Defining Plasmodium falciparum Treatment in South West Asia: A Randomized Trial Comparing Artesunate or Primaquine Combined with Chloroquine or SP
|
|
|
- Neal McCormick
- 6 years ago
- Views:
Transcription
1 Defining Plasmodium falciparum Treatment in South West Asia: A Randomized Trial Comparing Artesunate or Primaquine Combined with Chloroquine or SP Kate Kolaczinski 1,2 *, Toby Leslie 1,2, Iftikhar Ali 2, Naeem Durrani 2, Sue Lee 3,4, Marion Barends 5, Khalid Beshir 1, Rosalynn Ord 1, Rachel Hallett 1, Mark Rowland 1 1 London School of Hygiene and Tropical Medicine, London, United Kingdom, 2 HealthNet TPO, Peshawar, Pakistan, 3 Faculty of Tropical Medicine, Mahidol University, Bangkok, Thailand, 4 Centre for Clinical Vaccinology and Tropical Medicine, Churchill Hospital, Oxford, United Kingdom, 5 Shoklo Malaria Research Unit, Mae Sot, Thailand Abstract Introduction: Antimalarial resistance has led to a global policy of artemisinin-based combination therapy. Despite growing resistance chloroquine (CQ) remained until recently the official first-line treatment for falciparum malaria in Pakistan, with sulfadoxine-pyrimethamine (SP) second-line. Co-treatment with the gametocytocidal primaquine (PQ) is recommended for transmission control in South Asia. The relative effect of artesunate (AS) or primaquine, as partner drugs, on clinical outcomes and gametocyte carriage in this setting were unknown. Methods: A single-blinded, randomized trial among Afghan refugees in Pakistan compared six treatment arms: CQ; CQ+(single-dose)PQ; CQ+(3 d)as; SP; SP+(single-dose)PQ, and SP+(3 d)as. The objectives were to compare treatment failure rates and effect on gametocyte carriage, of CQ or SP monotherapy against the respective combinations (PQ or AS). Outcomes included trophozoite and gametocyte clearance (read by light microscopy), and clinical and parasitological failure. Findings: A total of 308 (87%) patients completed the trial. Failure rates by day 28 were: CQ 55/68 (81%); CQ+AS 19/67 (28%), SP 4/41 (9.8%), SP+AS 1/41 (2.4%). The addition of PQ to CQ or SP did not affect failure rates (CQ+PQ 49/67 (73%) failed; SP+PQ 5/33 (16%) failed). AS was superior to PQ at clearing gametocytes; gametocytes were seen on d7 in 85% of CQ, 40% of CQ+PQ, 21% of CQ+AS, 91% of SP, 76% of SP+PQ and 23% of SP+AS treated patients. PQ was more effective at clearing older gametocyte infections whereas AS was more effective at preventing emergence of mature gametocytes, except in cases that recrudesced. Conclusions: CQ is no longer appropriate by itself or in combination. These findings influenced the replacement of CQ with SP+AS for first-line treatment of uncomplicated falciparum malaria in the WHO Eastern Mediterranean Region. The threat of SP resistance remains as SP monotherapy is still common. Three day AS was superior to single-dose PQ for reducing gametocyte carriage. Trial Registration: ClinicalTrials.gov NCT Citation: Kolaczinski K, Leslie T, Ali I, Durrani N, Lee S, et al. (2012) Defining Plasmodium falciparum Treatment in South West Asia: A Randomized Trial Comparing Artesunate or Primaquine Combined with Chloroquine or SP. PLoS ONE 7(1): e doi: /journal.pone Editor: Ivo Mueller, Walter & Eliza Hall Institute, Australia Received April 26, 2011; Accepted November 17, 2011; Published January 31, 2012 Copyright: ß 2012 Kolaczinski et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Funding: This manuscript was supported by UNDP/World Bank/WHO Special Programme for Research on Tropical Diseases (A00017)( The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. Competing Interests: The authors have declared that no competing interests exist. * k.kolaczinski@gmail.com Introduction Antimalarial drug resistance is an ongoing threat to malaria control [1]. Despite widespread documented resistance, chloroquine remained widely used in Pakistan and Afghanistan for first line treatment of falciparum malaria at the time of this study ( ) [2 4]. In many other parts of the world including Pakistan and Afghanistan the antifolate drug sulfadoxinepyrimethamine (SP) is comparatively effective against falciparum malaria in contrast to the situation in South East Asia and many African settings. In Pakistan and Afghanistan transmission is seasonal, strong immunity seldom develops, infected individuals are symptomatic and it is thought that the majority seek treatment [2,3,5]. These conditions expose the majority of infections to antimalarial drugs and would be expected to exert strong selection for resistance [6]. SP has a long plasma half-life which may further contribute to selection. In such areas of low seasonal transmission the operational effectiveness of SP before resistance arises appears to be short [7]. Whilst current effectiveness remains comparatively good in the region low level in vivo resistance to SP has been demonstrated [5,8,9]. Wide-scale adoption of effective SP based combinations, rather than SP monotherapy, which was being considered as an option to replace chloroquine at the time of the study, could delay the selection of resistance and prolong the useful life of SP across the subcontinent. PLoS ONE 1 January 2012 Volume 7 Issue 1 e28957
2 In areas of low or medium endemicity co-treatment of infections with a gametocytocidal drug may help to reduce transmission and may be particularly important when considering strategies for malaria elimination. In South Asia, the standard policy has been to co-treat with a single dose of primaquine to reduce gametocyte carriage. Primaquine is known to have poor efficacy as a direct treatment but has repeatedly been shown to be highly gametocytocidal [10 14]. Reduction in gametocyte carriage and infectivity to mosquitoes after artesunate treatment is widely documented [15,16]. It appears to be due to a combination of rapid clearance of asexual stages, direct activity on immature gametocytes (either killing them or preventing their maturation) and possibly reduction in the infectivity of mature gametocytes [17,18]. Use of ACTs has been shown to reduce transmission [19 23] and is recommended for epidemic response [24], as too is primaquine [25]. There is increasing interest in using primaquine with ACTs to accelerate gametocyte clearance [14]. SP treatment of clinical infections can lead to high gametocyte loads which persist for 10 days or more [15] with latent gametocytaemia detected by PCR for up to a year [26]. A direct comparison of artesunate and primaquine on treatment failure and gametocyte carriage has not been conducted before. Many Afghan refugee communities in Pakistan have a history of falciparum malaria and are prone to outbreaks [27 29]. A trial examining the comparative efficacy of chloroquine and SP combined with either artesunate or primaquine was therefore carried out in refugee villages in North-western Pakistan. Materials and Methods The protocol for this trial and supporting CONSORT checklist are available as supporting information; see Checklist S1 and Protocol S1. Study area and population The study recruited patients from five Afghan refugee villages within an 80 km radius of Peshawar, Khyber Province (formerly North West Frontier Province), Pakistan. The 5 villages were established in the early 1980s and each has a history of falciparum transmission. Three (Adizai, Naguman and Yakka Ghund) are situated on the banks of the Kabul river, and two (Mohammed Khoja and Kotki) are situated to the south of Peshawar in Kohat district. Malaria transmission is seasonal with vivax malaria occurring from March to November and falciparum from July to December. Participants were Afghan refugees who were permanently resident in the Pakistan villages. A minority might have acquired their infections in Afghanistan, but admission criteria required 4 6 weeks of follow-up which would have excluded the more regular travellers. Study sites The study was conducted through three sites with well-managed clinics run by Non-Governmental Organisations (NGO) and government agencies. Site 1 was Adizai village which also served the population of nearby Naguman. Site 2 was Yakka Ghund village. Site 3 was Kotki which also serviced Mohammed Khoja village. Health staff from the NGO HealthNet TPO were seconded to each clinic to manage the recruitment and followup of patients. The study took place over three malaria seasons from 2000 to In the first season only site 1 was used, in the second season site 2 was added, and in the third season site 3 was added. The stepped inclusion of sites resulted from unexpectedly low recruitment rates at the first study site, and is summarized in Table 1. An earlier in vivo survey across all refugee camps along the length of the 1000 km North-South axis of Khyber Province showed little heterogeneity in resistance frequency to chloroquine and SP [30]. (Note that SP is the only drug name abbreviated throughout the text. Abbreviations for chloroquine (CQ), primaquine (PQ) and artesunate (AS) are used when referring to specific study arms (e.g. CQ+PQ) but not at other points in the text.) Study design and procedures. Individuals presenting with clinical symptoms and diagnosed microscopically with falciparum malaria were referred to trial staff for further assessment. Inclusion criteria were: over two years of age, not pregnant, P. falciparum mono-infection, more than 1 asexual parasite per 10 fields, no other serious disease, resident in the refugee village for the full period of follow-up, no verbal report of antimalarial use during the last 21 days, and no signs of severe malaria. Individuals meeting the inclusion criteria and giving informed consent were allocated using randomization tables stratified by age and sex to the following treatment arms: chloroquine (CQ 1 ) (25 mg/kg) over 3 days; CQ (25 mg/kg) over 3 days plus primaquine (PQ) (0.5 mg/kg) on the last day of treatment; CQ (25 mg/kg) over 3 days plus artesunate (AS) (4 mg/kg per day) over 3 days; sulfadoxine (25 mg/kg) and pyrimethamine (1.25 mg/kg) (SP) on day 0; SP (25:1.25 mg/kg) plus PQ (0.5 mg/kg) on day 0; SP (25:1.25 mg/kg) on day 0 plus AS (4 mg/kg per day) over 3 days. The primaquine co-treatment regimens were based on recommendations for use of primaquine as a gametocytocide treatment for falciparum malaria [31]. On treatment days when any specific arm did not require a partner drug, a placebo was substituted. Patients were not allocated to all six treatment arms at each site (Table 1). During years two and three, at any one site, patients were allocated to either one of the three SP treatment arms or one of the three chloroquine treatment arms; only in year one were patients allocated to all six treatment arms in the original site. For each of the study sites patients were stratified by age and sex and assigned consecutive patient numbers at enrolment. Treatment groups were pre-assigned to patient numbers using simple randomization lists generated using Excel (Microsoft Corp., Seattle, USA). The assignment of treatment group to patient Table 1. Summary of treatment arms tested at each of the study sites over the three transmission seasons. Study site Transmission season (July January) Site 1 (Adizai) Site 2 (Yakka Ghund) Site 3 (Kotki) Season 1: CQ, CQ+PQ, CQ+AS, SP, SP+PQ, SP+AS Season 2: SP, SP+PQ, SP+AS CQ, CQ+PQ, CQ+AS Season 3: CQ, CQ+PQ, CQ+AS SP, SP+PQ, SP+AS CQ, CQ+PQ, CQ+AS doi: /journal.pone t001 PLoS ONE 2 January 2012 Volume 7 Issue 1 e28957
3 number was concealed until after enrolment. The random allocation sequence was generated by two of the investigators (KK, MR) neither of whom enrolled or assessed patients. The brands and manufacturers/suppliers were: SP (Fansidar H, Roche), chloroquine (Nivaquine H, Beacon), primaquine (IDA), artesunate (Plasmotrim TM, Mepha). Although chloroquine resistance was known to exist in the study area, chloroquine was the first line treatment policy of the Government of Pakistan and the UN refugee agency (UNHCR) at the time and was therefore included. The trial manager, who allocated the treatment arms and administered treatment, was not blind to the study drugs and allocations. Recruited patients, microscopists and health workers were partially blinded; full blinding was not achieved given (i) the appearance of the different drugs, and (ii) the different times of follow up for the SP arms compared to the chloroquine arms. Patients were given directly observed treatment (by the trial manager), monitored for 30 minutes and re-dosed if vomiting occurred. Health workers then recorded the other day 0 biomedical parameters. Patients were asked to return on each day of treatment (days 0, 1, 2) and on days 3, 7, 14, 21 and 28 post treatment. Patients in the three SP arms were also followed up on days 35 and 42 for detection of late recrudescence [32]. On each day of follow up thick and thin smears were taken, clinical symptoms recorded and blood spots collected on Whatman No. 1 filter paper for parasite typing and differentiation of recrudescent from new infections. Haematocrits and blood spots were taken either on the day of failure or on day 28. Patients not presenting at the clinic were followed up at home. Criteria for withdrawal were reported administration of additional anti-malarial drugs (protocol violation), emergence of any concomitant febrile illness that interfered with outcome classification (including a non-falciparum malaria, for which the withdrawn study patient would be given appropriate first line treatment), parasitaemia still present on day 7, or signs of severe malaria developing before completing the initial treatment course. Patients found to be parasitaemic on any day after day 3 were treated with SP (the official second line treatment) or with SP and mefloquine (Fansimef, Roche) for those whose initial treatment was SP based. SP resistant parasites were sensitive to the mefloquine component of Fansimef, which was used in lieu of mefloquine monotherapy which was unavailable in the study area. Those who developed severe malaria, severe anaemia or other complications were referred to Khyber Hospital, Peshawar for treatment. Laboratory tests. Thick and thin blood smears were stained with 2% Giemsa solution. All slides were read on the day of collection by a microscopist based at each site. Differential diagnosis of vivax and falciparum (trophozoites and gametocytes) was by examination of thick and thin smears according to standard microscopy methods [33]. Trophozoites and gametocytes were counted against 200 white blood cells (WBC) from the thick blood smear on the assumption of a WBC count of 8000/ml. A smear was declared negative if no parasites were seen after examining 100 fields. Slides from sites 2 and 3 