Etiology of Rheumatoid Arthritis: A Historical and Evidence-Based Perspective
|
|
|
- Peregrine Gervais Fox
- 6 years ago
- Views:
Transcription
1 Etiology of Rheumatoid Arthritis: A Historical and Evidence-Based Perspective 2 David A. Fox Introduction Rheumatoid arthritis (RA) is a chronic, inflammatory, and destructive polyarthritis with numerous autoimmune features and the potential for extra-articular and systemic complications. Its etiology is still unknown but much progress has occurred in defining important mechanistic components of RA, leading to significant advances in its treatment. RA is a multifactorial and multistage disease, beginning with preclinical autoimmunity that arises in a genetically predisposed individual who encounters one or more environmental triggers, progressing to the clinical appearance of inflammation in joints and sometimes in other organs, and leading (if effective treatment is unavailable) to destruction of the articular cartilage and adjacent bone. This chapter will consider historical, epidemiologic, genetic, environmental, autoimmune, and inflammatory aspects of the development and progression of RA. D.A. Fox, MD (*) Internal Medicine, Division of Rheumatology, University of Michigan, 300 North Ingalls St., Suite 7C27, Ann Arbor, MI , USA dfox@med.umich.edu Epidemiology and Historical Aspects of RA In a Caucasian population sample in the United States, the incidence and prevalence of RA have fluctuated over the past five decades [1]. As of 2005, the incidence per year per 100,000 of population was 27.7 in men and 53.1 in women, with an overall prevalence of 0.72 %. The incidence of RA rises in frequency from early adulthood into the seventh decade, before declining in the eighth decade and beyond [1]. In this context, and in view of the lifelong persistence of RA in most affected individuals, the lifetime risk of developing RA is strikingly high: 3.64 % in women and 1.68 % in men [2]. Individuals with RA have an approximately 50 % increase in premature mortality (after adjustment for comorbidities and risk factors such as smoking), which equates to a reduction in life expectancy of 3 10 years [3]. Multiple factors appear to contribute to this mortality gap versus the general population, with accelerated cardiovascular disease identified as the most significant component [4]. The historical epidemiology of RA is intriguing and, if accurately understood, could provide clues to etiology [5]. Recognizable descriptions of RA in the medical literature are recent, beginning about 200 years ago, but some earlier European paintings show what appear to be RA-like deformities. A few skeletal remains from Springer International Publishing Switzerland 2016 K.C. Chung (ed.), Clinical Management of the Rheumatoid Hand, Wrist, and Elbow, DOI / _2 13
2 14 both the New World and the Old World, dated to points in time over the past four millennia, have shown damage interpreted as potentially due to RA (reviewed in [5]). RA may have been present in ancient times but was likely rarer than at present. If this assessment is correct, it may indicate changes in the presence of environmental triggers and/or genetic changes in the human population over time that have increased propensity to RA. Genetics of RA The importance of inherited risk alleles in the pathogenesis of RA is highlighted by increased concordance for RA in monozygotic compared to dizygotic twins and by the familial clustering of RA. The most important region of the human genome in RA susceptibility is the major histocompatibility complex (MHC), which encodes for genes that are essential to immune responses, notably the HLA-A, HLA-B, HLA-C, and HLA-D proteins. These structures are expressed on the surface of antigen-presenting cells and are required for recognition of peptide antigens by T lymphocytes, leading to initiation of immune responses. The RA-associated MHC allele was initially identified as HLA-DR4 [6] and later localized to a five-amino-acid sequence from residues of the beta chain of subtypes of HLA-DR4 and selected other DR alleles, termed the shared epitope, which is located within the MHC peptide-binding cleft [7]. More recently polymorphisms that govern additional amino acid variations in HLA-DR that are located outside the shared epitope have also been strongly associated with susceptibility to RA [8, 9]. The mechanism for MHC predisposition to RA remains to be established while presentation of a pathogenic autoantigen by RA-associated alleles is an attractive theory, other possibilities exist, for example, unique pro-inflammatory properties of the shared epitope itself [10]. Genome-wide association studies have identified more than 100 other loci that affect susceptibility to RA, each of which has a modest effect [8, 11]. The specific genes associated with these loci mostly function in cells that mediate immune responses, such as lymphocytes and antigen- presenting cells, Table 2.1 Examples of RA-associated genes Gene HLA-DR (shared epitope) PTPN 22 (proteintyrosine phosphatase non-receptor type 22) PADI4 (peptidyl arginine deiminase 4) CCR6 (chemokine receptor 6) STAT4 (signal transducer and activator of transcription 4) Function Antigen presentation, lymphocyte activation Regulation of T cell receptor signaling Posttranslational conversion of arginine to citrulline Attraction of Th17 cells to sites of inflammation Signaling downstream of cytokine receptors reinforcing the concept that RA is an autoimmune disease (Table 2.1). The known loci associated with RA, both MHC and non- MHC, are more strongly linked to seropositive RA, i.e., RA in which either rheumatoid factor (RF) or antibodies to citrullinecontaining proteins (ACPA) are present. The most influential RA-associated non-mhc gene is PTPN22, which encodes a tyrosine phosphatase that is expressed in lymphocytes, regulates signaling through the T cell receptor for antigen, and influences lymphocyte development [12]. Epigenetic mechanisms control gene expression in a potentially heritable manner and include DNA methylation, histone modifications such as acetylation, and microrna control of posttranscriptional stages of gene expression. Understanding of the role of epigenetics in RA is still in its infancy, but such mechanisms are likely to be of great importance, especially in the connection of environmental triggers to changes in gene expression [8, 13]. Epigenetic changes often occur distinctly in specific cell types, such as lymphocytes or synovial fibroblasts [13, 14], increasing the complexity of analysis in a disease such as RA that involves multiple cell populations. Environmental Triggers of RA D.A. Fox Smoking is the best-established environmental risk factor for RA and is receiving attention as a potential trigger for the development of RA-associated autoimmunity. Although the association of smoking with RA was suspected 25 years ago [15], this link has become much better
3 2 Etiology of Rheumatoid Arthritis: A Historical and Evidence-Based Perspective 15 established within the past decade [16, 17], with smoking shown to increase the risk for seropositive RA by more than twofold. Smoking synergizes with the presence and gene dosage of the MHC shared epitope allele to greatly increase the risk of developing RA [18]. Preliminary evidence suggests that cigarette smoking can induce expression in the lungs of the enzymes responsible for citrullination of various proteins, thus creating antigen targets of autoantibodies that are tightly associated with RA [18, 19]. Smoking is also associated with resistance to successful treatment of RA and more rapid disease progression [20]. Thus, smoking cessation should be viewed as part of both prevention and treatment of RA. Infection has long been viewed as a potential trigger of RA, even though direct infection of RA joints has not been demonstrated (reviewed in [21]). A variety of bacterial and viral pathogens have been implicated, but not definitively [21]. Recently attention has refocused on the clinical association of RA and periodontal disease [22, 23]. Porphyromonas gingivalis (Pg) is a gram- negative bacterium that is strongly linked to periodontal disease. Uniquely among bacteria, it possesses the enzymatic machinery to generate citrullinated proteins, and such RA autoantigens are indeed detected in the gingival tissue of subjects with periodontitis [22, 23]. Smoking and periodontal disease