Physiological effects of ECT
|
|
|
- Shanon Sims
- 6 years ago
- Views:
Transcription
1 Physiological effects of ECT
2 This is where I work Not where ECT is done usually
3 Broad Oak Hospital Liverpool (Mersey Care) Cottage hospital setting (no acute physicians or intensive care) At least 500 treatments a year Most done a Broadoak but some patients done at RLUH.
4 Aims of Today Physiological effects of ECT Physiological effects of Anaesthesia Effects that patient comorbidity has Broadly speaking) Effects that psychiatric drugs on Physiology (relevant to anaesthesia) What does the anaesthetist want to know about patient (what can the psychiatrist tell the anaesthetist)?
5 Scope of a problem ECT is inherently safe (1-3/100,000 mortality) This does not mean that we should be complacent: ECT is more commonly prescribed in the older population Comorbidity is more common in older people Physiological extremes more likely in older people ECT is repeated up to 12 times (or more), therefore anaesthesia is repeated, therefore risk is repeated. Also Consider morbidity of ECT.
6 Function of Anaesthetist in ECT Provide anaesthesia: Amnesia Modify muscular component of seizure (clonic can be abolished almost completely. Tonic less so) Effective Oxygenation But also need to support changes in physiology that we measure
7 Anaesthetic drugs used Oxygen Induction agents: Propofol, Etomidate, Thiopentone, Ketamine Muscle relaxant: Suxamethonium, Rocuronium/sugamadex (expensive!) Analgesia: Alfentanil, Remifentanil (short acting) Rescue drugs and fluids
8 Physiological effects of Anaesthesia CVS Hypotension (worse if dehydrated or cardiac disease) BP better maintained if using Etomidate (Ketamine) Possible Bradycardia RS Lose control of airway Apnoea, hypoxia Hypoxia and compromised airway is more likely if patient is morbidly obese or has acute respiratory problem
9 Physiological effects of Anaesthesia CNS Raise seizure threshold (Propofol). Use enough to produce anaesthesia Reduced cerebral oxygen consumption and blood flow CBF: Propofol,Etomidate Increased CBF and oxygen consumption (Ketamine) other Muscle pain (suxemothonium) Rise in potassium level (Suxamethonium) Catatonia Increased IOP (Sux again!) Adverse Drug reaction
10 Physiological Effect of ECT Autonomic effects: Initial stimulus: Direct stimulation of the hypothalamus Parasympathetic outflow (Vagus) Bradycardia Asystole (more common in young and fit,) More likely to be persistent if no clonic phase or unilateral stimulus More common in first tx (dose titration) Hypotension due to anaesthesia may be attenuated at this point May also get a sudden decrease in heart rate at end of tonic phase
11 Autonomic effects of ECT Sympathetic NS stimulated directly during clonic phase (Via spinal cord). Increased NA and A levels Tachycardia Hypertension and increase in venous pressure Worse if using Etomidate or Ketamine Oxygen demand in heart increased and supply of oxygen needs to increase otherwise Ischaemia develops. Continues after ECT and into recovery phase Transient arrhythmia Piloerection and pupillary dilation
12 CNS effects of Seizure Increased oxygen consumption during seizure Increased cerebral blood flow and cerebral vasodilatation. Increased blood volume Skull has a fixed volume and therefore if blood volume increases, ICP increases. (Monroe Kellie doctrine) Brain compensates ICP increases more rapidly if ICP raised already Increased (eg mass lesions) After ECT, CBF is reduced a while later (postulated mechanism of action) Increased intraocular pressure BUT Induction agents reduce oxygen consumption and CBF
13 CNS effects of seizure Brain dependent on oxygen and glucose (limited anaerobic capacity Brain maintains blood flow through a range of pressures to Maintain oxygen delivery In normal circumstances Auotoregulation is probably maintained during ECT unless severe hypo or hypertension (but we don t know)
14 Effect of hyperventilation May prolong fit Anaesthetist can reduce EtCO 2 by hyperventilation. (if they have the means to do so) Reduces CBF and oxygen delivery.?may not be a good thing if brain is relatively hypoxic
15 Neuro endocrine effects Hypothalamic Pituitary axis CRF and ACTH increased with increased cortisol (about one hours)? Stress related TSH increases after treatment (one hour) Prolactin (about one hour) But No effect on Growth Hormone, FSH or LH? increase in 5HT pathway Serotonin Is it clinically relevant? No evidence that increases in levels correlate with therapeutic response
16 Drugs used in psychiatry problems for ECT anaesthesia Interaction with anaesthetic drugs or accentuate CVS/RS side effects of anaesthesia and ECT Anticholinergic side effects (TCAs, antipsychotics) Prolonged QTc ( TCAs and antipsychotics) Cardiac toxicity (clozapine) Decreased T4 (lithium) Hepatotoxicity and interaction with drugs (MAOI) Hyponatraemia (SSRI) Weight gain (all)
17 Treatment of physiological compromise; Cardiac most common problem BRADYCARDIA Give Atropine or Glycopyrollate If Bradycrdia persistent If rate of change is significant If previous hx of Bradycardia with ECT Sometimes use this on first treatment. No evidence that patients taking B blockers more likely to cause a Bradycardia that needs treating HYPOTENSION Vasoconstrictors or sympathomimetic agents fluids
18 Cardiovascular effects : treatment TACHYCARDIA AND HYPERTENSION Treat If persistent or predictable Can treat before start of anaesthesia use B blockade. Esmolol has been used and attenuates out hypertension /tachycardia but doesn t abolish it. Also may shorten fit which may reduce efficacy of ECT. Therefore don t use it routinely. We use Atenolol Remifentanil has been used again does not abolish. (Max 100Ug). If use more leads to prolonged recovery. And hypotension. Arrhythmias: most do not need treating
19 Who is more likely to be at risk of cardiac problems during ECT? Normally only 7.5% most do not need treating BUT. Recent cardiac event IHD LV dysfunction. ECT has been reported repeatedly as safe in patients with stable IHD. Valvular disease: Aortic stenosis Effect of depression on cardiac function (unstable comorbidities, dehydration) Effect of antidepressants on cardiac function
20 Respiratory problems; Most at Acute problem (URTI, unstable COPD may cause airway sensitivity (laryngospasm and wheeze) Obese. (also more likely to aspirate) Airway problems. risk?
