Incidence of latex sensitization among latex glove users
|
|
|
- Magnus Norris
- 6 years ago
- Views:
Transcription
1 Incidence of latex sensitization among latex glove users Gordon L. Sussman MD, FRCPC, a Gary M. Liss, MD, MS, FRCPC, b, c Ken Deal, PhD, d Shirley Brown, RN, e Maureen Cividino, MD, CCFP, e Sidney Siu, MD, FRCPC, b Donald H. Beezhold, PhD, f Gordon Smith, b Mark C. Swanson, BA, g John Yunginger, MD, g Andrew Douglas, BSc, h D. Linn Holness, MD, FRCPC, i Phyllis Lebert, MD, FRCPC, j Paul Keith, MD, FRCPC, j Susan Waserman, MD, FRCPC, j and Kristiina Turjanmaa, MD k Toronto, Ontario, Canada, Hamilton, Ontario, Canada, Sayre, Pa., Rochester, Minn., Ottawa, Ontario, Canada, and Tampere, Finland Background: Although there are several reports of the prevalence of latex sensitization among health care workers, the incidence of sensitization is unknown. Objective: The objective of this study was to estimate the incidence of sensitization among latex glove users at a hospital in Hamilton, Ontario, Canada. Methods: Workers with negative results to the skin test at baseline were followed prospectively over 1 year, some wearing powdered gloves and others using powder-free gloves. They were reevaluated in 1995 with a questionnaire and skin prick test (SPT) sensitivity to latex reagents, three common inhalants, and six foods. A conversion was defined as a (new) latex SPT with wheal diameter at least 4 mm greater than saline control. Glove extracts were assayed for antigenic protein, and air samples were obtained to estimate exposure to airborne latex protein. Results: During powdered glove use, personal exposures ranged from 5 to 616 ng/m 3, whereas during powder-free glove use, all but two results for air samples were below the limit of detection (about 0.1 ng/m 3 ). During the study period, the protein concentration in the powdered gloves, initially mean 557 g/gm of sample, declined at a rate of 295 g/gm per year (p < ). Of the 1075 SPT-negative participants at baseline, 479 were working in eligible wards, and of these, 435 (91%) participated in follow-up, 227 using powder-free gloves and 208 using powdered gloves. We identified four conversions, two (1.0%) in the powdered glove group and two From a the Section of Allergy, Wellesley Hospital, University of Toronto, Toronto; b Ontario Ministry of Labour, Ontario; c the Department of Preventive Medicine and Biostatistics, University of Toronto, Toronto; d Michael G. DeGroot School of Business, McMaster University, Hamilton; e Employee Health Service, Hamilton Health Sciences Corp., Hamilton; f Guthrie Research Institute, Sayre; g Allergic Diseases Research Laboratory, Mayo Clinic, Rochester; h Medical Devices Bureau, Health Canada, Ottawa; i the Department of Occupational and Environmental Health, St. Michael s Hospital, University of Toronto, Toronto; j the Department of Medicine, McMaster University, Hamilton; and k the Department of Dermatology, University Hospital, Tampere. Supported in part by Aladan Corporation, Ansell Medical, and Regent Hospital Products. Received for publication May 19, 1997; revised Sept. 22, 1997; accepted for publication Sept. 24, Reprint requests: Gordon L. Sussman, MD, FRCPC, 202 St. Clair Ave. West, Toronto, ON, Canada M4V 1R2. Copyright 1998 by Mosby, Inc /98 $ /1/86357 (0.9%) in the powder-free group. The two participants using powdered gloves were the only converters who were symptomatic. The significance of skin test conversions identified in the powder-free group, both asymptomatic patients, is unclear. The limitations of the study are discussed, including the limited power, the declines in latex protein concentrations, and the possibility of information (observer) bias. Conclusion: To our knowledge, this represents the first reported estimate (about 1%) of incidence of sensitization in hospital personnel using latex gloves. (J Allergy Clin Immunol 1998;101:171-8.) Key words: Latex gloves, sensitization, powdered gloves, powderfree gloves, latex protein concentrations, prospective study, skin testing, airborne exposure Natural rubber latex (NRL) allergy has become an important occupational health concern in recent years, particularly among health care workers (HCWs). 1-5 The major source of workplace exposure has been powdered latex glove use by HCWs. Workers involved in glove manufacturing may also be affected. 6 Type I (IgEmediated) NRL allergy symptoms include urticaria, angioedema, rhinitis, conjunctivitis, bronchospasm, and anaphylaxis. Surveys of HCWs have demonstrated that the prevalence of sensitization to latex ranged from 2.9% in Finland 7 to 4.7% in Belgium 8 among hospital employees as a group and from 7% among operating room staff in Finland 7 to 9% to 10% among operating room nurses in France 9 and surgeons, anesthesiologists, and radiologists in Canada. 10 Recently, Grzybowski et al. 11 found that 8.9% of 741 registered nurses in Michigan had positive test results for anti-latex IgE antibodies, which may be less sensitive than skin testing. Vandenplas et al. 8 documented 2.5% of HCWs to have latex-induced occupational asthma confirmed with specific inhalation challenge. Sensitization of HCWs may involve high costs, both in terms of day-to-day risks at work as well as potentially fatal anaphylactic shock. Disability from latex sensitivity is an increasing problem caused by latex product substitution, personnel reassignments, and workers compensation claims. Turjanmaa and Lahti 12 found, as did we,
2 172 Sussman et al. J ALLERGY CLIN IMMUNOL FEBRUARY 1998 Abbreviations used HCW: Health care worker NRL: Natural rubber latex SPT: Skin prick test that individuals already sensitized to latex reacted less to an extract taken from a low-protein glove than to an extract from a regular glove. In addition, Vandenplas et al. 14 suggested that gloves with a lower protein content could be useful in reducing the risk of asthmatic reactions in subjects with latex-induced asthma. It is not known, however, if use of low-protein gloves will reduce the incidence of latex sensitization. Although the need for such a study has been noted, 5, 15 we are not aware that a prospective study has been published. During 1992 and 1993, a number of HCWs at a hospital with two sites in Hamilton, Ontario, Canada, developed allergic symptoms that were associated with exposure to NRL. This provided an opportunity to undertake the current investigation to test the hypothesis that high protein levels in latex gloves are related to the incidence of sensitization. Overall design The study design had two main components. The first phase was a cross-sectional investigation in which 1351 HCWs who used latex gloves at the two sites at Hamilton hospital were screened in 1994 to determine the baseline prevalence of sensitivity to NRL. We recently reported the findings of the baseline survey. 16 The prevalence of latex sensitization was 12.1% among participants, which was in the upper range of previous reports. There were significant associations with atopic status, positive skin test results to certain foods, work-related symptoms, and departmental use of gloves per HCW. The second phase involved following the cohort prospectively over 1 year. At one of the sites, some departments continued to use the same powdered moderate- to high-protein latex gloves as in the past, whereas at the other site, powder-free latex gloves were introduced. We then performed repeat testing in 1995 to identify newly sensitized individuals. The objectives of the present study were to determine (1) the incidence rate at which individuals with initially negative skin test results within this group became newly sensitized to NRL and (2) the association, if any, between the rate of sensitization and exposure, as reflected by the latex protein of the gloves worn and airborne latex protein. METHODS Eligible population Baseline. The details of the baseline study were reported previously. 16 All 2062 employees at both sites who used latex gloves on a regular basis (at least one to two times per week) were invited to participate in the baseline screening in April through May The assessment included administration of a questionnaire and latex skin testing. Informed signed consent was obtained from all participants, and the study protocol received approval from the institutional review board of the hospitals. Glove use over the year. During the year after the 1994 assessment, glove use was as follows. At site G, HCWs on the wards used powder-free gloves whereas those in the operating rooms used powdered gloves. At site H, the situation was reversed. Those on the wards used powdered gloves and those in the operating rooms used powder-free gloves. As shown in the Results section below, the powder-free gloves contained very low levels of protein, whereas the powdered gloves contained much higher levels. Follow-up. Follow-up testing was conducted in April and May 1995 and consisted of the same modalities (i.e., a questionnaire and latex skin testing). A negative-result latex SPT at baseline was defined as any individual with a 0 or 1 mm wheal to all latex reagents (i.e., none greater than 1 mm) in We also defined a priori that any skin test with a2or3mmwheal in 1994 would be considered equivocal and not included in the conversion data. Those who initially did not participate in retesting were contacted by the Employee Health Department to encourage participation. Two workers in the Labor and Delivery Unit at site H asssigned to wear powdered gloves became symptomatic in October 1994, 6 months into the study. They were retested at that time and both were identified as having latex conversions. These two HCWs switched to nonlatex gloves, and coworkers on the ward changed to powder-free gloves (see Results section). Skin test definitions at follow-up A positive SPT was defined as a wheal diameter at least 4 mm greater than that caused by the saline control in a subject who had negative results to the latex skin test the previous year. Atopy was defined as two or more SPTs with results positive to common inhalant aeroallergens (ragweed, dust mite, or timothy grass). A latex skin test conversion was defined as a subject whose status went from negative (as defined above) to positive at follow-up testing, that is, development of a4mmorgreater wheal (versus saline) to any latex reagent was considered a new positive skin test result and a conversion. Questionnaire The questionnaire, which was adapted from those used previously, 17, 18 was, with minor exceptions, identical to that used for the 1994 baseline evaluation 16 and was administered by four trained interviewers. The questionnaire obtained information on occupational history including job title, department, number of pairs of gloves and number of hours of glove use (over 3 days before the interview), years using latex gloves, types of glove worn during the past year, and exposure to chemical irritants at work. We also asked about smoking, past medical history, and allergies. Latex skin test reagents Skin testing was done with dilutions of commercially available ammoniated latex (Bencard Laboratory, Mississauga, Ontario, Canada). In vitro analyses of Bencard latex were done by Western blotting technique and contained all relevant proteins (7 to 10 mg/ml). 19 Skin test dilutions to 1:10, 1:100, 1:1000, 1:10,000, 1:100,000, and 1:1,000,000 of the stock latex extracts were prepared with saline diluent. In patients with suggestive histories of latex allergy (identified by questionnaire), skin tests were done beginning with the lowest dilution and progressing through increasing concentrations until a definite positive-
