Potential Pharmacologic Treatments for Cystinuria and for Calcium Stones Associated with Hyperuricosuria
|
|
|
- Cecil Bryan
- 5 years ago
- Views:
Transcription
1 Potential Pharmacologic Treatments for Cystinuria and for Calcium Stones Associated with Hyperuricosuria David S. Goldfarb Summary Two new potential pharmacologic therapies for recurrent stone disease are described. The role of hyperuricosuria in promoting calcium stones is controversial with only some but not all epidemiologic studies demonstrating associations between increasing urinary uric acid excretion and calcium stone disease. The relationship is supported by the ability of uric acid to salt out (or reduce the solubility of) calcium oxalate in vitro. A randomized, controlled trial of allopurinol in patients with hyperuricosuria and normocalciuria was also effective in preventing recurrent stones. Febuxostat, a nonpurine inhibitor of xanthine oxidase (also known as xanthine dehydrogenase or xanthine oxidoreductase) may have advantages over allopurinol and is being tested in a similar protocol, with the eventual goal of determining whether urate-lowering therapy prevents recurrent calcium stones. Treatments for cystinuria have advanced little in the past 30 years. Atomic force microscopy has been used recently to demonstrate that effective inhibition of cystine crystal growth is accomplished at low concentrations of L-cystine methyl ester and L-cystine dimethyl ester, structural analogs of cystine that provide steric inhibition of crystal growth. In vitro, L-cystine dimethyl ester had a significant inhibitory effect on crystal growth. The drug s safety and effectiveness will be tested in an Slc3a1 knockout mouse that serves as an animal model of cystinuria. Clin J Am Soc Nephrol 6: , doi: /CJN Nephrology Section, New York Harbor VA Medical Center, and Division of Nephrology, New York University School of Medicine, New York, New York Correspondence: Dr. David S. Goldfarb, Nephrology Section/ 111G, NY DVAMC, 423 E. 23 Street, New York, NY Phone: , ext. 3877; Fax: ; david.goldfarb@va.gov Introduction The current pharmacologic therapies for prevention of recurrent kidney stones all are relatively ancient (1). Only a handful of drugs are commonly used today, none of which is less than 30 years old. For prevention of recurrent calcium stones, available therapies include the thiazides (chlorthalidone, hydrochlorothiazide, and indapamide), potassium citrate, and allopurinol. Differences between pharmacologic therapy for calcium oxalate and calcium phosphate stones are not clearly delineated. Uric acid stones are treated with urinary alkalinization, usually with potassium citrate and less frequently with sodium citrate, and allopurinol has only a secondary role. For cystine stones, alkalinization as for uric acid stones and thiol therapy with tiopronin and d-penicillamine are appropriate. This review briefly considers two novel topics: Febuxostat for calcium stones and new inhibitors of cystine crystallization. Other pharmacologic therapies are in development; these are simply two topics of current interest to the author. Febuxostat Approximately one third of patients with recurrent calcium stones have hyperuricosuria as one of their urinary risk factors (2). Increasing the urate concentration of experimental solutions effectively halves the amount of oxalate required to provoke calcium oxalate crystallization and increases the size of particles deposited (3). The pathophysiology of this relationship has been attributed to the ability of uric acid to salt out calcium oxalate. Salting out is simply the ability of an electrolyte, in this case uric acid, to reduce the solubility of a nonelectrolyte, in this case calcium oxalate (4). For the purposes of this definition, nonelectrolytes and electrolytes are salts that have low and high solubilities, respectively. This phenomenon is distinct from epitaxy, whereby one crystal forms on another. (Although sodium urate can lead to crystallization of calcium oxalate in vitro, such an effect has not been demonstrated to occur in human urine and is now considered unimportant in explaining the ability of hyperuricosuria to promote calcium stone disease.) Although these in vitro data and phenomena are interesting, the epidemiologic data demonstrating that hyperuricosuria is an important risk factor for calcium stones is less compelling with variable results and conclusions. Most recently, three well characterized cohorts of prospectively followed participants were studied with regard to 24-hour uric acid excretion as a risk for kidney stone formation (5). In 3350 men and women, 2237 of whom had a history of nephrolithiasis, urinary uric acid had a significant inverse association with stone formation in men, a marginal inverse association with risk in younger women, and no association in older women. With many small and inadequately controlled trials in the literature suggesting that reducing uric acid excretion might reduce calcium stone recurrence, only one adequate randomized, controlled trial has dem- Vol 6 August, 2011 Copyright 2011 by the American Society of Nephrology 2093
2 2094 Clinical Journal of the American Society of Nephrology onstrated this effect (6). The hypothesis was that allopurinol, an inhibitor of xanthine oxidase (also known recently as xanthine dehydrogenase or xanthine oxidoreductase) would decrease the rate of recurrent calcium oxalate calculi in patients with hyperuricosuria ( 800 mg/d in men, 750 mg/d in women) and normocalciuria ( 300 mg/d in men, 250 mg/d in women). The patients were randomly assigned to either allopurinol 100 mg three times a day or placebo. Recurrent stone outcomes were determined either by recording of stone passage or by comparison of plain radiographs taken at yearly intervals with the baseline film. Allopurinol reduced uric acid excretion by 400 mg/d, whereas the placebo group had a variable reduction of 0 to 100 mg/d. Although both groups had a reduction in stone events, new stones occurred in 18 patients receiving placebo and nine receiving allopurinol, and the allopurinol group had a significantly longer time before recurrence. This study exists in the context of the heterogeneity of epidemiologic data that fail to demonstrate strongly that hyperuricosuria is a risk factor for calcium stones. It has therefore been suggested that the effect of allopurinol on calcium stone incidence is actually not related to its ability to lower uric acid production (5,7). Its effects could include other effects of xanthine oxidase inhibition, as the enzyme has been linked to oxidative stress and production of free radicals (8). How these pleiotropic effects of xanthine oxidase and its inhibition are linked to stone formation remain speculative and unproved. One interesting question is whether xanthine oxidase inhibition to reduce uric acid excretion is effective only in calcium stone formers with normocalciuria and not in patients with hypercalciuria. Review of this literature demonstrates a paucity of evidence. In one frequently cited article, a nonrandomized trial, 31 patients were treated with allopurinol, and 43 patients served as untreated controls for recurrent calcium stones (9). Overall, patients who were treated with allopurinol had a recurrence rate of 49% (15 of 31), whereas the control patients, who were not treated with allopurinol, had a recurrence rate of 40% (17 of 43). In other words, allopurinol had no effect on the aggregated group. Five of six with both hyperuricosuria and hypercalciuria had an episode of stone recurrence at 2 years, whereas only two of eight with hyperuricosuria and normocalciuria did; regardless of uric acid excretion, the patients with hypercalciuria had a 64% recurrence rate, whereas patients with normocalciuria had a 40% recurrence rate. This small, nonrandomized trial with smaller subgroups cannot serve as an adequate basis for concluding that urate-lowering therapy is not efficacious in the presence of hypercalciuria. In a review of the efficacy of allopurinol for calcium stones, Ettinger (7) tabulated 15 articles that either did or did not prescribe the drug in a selective manner, that is, excluding hypercalciuria. The studies are mostly small and nonrandomized. He concluded, Treatment has not been systematically evaluated for patients (with) hyperuricosuria combined with hypercalciuria. The school of selective treatment would suggest thiazide and allopurinol. However, this combination is thought to lead to a higher rate of allopurinol hypersensitivity, perhaps via increased reabsorption of the metabolite oxypurinol (10). Many such cases have occurred when allopurinol was given to treat asymptomatic hyperuricemia developing from thiazide use. Febuxostat is a newer xanthine oxidase inhibitor and, unlike allopurinol, is not a purine analog. It received approval by the Food and Drug Administration in 2009 for the long-term management of hyperuricemia in patients with gout. Its efficacy in reducing serum uric acid concentration and urinary uric acid excretion may be superior to allopurinol, although the two have not been properly tested head-to-head because allopurinol has not been titrated past 300 mg/d in studies performed in the United States (11 13). Whereas excretion of allopurinol is mainly via the kidneys, febuxostat is largely metabolized by the liver. It may therefore be particularly useful for urate lowering in patients with chronic kidney disease, a category that is not necessarily relevant to stone disease. Studies have concluded that the 80-mg dosage does not require adjustment in patients with impaired GFR, although the data for patients with estimated GFR 30 ml/min per 1.73 m 2 are limited (14,15). Febuxostat is currently used mostly in patients with allopurinol allergy or hypersensitivity and in patients who fail to achieve serum uric acid targets with allopurinol (13). In stone formers being treated for gout and hyperuricemia, it might be preferable, in the allopurinol-intolerant patient, to uricosuric agents. On the basis of the possibility that the drug could be as efficacious as or superior to allopurinol, I helped Takeda design a study to test the hypothesis that febuxostat, like allopurinol, could reduce hyperuricosuria and recurrent calcium stones. The study has completed enrollment at a number of kidney stone prevention programs and urology practices throughout the United States. Its title is Febuxostat Versus Allopurinol or Placebo in Subjects with Hyperuricosuria and Calcium Oxalate Stones (ClinicalTrials-.gov identifier NCT ). The preliminary design seeks essentially to replicate the allopurinol study of Ettinger et al. (6). Patients with a history of calcium stones and at least one 3-mm stone in place and with hyperuricosuria ( 700 mg/d) and normocalciuria ( 4 mg/kg) will be randomly assigned to one of three groups: febuxostat 80 mg/d, allopurinol 200 or 300 mg/d (depending on GFR), or placebo. Hyperuricemia is not required. The outcome is uric acid excretion and assessment of stones on computed tomography at 6 months. Although this period of time is likely too short to demonstrate a change in stone outcomes, the uric acid excretion results may serve as the basis for a possible longer study sufficient to replicate the findings of Ettinger (6). The study will generate data on the magnitude of reduction of uricosuria by this dosage of febuxostat. In a potential longer phase 3 study, with a primary outcome of stone burden as determined by computed tomography, febuxostat could be compared with allopurinol. Because allopurinol is available as a generic medication, it is significantly less expensive. Febuxostat may be more efficacious if greater reductions in serum uric acid correlate with lower urinary uric acid (11,12) and if that in turn correlates with less stone disease activity. Whereas allopurinol is associated with an incidence of rash of 2% and rare life-threatening hypersensitivity reactions (10), febuxostat seems thus far to be associated with fewer hypersensitivity events, with only two reported to Takeda via the
