Concussion Management Guidelines for Gaelic Games
|
|
|
- Amberly Briggs
- 6 years ago
- Views:
Transcription
1
2 Concussion Management Guidelines for Gaelic Games Updated January 2018 Introduction 3 What is Concussion? 3 Summary Principles 4 Signs and Symptoms 5 Pitch Assessment / Initial Management of a Concussion Injury 6 Sports Concussion Assessment Tool 5 (SCAT5) 7 Baseline Testing 7 Return to Play 8 Graduated Return to School Strategy 10 Factors that Influence the Investigation and Management of Concussion 10 Helping Players Cope with a Concussion Injury 11 References 11 2 Appendix 1: Appendix Pocket Concussion Recognition Tool
3 Introduction Gaelic Games are contact sports. While collisions occur, they are not the primary focus of our games. The GAA has led the way in concussion awareness and education since the publication of the association s first statement on concussion in Since the publication of the most recent concussion management guidelines in 2013, extensive education has taken place at all levels of the association through various programmes and initiatives including seminars, workshops, information sheets, posters and an e-learning course available to players, members, administrators, referees and coaches. The GAA has been represented at a number of conferences on the subject including the 5th International Consensus Statement in Berlin in The recent Concussion Symposiums, held in Croke Park in 2016 and 2017 in association with Bon Secours Health System and UPMC International have also further increased awareness in relation to ongoing research and advances in treatment in this area. This document is intended as a master guideline to those involved in the sport and as an assistance to players, coaches, referee s and medics in understanding and managing suspected concussion at all levels of the game. In this document, the GAA reaffirms its position that if there are any signs leading to a suspicion of a concussion for a player, at any level or any age, the player should be removed immediately from play, and not return to action on the same day (the impact itself may on occasion be considered an indicator in this context, even in the absence of any immediate symptoms). The player should be medically assessed and not return to full contact play without prior medical approval If In Doubt, Sit Them Out. In fact, research has shown that by withdrawing a player from play immediately following a potential concussive impact, this reduced players recovery time when compared with those who remained in games and required a longer spell out of action before making a full recovery. 3 What is Concussion? Concussion is a brain injury and can be caused by a direct or indirect hit to the player s head or body. Concussion typically results in an immediate onset of short lived signs and symptoms. However, in some cases, the signs and symptoms of concussion may evolve over a number of minutes or hours or even days. Concussion must be taken extremely seriously as there is potential for catastrophic brain injury with children and adolescents at most risk. This document sets out the GAA s Guidelines in relation to Concussion Management. The following recommendations are not protocols or a clinical standard of care.
4 SUMMARY PRINCIPLES Concussion is a brain injury that needs to be taken seriously to protect the short and long-term health and welfare of all players. If there are any signs leading to the suspicion of concussion, a player should be removed immediately from the field of play pending a full medical assessment (the impact itself may on occasion be considered an indicator even in the absence of any immediate symptoms). A player suspected of sustaining/having sustained a concussion should not return to play on the same day. Subsequently a satisfactory, supervised return to play protocol must be completed, followed by medical approval, prior to return to play. If In Doubt, Sit Them Out. Where a Team Doctor is present, he must advise the person in charge of the team (i.e. Team Manager) in this regard and the player must not be allowed to continue his participation in the game. Concussion diagnosis is a clinical judgement Use of the SCAT 5 can aid the doctor in his/her diagnosis. If a full SCAT 5 assement has been deemed necessary the player should not return to play on the day. Concussion is an evolving injury. It is important to monitor the player after the injury for hours. Adult players suspected of having a concussion, must have adequate rest of at least hours and then must follow a gradual return to play (GRTP) protocol. Players must receive written medical clearance (from a doctor) and present to the person in charge of the team before returning to full contact training. Adult players should not return to full contact training/matches for at least 1 week from when the injury has first been diagnosed. (The GRTP should take at least 7 days for adult players) Players under the age of 18 suspected of having a concussion must rest for a minimum of 48 hours and then must follow a GRTP protocol. Players must receive written medical clearance from a doctor) and present to the person in charge of the team before returning to full contact training. Players under the age of 18 should not return to full contact training/matches for at least 2 weeks from when the injury has first been diagnosed. (It is recommended that the GRTP should take at least 14 days for players under the age of 18.) 4 A graduated return to school/education strategy is also necessary. Communication between the doctor, parents and teachers is essential so that a flexible individualised plan alowing incremental progression from daily activities, school activities, return to school part time and return to school full time be implemented. No player should return to competitive sporting activity prior to being cleared to return to school. The vast majority of players can be managed locally by a doctor with the necessary skillsets, for example Team Doctor, GP, or Sports Medicine Doctor. A minority of players with prolonged symptoms (greater than 4 weeks for under-18s or greater than days for adult players, players with recurrent injuries or experiencing educational difficulties) should be referred to an appropriate specialist or multidisciplinary clinic. All coaches should be made aware by players and/or parents if a player under their care has received a concussion in another sport/event. In children and adolescents, there is a risk of catastrophic injury from second impact syndrome if players are returned to play before they are recovered from concussion.
5 SIGNS AND SYMPTOMS Contrary to popular belief, most (over 90%) concussions occur without a loss of consciousness and so it is important to recognise the other signs and symptoms. Concussion must be recognised as an evolving injury in the acute stage. Some symptoms may develop immediately while other symptoms may appear gradually over time. Monitoring of players - minutes, hours and days - after the injury is therefore an important aspect of concussion management. DIAGNOSIS OF ACUTE CONCUSSION SHOULD INVOLVE THE FOLLOWING: 1. Player s subjective report of his/her symptoms. 2. Observation of the player for physical signs of concussion. 3. Assessment of the player for cognitive change or decline. 4. Observation of players for behavioural change. 5. Players report of any sleep disturbance. CONCUSSION ASSESSMENT DOMAINS INDICATORS Symptoms Physical Signs Cognitive Impairment Behavioural Changes Sleep Disturbance *Most common symptom WHAT YOU WOULD EXPECT TO SEE Headaches* Dizziness Feeling in a fog. Fatigue Sensitivity to light or noise Loss of consciousness Vomiting Vacant Facial Expression Clutching Head Balance Disturbance (ataxia / unsteadiness) Motor In coordination Slurred speech Loss short term memory Difficulty with concentration Decreased attention Diminished work performance Irritability Anger Mood Swings Feeling Nervous Anxious Sadness or Depression Withdrawal Drowsiness Difficulty Falling Asleep 5
6 Pitch Assessment / Initial Management of a Concussion Injury* Knowledge of a player s history (has the player suffered a concussion previously?), visualizing the impact and performing an examination in the first 3 minutes may provide invaluable information The player should be assessed by a doctor on the field using standard emergency management principles. Particular attention should be given to excluding a cervical spine injury. If no doctor is present, the player should be assessed by a registered healthcare practitioner (Physiotherapist/ Nurse) on the field using standard emergency management principles. Particular attention should be given to excluding a cervical spine injury. If no healthcare practitioner is available the player should be removed from practice or play and urgent referral to a doctor is required. If there is a possibility of a potential neck or cervical spine injury the player should not be moved and an ambulance called immediately. While the diagnosis of concussion is a clinical judgement, made by a doctor on an individual basis, there are red flags that mandate the urgent removal of a player to urgent medical attention/request for an ambulance: - Prolonged Loss of consciousness - Deteriorating conscious state - Convulsions or tonic posturing - Increasingly restless, agitated or combative - Vomiting - Double Vision - Disorientation/Confusion - Severe or increasing headache - Abnormalities of balance, gait or coordination - Slurred or incoherent speech - Weakness or tingling/burning in arms or legs 6 If there is a possibility of a potential neck or cervical spine injury the player should not be moved and an ambulance called immediately. Once the above first aid issues are addressed, an assessment of the concussive injury should include clinical judgement and the use of the SCAT 5 The player should NOT be left alone for 24 hours following the injury. The player should not drive, take alcohol or any medication unless prescribed by a doctor. Regular observation for deterioration is essential over the initial 24 hours following injury. * There is a need to recognise that the appearance of symptoms might be delayed several hours following a concussive episode. For example, there may be no forgetfulness (retrograde amnesia) present at 0 mins post injury, yet forgetfulness (amnesia) may be present at 10 mins post injury. * Orientation tests (i.e. name, place, and person) have been shown to be an unreliable cognitive function test in the sporting situation.