are also positively associated [23]. Investigation of the microbiome is a new area of inquiry in RA and other autoimmune diseases, and is a complex task in view of the multiple microbiomes present on the skin and in the respiratory and gastrointestinal tracts and the multiple influences that can skew the composition of each microbiome. One report identified a higher level of Prevotella copri in feces of patients with new onset RA. This RA group was seropositive for RF and/or ACPA, and expansion of Prevotella was more pronounced in the subset that lacked the MHC shared epitope compared with those who were shared epitope positive [24]. This finding will require confirmation and further exploration of implications for the pathogenesis of RA. Stages of RA RA-associated autoimmunity precedes clinical onset of RA, and joint inflammation precedes damage to the cartilage and bone. The sequence of systemic and articular events in RA can be conceptualized as discrete stages of RA. Holmdahl et al. have delineated these stages as autoimmune priming, tissue attack, and chronic inflammation [25]. The hallmark of autoimmune priming is the appearance of RA-associated autoantibodies, especially RF and/or ACPA. Rheumatoid factors (RFs) are antibodies that recognize a domain of the IgG Fc portion as their target antigen. Recognized since the 1950s as present in about 70 % of patients with RA, RF is however highly nonspecific and is found in many other immune-mediated and infectious conditions as well as in some apparently healthy older individuals. The presence and titer of RF correlate positively with disease severity and extraarticular manifestations, and RF has plausible roles in the pathogenesis of RA synovitis (reviewed in [21]). ACPA recognize proteins that have undergone posttranslational conversion of arginine to citrulline at one or more arginine residues [26], a reaction that is catalyzed by peptidyl arginine deiminase (PAD). ACPA are much more specific for RA than in RF and are thus useful diagnostically [27]. The presence and titer of ACPA also predict disease severity, including the degree of joint destruction [28]. Both RF and ACPA can appear years before the clinical onset of RA [25, 29 31]. At this stage, elevated serum biomarkers of inflammation can also be detected, including pro-inflammatory cytokines [30, 31]. The high specificity of ACPA for RA has prompted consideration of a potential role for these autoantibodies in RA etiology and pathogenesis. As mentioned previously, citrullinated antigens can be formed in the lung and oral cavity as a result of cigarette smoking or by P. gingivalis, respectively, environmental triggers that are epidemiologically associated with risk of RA. Thus, local extra-articular inflammatory processes could create immunogens for development
4 16 D.A. Fox Table 2.2 Key elements in the pathogenesis of RA synovitis and tissue damage Autoantibodies T cells Cytokines Synovial fibroblasts Osteoclasts Endothelial cells RF, ACPA Th17 (?Th1) TNF, IL-6, IL-1, IL-17 Cartilage damage, interactions with lymphocytes Bone destruction Angiogenesis of RA-associated autoantibodies, capable of recognizing citrullinated proteins in the joint at a later stage of disease [32]. The second stage of RA is the appearance of clinical arthritis due to a level of joint inflammation that is sufficient to generate clinical symptoms and signs. The specific trigger or triggers that localize the systemic autoimmune process to the joint are unknown and could be heterogeneous, including local trauma, transient infection of the joint itself, systemic infection that alters permeability of the synovial microcirculation, noninfectious tissue damage that generates ligands of innate immune receptors, and increase in the magnitude and affinity of autoreactive B and T lymphocyte responses that react against articular antigens. A curious feature of RA is the tendency toward symmetry of joint involvement. This mapping of the disease, which differs from other forms of inflammatory and degenerative arthritis, can be interpreted to implicate pathogenic events in the local mesenchymal cells [synovial fibroblasts (FLS), also known as type B synoviocytes] in the control of disease onset in specific joints in RA. Synovitis is the hallmark of clinical RA (Table 2.2), and a detailed molecular understanding of this process has led to remarkable advances in the treatment of RA with both biologic and non-biologic pharmaceutical agents. The three most abundant cell populations in RA synovium are type A synoviocytes (of monocytemacrophage lineage), FLS, and T cells. Other important participants include dendritic cells (potent antigen-presenting cells), B lymphocytes, plasma cells, endothelial cells, mast cells, neutrophils (primarily in synovial fluid rather than synovial tissue), and osteoclasts. Normal synovium is Fig. 2.1 Photomicrograph (20 ) of chronic rheumatoid synovitis. Note the synovial fibroblast hyperplasia (lower right), extensive arterial and venous vascularity, and inflammatory cell infiltrate not known to be a location for initiation or propagation of immune responses, but in RA the synovium assumes characteristics of a tertiary lymphoid organ. The massive infiltration of leukocytes in RA synovium is accompanied by (and likely causes) marked hypertrophy of the synovial lining layer (Fig. 2.1). Numerous cytokines and other inflammatory mediators are produced in RA synovium as an outcome of the complex interactions between the various cellular constituents [33]. These interactions are both cognate (resulting from direct cell-cell contact mediated by various receptor-ligand pairings) and paracrine (due to local release of soluble pro- inflammatory mediators). Angiogenesis is a critical process in supporting synovial expansion and inflammation in RA, by providing avenues for the ingress of inflammatory cells and the nutrients to sustain them. The third stage of RA is chronic inflammation that is destructive of cartilage, bone, and other structures including tendons and ligaments, leading to deformities that may require surgical intervention. Cartilage is directly invaded by chronically inflamed synovial tissue termed pannus, with a key role for FLS. Although FLS can secrete a variety of proteases and other mediators that may contribute to tissue damage in RA, a critical role has emerged for the membraneanchored matrix metalloproteinase on the FLS surface known as MMP-14 or MT1-MMP in the
5 2 Etiology of Rheumatoid Arthritis: A Historical and Evidence-Based Perspective 17 invasion and destruction of collagenous structures [34]. Bone is eroded in RA through the activation of osteoclasts in the adjacent bone and through differentiation of monocyte precursors into osteoclasts in the inflamed synovial tissue, processes that are cytokine driven [35]. The distinctions between these three stages become blurred when one examines underlying mechanisms. Thus, ACPA can bind directly to citrullinated structures on the surface of osteoclasts, leading to osteoclast activation that would promote bone erosion. Sensitive imaging techniques confirm that joint damage can occur very early in clinically diagnosed RA and that osteopenia is present at the time of diagnosis in ACPApositive patients [35]. The concept that joint destruction begins as soon as (or even before) recognizable synovitis is present reinforces the necessity for early diagnosis and aggressive treatment to minimize cartilage loss, bone erosion, soft tissue disruption, deformity, and consequent functional disability. Cytokines and T Cells in RA An essential role for pro-inflammatory cytokines is well established in RA, and RA has become the prototypic autoimmune disease in which cytokine blockade by biologic agents has revolutionized disease management. Of the nine biologics approved in the United States for use in RA, seven neutralize key cytokines in RA synovium tumor necrosis factor (TNF), interleukin-1 (IL- 1), or interleukin-6 (IL-6). (Of the other two biologics approved for RA, one impairs T cell activation and one depletes B lymphocytes.) Moreover, other agents that are effective in RA, such as a Janus kinase inhibitor, act primarily by blocking signaling downstream of cytokine receptor activation [36]. Cytokines appear to be important at all stages of RA, although it is possible that shifts in cytokine networks occur as RA evolves. The search for additional