3 Clin J Am Soc Nephrol 6: , August, 2011 New Pharmacologic Therapies for Nephrolithiasis, Goldfarb 2095 Food and Drug Administration s Medwatch (Patricia Macdonald, RN, personal communication). Liver function abnormalities are seen at a slightly higher rate than in placebotreated patients. Other potential advantages of febuxostat, of unproven clinical significance thus far, is that, unlike allopurinol, it inhibits both the oxidized and reduced forms of xanthine oxidase and has fewer effects on other enzymes involved in purine and pyrimidine metabolism. It might also be worthwhile to test urate-lowering therapy with or without thiazides in patients with hypercalciuria and hyperuricosuria. Both allopurinol and febuxostat may be better tolerated than thiazides in many patients (16) and may have additional cardiovascular benefits related to either reduction of uric acid or inhibition of xanthine oxidase (17). The limitation to using allopurinol more widely because of the purported lack of efficacy in hypercalciuria and the risk for hypersensitivity when co-administered with thiazides leaves open the possibility of a range of studies with febuxostat. New Therapies for Cystinuria Cystinuria is an autosomal recessive disorder that occurs as the result of mutations in one of the two genes that code for the proteins that constitute the cystine and basic amino acid transporter expressed in the proximal tubule (18). The result is failure to reabsorb filtered cystine, a poorly soluble amino acid that crystallizes in the distal tubules and forms large and recurrent stones. Treatments for cystinuria have essentially not changed for more than 30 years (19). Fluids to increase urine volume and dilute excreted cystine are considered critical. Dietary therapy, which remains untested in actually changing stone activity, includes sodium and animal protein restriction. Reduction of sodium intake is associated with a reduction in cystine excretion, although the basis for this effect is not clear (20,21); the cystine transporter in the proximal tubule is not a sodium-dependent transporter. Restriction of animal protein ingestion facilitates urinary alkalinization to increase cystine solubility and reduces intake of the cystine precursor methionine, reducing urinary cystine excretion (22). Pharmacologic therapies are twofold. Urinary alkalinization increases cystine solubility and is achieved with administration of citrate or bicarbonate. Because cystine is a dimer of cysteine linked by a disulfide bridge, thiols, whether d-penicillamine or tiopronin, can break the disulfide bridge and form a more soluble complex with monomeric cysteine. Captopril, although also a thiol, is ineffective because its appearance in the urine is insufficient to have a meaningful effect. The thiols, however, are not particularly well tolerated and are associated with a significant incidence of allergy; gastrointestinal intolerance; and a broad variety of adverse effects that include elevation in hepatic enzymes, blood dyscrasias, skin disorders such as elastosis perforans serpiginosa, and proteinuria with membranous nephropathy (23). Tiopronin is better tolerated than d-penicillamine, with 30.6% and 69.4%, respectively, having reactions that required cessation of therapy in one nonrandomized study (23); however, adverse reactions to tiopronin were extremely common. The basis for the toxicity of thiols in general might result from the ability of thiols to produce superoxide radicals and hydrogen peroxide. Thiols can auto-oxidize to disulphides, whereas the latter can be reduced to thiols, and this potential for redox cycling can potentially produce these toxic byproducts (24). The reaction of thiol drugs with cystine might be a model for their interactions with disulfide bridge containing proteins throughout the body. The basis for their use in various other diseases includes their ability both to induce autoimmunity and inhibit T and B cells and to inhibit various enzymes including metalloproteinases. Other approaches to the treatment of cystinuria would therefore be welcome. Ward and his team in the Department of Chemistry at New York University recently reported a potential alternative approach to the prevention of cystine kidney stones based on crystal growth inhibition (25). The technique that allows crystal growth and the effect of inhibitors to be measured is atomic force microscopy (AFM) (26). This technique provides for in situ visualization of the early stages of growth of organic crystals in liquids. The result is the ability to observe nucleation events and topographic features of growing crystals that play an important role in crystal growth. It is then possible to quantify the velocity of growth under varying conditions and in the presence of changing concentrations of putative inhibitors. Real-time in situ AFM of l-cystine during growth in aqueous solutions containing l-cystine revealed expanding steps generating hexagonal hillocks in a spiral growth pattern. Examination of the crystal structure of l-cystine suggested several potential inhibitors of crystal growth. Among several that were tested, the most effective were l-cystine dimethyl ester (L-CDME) and l-cystine methylester (L-CME). These molecules serve as structural mimics of l-cystine in which one carboxylate group is replaced by a methylester group (L-CME), or in the symmetrical form, both carboxylates are replaced by methylester groups (L-CDME). Using these inhibitors resulted in roughening of the otherwise highly linear growing step edges and rounding of the hillock corners seen by AFM (25) (Figure 1). The step velocity decreased with increasing L-CDME concentration, becoming negligible above 30 mg/l. The inhibitor effect was reversible, with the rate of growth returning to the original value once the aqueous solution containing L-CDME was replaced with one containing only l-cystine. L-CDME was significantly more efficacious in inhibiting crystal growth than L-CME. Importantly, for consideration of whether L-CDME could be useful in people with cystinuria, the concentrations at which L-CDME was effective at a concentration of only 2 mg/l. Because l-cystine stone formers generally have urinary l-cystine concentrations ranging from 1 to 4 mm, comparable with the concentrations used for the AFM studies. Therefore, L-CDME concentrations near 2 mg/l ( 0.01 mm), at which inhibition of l-cystine growth was highly effective, may be adequate for therapeutic effect. The advantage of these inhibitors over the thiols in use today is that at the low concentrations at which they seem effective, they may have a better profile of adverse effects and be better tolerated. They may also be more effective. As structural mimics of l-cystine, they interfere with crystallization by providing a steric inhibitory effect rather
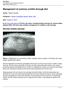
4 2096 Clinical Journal of the American Society of Nephrology Figure 1. (A and B) Real-time in situ AFM images of an L-cystine crystal, acquired 12 minutes apart. A pair of hexagonal hillocks generated by two closely spaced dislocations serve as landmarks. (C and D) AFM images of a single dislocation center of L-cystine (C) and D-cystine (D) crystal during growth. (E and F) AFM images of a hexagonal growth hillock on the face of L-cystine before (E) and after (F) addition of L-CDME (5 mg/l; 0.02 mm), revealing roughening of the steps as a result of step pinning. Images were acquired in aqueous solutions containing 2 mm L-cystine. AFM, atomic force microscopy. Reprinted, from reference 25, with permission. than the chemical reaction of disulfide exchange offered by tiopronin and d-penicillamine. However, the use of L-CDME is not without potential risk. Interestingly, incubation of LLC-PK1 cells, a model of proximal tubular epithelium, with L-CDME leads to lysosomal accumulation of cystine (27). The cells have impaired solute transport, oxygen utilization and substrate utilization (28 30). This loading with cystine serves as a model for cystinosis, an autosomal recessive disorder of lysosomal cystine accumulation as a result of abnormal cystine transport. Cystinosis is characterized by the Fanconi syndrome and frequently the development of kidney failure. The use of L-CDME as a treatment of cystinuria would then depend on its efficacy at dosages low enough to lead to inhibitory urine concentrations while not causing lysosomal accumulation and mimicking cystinosis. It may therefore be desirable to use AFM to find other possible inhibitors of cystine crystal growth to avoid this possible adverse effect. It is of course also possible that other molecules could be shown to be more effective than L-CDME. The further development and testing of L-CDME and its congeners is being undertaken by Dr. Amrik Sahota. Cystinuria has been replicated in three mouse models in which the mouse genes Slc3a1 and Slc7a9 are mutated, leading to a reasonable facsimile of the human disorder (31 33). In collaboration with Dr. Ward, Dr. Sahota and his co-workers are administering L-CDME to cystinuric mice and using micro-computed tomography to assess efficacy. Densitometric analysis of x-ray images has been successfully used to assess quantitatively stone growth in response to treatment of cystinuric mice with d-penicillamine (32). If L-CDME is effective and safe in knockout mice, then the eventual goal would be to study the drug or its congeners in humans with cystinuria. Ensuring that the dosages used to inhibit urinary stone formation are not associated with lysosomal accumulation of cystine as in cystinosis will be an important part of the safety monitoring. Acknowledgments The study of febuxostat described is funded by Takeda. Pat MacDonald, RN, of Takeda has been particularly supportive and enthusiastic in going forth with this project. Dr. Michael Ward s atomic force microscopy studies were supported primarily by National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) grant R01-DK068551, the NYU Molecular Design Institute, and the Advanced Photon Source, ChemMatCARS Sector 15, which is principally supported by the National Science Foundation/U.S. Department of Energy (CHE ). The Rare Kidney Stone Consortium is funded by NIDDK and Office of Rare Disease Research via the Rare Disease Clinical Research Network, grant 1U54DK I appreciate the thoughtful suggestions of Dr. Amrik Sahota. Disclosures Dr. Goldfarb is a consultant for Takeda. Takeda was not involved with the concept or writing of the manuscript and did not approve its contents.
