 2017 that participants in clinical trials be offered PrEP, the ECHO Study moved quickly to incorporate the offering of PrEP at the study sites in South Africa. PrEP continues to be available through referral at all ECHO sites; in addition, all South Africa ECHO sites offer PrEP on site. 18. Where is the study being conducted? The ECHO Study is being conducted at 12 trial sites in four countries: Kenya, South Africa, Swaziland and Zambia (see next question for full list of sites). These countries were selected because women in southern and East Africa continue to be among the hardest hit by HIV and maternity mortality. DMPA is also the most widely used modern method of contraception in the region. It is important to work with affected communities to ensure the study provides evidence based on the population most in need of guidance on hormonal contraceptive use and any possible link with HIV acquisition. 19. Who is conducting the ECHO Study? Leading global and national institutions are collaborating on the ECHO trial. The study is jointly sponsored by FHI 360, the Wits Reproductive Health and HIV Institute (WRHI) and the University of Washington, who are coordinating to implement the trial. The World Health Organization collaborates in study management and leads stakeholder engagement in reviewing the evidence on hormonal contraception and HIV acquisition. Other partners include investigators from the Kenya Coast Provincial Hospital/International Centre for Reproductive Health, the Kenya Medical Research Institute, the University of Fort Hare and the University of Zimbabwe. Collaborating study site partners include: in South Africa, the Aurum Institute in Klerksdorp, the Desmond Tutu Foundation Emavundleni Research Centre in Cape Town, the Effective Care Research Unit in East London, the Madibeng Centre for Research in Brits, Maternal, Adolescent and Child Health (MatCH) Research in Durban and Pietermaritzburg, the Qhakaza Mbokodo Research Clinic in Ladysmith, the Setshaba Research Centre in Shoshanguve and WRHI/University ECHO Study Q&A Revised 23 March
8 of the Witwatersrand in Johannesburg; in Kenya, the KEMRI-RCTP Study Centre, Lumumba Health Centre, in Kisumu; in Swaziland, the Family Life Association of Swaziland and ICAP-Columbia in Manzini; and in Zambia, the UNC Global Projects Zambia/Kamwala Clinic in Lusaka. 20. When did the study begin, and when will it end? The study began in December 2015, when two sites in South Africa started screening and enrolling participants. Enrolment was completed on 12 September 2017, and the total duration of the study in the field will be approximately 36 months from first enrolment. Data analysis will begin in early 2019, and results are expected in How is the study funded? A consortium of donors is funding the study. They include the Bill & Melinda Gates Foundation, the US Agency for International Development (USAID), the Swedish International Development Cooperation Agency (SIDA), the United Nations Population Fund (UNFPA) and the Medical Research Council of South Africa. In addition, USAID and the South African government are donating the contraceptives used in the study. 22. What approvals were required for this study? The ECHO Study was reviewed and approved by the institutional review board (IRB) of FHI 360 and by local research ethics committees in the countries where it is being conducted. In addition, national regulatory authorities, including the South African Health Products Regulatory Authority (formerly the Medicines Control Council) and Kenya s Pharmacy and Poisons Board, were notified of the study. 23. Who oversees the study? Several groups together oversee the ECHO Study. A stewardship committee composed of the funders oversees the ECHO Consortium, and their main role is to assure the financial resources and operational milestones of the trial. A management committee provides overall accountability of the ECHO Study, including meeting the timelines and major trial milestones; the management committee includes representatives from the three organisations sponsoring the study (FHI 360, WRHI and the University of Washington). Finally, the implementation team is responsible for overseeing the implementation of the protocol and has final responsibility for trial conduct, including Good Clinical Practice (GCP), quality assurance and regulatory oversight. In addition, an independent Data and Safety Monitoring Board (DSMB), comprised of global experts in reproductive health, HIV and biostatistics, oversees the well-being of participants. The DSMB reviewed the protocol before the study began and conducts regular reviews of the study data. The DSMB can recommend modifying or stopping the study if there is a safety concern, or if a reliable result is unlikely by the end of the study. This could happen in the event of low ECHO Study Q&A Revised 23 March
9 enrolment, low contraceptive continuation, poor retention or other potential operational challenges. 24. How does the study monitor participants safety and well-being? The study has several mechanisms for monitoring the safety of participants and implementation of the study. An independent Data and Safety Monitoring Board (see #23) is responsible for reviewing all safety study data and ensuring that participants well-being is protected. If the DSMB members have safety concerns, they can recommend that the study be modified or stopped. The study site investigators are responsible for continuous safety monitoring of all study participants and for alerting the safety monitor and protocol management team if unexpected concerns arise. The safety oversight committee reviews safety data from all sites monthly and is available 24-7 to the sites for clinical advice. 25. What happens if a participant acquires HIV during the study? The well-being of the women enrolled in the study is the ECHO Consortium s highest priority. ECHO researchers do their best to reduce each participant s risk by providing condoms and HIV prevention counselling. Even so, because the rates of HIV are high in their communities, some women are likely to acquire HIV during the study period. Women who seroconvert during the study receive counselling and are referred to local HIV care providers for on-going care, including assessment of CD4 cell counts and antiretroviral treatment according to local guidelines. They are asked to remain in the study until completion of the follow- up period. This gives participants the opportunity to continue receiving services at the clinical site and allows researchers to continue collecting data relevant to the additional study questions. 26. What happens to participants who become pregnant during the study? Study staff provide care or refer for further care women who become pregnant, according to their wishes. If a pregnancy continues, the woman discontinues her assigned method but remains in the study to the end of the follow-up period, which gives her the opportunity to continue receiving services at the clinical site. Should a pregnancy end prior to completion of study follow-up, the woman will be encouraged to resume her allocated method of contraception but will be offered a choice of any method available at the study site. If a pregnancy continues beyond the end of the study, the woman will be referred for further care of her pregnancy. ECHO Study Q&A Revised 23 March
