PDF hosted at the Radboud Repository of the Radboud University Nijmegen
|
|
|
- Ashlynn Shepherd
- 6 years ago
- Views:
Transcription
1 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. Please be advised that this information was generated on and may be subject to change.
2 Acta Derm Venereol 2011; 91: 5 11 REVIEW ARTICLE Genital Psoriasis: A Systematic Literature Review on this Hidden Skin Disease Kim A. P. Meeuwis 1,2, Joanne A. de Hullu 2, Leon F. A. G. Massuger 2, Peter C. M. van de Kerkhof 1 and Michelle M. van Rossum 1 Departments of 1 Dermatology and 2 Obstetrics and Gynaecology, Radboud University Nijmegen Medical Centre, Nijmegen, The Netherlands It is well known that the genital skin may be affected by psoriasis. However, little is known about the prevalence and clinical appearance of genital psoriasis, and genital skin is often neglected in the treatment of psoriatic patients. We performed an extensive systematic literature search for evidence-based data on genital psoriasis with respect to epidemiology, aetiology, clinical and histopathological presentation, diagnosis and treatment. Three bibliogra phical databases (PubMed, EMBASE and the Cochrane Library) were used as data sources. Fifty-nine articles on genital psoriasis were included. The results show that psoriasis frequently affects the genital skin, but that evidence-based data with respect to the efficacy and safety of treatments for genital psoriasis are extremely limited. An advised treatment paradigm for genital psoriasis, based on the levels of evidence, is: first-line: (weak) topical corticosteroids; second-line: vitamin D preparations or tar-based treatments. Key words: psoriasis; inverse psoriasis; flexural psoriasis; male/female genital diseases; genital; treatment. (Accepted June 29, 2010.) Acta Derm Venereol 2011; 91: Kim A. P. Meeuwis, Department of Dermatology (370), Radboud University Nijmegen Medical Centre, PO Box 9101, NL-6500 HB Nijmegen, The Netherlands. k.meeuwis@derma.umcn.nl A wide range of cutaneous diseases can affect the female and male genital skin. Some of these dermatoses are entirely or predominantly present in this region, while others, such as psoriasis, primarily involve non-genital skin. Psoriasis is a chronic, inflammatory epidermal skin disease with a high prevalence in the general population of approximately 2% (1 3). It is one of the most commonly seen dermatoses of genital skin, although often limited attention is paid to the genital presentation of this skin disease. In many cases, genital psoriasis is part of a more generalised plaque psoriasis, although the external genitalia may be the only area affected. However, the isolated presentation of psoriasis solely on genital skin seems to be rare and occurs in only 2 5% of the psoriatic patients (4, 5). Genital skin can also be affected in cases of inverse psoriasis (synonym: flexural or intertriginous psoriasis) (2, 4, 5). The external genital skin is generally classified as flexural skin, although it forms a unique area comprising different structures and types of epithelium. The epithelium covering the different structures of the vulva changes from stratified, keratinised squamous cell epithelium on the outer parts to mucosa on the innermost regions (5, 6). Similarly, the male genital epithelium has a different pattern of keratinisation throughout the genital area. The prepuce forms the anatomical covering of the glans penis and is the junction between the mucosal surface of the glans and coronal sulcus and the keratinised squamous cell epithelium of the remaining external genital skin (7). In general, the unique microenvironment of the genital region may have consequences for the clinical appearance of skin diseases. Genital skin folds are susceptible to maceration and fissuring due to the combination of moisture, warmth and friction. In addition, the genital area is often exposed to mechanical and chemical irritation. Consequently, the normal characteristics of common dermatoses may be lost or modified in the genital region. Moreover, as a result of their location, these dermatoses may be confused with sexually transmitted diseases. Because of the high sensitivity of the vulnerable, thin genital skin and the increased penetration of topical treatments applied to this site of the body, treatment of genital lesions is a challenge. Psoriasis affecting genital skin may be associated with considerable morbidity, discomfort and embarrassment and may considerably impair quality of life and psychosexual wellbeing. This review covers both female and male genital psoriatic lesions. Epidemiology, aetiology, clinical and histopathological findings, diagnosis and the various treatment options are described. MATERIALS AND METHODS An extensive literature search was performed to collect evidencebased data on genital psoriasis. Relevant literature published between January 1988 and June 2009 was obtained from three computerised bibliographical databases: PubMed, EMBASE and the Cochrane Library. Additional papers were identified using the related articles button in PubMed The Authors. doi: / Journal Compilation 2011 Acta Dermato-Venereologica. ISSN
3 6 K. A. P. Meeuwis et al. Key words and selection criteria As key words we used psoriasis or psoriatic, combined with inverse, inversa, intertriginous, flexural or flexures. Subsequently, these key words were combined with the following search terms: groin, groins, genital* (truncated), anogenital* (truncated), vulva* (truncated), penis, penile, foreskin, prepuce, preputial, penoscrotal, scrotal, scrotum, inguinal, anal, anus, diaper and napkin. The search and selection of the literature was restricted to publications written in English, Dutch, German or French. Because published data specific for genital psoriasis are extremely limited, we reviewed all available literature, including clinical trials, case reports, retrospective studies, and letters to the editor concerning all types of genital psoriasis. Study selection: inclusion and exclusion criteria The selection of studies involved a two-stage process. Titles and abstracts of all identified citations were screened; full-text articles were obtained if potentially relevant according to the abstract. Articles without information on flexural or genital psoriasis were excluded during this first selection step. Articles present in more than one database were included once. Subsequently, two reviewers (KM and MvR) independently and critically assessed the articles for inclusion or exclusion, using a checklist. Levels of evidence and grading recommendations were determined according to the Oxford Centre for Evidence-based Medicine Levels of Evidence guidelines, version March 2009 (adapted from The Oxford Centre for Evidence-based Medicine suggests levels of evidence (LoE) according to the study design. These levels vary between 1a and 5 the higher the number, the worse the quality of the evidence. Recommendations are graded from A (strong) to D (weak) based on the LoE. Articles covering all types of genital psoriatic lesions in all age groups were included. Articles on flexural psoriasis with inadequate/insufficient data on genital psoriasis (e.g. articles that did not discriminate between flexural and genital psoriasis or trials that did not assess the safety and efficacy of the investigated Citations obtained via manual search n=15 Total citations identified from electronic databases PubMed (345) Embase (434) Cochrane (19) n=798 Citations for first screening (potentially relevant) n=540 Full text articles for detailed evaluation n=184 Articles included in review n=59 Duplicate articles excluded n=258 Citations excluded after screening titles and abstracts n=356 Excluded after examination of full text manuscript n=140 - Unavailable (n=42) - Not relevant (n=98) No relevant information on genital psoriasis (n=60) No discrimination between flexural and genital psoriasis (n=22) Focus: secondary endpoint (n=12) Article only referring to other publications (n=4) Fig. 1. The selection process for relevant articles on genital psoriasis. therapy on genital skin) were excluded. In addition, articles that referred only to other publications were excluded and the source data were retrieved instead. Articles in which genital psoriasis cases were excluded from the analysis, as well as articles about secondary outcome measures, case reports without any supplementary information, and articles that were not available were also excluded. When there was disagreement about article selection, a third investigator (JdH) was consulted. Reference lists in the selected articles were scrutinised to identify other relevant articles that had been overlooked in the database search. Fig. 1 illustrates the complete selection process. RESULTS A total of 798 citations that were potentially relevant were identified. Of these, 184 articles seemed to be relevant according to their title and abstract and were selected for detailed evaluation. Forty-two articles were not available since they were published in journals that were unavailable via the libraries of nine European universities. For 98 articles the exclusion criteria appeared to be applicable on closer evaluation. These articles were excluded from further evaluation. In addition, a manual search of the reference lists retrieved a further 15 articles. Consequently, 59 full-text articles were considered appro priate for detailed evaluation (see references 8 