CLINICAL SCIENCES. Bilateral Simultaneous-Onset Nongranulomatous Acute Anterior Uveitis
|
|
|
- Cecily Mathews
- 6 years ago
- Views:
Transcription
1 ONLINE FIRST CLINICAL SCIENCES Bilateral Simultaneous-Onset Nongranulomatous Acute Anterior Uveitis Clinical Presentation and Etiology Andrea D. Birnbaum, MD, PhD; Yi Jiang, MD; Roshni Vasaiwala, MD; Howard H. Tessler, MD; Debra A. Goldstein, MD Objective: To describe the etiology and outcome of patients with simultaneous-onset nongranulomatous bilateral acute anterior uveitis. Methods: The medical records of patients who presented to a single tertiary care center with simultaneousonset nongranulomatous bilateral acute anterior uveitis between January 1990 and May 2010 were retrospectively reviewed; the clinical presentation, results of diagnostic testing, and outcome data are described. Results: A total of 4288 new patients with uveitis were evaluated by the Uveitis Service at the University of Illinois at Chicago Eye and Ear Infirmary between January 1990 and May Of these new patients, 44 (1%) presented with simultaneous-onset nongranulomatous bilateral acute anterior uveitis. The most common etiologies were postinfectious or drug-induced uveitis (23 of 44 patients [52%]) and idiopathic uveitis (15 patients [34%]). Tubulointerstitial nephritis and uveitis syndrome, HLA-B27 associated uveitis, inflammatory bowel disease, and Kawasaki disease each made up fewer than 5% of diagnoses. Overall, this group of patients was younger than the entire cohort of new patients with uveitis who were evaluated during the same time period (P=.002). For 14 of the 15 patients with at least a year of follow-up (93%), the disease duration was limited ( 3 months). Of these 14 patients, 7 (50%) developed recurrent disease, with an average time to first recurrence of 20 months (range, months) after resolution of the initial inflammatory episode. Conclusions: Simultaneous-onset nongranulomatous bilateral acute anterior uveitis is a rare clinical entity that is more common in younger patients and is most frequently associated with recent infection and/or systemic antibiotic use. Tubulointerstitial nephritis and uveitis syndrome should also be considered as a diagnosis. Diagnostic evaluation should include serum antistreptolysin-o titers, HLA-B27 antigen, and urine 2 microglobulin levels because these may reveal systemic disease that requires therapy. Arch Ophthalmol. 2012;130(11): Published online July 9, doi: /archophthalmol Author Affiliations: Department of Ophthalmology, Northwestern University (Dr Birnbaum), Rush University Medical School (Dr Jiang), and Department of Ophthalmology and Visual Sciences, University of Illinois at Chicago (Drs Vasaiwala, Tessler, and Goldstein), Chicago, Illinois. ANTERIOR UVEITIS REFERS TO inflammation located in the anterior chamber (iritis) or with associated anterior vitreousinvolvement(iridocyclitis), and is the most common presentationofuveitis. 1-3 Frequentdiagnoses,aside from idiopathic disease, include HLA-B27 associated disease, Fuchs heterochromic iridocyclitis, juvenileidiopathicarthritis, and herpetic disease. 1-3 Acute anterior uveitis describes episodic inflammation of sudden onset and limited duration ( 3 months). 4 Patients are symptomatic, usually experiencing pain, redness, photophobia, and decreased vision. The disease typically presents unilaterally, although episodes may alternate between eyes. Less well described is acute anterior uveitis that presents with bilateral, simultaneous onset. We present data on a series of patients with simultaneous-onset nongranulomatous bilateral acute anterior uveitis (BAAU) evaluated by the Uveitis Service at the University of Illinois at Chicago Eye and Ear Infirmary between 1990 and METHODS We were granted permission by the institutional review board of the University of Illinois at Chicago to retrospectively review existing medical records of patients evaluated by the Uveitis Service between January 1990 and May 2010 with a diagnosis of acute anterior uveitis. The charts of patients with acute anterior uveitis were then reviewed to identify those patients who presented with symptomatic simultaneous-onset BAAU. Patients with granulomatous inflammation (based on the presence of mutton fat keratic precipitates or granulomatous iris nodules) were excluded. To be considered symptomatic, patients had to have at least 1 ocular complaint consistent with Author Affil Department Northwester (Dr Birnbaum Medical Scho Department and Visual S of Illinois at (Drs Vasaiwa Goldstein), C 1389
2 acute anterior uveitis (pain, redness, or photophobia) at presentation. Simultaneous onset was defined as onset of symptomatic disease in the second eye within 4 weeks of the first. Patients with unilateral inflammation or bilateral anterior uveitis symptomatic in only 1 eye were excluded. Demographic information collected included age at presentation, self-reported race, and sex. The classification of uveitis was based on the Standardization of Uveitis Nomenclature criteria. 4 A diagnosis of postinfectious or drug-induced uveitis was made in patients who developed symptomatic inflammation in both eyes within 4 weeks of either documented systemic infection or treatment with systemic antibiotics, or in a patient with an elevated antistreptolysin-o (ASO) titer after vague systemic complaints. A diagnosis of HLA-B27 associated anterior uveitis was made for any patient who tested positive for the HLA-B27 antigen, either by serological testing or polymerase chain reaction (PCR). Tubulointerstitial nephritis and uveitis (TINU) syndrome was diagnosed in patients with elevated urine 2 microglobulin and associated kidney dysfunction or with confirmation of diagnosis by a nephrologist. Any patient younger than 17 years at initial presentation was considered part of the pediatric population. Comparisons between pediatric and adult patients were performed using the Fisher exact test. Additional comparisons of age at presentation were calculated using a 2-tailed t test. P.05 was considered statistically significant. Table 1. Demographic Distribution of Patients With BAAU Characteristic Nongranulomatous BAAU (n=44) No. (%) Nongranulomatous Unilateral Acute Uveitis (n=643) All Patients Without BAAU (n=4244) Age at presentation, y Mean Median (range) 37 (4-81) 41 (1-91) 43 (1-93) Female sex 28 (64) 361 (56) 2594 (61) Racial distribution a (n = 44) (n = 633) (n = 4184) White 26 (59) 420 (66) 2426 (58) African American 11 (25) 110 (17) 1090 (26) Hispanic 4 (9) 64 (10) 462 (11) Asian 3 (7) 39 (6) 206 (5) Abbreviation: BAAU, bilateral acute anterior uveitis. a Self-reported (based on uveitis questionnaire). Race was not reported in all patients. Patients with BAAU presented at a younger age relative to those with unilateral acute uveitis (P=.002) and when compared with all other patients with uveitis who were evaluated during the same time period (P=.002). RESULTS A total of 4288 new patients were evaluated by the Uveitis Service between January 1990 and May Acute nongranulomatous anterior uveitis was diagnosed in 687 patients (23 patients with granulomatous disease were excluded). Of these, 44 presented with simultaneous-onset nongranulomatous BAAU (1% of the total number of new patients [n=4288] and 6% of patients with nongranulomatous acute anterior uveitis [n=687]). All patients with BAAU developed symptomatic inflammation in the second eye within 7 days of the first eye; 36 patients (82%) presented with symptomatic bilateral inflammation at onset. The most common complaints at presentation included redness (38 patients [86%]), pain (35 patients [80%]), and photophobia (32 patients [73%]). Less common complaints were sudden-onset blurred vision (13 patients [30%]) and floaters (4 patients [9%]). Children younger than 17 years comprised 25% of BAAU patients (n=11), compared with 3% of all patients with unilateral acute anterior uveitis (P.001) and 10% of all new patients with uveitis evaluated during the same time period (.001). Patients with BAAU were younger than the cohort of other new patients with uveitis evaluated during the same time period (P=.002) and the cohort of new patients with unilateral acute anterior uveitis (P=.002). There was no difference in age at presentation