PATIENT INFORMATION FORM
|
|
|
- Kerrie Lawson
- 6 years ago
- Views:
Transcription
1 PATIENT INFORMATION FORM "I am going to ask you a number of questions about your asthma. The set of questions is somewhat long, but I will try to move through it fairly quickly so that we can complete this meeting in a reasonable amount of time. I may need to bring us back to the questions if we get off track, but if there is something I'm not asking about that you feel is really important to tell me, please let me know." ASTHMA BOTHER Question Probe Notes on patient responses How much does asthma get in the way of doing what you want to do or living the way you want to live -- how does it affect your daily life? Are there one or two things that you just mentioned that bother you the most, or that you would most like to change? How long have you had asthma? SYMPTOMS Probe for information about: activity level your finances your work and/or home life, your relationships with friends/ family how you think about or see yourself anything else? Question Probe Notes on patient responses In the past 4 weeks, did your asthma wake you up at night? (Includes asthma related coughing) In the past 4 weeks, did you miss any normal daily activity because of your asthma? How often do experience episodes in which your asthma is especially bad (we call these "asthma exacerbations" or flare-ups)? How often? How often? Years Awakened at night? Y N Frequency or # times? Miss daily activity? Y N Frequency or # times? Have you ever had to go to the ER or urgent care during an asthma exacerbation? Have you ever been hospitalized because of asthma? Do you experience a cough with your asthma? How well-controlled you do think your symptoms are? [go to control meter] [If yes] When was the last time? [If yes] When was the last time? How often? Can you tell me what the cough is like? Have patient draw arrow on Handout 1: "How wellcontrolled is your asthma?" to indicate perceived control. CHRONIC RHINOSINUSITIS: Do you usually have a stuffy, runny, or plugged nose for much of the year? Do you often have itchy, watery eyes? Do you have drainage in the back of your throat (also called post-nasal drip) most of the year? Has your health care provider told you that you have chronic sinus problems? When you have a head cold, do your nasal symptoms usually last for 3 months or more? Are you unable to smell scents? GERD: Do you have heartburn? Does food sometimes come up into your throat? In the past 4 weeks, have you had coughing, wheezing, or shortness of breath that was not relieved by taking albuterol? Y N Y N Y N Y N Y N Y N # Y Y N Y N Y N # Y FORM SDM-R1 Page 1 of 4
2 MEDICATION USE CONTINUED Question Probe Notes on patient responses Many people have a hard time taking their controller medication on the prescribed schedule. How often do you miss taking a dose of (any of) your controller medication(s) (your [or ])? Almost everyone tries cutting back on their controller medications at some point, or they don t take them as often or in the amount their doctor prescribes. What situations have led you to decrease any controller medications you use (your [or ], or asthma controllers you have used in the past)? Have you tried taking more of any controller medications than what was prescribed by your doctor? What is the reason? (e.g. forgetting, being tired or busy, deciding not to) What happened? Did you continue to take a decreased amount or stop altogether? How did that work out? What led you to do this? What happened when you did it? What asthma medications have you tried in the past that you feel did not help or that caused you problems? What happened when you took it? [Probe if reported problems are unlikely to be attributable to the medication] What did you do about that? Any other asthma medications that gave you problems? How do [would] you feel about taking asthma controller medications (your [and ]) on a regular basis? Are there other things that [would] bother you about taking asthma medication every day? ASK ONLY PATIENTS WHO DO NOT TAKE ASTHMA CONTROL MEDICATIONS OR Short Acting Beta Agonists REGULARLY: What are the worst things about taking asthma medication every day? Do you believe that taking your [controller] meds more regularly would make any difference in your asthma? Are you concerned about side effects of any asthma medications (ones you take, or others)? What things are you concerned about? Probe further if side effects mentioned have not been documented FORM SDM-R1 PAGE 3 of 4
3 MEDICATION USE If necessary for this section, show pictures on the Asthma Controllers/Relievers poster What are your current PRESCRIPTIONS for your asthma medications? Let s start with albuterol. For each medication: How often is it supposed to be taken? (Inhaled meds) How many puffs each time? How many days in the last week did you take your [insert name]? (Inhaled meds) How many puffs do you usually take? How do you think this medication works on your asthma? Med 1: ALBUTEROL Rx: # days taken last week: Usual # puffs: How patient thinks it works: Med 2: Rx: # days taken last week: Usual # puffs: How patient thinks it works: Med 3: Rx: # days taken last week: Usual # puffs: How patient thinks it works: Question Would you show me how you use your inhaler? [Examine technique, using appropriate Skills Checklist " below. Note errors, but do not correct technique until "Wrap up" section later in the session.] 1. Did the patient shake the inhaler vigorously (5-10 seconds) prior to use? 2. Did the patient exhale fully prior to inhalation? 3. Did the patient tip her/his chin up prior to inhalation? 4. Was the inhaler held level and discharged with the index or middle finger on top of the medication canister and the thumb supporting the inhaler's base? 5. *Did the patient have his/her lips closed and the spacer between his/her teeth during discharge? 6. Did the patient inhale slowly and deeply after inhaler discharge? 7. Did the patient hold his/her breath for 6 to 10 seconds after inhalation? 8. ASK THE PATIENT: If you were really using an inhaler, how long would you wait before taking a second puff? CHECK YES IF ANSWERED ONE OR MORE MINUTES, OTHERWISE CHECK NO. * If a spacer is not used: was the inhaler held 2-5 cm. (1-2 in.) from the patient's open mouth during discharge? FORM SDM-R1 Med 4: Rx: # days taken last week: Usual # puffs: How patient thinks it works: PAGE 2 of 4 Notes on patient technique MDI CHECKLIST SEREVENT & ADVAIR DISKUS CHECKLIST TURBUHALER CHECKLIST 1. Did the patient hold the DISKUS in one hand and use the thumb of the other hand to unveil the mouthpiece? 2. Did the patient hold the DISKUS in a level, horizontal position with the mouthpiece facing him/her? 3. Did the patient slide the lever away from him/her as far as it would go until it clicked? 4. Did the patient exhale while holding the DISKUS level and away from his/her mouth? 5. Did the patient put the mouthpiece to his/her lips and inhale quickly and deeply through his/her mouth? 6. Did the patient hold his/her breath for about 10 seconds after inhalation? 7. Did the patient exhale slowly after holding his/her breath? 8. Did the patient close the DISKUS by sliding the thumbgrip back towards him/her as far as it would go until it clicked shut? 1. Did the patient hold the turbuhaler in the upright position while loading the dose? 2. Did the patient twist the brown grip fully to the right and twist it back fully to the left until there was an audible click? 3. Did the patient turn his/her head away from the turbuhaler while exhaling prior to inhaling the dose? 4. Was the turbuhaler held in the horizontal position when the patient inhaled? 5. Did the patient have his/her lips closed and the mouthpiece between his/her teeth during the inhalation? 6. Did the patient inhale deeply and forcefully so as to activate the flow of medication? 7. Did the patient hold his/her breath for 5 to 10 seconds after inhalation? 8. Did the patient exhale slowly through pursed lips? 9. ASK THE PATIENT: If you were really using an turbuhaler, how long would you wait before taking a second inhalation?
