ICMR. Intensive eradication efforts against malaria led to its near BULLETIN. Antimalarial drug policy in India: Past, present & future
|
|
|
- Quentin Holland
- 5 years ago
- Views:
Transcription
1 ICMR BULLETIN ISSN Vol. 44, No January-December 2014 In This Issue... Antimalarial drug policy in India: Past, present & future Antimalarial drug policy in India: Past, present & future Editorial Board Chairman Editor Members Publisher : Dr. V.M. Katoch Director-General, ICMR and Secretary, DHR Ministry of Health and Family Welfare, Government of India : Dr. V.K. Srivastava : Dr. Rashmi Arora : Dr. D.K. Shukla : Dr. Malvika Roy : Dr. Vijay Kumar : Shri J.N. Mathur Intensive eradication efforts against malaria led to its near elimination in the mid s. That was a golden period of motivated men and women, a powerful insecticide and susceptible vectors, and the wonder drug chloroquine whose safety and efficacy against both Plasmodium falciparum and P. vivax formed the mainstay of antimalarial treatment. The success could not last. Reported malaria cases in India peaked in 1976 and although the overall incidence decreased, the incidence of P. falciparum has remained stable 1. The emergence and spread of antimalarial drug resistance in P. falciparum was a key contributor to this trend. The management of antimalarial drug resistance by control programmes consists of three primary activities: (i) reduce drug pressure, primarily through rational use, to prevent the emergence and subsequent spread of drug resistance, (ii) monitor the efficacy of current drug and future drugs under consideration, and (iii) create a robust pipeline, from research and development to regulatory registration, to ensure alternatives drugs in the future. Recently, Shah et al 2 systematically reviewed data from the monitoring of antimalarial drug resistance in India during However, the policy components related to all three activities are not well described. We discuss the evolution of antimalarial drug policy with the aim of evaluating the trends in policy changes. Past: historical perspectives There was no organized programme for malaria control in India in the pre-independence era; but there are records of epidemics and their control by the then Indian Medical Service. In 1912, a special malaria department was created in Mumbai (then Bombay). The department, apart from various surveillance and vector control activities, also distributed quinine and Cinchona febrifuge free of cost 3. Large epidemics, and their classic investigations, were reported from Punjab, Bombay, and Bengal 4. Quinine was the treatment Division of Publication & Information, ICMR, New Delhi
2 of choice for malaria and distribution measures for prophylaxis and treatment existed in several areas 5. In 1917, the Bengal Nagpur Railway and the East India Railways formed separate malaria control organizations for controlling malaria in and around stations. Similar programmes were undertaken in tea plantations of Assam and in Mysore by the Rockefeller Foundation 6. The first organized national programme in health - the National Malaria Control Programme was launched in In view of its initial successes, it was rechristened the National Malaria Eradication Programme (NMEP) in 1958 and developed organized surveillance for active case detection and treatment in A single dose of any 4-aminoquinoline was recommended as the presumptive treatment to all fever cases, while 8-aminoquinoline was added as the radical treatment to achieve gametocytocidal cure in falciparum and hypnozoiticidal cure in vivax malaria. By 1965, only 99,667 malaria cases were reported 2, but the situation deteriorated in subsequent years in the face of administrative, political, and technical challenges (Fig. 1). Hence, the Modified Plan of Operations was introduced in 1977 which emphasized the reduction of disease burden in a cost-effective and integrated manner. Fever treatment depots (FTDs), which obtained blood smears prior to presumptive treating, and drug distribution centres (DDCs), which did not, were established at the village level to ensure the availability of antimalarials in remote and inaccessible areas 1. Chloroquine resistant P. falciparum malaria was first reported in 1973 from the State of Assam in the northeast of the nation 7. Under the modified plan, the emphasis on chemotherapy was also supported by measures to strengthen operational research by mapping areas with chloroquine resistant strains. In 1978, NMEP created six regional monitoring teams to routinely Fig. 1. Reported malaria incidence and the evolution of the National Drug Policy for malaria in India, AS, artesunate; SP, sulphadoxine-pyrimethamine; ACT, artemisinin based combination therapy; AL, artemether lumefantrine; NE, North-East. Source: National Vector Borne Disease Control Programme, Delhi. conduct therapeutic efficacy studies of antimalarials drugs which expanded to 13 teams by Under the eradication era: During the early days of the malaria programme in the 1950s-1970s the reduction of transmission occurred through vector control, primarily indoor residual spray operations. Case detection was geared towards identifying foci of transmission and not providing health care per se. The treatment aspect of eradication work sought to reduce morbidity among detected cases with little emphasis on radical cure until the latter maintenance phase of the programme as re-infection was though likely. No formal drug policies existed but the treatment en vogue was a 4-aminoquinoline (chloroquine or amodiaquine 10 mg/kg single-dose) for presumptive therapy with the addition of five days of primaquine (0.25 mg/kg for five days) regardless of the species present. For mass treatment in special situations, such as temporary labour camps, pyrimethamine (50 mg adult dose) was added for its sporontocidal action 1. First antimalarial drug policy: 1982: The first antimalarial drug policy was drafted in 1982 following the initial report of chloroquine resistance 7 and the documentation of its presence in other States The policy recommended different regimens for different areas depending on the species prevalent and the chloroquine resistance status. Areas were designated as chloroquine-resistant based on the proportion of RIII cases (early treatment failure) found during sensitivity studies. In chloroquine sensitive areas, presumptive treatment was recommended in the form of single dose of chloroquine (10 mg/kg) for malaria cases detected by active case detection (ACD), DDCs, and FTDs. After confirmation of the diagnosis by microscopy, radical treatment in the form of single dose primaquine (0.75 mg/kg) was recommended for falciparum malaria with the use of sulphalene-pyrimethamine (SLP) (adult single dose 1000/50 mg) in cases where the patient did not respond to chloroquine. In chloroquine resistant areas, amodiaquine (10 mg/kg single dose) was recommended for presumptive treatment in patients detected through ACD, DDCs and FTDs while patients detected through passive case detection (PCD) were presumptively treated with SLP. In migrant labour, a single dose of primaquine would be added during presumptive treatment. Radical treatment for falciparum malaria was SLP plus single dose of primaquine 12. In all areas the radical treatment for vivax malaria was chloroquine (10 mg/kg) and primaquine (0.25 mg/kg for five days). The five day regimen of primaquine was developed by the NMEP for its operational ease and reduced toxicity 2
3 compared to the 14 days course and early reports of its comparable efficacy. The Table summarizes the revisions in the National Drug Policy for malaria in India. Modified presumptive treatment: 1995: The number of reported malaria cases dropped from 2.2 million in 1982 to 1.6 million in 1987 but again increased to 3 million by In light of several large epidemics of malaria with substantial mortality, the policy underwent a major revision in The NMEP stratified primary health centres (PHCs) into high and low risk areas based on the proportion of falciparum malaria cases, focus of chloroquine resistance in P. falciparum, slide positivity rate, and recorded malaria deaths. In low risk areas, presumptive and radical treatment and primaquine continued as recommended in the earlier policy 1. In high risk areas, the full dose of chloroquine (25 mg/kg over three days) as opposed to the single dose of chloroquine (10 mg/kg), along with single dose of primaquine was recommended as radical treatment for all fever cases. Additional primaquine (0.25 mg/kg for five days) was provided for all confirmed vivax malaria cases. In chloroquine-resistant areas, a single dose of sulphalene/ sulphadoxine-pyrimethamine (SP) (adult single dose 1500/75 mg) was recommended for the treatment of falciparum malaria. The SP dose was increased from the two-tablet adult dose (1000/50 mg) recommended earlier to the three tablet adult dose (1500/75 mg) after studies suggesting higher efficacy of the latter. Amodiaquine was withdrawn from the drug policy since it possessed no advantage over chloroquine due to cross-resistance and was considered more toxic 1. The World Health Organization (WHO) also recommended the withdrawal of amodiaquine at the time because of reported side effects 14. The policy also approved the use of mefloquine in the country but only by a registered medical practitioner in cases of confirmed P. falciparum with ring stages and in chloroquine resistance areas. Finally, a review of the national drug policy was recommended every two years to keep up with the complex scenario and changing patterns in the country. The stable millennium years: In 1998, the NMEP became the National Anti-Malaria Programme (NAMP) acknowledging the change of emphasis in the goals of control efforts. The 2001 review of the drug policy continued the recommendations of 1995 policy 13. The criteria for the designation of chloroquine-resistant areas, more than 25 per cent treatment failure (RI- RIII) in at least 30 patients of one PHC, were stated in the policy. In 2003, NAMP acquired additional responsibilities and emerged as the National Vector Borne Disease Control Programme (NVBDCP). In 2003, the short follow up (7 day) drug resistance studies were also ended 15. Artemisinin combination therapy (ACT) and treatment after confirmation: : The WHO technical advisory group, while meeting in India in 2004, recommended the use of combination antimalarial therapy, particularly with artemisinin derivatives, in member countries for treating P. falciparum to delay the emergence of drug resistance. Artemisinin combination therapy (ACT) consists of an artemisinin derivative combined with a long acting partner antimalarial drug. In the 2005 drug policy, in light of SP monotherapy resistance and WHO recommendations, artesunate (AS) + SP replaced SP alone in the national drug policy for the treatment of confirmed falciparum malaria cases in chloroquine resistant areas in Injection artemisinin was to be restricted to severe malaria cases only but oral artemisinin could be used in cases which were resistant to chloroquine and SP. The use of artemisinin related compounds was not recommended in infants. In 2007, several major changes occurred in the malaria drug policy. First, presumptive treatment, that is single dose chloroquine, was no longer recommended and the use of clinical diagnosis alone was rejected. The policy recommended investigating all suspected malaria cases by microscopy or with rapid diagnostic kits (RDK) 16. In situations where diagnosis was not possible or the delay would be great, clinical treatment should use the full-dose, three days, of chloroquine until diagnosis was obtained. Second, the cut-off for designating an area as chloroquine-resistant was now only 10 per cent treatment failure given the recognition of the rapid spread of drug resistance as well as new cost-effectiveness analysis. Furthermore, clusters of PHCs, with a high (>30%) proportion of falciparum cases, around the resistant focus became the unit used for adopting second-line drug. Third, the anti-relapse treatment for P. vivax was extended to 14 days of therapy after definitive studies demonstrating the poor efficacy of the five day course. Other notable points were for cases in whom chloroquine and AS+SP failed, oral quinine plus tetracycline or doxycycline would be used. The policy also dictated the disuse of single dose of primaquine along with AS+SP given that artesunate itself reduces gametocyte carriage. Another revision in 2008 added the treatment of patients negative by RDK with full-dose chloroquine as the NVBDCP kits are monovalent and only detect 3