7 Sports Concussion Assessment Tool 5 (SCAT5) While the diagnosis of concussion is a clinical judgment ideally made by a medical professional, the SCAT 5 provides a standardized tool assessing an injured player aged from 13 years and older for concussion. (Child SCAT 5 can be used for children aged 5-13). SCAT 5 is designed for use by registered medical practitioners and other clinical personnel that have appropriate training to use SCAT 5. It is recognised that the SCAT5 should not be used solely to make or exclude the diagnosis of concussion in the absence of clinical judgement. An athlete may have a concussion even if their SCAT5 is normal. SCAT 5 consists of two parts - the first part is an initial pitch side assessment of injury severity (Concussion signs, Glasgow Coma Scale and Maddocks Score). The second part of the SCAT 5 should be carried out after a minimum 15 minute rest period to avoid the influence of exertion and fatigue on the player s performance. This assessment consists of symptom checklist, symptom severity, as well as neuro cognitive and balance functions. The diagnosis of a concussion is a clinical judgement. If a full SCAT 5 assessment has been deemed necessary the player should not return to play on the same day. Any player with a suspected concussion should be REMOVED FROM PLAY, medically assessed, monitored for deterioration and should not drive a motor vehicle until cleared to do so by a registered medical practitioner. In Gaelic games, SCAT 5 can be used to perform a baseline assessment in the medical room/dressing room following removal from play and subsequently at 24 or 48 hours to monitor progress. Reliability is significantly diminished after 3 days. The SCAT 5 is available at the follow link for use by medical professionals only Sport Concussion Assessment Tool - 5th Edition 7 The Concussion Recognition Tool 5 is included as an Appendix to this document. A CRT 5 assessment can be used by non-medical professionals (Team mentors etc). A player should not be returned to play if a CRT 5 has been carried out. Baseline Testing Baseline or pre-season NP testing is not yet felt to be required as a mandatory aspect of every assessment; however, it may be helpful or add useful information to the overall interpretation of these tests. It also provides an additional educative opportunity to discuss the significance of this injury with the athlete subject to resources available within the county/club.
8 RETURN TO PLAY A player with a suspected/ concussion should NEVER be allowed to return to play on the day of injury. In addition, return to play must follow a medically supervised stepwise approach and a player SHOULD NEVER return to play while symptomatic A graded program of exertion prior to medical clearance and return to play (RTP is generally recommended. 1. There should be an initial minimum period of hours rest for adult players post a concussive injury. This rest period should be a minimum of 48 hours for players under the age of Following this rest period, players can be encouraged to become gradually and progressively more active while staying below their cognitive and physical symptom-exacerbation thresholds (ie, activity level should not bring on or worsen their symptoms) 3. RTP protocols following concussion follow a stepwise approach. With this stepwise progression, the players should only continue to proceed to the next level if asymptomatic at the current level. 4. Generally, for adults each step should take at least 24 hours so that the athlete would take approximately one week to proceed to full rehabilitation once they are asymptomatic at rest Generally, for players under the age of 18, steps 2-4 (inclusive) should take at least 4 days each to complete so that the player would take approximately two weeks to proceed to full rehabilitation once they are asymptomatic at rest. 6. If any post-concussion symptoms occur while in the RTP program, then the player should drop back to the previous asymptomatic level and try to progress again after a further 24 hours period of rest has passed. 7. Adult players should not return competitive action/full contact training without medical clearance. This should be at least 1 week from when a diagnosis has been made. 8. Players under the age of 18 should not return competitive action/full contact training without medical clearance. This should be at least 2 weeks from when a diagnosis has been made. 9. Medical clearance refers to clearance by a doctor, in writing, is required to be provided to the person in charge of the team prior to return to full contact sports.
9 GRTP FOR ADULT PLAYERS REHABILITATION STAGE FUNCTIONAL EXERCISE AT EACH STAGE OF REHABILITATION OBJECTIVE OF EACH STAGE 1. No Activity for hours Physical and Cognitive Rest Recovery 2. Light Activity (at least 1 day) Walking, swimming, cycling, keeping intensity <70% maximum permitted heart rate. (If Activity does worsen symptoms or bring on further symptoms return to previous stage. If no symptoms progress to next stage) Increase HR 3. Sports Specific Exercise (at least 1 day) 4. No Contact Training Drills (at least 1 day) 5. Full Contact Practice (at least 1 day) 6. Return to play (Minimum of 7 days since diagnosis) Running drills ((If Activity does worsen symptoms or bring on further symptoms return to previous stage. If no symptoms progress to next stage) Progress to more complex training drills - passing drills, progressive resistance training (If Activity does worsen symptoms or bring on further symptoms return to previous stage. If no symptoms progress to next stage) Following written medical clearance, participate in normal training activities. (If Activity does worsen symptoms or bring on further symptoms return to previous stage. If no symptoms progress to next stage) Normal game play Add Movement Exercise, coordination and cognitive load Restore confidence and assess functional skills by coaching staff Return to competitive action. If any increase in/development of further symptoms occur while in the RTP program, then the player should drop back to the previous asymptomatic level and try to progress again after a further 24 hours period of rest has passed GRTP FOR PLAYERS UNDER THE AGE OF 18 REHABILITATION STAGE 1. No Activity for a minimum of 48 hours 2. Light Activity (at least 4 days) 3. Sports Specific Exercise (at least 4 days) 4. No Contact Training Drills (at least 4 days) 5. Full Contact Practice (at least 1 day) 6. Return to play (Minimum of at least 15 days since diagnosis) FUNCTIONAL EXERCISE AT EACH STAGE OF REHABILITATION Physical and Cognitive Rest Walking, swimming, cycling, keeping intensity <70% maximum permitted heart rate - (If Activity does worsen symptoms or bring on further symptoms return to previous stage. If no symptoms progress to next stage) Running drills - (If Activity does worsen symptoms or bring on further symptoms return to previous stage. If no symptoms progress to next stage) Progress to more complex training drills- passing drills, progressive resistance training - (If Activity does worsen symptoms or bring on further symptoms return to previous stage. If no symptoms progress to next stage) Following written medical clearance, participate in normal training activities. (If Activity does worsen symptoms or bring on further symptoms return to previous stage. If no symptoms progress to next stage) Normal game play OBJECTIVE OF EACH STAGE Recovery Increase HR Add Movement Exercise, coordination and cognitive load Restore confidence and assess functional skills by coaching staff Return to competitive action. 9 If any increase in/development of further symptoms occur while in the RTP program, then the player should drop back to the previous asymptomatic level and try to progress again after a further 24 hours period of rest has passed In children and adolescents, there is a risk of catastrophic injury from second impact syndrome if players are returned to play before they are recovered from concussion.