4 ALTERNATIVE TREATMENTS Question Probe Notes on patient responses Have you ever tried any things other than prescription medications to help with your asthma: Vitamins? Herbs? Acupuncture? Deep breathing yoga? Seeing a chiropractor? Anything else? [For each] Did it help your asthma? Do you think any of these things were helpful in reducing your asthma symptoms? [If no ] Do you have any thoughts on why this didn t work for you? Did you add this/these treatments to your medications or did you try to use them as an alternative to taking medication? ENVIRONMENTAL TRIGGERS Question Probe Notes on patient responses Are there different times of the year that your asthma is better of worse? When is it worse? Worse at times? Y N When? Are there certain things in your surroundings that you know affect your asthma? What changes have you made in your surroungings in order to avoid asthma symptoms? Has that been helpful? Are there changes you think you should make that you haven t decided to or haven t been able to do? What are they? What gets in the way of these changes? Are you a smoker? [if yes] Have you tried to quit? I will give you some information on Kaiser's programs to help people quit and I want to encourage you to take advantage of them. This is particularly important because you have asthma. Check box indicating that you have recommended cessation and provided cessation resources for smokers. FORM SDM-R1 PAGE 4 of 4
5 FORM SDM-HO1A How well controlled is your asthma?
6 How well controlled is your asthma? Symptoms more than once a week but not daily Nighttime symptoms more than twice a month but not weekly Normal lung function between episodes Symptoms daily Asthma episodes may affect activity & sleep Nighttime symptoms weekly or more often FEV % of predicted OR PEF 60-80% of personal best Symptoms less than weekly Brief asthma episodes Nighttime symptoms no more that twice a month Normal lung function between episodes Symptoms daily Frequent asthma episodes Frequent nighttime asthma symptoms FEV1 < 60% predicted OR PEF < 60% of personal best FORM SDM-HO1B
7 MEDICATION OPTIONS TO CONTROL ASTHMA OPTIONS MILD PERSISTENT ASTHMA FEATURES QVAR puffs twice a day QVAR 80 1 puff twice a day Pulmicort 1 puff twice a day Aerobid 1-2 puffs twice a day QVAR puffs once a day Flovent puffs once a day Flovent puff once a day Pulmicort 2-3 puffs once a day Aerobid 2-4 puffs once a day Singulair 1 10-mg pill once a day Sustained release theophylline Gives optimal control Maximizes convenience Probably provides less control; not a corticosteroid OPTIONS QVAR puffs twice a day Flovent puffs twice a day Flovent puff twice a day Pulmicort 2-3 puffs twice a day Aerobid 3-4 puffs twice a day MODERATE PERSISTENT ASTHMA QVAR puffs twice a day + Serevent Diskus 1 inhalation twice a day Flovent puffs twice a day + Serevent Diskus 1 inhalation twice a day Flovent puff twice a day + Serevent Diskus 1 inhalation twice a day Pulmicort 2-3 puffs twice a day + Serevent Diskus 1 inhalation twice a day Aerobid 2-4 puffs twice a day + Serevent Diskus 1 inhalation twice a day Advair 250/50 two inhalations per day FEATURES Gives optimal control QVAR puffs twice a day Flovent puffs twice a day Flovent puff twice a day Pulmicort 2-3 puffs twice a day Aerobid 2-4 puffs twice a day QVAR puffs once a day + Serevent Diskus 1 inhalation once a day Flovent puffs once a day + Serevent Diskus 1 inhalation once a day Flovent puffs once a day + Serevent Diskus 1 inhalation once a day Pulmicort 3-4 puffs once a day + Serevent Diskus 1 inhalation once a day Aerobid 4 puffs once a day + Serevent Diskus 1 inhalation once a day Advair 500/50 one inhalation per day Inhaled corticosteroid plus another controller in tablet form; not a Long Acting Beta Agonist. Once a day; Inhaled corticosteroid plus a Long Acting Beta Agonist - maximizes convenience QVAR puffs once a day Flovent puffs once a day Flovent puffs once a day Pulmicort 3-4 puffs once a day Aerobid 4 puffs once a day Inhaled corticosteroid plus another controller in tablet form; once a day; not a Long Acting Beta Agonist. QVAR 80 4 puffs once a day Flovent puffs once a day Flovent puffs once a day Pulmicort 3-4 puffs once a day Aerobid 4 puffs once a day Sustained release theophylline 1 Probably provides less control SEVERE PERSISTENT ASTHMA OPTIONS QVAR 80 >4 puffs twice a day + Serevent Diskus 1 inhalation twice a day Flovent 110 >4 puffs twice a day + Serevent Diskus 1 inhalation twice a day Flovent 220 >2 puffs twice a day + Serevent Diskus 1 inhalation twice a day Pulmicort >4 puffs twice a day + Serevent Diskus 1 inhalation twice a day Aerobid >5 puffs twice a day + Serevent Diskus 1 inhalation twice a day Advair 500/50 two inhalations per day Flovent puffs once a day + Serevent Diskus 1 inhalation twice a day FEATURES Gives optimal control Provides less control. The inhaled corticosteroid only is taken once a day. FORM SDM-R4 rev 6/17/03 Prescribing Guidelines adapated from the National Asthma Education and Prevention Program NAEPP Expert Panel Report: Guidelines for the Diagnosis and Management of Asthma - Update on Selected Topics 2002.