were re-examined for accuracy by the site 1 microscopist. Comparison was made between the parasite counts made by the three microscopists. The mean variation in parasite count for trophozoites and gametocytes was less than 5%. Owing to electricity supply deficiency, the haematocrit microcentrifuge was only used at sites 1 and 3. Outcome measures. Patients completed the trial if treatment was administered fully and all follow-up appointments conducted, or if they failed treatment on any day of follow-up. The primary endpoint of the trial was any clinical or parasitological failure up to day 28, although a subset of patients in the SP treatment arms was also followed until day 42. Patient outcomes were classified under the WHO parasitological classification system of sensitive (S) or resistant (RI, RII, RIII) infections with those whose outcomes were classified as S (sensitive) being treatment successes and those with outcomes of RI, RII or RIII being classified as treatment failures [34]. This classification system was still commonly used at the time of the study and the ethical clearance for this study (received in 2000) was based on a protocol using this classification system. Patients were also classified against the newer WHO treatment outcome system [35,36]. Presenting the outcomes under both of these systems allows better comparability with data past and present [37]. For the WHO classification system standard definitions were applied: adequate clinical and parasitological response (ACPR), early treatment failure (ETF) or late treatment failure (LTF) which incorporated standard definitions of late clinical and parasitological response [35]. Those cases with ETF or LTF were classified as treatment failures, and ACPR was classified as treatment success if they completed the follow-up period. Other parameters examined were time to fever resolution (with fever defined as axillary temperature $37.5uC), asexual parasite clearance, gametocyte clearance and gametocyte carriage on or after day 7. Molecular characterisation. PCR genotyping was conducted on a subset of samples to distinguish recrudescent from new infections using the protocol described by Brockman et al [38]. P. falciparum genes msp-1, msp-2 and glurp were genotyped according to polymorphisms present at variable loci on day 0 and day of failure. Approximately 50% of cases were available for genotyping. PCR corrected outcomes were applied as a secondary analysis using redefined outcomes based on the number and frequency of true recrudescent infections and reclassifying cases with new infections as treatment successes, excluding those with indeterminate outcomes or negative PCR results. PCR testing was performed at the Shoklo Malaria Research Unit, Thailand. We also conducted an analysis at the London School of Hygiene and Tropical Medicine (LSHTM), UK, for known resistanceassociated mutations to chloroquine and antifolate drugs. Samples collected at enrolment were tested for known mutations in the pfcrt, pfmdr1, pfdhfr and pfdhps genes [39,40]. PCR and sequence specific oligonucleotide probe assays were used to analyse nucleotide polymorphisms at pfcrt codon 76, pfmdr1 codons 86 and 184, pfdhfr codons 16, 51, 59 and 108 and pfdhps codons 436, 437, 581 and 613 [41]. Sample size and data analysis The sample size required to detect a difference in treatment failure or gametocyte carriage with 80% power and 95% confidence (two-sided significance level for type 1 error of 0.05) were calculated using the following predictions. In the chloroquine arms (i) the estimated frequency of failure in chloroquine monotherapy arm was 30% and in each of the combination arms (CQ+PQ or CQ+AS) it was 10% or less; (ii) the estimated proportion of gametocyte positive individuals after 7 days in the chloroquine arm was 50% and in each of the combination arms it was 25%. In the SP arms (i) the estimated frequency of failure in the SP arm was 10% and in each of the combination arms (SP+PQ or SP+AS) it was 1%; (ii) the estimated frequency of gametocyte positive patients after 7 days in the SP arm was 50% and in each combination arm it was 25%. The estimated samples sizes were 64 per arm in the chloroquine arms and 121 per arm in the SP arms. For gametocyte carriage the required sample sizes were 65 per arm. The target sample sizes for the study were 65 for PLoS ONE 3 January 2012 Volume 7 Issue 1 e28957
4 Table 2. Enrolment characteristics of the treatment groups. Variable CQ CQ+PQ CQ+AS SP SP+PQ SP+AS Number enrolled Number evaluable at day 28 (%) 68 (89) 67 (88) 67 (91) 41 (91) 33 (82) 41 (93) Age [median (IQR) years] 12 (8 18) 12 (8 20) 12 (8 20) 17 (9 27) 14 (7 25) 18.5 (9.5 30) Percentage female Weight [median (IQR) kg] 29 (20 47) 30 (20 53) 33 (20 45) 48 (25 58) 42 (22 55) 41 (21 57) Temperature [mean (SD) uc] 37.3 (1.0) 37.5 (1.2) 37.4 (1.2) 37.5 (1.0) 37.5 (1.2) 37.5 (1.5) Temperature $37.5uCon 33 (43) 34 (45) 34 (46) 21 (47) 17 (43) 23 (52) presentation [n (%)] PCV [mean (SD) % haematocrit] (9.7) 40.8 (3.9) 41.5 (4.3) 44.2 (7.7) 45.5 (6.9) 44.3 (5.1) PCV,30% [n (%)] (2.2) 0 0 Asexual parasite density 5161 ( ) 5263 ( ) 7366 ( ,915) 7600 ( ,140) 8091 ( ,454) 12,134 ( ,982) [geometric mean (95% CI) per ml] Gametocyte positive [n (%)] 12 (15.8) 15 (19.7) 9 (12.2) 14 (31.1) 7 (17.5) 7 (15.9) Gametocyte density [geometric mean (95% CI) per ml] 1.3 ( ) 1.7 ( ) 0.6 ( ) 4.1 ( ) 1.6 ( ) 1.2 ( ) Notes: (1) PCV was not recorded for all patients; a microcentrifuge was only available at one of the 3 clinics. For PCV percentages in the 6 treatment groups: CQ n = 10; CQ+PQ n = 19; CQ+AS n = 13; SP n = 19; SP+PQ n = 15, SP+AS n = 15. doi: /journal.pone t002 the chloroquine arms and 121 for the SP arms. To allow for 15% loss to follow up the targets for recruitment were 76 for the chloroquine arms and 142 for the SP arms. The primary aims of the study were to evaluate: 1) the relative efficacy of the combination drugs in providing parasite clearance with no recrudescence compared to monotherapy, and 2) the effect on gametocyte clearance. The secondary aim was to determine the proportion of individuals in each arm with classifiable treatment failure. The primary outcome was the proportion of individuals in each treatment group classified as a treatment failure during the 28 days follow-up compared to the respective monotherapy. The odds of treatment failure between each of the study groups at day 28 were estimated after adjusting for potential confounders (age, sex, parasitaemia, PCV, study site) using logistic regression analysis or Mantel-Haenszel x 2 test. Treatment failure was also analysed using the definitions of ACPR and ETF or LTF, and parasitological classifications using the S-R scale in addition to the PCR corrected analysis [35]. Time to event data (time to treatment failure) were analysed with Kaplan Meier survival analysis. For assessing potential effects on gametocyte carriage, the primary outcome was the presence or absence of gametocytes on day 7 with a secondary analysis examining the presence or absence of gametocytes and the geometric mean gametocyte density on each day of follow-up. All data were entered in Microsoft Excel (1997) by one data clerk and the database checked patient by patient against paper records by a second data clerk. Analysis was performed using STATA 10.0 (STATA Corp, College Station, TX, USA). Ethics Statement The study protocol was approved by the ethics committees of the Pakistan Medical Research Council and LSHTM, UK. All patients or their guardians gave written informed consent to participate. The trial was registered under clinicaltrials.gov [NCT ]. Figure 1. Trial profile. doi: /journal.pone g001 PLoS ONE 4 January 2012 Volume 7 Issue 1 e28957
5 Table 3. Clinical and parasitological failure rates at 28 days follow-up and for gametocytaemia at day 7. Day 28 clinical or parasitological failure Day 7 gametocytaemia No./Total (%) Odds Ratio (95% CI) P No./Total (%) Odds Ratio (95% CI) P CQ 55/68 (81) Reference - 52/67 (78) Reference - CQ+PQ 49/67 (73) 0.64 ( ) /70 (39) 0.18 ( ),0.001 CQ+AS 19/67 (28) 0.09 ( ), /72 (17) 0.06 ( ),0.001 SP 4/41 (10) Reference - 37/43 (86.1) Reference - SP+PQ 5/33 (16) 1.6 ( ) /36 (66.7) 0.32 ( ) SP+AS 1/41 (2) 0.23 ( ) 0.2 9/44 (20.5) 0.04 ( ),0.001 doi: /journal.pone t003 Figure 2. Kaplan Meier survival analysis showing cumulative probability of failure in CQ treatment groups (A) and SP treatment groups (B). doi: /journal.pone g002 PLoS ONE 5 January 2012 Volume 7 Issue 1 e28957
6 Table 4. Clinical and parasitological outcomes after 28 days follow-up: n (%). CQ CQ+PQ CQ+AS SP SP+PQ SP+AS Clinical outcomes N = 56 N = 58 N = 67 N = 41 N = 30 N = 40 Adequate clinical response 13 (23) 18 (31) 48 (72) 37 (90) 28 (93) 40 (100) Early treatment failure 9 (16) 7 (12) 0 1 (2) 1 (3) 0 Late clinical failure 2 (4) 4 (7) 1 (2) Late Parasitological Failure 32 (57) 35 (50) 18 (26) 3 (7) 1 (3) 0 Parasitological outcomes N = 63 N = 65 N = 67 N = 40 N = 32 N = 41 S 13 (21) 18 (28) 48 (72) 37 (93) 28 (88) 40 (98) RI 35 (56) 33 (51) 19 (28) 3 (7) 1 (3) 0 RII 13 (21) 11 (16.9) (9) 1 (2) RIII 2 (3) 3 (5) doi: /journal.pone t004 Results Recruitment and follow-up A total of 355 cases of microscopically confirmed falciparum malaria were enrolled into the study between July 2000 and December Table 2 shows enrolment characteristics and Figure 1 shows the trial profile. Patients were recruited to the chloroquine arms in line with recruitment targets. Insufficient numbers were recruited to the SP arms. This was due to considerably lower than expected malaria cases occurring in these locations during the study period (in contrast to the years leading up to the study). Additional sites were added over the three-year study period to increase recruitment but it was not possible to continue the trial for longer because of resource constraints. chloroquine arms met the recruitment targets because of the site allocations and unexpected pattern of case loads in the third year. Characteristics of patients recruited into the 3 chloroquine arms were broadly similar, as were the three SP arms. The SP+AS arm showed slightly higher asexual parasite densities on enrolment than other groups (Table 2). Of 355 patients enrolled, 38 (10.7%) were either withdrawn or lost to follow up leaving 317 for possible inclusion (Figure 1). Of these 292 (82%) were evaluable for parasitological outcomes because 25 patients classified as RII parasitological failure did not meet the definition of clinical failure, i.e. they did not have fever on day 3. Likewise, 308 (87%) were evaluable for clinical outcomes because 9 patients who had classifiable Early Treatment Failure did not fit the definition for parasitological failures (they did not reach day 7 of the trial). Of the 266 patients followed up for 42 days, 221 (83%) were evaluable for clinical and parasitological outcomes. All treatments were well tolerated and no severe or serious adverse events were recorded during the study. Clinical Outcomes. The 28-day failure rate in the CQ and CQ+PQ arms was 81% and 73% respectively (Table 3, Figure 2A). The addition of artesunate improved the treatment response, with a treatment failure rate of 27%. The failure rates in the SP groups were 16% or less (Table 3) with the combination of SP+AS having the lowest failure rate (1/41 [2.4%]). Neither SP+AS nor SP+PQ arms were significantly different to the SP arm at the 28-day end point (Figure 2B). None of the potential confounding factors examined (age, sex, parasitaemia, study site, PCV) were associated with treatment outcome so adjustments were unnecessary in the final regression analysis. Crude odds ratios are presented. Clinical and parasitological outcomes are shown in Table 4. Only 32/133 (24%) of the individuals who failed had fever on the day of failure; the majority of late treatment failures therefore fell into the category of late parasitological failure. Some recent history of fever may have gone unreported. Trophozoite clearance time (days until negative smear) was lowest for the artesunate combination arms. Addition of primaquine to either chloroquine or SP did not appear to affect clearance times. Clearance times for each arm (median (interquartile range)) were: CQ, 3 days (2 7); CQ+PQ, 3 days (2 7); Table 5. Outcomes of PCR analysis, and projected adjusted failure rates by treatment group excluding indeterminate results. PCR Results [n (%)] Failure rates [n/n (%)] Reinfection Recrudescent Negative Total in vivo 1 PCR adjusted 2 CQ 6 (21) 20 (69) 3 (10) 29 55/68 (81) 42/68 (62) CQ+PQ 4 (21) 11 (58) 4 (21) 19 49/67 (73) 36/67 (54) CQ+AS 7 (64) 3 (27) 1 (9) 11 19/67 (28) 6/67 (9) SP 0 2 (100) 0 2 4/41 (10) 4/41 (10) SP+PQ 0 2 (100) 0 2 5/33 (16) 5/33 (16) SP+AS /41 (2) 1/41 (2) Notes: (1) Taken from Table 3 for 28 day failures; (2) Adjusted by the ratio of PCR recrudescent to PCR re-infected cases to estimate number of true recrudescent cases among the observed in vivo failures. doi: /journal.pone t005 PLoS ONE 6 January 2012 Volume 7 Issue 1 e28957
