Effect of the US National HIV/AIDS Strategy targets for improved HIV care engagement: a modelling study
|
|
|
- Steven Rogers
- 5 years ago
- Views:
Transcription
1 Effect of the US National HIV/AIDS Strategy targets for improved HIV care engagement: a modelling study Maunank Shah, Johns Hopkins University Allison Perry, Johns Hopkins University Kathryn Risher, Johns Hopkins University Sunaina Kapoor, Johns Hopkins University Jeremy Grey, Emory University Akshay Sharma, Emory University Eli Rosenberg, Emory University Carlos Del Rio, Emory University Patrick Sullivan, Emory University David W. Dowdy, Johns Hopkins University Journal Title: Lancet HIV Volume: Volume 3, Number 3 Publisher: Elsevier: Lancet , Pages E140-E146 Type of Work: Article Post-print: After Peer Review Publisher DOI: /S (16) Permanent URL: Final published version: Copyright information: 2016 Elsevier Ltd. This is an Open Access work distributed under the terms of the Creative Commons Attribution 4.0 International License ( Accessed August 20, :13 AM EDT
2 HHS Public Access Author manuscript Published in final edited form as: Lancet HIV March ; 3(3): e140 e146. doi: /s (16) Quantifying the impact of the National HIV/AIDS strategy targets for improved HIV care engagement in the US: a modelling study Maunank Shah 1, Allison Perry 2, Kathryn Risher 3, Sunaina Kapoor 1, Jeremy Grey 4, Akshay Sharma 4, Eli S Rosenberg 4, Carlos Del Rio 4,*, Patrick Sullivan 4,*, and David W. Dowdy 3 1 Johns Hopkins University School of Medicine, Baltimore, MD 2 Johns Hopkins University, Krieger School of Arts and Sciences, Baltimore, MD 3 Johns Hopkins Bloomberg School of Public Health, Baltimore, MD 4 Emory University Rollins School of Public Health, Atlanta, GA Structured Summary Background The recently updated White House National HIV/AIDS Strategy (NHAS) includes specific progress indicators for improving the HIV care continuum, but the economic and epidemiological impact of achieving those indicators remains unclear. This manuscript version is made available under the CC BY-NC-ND 4.0 license. Corresponding author: Maunank Shah, MD PhD, Johns Hopkins University, School of Medicine, Department of Medicine, Division of Infectious Diseases, 725 N. Wolfe St. PCTB building-224. Baltimore, MD, USA 21205, Phone: Fax: , mshah28@jhmi.edu. * Full professors Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain. Research in Context: Evidence before this study: We searched PubMed to identify studies related to the National HIV/AIDS strategy (NHAS), and mathematical models of the care continuum in the US. We searched terms ( HIV or AIDS ) and ( National HIV/AIDS strategy or model or continuum ) and included all studies published from 2010 (initial NHAS release) until November 16, 2015 without language restrictions. Our search identified no models or epidemiological studies related to the recently updated US National HIV/ AIDS strategy. Our search identified one cost-effectiveness analysis of the prior 2010 NHAS linkage to care target, that showed improved early linkage would cost an extra $62,200 per QALY-gained. Our prior mathematical model of HIV transmission in the US suggested that improving yearly rates of retention in care by 50% could avert 35% of new infections. Added Value of this Study Our results demonstrate that achieving the updated NHAS progress indicators of 90% awareness of HIV serostatus, 85% rapid linkage, and 90% of diagnosed individuals in care by 2020 could allow the United States to reach NHAS epidemiological goals and halve new infections over 10 years with eventual reductions in HIV prevalence. The primary driver of this achievement (and also the progress indicator furthest from being met) is retention in care. Meeting NHAS care targets would require an increase of $105 billion of HIV care costs compared to continuation of current practice; the majority of these additional costs represent ART costs for PLWH who are not currently virally suppressed. Implications of all the available evidence: The evidence suggests that continuous retention in care is critical for long term success in HIV treatment. Meeting the NHAS progress indicators for improved HIV screening, linkage, and care-engagement could alter the trajectory of the US HIV epidemic, but will require continued and increased investment. ART drug prices are the most influential drivers of cost in meeting the goals of improving HIV care engagement. Contributors: MS, ESR, DWD, and PS conceived and designed the study and led manuscript writing. CDR assisted with data interpretation and manuscript writing. MS, AP, KR and DD executed the study and performed data analysis. SK, AS and JG assisted with manuscript writing, literature search, and data collection. Declarations of interest: The authors declare they have no conflicts of interest or financial interests in connection to this work.
3 Shah et al. Page 2 Methods We constructed a dynamic transmission model of HIV progression and care engagement to project HIV incidence, prevalence, mortality, and costs among adults in the United States over ten years. We specifically considered achievement of the 2020 targets set forth in NHAS progress indicator 1 (90% awareness of serostatus), indicator 4 (85% linkage within one month), and indicator 5 (90% of diagnosed individuals in care). Finding At current rates of engagement in the HIV care continuum, we project 524,000 (95% Uncertainty Range 442, ,000) new HIV infections and 375,000 deaths (364, ,000) between 2016 and Achieving NHAS progress indicators 1 and 4 has modest epidemiologic impact (new infections reduced by 2 0% and 3 9%, respectively). By contrast, increasing the proportion of diagnosed individuals in care (indicator 5) averts 52% (47-56%) of new infections. Achieving all NHAS targets resulted in a 58% reduction (52%-61%) in new infections and 128,000 lives saved (106, ,000) at an incremental health system cost of $105 billion dollars. Interpretation Achievement of NHAS progress indicators for screening, linkage, and particularly improving retention in care, can substantially reduce the burden of HIV in the United States. Introduction Since the HIV care continuum in the United States (US) was first described 1, stakeholders at the federal, state and local levels have sought to identify and address gaps at each step of the cascade. These steps include HIV diagnosis, linkage to medical care, retention, prescription of antiretroviral therapy [ART], and viral suppression. Broader screening and early ART initiation have been shown to confer both therapeutic and preventive benefits 2, 3. However, 2012 figures from the Centers for Disease Control and Prevention (CDC) indicate that of the estimated 1 2 million people living with HIV (PLWH) in the US, approximately one out of eight remained unaware of their infection, and only three out of ten achieved viral suppression 4. Given that more than 90% of transmissions have been estimated to be attributable to PLWH who were either undiagnosed or not retained in medical care 5, the need for sustained and coordinated efforts along the continuum is tremendous. In 2013, the HIV Care Continuum Initiative was established to accelerate progress towards specific quantitative goals outlined in the first comprehensive National HIV/AIDS Strategy (NHAS) 6. The White House recently updated the NHAS care continuum targets to 90% of PLWH knowing their serostatus (progress indicator 1), 85% of newly diagnosed individuals linking to clinical care within one month of their diagnosis (progress indicator 4), and 90% of diagnosed individuals engaged in HIV medical care (progress indicator 5) 7. These align closely with the Joint United Nations Programme on HIV/AIDS (UNAIDS) ambitious targets seeking to end the epidemic as a major global health threat by The current 2015 NHAS additionally contains two epidemiological targets: reduction in the number of new HIV diagnoses of at least 25% by 2020 (progress indicator 2) and a reduction in mortality among persons diagnosed with HIV of 33% (progress indicator 8). However, the extent to which achieving revised NHAS progress indicators for improved screening, linkage, and care engagement would advance progress toward these
4 Shah et al. Page 3 Methods Model description Statistical Anlaysis epidemiological targets, and the magnitude of resources required to achieve desired levels of coverage have not yet been quantified. Therefore, we constructed a dynamic transmission model to project incident HIV infections, prevalence, mortality, and health care costs over the next ten years ( ). For each outcome, we modeled the impact of attaining the three 2020 national progress indicators for serostatus awareness, linkage to care, and retention. The Johns Hopkins HIV economic-epidemic model (JHHEM) 9, 10 is a compartmental model of the US HIV epidemic that incorporates transmission, disease progression, and health system engagement. A full description has been published previously 9. Briefly, our model partitions the adult population (18 to 78 years) of the US based on sex, age, HIV infection, and transmission category (heterosexuals, men who have sex with men [MSM], and people who inject drugs [PWID]). PLWH are further characterized by CD4 strata and location on the HIV care continuum (e.g. unaware of HIV status, aware but out of care, in care but not on ART, on ART but not virologically suppressed, and virologically suppressed). HIV infection, transition through the care continuum, and demographic changes are modeled dynamically as a system of ordinary differential equations 9. The model parameters (Table 1) 3, were updated and calibrated to reflect most recent CDC data on the US HIV epidemic and continuum of care 4, 9, 19 (Supplement). The model incorporates HIV transmission through sex (heterosexual or male homosexual) and through needle sharing. We explicitly modeled rates of annual HIV testing, initial linkage to care, discontinuation and reengagement in care, and ART initiation, calibrating those rates to reflect current national estimates of engagement in the continuum of care19, 20 (Supplemental Figure 3). To determine transmission probabilities during model calibration (average yearly partnerships and probability of transmission per partnership), we brought the model to equilibrium in 2006 and then allowed population growth, identifying parameter values in an iterative process for which the model outputs best reflected epidemiologic data on incidence and prevalence between (model projections and CDC estimates shown in Supplemental Figure 2 4, 19 ). Our primary outcomes were HIV incidence, prevalence, mortality and health care costs over a 10-year time horizon. In the base-case, we assumed implementation of updated guidelines that ART be initiated regardless of CD4 count 21, but with continuation of current trends in the HIV care continuum 19, 20. We then estimated the epidemiologic and economic impact of reaching targets set forth in the new NHAS progress indicators (indicators 1, 4, and 5 either individually or in combinations) by 2020 by comparing the following scenarios to the base-case: NHAS Indicator 1 Increase the percentage of PLWH who know their serostatus to at least 90% : We increased annual testing rates for high-risk individuals (MSM, PWID, and heterosexuals aged years old), with ongoing screening at current
5 Shah et al. Page 4 rates in the general population, to a level that would achieve 90% serostatus awareness by During model calibration of intervention scenarios, this corresponded to an approximate 50% increase compared to current annual testing rates among MSM, PWID, and young heterosexuals (Supplement). NHAS Indicator 4 Increase the percentage of newly diagnosed persons linked to HIV medical care within 1 month of their HIV diagnosis to at least 85% : We increased the proportion of newly diagnosed persons completing an HIV care visit within a month to 85% by NHAS Indicator 5 Increase the percentage of persons with diagnosed HIV infection who are retained in HIV medical care to at least 90% : We iteratively decreased the annual rate of disengagement in care (from 18-25% per year [depending on risk group] in the base-case to 4-6% per year), and increased the rate of reengagement in care among those out of care (from 12 5% per year to 50% per year), until the point that the proportion of serostatus-aware PLWH engaged in care was 90% in 2020 (Supplement). Costs were calculated from a health-system perspective with a unit-costing (Table 1) approach that considers the person-time spent in each model compartment (e.g., person-time on ART) and the number of transitions between compartments (e.g. transition from unaware to aware as a result of HIV testing). In the base-case, we considered costs related to HIV testing, linkage referrals, and clinical care (e.g. viral loads, genotypes, ART usage, hospitalizations). We additionally included costs of existing retention in care services, based on staffing for social work, nurse-managers, and case-managers at local HIV clinics (basecase, $300 per patient in care per year [range $50-$1500]) 9. All costs are reported in 2015 US dollars; future costs were discounted at an annual rate of 3% 22. Estimates of disease burden (e.g., infections or deaths) averted are reported without discounting. In primary analysis we did not consider infrastructural or programmatic costs of interventions to improve the HIV care continuum. However, costs related to increased health care utilization when achieving NHAS targets as a result of increased care-engagement were incorporated (e.g. increased numbers of tests, increased ART usage). We explored a range of intervention costs in secondary analyses. We conducted a probabilistic uncertainty analysis by simultaneously varying all parameter values over beta distributions bounded by their ranges (Table 1). We report 95% uncertainty ranges (URs) as the 2 5 th and 97 5 th percentile of those simulations. We performed all analyses using R version 3 0 1(R Foundation for Statistical Computing). Role of the funding source The sponsors of the study had no role in study design, data collection, data analysis, data interpretation, or writing of the report. The corresponding author had full access to all the data in the study and had final responsibility for the decision to submit for publication.
