INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
|
|
|
- Kerry Rose
- 6 years ago
- Views:
Transcription
1 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains an exposure to blood or other potentially infectious body fluids. All potentially infectious body fluids/substances are to be considered potentially infectious with blood-borne pathogens [e.g., human immunodeficiency virus (HIV), hepatitis B virus, and hepatitis C virus]. Any exposure to a potentially infectious body fluid/substance requires immediate evaluation for necessary management. 1. Definitions: Exposure: Percutaneous injury (e.g., a needle stick, cut with a sharp object, bite), contact of mucous membranes, tissue, non-intact skin (e.g., chapped, abraded, or afflicted with dermatitis), or prolonged or extensive skin contact with blood or tissue or body fluids as defined below. Potentially infectious body fluids: Blood, semen, vaginal secretions, cerebrospinal fluid, synovial fluid, pleural fluid, peritoneal fluid, pericardial fluid, amniotic fluid, peritoneal or hemodialysis waste, or other body fluid contaminated with visible blood; breast milk, (including an infant s inadvertent ingestion of milk from a woman other than natural mother); laboratory specimens that contain virus (e.g., suspensions of concentrated virus); any unfixed tissue. Source: Person whose blood, tissue, or body fluid accounted for exposure.* Exposed Person: Person who sustains an exposure.* *NOTE: The source and exposed person may be: an employee, patient, contract worker, visitor, voluntary worker, physician, student, volunteer, etc. 2. Procedures: After an exposure (as defined above) the following procedures are to be initiated as soon as possible:
2 Page 2 of The exposed area must be washed with soap and water (or, in the case of mucous membrane exposures, flushed with water) immediately or as soon as feasible following the exposure Procedures for Evaluation of Exposure and Source; and for Referral of Exposed Person for Medical Evaluation Reporting the exposure: a) Non-physician staff members: incident is to be reported to their supervisor. b) Physician staff members, medical students, patients, visitors, volunteers or any other individuals: incident is to be reported to the supervisor of the area where incident occurred. c) All exposed persons are to be informed of the exposure if they are unaware. If the exposed person is a patient, the responsible physician (attending and/or housestaff) is to inform her/him that an exposure has occurred Once informed, the supervisor will: a) Assure that the exposed area is cleansed appropriately (See 2.1). b) Contact the Needlestick Coordinator at pager 4118 (Monday-Friday, 9AM 5PM) or the Nursing Administrator (at all other times). c) Gather information for Blood/Body Fluid Exposure worksheet. d) Complete Accident Injury Report (for exposed employees) and Non- Employee Occurrence Report (for patients and all others). e) Refer the exposed person to the appropriate area for medical evaluation (see 2.2.4) The Needlestick Coordinator or Nursing Administrator will: a) Gather information for Blood/Body Fluid Exposure worksheet in conjunction with supervisor. b) Obtain bloodborne pathogen risk factor information from source (see Appendix I) and inform and confirm information by contacting the responsible physician (attending and/or housestaff) for the source. c) If not already done, refer exposed person for medical evaluation (see 2.2.4).
3 Page 3 of 11 d) If exposed person is a patient: Notify the responsible physician (attending and/or house-staff) immediately. Instruct responsible physician to contact ID Attending/Fellow on call through page operator (24 hours per day) for recommended management of exposure. Assure that recommendations have been followed through by the responsible physician. e) Obtain from the source HBsAg and Hepatitis C antibody (anti-hcv). Samples may be drawn without physician order, by Medical Board decision, but shall be documented in the medical record. An attempt should be made to notify the physician of record prior to drawing a sample. If prior notification is not possible, the physician of record should be informed after the fact. f) Request and perform (if consent provided) HIV counseling/expedited testing of source if not already known to be HIV-positive (can be performed by Needlestick Coordinator, physician, NP, PA, counselors/social workers) Referral of exposed persons for medical evaluation: Hospital staff and volunteers: Employee Health Service (Monday-Friday 8AM-4PM) or Emergency Department (all other times). Medical students: Jack Martin Fund Clinic (Monday-Friday 8:30AM- 4:30PM) or Emergency Department (all other times) All other students: Emergency Department at all times Agency, contract, or traveling staff: Emergency Department at all times 2.3. Procedures for the Employee Health Service, Jack Martin Fund Clinic and Emergency Department Determine that an exposure has occurred (see above definition). Determine extent of exposure (exposure risk (see 2.3.6).