5 Clin J Am Soc Nephrol 6: , August, 2011 New Pharmacologic Therapies for Nephrolithiasis, Goldfarb 2097 References 1. Moe OW, Pearle MS, Sakhaee K: Pharmacotherapy of urolithiasis: Evidence from clinical trials. Kidney Int 79: , Ettinger B: Hyperuricosuric calcium stone disease and mixed stones. In: Kidney Stones: Medical and Surgical Management, edited by Coe FL, Favus MJ, Pak CY, Parks JH, Preminger GM, Philadelphia, Lippincott-Raven, 1996, pp Ryall RL, Grover PK, Marshall VR: Urate and calcium stones: Picking up a drop of mercury with one s fingers? Am J Kidney Dis 17: , Grover PK, Marshall VR, Ryall RL: Dissolved urate salts out calcium oxalate in undiluted human urine in vitro: Implications for calcium oxalate stone genesis. Chem Biol 10: , Curhan GC, Taylor EN: 24-h uric acid excretion and the risk of kidney stones. Kidney Int 73: , Ettinger B, Tang A, Citron JT, Livermore B, Williams T: Randomized trial of allopurinol in the prevention of calcium oxalate calculi. N Engl J Med 315: , Ettinger B: Does hyperuricosuria play a role in calcium oxalate lithiasis? J Urol 141: , Guthikonda S, Sinkey C, Barenz T, Haynes WG: Xanthine oxidase inhibition reverses endothelial dysfunction in heavy smokers. Circulation 107: , Fellstrom B, Backman U, Danielson BG, Holmgren K, Johansson G, Lindsjo M, Ljunghall S, Wikstrom B: Allopurinol treatment of renal calcium stone disease. Br J Urol 57: , Arellano F, Sacristan JA: Allopurinol hypersensitivity syndrome: A review. Ann Pharmacother 27: , Becker MA, Schumacher HR Jr, Wortmann RL, MacDonald PA, Eustace D, Palo WA, Streit J, Joseph-Ridge N: Febuxostat compared with allopurinol in patients with hyperuricemia and gout. N Engl J Med 353: , Schumacher HR Jr, Becker MA, Wortmann RL, MacDonald PA, Hunt B, Streit J, Lademacher C, Joseph-Ridge N: Effects of febuxostat versus allopurinol and placebo in reducing serum urate in subjects with hyperuricemia and gout: A 28- week, phase III, randomized, double-blind, parallel-group trial. Arthritis Rheum 59: , Jansen TL, Richette P, Perez-Ruiz F, Tausche AK, Guerne PA, Punzi L, Leeb B, Barskova V, Uhlig T, Pimentao J, Zimmermann-Gorska I, Pascual E, Bardin T, Doherty M: International position paper on febuxostat. Clin Rheumatol 29: , Mayer MD, Khosravan R, Vernillet L, Wu JT, Joseph-Ridge N, Mulford DJ: Pharmacokinetics and pharmacodynamics of febuxostat, a new non-purine selective inhibitor of xanthine oxidase in subjects with renal impairment. Am J Ther 12: 22 34, Hoshide S, Takahashi Y, Ishikawa T, Kubo J, Tsuchimoto M, Komoriya K, Ohno I, Hosoya T: PK/PD and safety of a single dose of TMX-67 (febuxostat) in subjects with mild and moderate renal impairment. Nucleosides Nucleotides Nucleic Acids 23: , Huen SC, Goldfarb DS: Adverse metabolic side effects of thiazides: Implications for patients with calcium nephrolithiasis. J Urol 177: , Keenan RT, Pillinger MH: Hyperuricemia, gout, and cardiovascular disease: An important muddle. Bull NYU Hosp Jt Dis 67: , Chillaron J, Font-Llitjos M, Fort J, Zorzano A, Goldfarb DS, Nunes V, Palacin M: Pathophysiology and treatment of cystinuria. Nat Rev Nephrol 6: , Mattoo A, Goldfarb DS: Cystinuria. Semin Nephrol 28: , Rodriguez LM, Santos F, Malaga S, Martinez V: Effect of a low sodium diet on urinary elimination of cystine in cystinuric children. Nephron 71: , Goldfarb DS, Coe FL, Asplin JR: Urinary cystine excretion and capacity in patients with cystinuria. Kidney Int 69: , Rodman JS, Blackburn P, Williams JJ, Brown A, Pospischil MA, Peterson CM: The effect of dietary protein on cystine excretion in patients with cystinuria. Clin Nephrol 22: , Pak CY, Fuller C, Sakhaee K, Zerwekh JE, Adams BV: Management of cystine nephrolithiasis with alpha-mercaptopropionylglycine. J Urol 136: , Munday R: Toxicity of thiols and disulphides: Involvement of free-radical species. Free Radic Biol Med 7: , Rimer JD, An Z, Zhu Z, Lee MH, Goldfarb DS, Wesson JA, Ward MD: Crystal growth inhibitors for the prevention of L- cystine kidney stones through molecular design. Science 330: , Hillier AC, Ward MD: Atomic force microscopy of the electrochemical nucleation and growth of molecular crystals. Science 263: , Moran A, Ben-Nun A, Potashnik R, Bashan N: Renal cells in culture as a model for cystinosis. J Basic Clin Physiol Pharmacol 1: , Foreman JW, Benson L: Effect of cystine loading and cystine dimethylester on renal brushborder membrane transport. Biosci Rep 10: , Foreman JW, Benson LL: Effect of cystine loading on substrate oxidation by rat renal tubules. Pediatr Nephrol 4: , Foreman JW, Bowring MA, Lee J, States B, Segal S: Effect of cystine dimethylester on renal solute handling and isolated renal tubule transport in the rat: A new model of the Fanconi syndrome. Metabolism 36: , Ercolani M, Sahota A, Schuler C, Yang M, Evan AP, Reimer D, Barone JG, Tischfield JA, Levin RM: Bladder outlet obstruction in male cystinuria mice. Int Urol Nephrol 42: 57 63, Font-Llitjos M, Feliubadalo L, Espino M, Cleries R, Manas S, Frey IM, Puertas S, Colell G, Palomo S, Aranda J, Visa J, Palacin M, Nunes V: Slc7a9 knockout mouse is a good cystinuria model for antilithiasic pharmacological studies. Am J Physiol Renal Physiol 293: F732 F740, Peters T, Thaete C, Wolf S, Popp A, Sedlmeier R, Grosse J, Nehls MC, Russ A, Schlueter V: A mouse model for cystinuria type I. Hum Mol Genet 12: , 2003 Published online ahead of print. Publication date available at
24-h uric acid excretion and the risk of kidney stones