3 J ALLERGY CLIN IMMUNOL VOLUME 101, NUMBER 2, PART 1 Sussman et al. 173 TABLE I. Results of personal and area air sampling for latex, according to hospital, season, and glove type, Hamilton Hospitals Latex Study, Powdered gloves (ng/m 3 ) Powder-free gloves (ng/m 3 ) Summer Winter Summer Winter Personal samples Hospital H Ward Ward OR OR * * Hospital G OR OR Ward Ward samples (*) 5 samples (*) Area samples Hospital H Ward Ward OR OR * * Hospital G OR OR Ward Ward samples (*) * * OR, operating room. *Below limit of detection. results skin test was obtained. In patients with no symptoms suggestive of latex allergy, skin testing was done with all latex dilutions at one time. Another skin test reagent was extracted from noncompounded ammoniated latex as previously described (reconstituted to 1 mg/ml). 13 Glove extracts used for skin testing were prepared as reported previously. 20 Two grams of the palmar surface of latex rubber gloves used in the study (examination and surgical powdered gloves and examination and surgical powder-free gloves) were cut into 2 cm squares and submerged in 10 ml saline, agitated for 30 seconds to ensure all parts were wetted, and left for 15 minutes. The latex extracts were prepared in polypropylene tubes and containers. The final latex glove extracts were refrigerated and stored in 5 ml aliquots. The solution was labeled for date, glove brand, and glove lot number. The extract was assayed for antigenic protein with the use of an indirect ELISA technique. 21 Variability in the potency of the skin test materials was minimized by use of the same lots of gloves for skin testing at baseline and follow-up. Extracts were prepared for use in 1994, and additional gloves from the same lot were frozen. Fresh extracts were prepared from the frozen gloves for the repeat testing in The Bencard reagent was purchased separately for each year. The ammoniated latex protein was prepared fresh for each year from the same lot of lyophilized latex protein. Food and inhalant skin test extracts Commercially available food and inhalant extracts were used for skin testing. Food extracts (Bencard Laboratory) included avocado, banana, kiwi, potato (all 1:10 dilution), and chestnut and cow s milk (1:20 dilution). Inhalant extracts included ragweed, timothy grass, and dust mite (Bencard Laboratory). Histamine (1:1000) (Bencard Laboratory) and physiologic saline served as positive and negative controls, respectively. New skin test reagents were purchased each year. FIG. 1. Protein concentrations in powdered surgical gloves according to batch analysis date (squares represent mean, bars represent SEM). Skin test method The SPT was performed by trained registered nurses. They were not aware of the glove types worn by individual subjects, and as noted above, both powdered and powder-free gloves were in use at both hospitals. The same pair of nurses remained at each site throughout the skin testing procedure. Both forearms were wiped clean with alcohol. Skin test sites were clearly marked, a drop of extract was placed on the skin, and this was pricked with commercially available skin test lancets (Hollister Stier Laboratory, Etobicoke, Ontario). Skin tests were read at 15 minutes, and all positive test results were measured. All positive skin test wheal and flare responses were outlined with black pen and transferred to paper with the use of transparent tape for a permanent record. Exposure assessment Direct exposure. To provide estimates regarding the range of airborne latex concentrations, a limited number of area and personal air samples were obtained in both hospitals to characterize locations of frequent and low or no glove use. These were conducted on two occasions (winter and summer) to reflect different ventilation conditions. We present the results from sampling at locations for both powdered and powder-free gloves obtained during the 1-year prospective time interval. Air sampling method. Air samples assayed for airborne latex protein were collected by drawing air through Teflon (polytetrafluoroethylene) filters at a flow rate of 3.5 or 4.0 L/min for personal samples and 180 L/min for area samples. Analytical method. The immunoassay for latex aeroallergens has been previously described. 22, 23 Briefly, the latex allergens were extracted with buffer and quantified by inhibition immunoassay with the use of a concentrated latex glove extract adsorbed onto plastic microtiter plates and latex-specific IgE antibodies pooled from five latex-sensitive persons. The results were expressed as latex-allergenic protein per cubic meter of air. The lower analytical limit of detection of this method is approximately 2 ng or 40 ng/ml, allowing detection of 0.1 ng/m 3 in 20 m 3 of air. Indirect exposure measures. The following were declared in advance to be latex exposure metrics of interest: hospital; departmental use of gloves (obtained from hospital purchasing records over the previous year); job title; years since subject started using latex gloves; number of gloves per day averaged over the 3 days before the interview; number of hours per day wearing gloves; and exposure to chemical irritants at work.
4 174 Sussman et al. J ALLERGY CLIN IMMUNOL FEBRUARY 1998 TABLE II. Distribution of participants in follow-up study according to hospital site, Hamilton Hospitals Latex Study, Ontario, 1995 Site G Site H Total FIG. 2. Protein concentrations in surgical (circles) and examination (squares) powder-free gloves, according to batch analysis date (squares and circles represent mean, bars represent SEM). Latex protein content of gloves over time. Samples of gloves from consecutive lots used during the follow-up period were forwarded to the Guthrie Research Institute from the hospital as received. They were shipped in groups when several lots had accumulated and were assayed when received. For the purposes of analyses, glove protein concentrations less than the limit of detection were taken to be one half of the limit (e.g., 0.2 g/gm taken as 0.1 g/gm). Variability of the latex ELISA was found to be less than 25%. 22 Statistical analyses Estimates of sample size requirements for the powder-free and powdered glove groups were calculated before the baseline study, assuming an alpha level of 0.05 and 80% power. Although we were uncertain what the incidence rate of latex sensitization would be, on the basis of the approximate 10% latex sensitization prevalence observed in HCWs, we calculated sample sizes required for possible incidence rates among those HCWs using powdered gloves ranging from 0.5% to 5.0% and among those using powderfree gloves ranging from 0.01% to 0.5%. For example, given a 2.0% incidence rate in the powdered glove group, the sample size required in each group was 489, 551, or 989 if the incidence rate in the powder-free glove group was 0.01%, 0.1%, or 0.5%, respectively. On the basis of our knowledge that more than 2000 HCWs were initially eligible at baseline, 16 we anticipated during the design stage that there would be approximately 500 participants per group at follow-up. We compared categorical variables with chi-square tests or Fisher s exact test (two-tailed) as appropriate. We examined the change in protein concentration in gloves as a function of time by using linear regression models. The distribution of protein concentrations in each glove brand was examined to determine whether log-transformed data were closer than the untransformed data to a normal distribution, although the arithmetic and geometric means did not differ markedly. We computed the relative risk of conversion between glove groups adjusted for potentially confounding variables by using logistic regression. We used the SAS (Cary, N.C.), SPSS (Chicago, Ill.), and SYSTAT (Chicago, Ill.) statistical programs. A probability value of less than 0.05 was considered to be statistically significant. RESULTS Exposure Air sampling results. The results of personal and area air samples for latex protein during use of powdered and SPT negative at baseline Excluding those in nonparticipatory depts in 1994 Excluding wards that did not participate during the year Excluding those who floated, were transferred, or were absent during the year (leaving those eligible to participate) Participated in follow-up testing powder-free gloves are displayed in Table I. For the powdered gloves, the personal exposures ranged from 5 to 83 ng/m 3 in the summer and 40 to 616 ng/m 3 in the winter. The samples obtained at background locations where gloves were not in use showed nondetectable levels. During powder-free glove use, all but two results for air samples were below the limit of detection ( 0.1 ng/m 3, and these two results were 1 ng/m 3 ). Glove protein concentrations over time. The mean protein concentrations expressed as micrograms per gram of sample, according to the assay batch dates, are shown in Fig. 1 (for powdered surgical gloves) and Fig. 2 (for powder-free gloves). There were too few samples of the powdered examination gloves for a meaningful regression model. The latex content of the powdered surgical gloves declined (Fig. 1) at a rate of g/gm per year, and this was highly statistically significant (p ) whether untransformed or log-transformed. The decline was thus more than an order of magnitude over the time period under study; the regression model explained approximately 40% of the variation. There were very small changes over time in the powder-free gloves (Fig. 2). The protein content was less than 1% of that in the powdered gloves studied. Participants in follow-up testing Of the 1075 participants with negative results to the skin test at baseline testing in 1994, 947 were working at the time of the 1994 assessment in departments that were included in the prospective study (Table II). After excluding those working in wards that became ineligible for the study during the year of follow-up and those who floated between wards, were transferred, or were absent for more than 6 months during the year, there were 479 subjects with negative results to the SPTs at baseline who could have participated (Table II). Of these, 435 (91%) participated in the follow-up testing. These 435 HCWs were similar to the other 640 with negative skin test results who were not eligible for (or did not participate in) the follow-up with respect to sex, hospital, atopic status, and distribution of job titles, although they were more likely to be current or ex-smokers and less likely to be younger than 30 years old (data not shown).
