Urakawa et al. World Journal of Surgical Oncology (2018) 16:160
|
|
|
- Daniel Carter
- 5 years ago
- Views:
Transcription
1 Urakawa et al. World Journal of Surgical Oncology (2018) 16:160 RESEARCH Open Access Clinical outcome of primary giant cell tumor of bone after curettage with or without perioperative denosumab in Japan: from a questionnaire for JCOG 1610 study Hiroshi Urakawa 1*, Tsukasa Yonemoto 2, Seiichi Matsumoto 3, Tatsuya Takagi 4, Kunihiro Asanuma 5, Munenori Watanuki 6, Akira Takemoto 7, Norifumi Naka 8, Yoshihiro Matsumoto 9, Akira Kawai 10, Toshiyuki Kunisada 11, Tadahiko Kubo 12, Makoto Emori 13, Hiroaki Hiraga 14, Hiroshi Hatano 15, Satoshi Tsukushi 16, Yoshihiro Nishida 1, Toshihiro Akisue 17, Takeshi Morii 18, Mitsuru Takahashi 19, Akihito Nagano 20, Hideki Yoshikawa 21, Kenji Sato 22, Masanori Kawano 23, Koji Hiraoka 24, Kazuhiro Tanaka 25, Yukihide Iwamoto 26 and Toshifumi Ozaki 27 Abstract Background: Giant cell tumor of bone (GCTB) is an intermediate tumor known to be locally aggressive, but rarely metastasizing. To plan a prospective study of GCTB, we performed a questionnaire survey for institutions participating in the Bone and Soft Tissue Tumor Study Group (BSTTSG) in the Japan Clinical Oncology Group (JCOG) in Methods: We reviewed 158 consecutive patients with primary GCTB treated with curettage without perioperative denosumab from 2008 to 2010 in Japan. We investigated local and distant recurrence rates after definitive curettage. We also investigated the recurrence rate after treatment with preoperative and/or postoperative denosumab with curettage in recent years. There were 40 patients treated with perioperative denosumab, and the factors affecting recurrence in them were investigated. Results: Answers were available from 24 of 30 institutions (80.0%) participating in JCOG BSTTSG. Thirty (19.0%) and 4 (2.5%) of 158 patients developed local and distant recurrence after curettage without perioperative denosumab from 2008 to 2010, respectively. Campanacci grade and embolization before surgery were significantly associated with increasing incidence of local recurrence after curettage (p = and p = 0.022, respectively). In patients treated with perioperative desnosumab, 120 mg denosumab was administered subcutaneously for a median 6 (2 41) and 6 (1 14) times in preoperative and postoperative settings, respectively. The recurrence rates were 6 of 21 (28.6%), 2 of 9 (22.2%), and 0 of 10 (0.0%) in the preoperative, postoperative, and both pre- and postoperative denosumab treatment groups, respectively. With all of the preoperative treatments, administration exceeding five times was significantly associated with a decreased incidence of local recurrence after curettage (p <0.001). Conclusion: The recurrence rate of GCTB was still high after curettage, especially in Campanacci grade III, and improvements in the therapeutic strategy are needed in this cohort. There is a possibility that a sufficient dose of preoperative denosumab can reduce recurrence after curettage. Recently, we have started a clinical trial, JCOG1610, to investigate the efficacy of preoperative denosumab in patients who can be treated with curettage in GCTB. Keywords: Giantcelltumorofbone,Outcome,Denosumab,Japan * Correspondence: urakawa@med.nagoya-u.ac.jp 1 Department of Orthopaedic Surgery, Nagoya University, 65 Tsurumai, Showa-ku, Nagoya, Aichi , Japan Full list of author information is available at the end of the article The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Urakawa et al. World Journal of Surgical Oncology (2018) 16:160 Page 2 of 8 Background Giant cell tumor of bone (GCTB) is an intermediate tumor known to be locally aggressive, but rarely metastasizing in the WHO classification [1]. GCTB possibly originates from the metaphyseal region [2], and accounts for 4 5% of all skeletal neoplasms in Japan. Local and distant recurrence rates were reported in % [3 6] and 2% [7, 8] of the patients after curettage, respectively. To reduce local recurrence and preserve the adjacent joint, adjuvant treatments such as high-speed burr [3], phenol [5, 9], ethanol, liquid nitrogen [5], and polymethyl methacrylate (PMMA) [3, 5, 9] have been reported. Even though there were some reports of GCTB in Japan [7, 10, 11], the recent clinical results of GCTB after curettage in multiple institutions in Japan have not been well documented. Denosumab is a fully human monoclonal antibody that inhibits the receptor activator of NF-κB (RANK) ligand (RANKL) and then interrupts RANK-RANKL interactions. In GCTB, the stromal cells and osteoclast-like giant cells express RANKL and RANK, respectively, and the RANK-RANKL interaction is considered to be necessary for the differentiation and activation of osteoclasts [12]. Therefore, the RANK-RANKL interaction has a critical role for bone destruction in GCTB, and dramatic change was observed after treatment of denosumab in GCTB. Multinucleated osteoclast-like giant cells and stromal cells were decreased after denosumab treatment for GCTB [13]. A recent phase 2 study demonstrated the effects of denosumab for patients with unresectable GCTB and salvageable GCTB whose surgery was associated with severe morbidity [14]. Denosumab was accepted for health insurance coverage in Japan in However, the role of denosumab in patients with GCTB who can be treated by curettage has not been well defined. We performed a questionnaire survey for institutions participating in the Bone and Soft Tissue Tumor Study Group (BSTTSG) in the Japan Clinical Oncology Group (JCOG) in 2015 for planning a clinical trial of JCOG1610, a randomized phase III study of preoperative denosumab with curettage for GCTB. The first aim of the present study was to identify the historical outcome after curettage for GCTB without perioperative desnosumab in Japan. The second purpose was to identify the clinical use of perioperative denosumab and the factors influencing local recurrence after perioperative denosumab with curettage. Methods Patients We reviewed 158 patients with GCTB treated by curettage without perioperative desnosumab from 2008 to 2010 in institutions participating in the JCOG BSTTSG. We also reviewed 40 patients with GCTB treated with curettage and perioperative denosumab. Methods We performed a questionnaire survey for institutions participating in the BSTTSG in JCOG in April and June This questionnaire survey was performed for planning a clinical trial of JCOG 1610 (UMIN ), a randomized phase III study of preoperative denosumab with curettage for GCTB. We retrospectively reviewed clinical records and filled out the questionnaire. The questionnaire included standard treatments (e.g., local adjuvant, reconstruction) of curettage for GCTB in each institution, details (e.g., number of extremities, Campanacci grade, pathological fracture at presentation, and embolization before surgery) of GCTB treated with curettage from 2008 to 2010, and clinical results (e.g., number of local recurrences, distant recurrences, and death) after the curettage, and details (e.g., sites, Campanacci grade, pathological fracture at presentation, time to the recurrence, final joint preservation, and embolization before surgery) of the patients with local recurrence. We also asked about perioperative use of denosumab for GCTB. The questionnaire included the indications of denosumab for GCTB in each institution, the number of patients treated with preoperative, postoperative, and both pre- and postoperative denosumab, respectively, number of times of perioperative denosumab administration, and clinical results of local recurrence after the perioperative denosumab with curettage. This study was approved by the ethics committee of Nagoya University Graduate School and School of Medicine (Nagoya, Japan) and a waiver of informed consent was provided. Statistics A chi-square test was used to analyze the correlation of various clinical factors with recurrence. Clinical factors such as sites (extremity, trunk), Campanacci grade (I, II, III), pathological fracture at presentation (yes, no), timing of denosumab (preoperative only vs postoperative only, both preoperative and postoperative vs preoperative or postoperative, preoperative only vs both preoperative and postoperative, postoperative only vs both preoperative and postoperative), and number of times of denosumab administration (5>, 5 ) were analyzed as related to the frequency of recurrence. p values of < 0.05 were considered significant. Statistical analysis was done using IBM SPSS Statistics 24.0 software (IBM, Armonk, NY, USA). Results Responses to the questionnaire were available from 24 of 30 institutions (80.0%) participating to JCOG BSTTSG. Standard treatments of curettage for GCTB in the 24 institutions are summarized in Table 1. As a local adjuvant
3 Urakawa et al. World Journal of Surgical Oncology (2018) 16:160 Page 3 of 8 Table 1 Standard treatments with curettage for GCTB a in 24 institutions Treatments No. of institutions (%) Local adjuvants High-speed burr 22 (92%) Ethanol 8 (33%) Liquid nitrogen 6 (25%) Phenol 3 (13%) Reconstruction after curettage Autologous bone graft 18 (75%) PMMA b 17 (71%) β-tcp c 11 (46%) Hydroxyapatite 10 (42%) Allogeneic bone graft 2 (8%) a GCTB giant cell tumor of bone b PMMA, polymethyl methacrylate c β-tcp, β tricalcium phosphate; some of the replies by responded institutions are overlapped therapy, high-speed burr was used after curettage in 22 of 24 (92%) institutions followed by ethanol (8 of 24 institutions, 33%), liquid nitrogen (6 of 24 institutions, 25%), and phenol (3 of 24 institutions, 13%). Autologous bone graft and polymethyl methacrylate (PMMA) were used for reconstruction after curettage in 18 (75%) and 17 (71%) of 24 institutions, respectively. Characteristics of the patients with GCTB were summarized in Table 2. Primary tumor sites were in an extremity in 151 of 158 (96%) patients and trunk in 7 of 158 (4%). Sixteen of 158 Table 2 Characteristics of patients of GCTB a treated with curettage from 2008 to 2010 Characteristics No. of patients (%) Primary tumor site Extremity 151 (96%) Trunk 7 (4%) Campanacci grade Grade I 16 (10%) Grade II 97 (61%) Grade III 45 (29%) Pathological fracture at presentation Yes 26 (16%) No 132 (84%) Do you use denosumab for this case now? Yes 83 (52%) No 75 (48%) Embolization before surgery Yes 8 (5%) No 150 (95%) (10%) evaluated as Campanacci grade I, 97 of 158 (61%) as Campanacci grade II, and 45 of 158 (29%) as Campanacci grade III. Thirty of 158 (19.0%) developed local recurrence, and 4 of 158 (2.5%) developed distant recurrence after curettage without perioperative denosumab. In extremities, 29 of 151 (19.2%) developed local recurrence, and 4 of 151 (2.6%) developed distant