Mean Platelet Volume in Crohn s Disease Patients Predicts Sustained Response to a 52-Week Infliximab Therapy: A Pilot Study
|
|
|
- Helen Stafford
- 6 years ago
- Views:
Transcription
1 Dig Dis Sci (2016) 61: DOI /s ORIGINAL ARTICLE Mean Platelet Volume in Crohn s Disease Patients Predicts Sustained Response to a 52-Week Infliximab Therapy: A Pilot Study Aleksandra Sobolewska 1 Marcin Włodarczyk 1 Jakub Fichna 2 Maria Wiśniewska-Jarosińska 1 Krystyna Stec-Michalska 1 Received: 22 March 2015 / Accepted: 18 September 2015 / Published online: 6 October 2015 The Author(s) This article is published with open access at Springerlink.com Abstract Background The loss of response to infliximab in Crohn s disease (CD) patients is currently a major clinical problem. Recently, mean platelet volume (MPV) has been proposed as a new biomarker of CD activity. Here, we hypothesized that MPV may be used as cheap and efficient biomarker of subclinical inflammation during 52-week therapy in CD patients responding to infliximab induction treatment. Aims The aim of study was to establish whether MPV at baseline and pre-infusion at week 14 are good predictors of sustained response after week 14 in CD patients undergoing 52-week infliximab therapy. Methods A retrospective study of 30 adult CD patients who underwent a 52-week course of treatment with infliximab and achieved response at week 14 to induction treatment was performed. The association between MPV, baseline disease parameters and maintained clinical response or remission during infliximab therapy was assessed. Results Higher MPV at week 14 was observed in CD patients with sustained response to infliximab after week 14 than in patients with loss of response (p = ). In patients with loss of response to maintenance infliximab treatment, lower DMPV between baseline and week 14 was Aleksandra Sobolewska and Marcin Włodarczyk have contributed equally to this study. & Marcin Włodarczyk dr.mwlodarczyk@gmail.com 1 2 Department of Gastroenterology, Medical University of Lodz, Haller Sq. 1, Lodz, Poland Department of Biochemistry, Medical University of Lodz, Lodz, Poland calculated (p = ). MPV [ 10.3 fl at week 14 predicts sustained response with 67 % sensitivity and 80 % specificity. DMPV between baseline and week 14 [0.4 fl predicts sustained response with 87 % sensitivity and 93 % specificity. Conclusion MPV at week 14 and DMPV between baseline and week 14 are good predictors of sustained response to infliximab maintenance treatment in CD patients. Keywords Crohn s disease Infliximab Mean platelet volume Prognosis Treatment outcomes Introduction Crohn s disease (CD) is an inflammatory bowel disease (IBD) characterized by chronic, segmental granulomatous inflammation with periods of exacerbations and remissions, which may involve any part of the gastrointestinal (GI) tract [1]. The pathogenesis of the intestinal lesions in CD is not entirely understood. Elevated pro-inflammatory cytokine levels, mainly tumor necrosis factor alpha (TNF-a), have strong impact on the clinical manifestations and inflammatory lesions in the intestinal wall. The main target of IBD treatment is long-term remission. Attempts have been made to find an effective treatment biological therapy using anti-tnf-a antibodies, such as infliximab or adalimumab, is currently the most attractive form of treatment [1, 2]. The target of the anti-tnf-a therapy is mucosal healing and long-term clinical remission. Unfortunately, loss of response to biological agents is often observed in clinical practice, ranging from 23 to 46 % after 12 months in CD patients treated with infliximab or adalimumab [3]. The mechanism underlying clinical exacerbations during
2 Dig Dis Sci (2016) 61: biological treatment is not fully understood. The loss of response has been associated with the development of antibodies to anti-tnf-a agents and rapid drug clearance [3, 4]. It was also postulated that some other pathways involved in CD development may be responsible, for example those associated with pro-inflammatory cytokines, like IL-12, IL-17, and IL-23 [5 8]. Several blood parameters have been evaluated as potential indicators of disease activity and predictors of the risk of relapse in CD patients during biological treatment. The most commonly used are the following: C-reactive protein (CRP), erythrocyte sedimentation rate (ESR), white blood cell (WBC) count, acid glycoprotein, platelet count, albumin with fecal (calprotectin) and serologic markers [9]. Previous studies suggested that platelets might also be involved in the pathogenesis of CD [10 12]. The mean platelet volume (MPV) has been reported to be an independent laboratory marker of clinical IBD disease activity. It has been shown that decreased MPV correlates with increased disease activity in patients with ulcerative colitis (UC) and CD [12]. It was also demonstrated that treatment with anti-tnf-a agents, such as infliximab, significantly improves MPV in patients with inflammatory lesions in rheumatoid arthritis (RA) [13]. In this study, we hypothesized that MPV level may be a useful biomarker of subclinical inflammation in patients with CD responding to infliximab induction treatment and therefore may predict maintenance or loss of response to further treatment. The aim of the study was to establish whether MPV at baseline and pre-infusion at week 14 are good predictors of sustained response or remission after week 14 in CD patients undergoing 52-week anti-tnf-a therapy with infliximab. Methods Patients A retrospective study was conducted in 30 adult patients with CD of Caucasian origin (22 men and 8 women; mean age ± standard deviation 32.8 ± 8.7 years), who were qualified for 52-week therapy with infliximab from January 2008 to March 2014 at the Department of Gastroenterology of the Medical University of Lodz, Poland. The control group comprised 15 individuals students, staff, and patients with dyspepsia or irritable bowel syndrome, and was homogenous to the study group in terms of age, sex, and body mass index (BMI). CD was diagnosed and confirmed according to clinical, radiological, endoscopic, and histological criteria developed by the European Crohn s and Colitis Organisation (ECCO) [2]. The clinical state of each patient was classified at designated time points according to Crohn s Disease Activity Index (CDAI), which is a complex scoring system based on characteristic clinical symptoms, such as the number of liquid stools, severity of abdominal pain, general well-being, extraintestinal CD manifestations, abnormal abdominal mass, use of loperamide or opiates for diarrhea, hematocrit, and body weight [1, 2]. The CDAI is a validated clinical/laboratory scoring system, used largely in trial settings to assess the activity of disease and the response to treatment. Despite limitations, the score has been widely used to evaluate drug efficacy in CD over a 25-year period; secondly, and perhaps more importantly, it reflects and correlates with clinical assessment and patient well-being, which is the general basis on which treatments for CD are currently justified. Inclusion criteria for biological therapy were exacerbation of the underlying disease, CDAI over 300, and the ineffectiveness of previously used non-biological therapies, such as mesalazine, azathioprine, and corticosteroids. All patients had endoscopic activity of intestinal lesions with ulcers, seen at colonoscopy performed just prior to initiation of infliximab therapy. All CD patients enrolled to biological therapy received induction treatment with a 5 mg/kg infliximab infusion over 2 h at baseline and next infusion at dose of 5 mg/kg at 2 and 6 weeks. The maintenance treatment was administered at a dose of infliximab 5 mg/kg every 8 weeks. A 1 2 day departure from the scheme was allowed. The CD patients enrolled in the study were in response or clinical remission at week 14 (Scheme 