5 J ALLERGY CLIN IMMUNOL VOLUME 101, NUMBER 2, PART 1 Sussman et al. 175 However, neither smoking status nor age were significantly related to latex skin test status in our baseline study. 16 Characteristics of powdered and powder-free glove users There were 227 participants retested who had been using powder-free gloves (40 from the operating room at site H and 187 from the wards at site G) and 208 participants who had been using powdered gloves (36 from the operating room at site G and 172 from the wards at site H). The two glove groups were similar with respect to age, sex, atopic status, years of glove use, and smoking status (Table III). Among those using the powder-free gloves, the proportion of laboratory workers was smaller and the proportion of other occupations, including housekeepers, was greater than among those using the powdered gloves. Skin test conversions We identified four conversions or incident cases of latex skin test positivity: two (1.0%) of 208 in the powdered glove group and two (0.9%) of 227 in the low-protein group. This yielded a crude odds ratio (OR) for the powdered versus powder-free glove groups of 1.1 (95% CI, 0.2 to 7.7). In logistic regression models, the addition of sex (p 0.2), smoking status (p 0.4), or age (in four strata; p 0.7) was not significant, and these did not result in a material change in the OR. The addition of atopic status in 1995 to the model was significant (p 0.001; OR 26) though based on the small number of cases. The addition of atopy did not result in a change in the risk estimate for glove type (OR 1.04). The characteristics of the subjects with skin test conversions are tabulated in Table IV. Three were female, including two nurses and a ward clerk, and one was a male lab worker. The two converters using powdered gloves worked in the labor and delivery unit; one was a nurse, the other a ward clerk. These were the only converters who were symptomatic. One reported burning and itching eyes, itchy tongue, and respiratory symptoms, and the other reported sneezing, runny and stuffy nose, and persistent cough. Both of these converters from the labor and delivery unit were nonatopic and did not react to foods at baseline but at retesting in October 1994 were found to be atopic, and one reacted to a single food (avocado). One of the converters from the powderfree group had skin test results for the common inhalants ranging from 3 to 17 mm (Table V). Skin test results Table V displays the skin test results observed for the converters. One of the converters in the powder-free glove group reacted only to ammoniated latex (Guthrie, Inc.) but not to the Bencard latex reagent, and one converter in the powdered glove group also reacted only to one latex reagent (powdered examination glove extract) but not to Bencard. The other two converters reacted to the full-strength Bencard reagent. TABLE III. Characteristics of participants at follow-up by glove usage group, Hamilton Hospitals Latex Study, Ontario, 1995 Characteristic examined Glove type used Powdered Powder-free p Value Age Younger than 40 (%) 81 (39.3) 107 (47.6) to 49 (%) 75 (36.4) 72 (32.0) 50 and older (%) 50 (24.3) 46 (20.4) Total* Sex, no. F (%) 192 (92.3) 212 (93.4) 0.6 Atopic status Atopic (%) 9 (4.3) 9 (4.0) Not Atopic (%) 199 (95.7) 218 (96.0) 0.8 Total Smoking status Current (%) 53 (25.9) 59 (26.0) 0.9 Ex (%) 57 (27.8) 64 (28.2) Never (%) 95 (46.3) 104 (45.8) Total Occupation Nurses and physicians 120 (58.0) 148 (65.2) (%) Therapist and technician 25 (12.7) 24 (10.6) (%) Lab worker (%) 2 (1.0) 21 (9.3) Others (%) 60 (29.0) 34 (15.0) Total Years since first use of latex gloves at work (mean SD) Total *Data for some characteristics not available for all subjects. DISCUSSION We observed a skin test conversion rate among HCWs using powdered gloves of approximately 1% over the year of follow-up, which was in the middle of the range that we had estimated during the design of the study. Although unexpected, the conversion rate in the group using powdered gloves was only slightly greater than that among those using powder-free gloves. However, we documented marked differences in exposure as assessed by both the protein levels measured in the gloves and the results obtained from air sampling. The concentrations of latex aeroallergens measured during use of powdered gloves were comparable to those reported previously. 23, 24 Although the incidence of newly sensitized workers was relatively low, it should be emphasized that both of the converters identified in the powdered glove group were symptomatic, but those in the powder-free glove group were not. Interpretation of conversions The clinical significance of the skin test conversions, especially in the absence of symptoms, is not known. Whether these represent subjects who might have devel-
6 176 Sussman et al. J ALLERGY CLIN IMMUNOL FEBRUARY 1998 TABLE IV. Characteristics of skin test converters, Hamilton Hospitals Latex Study, Ontario, 1995 Converter Case No./Hospital site 122/Site G 778/Site G 1541/Site H 1629/Site H Date of follow-up testing April/May 95 April/May 95 October 94 October 94 Sex/age M/47 F/31 F/28 F/42 Latex glove group Powder-free Powder-free Powdered Powdered Smoking in 1994 Ex Never Never Never Latex reaction BL/FU Neg/Pos Neg/Pos Neg/Pos Neg/Pos Atopy BL/FU Neg/Neg Neg/Neg Neg/Pos Neg/Pos Food sensitivity BL/FU Neg/Neg Neg/Neg Neg/Neg Neg/Pos Ward Lab CCU L&D L&D Job title Lab worker Nurse Nurse Ward Clerk Hours/wk Year first wore latex gloves 1988/ /1990 NK/1990 NK/1978 (ever/at current hospital) Gloves per day (average over 3 94: 2/2/0 94: 23/23/0 94: 5.7/5.7/0 94: 4/4/0 days before survey): Total/ Latex/Vinyl 95: 0/0/0 95: 1.3/1.3/0 95:? 95:? Time gloves worn per day 94: (hrs, 3 days before survey) 95: ?? BL, baseline; FU, follow-up; L&D, labor and delivery; NK, not known. oped work-related asthma with further exposure is not clear, but latex challenges were not performed. In particular, the skin test conversions identified among the asymptomatic workers using powder-free gloves are difficult to interpret. However, it should be noted that one of these patients reacted only to the ammoniated latex reagent and not to the glove extract or to the Bencard reagent. This is unusual and possibly suggests sensitization to other components. In one of these (case 778), results of Western blot and Ala-stat (Diagnostic Products Corp., Los Angeles, Calif.) studies performed at baseline in 1994 and at follow-up in 1995 were both negative (data not shown). Moreover, since one cannot state definitively when the conversions to the sensitized state occurred, it is possible that these (as well as any of the other) conversions reflected a delayed manifestation of sensitization associated with previous glove use that was underway at the time of baseline testing. Alternatively, these conversions may have occurred from exposure to residual latex dust in adjacent crawl spaces that remained from powdered latex gloves that had been used previously. These conversions may also represent a reaction to an altered protein or another chemical constituent of the glove. Both of the converters using powdered gloves tested as atopic at follow-up; one reacted to full-strength Bencard reagent and the other reacted only to the powdered examination glove extract. This latter finding is unusual and may represent a reaction to nonprotein material or to protein modified during manufacturing, but this speculation has not been verified by immunoblotting. Of interest, one of the converters working in a powdered glove environment was a ward clerk. While an initial impression might be that this job should involve little exposure to latex, Vandenplas et al. 25 recently reported a case of occupational asthma caused by latex in an administrative hospital employee (medical secretary in an emergency room) who never used latex gloves, thought to be caused by indirect exposure to airborne latex. Cluster of converters in the labor and delivery unit Both converters using powdered gloves were identified when the workers in the labor and delivery unit became symptomatic halfway through the 1-year follow-up period, which led to the request for early retesting for this group. Whether there was unusual glove use or other circumstances in this department is unknown. The data regarding glove purchases indicated that this department used more examination (bulk) than sterile gloves and that an index of glove use per HCW during the year before the study (1178) was in the middle of the range across departments, which ranged from 0 to We previously observed in our baseline investigation that latex SPT results status was associated with an index of sterile glove use per HCW by department but not with bulk glove use. 16 Of interest, although Grzybowski et al. 11 did not find significant differences in anti-ige latex positivity in their study of nurses, the prevalence was highest among labor and delivery nurses (13.6%) and lowest among operating room nurses (6.4%). Limitations The power of this prospective phase was limited by the number of participants, which was only about half of that expected. This occurred in part because many hospital wards where baseline negative-results SPT participants were working did not participate in the prospective phase of the study or the HCWs did not remain in an eligible location throughout the year because of hospital restructuring that was underway. In addition, the sub-
7 J ALLERGY CLIN IMMUNOL VOLUME 101, NUMBER 2, PART 1 Sussman et al. 177 TABLE V. Results of skin testing among converters (in mm), Hamilton Hospitals Latex Study, Ontario, Skin test reagent Case No Glove group Powder-free Powder-free Powdered Powdered Saline/histamine 0/4 0/3 0/4 0/4 Glove brand A/B/C/D 0/0/0/0 0/2/0/0 4/0/0/0 0/0/0/0 Ammoniated latex Bencard full Bencard 1: Bencard 1: Bencard 1: Bencard 1:10, Bencard 1:100, Bencard 1:1,000, *Banana/avocado/potato/chestnut 0/0/0/0 0/0/0/0 0/0/0/2 2/4/2/0 Ragweed/dust mite/timothy grass 0/0/0 3/3/17 4/4/2 4/4/4 *All test results to kiwi and milk were negative. stantial declines in protein levels in the powdered latex gloves that we documented during the study period may have reduced the number of conversions that occurred and suggests that the glove manufacturers had already responded to concerns about latex, even in products not considered to be low protein. The small declines observed in the powder-free gloves are very unlikely to be clinically significant. The participation rate at follow-up was greater than 90% among those eligible, and thus selection bias was unlikely. Moreover, these participants at follow-up testing did not differ from those identified at baseline as having negative results to the skin test but who were not eligible for (or did not participate in) the prospective component with respect to a number of characteristics, including atopic status, that are strongly associated with latex sensitivity and were thus a potential confounder. Although there were differences between the follow-up participants and other subjects with negative results to the skin test in the distribution of smoking status and age, these factors were not associated with latex skin test status at baseline. Among the participants at follow-up, those using powdered gloves resembled those using low-protein powder-free gloves for all of these characteristics. However, information bias may have been present. The definition of a skin test converter was determined before analysis of the data and was based on objective findings (skin test measurement). Although the nurses performing the skin tests were trained in skin testing, they were divided among the two locations and thus may not have been blinded to exposure group in general. On the other hand, both types of gloves were in use at both sites. Thus it was possible that the skin test procedures and interpretation differed between sites, resulting in observer bias. This was strongly suggested by the difference in the number of equivocal skin test readings (latex minus saline skin test differences of 2 to 3 mm), which was not a primary outcome of interest. There were 22 such skin test results in the powder-free glove group compared with two in the powdered glove group. The observed low incidence could also be related to the nature of the study design. Although prospective and therefore better than many workplace studies that have been cross-sectional in design, many of the workers we studied had been working with latex for years. Thus this was not an inception cohort. Because the incidence of occupational asthma and sensitization is thought to be greatest during the first 1 to 2 years of exposure, 26 those who became symptomatic or were at risk for sensitization may have left the workforce, leaving survivors who are more resistant (the healthy worker survivor effect). That is, this represented a survivor population that might be expected to display a lower latex sensitization rate. The 1-year follow-up period may also contribute to the results. A naive patient population, larger sample size, and longer follow-up period would have been more ideal and may have produced different results. Food tests We and others have previously demonstrated food cross-reactivity, with a strong association between latex SPT results status and skin test reactions to certain foods. 16, 27, 28 This can make interpretation of skin tests difficult. However, given that only one of the converters had a positive test reaction to foods, cross-reactions to foods are unlikely to explain the findings. On the other hand, the interesting observation that the two symptomatic converters using powdered gloves changed status from nonatopic to atopic (and one of these also changed food skin test results status) raised the possibility that the subjects had heightened skin test reactivity or dermatographism. However, the wheal diameter for saline for these two subjects was recorded as 0 mm, which argues against this. Both of these individ-