4 Table. Summary of different revisions of the National Drug Policy for malaria in India, 1950s-Present Treatment after confirmation Special groups Year Presumptive treatment Late 1950s CQ or AQ (10mg/kg SD) 1982 CQS: CQ (10 mg/ kg SD) in ACD, DDCs, and FTDs P. falciparum malaria P. vivax malaria Severe malaria Malaria in pregnancy Chemoprophylaxis or MDA PQ (0.25mg/kg for 5 days) MDA: Presumptive + PYR (adult SD 50 mg) CQS: CQ (10 mg/kg SD) + PQ (0.75mg/kg SD) CQ (10 mg/kg SD) + PQ (0.25 mg/kg for 5 days) Parenteral CQ or quinine Contraindications: PQ MDA in migrants: CQ (10 mg/kg) + PQ (0.75 mg/kg) Criteria for CQR areas with established CQ resistance by in vivo tests CQR: AQ (10 mg/ kg SD) in ACD, DDCs, FTDs and SLP (adult SD 1000/50mg) in PCD 1995 Low risk: CQ (10 mg/kg SD) High risk: CQ (25 mg/kg over 3 days) + PQ (0.75 mg/kg SD) CQR: SLP (adult SD 1000/50 mg) + PQ (0.75mg/kg SD) Low risk: CQ (10mg/kg SD) + PQ (0.75mg/kg SD) High risk CQS: no further treatment Low: CQ (10mg/ kg SD) + PQ (0.25 mg/kg for 5 days) High risk: PQ (0.25 mg/kg for 5 days) Parenteral Artemisinin derivatives or quinine CQS: CQ (10 mg/kg LD then 5 mg/kg weekly) CQR: CQ (5 mg/ kg weekly) + proguanil (100 mg daily) High risk CQR: SP (adult dose 1500/75mg) with PQ (0.75 mg/kg SD) 2002 Contraindications: PQ; Artemisinins in first trimister n>30, failure more than 25% in a PHC 2004 Low risk: CQ (25 mg/kg over 3 days) + PQ (0.75 mg/kg SD) CQ (25 mg/kg over 3 days) + PQ (0.25 mg/kg for 5 days) 4
5 Treatment after confirmation Special groups Year Presumptive treatment P. falciparum malaria P. vivax malaria Severe malaria Malaria in pregnancy Chemoprophylaxis or MDA Criteria for CQR High risk CQS & high risk CQR: same 2005 Low risk & high risk CQS: same CQR: AS (4 mg/ kg daily for 3 days) + SP (adult dose 1500/75 mg SD) 2007 No presumptive therapy; CQ (25 mg/kg over 3 days) if lab diagnosis is not available within 24 h CQS & CQR: same CQ (25mg/kg over 3 days) + PQ (0.25 mg/kg for 14 days) n>50, failure more than 10% in clusters of PHCs Treatment failure: Oral QN + tetracycline or DOX 2008 Same but with full treatment for RDT negative cases also Short term: DOX daily Long term: MQ weekly n>50, failure more than 10% in clusters of blocks 2010 AS (4 mg/kg daily for 3 days) + SP (adult dose 1500/75 mg SD) + PQ (0.75 mg/kg SD) QN (1st trimester) or AS+SP (2nd and 3rd trimester) 2013 Same (AS+SP) for all over India except North Eastern States; artemether lumefantrine ( mg adult dose) in North Eastern States CQ, chloroquine; AS, artesunate; CQR, chloroquine resistant; CQS, chloroquine sensitive; ACD, active case detection; DDC, Drug distribution centres; ACD: active case detection; AS, artesunate; CQ, chloroquine; CQR, chloroquine resistant; CQS, chloroquine sensitive; DDC, drug distribution centres; DOX, doxycycline; FTD, fever treatment depot; LD, loading dose; MDA, mass drug administration; MQ, mefloquine; PHC, primary health centre; QN, quinine; RDT, rapid diagnostic test; SD, single dose; SP, sulfadoxine pyrimethamine; PYR, pyrimethamine; AQ, amodiaquine; PQ, primaquine; SLP, sulfalene-pyrimethamine; PCD, passive case detection; RDK, rapid diagnostic kit. Source : Ref. 1,12,13,15-17,18,20 5
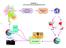
6 P. falciparum 17. The policy expanded the use of AS+SP to 117 districts across India which represented more than 90 per cent of the reported P. falciparum burden. The policy also recommended avoiding the use of mefloquine alone or in combination with artesunate in cerebral malaria. A flow diagram of the case management process was included for the first time to facilitate interpretation of the policy. Therapeutic efficacy studies continued to demonstrate a high prevalence of chloroquine resistance in falciparum malaria 2,19. In 2010, the drug policy was further reviewed and revised with the use of AS+SP for treating falciparum malaria cases made universal all across the country 18. For the first time the sulpha component of SP was specified as sulphadoxine instead of sulphalene/sulphadoxine. Single-dose primaquine was added to AS+SP, on day two, to reduce gametocyte carriage post-treatment since artesunate only acts against the immature forms. In 2013, there was another policy change in the seven North Eastern States (Arunachal Pradesh, Assam, Manipur, Meghalaya, Mizoram, Nagaland and Tipura) in view of the resistance to partner drug SP. The combination was replaced by artemether lumefantrine in these States 20. Severe malaria, pregnancy, and prophylaxis: Initially, only parenteral chloroquine and quinine were recommended for the treatment of severe malaria cases. Parenteral artemisinin derivatives were introduced in the national drug policy in 1995 for treating severe and complicated malaria in addition to quinine, particularly in areas of chloroquine resistance or during quinine shortages 1,13. Chloroquine was no longer recommended. Similarly, quinidine, under cardiac monitoring, was also recommended when quinine was not available. The 2002, the policy re-recommended injectable chloroquine for severe malaria, with precaution in children, in situations where injectable artesunate or quinine were unavailable. In 2005, the doses used for the artemisinin derivatives (artesunate, artemether, arteether, and artemisinin) were indicated, the minimum duration of treatment was seven days, followed by a full-course of ACT. In 2008, artemisinin was removed from the list of recommended derivatives 17. Till recently, quinine was the drug of choice for falciparum malaria in pregnancy though the emphasis of the national policy was on the drugs which were contraindicated rather than which were recommended. In 2001, the drug policy warned against the use of artemisinin derivatives in pregnant women. The present national drug policy recommends AS+SP in second and third trimesters though quinine is to be used in the first trimester until safety data for the artemisinin derivatives in the first trimester become available. For P. vivax malaria, chloroquine has been recommended 18. The national programme recommends chemoprophylaxis only for select groups from nonendemic areas (travelers, and military personnel) exposed to malaria in highly endemic areas. Among the population in endemic areas, chemoprophylaxis is only recommended in pregnant women. The 1995 drug policy recommended weekly chloroquine prophylaxis in chloroquine sensitive areas. In chloroquine resistant areas, besides weekly chloroquine, daily proguanil was recommended. Since 2008, the drug policy recommends daily doxycycline for short term prophylaxis (less than six weeks) and weekly mefloquine for long term prophylaxis 18 with treatment beginning two days or two week before and ending after four weeks of return, respectively. Among migrant labourers, weekly case detection instead of chemoprophylaxis was recommended on operational grounds. The maximum duration for chloroquine treatment was limited to three years because of concerns of toxicity. Present: SWOT analysis Strengths: Artemisinin monotherapy was banned in India in The drug policy recommends antimalarial therapy only after parasitological confirmation of the diagnosis which will reduce drug pressure for resistance, prevent side-effects, decrease drug costs, and improve the management of other causes of febrile illness. The current first-line therapy for P. falciparum, AS+SP, showed 98.8 per cent treatment success across 25 sites in India during 2009 and 2010 over 28 days of follow up 21. The programme has changed the ACT in North Eastern States to artemether lumefantrine in view of the resistance to partner drug SP 20. Chloroquine continues to be recommended for P. vivax malaria. Though there were reports of chloroquine resistance in P. vivax 22, the therapeutic efficacy studies showed a 100 per cent efficacy. The joint NIMR- NVBDCP National Drug Resistance Monitoring System conducts both widespread and longitudinal measurement of the treatments used in both species through simultaneous in vivo and molecular methods. The policy process is now well-defined, consultative, and evidence-based in addition to expert opinion. Fig. 2 outlines the policy process for the formation of National Drug Policy for Malaria in India. The frequency of drug policy updates has also increased with three policy changes in the last five years. Finally, the policy has been translated into easy to follow case management guidelines for use by clinicians 18. 6
7 Weaknesses: The present ACT (AS+SP) being recommended all over India except North Eastern States is a blister pack. Compared to fixed-dose combinations (FDCs), blister packs where the individual drugs are co-packaged may have poorer adherence, the potential for monotherapy use, and even poorer bioavailability. Another challenge for the drug policy is access to the delivery systems used for malaria diagnosis and treatment in India. Citizens living in remote, inaccessible, or disturbed areas may have to undergo considerable hardship to reach publicly provided care and turn to self-treatment or the formal and, more often, informal private sector for care. Communitybased care, while introduced in some places, is not available everywhere. On the provider side, there is lack of awareness of the National Drug Policy, and best practice in general, among the private sector. A host of available therapies (Box) shows a wide variation in treatment choice along with dose, duration, and coadministered drugs such as antibiotics. Physician and patient compliance to radical treatment (primaquine) is poor and may be contributing unnecessary burden in terms of additional transmission or relapses. Opportunities: New ACTs have recently completed or are undergoing phase III studies 23 and some are now registered. Phase III clinical trials have been completed for fixed dose ACTs including artesunate + mefloquine, dihydroartemisinin + piperaquine 24, arterolane + piperaquine 25, and pyronaridine + artesunate 26. Arterolane is a synthetic analogue of artemisinin and has the potential to replace plant-derived artemisinin 27. Trials are underway for combinations of current ACTs like artesunate + lumefantrine, artesunate+piperaquine, etc. Pharmacovigilance of antimalarial drugs is generating data on adverse events in patients which will help improve future policy. The case management of malaria has been extended to the village level in many areas through the use of community-based health workers. This should help promote more access and quicker treatment for suffering patients. The bivalent RDKs have recently been introduced and will improve the diagnosis. Threats: Emerging resistance to antimalarial drugs poses the greatest threat to the National Drug Policy on malaria. While the results of in vitro sensitivity testing of antimalarial drugs in India have not shown any evidence of decreased sensitivity to artemisinin derivatives 28, clinical resistance to artemisinin drugs has emerged along the nearby Thai-Myanmar and Thai-Cambodia borders 29. The spread of resistance westwards, as happened with chloroquine, could jeopardize the most effective class of compounds we have for malaria treatment today. There is considerable evidence (clinical, in vitro, and molecular) of drug resistance to the partner drug used in the first-line