6 Shah et al. Page 5 Results If the current rates of screening, linkage, and retention in care as part of the US HIV care continuum persists, approximately 524,000 (95%UR 442, ,000) new HIV infections would occur between 2016 and 2025 (Figure 1), with approximately 375,000 deaths (from all causes) among PLWH (95%UR 364, ,000). This results in a projected prevalence of 1 47 million PLWH in 2025, of whom 39 7% (582,000) would be virally suppressed. HIV care would cost the US health system $254 billion (95%UR $186 billion - $297 billion) with 3% discounting (Table 2) over the next decade ($295 billion without discounting). The epidemiologic and economic impact of achieving the three 2020 NHAS targets for improving HIV awareness (progress indicator 1), linkage to care (progress indicator 4), and retention in care (progress indicator 5) is shown in Table 2 and Figure 1. Increasing screening rates to allow achievement of NHAS indicator 1 (90% serostatus awareness by 2020) would avert 10,600 new HIV infections (95%UR 6,000-18,000), or a 2 0% reduction (95%UR 1 1%-2 8%) over the next 10 years. However, improved screening alone has little impact on overall number of PLWH achieving viral suppression (589,000 of 1 46 million PLWH, 40 3%) in Consequently, enhanced screening would avert only 0 4% (1400) of deaths among PLWH during the analysis period, if current rates of care retention persist. If 85% of those newly diagnosed with HIV were linked to care within 1 month (NHAS indicator 4), with current rates of screening and retention in care, the US would avert an estimated 20,600 (95%UR 14,000-35,000) HIV infections (3 9% reduction, 95%UR ), and would avert 11,600 (95%UR 8,000-25,000) deaths (3 1% reduction; 95%UR 2 0%-4 9). In isolation, improved linkage would increase the percent of total PLWH that are virally suppressed to 41 1% (598,000 of 1 46 million PLWH). Achieving the retention in care targets in NHAS progress indicator 5 (90% of diagnosed persons in care) was projected to avert a much larger disease burden: a 52 3% reduction (95%UR 47-56%) in HIV infections (274,000 infections averted, 95%UR 220, ,000) and a 31 7% reduction (95%UR 24%-39%) in deaths (119,000 lives saved, 95%UR 94, ,000) over 10 years (with 76 6% [999,000 of 1 30 million] of all PLWH virally suppressed), even at current rates of serostatus awareness and linkage to care. Simultaneously improving all aspects of the HIV care continuum to reach all three NHAS care targets increased the estimated point prevalence of virological suppression among all PLWH (1.01 million of 1.29million PLWH) in 2025 from the base-case of 39 7% to 78 8% (82% of those diagnosed [1.24million]). Consequently, this scenario resulted in a 57 7% reduction (95%UR 52%-61%) in HIV infections (302,000 HIV infections averted, 95%UR 240, ,000) and a 34 3% reduction (95% UR 26%-41%) in deaths (128,000 lives saved, 95%UR 106, ,000) (Table 2, Supplemental Figure 5). The increased testing, care-engagement, and ART usage if all NHAS care targets are met is projected to cost $105 billion more over 10 years (with 3% discounting; $124 billion incremental increase without discounting) than if current levels of the HIV care continuum persisted (Table 2, Supplemental Figure 6).
7 Shah et al. Page 6 DISCUSSION In one-way sensitivity analysis, total costs were most influenced by ART prices (Supplemental Figure 7 and 8). If ART prices could be reduced to the $10,000 per personyear, costs in the current care continuum scenario dropped from $254 billion to $107 billion dollars; alternatively, if ART regimen costs rose to $45,000 per person-year, costs increased to $341 billion over 10 years. The incremental cost to achieve all NHAS care continuum targets likewise primarily reflected the costs related to increased ART usage (range of incremental NHAS achievement cost of $26 billion to $152 billion, for ART costs of $10,000 to $45,000 per person-year, respectively). In a secondary analysis, we estimated health system costs inclusive of hypothetical intervention costs that would allow increased care engagement to achieve NHAS progress indicators. We explored up to a 20% increase in testing costs, along with an additional $500 per person linking to care, additional $5,000 per person-year to improve retention in care (above current retention costs), and $1,000 per person re-engaged in care. In this scenario, the total costs (with 3% discounting) of achieving all three NHAS care targets (NHAS 1, 4 and 5) was $408 billion (an increase of $49 billion [13 6% increase] compared to our primary NHAS analysis [without intervention costs], and an incremental increase of $154 billion over the scenario of continued current continuum of care). The US NHAS was updated in July 2015 with a vision to reduce new infections and provide high quality care for PLWH. Our model projects that there will be more than half million new HIV infections in the next decade if improvements to diagnosis and care are not realized. By contrast, our results suggest that this number can be cut by almost 60%, resulting in over 125,000 lives saved, if comprehensive steps are taken to achieve 2020 targets for screening, linkage and care-engagement set forth in NHAS progress indicators. The primary gap in the current continuum of care is in care retention, which is needed to realize the prevention and health benefits of ART usage and viral suppression; achieving the NHAS goal of engaging 90% of those diagnosed in care could halve the number of HIV infections over the next 10 years. These results offer credence to the importance of achieving the NHAS progress indicators in order to bend the curve of the HIV epidemic. Currently, CDC estimates that over 85% of PLWH are aware of their serostatus, and there are recommendations to increase HIV screening among high-risk groups 19, 23. As such, our modeling efforts found that incrementally increasing HIV diagnoses alone to meet NHAS targets (90% awareness by 2020), has relatively little impact on the overall HIV epidemic. The NHAS additionally outlines the need to increase the percentage of diagnosed PLWH who are virally suppressed to at least 80%. We found that increased screening and linkage alone is insufficient to meet this goal, due to inadequate long-term ART usage. By contrast, the effects of improved HIV screening and linkage could be greatly enhanced if coupled with improved care retention. Under the most intensive scenario, wherein screening, linkage, and proportion of PLWH in care are improved to meet the NHAS goals, nearly 82% of diagnosed PLWH are expected to be virally suppressed, exceeding the NHAS targets for viral suppression.
8 Shah et al. Page 7 The NHAS has also set ambitious epidemiological goals, including a 25% reduction in HIV diagnoses (as a surrogate for incident infections) and a 33% reduction in mortality among (diagnosed) PLWH by Our results suggest that both of these goals are within reach, but only by redoubling efforts to improve care retention. In particular, only when incorporating scenarios with a high proportion of PLWH in care do we observe significant declines in incidence (and mortality), with eventual reductions in the total number of PLWH over time. These results suggest that a change in thinking about the HIV response is necessary if we are to meaningfully bend the curve of HIV transmission. To date, most studies have evaluated the HIV care continuum cross-sectionally. However, continuous retention is required for long-term success in HIV treatment 24. Specifically identifying evidence-based interventions to improve long term retention and close this gap in the HIV care continuum 25 must be recognized as an urgent priority. Interventions such as housing assistance, case management, or opioid substitution therapy can be helpful, but ultimately we must develop a comprehensive, patient-centered approach to retention and reengagement in care that considers the diverse needs of PLWH and seeks to meet those needs in holistic fashion. Losing a patient to HIV care should be considered a sentinel event, with necessary structures put in place to prevent such events from ever occurring. Our results also highlight the financial resources that are likely required to achieve these ambitious goals. Currently, the federal domestic HIV budget is $25 3 billion for fiscal year 2016 (21% increase since 2010) 26, a funding rate consistent with model projections of total HIV health system costs ($254 billion) over the next decade if the current HIV care continuum persists. In order to achieve levels of care retention necessary to change the trajectory of HIV epidemiology in the US, a similar restructuring in thinking regarding funding of the HIV/AIDS response may be required. Specifically, we estimate that achieving NHAS targets for serostatus awareness, linkage to care, and retention in care would cost an incremental $105 billion in health care costs alone over 10 years, representing an over 40% increase in expenditures the vast majority of which represent additional costs of ART associated with a greater number of PLWH engaged in care. Thus, if we are to succeed in curbing transmission, we must also reframe our approach to funding the HIV response, seeking innovative and targeted funding mechanisms to facilitate this long term treatment and retention. Reducing ART costs through such mechanisms as 430B pricing, ADAP programs, and generic manufacturing of key drugs could offer marked health system cost savings.. Efforts to both expand funding for HIV care, including ancillary services and interventions to promote long term retention, and lower the costs of ART must both be prioritized. Our results build on other models of HIV transmission in the US. A study assessing the impact of the original NHAS (2010) linkage goals found a similarly small impact of linkage interventions on transmission 27. Compared to other authors 28, our results suggest a relatively more modest impact on HIV incidence of expanded screening interventions. The current results also expand on prior efforts by our group to evaluate the impact of the care continuum on HIV transmission in the US 5, 9. We now provide updated projections of incidence and prevalence incorporating recently revised estimates of HIV epidemiology and the care continuum 4, 19, and quantify the economic and epidemiologic impact of achieving targets for care engagement within NHAS progress indicators.