between patients with postinfectious or drug-induced uveitis and patients with other diagnoses in the BAAU cohort (P=.74). For all patients, BAAU was the first documented episode of ocular inflammation. Two patients reported previous episodes of bilateral anterior uveitis that had resolved in less than 3 months with topical and oral corticosteroids. For the other 42 patients, the presentation with BAAU to the Uveitis Service at the University of Illinois at Chicago Eye and Ear Infirmary represented the first episode of ocular inflammation. For all patients, follow-up time was based on the episode for which they were treated at the University of Illinois at Chicago Eye and Ear Infirmary. Demographic data are presented in Table 1. Comparison data are provided for patients with unilateral nongranulomatous acute anterior uveitis and for all other patients evaluated by the Uveitis Service during the same time period. Aside from age at presentation, the demographic profiles were similar between the patients with BAAU and the patients with unilateral acute anterior uveitis. Table 2. Results of Diagnostic Testing a No. Positive/Total No. (%), Patients From Each Group Postinfectious Test Total Adult Children or Drug-Induced Uveitis Idiopathic Uveitis Angiotensin-converting enzyme 3/36 (8) 1/27 (4) 2/9 (22) 2/19 (11) 1/13 (8) Lysozyme 2/29 (7) 1/21 (5) 1/8 (13) 2/19 (11) 0/8 (0) Antistreptolysin-O 4/13 (31) 1/8 (13) 3/5 (60) 4/11 (36) 0/0 (0) HLA-B27 5/34 (15) 5/30 (17) 0/4 (0) 2/17 (12) 0/12 (0) Urine 2 microglobulin 3/17 (18) 2/12 (17) 1/5 (20) 0/12 (0) 1/2 (50) Chest radiography 0/33 (0) 0/25 (0) 0/8 (0) 0/17 (0) 0/12 (0) a Antistreptolysin-O titers were elevated in 60% of children tested, and 36% of all patients diagnosed with postinfectious or drug-induced uveitis. Three patients had elevated urine 2 microglobulin levels; these elevated levels were associated with tubulointerstitial nephritis and uveitis syndrome in 2 patients and a kidney stone in 1 patient. 1390
3 Table 3. Etiologies of Simultaneous-Onset Bilateral Acute Anterior Uveitis a No. (%) Etiology Total (n=44) Adults (n=33) Children (n=11) Postinfectious or drug-induced 23 (52) 16 (48) 7 (64) uveitis Postinfectious or drug-induced 2 (5) 2 (6) 0 (0) uveitis with HLA-B27 positivity Idiopathic uveitis 15 (34) 13 (39) 2 (18) TINU syndrome 2 (5) 1 (3) 1 (9) TINU syndrome with HLA-B27 1 (2) 1 (3) 0 (0) positivity HLA-B27 associated uveitis 2 (5) 2 (6) 0 (0) HLA-B27 associated uveitis with 3 (7) 3 (9) 0 (0) other diagnosis Inflammatory bowel disease 1 (2) 1 (3) 0 (0) Kawasaki disease 1 (2) 0 (0) 1 (9) Abbreviation: TINU, tubulointerstitial nephritis and uveitis. a The majority of cases were attributed to recent infection, and many patients were treated with oral antibiotics. Three of the HLA-B27 positive patients fit into other categories: 2 with postinfectious or drug-induced disease and 1 with TINU syndrome. Diagnostic testing was variable, and no test result was positive for more than 30% of patients (Table 2). Serum angiotensin-converting enzyme was elevated in 3 of 36 patients tested (8%), and lysozyme was elevated in 2 of 29 patients tested (7%). Five of 34 patients (15%) tested were positive for HLA-B27. None of the 33 patients undergoing chest radiography had a significant finding, such as hilar lymphadenopathy, suggestive of sarcoidosis. Antistreptolysin-O titers were elevated in 4 of 13 patients tested (31%). Elevated urine 2 microglobulin was present in 3 of 17 patients tested (18%). This test was not obtained for the 15 patients evaluated before The etiologies of BAAU are shown in Table 3. The most common association was postinfectious or druginduced uveitis (23 patients [52%]). The profile of these patients is shown in Table 4. Of these 23 patients, 10 (43%) had received systemic antibiotics prior to presentation, and 13 (57%) had systemic infection without antibiotic therapy. No difference was noted between adults and children (P=.75). Seven patients (30%) with this diagnosis had only 1 evaluation by the Uveitis Service. Two patients were positive for HLA-B27, and both had recently been treated with oral antibiotics for throat infections (1 patient with confirmed infection with group A Streptococcus). The median duration from the onset of illness to the onset of eye symptoms for patients with postinfectious uveitis was 7 days (range, 1-30 days). Six patients specifically recalled the onset of eye symptoms after the termination of treatment with antibiotics at a mean duration of 8.5 days (range, 4-14 days). Two patients were taking oral antibiotics when ocular symptoms began: 1 patient on the fifth day of treatment and the other on the seventh. The other 5 patients did not recall their treatment timeline. The second most common diagnosis was idiopathic disease (15 of 44 patients [34%]). Tubulointerstitial nephritis and uveitis syndrome was diagnosed in 2 of 14 patients tested, one at 5 years of age and one at 51 years of age. Both had elevated urine 2 microglobulin and con- Table 4. Profile of Patients Diagnosed With Postinfectious or Drug-Induced Uveitis a Patient No./ Sex Age at Presentation to Uveitis Service, y Race Site Antibiotics ASO B 2 1/F 4 White Cellulitis (MRSA) Sulfamethoxazole/trimethoprim sulfate 2/F 4 White URI Unspecified 3/M 5 Black URI 4/F 8 White Throat (S) 5/M 11 Asian Throat 6/F 11 Hispanic URI 7/F 16 White Sinus 8/M 17 Black Throat (S) Penicillin 9/M 18 Hispanic Ear Levaquin 10/M 35 White 11/F 38 Asian 12/F 39 White 13/M 39 White Throat (S) Amoxicillin, erythromycin stearate 14/F 41 White URI 15/F 41 Hispanic 16/M 43 White Throat 17/F 43 White Throat Erythromycin 18/F 55 Asian Lung Unspecified intravenous antibiotics 19/M 56 White 20/F 58 White Throat Penicillin 21/M 59 Black Prostate Sulfamethoxazole/trimethoprim 22/M 60 White Middle ear 23/M 62 White Cellulitis Moxifloxacin Abbreviations: ASO, antistreptolysin-o antibody; B 2, urine 2 microglobulin; MRSA, methicillin-resistant Staphylococcus aureus; S, confirmed streptococcal throat infection; URI, upper respiratory tract infection;, negative (laboratory value within the normal range);, positive (elevated laboratory value). a A specific site of infection was identified in all but 5 patients (ie, patients 10, 11, 12, 15, and 19). These patients all reported generalized malaise and/or flulike symptoms prior to the development of ocular symptoms. Ten patients also received systemic antibiotic therapy. All antibiotics were given orally, unless specified otherwise. 1391
4 Table 5. Systemic Complaints of Patients at Initial Presentation to Uveitis Service No. (%) Disease Rash Oral Ulcers Back Pain Arthritis Total (n=44) 7 (16) 7 (16) 9 (20) 3 (7) Postinfectious or drug-induced uveitis (n=23) 2 (9) 4 (17) 6 (26) 2 (9) Idiopathic uveitis (n=15) 3 (20) 3 (20) 3 (20) 1 (7) TINU syndrome (n=2) 1 (50) 0 (0) 0 (0) 0 (0) Kawasaki disease (n=1) 1 (100) 0 (0) 0 (0) 0 (0) Inflammatory bowel disease (n=1) 0 (0) 0 (0) 0 (0) 0 (0) Abbreviation: TINU, tubulointerstitial nephritis and uveitis. Table 6. Disease Course in Patients With Simultaneous-Onset Nongranulomatous BAAU a Patients, No./Total No. (%) Patients, Acute Etiology Total No. Total Recurrent Chronic All 15 14/15 (93) 7/14 (50) 1/15 (7) Postinfectious or drug-induced uveitis 7 6/7 (86) 3/6 (50) 1/7 (14) Idiopathic uveitis 7 7/7 (100) 3/7 (43) 0/7 (0) HLA-B27 associated uveitis 2 2/2 (100) 1/2 (50) 0/2 (0) Abbreviation: BAAU, bilateral acute anterior uveitis. a Fifteen patients had at least 1 year of follow-up, and only one of these patients had chronic disease. Of the patients whose disease was initially acute in duration, 50% subsequently developed recurrences of inflammation between 7.5 to 40 months after resolution of first episode. firmation of diagnosis by a nephrologist. One patient with TINU syndrome tested positive for HLA-B27. Kawasaki disease and inflammatory bowel disease were each diagnosed in 1 patient, and both of these patients had been referred with the diagnosis. Systemic symptoms at presentation are shown in Table 5. The most common complaint was back pain, which was present in 9 of 44 patients with BAAU (20%) and 6 of 23 patients with postinfectious or druginduced uveitis (26%). Of the 44 patients with BAAU, 8 (18%) had a history of oral ulcers, and 7 (16%) had a recent