recurrence after curettage. There were no deaths after curettage. Campanacci grade and embolization before surgery were significantly associated with an increased incidence of local recurrence after curettage (p = and p = 0.022, respectively) (Table 3). Demographics of local recurrent patients after curettage for GCTB were summarized in Table 4. Local recurrence occurred in 1 of 16 (6.2%) in Campanacci grade I, 15 of 97 (15.5%) in Campanacci grade II, and 14 of 45 (31.1%) in Campanacci grade III. Median time to local recurrence was 15.5 months (5 69 months) after curettage, and joint preservation was achieved in 26 of 30 patients (86.7%). The indications of denosumab for GCTB at the 24 institutions are summarized in Table 5. As a general policy, denosumab was used perioperatively at 6 of 24 (25%) institutions. Actually, 40 patients were treated with perioperative denosumab in 16 institutions. The number of GCTB patients treated with perioperative denosumab and that of the institutions where they were treated were listed in Table 6. Denosumab was administered subcutaneously Table 3 Univariate analysis of local recurrence in patients with GCTB a treated with curettage from 2008 to (n = 158) Clinical factors No. of local recurrence (%) Univariate analysis p value b Site Extremity 29/151 (19.2%) p = Trunk 1/7 (14.3%) Campanacci grade Grade I 1/16 (6.3%) p = Grade II 15/97 (15.5%) Grade III 14/45 (31.1%) Pathological fracture at presentation Yes 5/26 (16.7%) p=0.972 No 25/132 (18.9%) Do you use denosumab for this case now? Yes 15/83 (18.1%) p=0.758 No 15/75 (20.0%) Embolization before surgery Yes 4/8 (50%) p=0.022 No 26/150 (17.3%) b Chi-square test
4 Urakawa et al. World Journal of Surgical Oncology (2018) 16:160 Page 4 of 8 Table 4 Characteristics of local recurrent patients after curettage for GCTB a from 2008 to 2010 Sites Campanacci grade Pathological fracture at presentation Time to recurrence (months) Final joint preservation Tibia II No 25 Possible No Femur II No 60 Possible Yes Metatarsal bone II No 60 Impossible Yes Femur III No 6 Impossible No Tibia III No 36 Possible Yes Tibia II No 27 Possible No Fibula II No 6 Possible No Femur III No 11 Possible No Femur II No 28 Possible No Ulna III No 6 Possible No Femur II No 9 Possible No Tibia II No 21 Possible No Femur II No 24 Impossible No Femur III No 6 Possible No Radius II No 6 Impossible No Tibia III Yes 24 Possible Yes Tibia III Yes 14 Possible No Fibula II No 35 Possible No Femur III Yes 21 Possible No Lumbar spine III No 60 Not available No Femur II No 12 Possible No Femur III Yes 5 Possible No Femur II No 6 Possible No Talus II No 12 Possible No Femur III Yes 30 Possible No Femur III No 6 Possible No Femur III No 22 Possible No Femur III No 7 Possible No Femur II No 17 Possible No Femur I No 7 Possible No Embolization before curettage Table 5 Indication of denosumab for GCTB a in 24 institutions Indications of denosumab No. of institutions (%) Unresectable 21 (88%) Difficult to joint preservation 17 (71%) Expanding to soft tissue 11 (46%) Adjusting the time of operation 7 (29%) Perioperative use with curettage 6 (25%) No experience of denosumab use 3 (13%) ; some of the replies by responded institutions are overlapped at 120 mg, but the dosing interval was not included in the questionnaire. Median number of times of denosumab administration were 6 (2 41) and 6 (1 14) in the preoperative and postoperative settings, respectively. The local recurrences were observed in 6 of 21 (28.6%), 2 of 9 (22.2%), and 0 of 10 (0.0%) patients treated with the preoperative, postoperative, and both preoperative and postoperative denosumab, respectively. In 31 patients treated with any preoperative denosumab, administration exceeding 5 times was significantly associated with a decreased incidence of local recurrence after curettage (p <0.001) (Table 7). Question for toxicity or side effects during perioperative denosumab were not included in the questionnaire survey.
5 Urakawa et al. World Journal of Surgical Oncology (2018) 16:160 Page 5 of 8 Table 6 No. of patients and institutions treated with perioperative denosumab for GCTB a Timing of perioperative denosumab No. of patients (%) No. of institutions (%) Preoperative only 21 (53%) 10 (63%) Postoperative only 9 (23%) 5 (31%) Both pre- and postoperative 10 (25%) 5 (31%) Total * *Some institutions performed denosumab at different timing Discussion To plan a clinical trial JCOG 1610, a randomized phase III study of preoperative denosumab with curettage for GCTB, we conducted a questionnaire survey to comprehend the historical clinical results after curettage of GCTB without perioperative denosumab. Although the clinical outcomes after curettage of GCTB have been reported sporadically in Japan [7, 10, 11], the more recent clinical results of GCTB after curettage in multiple institutions in Japan are not as clear. To determine the recent perioperative use in Japan, we also reviewed patients with GCTB Table 7 Univariate analysis of local recurrence in patients treated with perioperative denosumab and curettage for GCTB a (n =40) Comparison of factors No. of local recurrence (%) Univariate analysis p value b All patients (n = 40) Timing of denosumab Preoperative only 6/21 (28.6%) p = Postoperative only 2/9 (22.2%) Timing of denosumab Both pre- and postoperative 0/10 (0.0%) p=0.068 Pre- or postoperative only 8/30 (26.7%) Preoperative (n = 31) Times of denosumab administration 5> 5/7 (71.4%) p< /24 (4.2%) Timing of denosumab Preoperative only 6/21 (28.6%) p=0.060 Both pre- and postoperative 0/10 (18.9%) Postoperative (n = 19) Times of denosumab administration 5> 0/7 (0.0%) p= /12 (16.7%) Embolization before surgery Postoperative only 2/9 (22.2%) p=0.115 Both pre- and postoperative 0/10 (0.0%) Chi-square test treated with curettage and perioperative denosumab. Even though denosumab was accepted for health insurance coverage in Japan in 2014, the risk/benefit ratio of denosumab when used for patients with GCTB who are treatable by curettage is not well defined. There are some limitations in our study. First, because of its questionnaire format, we did not have data regarding the follow-up period after curettage. We investigated GCTB patients treated from 2008 to 2010 and performed this questionnaire survey in 2015, meaning that the follow-up period can be considered adequate given that most recurrences in GCTB occur within 5 years [3 6] and recurrent GCTB is usually treated at the same institution where the first surgery was performed. Second, there was a lack of important data such as size of tumor, detailed sites, and Campanacci grade of GCTB treated with perioperative denosumab, which could act as confounding factors. Because our study is a questionnaire survey, we could not conduct an additional survey due to unlinkable anonymizing of our data. Third, we could not perform multivariate analysis because of the small number of recurrences and lack of information regarding other important clinical factors. Finally, we could not determine whether the patients treated with preoperative denosumab were all suitable for curettage from the time of their initial consultation. As a local adjuvant therapy, a high-speed burr was used after curettage in 92% of institutions followed by ethanol (33%), liquid nitrogen (25%), and phenol (13%) in our study. Clinical results of these local adjuvant therapies have been reported [3, 5, 9], but it is difficult to determine the advantage of each treatment. Generally, the high-speed burr is easier to use than drug therapies such as ethanol, liquid nitrogen, and phenol, accounting for its extensive use in Japan. In our study, autologous bone graft and PMMA were used for reconstruction after curettage in 75% and 71% of institutions, respectively. Some reports demonstrated the clinical benefit of PMMA for decreasing local recurrence after curettage of GCTB [3, 4, 6, 9]. Autologous bone graft is widely used in Japan because the lack of a bone bank precludes routine use of allogenic bone. In our study, the local recurrence rate after curettage was 19.0%. Previous reports showed local recurrence of GCTB in % after curettage [3 6], and so our local recurrence rate is slightly better than that documented in these previous reports. Past reports have shown some clinical factors affecting local recurrence such as tumor extension, surgical margin, local adjuvant therapy, Campanacci grade, use of PMMA, and soft tissue progression on multivariate analyses [4, 5, 9]. In our study, Campanacci grade was well balanced similar to previous studies [9, 15], and we ascribe the better local recurrence rate achieved in our study to the wide use of
6 Urakawa et al. World Journal of Surgical Oncology (2018) 16:160 Page 6 of 8 local adjuvant treatments as well as PMMA in many institutions. In our study, Campanacci grade was significantly associated with increasing incidence of local recurrence after curettage, and this result was similar to that noted in previous studies [4]. Embolization before surgery was also significantly associated with the increasing incidence of local recurrence after curettage, but it was difficult to interpret. Since the embolization is usually used for patients with GCTB which is large and expected bleeding, there was a possibility that these factors had affected the result. However, in the present study, one of the recurrent cases after embolization had GCTB in metatarsal bone (Table 4). Our study included only a small number of cases of GCTB in the trunk and a previous report showed a high local recurrence rate of 43.3% in axial cases after curettage [4]. However, there was no difference in the local recurrence rate between location in the trunk (1 of 7 patients, 14.3%) and extremity (29 of 151 patients, 19.2%) in our study. There was no significant relation between pathological fracture at first visit and local recurrence in our study. A past report also could not demonstrate an effect of pathological fracture on local recurrence in a meta-analysis [16]. Local recurrent GCTB is known to be highly re-recurrent after curettage with rates of re-recurrence of 32 to 34% [17, 18]. Our study included no patients after recurrence, and our analysis was limited to primary tumors. Distant recurrence rate was 2.6% after curettage in our study, and this result was similar to that noted in previous studies [7, 8]. In our study, 16 of 24 (67%) institutions actually performed perioperative use of denosumab with curettage, and the recurrence rates were 6 of 21 (28.6%), 2 of 9 (22.2%), and 0 of 10 (0.0%) with preoperative, postoperative, and both pre- and postoperative treatments with curettage, respectively. One study on the perioperative use of denosumab for GCTB with curettage demonstrated