9 Shah et al. Page 8 Our study has several limitations. For all scenarios, we assume that PLWH will have timely access to ART after entry into care, as per current guidelines. Delays or gaps in therapy would lessen the impact of increased care engagement. Our model is also calibrated to currently available national estimates of engagement in the care continuum 19. Data from large city and county programs have generally suggested more optimistic estimates of current HIV care engagement and viral suppression 29, 30. To the extent that engagement in care and viral suppression in our base-case scenario are underestimated, the incremental impact of achieving NHAS targets may be more modest, and our model may be optimistically biased. Bias in our model estimates may also result from applying nationally representative numbers to any specific city or locale. Nonetheless, our model provides absolute, in addition to relative, projections on incidence and prevalence with uncertainty ranges under various engagement in care scenarios, while reinforcing the importance of accurate national continuum of care estimates. Our model did not evaluate specific interventions (or associated costs) that will likely be needed to achieve NHAS targets. Efforts to improve testing, linkage, and improve adherence or care-engagement will almost certainly require a combination of health system, policy, and clinical innovations. Nonetheless, we conducted secondary analyses to explore costs inclusive of hypothetical HIV care continuum interventions and found modest relative to the health system costs attributable to increased ART usage and clinical care expected to incur with achieving NHAS targets. Our model also found a significant number of new infections despite achievement of comprehensive improvements to screening, linkage, and care engagement, suggesting that additional prevention strategies may be needed to reduce transmissions further. Our model does not address the potential costs and effects of scale up of preexposure prophylaxis (PrEP), or other such prevention interventions that fall outside the care continuum. Improved HIV serostatus awareness with consequent consistent PrEP utilization could further decrease transmission among high risk groups, but could also substantially increase prevention costs. In conclusion, our results offer quantitative evidence of the extent to which achievement of NHAS targets for improving HIV testing, linkage, and care-engagement impacts the parallel NHAS goals of reducing HIV incidence and prevalence. As the US moves to implement the new NHAS, our model suggests that sustained improvements to retention in care must be the highest priority to reach the ambitious epidemiological targets for reduced HIV incidence and prevalence. Supplementary Material Acknowledgments Refer to Web version on PubMed Central for supplementary material. Funding The authors declare that they have no conflicts of interest or relevant financial interests or activities in relationship to this manuscript. This work was supported by funds from the National Institute of Allergy and Infectious Diseases, National Institutes of Health, under grant # K23AI089259, and T32AI102623, the B. Frank and Kathleen Polk Assistant Professorship in Epidemiology, and the Emory University Center for AIDS Research (P30 AI050409). Funders had no role in the design or conduct of the study, analysis or interpretation of the results,
10 Shah et al. Page 9 REFERENCES manuscript writing or decision to publish results. We acknowledge support from the CDC/NCHHSTP Epidemiological and Economic Modeling Agreement (5U38PS004646). The findings and conclusions in this report are those of the authors and do not necessarily represent the views of the Centers for Disease Control and Prevention. 1. Gardner EM, McLees MP, Steiner JF, del Rio C, Burman WJ. The Spectrum of Engagement in HIV Care and its Relevance to Test-and-Treat Strategies for Prevention of HIV Infection. Clinical Infectious Diseases. 2011; 52(6): [PubMed: ] 2. Quinn TC, Wawer MJ, Sewankambo N, et al. Viral load and heterosexual transmission of human immunodeficiency virus type 1. New England Journal of Medicine. 2000; 342(13): [PubMed: ] 3. Cohen, M. Final results of the HPTN 052 randomized controlled trial: antiretroviral therapy prevents HIV transmission Program number MOAC0106LB, Track C. International AIDS Society; Vancouver; Centers for Disease Control and Prevention. [Sept ] Monitoring selected national HIV prevention and care objectives by using HIV surveillance data-united States and 6 dependent areas HIV surveillance Supplemental Report reports/surveillance/ 5. Skarbinski J, Rosenberg E, Paz-Bailey G, et al. Human immunodeficiency virus transmission at each step of the care continuum in the United States. JAMA internal medicine. 2015; 175(4): [PubMed: ] 6. White House Office of National AIDS Policy. [06/25/2015] National HIV/AIDS Strategy for the United States White House Office of National AIDS Policy. [October 19, 2015] National HIV/AIDS Strategy for the United States UNAIDS. [06/30/2015] : An ambitious treatment target to help end the AIDS epidemic Shah M, Risher K, Berry SA, Dowdy DW. The epidemiologic and economic impact of improving HIV testing, linkage, and retention in care in the United States. Clin Infect Dis Maddali MV, Dowdy DW, Gupta A, Shah M. Economic and epidemiological impact of early antiretroviral therapy initiation in India. J Int AIDS Soc. 2015; 18(1): [PubMed: ] 11. Currie S, Rogstad KE, Piyadigamage A, Herman S. Time taken to undetectable viral load, following the initiation of HAART. Int J STD AIDS. 2009; 20(4): [PubMed: ] 12. Hollingsworth TD, Anderson RM, Fraser C. HIV-1 transmission, by stage of infection. J Infect Dis. 2008; 198(5): [PubMed: ] 13. Fleishman JA, Yehia BR, Moore RD, Korthuis PT, Gebo KA. Network HIVR. Establishment, retention, and loss to follow-up in outpatient HIV care. J Acquir Immune Defic Syndr. 2012; 60(3): [PubMed: ] 14. Udeagu CC, Webster TR, Bocour A, Michel P, Shepard CW. Lost or just not following up: public health effort to re-engage HIV-infected persons lost to follow-up into HIV medical care. Aids. 2013; 27(14): [PubMed: ] 15. Cunningham CO, Buck J, Shaw FM, Spiegel LS, Heo M, Agins BD. Factors Associated With Returning to HIV Care After a Gap in Care in New York State. J Acquir Immune Defic Syndr. 2014; 66(4): [PubMed: ] 16. Centers for Medicaid and Medicare Services. Medicaid Fee Schedule Gebo KA, Fleishman JA, Conviser R, et al. Contemporary costs of HIV healthcare in the HAART era. Aids. 2010; 24(17): [PubMed: ] 18. AIDSinfo. [Sept 29, 2015] Clinical Guidelines Portal--Cost considerations and Antiretroviral Therapy cost-considerations-and-antiretroviral-therapy
11 Shah et al. Page Bradley H, Hall HI, Wolitski RJ, et al. Vital Signs: HIV diagnosis, care, and treatment among persons living with HIV--United States, MMWR Morb Mortal Wkly Rep. 2014; 63(47): [PubMed: ] 20. Centers for Disease Control and Prevention. Vital signs: HIV prevention through care and treatment--united States. MMWR Morb Mortal Wkly Rep. 2011; 60(47): [PubMed: ] 21. DHHS Panel on Antiretroviral Guidelines for Adults and Adolescents. [Sept 29, 2015] Guidelines for the Use of Antiretroviral Agents in HIV-1-Infected Adults and Adolescents aidsinfo.nih.gov/guidelines 22. Weinstein MC, Siegel JE, Gold MR, Kamlet MS, Russell LB. Recommendations of the Panel on Cost-effectiveness in Health and Medicine. Jama. 1996; 276(15): [PubMed: ] 23. United States Preventive Services Task Force. Human Immunodeficiency Virus (HIV) Infection: Screening. Apr RecommendationStatementFinal/human-immunodeficiency-virus-hiv-infection-screening 24. Colasanti J, Kelly J, Pennisi E, et al. Continuous retention and viral suppression provide further insights into the HIV care continuum compared to the cross-sectional HIV care cascade. Clin Infect Dis Higa DH, Crepaz N, Mullins MM, Prevention Research Synthesis P. Identifying Best Practices for Increasing Linkage to, Retention, and Re-engagement in HIV Medical Care: Findings from a Systematic Review, AIDS Behav Kaiser Family Foundation. [Oct 2, 2015] US Federal Funding for HIV/AIDS: The president's FY 2016 budget request Gopalappa C, Farnham PG, Hutchinson AB, Sansom SL. Cost effectiveness of the National HIV/ AIDS Strategy goal of increasing linkage to care for HIV-infected persons. J Acquir Immune Defic Syndr. 2012; 61(1): [PubMed: ] 28. Long EF, Brandeau ML, Owens DK. The cost-effectiveness and population outcomes of expanded HIV screening and antiretroviral treatment in the United States. Annals of internal medicine. 2010; 153(12): [PubMed: ] 29. Laffoon BT, Hall HI, Surendera Babu A, et al. HIV Infection and Linkage to HIV-Related Medical Care in Large Urban Areas in the United States, J Acquir Immune Defic Syndr. 2015; 69(4): [PubMed: ] 30. Gray KM, Cohen SM, Hu X, Li J, Mermin J, Hall HI. Jurisdiction level differences in HIV diagnosis, retention in care, and viral suppression in the United States. J Acquir Immune Defic Syndr. 2014; 65(2): [PubMed: ]
12 Shah et al. Page 11 Figure 1. Total new HIV infections over the next decade, by achievement of NHAS targets Cumulative new HIV infections at varying levels of HIV care engagement. In the base-case scenario, the current rates of HIV care engagement (screening, linkage, retention in care) persist. In the NHAS scenarios, we project improvements in care engagement (through increased yearly screening, improved linkage to care after diagnosis, and reduced care disengagement) that allows achievement of NHAS indicators 1, 4, and 5 by 2020.
13 Shah et al. Page 12 Table 1 Key model parameters Variable Value Range for sensitivity analysis References HIV Disease Dynamics with ART Reduction in rate of transmission 93% % 3 Time to viral suppression on ART 6 months 2-12 months 11 Transmission Dynamics * Annual partnerships per year Transmission per partnership (male to female) % % Transmission per partnership (female to male) 2-2 7% % Transmission per partnership (MSM) 2 9% % Transmission probability per needle sharing partnership (PWID) Relative risk increase in transmission probability during acute HIV Engagement in Care dynamics, base-case % HIV test in past 12 months % 5-35% Calibrated * Calibrated * Calibrated * Calibrated * Calibrated * Calibrated Rate of disengagement from care annually , Calibrated Rate of reengagement in care annually per year , 15, Calibrated COSTS HIV test $33 $ HIV viral load $116 $ Outpatient Visit $129 $ CD4 Test $49 $20-$90 17 Annual ART $32,000 $10000-$ * Transmission in the model is a function of average partnerships per year and average probability of transmission per partnership within risk groups. We began with published estimates and then calibrated these parameters (Supplement for additional details and references) to fit observed HIV incidence and prevalence in the US and varied by gender and risk group 4, 19. Annual HIV screening rates, percent linkage, and disengagement from care were varied by gender and risk group. To obtain parameter estimates, we began with published data and calibrated model to fit published estimates of HIV care engagement in the US 4, 19 (Supplement for additional details and references). Individuals without initial linkage to care were eligible to engage in care at later times. We additionally included annual health care utilization costs for individuals not in care or on ART (e.g. hospitalizations, ED visits). ART regimen costs shown are for first line integrase inhibitor-based regimens 21 ( Additional cost details and references are in Supplement). All populations eligible for ART initiation regardless of CD4 count 21.