66). Epidemiology Table I recapitulates the results of several questionnaire-based surveys, showing that involvement of the genital skin occurs in 29 40% of patients with psoriasis (8 12) [LoE: 4]. The genital area may frequently be involved in cases of inverse psoriasis. Of 48 patients with inverse psoriasis, the external genitalia were involved in 38 (79.2%). All the cases concerned were diagnosed by two dermatologists (13) [LoE: 4]. Vulvar psoriasis [LoE: 4]. Psoriasis of the vulva was found in 25 of 1,000 women referred to special vulval clinics (14). In addition, in a group of 101 patients with chronic symptomatic (predominantly itching) vulvar disorders, two (2%) were caused by psoriasis (15). Two articles focused on non-neoplastic vulvar biopsies. Two biopsies from 114 women who visited a multidisciplinary clinic specialising in non-neoplastic diseases of the vagina and vulva were histologically diagnosed as vulvar psoriasis (16). Of 43 cases with clinical and pathological diagnoses of non-neoplastic alterations of the vulva, three were found to be suffering from psoriasis (17). An investigation into the pattern of non-venereal dermatoses of the female external genitalia, conducted in a dermatology and gynaecology outpatient department in South India, revealed that five patients out of a total of 120 (4.2%) had psoriasis (18). Vulvar psoriasis is also frequently seen in children. In an evaluation of 130 prepubertal girls with vulvar
4 Genital psoriasis 7 Table I. Involvement of the genital skin in patients with psoriasis Source Number of patients Genital involvement Author, year (ref.) Total Male Female n % Male: Female (%) Hellgren, 1964 (8) :10 (32.9:21.7) Farber et al., 1968 (9) :247 (43.0:21.0) Farber & Nall, 1974 (10) :994 (48.8:32.7) van de Kerkhof et al., 2000 (11) N/A Fouéré et al., 2005 (12) 1281 N/A N/A N/A N/A: not applicable. complaints, psoriasis (17%) was the third most common cutaneous condition, after atopic or irritant dermatitis (33%) and lichen sclerosus (18%) (19). Additionally, others found psoriasis to be one of the most common non-venereal dermatoses in a group of prepubertal girls, affecting two (9.5%) of the 21 patients studied (18). Penile psoriasis [LoE: 5]. One report stated that psoriasis of the penis can be diagnosed in 3% of male patients with alterations of the penile skin who visit specialised clinics (20). Aetiology No articles describing or discussing the aetiology of genital psoriasis were retrieved in this systematic review of the literature. Clinical presentation [LoE: 5] Psoriatic lesions on the genital skin often present as well-demarcated, brightly erythematous, thin plaques and usually lack, due to maceration, the typical scaling that is apparent on other parts of the body (21 39). However, scales may be seen on the more keratinised regions of the genital skin (34, 40, 41). When scaling is present, it is often minimal and can easily be scraped off, leaving pinpoint bleedings (26, 27, 38, 42). The appearance of vulvar psoriasis is often symmetrical and can vary from silvery, scaling patches adjacent to the outer parts of the labia majora to moist greyish plaques or glossy red plaques without scaling in the skin folds (33, 35, 40, 42 45). In male patients, both scrotal and penile skin may be affected. The glans penis is the area of male genital skin that is most commonly affected. Occasionally the entire penis, scrotum, and inguinal folds are involved (25, 26, 30, 41, 46). Whereas in uncircumcised males the welldefined non-scaling plaques are most common under the prepuce and on the proximal glans, in circumcised male patients the red lesions are usually present on the glans and corona (25, 30, 41). Psoriatic genital lesions of the glans and corona in circumcised males can be more scaly than those usually seen in genital skin (25, 41, 47). Some authors suggest that involvement of the genital mucosa may be diagnosed less frequently in women than in men (32, 34, 36). Genital lesions may be accompanied by rhagades or fissures, which can cause definite soreness (28, 48). Patients with genital psoriasis may also experience pruritus and/or a burning sensation in the affected area, which can range from minimal to marked (23, 26, 30, 36, 42, 49). Psoriasis is generally not associated with scarring. However, one case report described two patients with long-standing severe anogenital psoriasis that was associated with loss of the labia minora. Clinically, this mimicked the scarring associated with lichen sclerosus, but histopathologically the lesions were diagnosed as psoriasis (50). No other reports of genital scarring due to psoriasis were found in our systematic review of the literature. Due to the Koebner phenomenon, genital psoriasis may be worsened by irritation from urine and faeces, tightfitting clothes and sexual intercourse (26, 38, 40, 47). Pustular psoriasis. Although most genital psoriatic lesions represent plaque-type psoriasis, the genital area may also be affected by pustular psoriasis. Both generalised and localised pustular psoriatic eruptions may affect the genital skin (51 53). A case of a 23-year-old man with pustular psoriasis limited to the penis was described. The lesions presented as numerous white papules and pustules on an erythematous base (52). Another patient with recurrent episodes of multiple, painless, circinate, pustular eruptions over the glans penis was found to be suffering from pustular psoriasis on histopathological examination (53). No reports of female genital pustular psoriasis were found in our systematic review of the literature. Children. Although there is no difference in the presentation of genital psoriasis between children and adults, psoriatic napkin eruption deserves special attention in this review. It has been debated whether this condition should be regarded as psoriasis, seborrhoeic dermatitis or a Candida infection, although it is currently assumed that both localised and disseminated psoriatic napkin eruptions may represent psoriasis or a precursor to psoriasis in some children (37, 54 58) [LoE: 4]. The eruption is characterised by confluent erythematous, and sometimes silvery-squamous, plaques with welldefined borders in the napkin area, with the genitals possibly also being affected. Most often the lesions are surrounded by psoriasis-like papules, and may spread to the trunk, limbs and, very frequently, the scalp and
5 8 K. A. P. Meeuwis et al. face (37, 55, 56, 58 61) [LoE: 4 and 5]. In a clinical review of 1,262 cases of childhood psoriasis, 13% of the children studied had a psoriatic napkin eruption with dissemination and approximately 4% had a localised psoriatic napkin eruption. In children younger than two years of age psoriatic napkin eruption with dissemination was the most common type of psoriasis. Moreover, anogenital psoriasis occurred four times more often in children over two years of age than in children under two years of age (37) [LoE: 4]. Diagnosis [LoE: 4 and 5] The diagnosis of genital psoriasis can usually be made on the basis of its clinical appearance. Genital psoriatic lesions may be the only psoriatic features in a particular patient, but more often they are part of a more generalised form of psoriasis. Confirmatory lesions elsewhere or other clinical signs of psoriasis (such as nail deformities or joint complaints) may be present (19, 22 25, 27, 28, 30, 31, 33, 35, 36, 41 43, 45, 46). Skin biopsies are therefore rarely needed, but should not be omitted in inconclusive cases. Table II shows the possible differential diagnoses in cases of genital psoriasis, as mentioned in source articles. Histologically there is no apparent difference between genital and non-genital psoriasis (14, 16, 17, 22, 23, 27, 28, 34, 41). However, the typical characteristics of psoriasis may be less evident in vulvar and penile psoriatic lesions, which may necessitate a careful search for subtle signs in these cases (17, 50). Therapy Case reports [LoE: 4 and 5]. The current literature provides extremely limited evidence for the efficacy and safety of treatment options for genital psoriasis. Table II. Possible differential diagnoses in cases of genital psoriasis, as mentioned in source articles Differential diagnosis Dermatitis (variants: seborrhoeic dermatitis, contact dermatitis, atopic dermatitis, spongiotic dermatitis) References 16, 22, 23, 34, 35, 42, 45, 52, 55, 59 Dermatophytosis or candidiasis 16, 22, 34, 40, 42, 47, 59 Squamous cell carcinoma (in situ) (variants: 21, 26, 30, 34, 41, 46, 52 morbus Bowen, Bowenoid papulosis, erythroplasia de Queyrat) Plasma-cell balanitis or vulvitis 21, 34, 40, 41, 46, 52 Lichen planus 22, 41, 42, 46, 52 Secondary or tertiary (pustular) syphilis 22, 42, 46, 52, 53 Reiter s syndrome (balanitis circinata) 41, 47, 52, 53 Lichen simplex chronicus (excoriated) 16, 23, 42 Extramammary Paget disease 21, 42 Intertrigo 22, 34 Fixed drug eruption 41, 52 Lichen nitidus 52 Lichen sclerosus 23 Scabies or pediculosis pubis 42 Only six casuistic reports and one open-label study have roughly described the effects of therapies used. An overview of these reports can be found in Table III. Based on these reports, 1% pimecrolimus cream and topical cyclosporine may produce beneficial effects when used to treat plaque psoriasis of the glans penis and prepuce (62, 63). The application of an ointment containing betamethasone-17-valerate (a potent corticosteroid) three times a day was useful for psoriasis of the labium majus