8 178 Sussman et al. J ALLERGY CLIN IMMUNOL FEBRUARY 1998 uals were subsequently accommodated in an environment in which coworkers used powder-free gloves, consistent with the diagnosis of latex allergy and with other reports. We are not aware that any other prospective study has estimated the incidence of sensitization to latex. Newman Taylor 26 recently noted that such studies are few, with the exception of enzyme studies and current studies of laboratory animals, flour and acid anhydride workers, no other investigation has estimated the incidence of sensitization and asthma in relation to measured exposure. In conclusion, in this prospective study of latex sensitization, we observed a conversion rate for latex sensitization of approximately 1%. The incidence rate was not significantly related to glove type used, which was an unexpected finding. This may have resulted from observer bias between sites, limited study power, reactions to altered proteins or other materials in the low-protein gloves, other factors, or combination of these factors. Converters using powdered gloves were the only symptomatic ones. Importantly, we have also documented a sharp decline in latex protein concentrations in powdered latex gloves over the study period, which may have reduced the sensitization rate in this group. These results should not be interpreted to suggest that lowprotein powder-free gloves have no effect on reducing latex sensitization. Additional studies involving larger populations for longer periods of follow-up are required. We would recommend that low-protein powder-free gloves be used. The cooperation of Aladan Corporation (Dothan, Ala.), Ansell Medical (Eatontown, N.J.), Johnson and Johnson (Arlington, Tex.), Page Products (Burlington, Ontario), and Regent Hospital Products (Greenville, S.C.) is appreciated. We thank the participants and the hospital administration. We also thank Marlene Vaz for assistance with preparation of the tables. REFERENCES 1. Sussman GL, Beezhold DH. Allergy to latex rubber [editorial]. Ann Intern Med 1995;122: Slater JE. Latex allergy. J Allergy Clin Immunol 1994;94: Sussman GL, Tarlo S, Dolovich J. The spectrum of IgE-mediated responses to latex. JAMA 1991;265: Charous BL. The puzzle of latex allergy: some answers, still more questions [editorial]. Ann Allergy 1994;73: Hunt LW, Fransway AF, Reed CE, Miller LK, Jones RT, Swanson MC, et al. An epidemic of occupational allergy to latex involving health care workers. J Occup Environ Med 1995;37: Tarlo SM, Wong L, Roos J, Booth N. Occupational asthma caused by latex in a surgical glove manufacturing plant. J Allergy Clin Immunol 1990;85: Turjanmaa K. Incidence of immediate allergy to latex gloves in hospital personnel. Contact Dermatitis 1987;17: Vandenplas O, Delwiche JP, Evrard G, Aimont P, Van der Brempt X, Jamart J, et al. Prevalence of occupational asthma due to latex among hospital personnel. Am J Respir Crit Care Med 1995;151: Lagier F, Vervloet D, Lhermet I, Poyen D, Charpin D. Prevalence of latex allergy in operating room nurses. J Allergy Clin Immunol 1992;319: Arellano R, Bradley J, Sussman G. Prevalence of latex sensitization among hospital physicians occupationally exposed to latex gloves. Anesthesiology 1992;77: Grzybowski M, Ownby DR, Peyser PA, Johnson CC, Schork MA. The prevalence of anti-latex IgE antibodies among registered nurses. J Allergy Clin Immunol 1996;98: Turjanmaa K, Lahti A. Prick and use tests with 6 glove brands in patients with immediate allergy to rubber proteins. Contact Dermatitis 1992;26: Beezhold DH, Pugh B, Liss GM, Sussman GL. Correlation of protein levels with skin prick reactions in latex allergic patients. J Allergy Clin Immunol 1996;98: Vandenplas O, Delwiche JP, Depelchin S, Sibille Y, Vande Weyer R, Delaunois L. Latex gloves with a lower protein content reduce bronchial reactions in subjects with occupational asthma caused by latex. Am J Respir Crit Care Med 1995;151: Hamann CP. Natural rubber latex protein sensitivity in review. Am J Contact Dermatol 1993;4: Liss GM, Sussman GL, Deal K, Brown S, Cividino M, Sui S, et al. Latex allergy: epidemiologic study of 1351 hospital workers. Occup Environ Med 1997;54: Liss GM, Bernstein D, Genesove L, Roos JO, Lim J. Assessment of risk factors for IgE-mediated sensitization to tetrachlorophthalic anhydride. J Allergy Clin Immunol 1993;92: Smith BA, Bernstein D, Aw TC, Gallagher JS, London M, Kopp S, et al. Occupational asthma from inhaled egg protein. Am J Ind Med 1987;12: Beezhold DH, Chang NS, Kostyal DA, Sussman GL. Identification of a 46 kilodalton latex protein allergen in healthcare workers. Clin Exp Immunol 1994;98: Turjanmaa K. Contact urticaria from latex gloves. In: Mellstrom GA, Wahlberg JE, Maibach HI, editors. Protective gloves for occupational use. Boca Raton (FL): CRC Press; p Beezhold D. LEAP: latex ELISA for antigenic protein. Guthrie J 1992;61: Zehr BD, Beezhold DH. Antigenic proteins in latex glove extracts: sources of variability. Biomed Instrum Technol 1995;29: Swanson MC, Bubak ME, Hunt LW, Yunginger JW, Warner MA, Reed CE. Quantification of occupational latex aeroallergens in a medical center. J Allergy Clin Immunol 1994;94: Tarlo SM, Sussman G, Contala A, Swanson MC. Control of airborne latex by use of powder-free latex gloves. J Allergy Clin Immunol 1994;93: Vandenplas O, Delwiche JP, Sibille Y. Occupational asthma due to latex in a hospital administrative employee. Thorax 1996;51: Newman Taylor A. Asthma. In: McDonald C, editor. Epidemiology of work related diseases. London: BMJ Publishing Group; p Beezhold DH, Sussman GL, Liss GM, Chang NS. Latex allergy can induce clinical reactions to specific foods. Clin Exp Allergy 1996;26: Blanco C, Carillo T, Castillo R, Quiralte J, Cuevas M. Latex allergy: clinical features and cross-reactivity with fruits. Ann Allergy 1994; 73:
hospital workers Latex allergy: epidemiological study of 1351 (16.9%), and nurses and physicians
 Occupational and Environmental Medicine 1997;54:335-342 Ontario Ministry of Labour, Ontario, G M Liss S Siu G Smith Department of Preventive Medicine and Biostatistics, University of Toronto, Toronto,
Occupational and Environmental Medicine 1997;54:335-342 Ontario Ministry of Labour, Ontario, G M Liss S Siu G Smith Department of Preventive Medicine and Biostatistics, University of Toronto, Toronto,
A prospective, controlled study showing that rubber gloves are the major contributor to latex aeroallergen levels in the operating room
 A prospective, controlled study showing that rubber gloves are the major contributor to latex aeroallergen levels in the operating room Dann K. Heilman, MD, a Richard T. Jones, BS, b Mark C. Swanson, BA,
A prospective, controlled study showing that rubber gloves are the major contributor to latex aeroallergen levels in the operating room Dann K. Heilman, MD, a Richard T. Jones, BS, b Mark C. Swanson, BA,
Natural rubber latex (NRL) is used to manufacture
 FEATURE ARTICLE Research Impact of Converting to Powder-Free Gloves Decreasing the Symptoms of Latex Exposure in Operating Room Personnel by Denise M. Korniewicz, DNSc, RN, FAAN, Nantiya Chookaew, MSN,
FEATURE ARTICLE Research Impact of Converting to Powder-Free Gloves Decreasing the Symptoms of Latex Exposure in Operating Room Personnel by Denise M. Korniewicz, DNSc, RN, FAAN, Nantiya Chookaew, MSN,
Dental surgeons with natural rubber latex allergy: a report of 20 cases
 Occup. od. Vol. 49,. 2, pp. 103-107, 1999 Copyright C 1999 LJpptncott Williams 4 WilkJns for SO Printed In Great Britain. AH rights reserved 0962-7480/99 Dental surgeons with natural rubber latex allergy:
Occup. od. Vol. 49,. 2, pp. 103-107, 1999 Copyright C 1999 LJpptncott Williams 4 WilkJns for SO Printed In Great Britain. AH rights reserved 0962-7480/99 Dental surgeons with natural rubber latex allergy:
Prevalence and Risk Factors for Latex-Related Diseases Among Healthcare Workers in an Italian General Hospital
 184 Annals of Clinical & Laboratory Science, vol. 33, no. 2, 2003 Prevalence and Risk Factors for Latex-Related Diseases Among Healthcare Workers in an Italian General Hospital Nicola Verna, 1 Luca Di
184 Annals of Clinical & Laboratory Science, vol. 33, no. 2, 2003 Prevalence and Risk Factors for Latex-Related Diseases Among Healthcare Workers in an Italian General Hospital Nicola Verna, 1 Luca Di
Adverse Reactions to Latex Gloves Among Dentists in Bhubaneswar, Odisha
 Research Article J Res Adv Dent 2014; 3:1:55-59. Adverse Reactions to Latex Gloves Among Dentists in Bhubaneswar, Odisha Gunjan Kumar 1* Md Jalaluddin 2 Dhirendra K Singh 3 CL Dileep 4 Purnendu Rout 5
Research Article J Res Adv Dent 2014; 3:1:55-59. Adverse Reactions to Latex Gloves Among Dentists in Bhubaneswar, Odisha Gunjan Kumar 1* Md Jalaluddin 2 Dhirendra K Singh 3 CL Dileep 4 Purnendu Rout 5
Latex Allergy - the Australian experience Where are we now Prof CH Katelaris University of Western Sydney and Campbelltown Hospital
 Latex Allergy - the Australian experience Where are we now Prof CH Katelaris University of Western Sydney and Campbelltown Hospital Latex conf Dec Latex Allergy - Australian Experience Clinical studies
Latex Allergy - the Australian experience Where are we now Prof CH Katelaris University of Western Sydney and Campbelltown Hospital Latex conf Dec Latex Allergy - Australian Experience Clinical studies
Long-term outcome of 160 adult patients with natural rubber latex allergy
 Long-term outcome of 160 adult patients with natural rubber latex allergy Kristiina Turjanmaa, MD, a Mikko Kanto, CM, a Hannu Kautiainen, BA, b Timo Reunala, MD, a and Timo Palosuo, MD c Tampere, Heinola,
Long-term outcome of 160 adult patients with natural rubber latex allergy Kristiina Turjanmaa, MD, a Mikko Kanto, CM, a Hannu Kautiainen, BA, b Timo Reunala, MD, a and Timo Palosuo, MD c Tampere, Heinola,
health care workers effectiveness of laminar flow HEPA filtered helmets in reducing rhinoconjunctival and asthmatic reactions
 Inhalation challenge testing of latexsensitive health care workers and the effectiveness of laminar flow HEPA filtered helmets in reducing rhinoconjunctival and asthmatic reactions Nunthaporn Laoprasert,
Inhalation challenge testing of latexsensitive health care workers and the effectiveness of laminar flow HEPA filtered helmets in reducing rhinoconjunctival and asthmatic reactions Nunthaporn Laoprasert,
Primary prevention of natural rubber latex allergy in the German health care system through education and intervention