4 Page 4 of Review history of and risk factors for HIV, hepatitis B, and hepatitis C of source provided by Needlestick Coordinator or Nursing Administrator. (See Appendix I) Obtain HBV vaccination and immunity status of exposed person. Collect baseline serologies of exposed person for hepatitis B and C. Also, a baseline ALT will be obtained from the person exposed to blood/body fluid from a HCV positive source or source of unknown HCV status. (Refer to section 19.0 EHS Hepatitis Guidelines.) Obtain a baseline CBC with platelets and differential, Chem 7, and patient monitoring panel on exposed person if anti-retroviral post-exposure prophylaxis (PEP) is initiated Hepatitis/Management/Prophylaxis: a) Hepatitis B: Initiate hepatitis B prophylaxis, when indicated, as per Infection Control Guidelines, Hepatitis Guidelines Pre-exposure and Post-exposure Management and Prophylaxis in the Health Care Setting. This guideline is available in Employee Health Services, Emergency Department and the Jack Martin Fund Clinic. For any question, contact Infection Control (ext ) or the Infectious Diseases Attending or Fellow on call through the page operator. b) Hepatitis C: Refer to Hepatitis Guidelines - Pre exposure and Post exposure Management and Prophylaxis in the Health Care Setting as above Antiretroviral Prophylaxis: a) Recommendations for anti-retroviral post-exposure prophylaxis (PEP) are to be made in consultation with the Infectious Diseases Physician (Attending/ Fellow) on call. ID Attending/Fellow should be called for all exposures when anti-retroviral PEP is being considered. The ID physician on call can be paged through the Page Operator. The following are to be considered in the evaluation regarding recommendations.
5 Page 5 of Type/Extent of Exposure (Exposure Risk) a) Percutaneous Blood exposure Highest risk for HIV transmission (if HIV infected source) associated with deep injury, larger diameter hollow bore needle previously in source patient s vein or artery, especially involving injection of source patient s blood, and blood containing a high titer of HIV (e.g., source with acute retroviral illness or end-stage AIDS). Viral load measurement may be considered, but its use in relation to PEP has not been evaluated. Increased risk - exposure to large volume of blood. No increased risk - neither exposure to a larger volume of blood nor blood with a high titer of HIV (e.g., solid suture needle injury from source patient with asymptomatic HIV infection). b) Mucous Membrane c) Skin Determine volume and time exposed. Increased risk - Risk is increased for blood exposures involving a high titer of HIV, prolonged contact, an extensive area, or an area in which skin integrity is visibly compromised HIV status of source. a) In known HIV positive patients recommendations regarding anti-retroviral prophylaxis are made according to the exposure risk (as above).
6 Page 6 of 11 b) If the source patient or the patient s HIV status is unknown, recommendations regarding anti-retroviral PEP are to be made on a case by case basis, based on the exposure risk and likelihood of HIV infection in known or possible source patient (see Appendix I). If additional information becomes available, recommendations regarding anti-retroviral PEP may be modified (see EHS - Infection Control Policy Postexposure Management following Exposure to Blood Body Fluids of HIV -positive or potential HIV positive source) In all cases of a determined exposure to blood or other potentially infectious body fluid antiretroviral PEP will be offered, unless source patient is known to be HIV-negative Antiretroviral PEP consists of combination therapy, generally 2-3 antiretroviral agents. [The standard empiric post-occupational exposure prophylaxis regimen is currently tenofovir plus emtricitabine (together as Truvada) and atazanavir (Reyataz) and ritonavir (Norvir) The source patients current and previous antiretroviral therapy should be considered when making post-exposure prophylaxis regimen recommendations. Infectious Diseases should be consulted for all such cases For women of child bearing age, a stat pregnancy test will be done prior to initiating PEP. For pregnant patients, obstetrics physician on call or patient s obstetrician should be consulted The final decision to take antiretroviral PEP rests with the exposed person HIV pre-test counseling and a baseline specimen for HIV antibodies in the exposed person should be obtained at the time of exposure (or within hours after exposure) after New York State Consent form is signed. This may be done at initial or follow-up contact at EHS, Jack Martin Fund Clinic or personal physician.