cytokine targets in RA has focused in part on the cytokines secreted by differentiated effector cell subsets of CD4+ T lymphocytes. T cells have long been viewed as central to the pathogenesis of RA (reviewed in [21]). T cells in the joint respond to various local tissue antigens and interact with FLS in ways that can promote activation of both cell types [33]. Activated subsets of CD4+ cells can be defined by their cytokine products: Th1 cells secrete interferon-gamma, Th2 cells secrete interleukin 4, and Th17 cells secrete various isoforms of interleukin 17. Though Th2 cells are critical for allergic diseases, many autoimmune conditions, including RA, appeared to be driven by Th17 cells, Th1 cells, or by cells that overlap the Th1/ Th17 subsets [37]. Manipulation of the function of these cells and neutralization of their secreted cytokines are current areas of clinical investigation that may shed further light on disease pathogenesis. Future Directions Although the cause, cure, and prevention of RA are not yet known, significant and accelerating progress has been achieved toward each of these goals. Plausible models for the development of RA that integrate genetic predisposition, environmental triggers, autoimmunity, synovial inflammation, and tissue damage have been proposed [29 32, 38]. At the same time, the notion of molecular heterogeneity of RA is gaining traction, based on distinct patterns of synovial gene expression that can predict clinical response or lack of response to various biologics and ultimately guide individualized treatment approaches [39]. Perhaps most exciting, the improving ability to define risk for RA before onset of disease is laying the groundwork for clinical trials of RA prevention [40, 41]. References 1. Myasoedova E, Crowson CS, Kremers HM, Therneau TM, Gabriel SE. Is the incidence of rheumatoid arthritis rising?: results from Olmsted County, Minnesota, Arthritis Rheum. 2010;62(6): Pubmed Central PMCID: Crowson CS, Matteson EL, Myasoedova E, Michet CJ, Ernste FC, Warrington KJ, et al. The lifetime risk
6 18 of adult-onset rheumatoid arthritis and other inflammatory autoimmune rheumatic diseases. Arthritis Rheum. 2011;63(3): Pubmed Central PMCID: Myasoedova E, Davis 3rd JM, Crowson CS, Gabriel SE. Epidemiology of rheumatoid arthritis: rheumatoid arthritis and mortality. Curr Rheumatol Rep. 2010;12(5): Crowson CS, Liao KP, Davis 3rd JM, Solomon DH, Matteson EL, Knutson KL, et al. Rheumatoid arthritis and cardiovascular disease. Am Heart J. 2013;166(4):622 8.e621. Pubmed Central PMCID: Entezami P, Fox DA, Clapham PJ, Chung KC. Historical perspective on the etiology of rheumatoid arthritis. Hand Clin. 2011;27(1):1 10. Pubmed Central PMCID: Stastny P. Association of the B-cell alloantigen DRw4 with rheumatoid arthritis. N Engl J Med. 1978; 298(16): Gregersen PK, Silver J, Winchester RJ. The shared epitope hypothesis. An approach to understanding the molecular genetics of susceptibility to rheumatoid arthritis. Arthritis Rheum. 1987;30(11): Viatte S, Plant D, Raychaudhuri S. Genetics and epigenetics of rheumatoid arthritis. Nat Rev Rheumatol. 2013;9(3): Pubmed Central PMCID: Okada Y, Kim K, Han B, Pillai NE, Ong RT, Saw WY, et al. Risk for ACPA-positive rheumatoid arthritis is driven by shared HLA amino acid polymorphisms in Asian and European populations. Hum Mol Genet. 2014;23(25): Pubmed Central PMCID: Ling S, Cline EN, Haug TS, Fox DA, Holoshitz J. Citrullinated calreticulin potentiates rheumatoid arthritis shared epitope signaling. Arthritis Rheum. 2013;65(3): Pubmed Central PMCID: Kochi Y, Suzuki A, Yamamoto K. Genetic basis of rheumatoid arthritis: a current review. Biochem Biophys Res Commun. 2014;452(2): Stanford SM, Bottini N. PTPN22: the archetypal non- HLA autoimmunity gene. Nat Rev Rheumatol. 2014;10(10): Klein K, Gay S. Epigenetics in rheumatoid arthritis. Curr Opin Rheumatol. 2015;27(1): Nakano K, Whitaker JW, Boyle DL, Wang W, Firestein GS. DNA methylome signature in rheumatoid arthritis. Ann Rheum Dis. 2013;72(1): Pubmed Central PMCID: Hernandez Avila M, Liang MH, Willett WC, Stampfer MJ, Colditz GA, Rosner B, et al. Reproductive factors, smoking, and the risk for rheumatoid arthritis. Epidemiology. 1990;1(4): Padyukov L, Silva C, Stolt P, Alfredsson L, Klareskog L. A gene-environment interaction between smoking and shared epitope genes in HLA-DR provides a high risk of seropositive rheumatoid arthritis. Arthritis Rheum. 2004;50(10): D.A. Fox 17. Klareskog L, Stolt P, Lundberg K, Kallberg H, Bengtsson C, Grunewald J, et al. A new model for an etiology of rheumatoid arthritis: smoking may trigger HLA-DR (shared epitope)-restricted immune reactions to autoantigens modified by citrullination. Arthritis Rheum. 2006;54(1): Makrygiannakis D, Hermansson M, Ulfgren AK, Nicholas AP, Zendman AJ, Eklund A, et al. Smoking increases peptidylarginine deiminase 2 enzyme expression in human lungs and increases citrullination in BAL cells. Ann Rheum Dis. 2008;67(10): Kilsgard O, Andersson P, Malmsten M, Nordin SL, Linge HM, Eliasson M, et al. Peptidylarginine deiminases present in the airways during tobacco smoking and inflammation can citrullinate the host defense peptide LL-37, resulting in altered activities. Am J Respir Cell Mol Biol. 2012;46(2): Saevarsdottir S, Rezaei H, Geborek P, Petersson I, Ernestam S, Albertsson K, et al. Current smoking status is a strong predictor of radiographic progression in early rheumatoid arthritis: results from the SWEFOT trial. Ann Rheum Dis. 2014; Fox DA. Etiology and pathogenesis of rheumatoid arthritis. In: Koopman WJ, Moreland LW, editors. Arthritis and allied conditions. Philadelphia: LWW; p Bingham 3rd CO, Moni M. Periodontal disease and rheumatoid arthritis: the evidence accumulates for complex pathobiologic interactions. Curr Opin Rheumatol. 2013;25(3): Scher JU, Bretz WA, Abramson SB. Periodontal disease and subgingival microbiota as contributors for rheumatoid arthritis pathogenesis: modifiable risk factors? Curr Opin Rheumatol. 2014;26(4): Pubmed Central PMCID: Scher JU, Sczesnak A, Longman RS, Segata N, Ubeda C, Bielski C, et al. Expansion of intestinal Prevotella copri correlates with enhanced susceptibility to arthritis. elife. 2013;2:e Pubmed Central PMCID: Holmdahl R, Malmstrom V, Burkhardt H. Autoimmune priming, tissue attack and chronic inflammation the three stages of rheumatoid arthritis. Eur J Immunol. 2014;44(6): Schellekens GA, de Jong BA, van den Hoogen FH, van de Putte LB, van Venrooij WJ. Citrulline is an essential constituent of antigenic determinants recognized by rheumatoid arthritis-specific autoantibodies. J Clin Invest. 1998;101(1): Pubmed Central PMCID: van Jaarsveld CH, ter Borg EJ, Jacobs JW, Schellekens GA, Gmelig-Meyling FH, van Booma-Frankfort C, et al. The prognostic value of the antiperinuclear factor, anti-citrullinated peptide antibodies and rheumatoid factor in early rheumatoid arthritis. Clin Exp Rheumatol. 1999;17(6): Schellekens GA, Visser H, de Jong BA, van den Hoogen FH, Hazes JM, Breedveld FC, et al. The diagnostic properties of rheumatoid arthritis antibodies
7 2 Etiology of Rheumatoid Arthritis: A Historical and Evidence-Based Perspective 19 recognizing a cyclic citrullinated peptide. Arthritis Rheum. 2000;43(1): Demoruelle MK, Deane KD, Holers VM. When and where does inflammation begin in rheumatoid arthritis? Curr Opin Rheumatol. 2014;26(1): Pubmed Central PMCID: Holers VM. Autoimmunity to citrullinated proteins and the initiation of rheumatoid arthritis. Curr Opin Immunol. 2013;25(6): Pubmed Central PMCID: Deane KD. Preclinical rheumatoid arthritis (autoantibodies): an updated review. Curr Rheumatol Rep. 2014;16(5):419. Pubmed Central PMCID: Klareskog L, Malmstrom V, Lundberg K, Padyukov L, Alfredsson L. Smoking, citrullination and genetic variability in the immunopathogenesis of rheumatoid arthritis. Semin Immunol. 2011;23(2): Fox DA, Gizinski A, Morgan R, Lundy SK. Cell-cell interactions in rheumatoid arthritis synovium. Rheum Dis Clin North Am. 2010;36(2): Pubmed Central PMCID: Sabeh F, Fox D, Weiss SJ. Membrane-type I matrix metalloproteinase-dependent regulation of rheumatoid arthritis synoviocyte function. J Immunol. 2010;184(11): Schett G, Gravallese E. Bone erosion in rheumatoid arthritis: mechanisms, diagnosis and treatment. Nat Rev Rheumatol. 2012;8(11): Pubmed Central PMCID: Fox DA. Kinase inhibition a new approach to the treatment of rheumatoid arthritis. N Engl J Med. 2012;367(6): Sarkar S, Fox DA. Targeting IL-17 and Th17 cells in rheumatoid arthritis. Rheum Dis Clin North Am. 2010;36(2): Boissier MC, Semerano L, Challal S, Saidenberg- Kermanac'h N, Falgarone G. Rheumatoid arthritis: from autoimmunity to synovitis and joint destruction. J Autoimmun. 2012;39(3): Dennis Jr G, Holweg CT, Kummerfeld SK, Choy DF, Setiadi AF, Hackney JA, et al. Synovial phenotypes in rheumatoid arthritis correlate with response to biologic therapeutics. Arthritis Res Ther. 2014;16(2):R90. Pubmed Central PMCID: Karlson EW, van Schaaardenburg D, van der Helmvan Mil AH. Strategies to predict rheumatoid arthritis development in at-risk populations. Rheumatology (Oxford). 2016;55(1): Hunt L, Emery P. Defining populations at risk of rheumatoid arthritis: the first steps to prevention. Nat Rev Rheumatol. 2014;10(9):
