The Use of Early Postoperative MR in Detecting Residual Juvenile Cerebellar Pilocytic Astrocytoma
|
|
|
- Darcy Short
- 6 years ago
- Views:
Transcription
1 AJNR Am J Neuroradiol 19: , January 1998 The Use of Early Postoperative MR in Detecting Residual Juvenile Cerebellar Pilocytic Astrocytoma Nancy K. Rollins, Perry Nisen, and Kenneth N. Shapiro PURPOSE: We compared visibility of residual juvenile cerebellar pilocytic astrocytomas (JPAs) on early postoperative and follow-up MR studies to determine whether early postoperative MR imaging has a valid role as a baseline study. METHODS: We reviewed the MR images of 21 consecutive children who had undergone resection of cerebellar JPA. The diagnosis of residual tumor was made on the basis of nodular enhancement that corresponded to enhancing tumor on the preoperative MR studies and/or nonenhancing nodular T2 signal that corresponded to nonenhancing tumor. Because no patient received chemotherapy or radiation therapy, abnormal T2 signal or enhancement on the early postoperative study that resolved on the follow-up study was presumed to be due to peritumoral edema and/or surgical manipulation. Nodular T2 signal and/or enhancement in the tumor bed not seen on the initial postoperative MR study but present on the subsequent MR study and unchanged on serial follow-up MR studies was presumed to represent residual tumor rather than tumor that had recurred. RESULTS: Compared with follow-up studies, the initial postoperative MR images were true-positive for residual tumor in six patients, false-positive in five, equivocal for residual tumor in four, true-negative in five, and false-negative in one. Residual tumor did not consistently enhance, and peritumoral edema and changes resulting from surgical manipulation tended to mask or simulate residual tumor. CONCLUSION: Early postoperative MR imaging is not accurate in differentiating residual JPA from postoperative changes, and the role of early postoperative MR imaging as a baseline study for comparison with further studies is questionable. Juvenile pilocytic astrocytomas (JPAs) are among the most common brain tumors of childhood. Although histologically similar to JPAs arising from other parts of the brain, JPAs that arise from the cerebellum act biologically more benign than those that arise in other locations (1, 2). Cerebellar JPAs have the best long-term prognosis when total resection is achieved (1). Magnetic resonance (MR) imaging has, for the most part, replaced computed tomography (CT) in the radiologic evaluation of posterior fossa tumors, such as JPAs. The optimal timing for postoperative MR imaging to detect residual tumor is controversial (3, 4). The literature recommends CT as Received February 26, 1997; accepted after revision June 30. From the Departments of Radiology (N.K.R.) and Pediatrics (P.N.), Divisions of Pediatric Radiology and Hematology and Oncology, University of Texas Southwestern Medical Center and Neurosurgeons for Children (K.N.S.), Dallas. Address reprint requests to Nancy Rollins, MD, Department of Radiology, Children s Medical Center of Dallas, 1935 Motor St, Dallas, TX American Society of Neuroradiology soon as possible after surgery, preferably within 24 hours before nonneoplastic contrast enhancement resulting from surgical manipulation becomes radiologically apparent (3, 4). Although CT and MR imaging differ considerably in sensitivity to abnormal tissue on precontrast and postcontrast studies (5), clinical recommendations based on the CT literature have been applied to MR imaging, as in our institution, where cranial MR studies have traditionally been obtained as soon as possible after surgical resection of lowgrade cerebellar astrocytomas. We examined the role of early postoperative MR studies as a baseline for comparison with subsequent studies; specifically, to determine how accurate the early postoperative MR studies are in differentiating residual tumor from nonneoplastic edema and changes resulting from surgical manipulation. Methods From January 1991 through November 1996, 43 children with de novo intracranial neoplasms histologically confirmed as JPA were seen at our institution. In 24 of these patients, the 151
