Corneal Epithelial Wound Healing in the Absence of Limbal Epithelium
|
|
|
- Michael Jefferson
- 5 years ago
- Views:
Transcription
1 Investigative Ophthalmology & Visual Science, Vol. 32, No. 1, January 1991 Copyright Association for Research in Vision and Ophthalmology Corneal Epithelial Wound Healing in the Absence of Limbal Epithelium Andrew J. W. Huang and Scheffer C. G. Tseng Corneal epithelial stem cells are thought to be at the limbus. The limbal epithelium was surgically removed in 12 New Zealand white rabbits. After 6 months, four showed mild vascularization. To challenge the remaining proliferative reserve, two consecutive 7.5-mm epithelial woundings were created 3 weeks apart in 11 limbal-deficient corneas and 11 controls. After the first wounding, five of the limbal-deficient corneas showed delayed healing, and seven became moderately vascularized; the controls healed normally. After the second wounding, eight experimental corneas showed intense vascularization; the controls did not. Recurrent erosions with delays in healing were noted in nine experimental animals but not in controls. Flat-mount preparation and impression cytology revealed centripetal migration of conjunctival epithelium with goblet cells onto the experimental corneas. These results indicate that only limited proliferative capacity of corneal epithelium remains in the absence of limbus. The constellation of delayed healing with recurrent erosion, corneal vascularization, and conjunctival epithelial ingrowth can be considered possible signs of limbal stem cell dysfunction. Invest Ophthalmol Vis Sci 32:96-105,1991 In postnatal development, cells in any denned tissue that has active cellular renewal and differentiation can be classified into either of the two cellular compartments, proliferative or nonproliferative, depending on the presence or absence of mitotic activity. 12 Numerous cell-kinetic studies of hematopoietic systems and such epithelial tissues as intestinal epithelium, epidermis, and seminiferous epithelium indicate that the proliferative compartment includes stem cells and transient amplifying cells. 3 " 6 Stem cells are slow cycling and quiescent with a low mitotic activity in the normal steady state. However, they are long lived and can be activated by tissue demand for cellular regeneration. After a round of mitosis, stem cells give rise to transient amplifying cells, which are rapid cycling and can amplify cell mass effectively by limited rounds of mitosis. At a critical point, transient amplifying cells will cease mitosis and enter a nonproliferative compartment, committed to termi- From the Department of Ophthalmology, Bascom Palmer Eye Institute, University of Miami School of Medicine, Miami, Florida. Supported in part by U.S. Public Health Service Research Grant EY06819 (S.C.G.T.) and Core Grant EY02180, each awarded by the National Eye Institute, National Institutes of Health, Bethesda, Maryland. Presented in part at the annual meeting of the Association for Research in Vision and Ophthalmology, Sarasota, FL, May 1-6, Submitted for publication: January 11, 1990; accepted July 30, Reprint requests: Scheffer C. G. Tseng, MD, PhD, Bascom Palmer Eye Institute, P. O. Box , Miami, FL nal cellular differentiation. Therefore, in all self-renewing tissues, stem cells can be regarded as the origin of cell lineage and the ultimate source of cellular proliferation and differentiation. It is well known that corneal epithelium is well differentiated and has a rapid self-renewing capacity. Previous studies thought that the proliferative source of this tissue resided at the basal cell layer 7-8 or in the corneal periphery, based on the observation of centripetal cellular movement. 9 " 13 The exact location of the stem cells of corneal epithelium was unclear until Schermer et al. 14 showed the absence of a differentiation marker, a 64-kD corneal epithelial keratin, in the limbal basal cells, which suggested that limbal basal epithelium may contain the corneal stem cell. Additional evidence was provided by Ebato et al. 15 who showed that limbal epithelial cells grow better than peripheral or central corneal epithelia in explant cultures and by Cotsarelis et al. 16 who showed that limbal basal cells can be selectively stimulated by the topical application of a tumor promoter and by wounding the central corneal epithelium. Extrapolating from these data, we hypothesized that while the stem cells are in the limbus, the corneal basal epithelium contains the transient amplifying cells and that all the suprabasal cells of the cornea are postmitotic and committed to terminal differentiation. To examine this concept, we chose to compare the wound healing of central corneal epithelial defects when the limbal epithelium was either intact or removed.
2 No. 1 CORNEAL WOUND HEALING WITHOUT LIMDUS / Huong ond Tseng 97 Materials and Methods All animal experiments conducted in this study conformed to the ARVO Resolution on the Use of Animals in Research. Surgical Limbal Removal in Rabbits To ensure complete removal of the limbal epithelium, a ring lamellar dissection including 2 mm of peripheral cornea and 3 mm of perilimbal conjunctiva was done on one eye of 12 New Zealand albino rabbits. After marking with a trephine, a No. 69 Beaver blade (Boston, MA) was used to create a partial-thickness, circular corneal incision at the peripheral cornea, 2 mm within the limbus. Lamellar dissection toward the limbus was then done with a No. 66 Beaver blade. A 360 conjunctival peritomy was made 3 mm beyond the corneolimbal junction and dissected toward the limbus. The entire limbal zone was then excised with a pair of scissors in a ring. Topical gentamicin sulfate ointment was applied daily for 3 days. All rabbits were examined weekly and photographed monthly for evidence of corneal vascularization or recurrent epithelial erosion over 6 months. At the end of 6 months, one representative rabbit was killed, and the corneo-scleral button was removed for flat-mount preparation. Central Corneal Epithelial Wounding To investigate corneal epithelial wound healing in the absence of limbal epithelium, a central 7.5-mm corneal epithelial defect was created 6 months after limbal removal in the remaining 11 corneas of the experimental group and in another 11 control corneas with normal, intact limbus. After marking with a trephine into the superficial stroma, the central corneal epithelium was debrided with a surgical blade. The wounds were examined daily after 1% fluorescein staining. Three weeks after the first debridement, a second 7.5-mm central corneal wound was made in the same manner in both groups. Wound healing was again examined daily with fluorescein staining. Photographs were taken daily for the first 3 days, on day 7 of the first wounding, and on day 10 of the second wounding. Recurrent epithelial erosions were recorded if the previously healed area became enlarged or eroded based on serial fluorescein stainings. Studies of Wound Healing To examine the occurrence of corneal vascularization, external photographs taken before and after each of the two consecutive debridements were compared in both the experimental and control groups. To measure the healing rate, serial fluorescein external photographs of both groups were projected onto a screen at a fixed distance. The area of the subepithelial trephine mark and the area of epithelial defect outlined by the fluorescein staining were measured with a Zeiss Videoplan 2 image analyzer (Kontron, Eching, Germany). Using the 7.5-mm trephinemarked area as an internal standard, the area of epithelial defect was derived for each cornea. The data of each group were pooled and analyzed by paired student t-test and by Wilcoxon rank-sum test, with the assistance of William Feuer. To detect the emergence of conjunctival epithelial ingrowth on the corneas, corneal flat-mount preparations 17 and impression cytologies 18 were done as previously described. Flat-mount preparations were stained with periodic acid-schiff (PAS) to detect the presence of conjunctival goblet cells on the corneas. Impression cytology was stained with a combination of PAS and Papanicolaou staining to study the epithelial phenotype. Results After surgical removal of the limbal tissue, including 2 mm of the peripheral cornea and 3 mm of the perilimbal conjunctiva, the wounds of all 12 rabbit eyes healed in 3-5 days without any complications. To determine if the remaining central corneal epithelium would have any problem in maintaining the ocular surface integrity, these rabbits were followed for 6 months. During this time, no evidence of epithelial breakdowns such as erosions or epithelial defects was noted. At the end of 6 months, four of 12 (33%) corneas showed vascularization, one with dense pannus formation and three with mild peripheral vascularization. A flat mount of the corneoscleral button of one of the three rabbits with mild vascularization was prepared at the end of the 6-month follow-up period. The result revealed the emergence of goblet cells at the peripheral cornea (Fig. 1 A). In contrast, no goblet cells were found on the cornea of a normal control, which did not have surgical removal of the limbus (data not shown). To challenge the proliferative capacity of the residual corneal epithelium, two consecutive 7.5-mm central corneal epithelial defects were created in both the experimental and control groups (n = 11, each). After the first debridement, the pooled data of the residualdefect areas of the corneas with limbal removal was significantly larger than those of the control corneas with intact limbus (Fig. 2). This difference could be detected from days 2-7 after debridement (P < 0.05, Fig. 2). The healing rate derived from the linear re-
3 98 INVESTIGATIVE OPHTHALMOLOGY 6 VISUAL SCIENCE / Januory 1991 Vol. 32 I» - * X '/"? Fig. I. Rat preparation of the corneal button 6 months after limbal removal (a) showing migration of the goblet cells onto the peripheral cornea. Progressive migration of goblet cells onto the central cornea was noted 3 weeks after the second wounding (b). Arrows indicate the corneolimbal junction. gression of the kinetic curves shown in Figure 2 was 0.43 mm 2 /hr and 0.50 mm 2 /hr for the experimental and control corneas, respectively. As demonstrated in the serial photographs of one representative case of each group (Fig. 3), the normal control cornea healed uneventfully without any erosion in 7 days, but the experimental cornea with limbal removal showed delayed healing and corneal epithelial erosion. Recurrent epithelial erosion was noted in five of 11 (45%) experimental corneas but in none of the controls (P <0.1). Three weeks after the first wounding, a second 7.5- mm central epithelial debridement was done. The wound-healing rate was also noted to be significantly slower in the corneas with limbal removal compared with the control group from postoperative days 2-10 (P < 0.05, Fig. 4). The kinetic healing curve after the second wounding was biphasic, which differed from the linear healing pattern of the first wounding (Fig. 4). In the second wounding, the healing rate was rapid during the first 3 days in both the experimental and control groups but slowed thereafter in the experimental group. The healing rate of the first phase of the second wounding healed faster than that of the first wounding in both the experimental and control groups (Fig. 2 compared with Fig. 4). When the linear portion of the second wound healing curve (from days 0-3) was subjected to linear regression, the healing rate was calculated to be 0.60 mm 2 /hr and 0.79 mm 2 /hr for the experimental and control corneas, respectively (Fig. 4). The delayed healing noted in the second phase after day 3 in the experimental group could be attributed to the recurrent epithelial breakdowns that were frequently observed in the experi-