8 My Asthma Treatment Goals is/are: Activities: Other concerns: Features of Asthma Medications Control over inflammation and symptoms Side effects Cost Convenience FORM SDM-HO2
9 Medication Planner Features that matter to me How these options measure up Current Plan Option 1 Option 2 Option 3 Option 4 FORM SDM-HO5
10 Asthma Management and Action Plan Controller Medicines (Use every day to stay healthy) How much to take Date: Patient Name Care Provider's Name: Care Provider's Phone #: Other Instructions How often (such as spacers/masks, nebulizers) times per day EVERY DAY! times per day EVERY DAY! times per day EVERY DAY! times per day EVERY DAY! Quick-Relief Medicines How much to take How often Other Instructions Take ONLY as needed NOTE: If this medicine is needed often ( times per week), call physician. Green Zone I feel good No asthma symptoms, even when I'm active Peak flow above 80% Yellow Zone I do not feel good and have asthma symptoms that may include: Wheezing Tight chest Cough Shortness of breath Awakening due to coughing or difficulty breathing Decreased ability to do usual activities My peak flow is 50-80% _ _ Red Zone I feel awful! Warning signs may include: Wheezing, coughing, or difficulty breathing continues or worsens even after taking everyday and extra "yellow zone" medications listed above Unable to sleep or do activites because of trouble breathing My peak flow is below 50% Danger! Get help immediately PREVENT asthma symptoms every day: Take my controller medicines every day. Before exercise, take puffs of. Avoid things that make my asthma worse Avoid exposure to tobacco smoke CAUTION. Take action by continuing to take asthma controller medicines every day AND: Take Albuterol: puffs If I do not feel good and still have symptoms within one hour, then: Increase Add Call MEDICAL ALERT! Get Help! Take until I get help Take Call Call 911 if you have trouble walking or talking due to shortness of breath, OR lips or fingernails are grey or blue. I have discussed the treatment options for my asthma with my Care Manager. We have agreed that I will try the treatment regimen outlined above. I will inform my Asthma Care Manager about changes in my asthma symptoms so that adjustments can be made as needed. Signed: This plan is adapted from an action plan developed by the Regional Asthma Management and Prevention (RAMP) Initiative, a program of the Public Health Institute (
Kickin Asthma. Workbook for Children with Asthma. Name:
 Kickin Asthma Workbook for Children with Asthma Name: Why Have You Been Invited to Kickin Asthma? You have been invited to Kickin Asthma because you have asthma. Asthma is a disease of your air tubes that
Kickin Asthma Workbook for Children with Asthma Name: Why Have You Been Invited to Kickin Asthma? You have been invited to Kickin Asthma because you have asthma. Asthma is a disease of your air tubes that
Sources. Taking Charge of Your Asthma. Asthma Action Plan (to be completed with your doctor) UnitedHealthcare Insurance Company
 Asthma Action Plan (to be completed with your doctor) Green Zone: (80 to 00% of my personal best) Peak Flow between and (00% = personal best) You can do all the things you usually do. Your asthma medicine
Asthma Action Plan (to be completed with your doctor) Green Zone: (80 to 00% of my personal best) Peak Flow between and (00% = personal best) You can do all the things you usually do. Your asthma medicine
Breathe Easy. Tips for controlling your Asthma
 Breathe Easy Tips for controlling your Asthma Have you or a family member been told you have asthma? Are you or a family member coughing or wheezing? Do you or a family member have tightness in your chest?
Breathe Easy Tips for controlling your Asthma Have you or a family member been told you have asthma? Are you or a family member coughing or wheezing? Do you or a family member have tightness in your chest?
Nancy Davis, RRT, AE-C
 Nancy Davis, RRT, AE-C Asthma Statistics 25.6 million Americans diagnosed with asthma 6.8 million are children 10.5 million missed school days per year 14.2 lost work days for adults Approximately 10%
Nancy Davis, RRT, AE-C Asthma Statistics 25.6 million Americans diagnosed with asthma 6.8 million are children 10.5 million missed school days per year 14.2 lost work days for adults Approximately 10%
MANAGING ASTHMA. Nancy Davis, RRT, AE-C
 MANAGING ASTHMA Nancy Davis, RRT, AE-C What is asthma? Asthma is a chronic respiratory disease characterized by episodes or attacks of inflammation and narrowing of small airways in response to asthma
MANAGING ASTHMA Nancy Davis, RRT, AE-C What is asthma? Asthma is a chronic respiratory disease characterized by episodes or attacks of inflammation and narrowing of small airways in response to asthma
Because the more you know, the better you ll feel.
 ABOUT ASTHMA Because the more you know, the better you ll feel. This booklet is designed to help you understand asthma and the things you can do every day to help control symptoms. As always, talk to your
ABOUT ASTHMA Because the more you know, the better you ll feel. This booklet is designed to help you understand asthma and the things you can do every day to help control symptoms. As always, talk to your
CARE AT HOME: ASTHMA. A guide for parents. childrensmn.org
 CARE AT HOME: ASTHMA A guide for parents childrensmn.org Content Your child has asthma a chronic lung disease. To best control the symptoms of asthma, it is important that you learn all you can about asthma.
CARE AT HOME: ASTHMA A guide for parents childrensmn.org Content Your child has asthma a chronic lung disease. To best control the symptoms of asthma, it is important that you learn all you can about asthma.
Because the more you know, the better you ll feel.
 ABOUT ASTHMA Because the more you know, the better you ll feel. What You ll Find Attitudes and Beliefs Asthma What Is It? Where You ll Find It Page 4-5 This booklet is designed to help you understand asthma
ABOUT ASTHMA Because the more you know, the better you ll feel. What You ll Find Attitudes and Beliefs Asthma What Is It? Where You ll Find It Page 4-5 This booklet is designed to help you understand asthma
How to Use Inhaled Medications for Asthma and COPD
 How to Use Inhaled Medications for Asthma and COPD This information is not intended to diagnose health problems or to take the place of medical advice or care you receive from your physician or other health
How to Use Inhaled Medications for Asthma and COPD This information is not intended to diagnose health problems or to take the place of medical advice or care you receive from your physician or other health
Breathe Easy. Living with Asthma
 Breathe Easy Living with Asthma Got Asthma? You re Not Alone! More than 300 million people around the world have asthma. But having asthma doesn t have to limit what you can do. With education and treatment,
Breathe Easy Living with Asthma Got Asthma? You re Not Alone! More than 300 million people around the world have asthma. But having asthma doesn t have to limit what you can do. With education and treatment,
Get Healthy Stay Healthy
 Asthma Management WHAT IS ASTHMA? Asthma causes swelling and inflammation in the breathing passages that lead to your lungs. When asthma flares up, the airways tighten and become narrower. This keeps the
Asthma Management WHAT IS ASTHMA? Asthma causes swelling and inflammation in the breathing passages that lead to your lungs. When asthma flares up, the airways tighten and become narrower. This keeps the
How can I benefit most from my COPD medications?
 Fact Sheet: COPD Medications and Delivery Devices How can I benefit most from my COPD medications? COPD medications can improve your symptoms. By taking the right medication at the right time, you can
Fact Sheet: COPD Medications and Delivery Devices How can I benefit most from my COPD medications? COPD medications can improve your symptoms. By taking the right medication at the right time, you can
ASTHMA IN THE PEDIATRIC POPULATION
 ASTHMA IN THE PEDIATRIC POPULATION SEARCH Rotation 2 August 23, 2010 Objectives Define asthma as a chronic disease Discuss the morbidity of asthma in pediatrics Discuss a few things that a health center
ASTHMA IN THE PEDIATRIC POPULATION SEARCH Rotation 2 August 23, 2010 Objectives Define asthma as a chronic disease Discuss the morbidity of asthma in pediatrics Discuss a few things that a health center
DOCTOR: The last time I saw you and your 6-year old son Julio was about 2 months ago?