2 152 ROLLINS AJNR: 19, January 1998 TABLE 1: Comparison of perioperative and follow-up MR studies Case Age, y/ Sex Follow-up, mo Time to Initial MR, d Early Postoperative MR Findings Follow-up MR Findings 1 7/F* 54 6 Residual Residual 2 12/M 38 3 Residual No tumor 3 6/F 52 5 Residual Residual 4 5/F 62 3 Residual Residual 5 3/F 44 5 Residual No tumor 6 2/M 29 2 Residual No tumor 7 4/M 46 4 Residual No tumor 8 7/F 16 3 Residual Residual 9 3/F 29 4 Residual Residual 10 5/M 14 1 Residual No tumor 11 15/F 29 2 Residual Residual 12 5/F 29 1? Residual No tumor 13 7/M 28 2? Residual No tumor 14 4/F 40 5? Residual Residual 15 8/F 14 3? Residual No tumor 16 4/M 34 1 No tumor No tumor 17 4/F 48 5 No tumor Residual 18 5/F 58 6 No tumor No tumor 19 5/F 38 2 No tumor No tumor 20 4/M 8 3 No tumor No tumor 21 7/M 57 3 No tumor No tumor * Figure 3. Figure 1. Figure 2. tumors arose from the cerebellar hemisphere or vermis. Our study group consisted of 21 of these 24 consecutive children, ages 3 to 16 years, who had undergone posterior fossa craniectomy or craniotomy at our institution over this time interval. Criteria for inclusion in the study were as follows: availability of preoperative contrast-enhanced MR images (n 20) or CT scans (n 1), postoperative MR images obtained within 7 days of surgery, follow-up MR studies from this (n 17) or an outside (n 4) institution, and no chemotherapy or radiation therapy. After the posterior fossa tumors were identified radiologically, the patients had been started on high-dose dexamethasone, which was tapered postoperatively. At the time of follow-up, therefore, no patient was receiving exogenous steroids. MR imaging was done on a 0.5-T superconducting unit in 13 patients and on a 1.5-T unit in eight. Precontrast and postcontrast T1-weighted (525/20/2 [repetition time/echo time/excitations]) spin-echo sequences were obtained in the sagittal and axial planes, and proton density and heavily T2-weighted ( /35,90/1) conventional spin-echo sequences were obtained in the axial plane. The early postoperative and all subsequent follow-up MR images were assessed for abnormal contrast enhancement and T2 changes. The diagnosis of residual tumor was made on the basis of nodular enhancement that corresponded to enhancing tumor and/or nonenhancing nodular T2 signal that corresponded to nonenhancing tumor on the preoperative MR study. Findings on the initial postoperative MR study were compared with those on follow-up MR studies. Because no patient received chemotherapy or radiation therapy, abnormal T2 signal or enhancement observed on the early postoperative study that resolved on follow-up studies was presumed to be due to peritumoral edema and/or surgical manipulation. Nodular T2 signal and/or enhancement in the tumor bed not seen on the initial postoperative MR study but present on the subsequent MR images and unchanged on serial follow-up MR studies was presumed to represent residual tumor rather than tumor that had recurred. Results Early postoperative MR images were obtained a mean of 3 days after surgery (range, 1 to 6 days) (Table 1). Thirteen patients were imaged within 72 hours of surgery, including one at 16 hours and one at 24 hours after surgery. Three patients were restudied 5 weeks after surgery, and eight patients at 12 weeks after surgery for a variety of clinical indications, including nonspecific neurologic symptoms (n 3), possible hydrocephalus (n 3), and suspicion of residual tumor (n 5). The remaining 10 patients underwent follow-up MR imaging 6 months after surgery as per in-house protocol. The total duration of neuroradiologic follow-up was 8 to 62 months (mean, 37 months), during which time MR studies were obtained at 6-month intervals. The early postoperative MR images showed confluent increased T2 signal around the tumor bed in 16 patients. Eleven of the 14 patients with abnormal T2 signal around the tumor bed also had areas of abnormal enhancement. Eight patients had curvilinear or punctate enhancement while in three patients the enhancement was nodular. Five patients had no areas of abnormal T2 signal and no abnormal enhancement at the tumor bed. Overall, the early postoperative MR studies were interpreted as showing no residual tumor in six patients, equivocal for tumor in four patients, and positive for residual tumor in 11 patients. One patient was reexamined 3 days later; residual tumor was found but incompletely resected. Eight patients had evidence of residual tumor on follow-up MR images; in six, tumor was correctly identified on the initial postoperative MR study while
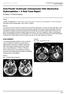