1); in these patients, infliximab induction had been effective and maintenance treatment began. Response to anti-tnf-a treatment was defined as a reduction in CDAI score by C25 % and C70 points from baseline, and maintenance of response as a sustained response at each visit after infliximab induction treatment. Clinical remission of CD was defined as a CDAI score of \150. If response or remission was achieved at each visit after week 14, during the whole 52-week therapy, the patient was considered to have sustained response or remission in 52-week therapy. Loss of infliximab response after week 14 was defined as meeting one of the following criteria: (1) a CDAI score of C175 and an increase in CDAI score of C35 % and C70 points for at least two following clinic visits (C21 days); (2) undergoing CD-related surgery; and (3) crossover from scheduled therapy to episodic retreatment. The clinical status of each patient was assessed at each visit associated with drug administration, at 0, 2, 6 weeks, and every 8 week during maintenance treatment. Current smokers, obese patients (BMI [ 25 kg/m 2 ), patients with a history of cardiovascular disease, pulmonary and kidney disease, allergy, diabetes, lichen planus, psoriasis, atopic dermatitis and other autoimmune skin lesions and those treated with anti-inflammatory drugs
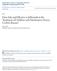
3 544 Dig Dis Sci (2016) 61: Inclusion criteria for biological therapy were exacerbation of the underlying disease, CDAI over 300 and the ineffectiveness of previously used non-biological therapies, such as mesalazine, azathioprine and corticosteroids. CD confirmed in colonoscopy specimens with histopathological examination. n= 95 Exclusion criteria: current smokers, obese patients (BMI >25 kg/m 2 ), patients with a history of cardiovascular disease, pulmonary and kidney disease, allergy, diabetes, lichen planus, psoriasis, atopic dermatitis and other autoimmune skin lesions and those treated with anti-inflammatory drugs (except azathioprine and corticosteroids), antioxidants, or statins, which can affect the inflammation process and MPV. n= 37 Response or clinical remission at week 14; reduction in CDAI score by 25% and 70 points from baseline. Clinical remission of CD was defined as a CDAI score of <150. NO n= 28 YES Response or clinical remission at each visit after week 14 during 52 week treatment ; reduction in CDAI score by 25% and 70 points from baseline. Clinical remission of CD was defined as a CDAI score of <150. n= 15 n= 30 Loss of infliximab response after week 14: meeting one of the following criteria: (i) a CDAI score of 175 and an increase of CDAI score of 35% and 70 points for at least two following clinic visits ( 21 days); (ii) undergoing CD-related surgery; (iii) crossover from scheduled therapy to episodic retreatment. n=15 Scheme 1 The flow chart for patients enrollment in the study (except azathioprine and corticosteroids), antioxidants, or statins, which can affect the inflammation process and MPV [14 16], were excluded from the study. Collection of Blood Samples and Blood Analysis From all patients, 2 ml venous blood was taken into standardized tubes containing ethylenediaminetetraacetic acid (EDTA) to determine MPV and white blood cell count (WBC). In CD patients, blood samples for analysis were obtained before initiation of 52-week infliximab therapy and after induction treatment at week 14. Blood analysis was performed within 2 h after collection using the same automatic analyser. The adult normal reference range for MPV is fl and for WBC /l. Also, 2 ml blood samples were collected into serum tube and CRP was determined using automatic devices (adult normal reference range for CRP: \0.5 mg/dl). Statistical Analysis The data were analyzed using the Statistica 10.0 software (StatSoft, Inc., United States). Results were expressed as mean ± standard deviation. Receiver operating characteristic (ROC) curves were constructed for the MPV analysis, and the areas under the ROC curves with 95 % CIs were calculated and compared with each other. Optimal cutoff values for MPV, used to discriminate between patients with and without sustained response to infliximab, were calculated by ROC curves. Sensitivity, specificity, and positive and negative predictive values (PPV, NPV, respectively) of the cutoff values and association were analyzed. Shapiro Wilk s test was used to test the distribution of the variables. Comparisons between groups were performed using the Student s t test (or nonparametric Mann Whitney U test) and Chi-square test. Correlations were evaluated using the Pearson s test or Spearman s rank correlation coefficient (r) test depending on normality of distribution. A p \ 0.05 was considered significant. Ethical Considerations The study was conducted in accordance with the ethical principles of the 1975 Declaration of Helsinki and the study protocol was approved by the Committee of Bioethics of Medical University of Lodz. Results The baseline characteristics of all 30 CD patients who underwent 52-week biological therapy with infliximab and 15 healthy controls are presented in Table 1. Nearly 50 % (n = 15) of the CD patients enrolled in the study had ileocolonic disease. Laboratory tests revealed that CD patients had significantly lower baseline MPV (10.25 ± 0.99 vs ± 1.08 fl; p = 0.003) and hematocrit (Ht) levels (37.4 ± 6.4 vs ± 11.4 %; p = 0.025), as well as significantly higher platelet counts (PLT) (329 ± 150 vs.
4 Dig Dis Sci (2016) 61: Table 1 Baseline clinical characteristics and laboratory findings in the Crohn s disease (CD) patients enrolled to a 52-week infliximab therapy and healthy controls Crohn s disease Control group p* Subjects, n (%) NA Sex Women, n (%) 8 (26.7 %) 5 (35.7 %) Men, n (%) 22 (73.3 %) 9 (64.3 %) Age, year 32.8 ± ± BMI, kg/m ± ± Duration of disease, year 5.9 ± 2.9 NA NA Location of lesions, n (%) Ileum lesions 2 (%) NA NA Colon lesions 9 (%) Ileum and colon lesions 19 (%) Perianal lesions 14 (%) CDAI, points ± 50.7 NA NA Corticosteroid history, n (%) Never used 1 (3.3 %) NA NA B1 year 3 (10.0 %) [1 tob2 years 11 (36.7 %) [2 years 15 (50.0 %) Hematocrit, % 37.4 ± ± White blood cell count, /ll 9.37 ± ± 2.59 \0.001 Platelet count, /ll 329 ± ± Mean platelet volume, fl ± ± CRP, mg/dl 19.7 ± ± Data are presented as mean ± standard deviation or number (percentage) BMI Body mass index, CDAI Crohn s Disease Activity Index, CRP C-reactive protein, NA not applicable p* statistical significance between CD patients and healthy control group 247 ± /ll; p = 0.049) compared with the healthy control group. The study showed a negative correlation of moderate strength in CD patients between baseline CDAI and MPV (r =-0.522; p = 0.003; Fig. 1), and Ht (r =-0.438; p = 0.015). There was no significant correlation between the CDAI and CRP, WBC, and PLT levels (r = 0.267; p = 0.153; r = 059; p = 0.757; r = 0.168; p = 0.375; respectively). CRP levels in CD patient were significantly increased at baseline compared with healthy controls (19.7 ± 25.3 vs. 1.1 ± 0.8; p = 0.009). However, seven CD patients (n = 7; 23.3 %) had persistent low CRP levels (CPR level under 5 mg/dl) despite clinical and endoscopic disease activity. In all CD patients, there was no significant association between infliximab sustained response and gender (p = 0.099) or age at diagnosis (31.3 ± 9.2 vs ± 8.6; p = 0.385) (Table 2). No significant relationship was found between location and response to infliximab (p = 0.507), and disease duration (p = 0.410) (Table 2). Baseline MPV and week 14 MPV levels in CD patients were not influenced by perianal disease (p = and Fig. 1 Correlation between the mean platelet volume (MPV) level and Crohn s Disease Activity Index (CDAI) score (r =-0.52; p = 0.003) p = 0.721, respectively), disease location (p = and p = 0.224, respectively), or disease duration (p = and p = 0.398, respectively).