rash. Only 3 of the 44 patients (7%) reported arthritis or joint pain, 2 of whom were diagnosed with postinfectious or drug-induced uveitis. Fifteen patients had at least 1 year of follow-up, with a mean follow-up time of 33.5 months (range, months) (Table 6). Of these 15 patients, 14 (93%) had acute disease that resolved within 3 months, and 1 (7%) had chronic disease with ultimate resolution by 6 months. Of the 14 patients with acute disease and at least a year of follow-up, 7 (50%) developed recurrent inflammation. The second episode of inflammation was bilateral in 6 of the 7 patients and occurred, on average, 20 months (range, 5-49 months) after resolution of the initial episode. Finally, 9 of the patients had more than 2 years of follow-up (range, months). None had active chronic disease. Four of the 8 patients with acute disease (50%) developed a recurrent but limited episode of inflammation. COMMENT Nongranulomatous acute anterior uveitis with bilateral simultaneous onset is a rare presentation of ocular inflammation, even at our tertiary referral service. In this series, it comprised 44 of 4288 new patients with uveitis (1%), which was only 6% of the 687 new patients with nongranulomatous acute anterior uveitis. Other series 5-7 have reported somewhat higher percentages of simultaneous-onset BAAU. In one study 5 from the United States, 4% of all patients with uveitis had this presentation, although this study 5 included patients who developed bilateral involvement within 16 weeks of initial onset of unilateral inflammation vs 4 weeks in our study. In Turkey, simultaneous-onset BAAU was reported in 7% of patients who tested positive for HLA-B27 and in 26% of patients who tested negative. 6 This patient population was different, however, because only those retrospectively determined to have iridocyclitis of sudden onset and limited duration were included in the study, 6 whereas our series included patients with uveitis of both limited and persistent duration. Finally, a study 7 of patients with uveitis in Spain reported 2.7% of patients with this presentation (ie, BAAU), which is similar to that reported in our study. More than half (52%) of the patients in this series were diagnosed with postinfectious or drug-induced anterior uveitis. Within the spectrum of postinfectious disease is the clinical entity poststreptococcal syndrome uveitis. First described in 1991, the syndrome is common in younger patients ( 40 years) and usually presents 1 to 6 weeks after onset of systemic symptoms. 8 The disease is typically bilateral and associated with elevated serum ASO titers in more than 95% of cases. 8 Titers are normally elevated 1 week after infection with group A Streptococcus and peak between 3 to 6 weeks. A decrease begins after 6 to 8 weeks, but some patients maintain elevated levels for longer periods of time. 9 Posterior segment involve- 1392
5 ment has been described, including vitritis, vascular sheathing, and retinitis. 10 Interestingly, approximately 12% of patients deny a preceding systemic illness. 8 In this series, patients without systemic complaints did not have ASO titers measured; therefore, this condition may have been underdiagnosed. Also, cutaneous streptococcal infection is not always associated with increased ASO titers. 11 One patient with postinfectious or drug-induced uveitis in our series had a history of cellulitis and normal ASO titers. This patient may, in fact, have had recent streptococcal skin infection without an increase in ASO titers. Postinfectious uveitis is not limited to anterior segment inflammation, as was shown in a series of patients with poststreptococcal inflammation. 10 Frosted branch angiitis is a type of retinal vasculitis that is often associated with inflammation in the anterior segment and vitreous. Much like the patients with postinfectious or druginduced BAAU in our study, the condition is often bilateral (75% of patients) and may be preceded by a systemic illness. 12 Simultaneous-onset nongranulomatous BAAU was more common in young patients in our series. The younger age cannot be attributed entirely to a presumed increased risk of infection associated with the immature immune systems of younger patients leading to a predominance of postinfectious or drug-induced uveitis. The ages at presentation between the group of patients with postinfectious or drug-induced uveitis and the group of patients with BAAU were not different. However, as stated previously, our results may underestimate cases of postinfectious or drug-induced disease because ASO titers were not obtained for patients who did not present with a history of a recent infection. Perhaps more of the younger patients had a preceding subclinical infection. The HLA-B27 allele is present in approximately 50% of patients with acute anterior uveitis. 13,14 HLA-B27 associated uveitis is most often characterized by recurrent anterior ocular inflammation in one eye at a time. Bilateral simultaneous disease is much less common and behaves differently from unilateral disease, with fewer recurrences. 15 In our series, HLA-B27 was not a common etiology of BAAU; only 5 of 35 patients tested (14%) were positive for the allele. Two of these patients had postinfectious or drug-induced uveitis, and one was classified as having TINU syndrome. It is possible that this association occurred by chance because approximately 8% of whites and 2% of African Americans are positive for HLA- B27. 16,17 However, bacterial infection is known to be a trigger for acute anterior uveitis in patients with the HLA-B27 allele. Antibodies targeting endotoxin lipopolysaccharides of gram-negative bacteria have been found to be elevated in patients positive for HLA-B27 during their first attack of anterior acute uveitis, relative to levels during relapses. 15 Patients with bilateral disease had higher antibody levels but lower recurrence rates than patients with unilateral disease. 18 This is in keeping with our finding that the HLA-B27 positive patient with acute disease and 15 months of follow-up did not have a relapse. Also, endotoxin-induced uveitis, characterized by transient bilateral anterior segment inflammation, is a disease that was originally described in an animal model after injection of lipopolysaccharides or endotoxin of gram-negative bacteria into foot pads of rats. 18 The similarity in presentation (bilateral acute inflammation with eventual resolution) may suggest a similar triggering mechanism to what is seen clinically in HLA-B27 positive patients. Of the 15 patients with more than a year of followup, 14 (93%) had a disease course of limited duration. Of these 14 patients, 7 (50%) developed recurrent acute disease. With longer clinical follow-up, the number of patients with recurrent disease would likely have increased. However, the real rate of recurrence may be much lower than ascertained because many patients with acute disease (sudden onset, limited duration) did not come for follow-up after disease resolution. This may be because they had no further episodes. Depending on the outcomes of the patients who did not return for followup, the true recurrence rate could be anywhere from 26% (10 of 39 patients) to 82% (32 of 39 patients). The actual recurrence rate for patients with BAAU would thus be better assessed in a prospective fashion. In our study, patients with bilateral inflammation tended to have a recurrence of disease at approximately 20 months, similar to or slightly earlier than reported in a series 19 of patients with acute anterior uveitis, with a median time to first recurrence of 24 months. This same study 19 also reported a significant decrease in time to first recurrence for patients with bilateral disease. A diagnosis of TINU syndrome was made for 2 patients. First described in 1975, 20 TINU syndrome is a rare cause of uveitis originally thought to be more common in young women, 20 with a more recent series reporting an equal sex distribution or even a preponderance of male patients. 21 Urine 2 microglobulin is often used as a screening test and was elevated in 11 of 12 patients in a series of patients with biopsy-confirmed TINU syndrome. 