10 27. What happens to participants who want to switch to a different contraceptive method during the study? The study team pays close attention to the eligibility criteria and conducts thorough counselling before enrolling women in the study, to ensure that participants are comfortable with random assignment to a method and are willing to continue using that method throughout the study. If a woman experiences side effects or concerns regarding her assigned method, she will be advised to come to the clinic to discuss her questions and experience with the method. Trained clinicians work closely with participants to resolve any challenges faced. Some women may wish to switch to another contraceptive method despite receiving counselling and treatment for any side effects. Participants are free to change methods at any time during the study. If a participant prefers a non-study contraceptive method, she will receive that method either on site or by referral. All women who switch methods remain in the study and are seen according to the same schedule as other participants. Women who choose not to use any contraceptive method also continue to be followed according to the same schedule as all other participants. 28. What will happen to study participants contraception when the trial is over? When a participant exits the ECHO Study, she is given the option to remain on the same contraceptive to which she was randomly assigned at the beginning of the study. Any woman who wishes to switch methods can have her study-assigned method removed (if she was assigned to an IUD or implant) and have any new method provided by the site at no cost. Participants who had been assigned to an IUD or implant who wish to stop using contraception can also have the device removed. 29. How is the operational feasibility of the study being monitored? As with all clinical trials, the ECHO Study has a set of challenges which are being monitored closely. One anticipated challenge was whether women would accept randomisation. Several studies had successfully randomised women to use either an IUD or an injectable contraceptive. 3 The ECHO Study team took great care to ensure women were properly selected and counselled appropriately, which has resulted in very few participants refusing to start the method to which they were assigned. 3 Hubacher D, Raymond ER, Beksinka M, et al. Hormonal contraception and the risks of STI acquisition: results of a feasibility study to plan a future randomized trial. Contraception 2008; 77: ; Feldblum PJ, Caraway J, Bahamondes L, et al. Randomized assignment to copper IUD or depot-medroxyprogesterone acetate: feasibility of enrollment, continuation, and disease ascertainment. Contraception 2005; 72: ; Hofmeyr J. A randomized trial of DMPA and the Cu-IUD. Presented at the WHO Expert Group to Examine Hormonal Contraception and HIV. Geneva: January 31, ECHO Study Q&A Revised 23 March
11 Method continuation is also critical to the success of the trial, because a high percentage of women must continue their assigned methods to ensure sufficient statistical power to detect any differences in HIV acquisition among the groups. To promote and support method continuation, study staff received intensive training in contraceptive method delivery and management, and women were carefully screened prior to study entry. The study sites are closely monitored to ensure that the study team responds quickly if retention is low or contraceptive discontinuation rates are higher than anticipated. This monitoring will allow the study leadership to intervene with sites that have difficulty in the conduct of the study, and to modify or discontinue the study if required. About the Products 30. How do the contraceptives being tested work? DMPA is given by injection every three months and is slowly absorbed into the blood stream to prevent pregnancy. DMPA contains a synthetic progestogen that acts like the hormone progesterone, which occurs naturally in a woman s body. It works primarily by preventing the release of eggs from the ovaries (ovulation) and by thickening the cervical mucus, which prevents sperm from penetrating into the uterus (womb) and fallopian tubes and meeting an egg. Once a woman stops using DMPA, there may be a six- to nine-month delay before she is able to conceive. Levonorgestrel implant (Jadelle) consists of two thin, flexible rods that are inserted just under the skin of a woman s upper arm, where they continuously release low doses of the synthetic progestogen levonorgestrel into the bloodstream. Once inserted, Jadelle protects against pregnancy for up to five years but can be removed at any time. Like DMPA, it works primarily by preventing ovulation and thickening the cervical mucus. Implants do not delay the return of a woman's fertility after they are removed. Women who stop using implants can become pregnant as quickly as women who stop non-hormonal methods. The copper IUD is a small, flexible, plastic frame with copper sleeves or wire around it. Once inserted in the uterus, it provides contraceptive protection for years but can be removed at any time. The copper IUD prevents pregnancy mainly by preventing fertilisation. Once the IUD is removed, fertility returns quickly. All the contraceptives being tested in the ECHO Study are highly effective, long-acting, reversible, private methods that do not interfere with sex. ECHO Study Q&A Revised 23 March
12 Contraceptives used in the ECHO Study Family Planning What it is DMPA Depot medroxyprogesterone acetate, also known as DMPA or Depo Provera, is the most widely used progestogen-only injectable. It is injected deep into the muscle of the upper arm, buttocks or hip. Levonorgestrel Implant (Jadelle) This implant consists of 2 thin, flexible rods filled with a progestogen (levonorgestrel) that are inserted just under the skin of a woman s upper arm. Frequency Given every 3 months Once inserted, lasts up to 5 years; can have it removed at any time Benefits Side Effects Long-acting and privacy of use No interference with sex Often stops monthly periods Can be used during breastfeeding Protects against endometrial cancer (cancer of the lining of the uterus) and uterine fibroids May protect against irondeficiency anaemia Most users report irregular or prolonged menstrual bleeding initially, followed by infrequent, irregular or no bleeding, Some users report: Weight gain Headaches Dizziness Abdominal bloating and discomfort Mood changes Reduced sex drive Long-acting and privacy of use No interference with sex May stop monthly periods while being used Can be used during breastfeeding Protects again symptomatic pelvic inflammatory disease May protect against irondeficiency anaemia Some users report: Lighter, irregular, infrequent, prolonged or no menstrual bleeding initially, followed by infrequent, light, irregular or no bleeding Headaches Mood changes Dizziness Acne (can improve or worsen) Breast tenderness Nausea Abdominal pain Weight changes Copper IUD The copper-bearing intrauterine device is shaped like a T and is the size of a matchstick. It is made of soft but strong plastic with copper bands and has a tail made of 2 strings. A doctor or nurse places it in the womb. Once inserted, lasts up to years; can have it removed at any time Long-acting and privacy of use No interference with sex Can be used during breastfeeding May protect against endometrial and cervical cancer Reduces risk of ectopic pregnancy Some users report: Heavier and longer menstrual bleeding and more cramps and pain during monthly bleeding, especially in the first 3 6 months of use Irregular bleeding during the first 1 2 months after insertion. Return to Fertility Return of fertility is often delayed by 6 9 months after the last injection. Rapid return to fertility once removed Rapid return to fertility once removed Source: World Health Organization (WHO) Department of Reproductive Health and Research and Johns Hopkins Bloomberg School of Public Health/Center for Communication Programs (CCP). Family Planning: A Global Handbook for Providers (2018 update). Baltimore and Geneva: CCP and WHO; Available at: ECHO Study Q&A Revised 23 March