ACT. Studies suggested the presence of double mutations in dhfr and single/double mutations in dhps 30. Changes in these drug resistance markers are currently being monitored among patients enrolled in therapeutic efficacy studies in sentinel sites across the country 31. The spread and increase in SP resistance, which is likely inevitable, may decrease the present high efficacy of AS+SP in India and necessitate the switch to a different combination therapy. Though data on the efficacy of AS+SP on mixed infections are sparse, we know that SP is not very effective against vivax malaria. Finally, the emergence of chloroquine resistance in P. vivax, as has happened elsewhere in the not too distant Western Pacific region 32, would complicate the control of the species responsible for half of the national malaria burden. Future: unresolved challenges From antimalarial treatment to case management: A key transition from the malaria eradication era towards a modern malaria control programme is moving from drug distribution to case management. The former is concerned with an output, supplying drug, while the latter is an entire process from diagnosis to care to referrals and is concerned with quality. The change to the case management can be challenging where activities are influenced by many interconnected factors. While the process has been long initiated, and strengthened by policy changes such as the end of presumptive treatment, quality has room to improve. To begin with, indicators such as the time from fever to diagnosis and treatment need to be monitored. Another goal should be increasing the proportion of malaria cases from passive Fig. 2. The policy process for the formation of National Drug Policy for malaria in India, 2001-onwards. NIMR, National Institute of Malaria Research (ICMR), New Delhi; NVBDCP, Natiional Vector Borne Disease Control Programme, Government of India, Delhi. 7
8 Box. Currently registered antimalarial drugs in India Amodiaquine Artemether + Lumefantrine FDC Arterolane + Piperaquine FDC Artesunate + Amodiaquine FDC Artesunate + Mefloquine blister pack and FDC Artesunate + Sulphadoxine-Pyrimethamine blister pack Chloroquine Injectable artemisinin derivatives Mefloquine Primaquine Proguanil Pyrimethamine Quinine 14. Sulphadoxine-Pyrimethamine Source: Refs 18, 23 detection, which is better suited to quality care, than from active detection, which is needed when health systems are not available or accessible. Finally, at present there are no protocols for the management of malaria-negative fever patients who seek care. Private sector treatment practices: The universe of malaria treatment practices in India is wide and diverse. The National Drug Policy for malaria seeks to be evidence-based best practice. However, the adherence of the private sector to correct treatment of malaria, according to species or severity, is generally poor though more extensive surveys are needed. In 2008, private sector treatment was the largest risk factor for receiving artemisinin monotherapy in a six State survey 33. In 2009, the Drugs Controller General of India has banned the use, manufacture, sell and export of oral artemisinin monotherapy in the country. However, injectable artemisinin derivatives remain a preferred antimalarial treatment in rural areas 33 for treating uncomplicated malaria. There is a need to rationalize the use of injectable artemisinin derivatives by limiting to severe malaria. While at present 80 per cent of medical care in India is privately provided, household survey data suggest that in rural areas of malaria endemic States only half of patients with fever seek private sector care 34. This is still a substantial proportion. Strategies for communicating and promoting the quality of care, including print media, workshops, and even one-to-one interaction, in the private sector are needed. Selecting future ACTs: The choice of optimal ACT for future use is not clear. Artesunate amodiaquine has the disadvantage of cross-resistance with chloroquine whose sensitivity is decreased nationwide in P. falciparum 1,28. Artemether+lumefantrine is effective 35 in India but has to be administered twice daily and can have erratic absorption. Arterolane+piperaquine is promising as a treatment for both species and has a long half-life but more data need to be generated 25. AS+mefloquine was also effective 36, India is largely mefloquine naïve from a resistance point of view, but has the disadvantage of neuropsychiatric complications and a higher cost than other ACTs. Evolutionaryepidemiological modeling suggests that the use of multiple first-line therapies may slow the spread of resistance although there is no empirical validation of the idea 37. Switching to multiple ACTs, or regionwise ACTs, in the public sector may be beneficial, but there are several operational barriers for doing so from procurement and supply chain difficulties to training multiple levels, including community-based staff. One step regarding the regional policy has been taken by the programme by replacing AS+SP with artemether lumefantrine. Gametocytocidal and antirelapse considerations: Current policy recommends a single dose of primaquine on the second day in falciparum and for 14 days in vivax malaria. For the former, the efficacy, optimal day of administration, dose, and safety are not well known though these are being evaluated in an on-going randomized controlled trial (CTRI/2012/12/003273). For the latter, the course is long and compliance, by both provider and patient, is not well-known though suspected to be poor. It is important to improve compliance to antirelapse therapy since upto 40 per cent P. vivax infections are known to relapse 38. Strategies to improve anti-relapse primaquine treatment could include directly observed therapy or administering the same total dose over a short duration. Tafenoquine, a long half-life 8-aminoquinoline resulting in a quicker treatment course, could become an alternative choice of drug and is in clinical development 39. Finally, there is a need to assess both the risks and benefits of primaquine therapy given its haemolytic potential. While glucose- 6-phosphate dehydrogenase (G6PD) deficiency is rare in the general population, studies have documented its prevalence in up to per cent of certain ethnic groups including tribal populations at higher risk for malaria 40. However, primaquine is being used since several decades and no significant adverse events have been documented till date though these are not well monitored either. Tools for G6PD testing at the primary healthcare level could help address this challenge. Preventing malaria during pregnancy: In the present National Drug Policy on malaria, personal protection measures are recommended for preventing malaria during pregnancy. There is a need to assess other 8
9 methods of preventing malaria in this vulnerable group, particularly in regions where the burden may be high. Strategies for evaluation include intermittent screening and treatment, intermittent preventive treatment, and other protection measures during antenatal care. The first strategy is currently being evaluated (CTRI/2012/08/002921). Finally, more data on the safety and efficacy of different drugs are also needed. Trials are underway in India to compare two ACTs (AS+SP versus AS+mefloquine) for treating malaria during pregnancy 23. Data from these efforts will be useful for future revisions. Counterfeit antimalarials: Counterfeit and substandard antimalarials may pose a risk to patient health and antimalarial drug resistance in the country, with the North Eastern States near the China and Myanmar borders being particularly vulnerable 41. In a limited study of chemist shops in two sites of India, 12 per cent of essential drugs, including antimalarial drugs, were of substandard quality 42. Pre-procurement quality checks of antimalarial drugs are conducted by the procuring agency for public sector supply, but similar monitoring does not exist in the general retail market. Routine monitoring of the quality of drugs available on the market should be conducted, ideally by the drug regulatory agencies, in India. Even for public sector drugs, there is a need to check drug quality after dispatch and storage in field conditions where temperature, humidity, and physical placement may be adverse. Conclusion The National Drug Policy on malaria in India has evolved frequently and substantively since its inception in The current policy is up to date with the available evidence, both in India and from abroad. In addition to the policy document, a set of easy to use guidelines, in a frequently-asked-questions format is available in print and for download to be used by practitioners ( Addendum.pdf). Several unrealized opportunities and possible threats to the policy have been identified. Improving the National Drug Policy will require considerable participation and effort by, in addition to the national control programme, numerous other groups - academia, medical colleges, research institutes, regulatory agencies, the pharmaceutical industry, etc. - invested in malaria control for the country. References 1. Sharma RS, Sharma GK, Dhillon GPS. Epidemiology and control of malaria in India New Delhi: Ministry of Health and Family Welfare, National Malaria Eradication Programme, Directorate General of Health Services, Government of India; Shah NK, Dhillon GP, Dash AP, Arora U, Meshnick SR, Valecha N. Antimalarial drug resistance of Plasmodium falciparum in India: changes over time and space. Lancet Infect Dis 2011; 11 : Covell G. Malaria in Bombay, Bombay: Government Central Press; Watts S. British development policies and malaria in India: 1897-c Past Present 1999; 165 : Muraleedharan VR. Quinine (Cinchona) and the incurable malaria: Indiac s. Parasitologia 2000; 42 : Stapleton DH. Lessons of history? Anti-malaria strategies of the International Health Board and the Rockefeller Foundation from the 1920s to the era of DDT. Public Health Rep 2004; 119 : Sehgal PN, Sharma MID, Sharma SL, Gogai S. Resistance to chloroquine in falciparum malaria in Assam state, India. J Commun Dis 1973; 5 : Guha AK, Roy JR, Das S, Roy RG, Pattanayak S. Results of chloroquine sensitivity tests in Plasmodium falciparum in Orissa State. Indian J Med Res 1979; 70 (Suppl): Chakravarty SC, Dwivedi SR, Das S, Phukan D, Roy RG, Pattanayak S. Response of Plasmodium falciparum to chloroquine in the Meghalaya State. Indian J Med Res 1979; 70 (Suppl): Dwivedi SR, Sahu H, Yadava RL, Roy RG, Pattanayak S. In vivo chloroquine sensitivity tests of Plasmodium falciparum in some parts of Uttar Pradesh and Haryana States. Indian J Med Res 1979; 70 (Suppl): Choudhury B, Dutt SC, Roy RG, Pattanayak S. Chloroquine resistant P. falciparum in Chandrapur district of Maharastra state. J Commun Dis 1981; 13 : Directorate of the National Malaria Eradication Programme. Malaria and its control in India. New Delhi: National Malaria Eradication Programme, Directorate General of Health Services, Ministry of Health and Family Welfare, Government of India; National Anti Malaria Programme. National drug policy on malaria. Delhi: National Anti Malaria Programme, Directorate of Health Services, Government of India, Delhi; Practical chemotherapy of malaria: Report of a WHO Scientific Group, WHO Tech Rep Ser; 805. Geneva: WHO; p National Anti Malaria Programme. National Drug Policy on malaria. Delhi: National Anti Malaria Programme, Directorate of Health Services, Government of India, National Vector Borne Disease Control Programme (NVBDCP). National Drug Policy on malaria. Directorate of Health Services, Government of India, Delhi : NVBDCP, National Vector Borne Disease Control Programme (NVBDCP). National Drug Policy on malaria. (Delhi: NBVDCP), Directorate of Health Services, Government of India, Delhi; National Institute of Malaria Research (NIMR). Guidelines for diagnosis and treatment of malaria in India, 2 nd ed. New Delhi: NIMR; Valecha N, Joshi H, Mallick PK, Sharma SK, Kumar A, Tyagi PK, et al. Low efficacy of chloroquine: time to switch over to artemisinin-based combination therapy for falciparum malaria in India. Acta Trop 2009; 111 :