7 Page 7 of The Blood and Body Fluid Exposure Form will be completed by the initial evaluating physician or practitioner in EHS or the Emergency Department and copies sent to EHS (for employee), Jack Martin Fund Clinic (medical students and others). Documentation of post-exposure management, counseling, and discussion regarding risks/benefits of Post- Exposure Prophylaxis (PEP) will be included on the form and signed by the evaluating physician/practitioner The Healthcare Provider s Written Opinion will be signed by the evaluating physician/practitioner and the exposed person FOR FOLLOW-UP OF POST-EXPOSURE MANAGEMENT: Hospital employees and volunteers will be referred to Employee Health Service Medical students will be referred to Jack Martin Fund Clinic Other students and contract, agency, or traveling staff will be referred to Jack Martin Fund Clinic, FPA Infectious Diseases Clinic, private Infectious Disease group, or personal physician (depending upon exposed person s preference) Refer to the following Guidelines for follow-up Procedures and Management: a) Employee Health Service - Infection Control - Hepatitis Pre-exposure and Post-exposure Management and Prophylaxis in the Healthcare setting. b) Infection Control Policy for Post Exposure Management Following Exposure to Blood -Body Fluids of HIV positive or potential HIV potential source.
8 Page 8 of 11 APPENDIX I Risk Factors a) Risk Factors for HIV: Known Risk: High Risk: Potential Risk: Low Risk: AIDS/HIV infected patient. Men who have or have had sex with men, users or past users of illicit parenteral drugs, hemophiliacs or persons with coagulation disorders who have received blood products, recipients of blood transfusions ( ), prisoners, commercial sex workers, persons with a medical condition suggestive of AIDS or HIV infection; sexual partners or children of person with AIDS or HIV infection or in any of above high risk groups; persons from sub-saharan Africa. Person who has had a sexual partner whose history is unknown, recipients of blood after All other persons. b) Risk Factors for Hepatitis B: Known Risk: High Risk: Low Risk: Hepatitis B (HBV) carrier (i.e., HBsAg positive). Persons with multiple sex partners or history of sexually transmitted disease, residents of institutions for the mentally retarded or developmentally disabled, hemophiliacs or persons with coagulation disorders or others who have received blood products, history of hemodialysis, men who have or have had sex with men, immigrants or refugees from areas of high HBV frequency (e.g. Asia, Africa), Alaskan natives or Pacific Islanders, sexually active individuals, household contacts or children of HBV carriers. All other persons.
9 Page 9 of 11 c) Risk factors for Hepatitis C: Known Risk: Hepatitis C (HCV) carrier High Risk: Hemophiliacs or persons with coagulation disorders or others who have received blood products (particularly prior to 1990), injection drug users Intermediate Risk: Hemodialysis patients, recipients of blood or solid organs prior to 1992, persons with undiagnosed liver disease, infants born to infected mothers
10 MT. SINAI HOSPITAL Page 10 of 11 APPENDIX II Post-exposure Counseling Following known/unknown HIV positive Exposures A. Provide information regarding: 1. The risk of occupationally-acquired HIV infection due to exposure to known HIVpositive blood is estimated at approximately 0.3% following a percutaneous exposure and 0.09% following a mucous membrane exposure. Factors associated with a higher risk of HIV transmission include: a deep injury, a device visibly contaminated with the source patient s blood, procedures involving a needle placed directly in a vein or artery, or advanced HIV disease (i.e., high viral load) in the source patient. 2. The theoretical rationale for post-exposure prophylaxis (PEP). 3. Current knowledge of the toxicity of anti-retroviral therapy and the limitations of this knowledge in predicting toxicity in uninfected individuals who take the drug after occupational exposures. 4. A case-control study of HIV seroconversion in health care workers after percutaneous exposure to HIV-positive blood showed that health care workers that seroconverted to HIV positive were significantly less likely to have received AZT post-exposure prophylaxis than those who did not seroconvert (79% reduction in HIV seroconversion with the use of AZT post-exposure prophylaxis). 5. Precautions to prevent transmission of HIV infection including refraining from blood, semen, or organ donation; refraining from breast feeding and either abstaining from sexual intercourse or using latex condoms during sexual intercourse during the followup period (at least six months). 6. Pregnancy/Nursing: It is not known whether PEP can cause harm to the human fetus. If a pregnant woman is considering the use of PEP, in addition to the Infectious Diseases Attending/Fellow, also call Obstetrics for further consultation. Mothers will be asked to discontinue breast feeding while receiving anti-retroviral prophylaxis. 7. The need for post-exposure follow-up (including HIV serologic testing) (see EHS Guidelines, Infection Control Policy for Post Exposure Management following Exposure to Blood-Body Fluids of HIV positive/or potential HIV-potential source).