21 CNS compromise; who is more likely to be at risk? Mass lesions (increased ICP) Recent stroke (autoregulation ) Cerebral aneurism (?) Most common is agitation or memory issue (dose titration) Can we predict? We do not routinely measure effects of cerebral blood flow in ECT (unlike cardiac monitors so we do not treat problems directly and we have limited drugs to treat problems. Many anecdotal case reports where ECT has been done in CNS compromised patients
22 Reducing the risk; Role of Psychiatrist Some Knowledge of what increases risk of morbidity in ECT Importance of psychiatrist being able to obtain clinical information from relatives, other hospitals and GP (deteriorating comorbidity) And communicating them to anaesthetist: Usually in the form of a questionnaire to fill in before ECT commences. This is usually delegated to junior doctor. Sometimes, verbal communication is best! Direct Access to physicians in medicine/ cardiologists to stabilise where appropriate. Family should be aware that although ECT carries a small risk, this is increased if they have severe depression, have unstable or severe comorbidity and are dehydrated.
23 Reducing the risk Preanaesthetic assessment History from patient/nurses/psychiatrists history Patient cant always give a coherent history (depression, dementia etc) Patient doesn t always arrive at ECT with anyone who knows about their condition. Psychiatric history very important! Access to relatives very useful Clues from drug history Results from routine screening helps with decision making process Problems more likely if patient is prepared for ECT urgently, but this is when patients are most unfit.
24 Reducing the risk Decisions for anaesthetist and Psychiatrist Is comorbidity stable? Is comorbidity likely to cause physiological problems? Have I got the bigger picture? Is ECT in patients best interests? Refer patient to acute care physician to treat acute problems (e.g. renal failure, dysrythmia). AN EXPERT? Defer ECT until stable (risk vs. benefit)? Treat in acute care setting Terminal illness is not a reason not to go ahead Decision made on a CASE BY CASE BASIS Patient Centred Care Remember that ECT needs to be repeated.
25 Conclusion Anaesthesia for ECT is inherently safe; short procedure, no fluid shifts Physiological changes need to be monitored where possible. Treated if necessary Most problems with ECT relate to CVS compromise Anaesthetic and psychiatric assessment is aimed at reducing the risk with the knowledge of physiological impact on patient. Need to repeat to produce clinical effect Treat patients on a case by case basis (and relatives) Communication and a good working relationship with the ECT team is essential to ensure that risks of ECT are minimised
26
27 Acute care setting? Access to ICU and AMU May delay treatment If decision is made to start treatment in an acute care setting, this will need careful organisation Can reassess the need for acute care setting after a few treatment sessions
28 Reducing risk on the day Pre treatment assessment (nurse lead) including NBM. Any change form last time? AAGBI monitors Records of previous anaesthetic and communication Skilled staff (inc. appropriate dose titration) Recovery
29 So what? Risk reduction Choice of patients, stable co morbid state Monitors (AAGBI) to treat side effects' of physiology
30 Assessing the risk Should we do ECT? Absolute contraindications are few : Risk benefit assessments E.g. Recent MI, Severe Aortic stenosis, recent CVA, raised ICP Having terminal illness does not necessarily preclude treatment IMPORTANT. Do patient and/or relatives understand risk?
31 Incidents in ECT Higher incidence if Dehydrated Unstable CVS especially; Aortic stenosis, untreated heart failure, uncontrolled hypertension, uncontrolled dysrythmia Unstable RS (i.e. acute problem) Unstable endocrine; Diabetes, thyroid Difficult airway: Morbid obesity, SOL in mouth, neck
32 Cardiovascular response ; treatment heart rate heart rate Often no treatment needed Can sometimes preempt problems Atropine/ Glycopyrollate. Ephedrine Fluids Atenolol (B blockers)
33 Other effects Succinylcholine Hyperkalaemia (care in catatonia). Intragastric pressure (due to fir) and succ Intraocular pressure (due to fir as well) and succ
34 Drugs used in psychiatry Effects that can cause problem for patient and anaesthetic during ECT NMS, Serotonin syndrome () QT prolongation and arrhythmia () Tachycardia (anticholinergic side effects) Electrolyte disturbances (hyponatraemia) Thyroid and renal function (Lithium): MAOI (we cannot give certain drugs )
35 Common Acute changes which may need treatment Autonomic Bradycardia more likely if no clonic seizure (anticholinergic agents) Tachycardia and hypertension (B Blockers) Dysrythmia usually resolves but may need treating Hypotension (Fluids, sympathomimetic agents) Salivation not usually a problem RS Acute Wheeze CNS Delirium may need treating (midazolam)
Anaesthesia for ECT. Session 1. Dr Richard Cree Consultant in Anaesthesia & ICU. Roseberry Park Hospital and The James Cook Hospital, Middlesbrough
 Anaesthesia for ECT Session 1 Dr Richard Cree Consultant in Anaesthesia & ICU Roseberry Park Hospital and The James Cook Hospital, Middlesbrough Anaesthesia for ECT CHAPTERS 1. The principles of anaesthesia
Anaesthesia for ECT Session 1 Dr Richard Cree Consultant in Anaesthesia & ICU Roseberry Park Hospital and The James Cook Hospital, Middlesbrough Anaesthesia for ECT CHAPTERS 1. The principles of anaesthesia
ECT Workshop. Rahul Bajekal Consultant Anaesthetist Newcastle upon Tyne 23 November 2017
 ECT Workshop Rahul Bajekal Consultant Anaesthetist Newcastle upon Tyne 23 November 2017 My role To attenuate seizure appropriately Manage comorbidity Best place to treat? What we don t like Complex comorbidity
ECT Workshop Rahul Bajekal Consultant Anaesthetist Newcastle upon Tyne 23 November 2017 My role To attenuate seizure appropriately Manage comorbidity Best place to treat? What we don t like Complex comorbidity
Pain: 1-2µg/kg q30-60min prn. effects in 10 minutes. Contraindications: Morphine is preferred in. Duration of Action: minutes. renal failure.
