Endpoints of hepatitis B treatment
|
|
|
- May Adams
- 5 years ago
- Views:
Transcription
1 Journal of Viral Hepatitis, 2010, 17, doi: /j x REVIEW Endpoints of hepatitis B treatment W. Chotiyaputta and A. S. F. Lok Division of Gastroenterology, Department of Internal Medicine, University of Michigan Health System, Ann Arbor, MI, USA Received April 2010; accepted for publication April 2010 SUMMARY. The goal of hepatitis B treatment is to prevent the development of cirrhosis, liver failure, and hepatocellular carcinoma. Ideally, clinical studies should demonstrate that hepatitis B therapies can prevent liver-related complications; however, these clinical endpoints evolve over years or decades. Therefore, clinical trials have relied on intermediate endpoints to evaluate the efficacy of treatment and to determine when treatment can be stopped. Intermediate endpoints that have been used include biochemical, histological, virological, and serological endpoints. This review will discuss the validity of these intermediate endpoints as surrogates of clinical endpoints, and the rates at which these intermediate endpoints can be achieved with currently available therapies. Keywords: alanine aminotransferase, HBeAg seroconversion, HBsAg loss, HBV DNA, liver histology. INTRODUCTION The ultimate goal of chronic infectious disease treatment is the eradication of the infectious agent; however, eradication of hepatitis B virus (HBV) is not a realistic goal of hepatitis B treatment. Currently available nucleos(t)ide analogues (NUCs) act mainly as inhibitors of the reverse transcription of the pregenomic RNA to HBV DNA and have no direct effect on the covalently closed circular DNA (cccdna) the template for the transcription of the pregenomic RNA as well as for the translation of viral proteins. This accounts for the high rate of viral relapse when treatment is stopped. Indeed, even in persons who have serological recovery from an acute HBV infection, HBV DNA remains detectable in the liver and reactivation of HBV replication can occur when those persons receive immunosuppressive therapy [1]. Recent studies suggest that clearance of cccdna relies on the turnover of infected hepatocytes [2,3]. This may explain the higher rate of sustained off-treatment response to interferon (IFN) therapy even though IFN has weaker antiviral activity compared to NUCs. Abbreviations: ALT, alanine aminotransferase; Anti-HBe, hepatitis B e antibody; cccdna, covalently closed circular DNA; CTP, Child- Turcotte-Pugh; HAI, histology activity index; HBeAg, hepatitis B e antigen; HBV, hepatitis B virus; HCC, hepatocellular carcinoma; HR, hazard ratio; IFN, interferon; NUCs, nucleos(t)ide analogues; Peg-IFN, pegylated interferon; RCTs, randomized controlled trials; ULN, upper limit of normal. Correspondence: Anna S. F. Lok, MD, Division of Gastroenterology, University of Michigan Health System, 3912 Taubman Center, SPC 5362, Ann Arbor 48109, MI, USA. aslok@med.umich.edu CLINICAL ENDPOINTS VS INTERMEDIATE (SURROGATE) ENDPOINTS The goal of hepatitis B treatment is to prevent the development of cirrhosis, liver failure, and hepatocellular carcinoma (HCC). These clinical endpoints take decades to evolve. Clinical trials designed to demonstrate a benefit on clinical outcomes would need to enrol hundreds or thousands of patients at risk for these events followed for many years or decades; therefore, clinical trials of hepatitis B treatment have relied on intermediate endpoints that reflect viral replication and liver disease activity as surrogates for clinical benefit. The intermediate endpoints used include virological endpoint (suppression of serum HBV DNA to undetectable by a sensitive PCR assay), serological endpoint [loss of hepatitis B e antigen (HBeAg) with or without seroconversion to hepatitis B e antibody (anti-hbe)], biochemical endpoint [normalization of alanine aminotransferase (ALT)], as well as histological endpoint (decrease in necrosis and inflammation score by 2 points with no worsening of fibrosis). The criteria for surrogate endpoints are summarized in Table 1. An expert review panel questioned the validity of these intermediate endpoints as surrogates for clinical outcomes [4]. The panel cited the lack of data from randomized controlled trials (RCTs) demonstrating that achievement of the intermediate endpoints translates into decreased clinical outcomes. While data from RCTs are more vigorous, evidence supporting the validity of intermediate endpoints as surrogates for clinical outcomes can be deduced from natural history studies linking cirrhosis, liver failure, HCC, or liver-related mortality with elevated ALT, high HBV DNA, or persistent presence of HBeAg. In addition, long-term followup studies of patients who received antiviral treatment can
2 676 W. Chotiyaputta & A. S. F. Lok Table 1 Definition of clinical endpoints and surrogate endpoints Term Clinical endpoint Surrogate endpoint Criteria for surrogate endpoint Definition A characteristic or variable that reflects how a patient feels, functions, or survives A biomarker that is intended to substitute for a clinical endpoint that should predict clinical benefit or harm or lack of both Should be easier to assess and occur more often than the corresponding clinical endpoint Should be in the causal pathway to the outcome The effect of an intervention on the surrogate endpoint must explain the effect on subsequent clinical outcomes References: [60], [61]. be used to show that patients who have intermediate responses have improved clinical outcomes. Therefore, regulatory authorities have relied on intermediate endpoints to evaluate the benefits of new HBV treatment, and professional guidelines have recommended the use of intermediate endpoints to determine treatment response and when treatment can be stopped [5 7]. This review will discuss evidence supporting the validity of the intermediate endpoints as surrogates for clinical endpoints in HBV treatment and the rate at which these endpoints can be achieved with currently available treatments. BIOCHEMICAL ENDPOINT Serum ALT is a cheap and readily available marker of liver inflammation. Phase III clinical trials of HBV treatment have included ALT normalization as an indicator of efficacy. ALT normalization has been observed in 34 51% of patients at the end of a week course of pegylated interferon (peg- IFN) with or without lamivudine and in 41 78% of patients after 1 year of NUC therapy [8 17] (Table 2). Studies of long-term NUC therapy found that ALT normalization increased to 66 80% after 5 years of treatment [18 21]. These data indicate that antiviral treatment can result in ALT normalization in most patients, but follow-up studies showed that ALT remained normal in only 32 60% of patients within 6 months of discontinuing a 1-year course of peg-ifn [8,9,21] and in 32 49% of patients 6 12 months after completing a 1-year course of NUC therapy [22,23]. Furthermore, ALT flares have been reported in 1 29% of patients 4 6 months after completing a 1-year course of NUC therapy, and in some instances, these flares have resulted in liver failure [11,14,15,24]. Thus, ALT normalization, particularly if short-lived, is not a reliable surrogate of clinical outcome. Recent data from studies of patients not receiving antiviral therapy found that persons with normal ALT can have abnormal liver histology, liver complications and liver-related deaths. These studies showed that up to 37% of persons with chronic HBV infection and normal ALT had significant inflammation and/or fibrosis on liver biopsy [25,26]. One study followed persons, aged years for a mean of 8 years after a health examination. Compared to those with baseline ALT <20 IU/L, persons with ALT at enrolment of IU/L and IU/L had a 2.5-fold and eightfold risk of deaths from liver disease, respectively, for men and a 3.3-fold and 18.2-fold risk of deaths from liver disease, respectively, for women [27]. Another study of 3233 patients with chronic hepatitis B found that patients with ALT 1 2 times the upper limit of normal ( ULN) and those with ALT ULN had higher cumulative risks of liver complications compared to patients with ALT < 0.5 ULN [28]. Thus, data from patients not on treatment indicate that lower ALT is associated with improved clinical outcome, but decreasing ALT to the normal range defined by most clinical diagnostic laboratories may not be sufficient to prevent liver complications and liver-related deaths. These findings have led to a re-examination of the true ULN for ALT. A study of Italian blood donors suggested that the ULN for ALT should be 30 IU/L for men and 19 IU/L for women [29], while a recent study of 1105 potential liver donors in Korea all of whom had a biopsy-proven normal liver found that the ULN for ALT should be 35 IU/L for men and 26 IU/L for women [30]. Given the uncertainty regarding the upper limit for ALT in persons with normal livers, the legitimacy of ALT normalization as an intermediate endpoint is questionable. HISTOLOGICAL ENDPOINT Improvement in liver histology was used as the primary endpoint in many phase III clinical trials of HBV treatment because traditionally liver histology is considered to be the most accurate assessment of liver disease. In most studies, histological improvement was defined as a 2-point decrease in the histology activity index (HAI) with no worsening of fibrosis between the pretreatment and end-of-treatment biopsies. Using this definition, histological improvement has been reported to occur in 38 48% of patients after a 1-year course of peg-ifn treatment [8,9] and in 49 74% of patients
3 Endpoints of HBV treatment 677 Table 2 Rates of intermediate endpoints during or after antiviral treatment in (a) HBeAg-positive patients (b) HBeAg-negative patients Peg-IFN Peg-IFN + LAM LAM ADV ETV LdT TDF (a) HBeAg-positive patients Responses at year 1 ALT normalization (32 41)* (35 39)* (28)* Histologic improvement 22 (38)* 33 (41)* (34)* Undetectable HBV DNA (7 14)* (9 14)* (5)* HBeAg seroconversion (29 32)* (27 29)* ( )* (15.3)* HBsAg loss 5 (3 5)* 7 (3 7)* 1 (0)* Responses at year 3 5 ALT normalization N/A Undetectable HBV DNA N/A HBeAg seroconversion HBsAg loss 8 15 N/A (b) HBeAg-negative patients Responses at year 1 ALT normalization 38 (59)* 49 (60)* (39 44)* 72 (32)* 78 (49)* Histologic improvement N/A (48)* N/A (38)* (40)* Undetectable HBV DNA 63 (19)* 87 (20)* (5 7)* 51 (8)* 90 (3)* HBsAg loss N/A (4)* N/A (3)* 1 (0)* 0 (0)* <1 <1 0 Responses at year 3 5 ALT normalization N/A 69 N/A 91 N/A Undetectable HBV DNA N/A 67 N/A HBsAg loss 8 8 N/A 5 N/A N/A N/A Data expressed as percent. References: [8 18], [20 23], [34,35], [38,39], [51], [62], [63], [64]. Peg-IFN, pegylated interferon; LAM, lamivudine; ADV, adefovir; ETV, entecavir; LdT, telbivudine; TDF, tenofovir, ALT, alanine aminotransferase; N/A, not available; HBeAg, hepatitis B e antigen; HBsAg, hepatitis B surface antigen; HBV, hepatitis B virus. *Data in bracket show responses 6 months after stopping treatment. Off-treatment response. after a 1-year course of NUC treatment [10 17] compared to 24 33% of patients who received placebo or no treatment [10 13] (Table 2). These data demonstrated that antiviral therapy can result in improvement in liver histology, but it should be noted that fibrosis scores remained largely unchanged with these short courses of treatment, and in studies of NUCs, follow-up biopsies were performed while the patients were still receiving treatment. Studies of patients receiving longer courses of NUC showed that necrosis and inflammation continued to decrease and fibrosis regressed in patients with maintained viral suppression. One study compared liver histology pretreatment, after 1 year of lamivudine and after 3 years of lamivudine. Compared to the year-1 biopsy, further reduction in necrosis and inflammation on the year-3 biopsy was observed in 19% of patients. Of note, eight of 11 patients had regression of cirrhosis, while only one of 52 had progression to cirrhosis after 3 years of lamivudine treatment [31]. In another study of 45 HBeAg-negative patients treated with adefovir, the proportion of patients with regression of fibrosis as measured by a 1 point decrease in Ishak fibrosis score increased from 35% at 1 year to 71% after 5 years of treatment and seven of the 12 patients (58%) with bridging fibrosis or cirrhosis on the pretreatment biopsy had decrease in Ishak fibrosis score by 2 points [19]. In a third study of 63 patients treated with entecavir for a median of 6 years (range 3 7), a 1 point decrease in Ishak fibrosis score was observed in 88% of the patients and cirrhosis was no longer demonstrated in three of four patients who had cirrhosis before treatment [32]. Thus, antiviral therapy has been shown not only to prevent progression of liver disease but also to reverse fibrosis. Although liver histology is the most direct assessment of liver disease, histology is not a practical endpoint of HBV treatment in clinical practice. Assessment of histological endpoint will require at least two biopsies. Liver biopsy is an invasive and expensive procedure that may be associated with a small risk of serious complications. Furthermore, liver histology is not always accurate because of sampling error, particularly when the biopsy samples are small [33].
