NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
|
|
|
- Warren Wiggins
- 6 years ago
- Views:
Transcription
1 Last Updated: Version 4.3a NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set Measure ID#: MORT-30-COPD Performance Measure Name: Hospital 30-day, all-cause, risk-standardized mortality rate following acute exacerbation of Chronic Obstructive Pulmonary Disease (COPD). Description: The measure estimates a hospital-level, risk-standardized mortality rate for patients discharged from the hospital with a principal diagnosis of COPD, as well as those with a principal diagnosis of respiratory failure who had a secondary diagnosis of an acute exacerbation of COPD (AECOPD). Rationale: Risk-standardized mortality rates (RSMRs) can provide important information about quality of care that is currently unavailable to hospitals. Variation in mortality, after adjusting for case-mix, may reflect differences in hospitals' general environments (such as coordination of care, patient safety policies, and staffing) or variation in care processes. Outcome measures can focus attention on a broad set of healthcare activities that affect patients well-being. Moreover, improving outcomes is the ultimate goal of quality improvement, and so the inclusion of outcomes measures assists in attaining improvement goals. COPD is a common condition with substantial mortality and morbidity. The condition imposes a substantial burden on patients and the health care system, and there is marked variation in outcomes by institution. Type of Measure: Outcome Improvement Noted As: A decrease in the RSMR. Numerator Statement: This outcome measure does not have a traditional numerator and denominator like a core process measure (e.g., percentage of adult patients with diabetes aged years receiving one or more hemoglobin A1c tests per year); thus, we are using this field to define our outcome. The calculation of the rate is defined below under Measure Calculation. The outcome for this measure is 30-day all-cause mortality. We define mortality as death from any cause within 30 days after the index admission date. Discharges (1Q15) through (3Q15) 10-20
2 Denominator Statement: The target population for this measure includes admissions for Medicare Fee-for- Service (FFS) beneficiaries aged 65 years discharged from acute care non-federal hospitals, having a principal discharge diagnosis of COPD, as well as those with a principal diagnosis of respiratory failure who had a secondary diagnosis of AECOPD. Included Populations: Admissions for Medicare FFS beneficiaries aged 65 years discharged from non-federal acute care hospitals, having a principal discharge diagnosis of COPD, as well as those with a principal diagnosis of respiratory failure who had a secondary diagnosis of AECOPD. CMS FFS beneficiaries hospitalized within an acute care non-federal hospital are included if they have been enrolled in Part A and Part B Medicare for the 12 months prior to the date of admission to ensure a full year of administrative data for riskadjustment. For patients with more than one admission in a given year for a given condition, only one admission is randomly selected to include in the cohort (others are excluded). The measure includes patients who are admitted to an acute care hospital with a diagnosis of COPD and then transferred to another acute facility if the primary discharge diagnosis is COPD at the second hospital. The measure considers admission to the first hospital as the start of an acute episode of care and assigns the patient s outcome to the hospital that initially admitted them. ICD-9-CM codes that define the patient cohort Obstructive chronic bronchitis; with (acute) exacerbation; acute exacerbation of COPD, decompensated COPD, decompensated COPD with exacerbation Obstructive chronic bronchitis; with acute bronchitis Other chronic bronchitis. Chronic: tracheitis, tracheobronchitis Unspecified chronic bronchitis Other emphysema; emphysema (lung or pulmonary): NOS, centriacinar, centrilobular, obstructive, panacinar, panlobular, unilateral, vesicular. MacLeod's syndrome; Swyer-James syndrome; unilateral hyperlucent lung Chronic obstructive asthma; asthma with COPD, chronic asthmatic bronchitis, unspecified Chronic obstructive asthma; asthma with COPD, Chronic asthmatic bronchitis, with status asthmaticus Chronic obstructive asthma; asthma with COPD, chronic asthmatic bronchitis, with (acute) exacerbation 496 Chronic: nonspecific lung disease, obstructive lung disease, obstructive pulmonary disease (COPD) NOS. NOTE: This code is not to be used with any code from categories * Other diseases of lung; acute respiratory failure; respiratory failure NOS * Other diseases of lung; acute respiratory failure; other pulmonary insufficiency, acute respiratory distress * Other diseases of lung; acute respiratory failure; acute and chronic respiratory failure Discharges (1Q15) through (3Q15) 10-21
3 799.1* Other ill-defined and unknown causes of morbidity and mortality; respiratory arrest, cardiorespiratory failure *Patients with a principal diagnosis represented by these codes are included in the measure if the code is accompanied by a secondary diagnosis of AECOPD (491.21, , , or ) Excluded Populations: The measure excludes admissions for patients: with inconsistent or unknown mortality status or other unreliable data (e.g. date of death precedes admission date) who were transferred from another acute care hospital (because the death is attributed to the hospital where the patient was initially admitted) enrolled in the Medicare Hospice program any time in the 12 months prior to the index hospitalization including the first day of the index admission (since it is likely these patients are continuing to seek comfort measures only) who were discharged against medical advice (AMA) (because providers did not have the opportunity to deliver full care and prepare the patient for discharge) Risk Adjustment: For each patient, covariates are obtained from administrative data extending 12 months prior to, and including, the index admission. For all patients, information from Medicare inpatient claims, physician Part B claims and hospital outpatient claims are used for risk adjustment. Inpatient claim records have data on hospitalization for and include demographic information, principal and secondary diagnosis codes, and procedure codes. Diagnosis codes for comorbidities are also collected from physician and hospital outpatient files. These data are captured from the claim(s) for the index admission and from all inpatient and outpatient claims for the entire year before the patient s index COPD hospitalization to be utilized in the riskadjustment model. Only variables that convey information about patients clinical status at the time of admission are used for the risk-adjustment, while complications that arise during the course of patients index hospitalization are not included in the model. Full details of the development of the risk-standardization model for this measure are available at: Discharges (1Q15) through (3Q15) 10-22
4 The final set of risk-adjustment variables included: Demographics Age Cardiovascular/ Respiratory Comorbidity Sleep Apnea History of Mechanical Ventilation Respirator Dependence/Respiratory Failure Cardio-Respiratory Failure and Shock Congestive Heart Failure Chronic Atherosclerosis Arrhythmias Vascular or Circulatory Disease Fibrosis of Lung and Other Chronic Lung Disorder Asthma Pneumonia Pleural Effusion/Pneumothorax Other Lung Disorders Metastatic Cancer and Acute Leukemia Lung, Upper Digestive Tract, and Other Severe Cancers Lymphatic, Head and Neck, Brain, and Other Major Cancers; Breast, Prostate, Colorectal and Other Cancers and Tumors; Other Respiratory and Heart Neoplasms Other Digestive and Urinary Neoplasms Diabetes and DM Complications Protein-calorie Malnutrition Disorders of Fluid/Electrolyte/Acid-Base Other Endocrine/Metabolic/Nutritional Disorders Other Gastrointestinal Disorders Osteoarthritis of Hip or Knee Other Musculoskeletal and Connective Tissue Disorders Iron Deficiency and Other/Unspecified Anemias and Blood Disease Dementia and Senility Drug/Alcohol Abuse, Without Dependence Other Psychiatric Disorders Quadriplegia, Paraplegia, Functional Disability Mononeuropathy, Other Neurological Conditions/Injuries Hypertension and Hypertensive Disease Stroke Retinal Disorders, Except Detachment and Vascular Retinopathies Other Eye Disorders Other Ear, Nose, Throat, and Mouth Disorders Renal Failure Decubitus Ulcer or Chronic Skin Ulcer Other Dermatological Disorders Trauma Vertebral Fractures Major Complications of Medical Care and Trauma Discharges (1Q15) through (3Q15) 10-23
