Genitourinary Imaging Original Research
|
|
|
- Ernest Potter
- 6 years ago
- Views:
Transcription
1 Genitourinary Imaging Original Research Woodfield et al. DWI of Prostate Cancer Genitourinary Imaging Original Research Courtney A. Woodfield 1,2 Glenn A. Tung 1,2 David J. Grand 1,2 John A. Pezzullo 1,2 Jason T. Machan 3 Joseph F. Renzulli II 2,4 Woodfield CA, Tung GA, Grand DJ, Pezzullo JA, Machan JT, Renzulli JF II Keywords: diffusion-weighted imaging, Gleason score, MRI, prostate cancer, tumor volume DOI: /AJR Received February 24, 2009; accepted after revision October 9, Department of Diagnostic Imaging, Rhode Island Hospital, 593 Eddy St., Providence, RI Address correspondence to C. A. Woodfield (courtneywoodfield@ yahoo.com). 2 The Warren Alpert Medical School of Brown University, Providence, RI. 3 Department of Biostatistics, Rhode Island Hospital, Providence, RI. 4 Division of Urology, Rhode Island Hospital, Providence, RI. WEB This is a Web exclusive article. AJR 2010; 194:W316 W X/10/1944 W316 American Roentgen Ray Society Diffusion-Weighted MRI of Peripheral Zone Prostate Cancer: Comparison of Tumor Apparent Diffusion Coefficient With Gleason Score and Percentage of Tumor on Core Biopsy OBJECTIVE. The objective of our study was to determine the relationship between the apparent diffusion coefficient (ADC) value on diffusion-weighted imaging (DWI) and Gleason score of prostate cancer and percentage of tumor involvement on prostate core biopsy. MATERIALS AND METHODS. We performed a retrospective study of 57 patients with biopsy-proven prostate cancer who underwent endorectal MRI with DWI between July 2007 and March Regions of interest (ROIs) were drawn on ADC maps at sites of visible tumor on DW images and ADC maps. A hierarchic mixed linear model was used to compare the ADC value of prostate cancer with the Gleason score and the percentage of tumor on core biopsy. RESULTS. Eighty-one sites of biopsy-proven prostate cancer were visible on DW images and ADC maps. The least-squares mean ADC for disease with a Gleason score of 6 was mm 2 /s (standard error of the mean [SEM], 0.036); Gleason score of 7, mm 2 /s (SEM, 0.030); Gleason score of 8, mm 2 /s (SEM, 0.057); and Gleason score of 9, mm 2 /s (SEM, 0.067). Differences between the mean ADC values for a prostate tumor with a Gleason score of 6 and one with a Gleason score of 7 (p = ) and for a prostate tumor with a Gleason score of 6 and one with a Gleason score of 8 (p = ) were significant. Comparison between the ADC and percentage of tumor on core biopsy showed a mean ADC decrease of (range, mm 2 /s) for every 1% increase in tumor in the core biopsy specimen. CONCLUSION. DWI may help differentiate between low-risk (Gleason score, 6) and intermediate-risk (Gleason score, 7) prostate cancer and between low-risk (Gleason score, 6) and high-risk (Gleason score > 7) prostate cancer. There is an inverse relationship between the ADC and the percentage of tumor involvement on prostate core biopsies. M RI of prostate cancer with conventional T2-weighted imaging is predominantly limited to staging for the presence of extracapsular extension and seminal vesicle invasion. However, the more recent application of functional MRI techniques, including diffusion-weighted imaging (DWI), has the potential to expand the role of MRI to noninvasive characterization of prostate cancer by providing more specific information regarding tumor location, size, and aggressiveness [1 6]. Several recent studies have shown that DWI can help differentiate between malignant and benign prostatic tissue on the basis of lower apparent diffusion coefficient (ADC) values of prostate carcinoma compared with normal prostate tissue [2 4, 7 12]. Decreased diffusion in prostate carcinoma is believed to be caused, at least partly, by the more highly cellular environment of neoplastic tissue, which restricts water molecule movement in the ex- tracellular space. The reported ADC values of prostate cancer in the peripheral zone range between 0.93 and mm 2 /s [2 4, 8 13]. This variability in ADC values may be related, at least in part, to the heterogeneous tissue composition of prostate cancer [14]. The histopathologic reference standard for measuring and reporting prostate cancer aggressiveness is the Gleason grading system. Gleason grades 1 5 correspond to progressively more poorly differentiated prostate cancer. A given tumor is assigned both a primary (most prevalent) and a secondary (second most prevalent) Gleason grade, and the sum of these grades yields the Gleason score. Gleason scores are also used to describe tumors as low grade (Gleason score, 6), intermediate grade (Gleason score, 7), or high grade (Gleason score, > 7) with respect to tumor aggressiveness. More aggressive tumors are associated with an increased likelihood of prostate cancer recurrence [15]. A larger tumor volume is also W316 AJR:194, April 2010
2 DWI of Prostate Cancer associated with an increased risk of tumor recurrence [16]. The purpose of this study was to investigate the relationship between the ADC value of prostate cancer on MRI and the Gleason score and tumor volume of prostate cancer on transrectal ultrasound guided prostate core biopsy. Further understanding of the restricted diffusion characteristics of prostate cancer may allow improved assessment of tumor aggressiveness with MRI. Materials and Methods Patients This retrospective study was approved by our institutional review board (IRB) and was compliant with HIPAA. The IRB waived the requirement for informed patient consent. Between July 2007 and March 2008, 90 men underwent endorectal prostate MRI at our institution. Thirty-three of these men were excluded from this study because one or more of the following inclusion criteria were not met: MRI examination included DWI; transrectal ultrasound guided biopsy results were available for review; MRI was performed 3 weeks to less than 6 months after prostate biopsy; and no treatment of prostate cancer had been received before MRI. In all subjects, a tissue diagnosis of prostate cancer was determined from analysis of transrectal ultrasound guided biopsy specimens. Patient age, serum prostate-specific antigen (PSA) level, biopsy results for Gleason score, and percentage of tumor involvement of the biopsy core were recorded from review of the medical records. MRI Technique All prostate MRI examinations were performed on a 1.5-T system (Signa Excite, GE Healthcare) with a gradient strength of 120 mt/m and using both a pelvic phased-array coil and balloon-covered expandable endorectal coil. Glucagon, 1 mg, was administered subcutaneously immediately before the start of the examination. All patients were imaged in the supine position. After the acquisition of localizing images, sagittal T2-weighted singleshot fast spin-echo imaging through the pelvis was performed to confirm the position of the endorectal coil. Axial, coronal, and sagittal thin-section, high-spatial-resolution T2-weighted fast spin-echo (FSE) images through the prostate and seminal vesicles were obtained using the following parameters: TR range, 3,000 4,000 milliseconds; TE, 120 milliseconds; echo-train length, 16; field of view (FOV), 12 cm; section thickness, 3 mm; intersection gap, 0 mm; matrix, ; and number of excitations (NEX), 4. Transverse axial T1-weighted spoiled gradient-echo images with a TR/TE of 325/4.2 and all other parameters matched to the axial high-resolution T2-weighted FSE sequence were obtained. Transverse axial T1-weighted spoiled gradient-echo images were also obtained from the aortic bifurcation to the symphysis pubis using the following parameters: 100/4.2; FOV, 38 cm; section thickness, 5 mm; intersection gap, 1 mm; matrix, ; and NEX, 1. DWI was performed using a single-shot echoplanar imaging technique with a TR of 3,000 milliseconds and a minimum TE; FOV, 18 cm; section thickness, 3 mm; intersection gap, 0 mm; matrix, ; NEX, 6; and b values, 0 and 1,000 s/ mm 2. Before this study, we established that a b value of 1,000 s/mm 2 provided the highest image contrast between normal and malignant prostate tissue on our 1.5-T system. In addition, a larger FOV (18 cm) was used for the DWI sequences than for the T1- and T2-weighted sequences (FOV, 12 cm) to optimize the signal-to-noise ratio on the DWI images. In other studies, the highest b values used for DWI of prostate cancer range between 500 and 1,000 s/mm 2 [1 12]. The use of b values higher than 1,000 s/mm 2 has not been shown to further improve differentiation between normal and malignant prostate tissues [17]. ADC values were obtained from the DWI sequences performed with b values of 0 and 1,000 s/mm 2, and the ADC maps were generated by calculating the ADC value in each pixel of each slice. MR Image Analysis MRI was analyzed by a radiologist blinded to Gleason score and tumor volume but with knowledge of the location of prostate cancer from transrectal ultrasound guided prostate biopsy results. The transverse, longitudinal, and lateral locations of the prostate biopsy were described by the urologist who performed the biopsy as right or left side of gland; base of gland, mid gland, or apex of gland; and medial, central, or lateral, respectively, to help determine the biopsy locations on MR images. All of the biopsied tumors were located in the prostatic peripheral zone. None of the patients had central gland biopsies. All sequences of the MR examination were reviewed for each patient by a radiologist with 5 years of experience interpreting prostate MR examinations and 2 years of experience interpreting DWI of the prostate. The criteria for tumor visibility were focal hyperintensity on DW images and corresponding hypointensity on ADC maps relative to the rest of the prostate gland and at a site of biopsy-proven carcinoma. Focal hypointensity at a site of biopsyproven carcinoma on both T1- and T2-weighted images was not a criterion for tumor visibility. The T1- and T2-weighted sequences were reviewed only to confirm findings on other sequences and to ensure that any measured areas of restricted diffusion were not due to the presence of blood products. If an area of decreased signal intensity was detected on a T1- and T2-weighted image at a site of biopsy-proven carcinoma, it still did not meet criteria for tumor visibility if there was no corresponding restricted diffusion. The FOVs were different for the T2- weighted and DWI sequences. Therefore, a region of interest (ROI) placed in the center of the tumor on T2-weighted imaging could not be precisely crossreferenced to the corresponding DW image. Similarly, biopsy-proven sites of carcinoma that were not visible on T2-weighted imaging or DWI were not analyzed because we believe that estimated ROI measurements based on biopsy site