4 No. 1 CORNEAL WOUND HEALING WITHOUT LIMDUS / Huong ond Tseng 99 FIRST CENTRAL CORNEAL WOUNDING controls (Figs. 7A-B). However, goblet cells were found in a high number after the first (Fig. 7C) and the second wounding in corneas with limbal removal (Fig. 7E). Additionally, both goblet and nongoblet conjunctival epithelial cells were found on the central corneal area after the second wounding in these corneas (Figs. 7D,F). Discussion TIME (DAY) Fig. 2. Areas of remaining epithelial defect during 1 week of healing after the first 7.5 mm diameter circular wound of corneal epithelium in the experimental group with limbal removal ( ) and the normal control (O). The extension bar represents the standard error. P values were derived from the analysis by Wilcoxon Rank Sum Test. A significant delay of wound healing was noted in the experimental group from day 3 to day 7. mental corneas with limbal removal (Fig. 5). Delayed healing due to recurrent epithelial erosion was noted in ten (90%) of 11 experimental corneas compared with none in the controls (P < 0.01). As stated, peripheral vascularization was observed in four corneas (33%) 6 months after limbal removal (Figs. 6D,G,J). However, 1 week after the first central corneal epithelial wounding, the extent of vascularization progressed toward the central cornea (Figs. 6E,H,K) and advanced further 1 week after the second corneal debridement (Figs. 6F,I,L). Progression of corneal vascularization was noted in seven (64%) of 11 corneas with limbal removal after the first wounding and increased to eight (73%) after the second wounding. No vascularization was noted in the control corneas after either the first or second woundings (Figs. 6A-C). When the incidence of corneal vascularization in the experimental group was compared with that of the control, it was statistically significant for the first and second woundings (P < 0.05, respectively). To study if there was any progression of conjunctival epithelial ingrowth, both corneal flat-mount preparations and impression cytology were done. The flat-mount preparations of the experimental corneas obtained 2 weeks after the second corneal wounding showed that goblet cells had migrated onto the central cornea with an increasing density (Fig. 1B). Impression cytology taken from the limbal region confirmed that after the two consecutive woundings, no goblet cells migrated to the corneal surface of the normal The limbal location of corneal epithelial stem cells is a new concept. It implies that limbal basal epithelium serves as the ultimate source of cellular proliferation and differentiation by providing an unlimited supply of transient amplifying cells. Through a high, although limited, proliferative capacity of the transient amplifying cells, the demand for rapid self-renewal of the corneal epithelium can be achieved. Because of such a unique feature, the perilimbal zone also precludes the invasion of conjunctival epithelium onto the corneal surface under normal circumstances. A similar concept of growth pressure was first mentioned by Friedenwald. 19 When the limbal zone was surgically removed as shown in our study, the features of abnormal wound healing ensued and encompassed delayed healing with recurrent epithelial erosion, corneal vascularization, and conjunctival epithelial ingrowth. These results also substantiate the belief that the limbal epithelium is the location of the stem cells for corneal epithelial proliferation and differentiation, a concept first proposed by Schermer etal. 14 As we demonstrated, initial removal of the limbal stem cells does not lead to a notable difficulty in corneal epithelial wound healing. The remaining transient amplifying cells, presumably the corneal basal cells, were evidently still able to maintain the central corneal epithelial cell mass and integrity for at least 6 months. To explain the duration of time required for the corneal epithelium to show possible decompensation under such a circumstance, we refer to several previous investigations. 10 " 13 Centripetal cellular movement by the peripheral corneal epithelium is responsible for the healing of traumatic loss of central corneal epithelium, such as an epithelial defect. 7 " 9 However, even in a less traumatic situation, eg, penetrating keratoplasty or lamellar keratoplasty in which the central corneal epithelium is substituted by the donor tissue, the centripetal movement of the surrounding host epithelium to replace the donor derivatives is well documented by the elegant work of Kinoshita et al. 1 ' They observed a gradual dilution of sex chromatin on the female donor graft by the male recipient over 12 weeks. When their data are extrapolated to the end point of complete replacement, it is
5 Fig. 3. Comparison of external photographs of corneal epithelial wound healing with fluorescein staining after the first 7.5 mm central corneal wounding between one representative case of the control (left column) and of the experimental group (right column). Delayed healing was noted in the experimental group.
6 No. 1 CORNEAL WOUND HEALING WITHOUT LIMDUS / Huong ond Tseng 101 SECOND CENTRAL CORNEAL WOUNDING 3 4 TIME (DAY) Fig. 4. Areas of remaining epithelial defect after the second 7.5 mm diameter circular wounding of corneal epithelium in the experimental group with limbal removal ( ) and the normal control (O). The extension bar represents the standard error. P values were derived from the analysis by Wilcoxon Rank Sum Test. A significant delay of wound healing was noted in the experimental group from day 3 to day 7. interesting to note that the entire process might have taken about 1 yr. These data are also consistent with the clinical observations of centripetal migration of the epithelial dots in penetrating keratoplasty 10 and with the relatively low incidence of epithelial rejection compared with other types of graft rejection 1 yr after penetrating keratoplasty. 12 Even under normal atraumatic desquamation, Buck 13 also detected centripetal migration of superficial corneal epithelial cells in mice and measured a rate of 17 /xm per day. Variations among different species may exist. Nonetheless, when this migration rate (17 /um/day) is applied to the rabbit" and human 1012 conditions, the total replacement of a corneal epithelium with a diameter of mm is estimated at about 1 yr. Therefore, in the present experiment, we could expect that the epithelial breakdown might begin in 1 yr when the remaining proliferative reserves of the transient amplifying cells are exhausted and no such new cells have been generated by the limbal stem cells. The fact that the corneal flat mount prepared 6 months after limbal removal showed the emergence of conjunctival goblet cells at the peripheral cornea (Fig. 1A) further suggests a deficiency of limbal stem cells that might later lead to inadequate corneal epithelial regeneration. To substantiate that limbal basal epithelium, instead of peripheral corneal epithelium, contains the stem cell population and to distinguish the functional role between stem cells and transient amplifying cells in wound healing, we challenged the remaining cellular reserve by creating two consecutive 7.5-mm central epithelial debridements. With respect to the proliferative reserve, there was a statistically significant delay of wound healing and recurrent erosion in the experimental group compared with the normal controls (Figs. 2,4). This result indicates that the residual transient amplifying cells in the peripheral cornea were not sufficient to maintain the entire corneal epithelial cell mass. Since transient amplifying cells are known to have a high mitotic activity and a short cell cycle, their insufficiency to attain the proliferative goal can be explained by their shorter limited life span. We also observed that there was a statistically significant delay of wound healing and worsening of recurrent erosions when the second wounding was compared with the first. This suggests that there is further depletion of transient amplifying cells after the first wounding in the experimental group, which could not be replenished due to the removal of limbal stem cells. The fact that the normal controls could withstand two such consecutive epithelial debridements indicates that the proliferative source had not been violated. It is also interesting that the initial healing rate of the second wounding was faster than that of the first in both groups. This finding indicates that the residual proliferative cellular compartment had been activated by the first wounding and the newly (younger) regenerated cells are more readily responsive to the demand for cellular proliferation when the second wounding was induced. Similar findings have also been observed by Srinivasan et al. 20 when they measured the healing rate in rabbit corneas receiving repetitive corneal epithelial trauma. The fact that this initial rapid healing could only last for 3 days in the experimental group and was immediately followed by markedly delayed healing further supports the notion that the residual proliferative cells were indeed transient amplifying cells and not stem cells. With respect to the differentiative reserve, we also observed that limbal removal led to a significant increase of conjunctival epithelial ingrowth, which was characterized by the invasion of conjunctival goblet cells onto the central cornea (Figs. 1,7). The progressive centripetal ingrowth of conjunctival epithelium with goblet cells signifies the deranged junctional epithelial barriers between corneal and conjunctival epithelia. Under normal circumstances, such an epithelial barrier is presumably operated by the high mitotic activity of transient amplifying cells derived from limbal stem cells. Due to the limited life span of these cells, the growth pressure of the perilimbal zone will eventually rely on the limbal stem cells, which can continuously generate newer and more active proliferative transient amplifying cells. In the absence of
7 Fig. S. Comparison of external photographs of corneal epithelial wound healing withfluoresceinstaining after the second 7.5 mm central corneal wounding, between one representative case of the control (left column) and of the experimental group (right column). Delayed healing with recurrent epithelial breakdown was frequently noted in the experimental group. The latter can be illustrated by enlarged area of fluorescein staining in 10 d as compared to 3 d.