The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Study Questions and Answers
 The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Study Questions and Answers About the ECHO Study Background and Implications for the Field How the Study Works About the Products About the
The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Study Questions and Answers About the ECHO Study Background and Implications for the Field How the Study Works About the Products About the
Update on the Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial
 Update on the Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial A Multi-Center, Open-Label, Randomised Clinical Trial Comparing HIV Incidence and Contraceptive Benefits in Women using Depot
Update on the Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial A Multi-Center, Open-Label, Randomised Clinical Trial Comparing HIV Incidence and Contraceptive Benefits in Women using Depot
Nelly Mugo, MBChB, MMed, MPH Kenya Medical Research Institute. May 2015
 Nelly Mugo, MBChB, MMed, MPH Kenya Medical Research Institute May 2015 Outline Rationale for the trial Design and objectives Contraceptive methods to be evaluated Study population and follow-up Potential
Nelly Mugo, MBChB, MMed, MPH Kenya Medical Research Institute May 2015 Outline Rationale for the trial Design and objectives Contraceptive methods to be evaluated Study population and follow-up Potential
The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial
 The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial A Multi-Center, Open-Label, Randomised Clinical Trial Comparing HIV Incidence and Contraceptive Benefits in Women using Depot Medroxyprogesterone
The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial A Multi-Center, Open-Label, Randomised Clinical Trial Comparing HIV Incidence and Contraceptive Benefits in Women using Depot Medroxyprogesterone
Hormonal contraception and HIV risk
 Hormonal contraception and HIV risk Jared Baeten, MD, PhD Departments of Global Health, Medicine, and Epidemiology, University of Washington On behalf of the ECHO Consortium HPTN Annual Meeting Washington
Hormonal contraception and HIV risk Jared Baeten, MD, PhD Departments of Global Health, Medicine, and Epidemiology, University of Washington On behalf of the ECHO Consortium HPTN Annual Meeting Washington
Hormonal contraceptive methods & HIV acquisition in women: updated systematic review of epidemiological evidence
 Hormonal contraceptive methods & HIV acquisition in women: updated systematic review of epidemiological evidence CHELSEA B. POLIS, PHD SEPTEMBER 16, 2016 AVAC WEBINAR GUTTMACHER INSTITUTE 2016 Acknowledgements
Hormonal contraceptive methods & HIV acquisition in women: updated systematic review of epidemiological evidence CHELSEA B. POLIS, PHD SEPTEMBER 16, 2016 AVAC WEBINAR GUTTMACHER INSTITUTE 2016 Acknowledgements
Family Planning UNMET NEED. The Nurse Mildred Radio Talk Shows
 Family Planning UNMET NEED The Nurse Mildred Radio Talk Shows TOPIC 9: IUD/COIL Guests FP counsellor from MSU, RHU& UHMG Nurse Mildred Nurse Betty Objectives of the programme: To inform listeners about
Family Planning UNMET NEED The Nurse Mildred Radio Talk Shows TOPIC 9: IUD/COIL Guests FP counsellor from MSU, RHU& UHMG Nurse Mildred Nurse Betty Objectives of the programme: To inform listeners about
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system)
 FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
Information for Informed Consent for Insertion of a Mirena IUD
 Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
WHAT ARE CONTRACEPTIVES?
 CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
Contraceptives. Kim Dawson October 2010
 Contraceptives Kim Dawson October 2010 Objectives: You will learn about: The about the different methods of birth control. How to use each method of birth control. Emergency contraception What are they?
Contraceptives Kim Dawson October 2010 Objectives: You will learn about: The about the different methods of birth control. How to use each method of birth control. Emergency contraception What are they?
Hormonal Contraception and HIV Acquisition: Getting on the Same Page. Zambia October 2015
 Hormonal Contraception and HIV Acquisition: Getting on the Same Page Zambia October 2015 Key questions for three populations HIV-negative men Whether HIV-negative men are at higher risk of acquiring HIV
Hormonal Contraception and HIV Acquisition: Getting on the Same Page Zambia October 2015 Key questions for three populations HIV-negative men Whether HIV-negative men are at higher risk of acquiring HIV
100% Highly effective No cost No side effects
 effective? Advantages Disadvantages How do I get Cost Abstinence For some it can mean no sexual contact. For others it is no sexual intercourse or vaginal penetration. A permanent surgical procedure available
effective? Advantages Disadvantages How do I get Cost Abstinence For some it can mean no sexual contact. For others it is no sexual intercourse or vaginal penetration. A permanent surgical procedure available
About FEM-PrEP. FEM-PrEP is also studying various behaviors, clinical measures, and health outcomes among the trial s participants.
 Fact Sheet About FEM-PrEP What is the FEM-PrEP clinical trial? FEM-PrEP is a Phase III randomized, placebo-controlled, clinical trial designed to assess the safety and effectiveness of a daily oral dose
Fact Sheet About FEM-PrEP What is the FEM-PrEP clinical trial? FEM-PrEP is a Phase III randomized, placebo-controlled, clinical trial designed to assess the safety and effectiveness of a daily oral dose
Informed Consent Flipchart. Version 1.0, 30 Jan 2018
 Informed Consent Flipchart Version 1.0, 30 Jan 2018 Knowledge is Power Did you know? Across the world, young women are at high risk of getting HIV. In Africa, more than half of people living with HIV are
Informed Consent Flipchart Version 1.0, 30 Jan 2018 Knowledge is Power Did you know? Across the world, young women are at high risk of getting HIV. In Africa, more than half of people living with HIV are
the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD your guide to
 your guide to Helping you choose the method of contraception that s best for you IUD IUD the e IUD IU IUD the IUD 2 3 The intrauterine device (IUD) An IUD is a small plastic and copper device that s put
your guide to Helping you choose the method of contraception that s best for you IUD IUD the e IUD IU IUD the IUD 2 3 The intrauterine device (IUD) An IUD is a small plastic and copper device that s put
Birth Control Options Chart
 Hormonal Methods Birth control pills also known as mini-pills 91-99% A daily pill containing hormones that stops you from ovulating. There are combination estrogen or progestin-only (mini-pill) options.
Hormonal Methods Birth control pills also known as mini-pills 91-99% A daily pill containing hormones that stops you from ovulating. There are combination estrogen or progestin-only (mini-pill) options.
The Balanced Counseling Strategy Plus: A Toolkit for Family Planning Service Providers Working in High STI/HIV Prevalence Settings.