description alone would not be accurate. The criterion for benign prostate tissue was the absence of hyperintensity on the DWI sequence and absence of hypointensity on T2-weighted images in the peripheral zone at a site of biopsy-proven benign tissue. ROIs were drawn manually by the reviewing radiologist on ADC maps in the center of each visible tumor and at sites of biopsy-proven benign tissue. The ROIs were drawn to encompass the largest area of prostate cancer or benign tissue without including the tumor margins, the prostate capsule, or the urethra (Figs. 1 and 2). The areas of ROIs ranged from 3 to 20 mm 2. The wide range of areas was due to the wide range in the sizes of prostate glands and prostate carcinomas. The size and location of all biopsyproven tumor foci visible on DW images and ADC maps were also recorded. Tumor size was measured on ADC maps. Mean signal intensity values and SDs in the ROI were automatically determined by the PACS (Synpase, Fuji Medical Systems). Biopsyrelated hemorrhage in the prostate gland was also scored on a 4-point scale: 0, no blood; 1, blood in less than 25% of the peripheral zone; 2, blood in 25 50% of the peripheral zone; and 3, blood in more than 50% of the peripheral zone. Statistical Analysis A generalized estimating equation was used first to determine whether there was a relationship between tumor visibility on DW images and ADC maps and pathologic Gleason score. An unstructured variance covariance structure was used. To further evaluate the relationship between ADC values of visible tumor and pathologic Gleason score and between ADC values of visible tumor and the percentage of tumor on core biopsy, a hierarchic mixed linear model was used to predict ADC, in which Gleason score was a categoric fixed and random effect and percentage of tumor involvement on core biopsy as a continuous fixed and random effect. This model was chosen to account for the clustered nature of multiple samples from the same patient. In addition, a Bonferroni adjustment was used to adjust p values on the basis of the number of follow-up comparisons performed if necessary. An AJR:194, April 2010 W317
3 Woodfield et al. unstructured variance covariance structure was also used. A linear trend was tested for increases in ADC as a function of increasing Gleason score. A chi-square test was used to assess the effect of biopsy-related hemorrhage on tumor visibility, where only one observation was made per patient. A hierarchic model was also used to compare the percentage of tumor involvement on core biopsy for DWI and ADC value for tumors visible on DW images and ADC maps and tumors not visible on DW images and ADC maps. Results In this study, 57 men (mean age, 66 years; SD, 10.9; range, years) had a total of 342 transrectal ultrasound guided core prostate biopsies and 185 (54%) of these sextant biopsies yielded prostate cancer. Forty-four A Fig year-old man with prostate cancer with Gleason score of 6 in peripheral zone of right mid gland involving 50% of core biopsy. A, Axial diffusion-weighted image (b = 1,000 s/mm 2 ) shows area of slightly rounded hyperintensity (arrow) at site of biopsy-proven carcinoma. Note similar increased signal intensity at contralateral base due to coil artifact. B, Isotropic axial apparent diffusion coefficient (ADC) map shows area of hypointensity (arrow) corresponding to that shown in A. C, Isotropic axial ADC map with region of interest (circle) placed in center of hypointense signal yields ADC of mm 2 /s. A Fig year-old man with prostate cancer with Gleason score of 8 in peripheral zone of right mid gland involving 53% of prostate core biopsy. A, Axial diffusion-weighted image (b = 1,000 s/mm 2 ) shows area of increased signal intensity (arrow) at site of biopsy-proven carcinoma. B, Isotropic axial apparent diffusion coefficient (ADC) map shows area of hypointensity (arrow) corresponding to that shown in A. C, Isotropic axial ADC map with region of interest (circle) placed in center of hypointense signal yields measured ADC of mm 2 /s. subjects (77%) had more than one site of tumor on sextant biopsy: seven subjects had two sites; 15, three sites; six, four sites; seven, five sites; and nine, six sites. All transrectal ultrasound guided biopsies and sites of tumor were in the peripheral zone of the prostate gland. None of the patients who met inclusion criteria for this study had biopsy of TABLE 1: Probability of Prostate Tumor Being Visible on Diffusion-Weighted Imaging (DWI) by Gleason Score Gleason Score No. (%) of Tumors Odds That Tumor Is Visible on DWI a 95% CI Visible on DWI Not Visible on DWI Mean Lower Limit Upper Limit 6 25 (37) 43 (63) (44) 48 (56) (43) 13 (57) (100) 0 (0) Note Increase in odds was 8.44 (linear trend) with a 95% CI of (p = ). a Generalized estimating equation with biopsy location nested within patient. B B C C W318 AJR:194, April 2010
4 DWI of Prostate Cancer the central or transitional zone. The mean PSA level was 10.3 ng/ml (SD, 7.2; range, ng/ml). Diffusion-Weighted MRI The mean number of days between transrectal ultrasound guided prostate biopsy and MRI was 44 days (SD, 15; range, days). Most of the biopsy-proven sites of prostate cancer were not visible on DWI. Eightyone biopsy-proven sites of prostate carcinoma (44%) were detected on DWI. The remaining 104 biopsy-proven sites of cancer (56%) were not visible on DWI. Five of these 104 sites of cancer were visible as focal hypointensity on T2-weighted images, but the remaining 99 tumors were not visible on DWI or T2-weighted imaging. The Gleason scores for the 81 tumors visible on DWI and ADC maps and the 104 nonvisible tumors are outlined in Table 1. In 62 of the prostate cancers that were visible A D Fig year-old man with biopsy-proven prostate cancer with Gleason score of 7 in peripheral zone of left base (60% of core) and peripheral zone of right mid gland (20% of core). A, Axial T2-weighted image illustrates focal low-signal-intensity nodule (arrow) in peripheral zone of left base at site of biopsy-proven carcinoma. B and C, Restricted diffusion (arrow) is shown on axial diffusion-weighted image (B) (b = 1,000 s/mm 2 ) and isotropic axial ADC map (C). D, Axial T2-weighted image through mid gland shows heterogeneous signal intensity (arrows) in peripheral zone bilaterally, but no discrete right midgland tumor nodule. E and F, There is no evidence of restricted diffusion in mid gland on corresponding axial diffusion-weighted image (E) (b = 1,000 s/mm 2 ) and isotropic axial ADC map (F). on DWI (77%) and 91 of those that were not visible (88%), disease was characterized as a Gleason score of 6 or 7 on prostate biopsy. The odds of tumor being visible on DWI increased with increasing Gleason score (linear trend, p = ). There was also a statistically significant difference (p ) between the percentage of tumor involvement on core biopsy between the tumors not visible on DWI and those that were visible on DWI (Fig. 3). The mean percentage of tumor on core biopsy for tumors not visible on DWI was 19% (SD, 25.2; range, 1 95%) versus 52% (SD, 19.9; range, 1 100%) for those visible on DWI. For the 81 tumors that were visible on DWI, the amount of blood in the peripheral zone was a score of 0 for four tumors (5%), a score of 1 for 26 (32%), a score of 2 for 24 (30%), and a score of 3 for 27 (33%). For the 104 tumors not visible on DWI, the amount of blood in the peripheral zone was a score B E of 0 for three tumors (3%), a score of 1 for 36 (35%), a score of 2 for 15 (14%), and a score of 3 for 50 (48%). There was no statistically significant difference in the amount of hem- Fig. 4 Venn diagram illustrates number of biopsyproven prostate carcinomas visible on only diffusionweighted images and ADC maps (blue); on only T2- weighted images (yellow); and on diffusion-weighted images, ADC maps, and T2-weighted images (green). C F AJR:194, April 2010 W319
5 Woodfield et al. TABLE 2: Apparent Diffusion Coefficient (ADC) Values for Tumors Visible on Diffusion-Weighted Imaging According to Gleason Score Gleason Score ADC ( 10 3 mm 2 /s) No. of Tumors ADC ( 10 3 mm 2 /s) Least-Squares Mean Standard Error of Mean Range Gleason Score Fig. 5 Scatterplot shows relationship between apparent diffusion coefficient (ADC) values in diffusion-weighted image and ADC visible tumors and tumor Gleason score. Data shown are multiple observations from same patients accounted for in analysis estimating mean ADC values. Differences between mean ADC values of tumors with Gleason score of 6 and those with Gleason score of 7 and of tumors with Gleason score of 6 and those with Gleason score of > 7 are significant. orrhage in the peripheral zone for the tumors that were visible and those that were not visible on DW images. Twenty-three tumors were visible on DWI only, five on T2-weighted imaging only, and 58 tumors were visible on both (Fig. 4). There was no significant difference in the estimated odds of tumor visibility on T2-weighted images compared with DW images. The odds ratio for visualizing tumor on T2-weighted imaging was (95% CI, ), which overlaps with the CIs for the odds ratio of visualizing tumor on DWI, (95% CI, ). One-hundred forty-eight of the 157 sites of biopsy-proven benign prostate tissue met visibility criteria. Nine biopsy-proven sites of benign peripheral zone tissue had focal hyperintensity in the peripheral zone on DWI with corresponding hypointensity on the ADC map, but there was no corresponding low signal intensity on T1- and T2-weighted images for these cases. None of the biopsyproven sites of benign peripheral zone tissue had DWI hyperintensity with corresponding ADC map hypointensity and corresponding T1- and T2-weighted hypointensity. Eleven sites of restricted diffusion with corresponding low signal intensity on T1- and T2- weighted images were detected in the central gland of nine patients; these sites are suspicious for central gland tumor, but to date none of these patients has undergone additional biopsy or surgery for confirmation. For the 81 tumors visible on DWI, the mean tumor volume was 1.4 cm 3 (SD, 1.2; range, cm 3 ). All were identified in the peripheral zone of the prostate gland, with 31 (38%) in the base of the gland, 19 (23%) in the mid gland, and 31 (38%) in the apex of the gland. The mean ADC (± SD) for 148 measurements of biopsy-proven benign peripheral zone tissue was ± mm 2 /s (range, mm 2 /s), and the mean ADC for the 81 visible sites of biopsy- ADC ( 10 3 mm 2 /s) proven tumor was ± mm 2 /s (range, mm 2 /s). The ADC values and the mean ADC values for visible tumor with disease characterized as a Gleason score of 6 9 are indicated in Table 2 and Figure 5. Differences between the mean ADC values of tumors with a Gleason score of 6 and those with a Gleason score of 7 (p = ) and tumors with a Gleason score of 6 and those with a Gleason score of 8 (p = ) were statistically significant. The difference between the mean ADC value of tumor with a Gleason score of 6 and that of tumor with a Gleason score of 9 was also initially statistically significant (p = ); however, after the Bonferroni adjustment was used to adjust for multiple comparisons, this difference was not significant (p = ). The differences between the mean ADC values of tumors with a Gleason score of 7, 8, and 9 were not significantly different with or without adjustment. A mean ADC decrease of mm 2 /s (range, mm 2 /s) was detected for every 1% increase in tumor in the core biopsy specimen (Fig. 6). Discussion A significant reduction in the diffusion properties of water protons in prostate cancer and the resulting reduction in the measured ADC value of prostate cancer relative to normal prostatic tissue have been well documented [3, 4, 7 9, 11, 12] and are supported by our Percentage of Tumor at Core Biopsy Fig. 6 Scatterplot shows relationship between apparent diffusion coefficient (ADC) values in diffusion-weighted image and ADC visible tumors and percentage of tumor involvement of core biopsy. Figure contains multiple observations from same patients which were accounted for in analysis which estimated plotted linear function. There is correlation between increasing percent core involvement and decreasing ADC value. W320 AJR:194, April 2010