14 Shah et al. Page 13 Table 2 Economic and epidemiologic impact from of achieving NHAS targets for care engagement by 2020 HIV Prevalence * Deaths Costs HIV Incidence NHAS targets within progress indicators Total (% Δ from base-case) Tota(% Δ from base-case) Total (% Δ from base-case) Total (% Δ from base-case) Base-case: No change in care 524,000 (0%) 1 47 million (0 0%) 375,000 (0 0%) $254 billion (0 0%) NHAS 1: 90% awareness by ,000 ( 2 0%) 1-46 million ( 0 5%) 373,000 ( 0 4%) $258 billion (+1 5%) 503,000 ( 3 9%) 1 46 million ( 0 7%) 363,000 ( 3 1%) $261 billion (+2 6%) NHAS 4: 85% linkage within 1 month 250,000 ( 52 3%) 1 30 million ( 11 1%) 256,000 ( 31 7%) $350 billion (+37 9%) NHAS 5: 90% in care by 2020 NHAS 1 and 4: 90% awareness and 85% linkage 490,000 ( 6 4%) 1 45 million ( 1 3%) 361,000 ( 3 5%) $265 billion (+4 3%) NHAS 4 and 5: 85% linkage, and 90% in care 235,000 ( 55 1%) 1 30 million ( 11 6%) 249,000 ( 33 7%) $355 billion (+39 7%) NHAS 1 and 4 and 5: 90% awareness, 85% linkage, and 90% in care 221,000 ( 57 7%) 1 29 million ( 12 3%) 246,000 ( 34 3%) $359 billion (+41 3%) Table legend: Abbreviations: SOC, standard of care; NHAS, National HIV/AIDS strategy; PLWH: People Living with HIV. Incremental percent reductions are based on precise model outputs; total values rounded to three significant digits. We modeled scenarios of achieving the targets set forth in the NHAS progress indicators independently, and in combination. In all scenarios, individuals that do not link to care initially are eligible to engage in care at any later time point. NHAS 4 independent scenarios utilizes current rates of HIV screening, but improves linkage to care within 1 month to 85%. NHAS 5 independent scenario enhances care-retention (reduced rates of yearly loss from care, and improved reengagement rates for those out of care) such that 90% of those aware of their diagnosis are in care in 2020; in this scenario, the yearly rates of HIV screening and linkage to care after HIV diagnosis are the same as the base-case. Costs represent 3% discounting of future costs. For the NHAS scenarios, costs represent total health system costs accounting for increased HIV tests and health care engagement and ART usage, but do not include costs related to potential interventions needed to achieve improved HIV care continuum engagement. * Projected number of people living with HIV in 2025.Yearly prevalence is shown in Supplemental figure 5.
Implementation of testing (and other interventions along the Continuum of Care)
 Implementation of testing (and other interventions along the Continuum of Care) Jonathan Mermin, MD, MPH National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention U.S. Centers for Disease Control
Implementation of testing (and other interventions along the Continuum of Care) Jonathan Mermin, MD, MPH National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention U.S. Centers for Disease Control
High Impact Prevention: Science, Practice, and the Future of HIV
 High Impact Prevention: Science, Practice, and the Future of HIV Jonathan Mermin, MD, MPH National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention Centers for Disease Control and Prevention
High Impact Prevention: Science, Practice, and the Future of HIV Jonathan Mermin, MD, MPH National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention Centers for Disease Control and Prevention
Home testing and counselling with linkage to care. Becky L Genberg, Joseph W Hogan and Paula Braitstein
 Home testing and counselling with linkage to care Becky L Genberg, Joseph W Hogan and Paula Braitstein Globally, researchers and programme implementers strive towards the ambitious UNAIDS goal of 90-90-90
Home testing and counselling with linkage to care Becky L Genberg, Joseph W Hogan and Paula Braitstein Globally, researchers and programme implementers strive towards the ambitious UNAIDS goal of 90-90-90
High Impact HIV Prevention Services and Best Practices
 High Impact HIV Prevention Services and Best Practices David W. Purcell, JD, PhD Deputy Director for Behavioral and Social Science Division of HIV/AIDS Prevention Centers for Disease Control and Prevention
High Impact HIV Prevention Services and Best Practices David W. Purcell, JD, PhD Deputy Director for Behavioral and Social Science Division of HIV/AIDS Prevention Centers for Disease Control and Prevention
Supplementary Material. In this supplement we derive the full form of the monetary and health costs of testing
 Supporting document Supplementary Material In this supplement we derive the full form of the monetary and health costs of testing every years, and ; we derive the approximation shown in (1); and we justify
Supporting document Supplementary Material In this supplement we derive the full form of the monetary and health costs of testing every years, and ; we derive the approximation shown in (1); and we justify
From Africa to Georgia: What We Have Learned From the Treatment for All Initiative
 From Africa to Georgia: What We Have Learned From the 90-90-90 Treatment for All Initiative Carlos del Rio, MD Professor of Global Health Rollins School of Public Health Professor of Medicine Emory University
From Africa to Georgia: What We Have Learned From the 90-90-90 Treatment for All Initiative Carlos del Rio, MD Professor of Global Health Rollins School of Public Health Professor of Medicine Emory University
Potential Impact on HIV Incidence of Increasing Viral Suppression among HIV-positive MSM in Baltimore: Mathematical Modelling for HPTN 078
 Potential Impact on HIV Incidence of Increasing Viral Suppression among HIV-positive MSM in Baltimore: Mathematical Modelling for HPTN 078 Kate M Mitchell, Brooke Hoots, Dobromir Dimitrov, Jason Farley,
Potential Impact on HIV Incidence of Increasing Viral Suppression among HIV-positive MSM in Baltimore: Mathematical Modelling for HPTN 078 Kate M Mitchell, Brooke Hoots, Dobromir Dimitrov, Jason Farley,
Return on Public Health Investment: CDC s Expanded HIV Testing Initiative ACCEPTED
 JAIDS Journal of Acquired Immune Deficiency Syndromes Publish Ahead of Print DOI: 10.1097/QAI.0b013e31823e5bee 10.7.11 Return on Public Health Investment: CDC s Expanded HIV Testing Initiative Angela B
JAIDS Journal of Acquired Immune Deficiency Syndromes Publish Ahead of Print DOI: 10.1097/QAI.0b013e31823e5bee 10.7.11 Return on Public Health Investment: CDC s Expanded HIV Testing Initiative Angela B
HIV Prevention in Clinical Care Settings
 NORTHWEST AIDS EDUCATION AND TRAINING CENTER HIV Prevention in Clinical Care Settings Jeanne Marrazzo, MD, MPH Professor, Division of Allergy and Infectious Diseases University of Washington HIV Prevention
NORTHWEST AIDS EDUCATION AND TRAINING CENTER HIV Prevention in Clinical Care Settings Jeanne Marrazzo, MD, MPH Professor, Division of Allergy and Infectious Diseases University of Washington HIV Prevention
Zero HIV infections Zero HIV deaths Zero HIV stigma. Stephanie Cohen, MD, MPH on behalf of the Getting to Zero Consortium
 Zero HIV infections Zero HIV deaths Zero HIV stigma Stephanie Cohen, MD, MPH on behalf of the Getting to Zero Consortium Number of New HIV Diagnoses Overall decline in new HIV diagnoses and death in San
Zero HIV infections Zero HIV deaths Zero HIV stigma Stephanie Cohen, MD, MPH on behalf of the Getting to Zero Consortium Number of New HIV Diagnoses Overall decline in new HIV diagnoses and death in San
Tying it all together health economic modeling
 Tying it all together health economic modeling Ruanne V Barnabas, MD, DPhil Associate Professor, Global Health, Allergy & Infectious Disease University of Washington How models can be used with cost-effectiveness
Tying it all together health economic modeling Ruanne V Barnabas, MD, DPhil Associate Professor, Global Health, Allergy & Infectious Disease University of Washington How models can be used with cost-effectiveness
Why are the targets a game-changer? What is the Fast-Track Cities Initiative and its connection to ?
 Frequently Asked Questions about 90-90-90 Targets, the HIV Care Continuum, the Updated National HIV AIDS Strategy (NHAS), and the Fast-Track Cities Initiative What is the origin of the 90-90-90 targets?
Frequently Asked Questions about 90-90-90 Targets, the HIV Care Continuum, the Updated National HIV AIDS Strategy (NHAS), and the Fast-Track Cities Initiative What is the origin of the 90-90-90 targets?
Receptive Anal Intercourse and HIV Infection
 World Journal of AIDS, 2017, 7, 269-278 http://www.scirp.org/journal/wja ISSN Online: 2160-8822 ISSN Print: 2160-8814 Receptive Anal Intercourse and HIV Infection Gilbert R. Lavoie 1, John F. Fisher 2
World Journal of AIDS, 2017, 7, 269-278 http://www.scirp.org/journal/wja ISSN Online: 2160-8822 ISSN Print: 2160-8814 Receptive Anal Intercourse and HIV Infection Gilbert R. Lavoie 1, John F. Fisher 2
We Are Going to Need a Bigger Wrench: Improving Linkage and Retention in HIV Care
 Slide 1 of XX We Are Going to Need a Bigger Wrench: Improving Linkage and Retention in HIV Care Carlos del Rio, MD Hubert Professor of Global Health Rollins School of Public Health Professor of Medicine
Slide 1 of XX We Are Going to Need a Bigger Wrench: Improving Linkage and Retention in HIV Care Carlos del Rio, MD Hubert Professor of Global Health Rollins School of Public Health Professor of Medicine
Cost Effectiveness of HIV Prevention Interventions in the U.S.
 Cost Effectiveness of HIV Prevention Interventions in the U.S. Feng Lin, PhD, Paul G. Farnham, PhD, Ram K. Shrestha, PhD, Jonathan Mermin, MD, Stephanie L. Sansom, PhD Introduction: The purpose of this
Cost Effectiveness of HIV Prevention Interventions in the U.S. Feng Lin, PhD, Paul G. Farnham, PhD, Ram K. Shrestha, PhD, Jonathan Mermin, MD, Stephanie L. Sansom, PhD Introduction: The purpose of this
The cost-effectiveness of expanded testing for primary HIV infection Coco A
 The cost-effectiveness of expanded testing for primary HIV infection Coco A Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract
The cost-effectiveness of expanded testing for primary HIV infection Coco A Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract
The HIV Medicine Association (HIVMA) of the Infectious Diseases Society of America (IDSA)
 Written Testimony for the Record to the House Subcommittee on Labor, Health and Human Services, Education and Related Agencies regarding FY 2018 Appropriations for HIV/AIDS Programs Submitted by Dr. Wendy
Written Testimony for the Record to the House Subcommittee on Labor, Health and Human Services, Education and Related Agencies regarding FY 2018 Appropriations for HIV/AIDS Programs Submitted by Dr. Wendy
Connecting the Community. Advancing the HIV Response in Baltimore and Jackson.
