MiR-181b modulates chemosensitivity of glioblastoma multiforme cells to temozolomide by targeting the epidermal growth factor receptor
|
|
|
- Horace Gilbert
- 5 years ago
- Views:
Transcription
1 DOI /s LABORATORY INVESTIGATION MiR-181b modulates chemosensitivity of glioblastoma multiforme cells to temozolomide by targeting the epidermal growth factor receptor Yunxiang Chen 1 Rui Li 1 Minhong Pan 2 Zhumei Shi 1 Wei Yan 1 Ning Liu 1 Yongping You 1 Junxia Zhang 1 Xiefeng Wang 1 Received: 17 September 2016 / Accepted: 6 May 2017 Springer Science+Business Media New York 2017 Abstract Temozolomide (TMZ) is a promising chemotherapeutic agent to treat Glioblastoma multiforme (GBM). However, resistance to TMZ develops quickly with a high frequency. The mechanisms underlying GBM cells resistance to TMZ are not fully understood. MicroRNAs (mir- NAs) are small, non-coding RNA molecules that regulate protein expression by cleaving or repressing the translation of target mrnas. Recently, mirnas have been discovered to play important roles in drug resistance. A previous study showed that mir-181b in involved in glioma tumorigenesis. Thus, it would be valuable to explore the functions and mechanisms of mir-181b in regulating GMB cells sensitivity to TMZ. In this study, quantitative real-time reverse transcription PCR (qrt-pcr) data indicated that mir- 181b was significantly downregulated in recurrent GBM tissues compared with initial GBM tissues. We also found that mir-181b overexpression increased the chemo-sensitivity of GBM cells to TMZ and potentiated TMZ-induced apoptosis in vitro and in vivo. Moreover, we demonstrated that the epidermal growth factor receptor (EGFR) was a direct target of mir-181b: restoration of EGFR rescued the Yunxiang Chen, Rui Li and Minhong Pan have contributed equally to this work. * Junxia Zhang zjx2032@126.com * Xiefeng Wang xiefeng@njmu.edu.cn 1 Department of Neurosurgery, The First Affiliated Hospital of Nanjing Medical University, 300, Guangzhou road, Nanjing, People s Republic of China 2 Department of Pathology, The First Affiliated Hospital of Nanjing Medical University, 300, Guangzhou road, Nanjing, People s Republic of China inhibitory effects of mir-181b and TMZ treatment. Taken together, our data support strongly an important role for mir-181b in conferring TMZ resistance by targeting EGFR expression. Keywords MiR-181b Glioblastoma multiforme Temozolomide Epidermal growth factor receptor Introduction Glioblastoma multiforme (GBM), a Grade IV brain tumor according to the World Health Organization (WHO) classification, is one of the most aggressive human cancers [1, 2]. Current treatments include surgical resection and radio/chemotherapy; however, the median survival remains months from time of diagnosis and a nearly 100% local recurrence rate following maximal therapy has been reported [3, 4]. One of the most common reasons for GBM recurrence is resistance to therapeutic drugs [5, 6]. Furthermore, treatment of drug resistant-gbm is more difficult because of its limited repair mechanisms and anatomical complexities [7 9]. Therefore, it is urgent to explore the molecular mechanisms involved in GBM to develop effective therapeutic interventions. The epidermal growth factor receptor (EGFR, also referred to as ERBB1 or HER1) is a member of the HER superfamily of receptor tyrosine kinases, together with ERBB2, ERBB3, and ERBB4 [10, 11]. Binding of growth factors to EGFR leads to autophosphorylation of receptor tyrosine kinase and activation of the downstream signal transduction pathways, which are involved in regulating cellular proliferation, differentiation, and survival [12, 13]. EGFR is commonly overexpressed and amplified in gliomas, and contributes to uncontrolled Vol.:( )
2 proliferation and survival of GBM cells [14, 15]. Multiple EGFR inhibitors have been developed that can inhibit tumor growth, such as erlotinib and gefitinib; however, many patients do not respond well to EGFR inhibitors, including those with non-small-cell lung cancer or GBM [16 18]. Meanwhile, EGFR inhibition can cooperate in a schedule-dependent manner with low doses of temozolomide (TMZ) to reduce GBM cell growth [19, 20]. Unfortunately, the mechanisms related to resistance to EGFR inhibitors remain unclear; however, evidence of the roles for micrornas (mirnas) in determining drug-sensitivity/resistance is emerging. MiRNAs are small regulatory RNA molecules that have been identified recently in the progression of various cancers and are proposed as novel targets for anticancer therapies [21, 22]. MiRNAs target the 3 untranslated regions (UTRs) of oncogenes and tumor suppressor genes, thus contributing to the tumorigenesis of various human cancers [23, 24]. Previous studies demonstrated that mirnas could mediate EGFR signaling to influence tumor growth and drug resistance [25 27]. For example, mirna-556 regulates EGFR directly and enhances drug-resistance, correlating significantly with the clinical response and survival following anti-egfr therapy [28]. Our previous studies demonstrated that mir-181b functions as a tumor suppressor gene by inhibiting tumor cell growth, migration, and invasion [29]. However, the detailed role and underlying mechanism of mir-181b s regulation of GMB cells sensitivity to TMZ is unclear. In the present study, overexpression of mir-181b downregulated EGFR and enhanced the apoptosis induced by TMZ. We confirmed that mir-181b influences the EGFR pathway and enhances the sensitivity of GBM cells to TMZ in vitro and in vivo. Therefore, mir-181b may serve as a potential target for overcoming TMZ resistance in human GBM treatment. Materials and methods Tissue collection Twenty Human GBM tissue samples, eight normal brain tissues, and ten paired initial and recurrent GBM tissues with particular clinical data were obtained from the Department of Neurosurgery at the first affiliated hospital of Nanjing medical university. All the tissues were immediately snap-frozen and stored in liquid nitrogen after surgical removal. This study was approved by the hospital Ethics Committee, and written informed consent was obtained from all patients. Cell culture and treatment Human U87 and U251 GBM cells were purchased from ATCC (the American Type Culture Collection, USA) and maintained in Dulbecco s modified Eagle medium (DMEM, Gibco, USA) supplemented with 10% fetal bovine serum (FBS) (Gibco, USA), 2 mm glutamine (Sigma, USA), 100 µg/ml penicillin (Sigma, USA), and 100 µg/ml streptomycin (Sigma, USA), and incubated at 37 C with 5% CO 2. For cell transfection, Lipofectamine 2000 (Invitrogen, USA) was used according to the manufacturer s instruction. Cell transfection Cells at 50 70% confluence were transfected using Lipofectamine 2000 (Invitrogen). A vector expressing EGFR or the empty vector (both 2 μg) were transfected into U87 and U251 cells according to the manufacturer s instructions. Chemo sensitivity assay The cells were seeded into 96-well plates at per well. After 24 h, the cells were treated with different concentrations of TMZ. The absorption of the cells were measured after 48h using a Cell Counting Kit-8 (CCK-8) (Dojindo Laboratories, Kumamoto, Japan). Lentivirus packaging and stable cell lines The lentiviral packaging kit was purchased from Open Biosystems (Huntsville, AL, USA). Lentiviruses carrying hsa-mir-181b or hsa-mir-negative control (mir-nc) were packaged following the manufacturer s manual. Lentiviruses were packaged in HEK293T cells and collected from the medium supernatant. Stable cell lines were established by infecting lentiviruses into U87 and U251 cells and selecting them using puromycin. Cell apoptosis assay To measure cell apoptosis, cells in the log phase of growth were harvested by centrifugation for 5 min at 500 g and subjected to annexin V/propidium iodide (PI) staining using an annexin V-FITC Apoptosis Detection Kit (Bio- Vision, CA), according to the manufacturer s protocol. Annexin V and PI cells were used as controls. Annexin V + and PI cells were designated as apoptotic, and Annexin V + and PI + cells displayed necrotic features. The
3 results were evaluated by fluorescence activated cell sorting (FACS) flow cytometry. Western blotting analysis The total proteins of cells were extracted using protein lysis buffer (20 mm Tris HCL, ph 8.0, 120 mm NaCl, 1% Nonidet P-40, 10% glycerol, 1 mm CaCl 2, 1 mm MgCl 2, 1 mm phenylmethylsulfonyl fluoride, 1 mm sodium fluoride, 1 mm sodium orthovanadate, and a protease inhibitor mixture). Lysates containing 20 μg of total protein were separated on 8 or 10% SDS-PAGE gels. Proteins were then transferred onto a polyvinylidenedifluoride (PVDF) membrane (Bio-Rad) using a semidry transfer unit (Bio-Rad). Membranes were blocked with 5% nonfat dried milk for 2 h and then incubated with primary antibodies followed by mouse anti-rabbit secondary antibodies. The following primary antibodies were used: EGFR (1:1000, Cell Signaling Technology, USA), and glyceraldehyde-3-phosphate dehydrogenase (GAPDH) (1:3000, Abcam, UK). An ECL Western Blotting Kit (Pierce) and X-ray film were used, and signal intensities were determined using Image J software (NIH). Luciferase assay A luciferase assay was performed as described in our previous study [29]. The 3 UTR of EGFR was amplified by PCR from human cdna using the following primers: EGFR forward primer: ccgag CTC AAT AAT AAC TCG GAT TCC AGCCC, EGFR reverse primer: ccctc GAG TTC TGA ACC ATT TCT TCC TTGAT. The complementary sequence in the 3 UTR of EGFR (GAA TGT ) was replaced by (GCA CGC ). The PCR products were digested using SacI and HindIII and inserted into pmirreporter. These constructs were then validated by sequencing. HEK-293 cells were seeded into 24-well plates and co-transfected with the wild-type or mutated EGFR 3 -UTR reporter plasmids and prl-tk, or transfected with mir-181b and mir-nc. Luciferase assays were performed 24 h after transfection using the Dual Luciferase Reporter Assay System (Promega). Tumorigenesis in nude mice Nude mice (male BALB/cA-nu, 6 weeks old) were purchased from the Shanghai Experimental Animal Center (Chinese Academy of Sciences, Shanghai, China) and maintained in specific pathogen-free conditions. Sixteen mice were randomly divided into two groups. In one group, U87 cells stably expressing mir-181b were injected subcutaneously into both flanks of each mouse ( cells in 100 μl), and in the other group, U87 cells stably expressing mir-nc (as a negative control) were similarly injected. When tumors became visible, half of the mice of each group were treated with TMZ by intraperitoneal injection and the other half were not; the tumor sizes were measured using vernier calipers every 2 days. The tumor volume was calculated according to the formula: volume = 0.5 length width 2. The mice were euthanized after 18 days, and tumors were photographed and weighed. Statistical analysis Results showed in figures are expressed as mean ± SD. Data was analyzed using Student s t test in GraphPad Prism (GraphPad Software Inc. La Jolla, CA). P values less than 0.05 were considered to be statistically significant. Results MiR 181b levels are downregulated in human GBM tissues and are especially low in recurrent tissues In our previous research, we showed that mir-181b had a markedly low expression in human glioma tissues. To further investigate the expression of mir-181b in human GBM tissues, we tested new samples and performed a qrt-pcr analysis. The results showed that mir-181b had very low expression in GBM compared with normal brain tissues (Fig. 1a). To evaluate the roles of mir-181b in neoplasm recurrence, ten paired initial and recurrent GBM tissues were collected and analyzed for their mir-181b expression levels. As shown in Fig. 1b, mir-181b expression was significantly downregulated in the recurrent GBM tissues, which suggested that mir-181b has important biological functions in tumor recurrence. Overexpression of mir 181b sensitizes GBM cells to TMZ and induced apoptosis To explore the potential role of mir-181b in chemotherapy, we treated U87 and U251 cells stably expressing mir- 181b or mir-nc with different concentrations of TMZ. As shown in Fig. 2a, b, overexpression of mir-181b in GBM cells significantly increased their chemo-sensitivity to TMZ treatment, and cell viability was reduced significantly with increasing concentrations of TMZ compared with the mir-nc group. To further investigate the effect of mir-181b on apoptosis in the presence of TMZ treatment, FACS analysis was performed to detect cell apoptosis rates. The combination of mir-181b and TMZ treatment induced significant apoptosis (Fig. 2c, d). These findings implied that mir-181b overexpression increases the chemo-sensitivity of GBM cells to TMZ and potentiates TMZ-induced apoptosis.