4 678 W. Chotiyaputta & A. S. F. Lok VIROLOGICAL ENDPOINT Suppression of HBV replication with undetectable serum HBV DNA when tested by a sensitive PCR assay has been used as an endpoint in all clinical trials of HBV treatment. Phase III clinical trials of peg-ifn showed that virological response could be achieved in 10 69% of HBeAg-positive and in 63 87% of HBeAg-negative patients at the end of a 1-year course of peg-ifn alone or in combination with lamivudine [8,9] (Table 2). A higher rate of virological response was observed in patients who received combination therapy of peg-ifn and lamivudine [8,9,21]. However, serum HBV DNA remained undetectable in only 7 14% of HBeAg-positive patients and in 19 20% of HBeAg-negative patients 6 months after stopping treatment, and the response rates were similar in patients who received peg-ifn alone or peg-ifn plus lamivudine (Table 2). Long-term follow-up studies showed that only 19% of HBeAg-positive patients and 15.6% of HBeAg-negative patients had sustained viral suppression 3 5 years after completing a 1-year course of peg-ifn treatment [34,35]. NUC therapy has more potent antiviral activity than IFN. Phase III clinical trials of NUCs showed that virological response could be achieved in 21 76% of HBeAg-positive and in 51 93% of HBeAg-negative patients at the end of a 1-year course of treatment [10 17] (Table 2). Of the five approved HBV NUCs, entecavir, telbivudine, and tenofovir were associated with higher rates of virological response, followed by lamivudine and then adefovir. Withdrawal of therapy after a 1-year course is associated with rapid viral relapse, and serum HBV DNA remained undetectable in only 5% of HBeAg-positive patients and in 3 8% of HBeAgnegative patients 6 12 months after stopping treatment [8,9,22,23,36]. By contrast, follow-up of patients who received long-term NUCs that have modest-high genetic barrier to resistance showed that an increasing proportion of patients achieved virological response. In a study of 125 HBeAg-negative patients who had received adefovir for 4 5 years, 72% had undetectable serum HBV DNA compared to 67% after 1 year of treatment [13,19]. In another study of 354 HBeAg-positive patients receiving entecavir, virological response increased from 67% at the end of 1 -year to 94% at the end of 5- year treatment [20]. Virological breakthrough was observed in only 28 patients (approximately 2%/year) through the 5-year course of treatment [37]. In a third study of 176 HBeAg-positive and 250 HBeAg-negative patients receiving tenofovir, virological response increased from 76% at the end of 1- year to 95% at the end of 3- year treatment among the HBeAg-positive patients and from 93% to 99% among the HBeAg-negative patients. Virological breakthrough was observed in only 14 patients through the 3-year course of treatment [17,38,39]. These studies showed that viral suppression is maintained in the vast majority of patients receiving long-term NUCs that have high genetic barrier to resistance. The clinical benefit of treatment-related viral suppression was demonstrated in a prospective, double-blind RCT of lamivudine in 651 patients with advanced fibrosis or cirrhosis [40]. After a median of 32 months, a statistically significant difference in the incidence of the primary endpoint defined as an increase in Child-Turcotte-Pugh (CTP) score of 2 points, variceal haemorrhage, spontaneous bacterial peritonitis, or HCC was observed between the treated patients and controls [7.8% vs 17.7%, hazard ratio (HR) 0.45, 95% CI , P = 0.001]. This trial also demonstrated a statistically significant decrease in the incidence of HCC among the treated patients, 3.9% vs 7.4% in the controls (P = 0.047). In this study, a clinical endpoint was observed in 11% of treated patients with and in 5% of patients without lamivudine resistance mutations compared to 18% of those on placebo. The benefit of treatment-related viral suppression was also shown in a retrospective study of 656 patients (46% had cirrhosis) who had received lamivudine for a median of 22 (range 1 66) months [41]. Among the patients with cirrhosis, HCC and death occurred less frequently in those who had maintained viral suppression compared to those with virological breakthrough. Virological response had also been shown to be associated with histologic improvement. A review of 26 prospective clinical studies of antiviral therapy involving 3428 patients who had pretreatment and post-treatment liver biopsies found that treatment-associated decrease in necrosis and inflammation was directly proportional to the reduction in serum HBV DNA levels [42]. Several large cohort studies of patients not receiving antiviral treatment have demonstrated a strong association between high serum HBV DNA level and an increased risk of developing cirrhosis, HCC, and liver-related death. In one study of 3653 hepatitis B surface antigen (HBsAg)-positive persons followed for 11.4 years in whom HBV DNA levels at baseline and the last follow-up visit were available, the adjusted HR for HCC was (95% CI ) among those with both HBV DNA values more than copies/ml and 1.9 (95% CI ) for those with HBV DNA more than copies/ml at enrolment and < copies/ml at the last follow-up visit, when compared to those who had HBV DNA < copies/ml at enrolment. This study showed that persistently high serum HBV DNA was associated with an increased risk of HCC development and decrease in serum HBV DNA during follow-up was associated with a reduction in risk of HCC [43]. In another analysis of this cohort, the cumulative incidence of cirrhosis was reported to be 4.5% and 36.2% for patients with baseline HBV DNA level <300 copies/ml and copies/ml, respectively [44]. Substantial data support that persistently high serum HBV DNA is associated with an increased risk of clinical outcome and suppression of serum HBV DNA as a result of host immune response or antiviral treatment results in improved liver histology and decreased risk of clinical outcome.
5 Endpoints of HBV treatment 679 Clinical trials showed that approved treatments for hepatitis B are effective in suppressing HBV replication, but only a small percent of patients achieved sustained virological response when treatment is discontinued. Therefore, while virological endpoint is an important parameter of success of hepatitis B treatment, it is not a reliable surrogate for clinical outcome unless viral suppression is sustained after discontinuation of treatment or maintained during continued treatment. [22]. SEROLOGICAL ENDPOINTS Hepatitis B e antigen seroconversion Hepatitis B e antigen seroconversion is an important endpoint in clinical trials of antiviral therapy in HBeAg-positive patients. Phase III clinical trials showed that a 1-year course of peg-ifn resulted in HBeAg seroconversion in 24 30% of patients at the end of treatment, and addition of lamivudine did not increase the rate of HBeAg seroconversion (Table 2). HBeAg seroconversion was durable in most (81%) patients after peg-ifn was stopped, and incremental HBeAg seroconversion was observed during post-treatment follow-up [34]. Phase III clinical trials showed that a 1-year course of NUC resulted in HBeAg seroconversion rates of 16 22% (Table 2a). The durability of NUC-induced HBeAg seroconversion has been reported to vary from 62 to 77% when treatment was stopped after 1 year [45,46]. Factors associated with durability of HBeAg seroconversion include a longer duration of consolidation therapy (12 months), younger age of the patient (<40 years), HBV genotype B (vs C), and lower HBV DNA level at the time treatment was stopped [47 50]. Continued treatment with NUC resulted in increasing rates of HBeAg seroconversion to 26 31% after 2 years and to 40 50% after 5 years of treatment [20,35,51]. Studies of patients not receiving antiviral therapy showed that presence of HBeAg was associated with a higher risk of development of cirrhosis and HCC. In a prospective study of 2361 HBsAg-positive men followed for person-years, those who were HBeAg positive at enrolment had a relative risk of HCC sixfold higher than those who were HBeAg negative [52]. Cohort follow-up studies showed that patients who underwent spontaneous HBeAg seroconversion had favourable outcome particularly if the HBeAg seroconversion occurred early in the course of chronic HBV infection and was durable, and the outcome was improved compared to patients who remained HBeAg positive. In one study, 88% of 223 patients who underwent HBeAg seroconversion had sustained normalization of ALT and 79% had histologic improvement [53]. In a follow-up report of the same cohort, 66% remained as inactive carriers after a median follow-up of 25 years [54]. The 25-year probability of survival was 40% for those who remained HBeAg positive, 50% for those progressing to HBeAg-negative chronic hepatitis or reverting to HBeAg positive, and 95% for those whose HBeAg seroconversion was maintained. In another study, 283 patients underwent spontaneous HBeAg seroconversion. Of the 269 patients who had no evidence of cirrhosis at the time of HBeAg seroconversion, 21 developed cirrhosis during a mean follow-up of 9 years, 14 of 62 patients who progressed to HBeAg-negative hepatitis, five of nine who had HBeAg reversion, one of 14 patients who had active hepatitis of undetermined causes, and one of 184 who had sustained HBeAg seroconversion [55]. A third study of 483 patients followed for a mean of 11.7 years found that patients who underwent HBeAg seroconversion before age 30 had excellent prognosis when compared to those who did so at an older age. The cumulative incidence of cirrhosis was 3.7%, 12.9%, and 42.9% and for HCC 2.1%, 3.2%, and 7.7% in patients who underwent HBeAg seroconversion before age 30 years, at age years and after age 40 years, respectively [56]. Follow-up studies of patients who received HBV treatment also support the use of HBeAg seroconversion as a surrogate marker for clinical outcome. In a study by Niederau et al., 103 patients who were treated with IFN alfa and 53 untreated controls were followed for a mean of 50.0 ± 19.8 months. Fifty (49%) of the IFN-treated patients lost HBeAg compared to 7 (13%) of the untreated controls. Liverrelated complications occurred in 16 (16%) treated patients all but one of whom failed to lose HBeAg and in 13 (25%) controls. Survival until liver transplantation or death and lack of clinical complications was significantly better in treated patients who cleared HBeAg than in patients who did not (P = for survival and P = for absence of clinical complications). In another study, Lau et al. [57] followed 103 patients who received IFN treatment for a mean of 6.2 years. Patients who did not clear HBeAg had higher rates of liver-related complications and mortality (HR = 13.7, 95% CI ) compared to those who lost HBeAg within 1 year of treatment. These studies demonstrate that HBeAg seroconversion, spontaneous or treatment related, is associated with improvement in liver histology and clinical outcomes including survival. Therefore, HBeAg seroconversion is a valid surrogate endpoint for clinical outcome, and treatment guidelines have recommended that NUC treatment can be stopped in patients who completed at least 6- month consolidation therapy after confirmed HBeAg seroconversion. Many experts have questioned the validity of HBeAg seroconversion as an endpoint of HBV treatment citing that HBV DNA remains detectable in most patients albeit at lower levels and reactivation of HBV replication with recrudescence of hepatitis leading to progressive liver disease will ultimately occur in most patients. However, one study involving 283 patients followed for a median of 8.6 years (range, years) after HBeAg seroconversion found that only 4.2% had HBeAg reversion and 24% developed HBeAg-negative hepatitis with detectable HBV DNA, while
6 680 W. Chotiyaputta & A. S. F. Lok Table 3 Validity of intermediate endpoints of chronic hepatitis B treatment as surrogates for clinical outcomes Randomized controlled trials Cohort studies of untreated patients Cohort studies of treated patients Retrospective studies of untreated patients Retrospective studies of treated patients Biochemical improvement Histologic improvement Undetectable HBV DNA HBeAg seroconversion Liaw YF 2004 [40] Tai DI et al [65] Lau DT 1997 [57], Wong VW 2009 [66] N/A N/A Dienstag JL 2003 [31], Hadziyannis SJ 2006[19], Liaw YF 2008 [32], Hui CK et al [70], Wong VW et al [66] Liaw YF 2004 [40] Chen CJ 2006 [43], Iloeje UH 2006 [44], Chen G 2006 [71] N/A Yang HI 2002 [52], Hsu YS 2002[55], Fattovich G 2008[54], Fattovich G et al [53] HBsAg loss N/A Chen YC 2002 [58], Arase Y et al [74] Lau DT 1997 [57], Niederau C 1996[72] Niederau C et al [72], Lau DT 1997 [57] Park BY et al [67] N/A N/A Fattovich G et al [68], Papatheodoridis GV et al [69] N/A Di Marco V 2004 [41], Papatheodoridis GV et al. 2005[69] Lin SM et al [73] Lau DT 1997 [57] Yuen MF 2008 [59] Fattovich G et al [68] Fattovich G et al [75] HBV, hepatitis B virus; HBeAg, hepatitis B e antigen; HBsAg, hepatitis B s antigen; N/A, not available.