in one patient (42). Corticosteroid ointment was effective in only three out of 67 children with napkin plaque psoriasis, while coal-tar preparations were helpful in the remaining 64 patients. Therapy with zinc paste and salicylic acid was ineffective in these patients (54). Ketoconazole cream was effective against lesions in the napkin area of a four-month-old boy suffering from napkin psoriasis with pustular dissemination, where examination of the scales was positive for fungal infection (64). Two case reports of pustular psoriasis of the glans and penile shaft were included in our study. One of these suggests a minor effect of the combination of a weak corticosteroid with coal-tar. Systemic treatment with itraconazole (200 mg twice daily for 6 weeks) demonstrated some effect, whereas dapsone (100 mg daily for 4 weeks) was very effective (52, 53). Expert opinions [LoE: 5].Twenty-four articles reflected merely the opinions of experts on the preferred treatments for genital psoriasis. We have summarised these different opinions in Table SI ( Corticosteroids. All authors advise the use of topical corticosteroids. Most of the authors are reluctant in the prescription of corticosteroids for genital psoriasis and only recommend the use of weak (and sometimes, if necessary, moderate) steroids, which may be combined with vitamin D analogues or mild tar preparations (25, 26, 32 34, 40, 41, 47, 60, 61). Although weak cortico steroids are preferable because of their mild sideeffects, they often seem insufficiently potent to induce a response. Some experts therefore advise short-term, intermittent use of moderate-to-potent corticosteroids to induce a response, followed by a subsequent gradual shift towards a weaker steroid preparation (14, 35, 36, 43 45, 65). On the contrary, other authors advise intensive, short-term, intermittent use of potent corticosteroids (22, 23, 29, 30, 46, 59, 66). Coal-tar preparations. The use of mild topical tar preparations (i.e. 1 5% liquor carbonis detergens in aqueous cream) for the treat ment of genital psoriasis is frequently recommended and is the second most advised topical therapy after corticosteroids. Tar may be used as an individual topical therapy or, when (maintenance) treatment with weak potent corticosteroids is insufficient, be combined or alternated with topical steroids (25, 35, 36, 40, 41, 44, 45, 65). Tar may also be used
6 Genital psoriasis 9 Table III. Case reports/series on treatment of genital psoriasis Study characteristics Treatments and outcomes Cohort No. patients (M/F, age group) Site LoE Therapy 1 Therapy 2 Conclusion/remarks Type of psoriasis Source First author, year (ref.) Study design Treatment was effective and recurrence was treated successfully Amichai, 2004 (62) Case report Plaque 1 (1/0, C) Glans penis 5 1% pimecrolimus cream, 3 weeks, topical Marked local improvement within 4 weeks; no side effects 4 Topical cyclosporine (100 mg/ml) as a wet dressing, 3 times a day Open label Plaque 3 (3/0, A) Glans penis & inner fold prepuce (=mucosal skin) Jemec & Baadsgaard, 1993 (63) Lesions disappeared in several days Case report Plaque 1 (0/1, A) Labium majus 5 Betamethasone-17-valerate ointment, 3 times a day Weinrauch & Katz, 1986 (42) Zinc paste and salicylic acid ointment were ineffective Coal-tar: effective in the remaining 64 patients Case series Plaque 67 (35/32, C) Napkin area 4 Corticosteroid ointment: only effective in three patients Andersen & Thomsen, 1971 (54) Case report Plaque 1 (1/0, C) Napkin area 5 0.2% ketoconazole cream Lesions gradually resolved (complete clearance within one month) Watanabe et al., 2002 (64) Itraconazole was directed towards possible Candida colonization Oral itraconazole 200 mg, twice daily for 6 weeks: some improvement 5 1% hydrocortisone and 2% coaltar: little improvement Case report Pustular 1 (1/0, A) Glans penis and distal penile shaft Quan & Ruben, 1996 (52) Case report Pustular 1 (1/0, A) Glans 5 Dapsone, 100 mg daily Lesions subsided completely in 4 weeks Singh & Thappa, 2008 (53) M: male; F: female; LoE: level of evidence; C: children; A: adults. for napkin psoriasis, for example mixed with zinc oxide (60, 61). Despite these positive opinions regarding the use of coal-tar preparations, there are also reports that advise against the use of tar preparations because of their potential to cause irritation (22, 29, 32, 33). Others point out the importance of the choice of the vehicle, as tar gels may be too irritating to sensitive genital skin and tar ointment may cause folliculitis in hairy areas. They suggest that mixing a tar preparation with a steroid preparation may reduce irritation (40). Vitamin D analogues.vitamin D analogues are another possible non-steroidal treatment for genital psoriatic lesions, in particular those affecting male genital skin (25, 26, 30, 46). They can be prescribed as mo notherapy or in combination with steroid preparations (25). Vitamin D analogues may cause irritation, which may be minimised by their combination with steroids (25, 46). Nevertheless, some authors advise against the use of vitamin D analogues, as these may be too irritating to apply to the genital area (33, 60). Immunomodulators. One author expressed the opinion that the use of pimecrolimus ointment or tacrolimus cream may be useful (33), while acknowledging that they may cause local irritation and stinging. Monitoring of possible complications of immunomodulators is advised, as they can cause irritant or allergic contact dermatitis, candidiasis, or (re)activation of viral skin infections. Other modalities/general advice. Suspected concurrent bacterial or fungal infections of the genital area should be treated with topical antibiotics or ketoconazole/miconazole, respectively, to eliminate the possible Koebner effect (23, 26, 30, 32, 35, 36, 40, 46, 60). Moreover, minimising contact with local irritating factors and the use of mild emollients may be useful in the treatment of genital psoriasis (29, 40, 46, 59). Systemic therapy is no common practice for isolated genital psoriasis. Nevertheless, such treatment modalities may also be beneficial for genital lesions if prescribed because of severe and extensive psoriasis (32, 33). Anthralin, tazarotene, ultraviolet (UV)-light and laser therapy should be avoided in the genital area (22, 33, 40). Therapy-resistant penile and vulvar plaques should always be clinically and histologically re-evaluated to rule out malignancy (26, 30, 42). CONCLUSION An extensive, systematic literature search revealed data concerning the epidemiology, clinical presentation and therapy of psoriasis of the genital skin. Remarkably few studies have been published on this topic. Our literature review demonstrates that this hidden skin disease will affect a significant proportion of patients with psoriasis at some time during their disease and is a frequent cause of genital complaints.
7 10 K. A. P. Meeuwis et al. It remains to be established whether genital discomfort in psoriatic patients is caused by genital psoriasis or by a comorbidity of the genital skin/mucosa. Examination of the whole skin, including the genital region, is important and should be implemented in daily clinical practice. Unfortunately, there is often no discrimination between flexural and genital psoriasis in existing publications. Moreover, the current literature often lacks data on the efficacy and safety of investigated treatments for genital skin, and therefore the treatment of genital psoriasis is often empirical. Based on the available literature, the following treatment paradigm is advised for genital psoriasis: First-line treatment: topical corticosteroid. Secondline treatment: vitamin D preparation or tar-based treatment. The general advice is to start with weak corticos teroids and, in cases of resistance to treatment, to increase the strength of the corticosteroid preparation. Treatment with potent corticosteroids should be limited to a few weeks in view of their atrophic effects, in particular on genital skin. The addition of topical vitamin D or coal-tar preparations has been suggested to be effective. They can reduce the side-effects of cortico steroids, although irritation may restrict their application. Evidence for the use of immunomodulators on genital skin is scarce. They should be regarded as third-line treatment options. These recommendations are based on case series and expert opinions only (grade of recommendation: D). Further studies are urgently needed to determine the efficacy and safety of potential treatments and to improve care for patients with genital psoriasis. ACKNOWLEDGEMENTS This systematic review was funded by LEO Pharma. LEO Pharma played no role in the design and conduct of the study or in data collection, data management, data analysis, interpretation of the data, manuscript preparation, manuscript review or manuscript approval. The authors declare no conflicts of interest. REFERENCES 1. Christophers E. Psoriasis epidemiology and clinical spectrum. Clin Exp Dermatol 2001; 26: Myers WA, Gottlieb AB, Mease P. Psoriasis and psoriatic arthritis: clinical features and disease mechanisms. Clin Dermatol 2006; 24: Raychaudhuri SP, Farber EM. The prevalence of psoriasis in the world. J Eur Acad Dermatol Venereol 2001; 15: van de Kerkhof PCM. Clinical Features. In: van de Kerkhof PCM, editor. Textbook of Psoriasis. Oxford: Blackwell Publishing Ltd, 2003: p Stoof TJ, van der Meijden WI. Psoriasis. In: van der Meijden