4 A B Relative mir-181b expression (Normalized by U6) Initial (n=10) ** Recurrent (n=10) Fig. 1 MiR-181b levels are downregulated in human glioblastoma multiforme (GBM) tissues and are especially low in recurrent tissues. a Relative mir-181b expression levels were analyzed by quantitative real-time reverse transcription PCR (qrt-pcr) in normal (n = 8) and GBM tissues (n = 20). U6 RNA levels were used as an internal control. **p < 0.01 indicates a significant difference. b Relative expression levels of mir-181b in initial and recurrent cancer tissues; **p < 0.01 Fig. 2 Overexpression of mir-181b sensitizes glioblastoma multiforme (GBM) cells to temozolomide (TMZ) and induces apoptosis. The GBM cell lines U87 and U251 were infected with mir-181b or mir-nc lentivirus to establish stable cell lines. a and b TMZ sensitivity in U87/miR-NC, U87/miR-181b, U251/miR-NC, and U251/ mir-181b cell lines were tested using a Cell Counting Kit-8 (CCK-8) assay. Data are presented as the mean ± SD from three independent experiments with triple replicates per experiment. **p < c and d Cells were treated with 200 μm TMZ or not, and cell apoptosis was analyzed by flow cytometry after 48 h; **p < 0.01
5 MiR 181b directly targets and inhibits EGFR expression EGFR was reported to be overexpressed and amplified in GBM, in which it promotes GBM cell proliferation, apoptosis and invasion. Using bioinformatics analysis (microrna.org), we found that EGFR is a potential target of mir-181b (Fig. 3a). To confirm this, reporter constructs were made containing the putative mir-181b binding sites from the EGFR 3 -UTR regions (WT), or a mutated version of the same binding site (Mut), as indicated in Fig. 3b. Overexpression of mir-181b inhibited EGFR WT, but not Mut reporter activities (Fig. 3b), demonstrating that mir-181b can specifically target the EGFR 3 -UTR via the binding site sequences. Next, we used western blotting to show that the EGFR protein expression was decreased in U87 cells overexpressing mir-181b compared with cells expressing mir-nc (Fig. 3c). In addition, we found that the expression levels of EGFR were significantly upregulated in human GBM tissues compared with those in normal brain tissues using qrt-pcr (Fig. 3d). Furthermore, there was a significant inverse correlation between EGFR and mir- 181b in the GBM tissues (Fig. 3e, Spearman s correlation r = ). This inverse correlation indicated a possible relationship between mir-181b and EGFR. Fig. 3 mir-181b directly targets and inhibits epidermal growth factor receptor (EGFR) expression. a Putative seed-matching sites or mutant sites (red) between mir-181b and the 3 -untranslated region (UTR) of EGFR. b A luciferase reporter assay was performed on U87 cells to detect the relative luciferase activities of the wild-type (WT) and mutant (Mut) EGFR reporters. A renilla luciferase vector was used as an internal control; **p < c Total proteins of mir- 181b and mir-nc-expressing cells were subjected to western blotting and detected for EGFR expression levels. d The expression levels of EGFR in normal and human GBM tissues were determined by quantitative real-time reverse transcription PCR (qrt-pcr) analysis, and the fold changes were obtained from the ratio of EGFR to glyceraldehyde-3-phosphate dehydrogenase (GAPDH) levels; **p < e Spearman s correlation analysis was used to determine the correlation between the expression levels of EGFR and mir-181b in human glioblastoma multiforme (GBM) specimens
6 Overexpression of EGFR reverses the inhibitory effects of mir 181b and its apoptotic induction effect in the presence of TMZ To further investigate whether the effects of mir-181b and TMZ in chemotherapy are mediated via EGFR, a plasmid expressing the EGFR cdna was transfected into mir- 181b- or mir-nc-expressing cells. Cell viability under different concentrations of TMZ was assayed using the CCK-8 proliferation assay. The results showed that overexpression of EGFR reversed the mir-181b-induced chemo-sensitivity of GBM cells to TMZ (Fig. 4a, b). We then examined whether the restoration of EGFR could rescue the anti-apoptotic effects of mir-181b. As shown in Fig. 4c, d, the cell apoptosis rate of mir-181b-overexpression plus TMZ treatment was rescued by overexpression of EGFR compared with control cells. Based on these findings, our results indicated that mir-181b sensitizes GBM cells to TMZ, and induces an apoptotic effect combined with TMZ by targeting EGFR. MiR 181b enhances the chemo sensitivity of TMZ in vivo To assess the functions of mir-181b in GBM chemo-sensitivity in vivo, a subcutaneous xenotransplanted GBM model was employed. U87 cells overexpressing mir-nc or mir-181b were collected and injected subcutaneously into both posterior flanks of male BALB/c nude mice, respectively. After 8 days, the mir-nc group was randomly divided into two groups: mir-nc and mir-nc+tmz. TMZ was delivered to the mir-nc+tmz group by peritoneal injection. The same procedure was also applied to the mir-181b group and the tumor volumes were monitored every 2 days during the tumor progression (Fig. 5a). The mice were sacrificed on day 18 and the tumors were excised, after which the tumors were photographed and weighed (Fig. 5b, c). The mir-181b-treated xenografts group had a significant decrease in tumor volume and weight when treated with TMZ compared with the mir-nc group. To reveal the molecular mechanisms of mir-181 in tumor growth, total protein was extracted to perform western blotting analysis to analyze the EGFR expression levels. The results demonstrated the EGFR levels were significantly downregulated in mir-181b overexpressing tumors (Fig. 5d). Thus, mir-181b not only inhibits tumor growth, but also enhances the sensitivity of TMZ chemotherapy via its target EGFR in vivo. Discussion TMZ is the most widely used alkylating agent to treat GBM; however, drug resistance often leads to tumor Fig. 4 Overexpression of EGFR reversed the mir- 181b-induced chemo-sensitivity of GBM cells to TMZ. mir- 181b- or mir-nc-overexpressing cells were transfected with vector or epidermal growth factor receptor (EGFR). a and b TMZ sensitivity were tested using a Counting Kit-8 (CCK- 8) assay; **p < 0.01 indicates significant difference compared with the mir-nc+vector group # p < 0.05, ## p < 0.01 indicate significant differences compared with the mir-181b+ vector group. c and d Cells were treated with 200 μm TMZ or not, and cell apoptosis was analyzed by flow cytometry after 48 h; **p < 0.01
7 Fig. 5 MiR-181b enhances the chemo-sensitivity of temozolomide (TMZ) in vivo. mir-181b- or mir-nc-overexpression cells were dispersed in 100 μl of serum-free DMEM medium and were subcutaneously injected into each side of posterior flank of nude mice (n = 4), then half the mice in each group were treated with TMZ by peritoneal injection. a, b and c Tumors were measured every 2 days after they were observed by the naked eye and their volumes were calculated using the following formula: volume = 0.5 Length Width2. The tumor was excised and weighed after 18 days with representative pictures of tumors shown (Bar 10 mm). d Whole proteins were extracted from xenografts and subjected to western blotting assay for epidermal growth factor receptor (EGFR) expression. Glyceraldehyde-3-phosphate dehydrogenase (GAPDH) expression served as an internal control recurrence and poor outcome [30, 31]. Therefore, it is pivotal to improve current chemotherapy regimens by identifying new predictive biomarkers based on the existing treatment. Accumulating evidence indicates that the aberrant expression of mirnas is associated with human GBM chemotherapy resistance and sensitivity. Wang et al. confirmed that inhibition of mir-381 enhanced the sensitivity of neurofilament, light polypeptide (NEFL)-mediated stemness factors to TMZ in GBM. MiR-125b has been reported to control apoptosis and TMZ resistance by targeting TNFAIP3 and NKIRAS2 in GBM [32]. Our previous studies focused on the roles of mir-181b in glioma. Meanwhile, mir-181b has also been reported to affect tumor chemo-sensitivity. For example, the suppression of mir181b enhanced the sensitivity of hepatocellular carcinoma cells to doxorubicin. In addition, Wang et al. showed that increased mir-181b modulated GBM cells sensitivity to TMZ by targeting MEK1 [33]. In the present study, we found that mir-181b was decreased between paired initial and recurrent GBMs that were insensitive to TMZ treatment. Moreover, overexpression of mir-181b enhanced the chemo-sensitivity of GBM cells to TMZ by inducing cell apoptosis. These data were further supported by the finding that mir-181b-treated xenografts group had a significant decrease in tumor volume and weight when treated with TMZ compared with the mir-nc group. Therefore, overexpression of mir-181b might not only limit cancer growth, but also sensitize cells to TMZ in vitro and in vivo. Most mirnas function by inhibiting effective mrna translation of target genes. To date, several targets of 13