 Procedural Sedation / Analgesia / Anaesthesia Chart - Page 1 Diazepam (Valium) Anxiolytic / Sedative Etomidate (Amidate) Hypnotic / Anesthetic Fentanyl Citrate (Sublimaze) Narcotic Analgesic Dose Pediatric:
Procedural Sedation / Analgesia / Anaesthesia Chart - Page 1 Diazepam (Valium) Anxiolytic / Sedative Etomidate (Amidate) Hypnotic / Anesthetic Fentanyl Citrate (Sublimaze) Narcotic Analgesic Dose Pediatric:
Core Safety Profile. Pharmaceutical form(s)/strength: 5mg/ml and 25 mg/ml, Solution for injection, IM/IV FI/H/PSUR/0010/002 Date of FAR:
 Core Safety Profile Active substance: Esketamine Pharmaceutical form(s)/strength: 5mg/ml and 25 mg/ml, Solution for injection, IM/IV P-RMS: FI/H/PSUR/0010/002 Date of FAR: 29.05.2012 4.3 Contraindications
Core Safety Profile Active substance: Esketamine Pharmaceutical form(s)/strength: 5mg/ml and 25 mg/ml, Solution for injection, IM/IV P-RMS: FI/H/PSUR/0010/002 Date of FAR: 29.05.2012 4.3 Contraindications
Sedation For Cardiac Procedures A Review of
 Sedation For Cardiac Procedures A Review of Sedative Agents Dr Simon Chan Consultant Anaesthesiologist Department of Anaesthesia and Intensive Care Prince of Wales Hospital Hong Kong 21 February 2009 Aims
Sedation For Cardiac Procedures A Review of Sedative Agents Dr Simon Chan Consultant Anaesthesiologist Department of Anaesthesia and Intensive Care Prince of Wales Hospital Hong Kong 21 February 2009 Aims
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Postpartum Period. Dr Ann Roberts Consultant Psychiatrist
 ECT in Pregnancy and the Postpartum Period Dr Ann Roberts Consultant Psychiatrist Thumbswood MBU Hertfordshire ECT searches/overview of evidence e Medline, Embase, Psychinfo, Pubmed No prospective randomised
ECT in Pregnancy and the Postpartum Period Dr Ann Roberts Consultant Psychiatrist Thumbswood MBU Hertfordshire ECT searches/overview of evidence e Medline, Embase, Psychinfo, Pubmed No prospective randomised
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS)
 Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
THE PRACTICE OF ECT. Kiran Rabheru
 THE PRACTICE OF ECT Kiran Rabheru MD, CCFP, FRCP Geriatric Psychiatrist Professor University of Ottawa February 11, 2015 U of Ottawa Review Course in Psychiatry: Dr. K. Rabheru 1 Disclosures n NONE 2 Learning
THE PRACTICE OF ECT Kiran Rabheru MD, CCFP, FRCP Geriatric Psychiatrist Professor University of Ottawa February 11, 2015 U of Ottawa Review Course in Psychiatry: Dr. K. Rabheru 1 Disclosures n NONE 2 Learning
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED
 ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
Airway management problem during anaesthesia. Airway management problem in ICU / HDU. Airway management problem occurring in the Emergency Department
 4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Kelowna June 2011 Airway Assessment and Management. Golden, BC
 Kelowna June 2011 Airway Assessment and Management Dr. Bruce Starke Golden, BC Not really... I am unable to identify any potential conflict of interest and I am unable to identify any potential conflict
Kelowna June 2011 Airway Assessment and Management Dr. Bruce Starke Golden, BC Not really... I am unable to identify any potential conflict of interest and I am unable to identify any potential conflict
Hearts and Minds An ECG Update. Tuesday 18 th November The Met Hotel, Leeds
 Hearts and Minds An ECG Update Tuesday 18 th November The Met Hotel, Leeds Ashleigh Bradley Specialist Clinical Pharmacist for Mental Health and Lithium Clinic Airedale NHS Foundation Trust Introduction
Hearts and Minds An ECG Update Tuesday 18 th November The Met Hotel, Leeds Ashleigh Bradley Specialist Clinical Pharmacist for Mental Health and Lithium Clinic Airedale NHS Foundation Trust Introduction
1 Recognition. 2 Immediate management. 3 Treatment. 4 Follow-up. AAGBI Safety Guideline. Management of Severe Local Anaesthetic Toxicity
 AAGBI Safety Guideline Management of Severe Local Anaesthetic Toxicity 1 Recognition 2 Immediate management 3 Treatment Signs of severe toxicity: Sudden alteration in mental status, severe agitation or
AAGBI Safety Guideline Management of Severe Local Anaesthetic Toxicity 1 Recognition 2 Immediate management 3 Treatment Signs of severe toxicity: Sudden alteration in mental status, severe agitation or
Anaesthesia and Morbid Obesity
 Anaesthesia and Morbid Obesity Facts 20% adults Obese (1% Morbidly Obese) BMI >35 with comorbidity / BMI >40 without comorbidity = morbidly obese BMI > 55 = super-morbidly obese BMI > 30 rapid increase
Anaesthesia and Morbid Obesity Facts 20% adults Obese (1% Morbidly Obese) BMI >35 with comorbidity / BMI >40 without comorbidity = morbidly obese BMI > 55 = super-morbidly obese BMI > 30 rapid increase
Preoperative Assessment. Block Prof JLA Rantloane Department of Anaesthesiology
 Preoperative Assessment Block 18 2013 Prof JLA Rantloane Department of Anaesthesiology!1 Principles All patients scheduled to undergo surgery should have a preoperative evaluation to assist in planning
Preoperative Assessment Block 18 2013 Prof JLA Rantloane Department of Anaesthesiology!1 Principles All patients scheduled to undergo surgery should have a preoperative evaluation to assist in planning
General Anesthesia. Mohamed A. Yaseen
 General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
Drugs for Emotional and Mood Disorders Chapter 16
 Drugs for Emotional and Mood Disorders Chapter 16 NCLEX-RN Review Question 1 Choices Please note Question #1 at the end of Ch 16 pg 202 & Key pg 805 answer is #4 1. Psychomotor symptoms 2. Tachycardia,
Drugs for Emotional and Mood Disorders Chapter 16 NCLEX-RN Review Question 1 Choices Please note Question #1 at the end of Ch 16 pg 202 & Key pg 805 answer is #4 1. Psychomotor symptoms 2. Tachycardia,
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
General anesthesia. No single drug capable of achieving these effects both safely and effectively.