11 MT. SINAI HOSPITAL Page 11 of 11 References: Centers for Disease Control and Prevention. Updated US Public Health Service guidelines for the management of occupational exposures to HIV and recommendations for postexposure prophylaxis. MMWR 2005;54(RR9):1-17 Centers for Disease Control and Prevention. Updated US Public Health Service guidelines for the management of occupational exposures to HBV, HCV, and HIV and recommendations for postexposure prophylaxis. MMWR 2001;50(RR11):1-53 AIDS/TB Committee of the Society for Healthcare Epidemiology of America. Management of Healthcare Workers Infected with Hepatitis B Virus, Hepatitis C Virus, Human Immunodeficiency Virus, or Other Bloodborne Pathogens. Infect Control Hosp Epidemiol 1997;18: Centers for Disease Control and Prevention. Guidelines for Environmental Infection Control in Health-Care Facilities: recommendations of CDC and the Healthcare Infection Control Practices Advisory Committee (HICPAC). MMWR 2003; 52 (RR10): New York State Department of Health- Managing Regulated Medical Waste- Revised January, New York State Dept. Of Health (1995). Managing Regulated Medical Waste, Public Health Law 1389 AA-GG, 1-9 U.S. Department of Labor, Occupational Safety and Health Administration. (1991, revised 2001) Occupational Safety and Health Standards. Subpart Z. Toxic and hazardous substances. Standard Bloodborne pathogens.
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS
 STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Bloodborne Pathogens. Exposure Control Plan
 Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
BAY-ARENAC BEHAVIORAL HEALTH AUTHORITY POLICIES AND PROCEDURES MANUAL
 Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Management
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Contamination Incidents Frequently Asked Questions
 Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May Contains information for:
 APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Prophylaxis
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Establish protocol for management of occupational exposures to blood or potentially infectious materials. All employees of
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Establish protocol for management of occupational exposures to blood or potentially infectious materials. All employees of
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogen Exposure STUDENT. Blood Borne Pathogen Exposure. Student. Rev:
 Blood Borne Pathogen Exposure Student INSTRUCTIONS 1. Student: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Blood Borne Pathogen Exposure Student INSTRUCTIONS 1. Student: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
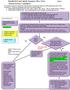 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
Hepatitis STARS Program. Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003
 Hepatitis 2003 STARS Program Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003 Outline n Hepatitis A Epidemiology and screening Transmission n Hepatitis B Epidemiology
Hepatitis 2003 STARS Program Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003 Outline n Hepatitis A Epidemiology and screening Transmission n Hepatitis B Epidemiology
Colgate University. Bloodborne Pathogens Exposure Control Plan
 Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
OB Provider Guide to Alaska s Perinatal Hepatitis B Prevention Program
 OB Provider Guide to Alaska s Perinatal Hepatitis B Prevention Program Dear Colleague, This letter is to introduce myself and explain the role I play with the Alaska Perinatal Hepatitis B Program. Alaska
OB Provider Guide to Alaska s Perinatal Hepatitis B Prevention Program Dear Colleague, This letter is to introduce myself and explain the role I play with the Alaska Perinatal Hepatitis B Program. Alaska
Blood-borne Pathogens Exposure Policy
 Blood-borne Pathogens Exposure Policy Contents Blood Borne Pathogen(s) Exposure (BBPE) -Post-Exposure Prophylaxis... 1 STUDENT CHECKLIST... 3 PROGRAM CHECKLIST... 4 PROVIDER CHECKLIST... 5 POST-EXPOSURE
Blood-borne Pathogens Exposure Policy Contents Blood Borne Pathogen(s) Exposure (BBPE) -Post-Exposure Prophylaxis... 1 STUDENT CHECKLIST... 3 PROGRAM CHECKLIST... 4 PROVIDER CHECKLIST... 5 POST-EXPOSURE
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
HEPATITIS B INFECTION and Pregnancy. Caesar Mensah Communicable Diseases & Infection Control Specialist, UK June 2011
 HEPATITIS B INFECTION and Pregnancy Caesar Mensah Communicable Diseases & Infection Control Specialist, UK June 2011 HEPATITIS B 26/07/2011 What is Hepatitis B? It is inflammation (infection) of the liver