7 CQ+AS, 2 days (1 2); SP, 2 days (2 3); SP+PQ, 2 days (1.5 3); SP+AS, 1 day (1 2). Of the 133 failures, 79 (47%) matched pairs were available for PCR evaluation of MSP-1, MSP-2 and GLURP. Matched pairs were collected on day 0 and on the day of failure. Outcomes of the PCR are shown in Table 5, which excludes those with indeterminate results. Most re-infections took place at one site (Site 3, Yakka Ghund) where malaria transmission was higher than in the other villages. Treatment outcomes were reclassified for those failures where matched pairs were available and used to give adjusted failure rates for the sample (Table 5). Although the number of failures in the chloroquine arms was reduced by the correction, the failure rates remained high at.50% for chloroquine monotherapy. The PCR adjusted treatment failure rate of the CQ+AS combination (9%) was considerably lower that the in vivo rate (28%). In the subset of patients followed-up for 42 days, recrudescence between day 28 and 42 was rare: only 8/317 (2.5%) of individuals classified as adequate clinical and parasitological response (ACPR) or sensitive (S) at day 28 went on to fail by day 42 (1 in the CQ arm, 2 in the CQ+PQ arm, 3 in the CQ+AS arm, 1 in the SP arm and 1 in the SP+PQ arm). Failure rates at day 42 were therefore similar to day 28. The failures between 28-day and 42-day rates were not corrected by PCR and hence could have resulted from new infections. Molecular outcomes. Molecular analysis of drug resistanceassociated alleles was conducted on samples taken on day 0 (Table 6). The major marker of chloroquine resistance, pfcrt-76t, was fixed at 100%. Mutations in pfmdr1 are known to modulate resistance to quinoline and other drugs. The prevalence of chloroquine-resistance associated allele pfmdr1-86y was 13.6% in this sample. Mutations associated with pyrimethamine resistance (on the pfdhfr gene) were seen frequently; 108 N was found in all but one of 74 typable samples (98.6%) and 59R occurred in 66/76 (86.8%) samples. However, 51I was only detected in 5/75 (6.7%) Table 6. Drug resistance alleles in a sub-set collected at enrolment. Locus Allele Number (%) Pfcrt 76 K 0 76 T 63 (100) Pfmdr1 86 N 76 (86) 86 Y 12 (14) 184 Y 22 (27) 184 F 60 (73) DHFR 16 A 76 (99) 16 V 1 (1) 50/51 CN1 70 (93) 50/51 C1 5 (7) 59 C 10 (13) 59 R 66 (67) 108 N 73 (99) 108 T 1 (1) DHPS 436/437 SA 43 (100) 581 A 41 (100) 613 A 43 (100) doi: /journal.pone t006 samples. Therefore pfdhfr double mutants were common (at codons ) but triple mutants were rare. Interestingly, we observed one sample with the pfdhfr mutations 16V+108T. These are reportedly selected by the antifolate drug cycloguanil, rather than pyrimethamine [42]. No mutations on the dhps gene were seen. These PCR results broadly match what would be expected from the clinical outcomes. The pfdhr/pfdhps mutation profile suggests that the parasites would be killed by a full therapeutic dose of SP, but that some tolerance to lower doses existed. Effect on Gametocytes The addition of artesunate or primaquine to chloroquine or SP reduced gametocyte carriage on day 7 (Table 3). Combining chloroquine or SP with artesunate succeeded in eliminating gametocytaemia from more individuals by day 7 compared to monotherapy or co-treatment with a single-dose of primaquine. Figure 3 shows the proportion of individuals with patent gametocytaemia over 28 days of follow-up. In the chloroquine and SP arms, gametocyte carriage persisted at day 28 in.30% of individuals in the CQ arm and.70% of individuals in the SP arm. The addition of primaquine reduced gametocyte carriage; the effect was more pronounced with chloroquine than with SP. The proportion of gametocytaemic individuals was lowest in the artesunate arms and the difference was evident within two days of the start of treatment. Peak gametocyte densities occurred 7 days after the start of treatment (Figure 4). Gametocyte density was higher after SP than after chloroquine treatment. Both primaquine and artesunate reduced density to low levels by day 7. Most patients did not have gametocytaemia on day 0 (291/355 (82.0%) had no gametocytes on day 0). However, the presence or absence of sexual stage parasites on day 0 was an important explanatory variable in the secondary analysis; patients who presented with gametocytes on day 0 were more likely to be gametocytaemic on day 7 than individuals who were not gametocytaemic on day 0 regardless of treatment group (Mantel- Haenszel OR: 3.5 [95%CI: ], p,0.001). We therefore conducted further analysis comparing those who presented with gametocytes on day 0 and those who did not. The artesunate treatments were more effective at preventing the emergence of gametocytaemia between day 0 and 7 than in removing established gametocytaemia already present on day 0 (Table 7). For example, among the CQ+AS group who did have patent gametocytaemia on day 0, 8/9 were still gametocytaemic on day 7 after treatment. This was not significantly different from the proportion gametocytaemic on day 7 (11/12) after treatment with chloroquine monotherapy (Fisher s exact test p = 1.0). By contrast, in the chloroquine arms of the patients who did not have patent gametocytaemia on day 0, only 11% (7/63) were gametocytaemic on day 7 when treated with CQ+AS as compared to 47/56 (84%) among those treated with chloroquine monotherapy (x 2 p,0.001). Similar trends were evident in the SP arms treated with artesunate; prevalence of gametocytaemia on day 7 was significantly lower in the SP+AS group that was not gametocytaemic on day 0 than in the group that was (Fisher s exact test p,0.001). This indicates that artesunate is less active against older gametocytes than against those newly emerged or immature forms that are not yet emerged. Primaquine showed no such trend: the proportion of patients gametocytaemic on day 7 was not significantly different for patients who were or were not gametocytaemic on day 0. Primaquine therefore appears to be active against gametocytes of all ages. Primaquine was more effective at controlling gametocytaemia when combined with CQ than with SP, regardless of whether individuals were gametocytaemic at the start of treatment (MH- PLoS ONE 7 January 2012 Volume 7 Issue 1 e28957
8 Figure 3. Percentage of patients (+CI) carrying gametocytes on specified days after treatment in CQ (A) and SP (B) treatment arms. doi: /journal.pone g003 OR = 0.22, P = 0.001) (Table 7). By contrast, artesunate seemed as effective when combined with chloroquine as it was when combined with SP (MH-OR = 1.04, P = 0.83). Though, as discussed, artesunate was more effective at preventing development of patent gametocytaemia than in clearing existing gametocytaemia. Artesunate was better than primaquine at preventing patent gametocytaemia among those that were not gametocytaemic at day 0 enrolment (CQ: OR = 0.30, P,0.001; SP: OR = 0.18, P,0.001). Using the presence of gametocytes on day 7 as the secondary endpoint, adjusted for the presence of gametocytes at day 0, both primaquine and artesunate with chloroquine or SP were more effective than their respective monotherapies at reducing the presence of gametocytes (Table 8). Compared to monotherapy with chloroquine or SP, cotreatment with artesunate was negatively associated with having gametocytes on day 28 whether the accompanying drug was chloroquine or SP (Table 8). The presence of gametocytes on day 0 was not associated with the presence of gametocytes on day 28 (MH-OR, adjusted for treatment arm: 1.0, p = 1.0) suggesting that older gametocytes had cleared by day 28, regardless of treatment. PLoS ONE 8 January 2012 Volume 7 Issue 1 e28957
9 Figure 4. Geometric mean gametocyte density (+CI) after treatment in chloroquine (A) and SP treatment arms (B). Note the different scales on the Y-axis. Where the CI bars are absent, only 1 patient had gametocytes. doi: /journal.pone g004 Discussion The present study was designed to inform decision-making at several levels: to guide UNHCR on appropriate treatment in the Afghan refugee communities in Pakistan, to build evidence for national treatment policy in the Pakistan Directorate of Malaria Control and in the Afghanistan Ministry of Public Health, to guide the WHO Eastern Mediterranean Region Office (EMRO) on regional treatment recommendations, and to build evidence for international epidemic response guidelines. The findings of this study, when presented at an inter-country meeting of national malaria control managers coordinated by WHO/EMRO in 2004, contributed to a shift in policy from chloroquine monotherapy to ACT in South and West Asia [43], influencing the defining of PLoS ONE 9 January 2012 Volume 7 Issue 1 e28957
10 Table 7. Numbers and percentages of individuals with gametocytes on day 7 post treatment. No (%) parasitaemic on day 7 Amongst those who had gametocytes on day 0 Amongst those who did not have gametocytes on day 0 CQ 11/12 (91.7%) a, 1 47/56 (83.9%) a, 1 CQ+PQ 7/14 (50%) b, 1 21/56 (37.5%) b, 1 CQ+AS 8/9(88.9%) a, 1 7/63(11.1%) c, 2 SP 14/14 (100%) a, 1 25/29 (86.2%) a, 1 SP+PQ 5/7 (71.4%) b, 1 23/30 (76.7%) a, 1 SP+AS 5/7 (71.4%) b, 1 5/37 (13.5) b, 2 Chloroquine or SP treatments in the same column that share the same superscript letter are not significantly different. Treatments in the same row that share the same numeric superscript are not significantly different. doi: /journal.pone t007 SP+AS as the first line treatment of choice for the WHO Eastern Mediterranean Region. India is the latest neighbouring country to adopt SP+AS as first line treatment with the support of WHO [37]. The SP+AS combination is also effective against vivax malaria [44], although not as an approved treatment. SP monotherapy was effective in the study population, with treatment failure rates remaining in the 5 10% range, similar to that seen in other studies in the region [5,8,45]. Molecular studies in the region show that genetic markers for SP resistance are still at low levels in the parasite population [46,47]. However, the South East Asian experience of rapid rise in SP resistance in settings of similar endemicity [7] points to SP resistance spreading rapidly if ACT policy is not implemented rigorously in both public and private sectors across the region [37]. The complete failure of chloroquine (which at the time of the study remained the officially sanctioned first line treatment) convinced policy makers of the need to redefine treatment practices in South Asia. The new data demonstrated higher levels of resistance than in previous studies dating back to the 1980s and 1990s [2,3,5,48,49] and emphasised the need for change to national treatment guidelines. The addition of artesunate to chloroquine did reduce treatment failure rates, but if this regimen was used as policy it would, in effect, constitute artesunate monotherapy in the majority of infections and accelerate the development of artesunate tolerance, as reported in South East Asia [50]. A constraint on the study design was that not all 6 arms could be included at each of the three study sites. Site is therefore a potential confounding covariate that cannot be fully controlled for in the data analysis. Differences in transmission could, for example, affect the risk of re-infection between sites but this was corrected for by the PCR analysis. At each site in any one year each triplet of treatment arms (all the SP arms or all the chloroquine arms) were examined at the same time, and it is comparisons within these triplets which are of greatest interest. The study did not complete its target sample size for the SP arms because of low recruitment rates. PCR corrected outcomes were not attainable for all failures, and higher numbers of patients were reinfected at one site where only the chloroquine arms were being tested. Low rates of transmission at the other sites make it unlikely that failing cases were due to reinfection. The secondary analysis with PCR-corrected outcomes did not change the overall conclusions on the suitability of the combinations for revised treatment policy. Treatment with either the clinically effective SP monotherapy or the failing chloroquine monotherapy resulted in persistence of gametocytaemia into the second and third weeks in the majority of individuals. This effect was more evident for SP than for chloroquine, SP being well known for high rates of gametocyte carriage post treatment [32]. This contrasts with situations of lowfrequency chloroquine resistance where the proportion of gametocytaemic patients post treatment also tends to be lower [16,51]. The effect of artemisinin derivatives on reducing gametocyte carriage is already documented [16,52]. Artesunate also proved highly effective in reducing the prevalence of gametocytaemia in the present study. Regimens combining artesunate with chloroquine or SP saw marked reductions in gametocyte carriage and few cases had persisting gametocytaemia. As demonstrated with SP+AS in The Gambia [16] the SP+AS and CQ+AS combina- Table 8. Effect of treatment on gametocyte carriage at day 7 and day 28, for those patients who were gametocytaemic on enrolment. AOR for presence of gametocytes on day 7, (95% CI), p-value 1 AOR for presence of gametocytes on day 28, (95% CI), p-value 1 CQ Reference Reference CQ+PQ 0.15 ( ), p, ( ), p = 0.3 CQ+AS 0.05 ( ), p, ( ), p = SP Reference Reference SP+PQ 0.37 ( ), p = ( ), p,0.001 SP+AS 0.04 ( ), p, ( ), p,0.001 Notes: (1) AOR: Odds ratios using logistic regression analysis adjusted for presence of gametocytes on day 0 (CQ and SP arms analysed separately). doi: /journal.pone t008 PLoS ONE 10 January 2012 Volume 7 Issue 1 e28957
11 tions appear to have limited activity against mature circulating gametocytes [53]. Co-treatment with a single dose of primaquine was more effective against older gametocyte infections. Both primaquine and, more markedly, artesunate reduced the odds of persisting gametocytes from that seen post treatment with either chloroquine or SP monotherapy. Primaquine is more rapidly excreted than artesunate and this may account for the fact that the single dose of primaquine used in this study had a lower impact on gametocyte carriage than the artesunate regimens. The usefulness of primaquine as a gametocytocidal treatment may be improved by administering it after the ACT course [14,54]. In our study, a key factor in the clearance of gametocytes was the presence or absence of gametocytes on day 0. Those who presented with gametocytes were more likely to have gametocytes on day 7, an effect which was independent of the treatment given. Although the majority of patients (80%) presented without gametocytaemia, artesunate appeared to be less active against these older parasites whereas primaquine appeared to be effective against all ages. The proportion presenting with gametocytes may vary according to background transmission levels. If gametocytes persist after treatment with ACTs, the effect on transmission in areas where a high proportion of cases present with gametocytes may prove suboptimal and justify the simultaneous use of primaquine. Primaquine is more rapidly excreted than artesunate and this may account for the fact that the single dose of primaquine used in this study had a lower impact on gametocyte carriage than the artesunate regimens. The usefulness of primaquine as a gametocytocidal treatment may be improved by administering it after the ACT [14,54]. For treatment policy to have a major impact on transmission several criteria need to be met: i) transmission is low to moderate; ii) the majority of people use public health rather than private facilities, or effective private sector interventions ensure adherence to policy; iii) public health facilities correctly prescribe the approved regimen, and iv) patients take the full course. These conditions are largely met in the refugee villages of Pakistan. The region is characterized by low endemicity and low immunity, well supported health care facilities are available in the Afghan refugee villages, and diagnosis of malaria to species level is maintained to a high standard [28]. The health facilities are well utilized by the Afghan refugees and Pakistanis living nearby. The effect of this policy is evident in the refugee populations: since 2005 falciparum malaria has virtually disappeared in all but a handful of the refugee villages [International