Lumacaftor Ivacaftor in Patients with Cystic Fibrosis Homozygous for Phe508del CFTR
|
|
|
- Morris Berry
- 6 years ago
- Views:
Transcription
1 The new england journal of medicine Original Article Lumacaftor Ivacaftor in Patients with Cystic Fibrosis Homozygous for Phe508del CFTR C.E. Wainwright, J.S. Elborn, B.W. Ramsey, G. Marigowda, X. Huang, M. Cipolli, C. Colombo, J.C. Davies, K. De Boeck, P.A. Flume, M.W. Konstan, S.A. McColley, K. McCoy, E.F. McKone, A. Munck, F. Ratjen, S.M. Rowe, D. Waltz, and M.P. Boyle, for the TRAFFIC and TRANSPORT Study Groups* ABSTRACT The authors full names, academic degrees, and affiliations are listed in the Appendix. Address reprint requests to Dr. Wainwright at the Department of Respiratory and Sleep Medicine, Lady Cilento Children s Hospital, 501 Stanley St., South Brisbane, QLD 4101, Australia, or at claire. wainwright@ health. qld. gov. au. * A complete list of the investigators in the TRAFFIC and TRANSPORT studies is provided in the Supplementary Appendix, available at NEJM.org. Drs. Wainwright, Elborn, Ramsey, and Boyle contributed equally to this article. This article was published on May 17, 2015, and updated on February 4, 2016, at NEJM.org. N Engl J Med 2015;373: DOI: /NEJMoa Copyright 2015 Massachusetts Medical Society. BACKGROUND Cystic fibrosis is a life-limiting disease that is caused by defective or deficient cystic fibrosis transmembrane conductance regulator (CFTR) protein activity. Phe508del is the most common CFTR mutation. METHODS We conducted two phase 3, randomized, double-blind, placebo-controlled studies that were designed to assess the effects of lumacaftor (VX-809), a CFTR corrector, in combination with ivacaftor (VX-770), a CFTR potentiator, in patients 12 years of age or older who had cystic fibrosis and were homozygous for the Phe508del CFTR mutation. In both studies, patients were randomly assigned to receive either lumacaftor (600 mg once daily or 400 mg every 12 hours) in combination with ivacaftor (250 mg every 12 hours) or matched placebo for 24 weeks. The primary end point was the absolute change from baseline in the percentage of predicted forced expiratory volume in 1 second (FEV 1 ) at week 24. RESULTS A total of 1108 patients underwent randomization and received study drug. The mean baseline FEV 1 was 61% of the predicted value. In both studies, there were significant improvements in the primary end point in both lumacaftor ivacaftor dose groups; the difference between active treatment and placebo with respect to the mean absolute improvement in the percentage of predicted FEV 1 ranged from 2.6 to 4.0 percentage points (P<0.001), which corresponded to a mean relative treatment difference of 4.3 to 6.7% (P<0.001). Pooled analyses showed that the rate of pulmonary exacerbations was 30 to 39% lower in the lumacaftor ivacaftor groups than in the placebo group; the rate of events leading to hospitalization or the use of intravenous antibiotics was lower in the lumacaftor ivacaftor groups as well. The incidence of adverse events was generally similar in the lumacaftor ivacaftor and placebo groups. The rate of discontinuation due to an adverse event was 4.2% among patients who received lumacaftor ivacaftor versus 1.6% among those who received placebo. CONCLUSIONS These data show that lumacaftor in combination with ivacaftor provided a benefit for patients with cystic fibrosis homozygous for the Phe508del CFTR mutation. (Funded by Vertex Pharmaceuticals and others; TRAFFIC and TRANSPORT ClinicalTrials.gov numbers, NCT and NCT ) 220 n engl j med 373;3 nejm.org July 16, 2015
2 Lumacaftor with Ivacaftor for Cystic Fibrosis Cystic fibrosis is a genetic disease that is associated with high rates of premature death. 1-4 It is a multisystem disease that is characterized by pancreatic insufficiency and chronic airway infections associated with loss of lung function, repeated pulmonary exacerbations, and, ultimately, respiratory failure. 5 Cystic fibrosis is caused by gene mutations that result in deficient or dysfunctional cystic fibrosis transmembrane conductance regulator (CFTR) protein, an anion channel that is normally present in the epithelial membrane. Phe508del (c.1521_1523delctt; formerly F508del) is the most common CFTR mutation; approximately 45% of patients with cystic fibrosis are homozygous for this allele. 1 Cystic fibrosis is a progressive disease; despite advances in therapies designed to address the symptoms of the disease, the median predicted survival among patients who are homozygous for Phe508del in the United States is 37 years. 6 The Phe508del CFTR mutation causes a processing defect that severely reduces protein levels at the epithelial membrane; for the few channels that reach the cell surface, the mutation also disrupts channel opening; together, these effects lead to minimal CFTR chloride transport activity One approach to treating cystic fibrosis is to address the underlying cause of the disease by targeting the CFTR protein dysfunction. Restoring chloride transport to p.phe508del CFTR (formerly F508del CFTR) is therefore thought to require at least two steps: correction of cellular misprocessing to increase the amount of functional mutated CFTR and potentiation to further increase channel opening. Lumacaftor is an investigational CFTR corrector that has been shown in vitro to correct p.phe508del CFTR misprocessing and increase the amount of cell surface localized protein. 11 Ivacaftor is an approved CFTR potentiator that increases the open probability of CFTR channels (i.e., the fraction of time that the channels are open) in vitro and improves clinical outcomes in patients 6 years of age or older who have cystic fibrosis and at least one copy of most class III (gating) mutations In vitro studies have shown that ivacaftor also potentiates surface-localized p.phe508del CFTR, 18 and the combination of lumacaftor with ivacaftor has been associated with a greater increase in chloride transport than has either agent alone. 11 Although neither ivacaftor nor lumacaftor monotherapy has been shown to have meaningful clinical efficacy in patients who are homozygous for the Phe508del CFTR mutation, 19,20 a phase 2 study suggested that the combination of lumacaftor and ivacaftor increased CFTR activity to a degree that may be sufficient to improve clinical outcomes in these patients. 21 Therefore, two phase 3 trials (TRAFFIC and TRANSPORT) were conducted to evaluate the efficacy and safety of two different doses of lumacaftor in combination with ivacaftor in patients with cystic fibrosis who were homozygous for the Phe508del CFTR mutation. Methods Study Design and Oversight The TRAFFIC and TRANSPORT trials were two phase 3, multinational, randomized, doubleblind, placebo-controlled, parallel-group studies in which lumacaftor (VX-809, Vertex Pharmaceuticals) was orally administered in combination with ivacaftor (VX-770, Vertex Pharmaceuticals) for 24 weeks; the studies were conducted from April 2013 through April The study design and methods of data analysis were identical for the two studies, with the exception of the inclusion of ambulatory electrocardiography (TRAFFIC only) and adolescent pharmacokinetic assessments (TRANSPORT only) for a subgroup of patients. The studies were designed to evaluate the efficacy of lumacaftor ivacaftor in patients with cystic fibrosis who were homozygous for the Phe508del CFTR mutation; the evaluation of safety was a secondary objective. The protocols (available with the full text of this article at NEJM.org) were reviewed and approved by an ethics committee at each of the 187 participating centers; all patients provided written informed consent. Patients were randomly assigned (in a 1:1:1 ratio) to one of three study groups (Fig. S1 in the Supplementary Appendix, available at NEJM.org): 600 mg of lumacaftor once daily in combination with 250 mg of ivacaftor every 12 hours (LUM [600 mg/day] IVA), 400 mg of lumacaftor every 12 hours in combination with 250 mg of ivacaftor every 12 hours (LUM [400 mg every 12 hr] IVA), or lumacaftor-matched placebo every 12 hours in combination with ivacaftor-matched placebo every 12 hours. All regimens were given for 24 weeks. Randomization was stratified according to age (<18 years vs. 18 years), sex, and pulmonary function (percentage of predicted forced expiratory volume in 1 second [FEV 1 ] at screening, <70 vs. 70). n engl j med 373;3 nejm.org July 16,
3 The new england journal of medicine The sponsor of the studies (Vertex Pharmaceuticals) designed the protocol in collaboration with the authors. Site investigators collected the data, which were analyzed by the sponsor. All the authors had full access to the study data after the study periods were complete and the data were unblinded. The authors vouch for the accuracy and completeness of the data and for the fidelity of this report to the study protocols, which are available at NEJM.org. Study Participants Eligibility criteria included a confirmed diagnosis of cystic fibrosis, homozygosity for the Phe- 508del CFTR mutation, an age of 12 years or older, a percentage of predicted FEV 1 at the time of screening that was 40 to 90% of the predicted normal values, 22,23 and stable cystic fibrosis disease. Between the screening and baseline visits ( 4 weeks), fluctuation in FEV 1 occurred in some cases and was documented; 81 patients had an FEV 1 that fell to below 40% of the predicted value at baseline. Patients continued to take their prestudy medications. Study Assessments All assessments were prespecified in the study protocols and statistical analysis plans unless otherwise noted. The primary end point was the absolute change from baseline at week 24 in the percentage of predicted FEV 1, calculated by averaging the mean absolute change at week 16 and the mean absolute change at week 24; this approach was used because we anticipated that it would reduce variability, as compared with using the point estimate at week 24 alone. Key secondary end points included the relative change from baseline in the percentage of predicted FEV 1 (calculated by averaging the mean values for weeks 16 and 24), the absolute change from baseline at week 24 in body-mass index (BMI), the absolute change from baseline at week 24 in the patient-reported Cystic Fibrosis Questionnaire Revised (CFQ-R) respiratory domain score (scores range from 0 to 100, with higher scores indicating a higher patient-reported quality of life with regard to respiratory status), 24 the percentage of patients with a relative increase from baseline of 5% or higher in the percentage of predicted FEV 1 (calculated by averaging the mean values for weeks 16 and 24), and the number of pulmonary exacerbations through week 24. The time to the first pulmonary exacerbation was assessed, as was the absolute change in body weight. The safety of the study regimens was also evaluated. Subgroup analyses and additional assessments of exacerbation, including assessments of the numbers of patients requiring hospitalization and those requiring treatment with intravenous antibiotics, were also performed. Statistical Analyses All patients who underwent randomization and received at least one dose of study drug were included in the efficacy analysis, in which patients were analyzed as part of the study group to which they were randomly assigned (full analysis set). In the primary analysis, we evaluated the treatment difference in the percentage of predicted FEV 1 at week 24, which was assessed as the difference between the treatment groups and the placebo group in the primary end point. The safety set included all patients who received any amount of study drug; data were analyzed according to the patients actual study group (regardless of the group to which they had been randomly assigned). The reported adverse events are those that either developed or increased in severity at or after the time patients received the initial dose of study drug, up to 28 days after receipt of the last dose. Additional details regarding the statistical analysis, including the hierarchical testing procedure for the multiple end points and the criteria for the assessment of statistical significance, are provided in the Supplementary Appendix. Results Participants Of the 1122 patients who underwent randomization (559 in the TRAFFIC study and 563 in the TRANSPORT study), 1108 received at least one dose of study drug or placebo (Fig. S2 in the Supplementary Appendix). The baseline demographic and other characteristics were well balanced across study groups (Table 1, and Table S1 in the Supplementary Appendix). The mean baseline FEV 1 was 61% of the predicted value. At baseline, a high percentage of patients reported maintenance use of multiple pulmonary, nutritional, and other cystic fibrosis therapies. The majority of patients completed their assigned study regimens: 348 patients in the LUM ( n engl j med 373;3 nejm.org July 16, 2015