HEPATITIS B INFECTION and Pregnancy Caesar Mensah Communicable Diseases & Infection Control Specialist, UK June 2011 HEPATITIS B 26/07/2011 What is Hepatitis B? It is inflammation (infection) of the liver
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Bloodborne Pathogens. Montclair Kimberley Academy 1
 Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1
 PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
NEOMED ACADEMIC POLICY
 (A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
(A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital
 HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
OVERVIEW OF PRESENTATION
 OVERVIEW OF PRESENTATION This training is required by the Texas Department of Health Ch. 96, Bloodborne Pathogen Control. Every employee of the district will be required to have some training on bloodborne
OVERVIEW OF PRESENTATION This training is required by the Texas Department of Health Ch. 96, Bloodborne Pathogen Control. Every employee of the district will be required to have some training on bloodborne
CONTINUING CARE ADMINISTRATIVE MANUAL POLICY
 CONTINUING CARE ADMINISTRATIVE MANUAL POLICY NUMBER III-10 DATE Draft June 8, 2010 PAGE 1 OF 3 APPROVED BY: SITE: CATEGORY TITLE: Vice President & Senior Operating Officer, Rehab & Continuing Care Edmonton
CONTINUING CARE ADMINISTRATIVE MANUAL POLICY NUMBER III-10 DATE Draft June 8, 2010 PAGE 1 OF 3 APPROVED BY: SITE: CATEGORY TITLE: Vice President & Senior Operating Officer, Rehab & Continuing Care Edmonton
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK)
 POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
Post Blood & Body Fluid Exposure Checklist
 Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
WVU Occupational Medicine Program for evaluation and treatment of persons exposed to Lentivirus Vectors
 Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Blood Borne Pathogen Exposure Employee
 Blood Borne Pathogen Exposure Employee INSTRUCTIONS 1. Employee: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Blood Borne Pathogen Exposure Employee INSTRUCTIONS 1. Employee: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV
 Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
B. Tasks and Procedures where employees, students or contractors can be exposed to bloodborne pathogens:
 Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
SUBJECT: Hepatitis C Virus (HCV) Counseling/Education, Testing, Referral, and Partner Notification
 SUBJECT: Hepatitis C Virus (HCV) Counseling/Education, Testing, Referral, and Partner Notification Hepatitis C virus (HCV) infection is the most common chronic bloodborne infection in the United States.
SUBJECT: Hepatitis C Virus (HCV) Counseling/Education, Testing, Referral, and Partner Notification Hepatitis C virus (HCV) infection is the most common chronic bloodborne infection in the United States.
TRANSMISSION OF BLOODBORNE PATHOGENS: HIV,HBV,HCV. Dr Daniel Kimani HIV Prevention Medical Transmission CDC, Kenya.
 TRANSMISSION OF BLOODBORNE PATHOGENS: HIV,HBV,HCV Dr Daniel Kimani HIV Prevention Medical Transmission CDC, Kenya. Nevada Hepatitis C Outbreak Tied to Las Vegas Clinic. Thousands Now At Risk for Hepatitis,
TRANSMISSION OF BLOODBORNE PATHOGENS: HIV,HBV,HCV Dr Daniel Kimani HIV Prevention Medical Transmission CDC, Kenya. Nevada Hepatitis C Outbreak Tied to Las Vegas Clinic. Thousands Now At Risk for Hepatitis,
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
Post-Sexual Exposure Prophylaxis (npep)
 Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Exposure. Blood. Department of Health & Human Services
 Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
CHAPTER Committee Substitute for Committee Substitute for House Bill No. 321
 CHAPTER 2015-110 Committee Substitute for Committee Substitute for House Bill No. 321 An act relating to HIV testing; amending s. 381.004, F.S.; revising and providing definitions; specifying the notification
CHAPTER 2015-110 Committee Substitute for Committee Substitute for House Bill No. 321 An act relating to HIV testing; amending s. 381.004, F.S.; revising and providing definitions; specifying the notification
EMPLOYEE HEALTH TABLE OF CONTENTS
 EMPLOYEE HEALTH TABLE OF CONTENTS PHYSICAL ASSESSMENT.2 REPORTING EMPLOYEE INFECTIONS...3 SUMMARY OF IMPORTANT RECOMMENDATIONS AND WORK RESTRICTIONS FOR PERSONNEL WITH INFECTIOUS DISEASES.4 HEPATITIS B
EMPLOYEE HEALTH TABLE OF CONTENTS PHYSICAL ASSESSMENT.2 REPORTING EMPLOYEE INFECTIONS...3 SUMMARY OF IMPORTANT RECOMMENDATIONS AND WORK RESTRICTIONS FOR PERSONNEL WITH INFECTIOUS DISEASES.4 HEPATITIS B
Management of Exposure to Needlestick Injuries & Body Fluids
 Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Bloodborne Pathogens Training (OHS_BIO500) Course Material
 Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis).
 LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
Emergency Department Blood/Body Fluid Exposure Instructions
 Emergency Department Blood/Body Fluid Exposure Instructions For employees sent to the Emergency Department after hours to be evaluated for needle stick / body fluid exposure 1. Floor or unit Charge RN
Emergency Department Blood/Body Fluid Exposure Instructions For employees sent to the Emergency Department after hours to be evaluated for needle stick / body fluid exposure 1. Floor or unit Charge RN
Occupational Exposures to Bloodborne Pathogen (BBP) Training
 Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Revised April WGH ER #5 Hospital Rd. Whitehorse Phone: (867) Outside of Whitehorse: Local Community Health Centre/Clinic/ER
 Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Policy S- 15 FLORIDA STATE UNIVERSITY COLLEGE OF NURSING BLOODBORNE PATHOGEN EXPOSURE CONTROL PLAN FOR NURSING STUDENTS
 TITLE: Policy S- 15 FLORIDA STATE UNIVERSITY COLLEGE OF NURSING BLOODBORNE PATHOGEN EXPOSURE CONTROL PLAN FOR NURSING STUDENTS Page 1 of 2 POLICY: The College of Nursing shall maintain a bloodborne pathogen
TITLE: Policy S- 15 FLORIDA STATE UNIVERSITY COLLEGE OF NURSING BLOODBORNE PATHOGEN EXPOSURE CONTROL PLAN FOR NURSING STUDENTS Page 1 of 2 POLICY: The College of Nursing shall maintain a bloodborne pathogen
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: F:
 University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
2017 BLOODBORNE PATHOGENS
 2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
Blood Borne Pathogens (BBP)
 Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Hepatitis C Best Practice Guidelines For Local Health Departments
 Hepatitis C Best Practice Guidelines For Local Health Departments LHDs are responsible for investigating and reporting all physician reported cases of acute hepatitis C (HCV). For clients known to have
Hepatitis C Best Practice Guidelines For Local Health Departments LHDs are responsible for investigating and reporting all physician reported cases of acute hepatitis C (HCV). For clients known to have
Greenwood School District 50 OSHA UPDATE BLOODBORNE PATHOGENS
 Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Blood borne Pathogen
 Blood borne Pathogen Training For Certified Nursing Assistants Meets the Blood borne Pathogens & Infection Control Update (Formerly HIV/AIDS) 1 0 In-service Hour Meets the Blood borne Pathogens & Infection
Blood borne Pathogen Training For Certified Nursing Assistants Meets the Blood borne Pathogens & Infection Control Update (Formerly HIV/AIDS) 1 0 In-service Hour Meets the Blood borne Pathogens & Infection
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses
 Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Chapter 5 Serology Testing
 Chapter 5 Serology Testing 49 50 This page intentionally left blank. Diagnostic Tests for Hepatitis B Virus (HBV) Diagnosis of HBV infection (acute vs. chronic) is based on clinical, laboratory, and epidemiologic
Chapter 5 Serology Testing 49 50 This page intentionally left blank. Diagnostic Tests for Hepatitis B Virus (HBV) Diagnosis of HBV infection (acute vs. chronic) is based on clinical, laboratory, and epidemiologic
What is hepatitis? What is hepatitis A? How is it spread? What are the symptoms? How soon do symptoms appear? How is hepatitis A diagnosed?
 Hepatitis A Massachusetts Department of Public Health, 305 South Street, Jamaica Plain, MA 02130 What is hepatitis? Hepatitis is any kind of inflammation (a reaction which can include swelling and pain)
Hepatitis A Massachusetts Department of Public Health, 305 South Street, Jamaica Plain, MA 02130 What is hepatitis? Hepatitis is any kind of inflammation (a reaction which can include swelling and pain)
How does HBV affect the liver?