8 mir-181b have been identified, such as NOVA1, MDM2, LATS2, HMGB1, and MCL-1 [34 36]. Our previous research showed that mir-181b inhibited GBM cell growth by targeting IGF1R [29]. In the present study, we uncovered a novel role of mir-181b for TMZ resistance in GBM and identified EGFR as a direct target of mir-181b. Aberrant expression of EGFR occurs in the majority of gliomas, and activation of EGFR signaling plays a central role in GBM and other human cancers, including lung, breast, and colorectal [37 40]. Accumulating evidence suggests that mirnas can regulate EGFR signaling, correlate with EGFR expression, and influence chemotherapy resistance. For example, mir-21 is responsible for modulating EGFR signaling and is involved in the responses of GBM cells to anti-egfr treatment [41]. Furthermore, mir-146b-5p could target EGFR and reduce the in vitro migration and invasion of glioma [42]. Here, we found that the relative luciferase level for EGFR was significantly decreased in the mir-181b-overexpression group compared with that in the mir-nc group, and western blotting analysis further confirmed these findings. Additionally, overexpression of EGFR partially abolished the effect induced by mir- 181b plus TMZ treatment. Meanwhile, the xenograft data showed that the expression of EGFR in mir-181b-overexpressing cells treated with TMZ was lower that that in the non-treated cells, suggesting that mir-181b is a potential strategy for EGFR-targeted therapy. In conclusion, this study demonstrated that EGFR, as a direct target of mir-181b, might be involved in the mir- 181b-mediated chemo-resistance of GBM cells to TMZ. Further studies are required to verify this association. Acknowledgements This work was supported in part by the National Natural Science Foundation of China [Grant Nos , , , , ], and the Priority Academic Program Development of Jiangsu Higher Education Institutions (PAPD). Compliance with ethical standards Conflict of interest The authors declare that they have no conflict of interest. Ethical approval This study was approved by the Hospital Ethics Committee. Informed consent For the glioma tissues, written informed consent was obtained from all patients. References 1. Cloughesy TF, Cavenee WK, Mischel PS (2014) Glioblastoma: from molecular pathology to targeted treatment. Ann Rev Pathol 9:1 25. doi: /annurev-pathol Aldape K, Zadeh G, Mansouri S, Reifenberger G, von Deimling A (2015) Glioblastoma: pathology, molecular mechanisms and markers. Acta Neuropathol 129: doi: / s Wen PY, Reardon DA (2016) Neuro-oncology in 2015: progress in glioma diagnosis, classification and treatment. Nat Rev Neurol 12: doi: /nrneurol Omuro A, DeAngelis LM (2013) Glioblastoma and other malignant gliomas: a clinical review. Jama 310: doi: /jama Messaoudi K, Clavreul A, Lagarce F (2015) Toward an effective strategy in glioblastoma treatment: part I: resistance mechanisms and strategies to overcome resistance of glioblastoma to temozolomide. Drug Discov Today 20: doi: /j. drudis Fan CH, Liu WL, Cao H, Wen C, Chen L, Jiang G (2013) O6-methylguanine DNA methyltransferase as a promising target for the treatment of temozolomide-resistant gliomas. Cell Death Dis 4:e876. doi: /cddis Furnari FB, Fenton T, Bachoo RM, Mukasa A, Stommel JM, Stegh A, Hahn WC, Ligon KL, Louis DN, Brennan C, Chin L, DePinho RA, Cavenee WK (2007) Malignant astrocytic glioma: genetics, biology, and paths to treatment. Genes Dev 21: doi: /gad Stupp R, Hegi ME, Gilbert MR, Chakravarti A (2007) Chemoradiotherapy in malignant glioma: standard of care and future directions. J Clin Oncol 25: doi: / JCO Van Meir EG, Hadjipanayis CG, Norden AD, Shu HK, Wen PY, Olson JJ (2010) Exciting new advances in neuro-oncology: the avenue to a cure for malignant glioma. CA Cancer J Clin 60: doi: /caac Dancey JE, Freidlin B (2003) Targeting epidermal growth factor receptor are we missing the mark? Lancet 362: doi: /s (03)13810-x 11. Ohashi K, Maruvka YE, Michor F, Pao W (2013) Epidermal growth factor receptor tyrosine kinase inhibitor-resistant disease. J Clin Oncol 31: doi: /jco Blobel CP (2005) ADAMs: key components in EGFR signalling and development. Nat Rev Mol Cell Biol 6: doi: / nrm Ciardiello F, Tortora G (2008) EGFR antagonists in cancer treatment. N Engl J Med 358: doi: / NEJMra Maire CL, Ligon KL (2014) Molecular pathologic diagnosis of epidermal growth factor receptor. Neuro-Oncol. doi: / neuonc/nou Huang PH, Xu AM, White FM (2009) Oncogenic EGFR signaling networks in glioma. Sci Signal. doi: /scisignal.287re6 16. Chong CR, Janne PA (2013) The quest to overcome resistance to EGFR-targeted therapies in cancer. Nat Med 19: doi: /nm Pao W, Chmielecki J (2010) Rational, biologically based treatment of EGFR-mutant non-small-cell lung cancer. Nat Rev Cancer 10: doi: /nrc Wheeler DL, Dunn EF, Harari PM (2010) Understanding resistance to EGFR inhibitors-impact on future treatment strategies. Nat Rev Clin Oncol 7: doi: /nrclinonc Munoz JL, Rodriguez-Cruz V, Greco SJ, Ramkissoon SH, Ligon KL, Rameshwar P (2014) Temozolomide resistance in glioblastoma cells occurs partly through epidermal growth factor receptor-mediated induction of connexin 43. Cell Death Dis 5:e1145. doi: /cddis Hobbs J, Nikiforova MN, Fardo DW, Bortoluzzi S, Cieply K, Hamilton RL, Horbinski C (2012) Paradoxical relationship between the degree of EGFR amplification and outcome in
9 glioblastomas. Am J Surg Pathol 36: doi: / PAS.0b013e e Hammond SM (2015) An overview of micrornas. Adv Drug Deliv Rev 87:3 14. doi: /j.addr Cheng G (2015) Circulating mirnas: roles in cancer diagnosis, prognosis and therapy. Adv Drug Deliv Rev 81: doi: /j.addr Ling H, Fabbri M, Calin GA (2013) MicroRNAs and other noncoding RNAs as targets for anticancer drug development. Nat Rev Drug Discov 12: doi: /nrd Squadrito ML, Etzrodt M, De Palma M, Pittet MJ (2013) MicroRNA-mediated control of macrophages and its implications for cancer. Trends Immunol 34: doi: /j. it Garofalo M, Romano G, Di Leva G, Nuovo G, Jeon YJ, Ngankeu A, Sun J, Lovat F, Alder H, Condorelli G, Engelman JA, Ono M, Rho JK, Cascione L, Volinia S, Nephew KP, Croce CM (2012) EGFR and MET receptor tyrosine kinase-altered microrna expression induces tumorigenesis and gefitinib resistance in lung cancers. Nat Med 18: doi: /nm De Cola A, Volpe S, Budani MC, Ferracin M, Lattanzio R, Turdo A, D Agostino D, Capone E, Stassi G, Todaro M, Di Ilio C, Sala G, Piantelli M, Negrini M, Veronese A, De Laurenzi V (2015) mir-205-5p-mediated downregulation of ErbB/HER receptors in breast cancer stem cells results in targeted therapy resistance. Cell Death Dis 6: e1823. doi: /cddis Zhou JY, Chen X, Zhao J, Bao Z, Chen X, Zhang P, Liu ZF, Zhou JY (2014) MicroRNA-34a overcomes HGF-mediated gefitinib resistance in EGFR mutant lung cancer cells partly by targeting MET. Cancer Lett 351: doi: /j. canlet Zhang KL, Zhou X, Han L, Chen LY, Chen LC, Shi ZD, Yang M, Ren Y, Yang JX, Frank TS, Zhang CB, Zhang JX, Pu PY, Zhang JN, Jiang T, Wagner EJ, Li M, Kang CS (2014) Micro- RNA-566 activates EGFR signaling and its inhibition sensitizes glioblastoma cells to nimotuzumab. Mol Cancer 13:63. doi: / Shi ZM, Wang XF, Qian X, Tao T, Wang L, Chen QD, Wang XR, Cao L, Wang YY, Zhang JX, Jiang T, Kang CS, Jiang BH, Liu N, You YP (2013) MiRNA-181b suppresses IGF-1R and functions as a tumor suppressor gene in gliomas. Rna 19: doi: /rna Detry JM (1993) Clinical features of an anti-anginal drug in angina pectoris. Eur Heart J 14(Suppl G): Tatar Z, Thivat E, Planchat E, Gimbergues P, Gadea E, Abrial C, Durando X (2013) Temozolomide and unusual indications: review of literature. Cancer Treat Rev 39: doi: /j.ctrv Wang Z, Yang J, Xu G, Wang W, Liu C, Yang H, Yu Z, Lei Q, Xiao L, Xiong J, Zeng L, Xiang J, Ma J, Li G, Wu M (2015) Targeting mir-381-nefl axis sensitizes glioblastoma cells to temozolomide by regulating stemness factors and multidrug resistance factors. Oncotarget 6: doi: / oncotarget Wang J, Sai K, Chen FR, Chen ZP (2013) mir-181b modulates glioma cell sensitivity to temozolomide by targeting MEK1. Cancer Chemother Pharmacol 72: doi: / s Zhi F, Wang Q, Deng D, Shao N, Wang R, Xue L, Wang S, Xia X, Yang Y (2014) MiR-181b-5p downregulates NOVA1 to suppress proliferation, migration and invasion and promote apoptosis in astrocytoma. PLoS ONE 9:e doi: /journal. pone Sun YC, Wang J, Guo CC, Sai K, Wang J, Chen FR, Yang QY, Chen YS, Wang J, To TS, Zhang ZP, Mu YG, Chen ZP (2014) MiR-181b sensitizes glioma cells to teniposide by targeting MDM2. BMC Cancer 14:611. doi: / Lu F, Zhang J, Ji M, Li P, Du Y, Wang H, Zang S, Ma D, Sun X, Ji C (2014) mir-181b increases drug sensitivity in acute myeloid leukemia via targeting HMGB1 and Mcl-1. Int J Oncol 45: doi: /ijo Sezeur A, Leandri J, Rey P, Daumet P, Vouron J (1982) An experimental study of slowly resorbed suture material in the tracheal sutures (author s transl). Ann Chir 36: Ramalingam SS, Owonikoko TK, Khuri FR (2011) Lung cancer: New biological insights and recent therapeutic advances. CA Cancer J Clin 61: doi: /caac Nicholson S, Sainsbury JR, Halcrow P, Chambers P, Farndon JR, Harris AL (1989) Expression of epidermal growth factor receptors associated with lack of response to endocrine therapy in recurrent breast cancer. Lancet 1: Messersmith WA, Ahnen DJ (2008) Targeting EGFR in colorectal cancer. N Engl J Med 359: doi: / NEJMe Zhang KL, Han L, Chen LY, Shi ZD, Yang M, Ren Y, Chen LC, Zhang JX, Pu PY, Kang CS (2014) Blockage of a mir-21/ EGFR regulatory feedback loop augments anti-egfr therapy in glioblastomas. Cancer Lett 342: doi: /j. canlet Katakowski M, Zheng X, Jiang F, Rogers T, Szalad A, Chopp M (2010) MiR-146b-5p suppresses EGFR expression and reduces in vitro migration and invasion of glioma. Cancer Invest 28: doi: /
10 本文献由 学霸图书馆 - 文献云下载 收集自网络, 仅供学习交流使用 学霸图书馆 ( 是一个 整合众多图书馆数据库资源, 提供一站式文献检索和下载服务 的 24 小时在线不限 IP 图书馆 图书馆致力于便利 促进学习与科研, 提供最强文献下载服务 图书馆导航 : 图书馆首页文献云下载图书馆入口外文数据库大全疑难文献辅助工具
Supporting Information. Electrochemiluminescence for Electric-Driven Antibacterial. Therapeutics
 Supporting Information Electrochemiluminescence for Electric-Driven Antibacterial Therapeutics Shanshan Liu, a,b Huanxiang Yuan, a Haotian Bai, a Pengbo Zhang, a Fengting Lv, a Libing Liu, a Zhihui Dai,
Supporting Information Electrochemiluminescence for Electric-Driven Antibacterial Therapeutics Shanshan Liu, a,b Huanxiang Yuan, a Haotian Bai, a Pengbo Zhang, a Fengting Lv, a Libing Liu, a Zhihui Dai,
Optimization of Processing Parameters of Stabilizers After Enzymes Hydrolysis for Cloudy Ginkgo Juice
 Optimization of Processing Parameters of Stabilizers After Enzymes Hydrolysis for Cloudy Ginkgo Juice Haifeng Yu, Junyan Liu and Jingxi Yang 1 Introduction Ginkgo biloba, dating back 300 million years,
Optimization of Processing Parameters of Stabilizers After Enzymes Hydrolysis for Cloudy Ginkgo Juice Haifeng Yu, Junyan Liu and Jingxi Yang 1 Introduction Ginkgo biloba, dating back 300 million years,
Racial disparities in the management of acne: evidence from the National Ambulatory Medical Care Survey,
 Journal of Dermatological Treatment ISSN: 0954-6634 (Print) 1471-1753 (Online) Journal homepage: http://www.tandfonline.com/loi/ijdt20 Racial disparities in the management of acne: evidence from the National