10 20. National Vector Borne Disease Control Programme. National Drug Policy on malaria. Directorate of National Vector Borne Disease Control Programme, Directorate General of Health Services, Ministry of Health and Family Welfare, Government of India, Available from: National-Drug-Policy-2013.pdf, accessed on December 21, Mishra N, Singh JP, Srivastava B, Arora U, Shah NK, Ghosh SK, et al. Monitoring antimalarial drug resistance in India via sentinel sites: outcomes and risk factors for treatment failure, Bull World Health Organ 2012; 90 : Dua VK, Kar PK, Sharma VP. Chloroquine resistant Plasmodium vivax malaria in India. Trop Med Int Health 1996; 1 : Clinical Trials Registry of India. Available from: in/clinicaltrials/do/login1, accessed on November 22, Valecha N, Phyo AP, Mayxay M, Newton PN, Krudsood S, Keomany S, et al. An open-label, randomised study of dihydroartemisinin-piperaquine versus artesunate-mefloquine for falciparum malaria in Asia. PLoS One 2010; 5 : e Valecha N, Krudsood S, Tangpukdee N, Mohanty S, Sharma SK, Tyagi PK, et al. Arterolane maleate plus piperaquine phosphate for treatment of uncomplicated Plasmodium falciparum malaria: a comparative, multicenter, randomized clinical trial. Clin Infect Dis 2012; 55 : Poravuth Y, Socheat D, Rueangweerayut R, Uthaisin C, Phyo A, Valecha N, et al. Pyronaridine-artesunate versus chloroquine in patients with acute Plasmodium vivax malaria: a randomized, double-blind, non-inferiority trial. PLoS One 2011; 6 : e Valecha N, Looareesuwan S, Martensson A, Abdulla SM, Krudsood S, Tangpukdee N, et al. Arterolane, a new synthetic trioxolane for treatment of uncomplicated Plasmodium falciparum malaria: a phase II, multicenter, randomized, dosefinding clinical trial. Clin Infect Dis 2010; 51 : Anvikar AR, Sharma B, Sharma SK, Ghosh SK, Bhatt RM, Kumar A, et al. In vitro assessment of drug resistance in Plasmodium falciparum in five States of India. Indian J Med Res 2012; 135 : Dondorp AM, Nosten F, Yi P, Das D, Phyo AP, Tarning J, et al. Artemisinin resistance in Plasmodium falciparum malaria. N Engl J Med 2009; 361 : Ahmed A, Bararia D, Vinayak S, Yameen M, Biswas S, Dev V, et al. Plasmodium falciparum isolates in India exhibit a progressive increase in mutations associated with sulfadoxine - pyrimethamine resistance. Antimicrob Agents Chemother 2004; 48 : National Institute of Malaria Research. Annual Report National Institute of Malaria Research (Indian Council of Medical Research), New Delhi, Available from: accessed on May 6, Baird JK. Chloroquine resistance in Plasmodium vivax. Antimicrob Agents Chemother 2004; 48 : Mishra N, Anvikar AR, Shah NK, Kamal VK, Sharma SK, Srivastava HC, et al. Prescription practices and availability of artemisinin monotherapy in India: where do we stand? Malar J 2011; 10 : National Institute of Malaria Research. Household Survey and Health Facility Survey for In-depth Review of NVBDCP (Malaria) Available from: Annexure-10%20%20IDR_Mal.pdf, accessed on December 17, Valecha N, Srivastava P, Mohanty SS, Mitra P, Sharma SK, Tyagi PK, et al. Therapeutic efficacy of artemetherlumefantrine in uncomplicated falciparum malaria in India. Malaria J 2009; 8 : Valecha N, Srivastava B, Dubhashi NG, Krishnamoorthy Rao BHK, Kumar A, Ghosh SK, et al. Safety and efficacy and population pharmacokinetics of fixed-dose combination of artesunate-mefloquine in the treatment of acute uncomplicated Plasmodium falciparum malaria in India. J Vector Borne Dis 2013; 50 : Boni MF, Smith DL, Laxminarayan R. Benefits of using multiple first - line therapies against malaria. Proc Natl Acad Sci USA 2008; 105 : Adak T, Valecha N, Sharma VP. Plasmodium vivax polymorphism in a clinical drug trial. Clin Diagn Lab Immunol 2001; 8 : Llanos-Cuentas A, Lacerda MV, Rueangweerayut R, Krudsood S, Gupta SK, Kochar SK, et al. Tafenoquine plus chloroquine for the treatment and relapse prevention of Plasmodium vivax malaria (DETECTIVE): multicentre, double-blind, randomised, phase 2b dose-selection study. Lancet 2013; pii. S (13) Mohanty D, Mukherjee MB, Colah RB. Glucose-6-phosphate dehydrogenase deficiency in India. Indian J Pediatr 2004; 71 : Dash AP, Valecha N, Anvikar AR, Kumar A. Malaria in India: challenges and opportunities. J Biosci 2008; 33 : Bate R, Tren R, Mooney L, Hess K, Mitra B, Debroy B, et al. Pilot study of essential drug quality in two major cities in India. PLoS One 2009; 4 : e6003. This write-up contributed by Dr. AnupKumar, R. Anvikar, National Institute of Malaria Research (NIMR), New Delhi, Dr. Usha Arora and Dr. G.S. Sonal, National Vector-borne Disease Control Programme, Delhi, Dr. Neelima Mishra, Dr. B. Shahi, Dr. Deepali Savargaonkar, Scientist, Dr. Navin Kumar Dr. Nornan K Shah, and Dr. Neena Voleaha, NIMR, New Delhi, has been adopted from Indian Journal of Medical Research, Vol. 139, February 2014, pp Published by Division of Publication & Information on behalf of Director-General, Indian Council of Medical Research, New Delhi R.N /71 10
Interpretation of the World Malaria Report Country Profile
 Interpretation of the World Malaria Report Country Profile Acknowledgements This presentation was developed to help explain the components of the World Malaria Report Country Profile. The 2017 World Malaria
Interpretation of the World Malaria Report Country Profile Acknowledgements This presentation was developed to help explain the components of the World Malaria Report Country Profile. The 2017 World Malaria
Directorate of National Vector Borne Disease Control Programme
 NATIONAL DRUG POLICY ON MALARIA (2008) Directorate of National Vector Borne Disease Control Programme (Directorate General of Health Services) Ministry of Health and Family Welfare 22-Shamnath Marg,, Delhi-110054..
NATIONAL DRUG POLICY ON MALARIA (2008) Directorate of National Vector Borne Disease Control Programme (Directorate General of Health Services) Ministry of Health and Family Welfare 22-Shamnath Marg,, Delhi-110054..
38 Current Concepts in
 38 Current Concepts in Management of Falciparum Malaria Abstract: Artemisinin based Combination Therapy (ACT) is the preferred agent to treat drug resistance uncomplicated Plasmodium Falciparum (PF) Malaria.
38 Current Concepts in Management of Falciparum Malaria Abstract: Artemisinin based Combination Therapy (ACT) is the preferred agent to treat drug resistance uncomplicated Plasmodium Falciparum (PF) Malaria.
Combination Anti-malarial Therapy and WHO Recommendations
 Prakaykaew Charunwatthana 2, and Sasithon Pukrittayakamee 1,2 1 Associate Fellow of the Royal Institute, Academy of Science 2 Department of Clinical Tropical Medicine, Faculty of Tropical Medicine, Mahidol
Prakaykaew Charunwatthana 2, and Sasithon Pukrittayakamee 1,2 1 Associate Fellow of the Royal Institute, Academy of Science 2 Department of Clinical Tropical Medicine, Faculty of Tropical Medicine, Mahidol
Antimalarial drug resistance
 Antimalarial drug resistance Md Mushfiqur Rahman*, Leonard Ortega**, R M Rastogi* and Krongthong Thimasarn* Abstract Antimalarial drug resistance is of great concern in the WHO South-East Asia (SEA) Region.
Antimalarial drug resistance Md Mushfiqur Rahman*, Leonard Ortega**, R M Rastogi* and Krongthong Thimasarn* Abstract Antimalarial drug resistance is of great concern in the WHO South-East Asia (SEA) Region.
Operational feasibility of rapid diagnostic kits & blister packs use for malaria control in high transmission areas of Orissa & Chhattisgarh
 Indian J Med Res 125, January 2007, pp 65-72 Operational feasibility of rapid diagnostic kits & blister packs use for malaria control in high transmission areas of Orissa & Chhattisgarh A.M. Reetha, S.K.
Indian J Med Res 125, January 2007, pp 65-72 Operational feasibility of rapid diagnostic kits & blister packs use for malaria control in high transmission areas of Orissa & Chhattisgarh A.M. Reetha, S.K.
Malaria Symposia Myanmar Medical Association. Dr Aung Thi National Malaria Control Program 04 March 2017
 Malaria Symposia Myanmar Medical Association Dr Aung Thi National Malaria Control Program 04 March 2017 OUTLINE OF THE PRESENTATION Country profile Programmatic achievements Challenges Lessons learnt Way
Malaria Symposia Myanmar Medical Association Dr Aung Thi National Malaria Control Program 04 March 2017 OUTLINE OF THE PRESENTATION Country profile Programmatic achievements Challenges Lessons learnt Way
Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1
 Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1 Part I: Evaluation of the current list Proposed grouping from the March 2007 meeting 6.5.3 Antimalarial medicines 6.5.3.1 For curative
Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1 Part I: Evaluation of the current list Proposed grouping from the March 2007 meeting 6.5.3 Antimalarial medicines 6.5.3.1 For curative
Progress on the Containment of Artemisinin Tolerant Malaria Parasites in South-East Asia (ARCE) Initiative
 Progress on the Containment of Artemisinin Tolerant Malaria Parasites in South-East Asia (ARCE) Initiative I. Background For many years, the border area between Cambodia and Thailand has been the source
Progress on the Containment of Artemisinin Tolerant Malaria Parasites in South-East Asia (ARCE) Initiative I. Background For many years, the border area between Cambodia and Thailand has been the source
Summary World Malaria Report 2010
 Summary The summarizes information received from 106 malaria-endemic countries and other partners and updates the analyses presented in the 2009 Report. It highlights continued progress made towards meeting
Summary The summarizes information received from 106 malaria-endemic countries and other partners and updates the analyses presented in the 2009 Report. It highlights continued progress made towards meeting
ISSN X (Print) Original Research Article. DOI: /sjams India
 DOI: 10.21276/sjams.2016.4.6.22 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(6B):1981-198 5 Scholars Academic and Scientific Publisher (An International Publisher
DOI: 10.21276/sjams.2016.4.6.22 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(6B):1981-198 5 Scholars Academic and Scientific Publisher (An International Publisher
Clinical Drug Trials
 Clinical Drug Trials Drug resistance to chloroquine in P. falciparum was reported in India for the first time from Assam in 1973. Since then the foci of resistance have spread to many more states all over
Clinical Drug Trials Drug resistance to chloroquine in P. falciparum was reported in India for the first time from Assam in 1973. Since then the foci of resistance have spread to many more states all over
A New Class of Malaria Drugs: The Coartem Breakthrough from Novartis
 A New Class of Malaria Drugs: The Coartem Breakthrough from Novartis and its Chinese Partners Hans Rietveld, Director, Global Access and Marketing, Malaria Initiative, Novartis Pharma AG Workshop on Access
A New Class of Malaria Drugs: The Coartem Breakthrough from Novartis and its Chinese Partners Hans Rietveld, Director, Global Access and Marketing, Malaria Initiative, Novartis Pharma AG Workshop on Access
Disclosure Information
 Malaria Medications Charlie Mosler, RPh, PharmD, CGP, FASCP Assistant Professor of Pharmacy Practice The University of Findlay College of Pharmacy Findlay, OH mosler@findlay.edu Disclosure Information
Malaria Medications Charlie Mosler, RPh, PharmD, CGP, FASCP Assistant Professor of Pharmacy Practice The University of Findlay College of Pharmacy Findlay, OH mosler@findlay.edu Disclosure Information
Box 1. Recommendations unchanged from the first edition of the Guidelines (2006)
 Executive summary Executive Summary Malaria case management remains a vital component of the malaria control strategies. This entails early diagnosis and prompt treatment with effective antimalarial medicines.