8 No. 1 CORNEAL WOUND HEALING WITHOUT LIMDUS / Huong and Tseng 103 Fig. 6. External photographs of one control normal cornea (upper panel), and three representative experimental corneas with limbal removal (bottom three panels). No vasculanzation was noted in the control cornea 1 week following the first (b) and second (c) wounding as compared to the preoperative state (a). Minimal vasculanzation indicated by arrows was noted in some experimental corneas (d, g, j) 6 months following the limbal removal, progression of the corneal vasculanzation towards the central cornea became apparent 1 week after the first wounding (middle panel, e, h, k) and 1 week after the second wounding (right panel, f, i, 1). limbal stem cells, the healing of the central corneal epithelial defect triggers the ingrowth of surrounding conjunctival epithelium. In this study, we observed corneal vasculanzation 6 months after limbal removal in four of 12 (33%) rabbits. After the first and second wounding, the incidence of vascularization increased to 64% and 73%, respectively, as did the severity. This result indicates that the deficiency or dysfunction of limbal stem cells would also lead to increasing corneal vascularization. It has long been recognized that corneal epithelial defects in the limbus invariably heal without any vascularization. But if the defects extend beyond the limbus, variable incidences, ranging from 14-65%, of
9 104 INVESTIGATIVE OPHTHALMOLOGY G VISUAL SCIENCE / January 1991 Vol. 32 I e Fig. 7. Impression cytology specimen from the peripheral corneal/limbal region (left column) and the central cornea (right column) of the normal control (a, b) and of the experimental corneas (c-f) following two woundings, The normal control did not show any goblet cell migration to either the peripheral (a) or central (b) cornea. In contrast, the centripetal migration of numerous goblet cells (GC), indicated by large open arrows, onto the peripheral and central corneas was noted in the experimental corneas following the first (c, d) and second (e, f) wounding. The solid arrows in (a), (c), and (c) indicate the anatomic function of cornea and limbus. corneal vascularization and conjunctival epithelial ingrowth have been reported " 24 Recently, we noted that the total removal of limbal and corneal epithelia resulted in a high (96%) incidence of corneal vascularization in 54 rabbit eyes. 25 Furthermore, conjunctival transplantation including the limbal epithelium, a procedure called limbal transplantation, could restore the corneal epithelial phenotype in the
10 No. 1 CORNEAL WOUND HEALING WITHOUT LIMBUS / Huong and Tseng 105 damaged corneal surface more effectively than conjunctival transplantation alone. 26 After limbal transplantation, the previously vascularized corneas showed a progressive decrease of vascularization, 26 a phenomenon also observed in human patients. 27 Taken together, these observations suggest that on the corneal surface, conjunctival epithelial ingrowth is accompanied by corneal vascularization. This concept is also supported in our recent study of partial limbal deficiency. 28 To explain this association, one can speculate that conjunctival epithelium may produce certain inflammatory or angiogenic mediator(s) that are essential to maintain its phenotypic expression. In summary, we showed that corneal epithelial wound healing was impaired in the absence of limbal stem cells. Total removal of limbal stem cells can lead to (1) delayed wound healing with recurrent epithelial breakdowns, (2) corneal vascularization, and (3) conjunctival epithelial ingrowth (conjunctivalization). This constellation of abnormal features can thus be regarded as typical signs of limbal stem cell deficiency (dysfunction). Similar findings have been observed clinically in such ocular surface disorders as chemical injuries, Stevens-Johnson syndrome, aniridia, and some contact lens-induced keratopathy. We speculated that dysfunction of the limbal stem cells might be the basis for these disorders. 29 Clinically, it is therefore important to recognize such a disease entity and its pathophysiology. Use of the unique property of limbal stem cells, eg, limbal transplantation, can enhance our ability to manage these disorders. Further exploration of the regulatory mechanism of the limbal stem cells will help our understanding of other ocular surface disorders that have various other manifestations of stem cell dysfunction. Key words: cornea, epithelium, limbus, stem cells, wound healing References 1. Cairnie AB, Lala PK, and Osmond DG, editors: Stem Cells of Renewing Cell Populations. New York, Academic Press, Leblond CP: The life history of cells in renewing systems. Am J Anat 160:114, Clausen OPF, Aarnaes E, Kirkhus B, Pedersen S, Thorud E, and Bolund L: Subpopulations of slowly cycling cells in S and G2 phase in mouse epidermis. Cell Tissue Kinet 17:351, Jensen PICA, Pedersen S, and Bolund L: Basal-cell subpopulations and cell-cycle kinetics in human epidermal explant cultures. Cell Tissue Kinet 18:201, Lajtha LG: Stem cell concepts. Differentiation 14:23, Potten CS: Epithelial proliferation subpopulations. In Stem Cells and Tissue Homeostasis, Lord BI, Potten CS, and Cole RJ, editors. New York, Cambridge University Press, 1978, pp Friedenwald JS and Buschke W: Some factors concerned in the mitotic and wound-healing activities of the corneal epithelium. Trans Am Ophthalmol Soc 42:371, Kuwabara T, Perkins DG, and Cogan DG: Sliding of the epithelium in experimental corneal wounds. Invest Ophthalmol 15:4, Buck RC: Cell migration in repair of mouse corneal epithelium. Invest Ophthalmol Vis Sci 18:767, Kaye DB: Epithelial response in penetrating keratoplasty. Am J Ophthalmol 89:381, Kinoshita S, Friend J, and Thoft RA: Sex chromatin of donor corneal epithelium in rabbits. Invest Ophthalmol Vis Sci 21:434, Alldredge OC and Kxachmer JH: Clinical types of corneal transplant rejection: Their manifestations, frequency, preoperative correlates, and treatment. Arch Ophthalmol 99:599, Buck RC: Measurement of centripetal migration of normal corneal epithelial cells in the mouse. Invest Ophthalmol Vis Sci 26:1296, Schermer A, Galvin S, and Sun T-T: Differentiation-related expression of a major 64K corneal keratin in vivo and in culture suggests limbal location of corneal epithelial stem cells. J Cell Biol 103:49, Ebato B, Friend J, and Thoft RA: Comparison of central and peripheral human corneal epithelium in tissue culture. Invest Ophthalmol Vis Sci 28:1450, Cotsarelis G, Cheng S-Z, Dong G, Sun T-T, and Lavker RM: Existence of slow-cycling limbal epithelial basal cells that can be preferentially stimulated to proliferate: Implications on epithelial stem cells. Cell 57:201, Tseng SCG, Hirst LW, Farazdaghi M, and Green WR: Goblet cell density and vascularization during conjunctival transdifferentiation. Invest Ophthalmol Vis Sci 25:1168, Tseng SCG: Staging of conjunctival squamous metaplasia by impression cytology. Ophthalmology 92:728, Friedenwald JS: Growth pressure and metaplasia of conjunctival and corneal epithelium. Doc Ophthalmol 5-6:184, Srinivasan BD and Eakins ICE: The reepithelialization of rabbit cornea following single and multiple denudation. Exp Eye Res 29:595, Shapiro MS, Friend J, and Thoft RA: Corneal re-epithelialization from the conjunctiva. Invest Ophthalmol Vis Sci 21:135, Kinoshita S, Friend J, and Thoft RA: Biphasic cell proliferation in transdifferentiation of conjunctival to corneal epithelium in rabbits. Invest Ophthalmol Vis Sci 24:1008, Tseng SCG, Farazdaghi M, and Ryder AA: Conjunctival transdifferentiation induced by systemic vitamin A deficiency in vascularized rabbit corneas. Invest Ophthalmol Vis Sci 28:1497, Huang AJW, Watson BD, Hernandez E, and Tseng SCG: Induction of conjunctival transdifferentiation on vascularized corneas by photothrombotic occlusion of corneal neovascularization. Ophthalmology 95:228, Kruse FE, Chen JJY, Tsai RJF, and Tseng SCG: Conjunctival transdifferentiation is due to incomplete removal of limbal basal epithelium. Invest Ophthalmol Vis Sci 31:1903, Tsai RJF, Sun T-T, and Tseng SCG: Comparison of limbal and conjunctival autograft transplantation in corneal surface reconstruction in rabbits. Ophthalmology 97:446, Kenyon KR and Tseng SCG: Limbal autograft transplantation for ocular surface disorders. Ophthalmology 96:709, Chen JJY and Tseng SCG: Corneal epithelial wound healing in partial limbal deficiency. Invest Ophthalmol Vis Sci 31:107, Tseng SCG: Concept and application of limbal stem cells. Eye 3:141, 1989.
Change of Paracellular Permeability of Ocular Surface Epithelium by Vitamin A Deficiency
 Investigative Ophthalmology & Visual Science, Vol. 32, No. 3, March 1991 Copyright Association for Research in Vision and Ophthalmology Change of Paracellular Permeability of Ocular Surface Epithelium
Investigative Ophthalmology & Visual Science, Vol. 32, No. 3, March 1991 Copyright Association for Research in Vision and Ophthalmology Change of Paracellular Permeability of Ocular Surface Epithelium
LIMBAL TRANSPLANTATION IN THE MANAGEMENT OF CHRONIC CONTACT-LENS-ASSOCIATED EPITHELIOPATHY
 LIMBAL TRANSPLANTATION IN THE MANAGEMENT OF CHRONIC CONTACT-LENS-ASSOCIATED EPITHELIOPATHY CHRISTOPHER JENKINS, STEPHEN TUFT, CHRISTOPHER LIU and ROGER BUCKLEY London SUMMARY We describe the clinical management
LIMBAL TRANSPLANTATION IN THE MANAGEMENT OF CHRONIC CONTACT-LENS-ASSOCIATED EPITHELIOPATHY CHRISTOPHER JENKINS, STEPHEN TUFT, CHRISTOPHER LIU and ROGER BUCKLEY London SUMMARY We describe the clinical management
STEM CELLS AND CORNEAL EPITHELIAL REGENERATION
 STEM CELLS AND CORNEAL EPITHELIAL REGENERATION FRIEDRICH E. KRUSE Heidelberg, Germany SUMMARY Self-renewing tissues such as the corneal epithelium contain stem cells which represent the proliferative reserve.