 DOCTOR: The last time I saw you and your 6-year old son Julio was about 2 months ago? MOTHER: Um, ya, I think that was our first time here. DOCTOR: Do you remember if you got an Asthma Action Plan? MOTHER:
DOCTOR: The last time I saw you and your 6-year old son Julio was about 2 months ago? MOTHER: Um, ya, I think that was our first time here. DOCTOR: Do you remember if you got an Asthma Action Plan? MOTHER:
Breathe Easy ACTIVITIES. A Family Guide to Living with Asthma F O R T H E K ! I D S
 Breathe Easy A Family Guide to Living with Asthma ACTIVITIES FUN & EDUCATIONAL F O R T H E K! I D S What Is Asthma? Asthma is a disease of the lungs. It s a chronic (long-term) condition that affects the
Breathe Easy A Family Guide to Living with Asthma ACTIVITIES FUN & EDUCATIONAL F O R T H E K! I D S What Is Asthma? Asthma is a disease of the lungs. It s a chronic (long-term) condition that affects the
Date of Assessment: Assessed By: Questionnaire: Assessing Student Readiness to Self- Carry
 Student Name: Score: Date of Assessment: Assessed By: naire: Assessing Student Readiness to Self- Carry Having immediate access to quick- relief medicine is critical for people with asthma. The purpose
Student Name: Score: Date of Assessment: Assessed By: naire: Assessing Student Readiness to Self- Carry Having immediate access to quick- relief medicine is critical for people with asthma. The purpose
MANAGEMENT OF ASTHMA SPRING Presented by:
 MEDS@Work MANAGEMENT OF ASTHMA SPRING 2013 Presented by: Lusia Fomuso PharmD candidate 2014 Olivia Sibailly PharmD candidate 2014 Kimberly Biedka PharmD candidate 2014 Dr. Donna Bartlett PharmD CGP RPh
MEDS@Work MANAGEMENT OF ASTHMA SPRING 2013 Presented by: Lusia Fomuso PharmD candidate 2014 Olivia Sibailly PharmD candidate 2014 Kimberly Biedka PharmD candidate 2014 Dr. Donna Bartlett PharmD CGP RPh
Appendix E: Device Technique
 Adult Asthma Care Guidelines for Nurses: Promoting Control of Asthma Appendix E: Device Technique Medications: Inhalation Devices Adapted with permission from The Lung Association: www.lung.ca/asthma/manage/devices.html
Adult Asthma Care Guidelines for Nurses: Promoting Control of Asthma Appendix E: Device Technique Medications: Inhalation Devices Adapted with permission from The Lung Association: www.lung.ca/asthma/manage/devices.html
Using an Inhaler and Nebulizer
 Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
In case of an urgent concern or emergency, call 911 or go to the nearest emergency department right away.
 Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Asthma Education. The Keys to Asthma Prevention and Control. what to do when one s asthma is flared! Lucile Packard Children s Hospital.
 Asthma Education Lucile Packa r d Children s H o spit al Created by Rachel Lawler RN, MSN, cpnp, AE-C, NPAT Pulmonary Pediatric Nurse Practitioner Lucile Packard Children s Hospital The Keys to Asthma
Asthma Education Lucile Packa r d Children s H o spit al Created by Rachel Lawler RN, MSN, cpnp, AE-C, NPAT Pulmonary Pediatric Nurse Practitioner Lucile Packard Children s Hospital The Keys to Asthma
Welcome to our Asthma Program
 Welcome to our Asthma Program We re here to help you be your healthiest through information, education and support for your asthma. We ll work with you by: Partnering with your health care team to make
Welcome to our Asthma Program We re here to help you be your healthiest through information, education and support for your asthma. We ll work with you by: Partnering with your health care team to make
My Asthma Log. Tommy Traffic Light. NHS Number: Name:
 My Asthma Log Tommy Traffic Light NHS Number: Name: My Asthma Log Book This book is designed to help you understand and learn about managing your asthma. You should take your book with you to all your
My Asthma Log Tommy Traffic Light NHS Number: Name: My Asthma Log Book This book is designed to help you understand and learn about managing your asthma. You should take your book with you to all your
Medications. prescribed. Use as. A s t h m a B a s i c s # 3
 Medications A s t h m a B a s i c s # 3 Use as prescribed The Asthma Basics Booklet Series was developed to provide Canadians with asthma, current and accurate information about asthma management. This
Medications A s t h m a B a s i c s # 3 Use as prescribed The Asthma Basics Booklet Series was developed to provide Canadians with asthma, current and accurate information about asthma management. This
Asthma Medications: Information for Children and Families. What You Need to Know about Medicines for Asthma
 Page 1 of 8 PED-ALL-005-1992 Asthma Medications: Information for Children and Families What You Need to Know about Medicines for Asthma What Medicines Are used to Treat Asthma? There are two kinds of medicines:
Page 1 of 8 PED-ALL-005-1992 Asthma Medications: Information for Children and Families What You Need to Know about Medicines for Asthma What Medicines Are used to Treat Asthma? There are two kinds of medicines:
Inhaler Devices. Ask the patient/carer to demonstrate the technique and correct accordingly at every opportunity.
 Inhaler Devices The most effective way of taking most asthma medicines is to inhale them so they get straight into the lungs. The best inhaler device is one that the patient can and will use. The correct
Inhaler Devices The most effective way of taking most asthma medicines is to inhale them so they get straight into the lungs. The best inhaler device is one that the patient can and will use. The correct
Appendix 1: Shared decision making Intervention description: Carolinas Asthma Coach
 Appendix 1: Shared decision making Intervention description: Carolinas Asthma Coach Based on the platform of motivational interviewing and shared decision making, the ipad version of the Asthma Coach was
Appendix 1: Shared decision making Intervention description: Carolinas Asthma Coach Based on the platform of motivational interviewing and shared decision making, the ipad version of the Asthma Coach was
ASTHMA CONTROL. Asthma is a chronic airway disease. You cannot cure asthma, but you can control it. Treatment can improve asthma symptoms.
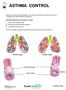 ASTHMA CONTROL Asthma is a chronic airway disease. You cannot cure asthma, but you can control it. Treatment can improve asthma symptoms. Asthma changes the lung airways in 3 ways: 1. Lining of the airways
ASTHMA CONTROL Asthma is a chronic airway disease. You cannot cure asthma, but you can control it. Treatment can improve asthma symptoms. Asthma changes the lung airways in 3 ways: 1. Lining of the airways
Medications. prescribed. Use as. Your Asthma Basics series: Asthma Basics #3. Diagnosis Triggers Medications Kids
 Medications Asthma Basics #3 Your Asthma Basics series: 1 2 3 Diagnosis Triggers Medications Kids Use as prescribed Supported by unrestricted educational grants from: For more information from the Asthma
Medications Asthma Basics #3 Your Asthma Basics series: 1 2 3 Diagnosis Triggers Medications Kids Use as prescribed Supported by unrestricted educational grants from: For more information from the Asthma
EARLY warning signs. Coughing (may be worse at night or with exercise) Wheezing
 Breathing Easier What is asthma? Asthma is a disease of the lungs that often leads to repeated episodes of wheezing, chest tightness, breathlessness, and early morning or nighttime coughing. Asthma currently
Breathing Easier What is asthma? Asthma is a disease of the lungs that often leads to repeated episodes of wheezing, chest tightness, breathlessness, and early morning or nighttime coughing. Asthma currently
Explain purpose of peak flow meter (To measure how well their lungs are working)
 Peak Flow Technique Explain purpose of peak flow meter (To measure how well their lungs are working) Review student s peak flow expected rates based on height and plot into Red, Yellow, and Green zones
Peak Flow Technique Explain purpose of peak flow meter (To measure how well their lungs are working) Review student s peak flow expected rates based on height and plot into Red, Yellow, and Green zones
Your Guide to MANAGING ASTHMA
 Your Guide to MANAGING ASTHMA Asthma affects more than 24 MILLION AMERICANS. It is a chronic disease that causes your airways to become inflamed, making it hard to breathe. There is no cure for asthma.