10 GRADUATED RETURN TO SCHOOL STRATEGY Concussion may affect the ability to learn at school. Initially, the player may need to miss a few days of school, followed by a gradual return, avoiding activities that exacerbate symptoms MENTAL ACTIVITY ACTIVITY AT EACH STEP GOAL OF EACH STEP 1. Daily activities that do not give the athlete symptoms Typical activities that the athlete does during the day as long as they do not increase symptoms (e.g. reading, texting, screen time). Start with 5-15 minutes at a time and gradually build up. 2. School activities Homework, reading or other cognitive activities outside of the classroom. 3. Return to school full-time Gradual introduction of schoolwork. May need to start with a partial school day or with increased breaks during the day. 4. Return to school full-time Gradually progress school activities until a full day can be tolerated. Gradual return to typical activities. Increase tolerance to cognitive work. Increase academic activities. Return to full academic activities and catch up on missed work. Factors that Influence the Investigation and Management of Concussion A range of modifying factors may influence the investigation and management of concussion and, in some cases, may predict the potential for prolonged or persistent symptoms. Examples of modifiers would be children and adolescents under the age of 18 or players with previous concussions. Medical personnel should be mindful of these modifiers when managing a player s concussive injury. Most players with concussion can be managed locally. Players with prolonged symptoms (adults over 10 days, children more than 4 weeks), players with intractable symptoms or experiencing difficulty returning to education will require referral to an appropriate specialist. The following factors predispose to, or influence the course of a concussive episode. 10 CONCUSSION MODIFIERS FACTORS MODIFIERS Symptoms Number Duration(>10days) Severity Signs Prolonged loss of consciousness (LOC) (>1 min), Amnesia Sequelae Concussive convulsions Temporal Frequency repeated concussions over time Timing injuries close together in time Recency recent concussion or traumatic brain injury Threshold Repeated concussions occurring with progressively less impact force or slower recovery after each successive concussion Age Child and adolescent (<18 years) Comorbidities and premorbidities Migraine, depression or other mental health disorders, attention deficit hyperactive disorder (ADHD), learning disabilities (LD), sleep disorders, vestibular disorder (e.g., motion sickness), pre-existing oculo-motor dysfunction Medication Psychoactive drugs, anticoagulants Behaviour Dangerous style of play Sport High risk activity, contact with collision sport, high sporting level
11 Helping Players Cope with a Concussion Injury Players often feel tired and may experience difficulties at work or school when carrying out a task which requires concentration. Players may also encounter mood difficulties and feel depressed, anxious or irritable with family or team mates. The following actions can help players cope: Once symptoms initially resolve a light exercise programme (See GRTP) appears to speed up recovery. Support should be provided to players during this recovery period. Parents, Coaches and Team-mates should reassure the player to follow the recovery protocols and ask the player if he has any questions or concerns regarding the injury. The player should be included in social activities which do not put the player at risk of a further concussion. Alcohol should be avoided as it may delay recovery and put the player at increased risk for further injury. Minimise exposure to TV, PC, Laptops, Smartphone, Tablet, Video Games etc These items should be avoided two hours before sleep as they can cause sleep disturbance. Sleep disturbance is common and hence restoring normal sleep patterns and Circadian rhythms is essential. Napping is generally not recommended during recovery from concussion, as it can disrupt the circadian cycle of sleep and wakefulness. Attention to hydration and nutrition is important (dehydration exacerbates and prolongs headaches and other symptoms). When dealing with persistent symptoms, it is essential that players only take medications prescribed by their doctor. Recovery from concussion should not be rushed nor pressure applied to players to resume playing until recovery is complete. The risk of re injury is high and may lead to recurrent concussion injuries. It is better to have missed one game than the whole season. 11 Remember In children and adolescents, there is a risk of catastrophic injury from second impact if players are returned before they have recovered. References Elbin RJ. et al (2016). Removal from play after concussion and recovery time. Pediatrics; 2016; 138(3). Epub ahead of print (June 6,2016) DOI: /peds GAA. (2015) GAA Concussion Management Guidelines ( ). Available at: Mc Crory, P. et al (2017) Consensus statement on concussion in sport: the 4th International Conference on Concussion in Sport held in Berlin, October Br J Sports Med; Published Online First April 26, 2017 DOI: / bjsports ALL CORRESPONDENCE SHOULD BE DIRECTED TO: GAA MEDICAL, SCIENTIFIC AND WELFARE COMMITTEE, GAA, CROKE PARK. DUBLIN 3
12 Appendix CONCUSSION RECOGNITION TOOL 5 To help identify concussion in children, adolescents and adults RECOGNISE & REMOVE Head impacts can be associated with serious and potentially fatal brain injuries. The Concussion Recognition Tool 5 (CRT5) is to be used for the identification of suspected concussion. It is not designed to diagnose concussion. STEP 1: RED FLAGS CALL AN AMBULANCE If there is concern after an injury including whether ANY of the following signs are observed or complaints are reported then the player should be safely and immediately removed from play/game/activity. If no licensed healthcare professional is available, call an ambulance for urgent medical assessment: Neck pain or tenderness Severe or increasing headache Deteriorating conscious state Weakness or tingling/burning in arms or legs Seizure or convulsion Vomiting Increasingly restless, agitated or combative Loss of consciousness Remember: In all cases, the basic principlesof first aid (danger, response, airway, breathing, circulation) should be followed. Assessment for a spinal cord injury is critical. Do not attempt to move the player (other than required for airway support) unless trained to so do. Do not remove a helmet or any other equipment unless trained to do so safely. If there are no Red Flags, identification of possible concussion should proceed to the following steps: STEP 2: OBSERVABLE SIGNS Visual clues that suggest possible concussion include: Lying motionless on Disorientation or Balance, gait difficulties, the playing surface confusion, or an inability motor incoordination, to respond appropriately stumbling, slow Slow to get up after to questions laboured movements a direct or indirect hit to the head Blank or vacant look Facial injury after head trauma 12 STEP 3: SYMPTOMS Headache Pressure in head Balance problems Nausea or vomiting Drowsiness Dizziness Blurred vision STEP 4: MEMORY ASSESSMENT (In Athletes older than 12 years) Failure to answer any of these questions (modified appropriately for each sport) correctly may suggest a concussion: Sensitivity to light Sensitivity to noise Fatigue or low energy Don t feel right More emotional More Irritable Sadness What venue are we at today? Which half is it now? Who scored last in this game? Nervous or anxious Neck Pain Difficulty concentrating Difficulty remembering Feeling slowed down Feeling like in a fog What team did you play last week/game? Did your team win the last game? Athletes with suspected concussion should: Not be left alone initially (at least for the first 1-2 hours) Not drink alcohol. Not use recreational/ prescription drugs. Not be sent home by themselves. They need to be with a responsible adult. Not drive a motor vehicle until cleared to do so by a healthcare professional. ANY ATHLETE WITH A SUSPECTED CONCUSSION SHOULD BE IMMEDIATELY REMOVED FROM PRACTICE OR PLAY AND SHOULD NOT RETURN TO ACTIVITY UNTIL ASSESSED MEDICALLY, EVEN IF THE SYMPTOMS RESOLVE
and present Date: Amended January 2015
 and present Concussionn Guidelines in the GAA 2013 2016 Adopted by LGFA Date: Amended January 2015 Table of Contents Summary Principles... 2 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
and present Concussionn Guidelines in the GAA 2013 2016 Adopted by LGFA Date: Amended January 2015 Table of Contents Summary Principles... 2 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
Concussion Guidelines in the GAA
 And present Concussion Guidelines in the GAA 2013 2016 Page 1 of 13 Position Statement Concussion Guidelines 2013 2016 Summary Principles... 3 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
And present Concussion Guidelines in the GAA 2013 2016 Page 1 of 13 Position Statement Concussion Guidelines 2013 2016 Summary Principles... 3 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
Dhiren J. Naidu MD FRCPC Dip. Sport Med.