5 Model Validation: We computed several summary statistics for assessing logistic regression (patient-level) model performance, which included over-fitting indices, predictive ability, area under the receiver operating characteristic (ROC) curve, distribution of residuals, and model chi-square. Model performance is similar in the development and validation samples, with strong model discrimination and fit. Predictive ability is also similar in both samples. The C statistic (area under the receiver operator curve) is 0.72 when the model is applied to either the development or validation sample. Data Accuracy: The administrative claims data used to calculate the measure are maintained by CMS' Office of Information Services. These data undergo additional quality assurance checks during measure development and maintenance. Measure Analysis Suggestions: None Sampling: No. Data Reported As: Hospital 30-day, all-cause, risk-standardized mortality rate (RSMR) following acute exacerbation of Chronic Obstructive Pulmonary Disease (COPD). Measure Calculation: The measure estimates hospital-level 30-day all-cause RSMR for COPD using hierarchical logistic regression modeling. In brief, the approach simultaneously models two levels (patient and hospital) to account for the variance in patient outcomes within and between hospitals. At the patient level, the model adjusts the log-odds of mortality within 30 days of admission for age, sex, selected clinical covariates, and a hospitalspecific intercept. At the hospital level, it models the hospital-specific intercepts as arising from a normal distribution. The hospital intercept represents the underlying risk of mortality at the hospital, after accounting for patient risk. The hospital-specific intercepts are given a distribution in order to account for the clustering (nonindependence) of patients within the same hospital. If there were no differences among hospitals, then after adjusting for patient risk, the hospital intercepts should be identical across all hospitals. The RSMR is calculated as the ratio of the number of predicted deaths to the number of expected deaths, multiplied by the national unadjusted mortality rate. For each hospital, the numerator of the ratio is the number of deaths within 30 days predicted on the basis of the hospital s performance with its observed case-mix, and the denominator is the number of deaths expected on the basis of the nation s performance with that hospital s case-mix. This approach is analogous to a ratio of observed to expected used in other types of statistical analyses. It conceptually allows for a comparison of a particular hospital s performance given its case-mix to an average hospital s performance with the same case-mix. Thus, a lower ratio indicates lower-than-expected mortality or better quality, and a higher ratio indicates higher-thanexpected mortality or worse quality. The predicted number of deaths (the numerator) is calculated by regressing the risk factors and the hospital-specific intercept on the risk of mortality, multiplying the estimated regression coefficients by the patient characteristics in the hospital, Discharges (1Q15) through (3Q15) 10-24
6 transforming, and then summing over all patients attributed to the hospital to get a value. The expected number of deaths (the denominator) is obtained by regressing the risk factors and a common intercept on the mortality outcome using all hospitals in our sample, multiplying the subsequent estimated regression coefficients by the patient characteristics observed in the hospital, transforming, and then summing over all patients in the hospital to get a value. To assess hospital performance in any reporting period, we re-estimate the model coefficients using the years of data in that period. The statistical modeling approach is described fully in the original methodology report. Selected References: Drye EE, Lindenauer P, Wang C, et al Version Measure Updates and Specifications Report: Hospital-level 30-day Mortality Following an Admission for an Acute Exacerbation of Chronic Obstructive Pulmonary Disease. Faustini A, Marino C, D'Ippoliti D, Forastiere F, Belleudi V, Purcci CA. The impact on risk-factor analysis of different mortality outcomes in COPD patients. European Respiratory Journal. September 2008;32(3): Grosso LM, Lindenauer P, Wang C, et al Hospital-level 30-day Mortality Following Admission for an Acute Exacerbation of Chronic Obstructive Pulmonary Disease: Measure Methodology Report. Krumholz HM, Brindis RG, Brush JE, et al Standards for Statistical Models Used for Public Reporting of Health Outcomes: An American Heart Association Scientific Statement From the Quality of Care and Outcomes Research Interdisciplinary Writing Group: Cosponsored by the Council on Epidemiology and Prevention and the Stroke Council Endorsed by the American College of Cardiology Foundation. Circulation 113: Lindenauer PK, Oekow P, Gao S, Crawford AS, Gutierrez B, Benjamin EM. Quality of care for patients hospitalized for acute exacerbations of chronic obstructive pulmonary disease. Ann Intern Med. June ;144(12): Normand S-LT, Shahian DM Statistical and clinical aspects of hospital outcomes profiling. Stat Sci 22(2): Patil SP, Krishnan JA, Lichtzin N, Diette GB. In-Hospital Mortality Following Acute Exacerbations of Chronic Obustructive Pulmonary Disease. Archives of Interanl Medicine. 2003;163(10). Tabak YP, Sun X, Johannes RS, et al. Mortality and need for mechanical ventilation in acute exacerbations of chronic obstructive pulmonary disease: development and validation of a simple risk score. Archives of Internal Medicine. 2009;169(17). Discharges (1Q15) through (3Q15) 10-25
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Supplementary Online Content
 Supplementary Online Content Dharmarajan K, Wang Y, Lin Z, et al. Association of changing hospital readmission rates with mortality rates after hospital discharge. JAMA. doi:10.1001/jama.2017.8444 etable
Supplementary Online Content Dharmarajan K, Wang Y, Lin Z, et al. Association of changing hospital readmission rates with mortality rates after hospital discharge. JAMA. doi:10.1001/jama.2017.8444 etable
Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: New Measure Version 4.4a Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Episode-of-Care Payment Measures Set Measure ID #: PAYM-30-HF Performance
Last Updated: New Measure Version 4.4a Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Episode-of-Care Payment Measures Set Measure ID #: PAYM-30-HF Performance
NATIONAL QUALITY FORUM
 TO: NQF Members and Public FR: NQF Staff RE: Pre-comment review of an addendum to National Voluntary Consensus Standards: Cardiovascular Endorsement Maintenance 2010: A Consensus Report DA: October 6,
TO: NQF Members and Public FR: NQF Staff RE: Pre-comment review of an addendum to National Voluntary Consensus Standards: Cardiovascular Endorsement Maintenance 2010: A Consensus Report DA: October 6,
Appendix Identification of Study Cohorts
 Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
APPENDIX EXHIBITS. Appendix Exhibit A2: Patient Comorbidity Codes Used To Risk- Standardize Hospital Mortality and Readmission Rates page 10
 Ross JS, Bernheim SM, Lin Z, Drye EE, Chen J, Normand ST, et al. Based on key measures, care quality for Medicare enrollees at safety-net and non-safety-net hospitals was almost equal. Health Aff (Millwood).