STEM CELLS AND CORNEAL EPITHELIAL REGENERATION FRIEDRICH E. KRUSE Heidelberg, Germany SUMMARY Self-renewing tissues such as the corneal epithelium contain stem cells which represent the proliferative reserve.
Ocular Surface Reconstruction
 OCULAR SURFACE From Tissue Transplantation to Cell Therapy Abraham Solomon, MD Abstract: The most difficult part in ocular surface reconstruction for total limbal stem cell deficiency is restoring a healthy
OCULAR SURFACE From Tissue Transplantation to Cell Therapy Abraham Solomon, MD Abstract: The most difficult part in ocular surface reconstruction for total limbal stem cell deficiency is restoring a healthy
Regional Heterogeneity in Human Corneal and Limbal Epithelia: An Innmunohistochemical Evaluation
 Investigative Ophthalmology & Visual Science, Vol. 32, No. 3, March 1991 Copyright Association for Research in Vision and Ophthalmology Regional Heterogeneity in Human Corneal and Limbal Epithelia: An
Investigative Ophthalmology & Visual Science, Vol. 32, No. 3, March 1991 Copyright Association for Research in Vision and Ophthalmology Regional Heterogeneity in Human Corneal and Limbal Epithelia: An
Mucocutaneous Junction As the Major Source of Replacement Palpebral Conjunctival Epithelial Cells
 Mucocutaneous Junction As the Major Source of Replacement Palpebral Conjunctival Epithelial Cells Jonathan D. Wirtschafter, 1,2,3 Jeffrey M. Ketcham, 1 Robert J. Weinstock, 1 Tara Tabesh, 1 and Linda K.
Mucocutaneous Junction As the Major Source of Replacement Palpebral Conjunctival Epithelial Cells Jonathan D. Wirtschafter, 1,2,3 Jeffrey M. Ketcham, 1 Robert J. Weinstock, 1 Tara Tabesh, 1 and Linda K.
Original Research Article
 STUDY OF EPITHELIAL PHENOTYPE AFTER PTERYGIUM EXCISION BY USING CONJUNCTIVAL IMPRESSION CYTOLOGY. Dr. Sachin O. Agrawal*, Dr. Sudhir Pendke, Dr. Ravi Chauhan Department of Ophthalmology, Indira Gandhi
STUDY OF EPITHELIAL PHENOTYPE AFTER PTERYGIUM EXCISION BY USING CONJUNCTIVAL IMPRESSION CYTOLOGY. Dr. Sachin O. Agrawal*, Dr. Sudhir Pendke, Dr. Ravi Chauhan Department of Ophthalmology, Indira Gandhi
TISSUE-SPECIFIC PROGENITOR AND STEM CELLS
 SM TISSUE-SPECIFIC PROGENITOR AND STEM CELLS Concise Review: Limbal Stem Cell Deficiency, Dysfunction, and Distress SAJJAD AHMAD Key Words. Cornea Corneal epithelium Limbal stem cell Limbal stem cell deficiency
SM TISSUE-SPECIFIC PROGENITOR AND STEM CELLS Concise Review: Limbal Stem Cell Deficiency, Dysfunction, and Distress SAJJAD AHMAD Key Words. Cornea Corneal epithelium Limbal stem cell Limbal stem cell deficiency
Ocular Surface Stem Cells and Disease: Current Concepts and Clinical Applications
 576 Review Article Ocular Surface Stem Cells and Disease: Current Concepts and Clinical Applications LPK Ang, 1,2,3 FRCS (Edin), MRCOphth, M Med (Ophth), DTH Tan, 1,2,3 FRCS (Glas), FRCOphth, FAMS Abstract
576 Review Article Ocular Surface Stem Cells and Disease: Current Concepts and Clinical Applications LPK Ang, 1,2,3 FRCS (Edin), MRCOphth, M Med (Ophth), DTH Tan, 1,2,3 FRCS (Glas), FRCOphth, FAMS Abstract
PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL
 PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL Endothelial keratoplasty (EK) has evolved at a brisk pace and the volume of data accumulated over the past 10 years has demonstrated that
PRE-DESCEMET S ENDOTHELIAL KERATOPLASTY (PDEK) DR ASHVIN AGARWAL Endothelial keratoplasty (EK) has evolved at a brisk pace and the volume of data accumulated over the past 10 years has demonstrated that
Existence of Slow-Cycling Limbal Epithelial Basal Cells That Can Be Preferentially Stimulated to Proliferate: Implications on Epithelial Stem Cells
 Cell, Vol. 57, 201-209. April 21, 1989, Copyright 0 1989 by Cell Press Existence of Slow-Cycling Limbal Epithelial Basal Cells That Can Be Preferentially Stimulated to Proliferate: Implications on Epithelial
Cell, Vol. 57, 201-209. April 21, 1989, Copyright 0 1989 by Cell Press Existence of Slow-Cycling Limbal Epithelial Basal Cells That Can Be Preferentially Stimulated to Proliferate: Implications on Epithelial
T he normal ocular surface is covered with highly
 1280 EXTENDED REPORT Transplantation of cultivated autologous oral mucosal epithelial cells in patients with severe ocular surface disorders T Nakamura, T Inatomi, C Sotozono, T Amemiya, N Kanamura, S
1280 EXTENDED REPORT Transplantation of cultivated autologous oral mucosal epithelial cells in patients with severe ocular surface disorders T Nakamura, T Inatomi, C Sotozono, T Amemiya, N Kanamura, S
Keratin-like Proteins in Corneal and Conjunctival Epithelium are Different
 Keratin-like Proteins in Corneal and Conjunctival Epithelium are Different Shigeru Kinoshiro,* Judith Friend, Timothy C. Kiorpes, and Richard A. Thoft Using SDS polyacrylamide slab-gel electrophoresis,
Keratin-like Proteins in Corneal and Conjunctival Epithelium are Different Shigeru Kinoshiro,* Judith Friend, Timothy C. Kiorpes, and Richard A. Thoft Using SDS polyacrylamide slab-gel electrophoresis,
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 340 J UNE 3, 1999 NUMBER TREATMENT OF SEVERE OCULAR-SURFACE DISORDERS WITH CORNEAL EPITHELIAL STEM-CELL
The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 340 J UNE 3, 1999 NUMBER TREATMENT OF SEVERE OCULAR-SURFACE DISORDERS WITH CORNEAL EPITHELIAL STEM-CELL
Rabbit Conjunctival and Corneal Epithelial Cells Belong to Two Separate Lineages
 Rabbit Conjunctival and Corneal Epithelial Cells Belong to Two Separate Lineages Zhi-Gang Wei,* Tung-Tien Sun,-\ and Robert M. Lavker* Purpose. This study investigated rabbit conjunctival and corneal epithelial
Rabbit Conjunctival and Corneal Epithelial Cells Belong to Two Separate Lineages Zhi-Gang Wei,* Tung-Tien Sun,-\ and Robert M. Lavker* Purpose. This study investigated rabbit conjunctival and corneal epithelial
The recurrence of pterygium after different modalities of surgical treatment
 Saudi Journal of Ophthalmology (2011) 25, 411 415 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE The recurrence of
Saudi Journal of Ophthalmology (2011) 25, 411 415 King Saud University Saudi Journal of Ophthalmology www.saudiophthaljournal.com www.ksu.edu.sa www.sciencedirect.com ORIGINAL ARTICLE The recurrence of
OPTOMETRY. Corneal conjunctivalisation in long-standing contact lens wearers
 C L I N I C A L A N D E X P E R I M E N T A L OPTOMETRY Corneal conjunctivalisation in long-standing contact lens wearers Clin Exp Optom 2007; 90: 1: 26 30 Raul Martin OD IOBA Eye Institute, School of
C L I N I C A L A N D E X P E R I M E N T A L OPTOMETRY Corneal conjunctivalisation in long-standing contact lens wearers Clin Exp Optom 2007; 90: 1: 26 30 Raul Martin OD IOBA Eye Institute, School of
Corneal blood staining after hyphaema
 Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Fate of Corneal Epithelial Cells Separated from Limbus In Vivo METHODS
 Cornea Fate of Corneal Epithelial Cells Separated from Limbus In Vivo Tetsuya Kawakita, 1,2,3 Kazunari Higa, 1,2,3 Shigeto Shimmura, 1,2 Machiko Tomita, 1 Kazuo Tsubota, 1,2 and Jun Shimazaki 1,2 PURPOSE.
Cornea Fate of Corneal Epithelial Cells Separated from Limbus In Vivo Tetsuya Kawakita, 1,2,3 Kazunari Higa, 1,2,3 Shigeto Shimmura, 1,2 Machiko Tomita, 1 Kazuo Tsubota, 1,2 and Jun Shimazaki 1,2 PURPOSE.