4 Lumacaftor with Ivacaftor for Cystic Fibrosis Table 1. Baseline Characteristics and Demographic Data.* Characteristic (N = 371) LUM (600 mg/day) IVA (N = 368) (N = 369) Female sex no. (%) 181 (48.8) 182 (49.5) 182 (49.3) Mean age (range) yr 25.4 (12 64) 24.5 (12 54) 25.3 (12 57) Age group no. (%) 12 to <18 yr 96 (25.9) 96 (26.1) 98 (26.6) 18 yr 275 (74.1) 272 (73.9) 271 (73.4) Percentage of predicted FEV 1 at baseline Mean (range) 60.4 ( ) 60.8 ( ) 60.5 ( ) Subgroup no. (%) <40 28 (7.5) 24 (6.5) 29 (7.9) 40 to < (64.2) 241 (65.5) 233 (63.1) 70 to (26.1) 98 (26.6) 100 (27.1) >90 3 (0.8) 3 (0.8) 3 (0.8) Mean BMI (range) 21.0 ( ) 21.0 ( ) 21.5 ( ) Maintenance use of pulmonary or respiratory cystic fibrosis therapy at baseline no. (%) Bronchodilators 342 (92.2) 342 (92.9) 344 (93.2) Dornase alfa 281 (75.7) 289 (78.5) 273 (74.0) Inhaled antibiotics 258 (69.5) 232 (63.0) 225 (61.0) Azithromycin 233 (62.8) 233 (63.3) 215 (58.3) Inhaled hypertonic saline 220 (59.3) 197 (53.5) 227 (61.5) Inhaled glucocorticoids 220 (59.3) 213 (57.9) 212 (57.5) * The LUM (600 mg/day) IVA group received 600 mg of lumacaftor (LUM) once daily in combination with 250 mg of ivacaftor (IVA) every 12 hours; the group received 400 mg of lumacaftor every 12 hours in combination with 250 mg of ivacaftor every 12 hours. FEV 1 denotes forced expiratory volume in 1 second. The body-mass index (BMI) is the weight in kilograms divided by the square of the height in meters. mg/day) IVA group (94.6%), 344 patients in the group (93.2%), and 362 patients in the placebo group (97.6%). Clinical Efficacy In both studies, FEV 1 improvements were observed as early as day 15 and were sustained through 24 weeks in both lumacaftor ivacaftor dose groups (Fig. 1A, and Fig. S3 and S4 in the Supplementary Appendix). The difference between lumacaftor ivacaftor and placebo with respect to the mean absolute change in the percentage of predicted FEV 1 from baseline at week 24 was significant in all dose groups and ranged from 2.6 to 4.0 percentage points (P<0.001 for all comparisons) (Table 2). The difference between lumacaftor ivacaftor and placebo with respect to the mean relative change in FEV 1 was also significant and ranged from 4.3 to 6.7% (P<0.001 for all groups) (Table 2). In each study, the percentage of patients who had a relative improvement in the percentage of predicted FEV 1 of 5% or higher was greater in the lumacaftor ivacaftor groups than in the placebo group (P<0.001 to P = for the odds ratio) but was not significant in the testing hierarchy (Table 2, and Table S2 in the Supplementary Appendix). In the pooled analysis, approximately twice as many patients in the lumacaftor ivacaftor groups as in the placebo group had a relative improvement in the percentage of predicted FEV 1 of 5% or higher (39 to 46% vs. 22%) and 10% or higher (24 to 27% vs. 13%) (Table 2, and Table S2 and Fig. S5 in the Supplementary Appendix). The mean absolute change in the percentage of predicted FEV 1 was also assessed in a variety of subgroups (e.g., subgroups defined according to various baseline characteristics and concomitant n engl j med 373;3 nejm.org July 16,
5 The new england journal of medicine A Change from Baseline in Percentage of Predicted FEV 1 6 LUM (600 mg/day) IVA Absolute Change in Percentage of Predicted FEV 1 (percentage points) Baseline Day 15 Wk 4 Wk 8 Visit B Subgroup Analysis of the Change from Baseline in Percentage of Predicted FEV 1 LUM (600 mg/day) IVA Difference in Absolute Change from Baseline Subgroup No. of Patients (percentage points) Overall Age 12 to <18 yr 18 yr Percentage of predicted FEV 1 at screening <70% 70% Percentage of predicted FEV 1 at baseline <40% 40% Sex Male Female Pseudomonas aeruginosa infection status Positive Negative Better Wk 16 Wk Treatment Better medications); the improvement in the percentage of predicted FEV 1 in the lumacaftor ivacaftor groups versus the placebo group was consistent Figure 1. Absolute Changes from Baseline in the Percentage of Predicted Forced Expiratory Volume in 1 Second (FEV 1 ) According to Study Group. The LUM (600 mg/day) IVA group received 600 mg of lumacaftor (LUM) once daily in combination with 250 mg of ivacaftor (IVA) every 12 hours; the group received 400 mg of lumacaftor every 12 hours in combination with 250 mg of ivacaftor every 12 hours. Panel A shows the mean absolute change in the percentage of predicted FEV 1 over time in each study group; the difference between each active-treatment group and the placebo group at each time point was significant (P<0.025). Panel B shows subgroup analyses of the differences between the active treatment and placebo in the absolute change from baseline in the percentage of predicted FEV 1 at week 24. Data in both panels are least-squares means; I bars indicate 95% confidence intervals. The results represent pooled data from the TRAFFIC and TRANSPORT studies. across all subgroups (Fig. 1B, and Fig. S6 in the Supplementary Appendix). Additional details are provided in the Supplementary Appendix. Clinically meaningful reductions in the rates of protocol-defined pulmonary exacerbations were seen in both lumacaftor ivacaftor dose groups. The rate ratio (lumacaftor ivacaftor vs. placebo) ranged from 0.57 to 0.72 (P<0.001 to P = 0.05; none of the rate ratios were considered significant in the testing hierarchy) (Table 2, and Table S2 in the Supplementary Appendix). In the pooled analysis, the rate of exacerbations was significantly lower in both lumacaftor ivacaftor dose groups than in the placebo group: 30% lower in the LUM (600 mg/day) IVA group and 39% lower in the every 12 hr) IVA group (P = and P<0.001, respectively) (Table 2, and Table S2 in the Supplementary Appendix). Through week 24, the proportion of patients who remained free from exacerbations in the pooled analysis was significantly higher in both lumacaftor ivacaftor groups than in the placebo group, and the risk of having an exacerbation was significantly lower in the lumacaftor ivacaftor groups (Fig. 2A and Table 2). Additional analyses revealed significant reductions with lumacaftor ivacaftor therapy in the number of exacerbations leading to hospitalizations and those necessitating the administration of intravenous antibiotics (Fig. 2B). Over the course of the 24-week period, the mean BMI (the weight in kilograms divided by the square of the height in meters) increased steadily in both lumacaftor ivacaftor dose groups (Fig. S7 in the Supplementary Appendix). 224 n engl j med 373;3 nejm.org July 16, 2015
6 Lumacaftor with Ivacaftor for Cystic Fibrosis In the analysis of the individual trials, the difference between lumacaftor ivacaftor and placebo with respect to the absolute change in BMI was significant for both dose groups in the TRANS- PORT study but for neither dose group in the TRAFFIC study (Table 2). In the pooled analysis at week 24, the treatment difference versus placebo with respect to the absolute change in BMI was 0.24 to 0.28 (P<0.001) (Table 2, and Table S2 and Fig. S7 in the Supplementary Appendix); this represents an improvement of approximately 1% with lumacaftor ivacaftor. Across the lumacaftor ivacaftor dose groups in TRAFFIC and TRANSPORT, the least-squares mean change from baseline in body weight at week 24 ranged from 1.23 to 1.57 kg. The CFQ-R is a cystic fibrosis specific instrument that is designed to evaluate patient-reported assessments of various health-related measures. In both lumacaftor ivacaftor dose groups, there were improvements in the within-group CFQ-R respiratory domain score; the treatment difference versus placebo was nominally significant (on the basis of the testing hierarchy) in the analysis of the individual trials only for the LUM (600 mg/day) IVA group in the TRAFFIC study; the treatment difference reached significance in the LUM (600 mg/day) IVA group in the pooled analysis (Table 2, and Fig. S8 in the Supplementary Appendix). Safety Overall, the proportion of patients reporting adverse events was similar across the lumacaftor ivacaftor groups and the placebo group (Table 3). Pooled across the studies, serious adverse events were reported in 28.6% of the patients in the placebo group and in 17.3 to 22.8% of the patients in the lumacaftor ivacaftor groups. In all the groups, infective pulmonary exacerbation was the most common serious adverse event (occurring in 24.1% of the patients in the placebo group and in 13.0% of those in the pooled lumacaftor ivacaftor groups). The proportion of patients who discontinued the study regimen because of an adverse event was higher in the lumacaftor ivacaftor groups than in the placebo group (4.2% [31 of 738 patients] vs. 1.6% [6 of 370 patients]). Among the patients receiving lumacaftor ivacaftor, the adverse events that led to discontinuation of the study regimen in two or more patients were elevation of the creatine kinase level (4 patients), hemoptysis (3), bronchospasm (2), dyspnea (2), pulmonary exacerbation (2), and rash (2). No deaths were reported. The adverse events reported more frequently in the lumacaftor ivacaftor groups were generally respiratory in nature. The majority were of mild-to-moderate severity and included dyspnea and chest tightness (Table 3, and Table S3 in the Supplementary Appendix). Two patients in the placebo group (one with dyspnea and one with chest discomfort) and four patients in the LUM (600 mg/day) IVA group (two with dyspnea and two with bronchospasm) had adverse events of respiratory symptoms or reactive airways that were severe. In patients who had respiratorysymptom adverse events within 1 to 2 days after the initiation of therapy and who did not discontinue the study regimen, the events generally resolved within the first 2 to 3 weeks of therapy. Beyond the first week of therapy, the incidence of respiratory events was similar in the lumacaftor ivacaftor and placebo groups. In addition, the pattern of adverse events according to the severity of lung disease at baseline was generally similar across the groups. Elevations in levels of alanine or aspartate aminotransferase to more than 3 times the upper limit of the normal range were observed in 5.1% of the patients in the placebo group and in 5.2% of those in the lumacaftor ivacaftor groups (Table S4 in the Supplementary Appendix). Serious adverse events related to abnormal liver function were not observed in the placebo group and were reported for seven patients in the lumacaftor ivacaftor groups. After discontinuation or interruption of lumacaftor ivacaftor therapy, liver function in all patients improved substantially, and results of liver-function tests returned to baseline in the case of six patients. Details regarding these events, including concomitant elevations in bilirubin, are provided in the Supplementary Appendix. Discussion Significant improvements in the percentage of predicted FEV 1 were seen in all four lumacaftor ivacaftor treatment groups in the TRAFFIC and TRANSPORT studies. In both dose groups in each study, improvements in FEV 1 were seen by day 15 and were sustained throughout the 24- week study period. Lumacaftor ivacaftor combination therapy n engl j med 373;3 nejm.org July 16,