3 AJNR: 19, January 1998 JUVENILE ASTROCYTOMA 153 in two patients the tumor was missed (Table 2). Compared with the follow-up MR studies, the initial postoperative MR study was true-positive for residual tumor in six patients (Fig 1), false-positive in five (Fig 2), suspicious for residual tumor where none was TABLE 2: Sensitivity and specificity of early postoperative MR Residual Tumor at Follow-up No Residual Tumor Total Residual tumor on early MR No residual tumor Questionable tumor Total Sensitivity: TP/TP FN 6/ Specificity: TN/TN FP 5/ Positive predictive value: TP/TP FP 6/ Negative predictive value: TN/TN FN 5/ Note. TN indicates true negative; TP, true positive; FP, false positive; and FN, false negative. present at follow-up in three, suspicious for residual tumor confirmed at follow-up in one, true-negative in five, and false-negative in one (Fig 3). In eight patients, the enhancement seen on the initial postoperative MR study had resolved on subsequent MR studies and was presumably nonneoplastic. Nonneoplastic enhancement was either curvilinear or curvilinear with punctate nodules and was seen as early as 16 hours after surgery. Neoplastic enhancement was curvilinear in one patient. Discussion On the basis of this study, we conclude that early postoperative MR imaging is not accurate in differentiating residual JPA from postoperative changes and suggest that early postoperative MR imaging should not be used as a baseline examination. Residual tumor does not consistently enhance and peritumoral edema and changes resulting from surgical manipulation may mask or simulate residual tumor. Documentation of residual cerebellar JPA in the FIG 1. A 6-year-old girl with JPA arising from the cerebellar vermis. This case illustrates the importance of T2-weighted MR sequences in the detection of residual JPA, as residual tumor may not enhance. A, Preoperative proton density weighted image (3250/35/1) shows well-defined hyperintense tumor with no peritumoral edema. B, Preoperative contrast-enhanced T1-weighted image shows predominantly solid tumor mass with areas of cystic change. Notice that the periphery of the tumor mass has minimal enhancement (short arrows). Long arrow indicates enhancing nodule surrounded by nonenhancing tumor. C, Contrast-enhanced T1-weighted image 72 hours after surgery shows minimal residual enhancing tumor (arrow). D, Postoperative proton density weighted image shows more tumor (arrows) than is identifiable on the contrast-enhanced images.
4 154 ROLLINS AJNR: 19, January 1998 FIG 2. A 4-year-old boy with right cerebellar JPA in whom abnormal T2 signal mimicked residual tumor on perioperative MR images. In this case, absence of significant enhancement on the postoperative MR study was an accurate indication of total tumor resection. A, Preoperative proton density weighted image shows large hyperintense mass with extensive peritumoral edema extending into brain stem (arrow). B, Proton density weighted image 72 hours after craniectomy shows considerable abnormal signal within the right cerebellum, suggestive of residual tumor. C, Contrast-enhanced T1-weighted image shows minimal enhancement around the periphery of the tumor bed. D, Proton density weighted image 3 months later shows complete resolution of abnormal T2 signal. Patient was tumor-free 46 months later. immediate postoperative period does not influence clinical management (1, 2). The tumor is not usually treated with irradiation, the role of adjuvant chemotherapy in this setting is controversial, and in the absence of bulky residual disease most neurosurgeons will defer reexploration. Nonetheless, it is a common clinical practice to obtain MR images as soon as possible after surgery. In fact, patient enrollment into the Children s Cancer Group (CCG) and Pediatric Oncology Group (POG) protocols 9891 and 9130, respectively, which studied the natural history of newly diagnosed low-grade astrocytomas in children receiving radical surgical resection as the sole treatment, stipulated imaging, preferably MR, within 72 hours of surgery (Study Committee Progress Report CCG-9891/POG-9130). The rationale for early postoperative imaging after resection of cerebellar JPA is based on reports that nonneoplastic postsurgical changes do not enhance by CT before 5 days, whereas residual neoplastic disease shows enhancement immediately after surgery (3, 6 8). Steinbok et al (6) studied 21 children with a variety of benign and malignant tumors in different locations, eight of whom had cerebellar astrocytomas. All the patients in this study had