WI, ter Harmsel WA, editors. Vulvapathologie. Assen: Koninklijke Van Gorcum BV, 2007: Bunker CB, Neill SM. The genital, perianal and umbilical regions. In: Rook A, Burns T, Breathnach SM, Cox N, Griffiths CE, editors. Rook s textbook of dermatology. Oxford: Blackwell Publishing, 2004: Cold CJ, Taylor JR. The prepuce. BJU Int 1999; 83 Suppl 1: Hellgren L. Psoriasis. A statistical, clinical and laboratory investigation of 255 psoriatics and matched healthy controls. Acta Derm Venereol 1964; 44: Farber EM, Bright RD, Nall ML. Psoriasis. A questionnaire survey of 2,144 patients. Arch Dermatol 1968; 98: Farber EM, Nall ML. The natural history of psoriasis in 5,600 patients. Dermatologica 1974; 148: van de Kerkhof PCM, de Hoop D, de Korte J, Cobelens SA, Kuipers MV. Patient compliance and disease management in the treatment of psoriasis in the Netherlands. Dermatology 2000; 200: Fouéré S, Adjadj L, Pawin H. How patients experience psoriasis: results from a European survey. J Eur Acad Dermatol Venereol 2005; 19 Suppl 3: Wang G, Li C, Gao T, Liu Y. Clinical analysis of 48 cases of inverse psoriasis: a hospital-based study. Eur J Dermatol 2005; 15: MacLean AB, Roberts DT, Reid WMN. Review of 1000 women seen at two specially designated vulval clinics. Curr Obstet Gynaecol 1998; 8: Fischer G, Spurrett B, Fischer A. The chronically symptomatic vulva: aetiology and management. Br J Obstet Gynaecol 1995; 102: O Keefe RJ, Scurry JP, Dennerstein G, Sfameni S, Brenan J. Audit of 114 non-neoplastic vulvar biopsies. Br J Obstet Gynaecol 1995; 102: Ambros RA, Malfetano JH, Carlson JA, Mihm MC Jr. Nonneoplastic epithelial alterations of the vulva: recognition assessment and comparisons of terminologies used among the various specialties. Mod Pathol 1997; 10: Singh N, Thappa DM, Jaisankar TJ, Habeebullah S. Pattern of non-venereal dermatoses of female external genitalia in South India. Dermatol Online J 2008; 14: Fischer G, Rogers M. Vulvar disease in children: a clinical audit of 130 cases. Pediatr Dermatol 2000; 17: Kohn FM. Hautveränderungen des Penis. Differenzieren Sie den Lokalbefund von gereralisierten Erkrankungen! MMW Fortschr Med 2002; 144: Lisi P. Differential diagnosis of psoriasis. Reumatismo 2007; 59 Supp 1: Mroczkowski TF. Common nonvenereal genital lesions. Med Clin North Am 1990; 74: Pincus SH. Vulvar dermatoses and pruritus vulvae. Dermatol Clin 1992; 10: Apgar BS, Cox JT. Differentiating normal and ab normal findings of the vulva. Am Fam Physician 1996; 53: Buechner SA. Common skin disorders of the penis. BJU Int 2002; 90: Goldman BD. Common dermatoses of the male genitalia. Recognition of differences in genital rashes and lesions is essential and attainable. Postgrad Med 2000; 108: Golombowski G, Anthuber S, Anthuber C. Vulvaerkran- kungen im Kindesalter. Gynakologe 1998; 31: Gross G. Dermatologische Befunde an Mamma und Genitale. Gynakologe 2001; 34: Nunns D. Pruritus vulvae. Curr Obs Gynaecol 2002; 12: van Dijk F, Thio HB, Neumann HAM. Non-oncological and non-infectious diseases of the penis (penile lesions). EAU- EBU Update Series 2006; 4:
8 Genital psoriasis Rosen T. Update on genital lesions. JAMA 2003; 290: Salim A, Wojnarowska F. Skin diseases affecting the vulva. Curr Obstet Gynaecol 2002; 12: Trager JDK. What s your diagnosis? Well-demarcated vulvar erythema in two girls. J Pediatr Adolesc Gynecol 2005; 18: Varghese M, Kindel S. Pigmentary disorders and inflammatory lesions of the external genitalia. Urol Clin North Am 1992; 19: Welsh B, Howard A, Cook K. Vulval itch. Aust Fam Physician 2004; 33: Fischer GO. Vulval disease in pre-pubertal girls. Australas J Dermatol 2001; 42: Morris A, Rogers M, Fischer G, Williams K. Childhood psoriasis: a clinical review of 1262 cases. Pediatr Dermatol 2001; 18: Fiumara NJ. Psoriasis of the penis: Koebner reaction. Following oral genital exposure. J Am Vener Dis Assoc 1976; 3: Eichmann AR. Dermatoses of the male genital area. Dermatology 2005; 210: Farber EM, Nall L. Genital psoriasis. Cutis 1992; 50: Coldiron BM, Jacobson C. Common penile lesions. Urol Clin North Am 1988; 15: Weinrauch L, Katz M. Psoriasis vulgaris of labium majus. Cutis 1986; 38: McKay M. Vulvitis and vulvovaginitis: cutaneous considerations. Am J Obstet Gynecol 1991; 165: Paek SC, Merritt DF, Mallory SB. Pruritus vulvae in prepubertal children. J Am Acad Dermatol 2001; 44: Welsh BM, Berzins KN, Cook KA, Fairley CK. Management of common vulval conditions. Med J Aust 2003; 178: Bonnetblanc J-M. Psoriasis. Ann Dermatol Venereol 2006; 133: Shenenberger DW. Curbing the psoriasis cascade: Therapies to minimize flares and frustration. Postgrad Med 2005; 117: Porter WM, Bunker CB. The dysfunctional foreskin. Int J STD AIDS 2001; 12: Zamirska A, Reich A, Berny-Moreno J, Salomon J, Szepie- towski JC. Vulvar pruritus and burning sensation in women with psoriasis. Acta Derm Venereol 2008; 88: Albert S, Neill S, Derrick EK, Calonje E. Psoriasis associated with vulval scarring. Clin Exp Dermatol 2004; 29: Tolman MM, Moschella SL. Pustular psoriasis (Zumbusch). Arch Dermatol 1960; 81: Quan MB, Ruben BS. Pustular psoriasis limited to the penis. Int J Dermatol 1996; 35: Singh N, Thappa DM. Circinate pustular psoriasis localized to glans penis mimicking circinate balanitis and responsive to dapsone. Indian J Dermatol Venereol Leprol 2008; 74: Andersen SL, Thomsen K. Psoriasiform napkin dermatitis. Br J Dermatol 1971; 84: Warin RP, Faulkner KE. Napkin psoriasis. Br J Dermatol 1961; 73: de Raeve L. Etiology, diagnosis and treatment of diaper dermatitis. [Dutch]. Tijdschrift voor Geneeskunde 1991; 47: Neville EA, Finn OA. Psoriasiform napkin dermatitis a follow-up study. Br J Dermatol 1975; 92: Boje Rasmussen H, Hagdrup H, Schmidt H. Psoriasiform napkin dermatitis. Acta Derm Venereol 1986; 66: Fond L, Michel JL, Gentil-Perret A, Eve B, Montelimard N, Perrot JL, et al. Psoriasis chez l enfant. Arch Pediatr 1999; 6: Camilleri MJ, Calobrisi SD. Skin eruptions in the diaper area. Curr Problems Dermatol 1999; 11: Hogan P. Irritant napkin dermatitis. Aust Fam Physician 1999; 28: Amichai B. Psoriasis of the glans penis in a child successfully treated with Elidel (pimecrolimus) cream. J Eur Acad Dermatol Venereol 2004; 18: Jemec GB, Baadsgaard O. Effect of cyclosporine on genital psoriasis and lichen planus. J Am Acad Dermatol 1993; 29: Watanabe M, Tabata N, Tagami H. Explosive diaper pustular psoriasis. Pediatr Dermatol 2002; 19: Siddha SK, Burden AD. Recognition and treatment of psoriasis in children. Paediatr Child Health 2007; 17: Quint EH, Smith YR. Vulvar disorders in adolescent patients. Pediatr Clin North Am 1999; 46:
Psoriasis Penis - A Two Case Report
 Article ID: WMC003176 ISSN 2046-1690 Psoriasis Penis - A Two Case Report Corresponding Author: Dr. Ilko Bakardzhiev, MD, PhD, Medical College, Medical University of Varna, 9000 - Bulgaria Submitting Author:
Article ID: WMC003176 ISSN 2046-1690 Psoriasis Penis - A Two Case Report Corresponding Author: Dr. Ilko Bakardzhiev, MD, PhD, Medical College, Medical University of Varna, 9000 - Bulgaria Submitting Author:
Disorders of the vulva
 Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
Vulval dermatoses. Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough
 Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Clearance in vulvar lichen sclerosus: a realistic treatment endpoint or a chimera?
 DOI: 10.1111/jdv.14516 JEADV SHORT REPORT Clearance in vulvar lichen sclerosus: a realistic treatment endpoint or a chimera? A. Borghi,* A. Virgili, S. Minghetti, G. Toni, M. Corazza Dipartimento di Scienze
DOI: 10.1111/jdv.14516 JEADV SHORT REPORT Clearance in vulvar lichen sclerosus: a realistic treatment endpoint or a chimera? A. Borghi,* A. Virgili, S. Minghetti, G. Toni, M. Corazza Dipartimento di Scienze
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/3640
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/3640
Vaginal involvement in genital erosive lichen planus
 Acta Obstetricia et Gynecologica. 2010; 89: 966 970 SHORT REPORT Vaginal involvement in genital erosive lichen planus ANNE LISE ORDING HELGESEN 1,2,3, PETTER GJERSVIK 3,4, PETER JEBSEN 5, ROLF KIRSCHNER
Acta Obstetricia et Gynecologica. 2010; 89: 966 970 SHORT REPORT Vaginal involvement in genital erosive lichen planus ANNE LISE ORDING HELGESEN 1,2,3, PETTER GJERSVIK 3,4, PETER JEBSEN 5, ROLF KIRSCHNER
Effectiveness of treating non-specific pruritus vulvae with topical steroids: A randomized controlled trial
 European Journal of General Practice. 2009; 15: 2933 ORIGINAL ARTICLE Effectiveness of treating non-specific pruritus vulvae with topical steroids: A randomized controlled trial ANTOINE L. M. LAGRO-JANSSEN
European Journal of General Practice. 2009; 15: 2933 ORIGINAL ARTICLE Effectiveness of treating non-specific pruritus vulvae with topical steroids: A randomized controlled trial ANTOINE L. M. LAGRO-JANSSEN
Psoriasis is a chronic, inflammatory, Prescribing in children
 Psoriasis in children: current approaches to management Laura Proudfoot BSc, MRCP, Elisabeth Higgins MA, FRCP and Judy Davids RGN Our series Prescribing in children gives practical advice for successful
Psoriasis in children: current approaches to management Laura Proudfoot BSc, MRCP, Elisabeth Higgins MA, FRCP and Judy Davids RGN Our series Prescribing in children gives practical advice for successful
KEY MESSAGES. Psoriasis patients are more prone to cardiovascular diseases, stroke, lymphoma and non-melanoma skin cancers, and increased mortality.
 KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
Lichen planus. Information for patients Gynaecology
 Lichen planus Information for patients Gynaecology page 2 of 8 What is lichen planus? Lichen planus is a non-cancerous, inflammatory skin condition that causes an itchy, non-infectious rash (small purple
Lichen planus Information for patients Gynaecology page 2 of 8 What is lichen planus? Lichen planus is a non-cancerous, inflammatory skin condition that causes an itchy, non-infectious rash (small purple
Conflicts of interest
 Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
Asymptomatic Undiagnosed Lichen Sclerosus
 Asymptomatic Undiagnosed Lichen Sclerosus Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology) Geisel School of Medicine at Dartmouth Lebanon, NH, USA Disclosures
Asymptomatic Undiagnosed Lichen Sclerosus Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology) Geisel School of Medicine at Dartmouth Lebanon, NH, USA Disclosures
MALE GENITAL (PENIS) LICHEN SCLEROSUS
 MALE GENITAL (PENIS) LICHEN SCLEROSUS What are the aims of this leaflet? This leaflet has been written to help you understand more about male genital lichen sclerosus (also known as balanitis xerotica
MALE GENITAL (PENIS) LICHEN SCLEROSUS What are the aims of this leaflet? This leaflet has been written to help you understand more about male genital lichen sclerosus (also known as balanitis xerotica
This PDF is available for free download from a site hosted by Medknow Publications
 Net Study Comparison of clinical efficacy of topical tazarotene.1% cream with topical clobetasol propionate.5% cream in chronic plaque psoriasis: A double-blind, randomized, right-left comparison study
Net Study Comparison of clinical efficacy of topical tazarotene.1% cream with topical clobetasol propionate.5% cream in chronic plaque psoriasis: A double-blind, randomized, right-left comparison study
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA)
 Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
4/3/2017 DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS BACTERIAL VAGINOSIS EPIDEMIOLOGY OBJECTIVES
 DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS KELLY HODGES, MD (NO DISCLOSURES) OBJECTIVES REVIEW THE TWO MOST COMMON CAUSES OF RECURRENT ABNORMAL DISCHARGE (CANDIDA AND BV) REVIEW THE MOST
DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS KELLY HODGES, MD (NO DISCLOSURES) OBJECTIVES REVIEW THE TWO MOST COMMON CAUSES OF RECURRENT ABNORMAL DISCHARGE (CANDIDA AND BV) REVIEW THE MOST
Kelly H. Tyler, MD, FACOG, FAAD S052 Gender Dermatology: Diagnosis and Treatment of Genital Skin Disorders Vulvar Dermatitis
 Vulvar Dermatitis Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics and Gynecology Center for
Vulvar Dermatitis Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics and Gynecology Center for
Lichen sclerosus. Lichen planus
 Lichen sclerosus Lichen planus Dr Fiona Lewis, Consultant Dermatologist, Heatherwood and Wexham Park NHS Foundation Trust & St John s Institute of Dermatology, GSTT Outline Typical features of lichen sclerosus
Lichen sclerosus Lichen planus Dr Fiona Lewis, Consultant Dermatologist, Heatherwood and Wexham Park NHS Foundation Trust & St John s Institute of Dermatology, GSTT Outline Typical features of lichen sclerosus
Topical Calcipotriol Algorithm
 Topical Calcipotriol Algorithm Is this patient an adult previously diagnosed with psoriasis by a doctor? Do the skin patches look the same as those diagnosed as psoriasis? Is this psoriasis covering an
Topical Calcipotriol Algorithm Is this patient an adult previously diagnosed with psoriasis by a doctor? Do the skin patches look the same as those diagnosed as psoriasis? Is this psoriasis covering an
Lichen sclerosus (LS) is an uncommon inflammatory. Constipation as a Feature of Anogenital Lichen Sclerosus in Children
 Mandi L. Maronn, MD*, and Nancy B. Esterly, MD ABSTRACT. Objective. To call attention to constipation as a frequent sign of lichen sclerosus (LS) in girls. Methods. A focused questionnaire was sent to
Mandi L. Maronn, MD*, and Nancy B. Esterly, MD ABSTRACT. Objective. To call attention to constipation as a frequent sign of lichen sclerosus (LS) in girls. Methods. A focused questionnaire was sent to
Topical Immunomodulator Step Therapy Program
 Topical Immunomodulator Step Therapy Program Policy Number: 5.01.557 Last Review: 8/2017 Origination: 7/2013 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) BCBSKC will provide
Topical Immunomodulator Step Therapy Program Policy Number: 5.01.557 Last Review: 8/2017 Origination: 7/2013 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) BCBSKC will provide
Psoriasis. What is Psoriasis? What causes psoriasis? Medical Topics Psoriasis
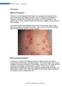 1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
Non venereal benign dermatoses of vulva in sexually active women: a clinical study
 International Journal of Research in Dermatology Singh G et al. Int J Res Dermatol. 2016 Jun;2(2):25-29 http://www.ijord.com Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20162419
International Journal of Research in Dermatology Singh G et al. Int J Res Dermatol. 2016 Jun;2(2):25-29 http://www.ijord.com Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20162419
Psoriasis: Causes, Symptoms, And Treatment
 Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Psoriasis the latest recommendations for management: where can primary care make a real difference?
 Dermatology Psoriasis the latest recommendations for management: where can primary care make a real difference? Dr Stephen Kownacki Executive chair, Primary Care Dermatology Society (PCDS) This session
Dermatology Psoriasis the latest recommendations for management: where can primary care make a real difference? Dr Stephen Kownacki Executive chair, Primary Care Dermatology Society (PCDS) This session
Difference Between Seborrheic Dermatitis and Psoriasis
 Difference Between Seborrheic Dermatitis and Psoriasis www.differencebetween.com Key Difference Seborrheic Dermatitis vs Psoriasis Dermatological conditions are perhaps the most worrisome diseases in the
Difference Between Seborrheic Dermatitis and Psoriasis www.differencebetween.com Key Difference Seborrheic Dermatitis vs Psoriasis Dermatological conditions are perhaps the most worrisome diseases in the
British Association of Dermatologists Undergraduate Award Essay Prize Who should look after genital skin disease in the 21 st century?
 Who should look after genital skin disease in the 21 st century? Sethuparvathy Jayakumar, 4 th year medical student, King s College London GKT School of Medical Education Genital skin disease is a broad
Who should look after genital skin disease in the 21 st century? Sethuparvathy Jayakumar, 4 th year medical student, King s College London GKT School of Medical Education Genital skin disease is a broad
Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])
![Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV]) Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])](/thumbs/89/99382632.jpg) Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Common Superficial Fungal Infections
 How to recognise and treat Common Superficial Fungal Infections Dr Lilianne Scholtz (MBBCh) Types of superficial fungal infections Ringworm (Tinea) Candida (Thrush) Body Groin Feet Skin Nappy rash Vagina
How to recognise and treat Common Superficial Fungal Infections Dr Lilianne Scholtz (MBBCh) Types of superficial fungal infections Ringworm (Tinea) Candida (Thrush) Body Groin Feet Skin Nappy rash Vagina
Non-Venereal Female Genital Dermatoses A Clinical Study
 JMSCR Volume 2 Issue 11 Page 2864-2873 November-2014 2864-2902 November-2014 2014 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x ABSTRACT Non-Venereal Female Genital Dermatoses A Clinical
JMSCR Volume 2 Issue 11 Page 2864-2873 November-2014 2864-2902 November-2014 2014 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x ABSTRACT Non-Venereal Female Genital Dermatoses A Clinical
Treatment of Genital Psoriasis: A Systematic Review
 Dermatol Ther (Heidelb) (2018) 8:09 2 https://doi.org/10.1007/s13-018-027-y REVIEW Treatment of Genital Psoriasis: A Systematic Review Kristen M. Beck. Eric J. Yang. Isabelle M. Sanchez. Wilson Liao Received:
Dermatol Ther (Heidelb) (2018) 8:09 2 https://doi.org/10.1007/s13-018-027-y REVIEW Treatment of Genital Psoriasis: A Systematic Review Kristen M. Beck. Eric J. Yang. Isabelle M. Sanchez. Wilson Liao Received:
Prescribing Information
 Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
The use of CO2 laser for patients with Lichen sclerosus
 The use of CO2 laser for patients with Lichen sclerosus Dr. Christina Kuhler-Obbarius, Elisabeth Kunkel, Dr. Matthias Theden-Schow, Hamburg, Germany Our clinical center located in Hamburg includes eight
The use of CO2 laser for patients with Lichen sclerosus Dr. Christina Kuhler-Obbarius, Elisabeth Kunkel, Dr. Matthias Theden-Schow, Hamburg, Germany Our clinical center located in Hamburg includes eight
Eczema & Dermatitis Clinical features: Histopathological features: Classification:
 Eczema & Dermatitis Eczema is an inflammatory reactive pattern of skin to many and different stimuli characterized by itching, redness, scaling and clustered papulovesicles. Eczema and dermatitis are synonymous
Eczema & Dermatitis Eczema is an inflammatory reactive pattern of skin to many and different stimuli characterized by itching, redness, scaling and clustered papulovesicles. Eczema and dermatitis are synonymous
Supplementary Table 1: Study and sample characteristics of the included studies
 Supplementary Table 1: Study and sample characteristics of the included studies First author, Imiquimod 5% cream vs. placebo Arican et al. 2004 34 Beutner et al. 1998a 35 Tyring et al. 1998a 36 Beutner
Supplementary Table 1: Study and sample characteristics of the included studies First author, Imiquimod 5% cream vs. placebo Arican et al. 2004 34 Beutner et al. 1998a 35 Tyring et al. 1998a 36 Beutner
50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate).