7 The new england journal of medicine Table 2. Efficacy Results at Week 24.* Result TRAFFIC TRANSPORT Pooled (N = 184) LUM (600 mg/ day) IVA (N = 183) (N = 182) (N = 187) LUM (600 mg/ day) IVA (N = 185) (N = 187) (N = 371) LUM (600 mg/ day) IVA (N = 368) (N = 369) Change in percentage of predicted FEV 1 from baseline Difference vs. placebo in the absolute change percentage points Mean (95% CI) 4.0 (2.6 to 5.4) 2.6 (1.2 to 4.0) 2.6 (1.2 to 4.1) 3.0 (1.6 to 4.4) 3.3 (2.3 to 4.3) 2.8 (1.8 to 3.8) P value <0.001 <0.001 <0.001 <0.001 <0.001 <0.001 Difference vs. placebo in the relative change % Mean (95% CI) 6.7 (4.3 to 9.2) 4.3 (1.9 to 6.8) 4.4 (1.9 to 7.0) 5.3 (2.7 to 7.8) 5.6 (3.8 to 7.3) 4.8 (3.0 to 6.6) P value <0.001 <0.001 <0.001 <0.001 <0.001 <0.001 Difference vs. placebo in absolute change from baseline in BMI Mean (95% CI) 0.16 ( 0.04 to 0.35) 0.13 ( 0.07 to 0.32) 0.41 (0.23 to 0.59) 0.36 (0.17 to 0.54) 0.28 (0.15 to 0.41) 0.24 (0.11 to 0.37) P value <0.001 <0.001 <0.001 <0.001 Difference vs. placebo in absolute change from baseline in CFQ-R respiratory domain Mean (95% CI) points 3.9 (0.7 to 7.1) 1.5 ( 1.7 to 4.7) 2.2 ( 0.9 to 5.3) 2.9 ( 0.3 to 6.0) 3.1 (0.8 to 5.3) P value Odds ratio for a relative increase of 5% from baseline in the percentage of predicted FEV1 Odds ratio (95% CI) 2.9 (1.9 to 4.6) 2.1 (1.3 to 3.3) 3.0 (1.9 to 4.6) 2.4 (1.5 to 3.7) 2.9 (2.1 to 4.0) 2.2 (0.0 to 4.5) 2.2 (1.6 to 3.1) P value < <0.001 <0.001 <0.001 <0.001 Pulmonary exacerbations Events no. (rate per 48 wk) 112 (1.07) 79 (0.77) 73 (0.71) 139 (1.18) 94 (0.82) 79 (0.67) 251 (1.14) 173 (0.80) 152 (0.70) 226 n engl j med 373;3 nejm.org July 16, 2015
8 Lumacaftor with Ivacaftor for Cystic Fibrosis Result TRAFFIC TRANSPORT Pooled (N = 369) LUM (600 mg/ day) IVA (N = 368) (N = 371) (N = 187) LUM (600 mg/ day) IVA (N = 185) (N = 187) (N = 182) LUM (600 mg/ day) IVA (N = 183) (N = 184) 0.61 (0.49 to 0.76) 0.70 (0.56 to 0.87) 0.57 (0.42 to 0.76) 0.69 (0.52 to 0.92) 0.66 (0.47 to 0.93) Rate ratio (95% CI) 0.72 (0.52 to 1.00) P value for the rate ratio < <0.001 * Reported means are least-squares means. For individual studies, within each active-treatment group and between the active-treatment groups and the placebo group, a hierarchical testing procedure was performed to control for multiplicity across primary and key secondary end points; P in the current test and all previous tests was required to claim significance in the hierarchy. CFQ-R denotes Cystic Fibrosis Questionnaire Revised. Changes in the percentage of predicted FEV 1 are calculated by averaging the means at weeks 16 and 24. The difference versus placebo was significant. The number of pulmonary exacerbations was reported through week 24 and is expressed as a rate per patient over 48 weeks. resulted in improvements in multiple clinical end points, and the findings were generally consistent across dose groups and studies. Clinically important reductions in the rate of pulmonary exacerbations were also observed in association with lumacaftor ivacaftor therapy. Through 24 weeks, the lumacaftor ivacaftor groups had reductions in the rate of pulmonary exacerbations, with decreases in the numbers of events leading to hospitalization or intravenous antibiotic treatment. FEV 1 and rates of pulmonary exacerbations are strong predictors of survival and thus remain important for the evaluation of new therapies for cystic fibrosis. 25 Significant improvements (i.e., increases) in BMI were observed in the TRANSPORT study and in the pooled analyses but not in the TRAF- FIC study. Across both studies, BMI continued to increase during the study period in both lumacaftor ivacaftor groups. Although the mechanisms for improvement in the nutritional status of patients with cystic fibrosis are not fully defined, the gains are hypothesized to reflect either better caloric absorption, possibly due to normalized intestinal ph, 17 or a reduction in energy expenditure resulting from amelioration of lung disease. 17,26 Numerical increases in the CFQ-R respiratory domain score favoring active treatment were seen in both dose groups in both studies; however, in the pooled analysis of that score, the treatment difference was significant only in the LUM (600 mg/day) IVA group and did not meet the requirement for a minimum clinically important difference (4 points). 24 It is challenging to interpret these results, given the significant improvements in FEV 1. The CFQ-R instrument is valuable for assessing patient-reported outcomes; however, there is precedent for a lack of correlation with FEV 1. Studies of tobramycin showed no correlation between changes in CFQ-R and FEV It is also worth noting that the CFQ-R minimum clinically important difference was established as a within-group change in patients who had markers of advanced disease, which complicates its application to other populations. 24 The TRAFFIC and TRANSPORT study cohorts were a population with well-managed cystic fibrosis, as evidenced by the minimal FEV 1 deterioration in the placebo group and the high rates of the use of standard cystic fibrosis therapy. The magnitude of the change in FEV 1 was sig- n engl j med 373;3 nejm.org July 16,
9 The new england journal of medicine A Time to First Pulmonary Exacerbation 100 Patients without an Event (%) Baseline Day 15 B Pulmonary Exacerbations through Wk 24 Events Leading to Hospitalization 0.7 Event Rate per Patient over 48 Wk LUM (600 mg/day) IVA LUM (600 mg/day) IVA Week 39% P= % P<0.001 Events Leading to Intravenous Antibiotic Treatment LUM (600 mg/day) IVA 45% P< % P<0.001 Figure 2. Pulmonary Exacerbations. The time to first pulmonary exacerbation and number of pulmonary exacerbations leading to hospitalization or treatment with intravenous antibiotics are shown. In Panel B, the number of pulmonary exacerbations observed through week 24 is expressed as a rate per patient over 48 weeks. The results represent pooled data from the TRAFFIC and TRANSPORT studies. nificant and was in the range of the magnitudes of change seen in studies of other cystic fibrosis therapeutics The changes due to treatment in the percentage of predicted FEV 1 were largely consistent across studies, dose groups, and all subgroups analyzed, including subgroups defined according to age, baseline FEV 1 (<40 vs. 40), and status with respect to Pseudomonas aeruginosa infection. Improvements in FEV 1 and BMI and reductions in exacerbations were observed while patients continued to use their prescribed cystic fibrosis therapies; lumacaftor ivacaftor is therefore expected to provide a clinically meaningful benefit in addition to the standard of care. The determination of the potential for lumacaftor ivacaftor mediated CFTR modulation to modify the course of disease will require additional analyses and longer-term data. Although the improvements in FEV 1 associated with lumacaftor ivacaftor were significant and consistent with in vitro 11 and phase 2 sweat chloride and FEV 1 results, 21 the effect of lumacaftor ivacaftor on sweat chloride and FEV 1 was smaller than that observed in patients with the Gly551Asp mutation who were treated with ivacaftor monotherapy. 13,14 Whereas CFTR with the p.gly551asp mutation has a gating defect but is found at the cell surface, CFTR with the p.phe- 508del mutation has multiple defects, which makes addressing the underlying cause of disease in patients homozygous for this mutation more complex. The most important of these defects is a substantial reduction in processing and transport to the cell surface, plus a reduced stability and channel gating of the few surfacelocalized proteins. These multiple defects make restoring p.phe508del CFTR activity and subsequent observation of a clinical benefit more challenging than addressing the p.gly551asp gating defect. The smaller changes in sweat chloride and FEV 1 seen in association with lumacaftor ivacaftor therapy in patients homozygous for Phe508del, as compared with the changes seen in association with ivacaftor monotherapy in patients with Gly551Asp, was predicted in vitro and may be due in part to the fact that lumacaftor only partially rescues the p.phe508del CFTR processing defect, 11 which results in fewer p.phe508del CFTR channels at the cell surface than are seen with p.gly551asp CFTR. Two in vitro studies have suggested that treatment (for 48 hours) with potentiators, including ivacaftor, may reduce the stability and expression of corrected p.phe508del. 32,33 Although it is possible that ivacaftor affects the steady-state levels of corrected p.phe508del CFTR in vitro, the results of the TRAFFIC and TRANSPORT studies, which included more than 1100 patients, suggest that lumacaftor ivacaftor provides a clinical benefit that is greater than that previously observed with either agent alone. 20,21 Moreover, the clinical benefit was sustained for the entire duration of the studies. 228 n engl j med 373;3 nejm.org July 16, 2015
10 Lumacaftor with Ivacaftor for Cystic Fibrosis Table 3. Adverse Events Associated with the Study Regimens.* Event (N = 370) Nevertheless, the differences between the results of treatment with lumacaftor ivacaftor in patients with the Phe508del mutation and treatment with ivacaftor in patients with the Gly551Asp mutation point to the need for continued development of CFTR modulators that will further improve on the meaningful FEV 1 benefits observed in the TRAFFIC and TRANS- PORT studies. Lumacaftor ivacaftor therapy at both dosing regimens generally had an acceptable side-effect profile. The proportion of patients who discontinued the study regimen for reasons related to an adverse event was higher among those who received lumacaftor ivacaftor than among those who received placebo, and dyspnea and chest LUM (600 mg/day) IVA (N = 369) number of patients (percent) (N = 369) Any adverse event reported 355 (95.9) 356 (96.5) 351 (95.1) Discontinuation of the study regimen 6 (1.6) 14 (3.8) 17 (4.6) because of an adverse event At least one serious adverse event 106 (28.6) 84 (22.8) 64 (17.3) Most common adverse events Infective pulmonary exacerbation of 182 (49.2) 145 (39.3) 132 (35.8) cystic fibrosis Cough 148 (40.0) 121 (32.8) 104 (28.2) Headache 58 (15.7) 58 (15.7) 58 (15.7) Increase in sputum production 70 (18.9) 55 (14.9) 54 (14.6) Dyspnea 29 (7.8) 55 (14.9) 48 (13.0) Hemoptysis 50 (13.5) 52 (14.1) 50 (13.6) Diarrhea 31 (8.4) 36 (9.8) 45 (12.2) Nausea 28 (7.6) 29 (7.9) 46 (12.5) Abnormal respiration (chest tightness) 22 (5.9) 40 (10.8) 32 (8.7) Nasopharyngitis 40 (10.8) 23 (6.2) 48 (13.0) Oropharyngeal pain 30 (8.1) 44 (11.9) 24 (6.5) Upper respiratory tract infection 20 (5.4) 24 (6.5) 37 (10.0) Nasal congestion 44 (11.9) 33 (8.9) 24 (6.5) Serious adverse events occurring in at least 3 patients in any treatment group Infective pulmonary exacerbation of 89 (24.1) 55 (14.9) 41 (11.1) cystic fibrosis Hemoptysis 3 (0.8) 4 (1.1) 5 (1.4) Distal intestinal obstruction syndrome 5 (1.4) 2 (0.5) 2 (0.5) * The reported adverse events are those that either developed or increased in severity at or after the time patients received the initial dose of study drug (placebo or active agent), up to 28 days after receipt of the last dose. The most common adverse events were defined as those that occurred in at least 10% of patients in any treatment group. tightness were reported more frequently in the active-treatment groups. In a phase 2 study, treatment with lumacaftor monotherapy was associated with an initial increased risk of dyspnea or chest tightness, although these symptoms were uncommon after the addition of ivacaftor to lumacaftor. 21 Elevated levels of liver enzymes were observed in a similar number of patients in the active-treatment groups and the placebo group; however, serious adverse events related to elevation of liver enzymes were reported only in the active-treatment group. The TRAFFIC and TRANSPORT studies included the same two doses of lumacaftor so that we could ascertain whether there was a dose response for the CFTR corrector. Pooled across the two n engl j med 373;3 nejm.org July 16,