 The Balanced Counseling Strategy Plus: A Toolkit for Family Planning Service Providers Working in High STI/HIV Prevalence Settings Counseling Cards Checklist to be reasonably sure a woman is not pregnant
The Balanced Counseling Strategy Plus: A Toolkit for Family Planning Service Providers Working in High STI/HIV Prevalence Settings Counseling Cards Checklist to be reasonably sure a woman is not pregnant
International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage:
 Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
Strategic Communication for Hormonal Contraception and HIV: An Evidence Review
 Strategic Communication for Hormonal Contraception and HIV: An Evidence Review 2016 Laura Wando, WellShare International Uganda, Courtesy of Photoshare Elizabeth C. Mallalieu, MPH; Lynn M. Van Lith, MPA;
Strategic Communication for Hormonal Contraception and HIV: An Evidence Review 2016 Laura Wando, WellShare International Uganda, Courtesy of Photoshare Elizabeth C. Mallalieu, MPH; Lynn M. Van Lith, MPA;
The following lesson on contraception (birth control) is not intended to infer that you will be sexually active as a teen. This is information that
 The following lesson on contraception (birth control) is not intended to infer that you will be sexually active as a teen. This is information that may be used in the future Abstinence Choosing not to
The following lesson on contraception (birth control) is not intended to infer that you will be sexually active as a teen. This is information that may be used in the future Abstinence Choosing not to
Management of Emergency Contraception (EC)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Management of Emergency Contraception (EC) The risks and benefits of an IUD or oral EC should be discussed and documented (see appendix). Reasonable measures
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Management of Emergency Contraception (EC) The risks and benefits of an IUD or oral EC should be discussed and documented (see appendix). Reasonable measures
Contraception for Women and Couples with HIV. Knowledge Test
 Contraception for Women and Couples with HIV Knowledge Test Instructions: For each question below, check/tick all responses that apply. 1. Which statements accurately describe the impact of HIV/AIDS in
Contraception for Women and Couples with HIV Knowledge Test Instructions: For each question below, check/tick all responses that apply. 1. Which statements accurately describe the impact of HIV/AIDS in
LARC. sample. ask brook about. Are any of them right for me? How effective is it? How long does it last? long acting reversible contraception
 72888_LARC:Layout 1 9/11/09 11:47 Page 1 Are any of them right for me? ask brook about LARC How effective is it? long acting reversible contraception How long does it last? 72888_LARC:Layout 1 9/11/09
72888_LARC:Layout 1 9/11/09 11:47 Page 1 Are any of them right for me? ask brook about LARC How effective is it? long acting reversible contraception How long does it last? 72888_LARC:Layout 1 9/11/09
Contraception Choices: An Evidence Based Approach Case Study Approach. Susan Hellier PhD, DNP, FNP-BC, CNE
 Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
Welcome to Mirena. The Mirena Handbook: A Personal Guide to Your New Mirena. mirena.com. Mirena is the #1 prescribed IUD * in the U.S.
 Mirena is the #1 prescribed IUD * in the U.S. Welcome to Mirena The Mirena Handbook: A Personal Guide to Your New Mirena *Intrauterine Device Supported by 2015-2016 SHS data INDICATIONS FOR MIRENA Mirena
Mirena is the #1 prescribed IUD * in the U.S. Welcome to Mirena The Mirena Handbook: A Personal Guide to Your New Mirena *Intrauterine Device Supported by 2015-2016 SHS data INDICATIONS FOR MIRENA Mirena
Contraception for Adolescents: What s New?
 Contraception for Adolescents: What s New? US Medical Eligibility Criteria for Contraceptive Use Kathryn M. Curtis, PhD Division of Reproductive Health, CDC Expanding Our Experience and Expertise: Implementing
Contraception for Adolescents: What s New? US Medical Eligibility Criteria for Contraceptive Use Kathryn M. Curtis, PhD Division of Reproductive Health, CDC Expanding Our Experience and Expertise: Implementing
Unintended Pregnancy is Common LEARNING OBJECTIVES. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy And Contraceptive Use
 3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
Contraception Effective Methods of Birth Control
 Contraception Effective Methods of Birth Control Abstinence Means choosing NOT to have sex It is the ONLY method that is 100% effective It is your right to be in control of your body and say NO What are
Contraception Effective Methods of Birth Control Abstinence Means choosing NOT to have sex It is the ONLY method that is 100% effective It is your right to be in control of your body and say NO What are
Hormonal Contraception and HIV: The WHO Responds. Ward Cates MTN Annual Meeting February 21, 2012
 Hormonal Contraception and HIV: The WHO Responds Ward Cates MTN Annual Meeting February 21, 2012 Acknowledgments Colleagues from: FHI 360 The MTN USAID University of Washington WHO And many more Woman
Hormonal Contraception and HIV: The WHO Responds Ward Cates MTN Annual Meeting February 21, 2012 Acknowledgments Colleagues from: FHI 360 The MTN USAID University of Washington WHO And many more Woman
Fitting of an Intrauterine Device (IUD)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an IUD? An IUD is a small T-shaped plastic and copper device that is put into
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an IUD? An IUD is a small T-shaped plastic and copper device that is put into
What s New in Adolescent Contraception?
 What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
Contraception. Objectives. Unintended Pregnancy. Unintended Pregnancy in the US. What s the Impact? 10/7/2014
 Contraception Tami Allen, RNC OB, MHA Robin Petersen, RN, MSN Perinatal Clinical Nurse Specialist Objectives Discuss the impact of unintended pregnancy in the United States Discuss the risks and benefits
Contraception Tami Allen, RNC OB, MHA Robin Petersen, RN, MSN Perinatal Clinical Nurse Specialist Objectives Discuss the impact of unintended pregnancy in the United States Discuss the risks and benefits
FACT SHEET: Copper IUD
 FACT SHEET: Copper IUD How does the copper IUD help me? The copper IUD is a hormone-free option. If you don t like the copper IUD or you decide to get pregnant, your health care provider can remove the
FACT SHEET: Copper IUD How does the copper IUD help me? The copper IUD is a hormone-free option. If you don t like the copper IUD or you decide to get pregnant, your health care provider can remove the
17. Preventing pregnancy
 17. Preventing pregnancy Objectives By the end of this session, group members will be able to: Define contraception. List ways young people can prevent pregnancy. Background notes What is contraception?
17. Preventing pregnancy Objectives By the end of this session, group members will be able to: Define contraception. List ways young people can prevent pregnancy. Background notes What is contraception?
Expanding Access to Birth Control: Will Women Get the Care They Need?
 Expanding Access to Birth Control: Will Women Get the Care They Need? Target Audience: Pharmacists ACPE#: 0202-0000-18-045-L01-P Activity Type: Application-based Target Audience: ACPE#: Activity Type:
Expanding Access to Birth Control: Will Women Get the Care They Need? Target Audience: Pharmacists ACPE#: 0202-0000-18-045-L01-P Activity Type: Application-based Target Audience: ACPE#: Activity Type:
An Illustrative Communication Strategy for Contraceptive Implants
 An Illustrative Communication Strategy for Contraceptive Implants: Step 1 (Analyze the Situation) 1 An Illustrative Communication Strategy for Contraceptive Implants Step 1: Analyze the Situation Health
An Illustrative Communication Strategy for Contraceptive Implants: Step 1 (Analyze the Situation) 1 An Illustrative Communication Strategy for Contraceptive Implants Step 1: Analyze the Situation Health
LEARNING OBJECTIVES. Beyond the Pill: Long Acting Contraception. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy is Common
 4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
Instruction for the patient
 WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
Contraceptive. Ready Lessons II. What Can a Contraceptive Security Champion Do?