 Connecting the Community. Advancing the HIV Response in Baltimore and Jackson. Connecting the Community. Advancing the HIV Response in Baltimore and Jackson. The Motivation: What the Numbers Say ACCELERATE!
Connecting the Community. Advancing the HIV Response in Baltimore and Jackson. Connecting the Community. Advancing the HIV Response in Baltimore and Jackson. The Motivation: What the Numbers Say ACCELERATE!
Federal AIDS Policy Partnership March 29, 2017
 Federal AIDS Policy Partnership March 29, 2017 Laura Cheever, MD, ScM Associate Administrator HIV/AIDS Bureau (HAB) Health Resources and Services Administration (HRSA) HIV/AIDS Bureau Vision and Mission
Federal AIDS Policy Partnership March 29, 2017 Laura Cheever, MD, ScM Associate Administrator HIV/AIDS Bureau (HAB) Health Resources and Services Administration (HRSA) HIV/AIDS Bureau Vision and Mission
PS : Comprehensive HIV Prevention Programs for Health Departments
 PS12-1201: Comprehensive HIV Prevention Programs for Health Departments Program Overview Erica K. Dunbar, MPH Program Leader, Health Department Initiatives National Center for HIV/AIDS, Viral Hepatitis,
PS12-1201: Comprehensive HIV Prevention Programs for Health Departments Program Overview Erica K. Dunbar, MPH Program Leader, Health Department Initiatives National Center for HIV/AIDS, Viral Hepatitis,
Didactic Series. Update on DHHS Guidelines for HIV Treatment: Adherence to the Care Continuum
 Didactic Series Update on DHHS Guidelines for HIV Treatment: Adherence to the Care Continuum Daniel Lee, MD UCSD Medical Center Owen Clinic March 8 th, 2018 1 Adherence to the Care Continuum Revised from
Didactic Series Update on DHHS Guidelines for HIV Treatment: Adherence to the Care Continuum Daniel Lee, MD UCSD Medical Center Owen Clinic March 8 th, 2018 1 Adherence to the Care Continuum Revised from
Fulton County Board of Health Strategy to End the HIV Epidemic in Fulton County
 Fulton County Board of Health Strategy to End the HIV Epidemic in Fulton County April 25, 2018 Derick B. Wilson, MHA Administrator FCBOH HIV Strategy Overview Increase Testing and Supplies availability
Fulton County Board of Health Strategy to End the HIV Epidemic in Fulton County April 25, 2018 Derick B. Wilson, MHA Administrator FCBOH HIV Strategy Overview Increase Testing and Supplies availability
Care Coach Collaborative Model Bridging Gap of Medical Linkage for HIV Positive Inmates Go home, kiss your Mother, and come into our offices. (Patsy F
 Care Coach Collaborative Model Bridging Gap of Medical Linkage for HIV Positive Inmates Go home, kiss your Mother, and come into our offices. (Patsy Fitzgerald) 93% of participants in the Care Coach program
Care Coach Collaborative Model Bridging Gap of Medical Linkage for HIV Positive Inmates Go home, kiss your Mother, and come into our offices. (Patsy Fitzgerald) 93% of participants in the Care Coach program
HIV & AIDS IN SOUTH AFRICA: WHERE ARE WE AND WHAT ARE
 HIV & AIDS IN SOUTH AFRICA: WHERE ARE WE AND WHAT ARE THE REMAINING CHALLENGES DR YOGAN PILLAY, NDOH SA HIV CLINICIANS SOCIETY CONFERENCE, CAPE TOWN 25 NOVEMBER, 2012 GLOBAL DATA 34m people living with
HIV & AIDS IN SOUTH AFRICA: WHERE ARE WE AND WHAT ARE THE REMAINING CHALLENGES DR YOGAN PILLAY, NDOH SA HIV CLINICIANS SOCIETY CONFERENCE, CAPE TOWN 25 NOVEMBER, 2012 GLOBAL DATA 34m people living with
ViiV Healthcare s Position on Continuous Innovation in Prevention, Testing, Treatment & Care of HIV
 ViiV Healthcare s Position on Continuous Innovation in Prevention, Testing, Treatment & Care of HIV ViiV Healthcare is a company 100% committed to HIV, and we are always looking to move beyond the status
ViiV Healthcare s Position on Continuous Innovation in Prevention, Testing, Treatment & Care of HIV ViiV Healthcare is a company 100% committed to HIV, and we are always looking to move beyond the status
2016 NYS HIV Quality of Care Review
 2016 NYS HIV Quality of Care Review A new way forward in four parts Bruce Agins, MD, MPH Medical Director NYSDOH AIDS Institute December 15, 2016 Ending the Epidemic: update! A 3-Point plan announced by
2016 NYS HIV Quality of Care Review A new way forward in four parts Bruce Agins, MD, MPH Medical Director NYSDOH AIDS Institute December 15, 2016 Ending the Epidemic: update! A 3-Point plan announced by
HIV in Russia. Cost-effectiveness of Treating Injection Drug Users with Antiretroviral Therapy
 HIV in Russia Cost-effectiveness of Treating Injection Drug Users with Antiretroviral Therapy Elisa F. Long, M.S. Margaret L. Brandeau, Ph.D. Tatyana Vinichenko, M.D., M.P.A. Cristina M. Galvin, M.S. Swati
HIV in Russia Cost-effectiveness of Treating Injection Drug Users with Antiretroviral Therapy Elisa F. Long, M.S. Margaret L. Brandeau, Ph.D. Tatyana Vinichenko, M.D., M.P.A. Cristina M. Galvin, M.S. Swati
Financial Resources for HIV: PEPFAR s Contributions to the Global Scale-up of Treatment
 Financial Resources for HIV: PEPFAR s Contributions to the Global Scale-up of Treatment Joint WHO & UNAIDS Consultation with Pharmaceuticals and Stakeholders November 05 2012 Lara Stabinski, MD, MPH Medical
Financial Resources for HIV: PEPFAR s Contributions to the Global Scale-up of Treatment Joint WHO & UNAIDS Consultation with Pharmaceuticals and Stakeholders November 05 2012 Lara Stabinski, MD, MPH Medical
State of Alabama HIV Surveillance 2014 Annual Report
 State of Alabama HIV Surveillance 2014 Annual Report Prepared by: Division of STD Prevention and Control HIV Surveillance Branch Contact Person: Richard P. Rogers, MS, MPH richard.rogers@adph.state.al.us
State of Alabama HIV Surveillance 2014 Annual Report Prepared by: Division of STD Prevention and Control HIV Surveillance Branch Contact Person: Richard P. Rogers, MS, MPH richard.rogers@adph.state.al.us
Ending the Epidemic in New York State
 Ending the Epidemic in New York State HIV Quality of Care Clinical and Consumer Advisory Committee Joint Meeting September 8, 2015 September 10, 2015 Defining the End of AIDS Goal Reduce from 3,000 to
Ending the Epidemic in New York State HIV Quality of Care Clinical and Consumer Advisory Committee Joint Meeting September 8, 2015 September 10, 2015 Defining the End of AIDS Goal Reduce from 3,000 to
Thresia Sebastian MD, MPH University of Colorado, Denver Global Health Disasters Course October 2016
 Thresia Sebastian MD, MPH University of Colorado, Denver Global Health Disasters Course October 2016 1 Objectives of today s lecture Describe global goals in the fight against HIV Review the epidemiology
Thresia Sebastian MD, MPH University of Colorado, Denver Global Health Disasters Course October 2016 1 Objectives of today s lecture Describe global goals in the fight against HIV Review the epidemiology
Treat All : From Policy to Action - What will it take?
