A randomized trial comparing the efficacy of cognitive behavioral therapy for bulimia nervosa delivered via telemedicine versus face-to-face $
|
|
|
- Lindsey Scott
- 5 years ago
- Views:
Transcription
1 Behaviour Research and Therapy 46 (2008) A randomized trial comparing the efficacy of cognitive behavioral therapy for bulimia nervosa delivered via telemedicine versus face-to-face $ James E. Mitchell a,b,, Ross D. Crosby a,b, Stephen A. Wonderlich a,b, Scott Crow c, Kathy Lancaster b, Heather Simonich a,b, Lorraine Swan-Kremeier a,b, Christianne Lysne a,b, Tricia Cook Myers a,b a Department of Clinical Neuroscience, University of North Dakota School of Medicine and Health Sciences, ND, USA b Neuropsychiatric Research Institute, 120 8th Street South, Box 1415, Fargo, ND 58107, USA c Department of Psychiatry, University of Minnesota Medical School, Minneapolis, MN, USA Received 2 July 2007; received in revised form 26 December 2007; accepted 4 February 2008 Abstract Objective: A major problem in the delivery of mental health services is the lack of availability of empirically supported treatment, particularly in rural areas. To date no studies have evaluated the administration of an empirically supported manual-based psychotherapy for a psychiatric condition via telemedicine. The aim of this study was to compare the relative efficacy and acceptability of a manual-based cognitive behavioral therapy (CBT) for bulimia nervosa (BN) delivered in person to a comparable therapy delivered via telemedicine. Method: One hundred twenty-eight adults meeting DSM-IV criteria for BN or eating disorder not otherwise specified with binge eating or purging at least once per week were recruited through referrals from clinicians and media advertisements in the targeted geographical areas. Participants were randomly assigned to receive 20 sessions of manualbased, CBT for BN over 16 weeks delivered either face-to-face (FTF-CBT) or via telemedicine (TV-CBT) by trained therapists. The primary outcome measures were binge eating and purging frequency as assessed by interview at the end of treatment, and again at 3- and 12-month follow-ups. Secondary outcome measures included other bulimic symptoms and changes in mood. Results: Retention in treatment was comparable for TV-CBT and FTF-CBT. Abstinence rates at end-of-treatment were generally slightly higher for FTF-CBT compared with TV-CBT, but differences were not statistically significant. FTF-CBT patients also experienced significantly greater reductions in eating disordered cognitions and interview-assessed depression. However, the differences overall were few in number and of marginal clinical significance. $ Funding for this study was provided by a grant funded jointly by the National Institute of Mental Health and the National Institute of Diabetes and Digestive and Kidney Diseases (R01-MHDK-58820), the National Institute of Mental Health (KO2 MH65919) and the Neuropsychiatric Research Institute. Corresponding author at. Neuropsychiatric Research Institute, 120 8th Street South, Box 1415, Fargo, ND 58107, USA. Tel.: ; fax: address: jmitchell@nrifargo.com (J.E. Mitchell) /$ - see front matter r 2008 Elsevier Ltd. All rights reserved. doi: /j.brat
2 582 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Conclusions: CBT for BN delivered via telemedicine was both acceptable to participants and roughly equivalent in outcome to therapy delivered in person. r 2008 Elsevier Ltd. All rights reserved. Keywords: Bulimia nervosa; Cognitive behavioral therapy; Telemedicine Introduction There is general consensus among researchers in the field of eating disorders that at this time cognitive behavioral therapy (CBT) is the treatment of choice for individuals with bulimia nervosa (BN) (Mitchell, Agras, & Wonderlich, 2007). Although undoubtedly not the final stage in the development of effective therapies for BN, CBT remains the most widely studied and the best-supported treatment for BN. Despite this finding there is considerable evidence that most patients who are treated for BN do not receive an empirically supported psychotherapy for their condition (Arnow, 1999). In a survey of psychologists, Mussell, Crosby, Knopke, Peterson, and Mitchell (2000) found that the vast majority of clinicians who said that at least 5% of their practice included eating disorders reported not using CBT as the treatment of choice, and only 21.7% reported any significant training experience in CBT for any condition. In another study (Crow, Mussell, Peterson, Knopke, & Mitchell, 1999), a cohort of 353 potential subjects who called an eating disorders research program requesting treatment were asked about prior therapy. Of these, 65.4% had received treatment before and 96.7% of these had received psychotherapy but only 6.9% reported that the treatment they received included even minimal elements of CBT. Most recently, von Ransom and Robinson (2006) found that clinicians who work with eating disorders reported that they prefered to tailor their treatment to the patient rather than choose an approach based on the level of empirical support. Therefore, although CBT may be the treatment of choice for these patients, many therapists working with BN patients choose not to use it, and do not know how to deliver it. Furthermore, most patients who have been treated for BN have not received it. A related problem is the lack of availability of empirically supported treatments for patients with BN and other forms of psychopathology in rural areas. This is particularly true in the region in which this study was conducted (e.g., North Dakota and Minnesota), where much of the population lives in smaller urban and rural settings. In attempting to identify ways to deliver therapies to this population, several possibilities exist. One would be to train therapists in these areas; however, this would be expensive and impractical and many therapists would not have the time or economic resources to undertake such training. Also, their skills would likely atrophy over time if they were not seeing a critical number of such patients. A second possibility would be to utilize a traveling therapist who would periodically go to various rural areas to provide treatment. However, this would typically be considered undesirable work and third party payors would not reimburse for travel time, resulting in a major financial disincentive. A third possibility, and the one we studied in this protocol, is to deliver therapy through new technologies such as telemedicine. Two prior studies have examined the utility of telemedicine in treating psychiatric patients. A modest study by Nelson, Barnard, and Cain (2003) assigned a series of 28 depressed children to in-person therapy or telemedicine therapy and found no evidence of a difference in outcomes. A second, larger study by Ruskin et al. (2004) was reported in which a series of 119 depressed patients were randomized to in-person versus telemedicine-delivered therapy. The therapy delivered was supportive psychotherapy, psycho-education and medication management. Again, no significant differences were found in outcome and both approaches were helpful. Although, several reports have detailed the use of psychotherapy via telemedicine (see for example, Frueh, Henderson, & Myrick, 2005; Cluver, Schuyler, Frueh, Brescia, & Arana, 2005; Griffiths, Blignault, & Yellowlees, 2006; Metropolitan Life Insurance Table, 1983; Passik et al., 2004; Shepherd et al., 2006; Ugarriza & Schmidt, 2006), to our knowledge there have been no studies testing telemedicine administration of an empirically supported manual-based psychotherapy for a psychiatric condition. In this research, we studied the relative efficacy and acceptability of a manual-based psychotherapy for BN, CBT, delivered in person by a
3 therapist who traveled to the local community, compared with CBT delivered via telemedicine wherein the treated subject never actually met the therapist in person. Method Participants This study was conducted at nine regions in eastern North Dakota and northwestern Minnesota (which adjoins North Dakota to the east). Participants were recruited in waves through mailings to local physicians and psychologists and through advertisements in the media. Recruitment took place between October 1999 and September This study was approved by institutional review boards at the University of North Dakota (Grand Forks, North Dakota) and MeritCare Health System (Fargo, North Dakota). Written informed consent was obtained from all participants. Participants were eligible for this study if they were at least 18 years of age, met DSM-IV criteria for BN (purging or non-purging subtype) or eating disorder-not otherwise specified (EDNOS) with one of the following: (1) DSM-IV criteria for BN except binge eating/purging at a minimum frequency of once per week; (2) DSM-IV criteria for BN with only subjective binge eating episodes. Participants were ineligible for the study if their body weight was less than 85% of ideal weight (Metropolitan Life Insurance Table, 1983), if they received a change in prescribed psychotropic medication in the previous 6 weeks, had ever received eight or more sessions of CBT, abused alcohol or drugs as defined by DSM-IV in the previous 6 months or were dependent in the previous 1 month, were pregnant, had a significant active medical illness that would jeopardize safe study participation (e.g., type I diabetes mellitus), had a significant risk of suicide as determined by a trained assessor, were actively psychotic, or had a current or past DSM-IV diagnosis of schizophrenia or bipolar disorder. Interventions J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Cognitive behavioral therapy The therapy used in this study was the manual-based CBT developed by Fairburn and colleagues (Fairburn & Cooper, 1993; Fairburn, Kirl, O Connor, & Cooper, 1986). This therapy has been used in a variety of trials including two large multi-center studies in the United States, one funded by the National Institute of Mental Health (Agras, Walsh, Fairburn, Wilson, & Kraemer, 2000) and one funded by the McKnight Foundation (Mitchell et al., 2002). The therapy consisted of 20 sessions delivered over a 16 weeks period. TV-CBT was delivered using a telemedicine system linking a regional healthcare system facility using T1 lines. Subjects interacted with the therapist only through telemedicine. Units were placed so as to mimic the interpersonal distance and height equality used in face-to-face (FTF) therapy. Rooms at distal sites were chosen for their privacy and lack of excessive noise. Therapists and assessors CBT was delivered by six doctoral-level psychologists with training and prior experience in delivering therapy with this manual. Training consisted of coursework, readings and supervised practice cases. All therapists treated both FTF-CBT and TV-CBT patients. Assessments were conduct by four masters or doctoral-level individuals all of whom had used the assessment instruments in previous studies. Weekly separate supervisory sessions were held with assessors and therapists and monitoring tapes were discussed. Treatment fidelity All therapy sessions were audiotaped. Sessions tapes were evaluated by the PI and feedback was provided to the therapists. In therapy supervision, each patient s progress was reviewed and therapists adherence to the treatment protocol was discussed. A random sample of patients tapes were audited and scored by alternative therapists. Detailed feedback on all tapes was provided to the PI and the therapists. The results of the therapy tape auditing and the process measures will be reported separately, and treatment fidelity was high.