 Dhiren J. Naidu MD FRCPC Dip. Sport Med. Associate Professor, Division of Physical Medicine & Rehabilitation Faculty of Medicine & Dentistry Varsity Health, University of Alberta Team Physician - Oilers,
Dhiren J. Naidu MD FRCPC Dip. Sport Med. Associate Professor, Division of Physical Medicine & Rehabilitation Faculty of Medicine & Dentistry Varsity Health, University of Alberta Team Physician - Oilers,
May 2016 accsportsmart.co.nz
 SPORT CONCUSSION IN NEW ZEALAND: ACC NATIONAL GUIDELINES May 2016 accsportsmart.co.nz This guideline document has been produced to inform National Sports Organisations (NSOs), and recreation, education
SPORT CONCUSSION IN NEW ZEALAND: ACC NATIONAL GUIDELINES May 2016 accsportsmart.co.nz This guideline document has been produced to inform National Sports Organisations (NSOs), and recreation, education
CONCUSSION GUIDELINES
 CONCUSSION GUIDELINES EDITION 2017 Table of Content 11.1 Summary Principles... 2 11.2 Introduction... 3 11.3 What is Concussion?... 3 11.3.1 Concussion must be taken extremely seriously... 4 11.4 What
CONCUSSION GUIDELINES EDITION 2017 Table of Content 11.1 Summary Principles... 2 11.2 Introduction... 3 11.3 What is Concussion?... 3 11.3.1 Concussion must be taken extremely seriously... 4 11.4 What
INTERNATIONAL RUGBY BOARD Putting players first
 CONCUSSION FACTS A concussion is a brain injury. All concussions are serious. Concussions can occur without loss of consciousness. All athletes with any symptoms following a head injury must be removed
CONCUSSION FACTS A concussion is a brain injury. All concussions are serious. Concussions can occur without loss of consciousness. All athletes with any symptoms following a head injury must be removed
Concussion guidance. Introduction CONCUSSION FACTS
 Introduction This World Rugby Concussion Guidance document has been developed to provide guidance and information to persons involved in the non-elite level of the game of Rugby regarding concussion and
Introduction This World Rugby Concussion Guidance document has been developed to provide guidance and information to persons involved in the non-elite level of the game of Rugby regarding concussion and
CONCUSSION RECOGNISING THE SIGNS STARTS WITH YOU. co.nz
 CONCUSSION RECOGNISING THE SIGNS STARTS Malcolm.Francis@acc. co.nz WITH YOU. A step-by-step guide to concussion and your role in recognising the signs, removing players from play and referring them to
CONCUSSION RECOGNISING THE SIGNS STARTS Malcolm.Francis@acc. co.nz WITH YOU. A step-by-step guide to concussion and your role in recognising the signs, removing players from play and referring them to
ETA STAFF - concussion
 These guidelines are designed to be used by Referees, Coaching staff and Managers This guideline has been adapted from the Rugby Football Union (RFU) guidance, World rugby guidance and the Zurich Consensus
These guidelines are designed to be used by Referees, Coaching staff and Managers This guideline has been adapted from the Rugby Football Union (RFU) guidance, World rugby guidance and the Zurich Consensus
Director of Athletics
 3341-8-1 Concussion Management Policy. Applicability Intercollegiate Athletics Responsible Unit Policy Administrator Intercollegiate Athletics/Director of Athletics Director of Athletics (A) Policy Purpose
3341-8-1 Concussion Management Policy. Applicability Intercollegiate Athletics Responsible Unit Policy Administrator Intercollegiate Athletics/Director of Athletics Director of Athletics (A) Policy Purpose
IF IN DOUBT, SIT THEM OUT.
 IF IN DOUBT, SIT THEM OUT. Scottish Sports Concussion Guidance: grassroots sport and general public 2018 version. Adapted from the Berlin 5th International concussion consensus statement 2016. Contents
IF IN DOUBT, SIT THEM OUT. Scottish Sports Concussion Guidance: grassroots sport and general public 2018 version. Adapted from the Berlin 5th International concussion consensus statement 2016. Contents
CONCUSSION AWARENESS, MANAGEMENT, AND ASSESSMENT FROM AN ATHLETIC TRAINER
 CONCUSSION AWARENESS, MANAGEMENT, AND ASSESSMENT FROM AN ATHLETIC TRAINER Dr. Ryan Krzyzanowicz, DAT, ATC Clinical Associate Professor Program Director - Athletic Training Education University at Buffalo
CONCUSSION AWARENESS, MANAGEMENT, AND ASSESSMENT FROM AN ATHLETIC TRAINER Dr. Ryan Krzyzanowicz, DAT, ATC Clinical Associate Professor Program Director - Athletic Training Education University at Buffalo
Australian Canoeing Limited Concussion Guidelines
 Australian Canoeing Limited Concussion Guidelines Date 5 th January 2016 Australian Canoeing PO Box 6805 Silverwater, NSW 2128 T: (02) 9763 0670 W: canoe.org.au CONTENTS 1. Overview... 1 2. Introduction...
Australian Canoeing Limited Concussion Guidelines Date 5 th January 2016 Australian Canoeing PO Box 6805 Silverwater, NSW 2128 T: (02) 9763 0670 W: canoe.org.au CONTENTS 1. Overview... 1 2. Introduction...
Concussion Policy. Guideline summary
 Guideline summary RECOGNISE AND REMOVE - learn to recognise the signs and symptoms of concussion and remove a player from the field if ANY doubt. PROTECT OUR YOUNG ATHLETES England & GB Hockey recommends
Guideline summary RECOGNISE AND REMOVE - learn to recognise the signs and symptoms of concussion and remove a player from the field if ANY doubt. PROTECT OUR YOUNG ATHLETES England & GB Hockey recommends
MANITOBA SOCCER ASSOCIATION YOUTH CONCUSSION PROTOCOL SUMMARY
 MANITOBA SOCCER ASSOCIATION YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the MANITOBA SOCCER ASSOCIATION (MSA) YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
MANITOBA SOCCER ASSOCIATION YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the MANITOBA SOCCER ASSOCIATION (MSA) YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
Sports Related Concussion. Joshua T. Williams, PT, DPT, OCS, SCS, CSCS
 Sports Related Concussion Joshua T. Williams, PT, DPT, OCS, SCS, CSCS Concussion & Traumatic Brain Injury Glasgow Coma Scale Minimal Mild Mod Severe? Sports concussion Severe GCS 8 Moderate GCS 9-12 Mild
Sports Related Concussion Joshua T. Williams, PT, DPT, OCS, SCS, CSCS Concussion & Traumatic Brain Injury Glasgow Coma Scale Minimal Mild Mod Severe? Sports concussion Severe GCS 8 Moderate GCS 9-12 Mild
UNIVERSITY OF MASSACHUSETTS SPORTS MEDICINE PROGRAM Concussion Management Plan
 UNIVERSITY OF MASSACHUSETTS SPORTS MEDICINE PROGRAM Concussion Management Plan University of Massachusetts Sports Medicine personnel will evaluate student-athletes with a suspected concussion as follows:
UNIVERSITY OF MASSACHUSETTS SPORTS MEDICINE PROGRAM Concussion Management Plan University of Massachusetts Sports Medicine personnel will evaluate student-athletes with a suspected concussion as follows:
PRE-SEASON INFORMATION SHEET CONCUSSIONS
 PRE-SEASON INFORMATION SHEET CONCUSSIONS HOW TO USE THIS EDUCATION SHEET: Distribute this pre-season concussion education sheet to your athletes and their parents or legal guardians during a pre-season
PRE-SEASON INFORMATION SHEET CONCUSSIONS HOW TO USE THIS EDUCATION SHEET: Distribute this pre-season concussion education sheet to your athletes and their parents or legal guardians during a pre-season
Review of: NATA Position Statement Management of Sport Concussion.
 Review of: NATA Position Statement Management of Sport Concussion www.csm-institute.com Topics: Education and Prevention Documentation and Legal Aspects Evaluation and RTP Other Considerations Strength
Review of: NATA Position Statement Management of Sport Concussion www.csm-institute.com Topics: Education and Prevention Documentation and Legal Aspects Evaluation and RTP Other Considerations Strength
Page I
 Page 2 How to manage concussion? World Rugby standard: Recognize and Remove Protocol (6Rs). RECOGNIZE - Learn the signs and symptoms of concussion so you understand when an athlete might have a concussion.
Page 2 How to manage concussion? World Rugby standard: Recognize and Remove Protocol (6Rs). RECOGNIZE - Learn the signs and symptoms of concussion so you understand when an athlete might have a concussion.