8
PATHOGENESIS OF RHEUMATOID ARTHRITIS
 PATHOGENESIS OF RHEUMATOID ARTHRITIS Division of Rheumatology Department of Internal Medicine College of Medicine Seoul National University Seoul National University Bundang Hospital Yun Jong Lee Rheumatoid
PATHOGENESIS OF RHEUMATOID ARTHRITIS Division of Rheumatology Department of Internal Medicine College of Medicine Seoul National University Seoul National University Bundang Hospital Yun Jong Lee Rheumatoid
PATHOGENESIS OF RHEUMATOID ARTHRITIS
 PATHOGENESIS OF RHEUMATOID ARTHRITIS Division of Rheumatology Department of Internal Medicine College of Medicine Seoul National University Seoul National University Bundang Hospital Yun Jong Lee Rheumatoid
PATHOGENESIS OF RHEUMATOID ARTHRITIS Division of Rheumatology Department of Internal Medicine College of Medicine Seoul National University Seoul National University Bundang Hospital Yun Jong Lee Rheumatoid
AUTOIMMUNITY CLINICAL CORRELATES
 AUTOIMMUNITY CLINICAL CORRELATES Pamela E. Prete, MD, FACP, FACR Section Chief, Rheumatology VA Healthcare System, Long Beach, CA Professor of Medicine, Emeritus University of California, Irvine Colonel
AUTOIMMUNITY CLINICAL CORRELATES Pamela E. Prete, MD, FACP, FACR Section Chief, Rheumatology VA Healthcare System, Long Beach, CA Professor of Medicine, Emeritus University of California, Irvine Colonel
AUTOIMMUNITY TOLERANCE TO SELF
 AUTOIMMUNITY CLINICAL CORRELATES Pamela E. Prete, MD, FACP, FACR Section Chief, Rheumatology VA Healthcare System, Long Beach, CA Professor of Medicine, Emeritus University of California, Irvine Colonel
AUTOIMMUNITY CLINICAL CORRELATES Pamela E. Prete, MD, FACP, FACR Section Chief, Rheumatology VA Healthcare System, Long Beach, CA Professor of Medicine, Emeritus University of California, Irvine Colonel
MAF Shalaby Prof. Rheumatology Al Azhar University, Cairo, Egypt.
 MAF Shalaby Prof. Rheumatology Al Azhar University, Cairo, Egypt. AUTOIMMUNE DISEASE RA SLE VASCULITIS RELAPSING POLYCHONDRITIS SS DM/PM SJOGREN S SYNDROME RHEUMATOID ARTHRITIS Classically immune mediated
MAF Shalaby Prof. Rheumatology Al Azhar University, Cairo, Egypt. AUTOIMMUNE DISEASE RA SLE VASCULITIS RELAPSING POLYCHONDRITIS SS DM/PM SJOGREN S SYNDROME RHEUMATOID ARTHRITIS Classically immune mediated
Autoimmune Diseases. Betsy Kirchner CNP The Cleveland Clinic
 Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Rheumatoid Arthritis. Manish Relan, MD FACP RhMSUS Arthritis & Rheumatology Care Center. Jacksonville, FL (904)
 Rheumatoid Arthritis Manish Relan, MD FACP RhMSUS Arthritis & Rheumatology Care Center. Jacksonville, FL (904) 503-6999. 1 Disclosures Speaker Bureau: Abbvie 2 Objectives Better understand the pathophysiology
Rheumatoid Arthritis Manish Relan, MD FACP RhMSUS Arthritis & Rheumatology Care Center. Jacksonville, FL (904) 503-6999. 1 Disclosures Speaker Bureau: Abbvie 2 Objectives Better understand the pathophysiology
Immunological Aspect of Ozone in Rheumatic Diseases
 Immunological Aspect of Ozone in Rheumatic Diseases Prof. Dr. med. Z. Fahmy Chief Consulting Rheumatologist Augusta Clinic for Rheumatic Diseases And Rehabilitation Bad Kreuznach Germany Rheumatoid arthritis
Immunological Aspect of Ozone in Rheumatic Diseases Prof. Dr. med. Z. Fahmy Chief Consulting Rheumatologist Augusta Clinic for Rheumatic Diseases And Rehabilitation Bad Kreuznach Germany Rheumatoid arthritis
B cells: a fundamental role in the pathogenesis of rheumatoid arthritis?
 Rheumatology 2005;44(Suppl. 2):ii3 ii7 B cells: a fundamental role in the pathogenesis of rheumatoid arthritis? doi:10.1093/rheumatology/keh616 The role of T cells in the pathogenesis of RA is well established,
Rheumatology 2005;44(Suppl. 2):ii3 ii7 B cells: a fundamental role in the pathogenesis of rheumatoid arthritis? doi:10.1093/rheumatology/keh616 The role of T cells in the pathogenesis of RA is well established,
Requirements in the Development of an Autoimmune Disease Amino Acids in the Shared Epitope
 + T cell MHC/self-peptide MHC/Vβ Induction of + T H 1 mediated autoimmunity: A paradigm for the pathogenesis of rheumatoid arthritis, multiple sclerosis and type I diabetes APC Activated autoreactive +
+ T cell MHC/self-peptide MHC/Vβ Induction of + T H 1 mediated autoimmunity: A paradigm for the pathogenesis of rheumatoid arthritis, multiple sclerosis and type I diabetes APC Activated autoreactive +
The Pathogenesis of Bone Erosions in RA FULL VERSION
 The Pathogenesis of Bone Erosions in RA FULL VERSION 1 Key Learning Objectives Understand the role of osteoclasts in normal bone remodeling Comprehend the key processes in pathologic osteoclast functions
The Pathogenesis of Bone Erosions in RA FULL VERSION 1 Key Learning Objectives Understand the role of osteoclasts in normal bone remodeling Comprehend the key processes in pathologic osteoclast functions
Immunology for the Rheumatologist
 Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Anti-CCP antibody testing as a diagnostic and prognostic tool in rheumatoid arthritis
 Q J Med 2007; 100:193 201 doi:10.1093/qjmed/hcm015 Review Anti-CCP antibody testing as a diagnostic and prognostic tool in rheumatoid arthritis T.B. NIEWOLD, M.J. HARRISON and S.A. PAGET From the Department
Q J Med 2007; 100:193 201 doi:10.1093/qjmed/hcm015 Review Anti-CCP antibody testing as a diagnostic and prognostic tool in rheumatoid arthritis T.B. NIEWOLD, M.J. HARRISON and S.A. PAGET From the Department
Potential Role of Sphingosine 1-Phosphate in the. Pathogenesis of Rheumatoid Arthritis
 Potential Role of Sphingosine 1-Phosphate in the Pathogenesis of Rheumatoid Arthritis COMMENTARY for Zhao, C., Fernandes, M.J., Turgeon, M., Tancrede, S., Di Battista, J., Poubelle, P.E. and Bourgoin,
Potential Role of Sphingosine 1-Phosphate in the Pathogenesis of Rheumatoid Arthritis COMMENTARY for Zhao, C., Fernandes, M.J., Turgeon, M., Tancrede, S., Di Battista, J., Poubelle, P.E. and Bourgoin,
Treating Rheumatologic Disease in Arizona: Good News, Bad News
 Treating Rheumatologic Disease in Arizona: Good News, Bad News Jeffrey R. Lisse, M.D. Ethel P. McChesney Bilby Professor of Medicine Chief, Section of Rheumatology University of Arizona School of Medicine
Treating Rheumatologic Disease in Arizona: Good News, Bad News Jeffrey R. Lisse, M.D. Ethel P. McChesney Bilby Professor of Medicine Chief, Section of Rheumatology University of Arizona School of Medicine
Amino acid sequences in the β chain HLA- DRB*0401 molecules dictate susceptibility to RA Amino Acids in the Shared Epitope
 MHC/self-peptide MHC/Vβ TCR Vβx + Vβx T cell Induction of + TH1 mediated autoimmunity: A paradigm for the pathogenesis of rheumatoid arthritis, multiple sclerosis and APC type I diabetes TCR Vβx Activated
MHC/self-peptide MHC/Vβ TCR Vβx + Vβx T cell Induction of + TH1 mediated autoimmunity: A paradigm for the pathogenesis of rheumatoid arthritis, multiple sclerosis and APC type I diabetes TCR Vβx Activated
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/38506 holds various files of this Leiden University dissertation. Author: Nies, Jessica Annemarie Bernadette van Title: Early identification of rheumatoid
Cover Page The handle http://hdl.handle.net/1887/38506 holds various files of this Leiden University dissertation. Author: Nies, Jessica Annemarie Bernadette van Title: Early identification of rheumatoid
Use of Serological markers for evaluation of patients with Rheumatoid arthritis
 ISSN: 2319-7706 Volume 4 Number 9 (2015) pp. 61-66 http://www.ijcmas.com Original Research Article Use of Serological markers for evaluation of patients with Rheumatoid arthritis G. Sucilathangam*, G.