Rescue Committee, Final Report, unpublished]. This reduction is attributed to prompt and accurate diagnosis and wider access to ACTs as prevention interventions were minimal. The operational data from this region and elsewhere suggest that drugs showing faster gametocyte clearance in clinical trials do help to reduce transmission [20 23]. However, it is also important to note the results of recent research which suggest that drawing conclusions about the potential impact on transmission is not straightforward, for the following reasons: i. The effect of drugs on gametocyte carriage cannot be fully determined if only standard light microscopy (LM) is used. Research in the last decade shows that LM gives starkly different indications of gametocyte prevalence and densities compared to other techniques [55] and that sub-microscopic ii. iii. iv. levels of gametocytes likely play an important role in transmission, perhaps particularly in low transmission settings [56]. Gametocytes that are readily identified in blood following treatment may or may not be viable. Gametocytes may not be infective to mosquitoes either because they are recently emerged (naturally, gametocytes are not infectious to mosquitoes in the first 1 2 d of emergence [57]) or because the effect of the drug regimens have rendered them sterile [58]. It is unclear how the density of gametocytes in the blood links to potential for transmission success to blood feeding mosquitoes. Bousema & Drakeley [57] summarise the available data from membrane feeding studies showing that whilst there is an overall correlation, the variations within it are confusing; high density gametocytaemia can lead to minimal mosquito infection and very low densities lead to reasonable rates of infection. Even if solid data show that a particular drug does reduce the number of gametocytes which successfully infect, and lead to infectious, mosquitoes; the effect of this on malaria transmission cannot be stated with certainty. This effect would depend on what proportion of the gametocyte reservoir these patients would otherwise make up [56]. The comparative performance of artesunate and primaquine on gametocyte carriage in this study did not influence policy. The decision to use SP+AS was based on treatment efficacy and the need to protect against SP resistance through the use of an ACT combination. The fact that SP+AS led to reduced gametocyte carriage compared to the previous policy of chloroquine montherapy was reassuring, and raised the possibility of the regimen reducing transmission too. SP+AS is now the first line treatment policy in Pakistan, Iran, Afghanistan and India. The continuing collection of molecular data on SP resistance in this region will be vital, given that the treatment efficacy of artesunate could mask the emergence of SP resistance by acting alone to provide a degree of clinical cure in the presence of a failing companion drug [59]. This risk could be reduced by introduction of a co-blister of SP plus artesunate. Supporting Information Protocol S1 (DOC) Checklist S1 (DOC) Trial Protocol. Acknowledgments CONSORT Checklist. The authors acknowledge with thanks the support of Dr Naveeda Rehman of the United Nations High Commissioner for Refugees, Pakistan, and Dr M. Abdur Rab and staff of HealthNet International (now, HealthNet TPO) for their assistance. Author Contributions Conceived and designed the experiments: MR KK. Performed the experiments: KK SL MB KB RO IA ND. Analyzed the data: KK MR TL SL RH. Contributed reagents/materials/analysis tools: KK RH RO KB MB SL. Wrote the paper: KK MR TL RH. PLoS ONE 11 January 2012 Volume 7 Issue 1 e28957
12 References 1. White NJ (2008) Qinghaosu (artemisinin): the price of success. Science 320: Shah I, Rowland M, Mehmood P, Mujahid C, Razique F, et al. (1997) Chloroquine resistance in Pakistan and the upsurge of falciparum malaria in Pakistani and Afghan refugee populations. Ann Trop Med Parasitol 91: Rab MA, Freeman TW, Durrani N, De Poerck D, Rowland MW (2001) Resistance of Plasmodium falciparum malaria to chloroquine is widespread in eastern Afghanistan. Ann Trop Med Parasitol 95: Khan MA, Smego RAJ, Razi ST, Beg A (2004) Emerging drug resistance and guidelines for treatment of malaria. J Coll Physicians Surg Pak 14: Rowland M, Durrani N, Hewitt S, Sondorp E (1997) Resistance of falciparum malaria to chloroquine and sulfadoxine-pyrimethamine in Afghan refugee settlements in western Pakistan: surveys by the general health services using a simplified in vivo test. Trop Med Int Health 2: Bloland PB, Ettling M, Meek S (2000) Combination therapy for malaria in Africa: hype or hope? Bull World Health Organ 78: Nosten F, Ashley E (2004) The detection and treatment of Plasmodium falciparum malaria: time for a change. J Postgrad Med 50: Ezard N, Nellepalli P, Asha AW (2004) Sulfadoxine-pyrimethamine remains efficacious against uncomplicated Plasmodium falciparum malaria in northeastern Afghanistan. Ann Trop Med Parasitol 98: Campbell P, Baruah S, Narain K, Rogers CC (2006) A randomized trial comparing the efficacy of four treatment regimens for uncomplicated falciparum malaria in Assam state, India. Trans R Soc Trop Med Hyg 100: Reickmann KH, McNamara JV, Kass L, Powell RD (1969) Gametocytocidal and sporontocidal effects of primaquine upon two strains of Plasmodium falciparum. Mil Med 134(10): Chomcharn Y, Surathin K, Bunnag D, Sucharit S, Harinasuta T (1980) Effect of a single dose of primaquine on a Thai strain of Plasmodium falciparum. Southeast Asian J Trop Med Public Health 11: Kaneko A, Kamei K, Suzuki T, Ishii A, Siagian R, et al. (1989) Gametocytocidal effect of primaquine in a chemotherapeutic malaria control trial in North Sumatra, Indonesia. Southeast Asian J Trop Med Public Health 20: Pukrittayakamee S, Chotivanich K, Chantra A, Clemens R, Looareesuwan S, et al. (2004) Activities of artesunate and primaquine against asexual- and sexualstage parasites in falciparum malaria. Antimicrob Agents Chemother 48: Smithuis F, Kyaw MK, Phe O, Win T, Aung PP, et al. (2010) Effectiveness of five artemisinin combination regimens with or without primaquine in uncomplicated falciparum malaria: an open-label randomised trial. Lancet Infect Dis 10: Targett G, Drakeley C, Jawara M, Von Seidlein L, Coleman R, et al. (2001) Artesunate reduces but does not prevent post-treatment transmission of Plasmodium falciparum to Anopheles gambiae. J Infect Dis 183: Von Seidlein L, Jawara M, Coleman R, Doherty T, Walraven G, et al. (2001) Parasitaemia and gametocytaemia after treatment with chloroquine, pyrimethamine/sulfadoxine, and pyrimethamine/sulfadoxine combined with artesunate in young Gambians with uncomplicated malaria. Trop Med Int Health 6: Chotivanich K, Sattabongkot J, Udomsangpetch R, Looareesuwan S, Day NP, et al. (2006) Transmission-blocking activities of quinine, primaquine, and artesunate. Antimicrob Agents Chemother 50: Sutherland CJ, Drakeley CJ, Obisike U, Coleman R, Jawara M, et al. (2003) The addition of artesunate to chloroquine for treatment of Plasmodium falciparum malaria in Gambian children delays, but does not prevent treatment failure. Am J Trop Med Int Health 69: Nosten F, Van vugt M, Price R, Luxemburger C, Thwai KL, et al. (2000) Effects of artesunate-mefloquine combination on incidence of Plasmodium falciparum malaria and mefloquine resistance in western Thailand: a prospective study. Lancet 365: Barnes KI, Durrheim DN, Little F, Jackson A, Mehta U, et al. (2005) Effect of artemether-lumefantrine policy and improved vector control on malaria burden in KwaZulu-Natal, South Africa. PLoS Med 2: e Barnes KI, Chanda P, Ab Barnabas G (2009) Impact of the large-scale deployment of artemether/lumefantrine on the malaria disease burden in Africa: case studies of South Africa, Zambia and Ethiopia. Malar J 8 Suppl 1: S Bhattarai A, Ali AS, Kachur SP, Martensson A, Abbas AK, et al. (2007) Impact of artemisinin-based combination therapy and insecticide-treated nets on malaria burden in Zanzibar. PLoS Med 4: e O Meara WP, Mwangi TW, Williams TN, McKenzie FE, Snow RW, et al. (2008) Relationship between exposure, clinical malaria, and age in an area of changing transmission intensity. Am J Trop Med Hyg 79: WHO (2004) Prevention and Control of Malaria Epidemics: Forcasting, preventions, early detection and control From policy to practice. Report of an informal consultation. Geneva: World Health Organisation. 25. Najera JA, Kouznetsov RL, Delacollete C (1998) Malaria epidemics: Detection and Control, Forecasting and Prevention. Geneva: World Health Organisation. 26. Shekalaghe SA, Bousema JT, Kunei KK, Lushino P, Masokoto A, et al. (2007) Submicroscopic Plasmodium falciparum gametocyte carriage is common in an area of low and seasonal transmission in Tanzania. Trop Med Int Health 12: Suleman M (1988) Malaria in Afghan refugees in Pakistan. Trans R Soc Trop Med Hyg 82: Rowland M, Rab MA, Freeman T, Durrani N, Rehman N (2002) Afghan refugees and the temporal and spatial distribution of malaria in Pakistan. Soc Sci Med 55: Leslie T, Kaur H, Mohammed N, Kolaczinski K, Ord R, et al. (2009) An epidemic of Plasmodium falciparum malaria in Afghan refugees in Pakistan involving substandard antimalarial drugs. Emerg Infect Dis 15: Rowland M, Durrani N, Hewitt S, Sondorp E (1997) Resistance of falciparum malaria to chloroquine and sulfadoxine-pyrimethamine in Afghan refugee settlements in western Pakistan: surveys by the general health services using a simplified in vivo test. Trop Med Int Health 2: WHO (2001) The use of antimalarial drugs. Report of a WHO informal consultation. (WHO/CDSRBM/200133). Geneva: World Health Organisation. 32. Myint HY, Tipmanee P, Nosten F, Day NP, Pukrittayakamee S, et al. (2004) A systematic overview of published antimalarial drug trials. Trans R Soc Trop Med Hyg 98: WHO (2010) Basic malaria microscopy 2nd edition. Part 1: Learner s guide - Part 2: Tutor s guide. World Health Organisation, Geneva, Switzerland. 34. WHO (1991) Practical Chemotherapy of Malaria. WHO Technical Report Series No Geneva: World Health Organisation. 35. WHO (2002) Monitoring Antimalarial Drug Resistance. Report of a WHO consultation. (WHO/CDS/RBM/200239). Geneva: World Health Organisation. 36. WHO (2009) Methods for surveillance of antimalarial drug efficacy. Geneva: World Health Organisation. 37. Shah NK, Dhillon GPS, Dash AP, Meshnick SR, Valecha N (2011) Antimalarial drug resistance of Plasmodium falciparum in India: changes in time and space. Lancet 11: Brockman A, Paul RE, Anderson TJC, Hackford I, Phaiphun L, et al. (2000) Application of genetic markers to the identification of recrudescent Plasmodium falciparum infections on the north western border of Thailand. Am J Trop Med Hyg 60: Humphreys GS, Merinopoulos I, Ahmed J, Whitty CJ, Mutabingwa TK, et al. (2007) Amodiaquine and artemether-lumefantrine select distinct alleles of the Plasmodium falciparum mdr1 gene in Tanzanian children treated for uncomplicated malaria. Antimicrob Agents Chemother 51: Pearce RJ, Drakeley C, Chandramohan D, Mosha F, Roper C (2003) Molecular determination of point mutation haplotypes in the dihydrofolate reductase and dihydropteroate synthase of Plasmodium falciparum in three districts of northern Tanzania. Antimicrob Agents Chemother 47: Plowe CV, Djimde A, Bouare M, Doumbo O, Wellems TE (1995) Pyrimethamine and proguanil resistance-conferring mutations in Plasmodium falciparum dihydrofolate reductase: polymerase chain reaction methods for surveillance in Africa. Am J Trop Med Hyg 52: Peterson DS, Milhous WK, Wellems TE (1990) Molecular basis of differential resistance to cycloguanil and pyrimethamine in Plasmodium falciparum malaria. Proc Natl Acad Sci U S A 87: WHO (2004) Report of the Third Intercountry Meeting of National Malaria Control Managers, Lahore, Pakistan. (WHO-EM/MAL/297/E/0504/140). Geneva: World Health Organisation. 44. Kolaczinski K, Durrani N, Rahim S, Rowland M (2007) Sulfadoxinepyrimethamine plus artesunate compared with chloroquine for the treatment of vivax malaria in areas co-endemic for Plasmodium falciparum and P. vivax: a randomised non-inferiority trial in eastern Afghanistan. Trans R Soc Trop Med Hyg 101: Durrani N, Leslie T, Rahim S, Graham K, Ahmad F, et al. (2005) Efficacy of combination therapy with artesunate plus amodiaquine compared to monotherapy with chloroquine, amodiaquine or sulfadoxine-pyrimethamine for treatment of uncomplicated Plasmodium falciparum in Afghanistan. Trop Med Int Health 10: Ghanchi NK, Ursing J, Beg MA, Veiga MI, Jafri S, et al. (2011) Prevalence of resistance associated polymorphisms in Plasmodium falciparum field isolates from southern Pakistan. Malar J 10: Khatoon L, Baliraine FN, Bonizzoni M, Malik SA, Yan G (2009) Prevalence of antimalarial drug resistance mutations in Plasmodium vivax and P. falciparum from a malaria-endemic area of Pakistan. Am J Trop Med Hyg 81: Fox E, Khaliq AA, Sarwar M, Strickland GT (1985) Chloroquine-resistant Plasmodium falciparum: now in Pakistani Punjab. Lancet. pp Khaliq AA, Sarwar M, Fox E, Strickland ST (1985) Chloroquine resistant Plasmodium falciparum in the Punjab. Pak J Med Res Dondorp AM, Nosten F, Poravuth Y (2009) Artemisinin Resistance in Plasmodium falciparum Malaria. N Engl J Med 361: Robert V, Awono-Ambene HP, Le Hesran JY, Trape JF (2000) Gametocytaemia and infectivity to mosquitoes of patients with uncomplicated Plasmodium falciparum malaria attacks treated with chloroquine or sulfadoxine plus pyrimethamine. Am J Trop Med Hyg 62: International Artemisinin Study Group (2004) Artesunate combinations for treatment of malaria: a meta-analysis. Lancet 363: Butcher GA (1997) Antimalarial drugs and the mosquito transmission of Plasmodium. Int J Parasitol 27: PLoS ONE 12 January 2012 Volume 7 Issue 1 e28957
Statistical Analysis Plan (SAP)
 Statistical Analysis Plan (SAP) Comparison of artemether-lumefantrine and chloroquine with and without primaquine for the treatment of Plasmodium vivax in Ethiopia: a randomized controlled trial Contents
Statistical Analysis Plan (SAP) Comparison of artemether-lumefantrine and chloroquine with and without primaquine for the treatment of Plasmodium vivax in Ethiopia: a randomized controlled trial Contents
MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND C Rojanawatsirivej 1, S Vijaykadga 1, I Amklad 1, P Wilairatna
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND C Rojanawatsirivej 1, S Vijaykadga 1, I Amklad 1, P Wilairatna
Antimalarial drug resistance
 Antimalarial drug resistance Md Mushfiqur Rahman*, Leonard Ortega**, R M Rastogi* and Krongthong Thimasarn* Abstract Antimalarial drug resistance is of great concern in the WHO South-East Asia (SEA) Region.