6 DWI of Prostate Cancer investigation. The diffusion characteristics of any biologic tissue are based on the relative combination of water proton movement in the extracellular environment, across cell membranes, and within the cells of that tissue [18, 19]. Any change in the architecture of a tissue such as an increase in the proportion of intracellular to extracellular water protons, which occurs with the replacement of less cellular normal prostate tissue with more highly cellular neoplastic tissue, results in more restricted movement of water protons. This more restricted movement is due to a combination of decreased extracellular space and a more viscous and complex intracellular environment [20 22]. Although the more restricted movement of water protons and resulting lower ADC values in prostate cancer have been well described, only a few prior studies to date have investigated the relationship between prostate cancer ADC values and tumor aggressiveness [1 4, 6]. In our investigation of the relationship between the diffusion characteristics and aggressiveness of prostate cancer, we found that lower ADC values were associated with higher Gleason scores and that ADC values may help to differentiate between low-risk (Gleason score, 6) and intermediate-risk (Gleason score, 7) prostate cancer and between lowrisk (Gleason score, 6) and high-risk (Gleason score, > 7) prostate cancer if the tumor is visible on DW images and ADC maps. However, because of the retrospective nature of this study and overlap in the ADC values of tumors with different Gleason scores, we did not find that ADC values alone can always differentiate between tumors with low Gleason scores and those with high Gleason scores. The overlap of ADC values for tumors with Gleason scores of 7, 8, and 9 in our study may have been partly related to tumor heterogeneity, similarity in the cellular density of prostate cancers with a Gleason score of 7 or greater, or both. Investigators have reported that prostate cancer may be heterogeneous at histopathology, with one tumor composed of more than one Gleason grade and score [23]. The lower mean ADC values in the more aggressive tumors in our study may be due to higher cellular density in poorly differentiated tumors, resulting in more restricted movement of water protons. Zelhof et al. [24] recently reported that ADC values of prostate cancer correlate with cellular density and described a significant correlation between decreasing ADC values and increasing cellular density of prostate cancer. For the tumors visible on DWI, we also found a relationship between decreasing ADC values and increasing percentage of tumor involvement on prostate core biopsies, another measure of tumor aggressiveness. This tendency for ADC to decrease as tumor volume increases is likely due, at least partly, to better visibility of denser tumors on DW images and ADC maps compared with less dense tumors. This greater visibility facilitates larger and more accurate ROI placement on ADC maps. In contrast, in earlier studies of patients with prostate cancer imaged on a 3-T magnet without an endorectal coil and using maximal b values of 500 s/mm 2 [3, 4] and 1,000 s/mm 2 [2], Gibbs et al. [3], Pickles et al. [4], and Kim et al. [2] found no correlation between ADC values and Gleason scores. A more recent study by Yoshimitsu et al. [1] of 37 patients imaged on a 1.5-T magnet without the use of an endorectal coil and using b values of 0, 500, and 1,000 s/mm 2 found an inverse correlation between ADC values and Gleason scores, which is similar to the results of our study. Also similar to our study is that this difference was significant only between well-differentiated carcinomas (mean ADC, 1.19 ± mm 2 /s) and poorly differentiated carcinomas (mean ADC, 0.93 ± mm 2 /s) [1]. Tamada et al. [6] also recently reported a correlation between decreasing ADC values of peripheral zone prostate cancer and increasing Gleason score on prostate biopsy. In their series of patients with prostate cancer, imaging was performed on a 1.5-T magnet without the use of an endorectal coil and using 800 s/mm 2 as the highest b value. No other previous studies, to our knowledge, have compared the ADC values of prostate cancer with the percentage of tumor involvement on core biopsy or tumor volume at histopathology. The reported sensitivity and specificity of DWI with ADC maps for detecting prostate cancer range from 54% to 94% and from 61% to 100%, respectively [1 3]. These variable detection rates and the low detection rate in our study may be attributed in part to the use of biopsy and pathology results that include even small foci of tumor as gold standards. Langer et al. [14] recently reported that sparse tumors (i.e., those with > 50% of cross-sectional tumor area composed of normal peripheral zone) have ADC and T2 values similar to normal peripheral zone tissue. We found a similar trend in that the smaller the percentage of tumor involvement in a core biopsy, the less likely was the tumor to be visible on DW images and ADC maps. In addition, tumors with a low Gleason score (Gleason score, 6) comprised 72% of the tumors in our study, and we also found that these tumors were less likely to be visible on DW images and ADC maps. DW images and ADC maps also did not significantly improved tumor visibility compared with T2-weighted images alone. One of the limitations of this study is that step-section histopathology was not used as the gold standard for comparing ADC values with Gleason scores. Gleason scores are known to be prone to sampling error, and the final Gleason score at histopathology may differ from that determined by transrectal ultrasound guided biopsy. In general, there may be a 20 30% upstaging of Gleason score from core biopsy to surgical pathology. Similarly, the volume of disease may have been underestimated on core biopsy, which might also account for the high mean PSA value of 10.3 ng/ml in our study. However, because of the retrospective nature of this study, we included all patients scheduled for prostate MRI regardless of ultimate treatment and only eight of the 57 study patients had undergone radical prostatectomy at the time of study completion. An additional limitation of the study is the relatively small number of high-risk tumors with Gleason scores of 8 or 9, which reduces confidence in findings both within these groups and between these scores and other scores. All of the patients had also undergone prostate biopsy before the MRI examination. In a recent study, Tamada et al. [25] found that the degree of hemorrhage in the prostate gland did not correlate significantly with the time between biopsy and MRI. Although we did not find a significant difference between the amount of blood products in the peripheral zone of tumors not visible on DW images and ADC maps compared with visible tumors, blood products may still have affected measured ADC values. In conclusion, we found that the ADC values of prostate carcinoma on MRI performed at 1.5 T and using an endorectal coil and b values of 0 and 1,000 s/mm 2 may help differentiate between low-risk (Gleason score, 6) and intermediate-risk (Gleason score, 7) disease and between low-risk and high-risk (Gleason score > 7) disease. In addition, we found an inverse relationship between the ADC value and the percentage of tumor involvement on prostate core biopsies. The finding that lower ADC values are associat- AJR:194, April 2010 W321
7 Woodfield et al. ed with a higher percentage of tumor on core biopsy and higher Gleason score may help to identify more aggressive tumors and may help to further direct patient treatment. Future studies with larger numbers of patients and with comparison with prostatectomy whole-mount histopathology are warranted to confirm our findings. References 1. Yoshimitsu K, Kiyoshima K, Irie H, et al. Usefulness of apparent diffusion coefficient map in diagnosing prostate carcinoma: correlation with stepwise histopathology. J Magn Reson Imaging 2008; 27: Kim CK, Park BK, Han JJ, Kang TW, Lee HM. Diffusion-weighted imaging of the prostate at 3 T for differentiation of malignant and benign tissue in transition and peripheral zones: preliminary results. J Comput Assist Tomogr 2007; 31: Gibbs P, Pickles MD, Turnbull LW. Diffusion imaging of the prostate at 3.0 Tesla. Invest Radiol 2006; 41: Pickles MD, Gibbs P, Sreenivas M, Turnbull LW. Diffusion-weighted imaging of normal and malignant prostate tissue at 3.0 T. J Magn Reson Imaging 2006; 23: Sato C, Naganawa S, Nakamura T, et al. Differentiation of noncancerous tissue and cancer lesions by apparent diffusion coefficient values in transition and peripheral zone of the prostate. J Magn Reson Imaging 2005; 21: Tamada T, Sone T, Yoshimasa J, et al. Apparent diffusion coefficient values in peripheral and transition zones of the prostate: comparison between normal and malignant prostatic tissue and correlation with histologic grade. J Magn Reson Imaging 2008; 28: Kumar V, Jagannathan NR, Kumar R, et al. Apparent diffusion coefficient of the prostate in men prior to biopsy: determination of a cut-off value to predict malignancy of the peripheral zone. NMR Biomed 2007; 20: Tanimoto A, Nakashima J, Kohno H, Shinmoto H, Kuribayashi S. Prostate cancer screening: the clinical value of diffusion-weighted imaging