 Hepatitis B Why is the liver important? Your liver is a vital organ that performs many essential functions. It s the largest solid organ in the body and is located under your rib cage on the upper right
Hepatitis B Why is the liver important? Your liver is a vital organ that performs many essential functions. It s the largest solid organ in the body and is located under your rib cage on the upper right
Bloodborne Pathogens Training
 Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Bloodborne Pathogens: Recognition and Treatment 2011
 Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
Blood and Body Fluid Exposure
 Blood and Body Fluid Exposure Infection Prevention and Control Contents Policy... 1 Purpose... 1 Scope/Audience... 1 Definitions... 2 Associated documents... 2 1.1 Indications for BBFE reporting... 2 1.2
Blood and Body Fluid Exposure Infection Prevention and Control Contents Policy... 1 Purpose... 1 Scope/Audience... 1 Definitions... 2 Associated documents... 2 1.1 Indications for BBFE reporting... 2 1.2
The Bloodborne Pathogen Standard. An Overview
 The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
Blood borne Pathogen Exposure Policy for Students
 Blood borne Pathogen Exposure Policy for Students A University of Rhode Island (URI) student or intern who sustains an exposure from a needle stick, instrument stick, or mucous membranes to non-intact
Blood borne Pathogen Exposure Policy for Students A University of Rhode Island (URI) student or intern who sustains an exposure from a needle stick, instrument stick, or mucous membranes to non-intact
FAMILY HIV CENTER NJ CARES SANE
 HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
Village By Village HIV/AIDS Policy
 The Old Sweet Shop Teme Street, Tenbury Wells, Worcs. WR15 8BB Phone: 07887 870090 Web: villagebyvillage.org.uk Email: neil@villagebyvillage.org.uk Registered Charity Number 1116952 18/9/07 Village By
The Old Sweet Shop Teme Street, Tenbury Wells, Worcs. WR15 8BB Phone: 07887 870090 Web: villagebyvillage.org.uk Email: neil@villagebyvillage.org.uk Registered Charity Number 1116952 18/9/07 Village By
Infection/Disease Control HEPATITIS CONTROL PROGRAM
 OPERATING PROCEDURE NO. 153-29 Florida State Hospital Chattahoochee, Florida July 8, 2009 Infection/Disease Control HEPATITIS CONTROL PROGRAM 1. Purpose: To establish consistent surveillance, reporting,
OPERATING PROCEDURE NO. 153-29 Florida State Hospital Chattahoochee, Florida July 8, 2009 Infection/Disease Control HEPATITIS CONTROL PROGRAM 1. Purpose: To establish consistent surveillance, reporting,
Chapter 2 Hepatitis B Overview
 Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
HEPATITIS C, ACUTE CRUDE DATA. Number of Cases 5 Annual Incidence a LA County 0.05 California b 0.10 United States b 0.68 Age at Diagnosis Mean 38
 2016 Annual Morbidity Report HEPATITIS C, ACUTE a Rates calculated based on less than 19 cases or events are considered unreliable b Calculated from: CDC. Notice to Readers: Final 2016 Reports of Nationally
2016 Annual Morbidity Report HEPATITIS C, ACUTE a Rates calculated based on less than 19 cases or events are considered unreliable b Calculated from: CDC. Notice to Readers: Final 2016 Reports of Nationally
Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
 PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
Self-Instructional Packet (SIP)
 Self-Instructional Packet (SIP) Advanced Infection Prevention and Control Training Module 1 Intro to Infection Prevention Control February 11, 2013 Page 1 Learning Objectives Module One Introduction to
Self-Instructional Packet (SIP) Advanced Infection Prevention and Control Training Module 1 Intro to Infection Prevention Control February 11, 2013 Page 1 Learning Objectives Module One Introduction to
MONTANA STATE UNIVERSITY-BOZEMAN COLLEGE OF NURSING POLICY # D-3
 MONTANA STATE UNIVERSITY-BOZEMAN COLLEGE OF NURSING POLICY # D-3 TITLE: POLICY: COMMUNICABLE DISEASE PREVENTION POLICIES Nursing students are required to adhere to College of Nursing policies on health
MONTANA STATE UNIVERSITY-BOZEMAN COLLEGE OF NURSING POLICY # D-3 TITLE: POLICY: COMMUNICABLE DISEASE PREVENTION POLICIES Nursing students are required to adhere to College of Nursing policies on health