Various therapies for ocular surface diseases
 Romanian Journal of Ophthalmology, Volume 62, Issue 1, January-March 2018. pp:83-87 CASE REPORT Various therapies for ocular surface diseases Gheorghe Alina*, Rosoga Ancuţa Teodora**, Mrini Fildys*, Vărgău
Romanian Journal of Ophthalmology, Volume 62, Issue 1, January-March 2018. pp:83-87 CASE REPORT Various therapies for ocular surface diseases Gheorghe Alina*, Rosoga Ancuţa Teodora**, Mrini Fildys*, Vărgău
PATIENT INFORMATION ON CORNEAL GRAFT
 PATIENT INFORMATION ON CORNEAL GRAFT (TRANSPLANT) SURGERY M ANANDAN What is the cornea? The clear window of the eye approximately 0.5mm thick and 12mm across. It lies in front of the fluid filled anterior
PATIENT INFORMATION ON CORNEAL GRAFT (TRANSPLANT) SURGERY M ANANDAN What is the cornea? The clear window of the eye approximately 0.5mm thick and 12mm across. It lies in front of the fluid filled anterior
Paracellular Permeability of Corneal and Conjunctiva! Epithelia
 Investigative Ophthalmology & Visual Science, Vol. 30, No. 4, April 1989 Copyright Association for Research in Vision and Ophthalmology Paracellular Permeability of Corneal and Conjunctiva! Epithelia Andrew
Investigative Ophthalmology & Visual Science, Vol. 30, No. 4, April 1989 Copyright Association for Research in Vision and Ophthalmology Paracellular Permeability of Corneal and Conjunctiva! Epithelia Andrew
Subject Index. Atopic keratoconjunctivitis (AKC) management 16 overview 15
 Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Observation of corneal transplantation in peripheral corneal disease postoperatively
 EXPERIMENTAL AND THERAPEUTIC MEDICINE Observation of corneal transplantation in peripheral corneal disease postoperatively YIBING ZHANG 1, YUAN HU 2, XIAODONG LI 3, XIAORU SHI 1, FEIHONG XU 2 and HUI JIA
EXPERIMENTAL AND THERAPEUTIC MEDICINE Observation of corneal transplantation in peripheral corneal disease postoperatively YIBING ZHANG 1, YUAN HU 2, XIAODONG LI 3, XIAORU SHI 1, FEIHONG XU 2 and HUI JIA
FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM
 FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM ΙΟΑΝΝΙS Α. MALLIAS, MD, PHD Director of the Dept. of Ophthalmology, Mediterraneo Hospital, Glyfada, Athens, Greece Clinical Fellow in Cornea and
FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM ΙΟΑΝΝΙS Α. MALLIAS, MD, PHD Director of the Dept. of Ophthalmology, Mediterraneo Hospital, Glyfada, Athens, Greece Clinical Fellow in Cornea and
Sclerokeratoplasty David S. Chu, M.D. Cases
 Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Relationship between limbal incisions. angle. and the structures of the anterior chamber
 Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
Table 1. Characteristics of patients. Postoperative Comorbidity acuity band keratopathy. Visual Cause of. Case Age (Yr) Sex F/U (Month)
 착색양막을이용한띠각막병증의미용적치료 1459 Table 1. Characteristics of patients Case Age (Yr) Sex F/U (Month) Visual Cause of Postoperative Comorbidity acuity band keratopathy complications 1 19 M 13 NLP * PHPV Injection,
착색양막을이용한띠각막병증의미용적치료 1459 Table 1. Characteristics of patients Case Age (Yr) Sex F/U (Month) Visual Cause of Postoperative Comorbidity acuity band keratopathy complications 1 19 M 13 NLP * PHPV Injection,
Dystrophies. Molecular Causes. Anterior Membrane Dystrophies (epithelium, basement membrane and Bowman s layer)
 Dystrophies Characteristics of corneal dystrophies About half the members of appropriate age to have the dystrophy( usually autosomal dominant): inherited Usually seen in the first or second decade of
Dystrophies Characteristics of corneal dystrophies About half the members of appropriate age to have the dystrophy( usually autosomal dominant): inherited Usually seen in the first or second decade of
Human lamellar tendon graft in corneal surgery
 Human lamellar tendon graft in corneal surgery Armando Signorelli, Jr, MD, Carlos Roberto Signorelli, MD, Ernest Rifgatovich Muldashev, MD Refractive and Corneal surgery - 1993 - V.9(2) - P. 135-139 ABSTRACT
Human lamellar tendon graft in corneal surgery Armando Signorelli, Jr, MD, Carlos Roberto Signorelli, MD, Ernest Rifgatovich Muldashev, MD Refractive and Corneal surgery - 1993 - V.9(2) - P. 135-139 ABSTRACT
Limbal-Conjunctival Autograft Transplantation for the Management of Primary Pterygium
 Limbal-Conjunctival Autograft Transplantation for the Management of Primary Pterygium Mahmoud Jabbarvand, MD, 1 Mohammad-Reza Khalili, MD 2 Mohammad-Taher Rajabi, MD 3 Abstract Purpose: To investigate
Limbal-Conjunctival Autograft Transplantation for the Management of Primary Pterygium Mahmoud Jabbarvand, MD, 1 Mohammad-Reza Khalili, MD 2 Mohammad-Taher Rajabi, MD 3 Abstract Purpose: To investigate
Corneal Epithelial Cell Movement in Humans
 Eye (1989) 3, 438-445 Corneal Epithelial Cell Movement in Humans M. A. LEMP and W. D. MATHERS Washington, DC Summary Evidence is presented which supports the centripetal movement of epithelial cells in
Eye (1989) 3, 438-445 Corneal Epithelial Cell Movement in Humans M. A. LEMP and W. D. MATHERS Washington, DC Summary Evidence is presented which supports the centripetal movement of epithelial cells in
INTRA-CORNEAL LAMELLAR KERATOPLASTY*
 Brit. J. Ophthal. (1960) 44, 629. INTRA-CORNEAL LAMELLAR KERATOPLASTY* BY TADEUSZ KRWAWICZ Ophthalmological Clinic, Medical Academy, Lublin, Poland THE operative technique of lamellar keratoplasty is still
Brit. J. Ophthal. (1960) 44, 629. INTRA-CORNEAL LAMELLAR KERATOPLASTY* BY TADEUSZ KRWAWICZ Ophthalmological Clinic, Medical Academy, Lublin, Poland THE operative technique of lamellar keratoplasty is still
JMSCR Volume 03 Issue 01 Page January 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pterygium Excision and Conjunctival Autograft A Study Authors Dr. M. Premanandam 1, Dr. A. Geetha 2, Dr. Himabindu 3 1 MS, Associate Professor,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pterygium Excision and Conjunctival Autograft A Study Authors Dr. M. Premanandam 1, Dr. A. Geetha 2, Dr. Himabindu 3 1 MS, Associate Professor,
D JO. Conjunctivolimbal Autograft versus Cadaveric Keratolimbal Allograft in Ocular Surface Disorder: A Comparison
 20 Conjunctivolimbal Autograft versus Cadaveric Keratolimbal Allograft in Ocular Surface Disorder: A Comparison Jaya Kaushik 1-2, Jitendra Kumar Singh Parihar 1, Vaibhav Kumar Jain 3, Vijay Mathur 1 1
20 Conjunctivolimbal Autograft versus Cadaveric Keratolimbal Allograft in Ocular Surface Disorder: A Comparison Jaya Kaushik 1-2, Jitendra Kumar Singh Parihar 1, Vaibhav Kumar Jain 3, Vijay Mathur 1 1
Transplantation of Human Limbal Epithelium Cultivated on Amniotic Membrane for the Treatment of Severe Ocular Surface Disorders
 Transplantation of Human Limbal Epithelium Cultivated on Amniotic Membrane for the Treatment of Severe Ocular Surface Disorders Jun Shimazaki, MD, Masayo Aiba, BS, Eiki Goto, MD, Naoko Kato, MD, Shigeto
Transplantation of Human Limbal Epithelium Cultivated on Amniotic Membrane for the Treatment of Severe Ocular Surface Disorders Jun Shimazaki, MD, Masayo Aiba, BS, Eiki Goto, MD, Naoko Kato, MD, Shigeto
Deep Anterior Lamellar Keratoplasty - Techniques
 Deep Anterior Lamellar Keratoplasty - Techniques SHERAZ DAYA MD FACP FACS FRCS(Ed) FRCOphth Financial Disclosure Company Code 1. Abbott Medical Optics Inc. S 2. Bausch + Lomb C,L 3. Carl Zeiss Meditec
Deep Anterior Lamellar Keratoplasty - Techniques SHERAZ DAYA MD FACP FACS FRCS(Ed) FRCOphth Financial Disclosure Company Code 1. Abbott Medical Optics Inc. S 2. Bausch + Lomb C,L 3. Carl Zeiss Meditec
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endothelial_keratoplasty 9/2009 6/2018 6/2019 6/2018 Description of Procedure or Service Endothelial keratoplasty
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endothelial_keratoplasty 9/2009 6/2018 6/2019 6/2018 Description of Procedure or Service Endothelial keratoplasty
Corneal epithelial wound healing
 BritishJournal ofophthalmology 1994; 78: 401-408 401 PERSPECTIVE Corneal epithelial wound healing H S Dua, J A P Gomes, A Singh The corneal surface is, without question, the most specialised 123 mm2* of
BritishJournal ofophthalmology 1994; 78: 401-408 401 PERSPECTIVE Corneal epithelial wound healing H S Dua, J A P Gomes, A Singh The corneal surface is, without question, the most specialised 123 mm2* of
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique
 Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
A new classification of ocular surface burns
 Br J Ophthalmol 2001;85:1379 1383 1379 PERSPECTIVE A new classification of ocular surface burns Harminder S Dua, Anthony J King, Annie Joseph Ocular burns constitute true ocular emergencies and both thermal
Br J Ophthalmol 2001;85:1379 1383 1379 PERSPECTIVE A new classification of ocular surface burns Harminder S Dua, Anthony J King, Annie Joseph Ocular burns constitute true ocular emergencies and both thermal
Amniotic Membrane Transplantation In Ocular Surface Disorders
 Orginal Article Amniotic Membrane Transplantation In Ocular Surface Disorders Khalid Iqbal Talpur, Faiz Muhammad Halepota, Muhammad Pak J Ophthalmol 2005, Vol. 22 No. 3.................................................................................................