22 HLA-DRB1*0102 has also been associated with TINU syndrome, 23 and the allele may be an independent risk factor for simultaneous-onset BAAU. 5 This marker was not tested for in our series. Although TINU syndrome is a diagnosis of exclusion, diagnostic criteria have been proposed. 20,22 A series by Mackensen et al 21 from a tertiary referral center identified TINU syndrome in 1.7% of all new uveitis referrals and 10% of patients presenting with BAAU. A subgroup analysis on patients 20 years of age or younger identified TINU syndrome in 32% of them. 21 These rates are higher than reported in the present study. However, only 40% of our patients underwent urine analysis for 2 microglobulin, and we suspect that TINU syndrome may have been underdiagnosed. Three of the 17 patients tested had elevated urine 2 microglobulin levels. One of these patients was presumed to have an elevated level owing to a kidney stone. The other 2 patients had confirmation of the diagnosis of TINU syndrome by a nephrologist, resulting in a diagnosis of TINU syndrome in 12% of the tested patients with BAAU, similar to the rate reported by Mackensen et al. 21 Tubulointerstitial nephritis and uveitis syndrome is associated with the use of numerous systemic drugs. In one review of TINU syndrome, 17 24% of cases occurred in patients after antibiotic use, often to treat respiratory infections, and 18% of patients reported recent use of a non- 1393
6 steroidal anti-inflammatory drug. A spectrum of postinfectious and drug-induced uveitis may therefore exist that includes postinfectious or drug-induced uveitis without renal disease and TINU syndrome. In our study, the use of systemic nonsteroidal anti-inflammatory drugs prior to presentation was not documented. However, in light of their possible role as a trigger for inflammation, we now ask all uveitis patients about recent use of systemic nonsteroidal anti-inflammatory drugs. The other diagnoses in this series were inflammatory bowel disease and Kawasaki disease, and both were diagnosed prior to the onset of uveitis. Up to 14% of patients with inflammatory bowel disease develop ocular inflammation, 20 but, unlike the patient in our study, the most common presentation is chronic anterior uveitis. Kawasaki disease is a known cause of BAAU. One study 24 reported that 66% of children with Kawasaki disease developed anterior uveitis; 97% of them had bilateral disease. This type of systemic vasculitis typically presents with high fevers and a red tongue, which has been coined strawberry tongue. 24 Patients with this presentation should be referred for immediate care to decrease the risk of coronary artery aneurysm. In summary, symptomatic BAAU is an unusual presentation of uveitis that is more common in young patients. It must be distinguished from the insidious onset of anterior uveitis seen in children with juvenile idiopathic arthritis. Obtaining a detailed and thorough history, including queries regarding recent infection and use of systemic antibiotics or nonsteroidal anti-inflammatory drugs, may help elucidate a diagnosis. A complete review of systems, specifically focusing on possible systemic infection, gastrointestinal dysfunction, or signs of systemic vasculitis in a child, should be included. Diagnoses to consider include postinfectious or drug-induced uveitis and TINU syndrome. Diagnostic testing should include urine 2 microglobulin testing, HLA-B27 antigen testing, and ASO titers. Making an appropriate diagnosis is important in these young patients because each disease has its own set of associated systemic implications. Submitted for Publication: February 21, 2012; final revision received April 24, 2012; accepted May 1, Published Online: July 9, doi: /archophthalmol Correspondence: Debra A. Goldstein, MD, Department of Ophthalmology and Visual Sciences, University of Illinois at Chicago, 1855 W Taylor St, Chicago, IL (debrgold@uic.edu). Financial Disclosure: None reported. Funding/Support: This work was supported by an unrestricted grant from Research to Prevent Blindness, New York, New York (to Dr Goldstein). REFERENCES 1. McCannel CA, Holland GN, Helm CJ, Cornell PJ, Winston JV, Rimmer TG; UCLA Community-Based Uveitis Study Group. Causes of uveitis in the general practice of ophthalmology. Am J Ophthalmol. 1996;121(1): Suhler EB, Lloyd MJ, Choi D, Rosenbaum JT, Austin DF. Incidence and prevalence of uveitis in Veterans Affairs Medical Centers of the Pacific Northwest. Am J Ophthalmol. 2008;146(6):890.e8-896.e8. 3. Rodriguez A, Calonge M, Pedroza-Seres M, et al. Referral patterns of uveitis in a tertiary eye care center. Arch Ophthalmol. 1996;114(5): Jabs DA, Nussenblatt RB, Rosenbaum JT; Standardization of Uveitis Nomenclature (SUN) Working Group. Standardization of uveitis nomenclature for reporting clinical data: results of the First International Workshop. Am J Ophthalmol. 2005;140(3): Mackensen F, David F, Schwenger V, et al. HLA-DRB1*0102 is associated with TINU syndrome and bilateral, sudden-onset anterior uveitis but not with interstitial nephritis alone. Br J Ophthalmol. 2011;95(7): Tuncer S, Adam YS, Urgancioglu M, Tugal-Tutkun I. Clinical features and outcomes of HLA-b27-positive and HLA-B27-negative acute anterior uveitis in a Turkish patient population. Ocul Immunol Inflamm. 2005;13(5): Bañares A, Jover JA, Fernández-Gutiérrez B, et al. Patterns of uveitis as a guide in making rheumatologic and immunologic diagnoses. Arthritis Rheum. 1997; 40(2): Cokingtin CD, Han DP. Bilateral nongranulomatous uveitis and a poststreptococcal syndrome. Am J Ophthalmol. 1991;112(5): Shet A, Kaplan EL. Clinical use and interpretation of group A streptococcal antibody tests: a practical approach for the pediatrician or primary care physician. Pediatr Infect Dis J. 2002;21(5): , quiz Ur Rehman S, Anand S, Reddy A, et al. Poststreptococcal syndrome uveitis: a descriptive case series and literature review. Ophthalmology. 2006;113(4): Amigo MC, Martínez-Lavín M, Reyes PA. Acute rheumatic fever. Rheum Dis Clin North Am. 1993;19(2): Walker S, Iguchi A, Jones NP. Frosted branch angiitis: a review. Eye (Lond). 2004; 18(5): Feltkamp TE. Ophthalmological significance of HLA associated uveitis. Eye (Lond). 1990;4(Pt 6): Mapstone R, Woodrow JC. HL-A 27 and acute anterior uveitis. Br J Ophthalmol. 1975;59(5): Misiuk-Hojło M, Międzybrodzki R, Grzybowski A, et al. Elevated levels of antiendotoxin antibodies in patients with bilateral idiopathic acute anterior uveitis. Acta Ophthalmol. 2011;89(3):e283-e Khan MA, Braun WE, Kushner I, Grecek DE, Muir WA, Steinberg AG. HLA B27 in ankylosing spondylitis: differences in frequency and relative risk in American Blacks and Caucasians. J Rheumatol Suppl. 1977;3: Dobrin RS, Vernier RL, Fish AL. Acute eosinophilic interstitial nephritis and renal failure with bone marrow-lymph node granulomas and anterior uveitis: a new syndrome. Am J Med. 1975;59(3): Rosenbaum JT, McDevitt HO, Guss RB, Egbert PR. Endotoxin-induced uveitis in rats as a model for human disease. Nature. 1980;286(5773): Natkunarajah M, Kaptoge S, Edelsten C. Risks of relapse in patients with acute anterior uveitis. Br J Ophthalmol. 2007;91(3): Mandeville JT, Levinson RD, Holland GN. The tubulointerstitial nephritis and uveitis syndrome. Surv Ophthalmol. 2001;46(3): Mackensen F, Smith JR, Rosenbaum JT. Enhanced recognition, treatment, and prognosis of tubulointerstitial nephritis and uveitis syndrome. Ophthalmology. 2007;114(5): Goda C, Kotake S, Ichiishi A, Namba K, Kitaichi N, Ohno S. Clinical features in tubulointerstitial nephritis and uveitis (TINU) syndrome. Am J Ophthalmol. 2005; 140(4): Levinson RD, Park MS, Rikkers SM, et al. Strong associations between specific HLA-DQ and HLA-DR alleles and the tubulointerstitial nephritis and uveitis syndrome. Invest Ophthalmol Vis Sci. 2003;44(2): Burns JC, Joffe L, Sargent RA, Glode MP. Anterior uveitis associated with Kawasaki syndrome. Pediatr Infect Dis. 1985;4(3):
Uveitis of spondyloarthritis in Indian subcontinent: a cross sectional study
 International Journal of Advances in Medicine Ninan F et al. Int J Adv Med. 2017 Oct;4(5):1441-1446 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174300
International Journal of Advances in Medicine Ninan F et al. Int J Adv Med. 2017 Oct;4(5):1441-1446 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174300
A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D.