 Contraceptive Lesson Security Ready Lessons II Expand client choice and contraceptive security by supporting access to underutilized family planning methods. What Can a Contraceptive Security Champion
Contraceptive Lesson Security Ready Lessons II Expand client choice and contraceptive security by supporting access to underutilized family planning methods. What Can a Contraceptive Security Champion
Notes to Teacher continued Contraceptive Considerations
 Abstinence a conscious decision to refrain from sexual intercourse 100% pregnancy will not occur if close contact between the penis and vagina does not take place. The risk of a number of STDs, including
Abstinence a conscious decision to refrain from sexual intercourse 100% pregnancy will not occur if close contact between the penis and vagina does not take place. The risk of a number of STDs, including
Linda Gregg NP, Janet Isabell NP, Sue Montei NP Clinical Reviewers Reproductive Health Unit
 Linda Gregg NP, Janet Isabell NP, Sue Montei NP Clinical Reviewers Reproductive Health Unit What We Plan To Do Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC) Explain
Linda Gregg NP, Janet Isabell NP, Sue Montei NP Clinical Reviewers Reproductive Health Unit What We Plan To Do Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC) Explain
Discover the birth control you ve been looking for. Highly reliable. Virtually hassle-free. Totally hormone-free.
 Discover the birth control you ve been looking for Highly reliable. Virtually hassle-free. Totally hormone-free. Over 70 million women worldwide use a nonhormonal IUC like ParaGard. Millions of women with
Discover the birth control you ve been looking for Highly reliable. Virtually hassle-free. Totally hormone-free. Over 70 million women worldwide use a nonhormonal IUC like ParaGard. Millions of women with
Essure By Mayo Clinic staff
 Page 1 of 5 Reprints A single copy of this article may be reprinted for personal, noncommercial use only. Essure By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/essure/my00999 Definition
Page 1 of 5 Reprints A single copy of this article may be reprinted for personal, noncommercial use only. Essure By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/essure/my00999 Definition
QUESTIONS AND ANSWERS ABOUT PARTNERS PrEP AND VOICE
 CONTACT: Lisa Rossi +1-412-641-8940 +1-412- 916-3315 (mobile) rossil@upmc.edu QUESTIONS AND ANSWERS ABOUT PARTNERS PrEP AND VOICE 1. What is the Partners PrEP study? The Partners PrEP Study is a double-blind,
CONTACT: Lisa Rossi +1-412-641-8940 +1-412- 916-3315 (mobile) rossil@upmc.edu QUESTIONS AND ANSWERS ABOUT PARTNERS PrEP AND VOICE 1. What is the Partners PrEP study? The Partners PrEP Study is a double-blind,
Implants and ART: weighing the evidence to guide programs
 Implants and ART: weighing the evidence to guide programs Presented by: Jennifer Mason, MPH; Tabitha Sripipitana, MPH; and Sarah Yeiser, MPH Office of Population & Reproductive Health, USAID Office of
Implants and ART: weighing the evidence to guide programs Presented by: Jennifer Mason, MPH; Tabitha Sripipitana, MPH; and Sarah Yeiser, MPH Office of Population & Reproductive Health, USAID Office of
Strategic Communication Framework for Hormonal Contraceptive Methods and Potential HIV-Related Risks. Beth Mallalieu October 22, 2015
 Strategic Communication Framework for Hormonal Contraceptive Methods and Potential HIV-Related Risks Beth Mallalieu October 22, 2015 SHC vs. SBCC Strategic health communication (SHC) and social and behavior
Strategic Communication Framework for Hormonal Contraceptive Methods and Potential HIV-Related Risks Beth Mallalieu October 22, 2015 SHC vs. SBCC Strategic health communication (SHC) and social and behavior
Contraception and gynecological pathologies
 1 Contraception and gynecological pathologies 18 years old, 2 CMI normal First menstruation at 14 years old Irregular (every 2/3 months), painful + She does not need contraception She is worried about
1 Contraception and gynecological pathologies 18 years old, 2 CMI normal First menstruation at 14 years old Irregular (every 2/3 months), painful + She does not need contraception She is worried about
Medical Eligibility for Contraception Use
 Medical Eligibility for Contraception Use DIVISION OF REPRODUCTIVE HEALTH CENTERS FOR DISEASE CONTROL AND PREVENTION 2016 US Medical Eligibility Criteria for Contraceptive Use (US MEC) Purpose To assist
Medical Eligibility for Contraception Use DIVISION OF REPRODUCTIVE HEALTH CENTERS FOR DISEASE CONTROL AND PREVENTION 2016 US Medical Eligibility Criteria for Contraceptive Use (US MEC) Purpose To assist
Emergency Contraception THE FACTS
 Emergency Contraception Quick Facts What is it? Emergency contraception is birth control that you use after you have had unprotected sex--if you didn t use birth control or your regular birth control failed.
Emergency Contraception Quick Facts What is it? Emergency contraception is birth control that you use after you have had unprotected sex--if you didn t use birth control or your regular birth control failed.