Ross JS, Bernheim SM, Lin Z, Drye EE, Chen J, Normand ST, et al. Based on key measures, care quality for Medicare enrollees at safety-net and non-safety-net hospitals was almost equal. Health Aff (Millwood).
2011 Measures Maintenance Technical Report: Acute Myocardial Infarction, Heart Failure, and Pneumonia 30 Day Risk Standardized Readmission Measures
 2011 Measures Maintenance Technical Report: Acute Myocardial Infarction, Heart Failure, and Pneumonia 30 Day Risk Standardized Readmission Measures Submitted By Yale New Haven Health Services Corporation
2011 Measures Maintenance Technical Report: Acute Myocardial Infarction, Heart Failure, and Pneumonia 30 Day Risk Standardized Readmission Measures Submitted By Yale New Haven Health Services Corporation
Supplementary Online Content
 Supplementary Online Content Khera R, Dharmarajan K, Wang Y, et al. Association of the hospital readmissions reduction program with mortality during and after hospitalization for acute myocardial infarction,
Supplementary Online Content Khera R, Dharmarajan K, Wang Y, et al. Association of the hospital readmissions reduction program with mortality during and after hospitalization for acute myocardial infarction,
Hu J, Gonsahn MD, Nerenz DR. Socioeconomic status and readmissions: evidence from an urban teaching hospital. Health Aff (Millwood). 2014;33(5).
 Appendix Definitions of Index Admission and Readmission Definitions of index admission and readmission follow CMS hospital-wide all-cause unplanned readmission (HWR) measure as far as data are available.
Appendix Definitions of Index Admission and Readmission Definitions of index admission and readmission follow CMS hospital-wide all-cause unplanned readmission (HWR) measure as far as data are available.
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Appendix 1: Supplementary tables [posted as supplied by author]
![Appendix 1: Supplementary tables [posted as supplied by author] Appendix 1: Supplementary tables [posted as supplied by author]](/thumbs/81/83505567.jpg) Appendix 1: Supplementary tables [posted as supplied by author] Table A. International Classification of Diseases, Ninth Revision, Clinical Modification Codes Used to Define Heart Failure, Acute Myocardial
Appendix 1: Supplementary tables [posted as supplied by author] Table A. International Classification of Diseases, Ninth Revision, Clinical Modification Codes Used to Define Heart Failure, Acute Myocardial
2016 Condition-Specific Measures Updates and Specifications Report Hospital-Level 30-Day Risk-Standardized Readmission Measures
 2016 Condition-Specific Measures Updates and Specifications Report Hospital-Level 30-Day Risk-Standardized Readmission Measures Acute Myocardial Infarction Version 9.0 Chronic Obstructive Pulmonary Disease
2016 Condition-Specific Measures Updates and Specifications Report Hospital-Level 30-Day Risk-Standardized Readmission Measures Acute Myocardial Infarction Version 9.0 Chronic Obstructive Pulmonary Disease
Objectives. Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers
 Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Supplementary Online Content
 Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Writing Committee. ACP Performance Measurement Committee Members*
 Performance Measurement Coronary Artery Bypass Graft Surgery: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem,
Performance Measurement Coronary Artery Bypass Graft Surgery: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Krumholz HM, Wang K, Lin Z, et al. Hospital-readmission risk
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Krumholz HM, Wang K, Lin Z, et al. Hospital-readmission risk
National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 2 As of March 5, 2010
 National Voluntary Consensus Standards for Patient Outcomes Table of s Submitted-Phase 2 As of March 5, 2010 Note: This information is for personal and noncommercial use only. You may not modify, reformat,
National Voluntary Consensus Standards for Patient Outcomes Table of s Submitted-Phase 2 As of March 5, 2010 Note: This information is for personal and noncommercial use only. You may not modify, reformat,
TOTAL HIP AND KNEE REPLACEMENTS. FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES
 TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
ACOFP 55th Annual Convention & Scientific Seminars. How Complicated is Your Panel? Effective Risk Coding in Primary Care. Alison Mancuso, DO, FACOFP
 8 ACOFP 55th Annual Convention & Scientific Seminars How Complicated is Your Panel? Effective Risk Coding in Primary Care Alison Mancuso, DO, FACOFP How Complicated is Your Panel?: Effective Risk Coding
8 ACOFP 55th Annual Convention & Scientific Seminars How Complicated is Your Panel? Effective Risk Coding in Primary Care Alison Mancuso, DO, FACOFP How Complicated is Your Panel?: Effective Risk Coding
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes Acute COPD exacerbation (COPD); Screening and surveillance colonoscopy (COL); and Outpatient and non-acute
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes Acute COPD exacerbation (COPD); Screening and surveillance colonoscopy (COL); and Outpatient and non-acute
Mortality Risk Adjustment and HCCs: Is This the New 'Sweet Spot' for Physician Buy In?
 Mortality Risk Adjustment and HCCs: Is This the New 'Sweet Spot' for Physician Buy In? Kyra Brown, RHIA, CCS, CCDS Clinical Documentation Manager/Educator Erlanger Chattanooga, TN 1 Learning Objectives
Mortality Risk Adjustment and HCCs: Is This the New 'Sweet Spot' for Physician Buy In? Kyra Brown, RHIA, CCS, CCDS Clinical Documentation Manager/Educator Erlanger Chattanooga, TN 1 Learning Objectives
Episodes of Care Risk Adjustment
 Episodes of Care Risk Adjustment Episode Types Wave 1 Asthma Acute Exacerbation Perinatal Total Joint Replacement Wave 2 Acute Percutaneous Coronary Intervention COPD Acute Exacerbation Non-acute Percutaneous
Episodes of Care Risk Adjustment Episode Types Wave 1 Asthma Acute Exacerbation Perinatal Total Joint Replacement Wave 2 Acute Percutaneous Coronary Intervention COPD Acute Exacerbation Non-acute Percutaneous
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments
 Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis
 Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes Respiratory Infection (RI); Pneumonia (PNA); Inpatient Urinary Tract Infection (UTI-I; Outpatient Urinary
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes Respiratory Infection (RI); Pneumonia (PNA); Inpatient Urinary Tract Infection (UTI-I; Outpatient Urinary
TECHNICAL NOTES APPENDIX SUMMER
 TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM JULY 1, 2006 THROUGH JUNE 30, 2007 The Pennsylvania Health Care Cost Containment
TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM JULY 1, 2006 THROUGH JUNE 30, 2007 The Pennsylvania Health Care Cost Containment
An Introduction to MPRO. Harolyn Baker, MPH Director Applied Epidemiology and Evaluation
 An Introduction to MPRO Harolyn Baker, MPH Director Applied Epidemiology and Evaluation 2 MISSION & VISION Mission: Improving quality, safety and efficiency across the healthcare continuum. Vision: To
An Introduction to MPRO Harolyn Baker, MPH Director Applied Epidemiology and Evaluation 2 MISSION & VISION Mission: Improving quality, safety and efficiency across the healthcare continuum. Vision: To
JAMA, January 11, 2012 Vol 307, No. 2
 JAMA, January 11, 2012 Vol 307, No. 2 Dementia is associated with increased rates and often poorer outcomes of hospitalization Worsening cognitive status Adequate chronic disease management is more difficult
JAMA, January 11, 2012 Vol 307, No. 2 Dementia is associated with increased rates and often poorer outcomes of hospitalization Worsening cognitive status Adequate chronic disease management is more difficult
THE NATIONAL QUALITY FORUM
 THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
Arkansas Health Care Payment Improvement Initiative COPD Algorithm Summary
 Arkansas Health Care Payment Improvement Initiative COPD Algorithm Summary Chronic Obstructive Pulmonary Disease (COPD) Algorithm Summary v1.6 Page 2 of 6 Triggers PAP Assignment Exclusions Episode Time
Arkansas Health Care Payment Improvement Initiative COPD Algorithm Summary Chronic Obstructive Pulmonary Disease (COPD) Algorithm Summary v1.6 Page 2 of 6 Triggers PAP Assignment Exclusions Episode Time
Session Guidelines. This is a 15 minute webinar session for CNC physicians and staff
 Respiratory Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars monthly to address topics related to risk adjustment documentation and coding
Respiratory Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars monthly to address topics related to risk adjustment documentation and coding
79 HCCs CMS-HCC Risk Adjustment Model. ICD-10-CM to CMS-HCC Crosswalk. Over 9,500 ICD-10-CM codes map to one or more.
 2017 CMS-HCC Risk Adjustment Model Over 9,500 ICD-10-CM codes map to one or more 79 HCCs ICD-10-CM to CMS-HCC Crosswalk CMS-HCC Model On April 4, 2016, the Centers for Medicare & Medicaid Services (CMS)
2017 CMS-HCC Risk Adjustment Model Over 9,500 ICD-10-CM codes map to one or more 79 HCCs ICD-10-CM to CMS-HCC Crosswalk CMS-HCC Model On April 4, 2016, the Centers for Medicare & Medicaid Services (CMS)
Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians
 Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
A chapter by chapter look at the ICD-10-CM code set Coding Tip Sheet
 Coding Tip Sheet Chapter 1 - Certain Infectious and Parasitic Diseases Terminology changes: The term Sepsis (ICD-10-CM) has replaced the term Septicemia (ICD-9-CM) Urosepsis is a nonspecific term and is
Coding Tip Sheet Chapter 1 - Certain Infectious and Parasitic Diseases Terminology changes: The term Sepsis (ICD-10-CM) has replaced the term Septicemia (ICD-9-CM) Urosepsis is a nonspecific term and is
DRG Code DRG Description FY18 Average Charge
 DRG Code DRG Description FY18 Average Charge 3 ECMO OR TRACH W MV 96+ HRS OR PDX EXC FACE, MOUTH & NECK W MAJ O $ 665,511 4 TRACH W MV 96+ HRS OR PDX EXC FACE, MOUTH & NECK W/O MAJ O.R. $ 422,497 37 EXTRACRANIAL
DRG Code DRG Description FY18 Average Charge 3 ECMO OR TRACH W MV 96+ HRS OR PDX EXC FACE, MOUTH & NECK W MAJ O $ 665,511 4 TRACH W MV 96+ HRS OR PDX EXC FACE, MOUTH & NECK W/O MAJ O.R. $ 422,497 37 EXTRACRANIAL
ICD-9-CM CODING FUNDAMENTALS CODING EXERCISES
 Steps to Accurate Coding Underline the main term, then locate code: Stenosis of Carotid Artery Transient Ischemic Attack Gastrointestinal hemorrhage Degenerative Joint Disease Coronary Artery Disease Alcoholic
Steps to Accurate Coding Underline the main term, then locate code: Stenosis of Carotid Artery Transient Ischemic Attack Gastrointestinal hemorrhage Degenerative Joint Disease Coronary Artery Disease Alcoholic
WORKING P A P E R. Comparative Performance of the MS-DRGS and RDRGS in Explaining Variation in Cost for Medicare Hospital Discharges BARBARA O.
 WORKING P A P E R Comparative Performance of the MS-DRGS and RDRGS in Explaining Variation in Cost for Medicare Hospital Discharges BARBARA O. WYNN WR-606 This product is part of the RAND Health working
WORKING P A P E R Comparative Performance of the MS-DRGS and RDRGS in Explaining Variation in Cost for Medicare Hospital Discharges BARBARA O. WYNN WR-606 This product is part of the RAND Health working
APR-DRG Description Ave Charge
 Abdominal Pain 16,500.25 2.8 6,000.09 Acute & Subacute Endocarditis 15,339.30 3.0 5,113.10 Acute Myocardial Infarction 17,687.46 2.6 6,802.87 Alcohol Abuse & Dependence 19,126.64 4.2 4,553.96 Alcoholic
Abdominal Pain 16,500.25 2.8 6,000.09 Acute & Subacute Endocarditis 15,339.30 3.0 5,113.10 Acute Myocardial Infarction 17,687.46 2.6 6,802.87 Alcohol Abuse & Dependence 19,126.64 4.2 4,553.96 Alcoholic
Policy Brief June 2014
 Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
In your own words, please write the reason you are here. Please be specific, putting in dates as necessary. Use the back of the form if needed.
 Name: SS# In your own words, please write the reason you are here. Please be specific, putting in dates as necessary. Use the back of the form if needed. Patient Medical, Surgical and Family History Review
Name: SS# In your own words, please write the reason you are here. Please be specific, putting in dates as necessary. Use the back of the form if needed. Patient Medical, Surgical and Family History Review
JAWDA Performance Quarterly KPI Profile (Clinic & Centers) March 2018
 JAWDA Performance KPI Profile (Clinic & Centers) March 2018 1 P a g e Introduction: Physician office, clinic, and healthcare centers provide primary care function including health education, prevention,
JAWDA Performance KPI Profile (Clinic & Centers) March 2018 1 P a g e Introduction: Physician office, clinic, and healthcare centers provide primary care function including health education, prevention,
TECHNICAL NOTES APPENDIX SUMMER
 TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM July 1, 2005 through June 30, 2006 The Pennsylvania Health Care Cost Containment
TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM July 1, 2005 through June 30, 2006 The Pennsylvania Health Care Cost Containment
North Carolina Inpatient Hospital Discharge Data - Data Dictionary FY 2016 Alphabetic List of Variables and Attributes Standard Research File
 North Carolina Inpatient Hospital Discharge Data - Data Dictionary FY 2016 Alphabetic List of Variables and Attributes Standard Research File For a standard research file request one of three variables
North Carolina Inpatient Hospital Discharge Data - Data Dictionary FY 2016 Alphabetic List of Variables and Attributes Standard Research File For a standard research file request one of three variables
At the completion of this educational activity, the learner will be able to understand:
 Claims vs. Submission: Understanding the Difference Sonia Trepina, MPA Director, Risk Adjustment & Ambulatory CDI Services Enjoin Asheville, NC Brett Senor, MD, CRC, CCDS Physician Associate, CDI Quality
Claims vs. Submission: Understanding the Difference Sonia Trepina, MPA Director, Risk Adjustment & Ambulatory CDI Services Enjoin Asheville, NC Brett Senor, MD, CRC, CCDS Physician Associate, CDI Quality
3. Correct coding practice is to select the code with the greater number of characters available.
 Final Exam Part I: Chapters 1 6, Understanding the Fundamentals 1. ICD-10 codes are issued by the World Health Organization (WHO), and updates are published by the Centers for Medicare & Medicaid Services
Final Exam Part I: Chapters 1 6, Understanding the Fundamentals 1. ICD-10 codes are issued by the World Health Organization (WHO), and updates are published by the Centers for Medicare & Medicaid Services
Yale New Haven Health Services Corporation/Center for Outcomes Research and Evaluation (YNHHSC/CORE)
 701 Pennsylvania Avenue, Ste. 800 Washington, DC 20004 2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org July 8, 2011 Yale New Haven Health Services Corporation/Center for Outcomes Research and
701 Pennsylvania Avenue, Ste. 800 Washington, DC 20004 2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org July 8, 2011 Yale New Haven Health Services Corporation/Center for Outcomes Research and
Surgical Outcomes: A synopsis & commentary on the Cardiac Care Quality Indicators Report. May 2018
 Surgical Outcomes: A synopsis & commentary on the Cardiac Care Quality Indicators Report May 2018 Prepared by the Canadian Cardiovascular Society (CCS)/Canadian Society of Cardiac Surgeons (CSCS) Cardiac
Surgical Outcomes: A synopsis & commentary on the Cardiac Care Quality Indicators Report May 2018 Prepared by the Canadian Cardiovascular Society (CCS)/Canadian Society of Cardiac Surgeons (CSCS) Cardiac
ACO #44 Use of Imaging Studies for Low Back Pain
 Measure Information Form (MIF) DATA SOURCE Medicare Claims Medicare beneficiary enrollment data MEASURE SET ID ACO #44 VERSION NUMBER AND EFFECTIVE DATE Version 1, effective 01/01/18 CMS APPROVAL DATE
Measure Information Form (MIF) DATA SOURCE Medicare Claims Medicare beneficiary enrollment data MEASURE SET ID ACO #44 VERSION NUMBER AND EFFECTIVE DATE Version 1, effective 01/01/18 CMS APPROVAL DATE
Technical Appendix for Outcome Measures
 Study Overview Technical Appendix for Outcome Measures This is a report on data used, and analyses done, by MPA Healthcare Solutions (MPA, formerly Michael Pine and Associates) for Consumers CHECKBOOK/Center
Study Overview Technical Appendix for Outcome Measures This is a report on data used, and analyses done, by MPA Healthcare Solutions (MPA, formerly Michael Pine and Associates) for Consumers CHECKBOOK/Center
A Population-Based Study of the Effectiveness of Bisphosphonates at Reducing Hip Fractures among High Risk Women
 A Population-Based Study of the Effectiveness of Bisphosphonates at Reducing Hip Fractures among High Risk Women APHA Conference Washington, DC November 2, 2011 Presenter Disclosures Kathy Schneider, PhD
A Population-Based Study of the Effectiveness of Bisphosphonates at Reducing Hip Fractures among High Risk Women APHA Conference Washington, DC November 2, 2011 Presenter Disclosures Kathy Schneider, PhD
Appendix 1. Frailty as a confounder of the effectiveness of preventive treatment. Abbreviations: t1 = time one. t2 = time 2. This model indicates the
 Appendix 1. Frailty as a confounder of the effectiveness of preventive treatment. Abbreviations: t1 = time one. t2 = time 2. This model indicates the interrelatedness of comorbidity, frailty, and ADL dependency,
Appendix 1. Frailty as a confounder of the effectiveness of preventive treatment. Abbreviations: t1 = time one. t2 = time 2. This model indicates the interrelatedness of comorbidity, frailty, and ADL dependency,
Bundle Payments. Healthcare Systems & Services Presenters: Larry Litman, Tyler Litman
 Bundle Payments Healthcare Systems & Services Presenters: Larry Litman, Tyler Litman To determine the average cost of the SNF portion of a bundle through the analysis of our client data-base. Our Objective:
Bundle Payments Healthcare Systems & Services Presenters: Larry Litman, Tyler Litman To determine the average cost of the SNF portion of a bundle through the analysis of our client data-base. Our Objective:
ERRATA. To: Recipients of TR-213-CMS, RAND Corporation Publications Department
 ERRATA To: Recipients of TR-213-CMS, 2005 From: RAND Corporation Publications Department Date: July 2006 (Please note that this incorporates an Errata from December 2005) Re: Corrected page (p. iii); updated
ERRATA To: Recipients of TR-213-CMS, 2005 From: RAND Corporation Publications Department Date: July 2006 (Please note that this incorporates an Errata from December 2005) Re: Corrected page (p. iii); updated
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Risk Adjustment and Hierarchical Condition Category Coding
 Risk Adjustment 101 Agenda Risk Adjustment Model Hierarchical Condition Categories (HCC) Patient Example Documentation MEAT Documentation Guidance Chronic Conditions Risk Score Calculations Steps for Physician
Risk Adjustment 101 Agenda Risk Adjustment Model Hierarchical Condition Categories (HCC) Patient Example Documentation MEAT Documentation Guidance Chronic Conditions Risk Score Calculations Steps for Physician
Documentation Tips for Pulmonary/Critical Care
 Documentation Tips for Pulmonary/Critical Care ICD-10 classifications: The HARD WAY! J44 Other chronic obstructive pulmonary disease Includes: asthma with chronic obstructive pulmonary disease chronic
Documentation Tips for Pulmonary/Critical Care ICD-10 classifications: The HARD WAY! J44 Other chronic obstructive pulmonary disease Includes: asthma with chronic obstructive pulmonary disease chronic
Drug prescriptions (Pharm) Exposure (36/48 months)
 ANNEX SECTION PART A - Study design: Figure 1 overview of the study design Drug prescriptions (Pharm) 2006-2010 Exposure (36/48 months) flexible time windows (e.g. 90 days) time index date (hospital discharge)
ANNEX SECTION PART A - Study design: Figure 1 overview of the study design Drug prescriptions (Pharm) 2006-2010 Exposure (36/48 months) flexible time windows (e.g. 90 days) time index date (hospital discharge)
Combining Risk Adjustment and HEDIS to Improve Quality of Care. Colleen Gianatasio, CPC, CPC-P, CPMA, CPC-I, CRC
 Combining Risk Adjustment and HEDIS to Improve Quality of Care Colleen Gianatasio, CPC, CPC-P, CPMA, CPC-I, CRC Agenda Improving primary care in today s health care environment Risk adjustment basics (using
Combining Risk Adjustment and HEDIS to Improve Quality of Care Colleen Gianatasio, CPC, CPC-P, CPMA, CPC-I, CRC Agenda Improving primary care in today s health care environment Risk adjustment basics (using
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form
 Last Updated: Version 3.2 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Pneumonia (PN) Set Measure ID #: Measure Information Form Performance Measure Name: Pneumococcal Vaccination
Last Updated: Version 3.2 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Pneumonia (PN) Set Measure ID #: Measure Information Form Performance Measure Name: Pneumococcal Vaccination
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 8 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 8 Episodes Acute Seizure, Syncope, Acute Gastroenteritis, Pediatric Pneumonia, Bronchiolitis, Colposcopy, Hysterectomy,
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 8 Episodes Acute Seizure, Syncope, Acute Gastroenteritis, Pediatric Pneumonia, Bronchiolitis, Colposcopy, Hysterectomy,
In each hospital-year, we calculated a 30-day unplanned. readmission rate among patients who survived at least 30 days
 Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Patient Navigator Program: Focus MI Diplomat Hospital Metrics
 Patient Navigator Program: Focus MI Diplomat Hospital Metrics Goal Statement: To reduce avoidable hospital readmissions for patients discharged with acute myocardial infarction (AMI) by supporting a culture
Patient Navigator Program: Focus MI Diplomat Hospital Metrics Goal Statement: To reduce avoidable hospital readmissions for patients discharged with acute myocardial infarction (AMI) by supporting a culture
Heart Attack Readmissions in Virginia
 Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Polling Question #1. Risk Adjustment in the Inpatient Hospital Setting
 1 Risk Adjustment in the Inpatient Hospital Setting Mark N. Dominesey, RN, BSN, MBA, CCDS, CDIP, CHTS CP Manager of CDI Children s National Medical Center Washington, DC 2 Polling Question #1 Does your
1 Risk Adjustment in the Inpatient Hospital Setting Mark N. Dominesey, RN, BSN, MBA, CCDS, CDIP, CHTS CP Manager of CDI Children s National Medical Center Washington, DC 2 Polling Question #1 Does your
Quality measures a for measurement year 2016
 Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
Methodological Issues
 Methodological Issues Presentation by Ian Brownwood for the meeting of Health Promotion, Prevention and Primary Care Subgroup 22 October, 2009, Paris The Indicators Asthma* Chronic Obstructive Pulmonary
Methodological Issues Presentation by Ian Brownwood for the meeting of Health Promotion, Prevention and Primary Care Subgroup 22 October, 2009, Paris The Indicators Asthma* Chronic Obstructive Pulmonary
ICD-10 Physician Education. Palliative Care SIP
 ICD-10 Physician Education Palliative Care SIP 1 Training Objectives ICD-9 to ICD-10 Comparison Documentation Tips Additional Educational Opportunities Questions 2 ICD-9 to ICD-10 Comparison Code Structure
ICD-10 Physician Education Palliative Care SIP 1 Training Objectives ICD-9 to ICD-10 Comparison Documentation Tips Additional Educational Opportunities Questions 2 ICD-9 to ICD-10 Comparison Code Structure
ABF and Implications for Coding Helen Nolan
 ABF and Implications for Coding Helen Nolan 11 th May 2017 1 ABF explained What is ABF What are DRGs What are MDCs 2 What is Activity Based Funding (ABF) ABF is a way of funding hospitals for the number
ABF and Implications for Coding Helen Nolan 11 th May 2017 1 ABF explained What is ABF What are DRGs What are MDCs 2 What is Activity Based Funding (ABF) ABF is a way of funding hospitals for the number
Arkansas Health Care Payment Improvement Initiative Percutaneous Coronary Intervention Algorithm Summary
 Arkansas Health Care Payment Improvement Initiative Percutaneous Coronary Intervention Algorithm Summary Percutaneous Coronary Intervention (PCI) Algorithm Summary v1.0 Page 2 of 8 Triggers PAP assignment
Arkansas Health Care Payment Improvement Initiative Percutaneous Coronary Intervention Algorithm Summary Percutaneous Coronary Intervention (PCI) Algorithm Summary v1.0 Page 2 of 8 Triggers PAP assignment
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes Attention deficit hyperactivity disorder (ADHD); Opposition defiance disorder (ODD); Coronary artery bypass
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes Attention deficit hyperactivity disorder (ADHD); Opposition defiance disorder (ODD); Coronary artery bypass
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual
 Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Top 10 ICD-10 Coding Errors (and how to fix them!) Presented by Jennifer Warfield, BSN, HCS-D, COS-C Education Director, PPS Plus
 (and how to fix them!) Presented by Jennifer Warfield, BSN, HCS-D, COS-C Education Director, PPS Plus Top 10 ICD-10 Coding Errors (and how to fix them!) Top 10 Primary Diagnoses In ICD-10 ICD-10 Codes
(and how to fix them!) Presented by Jennifer Warfield, BSN, HCS-D, COS-C Education Director, PPS Plus Top 10 ICD-10 Coding Errors (and how to fix them!) Top 10 Primary Diagnoses In ICD-10 ICD-10 Codes
Pulmonary and Critical Care
 Pulmonary and Critical Care 2015-2016 DRAFT REPORT FOR COMMENT April 21, 2016 This report is funded by the Department of Health and Human Services under contract HHSM-500-2012-00009I Task Order HHSM-500-T0000
Pulmonary and Critical Care 2015-2016 DRAFT REPORT FOR COMMENT April 21, 2016 This report is funded by the Department of Health and Human Services under contract HHSM-500-2012-00009I Task Order HHSM-500-T0000
ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS
 R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
TN Bundled Payment Initiative: Overview of Episode Risk Adjustment
 TN Bundled Payment Initiative: Overview of Episode Risk Adjustment United Healthcare, April 2014 The State of Tennessee has implemented an episode-based approach to reimburse providers for the care delivered
TN Bundled Payment Initiative: Overview of Episode Risk Adjustment United Healthcare, April 2014 The State of Tennessee has implemented an episode-based approach to reimburse providers for the care delivered
PRINCIPAL ACCOUNTABLE PROVIDER MANUAL
 Health Care Payment Improvement Building a healthier future for all Arkansans Arkansas Payment Improvement Initiative Episodes of Care PRINCIPAL ACCOUNTABLE PROVIDER MANUAL COPD Episode Reimbursement Program
Health Care Payment Improvement Building a healthier future for all Arkansans Arkansas Payment Improvement Initiative Episodes of Care PRINCIPAL ACCOUNTABLE PROVIDER MANUAL COPD Episode Reimbursement Program
Understanding Hierarchical Condition Categories (HCC)
 Understanding Hierarchical Condition Categories (HCC) How hierarchical condition category coding will impact your practice and how you can use these codes to increase quality, improve the patient experience,
Understanding Hierarchical Condition Categories (HCC) How hierarchical condition category coding will impact your practice and how you can use these codes to increase quality, improve the patient experience,
Risk of Fractures Following Cataract Surgery in Medicare Beneficiaries
 Risk of Fractures Following Cataract Surgery in Medicare Beneficiaries Victoria L. Tseng, MD, Fei Yu, PhD, Flora Lum, MD, Anne L. Coleman, MD, PhD JAMA. 2012;308(5):493-501 Background Visual impairment
Risk of Fractures Following Cataract Surgery in Medicare Beneficiaries Victoria L. Tseng, MD, Fei Yu, PhD, Flora Lum, MD, Anne L. Coleman, MD, PhD JAMA. 2012;308(5):493-501 Background Visual impairment
University of Bristol - Explore Bristol Research
 Hunt, L., Ben-Shlomo, Y., Whitehouse, M., Porter, M., & Blom, A. (2017). The Main Cause of Death Following Primary Total Hip and Knee Replacement for Osteoarthritis: A Cohort Study of 26,766 Deaths Following
Hunt, L., Ben-Shlomo, Y., Whitehouse, M., Porter, M., & Blom, A. (2017). The Main Cause of Death Following Primary Total Hip and Knee Replacement for Osteoarthritis: A Cohort Study of 26,766 Deaths Following
SUPPLEMENTARY MATERIAL
 SUPPLEMENTARY MATERIAL Deep Patient: An Unsupervised Representation to Predict the Future of Patients from the Electronic Health Records Riccardo Miotto 1,2, Li Li 1,2, Brian A. Kidd 1,2, and Joel T. Dudley
SUPPLEMENTARY MATERIAL Deep Patient: An Unsupervised Representation to Predict the Future of Patients from the Electronic Health Records Riccardo Miotto 1,2, Li Li 1,2, Brian A. Kidd 1,2, and Joel T. Dudley
Chapter 1 Certain Infectious and Parasitic Diseases
 Chapter 1 Certain Infectious and Parasitic Diseases 1.1 A patient is seen for right lower leg muscle atrophy that is the result of a previous bout of polio. Chapter 2 Neoplasms 2.1 Small cell carcinoma
Chapter 1 Certain Infectious and Parasitic Diseases 1.1 A patient is seen for right lower leg muscle atrophy that is the result of a previous bout of polio. Chapter 2 Neoplasms 2.1 Small cell carcinoma
2014 Physician Quality Reporting System (PQRS) Measure Applicability-Validation (MAV) Process for Claims-Based Reporting Release Notes
 2014 Physician Quality Reporting System (PQRS) Measure Applicability-Validation (MAV) Process Version 8.0 Page 1 of 7 The following are the release notes for changes occurring for the 2014 PQRS Measure-
2014 Physician Quality Reporting System (PQRS) Measure Applicability-Validation (MAV) Process Version 8.0 Page 1 of 7 The following are the release notes for changes occurring for the 2014 PQRS Measure-
ICD-10-CM. International Classification of Diseases, 10th Revision, Clinical Modification
 ICD-10-CM International Classification of Diseases, 10th Revision, Clinical Modification ICD-10 stands for the International Statistical Classification of Diseases and Related Health Problems, 10 th revision
ICD-10-CM International Classification of Diseases, 10th Revision, Clinical Modification ICD-10 stands for the International Statistical Classification of Diseases and Related Health Problems, 10 th revision
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form
 Last Updated: Version 3.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Pneumonia (PN) Set Measure ID #: Measure Information Form Performance Measure Name: Pneumococcal Vaccination
Last Updated: Version 3.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Pneumonia (PN) Set Measure ID #: Measure Information Form Performance Measure Name: Pneumococcal Vaccination
Chapter 10 Respiratory System J00-J99. Presented by: Jesicca Andrews
 Chapter 10 Respiratory System J00-J99 Presented by: Jesicca Andrews 1 Respiratory System 2 Respiratory Infections A respiratory infection cannot be assumed from a laboratory report alone; physician concurrence