 General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
PAEDIATRIC ANAESTHETIC EMERGENCIES PART I. Dr James Cockcroft, South West School of Anaesthesia. Dr Sarah Rawlinson, Derriford Hospital, Plymouth, UK
 PAEDIATRIC ANAESTHETIC EMERGENCIES PART I Original Article by: Dr Claire Todd, South West School of Anaesthesia Dr James Cockcroft, South West School of Anaesthesia Dr Sarah Rawlinson, Derriford Hospital,
PAEDIATRIC ANAESTHETIC EMERGENCIES PART I Original Article by: Dr Claire Todd, South West School of Anaesthesia Dr James Cockcroft, South West School of Anaesthesia Dr Sarah Rawlinson, Derriford Hospital,
VO- PMHP Treatment Guideline 102: Electroconvulsive Therapy (ECT)
 VO- PMHP Treatment Guideline 102: Electroconvulsive Therapy (ECT) Diagnostic Guidelines: Introduction: Electroconvulsive Therapy has been in continuous use for more than 60 years. The clinical literature
VO- PMHP Treatment Guideline 102: Electroconvulsive Therapy (ECT) Diagnostic Guidelines: Introduction: Electroconvulsive Therapy has been in continuous use for more than 60 years. The clinical literature
10. Severe traumatic brain injury also see flow chart Appendix 5
 10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
Neurocardiogenic syncope
 Neurocardiogenic syncope Syncope Definition Collapse,Blackout A sudden, transient loss of consciousness and postural tone, with spontaneous recovery Very common Syncope Prevalence All age groups (particularly
Neurocardiogenic syncope Syncope Definition Collapse,Blackout A sudden, transient loss of consciousness and postural tone, with spontaneous recovery Very common Syncope Prevalence All age groups (particularly
Analgesic-Sedatives Drug Dose Onset
 Table 4. Commonly used medications in procedural sedation and analgesia Analgesic-Sedatives Fentanyl Morphine IV: 1-2 mcg/kg Titrate 1 mcg/kg q3-5 minutes prn IN: 2 mcg/kg Nebulized: 3 mcg/kg IV: 0.05-0.15
Table 4. Commonly used medications in procedural sedation and analgesia Analgesic-Sedatives Fentanyl Morphine IV: 1-2 mcg/kg Titrate 1 mcg/kg q3-5 minutes prn IN: 2 mcg/kg Nebulized: 3 mcg/kg IV: 0.05-0.15
Management Of Medical Emergencies
 Management Of Medical Emergencies U.S. Aging Population 35 million people (12%) 65 years or older Number will increase by nearly 75% by year 2030 The number of people more than 85 years old will approach
Management Of Medical Emergencies U.S. Aging Population 35 million people (12%) 65 years or older Number will increase by nearly 75% by year 2030 The number of people more than 85 years old will approach
What the s wrong with this person?
 Ketamine for Prehospital Management of Excited Delirium Syndrome: Is it all just a bunch of hype?!? Financial Disclosure Asa M. Margolis, DO, MPH, MS, FACEP Assistant Professor Division of Special Operation
Ketamine for Prehospital Management of Excited Delirium Syndrome: Is it all just a bunch of hype?!? Financial Disclosure Asa M. Margolis, DO, MPH, MS, FACEP Assistant Professor Division of Special Operation
WHAT DO YOU SEE WHEN YOU STIMULATE BETA
 CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
SEDATION / ANALGESIA for Brain Failure Patient INASNACC
 SEDATION / ANALGESIA for Brain Failure Patient INASNACC Neuroendocrinological metabolic responses to surgical or traumatic injury Endocrine : increase in ACTH, cortisol, ADH, GH, glucagon, renin, aldosteron,
SEDATION / ANALGESIA for Brain Failure Patient INASNACC Neuroendocrinological metabolic responses to surgical or traumatic injury Endocrine : increase in ACTH, cortisol, ADH, GH, glucagon, renin, aldosteron,
Non Thyroid Surgery. In patients with Thyroid disorders
 Non Thyroid Surgery In patients with Thyroid disorders The Thyroid disease problem. Is Thyroid disease a problem with anaesthetic? Why worry? The Physiology The evidence. A pragmatic approach From: The
Non Thyroid Surgery In patients with Thyroid disorders The Thyroid disease problem. Is Thyroid disease a problem with anaesthetic? Why worry? The Physiology The evidence. A pragmatic approach From: The
A Successful RSI Program
 RSI A Successful RSI Program Requires understanding of: Indications Contraindications Limitations Requires knowledge of: Physiology Pharmacology Airway techniques Goals of RSI Success rates comparable
RSI A Successful RSI Program Requires understanding of: Indications Contraindications Limitations Requires knowledge of: Physiology Pharmacology Airway techniques Goals of RSI Success rates comparable
MAKING RSI SAFER. Nick Taylor ETU THK 2015
 MAKING RSI SAFER Nick Taylor ETU THK 2015 GOALS 1. AIRWAY ASSESSMENT AND PLAN 2. MAXIMALLY PREOXYGENATE 3. HAEMODYNAMIC STABILITY PART 1 : AIRWAY ASSESSMENT AND PLAN LEMON: AIRWAY ASSESS AND PLAN Look
MAKING RSI SAFER Nick Taylor ETU THK 2015 GOALS 1. AIRWAY ASSESSMENT AND PLAN 2. MAXIMALLY PREOXYGENATE 3. HAEMODYNAMIC STABILITY PART 1 : AIRWAY ASSESSMENT AND PLAN LEMON: AIRWAY ASSESS AND PLAN Look
ANESTHESIA DRUG REVIEW
 ANESTHESIA REVIEW CAPA S 39 TH ANNUAL CONFERENCE PALM SPRINGS OCTOBER 10, 2015 ROBERT F. KOPEL, MD, FACP, FCCP HOAG HOSPITAL CARDIAC ANESTHESIOLOGIST ASSISTANT CLINICAL PROFESSOR UCLA SCHOOL OF MEDICINE
ANESTHESIA REVIEW CAPA S 39 TH ANNUAL CONFERENCE PALM SPRINGS OCTOBER 10, 2015 ROBERT F. KOPEL, MD, FACP, FCCP HOAG HOSPITAL CARDIAC ANESTHESIOLOGIST ASSISTANT CLINICAL PROFESSOR UCLA SCHOOL OF MEDICINE
Anaesthesia In Thyroid Disorder. Dr. Umme Salma Ayesha Hoque MBBS, DA Medical Officer Department of Anaesthesiology and SICU BIRDEM General Hospital
 Anaesthesia In Thyroid Disorder Dr. Umme Salma Ayesha Hoque MBBS, DA Medical Officer Department of Anaesthesiology and SICU BIRDEM General Hospital Anatomy Endocrine gland : Consist of two lobe Located
Anaesthesia In Thyroid Disorder Dr. Umme Salma Ayesha Hoque MBBS, DA Medical Officer Department of Anaesthesiology and SICU BIRDEM General Hospital Anatomy Endocrine gland : Consist of two lobe Located
Procedural Sedation in the Rural ER
 Procedural Sedation in the Rural ER Hal Irvine MD FCFP Rural FP Anesthetist Sundre, Alberta June 17, 2011 Disclosure I do not have any affiliations (financial or otherwise) with a commercial organization
Procedural Sedation in the Rural ER Hal Irvine MD FCFP Rural FP Anesthetist Sundre, Alberta June 17, 2011 Disclosure I do not have any affiliations (financial or otherwise) with a commercial organization
Fundamental Knowledge: List of topics relevant to PIC that will have been covered in membership examinations. They will not be repeated here.