 A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D. I. Introduction II. III. IV. A. Why I am giving this talk B. What to take from lecture Diagnosis 1. Better understanding
A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D. I. Introduction II. III. IV. A. Why I am giving this talk B. What to take from lecture Diagnosis 1. Better understanding
Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior Uveitis in a Korean Population
 J Korean Med Sci 2009; 24: 722-8 ISSN 1011-8934 DOI: 10.3346/jkms.2009.24.4.722 Copyright The Korean Academy of Medical Sciences Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior
J Korean Med Sci 2009; 24: 722-8 ISSN 1011-8934 DOI: 10.3346/jkms.2009.24.4.722 Copyright The Korean Academy of Medical Sciences Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior
JOURNAL OF OPHTHALMOLOGY AND RELATED SCIENCES
 JOURNAL OF OPHTHALMOLOGY AND RELATED SCIENCES BILATERAL ACUTE TRANSILLUMINATION OF THE IRIS Kavitha Avadhani 1, MD, MS, Jay Kalliath 1, MS, FRCS 1 Department of Ophthalmology, NMC Speciality Hospital,
JOURNAL OF OPHTHALMOLOGY AND RELATED SCIENCES BILATERAL ACUTE TRANSILLUMINATION OF THE IRIS Kavitha Avadhani 1, MD, MS, Jay Kalliath 1, MS, FRCS 1 Department of Ophthalmology, NMC Speciality Hospital,
Nausheen Khuddus, MD Melissa Elder, MD, PhD
 Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
Approach to Pediatric Uveitis. Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Service
 Approach to Pediatric Uveitis Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Service Epidemiology Uveitis is the 3 rd leading cause of blindness in USA 5-10% of uveitis cases involve children
Approach to Pediatric Uveitis Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Service Epidemiology Uveitis is the 3 rd leading cause of blindness in USA 5-10% of uveitis cases involve children
Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient
 CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
Review Article Gender and Spondyloarthropathy-Associated Uveitis
 Ophthalmology Volume 2013, Article ID 928264, 6 pages http://dx.doi.org/10.1155/2013/928264 Review Article Gender and Spondyloarthropathy-Associated Uveitis Wendy M. Smith MayoClinic,200FirstStreetSW,Rochester,MN55905,USA
Ophthalmology Volume 2013, Article ID 928264, 6 pages http://dx.doi.org/10.1155/2013/928264 Review Article Gender and Spondyloarthropathy-Associated Uveitis Wendy M. Smith MayoClinic,200FirstStreetSW,Rochester,MN55905,USA
A Clinical Study of Anterior Uveitis in a Rural Hospital
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
Patterns of Uveitis at a Tertiary Referral Center in Southern Iran
 Original Article Patterns of Uveitis at a Tertiary Referral Center in Southern Iran Mansour Rahimi, MD; Ghazaleh Mirmansouri, MD Poustchi Eye Research Center and Ophthalmology Department, Shiraz University
Original Article Patterns of Uveitis at a Tertiary Referral Center in Southern Iran Mansour Rahimi, MD; Ghazaleh Mirmansouri, MD Poustchi Eye Research Center and Ophthalmology Department, Shiraz University
Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia
 JKAU: Med. Sci., Vol. 19 No. 3, pp: 73-83 (2012 A.D. / 1433 A.H.) DOI: 10.4197/Med. 19-3.6 Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia Nizamuddin Shaik Hakim Mohammad
JKAU: Med. Sci., Vol. 19 No. 3, pp: 73-83 (2012 A.D. / 1433 A.H.) DOI: 10.4197/Med. 19-3.6 Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia Nizamuddin Shaik Hakim Mohammad
HLA-B27-related anterior Uveitis
 HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
REFRESHER: ANTERIOR UVEITIS
 REFRESHER: ANTERIOR UVEITIS 2. SAoO Kongress 28.2.2018 Messe Luzern Dr. med. Christian Böni Augenklinik Universitätsspital Zürich Christian Böni Seite 1 Anterior Uveitis: Clinical Issues Diagnostics: yes
REFRESHER: ANTERIOR UVEITIS 2. SAoO Kongress 28.2.2018 Messe Luzern Dr. med. Christian Böni Augenklinik Universitätsspital Zürich Christian Böni Seite 1 Anterior Uveitis: Clinical Issues Diagnostics: yes
High-speed optical coherence tomography as a reliable adjuvant tool to grade ocular anterior chamber inflammation.
 Thomas Jefferson University Jefferson Digital Commons Wills Eye Institute Papers Wills Eye Institute 3-2014 High-speed optical coherence tomography as a reliable adjuvant tool to grade ocular anterior
Thomas Jefferson University Jefferson Digital Commons Wills Eye Institute Papers Wills Eye Institute 3-2014 High-speed optical coherence tomography as a reliable adjuvant tool to grade ocular anterior
Diagnosis of uveitis, how to proceed?
 EOS meeting Cairo, 2018 Diagnosis of uveitis, how to proceed? Mohamed G.A Saleh Lecturer of Ophthalmology Assiut University Size of the problem 15/100000 in US every year. 10% of blindness Prevalence varies
EOS meeting Cairo, 2018 Diagnosis of uveitis, how to proceed? Mohamed G.A Saleh Lecturer of Ophthalmology Assiut University Size of the problem 15/100000 in US every year. 10% of blindness Prevalence varies
Anthony DeWilde, O.D Linwood Blvd. Kansas City, MO x
 Anthony DeWilde, O.D. 4801 Linwood Blvd. Kansas City, MO 64128 816-861-4700 x 57411 anthony.dewilde@va.gov Uveitis and Glaucoma: The Seven Reasons Why IOP Can Increase in Uveitis (and What to do About
Anthony DeWilde, O.D. 4801 Linwood Blvd. Kansas City, MO 64128 816-861-4700 x 57411 anthony.dewilde@va.gov Uveitis and Glaucoma: The Seven Reasons Why IOP Can Increase in Uveitis (and What to do About
Association of Cryptogenic Organizing Pneumonia in Bilateral Anterior Uveitis
 Published online: November 13, 2014 1663 2699/14/0053 0365$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: November 13, 2014 1663 2699/14/0053 0365$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Intravitreal Triamcinolone Acetonide for Macular Edema in HLA-B27 Negative Ankylosing Spondylitis
 105 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
105 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
o White dot syndromes pattern recognition o Activity and damage o Quality of life o Key points o Idiopathic o Sarcoidosis o Multiple sclerosis
 Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Rheumatic Fever And Post-streptococcal Reactive Arthritis
 www.printo.it/pediatric-rheumatology/ie/intro Rheumatic Fever And Post-streptococcal Reactive Arthritis Version of 2016 2. DIAGNOSIS AND THERAPY 2.1 How is it diagnosed? Clinical signs and investigations
www.printo.it/pediatric-rheumatology/ie/intro Rheumatic Fever And Post-streptococcal Reactive Arthritis Version of 2016 2. DIAGNOSIS AND THERAPY 2.1 How is it diagnosed? Clinical signs and investigations
Head prof. MUDr. E. Vlková, CSc.
 MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Cases CFEH. CFEH Facebook Case #4
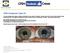 CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
WHAT IS YOUR DIAGNOSIS? By ADREA R. BENKOFF M.D.