Your Guide to MANAGING ASTHMA Asthma affects more than 24 MILLION AMERICANS. It is a chronic disease that causes your airways to become inflamed, making it hard to breathe. There is no cure for asthma.
PATIENT INFORMATION. ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation
![PATIENT INFORMATION. ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation PATIENT INFORMATION. ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation](/thumbs/74/71128680.jpg) PATIENT INFORMATION ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation What is ADVAIR DISKUS? ADVAIR DISKUS combines the inhaled corticosteroid
PATIENT INFORMATION ADVAIR DISKUS [AD vair DISK us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation What is ADVAIR DISKUS? ADVAIR DISKUS combines the inhaled corticosteroid
Asthma. January 2011
 Asthma January 2011 What is Asthma? Asthma is a lung disease that affects the breathing tubes (airways) that allow air to go in and out of the lungs. Normal airways are wide open, so air can go in and
Asthma January 2011 What is Asthma? Asthma is a lung disease that affects the breathing tubes (airways) that allow air to go in and out of the lungs. Normal airways are wide open, so air can go in and
Asthma in Pregnancy. Asthma. Chronic Airway Inflammation. Objective Measures of Airflow. Peak exp. flow rate (PEFR)
 Chronic Airway Inflammation Asthma in Pregnancy Robin Field, MD Maternal Fetal Medicine Kaiser Permanente San Francisco Asthma Chronic airway inflammation increased airway responsiveness to a variety of
Chronic Airway Inflammation Asthma in Pregnancy Robin Field, MD Maternal Fetal Medicine Kaiser Permanente San Francisco Asthma Chronic airway inflammation increased airway responsiveness to a variety of
Asthma Action Plan and Education
 Acute Services Division Asthma Action Plan and Education Name: Date: Index What is Asthma? Page 4 Asthma Triggers Page 5 Peak Expiratory Flow Rate (Peak Flow) Page 6 Asthma Treatments Page 7 Asthma Action
Acute Services Division Asthma Action Plan and Education Name: Date: Index What is Asthma? Page 4 Asthma Triggers Page 5 Peak Expiratory Flow Rate (Peak Flow) Page 6 Asthma Treatments Page 7 Asthma Action
Appendix M: Device Technique
 Nursing Care of Dyspnea: The 6th Vital Sign in Individuals with Chronic Obstructive Pulmonary Disease (COPD) Appendix M: Device Technique Medications: Inhalation Devices Medications come in many forms.
Nursing Care of Dyspnea: The 6th Vital Sign in Individuals with Chronic Obstructive Pulmonary Disease (COPD) Appendix M: Device Technique Medications: Inhalation Devices Medications come in many forms.
Asthma and COPD Awareness
 Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Texas Newsletter Spring 2011 Asthma Warning Signs In This Issue Asthma Warning Signs pg 1 Working with the Provider
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Texas Newsletter Spring 2011 Asthma Warning Signs In This Issue Asthma Warning Signs pg 1 Working with the Provider
Asthma By Mayo Clinic staff
 MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
Chronic Obstructive Pulmonary Disease
 Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Home Management Plan. Cover Page
 Home Management Plan Cover Page What is Asthma? Asthma is a chronic disease of the lungs caused by swelling and irritation in the lining of airways Tightness of the airway muscles Excess mucus in the airways
Home Management Plan Cover Page What is Asthma? Asthma is a chronic disease of the lungs caused by swelling and irritation in the lining of airways Tightness of the airway muscles Excess mucus in the airways
Metered Dose Inhaler (MDI)
 Metered Dose Inhaler (MDI) If the inhaler has not been used before, a test dose should be fired into the air to prime the system. 1. Remove cap. 2. Shake well. 3. Breathe out fully. 4. Holding inhaler
Metered Dose Inhaler (MDI) If the inhaler has not been used before, a test dose should be fired into the air to prime the system. 1. Remove cap. 2. Shake well. 3. Breathe out fully. 4. Holding inhaler
How to get the most out of your medical appointments. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 How to get the most out of your medical appointments Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital Objectives Discuss who works in the typical doctors office Discuss things you
How to get the most out of your medical appointments Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital Objectives Discuss who works in the typical doctors office Discuss things you
Adult Asthma My Days of Living in Tension with Asthma are Over!
 Published on: 9 Jul 2014 Adult Asthma My Days of Living in Tension with Asthma are Over! Introduction This is a recent picture, taken when we went on a family picnic. We climbed up this big hill and I
Published on: 9 Jul 2014 Adult Asthma My Days of Living in Tension with Asthma are Over! Introduction This is a recent picture, taken when we went on a family picnic. We climbed up this big hill and I
Asthma and COPD Awareness
 Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Washington Newsletter Spring 2011 Asthma Warning Signs In This Issue Asthma Warning Signs pg 1 Working with the
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Washington Newsletter Spring 2011 Asthma Warning Signs In This Issue Asthma Warning Signs pg 1 Working with the
OXEZE TURBUHALER formoterol fumarate dihydrate dry powder for oral inhalation
 IMPORTANT: PLEASE READ PART III: CONSUMER INFORMATION OEZE TURBUHALER formoterol fumarate dihydrate dry powder for oral inhalation This leaflet is part III of a three-part Product Monograph published when
IMPORTANT: PLEASE READ PART III: CONSUMER INFORMATION OEZE TURBUHALER formoterol fumarate dihydrate dry powder for oral inhalation This leaflet is part III of a three-part Product Monograph published when
Recommended Component: Manage Physical Activity for Students with Asthma
 Recommended Component: Manage Physical Activity for Students with Asthma Individuals with exercise-induced asthma do not necessarily have other asthma triggers. For others with asthma, exercise may be
Recommended Component: Manage Physical Activity for Students with Asthma Individuals with exercise-induced asthma do not necessarily have other asthma triggers. For others with asthma, exercise may be
CHILDREN S HEALTH SURVEY
 CHILDREN S HEALTH SURVEY FOR ASTHMA CHILD VERSION The purpose of this survey is to find out how much asthma affects the everyday life of both you and your family. THERE ARE NO RIGHT OR WRONG ANSWERS!!
CHILDREN S HEALTH SURVEY FOR ASTHMA CHILD VERSION The purpose of this survey is to find out how much asthma affects the everyday life of both you and your family. THERE ARE NO RIGHT OR WRONG ANSWERS!!