ISSN: 2319-7706 Volume 4 Number 9 (2015) pp. 61-66 http://www.ijcmas.com Original Research Article Use of Serological markers for evaluation of patients with Rheumatoid arthritis G. Sucilathangam*, G.
Cytokines modulate the functional activities of individual cells and tissues both under normal and pathologic conditions Interleukins,
 Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Self-tolerance. Lack of immune responsiveness to an individual s own tissue antigens. Central Tolerance. Peripheral tolerance
 Autoimmunity Self-tolerance Lack of immune responsiveness to an individual s own tissue antigens Central Tolerance Peripheral tolerance Factors Regulating Immune Response Antigen availability Properties
Autoimmunity Self-tolerance Lack of immune responsiveness to an individual s own tissue antigens Central Tolerance Peripheral tolerance Factors Regulating Immune Response Antigen availability Properties
Pathophysiologic Basis of Autoimmune Disorders
 Pathophysiologic Basis of Autoimmune Disorders Linda Felver, Ph.D., R.N. Associate Professor School of Nursing Oregon Health & Science University The immune system has two arms: Adaptive (Acquired) Immune
Pathophysiologic Basis of Autoimmune Disorders Linda Felver, Ph.D., R.N. Associate Professor School of Nursing Oregon Health & Science University The immune system has two arms: Adaptive (Acquired) Immune
Rheumatoid Arthritis
 Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
Topic (Final-03): Immunologic Tolerance and Autoimmunity-Part II
 Topic (Final-03): Immunologic Tolerance and Autoimmunity-Part II MECHANISMS OF AUTOIMMUNITY The possibility that an individual s immune system may react against autologous antigens and cause tissue injury
Topic (Final-03): Immunologic Tolerance and Autoimmunity-Part II MECHANISMS OF AUTOIMMUNITY The possibility that an individual s immune system may react against autologous antigens and cause tissue injury
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Disruption of Healthy Tissue by the Immune Response Autoimmune diseases: Inappropriate immune response against self-components
 Chapter 13 Disruption of Healthy Tissue by the Immune Response Autoimmune diseases: Inappropriate immune response against self-components Humoral imm 胞外 胞內 CMI: CD8 T Self Ag Self(Auto) antigen (encoded
Chapter 13 Disruption of Healthy Tissue by the Immune Response Autoimmune diseases: Inappropriate immune response against self-components Humoral imm 胞外 胞內 CMI: CD8 T Self Ag Self(Auto) antigen (encoded
Lack of association of IL-2RA and IL-2RB polymorphisms with rheumatoid arthritis in a Han Chinese population
 Lack of association of IL-2RA and IL-2RB polymorphisms with rheumatoid arthritis in a Han Chinese population J. Zhu 1 *, F. He 2 *, D.D. Zhang 2 *, J.Y. Yang 2, J. Cheng 1, R. Wu 1, B. Gong 2, X.Q. Liu
Lack of association of IL-2RA and IL-2RB polymorphisms with rheumatoid arthritis in a Han Chinese population J. Zhu 1 *, F. He 2 *, D.D. Zhang 2 *, J.Y. Yang 2, J. Cheng 1, R. Wu 1, B. Gong 2, X.Q. Liu
The lung may play a role in the pathogenesis of rheumatoid arthritis
 of International Journal of Clinical Rheumatology The lung may play a role in the pathogenesis of rheumatoid arthritis Multiple studies have identified strong associations between the lung and rheumatoid
of International Journal of Clinical Rheumatology The lung may play a role in the pathogenesis of rheumatoid arthritis Multiple studies have identified strong associations between the lung and rheumatoid
How the Innate Immune System Profiles Pathogens
 How the Innate Immune System Profiles Pathogens Receptors on macrophages, neutrophils, dendritic cells for bacteria and viruses Broad specificity - Two main groups of bacteria: gram positive, gram-negative
How the Innate Immune System Profiles Pathogens Receptors on macrophages, neutrophils, dendritic cells for bacteria and viruses Broad specificity - Two main groups of bacteria: gram positive, gram-negative
Rheumatoid Arthritis in Asians
 NO DISCLOSURES Rheumatoid rthritis in sians Mary C. Nakamura M.D. Professor of Medicine, UCSF Rheumatoid rthritis Rheumatoid rthritis Polyarthritis of synovial lined joints Inflammatory Characteristic
NO DISCLOSURES Rheumatoid rthritis in sians Mary C. Nakamura M.D. Professor of Medicine, UCSF Rheumatoid rthritis Rheumatoid rthritis Polyarthritis of synovial lined joints Inflammatory Characteristic
Immunology Lecture 4. Clinical Relevance of the Immune System
 Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
IL-17 in health and disease. March 2014 PSO13-C051n
 IL-17 in health and disease March 2014 PSO13-C051n Originally Researchers Suggested That IL-12 and IL-4 drove Th Cell Differentiation Naïve CD4 + T cell Question: Which of these cell types is responsible
IL-17 in health and disease March 2014 PSO13-C051n Originally Researchers Suggested That IL-12 and IL-4 drove Th Cell Differentiation Naïve CD4 + T cell Question: Which of these cell types is responsible
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Clinical and pathophysiologic relevance of autoantibodies in rheumatoid arthritis
 Brito Rocha et al. Advances in Rheumatology (2019) 59:2 https://doi.org/10.1186/s42358-018-0042-8 Advances in Rheumatology REVIEW Clinical and pathophysiologic relevance of autoantibodies in rheumatoid
Brito Rocha et al. Advances in Rheumatology (2019) 59:2 https://doi.org/10.1186/s42358-018-0042-8 Advances in Rheumatology REVIEW Clinical and pathophysiologic relevance of autoantibodies in rheumatoid
HLA and antigen presentation. Department of Immunology Charles University, 2nd Medical School University Hospital Motol
 HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
Autoimmunity. Autoimmunity arises because of defects in central or peripheral tolerance of lymphocytes to selfantigens
 Autoimmunity Autoimmunity arises because of defects in central or peripheral tolerance of lymphocytes to selfantigens Autoimmune disease can be caused to primary defects in B cells, T cells and possibly
Autoimmunity Autoimmunity arises because of defects in central or peripheral tolerance of lymphocytes to selfantigens Autoimmune disease can be caused to primary defects in B cells, T cells and possibly
MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism
 MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism SCHMAIEL SHIRDEL CONTENT 2 Introduction Autoimmune diseases Classification Involved components Autoimmune
MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism SCHMAIEL SHIRDEL CONTENT 2 Introduction Autoimmune diseases Classification Involved components Autoimmune
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases. Abul K. Abbas UCSF
 Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Third line of Defense
 Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Patient #1. Rheumatoid Arthritis. Rheumatoid Arthritis. 45 y/o female Morning stiffness in her joints >1 hour
 Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Clinic of Neurology, Carol Davila University of Medicine and Pharmacy, Colentina Clinical Hospital, Bucharest, Romania c
 Mædica - a Journal of Clinical Medicine EDITORIALS Autoimmunity to cyclic citrullinated peptide in rheumatoid arthritis Manole COJOCARU, MD, PhD a, Inimioara Mihaela COJOCARU MD, PhD b, Isabela SILOSI
Mædica - a Journal of Clinical Medicine EDITORIALS Autoimmunity to cyclic citrullinated peptide in rheumatoid arthritis Manole COJOCARU, MD, PhD a, Inimioara Mihaela COJOCARU MD, PhD b, Isabela SILOSI
The Immune System. These are classified as the Innate and Adaptive Immune Responses. Innate Immunity
 The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
Diagnostic and prognostic serological analyses in RA
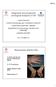 9/9/ Diagnostic and prognostic serological analyses in RA Johan Rönnelid Clinical Immunology and Transfusion medicine Akademiska sjukhuset, Uppsala Department of Immunology, Genetics and Pathology Uppsala
9/9/ Diagnostic and prognostic serological analyses in RA Johan Rönnelid Clinical Immunology and Transfusion medicine Akademiska sjukhuset, Uppsala Department of Immunology, Genetics and Pathology Uppsala
Types of osteoarthritis
 ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
Association of anti-mcv autoantibodies with SLE (Systemic Lupus Erythematosus) overlapping with various syndromes
 International Journal of Medicine and Medical Sciences Vol. () pp. 21-214, June 211 Available online http://www.academicjournals.org/ijmms ISSN 2-972 211 Academic Journals Full Length Research Paper Association
International Journal of Medicine and Medical Sciences Vol. () pp. 21-214, June 211 Available online http://www.academicjournals.org/ijmms ISSN 2-972 211 Academic Journals Full Length Research Paper Association
Supplementary Figure 1 Dosage correlation between imputed and genotyped alleles Imputed dosages (0 to 2) of 2-digit alleles (red) and 4-digit alleles
 Supplementary Figure 1 Dosage correlation between imputed and genotyped alleles Imputed dosages (0 to 2) of 2-digit alleles (red) and 4-digit alleles (green) of (A) HLA-A, HLA-B, (C) HLA-C, (D) HLA-DQA1,
Supplementary Figure 1 Dosage correlation between imputed and genotyped alleles Imputed dosages (0 to 2) of 2-digit alleles (red) and 4-digit alleles (green) of (A) HLA-A, HLA-B, (C) HLA-C, (D) HLA-DQA1,
Unit 5 The Human Immune Response to Infection
 Unit 5 The Human Immune Response to Infection Unit 5-page 1 FOM Chapter 21 Resistance and the Immune System: Innate Immunity Preview: In Chapter 21, we will learn about the branch of the immune system
Unit 5 The Human Immune Response to Infection Unit 5-page 1 FOM Chapter 21 Resistance and the Immune System: Innate Immunity Preview: In Chapter 21, we will learn about the branch of the immune system
11/25/2017. THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS BARRIER DEFENSES INNATE IMMUNITY OF VERTEBRATES
 THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
Rheumatoid Arthritis. Improving Outcomes in RA: Three Pillars. RA: Chronic Joint Destruction and Disability What We Try to Prevent
 Rheumatoid Arthritis Modern Management of Common Problems in Rheumatology: Rheumatoid Arthritis Jonathan Graf, M.D. Associate Professor of Medicine, UCSF Division of Rheumatology, SFGH Director, UCSF Rheumatoid
Rheumatoid Arthritis Modern Management of Common Problems in Rheumatology: Rheumatoid Arthritis Jonathan Graf, M.D. Associate Professor of Medicine, UCSF Division of Rheumatology, SFGH Director, UCSF Rheumatoid
Inflammation in the clinic
 Inflammation in the clinic Stephen T. Holgate MRC Clinical Professor of Immunopharmacology ILSI Europe Workshop, Seville, May 14-15 2012 The immune system acts in four general ways to ensure host defence
Inflammation in the clinic Stephen T. Holgate MRC Clinical Professor of Immunopharmacology ILSI Europe Workshop, Seville, May 14-15 2012 The immune system acts in four general ways to ensure host defence
Immune System. Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka
 Immune System Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka Content Standards 35.1 In innate immunity, recognition and response rely on traits common to groups of pathogens 35.2
Immune System Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka Content Standards 35.1 In innate immunity, recognition and response rely on traits common to groups of pathogens 35.2
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION
 CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
Immune system. Aims. Immune system. Lymphatic organs. Inflammation. Natural immune system. Adaptive immune system
 Aims Immune system Lymphatic organs Inflammation Natural immune system Adaptive immune system Major histocompatibility complex (MHC) Disorders of the immune system 1 2 Immune system Lymphoid organs Immune
Aims Immune system Lymphatic organs Inflammation Natural immune system Adaptive immune system Major histocompatibility complex (MHC) Disorders of the immune system 1 2 Immune system Lymphoid organs Immune
The Genetic Epidemiology of Rheumatoid Arthritis. Lindsey A. Criswell AURA meeting, 2016
 The Genetic Epidemiology of Rheumatoid Arthritis Lindsey A. Criswell AURA meeting, 2016 Overview Recent successes in gene identification genome wide association studies (GWAS) clues to etiologic pathways
The Genetic Epidemiology of Rheumatoid Arthritis Lindsey A. Criswell AURA meeting, 2016 Overview Recent successes in gene identification genome wide association studies (GWAS) clues to etiologic pathways
Concept of Spondyloarthritis (SpA)
 Concept of Spondyloarthritis (SpA) Spondyloarthritis: Characteristic Parameters Used for Diagnosis I Symptoms Inflammatory back pain Imaging Lab ESR/CRP Patient s history Good response to NSAIDs Spondyloarthritis-Characteristic
Concept of Spondyloarthritis (SpA) Spondyloarthritis: Characteristic Parameters Used for Diagnosis I Symptoms Inflammatory back pain Imaging Lab ESR/CRP Patient s history Good response to NSAIDs Spondyloarthritis-Characteristic
Introduction to Immunology and the Immune System
 Introduction to Immunology and the Immune System Assistant professor Dr. Aida R. Al-Derzi M.B.Ch.B; M.Sc; FICM/Path Dept. of Microbiology/College of Medicine/Baghdad University Introduction to Immunology
Introduction to Immunology and the Immune System Assistant professor Dr. Aida R. Al-Derzi M.B.Ch.B; M.Sc; FICM/Path Dept. of Microbiology/College of Medicine/Baghdad University Introduction to Immunology
The Innate Immune Response
 The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
Blood and Immune system Acquired Immunity
 Blood and Immune system Acquired Immunity Immunity Acquired (Adaptive) Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated
Blood and Immune system Acquired Immunity Immunity Acquired (Adaptive) Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated
T Cell Effector Mechanisms I: B cell Help & DTH
 T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
Immunity. Chapter 38 Part 1
 Immunity Chapter 38 Part 1 Impacts, Issues Frankie s Last Wish Infection with a common, sexually transmitted virus (HPV) causes most cervical cancers including the one that killed Frankie McCullogh 38.1
Immunity Chapter 38 Part 1 Impacts, Issues Frankie s Last Wish Infection with a common, sexually transmitted virus (HPV) causes most cervical cancers including the one that killed Frankie McCullogh 38.1
Genetics and the Path Towards Targeted Therapies in Systemic Lupus
 Genetics and the Path Towards Targeted Therapies in Systemic Lupus Emily Baechler Gillespie, Ph.D. University of Minnesota Department of Medicine Division of Rheumatic and Autoimmune Diseases Disclosures
Genetics and the Path Towards Targeted Therapies in Systemic Lupus Emily Baechler Gillespie, Ph.D. University of Minnesota Department of Medicine Division of Rheumatic and Autoimmune Diseases Disclosures
1.0 Abstract. Title. Keywords. Rationale and Background
 1.0 Abstract Title A Prospective, Multi-Center Study in Rheumatoid Arthritis Patients on Adalimumab to Evaluate its Effect on Synovitis Using Ultrasonography in an Egyptian Population Keywords Synovitis
1.0 Abstract Title A Prospective, Multi-Center Study in Rheumatoid Arthritis Patients on Adalimumab to Evaluate its Effect on Synovitis Using Ultrasonography in an Egyptian Population Keywords Synovitis
Autoimmune diseases. Autoimmune diseases. Autoantibodies. Autoimmune diseases relatively common
 Autoimmune diseases Fundamental abnormality: the adaptive immune system is triggered by self antigens to initiate a sustained immune response against self molecules that results in tissue injury Specificity
Autoimmune diseases Fundamental abnormality: the adaptive immune system is triggered by self antigens to initiate a sustained immune response against self molecules that results in tissue injury Specificity
Determinants of Immunogenicity and Tolerance. Abul K. Abbas, MD Department of Pathology University of California San Francisco
 Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Disclosures. Objectives. Inhaled risk factors for RA 11/7/2011. The Lung as a Site of Initiation of Rheumatoid Arthritis-related Autoimmunity
 Disclosures The Lung as a Site of Initiation of Rheumatoid Arthritis-related Autoimmunity No conflicts of interest Kevin Deane, MD/PhD University of Colorado Rheumatoid Arthritis: Where Does it Begin?