 DUPISOR Composition Gel 50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate). Action Calcipotriol is a non-steroidal antipsoriatic agent, derived from vitamin D. Calcipotriol
DUPISOR Composition Gel 50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate). Action Calcipotriol is a non-steroidal antipsoriatic agent, derived from vitamin D. Calcipotriol
It is estimated that about 26,000 new cases of
 Focus on CME at Dalhousie University Set On Soothing Psoriasis A. H. Murray, MD, FRCP(C) Presented at the 76th Annual Dalhousie Refresher Course It is estimated that about 26,000 new cases of psoriasis
Focus on CME at Dalhousie University Set On Soothing Psoriasis A. H. Murray, MD, FRCP(C) Presented at the 76th Annual Dalhousie Refresher Course It is estimated that about 26,000 new cases of psoriasis
11/1/18. Age and Vulvar Pathology ANATOMY. Prepuce Clitoris Vestibule Hart line. Labia. minora. Labia. majora. Fourchette.
 Age and Vulvar Pathology Maria Angelica Selim, MD Professor of Pathology and Dermatology Director Dermatopathology Unit Duke University Medical Center Labia minora Labia majora Bartholin s duct Prepuce
Age and Vulvar Pathology Maria Angelica Selim, MD Professor of Pathology and Dermatology Director Dermatopathology Unit Duke University Medical Center Labia minora Labia majora Bartholin s duct Prepuce
Conflicts of interest. Genital Lichen Planus. Objectives. Lichen Planus. Genital Lichen Planus. Author Up To Date. Vulvar Lichen Planus Patterns
 Genital Lichen Planus Lynette J. Margesson MD FRCPC AAD Washington Mucous Membrane Symposium Saturday, March 2, 2019 Conflicts of interest Author Up To Date Little evidence based treatment Too few studies
Genital Lichen Planus Lynette J. Margesson MD FRCPC AAD Washington Mucous Membrane Symposium Saturday, March 2, 2019 Conflicts of interest Author Up To Date Little evidence based treatment Too few studies
Disclosures Dr. Lynette Margesson
 Management of Vulvar Pruritus 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and
Management of Vulvar Pruritus 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and
Management of benign vulval dermatoses in primary care
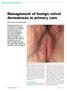 PRESCRIBING IN PRACTICE Management of benign vulval dermatoses in primary care MITESH PATEL AND DAVID NUNNS SPL Vulval dermatoses can be difficult to manage in primary care, and GPs need to be aware of
PRESCRIBING IN PRACTICE Management of benign vulval dermatoses in primary care MITESH PATEL AND DAVID NUNNS SPL Vulval dermatoses can be difficult to manage in primary care, and GPs need to be aware of
Lichen Sclerosus. Exceptional healthcare, personally delivered
 Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis
 Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
Site and distribution: symmetrical, asymmetrical. Surface characteristics: smooth, scaly, warty
 B I O T E R R O R I S M PRINCIPLES AND PRACTICE OF DERMATOLOGY Dr Matthew Ng Joo Ming INTRODUCTION Medical schools and textbooks teach us dermatology by subjects such as eczema and psoriasis. This is useful
B I O T E R R O R I S M PRINCIPLES AND PRACTICE OF DERMATOLOGY Dr Matthew Ng Joo Ming INTRODUCTION Medical schools and textbooks teach us dermatology by subjects such as eczema and psoriasis. This is useful
A study of treatment modalities in psoriasis in dermatology outpatient department of a tertiary care teaching hospital
 Original article A study of treatment modalities in psoriasis in dermatology outpatient department of a tertiary care teaching hospital 1Y Roja Ramani, 2 Benu Panigrahy, 3 Sailenkumar Mishra, 4 BTPS Singh
Original article A study of treatment modalities in psoriasis in dermatology outpatient department of a tertiary care teaching hospital 1Y Roja Ramani, 2 Benu Panigrahy, 3 Sailenkumar Mishra, 4 BTPS Singh
The role of the practice nurse in managing psoriasis in primary care
 The role of the practice nurse in managing psoriasis in primary care Item type Authors Publisher Journal Article Buckley, David Nursing in General Practice Nursing in general practice Downloaded 16-Sep-2016
The role of the practice nurse in managing psoriasis in primary care Item type Authors Publisher Journal Article Buckley, David Nursing in General Practice Nursing in general practice Downloaded 16-Sep-2016
VIN/VAIN O C T O B E R 3 RD J M O R G A N
 VIN/VAIN O C T O B E R 3 RD 2 0 1 8 J M O R G A N Vaginal Intraepithelial Neoplasia VAIN I, II, III Incidence 0.1/100,000 women in US Mean age 50s (J Womens Health (Larchmt) 2009:18:1731) (J Obstet Gynaecol
VIN/VAIN O C T O B E R 3 RD 2 0 1 8 J M O R G A N Vaginal Intraepithelial Neoplasia VAIN I, II, III Incidence 0.1/100,000 women in US Mean age 50s (J Womens Health (Larchmt) 2009:18:1731) (J Obstet Gynaecol
sclerosus, lichen simplex, or threadworm infestation (particularly if combined with peri-anal itch).
 Pruritus vulvae - Management View full scenario How should I assess a woman with pruritus vulvae? There is an identifiable cause for pruritus vulvae in most women. Confirm that the woman is experiencing
Pruritus vulvae - Management View full scenario How should I assess a woman with pruritus vulvae? There is an identifiable cause for pruritus vulvae in most women. Confirm that the woman is experiencing
EFFICACY AND SAFETY OF CLOBETASOL PROPIONATE SHAMPOO IN THERAPY OF PSORIASIS OF THE SCALP
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Platonova et al. SJIF Impact Factor 2.786 Volume 4, Issue 04, 238-246. Research Article ISSN 2278 4357 EFFICACY AND SAFETY OF CLOBETASOL PROPIONATE
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Platonova et al. SJIF Impact Factor 2.786 Volume 4, Issue 04, 238-246. Research Article ISSN 2278 4357 EFFICACY AND SAFETY OF CLOBETASOL PROPIONATE
JMSCR Vol 05 Issue 10 Page October 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i10.125 Histomorphological Study of Lichen Planus
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i10.125 Histomorphological Study of Lichen Planus
2/19/2018. Vulvar Infections and Infestations
 Vulvar Infections and Infestations Bethanee J. Schlosser, MD, PhD bschloss@nm.org Women s Skin Health Program Vulvar Mucosal Specialty Clinic Northwestern University February 19, 2018 Disclosure of Relationships
Vulvar Infections and Infestations Bethanee J. Schlosser, MD, PhD bschloss@nm.org Women s Skin Health Program Vulvar Mucosal Specialty Clinic Northwestern University February 19, 2018 Disclosure of Relationships
GROUP 15 TOPICAL PREPARATIONS
 - 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
- 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
Time to Learn. 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service
 Time to Learn 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service The Red Face Rosacea Acne Seborrhoeic eczema eczema Psoriasis Slapped cheek syndrome Fungal infection Erysipelas...
Time to Learn 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service The Red Face Rosacea Acne Seborrhoeic eczema eczema Psoriasis Slapped cheek syndrome Fungal infection Erysipelas...