7 Endpoints of HBV treatment 681 the other 71.8% remained in remission [55]. Given the high costs of NUCs and the risks of adverse events and antiviral resistance during long-term therapy, withdrawal of treatment in patients who have completed 12 months of consolidation therapy after confirmed HBeAg seroconversion and who have undetectable serum HBV DNA is a reasonable approach as long as the patients continue to be monitored. A recent study of patients who achieved HBeAg seroconversion during lamivudine treatment showed that durability of HBeAg seroconversion was 92% after 5 years of post-treatment follow-up among the patients who completed at least 12 months of consolidation therapy [48]. These data indicate that durable HBeAg seroconversion can be accomplished with NUC treatment. Hepatitis B surface antigen loss Hepatitis B surface antigen is the hallmark of HBV infection. Clinical trials showed that HBsAg loss can be observed in 5 7% of patients at the end of a 1-year course of peg-ifn with or without lamivudine [8,9] and in 0 3.2% of patients at the end of a 1-year course of NUC therapy [10 17] (Table 2). Long-term follow-up of patients who received peg-ifn with or without lamivudine found that the rate of HBsAg loss increased to 8 15% in HBeAg-positive patients and 8% in HBeAg-negative patients 3 years after completion of a 1-year course of peg-ifn [34,35]. However, it should be noted that the rate of HBsAg loss was not uniform across HBV genotypes. In a study of HBeAg-positive patients, HBsAg loss at 3 years was observed in 28% patients with genotype A but in only 3% of patients with other HBV genotypes [34]. Another study of 230 HBeAgnegative patients followed for 3 years after peg-ifn treatment found that HBsAg loss was observed in 9.4% of patients who had undetectable HBV DNA (<400 copies/ml) at the end of treatment compared to only 2% of those who remained viremic at the end of treatment [35]. NUCs have been reported to be associated with lower rates of HBsAg loss compared to peg-ifn. HBsAg loss has been reported to occur in 0 2% of HBeAg-positive patients and in <1% of HBeAg-negative patients at the end of year 1 increasing to 2 8% among HBeAg-positive patients and to 0 5% in HBeAg-negative patients after 3 5 years of continuous treatment [10 20,39] (Table 2). Cohort studies have demonstrated that patients with chronic HBV infection who lost HBsAg spontaneously have a reduced risk of cirrhosis, HCC, and liver-related mortality compared with patients who remained HBsAg positive. In a prospective cohort study of 218 patients who were followed up for a mean of 63 months after spontaneous HBsAg clearance, of the 146 patients who had HBV monoinfection and who did not have evidence of cirrhosis at the time of HBsAg loss, none developed cirrhosis or HCC during followup compared to an incidence of cirrhosis of 3.4% and an incidence of HCC of 0.7% in those who remained HBsAg positive [58]. Another study of 298 patients found that patients with HBsAg loss before age 50 years was associated with a lower risk of HCC [59]. These data indicate that HBsAg loss is a valid surrogate for clinical outcome and a desired goal during antiviral treatment; however, except for HBV genotype A HBeAg-positive patients receiving peg-ifn therapy, the low rate of treatment-related HBsAg loss makes HBsAg loss an unrealistic endpoint in HBV treatment. CONCLUSIONS The goal of HBV treatment is to prevent the development of cirrhosis, HCC, and liver failure. Because clinical outcomes take decades to evolve, intermediate endpoints have to be used as surrogates to evaluate the benefits of treatment and to determine when treatment can be stopped. Data from clinical trials as well as cohort studies showed that ALT normalization and HBV DNA suppression are associated with improved clinical outcomes and are valid surrogates for assessing the benefits of treatment, but the durability of these responses is low, and these endpoints cannot be used as indicators to stop treatment (Table 3). For HBeAg-positive patients, HBeAg seroconversion is a valid clinical endpoint and can be used as an indicator for stopping NUC treatment provided that serum HBV DNA was undetectable and consolidation therapy was completed. For HBeAg-negative patients, HBsAg loss would be an ideal endpoint but the low rate at which this occurs makes it an unrealistic goal and other endpoints or predictors of sustained response after NUC treatment must be sought. ACKNOWLEDGEMENTS WC was supported in part by the Tuktawa Foundation (ASL) and the Siriraj Hospital, Mahidol University Foundation, Bangkok, Thailand (WC). DISCLOSURES W Chotiyaputta: Nothing to disclosure; Anna S. F. Lok: Receives research support from Bristol-Myers Squibb, Gilead Sciences, GlaxoSmithKline, Schering, and Roche and serves on advisory panels of Gilead Sciences, Roche Pharmaceuticals, and Bristol-Myers Squibb. REFERENCES 1 Lok AS, Liang RH, Chiu EK, Wong KL, Chan TK, Todd D. Reactivation of hepatitis B virus replication in patients receiving cytotoxic therapy. Report of a prospective study. Gastroenterology 1991; 100(1): Summers J, Jilbert AR, Yang W et al. Hepatocyte turnover during resolution of a transient hepadnaviral infection. Proc Natl Acad Sci USA 2003; 100(20):
8 682 W. Chotiyaputta & A. S. F. Lok 3 Moraleda G, Saputelli J, Aldrich CE, Averett D, Condreay L, Mason WS. Lack of effect of antiviral therapy in nondividing hepatocyte cultures on the closed circular DNA of woodchuck hepatitis virus. J Virol 1997; 71(12): Shamliyan TA, MacDonald R, Shaukat A et al. Antiviral therapy for adults with chronic hepatitis B: a systematic review for a National Institutes of Health Consensus Development Conference. Ann Intern Med 2009; 150(2): Lok AS, McMahon BJ. Chronic hepatitis B. Hepatology 2007; 45(2): Liaw YF, Leung N, Kao JH et al. Asian-Pacific consensus statement on the management of chronic hepatitis B: a 2008 update. Hepatol Int 2008; 2(3): European Association For The Study Of The L. EASL Clinical Practice Guidelines: management of chronic hepatitis B. J Hepatol 2009; 50(2): Lau GK, Piratvisuth T, Luo KX et al. Peginterferon Alfa-2a, lamivudine, and the combination for HBeAg-positive chronic hepatitis B. N Engl J Med 2005; 352(26): Marcellin P, Lau GK, Bonino F et al. Peginterferon alfa-2a alone, lamivudine alone, and the two in combination in patients with HBeAg-negative chronic hepatitis B. N Engl J Med 2004; 351(12): Lai CL, Chien RN, Leung NW et al. A one-year trial of lamivudine for chronic hepatitis B. Asia Hepatitis Lamivudine Study Group. N Engl J Med 1998; 339(2): Dienstag JL, Schiff ER, Wright TL et al. Lamivudine as initial treatment for chronic hepatitis B in the United States. N Engl J Med 1999; 341(17): Marcellin P, Chang TT, Lim SG et al. Adefovir dipivoxil for the treatment of hepatitis B e antigen-positive chronic hepatitis B. N Engl J Med 2003; 348(9): Hadziyannis SJ, Tassopoulos NC, Heathcote EJ et al. Adefovir dipivoxil for the treatment of hepatitis B e antigen-negative chronic hepatitis B. N Engl J Med 2003; 348(9): Chang TT, Gish RG, de Man R et al. A comparison of entecavir and lamivudine for HBeAg-positive chronic hepatitis B. N Engl J Med 2006; 354(10): Lai CL, Shouval D, Lok AS et al. Entecavir versus lamivudine for patients with HBeAg-negative chronic hepatitis B. N Engl J Med 2006; 354(10): Lai CL, Gane E, Liaw YF et al. Telbivudine versus lamivudine in patients with chronic hepatitis B. N Engl J Med 2007; 357(25): Marcellin P, Heathcote EJ, Buti M et al. Tenofovir disoproxil fumarate versus adefovir dipivoxil for chronic hepatitis B. N Engl J Med 2008; 359(23): Marcellin P, Chang TT, Lim SG et al. Long-term efficacy and safety of adefovir dipivoxil for the treatment of hepatitis B e antigen-positive chronic hepatitis B. Hepatology 2008; 48(3): Hadziyannis SJ, Tassopoulos NC, Heathcote EJ et al. Longterm therapy with adefovir dipivoxil for HBeAg-negative chronic hepatitis B for up to 5 years. Gastroenterology 2006; 131(6): Chang TT, Lai CL, Kew Yoon S et al. Entecavir treatment for up to 5 years in patients with hepatitis B e antigen-positive chronic hepatitis B. Hepatology 2010; 51(2): Janssen HL, van Zonneveld M, Senturk H et al. Pegylated interferon alfa-2b alone or in combination with lamivudine for HBeAg-positive chronic hepatitis B: a randomised trial. Lancet 2005; 365(9454): Hadziyannis SJ, Tassopoulos NC, Heathcote EJ et al. Longterm therapy with adefovir dipivoxil for HBeAg-negative chronic hepatitis B. N Engl J Med 2005; 352(26): Shouval D, Lai CL, Chang TT et al. Relapse of hepatitis B in HBeAg-negative chronic hepatitis B patients who discontinued successful entecavir treatment: the case for continuous antiviral therapy. J Hepatol 2009; 50(2): Honkoop P, de Man RA, Niesters HG, Zondervan PE, Schalm SW. Acute exacerbation of chronic hepatitis B virus infection after withdrawal of lamivudine therapy. Hepatology 2000; 32(3): Lai M, Hyatt BJ, Nasser I, Curry M, Afdhal NH. The clinical significance of persistently normal ALT in chronic hepatitis B infection. J Hepatol 2007; 47(6): Kumar M, Sarin SK, Hissar S et al. Virologic and histologic features of chronic hepatitis B virus-infected asymptomatic patients with persistently normal ALT. Gastroenterology 2008; 134(5): Kim HC, Nam CM, Jee SH, Han KH, Oh DK, Suh I. Normal serum aminotransferase concentration and risk of mortality from liver diseases: prospective cohort study. BMJ 2004; 328(7446): Yuen MF, Yuan HJ, Wong DK et al. Prognostic determinants for chronic hepatitis B in Asians: therapeutic implications. Gut 2005; 54(11): Prati D, Taioli E, Zanella A et al. Updated definitions of healthy ranges for serum alanine aminotransferase levels. Ann Intern Med 2002; 137(1): Lee JK, Shim JH, Lee HC et al. Estimation of the healthy upper limits for serum alanine aminotransferase in Asian populations with normal liver histology. Hepatology 2010; 51: Dienstag JL, Goldin RD, Heathcote EJ et al. Histological outcome during long-term lamivudine therapy. Gastroenterology 2003; 124(1): Liaw YF, Chang TT, Wu SS et al. Long-term entecavir therapy results in reversal of fibrosis/cirrhosis and continued histologic improvement in patients with HBeAg (+) and (-) chronic hepatitis B: results from studies ETV-022, -027 and Hepatology 2008; 48(Suppl. 1): 706A. 33 Bedossa P, Dargere D, Paradis V. Sampling variability of liver fibrosis in chronic hepatitis C. Hepatology 2003; 38(6): Buster EH, Flink HJ, Cakaloglu Y et al. Sustained HBeAg and HBsAg loss after long-term follow-up of HBeAg-positive patients treated with peginterferon alpha-2b. Gastroenterology 2008; 135(2): Marcellin P, Bonino F, Lau GK et al. Sustained response of hepatitis B e antigen-negative patients 3 years after treatment with peginterferon alpha-2a. Gastroenterology 2009; 136(7): Liaw YF, Leung NW, Chang TT et al. Effects of extended lamivudine therapy in Asian patients with chronic hepatitis