Chapter 10 Respiratory System J00-J99 Presented by: Jesicca Andrews 1 Respiratory System 2 Respiratory Infections A respiratory infection cannot be assumed from a laboratory report alone; physician concurrence
Predictors of Rehospitalization After Admission for Pneumonia in the Veterans Affairs Healthcare System
 ORIGINAL RESEARCH Predictors of Rehospitalization After Admission for Pneumonia in the Veterans Affairs Healthcare System Victoria L. Tang, MD 1,2, Ethan A. Halm, MD, MPH 2, Michael J. Fine, MD, MSc 3,
ORIGINAL RESEARCH Predictors of Rehospitalization After Admission for Pneumonia in the Veterans Affairs Healthcare System Victoria L. Tang, MD 1,2, Ethan A. Halm, MD, MPH 2, Michael J. Fine, MD, MSc 3,
UnitedHealth Premium Physician Designation Program Episode Treatment Groups (ETG ) Description and Specialty
 UnitedHealth Premium Physician Designation Program Episode Treatment Groups (ETG ) Description and Specialty 666700 Acne Family Medicine, Internal Medicine, Pediatrics 438300 Acute Bronchitis Allergy,
UnitedHealth Premium Physician Designation Program Episode Treatment Groups (ETG ) Description and Specialty 666700 Acne Family Medicine, Internal Medicine, Pediatrics 438300 Acute Bronchitis Allergy,
Balancing Glycemic Overtreatment and Undertreatment for Seniors: An Out of Range (OOR) Population Health Safety Measure
 Balancing Glycemic Overtreatment and Undertreatment for Seniors: An Out of Range (OOR) Population Health Safety Measure Leonard Pogach, 1,2 Orysya Soroka, 1 Chin Lin Tseng, 1,2 Miriam Maney, 1 and David
Balancing Glycemic Overtreatment and Undertreatment for Seniors: An Out of Range (OOR) Population Health Safety Measure Leonard Pogach, 1,2 Orysya Soroka, 1 Chin Lin Tseng, 1,2 Miriam Maney, 1 and David
Measure Applications Partnership. Hospital Workgroup In-Person Meeting Follow- Up Call
 Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
Isle of Wight Joint Strategic Needs Assessment: Core Dataset 2009
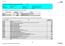 Isle of Wight Joint Strategic Needs Assessment: Core Dataset 2009 Domain: Burden of Ill Health Indicator: Hospital Admissions - Top 10 Causes Sub-Domain: Misc Indicator References: JSNA Core Dataset number
Isle of Wight Joint Strategic Needs Assessment: Core Dataset 2009 Domain: Burden of Ill Health Indicator: Hospital Admissions - Top 10 Causes Sub-Domain: Misc Indicator References: JSNA Core Dataset number
Archived SECTION 18 - DIAGNOSIS CODES. Section 18 - Diagnosis Codes 18.1 GENERAL INFORMATION PRIOR CONTENTS NO LONGER APPLICABLE...
 SECTION 18 - DIAGNOSIS CODES 18.1 GENERAL INFORMATION... 2 18.2 PRIOR CONTENTS NO LONGER APPLICABLE... 2 18.3 DIAGNOSIS CODE LISTING... 2 Ambulance Manual 1 SECTION 18 DIAGNOSIS CODES 18.1 GENERAL INFORMATION
SECTION 18 - DIAGNOSIS CODES 18.1 GENERAL INFORMATION... 2 18.2 PRIOR CONTENTS NO LONGER APPLICABLE... 2 18.3 DIAGNOSIS CODE LISTING... 2 Ambulance Manual 1 SECTION 18 DIAGNOSIS CODES 18.1 GENERAL INFORMATION
Results of the liberalisation of Medisave for a population-based diabetes management programme in Singapore
 Results of the liberalisation of Medisave for a population-based diabetes management programme in Singapore Woan Shin TAN 1, Yew Yoong DING 1, 2, Christine WU 3, Bee Hoon HENG 1 1 Health Services and Outcomes
Results of the liberalisation of Medisave for a population-based diabetes management programme in Singapore Woan Shin TAN 1, Yew Yoong DING 1, 2, Christine WU 3, Bee Hoon HENG 1 1 Health Services and Outcomes
Patient is unable to communicate and caregiver/informant is unavailable to provide information. Risk
 Falls Outcome for Patients with Parkinson s Disease Measure Description Percentage of patients with PD who experienced a fall in the preceding six months. Note: A lower score is desirable. Measure Components
Falls Outcome for Patients with Parkinson s Disease Measure Description Percentage of patients with PD who experienced a fall in the preceding six months. Note: A lower score is desirable. Measure Components
Hierarchical Generalized Linear Models for Behavioral Health Risk-Standardized 30-Day and 90-Day Readmission Rates
 Hierarchical Generalized Linear Models for Behavioral Health Risk-Standardized 30-Day and 90-Day Readmission Rates Allen Hom PhD, Optum, UnitedHealth Group, San Francisco, California Abstract The Achievements
Hierarchical Generalized Linear Models for Behavioral Health Risk-Standardized 30-Day and 90-Day Readmission Rates Allen Hom PhD, Optum, UnitedHealth Group, San Francisco, California Abstract The Achievements
Submitted By Yale New Haven Health Services Corporation/Center for Outcomes Research and Evaluation (YNHHSC/CORE)
 - - Submitted By Yale New Haven Health Services Corporation/Center for Outcomes Research and Evaluation (YNHHSC/CORE) CMS Contract # HHSM-500-2008-00025I/HHSM-500-T0001, Modification No. 000007 September
- - Submitted By Yale New Haven Health Services Corporation/Center for Outcomes Research and Evaluation (YNHHSC/CORE) CMS Contract # HHSM-500-2008-00025I/HHSM-500-T0001, Modification No. 000007 September
patients actual drug exposure for every single-day of contribution to monthly cohorts, either before or
 SUPPLEMENTAL MATERIAL Methods Monthly cohorts and exposure Exposure to generic or brand-name drugs were captured at an individual level, reflecting each patients actual drug exposure for every single-day
SUPPLEMENTAL MATERIAL Methods Monthly cohorts and exposure Exposure to generic or brand-name drugs were captured at an individual level, reflecting each patients actual drug exposure for every single-day
Care Pathways: Conditions most likely to cause blockages within emergency hospital care
 Care Pathways: Conditions most likely to cause blockages within emergency hospital care Dr Rod Jones (ACMA) Statistical Advisor www.hcaf.biz Executive Summary Conditions scoring high across various dimensions
Care Pathways: Conditions most likely to cause blockages within emergency hospital care Dr Rod Jones (ACMA) Statistical Advisor www.hcaf.biz Executive Summary Conditions scoring high across various dimensions
Medicare and Medicaid Payments
 and Payments The following table includes information about payments made by and for the 17 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on
and Payments The following table includes information about payments made by and for the 17 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