11 The new england journal of medicine studies, the dose regimens appeared to have similar efficacy and safety profiles, with no clear differentiation except with respect to pulmonary exacerbation related outcomes, which consistently favored the group. In conclusion, in the TRAFFIC and TRANSPORT studies, lumacaftor in combination with ivacaftor improved FEV 1 and reduced the rate of pulmonary exacerbations in patients with cystic fibrosis who were homozygous for the Phe508del CFTR mutation. Lumacaftor ivacaftor therapy generally had an acceptable side-effect profile, with more than 93% of patients completing the assigned therapy regimen. These data show that the combination of a CFTR corrector and potentiator, designed to address the underlying cause of cystic fibrosis by targeting CFTR, can benefit patients who are homozygous for the Phe508del CFTR mutation and represents a treatment milestone for the 45% of patients with cystic fibrosis who are homozygous for this mutation. Supported by Vertex Pharmaceuticals; a program grant from the Children s Hospital Foundation, Brisbane, Queensland, Australia (to Dr. Wainwright); the Northern Ireland Clinical Research Network (Respiratory Health) in Belfast Health and Social Care Trust (to Dr. Elborn); grants from the Institute of Translational Health Sciences, National Institutes of Health (NIH) (UL1TR000423) and the Cystic Fibrosis Translational Research Center, NIH (P30DK089507, both to Dr. Ramsey); the National Institute for Health Research Respiratory Biomedical Research Unit at the Royal Brompton and Harefield NHS Foundation Trust and Imperial College London (to Dr. Davies); the South Carolina Clinical and Translational Research Institute, Medical University of South Carolina (UL1TR to Dr. Flume); the Clinical and Translational Science Collaborative of Cleveland (UL1TR000439), a grant from the Cystic Fibrosis Core Center (DK027651), and a grant from the Cystic Fibrosis Foundation Therapeutics Development Network to Case Western Reserve University School of Medicine (all to Dr. Konstan); grants from the Northwestern University Clinical and Translational Sciences Institute (UL1RR025741) and the Cystic Fibrosis Foundation Therapeutics Development Network (MCCOLL14YO) (both to Dr. McColley); grants from the UAB Center for Clinical and Translational Science (UL1TR000165), the UAB Cystic Fibrosis Research Center (DK072482), and the Cystic Fibrosis Foundation (all to Dr. Rowe); and the Johns Hopkins Institute for Clinical and Translational Research, which is funded in part by a grant from the NIH (UL1TR001079, to Dr. Boyle). Dr. Wainwright reports receiving consulting fees from Medscape and Vertex, lecture fees and travel support from Vertex and Novartis, grant support from Vertex, GlaxoSmithKline, and Novo Nordisk, and fees on a per patient basis as principal investigator of a clinical study from Boehringer Ingelheim. Dr. Ramsey reports receiving grant support from Achaogen, Apartia, Bayer Healthcare, Breathe Easy, Bristol-Myers Squibb, Catabasis, 12th Man Technologies, Caltaxsys, Corbus Pharmaceuticals, Cornerstone Therapeutics, CSL Behring, CURx Pharmaceuticals, Eli Lilly, Flatley Discovery Lab, Genentech, Gilead Sciences, GlycoMimetics, Grifols Therapeutics, INC Research, Insmed, KaloBios, Kamada, Mpex Pharmaceuticals, N30 Pharmaceuticals, Nordmark, Novartis, Parion Sciences, Pharmagenesis (Cornerstone 281), Pharmaxis, ProQR Therapeutics, Pulmatrix, PulmoFlow, Respira Therapeutics, Savara Pharmaceuticals, and Vertex. Dr. Colombo reports receiving fees for serving on advisory boards from Vertex. Dr. Davies reports receiving fees through her institution for serving on advisory boards for Vertex, Proteostasis, Novartis, and Gilead; she has also received fees through her institution from Vertex for participation in educational activities and acting as lead investigator in other trials. Dr. De Boeck reports receiving fees for serving on an advisory board from Pharmaxis and KaloBios, fees for serving on a data monitoring committee from Aptalis, and consulting fees from Ablynx, Galapagos, Gilead, PTC Therapeutics, Celtaxys, and Boehringer Ingelheim; she has also served as principal investigator in studies funded by Gilead, Pharmaxis, and PTC Therapeutics. Dr. Flume reports receiving consulting fees and grant support from Vertex. Dr. Konstan reports receiving fees for serving on advisory boards from Genentech, Gilead Sciences, Insmed, and Savara Pharmaceuticals, consulting fees from Digestive Care, Novartis, PTC Therapeutics, Chiesi, KaloBios, and Celtaxsys, lecture fees from Novartis, travel support from Genentech, Gilead Sciences, Insmed, Novartis, PTC Therapeutics, and Celtaxsys, and grant support through his institution from Genentech, Insmed, Novartis, PTC Therapeutics, Savara Pharmaceuticals, and KaloBios. Dr. McCoy reports receiving travel support from Novartis and Pharmaxis, and grant support through her institution from Aptalis, KaloBios, Novartis, Gilead Sciences, Pharmaxis, Savara Pharmaceuticals, Genentech, AbbVie, Janssen, and N30 Pharmceuticals. Dr. McKone reports receiving fees for serving on advisory boards from Novartis and Vertex, consulting fees from Vertex, lecture fees from Gilead Sciences, travel support from Gilead Sciences and Novartis, and grant support from Vertex. Dr. Munck reports receiving fees for serving on advisory boards from Novartis. Dr. Ratjen reports receiving consulting fees from Bayer, Talecris, CSL Behring, Roche, Gilead Sciences, Genentech, and KaloBios, travel support from PARI Pharma, and grant support from Novartis. Dr. Rowe reports receiving grant support from Vertex, PTC Therapeutics, Novartis, and the Forest Research Institute. Dr. Boyle reports receiving fees for serving on advisory boards for Savara Pharmaceuticals, Vertex, Genentech, and Novartis. Dr. Marigowda, Dr. Huang, and Dr. Waltz are employees of and hold stock or stock options in Vertex. No other potential conflict of interest relevant to this article was reported. Disclosure forms provided by the authors are available with the full text of this article at NEJM.org. We thank all the patients, study coordinators, and study investigators; members of the Cystic Fibrosis Foundation, the United States Cystic Fibrosis Foundation Therapeutics Development Network, the European Clinical Trials Network, and the Cystic Fibrosis Foundation Data and Safety Monitoring Board for their support of this trial; Elizabeth Dorn, Ph.D. (Vertex Pharmaceuticals), for providing medical writing, editorial, and coordination support; and Jonathan Kirk (Vertex Pharmaceuticals) for providing graphic design support. 230 Appendix The authors full names and academic degrees are as follows: Claire E. Wainwright, M.B., B.S., M.D., J. Stuart Elborn, M.D., Bonnie W. Ramsey, M.D., Gautham Marigowda, M.D., Xiaohong Huang, Ph.D., Marco Cipolli, M.D., Carla Colombo, M.D., Jane C. Davies, M.D., Kris De Boeck, M.D., Patrick A. Flume, M.D., Michael W. Konstan, M.D., Susanna A. McColley, M.D., Karen McCoy, M.D., Edward F. McKone, M.D., Anne Munck, M.D., Felix Ratjen, M.D., Steven M. Rowe, M.D., M.S.P.H., David Waltz, M.D., and Michael P. Boyle, M.D., for the TRAFFIC and TRANSPORT Study Groups. The authors affiliations are as follows: Queensland Children s Medical Research Institute, Royal Children s Hospital, Lady Cilento Children s Hospital, and University of Queensland School of Medicine, Brisbane, Australia (C.E.W.); Queens University of Belfast, Belfast (J.S.E.), and Royal Brompton and Harefield NHS Foundation Trust and Imperial College London, London (J.C.D.) all in the n engl j med 373;3 nejm.org July 16, 2015
12 Lumacaftor with Ivacaftor for Cystic Fibrosis United Kingdom; Seattle Children s Hospital and University of Washington School of Medicine, Seattle (B.W.R.); Vertex Pharmaceuticals, Boston (G.M., X.H., D.W.); Cystic Fibrosis Center, Azienda Ospedaliera Universitaria Integrata, Verona (M.C.), and Fondazione IRCCS Ca Granda, Ospedale Maggiore Policlinico, University of Milan, Milan (C.C.) both in Italy; University Hospital Gasthuisberg, Leuven, Belgium (K.D.B.); Medical University of South Carolina, Charleston (P.A.F.); Case Western Reserve University School of Medicine, Rainbow Babies and Children s Hospital, Cleveland (M.W.K.), and the Department of Pediatrics, Pulmonary Division, Nationwide Children s Hospital and Ohio State University, Columbus (K.M.) both in Ohio; Stanley Manne Children s Research Institute, Northwestern University Feinberg School of Medicine, Chicago (S.A.M.); St. Vincent s University Hospital and University College Dublin School of Medicine, Dublin (E.F.M.); Hôpital Robert Debré, Paediatric Gastroenterology and Respiratory Department, CF Center, Assistance Publique Hôpitaux de Paris, Université Paris 7, Paris (A.M.); Division of Respiratory Medicine, Department of Pediatrics, Physiology, and Experimental Medicine, Hospital for Sick Children, University of Toronto, Toronto (F.R.); University of Alabama at Birmingham, Birmingham (S.M.R.); and Johns Hopkins Medicine, Baltimore (M.P.B.). References 1. US CF Foundation, Johns Hopkins University, the Hospital for Sick Children. The clinical and functional translation of CFTR (CFTR2) ( 2. Cystic Fibrosis Foundation. Patient registry: annual data report, Bethesda, MD: Cystic Fibrosis Foundation, 2013 ( UploadedFiles/ research/ ClinicalResearch/ PatientRegistryReport/ 2012-CFF-Patient-Registry.pdf). 3. European Cystic Fibrosis Patient Registry: annual data report, Denmark: European Cystic Fibrosis Society, 2014 ( / files/ webfm/ webfiles/ File/ ecfs_registry/ ECFSPR_Report10_ v12014_final_ pdf). 