5 546 Dig Dis Sci (2016) 61: Table 2 Baseline clinical characteristics in the Crohn s disease (CD) patients with and without sustained response to maintenance infliximab treatment Sustained response Loss of response p* Subjects, n (%) NA Sex Women, n (%) 2 (25 %) 6 (75 %) Men, n (%) 13 (59 %) 9 (41 %) Age at diagnosis, year 31.3 ± ± BMI, kg/m ± ± Duration of disease, year 5.4 ± ± Location of lesions, n (%) Ileum lesions 1 (50 %) 1 (50 %) Colon lesions 3 (33 %) 6 (67 %) Ileum and colon lesions 11 (58 %) 8 (42 %) Baseline CDAI, points ± ± Data are presented as mean ± standard deviation or number (percentage) BMI Body mass index, CDAI Crohn s Disease Activity Index, NA not applicable p* statistical significance between sustained response and loss of response In the study, only patients with CD who responded or achieved remission under infliximab induction treatment at week 14 were enrolled. Fifteen (50.0 %) of these patients have not reached a 1-year maintenance treatment without loss of response (short-term response): eleven (37.0 %) manifested clinical exacerbation of disease activity at 52-week maintenance treatment with infliximab (CDAI score of C175 and an increase from the induction CDAI score of C35 % and C70 points for at least two following clinical visits), two (6.5 %) underwent surgery, and two (6.5 %) had to crossover from scheduled therapy to episodic retreatment. The CD patients with sustained response had significantly higher MPV at week 14 compared with those who lost response to maintenance infliximab treatment (11.31 ± 1.16 vs ± 0.52 fl; p = ; Fig. 2). Furthermore, the MPV at baseline in CD patients with sustained response was higher than in the patients who relapsed; however, the association between baseline MPV and the maintenance of response was not significant (10.53 ± 1.28 vs ± 0.48 fl; p = ). DMPV, which signifies a change of MPV between baseline and week 14, was lower in patients with loss of response to infliximab versus patients with sustained response (0.227 ± vs ± fl; p = ; Fig. 3). ROC curves were constructed to assign optimal cutoff values associated with sustained response to infliximab maintenance treatment. Areas under curves were 0.82 for MPV at week 14 and 0.92 for DMPV. The analysis showed that MPV [ 10.3 fl at week 14 predicts sustained response to infliximab treatment with 67 % sensitivity and 80 % specificity (Fig. 4). The negative predictive value (NPV) was 71 %. DMPV between baseline and week 14 higher than 0.4 fl Fig. 2 Difference between mean platelet volume (MPV) levels in Crohn s disease (CD) patients with sustained and lost response to infliximab maintenance treatment (p = ) predicted sustained response during 52-week treatment with 87 % sensitivity and 93 % specificity; the NPV was 88 %. At week 14, twenty (20/30) CD patients had MPV C 10.3 fl and 65 % of them (13/20) had sustained response to maintenance infliximab treatment. Ten (10/30) CD patients had \10.3 fl and 20 % (2/10) had sustained response to infliximab (p = 0.01; Fig. 5). Twenty-one (21/ 30) CD patients had C0.4 fl DMPV (an increase in MPV value between baseline and week 14) and 71 % of them (15/21) had sustained response to infliximab. None of nine (9/30) CD patients with\0.4 fl DMPV had sustained response to maintenance treatment (p = ). The ROC curves were also constructed for Hct, CRP, PLT, and WBC at week 14; however, the results were insignificant (WBC AUC = 0.524; Hct
6 Dig Dis Sci (2016) 61: Fig. 3 Relationship between D mean platelet volume (DMPV) levels (difference between baseline MPV levels and at week 14) in Crohn s disease (CD) patients with sustained and lost response to infliximab maintenance treatment (p = ) Fig. 4 Receiver operating characteristic curve for mean platelet volume (MPV) levels at week 14 and the loss of response to infliximab maintenance treatment in Crohn s disease (CD) patients during a 52-week therapy AUC = 0.542; CRP AUC = 0.567; PLT AUC = 0.598; compared to MPV at week 14 AUC = 0.818). Discussion We observed that higher MPV is a good indicator of a sustained response to maintenance treatment during 52-week infliximab therapy. Observation of MPV during Fig. 5 Association between sustained response to infliximab 52-week maintenance therapy and mean platelet volume (MPV) levels at week 14 in Crohn s disease (CD) patients induction treatment may become a useful tool in personalized therapy and result in better control of CD. Infliximab, which is widely used in CD patients, effectively controls clinical symptoms, maintains remission, prevents relapses, improves quality of life, and reduces mortality. Furthermore, most CD patients respond positively to infliximab and clinical response after induction of remission is often achieved. Nevertheless, loss of response in CD patients under maintenance treatment with infliximab is still a common problem. Therefore, a predictor of response to anti-tnf-a therapy is essential in clinical practice [4, 15, 16]. MPV is an automated measurement of the average size of platelets in whole blood that adds no extra cost or effort to a full blood count. The relationship between MPV and inflammatory process has been investigated [4, 7, 10, 11, 13, 17]. Currently, platelets with higher volume are considered to be involved in the infiltration of tissues with inflammation [11]. Also, b-thromboglobulin (b-tg) and platelet factor 4 (PF4), specific proteins discharged from platelet a-granules, have been suggested to be markers of platelet activation and influence platelet production [18]. Recent studies showed a possible relationship between MPV and some inflammatory diseases, such as acute appendicitis, chronic hepatitis B, myocardial infarction, diabetes mellitus, RA, and IBD [17, 19, 20]. For IBD, increased count and low size of platelets, as well as prothrombotic state were observed [10]. Also, increased b-tg and PF4 plasma levels have been reported [18]. Of note, a decreased MPV was evidenced as an important and useful biomarker of CD exacerbations [11]. The possible explanation for this phenomenon is that the excessive production of pro-inflammatory cytokines and acute-phase reactants may suppress the size of the platelets by interfering with megakaryopoiesis, which is followed by the release of small size platelets from the bone marrow [4].
7 548 Dig Dis Sci (2016) 61: Another possible explanation of the decreased size of circulating platelets in exacerbation of CD relates to the intensive infiltration of large platelets at sites of inflammation. It is known that large platelets are more active in releasing a variety of pro-inflammatory and thrombotic agents than smaller size platelets, and their circulating count may thus be decreased by the consumption by peripheral tissues during the acute stage of inflammation [13]. In line with these hypotheses, Gasparyan et al. [10] suggested that microaggregates and microinfarction of mesenteric vessels unveil a potential role of platelets as pro-inflammatory cells in pathogenesis of CD. Others showed that platelets and their MPV are associated with thromboembolic risk in IBD patients and may play a role in pathogenesis of inflammation in the intestine wall. In some studies, a significant negative correlation between MPV and disease activity was observed [15], and it was suggested that a decreased MPV is an independent marker of increased disease activity in CD [21]. Similar results were demonstrated in clinical observations [20]. In our study, a significantly lower MPV was observed in CD patients than in healthy controls, which supports the hypothesis about the possible role of MPV in monitoring disease status. We also observed that the clinical activity of CD, expressed on CDAI scale, at time of enrollment to infliximab therapy significantly correlates with MPV. Anti-TNF-a drugs are used in the treatment of other immunological disorders, such as RA. Gasparyan et al. [13] suggested that MPV increases during anti-tnf-a therapy and may be a good predictor of clinical response to biological treatment in RA patients. However, to the best of our knowledge, earlier studies have not analyzed MPV as a possible predictor of sustained response to biological therapy with infliximab in CD patients. Here, we observed that higher MPV at week 14 in clinical responders to infliximab induction treatment is a good indicator of a sustained response to maintenance treatment during 52-week therapy. Furthermore, CD patients with a [0.4 fl increase in MPV after an induction infliximab treatment (between week 0 and 14) were more likely to maintain response and remission. Since MPV [ 10.3 fl at week 14 predicts sustained response with 67 % sensitivity and 80 % specificity, and DMPV (difference between baseline and week 14) higher than 0.4 fl predicts sustained response with 87 % sensitivity and 93 % specificity, we suggest for the first time that the MPV could be a useful predictor in medical practice. Conclusion In conclusion, our study showed that MPV may be a useful biomarker predicting a sustained response in the 52-week treatment in CD patients receiving infliximab. We suggest that MPV, as an easily accessible biomarker, will allow clinicians to select the most appropriate individual treatment. In case of possible loss of response, physicians will be able to increase the dose of anti-tnf-a antibodies, change drugs or consider other treatments (i.e., antibodies against cell adhesion molecules). This pilot study was performed on a small group of IBD patients. Further studies are warranted to confirm our observations on the predicting role of MPV and to establish the cutoff points in a larger cohort. Also, the possible application of this parameter in CD patients treated with other anti-tnf-a agents needs verification. Acknowledgments Supported by grant from the Medical University of Lodz (#503/ / to JF) and grants from National Science Centre (#UMO-2013/11/B/NZ7/01301 and UMO-2014/13/B/ NZ4/01179 to JF). Compliance with ethical standards Conflict of interest None. Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License ( which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. References 1. Dignass A, Van AG, Lindsay JO, et al. The second European evidence-based consensus on the diagnosis and management of Crohn s disease: current management. J Crohns Colitis. 2010;4: Van AG, Dignass A, Panes J, et al. The second European evidence-based consensus on the diagnosis and management of Crohn s disease: definitions and diagnosis. J Crohns Colitis. 2010;4: Ben-Horin S, Chowers Y. Review article: loss of response to anti- TNF treatments in Crohn s disease. Aliment Pharmacol Ther. 2011;33: Cornillie F, Hanauer SB, Diamond RH, et al. Postinduction serum infliximab trough level and decrease of C-reactive protein level are associated with durable sustained response to infliximab: a retrospective analysis of the ACCENT I trial. Gut. 2014;63: Monteleone I, Sarra M, Pallone F, Monteleone G. Th17-related cytokines in inflammatory bowel diseases: friends or foes? Curr Mol Med. 2012;12: Truchetet ME, Beven L, Renaudin H, et al. Potential role of Mycoplasma hominis in interleukin (IL)-17-producing CD4? T-cell generation via induction of IL-23 secretion by human dendritic cells. J Infect Dis. 2011;204: Verdier J, Begue B, Cerf-Bensussan N, Ruemmele FM. Compartmentalized expression of Th1 and Th17 cytokines in pediatric inflammatory bowel diseases. Inflamm Bowel Dis. 2012;18: Xin L, Li Y, Soong L. Role of interleukin-1beta in activating the CD11c(high) CD. Infect Immun. 2007;75: Mack DR, Langton C, Markowitz J, et al. Laboratory values for children with newly diagnosed inflammatory bowel disease. Pediatrics. 2007;119:
8 Dig Dis Sci (2016) 61: Gasparyan AY, Ayvazyan L, Mikhailidis DP, Kitas GD. Mean platelet volume: a link between thrombosis and inflammation? Curr Pharm Des. 2011;17: Kapsoritakis AN, Koukourakis MI, Sfiridaki A, et al. Mean platelet volume: a useful marker of inflammatory bowel disease activity. Am J Gastroenterol. 2001;96: Ozturk ZA, Dag MS, Kuyumcu ME, et al. Could platelet indices be new biomarkers for inflammatory bowel diseases? Eur Rev Med Pharmacol Sci. 2013;17: Gasparyan AY, Sandoo A, Stavropoulos-Kalinoglou A, Kitas GD. Mean platelet volume in patients with rheumatoid arthritis: the effect of anti-tnf-alpha therapy. Rheumatol Int. 2010;30: Bath PM, Butterworth RJ. Platelet size: measurement, physiology and vascular disease. Blood Coagul Fibrinolysis. 1996;7: Jaremo P, Sandberg-Gertzen H. Platelet density and size in inflammatory bowel disease. Thromb Haemost. 1996;75: Peyrin-Biroulet L, Reinisch W, Colombel JF, et al. Clinical disease activity, C-reactive protein normalisation and mucosal healing in Crohn s disease in the SONIC trial. Gut. 2014;63: Kisacik B, Tufan A, Kalyoncu U, et al. Mean platelet volume (MPV) as an inflammatory marker in ankylosing spondylitis and rheumatoid arthritis. Joint Bone Spine. 2008;75: Lecomte-Raclet L, Alemany M, Sequira-Le GA, et al. New insights into the negative regulation of hematopoiesis by chemokine platelet factor 4 and related peptides. Blood. 1998;91: Turhan O, Coban E, Inan D, Yalcin AN. Increased mean platelet volume in chronic hepatitis B patients with inactive disease. Med Sci Monit. 2010;16:CR202 CR Yuksel O, Helvaci K, Basar O, et al. An overlooked indicator of disease activity in ulcerative colitis: mean platelet volume. Platelets. 2009;20: Douda T, Bures J, Rejchrt S, Kopácová M, Pecka M, Malý J. Mean platelet volume (MPV) in Crohn s disease patients. Cas Lek Cesk. 2006;145:
The Best of IBD at UEGW (Crohn s)
 The Best of IBD at UEGW (Crohn s) Iyad Issa MD Head of Gastroenterology, Rafik Hariri Univ Hosp Adjunct Faculty, School of Medicine, Leb Univ Founding Faculty, School Of Medicine, Leb Am Univ 1 The Best
The Best of IBD at UEGW (Crohn s) Iyad Issa MD Head of Gastroenterology, Rafik Hariri Univ Hosp Adjunct Faculty, School of Medicine, Leb Univ Founding Faculty, School Of Medicine, Leb Am Univ 1 The Best
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease
 Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
Disclosures. What Do I Do When Anti-TNF Therapy Is Not Working Anymore? Fadi Hamid, M.D. Saint Luke s GI Specialists
 What Do I Do When Anti-TNF Therapy Is Not Working Anymore? Fadi Hamid, M.D. Saint Luke s GI Specialists Disclosures No financial relationships to disclose. 1 Learning Objectives Case 24M with ileocolonic
What Do I Do When Anti-TNF Therapy Is Not Working Anymore? Fadi Hamid, M.D. Saint Luke s GI Specialists Disclosures No financial relationships to disclose. 1 Learning Objectives Case 24M with ileocolonic
An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease. David A. Schwartz, MD
 An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University
An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University
September 12, 2015 Millie D. Long MD, MPH, FACG
 Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
Anne Griffiths MD, FRCPC. SickKids Hospital, University of Toronto. Buenos Aires, August 16, 2014
 Management and Medical Therapies for Crohn disease: strategies to enhance mucosal healing Anne Griffiths MD, FRCPC SickKids Hospital, University of Toronto Buenos Aires, August 16, 2014 New onset Crohn
Management and Medical Therapies for Crohn disease: strategies to enhance mucosal healing Anne Griffiths MD, FRCPC SickKids Hospital, University of Toronto Buenos Aires, August 16, 2014 New onset Crohn
PEDIATRIC INFLAMMATORY BOWEL DISEASE
 PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
Recent Advances in the Management of Refractory IBD
 Recent Advances in the Management of Refractory IBD Raina Shivashankar, M.D. Assistant Professor of Medicine Division of Gastroenterology and Hepatology Thomas Jefferson University Philadelphia, PA Outline
Recent Advances in the Management of Refractory IBD Raina Shivashankar, M.D. Assistant Professor of Medicine Division of Gastroenterology and Hepatology Thomas Jefferson University Philadelphia, PA Outline
Biologics in IBD. Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College
 Biologics in IBD Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College Case 30 year old man diagnosed with ulcerative proctitis diagnosed in 2003 Had been maintained
Biologics in IBD Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College Case 30 year old man diagnosed with ulcerative proctitis diagnosed in 2003 Had been maintained
5/2/2018 SHOULD DEEP REMISSION BE A TREATMENT GOAL? YES! Disclosures: R. Balfour Sartor, MD
 5/2/218 SHOULD DEEP REMISSION BE A TREATMENT GOAL? YES! Disclosures: R. Balfour Sartor, MD Grant support for preclinical studies: Janssen, Gusto Global, Vedanta, Artizan BALFOUR SARTOR, MD DISTINGUISHED
5/2/218 SHOULD DEEP REMISSION BE A TREATMENT GOAL? YES! Disclosures: R. Balfour Sartor, MD Grant support for preclinical studies: Janssen, Gusto Global, Vedanta, Artizan BALFOUR SARTOR, MD DISTINGUISHED
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Personalized Medicine in IBD: Where Are We in 2013
 Personalized Medicine in IBD: Where Are We in 2013 David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University Medical Center What is Personalized
Personalized Medicine in IBD: Where Are We in 2013 David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University Medical Center What is Personalized
Positioning Biologics in Ulcerative Colitis
 Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Department of Gastroenterology, Human Nutrition and Internal Diseases, Poznan University of Medical Sciences, Poznan, Poland
 Original paper Intestinal healing after anti-tnf induction therapy predicts long-term response to one-year treatment in patients with ileocolonic Crohn s disease naive to anti-tnf agents Piotr Eder 1,
Original paper Intestinal healing after anti-tnf induction therapy predicts long-term response to one-year treatment in patients with ileocolonic Crohn s disease naive to anti-tnf agents Piotr Eder 1,
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 3 October 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
Mucosal healing: does it really matter?
 Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Join the conversation at #GIFORUMCCFA
 1 Join the conversation at #GIFORUMCCFA 2 Disclosures In accordance with the ACCME Standards for Commercial Support of CME, the speakers for this course have been asked to disclose to participants the
1 Join the conversation at #GIFORUMCCFA 2 Disclosures In accordance with the ACCME Standards for Commercial Support of CME, the speakers for this course have been asked to disclose to participants the
Mono or Combination Therapy with. Individualized Approach
 Mono Combination Therapy with Biologics i in IBD: Developing an Individualized Approach David T. Rubin, MD, FACG Co-Direct, Inflammaty Bowel Disease Center Fellowship Program Direct University of Chicago
Mono Combination Therapy with Biologics i in IBD: Developing an Individualized Approach David T. Rubin, MD, FACG Co-Direct, Inflammaty Bowel Disease Center Fellowship Program Direct University of Chicago
Implementation of disease and safety predictors during disease management in UC
 Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Initiation of Maintenance Treatment in Moderate to Severe New Onset Crohn s Disease
 Initiation of Maintenance Treatment in Moderate to Severe New Onset Crohn s Disease The Case for Starting with Anti-TNFα Agents Maria Oliva-Hemker, M.D. Chief, Division of Pediatric Gastroenterology &
Initiation of Maintenance Treatment in Moderate to Severe New Onset Crohn s Disease The Case for Starting with Anti-TNFα Agents Maria Oliva-Hemker, M.D. Chief, Division of Pediatric Gastroenterology &
Faecal Calprotectin. Reliable Non-Invasive Discrimination Between Inflammatory Bowel Disease (IBD) & Irritable Bowel Syndrome (IBS)
 Faecal Calprotectin Reliable Non-Invasive Discrimination Between Inflammatory Bowel Disease (IBD) & Irritable Bowel Syndrome (IBS) Reliable, Non Invasive Identification of IBD vs IBS Available from Eurofins
Faecal Calprotectin Reliable Non-Invasive Discrimination Between Inflammatory Bowel Disease (IBD) & Irritable Bowel Syndrome (IBS) Reliable, Non Invasive Identification of IBD vs IBS Available from Eurofins
Mucosal Healing in Crohn s Disease. Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium
 Mucosal Healing in Crohn s Disease Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium Mucosal Lesions in CD: General Features CD can affect the entire GI tract
Mucosal Healing in Crohn s Disease Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium Mucosal Lesions in CD: General Features CD can affect the entire GI tract
Evaluation of Mean Thrombocyte Volumes in Asthma Patients During Acute Exacerbations and Stable Periods
 Research Article Evaluation of Mean Thrombocyte Volumes in Asthma Patients During Acute Exacerbations and Stable Periods Uysal Dolap 1, Tuncer Tuğ 2, Suat Konuk 2* 1 Şırnak State Hospital, Şırnak, Turkey
Research Article Evaluation of Mean Thrombocyte Volumes in Asthma Patients During Acute Exacerbations and Stable Periods Uysal Dolap 1, Tuncer Tuğ 2, Suat Konuk 2* 1 Şırnak State Hospital, Şırnak, Turkey
Common Questions in Crohn s Disease Therapy. Case
 Common Questions in Crohn s Disease Therapy Jean-Paul Achkar, MD, FACG Kenneth Rainin Chair for IBD Research Cleveland Clinic Case 23 yo male with 1 year history of diarrhea, abdominal pain and 15 pound
Common Questions in Crohn s Disease Therapy Jean-Paul Achkar, MD, FACG Kenneth Rainin Chair for IBD Research Cleveland Clinic Case 23 yo male with 1 year history of diarrhea, abdominal pain and 15 pound
Optimizing the effectiveness of anti-tnf therapy in paediatric IBD
 Optimizing the effectiveness of anti-tnf therapy in paediatric IBD Anne Griffiths MD, FRCPC Co-Lead, Inflammatory Bowel Disease Center Northbridge Chair in IBD Hospital for Sick Children, Professor of
Optimizing the effectiveness of anti-tnf therapy in paediatric IBD Anne Griffiths MD, FRCPC Co-Lead, Inflammatory Bowel Disease Center Northbridge Chair in IBD Hospital for Sick Children, Professor of
Use of extrapolation in small clinical trials:
 Use of extrapolation in small clinical trials: Infliximab for pediatric ulcerative colitis Jessica J. Lee, MD, MMSc Medical Officer Division of Gastroenterology and Inborn Errors Products CDER/ FDA 1 Learning
Use of extrapolation in small clinical trials: Infliximab for pediatric ulcerative colitis Jessica J. Lee, MD, MMSc Medical Officer Division of Gastroenterology and Inborn Errors Products CDER/ FDA 1 Learning
Efficacy and Safety of Treatment for Pediatric IBD
 Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Assistant Professor of Clinical Pediatrics Division of Gastroenterology,
Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Assistant Professor of Clinical Pediatrics Division of Gastroenterology,
Can fecal calprotectin better stratify Crohn s disease activity index?
 ORIGINAL ARTICLE Annals of Gastroenterology (215) 28, 1-6 Can fecal calprotectin better stratify Crohn s disease activity index? Eleonora Scaioli a, Carla Cardamone a, Michele Scagliarini b, Rocco Maurizio
ORIGINAL ARTICLE Annals of Gastroenterology (215) 28, 1-6 Can fecal calprotectin better stratify Crohn s disease activity index? Eleonora Scaioli a, Carla Cardamone a, Michele Scagliarini b, Rocco Maurizio
Principal Investigator. General Information. Certification Published on The YODA Project (
 Principal Investigator First Name: William J. Last Name: Sandborn Degree: M.D. Primary Affiliation: University of California San Diego E-mail: wsandborn@ucsd.edu Phone number: 8586575284 Address: 9500
Principal Investigator First Name: William J. Last Name: Sandborn Degree: M.D. Primary Affiliation: University of California San Diego E-mail: wsandborn@ucsd.edu Phone number: 8586575284 Address: 9500
I nflammatory bowel diseases (IBD) are chronic intestinal
 364 INFLAMMATORY BOWEL DISEASE Calprotectin is a stronger predictive marker of relapse in ulcerative colitis than in Crohn s disease F Costa, M G Mumolo, L Ceccarelli, M Bellini, M R Romano, C Sterpi,
364 INFLAMMATORY BOWEL DISEASE Calprotectin is a stronger predictive marker of relapse in ulcerative colitis than in Crohn s disease F Costa, M G Mumolo, L Ceccarelli, M Bellini, M R Romano, C Sterpi,
Crohn's Disease. The What, When, and Why of Treatment
 Crohn's Disease The What, When, and Why of Treatment Brian Feagan, MD, FACG Professor of Medicine and Epidemiology and Biostatistics Director, Robarts Clinical Trials Robarts Research Institute University
Crohn's Disease The What, When, and Why of Treatment Brian Feagan, MD, FACG Professor of Medicine and Epidemiology and Biostatistics Director, Robarts Clinical Trials Robarts Research Institute University
Efficacy and Safety of Treatment for Pediatric IBD
 Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Associate Professor of Clinical Pediatrics Division of Gastroenterology,
Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Associate Professor of Clinical Pediatrics Division of Gastroenterology,
Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals
 Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals Stephen Hanauer, MD Professor of Medicine Medical Director, Digestive Disease Center Northwestern Medicine Chicago, Illinois Speaker
Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals Stephen Hanauer, MD Professor of Medicine Medical Director, Digestive Disease Center Northwestern Medicine Chicago, Illinois Speaker
Dr David Epstein Vincent Pallotti Hospital and University of Cape Town
 Inflammatory Bowel Disease Management in South Africa in 2016 Pharmaceutical Care Management Association Dr David Epstein Vincent Pallotti Hospital and University of Cape Town Inflammatory Bowel Disease
Inflammatory Bowel Disease Management in South Africa in 2016 Pharmaceutical Care Management Association Dr David Epstein Vincent Pallotti Hospital and University of Cape Town Inflammatory Bowel Disease
Indications for use of Infliximab
 Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Efficacy of Adalimumab in Korean Patients with Crohn s Disease
 Gut and Liver, Vol. 10, No. 2, March 2016, pp. 255-261 ORiginal Article Efficacy of Adalimumab in Korean Patients with Crohn s Disease Il Woong Sohn, Sung Tae Kim, Bun Kim, Hyun Jung Lee, Soo Jung Park,
Gut and Liver, Vol. 10, No. 2, March 2016, pp. 255-261 ORiginal Article Efficacy of Adalimumab in Korean Patients with Crohn s Disease Il Woong Sohn, Sung Tae Kim, Bun Kim, Hyun Jung Lee, Soo Jung Park,
Outcomes of immunosuppressors and biologic drugs in inflammatory bowel diseases: a real life experience
 Outcomes of immunosuppressors and biologic drugs in inflammatory bowel Treatments and therapeutic approaches in IBD are constantly evolving. The newly emerged biologic treatments are one such evolving
Outcomes of immunosuppressors and biologic drugs in inflammatory bowel Treatments and therapeutic approaches in IBD are constantly evolving. The newly emerged biologic treatments are one such evolving
John F. Valentine, MD Inflammatory Bowel Disease Program University of Utah
 John F. Valentine, MD Inflammatory Bowel Disease Program University of Utah Hawaii 1/20/2017 DISCLOSURES Research Support: NIH, Pfizer, Celgene, AbbVie, Roche/Genentech, Takeda, CCFA OBJECTIVES Review
John F. Valentine, MD Inflammatory Bowel Disease Program University of Utah Hawaii 1/20/2017 DISCLOSURES Research Support: NIH, Pfizer, Celgene, AbbVie, Roche/Genentech, Takeda, CCFA OBJECTIVES Review
Crohn s Disease: Should We Treat Based on Symptoms or Based on Objective Markers of Inflammation?
 Crohn s Disease: Should We Treat Based on Symptoms or Based on Objective Markers of Inflammation? Edward V. Loftus, Jr., M.D. Professor of Medicine Division of Gastroenterology and Hepatology Mayo Clinic
Crohn s Disease: Should We Treat Based on Symptoms or Based on Objective Markers of Inflammation? Edward V. Loftus, Jr., M.D. Professor of Medicine Division of Gastroenterology and Hepatology Mayo Clinic
Beyond Anti TNFs: positioning of other biologics for Crohn s disease. Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center
 Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Policy #: 472 Latest Review Date: May 2017
 Name of Policy: Fecal Calprotectin Testing Policy #: 472 Latest Review Date: May 2017 Category: Laboratory Policy Grade: A Background/Definitions: As a general rule, benefits are payable under Blue Cross
Name of Policy: Fecal Calprotectin Testing Policy #: 472 Latest Review Date: May 2017 Category: Laboratory Policy Grade: A Background/Definitions: As a general rule, benefits are payable under Blue Cross
Differentiation Between Ileocecal Tuberculosis and Crohn s Disease using a Combination of Clinical, Endoscopic and Histological Characteristics
 38 Original Article Differentiation Between Ileocecal Tuberculosis and Crohn s Disease using a Combination of Clinical, Endoscopic and Histological Characteristics Anuchapreeda S Leelakusolvong S Charatcharoenwitthaya
38 Original Article Differentiation Between Ileocecal Tuberculosis and Crohn s Disease using a Combination of Clinical, Endoscopic and Histological Characteristics Anuchapreeda S Leelakusolvong S Charatcharoenwitthaya
Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R.
 UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
Response to First Intravenous Steroid Therapy Determines the Subsequent Risk of Colectomy in Ulcerative Colitis Patients
 Response to First Intravenous Steroid Therapy Determines the Subsequent Risk of Colectomy in Ulcerative Colitis Patients Tamás Molnár 1, Klaudia Farkas 1, Tibor Nyári 2, Zoltán Szepes 1, Ferenc Nagy 1,
Response to First Intravenous Steroid Therapy Determines the Subsequent Risk of Colectomy in Ulcerative Colitis Patients Tamás Molnár 1, Klaudia Farkas 1, Tibor Nyári 2, Zoltán Szepes 1, Ferenc Nagy 1,
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy
 Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
IBD Updates. Themes in IBD IBD management journey. New tools for therapeutic monitoring. First-line treatment in IBD
 IBD Updates Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Themes in IBD 213 First-line treatment in IBD New tools for therapeutic monitoring Biologic therapy for CD and
IBD Updates Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Themes in IBD 213 First-line treatment in IBD New tools for therapeutic monitoring Biologic therapy for CD and
Available Data on Pediatric Exposure Response a Clinician s Perspective
 Available Data on Pediatric Exposure Response a Clinician s Perspective Marla Dubinsky, MD Professor of Pediatrics and Medicine Chief Pediatric GI and Nutrition Co-Director Susan and Leonard Feinstein
Available Data on Pediatric Exposure Response a Clinician s Perspective Marla Dubinsky, MD Professor of Pediatrics and Medicine Chief Pediatric GI and Nutrition Co-Director Susan and Leonard Feinstein
Mean Platelet volume in diagnosis of acute appendicitis in children
 Mean Platelet volume in diagnosis of acute appendicitis in children *Bilici S 1, Sekmenli T 2, Göksu M 1, Melek M 1, Avci V 1 1. Department of Pediatric Surgery, Medical Faculty, Yuzuncu Yil University,
Mean Platelet volume in diagnosis of acute appendicitis in children *Bilici S 1, Sekmenli T 2, Göksu M 1, Melek M 1, Avci V 1 1. Department of Pediatric Surgery, Medical Faculty, Yuzuncu Yil University,
Il ruolo degli anticorpi anti farmaco nella pratica clinica
 Il ruolo degli anticorpi anti farmaco nella pratica clinica Daniela Pugliese, MD IBD Unit Complesso Integrato Columbus Gemelli Hospital Catholic University Foundation, Rome - Italy Therapeutic Drug monitoring
Il ruolo degli anticorpi anti farmaco nella pratica clinica Daniela Pugliese, MD IBD Unit Complesso Integrato Columbus Gemelli Hospital Catholic University Foundation, Rome - Italy Therapeutic Drug monitoring
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
The importance of the mean platelet volume in the diagnosis of supraventricular tachycardia
 The importance of the mean platelet volume in the diagnosis of supraventricular tachycardia Ocak T 1, Erdem A 2, Duran A 1, Tekelioglu U 3, Öztürk S 2, Ayhan S 2, Özlü FM 2, Yazici M 2 1. Department of
The importance of the mean platelet volume in the diagnosis of supraventricular tachycardia Ocak T 1, Erdem A 2, Duran A 1, Tekelioglu U 3, Öztürk S 2, Ayhan S 2, Özlü FM 2, Yazici M 2 1. Department of
Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort
 Alimentary Pharmacology and Therapeutics Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort N. Gies, K. I. Kroeker, K. Wong & R. N. Fedorak Division
Alimentary Pharmacology and Therapeutics Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort N. Gies, K. I. Kroeker, K. Wong & R. N. Fedorak Division
Choosing and Positioning Biologic Therapy for Crohn s Disease: (Still) Looking for the Crystal Ball
 Choosing and Positioning Biologic Therapy for Crohn s Disease: (Still) Looking for the Crystal Ball Siddharth Singh, MD, MS Assistant Professor of Medicine Division of Gastroenterology Division of Biomedical
Choosing and Positioning Biologic Therapy for Crohn s Disease: (Still) Looking for the Crystal Ball Siddharth Singh, MD, MS Assistant Professor of Medicine Division of Gastroenterology Division of Biomedical
Perianal and Fistulizing Crohn s Disease: Tough Management Decisions. Jean-Paul Achkar, M.D. Kenneth Rainin Chair for IBD Research Cleveland Clinic
 Perianal and Fistulizing Crohn s Disease: Tough Management Decisions Jean-Paul Achkar, M.D. Kenneth Rainin Chair for IBD Research Cleveland Clinic Talk Overview Background Assessment and Classification
Perianal and Fistulizing Crohn s Disease: Tough Management Decisions Jean-Paul Achkar, M.D. Kenneth Rainin Chair for IBD Research Cleveland Clinic Talk Overview Background Assessment and Classification
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: fecal_calprotectin_test 8/2009 11/2017 11/2018 11/2017 Description of Procedure or Service Fecal calprotectin
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: fecal_calprotectin_test 8/2009 11/2017 11/2018 11/2017 Description of Procedure or Service Fecal calprotectin
Crohn's Disease. The What, When, and Why of Treatment
 Crohn's Disease The What, When, and Why of Treatment Gary R. Lichtenstein, MD, FACG Professor of Medicine Director, Inflammatory Bowel Disease Program University of Pennsylvania Philadelphia, PA In my
Crohn's Disease The What, When, and Why of Treatment Gary R. Lichtenstein, MD, FACG Professor of Medicine Director, Inflammatory Bowel Disease Program University of Pennsylvania Philadelphia, PA In my
Blood mean platelet volume may be predictive for disease course in the cases with pemphigus vulgaris.
 Biomedical Research 2017; 28 (9): 4223-4227 ISSN 0970-938X www.biomedres.info Blood mean platelet volume may be predictive for disease course in the cases with pemphigus vulgaris. Sibel Berksoy Hayta,
Biomedical Research 2017; 28 (9): 4223-4227 ISSN 0970-938X www.biomedres.info Blood mean platelet volume may be predictive for disease course in the cases with pemphigus vulgaris. Sibel Berksoy Hayta,
IBD Tools to Aid in the Accurate Diagnosis of Inflammatory Bowel Disease
 IBD Tools to Aid in the Accurate Diagnosis of Inflammatory Bowel Disease Inflammatory Bowel Disease Experts in Autoimmunity Inova Diagnostics offers a complete array of methods to aid in the diagnosis
IBD Tools to Aid in the Accurate Diagnosis of Inflammatory Bowel Disease Inflammatory Bowel Disease Experts in Autoimmunity Inova Diagnostics offers a complete array of methods to aid in the diagnosis
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
Severe IBD: What to Do When Anti- TNFs Don t Work?
 Severe IBD: What to Do When Anti- TNFs Don t Work? David T. Rubin, MD, FACG Professor of Medicine Co-Director, Inflammatory Bowel Disease Center Interim Chief, Section of Gastroenterology, Hepatology and
Severe IBD: What to Do When Anti- TNFs Don t Work? David T. Rubin, MD, FACG Professor of Medicine Co-Director, Inflammatory Bowel Disease Center Interim Chief, Section of Gastroenterology, Hepatology and
Treating to Achieve a Target and Disease Monitoring in 2015: State of the Art
 Treating to Achieve a Target and Disease Monitoring in 2015: State of the Art David T. Rubin, MD The Joseph B. Kirsner Professor of Medicine Chief, Section of Gastroenterology, Hepatology and Nutrition
Treating to Achieve a Target and Disease Monitoring in 2015: State of the Art David T. Rubin, MD The Joseph B. Kirsner Professor of Medicine Chief, Section of Gastroenterology, Hepatology and Nutrition
Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R.
 UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital
 IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital Aims To understand the aetiology of IBD To understand the impact that
IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital Aims To understand the aetiology of IBD To understand the impact that
Treatment of Pediatric IBD: What is Different?