4 584 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Assessments Individuals requesting information about the study called a toll-free number at the research center (the Neuropsychiatric Research Institute in Fargo) where they were given additional information about the study, screened via phone to see if they were likely to meet eligibility criteria, and scheduled for an informational meeting to be held in their geographic area within the next few weeks. Project staff, including one of the investigators and a research coordinator, would then travel to that site to hold an evening informational meeting. Participants were seen individually to obtain informed consent and were then scheduled to complete self-report measures and meet with an assessor, who would travel to that site to administer interviews. Eligibility for the study in terms of eating disorder diagnosis was determined using the Eating Disorder Examination (EDE) (Fairburn & Cooper, 1993). The EDE is an investigator-administered interview used to determine DSM-IV eating disorder diagnosis and assess current eating disorder symptoms. The EDE provides frequency measures of binge eating and compensatory behaviors, which were used as the primary measures of treatment outcome. The EDE also contains four subscales (Dietary Restraint, Eating Concerns, Shape Concerns and Weight Concerns) associated with core psychopathology of eating disorders. The validity and reliability of EDE have been well documented and the instrument has been used extensively in treatment outcome studies of BN. The EDE was administered at baseline, end of treatment, and at 3- and 12-month follow-ups. Subjects also rated the suitability of the therapy and the likelihood that they would be successful in the assigned therapy after three sessions. Comorbid DSM-IV Axis I disorders were determined using the Structured Clinical Interview for DSM-IV, Patient Edition (SCID-P) (First, Spitzer, Gibbon, & Williams, 1995). An addendum was added to the SCID-P to assess impulse control disorders. Standard questions were added to assess suicidality. The SCID-P was administered only at baseline. A self-assessment battery was administered at baseline, end-of-treatment, and 3- and 12-month follow-ups. This battery included the Medical Outcomes Study Short-Form 36 (SF-36) (Ware, Gandek, & The IQOLA Project Group, 1994) to measure social functioning, the Rosenberg Self-Esteem (RSE) scale (Rosenberg, 1965) to measure self-esteem, and the Hamilton Rating Scale for Depression (HAM-D) (Hamilton, 1960). The Beck Depression Inventory (BDI) (Beck, Ward, Mendelson, Mock, & Erbaugh, 1961) and a Binge-Purge Recall form were completed bi-weekly during treatment and at 3- and 12-month follow-ups. Subjects also rated the suitability of the therapy and the likelihood that they would be successful in the assigned therapy after three sessions. Data were obtained on other psychiatric treatments received at the 3- and 12-month follow-up assessments using the McKnight Longitudinal Follow-up for Eating Disorders Interview (M-FED), an instrument used in several multi-center BN treatment and longitudinal studies (see for example, Crow, Agras, Halmi, Mitchell, & Kraemer, 2002; Mitchell et al., 2002). The Working Alliance Inventory (WAI) (Horvath, 1982; Horvath & Greenberg, 1989) was used to study the therapeutic relationship. The WAI was completed by both participant (WAI-C) and therapist (WAI-T) at weeks 2, 8 and 16 (end-of-treatment). The Hill Process Rating System (Hill, 1978, 1986, 1989, 1992) was used to assess treatment integrity and process. The HPRS contains measures of overt and covert behavior variables. The WAI data and the HPRS data will be the subject of a separate report. Randomization Participants were randomized to receive CBT in person (FTF-CBT) or via telemedicine (TV-CBT). The randomization sequence was generated by an independent statistician. Randomization was stratified by eating disorder diagnosis (BN vs. eating disorder-not otherwise specified) and antidepressant medication history (never/previous vs. current) to achieve balance on these variables, resulting in four allocation strata. Within each stratum, randomization was performed in blocks of four to control for potential changes in participant characteristics or study conduct (e.g., personnel changes) over time. Treatment assignment codes were concealed from study personnel until time of randomization and assessors were blinded to therapy administration technique throughout, although this was at times difficult to achieve because of statements made about this therapy when being assessed.
5 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Statistical analysis Power calculations for this study were based upon the methods described by Hedeker and colleagues (Hedeker, Gibbons, & Waternaux, 1999) for two-group longitudinal designs with attrition. Based upon a twotailed a of.05 and an attrition rate of 15% during therapy and 10% at follow-up, a randomized sample size of 65 per group (130 total) would provide a power of.80 to detect a difference of.50 standard deviations between FTF-CBT and TV-CBT in binge eating and purging frequencies (Hedeker et al., 1999). The proportion of participants completing EDE assessments at end-of-treatment, 3- and 12-month followups were compared between treatment conditions using Fisher s Exact test. Treatment groups were compared at baseline on demographic and clinical characteristics using Fisher s Exact test for dichotomous variables, independent samples t-tests for symmetrically distributed continuous measures, and Mann Whitney nonparametric tests for binge eating and purging frequencies. All primary analyses were based upon intention-to-treat and were conducted using SPSS for Windows Version 15.0 (SPSS Inc., Chicago, Illinois) or SAS Version 8.0 (SAS Institute, Cary, North Carolina). Primary outcome variables were abstinence rates from binge eating and purging and binge-purge episode frequencies as determined from the EDE at end-of-treatment and 3- and 12-month follow-ups. Treatment groups were compared on rates of abstinence from objective binge eating, purging, and combined binge eating/purging at end-of-treatment, 3- and 12-month follow-up using Fisher s Exact test. Mixed-effected linear regression models (Hedeker, Gibbons, & Waternaux, 2006) were used to compare FTF-CBT and TV-CBT participants on binge eating and purging episode frequencies at end-of-treatment, and 3- and 12-month follow-up controlling for baseline levels, with assessment points coded as class variables to allow post-hoc comparisons between groups at each assessment. Analyses were performed on log-transformed frequencies due to positive skew, with raw (i.e., untransformed) means and standard deviations reported in tables. Comparisons between groups were based upon the main effect for group with a two-tailed a of.05. Post-hoc comparisons between groups at specific time points were based upon a two-tailed Bonferroni-corrected a of.017 (.05/3). Secondary measures of outcome included EDE scale scores, SF-36, RSE, and HAM-D were analyzed with mixed effects regression models comparable to those described above. Analyses for BDI and binge/purge frequencies from the Binge-Purge Recall were analyzed with a mixed effects curvilinear trend model (Hedeker et al., 2006) controlling for baseline assessment, which included a random intercept and linear and quadratic trend components. This model allowed for the comparison between FTF-CBT and TV-CBT both in overall level and trajectories over time. Results Study flow Fig. 1 presents the participant flow through the study. The proportion of participants completing EDE assessments did not differ between TV-CBT and FTF-CBT at end of treatment (Fisher s Exact p ¼.467), 3- month follow-up (Fisher s Exact p ¼.480), or 12-month follow-up (Fisher s Exact p ¼.590). Participant characteristics at baseline Participants in the treatment groups were similar in baseline sociodemographic and clinical characteristics (Table 1). Most participants were female and Caucasian, with an average age in the late 20 s. The only significantly difference at baseline between treatment groups was in terms of current mood disorder, where 36% of TV-CBT participants met criteria compared with only 20% of FTF-CBT participants (Fisher s Exact p ¼.05). A minority of participants reported laxative (n ¼ 31, 24.2%) or diuretic use (n ¼ 10, 7.8%) at baseline. Treatment exposure A participant was considered to have completed a treatment session if they participated in therapy for at least 30 min. The average length of completed sessions was 50.5 min (SD ¼ 7.4). The range of completed
6 586 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Assessed for Eligibility (N = 142) Randomized (n = 128) Excluded (n = 14) 5 failed to meet BN/EDNOS criteria 7 alcohol abuse 1 drug abuse 1 lifetime bipolar disorder Assigned to FTF-CBT (n = 66) Did not receive treatment (n = 8) Received 1-5 sessions (n = 6) Received 6-10 sessions (n = 7) Received sessions (n = 5) Received sessions (n = 40) Assigned to TV-CBT (n = 62) Did not receive treatment (n = 4) Received 1-5 sessions (n = 4) Received 6-10 sessions (n = 7) Received sessions (n = 10) Received sessions (n = 37) End-of-Treatment Assessment (n = 39, 59.1%) End-of-Treatment Assessment (n = 41, 66.1%) 3-Month Follow-Up (n = 35, 53.0%) 3-Month Follow-Up (n = 37, 59.7%) 12-Month Follow-Up (n = 25, 37.9%) 12-Month Follow-Up (n = 27, 43.5%) Included in Primary Analyses (n = 66) Included in Primary Analyses (n = 62) Fig. 1. Flowchart of study participants. treatment sessions for FTF-CBT and TV-CBT participants is presented in Fig. 1. The mean number of completed sessions for FTF-CBT participants was 13.4 (SD ¼ 7.1) compared with 14.2 (SD ¼ 6.0) for TV- CBT participants (t ¼.68; df ¼ 126; p ¼.495). Primary outcomes Abstinence Abstinence rates for objective binge eating, purging (vomiting, laxative abuse, and diuretic abuse), and combined objective binge eating and purging based upon the EDE interview are presented in Table 2. Abstinence was defined as none of these behaviors reported in the previous 28 days. Abstinence rates were
7 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Table 1 Baseline demographic and clinical characteristics for participants receiving FTF-CBT and TV-CBT Characteristic Treatment group FTF-CBT (n ¼ 66) TV-CBT (n ¼ 62) n % n % Current diagnosis Bulimia nervosa Eating disorder not otherwise specified Comorbid disorders Lifetime mood disorder Current mood disorder a Lifetime anxiety disorder Current anxiety disorder Lifetime substance abuse/dependence Current anti-depressant medication Female Caucasian Post high school education Mean SD Mean SD Age Body mass index (kg/m 2 ) Objective binge episodes previous 28 days b Vomiting episodes previous 28 days c a TV-CBT4FTF-CBT: Fisher s Exact p ¼.050. b Binge eating episode frequency reported as too great to calculate (n ¼ 1) recoded to maximum reported value (132). c Vomiting episode frequency reported as too great to calculate (n ¼ 3) recoded to maximum reported value (132). determined in three different ways to allow comparisons to previous reports: (1) intention-to-treat based upon last observation carried forward (LOCF) replaces missing observations with the last valid observation for that participant; (2) intention-to-treat based upon baseline observation carried forward (BOCF) replaces missing observations with the baseline assessment for that participant (see for example, Agras et al., 2000); (3) completer analysis calculates rates of remission using only the valid observations for a given assessment (see for example, Bakke, Mitchell, Wonderlich, & Erickson, 2001). Abstinence rates from objective binge eating, purging, and combined binge eating/purging were generally slightly higher for FTF-CBT (with the exception of OBE based upon BOCF at 3- and 12-month follow-ups and OBE+Purging based upon BOCF at 12-month follow-up) compared with TV-CBT. However, none of these differences in abstinence rates approached statistical significance, regardless of how abstinence was calculated. Binge eating and purging frequencies Significant differences were found between FTF-CBT and TV-CBT on the frequency of binge eating episodes (F ¼ 6.76; df ¼ 1, 79; p ¼.011) (see Table 2). Fig. 2 shows changes in binge eating and purging frequencies over time. Of note, response in the FTF-CBT group appear to occur rapidly, while response in the TV-CBT group appear delayed. Post-hoc comparisons revealed that purging frequency at the 12-month follow-up was significantly lower for the FTF-CBT group (t ¼ 2.59; df ¼ 118; p ¼.011). No differences were found between groups in the frequency of binge eating episodes (F ¼ 2.66; df ¼ 1, 79; p ¼.107). There was evidence of some relapse/deterioration between 3 and 12 months follow-up. However, FTF-CBT participants report significantly lower levels (but comparable trajectories) for both binge eating (F ¼ 9.10; df ¼ 1, 113; p ¼.003) and purging (F ¼ 7.79; df ¼ 1, 113; p ¼.006). While binge eating rates between FTF-CBT and
8 588 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Table 2 Primary outcomes: abstinence rates and binge eating and purging rates by group from EDE interview Outcome variable Treatment group FTF-CBT TV-CBT Baseline (n ¼ 66) End of Tx (n ¼ 39) 3-month FU (n ¼ 35) 12-month FU (n ¼ 25) Baseline (n ¼ 62) End of Tx (n ¼ 41) 3-month FU (n ¼ 37) 12-month FU (n ¼ 27) n % n % n % n % n % n % n % n % Abstinence: LOCF OBE Purging a OBE and Purging a Abstinence: BOCF OBE Purging a OBE & Purging a Abstinence: completer OBE Purging a OBE and Purging a Mean SD Mean SD Mean SD Mean SD Mean SD Mean SD Mean SD Mean SD OBE episodes Purging episodes Abstinence: no behaviors reported in previous 28 days based upon EDE interview. OBE: objective binge-eating episode; LOCF: last observation carried forward; BOCF: baseline observation carried forward. a Purging is defined as vomiting, laxative abuse, and diuretic abuse. TV-CBT participants were comparable at 3- and 12-month follow-up, differences in purging frequencies between groups at follow-up assessment were maintained. Secondary outcomes Table 3 presents means and standard deviations of secondary outcomes across assessment times by group. No differences between groups were found for EDE Restraint and Weight Concern scales, Rosenberg Self- Esteem, or SF-36 scores. However, FTF-CBT participants reported significantly greater reductions from baseline in EDE Eating Concerns (F ¼ 6.5; df ¼ 1, 79; p ¼.012), with significant post-hoc differences at 3- month follow-up (t ¼ 3.09, df ¼ 118, p ¼.003). There was also a significant group difference in EDE Shape Concerns (F ¼ 4.66, df ¼ 1, 79; p ¼.030), with significant post-hoc differences at 12-month follow-up. The FTF-CBT also resulted in greater reductions in Ham-D scores (F ¼ 4.53, df ¼ 1, 72, p ¼.037, with significant post-hoc differences between groups at end-of-treatment (t ¼ 4.35, df ¼ 105, p ¼.008). No differences were found between groups on level or pattern of change in BDI scores (Fig. 3). The selfrated suitability of treatment and likelihood of response were not different between groups. Discussion This randomized trial, comparing CBT for BN delivered via telemedicine versus in person, demonstrated that telemedicine-delivered CBT was both acceptable to patients and roughly equivalent in outcome to therapy delivered in person. The strengths of this study include a relatively large sample size, careful training and supervision of assessors and therapists, the use of a manual-based approach for psychotherapy and the broadening of inclusion criteria to include subthreshhold cases that are frequently seen in clinical practice.