Orginal Article Amniotic Membrane Transplantation In Ocular Surface Disorders Khalid Iqbal Talpur, Faiz Muhammad Halepota, Muhammad Pak J Ophthalmol 2005, Vol. 22 No. 3.................................................................................................
Novel therapies for the treatment of persistent corneal epithelial defects
 Novel therapies for the treatment of persistent corneal epithelial defects Disclosures I have no financial interests in any of the techniques or products discussed. Bennie H. Jeng, M.D. Associate Professor
Novel therapies for the treatment of persistent corneal epithelial defects Disclosures I have no financial interests in any of the techniques or products discussed. Bennie H. Jeng, M.D. Associate Professor
Long-term results of autologous cultivated oral mucosal epithelial transplantation in the scar phase of severe ocular surface disorders
 1 Department of Ophthalmology, Kyoto Prefectural University of Medicine, Graduate School of Medicine, Kyoto, Japan 2 Research Center for Inflammation and Regenerative Medicine, Doshisha University, Kyoto,
1 Department of Ophthalmology, Kyoto Prefectural University of Medicine, Graduate School of Medicine, Kyoto, Japan 2 Research Center for Inflammation and Regenerative Medicine, Doshisha University, Kyoto,
Lamellar Keratoplasty for the Treatment of Fungal Keratitis
 Cornea 21(1): 33 37, 2002. 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Lamellar Keratoplasty for the Treatment of Fungal Keratitis Lixin Xie, M.D., Weiyun Shi, M.D., Zhaosheng Liu, M.D., and
Cornea 21(1): 33 37, 2002. 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Lamellar Keratoplasty for the Treatment of Fungal Keratitis Lixin Xie, M.D., Weiyun Shi, M.D., Zhaosheng Liu, M.D., and
The epidermis of the skin contains a subpopulation of basal
 Propagation and Phenotypic Preservation of Rabbit Limbal Epithelial Cells on Amniotic Membrane Der-Yuan Wang, 1,2 Yi-Jen Hsueh, 1 Vivian C. Yang, 3 and Jan-Kan Chen 1 PURPOSE. To describe the phenotypic
Propagation and Phenotypic Preservation of Rabbit Limbal Epithelial Cells on Amniotic Membrane Der-Yuan Wang, 1,2 Yi-Jen Hsueh, 1 Vivian C. Yang, 3 and Jan-Kan Chen 1 PURPOSE. To describe the phenotypic
Introduction. Donor tissue preparation for Descemet Membrane Endothelial ASCRS Aim of dissection. DMEK graft preparation
 Introduction Donor tissue preparation for Descemet Membrane Endothelial keratoplasty (DMEK) ASCRS - 2015 Endothelial Keratoplasty DSAEK / DSEK DMEK Donor lamellae stroma + DM + endothelium DM + endothelium
Introduction Donor tissue preparation for Descemet Membrane Endothelial keratoplasty (DMEK) ASCRS - 2015 Endothelial Keratoplasty DSAEK / DSEK DMEK Donor lamellae stroma + DM + endothelium DM + endothelium
Medical Affairs Policy
 Medical Affairs Policy Service: Corneal Treatments and Specialized Contact Lenses (Corneal remodeling, Corneal transplant, Corneal collagen crosslinking, Intrastromal Rings- INTACS, Keratoconus treatments,
Medical Affairs Policy Service: Corneal Treatments and Specialized Contact Lenses (Corneal remodeling, Corneal transplant, Corneal collagen crosslinking, Intrastromal Rings- INTACS, Keratoconus treatments,
Mooren s ulcer in China: a study of clinical characteristics and treatment
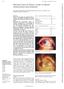 1244 Zhongshan Ophthalmic Center, Sun Yat-sen University of Medical Sciences, Guangzhou, PR China J Chen H Xie Z Wang B Yang Z Liu L Chen X Gong Y Lin Correspondence to: Dr Jiaqi Chen, Zhongshan Ophthalmic
1244 Zhongshan Ophthalmic Center, Sun Yat-sen University of Medical Sciences, Guangzhou, PR China J Chen H Xie Z Wang B Yang Z Liu L Chen X Gong Y Lin Correspondence to: Dr Jiaqi Chen, Zhongshan Ophthalmic
Corneal Re-epithelialization in Galactosemic Rats
 Corneal Re-epithelialization in Galactosemic Rats Manuel B. Doriles, Perer F. Kador, Henry N. Fukui, Tian-Sheng Hu, and Jin H. Kinoshiro Abnormalities in corneal epithelial healing in diabetic patients
Corneal Re-epithelialization in Galactosemic Rats Manuel B. Doriles, Perer F. Kador, Henry N. Fukui, Tian-Sheng Hu, and Jin H. Kinoshiro Abnormalities in corneal epithelial healing in diabetic patients
NEW OPPORTUNITIES OF USING THERAPEUTICAL CONTACT LENSES IN OCULAR SURGERY
 NEW OPPORTUNITIES OF USING THERAPEUTICAL CONTACT LENSES IN OCULAR SURGERY Authors: Prof univ. dr. Adriana Stănilă, Dr. Elena Mihai, Dr. Adrian Teodoru, Dr. IonuŃ Costache The Clinical Department of Op
NEW OPPORTUNITIES OF USING THERAPEUTICAL CONTACT LENSES IN OCULAR SURGERY Authors: Prof univ. dr. Adriana Stănilă, Dr. Elena Mihai, Dr. Adrian Teodoru, Dr. IonuŃ Costache The Clinical Department of Op
INDOLENT ULCER IN BOXER. Dr n. wet. Przemysław K. Bryla Przychodnia weterynaryjna w Warszawie INTRODUCTION
 Dr n. wet. Przemysław K. Bryla Przychodnia weterynaryjna w Warszawie brylapik@wp.pl SUMMARY A case of indolent ulcer in a Boxer is described. An indolent ulcer is a ulcer which fails to heal in the expected
Dr n. wet. Przemysław K. Bryla Przychodnia weterynaryjna w Warszawie brylapik@wp.pl SUMMARY A case of indolent ulcer in a Boxer is described. An indolent ulcer is a ulcer which fails to heal in the expected
Genetic susceptibility for Stevens-Johnson syndrome/toxic epidermal necrolysis with mucosal involvements
 249 Special Issue: Inflammation in Ophthalmology Review Article Genetic susceptibility for Stevens-Johnson syndrome/toxic epidermal necrolysis with mucosal involvements 1, 2, ) Mayumi Ueta 1) Department
249 Special Issue: Inflammation in Ophthalmology Review Article Genetic susceptibility for Stevens-Johnson syndrome/toxic epidermal necrolysis with mucosal involvements 1, 2, ) Mayumi Ueta 1) Department
Medicine HUMAN AMNIOTIC MEMBRANE FOR ACUTE SEVERE ALKALI BURN % VISUAL ACUITY RECOVERY
 Research and Science Today No. 2(10)/2015 Medicine HUMAN AMNIOTIC MEMBRANE FOR ACUTE SEVERE ALKALI BURN - 100 % VISUAL ACUITY RECOVERY Alina GHEORGHE * Monica Daniela POP 1 Calin- Petru TATARU 2 Constantin
Research and Science Today No. 2(10)/2015 Medicine HUMAN AMNIOTIC MEMBRANE FOR ACUTE SEVERE ALKALI BURN - 100 % VISUAL ACUITY RECOVERY Alina GHEORGHE * Monica Daniela POP 1 Calin- Petru TATARU 2 Constantin
Edinburgh Research Explorer
 Edinburgh Research Explorer Stem cells and corneal epithelial maintenance Citation for published version: Mort, RL, Douvaras, P, Morley, SD, Dorà, N, Hill, RE, Collinson, JM & West, JD 2012, 'Stem cells
Edinburgh Research Explorer Stem cells and corneal epithelial maintenance Citation for published version: Mort, RL, Douvaras, P, Morley, SD, Dorà, N, Hill, RE, Collinson, JM & West, JD 2012, 'Stem cells
Ascorbic acid prevents corneal ulceration and perforation following experimental alkali burns
 1 Ascorbic acid prevents corneal ulceration and perforation following experimental alkali burns Richard A. Levinson, Christopher A. Paterson, and Roswell R. Pfister* Depressed aqueous humor glucose and
1 Ascorbic acid prevents corneal ulceration and perforation following experimental alkali burns Richard A. Levinson, Christopher A. Paterson, and Roswell R. Pfister* Depressed aqueous humor glucose and
A Case Report of Recurrent Conjunctival Squamous Cell Carcinoma M Zhao 1, W Lin 2 *, Z Liu 2 ABSTRACT
 A Case Report of Recurrent Conjunctival Squamous Cell Carcinoma M Zhao 1, W Lin 2 *, Z Liu 2 ABSTRACT A case of recurrent squamous cell carcinoma of the conjunctiva is presented here. A 13-yearsold male
A Case Report of Recurrent Conjunctival Squamous Cell Carcinoma M Zhao 1, W Lin 2 *, Z Liu 2 ABSTRACT A case of recurrent squamous cell carcinoma of the conjunctiva is presented here. A 13-yearsold male
Ocular Surface Management in Corneal Transplantation, a Review
 CLINICAL INVESTIGATIONS Ocular Surface Management in Corneal Transplantation, a Review Kazuo Tsubota* *Departments of Ophthalmology, Tokyo Dental College, Chiba, and Keio University School of Medicine,
CLINICAL INVESTIGATIONS Ocular Surface Management in Corneal Transplantation, a Review Kazuo Tsubota* *Departments of Ophthalmology, Tokyo Dental College, Chiba, and Keio University School of Medicine,
Ocular Resurfacing and Alloepithelial Rejection in a Murine Keratoepithelioplasty Model
 Ocular Resurfacing and Alloepithelial Rejection in a Murine Keratoepithelioplasty Model Yu-Feng Yao,* Yoshitsugu Inoue,* Dai Miyazaki,* Yoshikazu Shimomura,* Yuichi Ohashi,^ and Yasuo Tano* Purpose. To