 http://www.kidney-international.org & 2008 International Society of Nephrology original article 24-h uric acid excretion and the risk of kidney stones GC Curhan 1,2,3 and EN Taylor 1,2 1 Department of
http://www.kidney-international.org & 2008 International Society of Nephrology original article 24-h uric acid excretion and the risk of kidney stones GC Curhan 1,2,3 and EN Taylor 1,2 1 Department of
Randomized Controlled Trial of Febuxostat Versus Allopurinol or Placebo in Individuals with Higher Urinary Uric Acid Excretion and Calcium Stones
 CJASN epress. Published on August 8, 2013 as doi: 10.2215/CJN.01760213 Article Randomized Controlled Trial of Febuxostat Versus Allopurinol or Placebo in Individuals with Higher Urinary Uric Acid Excretion
CJASN epress. Published on August 8, 2013 as doi: 10.2215/CJN.01760213 Article Randomized Controlled Trial of Febuxostat Versus Allopurinol or Placebo in Individuals with Higher Urinary Uric Acid Excretion
NEPHROLITHIASIS Etiology, stone composition, medical management, and prevention
 NEPHROLITHIASIS Etiology, stone composition, medical management, and prevention Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Epidemiology Prevalence 2-3%, maybe in
NEPHROLITHIASIS Etiology, stone composition, medical management, and prevention Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Epidemiology Prevalence 2-3%, maybe in
Medical Approach to Nephrolithiasis. Seth Goldberg, MD September 15, 2017 ACP Meeting
 Medical Approach to Nephrolithiasis Seth Goldberg, MD September 15, 2017 ACP Meeting DISCLOSURES Seth Goldberg, MD Assistant Professor of Medicine Research support Abbott Kadmon Otsuka Pfizer Introduction
Medical Approach to Nephrolithiasis Seth Goldberg, MD September 15, 2017 ACP Meeting DISCLOSURES Seth Goldberg, MD Assistant Professor of Medicine Research support Abbott Kadmon Otsuka Pfizer Introduction
The Nuts and Bolts of Kidney Stones. Soha Zouwail Consultant Chemical Pathology UHW Renal Training Day 2019
 The Nuts and Bolts of Kidney Stones Soha Zouwail Consultant Chemical Pathology UHW Renal Training Day 2019 Urinary Calculi Prevalence and incidence of kidney stones increasing across the world Environmental
The Nuts and Bolts of Kidney Stones Soha Zouwail Consultant Chemical Pathology UHW Renal Training Day 2019 Urinary Calculi Prevalence and incidence of kidney stones increasing across the world Environmental
Uloric Step Therapy Program
 Uloric Step Therapy Program Policy Number: 5.01.584 Last Review: 7/2017 Origination: 7/2014 Next Review: 7/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for brand
Uloric Step Therapy Program Policy Number: 5.01.584 Last Review: 7/2017 Origination: 7/2014 Next Review: 7/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for brand
Metabolic Stone Work-Up For Stone Prevention. Dr. Hazem Elmansy, MD, MSC, FRCSC Assistant Professor, NOSM, Urology Department
 Metabolic Stone Work-Up For Stone Prevention Dr. Hazem Elmansy, MD, MSC, FRCSC Assistant Professor, NOSM, Urology Department Faculty/Presenter Disclosure Slide Faculty: Hazem Elmansy Relationships with
Metabolic Stone Work-Up For Stone Prevention Dr. Hazem Elmansy, MD, MSC, FRCSC Assistant Professor, NOSM, Urology Department Faculty/Presenter Disclosure Slide Faculty: Hazem Elmansy Relationships with
School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR
 1 School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR URINARY (RENAL) STONE FORMATION An Overview What are Urinary (Renal)
1 School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR URINARY (RENAL) STONE FORMATION An Overview What are Urinary (Renal)
COMPARATIVE EVALUATION OF EFFICACY AND SAFETY PROFILE OF FEBUXOSTAT WITH ALLOPURINOL IN PATIENTS WITH HYPERURICEMIA AND GOUT
 Int. J. Pharm. Med. & Bio. Sc. 2013 P K Agarwal and Bijay Kumar, 2013 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 2, No. 4, October 2013 2013 IJPMBS. All Rights Reserved COMPARATIVE EVALUATION OF
Int. J. Pharm. Med. & Bio. Sc. 2013 P K Agarwal and Bijay Kumar, 2013 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 2, No. 4, October 2013 2013 IJPMBS. All Rights Reserved COMPARATIVE EVALUATION OF
Quaseem et coll. Ann Intern Med 2014
 Dietary and Pharmacologic Management to prevent Recurrent Nephrolithiasis in Adults A Clinical Practice Guideline From the American College of Physicians Introduction Approximately 80% of adults with kidney
Dietary and Pharmacologic Management to prevent Recurrent Nephrolithiasis in Adults A Clinical Practice Guideline From the American College of Physicians Introduction Approximately 80% of adults with kidney
Identification and qualitative Analysis. of Renal Calculi
 Identification and qualitative Analysis of Renal Calculi 1 -Renal Calculi: Kidney stones, renal calculi or renal lithiasis (stone formation) are small, hard deposits that form inside your kidneys. The
Identification and qualitative Analysis of Renal Calculi 1 -Renal Calculi: Kidney stones, renal calculi or renal lithiasis (stone formation) are small, hard deposits that form inside your kidneys. The
Urate Lowering Efficacy of Febuxostat Versus Allopurinol in Hyperuricemic Patients with Gout
 Philippine Journal of Internal Medicine Meta-Analysis Urate Lowering Efficacy of Febuxostat Versus Allopurinol in Hyperuricemic Patients with Gout Erika Bianca S. Villazor-Isidro, M.D.*; John Carlo G.
Philippine Journal of Internal Medicine Meta-Analysis Urate Lowering Efficacy of Febuxostat Versus Allopurinol in Hyperuricemic Patients with Gout Erika Bianca S. Villazor-Isidro, M.D.*; John Carlo G.