9 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Mean Binge Eating Episodes per Week TV-CBT (n = 62) FTF-CBT (n = 66) mo 12 mo 9 8 Mean Purging Episodes per Week TV-CBT (n = 62) FTF-CBT (n = 66) mo 12 mo Fig. 2. Binge eating and purging recall by group.
10 590 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Table 3 Secondary outcomes measures by group Outcome variable Treatment group FTF-CBT TV-CBT Baseline (n ¼ 66) End of Tx (n ¼ 39) 3-month FU (n ¼ 35) 12-month FU (n ¼ 25) Baseline (n ¼ 62) End of Tx (n ¼ 41) 3-month FU (n ¼ 37) 12-month FU (n ¼ 27) Mean SD Mean SD Mean SD Mean SD Mean SD Mean SD Mean SD Mean SD EDE Restraint Eating concerns Shape concerns Weight concerns Hamilton depression Rosenberg self-esteem SF-36 Physical component Mental component Mean Beck Depression Inventory Score TV-CBT (n = 62) FTF-CBT (n = 66) mo 12 mo Fig. 3. Beck Depression Inventory scores by group. One finding in this study was the substantial drop-out rate, which is unfortunately common in BN treatment trials but was particularly important here. This higher than anticipated drop-out rate likely reduced the statistical power of this study, thereby reducing our ability to detect differences in outcome between TV-CBT and FTF-CBT. In this trial, the drop-out rate may be attributable in part to the nature of the therapy delivery. First therapists in FTF-CBT were traveling to distal sites at preset times and telemedicine visits were at times
11 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) difficult to arrange; consequently there was very little flexibility in scheduling. If scheduling conflicts arose sessions could not always be rescheduled. The fallback was usually to do a brief therapy session by phone. Second, there were technical problems at times, which also impacted adversely on therapy involving the telemedicine equipment. Third, weather conditions during winter in the upper Midwest were problematic and at times sessions would have to be canceled because it was deemed unsafe for the research personnel to travel across long distances. None-the-less the abstinence rates at end-of-treatment were very similar to the rates in two recent large multi-center trials using CBT (17, 18: ITT abstinence rate McKnight trial ¼ 31%, NIMH trial ¼ 29%, this trial ¼ 28%; completer abstinence rates: McKnight trial ¼ 41%; NIMH trial ¼ 40%; this trial ¼ 41%). Anecdotally, the therapists in the study were more concerned about doing therapy via telemedicine versus in person than the subjects early on in the study. However, in general they noted that after a few sessions with each patient this did not seem to be a particularly important issue. The study also demonstrated a number of logistical issues and practical considerations that need to be addressed when using telemedicine to deliver psychotherapy. We have discussed some of these in detail in prior publications (Bakke et al., 2001; Mitchell, Swan-Kremeier, & Myers, 2003). First, in terms of the use of the equipment, lighting must be addressed, as well as monitor and chair placement so as not to have the intervention seem dominated by one party, or overly distant. Also, the rooms where telemedicine equipment is used at distal sites are often not optimal for psychotherapy, and not uncommonly are conference rooms. For this reason some of the rooms used were less than optimal. Another issue to consider is that some insurance companies will now reimburse for telemedicine-delivered psychotherapy and other psychiatric therapies in some states, but not in others. This remains in transition. The problem of therapy homework can usually be solved by simply faxing materials from the site to the center. Of particular concern are issues related to suicidality, in that the therapist may discover that the patient at the distal site is in need of some emergency intervention. In this particular study, we dealt with this by always having a research coordinator on site trained to assist the therapist in handling these emergencies; however, if the system were used in routine clinical care, some sort of emergency backup would need to be in place. The results of the study suggest that a manual-based form of psychotherapy for a specific psychiatric disorder can be effectively delivered via telemedicine. We believe this has implications for delivery of other manual-based, empirically supported psychotherapies for other psychiatric conditions, and that this may help to address the lack of dissemination of such therapies, particularly to rural areas. References Agras, W. S., Walsh, T., Fairburn, C. B., Wilson, G. T., & Kraemer, H. C. (2000). A multicenter comparison of cognitive behavioral therapy and interpersonal psychotherapy for bulimia nervosa. Archives of General Psychiatry, 57, Arnow, B. A. (1999). Why are empirically supported treatments for bulimia nervosa underutilized and what can we do about it? Journal of Clinical Psychology, 55, Bakke, B., Mitchell, J. E., Wonderlich, S., & Erickson, R. (2001). Administering cognitive behavioral therapy for bulimia nervosa via telemedicine in rural settings. International Journal of Eating Disorders, 30, Beck, A. T., Ward, C. M., Mendelson, M., Mock, J. E., & Erbaugh, J. K. (1961). An inventory for measuring depression. Archives of General Psychiatry, 44, Cluver, J. S., Schuyler, D., Frueh, B. C., Brescia, F., & Arana, G. W. (2005). Remote pspychotherapy for terminally ill cancer patients. Journal of Telemedicine and Telecare, 11, Crow, S., Agras, S., Halmi, K., Mitchell, J. E., & Kraemer, H. (2002). Full syndromal versus subthreshold anorexia nervosa, bulimia nervosa, and binge eating disorder: A multicenter study. International Journal of Eating Disorders, 232, Crow, S., Mussell, M. P., Peterson, C., Knopke, A., & Mitchell, J. (1999). Prior treatment received by patients with bulimia nervosa. International Journal of Eating Disorders, 25, Fairburn, C. G., & Cooper, Z. (1993). The eating disorders examination. In C. G. Fairburn, & G. T. Wilson (Eds.), Binge eating: Nature, assessment and treatment (12th ed, pp ). New York: Guilford Press. Fairburn, C. G., Kirl, H., O Connor, M., & Cooper, P. J. (1986). A comparison of two psychological treatments for bulimia nervosa. Behaviour Research and Therapy, 24, First, M. G., Spitzer, R. L., Gibbon, M., & Williams, J. B. (1995). Structured Clinical Interview for DSM-IV Axis I Disorders Patient edition (SCID ¼ I/P, version 2). New York: Biometrics Research Department. Frueh, B. C., Henderson, S., & Myrick, H. (2005). Telehealth service delivery for persons with alcoholism. Journal of Telemedicine and Telecare, 11,
12 592 J.E. Mitchell et al. / Behaviour Research and Therapy 46 (2008) Griffiths, L., Blignault, I., & Yellowlees, P. (2006). Telemedicine as a means of delivering cognitive behavioral therapy to rural and remote mental health clients. Journal of Telemedicine and Telecare, 12, Hamilton, M. (1960). A rating scale for depression. Journal of Neurology Neurosurgery and Psychiatry, 23, Hedeker, D., Gibbons, R. D., & Waternaux, C. (1999). Sample size estimation for longitudinal designs with attrition: Comparing timerelated contrasts between two groups. Journal of Educational and Behavioral Statistics, 24, Hedeker, D., Gibbons, R. D., & Waternaux, C. (2006). Sample size estimation for longitudinal designs with attrition: Comparing timerelated contrasts between two groups. Journal of Educational and Behavioral Statistics, 24, Hill, C. E. (1978). Development of a counselor verbal response category system. Journal of Counseling Psychology, 25, Hill, C. E. (1986). An overview of the Hill counselor and client verbal response modes category systems. In L. S. Greenberg, & W. M. Pinsof (Eds.), The psychotherapeutic process: A research handbook (pp ). New York: Guilford Press. Hill, C. E. (1989). In C. E. Hill (Ed.), Psychologist techniques and client outcomes: Eight cases of brief psychotherapy. Newbury Park, CA: Sage. Hill, C. E. (1992). An overview of four measures developed to test the Hill process model: Psychologist intentions, psychologist response modes, client reactions, and client behaviors. Journal of Counseling and Development, 70, Horvath, A. O. (1982). Working Alliance Inventory (revised). Instructional Psychology Research Group 82(1). Burnaby, British Columbia: Simon Fraser University. Horvath, A. O., & Greenberg, L. S. (1989). Development and validation of the working alliance inventory. Journal of Counseling Psychology, 36, Metropolitan Life Insurance Table (1983). Height and weight tables. Statistical Bulletin, 64, 3 9. Mitchell, J. E., Agras, S., & Wonderlich, S. (2007). Treatment of bulimia nervosa. Where are we and where are we going? International Journal of Eating Disorders, 40, Mitchell, J. E., Halmi, K., Wilson, G., Agras, S., Kraemer, H., & Crow, S. (2002). A randomized secondary treatment study of women with bulimia nervosa who fail to respond to CBT. International Journal of Eating Disorders, 32, 271. Mitchell, J. E., Swan-Kremeier, L., & Myers, T. (2003). Delivering psychotherapy to patients with bulimia nervosa via telemedicine. Eating Disorders Review, 11, Mussell, M. P., Crosby, R. D., Knopke, A. J., Peterson, C. B., & Mitchell, J. E. (2000). Utilization of empirically supported psychotherapy treatments for individuals with eating disorders: A survey of psychologists. International Journal of Eating Disorders, 22, Nelson, El., Barnard, M., & Cain, S. (2003). Treating childhood depression over videoconferencing. Telemedicine Journal and E-Health, 9, Passik, S. D., Kirsh, K. L., Leibee, S., Kaplan, L. S., Love, C., Napier, E., et al. (2004). A feasibility study of dignity psychotherapy delivered via telemedicine. Palliat Support Care, 2, Rosenberg, J. (1965). Society and the adolescent self-image. Princeton, NJ: Princeton University Press. Ruskin, P. E., Silver-Aylaian, M., Kling, M. A., Reed, S. A., Bradham, D. D., Hebel, J. R., et al. (2004). Treatment outcomes in depression: Comparison of remote treatment through telepsychiatry to in-person treatment. American Journal of Psychiatry, 161, Shepherd, L., Goldstein, D., Whitford, H., Thewes, B., Brummell, V., & Hicks, M. (2006). The utility of videoconferencing to provide innovative delivery of psychological treatment for rural cancer patients: Results of a pilot study. Journal of Pain and Symptom Management, 32, Ugarriza, D. N., & Schmidt, L. (2006). Telecare for women with postpartum depression. Journal of Psychosocial Nursing and Mental Health Services, 44, von Ransom, K. M., & Robinson, K. E. (2006). Who is providing what type of psychotherapy to eating disorder clients? A survey. International Journal of Eating Disorders, 39, Ware, J. E., Gandek, B., & The IQOLA Project Group (1994). The SF-36 Health Survey: Development and use in mental health research and the IQOLA Project. International Journal of Mental Health, 23,