 Strategy Finance Integration Cascade of services People centred Political Will Treat All : From Policy to Action - What will it take? Thursday, 9 June, 13.00 14.30 Conference Room 11, United Nations Questions
Strategy Finance Integration Cascade of services People centred Political Will Treat All : From Policy to Action - What will it take? Thursday, 9 June, 13.00 14.30 Conference Room 11, United Nations Questions
and Future Directions
 Involve[men]t PrEP, Health Disparities, A Study of Race and Age in HIV/STI Incidence and Prevalence Among MSM in Atlanta, and Future Directions GA: 2009-2014 Patrick Sullivan, DVM, PhD Rollins School of
Involve[men]t PrEP, Health Disparities, A Study of Race and Age in HIV/STI Incidence and Prevalence Among MSM in Atlanta, and Future Directions GA: 2009-2014 Patrick Sullivan, DVM, PhD Rollins School of
Using anti-hiv drugs for prevention
 Using anti-hiv drugs for prevention Highlights from AIDS 2012 (and 2 nd International Workshops on Treatment as Prevention) Tim Rogers, trogers@catie.ca Using anti-hiv Drugs for Prevention Outline Treatment
Using anti-hiv drugs for prevention Highlights from AIDS 2012 (and 2 nd International Workshops on Treatment as Prevention) Tim Rogers, trogers@catie.ca Using anti-hiv Drugs for Prevention Outline Treatment
HIV - Preventing New Infections: New Options, Readjusted Approaches
 HIV - Preventing New Infections: New Options, Readjusted Approaches Ronald P. Hattis, MD, MPH Beyond AIDS Foundation Presented at Loma Linda University December 6, 2013 1 Thesis (Summary) As of 2013-14,
HIV - Preventing New Infections: New Options, Readjusted Approaches Ronald P. Hattis, MD, MPH Beyond AIDS Foundation Presented at Loma Linda University December 6, 2013 1 Thesis (Summary) As of 2013-14,
Using HIV Surveillance Laboratory Data to Identify Out-of-Care Patients
 DOI 10.1007/s10461-017-1742-5 ORIGINAL PAPER Using HIV Surveillance Laboratory Data to Identify Out-of-Care Patients John Christian Hague 1 Betsey John 1 Linda Goldman 1 Kshema Nagavedu 1 Sophie Lewis
DOI 10.1007/s10461-017-1742-5 ORIGINAL PAPER Using HIV Surveillance Laboratory Data to Identify Out-of-Care Patients John Christian Hague 1 Betsey John 1 Linda Goldman 1 Kshema Nagavedu 1 Sophie Lewis
Bidders Conference. Amendment to Request For Proposals for Provision of HIV Prevention Services July 28, 2011
 Chicago Department of Public Health Bidders Conference Amendment to Request For Proposals 11-03 for Provision of HIV Prevention Services July 28, 2011 Chicago Department of Public Health Division of STI/HIV
Chicago Department of Public Health Bidders Conference Amendment to Request For Proposals 11-03 for Provision of HIV Prevention Services July 28, 2011 Chicago Department of Public Health Division of STI/HIV
State of Alabama HIV Surveillance 2013 Annual Report Finalized
 State of Alabama HIV Surveillance 2013 Annual Report Finalized Prepared by: Division of STD Prevention and Control HIV Surveillance Branch Contact Person: Allison R. Smith, MPH Allison.Smith@adph.state.al.us
State of Alabama HIV Surveillance 2013 Annual Report Finalized Prepared by: Division of STD Prevention and Control HIV Surveillance Branch Contact Person: Allison R. Smith, MPH Allison.Smith@adph.state.al.us
Submitted electronically to:
 Submitted electronically to: ODOARRFI19@nih.gov Maureen Goodenow, PhD Associate Director of AIDS Research, NIH Director, Office of AIDS Research (OAR) National Institutes of Health 5601 Fishers Lane. Room
Submitted electronically to: ODOARRFI19@nih.gov Maureen Goodenow, PhD Associate Director of AIDS Research, NIH Director, Office of AIDS Research (OAR) National Institutes of Health 5601 Fishers Lane. Room
Human Immunodeficiency Virus Transmission at Each Step of the Care Continuum in the United States
 Research Original Investigation Human Immunodeficiency Virus Transmission at Each Step of the Care Continuum in the United States Jacek Skarbinski, MD; Eli Rosenberg, PhD; Gabriela Paz-Bailey, MD, MSc,
Research Original Investigation Human Immunodeficiency Virus Transmission at Each Step of the Care Continuum in the United States Jacek Skarbinski, MD; Eli Rosenberg, PhD; Gabriela Paz-Bailey, MD, MSc,
California Department of Public Health (CDPH), Office of AIDS (OA) Monthly Report April 2018
 California Department of Public Health (CDPH), Office of AIDS (OA) Monthly Report April 2018 Please note: As part of OA s ongoing work to align all of our work and communications with Laying a Foundation
California Department of Public Health (CDPH), Office of AIDS (OA) Monthly Report April 2018 Please note: As part of OA s ongoing work to align all of our work and communications with Laying a Foundation
Regional program of the East Europe and Central Asia Union of PLWH within the framework of the Global Fund New Funding Model
 Regional program of the East Europe and Central Asia Union of PLWH within the framework of the Global Fund New Funding Model Background for the program development Problem areas Access to the whole HIV-care
Regional program of the East Europe and Central Asia Union of PLWH within the framework of the Global Fund New Funding Model Background for the program development Problem areas Access to the whole HIV-care
Modelling HIV Transmission and Treatment for US MSM to Estimate the Impact of HPTN 078 on HIV Incidence
 Modelling HIV Transmission and Treatment for US MSM to Estimate the Impact of HPTN 078 on HIV Incidence Kate Mitchell, PhD Imperial College London London, UK 14 th June 2016 Introduction: HPTN 078 Enhancing
Modelling HIV Transmission and Treatment for US MSM to Estimate the Impact of HPTN 078 on HIV Incidence Kate Mitchell, PhD Imperial College London London, UK 14 th June 2016 Introduction: HPTN 078 Enhancing
Stuck : Contextualizing the U.S. HIV epidemic among black MSM. Greg Millett amfar April 2, 2015
 Stuck : Contextualizing the U.S. HIV epidemic among black MSM Greg Millett amfar April 2, 2015 New HIV Infections, 2010 2008-2010 Women: 21% decrease MSM: 12% increase Young MSM: 22% increase Lifetime
Stuck : Contextualizing the U.S. HIV epidemic among black MSM Greg Millett amfar April 2, 2015 New HIV Infections, 2010 2008-2010 Women: 21% decrease MSM: 12% increase Young MSM: 22% increase Lifetime
hiv/aids Programme Use of Antiretroviral Drugs for Treating Pregnant Women and Preventing HIV Infection in Infants
 hiv/aids Programme Programmatic update Use of Antiretroviral Drugs for Treating Pregnant Women and Preventing HIV Infection in Infants EXECUTIVE SUMMARY April 2012 EXECUTIVE SUMMARY Recent developments
hiv/aids Programme Programmatic update Use of Antiretroviral Drugs for Treating Pregnant Women and Preventing HIV Infection in Infants EXECUTIVE SUMMARY April 2012 EXECUTIVE SUMMARY Recent developments
Health Resources and Services Administration and HIV/AIDS Bureau Update
 Health Resources and Services Administration and HIV/AIDS Bureau Update Presented to the CDC/HRSA Advisory Committee on HIV, Viral Hepatitis and STD Prevention and Treatment Laura Cheever, MD ScM Associate
Health Resources and Services Administration and HIV/AIDS Bureau Update Presented to the CDC/HRSA Advisory Committee on HIV, Viral Hepatitis and STD Prevention and Treatment Laura Cheever, MD ScM Associate
Disparities in HIV Care. Slides prepared by Kirk Fergus, Intern National Quality Center
 Disparities in HIV Care Slides prepared by Kirk Fergus, Intern National Quality Center At a glance At a glance MSM accounted for 61% of all new HIV infections in the U.S. in 2009, as well as nearly half
Disparities in HIV Care Slides prepared by Kirk Fergus, Intern National Quality Center At a glance At a glance MSM accounted for 61% of all new HIV infections in the U.S. in 2009, as well as nearly half
Bruce D. Agins, MD MPH Medical Director, AIDS Institute Adherence 2017; Miami
 1 1 Bruce D. Agins, MD MPH Medical Director, AIDS Institute Adherence 2017; Miami 3 Defining the End of AIDS Reduce new infections to 750 annually by the end of 2020 Three Point Plan 1. Identify all persons
1 1 Bruce D. Agins, MD MPH Medical Director, AIDS Institute Adherence 2017; Miami 3 Defining the End of AIDS Reduce new infections to 750 annually by the end of 2020 Three Point Plan 1. Identify all persons
Response to HIV LOGISTICAL AND OTHER PERSPECTIVES
 Response to HIV LOGISTICAL AND OTHER PERSPECTIVES Margaret Brandeau Department of Management Science and Engineering Department of Medicine Stanford University Topics HIV: A humanitarian crisis Planning
Response to HIV LOGISTICAL AND OTHER PERSPECTIVES Margaret Brandeau Department of Management Science and Engineering Department of Medicine Stanford University Topics HIV: A humanitarian crisis Planning
U.S. Counties Vulnerability to Rapid Dissemination of HIV/HCV Infections Among People Who Inject Drugs
 U.S. Counties Vulnerability to Rapid Dissemination of HIV/HCV Infections Among People Who Inject Drugs Michelle Van Handel, MPH Health Scientist National Center for HIV/AIDS, Viral Hepatitis, STDs and
U.S. Counties Vulnerability to Rapid Dissemination of HIV/HCV Infections Among People Who Inject Drugs Michelle Van Handel, MPH Health Scientist National Center for HIV/AIDS, Viral Hepatitis, STDs and
Advancing the National HIV/AIDS Strategy: Housing and the HCCI. Housing Summit Los Angeles, CA
 Advancing the National HIV/AIDS Strategy: Housing and the HCCI Housing Summit Los Angeles, CA October 21, 2014 The National HIV/AIDS Strategy Facets of the Strategy Limited number of action steps Sets
Advancing the National HIV/AIDS Strategy: Housing and the HCCI Housing Summit Los Angeles, CA October 21, 2014 The National HIV/AIDS Strategy Facets of the Strategy Limited number of action steps Sets
Strategic use of antiretroviral drugs to prevent HIV transmission
 Strategic use of antiretroviral drugs to prevent HIV transmission 22th Tunisian Congress of Infectious Diseases 2nd Congress of Federation of Arab Societies of Clinical Microbiology and Infectious Diseases
Strategic use of antiretroviral drugs to prevent HIV transmission 22th Tunisian Congress of Infectious Diseases 2nd Congress of Federation of Arab Societies of Clinical Microbiology and Infectious Diseases
Improving HIV Prevention and Care in New Mexico Through Integrated Planning
 Improving HIV Prevention and Care in New Mexico Through Integrated Planning Andrew Gans, MPH HIV, STD and Hepatitis Section Manager National Goals 1 Goals in the National HIV/AIDS Strategy (NHAS) 1. Reduce
Improving HIV Prevention and Care in New Mexico Through Integrated Planning Andrew Gans, MPH HIV, STD and Hepatitis Section Manager National Goals 1 Goals in the National HIV/AIDS Strategy (NHAS) 1. Reduce
Global health sector strategies on HIV, viral hepatitis and sexually transmitted infections ( )
 Regional Committee for Europe 65th session EUR/RC65/Inf.Doc./3 Vilnius, Lithuania, 14 17 September 2015 2 September 2015 150680 Provisional agenda item 3 ORIGINAL: ENGLISH Global health sector strategies
Regional Committee for Europe 65th session EUR/RC65/Inf.Doc./3 Vilnius, Lithuania, 14 17 September 2015 2 September 2015 150680 Provisional agenda item 3 ORIGINAL: ENGLISH Global health sector strategies
State of Alabama HIV Surveillance 2012 Annual Report Finalized
 State of Alabama HIV Surveillance 2012 Annual Report Finalized Prepared by: Division of HIV/AIDS Prevention and Control HIV Surveillance Branch Contact Person: Allison R. Smith, MPH Allison.Smith@adph.state.al.us
State of Alabama HIV Surveillance 2012 Annual Report Finalized Prepared by: Division of HIV/AIDS Prevention and Control HIV Surveillance Branch Contact Person: Allison R. Smith, MPH Allison.Smith@adph.state.al.us
The Geography of Infectious Diseases Related to the Opioid Epidemic. Patrick Sullivan, DVM, PhD Emory University March 12, 2018
 The Geography of Infectious Diseases Related to the Opioid Epidemic Patrick Sullivan, DVM, PhD Emory University March 12, 2018 Presentation Outline The importance of infectious diseases in the opioid epidemic
The Geography of Infectious Diseases Related to the Opioid Epidemic Patrick Sullivan, DVM, PhD Emory University March 12, 2018 Presentation Outline The importance of infectious diseases in the opioid epidemic
HIV/AIDS Epi Update Public Health Agency of Canada
 1 HIV/AIDS Epi Update Public Health Agency of Canada www.phac-aspc.gc.ca/hast-vsmt/ JULY 21 National HIV Prevalence and Incidence Estimates in Canada for 28 At a Glance More Canadians are living with HIV
