Drug Formulary Update, January 2017 Commercial and State Programs
|
|
|
- Ann Johnston
- 6 years ago
- Views:
Transcription
1 Drug Formulary Update, January 2017 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx, GenericsPlusRx, EnhancedRx, and GenericsAdvantageRx) and to HealthPartners Minnesota Health Care Programs (Medicaid and Minnesota Care State Programs ) Drug Formulary. Please see for details. Positive changes (additions) are generally effective January 1st, and negative changes (deletions) are generally effective April 1st. Additional communications are sent to all affected members and their providers. Acyclovir (Zovirax), Aripiprazole (Abilify), NF NF PA 4/1/2017 Zovirax Brands will be reserved for: 1. patients who have tried and failed the equivalent generic due to a documented allergic reaction, and 2. patients who have tried and failed at least one additional preferred alternative such as valacyclovir and famciclovir. Acyclovir remains on formulary. NF NF PA 4/1/2017 Abilify Brand is reserved for patients who Aripiprazole (generic Abilify) remains on formulary). Canakinumab (Ilaris) F PA F PA 1/1/2017 Coverage criteria have been updated.
2 Drug Formulary Update, January 2017, page 2 of 7 Coenzyme Q10 powder Desvenlafaxine (Khedezla) Dexamethasone dose pack (Dexpak) Dexmethylphenidate XR Dextroamphetamine (Dexedrine), Brandonly Doxycycline monohydrate 40mg NF NF PA 4/1/2017 Coenzyme Q10 powder has been added to the PA required compounding list. NF PA NF 1/1/2017 Desvenlafaxine (Khedezla) prior authorization criteria have been removed for State Programs, and desvenlafaxine is nonformulary for all formularies. NF NF PA 4/1/2017 Dexpak is reserved for: patients who have tried and failed generic dexamethasone due to a documented allergic reaction. NF F 1/1/2017 Dexmethylphenidate XR (generic Focalin XR) has been added to formulary. NF NF PA 4/1/2017 Dexedrine Brand is reserved for 1. patients who have tried and failed the equivalent generic due to a documented allergic reaction, and 2. patients who have tried and failed at least one additional preferred alternative such as amphetamine/ dextroamphetamine and Vyvanse. Dextroamphetamine (generic Dexedrine) remains on formulary. NF NF PA 4/1/2017 Doxycycline monohydrate 40mg (Brand Oracea and generic) are non formulary with prior authorization. Oracea Brand is reserved for patients who Doxycycline monohydrate 40mg (generic Oracea) is reserved for patients who have tried preferred generic doxycycline products, with significant clinical rationale suggesting improved outcomes.
3 Drug Formulary Update, January 2017, page 3 of 7 Dutasteride NF F 1/1/2017 Dutasteride (generic Avodart) has been added to State Programs, and is now on all Drug Formularies. Dutoprol (metoprolol/ HCTZ) ER Efinaconazole (Jublia) Epiduo Forte (adapalene 0.3%/ benzoyl peroxide 2.5%) gel NF NF PA 4/1/2017 Dutoprol (Brand and generic) are reserved for patients who have tried and failed metoprolol and hydrochlorothiazide given separately, due to a documented allergic reaction. NF PA NF PA 1/1/2017 Jublia coverage criteria have been updated. NF PA NF PA 1/1/2017 Epiduo Forte coverage criteria have been updated. Epiduo Forteo is reserved for patients who have tried and failed adapalene 0.3% and benzoyl peroxide given separately, Eplerenone F PA F 1/1/2017 Eplerenone (generic Inspra) coverage criteria have been removed, and eplerenone is on formulary with no restrictions. Fluoxetine (Prozac), NF NF PA 4/1/2017 Prozac Brand is reserved for patients who Fluoxetine remains on formulary. Hepatitis C 1/1/2017 Coverage criteria have been updated, removing fibrosis requirements. Preferred products have been updated for State Programs. Zepatier (elbasvir/ grazoprevir) is preferred for genotypes 1 and 4. Insulin glargine (Basaglar) NF F 1/1/2017 Basaglar has been added to formulary, and will replace Lantus and Toujeo.
4 Drug Formulary Update, January 2017, page 4 of 7 Insulin glargine (Lantus and Toujeo) F NF PA 2/1/2017 Lantus and Toujeo are being removed from the formulary. Basaglar will be preferred. Lantus and Toujeo will be reserved for patients who have tried and failed Basaglar due to documented allergic reactions. Itraconazole F PA F PA 1/1/2017 Itraconazole coverage criteria have been updated. Ivermectin (Soolantra) cream Levetiracetam (Keppra), NF NF PA 4/1/2017 Soolantra will be reserved for patients with an inadequate response to topical tretinoin or adapalene. NF NF PA 4/1/2017 Keppra Brands will be reserved for patients who have tried and failed the equivalent generic, due to a documented allergic reaction. Levetiracetam (generic Keppra) remains on formulary. Levetiracetam XR NF F 1/1/2017 Levetiracetam XR (generic Keppra XR) has been added to formulary. Lidocaine ointment F NF 4/1/2017 Lidocaine ointment has been removed from the formulary. Metformin GR NF NF PA 4/1/2017 Metformin GR (Glumetza and generics) requires prior authorization. Naproxen sodium F NF 4/1/2017 Naproxen sodium (generic Anaprox) has been removed from the formulary. Novacort (hydrocortisone/ pramoxine) gel NF NF PA 4/1/2017 Novacort will be reserved for patients with an inadequate response to two or more topical steroids, with significant clinical rationale suggesting improved outcomes.
5 Drug Formulary Update, January 2017, page 5 of 7 Orkambi (lumacaftor/ ivacaftor) Paliperidone (Invega) Pantoprazole (Protonix), Brandonly Quetiapine (Seroquel), Brandonly Quetiapine XR (Seroquel XR), F PA F PA 1/1/2017 Orkambi coverage criteria have been updated. NF PA NF PA 1/1/2017 Paliperidone (Brand Invega) coverage criteria have been updated. Invega is reserved for patients who have tried and failed the equivalent generic due to a documented allergic reaction. Paliperidone remains non formulary with prior authorization. NF NF PA 4/1/2017 Protonix Brand is reserved for patients who have tried the equivalent generic, due to a documented allergic reaction. Pantoprazole (generic Protonix) remains on formulary. Protonix (and all PPIs) remain excluded for the GenericsPlusRx Drug formulary. NF NF PA 4/1/2017 Seroquel Brand is reserved for patients who have tried the equivalent generic, due to a documented allergic reaction. Quetiapine remains on formulary. NF PA NF PA 1/1/2017 Coverage criteria have been updated. Seroquel XR is reserved for patients with significant documented compliance concerns with quetiapine regular release, or patients currently stable on this medication. Approvals are given for 3 years.
6 Drug Formulary Update, January 2017, page 6 of 7 Quetiapine XR F PA F PA 1/1/2017 Quetiapine XR (Seroquel XR) coverage criteria have been updated. Quetiapine XR is reserved for patients with significant documented compliance concerns with quetiapine regular release, or patients currently stable on this medication. Approvals are given for 3 years. Rabeprazole NF F 1/1/2017 Rabeprazole (generic Aciphex) has been added to the formulary. Rabeprazole (and all PPIs) remain excluded for the GenericsPlusRx Drug formulary. Rabeprazole (Aciphex), Brandonly NF NF PA 4/1/2017 Aciphex Brand is reserved for patients who Rabeprazole is on formulary. Aciphex (and all PPIs) remain excluded for the GenericsPlusRx Drug formulary. Rifaximin (Xifaxan) F PA F PA 1/1/2017 Coverage criteria have been updated. Tavaborole (Kerydin) NF PA NF PA 1/1/2017 Kerydin coverage criteria have been updated. Testosterone (Androgel and generics, Androderm, cypionate, and enanthate) F PA F PA 1/1/2017 The prior authorization criteria for preferred testosterone products have been updated. These are reserved for: 1. Members with a diagnosis of gender dysphoria, or 2. Male patients with a documented testosterone deficiency of less than 300 ng/ dl. Renewal Criteria: Reauthorizations are given for members who have been examined by the provider within the previous 14 months, have a positive response, and continue to require this medication. Coverage Duration: Approvals are given for three years.
7 Drug Formulary Update, January 2017, page 7 of 7 Testosterone (Axiron, Fortesta, Testim, Vogelxo) NF PA NF PA 1/1/2017 The prior authorization criteria for nonpreferred forms of testosterone have been updated. These are reserved for the following indications: 1. Members with a diagnosis of gender dysphoria, or 2. Male patients with a documented testosterone deficiency of less than 300 ng/ dl, AND an inadequate response to both Androderm AND Androgel. Renewal Criteria: Reauthorizations are given for members who have been examined by the provider within the previous 14 months, have a positive response, and continue to require this medication. Coverage Duration: Approvals are given for three years. Tolmetin F NF 4/1/2017 Tolmetin has been removed from the formulary. VGo DS PA DS 1/1/2017 Coverage criteria have been removed. V Go is a wearable insulin delivery device used with insulin, covered as a diabetic supply.
Drug Formulary Update, April 2017 Commercial and State Programs
 Drug Formulary Update, April 2017 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Drug Formulary Update, April 2017 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Drug Formulary Update, July 2016 Commercial and State Programs
 Drug Formulary Update, July 2016 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Drug Formulary Update, July 2016 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Drug Formulary Update, October 2016 Commercial and State Programs
 Drug Formulary Update, October 2016 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Drug Formulary Update, October 2016 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Drug Formulary Update, January 2018 Commercial and State Programs
 Drug Formulary Update, January 2018 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Drug Formulary Update, January 2018 Commercial and State Programs Updates to the HealthPartners Commercial and State Program Drug Formularies are listed below. Updates apply to all Commercial groups (PreferredRx,
Relative Cost/Month. Less than $10. Loratadine Liquid* $10-$15 Cetirizine liquid 1mg/mL*
 Allergy Chlorpheniramine Tablet* Diphenhydramine Tablet* Diphenhydramine Liquid* Loratadine Tablet* Cetirizine Tablet* Loratadine 10mg ODT* Less than $10 Loratadine Liquid* $10-$15 Cetirizine liquid 1mg/mL*
Allergy Chlorpheniramine Tablet* Diphenhydramine Tablet* Diphenhydramine Liquid* Loratadine Tablet* Cetirizine Tablet* Loratadine 10mg ODT* Less than $10 Loratadine Liquid* $10-$15 Cetirizine liquid 1mg/mL*
Step Therapy Requirements
 An Independent Licensee of the Blue Cross and Blue Shield Association Step Therapy Requirements Effective: 12/01/2017 Updated 11/2017 H0302_2_2014 CMS Accepted 05/05/2014 1 ABILIFY Abilify 10 mg tablet
An Independent Licensee of the Blue Cross and Blue Shield Association Step Therapy Requirements Effective: 12/01/2017 Updated 11/2017 H0302_2_2014 CMS Accepted 05/05/2014 1 ABILIFY Abilify 10 mg tablet
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES
 PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Generic Additions These generic drugs recently became available in the marketplace. When these generic drugs became available, we began covering them at the
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Generic Additions These generic drugs recently became available in the marketplace. When these generic drugs became available, we began covering them at the
2015 Step Therapy Prior Authorization Medical Necessity Guidelines
 Tufts Health Unify 2015 Step Therapy Prior Authorization Medical Necessity Guidelines Effective: 01/01/2015 Updated: 10/01/2015 Tufts Health Plan P.O. Box 9194 Watertown, MA 02471-9194 Phone: 855-393-3154
Tufts Health Unify 2015 Step Therapy Prior Authorization Medical Necessity Guidelines Effective: 01/01/2015 Updated: 10/01/2015 Tufts Health Plan P.O. Box 9194 Watertown, MA 02471-9194 Phone: 855-393-3154
Aetna Better Health of Illinois Medicaid Formulary Updates
 October 2017 o DOXYLAMINE SUCCINATE 25mg-QL o DULOXETINE CAP 40MG DR-QL o GUANFACIN ER TABS (all strengths)-ql o TOBRAMYCIN NEBU SOLUTION- PA August 2017 Aetna Better Health of Illinois Medicaid 2017 Formulary
October 2017 o DOXYLAMINE SUCCINATE 25mg-QL o DULOXETINE CAP 40MG DR-QL o GUANFACIN ER TABS (all strengths)-ql o TOBRAMYCIN NEBU SOLUTION- PA August 2017 Aetna Better Health of Illinois Medicaid 2017 Formulary
1/1/2019 FORMULARY CHANGES CIGNA COMMERCIAL CUSTOMERS
 1/1/2019 FORMULARY CHANGES CIGNA COMMERCIAL CUSTOMERS Effective 1/1/19, Cigna is making changes to our formularies that may impact medication coverage for customers at your pharmacy. We have included a
1/1/2019 FORMULARY CHANGES CIGNA COMMERCIAL CUSTOMERS Effective 1/1/19, Cigna is making changes to our formularies that may impact medication coverage for customers at your pharmacy. We have included a
Attention: Behavioral Health Providers, Pharmacists and Prescribers N.C. Medicaid and N.C. Health Choice Preferred Drug List Changes - UPDATE
 Attention: Behavioral Health Providers, Pharmacists and Prescribers N.C. Medicaid and N.C. Health Choice Drug List Changes - UPDATE Note: This article was previously published in the December 2014 Medicaid
Attention: Behavioral Health Providers, Pharmacists and Prescribers N.C. Medicaid and N.C. Health Choice Drug List Changes - UPDATE Note: This article was previously published in the December 2014 Medicaid
Alprazolam 0.25mg, 0.5mg, 1mg tablets
 Presbyterian Senior Care (HMO) / Presbyterian MediCare PPO Quantity Limits Effective November 1, 2014 For the most recent list of drugs or other questions, please contact the Presbyterian Customer Service
Presbyterian Senior Care (HMO) / Presbyterian MediCare PPO Quantity Limits Effective November 1, 2014 For the most recent list of drugs or other questions, please contact the Presbyterian Customer Service
Step Therapy Criteria 2019
 Step Therapy 2019 For information on obtaining an updated coverage determination or an exception to a coverage determination please call Freedom Health Member Services at 1-800-401-2740 or, for TTY/TDD
Step Therapy 2019 For information on obtaining an updated coverage determination or an exception to a coverage determination please call Freedom Health Member Services at 1-800-401-2740 or, for TTY/TDD
2018 PDP Premier Step Therapy Document September 2018 Y0114_18_33144_I_009
 2018 PDP Premier Step Therapy Document September 2018 Aggrenox Y0114_18_33144_I_009 aspirin 25 mg-dipyridamole 200 mg capsule,ext.release 12 hr multiphase drug may be given. Step 1 Drug(s): clopidigrel.
2018 PDP Premier Step Therapy Document September 2018 Aggrenox Y0114_18_33144_I_009 aspirin 25 mg-dipyridamole 200 mg capsule,ext.release 12 hr multiphase drug may be given. Step 1 Drug(s): clopidigrel.
Updates to your prescription benefits
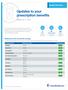 Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Drug Formulary Update, January 2013
 Drug Formulary Update, January 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
Drug Formulary Update, January 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
Drug Formulary Update, April 2013
 Drug Formulary Update, April 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
Drug Formulary Update, April 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
DEPARTMENT OF DEFENSE PHARMACY AND THERAPEUTICS COMMITTEE RECOMMENDATIONS INFORMATION FOR THE UNIFORM FORMULARY BENEFICIARY ADVISORY PANEL
 DEPARTMENT OF DEFENSE PHARMACY AND THERAPEUTICS COMMITTEE RECOMMENDATIONS INFORMATION FOR THE UNIFORM FORMULARY BENEFICIARY ADVISORY PANEL I. UNIFORM FORMULARY REVIEW PROCESS Under 10 United States Code
DEPARTMENT OF DEFENSE PHARMACY AND THERAPEUTICS COMMITTEE RECOMMENDATIONS INFORMATION FOR THE UNIFORM FORMULARY BENEFICIARY ADVISORY PANEL I. UNIFORM FORMULARY REVIEW PROCESS Under 10 United States Code
Step Therapy Requirements
 An Independent Licensee of the Blue Cross and Blue Shield Association Step Therapy Requirements Effective: 05/01/2018 Updated 4/2018 H0302_2_2014 CMS Accepted 05/05/2014 1 BETA-BLOCKERS BYSTOLIC 10 MG
An Independent Licensee of the Blue Cross and Blue Shield Association Step Therapy Requirements Effective: 05/01/2018 Updated 4/2018 H0302_2_2014 CMS Accepted 05/05/2014 1 BETA-BLOCKERS BYSTOLIC 10 MG
SmithRx Standard Formulary Step Therapy List
 SmithRx Standard Formulary Step Therapy List Revised: January 27, 2017 The following medications require prior use of at least one other medication for coverage. Please note that any plan-specific customizations
SmithRx Standard Formulary Step Therapy List Revised: January 27, 2017 The following medications require prior use of at least one other medication for coverage. Please note that any plan-specific customizations
ABILIFY INJ. Products Affected Step 2: ABILIFY MAINTENA PREFILLED SYRINGE 300 MG INTRAMUSCULAR ABILIFY MAINTENA PREFILLED SYRINGE 400 MG INTRAMUSCULAR
 ABILIFY INJ ABILIFY MAINTENA PREFILLED SYRINGE 300 MG ABILIFY MAINTENA PREFILLED SYRINGE 400 MG ABILIFY MAINTENA SUSPENSION RECONSTITUTED ER 300 MG Claim will pay automatically for ABILIFY MAINTENA if
ABILIFY INJ ABILIFY MAINTENA PREFILLED SYRINGE 300 MG ABILIFY MAINTENA PREFILLED SYRINGE 400 MG ABILIFY MAINTENA SUSPENSION RECONSTITUTED ER 300 MG Claim will pay automatically for ABILIFY MAINTENA if
Step Therapy Requirements. Effective: 1/1/2019
 Effective: 1/1/2019 Updated 1/2019 AMANTADINE ER Sharp Health Plan (HMO) OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED RELEASE PRIOR CLAIM FOR AMANTADINE
Effective: 1/1/2019 Updated 1/2019 AMANTADINE ER Sharp Health Plan (HMO) OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED RELEASE PRIOR CLAIM FOR AMANTADINE
Alameda Alliance for Health Pharmacy & Therapeutics (P&T) Committee Decisions
 Alameda Alliance for Health FORMULARY UPDATE Effective: October 27, 2017. Drugs notated with an * have an undetermined implementation date Alameda Alliance for Health Pharmacy & Therapeutics (P&T) Committee
Alameda Alliance for Health FORMULARY UPDATE Effective: October 27, 2017. Drugs notated with an * have an undetermined implementation date Alameda Alliance for Health Pharmacy & Therapeutics (P&T) Committee
BLUE SHIELD OF CALIFORNIA JUNE 2016 PLUS DRUG FORMULARY CHANGES
 BLUE SHIELD OF CALIFORNIA JUNE 2016 PLUS DRUG FORMULARY CHANGES Blue Shield is committed to covering safe, effective and affordable medications, so we regularly review and update our drug formularies.
BLUE SHIELD OF CALIFORNIA JUNE 2016 PLUS DRUG FORMULARY CHANGES Blue Shield is committed to covering safe, effective and affordable medications, so we regularly review and update our drug formularies.
Formulary Change Notice
 Formulary Change Notice HealthPartners may remove drugs from our formulary (list of covered drugs) or add rules about whether and when certain drugs are covered during the year. The chart below contains
Formulary Change Notice HealthPartners may remove drugs from our formulary (list of covered drugs) or add rules about whether and when certain drugs are covered during the year. The chart below contains
2017 Step Therapy Criteria
 FRESENIUS TOTAL HEALTH 2017 Step Therapy Updated 07/01/2017. For more recent information or other questions, please contact Fresenius Total Health Customer Service at 1-855-598-6774 / TTY 1-844-209-9094.
FRESENIUS TOTAL HEALTH 2017 Step Therapy Updated 07/01/2017. For more recent information or other questions, please contact Fresenius Total Health Customer Service at 1-855-598-6774 / TTY 1-844-209-9094.
AMANTADINE ER. Products Affected Step 2: OSMOLEX ER 129 MG TABLET, EXTENDED RELEASE OSMOLEX ER 193 MG TABLET, Details
 AMANTADINE ER OSMOLEX ER 129 MG TABLET, EXTENDED RELEASE OSMOLEX ER 193 MG TABLET, EXTENDED RELEASE OSMOLEX ER 258 MG TABLET, PRIOR CLAIM FOR AMANTADINE HCL IMMEDIATE RELEASE WITHIN THE PAST 120 DAYS.
AMANTADINE ER OSMOLEX ER 129 MG TABLET, EXTENDED RELEASE OSMOLEX ER 193 MG TABLET, EXTENDED RELEASE OSMOLEX ER 258 MG TABLET, PRIOR CLAIM FOR AMANTADINE HCL IMMEDIATE RELEASE WITHIN THE PAST 120 DAYS.
Oregon Health Plan prescription benefit updates
 Oregon Health Plan prescription benefit updates EOCCO s prescription program is a pharmacy benefit that offers members a choice of safe and effective medication treatments. The program also helps you save
Oregon Health Plan prescription benefit updates EOCCO s prescription program is a pharmacy benefit that offers members a choice of safe and effective medication treatments. The program also helps you save
2017 Formulary Changes Year to Date
 2017 Formulary Changes Year to Date Health Choice Arizona may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, add prior authorization, quantity limits and/or
2017 Formulary Changes Year to Date Health Choice Arizona may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, add prior authorization, quantity limits and/or
AMANTADINE ER. Products Affected Step 2: OSMOLEX ER 129 MG TABLET, EXTENDED RELEASE OSMOLEX ER 193 MG TABLET, Details
 AMANTADINE ER OSMOLEX ER 129 MG TABLET, EXTENDED RELEASE OSMOLEX ER 193 MG TABLET, EXTENDED RELEASE OSMOLEX ER 258 MG TABLET, PRIOR CLAIM FOR AMANTADINE HCL IMMEDIATE RELEASE WITHIN THE PAST 120 DAYS.
AMANTADINE ER OSMOLEX ER 129 MG TABLET, EXTENDED RELEASE OSMOLEX ER 193 MG TABLET, EXTENDED RELEASE OSMOLEX ER 258 MG TABLET, PRIOR CLAIM FOR AMANTADINE HCL IMMEDIATE RELEASE WITHIN THE PAST 120 DAYS.
ALLERGIC CONJUNCTIVITIS AGENTS
 2018 5 Tier Standard- Keystone First VIP Choice Document: 2018 Step Therapy Formulary ID: 18390 Last Updated: 04/2018 Effective Date: 05-01-2018 ALLERGIC CONJUNCTIVITIS AGENTS epinastine 0.05 % eye drops
2018 5 Tier Standard- Keystone First VIP Choice Document: 2018 Step Therapy Formulary ID: 18390 Last Updated: 04/2018 Effective Date: 05-01-2018 ALLERGIC CONJUNCTIVITIS AGENTS epinastine 0.05 % eye drops
OHIO MEDICAID PHARMACY COVERAGE
 OHIO MEDICAID PHARMACY COVERAGE This information is intended for use by providers to help select the most appropriate cost-effective medication and formulation for their patients. Prescribers should utilize
OHIO MEDICAID PHARMACY COVERAGE This information is intended for use by providers to help select the most appropriate cost-effective medication and formulation for their patients. Prescribers should utilize
Updates to the Alberta Drug Benefit List. Effective September 1, 2018
 Updates to the Alberta Drug Benefit List Effective September 1, 2018 Inquiries should be directed to: Pharmacy Services Alberta Blue Cross 10009 108 Street NW Edmonton AB T5J 3C5 Telephone Number: (780)
Updates to the Alberta Drug Benefit List Effective September 1, 2018 Inquiries should be directed to: Pharmacy Services Alberta Blue Cross 10009 108 Street NW Edmonton AB T5J 3C5 Telephone Number: (780)
Prescription benefit updates Large group
 Prescription benefit updates Large group Moda Health s prescription program is a pharmacy benefit that offers members a choice of safe and effective medication treatments. The program also helps you save
Prescription benefit updates Large group Moda Health s prescription program is a pharmacy benefit that offers members a choice of safe and effective medication treatments. The program also helps you save
Simply Step Therapy Document September 2018 Y0114_18_33074_I_009
 2018 2018 Simply Step Therapy Document September 2018 Aptiom APTIOM 200 MG TABLET APTIOM 400 MG TABLET Y0114_18_33074_I_009 APTIOM 600 MG TABLET APTIOM 800 MG TABLET Criteria If the patient has tried a
2018 2018 Simply Step Therapy Document September 2018 Aptiom APTIOM 200 MG TABLET APTIOM 400 MG TABLET Y0114_18_33074_I_009 APTIOM 600 MG TABLET APTIOM 800 MG TABLET Criteria If the patient has tried a
Pharmacy Program Updates: Quarterly Pharmacy Changes Effective July 1, 2017
 Pharmacy Program Updates: Quarterly Pharmacy Changes Effective July 1, 2017 DRUG LIST CHANGES Based on the availability of new prescription medications and Prime s National Pharmacy and Therapeutics Committee
Pharmacy Program Updates: Quarterly Pharmacy Changes Effective July 1, 2017 DRUG LIST CHANGES Based on the availability of new prescription medications and Prime s National Pharmacy and Therapeutics Committee
UF Decision Report FY06-07 Beneficiary Advisory Panel 10 Jan 2008
 UF Decision Report FY06-07 Beneficiary Advisory Panel 10 Jan 2008 Promoting high quality, cost effective drug therapy throughout the Military Health System UF Decisions, May 07 Class FY05 rank, total $
UF Decision Report FY06-07 Beneficiary Advisory Panel 10 Jan 2008 Promoting high quality, cost effective drug therapy throughout the Military Health System UF Decisions, May 07 Class FY05 rank, total $
Table 1: Price increases for Brand Name Drugs with Generic Equivalents
 Table 1: Price increases for Brand Name Drugs with Generic Equivalents Brand Name Medication and Dose Total % Change Since 10/2012 ACTOS 15 MG TABLET 6.36 11.03 73.39% ACTOS 30 MG TABLET 9.7 16.80 73.23%
Table 1: Price increases for Brand Name Drugs with Generic Equivalents Brand Name Medication and Dose Total % Change Since 10/2012 ACTOS 15 MG TABLET 6.36 11.03 73.39% ACTOS 30 MG TABLET 9.7 16.80 73.23%
FirstCarolinaCare Insurance Company Step Therapy Requirements
 ANALGESICS, NARCOTICS KADIAN MORPHINE SULFATE ER PRIOR CLAIM FOR MORPHINE SULFATE SUSTAINED ACTION TABLET (MS CONTIN) WITHIN THE PAST 120 DAYS. ANTIBACTERIALS (EENT) BESIVANCE PRIOR CLAIM FOR CIPROFLOXACIN
ANALGESICS, NARCOTICS KADIAN MORPHINE SULFATE ER PRIOR CLAIM FOR MORPHINE SULFATE SUSTAINED ACTION TABLET (MS CONTIN) WITHIN THE PAST 120 DAYS. ANTIBACTERIALS (EENT) BESIVANCE PRIOR CLAIM FOR CIPROFLOXACIN
Pharmacy Benefit Management (PBM) Program FORMULARY/PRODUCT RESTRICTIONS
 Workforce Safety & Insurance Revised Document Date: 07/21/2015 1600 E Century Ave Ste 1 PO Box 5585 Bismarck, ND 58506-5585 701.328.3800 1.800.777.5033 www.workforcesafety.com Pharmacy Benefit Management
Workforce Safety & Insurance Revised Document Date: 07/21/2015 1600 E Century Ave Ste 1 PO Box 5585 Bismarck, ND 58506-5585 701.328.3800 1.800.777.5033 www.workforcesafety.com Pharmacy Benefit Management
ANGIOTENSIN RECEPTOR BLOCKERS STEP THERAPY
 South Country Health Alliance 2017 Step Therapy Formulary ID: 17431 Last Updated: 10/20/2017 Effective Date: 11-01-2017 ANGIOTENSIN RECEPTOR BLOCKERS STEP THERAPY BENICAR 20 MG BENICAR 40 MG BENICAR 5
South Country Health Alliance 2017 Step Therapy Formulary ID: 17431 Last Updated: 10/20/2017 Effective Date: 11-01-2017 ANGIOTENSIN RECEPTOR BLOCKERS STEP THERAPY BENICAR 20 MG BENICAR 40 MG BENICAR 5
Step Therapy Requirements. Effective: 03/01/2015
 Effective: 03/01/2015 Updated 02/2015 ANTI-INFLAMMATORY AGENTS - GI DIPENTUM PRIOR CLAIM FOR BALSALAZIDE OR APRISO WITHIN THE PAST 120 DAYS. ANTICONVULSANTS APTIOM BANZEL FYCOMPA OXTELLAR XR POTIGA QUDEXY
Effective: 03/01/2015 Updated 02/2015 ANTI-INFLAMMATORY AGENTS - GI DIPENTUM PRIOR CLAIM FOR BALSALAZIDE OR APRISO WITHIN THE PAST 120 DAYS. ANTICONVULSANTS APTIOM BANZEL FYCOMPA OXTELLAR XR POTIGA QUDEXY
Step Therapy Medications
 Step Therapy Medications Step Therapy Group APTIOM Step-2: APTIOM 200 MG TABLET or APTIOM 400 MG TABLET or APTIOM 600 MG TABLET or APTIOM 800 MG TABLET Step 1 Drug(s): Oxcarbazepine immediate-release,
Step Therapy Medications Step Therapy Group APTIOM Step-2: APTIOM 200 MG TABLET or APTIOM 400 MG TABLET or APTIOM 600 MG TABLET or APTIOM 800 MG TABLET Step 1 Drug(s): Oxcarbazepine immediate-release,
Your prescription benefit updates Formulary Updates - Effective January 1, 2019
 Your prescription benefit updates Formulary Updates - Effective January 1, 2019 Medications are grouped by the conditions they treat. Each medication is placed in a tier that shows the amount you will
Your prescription benefit updates Formulary Updates - Effective January 1, 2019 Medications are grouped by the conditions they treat. Each medication is placed in a tier that shows the amount you will
Drug Formulary Update, October 2013
 Drug Formulary Update, October 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
Drug Formulary Update, October 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select Formulary April 1, 2018 Updates. Formulary Alternatives
 PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select April 1, 2018 Updates Drug Name adapalene-benzoyl-peroxide Gel 0.1-2.5% (Brand = Epiduo ) prasugrel hcl (Brand = Effient ) vigabatrin pak 500 mg (Brand
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select April 1, 2018 Updates Drug Name adapalene-benzoyl-peroxide Gel 0.1-2.5% (Brand = Epiduo ) prasugrel hcl (Brand = Effient ) vigabatrin pak 500 mg (Brand
Medicare Part D 2016 Formulary Changes Service To Senior and OC Preferred
 Medicare Part D 2016 Formulary s Service To Senior and OC Preferred Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior
Medicare Part D 2016 Formulary s Service To Senior and OC Preferred Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior
Drug Therapy Guidelines
 Classes of medications may be targeted for preferred products when there are multiple entries into the market in the same therapeutic category. Coverage of any non-preferred medication can be granted when
Classes of medications may be targeted for preferred products when there are multiple entries into the market in the same therapeutic category. Coverage of any non-preferred medication can be granted when
New Generics: Specialty Network: Retail Pharmacies Dispensing Specialty Products
 SUPPORTING OUR PROVIDER PARTNERS THROUGH COMMUNICATION AND COLLABORATION. DATE JANUARY 2016 ISSUE 1 HELPFUL NUMBERS FOR PROVIDERS Magellan: 1-800-846-7971 Bin: 016523 Processor control: 747 HELPFUL NUMBERS
SUPPORTING OUR PROVIDER PARTNERS THROUGH COMMUNICATION AND COLLABORATION. DATE JANUARY 2016 ISSUE 1 HELPFUL NUMBERS FOR PROVIDERS Magellan: 1-800-846-7971 Bin: 016523 Processor control: 747 HELPFUL NUMBERS
PRESCRIPTION SAVINGS CLUB FLAT- PRICED GENERIC DRUG LIST (EMDEON) Effective August 20, 2014
 PRESCRIPTION SAVINGS CLUB FLAT- PRICED GENERIC DRUG LIST (EMDEON) Effective August 20, 2014 The Prescription Savings Club provides its members with significant savings on prescription medications. The
PRESCRIPTION SAVINGS CLUB FLAT- PRICED GENERIC DRUG LIST (EMDEON) Effective August 20, 2014 The Prescription Savings Club provides its members with significant savings on prescription medications. The
Drug Therapy Guidelines
 Classes of medications may be targeted for preferred products when there are multiple entries into the market in the same therapeutic category. Coverage of any non-preferred medication can be granted when
Classes of medications may be targeted for preferred products when there are multiple entries into the market in the same therapeutic category. Coverage of any non-preferred medication can be granted when
CRITERIA Trial of two generic formulary products from the following: atomoxetine or ADHD stimulant medication.
 ADHD STIMULANTS ATOMOXETINE HCL, DEXEDRINE 10 MG TABLET, DEXEDRINE 5 MG TABLET, DEXMETHYLPHENIDATE HCL, DEXMETHYLPHENIDATE HCL ER, DEXTROAMPHETAMINE 10 MG TAB, DEXTROAMPHETAMINE 5 MG TAB, DEXTROAMPHETAMINE
ADHD STIMULANTS ATOMOXETINE HCL, DEXEDRINE 10 MG TABLET, DEXEDRINE 5 MG TABLET, DEXMETHYLPHENIDATE HCL, DEXMETHYLPHENIDATE HCL ER, DEXTROAMPHETAMINE 10 MG TAB, DEXTROAMPHETAMINE 5 MG TAB, DEXTROAMPHETAMINE
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select Formulary April 1, 2018 Updates. Formulary Alternatives
 PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select April 1, 2018 Updates Drug Name adapalene-benzoyl-peroxide Gel 0.1-2.5% (Brand = Epiduo ) prasugrel hcl (Brand = Effient ) vigabatrin pak 500 mg (Brand
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select April 1, 2018 Updates Drug Name adapalene-benzoyl-peroxide Gel 0.1-2.5% (Brand = Epiduo ) prasugrel hcl (Brand = Effient ) vigabatrin pak 500 mg (Brand
2017 Formulary Exclusions Drug List
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2017 Formulary Exclusions Drug List aetna.com 05.03.912.1 H (3/17) These drugs are not covered under your plan.
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2017 Formulary Exclusions Drug List aetna.com 05.03.912.1 H (3/17) These drugs are not covered under your plan.
Prepared for Regence BlueCross BlueShield of Oregon Producers Only. Not intended for distribution to Regence consumers or members.
 Revised date: 10/17/16 Issue Brief: Jan. 1, 2017, Formulary Changes OmedaRx regularly evaluates the performance and impact of medications using one of the most rigorous, evidence-based assessment processes
Revised date: 10/17/16 Issue Brief: Jan. 1, 2017, Formulary Changes OmedaRx regularly evaluates the performance and impact of medications using one of the most rigorous, evidence-based assessment processes
Neighborhood Medicaid Formulary Changes: June 2017
 Neighborhood Medicaid Formulary Changes: June 2017 The following changes to the Neighborhood Medicaid Formulary were recently approved by the Pharmacy and Therapeutics (P&T) Committee. All changes were
Neighborhood Medicaid Formulary Changes: June 2017 The following changes to the Neighborhood Medicaid Formulary were recently approved by the Pharmacy and Therapeutics (P&T) Committee. All changes were
Judges Reference Table for the March 2016 Psychotropic Medication Utilization Parameters for Foster Children
 Judges Reference Table for the Psychotropic Medication Utilization Parameters for Foster Children Stimulants for treatment of ADHD Preschool (Ages 3-5 years) Child (Ages 6-12 years) Adolescent (Ages 13-17
Judges Reference Table for the Psychotropic Medication Utilization Parameters for Foster Children Stimulants for treatment of ADHD Preschool (Ages 3-5 years) Child (Ages 6-12 years) Adolescent (Ages 13-17
A Brief Overview of Psychiatric Pharmacotherapy. Joel V. Oberstar, M.D. Chief Executive Officer
 A Brief Overview of Psychiatric Pharmacotherapy Joel V. Oberstar, M.D. Chief Executive Officer Disclosures Some medications discussed are not approved by the FDA for use in the population discussed/described.
A Brief Overview of Psychiatric Pharmacotherapy Joel V. Oberstar, M.D. Chief Executive Officer Disclosures Some medications discussed are not approved by the FDA for use in the population discussed/described.
CONTRAINDICATIONS TABLE
 CONTRAINDICATIONS TABLE Generic Name Brand Name Contraindications Amphetamine Salts Adderall, Adderall XR Hypersensitivity to amphetamine, dextroamphetamine, or other sympathomimetic amines Advanced arteriosclerosis
CONTRAINDICATIONS TABLE Generic Name Brand Name Contraindications Amphetamine Salts Adderall, Adderall XR Hypersensitivity to amphetamine, dextroamphetamine, or other sympathomimetic amines Advanced arteriosclerosis
Medications and Children Disorders
 Mental Health Comprehensive Services Providing Family Stability and Developing Life Coping Skills Medications and Children Disorders Psychiatric medications can be an effective part of the treatment for
Mental Health Comprehensive Services Providing Family Stability and Developing Life Coping Skills Medications and Children Disorders Psychiatric medications can be an effective part of the treatment for
Schedule FDA & literature based indications
 Psychotropic Medication List Recommended dosages are intended to serve only as a guide for children. Recommended doses are literature based. Clinicians should consult package insert of medications for
Psychotropic Medication List Recommended dosages are intended to serve only as a guide for children. Recommended doses are literature based. Clinicians should consult package insert of medications for
HEALTHTEAM ADVANTAGE 2018 Step Therapy Criteria
 GLP1-INSULIN XULTOPHY SOLUTION PEN- INJECTOR 100-3.6 UNIT-MG/ML HEALTHTEAM ADVANTAGE Claim will pay automatically for Xultophy if enrollee has a paid claim for at least a one day supply for step level
GLP1-INSULIN XULTOPHY SOLUTION PEN- INJECTOR 100-3.6 UNIT-MG/ML HEALTHTEAM ADVANTAGE Claim will pay automatically for Xultophy if enrollee has a paid claim for at least a one day supply for step level
HEALTHTEAM ADVANTAGE PLAN 2017 Step Therapy Criteria Pending CMS Approval
 ARISTADA - ARISTADA INJ 441MG/1.6 ARISTADA INJ 662MG/2.4 ARISTADA INJ 882MG/3.2 CLAIM WILL PAY AUTOMATICALLY FOR ARISTADA IF ENROLLEE HAS A PAID CLAIM FOR AT LEAST A 1 DAYS SUPPLY OF ABILIFY MAINTENA AND
ARISTADA - ARISTADA INJ 441MG/1.6 ARISTADA INJ 662MG/2.4 ARISTADA INJ 882MG/3.2 CLAIM WILL PAY AUTOMATICALLY FOR ARISTADA IF ENROLLEE HAS A PAID CLAIM FOR AT LEAST A 1 DAYS SUPPLY OF ABILIFY MAINTENA AND
TABLE OF CONTENTS (Click on a link below to view the section.)
 Follow the links below to access the complete formularies for Plans: Health Plan Acne Allergy Allergic Anaphylactic Reaction Allergic Conjunctivitis Allergic Rhinitis Asthma Atopic Dermatitis Behavioral
Follow the links below to access the complete formularies for Plans: Health Plan Acne Allergy Allergic Anaphylactic Reaction Allergic Conjunctivitis Allergic Rhinitis Asthma Atopic Dermatitis Behavioral
HEALTHTEAM ADVANTAGE 2018 Step Therapy Criteria
 GLP1-INSULIN XULTOPHY SOLUTION PEN- INJECTOR 100-3.6 UNIT-MG/ML Claim will pay automatically for Xultophy if enrollee has a paid claim for at least a one day supply for step level 1 agent (LANTUS, LEVEMIR,
GLP1-INSULIN XULTOPHY SOLUTION PEN- INJECTOR 100-3.6 UNIT-MG/ML Claim will pay automatically for Xultophy if enrollee has a paid claim for at least a one day supply for step level 1 agent (LANTUS, LEVEMIR,
2018 Step Therapy FID 18088
 2018 Step Therapy FID 18088 Step Therapy ANTIDEPRESSANTS, SEROTONIN/NOREPINEPHRINE REUPTAKE INHIBITORS LEON 2018 Desvenlafaxine Er Fetzima Fetzima Titration Pack Khedezla Paxil SUSP Pristiq Trintellix
2018 Step Therapy FID 18088 Step Therapy ANTIDEPRESSANTS, SEROTONIN/NOREPINEPHRINE REUPTAKE INHIBITORS LEON 2018 Desvenlafaxine Er Fetzima Fetzima Titration Pack Khedezla Paxil SUSP Pristiq Trintellix
Antipsychotic Medications Age and Step Therapy
 Market DC *- Florida Healthy Kids Antipsychotic Medications Age and Step Therapy Override(s) Approval Duration Prior Authorization 1 year Quantity Limit *Virginia Medicaid See State Specific Mandates *Indiana
Market DC *- Florida Healthy Kids Antipsychotic Medications Age and Step Therapy Override(s) Approval Duration Prior Authorization 1 year Quantity Limit *Virginia Medicaid See State Specific Mandates *Indiana
T Informatics recently released its
 Volume 25, Number 5 May 2011 Drugs & Therapy B U L L E T I N FORMULARY UPDATE The Pharmacy and Therapeutics Committee met April 19, 2011. 7 products were added in the Formulary; 7 were deleted, while 13
Volume 25, Number 5 May 2011 Drugs & Therapy B U L L E T I N FORMULARY UPDATE The Pharmacy and Therapeutics Committee met April 19, 2011. 7 products were added in the Formulary; 7 were deleted, while 13
ANTIDEPRESSANTS. Details. dose pack Viibryd 10 mg tablet Viibryd 20 mg tablet Viibryd 40 mg tablet. Criteria
 ANTIDEPRESSANTS Trintellix 10 mg tablet Trintellix 20 mg tablet Trintellix 5 mg tablet Viibryd 10 mg (7)-20 mg (23) tablets in a dose pack Viibryd 10 mg tablet Viibryd 20 mg tablet Viibryd 40 mg tablet
ANTIDEPRESSANTS Trintellix 10 mg tablet Trintellix 20 mg tablet Trintellix 5 mg tablet Viibryd 10 mg (7)-20 mg (23) tablets in a dose pack Viibryd 10 mg tablet Viibryd 20 mg tablet Viibryd 40 mg tablet
Beneficiary Advisory Panel Handout Uniform Formulary Decisions 23 June 2011
 Beneficiary Advisory Panel Handout Uniform Formulary Decisions 23 June 211 PURPOSE: The purpose of this handout is to provide BAP Committee members with a reference document for the relative clinical effectiveness
Beneficiary Advisory Panel Handout Uniform Formulary Decisions 23 June 211 PURPOSE: The purpose of this handout is to provide BAP Committee members with a reference document for the relative clinical effectiveness
AMANTADINE ER. Products Affected Step 2: OSMOLEX ER 129 MG TABLET, EXTENDED RELEASE OSMOLEX ER 193 MG TABLET, Details
 AMANTADINE ER OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED RELEASE PRIOR CLAIM FOR AMANTADINE HCL IMMEDIATE RELEASE WITHIN THE PAST 120 DAYS. 1 ANTICONVULSANTS
AMANTADINE ER OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED RELEASE PRIOR CLAIM FOR AMANTADINE HCL IMMEDIATE RELEASE WITHIN THE PAST 120 DAYS. 1 ANTICONVULSANTS
FORMULARY UPDATES TO DENVER HEALTH MEDICAID CHOICE (DHMC) AND CHILD HEALTH PLAN PLUS (CHP+) PLANS
 FORMULARY UPDATES TO DENVER HEALTH MEDICAID CHOICE (DHMC) AND CHILD HEALTH PLAN PLUS (CHP+) PLANS DHMC/CHP+ may add or remove drugs from the formulary or make changes to restrictions on formulary drugs
FORMULARY UPDATES TO DENVER HEALTH MEDICAID CHOICE (DHMC) AND CHILD HEALTH PLAN PLUS (CHP+) PLANS DHMC/CHP+ may add or remove drugs from the formulary or make changes to restrictions on formulary drugs
JULY 2017 ADDITIONS. NP Thyroid 120mg NP Thyroid 15mg JUNE 2017 CHANGES
 APRIL 2017 Ivermectin, Pin-X and Reeses (Pyrantel Pamoate) Selzentry 25mg and 75mg tablets Linzess 72 mcg capsule-with QLL Levalbuterol Tartrate Inhal Aerosol (Generic Xopenex HFA) with ST & QLL Jentadueto
APRIL 2017 Ivermectin, Pin-X and Reeses (Pyrantel Pamoate) Selzentry 25mg and 75mg tablets Linzess 72 mcg capsule-with QLL Levalbuterol Tartrate Inhal Aerosol (Generic Xopenex HFA) with ST & QLL Jentadueto
Recommended Exclusion of Selected Discretionary Drugs
 7100 N High Street Office Suite 305 Worthington, Ohio 43085 pharmaceuticalhorizons.com p 614.781.6500 f 614.781.6503 FROM: RE: Allan Zaenger R.Ph., MS Pharmaceutical Horizons, Inc. Recommended Exclusion
7100 N High Street Office Suite 305 Worthington, Ohio 43085 pharmaceuticalhorizons.com p 614.781.6500 f 614.781.6503 FROM: RE: Allan Zaenger R.Ph., MS Pharmaceutical Horizons, Inc. Recommended Exclusion
Pharmacy and Therapeutics (P&T) Committee Provider Update
 Pharmacy and Therapeutics (P&T) Committee Provider Update FIRST QUARTER 2017 P&T Committee Decisions effective March 1, 2017 Dear Healthcare Practitioner: The Presbyterian Health Plan, Inc., and Presbyterian
Pharmacy and Therapeutics (P&T) Committee Provider Update FIRST QUARTER 2017 P&T Committee Decisions effective March 1, 2017 Dear Healthcare Practitioner: The Presbyterian Health Plan, Inc., and Presbyterian
2018 Step Therapy Criteria
 2018 Step Therapy Criteria ANGIOTENSIN RECEPTOR BLOCKERS... 2 ANTIDEPRESSANTS... 3 ANTIDEPRESSANTS, MISCELLANEOUS... 4 ANTIDEPRESSANTS, OTHER... 5 ANTIDIABETIC AGENTS... 6 ANTIGOUT AGENTS... 7 ANTIHYPERTENSIVE
2018 Step Therapy Criteria ANGIOTENSIN RECEPTOR BLOCKERS... 2 ANTIDEPRESSANTS... 3 ANTIDEPRESSANTS, MISCELLANEOUS... 4 ANTIDEPRESSANTS, OTHER... 5 ANTIDIABETIC AGENTS... 6 ANTIGOUT AGENTS... 7 ANTIHYPERTENSIVE
Step Therapy Requirements. Effective: 05/01/2018
 Step Therapy Requirements Effective: 05/01/2018 ANTIDEPRESSANTS TRINTELLIX 10 MG TABLET TRINTELLIX 20 MG TABLET TRINTELLIX 5 MG TABLET VIIBRYD 10 MG (7)-20 MG (23) TABLETS IN A DOSE PACK VIIBRYD 10 MG
Step Therapy Requirements Effective: 05/01/2018 ANTIDEPRESSANTS TRINTELLIX 10 MG TABLET TRINTELLIX 20 MG TABLET TRINTELLIX 5 MG TABLET VIIBRYD 10 MG (7)-20 MG (23) TABLETS IN A DOSE PACK VIIBRYD 10 MG
Pharmacy Benefit Management (PBM) Program FORMULARY/PRODUCT RESTRICTIONS
 Workforce Safety & Insurance Revised Document Date: 07/23/2015 1600 E Century Ave Ste 1 PO Box 5585 Bismarck, ND 58506-5585 701.328.3800 1.800.777.5033 www.workforcesafety.com Pharmacy Benefit Management
Workforce Safety & Insurance Revised Document Date: 07/23/2015 1600 E Century Ave Ste 1 PO Box 5585 Bismarck, ND 58506-5585 701.328.3800 1.800.777.5033 www.workforcesafety.com Pharmacy Benefit Management
Avoid paying too much for your prescriptions
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2017 Aetna Rx Step Program Medicine List Avoid paying too much for your prescriptions It s important to try to
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2017 Aetna Rx Step Program Medicine List Avoid paying too much for your prescriptions It s important to try to
Special Generic Drug Pricing Program
 FREE PICK-UP & DELIVERY Flu-Shots Specialty prescription Compounding Wellness center providing health screenings for hypertension and diabetes $3 Special Generic Prescription Drug Program only offered
FREE PICK-UP & DELIVERY Flu-Shots Specialty prescription Compounding Wellness center providing health screenings for hypertension and diabetes $3 Special Generic Prescription Drug Program only offered
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Step Therapy Reference Number: HIM.PA.109 Effective Date: 08.01.17 Last Review Date: 05.18 Line of Business: Health Insurance Marketplace Revision Log See Important Reminder at the end
Clinical Policy: Step Therapy Reference Number: HIM.PA.109 Effective Date: 08.01.17 Last Review Date: 05.18 Line of Business: Health Insurance Marketplace Revision Log See Important Reminder at the end
Date: October 3, 2017 To: Participating Providers From: YourCare Health Plan Provider Relations Subject: 2018 Formulary Changes
 Date: October 3, 2017 To: Participating Providers From: YourCare Health Plan Provider Relations Subject: 2018 Formulary Changes 2018 Formulary-UM Changes What does this mean now, and for 2018? A number
Date: October 3, 2017 To: Participating Providers From: YourCare Health Plan Provider Relations Subject: 2018 Formulary Changes 2018 Formulary-UM Changes What does this mean now, and for 2018? A number
High-Cost Drug Exclusions
 Pharmacy Services High-Cost Exclusions The high cost medications listed below are excluded from coverage because lower cost similar alternatives are available. To help you get the best health benefit at
Pharmacy Services High-Cost Exclusions The high cost medications listed below are excluded from coverage because lower cost similar alternatives are available. To help you get the best health benefit at
VNSNY CHOICE FIDA Complete Step Therapy Requirements. Effective: 04/01/2019
 VNSNY CHOICE FIDA Complete Step Therapy Requirements Effective: 04/01/2019 Updated 03/2019 AMANTADINE ER OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED
VNSNY CHOICE FIDA Complete Step Therapy Requirements Effective: 04/01/2019 Updated 03/2019 AMANTADINE ER OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED
Network Health Insurance Corporation Upcoming Negative Changes to the Medicare Part D Formulary
 Requesting an Exception to the Formulary You can ask Network Health Insurance Corporation to make an exception to our coverage rules. Generally, we will only approve your request for an exception if alternative
Requesting an Exception to the Formulary You can ask Network Health Insurance Corporation to make an exception to our coverage rules. Generally, we will only approve your request for an exception if alternative
ANTICONVULSANTS. Details
 ANTICONVULSANTS Aptiom 200 mg tablet Aptiom 400 mg tablet Aptiom 600 mg tablet Aptiom 800 mg tablet Banzel 200 mg tablet Banzel 40 mg/ml oral suspension Banzel 400 mg tablet Fycompa 0.5 mg/ml oral suspension
ANTICONVULSANTS Aptiom 200 mg tablet Aptiom 400 mg tablet Aptiom 600 mg tablet Aptiom 800 mg tablet Banzel 200 mg tablet Banzel 40 mg/ml oral suspension Banzel 400 mg tablet Fycompa 0.5 mg/ml oral suspension
Pharmacy Coverage Guidelines are subject to change as new information becomes available.
 TESTOSTERONE REPLACEMENT THERAPY: ANDRODERM transdermal patch ANDROGEL pump transdermal gel and transdermal gel AXIRON transdermal solution FORTESTA transdermal gel NATESTO nasal gel STRIANT buccal mucoadhesive
TESTOSTERONE REPLACEMENT THERAPY: ANDRODERM transdermal patch ANDROGEL pump transdermal gel and transdermal gel AXIRON transdermal solution FORTESTA transdermal gel NATESTO nasal gel STRIANT buccal mucoadhesive
UnitedHealthcare Community Plan PDL Modifications. Added as an alternative agent for the 9/1/ /1/2012
 Avonex Pen Interferon beta-1a Added as alternative dosing formulation for the treatment of multiple sclerosis. Prior Korlym Mifepristone Added as alternative agent to control hyperglycemia secondary to
Avonex Pen Interferon beta-1a Added as alternative dosing formulation for the treatment of multiple sclerosis. Prior Korlym Mifepristone Added as alternative agent to control hyperglycemia secondary to
Step Therapy Requirements. Effective: 11/01/2018
 Effective: 11/01/2018 Updated 10/2018 ANTIDEPRESSANTS Sharp Health Plan (HMO) TRINTELLIX 10 MG TABLET TRINTELLIX 20 MG TABLET TRINTELLIX 5 MG TABLET VIIBRYD 10 MG (7)-20 MG (23) TABLETS IN A DOSE PACK
Effective: 11/01/2018 Updated 10/2018 ANTIDEPRESSANTS Sharp Health Plan (HMO) TRINTELLIX 10 MG TABLET TRINTELLIX 20 MG TABLET TRINTELLIX 5 MG TABLET VIIBRYD 10 MG (7)-20 MG (23) TABLETS IN A DOSE PACK
Medicare Part D Drugs that Require Step Therapy Effective 12/01/2017
 Medicare Part D Drugs that Require Step Therapy Effective 12/01/2017 Providers may call the Pharmacy Help Desk at 800-641-8921 for more information or questions about criteria. The formulary may change
Medicare Part D Drugs that Require Step Therapy Effective 12/01/2017 Providers may call the Pharmacy Help Desk at 800-641-8921 for more information or questions about criteria. The formulary may change
Updates to your prescription benefits
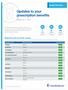 Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
FORMULARY UPDATES TO DENVER HEALTH MEDICAID CHOICE (DHMC) AND CHILD HEALTH PLAN PLUS (CHP+) PLANS
 FORMULARY UPDATES TO DENVER HEALTH MEDICAID CHOICE (DHMC) AND CHILD HEALTH PLAN PLUS (CHP+) PLANS DHMC/CHP+ may add or remove drugs from the formulary or make changes to restrictions on formulary drugs
FORMULARY UPDATES TO DENVER HEALTH MEDICAID CHOICE (DHMC) AND CHILD HEALTH PLAN PLUS (CHP+) PLANS DHMC/CHP+ may add or remove drugs from the formulary or make changes to restrictions on formulary drugs