Asthma. Definition. Symptoms
 Asthma Definition Asthma is a condition in which your airways narrow and swell and produce extra mucus. This can make breathing difficult and trigger coughing, wheezing and shortness of breath. For some
Asthma Definition Asthma is a condition in which your airways narrow and swell and produce extra mucus. This can make breathing difficult and trigger coughing, wheezing and shortness of breath. For some
Pediatric Allergies in America: A Landmark Survey of Nasal Allergy Sufferers
 Pediatric Allergies in America: A Landmark Survey of Nasal Allergy Sufferers EXECUTIVE SUMMARY Prepared for Nycomed Conducted by Schulman, Ronca and Bucuvalas, Inc. May 8, 2007 Supported by: Study Design
Pediatric Allergies in America: A Landmark Survey of Nasal Allergy Sufferers EXECUTIVE SUMMARY Prepared for Nycomed Conducted by Schulman, Ronca and Bucuvalas, Inc. May 8, 2007 Supported by: Study Design
UNDERSTANDING & MANAGING
 UNDERSTANDING & MANAGING YOUR CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)* *Includes chronic bronchitis, emphysema, or both Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any
UNDERSTANDING & MANAGING YOUR CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)* *Includes chronic bronchitis, emphysema, or both Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any
1 I *********IF YOU ARE NOT ON ALLERGY SHOTS PLEASE SKIP THIS SECTION AND MOVE TO PAGE 2********* NAME: AGE: ---- ID (For Office Use Only):
 NAME: AGE: ---- Date of Appointment:. ID (For Office Use Only): RETURN VISIT Date of Visit: Main Reason for visit: Reevaluation Family Doctor: Symptoms worse _ New problem _ Yearly follow up _ Follow up/office
NAME: AGE: ---- Date of Appointment:. ID (For Office Use Only): RETURN VISIT Date of Visit: Main Reason for visit: Reevaluation Family Doctor: Symptoms worse _ New problem _ Yearly follow up _ Follow up/office
A patient educational resource provided by Boehringer Ingelheim Pharmaceuticals, Inc.
 Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets its disease management products and services. A patient educational resource provided
Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets its disease management products and services. A patient educational resource provided
Respiratory Care 2. Clinical Skills School of Medicine 2015/16
 Respiratory Care 2 Clinical Skills School of Medicine 2015/16 Learning Objectives Identify the different types of inhalers and demonstrate the correct inhaler techniques for the different inhalers. Demonstrate
Respiratory Care 2 Clinical Skills School of Medicine 2015/16 Learning Objectives Identify the different types of inhalers and demonstrate the correct inhaler techniques for the different inhalers. Demonstrate
Breezhaler. Open to see clear capsule. How do I use my Breezhaler? Care of my Breezhaler
 Breezhaler 3 Pull cap off Press buttons once and release Breathe in rapidly and steadily. Hold. Open. Place capsule in chamber. Close (click). Breathe out 4 Open to see clear capsule. If not all clear
Breezhaler 3 Pull cap off Press buttons once and release Breathe in rapidly and steadily. Hold. Open. Place capsule in chamber. Close (click). Breathe out 4 Open to see clear capsule. If not all clear
PACKAGE LEAFLET: INFORMATION FOR THE USER Pulmicort Turbohaler budesonide. 1. What Pulmicort Turbohaler is and what it is used for
 PACKAGE LEAFLET: INFORMATION FOR THE USER Pulmicort Turbohaler budesonide Read all of this leaflet carefully before you start taking this medicine. Keep this leaflet. You may need to read it again. If
PACKAGE LEAFLET: INFORMATION FOR THE USER Pulmicort Turbohaler budesonide Read all of this leaflet carefully before you start taking this medicine. Keep this leaflet. You may need to read it again. If
Staying Healthy. with Asthma. Illustrations by paulsharp.com
 Staying Healthy with Asthma Illustrations by paulsharp.com Lungs & Asthma What is Asthma? Inflammation or swelling of airways that leads to: 1) Mucous production deep inside the airways. 2) Temporary difficulty
Staying Healthy with Asthma Illustrations by paulsharp.com Lungs & Asthma What is Asthma? Inflammation or swelling of airways that leads to: 1) Mucous production deep inside the airways. 2) Temporary difficulty
You Can Control Your Asthma
 asthma_brochureprint_v2.qxd 9/5/06 9:54 AM Page 2 For More Information on Controlling Asthma: Centers for Disease Control and Prevention National Center for Environmental Health, MS F52 4770 Buford Highway,
asthma_brochureprint_v2.qxd 9/5/06 9:54 AM Page 2 For More Information on Controlling Asthma: Centers for Disease Control and Prevention National Center for Environmental Health, MS F52 4770 Buford Highway,
MANAGING COPD AT HOME. Karla Schlichtmann, RRT
 MANAGING COPD AT HOME Karla Schlichtmann, RRT Chronic Obstructive Pulmonary Disease (COPD) is a progressive lung disease. WHAT IS COPD? The airways in your lungs become inflamed and thickens. This results
MANAGING COPD AT HOME Karla Schlichtmann, RRT Chronic Obstructive Pulmonary Disease (COPD) is a progressive lung disease. WHAT IS COPD? The airways in your lungs become inflamed and thickens. This results
Serevent Diskus 50 microgram per metered dose inhalation powder, pre-dispensed
 Agency Approval Date: Not applicable as IA Text Date: 27 April 2015 CO-0111149 GSK Logo Package Leaflet: Information for the User Serevent Diskus 50 microgram per metered dose inhalation powder, pre-dispensed
Agency Approval Date: Not applicable as IA Text Date: 27 April 2015 CO-0111149 GSK Logo Package Leaflet: Information for the User Serevent Diskus 50 microgram per metered dose inhalation powder, pre-dispensed
Asthma. If an Ambulance is required - call immediately - do not delay. H & A Training PL RTO No:90871
 Asthma is a reversible breathing problem caused from sudden or progressive narrowing and spasming of the smaller airways and includes mucus production, which interferes with oxygen exchange. People who
Asthma is a reversible breathing problem caused from sudden or progressive narrowing and spasming of the smaller airways and includes mucus production, which interferes with oxygen exchange. People who
OXEZE TURBUHALER formoterol fumarate dihydrate
 IMPORTANT: PLEASE READ PART III: CONSUMER INFORMATION OEZE TURBUHALER formoterol fumarate dihydrate This leaflet is part III of a three-part Product Monograph published when OEZE TURBUHALER was approved
IMPORTANT: PLEASE READ PART III: CONSUMER INFORMATION OEZE TURBUHALER formoterol fumarate dihydrate This leaflet is part III of a three-part Product Monograph published when OEZE TURBUHALER was approved
Sample blf.org.uk/copd
 Your COPD self-management plan blf.org.uk/copd Thank you to the people with lung conditions and leading health care professionals who helped to develop this plan. This resource has been developed in partnership
Your COPD self-management plan blf.org.uk/copd Thank you to the people with lung conditions and leading health care professionals who helped to develop this plan. This resource has been developed in partnership
10/18/2012. Penn State University Children s Hospital JODIE STABINSKI CRNP MSN AE-C
 Penn State University Children s Hospital JODIE STABINSKI CRNP MSN AE-C Daily: Long-Term Control Corticosteroids (inhaled and systemic) Long-acting beta 2 -agonists (Serevent, Foradil) Methylxanthines