1 HIV/AIDS Epi Update Public Health Agency of Canada www.phac-aspc.gc.ca/hast-vsmt/ JULY 21 National HIV Prevalence and Incidence Estimates in Canada for 28 At a Glance More Canadians are living with HIV
Funding the Ryan White Program: Now and in the Future
 Funding the Ryan White Program: Now and in the Future Carl Schmid United States Conference on AIDS San Diego, CA October 4, 2014 Outline The Fiscal Environment Recent Ryan White Funding Levels Impact of
Funding the Ryan White Program: Now and in the Future Carl Schmid United States Conference on AIDS San Diego, CA October 4, 2014 Outline The Fiscal Environment Recent Ryan White Funding Levels Impact of
HIV Modelling Consortium
 HIV Modelling Consortium Review of allocative efficiency tools Improving Efficiency in Health Conference Professor Timothy Hallett Ellen McRobie Aim & objectives of the HIV Modelling Consortium The HIV
HIV Modelling Consortium Review of allocative efficiency tools Improving Efficiency in Health Conference Professor Timothy Hallett Ellen McRobie Aim & objectives of the HIV Modelling Consortium The HIV
ACHAP LESSONS LEARNED IN BOTSWANA KEY INITIATIVES
 ACHAP Together with our company s foundation, a U.S.-based, private foundation, and the Bill & Melinda Gates Foundation, we established the African Comprehensive HIV/AIDS Partnerships (ACHAP) in 2000 to
ACHAP Together with our company s foundation, a U.S.-based, private foundation, and the Bill & Melinda Gates Foundation, we established the African Comprehensive HIV/AIDS Partnerships (ACHAP) in 2000 to
How has the Polio Eradication Initiative influenced the global AIDS response? Bradley S. Hersh, MD, MPH
 How has the Polio Eradication Initiative influenced the global AIDS response? Bradley S. Hersh, MD, MPH Presentation Outline Big history of global HIV epidemic Current status of HIV and the global AIDS
How has the Polio Eradication Initiative influenced the global AIDS response? Bradley S. Hersh, MD, MPH Presentation Outline Big history of global HIV epidemic Current status of HIV and the global AIDS
Repositioning AIDS: The World Bank s Approach to Improved Efficiency and Effectiveness Using HIV Program Science Principles
 Repositioning AIDS: The World Bank s Approach to Improved Efficiency and Effectiveness Using HIV Program Science Principles Marelize Gorgens mgorgens@worldbank.org The World Bank s Global HIV/AIDS Program
Repositioning AIDS: The World Bank s Approach to Improved Efficiency and Effectiveness Using HIV Program Science Principles Marelize Gorgens mgorgens@worldbank.org The World Bank s Global HIV/AIDS Program
Towards universal access
 Key messages Towards universal access Scaling up priority HIV/AIDS interventions in the health sector September 2009 Progress report Towards universal access provides a comprehensive global update on progress
Key messages Towards universal access Scaling up priority HIV/AIDS interventions in the health sector September 2009 Progress report Towards universal access provides a comprehensive global update on progress
HIV/AIDS MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: HIV/AIDS MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN HIV/AIDS MEASURES GROUP: #159. HIV/AIDS: CD4+ Cell Count or CD4+ Percentage Performed #160. HIV/AIDS: Pneumocystis
2014 PQRS OPTIONS F MEASURES GROUPS: HIV/AIDS MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN HIV/AIDS MEASURES GROUP: #159. HIV/AIDS: CD4+ Cell Count or CD4+ Percentage Performed #160. HIV/AIDS: Pneumocystis
Ending AIDS in Gabon: How long will it take? How much will it cost?
 Ending AIDS in Gabon: How long will it take? How much will it cost? Brian G. Williams, Eleanor Gouws* and David Ginsburg South African Centre for Epidemiological Modelling and Analysis (SACEMA), Stellenbosch,
Ending AIDS in Gabon: How long will it take? How much will it cost? Brian G. Williams, Eleanor Gouws* and David Ginsburg South African Centre for Epidemiological Modelling and Analysis (SACEMA), Stellenbosch,
NAMIBIA INVESTMENT CASE
 NAMIBIA INVESTMENT CASE OUTLINE Why an Investment Case for HIV Response in Namibia? Investment Scenarios Can we achieve Fast Track and End AIDS as public health threat by 2030? Can we afford it? Efficiencies:
NAMIBIA INVESTMENT CASE OUTLINE Why an Investment Case for HIV Response in Namibia? Investment Scenarios Can we achieve Fast Track and End AIDS as public health threat by 2030? Can we afford it? Efficiencies:
Impact of Pharmaceutical Innovation in HIV/AIDS Treatment during the Highly Active Antiretroviral Therapy (HAART) Era in the US, :
 White Paper Impact of Pharmaceutical Innovation in HIV/AIDS Treatment during the Highly Active Antiretroviral Therapy (HAART) Era in the US, 1987-2010: An Epidemiologic and Cost-impact Modeling Case Study
White Paper Impact of Pharmaceutical Innovation in HIV/AIDS Treatment during the Highly Active Antiretroviral Therapy (HAART) Era in the US, 1987-2010: An Epidemiologic and Cost-impact Modeling Case Study
March XX, Washington, DC Washington, DC Washington, DC Washington, DC 20515
 March XX, 2017 The Honorable Thad Cochran The Honorable Patrick Leahy Chairman Vice Chairman United States Senate United States Senate Washington, DC 20510 Washington, DC 20510 The Honorable Rodney Frelinghuysen
March XX, 2017 The Honorable Thad Cochran The Honorable Patrick Leahy Chairman Vice Chairman United States Senate United States Senate Washington, DC 20510 Washington, DC 20510 The Honorable Rodney Frelinghuysen
Getting to Zero in California: Integration of HIV Prevention and Surveillance
 Getting to Zero in California: Integration of HIV Prevention and Surveillance Steve Gibson, MSW and Deanna Sykes, PhD CDPH, Office of AIDS November 27, 2017 Learning Objectives Understand reasons for integrated
Getting to Zero in California: Integration of HIV Prevention and Surveillance Steve Gibson, MSW and Deanna Sykes, PhD CDPH, Office of AIDS November 27, 2017 Learning Objectives Understand reasons for integrated
HIV PREVENTION: NHAS TO HIP
 HIV PREVENTION: NHAS TO HIP Vasavi Thomas, RPh, MPH Public Health Advisor, Prevention Program Branch Division of HIV/AIDS Prevention Centers for Disease Control OVERVIEW National HIV/AIDS Strategy (NHAS)
HIV PREVENTION: NHAS TO HIP Vasavi Thomas, RPh, MPH Public Health Advisor, Prevention Program Branch Division of HIV/AIDS Prevention Centers for Disease Control OVERVIEW National HIV/AIDS Strategy (NHAS)
Unmet Oral Health Needs of Persons Living With HIV/AIDS in the United States
 Unmet Oral Health Needs of Persons Living With HIV/AIDS in the United States What Can We Do To Improve Services? Nicholas G. Mosca, DDS, DrPH CrescentCare Health/NO AIDS Task Force April 25, 2017 National
Unmet Oral Health Needs of Persons Living With HIV/AIDS in the United States What Can We Do To Improve Services? Nicholas G. Mosca, DDS, DrPH CrescentCare Health/NO AIDS Task Force April 25, 2017 National
Modernization of North Carolina s HIV control measures
 Modernization of North Carolina s HIV control measures North Carolina Division of Public Health Victoria Mobley, MD MPH Evelyn Foust, MPH CPM Agenda Introduction Summary of scientific evidence used to
Modernization of North Carolina s HIV control measures North Carolina Division of Public Health Victoria Mobley, MD MPH Evelyn Foust, MPH CPM Agenda Introduction Summary of scientific evidence used to
Here are some of the steps (greatly simplified) and gaps that can occur in the HIV Treatment Cascade:
 CATIE-News CATIE s bite-sized HIV and hepatitis C news bulletins. Alberta Reducing deaths by strengthening the HIV Treatment Cascade 20 May 2014 In Canada and other high-income countries, deaths from AIDS-related
CATIE-News CATIE s bite-sized HIV and hepatitis C news bulletins. Alberta Reducing deaths by strengthening the HIV Treatment Cascade 20 May 2014 In Canada and other high-income countries, deaths from AIDS-related
The New HIV Epidemic Challenges: Policy, Politics, and Poor Patients
 The New HIV Epidemic Challenges: Policy, Politics, and Poor Patients John T. Carlo, MD, MS Chief Executive Officer AIDS ARMS, INC. https://twitter.com/jtcarlo Conflict of Interest None 2 Learning Objectives
The New HIV Epidemic Challenges: Policy, Politics, and Poor Patients John T. Carlo, MD, MS Chief Executive Officer AIDS ARMS, INC. https://twitter.com/jtcarlo Conflict of Interest None 2 Learning Objectives
Ryan White HIV/AIDS Program Part B Proposal Q & A
 Ryan White HIV/AIDS Program Part B Proposal Q & A Why is this being considered? In response to requests by community members and legislators and in accordance with the new National HIV/AIDS Strategy, two
Ryan White HIV/AIDS Program Part B Proposal Q & A Why is this being considered? In response to requests by community members and legislators and in accordance with the new National HIV/AIDS Strategy, two
Elements of the Care Continuum
 Elements of the Care Continuum Michael J. Mugavero, MD, MHSc Associate Professor of Medicine University of Alabama at Birmingham Birmingham, Alabama FORMATTED: 12/09/15 Slide 3 of 38 Learning Objectives
Elements of the Care Continuum Michael J. Mugavero, MD, MHSc Associate Professor of Medicine University of Alabama at Birmingham Birmingham, Alabama FORMATTED: 12/09/15 Slide 3 of 38 Learning Objectives
IFMSA Policy Statement Ending AIDS by 2030
 IFMSA Policy Statement Ending AIDS by 2030 Proposed by IFMSA Team of Officials Puebla, Mexico, August 2016 Summary IFMSA currently acknowledges the HIV epidemic as a major threat, which needs to be tackled
IFMSA Policy Statement Ending AIDS by 2030 Proposed by IFMSA Team of Officials Puebla, Mexico, August 2016 Summary IFMSA currently acknowledges the HIV epidemic as a major threat, which needs to be tackled
State of Alabama AIDS Drug Assistance Program (ADAP) Quarterly Report
 State of Alabama AIDS Drug Assistance Program (ADAP) Quarterly Report This report reflects active clients currently enrolled in ADAP Full-pay Prescription Program (ADAP-Rx), Alabama s Insurance Assistance
State of Alabama AIDS Drug Assistance Program (ADAP) Quarterly Report This report reflects active clients currently enrolled in ADAP Full-pay Prescription Program (ADAP-Rx), Alabama s Insurance Assistance
Health Care Reform Update and Advocacy Priorities
 Health Care Reform Update and Advocacy Priorities Robert Greenwald Clinical Professor of Law Director, Center for Health Law and Policy Innovation of Harvard Law School October 2012 PRESENTATION OUTLINE
Health Care Reform Update and Advocacy Priorities Robert Greenwald Clinical Professor of Law Director, Center for Health Law and Policy Innovation of Harvard Law School October 2012 PRESENTATION OUTLINE
INTERNAL QUESTIONS AND ANSWERS DRAFT
 WHO CONSOLIDATED GUIDELINES ON THE USE OF ANTIRETROVIRAL DRUGS FOR TREATING AND PREVENTING HIV INFECTION Background: INTERNAL QUESTIONS AND ANSWERS DRAFT At the end of 2012, 9.7 million people were receiving
WHO CONSOLIDATED GUIDELINES ON THE USE OF ANTIRETROVIRAL DRUGS FOR TREATING AND PREVENTING HIV INFECTION Background: INTERNAL QUESTIONS AND ANSWERS DRAFT At the end of 2012, 9.7 million people were receiving
Implementation of the National HIV/AIDS Strategy to Improve HIV Prevention and Care Grant Colfax, MD Office of National AIDS Policy
 Implementation of the National HIV/AIDS Strategy to Improve HIV Prevention and Care Grant Colfax, MD Office of National AIDS Policy 7 th International Conference of HIV Treatment and Prevention Adherence
Implementation of the National HIV/AIDS Strategy to Improve HIV Prevention and Care Grant Colfax, MD Office of National AIDS Policy 7 th International Conference of HIV Treatment and Prevention Adherence
Billing Code: P DEPARTMENT OF HEALTH AND HUMAN SERVICES. Centers for Disease Control and Prevention. [30Day-18-17AUZ]
![Billing Code: P DEPARTMENT OF HEALTH AND HUMAN SERVICES. Centers for Disease Control and Prevention. [30Day-18-17AUZ] Billing Code: P DEPARTMENT OF HEALTH AND HUMAN SERVICES. Centers for Disease Control and Prevention. [30Day-18-17AUZ]](/thumbs/89/98265456.jpg) This document is scheduled to be published in the Federal Register on 06/18/2018 and available online at https://federalregister.gov/d/2018-12971, and on FDsys.gov Billing Code: 4163-18-P DEPARTMENT OF
This document is scheduled to be published in the Federal Register on 06/18/2018 and available online at https://federalregister.gov/d/2018-12971, and on FDsys.gov Billing Code: 4163-18-P DEPARTMENT OF
Getting to zero HIV new infections in Asia and the Pacific region: Possible or impossible dream?