 Primary prevention of natural rubber latex allergy in the German health care system through education and intervention Henning Allmers, Dr med, a,b Jörg Schmengler, MD, c and Christoph Skudlik, Dr med
Primary prevention of natural rubber latex allergy in the German health care system through education and intervention Henning Allmers, Dr med, a,b Jörg Schmengler, MD, c and Christoph Skudlik, Dr med
METHODS Study setting The study period lasted from September 1996 to September Participants
 Reduction of latex aeroallergens and latex-specific IgE antibodies in sensitized workers after removal of powdered natural rubber latex gloves in a hospital Henning Allmers, Dr. med., a Randolph Brehler,
Reduction of latex aeroallergens and latex-specific IgE antibodies in sensitized workers after removal of powdered natural rubber latex gloves in a hospital Henning Allmers, Dr. med., a Randolph Brehler,
The National Institute for Occupational Safety and Health (NIOSH) requests assistance
 By: R.E. Biagini, S. Deitchman, E.J. Esswein, J. Fedan, J.P. Flesch, P.K. Hodgins, T.K. Hodous, R.D. Hull, W.R. Jarvis, D.M Lewis, J.A. Lipscomb, B.D. Lushniak, M.L. Pearson, E.L. Petsonk, L. Pinkerton,
By: R.E. Biagini, S. Deitchman, E.J. Esswein, J. Fedan, J.P. Flesch, P.K. Hodgins, T.K. Hodous, R.D. Hull, W.R. Jarvis, D.M Lewis, J.A. Lipscomb, B.D. Lushniak, M.L. Pearson, E.L. Petsonk, L. Pinkerton,
A hospital-based screening study of latex allergy and latex sensitization among medical workers in Taiwan
 J Microbiol Immunol Infect. 2008;4:499-506 A hospital-based screening study of latex allergy and latex sensitization among medical workers in Taiwan Ching-Tsai Lin, Dong-Zong Hung 2,3, Der-Yuan Chen,3,
J Microbiol Immunol Infect. 2008;4:499-506 A hospital-based screening study of latex allergy and latex sensitization among medical workers in Taiwan Ching-Tsai Lin, Dong-Zong Hung 2,3, Der-Yuan Chen,3,
Measurement of natural rubber proteins in latex glove extracts: comparison of the methods
 Measurement of natural rubber proteins in latex glove extracts: comparison of the methods Donald Beezhold*, PhD; Mark Swanson ; Bradley D Zehr*; and David Kostyal*, PhD Background: Healthcare workers and
Measurement of natural rubber proteins in latex glove extracts: comparison of the methods Donald Beezhold*, PhD; Mark Swanson ; Bradley D Zehr*; and David Kostyal*, PhD Background: Healthcare workers and
Allergy Skin Prick Testing
 Allergy Skin Prick Testing What is allergy? The term allergy is often applied erroneously to a variety of symptoms induced by exposure to a wide range of environmental or ingested agents. True allergy
Allergy Skin Prick Testing What is allergy? The term allergy is often applied erroneously to a variety of symptoms induced by exposure to a wide range of environmental or ingested agents. True allergy
New Test ANNOUNCEMENT
 March 2003 W New Test ANNOUNCEMENT A Mayo Reference Services Publication Pediatric Allergy Screen
March 2003 W New Test ANNOUNCEMENT A Mayo Reference Services Publication Pediatric Allergy Screen
LATEX ALLERGY ASCIA Education Resources patient information
 LATEX ALLERGY ASCIA Education Resources patient information Allergies to latex rubber have only been recognised in the last 20 years. The reasons are uncertain, although increased use of latex gloves in
LATEX ALLERGY ASCIA Education Resources patient information Allergies to latex rubber have only been recognised in the last 20 years. The reasons are uncertain, although increased use of latex gloves in
GLOVE ALLERGIES AND HAND HEALTH
 GLOVE ALLERGIES AND HAND HEALTH INTRODUCTION Skin conditions caused by chemical, physical or biological agents in the workplace are common among disposable glove wearers in the industrial sector. Understanding
GLOVE ALLERGIES AND HAND HEALTH INTRODUCTION Skin conditions caused by chemical, physical or biological agents in the workplace are common among disposable glove wearers in the industrial sector. Understanding
estimated exposure in workers not previously exposed to flour
 Occupational and Environmental Medicine 1994;51:579-583 Department of Occupational and Environmental Medicine, National Heart and Lung Institute, London SW3, UK P Cullinan D Lowson M J Nieuwenhuijsen C
Occupational and Environmental Medicine 1994;51:579-583 Department of Occupational and Environmental Medicine, National Heart and Lung Institute, London SW3, UK P Cullinan D Lowson M J Nieuwenhuijsen C
Textile Chemist and Colorist & American Dyestuff Reporter. Vol. 32, No. 1, January Safe Handling of Enzymes
 Textile Chemist and Colorist & American Dyestuff Reporter Vol. 32, No. 1, January 2000 Safe Handling of Enzymes By the Enzyme Technical Association, Washington, D.C. Enzymes have been used for over 35
Textile Chemist and Colorist & American Dyestuff Reporter Vol. 32, No. 1, January 2000 Safe Handling of Enzymes By the Enzyme Technical Association, Washington, D.C. Enzymes have been used for over 35
Assessing the Risk of Laboratory Acquired Allergies
 Guideline Created By: Stephanie Thomson, Kelly Eaton, Sonam Uppal & Hollie Burrage Edited By: N/A Workplace Health Services Occupational & Preventive Health Unit Effective date: January 8, 2015 Review
Guideline Created By: Stephanie Thomson, Kelly Eaton, Sonam Uppal & Hollie Burrage Edited By: N/A Workplace Health Services Occupational & Preventive Health Unit Effective date: January 8, 2015 Review
ALERT. Preventing Allergic Reactions to Natural Rubber Latex in the Workplace WARNING! BACKGROUND. June 1997 DHHS (NIOSH) Publication No.
 ALERT Preventing Allergic Reactions to Natural Rubber Latex in the Workplace June 1997 DHHS (NIOSH) Publication No. 97-135 (DISCLAIMER) WARNING! Workers exposed to latex gloves and other products containing
ALERT Preventing Allergic Reactions to Natural Rubber Latex in the Workplace June 1997 DHHS (NIOSH) Publication No. 97-135 (DISCLAIMER) WARNING! Workers exposed to latex gloves and other products containing
American Journal of EPIDEMIOLOGY
 American Journal of EPIDEMIOLOGY Volume 153 Number 6 March 15, 2001 Copyright 2001 by The Johns Hopkins University School of Hygiene and Public Health Sponsored by the Society for Epidemiologic Research
American Journal of EPIDEMIOLOGY Volume 153 Number 6 March 15, 2001 Copyright 2001 by The Johns Hopkins University School of Hygiene and Public Health Sponsored by the Society for Epidemiologic Research
Section A: Evidence-based Environmental Control of Latex Allergens. METHODS Latex allergen immunoassays
 Management of occupational allergy to natural rubber latex in a medical center: The importance of quantitative latex allergen measurement and objective follow-up Loren W. Hunt, MD, Pramod Kelkar, MD, Charles
Management of occupational allergy to natural rubber latex in a medical center: The importance of quantitative latex allergen measurement and objective follow-up Loren W. Hunt, MD, Pramod Kelkar, MD, Charles
A Review of Natural-Rubber Latex Allergy in Health Care Workers
 HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor INVITED ARTICLE A Review of Natural-Rubber Latex Allergy in Health Care Workers Peter M. Ranta and Dennis R. Ownby Departments of Pediatrics
HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor INVITED ARTICLE A Review of Natural-Rubber Latex Allergy in Health Care Workers Peter M. Ranta and Dennis R. Ownby Departments of Pediatrics
O ccupational asthma (OA) is the most commonly
 58 ORIGINAL ARTICLE Changes in rates and severity of compensation claims for asthma due to diisocyanates: a possible effect of medical surveillance measures S M Tarlo, G M Liss, K S Yeung... See end of
58 ORIGINAL ARTICLE Changes in rates and severity of compensation claims for asthma due to diisocyanates: a possible effect of medical surveillance measures S M Tarlo, G M Liss, K S Yeung... See end of
Latex allergy in health care workers: prevalence and knowledge at a tertiary teaching hospital in a developing country
 International Journal of Infection Control www.ijic.info ISSN 1996-9783 original article Latex allergy in health care workers: prevalence and knowledge at a tertiary teaching hospital in a developing country
International Journal of Infection Control www.ijic.info ISSN 1996-9783 original article Latex allergy in health care workers: prevalence and knowledge at a tertiary teaching hospital in a developing country
Guidance for the Control of Animal Allergens
 Environmental & Occupational Health Guidance for the Control of Animal Allergens I. Background Laboratory animal allergy (LAA) is an occupationally acquired condition that affects up to 1/3 of laboratory
Environmental & Occupational Health Guidance for the Control of Animal Allergens I. Background Laboratory animal allergy (LAA) is an occupationally acquired condition that affects up to 1/3 of laboratory
ADVERSE REACTION TO LATEX CONTAINING MATERIALS IN HEALTH CARE WORKERS
 ORIGINAL REPORT ADVERSE REACTION TO LATEX CONTAINING MATERIALS IN HEALTH CARE WORKERS Gh. Pouryaghoub, R. Mehrdad and M. M. Mazhari Department of Occupational and Environmental Medicine, School of Medicine,
ORIGINAL REPORT ADVERSE REACTION TO LATEX CONTAINING MATERIALS IN HEALTH CARE WORKERS Gh. Pouryaghoub, R. Mehrdad and M. M. Mazhari Department of Occupational and Environmental Medicine, School of Medicine,
Test Name Results Units Bio. Ref. Interval ALLERGY, INDIVIDUAL MARKER, BANANA, SERUM (FEIA) 0.42 kua/l
 LL - LL-ROHINI (NATIONAL REFERENCE 135091547 Age 28 Years Gender Female 1/9/2017 120000AM 1/9/2017 103610AM 1/9/2017 14658M Ref By Final ALLERGY, INDIVIDUAL MARKER, BANANA, SERUM 0.42 kua/l QUANTITATIVE
LL - LL-ROHINI (NATIONAL REFERENCE 135091547 Age 28 Years Gender Female 1/9/2017 120000AM 1/9/2017 103610AM 1/9/2017 14658M Ref By Final ALLERGY, INDIVIDUAL MARKER, BANANA, SERUM 0.42 kua/l QUANTITATIVE
Test Name Results Units Bio. Ref. Interval ALLERGY, INDIVIDUAL MARKER, BAHIA GRASS (PASPALUM NOTATUM), SERUM (FEIA) 0.39 kua/l <0.
 135091546 Age 32 Years Gender Female 1/9/2017 120000AM 1/9/2017 103949AM 1/9/2017 14702M Ref By Final ALLERGY, INDIVIDUAL MARKER, BAHIA GRASS (ASALUM NOTATUM), SERUM QUANTITATIVE RESULT LEVEL OF ALLERGEN
135091546 Age 32 Years Gender Female 1/9/2017 120000AM 1/9/2017 103949AM 1/9/2017 14702M Ref By Final ALLERGY, INDIVIDUAL MARKER, BAHIA GRASS (ASALUM NOTATUM), SERUM QUANTITATIVE RESULT LEVEL OF ALLERGEN
Protective Glove Standard: Selection and Use
 Protective Glove Standard: Selection and Use In many University workplaces, exposure to chemicals, infectious agents, sharp objects, extreme temperatures and other hazards can create a potential for injury
Protective Glove Standard: Selection and Use In many University workplaces, exposure to chemicals, infectious agents, sharp objects, extreme temperatures and other hazards can create a potential for injury
Formulating hypotheses and implementing research in allergic disorders in rural Crete, Greece
 Formulating hypotheses and implementing research in allergic disorders in rural Crete, Greece Christos Lionis and Leda Chatzi, Clinic of Social and Family Medicine, School of Medicine, University of Crete,
Formulating hypotheses and implementing research in allergic disorders in rural Crete, Greece Christos Lionis and Leda Chatzi, Clinic of Social and Family Medicine, School of Medicine, University of Crete,
Cross Country University s Caregiver Safety Series. Latex Allergy. Background to Latex Allergy
 Latex Allergy Background to Latex Allergy What is latex? Latex is a rubber compound found in many products that you use on your job. It is produced from rubber trees in the Tropics. The most common medical
Latex Allergy Background to Latex Allergy What is latex? Latex is a rubber compound found in many products that you use on your job. It is produced from rubber trees in the Tropics. The most common medical
Prevalence and risk factors of latex sensitization in an unselected pediatric population
 Prevalence and risk factors of latex sensitization in an unselected pediatric population Roberto Bernardini, MD, Elio Novembre, MD, Anna Ingargiola, MD, Marinella Veltroni, MD, Luca Mugnaini, MD, Antonella
Prevalence and risk factors of latex sensitization in an unselected pediatric population Roberto Bernardini, MD, Elio Novembre, MD, Anna Ingargiola, MD, Marinella Veltroni, MD, Luca Mugnaini, MD, Antonella
Latex allergy: what has the epidemic taught us?