Disclosures The Lung as a Site of Initiation of Rheumatoid Arthritis-related Autoimmunity No conflicts of interest Kevin Deane, MD/PhD University of Colorado Rheumatoid Arthritis: Where Does it Begin?
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
Overview of the Lymphoid System
 Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
Bibliografia Microbiota
 Bibliografia Microbiota Systematic Review: Gut Microbiota in Fecal Samples and Detection of Colorectal Neoplasms. The role of the intestinal microbiome in ocular inflammatory disease. The gut microbiome
Bibliografia Microbiota Systematic Review: Gut Microbiota in Fecal Samples and Detection of Colorectal Neoplasms. The role of the intestinal microbiome in ocular inflammatory disease. The gut microbiome
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology
 Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Cellular Pathology of immunological disorders
 Cellular Pathology of immunological disorders SCBM344 Cellular and Molecular Pathology Witchuda Payuhakrit, Ph.D (Pathobiology) witchuda.pay@mahidol.ac.th Objectives Describe the etiology of immunological
Cellular Pathology of immunological disorders SCBM344 Cellular and Molecular Pathology Witchuda Payuhakrit, Ph.D (Pathobiology) witchuda.pay@mahidol.ac.th Objectives Describe the etiology of immunological
NTD Vaccine Design Toolkit and Training Workshop Providence, RI January 05, 2011 Cytokines Leslie P. Cousens, PhD EpiVax, Inc.
 NTD Vaccine Design Toolkit and Training Workshop Providence, RI January 05, 2011 Cytokines Leslie P. Cousens, PhD EpiVax, Inc. Cytokines Properties of Cytokines Cytokines are proteins with specific roles
NTD Vaccine Design Toolkit and Training Workshop Providence, RI January 05, 2011 Cytokines Leslie P. Cousens, PhD EpiVax, Inc. Cytokines Properties of Cytokines Cytokines are proteins with specific roles
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Third line of Defense. Topic 8 Specific Immunity (adaptive) (18) 3 rd Line = Prophylaxis via Immunization!
 Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
Rheumatologic Lab Tests
 Rheumatologic Lab Tests What the Practitioner Needs to Know Mary Nakamura M.D. 2008 Rheumatologic Lab Tests Are rarely diagnostic of any specific disease If you do not have in mind a rheumatologic disease
Rheumatologic Lab Tests What the Practitioner Needs to Know Mary Nakamura M.D. 2008 Rheumatologic Lab Tests Are rarely diagnostic of any specific disease If you do not have in mind a rheumatologic disease
HLA and antigen presentation. Department of Immunology Charles University, 2nd Medical School University Hospital Motol
 HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
Helminth worm, Schistosomiasis Trypanosomes, sleeping sickness Pneumocystis carinii. Ringworm fungus HIV Influenza
 Helminth worm, Schistosomiasis Trypanosomes, sleeping sickness Pneumocystis carinii Ringworm fungus HIV Influenza Candida Staph aureus Mycobacterium tuberculosis Listeria Salmonella Streptococcus Levels
Helminth worm, Schistosomiasis Trypanosomes, sleeping sickness Pneumocystis carinii Ringworm fungus HIV Influenza Candida Staph aureus Mycobacterium tuberculosis Listeria Salmonella Streptococcus Levels
DOI /art.39832
 Letter to the Editor DOI 10.1002/art.39832 David Hutchinson MD 1 2, Daniel Murphy BmBs 1, Alex Clarke BSc 2 and Paul Eggleton MPhil, PhD 2 1 Department of Rheumatology, Royal Cornwall Hospital Trust, Truro,
Letter to the Editor DOI 10.1002/art.39832 David Hutchinson MD 1 2, Daniel Murphy BmBs 1, Alex Clarke BSc 2 and Paul Eggleton MPhil, PhD 2 1 Department of Rheumatology, Royal Cornwall Hospital Trust, Truro,
Immunological Tolerance
 Immunological Tolerance Introduction Definition: Unresponsiveness to an antigen that is induced by exposure to that antigen Tolerogen = tolerogenic antigen = antigen that induces tolerance Important for
Immunological Tolerance Introduction Definition: Unresponsiveness to an antigen that is induced by exposure to that antigen Tolerogen = tolerogenic antigen = antigen that induces tolerance Important for
Physiology Unit 3. ADAPTIVE IMMUNITY The Specific Immune Response
 Physiology Unit 3 ADAPTIVE IMMUNITY The Specific Immune Response In Physiology Today The Adaptive Arm of the Immune System Specific Immune Response Internal defense against a specific pathogen Acquired
Physiology Unit 3 ADAPTIVE IMMUNITY The Specific Immune Response In Physiology Today The Adaptive Arm of the Immune System Specific Immune Response Internal defense against a specific pathogen Acquired
Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics
 Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics Dr Sarah Sasson SydPATH Registrar 23 rd June 2014 TLRs: Introduction Discovered in 1990s Recognise conserved structures in pathogens Rely
Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics Dr Sarah Sasson SydPATH Registrar 23 rd June 2014 TLRs: Introduction Discovered in 1990s Recognise conserved structures in pathogens Rely
The Major Histocompatibility Complex (MHC)
 The Major Histocompatibility Complex (MHC) An introduction to adaptive immune system before we discuss MHC B cells The main cells of adaptive immune system are: -B cells -T cells B cells: Recognize antigens
The Major Histocompatibility Complex (MHC) An introduction to adaptive immune system before we discuss MHC B cells The main cells of adaptive immune system are: -B cells -T cells B cells: Recognize antigens
Chapter 2. Overview of ankylosing spondylitis
 Chapter 2 Overview of ankylosing spondylitis The concept and classification of spondyloarthritis The term spondyloarthritis (SpA) comprises AS, reactive arthritis, arthritis/spondylitis associated with
Chapter 2 Overview of ankylosing spondylitis The concept and classification of spondyloarthritis The term spondyloarthritis (SpA) comprises AS, reactive arthritis, arthritis/spondylitis associated with
Rheumatoid Arthritis: An update for non rheumatologists
 Rheumatoid Arthritis: An update for non rheumatologists Dimitrios Pappas, M.D., M.P.H. Assistant Professor of Medicine Columbia University, College of Physicians & Surgeons Director of Rheumatology Athens
Rheumatoid Arthritis: An update for non rheumatologists Dimitrios Pappas, M.D., M.P.H. Assistant Professor of Medicine Columbia University, College of Physicians & Surgeons Director of Rheumatology Athens
Microbiology 204: Cellular and Molecular Immunology
 Microbiology 204: Cellular and Molecular Immunology Class meets MWF 1:00-2:30PM (*exceptions: no class Fri Sept 23, Fri Oct 14, Nov 11, or Wed Nov 23) Lectures are open to auditors and will be live-streamed