RISK FACTORS AND TREATMENT STRATEGIES FOR URINARY STONES Review of NASA s Evidence Reports on Human Health Risks
 Mayo Clinic O Brien Urology Research Center RISK FACTORS AND TREATMENT STRATEGIES FOR URINARY STONES 2017 Review of NASA s Evidence Reports on Human Health Risks John C Lieske, MD July 27, 2017 What types
Mayo Clinic O Brien Urology Research Center RISK FACTORS AND TREATMENT STRATEGIES FOR URINARY STONES 2017 Review of NASA s Evidence Reports on Human Health Risks John C Lieske, MD July 27, 2017 What types
MEDICAL STONE MANAGEMENT MADE EASY PRACTICAL ADVICE
 MEDICAL STONE MANAGEMENT MADE EASY PRACTICAL ADVICE Comprehensive Kidney Stone Center at Duke University Medical Center Durham, North Carolina Glenn M. Preminger, M.D. UCLA State-of-the Art Urology 02
MEDICAL STONE MANAGEMENT MADE EASY PRACTICAL ADVICE Comprehensive Kidney Stone Center at Duke University Medical Center Durham, North Carolina Glenn M. Preminger, M.D. UCLA State-of-the Art Urology 02
Journal of Advanced Scientific Research
 Bijoy Kumar Panda et al, J Adv Scient Res, 2012, 3(2): 03-11 3 Journal of Advanced Scientific Research Available online through http://www.sciensage.info/jasr ISSN 0976-9595 Review Article Febuxostat,
Bijoy Kumar Panda et al, J Adv Scient Res, 2012, 3(2): 03-11 3 Journal of Advanced Scientific Research Available online through http://www.sciensage.info/jasr ISSN 0976-9595 Review Article Febuxostat,
Management of common uroliths through diet
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Management of common uroliths through diet Author : Marge Chandler Categories : Canine, Companion animal, Feline, Vets Date
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Management of common uroliths through diet Author : Marge Chandler Categories : Canine, Companion animal, Feline, Vets Date
Febuxostat: a new treatment for hyperuricaemia in gout
 Rheumatology 2009;48:ii15 ii19 doi:10.1093/rheumatology/kep088 Febuxostat: a new treatment for hyperuricaemia in gout N. Lawrence Edwards 1 Febuxostat is a new non-purine xanthine oxidase inhibitor that
Rheumatology 2009;48:ii15 ii19 doi:10.1093/rheumatology/kep088 Febuxostat: a new treatment for hyperuricaemia in gout N. Lawrence Edwards 1 Febuxostat is a new non-purine xanthine oxidase inhibitor that
Clinical Biochemistry department/ College of medicine / AL-Mustansiriyah University
 Clinical Biochemistry department/ College of medicine / AL-Mustansiriyah University Dr. Ali al-bayati NUCLEOTIDE METABOLISM Lec. 3 The salvage pathway of purine synthesis Purines that result from the normal
Clinical Biochemistry department/ College of medicine / AL-Mustansiriyah University Dr. Ali al-bayati NUCLEOTIDE METABOLISM Lec. 3 The salvage pathway of purine synthesis Purines that result from the normal
2015 OPSC Annual Convention. syllabus. February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California
 2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California FRIDAY, FEBRUARY 6, 2015: 4:00pm - 5:00pm Stone Disease^ Presented by John Grimaldi, DO ^ California
2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California FRIDAY, FEBRUARY 6, 2015: 4:00pm - 5:00pm Stone Disease^ Presented by John Grimaldi, DO ^ California
Effective Health Care Program
 Comparative Effectiveness Review Number 61 Effective Health Care Program Recurrent Nephrolithiasis in Adults: Comparative Effectiveness of Preventive Medical Strategies Executive Summary Introduction Nephrolithiasis
Comparative Effectiveness Review Number 61 Effective Health Care Program Recurrent Nephrolithiasis in Adults: Comparative Effectiveness of Preventive Medical Strategies Executive Summary Introduction Nephrolithiasis
EQUILIBRIUM VERSUS SUPERSATURATED URINE HYPOTHESIS IN CALCIUM SALT UROLITHIASIS: A NEW THEORETICAL AND PRACTICAL APPROACH TO A CLINICAL PROBLEM
 Scanning Microscopy Vol. 13, No. 2-3, 1999 (Pages 261-265) 0891-7035/99$5.00+.25 Scanning Microscopy International, Chicago Equilibrium (AMF O Hare), model for IL calcium 60666 USA salt urolithiasis EQUILIBRIUM
Scanning Microscopy Vol. 13, No. 2-3, 1999 (Pages 261-265) 0891-7035/99$5.00+.25 Scanning Microscopy International, Chicago Equilibrium (AMF O Hare), model for IL calcium 60666 USA salt urolithiasis EQUILIBRIUM
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics
 This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
Diet and fluid prescription in stone disease
 http://www.kidney-international.org & 2006 International Society of Nephrology mini review Diet and fluid prescription in stone disease EN Taylor 1 and GC Curhan 1,2 1 Renal Division, Department of Medicine,
http://www.kidney-international.org & 2006 International Society of Nephrology mini review Diet and fluid prescription in stone disease EN Taylor 1 and GC Curhan 1,2 1 Renal Division, Department of Medicine,
Urinary Calculus Disease. Urinary Stones: Simplified Metabolic Evaluation. Urinary Calculus Disease. Urinary Calculus Disease 2/8/2008
 Urinary Stones: Simplified Metabolic Evaluation Marshall L. Stoller, M.D. Professor and Vice Chairman Department of Urology University of California San Francisco Incidence: 7-21/10,000 3 men: 1 woman
Urinary Stones: Simplified Metabolic Evaluation Marshall L. Stoller, M.D. Professor and Vice Chairman Department of Urology University of California San Francisco Incidence: 7-21/10,000 3 men: 1 woman
University Journal of Pre and Para Clinical Sciences
 ISSN 2455 2879 Volume 3 Issue 1 2017 To evaluate the uric acid lowering efficacy of Febuxostat in patients with chronic renal failure stage III SHANKARESWARI SHANMUGARAJ Department of Pharmacology, MADURAI
ISSN 2455 2879 Volume 3 Issue 1 2017 To evaluate the uric acid lowering efficacy of Febuxostat in patients with chronic renal failure stage III SHANKARESWARI SHANMUGARAJ Department of Pharmacology, MADURAI
Part I: On-line web-based survey of Dalmatian owners GENERAL INFORMATION
 Dr. Bartges' final report on the Dal stone survey: Commissioned by the Dalmatian Club of America Foundation (DCAF) Published in the DCA magazine, The Spotter, Summer 2006 Part I: On-line web-based survey
Dr. Bartges' final report on the Dal stone survey: Commissioned by the Dalmatian Club of America Foundation (DCAF) Published in the DCA magazine, The Spotter, Summer 2006 Part I: On-line web-based survey
Pharmacological Treatment of Endocrinopathies
 Pharmacological Treatment of Endocrinopathies Progress in Basic and Clinical Pharmacology Vol. 5 Series Editors P. Lomax, Los Angeles, Calif. E.S. Vesell, Hershey, Pa. KARGER Basel München Paris. London
Pharmacological Treatment of Endocrinopathies Progress in Basic and Clinical Pharmacology Vol. 5 Series Editors P. Lomax, Los Angeles, Calif. E.S. Vesell, Hershey, Pa. KARGER Basel München Paris. London
Febuxostat: a safe and effective therapy for hyperuricemia and gout
 DRUG EVALUATIO Febuxostat: a safe and effective therapy for hyperuricemia and gout atasha Jordan & Geraldine M McCarthy Author for correspondence Mater Misericordiae University Hospital, Eccles St. Dublin
DRUG EVALUATIO Febuxostat: a safe and effective therapy for hyperuricemia and gout atasha Jordan & Geraldine M McCarthy Author for correspondence Mater Misericordiae University Hospital, Eccles St. Dublin
Case presentation. serum uric acid = 11.5 mg/dl 24-hour uric acid excretion = 300 mg
 GOUT 55 y/o male 12 hours pain in my big toe & ankle went to bed last night feeling fine felt as if had broken toe this morning similar problems in right ankle & left wrist Case presentation lab studies
GOUT 55 y/o male 12 hours pain in my big toe & ankle went to bed last night feeling fine felt as if had broken toe this morning similar problems in right ankle & left wrist Case presentation lab studies
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Renal Tubular Acidosis
 1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
Drugs Used to Treat Gout. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Drugs Used to Treat Gout Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Gout is a metabolic disease characterized by recurrent episodes of acute arthritis
Drugs Used to Treat Gout Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Gout is a metabolic disease characterized by recurrent episodes of acute arthritis
ORIGINAL ARTICLE INTRODUCTION
 Arthritis & Rheumatism (Arthritis Care & Research) Vol. 59, No. 11, November 15, 2008, pp 1540 1548 DOI 10.1002/art.24209 2008, American College of Rheumatology ORIGINAL ARTICLE Effects of Versus Allopurinol
Arthritis & Rheumatism (Arthritis Care & Research) Vol. 59, No. 11, November 15, 2008, pp 1540 1548 DOI 10.1002/art.24209 2008, American College of Rheumatology ORIGINAL ARTICLE Effects of Versus Allopurinol
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics
 This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
Prevention of recurrent calcium stones in adults
 Official reprint from UpToDate www.uptodate.com Print Back Prevention of recurrent calcium stones in adults Author Gary C Curhan, MD, ScD Section Editor Stanley Goldfarb, MD Deputy Editor Theodore W Post,
Official reprint from UpToDate www.uptodate.com Print Back Prevention of recurrent calcium stones in adults Author Gary C Curhan, MD, ScD Section Editor Stanley Goldfarb, MD Deputy Editor Theodore W Post,
Uric acid and CKD. Sunil Badve Conjoint Associate Professor, UNSW Staff Specialist, St George
 Uric acid and CKD Sunil Badve Conjoint Associate Professor, UNSW Staff Specialist, St George Hospital @Badves Case Mr J, 52 Male, referred in June 2015 DM type 2 (4 years), HTN, diabetic retinopathy, diabetic
Uric acid and CKD Sunil Badve Conjoint Associate Professor, UNSW Staff Specialist, St George Hospital @Badves Case Mr J, 52 Male, referred in June 2015 DM type 2 (4 years), HTN, diabetic retinopathy, diabetic
THIOLA (tiopronin) oral tablet
 THIOLA (tiopronin) oral tablet Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
THIOLA (tiopronin) oral tablet Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
Kidney Stone Update. Epidemiology of Kidney Stones. Lifetime Risk of Kidney Stone
 Kidney Stone Update Michael Emmett MD Baylor University Medical Center Dallas, Texas Epidemiology of Kidney Stones Incidence About 0.3% Prevalence 10% Men 12% Women 8% Hospitalization Peak Age Stone Composition
Kidney Stone Update Michael Emmett MD Baylor University Medical Center Dallas, Texas Epidemiology of Kidney Stones Incidence About 0.3% Prevalence 10% Men 12% Women 8% Hospitalization Peak Age Stone Composition
HHS Public Access Author manuscript Hepatology. Author manuscript; available in PMC 2017 March 01.