undergone contrast-enhanced CT within 72 hours of tumor resection. Enhancement was seen within the tumor bed in three of the eight patients with cerebellar astrocytomas, although none had evidence of tumor on subsequent follow-up CT studies. One patient had biopsy-proved residual cerebellar astrocytoma that did not enhance on the CT study done early in the postoperative period. The authors concluded that the presence of contrast enhancement on the immediate postoperative CT scan does not distinguish residual tumor from changes due to surgical manipulation. The editor s brief commentary, which followed, suggested that the patients were not imaged early enough and stressed the need for CT within 12 to 24 hours after surgery (6). Nonneoplastic enhancement within the tumor bed is detectable much earlier with MR imaging than with CT because of the superior sensitivity of MR imaging to small amounts of extravascular contrast material
5 AJNR: 19, January 1998 JUVENILE ASTROCYTOMA 155 FIG 3. A 5-year-old girl with left cerebellar JPA. Residual tumor failed to enhance on the perioperative MR study, presumably because of exogenous steroids. A, Preoperative proton density weighted image shows extensive peritumoral edema involving left middle cerebellar peduncle. B, Proton density weighted image 3 days after craniectomy shows considerable residual edema. Arrow indicates nodule, suggestive of residual tumor. C, Contrast-enhanced MR image 3 days after surgery shows minimal enhancement in the tumor bed. D, Contrast-enhanced MR image 5 weeks later shows interval development of an enhancing nodule along the ventral aspect of the tumor bed (arrow). E, Another enhancing nodule is seen studding the lateral aspect of the tumor bed (arrow). F, Proton density weighted image 5 weeks after surgery shows the peritumoral edema has resolved, revealing two nodules (arrows), corresponding to the abnormal enhancement seen on the contrast-enhanced MR study but differing in location from the apparent tumor nodule seen on the proton density weighted image from the early postoperative MR study. Presumably, the residual tumor was masked on the perioperative MR study by edema. The tumor has remained stable over the ensuing 60 months. (5). Nonneoplastic enhancement may be seen on MR images within 24 hours of surgery (5). We frequently observed contrast enhancement at the tumor bed on the initial postoperative MR study; enhancement was seen in nine of the 12 patients imaged within 72 hours of surgery and as early as 16 hours after surgery. We found that nonneoplastic enhancement was usually but not invariably curvilinear and/or punctate while neoplastic enhancement was nodular, but that the absence of nodular enhancement did not always correlate with absence of tumor. Of the eight patients with residual tumor, three had minimal or no enhancement on the early postoperative MR studies despite the fact that the tumor had enhanced on the preoperative study and showed enhancement on follow-up studies. Lack of neoplastic enhancement on the initial postoperative MR study that was clearly visible at follow-up may have been due to the effects of the high-dose exogenous steroids routinely given in the perioperative period. Increased T2 signal at the surgical site may be due to edema, surgical manipulation, or residual tumor (4, 9). The use of contrast material increases the sensitivity of MR imaging but does not necessarily differentiate abnormal T2 signal due to tumor from that due to surgical manipulation (10 12). Moreover,
6 156 ROLLINS AJNR: 19, January 1998 areas of abnormal enhancement may not correlate with tumor margins; nonenhancing tumor may be visible only on the T2-weighted images (11, 12). While abnormal T2 signal due to neoplastic disease should persist on sequential MR studies, abnormal T2 signal due to surgical manipulation or peritumoral edema should resolve. We found that nonneoplastic edema was maximal on the initial postoperative MR study but resolved by 4 to 6 weeks. However, in the absence of abnormal enhancement, nodular T2 signal due to tumor cannot reliably be differentiated from gliosis. In our study, the neurosurgeons reported gross total resection of tumor in 17 of 21 patients and were correct in 12 of the 17. There were no cases in which the surgeon thought tumor was left but none was found by MR imaging. We agree with Schneider et al (2), who stated that surgeons tend to overestimate the extent of resection; a conclusion