4. The molecular genetic epidemiology of cystic fibrosis: report of a joint meeting of WHO/ECFTN/ICF(M)A/ECFS. Genoa, Italy: World Health Organization, June 2002: O Sullivan BP, Freedman SD. Cystic fibrosis. Lancet 2009; 373: MacKenzie T, Gifford AH, Sabadosa KA, et al. Longevity of patients with cystic fibrosis in 2000 to 2010 and beyond: survival analysis of the Cystic Fibrosis Foundation patient registry. Ann Intern Med 2014; 161: Farinha CM, Amaral MD. Most F508del-CFTR is targeted to degradation at an early folding checkpoint and independently of calnexin. Mol Cell Biol 2005; 25: Jensen TJ, Loo MA, Pind S, Williams DB, Goldberg AL, Riordan JR. Multiple proteolytic systems, including the proteasome, contribute to CFTR processing. Cell 1995; 83: Lukacs GL, Chang XB, Bear C, et al. The delta F508 mutation decreases the stability of cystic fibrosis transmembrane conductance regulator in the plasma membrane: determination of functional half-lives on transfected cells. J Biol Chem 1993; 268: Sharma M, Benharouga M, Hu W, Lukacs GL. Conformational and temperature-sensitive stability defects of the delta F508 cystic fibrosis transmembrane conductance regulator in post-endoplasmic reticulum compartments. J Biol Chem 2001; 276: Van Goor F, Hadida S, Grootenhuis PD, et al. Correction of the F508del-CFTR protein processing defect in vitro by the investigational drug VX-809. Proc Natl Acad Sci U S A 2011; 108: Yu H, Burton B, Huang CJ, et al. Ivacaftor potentiation of multiple CFTR channels with gating mutations. J Cyst Fibros 2012; 11: Ramsey BW, Davies J, McElvaney NG, et al. A CFTR potentiator in patients with cystic fibrosis and the G551D mutation. N Engl J Med 2011; 365: Davies JC, Wainwright CE, Canny GJ, et al. Efficacy and safety of ivacaftor in patients aged 6 to 11 years with cystic fibrosis with a G551D mutation. Am J Respir Crit Care Med 2013; 187: De Boeck K, Munck A, Walker S, et al. Efficacy and safety of ivacaftor in patients with cystic fibrosis and a non-g551d gating mutation. J Cyst Fibros 2014; 13: McKone EF, Borowitz D, Drevinek P, et al. Long-term safety and efficacy of ivacaftor in patients with cystic fibrosis who have the Gly551Asp-CFTR mutation: a phase 3, open-label extension study (PERSIST). Lancet Respir Med 2014; 2: Rowe SM, Heltshe SL, Gonska T, et al. Clinical mechanism of the cystic fibrosis transmembrane conductance regulator potentiator ivacaftor in G551D-mediated cystic fibrosis. Am J Respir Crit Care Med 2014; 190: Van Goor F, Hadida S, Grootenhuis PD, et al. Rescue of CF airway epithelial cell function in vitro by a CFTR potentiator, VX-770. Proc Natl Acad Sci U S A 2009; 106: Flume PA, Liou TG, Borowitz DS, et al. Ivacaftor in subjects with cystic fibrosis who are homozygous for the F508del-CFTR mutation. Chest 2012; 142: Clancy JP, Rowe SM, Accurso FJ, et al. Results of a phase IIa study of VX-809, an investigational CFTR corrector compound, in subjects with cystic fibrosis homozygous for the F508del-CFTR mutation. Thorax 2012; 67: Boyle MP, Bell SC, Konstan MW, et al. A CFTR corrector (lumacaftor) and a CFTR potentiator (ivacaftor) for treatment of patients with cystic fibrosis who have a phe508del CFTR mutation: a phase 2 randomised controlled trial. Lancet Respir Med 2014; 2: Hankinson JL, Odencrantz JR, Fedan KB. Spirometric reference values from a sample of the general U.S. population. Am J Respir Crit Care Med 1999; 159: Wang X, Dockery DW, Wypij D, Fay ME, Ferris BG Jr. Pulmonary function between 6 and 18 years of age. Pediatr Pulmonol 1993; 15: Quittner AL, Modi AC, Wainwright C, Otto K, Kirihara J, Montgomery AB. Determination of the minimal clinically important difference scores for the Cystic Fibrosis Questionnaire-Revised respiratory symptom scale in two populations of patients with cystic fibrosis and chronic Pseudomonas aeruginosa airway infection. Chest 2009; 135: Liou TG, Adler FR, Fitzsimmons SC, Cahill BC, Hibbs JR, Marshall BC. Predictive 5-year survivorship model of cystic fibrosis. Am J Epidemiol 2001; 153: Vaisman N, Pencharz PB, Corey M, Canny GJ, Hahn E. Energy expenditure of patients with cystic fibrosis. J Pediatr 1987; 111: Castellani C, Cuppens H, Macek M Jr, et al. Consensus on the use and interpretation of cystic fibrosis mutation analysis in clinical practice. J Cyst Fibros 2008; 7: Saiman L, Marshall BC, Mayer-Hamblett N, et al. Azithromycin in patients with cystic fibrosis chronically infected with Pseudomonas aeruginosa: a randomized controlled trial. JAMA 2003; 290: Elkins MR, Robinson M, Rose BR, et al. A controlled trial of long-term inhaled hypertonic saline in patients with cystic fibrosis. N Engl J Med 2006; 354: Konstan MW, Schluchter MD, Xue W, Davis PB. Clinical use of Ibuprofen is associated with slower FEV1 decline in children with cystic fibrosis. Am J Respir Crit Care Med 2007; 176: Mogayzel PJ Jr, Naureckas ET, Robinson KA, et al. Cystic fibrosis pulmonary guidelines: chronic medications for maintenance of lung health. Am J Respir Crit Care Med 2013; 187: Veit G, Avramescu RG, Perdomo D, et al. Some gating potentiators, including VX-770, diminish ΔF508-CFTR functional expression. Sci Transl Med 2014; 6: 46ra Cholon DM, Quinney NL, Fulcher ML, et al. Potentiator ivacaftor abrogates pharmacological correction of ΔF508 CFTR in cystic fibrosis. Sci Transl Med 2014; 6: 46ra96. Copyright 2015 Massachusetts Medical Society. n engl j med 373;3 nejm.org July 16,
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Moss RB, Flume PA, Elborn JS, et al, on behalf
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Moss RB, Flume PA, Elborn JS, et al, on behalf
(<40 and 40) and screening ppfev 1. , were done for patients with baseline ppfev 1
 Efficacy and safety of lumacaftor/ivacaftor combinion therapy in pients with cystic fibrosis homozygous for Phe508del CFTR by pulmonary function subgroup: a pooled analysis J Stuart Elborn, Bonnie W Ramsey,
Efficacy and safety of lumacaftor/ivacaftor combinion therapy in pients with cystic fibrosis homozygous for Phe508del CFTR by pulmonary function subgroup: a pooled analysis J Stuart Elborn, Bonnie W Ramsey,
A CFTR Potentiator in Patients with Cystic Fibrosis and the G551D Mutation A BS TR AC T
 The new england journal of medicine established in 112 november 3, 2011 vol. 365 no. 1 A CFTR Potentiator in Patients with Cystic Fibrosis and the G551D Mutation Bonnie W. Ramsey, M.D., Jane Davies, M.D.,
The new england journal of medicine established in 112 november 3, 2011 vol. 365 no. 1 A CFTR Potentiator in Patients with Cystic Fibrosis and the G551D Mutation Bonnie W. Ramsey, M.D., Jane Davies, M.D.,
Cystic Fibrosis: Progress in Treatment Management. Patrick A. Flume, M.D. Medical University of South Carolina
 Cystic Fibrosis: Progress in Treatment Management Patrick A. Flume, M.D. Medical University of South Carolina Disclosures Grant support Mpex Pharmaceuticals, Inc Gilead Sciences, Inc Bayer Healthcare AG
Cystic Fibrosis: Progress in Treatment Management Patrick A. Flume, M.D. Medical University of South Carolina Disclosures Grant support Mpex Pharmaceuticals, Inc Gilead Sciences, Inc Bayer Healthcare AG
Pharmacy Policy Bulletin
 Pharmacy Policy Bulletin Title: Policy #: Cystic Fibrosis Agents (Kalydeco, Orkambi ) Rx.01.117 Application of pharmacy policy is determined by benefits and contracts. Benefits may vary based on product
Pharmacy Policy Bulletin Title: Policy #: Cystic Fibrosis Agents (Kalydeco, Orkambi ) Rx.01.117 Application of pharmacy policy is determined by benefits and contracts. Benefits may vary based on product
Transformational Treatments. PRESTON W. CAMPBELL, III, M.D. Executive Vice President for Medical Affairs
 Transformational Treatments PRESTON W. CAMPBELL, III, M.D. Executive Vice President for Medical Affairs Symptom-based CF Therapies 45 Median Predicted Survival Age of US Patients with Cystic Fibrosis 41
Transformational Treatments PRESTON W. CAMPBELL, III, M.D. Executive Vice President for Medical Affairs Symptom-based CF Therapies 45 Median Predicted Survival Age of US Patients with Cystic Fibrosis 41
A Quick Guide to the. I507del. Mutation CFTR SCIENCE
 A Quick Guide to the I507del Mutation CFTR SCIENCE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of CFTR activity is the underlying cause of cystic fibrosis (CF) 1 Spectrum
A Quick Guide to the I507del Mutation CFTR SCIENCE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of CFTR activity is the underlying cause of cystic fibrosis (CF) 1 Spectrum
Lumacaftor and ivacaftor in the management of patients with cystic fibrosis: current evidence and future prospects
 601934TAR0010.1177/1753465815601934Therapeutic Advances in Respiratory DiseaseKuk and Taylor-Cousar research-article2015 Therapeutic Advances in Respiratory Disease Review Lumacaftor and ivacaftor in the
601934TAR0010.1177/1753465815601934Therapeutic Advances in Respiratory DiseaseKuk and Taylor-Cousar research-article2015 Therapeutic Advances in Respiratory Disease Review Lumacaftor and ivacaftor in the
Cystic Fibrosis Foundation Patient Registry 2013
 5/9/2015 Targeting CFTR to Treat Cystic Fibrosis: Small Molecule Therapy Mary Ellen Kleinhenz, MD Director, UCSF Adult Cystic Fibrosis Program Professor of Medicine UCSF Division of Pulmonary, Critical
5/9/2015 Targeting CFTR to Treat Cystic Fibrosis: Small Molecule Therapy Mary Ellen Kleinhenz, MD Director, UCSF Adult Cystic Fibrosis Program Professor of Medicine UCSF Division of Pulmonary, Critical
Class Update with New Drug Evaluation: Oral Cystic Fibrosis Modulators
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Class Update: Oral Cystic Fibrosis Modulators
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Cystic fibrosis (CF) is the most frequent. Ivacaftor treatment in patients with cystic REVIEW. Isabelle Sermet-Gaudelus
 Eur Respir Rev 2013; 22: 127, 66 71 DOI: 10.1183/09059180.00008512 CopyrightßERS 2013 REVIEW Ivacaftor treatment in patients with cystic fibrosis and the G551D-CFTR mutation Isabelle Sermet-Gaudelus ABSTRACT:
Eur Respir Rev 2013; 22: 127, 66 71 DOI: 10.1183/09059180.00008512 CopyrightßERS 2013 REVIEW Ivacaftor treatment in patients with cystic fibrosis and the G551D-CFTR mutation Isabelle Sermet-Gaudelus ABSTRACT:
Brand Name: Kalydeco. Generic: ivacaftor. Manufacturer 1 : Vertex Pharmaceuticals Incorporated
 Brand Name: Kalydeco Generic: ivacaftor Manufacturer 1 : Vertex Pharmaceuticals Incorporated Drug Class 2,3 : Cystic Fibrosis Transmembrane Conductance Regulator (CFTR) Potentiator Uses: Labeled Uses 1,2,3,4,5
Brand Name: Kalydeco Generic: ivacaftor Manufacturer 1 : Vertex Pharmaceuticals Incorporated Drug Class 2,3 : Cystic Fibrosis Transmembrane Conductance Regulator (CFTR) Potentiator Uses: Labeled Uses 1,2,3,4,5
Orkambi. Orkambi (lumacaftor/ivacaftor) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.45.06 Subject: Orkambi Page: 1 of 6 Last Review Date: November 30, 2018 Orkambi Description Orkambi (lumacaftor/ivacaftor)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.45.06 Subject: Orkambi Page: 1 of 6 Last Review Date: November 30, 2018 Orkambi Description Orkambi (lumacaftor/ivacaftor)
The Future of CF Therapy
 The Future of CF Therapy Peter J. Mogayzel, Jr., M.D., Ph.D. Eudowood Division of Pediatric Respiratory Sciences The Johns Hopkins School of Medicine Overview The Future of CF Therapy Personalized therapy
The Future of CF Therapy Peter J. Mogayzel, Jr., M.D., Ph.D. Eudowood Division of Pediatric Respiratory Sciences The Johns Hopkins School of Medicine Overview The Future of CF Therapy Personalized therapy
New Drug Evaluation: Lumacaftor/Ivacaftor
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Disclosures. Advances in the Management of Cystic Fibrosis: A Closer Look at the Roles of CFTR Modulation Therapy 10/28/2016
 Advances in the Management of Cystic Fibrosis: A Closer Look at the Roles of CFTR Modulation Therapy Susanna A McColley, MD Associate Chief Research Officer Stanley Manne Children s Research Institute