local recurrence in 17 of 116 patients (15%) with a median follow-up period of 13.0 months [19]. However, the study included patients with unresectable GCTB and salvageable GCTB whose surgery was associated with severe morbidity, and the effect of denosumab for patients with GCTB who can be treated by curettage at the first visit was not clear. Our study may have also included some patients who could not be treated by curettage at first, but we could not identify those patients due to the questionnaire format used. Median numbers of administration times of denosumab were 6 (2 41) and 6 (1 14) in the preoperative and postoperative settings, respectively in our study. Some reports demonstrated histopathological changes after 6 months treatment with denosumab [20, 21], but 6 months are thought to be too long to use it as a postand/or preoperative treatment in patients with GCTB which can be treated by curettage. In our study, more than five administration times was significantly associated with a decreased incidence of local recurrence after curettage in 31 patients treated with preoperative or both pre- and postoperative denosumab, meaning that a sufficiently high dose of preoperative denosumab can suppress local recurrence after curettage. When used as a running dose, five times administration of denosumab takes 3 months. This relatively short administration period is associated with major benefits, both economic and social, for patients, and this dose is specified in JCOG1610. The clinical use of perioperative denosumab is complicated by various issues such as economic problem, side effects, and pregnancy. The cost of one-shot denosumab (120 mg) for GCTB is 46,685 yen (approximately 420 dollar) in Japan as of October In the previous phase 2 trial of GCTB, denosumab caused diverse side effects such as arthralgia (20%), headache (18%), nausea (17%), fatigue (16%), back pain (15%), extremity pain (15%), hypocalcemia (5%), and osteonecrosis of jaw (1%) of any grade [14]. The use of denosumab for pregnant women should be avoided because it was reported to increase postnatal mortality, decreased body weight gain, and decreased growth/development in a study of infants exposed in utero in cynomolgus monkeys [22]. This may affect the clinical use of denosumab for premenopausal women. In addition, there is a report that denosumab treatment in postmenopausal women with osteoporosis did not interfere with fracture healing [23], but the effects of denosumab on pathological fracture healing and final joint preservation have not been well understood in GCTB patients. Malignant transformation occurs in less than 1% of GCTB [1], and recently, malignant transformation was reported after treatment with denosumab [24] and requires particular caution. In addition, recent study showed a higher rate of recurrence in the GCTB treated with denosumab and curettage compared to historical control without denosumab in retrospective study [25]. For these reasons, perioperative treatment of denosumab should not be done unless an advantage is considered or proved in GCTB which can be treated by curettage. At present, we have started a clinical trial, JCOG1610 (UMIN ), to investigate the efficacy of preoperative denosumab in patients with GCTB which can be treated with curettage. The primary aim of JCOG1610 is to confirm the effects of preoperative denosumab on recurrence after curettage. A previous report demonstrated that proliferation of stromal cells cultured from clinical specimens following denosumab treatment was approximately 50% slower than that of specimens from untreated patients [20]. Even though denosumab did not completely
7 Urakawa et al. World Journal of Surgical Oncology (2018) 16:160 Page 7 of 8 prevent proliferation of stromal cells which have been considered as genuine tumor cells [20], there is a possibility that preoperative denosumab may decrease local and distant recurrences after the curettage of the tumor stromal cells biologically suppressed by denosumab. Secondary endpoints of JCOG1610 include overall survival, joint-preserved survival, local relapse-free survival, metastasis-free survival, adverse events, serious adverse events, surgical and postoperative complications, and discontinuance of denosumab. Systemic denosumab treatment can affect joint-preserved survival, and both local and distant recurrence. Conclusions In conclusion, the recurrence rate of GCTB after curettage was 19.0% in Japan and especially high in Campanacci grade III; therefore, improvements in the therapeutic strategy are needed in this cohort. There is a possibility that a sufficient dose of preoperative denosumab can reduce recurrence after curettage. Recently, we have started JCOG1610 to investigate the efficacy of preoperative denosumab in patients with GCTB which can be treated with curettage. Abbreviations BSTTSG: Bone and Soft Tissue Tumor Study Group; GCTB: Giant cell tumor of bone; JCOG: Japan clinical oncology group; PMMA: Polymethyl methacrylate; RANK: Receptor activator of NF-κB; RANKL: Receptor activator of NF-κB ligand Acknowledgements We thank young researchers in JCOG BSTTSG, Dr. Shintaro Iwata, Dr. Makoto Endo, Dr. Tomoya Matsunobu, Dr. Tomoki Nakamura, Dr. Fumihiko Nakatani, and Dr. Kazuya Oshima for the kind advice regarding this questionnaire survey. Funding We do not have a funding for this questionnaire study. Availability of data and materials The datasets supporting the conclusions of the article are included within the article. Authors contributions HU was involved in the conception and design of the study. TY, SM, TT, KA, MW, AT, NN, YM, AK, TK, TK, ME, HH, HH, ST, YN, TA, TM, MT, AN, HY, KS, MK, and KH were responsible in the acquisition of data and HU in the analysis of data. HU drafted the article, and all authors edited and revised it for important intellectual content. HU, KT, HH, YI, and TO take responsibility for the integrity of the work as a whole, from inception to finished article. All authors approved the final version to be published. Ethics approval and consent to participate This study was approved by the ethics committee of Nagoya University Graduate School and School of Medicine (Nagoya, Japan) and a waiver of informed consent was provided. Consent for publication Not applicable. Competing interests None of the authors have any financial or personal relationships with any other persons or organizations that could potentially and/or inappropriately influence their work and conclusion. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Department of Orthopaedic Surgery, Nagoya University, 65 Tsurumai, Showa-ku, Nagoya, Aichi , Japan. 2 Division of Orthopaedic Surgery, Chiba Cancer Center, Chiba, Japan. 3 Department of Orthopaedic Surgery, Cancer Institute Hospital, Japanese Foundation for Cancer Research, Tokyo, Japan. 4 Department of Orthopaedic Surgery, Juntendo University, Tokyo, Japan. 5 Department of Orthopaedic Surgery, Graduate School of Medicine, Mie University, Tsu, Japan. 6 Department of Orthopaedic Surgery, Tohoku University Hospital, Sendai, Japan. 7 Department of Orthopaedic Surgery, School of Medicine, Yokohama City University, Yokohama, Japan. 8 Musculoskeletal Oncology Service, Osaka International Cancer Institute, Osaka, Japan. 9 Department of Orthopaedic Surgery, Kyushu University, Fukuoka, Japan. 10 Department of Orthopaedic Surgery, National Cancer Center, Tokyo, Japan. 11 Department of Medical Materials for Musculoskeletal Reconstruction, Graduate School of Medicine, Dentistry, and Pharmaceutical Sciences, Okayama University, Okayama, Japan. 12 Department of Orthopaedic Surgery, Hiroshima University, Hiroshima, Japan. 13 Department of Orthopaedic Surgery, Sapporo Medical University, Sapporo, Japan. 14 Department of Orthopaedic Surgery, Hokkaido Cancer Center, Sapporo, Japan. 15 Department of Orthopaedic Surgery, Niigata Cancer Center Hospital, Niigata, Japan. 16 Department of Orthopaedic Surgery, Aichi Cancer Center, Nagoya, Japan. 17 Department of Orthopaedic Surgery, Kobe University, Kobe, Japan. 18 Department of Orthopaedic Surgery, Kyorin University, Mitaka, Japan. 19 Department of Orthopaedic Surgery, Shizuoka Cancer Center, Shizuoka, Japan. 20 Department of Orthopaedic Surgery, Gifu University, Gifu, Japan. 21 Department of Orthopaedic Surgery, Osaka University, Osaka, Japan. 22 Department of Orthopaedic Surgery, Teikyo University, Tokyo, Japan. 23 Department of Orthopaedic Surgery, Oita University, Oita, Japan. 24 Department of Orthopaedic Surgery, Kurume University, Kurume, Japan. 25 Department of Endoprosthetic Surgery, Oita University, Oita, Japan. 26 Kyushu Rosai Hospital, Kitakyushu, Japan. 27 Department of Orthopaedic Surgery, Graduate School of Medicine, Dentistry, and Pharmaceutical Sciences, Okayama University, Okayama, Japan. Received: 6 June 2018 Accepted: 1 August 2018 References 1. Fletcher CDM. WHO classification of tumours of soft tissue and bone. 4th ed. Lyon: IARC Press; Futamura N, Urakawa H, Tsukushi S, Arai E, Kozawa E, Ishiguro N, Nishida Y. Giant cell tumor of bone arising in long bones possibly originates from the metaphyseal region. Oncol Lett. 2016;11: Balke M, Schremper L, Gebert C, Ahrens H, Streitbuerger A, Koehler G, Hardes J, Gosheger G. Giant cell tumor of bone: treatment and outcome of 214 cases. J Cancer Res Clin Oncol. 2008;134: Gaston CL, Bhumbra R, Watanuki M, Abudu AT, Carter SR, Jeys LM, Tillman RM, Grimer RJ. Does the addition of cement improve the rate of local recurrence after curettage of giant cell tumours in bone? J Bone Joint Surg Br. 2011;93: van der Heijden L, van der Geest IC, Schreuder HW, van de Sande MA, Dijkstra PD. Liquid nitrogen or phenolization for giant cell tumor of bone?: a comparative cohort study of various standard treatments at two tertiary referral centers. J Bone Joint Surg Am. 2014;96:e Gao ZH, Yin JQ, Xie XB, Zou CY, Huang G, Wang J, Shen JN. Local control of giant cell tumors of the long bone after aggressive curettage with and without bone cement. BMC Musculoskelet Disord. 2014;15: Masui F, Ushigome S, Fujii K. Giant cell tumor of bone: a clinicopathologic study of prognostic factors. Pathol Int. 1998;48: Siebenrock KA, Unni KK, Rock MG. Giant-cell tumour of bone metastasising to the lungs. A long-term follow-up. J Bone Joint Surg Br. 1998;80: Arbeitsgemeinschaft K, Becker WT, Dohle J, Bernd L, Braun A, Cserhati M, Enderle A, Hovy L, Matejovsky Z, Szendroi M, et al. Local recurrence of giant cell tumor of bone after intralesional treatment with and without adjuvant therapy. J Bone Joint Surg Am. 2008;90: Muramatsu K, Ihara K, Taguchi T. Treatment of giant cell tumor of long bones: clinical outcome and reconstructive strategy for lower and upper limbs. Orthopedics. 2009;32:491.