that underscores the need for postoperative imaging. However, because findings on immediate postoperative MR images may be false-positive or false-negative for tumor, we defer MR imaging until 4 to 6 weeks after surgery in this clinical setting. Although gross total resection of cerebellar JPA is associated with the best clinical outcome, even patients with subtotally resected tumor tend to have long event-free survivals. Schneider et al (2) followed up 23 patients with JPA over 5 years, during which time no patient had CT evidence of tumor progression. The follow-up period for the eight patients with residual tumor in our study was 8 to 62 months, during which time no patient had demonstrable tumor growth, underwent reexploration, or required chemotherapy or radiation therapy. However, as small nodules of residual JPA may grow and require further therapy, radiologic surveillance to detect clinically asymptomatic tumor growth is indicated. The duration and frequency of neuroradiologic surveillance may vary depending on the appearance of the tumor bed on baseline MR studies. Patients with no abnormal T2 signal or enhancement at the tumor bed are probably at less risk for recurrence than those with equivocal MR findings. Surveillance protocols should evaluate the cost of sequential MR studies and the benefits obtained from early detection of recurrence, and recommendations or guidelines should be revised accordingly. Acknowledgments We thank Kathryn Fletcher for manuscript preparation, Alison Russell for photography, and Naomi Winick for manuscript review. References 1. Undjian S, Marinov M, Georgiev K. Long-term follow-up after surgical treatment of cerebellar astrocytomas in 100 children. Childs Nerv Syst 1989;5: Schneider JH, Raffel C, McComb JG. Benign cerebellar astrocytomas of childhood. Neurosurgery 1992;30: Cairncross JG, Pexman JHW, Rathbone MP, DelMaestro RF. Postoperative contrast enhancement in patients with brain tumor. Ann Neurol 1985;17: Dickman CA, Rekate HL, Bird CR, Drayer BP, Medina M. Nonenhanced and gadolinium-dtpa-enhanced MR imaging in postoperative evaluation in pediatric brain tumors. J Neurosurg 1989; 71: Elster AD, DiPersio DA. Cranial postoperative site: assessment with contrast-enhanced MR imaging. Radiology 1990;174: Steinbok P, Poskitt K, Cochrane DD, Flodmark OO. Early computed tomographic scanning after resection of brain tumors in children. Childs Nerv Syst 1991;7: Rao CVGK, Kishore PRS, Bartlett J, Brennan TG. Computed tomography in the postoperative patient. Neuroradiology 1980;19: Jeffries BF, Kishore PRS, Singh KS, Ghatak NR, Krempa J. Contrast enhancement in the postoperative brain. Radiology 1981;139: Bird CR, Drayer BP, Medina J, Rekate HL, Flom RA, Hodak JA. Gd-DTPA enhanced MR imaging in pediatric patients after brain tumor resection. Radiology 1988;169: Atlas SW. Intraaxial brain tumors. In: Atlas SW, ed. Magnetic Resonance Imaging of the Brain and Spine. New York, NY: Raven Press; 1991; Brant-Zawadzki M, Norman D, Newton T, et al. Magnetic resonance of the brain: the optimal screening technique. Radiology 1984;152: Felix R, Scherner W, Laniado M, et al. Brain tumors: MR imaging with gadolinium-dtpa. Radiology 1985;156:
Value of Subtraction Images in the Detection of Hemorrhagic Brain Lesions on Contrast-Enhanced MR Images
 681 Value of Subtraction Images in the Detection of Hemorrhagic Brain Lesions on Contrast-Enhanced MR Images Soheil L. Hanna 1 James W. Langston Suzanne A. Gronemeyer Contrast-enhanced T1-weighted MR images
681 Value of Subtraction Images in the Detection of Hemorrhagic Brain Lesions on Contrast-Enhanced MR Images Soheil L. Hanna 1 James W. Langston Suzanne A. Gronemeyer Contrast-enhanced T1-weighted MR images
The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease
 AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Cranial Postoperative Site: MR Imaging Appearance
 27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
Early Post-Operative MRI: Correlation with Progression-Free Survival and Overall Survival Time in Malignant Gliomas
 J. Exp. Clin. Cancer Res., 25, 2, 2006 Early Post-Operative MRI: Correlation with Progression-Free Survival and Overall Survival Time in Malignant Gliomas A. Vidiri 1, C. M. Carapella 2, A. Pace 3, A.
J. Exp. Clin. Cancer Res., 25, 2, 2006 Early Post-Operative MRI: Correlation with Progression-Free Survival and Overall Survival Time in Malignant Gliomas A. Vidiri 1, C. M. Carapella 2, A. Pace 3, A.