Antimalarial drug resistance Md Mushfiqur Rahman*, Leonard Ortega**, R M Rastogi* and Krongthong Thimasarn* Abstract Antimalarial drug resistance is of great concern in the WHO South-East Asia (SEA) Region.
Combination Anti-malarial Therapy and WHO Recommendations
 Prakaykaew Charunwatthana 2, and Sasithon Pukrittayakamee 1,2 1 Associate Fellow of the Royal Institute, Academy of Science 2 Department of Clinical Tropical Medicine, Faculty of Tropical Medicine, Mahidol
Prakaykaew Charunwatthana 2, and Sasithon Pukrittayakamee 1,2 1 Associate Fellow of the Royal Institute, Academy of Science 2 Department of Clinical Tropical Medicine, Faculty of Tropical Medicine, Mahidol
Is there Artemisinin Resistance in Western Cambodia?
 Is there Artemisinin Resistance in Western Cambodia? Preliminary results, February 2008 Arjen Dondorp on behalf of the Task Force on Antimalarial Drug Resistance in Cambodia S769N PfATPase6 mutation Artemether
Is there Artemisinin Resistance in Western Cambodia? Preliminary results, February 2008 Arjen Dondorp on behalf of the Task Force on Antimalarial Drug Resistance in Cambodia S769N PfATPase6 mutation Artemether
DECLINING MEFLOQUINE SENSITIVITY OF PLASMODIUM FALCIPARUM ALONG THE THAI-MYANMAR BORDER
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH DECLINING MEFLOQUINE SENSITIVITY OF PLASMODIUM FALCIPARUM ALONG THE THAI-MYANMAR BORDER Chaiporn Rojanawatsirivet 1, Kanungnit Congpuong 1, Saowanit Vijaykadga
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH DECLINING MEFLOQUINE SENSITIVITY OF PLASMODIUM FALCIPARUM ALONG THE THAI-MYANMAR BORDER Chaiporn Rojanawatsirivet 1, Kanungnit Congpuong 1, Saowanit Vijaykadga
Clinical Analysis Report For Study Sample Study
 Clinical Analysis Report For Study Sample Study Automated report generated by WWARN May 9, 2014 Falciparum class org.wwarn.csr.clinicalstudyreport Version 1.020140508-1558 1 Contents 1 Executive Summary
Clinical Analysis Report For Study Sample Study Automated report generated by WWARN May 9, 2014 Falciparum class org.wwarn.csr.clinicalstudyreport Version 1.020140508-1558 1 Contents 1 Executive Summary
Chloroquine/sulphadoxinepyrimethamine. Children with Malaria: Transmission to Mosquitoes of Multidrug-Resistant Plasmodium falciparum
 Chloroquine/Sulphadoxine-Pyrimethamine for Gambian Children with Malaria: Transmission to Mosquitoes of Multidrug-Resistant Plasmodium falciparum Rachel L. Hallett 1, Samuel Dunyo 2, Rosalynn Ord 1, Musa
Chloroquine/Sulphadoxine-Pyrimethamine for Gambian Children with Malaria: Transmission to Mosquitoes of Multidrug-Resistant Plasmodium falciparum Rachel L. Hallett 1, Samuel Dunyo 2, Rosalynn Ord 1, Musa
Risk associated with asymptomatic parasitaemia occurring post-antimalarial treatment
 Tropical Medicine and International Health doi:10.1111/j.1365-3156.2007.01977.x volume 13 no 1 pp 83 90 january 2008 Risk associated with asymptomatic parasitaemia occurring post-antimalarial treatment
Tropical Medicine and International Health doi:10.1111/j.1365-3156.2007.01977.x volume 13 no 1 pp 83 90 january 2008 Risk associated with asymptomatic parasitaemia occurring post-antimalarial treatment
Downloaded from:
 Dunyo, S; Ord, R; Hallett, R; Jawara, M; Walraven, G; Mesa, E; Coleman, R; Sowe, M; Alexander, N; Targett, GA; Pinder, M; Sutherland, CJ (2006) Randomised Trial of Chloroquine/Sulphadoxine-Pyrimethamine
Dunyo, S; Ord, R; Hallett, R; Jawara, M; Walraven, G; Mesa, E; Coleman, R; Sowe, M; Alexander, N; Targett, GA; Pinder, M; Sutherland, CJ (2006) Randomised Trial of Chloroquine/Sulphadoxine-Pyrimethamine
Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1
 Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1 Part I: Evaluation of the current list Proposed grouping from the March 2007 meeting 6.5.3 Antimalarial medicines 6.5.3.1 For curative
Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1 Part I: Evaluation of the current list Proposed grouping from the March 2007 meeting 6.5.3 Antimalarial medicines 6.5.3.1 For curative
Single dose primaquine as a P.falciparum gametocytocide
 Single dose primaquine as a P.falciparum gametocytocide Cochrane Review Agreements and disagreements with other studies or reviews The findings of this review provide very little support for current WHO
Single dose primaquine as a P.falciparum gametocytocide Cochrane Review Agreements and disagreements with other studies or reviews The findings of this review provide very little support for current WHO
Interpretation of the World Malaria Report Country Profile
 Interpretation of the World Malaria Report Country Profile Acknowledgements This presentation was developed to help explain the components of the World Malaria Report Country Profile. The 2017 World Malaria
Interpretation of the World Malaria Report Country Profile Acknowledgements This presentation was developed to help explain the components of the World Malaria Report Country Profile. The 2017 World Malaria
38 Current Concepts in
 38 Current Concepts in Management of Falciparum Malaria Abstract: Artemisinin based Combination Therapy (ACT) is the preferred agent to treat drug resistance uncomplicated Plasmodium Falciparum (PF) Malaria.
38 Current Concepts in Management of Falciparum Malaria Abstract: Artemisinin based Combination Therapy (ACT) is the preferred agent to treat drug resistance uncomplicated Plasmodium Falciparum (PF) Malaria.
DOUBLE BLIND RANDOMISED CLINICAL TRIAL OF TWO DIFFERENT REGIMENS OF ORAL ARTESUNATE IN FALCIPARUM MALARIA
 DOUBLE BLIND RANDOMISED CLINICAL TRIAL OF TWO DIFFERENT REGIMENS OF ORAL ARTESUNATE IN FALCIPARUM MALARIA Danai Bunnag, Chaisin Viravan, Sornchai Looareesuwan, Juntra Karbwang and T-ranakchit Harinasuta
DOUBLE BLIND RANDOMISED CLINICAL TRIAL OF TWO DIFFERENT REGIMENS OF ORAL ARTESUNATE IN FALCIPARUM MALARIA Danai Bunnag, Chaisin Viravan, Sornchai Looareesuwan, Juntra Karbwang and T-ranakchit Harinasuta
Activities of amodiaquine, artesunate, and artesunate-amodiaquine against asexualand -sexual stage parasites in falciparum malaria in children
 AAC Accepts, published online ahead of print on 26 February 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.00077-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 26 February 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.00077-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
Gametocyte Clearance in Uncomplicated and Severe Plasmodium falciparum Malaria after Artesunate-Mefloquine Treatment in Thailand
 Korean J Parasitol. Vol. 46, No. 2: 65-70, June 2008 DOI: 10.3347/kjp.2008.46.2.65 Gametocyte Clearance in Uncomplicated and Severe Plasmodium falciparum Malaria after Artesunate-Mefloquine Treatment in
Korean J Parasitol. Vol. 46, No. 2: 65-70, June 2008 DOI: 10.3347/kjp.2008.46.2.65 Gametocyte Clearance in Uncomplicated and Severe Plasmodium falciparum Malaria after Artesunate-Mefloquine Treatment in
Anti-Malaria Chemotherapy
 Anti-Malaria Chemotherapy Causal Prophylaxis prevent infection (ie, liver stage) Suppressive Prophylaxis prevent clinical disease (ie, blood stages) Treatment Therapy (or clinical cure) relieve symptoms
Anti-Malaria Chemotherapy Causal Prophylaxis prevent infection (ie, liver stage) Suppressive Prophylaxis prevent clinical disease (ie, blood stages) Treatment Therapy (or clinical cure) relieve symptoms
Clinical Study Therapeutic Efficacy of Artemether-Lumefantrine for the Treatment of Uncomplicated Plasmodium falciparum Malaria in Northern Ethiopia
 Malaria Research and Treatment Volume 2012, Article ID 548710, 6 pages doi:10.1155/2012/548710 Clinical Study Therapeutic Efficacy of Artemether-Lumefantrine for the Treatment of Uncomplicated Plasmodium
Malaria Research and Treatment Volume 2012, Article ID 548710, 6 pages doi:10.1155/2012/548710 Clinical Study Therapeutic Efficacy of Artemether-Lumefantrine for the Treatment of Uncomplicated Plasmodium
Summary World Malaria Report 2010
 Summary The summarizes information received from 106 malaria-endemic countries and other partners and updates the analyses presented in the 2009 Report. It highlights continued progress made towards meeting
Summary The summarizes information received from 106 malaria-endemic countries and other partners and updates the analyses presented in the 2009 Report. It highlights continued progress made towards meeting
Against intervention No recommendation Strong Conditional Conditional Strong. For intervention. High Moderate Low Very low
 Draft recommendation: Consider using MDA as an additional tool for the elimination of malaria in low prevalence island or nonisland settings where the risk of imported malaria is low Balance of desirable
Draft recommendation: Consider using MDA as an additional tool for the elimination of malaria in low prevalence island or nonisland settings where the risk of imported malaria is low Balance of desirable
Eighth intercountry meeting of national malaria programme managers from HANMAT and PIAM-Net countries
 Summary report on the Eighth intercountry meeting of national malaria programme managers from HANMAT and PIAM-Net countries WHO-EM/MAL/384/E Islamabad, Pakistan 12 14 December 2016 Summary report on the
Summary report on the Eighth intercountry meeting of national malaria programme managers from HANMAT and PIAM-Net countries WHO-EM/MAL/384/E Islamabad, Pakistan 12 14 December 2016 Summary report on the
Sponsor / Company: Sanofi Drug substance(s): SSR103371
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Downloaded from:
 Abreha, T; Alemayehu, B; Assefa, A; Awab, GR; Baird, JK; Bezabih, B; Cheah, PY; Day, NP; Devine, A; Dorda, M; Dondorp, AM; Girma, S; Hien, TT; Jima, D; Kassa, M; Kebende, A; Khu, NH; Leslie, T; Ley, B;
Abreha, T; Alemayehu, B; Assefa, A; Awab, GR; Baird, JK; Bezabih, B; Cheah, PY; Day, NP; Devine, A; Dorda, M; Dondorp, AM; Girma, S; Hien, TT; Jima, D; Kassa, M; Kebende, A; Khu, NH; Leslie, T; Ley, B;
Progress on the Containment of Artemisinin Tolerant Malaria Parasites in South-East Asia (ARCE) Initiative
 Progress on the Containment of Artemisinin Tolerant Malaria Parasites in South-East Asia (ARCE) Initiative I. Background For many years, the border area between Cambodia and Thailand has been the source
Progress on the Containment of Artemisinin Tolerant Malaria Parasites in South-East Asia (ARCE) Initiative I. Background For many years, the border area between Cambodia and Thailand has been the source
INTRODUCTION. falciparum malaria (WHO, 2006). In Southeast Asia, where P. falciparum is the most drug resistant
 OPTIMUM DOSE OF ARTMISININ-PIPERAQUINE COMBINATIONS DOSE RANGING STUDIES OF NEW ARTEMISININ-PIPERAQUINE FIXED COMBINATIONS COMPARED TO STANDARD REGIMENS OF ARTEMISISNIN COMBINATION THERAPIES FOR ACUTE
OPTIMUM DOSE OF ARTMISININ-PIPERAQUINE COMBINATIONS DOSE RANGING STUDIES OF NEW ARTEMISININ-PIPERAQUINE FIXED COMBINATIONS COMPARED TO STANDARD REGIMENS OF ARTEMISISNIN COMBINATION THERAPIES FOR ACUTE
Malaria Updates. Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine
 Malaria Updates Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine Outline General epidemiology of malaria in the Philippines P falciparum Updates in treatment Recognizing
Malaria Updates Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine Outline General epidemiology of malaria in the Philippines P falciparum Updates in treatment Recognizing
A Simple Dose Regimen of Artesunate and Amodiaquine Based on Arm Span- or Age Range for Childhood Falciparum Malaria: A Preliminary Evaluation
 JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 4, 2012 A Simple Dose Regimen of Artesunate and Amodiaquine Based on Arm Span- or Age Range for Childhood Falciparum Malaria: A Preliminary Evaluation by Akintunde
JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 4, 2012 A Simple Dose Regimen of Artesunate and Amodiaquine Based on Arm Span- or Age Range for Childhood Falciparum Malaria: A Preliminary Evaluation by Akintunde
S Krudsood 1, K Chalermrut 2, C Pengruksa 2, S Srivilairit 2, U Silachamroon 3, S Treeprasertsuk 3, S Kano 4, GM Brittenham 5 and S Looareesuwan 3
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH COMPARATIVE CLINICAL TRIAL OF TWO-FIXED COMBINATIONS DIHYDROARTEMISININ-NAPTHOQUINE- TRIMETHOPRIM (DNP ) AND ARTEMETHER-LUMEFANTRINE (COARTEM / RIAMET ) IN THE