 Treatment of Pediatric IBD: What is Different? January 13, 2017 Michael Kappelman MD, MPH University of North Carolina at Chapel Hill Overview Is Pediatric IBD the same disease? Treatment considerations
Treatment of Pediatric IBD: What is Different? January 13, 2017 Michael Kappelman MD, MPH University of North Carolina at Chapel Hill Overview Is Pediatric IBD the same disease? Treatment considerations
Selby Inflamm Bowel Dis. 2008:14:
 Medical Management of Inflammatory Bowel Disease Freddy Caldera D.O. Assistant Professor Division of Gastroenterology Objectives Discuss Crohn s disease and Ulcerative Colitis Discuss Medications for Inflammatory
Medical Management of Inflammatory Bowel Disease Freddy Caldera D.O. Assistant Professor Division of Gastroenterology Objectives Discuss Crohn s disease and Ulcerative Colitis Discuss Medications for Inflammatory
New treatment options in IBD: today and the future. Silvio Danese Istituto Clinico Humanitas, Milan, Italy
 New treatment options in IBD: today and the future Silvio Danese Istituto Clinico Humanitas, Milan, Italy Date of preparation: October 2014 GLO/EYV/2014-00010h Overview of the late-stage IBD drug pipeline*
New treatment options in IBD: today and the future Silvio Danese Istituto Clinico Humanitas, Milan, Italy Date of preparation: October 2014 GLO/EYV/2014-00010h Overview of the late-stage IBD drug pipeline*
Infliximab Therapy in Pediatric Patients 7 Years of Age and Younger
 ORIGINAL ARTICLE: GASTROENTEROLOGY Infliximab Therapy in Pediatric Patients 7 Years of Age and Younger Judith R. Kelsen, Andrew B. Grossman, Helen Pauly-Hubbard, Kernika Gupta, Robert N. Baldassano, and
ORIGINAL ARTICLE: GASTROENTEROLOGY Infliximab Therapy in Pediatric Patients 7 Years of Age and Younger Judith R. Kelsen, Andrew B. Grossman, Helen Pauly-Hubbard, Kernika Gupta, Robert N. Baldassano, and
Drug Level Monitoring in IBD. Objectives
 Drug Level Monitoring in IBD Corey A. Siegel, MD, MS Director, Dartmouth-Hitchcock IBD Center Associate Professor of Medicine, Geisel School of Medicine at Dartmouth Objectives Review non-biologic drug
Drug Level Monitoring in IBD Corey A. Siegel, MD, MS Director, Dartmouth-Hitchcock IBD Center Associate Professor of Medicine, Geisel School of Medicine at Dartmouth Objectives Review non-biologic drug
INFLAMMATORY BOWEL DISEASE
 1. Medical Condition INFLAMMATORY BOWEL DISEASE (IBD) specifically includes Crohn s disease (CD) and ulcerative colitis (UC) but also includes IBD unclassified (IBDu), seen in about 10% of cases. These
1. Medical Condition INFLAMMATORY BOWEL DISEASE (IBD) specifically includes Crohn s disease (CD) and ulcerative colitis (UC) but also includes IBD unclassified (IBDu), seen in about 10% of cases. These
Evaluation of treatment effect in UC and CD (children)
 Evaluation of treatment effect in UC and CD (children) Dr Nick Croft Digestive Diseases, Centre for Immunobiology, Blizard Institute & Barts Health NHS Trust Blizard Institute Disclosures Dr Nick Croft
Evaluation of treatment effect in UC and CD (children) Dr Nick Croft Digestive Diseases, Centre for Immunobiology, Blizard Institute & Barts Health NHS Trust Blizard Institute Disclosures Dr Nick Croft
Guided by Dr. Michal Amitai Head of Abdominal Imaging Department of Diagnostic Imaging Sheba Medical Center Sackler School of Medicine, Tel Aviv
 Guided by Dr. Michal Amitai Head of Abdominal Imaging Department of Diagnostic Imaging Sheba Medical Center Sackler School of Medicine, Tel Aviv University 1 SHARE study My year Collaboration between gastroenterology
Guided by Dr. Michal Amitai Head of Abdominal Imaging Department of Diagnostic Imaging Sheba Medical Center Sackler School of Medicine, Tel Aviv University 1 SHARE study My year Collaboration between gastroenterology
Case Report: Induction of Remission in Drug-Resistant Pediatric Inflammatory Bowel Disease with Cannabinoid Therapy
 Case Report: Induction of Remission in Drug-Resistant Pediatric Inflammatory Bowel Disease with Cannabinoid Therapy Natasha R. Ryz, PhD*, Caroline MacCallum, MD (FRCPC Internal Medicine)**, Robert T. Brooke*
Case Report: Induction of Remission in Drug-Resistant Pediatric Inflammatory Bowel Disease with Cannabinoid Therapy Natasha R. Ryz, PhD*, Caroline MacCallum, MD (FRCPC Internal Medicine)**, Robert T. Brooke*
Clinical Use of Measuring Trough Levels and Antibodies against Infliximab in Patients with Pediatric Inflammatory Bowel Disease
 Gut and Liver, Published online September 9, 2016 ORiginal Article Clinical Use of Measuring Trough Levels and Antibodies against Infliximab in Patients with Pediatric Inflammatory Bowel Disease So Yoon
Gut and Liver, Published online September 9, 2016 ORiginal Article Clinical Use of Measuring Trough Levels and Antibodies against Infliximab in Patients with Pediatric Inflammatory Bowel Disease So Yoon
Original Policy Date
 MP 2.04.57 Fecal Calprotectin Testing Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy
MP 2.04.57 Fecal Calprotectin Testing Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy
Personalized Medicine in IBD
 Personalized Medicine in IBD Anita Afzali MD, MPH Assistant Professor of Medicine Director, Inflammatory Bowel Diseases Program University of Washington Harborview Medical Center CCFA April 2 nd, 2016
Personalized Medicine in IBD Anita Afzali MD, MPH Assistant Professor of Medicine Director, Inflammatory Bowel Diseases Program University of Washington Harborview Medical Center CCFA April 2 nd, 2016
How Safe and Effective is Infliximab in the Treatment of Children with Moderate to Severe Crohn s disease?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2011 How Safe and Effective is Infliximab
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2011 How Safe and Effective is Infliximab
Update on Biologics in Ulcerative Colitis. Scott Plevy, MD University of North Carolina Chapel Hill, NC
 Update on Biologics in Ulcerative Colitis Scott Plevy, MD University of North Carolina Chapel Hill, NC Objectives Discuss the latest advances in the pharmacologic management of ulcerative colitis Describe
Update on Biologics in Ulcerative Colitis Scott Plevy, MD University of North Carolina Chapel Hill, NC Objectives Discuss the latest advances in the pharmacologic management of ulcerative colitis Describe
Indian Journal of Basic and Applied Medical Research; June 2015: Vol.-4, Issue- 3, P
 Original article Evaluation of platelet morphology and C-reactive protein in patients of systemic lupus erythematosus attending dermatology outpatient department ( OPD ) of a rural hospital in south India
Original article Evaluation of platelet morphology and C-reactive protein in patients of systemic lupus erythematosus attending dermatology outpatient department ( OPD ) of a rural hospital in south India
Biologic Therapy for Inflammatory. Is Top-Down Too Top-Heavy? S. Devi Rampertab, MD, FACG, AGAF Associate Professor of Medicine University of Florida
 Biologic Therapy for Inflammatory Bowel Disease: Is Top-Down Too Top-Heavy? S. Devi Rampertab, MD, FACG, AGAF Associate Professor of Medicine University of Florida Learning Objectives Evaluate evidence
Biologic Therapy for Inflammatory Bowel Disease: Is Top-Down Too Top-Heavy? S. Devi Rampertab, MD, FACG, AGAF Associate Professor of Medicine University of Florida Learning Objectives Evaluate evidence
Treatment Goals. Current Therapeutic Pyramids Crohn s Disease Ulcerative Colitis 11/14/10
 Current Management of IBD: From Conventional Agents to Biologics Stephen B. Hanauer, M.D. University of Chicago Treatment Goals Induce and maintain response/ remission Prevent complications Improve quality
Current Management of IBD: From Conventional Agents to Biologics Stephen B. Hanauer, M.D. University of Chicago Treatment Goals Induce and maintain response/ remission Prevent complications Improve quality
Definitions. Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency)
 CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
Jonathan R. Dillman, MD, MSc. Associate Professor Department of Radiology Cincinnati Children s Hospital Medical Center