Penn State University Children s Hospital JODIE STABINSKI CRNP MSN AE-C Daily: Long-Term Control Corticosteroids (inhaled and systemic) Long-acting beta 2 -agonists (Serevent, Foradil) Methylxanthines
Asthma and COPD Awareness
 Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Washington Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Washington Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
A Guide to Help You Reduce and Stop Using Tobacco
 Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
MEDICATION GUIDE. ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol
![MEDICATION GUIDE. ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol MEDICATION GUIDE. ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol](/thumbs/78/76835983.jpg) MEDICATION GUIDE ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol ADVAIR HFA 115/21 (fluticasone propionate 115 mcg and salmeterol 21 mcg) Inhalation
MEDICATION GUIDE ADVAIR [ad vair] HFA 45/21 (fluticasone propionate 45 mcg and salmeterol 21 mcg) Inhalation Aerosol ADVAIR HFA 115/21 (fluticasone propionate 115 mcg and salmeterol 21 mcg) Inhalation
Chronic Obstructive Pulmonary Disease. Information about medication and an Action Plan to use if your condition gets worse due to an infection
 Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
Asthma medications: Know your options - MayoClinic.com. Asthma medications: Know your options
 MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
Asthma and COPD Awareness
 Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Ohio Fall 2012 Importance of Controller Medicines Asthma is a disease that causes swelling
Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Ohio Fall 2012 Importance of Controller Medicines Asthma is a disease that causes swelling
Skills Checklist Manual
 Skills Checklist Manual Alexandra L. Quittner, Ph.D. Kristen K. Marciel, Ph.D. Ivette Cruz, M.S. University of Miami Quittner, Marciel, & Cruz, 2009 i revised 2/5/09 Table of Contents Instructions 1 Airway
Skills Checklist Manual Alexandra L. Quittner, Ph.D. Kristen K. Marciel, Ph.D. Ivette Cruz, M.S. University of Miami Quittner, Marciel, & Cruz, 2009 i revised 2/5/09 Table of Contents Instructions 1 Airway
Asthma and COPD Awareness
 Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Texas Summer 2013 Asthma Triggers You may not always know when an asthma attack will
Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Texas Summer 2013 Asthma Triggers You may not always know when an asthma attack will
Ventolin Accuhaler 200 micrograms salbutamol sulfate
 Package Leaflet: Information for the User Ventolin Accuhaler 200 micrograms salbutamol sulfate Read all of this leaflet carefully before you start taking this medicine because it contains important information
Package Leaflet: Information for the User Ventolin Accuhaler 200 micrograms salbutamol sulfate Read all of this leaflet carefully before you start taking this medicine because it contains important information
Commonwealth of Massachusetts Department of Early Education and Care
 Commonwealth of Massachusetts Department of Early Education and Care MEDICATION CONSENT FORM 606 CMR 7.11(2)(b) Name of child: Name of medication: Please one of the following: Prescription: Oral/Non-Prescription:
Commonwealth of Massachusetts Department of Early Education and Care MEDICATION CONSENT FORM 606 CMR 7.11(2)(b) Name of child: Name of medication: Please one of the following: Prescription: Oral/Non-Prescription:
Ventamol CFC-Free 100 micrograms, Pressurised Inhalation, Suspension (Salbutamol)
 Ventamol CFC-Free 100 micrograms, Pressurised Inhalation, Suspension (Salbutamol) For inhalation use Important: Read instructions carefully Wash your inhaler once a week and allow to dry What you need
Ventamol CFC-Free 100 micrograms, Pressurised Inhalation, Suspension (Salbutamol) For inhalation use Important: Read instructions carefully Wash your inhaler once a week and allow to dry What you need
Beclazone 50, 100, 250 micrograms CFC-Free Inhaler
 NEW ZEALAND CONSUMER MEDICINE INFORMATION Beclazone 50, 100, 250 micrograms CFC-Free Inhaler Beclometasone dipropionate 50, 100, or 250 micrograms per metered dose ( puff ) Please read this leaflet carefully
NEW ZEALAND CONSUMER MEDICINE INFORMATION Beclazone 50, 100, 250 micrograms CFC-Free Inhaler Beclometasone dipropionate 50, 100, or 250 micrograms per metered dose ( puff ) Please read this leaflet carefully
HealthPartners Care Coordination Clinical Care Planning and Resource Guide ASTHMA
 The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Heart, Lung, and Blood Institute (NHLBI) and American Academy of Allergy,
The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Heart, Lung, and Blood Institute (NHLBI) and American Academy of Allergy,
Alberta Childhood Asthma Pathway for Primary Care
 Asthma Diagnosis Box 1 Diagnosis: Based on symptom pattern, careful and thorough history of symptoms (wheeze, cough, night waking and activity limitations), and assessment of family history of asthma and
Asthma Diagnosis Box 1 Diagnosis: Based on symptom pattern, careful and thorough history of symptoms (wheeze, cough, night waking and activity limitations), and assessment of family history of asthma and
HARRISON COUNTY SCHOOLS OFFICE OF HEALTH SERVICES 445 W. Main Street Clarksburg, WV (304) FAX (304)
 HARRISON COUNTY SCHOOLS OFFICE OF HEALTH SERVICES 44 W. Main Street Clarksburg, WV 6 (4) 6-769 FAX (4) 6-769 Dear Parent, Date Please complete the enclosed forms and return them to your school nurse. This
HARRISON COUNTY SCHOOLS OFFICE OF HEALTH SERVICES 44 W. Main Street Clarksburg, WV 6 (4) 6-769 FAX (4) 6-769 Dear Parent, Date Please complete the enclosed forms and return them to your school nurse. This
How to Use Inhaled Medications
 How to Use Inhaled Medications FOR ASTHMA AND COPD introduction Inhaled medications are an important part of controlling and treating asthma and chronic obstructive pulmonary disease (COPD). The medication
How to Use Inhaled Medications FOR ASTHMA AND COPD introduction Inhaled medications are an important part of controlling and treating asthma and chronic obstructive pulmonary disease (COPD). The medication
Asthma. Questions and Answers about. Information for Parents
 Questions and Answers about Asthma Information for Parents This booklet is written for parents to help explain the basics of childhood asthma and asthma management. Acknowledgements The Lung Association
Questions and Answers about Asthma Information for Parents This booklet is written for parents to help explain the basics of childhood asthma and asthma management. Acknowledgements The Lung Association
Controlling Your Asthma Patient Education Guide
 Controlling Your Asthma Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S A N D T H E C H E S T F O U N D A T I O N Controlling Your Asthma Patient Education Guide
Controlling Your Asthma Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S A N D T H E C H E S T F O U N D A T I O N Controlling Your Asthma Patient Education Guide
Asthma Basic Facts. Staying safe and well with asthma. For people with asthma and their carers.