Introducing the Contraceptive Sino Implant II (Zarin) in Sierra Leone. Background
 Introducing the Contraceptive Sino Implant II (Zarin) in Sierra Leone Background Maternal mortality in Sierra Leone is amongst the highest in the world. A decade-long civil war and severe underdevelopment
Introducing the Contraceptive Sino Implant II (Zarin) in Sierra Leone Background Maternal mortality in Sierra Leone is amongst the highest in the world. A decade-long civil war and severe underdevelopment
2
 1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
QUESTIONS AND ANSWERS
 CONTACT: Lisa Rossi +1-412-641-8940 +1-412- 916-3315 (mobile) rossil@upmc.edu QUESTIONS AND ANSWERS ASPIRE A Study to Prevent Infection with a Ring for Extended Use The Big Picture 1. What is the aim of
CONTACT: Lisa Rossi +1-412-641-8940 +1-412- 916-3315 (mobile) rossil@upmc.edu QUESTIONS AND ANSWERS ASPIRE A Study to Prevent Infection with a Ring for Extended Use The Big Picture 1. What is the aim of
QUESTIONS AND ANSWERS ASPIRE A Study to Prevent Infection with a Ring for Extended Use
 CONTACT: Lisa Rossi +1-412-641-8940 +1-412- 916-3315 (mobile) rossil@upmc.edu QUESTIONS AND ANSWERS ASPIRE A Study to Prevent Infection with a Ring for Extended Use I. ASPIRE and The Ring Study: The Basics
CONTACT: Lisa Rossi +1-412-641-8940 +1-412- 916-3315 (mobile) rossil@upmc.edu QUESTIONS AND ANSWERS ASPIRE A Study to Prevent Infection with a Ring for Extended Use I. ASPIRE and The Ring Study: The Basics
Transcervical Sterilization
 Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
Review of IUCD Complications: Lessons from CAT. Dr FG Mhlanga CAT Meeting 24 September 2016
 Review of IUCD Complications: Lessons from CAT Dr FG Mhlanga CAT Meeting 24 September 2016 INTRODUCTION The intrauterine device (IUD) is a reliable long term reversible, cost-effective,easy to use and
Review of IUCD Complications: Lessons from CAT Dr FG Mhlanga CAT Meeting 24 September 2016 INTRODUCTION The intrauterine device (IUD) is a reliable long term reversible, cost-effective,easy to use and
levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer
 levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer 6 March 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer 6 March 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
LESSON 5. Counseling clients about DMPA and Sayana Press
 LESSON 5 Counseling clients about DMPA and Sayana Press 1 LESSON 5 Learning objectives List possible side effects of DMPA. Describe what to do if a client has concerns or is experiencing side effects.
LESSON 5 Counseling clients about DMPA and Sayana Press 1 LESSON 5 Learning objectives List possible side effects of DMPA. Describe what to do if a client has concerns or is experiencing side effects.
How to use WHO's family planning guidelines and tools
 How to use WHO's family planning guidelines and tools Mary Eluned Gaffield Promoting Family Planning Team Department of Reproductive Health and Research Training Course in Sexual and Reproductive Health
How to use WHO's family planning guidelines and tools Mary Eluned Gaffield Promoting Family Planning Team Department of Reproductive Health and Research Training Course in Sexual and Reproductive Health
MTN-020. Jared Baeten, MD PhD Thesla Palanee, PhD On behalf of the ASPIRE team MTN Annual Meeting, Bethesda 21 February 2012
 MTN-020 Jared Baeten, MD PhD Thesla Palanee, PhD On behalf of the ASPIRE team MTN Annual Meeting, Bethesda 21 February 2012 MTN-020 / ASPIRE A Multi-Center, Randomized, Double- Blind, Placebo-Controlled
MTN-020 Jared Baeten, MD PhD Thesla Palanee, PhD On behalf of the ASPIRE team MTN Annual Meeting, Bethesda 21 February 2012 MTN-020 / ASPIRE A Multi-Center, Randomized, Double- Blind, Placebo-Controlled
Sterilisation for women at the RD&E: what you need to know Reference Number: CW
 Sterilisation for women at the RD&E: what you need to know Royal Devon and Exeter NHS Foundation Trust Patient Information Sterilisation for Women at The Royal Devon and Exeter Hospital What you need to
Sterilisation for women at the RD&E: what you need to know Royal Devon and Exeter NHS Foundation Trust Patient Information Sterilisation for Women at The Royal Devon and Exeter Hospital What you need to
Package leaflet: Information for the user. Levonorgestrel 1.5 mg Tablet. levonorgestrel
 Package leaflet: Information for the user Levonorgestrel 1.5 mg Tablet levonorgestrel Read all of this leaflet carefully before you start taking this medicine because it contains important information
Package leaflet: Information for the user Levonorgestrel 1.5 mg Tablet levonorgestrel Read all of this leaflet carefully before you start taking this medicine because it contains important information
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
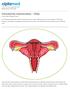 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
WOLFSON FERTILITY CENTRE. Wolfson Fertility Centre
 WOLFSON FERTILITY CENTRE Wolfson Fertility Centre Innovative, expert care The Wolfson Fertility Centre at Hammersmith Hospital is one of the leading centres for reproductive medicine in the world, with
WOLFSON FERTILITY CENTRE Wolfson Fertility Centre Innovative, expert care The Wolfson Fertility Centre at Hammersmith Hospital is one of the leading centres for reproductive medicine in the world, with
Reproductive health research at WHO
 Reproductive health research at WHO Paul F.A. Van Look, MD PhD Department of Reproductive Health and Research World Health Organization Geneva, 11 March 2004 PVL_GE_StudCourse_MAR04/1 Health is a state
Reproductive health research at WHO Paul F.A. Van Look, MD PhD Department of Reproductive Health and Research World Health Organization Geneva, 11 March 2004 PVL_GE_StudCourse_MAR04/1 Health is a state
Supplmentary File 1: ECHO Trial Protocol
 Supplmentary File 1: ECHO Trial Protocol A Multi Center, Open-Label, Randomised Clinical Trial Comparing HIV Incidence and Contraceptive Benefits in Women using Depot Medroxyprogesterone Acetate (DMPA),
Supplmentary File 1: ECHO Trial Protocol A Multi Center, Open-Label, Randomised Clinical Trial Comparing HIV Incidence and Contraceptive Benefits in Women using Depot Medroxyprogesterone Acetate (DMPA),
BIRTH CONTROL METHOD COMPARISON CHART
 BIRTH CONTROL METHOD COMPARISON CHART Abstinence 100% Yes Male latex condom 86%-95% Can increase to 98% by using with a contraceptive jelly Yes Highly effective No side effects, as with other methods No
BIRTH CONTROL METHOD COMPARISON CHART Abstinence 100% Yes Male latex condom 86%-95% Can increase to 98% by using with a contraceptive jelly Yes Highly effective No side effects, as with other methods No
Cue Cards for Counseling Adolescents on Contraception
 Cue Cards for Counseling Adolescents on Contraception About the Cue Cards This set of contraceptive counseling cue cards was developed to support a range of providers (such as facility-based providers,
Cue Cards for Counseling Adolescents on Contraception About the Cue Cards This set of contraceptive counseling cue cards was developed to support a range of providers (such as facility-based providers,
QUESTIONS AND ANSWERS
 CONTACTS: Clare Collins Lisa Rossi +1-412-641-7299 +1-412-641-8940 +1-412-770-8643 (mobile) +1-412-916-3315 (mobile) collcx@upmc.edu rossil@upmc.edu QUESTIONS AND ANSWERS MTN-016: HIV Prevention Agent
CONTACTS: Clare Collins Lisa Rossi +1-412-641-7299 +1-412-641-8940 +1-412-770-8643 (mobile) +1-412-916-3315 (mobile) collcx@upmc.edu rossil@upmc.edu QUESTIONS AND ANSWERS MTN-016: HIV Prevention Agent
Contraceptive Updates and Recommendations
 Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Contraceptive Updates and Recommendations
 Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
HIV and contraception the latest recommendations
 1 8-11 June 2015, Chiang-Mai HIV and contraception the latest recommendations Mary Lyn Gaffield, Sharon Phillips, Rachel Baggaley, Petrus Steyn, and Marleen Temmerman 2 Medical eligibility criteria for
1 8-11 June 2015, Chiang-Mai HIV and contraception the latest recommendations Mary Lyn Gaffield, Sharon Phillips, Rachel Baggaley, Petrus Steyn, and Marleen Temmerman 2 Medical eligibility criteria for
Birth Control -- Especially for Teens
 AP112, June 2011 Birth Control -- Especially for Teens Making the decision whether to have sex can be difficult. You should make up your own mind when the time is right for you. If you are not ready for
AP112, June 2011 Birth Control -- Especially for Teens Making the decision whether to have sex can be difficult. You should make up your own mind when the time is right for you. If you are not ready for
LONG-ACTING REVERSIBLE CONTRACEPTION. Summary Tables
 LONG-ACTING REVERSIBLE CONTRACEPTION Summary Tables Bridging the Divide: A Project of the Jacobs Institute of Women s Health June 2016 Table 1. Summary of LARC Methods Available Years Since Effective Copper
LONG-ACTING REVERSIBLE CONTRACEPTION Summary Tables Bridging the Divide: A Project of the Jacobs Institute of Women s Health June 2016 Table 1. Summary of LARC Methods Available Years Since Effective Copper
Product Information. Confidence that lasts
 Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
Can you imagine reversible birth control that s more than 99% effective and 100% hormone free, too?