9 Endpoints of HBV treatment 683 B. Asia Hepatitis Lamivudine Study Group. Gastroenterology 2000; 119(1): Tenney DJ, Rose RE, Baldick CJ et al. Long-term monitoring shows hepatitis B virus resistance to entecavir in nucleosidenaive patients is rare through 5 years of therapy. Hepatology 2009; 49(5): Marcellin P, Maria B, Krastev Z et al. Three years of tenofovir disoproxil fumarate (TDF) treatment in HBeAg-negative patients with chronic hepatitis B (study 102); preliminary analysis. Hepatology 2009; 50(Suppl. 4): 532A 533A. 39 Heathcote EJ, Gane EJ, De Man RA et al. Three years of tenofovir disoproxil (TDF) treatment in HBeAg-positive patients (HBeAg+) with chronic hepatitis B (study 103), preliminary analysis. Hepatology 2009; 50(Suppl. 4): 533A 534A. 40 Liaw YF, Sung JJ, Chow WC et al. Lamivudine for patients with chronic hepatitis B and advanced liver disease. N Engl J Med 2004; 351(15): Di Marco V, Marzano A, Lampertico P et al. Clinical outcome of HBeAg-negative chronic hepatitis B in relation to virological response to lamivudine. Hepatology 2004; 40(4): Mommeja-Marin H, Mondou E, Blum MR, Rousseau F. Serum HBV DNA as a marker of efficacy during therapy for chronic HBV infection: analysis and review of the literature. Hepatology 2003; 37(6): Chen CJ, Yang HI, Su J et al. Risk of hepatocellular carcinoma across a biological gradient of serum hepatitis B virus DNA level. JAMA 2006; 295(1): Iloeje UH, Yang HI, Su J, Jen CL, You SL, Chen CJ. Predicting cirrhosis risk based on the level of circulating hepatitis B viral load. Gastroenterology 2006; 130(3): Song BC, Suh DJ, Lee HC, Chung YH, Lee YS. Hepatitis B e antigen seroconversion after lamivudine therapy is not durable in patients with chronic hepatitis B in Korea. Hepatology 2000; 32(4): Dienstag JL, Cianciara J, Karayalcin S et al. Durability of serologic response after lamivudine treatment of chronic hepatitis B. Hepatology 2003; 37(4): Ryu SH, Chung YH, Choi MH et al. Long-term additional lamivudine therapy enhances durability of lamivudine-induced HBeAg loss: a prospective study. J Hepatol 2003; 39(4): Lee HW, Lee HJ, Hwang JS et al. Lamivudine maintenance beyond one year after HBeAg seroconversion is a major factor for sustained virologic response in HBeAg-positive chronic hepatitis B. Hepatology 2010; 51(2): Chien RN, Yeh CT, Tsai SL, Chu CM, Liaw YF. Determinants for sustained HBeAg response to lamivudine therapy. Hepatology 2003; 38(5): Lee KM, Cho SW, Kim SW, Kim HJ, Hahm KB, Kim JH. Effect of virological response on post-treatment durability of lamivudine-induced HBeAg seroconversion. J Viral Hepat 2002; 9(3): Gish RG, Lok AS, Chang TT et al. Entecavir therapy for up to 96 weeks in patients with HBeAg-positive chronic hepatitis B. Gastroenterology 2007; 133(5): Yang HI, Lu SN, Liaw YF et al. Hepatitis B e antigen and the risk of hepatocellular carcinoma. N Engl J Med 2002; 347(3): Fattovich G, Rugge M, Brollo L et al. Clinical, virologic and histologic outcome following seroconversion from HBeAg to anti-hbe in chronic hepatitis type B. Hepatology 1986; 6(2): Fattovich G, Olivari N, Pasino M, DÕOnofrio M, Martone E, Donato F. Long-term outcome of chronic hepatitis B in Caucasian patients: mortality after 25 years. Gut 2008; 57(1): Hsu YS, Chien RN, Yeh CT et al. Long-term outcome after spontaneous HBeAg seroconversion in patients with chronic hepatitis B. Hepatology 2002; 35(6): Chen YC, Chu CM, Liaw YF. Age-specific prognosis following spontaneous hepatitis B e antigen seroconversion in chronic hepatitis B. Hepatology 2010; 51(2): Lau DT, Everhart J, Kleiner DE et al. Long-term follow-up of patients with chronic hepatitis B treated with interferon alfa. Gastroenterology 1997; 113(5): Chen YC, Sheen IS, Chu CM, Liaw YF. Prognosis following spontaneous HBsAg seroclearance in chronic hepatitis B patients with or without concurrent infection. Gastroenterology 2002; 123(4): Yuen MF, Wong DK, Fung J et al. HBsAg Seroclearance in chronic hepatitis B in Asian patients: replicative level and risk of hepatocellular carcinoma. Gastroenterology 2008; 135(4): Biomarkers Definitions Working Group. Biomarkers and surrogate endpoints: preferred definitions and conceptual framework. Clin Pharmacol Ther 2001; 69(3): Boissel JP, Collet JP, Moleur P, Haugh M. Surrogate endpoints: a basis for a rational approach. Eur J Clin Pharmacol 1992; 43(3): Chang TT, Lai CL, Chien RN et al. Four years of lamivudine treatment in Chinese patients with chronic hepatitis B. J Gastroenterol Hepatol 2004; 19(11): Hsu CW, Chen YC, Liaw YF et al. Prolonged efficacy and safety of 3 years of continuous telbivudine treatment in pooled data from Globe and 015 studies in chronic hepatitis B patients. J Hepatol 2009; 50(Suppl. 1): S Wang Y, Thongsawat S, Gane EJ et al. Efficacy and safety outcomes after 4 years of telbivudine treatment in patients with chronic hepatitis B (CHB). Hepatology 2009; 50(Suppl. 4): 533A. 65 Tai DI, Lin SM, Sheen IS, Chu CM, Lin DY, Liaw YF. Longterm outcome of hepatitis B e antigen-negative hepatitis B surface antigen carriers in relation to changes of alanine aminotransferase levels over time. Hepatology 2009; 49(6): Wong VW, Wong GL, Chim AM et al. Surrogate end points and long-term outcome in patients with chronic hepatitis B. Clin Gastroenterol Hepatol 2009; 7(10): Park BK, Park YN, Ahn SH et al. Long-term outcome of chronic hepatitis B based on histological grade and stage. J Gastroenterol Hepatol 2007; 22(3): Fattovich G, Giustina G, Realdi G, Corrocher R, Schalm SW. Long-term outcome of hepatitis B e antigen-positive patients with compensated cirrhosis treated with interferon alfa. European Concerted Action on Viral Hepatitis (EUROHEP). Hepatology 1997; 26(5):
10 684 W. Chotiyaputta & A. S. F. Lok 69 Papatheodoridis GV, Dimou E, Dimakopoulos K et al. Outcome of hepatitis B e antigen-negative chronic hepatitis B on long-term nucleos(t)ide analog therapy starting with lamivudine. Hepatology 2005; 42(1): Hui CK, Leung N, Shek WH et al. Changes in liver histology as a surrogate end point of antiviral therapy for chronic HBV can predict progression to liver complications. J Clin Gastroenterol 2008; 42(5): Chen G, Lin W, Shen F, Iloeje UH, London WT, Evans AA. Past HBV viral load as predictor of mortality and morbidity from HCC and chronic liver disease in a prospective study. Am J Gastroenterol 2006; 101(8): Niederau C, Heintges T, Lange S et al. Long-term follow-up of HBeAg-positive patients treated with interferon alfa for chronic hepatitis B. N Engl J Med 1996; 334(22): Lin SM, Yu ML, Lee CM et al. Interferon therapy in HBeAg positive chronic hepatitis reduces progression to cirrhosis and hepatocellular carcinoma. J Hepatol 2007; 46(1): Arase Y, Ikeda K, Suzuki F et al. Long-term outcome after hepatitis B surface antigen seroclearance in patients with chronic hepatitis B. Am J Med 2006; 119(1): 71.e9 71.e Fattovich G, Giustina G, Sanchez-Tapias J et al. Delayed clearance of serum HBsAg in compensated cirrhosis B: relation to interferon alpha therapy and disease prognosis. European Concerted Action on Viral Hepatitis (EUROHEP). Am J Gastroenterol 1998; 93(6):
Hepatitis B Virus therapy. Maria Buti Hospital Universitario Valle Hebron Barcelona Spain
 Hepatitis B Virus therapy Maria Buti Hospital Universitario Valle Hebron Barcelona Spain Disclosures Advisor: AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp &
Hepatitis B Virus therapy Maria Buti Hospital Universitario Valle Hebron Barcelona Spain Disclosures Advisor: AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp &
29th Viral Hepatitis Prevention Board Meeting
 29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis B José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HBV INFECTION
29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis B José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HBV INFECTION
Prediction of HBsAg Loss by Quantitative HBsAg Kinetics during Long-Term 2015
 THAI J 16 GASTROENTEROL Treatment with Nucleos(t)ide Original Analogues Article Prediction of HBsAg Loss by Quantitative HBsAg Kinetics during Long-Term Treatment with Nucleos(t)ide Analogues Sombutsook
THAI J 16 GASTROENTEROL Treatment with Nucleos(t)ide Original Analogues Article Prediction of HBsAg Loss by Quantitative HBsAg Kinetics during Long-Term Treatment with Nucleos(t)ide Analogues Sombutsook
The Impact of HBV Therapy on Fibrosis and Cirrhosis
 The Impact of HBV Therapy on Fibrosis and Cirrhosis Jordan J. Feld, MD, MPH Associate Professor of Medicine University of Toronto Hepatologist Toronto Centre for Liver Disease Sandra Rotman Centre for
The Impact of HBV Therapy on Fibrosis and Cirrhosis Jordan J. Feld, MD, MPH Associate Professor of Medicine University of Toronto Hepatologist Toronto Centre for Liver Disease Sandra Rotman Centre for
Hepatitis B Virus therapy. Maria Buti Hospital Universitario Valle Hebron Barcelona Spain
 Hepatitis B Virus therapy Maria Buti Hospital Universitario Valle Hebron Barcelona Spain Disclosures Advisor: AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp &
Hepatitis B Virus therapy Maria Buti Hospital Universitario Valle Hebron Barcelona Spain Disclosures Advisor: AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp &
Chronic hepatitis B - New goals, new treatment. New England Journal Of Medicine, 2008, v. 359 n. 23, p
 Title Chronic hepatitis B - New goals, new treatment Author(s) Lai, CL; Yuen, MF Citation New England Journal Of Medicine, 2008, v. 359 n. 23, p. 2488-2491 Issued Date 2008 URL http://hdl.handle.net/10722/59270
Title Chronic hepatitis B - New goals, new treatment Author(s) Lai, CL; Yuen, MF Citation New England Journal Of Medicine, 2008, v. 359 n. 23, p. 2488-2491 Issued Date 2008 URL http://hdl.handle.net/10722/59270
Response-guided antiviral therapy in chronic hepatitis B: nucleot(s)ide analogues vs. pegylated interferon
 Response-guided antiviral therapy in chronic hepatitis B: Sang Hoon Ahn, M.D., Ph.D. Department of Internal Medicine, Yonsei University College of Medicine, Institute of Gastroenterology, Liver Cirrhosis
Response-guided antiviral therapy in chronic hepatitis B: Sang Hoon Ahn, M.D., Ph.D. Department of Internal Medicine, Yonsei University College of Medicine, Institute of Gastroenterology, Liver Cirrhosis
Cornerstones of Hepatitis B: Past, Present and Future
 Cornerstones of Hepatitis B: Past, Present and Future Professor Man-Fung Yuen Queen Mary Hospital The University of Hong Kong Hong Kong 1 Outline Past Natural history studies Development of HBV-related
Cornerstones of Hepatitis B: Past, Present and Future Professor Man-Fung Yuen Queen Mary Hospital The University of Hong Kong Hong Kong 1 Outline Past Natural history studies Development of HBV-related
HBeAg-positve chronic hepatts B: Why do I treat my patent with a NA? Maria But
 HBeAg-positve chronic hepatts B: Why do I treat my patent with a NA? Maria But Hospital Universitario Valle Hebron and Ciberehd del Insttuto Carlos III. Barcelona. Spain Disclosures Advisory board of,
HBeAg-positve chronic hepatts B: Why do I treat my patent with a NA? Maria But Hospital Universitario Valle Hebron and Ciberehd del Insttuto Carlos III. Barcelona. Spain Disclosures Advisory board of,
Pros and Cons of Peginterferon Versus Nucleos(t)ide Analogues for Treatment of Chronic Hepatitis B
 Curr Hepatitis Rep (2010) 9:91 98 DOI 10.1007/s11901-010-0041-7 Pros and Cons of Peginterferon Versus Nucleos(t)ide Analogues for Treatment of Chronic Hepatitis B Milan J. Sonneveld & Harry L. A. Janssen
Curr Hepatitis Rep (2010) 9:91 98 DOI 10.1007/s11901-010-0041-7 Pros and Cons of Peginterferon Versus Nucleos(t)ide Analogues for Treatment of Chronic Hepatitis B Milan J. Sonneveld & Harry L. A. Janssen
NUCs for Chronic Hepatitis B. Rafael Esteban Hospital Universitario Valle Hebron and Ciberehd del Instituto Carlos III. Barcelona.