 Latex allergy: what has the epidemic taught us? Dr Michael Sutherland MBBS, FRACP, PhD Department of Allergy Immunology and Respiratory Medicine The Alfred Hospital and Monash University History of Latex
Latex allergy: what has the epidemic taught us? Dr Michael Sutherland MBBS, FRACP, PhD Department of Allergy Immunology and Respiratory Medicine The Alfred Hospital and Monash University History of Latex
Clinical aspects of allergic disease. Quantification of occupational latex aeroallergens in a medical center
 Clinical aspects of allergic disease Quantification of occupational latex aeroallergens in a medical center Mark C. Swanson, BA, Mark E. Bubak, MD, Loren W. Hunt, MD, John W. Yunginger, MD, Mark A. Warner,
Clinical aspects of allergic disease Quantification of occupational latex aeroallergens in a medical center Mark C. Swanson, BA, Mark E. Bubak, MD, Loren W. Hunt, MD, John W. Yunginger, MD, Mark A. Warner,
BOHRF BOHRF. Occupational Asthma. A Guide for Occupational Health Professionals, Safety Professionals and Safety Representatives BOHRF
 Occupational Asthma A Guide for Occupational Health Professionals, Safety Professionals and Safety Representatives March 2010 British O Occupational Health Research Foundation This leaflet summarises the
Occupational Asthma A Guide for Occupational Health Professionals, Safety Professionals and Safety Representatives March 2010 British O Occupational Health Research Foundation This leaflet summarises the
Prevention of occupational allergies
 15 Prevention of occupational allergies H. de Groot,, G.C.M. Groenewoud, A.M.H. Bijl, N.W. de Jong, A. Burdorf, A.W. van Toorenenbergen, T. Blacquiere, C.C. Smeekens and R. Gerth van Wijk Abstract In this
15 Prevention of occupational allergies H. de Groot,, G.C.M. Groenewoud, A.M.H. Bijl, N.W. de Jong, A. Burdorf, A.W. van Toorenenbergen, T. Blacquiere, C.C. Smeekens and R. Gerth van Wijk Abstract In this
Skin prick testing: Guidelines for GPs
 INDEX Summary Offered testing but where Allergens precautions are taken Skin prick testing Other concerns Caution Skin testing is not useful in these following conditions When skin testing is uninterpretable
INDEX Summary Offered testing but where Allergens precautions are taken Skin prick testing Other concerns Caution Skin testing is not useful in these following conditions When skin testing is uninterpretable
Work related asthma: a brief review. October 12, 2015 Mike Pysklywec MD MSc CCFP(EM) DOHS FCBOM
 Work related asthma: a brief review October 12, 2015 Mike Pysklywec MD MSc CCFP(EM) DOHS FCBOM Work-related asthma Occupational Asthma Work-aggravated Asthma Sensitizer-induced (allergic) Irritant-induced
Work related asthma: a brief review October 12, 2015 Mike Pysklywec MD MSc CCFP(EM) DOHS FCBOM Work-related asthma Occupational Asthma Work-aggravated Asthma Sensitizer-induced (allergic) Irritant-induced
The worry-free choice...
 Healthcare-Associated Infection Solutions KIMBERLY-CLARK* STERLING* Nitrile Exam Gloves The worry-free choice...... designed for use by everyone, everywhere. Latex-quality Performance in a Worry-free,
Healthcare-Associated Infection Solutions KIMBERLY-CLARK* STERLING* Nitrile Exam Gloves The worry-free choice...... designed for use by everyone, everywhere. Latex-quality Performance in a Worry-free,
Lab Animal Allergens: Exposure Control Plan Revised November 2016
 Lab Animal Allergens: Exposure Control Plan Revised November 2016 Contents Purpose of Document... 2 Lab Animal Allergies... 2 Roles and Responsibilities... 2 UBC Departmental Managers/Supervisors/PIs will:...
Lab Animal Allergens: Exposure Control Plan Revised November 2016 Contents Purpose of Document... 2 Lab Animal Allergies... 2 Roles and Responsibilities... 2 UBC Departmental Managers/Supervisors/PIs will:...
Food Diversity in the First Year of Life and the Development of Allergic Disease in High-Risk Children. By Cheryl Hirst. Supervisor: Dr.
 Food Diversity in the First Year of Life and the Development of Allergic Disease in High-Risk Children By Cheryl Hirst Supervisor: Dr. Meghan Azad A Capstone Project Submitted to the Faculty of Graduate
Food Diversity in the First Year of Life and the Development of Allergic Disease in High-Risk Children By Cheryl Hirst Supervisor: Dr. Meghan Azad A Capstone Project Submitted to the Faculty of Graduate
Accommodation and Compliance Series. Employees with Latex Allergy
 Accommodation and Compliance Series Employees with Latex Allergy Preface The Job Accommodation Network (JAN) is a service of the Office of Disability Employment Policy of the U.S. Department of Labor.
Accommodation and Compliance Series Employees with Latex Allergy Preface The Job Accommodation Network (JAN) is a service of the Office of Disability Employment Policy of the U.S. Department of Labor.
Shumani Makwarela Phaswana, Saloshni Naidoo
 To cite: Phaswana SM, Naidoo S. The prevalence of latex sensitisation and allergy and associated risk factors among healthcare workers using hypoallergenic latex gloves at King Edward VIII Hospital, KwaZulu-Natal
To cite: Phaswana SM, Naidoo S. The prevalence of latex sensitisation and allergy and associated risk factors among healthcare workers using hypoallergenic latex gloves at King Edward VIII Hospital, KwaZulu-Natal
Environmental and occupational disorders. A cross-sectional survey of sensitization to Aspergillus oryzae derived lactase in pharmaceutical workers
 Environmental and occupational disorders A cross-sectional survey of sensitization to Aspergillus oryzae derived lactase in pharmaceutical workers Jonathan A. Bernstein, MD, David I. Bernstein, MD, Tom
Environmental and occupational disorders A cross-sectional survey of sensitization to Aspergillus oryzae derived lactase in pharmaceutical workers Jonathan A. Bernstein, MD, David I. Bernstein, MD, Tom
NATURAL RUBBER LATEX ALLERGY: ANTIGEN SPECIFIC IgE IN POLISH BLOOD DONORS, PREVALENCE AND RISK FACTORS PRELIMINARY DATA
 International Journal of Occupational Medicine and Environmental Health, 2005;18(1):35 42 NATURAL RUBBER LATEX ALLERGY: ANTIGEN SPECIFIC IgE IN POLISH BLOOD DONORS, PREVALENCE AND RISK FACTORS PRELIMINARY
International Journal of Occupational Medicine and Environmental Health, 2005;18(1):35 42 NATURAL RUBBER LATEX ALLERGY: ANTIGEN SPECIFIC IgE IN POLISH BLOOD DONORS, PREVALENCE AND RISK FACTORS PRELIMINARY
A Review of the Expert Opinion on Latex Allergy
 A Review of the Expert Opinion on Latex Allergy Author(s) Pete Phillips BPharm, MRPharmS, DMS (Health) Deputy Director Surgical Materials Testing Laboratory Princess of Wales Hospital, Bridgend, Wales.
A Review of the Expert Opinion on Latex Allergy Author(s) Pete Phillips BPharm, MRPharmS, DMS (Health) Deputy Director Surgical Materials Testing Laboratory Princess of Wales Hospital, Bridgend, Wales.
LATEX ALLERGIES. As with many other natural products, natural rubber latex contains proteins to which some individuals may develop an allergy.