The Effect of Contrast Dose, Imaging Time, and Lesion Size in the MR Detection of Intracerebral Metastasis
 The Effect of Contrast Dose, Imaging Time, and Lesion Size in the MR Detection of Intracerebral Metastasis William T. C. Yuh, E. Turgut Tali, Hoang D. Nguyen, Tereasa M. Simonson, Nina A. Mayr, and David
The Effect of Contrast Dose, Imaging Time, and Lesion Size in the MR Detection of Intracerebral Metastasis William T. C. Yuh, E. Turgut Tali, Hoang D. Nguyen, Tereasa M. Simonson, Nina A. Mayr, and David
Original Research Article
 Original Research Article Study Determining Correlation between Histopathological Diagnosis and MRI Findings of Posterior Fossa Tumors Srinivasarao S. Gummadidala 1, B. Jyothi 2 1 Assistant Professor,
Original Research Article Study Determining Correlation between Histopathological Diagnosis and MRI Findings of Posterior Fossa Tumors Srinivasarao S. Gummadidala 1, B. Jyothi 2 1 Assistant Professor,
Intracranial Ganglioglioma: MR, CT,
 109 Intracranial Ganglioglioma: MR, CT, and Clinical Findings in 18 Patients Mauricio Castillo 1 Patricia C. Davis 1 Yoshii Takei 2 James C. Hoffman, Jr. 1 Eighteen cases of pathologically proved intracranial
109 Intracranial Ganglioglioma: MR, CT, and Clinical Findings in 18 Patients Mauricio Castillo 1 Patricia C. Davis 1 Yoshii Takei 2 James C. Hoffman, Jr. 1 Eighteen cases of pathologically proved intracranial
MR of Recurrent High-Grade Astrocytomas after Intralesional Immunotherapy
 MR of Recurrent High-Grade Astrocytomas after Intralesional Immunotherapy Michelle M. Smith, Jill E. Thompson, Mauricio Castillo, Sharon Cush, Suresh K. Mukherji, Claramae H. Miller, and Keith B. Quattrocchi
MR of Recurrent High-Grade Astrocytomas after Intralesional Immunotherapy Michelle M. Smith, Jill E. Thompson, Mauricio Castillo, Sharon Cush, Suresh K. Mukherji, Claramae H. Miller, and Keith B. Quattrocchi
Adult intramedullary astrocytomas of the spinal cord
 J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
Radiation-induced Brachial Plexopathy: MR Imaging
 Radiation-induced Brachial Plexopathy 85 Chapter 5 Radiation-induced Brachial Plexopathy: MR Imaging Neurological symptoms and signs of brachial plexopathy may develop in patients who have had radiation
Radiation-induced Brachial Plexopathy 85 Chapter 5 Radiation-induced Brachial Plexopathy: MR Imaging Neurological symptoms and signs of brachial plexopathy may develop in patients who have had radiation
Posterior Fossa Glioblastoma Multiforme: MR Findings
 Posterior Fossa Glioblastoma Multiforme: MR Findings Toshiro Kuroiwa, Yuji Numaguchi, Michael I. Rothman, Gregg H. Zoarski, Minoru Morikawa, Michael T. Zagardo, and Donald A. Kristt PURPOSE: To characterize
Posterior Fossa Glioblastoma Multiforme: MR Findings Toshiro Kuroiwa, Yuji Numaguchi, Michael I. Rothman, Gregg H. Zoarski, Minoru Morikawa, Michael T. Zagardo, and Donald A. Kristt PURPOSE: To characterize
Pleomorphic xanthoastrocytomas (PXAs) are rare neoplasms. Pleomorphic Xanthoastrocytoma of Childhood: MR Imaging and Diffusion MR Imaging Features
 Published July 3, 2014 as 10.3174/ajnr.A4011 ORIGINAL RESEARCH PEDIATRICS Pleomorphic Xanthoastrocytoma of Childhood: MR Imaging and Diffusion MR Imaging Features W. Moore, D. Mathis, L. Gargan, D.C. Bowers,
Published July 3, 2014 as 10.3174/ajnr.A4011 ORIGINAL RESEARCH PEDIATRICS Pleomorphic Xanthoastrocytoma of Childhood: MR Imaging and Diffusion MR Imaging Features W. Moore, D. Mathis, L. Gargan, D.C. Bowers,
The Utility of MR in Planning the Radiation Therapy of Oligodendroglioma