8 Urakawa et al. World Journal of Surgical Oncology (2018) 16:160 Page 8 of Oda Y, Miura H, Tsuneyoshi M, Iwamoto Y. Giant cell tumor of bone: oncological and functional results of long-term follow-up. Jpn J Clin Oncol. 1998;28: Atkins GJ, Haynes DR, Graves SE, Evdokiou A, Hay S, Bouralexis S, Findlay DM. Expression of osteoclast differentiation signals by stromal elements of giant cell tumors. J Bone Miner Res. 2000;15: Branstetter DG, Nelson SD, Manivel JC, Blay JY, Chawla S, Thomas DM, Jun S, Jacobs I. Denosumab induces tumor reduction and bone formation in patients with giant-cell tumor of bone. Clin Cancer Res. 2012;18: Chawla S, Henshaw R, Seeger L, Choy E, Blay JY, Ferrari S, Kroep J, Grimer R, Reichardt P, Rutkowski P, et al. Safety and efficacy of denosumab for adults and skeletally mature adolescents with giant cell tumour of bone: interim analysis of an open-label, parallel-group, phase 2 study. Lancet Oncol. 2013;14: Campanacci M, Baldini N, Boriani S, Sudanese A. Giant-cell tumor of bone. J Bone Joint Surg Am. 1987;69: Salunke AA, Chen Y, Chen X, Tan JH, Singh G, Tai BC, Khin LW, Puhaindran ME. Does pathological fracture affect the rate of local recurrence in patients with a giant cell tumour of bone?: a meta-analysis. Bone Joint J. 2015;97-B: Takeuchi A, Tsuchiya H, Niu X, Ueda T, Jeon DG, Wang EH, Asavamongkolkul A, Kusuzaki K, Sakayama K, Kang YK. The prognostic factors of recurrent GCT: a cooperative study by the Eastern Asian Musculoskeletal Oncology Group. J Orthop Sci. 2011;16: Klenke FM, Wenger DE, Inwards CY, Rose PS, Sim FH. Recurrent giant cell tumor of long bones: analysis of surgical management. Clin Orthop Relat Res. 2011;469: Rutkowski P, Ferrari S, Grimer RJ, Stalley PD, Dijkstra SP, Pienkowski A, Vaz G, Wunder JS, Seeger LL, Feng A, et al. Surgical downstaging in an open-label phase II trial of denosumab in patients with giant cell tumor of bone. Ann Surg Oncol. 2015;22: Mak IW, Evaniew N, Popovic S, Tozer R, Ghert M. A translational study of the neoplastic cells of Giant cell tumor of bone following neoadjuvant denosumab. J Bone Joint Surg Am. 2014;96:e Thomas D, Henshaw R, Skubitz K, Chawla S, Staddon A, Blay JY, Roudier M, Smith J, Ye Z, Sohn W, et al. Denosumab in patients with giant-cell tumour of bone: an open-label, phase 2 study. Lancet Oncol. 2010;11: Bussiere JL, Pyrah I, Boyce R, Branstetter D, Loomis M, Andrews-Cleavenger D, Farman C, Elliott G, Chellman G. Reproductive toxicity of denosumab in cynomolgus monkeys. Reprod Toxicol. 2013;42: Adami S, Libanati C, Boonen S, Cummings SR, Ho PR, Wang A, Siris E, Lane J, Group FF-HW, Adachi JD, et al. Denosumab treatment in postmenopausal women with osteoporosis does not interfere with fracture-healing: results from the FREEDOM trial. J Bone Joint Surg Am. 2012;94: Aponte-Tinao LA, Piuzzi NS, Roitman P, Farfalli GL. A high-grade sarcoma arising in a patient with recurrent benign giant cell tumor of the proximal tibia while receiving treatment with denosumab. Clin Orthop Relat Res. 2015;473: Errani C, Tsukamoto S, Leone G, Righi A, Akahane M, Tanaka Y, Donati DM. Denosumab may increase the risk of local recurrence in patients with giant-cell tumor of bone treated with curettage. J Bone Joint Surg Am. 2018;100:
Giant cell tumour of the proximal femur
 ONCOLOGY Giant cell tumour of the proximal femur IS JOINT-SPARING MANAGEMENT EVER SUCCESSFUL? A. E. Wijsbek, B. L. Vazquez- Garcia, R. J. Grimer, S. R. Carter, A. A. Abudu, R. M. Tillman, L. Jeys From
ONCOLOGY Giant cell tumour of the proximal femur IS JOINT-SPARING MANAGEMENT EVER SUCCESSFUL? A. E. Wijsbek, B. L. Vazquez- Garcia, R. J. Grimer, S. R. Carter, A. A. Abudu, R. M. Tillman, L. Jeys From
Therapeutic benefits of neoadjuvant and post-operative denosumab on sacral giant cell tumor: a retrospective cohort study of 30 cases
 JBUON 2018; 23(2): 453-459 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic benefits of neoadjuvant and post-operative denosumab on
JBUON 2018; 23(2): 453-459 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic benefits of neoadjuvant and post-operative denosumab on
Does the addition of cement improve the rate of local recurrence after curettage of giant cell tumours in bone?
 ONCOLOGY Does the addition of cement improve the rate of local recurrence after curettage of giant cell tumours in bone? C. L. Gaston, R. Bhumbra, M. Watanuki, A. T. Abudu, S. R. Carter, L. M. Jeys, R.
ONCOLOGY Does the addition of cement improve the rate of local recurrence after curettage of giant cell tumours in bone? C. L. Gaston, R. Bhumbra, M. Watanuki, A. T. Abudu, S. R. Carter, L. M. Jeys, R.
British Journal of Cancer Research
 222 Review 2019; 1(4): 222-227. doi: 10.31488/bjcr.120 Treatment of giant cell tumor of bone: focus on denosumab Atrayee Basu Mallick MD *1, Sant P Chawla MD 2, John A Abraham MD 3, Ravi K Gupta MD 4,
222 Review 2019; 1(4): 222-227. doi: 10.31488/bjcr.120 Treatment of giant cell tumor of bone: focus on denosumab Atrayee Basu Mallick MD *1, Sant P Chawla MD 2, John A Abraham MD 3, Ravi K Gupta MD 4,
p53 Expression Immuno-histochemistry Index in Stage III Giant Cell Tumor of the Bone
 IBIMA Publishing JMED Research http://www.ibimapublishing.com/journals/jmed/jmed.html Vol. 2014 (2014), Article ID 675393, 7 pages DOI: 10.5171/2014.675393 Research Article p53 Expression Immuno-histochemistry
IBIMA Publishing JMED Research http://www.ibimapublishing.com/journals/jmed/jmed.html Vol. 2014 (2014), Article ID 675393, 7 pages DOI: 10.5171/2014.675393 Research Article p53 Expression Immuno-histochemistry
Surgery methods and soft tissue extension are the potential risk factors of local recurrence in giant cell tumor of bone
 Li et al. World Journal of Surgical Oncology (2016) 14:114 DOI 10.1186/s12957-016-0871-z RESEARCH Open Access Surgery methods and soft tissue extension are the potential risk factors of local recurrence
Li et al. World Journal of Surgical Oncology (2016) 14:114 DOI 10.1186/s12957-016-0871-z RESEARCH Open Access Surgery methods and soft tissue extension are the potential risk factors of local recurrence
Outcome of Treatment of Giant-Cell Tumor of Bone: a Single-Institutional Retrospective Study
 Original Article Research in Oncology 2019; Vol. X, No. X: X-X. DOI: 10.21608/resoncol.2019.7254.1072 Outcome of Treatment of Giant-Cell Tumor of Bone: a Single-Institutional Retrospective Study Mahmoud
Original Article Research in Oncology 2019; Vol. X, No. X: X-X. DOI: 10.21608/resoncol.2019.7254.1072 Outcome of Treatment of Giant-Cell Tumor of Bone: a Single-Institutional Retrospective Study Mahmoud
Management of Campanacci type III giant cell tumor
 2017; 3(1): 836-841 ISSN: 2395-1958 IJOS 2017; 3(1): 836-841 2017 IJOS www.orthopaper.com Received: 15-11-2016 Accepted: 16-12-2016 Brig. Muhammad Suhail Amin Head of Orthopedics Surgery Department, Combined
2017; 3(1): 836-841 ISSN: 2395-1958 IJOS 2017; 3(1): 836-841 2017 IJOS www.orthopaper.com Received: 15-11-2016 Accepted: 16-12-2016 Brig. Muhammad Suhail Amin Head of Orthopedics Surgery Department, Combined
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/28526 holds various files of this Leiden University dissertation. Author: Heijden, Lizz van der Title: Giant cell tumor of bone and tenosynovial tissue
Cover Page The handle http://hdl.handle.net/1887/28526 holds various files of this Leiden University dissertation. Author: Heijden, Lizz van der Title: Giant cell tumor of bone and tenosynovial tissue
Takafumi Ueda Akira Kawai Editors. Osteosarcoma. A Multidisciplinary Approach to Treatment
 Takafumi Ueda Akira Kawai Editors Osteosarcoma A Multidisciplinary Approach to Treatment 123 Osteosarcoma ThiS is a FM Blank Page Takafumi Ueda Akira Kawai Editors Osteosarcoma A Multidisciplinary Approach
Takafumi Ueda Akira Kawai Editors Osteosarcoma A Multidisciplinary Approach to Treatment 123 Osteosarcoma ThiS is a FM Blank Page Takafumi Ueda Akira Kawai Editors Osteosarcoma A Multidisciplinary Approach
A High-grade Sarcoma Arising in a Patient With Recurrent Benign Giant Cell Tumor of the Proximal Tibia While Receiving Treatment With Denosumab
 Clin Orthop Relat Res (2015) 473:3050 3055 DOI 10.1007/s11999-015-4249-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CASE REPORT A High-grade
Clin Orthop Relat Res (2015) 473:3050 3055 DOI 10.1007/s11999-015-4249-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons CASE REPORT A High-grade
Giant cell tumor of bone arising in long bones possibly originates from the metaphyseal region
 ONCOLOGY LETTERS 11: 2629-2634, 2016 Giant cell tumor of bone arising in long bones possibly originates from the metaphyseal region NAOHISA FUTAMURA, HIROSHI URAKAWA, SATOSHI TSUKUSHI, EISUKE ARAI, EIJI
ONCOLOGY LETTERS 11: 2629-2634, 2016 Giant cell tumor of bone arising in long bones possibly originates from the metaphyseal region NAOHISA FUTAMURA, HIROSHI URAKAWA, SATOSHI TSUKUSHI, EISUKE ARAI, EIJI
Simret Singh Randhawa, Angel Khor Nee Kwan, Chee Kidd Chiu, Chris Yin Wei Chan, Mun Keong Kwan. 1. Case 1
 Asian Spine Journal Asian Spine Case Journal Report Asian Spine J 2016;10(5):945-949 Treatment of https://doi.org/10.4184/asj.2016.10.5.945 denosumab without surgery Neurological Recovery in Two Patients
Asian Spine Journal Asian Spine Case Journal Report Asian Spine J 2016;10(5):945-949 Treatment of https://doi.org/10.4184/asj.2016.10.5.945 denosumab without surgery Neurological Recovery in Two Patients
Symptoms and signs associated with benign and malignant proximal fibular tumors: a clinicopathological analysis of 52 cases
 Sun et al. World Journal of Surgical Oncology (2017) 15:92 DOI 10.1186/s12957-017-1162-z RESEARCH Open Access Symptoms and signs associated with benign and malignant proximal fibular tumors: a clinicopathological
Sun et al. World Journal of Surgical Oncology (2017) 15:92 DOI 10.1186/s12957-017-1162-z RESEARCH Open Access Symptoms and signs associated with benign and malignant proximal fibular tumors: a clinicopathological
Case Report Two Cases of Sarcoma Arising in Giant Cell Tumor of Bone Treated with Denosumab
 Case Reports in Medicine Volume 2015, Article ID 767198, 6 pages http://dx.doi.org/10.1155/2015/767198 Case Report Two Cases of Sarcoma Arising in Giant Cell Tumor of Bone Treated with Denosumab Cory Julian
Case Reports in Medicine Volume 2015, Article ID 767198, 6 pages http://dx.doi.org/10.1155/2015/767198 Case Report Two Cases of Sarcoma Arising in Giant Cell Tumor of Bone Treated with Denosumab Cory Julian
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.140 A Case Report of Recurrent
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.140 A Case Report of Recurrent
Denosumab et Tumeurs à Cellules Géantes:
 Denosumab et Tumeurs à Cellules Géantes: «La preuve du concept» Axel Le Cesne Institut Gustave Roussy, Villejuif Strasbourg, 27 Juin 2013 GCT of bone Common bone tumour Typically in young adults More in
Denosumab et Tumeurs à Cellules Géantes: «La preuve du concept» Axel Le Cesne Institut Gustave Roussy, Villejuif Strasbourg, 27 Juin 2013 GCT of bone Common bone tumour Typically in young adults More in
SICOT Online Report E057 Accepted April 23th, in Fibula and Rib
 Metachronous, multicentric giant cell tumors in Fibula and Rib Toshihiro Akisue, Tetsuji Yamamoto ( ), Teruya Kawamoto, Toshiaki Hitora, Takashi Marui, Tetsuya Nakatani, Takafumi Onga, and Masahiro Kurosaka
Metachronous, multicentric giant cell tumors in Fibula and Rib Toshihiro Akisue, Tetsuji Yamamoto ( ), Teruya Kawamoto, Toshiaki Hitora, Takashi Marui, Tetsuya Nakatani, Takafumi Onga, and Masahiro Kurosaka
Denosumab treatment of inoperable or locally advanced giant cell tumor of bone
 4312 Denosumab treatment of inoperable or locally advanced giant cell tumor of bone ANETA BORKOWSKA 1*, TOMASZ GORYŃ 2*, ANDRZEJ PIEŃKOWSKI 2, MICHAŁ WĄGRODZKI 3, EWELINA JAGIEŁŁO WIECZOREK 2, PAWEŁ ROGALA
4312 Denosumab treatment of inoperable or locally advanced giant cell tumor of bone ANETA BORKOWSKA 1*, TOMASZ GORYŃ 2*, ANDRZEJ PIEŃKOWSKI 2, MICHAŁ WĄGRODZKI 3, EWELINA JAGIEŁŁO WIECZOREK 2, PAWEŁ ROGALA
Surveillance for lung metastasis from giant cell tumor of bone
 Received: 2 March 2017 Accepted: 29 May 2017 DOI: 10.1002/jso.24739 RESEARCH ARTICLE Surveillance for lung metastasis from giant cell tumor of bone Mamer Rosario MD 1,2 Han-Soo Kim MD PhD 1 Ji Yeon Yun
Received: 2 March 2017 Accepted: 29 May 2017 DOI: 10.1002/jso.24739 RESEARCH ARTICLE Surveillance for lung metastasis from giant cell tumor of bone Mamer Rosario MD 1,2 Han-Soo Kim MD PhD 1 Ji Yeon Yun
Case Report Denosumab Chemotherapy for Recurrent Giant-Cell Tumor of Bone: A Case Report of Neoadjuvant Use Enabling Complete Surgical Resection
 Case Reports in Oncological Medicine Volume 2013, Article ID 496351, 4 pages http://dx.doi.org/10.1155/2013/496351 Case Report Denosumab Chemotherapy for Recurrent Giant-Cell Tumor of Bone: A Case Report
Case Reports in Oncological Medicine Volume 2013, Article ID 496351, 4 pages http://dx.doi.org/10.1155/2013/496351 Case Report Denosumab Chemotherapy for Recurrent Giant-Cell Tumor of Bone: A Case Report
Tartrate-Resistant Acid Phosphatase 5b is a Useful Serum Marker for Diagnosis and Recurrence Detection of Giant Cell Tumor of Bone
 392 The Open Orthopaedics Journal, 2012, 6, 392-399 Open Access Tartrate-Resistant Acid Phosphatase 5b is a Useful Serum Marker for Diagnosis and Recurrence Detection of Giant Cell Tumor of Bone Tetsuya
392 The Open Orthopaedics Journal, 2012, 6, 392-399 Open Access Tartrate-Resistant Acid Phosphatase 5b is a Useful Serum Marker for Diagnosis and Recurrence Detection of Giant Cell Tumor of Bone Tetsuya
Evaluation of prognostic scoring systems for bone metastases using single center data
 MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
Giant cell tumor of the patella: An uncommon cause of anterior knee pain
 MOLECULAR AND CLINICAL ONCOLOGY 3: 207-211, 2015 Giant cell tumor of the patella: An uncommon cause of anterior knee pain TATSUYA SHIBATA 1, JUN NISHIO 1, TAIKI MATSUNAGA 1, MIKIKO AOKI 2, HIROSHI IWASAKI
MOLECULAR AND CLINICAL ONCOLOGY 3: 207-211, 2015 Giant cell tumor of the patella: An uncommon cause of anterior knee pain TATSUYA SHIBATA 1, JUN NISHIO 1, TAIKI MATSUNAGA 1, MIKIKO AOKI 2, HIROSHI IWASAKI
Analysis of the outcome of young age tongue squamous cell carcinoma
 Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Name of Active Ingredient: Fully human monoclonal antibody to receptor activator for nuclear factor-κb ligand
 Page 2 of 1765 2. SYNOPSIS Name of Sponsor: Amgen Inc. Name of Finished Product: Denosumab (AMG 162) Name of Active Ingredient: Fully human monoclonal antibody to receptor activator for nuclear factor-κb
Page 2 of 1765 2. SYNOPSIS Name of Sponsor: Amgen Inc. Name of Finished Product: Denosumab (AMG 162) Name of Active Ingredient: Fully human monoclonal antibody to receptor activator for nuclear factor-κb
We have previously reported good clinical results
 J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication for Repeat Metastasectomy
 Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
The gastrocnemius with soleus bi-muscle flap
 The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
The British Association of Plastic Surgeons (2004) 57, 77 82 The gastrocnemius with soleus bi-muscle flap Ikuo Hyodo a, *, Bin Nakayama b, Mitsuru Takahashi c, Kazuhiro Toriyama d, Yuzuru Kamei d, Shuhei
Clear Cell Chondrosarcoma of the Sacrum
 Clear Cell Chondrosarcoma of the Sacrum Yasunobu Iwasaki MD 1, Tetsuji Yamamoto MD (!) 2, Mitsuo Tsuji MD 1, Akira Kurihara MD 1, Masaaki Uratsuji MD 1, Norihide Sha MD 1, and Shinichi Yoshiya MD 2 1 Department
Clear Cell Chondrosarcoma of the Sacrum Yasunobu Iwasaki MD 1, Tetsuji Yamamoto MD (!) 2, Mitsuo Tsuji MD 1, Akira Kurihara MD 1, Masaaki Uratsuji MD 1, Norihide Sha MD 1, and Shinichi Yoshiya MD 2 1 Department
Pulmonary metastasis of giant cell tumor of bones
 Muheremu and Niu World Journal of Surgical Oncology 2014, 12:261 WORLD JOURNAL OF SURGICAL ONCOLOGY REVIEW Pulmonary metastasis of giant cell tumor of bones Aikeremujiang Muheremu and Xiaohui Niu * Open
Muheremu and Niu World Journal of Surgical Oncology 2014, 12:261 WORLD JOURNAL OF SURGICAL ONCOLOGY REVIEW Pulmonary metastasis of giant cell tumor of bones Aikeremujiang Muheremu and Xiaohui Niu * Open
Surgical management of Grade I chondrosarcoma of the long bones
 Acta Orthop. Belg., 2013, 79, 331-337 ORIGINAL STUDY Surgical management of Grade I chondrosarcoma of the long bones Cuneyd Gunay, Hakan Atalar, Onur Hapa, Kerem Basarir, Yusuf Yildiz, Yener Saglik From
Acta Orthop. Belg., 2013, 79, 331-337 ORIGINAL STUDY Surgical management of Grade I chondrosarcoma of the long bones Cuneyd Gunay, Hakan Atalar, Onur Hapa, Kerem Basarir, Yusuf Yildiz, Yener Saglik From
Current status and unanswered questions on the use of Denosumab in giant cell tumor of bone
 DOI 10.1186/s13569-016-0056-0 Clinical Sarcoma Research REVIEW Open Access Current status and unanswered questions on the use of Denosumab in giant cell tumor of bone Czar Louie Gaston 1*, Robert J. Grimer
DOI 10.1186/s13569-016-0056-0 Clinical Sarcoma Research REVIEW Open Access Current status and unanswered questions on the use of Denosumab in giant cell tumor of bone Czar Louie Gaston 1*, Robert J. Grimer
News Release. Identification of the cause of chronic active Epstein Barr virus (EBV) infection and the mechanism by which EBV causes cancer
 News Release Title Identification of the cause of chronic active Epstein Barr virus (EBV) infection and the mechanism by which EBV causes cancer Key Points A research group in Japan, led by Dr. Hiroshi
News Release Title Identification of the cause of chronic active Epstein Barr virus (EBV) infection and the mechanism by which EBV causes cancer Key Points A research group in Japan, led by Dr. Hiroshi
Chondroblastoma of bone
 Chronology Chondroblastoma of bone LONG-TERM RESULTS AND FUNCTIONAL OUTCOME AFTER INTRALESIONAL CURETTAGE R. Suneja, R. J. Grimer, M. Belthur, L. Jeys, S. R. Carter, R. M. Tillman, A. M. Davies From The
Chronology Chondroblastoma of bone LONG-TERM RESULTS AND FUNCTIONAL OUTCOME AFTER INTRALESIONAL CURETTAGE R. Suneja, R. J. Grimer, M. Belthur, L. Jeys, S. R. Carter, R. M. Tillman, A. M. Davies From The
Giant cell tumour of bone: A demographic study from a tumour unit in South Africa
 SA Orthopaedic Journal Summer 2016 Vol 15 No 4 Page 17 Giant cell tumour of bone: A demographic study from a tumour unit in South Africa Dr A Zanati MBChB, HDip Orth(SA) Dr N Ferreira BSc, MBChB, HDip
SA Orthopaedic Journal Summer 2016 Vol 15 No 4 Page 17 Giant cell tumour of bone: A demographic study from a tumour unit in South Africa Dr A Zanati MBChB, HDip Orth(SA) Dr N Ferreira BSc, MBChB, HDip
Osteosarcoma Arising from Giant Cell Tumor of Bone Ten Years After Primary Surgery: A Case Report and Review of the Literature
 Tohoku J. Exp. Med., 2006, Osteosarcoma 208, 157-162 Arising from Giant Cell Tumor of Bone 157 Osteosarcoma Arising from Giant Cell Tumor of Bone Ten Years After Primary Surgery: A Case Report and Review
Tohoku J. Exp. Med., 2006, Osteosarcoma 208, 157-162 Arising from Giant Cell Tumor of Bone 157 Osteosarcoma Arising from Giant Cell Tumor of Bone Ten Years After Primary Surgery: A Case Report and Review
Xgeva. Xgeva (denosumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.18 Subject: Xgeva Page: 1 of 5 Last Review Date: March 16, 2018 Xgeva Description Xgeva (denosumab)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.18 Subject: Xgeva Page: 1 of 5 Last Review Date: March 16, 2018 Xgeva Description Xgeva (denosumab)
Xgeva. Xgeva (denosumab) Description. Section: Prescription Drugs Effective Date: January 1, 2016
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.18 Subject: Xgeva Page: 1 of 5 Last Review Date: December 3, 2015 Xgeva Description Xgeva (denosumab)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.18 Subject: Xgeva Page: 1 of 5 Last Review Date: December 3, 2015 Xgeva Description Xgeva (denosumab)
Clinical factors affecting pathological fracture and healing of unicameral bone cysts
 Urakawa et al. BMC Musculoskeletal Disorders 2014, 15:159 RESEARCH ARTICLE Open Access Clinical factors affecting pathological fracture and healing of unicameral bone cysts Hiroshi Urakawa 1*, Satoshi
Urakawa et al. BMC Musculoskeletal Disorders 2014, 15:159 RESEARCH ARTICLE Open Access Clinical factors affecting pathological fracture and healing of unicameral bone cysts Hiroshi Urakawa 1*, Satoshi
CASE PRESENTATION. Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN
 CASE PRESENTATION Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN CASE PRESENTATION - History Ms. SB, 30yo Afghan National Presented with 3 months history of Swelling
CASE PRESENTATION Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN CASE PRESENTATION - History Ms. SB, 30yo Afghan National Presented with 3 months history of Swelling
Functional Results after Giant Cell Tumor Operation near Knee Joint and the Cement Radiolucent Zone as Indicator of Recurrence
 Functional Results after Giant Cell Tumor Operation near Knee Joint and the Cement Radiolucent Zone as Indicator of Recurrence K. KAFCHITSAS 1, B. HABERMANN 1, D. PROSCHEK 1, A. KURTH 1 and C. EBERHARDT
Functional Results after Giant Cell Tumor Operation near Knee Joint and the Cement Radiolucent Zone as Indicator of Recurrence K. KAFCHITSAS 1, B. HABERMANN 1, D. PROSCHEK 1, A. KURTH 1 and C. EBERHARDT
The other bone sarcomas
 ONCOLOGY The other bone sarcomas PROGNOSTIC FACTORS AND OUTCOMES OF SPINDLE CELL SARCOMAS OF BONE E. E. Pakos, R. J. Grimer, D. Peake, D. Spooner, S. R. Carter, R. M. Tillman, S. Abudu, L. Jeys From Royal
ONCOLOGY The other bone sarcomas PROGNOSTIC FACTORS AND OUTCOMES OF SPINDLE CELL SARCOMAS OF BONE E. E. Pakos, R. J. Grimer, D. Peake, D. Spooner, S. R. Carter, R. M. Tillman, S. Abudu, L. Jeys From Royal
GIANT CELL TUMOR OF BONES: MANAGEMENT BY DIFFERENT SURGICAL TECHNIQUES
 GIANT CELL TUMOR OF BONES: MANAGEMENT BY DIFFERENT SURGICAL TECHNIQUES Sudqi A. Hamed MD*, Falah Z. Harfoushi MD* ABSTRACT Objective: To evaluate the clinical outcome of different surgical techniques used
GIANT CELL TUMOR OF BONES: MANAGEMENT BY DIFFERENT SURGICAL TECHNIQUES Sudqi A. Hamed MD*, Falah Z. Harfoushi MD* ABSTRACT Objective: To evaluate the clinical outcome of different surgical techniques used
CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT
 Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
Conservative surgical management of simple monostotic fibrous dysplasia of the proximal femur in a 19-year-old basketballer: a case report
 Yung et al. Journal of Medical Case Reports (2018) 12:240 https://doi.org/10.1186/s13256-018-1763-3 CASE REPORT Open Access Conservative surgical management of simple monostotic fibrous dysplasia of the
Yung et al. Journal of Medical Case Reports (2018) 12:240 https://doi.org/10.1186/s13256-018-1763-3 CASE REPORT Open Access Conservative surgical management of simple monostotic fibrous dysplasia of the
DENOSUMAB (PROLIA & XGEVA )
 DENOSUMAB (PROLIA & XGEVA ) UnitedHealthcare Oxford Clinical Policy Policy Number: PHARMACY 306.3 T2 Effective Date: July 2, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
DENOSUMAB (PROLIA & XGEVA ) UnitedHealthcare Oxford Clinical Policy Policy Number: PHARMACY 306.3 T2 Effective Date: July 2, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
ARMS. Reconstruction of Large Femur and Tibia Defect with Free Vascularized Fibula Graft and Locking Plate INTRODUCTION.
 Original Article ARMS Archieves of Reconstructive Microsurgery pissn 2383-5257 eissn 2288-6184 Arch Reconstr Microsurg 2015;24(2):68-74 http://dx.doi.org/10.15596/arms.2015.24.2.68 Reconstruction of Large
Original Article ARMS Archieves of Reconstructive Microsurgery pissn 2383-5257 eissn 2288-6184 Arch Reconstr Microsurg 2015;24(2):68-74 http://dx.doi.org/10.15596/arms.2015.24.2.68 Reconstruction of Large
CURRICULUM VITAE (MALE, FEMALE) Photo 4.5 x 3.5 cm DATE & PLACE OF BIRTH: PRESENT ADDRESS: HOME: TEL: OFFICE: EDUCATION:
 CURRICULUM VITAE NAME: (MALE, FEMALE) DATE & PLACE OF BIRTH: Photo 4.5 x 3.5 cm PRESENT ADDRESS: HOME: TEL: OFFICE: TEL: E-mail: FAX: EDUCATION: LICENSURE & CERTIFICATION: FELLOWSHIP OR STUDY ABROAD: ACADEMIC
CURRICULUM VITAE NAME: (MALE, FEMALE) DATE & PLACE OF BIRTH: Photo 4.5 x 3.5 cm PRESENT ADDRESS: HOME: TEL: OFFICE: TEL: E-mail: FAX: EDUCATION: LICENSURE & CERTIFICATION: FELLOWSHIP OR STUDY ABROAD: ACADEMIC
MARK D. MURPHEY MD, FACR. Physician-in-Chief, AIRP. Chief, Musculoskeletal Imaging
 ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
Soluble N-cadherin as a Biomarker for Malignant Bone and Soft Tissue Tumors
 Soluble N-cadherin as a Biomarker for Malignant Bone and Soft Tissue Tumors Akihiko Matsumine, Rui Niimi, Takahiro Iino, Tomoki Nakamura, Takao Matsubara, Kunihiro Asanuma, Akihiro Sudo, Prof.. Mie University
Soluble N-cadherin as a Biomarker for Malignant Bone and Soft Tissue Tumors Akihiko Matsumine, Rui Niimi, Takahiro Iino, Tomoki Nakamura, Takao Matsubara, Kunihiro Asanuma, Akihiro Sudo, Prof.. Mie University
In Vivo Heat-stimulus Triggered Osteogenesis
 In Vivo Heat-stimulus Triggered Osteogenesis Kunihiro Ikuta 1, Hiroshi Urakawa 1, Eiji Kozawa 1, Shunsuke Hamada 1, Naoki Ishiguro 2, Yoshihiro Nishida 1. 1 Nagoya University, Nagoya, Japan, 2 Nagoya Graduated
In Vivo Heat-stimulus Triggered Osteogenesis Kunihiro Ikuta 1, Hiroshi Urakawa 1, Eiji Kozawa 1, Shunsuke Hamada 1, Naoki Ishiguro 2, Yoshihiro Nishida 1. 1 Nagoya University, Nagoya, Japan, 2 Nagoya Graduated
Functional Outcome Study of Mega-Endoprosthetic Reconstruction in Limbs With Bone Tumour Surgery
 192 Original Article Functional Outcome Study of Mega-Endoprosthetic Reconstruction in Limbs With Bone Tumour Surgery Peh Khee Tan, 1 MBBS, MRCS (Edin), MMed (Orthop), Mann Hong Tan, 1 MBBS, FRCS (Edin
192 Original Article Functional Outcome Study of Mega-Endoprosthetic Reconstruction in Limbs With Bone Tumour Surgery Peh Khee Tan, 1 MBBS, MRCS (Edin), MMed (Orthop), Mann Hong Tan, 1 MBBS, FRCS (Edin
Giant cell tumor of the distal ulna: a case report
 Vanni et al. Journal of Medical Case Reports 2012, 6:143 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant cell tumor of the distal ulna: a case report Daniele Vanni 1, Andrea Pantalone 1,
Vanni et al. Journal of Medical Case Reports 2012, 6:143 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant cell tumor of the distal ulna: a case report Daniele Vanni 1, Andrea Pantalone 1,
Giant cell tumours of the small bones of the hands and feet
 ONCOLOGY Giant cell tumours of the small bones of the hands and feet LONG-TERM RESULTS OF 30 PATIENTS AND A SYSTEMATIC LITERATURE REVIEW V. C. Oliveira, L. van der Heijden, I. C. M. van der Geest, D. A.
ONCOLOGY Giant cell tumours of the small bones of the hands and feet LONG-TERM RESULTS OF 30 PATIENTS AND A SYSTEMATIC LITERATURE REVIEW V. C. Oliveira, L. van der Heijden, I. C. M. van der Geest, D. A.
Clinical Study Primary Malignant Tumours of Bone Following Previous Malignancy
 Sarcoma Volume 2008, Article ID 418697, 4 pages doi:10.1155/2008/418697 Clinical Study Primary Malignant Tumours of Bone Following Previous Malignancy J. T. Patton, S. M. M. Sommerville, and R. J. Grimer
Sarcoma Volume 2008, Article ID 418697, 4 pages doi:10.1155/2008/418697 Clinical Study Primary Malignant Tumours of Bone Following Previous Malignancy J. T. Patton, S. M. M. Sommerville, and R. J. Grimer
Upper extremity open fractures in hospitalized road traffic accident patients: adult versus pediatric cases
 Rubin et al. Journal of Orthopaedic Surgery and Research (2017) 12:157 DOI 10.1186/s13018-017-0657-1 RESEARCH ARTICLE Open Access Upper extremity in hospitalized road traffic accident : adult versus pediatric
Rubin et al. Journal of Orthopaedic Surgery and Research (2017) 12:157 DOI 10.1186/s13018-017-0657-1 RESEARCH ARTICLE Open Access Upper extremity in hospitalized road traffic accident : adult versus pediatric
Soft-tissue Recurrence of Giant Cell tumor of Bone Associated with Pulmonary Metastases.
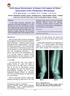 Soft-tissue Recurrence of Giant Cell tumor of Bone Associated with Pulmonary Metastases. M. M. Abdel- Motaal 1, A. S. Othman 1, M. K. C. Katchy 2, A. K. Jassar 3 1 Al-Razi Orthopaedic Hospital, Kuwait,
Soft-tissue Recurrence of Giant Cell tumor of Bone Associated with Pulmonary Metastases. M. M. Abdel- Motaal 1, A. S. Othman 1, M. K. C. Katchy 2, A. K. Jassar 3 1 Al-Razi Orthopaedic Hospital, Kuwait,
EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence
 102 Journal of Cancer Research Updates, 2012, 1, 102-107 EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence Kenichi
102 Journal of Cancer Research Updates, 2012, 1, 102-107 EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence Kenichi
GIANT CELL TUMOR OF BONE
 GIANT CELL TUMOR OF BONE Definition. First described by Jaffe et al. 1, giant cell tumor of bone is a locally aggressive primary neoplasm of bone that is composed of proliferation of bland looking oval
GIANT CELL TUMOR OF BONE Definition. First described by Jaffe et al. 1, giant cell tumor of bone is a locally aggressive primary neoplasm of bone that is composed of proliferation of bland looking oval
PHYSICIAN OFFICE BILLING INFORMATION SHEET FOR XGEVA. Notes
 For prevention of skeletal-related events XGEVA is indicated for the prevention of skeletal-related events in patients with bone metastases from solid tumors. XGEVA is not indicated for the prevention
For prevention of skeletal-related events XGEVA is indicated for the prevention of skeletal-related events in patients with bone metastases from solid tumors. XGEVA is not indicated for the prevention
A prediction model of survival for patients with bone metastasis from uterine corpus cancer
 JJCO Japanese Journal of Clinical Oncology Japanese Journal of Clinical Oncology, 2016, 46(11) 973 978 doi: 10.1093/jjco/hyw120 Advance Access Publication Date: 21 September 2016 Original Article Original
JJCO Japanese Journal of Clinical Oncology Japanese Journal of Clinical Oncology, 2016, 46(11) 973 978 doi: 10.1093/jjco/hyw120 Advance Access Publication Date: 21 September 2016 Original Article Original
Endovascular and surgical treatment of giant pelvic tumor
 Endovascular and surgical treatment of giant pelvic tumor Mitrev Z., MD FETCS; Anguseva T., MD; Milev I., MD; Zafiroski G., PhD MD Center for Cardiosurgery, Filip the II, Skopje, Macedonia Background Giant
Endovascular and surgical treatment of giant pelvic tumor Mitrev Z., MD FETCS; Anguseva T., MD; Milev I., MD; Zafiroski G., PhD MD Center for Cardiosurgery, Filip the II, Skopje, Macedonia Background Giant
Genetic variability of genes involved in DNA repair influence treatment outcome in osteosarcoma
 Genetic variability of genes involved in DNA repair influence treatment outcome in osteosarcoma M.J. Wang, Y. Zhu, X.J. Guo and Z.Z. Tian Department of Orthopaedics, Xinxiang Central Hospital, Xinxiang,
Genetic variability of genes involved in DNA repair influence treatment outcome in osteosarcoma M.J. Wang, Y. Zhu, X.J. Guo and Z.Z. Tian Department of Orthopaedics, Xinxiang Central Hospital, Xinxiang,
Treatment of the benign lytic lesions of the proximal femur with synthetic bone graft
 Zekry et al. Journal of Orthopaedic Surgery and Research (2018) 13:270 https://doi.org/10.1186/s13018-018-0982-z RESEARCH ARTICLE Open Access Treatment of the benign lytic lesions of the proximal femur
Zekry et al. Journal of Orthopaedic Surgery and Research (2018) 13:270 https://doi.org/10.1186/s13018-018-0982-z RESEARCH ARTICLE Open Access Treatment of the benign lytic lesions of the proximal femur
Introduction. Original Article
 pissn : 2093-582X, eissn : 2093-5641 J Gastric Cancer 2016;16(2):93-97 http://dx.doi.org/10.5230/jgc.2016.16.2.93 Original Article Non-Randomized Confirmatory Trial of Laparoscopy-Assisted Total Gastrectomy
pissn : 2093-582X, eissn : 2093-5641 J Gastric Cancer 2016;16(2):93-97 http://dx.doi.org/10.5230/jgc.2016.16.2.93 Original Article Non-Randomized Confirmatory Trial of Laparoscopy-Assisted Total Gastrectomy
ORIGINAL PAPER. Marginal pulmonary function is associated with poor short- and long-term outcomes in lung cancer surgery
 Nagoya J. Med. Sci. 79. 37 ~ 42, 2017 doi:10.18999/nagjms.79.1.37 ORIGINAL PAPER Marginal pulmonary function is associated with poor short- and long-term outcomes in lung cancer surgery Naoki Ozeki, Koji
Nagoya J. Med. Sci. 79. 37 ~ 42, 2017 doi:10.18999/nagjms.79.1.37 ORIGINAL PAPER Marginal pulmonary function is associated with poor short- and long-term outcomes in lung cancer surgery Naoki Ozeki, Koji
Chondrosarcoma with a late local relapse
 Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Total en bloc spondylectomy of the eleventh thoracic vertebra following denosumab therapy for the treatment of a giant cell tumor
 ONCOLOGY LETTERS 14: 4005-4010, 2017 Total en bloc spondylectomy of the eleventh thoracic vertebra following denosumab therapy for the treatment of a giant cell tumor GEN INOUE, TAKAYUKI IMURA, MASAYUKI
ONCOLOGY LETTERS 14: 4005-4010, 2017 Total en bloc spondylectomy of the eleventh thoracic vertebra following denosumab therapy for the treatment of a giant cell tumor GEN INOUE, TAKAYUKI IMURA, MASAYUKI
Product: Denosumab (AMG 162) Abbreviated Clinical Study Report: (Extension Phase Results) Date: 24 August 2010 Page Page 2 of 2 of
 Product: Denosumab (MG 162) bbreviated Clinical Study Report: 20040114 (Extension Phase Results) Date: 24 ugust 2010 Page Page 2 of 2 of 1314 55 2. SYNOPSIS Name of Sponsor: mgen Inc. Name of Finished
Product: Denosumab (MG 162) bbreviated Clinical Study Report: 20040114 (Extension Phase Results) Date: 24 ugust 2010 Page Page 2 of 2 of 1314 55 2. SYNOPSIS Name of Sponsor: mgen Inc. Name of Finished
The choice of internal fixator for fractures around the femoral trochanter depends on area classification
 DOI 10.1186/s40064-016-3206-1 RESEARCH Open Access The choice of internal fixator for fractures around the femoral trochanter depends on area classification Hiroaki Kijima 1,2*, Shin Yamada 1,2, Natsuo
DOI 10.1186/s40064-016-3206-1 RESEARCH Open Access The choice of internal fixator for fractures around the femoral trochanter depends on area classification Hiroaki Kijima 1,2*, Shin Yamada 1,2, Natsuo
Treatment of bone defect with calcium phosphate cement subsequent to tumor curettage in pediatric patients
 ONCOLOGY LETTERS 11: 247-252, 2016 Treatment of bone defect with calcium phosphate cement subsequent to tumor curettage in pediatric patients TOMOKI NAKAMURA, AKIHIKO MATSUMINE, KUNIHIRO ASANUMA, TAKAO
ONCOLOGY LETTERS 11: 247-252, 2016 Treatment of bone defect with calcium phosphate cement subsequent to tumor curettage in pediatric patients TOMOKI NAKAMURA, AKIHIKO MATSUMINE, KUNIHIRO ASANUMA, TAKAO
Limb Salvage Surgery for Musculoskeletal Oncology
 Editorial Limb Salvage Surgery for Musculoskeletal Oncology Wan Faisham Nu man Bin Wan Ismail Submitted: 2 May 2015 Accepted: 18 June 2015 Orthopaedic Oncology Unit, Orthopaedic Department, School of Medical
Editorial Limb Salvage Surgery for Musculoskeletal Oncology Wan Faisham Nu man Bin Wan Ismail Submitted: 2 May 2015 Accepted: 18 June 2015 Orthopaedic Oncology Unit, Orthopaedic Department, School of Medical
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
Frozen recapping laminoplasty: a new technique to treat spinal tumor
 EUROSPINE 2018 19-21 September, Barcelona, Spain Frozen recapping laminoplasty: a new technique to treat spinal tumor Noritaka Yonezawa, Hideki Murakami, Satoru Demura, Satoshi Kato, Katsuhito Yoshioka,
EUROSPINE 2018 19-21 September, Barcelona, Spain Frozen recapping laminoplasty: a new technique to treat spinal tumor Noritaka Yonezawa, Hideki Murakami, Satoru Demura, Satoshi Kato, Katsuhito Yoshioka,
Long-term administration of bisphosphonate to reduce local recurrence of sacral giant cell tumor after nerve-sparing surgery
 CLINICAL ARTICLE J Neurosurg Spine 26:716 721, 2017 Long-term administration of bisphosphonate to reduce local recurrence of sacral giant cell tumor after nerve-sparing surgery *Wei Xu, MD, 1 Yu Wang,
CLINICAL ARTICLE J Neurosurg Spine 26:716 721, 2017 Long-term administration of bisphosphonate to reduce local recurrence of sacral giant cell tumor after nerve-sparing surgery *Wei Xu, MD, 1 Yu Wang,
Akiko Serizawa *, Kiyoaki Taniguchi, Takuji Yamada, Kunihiko Amano, Sho Kotake, Shunichi Ito and Masakazu Yamamoto
 Serizawa et al. Surgical Case Reports (2018) 4:88 https://doi.org/10.1186/s40792-018-0494-4 CASE REPORT Successful conversion surgery for unresectable gastric cancer with giant paraaortic lymph node metastasis
Serizawa et al. Surgical Case Reports (2018) 4:88 https://doi.org/10.1186/s40792-018-0494-4 CASE REPORT Successful conversion surgery for unresectable gastric cancer with giant paraaortic lymph node metastasis
Yoshihisa Fujita 1*, Kumi Shimada 1, Tomohiko Sato 1, Masahiko Akatsu 1, Koichi Nishikawa 2, Atsuko Kanno 3 and Toshitake Aizawa 3
 Fujita et al. JA Clinical Reports (2018) 4:36 https://doi.org/10.1186/s40981-018-0172-3 CLINICAL RESEARCH LETTER Open Access In-hospital mortality does not increase in patients aged over 85 years after
Fujita et al. JA Clinical Reports (2018) 4:36 https://doi.org/10.1186/s40981-018-0172-3 CLINICAL RESEARCH LETTER Open Access In-hospital mortality does not increase in patients aged over 85 years after
Trends of kidney transplantation in Japan in 2018: data from the kidney transplant registry
 Yagisawa et al. Renal Replacement Therapy (2019) 5:3 https://doi.org/10.1186/s41100-019-0199-6 POSITION STATEMENT Trends of kidney transplantation in Japan in 2018: data from the kidney transplant registry
Yagisawa et al. Renal Replacement Therapy (2019) 5:3 https://doi.org/10.1186/s41100-019-0199-6 POSITION STATEMENT Trends of kidney transplantation in Japan in 2018: data from the kidney transplant registry
Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing Tumor Resections
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 426, pp. 97 102 2004 Lippincott Williams & Wilkins Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 426, pp. 97 102 2004 Lippincott Williams & Wilkins Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing
A multiplanar complex resection of a low-grade chondrosarcoma of the distal femur guided by K-wires previously inserted under CT-guide: a case report
 Zoccali et al. BMC Surgery 2014, 14:52 CASE REPORT Open Access A multiplanar complex resection of a low-grade chondrosarcoma of the distal femur guided by K-wires previously inserted under CT-guide: a
Zoccali et al. BMC Surgery 2014, 14:52 CASE REPORT Open Access A multiplanar complex resection of a low-grade chondrosarcoma of the distal femur guided by K-wires previously inserted under CT-guide: a
Risk factors affecting inhospital mortality after hip fracture: retrospective analysis using the Japanese Diagnosis Procedure Combination Database
 Open Access To cite: Shoda N, Yasunaga H, Horiguchi H, et al. Risk factors affecting inhospital mortality after hip fracture: retrospective analysis using the Japanese Diagnosis Procedure Combination Database.
Open Access To cite: Shoda N, Yasunaga H, Horiguchi H, et al. Risk factors affecting inhospital mortality after hip fracture: retrospective analysis using the Japanese Diagnosis Procedure Combination Database.
Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study
 Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
CASE STUDY: PRO-DENSE Injectable Regenerative Graft Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor
 : PRO-DENSE Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor Contributed by: Matthew J. Seidel, MD* Lauren A. Schwartz, NP Scottsdale, AZ *Dr. Seidel is a paid consultant for Wright
: PRO-DENSE Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor Contributed by: Matthew J. Seidel, MD* Lauren A. Schwartz, NP Scottsdale, AZ *Dr. Seidel is a paid consultant for Wright
Clinical statistics of gynecologic cancers in Japan
 J Gynecol Oncol. 2017 Mar;28(2):e32 pissn 2005-0380 eissn 2005-0399 Review Article Clinical statistics of gynecologic cancers in Japan Wataru Yamagami, 1,7 Satoru Nagase, 2,7 Fumiaki Takahashi, 3 Kazuhiko
J Gynecol Oncol. 2017 Mar;28(2):e32 pissn 2005-0380 eissn 2005-0399 Review Article Clinical statistics of gynecologic cancers in Japan Wataru Yamagami, 1,7 Satoru Nagase, 2,7 Fumiaki Takahashi, 3 Kazuhiko
A 42-year-old patient presenting with femoral
 Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Pregabalin prescription for terminally ill cancer patients receiving specialist palliative care in an acute hospital
 Yajima et al. Journal of Pharmaceutical Health Care and Sciences (2016) 2:29 DOI 10.1186/s40780-016-0063-6 RESEARCH ARTICLE Open Access Pregabalin prescription for terminally ill cancer patients receiving
Yajima et al. Journal of Pharmaceutical Health Care and Sciences (2016) 2:29 DOI 10.1186/s40780-016-0063-6 RESEARCH ARTICLE Open Access Pregabalin prescription for terminally ill cancer patients receiving
Efficacy of Trabectedin in Patients With Advanced Translocation- Related Sarcomas: Pooled Analysis of Two Phase II Studies
 Sarcomas Efficacy of Trabectedin in Patients With Advanced Translocation- Related Sarcomas: Pooled Analysis of Two Phase II Studies MITSURU TAKAHASHI, a SHUNJI TAKAHASHI, b NOBUHITO ARAKI, c HIDESHI SUGIURA,
Sarcomas Efficacy of Trabectedin in Patients With Advanced Translocation- Related Sarcomas: Pooled Analysis of Two Phase II Studies MITSURU TAKAHASHI, a SHUNJI TAKAHASHI, b NOBUHITO ARAKI, c HIDESHI SUGIURA,
Lung cancer is one of the leading causes of death in most
 ORIGINAL ARTICLE Japanese Lung Cancer Registry Study of 11,663 Surgical Cases in Demographic and Prognosis Changes Over Decade Noriyoshi Sawabata, MD, PhD,* Etsuo Miyaoka, PhD, Hisao Asamura, MD, PhD,
ORIGINAL ARTICLE Japanese Lung Cancer Registry Study of 11,663 Surgical Cases in Demographic and Prognosis Changes Over Decade Noriyoshi Sawabata, MD, PhD,* Etsuo Miyaoka, PhD, Hisao Asamura, MD, PhD,
Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft
 900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
We have studied 560 patients with osteosarcoma of a
 Osteosarcoma of the limb AMPUTATION OR LIMB SALVAGE IN PATIENTS TREATED BY NEOADJUVANT CHEMOTHERAPY G. Bacci, S. Ferrari, S. Lari, M. Mercuri, D. Donati, A. Longhi, C. Forni, F. Bertoni, M. Versari, E.
Osteosarcoma of the limb AMPUTATION OR LIMB SALVAGE IN PATIENTS TREATED BY NEOADJUVANT CHEMOTHERAPY G. Bacci, S. Ferrari, S. Lari, M. Mercuri, D. Donati, A. Longhi, C. Forni, F. Bertoni, M. Versari, E.
Metastatic Disease of the Proximal Femur
 CASE REPORT Metastatic Disease of the Proximal Femur WI Faisham, M.Med{Ortho)*, W Zulmi, M.S{Ortho)*, B M Biswal, MBBS** 'Department of Orthopaedic, "Department of Oncology and Radiotherapy, School of
CASE REPORT Metastatic Disease of the Proximal Femur WI Faisham, M.Med{Ortho)*, W Zulmi, M.S{Ortho)*, B M Biswal, MBBS** 'Department of Orthopaedic, "Department of Oncology and Radiotherapy, School of
Surgical Management for Giant Cell Tumor of Bones
 Journal of the Egyptian Nat. Cancer Inst., Vol. 6, No., September: 5-5, 00 Surgical Management for Giant Cell Tumor of Bones EL SAYED ASHRAF KHALIL, M.D. FRCS; ALAA YOUNIS, M.D.; SHERIF A. AZIZ, M.D and
Journal of the Egyptian Nat. Cancer Inst., Vol. 6, No., September: 5-5, 00 Surgical Management for Giant Cell Tumor of Bones EL SAYED ASHRAF KHALIL, M.D. FRCS; ALAA YOUNIS, M.D.; SHERIF A. AZIZ, M.D and
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Factors predictive of myoinvasion in cases of Complex Atypical Hyperplasia diagnosed on endometrial biopsy or curettage
 Factors predictive of myoinvasion in cases of Complex Atypical Hyperplasia diagnosed on endometrial biopsy or curettage Jessica Johns, MD Jeffrey Killeen, MD Robert Kim, MD Hyeong Jun Ahn, PhD None Disclosures
Factors predictive of myoinvasion in cases of Complex Atypical Hyperplasia diagnosed on endometrial biopsy or curettage Jessica Johns, MD Jeffrey Killeen, MD Robert Kim, MD Hyeong Jun Ahn, PhD None Disclosures
ORIGINAL ARTICLE. Adult Soft Tissue Ewing Sarcoma or Primitive Neuroectodermal Tumors
 Adult Soft Tissue Ewing Sarcoma or Primitive Neuroectodermal Tumors Predictors of Survival? Robert C. G. Martin II, MD; Murray F. Brennan, MD ORIGINAL ARTICLE Background: Ewing sarcoma (ES) is the second
Adult Soft Tissue Ewing Sarcoma or Primitive Neuroectodermal Tumors Predictors of Survival? Robert C. G. Martin II, MD; Murray F. Brennan, MD ORIGINAL ARTICLE Background: Ewing sarcoma (ES) is the second
Impact of a new medical network system on the efficiency of treatment for eating disorders in Japan: a retrospective observational study
 Moriya et al. BioPsychoSocial Medicine (2017) 11:27 DOI 10.1186/s13030-017-0113-9 RESEARCH Open Access Impact of a new medical network system on the efficiency of treatment for eating disorders in Japan:
Moriya et al. BioPsychoSocial Medicine (2017) 11:27 DOI 10.1186/s13030-017-0113-9 RESEARCH Open Access Impact of a new medical network system on the efficiency of treatment for eating disorders in Japan:
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: denosumab_prolia_xgeva 3/2011 9/2017 9/2018 9/2017 Description of Procedure or Service Receptor activator
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: denosumab_prolia_xgeva 3/2011 9/2017 9/2018 9/2017 Description of Procedure or Service Receptor activator
Surgical treatment is decisive for outcome in chondrosarcoma of the chest wall: A population-based Scandinavian Sarcoma Group study of 106 patients
 Surgical treatment is decisive for outcome in chondrosarcoma of the chest wall: A population-based Scandinavian Sarcoma Group study of 106 patients Björn Widhe, MD, and Prof. Henrik C. F. Bauer, MD, PhD
Surgical treatment is decisive for outcome in chondrosarcoma of the chest wall: A population-based Scandinavian Sarcoma Group study of 106 patients Björn Widhe, MD, and Prof. Henrik C. F. Bauer, MD, PhD
Synovial Sarcoma of Extremities: Evaluation of Prognostic Factors and Clinical Outcomes
 Med. J. Cairo Univ., Vol. 81, No. 1, December: 1093-1097, 2013 www.medicaljournalofcairouniversity.net Synovial Sarcoma of Extremities: Evaluation of Prognostic Factors and Clinical Outcomes SEHAM E. ABDELKHALEK,
Med. J. Cairo Univ., Vol. 81, No. 1, December: 1093-1097, 2013 www.medicaljournalofcairouniversity.net Synovial Sarcoma of Extremities: Evaluation of Prognostic Factors and Clinical Outcomes SEHAM E. ABDELKHALEK,