 What is Natural Rubber Latex? LATEX ALLERGIES Natural rubber latex (NRL) is a milky fluid obtained from the Heva barsiliensis tree, which is widely grown in South East Asia and other countries. NRL is
What is Natural Rubber Latex? LATEX ALLERGIES Natural rubber latex (NRL) is a milky fluid obtained from the Heva barsiliensis tree, which is widely grown in South East Asia and other countries. NRL is
An Insight into Allergy and Allergen Immunotherapy Co-morbidities of allergic disease
 An Insight into Allergy and Allergen Immunotherapy Co-morbidities of allergic disease Carmen Vidal Athens, September 11, 2014 Pucci S & Incorvaia C, 2008; 153:1-2 1. The major player in driving the immune
An Insight into Allergy and Allergen Immunotherapy Co-morbidities of allergic disease Carmen Vidal Athens, September 11, 2014 Pucci S & Incorvaia C, 2008; 153:1-2 1. The major player in driving the immune
Exposure-response relations of α-amylase sensitisation in British bakeries and flour mills
 Occup Environ Med 1999;56:197 201 197 T H Huxley School of Environment, Earth Sciences and Engineering, Centre for Environmental Technology, Imperial College of Science, Technology and Medicine, London
Occup Environ Med 1999;56:197 201 197 T H Huxley School of Environment, Earth Sciences and Engineering, Centre for Environmental Technology, Imperial College of Science, Technology and Medicine, London
Atopic status and latex sensitization in a cohort of 1,628 students of health care faculties
 Atopic status and latex sensitization in a cohort of 1,628 students of health care faculties Anna Elena Wudy, MD; Corrado Negro, MD; Alessandro Adami, MD; Francesca Larese Filon, MD Unit of Occupational
Atopic status and latex sensitization in a cohort of 1,628 students of health care faculties Anna Elena Wudy, MD; Corrado Negro, MD; Alessandro Adami, MD; Francesca Larese Filon, MD Unit of Occupational
Quantified environmental challenge with absorbable dusting powder aerosol from natural rubber latex gloves
 Quantified environmental challenge with absorbable dusting powder aerosol from natural rubber latex gloves Santiago Quirce, MD, PhD, a Mark C. Swanson, BA, b Mar Fernández-Nieto, MD, a Manuel de las Heras,
Quantified environmental challenge with absorbable dusting powder aerosol from natural rubber latex gloves Santiago Quirce, MD, PhD, a Mark C. Swanson, BA, b Mar Fernández-Nieto, MD, a Manuel de las Heras,
Volunteer Applicant Health Clearance Checklist
 Volunteer Applicant Health Clearance Checklist Employee Health Contact Information Office Phone: (202) 715-4275; Fax: (202) 715-4587; Email: gwuehs@medcor.com Walk-in hours: M-F 8:00 a.m. 12:00 p.m. &
Volunteer Applicant Health Clearance Checklist Employee Health Contact Information Office Phone: (202) 715-4275; Fax: (202) 715-4587; Email: gwuehs@medcor.com Walk-in hours: M-F 8:00 a.m. 12:00 p.m. &
Clinical Study Report SLO-AD-1 Final Version DATE: 09 December 2013
 1. Clinical Study Report RANDOMIZED, OPEN, PARALLEL GROUP, PHASE IIIB STUDY ON THE EVALUATION OF EFFICACY OF SPECIFIC SUBLINGUAL IMMUNOTHERAPY IN PAEDIATRIC PATIENTS WITH ATOPIC DERMATITIS, WITH OR WITHOUT
1. Clinical Study Report RANDOMIZED, OPEN, PARALLEL GROUP, PHASE IIIB STUDY ON THE EVALUATION OF EFFICACY OF SPECIFIC SUBLINGUAL IMMUNOTHERAPY IN PAEDIATRIC PATIENTS WITH ATOPIC DERMATITIS, WITH OR WITHOUT
HealthStream Regulatory Script
 HealthStream Regulatory Script Latex Allergy Release Date: August 2009 HLC Version: 602 Lesson 1: Introduction Lesson 2: Risk Factors & Diagnosis Lesson 3: Types of Latex Reactions Lesson 4: Managing Latex
HealthStream Regulatory Script Latex Allergy Release Date: August 2009 HLC Version: 602 Lesson 1: Introduction Lesson 2: Risk Factors & Diagnosis Lesson 3: Types of Latex Reactions Lesson 4: Managing Latex
Predictors of obstructive lung disease among seafood processing workers along the West Coast of the Western Cape Province
 Predictors of obstructive lung disease among seafood processing workers along the West Coast of the Western Cape Province Adams S 1, Jeebhay MF 1, Lopata AL 2, Bateman ED 3, Smuts M 4, Baatjies R 1, Robins
Predictors of obstructive lung disease among seafood processing workers along the West Coast of the Western Cape Province Adams S 1, Jeebhay MF 1, Lopata AL 2, Bateman ED 3, Smuts M 4, Baatjies R 1, Robins
Latex and Occupational Dermatitis Policy Incorporating Glove Selection
 Latex and Occupational Dermatitis Policy Incorporating Glove Selection DOCUMENT CONTROL: Version: 3 Ratified by: Risk Management Sub Group Date ratified: 17 July 2013 Name of originator/author: Health
Latex and Occupational Dermatitis Policy Incorporating Glove Selection DOCUMENT CONTROL: Version: 3 Ratified by: Risk Management Sub Group Date ratified: 17 July 2013 Name of originator/author: Health
OCCUPATIONAL ASTHMA A GUIDE FOR OCCUPATIONAL PHYSICIANS AND OCCUPATIONAL HEALTH PRACTITIONERS
 OCCUPATIONAL ASTHMA A GUIDE FOR OCCUPATIONAL PHYSICIANS AND OCCUPATIONAL HEALTH PRACTITIONERS OCCUPATIONAL ASTHMA A guide for occupational physicians and occupational health practitioners Occupational
OCCUPATIONAL ASTHMA A GUIDE FOR OCCUPATIONAL PHYSICIANS AND OCCUPATIONAL HEALTH PRACTITIONERS OCCUPATIONAL ASTHMA A guide for occupational physicians and occupational health practitioners Occupational
CONTENTS. STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1
 CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
Myth: Prior Episodes Predict Future Reactions REALITY: No predictable pattern Severity depends on: Sensitivity of the individual Dose of the allergen
 Myth: Prior Episodes Predict Future Reactions REALITY: No predictable pattern Severity depends on: Sensitivity of the individual Dose of the allergen Anaphylaxis Fatalities Estimated 500 1000 deaths annually
Myth: Prior Episodes Predict Future Reactions REALITY: No predictable pattern Severity depends on: Sensitivity of the individual Dose of the allergen Anaphylaxis Fatalities Estimated 500 1000 deaths annually
PROTECT YOURSELF FROM TYPE I ALLERGIES.
 PROTECT YOURSELF FROM TYPE I ALLERGIES. 1 PROTECT YOURSELF FROM TYPE I ALLERGIES. Occasionally wearing glove products can cause issues with the health of our skin. This predominantly manifests itself in
PROTECT YOURSELF FROM TYPE I ALLERGIES. 1 PROTECT YOURSELF FROM TYPE I ALLERGIES. Occasionally wearing glove products can cause issues with the health of our skin. This predominantly manifests itself in
Ear, Nose & Throat (ENT) - Head & Neck Surgery. Allergic Rhinitis (Sinus)
 Ear, Nose & Throat (ENT) - Head & Neck Surgery Allergic Rhinitis (Sinus) The Department of Ear, Nose & Throat (ENT) - Head & Neck Surgery provides a wide range of surgical services for adult patients with
Ear, Nose & Throat (ENT) - Head & Neck Surgery Allergic Rhinitis (Sinus) The Department of Ear, Nose & Throat (ENT) - Head & Neck Surgery provides a wide range of surgical services for adult patients with
A llergy is a common occupational hazard for workers
 766 ORIGINAL ARTICLE Incidence of allergy and allergy symptoms among workers exposed to laboratory animals L Elliott, D Heederik, S Marshall, D Peden, D Loomis... See end of article for authors affiliations...
766 ORIGINAL ARTICLE Incidence of allergy and allergy symptoms among workers exposed to laboratory animals L Elliott, D Heederik, S Marshall, D Peden, D Loomis... See end of article for authors affiliations...
Allergy in Personnel with Laboratory Animal Contact. Horatiu V. Vinerean DVM, DACLAM Director, Laboratory Animal Research Attending Veterinarian
 Allergy in Personnel with Laboratory Animal Contact Horatiu V. Vinerean DVM, DACLAM Director, Laboratory Animal Research Attending Veterinarian Significance Allergy incidence - some estimate that as many
Allergy in Personnel with Laboratory Animal Contact Horatiu V. Vinerean DVM, DACLAM Director, Laboratory Animal Research Attending Veterinarian Significance Allergy incidence - some estimate that as many
VELINDRE NHS TRUST. REF: Black 46. Trust Policy
 VELINDRE NHS TRUST REF: Black 46 POLICY FOR THE MANAGEMENT OF LATEX AND LATEX ALLERGY Health and Safety Manager Ref: Black 46 Page 1 of 14 CONTENTS Executive Summary Page 3 1. Introduction Page 4 2. Scope
VELINDRE NHS TRUST REF: Black 46 POLICY FOR THE MANAGEMENT OF LATEX AND LATEX ALLERGY Health and Safety Manager Ref: Black 46 Page 1 of 14 CONTENTS Executive Summary Page 3 1. Introduction Page 4 2. Scope
latex allergy Safety in the OR Pat Lawson, CST
 latex allergy Safety in the OR Pat Lawson, CST EDITOR S NOTE This is the first of two articles discussing latex allergy.in this issue, the author covers general information regarding latex allergy and
latex allergy Safety in the OR Pat Lawson, CST EDITOR S NOTE This is the first of two articles discussing latex allergy.in this issue, the author covers general information regarding latex allergy and
Environmental and occupational disorders
 Environmental and occupational disorders Effectiveness of a medical surveillance program for the prevention of occupational asthma caused by platinum salts: A nested case-control study Rolf Merget, MD,
Environmental and occupational disorders Effectiveness of a medical surveillance program for the prevention of occupational asthma caused by platinum salts: A nested case-control study Rolf Merget, MD,
Sensitisation to natural rubber latex: an epidemiological study of workers exposed during tapping and glove manufacture in Thailand
 386 Community Medicine Department, Faculty of Medicine, Khon Kaen University, Khon Kaen 40002, Thailand N Chaiear Institute of Occupational Health, The University of Birmingham, Birmingham B15 2TT, UK
386 Community Medicine Department, Faculty of Medicine, Khon Kaen University, Khon Kaen 40002, Thailand N Chaiear Institute of Occupational Health, The University of Birmingham, Birmingham B15 2TT, UK
Natural rubber latex allergy
 I Allerg! 1996: 51: 593-602 Printed in L'K ~ crll ri%ghfs reserved Review article Natural rubber latex allergy Turjanmaa K, Alenius H, Makinen-Kiljunen S, Reunala T. Palosuo T. Natural rubber latex allergy.
I Allerg! 1996: 51: 593-602 Printed in L'K ~ crll ri%ghfs reserved Review article Natural rubber latex allergy Turjanmaa K, Alenius H, Makinen-Kiljunen S, Reunala T. Palosuo T. Natural rubber latex allergy.
Ward/Unit/Team managers to carry out an occupational skin disease risk assessment for their area
 Policy Title: Prevention and Management of Occupational Skin Disease Reference and Version No: RM26 Version 3 Author and Job Title: Jude Cooper Head of Occupational Health and Wellbeing Executive Lead
Policy Title: Prevention and Management of Occupational Skin Disease Reference and Version No: RM26 Version 3 Author and Job Title: Jude Cooper Head of Occupational Health and Wellbeing Executive Lead
Cat and dog sensitization in pet shop workers
 Occupational Medicine 2013;63:563 567 Advance Access publication 30 October 2013 doi:10.1093/occmed/kqt116 Cat and dog sensitization in pet shop workers I. Yilmaz 1, F. Oner Erkekol 2, D. Secil 1, Z. Misirligil
Occupational Medicine 2013;63:563 567 Advance Access publication 30 October 2013 doi:10.1093/occmed/kqt116 Cat and dog sensitization in pet shop workers I. Yilmaz 1, F. Oner Erkekol 2, D. Secil 1, Z. Misirligil
Food allergy in children. nice bulletin. NICE Bulletin Food Allergy in Chlidren.indd 1
 nice bulletin Food allergy in children NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin Food Allergy in Chlidren.indd 1 23/01/2012 11:04
nice bulletin Food allergy in children NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin Food Allergy in Chlidren.indd 1 23/01/2012 11:04
Threshold levels in food challenge and specific IgE in patients with egg allergy: Is there a relationship?
 Threshold levels in food challenge and specific IgE in patients with egg allergy: Is there a relationship? Morten Osterballe, MD, and Carsten Bindslev-Jensen, MD, PhD, DSc Odense, Denmark Background: Previously
Threshold levels in food challenge and specific IgE in patients with egg allergy: Is there a relationship? Morten Osterballe, MD, and Carsten Bindslev-Jensen, MD, PhD, DSc Odense, Denmark Background: Previously
Tony Gray Head of Safety and Security. Tony Gray Head of Safety and Security. Contents Section Description Page No.
 Health and Safety Policy Practice Guidance Note Latex Sensitivity V04 Date Issued Planned Review Issue 1 Oct 17 Oct 2020 HS-PGN-10 Part of NTW(O)20 Health and Safety Policy Author/Designation Tony Gray
Health and Safety Policy Practice Guidance Note Latex Sensitivity V04 Date Issued Planned Review Issue 1 Oct 17 Oct 2020 HS-PGN-10 Part of NTW(O)20 Health and Safety Policy Author/Designation Tony Gray
SLIT: Review and Update
 SLIT: Review and Update Disclosure Speaker: ISTA Pharmaceuticals Speaker: GlaxoSmithKline Allergen IT - Evidence Based Evaluation: Rescue Medications Meta-analysis Disease IT # of Patients Rescue Medication
SLIT: Review and Update Disclosure Speaker: ISTA Pharmaceuticals Speaker: GlaxoSmithKline Allergen IT - Evidence Based Evaluation: Rescue Medications Meta-analysis Disease IT # of Patients Rescue Medication
Dr. Janice M. Joneja, Ph.D. FOOD ALLERGIES - THE DILEMMA
 Dr. Janice M. Joneja, Ph.D. FOOD ALLERGIES - THE DILEMMA 2002 The Dilemma Accurate identification of the allergenic food is crucial for correct management of food allergy Inaccurate identification of the
Dr. Janice M. Joneja, Ph.D. FOOD ALLERGIES - THE DILEMMA 2002 The Dilemma Accurate identification of the allergenic food is crucial for correct management of food allergy Inaccurate identification of the
Introduction. Methods. Results 12/7/2012. Immunotherapy in the Pediatric Population
 12/7/212 Introduction Immunotherapy in the Pediatric Population Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine University of Tennessee Health Science Center Memphis, Tennessee Allergen
12/7/212 Introduction Immunotherapy in the Pediatric Population Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine University of Tennessee Health Science Center Memphis, Tennessee Allergen
Revised Protocol: Criteria for Designating Substances as. Occupational Asthmagens on the AOEC List of. Exposure Codes
 Revised Protocol: Criteria for Designating Substances as Occupational Asthmagens on the AOEC List of Exposure Codes Revised September 2008 1 I. Introduction This is a project to evaluate the current AOEC
Revised Protocol: Criteria for Designating Substances as Occupational Asthmagens on the AOEC List of Exposure Codes Revised September 2008 1 I. Introduction This is a project to evaluate the current AOEC
Enzyme Safety Management: Thanks for joining us today!
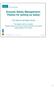 Enzyme Safety Management: Thanks for joining us today!.the webinar will begin shortly. The webinar will be recorded. Please make sure to be on mute so that we can ensure a good quality of the audio. 1
Enzyme Safety Management: Thanks for joining us today!.the webinar will begin shortly. The webinar will be recorded. Please make sure to be on mute so that we can ensure a good quality of the audio. 1
FinTest IgG4 Screen 20 ELISA KIT
 FinTest IgG4 Screen 20 ELISA KIT Cat. No.:DEIA6196 Pkg.Size:96T Intended use Enzyme immunoassay (microtiter strips) for the detection and the quantitative determination of IgG4 antibodies against 20 Food
FinTest IgG4 Screen 20 ELISA KIT Cat. No.:DEIA6196 Pkg.Size:96T Intended use Enzyme immunoassay (microtiter strips) for the detection and the quantitative determination of IgG4 antibodies against 20 Food
Allergic Disorders. Allergic Disorders. IgE-dependent Release of Inflammatory Mediators. TH1/TH2 Paradigm
 Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Allergic Disorders. Allergic Disorders. IgE-dependent Release of Inflammatory Mediators. TH1/TH2 Paradigm
 Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Protein and allergen assays for natural rubber latex products
 Protein and allergen assays for natural rubber latex products Vesna J. Tomazic-Jezic, PhD, and Anne D. Lucas, PhD Rockville, Md The major issues in the efforts to alleviate allergy to natural rubber latex
Protein and allergen assays for natural rubber latex products Vesna J. Tomazic-Jezic, PhD, and Anne D. Lucas, PhD Rockville, Md The major issues in the efforts to alleviate allergy to natural rubber latex
FDA/NSTA Web Seminar: Teach Science Concepts and Inquiry with Food
 LIVE INTERACTIVE LEARNING @ YOUR DESKTOP FDA/NSTA Web Seminar: Teach Science Concepts and Inquiry with Food Thursday, November 15, 2007 Food allergy Stefano Luccioli, MD Office of Food Additive Safety
LIVE INTERACTIVE LEARNING @ YOUR DESKTOP FDA/NSTA Web Seminar: Teach Science Concepts and Inquiry with Food Thursday, November 15, 2007 Food allergy Stefano Luccioli, MD Office of Food Additive Safety
The worry-free choice...
 Healthcare-Associated Infection Solutions KIMBERLY-CLARK* STERLING* Nitrile Exam Gloves The worry-free choice...... designed for use by everyone, everywhere. Latex-quality Performance in a Worry-free,
Healthcare-Associated Infection Solutions KIMBERLY-CLARK* STERLING* Nitrile Exam Gloves The worry-free choice...... designed for use by everyone, everywhere. Latex-quality Performance in a Worry-free,
GUIDE TO... Latex allergy. Learning outcomes. This guide is supported by an educational grant from
 GUIDE Janet Pickles is Chairwoman, RA Medical Services Ltd, Steeton, West Yorkshire Email: janet@ramedical.com TO... Learning outcomes After reading this Guide to Latex Allergy you should: n Understand
GUIDE Janet Pickles is Chairwoman, RA Medical Services Ltd, Steeton, West Yorkshire Email: janet@ramedical.com TO... Learning outcomes After reading this Guide to Latex Allergy you should: n Understand
Latex Allergy Management Guidelines
 Latex Allergy Management Guidelines Overview Definition of Latex Allergy In recent years, natural rubber latex (NRL or latex) allergy has been recognized as a significant problem for both patients and
Latex Allergy Management Guidelines Overview Definition of Latex Allergy In recent years, natural rubber latex (NRL or latex) allergy has been recognized as a significant problem for both patients and
Sergio Bonini. Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy.
 Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Immediate hypersensitivity to natural rubber latex (NRL) has become increasingly common during
 NATURAL RUBBER LATEX ALLERGY c SYMPTOMS Correspondence to: Dr Harri Alenius, Department of Industrial Hygiene and Toxicology, Finnish Institute of Occupational Health, Topeliuksenkatu 41b, FIN-00250 Helsinki,
NATURAL RUBBER LATEX ALLERGY c SYMPTOMS Correspondence to: Dr Harri Alenius, Department of Industrial Hygiene and Toxicology, Finnish Institute of Occupational Health, Topeliuksenkatu 41b, FIN-00250 Helsinki,
Evaluation of a Dipstick Test (Allergodip -Latex) for in vitro Diagnosis of Natural Rubber Latex Allergy
 Original Paper Int Arch Allergy Immunol 2001;126:226 230 Received: November 7, 2000 Accepted after revision: July 18, 2001 Evaluation of a Dipstick Test (Allergodip -Latex) for in vitro Diagnosis of Natural
Original Paper Int Arch Allergy Immunol 2001;126:226 230 Received: November 7, 2000 Accepted after revision: July 18, 2001 Evaluation of a Dipstick Test (Allergodip -Latex) for in vitro Diagnosis of Natural
NIOSH FIELD STUDIES ON DAMPNESS AND MOLD AND RELATED HEALTH EFFECTS
 NIOSH FIELD STUDIES ON DAMPNESS AND MOLD AND RELATED HEALTH EFFECTS Jean Cox-Ganser, Ph.D. Division of Respiratory Disease Studies The findings and conclusions in this presentation are those of the author
NIOSH FIELD STUDIES ON DAMPNESS AND MOLD AND RELATED HEALTH EFFECTS Jean Cox-Ganser, Ph.D. Division of Respiratory Disease Studies The findings and conclusions in this presentation are those of the author
Glove Selection as Personal Protective Equipment and Occupational Dermatitis among Japanese Midwives
 J Occup Health 2006; 48: 35 43 Journal of Occupational Health Glove Selection as Personal Protective Equipment and Occupational Dermatitis among Japanese Midwives Minako SASAKI and Katsuya KANDA Department
J Occup Health 2006; 48: 35 43 Journal of Occupational Health Glove Selection as Personal Protective Equipment and Occupational Dermatitis among Japanese Midwives Minako SASAKI and Katsuya KANDA Department
Care. Every day, health care workers are confronted OF THE LATEX ALLERGIC PATIENT. with situations that could
 Care OF THE LATEX ALLERGIC PATIENT Every day, health care workers are confronted with situations that could compromise their patients safety. Natural rubber latex allergy (NRLA or latex allergy) is one
Care OF THE LATEX ALLERGIC PATIENT Every day, health care workers are confronted with situations that could compromise their patients safety. Natural rubber latex allergy (NRLA or latex allergy) is one
LATEX sensitization in elderly: allergological study and diagnostic protocol
 Grieco et al. Immunity & Ageing 2014, 11:7 IMMUNITY & AGEING METHODOLOGY Open Access LATEX sensitization in elderly: allergological study and diagnostic protocol Teresa Grieco *, Valentina Faina, Laura
Grieco et al. Immunity & Ageing 2014, 11:7 IMMUNITY & AGEING METHODOLOGY Open Access LATEX sensitization in elderly: allergological study and diagnostic protocol Teresa Grieco *, Valentina Faina, Laura
SARASOTA MEMORIAL HEALTH CARE SYSTEM CORPORATE POLICY
 SARASOTA MEMORIAL HEALTH CARE SYSTEM CORPORATE POLICY TITLE: LATEX ALLERGY POLICY #: EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY TYPE: 5/28/97 08/25/17 Clinical 1 of 5 Non-Clinical Job Title of Responsible
SARASOTA MEMORIAL HEALTH CARE SYSTEM CORPORATE POLICY TITLE: LATEX ALLERGY POLICY #: EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY TYPE: 5/28/97 08/25/17 Clinical 1 of 5 Non-Clinical Job Title of Responsible
Prevention of occupational asthma practical implications for occupational physicians
 IN-DEPTH REVIEW Occupational Medicine 2005;55:588 594 doi:10.1093/occmed/kqi182... Prevention of occupational asthma practical implications for occupational physicians Susan M. Tarlo 1,2,3,4 and Gary M.
IN-DEPTH REVIEW Occupational Medicine 2005;55:588 594 doi:10.1093/occmed/kqi182... Prevention of occupational asthma practical implications for occupational physicians Susan M. Tarlo 1,2,3,4 and Gary M.
GEORGE WASHINGTON UNIVERSITY HOSPITAL EMPLOYEE HEALTH SERVICES REQUIREMENTS FOR CLEARANCE:
 GEORGE WASHINGTON UNIVERSITY HOSPITAL EMPLOYEE HEALTH SERVICES Office: 202 715 4275 Fax: 202 715 4587 Email: gwuehs@medcor.com Walk-in hours: M-F 8am-12pm and 1pm-4pm REQUIREMENTS FOR CLEARANCE: Physical
GEORGE WASHINGTON UNIVERSITY HOSPITAL EMPLOYEE HEALTH SERVICES Office: 202 715 4275 Fax: 202 715 4587 Email: gwuehs@medcor.com Walk-in hours: M-F 8am-12pm and 1pm-4pm REQUIREMENTS FOR CLEARANCE: Physical