2017 Concussion Management Program
 2017 Concussion Management Program Michael Stuart MD Alan Ashare MD Kevin Margarucci ATC The standard of care for current medical practice and the law in most states requires that any athlete with a suspected
2017 Concussion Management Program Michael Stuart MD Alan Ashare MD Kevin Margarucci ATC The standard of care for current medical practice and the law in most states requires that any athlete with a suspected
When a concussion occurs:
 When a concussion occurs: Once an athlete has experienced any type of potential head injury initiate the following checklist: 1. n Remove athlete from all activity and use the Concussion Recognition Tool
When a concussion occurs: Once an athlete has experienced any type of potential head injury initiate the following checklist: 1. n Remove athlete from all activity and use the Concussion Recognition Tool
Signs and Symptoms of Concussion
 Signs and Symptoms of Concussion These signs and symptoms following a witnessed or suspected blow to the head or body are indicative of probable concussion. Signs (observed by others) Appears dazed or
Signs and Symptoms of Concussion These signs and symptoms following a witnessed or suspected blow to the head or body are indicative of probable concussion. Signs (observed by others) Appears dazed or
Please feel free to contact me if you have any questions. HOME INSTRUCTIONS FOR CONCUSSION. Recommendations for monitoring symptoms at home:
 Recommendations for monitoring symptoms at home: What should I do when I m recovering? Physical and mental rest are very important to your recovery. Keep your heart rate low and do not do any physical
Recommendations for monitoring symptoms at home: What should I do when I m recovering? Physical and mental rest are very important to your recovery. Keep your heart rate low and do not do any physical
The Kansas Legislature has enacted the School Sports Head Injury Prevention Act (hereinafter the Kansas Act ) effective July 1, 2011:
 KANSAS STATE HIGH SCHOOL ACTIVITIES ASSOCIATION RECOMMENDATIONS FOR COMPLIANCE WITH THE KANSAS SCHOOL SPORTS HEAD INJURY PREVENTION ACT AND IMPLEMENTATION OF THE NATIONAL FEDERATION SPORTS PLAYING RULES
KANSAS STATE HIGH SCHOOL ACTIVITIES ASSOCIATION RECOMMENDATIONS FOR COMPLIANCE WITH THE KANSAS SCHOOL SPORTS HEAD INJURY PREVENTION ACT AND IMPLEMENTATION OF THE NATIONAL FEDERATION SPORTS PLAYING RULES
Texas State University Concussion Program for Varsity Athletes
 Administrative Considerations o Emergency Action Plan placed in all venues including the Concussion Plan for all high risk sports. o Coaching education regarding EAP & Concussion Plan including signs &
Administrative Considerations o Emergency Action Plan placed in all venues including the Concussion Plan for all high risk sports. o Coaching education regarding EAP & Concussion Plan including signs &
Concussion Management Protocol
 Concussion Management Protocol We at Total Sports Experience desire a safe return to play for all sick or injured athletes. Research has shown that an athlete's coordination, balance and/or cognitive functioning
Concussion Management Protocol We at Total Sports Experience desire a safe return to play for all sick or injured athletes. Research has shown that an athlete's coordination, balance and/or cognitive functioning
Return-to-Play Protocol After Concussion/mild TBI
 Return-to-Play Protocol After Concussion/mild TBI Return to activity and play is a medical decision. The athlete must meet all of the following criteria to progress to activity: Asymptomatic at rest and
Return-to-Play Protocol After Concussion/mild TBI Return to activity and play is a medical decision. The athlete must meet all of the following criteria to progress to activity: Asymptomatic at rest and
Carleton College Concussion Safety Protocol
 Carleton College Introduction Carleton College is committed to ensuring the health and safety of its student-athletes. To this end, and in accordance with NCAA legislation [Division III Constitution 3.2.4.16],
Carleton College Introduction Carleton College is committed to ensuring the health and safety of its student-athletes. To this end, and in accordance with NCAA legislation [Division III Constitution 3.2.4.16],
Concussion Assessment, Management, and Return to Play Guidelines
 Concussion Assessment, Management, and Return to Play Guidelines The following policy and procedures on neurocognitive baseline testing and subsequent assessment and management of concussions as well as
Concussion Assessment, Management, and Return to Play Guidelines The following policy and procedures on neurocognitive baseline testing and subsequent assessment and management of concussions as well as
Eagle High School Lacrosse Concussion Management Plan
 ! Eagle High School Lacrosse Concussion Management Plan August 2018 Contents (1) Mandatory Parent/Athlete Meeting 1 (2) Recommended Baseline Testing 2 (3) Concussion Training for Athletic Trainers and
! Eagle High School Lacrosse Concussion Management Plan August 2018 Contents (1) Mandatory Parent/Athlete Meeting 1 (2) Recommended Baseline Testing 2 (3) Concussion Training for Athletic Trainers and
HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL SUMMARY
 2018-2019 HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
2018-2019 HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
Page
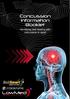 Page 2 Concussion step by step guide Name: Date 1.Education 2.Baseline testing 3.Immediate medical evaluation Post-concussion by a medical doctor 4.Follow up Computer testing 5. Return-to-play protocol
Page 2 Concussion step by step guide Name: Date 1.Education 2.Baseline testing 3.Immediate medical evaluation Post-concussion by a medical doctor 4.Follow up Computer testing 5. Return-to-play protocol
LACROSSE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY
 LACROSSE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the Manitoba Lacrosse Association s Youth Concussion Protocol 1. All youth athletes (
LACROSSE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the Manitoba Lacrosse Association s Youth Concussion Protocol 1. All youth athletes (
1. Begin light aerobic exercise such as walking, stationary bike, etc. No resistance training.
 POLICY: Any athlete displaying signs or symptoms of a concussion, or if there is a high suspicion for concussion, an athlete will not be returned to competition or practice until they have written clearance
POLICY: Any athlete displaying signs or symptoms of a concussion, or if there is a high suspicion for concussion, an athlete will not be returned to competition or practice until they have written clearance
COS SPORTS MEDICINE CONCUSSION ASSESSMENT FORM BASELINE TEST Adapted from SCAT3
 COS SPORTS MEDICINE CONCUSSION ASSESSMENT FORM BASELINE TEST Adapted from SCAT3 Name Sport Examiner Name: Date of BASELINE TEST: Age Gender M / F COGNITIVE ASSESSMENT Orientation (1 pt each) What month
COS SPORTS MEDICINE CONCUSSION ASSESSMENT FORM BASELINE TEST Adapted from SCAT3 Name Sport Examiner Name: Date of BASELINE TEST: Age Gender M / F COGNITIVE ASSESSMENT Orientation (1 pt each) What month
POLICY / PROCEDURE DOCUMENT Effective Date 08/19/2010. Concussion Assessment, Management, and Return to Play Guidelines
 Beacon Medical Group Sports Medicine POLICY / PROCEDURE DOCUMENT Effective Date 08/19/2010 TITLE: Document of (Entity) POLICY: PATIENT POPULATION: Concussion Assessment, Management, and Return to Play
Beacon Medical Group Sports Medicine POLICY / PROCEDURE DOCUMENT Effective Date 08/19/2010 TITLE: Document of (Entity) POLICY: PATIENT POPULATION: Concussion Assessment, Management, and Return to Play
UPPER PERKIOMEN HIGH SCHOOL
 UPPER PERKIOMEN HIGH SCHOOL Concussion Management and Return to Play Protocol Recognizing that sport related concussions pose a significant health risk for studentathletes, the Upper Perkiomen School District
UPPER PERKIOMEN HIGH SCHOOL Concussion Management and Return to Play Protocol Recognizing that sport related concussions pose a significant health risk for studentathletes, the Upper Perkiomen School District
Bump to Head, Head Injury and Concussion Policy
 Bump to Head, Head Injury and Concussion Policy Policy Type Non-regulatory Last Review Summer 2018 Next Review Autumn 2018 Bump to Head, Head Injury & Concussion Policy See Appendix 1 for a flow chart
Bump to Head, Head Injury and Concussion Policy Policy Type Non-regulatory Last Review Summer 2018 Next Review Autumn 2018 Bump to Head, Head Injury & Concussion Policy See Appendix 1 for a flow chart
CONCUSSION PROTOCOL STEPS FOR RETURN TO PLAY
 Winnacunnet High School Concussion Protocol All coaches must take the NFHS Concussion course prior to working with students in their coaching season. Coaches must retake the course on even numbered years.
Winnacunnet High School Concussion Protocol All coaches must take the NFHS Concussion course prior to working with students in their coaching season. Coaches must retake the course on even numbered years.
IT S ALL IN YOUR HEAD!