 NUCs for Chronic Hepatitis B Rafael Esteban Hospital Universitario Valle Hebron and Ciberehd del Instituto Carlos III. Barcelona. Spain Disclosures Advisory board of, and/or, received speaker fee from
NUCs for Chronic Hepatitis B Rafael Esteban Hospital Universitario Valle Hebron and Ciberehd del Instituto Carlos III. Barcelona. Spain Disclosures Advisory board of, and/or, received speaker fee from
Management of chronic hepatitis B : recent advance in the treatment of antiviral resistance
 anagement of chronic hepatitis B : recent advance in the treatment of antiviral resistance / 김강모 연수강좌 anagement of chronic hepatitis B : recent advance in the treatment of antiviral resistance 김강모 울산대학교의과대학서울아산병원소화기내과
anagement of chronic hepatitis B : recent advance in the treatment of antiviral resistance / 김강모 연수강좌 anagement of chronic hepatitis B : recent advance in the treatment of antiviral resistance 김강모 울산대학교의과대학서울아산병원소화기내과
Treatment as a form of liver cancer prevention The clinical efficacy and cost effectiveness of treatment across Asia
 Treatment as a form of liver cancer prevention The clinical efficacy and cost effectiveness of treatment across Asia Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute
Treatment as a form of liver cancer prevention The clinical efficacy and cost effectiveness of treatment across Asia Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute
HBV Diagnosis and Treatment
 HBV Diagnosis and Treatment Anna S. F. Lok, MD Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research University of Michigan Ann Arbor, MI, USA
HBV Diagnosis and Treatment Anna S. F. Lok, MD Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research University of Michigan Ann Arbor, MI, USA
Chronic hepatitis B is one of the leading causes of hepatocellular. Surrogate End Points and Long-Term Outcome in Patients With Chronic Hepatitis B
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1113 1120 Surrogate End Points and Long-Term Outcome in Patients With Chronic Hepatitis B VINCENT WAI SUN WONG,*, GRACE LAI HUNG WONG,*, ANGEL MEI LING CHIM,*,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1113 1120 Surrogate End Points and Long-Term Outcome in Patients With Chronic Hepatitis B VINCENT WAI SUN WONG,*, GRACE LAI HUNG WONG,*, ANGEL MEI LING CHIM,*,
Who to Treat? Consider biopsy Treat. > 2 ULN Treat Treat Treat Treat CIRRHOTIC PATIENTS Compensated Treat HBV DNA detectable treat
 Who to Treat? Parameter AASLD US Algorithm EASL APASL HBV DNA CRITERIA HBeAg+ >, IU/mL > 2, IU/mL > 2, IU/mL >, IU/mL HBeAg- > 2, IU/mL > 2, IU/mL > 2, IU/mL > 2, IU/mL ALT CRITERIA PNALT 1-2 ULN Monitor
Who to Treat? Parameter AASLD US Algorithm EASL APASL HBV DNA CRITERIA HBeAg+ >, IU/mL > 2, IU/mL > 2, IU/mL >, IU/mL HBeAg- > 2, IU/mL > 2, IU/mL > 2, IU/mL > 2, IU/mL ALT CRITERIA PNALT 1-2 ULN Monitor
Viral Hepatitis The Preventive Potential of Antiviral Therapy. Thomas Berg
 Viral Hepatitis The Preventive Potential of Antiviral Therapy Thomas Berg Therapeutic and preventive strategies in patients with hepatitis virus infection Treatment of acute infection Treatment of chronic
Viral Hepatitis The Preventive Potential of Antiviral Therapy Thomas Berg Therapeutic and preventive strategies in patients with hepatitis virus infection Treatment of acute infection Treatment of chronic
Management of hepatitis B virus
 Journal of Antimicrobial Chemotherapy Advance Access published May 14, 2008 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkn188 Management of hepatitis B virus Nidhi A. Singh and Nancy Reau* Section
Journal of Antimicrobial Chemotherapy Advance Access published May 14, 2008 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkn188 Management of hepatitis B virus Nidhi A. Singh and Nancy Reau* Section
New therapeutic perspectives in HBV: when to stop NAs
 Liver International ISSN 1478-3223 REVIEW ARTICLE New therapeutic perspectives in HBV: when to stop NAs Cristina Perez-Cameo, Monica Pons and Rafael Esteban Liver Unit, Department of Internal Medicine,
Liver International ISSN 1478-3223 REVIEW ARTICLE New therapeutic perspectives in HBV: when to stop NAs Cristina Perez-Cameo, Monica Pons and Rafael Esteban Liver Unit, Department of Internal Medicine,
Treatment of chronic hepatitis B: Evolution over two decades_
 doi:10.1111/j.1440-1746.2010.06545.x REVIEW Treatment of chronic hepatitis B: Evolution over two decades_6545 138..143 Man-Fung Yuen and Ching-Lung Lai Department of Medicine, the University of Hong Kong,
doi:10.1111/j.1440-1746.2010.06545.x REVIEW Treatment of chronic hepatitis B: Evolution over two decades_6545 138..143 Man-Fung Yuen and Ching-Lung Lai Department of Medicine, the University of Hong Kong,
Management of Decompensated Chronic Hepatitis B
 Management of Decompensated Chronic Hepatitis B Dr James YY Fung, FRACP, MD Department of Medicine The University of Hong Kong Liver Transplant Center Queen Mary Hospital State Key Laboratory for Liver
Management of Decompensated Chronic Hepatitis B Dr James YY Fung, FRACP, MD Department of Medicine The University of Hong Kong Liver Transplant Center Queen Mary Hospital State Key Laboratory for Liver
Consensus AASLD-EASL HBV Treatment Endpoint and HBV Cure Definition
 Consensus AASLD-EASL HBV Treatment Endpoint and HBV Cure Definition Anna S. Lok, MD, DSc Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research
Consensus AASLD-EASL HBV Treatment Endpoint and HBV Cure Definition Anna S. Lok, MD, DSc Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research
HBV (AASLD) CHB, HBV, CHB , ( < 5% ) 11 ( immune tolerant phase) : 21 ( immune clearance phase ) : 31 ( inactive phase) : HBeAg - HBe HBV DNA ALT
 2010262 125 R51216 + 2 C 1001-5256 (2010) 02-0125 - 06 2005 12 [ 1 ], (HBV ) (APASL) ( EASL ) (AASLD) (CHB) [ 2 4 ], ( ) ( ), CHB,, CHB CHB,, CHB,, 2 1 HBV hepatitis B virus CHB chronic hepatitis B HB
2010262 125 R51216 + 2 C 1001-5256 (2010) 02-0125 - 06 2005 12 [ 1 ], (HBV ) (APASL) ( EASL ) (AASLD) (CHB) [ 2 4 ], ( ) ( ), CHB,, CHB CHB,, CHB,, 2 1 HBV hepatitis B virus CHB chronic hepatitis B HB
Novedades en el tratamiento de la hepatitis B: noticias desde la EASL. Maria Buti Hospital Universitario Valle Hebrón Barcelona
 Novedades en el tratamiento de la hepatitis B: noticias desde la EASL Maria Buti Hospital Universitario Valle Hebrón Barcelona Milestones in CHB treatment Conventional IFN 1991 Lamivudine (LAM) 1998 Adefovir
Novedades en el tratamiento de la hepatitis B: noticias desde la EASL Maria Buti Hospital Universitario Valle Hebrón Barcelona Milestones in CHB treatment Conventional IFN 1991 Lamivudine (LAM) 1998 Adefovir
Disclaimer. Presenter Release are for reactive use by Medical Information only internal learning/educational use only
 Disclaimer Presenter Release are for reactive use by Medical Information only internal learning/educational use only Any unsolicited request from HCP must be forwarded to Medical Information Housekeeping
Disclaimer Presenter Release are for reactive use by Medical Information only internal learning/educational use only Any unsolicited request from HCP must be forwarded to Medical Information Housekeeping
Individualizing Treatment in the Patient With Chronic HBV Infection: When to Start, What to Use, and When to Stop CME
 Individualizing Treatment in the Patient With Chronic HBV Infection: When to Start, What to Use, and When to Stop CME Chia C. Wang, MD, MS Anna S. F. Lok, MD Kris V. Kowdley, MD Supported by an independent
Individualizing Treatment in the Patient With Chronic HBV Infection: When to Start, What to Use, and When to Stop CME Chia C. Wang, MD, MS Anna S. F. Lok, MD Kris V. Kowdley, MD Supported by an independent
The presence of hepatitis B e antigen (HBeAg) is
 Assessment of Current Criteria for Primary Nonresponse in Chronic Hepatitis B Patients Receiving Entecavir Therapy Young-Joo Yang, 1 Ju Hyun Shim, 2 Kang Mo Kim, 2 Young-Suk Lim, 2 and Han Chu Lee 2 A
Assessment of Current Criteria for Primary Nonresponse in Chronic Hepatitis B Patients Receiving Entecavir Therapy Young-Joo Yang, 1 Ju Hyun Shim, 2 Kang Mo Kim, 2 Young-Suk Lim, 2 and Han Chu Lee 2 A
Does Viral Cure Prevent HCC Development
 Does Viral Cure Prevent HCC Development Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute of Digestive Disease Director, Center for Liver Health Assistant Dean,
Does Viral Cure Prevent HCC Development Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute of Digestive Disease Director, Center for Liver Health Assistant Dean,
Choice of Oral Drug for Hepatitis B: Status Asokananda Konar
 Choice of Oral Drug for Hepatitis B: Status 2011 Asokananda Konar Chronic hepatitis B (CHB) is a global public health challenge with an estimated 350 to 400 million people with chronic HBV infection, despite
Choice of Oral Drug for Hepatitis B: Status 2011 Asokananda Konar Chronic hepatitis B (CHB) is a global public health challenge with an estimated 350 to 400 million people with chronic HBV infection, despite
HBV Therapy in Special Populations: Liver Cirrhosis
 HBV Therapy in Special Populations: Liver Cirrhosis Universitätsklinikum Leipzig Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber- und Studienzentrum
HBV Therapy in Special Populations: Liver Cirrhosis Universitätsklinikum Leipzig Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber- und Studienzentrum
How to use pegylated Interferon for Chronic Hepatitis B in 2015
 How to use pegylated Interferon for Chronic Hepatitis B in 215 Teerha Piratvisuth NKC Institute of Gastroenterology and Hepatology Prince of Songkla University, Thailand ASIAN-PACIFIC CLINICAL PRACTICE
How to use pegylated Interferon for Chronic Hepatitis B in 215 Teerha Piratvisuth NKC Institute of Gastroenterology and Hepatology Prince of Songkla University, Thailand ASIAN-PACIFIC CLINICAL PRACTICE
The role of entecavir in the treatment of chronic hepatitis B
 REVIEW The role of entecavir in the treatment of chronic hepatitis B Evangelini Dimou Vasilios Papadimitropoulos Stephanos J Hadziyannis Department of Medicine and Liver Unit, Henry Dunant Hospital, Athens,
REVIEW The role of entecavir in the treatment of chronic hepatitis B Evangelini Dimou Vasilios Papadimitropoulos Stephanos J Hadziyannis Department of Medicine and Liver Unit, Henry Dunant Hospital, Athens,
CURRENT TREATMENT. Mitchell L Shiffman, MD Director Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, Virginia
 CURRENT TREATMENT OF HBV Mitchell L Shiffman, MD Director Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, Virginia CHRONIC HBV INFECTION DEMOGRAPHICS IN THE USA Estimated
CURRENT TREATMENT OF HBV Mitchell L Shiffman, MD Director Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, Virginia CHRONIC HBV INFECTION DEMOGRAPHICS IN THE USA Estimated
The advent of sensitive assays for the detection of hepatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;-:1 10 All studies published in Clinical Gastroenterology and Hepatology are embargoed until 3PM ET of the day they are published as corrected proofs on-line.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;-:1 10 All studies published in Clinical Gastroenterology and Hepatology are embargoed until 3PM ET of the day they are published as corrected proofs on-line.