 Disclaimer: The Great Ormond Street Paediatric Intensive Care Training Programme was developed in 2004 by the clinicians of that Institution, primarily for use within Great Ormond Street Hospital and the
Disclaimer: The Great Ormond Street Paediatric Intensive Care Training Programme was developed in 2004 by the clinicians of that Institution, primarily for use within Great Ormond Street Hospital and the
Addendum D. Procedural Sedation Test MERCY MEDICAL CENTER- SIOUX CITY. Procedural Sedation Questions
 Addendum D. Procedural Sedation Test MERCY MEDICAL CENTER- SIOUX CITY Procedural Sedation Questions Individuals applying for moderate sedation privileges must achieve a score of 80%. PRACTITIONER NAME
Addendum D. Procedural Sedation Test MERCY MEDICAL CENTER- SIOUX CITY Procedural Sedation Questions Individuals applying for moderate sedation privileges must achieve a score of 80%. PRACTITIONER NAME
Induction Agents 2013/05/28 1
 Induction Agents 2013/05/28 1 Basic concepts One arm-brain circulation time Compartments Protein binding Redistribution vs. Metabolism Receptor binding 2013/05/28 2 One arm-brain circulation time From
Induction Agents 2013/05/28 1 Basic concepts One arm-brain circulation time Compartments Protein binding Redistribution vs. Metabolism Receptor binding 2013/05/28 2 One arm-brain circulation time From
Diabetes. & Mental Health. David J. Robinson MD, FRCPC. This slide is for review purposes only and not for presentations.
 Diabetes This slide is for review purposes only and not for presentations & Mental Health David J. Robinson MD, FRCPC CMHA - London, ON In the past 2 years, I have received speaking honoraria from, and
Diabetes This slide is for review purposes only and not for presentations & Mental Health David J. Robinson MD, FRCPC CMHA - London, ON In the past 2 years, I have received speaking honoraria from, and
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire)
 Best Practice Guidance Sedation These recommendations are bound by the current evidence and best practice at the time of writing and so will be subject to change as further developments are made in this
Best Practice Guidance Sedation These recommendations are bound by the current evidence and best practice at the time of writing and so will be subject to change as further developments are made in this
JMSCR Vol 04 Issue 01 Page January 2016
 www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i1.04 Haemodynamic Effects during Induction in
www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i1.04 Haemodynamic Effects during Induction in
PRE Operative Care of the High Risk Surgical Patient. Dr A T Dewhurst Consultant Anaesthetist St George s Hospital London
 PRE Operative Care of the High Risk Surgical Patient Dr A T Dewhurst Consultant Anaesthetist St George s Hospital London Perioperative Optimization Shoemaker oxygen delivery goal directed therapy ITS NOT
PRE Operative Care of the High Risk Surgical Patient Dr A T Dewhurst Consultant Anaesthetist St George s Hospital London Perioperative Optimization Shoemaker oxygen delivery goal directed therapy ITS NOT
Dr. Vishaal Bhat. anti-adrenergic drugs
 Dr. Vishaal Bhat anti-adrenergic drugs Divisions of human nervous system Human Nervous system Central Nervous System Peripheral Nervous System Autonomic Nervous System Nervous system Includes neurons and
Dr. Vishaal Bhat anti-adrenergic drugs Divisions of human nervous system Human Nervous system Central Nervous System Peripheral Nervous System Autonomic Nervous System Nervous system Includes neurons and
PRACTICAL MANAGEMENT OF DEPRESSION IN OLDER ADULTS. Lee A. Jennings, MD MSHS Assistant Professor Division of Geriatrics, UCLA
 CASE #1 PRACTICAL MANAGEMENT OF DEPRESSION IN OLDER ADULTS Lee A. Jennings, MD MSHS Assistant Professor Division of Geriatrics, UCLA OBJECTIVES Epidemiology Presentation in older adults Assessment Treatment
CASE #1 PRACTICAL MANAGEMENT OF DEPRESSION IN OLDER ADULTS Lee A. Jennings, MD MSHS Assistant Professor Division of Geriatrics, UCLA OBJECTIVES Epidemiology Presentation in older adults Assessment Treatment
Antidepressants: Prof. Riyadh Al_Azzawi F.R.C.Psych
 Antidepressants: Prof. Riyadh Al_Azzawi F.R.C.Psych A. Heterocyclic antidepressants: (tricyclic and tetracyclic ), e.g.amitryptaline,imipramine. B. Monoamine oxidase inhibitors(m.a.o.i), e.g.phenelzine.
Antidepressants: Prof. Riyadh Al_Azzawi F.R.C.Psych A. Heterocyclic antidepressants: (tricyclic and tetracyclic ), e.g.amitryptaline,imipramine. B. Monoamine oxidase inhibitors(m.a.o.i), e.g.phenelzine.