 IT S ALL IN YOUR HEAD! CARING FOR CONCUSSIONS IN YOUR COMMUNITY Stephen K Stacey, DO CPT, MC, USA OUTLINE Definition Epidemiology Diagnosis Evaluation Recovery Sequelae Prevention Resources for providers
IT S ALL IN YOUR HEAD! CARING FOR CONCUSSIONS IN YOUR COMMUNITY Stephen K Stacey, DO CPT, MC, USA OUTLINE Definition Epidemiology Diagnosis Evaluation Recovery Sequelae Prevention Resources for providers
University of Central Arkansas Concussion Protocol and Management Plan
 University of Central Arkansas Concussion Protocol and Management Plan 5/2018 It is often reported that there is no universal agreement on the standard definition or nature of concussion; however, agreement
University of Central Arkansas Concussion Protocol and Management Plan 5/2018 It is often reported that there is no universal agreement on the standard definition or nature of concussion; however, agreement
Wisconsin Lacrosse Federation
 The purpose of this policy is to insure the safety of the players and to limit the liability of those protecting the safety of the players. The responsibility of player safety falls on everyone involved
The purpose of this policy is to insure the safety of the players and to limit the liability of those protecting the safety of the players. The responsibility of player safety falls on everyone involved
Departmental Concussion Guidelines
 Concussion Plan Departmental Concussion Guidelines The following guidelines have been developed in accordance with Alabama A&M s Mission Statement and service goal of providing quality healthcare services
Concussion Plan Departmental Concussion Guidelines The following guidelines have been developed in accordance with Alabama A&M s Mission Statement and service goal of providing quality healthcare services
Notre Dame of Maryland University Athletics Concussion Management Protocol
 Notre Dame of Maryland University Athletics Concussion Management Protocol Neuropsychological (NP) Baseline Testing: All NCAA sports will utilize baseline NP testing. All athletes will receive baseline
Notre Dame of Maryland University Athletics Concussion Management Protocol Neuropsychological (NP) Baseline Testing: All NCAA sports will utilize baseline NP testing. All athletes will receive baseline
Concussion Management and Update. Objectives
 Concussion Management and Update Ricardo Guirola MD M Ed Pediatric Rheumatology Primary Care Sports Medicine Objectives Review definition, signs and symptoms Discuss the initial evaluation of a patient
Concussion Management and Update Ricardo Guirola MD M Ed Pediatric Rheumatology Primary Care Sports Medicine Objectives Review definition, signs and symptoms Discuss the initial evaluation of a patient
BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY
 BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
Little League Concussion Information Sheet
 Little League Concussion Information Sheet Why am I getting this information sheet? You are receiving this information sheet about concussion because of California Assembly Bill 2007 (2016), which added
Little League Concussion Information Sheet Why am I getting this information sheet? You are receiving this information sheet about concussion because of California Assembly Bill 2007 (2016), which added
CONCUSSION/HEAD INJURY AND HEAT ILLNESS GUIDELINES
 CONCUSSION/HEAD INJURY AND HEAT ILLNESS GUIDELINES WHAT IS A CONCUSSION? A concussion is a type of traumatic brain injury caused by a bump, blow, or jolt to the head, or by a blow to the body with the
CONCUSSION/HEAD INJURY AND HEAT ILLNESS GUIDELINES WHAT IS A CONCUSSION? A concussion is a type of traumatic brain injury caused by a bump, blow, or jolt to the head, or by a blow to the body with the
INTERCOLLEGIATE ATHLETICS CONCUSSION ACKNOWLEDGEMENT AND STATEMENT
 ACKNOWLEDGEMENT AND STATEMENT A FACT SHEET FOR STUDENT-ATHLETES WHAT IS A? A concussion is a brain injury that: Is caused by a blow to the head or body -From contact with another player, hitting a hard
ACKNOWLEDGEMENT AND STATEMENT A FACT SHEET FOR STUDENT-ATHLETES WHAT IS A? A concussion is a brain injury that: Is caused by a blow to the head or body -From contact with another player, hitting a hard
North Thurston Public Schools Concussion Information Sheet
 North Thurston Public Schools Concussion Information Sheet Definition A concussion is a brain injury that may be caused either by a direct blow to the head, face, neck or elsewhere on the body with an
North Thurston Public Schools Concussion Information Sheet Definition A concussion is a brain injury that may be caused either by a direct blow to the head, face, neck or elsewhere on the body with an
SAIL CANADA CONCUSSION PROTOCOL
 SAIL CANADA CONCUSSION PROTOCOL Sail Canada has developed the Sail Canada Concussion Protocol to help guide the management of Sailing Sport Participants (athletes, coaches, instructors, officials & volunteers)
SAIL CANADA CONCUSSION PROTOCOL Sail Canada has developed the Sail Canada Concussion Protocol to help guide the management of Sailing Sport Participants (athletes, coaches, instructors, officials & volunteers)
CONCUSSION POLICY STATEMENT AND MANAGEMENT GUIDELINES
 INTRODUCTION It is clear that a persuasive argument can be made that a comprehensive and systematic approach to concussion injury utilizing an evidence based method holds potential benefit for both the
INTRODUCTION It is clear that a persuasive argument can be made that a comprehensive and systematic approach to concussion injury utilizing an evidence based method holds potential benefit for both the
Paramus Athletics. Paramus High School Athletic Department Protocol and Procedures for Management of Sports - Related Concussion
 Paramus Athletics Paramus High School Athletic Department Protocol and Procedures for Management Medical management of sports-related concussions is evolving. In recent years, there has been significant
Paramus Athletics Paramus High School Athletic Department Protocol and Procedures for Management Medical management of sports-related concussions is evolving. In recent years, there has been significant
The Master s Academy Concussion Policy
 The Master s Academy Concussion Policy Ann Williams,M.S.N., R.N. Robert O Quinn, MS, ATC, LAT Updated 2/6/2018 Outline I. Abbreviated policy II. Introduction III. Prevention and Education IV. Recognition
The Master s Academy Concussion Policy Ann Williams,M.S.N., R.N. Robert O Quinn, MS, ATC, LAT Updated 2/6/2018 Outline I. Abbreviated policy II. Introduction III. Prevention and Education IV. Recognition
RECOGNISE AND REMOVE
 RECOGNISE AND REMOVE Remember the 4 R s of concussion management: RECOGNISE REMOVE RECOVER RETURN Identifying concussion is not always easy, and players may not exhibit the signs or symptoms immediately
RECOGNISE AND REMOVE Remember the 4 R s of concussion management: RECOGNISE REMOVE RECOVER RETURN Identifying concussion is not always easy, and players may not exhibit the signs or symptoms immediately
Loss of consciousness (LOC) Poor recall for events prior to injury or after injury
 NAIA Championship Concussion Policy Concussions can be serious and potentially life threatening injuries in sports. Research indicates that if concussion symptoms are appropriately managed, an individual
NAIA Championship Concussion Policy Concussions can be serious and potentially life threatening injuries in sports. Research indicates that if concussion symptoms are appropriately managed, an individual
Bishop Kelly High School s Concussion Management Plan
 Bishop Kelly High School s Concussion Management Plan September 2016 Contents (1) Mandatory Parent/Athlete Meeting, Parent/Athlete Consent Form... 1 (2) Baseline Testing... 2 (3) Concussion Training for
Bishop Kelly High School s Concussion Management Plan September 2016 Contents (1) Mandatory Parent/Athlete Meeting, Parent/Athlete Consent Form... 1 (2) Baseline Testing... 2 (3) Concussion Training for
RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY
 RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
The University of Nebraska Omaha Concussion Management Plan
 Definition: The University of Nebraska Omaha Concussion Management Plan A concussion is a complex pathophysiological process affecting the brain, induced by traumatic biomechanical forces secondary to
Definition: The University of Nebraska Omaha Concussion Management Plan A concussion is a complex pathophysiological process affecting the brain, induced by traumatic biomechanical forces secondary to
RIDGEWOOD BOARD OF EDUCATION PROGRAM /page 1 of 8 Management of Sports-Related Concussion M Management of Sports-Related Concussion
 2431.4/page 1 of 8 M 2431.4 Medical management of sports-related concussions is evolving. In recent years, there has been significant research into sports-related concussions in high school athletes. As
2431.4/page 1 of 8 M 2431.4 Medical management of sports-related concussions is evolving. In recent years, there has been significant research into sports-related concussions in high school athletes. As
TMPW Xplorers Basketball Concussion Management Plan
 TMPW Xplorers Basketball Concussion Management Plan November 2017 Contents (1) Mandatory Parent / Athlete Education 1 & 2 (2) Recommended Baseline Testing 3 (3) Concussion Training for Athletic Trainers
TMPW Xplorers Basketball Concussion Management Plan November 2017 Contents (1) Mandatory Parent / Athlete Education 1 & 2 (2) Recommended Baseline Testing 3 (3) Concussion Training for Athletic Trainers
CONCUSSION INFORMATION When in Doubt, Sit Them Out!
 CONCUSSION INFORMATION When in Doubt, Sit Them Out! A concussion is a type of traumatic brain injury that interferes with normal function of the brain. All concussions are brain injuries. The WIAA recommends
CONCUSSION INFORMATION When in Doubt, Sit Them Out! A concussion is a type of traumatic brain injury that interferes with normal function of the brain. All concussions are brain injuries. The WIAA recommends
Post Concussion Instructions and Return to Play Clearance Form. To: Parent/Guardian: Page 1. From:, at School
 Post Concussion Instructions and Return to Play Clearance Form To: Parent/Guardian: From:, at School Name of School Representative* Name of School, Position of School Representative* Phone Number of School
Post Concussion Instructions and Return to Play Clearance Form To: Parent/Guardian: From:, at School Name of School Representative* Name of School, Position of School Representative* Phone Number of School
Hockey New South Wales Head Injury Guidelines Effective November
 Hockey New South Wales Effective November 2011 1 Table of Contents Part 1: Guidelines Statement 3 Head Injuries 3 Two Types of Head Injuries 3 Symptoms of Head Injuries 3 Head Injury Notifications 3 Important
Hockey New South Wales Effective November 2011 1 Table of Contents Part 1: Guidelines Statement 3 Head Injuries 3 Two Types of Head Injuries 3 Symptoms of Head Injuries 3 Head Injury Notifications 3 Important
Concussion: A Treatable Injury MELISSA N. WOMBLE, PHD NEUROPSYCHOLOGIST, DIRECTOR INOVA SPORTS MEDICINE CONCUSSION PROGRAM
 Concussion: A Treatable Injury MELISSA N. WOMBLE, PHD NEUROPSYCHOLOGIST, DIRECTOR INOVA SPORTS MEDICINE CONCUSSION PROGRAM THE CURRENT PROBLEM 1. WHAT IS A CONCUSSION? 2. ACUTE/SIDELINE EVALUATION 3. AT
Concussion: A Treatable Injury MELISSA N. WOMBLE, PHD NEUROPSYCHOLOGIST, DIRECTOR INOVA SPORTS MEDICINE CONCUSSION PROGRAM THE CURRENT PROBLEM 1. WHAT IS A CONCUSSION? 2. ACUTE/SIDELINE EVALUATION 3. AT
Concussion Information Sheet
 Concussion Information Sheet A concussion is a brain injury and all brain injuries are serious. They are caused by a bump, blow, or jolt to the head, or by a blow to another part of the body with the force
Concussion Information Sheet A concussion is a brain injury and all brain injuries are serious. They are caused by a bump, blow, or jolt to the head, or by a blow to another part of the body with the force
Lee County School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion
 Lee County School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Medical management of sports-related concussions are evolving. In recent years, there
Lee County School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Medical management of sports-related concussions are evolving. In recent years, there
Excerpt from the CONCUSSION. KiT. Understanding and Managing Concussion in Youth
 Excerpt from the KiT CONCUSSION Understanding and Managing Concussion in Youth What Is a Concussion õõ A concussion is a type of brain injury. õõ A concussion is also referred to as a mild traumatic brain
Excerpt from the KiT CONCUSSION Understanding and Managing Concussion in Youth What Is a Concussion õõ A concussion is a type of brain injury. õõ A concussion is also referred to as a mild traumatic brain
INTERCOLLEGIATE ATHLETICS CONCUSSION MANAGEMENT PLAN
 INTERCOLLEGIATE ATHLETICS CONCUSSION MANAGEMENT PLAN I. PURPOSE In an effort to better serve the healthcare needs of its student athletes, as well as to adhere to best practices recommended by the National
INTERCOLLEGIATE ATHLETICS CONCUSSION MANAGEMENT PLAN I. PURPOSE In an effort to better serve the healthcare needs of its student athletes, as well as to adhere to best practices recommended by the National
When it comes to concussions, is critical.
 When it comes to concussions, knowledge is critical. 1 Be Smart About the Brain Know the Facts A concussion is a traumatic injury to the brain that affects how the brain functions. Early diagnosis and
When it comes to concussions, knowledge is critical. 1 Be Smart About the Brain Know the Facts A concussion is a traumatic injury to the brain that affects how the brain functions. Early diagnosis and
Definition and causes:
 Up2Date September 2014 Concussion by Wendy Quick Definition and causes: A concussion is not just a "bump on the head." It is a traumatic brain injury that needs proper treatment whether it is mild or severe.
Up2Date September 2014 Concussion by Wendy Quick Definition and causes: A concussion is not just a "bump on the head." It is a traumatic brain injury that needs proper treatment whether it is mild or severe.
STAMFORD CENTRAL SCHOOL CONCUSSION POLICY
 STAMFORD CENTRAL SCHOOL CONCUSSION POLICY Revised October 14, 2015 Page 1 Management of Sports-Related Concussions StamfordCentralSchool District Medical management of sports-related concussion continues
STAMFORD CENTRAL SCHOOL CONCUSSION POLICY Revised October 14, 2015 Page 1 Management of Sports-Related Concussions StamfordCentralSchool District Medical management of sports-related concussion continues
SPRINGFIELD CLINIC S
 SPRINGFIELD CLINIC S HEAD INJURY MANAGEMENT GUIDE FOR PARENTS Given the complexities of concussion management, Springfield Clinic recognizes the importance of managing concussions on an individualized
SPRINGFIELD CLINIC S HEAD INJURY MANAGEMENT GUIDE FOR PARENTS Given the complexities of concussion management, Springfield Clinic recognizes the importance of managing concussions on an individualized
Your guide to recovery. Treating concussions
 Your guide to recovery Treating concussions About concussions A concussion is a condition, usually caused when a blow to the head or body causes the brain to move rapidly within the skull, that can temporarily
Your guide to recovery Treating concussions About concussions A concussion is a condition, usually caused when a blow to the head or body causes the brain to move rapidly within the skull, that can temporarily
Concussion. Introduction
 Concussion Introduction Concussion is unlike most injuries that athlete s experience. As concussion is an injury to the brain, it cannot be seen and the effects can be either subtle or devastating or cumulatively
Concussion Introduction Concussion is unlike most injuries that athlete s experience. As concussion is an injury to the brain, it cannot be seen and the effects can be either subtle or devastating or cumulatively
The Greenville Hurricanes Athletic Association. Concussion Policy. Injury Prevention and Control. What is a concussion?
 The Greenville Hurricanes Athletic Association Concussion Policy Injury Prevention and Control What is a concussion? How do I recognize a possible concussion? Know your concussion ABCs! What can I do to
The Greenville Hurricanes Athletic Association Concussion Policy Injury Prevention and Control What is a concussion? How do I recognize a possible concussion? Know your concussion ABCs! What can I do to
Lower Moreland School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion
 Lower Moreland School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Preamble: Medical management of sports-related concussion is evolving. In recent
Lower Moreland School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Preamble: Medical management of sports-related concussion is evolving. In recent
What Is A Concussion?
 What Is A Concussion? A concussion is a brain injury, and all brain injuries are serious. Concussions can range from mild to severe, and they can change the way your brain normally functions. Symptoms
What Is A Concussion? A concussion is a brain injury, and all brain injuries are serious. Concussions can range from mild to severe, and they can change the way your brain normally functions. Symptoms
PEDIATRIC SPORTS RELATED CONCUSSIONS
 Anna Mazur, PhD PEDIATRIC SPORTS RELATED CONCUSSIONS Disclosure No financial interests or funding 1 Presentation Outline Prevalence Predicting recovery: Post Traumatic Amnesia and Loss of Consciousness
Anna Mazur, PhD PEDIATRIC SPORTS RELATED CONCUSSIONS Disclosure No financial interests or funding 1 Presentation Outline Prevalence Predicting recovery: Post Traumatic Amnesia and Loss of Consciousness
VENUS ISD CONCUSSION POLICY
 VENUS ISD CONCUSSION POLICY Introduction The Centers for Disease Control (CDC) estimates that there are approximately 300,000 cases of mild traumatic brain injury (MTBI) or concussions annually in the
VENUS ISD CONCUSSION POLICY Introduction The Centers for Disease Control (CDC) estimates that there are approximately 300,000 cases of mild traumatic brain injury (MTBI) or concussions annually in the
CEDARVILLE UNIVERSITY CONCUSSION MANAGEMENT GUIDELINES
 Concussion Management CEDARVILLE UNIVERSITY CONCUSSION MANAGEMENT GUIDELINES Aug. 2015 1. Cedarville University will require all student-athletes to sign a statement in which studentathletes accept the
Concussion Management CEDARVILLE UNIVERSITY CONCUSSION MANAGEMENT GUIDELINES Aug. 2015 1. Cedarville University will require all student-athletes to sign a statement in which studentathletes accept the
University of Notre Dame Sports Medicine Department Intercollegiate Athletics Concussion Management Plan
 ! Purpose: University of Notre Dame Sports Medicine Department Intercollegiate Athletics Concussion Management Plan Head injuries can pose a significant health risk for student-athletes competing in intercollegiate
! Purpose: University of Notre Dame Sports Medicine Department Intercollegiate Athletics Concussion Management Plan Head injuries can pose a significant health risk for student-athletes competing in intercollegiate
Coach s name: Please print. Coach s signature: Please sign. Today s date: Witness: Print name. Title: Please print. Signature:
 I have been provided the MAHA / USA Hockey Concussion Management educational materials. I have read and understand the information. I agree to comply with the requirement to remove a youth athlete who
I have been provided the MAHA / USA Hockey Concussion Management educational materials. I have read and understand the information. I agree to comply with the requirement to remove a youth athlete who
NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY
 NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY February 2015 New Zealand Rugby League Medical panel The aim of the policy is to provide information on concussion to all those involved in rugby
NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY February 2015 New Zealand Rugby League Medical panel The aim of the policy is to provide information on concussion to all those involved in rugby
Coastal Carolina University Athletic Training Department Policy and Procedure Manual Concussion Management Revised/Reviewed 6/2012
 Coastal Carolina University Athletic Training Department Policy and Procedure Manual Concussion Management Revised/Reviewed 6/2012 INTRODUCTION: Concussion classification, management, and protocols have
Coastal Carolina University Athletic Training Department Policy and Procedure Manual Concussion Management Revised/Reviewed 6/2012 INTRODUCTION: Concussion classification, management, and protocols have
 www.dylansteigersconcussionproject.com What is a Concussion? A concussion (kun-kush-un) is an injury to the tissue or blood vessels of the brain. It is also called a closed head injury or mild traumatic
www.dylansteigersconcussionproject.com What is a Concussion? A concussion (kun-kush-un) is an injury to the tissue or blood vessels of the brain. It is also called a closed head injury or mild traumatic
CONCUSSION MANAGEMENT PROTOCOL 2015
 301-333 Terminal Avenue, Vancouver, BC Canada V6A 4C1 t: 604.568.1135 f: 604.568.1639 e: info@canadasnowboard.ca www.canadasnowboard.ca CONCUSSION MANAGEMENT PROTOCOL 2015 A CONCUSSION is a disturbance
301-333 Terminal Avenue, Vancouver, BC Canada V6A 4C1 t: 604.568.1135 f: 604.568.1639 e: info@canadasnowboard.ca www.canadasnowboard.ca CONCUSSION MANAGEMENT PROTOCOL 2015 A CONCUSSION is a disturbance
Eagle High School Lacrosse Concussion Management Plan
 ! Eagle High School Lacrosse Concussion Management Plan October 2017 Contents (1) Mandatory Parent/Athlete Meeting 1 (2) Recommended Baseline Testing 2 (3) Concussion Training for Athletic Trainers and
! Eagle High School Lacrosse Concussion Management Plan October 2017 Contents (1) Mandatory Parent/Athlete Meeting 1 (2) Recommended Baseline Testing 2 (3) Concussion Training for Athletic Trainers and
spontaneous localises pain withdraws to pain abnormal flexion abnormal extension none > 5 years 2 5 years 0 2 years
 APPENDIX. GLASGOW COMA SCALES (GCS) For Adults Alert patients have a total score of 5 Eye Opening: to voice to pain Verbal Score: 5 oriented confused but answers questions inappropriate words: recognises
APPENDIX. GLASGOW COMA SCALES (GCS) For Adults Alert patients have a total score of 5 Eye Opening: to voice to pain Verbal Score: 5 oriented confused but answers questions inappropriate words: recognises
Forney ISD Protocol and Procedures for the Management of the Sports-Related Concussion
 Forney ISD Protocol and Procedures for the Management of the Sports-Related Concussion Medical management of sports-related concussion is evolving. Recently, there has been a significant amount of research
Forney ISD Protocol and Procedures for the Management of the Sports-Related Concussion Medical management of sports-related concussion is evolving. Recently, there has been a significant amount of research
Head Injury Guidelines POL 5700
 Issued by: WHS Effective Date: 1 st Oct 13 Rev: A Page 1 of 5 1. PURPOSE Concussion - Important information What is a concussion? A concussion is an injury to the brain. A blow to the head usually causes
Issued by: WHS Effective Date: 1 st Oct 13 Rev: A Page 1 of 5 1. PURPOSE Concussion - Important information What is a concussion? A concussion is an injury to the brain. A blow to the head usually causes
Diagnosis Players, coaches, parents and heath care providers should be able to recognize the symptoms and signs of a concussion:
 USA Hockey Concussion Management Program (as adopted by MAHA, with revisions 12/7/12) 1 Michael Stuart MD Alan Ashare MD A concussion is a traumatic brain injury- there is no such thing as a minor brain
USA Hockey Concussion Management Program (as adopted by MAHA, with revisions 12/7/12) 1 Michael Stuart MD Alan Ashare MD A concussion is a traumatic brain injury- there is no such thing as a minor brain
BRSC Concussion Policy & Protocol
 BRSC Concussion Policy & Protocol January 2018 BRSC has a full-time, certified Athletic Trainer on staff that provides immediate care for concussed athletes. BRSC also requires coaches at our competitive
BRSC Concussion Policy & Protocol January 2018 BRSC has a full-time, certified Athletic Trainer on staff that provides immediate care for concussed athletes. BRSC also requires coaches at our competitive
2016 Concussion Management Plan
 2016 Concussion Management Plan For: Dane County Area Youth Football League Date: August 9, 2013 Prepared by: Dr. Brian Reeder, MD (Reviewed 08/02/16) 1. Overview 1.1. In response to the growing concern
2016 Concussion Management Plan For: Dane County Area Youth Football League Date: August 9, 2013 Prepared by: Dr. Brian Reeder, MD (Reviewed 08/02/16) 1. Overview 1.1. In response to the growing concern
WISD Athletic Department Guidelines for Concussion Management
 WISD Athletic Department Guidelines for Concussion Management Introduction Approximately 10 percent of all athletes involved in contact sports suffer a Mild Traumatic Brain Injury (concussion) each season;
WISD Athletic Department Guidelines for Concussion Management Introduction Approximately 10 percent of all athletes involved in contact sports suffer a Mild Traumatic Brain Injury (concussion) each season;
Concussion Management Plan
 Concussion Management Plan Table of Contents Purpose of the plan 2 Definition of concussion 2 Common signs and symptoms of concussion 3 Prior Education 3 Baseline testing 3 Management and return to play
Concussion Management Plan Table of Contents Purpose of the plan 2 Definition of concussion 2 Common signs and symptoms of concussion 3 Prior Education 3 Baseline testing 3 Management and return to play
The NOJHL Sport Concussion Policy and Management Protocol. Developed by Dr. Chris Myers, D.C., BMSc. Updated as of August 2018
 The NOJHL Sport Concussion Policy and Management Protocol Developed by Dr. Chris Myers, D.C., BMSc Updated as of August 2018 The NOJHL concussion policy and concussion management protocol have been developed
The NOJHL Sport Concussion Policy and Management Protocol Developed by Dr. Chris Myers, D.C., BMSc Updated as of August 2018 The NOJHL concussion policy and concussion management protocol have been developed
Gilbert Public Schools (High School) Athletic Department Protocol and Procedures for Management of Sports-Related Concussion
 Gilbert Public Schools (High School) Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Medical management of sports-related concussion is evolving. In recent years,
Gilbert Public Schools (High School) Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Medical management of sports-related concussion is evolving. In recent years,
CCYFL Concussion Information Sheet
 CCYFL Concussion Information Sheet Why am I getting this information sheet? You are receiving this information sheet about concussions because of California state law AB 2007, (effective January 1, 2017),
CCYFL Concussion Information Sheet Why am I getting this information sheet? You are receiving this information sheet about concussions because of California state law AB 2007, (effective January 1, 2017),