Ocular Resurfacing and Alloepithelial Rejection in a Murine Keratoepithelioplasty Model Yu-Feng Yao,* Yoshitsugu Inoue,* Dai Miyazaki,* Yoshikazu Shimomura,* Yuichi Ohashi,^ and Yasuo Tano* Purpose. To
SCLERAL CONTACT LENSES 1. EPSILON SCLERAL
 SCLERAL CONTACT LENSES 1. EPSILON SCLERAL - Out stands due to multi aspheric variable eccentricity design - Fitted in two steps due to it s novel philosophy and diagnostic set - Reassures limbal stem cells
SCLERAL CONTACT LENSES 1. EPSILON SCLERAL - Out stands due to multi aspheric variable eccentricity design - Fitted in two steps due to it s novel philosophy and diagnostic set - Reassures limbal stem cells
Amniotic membrane transplantation for partial limbal stem cell deficiency
 Br J Ophthalmol 2001;85:567 575 567 ORIGINAL ARTICLES Clinical science Amniotic membrane transplantation for partial limbal stem cell deficiency David F Anderson, Pierre Ellies, Renato T F Pires, ScheVer
Br J Ophthalmol 2001;85:567 575 567 ORIGINAL ARTICLES Clinical science Amniotic membrane transplantation for partial limbal stem cell deficiency David F Anderson, Pierre Ellies, Renato T F Pires, ScheVer
Fitting Keratoconus and Other Complicated Corneas
 Fitting Keratoconus and Other Complicated Corneas Christine W Sindt OD FAAO Professor, Clinical Ophthalmology Director, Contact Lens Service University of Iowa Disclosure Consultant: ALCON Vision Care
Fitting Keratoconus and Other Complicated Corneas Christine W Sindt OD FAAO Professor, Clinical Ophthalmology Director, Contact Lens Service University of Iowa Disclosure Consultant: ALCON Vision Care
April 1962 Volume 1, Number 2 INVESTIGATIVE OPHTHALMOLOGY. Symposium on the cornea. Introduction: Factors influencing corneal hydration
 April 1962 Volume 1, Number 2 INVESTIGATIVE OPHTHALMOLOGY Symposium on the cornea Introduction: Factors influencing corneal hydration John E. Harris The swelling of the corneal buttons in aqueous solution
April 1962 Volume 1, Number 2 INVESTIGATIVE OPHTHALMOLOGY Symposium on the cornea Introduction: Factors influencing corneal hydration John E. Harris The swelling of the corneal buttons in aqueous solution
GENERAL INFORMATION CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL TRANSPLANTATION WHAT IS CORNEAL TRANSPLANTATION? A corneal transplant is an operation where a damaged or diseased cornea is replaced with donated, healthy tissue. Also called
GENERAL INFORMATION CORNEAL TRANSPLANTATION WHAT IS CORNEAL TRANSPLANTATION? A corneal transplant is an operation where a damaged or diseased cornea is replaced with donated, healthy tissue. Also called
Disease caused by herpes simplex virus
 Recurrence of herpes simplex virus in rabbit eyes: Results of a three-year study Peter R. Laibson and Sidney Kibrick Spontaneous reactivation of herpes simplex virus in rabbit ocular tissue was found on
Recurrence of herpes simplex virus in rabbit eyes: Results of a three-year study Peter R. Laibson and Sidney Kibrick Spontaneous reactivation of herpes simplex virus in rabbit ocular tissue was found on
Amniotic membrane transplantation for partial limbal stem cell deficiency
 Br J Ophthalmol 2001;85:567 575 567 ORIGINAL ARTICLES Clinical science Ocular Surface and Tear Center, Department of Ophthalmology, Bascom Palmer Eye Institute, Miami, Florida, USA D F Anderson P Ellies
Br J Ophthalmol 2001;85:567 575 567 ORIGINAL ARTICLES Clinical science Ocular Surface and Tear Center, Department of Ophthalmology, Bascom Palmer Eye Institute, Miami, Florida, USA D F Anderson P Ellies
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW
 MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
Differential Staining of Ocular Goblet Cells
 Eye (1989) 3, 840--844 Differential Staining of Ocular Goblet Cells G. G. W. ADAMS and P. N. DILLY London Summary Millipore filters were used to obtain sheets of cells from the ocular surface. Using Periodic
Eye (1989) 3, 840--844 Differential Staining of Ocular Goblet Cells G. G. W. ADAMS and P. N. DILLY London Summary Millipore filters were used to obtain sheets of cells from the ocular surface. Using Periodic
Specialist Referral Service Willows Information Sheets. Recurrent corneal erosions (indolent ulcers)
 Specialist Referral Service Willows Information Sheets Recurrent corneal erosions (indolent ulcers) A rabbit s cornea undergoing debridement under topical anaesthesia Recurrent corneal erosions (indolent
Specialist Referral Service Willows Information Sheets Recurrent corneal erosions (indolent ulcers) A rabbit s cornea undergoing debridement under topical anaesthesia Recurrent corneal erosions (indolent
BY N. N. SOODt AND V. J. MARMION- St. Paul's Eye Hospital, Liverpool
 Brit. J. Ophthal. (1964) 48, 609. SUPERFICIAL HERPETIC KERATITIS TREATED WITH 5-IODO-2'-DEOXYURIDINE* BY N. N. SOODt AND V. J. MARMION- St. Paul's Eye Hospital, Liverpool THE results of treating herpetic
Brit. J. Ophthal. (1964) 48, 609. SUPERFICIAL HERPETIC KERATITIS TREATED WITH 5-IODO-2'-DEOXYURIDINE* BY N. N. SOODt AND V. J. MARMION- St. Paul's Eye Hospital, Liverpool THE results of treating herpetic
Studies of mitotic activity in the lens
 Effect of age on cell division, 3 H-thymidine incorporation, and diurnal rhythm in the lens epithelium of rats Ludtvig von Sallmann and Patricia Grimes The rapid growth of the rat lens during the first
Effect of age on cell division, 3 H-thymidine incorporation, and diurnal rhythm in the lens epithelium of rats Ludtvig von Sallmann and Patricia Grimes The rapid growth of the rat lens during the first
Therapeutic keratoplasty in
 Brit. J. Ophthal. (I 97 I) 55, 326 Therapeutic keratoplasty in Pseudomonas pyocyaneus corneal ulcers S. R. K. MALIK AND GURBAX SINGH Maulana Azad Medical College and Associated Irwin and G.B. Pant Hospital,
Brit. J. Ophthal. (I 97 I) 55, 326 Therapeutic keratoplasty in Pseudomonas pyocyaneus corneal ulcers S. R. K. MALIK AND GURBAX SINGH Maulana Azad Medical College and Associated Irwin and G.B. Pant Hospital,
Mustard Gas Induced Ocular Surface Disorders
 Challenging Case Mustard Gas Induced Ocular Surface Disorders Section Editor: Alireza Baradaran-Rafii, MD Ophthalmic Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran Sulfur
Challenging Case Mustard Gas Induced Ocular Surface Disorders Section Editor: Alireza Baradaran-Rafii, MD Ophthalmic Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran Sulfur
Amniotic membrane transplantation (AMT) without the use of sutures/fibrin glue
 Original article Amniotic membrane transplantation (AMT) without the use of sutures/fibrin glue Ajai Agrawal 1, VB Pratap 2 1 Department of Ophthalmology, Kalpana Chawla Government Medical College, Karnal,
Original article Amniotic membrane transplantation (AMT) without the use of sutures/fibrin glue Ajai Agrawal 1, VB Pratap 2 1 Department of Ophthalmology, Kalpana Chawla Government Medical College, Karnal,
Protocol. Endothelial Keratoplasty
 Protocol Endothelial Keratoplasty (90322) Medical Benefit Effective Date: 04/01/14 Next Review Date: 11/18 Preauthorization No Review Dates: 01/14, 11/14, 11/15, 11/16, 11/17 Preauthorization is not required.
Protocol Endothelial Keratoplasty (90322) Medical Benefit Effective Date: 04/01/14 Next Review Date: 11/18 Preauthorization No Review Dates: 01/14, 11/14, 11/15, 11/16, 11/17 Preauthorization is not required.
Senile: flattening of vertical meridian, thinning of periphery, lack of luster
 Pterygia Etiology: triangular, fibrovascular, connective tissue overgrowths of bulbar conjunctiva onto cornea; distribution of ultraviolet energy- heat, wind, dust, dry atmosphere,higher prevalence nearer
Pterygia Etiology: triangular, fibrovascular, connective tissue overgrowths of bulbar conjunctiva onto cornea; distribution of ultraviolet energy- heat, wind, dust, dry atmosphere,higher prevalence nearer
 Traumatic Cataract Orbital Wall Fracture Vitreous Hemorrhage Optic Disc Hemorrhage a) Amblyopia b) Strabismus c) Trauma Playing with other children Sports Fire works BB gun Injecting needles .
Traumatic Cataract Orbital Wall Fracture Vitreous Hemorrhage Optic Disc Hemorrhage a) Amblyopia b) Strabismus c) Trauma Playing with other children Sports Fire works BB gun Injecting needles .