Access from the University of Nottingham repository:
 Simpson, Rosalind C. and Nunns, David (2017) Skin diseases affecting the vulva. Obstetrics, Gynaecology and Reproductive Medicine, 27 (3). pp. 77-85. ISSN 1879-3622 Access from the University of Nottingham
Simpson, Rosalind C. and Nunns, David (2017) Skin diseases affecting the vulva. Obstetrics, Gynaecology and Reproductive Medicine, 27 (3). pp. 77-85. ISSN 1879-3622 Access from the University of Nottingham
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Psoriasis: the management of psoriasis 1.1 Short title Psoriasis 2 The remit The Department of Health has asked NICE: 'to produce
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Psoriasis: the management of psoriasis 1.1 Short title Psoriasis 2 The remit The Department of Health has asked NICE: 'to produce
Vulval disease in children
 Vulval disease in children SYDNEY MEDICAL SCHOOL NORTHERN Associate Professor Gayle Fischer MBBS MD FACD gayle.fischer@sydney.edu.au I have no conflict of interests Range of vulval diseases in children
Vulval disease in children SYDNEY MEDICAL SCHOOL NORTHERN Associate Professor Gayle Fischer MBBS MD FACD gayle.fischer@sydney.edu.au I have no conflict of interests Range of vulval diseases in children
OCCG SERVICE SPECIFICATION (2017/18)
 OCCG SERVICE SPECIFICATION (2017/18) Primary Care Service for Skin Cancers: Dermatology Shared Care Monitoring for Melanoma, Lichen Sclerosus and Squamos Cell Carcinoma 1. Background For patients who have
OCCG SERVICE SPECIFICATION (2017/18) Primary Care Service for Skin Cancers: Dermatology Shared Care Monitoring for Melanoma, Lichen Sclerosus and Squamos Cell Carcinoma 1. Background For patients who have
PACKAGE LEAFLET: INFORMATION FOR THE USER. Flutarzole 0,05% w/w cream, Fluticasone propionate
 PACKAGE LEAFLET: INFORMATION FOR THE USER Flutarzole 0,05% w/w cream, Fluticasone propionate 1. IDENTIFICATION OF THE MEDICINAL PRODUCT 1.1. Trade name Flutarzole 1.2. Composition Active substance: Fluticasone
PACKAGE LEAFLET: INFORMATION FOR THE USER Flutarzole 0,05% w/w cream, Fluticasone propionate 1. IDENTIFICATION OF THE MEDICINAL PRODUCT 1.1. Trade name Flutarzole 1.2. Composition Active substance: Fluticasone
COMMON SKIN CONDITIONS IN PRIMARY CARE. Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio
 COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
Dermatology elective for yr. 5. Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015
 Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
The Case of Mrs. Virginia Jones* Asst. Professor Division of Gyne-Oncology University of British Columbia, Department of Gynecology Vancouver, Canada
 Case title: Case authors: Case synopsis: The Case of Mrs. Virginia Jones* Dr. Leslie A. Sadownik Asst. Professor Division of Gyne-Oncology University of British Columbia, Department of Gynecology Vancouver,
Case title: Case authors: Case synopsis: The Case of Mrs. Virginia Jones* Dr. Leslie A. Sadownik Asst. Professor Division of Gyne-Oncology University of British Columbia, Department of Gynecology Vancouver,
Psoriasis is an inflammatory condition of the skin that
 Mayo Clin Proc, September 2001, Vol 76 Topical Therapies for Localized Psoriasis 943 Concise Review for Clinicians Concise Review for Clinicians Topical Therapies for Localized Psoriasis PATRICIA M. WITMAN,
Mayo Clin Proc, September 2001, Vol 76 Topical Therapies for Localized Psoriasis 943 Concise Review for Clinicians Concise Review for Clinicians Topical Therapies for Localized Psoriasis PATRICIA M. WITMAN,
My ear won t stop hurting!
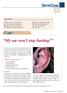 This month: 1. My ear won t stop hurting! 5. Cortisone Cream Didn t Help! 2. What are these red bumps? 6. Can my girlfriend get it? 3. Why won t this rash leave? 7. My wife noticed it! 4. What s the cause
This month: 1. My ear won t stop hurting! 5. Cortisone Cream Didn t Help! 2. What are these red bumps? 6. Can my girlfriend get it? 3. Why won t this rash leave? 7. My wife noticed it! 4. What s the cause
STUDY. Circumcision and Genital Dermatoses
 STUDY Circumcision and Genital Dermatoses Eleanor Mallon, MRCP; David Hawkins, FRCP; Michael Dinneen, FRCS; Nicholas Francis, FRCPath; Louise Fearfield, MRCP; Roger Newson, DPhil; Christopher Bunker, FRCP
STUDY Circumcision and Genital Dermatoses Eleanor Mallon, MRCP; David Hawkins, FRCP; Michael Dinneen, FRCS; Nicholas Francis, FRCPath; Louise Fearfield, MRCP; Roger Newson, DPhil; Christopher Bunker, FRCP
Month/Year of Review: January 2015 Date of Last Review: January 2010
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119 Copyright 2012 Oregon State University. All Rights
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119 Copyright 2012 Oregon State University. All Rights
What is Psoriasis? Common Areas Affected. Type Who Does it Affect Characteristics
 What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
An otherwise healthy 12-year-old
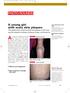 1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
Lichen sclerosus. Information for patients Gynaecology
 Lichen sclerosus Information for patients Gynaecology page 2 of 8 What is lichen sclerosus? Lichen sclerosus is a skin condition that most often affects the vulva (the outer folds of skin around your vagina).
Lichen sclerosus Information for patients Gynaecology page 2 of 8 What is lichen sclerosus? Lichen sclerosus is a skin condition that most often affects the vulva (the outer folds of skin around your vagina).
Acitretin for Severe Lichen Sclerosus of Male Genitalia: A Randomized, Placebo Controlled Study
 Acitretin for Severe Lichen Sclerosus of Male Genitalia: A Randomized, Placebo Controlled Study D. Ioannides, E. Lazaridou,* Z. Apalla, E. Sotiriou, S. Gregoriou and D. Rigopoulos From the First Department
Acitretin for Severe Lichen Sclerosus of Male Genitalia: A Randomized, Placebo Controlled Study D. Ioannides, E. Lazaridou,* Z. Apalla, E. Sotiriou, S. Gregoriou and D. Rigopoulos From the First Department
Eczema. By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University
 Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
Treatment of Bowenoid and Basaloid Vulvar Intraepithelial Neoplasia 2/3 with Imiquimod 5% Cream DO NOT DUPLICATE
 The Journal of Reproductive Medicine Treatment of Bowenoid and Basaloid Vulvar Intraepithelial Neoplasia 2/3 with Imiquimod 5% Cream Claudia Marchitelli, M.D., Graciela Secco, M.D., Myriam Perrotta, M.D.,
The Journal of Reproductive Medicine Treatment of Bowenoid and Basaloid Vulvar Intraepithelial Neoplasia 2/3 with Imiquimod 5% Cream Claudia Marchitelli, M.D., Graciela Secco, M.D., Myriam Perrotta, M.D.,
Prescribing Information. Taro-Clobetasol. Taro-Clobetasol
 Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Clinical Scoring System to Detect Malignant and Premalignant Vulval Lesions
 The Journal of Obstetrics and Gynecology of India (January February 2014) 64(1):41 46 DOI 10.1007/s13224-013-0458-3 ORIGINAL ARTICLE Clinical Scoring System to Detect Malignant and Premalignant Vulval
The Journal of Obstetrics and Gynecology of India (January February 2014) 64(1):41 46 DOI 10.1007/s13224-013-0458-3 ORIGINAL ARTICLE Clinical Scoring System to Detect Malignant and Premalignant Vulval
ONCOGENIC BALANITIS. G. Tchernev 1, J. Ananiev 2, J. C. Cardoso 3, S. Philipov 4 and U. Wollina 5
 ONCOGENIC BALANITIS G. Tchernev 1, J. Ananiev 2, J. C. Cardoso 3, S. Philipov 4 and U. Wollina 5 1 Polyclinic for Dermatology and Venerology, University Hospital Lozenetz, Saint Kliment Ohridski University,
ONCOGENIC BALANITIS G. Tchernev 1, J. Ananiev 2, J. C. Cardoso 3, S. Philipov 4 and U. Wollina 5 1 Polyclinic for Dermatology and Venerology, University Hospital Lozenetz, Saint Kliment Ohridski University,
Clinical profile of skin diseases in accident and emergency department attenders
 Hong Kong J. Dermatol. Venereol. (2007) 15, 4-9 Original Article Clinical profile of skin diseases in accident and emergency department attenders CY Chan, KL Kam, CA Graham, TH Rainer, NM Luk Skin problems
Hong Kong J. Dermatol. Venereol. (2007) 15, 4-9 Original Article Clinical profile of skin diseases in accident and emergency department attenders CY Chan, KL Kam, CA Graham, TH Rainer, NM Luk Skin problems
Genital Psoriasis Awareness Program: Physical and Psychological Care for Patients with Genital Psoriasis
 Acta Derm Venereol 2015; 95: 211 216 CLINICAL REPORT Genital Psoriasis Awareness Program: Physical and Psychological Care for Patients with Genital Psoriasis Kim A. P. Meeuwis 1,2, Joanne A. de Hullu 2,
Acta Derm Venereol 2015; 95: 211 216 CLINICAL REPORT Genital Psoriasis Awareness Program: Physical and Psychological Care for Patients with Genital Psoriasis Kim A. P. Meeuwis 1,2, Joanne A. de Hullu 2,
STUDY. 1% Pimecrolimus, 0.005% Calcipotriol, and 0.1% Betamethasone in the Treatment of Intertriginous Psoriasis
 STUDY 1% Pimecrolimus, 0.005% Calcipotriol, and 0.1% Betamethasone in the Treatment of Intertriginous Psoriasis A Double-blind, Randomized Controlled Study Alexander Kreuter, MD; Anna Sommer, MD; Julia
STUDY 1% Pimecrolimus, 0.005% Calcipotriol, and 0.1% Betamethasone in the Treatment of Intertriginous Psoriasis A Double-blind, Randomized Controlled Study Alexander Kreuter, MD; Anna Sommer, MD; Julia
A giant skin Tag over labium majus: An unusual location of skin tag
 A giant skin Tag over labium majus: An unusual location of skin tag Garima Gupta 1, Ruchi Sinha 2, Sulekha Pandey 3, L. K. Pandey 3 Department of Obstetrics and Gynecology, Institute of Medical Sciences,
A giant skin Tag over labium majus: An unusual location of skin tag Garima Gupta 1, Ruchi Sinha 2, Sulekha Pandey 3, L. K. Pandey 3 Department of Obstetrics and Gynecology, Institute of Medical Sciences,
New Medicine Report. Pimecrolimus. RED- Hospital only Date of Last Revision 6 th March 2003
 New Medicine Report Document Status Pimecrolimus Reviewed by Suffolk D&T RED- Hospital only Date of Last Revision 6 th March 2003 Approved Name Pimecrolimus Trade Name Elidel Manufacturer Novartis Legal
New Medicine Report Document Status Pimecrolimus Reviewed by Suffolk D&T RED- Hospital only Date of Last Revision 6 th March 2003 Approved Name Pimecrolimus Trade Name Elidel Manufacturer Novartis Legal
Diseases of the vulva
 Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Skin disorders. Seborrhoeic dermatitis Search date April 2010 Luigi Naldi ...