Journal of Dermatological Treatment ISSN: 0954-6634 (Print) 1471-1753 (Online) Journal homepage: http://www.tandfonline.com/loi/ijdt20 Racial disparities in the management of acne: evidence from the National
Accepted Manuscript. Hemorrhagic cystitis associated with gefitinib treatment: a case report. Peng Zhang, Jinjing Tu, Tieding Chen, Rubing Li
 Accepted Manuscript Hemorrhagic cystitis associated with gefitinib treatment: a case report Peng Zhang, Jinjing Tu, Tieding Chen, Rubing Li PII: S0090-4295(18)30555-7 DOI: 10.1016/j.urology.2018.05.035
Accepted Manuscript Hemorrhagic cystitis associated with gefitinib treatment: a case report Peng Zhang, Jinjing Tu, Tieding Chen, Rubing Li PII: S0090-4295(18)30555-7 DOI: 10.1016/j.urology.2018.05.035
Fetal Response to Intramuscular Epinephrine for Anaphylaxis during Maternal Penicillin Desensitization for Secondary Syphilis
 The Journal of Maternal-Fetal & Neonatal Medicine ISSN: 1476-7058 (Print) 1476-4954 (Online) Journal homepage: http://www.tandfonline.com/loi/ijmf20 Fetal Response to Intramuscular Epinephrine for Anaphylaxis
The Journal of Maternal-Fetal & Neonatal Medicine ISSN: 1476-7058 (Print) 1476-4954 (Online) Journal homepage: http://www.tandfonline.com/loi/ijmf20 Fetal Response to Intramuscular Epinephrine for Anaphylaxis
Chapter 5 Trimalleolar Ankle Fracture: Posterior Plate for Posterior Malleolus Fractures
 Chapter 5 Trimalleolar Ankle Fracture: Posterior Plate for Posterior Malleolus Fractures Roy I. Davidovitch and Alexander M. Crespo Introduction Trimalleolar ankle fractures with a posterior malleolus
Chapter 5 Trimalleolar Ankle Fracture: Posterior Plate for Posterior Malleolus Fractures Roy I. Davidovitch and Alexander M. Crespo Introduction Trimalleolar ankle fractures with a posterior malleolus
ACCEPTED ARTICLE PREVIEW. Accepted manuscript
 First in Class Angiotensin Receptor Neprilysin Inhibitor in Heart Failure Orly Vardeny, PharmD, MS, Travis Tacheny, Scott D. Solomon, MD Cite this article as: Orly Vardeny, PharmD, MS, Travis Tacheny,
First in Class Angiotensin Receptor Neprilysin Inhibitor in Heart Failure Orly Vardeny, PharmD, MS, Travis Tacheny, Scott D. Solomon, MD Cite this article as: Orly Vardeny, PharmD, MS, Travis Tacheny,
Thinking & Reasoning Publication details, including instructions for authors and subscription information:
 This article was downloaded by: [Umeå University Library] On: 07 October 2013, At: 11:46 Publisher: Routledge Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered office: Mortimer
This article was downloaded by: [Umeå University Library] On: 07 October 2013, At: 11:46 Publisher: Routledge Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered office: Mortimer
Accepted Manuscript. Robotics in Orthopedics: A Brave New World. Brian S. Parsley, MD, Associate Professor
 Accepted Manuscript Robotics in Orthopedics: A Brave New World Brian S. Parsley, MD, Associate Professor PII: S0883-5403(18)30163-3 DOI: 10.1016/j.arth.2018.02.032 Reference: YARTH 56428 To appear in:
Accepted Manuscript Robotics in Orthopedics: A Brave New World Brian S. Parsley, MD, Associate Professor PII: S0883-5403(18)30163-3 DOI: 10.1016/j.arth.2018.02.032 Reference: YARTH 56428 To appear in:
How might treatment of ALK-positive non-small cell lung cancer change in the near future?
 Expert Review of Anticancer Therapy ISSN: 1473-7140 (Print) 1744-8328 (Online) Journal homepage: http://www.tandfonline.com/loi/iery20 How might treatment of ALK-positive non-small cell lung cancer change
Expert Review of Anticancer Therapy ISSN: 1473-7140 (Print) 1744-8328 (Online) Journal homepage: http://www.tandfonline.com/loi/iery20 How might treatment of ALK-positive non-small cell lung cancer change
Accepted Manuscript. Red yeast rice preparations: are they suitable substitutions for statins?
 Accepted Manuscript Red yeast rice preparations: are they suitable substitutions for statins? Carlos A. Dujovne, MD, Fellow NLA, Certified Clinical Lipidologist PII: S0002-9343(17)30591-0 DOI: 10.1016/j.amjmed.2017.05.013
Accepted Manuscript Red yeast rice preparations: are they suitable substitutions for statins? Carlos A. Dujovne, MD, Fellow NLA, Certified Clinical Lipidologist PII: S0002-9343(17)30591-0 DOI: 10.1016/j.amjmed.2017.05.013
Effects of idebenone on electroencephalograms of patients with cerebrovascular disorders
 Arch. Gerontol. Geriatr., 8 (1989) 355-366 355 Elsevier AGG 00266 Effects of idebenone on electroencephalograms of patients with cerebrovascular disorders Takashi Nakano a Matu6 Miyasaka a, Katsumi Mori
Arch. Gerontol. Geriatr., 8 (1989) 355-366 355 Elsevier AGG 00266 Effects of idebenone on electroencephalograms of patients with cerebrovascular disorders Takashi Nakano a Matu6 Miyasaka a, Katsumi Mori
uncorrected proof version
 Galley Proof 8/02/2017; 9:17 File: jcm 1-jcm708.tex; BOKCTP/ljl p. 1 Journal of Computational Methods in Sciences and Engineering -1 (2017) 1 10 1 DOI 10.3233/JCM-170708 IOS Press 1 2 3 Comparison of sliding
Galley Proof 8/02/2017; 9:17 File: jcm 1-jcm708.tex; BOKCTP/ljl p. 1 Journal of Computational Methods in Sciences and Engineering -1 (2017) 1 10 1 DOI 10.3233/JCM-170708 IOS Press 1 2 3 Comparison of sliding
Serum mir-182 and mir-331-3p as diagnostic and prognostic markers in patients with hepatocellular carcinoma
 Tumor Biol. (2015) 36:7439 7447 DOI 10.1007/s13277-015-3430-2 RESEARCH ARTICLE Serum mir-182 and mir-331-3p as diagnostic and prognostic markers in patients with hepatocellular carcinoma Lin Chen 1 & Feihu
Tumor Biol. (2015) 36:7439 7447 DOI 10.1007/s13277-015-3430-2 RESEARCH ARTICLE Serum mir-182 and mir-331-3p as diagnostic and prognostic markers in patients with hepatocellular carcinoma Lin Chen 1 & Feihu
Journal of Chromatography A 819 (1998)
 Journal of Chromatography A 89 (998) 33 42 Investigation of potential degradation products of a newly synthesised b-lactam antibiotic by multi-stage liquid chromatography electrospray mass spectrometry
Journal of Chromatography A 89 (998) 33 42 Investigation of potential degradation products of a newly synthesised b-lactam antibiotic by multi-stage liquid chromatography electrospray mass spectrometry
Yang S-S, Gao Y, Wang D-Y, Xia B-R, Liu Y-D, Qin Y, Ning X-M, Li G-Y, Hao L-X, Xiao M & Zhang Y-Y (2016) Histopathology. DOI: /his.
 Histopathology 2016 DOI: 10.1111/his.12933 Overexpression of eukaryotic initiation factor 5A2 (EIF5A2) is associated with cancer progression and poor prognosis in patients with early-stage cervical cancer
Histopathology 2016 DOI: 10.1111/his.12933 Overexpression of eukaryotic initiation factor 5A2 (EIF5A2) is associated with cancer progression and poor prognosis in patients with early-stage cervical cancer
Synthetic Tannins Structure by MALDI-TOF Mass Spectroscopy
 Synthetic Tannins Structure by MALDI-TOF Mass Spectroscopy S. Giovando, 1 A. Pizzi, 2 H. Pasch, 3,4 K. Rode 4 1 Centro Ricerche per la Chimica Fine Srl, S.Michele Mondovi, Italy 2 ENSTIB-LERMAB, Nancy
Synthetic Tannins Structure by MALDI-TOF Mass Spectroscopy S. Giovando, 1 A. Pizzi, 2 H. Pasch, 3,4 K. Rode 4 1 Centro Ricerche per la Chimica Fine Srl, S.Michele Mondovi, Italy 2 ENSTIB-LERMAB, Nancy
Pharmacokinetics of a Novel Orodispersible Tablet of Sildenafil in Healthy Subjects
 Clinical Therapeutics/Volume 36, Number 2, 2014 Pharmacokinetics of a Novel Orodispersible Tablet of Sildenafil in Healthy Subjects Bharat Damle, PhD 1 ; Gregory Duczynski, MS 2 ; Barrett W. Jeffers, PhD
Clinical Therapeutics/Volume 36, Number 2, 2014 Pharmacokinetics of a Novel Orodispersible Tablet of Sildenafil in Healthy Subjects Bharat Damle, PhD 1 ; Gregory Duczynski, MS 2 ; Barrett W. Jeffers, PhD
SOME PRACTICAL IMPROVEMENTS IN THE CONTINUAL REASSESSMENT METHOD FOR PHASE I STUDIES
 STATISTICS IN MEDICINE, VOL. 14, 1149-1161 (1995) SOME PRACTICAL IMPROVEMENTS IN THE CONTINUAL REASSESSMENT METHOD FOR PHASE I STUDIES STEVEN N. GOODMAN, MARIANNA L. ZAHURAK AND STEVEN PIANTADOSI Johns
STATISTICS IN MEDICINE, VOL. 14, 1149-1161 (1995) SOME PRACTICAL IMPROVEMENTS IN THE CONTINUAL REASSESSMENT METHOD FOR PHASE I STUDIES STEVEN N. GOODMAN, MARIANNA L. ZAHURAK AND STEVEN PIANTADOSI Johns
The conundrum of hodgkin lymphoma nodes: To be or not to be included in the involved node radiation fields. The EORTC-GELA lymphoma group guidelines
 Radiotherapy and Oncology 88 (2008) 202 210 www.thegreenjournal.com Hodgkin guidelines The conundrum of hodgkin lymphoma nodes: To be or not to be included in the involved node radiation fields. The EORTC-GELA
Radiotherapy and Oncology 88 (2008) 202 210 www.thegreenjournal.com Hodgkin guidelines The conundrum of hodgkin lymphoma nodes: To be or not to be included in the involved node radiation fields. The EORTC-GELA
Accepted Manuscript. Dural arteriovenous fistula between the inferolateral trunk and cavernous sinus draining to the ophthalmic vein: a case report
 Accepted Manuscript Dural arteriovenous fistula between the inferolateral trunk and cavernous sinus draining to the ophthalmic vein: a case report Kan Xu, Kun Hou, Baofeng Xu, Yunbao Guo, Jinlu Yu PII:
Accepted Manuscript Dural arteriovenous fistula between the inferolateral trunk and cavernous sinus draining to the ophthalmic vein: a case report Kan Xu, Kun Hou, Baofeng Xu, Yunbao Guo, Jinlu Yu PII:
Indacaterol, a once-daily beta 2 -agonist, versus twice-daily beta-agonists or placebo for chronic obstructive pulmonary disease (Protocol)
 Indacaterol, a once-daily beta 2 -agonist, versus twice-daily beta-agonists or placebo for chronic obstructive pulmonary disease (Protocol) Geake JB, Dabscheck EJ, Wood-Baker R This is a reprint of a Cochrane
Indacaterol, a once-daily beta 2 -agonist, versus twice-daily beta-agonists or placebo for chronic obstructive pulmonary disease (Protocol) Geake JB, Dabscheck EJ, Wood-Baker R This is a reprint of a Cochrane
Characterization of a prototype MR-compatible Delta4 QA-system in a 1.5 tesla MR-linac
 Physics in Medicine and Biology ACCEPTED MANUSCRIPT Characterization of a prototype MR-compatible Delta QA-system in a. tesla MR-linac To cite this article before publication: J H Wilfred de Vries et al
Physics in Medicine and Biology ACCEPTED MANUSCRIPT Characterization of a prototype MR-compatible Delta QA-system in a. tesla MR-linac To cite this article before publication: J H Wilfred de Vries et al
The role of air plethysmography in the diagnosis of chronic venous insufficiency
 The role of air plethysmography in the diagnosis of chronic venous insufficiency Enrique Criado, MD, Mark A. Farber, MD, William A. Marston, MD, Patty F. Daniel, RN, RVT, Cynthia B. Burnham, RN, RVT, and
The role of air plethysmography in the diagnosis of chronic venous insufficiency Enrique Criado, MD, Mark A. Farber, MD, William A. Marston, MD, Patty F. Daniel, RN, RVT, Cynthia B. Burnham, RN, RVT, and
How Advertising Slogans
 How Advertising Slogans Can Prime Evaluations of Brand Extensions David M. Boush University of Oregon ABSTRACT Different versions of a brand slogan were presented to each of three treatment groups before
How Advertising Slogans Can Prime Evaluations of Brand Extensions David M. Boush University of Oregon ABSTRACT Different versions of a brand slogan were presented to each of three treatment groups before
Prevalence of different HIV-1 subtypes in sexual transmission in China: a systematic review and meta-analysis
 Epidemiol. Infect. (2016), 144, 2144 2153. Cambridge University Press 2016 doi:10.1017/s0950268816000212 Prevalence of different HIV-1 subtypes in sexual transmission in China: a systematic review and
Epidemiol. Infect. (2016), 144, 2144 2153. Cambridge University Press 2016 doi:10.1017/s0950268816000212 Prevalence of different HIV-1 subtypes in sexual transmission in China: a systematic review and
NON-NARCOTIC ORALLY EFFECTIVE, CENTRALLY ACTING ANALGESIC FROM AN AYURVEDIC DRUG
 Journal of Ethnopharmocology, ll(l984) 309-317 Elsevier Scientific Publishers Ireland Ltd. 309 NON-NARCOTIC ORALLY EFFECTIVE, CENTRALLY ACTING ANALGESIC FROM AN AYURVEDIC DRUG CX ATAL, M.A. SIDDIQUI, USHA
Journal of Ethnopharmocology, ll(l984) 309-317 Elsevier Scientific Publishers Ireland Ltd. 309 NON-NARCOTIC ORALLY EFFECTIVE, CENTRALLY ACTING ANALGESIC FROM AN AYURVEDIC DRUG CX ATAL, M.A. SIDDIQUI, USHA
Cost-Effectiveness of Adding Rh-Endostatin to First-Line Chemotherapy in Patients With Advanced Non-Small-Cell Lung Cancer in China
 Clinical Therapeutics/Volume 33, Number 10, 2011 Cost-Effectiveness of Adding Rh-Endostatin to First-Line Chemotherapy in Patients With Advanced Non-Small-Cell Lung Cancer in China Bin Wu, PhD 1, Huafeng
Clinical Therapeutics/Volume 33, Number 10, 2011 Cost-Effectiveness of Adding Rh-Endostatin to First-Line Chemotherapy in Patients With Advanced Non-Small-Cell Lung Cancer in China Bin Wu, PhD 1, Huafeng
Effects of Angle of Approach on Cursor Movement with a Mouse: Consideration of Fitts' Law
 Pergamon Computers in Human Behavior, Vol. 12, No. 3, pp. 481-495, 1996 Copyright 1996 Elsevier Science Ltd Printed in Great Britain. All rights reserved 0747-5632/96 $15.00 + 0.00 S0747-5632(96) 00020-9
Pergamon Computers in Human Behavior, Vol. 12, No. 3, pp. 481-495, 1996 Copyright 1996 Elsevier Science Ltd Printed in Great Britain. All rights reserved 0747-5632/96 $15.00 + 0.00 S0747-5632(96) 00020-9
mir-25 promotes metastasis via targeting FBXW7 in esophageal squamous cell carcinoma
 3030 ONCOLOGY REPORTS 38: 3030-3038, 2017 mir-25 promotes metastasis via targeting FBXW7 in esophageal squamous cell carcinoma Ye Hua 1,2*, Kai Zhao 3*, Gang Tao 4*, Chunhua Dai 1 and Yuting Su 1 1 Institute
3030 ONCOLOGY REPORTS 38: 3030-3038, 2017 mir-25 promotes metastasis via targeting FBXW7 in esophageal squamous cell carcinoma Ye Hua 1,2*, Kai Zhao 3*, Gang Tao 4*, Chunhua Dai 1 and Yuting Su 1 1 Institute
Comparison of Carotid Artery Stenting and Carotid Endarterectomy in Patients with Symptomatic Carotid Artery Stenosis: A Single Center Study
 Adv Ther (2013) 30:845 853 DOI 10.1007/s25-013-0058-8 ORIGINAL RESEARCH Comparison of Carotid Artery Stenting and Carotid Endarterectomy in Patients with Symptomatic Carotid Artery Stenosis: A Single Center
Adv Ther (2013) 30:845 853 DOI 10.1007/s25-013-0058-8 ORIGINAL RESEARCH Comparison of Carotid Artery Stenting and Carotid Endarterectomy in Patients with Symptomatic Carotid Artery Stenosis: A Single Center
Mastering the Initial Dissection and Cannulation: Making Ablation Easy and Safe
 Chapter 5 Mastering the Initial Dissection and Cannulation: Making Ablation Easy and Safe 1 INTRODUCTION A good initial dissection with wide mobilization of the left atrium (LA) by dividing its attachments
Chapter 5 Mastering the Initial Dissection and Cannulation: Making Ablation Easy and Safe 1 INTRODUCTION A good initial dissection with wide mobilization of the left atrium (LA) by dividing its attachments
THE RATIONALITY/EMOTIONAL DEFENSIVENESS SCALE- I. INTERNAL STRUCTURE AND STABILITY
 Joouml of Psychosomaric Research, Vol. 35. No. 4/S, pp. 545-554, 1991. 0534-3999191 $3.00+.00 Printed in Great Britain 0 1991 Pergamon Press plc THE RATIONALITY/EMOTIONAL DEFENSIVENESS SCALE- I. INTERNAL
Joouml of Psychosomaric Research, Vol. 35. No. 4/S, pp. 545-554, 1991. 0534-3999191 $3.00+.00 Printed in Great Britain 0 1991 Pergamon Press plc THE RATIONALITY/EMOTIONAL DEFENSIVENESS SCALE- I. INTERNAL
The Use of Transdermal Buprenorphine to Relieve Radiotherapy-Related Pain in Head and Neck Cancer Patients
 Cancer Investigation, 31:412 420, 2013 ISSN: 0735-7907 print / 1532-4192 online Copyright C 2013 Informa Healthcare USA, Inc. DOI: 10.3109/07357907.2013.800094 IMAGING, DIAGNOSIS, PROGNOSIS The Use of
Cancer Investigation, 31:412 420, 2013 ISSN: 0735-7907 print / 1532-4192 online Copyright C 2013 Informa Healthcare USA, Inc. DOI: 10.3109/07357907.2013.800094 IMAGING, DIAGNOSIS, PROGNOSIS The Use of
Berberine Sensitizes Human Ovarian Cancer Cells to Cisplatin Through mir-93/ PTEN/Akt Signaling Pathway
 Chen Accepted: et al.: February Berberine 24, Sensitizes 2015 Ovarian Cancer Cells to Cisplatin www.karger.com/cpb 956 1421-9778/15/0363-0956$39.50/0 Original Paper This is an Open Access article licensed
Chen Accepted: et al.: February Berberine 24, Sensitizes 2015 Ovarian Cancer Cells to Cisplatin www.karger.com/cpb 956 1421-9778/15/0363-0956$39.50/0 Original Paper This is an Open Access article licensed
ORIGINAL ARTICLE ABSTRACT SUMMARY AT A GLANCE INTRODUCTION
 bs_bs_banner ORIGINAL ARTICLE Budesonide/formoterol maintenance and reliever therapy via Turbuhaler versus fixed-dose budesonide/formoterol plus terbutaline in patients with asthma: Phase III study results
bs_bs_banner ORIGINAL ARTICLE Budesonide/formoterol maintenance and reliever therapy via Turbuhaler versus fixed-dose budesonide/formoterol plus terbutaline in patients with asthma: Phase III study results
Effects of regular exercise on asthma control in young adults
 Journal of Asthma ISSN: 0277-0903 (Print) 1532-4303 (Online) Journal homepage: http://www.tandfonline.com/loi/ijas20 Effects of regular exercise on asthma control in young adults Dr Sirpa A.M. Heikkinen,
Journal of Asthma ISSN: 0277-0903 (Print) 1532-4303 (Online) Journal homepage: http://www.tandfonline.com/loi/ijas20 Effects of regular exercise on asthma control in young adults Dr Sirpa A.M. Heikkinen,
Hard-tissue alterations following immediate implant placement in extraction sites
 J Clin Periodontol 2004; 31: 820 828 doi: 10.1111/j.1600-051X.2004.00565.x Copyright r Blackwell Munksgaard 2004 Printed in Denmark. All rights reserved Hard-tissue alterations following immediate implant
J Clin Periodontol 2004; 31: 820 828 doi: 10.1111/j.1600-051X.2004.00565.x Copyright r Blackwell Munksgaard 2004 Printed in Denmark. All rights reserved Hard-tissue alterations following immediate implant
Author s Accepted Manuscript
 Author s Accepted Manuscript Rheumatologic symptoms in oncologic patients on PD-1 inhibitors Wilson F. Kuswanto, Lindsey A. MacFarlane, Lydia Gedmintas, Alexandra Mulloy, Toni K. Choueiri, Bonnie Bermas
Author s Accepted Manuscript Rheumatologic symptoms in oncologic patients on PD-1 inhibitors Wilson F. Kuswanto, Lindsey A. MacFarlane, Lydia Gedmintas, Alexandra Mulloy, Toni K. Choueiri, Bonnie Bermas
RAVEN'S COLORED PROGRESSIVE MATRICES AND INTELLECTUAL IMPAIRMENT IN PATIENTS WITH FOCAL BRAIN DAMAGE
 RAVEN'S COLORED PROGRESSIVE MATRICES AND INTELLECTUAL IMPAIRMENT IN PATIENTS WITH FOCAL BRAIN DAMAGE Claudio Villardita (Neuropsychology Unit, Department of Neurology, University of Catania) INTRODUCTION
RAVEN'S COLORED PROGRESSIVE MATRICES AND INTELLECTUAL IMPAIRMENT IN PATIENTS WITH FOCAL BRAIN DAMAGE Claudio Villardita (Neuropsychology Unit, Department of Neurology, University of Catania) INTRODUCTION
Title: Clinical and histopathological features of immunoglobulin G4-associated autoimmune hepatitis in children
 Title: Clinical and histopathological features of immunoglobulin G4-associated autoimmune hepatitis in children Short title: Immunoglobulin G4-associated autoimmune hepatitis in children Yusuf Aydemir¹,
Title: Clinical and histopathological features of immunoglobulin G4-associated autoimmune hepatitis in children Short title: Immunoglobulin G4-associated autoimmune hepatitis in children Yusuf Aydemir¹,
Antiproliferative, antimigratory, and anticlonogenic effects of Hedyotis diffusa, Panax ginseng, and their combination on colorectal cancer cell lines
 Journal of Herbs, Spices & Medicinal Plants ISSN: 1049-6475 (Print) 1540-3580 (Online) Journal homepage: http://www.tandfonline.com/loi/whsm20 Antiproliferative, antimigratory, and anticlonogenic effects
Journal of Herbs, Spices & Medicinal Plants ISSN: 1049-6475 (Print) 1540-3580 (Online) Journal homepage: http://www.tandfonline.com/loi/whsm20 Antiproliferative, antimigratory, and anticlonogenic effects
Clinical investigation of chronic subdural hematoma with impending brain herniation on arrival
 DOI 10.1007/s10143-017-0861-9 ORIGINAL ARTICLE Clinical investigation of chronic subdural hematoma with impending brain herniation on arrival Hiroaki Matsumoto 1 & Hiroaki Hanayama 1 & Takashi Okada 1
DOI 10.1007/s10143-017-0861-9 ORIGINAL ARTICLE Clinical investigation of chronic subdural hematoma with impending brain herniation on arrival Hiroaki Matsumoto 1 & Hiroaki Hanayama 1 & Takashi Okada 1
Divergent Thinking and Evaluation Skills: Do They Always Go Together?
 Journal of Creative Behavior MAGDALENA GROHMAN ZOFIA WODNIECKA MARCIN KLUSAK Divergent Thinking and Evaluation Skills: Do They Always Go Together? ABSTRACT INTRODUCTION The aim of the present study was
Journal of Creative Behavior MAGDALENA GROHMAN ZOFIA WODNIECKA MARCIN KLUSAK Divergent Thinking and Evaluation Skills: Do They Always Go Together? ABSTRACT INTRODUCTION The aim of the present study was
Energy Metabolism in Oreochromis niloticus
 Aquuculture, 79 (1989) 283-291 Eisevier Science Pubhshers B.V., Amsterdam - Printed in The Netherlands 283 Energy Metabolism in Oreochromis niloticus K.-H. MEYER-BURGDORFF, M.F. OSMAN and K.D. GUNTHER
Aquuculture, 79 (1989) 283-291 Eisevier Science Pubhshers B.V., Amsterdam - Printed in The Netherlands 283 Energy Metabolism in Oreochromis niloticus K.-H. MEYER-BURGDORFF, M.F. OSMAN and K.D. GUNTHER
Parallel Stent Graft Techniques to Facilitate Endovascular Repair in the Aortic Arch
 Parallel Stent Graft Techniques to Facilitate Endovascular Repair in the Aortic Arch 35 Frank J. Criado Introduction Whether using a traditional open-chest approach or endovascular techniques, the arch
Parallel Stent Graft Techniques to Facilitate Endovascular Repair in the Aortic Arch 35 Frank J. Criado Introduction Whether using a traditional open-chest approach or endovascular techniques, the arch
Introduction. urinary erythropoietin, and the two are indistinguishable
 BIOPHARMACEUTICS & DRUG DISPOSITION Biopharm. Drug Dispos. 21: 211 219 (2000) DOI: 10.1002/bdd.231 Comparative Pharmacokinetics, Safety, and Tolerability After Subcutaneous Administration of Recombinant
BIOPHARMACEUTICS & DRUG DISPOSITION Biopharm. Drug Dispos. 21: 211 219 (2000) DOI: 10.1002/bdd.231 Comparative Pharmacokinetics, Safety, and Tolerability After Subcutaneous Administration of Recombinant
164 J.A.H. an Laarho en et al. / International Journal of Pharmaceutics 232 (2002) An example of a sustained release system is a contraceptive
 International Journal of Pharmaceutics 232 (2002) 163 173 www.elsevier.com/locate/ijpharm In vitro release properties of etonogestrel and ethinyl estradiol from a contraceptive vaginal ring J.A.H. van
International Journal of Pharmaceutics 232 (2002) 163 173 www.elsevier.com/locate/ijpharm In vitro release properties of etonogestrel and ethinyl estradiol from a contraceptive vaginal ring J.A.H. van
Nebulized Magnesium for Moderate and Severe Pediatric Asthma: A Randomized Trial
 50:1191 1199 (2015) Nebulized Magnesium for Moderate and Severe Pediatric Asthma: A Randomized Trial Khalid Alansari, MD, FRCPC, FAAP(PEM), 1,2,3 * Wessam Ahmed, 2 Bruce L. Davidson, MD, MPH, 4 Mohamed
50:1191 1199 (2015) Nebulized Magnesium for Moderate and Severe Pediatric Asthma: A Randomized Trial Khalid Alansari, MD, FRCPC, FAAP(PEM), 1,2,3 * Wessam Ahmed, 2 Bruce L. Davidson, MD, MPH, 4 Mohamed
HYDRONEPHROSIS DUE TO THE INFERIOR POLAR ARTERY :
 HYDRONEPHROSIS DUE TO THE INFERIOR POLAR ARTERY : LATE RESULTS AFTER NEPHROPLICATION. Appendix of Recent Cases By A. WILFRID ADAMS, F.R.C.S. Bristol Royal Infirmary FOR hydronephrosis due to an aberrant,
HYDRONEPHROSIS DUE TO THE INFERIOR POLAR ARTERY : LATE RESULTS AFTER NEPHROPLICATION. Appendix of Recent Cases By A. WILFRID ADAMS, F.R.C.S. Bristol Royal Infirmary FOR hydronephrosis due to an aberrant,
Validation of ATS clinical practice guideline cut-points for FeNO in asthma
 Accepted Manuscript Validation of ATS clinical practice guideline cut-points for FeNO in asthma Maria Jeppegaard, Sandra Veidal, Asger Sverrild, Vibeke Backer, Celeste Porsbjerg PII: S0954-6111(18)30296-8
Accepted Manuscript Validation of ATS clinical practice guideline cut-points for FeNO in asthma Maria Jeppegaard, Sandra Veidal, Asger Sverrild, Vibeke Backer, Celeste Porsbjerg PII: S0954-6111(18)30296-8
Journal of Chromatography B, 857 (2007)
 Journal of Chromatography B, 857 (2007) 287 295 Determination of serum uric acid using high-performance liquid chromatography (HPLC)/isotope dilution mass spectrometry (ID-MS) as a candidate reference
Journal of Chromatography B, 857 (2007) 287 295 Determination of serum uric acid using high-performance liquid chromatography (HPLC)/isotope dilution mass spectrometry (ID-MS) as a candidate reference
Increased T-helper 17 cell differentiation mediated by exosome-mediated microrna-451 redistribution in gastric cancer infiltrated T cells
 Received: 24 July 217 Revised: 14 October 217 Accepted: 18 October 217 DOI: 1.1111/cas.13429 ORIGINAL ARTICLE Increased T-helper 17 cell differentiation mediated by exosome-mediated microrna-451 redistribution
Received: 24 July 217 Revised: 14 October 217 Accepted: 18 October 217 DOI: 1.1111/cas.13429 ORIGINAL ARTICLE Increased T-helper 17 cell differentiation mediated by exosome-mediated microrna-451 redistribution
Ovarian cancer is the most lethal gynecologic malignancy
 Original Research Laparoscopy Compared With Laparotomy for Debulking Ovarian Cancer After Neoadjuvant Chemotherapy Alexander Melamed, MD, MPH, Roni Nitecki, MD, David M. Boruta II, MD, Marcela G. del Carmen,
Original Research Laparoscopy Compared With Laparotomy for Debulking Ovarian Cancer After Neoadjuvant Chemotherapy Alexander Melamed, MD, MPH, Roni Nitecki, MD, David M. Boruta II, MD, Marcela G. del Carmen,
Incidence and predictors of synchronous liver metastases in patients with gastrointestinal stromal tumors (GISTs)
 Accepted Manuscript Incidence and predictors of synchronous liver metastases in patients with gastrointestinal stromal tumors (GISTs) Apostolos Gaitanidis, Michail Alevizakos, Alexandra Tsaroucha, Constantinos
Accepted Manuscript Incidence and predictors of synchronous liver metastases in patients with gastrointestinal stromal tumors (GISTs) Apostolos Gaitanidis, Michail Alevizakos, Alexandra Tsaroucha, Constantinos
Marlowe Crowne Social Desirability Scale and Short Form C: Forensic Norms
 Marlowe Crowne Social Desirability Scale and Short Form C: Forensic Norms Paul Andrews Private Practice, Tyler, Texas Robert G. Meyer University of Louisville Marlowe Crowne Social Desirability Scale (MC)
Marlowe Crowne Social Desirability Scale and Short Form C: Forensic Norms Paul Andrews Private Practice, Tyler, Texas Robert G. Meyer University of Louisville Marlowe Crowne Social Desirability Scale (MC)
Contrasting timing of virological relapse after discontinuation of. tenofovir or entecavir in hepatitis B e antigen-negative patients.
 Contrasting timing of virological relapse after discontinuation of tenofovir or entecavir in hepatitis B e antigen-negative patients. Running title: Difference after stopping TDF or ETV Christoph Höner
Contrasting timing of virological relapse after discontinuation of tenofovir or entecavir in hepatitis B e antigen-negative patients. Running title: Difference after stopping TDF or ETV Christoph Höner
Effect of health Baduanjin Qigong for mild to moderate Parkinson s disease
 bs_bs_banner Geriatr Gerontol Int 2016; 16: 911 919 ORIGINAL ARTICLE: EPIDEMIOLOGY, CLINICAL PRACTICE AND HEALTH Effect of health Baduanjin Qigong for mild to moderate Parkinson s disease Chun-Mei Xiao
bs_bs_banner Geriatr Gerontol Int 2016; 16: 911 919 ORIGINAL ARTICLE: EPIDEMIOLOGY, CLINICAL PRACTICE AND HEALTH Effect of health Baduanjin Qigong for mild to moderate Parkinson s disease Chun-Mei Xiao
Computerized Quantitative Coronary Angiography Applied to Percutaneous Transluminal Coronary Angioplasty: Advantages and Limitations
 Computerized Quantitative Coronary Angiography Applied to Percutaneous Transluminal Coronary Angioplasty: Advantages and Limitations P.W. Serruys, F. Booman, G.J. Troost, J.H.C. Reiber, J.J. Gerbrands*,
Computerized Quantitative Coronary Angiography Applied to Percutaneous Transluminal Coronary Angioplasty: Advantages and Limitations P.W. Serruys, F. Booman, G.J. Troost, J.H.C. Reiber, J.J. Gerbrands*,
MicroRNA-30a-5p suppresses epithelial-mesenchymal transition by targeting profilin-2 in high invasive non-small cell lung cancer cell lines
 3146 ONCOLOGY REPORTS 37: 3146-3154, 2017 MicroRNA-30a-5p suppresses epithelial-mesenchymal transition by targeting profilin-2 in high invasive non-small cell lung cancer cell lines Jiliang Yan 1*, Chunyan
3146 ONCOLOGY REPORTS 37: 3146-3154, 2017 MicroRNA-30a-5p suppresses epithelial-mesenchymal transition by targeting profilin-2 in high invasive non-small cell lung cancer cell lines Jiliang Yan 1*, Chunyan
Pulmonary Vein Stenosis After Catheter Ablation of Atrial Fibrillation
 Pulmonary Vein Stenosis After Catheter Ablation of Atrial Fibrillation E.B. SAAD Introduction Catheter ablation around the pulmonary veins (PVs) has become the treatment of choice for symptomatic patients
Pulmonary Vein Stenosis After Catheter Ablation of Atrial Fibrillation E.B. SAAD Introduction Catheter ablation around the pulmonary veins (PVs) has become the treatment of choice for symptomatic patients
Splenomegaly and Hemolytic Anemia Induced in Rats by Methylcellulose - An electron microscopic study '
 Splenomegaly and Hemolytic Anemia Induced in Rats by Methylcellulose - An electron microscopic study ' EMMA WENNBERG AND LEON WEISS Department of Anatomy, The johns Hopkins University School of Medicine,
Splenomegaly and Hemolytic Anemia Induced in Rats by Methylcellulose - An electron microscopic study ' EMMA WENNBERG AND LEON WEISS Department of Anatomy, The johns Hopkins University School of Medicine,
ABSTRACT. questions in the version of NorAQ administered to men (m-noraq) against the interview model.
 GENDER MEDICINE/VOL. 8,NO. 2, 2011 NorVold Abuse Questionnaire for Men (m-noraq): Validation of New Measures of Emotional, Physical, and Sexual Abuse and Abuse in Health Care in Male Patients Katarina
GENDER MEDICINE/VOL. 8,NO. 2, 2011 NorVold Abuse Questionnaire for Men (m-noraq): Validation of New Measures of Emotional, Physical, and Sexual Abuse and Abuse in Health Care in Male Patients Katarina
SYSTEMATIC REVIEW PROTOCOL
 Effectiveness of Silexan oral lavender essential oil compared to inhaled lavender essential oil aromatherapy on sleep in adults: a systematic review protocol Martha J. Greenberg 1,2 Jason T. Slyer 1,2
Effectiveness of Silexan oral lavender essential oil compared to inhaled lavender essential oil aromatherapy on sleep in adults: a systematic review protocol Martha J. Greenberg 1,2 Jason T. Slyer 1,2
LONG-TERM RESULTS OF A PHASE III TRIAL COMPARING ONCE-DAILY RADIOTHERAPY WITH TWICE-DAILY RADIOTHERAPY IN LIMITED- STAGE SMALL-CELL LUNG CANCER
 doi:10.1016/j.ijrobp.2004.01.055 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 4, pp. 943 951, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
doi:10.1016/j.ijrobp.2004.01.055 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 4, pp. 943 951, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
A. Alonso-Burgos a, *, E. García-Tutor b, G. Bastarrika a, D. Cano a, A. Martínez-Cuesta a, L.J. Pina a
 Journal of Plastic, Reconstructive & Aesthetic Surgery (2006) 59, 585 593 Preoperative planning of deep inferior epigastric artery perforator flap reconstruction with multislice-ct angiography: imaging
Journal of Plastic, Reconstructive & Aesthetic Surgery (2006) 59, 585 593 Preoperative planning of deep inferior epigastric artery perforator flap reconstruction with multislice-ct angiography: imaging
A Diabetes Mobile App With In-App Coaching From a Certified Diabetes Educator Reduces A1C for Individuals With Type 2 Diabetes
 765650TDEXXX10.1177/0145721718765650Impact of a Diabetes App and Coaching Program on A1CKumar et al research-article2018 Impact of a Diabetes App and Coaching Program on A1C 1 A Diabetes Mobile App With
765650TDEXXX10.1177/0145721718765650Impact of a Diabetes App and Coaching Program on A1CKumar et al research-article2018 Impact of a Diabetes App and Coaching Program on A1C 1 A Diabetes Mobile App With
Electrical Acupoint Stimulation Changes Body Composition and the Meridian Systems in Postmenopausal Women with Obesity
 The American Journal of Chinese Medicine, Vol. 38, No. 4, 683 694 2010 World Scientific Publishing Company Institute for Advanced Research in Asian Science and Medicine DOI: 10.1142/S0192415X10008159 Electrical
The American Journal of Chinese Medicine, Vol. 38, No. 4, 683 694 2010 World Scientific Publishing Company Institute for Advanced Research in Asian Science and Medicine DOI: 10.1142/S0192415X10008159 Electrical
Low- vs. high-pressure suction drainage after total knee arthroplasty: a double-blind randomized controlled trial
 JAN JOURNAL OF ADVANCED NURSING ORIGINAL RESEARCH Low- vs. high-pressure suction drainage after total knee arthroplasty: a double-blind randomized controlled trial Rafael Calvo, M a José Martínez-Zapata,
JAN JOURNAL OF ADVANCED NURSING ORIGINAL RESEARCH Low- vs. high-pressure suction drainage after total knee arthroplasty: a double-blind randomized controlled trial Rafael Calvo, M a José Martínez-Zapata,
Colchicine for prevention and treatment of cardiac diseases: A meta-analysis
 DOI: 10.1111/1755-5922.12226 ORIGINAL RESEARCH ARTICLE Colchicine for prevention and treatment of cardiac diseases: A meta-analysis Nikolaos Papageorgiou 1,2, Alexandros Briasoulis 3, George Lazaros 2
DOI: 10.1111/1755-5922.12226 ORIGINAL RESEARCH ARTICLE Colchicine for prevention and treatment of cardiac diseases: A meta-analysis Nikolaos Papageorgiou 1,2, Alexandros Briasoulis 3, George Lazaros 2
Small pulmonary nodules in baseline and incidence screening rounds of low-dose CT lung cancer screening
 Review Article Small pulmonary nodules in baseline and incidence screening rounds of low-dose CT lung cancer screening Joan E. Walter, Marjolein A. Heuvelmans, Matthijs Oudkerk University Medical Center
Review Article Small pulmonary nodules in baseline and incidence screening rounds of low-dose CT lung cancer screening Joan E. Walter, Marjolein A. Heuvelmans, Matthijs Oudkerk University Medical Center
Absolute monocyte count predicts overall survival in mantle cell lymphomas: correlation with tumourassociated
 Hematological Oncology Hematol Oncol 2014; 32: 178 186 Published online 29 October 2013 in Wiley Online Library (wileyonlinelibrary.com).2106 Original Research Article Absolute monocyte count predicts
Hematological Oncology Hematol Oncol 2014; 32: 178 186 Published online 29 October 2013 in Wiley Online Library (wileyonlinelibrary.com).2106 Original Research Article Absolute monocyte count predicts
Natural Course of Peripartum Cardiomyopathy
 Natural Course of Peripartum Cardiomyopathy By JOHN G. DEMAKIS, M.D., SHAHBUDIN H. RAHIMTOOLA, M.B., M.R.C.P.E., GEORGE C. SUTrON, M.D., W. ROBERT MEADOWS, M.D., PAUL B. SZANTO, M.D., JoHN R. TOBIN, M.D.,
Natural Course of Peripartum Cardiomyopathy By JOHN G. DEMAKIS, M.D., SHAHBUDIN H. RAHIMTOOLA, M.B., M.R.C.P.E., GEORGE C. SUTrON, M.D., W. ROBERT MEADOWS, M.D., PAUL B. SZANTO, M.D., JoHN R. TOBIN, M.D.,
Hepatitis B virus (HBV) infection is a global health
 GASTROENTEROLOGY 2012;142:1140 1149 High Levels of Hepatitis B Surface Antigen Increase Risk of Hepatocellular Carcinoma in Patients With Low HBV Load TAI CHUNG TSENG,*,, ** CHUN JEN LIU,, HUNG CHIH YANG,,#
GASTROENTEROLOGY 2012;142:1140 1149 High Levels of Hepatitis B Surface Antigen Increase Risk of Hepatocellular Carcinoma in Patients With Low HBV Load TAI CHUNG TSENG,*,, ** CHUN JEN LIU,, HUNG CHIH YANG,,#
Glucose-lowering activity of the dipeptidyl peptidase-4 inhibitor saxagliptin in drug-naive patients with type 2 diabetes*
 ORIGINAL ARTICLE doi: 10.1111/j.1463-1326.2008.00876.x Glucose-lowering activity of the dipeptidyl peptidase-4 inhibitor saxagliptin in drug-naive patients with type 2 diabetes* J. Rosenstock, 1 S. Sankoh
ORIGINAL ARTICLE doi: 10.1111/j.1463-1326.2008.00876.x Glucose-lowering activity of the dipeptidyl peptidase-4 inhibitor saxagliptin in drug-naive patients with type 2 diabetes* J. Rosenstock, 1 S. Sankoh
Functional Outcome of Unstable Distal Radius Fractures: ORIF With a Volar Fixed-Angle Tine Plate Versus External Fixation
 Functional Outcome of Unstable Distal Radius Fractures: ORIF With a Volar Fixed-Angle Tine Plate Versus External Fixation Thomas W. Wright, MD, MaryBeth Horodyski, EdD, Gainesville, FL, Dean W. Smith,
Functional Outcome of Unstable Distal Radius Fractures: ORIF With a Volar Fixed-Angle Tine Plate Versus External Fixation Thomas W. Wright, MD, MaryBeth Horodyski, EdD, Gainesville, FL, Dean W. Smith,
A LABORATORY TASK FOR INDUCTION OF MOOD STATES*
 khav. Res. & Therapy. 1968. Vol. 6. pp. 473 to 462. Pergamon Press. Printed in Englmd A LABORATORY TASK FOR INDUCTION OF MOOD STATES* EMMETT VELTEN, JR.? University of Southern California (Received 15
khav. Res. & Therapy. 1968. Vol. 6. pp. 473 to 462. Pergamon Press. Printed in Englmd A LABORATORY TASK FOR INDUCTION OF MOOD STATES* EMMETT VELTEN, JR.? University of Southern California (Received 15
Efficacy, safety and impact on β
 J Endocrinol Invest (2016) 39:1061 1074 DOI 10.1007/s40618-016-0465-1 ORIGINAL ARTICLE Efficacy, safety and impact on β cell function of dipeptidyl peptidase 4 inhibitors plus metformin combination therapy
J Endocrinol Invest (2016) 39:1061 1074 DOI 10.1007/s40618-016-0465-1 ORIGINAL ARTICLE Efficacy, safety and impact on β cell function of dipeptidyl peptidase 4 inhibitors plus metformin combination therapy
A Motivational Intervention to Reduce Cigarette
 A Motivational Intervention to Reduce Cigarette Smoking Among College Students: Overview and Exploratory Investigation Keith C. Herman and Beth Fahnlander College counselors can play an important role
A Motivational Intervention to Reduce Cigarette Smoking Among College Students: Overview and Exploratory Investigation Keith C. Herman and Beth Fahnlander College counselors can play an important role
Lisfranc Arthrodesis for Chronic Pain: A Cannulated Screw Technique
 Lisfranc Arthrodesis for Chronic Pain: A Cannulated Screw Technique Nine patients with injury to the tarsometatarsal joint underwent fusion with cannulated screw fixation after conservative treatment had
Lisfranc Arthrodesis for Chronic Pain: A Cannulated Screw Technique Nine patients with injury to the tarsometatarsal joint underwent fusion with cannulated screw fixation after conservative treatment had
Development and psychometric evaluation of the Thirst Distress Scale for patients with heart failure
 728624CNU0010.1177/1474515117728624European Journal of Cardiovascular Nursing 0(0)Waldréus et al. research-article2017 Original Article Development and psychometric evaluation of the Thirst Distress Scale
728624CNU0010.1177/1474515117728624European Journal of Cardiovascular Nursing 0(0)Waldréus et al. research-article2017 Original Article Development and psychometric evaluation of the Thirst Distress Scale
Address: Department of General Surgery, Royal Bolton Hospital, Bolton, UK. ; tel:
 Article type : Systematic Review Accepted Article 875-2017.R1 Systematic Review Effect of mesalazine on recurrence of diverticulitis in patients with symptomatic uncomplicated diverticular disease: a meta-analysis
Article type : Systematic Review Accepted Article 875-2017.R1 Systematic Review Effect of mesalazine on recurrence of diverticulitis in patients with symptomatic uncomplicated diverticular disease: a meta-analysis
Pulley lesions in rotator cuff tears: prevalence, etiology, and concomitant pathologies
 Arch Orthop Trauma Surg (2017) 137:1097 1105 DOI 10.1007/s00402-017-2721-z ARTHROSCOPY AND SPORTS MEDICINE Pulley lesions in rotator cuff tears: prevalence, etiology, and concomitant pathologies Nael Hawi
Arch Orthop Trauma Surg (2017) 137:1097 1105 DOI 10.1007/s00402-017-2721-z ARTHROSCOPY AND SPORTS MEDICINE Pulley lesions in rotator cuff tears: prevalence, etiology, and concomitant pathologies Nael Hawi
Congenital absence of teeth is a common dental
 CASE REPORT Management of congenitally missing second premolars with orthodontics and single-tooth implants Roy Sabri, DDS, MS Beirut, Lebanon This article describes the treatment of an adolescent girl
CASE REPORT Management of congenitally missing second premolars with orthodontics and single-tooth implants Roy Sabri, DDS, MS Beirut, Lebanon This article describes the treatment of an adolescent girl
010059, China b First Affiliated Hospital, Inner Mongolia Medical University, Hohhot , China Published online: 06 Jan 2015.