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH COMPARATIVE CLINICAL TRIAL OF TWO-FIXED COMBINATIONS DIHYDROARTEMISININ-NAPTHOQUINE- TRIMETHOPRIM (DNP ) AND ARTEMETHER-LUMEFANTRINE (COARTEM / RIAMET ) IN THE
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centers: Indication: Treatment: Objective: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Sulfadoxine-Pyrimethamine, Chlorproguanil-Dapsone, or Chloroquine for the Treatment of Plasmodium vivax Malaria in Afghanistan and Pakistan
 ORIGINAL CONTRIBUTION Sulfadoxine-Pyrimethamine, Chlorproguanil-Dapsone, or for the Treatment of Plasmodium vivax Malaria in Afghanistan and Pakistan A Randomized Controlled Trial Toby Leslie, MSc M. Ismail
ORIGINAL CONTRIBUTION Sulfadoxine-Pyrimethamine, Chlorproguanil-Dapsone, or for the Treatment of Plasmodium vivax Malaria in Afghanistan and Pakistan A Randomized Controlled Trial Toby Leslie, MSc M. Ismail
Am. J. Trop. Med. Hyg., 60(2), 1999, pp Copyright 1999 by The American Society of Tropical Medicine and Hygiene
 Am. J. Trop. Med. Hyg., 60(2), 1999, pp. 238 243 Copyright 1999 by The American Society of Tropical Medicine and Hygiene A RANDOMIZED, DOUBLE-BLIND, COMPARATIVE TRIAL OF A NEW ORAL COMBINATION OF ARTEMETHER
Am. J. Trop. Med. Hyg., 60(2), 1999, pp. 238 243 Copyright 1999 by The American Society of Tropical Medicine and Hygiene A RANDOMIZED, DOUBLE-BLIND, COMPARATIVE TRIAL OF A NEW ORAL COMBINATION OF ARTEMETHER
ISSN X (Print) Original Research Article. DOI: /sjams India
 DOI: 10.21276/sjams.2016.4.6.22 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(6B):1981-198 5 Scholars Academic and Scientific Publisher (An International Publisher
DOI: 10.21276/sjams.2016.4.6.22 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(6B):1981-198 5 Scholars Academic and Scientific Publisher (An International Publisher
PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia)
 PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia) A 37-year-old woman, who had traveled to New Guinea for several weeks, presented to the medical clinic with fever, chills, and rigors within
PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia) A 37-year-old woman, who had traveled to New Guinea for several weeks, presented to the medical clinic with fever, chills, and rigors within
Efficacy and effectiveness of dihydroartemisinin-piperaquine versus artesunate-mefloquine in falciparum malaria: an open-label randomised comparison
 Efficacy and effectiveness of dihydroartemisinin-piperaquine versus artesunate-mefloquine in falciparum malaria: an open-label randomised comparison Frank Smithuis, Moe Kyaw Kyaw, Ohn Phe, Khin Zarli Aye,
Efficacy and effectiveness of dihydroartemisinin-piperaquine versus artesunate-mefloquine in falciparum malaria: an open-label randomised comparison Frank Smithuis, Moe Kyaw Kyaw, Ohn Phe, Khin Zarli Aye,
Output... Links... Efficacy of artesunate pl...
 Efficacy of artesunate plus pyrimethamine-sulphadoxine for uncomplicated malaria in Gambian children: a double-blind, randomised, controlled trial [Articles] von Seidlein, Lorenz; Milligan, Paul; Pinder,
Efficacy of artesunate plus pyrimethamine-sulphadoxine for uncomplicated malaria in Gambian children: a double-blind, randomised, controlled trial [Articles] von Seidlein, Lorenz; Milligan, Paul; Pinder,
REPORT OF THE TECHNICAL CONSULTATION BACKGROUND
 Defining and validating a measure of parasite resistance to sulfadoxinepyrimethamine (SP) that would be indicative of the protective efficacy of SP for intermittent preventive treatment in infancy (SP-IPTi)
Defining and validating a measure of parasite resistance to sulfadoxinepyrimethamine (SP) that would be indicative of the protective efficacy of SP for intermittent preventive treatment in infancy (SP-IPTi)
Artesunate Mefloquine (AsMq)
 Artesunate Mefloquine (AsMq) Introduction AsMq in Rakhine in 1996 AsMq FDC compared to other ACTs AZG (MSF-Holland) malaria activities in Western Myanmar 9 townships 25 DoH clinics with AZG support (area
Artesunate Mefloquine (AsMq) Introduction AsMq in Rakhine in 1996 AsMq FDC compared to other ACTs AZG (MSF-Holland) malaria activities in Western Myanmar 9 townships 25 DoH clinics with AZG support (area
A systematic approach to the development of a rational malaria treatment policy in Zambia
 Tropical Medicine and International Health volume 3 no 7 pp 535 542 july 1998 A systematic approach to the development of a rational malaria treatment policy in Zambia Lawrence M. Barat 1, Benson Himonga
Tropical Medicine and International Health volume 3 no 7 pp 535 542 july 1998 A systematic approach to the development of a rational malaria treatment policy in Zambia Lawrence M. Barat 1, Benson Himonga
HALOFANTRINE HYDROCHLORIDE - EFFICACY AND SAFETY IN CHILDREN WITH ACUTE MALARIA
 HALOFANTRINE HYDROCHLORIDE - EFFICACY AND SAFETY IN CHILDREN WITH ACUTE MALARIA Pages with reference to book, From 8 To 10 Mushtaq A. Khan, Gui Nayyer Rehman, S.A. Qazi ( Children Hospital, Pakistan Institute
HALOFANTRINE HYDROCHLORIDE - EFFICACY AND SAFETY IN CHILDREN WITH ACUTE MALARIA Pages with reference to book, From 8 To 10 Mushtaq A. Khan, Gui Nayyer Rehman, S.A. Qazi ( Children Hospital, Pakistan Institute
Effectiveness of five artemisinin combination regimens with or without primaquine in uncomplicated falciparum malaria: an open-label randomised trial
 Effectiveness of five artemisinin combination regimens with or without primaquine in uncomplicated falciparum malaria: an open-label randomised trial Frank Smithuis, Moe Kyaw Kyaw, Ohn Phe, Thein Win,
Effectiveness of five artemisinin combination regimens with or without primaquine in uncomplicated falciparum malaria: an open-label randomised trial Frank Smithuis, Moe Kyaw Kyaw, Ohn Phe, Thein Win,
Therapeutic efficacy and artemisinin resistance in northern Myanmar: evidence from in vivo and molecular marker studies
 DOI 10.1186/s12936-017-1775-2 Malaria Journal RESEARCH Open Access Therapeutic efficacy and artemisinin resistance in northern Myanmar: evidence from in vivo and molecular marker studies Moe Kyaw Myint
DOI 10.1186/s12936-017-1775-2 Malaria Journal RESEARCH Open Access Therapeutic efficacy and artemisinin resistance in northern Myanmar: evidence from in vivo and molecular marker studies Moe Kyaw Myint
METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY ISBN
 METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY ISBN 978 92 4 159753 1 METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY WHO Library Cataloguing-in-Publication
METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY ISBN 978 92 4 159753 1 METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY WHO Library Cataloguing-in-Publication
Directorate of National Vector Borne Disease Control Programme
 NATIONAL DRUG POLICY ON MALARIA (2008) Directorate of National Vector Borne Disease Control Programme (Directorate General of Health Services) Ministry of Health and Family Welfare 22-Shamnath Marg,, Delhi-110054..
NATIONAL DRUG POLICY ON MALARIA (2008) Directorate of National Vector Borne Disease Control Programme (Directorate General of Health Services) Ministry of Health and Family Welfare 22-Shamnath Marg,, Delhi-110054..
Malaria. Edwin J. Asturias, MD
 Malaria Edwin J. Asturias, MD Associate Professor of Pediatrics and Epidemiology Director for Latin America Center for Global Health, Colorado School of Public Health Global Health and Disasters Course
Malaria Edwin J. Asturias, MD Associate Professor of Pediatrics and Epidemiology Director for Latin America Center for Global Health, Colorado School of Public Health Global Health and Disasters Course
Clinical Drug Trials
 Clinical Drug Trials Drug resistance to chloroquine in P. falciparum was reported in India for the first time from Assam in 1973. Since then the foci of resistance have spread to many more states all over
Clinical Drug Trials Drug resistance to chloroquine in P. falciparum was reported in India for the first time from Assam in 1973. Since then the foci of resistance have spread to many more states all over
Artemether-lumefantrine (four-dose regimen) for treating uncomplicated falciparum malaria (Review)
 Artemether-lumefantrine (four-dose regimen) for treating uncomplicated falciparum malaria (Review) Omari AAA, Gamble CL, Garner P This is a reprint of a Cochrane review, prepared and maintained by The
Artemether-lumefantrine (four-dose regimen) for treating uncomplicated falciparum malaria (Review) Omari AAA, Gamble CL, Garner P This is a reprint of a Cochrane review, prepared and maintained by The
MESA research grants 2014
 MESA research grants 2014 MESA operational research grant Principal investigator Mopping up and getting to zero: mapping residual malaria transmission for targeted response in urban Lusaka, Zambia. Daniel
MESA research grants 2014 MESA operational research grant Principal investigator Mopping up and getting to zero: mapping residual malaria transmission for targeted response in urban Lusaka, Zambia. Daniel
Supplementary figures
 Weight, kg Lumefantrine concentration μg/ml Supplementary figures 8 7 6 5 4 3 2 model data 1 0 0 5 10 15 Days Supplementary Figure 1. Plasma lumefantrine concentrations in African children [1] and model-fitted
Weight, kg Lumefantrine concentration μg/ml Supplementary figures 8 7 6 5 4 3 2 model data 1 0 0 5 10 15 Days Supplementary Figure 1. Plasma lumefantrine concentrations in African children [1] and model-fitted
Artesunate combinations for treatment of malaria: meta-analysis
 Articles Artesunate combinations for treatment of malaria: meta-analysis International Artemisinin Study Group* Summary Background Addition of artemisinin derivatives to existing drug regimens for malaria
Articles Artesunate combinations for treatment of malaria: meta-analysis International Artemisinin Study Group* Summary Background Addition of artemisinin derivatives to existing drug regimens for malaria
Gametocytaemia after Drug Treatment of Asymptomatic Plasmodium falciparum
 Gametocytaemia after Drug Treatment of Asymptomatic Plasmodium falciparum Samuel Dunyo 1, Paul Milligan 2*, Tansy Edwards 2, Colin Sutherland 2, Geoffrey Targett 2, Margaret Pinder 1 1 Medical Research
Gametocytaemia after Drug Treatment of Asymptomatic Plasmodium falciparum Samuel Dunyo 1, Paul Milligan 2*, Tansy Edwards 2, Colin Sutherland 2, Geoffrey Targett 2, Margaret Pinder 1 1 Medical Research
Rectal artesunate for pre-referral treatment of severe malaria
 Global Malaria Programme Rectal artesunate for pre-referral treatment of severe malaria october 2017 information note Background Severe malaria is a medical emergency: mortality from untreated severe malaria
Global Malaria Programme Rectal artesunate for pre-referral treatment of severe malaria october 2017 information note Background Severe malaria is a medical emergency: mortality from untreated severe malaria
ACTs in East Africa REALITY CHECK. Nathan Mulure MD Novartis Pharma
 ACTs in East Africa REALITY CHECK Nathan Mulure MD Novartis Pharma 1 Agenda Introduction and background Drug resistance to antimalarials Policy change Antimalarial market Challenges 2 Malaria Burden 34,000
ACTs in East Africa REALITY CHECK Nathan Mulure MD Novartis Pharma 1 Agenda Introduction and background Drug resistance to antimalarials Policy change Antimalarial market Challenges 2 Malaria Burden 34,000
POLICY BRIEF Review of Antimalarial Medicines Available to Treat P. falciparum in the Amazon Region
 POLICY BRIEF Review of Antimalarial Medicines Available to Treat P. falciparum in the Amazon Region Background Malaria is a substantial public health threat in the Americas. In 2010, the Americas had approximately
POLICY BRIEF Review of Antimalarial Medicines Available to Treat P. falciparum in the Amazon Region Background Malaria is a substantial public health threat in the Americas. In 2010, the Americas had approximately
Comparison of light microscopy and nested PCR assay in detecting of malaria mixed species infections in an endemic area of Iran
 Comparison of light microscopy and nested PCR assay in detecting of malaria mixed species infections in an endemic area of Iran Aliehsan Heidari, Manizheh Nourian, Hossein Keshavarz Associate Prof. Dept.