Executive summary Executive Summary Malaria case management remains a vital component of the malaria control strategies. This entails early diagnosis and prompt treatment with effective antimalarial medicines.
Against intervention No recommendation Strong Conditional Conditional Strong. For intervention. High Moderate Low Very low
 Draft recommendation: Consider using MDA as an additional tool for the elimination of malaria in low prevalence island or nonisland settings where the risk of imported malaria is low Balance of desirable
Draft recommendation: Consider using MDA as an additional tool for the elimination of malaria in low prevalence island or nonisland settings where the risk of imported malaria is low Balance of desirable
From a one-size-fits-all to a tailored approach for malaria control
 From a one-size-fits-all to a tailored approach for malaria control MMV 12 th Stakeholders Meeting New Delhi, India 07 November 2012 Robert D. Newman, MD, MPH Director, Global Malaria Programme newmanr@who.int
From a one-size-fits-all to a tailored approach for malaria control MMV 12 th Stakeholders Meeting New Delhi, India 07 November 2012 Robert D. Newman, MD, MPH Director, Global Malaria Programme newmanr@who.int
Evaluation of Malaria Surveillance System in Hooghly district of West Bengal - India
 Original Research Article Evaluation of Malaria Surveillance System in Hooghly district of West Bengal - India Dan Amitabha 1,*, Kunal Kanti De 2, Pasi A R 3, Jalaluddeen M 4, Roy Bibhash 5 1 Airport Health
Original Research Article Evaluation of Malaria Surveillance System in Hooghly district of West Bengal - India Dan Amitabha 1,*, Kunal Kanti De 2, Pasi A R 3, Jalaluddeen M 4, Roy Bibhash 5 1 Airport Health
Rectal artesunate for pre-referral treatment of severe malaria
 Global Malaria Programme Rectal artesunate for pre-referral treatment of severe malaria october 2017 information note Background Severe malaria is a medical emergency: mortality from untreated severe malaria
Global Malaria Programme Rectal artesunate for pre-referral treatment of severe malaria october 2017 information note Background Severe malaria is a medical emergency: mortality from untreated severe malaria
MMV s Access & Product Management Strategy
 MMV s Access & Product Management Strategy Siem Reap, Cambodia 24-26 February 2015 George Jagoe, EVP, Access & Product Mgmt Defeating Malaria Together OUR MISSION to reduce the burden of malaria in disease-endemic
MMV s Access & Product Management Strategy Siem Reap, Cambodia 24-26 February 2015 George Jagoe, EVP, Access & Product Mgmt Defeating Malaria Together OUR MISSION to reduce the burden of malaria in disease-endemic
Scenario#1 Fever from Kenya. New Drugs for Malaria
 New Drugs for Malaria This talk may be politically incorrect or in bad 1 taste.viewer discretion is advised 2 Scenario#1 Fever from Kenya A 37 year old traveller returns from a one month vacation in rural
New Drugs for Malaria This talk may be politically incorrect or in bad 1 taste.viewer discretion is advised 2 Scenario#1 Fever from Kenya A 37 year old traveller returns from a one month vacation in rural
APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS
 APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS 97 Country/ area APPENDIX 2a DRUG REGIMENS SEA REGION, 2001 (dosage for adults) : P. falciparum Lab confirmed Treatment failure Severe malaria Pregnancy
APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS 97 Country/ area APPENDIX 2a DRUG REGIMENS SEA REGION, 2001 (dosage for adults) : P. falciparum Lab confirmed Treatment failure Severe malaria Pregnancy
MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND C Rojanawatsirivej 1, S Vijaykadga 1, I Amklad 1, P Wilairatna
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND C Rojanawatsirivej 1, S Vijaykadga 1, I Amklad 1, P Wilairatna
Briefing on Intensified Malaria Control Project-3 (IMCP-3)
 Briefing on Intensified Malaria Control Project-3 (IMCP-3) India CCM Induction and Orientation Workshop 3 rd -4 th December 2015 Directorate of National Vector Borne Diseases Control Programme, Delhi Plan
Briefing on Intensified Malaria Control Project-3 (IMCP-3) India CCM Induction and Orientation Workshop 3 rd -4 th December 2015 Directorate of National Vector Borne Diseases Control Programme, Delhi Plan
Eighth intercountry meeting of national malaria programme managers from HANMAT and PIAM-Net countries
 Summary report on the Eighth intercountry meeting of national malaria programme managers from HANMAT and PIAM-Net countries WHO-EM/MAL/384/E Islamabad, Pakistan 12 14 December 2016 Summary report on the
Summary report on the Eighth intercountry meeting of national malaria programme managers from HANMAT and PIAM-Net countries WHO-EM/MAL/384/E Islamabad, Pakistan 12 14 December 2016 Summary report on the
Evaluation of Antimalarial Drug use in Tertiary Care Teaching Hospital
 Research Article Evaluation of Antimalarial Drug use in Tertiary Care Teaching Hospital Anushree Shrikant Deshpande 1 *, Mallappa Hanamantappa Shalavadi 2, Harshitkumar Bhupendrabhai Patel 2, Arvind Dayalbhai
Research Article Evaluation of Antimalarial Drug use in Tertiary Care Teaching Hospital Anushree Shrikant Deshpande 1 *, Mallappa Hanamantappa Shalavadi 2, Harshitkumar Bhupendrabhai Patel 2, Arvind Dayalbhai
Testing for G6PD deficiency for safe use of primaquine in radical cure of P. vivax and P. ovale
 Testing for G6PD deficiency for safe use of primaquine in radical cure of P. vivax and P. ovale Webinar presentation to support the dissemination of the policy brief Silvia Schwarte, WHO/GMP e-mail: schwartes@who.int
Testing for G6PD deficiency for safe use of primaquine in radical cure of P. vivax and P. ovale Webinar presentation to support the dissemination of the policy brief Silvia Schwarte, WHO/GMP e-mail: schwartes@who.int
POLICY BRIEF Review of Antimalarial Medicines Available to Treat P. falciparum in the Amazon Region
 POLICY BRIEF Review of Antimalarial Medicines Available to Treat P. falciparum in the Amazon Region Background Malaria is a substantial public health threat in the Americas. In 2010, the Americas had approximately
POLICY BRIEF Review of Antimalarial Medicines Available to Treat P. falciparum in the Amazon Region Background Malaria is a substantial public health threat in the Americas. In 2010, the Americas had approximately
Epidemiological trends of malaria in an endemic district Tumkur, Karnataka
 International Journal of Community Medicine and Public Health Krishna C et al. Int J Community Med Public Health. 2017 Jun;4(6):2141-2145 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original
International Journal of Community Medicine and Public Health Krishna C et al. Int J Community Med Public Health. 2017 Jun;4(6):2141-2145 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original
Malaria. Edwin J. Asturias, MD
 Malaria Edwin J. Asturias, MD Associate Professor of Pediatrics and Epidemiology Director for Latin America Center for Global Health, Colorado School of Public Health Global Health and Disasters Course
Malaria Edwin J. Asturias, MD Associate Professor of Pediatrics and Epidemiology Director for Latin America Center for Global Health, Colorado School of Public Health Global Health and Disasters Course
Artesunate Mefloquine (AsMq)
 Artesunate Mefloquine (AsMq) Introduction AsMq in Rakhine in 1996 AsMq FDC compared to other ACTs AZG (MSF-Holland) malaria activities in Western Myanmar 9 townships 25 DoH clinics with AZG support (area
Artesunate Mefloquine (AsMq) Introduction AsMq in Rakhine in 1996 AsMq FDC compared to other ACTs AZG (MSF-Holland) malaria activities in Western Myanmar 9 townships 25 DoH clinics with AZG support (area
128th Session 25 November 2010 Provisional agenda item Malaria. Prevention and control: sustaining the gains and reducing transmission
 EXECUTIVE BOARD 128th Session 25 November 2010 Provisional agenda item 4.11 Malaria Prevention and control: sustaining the gains and reducing transmission Report by the Secretariat 1. Millennium Development
EXECUTIVE BOARD 128th Session 25 November 2010 Provisional agenda item 4.11 Malaria Prevention and control: sustaining the gains and reducing transmission Report by the Secretariat 1. Millennium Development
Strategy to move from accelerated burden reduction to malaria elimination in the GMS by 2030
 Strategy to move from accelerated burden reduction to malaria elimination in the GMS by 2030 Dr Walter M Kazadi Coordinator Regional Hub Emergency Response to Artemisinin Resistance Regional Hub GMS MMV
Strategy to move from accelerated burden reduction to malaria elimination in the GMS by 2030 Dr Walter M Kazadi Coordinator Regional Hub Emergency Response to Artemisinin Resistance Regional Hub GMS MMV
26/06/ NIMR 2018 Conference - Malaria - a reality
 Malaria Elimination: Reality or Myth? Wellington A. Oyibo ANDI CENTRE OF EXCELLENCE FOR MALARIA DIAGNOSIS WHO/FIND Malaria Specimen Collection Site The International Center for Malaria Microscopy and Malaria
Malaria Elimination: Reality or Myth? Wellington A. Oyibo ANDI CENTRE OF EXCELLENCE FOR MALARIA DIAGNOSIS WHO/FIND Malaria Specimen Collection Site The International Center for Malaria Microscopy and Malaria
New Partnerships The Development of ASMQ - FDC
 New Partnerships The Development of ASMQ - FDC Jean-René Kiechel Senior Product Manager DNDi January 2011 1 ACTs: World Health Organization Treatment Guidelines (2006) In order to fight resistance: 1.
New Partnerships The Development of ASMQ - FDC Jean-René Kiechel Senior Product Manager DNDi January 2011 1 ACTs: World Health Organization Treatment Guidelines (2006) In order to fight resistance: 1.