Advances in the Management of Cystic Fibrosis: A Closer Look at the Roles of CFTR Modulation Therapy Susanna A McColley, MD Associate Chief Research Officer Stanley Manne Children s Research Institute
PA Update: Oral Cystic Fibrosis Modulators
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
North American Cystic Fibrosis Conference 27 October Noreen R Henig, MD Chief Development Officer ProQR Therapeutics
 Proof of Concept Study to Demonstrate the Effects of QR-010 on Nasal Potential Difference in Subjects With Cystic Fibrosis with the F508del CFTR Mutation Noreen R Henig, MD Chief Development Officer ProQR
Proof of Concept Study to Demonstrate the Effects of QR-010 on Nasal Potential Difference in Subjects With Cystic Fibrosis with the F508del CFTR Mutation Noreen R Henig, MD Chief Development Officer ProQR
Chronic Stenotrophomonas maltophilia infection and mortality or lung transplantation in cystic fibrosis patients
 Journal of Cystic Fibrosis 12 (2013) 482 486 www.elsevier.com/locate/jcf Original Article Chronic Stenotrophomonas maltophilia infection and mortality or lung transplantation in cystic fibrosis patients
Journal of Cystic Fibrosis 12 (2013) 482 486 www.elsevier.com/locate/jcf Original Article Chronic Stenotrophomonas maltophilia infection and mortality or lung transplantation in cystic fibrosis patients
THE ROLE OF CFTR MUTATIONS IN CAUSING CYSTIC FIBROSIS (CF)
 THE ROLE OF CFTR MUTATIONS IN CAUSING CYSTIC FIBROSIS (CF) Vertex Pharmaceuticals Incorporated, 50 Northern Avenue, Boston, MA 02210. Vertex and the Vertex triangle logo are registered trademarks for Vertex
THE ROLE OF CFTR MUTATIONS IN CAUSING CYSTIC FIBROSIS (CF) Vertex Pharmaceuticals Incorporated, 50 Northern Avenue, Boston, MA 02210. Vertex and the Vertex triangle logo are registered trademarks for Vertex
Treatment complexity in cystic fibrosis: Trends over time and associations with site-specific outcomes
 Journal of Cystic Fibrosis 12 (2013) 461 467 www.elsevier.com/locate/jcf Original Article Treatment complexity in cystic fibrosis: Trends over time and associations with site-specific outcomes Gregory
Journal of Cystic Fibrosis 12 (2013) 461 467 www.elsevier.com/locate/jcf Original Article Treatment complexity in cystic fibrosis: Trends over time and associations with site-specific outcomes Gregory
You Can Observe a Lot By Just Watching. Wayne J. Morgan, MD, CM
 You Can Observe a Lot By Just Watching Wayne J. Morgan, MD, CM Disclosures Genentech Epidemiological Study of Cystic Fibrosis, Scientific Advisory Group CF Foundation Data Safety Monitoring Board Registry/Comparative
You Can Observe a Lot By Just Watching Wayne J. Morgan, MD, CM Disclosures Genentech Epidemiological Study of Cystic Fibrosis, Scientific Advisory Group CF Foundation Data Safety Monitoring Board Registry/Comparative
Kalydeco. Kalydeco (ivacaftor) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.45.03 Subject: Kalydeco Page: 1 of 6 Last Review Date: November 30, 2018 Kalydeco Description Kalydeco
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.45.03 Subject: Kalydeco Page: 1 of 6 Last Review Date: November 30, 2018 Kalydeco Description Kalydeco
Briefing Document. FDA Pulmonary - Allergy Drugs Advisory Committee
 FDA Advisory Committee Briefing Materials Page 1 of 157 Briefing Document FDA Pulmonary - Allergy Drugs Advisory Committee Ivacaftor for the Treatment of Cystic Fibrosis in Patients Age 6 Years and Older
FDA Advisory Committee Briefing Materials Page 1 of 157 Briefing Document FDA Pulmonary - Allergy Drugs Advisory Committee Ivacaftor for the Treatment of Cystic Fibrosis in Patients Age 6 Years and Older
Scottish Paediatric Cystic Fibrosis MCN. Protocols / Guidelines. Ivacaftor: A guideline for use in paediatric CF patients in Scotland
 Scottish Paediatric Cystic Fibrosis MCN Protocols / Guidelines Ivacaftor: A guideline for use in paediatric CF patients in Scotland Authors: Dr Carol Dryden Dr Jane Wilkinson Miss Julie Crocker, Registered
Scottish Paediatric Cystic Fibrosis MCN Protocols / Guidelines Ivacaftor: A guideline for use in paediatric CF patients in Scotland Authors: Dr Carol Dryden Dr Jane Wilkinson Miss Julie Crocker, Registered
THE ROLE OF CFTR MUTATIONS IN CAUSING CYSTIC FIBROSIS (CF)
 THE ROLE OF CFTR MUTATIONS IN CAUSING CYSTIC FIBROSIS (CF) Vertex Pharmaceuticals Incorporated, 50 Northern Avenue, Boston, MA 02210. Vertex and the Vertex triangle logo are registered trademarks of Vertex
THE ROLE OF CFTR MUTATIONS IN CAUSING CYSTIC FIBROSIS (CF) Vertex Pharmaceuticals Incorporated, 50 Northern Avenue, Boston, MA 02210. Vertex and the Vertex triangle logo are registered trademarks of Vertex
CADTH CANADIAN DRUG EXPERT COMMITTEE FINAL RECOMMENDATION
 CADTH CANADIAN DRUG EXPERT COMMITTEE FINAL RECOMMENDATION LUMACAFTOR / IVACAFTOR (Orkambi Vertex Pharmaceuticals [Canada] Inc.) Indication: Cystic Fibrosis, F508del-CFTR mutation Recommendation: The CADTH
CADTH CANADIAN DRUG EXPERT COMMITTEE FINAL RECOMMENDATION LUMACAFTOR / IVACAFTOR (Orkambi Vertex Pharmaceuticals [Canada] Inc.) Indication: Cystic Fibrosis, F508del-CFTR mutation Recommendation: The CADTH
A Genetic Approach to the Treatment of Cystic Fibrosis
 A Genetic Approach to the Treatment of Cystic Fibrosis Peter Mueller, PhD Chief Scientific Officer and Executive Vice President Global Research and Development Vertex Pharmaceuticals, Incorporated March
A Genetic Approach to the Treatment of Cystic Fibrosis Peter Mueller, PhD Chief Scientific Officer and Executive Vice President Global Research and Development Vertex Pharmaceuticals, Incorporated March
We strive to develop innovative solutions that improve and extend the lives of people with cystic fibrosis
 Nivalis Therapeutics, Inc., October 2015 Analyst Breakfast at NACFC We strive to develop innovative solutions that improve and extend the lives of people with cystic fibrosis Disclaimer Regarding Forward
Nivalis Therapeutics, Inc., October 2015 Analyst Breakfast at NACFC We strive to develop innovative solutions that improve and extend the lives of people with cystic fibrosis Disclaimer Regarding Forward
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Cystic Fibrosis Transmembrane Page 1 of 13 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Cystic Fibrosis Transmembrane Conductance Regulator (CFTR) Prime Therapeutics
Cystic Fibrosis Transmembrane Page 1 of 13 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Cystic Fibrosis Transmembrane Conductance Regulator (CFTR) Prime Therapeutics
ClinicalTrials.gov Protocol Registration and Results System (PRS) Receipt Release Date: October 3, ClinicalTrials.gov ID: NCT
 ClinicalTrials.gov Protocol Registration and Results System (PRS) Receipt Release Date: October 3, 2012 ClinicalTrials.gov ID: NCT00457821 Study Identification Unique Protocol ID: VX06-770-101 Brief Title:
ClinicalTrials.gov Protocol Registration and Results System (PRS) Receipt Release Date: October 3, 2012 ClinicalTrials.gov ID: NCT00457821 Study Identification Unique Protocol ID: VX06-770-101 Brief Title:
Enabling CF Therapeutic Development
 Enabling CF Therapeutic Development PRESTON W. CAMPBELL, III, M.D. Executive Vice President for Medical Affairs No Disclosures Cystic Fibrosis In 1955 In 1955 most children with CF did not live long enough
Enabling CF Therapeutic Development PRESTON W. CAMPBELL, III, M.D. Executive Vice President for Medical Affairs No Disclosures Cystic Fibrosis In 1955 In 1955 most children with CF did not live long enough
GLPG1837 in Subjects with Cystic Fibrosis (CF) and the G551D Mutation: results from a Phase II study (SAPHIRA1)
 GLPG1837 in Subjects with Cystic Fibrosis (CF) and the G551D Mutation: results from a Phase II study (SAPHIRA1) ECFS, Sevilla, Spain 9 June 2017 Jane Davies on behalf of the SAPHIRA1 Study Team Copyright
GLPG1837 in Subjects with Cystic Fibrosis (CF) and the G551D Mutation: results from a Phase II study (SAPHIRA1) ECFS, Sevilla, Spain 9 June 2017 Jane Davies on behalf of the SAPHIRA1 Study Team Copyright
Characterizing aggressiveness and predicting future progression of CF lung disease
 Journal of Cystic Fibrosis Volume 8 Suppl 1 (2009) S15 S19 www.elsevier.com/locate/jcf Characterizing aggressiveness and predicting future progression of CF lung disease Michael W. Konstan a, *, Jeffrey
Journal of Cystic Fibrosis Volume 8 Suppl 1 (2009) S15 S19 www.elsevier.com/locate/jcf Characterizing aggressiveness and predicting future progression of CF lung disease Michael W. Konstan a, *, Jeffrey
Cystic Fibrosis the future
 Cystic Fibrosis the future Pathophysiologic cascade Abnormal Gene Abnormal CFTR Therapy Gene replacement Protein replacement Gene read through therapy Abnormal sodium chloride & water movement through
Cystic Fibrosis the future Pathophysiologic cascade Abnormal Gene Abnormal CFTR Therapy Gene replacement Protein replacement Gene read through therapy Abnormal sodium chloride & water movement through
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions
 CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
Pediatrics Grand Rounds 18 Sept University of Texas Health Science Center. + Disclosure. + Learning Objectives.
 Disclosure Dr Donna Willey Courand receives research support from Cystic Fibrosis Therapeutics The Cystic Fibrosis Foundation Children with Special Health Care Needs Cystic Fibrosis 05: Improving Survival
Disclosure Dr Donna Willey Courand receives research support from Cystic Fibrosis Therapeutics The Cystic Fibrosis Foundation Children with Special Health Care Needs Cystic Fibrosis 05: Improving Survival
Recently, the cystic fibrosis (CF) community celebrated the 25th
 focused review A new era of personalized medicine for cystic fibrosis at last! Bradley S Quon MD MSc FRCPC 1,2, Pearce G Wilcox MD FRCPC 1,2 BS Quon, PG Wilcox. A new era of personalized medicine for cystic
focused review A new era of personalized medicine for cystic fibrosis at last! Bradley S Quon MD MSc FRCPC 1,2, Pearce G Wilcox MD FRCPC 1,2 BS Quon, PG Wilcox. A new era of personalized medicine for cystic
Phase 3 EVOLVE & EXPAND Studies of Tezacaftor/Ivacaftor Combination Show Statistically Significant Improvements in Lung Function and Other Measures
 Phase 3 EVOLVE & EXPAND Studies of Tezacaftor/Ivacaftor Combination Show Statistically Significant Improvements in Lung Function and Other Measures in CF Patients March 29, 2017 Agenda Introduction Michael
Phase 3 EVOLVE & EXPAND Studies of Tezacaftor/Ivacaftor Combination Show Statistically Significant Improvements in Lung Function and Other Measures in CF Patients March 29, 2017 Agenda Introduction Michael
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis
 Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
Drug Use Criteria: Ivacaftor (Kalydeco ) and Lumacaftor/Ivacaftor (Orkambi )
 Texas Vendor Program Use Criteria: (Kalydeco ) and Lumacaftor/ (Orkambi ) Publication History Developed: October 2012 Revised: December 2017; February 2016; June 2014. Notes: Information on indications
Texas Vendor Program Use Criteria: (Kalydeco ) and Lumacaftor/ (Orkambi ) Publication History Developed: October 2012 Revised: December 2017; February 2016; June 2014. Notes: Information on indications
Targeted therapies to improve CFTR function in cystic fibrosis
 Brodlie et al. Genome Medicine (2015) 7:101 DOI 10.1186/s13073-015-0223-6 REVIEW Targeted therapies to improve CFTR function in cystic fibrosis Malcolm Brodlie 1*, Iram J. Haq 2, Katie Roberts 2 and J.
Brodlie et al. Genome Medicine (2015) 7:101 DOI 10.1186/s13073-015-0223-6 REVIEW Targeted therapies to improve CFTR function in cystic fibrosis Malcolm Brodlie 1*, Iram J. Haq 2, Katie Roberts 2 and J.