 This article was downloaded by: [University of Nebraska, Lincoln] On: 05 April 2015, At: 06:57 Publisher: Taylor & Francis Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered
This article was downloaded by: [University of Nebraska, Lincoln] On: 05 April 2015, At: 06:57 Publisher: Taylor & Francis Informa Ltd Registered in England and Wales Registered Number: 1072954 Registered
Epithelial Barrier Defects in HT-29/B6 Colonic Cell Monolayers Induced by Tumor Necrosis Factor α
 Epithelial Barrier Defects in HT-29/B6 Colonic Cell Monolayers Induced by Tumor Necrosis Factor α ALFRED H. GITTER, a,b KERSTIN BENDFELDT, a HEINZ SCHMITZ, c JÖRG-DIETER SCHULZKE, c CARL J. BENTZEL, d
Epithelial Barrier Defects in HT-29/B6 Colonic Cell Monolayers Induced by Tumor Necrosis Factor α ALFRED H. GITTER, a,b KERSTIN BENDFELDT, a HEINZ SCHMITZ, c JÖRG-DIETER SCHULZKE, c CARL J. BENTZEL, d
Endoscopic resection therapies for rectal neuroendocrine tumors: A systematic review and meta-analysis
 bs_bs_banner doi:.1111/jgh.12395 META-ANALYSIS AND SYSTEMATIC REVIEW for rectal neuroendocrine tumors: A systematic review and meta-analysis Xin Zhou,* Haiting Xie,* Lingduo Xie,* Jing Li, Weihua Cao and
bs_bs_banner doi:.1111/jgh.12395 META-ANALYSIS AND SYSTEMATIC REVIEW for rectal neuroendocrine tumors: A systematic review and meta-analysis Xin Zhou,* Haiting Xie,* Lingduo Xie,* Jing Li, Weihua Cao and
Combining ECMO with IABP for the Treatment of Critically Ill Adult Heart Failure Patients
 Heart, Lung and Circulation (2014) 23, 363 368 1443-9506/04/$36.00 http://dx.doi.org/10.1016/j.hlc.2013.10.081 ORIGINAL ARTICLE Combining ECMO with IABP for the Treatment of Critically Ill Adult Heart
Heart, Lung and Circulation (2014) 23, 363 368 1443-9506/04/$36.00 http://dx.doi.org/10.1016/j.hlc.2013.10.081 ORIGINAL ARTICLE Combining ECMO with IABP for the Treatment of Critically Ill Adult Heart
EGC Diagnosis of Paroxysmal Supraventricular Tachycardias in Patients without Preexcitation
 REVIEW ARTICLE EGC Diagnosis of Paroxysmal Supraventricular Tachycardias in Patients without Preexcitation Esteban González-Torrecilla, M.D., Ph.D., Angel Arenal, M.D., Felipe Atienza, M.D., Ph.D., Tomás
REVIEW ARTICLE EGC Diagnosis of Paroxysmal Supraventricular Tachycardias in Patients without Preexcitation Esteban González-Torrecilla, M.D., Ph.D., Angel Arenal, M.D., Felipe Atienza, M.D., Ph.D., Tomás
available at journal homepage:
 Lung Cancer (2006) 54, 217 225 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/lungcan Eg5 expression is closely correlated with the response of advanced non-small cell lung
Lung Cancer (2006) 54, 217 225 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/lungcan Eg5 expression is closely correlated with the response of advanced non-small cell lung
Tumor Spread Through Air Spaces Identifies a Distinct Subgroup With Poor Prognosis in Surgically Resected Lung Pleomorphic Carcinoma
 1 2 3 4 5 6 7 8 9 1 11 12 13 14 15 16 17 18 19 21 22 23 24 25 26 27 28 29 3 31 32 33 34 35 36 37 38 39 41 42 43 44 45 46 47 48 49 5 51 52 53 54 55 Q15 Q1 Q6 Q2 [ Original Research ] Tumor Spread Through
1 2 3 4 5 6 7 8 9 1 11 12 13 14 15 16 17 18 19 21 22 23 24 25 26 27 28 29 3 31 32 33 34 35 36 37 38 39 41 42 43 44 45 46 47 48 49 5 51 52 53 54 55 Q15 Q1 Q6 Q2 [ Original Research ] Tumor Spread Through
Protective effect of HTK solution on postoperative pulmonary function in infants with CHD and PAH
 Bioscience Reports: this is an Accepted Manuscript, not the final Version of Record. You are encouraged to use the Version of Record that, when published, will replace this version. The most up-to-date
Bioscience Reports: this is an Accepted Manuscript, not the final Version of Record. You are encouraged to use the Version of Record that, when published, will replace this version. The most up-to-date
A disease- specific quality of life instrument for non- alcoholic fatty liver disease and non- alcoholic steatohepatitis: CLDQ- NAFLD
 Received: 10 November 2016 Accepted: 8 February 2017 DOI: 10.1111/liv.13391 METABOLIC LIVER DISEASE A disease- specific quality of life instrument for non- alcoholic fatty liver disease and non- alcoholic
Received: 10 November 2016 Accepted: 8 February 2017 DOI: 10.1111/liv.13391 METABOLIC LIVER DISEASE A disease- specific quality of life instrument for non- alcoholic fatty liver disease and non- alcoholic
Effects of Mattress Material on Body Pressure Profiles in Different Sleeping Postures
 Effects of Mattress Material on Body Pressure Profiles in Different Sleeping Postures Fan-Zhe Low, BEng, Matthew Chin-Heng Chua, PhD, Pan-Yin Lim, BEng, and Chen-Hua Yeow, PhD ABSTRACT Objectives: This
Effects of Mattress Material on Body Pressure Profiles in Different Sleeping Postures Fan-Zhe Low, BEng, Matthew Chin-Heng Chua, PhD, Pan-Yin Lim, BEng, and Chen-Hua Yeow, PhD ABSTRACT Objectives: This
The Comparison of Pedicle Screw and Cortical Screw in Posterior Lumbar Inter-body Fusion: a Prospective Randomized Non-inferiority Trial
 Accepted Manuscript The Comparison of Pedicle Screw and Cortical Screw in Posterior Lumbar Inter-body Fusion: a Prospective Randomized Non-inferiority Trial Gun Woo Lee, MD, Jung-Hwan Son, MD, Myun-Whan
Accepted Manuscript The Comparison of Pedicle Screw and Cortical Screw in Posterior Lumbar Inter-body Fusion: a Prospective Randomized Non-inferiority Trial Gun Woo Lee, MD, Jung-Hwan Son, MD, Myun-Whan
Gomputed tomography of the normal temporomaandibular joint
 Gomputed tomography of the normal temporomaandibular joint EDWIN h. GHRISTiANSENi, TERENCE T: CHAN^, JOSEPH R. THOMPSON^ ANTON N. HASSO', DAVID B. HINSHAW JR' AND SIGVARD KOPP* ^Department of Endodontics^
Gomputed tomography of the normal temporomaandibular joint EDWIN h. GHRISTiANSENi, TERENCE T: CHAN^, JOSEPH R. THOMPSON^ ANTON N. HASSO', DAVID B. HINSHAW JR' AND SIGVARD KOPP* ^Department of Endodontics^
Infectivity of HBV DNA positive donations identified in look-back studies in Hyogo-Prefecture, Japan
 Transfusion Medicine, 2011, 21, 107 115 doi: 10.1111/j.1365-3148.2010.01057.x ORIGINAL ARTICLE Infectivity of HBV DNA positive donations identified in look-back studies in Hyogo-Prefecture, Japan Y. Bouike,
Transfusion Medicine, 2011, 21, 107 115 doi: 10.1111/j.1365-3148.2010.01057.x ORIGINAL ARTICLE Infectivity of HBV DNA positive donations identified in look-back studies in Hyogo-Prefecture, Japan Y. Bouike,
Memory-based attentional capture by colour and shape contents in visual working memory
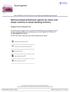 Visual Cognition ISSN: 1350-6285 (Print) 1464-0716 (Online) Journal homepage: http://www.tandfonline.com/loi/pvis20 Memory-based attentional capture by colour and shape contents in visual working memory
Visual Cognition ISSN: 1350-6285 (Print) 1464-0716 (Online) Journal homepage: http://www.tandfonline.com/loi/pvis20 Memory-based attentional capture by colour and shape contents in visual working memory
Lung cancer is one of the major tumors that causes human
 ORIGINAL RESEARCH Analysis of Contrast-Enhanced Ultrasound Perfusion Patterns and Time-Intensity Curves for Metastatic Lymph Nodes From Lung Cancer Preliminary Results Shanshan Yin, MD, Qiuli Cui, MSc,
ORIGINAL RESEARCH Analysis of Contrast-Enhanced Ultrasound Perfusion Patterns and Time-Intensity Curves for Metastatic Lymph Nodes From Lung Cancer Preliminary Results Shanshan Yin, MD, Qiuli Cui, MSc,
Efficacy and Safety of Saxagliptin Compared with Acarbose in Chinese. Patients with Type 2 Diabetes Mellitus Uncontrolled on Metformin
 Efficacy and Safety of Saxagliptin Compared with Acarbose in Chinese Patients with Type 2 Diabetes Mellitus Uncontrolled on Metformin Monotherapy: Results of a Phase IV Open-Label Randomized Controlled
Efficacy and Safety of Saxagliptin Compared with Acarbose in Chinese Patients with Type 2 Diabetes Mellitus Uncontrolled on Metformin Monotherapy: Results of a Phase IV Open-Label Randomized Controlled