Bloodborne Pathogens Training Lakeville Area Public Schools
 Bloodborne Pathogens Training Lakeville Area Public Schools Questions? Contact the District s Health & Safety Consultant Dan Fitch at IEA, Inc. 763-315-7900 dan.fitch@ieasafety.com OR District s Exposure
Bloodborne Pathogens Training Lakeville Area Public Schools Questions? Contact the District s Health & Safety Consultant Dan Fitch at IEA, Inc. 763-315-7900 dan.fitch@ieasafety.com OR District s Exposure
Introduction to Blood Borne Pathogens
 Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Public Employees Occupational Safety and Health Alert (Publication No. 21)
 Clifton R. Lacy, M.D. Commissioner Public Employees Occupational Safety and Health Alert (Publication No. 21) James E. McGreevey Governor Albert G. Kroll Commissioner OSHA Revises the Bloodborne Pathogens
Clifton R. Lacy, M.D. Commissioner Public Employees Occupational Safety and Health Alert (Publication No. 21) James E. McGreevey Governor Albert G. Kroll Commissioner OSHA Revises the Bloodborne Pathogens
C 肝職業暴露後之處置 衛福部疾病管制署 中區傳染病防治醫療網 王任賢指揮官
 C 肝職業暴露後之處置 衛福部疾病管制署 中區傳染病防治醫療網 王任賢指揮官 HCV:Structure and Classification Unclassified virus, Member of the flavivirus family (other members yellow fever and dengue) Enveloped single stranded RNA virus Humans
C 肝職業暴露後之處置 衛福部疾病管制署 中區傳染病防治醫療網 王任賢指揮官 HCV:Structure and Classification Unclassified virus, Member of the flavivirus family (other members yellow fever and dengue) Enveloped single stranded RNA virus Humans
(cf / / Exposure Control Plan for Bloodborne Pathogens)
 All Personnel BP 4119.43 UNIVERSAL PRECAUTIONS 4319.43 In order to protect employees from contact with potentially infectious blood or other body fluids, the Governing Board requires that universal precautions
All Personnel BP 4119.43 UNIVERSAL PRECAUTIONS 4319.43 In order to protect employees from contact with potentially infectious blood or other body fluids, the Governing Board requires that universal precautions
Bloodborne Pathogens. Kathleen Stefek, RN, MSN
 Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Drew University Bloodborne Pathogens Exposure Control Plan and Procedures
 PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
Post Exposure Prophylaxis (PEP)
 Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
QUALITY LIFE CONCEPTS Policy on Bloodborne Pathogens
 QUALITY LIFE CONCEPTS Policy on Bloodborne Pathogens A24 TUBERCULOSIS TESTING Quality Life Concepts is committed to protecting its employees and individuals who will be served by vigilance and regular
QUALITY LIFE CONCEPTS Policy on Bloodborne Pathogens A24 TUBERCULOSIS TESTING Quality Life Concepts is committed to protecting its employees and individuals who will be served by vigilance and regular
Bloodborne Pathogens and Universal Precautions
 Bloodborne Pathogens and Universal Precautions Parkway School District 2012-2013 Revised 9/19/2012 What Are Bloodborne Pathogens(BBPs) Bloodborne pathogens (BBPs) are disease causing microorganisms carried
Bloodborne Pathogens and Universal Precautions Parkway School District 2012-2013 Revised 9/19/2012 What Are Bloodborne Pathogens(BBPs) Bloodborne pathogens (BBPs) are disease causing microorganisms carried
Management of sharps injuries in the healthcare setting
 Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Hepatitis B Control. Table of Contents
 Control Table of Contents 1.0 INTRODUCTION... 1 2.0 GOALS... 1 3.0 DEFINITIONS... 1 4.0 CASE MANAGEMENT... 3 5.0 HEPATITIS B POST- EXPOSURE MANAGEMENT... 4 TABLE 1: HEPATITIS B POST EXPOSURE PROPHYLAXIS...
Control Table of Contents 1.0 INTRODUCTION... 1 2.0 GOALS... 1 3.0 DEFINITIONS... 1 4.0 CASE MANAGEMENT... 3 5.0 HEPATITIS B POST- EXPOSURE MANAGEMENT... 4 TABLE 1: HEPATITIS B POST EXPOSURE PROPHYLAXIS...
Needles and Sharps Exposure: How do We Proceed?
 Needles and Sharps Exposure: How do We Proceed? UMAYYA MUSHARRAFIEH,MD AMERICAN UNIVERSITY OF BEIRUT MEDICAL CENTER JUNE 14, 2013 Health care workers who use or may be exposed to needles are at increased
Needles and Sharps Exposure: How do We Proceed? UMAYYA MUSHARRAFIEH,MD AMERICAN UNIVERSITY OF BEIRUT MEDICAL CENTER JUNE 14, 2013 Health care workers who use or may be exposed to needles are at increased