 MR Enterography in Children: Interpretation & Value-Added Jonathan R. Dillman, MD, MSc Associate Professor Department of Radiology Cincinnati Children s Hospital Medical Center Disclosures Crohn s disease
MR Enterography in Children: Interpretation & Value-Added Jonathan R. Dillman, MD, MSc Associate Professor Department of Radiology Cincinnati Children s Hospital Medical Center Disclosures Crohn s disease
Effect of Adalimumab on an Enterocutaneous Fistula in Patients with Crohn s Disease: A Case Series
 CASE REPORT Effect of Adalimumab on an Enterocutaneous Fistula in Patients with Crohn s Disease: A Case Series Kaori Fujiwara, Takuya Inoue, Naoki Yorifuji, Munetaka Iguchi, Taisuke Sakanaka, Ken Narabayashi,
CASE REPORT Effect of Adalimumab on an Enterocutaneous Fistula in Patients with Crohn s Disease: A Case Series Kaori Fujiwara, Takuya Inoue, Naoki Yorifuji, Munetaka Iguchi, Taisuke Sakanaka, Ken Narabayashi,
Gionata Fiorino VEDOLIZUMAB E IBD. Un nuovo target terapeutico
 Gionata Fiorino VEDOLIZUMAB E IBD Un nuovo target terapeutico Anti cell adhesion molecules Danese S, NEJM 2011 6 Steps leukocyte recruitment Fiorino G. et al. 2010 Vedolizumab Blocks Fewer Biological Pathways
Gionata Fiorino VEDOLIZUMAB E IBD Un nuovo target terapeutico Anti cell adhesion molecules Danese S, NEJM 2011 6 Steps leukocyte recruitment Fiorino G. et al. 2010 Vedolizumab Blocks Fewer Biological Pathways
Association Between Plasma Concentrations of Certolizumab Pegol and Endoscopic Outcomes of Patients With Crohn's Disease
 Association Between Plasma Concentrations of Certolizumab Pegol and Endoscopic Outcomes of Patients With Crohn's Disease Jean Frédéric Colombel, William J. Sandborn, Matthieu Allez, Jean Louis Dupas, Olivier
Association Between Plasma Concentrations of Certolizumab Pegol and Endoscopic Outcomes of Patients With Crohn's Disease Jean Frédéric Colombel, William J. Sandborn, Matthieu Allez, Jean Louis Dupas, Olivier
Medical Therapy for Pediatric IBD: Efficacy and Safety
 Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
Consecutive monitoring of faecal calprotectin during mesalazine suppository therapy for active rectal inflammation in ulcerative colitis
 Alimentary Pharmacology and Therapeutics Consecutive monitoring of faecal calprotectin during mesalazine suppository therapy for active rectal inflammation in ulcerative colitis T. Yamamoto, T. Shimoyama
Alimentary Pharmacology and Therapeutics Consecutive monitoring of faecal calprotectin during mesalazine suppository therapy for active rectal inflammation in ulcerative colitis T. Yamamoto, T. Shimoyama
Novel anti-inflammatory compounds for ulcerative colitis and rheumatoid arthritis therapy
 Novel anti-inflammatory compounds for ulcerative colitis and rheumatoid arthritis therapy JANSA, P. 1, HOLÝ, A. 1, ZÍDEK, Z. 2, JANEBA, Z. 1, KOLMAN, V. 1 1 Institute of Organic Chemistry and Biochemistry
Novel anti-inflammatory compounds for ulcerative colitis and rheumatoid arthritis therapy JANSA, P. 1, HOLÝ, A. 1, ZÍDEK, Z. 2, JANEBA, Z. 1, KOLMAN, V. 1 1 Institute of Organic Chemistry and Biochemistry
RE: Title: Practical fecal calprotectin cut-off value for Japanese patients with ulcerative colitis
 September 10, 2018 Professor Xue-Jiao Wang, MD Science Editor Editorial Office 'World Journal of Gastroenterology' RE: 40814 Title: Practical fecal calprotectin cut-off value for Japanese patients with
September 10, 2018 Professor Xue-Jiao Wang, MD Science Editor Editorial Office 'World Journal of Gastroenterology' RE: 40814 Title: Practical fecal calprotectin cut-off value for Japanese patients with
IBD Understanding Your Medications. Thomas V. Aguirre, MD Santa Barbara GI Consultants
 IBD Understanding Your Medications Thomas V. Aguirre, MD Santa Barbara GI Consultants IBD Understanding Your Medications (& Your Doctor) Thomas V. Aguirre, MD Santa Barbara GI Consultants Disclosure I
IBD Understanding Your Medications Thomas V. Aguirre, MD Santa Barbara GI Consultants IBD Understanding Your Medications (& Your Doctor) Thomas V. Aguirre, MD Santa Barbara GI Consultants Disclosure I
Outline. Biologic Drugs in Inflammatory Bowel Disease Dr. Jason Etzel MD The Vancouver Clinic. Biologic Drugs. Biologic Drugs. Biologic Drugs Anti-TNF
 Outline Biologic Drugs in Inflammatory Bowel Disease Dr. Jason Etzel MD The Vancouver Clinic Types of biologic drugs How do they work? How effective are they? Safety/Toxicity concerns with biologics Biologic
Outline Biologic Drugs in Inflammatory Bowel Disease Dr. Jason Etzel MD The Vancouver Clinic Types of biologic drugs How do they work? How effective are they? Safety/Toxicity concerns with biologics Biologic
INFLAMMATORY BOWEL DISEASE. Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic
 INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
Biologic Therapy for Ulcerative Colitis in 2015
 5/6/215 Biologic Therapy for Ulcerative Colitis in 215 John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University Bressler B, Marshall JK, et al. Gastroenterology 215;148: 135-58
5/6/215 Biologic Therapy for Ulcerative Colitis in 215 John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University Bressler B, Marshall JK, et al. Gastroenterology 215;148: 135-58
1. Background: Infliximab is administered parenterally; therefore, it is not covered under retail pharmacy benefits.
 Subject: Infliximab (Remicade ) Original Original Committee Approval: October 13, 2006 Revised Last Committee Approval: December 3, 2008 Last Review: October 19, 2007 1. Background: Infliximab is a genetically
Subject: Infliximab (Remicade ) Original Original Committee Approval: October 13, 2006 Revised Last Committee Approval: December 3, 2008 Last Review: October 19, 2007 1. Background: Infliximab is a genetically
TREATMENT OF INPATIENTS WITH ACUTE SEVERE ULCERATIVE COLITIS
 TREATMENT OF INPATIENTS WITH ACUTE SEVERE ULCERATIVE COLITIS Target Audience: Physicians, Physician Assistants, Nurse Practitioners and Nurses impacted by the protocol. Scope/Patient Population: All adult
TREATMENT OF INPATIENTS WITH ACUTE SEVERE ULCERATIVE COLITIS Target Audience: Physicians, Physician Assistants, Nurse Practitioners and Nurses impacted by the protocol. Scope/Patient Population: All adult
Spectrum of Diverticular Disease. Outline
 Spectrum of Disease ACG Postgraduate Course January 24, 2015 Lisa Strate, MD, MPH Associate Professor of Medicine University of Washington, Seattle, WA Outline Traditional theories and updated perspectives
Spectrum of Disease ACG Postgraduate Course January 24, 2015 Lisa Strate, MD, MPH Associate Professor of Medicine University of Washington, Seattle, WA Outline Traditional theories and updated perspectives
Inflammatory Bowel Disease: Clinical updates. Dr Jeff Chao Princess Alexandra Hospital
 Inflammatory Bowel Disease: Clinical updates Dr Jeff Chao Princess Alexandra Hospital Inflammatory bowel disease 2017 Clinical updates and future directions Pathogenesis Treatment targets Therapeutic agents
Inflammatory Bowel Disease: Clinical updates Dr Jeff Chao Princess Alexandra Hospital Inflammatory bowel disease 2017 Clinical updates and future directions Pathogenesis Treatment targets Therapeutic agents
Clinical Policy Title: Fecal biomarkers in inflammatory bowel disease
 Clinical Policy Title: Fecal biomarkers in inflammatory bowel disease Clinical Policy Number: 08.01.08 Effective Date: April 1, 2017 Initial Review Date: October 19, 2016 Most Recent Review Date: November
Clinical Policy Title: Fecal biomarkers in inflammatory bowel disease Clinical Policy Number: 08.01.08 Effective Date: April 1, 2017 Initial Review Date: October 19, 2016 Most Recent Review Date: November
High Percentage of IBD Patients with Indefinite Fecal Calprotectin Levels: Additional Value of a Combination Score
 Dig Dis Sci (2017) 62:465 472 DOI 10.1007/s10620-016-4397-6 ORIGINAL ARTICLE High Percentage of IBD Patients with Indefinite Fecal Calprotectin Levels: Additional Value of a Combination Score Alexander
Dig Dis Sci (2017) 62:465 472 DOI 10.1007/s10620-016-4397-6 ORIGINAL ARTICLE High Percentage of IBD Patients with Indefinite Fecal Calprotectin Levels: Additional Value of a Combination Score Alexander