Update on HBV Treatment
 Update on HBV Treatment Calvin Q. Pan MD, FAASLD, FACG, MACP Professor of Medicine Division of Gastroenterology and Hepatology Department of Medicine, NYU Langone Health New York University School of Medicine,
Update on HBV Treatment Calvin Q. Pan MD, FAASLD, FACG, MACP Professor of Medicine Division of Gastroenterology and Hepatology Department of Medicine, NYU Langone Health New York University School of Medicine,
Optimized HBV Treatment Through Baseline and on-treatment Predictor Oral Antiviral Therapy. Watcharasak Chotiyaputta
 Optimized HBV Treatment Through Baseline and on-treatment Predictor Oral Antiviral Therapy Watcharasak Chotiyaputta Progression of Liver Disease Goal of HBV Treatment: prevention the development of cirrhosis
Optimized HBV Treatment Through Baseline and on-treatment Predictor Oral Antiviral Therapy Watcharasak Chotiyaputta Progression of Liver Disease Goal of HBV Treatment: prevention the development of cirrhosis
Hepatitis B Treatment Pearls. Agenda
 Hepatitis B Treatment Pearls Fredric D. Gordon, MD Vice Chair Dept. of Transplantation and Hepatobiliary Diseases Lahey Hospital & Medical Center Associate Professor of Medicine Tufts Medical School Boston,
Hepatitis B Treatment Pearls Fredric D. Gordon, MD Vice Chair Dept. of Transplantation and Hepatobiliary Diseases Lahey Hospital & Medical Center Associate Professor of Medicine Tufts Medical School Boston,
Our better understanding of the natural
 TREATMENT OF CHRONIC HEPATITIS B: MASTERING THE BASICS ON A COMPLEX TOPIC Ke-Qin Hu, MD* ABSTRACT The availability of newer antiviral agents, as well as comprehensive treatment recommendations, has equipped
TREATMENT OF CHRONIC HEPATITIS B: MASTERING THE BASICS ON A COMPLEX TOPIC Ke-Qin Hu, MD* ABSTRACT The availability of newer antiviral agents, as well as comprehensive treatment recommendations, has equipped
Personalized treatment of hepatitis B
 pissn 2287-2728 eissn 2287-285X Review Clinical and Molecular Hepatology 2015;21:1-6 Personalized treatment of hepatitis B Anna S. Lok Division of Gastroenterology and Hepatology, University of Michigan,
pissn 2287-2728 eissn 2287-285X Review Clinical and Molecular Hepatology 2015;21:1-6 Personalized treatment of hepatitis B Anna S. Lok Division of Gastroenterology and Hepatology, University of Michigan,
An estimated 400 million people worldwide are chronically
 GASTROENTEROLOGY 2010;139:1218 1229 Tenofovir and Entecavir Are the Most Effective Antiviral Agents for Chronic Hepatitis B: A Systematic Review and Bayesian Meta-analyses GLORIA WOO,*, GEORGE TOMLINSON,*,,
GASTROENTEROLOGY 2010;139:1218 1229 Tenofovir and Entecavir Are the Most Effective Antiviral Agents for Chronic Hepatitis B: A Systematic Review and Bayesian Meta-analyses GLORIA WOO,*, GEORGE TOMLINSON,*,,
Natural History of HBV Infection
 Natural History of HBV Infection Joseph JY Sung MD PhD Institute of Digestive Disease Department of Medicine & Therapeutics Prince of Wales Hospital The Chinese University of Hong Kong HBV Infection 2
Natural History of HBV Infection Joseph JY Sung MD PhD Institute of Digestive Disease Department of Medicine & Therapeutics Prince of Wales Hospital The Chinese University of Hong Kong HBV Infection 2
Natural History of Chronic Hepatitis B
 Natural History of Chronic Hepatitis B Anna SF Lok, MD Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research University of Michigan Ann Arbor,
Natural History of Chronic Hepatitis B Anna SF Lok, MD Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research University of Michigan Ann Arbor,
MedInform. HBsAg-guided extension of Peg-IFN therapy in HBeAg-negative responders. Original Article
 HBsAg-guided extension of Peg-IFN therapy in HBeAg-negative responders Nina Nikolova, Deian Jelev, Krassimir Antonov, Lyudmila Mateva, Zahariy Krastev. University Hospital St. Ivan Rilski Sofia, Clinic
HBsAg-guided extension of Peg-IFN therapy in HBeAg-negative responders Nina Nikolova, Deian Jelev, Krassimir Antonov, Lyudmila Mateva, Zahariy Krastev. University Hospital St. Ivan Rilski Sofia, Clinic
Journal of Antimicrobial Chemotherapy Advance Access published April 25, 2013
 Journal of Antimicrobial Chemotherapy Advance Access published April 25, 213 J Antimicrob Chemother doi:1.193/jac/dkt147 Virological response to entecavir reduces the risk of liver disease progression
Journal of Antimicrobial Chemotherapy Advance Access published April 25, 213 J Antimicrob Chemother doi:1.193/jac/dkt147 Virological response to entecavir reduces the risk of liver disease progression
Chronic Hepatitis B: management update.
 Chronic Hepatitis B: management update. E.O.Ogutu Department of clinical medicine & therapeutics, University of Nairobi. Physicians meeting,kisumu 2011. Background epidemiology Chronic hepatitis B (CHB)
Chronic Hepatitis B: management update. E.O.Ogutu Department of clinical medicine & therapeutics, University of Nairobi. Physicians meeting,kisumu 2011. Background epidemiology Chronic hepatitis B (CHB)
An Update HBV Treatment
 An Update HBV Treatment Epidemiology Natural history Treatment Daryl T.-Y. Lau, MD, MPH Associate Professor of Medicine Director of Translational Liver Research Division of Gastroenterology BIDMC, Harvard
An Update HBV Treatment Epidemiology Natural history Treatment Daryl T.-Y. Lau, MD, MPH Associate Professor of Medicine Director of Translational Liver Research Division of Gastroenterology BIDMC, Harvard
Hepatitis B: Future treatment developments
 Hepatitis B: Future treatment developments VIII International Update Workshop in Hepatology Curitiba, 27.08.2016 Christoph Sarrazin St. Josefs-Hospital Wiesbaden and Goethe-University, Frankfurt am Main
Hepatitis B: Future treatment developments VIII International Update Workshop in Hepatology Curitiba, 27.08.2016 Christoph Sarrazin St. Josefs-Hospital Wiesbaden and Goethe-University, Frankfurt am Main
Treatment of chronic hepatitis B 2013 update
 22 February 213 Treatment of chronic hepatitis B 213 update Pietro Lampertico 1st Gastroenterology Unit Fondazione IRCCS Cà Granda - Ospedale Maggiore Policlinico Università di Milano EASL 212 Clinical
22 February 213 Treatment of chronic hepatitis B 213 update Pietro Lampertico 1st Gastroenterology Unit Fondazione IRCCS Cà Granda - Ospedale Maggiore Policlinico Università di Milano EASL 212 Clinical
Is there a need for combination therapy? No. Maria Buti Hospital General Universitario Valle Hebron Barcelona. Spain
 Is there a need for combination therapy? No Maria Buti Hospital General Universitario Valle Hebron Barcelona. Spain No, No and No EASL Update HBV Guidelines 2012 The most potent drugs with the optimal
Is there a need for combination therapy? No Maria Buti Hospital General Universitario Valle Hebron Barcelona. Spain No, No and No EASL Update HBV Guidelines 2012 The most potent drugs with the optimal
Long-term lamivudine therapy reduces the risk of long-term complications of chronic hepatitis B infection even in patients without advanced disease
 Antiviral Therapy 12:1295 133 Long-term lamivudine therapy reduces the risk of long-term complications of chronic hepatitis B infection even in patients without advanced disease Man-Fung Yuen, Wai-Kay
Antiviral Therapy 12:1295 133 Long-term lamivudine therapy reduces the risk of long-term complications of chronic hepatitis B infection even in patients without advanced disease Man-Fung Yuen, Wai-Kay
Recent achievements in the treatment of hepatitis B by nucleosides and nucleotides. K. Zhdanov
 EASL endorsed conference White Nights of Hepatology 2012 Adverse events during antiviral therapy: how to predict, manage and monitor June 7-8 Saint-Petersburg Recent achievements in the treatment of hepatitis
EASL endorsed conference White Nights of Hepatology 2012 Adverse events during antiviral therapy: how to predict, manage and monitor June 7-8 Saint-Petersburg Recent achievements in the treatment of hepatitis
HBeAg-negative chronic hepatitis B. with a nucleos(t)ide analogue?
 4 th PARIS HEPATITIS CONFERENCE HBeAg-negative chronic hepatitis B Why do I treat my chronic hepatitis B patients with a nucleos(t)ide analogue? George V. Papatheodoridis, MD 2nd Department of Internal
4 th PARIS HEPATITIS CONFERENCE HBeAg-negative chronic hepatitis B Why do I treat my chronic hepatitis B patients with a nucleos(t)ide analogue? George V. Papatheodoridis, MD 2nd Department of Internal
Tenofovir as a drug of choice for the chronic hepatitis B treatment
 EASL endorsed conference White Nights of Hepatology 2013 Symposium Perspectives of chronic viral hepatitis B and C treatment June 6-7 Saint-Petersburg Tenofovir as a drug of choice for the chronic hepatitis
EASL endorsed conference White Nights of Hepatology 2013 Symposium Perspectives of chronic viral hepatitis B and C treatment June 6-7 Saint-Petersburg Tenofovir as a drug of choice for the chronic hepatitis
J.C. WANG, L.L. HE, Q. CHEN 1. Introduction. Abstract. BACKGROUND: Either combination. European Review for Medical and Pharmacological Sciences
 European Review for Medical and Pharmacological Sciences Comparison of re-treatment outcomes of lamivudine plus adefovir or entecavir in chronic hepatitis B patients with viral relapse after cessation
European Review for Medical and Pharmacological Sciences Comparison of re-treatment outcomes of lamivudine plus adefovir or entecavir in chronic hepatitis B patients with viral relapse after cessation
ESCMID Online Lecture Library. by author
 Pro-Con: To stop or not to stop hepatitis B treatment? To Stop HBV Treatment Resat Ozaras, MD, Professor Istanbul University, Cerrahpasa Medical School, Infection Dept. HBV Therapy Nucleos(t)ide analogues
Pro-Con: To stop or not to stop hepatitis B treatment? To Stop HBV Treatment Resat Ozaras, MD, Professor Istanbul University, Cerrahpasa Medical School, Infection Dept. HBV Therapy Nucleos(t)ide analogues
Meta-analysis: the impact of oral anti-viral agents on the incidence of hepatocellular carcinoma in chronic hepatitis B
 Alimentary Pharmacology and Therapeutics Meta-analysis: the impact of oral anti-viral agents on the incidence of hepatocellular carcinoma in chronic hepatitis B A. K. Singal*, H. Salameh, Y.-F. Kuo & R.