and dynamic MR imaging in combination with T2- weighted imaging. J Magn Reson Imaging 2007; 25: DeSouza NM, Reinsberg SA, Scurr ED, Brewster JM, Payne GS. Magnetic resonance imaging in prostate cancer: the value of apparent diffusion coefficients for identifying malignant nodules. Br J Radiol 2007; 80: Kumar V, Jagannathan NR, Kumar R, et al. Correlation between metabolite ratios and ADC values of prostate in men with increased PSA level. Magn Reson Imaging 2006; 24: Shimofusa R, Fujimoto H, Akamata H, et al. Diffusion-weighted imaging of prostate cancer. J Comput Assist Tomogr 2005; 29: Hosseinzadeh K, Schwarz SD. Endorectal diffusion-weighted imaging in prostate cancer to differentiate malignant and benign peripheral zone tissue. J Magn Reson Imaging 2004; 20: Kim CK, Park BK, Lee HM, Kwon GY. Value of diffusion-weighted imaging for the prediction of prostate cancer location at 3T using a phased-array coil. Invest Radiol 2007; 42: Langer DL, van der Kwast TH, Evans AJ, et al. Intermixed normal tissue within prostate cancer: effect on MR imaging measurements of apparent diffusion coefficient and T2 sparse versus dense cancers. Radiology 2008; 249: Bianco FJ Jr, Wood DP Jr, Cher ML, Powell IJ, Souza JW, Pontes JE. Ten-year survival after radical prostatectomy: specimen Gleason score is the predictor in organ-confined prostate cancer. Clin Prostate Cancer 2003; 1: Rampersaud EN, Sun L, Moul JW, Madden J, Freedland SJ. Percent tumor involvement and risk of biochemical progression after radical prostatectomy. J Urol 2008; 180: Kitajima K, Kaji Y, Kuroda K, Sugimura K. High b-value diffusion-weighted imaging in normal and malignant peripheral zone tissue of the prostate: effect of signal-to-noise ratio. Magn Reson Med Sci 2008; 7: Tanner JE. Intracellular diffusion of water. Arch Biochem Biophys 1983; 224: García-Pérez A, López-Beltrán E, Klüner P, Luque J, Ballesteros P, Cerdán S. Molecular crowding and viscosity as determinants of translational diffusion of metabolites in subcellular organelles. Arch Biochem Biophys 1999; 362: Latour LL, Svoboda K, Mitra PP, Sotak CH. Time-dependent diffusion of water in a biological model system. Proc Natl Acad Sci U S A 1994; 91: Szafer A, Zhong J, Gore JC. Theoretical model for water diffusion in tissues. Magn Reson Med 1995; 33: Le Bihan D. Molecular diffusion, tissue microdynamics and microstructure. NMR Biomed 1995; 8: Arora R, Koch MO, Eble JN, Ulbright TM, Li L, Cheng L. Heterogeneity of Gleason grade in multifocal adenocarcinoma of the prostate. Cancer 2004; 100: Zelhof B, Pickles M, Liney G, et al. Correlation of diffusion-weighted magnetic resonance data with cellularity in prostate cancer. BJU Int 2009; 103: Tamada T, Sone T, Jo Y, et al. Prostate cancer: relationships between postbiopsy hemorrhage and tumor detectability at MR diagnosis. Radiology 2008; 248: W322 AJR:194, April 2010
Shayan Sirat Maheen Anwar, 1 Zahid Anwar Khan, 2 Rana Shoaib Hamid, 3 Fahd Haroon, 4 Raza Sayani, 1 Madiha Beg, 1 and Yasir Jamil Khattak 1
 ISRN Radiology, Article ID 263417, 7 pages http://dx.doi.org/10.1155/2014/263417 Research Article Assessment of Apparent Diffusion Coefficient Values as Predictor of Aggressiveness in Peripheral Zone Prostate
ISRN Radiology, Article ID 263417, 7 pages http://dx.doi.org/10.1155/2014/263417 Research Article Assessment of Apparent Diffusion Coefficient Values as Predictor of Aggressiveness in Peripheral Zone Prostate
The diagnosis and localization of prostate cancer are based on a digital
 Diagn Interv Radiol 2011; 17:130 134 Turkish Society of Radiology 2011 ABDOMINAL IMAGING ORIGINAL ARTICLE The value of diffusion-weighted MRI for prostate cancer detection and localization Ahmet Baki Yağcı,
Diagn Interv Radiol 2011; 17:130 134 Turkish Society of Radiology 2011 ABDOMINAL IMAGING ORIGINAL ARTICLE The value of diffusion-weighted MRI for prostate cancer detection and localization Ahmet Baki Yağcı,
Diffusion Weighted Imaging in Prostate Cancer
 Diffusion Weighted Imaging in Prostate Cancer Disclosure Information Vikas Kundra, M.D, Ph.D. No financial relationships to disclose. Education Goals and Objectives To describe the utility of diffusion-weighted
Diffusion Weighted Imaging in Prostate Cancer Disclosure Information Vikas Kundra, M.D, Ph.D. No financial relationships to disclose. Education Goals and Objectives To describe the utility of diffusion-weighted
Prostate Cancer: Comparison of Tumor Visibility on Trace Diffusion- Weighted Images and the Apparent Diffusion Coefficient Map
 Genitourinary Imaging Original Research Rosenkrantz et al. Tumor Visibility in Prostate Cancer Genitourinary Imaging Original Research Andrew B. Rosenkrantz 1 Xiangtian Kong 2 Benjamin E. Niver 1 Douglas
Genitourinary Imaging Original Research Rosenkrantz et al. Tumor Visibility in Prostate Cancer Genitourinary Imaging Original Research Andrew B. Rosenkrantz 1 Xiangtian Kong 2 Benjamin E. Niver 1 Douglas
Diffusion-Weighted Imaging of Prostate Cancer
 ORIGINAL ARTICLE Diffusion-Weighted Imaging of Prostate Cancer Ryota Shimofusa, MD,* Hajime Fujimoto, MD, Hajime Akamata, MD, Ken Motoori, MD,* Seiji Yamamoto, MD,* Takuya Ueda, MD,* and Hisao Ito, MD*
ORIGINAL ARTICLE Diffusion-Weighted Imaging of Prostate Cancer Ryota Shimofusa, MD,* Hajime Fujimoto, MD, Hajime Akamata, MD, Ken Motoori, MD,* Seiji Yamamoto, MD,* Takuya Ueda, MD,* and Hisao Ito, MD*
Can Diffusion-Weighted Magnetic Resonance Imaging Predict a High Gleason Score of Prostate Cancer?
 www.kjurology.org http://dx.doi.org/.4/kju.3.54.4.34 Urological Oncology Can Diffusion-Weighted Magnetic Resonance Imaging Predict a High Gleason Score of Prostate Cancer? Katsumi Shigemura,, Nozomu Yamanaka,3,
www.kjurology.org http://dx.doi.org/.4/kju.3.54.4.34 Urological Oncology Can Diffusion-Weighted Magnetic Resonance Imaging Predict a High Gleason Score of Prostate Cancer? Katsumi Shigemura,, Nozomu Yamanaka,3,
Effect of intravenous contrast medium administration on prostate diffusion-weighted imaging
 Effect of intravenous contrast medium administration on prostate diffusion-weighted imaging Poster No.: C-1766 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit J. Bae, C. K. Kim, S.
Effect of intravenous contrast medium administration on prostate diffusion-weighted imaging Poster No.: C-1766 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit J. Bae, C. K. Kim, S.
Prostate MRI. Overview. Introduction 2/20/2015. Prostate cancer is most frequently diagnosed noncutaneous cancer in males (25%)
 Prostate MRI John Bell, MD Introduction Prostate Cancer Screening Staging Anatomy Prostate MRI overview Functional MRI Multiparametric Approach Indications Example Cases Overview Introduction Prostate
Prostate MRI John Bell, MD Introduction Prostate Cancer Screening Staging Anatomy Prostate MRI overview Functional MRI Multiparametric Approach Indications Example Cases Overview Introduction Prostate
The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (2), Page
 The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (2), Page 2490-2497 Role of ADC Map MR Imaging in Prediction of Local Aggressiveness of Prostate Cancer Asaad Gamal Asaad Sorial, Omar Farouk
The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (2), Page 2490-2497 Role of ADC Map MR Imaging in Prediction of Local Aggressiveness of Prostate Cancer Asaad Gamal Asaad Sorial, Omar Farouk
Recently, prostate-specific antigen (PSA) has been identified as a
 Diagn Interv Radiol 2011; 17:243 248 Turkish Society of Radiology 2011 ABDOMINAL IMAGING ORIGINAL ARTICLE Prostate cancer detection with MRI: is dynamic contrast-enhanced imaging necessary in addition
Diagn Interv Radiol 2011; 17:243 248 Turkish Society of Radiology 2011 ABDOMINAL IMAGING ORIGINAL ARTICLE Prostate cancer detection with MRI: is dynamic contrast-enhanced imaging necessary in addition
Genitourinary Imaging Original Research
 Genitourinary Imaging Original Research Tamada et al. Diagnostic Efficacy of Combined MRI in Detecting Prostate Cancer Genitourinary Imaging Original Research Tsutomu Tamada 1 Teruki Sone 1 Hiroki Higashi
Genitourinary Imaging Original Research Tamada et al. Diagnostic Efficacy of Combined MRI in Detecting Prostate Cancer Genitourinary Imaging Original Research Tsutomu Tamada 1 Teruki Sone 1 Hiroki Higashi
Department of Urology, II Clinic, Ankara Numune Education and Research Hospital, Ankara, Turkey 2
 International Scholarly Research Network ISRN Urology Volume 2012, Article ID 252846, 5 pages doi:10.5402/2012/252846 Clinical Study The Correlation between Diffusion-Weighted Imaging and Histopathological
International Scholarly Research Network ISRN Urology Volume 2012, Article ID 252846, 5 pages doi:10.5402/2012/252846 Clinical Study The Correlation between Diffusion-Weighted Imaging and Histopathological
Genitourinary Imaging Original Research
 Genitourinary Imaging Original Research Downloaded from www.ajronline.org by 1.1.3.3 on /7/1 from IP address 1.1.3.3. Copyright ARRS. For personal use only; all rights reserved Park et al. ADC in Prostate
Genitourinary Imaging Original Research Downloaded from www.ajronline.org by 1.1.3.3 on /7/1 from IP address 1.1.3.3. Copyright ARRS. For personal use only; all rights reserved Park et al. ADC in Prostate
High-Resolution Diffusion-Weighted Imaging of the Prostate
 Genitourinary Imaging Original Research Medved et al. High-Resolution DWI of the Prostate Genitourinary Imaging Original Research Milica Medved 1 Fatma N. Soylu-oy 1,2 Ibrahim Karademir 1,3 Ila Sethi 1,4
Genitourinary Imaging Original Research Medved et al. High-Resolution DWI of the Prostate Genitourinary Imaging Original Research Milica Medved 1 Fatma N. Soylu-oy 1,2 Ibrahim Karademir 1,3 Ila Sethi 1,4
11/10/2015. Prostate cancer in the U.S. Multi-parametric MRI of Prostate Diagnosis and Treatment Planning. NIH estimates for 2015.
 Multi-parametric MRI of Prostate Diagnosis and Treatment Planning Temel Tirkes, M.D. Associate Professor of Radiology Director, Genitourinary Radiology Indiana University School of Medicine Department
Multi-parametric MRI of Prostate Diagnosis and Treatment Planning Temel Tirkes, M.D. Associate Professor of Radiology Director, Genitourinary Radiology Indiana University School of Medicine Department
Prostate MRI: Who needs it?
 Prostate MRI: Who needs it? Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Abdominal Imaging Magnetic Resonance Science Center
Prostate MRI: Who needs it? Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Abdominal Imaging Magnetic Resonance Science Center
PI-RADS classification: prognostic value for prostate cancer grading
 PI-RADS classification: prognostic value for prostate cancer grading Poster No.: C-1622 Congress: ECR 2014 Type: Scientific Exhibit Authors: I. Platzek, A. Borkowetz, T. Paulus, T. Brauer, M. Wirth, M.