Anterior Stromal Puncture with the Nd:YAG Laser
 Investigative Ophthalmology & Visual Science, Vol. 31. No. 8, August 1990 Copyright Association foi Research in Vision and Ophthalmology Anterior Stromal Puncture with the Nd:YAG Laser Harry 5. Geggel
Investigative Ophthalmology & Visual Science, Vol. 31. No. 8, August 1990 Copyright Association foi Research in Vision and Ophthalmology Anterior Stromal Puncture with the Nd:YAG Laser Harry 5. Geggel
Corneal Transplants. Corneal transplants. What causes cornea problems? Full thickness corneal transplant
 Corneal transplants The cornea is the clear, front window of the eye. It helps focus light into the eye so that you can see. The cornea is made of layers of cells. These layers work together to protect
Corneal transplants The cornea is the clear, front window of the eye. It helps focus light into the eye so that you can see. The cornea is made of layers of cells. These layers work together to protect
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
Eye Care for Animals Micki Armour VMD DACVO THE CORNEA
 Eye Care for Animals Micki Armour VMD DACVO THE CORNEA ANATOMY 0.5-0.6mm thick 4 primary layers Epithelium (5-7 cell layers) Stroma (90% total thickness) Descemet s membrane Endothelium (1 layer) ANATOMY-
Eye Care for Animals Micki Armour VMD DACVO THE CORNEA ANATOMY 0.5-0.6mm thick 4 primary layers Epithelium (5-7 cell layers) Stroma (90% total thickness) Descemet s membrane Endothelium (1 layer) ANATOMY-
Corneal Transplants. Corneal transplants. What causes cornea problems? Full thickness corneal transplant
 2014 2015 Corneal transplants The cornea is the clear, front window of the eye. It helps focus light into the eye so that you can see. The cornea is made of layers of cells. These layers work together
2014 2015 Corneal transplants The cornea is the clear, front window of the eye. It helps focus light into the eye so that you can see. The cornea is made of layers of cells. These layers work together
T he corneal epithelium is a non-keratinised stratified
 393 EXTENDED REPORT Epithelial cell characteristics of cultured human limbal explants A Joseph, A O R Powell-Richards, V A Shanmuganathan, H S Dua... See end of article for authors affiliations... Correspondence
393 EXTENDED REPORT Epithelial cell characteristics of cultured human limbal explants A Joseph, A O R Powell-Richards, V A Shanmuganathan, H S Dua... See end of article for authors affiliations... Correspondence
Fleck. Pre-Descemet Dystrophies (generally good vision and comfort) Primary Pre-Descemet Dystrophy
 Fleck Etiology: bilateral, sometimes asymmetric, autosomal dominant opacities located in all levels of stroma as early as 1 st decade Slit lamp: well demarcated, small round gray-white doughnut-like, wreath-like
Fleck Etiology: bilateral, sometimes asymmetric, autosomal dominant opacities located in all levels of stroma as early as 1 st decade Slit lamp: well demarcated, small round gray-white doughnut-like, wreath-like
WARNING LETTER. According to the Indications and Usage section of the FDA approved product labeling (PI):
 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE David E.I. Pyott President and Chief Executive Officer PO Box 19534
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE David E.I. Pyott President and Chief Executive Officer PO Box 19534
Meibomian Gland Dysfunction
 Investigative Ophthalmology & Visual Science. Vol. 30. No. 5. May 1989 Copyright Association for Research in Vision and Ophthalmology Meibomian Gland Dysfunction //. The Role of Kerarinizarion in o Rabbit
Investigative Ophthalmology & Visual Science. Vol. 30. No. 5. May 1989 Copyright Association for Research in Vision and Ophthalmology Meibomian Gland Dysfunction //. The Role of Kerarinizarion in o Rabbit
Conjunctival Goblet Cell Frequency after Alkali Injury is not Accurately Reflected by Aqueous Tear Mucin Content
 Conjunctival Goblet Cell Frequency after Alkali Injury is not Accurately Reflected by Aqueous Tear Mucin Content Judith Friend, Timothy Kiorpes, and Richard A. Thoft Goblet cell counts have been used to
Conjunctival Goblet Cell Frequency after Alkali Injury is not Accurately Reflected by Aqueous Tear Mucin Content Judith Friend, Timothy Kiorpes, and Richard A. Thoft Goblet cell counts have been used to
SCLERAL CONTACT LENSES EPSILON SCLERAL
 SCLERAL CONTACT LENSES EPSILON SCLERAL - Outstands due to multi aspheric variable eccentricity design - Fitted in two steps due to it s novel philosophy and diagnostic set - Reassures limbal stem cells
SCLERAL CONTACT LENSES EPSILON SCLERAL - Outstands due to multi aspheric variable eccentricity design - Fitted in two steps due to it s novel philosophy and diagnostic set - Reassures limbal stem cells
What are some common conditions that affect the cornea?
 What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
Amodified penetrating keratoplasty procedure with a new lamellar configuration of the
 A New Lamellar Wound Configuration for Penetrating Keratoplasty Surgery Massimo Busin, MD SURGICAL TECHNIQUE Amodified penetrating keratoplasty procedure with a new lamellar configuration of the surgical
A New Lamellar Wound Configuration for Penetrating Keratoplasty Surgery Massimo Busin, MD SURGICAL TECHNIQUE Amodified penetrating keratoplasty procedure with a new lamellar configuration of the surgical
9/24/14. Anatomy of the Eye. Corneal Anatomy. The Cornea! Transparent Tough Biological Barrier Refractile. The Cornea is an ORGAN
 The Cornea! J Funderburgh Biology of Vision INTBP2100 24 Sep 2014 Transparent Tough Biological Barrier Refractile 1! Anatomy of the Eye www.ohiovalleyeye.com/eyeinfo_anatomy.htm The Cornea is an ORGAN
The Cornea! J Funderburgh Biology of Vision INTBP2100 24 Sep 2014 Transparent Tough Biological Barrier Refractile 1! Anatomy of the Eye www.ohiovalleyeye.com/eyeinfo_anatomy.htm The Cornea is an ORGAN
Basal cell carcinoma 5/28/2011
 Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
I nadequate corneal epithelial nutrition
 Corneal amino acid supply and distribution Richard A. Thoft and Judith Friend The distribution of nonmetabolized carbon ^'labelled aaminoisobutyric acid (aaib) in the anterior segment of the rabbit eye
Corneal amino acid supply and distribution Richard A. Thoft and Judith Friend The distribution of nonmetabolized carbon ^'labelled aaminoisobutyric acid (aaib) in the anterior segment of the rabbit eye
Efficacy of transepithelial corneal cross-linking using iontophoresis
 Efficacy of transepithelial corneal cross-linking using iontophoresis Experimental studies on eye-bank donor eyes and Preliminary results on the clinical trial NCT02117999 Marco Lombardo, MD, PhD Senior
Efficacy of transepithelial corneal cross-linking using iontophoresis Experimental studies on eye-bank donor eyes and Preliminary results on the clinical trial NCT02117999 Marco Lombardo, MD, PhD Senior
TGF- 2, Tenascin, and Integrin 1 Expression in Superior Limbic Keratoconjunctivitis
 LABORATORY INVESTIGATIONS TGF- 2, Tenascin, and Integrin 1 Expression in Superior Limbic Keratoconjunctivitis Akira Matsuda, Yoshitsugu Tagawa and Hidehiko Matsuda Department of Ophthalmology, Hokkaido
LABORATORY INVESTIGATIONS TGF- 2, Tenascin, and Integrin 1 Expression in Superior Limbic Keratoconjunctivitis Akira Matsuda, Yoshitsugu Tagawa and Hidehiko Matsuda Department of Ophthalmology, Hokkaido
Comparison of prognostic value of Roper Hall and Dua classification systems in acute ocular burns
 1 Cornea and Refractive Surgery Services, Dr Rajendra Prasad Centre for Ophthalmic Sciences, All India Institute of Medical Sciences, New Delhi, India 2 Department of Biostatistics, All India Institute
1 Cornea and Refractive Surgery Services, Dr Rajendra Prasad Centre for Ophthalmic Sciences, All India Institute of Medical Sciences, New Delhi, India 2 Department of Biostatistics, All India Institute
Innovative Iris Repair
 UNC Eye Symposium April 2, 2016 Chapel Hill, NC Innovative Iris Repair D Mark A. Terry, MD Director, Corneal Services Devers Eye Institute Scientific Director Lions VisionGift Research Lab Portland, Oregon,
UNC Eye Symposium April 2, 2016 Chapel Hill, NC Innovative Iris Repair D Mark A. Terry, MD Director, Corneal Services Devers Eye Institute Scientific Director Lions VisionGift Research Lab Portland, Oregon,
CONGENITAL CORNEAL OPACITIES*t IN A PATIENT WITH RIEGER'S ANOMALY AND DOWN'S SYNDROME
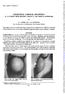 Brit. J. Ophthal. (1968) 52, 631 CONGENITAL CORNEAL OPACITIES*t IN A PATIENT WITH RIEGER'S ANOMALY AND DOWN'S SYNDROME BY From the Department of Ophthalmology, Royal Hospital, Sheffield THIS report concerns
Brit. J. Ophthal. (1968) 52, 631 CONGENITAL CORNEAL OPACITIES*t IN A PATIENT WITH RIEGER'S ANOMALY AND DOWN'S SYNDROME BY From the Department of Ophthalmology, Royal Hospital, Sheffield THIS report concerns
Title: Keeping Step with DEWS2: Clinical Applications Lecturer: Scott G. Hauswirth, OD
 Title: Keeping Step with DEWS2: Clinical Applications Lecturer: Scott G. Hauswirth, OD Course Description: The Dry Eye Workshop 2 was an assemblage of experts in dry eye disease from around the world,
Title: Keeping Step with DEWS2: Clinical Applications Lecturer: Scott G. Hauswirth, OD Course Description: The Dry Eye Workshop 2 was an assemblage of experts in dry eye disease from around the world,