 Febuxostat-Induced Acute Liver Injury Matt Bohm, DO, Raj Vuppalanchi, MD, Naga Chalasani, MD, and Drug Induced Liver Injury Network (DILIN) Department of Medicine, Indiana University School of Medicine,
Febuxostat-Induced Acute Liver Injury Matt Bohm, DO, Raj Vuppalanchi, MD, Naga Chalasani, MD, and Drug Induced Liver Injury Network (DILIN) Department of Medicine, Indiana University School of Medicine,
Gout 2.0. Scott Vogelgesang, M.D. Division of Immunology: Rheumatology & Allergy
 Gout 2.0 Scott Vogelgesang, M.D. Division of Immunology: Rheumatology & Allergy Case 48 year old man presents with swollen, painful left toe that started overnight. Didn t hurt when he went to bed. No
Gout 2.0 Scott Vogelgesang, M.D. Division of Immunology: Rheumatology & Allergy Case 48 year old man presents with swollen, painful left toe that started overnight. Didn t hurt when he went to bed. No
Diet for Kidney Stone Prevention
 Diet for Kidney Stone Prevention National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH How does diet affect the risk
Diet for Kidney Stone Prevention National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH How does diet affect the risk
Study of Febuxostat for the Management of Hyperuricemia in Gout
 Human Journals Review Article October 2015 Vol.:4, Issue:3 All rights are reserved by Sachin S. Shinde et al. Study of Febuxostat for the Management of Hyperuricemia in Gout Keywords: Febuxostat, Hyperuricemia,
Human Journals Review Article October 2015 Vol.:4, Issue:3 All rights are reserved by Sachin S. Shinde et al. Study of Febuxostat for the Management of Hyperuricemia in Gout Keywords: Febuxostat, Hyperuricemia,
Correspondence between stone composition and urine supersaturation in nephrolithiasis
 Kidney International, Vol. 51 (1997), pp. 894 900 Correspondence between stone composition and urine supersaturation in nephrolithiasis JOAN H. PARKS, MARK COWARD, and REDRIC L. COE Program in Nephrology,
Kidney International, Vol. 51 (1997), pp. 894 900 Correspondence between stone composition and urine supersaturation in nephrolithiasis JOAN H. PARKS, MARK COWARD, and REDRIC L. COE Program in Nephrology,
Evaluation of the Recurrent Stone Former
 Urol Clin N Am 34 (2007) 315 322 Evaluation of the Recurrent Stone Former Paramjit S. Chandhoke, MD, PhD* Department of Urology, Northwest Permanente, Portland, OR, USA At one time, metabolic kidney stone
Urol Clin N Am 34 (2007) 315 322 Evaluation of the Recurrent Stone Former Paramjit S. Chandhoke, MD, PhD* Department of Urology, Northwest Permanente, Portland, OR, USA At one time, metabolic kidney stone
Gout: Update in therapeutics
 Summary Gout: Update in therapeutics 29/11/14 Caroline van Durme CHU de Liège Maastricht University Medical Centre+ Why treating gout? Guidelines: ACR 12 Drugs: Colchicine Allopurinol: what about the kidney?
Summary Gout: Update in therapeutics 29/11/14 Caroline van Durme CHU de Liège Maastricht University Medical Centre+ Why treating gout? Guidelines: ACR 12 Drugs: Colchicine Allopurinol: what about the kidney?
Urologic Stone Disease. Urologic Stone Disease. Urologic Stone Disease. Urologic Stone Disease. Urologic Stone Disease 5/7/2010
 Diagnosis and Treatment Stephen E. Strup MD William Farish Professor and Chief of Urology Director of Minimally Invasive Urologic Surgery University of Kentucky I will not cut, even for the stone, but
Diagnosis and Treatment Stephen E. Strup MD William Farish Professor and Chief of Urology Director of Minimally Invasive Urologic Surgery University of Kentucky I will not cut, even for the stone, but
Kidney Stone Clinic Dr. Raymond Ko MB BS (Hons 1) FRACS (Urology) General Information about Kidney Stones
 Why do kidney stones form? General Information about Kidney Stones Kidney stones form from minerals and salts in the urine that clump together when the urine becomes highly concentrated. Normally these
Why do kidney stones form? General Information about Kidney Stones Kidney stones form from minerals and salts in the urine that clump together when the urine becomes highly concentrated. Normally these
uric acid Non electrolytes of the plasma
 73 uric acid Non electrolytes of the plasma 1 Purines and uric acid Fig 2 JFI Uric acid is the major product of catabolism of the purine nucleosides adenosine and guanosine, Uric acid is sparingly soluble
73 uric acid Non electrolytes of the plasma 1 Purines and uric acid Fig 2 JFI Uric acid is the major product of catabolism of the purine nucleosides adenosine and guanosine, Uric acid is sparingly soluble
AUA Guidelines. Medical Management of Kidney Stones: AUA Guideline
 AUA Guidelines Medical Management of Kidney Stones: AUA Guideline Margaret S. Pearle, David S. Goldfarb, Dean G. Assimos, Gary Curhan, Cynthia J. Denu-Ciocca, Brian R. Matlaga, Manoj Monga, Kristina L.
AUA Guidelines Medical Management of Kidney Stones: AUA Guideline Margaret S. Pearle, David S. Goldfarb, Dean G. Assimos, Gary Curhan, Cynthia J. Denu-Ciocca, Brian R. Matlaga, Manoj Monga, Kristina L.
Calcium Nephrolithiasis and Bone Health. Noah S. Schenkman, MD
 Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Oxalate (urine, plasma)
 Oxalate (urine, plasma) 1 Name and description of analyte 1.1 Name of analyte Oxalate 1.2 Alternative names 1.3 NLMC code To follow 1.4. Function of analyte Oxalate is a metabolic end product primarily
Oxalate (urine, plasma) 1 Name and description of analyte 1.1 Name of analyte Oxalate 1.2 Alternative names 1.3 NLMC code To follow 1.4. Function of analyte Oxalate is a metabolic end product primarily
Essence of the Revised Guideline for the Management of Hyperuricemia and Gout
 Research and Reviews Essence of the Revised Guideline for the Management of Hyperuricemia and Gout JMAJ 55(4): 324 329, 2012 Hisashi YAMANAKA,* 1 The Guideline Revising Committee of Japanese Society of
Research and Reviews Essence of the Revised Guideline for the Management of Hyperuricemia and Gout JMAJ 55(4): 324 329, 2012 Hisashi YAMANAKA,* 1 The Guideline Revising Committee of Japanese Society of
The CARI Guidelines Caring for Australasians with Renal Impairment. Uric acid GUIDELINES. No recommendations possible based on Level I or II evidence.
 Date written: July 2004 Final submission: July 2004 Author: David Johnson Uric acid GUIDELINES No recommendations possible based on Level I or II evidence. SUGGESTIONS FOR CLINICAL CARE (Suggestions are
Date written: July 2004 Final submission: July 2004 Author: David Johnson Uric acid GUIDELINES No recommendations possible based on Level I or II evidence. SUGGESTIONS FOR CLINICAL CARE (Suggestions are
A Rare Cause of Renal Stone Formation in Two Siblings. Chris Stockdale
 A Rare Cause of Renal Stone Formation in Two Siblings Chris Stockdale Index case-patient A Born 2000 Parents (first cousins) from Indian sub-continent Paternal Grandmother received dialysis for ESRF Possible
A Rare Cause of Renal Stone Formation in Two Siblings Chris Stockdale Index case-patient A Born 2000 Parents (first cousins) from Indian sub-continent Paternal Grandmother received dialysis for ESRF Possible
Dependence of upper limit of metastability on supersaturation in
 Kidney International, Vol. 52 (1997), pp. 162 168 CLINICAL NEPHROLOGY_- EPIDEMIOLOGY - CLINICAL TRIALS Dependence of upper limit of metastability on supersaturation in nephrolithiasis JOHN R. ASPLIN, JOAN
Kidney International, Vol. 52 (1997), pp. 162 168 CLINICAL NEPHROLOGY_- EPIDEMIOLOGY - CLINICAL TRIALS Dependence of upper limit of metastability on supersaturation in nephrolithiasis JOHN R. ASPLIN, JOAN
Dietary and medical management of recurrent nephrolithiasis
 REVIEW EDUCATIONAL OBJECTIVE: Readers will apply interventions to reduce the risk of recurrent nephrolithiasis SILVI SHAH, MD Department of Nephrology, University of Alabama at Birmingham JUAN CAMILO CALLE,
REVIEW EDUCATIONAL OBJECTIVE: Readers will apply interventions to reduce the risk of recurrent nephrolithiasis SILVI SHAH, MD Department of Nephrology, University of Alabama at Birmingham JUAN CAMILO CALLE,
URINARY CRYSTALS. by Geoffrey K. Dube and Robert S. Brown
 URINARY CRYSTALS by Geoffrey K. Dube and Robert S. Brown A 26 year-old man presents with a fever and weakness. His WBC is 133,000, with 83% blasts. Creatinine is 2.0 mg/dl and serum uric acid is 15.4 mg/dl.