Comparison of light microscopy and nested PCR assay in detecting of malaria mixed species infections in an endemic area of Iran Aliehsan Heidari, Manizheh Nourian, Hossein Keshavarz Associate Prof. Dept.
Primaquine or other 8-aminoquinoline for reducing Plasmodium falciparum transmission (Review)
 Primaquine or other 8-aminoquinoline for reducing Plasmodium falciparum transmission (Review) Graves PM, Gelband H, Garner P This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
Primaquine or other 8-aminoquinoline for reducing Plasmodium falciparum transmission (Review) Graves PM, Gelband H, Garner P This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
Implementing the Abuja Declaration and Plan of Action: the journey so far
 Implementing the Abuja Declaration and Plan of Action: the journey so far The Abuja Declaration African leaders who met on 25 April 2000 in Abuja, Nigeria, laid out the foundation for a sustained battle
Implementing the Abuja Declaration and Plan of Action: the journey so far The Abuja Declaration African leaders who met on 25 April 2000 in Abuja, Nigeria, laid out the foundation for a sustained battle
Checchi, F; Piola, P; Kosack, C; Ardizzoni, E; Klarkowski, D; Kwezi, E; Priotto, G; Balkan, S; Bakyaita, N; Brockman, A; Guthmann, J P
 MSF Field Research Antimalarial efficacy of sulfadoxine-pyrimethamine, amodiaquine and a combination of chloroquine plus sulfadoxinepyrimethamine in Bundi Bugyo, western Uganda. Authors Citation DOI Publisher
MSF Field Research Antimalarial efficacy of sulfadoxine-pyrimethamine, amodiaquine and a combination of chloroquine plus sulfadoxinepyrimethamine in Bundi Bugyo, western Uganda. Authors Citation DOI Publisher
Department of Pharmacology and Therapeutics and Institute for Medical Research and Training, University of Ibadan, Ibadan, Nigeria
 The Open Tropical Medicine Journal, 2011, 4, 33-38 33 Open Access Kinetics of Plasmodium falciparum Gametocyte Sex Ratios: Application to the Evaluation of the Potential of Antimalarial Drugs to Influence
The Open Tropical Medicine Journal, 2011, 4, 33-38 33 Open Access Kinetics of Plasmodium falciparum Gametocyte Sex Ratios: Application to the Evaluation of the Potential of Antimalarial Drugs to Influence
APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS
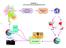 APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS 97 Country/ area APPENDIX 2a DRUG REGIMENS SEA REGION, 2001 (dosage for adults) : P. falciparum Lab confirmed Treatment failure Severe malaria Pregnancy
APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS 97 Country/ area APPENDIX 2a DRUG REGIMENS SEA REGION, 2001 (dosage for adults) : P. falciparum Lab confirmed Treatment failure Severe malaria Pregnancy
A New Class of Malaria Drugs: The Coartem Breakthrough from Novartis
 A New Class of Malaria Drugs: The Coartem Breakthrough from Novartis and its Chinese Partners Hans Rietveld, Director, Global Access and Marketing, Malaria Initiative, Novartis Pharma AG Workshop on Access
A New Class of Malaria Drugs: The Coartem Breakthrough from Novartis and its Chinese Partners Hans Rietveld, Director, Global Access and Marketing, Malaria Initiative, Novartis Pharma AG Workshop on Access
OF ANTIMALARIAL DRUGS
 THE USE OF ANTIMALARIAL DRUGS THE USE OF ANTIMALARIAL DRUGS Report of an Informal Consultation World Health Organization, Geneva WHO, 2001 Technical Review: A. Bosman, C. Delacollette, P. Olumese, R. G.
THE USE OF ANTIMALARIAL DRUGS THE USE OF ANTIMALARIAL DRUGS Report of an Informal Consultation World Health Organization, Geneva WHO, 2001 Technical Review: A. Bosman, C. Delacollette, P. Olumese, R. G.
Evidence Review Group on MDA, MSAT and FSAT Malaria Policy Advisory Committee Geneva, Switzerland September 2015
 Evidence Review Group on MDA, MSAT and FSAT Malaria Policy Advisory Committee Geneva, Switzerland 16-18 September 2015 Kevin Marsh Chairperson of the Evidence Review Group 1 Outline of the Presentation
Evidence Review Group on MDA, MSAT and FSAT Malaria Policy Advisory Committee Geneva, Switzerland 16-18 September 2015 Kevin Marsh Chairperson of the Evidence Review Group 1 Outline of the Presentation
Disclosure Information
 Malaria Medications Charlie Mosler, RPh, PharmD, CGP, FASCP Assistant Professor of Pharmacy Practice The University of Findlay College of Pharmacy Findlay, OH mosler@findlay.edu Disclosure Information
Malaria Medications Charlie Mosler, RPh, PharmD, CGP, FASCP Assistant Professor of Pharmacy Practice The University of Findlay College of Pharmacy Findlay, OH mosler@findlay.edu Disclosure Information
MALARIA IS ONE OF THE
 ORIGINAL CONTRIBUTION Combination Therapy for Uncomplicated Falciparum Malaria in Ugandan Children A Randomized Trial Grant Dorsey, MD, PhD Sarah Staedke, MD Tamara D. Clark, MPH Denise Njama-Meya, MB
ORIGINAL CONTRIBUTION Combination Therapy for Uncomplicated Falciparum Malaria in Ugandan Children A Randomized Trial Grant Dorsey, MD, PhD Sarah Staedke, MD Tamara D. Clark, MPH Denise Njama-Meya, MB
Artemisinin-based combination therapy reduces expenditure on malaria treatment in KwaZulu Natal, South Africa
 Tropical Medicine and International Health volume 9 no 9 pp 959 966 september 2004 Artemisinin-based combination therapy reduces expenditure on malaria treatment in KwaZulu Natal, South Africa Charlotte
Tropical Medicine and International Health volume 9 no 9 pp 959 966 september 2004 Artemisinin-based combination therapy reduces expenditure on malaria treatment in KwaZulu Natal, South Africa Charlotte
Stephan Duparc 1*, Isabelle Borghini-Fuhrer 1, J Carl Craft 1,2, Sarah Arbe-Barnes 3, Robert M Miller 3, Chang-Sik Shin 4 and Lawrence Fleckenstein 5
 Duparc et al. Malaria Journal 213, 12:7 http://www.malariajournal.com/content/12/1/7 RESEARCH Open Access Safety and efficacy of pyronaridine-artesunate in uncomplicated acute malaria: an integrated analysis
Duparc et al. Malaria Journal 213, 12:7 http://www.malariajournal.com/content/12/1/7 RESEARCH Open Access Safety and efficacy of pyronaridine-artesunate in uncomplicated acute malaria: an integrated analysis
Early rising asexual parasitaemia in Nigerian children following a first dose of artemisinin-based combination treatments of falciparum malaria
 Sowunmi et al. BMC Infectious Diseases (2017) 17:110 DOI 10.1186/s12879-016-2173-z RESEARCH ARTICLE Early rising asexual parasitaemia in Nigerian children following a first dose of artemisinin-based combination
Sowunmi et al. BMC Infectious Diseases (2017) 17:110 DOI 10.1186/s12879-016-2173-z RESEARCH ARTICLE Early rising asexual parasitaemia in Nigerian children following a first dose of artemisinin-based combination
Downloaded from:
 Bukirwa, H; Yeka, A; Kamya, MR; Talisuna, A; Banek, K; Bakyaita, N; Rwakimari, JB; Rosenthal, PJ; Wabwire-Mangen, F; Dorsey, G; Staedke, SG (2006) Artemisinin combination therapies for treatment of uncomplicated
Bukirwa, H; Yeka, A; Kamya, MR; Talisuna, A; Banek, K; Bakyaita, N; Rwakimari, JB; Rosenthal, PJ; Wabwire-Mangen, F; Dorsey, G; Staedke, SG (2006) Artemisinin combination therapies for treatment of uncomplicated
Sponsor / Company: Sanofi Drug substance(s): artesunate plus amodiaquine Title of the study:
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
14th Stakeholders Meeting
 14th Stakeholders Meeting Steady progress towards malaria elimination: Interventions for today and tomorrow Denpasar, Bali 11 12 October 2017 David Hughes, Novartis 12th October 2017 Defeating Malaria
14th Stakeholders Meeting Steady progress towards malaria elimination: Interventions for today and tomorrow Denpasar, Bali 11 12 October 2017 David Hughes, Novartis 12th October 2017 Defeating Malaria
EFFICACY OF PRIMAQUINE REGIMENS FOR PRIMAQUINE-RESISTANT PLASMODIUM VIVAX MALARIA IN THAILAND
 Am. J. Trop. Med. Hyg., 61(6), 1999, pp. 973 977 Copyright 1999 by The American Society of Tropical Medicine and Hygiene EFFICACY OF PRIMAQUINE REGIMENS FOR PRIMAQUINE-RESISTANT PLASMODIUM VIVAX MALARIA
Am. J. Trop. Med. Hyg., 61(6), 1999, pp. 973 977 Copyright 1999 by The American Society of Tropical Medicine and Hygiene EFFICACY OF PRIMAQUINE REGIMENS FOR PRIMAQUINE-RESISTANT PLASMODIUM VIVAX MALARIA
Downloaded from:
 Sutherland, CJ; Drakeley, CJ; Obisike, U; Coleman, R; Jawara, M; Targett, GA; Milligan, P; Pinder, M; Walraven, G (2003) The addition of artesunate to chloroquine for treatment of Plasmodium falciparum
Sutherland, CJ; Drakeley, CJ; Obisike, U; Coleman, R; Jawara, M; Targett, GA; Milligan, P; Pinder, M; Walraven, G (2003) The addition of artesunate to chloroquine for treatment of Plasmodium falciparum
Akintunde Sowunmi 1,2,5*, Kazeem Akano 1, Adejumoke I. Ayede 3, Godwin Ntadom 4, Temitope Aderoyeje 5, Elsie O. Adewoye 6 and Bayo Fatunmbi 7
 Sowunmi et al. BMC Infectious Diseases (2016) 16:240 DOI 10.1186/s12879-016-1565-4 RESEARCH ARTICLE Clinical illness and outcomes in Nigerian children with late-appearing anaemia after artemisinin-based
Sowunmi et al. BMC Infectious Diseases (2016) 16:240 DOI 10.1186/s12879-016-1565-4 RESEARCH ARTICLE Clinical illness and outcomes in Nigerian children with late-appearing anaemia after artemisinin-based
Pharmacokinetics of Mefloquine Combined with Artesunate in Children with Acute Falciparum Malaria
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 1999, p. 341 346 Vol. 43, No. 2 0066-4804/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Pharmacokinetics of Mefloquine
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 1999, p. 341 346 Vol. 43, No. 2 0066-4804/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Pharmacokinetics of Mefloquine
ARTEMISININ FOR TREATMENT OF UNCOMPLICATED FALCIPARUM MALARIA: IS THERE A PLACE FOR MONOTHERAPY?