PURPOSE The purpose of the Malaria Control Strategic Plan 2005/ /10 is to provide a common platform and detailed description of interventions
 PURPOSE The purpose of the Malaria Control Strategic Plan 2005/06-2009/10 is to provide a common platform and detailed description of interventions for all RBM partners and sectors of society. It encourages
PURPOSE The purpose of the Malaria Control Strategic Plan 2005/06-2009/10 is to provide a common platform and detailed description of interventions for all RBM partners and sectors of society. It encourages
Updating the Guidelines for the Treatment of Malaria
 Updating the Guidelines for the Treatment of Malaria Meeting of the Malaria Policy Advisory Committee Geneva, 13-15 March, 2013 Prof. Nick White Co-chair, Chemotherapy Technical Expert Group With thanks
Updating the Guidelines for the Treatment of Malaria Meeting of the Malaria Policy Advisory Committee Geneva, 13-15 March, 2013 Prof. Nick White Co-chair, Chemotherapy Technical Expert Group With thanks
Achieving Consensus on Malaria Recommendations: Is It Possible? Mary E. Wilson, MD May 28, 2015 CISTM14 Québec City, Canada
 Achieving Consensus on Malaria Recommendations: Is It Possible? Mary E. Wilson, MD May 28, 2015 CISTM14 Québec City, Canada I have no conflicts of interest to disclose. 2 Questions How do guidelines/recommendations
Achieving Consensus on Malaria Recommendations: Is It Possible? Mary E. Wilson, MD May 28, 2015 CISTM14 Québec City, Canada I have no conflicts of interest to disclose. 2 Questions How do guidelines/recommendations
Swaziland National Malaria Elimination Policy
 DRAFT 21 April 2010 Swaziland National Malaria Elimination Policy Version 1.0 May 2010 Kingdom of Swaziland Ministry of Health National Malaria Control Programme TABLE OF CONTENTS Acronyms... 3 Foreword...
DRAFT 21 April 2010 Swaziland National Malaria Elimination Policy Version 1.0 May 2010 Kingdom of Swaziland Ministry of Health National Malaria Control Programme TABLE OF CONTENTS Acronyms... 3 Foreword...
Malaria Updates. Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine
 Malaria Updates Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine Outline General epidemiology of malaria in the Philippines P falciparum Updates in treatment Recognizing
Malaria Updates Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine Outline General epidemiology of malaria in the Philippines P falciparum Updates in treatment Recognizing
Is there Artemisinin Resistance in Western Cambodia?
 Is there Artemisinin Resistance in Western Cambodia? Preliminary results, February 2008 Arjen Dondorp on behalf of the Task Force on Antimalarial Drug Resistance in Cambodia S769N PfATPase6 mutation Artemether
Is there Artemisinin Resistance in Western Cambodia? Preliminary results, February 2008 Arjen Dondorp on behalf of the Task Force on Antimalarial Drug Resistance in Cambodia S769N PfATPase6 mutation Artemether
Malaria Outbreak in District Korea, Chhattisgarh
 Malaria Outbreak in District Korea, Chhattisgarh A.K. Mishra, S.K. Chand Abstract Malaria is a major public health problem in India. Recently malaria, particularly that caused by Plasmodium falciparum
Malaria Outbreak in District Korea, Chhattisgarh A.K. Mishra, S.K. Chand Abstract Malaria is a major public health problem in India. Recently malaria, particularly that caused by Plasmodium falciparum
Resuming the fight against relapse of Plasmodium vivax
 Resuming the fight against relapse of Plasmodium vivax Professor J. Kevin Baird Head of Unit, Eijkman-Oxford Clinical Research Unit, Jakarta, Indonesia & Centre for Tropical Medicine Nuffield Department
Resuming the fight against relapse of Plasmodium vivax Professor J. Kevin Baird Head of Unit, Eijkman-Oxford Clinical Research Unit, Jakarta, Indonesia & Centre for Tropical Medicine Nuffield Department
Tolerability of Artemisinin based combination treatments - ACTs. Bob Taylor MD (Lond), FRCP (UK), DTM&H (Lond)
 Tolerability of Artemisinin based combination treatments - ACTs Bob Taylor MD (Lond), FRCP (UK), DTM&H (Lond) Main ACTs Artesunate + mefloquine Dihydroartemisinin + piperaquine Artemether + lumefantrine
Tolerability of Artemisinin based combination treatments - ACTs Bob Taylor MD (Lond), FRCP (UK), DTM&H (Lond) Main ACTs Artesunate + mefloquine Dihydroartemisinin + piperaquine Artemether + lumefantrine
Copyright by Population Services International and ACTwatch 2016.
 Malaria markets in the Greater Mekong Sub-Region: 2015-2016 1 Copyright by Population Services International and ACTwatch 2016. Suggested Citation: Malaria Markets in the Greater Mekong Sub-Region: 2015-2016.
Malaria markets in the Greater Mekong Sub-Region: 2015-2016 1 Copyright by Population Services International and ACTwatch 2016. Suggested Citation: Malaria Markets in the Greater Mekong Sub-Region: 2015-2016.
Anti-Malaria Chemotherapy
 Anti-Malaria Chemotherapy Causal Prophylaxis prevent infection (ie, liver stage) Suppressive Prophylaxis prevent clinical disease (ie, blood stages) Treatment Therapy (or clinical cure) relieve symptoms
Anti-Malaria Chemotherapy Causal Prophylaxis prevent infection (ie, liver stage) Suppressive Prophylaxis prevent clinical disease (ie, blood stages) Treatment Therapy (or clinical cure) relieve symptoms
Global Report on Antimalarial Drug. and the Global Plan for Artemisinin Resistance Containment (GPARC)
 Global Report on Antimalarial Drug Resistance and Drug Efficacy: 2-21 21 and the Global Plan for Artemisinin Resistance Containment (GPARC) MMV Stakeholders Meeting Dar es Salaam, Tanzania 2 June 211 Robert
Global Report on Antimalarial Drug Resistance and Drug Efficacy: 2-21 21 and the Global Plan for Artemisinin Resistance Containment (GPARC) MMV Stakeholders Meeting Dar es Salaam, Tanzania 2 June 211 Robert
Media centre Malaria. Key facts. Symptoms
 Media centre Malaria Fact sheet Updated November 2017 Key facts Malaria is a life-threatening disease caused by parasites that are transmitted to people through the bites of infected female Anopheles mosquitoes.
Media centre Malaria Fact sheet Updated November 2017 Key facts Malaria is a life-threatening disease caused by parasites that are transmitted to people through the bites of infected female Anopheles mosquitoes.
Malaria Initiative: Access
 Novartis Social Business Malaria Initiative: Access Improving affordability and availability of medicines Over the past decade, the Novartis Malaria Initiative has pioneered the pharmaceutical response
Novartis Social Business Malaria Initiative: Access Improving affordability and availability of medicines Over the past decade, the Novartis Malaria Initiative has pioneered the pharmaceutical response
Ending Malaria in Nigeria: The WHO Agenda
 Nigeria Institute of Medical Research 2016 World Malaria Day Lecture 27 April, 2016 Ending Malaria in Nigeria: The WHO Agenda Dr Tolu Arowolo Malaria Containment Programme, WHO, Nigeria arowolot@who.int
Nigeria Institute of Medical Research 2016 World Malaria Day Lecture 27 April, 2016 Ending Malaria in Nigeria: The WHO Agenda Dr Tolu Arowolo Malaria Containment Programme, WHO, Nigeria arowolot@who.int
Driving access to medicine
 Driving access to medicine An example from the Novartis Malaria Initiative Hans Rietveld Director, Market Access & Capacity Building Novartis Malaria Initiative Social Forum - Geneva February 20, 2015
Driving access to medicine An example from the Novartis Malaria Initiative Hans Rietveld Director, Market Access & Capacity Building Novartis Malaria Initiative Social Forum - Geneva February 20, 2015
Imported malaria: a possible threat to the elimination of malaria from Sri Lanka?
 Tropical Medicine and International Health doi:0./tmi.097 volume 8 no 6 pp 76 768 june 03 Imported malaria: a possible threat to the elimination of malaria from Sri Lanka? G. N. L. Galappaththy, S. D.
Tropical Medicine and International Health doi:0./tmi.097 volume 8 no 6 pp 76 768 june 03 Imported malaria: a possible threat to the elimination of malaria from Sri Lanka? G. N. L. Galappaththy, S. D.