 WHAT IS YOUR DIAGNOSIS? By ADREA R. BENKOFF M.D. Anterior Chamber Inflammation and Iris Depigmentation Noted 25 Years After Cataract Extraction Decreasing Vision Over a 5- Year Period 64 year old white
WHAT IS YOUR DIAGNOSIS? By ADREA R. BENKOFF M.D. Anterior Chamber Inflammation and Iris Depigmentation Noted 25 Years After Cataract Extraction Decreasing Vision Over a 5- Year Period 64 year old white
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO
 Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO brujic@prodigy.net Summary As optometry s role in health care increases, so does our responsibility to appropriately diagnose and appropriately
Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO brujic@prodigy.net Summary As optometry s role in health care increases, so does our responsibility to appropriately diagnose and appropriately
Sarcoidosis and Uveitis
 Sarcoidosis and Uveitis Nicholas Jones Royal Eye Hospital Manchester, UK Sarcoidosis a multisystem chronic inflammation causing multifocal non-caseating granulomas BUT Diagnosis often made indirectly (without
Sarcoidosis and Uveitis Nicholas Jones Royal Eye Hospital Manchester, UK Sarcoidosis a multisystem chronic inflammation causing multifocal non-caseating granulomas BUT Diagnosis often made indirectly (without
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Pauciarticular juvenile rheumatoid arthritis: clinical and immunogenetic aspects
 Ann. rheum. Dis. (1979), 38, Supplement p. 79 Pauciarticular juvenile rheumatoid arthritis: clinical and immunogenetic aspects CHESTER W. FINK, AND PETER STASTNY From the University of Texas Southwestern
Ann. rheum. Dis. (1979), 38, Supplement p. 79 Pauciarticular juvenile rheumatoid arthritis: clinical and immunogenetic aspects CHESTER W. FINK, AND PETER STASTNY From the University of Texas Southwestern
Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcus (PANDAS) Brittany Andry, MD PGY III Pediatric Resident LSUHSC
 Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcus (PANDAS) Brittany Andry, MD PGY III Pediatric Resident LSUHSC Objectives Learn the diagnostic criteria of Pediatric Autoimmune
Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcus (PANDAS) Brittany Andry, MD PGY III Pediatric Resident LSUHSC Objectives Learn the diagnostic criteria of Pediatric Autoimmune
Mycobacterial Ocular Inflammation. Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah
 Mycobacterial Ocular Inflammation Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah Financial Disclosure I have no financial interests or relationships to disclose. Applied anatomy What
Mycobacterial Ocular Inflammation Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah Financial Disclosure I have no financial interests or relationships to disclose. Applied anatomy What
Eye (2009) 23, & 2009 Macmillan Publishers Limited All rights reserved X/09 $32.00
 (2009) 23, 543 548 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Effects of the duration of initial oral corticosteroid treatment on the recurrence of inflammation
(2009) 23, 543 548 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye Effects of the duration of initial oral corticosteroid treatment on the recurrence of inflammation
KAWASAKI DISEASE. What is Kawasaki disease? Causes
 What is Kawasaki disease? Kawasaki disease is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict blood flow and damage vital organs and
What is Kawasaki disease? Kawasaki disease is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict blood flow and damage vital organs and
An Observational Descriptive Cross-Sectional Study of 200 Iraqi Adult Patients with Ankylosing Spondylitis: Analysis of Ocular Manifestations
 An Observational Descriptive Cross-Sectional Study of 200 Iraqi Adult Patients with Ankylosing Spondylitis: Analysis of Ocular Manifestations Khudair Al-Bedri 1 Najah K. Mohammad Al-Quriashi 2 Faiq I.
An Observational Descriptive Cross-Sectional Study of 200 Iraqi Adult Patients with Ankylosing Spondylitis: Analysis of Ocular Manifestations Khudair Al-Bedri 1 Najah K. Mohammad Al-Quriashi 2 Faiq I.
Juvenile Spondyloarthritis / Enthesitis Related Arthritis (SpA-ERA)
 www.printo.it/pediatric-rheumatology/gb/intro Juvenile Spondyloarthritis / Enthesitis Related Arthritis (SpA-ERA) Version of 2016 1. WHAT IS JUVENILE SPONDYLOARTHRITIS/ENTHESITIS- RELATED ARTHRITIS (SpA-ERA)
www.printo.it/pediatric-rheumatology/gb/intro Juvenile Spondyloarthritis / Enthesitis Related Arthritis (SpA-ERA) Version of 2016 1. WHAT IS JUVENILE SPONDYLOARTHRITIS/ENTHESITIS- RELATED ARTHRITIS (SpA-ERA)
RHEUMATIC FEVER RHF-1. Disease name. Basis of diagnosis
 RHF-1 RHEUMATIC FEVER Disease name Disease Indicate whether this is an initial (i.e first) attack of rheumatic fever or a recurrent attack (an episode in a person with known past history of acute rheumatic
RHF-1 RHEUMATIC FEVER Disease name Disease Indicate whether this is an initial (i.e first) attack of rheumatic fever or a recurrent attack (an episode in a person with known past history of acute rheumatic
Case Presentation. By Eman El Sharkawy Ass. Professor of cardiology Alexandria University
 Case Presentation By Eman El Sharkawy Ass. Professor of cardiology Alexandria University 6m old baby girl Past history : - At the age of 2m attack of fever, diarrhea, mouth ulcers, difficult breast feeding
Case Presentation By Eman El Sharkawy Ass. Professor of cardiology Alexandria University 6m old baby girl Past history : - At the age of 2m attack of fever, diarrhea, mouth ulcers, difficult breast feeding
*HSP is a common vasculitis of small vessels with cutaneous & systemic complications. Its etiology is unknown& often follows URTIs.
 BY Introduction The disease is eponymously named after Eduard heinrich Henoch (1820-1910), a German pediatrician, and his teacher Johann Lukas Schonlein (1793-1864), who described it in the 1860s. Cont
BY Introduction The disease is eponymously named after Eduard heinrich Henoch (1820-1910), a German pediatrician, and his teacher Johann Lukas Schonlein (1793-1864), who described it in the 1860s. Cont
LECOM Health Ophthalmology
 Patient Name: Date of Birth: New Patient Questionnaire Your answers will be used by your healthcare provider get an accurate history of your medical conditions and ocular concerns. If you are uncomfortable
Patient Name: Date of Birth: New Patient Questionnaire Your answers will be used by your healthcare provider get an accurate history of your medical conditions and ocular concerns. If you are uncomfortable
Two Cases of Uveitis with Tubulointerstitial Nephritis in HTLV-1 Carriers
 Two Cases of Uveitis with Tubulointerstitial Nephritis in HTLV-1 Carriers Hiroko Eida Deguchi and Tsugio Amemiya Department of Ophthalmology and Visual Sciences, Graduate School of Biomedical Sciences,
Two Cases of Uveitis with Tubulointerstitial Nephritis in HTLV-1 Carriers Hiroko Eida Deguchi and Tsugio Amemiya Department of Ophthalmology and Visual Sciences, Graduate School of Biomedical Sciences,
Uveitis associated with acute interstitial nephritis (AIN)
 Strong Associations between Specific HLA-DQ and HLA-DR Alleles and the Tubulointerstitial Nephritis and Uveitis Syndrome Ralph D. Levinson, 1,2 Min S. Park, 3 Sarah M. Rikkers, 1,2 Elaine F. Reed, 3 Justine
Strong Associations between Specific HLA-DQ and HLA-DR Alleles and the Tubulointerstitial Nephritis and Uveitis Syndrome Ralph D. Levinson, 1,2 Min S. Park, 3 Sarah M. Rikkers, 1,2 Elaine F. Reed, 3 Justine
Management of uveitis
 Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
hemolytic streptococci were
 THE RELATION OF THE SERUM ANTISTREPTOLYSIN TITER TO THE EXACERBATION IN CHRONIC GLOMERULONEPHRITIS By DAVID P. EARLE, JR., DAVID SEEGAL, JOHN D. LYTTLE, EMILY N. LOEB, AND ELIZABETH L. JOST (From the Research
THE RELATION OF THE SERUM ANTISTREPTOLYSIN TITER TO THE EXACERBATION IN CHRONIC GLOMERULONEPHRITIS By DAVID P. EARLE, JR., DAVID SEEGAL, JOHN D. LYTTLE, EMILY N. LOEB, AND ELIZABETH L. JOST (From the Research
10/18/2018. Unraveling Uveitis
 Unraveling Uveitis Trenton Cleghern, OD, FAAO VisionAmerica UAB School of Optometry 11/10/2018 1 Disclosure Statement: Nothing to disclose 2 Objectives Classify uveitis Current and new therapeutic options
Unraveling Uveitis Trenton Cleghern, OD, FAAO VisionAmerica UAB School of Optometry 11/10/2018 1 Disclosure Statement: Nothing to disclose 2 Objectives Classify uveitis Current and new therapeutic options
Bilateral multiple choroidal granulomas and systemic vasculitis as presenting features of tuberculosis in an immunocompetent patient
 Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
UVEITIS. Dr. Yılmaz ÖZYAZGAN
 UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
Laboratory Testing and Systemic Investigations in Uveitis
 Laboratory Testing and Systemic Investigations in Uveitis Investigating Uveitis A Tailored Approach Nicholas Jones The Royal Eye Hospital Manchester, UK Nicholas Jones Manchester Uveitis Clinic Manchester
Laboratory Testing and Systemic Investigations in Uveitis Investigating Uveitis A Tailored Approach Nicholas Jones The Royal Eye Hospital Manchester, UK Nicholas Jones Manchester Uveitis Clinic Manchester
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis
 Haddad and Reddy Journal of Ophthalmic Inflammation and Infection 2014, 4:28 BRIEF REPORT Open Access Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis Zeina
Haddad and Reddy Journal of Ophthalmic Inflammation and Infection 2014, 4:28 BRIEF REPORT Open Access Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis Zeina
Sarcoidosis. Julia Rhiannon Harborview/UW Rheumatology November 2010
 Sarcoidosis Julia Rhiannon Harborview/UW Rheumatology November 2010 julrhi@uw.edu outline Introduction/Epi/Genetics Clinical features Acute/Lofgren s vs chronic Pathogenesis Treatment sarc eidos osis flesh
Sarcoidosis Julia Rhiannon Harborview/UW Rheumatology November 2010 julrhi@uw.edu outline Introduction/Epi/Genetics Clinical features Acute/Lofgren s vs chronic Pathogenesis Treatment sarc eidos osis flesh
In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between
 In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between the two, we also propose a classification system for
In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between the two, we also propose a classification system for
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Uveitis Update DISCLOSURE STATEMENT. Featured Speaker: Dr. Kyle Cheatham, FAAO, DIP ABO
 Uveitis Update Featured Speaker: Dr. Kyle Cheatham, FAAO, DIP ABO DISCLOSURE STATEMENT We have no direct financial or proprietary interest in any companies, products or services mentioned in this presentation.