 Getting to zero HIV new infections in Asia and the Pacific region: Possible or impossible dream? Steven J. Kraus Director UNAIDS Regional Support Team, Asia and the Pacific Timothy D. Mastro Director,
Getting to zero HIV new infections in Asia and the Pacific region: Possible or impossible dream? Steven J. Kraus Director UNAIDS Regional Support Team, Asia and the Pacific Timothy D. Mastro Director,
San Francisco Medical Monitoring Project (MMP) Maree Kay Parisi Applied Research, Community Health Epidemiology and Surveillance
 San Francisco Medical Monitoring Project (MMP) Maree Kay Parisi Applied Research, Community Health Epidemiology and Surveillance Medical Monitoring Project Overview National prospective Local data and
San Francisco Medical Monitoring Project (MMP) Maree Kay Parisi Applied Research, Community Health Epidemiology and Surveillance Medical Monitoring Project Overview National prospective Local data and
The Affordable Care Act and HIV/AIDS: Implications for Coverage, Access to Care, and Payment
 The Affordable Care Act and HIV/AIDS: Implications for Coverage, Access to Care, and Payment for National and Global Health Law Overview This is a unique moment in our Nation s response to the HIV epidemic.
The Affordable Care Act and HIV/AIDS: Implications for Coverage, Access to Care, and Payment for National and Global Health Law Overview This is a unique moment in our Nation s response to the HIV epidemic.
MANITOBA HIV REPORT 2015
 MANITOBA HIV REPORT 2015 The Manitoba HIV Program provides information, specialized care, treatment, and support to approximately 1,250 people living with HIV across the province. The Program has two Winnipeg-based
MANITOBA HIV REPORT 2015 The Manitoba HIV Program provides information, specialized care, treatment, and support to approximately 1,250 people living with HIV across the province. The Program has two Winnipeg-based
WHO Strategy and Goals for Viral Hepatitis Elimination
 WHO Strategy and Goals for Viral Hepatitis Elimination No Disclosures Outline 1. Global strategy for elimination WHO targets and rationale 2. The global response so far Gaps in achieving the HBV and HCV
WHO Strategy and Goals for Viral Hepatitis Elimination No Disclosures Outline 1. Global strategy for elimination WHO targets and rationale 2. The global response so far Gaps in achieving the HBV and HCV
Viral Load Suppression/Any HIV Care 84%
 1 2 Viral Load Suppression/Any HIV Care 84% 3 Key Policy Advancements 4 Implementati on of 30% rent cap affordable housing project Expansion of data sharing Elimination of written consent for HIV Testing
1 2 Viral Load Suppression/Any HIV Care 84% 3 Key Policy Advancements 4 Implementati on of 30% rent cap affordable housing project Expansion of data sharing Elimination of written consent for HIV Testing
FULTON COUNTY GOVERNMENT RYAN WHITE PART A PROGRAM. Atlanta Eligible Metropolitan Area HIV/AIDS Unmet Need Estimate
 FULTON COUNTY GOVERNMENT RYAN WHITE PART A PROGRAM Atlanta Eligible Metropolitan Area HIV/AIDS Unmet Need Estimate Southeast AIDS Training and Education Center Department of Family and Preventative Medicine
FULTON COUNTY GOVERNMENT RYAN WHITE PART A PROGRAM Atlanta Eligible Metropolitan Area HIV/AIDS Unmet Need Estimate Southeast AIDS Training and Education Center Department of Family and Preventative Medicine
Aidspan Review of a Study on the Costs and Health Impact of Continued Global Fund Support for Antiretroviral Therapy
 An independent watchdog of the Global Fund, and publisher of Global Fund Observer P.O. Box 66869-00800, Nairobi, Kenya Web: www.aidspan.org Email: info@aidspan.org Phone: +254-20-418-0149 Fax: +254-20-418-0156
An independent watchdog of the Global Fund, and publisher of Global Fund Observer P.O. Box 66869-00800, Nairobi, Kenya Web: www.aidspan.org Email: info@aidspan.org Phone: +254-20-418-0149 Fax: +254-20-418-0156
Data inputs for HIV models and how they inform HIV prevention interventions Dobromir Dimitrov
 Data inputs for HIV models and how they inform HIV prevention interventions Dobromir Dimitrov Vaccine & Infectious Disease Division Fred Hutchinson Cancer Research Center Dynamic model integration The
Data inputs for HIV models and how they inform HIV prevention interventions Dobromir Dimitrov Vaccine & Infectious Disease Division Fred Hutchinson Cancer Research Center Dynamic model integration The
When PrEP fails. Laura Waters MD FRCP Mortimer Market Centre London
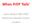 When PrEP fails Laura Waters MD FRCP Mortimer Market Centre London www.aidsunited.org PrEP works If people at risk take it If it s taken in the right way If it s available Commissioned/licensed Affordable
When PrEP fails Laura Waters MD FRCP Mortimer Market Centre London www.aidsunited.org PrEP works If people at risk take it If it s taken in the right way If it s available Commissioned/licensed Affordable
Title: Trends of the HIV/AIDS epidemic in Lyon University Hospitals from 1985 to 2011: continuous decrease since the introduction of HAART
 Title: Trends of the HIV/AIDS epidemic in Lyon University Hospitals from 1985 to 2011: continuous decrease since the introduction of HAART Author: Olivia Febvey Thomas Bénet Dominique Baratin Patrick Miailhes
Title: Trends of the HIV/AIDS epidemic in Lyon University Hospitals from 1985 to 2011: continuous decrease since the introduction of HAART Author: Olivia Febvey Thomas Bénet Dominique Baratin Patrick Miailhes
HRSA HIV/AIDS Bureau Updates
 HRSA HIV/AIDS Bureau Updates Minority AIDS Initiative (MAI): 15 Years Later What s Been Achieved? What Are the Ongoing Barriers to Success? October 2, 2014 Harold J. Phillips Deputy Director Division of
HRSA HIV/AIDS Bureau Updates Minority AIDS Initiative (MAI): 15 Years Later What s Been Achieved? What Are the Ongoing Barriers to Success? October 2, 2014 Harold J. Phillips Deputy Director Division of
Bukoba Combination Prevention Evaluation: Effective Approaches to Linking People Living with HIV to Care and Treatment Services in Tanzania
 Bukoba Combination Prevention Evaluation: Effective Approaches to Linking People Living with HIV to Care and Treatment Services in Tanzania COUNTRY: Tanzania Tanzania has successfully implemented the standard
Bukoba Combination Prevention Evaluation: Effective Approaches to Linking People Living with HIV to Care and Treatment Services in Tanzania COUNTRY: Tanzania Tanzania has successfully implemented the standard
Using a validated computer simulation to assess HIV prevention efforts in Connecticut
 Using a validated computer simulation to assess HIV prevention efforts in Connecticut R. Scott Braithwaite, MD, MS, FACP Professor of Medicine and Population Health CIRA/Yale and New York University Introduction
Using a validated computer simulation to assess HIV prevention efforts in Connecticut R. Scott Braithwaite, MD, MS, FACP Professor of Medicine and Population Health CIRA/Yale and New York University Introduction
The outlook for hundreds of thousands adolescents is bleak.
 Adolescents & AIDS Dr. Chewe Luo Chief HIV/AIDS, UNICEF Associate Director, Programmes Division 28/11/17 Professor Father Micheal Kelly Annual Lecture on HIV/AIDS Dublin, Ireland The outlook for hundreds
Adolescents & AIDS Dr. Chewe Luo Chief HIV/AIDS, UNICEF Associate Director, Programmes Division 28/11/17 Professor Father Micheal Kelly Annual Lecture on HIV/AIDS Dublin, Ireland The outlook for hundreds
EDMA HIV-AIDS TEAM Fact Sheet November 2007
 EDMA HIV-AIDS TEAM Fact Sheet November 2007 1. HIV Facts AIDS epidemic update UNAIDS Epidemic Update, November 2007 (1) 760,000 people to be living with HIV in Western and Central Europe in 2007. 31,000
EDMA HIV-AIDS TEAM Fact Sheet November 2007 1. HIV Facts AIDS epidemic update UNAIDS Epidemic Update, November 2007 (1) 760,000 people to be living with HIV in Western and Central Europe in 2007. 31,000