Microbiology 204: Cellular and Molecular Immunology Class meets MWF 1:00-2:30PM (*exceptions: no class Fri Sept 23, Fri Oct 14, Nov 11, or Wed Nov 23) Lectures are open to auditors and will be live-streamed
Understanding Autoimmune Diseases: Evolving Issues. Alvina D. Chu, M.D. April 23, 2009
 Understanding Autoimmune Diseases: Evolving Issues Alvina D. Chu, M.D. April 23, 2009 Objectives Define the key pathogenic characteristics of: Type I diabetes mellitus Multiple sclerosis Rheumatoid arthritis
Understanding Autoimmune Diseases: Evolving Issues Alvina D. Chu, M.D. April 23, 2009 Objectives Define the key pathogenic characteristics of: Type I diabetes mellitus Multiple sclerosis Rheumatoid arthritis
ROLE OF GENES AND ENVIRONMENT FOR THE DEVELOPMENT OF RHEUMATOID ARTHRITIS - RESULTS FROM THE SWEDISH EIRA STUDY
 From the Institute of Environmental Medicine, Division of Cardiovascular Epidemiology, Karolinska Institutet, Stockholm, Sweden in collaboration with the Rheumatology Unit, Department of Medicine, Karolinska
From the Institute of Environmental Medicine, Division of Cardiovascular Epidemiology, Karolinska Institutet, Stockholm, Sweden in collaboration with the Rheumatology Unit, Department of Medicine, Karolinska
Retrospective Genetic Analysis of Efficacy and Adverse Events in a Rheumatoid Arthritis Population Treated with Methotrexate and Anti-TNF-α
 Retrospective Genetic Analysis of Efficacy and Adverse Events in a Rheumatoid Arthritis Population Treated with Methotrexate and Anti-TNF-α Foti A 1, Lichter D 1, Shadick NA 2, Maher NE 2, Ginsburg GS
Retrospective Genetic Analysis of Efficacy and Adverse Events in a Rheumatoid Arthritis Population Treated with Methotrexate and Anti-TNF-α Foti A 1, Lichter D 1, Shadick NA 2, Maher NE 2, Ginsburg GS
Cell-mediated response (what type of cell is activated and what gets destroyed?)
 The Immune System Reading Guide (Chapter 43) Name Per 1. The immune response in animals can be divided into innate immunity and adaptive immunity. As an overview, complete this figure indicating the divisions
The Immune System Reading Guide (Chapter 43) Name Per 1. The immune response in animals can be divided into innate immunity and adaptive immunity. As an overview, complete this figure indicating the divisions
2017 Arizona United Rheumatology Alliance Annual Meeting. Overview of the Immune System and Memory B-cell Activity in RA
 2017 Arizona United Rheumatology Alliance Annual Meeting Overview of the Immune System and Memory B-cell Activity in RA Gregg J. Silverman, MD Professor of Medicine and Pathology Director, Laboratory of
2017 Arizona United Rheumatology Alliance Annual Meeting Overview of the Immune System and Memory B-cell Activity in RA Gregg J. Silverman, MD Professor of Medicine and Pathology Director, Laboratory of
Nonspecific External Barriers skin, mucous membranes
 Immune system Chapter 36 BI 103 Plant-Animal A&P Levels of Defense Against Disease Nonspecific External Barriers skin, mucous membranes Physical barriers? Brainstorm with a partner If these barriers are
Immune system Chapter 36 BI 103 Plant-Animal A&P Levels of Defense Against Disease Nonspecific External Barriers skin, mucous membranes Physical barriers? Brainstorm with a partner If these barriers are
The Role of IL-1 and Tumor Necrosis Factor-α in Pathogenesis of Rheumatoid Arthritis
 RHEUMATOID THE IRAQI POSTGRADUATE ARTHRITIS MEDICAL JOURNAL The Role of IL-1 and Tumor Necrosis Factor-α in Pathogenesis of Rheumatoid Arthritis Eman Sh.Al-Obeidy*, Shatha F. Abdullah** ABSTRACT: BACKGROUND:
RHEUMATOID THE IRAQI POSTGRADUATE ARTHRITIS MEDICAL JOURNAL The Role of IL-1 and Tumor Necrosis Factor-α in Pathogenesis of Rheumatoid Arthritis Eman Sh.Al-Obeidy*, Shatha F. Abdullah** ABSTRACT: BACKGROUND:
Biology of Immune Aging
 Biology of Immune Aging Jorg J. Goronzy Stanford University Immune deficiency Increase morbidity and mortality from infections Poor vaccine responses Cancer Immune Aging Chronic inflammation Coronary artery
Biology of Immune Aging Jorg J. Goronzy Stanford University Immune deficiency Increase morbidity and mortality from infections Poor vaccine responses Cancer Immune Aging Chronic inflammation Coronary artery
Role of BAFF in B cell Biology and Autoimmunity
 Role of BAFF in B cell Biology and Autoimmunity B cell development in health and disease: B-lymphocytes or B cells, and the antibodies they produce, are crucial mediators of humoral immunity, providing
Role of BAFF in B cell Biology and Autoimmunity B cell development in health and disease: B-lymphocytes or B cells, and the antibodies they produce, are crucial mediators of humoral immunity, providing
NOVEL BIOMARKERS AS RISK FACTORS FOR CARDIOVASCULAR DISEASE
 NOVEL BIOMARKERS AS RISK FACTORS FOR CARDIOVASCULAR DISEASE Amy Alman, PhD Assistant Professor of Epidemiology College of Public Health University of South Florida Causation is a concept central to epidemiology
NOVEL BIOMARKERS AS RISK FACTORS FOR CARDIOVASCULAR DISEASE Amy Alman, PhD Assistant Professor of Epidemiology College of Public Health University of South Florida Causation is a concept central to epidemiology
Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells
 ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
Immunology - Lecture 2 Adaptive Immune System 1
 Immunology - Lecture 2 Adaptive Immune System 1 Book chapters: Molecules of the Adaptive Immunity 6 Adaptive Cells and Organs 7 Generation of Immune Diversity Lymphocyte Antigen Receptors - 8 CD markers
Immunology - Lecture 2 Adaptive Immune System 1 Book chapters: Molecules of the Adaptive Immunity 6 Adaptive Cells and Organs 7 Generation of Immune Diversity Lymphocyte Antigen Receptors - 8 CD markers
Chapter 11 CYTOKINES
 Chapter 11 CYTOKINES group of low molecular weight regulatory proteins secreted by leukocytes as well as a variety of other cells in the body (8~30kD) regulate the intensity and duration of the immune
Chapter 11 CYTOKINES group of low molecular weight regulatory proteins secreted by leukocytes as well as a variety of other cells in the body (8~30kD) regulate the intensity and duration of the immune
chapter 17: specific/adaptable defenses of the host: the immune response
 chapter 17: specific/adaptable defenses of the host: the immune response defense against infection & illness body defenses innate/ non-specific adaptable/ specific epithelium, fever, inflammation, complement,
chapter 17: specific/adaptable defenses of the host: the immune response defense against infection & illness body defenses innate/ non-specific adaptable/ specific epithelium, fever, inflammation, complement,
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A
 HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