Eating Disorders: Clinical Features, Comorbidity, and Treatment
 Eating Disorders: Clinical Features, Comorbidity, and Treatment Carol B. Peterson, PhD Associate Professor Eating Disorders Research Program Department of Psychiatry University of Minnesota peter161@umn.edu
Eating Disorders: Clinical Features, Comorbidity, and Treatment Carol B. Peterson, PhD Associate Professor Eating Disorders Research Program Department of Psychiatry University of Minnesota peter161@umn.edu
The delineation of patient characteristics that usefully
 Article Outcome Predictors for the Cognitive Behavior Treatment of Bulimia Nervosa: Data From a Multisite Study W. Stewart Agras, M.D. Scott J. Crow, M.D. Katherine A. Halmi, M.D. James E. Mitchell, M.D.
Article Outcome Predictors for the Cognitive Behavior Treatment of Bulimia Nervosa: Data From a Multisite Study W. Stewart Agras, M.D. Scott J. Crow, M.D. Katherine A. Halmi, M.D. James E. Mitchell, M.D.
NIH Public Access Author Manuscript Behav Res Ther. Author manuscript; available in PMC 2012 October 1.
 NIH Public Access Author Manuscript Published in final edited form as: Behav Res Ther. 2011 October ; 49(10): 714 717. doi:10.1016/j.brat.2011.06.006. Ecological Momentary Assessment of Bulimia Nervosa:
NIH Public Access Author Manuscript Published in final edited form as: Behav Res Ther. 2011 October ; 49(10): 714 717. doi:10.1016/j.brat.2011.06.006. Ecological Momentary Assessment of Bulimia Nervosa:
DSM-IV Threshold Versus Subthreshold Bulimia Nervosa
 REGULAR ARTICLE DSM-IV Threshold Versus Subthreshold Bulimia Nervosa Daniel le Grange, PhD 1 * Roslyn B. Binford, PhD 1 Carol B. Peterson, PhD 2 Scott J. Crow, MD 2 Ross D. Crosby, PhD 3 Marjorie H. Klein,
REGULAR ARTICLE DSM-IV Threshold Versus Subthreshold Bulimia Nervosa Daniel le Grange, PhD 1 * Roslyn B. Binford, PhD 1 Carol B. Peterson, PhD 2 Scott J. Crow, MD 2 Ross D. Crosby, PhD 3 Marjorie H. Klein,
Mild, moderate, meaningful? Examining the psychological and functioning correlates of DSM-5 eating disorder severity specifiers
 Received: 9 August 2016 Revised: 14 April 2017 Accepted: 17 April 2017 DOI: 10.1002/eat.22728 ORIGINAL ARTICLE Mild, moderate, meaningful? Examining the psychological and functioning correlates of DSM-5
Received: 9 August 2016 Revised: 14 April 2017 Accepted: 17 April 2017 DOI: 10.1002/eat.22728 ORIGINAL ARTICLE Mild, moderate, meaningful? Examining the psychological and functioning correlates of DSM-5
ORIGINAL ARTICLE. A Multicenter Comparison of Cognitive-Behavioral Therapy and Interpersonal Psychotherapy for Bulimia Nervosa
 ORIGINAL ARTICLE A Multicenter Comparison of Cognitive-Behavioral Therapy and Interpersonal Psychotherapy for Bulimia Nervosa W. Stewart Agras, MD; B. Timothy Walsh, MD; Christopher G. Fairburn, MD; G.
ORIGINAL ARTICLE A Multicenter Comparison of Cognitive-Behavioral Therapy and Interpersonal Psychotherapy for Bulimia Nervosa W. Stewart Agras, MD; B. Timothy Walsh, MD; Christopher G. Fairburn, MD; G.
Does Interpersonal Therapy Help Patients With Binge Eating Disorder Who Fail to Respond to Cognitive-Behavioral Therapy?
 Journal of Consulting and Clinical Psychology 1995, Vol. 63, No. 3, 356-360 Copyright 1995 by the American Psychological Association, Inc. 0022-006X/95/S3.00 Does Interpersonal Therapy Help Patients With
Journal of Consulting and Clinical Psychology 1995, Vol. 63, No. 3, 356-360 Copyright 1995 by the American Psychological Association, Inc. 0022-006X/95/S3.00 Does Interpersonal Therapy Help Patients With
Internet-based interventions for eating disorders in adults: a systematic review
 Dölemeyer et al. BMC Psychiatry 2013, 13:207 RESEARCH ARTICLE Open Access Internet-based interventions for eating disorders in adults: a systematic review Ruth Dölemeyer 1,2*, Annemarie Tietjen 1, Anette
Dölemeyer et al. BMC Psychiatry 2013, 13:207 RESEARCH ARTICLE Open Access Internet-based interventions for eating disorders in adults: a systematic review Ruth Dölemeyer 1,2*, Annemarie Tietjen 1, Anette
State Self-Esteem Ratings in Women with Bulimia Nervosa and Bulimia Nervosa in Remission
 REGULAR ARTICLE State Self-Esteem Ratings in Women with and in Remission Karen A. Daley, MPH, MS 1 David C. Jimerson, MD 2 Todd F. Heatherton, PhD 3 Eran D. Metzger, MD 2 Barbara E. Wolfe, PhD 1 * ABSTRACT
REGULAR ARTICLE State Self-Esteem Ratings in Women with and in Remission Karen A. Daley, MPH, MS 1 David C. Jimerson, MD 2 Todd F. Heatherton, PhD 3 Eran D. Metzger, MD 2 Barbara E. Wolfe, PhD 1 * ABSTRACT
Comparison of DSM-IV Versus Proposed DSM-5 Diagnostic Criteria for Eating Disorders: Reduction of Eating Disorder Not Otherwise Specified and Validity
 CE ACTIVITY Comparison of DSM-IV Versus Proposed DSM-5 Diagnostic Criteria for Eating Disorders: Reduction of Eating Disorder Not Otherwise Specified and Validity Pamela K. Keel, PhD 1 * Tiffany A. Brown,
CE ACTIVITY Comparison of DSM-IV Versus Proposed DSM-5 Diagnostic Criteria for Eating Disorders: Reduction of Eating Disorder Not Otherwise Specified and Validity Pamela K. Keel, PhD 1 * Tiffany A. Brown,
Treatment Quad Cities Eating Disorders Consortium
 Treatment Quad Cities Eating Disorders Consortium James E. Mitchell, MD UND School of Medicine and Health Sciences Neuropsychiatric Research Institute ANOREXIA NERVOSA BULIMIA NERVOSA BINGE EATING DISORDER
Treatment Quad Cities Eating Disorders Consortium James E. Mitchell, MD UND School of Medicine and Health Sciences Neuropsychiatric Research Institute ANOREXIA NERVOSA BULIMIA NERVOSA BINGE EATING DISORDER
Maintenance Treatment for Anorexia Nervosa: A Comparison of Cognitive Behavior Therapy and Treatment as Usual
 REGULAR ARTICLE Maintenance Treatment for Anorexia Nervosa: A Comparison of Cognitive Behavior Therapy and Treatment as Usual Jacqueline C. Carter, PhD 1,2 * Traci L. McFarlane, PhD 1,2 Carmen Bewell,
REGULAR ARTICLE Maintenance Treatment for Anorexia Nervosa: A Comparison of Cognitive Behavior Therapy and Treatment as Usual Jacqueline C. Carter, PhD 1,2 * Traci L. McFarlane, PhD 1,2 Carmen Bewell,
Counseling College Women Experiencing Eating Disorder Not Otherwise Specified: A Cognitive Behavior Therapy Model
 Counseling College Women Experiencing Eating Disorder Not Otherwise Specified: A Cognitive Behavior Therapy Model Sarina: 1. Although the Counseling College Women article suggests utilizing CBT to treat
Counseling College Women Experiencing Eating Disorder Not Otherwise Specified: A Cognitive Behavior Therapy Model Sarina: 1. Although the Counseling College Women article suggests utilizing CBT to treat
Eating Disorders Detection and Treatment. Scott Crow, M.D. Professor of Psychiatry University of Minnesota Chief Research Officer The Emily Program
 Eating Disorders Detection and Treatment Scott Crow, M.D. Professor of Psychiatry University of Minnesota Chief Research Officer The Emily Program Obesity Trends* Among U.S. Adults BRFSS, 1990, 1995, 2005
Eating Disorders Detection and Treatment Scott Crow, M.D. Professor of Psychiatry University of Minnesota Chief Research Officer The Emily Program Obesity Trends* Among U.S. Adults BRFSS, 1990, 1995, 2005
Moderator Introduction
 DBT as a Stand-Alone or Adjunctive Treatment: Efficacy and Clinical Applications www.behavioraltech.org Moderator Introduction Alexis Karlson, MSSW Director of Business Operations Visit www.behavioraltech.org
DBT as a Stand-Alone or Adjunctive Treatment: Efficacy and Clinical Applications www.behavioraltech.org Moderator Introduction Alexis Karlson, MSSW Director of Business Operations Visit www.behavioraltech.org
Metacognitive therapy for generalized anxiety disorder: An open trial
 Journal of Behavior Therapy and Experimental Psychiatry 37 (2006) 206 212 www.elsevier.com/locate/jbtep Metacognitive therapy for generalized anxiety disorder: An open trial Adrian Wells a,, Paul King
Journal of Behavior Therapy and Experimental Psychiatry 37 (2006) 206 212 www.elsevier.com/locate/jbtep Metacognitive therapy for generalized anxiety disorder: An open trial Adrian Wells a,, Paul King
Developing a new treatment approach to binge eating and weight management. Clinical Psychology Forum, Number 244, April 2013.
 Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
NICE UPDATE - Eating Disorders: The 2018 Quality Standard. Dr A James London 2018
 NICE UPDATE - Eating Disorders: The 2018 Quality Standard Dr A James London 2018 Background Estimated number of people aged 16 years or older with eating disorders in England Description Percentage of
NICE UPDATE - Eating Disorders: The 2018 Quality Standard Dr A James London 2018 Background Estimated number of people aged 16 years or older with eating disorders in England Description Percentage of
The Current Status of Treatment for Anorexia Nervosa and Bulimia Nervosa
 The Current Status of Treatment for Anorexia Nervosa and Bulimia Nervosa David B. Herzog Martin B. Keller Michael Strober Christine Yeh Sung-Yun Pai (Accepted 1 March 1991) A survey investigating the current
The Current Status of Treatment for Anorexia Nervosa and Bulimia Nervosa David B. Herzog Martin B. Keller Michael Strober Christine Yeh Sung-Yun Pai (Accepted 1 March 1991) A survey investigating the current
Using Family-Based Treatments for Adolescent Eating Disorders: Empirical Support for Efficacy and Dissemination
 Using Family-Based Treatments for Adolescent Eating Disorders: Empirical Support for Efficacy and Dissemination Treatment Modalities for Eating Disorders: Consensus and Controversy Jerusalem, Israel Feb
Using Family-Based Treatments for Adolescent Eating Disorders: Empirical Support for Efficacy and Dissemination Treatment Modalities for Eating Disorders: Consensus and Controversy Jerusalem, Israel Feb
Mindfulness Action-Based Cognitive Behavioural Therapy for Concurrent Binge Eating Disorder and Substance Use Disorders
 Mindfulness Action-Based Cognitive Behavioural Therapy for Concurrent Binge Eating Disorder and Substance Use Disorders Leah Shapira, M.A. Christine M. Courbasson, Ph.D., C.Psych Yasunori Nishikawa, Hon.
Mindfulness Action-Based Cognitive Behavioural Therapy for Concurrent Binge Eating Disorder and Substance Use Disorders Leah Shapira, M.A. Christine M. Courbasson, Ph.D., C.Psych Yasunori Nishikawa, Hon.
New Directions, a psycho-educational program for adolescents with eating disorders: Stage two in a multi-step program evaluation
 New Directions, a psycho-educational program for adolescents with eating disorders: Stage two in a multi-step program evaluation Authors: Mary Kaye Lucier MSW, RSW, Executive Director, Bulimia Anorexia
New Directions, a psycho-educational program for adolescents with eating disorders: Stage two in a multi-step program evaluation Authors: Mary Kaye Lucier MSW, RSW, Executive Director, Bulimia Anorexia
Is laxative misuse associated with binge eating? Examination of laxative misuse among individuals seeking treatment for eating disorders
 Received: 3 March 2017 Revised: 13 July 2017 Accepted: 13 July 2017 DOI: 10.1002/eat.22745 BRIEF REPORT Is laxative misuse associated with binge eating? Examination of laxative misuse among individuals
Received: 3 March 2017 Revised: 13 July 2017 Accepted: 13 July 2017 DOI: 10.1002/eat.22745 BRIEF REPORT Is laxative misuse associated with binge eating? Examination of laxative misuse among individuals
Contents. Eating Disorders: Introduction. Who Gets Eating Disorders? What is Anorexia Nervosa?
 Contents Eating Disorders: Introduction Who Gets Eating Disorders? What is Anorexia Nervosa? Physical and Psychological Effects What is Bulimia Nervosa? Physical Effects What is Eating Disorders Not Otherwise
Contents Eating Disorders: Introduction Who Gets Eating Disorders? What is Anorexia Nervosa? Physical and Psychological Effects What is Bulimia Nervosa? Physical Effects What is Eating Disorders Not Otherwise
TELEPSYCHOLOGY FOR THE PSYCHOLOGIST IN PRIVATE PRACTICE
 TELEPSYCHOLOGY FOR THE PSYCHOLOGIST IN PRIVATE PRACTICE Dr. Madalina Sucala Icahn School of Medicine at Mount Sinai Department of Oncological Sciences OUTLINE Video conferencing as a delivery method Assessment
TELEPSYCHOLOGY FOR THE PSYCHOLOGIST IN PRIVATE PRACTICE Dr. Madalina Sucala Icahn School of Medicine at Mount Sinai Department of Oncological Sciences OUTLINE Video conferencing as a delivery method Assessment
Disorders and Symptoms
 Eating Disorders Eating disorders is the term used to describe a category of mental illnesses involving disordered eating and weight problems. This category can then generally be separated into four main
Eating Disorders Eating disorders is the term used to describe a category of mental illnesses involving disordered eating and weight problems. This category can then generally be separated into four main
Eating And Weight Related Disorders: Case Presentations of Multidisciplinary Care. Renee Gibbs, PhD Central Arkansas VA Healthcare System
 Eating And Weight Related Disorders: Case Presentations of Multidisciplinary Care Renee Gibbs, PhD Central Arkansas VA Healthcare System DISCLOSURES No disclosures of conflict of interest to report 2 OVERVIEW
Eating And Weight Related Disorders: Case Presentations of Multidisciplinary Care Renee Gibbs, PhD Central Arkansas VA Healthcare System DISCLOSURES No disclosures of conflict of interest to report 2 OVERVIEW
Telemedicine of family-based treatment for adolescent anorexia nervosa: A protocol of a treatment development study
 Anderson et al. Journal of Eating Disorders (2015) 3:25 DOI 10.1186/s40337-015-0063-1 STUDY PROTOCOL Open Access Telemedicine of family-based treatment for adolescent anorexia nervosa: A protocol of a
Anderson et al. Journal of Eating Disorders (2015) 3:25 DOI 10.1186/s40337-015-0063-1 STUDY PROTOCOL Open Access Telemedicine of family-based treatment for adolescent anorexia nervosa: A protocol of a
Submission to. MBS Review Taskforce Eating Disorders Working Group
 Submission to MBS Review Taskforce Eating Disorders Working Group Contact: Dr Vida Bliokas President ACPA President@acpa.org.au Introduction The Australian Clinical Psychology Association (ACPA) represents
Submission to MBS Review Taskforce Eating Disorders Working Group Contact: Dr Vida Bliokas President ACPA President@acpa.org.au Introduction The Australian Clinical Psychology Association (ACPA) represents
Paper s Information. Eating Disorder Diagnoses. Paper Type: Essay. Word Count: 1700 words. Referencing Style: APA Style
 1 Paper s Information Topic: Eating Disorder Diagnoses Paper Type: Essay Word Count: 1700 words Pages: 7pages Referencing Style: APA Style Education Level: Under Graduate 2 Running Head: EATING DISORDER
1 Paper s Information Topic: Eating Disorder Diagnoses Paper Type: Essay Word Count: 1700 words Pages: 7pages Referencing Style: APA Style Education Level: Under Graduate 2 Running Head: EATING DISORDER
A Pilot Study of Interpersonal Psychotherapy for Depressed Women with Breast Cancer
 A Pilot Study of Interpersonal Psychotherapy for Depressed Women with Breast Cancer CARLOS BLANCO, M.D., Ph.D.* JOHN C. MARKOWITZ, M.D.* DAWN L. HERSHMAN, M.D., M.S.# JON A. LEVENSON, M.D.* SHUAI WANG,
A Pilot Study of Interpersonal Psychotherapy for Depressed Women with Breast Cancer CARLOS BLANCO, M.D., Ph.D.* JOHN C. MARKOWITZ, M.D.* DAWN L. HERSHMAN, M.D., M.S.# JON A. LEVENSON, M.D.* SHUAI WANG,
Eating Disorders. Abnormal Psychology PSYCH Eating Disorders: An Overview. DSM-IV: Anorexia Nervosa
 Abnormal Psychology PSYCH 40111 Eating Disorders Eating Disorders: An Overview Two Major Types of DSM-IV Eating Disorders Anorexia nervosa and bulimia nervosa Severe disruptions in eating behavior Extreme
Abnormal Psychology PSYCH 40111 Eating Disorders Eating Disorders: An Overview Two Major Types of DSM-IV Eating Disorders Anorexia nervosa and bulimia nervosa Severe disruptions in eating behavior Extreme
Dealing with Feelings: The Effectiveness of Cognitive Behavioural Group Treatment for Women in Secure Settings
 Behavioural and Cognitive Psychotherapy, 2011, 39, 243 247 First published online 30 November 2010 doi:10.1017/s1352465810000573 Dealing with Feelings: The Effectiveness of Cognitive Behavioural Group
Behavioural and Cognitive Psychotherapy, 2011, 39, 243 247 First published online 30 November 2010 doi:10.1017/s1352465810000573 Dealing with Feelings: The Effectiveness of Cognitive Behavioural Group
Adolescent Coping with Depression (CWD-A)
 This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
An Exploratory Study of a. Meditation-Based Intervention. for Binge Eating Disorder. Jean L. Kristeller and C. Brendan Hallett. Dept.
 1 An Exploratory Study of a Meditation-Based Intervention for Binge Eating Disorder Jean L. Kristeller and C. Brendan Hallett Dept. of Psychology Indiana State University Journal of Health Psychology.
1 An Exploratory Study of a Meditation-Based Intervention for Binge Eating Disorder Jean L. Kristeller and C. Brendan Hallett Dept. of Psychology Indiana State University Journal of Health Psychology.
Heidi Clayards Lynne Cox Marine McDonnell
 Heidi Clayards Lynne Cox Marine McDonnell Introduction to Interpersonal Psychotherapy (IPT) Adaptations from IPT to IPT-A Theoretical framework Description of treatment Review of the manual and demonstration
Heidi Clayards Lynne Cox Marine McDonnell Introduction to Interpersonal Psychotherapy (IPT) Adaptations from IPT to IPT-A Theoretical framework Description of treatment Review of the manual and demonstration
Hafizullah Azizi M.D.
 Hafizullah Azizi M.D. Eating disorders Feeding and Eating Disorders of Infancy and Early Childhood and Obesity Anorexia Nervosa Bulimia Nervosa EDNOS Binge Eating Disorder Purging Disorder Night Eating
Hafizullah Azizi M.D. Eating disorders Feeding and Eating Disorders of Infancy and Early Childhood and Obesity Anorexia Nervosa Bulimia Nervosa EDNOS Binge Eating Disorder Purging Disorder Night Eating
Eating Disorders in Youth
 Eating Disorders in Youth Evaluating and Treating in the Medical Home February 27, 2017 Rebecca Marshall, MD, MPH Outline Anorexia Nervosa Bulimia Nervosa Binge Eating Disorder Avoidant Restrictive Food
Eating Disorders in Youth Evaluating and Treating in the Medical Home February 27, 2017 Rebecca Marshall, MD, MPH Outline Anorexia Nervosa Bulimia Nervosa Binge Eating Disorder Avoidant Restrictive Food
Title: Group therapy for binge eating in type 2 diabetes: A randomized trial.
 Group Treatment of Binge Eating 1 Title: Group therapy for binge eating in type 2 diabetes: A randomized trial. Authors: J. Kenardy 1, M. Mensch 2, K. Bowen 2, B. Green 2, J. Walton 2 Departments: 1 School
Group Treatment of Binge Eating 1 Title: Group therapy for binge eating in type 2 diabetes: A randomized trial. Authors: J. Kenardy 1, M. Mensch 2, K. Bowen 2, B. Green 2, J. Walton 2 Departments: 1 School
Self Evaluation. Bulimia Nervosa Diagnostic Criteria 30/08/2012. Client's Current Self-Evaluation Pie Chart Relationship
 Rachel Lawson Acting Clinical Head Project Leader Eating Disorders The Werry Centre ED and SUDS in Adolescence Background Research is limited Prevalence about a third Vast majority of those will have Bulimia
Rachel Lawson Acting Clinical Head Project Leader Eating Disorders The Werry Centre ED and SUDS in Adolescence Background Research is limited Prevalence about a third Vast majority of those will have Bulimia
BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES
 BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES Craig Johnson, PhD, FAED, CEDS, Chief Science Officer Emmett R. Bishop Jr., MD, FAED,
BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES BECOMING A DISCRIMINATING CONSUMER OF TREATMENT OUTCOMES Craig Johnson, PhD, FAED, CEDS, Chief Science Officer Emmett R. Bishop Jr., MD, FAED,
Eating Disorders: recognition and treatment
 National Guideline Alliance Version 1.0 Eating Disorders: recognition and treatment Appendix O - HE evidence checklists NICE Guideline Methods, evidence and recommendations December 2016 Draft for Consultation
National Guideline Alliance Version 1.0 Eating Disorders: recognition and treatment Appendix O - HE evidence checklists NICE Guideline Methods, evidence and recommendations December 2016 Draft for Consultation
Long-term efficacy of psychological treatments for binge eating disorder
 The British Journal of Psychiatry (212) 2, 232 237. doi: 1.1192/bjp.bp.11.894 Long-term efficacy of psychological treatments for binge eating disorder Anja Hilbert, Monica E. Bishop, Richard I. Stein,
The British Journal of Psychiatry (212) 2, 232 237. doi: 1.1192/bjp.bp.11.894 Long-term efficacy of psychological treatments for binge eating disorder Anja Hilbert, Monica E. Bishop, Richard I. Stein,
DSM-5 Reduces the Proportion of EDNOS Cases: Evidence from Community Samples
 REGULAR ARTICLE DSM-5 Reduces the Proportion of EDNOS Cases: Evidence from Community Samples Paulo P.P. Machado, PhD 1 * Sónia Gonçalves, PhD 1 Hans W. Hoek, MD, PhD 2,3,4 ABSTRACT Objective: Eating Disorder
REGULAR ARTICLE DSM-5 Reduces the Proportion of EDNOS Cases: Evidence from Community Samples Paulo P.P. Machado, PhD 1 * Sónia Gonçalves, PhD 1 Hans W. Hoek, MD, PhD 2,3,4 ABSTRACT Objective: Eating Disorder
Acute Stabilization In A Trauma Program: A Pilot Study. Colin A. Ross, MD. Sean Burns, MA, LLP
 In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
II3B GD2 Depression and Suicidality in Human Research
 Office of Human Research Protection University of Nevada, Reno II3B GD2 Depression and Suicidality in Human Research Overview Research studies that include measures for depression and suicidality should
Office of Human Research Protection University of Nevada, Reno II3B GD2 Depression and Suicidality in Human Research Overview Research studies that include measures for depression and suicidality should
Child and Adolescent Eating Disorders: Diagnoses and Treatment Innovations
 Child and Adolescent Eating Disorders: Diagnoses and Treatment Innovations Kamryn T. Eddy, Ph.D. Co-Director, Eating Disorders Clinical and Research Program, Massachusetts General Hospital Associate Professor
Child and Adolescent Eating Disorders: Diagnoses and Treatment Innovations Kamryn T. Eddy, Ph.D. Co-Director, Eating Disorders Clinical and Research Program, Massachusetts General Hospital Associate Professor
Online publication date: 24 February 2011 PLEASE SCROLL DOWN FOR ARTICLE
 This article was downloaded by: [Brewerton, Timothy D.] On: 24 February 2011 Access details: Access Details: [subscription number 933991272] Publisher Routledge Informa Ltd Registered in England and Wales
This article was downloaded by: [Brewerton, Timothy D.] On: 24 February 2011 Access details: Access Details: [subscription number 933991272] Publisher Routledge Informa Ltd Registered in England and Wales
Eating Disorders Are we doing enough? Tracey Wade Professor, School of Psychology
 Eating Disorders Are we doing enough? Tracey Wade Professor, School of Psychology 25 June 2013 Myth 1 Anorexia nervosa is the most serious eating disorder Isabelle Caro 1982-2010 Fact 1 All eating disorders
Eating Disorders Are we doing enough? Tracey Wade Professor, School of Psychology 25 June 2013 Myth 1 Anorexia nervosa is the most serious eating disorder Isabelle Caro 1982-2010 Fact 1 All eating disorders
Comparison of Long-Term Outcomes in Adolescents With Anorexia Nervosa Treated With Family Therapy
 Comparison of Long-Term Outcomes in Adolescents With Anorexia Nervosa Treated With Family Therapy JAMES LOCK, M.D., PH.D., JENNIFER COUTURIER, M.D., AND W. STEWART AGRAS, M.D. ABSTRACT Objective: To describe
Comparison of Long-Term Outcomes in Adolescents With Anorexia Nervosa Treated With Family Therapy JAMES LOCK, M.D., PH.D., JENNIFER COUTURIER, M.D., AND W. STEWART AGRAS, M.D. ABSTRACT Objective: To describe
Dose-Response Studies in Psychotherapy
 Dose-Response Studies in Psychotherapy Howard, K. I., Kopta, S. M., Krause, M. S., & Orlinsky, D. E. (1986). The dose-effect relationship in psychotherapy. The American Psychologist, 41, 159 164. Investigated
Dose-Response Studies in Psychotherapy Howard, K. I., Kopta, S. M., Krause, M. S., & Orlinsky, D. E. (1986). The dose-effect relationship in psychotherapy. The American Psychologist, 41, 159 164. Investigated
Taking Care: Child and Youth Mental Health TREATMENT OPTIONS
 Taking Care: Child and Youth Mental Health TREATMENT OPTIONS Open Learning Agency 2004 TREATMENT OPTIONS With appropriate treatment, more than 80% of people with depression get full relief from their symptoms
Taking Care: Child and Youth Mental Health TREATMENT OPTIONS Open Learning Agency 2004 TREATMENT OPTIONS With appropriate treatment, more than 80% of people with depression get full relief from their symptoms
2) Percentage of adult patients (aged 18 years or older) with a diagnosis of major depression or dysthymia and an
 Quality ID #370 (NQF 0710): Depression Remission at Twelve Months National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Prevention, Treatment, and Management of Mental Health
Quality ID #370 (NQF 0710): Depression Remission at Twelve Months National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Prevention, Treatment, and Management of Mental Health
A Randomized Controlled Trial of In-Person and Telephone Cognitive Behavioral Therapy for Major Depression after Traumatic Brain Injury
 A Randomized Controlled Trial of In-Person and Telephone Cognitive Behavioral Therapy for Major Depression after Traumatic Brain Injury Josh Dyer, PhD Department of Rehabilitation Medicine University of
A Randomized Controlled Trial of In-Person and Telephone Cognitive Behavioral Therapy for Major Depression after Traumatic Brain Injury Josh Dyer, PhD Department of Rehabilitation Medicine University of
Weight Suppression Predicts Time to Remission From Bulimia Nervosa
 Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 6, 772 776 0022-006X/11/$12.00 DOI: 10.1037/a0025714 Weight Suppression Predicts Time to Remission
Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 6, 772 776 0022-006X/11/$12.00 DOI: 10.1037/a0025714 Weight Suppression Predicts Time to Remission
HealthPartners Care Coordination Clinical Care Planning and Resource Guide EATING DISORDER
 The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Mental Health) and the National Eating Disorders Association
The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Mental Health) and the National Eating Disorders Association
Combining Pharmacotherapy with Psychotherapeutic Management for the Treatment of Psychiatric Disorders
 Combining Pharmacotherapy with Psychotherapeutic Management for the Treatment of Psychiatric Disorders Ira D. Glick, M.D. Stanford University School of Medicine Characteristics of Psychotherapy Received
Combining Pharmacotherapy with Psychotherapeutic Management for the Treatment of Psychiatric Disorders Ira D. Glick, M.D. Stanford University School of Medicine Characteristics of Psychotherapy Received
Do Adherence Variables Predict Outcome in an Online Program for the Prevention of Eating Disorders?
 Journal of Consulting and Clinical Psychology Copyright 2008 by the American Psychological Association 2008, Vol. 76, No. 2, 341 346 0022-006X/08/$12.00 DOI: 10.1037/0022-006X.76.2.341 BRIEF REPORTS Do
Journal of Consulting and Clinical Psychology Copyright 2008 by the American Psychological Association 2008, Vol. 76, No. 2, 341 346 0022-006X/08/$12.00 DOI: 10.1037/0022-006X.76.2.341 BRIEF REPORTS Do
CRITICAL ANALYSIS PROBLEMS
 CRITICAL ANALYSIS PROBLEMS MOCK EXAMINATION Paper II 2015 STIMULUS THIS STIMULUS IS NOT TO BE REMOVED FROM THE EXAMINATION ROOM DIRECTIONS To be used as a handout while answering questions. Do not answer
CRITICAL ANALYSIS PROBLEMS MOCK EXAMINATION Paper II 2015 STIMULUS THIS STIMULUS IS NOT TO BE REMOVED FROM THE EXAMINATION ROOM DIRECTIONS To be used as a handout while answering questions. Do not answer
The treatment of postnatal depression: a comprehensive literature review Boath E, Henshaw C
 The treatment of postnatal depression: a comprehensive literature review Boath E, Henshaw C Authors' objectives To evalute treatments of postnatal depression. Searching MEDLINE, PsycLIT, Sociofile, CINAHL
The treatment of postnatal depression: a comprehensive literature review Boath E, Henshaw C Authors' objectives To evalute treatments of postnatal depression. Searching MEDLINE, PsycLIT, Sociofile, CINAHL
Proceedings of the International Conference on RISK MANAGEMENT, ASSESSMENT and MITIGATION
 COGNITIVE-BEHAVIOURAL THERAPY EFFICACY IN MAJOR DEPRESSION WITH ASSOCIATED AXIS II RISK FACTOR FOR NEGATIVE PROGNOSIS DANIEL VASILE*, OCTAVIAN VASILIU** *UMF Carol Davila Bucharest, ** Universitary Military
COGNITIVE-BEHAVIOURAL THERAPY EFFICACY IN MAJOR DEPRESSION WITH ASSOCIATED AXIS II RISK FACTOR FOR NEGATIVE PROGNOSIS DANIEL VASILE*, OCTAVIAN VASILIU** *UMF Carol Davila Bucharest, ** Universitary Military
MEDICAL POLICY EFFECTIVE DATE: 04/28/11 REVISED DATE: 04/26/12, 04/25/13, 04/24/14, 06/25/15, 06/22/16, 06/22/17
 MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
TREATMENT OUTCOMES REPORT
 TREATMENT OUTCOMES REPORT 2016 EDITION Helping patients, families and professionals understand treatment results Eating Recovery Center Treatment Outcomes Report, 2016 Edition Helping patients, families
TREATMENT OUTCOMES REPORT 2016 EDITION Helping patients, families and professionals understand treatment results Eating Recovery Center Treatment Outcomes Report, 2016 Edition Helping patients, families
The strength of a multidisciplinary approach towards students with an eating problem.
 The strength of a multidisciplinary approach towards students with an eating problem. Sigrid Schoukens, psychologist Maura Sisk, general practitioner Student Health Center, KULeuven EUSUSHM CONGRESS 2017
The strength of a multidisciplinary approach towards students with an eating problem. Sigrid Schoukens, psychologist Maura Sisk, general practitioner Student Health Center, KULeuven EUSUSHM CONGRESS 2017
NIH Public Access Author Manuscript Int J Eat Disord. Author manuscript; available in PMC 2014 December 01.
 NIH Public Access Author Manuscript Published in final edited form as: Int J Eat Disord. 2013 December ; 46(8): 849 854. doi:10.1002/eat.22163. Restrictive Eating Behaviors are a Non-Weight-Based Marker
NIH Public Access Author Manuscript Published in final edited form as: Int J Eat Disord. 2013 December ; 46(8): 849 854. doi:10.1002/eat.22163. Restrictive Eating Behaviors are a Non-Weight-Based Marker
With the preparation for the fifth edition of the Diagnostic
 Article Diagnostic Crossover in Anorexia Nervosa and Bulimia Nervosa: Implications for DSM-V Kamryn T. Eddy, Ph.D. David J. Dorer, Ph.D. Debra L. Franko, Ph.D. Kavita Tahilani, B.S. Heather Thompson-Brenner,
Article Diagnostic Crossover in Anorexia Nervosa and Bulimia Nervosa: Implications for DSM-V Kamryn T. Eddy, Ph.D. David J. Dorer, Ph.D. Debra L. Franko, Ph.D. Kavita Tahilani, B.S. Heather Thompson-Brenner,
Research Studies on Eating Disorders:
 Research Studies on Eating Disorders: Chicago, IL Adolescent Bulimia Nervosa Study The University of Chicago seeks adolescents with bulimia nervosa and their families for participation in a 6-month outpatient
Research Studies on Eating Disorders: Chicago, IL Adolescent Bulimia Nervosa Study The University of Chicago seeks adolescents with bulimia nervosa and their families for participation in a 6-month outpatient
Interpersonal Psychotherapy and Ea2ng Disorders
 Interpersonal Psychotherapy and Ea2ng Disorders Christopher G Fairburn Centre for Research on Ea2ng Disorders at Oxford credo- oxford.com IPT AND EATING DISORDERS Structure of the Talk 1. What is IPT?
Interpersonal Psychotherapy and Ea2ng Disorders Christopher G Fairburn Centre for Research on Ea2ng Disorders at Oxford credo- oxford.com IPT AND EATING DISORDERS Structure of the Talk 1. What is IPT?
Kyle was a 22-year old, Caucasian, gay male undergraduate student in his junior year
 Introduction and Background CASE CONCEPTUALIZATION Kyle was a 22-year old, Caucasian, gay male undergraduate student in his junior year at a large southeastern university. Kyle first presented for intake
Introduction and Background CASE CONCEPTUALIZATION Kyle was a 22-year old, Caucasian, gay male undergraduate student in his junior year at a large southeastern university. Kyle first presented for intake
Feeding and Eating Disorders
 The Time is Here: Differential Diagnosis and Coding Using the DSM 5 and ICD 10 Diane Snow, PhD, RN, PMHNP-BC, FAANP, FIAAN University of Texas at Arlington College of Nursing and Health Innovation IntNSA
The Time is Here: Differential Diagnosis and Coding Using the DSM 5 and ICD 10 Diane Snow, PhD, RN, PMHNP-BC, FAANP, FIAAN University of Texas at Arlington College of Nursing and Health Innovation IntNSA
U.S. 1 February 22, 2013
 U.S. 1 February 22, 2013 A Placebo-controlled, Randomized, Blinded, Dose Finding Phase 2 Pilot Safety Study of MDMA-assisted Therapy for Social Anxiety in Autistic Adults Study Code: MAA-1 Sponsor: Multidisciplinary
U.S. 1 February 22, 2013 A Placebo-controlled, Randomized, Blinded, Dose Finding Phase 2 Pilot Safety Study of MDMA-assisted Therapy for Social Anxiety in Autistic Adults Study Code: MAA-1 Sponsor: Multidisciplinary
APS Submission to the MBS Review: Better Access to Psychiatrists, Psychologists and General Practitioners
 APS Submission to the MBS Review: Better Access to Psychiatrists, Psychologists and General Practitioners July 2018 The Australian Psychological Society Limited psychology.org.au 1 Contributors Professor
APS Submission to the MBS Review: Better Access to Psychiatrists, Psychologists and General Practitioners July 2018 The Australian Psychological Society Limited psychology.org.au 1 Contributors Professor
Supplementary Online Content
 Supplementary Online Content Janssen CW, Lowry CA, Mehl MR, et al. Whole-body hyperthermia for the treatment of major depressive disorder: a randomized clinical trial. JAMA Psychiatry. Published online
Supplementary Online Content Janssen CW, Lowry CA, Mehl MR, et al. Whole-body hyperthermia for the treatment of major depressive disorder: a randomized clinical trial. JAMA Psychiatry. Published online
DEPRESSION-FOCUSED INTERVENTION FOR PREGNANT SMOKERS 1. Supplemental Material For Online Use Only
 DEPRESSION-FOCUSED INTERVENTION FOR PREGNANT SMOKERS 1 Supplemental Material For Online Use Only Effects of an Intensive Depression-Focused Intervention for Smoking Cessation in Pregnancy DEPRESSION-FOCUSED
DEPRESSION-FOCUSED INTERVENTION FOR PREGNANT SMOKERS 1 Supplemental Material For Online Use Only Effects of an Intensive Depression-Focused Intervention for Smoking Cessation in Pregnancy DEPRESSION-FOCUSED
Cognitive-behavioral guided self-help for the treatment of recurrent binge eating
 Wesleyan University From the SelectedWorks of Ruth Striegel Weissman 2010 Cognitive-behavioral guided self-help for the treatment of recurrent binge eating Ruth Striegel Weissman Available at: https://works.bepress.com/ruth_striegel/67/
Wesleyan University From the SelectedWorks of Ruth Striegel Weissman 2010 Cognitive-behavioral guided self-help for the treatment of recurrent binge eating Ruth Striegel Weissman Available at: https://works.bepress.com/ruth_striegel/67/
UNIVERSITY OF CALGARY. A Randomized Wait-List Controlled Trial of Dialectical Behaviour Therapy Guided Self-
 UNIVERSITY OF CALGARY A Randomized Wait-List Controlled Trial of Dialectical Behaviour Therapy Guided Self- Help for Recurrent Binge Eating: A Pilot Study by Philip Christopher Masson A THESIS SUBMITTED
UNIVERSITY OF CALGARY A Randomized Wait-List Controlled Trial of Dialectical Behaviour Therapy Guided Self- Help for Recurrent Binge Eating: A Pilot Study by Philip Christopher Masson A THESIS SUBMITTED
Eating Disorders. Anorexia Nervosa. DSM 5:Eating Disorders. DSM 5: Feeding and Eating Disorders 9/24/2015
 DSM 5: Feeding and Eating Disorders Eating Disorders Marsha D. Marcus, PhD The North American Menopause Society October 3, 2015 Feeding and Eating Disorders are characterized by a persistent disturbance
DSM 5: Feeding and Eating Disorders Eating Disorders Marsha D. Marcus, PhD The North American Menopause Society October 3, 2015 Feeding and Eating Disorders are characterized by a persistent disturbance
Study Data Excluded Reason for Exclusions
 Data Supplement for Sharf, J., Primavera, L.H., and Diener, M. J. (2010). Dropout and Therapeutic Alliance: A Meta-Analysis of Adult Individual Psychotherapy, Psychotherapy Theory, Research, Practice,
Data Supplement for Sharf, J., Primavera, L.H., and Diener, M. J. (2010). Dropout and Therapeutic Alliance: A Meta-Analysis of Adult Individual Psychotherapy, Psychotherapy Theory, Research, Practice,
Care Team Training. Key Components of Collaborative Care. Collaborative Team Approach 4/21/2014 PCP. Core Program. New Roles. Psychiatric Consultant
 Team Training Key Components of Collaborative Collaborative Team Approach Patient PCP Manager New Roles Core Program Psychiatric Consultant Behavioral Health Clinicians Additional Clinic Resources Substance,
Team Training Key Components of Collaborative Collaborative Team Approach Patient PCP Manager New Roles Core Program Psychiatric Consultant Behavioral Health Clinicians Additional Clinic Resources Substance,
EATING DISORDERS AND SUBSTANCE ABUSE. Margot L. Waitz, DO October 7, 2017 AOAAM - OMED
 EATING DISORDERS AND SUBSTANCE ABUSE Margot L. Waitz, DO October 7, 2017 AOAAM - OMED OBJECTIVES Review criteria for diagnosis of several eating disorders Discuss co-morbidity of substance abuse in patients
EATING DISORDERS AND SUBSTANCE ABUSE Margot L. Waitz, DO October 7, 2017 AOAAM - OMED OBJECTIVES Review criteria for diagnosis of several eating disorders Discuss co-morbidity of substance abuse in patients
Department of Psychiatry, Hokkaido University Graduate School of Medicine North 15, West 7, Sapporo , JAPAN
 Title Clinical Study of Early-Onset Eating Disorders Authors Kenzo Denda, M.D., Ph.D. 1 Yuki Kako, M.D. 1 Nobuki Kitagawa, M.D. 1 Tsukasa Koyama, M.D., Ph.D. 1 Affiliation 1 Department of Psychiatry, Hokkaido
Title Clinical Study of Early-Onset Eating Disorders Authors Kenzo Denda, M.D., Ph.D. 1 Yuki Kako, M.D. 1 Nobuki Kitagawa, M.D. 1 Tsukasa Koyama, M.D., Ph.D. 1 Affiliation 1 Department of Psychiatry, Hokkaido
Description of intervention
 Helping to Overcome PTSD through Empowerment (HOPE) Johnson, D., Zlotnick, C. and Perez, S. (2011) Johnson, D. M., Johnson, N. L., Perez, S. K., Palmieri, P. A., & Zlotnick, C. (2016) Description of Helping
Helping to Overcome PTSD through Empowerment (HOPE) Johnson, D., Zlotnick, C. and Perez, S. (2011) Johnson, D. M., Johnson, N. L., Perez, S. K., Palmieri, P. A., & Zlotnick, C. (2016) Description of Helping
Summary ID#7029. Clinical Study Summary: Study F1D-MC-HGKQ
 CT Registry ID# 7029 Page 1 Summary ID#7029 Clinical Study Summary: Study F1D-MC-HGKQ Clinical Study Report: Versus Divalproex and Placebo in the Treatment of Mild to Moderate Mania Associated with Bipolar
CT Registry ID# 7029 Page 1 Summary ID#7029 Clinical Study Summary: Study F1D-MC-HGKQ Clinical Study Report: Versus Divalproex and Placebo in the Treatment of Mild to Moderate Mania Associated with Bipolar
 Does Practical Body Image with mirror exposure improve body image and increase acceptance of a healthy weight in adolescents with an eating disorder? Sarah Astbury Assistant Psychologist sarah.astbury@newbridge-health.org.uk
Does Practical Body Image with mirror exposure improve body image and increase acceptance of a healthy weight in adolescents with an eating disorder? Sarah Astbury Assistant Psychologist sarah.astbury@newbridge-health.org.uk
Cognitive Behavior Therapy And Eating Disorders By Christopher G. Fairburn READ ONLINE
 Cognitive Behavior Therapy And Eating Disorders By Christopher G. Fairburn READ ONLINE If you are searching for a book by Christopher G. Fairburn Cognitive Behavior Therapy and Eating Disorders in pdf
Cognitive Behavior Therapy And Eating Disorders By Christopher G. Fairburn READ ONLINE If you are searching for a book by Christopher G. Fairburn Cognitive Behavior Therapy and Eating Disorders in pdf
Dynamic Deconstructive Psychotherapy
 This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
USING BEHAVIOURAL ACTIVATION AS A PSYCHOLOGICAL INTERVENTION TO TREAT AND PREVENT DEPRESSION. Professor David Ekers PhD, MSc ENB 650, RMN
 USING BEHAVIOURAL ACTIVATION AS A PSYCHOLOGICAL INTERVENTION TO TREAT AND PREVENT DEPRESSION Professor David Ekers PhD, MSc ENB 650, RMN Aims for the session The problem-why are we interested in BA-what
USING BEHAVIOURAL ACTIVATION AS A PSYCHOLOGICAL INTERVENTION TO TREAT AND PREVENT DEPRESSION Professor David Ekers PhD, MSc ENB 650, RMN Aims for the session The problem-why are we interested in BA-what
Frequency of Binge Eating Episodes in Bulimia Nervosa and Binge Eating Disorder: Diagnostic Considerations
 SPECIAL SECTION REVIEW ARTICLE Frequency of Binge Eating Episodes in Bulimia Nervosa and Binge Eating Disorder: Diagnostic Considerations G. Terence Wilson, PhD 1 * Robyn Sysko, PhD 2 ABSTRACT Objective:
SPECIAL SECTION REVIEW ARTICLE Frequency of Binge Eating Episodes in Bulimia Nervosa and Binge Eating Disorder: Diagnostic Considerations G. Terence Wilson, PhD 1 * Robyn Sysko, PhD 2 ABSTRACT Objective:
Follow this and additional works at: Part of the Medicine and Health Sciences Commons
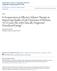 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Acupuncture an Effective Adjunct Therapy
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Acupuncture an Effective Adjunct Therapy
Is Major Depressive Disorder or Dysthymia More Strongly Associated with Bulimia Nervosa?
 Is Major Depressive Disorder or Dysthymia More Strongly Associated with Bulimia Nervosa? Marisol Perez, 1 Thomas E. Joiner, Jr., 1 * and Peter M. Lewinsohn 2 1 Department of Psychology, Florida State University,
Is Major Depressive Disorder or Dysthymia More Strongly Associated with Bulimia Nervosa? Marisol Perez, 1 Thomas E. Joiner, Jr., 1 * and Peter M. Lewinsohn 2 1 Department of Psychology, Florida State University,
MEDICAL POLICY No R8 EATING DISORDERS POLICY/CRITERIA
 EATING DISORDERS MEDICAL POLICY Effective Date: June 27, 2016 Review Dates: 1/93, 8/96, 4/99, 12/01, 12/02, 11/03, 11/04, 10/05, 10/06, 10/07, 8/08, 8/09, 8/10, 8/11, 8/12, 8/13, 5/14, 5/15, 5/16 Date
EATING DISORDERS MEDICAL POLICY Effective Date: June 27, 2016 Review Dates: 1/93, 8/96, 4/99, 12/01, 12/02, 11/03, 11/04, 10/05, 10/06, 10/07, 8/08, 8/09, 8/10, 8/11, 8/12, 8/13, 5/14, 5/15, 5/16 Date
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Drahota, A., Wood, J. J., Sze, K. M., & Van Dyke, M. (2011). Effects of cognitive behavioral therapy on daily living skills in children with high-functioning autism and
CRITICALLY APPRAISED PAPER (CAP) Drahota, A., Wood, J. J., Sze, K. M., & Van Dyke, M. (2011). Effects of cognitive behavioral therapy on daily living skills in children with high-functioning autism and
Relapse in anorexia nervosa: a survival analysis
 Psychological Medicine, 2004, 34, 671 679. f 2004 Cambridge University Press DOI: 10.1017/S0033291703001168 Printed in the United Kingdom Relapse in anorexia nervosa: a survival analysis J. C. CARTER,
Psychological Medicine, 2004, 34, 671 679. f 2004 Cambridge University Press DOI: 10.1017/S0033291703001168 Printed in the United Kingdom Relapse in anorexia nervosa: a survival analysis J. C. CARTER,
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centers: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Behaviour Research and Therapy
 Behaviour Research and Therapy 48 (2010) 187 193 Contents lists available at ScienceDirect Behaviour Research and Therapy journal homepage: www.elsevier.com/locate/brat The significance of overvaluation
Behaviour Research and Therapy 48 (2010) 187 193 Contents lists available at ScienceDirect Behaviour Research and Therapy journal homepage: www.elsevier.com/locate/brat The significance of overvaluation
CARE BUNDLE Robyn Girling-Butcher
 CARE BUNDLE Robyn Girling-Butcher Senior Clinical Psychologist Child, Adolescent & Family Service Mental Health MidCentral DHB Principles of Care AN has highest death rate of any mental health disorder
CARE BUNDLE Robyn Girling-Butcher Senior Clinical Psychologist Child, Adolescent & Family Service Mental Health MidCentral DHB Principles of Care AN has highest death rate of any mental health disorder
A Depression Management Program for Elderly Adults
 Program to Encourage Active, Rewarding Lives for Seniors (PEARLS) A Depression Management Program for Elderly Adults Illinois Governor s Conference on Aging Chicago, IL December 13, 2012 Amanda Timm Planning
Program to Encourage Active, Rewarding Lives for Seniors (PEARLS) A Depression Management Program for Elderly Adults Illinois Governor s Conference on Aging Chicago, IL December 13, 2012 Amanda Timm Planning
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI
 Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia Nervosa A. A refusal to maintain body weight
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia Nervosa A. A refusal to maintain body weight
Patient sample criteria for the Preventive Care Measure Group are patients aged 50 years and older with a specific patient encounter:
 2016 Physician Quality Reporting System Data Collection Form: Preventive Care (for patients aged 50 and older) NOTE: Individual measures may have more restrictive age and gender requirements. IMPORTANT:
2016 Physician Quality Reporting System Data Collection Form: Preventive Care (for patients aged 50 and older) NOTE: Individual measures may have more restrictive age and gender requirements. IMPORTANT:
NIH Public Access Author Manuscript J Consult Clin Psychol. Author manuscript; available in PMC 2013 October 01.
 NIH Public Access Author Manuscript Published in final edited form as: J Consult Clin Psychol. 2012 October ; 80(5): 897 906. doi:10.1037/a0027001. Predictors and Moderators of Response to Cognitive Behavioral
NIH Public Access Author Manuscript Published in final edited form as: J Consult Clin Psychol. 2012 October ; 80(5): 897 906. doi:10.1037/a0027001. Predictors and Moderators of Response to Cognitive Behavioral