PI-RADS classification: prognostic value for prostate cancer grading Poster No.: C-1622 Congress: ECR 2014 Type: Scientific Exhibit Authors: I. Platzek, A. Borkowetz, T. Paulus, T. Brauer, M. Wirth, M.
Diffusion-Weighted Magnetic Resonance Imaging for the Evaluation of Prostate Cancer: Optimal B Value at 3T
 Original Article http://dx.doi.org/10.3348/kjr.2013.14.1.61 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2013;14(1):61-69 Diffusion-Weighted Magnetic Resonance Imaging for the Evaluation of Prostate
Original Article http://dx.doi.org/10.3348/kjr.2013.14.1.61 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2013;14(1):61-69 Diffusion-Weighted Magnetic Resonance Imaging for the Evaluation of Prostate
FieldStrength. Multi-parametric 3.0T MRI provides excellent prostate imaging
 FieldStrength Publication for the Philips MRI Community Issue 35 September / October 2008 Multi-parametric 3.0T MRI provides excellent prostate imaging Three different centers show that advances in imaging
FieldStrength Publication for the Philips MRI Community Issue 35 September / October 2008 Multi-parametric 3.0T MRI provides excellent prostate imaging Three different centers show that advances in imaging
The role of T2-weighted imaging in detecting prostate cancer of the central zone in 3T multiparametric magnetic resonance examination
 The role of T2-weighted imaging in detecting prostate cancer of the central zone in 3T multiparametric magnetic resonance examination Poster No.: C-2317 Congress: ECR 2014 Type: Scientific Exhibit Authors:
The role of T2-weighted imaging in detecting prostate cancer of the central zone in 3T multiparametric magnetic resonance examination Poster No.: C-2317 Congress: ECR 2014 Type: Scientific Exhibit Authors:
Sensitivity and Specificity in Detection of Labral Tears with 3.0-T MRI of the Shoulder
 Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Prostate Cancer DFP Case of the Week
 Prostate Cancer DFP Case of the Week Antonio C. Westphalen, MD PhD Clinical Prostate MR Imaging Program, Director Associate Professor of Radiology and Urology University of California, San Francisco Case
Prostate Cancer DFP Case of the Week Antonio C. Westphalen, MD PhD Clinical Prostate MR Imaging Program, Director Associate Professor of Radiology and Urology University of California, San Francisco Case
Differentiation of Noncancerous Tissue and Cancer Lesions by Apparent Diffusion Coefficient Values in Transition and Peripheral Zones of the Prostate
 JOURNAL OF MAGNETIC RESONANCE IMAGING 21:258 262 (2005) Original Research Differentiation of Noncancerous Tissue and Cancer Lesions by Apparent Diffusion Coefficient Values in Transition and Peripheral
JOURNAL OF MAGNETIC RESONANCE IMAGING 21:258 262 (2005) Original Research Differentiation of Noncancerous Tissue and Cancer Lesions by Apparent Diffusion Coefficient Values in Transition and Peripheral
DTI fiber tracking at 3T MR using b-1000 value in the depiction of periprostatic nerve before and after nervesparing prostatectomy
 DTI fiber tracking at 3T MR using b-1000 value in the depiction of periprostatic nerve before and after nervesparing prostatectomy Poster No.: C-2328 Congress: ECR 2012 Type: Scientific Paper Authors:
DTI fiber tracking at 3T MR using b-1000 value in the depiction of periprostatic nerve before and after nervesparing prostatectomy Poster No.: C-2328 Congress: ECR 2012 Type: Scientific Paper Authors:
Diffusion-Weighted Magnetic Resonance Imaging Detects Local Recurrence After Radical Prostatectomy: Initial Experience
 EUROPEAN UROLOGY 61 (2012) 616 620 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Diffusion-Weighted Magnetic Resonance Imaging Detects Local Recurrence
EUROPEAN UROLOGY 61 (2012) 616 620 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Diffusion-Weighted Magnetic Resonance Imaging Detects Local Recurrence
Combined T2-Weighted and Diffusion-Weighted MRI for Localization of Prostate Cancer
 T2 Combined with DWI for Prostate Cancer Localization Genitourinary Imaging Original Research Masoom A. Haider 1 Theodorus H. van der Kwast 2,3 Jeff Tanguay 2 Andrew J. Evans 2 Ali-Tahir Hashmi 1 Gina
T2 Combined with DWI for Prostate Cancer Localization Genitourinary Imaging Original Research Masoom A. Haider 1 Theodorus H. van der Kwast 2,3 Jeff Tanguay 2 Andrew J. Evans 2 Ali-Tahir Hashmi 1 Gina
Mucinous Adenocarcinoma of the Prostate: MRI and MR Spectroscopy Features
 Genitourinary Imaging Clinical Observations Westphalen et al. MRI of Mucinous Adenocarcinoma of the Prostate Genitourinary Imaging Clinical Observations Antonio C. Westphalen 1 Fergus V. Coakley 1 John
Genitourinary Imaging Clinical Observations Westphalen et al. MRI of Mucinous Adenocarcinoma of the Prostate Genitourinary Imaging Clinical Observations Antonio C. Westphalen 1 Fergus V. Coakley 1 John
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017
 Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Diffusion weighted MRI in evaluation of transplanted kidney: Preliminary clinical experience
 African Journal of Nephrology (2009) 13: 26-30 Original Article AJN Diffusion weighted MRI in evaluation of transplanted kidney: Preliminary clinical experience Mohamed Abou El-Ghar; M.D, Huda Refaie;
African Journal of Nephrology (2009) 13: 26-30 Original Article AJN Diffusion weighted MRI in evaluation of transplanted kidney: Preliminary clinical experience Mohamed Abou El-Ghar; M.D, Huda Refaie;
Yahui Peng, PhD 2 Yulei Jiang, PhD Tatjana Antic, MD Maryellen L. Giger, PhD Scott E. Eggener, MD Aytekin Oto, MD. Purpose: Materials and Methods:
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Validation of Quantitative
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Validation of Quantitative
Apparent Diffusion Coefficient for Prostate Cancer Imaging: Impact of b Values
 Genitourinary Imaging Original Research Peng et al. Impact of b Value on Apparent Diffusion Coefficient in Prostate Cancer Imaging Genitourinary Imaging Original Research Yahui Peng 1 Yulei Jiang 2 Tatjana
Genitourinary Imaging Original Research Peng et al. Impact of b Value on Apparent Diffusion Coefficient in Prostate Cancer Imaging Genitourinary Imaging Original Research Yahui Peng 1 Yulei Jiang 2 Tatjana
D. J. Margolis 1, S. Natarajan 2, D. Kumar 3, M. Macairan 4, R. Narayanan 3, and L. Marks 4
 Biopsy Tracking and MRI Fusion to Enhance Imaging of Cancer Within the Prostate D. J. Margolis 1, S. Natarajan 2, D. Kumar 3, M. Macairan 4, R. Narayanan 3, and L. Marks 4 1 Dept. of Radiology, UCLA, Los
Biopsy Tracking and MRI Fusion to Enhance Imaging of Cancer Within the Prostate D. J. Margolis 1, S. Natarajan 2, D. Kumar 3, M. Macairan 4, R. Narayanan 3, and L. Marks 4 1 Dept. of Radiology, UCLA, Los
OASIS 1.2T: MULTIPARAMETRIC MRI OF PROSTATE CANCER
 OASIS 1.2T: MULTIPARAMETRIC MRI OF PROSTATE CANCER By Dr. John Feller, MD, Radiologist Desert Medical Imaging, Palm Springs, CA MRI is clinically accepted as the best imaging modality for displaying anatomical
OASIS 1.2T: MULTIPARAMETRIC MRI OF PROSTATE CANCER By Dr. John Feller, MD, Radiologist Desert Medical Imaging, Palm Springs, CA MRI is clinically accepted as the best imaging modality for displaying anatomical
Current Clinical Practice. MR Imaging Evaluations. MRI Anatomic Review. Imaging to Address Clinical Challenges. Prostate MR
 BETH ISRAEL DEACONESS MEDICAL CENTER Prostate MR Neil M. Rofsky, MD Harvard Medical School Current Clinical Practice DIGITAL RECTAL EXAMINATION PSA ( ~ 20% False negative) BIOPSY (18-25% False negative)
BETH ISRAEL DEACONESS MEDICAL CENTER Prostate MR Neil M. Rofsky, MD Harvard Medical School Current Clinical Practice DIGITAL RECTAL EXAMINATION PSA ( ~ 20% False negative) BIOPSY (18-25% False negative)
Genitourinary Imaging Original Research
 Genitourinary Imaging Original Research Tamada et al. Prostate Imaging After High-Dose-Rate Brachytherapy Genitourinary Imaging Original Research Tsutomu Tamada 1 Teruki Sone 1 Yoshimasa Jo 2 Junichi Hiratsuka
Genitourinary Imaging Original Research Tamada et al. Prostate Imaging After High-Dose-Rate Brachytherapy Genitourinary Imaging Original Research Tsutomu Tamada 1 Teruki Sone 1 Yoshimasa Jo 2 Junichi Hiratsuka
Effects of Post Biopsy Digital Rectal Compression on Improving Prostate Cancer Staging Using Magnetic Resonance Imaging in Localized Prostate Cancer
 Original Article http://dx.doi.org/10.3349/ymj.2013.54.1.81 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(1):81-86, 2013 Effects of Post Biopsy Digital Rectal Compression on Improving Prostate Cancer
Original Article http://dx.doi.org/10.3349/ymj.2013.54.1.81 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 54(1):81-86, 2013 Effects of Post Biopsy Digital Rectal Compression on Improving Prostate Cancer
Improved Detection of Clinically Significant Prostate Cancer Using a Structured Prostate Imaging Reporting Data System (PI-RADS) Template
 Improved Detection of Clinically Significant Prostate Cancer Using a Structured Prostate Imaging Reporting Data System (PI-RADS) Template Abstract #17-130 ACR Annual Meeting 2017 Presenting Author: Whitney
Improved Detection of Clinically Significant Prostate Cancer Using a Structured Prostate Imaging Reporting Data System (PI-RADS) Template Abstract #17-130 ACR Annual Meeting 2017 Presenting Author: Whitney
Int J Clin Exp Med 2016;9(2): /ISSN: /IJCEM Dong Yang 1, Nan Jin 2, Yan Guo 3, Huan-Jun Wang 3, Bi-Tao Pan 3
 Int J Clin Exp Med 2016;9(2):5127-5134 www.ijcem.com /ISSN:1940-5901/IJCEM0018844 Original Article Differentiation of prostate cancer and prostatitis in the peripheral zone with diffusion-weighted imaging:
Int J Clin Exp Med 2016;9(2):5127-5134 www.ijcem.com /ISSN:1940-5901/IJCEM0018844 Original Article Differentiation of prostate cancer and prostatitis in the peripheral zone with diffusion-weighted imaging:
Keywords Prostate, cancer, magnetic resonance imaging (MRI), diffusion-weighted imaging (DWI), Gleason score
 Original Article The value of ADC, T2 signal intensity, and a combination of both parameters to assess Gleason score and primary Gleason grades in patients with known prostate cancer Acta Radiologica 2016,
Original Article The value of ADC, T2 signal intensity, and a combination of both parameters to assess Gleason score and primary Gleason grades in patients with known prostate cancer Acta Radiologica 2016,
Multiparametric MRI diagnostic value in a case of prostate cancer
 CASE REPORT J. Transl. Med. Res 2015;20(3):162-167 Multiparametric MRI diagnostic value in a case of prostate cancer Gelu Adrian Popa 1,4, Ioana Gabriela Lupescu 1,4, Emi M. Preda 1,4, Cristina Nicolae
CASE REPORT J. Transl. Med. Res 2015;20(3):162-167 Multiparametric MRI diagnostic value in a case of prostate cancer Gelu Adrian Popa 1,4, Ioana Gabriela Lupescu 1,4, Emi M. Preda 1,4, Cristina Nicolae
Prostate Cancer: Role of Pretreatment Multiparametric 3-T MRI in Predicting Biochemical Recurrence After Radical Prostatectomy
 Genitourinary Imaging Original Research Park et al. MRI to Predict Biochemical Recurrence After Radical Prostatectomy Genitourinary Imaging Original Research Jung Jae Park 1,2 Chan Kyo Kim 1 Sung Yoon
Genitourinary Imaging Original Research Park et al. MRI to Predict Biochemical Recurrence After Radical Prostatectomy Genitourinary Imaging Original Research Jung Jae Park 1,2 Chan Kyo Kim 1 Sung Yoon
PROSTATE MRI. Dr. Margaret Gallegos Radiologist Santa Fe Imaging
 PROSTATE MRI Dr. Margaret Gallegos Radiologist Santa Fe Imaging Topics of today s talk How does prostate MRI work? Definition of multiparametric (mp) MRI Anatomy of prostate gland and MRI imaging Role
PROSTATE MRI Dr. Margaret Gallegos Radiologist Santa Fe Imaging Topics of today s talk How does prostate MRI work? Definition of multiparametric (mp) MRI Anatomy of prostate gland and MRI imaging Role
1 Uniform hyperintense signal intensity (normal). 2 Linear (arrow), wedge-shaped, or diffuse mild hypointensity, usually indistinct margin.
 Figure 3 PI-RADS assessment for peripheral zone on T2-weighted imaging. 1 Uniform hyperintense signal intensity (normal). 2 Linear (arrow), wedge-shaped, or diffuse mild hypointensity, usually indistinct
Figure 3 PI-RADS assessment for peripheral zone on T2-weighted imaging. 1 Uniform hyperintense signal intensity (normal). 2 Linear (arrow), wedge-shaped, or diffuse mild hypointensity, usually indistinct
Correlated diffusion imaging
 Wong et al. BMC Medical Imaging 2013, 13:26 RESEARCH ARTICLE Open Access Correlated diffusion imaging Alexander Wong 1*, Jeffrey Glaister 1,AndrewCameron 1 and Masoom Haider 2 Abstract Background: Prostate
Wong et al. BMC Medical Imaging 2013, 13:26 RESEARCH ARTICLE Open Access Correlated diffusion imaging Alexander Wong 1*, Jeffrey Glaister 1,AndrewCameron 1 and Masoom Haider 2 Abstract Background: Prostate
Abdominal applications of DWI
 Postgraduate course, SPR San Antonio (Texas), May 14-15, 2013 Abdominal applications of DWI Rutger A.J. Nievelstein Wilhelmina Children s s Hospital, Utrecht (NL) Outline What is DWI? How to perform? Challenges
Postgraduate course, SPR San Antonio (Texas), May 14-15, 2013 Abdominal applications of DWI Rutger A.J. Nievelstein Wilhelmina Children s s Hospital, Utrecht (NL) Outline What is DWI? How to perform? Challenges
Research Article Correlation of Gleason Scores with Diffusion-Weighted Imaging Findings of Prostate Cancer
 Hindawi Publishing Corporation Advances in Urology Volume 2012, Article ID 374805, 5 pages doi:10.1155/2012/374805 Research Article Correlation of Gleason Scores with Diffusion-Weighted Imaging Findings
Hindawi Publishing Corporation Advances in Urology Volume 2012, Article ID 374805, 5 pages doi:10.1155/2012/374805 Research Article Correlation of Gleason Scores with Diffusion-Weighted Imaging Findings
Essential Initial Activities and Clinical Outcomes
 Essential Initial Activities and Clinical Outcomes Crystal Farrell 1,2 & Sabrina L. Noyes 2, Joe Joslin 2, Manish Varma 2,3, Andrew Moriarity 2,3, Christopher Buchach 2,3, Leena Mammen 2,3, Brian R. Lane
Essential Initial Activities and Clinical Outcomes Crystal Farrell 1,2 & Sabrina L. Noyes 2, Joe Joslin 2, Manish Varma 2,3, Andrew Moriarity 2,3, Christopher Buchach 2,3, Leena Mammen 2,3, Brian R. Lane
Diffusion tensor imaging of normal prostate at 3 T: effect of number of diffusion-encoding directions on quantitation and image quality
 The British Journal of Radiology, 85 (2012), e279 e283 Diffusion tensor imaging of normal prostate at 3 T: effect of number of diffusion-encoding directions on quantitation and image quality C K KIM, MD,
The British Journal of Radiology, 85 (2012), e279 e283 Diffusion tensor imaging of normal prostate at 3 T: effect of number of diffusion-encoding directions on quantitation and image quality C K KIM, MD,
Genitourinary Imaging Original Research
 Genitourinary Imaging Original Research Kitajima et al. MRI of Local Recurrence After Prostatectomy Genitourinary Imaging Original Research Kazuhiro Kitajima 1,2 Robert P. Hartman 1 Adam T. Froemming 1
Genitourinary Imaging Original Research Kitajima et al. MRI of Local Recurrence After Prostatectomy Genitourinary Imaging Original Research Kazuhiro Kitajima 1,2 Robert P. Hartman 1 Adam T. Froemming 1
Essentials of Clinical MR, 2 nd edition. 73. Urinary Bladder and Male Pelvis
 73. Urinary Bladder and Male Pelvis Urinary bladder carcinoma is best locally staged with MRI. It is important however to note that a thickened wall (> 5 mm) is a non-specific finding seen in an underfilled
73. Urinary Bladder and Male Pelvis Urinary bladder carcinoma is best locally staged with MRI. It is important however to note that a thickened wall (> 5 mm) is a non-specific finding seen in an underfilled
Prostate MRI: Not So Difficult. Neil M. Rofsky, MD, FACR, FSCBTMR, FISMRM Dallas, TX
 Prostate MRI: Not So Difficult Neil M. Rofsky, MD, FACR, FSCBTMR, FISMRM Dallas, TX What is the biggest barrier to your practice incorporating prostate MRI? 1) I don t know how to read the cases 2) I don
Prostate MRI: Not So Difficult Neil M. Rofsky, MD, FACR, FSCBTMR, FISMRM Dallas, TX What is the biggest barrier to your practice incorporating prostate MRI? 1) I don t know how to read the cases 2) I don
Introduction. Key Words: high-grade prostatic intraepithelial neoplasia, HGPIN, radical prostatectomy, prostate biopsy, insignificant prostate cancer
 Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Magnetic resonance imaging predictors of extracapsular extension of prostate cancer: Do they accurately reflect pt3 staging?
 Magnetic resonance imaging predictors of extracapsular extension of prostate cancer: Do they accurately reflect pt3 staging? Poster No.: C-1399 Congress: ECR 2010 Type: Scientific Exhibit Topic: Genitourinary
Magnetic resonance imaging predictors of extracapsular extension of prostate cancer: Do they accurately reflect pt3 staging? Poster No.: C-1399 Congress: ECR 2010 Type: Scientific Exhibit Topic: Genitourinary
Cancer. Description. Section: Surgery Effective Date: October 15, 2016 Subsection: Original Policy Date: September 9, 2011 Subject:
 Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
Diffusion-Weighted Imaging to Evaluate for Changes From Androgen Deprivation Therapy in Prostate Cancer
 Genitourinary Imaging Original Research Kim et al. DWI of Prostate Cancer Patients Treated With ADT Genitourinary Imaging Original Research Ah Yeong Kim 1 Chan Kyo Kim Sung Yoon Park Byung Kwan Park Kim
Genitourinary Imaging Original Research Kim et al. DWI of Prostate Cancer Patients Treated With ADT Genitourinary Imaging Original Research Ah Yeong Kim 1 Chan Kyo Kim Sung Yoon Park Byung Kwan Park Kim
Genitourinary Imaging Original Research
 Genitourinary Imaging Original Research Roy et al. Detection of Prostate Cancer Recurrence With Different Functional MRI Sequences Genitourinary Imaging Original Research Catherine Roy 1 Fatah Foudi 1
Genitourinary Imaging Original Research Roy et al. Detection of Prostate Cancer Recurrence With Different Functional MRI Sequences Genitourinary Imaging Original Research Catherine Roy 1 Fatah Foudi 1
PI-RADS V2 IN PRACTICE A PICTORIAL REVIEW
 PI-RADS V2 IN PRACTICE A PICTORIAL REVIEW KP Murphy, A Walsh, C Donagh, R Aljurayyan, AC Harris, SD Chang Department of Abdominal and GU Radiology, Vancouver General Hospital & University of British Columbia,
PI-RADS V2 IN PRACTICE A PICTORIAL REVIEW KP Murphy, A Walsh, C Donagh, R Aljurayyan, AC Harris, SD Chang Department of Abdominal and GU Radiology, Vancouver General Hospital & University of British Columbia,
MRI IN THE CHARACTERIZATION OF SEMINOMATOUS AND NONSEMINOMATOUS GERM CELL TUMORS OF THE TESTIS
 MRI IN THE CHARACTERIZATION OF SEMINOMATOUS AND NONSEMINOMATOUS GERM CELL TUMORS OF THE TESTIS Ambesh Deshar *, Gyanendra KC and Zhang Lopsang *Department of Medical Imaging and Nuclear Medicine, First
MRI IN THE CHARACTERIZATION OF SEMINOMATOUS AND NONSEMINOMATOUS GERM CELL TUMORS OF THE TESTIS Ambesh Deshar *, Gyanendra KC and Zhang Lopsang *Department of Medical Imaging and Nuclear Medicine, First
Role of MRI Apparent Diffusion Coefficient Quantification in the Differentiation between Benign and Malignant Mediastinal and Pulmonary Lesions
 Med. J. Cairo Univ., Vol. 82, No. 2, March: 153-158, 2014 www.medicaljournalofcairouniversity.net Role of MRI Apparent Diffusion Coefficient Quantification in the Differentiation between Benign and Malignant
Med. J. Cairo Univ., Vol. 82, No. 2, March: 153-158, 2014 www.medicaljournalofcairouniversity.net Role of MRI Apparent Diffusion Coefficient Quantification in the Differentiation between Benign and Malignant
Accuracy of Multiparametric MRI for Prostate Cancer Detection: A Meta-Analysis
 Genitourinary Imaging Original Research de Rooij et al. Multiparametric MRI for Prostate Cancer Detection Genitourinary Imaging Original Research Maarten de Rooij 1,2 Esther H. J. Hamoen 1,3 Jurgen J.
Genitourinary Imaging Original Research de Rooij et al. Multiparametric MRI for Prostate Cancer Detection Genitourinary Imaging Original Research Maarten de Rooij 1,2 Esther H. J. Hamoen 1,3 Jurgen J.
I have no financial relationships to disclose. I WILL NOT include discussion of investigational or off-label use of a product in my presentation.
 Prostate t Cancer MR Report Disclosure Information Vikas Kundra, M.D, Ph.D. I have no financial relationships to disclose. I WILL NOT include discussion of investigational or off-label use of a g product
Prostate t Cancer MR Report Disclosure Information Vikas Kundra, M.D, Ph.D. I have no financial relationships to disclose. I WILL NOT include discussion of investigational or off-label use of a g product
Diffusion Restriction Precedes Contrast Enhancement in Glioblastoma Multiforme
 Diffusion Restriction Precedes Contrast Enhancement in Glioblastoma Multiforme Adil Bata 1, Jai Shankar 2 1 Faculty of Medicine, Class of 2017 2 Department of Diagnostic Radiology, Division of Neuroradiology,
Diffusion Restriction Precedes Contrast Enhancement in Glioblastoma Multiforme Adil Bata 1, Jai Shankar 2 1 Faculty of Medicine, Class of 2017 2 Department of Diagnostic Radiology, Division of Neuroradiology,
PCa Commentary. Executive Summary: The "PCa risk increased directly with increasing phi values."
 1101 Madison Street Suite 1101 Seattle, WA 98104 P 206-215-2490 www.seattleprostate.com PCa Commentary Volume 77 September October 2012 CONTENT Page The Prostate 1 Health Index Active Surveillance 2 A
1101 Madison Street Suite 1101 Seattle, WA 98104 P 206-215-2490 www.seattleprostate.com PCa Commentary Volume 77 September October 2012 CONTENT Page The Prostate 1 Health Index Active Surveillance 2 A
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
Q&A. Overview. Collecting Cancer Data: Prostate. Collecting Cancer Data: Prostate 5/5/2011. NAACCR Webinar Series 1
 Collecting Cancer Data: Prostate NAACCR 2010-2011 Webinar Series May 5, 2011 Q&A Please submit all questions concerning webinar content through the Q&A panel Overview NAACCR 2010-2011 Webinar Series 1
Collecting Cancer Data: Prostate NAACCR 2010-2011 Webinar Series May 5, 2011 Q&A Please submit all questions concerning webinar content through the Q&A panel Overview NAACCR 2010-2011 Webinar Series 1
Prostate biopsy: MR imaging to the rescue
 Prostate biopsy: MR imaging to the rescue Poster No.: C-1855 Congress: ECR 2014 Type: Educational Exhibit Authors: N. V. V. B. Marques 1, J. Ip 1, A. Loureiro 2, J. Niza 1, M. Palmeiro 2, Keywords: DOI:
Prostate biopsy: MR imaging to the rescue Poster No.: C-1855 Congress: ECR 2014 Type: Educational Exhibit Authors: N. V. V. B. Marques 1, J. Ip 1, A. Loureiro 2, J. Niza 1, M. Palmeiro 2, Keywords: DOI:
Prostate MRI: Access to and Current Practice of Prostate MRI in the United States
 Prostate MRI: Access to and Current Practice of Prostate MRI in the United States James L. Leake, MS a, Rulon Hardman, MD a, Vijayanadh Ojili, MD a, Ian Thompson, MD b, Alampady Shanbhogue, MD a, Javier
Prostate MRI: Access to and Current Practice of Prostate MRI in the United States James L. Leake, MS a, Rulon Hardman, MD a, Vijayanadh Ojili, MD a, Ian Thompson, MD b, Alampady Shanbhogue, MD a, Javier
The role of apparent diffusion coefficient (ADC) and relative ADC in the evaluation of breast masses
 The role of apparent diffusion coefficient (ADC) and relative ADC in the evaluation of breast masses Poster No.: C-1749 Congress: ECR 2014 Type: Scientific Exhibit Authors: U. Aksoy Ozcan 1, A. Öz 2, S.
The role of apparent diffusion coefficient (ADC) and relative ADC in the evaluation of breast masses Poster No.: C-1749 Congress: ECR 2014 Type: Scientific Exhibit Authors: U. Aksoy Ozcan 1, A. Öz 2, S.
Successful Breast MRI Program : The ingredients
 Successful Breast MRI Program : The ingredients Dr. Smriti Hari Associate Professor Deptt. Of Radiology All India Institute of Medical Sciences New Delhi How to perform Breast MRI Breast MRI descriptors
Successful Breast MRI Program : The ingredients Dr. Smriti Hari Associate Professor Deptt. Of Radiology All India Institute of Medical Sciences New Delhi How to perform Breast MRI Breast MRI descriptors
MRI-targeted, transrectal ultrasound-guided prostate biopsy for suspected prostate malignancy: A pictorial review
 MRI-targeted, transrectal ultrasound-guided prostate biopsy for suspected prostate malignancy: A pictorial review Poster No.: C-1208 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Murphy, M.
MRI-targeted, transrectal ultrasound-guided prostate biopsy for suspected prostate malignancy: A pictorial review Poster No.: C-1208 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Murphy, M.
Hospital, University of Bologna, Bologna, Italy. Department of Urology, University of Bologna, Sant Orsola-Malpighi Hospital, Bologna, Italy
 IBIMA Publishing International Journal of Research in Urology http://www.ibimapublishing.com/journals/urol/urol.html Vol. 2016(2016), Article ID 652137, 5 Pages DOI: 10.5171/2016.652137 Research Article
IBIMA Publishing International Journal of Research in Urology http://www.ibimapublishing.com/journals/urol/urol.html Vol. 2016(2016), Article ID 652137, 5 Pages DOI: 10.5171/2016.652137 Research Article
MOLECULAR MEDICINE REPORTS 9: , Provincial Hospital, Shandong University, Jinan , P.R. China
 MOLECULAR MEDICINE REPORTS 9: 1989-1997, 2014 Magnetic resonance imaging directed biopsy improves the prediction of prostate cancer aggressiveness compared with a 12 core transrectal ultrasound guided
MOLECULAR MEDICINE REPORTS 9: 1989-1997, 2014 Magnetic resonance imaging directed biopsy improves the prediction of prostate cancer aggressiveness compared with a 12 core transrectal ultrasound guided
Low risk. Objectives. Case-based question 1. Evidence-based utilization of imaging in prostate cancer
 Evidence-based utilization of imaging in prostate cancer Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Objectives State the modalities,
Evidence-based utilization of imaging in prostate cancer Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Objectives State the modalities,
Low-Risk Prostate Cancer: The Accuracy of Multiparametric MR Imaging for Detection 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Jin Young Kim, MD
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Jin Young Kim, MD
Genitourinary Imaging Original Research
 Genitourinary Imaging Original Research De Cobelli et al. Use of Apparent Diffusion Coefficient to Predict Prostate Cancer Grade Genitourinary Imaging Original Research Francesco De Cobelli 1 Silvia Ravelli
Genitourinary Imaging Original Research De Cobelli et al. Use of Apparent Diffusion Coefficient to Predict Prostate Cancer Grade Genitourinary Imaging Original Research Francesco De Cobelli 1 Silvia Ravelli
MR IMAGING OF THE PROSTATE AT 3.0T WITH EXTERNAL PHASED ARRAY COIL PRELIMINARY RESULTS
 EUROPEAN JOURNAL OF MEDICAL RESEARCH 287 Eur J Med Res (2008) 13: 287-291 I. Holzapfel Publishers 2008 MR IMAGING OF THE PROSTATE AT 3.0T WITH EXTERNAL PHASED ARRAY COIL PRELIMINARY RESULTS N. Morakkabati-Spitz
EUROPEAN JOURNAL OF MEDICAL RESEARCH 287 Eur J Med Res (2008) 13: 287-291 I. Holzapfel Publishers 2008 MR IMAGING OF THE PROSTATE AT 3.0T WITH EXTERNAL PHASED ARRAY COIL PRELIMINARY RESULTS N. Morakkabati-Spitz
Can diffusion weighted imaging distinguish between benign and malignant solid or predominantly solid gynecological adnexal masses?