 Asthma Basic Facts Staying safe and well with asthma. For people with asthma and their carers. Asthma App Contact your local Asthma Foundation asthmaaustralia.org.au Breathing Breathing is how we get air
Asthma Basic Facts Staying safe and well with asthma. For people with asthma and their carers. Asthma App Contact your local Asthma Foundation asthmaaustralia.org.au Breathing Breathing is how we get air
ASTHMA INFORMATION SHEET
 ASTHMA INFORMATION SHEET Name of student Name of parent/guardian School Year Grade Asthma Management Date or age of diagnosis Name of current physician Office number Please list ALL current medications,
ASTHMA INFORMATION SHEET Name of student Name of parent/guardian School Year Grade Asthma Management Date or age of diagnosis Name of current physician Office number Please list ALL current medications,
Your Inhaler Devices & You
 1 Your Inhaler Devices & You COUNSEL ON THE APPROPRIATE USE OF A: METERED DOSE INHALER (MDI) DRY POWDER INHALER (DPI) DISCUSS THE APPROPRIATE USAGE OF A PEAK FLOW METER AND SPACER/HOLDING CHAMBER DEVICE
1 Your Inhaler Devices & You COUNSEL ON THE APPROPRIATE USE OF A: METERED DOSE INHALER (MDI) DRY POWDER INHALER (DPI) DISCUSS THE APPROPRIATE USAGE OF A PEAK FLOW METER AND SPACER/HOLDING CHAMBER DEVICE
SAMPLE. mg by mouth every day for day(s) Prednisolone. Other Medicine: Medicine Dose How long Directions
 Pediatric Asthma Discharge Prescription and Short-Term Plan The doctor will fill out this form before your child is discharged. Please follow this plan until you see your usual doctor in 3 to 7 days. Hospital
Pediatric Asthma Discharge Prescription and Short-Term Plan The doctor will fill out this form before your child is discharged. Please follow this plan until you see your usual doctor in 3 to 7 days. Hospital
NUCALA. mepolizumab. Patient Support
 NUCALA mepolizumab Patient Support This booklet has been developed by GSK UK/NLA/0007/15(1) Date of preparation: November 2016 INTRODUCTION This informative guide is for people who have been prescribed
NUCALA mepolizumab Patient Support This booklet has been developed by GSK UK/NLA/0007/15(1) Date of preparation: November 2016 INTRODUCTION This informative guide is for people who have been prescribed
Student ASTHMA Record
 Student ASTHMA Record GENERAL INFORMATION SHEET (To be filled out by parent/guardian) The Asthma Foundation of Tasmania strongly advises parents/guardians to complete this form with the family doctor.
Student ASTHMA Record GENERAL INFORMATION SHEET (To be filled out by parent/guardian) The Asthma Foundation of Tasmania strongly advises parents/guardians to complete this form with the family doctor.
IMMACULATE HEART COLLEGE
 IMMACULATE HEART COLLEGE Through Mary to Jesus: The Way, the Truth and the Life John 14:6 ASTHMA FRIENDLY SCHOOL POLICY October 2017 This Policy will be reviewed by September 2018 1 Asthma Friendly School
IMMACULATE HEART COLLEGE Through Mary to Jesus: The Way, the Truth and the Life John 14:6 ASTHMA FRIENDLY SCHOOL POLICY October 2017 This Policy will be reviewed by September 2018 1 Asthma Friendly School
Package leaflet: Information for the user. Bricanyl Turbohaler 0.5 mg/dose terbutaline sulfate
 Package leaflet: Information for the user Bricanyl Turbohaler 0.5 mg/dose terbutaline sulfate Read all of this leaflet carefully before you start using this medicine because it contains important information
Package leaflet: Information for the user Bricanyl Turbohaler 0.5 mg/dose terbutaline sulfate Read all of this leaflet carefully before you start using this medicine because it contains important information
QUIT TODAY. It s EASIER than you think. DON T LET TOBACCO CONTROL YOUR LIFE. WE CAN HELP.
 QUIT TODAY. It s EASIER than you think. DON T LET TOBACCO CONTROL YOUR LIFE. WE CAN HELP. WHEN YOU RE READY TO QUIT, CALL THE SOUTH DAKOTA QUITLINE 1-866-SD-QUITS. IN THE BEGINNING, it s about freedom
QUIT TODAY. It s EASIER than you think. DON T LET TOBACCO CONTROL YOUR LIFE. WE CAN HELP. WHEN YOU RE READY TO QUIT, CALL THE SOUTH DAKOTA QUITLINE 1-866-SD-QUITS. IN THE BEGINNING, it s about freedom
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease
 Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Michigan Newsletter Spring 2012 Getting Rid of Mold There are many types of molds. Molds will not grow without water
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Michigan Newsletter Spring 2012 Getting Rid of Mold There are many types of molds. Molds will not grow without water
your breathing problems worsen quickly. you use your rescue inhaler, but it does not relieve your breathing problems.
 MEDICATION GUIDE ADVAIR DISKUS [ad vair disk us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation What is the most important information I should know about ADVAIR DISKUS?
MEDICATION GUIDE ADVAIR DISKUS [ad vair disk us] (fluticasone propionate and salmeterol inhalation powder) for oral inhalation What is the most important information I should know about ADVAIR DISKUS?
Asthma. & Older Adults. A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS
 Asthma & Older Adults A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS what is Asthma? Asthma is a disease of the airways, the small tubes which carry air in and out
Asthma & Older Adults A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS what is Asthma? Asthma is a disease of the airways, the small tubes which carry air in and out
Tiredness/Fatigue Mild Moderate to severe, especially at onset of symptoms Head and Body Aches and Pains
 What is the difference between a cold COLD FLU and the flu? How it starts Symptoms It s Cold and Flu Season in Snohomish County! Colds and Flu are respiratory illnesses caused by viruses. Our Immune Systems
What is the difference between a cold COLD FLU and the flu? How it starts Symptoms It s Cold and Flu Season in Snohomish County! Colds and Flu are respiratory illnesses caused by viruses. Our Immune Systems
Chronic Obstructive Pulmonary Disease (COPD)
 James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
Package leaflet: Information for the user
 Package leaflet: Information for the user Qvar Easi-Breathe 50 micrograms per actuation Inhaler Qvar Easi-Breathe 100 micrograms per actuation Inhaler Beclometasone Dipropionate Read all of this leaflet
Package leaflet: Information for the user Qvar Easi-Breathe 50 micrograms per actuation Inhaler Qvar Easi-Breathe 100 micrograms per actuation Inhaler Beclometasone Dipropionate Read all of this leaflet
Living Well with Asthma
 Living Well with Asthma Understanding Asthma Monitoring Your Breathing Using an Inhaler Reducing Triggers Staying Active Living with Asthma If you have asthma, there s good news. Today, people with asthma
Living Well with Asthma Understanding Asthma Monitoring Your Breathing Using an Inhaler Reducing Triggers Staying Active Living with Asthma If you have asthma, there s good news. Today, people with asthma
Glossary of Asthma Terms
 HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