 Am. J. Trop. Med. Hyg., 65(6), 2001, pp. 690 695 Copyright 2001 by The American Society of Tropical Medicine and Hygiene ARTEMISININ FOR TREATMENT OF UNCOMPLICATED FALCIPARUM MALARIA: IS THERE A PLACE
Am. J. Trop. Med. Hyg., 65(6), 2001, pp. 690 695 Copyright 2001 by The American Society of Tropical Medicine and Hygiene ARTEMISININ FOR TREATMENT OF UNCOMPLICATED FALCIPARUM MALARIA: IS THERE A PLACE
ACCEPTED. Diseases, Monash University, Commercial Road, Melbourne, Victoria 3004, Australia
 The Pediatric Infectious Disease Journal Publish Ahead of Print DOI : 10.1097/INF.0000000000000671 Plasmodium vivax malaria: challenges in diagnosis, treatment, and elimination James G Beeson 1,2, Cindy
The Pediatric Infectious Disease Journal Publish Ahead of Print DOI : 10.1097/INF.0000000000000671 Plasmodium vivax malaria: challenges in diagnosis, treatment, and elimination James G Beeson 1,2, Cindy
New Partnerships The Development of ASMQ - FDC
 New Partnerships The Development of ASMQ - FDC Jean-René Kiechel Senior Product Manager DNDi January 2011 1 ACTs: World Health Organization Treatment Guidelines (2006) In order to fight resistance: 1.
New Partnerships The Development of ASMQ - FDC Jean-René Kiechel Senior Product Manager DNDi January 2011 1 ACTs: World Health Organization Treatment Guidelines (2006) In order to fight resistance: 1.
University of Veterinary and Animal Sciences, Bikaner), V.P.O. Bajor, Dist. Sikar, Rajasthan, India
 REVIEW ARTICLE www.ijapc.com e-issn 2350-0204 Malaria, A Widely Prevalent Mosquito-Borne Infection in Humans and Recommended Herbal Therapy Subha Ganguly 1*, Satarupa Roy 2 1 Associate Department of Veterinary
REVIEW ARTICLE www.ijapc.com e-issn 2350-0204 Malaria, A Widely Prevalent Mosquito-Borne Infection in Humans and Recommended Herbal Therapy Subha Ganguly 1*, Satarupa Roy 2 1 Associate Department of Veterinary
Tolerability of Artemisinin based combination treatments - ACTs. Bob Taylor MD (Lond), FRCP (UK), DTM&H (Lond)
 Tolerability of Artemisinin based combination treatments - ACTs Bob Taylor MD (Lond), FRCP (UK), DTM&H (Lond) Main ACTs Artesunate + mefloquine Dihydroartemisinin + piperaquine Artemether + lumefantrine
Tolerability of Artemisinin based combination treatments - ACTs Bob Taylor MD (Lond), FRCP (UK), DTM&H (Lond) Main ACTs Artesunate + mefloquine Dihydroartemisinin + piperaquine Artemether + lumefantrine
Downloaded from:
 Wootton, DG; Opara, H; Biagini, GA; Kanjala, MK; Duparc, S; Kirby, PL; Woessner, M; Neate, C; Nyirenda, M; Blencowe, H; Dube- Mbeye, Q; Kanyok, T; Ward, S; Molyneux, M; Dunyo, S; Winstanley, PA (2008)
Wootton, DG; Opara, H; Biagini, GA; Kanjala, MK; Duparc, S; Kirby, PL; Woessner, M; Neate, C; Nyirenda, M; Blencowe, H; Dube- Mbeye, Q; Kanyok, T; Ward, S; Molyneux, M; Dunyo, S; Winstanley, PA (2008)
P. vivax P. falciparum coinfection and antimalarial drug resistance. Ric Price
 P. vivax P. falciparum coinfection and antimalarial drug resistance Ric Price Outline Global Burden Comparative biology of Pv and Pf Coinfections: Pv effect on Pf Relapses and the role post treatment prophylaxis
P. vivax P. falciparum coinfection and antimalarial drug resistance Ric Price Outline Global Burden Comparative biology of Pv and Pf Coinfections: Pv effect on Pf Relapses and the role post treatment prophylaxis
In several African countries in sub-saharan Africa, malaria is the leading cause of death in children under five.
 TECHNICAL SEMINAR - MALARIA SLIDE 1 Technical Seminar - Malaria Malaria is an extremely important cause of mortality in different parts of world. In this technical seminar, I ll discuss the rationale for
TECHNICAL SEMINAR - MALARIA SLIDE 1 Technical Seminar - Malaria Malaria is an extremely important cause of mortality in different parts of world. In this technical seminar, I ll discuss the rationale for
Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M.
 UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
UvA-DARE (Digital Academic Repository) Artemether-lumefantrine: a new treatment combination for multi-drug resistant falciparum malaria van Vugt, M. Link to publication Citation for published version (APA):
Grace Olusola Gbotosho, Akintunde Sowunmi/ +, Christian Tientcha Happi, Titilope Modupe Okuboyejo
 Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 106(6): 685-690, September 2011 685 Plasmodium falciparum gametocyte carriage, sex ratios and asexual parasite rates in Nigerian children before and after a
Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 106(6): 685-690, September 2011 685 Plasmodium falciparum gametocyte carriage, sex ratios and asexual parasite rates in Nigerian children before and after a
Imported malaria: a possible threat to the elimination of malaria from Sri Lanka?
 Tropical Medicine and International Health doi:0./tmi.097 volume 8 no 6 pp 76 768 june 03 Imported malaria: a possible threat to the elimination of malaria from Sri Lanka? G. N. L. Galappaththy, S. D.
Tropical Medicine and International Health doi:0./tmi.097 volume 8 no 6 pp 76 768 june 03 Imported malaria: a possible threat to the elimination of malaria from Sri Lanka? G. N. L. Galappaththy, S. D.
Pelagia Research Library
 Available online at www.pelagiaresearchlibrary.com European Journal of Experimental Biology, 2011, 1 (3):7-13 ISSN: 2248 9215 Polymorphisms in Plasmodium falciparum Adenosine Triphosphatase 6 (PfATPase6)
Available online at www.pelagiaresearchlibrary.com European Journal of Experimental Biology, 2011, 1 (3):7-13 ISSN: 2248 9215 Polymorphisms in Plasmodium falciparum Adenosine Triphosphatase 6 (PfATPase6)
History, Dynamics, and Public Health Importance of Malaria Parasite Resistance
 CLINICAL MICROBIOLOGY REVIEWS, Jan. 2004, p. 235 254 Vol. 17, No. 1 0893-8512/04/$08.00 0 DOI: 10.1128/CMR.17.1.235 254.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved. History,
CLINICAL MICROBIOLOGY REVIEWS, Jan. 2004, p. 235 254 Vol. 17, No. 1 0893-8512/04/$08.00 0 DOI: 10.1128/CMR.17.1.235 254.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved. History,
drug efficacy and drug resistance:
 Global report on antimalarial drug efficacy and drug resistance: 2000 2010 WHO Library Cataloguing-in-Publication Data Global report on antimalarial drug efficacy and drug resistance: 2000-2010. 1.Malaria
Global report on antimalarial drug efficacy and drug resistance: 2000 2010 WHO Library Cataloguing-in-Publication Data Global report on antimalarial drug efficacy and drug resistance: 2000-2010. 1.Malaria
PURPOSE The purpose of the Malaria Control Strategic Plan 2005/ /10 is to provide a common platform and detailed description of interventions
 PURPOSE The purpose of the Malaria Control Strategic Plan 2005/06-2009/10 is to provide a common platform and detailed description of interventions for all RBM partners and sectors of society. It encourages
PURPOSE The purpose of the Malaria Control Strategic Plan 2005/06-2009/10 is to provide a common platform and detailed description of interventions for all RBM partners and sectors of society. It encourages
CLINICAL TRIALS OF MEFLOQUINE WITH TETRACYCLINE
 CLINICAL TRIALS OF MEFLOQUINE WITH TETRACYCLINE Danai Bunnag, Juntra Karbwang, Chaisin Viravan, Sunee Chitamas and Tranakchit Harinasuta Department of Clinical Tropical Medicine and Hospital for Tropical
CLINICAL TRIALS OF MEFLOQUINE WITH TETRACYCLINE Danai Bunnag, Juntra Karbwang, Chaisin Viravan, Sunee Chitamas and Tranakchit Harinasuta Department of Clinical Tropical Medicine and Hospital for Tropical
Individual Pvmsp1 variants within polyclonal Plasmodium vivax infections
 JCM Accepts, published online ahead of print on 28 11 December January 2012 2011 J. Clin. Microbiol. doi:10.1128/jcm.06212-11 Copyright 2011, 2012, American Society for Microbiology. All Rights Reserved.
JCM Accepts, published online ahead of print on 28 11 December January 2012 2011 J. Clin. Microbiol. doi:10.1128/jcm.06212-11 Copyright 2011, 2012, American Society for Microbiology. All Rights Reserved.
OVERVIEW DRUG RESISTANT MALARIA ON THE THAI-MYANMAR AND THAI-CAMBODIAN BORDERS
 OVERVIEW DRUG RESISTANT MALARIA ON THE THAI-MYANMAR AND THAI-CAMBODIAN BORDERS Chansuda Wongsrichanalai 1, Jeeraphat Sirichaisinthop 2, Jerome J Karwacki 1, Kanungnit Congpuong 3, R Scott Miller, 1 Lorrin
OVERVIEW DRUG RESISTANT MALARIA ON THE THAI-MYANMAR AND THAI-CAMBODIAN BORDERS Chansuda Wongsrichanalai 1, Jeeraphat Sirichaisinthop 2, Jerome J Karwacki 1, Kanungnit Congpuong 3, R Scott Miller, 1 Lorrin
Dihydroartemisinin-piperaquine for treating uncomplicated Plasmodium falciparum malaria (Review)
 Dihydroartemisinin-piperaquine for treating uncomplicated Plasmodium falciparum malaria (Review) Zani B, Gathu M, Donegan S, Olliaro PL, Sinclair D This is a reprint of a Cochrane review, prepared and
Dihydroartemisinin-piperaquine for treating uncomplicated Plasmodium falciparum malaria (Review) Zani B, Gathu M, Donegan S, Olliaro PL, Sinclair D This is a reprint of a Cochrane review, prepared and
DETERMINANTS OF PARASITE CLEARANCE TIME AND RECRUDESCENCE IN PATIENTS TREATED FOR UNCOMPLICATED PLASMODIUM FALCIPARUM MALARIA IN SUB-SAHARAN AFRICA
 DETERMINANTS OF PARASITE CLEARANCE TIME AND RECRUDESCENCE IN PATIENTS TREATED FOR UNCOMPLICATED PLASMODIUM FALCIPARUM MALARIA IN SUB-SAHARAN AFRICA Mary A. Woessner A dissertation submitted to the faculty
DETERMINANTS OF PARASITE CLEARANCE TIME AND RECRUDESCENCE IN PATIENTS TREATED FOR UNCOMPLICATED PLASMODIUM FALCIPARUM MALARIA IN SUB-SAHARAN AFRICA Mary A. Woessner A dissertation submitted to the faculty
Artesunate plus pyronaridine for treating uncomplicated Plasmodium falciparum malaria (Review)
 Artesunate plus pyronaridine for treating uncomplicated Plasmodium falciparum malaria (Review) Bukirwa H, Unnikrishnan B, Kramer CV, Sinclair D, Nair S, Tharyan P This is a reprint of a Cochrane review,
Artesunate plus pyronaridine for treating uncomplicated Plasmodium falciparum malaria (Review) Bukirwa H, Unnikrishnan B, Kramer CV, Sinclair D, Nair S, Tharyan P This is a reprint of a Cochrane review,
Ph.D. Thesis: Protective immune response in P.falciparum malaria 2011 CHAPTER I: Introduction. S.D. Lourembam 16
 CHAPTER I: Introduction S.D. Lourembam 16 1. INTRODUCTION Malaria remains a major global health problem with 300 to 500 million clinical infections and more than a million deaths reported each year. In
CHAPTER I: Introduction S.D. Lourembam 16 1. INTRODUCTION Malaria remains a major global health problem with 300 to 500 million clinical infections and more than a million deaths reported each year. In
Phenotyping Plasmodium vivax in Indonesia using Standard Chloroquine Therapy. Puji Budi Setia Asih. Eijkman Institute for Molecular Biology
 Phenotyping Plasmodium vivax in Indonesia using Standard Chloroquine Therapy Puji Budi Setia Asih Eijkman Institute for Molecular Biology Background Plasmodium vivax threatens 2.6 billion people with a
Phenotyping Plasmodium vivax in Indonesia using Standard Chloroquine Therapy Puji Budi Setia Asih Eijkman Institute for Molecular Biology Background Plasmodium vivax threatens 2.6 billion people with a
Malaria: A Global Perspective and Prospects for Elimination. Rima Shretta
 Malaria: A Global Perspective and Prospects for Elimination Rima Shretta Background Spread by the female anopheles mosquito; caused by plasmodium parasite: P. falciparum, P. vivax, P. ovale, P. malariae,
Malaria: A Global Perspective and Prospects for Elimination Rima Shretta Background Spread by the female anopheles mosquito; caused by plasmodium parasite: P. falciparum, P. vivax, P. ovale, P. malariae,
Copyright The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY-NC-ND license.
 Comparison of artesunate mefloquine and artemether lumefantrine fixed-dose combinations for treatment of uncomplicated Plasmodium falciparum malaria in children younger than 5 years in sub-saharan Africa:
Comparison of artesunate mefloquine and artemether lumefantrine fixed-dose combinations for treatment of uncomplicated Plasmodium falciparum malaria in children younger than 5 years in sub-saharan Africa:
