Chronic Obstructive Pulmonary Disease (COPD)
|
|
|
- Gwenda Ferguson
- 6 years ago
- Views:
Transcription
1 โครงการประช มเช งปฏ บ ต การ งานเภส ชกรรมคล น ก คร งท 18/2557 เร อง Pharmaceutical Care f Patients with Chronic Diseases Chronic Obstructive Pulmonary Disease (COPD) GOLD, 2014: Definitions COPD, a common preventable and treatable disease, is characterized by persistent airflow limitation that is usually progressive and associated with an enhanced chronic inflammaty response in the airways and the lung to noxious particles gases. Exacerbations and combidities contribute to the overall severity in individual patients. 19 June 2014 Definitions (American Thacic Society, ATS) Asthma and COPD Overlap Syndrome (ACOS) A disease state characterized by the presence of airflow obstruction due to chronic bronchitis (and)/ emphysema; the airflow obstruction is generally progressive, may be accompanied by airway hyperreactivity, and may be partially reversible. 4 1
2 Pathogenesis of COPD Mechanism underlying airflow limitation in COPD Noxious particles & gases Anti-oxidants Antiproteinases Lung inflammation Oxidative stress Proteinases COPD pathology 5 6 Risk facts f COPD Host facts Gene (e.g., alpha-1 antitrypsin deficiency) Airway hyperresponsiveness Lung Growth Exposures Smoking Aging Populations Occupational dusts and chemicals Air pollution Infections Asthma / bronchial hyperreactivity Asthma Sensitizing agent Asthmatic airway inflammation CD4+ T-lymphocytes Eosinophils Small airway disease Airway inflammation Airway remodeling Completely reversible Airflow limitation COPD Noxious agent COPD airway inflammation CD8+ T-lymphocytes Macrophages Neutrophils Parenchymal destruction Loss of alveolar attachments Decrease of elastic recoil Completely irreversible 2
3 9 Key indicats f considering a Dx of COPD A clinical diagnosis of COPD should be considered in any patient who has dyspnea, chronic cough sputum production, and a histy of exposure to risk facts f the disease. Spirometry is required to make the diagnosis; the presence of a post-bronchodilat FEV 1 /FVC < 0.70 confirms the presence of persistent airflow limitation and thus of COPD. Diagnosis of COPD Symptoms of COPD Dyspnea: Progressive, persistent and wse with exercise. Chronic cough: May be intermittent and may be unproductive. Chronic sputum production: COPD patients commonly cough up sputum. Spirometry: FEV 1 /FVC ratio < 0.70 PLUS an FEV 1 < 80% predicted that is incompletely reversible with inhaled bronchodilat Absence of an alternative explanation f the symptoms and airflow limitation (Diff Dx) Assessment of COPD Assess symptoms Assess symptoms Assess degree of airflow limitation using spirometry Assess risk of exacerbations Assess combidities COPD Assessment Test (CAT) Clinical COPD Questionnaire (CCQ) mmrc Breathlessness scale COPD Assessment Test (CAT): An 8-item measure of health status impairment in COPD ( Clinical COPD Questionnaire (CCQ): Self-administered questionnaire developed to measure clinical control in patients with COPD ( Breathlessness Measurement using the Modified British Medical Research Council (mmrc) Questionnaire: relates well to other measures of health status and predicts future mtality risk. 12 3
4 mmrc (Modified Medical Research Council Dyspnea Sce) เกณฑ การให คะแนนภาวะหายใจล าบาก ซ งแบ งระด บความร นแรงของ ภาวะหายใจล าบากเป น 5 ระด บ ระด บ 0: ปกต ไม ม เหน อยง าย ระด บ 1: ม อาการเหน อยง ายเม อเด นเร ว ๆ ข นทางช น ระด บ 2: เด นในพ นราบไม ท นเพ อนท อย ในว ยเด ยวก น เพราะเหน อย หร อต องหย ดเด นเป นพ กๆ ระด บ 3 : เด นได น อยกว า 100 เมตร ระด บ 4 : เหน อยเวลาท าก จว ตรประจ าว น เช น ใส เส อผ า อาบน าแต งต ว จนไม สามารถออกนอกบ านได CAT (COPD Assessment Test) การประเม นผลกระทบของ COPD ต อผ ป วย ประกอบด วย ค าถาม 8 ข อ ข อละ 5 คะแนน เต ม 40 คะแนน คะแนน < 10 แสดงว าม ผลกระทบน อย คะแนน > 10 แสดงว าม ผลกระทบมาก Assessment of COPD Assess symptoms Assess degree of airflow limitation Use spirometry f grading severity accding to spirometry, using four grades split at 80%, 50% and 30% of predicted value Classification of severity of airflow limitation (based on postbronchodilat FEV 1 ) In patients with FEV 1 /FVC <0.70: Stage I: mild FEV 1 80% predicted Stage II: moderate 50% FEV 1 <80% predicted Stage III: severe 30% < FEV 1 < 50% predicted Stage IV: very severe FEV 1 < 30% predicted 4
5 Risk (GOLD Classification of Airflow Limitation)) Risk (Exacerbation histy) Assessment of COPD Assess symptoms Assess degree of airflow limitation Assess risk of exacerbations Use histy of exacerbations and spirometry. > 2 exacerbations within the last year an FEV 1 < 50 % of predicted value are indicats of high risk. > 1 hospitalization f a COPD exacerbation high risk Combined Assessment of COPD 2 4 > 1 leading (C) (D) to hospital admission (A) (B) CAT < 10 CAT > 10 Symptoms mmrc 0 1 mmrc > 2 Breathlessness 1 (not leading to hospital) admission) 0 Combined Assessment of COPD ASSESS Symptom first If CAT < 10 mmrc 0-1: Less Symptoms/breathlessness (A C) If CAT > 10 mmrc > 2: Me Symptoms/breathlessness (B D) C A D CAT<10 CAT >10 mmrc 0-1 mmrc >2 B Combined Assessment of COPD Assess risk of exacerbations next If GOLD exacerbations per year > 1 leading to hospital admission: High Risk (C D) If GOLD 1 2 and only 0 1 exacerbations per year (not leading to hospital admission): Low Risk (A B) C A D B >
6 Combined Assessment of COPD Patient Characteristic Spirometric Classification A B C D Low Risk Less Symptoms Low Risk Me Symptoms High Risk Less Symptoms High Risk Me Symptoms Exacerbations per year C CAT D mmrc GOLD < GOLD > 10 > 2 GOLD 3-4 > 2 < GOLD 3-4 > 2 > 10 >2 A B 0 CAT<10 CAT >10 mmrc 0-1 mmrc >2 1 > 2 Assess COPD Combidities COPD patients are at increased risk f: Cardiovascular diseases Osteoposis Respiraty infections Anxiety and Depression Diabetes Lung cancer Bronchiectasis These combid conditions may influence mtality and hospitalizations and should be looked f routinely, and treated appropriately. Differential Diagnosis: COPD and Asthma Therapeutic Options: Key Points COPD Onset in mid-life Symptoms slowly progressive Long smoking histy ASTHMA Onset early in life (often childhood) Symptoms vary from day to day Symptoms wse at night/early mning Allergy, rhinitis, and/ eczema also present Family histy of asthma Smoking cessation has the greatest capacity to influence the natural histy of COPD. Health care providers should encourage all patients who smoke to quit. All COPD patients benefit from regular physical activity and should repeatedly be encouraged to remain active. 6
7 Therapeutic Options: Key Points Appropriate pharmacologic therapy can reduce COPD symptoms reduce the frequency and severity of exacerbations improve health status and exercise tolerance. None of the existing medications f COPD has been shown conclusively to modify the long-term decline in lung function. Beta 2 -agonists Sht-acting beta 2 -agonists (SABA): salbutamol Long-acting beta 2 -agonists (LABA): salmeterol, fmoterol, indacaterol Anticholinergics (anti-muscarinic agents) Sht-acting anticholinergics (SAMA): ipratropium Long-acting anticholinergics (LAMA): tiotropium Combination SABA + SAMA in one inhaler Combination LABA + LAMA in one inhaler Methylxanthines: theophylline SR Inhaled cticosteroids (ICS) Combination LABA + ICS in one inhaler Systemic cticosteroids Phosphodiesterase-4 inhibits: roflumilast Pharmacotherapy: Bronchodilats Pharmacotherapy: Bronchodilats Bronchodilat medications are central to the symptomatic management of COPD. Bronchodilats are prescribed on an as-needed on a regular basis to prevent reduce symptoms. The principal bronchodilat treatments are beta 2 -agonists, anticholinergics, theophylline combination therapy. The choice of treatment depends on the availability of medications and each patient s individual response in terms of symptom relief and side effects.. Long-acting inhaled bronchodilats are convenient and me effective f symptom relief than sht-acting bronchodilats. Long-acting inhaled bronchodilats reduce exacerbations and related hospitalizations improve symptoms and health status. Combining bronchodilats of different pharmacological classes may improve efficacy and decrease the risk of side effects compared to increasing the dose of a single bronchodilat. 7
8 Bronchodilats: Theophylline Bronchodilats: Theophylline Mode of action: smooth muscle relaxation due to phosphodiesterase inhibition (PDE-IV), increases diaphragmatic contractility, may reduce inflammation All studies that have shown efficacy of theophylline in COPD were done with slow-release preparations. Theophylline is less effective and less well tolerated than inhaled long-acting bronchodilats and is not recommended if those drugs are available and affdable. 30 Addition of theophylline to salmeterol produces a greater increase in FEV 1 and breathlessness than salmeterol alone. Low dose theophylline reduces exacerbations but does not improve postbronchodilat lung function. Roflumilast highly selective PDE 4 inhibit Theophylline nonselective weak PDE inhibit ม ข อจำก ด: safety และควำมทนต อยำของผ ป วย PDE-4 = subtype ของ PDE พบมำกในบร เวณท ม กำรอ กเสบ และกล ำมเน อเร ยบของทำงเด นหำยใจ กำรย บย ง PDE-4 แบบ จำเพำะเจำะจงจะออกฤทธ ท งท mast cells และ neutrophils MOA: เพ มระด บของ camp โดยย บย งเอนไซม ท ทำลำย camp, ย บย ง mediat ท ก อให เก ดกำรอ กเสบในทำงเด นหำยใจ 31 Roflumilast highly selective PDE 4 inhibit severe and very severe COPD (GOLD 3 and 4) and a histy of exacerbations and chronic bronchitis 1 tab once daily. กำรส บบ หร ไม ม ผลต อค ำเภส ชจลนศำสตร ของยำ SE: ปวดศ รษะ คล นไส ท องเส ย ส บสน 32 DAXAS 8
9 Tiotropium bromide Specific M1 and M3 Muscarinic Blockade Indication: maintenance Tx of COPD not suitable f relief of acute bronchospasm Side effects: Tiotropium, like ipratropium (quaternary ammonium compounds), is poly absbed from the GI tract and has very low systemic bioavailability. --- wide therapeutic margin dryness of the mouth, a typical anticholinergic effect Tiotropium bromide GOLD guideline: recommend f moderate severe COPD use of regular tx of long acting bronchodilat, including tiotropium, rather than sht acting bronchodilat tiotropium 18 mcg OD with without salmeterol should not be use together with other ipratropium DPI (Handihaler) Tiotropium 470 patients - stable COPD 3 month, randomized, double blind, once daily tiotropium vs. placebo Conclusions: Increased FEV1 and FVC No tachyphylaxis Decreased rescue albuterol Decreased wheezing, SOB Dry mouth in 9.3% Casaburi et al. CHEST 118:1294, 2000 Tiotroprium 1207 patients, double blind, randomized trial, qd tiotropium vs. bid salmeterol vs. placebo Conclusions: Tiotropium Fewer exacerbations Increased time to first exacerbation Fewer admissions Increased QOL Brusasco et al. Thax 58:399:2003 9
10 Tiotropium versus LABA f stable COPD 7 clinical studies totaling 12,223 patients with COPD LABA: fmoterol, salmeterol, indacaterol Tiotropium was me effective than LABAs as a group in. preventing COPD exacerbations and diseaserelated hospitalisations no statistical differences between groups in overall hospitalisation rates mtality during the study periods (3-12 months). 37 Cochrane Database of Systematic Reviews 2012, Issue 9. Inhaled Cticosteroids (ICS) Regular treatment with ICS : improves symptoms, lung function and QoL reduces frequency of exacerbations f COPD patients with an FEV 1 < 60% predicted. ICS therapy is associated with an increased risk of pneumonia. Combination: ICS + bronchodilat To reduce the frequency of exacerbation ICS ให ร วมก บ LABA me effective than the individual components in reducing exacerbations and improving LF Combination therapy is associated with an increased risk of pneumonia. LABA/ICS combination + tiotropium appears to 39 provide additional benefits. Meta-analysis: efficacy of ICS and LABA in a single inhaler with mono-component LABA alone in adults with COPD trials involving 11,794 people with COPD ICS/LABA inhalers reduced (compared with their LABA component alone) frequency of exacerbations an average of one exacerbation per year on a LABA to an average of 0.76 exacerbations per year on a combined inhaler. risk of mtality was similar between the treatments Cochrane Database of Systematic Reviews 2012, Issue 9. 10
11 Meta-analysis: efficacy of ICS and LABA in a single inhaler with mono-component LABA alone in adults with COPD There was evidence of an overall increased risk of pneumonia with combined inhalers, from around 3/100 people/year on LABA to 4/100/ year on combined inhalers. There was no significant difference between treatments in terms of hospitalisations Systemic cticosteroids จำก meta-analysis พบผ ป วย stable COPD ท ได ร บ al cticosteroid ม ค ำ FEV 1 ด ข น > 20% ม มำกกว ำกล มท ได ร บ placebo ประมำณ 10% Chronic treatment with systemic cticosteroids should be avoided (an unfavable benefit-to-risk ratio. 41 Cochrane Database of Systematic Reviews 2012, Issue Manage Stable COPD: Key Points Manage Stable COPD: Key Points Identification and reduction of exposure to risk facts are imptant steps in prevention and treatment. Individualized assessment of symptoms, airflow limitation, and future risk of exacerbations should be incpated into the management strategy. Pharmacologic therapy is used to reduce symptoms, reduce frequency and severity of exacerbations, and improve health status and exercise tolerance. LABA and LAMA are preferred over sht-acting fmulations. Based on efficacy and side effects, inhaled bronchodilats are preferred over al bronchodilats. Long-term treatment with ICS added to longacting bronchodilats is recommended f patients with high risk of exacerbations. 11
12 Manage Stable COPD: Key Points Therapeutic Options: Other Pharmacologic Treatments Long-term monotherapy with OSC ICS is not recommended in COPD. The phospodiesterase-4 inhibit roflumilast may be useful to reduce exacerbations f patients with FEV 1 < 50% of predicted, chronic bronchitis, and frequent exacerbations. Influenza vaccines can reduce serious illness. Pneumococcal polysaccharide vaccine is recommended f COPD patients (>65 years) and f COPD patients younger than age 65 with an FEV 1 < 40% predicted. The use of antibiotics, other than f treating infectious exacerbations of COPD and other bacterial infections, is currently not indicated. Mucolytics: Patients with viscous sputum may benefit from mucolytics; overall benefits are very small. Antitussives: Not recommended. Manage Stable COPD: Non-pharmacologic Manage Stable COPD: Pharmacologic Therapy (Medications in each box are mentioned in alphabetical der, and therefe not necessarily in der of preference.) Patient Group Essential Recommended Depending on local guidelines A Smoking cessation Physical activity Flu vaccination Pneumococcal vaccination Patient A B Recommended First choice SAMA prn SABA prn LAMA LABA Alternative choice LAMA LABA SABA and SAMA LAMA and LABA Other Possible Treatments Theophylline SABA and/ SAMA Theophylline B, C, D Smoking cessation Pulmonary rehabilitation Physical activity Flu vaccination Pneumococcal vaccination C D ICS + LABA LAMA ICS + LABA and/ LAMA LAMA and LABA LAMA and PDE4-inh. LABA and PDE4-inh. ICS + LABA and LAMA ICS+LABA and PDE4-inh. LAMA and LABA LAMA and PDE4-inh. SABA and/ SAMA Theophylline Carbocysteine SABA and/ SAMA Theophylline 12
13 Manage Exacerbations: Key Points Manage Exacerbations: The most common causes of COPD exacerbations are viral upper respiraty tract infections and infection of the tracheobronchial tree. SABA with without SAMA are usually the preferred bronchodilats f tx of an exacerbation. Systemic cticosteroids and antibiotics can shten recovery time, improve lung function and arterial hypoxemia (PaO 2 ), and reduce the risk of early relapse, tx failure, and length of hospital stay. Antibiotics should be given to patients with: Three cardinal symptoms: increased dyspnea, increased sputum volume, and increased sputum purulence. Who require mechanical ventilation. Oxygen: titrate to improve the patient s hypoxemia with a target saturation of 88-92%. Manage Exacerbations: Assessments Summary Arterial blood gas measurements (in hospital): PaO 2 < 8.0 kpa with without PaCO 2 > 6.7 kpa when breathing room air indicates respiraty failure. Chest radiographs: useful to exclude alternative diagnoses. ECG: may aid in the diagnosis of coexisting cardiac problems. Whole blood count: identify polycythemia, anemia bleeding. Purulent sputum during an exacerbation: indication to begin empirical antibiotic treatment. Biochemical tests: detect electrolyte disturbances, diabetes, and po nutrition. Spirometric tests: not recommended during an exacerbation. Prevention of COPD is to a large extent possible and should have high priity Spirometry is required to make the diagnosis of COPD; the presence of a post-bronchodilat FEV 1 /FVC < 0.70 confirms the presence of persistent airflow limitation and thus of COPD Combined assessment of symptoms and risk of exacerbations is the basis f non-pharmacologic and pharmacologic management of COPD Treat COPD exacerbations to minimize their impact and to prevent the development of subsequent exacerbations 13
At-A-Glance Outpatient Management Reference for Chronic Obstructive Pulmonary Disease (COPD)
 At-A-Glance Outpatient Management Reference f Chronic Obstructive Pulmonary Disease (COPD) BASED ON THE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT AND PREVENTION OF COPD GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE
At-A-Glance Outpatient Management Reference f Chronic Obstructive Pulmonary Disease (COPD) BASED ON THE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT AND PREVENTION OF COPD GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE
Global Strategy for the Diagnosis, Management and Prevention of COPD 2016 Clinical Practice Guideline. MedStar Health
 Global Strategy f the Diagnosis, Management and Prevention of COPD 2016 Clinical Practice Guideline MedStar Health These guidelines are provided to assist physicians and other clinicians in making decisions
Global Strategy f the Diagnosis, Management and Prevention of COPD 2016 Clinical Practice Guideline MedStar Health These guidelines are provided to assist physicians and other clinicians in making decisions
Update on heterogeneity of COPD, evaluation of COPD severity and exacerbation
 Update on heterogeneity of COPD, evaluation of COPD severity and exacerbation Yung-Yang Liu, MD Taipei Veterans General Hospital Aug 29, 2015 G O lobal Initiative for Chronic bstructive L D ung isease
Update on heterogeneity of COPD, evaluation of COPD severity and exacerbation Yung-Yang Liu, MD Taipei Veterans General Hospital Aug 29, 2015 G O lobal Initiative for Chronic bstructive L D ung isease
COPD: Current Medical Therapy
 COPD: Current Medical Therapy Angela Golden, DNP, FNP-C, FAANP Owner, NP from Home, LLC Outcomes As a result of this activity, learners will be able to: 1. List the appropriate classes of medications for
COPD: Current Medical Therapy Angela Golden, DNP, FNP-C, FAANP Owner, NP from Home, LLC Outcomes As a result of this activity, learners will be able to: 1. List the appropriate classes of medications for
COPD is a syndrome of chronic limitation in expiratory airflow encompassing emphysema or chronic bronchitis.
 1 Definition of COPD: COPD is a syndrome of chronic limitation in expiratory airflow encompassing emphysema or chronic bronchitis. Airflow obstruction may be accompanied by airway hyper-responsiveness
1 Definition of COPD: COPD is a syndrome of chronic limitation in expiratory airflow encompassing emphysema or chronic bronchitis. Airflow obstruction may be accompanied by airway hyper-responsiveness
Global Strategy for the Diagnosis, Management and Prevention of COPD 2016 Clinical Practice Guideline. MedStar Health
 Global Strategy for the Diagnosis, Management and Prevention of COPD 2016 Clinical Practice Guideline MedStar Health These guidelines are provided to assist physicians and other clinicians in making decisions
Global Strategy for the Diagnosis, Management and Prevention of COPD 2016 Clinical Practice Guideline MedStar Health These guidelines are provided to assist physicians and other clinicians in making decisions
Defining COPD. Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist
 Defining COPD Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist Defining COPD Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disease
Defining COPD Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist Defining COPD Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disease
Advances in the management of chronic obstructive lung diseases (COPD) David CL Lam Department of Medicine University of Hong Kong October, 2015
 Advances in the management of chronic obstructive lung diseases (COPD) David CL Lam Department of Medicine University of Hong Kong October, 2015 Chronic obstructive pulmonary disease (COPD) COPD in Hong
Advances in the management of chronic obstructive lung diseases (COPD) David CL Lam Department of Medicine University of Hong Kong October, 2015 Chronic obstructive pulmonary disease (COPD) COPD in Hong
Improving Outcomes in COPD
 Neil MacIntyre MD Duke University Durham NC Current treatment guidelines f COPD focus Barriers to providing optimal treatment Diagnosis of COPD EXPOSURE TO RISK FACTORS AND/ OR SYMPTOMS sputum cough dyspnea
Neil MacIntyre MD Duke University Durham NC Current treatment guidelines f COPD focus Barriers to providing optimal treatment Diagnosis of COPD EXPOSURE TO RISK FACTORS AND/ OR SYMPTOMS sputum cough dyspnea
Disclosure and Conflict of Interest 8/15/2017. Pharmacist Objectives. At the conclusion of this program, the pharmacist will be able to:
 Digging for GOLD Rebecca Young, PharmD, BCACP, Roosevelt University College of Pharmacy Assistant Professor of Clinical Sciences Practice Site Advocate Medical Group-Nesset Pavilion Disclosure and Conflict
Digging for GOLD Rebecca Young, PharmD, BCACP, Roosevelt University College of Pharmacy Assistant Professor of Clinical Sciences Practice Site Advocate Medical Group-Nesset Pavilion Disclosure and Conflict
2/4/2019. GOLD Objectives. GOLD 2019 Report: Chapters
 GOLD Objectives To provide a non biased review of the current evidence for the assessment, diagnosis and treatment of patients with COPD. To highlight short term and long term treatment objectives organized
GOLD Objectives To provide a non biased review of the current evidence for the assessment, diagnosis and treatment of patients with COPD. To highlight short term and long term treatment objectives organized
COPD: A Renewed Focus. Disclosures
 COPD: A Renewed Focus Heath Latham, MD Assistant Professor Division of Pulmonary and Critical Care Medicine Disclosures No Business Interests No Consulting No Speakers Bureau No Off Label Use to Discuss
COPD: A Renewed Focus Heath Latham, MD Assistant Professor Division of Pulmonary and Critical Care Medicine Disclosures No Business Interests No Consulting No Speakers Bureau No Off Label Use to Discuss
AECOPD: Management and Prevention
 Neil MacIntyre MD Duke University Medical Center Durham NC Professor P.J. Barnes, MD, National Heart and Lung Institute, London UK Professor Peter J. Barnes, MD National Heart and Lung Institute, London
Neil MacIntyre MD Duke University Medical Center Durham NC Professor P.J. Barnes, MD, National Heart and Lung Institute, London UK Professor Peter J. Barnes, MD National Heart and Lung Institute, London
COPD. Breathing Made Easier
 COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
COPD/Asthma. Prudence Twigg, AGNP
 COPD/Asthma Prudence Twigg, AGNP COPD/Asthma Qualifying Diagnosis Known diagnosis of COPD/asthma or CXR showing COPD with hyperinflated lungs and no infiltrates + two or more: Wheezing, SOB, increased
COPD/Asthma Prudence Twigg, AGNP COPD/Asthma Qualifying Diagnosis Known diagnosis of COPD/asthma or CXR showing COPD with hyperinflated lungs and no infiltrates + two or more: Wheezing, SOB, increased
COPD: Preventable and Treatable. Lecture Outline. Diagnosis of COPD. COPD: Defining Terms
 COPD: Preventable and Treatable Christopher H. Fanta, M.D. Partners Asthma Center Pulmonary and Critical Care Division Brigham and Women s Hospital Harvard Medical School Lecture Outline I. Diagnosis and
COPD: Preventable and Treatable Christopher H. Fanta, M.D. Partners Asthma Center Pulmonary and Critical Care Division Brigham and Women s Hospital Harvard Medical School Lecture Outline I. Diagnosis and
Case approach in Asthma and COPD. Assoc.Prof.Sunee Lertsinudom BSc.Grad.Diplo.BCP. Department of Clinical pharmacy Khonkaen University
 Case approach in Asthma and COPD Assoc.Prof.Sunee Lertsinudom BSc.Grad.Diplo.BCP. Department of Clinical pharmacy Khonkaen University Asthma Diagnosis History and patterns of symptoms Physical examination
Case approach in Asthma and COPD Assoc.Prof.Sunee Lertsinudom BSc.Grad.Diplo.BCP. Department of Clinical pharmacy Khonkaen University Asthma Diagnosis History and patterns of symptoms Physical examination
CHRONIC OBSTRUCTIVE LUNG DISEASE (COPD), BRONCHIAL ASTHMA
 CHRONIC OBSTRUCTIVE LUNG DISEASE (COPD), BRONCHIAL ASTHMA GOLD GINA Chronic Obstructive Pulmonary Disease (COPD) COPD is currently the fourth leading cause of death in the world.1 COPD is projected to
CHRONIC OBSTRUCTIVE LUNG DISEASE (COPD), BRONCHIAL ASTHMA GOLD GINA Chronic Obstructive Pulmonary Disease (COPD) COPD is currently the fourth leading cause of death in the world.1 COPD is projected to
รศ. นพ. ว ชรา บ ญสว สด M.D., Ph.D. ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล ยขอนแก น
 รศ. นพ. ว ชรา บ ญสว สด M.D., Ph.D. ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล ยขอนแก น COPD Guideline Changing concept in COPD management Evidences that we can offer COPD patients better life COPD Guidelines
รศ. นพ. ว ชรา บ ญสว สด M.D., Ph.D. ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล ยขอนแก น COPD Guideline Changing concept in COPD management Evidences that we can offer COPD patients better life COPD Guidelines
COPD. Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS
 IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
Current concepts in the management of chronic obstructive pulmonary
 Earn 3 CPD Points online Current concepts in the management of chronic obstructive pulmonary disease (COPD) Based on presentations by Introduction The Global Initiative f Chronic Obstructive Lung Disease
Earn 3 CPD Points online Current concepts in the management of chronic obstructive pulmonary disease (COPD) Based on presentations by Introduction The Global Initiative f Chronic Obstructive Lung Disease
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES
 JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
Treatment Responses. Ronald Dahl, Aarhus University Hospital, Denmark
 Asthma and COPD: Are They a Spectrum Treatment Responses Ronald Dahl, Aarhus University Hospital, Denmark Pharmacological Treatments Bronchodilators Inhaled short-acting β -Agonist (rescue) Inhaled short-acting
Asthma and COPD: Are They a Spectrum Treatment Responses Ronald Dahl, Aarhus University Hospital, Denmark Pharmacological Treatments Bronchodilators Inhaled short-acting β -Agonist (rescue) Inhaled short-acting
OPTIMIZING MANAGEMENT OF COPD IN THE PRACTICE SETTING 10/16/2018 DISCLOSURES I have no financial or other disclosures
 OPTIMIZING MANAGEMENT OF COPD IN THE PRACTICE SETTING J. Michael Fuller, MD, MEd, FACP, FCCP Associate Professor of Medicine University of South Carolina Greenville DISCLOSURES I have no financial or other
OPTIMIZING MANAGEMENT OF COPD IN THE PRACTICE SETTING J. Michael Fuller, MD, MEd, FACP, FCCP Associate Professor of Medicine University of South Carolina Greenville DISCLOSURES I have no financial or other
You ve come a long way, baby.
 COPD Dr Badri Paudel Dept of Medicine GMC/CHRC 4/22/12 badri@gmc 2 You ve come a long way, baby. Wayne McLaren Former Marlboro Man 4/22/12 badri@gmc 3 Age 30 a robust young man Age 51 riding into the sunset
COPD Dr Badri Paudel Dept of Medicine GMC/CHRC 4/22/12 badri@gmc 2 You ve come a long way, baby. Wayne McLaren Former Marlboro Man 4/22/12 badri@gmc 3 Age 30 a robust young man Age 51 riding into the sunset
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MOUSTAPHA ABIDALI, DO CRITICAL CARE FELLOW UNIVERSITY OF ARIZONA- PHOENIX
 CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MOUSTAPHA ABIDALI, DO CRITICAL CARE FELLOW UNIVERSITY OF ARIZONA- PHOENIX COPD OUTLINE Definition and Overview Pathophysiology Diagnosis and Assessment Therapeutic
CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MOUSTAPHA ABIDALI, DO CRITICAL CARE FELLOW UNIVERSITY OF ARIZONA- PHOENIX COPD OUTLINE Definition and Overview Pathophysiology Diagnosis and Assessment Therapeutic
Doctor of Medicine. Alastair Stewart Dept. of Pharmacology 8 th Floor, Medical Building Rm. N802
 Doctor of Medicine Alastair Stewart Dept. of Pharmacology 8 th Floor, Medical Building Rm. N802 astew@unimelb.edu.au Drugs affecting airway structure and function 2 Objectives Understand and know the mechanism
Doctor of Medicine Alastair Stewart Dept. of Pharmacology 8 th Floor, Medical Building Rm. N802 astew@unimelb.edu.au Drugs affecting airway structure and function 2 Objectives Understand and know the mechanism
Disclosures. Case #1 - Asthma. Question #1 Asthma. Update on Asthma & COPD. No Pharma Consulting, Research, Lectures
 Update on Asthma & COPD Disclosures No Pharma Consulting, Research, Lectures NHLBI - Asthma Clinical Research Netwk Stephen C. Lazarus, M.D. Division of Pulmonary & Critical Care Medicine Cardiovascular
Update on Asthma & COPD Disclosures No Pharma Consulting, Research, Lectures NHLBI - Asthma Clinical Research Netwk Stephen C. Lazarus, M.D. Division of Pulmonary & Critical Care Medicine Cardiovascular
Improving Outcomes in COPD. Improving Outcomes in COPD 4/4/2018
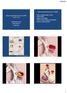 Updates 2018 Neil MacIntyre MD Duke University Durham NC. Barnes PJ. N Engl J Med. 2000;343:269-80. 1 COPD spectrum Proximal predominant (large airways) mucus gland hypertrophy (cough/sputum) reduced respiraty
Updates 2018 Neil MacIntyre MD Duke University Durham NC. Barnes PJ. N Engl J Med. 2000;343:269-80. 1 COPD spectrum Proximal predominant (large airways) mucus gland hypertrophy (cough/sputum) reduced respiraty
Curriculum Vitae. Head of Public Wing HCU - RSCM. Head of ICU Sari Asih Ciledug Hospital
 Curriculum Vitae Name : Dr. Ceva W. Pitoyo,SpPD,K-P,KIC,FINASIM POB / DOB : Jakarta, March 8th 1968 Education : o General Practitioner : FKUI 1993 o Internist : FKUI 2002 o Pulmonology Consultant : PAPDI-UI
Curriculum Vitae Name : Dr. Ceva W. Pitoyo,SpPD,K-P,KIC,FINASIM POB / DOB : Jakarta, March 8th 1968 Education : o General Practitioner : FKUI 1993 o Internist : FKUI 2002 o Pulmonology Consultant : PAPDI-UI
Chronic obstructive pulmonary disease
 0 Chronic obstructive pulmonary disease Implementing NICE guidance June 2010 NICE clinical guideline 101 What this presentation covers Background Scope Key priorities for implementation Discussion Find
0 Chronic obstructive pulmonary disease Implementing NICE guidance June 2010 NICE clinical guideline 101 What this presentation covers Background Scope Key priorities for implementation Discussion Find
Turning Science into Real Life Roflumilast in Clinical Practice. Roland Buhl Pulmonary Department Mainz University Hospital
 Turning Science into Real Life Roflumilast in Clinical Practice Roland Buhl Pulmonary Department Mainz University Hospital Therapy at each stage of COPD I: Mild II: Moderate III: Severe IV: Very severe
Turning Science into Real Life Roflumilast in Clinical Practice Roland Buhl Pulmonary Department Mainz University Hospital Therapy at each stage of COPD I: Mild II: Moderate III: Severe IV: Very severe
Provider Respiratory Inservice
 Provider Respiratory Inservice 2 Welcome Opening Remarks We will cover: Definition of Asthma & COPD Evidence based guidelines for diagnosis, evaluation, and management of asthma Evidence based guidelines
Provider Respiratory Inservice 2 Welcome Opening Remarks We will cover: Definition of Asthma & COPD Evidence based guidelines for diagnosis, evaluation, and management of asthma Evidence based guidelines
Chronic Obstructive Pulmonary Disease (COPD) Clinical Guideline
 Chronic Obstructive Pulmonary Disease (COPD) Clinical These clinical guidelines are designed to assist clinicians by providing an analytical framework for the evaluation and treatment of patients. They
Chronic Obstructive Pulmonary Disease (COPD) Clinical These clinical guidelines are designed to assist clinicians by providing an analytical framework for the evaluation and treatment of patients. They
What is COPD? COPD Pharmacotherapy. COPD Mortality Is Increasing
 COPD Pharmacotherapy Chronic Bronchitis What is COPD? 75% 17.5% Emphysema Laura C. Feemster, MD, MS Assistant Professor University of Washington Division of Pulmonary & Critical Care April 23,2015 COPD
COPD Pharmacotherapy Chronic Bronchitis What is COPD? 75% 17.5% Emphysema Laura C. Feemster, MD, MS Assistant Professor University of Washington Division of Pulmonary & Critical Care April 23,2015 COPD
Up in FLAMES: Stable Chronic Obstructive Pulmonary Disease (COPD) Management. Colleen Sakon, PharmD BCPS September 27, 2018
 Up in FLAMES: Stable Chronic Obstructive Pulmonary Disease (COPD) Management Colleen Sakon, PharmD BCPS September 27, 2018 Disclosures I have no actual or potential conflicts of interest 2 Objectives Summarize
Up in FLAMES: Stable Chronic Obstructive Pulmonary Disease (COPD) Management Colleen Sakon, PharmD BCPS September 27, 2018 Disclosures I have no actual or potential conflicts of interest 2 Objectives Summarize
COPD GOLD Guidelines & Barnet inhaler choices. Dr Dean Creer, Respiratory Consultant, Royal Free London NHS Foundation Trust
 COPD GOLD Guidelines & Barnet inhaler choices Dr Dean Creer, Respiratory Consultant, Royal Free London NHS Foundation Trust GOLD 2017 Report: Chapters 1. Definition and Overview 2. Diagnosis and Initial
COPD GOLD Guidelines & Barnet inhaler choices Dr Dean Creer, Respiratory Consultant, Royal Free London NHS Foundation Trust GOLD 2017 Report: Chapters 1. Definition and Overview 2. Diagnosis and Initial
If you require this document in another format such as Braille, large print, audio or another language please contact the Trusts Communications Team
 MANAGEMENT OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) IN ADULTS Summary statement: How does the document support patient care? Staff/stakeholders involved in development: Job titles only Division:
MANAGEMENT OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) IN ADULTS Summary statement: How does the document support patient care? Staff/stakeholders involved in development: Job titles only Division:
CARE OF THE ADULT COPD PATIENT
 CARE OF THE ADULT COPD PATIENT Target Audience: The target audience for this clinical guideline is all MultiCare providers and staff including those associated with our Clinically Integrated Network. The
CARE OF THE ADULT COPD PATIENT Target Audience: The target audience for this clinical guideline is all MultiCare providers and staff including those associated with our Clinically Integrated Network. The
Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984]
![Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984] Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984]](/thumbs/85/91889043.jpg) Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984] 1 st Appraisal Committee meeting Background & Clinical Effectiveness John McMurray 11 th January 2016 For
Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984] 1 st Appraisal Committee meeting Background & Clinical Effectiveness John McMurray 11 th January 2016 For
Lecture Notes. Chapter 4: Chronic Obstructive Pulmonary Disease (COPD)
 Lecture Notes Chapter 4: Chronic Obstructive Pulmonary Disease (COPD) Objectives Define COPD Estimate incidence of COPD in the US Define factors associated with onset of COPD Describe the clinical features
Lecture Notes Chapter 4: Chronic Obstructive Pulmonary Disease (COPD) Objectives Define COPD Estimate incidence of COPD in the US Define factors associated with onset of COPD Describe the clinical features
Chronic Obstructive Pulmonary Disease
 Chronic Obstructive Pulmonary Disease Catherine Whittaker (BPharm, MRPharmS) Abstract Chronic Obstructive Pulmonary Disease affects millions of people, has a major impact on quality of life and has become
Chronic Obstructive Pulmonary Disease Catherine Whittaker (BPharm, MRPharmS) Abstract Chronic Obstructive Pulmonary Disease affects millions of people, has a major impact on quality of life and has become
Newer Therapies in COPD
 C H A P T E R 50 Newer Therapies in COPD Prem Parkash Gupta INTRODUCTION Chronic Obstructive Pulmonary Disease (COPD), a common preventable and treatable disease, is characterized by persistent airflow
C H A P T E R 50 Newer Therapies in COPD Prem Parkash Gupta INTRODUCTION Chronic Obstructive Pulmonary Disease (COPD), a common preventable and treatable disease, is characterized by persistent airflow
Roflumilast (Daxas) for chronic obstructive pulmonary disease
 Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
SABA: VENTOLIN EVOHALER (SALBUTAMOL) SAMA: ATROVENT IPRATROPIUM. Offer LAMA (discontinue SAMA) OR LABA
 COPD GUIDELINES DIAGNOSIS >35 years of age Symptoms of cough, breathlessness, sputum, wheeze, Risk factor (SMOKING) Spirometry (post bronchodilator) FEV1/FVC = 0.7 ENCOURAGE PATIENTS TO BRING INHALERS
COPD GUIDELINES DIAGNOSIS >35 years of age Symptoms of cough, breathlessness, sputum, wheeze, Risk factor (SMOKING) Spirometry (post bronchodilator) FEV1/FVC = 0.7 ENCOURAGE PATIENTS TO BRING INHALERS
Take My Breath Away: COPD Update. Jason Henderson D.O. Warren Clinic Pulmonary & Critical Care
 Take My Breath Away: Update Jason Henderson D.O. Warren Clinic Pulmonary & Critical Care Objectives 1. Recognize clinical signs and symptoms associated with chronic bronchitis and emphysema. 2. Describe
Take My Breath Away: Update Jason Henderson D.O. Warren Clinic Pulmonary & Critical Care Objectives 1. Recognize clinical signs and symptoms associated with chronic bronchitis and emphysema. 2. Describe
Disclosure Statement. Epidemiological Data
 EVALUATION OF THE MEDICATION UTILIZATION OF COPD PATIENTS AT THE MIAMI VA HEALTHCARE SYSTEM Simone Edgerton, PharmD. PGY 1 Pharmacy Resident Miami VA Healthcare System Miami, Florida Simone.edgerton2@va.gov
EVALUATION OF THE MEDICATION UTILIZATION OF COPD PATIENTS AT THE MIAMI VA HEALTHCARE SYSTEM Simone Edgerton, PharmD. PGY 1 Pharmacy Resident Miami VA Healthcare System Miami, Florida Simone.edgerton2@va.gov
COPD, Asthma, Or Something In Between? Sharon R. Rosenberg Assistant Professor of Medicine Northwestern University December 4, 2013
 COPD, Asthma, Or Something In Between? Sharon R. Rosenberg Assistant Professor of Medicine Northwestern University December 4, 2013 None Disclosures Definitions Asthma Asthma is a chronic inflammatory
COPD, Asthma, Or Something In Between? Sharon R. Rosenberg Assistant Professor of Medicine Northwestern University December 4, 2013 None Disclosures Definitions Asthma Asthma is a chronic inflammatory
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease Abstract Whittaker C, BPharm, MRPharmS Amayeza Info Centre Chronic obstructive pulmonary disease affects millions of people, has a major impact on quality of life
Chronic obstructive pulmonary disease Abstract Whittaker C, BPharm, MRPharmS Amayeza Info Centre Chronic obstructive pulmonary disease affects millions of people, has a major impact on quality of life
COPD exacerbation. Chiara Maruggi, PGY2
 COPD exacerbation Chiara Maruggi, PGY2 Learning objectives At the end of this lecture students will be able to: 1) Critically assess patients for COPD and design a management plan. 2) Develop a step-wise
COPD exacerbation Chiara Maruggi, PGY2 Learning objectives At the end of this lecture students will be able to: 1) Critically assess patients for COPD and design a management plan. 2) Develop a step-wise
COPD Update. Plus New and Improved Products for Inhaled Therapy. Catherine Bourg Rebitch, PharmD, BCACP Clinical Associate Professor
 COPD Update Plus New and Improved Products for Inhaled Therapy Catherine Bourg Rebitch, PharmD, BCACP Clinical Associate Professor Disclosure The presenter has nothing to disclose concerning possible financial
COPD Update Plus New and Improved Products for Inhaled Therapy Catherine Bourg Rebitch, PharmD, BCACP Clinical Associate Professor Disclosure The presenter has nothing to disclose concerning possible financial
Chronic Obstructive Pulmonary Disease
 Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
Chronic Obstructive Pulmonary Disease (COPD) KAREN ALLEN MD PULMONARY & CRITICAL CARE MEDICINE VA HOSPITAL OKC / OUHSC
 Chronic Obstructive Pulmonary Disease (COPD) KAREN ALLEN MD PULMONARY & CRITICAL CARE MEDICINE VA HOSPITAL OKC / OUHSC I have no financial disclosures Definition COPD is a preventable and treatable disease
Chronic Obstructive Pulmonary Disease (COPD) KAREN ALLEN MD PULMONARY & CRITICAL CARE MEDICINE VA HOSPITAL OKC / OUHSC I have no financial disclosures Definition COPD is a preventable and treatable disease
CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) TREATMENT GUIDELINES
 CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) TREATMENT GUIDELINES Document Description Document Type Service Application Version Guidelines All healthcare professionals(hcps) caring for patients with asthma
CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) TREATMENT GUIDELINES Document Description Document Type Service Application Version Guidelines All healthcare professionals(hcps) caring for patients with asthma
THE CHALLENGES OF COPD MANAGEMENT IN PRIMARY CARE An Expert Roundtable
 THE CHALLENGES OF COPD MANAGEMENT IN PRIMARY CARE An Expert Roundtable This activity is supported by an educational grant from Sunovion Pharmaceuticals Inc. COPD in the United States Third leading cause
THE CHALLENGES OF COPD MANAGEMENT IN PRIMARY CARE An Expert Roundtable This activity is supported by an educational grant from Sunovion Pharmaceuticals Inc. COPD in the United States Third leading cause
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Exacerbations of COPD. Dr J Cullen
 Exacerbations of COPD Dr J Cullen Definition An AECOPD is a sustained worsening of the patient s clinical condition from their stable state that is beyond their usual day-to-day variation is acute in onset
Exacerbations of COPD Dr J Cullen Definition An AECOPD is a sustained worsening of the patient s clinical condition from their stable state that is beyond their usual day-to-day variation is acute in onset
Prescribing guidelines: Management of COPD in Primary Care
 Prescribing guidelines: Management of COPD in Primary Care Establish diagnosis of COPD in patients 35 years with appropriate symptoms with history, examination and spirometry (FEV1/FVC ratio < 70%) Establish
Prescribing guidelines: Management of COPD in Primary Care Establish diagnosis of COPD in patients 35 years with appropriate symptoms with history, examination and spirometry (FEV1/FVC ratio < 70%) Establish
Changing Landscapes in COPD New Zealand Respiratory Conference
 Changing Landscapes in COPD New Zealand Respiratory Conference Dr Robert Young BMedSc MBChB DPhil (Oxon) FRACP FRCP Associate Professor Consultant Physician Changing Landscapes in COPD: Summary 1. Overview
Changing Landscapes in COPD New Zealand Respiratory Conference Dr Robert Young BMedSc MBChB DPhil (Oxon) FRACP FRCP Associate Professor Consultant Physician Changing Landscapes in COPD: Summary 1. Overview
Chronic Obstructive Pulmonary Disease Guidelines and updates
 Chronic Obstructive Pulmonary Disease Guidelines and updates October 20, 2018 Saratoga Springs, NY COPD (Chronic obstructive pulmonary disease) is a major cause of mortality and morbidity in the United
Chronic Obstructive Pulmonary Disease Guidelines and updates October 20, 2018 Saratoga Springs, NY COPD (Chronic obstructive pulmonary disease) is a major cause of mortality and morbidity in the United
What s new in COPD? Apichart Khanichap MD. Department of Medicine, Faculty of Medicine, Thammasat university
 What s new in COPD? Apichart Khanichap MD. Department of Medicine, Faculty of Medicine, Thammasat university Management stable COPD Relieve symptoms Improve exercise tolerance Improve health status Prevent
What s new in COPD? Apichart Khanichap MD. Department of Medicine, Faculty of Medicine, Thammasat university Management stable COPD Relieve symptoms Improve exercise tolerance Improve health status Prevent
Early Identification and Diagnosis of Chronic Respiratory Diseases: The Primary Role in Improving Patient Outcomes in Asthma, COPD, and IPF