NERVOUS SYSTEM NERVOUS SYSTEM. Somatic nervous system. Brain Spinal Cord Autonomic nervous system. Sympathetic nervous system
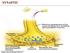 SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
Pediatric Procedural Sedation
 Pediatric Procedural Sedation Case 1: 2 year old complex facial laceration Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Department of Emergency Medicine Objectives: The
Pediatric Procedural Sedation Case 1: 2 year old complex facial laceration Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Department of Emergency Medicine Objectives: The
Chapter 161 Antipsychotics
 Chapter 161 Antipsychotics Episode Overview Extrapyramidal syndromes are a common complication of antipsychotic medications. First line treatment is benztropine or diphenhydramine. Lorazepam is used in
Chapter 161 Antipsychotics Episode Overview Extrapyramidal syndromes are a common complication of antipsychotic medications. First line treatment is benztropine or diphenhydramine. Lorazepam is used in
HTEC 91. Performing ECGs: Procedure. Normal Sinus Rhythm (NSR) Topic for Today: Sinus Rhythms. Characteristics of NSR. Conduction Pathway
 HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
Lujain Hamdan. Ayman Musleh & Yahya Salem. Mohammed khatatbeh
 12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
FOAM A New Style of Learning for a New Generation. Eric Einstein, M.D. Henry Ford Hospital Department of Emergency Medicine November 13, 2014
 FOAM A New Style of Learning for a New Generation Eric Einstein, M.D. Henry Ford Hospital Department of Emergency Medicine November 13, 2014 Objectives Define and discuss the basics Peer review a podcast
FOAM A New Style of Learning for a New Generation Eric Einstein, M.D. Henry Ford Hospital Department of Emergency Medicine November 13, 2014 Objectives Define and discuss the basics Peer review a podcast
INTRACRANIAL PRESSURE -!!
 INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
THE HEART OF THE MATTER MAYANNA LUND CMH
 THE HEART OF THE MATTER MAYANNA LUND CMH CARDIOLOGY ASSESSMENT AND WHEN TO REFER CHEST PAIN - ACUTE History Examination: vital signs are vital ECG Troponin Concerns: MI, unstable angina, PE, aortic dissection
THE HEART OF THE MATTER MAYANNA LUND CMH CARDIOLOGY ASSESSMENT AND WHEN TO REFER CHEST PAIN - ACUTE History Examination: vital signs are vital ECG Troponin Concerns: MI, unstable angina, PE, aortic dissection
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery
 Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Beta Blockade: Protection or Panacea
 Beta Blockade: Protection or Panacea Jason Axt Jason s Recommendations Perioperative β Blockade (BB) If on BB stay on If Vascular Sx + documented ischemia - start. 2+ risk factors - start Use in isolated
Beta Blockade: Protection or Panacea Jason Axt Jason s Recommendations Perioperative β Blockade (BB) If on BB stay on If Vascular Sx + documented ischemia - start. 2+ risk factors - start Use in isolated
May 2013 Anesthetics SLOs Page 1 of 5
 May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
Sleep and Heart Health: Consequences of OSA
 Sleep and Heart Health: Consequences of OSA Michelle Zetoony, DO, FCCP, FACOI Sleep Medicine Specialist Board Certified Pulmonary, Critical Care, Sleep and Internal Medicine 2014 Objectives Explain the
Sleep and Heart Health: Consequences of OSA Michelle Zetoony, DO, FCCP, FACOI Sleep Medicine Specialist Board Certified Pulmonary, Critical Care, Sleep and Internal Medicine 2014 Objectives Explain the
Anti-Depressant Medications
 Anti-Depressant Medications A Introduction: This topic may be a little bit underestimated here in Jordan, while in western countries it has more significance. The function of anti-depressants is to change
Anti-Depressant Medications A Introduction: This topic may be a little bit underestimated here in Jordan, while in western countries it has more significance. The function of anti-depressants is to change
POST-INTUBATION ANALGESIA AND SEDATION. August 2012 J Pelletier
 POST-INTUBATION ANALGESIA AND SEDATION August 2012 J Pelletier Intubated patients experience pain and anxiety Mechanical ventilation, endotracheal tube Blood draws, positioning, suctioning Surgical procedures,
POST-INTUBATION ANALGESIA AND SEDATION August 2012 J Pelletier Intubated patients experience pain and anxiety Mechanical ventilation, endotracheal tube Blood draws, positioning, suctioning Surgical procedures,
Approach to type 2 Respiratory Failure
 Approach to type 2 Respiratory Failure Changing Nature of NIV Not longer just the traditional COPD patients Increasingly Obesity Neuromuscular Pneumonias 3 fold increase in patients with Ph 7.25 and below
Approach to type 2 Respiratory Failure Changing Nature of NIV Not longer just the traditional COPD patients Increasingly Obesity Neuromuscular Pneumonias 3 fold increase in patients with Ph 7.25 and below
A Basic Approach to Mood and Anxiety Disorders in the Elderly
 A Basic Approach to Mood and Anxiety Disorders in the Elderly November 1 2013 Sarah Colman MD FRCPC Clinical Fellow, Geriatric Psychiatry Mount Sinai Hospital, University of Toronto Disclosure No conflict
A Basic Approach to Mood and Anxiety Disorders in the Elderly November 1 2013 Sarah Colman MD FRCPC Clinical Fellow, Geriatric Psychiatry Mount Sinai Hospital, University of Toronto Disclosure No conflict
P-RMS: NO/H/PSUR/0009/001
 Core Safety Profile Active substance: Propofol Pharmaceutical form(s)/strength: Emulsion for injection, infusion, 10mg/ml Emulsion for infusion, 20mg/ml P-RMS: NO/H/PSUR/0009/001 Date of FAR: 30.06.2011
Core Safety Profile Active substance: Propofol Pharmaceutical form(s)/strength: Emulsion for injection, infusion, 10mg/ml Emulsion for infusion, 20mg/ml P-RMS: NO/H/PSUR/0009/001 Date of FAR: 30.06.2011
GENERAL ANAESTHESIA AND FAILED INTUBATION
 GENERAL ANAESTHESIA AND FAILED INTUBATION INTRODUCTION The majority of caesarean sections in the UK are performed under regional anaesthesia. However, there are situations where general anaesthesia (GA)
GENERAL ANAESTHESIA AND FAILED INTUBATION INTRODUCTION The majority of caesarean sections in the UK are performed under regional anaesthesia. However, there are situations where general anaesthesia (GA)
Behavioral Interventions
 Behavioral Interventions Linda K. Shumaker, R.N.-BC, MA Pennsylvania Behavioral Health and Aging Coalition Behavioral Management is the key in taking care of anyone with a Dementia! Mental Health Issues
Behavioral Interventions Linda K. Shumaker, R.N.-BC, MA Pennsylvania Behavioral Health and Aging Coalition Behavioral Management is the key in taking care of anyone with a Dementia! Mental Health Issues
Without Background for printing as Pocket Reference
 Without Background for printing as Pocket Reference Diabetes Prevention Program 1 LOOK AHEAD 3 Multi-center trial in patients with impaired glucose tolerance Weight loss of 7% reduced the rate of progression
Without Background for printing as Pocket Reference Diabetes Prevention Program 1 LOOK AHEAD 3 Multi-center trial in patients with impaired glucose tolerance Weight loss of 7% reduced the rate of progression
INHALATION AGENTS 2013/05/28 1
 INHALATION AGENTS 2013/05/28 1 2013/05/28 Isn t it romantic? 2 Administration 3 Physics Critical temperature Vapour vs. Gas Vapour pressure Blood Gas Partition Coefficient BGPC MAC 2013/05/28 4 Critical
INHALATION AGENTS 2013/05/28 1 2013/05/28 Isn t it romantic? 2 Administration 3 Physics Critical temperature Vapour vs. Gas Vapour pressure Blood Gas Partition Coefficient BGPC MAC 2013/05/28 4 Critical
Michigan EMS. Medication In-Service: Ondansetron (Zofran) ODT
 Michigan EMS Medication In-Service: Ondansetron (Zofran) ODT Course Objectives Identify the location of ondansetron (Zofran) ODT in the SEM Drug Box, as well as how it may be packaged. Describe the pharmacokinetics
Michigan EMS Medication In-Service: Ondansetron (Zofran) ODT Course Objectives Identify the location of ondansetron (Zofran) ODT in the SEM Drug Box, as well as how it may be packaged. Describe the pharmacokinetics
Complicated Withdrawal
 Complicated Withdrawal Shamim Nejad, MD Director, Adult Burns & Trauma Psychiatry Division of Psychiatry and Medicine Medical Director, Addiction Consultation Team MGH Center for Addiction Medicine Massachusetts
Complicated Withdrawal Shamim Nejad, MD Director, Adult Burns & Trauma Psychiatry Division of Psychiatry and Medicine Medical Director, Addiction Consultation Team MGH Center for Addiction Medicine Massachusetts
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006.
 Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
R Adams Cowley Founder of the R Adams Cowley Shock Trauma Center and Maryland EMS System in Baltimore, Maryland.
 R Adams Cowley 1917 -- 1991 Founder of the R Adams Cowley Shock Trauma Center and Maryland EMS System in Baltimore, Maryland. ...That the primary purpose of medicine was to save lives, that every critically
R Adams Cowley 1917 -- 1991 Founder of the R Adams Cowley Shock Trauma Center and Maryland EMS System in Baltimore, Maryland. ...That the primary purpose of medicine was to save lives, that every critically
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Prehospital Care Bundles
 Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Update on Palpitations and AF February 28 th 2018
 Update on Palpitations and AF February 28 th 2018 Dr Mrinal Andrew Saha MA(Cantab) MBBS FRCP PhD Consultant Interventional Cardiologist GHNHSFT Dr Mrinal Saha Appointed 2010 Special interests: Angioplasty,
Update on Palpitations and AF February 28 th 2018 Dr Mrinal Andrew Saha MA(Cantab) MBBS FRCP PhD Consultant Interventional Cardiologist GHNHSFT Dr Mrinal Saha Appointed 2010 Special interests: Angioplasty,
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Traumatic Brain Injury
 Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to
 Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Total Intravenous Anaesthesia
 Total Intravenous Anaesthesia Balasubramanian Thiagarajan Stanley Medical College Abstract: Total intravenous anaesthesia (TIVA) is a technique of anaesthesia which involves use of intravenous drugs to
Total Intravenous Anaesthesia Balasubramanian Thiagarajan Stanley Medical College Abstract: Total intravenous anaesthesia (TIVA) is a technique of anaesthesia which involves use of intravenous drugs to
Blood Brain Barrier (BBB)
 Cerebral Blood Flow, Cerebral Spinal Fluid, and Brain Metabolism Part Two Guyton Chapter 61 Morgan & Mikhail, 4 th ed, Chapter 25 (or Morgan & Mikhail 5 th ed, Chapter 26) Blood Brain Barrier (BBB) Cerebral
Cerebral Blood Flow, Cerebral Spinal Fluid, and Brain Metabolism Part Two Guyton Chapter 61 Morgan & Mikhail, 4 th ed, Chapter 25 (or Morgan & Mikhail 5 th ed, Chapter 26) Blood Brain Barrier (BBB) Cerebral
Anaesthetic Plan And The Practical Conduct Of Anaesthesia. Dr.S.Vashisht Hillingdon Hospital
 Anaesthetic Plan And The Practical Conduct Of Anaesthesia Dr.S.Vashisht Hillingdon Hospital Anaesthetic Plan Is based on Age / physiological status of the patient (ASA) Co-morbid conditions that may be
Anaesthetic Plan And The Practical Conduct Of Anaesthesia Dr.S.Vashisht Hillingdon Hospital Anaesthetic Plan Is based on Age / physiological status of the patient (ASA) Co-morbid conditions that may be
Effective Shared Care Agreement (ESCA) for drugs used in dementia- Donepezil, Galantamine, Rivastigmine and Memantine
 Effective Shared Care Agreement (ESCA) for drugs used in dementia- Donepezil, Galantamine, Rivastigmine and Memantine for the treatment of dementia AREAS OF RESPONSIBILITY FOR THE SHARING OF CARE This
Effective Shared Care Agreement (ESCA) for drugs used in dementia- Donepezil, Galantamine, Rivastigmine and Memantine for the treatment of dementia AREAS OF RESPONSIBILITY FOR THE SHARING OF CARE This
W. Heath Giles, M.D. University of Tennessee College of Medicine Chattanooga Assistant Professor of Surgery Associate Residency Program Director
 W. Heath Giles, M.D. University of Tennessee College of Medicine Chattanooga Assistant Professor of Surgery Associate Residency Program Director It is our duty to each learner to honor your right to expect
W. Heath Giles, M.D. University of Tennessee College of Medicine Chattanooga Assistant Professor of Surgery Associate Residency Program Director It is our duty to each learner to honor your right to expect
DRUG GUIDELINE. HYDRALAZINE (Intravenous severe hypertension in pregnancy)
 DRUG GUIDELINE HYDRALAZINE (Intravenous severe hypertension SCOPE (Area): FOR USE IN: Labour Ward, HDU, Theatre and ED EXCLUSIONS: Paediatrics (seek Paediatrician advice) and other general wards. SCOPE
DRUG GUIDELINE HYDRALAZINE (Intravenous severe hypertension SCOPE (Area): FOR USE IN: Labour Ward, HDU, Theatre and ED EXCLUSIONS: Paediatrics (seek Paediatrician advice) and other general wards. SCOPE
a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure.