 Can you imagine reversible birth control that s more than 99% effective and 100% hormone free, too? BIRTH CONTROL THAT FITS YOUR LIFE, NATURALLY. ParaGard is a registered trademark of Teva Women s Health,
Can you imagine reversible birth control that s more than 99% effective and 100% hormone free, too? BIRTH CONTROL THAT FITS YOUR LIFE, NATURALLY. ParaGard is a registered trademark of Teva Women s Health,
The Doctor Is In. Brent N Davidson MD Vice Chair Women s Health Henry Ford Health System Medical Director Family Planning MDCH
 The Doctor Is In Brent N Davidson MD Vice Chair Women s Health Henry Ford Health System Medical Director Family Planning MDCH Contraception Resources from the CDC: 2016 U.S. Medical Eligibility Criteria
The Doctor Is In Brent N Davidson MD Vice Chair Women s Health Henry Ford Health System Medical Director Family Planning MDCH Contraception Resources from the CDC: 2016 U.S. Medical Eligibility Criteria
Reintroducing the IUD in Kenya
 Reintroducing the IUD in Kenya Background Between 1978 and 1998, the proportion of married Kenyan women using modern contraceptive methods rose from only 9 percent to 39 percent. However, use of the intrauterine
Reintroducing the IUD in Kenya Background Between 1978 and 1998, the proportion of married Kenyan women using modern contraceptive methods rose from only 9 percent to 39 percent. However, use of the intrauterine
The Johns Hopkins Bloomberg School of Public Health
 The Johns Hopkins Bloomberg School of Public Health CONSENT FORM A / NEW RESEARCH PROJECT Title of Research Project: A Randomized Trial of HAART in Acute/Early HIV Infection Version 3.0 Principal Investigator:
The Johns Hopkins Bloomberg School of Public Health CONSENT FORM A / NEW RESEARCH PROJECT Title of Research Project: A Randomized Trial of HAART in Acute/Early HIV Infection Version 3.0 Principal Investigator:
Fertility control: what do women want?
 FIAPAC 2018 Fertility control: what do women want? Dr. Raymond H.W. Li MBBS, MMedSC, FRCOG, FHKAM (O&G) Cert RCOG/HKCOG (Reprod Med) Department of O&G, The University of Hong Kong The Family Planning Association
FIAPAC 2018 Fertility control: what do women want? Dr. Raymond H.W. Li MBBS, MMedSC, FRCOG, FHKAM (O&G) Cert RCOG/HKCOG (Reprod Med) Department of O&G, The University of Hong Kong The Family Planning Association
Annex 2: GRADE evidence profiles
 Annex 2: GRADE evidence profiles GRADE table 1: Does the use of a particular method of hormonal contraception directly increase the risk of HIV acquisition in women? Outcome ( participants) Injectable
Annex 2: GRADE evidence profiles GRADE table 1: Does the use of a particular method of hormonal contraception directly increase the risk of HIV acquisition in women? Outcome ( participants) Injectable
Expanding access to injectable contraceptives
 Expanding access to injectable contraceptives Background Catherine d'arcangues World Health Organization Geneva, 15 June 2009 06_PVL_TURIN_APRIL1 Contraceptive prevalence by method: world and development
Expanding access to injectable contraceptives Background Catherine d'arcangues World Health Organization Geneva, 15 June 2009 06_PVL_TURIN_APRIL1 Contraceptive prevalence by method: world and development
HIV Prevention and Reproductive Choices
 HIV Prevention and Reproductive Choices Renee Heffron, PhD MPH University of Washington Virology Education International Workshop on HIV & Women Boston, 20-21 February 2016 Reproductive choices & pregnancy
HIV Prevention and Reproductive Choices Renee Heffron, PhD MPH University of Washington Virology Education International Workshop on HIV & Women Boston, 20-21 February 2016 Reproductive choices & pregnancy
ANALYZING CONTRACEPTION OPTIONS
 ANALYZING CONTRACEPTION OPTIONS LESSON INTRODUCTION: The purpose of this lesson is to identify and categorize the various forms of contraception and discuss influences on, and reasons why, students may
ANALYZING CONTRACEPTION OPTIONS LESSON INTRODUCTION: The purpose of this lesson is to identify and categorize the various forms of contraception and discuss influences on, and reasons why, students may
UNIVERSITY OF PENNSYLVANIA HEALTH SYSTEM
 White Blood Cell Collection by Leukapheresis in HIV-infected Individuals On Chemotherapy and Controls Not on Chemotherapy: A Study of HIV Reservoir Eradication CONSENT TO PARTICIPATE IN A RESEARCH STUDY
White Blood Cell Collection by Leukapheresis in HIV-infected Individuals On Chemotherapy and Controls Not on Chemotherapy: A Study of HIV Reservoir Eradication CONSENT TO PARTICIPATE IN A RESEARCH STUDY
Birth Control. Choosing the method that s right for you
 Birth Control Choosing the method that s right for you Contents Family planning services... 1 How to use this brochure... 2 Implant... 3 IUD/IUS... 5 Sterilization... 7 Depo-Provera : The shot...9 Pill/ring/patch...