URINARY CRYSTALS by Geoffrey K. Dube and Robert S. Brown A 26 year-old man presents with a fever and weakness. His WBC is 133,000, with 83% blasts. Creatinine is 2.0 mg/dl and serum uric acid is 15.4 mg/dl.
Tumor Lysis Syndrome Nephrology Grand Rounds Tuesday, July 27 th, 2010 Aditya Mattoo
 Tumor Lysis Syndrome Nephrology Grand Rounds Tuesday, July 27 th, 2010 Aditya Mattoo Outline Background/Definition Epidemiology/Risk Stratification Pathophysiology Treatment Renal Replacement Therapy Background/Definition
Tumor Lysis Syndrome Nephrology Grand Rounds Tuesday, July 27 th, 2010 Aditya Mattoo Outline Background/Definition Epidemiology/Risk Stratification Pathophysiology Treatment Renal Replacement Therapy Background/Definition
Approach to the Patient with Nephrolithiasis; The Stone Quiz. Farahnak Assadi* 1, MD
 Education Article Iran J Ped Sep 2007; Vol 17 (No 3), Pp:283-292 Approach to the Patient with Nephrolithiasis; The Stone Quiz Farahnak Assadi* 1, MD 1. Pediatric Nephrologist, Rush University Medical Center,
Education Article Iran J Ped Sep 2007; Vol 17 (No 3), Pp:283-292 Approach to the Patient with Nephrolithiasis; The Stone Quiz Farahnak Assadi* 1, MD 1. Pediatric Nephrologist, Rush University Medical Center,
Metabolism of Nucleotides
 Metabolism of Nucleotides Outline Nucleotide degradation Components of Nucleobases Purine and pyrimidine biosynthesis Hyperuricemia Sources Nucleotide degradation The nucleotides are among the most complex
Metabolism of Nucleotides Outline Nucleotide degradation Components of Nucleobases Purine and pyrimidine biosynthesis Hyperuricemia Sources Nucleotide degradation The nucleotides are among the most complex
Family History and Age at the Onset of Upper Urinary Tract Calculi
 Endourology and Stone Disease Family History and Age at the Onset of Upper Urinary Tract Calculi Yadollah Ahmadi Asr Badr, Samad Hazhir, Kamaleddin Hasanzadeh Introduction: The aim of this study was to
Endourology and Stone Disease Family History and Age at the Onset of Upper Urinary Tract Calculi Yadollah Ahmadi Asr Badr, Samad Hazhir, Kamaleddin Hasanzadeh Introduction: The aim of this study was to
Reviews in Clinical Medicine
 Mashhad University of Medical Sciences (MUMS) Reviews in Clinical Medicine Clinical Research Development Center Ghaem Hospital Evaluation of the effects of magnesium supplement in primary and secondary
Mashhad University of Medical Sciences (MUMS) Reviews in Clinical Medicine Clinical Research Development Center Ghaem Hospital Evaluation of the effects of magnesium supplement in primary and secondary
Urine Stone Screen requirements
 Urine Stone Screen requirements Unique Identifying Index Number LP/PA/CB/CBSP030 Version number 4 Issue Date (this version) 03.08.15 Document Type Accreditation or Licensing Standard to which this applies
Urine Stone Screen requirements Unique Identifying Index Number LP/PA/CB/CBSP030 Version number 4 Issue Date (this version) 03.08.15 Document Type Accreditation or Licensing Standard to which this applies
Alterations of Renal and Urinary Tract Function
 Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Secondary Gout Associated with Myeloproliferative Diseases* imt. Sinai Hospital
 Chapter VI Secondary Gout Associated with Myeloproliferative Diseases* By TS'AI-FAN Yu, M.D. imt. Sinai Hospital In a variety of disorders of hemopoiesis, the turnover of nucleic acids is greatly augmented,
Chapter VI Secondary Gout Associated with Myeloproliferative Diseases* By TS'AI-FAN Yu, M.D. imt. Sinai Hospital In a variety of disorders of hemopoiesis, the turnover of nucleic acids is greatly augmented,
The Urate-lowering Efficacy and Safety of Febuxostat in Korean Patients with Gout
 Journal of Rheumatic Diseases Vol. 2, No. 4, August 213 http://dx.doi.org/1.478/jrd.213.2.4.223 Original Article The Urate-lowering Efficacy and Safety of in Korean Patients with Gout Sung Hwan Park 1,
Journal of Rheumatic Diseases Vol. 2, No. 4, August 213 http://dx.doi.org/1.478/jrd.213.2.4.223 Original Article The Urate-lowering Efficacy and Safety of in Korean Patients with Gout Sung Hwan Park 1,
Limitations of Use: (1) Duzallo is not recommended for the treatment of asymptomatic hyperuricemia.
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.63 Subject: Duzallo Page: 1 of 5 Last Review Date: December 8, 2017 Duzallo Description Duzallo (lesinurad
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.63 Subject: Duzallo Page: 1 of 5 Last Review Date: December 8, 2017 Duzallo Description Duzallo (lesinurad
Urolithiasis. Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery
 Urolithiasis Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery Urolithiasis: Why should we care? Affects 5% of US men and women Men twice as
Urolithiasis Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery Urolithiasis: Why should we care? Affects 5% of US men and women Men twice as
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Renal Pharmacology. Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics BIMM118
 Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
Febuxostat now subsidised on Special Authority
 Gout update: Febuxostat now subsidised on Special Authority 38 Febuxostat was added to the New Zealand Pharmaceutical Schedule on 1 June, 2014. It is now available as a third-line preventive treatment
Gout update: Febuxostat now subsidised on Special Authority 38 Febuxostat was added to the New Zealand Pharmaceutical Schedule on 1 June, 2014. It is now available as a third-line preventive treatment
Recurrent stone formers-metabolic evaluation: a must investigation
 International Surgery Journal Bhangu GS et al. Int Surg J. 2017 Jan;4(1):86-90 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163972
International Surgery Journal Bhangu GS et al. Int Surg J. 2017 Jan;4(1):86-90 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163972
Guideline of guidelines: kidney stones
 Justin B. Ziemba and Brian R. Matlaga* Division of Urology, Department of Surgery, Perelman School of Medicine at the University of Pennsylvania, Philadelphia, PA, and *James Buchanan Brady Urological
Justin B. Ziemba and Brian R. Matlaga* Division of Urology, Department of Surgery, Perelman School of Medicine at the University of Pennsylvania, Philadelphia, PA, and *James Buchanan Brady Urological
Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari
![Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari](/thumbs/90/104323364.jpg) Pharmacology I [PHL 313] Diuretics Dr. Mohammad Nazam Ansari Renal Pharmacology Kidneys: Each adult kidney weighs 125-170g in males and 115-155g in females, represent 0.5% of total body weight, but receive
Pharmacology I [PHL 313] Diuretics Dr. Mohammad Nazam Ansari Renal Pharmacology Kidneys: Each adult kidney weighs 125-170g in males and 115-155g in females, represent 0.5% of total body weight, but receive
Dr. Mehmet Kanbay Department of Medicine Division of Nephrology Istanbul Medeniyet University School of Medicine Istanbul, Turkey.