 B. 10 Applied Respiratory Physiology a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure. Intermittent positive pressure ventilation
B. 10 Applied Respiratory Physiology a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure. Intermittent positive pressure ventilation
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Hyperglycaemic Emergencies GRI EDUCATION
 Hyperglycaemic Emergencies GRI EDUCATION LEARNING OUTCOMES Develop and describe your system of blood gas interpretation and recognise common patterns of acid-base abnormality. Describe the pathophysiology
Hyperglycaemic Emergencies GRI EDUCATION LEARNING OUTCOMES Develop and describe your system of blood gas interpretation and recognise common patterns of acid-base abnormality. Describe the pathophysiology
Pharmacists in Medication Adherence in Psychiatric Patients
 Pharmacists in Medication Adherence in Psychiatric Patients Mamta Parikh, PharmD, BCPS, BCPP Assistant Professor, Clinical and Administrative Sciences Notre Dame of Maryland University School of Pharmacy
Pharmacists in Medication Adherence in Psychiatric Patients Mamta Parikh, PharmD, BCPS, BCPP Assistant Professor, Clinical and Administrative Sciences Notre Dame of Maryland University School of Pharmacy
FHR Monitoring: Maternal Fetal Physiology
 FHR Monitoring: Maternal Fetal Physiology M. Sean Esplin, MD and Alexandra Eller, MD Maternal Fetal Medicine Intermountain Healthcare University of Utah Health Sciences Center Disclosures I have no financial
FHR Monitoring: Maternal Fetal Physiology M. Sean Esplin, MD and Alexandra Eller, MD Maternal Fetal Medicine Intermountain Healthcare University of Utah Health Sciences Center Disclosures I have no financial
Shaded areas=not MARKETED 24/2/09
 PACKAGE INSERT SCHEDULING STATUS Schedule 6 PROPRIETARY NAME AND DOSAGE FORM RAPIFEN 2 ml IV injection RAPIFEN 10 ml IV injection COMPOSITION Each ml contains alfentanil hydrochloride 0,544 mg (equivalent
PACKAGE INSERT SCHEDULING STATUS Schedule 6 PROPRIETARY NAME AND DOSAGE FORM RAPIFEN 2 ml IV injection RAPIFEN 10 ml IV injection COMPOSITION Each ml contains alfentanil hydrochloride 0,544 mg (equivalent
Homeostasis. Achievement Criteria. Excellence Criteria. Demonstrate understanding of how an animal maintains a stable internal environment 10/02/2016
 Homeostasis Demonstrate understanding of how an animal maintains a stable internal environment Biology 3.4 AS91604 Achievement Criteria Explain the purpose of the homeostatic mechanism Be able to explain
Homeostasis Demonstrate understanding of how an animal maintains a stable internal environment Biology 3.4 AS91604 Achievement Criteria Explain the purpose of the homeostatic mechanism Be able to explain
In our patients the cause of seizures can be broadly divided into structural and systemic causes.
 Guidelines for the management of Seizures Amalgamation and update of previous policies 7 (Seizure guidelines, ND, 2015) and 9 (Status epilepticus, KJ, 2011) Seizures can occur in up to 15% of the Palliative
Guidelines for the management of Seizures Amalgamation and update of previous policies 7 (Seizure guidelines, ND, 2015) and 9 (Status epilepticus, KJ, 2011) Seizures can occur in up to 15% of the Palliative
SYNCOPE. DEFINITION Syncope is defined as sudden and transient loss of consciousness which is secondary to period of cerebral ischemia CAUSES
 SYNCOPE INTRODUCTION Syncope is a symptom not a disease Syncope is the abrupt and transient loss of consciousness associated with absence of postural tone, followed by complete and usually rapid spontaneous
SYNCOPE INTRODUCTION Syncope is a symptom not a disease Syncope is the abrupt and transient loss of consciousness associated with absence of postural tone, followed by complete and usually rapid spontaneous
Status Epilepticus And Prolonged Seizures: Guideline For Management In Adults. Contents
 Status Epilepticus And Prolonged Seizures: Guideline For Management In Adults Classification: Clinical guideline Lead Author: Rajiv Mohanraj, Consultant Neurologist Additional author(s): Matt Jones, Consultant
Status Epilepticus And Prolonged Seizures: Guideline For Management In Adults Classification: Clinical guideline Lead Author: Rajiv Mohanraj, Consultant Neurologist Additional author(s): Matt Jones, Consultant
Procedural Sedation and Analgesia in the ED
 Overview Procedural Sedation and Analgesia in the ED Susan Lambe, MD Assistant Clinical Professor UCSF Division of Emergency Medicine Terminology Goals Indications Presedation Assessment Consent Issues
Overview Procedural Sedation and Analgesia in the ED Susan Lambe, MD Assistant Clinical Professor UCSF Division of Emergency Medicine Terminology Goals Indications Presedation Assessment Consent Issues
Preoperative tests (update)
 National Institute for Health and Care Excellence. Preoperative tests (update) Routine preoperative tests for elective surgery NICE guideline NG45 Appendix C: April 2016 Developed by the National Guideline
National Institute for Health and Care Excellence. Preoperative tests (update) Routine preoperative tests for elective surgery NICE guideline NG45 Appendix C: April 2016 Developed by the National Guideline
Obesity and Anaesthesia. Western General Hospital. Friday 10 th March 2006.
 Obesity and Anaesthesia Western General Hospital. Friday 10 th March 2006. Obesity: Topics Definition Incidence. Pathophysiology Pharmacokinetics. Anaesthesia. Bariatric Surgery. Definition 1 Body Mass
Obesity and Anaesthesia Western General Hospital. Friday 10 th March 2006. Obesity: Topics Definition Incidence. Pathophysiology Pharmacokinetics. Anaesthesia. Bariatric Surgery. Definition 1 Body Mass
Presentation of transient loss of consciousness
 Presentation of transient loss of consciousness Definition of transient loss of consciousness Transient loss of consciousness: sudden onset, complete loss of consciousness of brief duration with relatively
Presentation of transient loss of consciousness Definition of transient loss of consciousness Transient loss of consciousness: sudden onset, complete loss of consciousness of brief duration with relatively