 Seborrhoeic Search date April 21 Luigi Naldi.................................................. ABSTRACT INTRODUCTION: Seborrhoeic affects at least 1% of the population. Malassezia (Pityrosporum) ovale
Seborrhoeic Search date April 21 Luigi Naldi.................................................. ABSTRACT INTRODUCTION: Seborrhoeic affects at least 1% of the population. Malassezia (Pityrosporum) ovale
Case Study: The Surgical Management of Angiokeratoma Resulting from Radiotherapy for Penile Cancer
 Case Study TheScientificWorldJOURNAL (2009) 9, 339 342 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.23 Case Study: The Surgical Management of Angiokeratoma Resulting from Radiotherapy for Penile Cancer
Case Study TheScientificWorldJOURNAL (2009) 9, 339 342 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.23 Case Study: The Surgical Management of Angiokeratoma Resulting from Radiotherapy for Penile Cancer
PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN:
 PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN: 2072 1625 Pac. J. Med. Sci. (PJMS) www.pacjmedsci.com. Email: pacjmedsci@gmail.com. EROSIVE LICHEN PLANUS A CASE REPORT *Prathima
PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN: 2072 1625 Pac. J. Med. Sci. (PJMS) www.pacjmedsci.com. Email: pacjmedsci@gmail.com. EROSIVE LICHEN PLANUS A CASE REPORT *Prathima
Using Your ESP* in Pharmacy: How to Improve Treatment Adherence and Patient Outcomes in Psoriasis (*Expanded Scope of Practice)
 Using Your ESP* in Pharmacy: How to Improve Treatment Adherence and Patient Outcomes in Psoriasis (*Expanded Scope of Practice) Patient Case Study in Psoriasis Patient Case Study in Psoriasis William Smith,
Using Your ESP* in Pharmacy: How to Improve Treatment Adherence and Patient Outcomes in Psoriasis (*Expanded Scope of Practice) Patient Case Study in Psoriasis Patient Case Study in Psoriasis William Smith,
Derm quiz. Go to this link: goo.gl/forms/kchrhmtzl3vfnlv52. bit.ly/2a8asoy. Scan the QR code with your phone
 Dermatology quiz Derm quiz Go to this link: goo.gl/forms/kchrhmtzl3vfnlv52 OR bit.ly/2a8asoy OR Scan the QR code with your phone Contents Childhood rashes Pigmented lesions Sun damage Pityriasis References
Dermatology quiz Derm quiz Go to this link: goo.gl/forms/kchrhmtzl3vfnlv52 OR bit.ly/2a8asoy OR Scan the QR code with your phone Contents Childhood rashes Pigmented lesions Sun damage Pityriasis References
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Penile Conditions - Surgical Opinion and Treatment Policy including Circumcision in all male patients over the age of 18 years Prior Approval Policy Date
Commissioning Policy Individual Funding Request Penile Conditions - Surgical Opinion and Treatment Policy including Circumcision in all male patients over the age of 18 years Prior Approval Policy Date
Topical treatment of psoriasis in difficult to treat areas: Genital, folds and palmoplantar
 Topical treatment of psoriasis in difficult to treat areas: Genital, folds and palmoplantar Dr. Steven Feldman 1 Genital psoriasis: a questionnaire-based survey on a concealed skin disease in the Netherlands
Topical treatment of psoriasis in difficult to treat areas: Genital, folds and palmoplantar Dr. Steven Feldman 1 Genital psoriasis: a questionnaire-based survey on a concealed skin disease in the Netherlands
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Premalignant skin tumours
 Chapter 14: Premalignant skin tumours page: 434 Premalignant skin tumours page: 435 Solar keratoses (senile keratoses) Raised red and well-defined plaques with a rough surface covered in scales of varying
Chapter 14: Premalignant skin tumours page: 434 Premalignant skin tumours page: 435 Solar keratoses (senile keratoses) Raised red and well-defined plaques with a rough surface covered in scales of varying
Anne Arundel Medical Center Informed Consent
 Informed Consent Title: Exploratory Trial of Autologous Platelet Rich Plasma (PRP) Intradermal Injections for the Treatment of Vulvar Lichen Sclerosus Investigator: Andrew Goldstein, M.D. Telephone Study
Informed Consent Title: Exploratory Trial of Autologous Platelet Rich Plasma (PRP) Intradermal Injections for the Treatment of Vulvar Lichen Sclerosus Investigator: Andrew Goldstein, M.D. Telephone Study
Elements for a Public Summary
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
SELF-TEST QUESTIONNAIRE PSORIASIS. Plaque a raised lesion where the diameter is greater than the thickness. Number 2
 Number 2 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE AYERS ROCK, ULURU PSORIASIS NATIONAL PARK, AUSTRALIA Plaque a raised lesion where the diameter is greater than the thickness
Number 2 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE AYERS ROCK, ULURU PSORIASIS NATIONAL PARK, AUSTRALIA Plaque a raised lesion where the diameter is greater than the thickness
Advanced Training Skills Module August Vulval Disease
 Introduction Vulval Disease This module is designed to provide training in all aspects of vulval disease. Successful completion of the ATSM will equip an individual to develop this aspect of care in their
Introduction Vulval Disease This module is designed to provide training in all aspects of vulval disease. Successful completion of the ATSM will equip an individual to develop this aspect of care in their
Undergraduate Dermatology Curriculum July 2016
 Undergraduate Dermatology Curriculum July 2016 British Association of Dermatologists Introduction This document is the 2016 revised dermatology undergraduate curriculum (UK) from the British Association
Undergraduate Dermatology Curriculum July 2016 British Association of Dermatologists Introduction This document is the 2016 revised dermatology undergraduate curriculum (UK) from the British Association
COMPARATIVE STUDY OF THE EFFICACY OF VARIOUS TOPICAL TREATMENT MODALITIES AND PHOTOTHERAPY FOR PSORIASIS VULGARIS: A REVIEW
 COMPARATIVE STUDY OF THE EFFICACY OF VARIOUS TOPICAL TREATMENT MODALITIES AND PHOTOTHERAPY FOR PSORIASIS VULGARIS: A REVIEW Dr. Shweta Aryal *, Prof. Dr. Liu Jin Xian, Dr. Gong Shao Zhi and Dr. Jyoti Karki
COMPARATIVE STUDY OF THE EFFICACY OF VARIOUS TOPICAL TREATMENT MODALITIES AND PHOTOTHERAPY FOR PSORIASIS VULGARIS: A REVIEW Dr. Shweta Aryal *, Prof. Dr. Liu Jin Xian, Dr. Gong Shao Zhi and Dr. Jyoti Karki
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Psoriasis. Causes of Psoriasis
 Psoriasis Psoriasis is a common, chronic, relapsing/remitting, immune-mediated systemic disease characterized by skin lesions including red, scaly patches, papules, and plaques, which usually itch. The
Psoriasis Psoriasis is a common, chronic, relapsing/remitting, immune-mediated systemic disease characterized by skin lesions including red, scaly patches, papules, and plaques, which usually itch. The
Literature Scan: Topical Corticosteroids. Month/Year of Review: March 2015 Date of Last Review: March 2013 Source Document: OSU College of Pharmacy
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Epidemiological study of Lichen Planus
 Year: 2014; Volume: 1; Issue: 1 Article ID: MD14 20; Pages: 1-9 BioMed Research The Open Access Publisher BMR Medicine Research Article Epidemiological study of Lichen Planus Shankar Gouda Ireddy 1 and
Year: 2014; Volume: 1; Issue: 1 Article ID: MD14 20; Pages: 1-9 BioMed Research The Open Access Publisher BMR Medicine Research Article Epidemiological study of Lichen Planus Shankar Gouda Ireddy 1 and