Respiratory Pharmacology: Treatment of Cystic Fibrosis
 Respiratory Pharmacology: Treatment of Cystic Fibrosis Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
Respiratory Pharmacology: Treatment of Cystic Fibrosis Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
CYSTIC FIBROSIS CANADA S CF PHYSICIAN PANEL ON LUMACAFTOR/IVACAFTOR: RECOMMENDATIONS FOR CRITERIA FOR CLINICAL USE
 CYSTIC FIBROSIS CANADA S CF PHYSICIAN PANEL ON LUMACAFTOR/IVACAFTOR: RECOMMENDATIONS FOR CRITERIA FOR CLINICAL USE I - INTRODUCTION a) Cystic Fibrosis Cystic fibrosis (CF) is the most common fatal genetic
CYSTIC FIBROSIS CANADA S CF PHYSICIAN PANEL ON LUMACAFTOR/IVACAFTOR: RECOMMENDATIONS FOR CRITERIA FOR CLINICAL USE I - INTRODUCTION a) Cystic Fibrosis Cystic fibrosis (CF) is the most common fatal genetic
CYSTIC FIBROSIS OBJECTIVES NO CONFLICT OF INTEREST TO DISCLOSE
 CYSTIC FIBROSIS Madhu Pendurthi MD MPH Staff Physician, Mercy Hospital Springfield, MO NO CONFLICT OF INTEREST TO DISCLOSE OBJECTIVES Epidemiology of Cystic Fibrosis (CF) Genetic basis and pathophysiology
CYSTIC FIBROSIS Madhu Pendurthi MD MPH Staff Physician, Mercy Hospital Springfield, MO NO CONFLICT OF INTEREST TO DISCLOSE OBJECTIVES Epidemiology of Cystic Fibrosis (CF) Genetic basis and pathophysiology
A Quick Guide to the G A. Mutation CFTR SCIENCE
 A Quick Guide to the 1717-1G A Mutation FR SIENE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of FR activity is the underlying cause of cystic fibrosis (F) 1 Spectrum of Phenotypes
A Quick Guide to the 1717-1G A Mutation FR SIENE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of FR activity is the underlying cause of cystic fibrosis (F) 1 Spectrum of Phenotypes
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Cystic Fibrosis Transmembrane Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Cystic Fibrosis Transmembrane Conductance Regulator (CFTR) Prime Therapeutics
Cystic Fibrosis Transmembrane Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Cystic Fibrosis Transmembrane Conductance Regulator (CFTR) Prime Therapeutics
"Management and Treatment of Patients with Cystic fibrosis (CF)
 "Management and Treatment of Patients with Cystic fibrosis (CF) Dr. Malena Cohen-Cymberknoh Pediatric Pulmonology and CF Center Hadassah Hebrew-University Medical Center Jerusalem, Israel Afula, March
"Management and Treatment of Patients with Cystic fibrosis (CF) Dr. Malena Cohen-Cymberknoh Pediatric Pulmonology and CF Center Hadassah Hebrew-University Medical Center Jerusalem, Israel Afula, March
Opening Doors to CF Clinical Research: Change is Coming
 Opening Doors to CF Clinical Research: Change is Coming Disclosures Contracts with sponsors for clinical trials conducted at UNC-Chapel Hill: CFFT NIH/NHLBI AbbVie Inc. Aptalis Pharma US, Inc. Janssen
Opening Doors to CF Clinical Research: Change is Coming Disclosures Contracts with sponsors for clinical trials conducted at UNC-Chapel Hill: CFFT NIH/NHLBI AbbVie Inc. Aptalis Pharma US, Inc. Janssen
Clinical Commissioning Policy: Ivacaftor for Cystic Fibrosis (named mutations)
 Clinical Commissioning Policy: Ivacaftor for Cystic Fibrosis (named mutations) Reference: NHS England: A01/P/c NHS England INFORMATION READER BOX Directorate Medical Commissioning Operations Patients and
Clinical Commissioning Policy: Ivacaftor for Cystic Fibrosis (named mutations) Reference: NHS England: A01/P/c NHS England INFORMATION READER BOX Directorate Medical Commissioning Operations Patients and
North American Cystic Fibrosis Conference 27 October Noreen R Henig, MD Chief Development Officer ProQR Therapeutics
 Proof of Concept Study to Demonstrate the Effects of QR-010 on Nasal Potential Difference in Subjects With Cystic Fibrosis with the F508del CFTR Mutation Noreen R Henig, MD Chief Development Officer ProQR
Proof of Concept Study to Demonstrate the Effects of QR-010 on Nasal Potential Difference in Subjects With Cystic Fibrosis with the F508del CFTR Mutation Noreen R Henig, MD Chief Development Officer ProQR
CFTR Genotype as a Predictor of Prognosis in Cystic Fibrosis*
 Original Research CYSTIC FIBROSIS CFTR Genotype as a Predictor of Prognosis in Cystic Fibrosis* Edward F. McKone, MD, MS; Christopher H. Goss, MD, MS, FCCP; and Moira L. Aitken, MD, FCCP Study rationale:
Original Research CYSTIC FIBROSIS CFTR Genotype as a Predictor of Prognosis in Cystic Fibrosis* Edward F. McKone, MD, MS; Christopher H. Goss, MD, MS, FCCP; and Moira L. Aitken, MD, FCCP Study rationale:
NACFC investor meeting. Dr Katja Conrath, Therapeutic Head CF Dr Piet Wigerinck, CSO NACFC November 2017 Copyright 2017 Galapagos NV
 NACFC investor meeting Dr Katja Conrath, Therapeutic Head CF Dr Piet Wigerinck, CSO NACFC 2017 2 November 2017 Copyright 2017 Galapagos NV Disclaimer This presentation contains forward-looking statements,
NACFC investor meeting Dr Katja Conrath, Therapeutic Head CF Dr Piet Wigerinck, CSO NACFC 2017 2 November 2017 Copyright 2017 Galapagos NV Disclaimer This presentation contains forward-looking statements,
Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages)
 Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages) NHS England Reference: 1732P NHS England INFORMATION READER BOX Directorate
Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages) NHS England Reference: 1732P NHS England INFORMATION READER BOX Directorate
Oral Cystic Fibrosis Modulators
 Oral Cystic Fibrosis Modulators Goals: To ensure appropriate drug use and limit to patient populations in which they have demonstrated to be effective and safe. To monitor for clinical response for appropriate
Oral Cystic Fibrosis Modulators Goals: To ensure appropriate drug use and limit to patient populations in which they have demonstrated to be effective and safe. To monitor for clinical response for appropriate
A treatment option for patients with CF who have responsive mutations
 A treatment option for patients with CF who have responsive mutations INDICATIONS AND USAGE SYMDEKO is indicated for the treatment of patients with cystic fibrosis (CF) aged 12 years and older who are
A treatment option for patients with CF who have responsive mutations INDICATIONS AND USAGE SYMDEKO is indicated for the treatment of patients with cystic fibrosis (CF) aged 12 years and older who are
A Cure for All: Leaving No One Behind. Assuring Effective Therapies for All Patients with Cystic Fibrosis
 A Cure for All: Leaving No One Behind Assuring Effective Therapies for All Patients with Cystic Fibrosis Topics for Today s Presentation Demographics of the CF patient population in the modulator era
A Cure for All: Leaving No One Behind Assuring Effective Therapies for All Patients with Cystic Fibrosis Topics for Today s Presentation Demographics of the CF patient population in the modulator era
Clinical Commissioning Policy: Continuous aztreonam lysine for cystic fibrosis (all ages)
 Clinical Commissioning Policy: Continuous aztreonam lysine for cystic fibrosis (all ages) Reference: NHS England: 16001/P NHS England INFORMATION READER BOX Directorate Medical Operations and Information
Clinical Commissioning Policy: Continuous aztreonam lysine for cystic fibrosis (all ages) Reference: NHS England: 16001/P NHS England INFORMATION READER BOX Directorate Medical Operations and Information
ivacaftor 150mg film-coated tablets (Kalydeco ) SMC No. (1193/16) Vertex Pharmaceuticals (Europe) Ltd
 ivacaftor 150mg film-coated tablets (Kalydeco ) SMC No. (1193/16) Vertex Pharmaceuticals (Europe) Ltd 04 November 2016 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
ivacaftor 150mg film-coated tablets (Kalydeco ) SMC No. (1193/16) Vertex Pharmaceuticals (Europe) Ltd 04 November 2016 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
Cystic Fibrosis: KOL Insight [2017]
![Cystic Fibrosis: KOL Insight [2017] Cystic Fibrosis: KOL Insight [2017]](/thumbs/90/102403567.jpg) Cystic Fibrosis: KOL Insight [2017] Cystic Fibrosis: KOL Insight [2017] BioPortfolio has been marketing business and market research reports from selected publishers for over fifteen years. BioPortfolio
Cystic Fibrosis: KOL Insight [2017] Cystic Fibrosis: KOL Insight [2017] BioPortfolio has been marketing business and market research reports from selected publishers for over fifteen years. BioPortfolio
At-A-Glance report 2013
 At-A-Glance report 213 Cystic Fibrosis in Europe Facts and Figures 213 The European Cystic Fibrosis Society Patient Registry (ECFSPR) is happy to present this report with key information about how cystic
At-A-Glance report 213 Cystic Fibrosis in Europe Facts and Figures 213 The European Cystic Fibrosis Society Patient Registry (ECFSPR) is happy to present this report with key information about how cystic
Pulmonary Exacerbations:
 Pulmonary Exacerbations: Better Understanding Needed Michael Tracy, MD Clinical Assistant Professor Pediatric Pulmonary CF Pulmonary Exacerbations Definition Importance Causes Treatment Research opportunities
Pulmonary Exacerbations: Better Understanding Needed Michael Tracy, MD Clinical Assistant Professor Pediatric Pulmonary CF Pulmonary Exacerbations Definition Importance Causes Treatment Research opportunities
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Wells JM, Farris RF, Gosdin TA, et al. Pulmonary
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Wells JM, Farris RF, Gosdin TA, et al. Pulmonary
Symdeko. Symdeko (tezacaftor and ivacaftor) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.45.10 Subject: Symdeko Page: 1 of 5 Last Review Date: June 22, 2018 Symdeko Description Symdeko (tezacaftor
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.45.10 Subject: Symdeko Page: 1 of 5 Last Review Date: June 22, 2018 Symdeko Description Symdeko (tezacaftor
Opinion 7 November 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 7 November 2012 KALYDECO 150 mg film-coated tablets B/56 (CIP code: 34009 266 060 5 3) Applicant: VERTEX INN ATC Code
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 7 November 2012 KALYDECO 150 mg film-coated tablets B/56 (CIP code: 34009 266 060 5 3) Applicant: VERTEX INN ATC Code
Pharmacogenomics in Rare Diseases: Development Strategy for Ivacaftor as a Therapy for Cystic Fibrosis
 Pharmacogenomics in Rare Diseases: Development Strategy for Ivacaftor as a Therapy for Cystic Fibrosis Federico Goodsaid Vice President Strategic Regulatory Intelligence Vertex Pharmaceuticals Is there
Pharmacogenomics in Rare Diseases: Development Strategy for Ivacaftor as a Therapy for Cystic Fibrosis Federico Goodsaid Vice President Strategic Regulatory Intelligence Vertex Pharmaceuticals Is there
Tiotropium Respimat in cystic fibrosis: Phase 3 and Pooled phase 2/3 randomized trials
 Tiotropium Respimat in cystic fibrosis: Phase 3 and Pooled phase 2/3 randomized trials Ratjen, F., Koker, P., Geller, D. E., Langellier-Cocteaux, B., Le Maulf, F., Kattenbeck, S.,... Elborn, J. S. (2015).
Tiotropium Respimat in cystic fibrosis: Phase 3 and Pooled phase 2/3 randomized trials Ratjen, F., Koker, P., Geller, D. E., Langellier-Cocteaux, B., Le Maulf, F., Kattenbeck, S.,... Elborn, J. S. (2015).