World Health Organization Global Fund concept note development WHO POLICY BRIEF
 World Health Organization 2014 All rights reserved. Publications of the World Health Organization are available on the WHO website (www.who.int) or can be purchased from WHO Press, World Health Organization,
World Health Organization 2014 All rights reserved. Publications of the World Health Organization are available on the WHO website (www.who.int) or can be purchased from WHO Press, World Health Organization,
Issue 6: January - June 2016 National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana
 Issue 6: January - June 2016 National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana Contents Page Editorial and Report Highlights Page 1 Malaria Burden Page 2 Key Activities undertaken
Issue 6: January - June 2016 National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana Contents Page Editorial and Report Highlights Page 1 Malaria Burden Page 2 Key Activities undertaken
Sustained funding is crucial to malaria control
 Update on Malaria Chi Eziefula Senior Lecturer in Brighton and Sussex Centre for Global Health Research, Brighton and Sussex Medical School Honorary Consultant in Infection, Brighton and Sussex University
Update on Malaria Chi Eziefula Senior Lecturer in Brighton and Sussex Centre for Global Health Research, Brighton and Sussex Medical School Honorary Consultant in Infection, Brighton and Sussex University
Malaria: A Global Perspective and Prospects for Elimination. Rima Shretta
 Malaria: A Global Perspective and Prospects for Elimination Rima Shretta Background Spread by the female anopheles mosquito; caused by plasmodium parasite: P. falciparum, P. vivax, P. ovale, P. malariae,
Malaria: A Global Perspective and Prospects for Elimination Rima Shretta Background Spread by the female anopheles mosquito; caused by plasmodium parasite: P. falciparum, P. vivax, P. ovale, P. malariae,
Anas Raed. - Zaid Emad. - Malik Zuhlof
 - 6 - Anas Raed - Zaid Emad - Malik Zuhlof 1 P a g e - This lecture started with the excellent presentation of chronic fatigue syndrome and the role of Vitamin B12 in its treatment by our colleague Osama
- 6 - Anas Raed - Zaid Emad - Malik Zuhlof 1 P a g e - This lecture started with the excellent presentation of chronic fatigue syndrome and the role of Vitamin B12 in its treatment by our colleague Osama
DEATH AUDIT OF DEATHS DUE TO MALARIA AT LG HOSPITAL, AHMEDABAD (GUJARAT) DURING THE YEAR 2011
 ORIGINAL ARTICLE DEATH AUDIT OF DEATHS DUE TO MALARIA AT LG HOSPITAL, AHMEDABAD (GUJARAT) DURING THE YEAR 2011 Vyas Sheetal 1, Solanki Anand 2, Joshi Urvish 2, Nayak Himanshu 2 1 Professor and Head, 2
ORIGINAL ARTICLE DEATH AUDIT OF DEATHS DUE TO MALARIA AT LG HOSPITAL, AHMEDABAD (GUJARAT) DURING THE YEAR 2011 Vyas Sheetal 1, Solanki Anand 2, Joshi Urvish 2, Nayak Himanshu 2 1 Professor and Head, 2
Malaria treatment policy and drug resistance monitoring in countries of South-East Asia Region
 Malaria treatment policy and drug resistance monitoring in countries of South-East Asia Region Report of a Workshop Bali, Indonesia, 15-17 September 2010 Regional Office for South-East Asia SEA-MAL-267
Malaria treatment policy and drug resistance monitoring in countries of South-East Asia Region Report of a Workshop Bali, Indonesia, 15-17 September 2010 Regional Office for South-East Asia SEA-MAL-267
Programme and Treatment in Rural and Urban Baroda
 Operational Efficiency of Malaria Chapter 1 Programme and Treatment in Rural and Urban Baroda Evaluation of Operational Efficiency of the National Antimalaria Program in High- Risk Rural Areas of Vadodara
Operational Efficiency of Malaria Chapter 1 Programme and Treatment in Rural and Urban Baroda Evaluation of Operational Efficiency of the National Antimalaria Program in High- Risk Rural Areas of Vadodara
Statistical Analysis Plan (SAP)
 Statistical Analysis Plan (SAP) Comparison of artemether-lumefantrine and chloroquine with and without primaquine for the treatment of Plasmodium vivax in Ethiopia: a randomized controlled trial Contents
Statistical Analysis Plan (SAP) Comparison of artemether-lumefantrine and chloroquine with and without primaquine for the treatment of Plasmodium vivax in Ethiopia: a randomized controlled trial Contents
A I D S E p I D E m I c u p D A t E a S I a ASIA china India
 ASIA In Asia, national HIV prevalence is highest in South-East Asia, with wide variation in epidemic trends between different countries. While the epidemics in Cambodia, Myanmar and Thailand all show declines
ASIA In Asia, national HIV prevalence is highest in South-East Asia, with wide variation in epidemic trends between different countries. While the epidemics in Cambodia, Myanmar and Thailand all show declines
ACTs in East Africa REALITY CHECK. Nathan Mulure MD Novartis Pharma
 ACTs in East Africa REALITY CHECK Nathan Mulure MD Novartis Pharma 1 Agenda Introduction and background Drug resistance to antimalarials Policy change Antimalarial market Challenges 2 Malaria Burden 34,000
ACTs in East Africa REALITY CHECK Nathan Mulure MD Novartis Pharma 1 Agenda Introduction and background Drug resistance to antimalarials Policy change Antimalarial market Challenges 2 Malaria Burden 34,000
Implementing the Abuja Declaration and Plan of Action: the journey so far
 Implementing the Abuja Declaration and Plan of Action: the journey so far The Abuja Declaration African leaders who met on 25 April 2000 in Abuja, Nigeria, laid out the foundation for a sustained battle
Implementing the Abuja Declaration and Plan of Action: the journey so far The Abuja Declaration African leaders who met on 25 April 2000 in Abuja, Nigeria, laid out the foundation for a sustained battle
NATIONAL MALARIA ELIMINATION ACTION PLAN Ministry of Health Belize
 NATIONAL MALARIA ELIMINATION ACTION PLAN 2015-2020 Ministry of Health Belize October, 2015 Table of Content Contextual Analysis 1 Situation Analysis of Malaria in Belize 2 Malaria Program in Belize 3 Vision
NATIONAL MALARIA ELIMINATION ACTION PLAN 2015-2020 Ministry of Health Belize October, 2015 Table of Content Contextual Analysis 1 Situation Analysis of Malaria in Belize 2 Malaria Program in Belize 3 Vision
OF ANTIMALARIAL DRUGS
 THE USE OF ANTIMALARIAL DRUGS THE USE OF ANTIMALARIAL DRUGS Report of an Informal Consultation World Health Organization, Geneva WHO, 2001 Technical Review: A. Bosman, C. Delacollette, P. Olumese, R. G.
THE USE OF ANTIMALARIAL DRUGS THE USE OF ANTIMALARIAL DRUGS Report of an Informal Consultation World Health Organization, Geneva WHO, 2001 Technical Review: A. Bosman, C. Delacollette, P. Olumese, R. G.
WHO Global Malaria Programme. February 2009
 WHO Global Malaria Programme February 2009 Table of Contents 1. The world malaria situation 2. The critical role of WHO's Global Malaria Programme 3. Our programme of work explained 4. Situation analysis
WHO Global Malaria Programme February 2009 Table of Contents 1. The world malaria situation 2. The critical role of WHO's Global Malaria Programme 3. Our programme of work explained 4. Situation analysis
IDELINES FO R THE TREATMENT OF MALARIA. Second edition
 GU IDELINES FO R THE TREATMENT OF MALARIA Second edition Guidelines for the treatment of malaria Second edition Guidelines for the treatment of malaria 2 nd edition WHO Library Cataloguing-in-Publication
GU IDELINES FO R THE TREATMENT OF MALARIA Second edition Guidelines for the treatment of malaria Second edition Guidelines for the treatment of malaria 2 nd edition WHO Library Cataloguing-in-Publication
Evidence Review Group on MDA, MSAT and FSAT Malaria Policy Advisory Committee Geneva, Switzerland September 2015
 Evidence Review Group on MDA, MSAT and FSAT Malaria Policy Advisory Committee Geneva, Switzerland 16-18 September 2015 Kevin Marsh Chairperson of the Evidence Review Group 1 Outline of the Presentation
Evidence Review Group on MDA, MSAT and FSAT Malaria Policy Advisory Committee Geneva, Switzerland 16-18 September 2015 Kevin Marsh Chairperson of the Evidence Review Group 1 Outline of the Presentation
THE ROAD TO 2020: MOBILSING THE PRIVATE SECTOR IN NIGERIA S FIGHT AGAINST MALARIA- THE LAGOS STATE APPROACH.
 THE ROAD TO 2020: MOBILSING THE PRIVATE SECTOR IN NIGERIA S FIGHT AGAINST MALARIA- THE LAGOS STATE APPROACH. A PAPER PRESENTED AT THE 2015 CAMA ANNUAL TECHNICAL FORUM. Dr Modele Osunkiyesi Permanent Secretary
THE ROAD TO 2020: MOBILSING THE PRIVATE SECTOR IN NIGERIA S FIGHT AGAINST MALARIA- THE LAGOS STATE APPROACH. A PAPER PRESENTED AT THE 2015 CAMA ANNUAL TECHNICAL FORUM. Dr Modele Osunkiyesi Permanent Secretary
EPIDEMIOLOGICAL SURVEILLANCE REPORT Malaria in Greece, 2018, up to 22/10/2018
 Page 1 EPIDEMIOLOGICAL SURVEILLANCE REPORT Malaria in Greece, 2018, up to 22/10/2018 Introduction Greece was declared free from malaria in 1974, following an intense control program (1946-1960). Since
Page 1 EPIDEMIOLOGICAL SURVEILLANCE REPORT Malaria in Greece, 2018, up to 22/10/2018 Introduction Greece was declared free from malaria in 1974, following an intense control program (1946-1960). Since
ituation Analysis of Malaria Control in Five Selected Pilot Areas in the Country for the Implementation of Roll Back Malaria (RBM) Initiative
 S ituation Analysis of Malaria Control in Five Selected Pilot Areas in the Country for the Implementation of Roll Back Malaria (RBM) Initiative Roll Back Malaria (RBM) is a new global initiative against
S ituation Analysis of Malaria Control in Five Selected Pilot Areas in the Country for the Implementation of Roll Back Malaria (RBM) Initiative Roll Back Malaria (RBM) is a new global initiative against
Private sector role, readiness and performance for malaria case management in Uganda, 2015
 Malaria Journal Private sector role, readiness and performance for malaria case management in Uganda, 2015 ACTwatch Group et al. ACTwatch Group et al. Malar J (2017) 16:219 DOI 10.1186/s12936-017-1824-x
Malaria Journal Private sector role, readiness and performance for malaria case management in Uganda, 2015 ACTwatch Group et al. ACTwatch Group et al. Malar J (2017) 16:219 DOI 10.1186/s12936-017-1824-x
Overview of Malaria Epidemiology in Ethiopia
 Overview of Malaria Epidemiology in Ethiopia Wakgari Deressa, PhD School of Public Health Addis Ababa University Symposium on Neuro-infectious Disease United Nations Conference Center, AA February 28,
Overview of Malaria Epidemiology in Ethiopia Wakgari Deressa, PhD School of Public Health Addis Ababa University Symposium on Neuro-infectious Disease United Nations Conference Center, AA February 28,
Annex A: Impact, Outcome and Coverage Indicators (including Glossary of Terms)
 IMPACT INDICATORS (INDICATORS PER GOAL) HIV/AIDS TUBERCULOSIS MALARIA Reduced HIV prevalence among sexually active population Reduced HIV prevalence in specific groups (sex workers, clients of sex workers,
IMPACT INDICATORS (INDICATORS PER GOAL) HIV/AIDS TUBERCULOSIS MALARIA Reduced HIV prevalence among sexually active population Reduced HIV prevalence in specific groups (sex workers, clients of sex workers,
14th Stakeholders Meeting
 14th Stakeholders Meeting Steady progress towards malaria elimination: Interventions for today and tomorrow Denpasar, Bali 11 12 October 2017 Dr. Iriani Samad : INDONESIA S PROGRESS IN MALARIA ELIMINATION
14th Stakeholders Meeting Steady progress towards malaria elimination: Interventions for today and tomorrow Denpasar, Bali 11 12 October 2017 Dr. Iriani Samad : INDONESIA S PROGRESS IN MALARIA ELIMINATION