Alimentary Pharmacology and Therapeutics Meta-analysis: the impact of oral anti-viral agents on the incidence of hepatocellular carcinoma in chronic hepatitis B A. K. Singal*, H. Salameh, Y.-F. Kuo & R.
Currently status of HBV therapy: efficacy and limitations
 9 November 2016 Currently status of HBV therapy: efficacy and limitations Pietro Lampertico Gastroenterology and Hepatology Unit Fondazione IRCCS Cà Granda - Ospedale Maggiore Policlinico University of
9 November 2016 Currently status of HBV therapy: efficacy and limitations Pietro Lampertico Gastroenterology and Hepatology Unit Fondazione IRCCS Cà Granda - Ospedale Maggiore Policlinico University of
Management of Chronic Hepatitis B in Asian Americans
 Management of Chronic Hepatitis B in Asian Americans Myron J Tong; UCLA, CA Calvin Q. Pan; Mount Sinai, NY Hie-Won Hann; Thomas Jefferson, PA Kris V. Kowdley; Virginia Mason, WA Steven Huy B Han; UCLA,
Management of Chronic Hepatitis B in Asian Americans Myron J Tong; UCLA, CA Calvin Q. Pan; Mount Sinai, NY Hie-Won Hann; Thomas Jefferson, PA Kris V. Kowdley; Virginia Mason, WA Steven Huy B Han; UCLA,
Chronic hepatitis B virus (HBV) infection is an important. New and Emerging Treatment of Chronic Hepatitis B
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:285 294 New and Emerging Treatment of Chronic Hepatitis B EMMET B. KEEFFE* and PATRICK MARCELLIN *Division of Gastroenterology and Hepatology, Stanford University
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:285 294 New and Emerging Treatment of Chronic Hepatitis B EMMET B. KEEFFE* and PATRICK MARCELLIN *Division of Gastroenterology and Hepatology, Stanford University
Hepatitis B. Epidemiology and Natural History and Implications for Treatment
 Hepatitis B Epidemiology and Natural History and Implications for Treatment Norah Terrault, MD Professor of Medicine and Surgery Director, Viral Hepatitis Center University of California San Francisco
Hepatitis B Epidemiology and Natural History and Implications for Treatment Norah Terrault, MD Professor of Medicine and Surgery Director, Viral Hepatitis Center University of California San Francisco
Hepatitis B virus infection (HBV) is global epidemic. Current Treatment Strategies for the Management of Chronic Hepatitis B CHRONIC HEPATITIS B
 CHRONIC HEPATITIS B Current Treatment Strategies for the Management of Chronic Hepatitis B Case Study and Commentary, Robert J. Wong, MD, and Walid S. Ayoub, MD ABSTRACT Objective: To review current treatment
CHRONIC HEPATITIS B Current Treatment Strategies for the Management of Chronic Hepatitis B Case Study and Commentary, Robert J. Wong, MD, and Walid S. Ayoub, MD ABSTRACT Objective: To review current treatment
Need for long-term evaluation of therapy in Chronic Hepatitis B
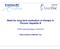 Need for long-term evaluation of therapy in Chronic Hepatitis B VHPB meeting Budapest 18/03/2010 Solko Schalm & Mehlika Toy Licensed Therapy Chronic hepatitis B Drug Date of Efficacy Disease Clinical Mortality
Need for long-term evaluation of therapy in Chronic Hepatitis B VHPB meeting Budapest 18/03/2010 Solko Schalm & Mehlika Toy Licensed Therapy Chronic hepatitis B Drug Date of Efficacy Disease Clinical Mortality
Antiviral Therapy 14:
 Antiviral Therapy 14:679 685 Original article Combination of baseline parameters and on-treatment hepatitis B virus DNA levels to start and continue patients with lamivudine therapy Man-Fung Yuen 1 *,
Antiviral Therapy 14:679 685 Original article Combination of baseline parameters and on-treatment hepatitis B virus DNA levels to start and continue patients with lamivudine therapy Man-Fung Yuen 1 *,
Perspective Hepatitis B Virus Infection: What Is Current and New
 Perspective Hepatitis B Virus Infection: What Is Current and New Hepatitis B virus (HBV) infection is a lifelong dynamic disease that can be controlled with treatment but cannot yet be cured. Risk of end-stage
Perspective Hepatitis B Virus Infection: What Is Current and New Hepatitis B virus (HBV) infection is a lifelong dynamic disease that can be controlled with treatment but cannot yet be cured. Risk of end-stage
Antiviral Therapy 2012; 17: (doi: /IMP1945)
 Antiviral Therapy 2012; 17:387 394 (doi: 10.3851/IMP1945) Original article HBV DNA level at 24 weeks is the best predictor of virological response to adefovir add-on therapy in patients with lamivudine
Antiviral Therapy 2012; 17:387 394 (doi: 10.3851/IMP1945) Original article HBV DNA level at 24 weeks is the best predictor of virological response to adefovir add-on therapy in patients with lamivudine
High Rates of Viral Suppression After Long-term Entecavir Treatment of Asian Patients With Hepatitis B e Antigen Positive Chronic Hepatitis B
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1047 1050 BRIEF COMMUNICATIONS High Rates of Viral Suppression After Long-term Entecavir Treatment of Asian Patients With Hepatitis B e Antigen Positive
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1047 1050 BRIEF COMMUNICATIONS High Rates of Viral Suppression After Long-term Entecavir Treatment of Asian Patients With Hepatitis B e Antigen Positive
Potential Efficacy of Pegylated Interferon-α and a Nucleos(t)ide Analogue as Combination Therapy for HBeAg-Positive Chronic Hepatitis B
 Gut and Liver, Vol. 10, No. 4, July 2016, pp. 611-616 ORiginal Article Potential Efficacy of Pegylated Interferon-α and a Nucleos(t)ide Analogue as Combination Therapy for HBeAg-Positive Chronic Hepatitis
Gut and Liver, Vol. 10, No. 4, July 2016, pp. 611-616 ORiginal Article Potential Efficacy of Pegylated Interferon-α and a Nucleos(t)ide Analogue as Combination Therapy for HBeAg-Positive Chronic Hepatitis
entecavir, 0.5mg and 1mg film-coated tablets and 0.05 mg/ml oral solution, Baraclude SMC No. (747/11) Bristol-Myers Squibb Pharmaceuticals Ltd
 entecavir, 0.5mg and 1mg film-coated tablets and 0.05 mg/ml oral solution, Baraclude SMC No. (747/11) Bristol-Myers Squibb Pharmaceuticals Ltd 09 December 2011 The Scottish Medicines Consortium (SMC) has
entecavir, 0.5mg and 1mg film-coated tablets and 0.05 mg/ml oral solution, Baraclude SMC No. (747/11) Bristol-Myers Squibb Pharmaceuticals Ltd 09 December 2011 The Scottish Medicines Consortium (SMC) has
Pegasys Hepatitis B. Pegasys (peginterferon alfa-2a) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.03.02 Subject: Pegasys Hepatitis B Page: 1 of 5 Last Review Date: September 18, 2015 Pegasys Hepatitis
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.03.02 Subject: Pegasys Hepatitis B Page: 1 of 5 Last Review Date: September 18, 2015 Pegasys Hepatitis
Relative predictive factors for hepatocellular carcinoma after HBeAg seroconversion in HBV infection
 PO Box 2345, Beijing 123, China World J Gastroenterol 25;11(43):6848-6852 www.wjgnet.com World Journal of Gastroenterology ISSN 17-9327 wjg@wjgnet.com E L S E V I E R 25 The WJG Press and Elsevier Inc.
PO Box 2345, Beijing 123, China World J Gastroenterol 25;11(43):6848-6852 www.wjgnet.com World Journal of Gastroenterology ISSN 17-9327 wjg@wjgnet.com E L S E V I E R 25 The WJG Press and Elsevier Inc.
Durability Of Lamivudine Associated HBe Antigen Seroconversion in Chinese-Canadian Patients with Chronic Hepatitis B Virus Infection
 ISPUB.COM The Internet Journal of Gastroenterology Volume 4 Number 2 Durability Of Lamivudine Associated HBe Antigen Seroconversion in Chinese-Canadian Patients with Chronic Hepatitis B Virus Infection
ISPUB.COM The Internet Journal of Gastroenterology Volume 4 Number 2 Durability Of Lamivudine Associated HBe Antigen Seroconversion in Chinese-Canadian Patients with Chronic Hepatitis B Virus Infection
Hepatitis B surface antigen levels: association with 5-year response to peginterferon alfa-2a in hepatitis B e-antigen-negative patients
 Hepatol Int (2013) 7:88 97 DOI 10.1007/s12072-012-9343-x ORIGINAL ARTICLE Hepatitis B surface antigen levels: association with 5-year response to peginterferon alfa-2a in hepatitis B e-antigen-negative
Hepatol Int (2013) 7:88 97 DOI 10.1007/s12072-012-9343-x ORIGINAL ARTICLE Hepatitis B surface antigen levels: association with 5-year response to peginterferon alfa-2a in hepatitis B e-antigen-negative
Beyond the Tip of the Iceberg: Strategies to Ensure Optimal HBV Screenin g, Diagnosis, and Initial Therapy
 : Strategies to Ensure Optimal HBV Screenin g, Diagnosis, and Initial Therapy Sunday, November 1, 2009 Back Bay Ballroom Sheraton Boston Hotel Boston, Massachusetts This program is supported by an educational
: Strategies to Ensure Optimal HBV Screenin g, Diagnosis, and Initial Therapy Sunday, November 1, 2009 Back Bay Ballroom Sheraton Boston Hotel Boston, Massachusetts This program is supported by an educational
Regression of fibrosis after HBV antiviral therapy. Is cirrhosis reversible?