 Early Identification and Diagnosis of Chronic Respiraty Diseases: Learning Objectives Early Identification and Diagnosis of Chronic Respiraty Diseases The Primary Role in Improving Patient Outcomes in
Early Identification and Diagnosis of Chronic Respiraty Diseases: Learning Objectives Early Identification and Diagnosis of Chronic Respiraty Diseases The Primary Role in Improving Patient Outcomes in
Medicines Management of Chronic Obstructive Pulmonary Disease (COPD)
 Medicines Management of Chronic Obstructive Pulmonary Disease (COPD) (Chronic & Acute) Guidelines for Primary Care Guideline Authors: Shaneez Dhanji (Wandsworth CCG) Samantha Prigmore (St George s Hospital)
Medicines Management of Chronic Obstructive Pulmonary Disease (COPD) (Chronic & Acute) Guidelines for Primary Care Guideline Authors: Shaneez Dhanji (Wandsworth CCG) Samantha Prigmore (St George s Hospital)
CHRONIC OBSTRUCTIVE PULMONARY DISEASE
 CHRONIC OBSTRUCTIVE PULMONARY DISEASE INCIDENCE UP TO 380,000 PEOPLE IN IRELAND HSE FIGURES 110,000 DIAGNOSED AND 200,000 UNDIAGNOSED. AFFECTS MORE MEN THAN WOMEN BUT RATES ARE RISING 1500 DEATHS PER YEAR
CHRONIC OBSTRUCTIVE PULMONARY DISEASE INCIDENCE UP TO 380,000 PEOPLE IN IRELAND HSE FIGURES 110,000 DIAGNOSED AND 200,000 UNDIAGNOSED. AFFECTS MORE MEN THAN WOMEN BUT RATES ARE RISING 1500 DEATHS PER YEAR
Pharmacotherapy for COPD
 10/3/2017 Topics to be covered Pharmacotherapy for chronic treatment Pharmacotherapy for COPD Dr. W C Yu 3rd September 2017 Commonly used drugs Guidelines for their use Inhaled corticosteroids (ICS) in
10/3/2017 Topics to be covered Pharmacotherapy for chronic treatment Pharmacotherapy for COPD Dr. W C Yu 3rd September 2017 Commonly used drugs Guidelines for their use Inhaled corticosteroids (ICS) in
Early Identification and Diagnosis of Chronic Respiratory Diseases: The Primary Role in Improving Patient Outcomes in Asthma, COPD, and IPF
 Learning Objectives The Primary Role in Improving Patient Outcomes in Asthma, COPD, and IPF Ellen H. Miller, MD Profess of Science Education & Medicine Hofstra Nthwell School of Medicine Seni Medical Direct
Learning Objectives The Primary Role in Improving Patient Outcomes in Asthma, COPD, and IPF Ellen H. Miller, MD Profess of Science Education & Medicine Hofstra Nthwell School of Medicine Seni Medical Direct
Global Initiative for Chronic Obstructive Lung Disease
 Global Initiative for Chronic Obstructive Lung Disease POCKET GUIDE TO COPD DIAGNOSIS, MANAGEMENT, AND PREVENTION A Guide for Health Care Professionals REVISED 2011 Global Initiative for Chronic Obstructive
Global Initiative for Chronic Obstructive Lung Disease POCKET GUIDE TO COPD DIAGNOSIS, MANAGEMENT, AND PREVENTION A Guide for Health Care Professionals REVISED 2011 Global Initiative for Chronic Obstructive
2017 GOLD Report. Is it worth its weight in GOLD??? CSHP-NB Fall Education Day September 30, 2017
 2017 GOLD Report Is it worth its weight in GOLD??? CSHP-NB Fall Education Day September 30, 2017 Lauren Munro; BSc(Pharm) Amanda Burns; BSc(Pharm) Pharmacy Residents The Moncton Hospital Objectives Explain
2017 GOLD Report Is it worth its weight in GOLD??? CSHP-NB Fall Education Day September 30, 2017 Lauren Munro; BSc(Pharm) Amanda Burns; BSc(Pharm) Pharmacy Residents The Moncton Hospital Objectives Explain
Advancing COPD treatment strategies with evidencebased. 17:15 19:15 Monday 11 September 2017 ERS 2017, Milan, Italy
 Advancing COPD treatment strategies with evidencebased approaches 17:15 19:15 Monday 11 September 2017 ERS 2017, Milan, Italy Increasing understanding of COPD and the effect on guideline evolution. GOLD
Advancing COPD treatment strategies with evidencebased approaches 17:15 19:15 Monday 11 September 2017 ERS 2017, Milan, Italy Increasing understanding of COPD and the effect on guideline evolution. GOLD
Chronic Obstructive Pulmonary Disease
 Chronic Obstructive Pulmonary Disease Practical Approaches to Diagnosis and Management MARCH 20, 2014 9:15 AM 10:30 AM Houston, Texas Sponsed by pmicme Educational Partner Session 2: Chronic Obstructive
Chronic Obstructive Pulmonary Disease Practical Approaches to Diagnosis and Management MARCH 20, 2014 9:15 AM 10:30 AM Houston, Texas Sponsed by pmicme Educational Partner Session 2: Chronic Obstructive
COPD Management in LTC: Presented By: Jessica Denney RRT
 COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
WINDY CITY WHEEZE: A PREVENTATIVE APPROACH TO COPD MANAGEMENT
 WINDY CITY WHEEZE: A PREVENTATIVE APPROACH TO COPD MANAGEMENT Thursday, October 25, 2018 Sarah Sungurlu DO Assistant Professor Division of Pulmonary and Critical Care Medicine Disclosures I have no actual
WINDY CITY WHEEZE: A PREVENTATIVE APPROACH TO COPD MANAGEMENT Thursday, October 25, 2018 Sarah Sungurlu DO Assistant Professor Division of Pulmonary and Critical Care Medicine Disclosures I have no actual
Chronic Obstructive Pulmonary Disease
 Chronic Obstructive Pulmonary Disease CareOregon Pharmacy Abridged sample of presentation content Home Equipment Pathophysiology Exacerbations Guidelines Lifestyle Modification Medication Management Sample
Chronic Obstructive Pulmonary Disease CareOregon Pharmacy Abridged sample of presentation content Home Equipment Pathophysiology Exacerbations Guidelines Lifestyle Modification Medication Management Sample
TORCH: Salmeterol and Fluticasone Propionate and Survival in COPD
 TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
COPD: GOLD guidelines Ijlal Babar, MD Medical Director Pulmonary CCM, Pulmonary Hypertension Center SRHS
 COPD: GOLD guidelines 2017 Ijlal Babar, MD Medical Director Pulmonary CCM, Pulmonary Hypertension Center SRHS Introduction The Global Initiative for Chronic Obstructive Lung Disease (GOLD) program was
COPD: GOLD guidelines 2017 Ijlal Babar, MD Medical Director Pulmonary CCM, Pulmonary Hypertension Center SRHS Introduction The Global Initiative for Chronic Obstructive Lung Disease (GOLD) program was
Guideline for the Diagnosis and Management of COPD
 Guideline for the Diagnosis and Management of COPD Introduction Chronic obstructive pulmonary disease (COPD) is a respiratory disorder largely caused by smoking. It is characterized by progressive, partially
Guideline for the Diagnosis and Management of COPD Introduction Chronic obstructive pulmonary disease (COPD) is a respiratory disorder largely caused by smoking. It is characterized by progressive, partially
Treatment. Assessing the outcome of interventions Traditionally, the effects of interventions have been assessed by measuring changes in the FEV 1
 58 COPD 59 The treatment of COPD includes drug therapy, surgery, exercise and counselling/psychological support. When managing COPD patients, it is particularly important to evaluate the social and family
58 COPD 59 The treatment of COPD includes drug therapy, surgery, exercise and counselling/psychological support. When managing COPD patients, it is particularly important to evaluate the social and family
Chronic Obstructive Pulmonary Disease (COPD).
 Chronic Obstructive Pulmonary Disease (COPD). Linde: Living healthcare 02 03 Chronic Obstructive Pulmonary Disease (COPD). A pocket guide for healthcare professionals. COPD the facts Moderate to severe
Chronic Obstructive Pulmonary Disease (COPD). Linde: Living healthcare 02 03 Chronic Obstructive Pulmonary Disease (COPD). A pocket guide for healthcare professionals. COPD the facts Moderate to severe
Surveillance report Published: 6 April 2016 nice.org.uk. NICE All rights reserved.
 Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
VA/DoD Clinical Practice Guideline Management of COPD Pocket Guide
 VA/DoD Clinical Practice Guideline Management of COPD Pocket Guide MODULE A: MAAGEMET OF COPD 1 2 Patient with suspected or confirmed COPD presents to primary care [ A ] See sidebar A Perform brief clinical
VA/DoD Clinical Practice Guideline Management of COPD Pocket Guide MODULE A: MAAGEMET OF COPD 1 2 Patient with suspected or confirmed COPD presents to primary care [ A ] See sidebar A Perform brief clinical
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
PFT s / 2017 Pulmonary Update. Eric S. Papierniak, DO University of Florida NF/SG VHA
 PFT s / 2017 Pulmonary Update Eric S. Papierniak, DO University of Florida NF/SG VHA Outline Overview of pulmonary function testing Uses/indications/limitations Technical aspects Basics of interpretation
PFT s / 2017 Pulmonary Update Eric S. Papierniak, DO University of Florida NF/SG VHA Outline Overview of pulmonary function testing Uses/indications/limitations Technical aspects Basics of interpretation
COPD in primary care: reminder and update
 COPD in primary care: reminder and update Managing COPD continues to be a major feature of primary care, particularly in practices with a high proportion of M ori and Pacific peoples. COPDX clinical practice
COPD in primary care: reminder and update Managing COPD continues to be a major feature of primary care, particularly in practices with a high proportion of M ori and Pacific peoples. COPDX clinical practice
Chronic Obstructive Pulmonary Disease
 Chronic Obstructive Pulmonary Disease Practical Approaches to Diagnosis and Management MAY 14, 2014 11:15 AM 12:30 PM Chicago, Illinois Sponsed by pmicme Educational Partner Session 3: Chronic Obstructive
Chronic Obstructive Pulmonary Disease Practical Approaches to Diagnosis and Management MAY 14, 2014 11:15 AM 12:30 PM Chicago, Illinois Sponsed by pmicme Educational Partner Session 3: Chronic Obstructive
COPD: From Hospital to Home October 5, 2015 Derek Linderman, MD Associate Professor COPD Center Pulmonary Nodule Clinic
 COPD: From Hospital to Home October 5, 2015 Derek Linderman, MD Associate Professor COPD Center Pulmonary Nodule Clinic Learning Objectives Know the adverse effects of COPD exacerbations Know mainstays
COPD: From Hospital to Home October 5, 2015 Derek Linderman, MD Associate Professor COPD Center Pulmonary Nodule Clinic Learning Objectives Know the adverse effects of COPD exacerbations Know mainstays
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
COPD/ Asthma. Dr Heather Lewis Honorary Clinical Lecturer
 COPD/ Asthma Dr Heather Lewis Honorary Clinical Lecturer Objectives To understand the pathogenesis of asthma/ COPD To recognise the clinical features of asthma/ COPD To know how to diagnose asthma/ COPD
COPD/ Asthma Dr Heather Lewis Honorary Clinical Lecturer Objectives To understand the pathogenesis of asthma/ COPD To recognise the clinical features of asthma/ COPD To know how to diagnose asthma/ COPD
What is this patient s diagnosis?
 Asthma and COPD KANTA VELAMURI, MD ASSOCIATE PROFESSOR OF MEDICINE PULMONARY, CRITICAL CARE AND SLEEP MEDICINE SECTION MICHAEL E. DEBAKEY VA MEDICAL CENTER BAYLOR COLLEGE OF MEDICINE Disclosures None Case
Asthma and COPD KANTA VELAMURI, MD ASSOCIATE PROFESSOR OF MEDICINE PULMONARY, CRITICAL CARE AND SLEEP MEDICINE SECTION MICHAEL E. DEBAKEY VA MEDICAL CENTER BAYLOR COLLEGE OF MEDICINE Disclosures None Case
Fact. Objectives 1/6/2016. Reducing Hospital Readmissions for Chronic Obstructive Pulmonary Disease (COPD)
 Reducing Hospital Readmissions for Chronic Obstructive Pulmonary Disease (COPD) Jin S. Oh, PharmD Larkin Community Hospital January 10, 2016 Fact COPD is the third leading cause of death in the United
Reducing Hospital Readmissions for Chronic Obstructive Pulmonary Disease (COPD) Jin S. Oh, PharmD Larkin Community Hospital January 10, 2016 Fact COPD is the third leading cause of death in the United
Advances in Chronic Obstructive Pulmonary Disease
 Advances in Chronic Obstructive Pulmonary Disease By Dave C. Todd, MD; and Darcy D. Marciniuk, MD, FRCPC The case of Nina Nina, 64, presents to the clinic with a three- to fouryear history of progressive,
Advances in Chronic Obstructive Pulmonary Disease By Dave C. Todd, MD; and Darcy D. Marciniuk, MD, FRCPC The case of Nina Nina, 64, presents to the clinic with a three- to fouryear history of progressive,
Objectives. Advances in Managing COPD Patients
 4:45 5:30pm Advances in Managing Patients SPEAKER Nicola Hanania, MD, FCCP, FRCP, FACP Presenter Disclosure Information The following relationships exist related to this presentation: Nicola Hanania, MD,
4:45 5:30pm Advances in Managing Patients SPEAKER Nicola Hanania, MD, FCCP, FRCP, FACP Presenter Disclosure Information The following relationships exist related to this presentation: Nicola Hanania, MD,
Integrated Cardiopulmonary Pharmacology Third Edition
 Integrated Cardiopulmonary Pharmacology Third Edition Chapter 13 Pharmacologic Management of Asthma, Chronic Bronchitis, and Emphysema Multimedia Directory Slide 7 Slide 12 Slide 60 COPD Video Passive
Integrated Cardiopulmonary Pharmacology Third Edition Chapter 13 Pharmacologic Management of Asthma, Chronic Bronchitis, and Emphysema Multimedia Directory Slide 7 Slide 12 Slide 60 COPD Video Passive
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A.
 aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
How to treat COPD? What is the mechanism of dyspnea? Smoking cessation
 : The Increasing Role of the FP Alan Kaplan, MD, CCFP(EM) Presented at the Primary Care Today: Education Conference and Medical Exposition, Toronto, Ontario, May 2006. Chronic obstructive pulmonary disease
: The Increasing Role of the FP Alan Kaplan, MD, CCFP(EM) Presented at the Primary Care Today: Education Conference and Medical Exposition, Toronto, Ontario, May 2006. Chronic obstructive pulmonary disease
Pharmacist Objectives. Pulmonary Update. Outline. Technician Objectives. GOLD Guidelines. COPD Diagnosis 9/22/2017
 Pharmacist Objectives Pulmonary Update Patty Marshik, PharmD Associate Professor University of New Mexico College of Pharmacy pmarshik@salud.unm.edu Discuss the new Global Initiative for Chronic Obstructive
Pharmacist Objectives Pulmonary Update Patty Marshik, PharmD Associate Professor University of New Mexico College of Pharmacy pmarshik@salud.unm.edu Discuss the new Global Initiative for Chronic Obstructive
Decramer 2014 a &b [21]
![Decramer 2014 a &b [21] Decramer 2014 a &b [21]](/thumbs/90/101390504.jpg) Buhl 2015 [19] Celli 2014 [20] Decramer 2014 a &b [21] D Urzo 2014 [22] Maleki-Yazdi 2014 [23] Inclusion criteria: Diagnosis of chronic obstructive pulmonary disease; 40 years of age or older; Relatively
Buhl 2015 [19] Celli 2014 [20] Decramer 2014 a &b [21] D Urzo 2014 [22] Maleki-Yazdi 2014 [23] Inclusion criteria: Diagnosis of chronic obstructive pulmonary disease; 40 years of age or older; Relatively
Presented by UIC College of Nursing
 Presented by UIC College of Nursing Describe COPD. Identify red flags for a COPD exacerbation. Identify COPD triggers or risk factors. Differentiate between long-acting inhalers and emergency use inhalers.
Presented by UIC College of Nursing Describe COPD. Identify red flags for a COPD exacerbation. Identify COPD triggers or risk factors. Differentiate between long-acting inhalers and emergency use inhalers.
Chronic Obstructive Pulmonary Disease 1/18/2018
 Presented by UIC College of Nursing Describe COPD. Identify red flags for a COPD exacerbation. Identify COPD triggers or risk factors. Differentiate between long acting inhalers and emergency use inhalers.
Presented by UIC College of Nursing Describe COPD. Identify red flags for a COPD exacerbation. Identify COPD triggers or risk factors. Differentiate between long acting inhalers and emergency use inhalers.
Current Approaches to Asthma & COPD
 10/11/18 Current Approaches to Asthma & COPD Lekshmi Santhosh, M.D. Assistant Professor, Pulm/Critical Care & Hosp Med Primary Care Medicine: Principles & Practice 10.11.2018 Revisiting the Dutch Hypothesis:
10/11/18 Current Approaches to Asthma & COPD Lekshmi Santhosh, M.D. Assistant Professor, Pulm/Critical Care & Hosp Med Primary Care Medicine: Principles & Practice 10.11.2018 Revisiting the Dutch Hypothesis:
