Chapter 28 Emerging Indications in Stereotactic Radiosurgery: The First Application of Cellular Surgery
|
|
|
- Marianna Cook
- 6 years ago
- Views:
Transcription
1 Chapter 28 Emerging Indications in Stereotactic Radiosurgery: The First Application of Cellular Surgery Douglas Kondziolka, M.D., M.Sc., F.R.C.S.C., L. Dade Lunsford, M.D., John C. Flickinger, M.D., and Ajay Niranjan, M.Ch. At this meeting of the Congress of Neurological Surgeons, the theme "Surgery at the Crossroads" was presented. Stereotactic radiosurgery reflects one important neurosurgical field that crosses the lines of multiple medical disciplines. To discuss the role of radiosurgery and its emerging indications in this context, it is important to first define surgery. We defined surgery as "definitive manipulation of an organ system or tissue to achieve a specific purpose, performed in a single-session, using energy. (19) Historically, the most common energy source was mechanical. The surgeon simply moved his or her arm that held an instrument. Over the years, other forms of energy were used as a surgical effector. These included light energy (laser surgery), thermal energy (radiofrequency lesioning), chemical energy (tissue manipulation with alcohol or chymopapain), and radiation energy (stereotactic radiosurgery). For decades, one focus of neurosurgery residency training has been to master microneurosurgical techniques using exposure augmented by the operating microscope. Radiosurgery represents the first way to truly perform microsurgery, that is, surgery on a submicroscopic level. Radiosurgery is the first surgery for disruption of tumor-cell membranes, surgery to disrupt the strands of DNA, surgery to eliminate protein biosynthesis, and surgery of endothelial cells. Radiosurgery truly has become the first broadly applied biologic surgery. Thus, it is important to evaluate its current and emerging uses and identify how surgeons will use this tool for the spectrum of disorders that they manage (28). Previously, newly emerging radiosurgical indications had their roots in our understanding of radiobiologic effects on different tissues. To date, radiosurgery has been used for both abnormal intracranial mass lesions and normal brain. Table 28.1 shows the current brain radiosurgery experience at the University of Pittsburgh. RADIOBIOLOGY AND THE BASIS OF THE RADIOSURGERY Borje Larsson, a radiobiologist working with Lars Leksell, performed the first basic science experiments in radiosurgery using protons and then photons. Their goal was to create small brain lesions in the hope of improving the care of patients with functional disorders. Subsequent animal studies in rabbits, cats, goats, rats, and later subhuman primates showed consistent effects on small-volume lesions using high radiation doses. A baboon model pioneered at the University of Pittsburgh studied effects between 1 and 24 months using maximum doses of 20, 50, 100, and 150 Gray and 8-mm collimators (17). Imaging studies identified the time course for lesion development and the resolution of imaging changes that followed (28). Histologic studies proved that the lesion was created sharply with a rapid follow-up of the histologic effect outside the lesion. The 50 Gray dose, more typically used in human clinical radiosurgery for arteriovenous malformations, was followed by complete target destruction if enough time elapsed. This indicated that arteriovenous malformation (AVM) obliteration could not only occur from a selective effect on the vessel wall, but also from total tissue destruction at the target. Such studies raised the hope for the use of radiosurgery in vascular malformations, neoplasms, and other functional targets such as tremor cells, pain pathways, and perhaps epileptic foci.
2 "NORMAL" BRAIN AS THE TARGET The most common functional indication is trigeminal neuralgia (3, 15, 16). The effects of trigeminal nerve radiosurgery have been evaluated in a subhuman primate model. Using maximum radiosurgery doses of 80 or 100 Gray, Kondziolka et al. (18) studied histologic and ultrastructural effects on the nerve target 6 months after irradiation. They found evidence of axonal degeneration at the 80-Gray human dose that was not specific to different kinds of nerve fibers. The 80-Gray dose led to a subtotal axonal degeneration with preservation of some axons. This indicated that the high rate of facial sensory preservation was because of the fact that the lesion was not complete, and pain relief likely occurred from degeneration of enough axons that blocked pain. Baboon studies using 100 or 150 Gray in the thalamus provided additional basis for the use of radiosurgery to create thalamotomy lesions in patients with movement disorders (11). To date, radiosurgical thalamotomy has been used in patients with tremors related to Parkinson's disease, essential tremor, and multiple sclerosis tremor (17). Published reports indicate that the rate of significant improvement is approximately 80% using maximum doses of 130 to 150 Gray with a single 4-mm collimator, targeted to the ventral intermediate nucleus (VIM) of the thalamus. Highresolution, stereotactic magnetic resonance imaging is crucial for targeting. For the most part, radiosurgical thalamotomy is used in patients who are elderly or medically infirm and who do not want to undergo deep brain stimulation with placement of hardware or radiofrequency thalamotomy. Radiosurgery for epilepsy has been used in increasing numbers of patients with a variety of different brain targets. The basis for the use of radiosurgery was the observation that irradiation could stop seizures in patients with brain tumors or vascular malformations (23). Animal studies (rat kainic acid or rat kindling models) showed a reduction or elimination of seizures after radiosurgery (25). Dr. Nicholas Barbaro and colleagues at the University of California at San Francisco conducted a multicenter study to evaluate the effects of radiosurgery for mesial temporal sclerosisrelated epilepsy. Patients were randomized to maximum doses of 40 or 48 Gray using target volumes between 5.5 and 7.5 ml. This work followed the pioneering efforts of Regis et al. (30), who first studied mesial temporal lobe sclerosis-related epilepsy in Marseille, France. Radiosurgery for hypothalamic hamartoma-related gelastic seizures is an important therapeutic alternative to hamartoma resection or to radiofrequency lesioning (30). An additional emerging indication is anterior capsulotomy for obsessive-compulsive disorder. Radiosurgical lesioning has been performed for depression (cingulotomy), chronic pain (medial thalamotomy), cancer pain (hypophysectomy) and other anxiety neuroses but requires additional research before any of these indications becomes more mainstream. "MALFORMED" BRAIN AS THE TARGET For several decades, perhaps the most frequent radiosurgical indication was the AVM (5, 23). When an AVM was located in a region of the brain associated with high risk for surgical resection, radiosurgery often was considered as the main therapeutic alternative. Particularly in patients with smaller-volume, critically located malformations, radiosurgery has proven a highly effective strategy. The various management options including conservative therapy, endovascular embolization, resection, and radiosurgery (sometimes alone or in combination) should be discussed with symptomatic patients. Larger-volume AVMs are occasionally selected for radiosurgery, usually using a staged-
3 volume approach (1), when no other option is feasible. Patients with dural arteriovenous fistulas may also be appropriate candidates for radiosurgery, sometimes followed by endovascular or open surgical approaches (37). Cerebral cavernous malformations are an emerging radiosurgical indication in patients with deep-seated lesions unsuitable for microsurgery. This common malformation, easily identified on magnetic resonance imaging scans, presents an ideal radiosurgical target for a number of reasons. First, these lesions usually are small and located in critical brain areas. Most patients have minimal symptoms, and natural history studies show a relatively infrequent annual hemorrhage rate in patients without previous symptomatic hemorrhage (0.6% per year). Only in patients with significant single hemorrhages or multiple hemorrhages should radiosurgery be considered. The University of Pittsburgh protocol initially included only patients with two imaging-defined symptomatic bleeding episodes in locations at high risk for neurologic deficits with resection. To date, we have performed radiosurgery on 112 patients whose median age was 39 years (10). The mean margin dose to the malformation was 16 Gray and the maximum dose 30 Gray. The mean number of previous symptomatic bleeding episodes was 2.6. After radiosurgery, at an average of 5 years, the 40% annual hemorrhage rate before radiosurgery (excluding the first hemorrhage) was reduced to 9.7% within 2 years and 0.56% after 2 years. Thus, radiosurgery may transform a malformation with a propensity to repeated symptomatic hemorrhage into one that is quiescent. Whether or not the lesion is truly obliterated completely cannot be determined using available imaging methods. NEOPLASTIC BRAIN AS THE TARGET There has been extensive experience in the use of stereotactic radiosurgery for patients with a wide array of benign and malignant brain tumors. Such work is based on the known radiobiologic effects of radiation on neoplastic tissue. Stereotactic precision and the overwhelming biologically effective single-procedure dose (compared with standard radiotherapy) have led to impressive results after tumor radiosurgery. Animal models, particularly using glial tumors in rat brain, have shown the benefits of focused radiation in comparison to animals that were not radiated. Additional research has been performed using human schwannoma and meningioma xenografts implanted into the sub-renal capsule of nude mice. Recently, we measured tumor apoptosis after radiosurgery in rats with malignant tumors (39). In an analysis of apoptosis performed in the immediate postirradiation period, the number of apoptotic bodies increased significantly compared with controls. Thus, the acute affects of radiation may not only be mediated through delayed tumor cell necrosis but by apoptotic pathways. Such work on the biologic effects of radiosurgery is the foundation for the observations seen in many thousands of patients managed with intracranial tumors. The most frequent benign tumor cared for by radiosurgery is the vestibular schwannoma (acoustic neuroma). Numerous studies have shown not only excellent short-term outcomes, but also consistent long-term effects now published with 15-year follow-up data (20). Kondziolka et al. (14) reported 5- to 10- year outcomes including information on patient-reported complications and satisfaction rates. Regis et al. (30) compared cohorts of patients who either underwent gamma-knife radiosurgery or microsurgical resection for their vestibular schwannoma. In that study, clinical outcomes were superior in the radiosurgery group. At the same time, imaging studies from numerous centers have clarified what can be expected after radiosurgery. Loss of central contrast enhancement followed by slow progressive tumor shrinkage is most frequently observed. In some patients, transient expansion of the tumor capsule (usually by 1 or 2 mm) can be seen if the internal biologic effect is
4 pronounced. Such tumors later regress in most instances. Imaging studies that show tumoral compression of the lateral brain stem surface may show regression completely off the brain stem over several years. In an earlier report from our center, we noted that over 70% of tumors were smaller once 5 years of follow-up had passed (14). The combination of high tumor control rates and low cranial neuropathy rates (less than 1% for facial weakness and less than 3% for facial numbness, as well as high rates of hearing preservation) have led to the emergence of radiosurgery as possibly the most frequent treatment choice for patients with vestibular schwannomas (24, 28). Other cranial nerve schwannomas are also appropriate for radiosurgery (29). Similar outcomes have been reported in patients with meningiomas, either managed primarily or after previous surgical resection (13). Radiosurgery has played its largest role in tumors of the skull base and those located close to dural sinuses or cranial nerves (6, 22). High tumor control rates (more than 90%) past 10 years of follow-up have been noted in evaluated patients, again with infrequent rates of associated cranial neuropathy when proper patient selection and judicious dose planning was performed. Another dural based tumor, the hemangiopericytoma, can respond dramatically to radiosurgery, and often marked tumor regression is noted on follow-up imaging studies (36). Radiosurgery in children is an under-used management approach. When it would be desirable to restrict radiation administration to much of the developing brain (as could be achieved in radiosurgery), this approach should be considered. Perhaps the most common indication in children is management of the recurrent or residual pilocytic astrocytoma located in a deep-brain location (4). Radiosurgery is usually performed under general anesthesia in patients younger than 12 years old. In more than half of the patients managed, significant reduction in tumor size was noted after pilocytic astrocytoma radiosurgery. Radiosurgery has also played a significant role in patients with small residual or recurrent solid craniopharyngiomas, ependymomas, medulloblastomas, and germ cell neoplasms (7, 9). Extracranial radiosurgery for tumors of the nasopharynx or skull base has proven effective for patients with recurrent tumors, particularly after previous resection or radiation therapy (2). Care of the patient with brain metastases has emerged as the most frequent indication for stereotactic radiosurgery (8, 21, 31 33, 35). It is believed that there may be more than 300,000 patients per year in the United States who develop a brain metastasis from systemic solid cancers. First, radiosurgery was evaluated in patients with solitary metastasis. Now, it has proven to be effective for patients with more than one metastasis. We routinely offer this approach for patients with up to eight tumors who remain in good neurologic condition and remain actively managed for their extracranial disease. Most such tumors are not associated with the significant mass effect that might cause marked neurologic disability. In such patients, surgical resection should be considered if appropriate based on brain location. The role of whole-brain radiation therapy remains controversial for patients with limited numbers of brain tumors but remains an important strategy for patients with multiple metastases, particularly in the setting of metastatic lung or breast cancer. In tumors that are often considered more radioresistant, such as melanoma or renal cell carcinoma, radiosurgery alone may be performed (32). Median survivals after radiosurgery have been noted in patients with lung cancer (11 mo), renal cell cancer (11 mo), breast cancer (13 mo), melanoma (7 mo), and gastrointestinal tract cancer (5 mo) after radiosurgery. Such outcomes vary depending on what can be offered for concomitant management of extracranial cancer. For example, it is infrequent that a patient with a gastrointestinal primary would develop a brain tumor without additional lung or liver metastases.
5 Other tumors suitable for radiosurgery include chordomas and chondrosarcomas (26), craniopharyngiomas, glomus tumors (34), hemangioblastomas, and pituitary adenomas. There are numerous reports on all of these indications that discuss the role of adjuvant or primary radiosurgery for properly selected patients. Radiosurgery can also play an important role for patients with malignant glial neoplasms, either as a boost to fractionated radiotherapy or for later recurrence (12, 27). It should be considered within a multi-modality strategy for these difficult tumors. TABLE Gamma-knife radiosurgery at the University of Pittsburgh (n = 7018) a Indication No. of procedures Arteriovenous malformation 1047 Cavernous malformation 119 AV fistula 21 Vestibular schwannoma 1075 Trigeminal schwannoma 36 Jugular foramen schwannoma 27 Other schwannoma 13 Meningioma 990 Pituitary adenoma 232 Craniopharyngioma 47 Chordoma 26 Chondrosarcoma 17 Hemangioblastoma 37 Pineal region tumor 25 Hemangiopericytoma 27
6 Hemangioma 7 Choroid plexus papilloma 7 Lymphoma 10 Glomus tumor Glioblastoma multiforme 277 Anaplastic astrocytoma 112 Astrocytoma/oligodendroglioma 105 Ependymoma 52 Medulloblastoma 19 Brain metastasis 1902 Other tumor 37 Skull base malignant tumors 28 Trigeminal neuralgia 625 Thalamotomy for tremor 57 Epilepsy 6 Capsulotomy for OCD 1 Ablation for cancer pain 2 a AV, arteriovenous. REFERENCES 1. Firlik A, Levy E, Kondziolka D, Yonas H: Staged volume radiosurgery and resection: A new treatment for a giant arteriovenous malformation. Neurosurgery 43: , 1998.
7 2. Firlik KS, Kondziolka D, Lunsford LD, Janecka IP, Flickinger JC: Radiosurgery for recurrent cranial base cancer arising from the head and neck. Head Neck 18: , Flickinger JC, Pollock BE, Kondziolka D, Phuang LK, Foote R, Stafford S, Lunsford LD: Does increased nerve length within the treatment volume improve trigeminal neuralgia radiosurgery? A prospective, blinded, randomized study. Int J Radiat Oncol Biol Phys 51: , Hadjipanayis C, Kondziolka D, Gardner P, Niranjan A, Dagam S, Flickinger JC, Lunsford LD: Stereotactic radiosurgery for pilocytic astrocytomas when multimodal therapy is necessary. J Neurosurg 97:56 64, Hadjipanayis C, Levy E, Niranjan A, Firlik A, Kondziolka D, Flickinger J, Lunsford LD: Stereotactic radiosurgery for motor cortex region arteriovenous malformations. Neurosurgery 48:70 77, Harris AE, Lee JYK, Omalu B, Flickinger JC, Kondziolka D, Lunsford LD: The effect of radiosurgery during management of aggressive meningiomas. Surg Neurol 60: , Hasegawa T, Kondziolka D, Hadjipanayis C, Flickinger J, Lunsford LD: Stereotactic radiosurgery for CNS nongerminomatous germ cell tumors. Pediatr Neurosurg 38: , Hasegawa T, Kondziolka D, Flickinger JC, Germanwala A, Lunsford LD: Brain metastases treated with radiosurgery alone: An alternative to whole brain radiotherapy? Neurosurgery 52: , Hasegawa T, Kondziolka D, Hadjipanayis C, Flickinger J, Lunsford LD: The role of radiosurgery for the treatment of pineal parenchymal tumors. Neurosurgery 51: , Hasegawa T, McInerney J, Kondziolka D, Lee JYK, Flickinger J, Lunsford LD: Long term results after stereotactic radiosurgery for patients with cavernous malformations. Neurosurgery 50: , Kondziolka D, Couce M, Niranjan A, Maesawa S, Fellows W. Histology of the 100 Gy thalamotomy in the baboon. Radiosurgery 4: , Kondziolka D, Flickinger JC, Bissonette DJ, Bozik M, Lunsford LD: Survival benefit of stereotactic radiosurgery for patients with malignant glial neoplasms. Neurosurgery 41: , Kondziolka D, Levy E, Niranjan A, Flickinger J, Lunsford LD: Long-term outcomes after meningioma radiosurgery: Physicians and patients perspective. J Neurosurg 91:44 50, Kondziolka D, Lunsford LD, McLaughlin M, Flickinger JC: Long-term outcomes after radiosurgery for acoustic neuromas. N Engl J Med 339: , Kondziolka D, Lunsford LD, Flickinger JC: Stereotactic radiosurgery for the treatment of trigeminal neuralgia. Clin J Pain 18:42 47, 2002.
8 16. Kondziolka D, Lunsford LD, Flickinger JC, Young RF, Vermeulen S, Duma CM, Jacques DB, Rand RW, Regis J, Peragut JC, Epstein M, Lindquist C: Stereotactic radiosurgery for trigeminal neuralgia: A multi-institution study using the gamma unit. J Neurosurg 84: , Kondziolka D, Lunsford LD, Witt TC, Flickinger JC. The future of radiosurgery: Radiobiology, technology, and applications. Surg Neurol 54: , Kondziolka D, Lacomis D, Niranjan A, Maesawa S, Mori Y, Fellows W, Lunsford LD: Histologic effects of trigeminal nerve radiosurgery in a primate model: Implications for trigeminal neuralgia radiosurgery. Neurosurgery 46: , Kondziolka D, Lunsford LD, Loeffler JS, Friedman W: Radiosurgery and radiotherapy: Observations and clarifications. J Neurosurg 101: , Kondziolka D, Nathoo N, Flickinger JC, Niranjan A, Maitz AH, Lunsford LD: Long-term results after radiosurgery for benign intracranial tumors. Neurosurgery 53: , Kondziolka D, Patel A, Lunsford LD, Kassam A, Flickinger JC: Stereotactic radiosurgery plus whole brain radiotherapy versus radiotherapy alone for patients with multiple brain metastases. Int J Radiat Oncol Biol Phys 45: , Lee JYK, Niranjan A, McInerney J, Kondziolka D, Flickinger JC, Lunsford LD: Stereotactic radiosurgery provides long term tumor control of cavernous sinus meningiomas. J Neurosurg 97:65 72, Lunsford LD, Kondziolka D, Flickinger JC, Bissonette D, Jungreis CA, Horton JA, Maitz AH, Coffey RJ: Stereotactic radiosurgery for arteriovenous malformations of the brain. J Neurosurg 75: , Lunsford LD, Niranjan A, Flickinger JC, Maitz A, Kondziolka D. Radiosurgery of vestibular schwannomas: Summary of experience in 829 cases. J Neurosurg 102: , Maesawa S, Kondziolka D, Dixon E, Balzer J, Fellows W, Lunsford LD: Subnecrotic stereotactic radiosurgery controlling epilepsy produced by kainic acid injection in rats. J Neurosurg 93: , Muthukumar N, Kondziolka D, Lunsford LD, et al: Stereotactic radiosurgery for chordoma and chondrosarcoma: Further experiences. Int J Radiat Oncol Biol Phys 41: , Nagai H, Kondziolka D, Niranjan A, Flickinger J, Lunsford LD: Results following stereotactic radiosurgery for patients with glioblastoma multiforme. Radiosurgery 5:91 99, Niranjan A, Gobbel G, Kondziolka D, Flickinger JC, Lunsford LD: Experimental radiobiological investigations into radiosurgery: Present understanding and future directions. Neurosurgery 55: , 2004.
9 29. Nettel B, Niranjan A, Martin JJ, Koebbe CJ, Kondziolka D, Flickinger JC, Lunsford LD: Gamma knife radiosurgery for trigeminal schwannomas. Surg Neurol 62: , Regis J, Bartolomei F, de Toffol B, Genton P, Kobayashi T, Mori Y, Takakura K, Hori T, Inoue H, Schrottner O, Pendl G, Wolf A, Arita K, Chauvel P: Gamma knife surgery for epilepsy related to hypothalamic hamartomas. Neurosurgery 47: , Rutigliano MJ, Lunsford LD, Kondziolka D, Strauss MJ, Khanna V: The cost-effectiveness of stereotactic radiosurgery versus surgical resection in the treatment of solitary metastatic brain tumors. Neurosurgery 37: , Sheehan J, Sun MH, Kondziolka D, Flickinger JC, Lunsford LD: Radiosurgery for patients with renal cell carcinoma metastatic to the brain: Long-term outcomes and prognostic factors influencing survival and local tumor control. J Neurosurg 98: , Sheehan J, Sun MH, Kondziolka D, Flickinger JC, Lunsford LD: Radiosurgery for patients with non-small cell lung carcinoma metastatic to the brain: Outcomes and prognostic factors. J Neurosurg 97: , Sheehan JS, Kondziolka D, Flickinger JC, Lunsford LD: Gamma knife surgery for glomus jugulare tumors: An intermediate report on efficacy and safety. J Neurosurg 102: , Sheehan J, Niranjan A, Flickinger JC, Kondziolka D, Lunsford LD: The expanding role of neurosurgeons in the management of brain metastases. Surg Neurol 62:32 41, Sheehan J, Kondziolka D, Flickinger JC, Lunsford LD: Stereotactic radiosurgery for intracranial hemangiopericytomas. Neurosurgery 51: , Singhal D, Sheehan J, Koebbe C, Jungreis C, Horowitz M, Kondziolka D, Flickinger J, Lunsford LD: Radiosurgery for dural arteriovenous fistulas. Surg Neurol. In press. 38. Subach B, Kondziolka D, Lunsford LD, Bissonette D, Flickinger JC, Maitz A: Stereotactic radiosurgery in the management of acoustic neuromas associated with neurofibromatosis - type II. J Neurosurg 90: , Witham T, Kondziolka D, Niranjan A, Fellows W, Chambers W: The characterization of tumor apoptosis after experimental radiosurgery. Stereotact Funct Neurosurg. In press.
Patients Treated with Leksell Gamma Knife
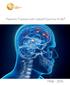 Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
IMAGE-GUIDED RADIOSURGERY USING THE GAMMA KNIFE
 IMAGE-GUIDED RADIOSURGERY USING THE GAMMA KNIFE L. D. LUNSFORD INTRODUCTION Image guided brain surgery became a reality in the mid-1970s after the introduction of the first methods to obtain axial imaging
IMAGE-GUIDED RADIOSURGERY USING THE GAMMA KNIFE L. D. LUNSFORD INTRODUCTION Image guided brain surgery became a reality in the mid-1970s after the introduction of the first methods to obtain axial imaging
Background Principles and Technical Development
 Contents Part I Background Principles and Technical Development 1 Introduction and the Nature of Radiosurgery... 3 Definitions of Radiosurgery... 5 Consequences of Changing Definitions of Radiosurgery...
Contents Part I Background Principles and Technical Development 1 Introduction and the Nature of Radiosurgery... 3 Definitions of Radiosurgery... 5 Consequences of Changing Definitions of Radiosurgery...
Dosimetry, see MAGIC; Polymer gel dosimetry. Fiducial tracking, see CyberKnife radiosurgery
 Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
Otolaryngologist s Perspective of Stereotactic Radiosurgery
 Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2015
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2015
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 03/01/2013 Section:
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 03/01/2013 Section:
Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary
 Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary László Bognár M.D., Ph.D., József G. Dobai M.D., Gábor Csiky and Imre Fedorcsák M.D., Ph.D. Department of Neurosurgery, Medical
Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary László Bognár M.D., Ph.D., József G. Dobai M.D., Gábor Csiky and Imre Fedorcsák M.D., Ph.D. Department of Neurosurgery, Medical
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/20/2015
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/20/2015
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017
Update on IGKRF Activities
 Stereotactic radiosurgery research, education and publishing for the purpose of improving public health Fall 2016 In this issue: Update on IGKRF Activities The IGKRF Recently Published Articles Topics
Stereotactic radiosurgery research, education and publishing for the purpose of improving public health Fall 2016 In this issue: Update on IGKRF Activities The IGKRF Recently Published Articles Topics
Chapter 5 Section 3.1
 Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Estimating the Risks of Adverse Radiation Effects After Gamma Knife Radiosurgery for Arteriovenous Malformations
 Estimating the Risks of Adverse Radiation Effects After Gamma Knife Radiosurgery for Arteriovenous Malformations Hideyuki Kano, MD, PhD; John C. Flickinger, MD; Daniel Tonetti, MD; Alan Hsu, MD; Huai-che
Estimating the Risks of Adverse Radiation Effects After Gamma Knife Radiosurgery for Arteriovenous Malformations Hideyuki Kano, MD, PhD; John C. Flickinger, MD; Daniel Tonetti, MD; Alan Hsu, MD; Huai-che
Stereotactic Radiosurgery and Stereotactic Body Radiotherapy
 Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Policy Number: 6.01.10 Last Review: 11/2018 Origination: 1/1989 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Policy Number: 6.01.10 Last Review: 11/2018 Origination: 1/1989 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 04/01/2014 Section:
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 04/01/2014 Section:
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: 6.01.10 Last Review: 11/2013 Origination: 1/1989 Next Review: 11/2014 Policy Blue Cross and Blue Shield of Kansas City (Blue
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: 6.01.10 Last Review: 11/2013 Origination: 1/1989 Next Review: 11/2014 Policy Blue Cross and Blue Shield of Kansas City (Blue
Medical Policy. MP Stereotactic Radiosurgery and Stereotactic Body Radiotherapy
 Medical Policy MP 6.01.10 BCBSA Ref. Policy: 6.01.10 Last Review: 10/18/2018 Effective Date: 10/18/2018 Section: Radiation Related Policies 8.01.10 Charged-Particle (Proton or Helium Ion) Radiotherapy
Medical Policy MP 6.01.10 BCBSA Ref. Policy: 6.01.10 Last Review: 10/18/2018 Effective Date: 10/18/2018 Section: Radiation Related Policies 8.01.10 Charged-Particle (Proton or Helium Ion) Radiotherapy
This LCD recognizes these two distinct treatment approaches and is specific to treatment delivery:
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: 77371, 77372, 77373 LCD ID Number: L33410 J-N FL Responsible
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: 77371, 77372, 77373 LCD ID Number: L33410 J-N FL Responsible
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Page 1 of 74 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Stereotactic Radiosurgery and Stereotactic
Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Page 1 of 74 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Stereotactic Radiosurgery and Stereotactic
LONG-TERM FOLLOW-UP OF ACOUSTIC SCHWANNOMA RADIOSURGERY WITH MARGINAL TUMOR DOSES OF 12 TO 13 Gy
 doi:10.1016/j.ijrobp.2007.01.001 Int. J. Radiation Oncology Biol. Phys., Vol. 68, No. 3, pp. 845 851, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front
doi:10.1016/j.ijrobp.2007.01.001 Int. J. Radiation Oncology Biol. Phys., Vol. 68, No. 3, pp. 845 851, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front
Description. Section: Therapy Effective Date: January 15, 2015 Subsection: Therapy Original Policy Date: September 13, 2012 Subject:
 Last Review Status/Date: December 2014 Page: 1 of 51 Description Stereotactic radiosurgery (SRS) and stereotactic body radiotherapy (SBRT) are radiotherapy methods that entail delivering highly focused,
Last Review Status/Date: December 2014 Page: 1 of 51 Description Stereotactic radiosurgery (SRS) and stereotactic body radiotherapy (SBRT) are radiotherapy methods that entail delivering highly focused,
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
Gamma Knife Radiosurgery
 Gamma Knife Radiosurgery A Team Approach to Treating Patients George Bovis, MD Patrick Sweeney, MD Jagan Venkatesan, MS Matt White, MS Illinois Gamma Knife Center Elk Grove Village, IL Disclosures Shareholders
Gamma Knife Radiosurgery A Team Approach to Treating Patients George Bovis, MD Patrick Sweeney, MD Jagan Venkatesan, MS Matt White, MS Illinois Gamma Knife Center Elk Grove Village, IL Disclosures Shareholders
CURRICULUM VITAE. John C. Flickinger, MD, FACR. Department of Radiation Oncology 200 Lothrop Street Pittsburgh, Pennsylvania 15213
 CURRICULUM VITAE John C. Flickinger, MD, FACR Office Address: Presbyterian-University Hospital Department of Radiation Oncology 200 Lothrop Street Pittsburgh, Pennsylvania 15213 Office Telephone: (412)
CURRICULUM VITAE John C. Flickinger, MD, FACR Office Address: Presbyterian-University Hospital Department of Radiation Oncology 200 Lothrop Street Pittsburgh, Pennsylvania 15213 Office Telephone: (412)
The New England Journal of Medicine LONG-TERM OUTCOMES AFTER RADIOSURGERY FOR ACOUSTIC NEUROMAS
 LONG-TERM OUTCOMES AFTER RADIOSURGERY FOR ACOUSTIC NEUROMAS DOUGLAS KONDZIOLKA, M.D., L. DADE LUNSFORD, M.D., MARK R. MCLAUGHLIN, M.D., AND JOHN C. FLICKINGER, M.D. ABSTRACT Background Stereotactic radiosurgery
LONG-TERM OUTCOMES AFTER RADIOSURGERY FOR ACOUSTIC NEUROMAS DOUGLAS KONDZIOLKA, M.D., L. DADE LUNSFORD, M.D., MARK R. MCLAUGHLIN, M.D., AND JOHN C. FLICKINGER, M.D. ABSTRACT Background Stereotactic radiosurgery
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report
 Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Original Date: April 2016 Page 1 of 7 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
Although histologically benign, tumors LONG-TERM RESULTS AFTER RADIOSURGERY FOR BENIGN INTRACRANIAL TUMORS CLINICAL STUDIES
 CLINICAL STUDIES LONG-TERM RESULTS AFTER RADIOSURGERY FOR BENIGN INTRACRANIAL TUMORS Douglas Kondziolka, M.D. Narendra Nathoo, M.D. John C. Flickinger, M.D. Ajay Niranjan, M.Ch. Ann H. Maitz, M.S. L. Dade
CLINICAL STUDIES LONG-TERM RESULTS AFTER RADIOSURGERY FOR BENIGN INTRACRANIAL TUMORS Douglas Kondziolka, M.D. Narendra Nathoo, M.D. John C. Flickinger, M.D. Ajay Niranjan, M.Ch. Ann H. Maitz, M.S. L. Dade
ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS
 ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS Dr. Maitri P Gandhi 1, Dr. Chandni P Shah 2 1 Junior resident, Gujarat Cancer & Research
ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS Dr. Maitri P Gandhi 1, Dr. Chandni P Shah 2 1 Junior resident, Gujarat Cancer & Research
Classification of Facial Pain. Surgical Treatment of Facial Pain. Typical trigeminal neuralgia. Atypical trigeminal neuralgia
 Surgical Treatment of Facial Pain Nicholas M. Barbaro, MD University of California at San Francisco Classification of Facial Pain Trigeminal neuralgia Atypical trigeminal neuralgia Neuropathic facial pain
Surgical Treatment of Facial Pain Nicholas M. Barbaro, MD University of California at San Francisco Classification of Facial Pain Trigeminal neuralgia Atypical trigeminal neuralgia Neuropathic facial pain
Results of acoustic neuroma radiosurgery: an analysis of 5 years experience using current methods
 See the Letter to the Editor and the Response in this issue in Neurosurgical Forum, pp 141 142. J Neurosurg 94:1 6, 2001 Results of acoustic neuroma radiosurgery: an analysis of 5 years experience using
See the Letter to the Editor and the Response in this issue in Neurosurgical Forum, pp 141 142. J Neurosurg 94:1 6, 2001 Results of acoustic neuroma radiosurgery: an analysis of 5 years experience using
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Clinical Commissioning Policy: Arteriovenous Malformations. December Reference : NHSCB/D5/4
 Clinical Commissioning Policy: Arteriovenous Malformations December 2012 Reference : NHSCB/D5/4 NHS Commissioning Board Clinical Commissioning Policy: Arteriovenous Malformations First published: December
Clinical Commissioning Policy: Arteriovenous Malformations December 2012 Reference : NHSCB/D5/4 NHS Commissioning Board Clinical Commissioning Policy: Arteriovenous Malformations First published: December
Evidence Based Medicine for Gamma Knife Radiosurgery. Metastatic Disease GAMMA KNIFE SURGERY
 GAMMA KNIFE SURGERY Metastatic Disease Evidence Based Medicine for Gamma Knife Radiosurgery Photos courtesy of Jean Régis, Timone University Hospital, Marseille, France Brain Metastases The first report
GAMMA KNIFE SURGERY Metastatic Disease Evidence Based Medicine for Gamma Knife Radiosurgery Photos courtesy of Jean Régis, Timone University Hospital, Marseille, France Brain Metastases The first report
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Brain tumors: tumor types
 Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Dr Eddie Mee. Neurosurgeon Auckland City Hospital, Ascot Integrated Hospital, MercyAscot Hospitals, Auckland
 Dr Eddie Mee Neurosurgeon Auckland City Hospital, Ascot Integrated Hospital, MercyAscot Hospitals, Auckland 16:30-17:25 WS #48: Current Management of Brain Bleeds and Tumours 17:35-18:30 WS #58: Current
Dr Eddie Mee Neurosurgeon Auckland City Hospital, Ascot Integrated Hospital, MercyAscot Hospitals, Auckland 16:30-17:25 WS #48: Current Management of Brain Bleeds and Tumours 17:35-18:30 WS #58: Current
Gamma Knife Radiosurgery A tool for treating intracranial conditions. CNSA Annual Congress 2016 Radiation Oncology Pre-congress Workshop
 Gamma Knife Radiosurgery A tool for treating intracranial conditions CNSA Annual Congress 2016 Radiation Oncology Pre-congress Workshop ANGELA McBEAN Gamma Knife CNC State-wide Care Coordinator Gamma Knife
Gamma Knife Radiosurgery A tool for treating intracranial conditions CNSA Annual Congress 2016 Radiation Oncology Pre-congress Workshop ANGELA McBEAN Gamma Knife CNC State-wide Care Coordinator Gamma Knife
Public Statement: Medical Policy Statement:
 Medical Policy Title: Stereotactic ARBenefits Approval: 07/25/2012 Radiosurgery Effective Date: 01/01/2012 Document: ARB0321 Revision Date: Code(s): 77371 Radiation treatment delivery, Stereotactic radiosurgery
Medical Policy Title: Stereotactic ARBenefits Approval: 07/25/2012 Radiosurgery Effective Date: 01/01/2012 Document: ARB0321 Revision Date: Code(s): 77371 Radiation treatment delivery, Stereotactic radiosurgery
Stereotactic Radiosurgery. Extracranial Stereotactic Radiosurgery. Linear accelerators. Basic technique. Indications of SRS
 Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Gamma Knife radiosurgery with CT image-based dose calculation
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 6, 2015 Gamma Knife radiosurgery with CT image-based dose calculation Andy (Yuanguang) Xu, 1a Jagdish Bhatnagar, 1 Greg Bednarz, 1 Ajay Niranjan,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 6, 2015 Gamma Knife radiosurgery with CT image-based dose calculation Andy (Yuanguang) Xu, 1a Jagdish Bhatnagar, 1 Greg Bednarz, 1 Ajay Niranjan,
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Radiation Oncology Study Guide
 Radiation Oncology Study Guide For the Initial CertificationQualifying (Computer-Based) Examination General and Radiation Oncology This examination is designed to assess your understanding of the entire
Radiation Oncology Study Guide For the Initial CertificationQualifying (Computer-Based) Examination General and Radiation Oncology This examination is designed to assess your understanding of the entire
The clinical significance of persistent trigeminal nerve contrast enhancement in patients who undergo repeat radiosurgery
 CLINICAL ARTICLE J Neurosurg 127:219 225, 2017 The clinical significance of persistent trigeminal nerve contrast enhancement in patients who undergo repeat radiosurgery Seyed H. Mousavi, MD, 1 Berkcan
CLINICAL ARTICLE J Neurosurg 127:219 225, 2017 The clinical significance of persistent trigeminal nerve contrast enhancement in patients who undergo repeat radiosurgery Seyed H. Mousavi, MD, 1 Berkcan
Gamma. Knife PERFEXION. care. World-class. The Gamma Knife Program at Washington Hospital
 The Gamma Knife Program at Washington Hospital PERFEXION Fast, precise, minimally invasive treatment for neurological conditions. Locally based care by internationally Gamma recognized experts. World-class
The Gamma Knife Program at Washington Hospital PERFEXION Fast, precise, minimally invasive treatment for neurological conditions. Locally based care by internationally Gamma recognized experts. World-class
Stereotactic Radiosurgery and Proton Beam Therapy
 Last Review Date: January 12, 2018 Number: MG.MM.RA.13i Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: January 12, 2018 Number: MG.MM.RA.13i Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Acoustic neuromas (vestibular schwannomas) are generally
 CHAPTER 6 Navigating Change and the Acoustic Neuroma Story: Methods, Outcomes, and Myths L. Dade Lunsford, M.D., F.A.C.S., Ajay Niranjan, M.B.B.S., M.Ch., John C. Flickinger, M.D., and Douglas Kondziolka,
CHAPTER 6 Navigating Change and the Acoustic Neuroma Story: Methods, Outcomes, and Myths L. Dade Lunsford, M.D., F.A.C.S., Ajay Niranjan, M.B.B.S., M.Ch., John C. Flickinger, M.D., and Douglas Kondziolka,
STEREOTACTIC RADIATION THERAPY. Monique Blanchard ANUM Radiation Oncology Epworth HealthCare
 STEREOTACTIC RADIATION THERAPY Monique Blanchard ANUM Radiation Oncology Epworth HealthCare Overview Stereotactic radiation therapy at Epworth Healthcare What is stereotactic radiation therapy? Delivery
STEREOTACTIC RADIATION THERAPY Monique Blanchard ANUM Radiation Oncology Epworth HealthCare Overview Stereotactic radiation therapy at Epworth Healthcare What is stereotactic radiation therapy? Delivery
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Medical Policy Manual Surgery, Policy No. 16 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Next Review: June 2019 Last Review: February 2019 Effective: February 15, 2019 IMPORTANT REMINDER
Medical Policy Manual Surgery, Policy No. 16 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Next Review: June 2019 Last Review: February 2019 Effective: February 15, 2019 IMPORTANT REMINDER
Pineal Region Tumors. Diagnosis and Treatment Options
 Pineal Region Tumors. Diagnosis and Treatment Options Progress in Neurological Surgery Vol. 23 Series Editor L. Dade Lunsford Pittsburgh, Pa. Pineal Region Tumors Diagnosis and Treatment Options Volume
Pineal Region Tumors. Diagnosis and Treatment Options Progress in Neurological Surgery Vol. 23 Series Editor L. Dade Lunsford Pittsburgh, Pa. Pineal Region Tumors Diagnosis and Treatment Options Volume
Medical Benefit Effective Date: 01/01/13 Next Review Date: 09/13 Preauthorization* No Review Dates: 11/07, 07/08, 01/09, 01/10, 03/11, 01/12, 09/12
 Protocol Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy (60110) Medical Benefit Effective Date: 01/01/13 Next Review Date: 09/13 Preauthorization* No Review Dates: 11/07, 07/08, 01/09,
Protocol Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy (60110) Medical Benefit Effective Date: 01/01/13 Next Review Date: 09/13 Preauthorization* No Review Dates: 11/07, 07/08, 01/09,
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
GAMMA KNIFE NEUROSURGERY A REVIEW
 GAMMA KNIFE NEUROSURGERY A REVIEW Michael Torrens Department of Gamma Knife Radiosurgery and Neurosurgery Clinic, Hygeia Hospital, Athens. ABSTRACT Gamma Knife radiosurgery has an established therapeutic
GAMMA KNIFE NEUROSURGERY A REVIEW Michael Torrens Department of Gamma Knife Radiosurgery and Neurosurgery Clinic, Hygeia Hospital, Athens. ABSTRACT Gamma Knife radiosurgery has an established therapeutic
Leksell Gamma Knife Icon. Treatment information
 Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
Neuro-oncology Update Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013
 Neuro-oncology Update 2013 Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013 Case 1 58 year old man with recent facial droop and HA s Thin, cachectic
Neuro-oncology Update 2013 Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013 Case 1 58 year old man with recent facial droop and HA s Thin, cachectic
MEDICAL POLICY SUBJECT: STEREOTACTIC RADIOSURGERY AND STEREOTACTIC BODY RADIATION THERAPY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: STEREOTACTIC RADIOSURGERY PAGE: 1 OF: 9 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: STEREOTACTIC RADIOSURGERY PAGE: 1 OF: 9 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Brain cancer survival rate mayo clinic
 Brain cancer survival rate mayo clinic Ed' s Guide to Alternative Therapies. Contents: Acai Berries Acupuncture Artemisinin for cancer Beta-mannan to reverse dysplasia of the cervix Anti-Malignin antibody.
Brain cancer survival rate mayo clinic Ed' s Guide to Alternative Therapies. Contents: Acai Berries Acupuncture Artemisinin for cancer Beta-mannan to reverse dysplasia of the cervix Anti-Malignin antibody.
Our experts who pioneered fractionated stereotactic
 INTRODUCTION Our experts who pioneered fractionated stereotactic radiosurgery in the Western Hemisphere have tremendous experience treating many kinds of primary and metastatic cancers as well as benign
INTRODUCTION Our experts who pioneered fractionated stereotactic radiosurgery in the Western Hemisphere have tremendous experience treating many kinds of primary and metastatic cancers as well as benign
Neuroimaging Core Curriculum
 Neuroimaging Core Curriculum Program Content The purpose of the training program is to prepare the physician for the independent practice of neuroimaging. Neuroimaging is the subspecialty of Neurology
Neuroimaging Core Curriculum Program Content The purpose of the training program is to prepare the physician for the independent practice of neuroimaging. Neuroimaging is the subspecialty of Neurology
Neurosurgical Management of Brain Tumours. Nicholas Little Neurosurgeon RNSH
 Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Acoustic Neuroma. Presenting Signs and Symptoms of an Acoustic Neuroma:
 Acoustic Neuroma An acoustic neuroma is a benign tumor which arises from the nerves behind the inner ear and which may affect hearing and balance. The incidence of symptomatic acoustic neuroma is estimated
Acoustic Neuroma An acoustic neuroma is a benign tumor which arises from the nerves behind the inner ear and which may affect hearing and balance. The incidence of symptomatic acoustic neuroma is estimated
Radiosurgery by Leksell gamma knife. Josef Novotny, Na Homolce Hospital, Prague
 Radiosurgery by Leksell gamma knife Josef Novotny, Na Homolce Hospital, Prague Radiosurgery - Definition Professor Lars Leksell The tools used by the surgeon must be adapted to the task and where the human
Radiosurgery by Leksell gamma knife Josef Novotny, Na Homolce Hospital, Prague Radiosurgery - Definition Professor Lars Leksell The tools used by the surgeon must be adapted to the task and where the human
Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined Approach
 Radiosurgery as part of the neurosurgical armamentarium: Educational Symposium November 24 th 2011 Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined
Radiosurgery as part of the neurosurgical armamentarium: Educational Symposium November 24 th 2011 Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR EPENDYMOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR EPENDYMOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR EPENDYMOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
Serial Follow-up MR Imaging after Gamma Knife Radiosurgery for Vestibular Schwannoma
 AJNR Am J Neuroradiol 21:1540 1546, September 2000 Serial Follow-up MR Imaging after Gamma Knife Radiosurgery for Vestibular Schwannoma Hiroyuki Nakamura, Hidefumi Jokura, Kou Takahashi, Nagatoshi Boku,
AJNR Am J Neuroradiol 21:1540 1546, September 2000 Serial Follow-up MR Imaging after Gamma Knife Radiosurgery for Vestibular Schwannoma Hiroyuki Nakamura, Hidefumi Jokura, Kou Takahashi, Nagatoshi Boku,
A lthough more than 90% of intracranial meningiomas are
 226 PAPER Complications after gamma knife radiosurgery for benign meningiomas J H Chang, J W Chang, J Y Choi, Y G Park, S S Chung... See end of article for authors affiliations... Correspondence to: Professor
226 PAPER Complications after gamma knife radiosurgery for benign meningiomas J H Chang, J W Chang, J Y Choi, Y G Park, S S Chung... See end of article for authors affiliations... Correspondence to: Professor
DECISION MAKING IN AVM TREATMENT STRATEGY TREATMENT BOARD SYSTEM AT TOHOKU UNIVERSITY
 Kitakanto Med. J. (S1) : 79-84, 1998 79 DECISION MAKING IN AVM TREATMENT STRATEGY TREATMENT BOARD SYSTEM AT TOHOKU UNIVERSITY Takashi Yoshimoto, Hidefumi Jokura Department of Neurosurgery, Tohoku University
Kitakanto Med. J. (S1) : 79-84, 1998 79 DECISION MAKING IN AVM TREATMENT STRATEGY TREATMENT BOARD SYSTEM AT TOHOKU UNIVERSITY Takashi Yoshimoto, Hidefumi Jokura Department of Neurosurgery, Tohoku University
STEREOTACTIC RADIOSURGERY & STEREOTACTIC BODY RADIATION THERAPY
 STEREOTACTIC RADIOSURGERY & STEREOTACTIC BODY RADIATION THERAPY Protocol: NEU017 Effective Date: November 1, 2017 Table of Contents Page COMMERCIAL & MEDICAID COVERAGE RATIONALE... 1 MEDICARE COVERAGE
STEREOTACTIC RADIOSURGERY & STEREOTACTIC BODY RADIATION THERAPY Protocol: NEU017 Effective Date: November 1, 2017 Table of Contents Page COMMERCIAL & MEDICAID COVERAGE RATIONALE... 1 MEDICARE COVERAGE
Stereotactic radiosurgery for idiopathic trigeminal neuralgia
 J Neurosurg 97:347 353, 2002 Stereotactic radiosurgery for idiopathic trigeminal neuralgia BRUCE E. POLLOCK, M.D., LOI K. PHUONG, M.D., DEBORAH A. GORMAN, R.N., ROBERT L. FOOTE, M.D., AND SCOTT L. STAFFORD,
J Neurosurg 97:347 353, 2002 Stereotactic radiosurgery for idiopathic trigeminal neuralgia BRUCE E. POLLOCK, M.D., LOI K. PHUONG, M.D., DEBORAH A. GORMAN, R.N., ROBERT L. FOOTE, M.D., AND SCOTT L. STAFFORD,
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Medical Policy Manual Surgery, Policy No. 16 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Next Review: June 2018 Last Review: August 2017 Effective: October 1, 2017 IMPORTANT REMINDER
Medical Policy Manual Surgery, Policy No. 16 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Next Review: June 2018 Last Review: August 2017 Effective: October 1, 2017 IMPORTANT REMINDER
Radiosurgery and fractionated radiation therapy: comparison of different techniques in an in vivo rat glioma model
 J Neurosurg 84:1033 1038, 1996 Radiosurgery and fractionated radiation therapy: comparison of different techniques in an in vivo rat glioma model DOUGLAS KONDZIOLKA, M.D., M.SC., F.R.C.S.(C), SALVADOR
J Neurosurg 84:1033 1038, 1996 Radiosurgery and fractionated radiation therapy: comparison of different techniques in an in vivo rat glioma model DOUGLAS KONDZIOLKA, M.D., M.SC., F.R.C.S.(C), SALVADOR
Extracranial doses in stereotactic and conventional radiotherapy for pituitary adenomas
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 7, NUMBER 2, SPRING 2006 Extracranial doses in stereotactic and conventional radiotherapy for pituitary adenomas Thomas Samuel Ram, a Paul B. Ravindran,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 7, NUMBER 2, SPRING 2006 Extracranial doses in stereotactic and conventional radiotherapy for pituitary adenomas Thomas Samuel Ram, a Paul B. Ravindran,
Imaging the Spinal Cord & Intradural Disease
 Department of Radiology University of California San Diego Imaging the Spinal Cord & Intradural Disease John R. Hesselink, M.D. Spinal Cord Diseases Tumors Syringohydromyelia Trauma Ischemia / Infarction
Department of Radiology University of California San Diego Imaging the Spinal Cord & Intradural Disease John R. Hesselink, M.D. Spinal Cord Diseases Tumors Syringohydromyelia Trauma Ischemia / Infarction
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Specialised Services Policy: CP22. Stereotactic Radiosurgery
 Specialised Services Policy: CP22 Document Author: Assistant Director of Planning Executive Lead: Director of Planning ad Performance Approved by: Management Group Issue Date: 01 July 2015 Review Date:
Specialised Services Policy: CP22 Document Author: Assistant Director of Planning Executive Lead: Director of Planning ad Performance Approved by: Management Group Issue Date: 01 July 2015 Review Date:
Cyberknife Radiotherapy for Vestibular Schwannoma
 Cyberknife Radiotherapy for Vestibular Schwannoma GordonT. Sakamoto, MD a, *, Nikolas Blevins, MD b, Iris C. Gibbs, MD c KEYWORDS Stereotactic radiosurgery Vestibular schwannomas Cyberknife Fractionation
Cyberknife Radiotherapy for Vestibular Schwannoma GordonT. Sakamoto, MD a, *, Nikolas Blevins, MD b, Iris C. Gibbs, MD c KEYWORDS Stereotactic radiosurgery Vestibular schwannomas Cyberknife Fractionation
Ac o u s t i c neuromas, also known as vestibular. Predictors of hearing preservation after stereotactic radiosurgery for acoustic neuroma
 J Neurosurg 111:863 873, 2009 Predictors of hearing preservation after stereotactic radiosurgery for acoustic neuroma Clinical article Hi d e y u k i Ka n o, M.D., Ph.D., 1,3 Do u g l a s Ko n d z i o
J Neurosurg 111:863 873, 2009 Predictors of hearing preservation after stereotactic radiosurgery for acoustic neuroma Clinical article Hi d e y u k i Ka n o, M.D., Ph.D., 1,3 Do u g l a s Ko n d z i o
Gamma Knife surgery for trigeminal schwannoma
 J Neurosurg 106:839 845, 2007 Gamma Knife surgery for trigeminal schwannoma JASON SHEEHAN, M.D., PH.D., CHUN PO YEN, M.D., YASSER ARKHA, M.D., DAVID SCHLESINGER, PH.D., AND LADISLAU STEINER, M.D., PH.D.
J Neurosurg 106:839 845, 2007 Gamma Knife surgery for trigeminal schwannoma JASON SHEEHAN, M.D., PH.D., CHUN PO YEN, M.D., YASSER ARKHA, M.D., DAVID SCHLESINGER, PH.D., AND LADISLAU STEINER, M.D., PH.D.
PITUITARY PARASELLAR LESIONS. Kim Learned, MD
 PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
Paraganglioma of the Skull Base. Ross Zeitlin, MD Medical College of Wisconsin Milwaukee, WI
 Paraganglioma of the Skull Base Ross Zeitlin, MD Medical College of Wisconsin Milwaukee, WI Case Presentation 63-year-old female presents with right-sided progressive conductive hearing loss for several
Paraganglioma of the Skull Base Ross Zeitlin, MD Medical College of Wisconsin Milwaukee, WI Case Presentation 63-year-old female presents with right-sided progressive conductive hearing loss for several
The impact of cobalt-60 source age on biologically effective dose in high-dose functional Gamma Knife radiosurgery
 laboratory investigation J Neurosurg (Suppl 1) 125:154 159, 2016 The impact of cobalt-60 source age on biologically effective dose in high-dose functional Gamma Knife radiosurgery Benjamin H. Kann, MD,
laboratory investigation J Neurosurg (Suppl 1) 125:154 159, 2016 The impact of cobalt-60 source age on biologically effective dose in high-dose functional Gamma Knife radiosurgery Benjamin H. Kann, MD,
brain talk brain talk IRSA Inside: Definition 2 Radiosurgery: First Choice for Many 3 Management Algorithm 7 SRS and FSR 8 Patient Story 9 Scanning 10
 brain talk brain talk An Educational Publication Volume 9, Number 2 ISSN 1086-427X Acoustic Neuroma & Patient Choice Inside: Definition 2 : First Choice for Many 3 Management Algorithm 7 SRS and FSR 8
brain talk brain talk An Educational Publication Volume 9, Number 2 ISSN 1086-427X Acoustic Neuroma & Patient Choice Inside: Definition 2 : First Choice for Many 3 Management Algorithm 7 SRS and FSR 8
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Despite recent progress in microsurgical techniques, endovascular
 Application of Single-Stage Stereotactic Radiosurgery for Cerebral Arteriovenous Malformations >10 cm 3 Shunya Hanakita, MD; Tomoyuki Koga, MD, PhD; Masahiro Shin, MD, PhD; Hiroshi Igaki, MD, PhD; Nobuhito
Application of Single-Stage Stereotactic Radiosurgery for Cerebral Arteriovenous Malformations >10 cm 3 Shunya Hanakita, MD; Tomoyuki Koga, MD, PhD; Masahiro Shin, MD, PhD; Hiroshi Igaki, MD, PhD; Nobuhito
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Tumor and Skull Base Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Tumor / Skull Base Neurosurgery
Introduction to Neurosurgical Subspecialties: Tumor and Skull Base Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Tumor / Skull Base Neurosurgery
Role of protons, heavy ions and BNCT in brain tumors
 Role of protons, heavy ions and BNCT in brain tumors Prof G K Rath Head, NCI (AIIMS-2) Chief, Dr. BRA IRCH, Professor Radiation Oncology All India Institute of Medical Sciences, New Delhi 1 Overview of
Role of protons, heavy ions and BNCT in brain tumors Prof G K Rath Head, NCI (AIIMS-2) Chief, Dr. BRA IRCH, Professor Radiation Oncology All India Institute of Medical Sciences, New Delhi 1 Overview of
ORIGINAL PAPER USEFUL BASE PLATE TO SUPPORT THE HEAD DURING LEKSELL SKULL FRAME PLACEMENT IN GAMMA KNIFE PERFEXION RADIOSURGERY
 Nagoya J. Med. Sci. 76. 27 ~ 33, 2014 ORIGINAL PAPER USEFUL BASE PLATE TO SUPPORT THE HEAD DURING LEKSELL SKULL FRAME PLACEMENT IN GAMMA KNIFE PERFEXION RADIOSURGERY HISATO NAKAZAWA 1,2, MSc; YOSHIMASA
Nagoya J. Med. Sci. 76. 27 ~ 33, 2014 ORIGINAL PAPER USEFUL BASE PLATE TO SUPPORT THE HEAD DURING LEKSELL SKULL FRAME PLACEMENT IN GAMMA KNIFE PERFEXION RADIOSURGERY HISATO NAKAZAWA 1,2, MSc; YOSHIMASA
ORIGINAL ARTICLE GAMMA KNIFE STEREOTACTIC RADIOSURGERY FOR SALIVARY GLAND NEOPLASMS WITH BASE OF SKULL INVASION FOLLOWING NEUTRON RADIOTHERAPY
 ORIGINAL ARTICLE GAMMA KNIFE STEREOTACTIC RADIOSURGERY FOR SALIVARY GLAND NEOPLASMS WITH BASE OF SKULL INVASION FOLLOWING NEUTRON RADIOTHERAPY James G. Douglas, MD, MS, 1,2 Robert Goodkin, MD, 1,2 George
ORIGINAL ARTICLE GAMMA KNIFE STEREOTACTIC RADIOSURGERY FOR SALIVARY GLAND NEOPLASMS WITH BASE OF SKULL INVASION FOLLOWING NEUTRON RADIOTHERAPY James G. Douglas, MD, MS, 1,2 Robert Goodkin, MD, 1,2 George
Microsurgical Resection of Incompletely Obliterated Intracranial Arteriovenous Malformations Following Stereotactic Radiosurgery
 II-2. Selection of Treatment Microsurgical Resection of Incompletely Obliterated Intracranial Arteriovenous Malformations Following Stereotactic Radiosurgery Steven D. CHANG*, Gary K. STEINBERG*, Richard
II-2. Selection of Treatment Microsurgical Resection of Incompletely Obliterated Intracranial Arteriovenous Malformations Following Stereotactic Radiosurgery Steven D. CHANG*, Gary K. STEINBERG*, Richard
Overview of radiosurgery for benign brain tumors
 Overview of radiosurgery for benign brain tumors Anuj V. Peddada, M.D. Department of Radiation Oncology Penrose Cancer Center Colorado Springs, CO Objectives Provide overview of benign brain tumors meningiomas
Overview of radiosurgery for benign brain tumors Anuj V. Peddada, M.D. Department of Radiation Oncology Penrose Cancer Center Colorado Springs, CO Objectives Provide overview of benign brain tumors meningiomas
Histopathological Study and Categorisation of Brain Tumors
 Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Stereotactic radiosurgery (SRS) is the least invasive
 » This article has been updated from its originally published version to correct Table 1 and terminology in the text. See the corresponding erratum notice, DOI: 10.3171/2017.3.JNS151624a. «CLINICAL ARTICLE
» This article has been updated from its originally published version to correct Table 1 and terminology in the text. See the corresponding erratum notice, DOI: 10.3171/2017.3.JNS151624a. «CLINICAL ARTICLE
Directorate Medical Operations Patients and Information Nursing Policy Commissioning Development. Clinical Reference Group Chairs
 Clinical Commissioning Policy: Stereotactic Radiosurgery/ Radiotherapy for Glomus Tumours (skull base paragangliomas, glomus jugulare tumours) September 2013 Reference: NHS ENGLAND D05/P/f England 1 NHS
Clinical Commissioning Policy: Stereotactic Radiosurgery/ Radiotherapy for Glomus Tumours (skull base paragangliomas, glomus jugulare tumours) September 2013 Reference: NHS ENGLAND D05/P/f England 1 NHS
Stereotactic radiosurgery in the management of acoustic neuromas associated with neurofibromatosis Type 2
 Stereotactic radiosurgery in the management of acoustic neuromas associated with neurofibromatosis Type 2 Brian R. Subach, M.D., Douglas Kondziolka, M.D., M. Sc., F.R.C.S.(C), L. Dade Lunsford, M.D., F.A.C.S.,
Stereotactic radiosurgery in the management of acoustic neuromas associated with neurofibromatosis Type 2 Brian R. Subach, M.D., Douglas Kondziolka, M.D., M. Sc., F.R.C.S.(C), L. Dade Lunsford, M.D., F.A.C.S.,
Long-term control of large pontine arteriovenous malformation using gamma knife therapy: a review with illustrative case
 Long-term control of large pontine arteriovenous malformation using gamma knife therapy: a review with illustrative case Martin M. Mortazavi 1, Daxa Patel 1, Christoph J. Griessenauer 1, R. Shane Tubbs
Long-term control of large pontine arteriovenous malformation using gamma knife therapy: a review with illustrative case Martin M. Mortazavi 1, Daxa Patel 1, Christoph J. Griessenauer 1, R. Shane Tubbs
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR HAEMANGIOBLASTOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR HAEMANGIOBLASTOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR HAEMANGIOBLASTOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