 The uric acid dilemma: causal risk factor for hypertension and CKD or mere bystander? Mehmet Kanbay, Istanbul, Turkey Chairs: Anton H. van den Meiracker, Rotterdam, The Netherlands Claudia R.C. Van Roeyen,
The uric acid dilemma: causal risk factor for hypertension and CKD or mere bystander? Mehmet Kanbay, Istanbul, Turkey Chairs: Anton H. van den Meiracker, Rotterdam, The Netherlands Claudia R.C. Van Roeyen,
Inborn errors of metabolism presenting with kidney stones: clinical aspects. Francesco Emma
 Inborn errors of metabolism presenting with kidney stones: clinical aspects Francesco Emma Division of Nephrology and Dialysis Bambino Gesù Children s Hospital, IRCCS Rome, Italy September 6, 2016 Palazzo
Inborn errors of metabolism presenting with kidney stones: clinical aspects Francesco Emma Division of Nephrology and Dialysis Bambino Gesù Children s Hospital, IRCCS Rome, Italy September 6, 2016 Palazzo
Alkaline citrate reduces stone recurrence and regrowth after shockwave lithotripsy and percutaneous nephrolithotomy
 Clinical Urology Alkaline citrate and stone recurrence International Braz J Urol Vol. 37 (5): 611-616, September - October, 2011 Alkaline citrate reduces stone recurrence and regrowth after shockwave lithotripsy
Clinical Urology Alkaline citrate and stone recurrence International Braz J Urol Vol. 37 (5): 611-616, September - October, 2011 Alkaline citrate reduces stone recurrence and regrowth after shockwave lithotripsy
PRINCIPLES OF DIURETIC ACTIONS:
 DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
Krystexxa. Krystexxa (pegloticase) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.14 Subject: Krystexxa Page: 1 of 5 Last Review Date: March 16, 2018 Krystexxa Description Krystexxa
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.14 Subject: Krystexxa Page: 1 of 5 Last Review Date: March 16, 2018 Krystexxa Description Krystexxa
Non-Protein Nitrogenous Compounds. Non-Protein Nitrogenous Compounds. NPN s. Urea (BUN) Creatinine NH 3. University of Cincinnati MLS Program 1
 Non-Protein Nitrogenous Compounds NPN s Urea (BUN) Creatinine NH 3 Uric Acid Ammonia University of Cincinnati MLS Program 1 Urea Metabolic product derived from catabolism of proteins Proteolysis of proteins
Non-Protein Nitrogenous Compounds NPN s Urea (BUN) Creatinine NH 3 Uric Acid Ammonia University of Cincinnati MLS Program 1 Urea Metabolic product derived from catabolism of proteins Proteolysis of proteins
Shlomi Albert, M.D., Inc Warner Avenue, Suite 423 Fountain Valley, Ca Tel (714) Fax (714) Kidney Stone Disease in Adults
 Shlomi Albert, M.D., Inc. 11160 Warner Avenue, Suite 423 Fountain Valley, Ca 92708 Tel (714)549-3333 Fax (714)549-3334 Kidney Stone Disease in Adults Overview Kidney stones are one of the most painful
Shlomi Albert, M.D., Inc. 11160 Warner Avenue, Suite 423 Fountain Valley, Ca 92708 Tel (714)549-3333 Fax (714)549-3334 Kidney Stone Disease in Adults Overview Kidney stones are one of the most painful
Investigating Potential Therapies to Decrease the Rate of Cystine Stone Growth in Slc3a1-/- Mice
 Dominican Scholar Graduate Master's Theses, Capstones, and Culminating Projects Student Scholarship 2015 Investigating Potential Therapies to Decrease the Rate of Cystine Stone Growth in Slc3a1-/- Mice
Dominican Scholar Graduate Master's Theses, Capstones, and Culminating Projects Student Scholarship 2015 Investigating Potential Therapies to Decrease the Rate of Cystine Stone Growth in Slc3a1-/- Mice
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 24 June 2009
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 24 June 2009 ADENURIC 80 mg, film-coated tablets B/28 (CIP code: 385 724-4) B/84 (CIP code: 572 820-3) ADENURIC 120
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 24 June 2009 ADENURIC 80 mg, film-coated tablets B/28 (CIP code: 385 724-4) B/84 (CIP code: 572 820-3) ADENURIC 120
GOUT disease spectrum including
 GOUT disease spectrum including *hyperuricemia, *recurrent attacks of acute arthritis associated with monosodium urate crystals in leukocytes found in synovial fluid, *deposits of monosodium urate crystals
GOUT disease spectrum including *hyperuricemia, *recurrent attacks of acute arthritis associated with monosodium urate crystals in leukocytes found in synovial fluid, *deposits of monosodium urate crystals
NIH Public Access Author Manuscript Expert Opin Pharmacother. Author manuscript; available in PMC 2013 September 13.
 NIH Public Access Author Manuscript Published in final edited form as: Expert Opin Pharmacother. 2013 March ; 14(4): 435 447. doi:10.1517/14656566.2013.775250. KIDNEY STONES: AN UPDATE ON CURRENT PHARMACOLOGICAL
NIH Public Access Author Manuscript Published in final edited form as: Expert Opin Pharmacother. 2013 March ; 14(4): 435 447. doi:10.1517/14656566.2013.775250. KIDNEY STONES: AN UPDATE ON CURRENT PHARMACOLOGICAL
Summary 255 Research Summary
 Chapter 10 Summary Nephrolithiasis remains a public health problem around the world, affecting 12% of the adult population. The prevalence and incidence of kidney stones are increasing with global warming,
Chapter 10 Summary Nephrolithiasis remains a public health problem around the world, affecting 12% of the adult population. The prevalence and incidence of kidney stones are increasing with global warming,
Excretory System. Biology 2201
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System. Excretory System
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
1. To review the diagnosis of gout and its differential. 2. To understand the four stages of gout
 Objectives 1. To review the diagnosis of gout and its differential GOUT 2. To understand the four stages of gout 3. To develop an approach for the acute treatment of gout Anthony Lim 9/13/12 Cycle 3 4.
Objectives 1. To review the diagnosis of gout and its differential GOUT 2. To understand the four stages of gout 3. To develop an approach for the acute treatment of gout Anthony Lim 9/13/12 Cycle 3 4.
Association of serum biochemical metabolic panel with stone composition
 bs_bs_banner International Journal of Urology (2015) 22, 195 199 doi: 10.1111/iju.12632 Original Article: Clinical Investigation Association of serum biochemical metabolic panel with stone composition
bs_bs_banner International Journal of Urology (2015) 22, 195 199 doi: 10.1111/iju.12632 Original Article: Clinical Investigation Association of serum biochemical metabolic panel with stone composition
For the past century, treatment for urolithiasis in
 ACVIM Consensus Statement J Vet Intern Med 2016;30:1564 1574 Consensus Statements of the American College of Veterinary Internal Medicine (ACVIM) provide the veterinary community with up-to-date information
ACVIM Consensus Statement J Vet Intern Med 2016;30:1564 1574 Consensus Statements of the American College of Veterinary Internal Medicine (ACVIM) provide the veterinary community with up-to-date information
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
COMPOSITION. A film coated tablet contains. Active ingredient: irbesartan 75 mg, 150 mg or 300 mg. Rotazar (Film coated tablets) Irbesartan
 Rotazar (Film coated tablets) Irbesartan Rotazar 75 mg, 150 mg, 300 mg COMPOSITION A film coated tablet contains Active ingredient: irbesartan 75 mg, 150 mg or 300 mg. Rotazar 75 mg, 150 mg, 300 mg PHARMACOLOGICAL
Rotazar (Film coated tablets) Irbesartan Rotazar 75 mg, 150 mg, 300 mg COMPOSITION A film coated tablet contains Active ingredient: irbesartan 75 mg, 150 mg or 300 mg. Rotazar 75 mg, 150 mg, 300 mg PHARMACOLOGICAL
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Pathogenesis and clinical course of mixed calcium oxalate and uric acid nephrolithiasis
 Kidney International, Vol. 22 (1982), pp. 366 3 70 Pathogenesis and clinical course of mixed calcium oxalate and uric acid nephrolithiasis STEPHANIE MILLMAN, AMY L. STRAUSS, JOAN H. PARKS, AND FREDRIC
Kidney International, Vol. 22 (1982), pp. 366 3 70 Pathogenesis and clinical course of mixed calcium oxalate and uric acid nephrolithiasis STEPHANIE MILLMAN, AMY L. STRAUSS, JOAN H. PARKS, AND FREDRIC
The 82 nd UWI/BAMP CME Conference November 18, Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist
 The 82 nd UWI/BAMP CME Conference November 18, 2017 Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist Disclosures Outline Index case Introduction Etiology Risk factors Acute stone event Conservative
The 82 nd UWI/BAMP CME Conference November 18, 2017 Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist Disclosures Outline Index case Introduction Etiology Risk factors Acute stone event Conservative
UC San Francisco UC San Francisco Previously Published Works
 UC San Francisco UC San Francisco Previously Published Works Title Effect of Diet Orange soda on urinary lithogenicity Permalink https://escholarship.org/uc/item/27x8w1h4 Journal Urological Research, 40(3)
UC San Francisco UC San Francisco Previously Published Works Title Effect of Diet Orange soda on urinary lithogenicity Permalink https://escholarship.org/uc/item/27x8w1h4 Journal Urological Research, 40(3)