Issue 9: January March, 2017 National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana
 Issue 9: January March, 2017 National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana Contents Page Editorial and Report Highlights 1 Malaria Burden 2 Key activities undertaken in First
Issue 9: January March, 2017 National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana Contents Page Editorial and Report Highlights 1 Malaria Burden 2 Key activities undertaken in First
METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY ISBN
 METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY ISBN 978 92 4 159753 1 METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY WHO Library Cataloguing-in-Publication
METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY ISBN 978 92 4 159753 1 METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY WHO Library Cataloguing-in-Publication
Treatment Outcome of Pulmonary and Extra Pulmonary Tuberculosis Patients in TB and Chest Disease Hospital DOT Centre, Goa, India
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 4 (2016) pp. 437-441 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.504.051
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 4 (2016) pp. 437-441 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.504.051
India's voice against AIDS. December 2012
 India's voice against AIDS December 2012 HIV Sentinel Surveillance 2010-11 A Technical Brief India's voice against AIDS December 2012 Contents Acronyms...4 Executive Summary...5 1. Introduction...8 Objectives
India's voice against AIDS December 2012 HIV Sentinel Surveillance 2010-11 A Technical Brief India's voice against AIDS December 2012 Contents Acronyms...4 Executive Summary...5 1. Introduction...8 Objectives
Cronfa - Swansea University Open Access Repository
 Cronfa - Swansea University Open Access Repository This is an author produced version of a paper published in: Malaria Journal Cronfa URL for this paper: http://cronfa.swan.ac.uk/record/cronfa40379 Paper:
Cronfa - Swansea University Open Access Repository This is an author produced version of a paper published in: Malaria Journal Cronfa URL for this paper: http://cronfa.swan.ac.uk/record/cronfa40379 Paper:
NOTABLE EVENTS IN NATIONAL POLICY AND FINANCING FOR MALARIA
 Malaria Policy Landscape PATH MACEPA JULY 2016 OVERVIEW API 2014 PATH MACEPA has been working in partnership with s Federal Ministry of Health (FMOH) since 2007 and the Amhara Regional Health Bureau (ARHB)
Malaria Policy Landscape PATH MACEPA JULY 2016 OVERVIEW API 2014 PATH MACEPA has been working in partnership with s Federal Ministry of Health (FMOH) since 2007 and the Amhara Regional Health Bureau (ARHB)
Malaria Control. Umberto D Alessandro
 Malaria Control Umberto D Alessandro Zanzibar - hospitalizations et malaria deaths 1999-2008 2 The Gambia - slide positivity rates 2003-2009 Under-5 mortality rate (per 1,000 live births) 300 250 200 150
Malaria Control Umberto D Alessandro Zanzibar - hospitalizations et malaria deaths 1999-2008 2 The Gambia - slide positivity rates 2003-2009 Under-5 mortality rate (per 1,000 live births) 300 250 200 150
Technical Guidance Note for Round 11 Global Fund HIV Proposals
 Technical Guidance Note for Round 11 Global Fund HIV Proposals UNAIDS I World Health Organization I 2011 Rationale for including HIVDR prevention and assessment in the proposal Situation analysis As access
Technical Guidance Note for Round 11 Global Fund HIV Proposals UNAIDS I World Health Organization I 2011 Rationale for including HIVDR prevention and assessment in the proposal Situation analysis As access
WHO Consultation on universal access to core malaria interventions in high burden countries: main conclusions and recommendations
 WHO Consultation on universal access to core malaria interventions in high burden countries: main conclusions and recommendations 12-15 February 2018 Salle XI, ILO Building, Geneva, Switzerland Country
WHO Consultation on universal access to core malaria interventions in high burden countries: main conclusions and recommendations 12-15 February 2018 Salle XI, ILO Building, Geneva, Switzerland Country
Asian Pacific Journal of Tropical Disease
 Asian Pac J Trop Dis 2014; 4(Suppl 1): S221-S225 S221 Contents lists available at ScienceDirect Asian Pacific Journal of Tropical Disease journal homepage: www.elsevier.com/locate/apjtd Document heading
Asian Pac J Trop Dis 2014; 4(Suppl 1): S221-S225 S221 Contents lists available at ScienceDirect Asian Pacific Journal of Tropical Disease journal homepage: www.elsevier.com/locate/apjtd Document heading
AFRICA FIGHTING MALARIA BULLETIN #3
 AFRICA FIGHTING MALARIA BULLETIN #3 March 2, 2009 Safe Medicines Project Phase II: The Zambian Case Study Summary A range of antimalarial drugs were procured from private pharmacies, shops and kiosks within
AFRICA FIGHTING MALARIA BULLETIN #3 March 2, 2009 Safe Medicines Project Phase II: The Zambian Case Study Summary A range of antimalarial drugs were procured from private pharmacies, shops and kiosks within
Repellent Soap. The Jojoo Mosquito. Africa s innovative solution to Malaria prevention. Sapphire Trading Company Ltd
 The Jojoo Mosquito Repellent Soap Africa s innovative solution to Malaria prevention Sapphire Trading Company Ltd P.O.Box: 45938-00100 Nairobi, Kenya. Tel: +254 735 397 267 +254 733 540 868 +254 700 550
The Jojoo Mosquito Repellent Soap Africa s innovative solution to Malaria prevention Sapphire Trading Company Ltd P.O.Box: 45938-00100 Nairobi, Kenya. Tel: +254 735 397 267 +254 733 540 868 +254 700 550
Issue 8: January December 2016 National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana
 Issue 8: January December National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana Contents Page Editorial and Report Highlights 1 Malaria Burden 2 Key Activities Undertaken in 2 Malaria
Issue 8: January December National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana Contents Page Editorial and Report Highlights 1 Malaria Burden 2 Key Activities Undertaken in 2 Malaria
MESA research grants 2014
 MESA research grants 2014 MESA operational research grant Principal investigator Mopping up and getting to zero: mapping residual malaria transmission for targeted response in urban Lusaka, Zambia. Daniel
MESA research grants 2014 MESA operational research grant Principal investigator Mopping up and getting to zero: mapping residual malaria transmission for targeted response in urban Lusaka, Zambia. Daniel
How to protect yourself against malaria
 World Health Organization 17 September, 2008 How to protect yourself against malaria Mine Action Technology Workshop 2008 co-hosted by the United Nations Mine Action Service (UNMAS) and the Geneva International
World Health Organization 17 September, 2008 How to protect yourself against malaria Mine Action Technology Workshop 2008 co-hosted by the United Nations Mine Action Service (UNMAS) and the Geneva International
Tuberculosis-HIV epidemic situation and emerging challenges in North India
 NTI Bulletin 2015,51 /1&4, 1 7 Tuberculosis-HIV epidemic situation and emerging challenges in North India Rajesh Deshmukh 1,3, Raghu Ram Rao 2, Shah A 2,3, Sreenivas A Nair 3, R S Gupta 1, SD Khaparde
NTI Bulletin 2015,51 /1&4, 1 7 Tuberculosis-HIV epidemic situation and emerging challenges in North India Rajesh Deshmukh 1,3, Raghu Ram Rao 2, Shah A 2,3, Sreenivas A Nair 3, R S Gupta 1, SD Khaparde
Jaderson Lima, MD On behalf of François Bompart, MD
 Challenges and Successes of the FACT Project through Innovative Partnerships for the Development of Artesunate Combination Therapies for Malaria 5º. ENIFarMed São Paulo Brazil August 2011 Public-private
Challenges and Successes of the FACT Project through Innovative Partnerships for the Development of Artesunate Combination Therapies for Malaria 5º. ENIFarMed São Paulo Brazil August 2011 Public-private
Mass drug Administration When Is It Useful
 Mass drug Administration When Is It Useful Kwaku Poku Asante, MD MPH PhD Kintampo Health Research Centre, Ghana Malaria Control and Elimination 8-9 December 2016, Congress Center Basel, Switzerland MDA
Mass drug Administration When Is It Useful Kwaku Poku Asante, MD MPH PhD Kintampo Health Research Centre, Ghana Malaria Control and Elimination 8-9 December 2016, Congress Center Basel, Switzerland MDA
FACTS. Approximately 2.48 million malaria cases are reported annually from South Asia. Of Which 75% cases are contributed by India alone.
 MALARIA 2 FACTS Approximately 2.48 million malaria cases are reported annually from South Asia. Of Which 75% cases are contributed by India alone. The magnitude of the problem is further enhanced by P
MALARIA 2 FACTS Approximately 2.48 million malaria cases are reported annually from South Asia. Of Which 75% cases are contributed by India alone. The magnitude of the problem is further enhanced by P
Situation Analysis of Malaria Control in Five Selected Pilot Areas in the Country for the Implementation of Roll Back Malaria Initiative
 Situation Analysis of Malaria Control in Five Selected Pilot Areas in the Country for the Implementation of Roll Back Malaria Initiative Roll Back Malaria (RBM) is a new global initiative against malaria.
Situation Analysis of Malaria Control in Five Selected Pilot Areas in the Country for the Implementation of Roll Back Malaria Initiative Roll Back Malaria (RBM) is a new global initiative against malaria.
National Treatment Guidelines for Malaria in Cambodia
 Kingdom of Cambodia Nation Religion King National Treatment Guidelines for Malaria in Cambodia December 2014 National Treatment Guidelines for Malaria in Cambodia i 1. PREFACE Malaria, which has plagued
Kingdom of Cambodia Nation Religion King National Treatment Guidelines for Malaria in Cambodia December 2014 National Treatment Guidelines for Malaria in Cambodia i 1. PREFACE Malaria, which has plagued
USE OF ROUTINELY COLLECTED PAST SURVEILLANCE DATA IN IDENTIFYING AND MAPPING HIGH-RISK AREAS IN A MALARIA ENDEMIC AREA OF SRI LANKA
 USE OF ROUTINELY COLLECTED PAST SURVEILLANCE DATA IN IDENTIFYING AND MAPPING HIGH-RISK AREAS IN A MALARIA ENDEMIC AREA OF SRI LANKA AR Wickremasinghe 1, DM Gunawardena 2 and STC Mahawithanage 3 1 Department
USE OF ROUTINELY COLLECTED PAST SURVEILLANCE DATA IN IDENTIFYING AND MAPPING HIGH-RISK AREAS IN A MALARIA ENDEMIC AREA OF SRI LANKA AR Wickremasinghe 1, DM Gunawardena 2 and STC Mahawithanage 3 1 Department
Minutes of the Drug Resistance and Containment Technical Expert Group
 Minutes of the Drug Resistance and Containment Technical Expert Group 28 30 April 2014 Starling Hotel, Geneva, Switzerland Contents Acknowledgments... 3 Abbreviations... 4 Summary and recommendations...
Minutes of the Drug Resistance and Containment Technical Expert Group 28 30 April 2014 Starling Hotel, Geneva, Switzerland Contents Acknowledgments... 3 Abbreviations... 4 Summary and recommendations...
Current knowledge and challenges of antimalarial drugs for treatment and prevention in pregnancy
 Expert Opinion on Pharmacotherapy ISSN: 1465-6566 (Print) 1744-7666 (Online) Journal homepage: http://www.tandfonline.com/loi/ieop20 Current knowledge and challenges of antimalarial drugs for treatment
Expert Opinion on Pharmacotherapy ISSN: 1465-6566 (Print) 1744-7666 (Online) Journal homepage: http://www.tandfonline.com/loi/ieop20 Current knowledge and challenges of antimalarial drugs for treatment