Uveitis Update Featured Speaker: Dr. Kyle Cheatham, FAAO, DIP ABO DISCLOSURE STATEMENT We have no direct financial or proprietary interest in any companies, products or services mentioned in this presentation.
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
2/23/18. Disclosures. Rheumatic Diseases of Childhood. Making Room for Rheumatology. I have nothing to disclose. James J.
 Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
2/16/17. 3 main underlying causes are:
 Definition Etiology Signs/Symptoms Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College
Definition Etiology Signs/Symptoms Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College
Learning about Lupus. Learning About Lupus. Lupus Society of Illinois
 Learning About Lupus Learning about Lupus Lupus Society of Illinois 525 W. Monroe Street, Suite 900 Chicago, Illinois 60661 Robert S. Katz, M.D. Professor of Medicine Rush University Medical Center Northwestern
Learning About Lupus Learning about Lupus Lupus Society of Illinois 525 W. Monroe Street, Suite 900 Chicago, Illinois 60661 Robert S. Katz, M.D. Professor of Medicine Rush University Medical Center Northwestern
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults
 Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Case Presentation VASCULITIS. Case Presentation. Case Presentation. Vasculitis
 Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Role of high-resolution computerized tomography chest in identifying tubercular etiology in patients diagnosed as Eales disease
 Kharel (Sitaula) et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:4 DOI 10.1186/s12348-016-0120-1 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Role of
Kharel (Sitaula) et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:4 DOI 10.1186/s12348-016-0120-1 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Role of
Clarithromycin versus penicillin in the treatment of streptococcal pharyngitis
 Journal of Antimicrobial Chemotherapy (1991) 27, Suppl. A, 67-74 Clarithromycin versus penicillin in the treatment of streptococcal pharyngitis Joseph H. Levenstein* South Africa Academy of Family Practice,
Journal of Antimicrobial Chemotherapy (1991) 27, Suppl. A, 67-74 Clarithromycin versus penicillin in the treatment of streptococcal pharyngitis Joseph H. Levenstein* South Africa Academy of Family Practice,
Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
VASCULITIS. Case Presentation. Case Presentation
 VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Optical coherence tomography findings in a child with posterior scleritis
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
3 main underlying causes are:
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu
Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu
5/2/2016 EYE EMERGENCIES. Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates. Anatomy. Tools
 EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
Acute (Tubulo-) Interstitial Nephritis (TIN)
 Acute (Tubulo-) Interstitial Nephritis (TIN) Rodney D Gilbert Case 1 16 year old girl with intractable psychosis Started Clozapine Monitored closely 6 weeks later: AKI Creatinine 200 How would you manage?
Acute (Tubulo-) Interstitial Nephritis (TIN) Rodney D Gilbert Case 1 16 year old girl with intractable psychosis Started Clozapine Monitored closely 6 weeks later: AKI Creatinine 200 How would you manage?
Evaluation of corneal endothelium and keratic precipitates by specular microscopy in anterior uveitis
 Br J Ophthalmol 2000;84:1367 1371 1367 Department of Ophthalmology, B Floor, South Block, University Hospital, Queen s Medical Centre, Nottingham NG7 2UH, UK C T Pillai H S Dua A Azuara-Blanco A R Sarhan
Br J Ophthalmol 2000;84:1367 1371 1367 Department of Ophthalmology, B Floor, South Block, University Hospital, Queen s Medical Centre, Nottingham NG7 2UH, UK C T Pillai H S Dua A Azuara-Blanco A R Sarhan
Oral azithromycin combined with topical anti-inflammatory agents in the treatment of blepharokeratoconjunctivitis in children
 Oral azithromycin combined with topical anti-inflammatory agents in the treatment of blepharokeratoconjunctivitis in children Daniel S. Choi, BA, and Ali Djalilian, MD Author affiliations: Department of
Oral azithromycin combined with topical anti-inflammatory agents in the treatment of blepharokeratoconjunctivitis in children Daniel S. Choi, BA, and Ali Djalilian, MD Author affiliations: Department of
DISCLOSURES. PEDIATRIC RED EYES Rachel M. Smith, OD, FCOVD HISTORY, HISTORY, HISTORY WHY RED EYES? EXAMINE THE EYE RED FLAGS TO REFER 3/25/2019
 DISCLOSURES Consultant/Speakers bureaus Research funding PEDIATRIC RED EYES Rachel M. Smith, OD, FCOVD Pediatric Optometrist Children s Hospital & Medical Center Stock ownership/corporate boards employment
DISCLOSURES Consultant/Speakers bureaus Research funding PEDIATRIC RED EYES Rachel M. Smith, OD, FCOVD Pediatric Optometrist Children s Hospital & Medical Center Stock ownership/corporate boards employment
ANCA associated vasculitis in China
 ANCA associated vasculitis in China Min Chen Renal Division, Peking University First Hospital, Beijing 100034, P. R. China 1 General introduction of AAV in China Disease spectrum and ANCA type Clinical
ANCA associated vasculitis in China Min Chen Renal Division, Peking University First Hospital, Beijing 100034, P. R. China 1 General introduction of AAV in China Disease spectrum and ANCA type Clinical
RARE JUVENILE PRIMARY SYSTEMIC VASCULITIS
 www.pediatric-rheumathology.printo.it RARE JUVENILE PRIMARY SYSTEMIC VASCULITIS WHAT IS IT? Vasculitis is an inflammation of blood vessels. Vasculitides cover a wide group of diseases. Primary vasculitis
www.pediatric-rheumathology.printo.it RARE JUVENILE PRIMARY SYSTEMIC VASCULITIS WHAT IS IT? Vasculitis is an inflammation of blood vessels. Vasculitides cover a wide group of diseases. Primary vasculitis
CLINICAL VIGNETTE Sarcoidosis: A Case Study Gloria Kim, M.D.