 The Egyptian Journal of Radiology and Nuclear Medicine (2013) 44, 113 119 Egyptian Society of Radiology and Nuclear Medicine The Egyptian Journal of Radiology and Nuclear Medicine www.elsevier.com/locate/ejrnm
The Egyptian Journal of Radiology and Nuclear Medicine (2013) 44, 113 119 Egyptian Society of Radiology and Nuclear Medicine The Egyptian Journal of Radiology and Nuclear Medicine www.elsevier.com/locate/ejrnm
GUIDELINES ON PROSTATE CANCER
 10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
Prostate tumour volumes: evaluation of the agreement between magnetic resonance imaging and histology using novel co-registration software
 Prostate tumour volumes: evaluation of the agreement between magnetic resonance imaging and histology using novel co-registration software Julien Le Nobin*, Clément Orczyk*, Fang-Ming Deng, Jonathan Melamed,
Prostate tumour volumes: evaluation of the agreement between magnetic resonance imaging and histology using novel co-registration software Julien Le Nobin*, Clément Orczyk*, Fang-Ming Deng, Jonathan Melamed,
Standards for MRI reporting the evolution to PI-RADS v 2.0
 Review Article Standards for MRI reporting the evolution to PI-RADS v 2.0 Michael Spektor, Mahan Mathur, Jeffrey C. Weinreb Department of Radiology and Biomedical Imaging, Yale New Haven Hospital, USA
Review Article Standards for MRI reporting the evolution to PI-RADS v 2.0 Michael Spektor, Mahan Mathur, Jeffrey C. Weinreb Department of Radiology and Biomedical Imaging, Yale New Haven Hospital, USA
MR-US Fusion Guided Biopsy: Is it fulfilling expectations?
 MR-US Fusion Guided Biopsy: Is it fulfilling expectations? Kenneth L. Gage MD, PhD Assistant Member Department of Diagnostic Imaging and Interventional Radiology 4 th Annual New Frontiers in Urologic Oncology
MR-US Fusion Guided Biopsy: Is it fulfilling expectations? Kenneth L. Gage MD, PhD Assistant Member Department of Diagnostic Imaging and Interventional Radiology 4 th Annual New Frontiers in Urologic Oncology
Research Article MR Imaging of Prostate Cancer: Diffusion Weighted Imaging and (3D) Hydrogen 1 ( 1 H) MR Spectroscopy in Comparison with Histology
 Radiology Research and Practice Volume 2011, Article ID 616852, 9 pages doi:10.1155/2011/616852 Research Article MR Imaging of Prostate Cancer: Diffusion Weighted Imaging and (3D) Hydrogen 1 ( 1 H) MR
Radiology Research and Practice Volume 2011, Article ID 616852, 9 pages doi:10.1155/2011/616852 Research Article MR Imaging of Prostate Cancer: Diffusion Weighted Imaging and (3D) Hydrogen 1 ( 1 H) MR
Prostate MRI for local staging and surgical planning in prostate cancer
 Prostate MRI for local staging and surgical planning in prostate cancer 15th Annual Floyd A. Fried Advances in Urology Symposium June 23, 2017 Ray Tan, MD, MSHPM Assistant Professor Disclosures None Objectives
Prostate MRI for local staging and surgical planning in prostate cancer 15th Annual Floyd A. Fried Advances in Urology Symposium June 23, 2017 Ray Tan, MD, MSHPM Assistant Professor Disclosures None Objectives
Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the
 Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the potential relation between whole-tumor apparent diffusion
Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the potential relation between whole-tumor apparent diffusion
The visualization of periprostatic nerve fibers using Diffusion Tensor Magnetic Resonance Imaging with tractography
 The visualization of periprostatic nerve fibers using Diffusion Tensor Magnetic Resonance Imaging with tractography Poster No.: C-0009 Congress: ECR 2014 Type: Scientific Exhibit Authors: K. Kitajima 1,
The visualization of periprostatic nerve fibers using Diffusion Tensor Magnetic Resonance Imaging with tractography Poster No.: C-0009 Congress: ECR 2014 Type: Scientific Exhibit Authors: K. Kitajima 1,
Post Radical Prostatectomy Radiation in Intermediate and High Risk Group Prostate Cancer Patients - A Historical Series
 Post Radical Prostatectomy Radiation in Intermediate and High Risk Group Prostate Cancer Patients - A Historical Series E. Z. Neulander 1, Z. Wajsman 2 1 Department of Urology, Soroka UMC, Ben Gurion University,
Post Radical Prostatectomy Radiation in Intermediate and High Risk Group Prostate Cancer Patients - A Historical Series E. Z. Neulander 1, Z. Wajsman 2 1 Department of Urology, Soroka UMC, Ben Gurion University,
MONA V. SANGHANI, DELRAY SCHULTZ, CLARE M. TEMPANY, DAVID TITELBAUM, ANDREW A. RENSHAW, MARIAN LOFFREDO, KERRI COTE, BETH MCMAHON,
 ADULT UROLOGY QUANTIFYING THE CHANGE IN ENDORECTAL MAGNETIC RESONANCE IMAGING-DEFINED TUMOR VOLUME DURING NEOADJUVANT ANDROGEN SUPPRESSION THERAPY IN PATIENTS WITH PROSTATE CANCER MONA V. SANGHANI, DELRAY
ADULT UROLOGY QUANTIFYING THE CHANGE IN ENDORECTAL MAGNETIC RESONANCE IMAGING-DEFINED TUMOR VOLUME DURING NEOADJUVANT ANDROGEN SUPPRESSION THERAPY IN PATIENTS WITH PROSTATE CANCER MONA V. SANGHANI, DELRAY
Interac(ve Experience with Prostate Imaging Repor(ng and Data System Version 2 (PI-RADS v2)
 Interac(ve Experience with Prostate Imaging Repor(ng and Data System Version 2 (PI-RADS v2) E Hassanzadeh 1,2, MD; E Velez 3, BS; F M Fennessy 1,4, MD, PhD; R M Dunne 1,2, MBBCh; M G Harisinghani 1,5,
Interac(ve Experience with Prostate Imaging Repor(ng and Data System Version 2 (PI-RADS v2) E Hassanzadeh 1,2, MD; E Velez 3, BS; F M Fennessy 1,4, MD, PhD; R M Dunne 1,2, MBBCh; M G Harisinghani 1,5,
Prostate Cancer MRI. Accurate Diagnosis and Treatment. PSA to Prostate MRI. for patients and curious doctors
 6 Prostate Cancer MRI Accurate Diagnosis and Treatment PSA to Prostate MRI for patients and curious doctors Samuel Aronson, M.D. Vincent Pelsser, M.D. Franck Bladou, M.D. Armen Aprikian, M.D. & Marc Emberton,
6 Prostate Cancer MRI Accurate Diagnosis and Treatment PSA to Prostate MRI for patients and curious doctors Samuel Aronson, M.D. Vincent Pelsser, M.D. Franck Bladou, M.D. Armen Aprikian, M.D. & Marc Emberton,
MR Imaging of Prostate Cancer: Present Limitations and Future Directions
 CASE PRESENTATION AND MINI-REVIEW MR Imaging of Prostate Cancer: Present Limitations and Future Directions David A. Boyajian HMS 4, Thursday, 18 September 2003 Beth Israel Deaconess Medical Center Prostate:
CASE PRESENTATION AND MINI-REVIEW MR Imaging of Prostate Cancer: Present Limitations and Future Directions David A. Boyajian HMS 4, Thursday, 18 September 2003 Beth Israel Deaconess Medical Center Prostate:
Stephen McManus, MD David Levi, MD
 Stephen McManus, MD David Levi, MD Prostate MRI Indications INITIAL DETECTION, STAGING, RECURRENT TUMOR LOCALIZATION, RADIATION THERAPY PLANNING INITIAL DETECTION Clinically suspected prostate cancer before
Stephen McManus, MD David Levi, MD Prostate MRI Indications INITIAL DETECTION, STAGING, RECURRENT TUMOR LOCALIZATION, RADIATION THERAPY PLANNING INITIAL DETECTION Clinically suspected prostate cancer before
Supplemental Information
 Supplemental Information Prediction of Prostate Cancer Recurrence using Quantitative Phase Imaging Shamira Sridharan 1, Virgilia Macias 2, Krishnarao Tangella 3, André Kajdacsy-Balla 2 and Gabriel Popescu
Supplemental Information Prediction of Prostate Cancer Recurrence using Quantitative Phase Imaging Shamira Sridharan 1, Virgilia Macias 2, Krishnarao Tangella 3, André Kajdacsy-Balla 2 and Gabriel Popescu
Whole Body MRI. Dr. Nina Tunariu. Prostate Cancer recurrence, progression and restaging
 Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
S1.04 PRINCIPAL CLINICIAN G1.01 COMMENTS S2.01 SPECIMEN LABELLED AS G2.01 *SPECIMEN DIMENSIONS (PROSTATE) S2.03 *SEMINAL VESICLES
 Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
The follow-up of uterine fibroids treated with HIFU: role of DWI and Dynamic contrast-study MRI
 The follow-up of uterine fibroids treated with HIFU: role of DWI and Dynamic contrast-study MRI Poster No.: C-1137 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit V. Zampa, V. Vallini,
The follow-up of uterine fibroids treated with HIFU: role of DWI and Dynamic contrast-study MRI Poster No.: C-1137 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit V. Zampa, V. Vallini,
Pathologists Perspective on Focal Therapy: The Role of Mapping Biopsies and Markers
 Pathologists Perspective on Focal Therapy: The Role of Mapping Biopsies and Markers M. Scott Lucia, MD Professor and Vice Chair of Anatomic Pathology Chief of Genitourinary and Renal Pathology Dept. of
Pathologists Perspective on Focal Therapy: The Role of Mapping Biopsies and Markers M. Scott Lucia, MD Professor and Vice Chair of Anatomic Pathology Chief of Genitourinary and Renal Pathology Dept. of
Preoperative Gleason score, percent of positive prostate biopsies and PSA in predicting biochemical recurrence after radical prostatectomy
 JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/35124 holds various files of this Leiden University dissertation. Author: Wokke, Beatrijs Henriette Aleid Title: Muscle MRI in Duchenne and Becker muscular
Cover Page The handle http://hdl.handle.net/1887/35124 holds various files of this Leiden University dissertation. Author: Wokke, Beatrijs Henriette Aleid Title: Muscle MRI in Duchenne and Becker muscular
First Clinical Experiences with Simultaneous Multi-Slice Accelerated Diffusion-Weighted Imaging Throughout the Body
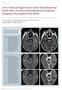 Clinical Oncological Imaging First Clinical Experiences with Simultaneous Multi-Slice Accelerated Diffusion-Weighted Imaging Throughout the Body Valentin Tissot, M.D. 1 ; Olivier Legeas, M.D. 1 ; Isabelle
Clinical Oncological Imaging First Clinical Experiences with Simultaneous Multi-Slice Accelerated Diffusion-Weighted Imaging Throughout the Body Valentin Tissot, M.D. 1 ; Olivier Legeas, M.D. 1 ; Isabelle