Birth Control Choosing the method that s right for you Contents Family planning services... 1 How to use this brochure... 2 Implant... 3 IUD/IUS... 5 Sterilization... 7 Depo-Provera : The shot...9 Pill/ring/patch...
Topic 24: Estrogens and Female Reproductive Drugs
 Topic 24: Estrogens and Female Reproductive Drugs I. Contraceptives A. Estrogen-Progestin Contraceptives Note all of these drugs contain one estrogen (listed first) and one progestin Drug to know: ethinyl
Topic 24: Estrogens and Female Reproductive Drugs I. Contraceptives A. Estrogen-Progestin Contraceptives Note all of these drugs contain one estrogen (listed first) and one progestin Drug to know: ethinyl
Ovarian Cancer. What you should know. making cancer less frightening by enlightening
 Ovarian Cancer What you should know making cancer less frightening by enlightening ovarian cancer the facts Over 360 cases are diagnosed in Ireland annually It is the 6th most common cancer in women 4
Ovarian Cancer What you should know making cancer less frightening by enlightening ovarian cancer the facts Over 360 cases are diagnosed in Ireland annually It is the 6th most common cancer in women 4
Contraception and Kidney Problems: Advice for Young Adults
 Contraception and Kidney Problems: Advice for Young Adults Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Contraception and Kidney Problems: Advice for Young Adults Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Birth Control- an Overview. Keith Merritt, MD. Remember, all methods of birth control are safer and have fewer side effects than pregnancy
 Birth Control- an Overview Keith Merritt, MD Basics Remember, all methods of birth control are safer and have fewer side effects than pregnancy Even with perfect use, each method of birth control has a
Birth Control- an Overview Keith Merritt, MD Basics Remember, all methods of birth control are safer and have fewer side effects than pregnancy Even with perfect use, each method of birth control has a
Effective Contraception Utilization. Sarah Laiosa, DO Family Physician Contract Medical Director, EOCCO
 Effective Contraception Utilization Sarah Laiosa, DO Family Physician Contract Medical Director, EOCCO Disclosures Contract Medical Director, EOCCO Objectives Illustrate how to best address contraception
Effective Contraception Utilization Sarah Laiosa, DO Family Physician Contract Medical Director, EOCCO Disclosures Contract Medical Director, EOCCO Objectives Illustrate how to best address contraception
Application for inclusion of levonorgestrel - releasing IUD for contraception in the WHO Model List of Essential Medicines
 Application for inclusion of levonorgestrel - releasing IUD for contraception in the WHO Model List of Essential Medicines 1. Summary statement of the proposal for inclusion LNG-IUS is an effective contraceptive;
Application for inclusion of levonorgestrel - releasing IUD for contraception in the WHO Model List of Essential Medicines 1. Summary statement of the proposal for inclusion LNG-IUS is an effective contraceptive;
What?! Why?! Emergency Contraception. physical consequences. emotional consequences
 HealthCHAT Emergency Contraception What?! Emergency contraception is a series of pills that can be taken by a woman to prevent pregnancy after having unprotected sex. Why?! Emergency contraception allows
HealthCHAT Emergency Contraception What?! Emergency contraception is a series of pills that can be taken by a woman to prevent pregnancy after having unprotected sex. Why?! Emergency contraception allows
MICROBICIDES DEVELOPMENT PROGRAMME
 The MDP 301 Trial - Q&A What is the MDP 301 trial? MDP 301 is a Phase III trial evaluating the safety and effectiveness of the investigational vaginal microbicide PRO 2000 for reducing the risk of HIV
The MDP 301 Trial - Q&A What is the MDP 301 trial? MDP 301 is a Phase III trial evaluating the safety and effectiveness of the investigational vaginal microbicide PRO 2000 for reducing the risk of HIV
Expanding Access to Injectable Contraception Geneva, June 2009
 Bangladesh Experience in Expanding the Delivery of Injectable Contraception A brief overview Presentation at Expanding Access to Injectable Contraception Geneva, 15-17 June 2009 Dr S. Thapa Reproductive
Bangladesh Experience in Expanding the Delivery of Injectable Contraception A brief overview Presentation at Expanding Access to Injectable Contraception Geneva, 15-17 June 2009 Dr S. Thapa Reproductive
Contraception and Risk of HIV Progression
 Contraception and Risk of HIV Progression Catherine Hankins BA MD MSc FRCPC Deputy Director, Science Amsterdam Institute for Global Health and Development Honorary Professor London School of Hygiene and
Contraception and Risk of HIV Progression Catherine Hankins BA MD MSc FRCPC Deputy Director, Science Amsterdam Institute for Global Health and Development Honorary Professor London School of Hygiene and
Guideline for Fertility Preservation for Patients with Cancer
 Guideline for Fertility Preservation for Patients with Cancer COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive Care Endorsed Guidelines. DISCLAIMER For Informational Purposes
Guideline for Fertility Preservation for Patients with Cancer COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive Care Endorsed Guidelines. DISCLAIMER For Informational Purposes
Power Point Use in EBPs. CAPP & PREP Learning Community May 15, 2018
 Power Point Use in EBPs CAPP & PREP Learning Community May 15, 2018 Objectives Best practices for power point use Why use power point for EBP delivery Examples: the Good, the Bad and the Ugly Recommendations
Power Point Use in EBPs CAPP & PREP Learning Community May 15, 2018 Objectives Best practices for power point use Why use power point for EBP delivery Examples: the Good, the Bad and the Ugly Recommendations
MTN-020 and IPM 027 and the MTN-020 DSMB. Jared Baeten, MD PhD Thesla Palanee, PhD ASPIRE Protocol Team Meeting 22 February 2012
 MTN-020 and IPM 027 and the MTN-020 DSMB Jared Baeten, MD PhD Thesla Palanee, PhD ASPIRE Protocol Team Meeting 22 February 2012 Developing a range of options for antiretroviral-based HIV prevention Pill
MTN-020 and IPM 027 and the MTN-020 DSMB Jared Baeten, MD PhD Thesla Palanee, PhD ASPIRE Protocol Team Meeting 22 February 2012 Developing a range of options for antiretroviral-based HIV prevention Pill
2. Studies of Cancer in Humans
 346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