 CLINICAL VIGNETTE Sarcoidosis: A Case Study Gloria Kim, M.D. Case Report A 56-year-old female presented to her primary care physician with complaints of dyspnea on exertion and increasing cough. She reported
CLINICAL VIGNETTE Sarcoidosis: A Case Study Gloria Kim, M.D. Case Report A 56-year-old female presented to her primary care physician with complaints of dyspnea on exertion and increasing cough. She reported
Cardiac Sarcoidosis. Millee Singh DO Non Invasive Cardiology First Coast Heart and Vascluar
 Cardiac Sarcoidosis Millee Singh DO Non Invasive Cardiology First Coast Heart and Vascluar Introduction Multisystem granulomatous disease of unknown etiology characterized by noncaseating granulomas in
Cardiac Sarcoidosis Millee Singh DO Non Invasive Cardiology First Coast Heart and Vascluar Introduction Multisystem granulomatous disease of unknown etiology characterized by noncaseating granulomas in
ACP Rheumatology Pearls. Adam Q Carlson MD Assistant Professor UVA Rheumatology
 ACP Rheumatology Pearls Adam Q Carlson MD Assistant Professor UVA Rheumatology Disclosures I have no personal or professional disclosures Case #1 27 yo woman with a history of systemic lupus complicated
ACP Rheumatology Pearls Adam Q Carlson MD Assistant Professor UVA Rheumatology Disclosures I have no personal or professional disclosures Case #1 27 yo woman with a history of systemic lupus complicated
Re-emerging infections: Syphilis & Tuberculosis
 Re-emerging infections: Syphilis & Tuberculosis Nicholas Jones Manchester Royal Eye Hospital Syphilis and TB - historical plagues? Syphilis incidence over 40yrs Manchester: Manchester: The Syphilis Capital
Re-emerging infections: Syphilis & Tuberculosis Nicholas Jones Manchester Royal Eye Hospital Syphilis and TB - historical plagues? Syphilis incidence over 40yrs Manchester: Manchester: The Syphilis Capital
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
!! Definition. !! Etiology. !! Signs/Symptoms. !! Classification/Diagnosis. !! Systemic Associations. !! Lab Testing. !! Treatment. !!
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu!!
Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu!!
Combined Infliximab and Rituximab in Necrotising Scleritis
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
RHEUMATIC FEVER AND POST-STREPTOCOCCAL REACTIVE ARTHRITIS
 www.pediatric-rheumathology.printo.it RHEUMATIC FEVER AND POST-STREPTOCOCCAL REACTIVE ARTHRITIS What is it? Rheumatic fever has been defined as a disease triggered by infection caused by streptococcus.
www.pediatric-rheumathology.printo.it RHEUMATIC FEVER AND POST-STREPTOCOCCAL REACTIVE ARTHRITIS What is it? Rheumatic fever has been defined as a disease triggered by infection caused by streptococcus.
CLINICAL SCIENCES. Antineutrophil Cytoplasmic Antibody Associated Active Scleritis
 CLINICAL SCIENCES Antineutrophil Cytoplasmic Antibody Associated Active Scleritis Lani T. Hoang, MD; Lyndell L. Lim, MBBS, FRANZCO; Brian Vaillant, MD; Dongseok Choi, PhD; James T. Rosenbaum, MD Objective:
CLINICAL SCIENCES Antineutrophil Cytoplasmic Antibody Associated Active Scleritis Lani T. Hoang, MD; Lyndell L. Lim, MBBS, FRANZCO; Brian Vaillant, MD; Dongseok Choi, PhD; James T. Rosenbaum, MD Objective:
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry
 doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
Behcet's Disease in Bahrain, Clinical and HLA Findings
 Bahrain Medical Bulletin, Vol.23, No., March 200 Behcet's Disease in Bahrain, Clinical and HLA Findings Reda Ali Ebrahim, MD, FRCP* Raed Al Alawi, MD** Eman Farid, MD,PhD*** Objective: To study the clinical
Bahrain Medical Bulletin, Vol.23, No., March 200 Behcet's Disease in Bahrain, Clinical and HLA Findings Reda Ali Ebrahim, MD, FRCP* Raed Al Alawi, MD** Eman Farid, MD,PhD*** Objective: To study the clinical
Rheumatic Fever And Post-streptococcal Reactive Arthritis
 www.printo.it/pediatric-rheumatology/gb/intro Rheumatic Fever And Post-streptococcal Reactive Arthritis Version of 2016 1. WHAT IS RHEUMATIC FEVER 1.1 What is it? Rheumatic fever is a disease caused by
www.printo.it/pediatric-rheumatology/gb/intro Rheumatic Fever And Post-streptococcal Reactive Arthritis Version of 2016 1. WHAT IS RHEUMATIC FEVER 1.1 What is it? Rheumatic fever is a disease caused by
Work Sheet And Course Hand Out
 Work Sheet And Course Hand Out This course provides the primary care health professional with a basic understanding of the eye, its function and the assessment of common sight- and non-sight threatening
Work Sheet And Course Hand Out This course provides the primary care health professional with a basic understanding of the eye, its function and the assessment of common sight- and non-sight threatening
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Case History. The SEVEN HABITS of Highly Effective Anterior Uveitis Management. SLEx findings: SLEx corneal findings: y.o.
 The SEVEN HABITS of Highly Effective Anterior Uveitis Management Case History! 68 y.o. Caucasian female of photophobia and blurred vision! As well as a headache over right eye for 2 days! Complains Paul
The SEVEN HABITS of Highly Effective Anterior Uveitis Management Case History! 68 y.o. Caucasian female of photophobia and blurred vision! As well as a headache over right eye for 2 days! Complains Paul
COVER FOCUS AT A GLANCE. BY LISA J. FAIA, MD, and KIMBERLY A. DRENSER, MD, PhD
 PEDIATRIC UVEITIS: CHALLENGING FOR OPHTHALMOLOGISTS, PATIENTS, AND PARENTS Management of these complicated diseases differs between pediatric and adult patient populations. BY LISA J. FAIA, MD, and KIMBERLY
PEDIATRIC UVEITIS: CHALLENGING FOR OPHTHALMOLOGISTS, PATIENTS, AND PARENTS Management of these complicated diseases differs between pediatric and adult patient populations. BY LISA J. FAIA, MD, and KIMBERLY
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
SYNOPSIS. Clinical Study Report IM Double-blind Period
 Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Abatacept () Name of Active Ingredient: Abatacept () Individual Study Table Referring to the Dossier SYNOPSIS (For National Authority
Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Abatacept () Name of Active Ingredient: Abatacept () Individual Study Table Referring to the Dossier SYNOPSIS (For National Authority
High Impact Rheumatology
 High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH)
 Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Case Presentation. Rafid Asfar, MD
 Case Presentation Rafid Asfar, MD Introduction ANCA associated vasculitis may be localized or systemic, and can involve the eyes Ocular manifestations can occur in the absence of systemic disease in persons
Case Presentation Rafid Asfar, MD Introduction ANCA associated vasculitis may be localized or systemic, and can involve the eyes Ocular manifestations can occur in the absence of systemic disease in persons
16.1 Risk of UTI recurrence in children
 16. UTI prognosis 16.1 Risk of UTI recurrence in children Key question: What is the risk of recurrent UTI in children with no known structural or functional abnormalities of the urinary tract with a first
16. UTI prognosis 16.1 Risk of UTI recurrence in children Key question: What is the risk of recurrent UTI in children with no known structural or functional abnormalities of the urinary tract with a first
Uveitis as an important ocular sign to help early diagnosis in Kawasaki disease
 Original article Choi Korean HS, J et Pediatr al. Uveitis 2015;58(10):374-379 in Kawasaki disease pissn 1738-1061 eissn 2092-7258 Korean J Pediatr Uveitis as an important ocular sign to help early diagnosis
Original article Choi Korean HS, J et Pediatr al. Uveitis 2015;58(10):374-379 in Kawasaki disease pissn 1738-1061 eissn 2092-7258 Korean J Pediatr Uveitis as an important ocular sign to help early diagnosis
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS. Myriam Farah, MD, FRCPC
 ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