 LIV Dispatch:.. CE: Malarvizhi Journal Code Manuscript No. No. of pages: PE: Prasanna Liver International ISSN - 0 0 0 ORIGINAL ARTICLE Regression of fibrosis after HBV antiviral therapy. Is cirrhosis
LIV Dispatch:.. CE: Malarvizhi Journal Code Manuscript No. No. of pages: PE: Prasanna Liver International ISSN - 0 0 0 ORIGINAL ARTICLE Regression of fibrosis after HBV antiviral therapy. Is cirrhosis
Challenges in therapy of chronic hepatitis B
 Journal of Hepatology 39 (2003) S230 S235 www.elsevier.com/locate/jhep Challenges in therapy of chronic hepatitis B Jay H. Hoofnagle* Division of Digestive Diseases and Nutrition, National Institute of
Journal of Hepatology 39 (2003) S230 S235 www.elsevier.com/locate/jhep Challenges in therapy of chronic hepatitis B Jay H. Hoofnagle* Division of Digestive Diseases and Nutrition, National Institute of
Chronic HBV Management in 2013
 Chronic HBV Management in 2013 Mohammad Hossein Somi MD Professor of Gastroentrology and hepatology Liver and Gastrointestinal Disease Research Center Tabriz University of Medical Sciences 1 HBV in 2013
Chronic HBV Management in 2013 Mohammad Hossein Somi MD Professor of Gastroentrology and hepatology Liver and Gastrointestinal Disease Research Center Tabriz University of Medical Sciences 1 HBV in 2013
Entecavir Maintains a High Genetic Barrier to HBV Resistance Through 6 Years in Naïve Patients
 Entecavir Maintains a High Genetic Barrier to HBV Resistance Through 6 Years in Naïve Patients D.J. Tenney 1, K.A. Pokorowski 1, R.E. Rose 1, C.J. Baldick 1, B.J. Eggers 1, J. Fang 1, M.J. Wichroski 1,
Entecavir Maintains a High Genetic Barrier to HBV Resistance Through 6 Years in Naïve Patients D.J. Tenney 1, K.A. Pokorowski 1, R.E. Rose 1, C.J. Baldick 1, B.J. Eggers 1, J. Fang 1, M.J. Wichroski 1,
Off-Therapy Durability of Response to Entecavir Therapy in Hepatitis B e Antigen-Negative Chronic Hepatitis B Patients
 VIRAL HEPATITIS Off-Therapy Durability of Response to Entecavir Therapy in Hepatitis B e Antigen-Negative Chronic Hepatitis B Patients Wen-Juei Jeng, 1,2 I-Shyan Sheen, 1,2 Yi-Cheng Chen, 1,2 Chao-Wei
VIRAL HEPATITIS Off-Therapy Durability of Response to Entecavir Therapy in Hepatitis B e Antigen-Negative Chronic Hepatitis B Patients Wen-Juei Jeng, 1,2 I-Shyan Sheen, 1,2 Yi-Cheng Chen, 1,2 Chao-Wei
Alam MM 1, Mahtab MA 1, Akbar SMF 2, Kamal M 3, Rahman S 1
 Bangladesh Med Res Counc Bull 2014; 40: 92-56 Hepatic necroinflammation and severe liver fibrosis in patients with chronic hepatitis B with undetectable HBV DNA and persistently normal alanine aminotransferase
Bangladesh Med Res Counc Bull 2014; 40: 92-56 Hepatic necroinflammation and severe liver fibrosis in patients with chronic hepatitis B with undetectable HBV DNA and persistently normal alanine aminotransferase
Gish RG and AC Gadano. J Vir Hep
 Treatment in Hepatitis B and C There are options! Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s Hepatitis B Virus Epidemiology and natural history 400
Treatment in Hepatitis B and C There are options! Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s Hepatitis B Virus Epidemiology and natural history 400
New therapeutic strategies in HBV patients
 New therapeutic strategies in HBV patients Philippe HALFON MD, PhD Associate Professor of Medecine Internal Medecine and Infectious Diseases, Hopital Europeen, Marseille, France. NUC + PEG IFN, HBsAg Clearance
New therapeutic strategies in HBV patients Philippe HALFON MD, PhD Associate Professor of Medecine Internal Medecine and Infectious Diseases, Hopital Europeen, Marseille, France. NUC + PEG IFN, HBsAg Clearance
Hepatitis B therapy FOCUS ON VIRAL HEPATITIS. Hellan Kwon and Anna S. Lok
 FOCUS ON VIRAL HEPATITIS Hepatitis B therapy Hellan Kwon and Anna S. Lok Abstract The goal of hepatitis B treatment is to prevent cirrhosis, liver decompensation and hepatocellular carcinoma. In clinical
FOCUS ON VIRAL HEPATITIS Hepatitis B therapy Hellan Kwon and Anna S. Lok Abstract The goal of hepatitis B treatment is to prevent cirrhosis, liver decompensation and hepatocellular carcinoma. In clinical
Clinical impact of the early alanine amininotransferase flare during tenofovir monotherapy in treatment-naïve patients with chronic hepatitis B
 pissn 2287-2728 eissn 2287-285X Original Article Clinical and Molecular Hepatology 217;23:154-159 Clinical impact of the early alanine amininotransferase flare during tenofovir monotherapy in treatment-naïve
pissn 2287-2728 eissn 2287-285X Original Article Clinical and Molecular Hepatology 217;23:154-159 Clinical impact of the early alanine amininotransferase flare during tenofovir monotherapy in treatment-naïve
Title: Off therapy durability of response to Entecavir therapy in hepatitis B e
 Title: Off therapy durability of response to Entecavir therapy in hepatitis B e antigen negative chronic hepatitis B patients Wen-Juei Jeng, MD 1,3, I-Shyan Sheen, MD 1-3, Yi-Cheng Chen, MD 1,3, Chao-Wei
Title: Off therapy durability of response to Entecavir therapy in hepatitis B e antigen negative chronic hepatitis B patients Wen-Juei Jeng, MD 1,3, I-Shyan Sheen, MD 1-3, Yi-Cheng Chen, MD 1,3, Chao-Wei
Hepatitis B virus (HBV) is a major public health
 Hepatocellular Carcinoma Risk in Chronic Hepatitis B Virus Infected Compensated Cirrhosis Patients With Low Viral Load Dong Hyun Sinn, 1 Junggyu Lee, 1 Juna Goo, 2 Kyunga Kim, 2 Geum-Youn Gwak, 1 Yong-Han
Hepatocellular Carcinoma Risk in Chronic Hepatitis B Virus Infected Compensated Cirrhosis Patients With Low Viral Load Dong Hyun Sinn, 1 Junggyu Lee, 1 Juna Goo, 2 Kyunga Kim, 2 Geum-Youn Gwak, 1 Yong-Han
Hepatitis B Update. Jorge L. Herrera, M.D. University of South Alabama Mobile, AL. Gastroenterology
 Hepatitis B Update Jorge L. Herrera, M.D. University of South Alabama Mobile, AL Deciding Who to Treat Is hepatitis B a viral disease or a liver disease? Importance of HBV-DNA Levels in the Natural History
Hepatitis B Update Jorge L. Herrera, M.D. University of South Alabama Mobile, AL Deciding Who to Treat Is hepatitis B a viral disease or a liver disease? Importance of HBV-DNA Levels in the Natural History
Drug Class Monograph
 Drug Class Monograph Class: Chronic Hepatitis B Drug: Baraclude (entecavir), Epivir (lamivudine), Hepsera (adefovir), Intron A (interferon alfa- 2b), Pegasys (peginterferon alfa-2a), Tyzeka (telbivudine),
Drug Class Monograph Class: Chronic Hepatitis B Drug: Baraclude (entecavir), Epivir (lamivudine), Hepsera (adefovir), Intron A (interferon alfa- 2b), Pegasys (peginterferon alfa-2a), Tyzeka (telbivudine),
MedInform. HBV DNA loss in Bulgarian patients on NUC therapy. Speed related factors. (NUC related speed of HBV DNA loss in Bulgaria) Original Article
 DOI: 10.18044/Medinform.201852.897 ISSUE 3, 2018 HBV DNA loss in Bulgarian patients on NUC therapy. Speed related factors. (NUC related speed of HBV DNA loss in Bulgaria) Donika Krasteva, Radosveta Tomova,
DOI: 10.18044/Medinform.201852.897 ISSUE 3, 2018 HBV DNA loss in Bulgarian patients on NUC therapy. Speed related factors. (NUC related speed of HBV DNA loss in Bulgaria) Donika Krasteva, Radosveta Tomova,
C hronic hepatitis B (CHB) virus infection affects more
 161 HEPATITIS Prognostic determinants for chronic hepatitis B in Asians: therapeutic implications MF Yuen, HJ Yuan, D KH Wong, J CH Yuen, WM Wong, A OO Chan, B CY Wong, KC Lai, CL Lai... See end of article
161 HEPATITIS Prognostic determinants for chronic hepatitis B in Asians: therapeutic implications MF Yuen, HJ Yuan, D KH Wong, J CH Yuen, WM Wong, A OO Chan, B CY Wong, KC Lai, CL Lai... See end of article
Despite the availability of highly effective and safe vaccines REVIEW
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:890 897 REVIEW Report of an International Workshop: Roadmap for Management of Patients Receiving Oral Therapy for Chronic Hepatitis B EMMET B. KEEFFE,* STEFAN
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:890 897 REVIEW Report of an International Workshop: Roadmap for Management of Patients Receiving Oral Therapy for Chronic Hepatitis B EMMET B. KEEFFE,* STEFAN
Hepatitis B Prior Authorization Policy
 Hepatitis B Prior Authorization Policy Line of Business: Medi-Cal P&T Approval Date: November 15, 2017 Effective Date: January 1, 2018 This policy has been developed through review of medical literature,
Hepatitis B Prior Authorization Policy Line of Business: Medi-Cal P&T Approval Date: November 15, 2017 Effective Date: January 1, 2018 This policy has been developed through review of medical literature,
Original article Partial virological response to entecavir in treatment-naive patients with chronic hepatitis B
 Antiviral Therapy 2011; 16:469 477 (doi: 10.3851/IMP1772) Original article Partial virological response to entecavir in treatment-naive patients with chronic hepatitis B Young Eun Chon 1, Seung Up Kim
Antiviral Therapy 2011; 16:469 477 (doi: 10.3851/IMP1772) Original article Partial virological response to entecavir in treatment-naive patients with chronic hepatitis B Young Eun Chon 1, Seung Up Kim
Landmarks for Prevention and Treatment
 HBeAg-positive chronic hepatitis B Why do I treat my patient with a nucleos(t)ide analogue? Dr. Nancy Leung BSc(Lon) MSc(Lon) MBBS(Lon) MD(Lon), FRCP(Lon) FRCP(Edin) FHKCP FHKAM Consultant Physician, Alice
HBeAg-positive chronic hepatitis B Why do I treat my patient with a nucleos(t)ide analogue? Dr. Nancy Leung BSc(Lon) MSc(Lon) MBBS(Lon) MD(Lon), FRCP(Lon) FRCP(Edin) FHKCP FHKAM Consultant Physician, Alice
Hepatitis B and D Update on clinical aspects
 Hepatitis B and D Update on clinical aspects B. Müllhaupt Gastroenterology and Hepatology Swiss Transplant and HPB-Center University Hospital Zurich beat.muellhaupt@usz.ch B.M. 11.11.17 Hepatitis Strategy
Hepatitis B and D Update on clinical aspects B. Müllhaupt Gastroenterology and Hepatology Swiss Transplant and HPB-Center University Hospital Zurich beat.muellhaupt@usz.ch B.M. 11.11.17 Hepatitis Strategy
Hepatitis B virus (HBV) infection is a global
 VIRAL HEPATITIS Serum Hepatitis B Surface Antigen Levels Help Predict Disease Progression in Patients With Low Hepatitis B Virus Loads Tai-Chung Tseng, 1,3,8 Chun-Jen Liu, 2,3 Hung-Chih Yang, 2,6 Tung-Hung
VIRAL HEPATITIS Serum Hepatitis B Surface Antigen Levels Help Predict Disease Progression in Patients With Low Hepatitis B Virus Loads Tai-Chung Tseng, 1,3,8 Chun-Jen Liu, 2,3 Hung-Chih Yang, 2,6 Tung-Hung
Dual Therapy for Chronic Hepatitis B Virus
 Dual Therapy for Chronic Hepatitis B Virus Hussien Elsiesy, MD, and Douglas Dieterich, MD Corresponding author Douglas Dieterich, MD Division of Liver Diseases, Mount Sinai School of Medicine, One Gustave
Dual Therapy for Chronic Hepatitis B Virus Hussien Elsiesy, MD, and Douglas Dieterich, MD Corresponding author Douglas Dieterich, MD Division of Liver Diseases, Mount Sinai School of Medicine, One Gustave
Chronic hepatitis B virus (HBV) infection remains a major
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:541 545 Hepatitis B Virus DNA Level Predicts Hepatic Decompensation in Patients With Acute Exacerbation of Chronic Hepatitis B WEN JUEI JENG, I SHYAN SHEEN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:541 545 Hepatitis B Virus DNA Level Predicts Hepatic Decompensation in Patients With Acute Exacerbation of Chronic Hepatitis B WEN JUEI JENG, I SHYAN SHEEN,
Don t interfere My first choice is always nucs!
 Don t interfere My first choice is always nucs! Robert G Gish MD Professor Consultant Stanford University Medical Director, Hepatitis B Foundation Singapore Viral Hepatitis Meeting 2014 1 Disclosures Dr
Don t interfere My first choice is always nucs! Robert G Gish MD Professor Consultant Stanford University Medical Director, Hepatitis B Foundation Singapore Viral Hepatitis Meeting 2014 1 Disclosures Dr
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance
 Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
Hepatocellular Carcinoma: Can We Slow the Rising Incidence?
 Hepatocellular Carcinoma: Can We Slow the Rising Incidence? K.Rajender Reddy M.D. Professor of Medicine Director of Hepatology Medical Director of Liver Transplantation University of Pennsylvania Outline
Hepatocellular Carcinoma: Can We Slow the Rising Incidence? K.Rajender Reddy M.D. Professor of Medicine Director of Hepatology Medical Director of Liver Transplantation University of Pennsylvania Outline