TRANSPARENCY COMMITTEE
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 5 November 2014 KALYDECO 150 mg, film-coated tablet B/56 (CIP: 34009 266 060 5 3) Applicant: VERTEX INN ATC code Reason
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 5 November 2014 KALYDECO 150 mg, film-coated tablet B/56 (CIP: 34009 266 060 5 3) Applicant: VERTEX INN ATC code Reason
At-A-Glance report 2014
 At-A-Glance report 14 Cystic Fibrosis in Europe Facts and Figures 14 The European Cystic Fibrosis Society Patient Registry (ECFSPR) is happy to present this report with key information about how cystic
At-A-Glance report 14 Cystic Fibrosis in Europe Facts and Figures 14 The European Cystic Fibrosis Society Patient Registry (ECFSPR) is happy to present this report with key information about how cystic
Cystic fibrosis: From childhood to adulthood. Eitan Kerem Department of Pediatrics and CF Center Hadassah University Hospital Jerusalem Israel
 Cystic fibrosis: From childhood to adulthood Eitan Kerem Department of Pediatrics and CF Center Hadassah University Hospital Jerusalem Israel Vas deference H 2 O Cl - Na + H 2 O Na + Cl - Cl - Cl -
Cystic fibrosis: From childhood to adulthood Eitan Kerem Department of Pediatrics and CF Center Hadassah University Hospital Jerusalem Israel Vas deference H 2 O Cl - Na + H 2 O Na + Cl - Cl - Cl -
National Horizon Scanning Centre. Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis. April 2008
 Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
Outcome measures for clinical trials assessing treatment of cystic fibrosis lung disease
 Review: Clinical Trial Methodology Outcome measures for clinical trials assessing treatment of cystic fibrosis lung disease Clin. Invest. (2012) 2(2), 163 175 Cystic fibrosis (CF) is a complex genetic
Review: Clinical Trial Methodology Outcome measures for clinical trials assessing treatment of cystic fibrosis lung disease Clin. Invest. (2012) 2(2), 163 175 Cystic fibrosis (CF) is a complex genetic
A Quick Guide to the 621+1G T. Mutation CFTR SCIENCE
 Quick uide to the 621+1 Mutation FR SIENE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of FR activity is the underlying cause of cystic fibrosis (F) 1 Spectrum of Phenotypes
Quick uide to the 621+1 Mutation FR SIENE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of FR activity is the underlying cause of cystic fibrosis (F) 1 Spectrum of Phenotypes
Improving rate of decline of FEV1 in young adults with cystic
 Thorax Online First, published on December 29, 2005 as 10.1136/thx.2005.043372 Improving rate of decline of FEV1 in young adults with cystic fibrosis Chengli Que, Paul Cullinan, Duncan Geddes Department
Thorax Online First, published on December 29, 2005 as 10.1136/thx.2005.043372 Improving rate of decline of FEV1 in young adults with cystic fibrosis Chengli Que, Paul Cullinan, Duncan Geddes Department
C.S. HAWORTH 1, A. WANNER 2, J. FROEHLICH 3, T. O'NEAL 3, A. DAVIS 4, I. GONDA 3, A. O'DONNELL 5
 Inhaled Liposomal Ciprofloxacin in Patients With Non-Cystic Fibrosis Bronchiectasis and Chronic Pseudomonas aeruginosa: Results From Two Parallel Phase III Trials (ORBIT-3 and -4) C.S. HAWORTH 1, A. WANNER
Inhaled Liposomal Ciprofloxacin in Patients With Non-Cystic Fibrosis Bronchiectasis and Chronic Pseudomonas aeruginosa: Results From Two Parallel Phase III Trials (ORBIT-3 and -4) C.S. HAWORTH 1, A. WANNER
Plenary III: Without Mental Health
 Plenary III: There is No Health Without Mental Health Alexandra Quittner Disclosures Investigator initiated grants: Novartis & Insmed Consultant to Vertex, AbbVie, and Novartis Research support from CF
Plenary III: There is No Health Without Mental Health Alexandra Quittner Disclosures Investigator initiated grants: Novartis & Insmed Consultant to Vertex, AbbVie, and Novartis Research support from CF
Phase 1 and 2 Data for Triple Combination Regimens Demonstrate Improvements in Lung Function and Other Measures in CF Patients
 Phase 1 and 2 Data for Triple Combination Regimens Demonstrate Improvements in Lung Function and Other Measures in CF Patients July 18, 2017 Agenda Introduction Michael Partridge, VP Investor Relations
Phase 1 and 2 Data for Triple Combination Regimens Demonstrate Improvements in Lung Function and Other Measures in CF Patients July 18, 2017 Agenda Introduction Michael Partridge, VP Investor Relations
Cavosonstat Phase 2 Trial Results. November 28 th, 2016
 Phase 2 Trial Results November 28 th, 2016 Nivalis Therapeutics 2016 Agenda Introduction Mike Carruthers, Chief Financial Officer Initial Remarks Jon Congleton, President and CEO Data Highlights David
Phase 2 Trial Results November 28 th, 2016 Nivalis Therapeutics 2016 Agenda Introduction Mike Carruthers, Chief Financial Officer Initial Remarks Jon Congleton, President and CEO Data Highlights David
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Donaldson SH, Bennett WD, Zeman KL, et al. Mucus clearance
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Donaldson SH, Bennett WD, Zeman KL, et al. Mucus clearance
Efficacy of NaCl nebulized hypertonic solutions in cystic fibrosis
 Acta Biomed 2014; Vol. 85, Supplement 4: 10-18 Mattioli 1885 Original article Efficacy of NaCl nebulized hypertonic solutions in cystic fibrosis Azienda Ospedaliero Universitaria Policlinico, DAI Scienze
Acta Biomed 2014; Vol. 85, Supplement 4: 10-18 Mattioli 1885 Original article Efficacy of NaCl nebulized hypertonic solutions in cystic fibrosis Azienda Ospedaliero Universitaria Policlinico, DAI Scienze
A Quick Guide to the. CFTRdele2,3. Mutation CFTR SCIENCE
 Quick uide to the FRdele2,3 Mutation FR SIENE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of FR activity is the underlying cause of cystic fibrosis (F) 1 Spectrum of Phenotypes
Quick uide to the FRdele2,3 Mutation FR SIENE 2016 Vertex Pharmaceuticals Incorporated VXR-HQ-02-00045a(1) 03/2016 Loss of FR activity is the underlying cause of cystic fibrosis (F) 1 Spectrum of Phenotypes
Cost-effectiveness of Ivacaftor (Kalydeco ) for the treatment of cystic fibrosis in patients age 6 years and older who have the G551D mutation
 Cost-effectiveness of Ivacaftor (Kalydeco ) for the treatment of cystic fibrosis in patients age 6 years and older who have the G551D mutation January 2013 1. A rapid review submission on the drug ivacaftor
Cost-effectiveness of Ivacaftor (Kalydeco ) for the treatment of cystic fibrosis in patients age 6 years and older who have the G551D mutation January 2013 1. A rapid review submission on the drug ivacaftor
Clinical Commissioning Policy Proposition: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (Adults)
 Clinical Commissioning Policy Proposition: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (Adults) Reference: NHS England 1621 First published: Month Year Prepared
Clinical Commissioning Policy Proposition: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (Adults) Reference: NHS England 1621 First published: Month Year Prepared
A contemporary survival analysis of individuals with cystic fibrosis: a cohort study
 ORIGINAL ARTICLE CYSTIC FIBROSIS A contemporary survival analysis of individuals with cystic fibrosis: a cohort study Anne L. Stephenson 1 4, Melissa Tom 2, Yves Berthiaume 5, Lianne G. Singer 4,6, Shawn
ORIGINAL ARTICLE CYSTIC FIBROSIS A contemporary survival analysis of individuals with cystic fibrosis: a cohort study Anne L. Stephenson 1 4, Melissa Tom 2, Yves Berthiaume 5, Lianne G. Singer 4,6, Shawn
Azithromycin may antagonize inhaled tobramycin when targeting P. aeruginosa in cystic fibrosis
 Data Supplement Azithromycin may antagonize inhaled tobramycin when targeting P. aeruginosa in cystic fibrosis Jerry A. Nick 1, Samuel M. Moskowitz 2, James F. Chmiel 3, Anna V. Forssén 4, Sun Ho Kim 2,
Data Supplement Azithromycin may antagonize inhaled tobramycin when targeting P. aeruginosa in cystic fibrosis Jerry A. Nick 1, Samuel M. Moskowitz 2, James F. Chmiel 3, Anna V. Forssén 4, Sun Ho Kim 2,
A BS TR AC T. n engl j med 363;21 nejm.org november 18,
 The new england journal of medicine established in 1812 november 18, 21 vol. 363 no. 21 Effect of VX-77 in Persons with Cystic Fibrosis and the G551D-CFTR Mutation Frank J. Accurso, M.D., Steven M. Rowe,
The new england journal of medicine established in 1812 november 18, 21 vol. 363 no. 21 Effect of VX-77 in Persons with Cystic Fibrosis and the G551D-CFTR Mutation Frank J. Accurso, M.D., Steven M. Rowe,
Macrolide therapy in cystic fibrosis: new developments in clinical use
 Macrolide therapy in cystic fibrosis: new developments in clinical use Clin. Invest. (2013) 3(12), 1179 1186 Macrolide therapy, in particular azithromycin, has been shown to improve aspects of lung health
Macrolide therapy in cystic fibrosis: new developments in clinical use Clin. Invest. (2013) 3(12), 1179 1186 Macrolide therapy, in particular azithromycin, has been shown to improve aspects of lung health
Case Study What is the Relationship Between the Cell Membrane and Cystic Fibrosis?
 Names: Date: Case Study What is the Relationship Between the Cell Membrane and Cystic Fibrosis? Dr. Weyland examined a six month old infant that had been admitted to University Hospital earlier in the
Names: Date: Case Study What is the Relationship Between the Cell Membrane and Cystic Fibrosis? Dr. Weyland examined a six month old infant that had been admitted to University Hospital earlier in the
Key Points: References: Canadian data from the Canadian Cystic Fibrosis Registry 2015 Annual Report normal
 1 2 3 Cystic fibrosis is a rare life-long genetic disease that affects approximately 4,000 people in Canada and about 70,000 worldwide regardless of race or ethnicity but is more common in Caucasians 1,2
1 2 3 Cystic fibrosis is a rare life-long genetic disease that affects approximately 4,000 people in Canada and about 70,000 worldwide regardless of race or ethnicity but is more common in Caucasians 1,2
Arikace (Preclinical Summary)
 Full analyses of data from two phase II blinded and placebo-controlled studies of nebulized liposomal amikacin for inhalation (Arikace ) in the treatment of cystic fibrosis patients with chronic Pseudomonas
Full analyses of data from two phase II blinded and placebo-controlled studies of nebulized liposomal amikacin for inhalation (Arikace ) in the treatment of cystic fibrosis patients with chronic Pseudomonas
Supplementary Appendix
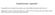 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Accurso FJ, Rowe SM, Clancy JP, et al. Effect of VX-77 in persons
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Accurso FJ, Rowe SM, Clancy JP, et al. Effect of VX-77 in persons
A Case of Cystic Fibrosis
 Name(s) Date A Case of Cystic Fibrosis Dr. Weyland examined a six month old infant that had been admitted to University Hospital earlier in the day. The baby's parents had brought young Zoey to the emergency
Name(s) Date A Case of Cystic Fibrosis Dr. Weyland examined a six month old infant that had been admitted to University Hospital earlier in the day. The baby's parents had brought young Zoey to the emergency
The management of cystic fibrosis (CF) has improved. clinical investigations. Factors Influencing Outcomes in Cystic Fibrosis* A Center-Based Analysis
 clinical investigations Factors Influencing Outcomes in Cystic Fibrosis* A Center-Based Analysis Charles Johnson, MB, ChB; Steven M. Butler, PhD; Michael W. Konstan, MD; Wayne Morgan, MD; and Mary Ellen
clinical investigations Factors Influencing Outcomes in Cystic Fibrosis* A Center-Based Analysis Charles Johnson, MB, ChB; Steven M. Butler, PhD; Michael W. Konstan, MD; Wayne Morgan, MD; and Mary Ellen
Respiratory Research Newsletter
 Date Published: September 2012 Respiratory Research Newsletter Contents Research at the Belfast Trust 1 NICRN Respiratory Health 2 The Respiratory Research Team 3 Our Partners 4 Getting Involved in Upcoming
Date Published: September 2012 Respiratory Research Newsletter Contents Research at the Belfast Trust 1 NICRN Respiratory Health 2 The Respiratory Research Team 3 Our Partners 4 Getting Involved in Upcoming
Cystic Fibrosis. Jennifer McDaniel, BS, RRT-NPS
 Cystic Fibrosis Jennifer McDaniel, BS, RRT-NPS Overview Cystic fibrosis is the most common fatal, inherited disease in the U. S. CF results from a defective autosomal recessive gene One copy of gene =
Cystic Fibrosis Jennifer McDaniel, BS, RRT-NPS Overview Cystic fibrosis is the most common fatal, inherited disease in the U. S. CF results from a defective autosomal recessive gene One copy of gene =
CYSTIC FIBROSIS (CF): THE CHALLENGE OF EARLY, SYSTEMIC PROGRESSION
 CYSTIC FIBROSIS (CF): THE CHALLENGE OF EARLY, SYSTEMIC PROGRESSION A Program for the CF Center Care Team Vertex Pharmaceuticals Incorporated, 50 Northern Avenue, Boston, MA 02210. Vertex and the Vertex
CYSTIC FIBROSIS (CF): THE CHALLENGE OF EARLY, SYSTEMIC PROGRESSION A Program for the CF Center Care Team Vertex Pharmaceuticals Incorporated, 50 Northern Avenue, Boston, MA 02210. Vertex and the Vertex
RESEARCH. Improved survival at low lung function in cystic fibrosis: cohort study from 1990 to 2007
 Improved survival at low lung function in cystic fibrosis: cohort study from 199 to 27 P M George, academic registrar in respiratory medicine, 1 W Banya, medical statistician, 2 N Pareek, specialist trainee
Improved survival at low lung function in cystic fibrosis: cohort study from 199 to 27 P M George, academic registrar in respiratory medicine, 1 W Banya, medical statistician, 2 N Pareek, specialist trainee
CYSTIC FIBROSIS (CF) COMPLICATIONS BEYOND THE LUNGS. A Resource for the CF Center Care Team
 CYSTIC FIBROSIS (CF) COMPLICATIONS BEYOND THE LUNGS A Resource for the CF Center Care Team Vertex Pharmaceuticals Incorporated, 50 Northern Avenue, Boston, MA 02210. Vertex and the Vertex triangle logo
CYSTIC FIBROSIS (CF) COMPLICATIONS BEYOND THE LUNGS A Resource for the CF Center Care Team Vertex Pharmaceuticals Incorporated, 50 Northern Avenue, Boston, MA 02210. Vertex and the Vertex triangle logo
Effect of pulmonary exacerbations on long-term lung function. decline in cystic fibrosis
 ERJ Express. Published on December 1, 2011 as doi: 10.1183/09031936.00159111 Effect of pulmonary exacerbations on long-term lung function decline in cystic fibrosis Valerie Waters 1*, MD, MSc, Sanja Stanojevic
ERJ Express. Published on December 1, 2011 as doi: 10.1183/09031936.00159111 Effect of pulmonary exacerbations on long-term lung function decline in cystic fibrosis Valerie Waters 1*, MD, MSc, Sanja Stanojevic