 93 The Utility of MR in Planning the Radiation Therapy of Oligodendroglioma William P. Shuman' Brian R. Griffin2 David R. Haynor' David C. Jones 2 J. Steve Johnson 2 Laurence D. Cromwell' George E. Laramore
93 The Utility of MR in Planning the Radiation Therapy of Oligodendroglioma William P. Shuman' Brian R. Griffin2 David R. Haynor' David C. Jones 2 J. Steve Johnson 2 Laurence D. Cromwell' George E. Laramore
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Enormous effort has been invested in clinical trials for malignant
 Published February 13, 2008 as 10.3174/ajnr.A0963 REVIEW ARTICLE J.W. Henson S. Ulmer G.J. Harris Brain Tumor Imaging in Clinical Trials SUMMARY: There are substantial challenges in the radiologic evaluation
Published February 13, 2008 as 10.3174/ajnr.A0963 REVIEW ARTICLE J.W. Henson S. Ulmer G.J. Harris Brain Tumor Imaging in Clinical Trials SUMMARY: There are substantial challenges in the radiologic evaluation
Prior to 1993, the only data available in the medical
 Neuro-Oncology Prospective clinical trials of intracranial low-grade glioma in adults and children Edward G. Shaw 1 and Jeffrey H. Wisoff Department of Radiation Oncology, Wake Forest University School
Neuro-Oncology Prospective clinical trials of intracranial low-grade glioma in adults and children Edward G. Shaw 1 and Jeffrey H. Wisoff Department of Radiation Oncology, Wake Forest University School
Neuroradiology Case of the Day
 Neuroradiology Case of the Day 76 th CAR Annual Meeting, Montreal, Quebec April 27, 2013 Eugene Yu, MD Assistant Professor of Radiology and Otolaryngology-Head and Neck Surgery Head and Neck Imaging Princess
Neuroradiology Case of the Day 76 th CAR Annual Meeting, Montreal, Quebec April 27, 2013 Eugene Yu, MD Assistant Professor of Radiology and Otolaryngology-Head and Neck Surgery Head and Neck Imaging Princess
High Signal Intensity of the Infundibular Stalk on Fluid-Attenuated Inversion Recovery MR
 High Signal Intensity of the Infundibular Stalk on Fluid-Attenuated Inversion Recovery MR Yutaka Araki, Ryuichirou Ashikaga, Satoru Takahashi, Jun Ueda, and Osamu Ishida PURPOSE: To determine the MR imaging
High Signal Intensity of the Infundibular Stalk on Fluid-Attenuated Inversion Recovery MR Yutaka Araki, Ryuichirou Ashikaga, Satoru Takahashi, Jun Ueda, and Osamu Ishida PURPOSE: To determine the MR imaging
Role of Diffusion Mri In Differentiation Between The Common Pediatric Posterior Fossa Brain Tumors.
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 73 (2), Page 6090-6096 Role of Diffusion Mri In Differentiation Between The Common Pediatric Posterior Fossa Brain Tumors. HanaaAbdelkader Ahmed
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 73 (2), Page 6090-6096 Role of Diffusion Mri In Differentiation Between The Common Pediatric Posterior Fossa Brain Tumors. HanaaAbdelkader Ahmed
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
MRI Of Locally Recurrent Soft Tissue Tumors Of The Musculoskeletal System
 ISPUB.COM The Internet Journal of Radiology Volume 5 Number 2 MRI Of Locally Recurrent Soft Tissue Tumors Of The Musculoskeletal System C Costelloe, A Yasko, W Murphy, R Kumar, V Lewis, P Lin, R Stafford,
ISPUB.COM The Internet Journal of Radiology Volume 5 Number 2 MRI Of Locally Recurrent Soft Tissue Tumors Of The Musculoskeletal System C Costelloe, A Yasko, W Murphy, R Kumar, V Lewis, P Lin, R Stafford,
Pediatric and Adolescent Oligodendrogliomas
 Pediatric and Adolescent Oligodendrogliomas Harold Tice, 1 Patrick D. Barnes, 1 Liliana Goumnerova, 2 R. Michael Scott, 2 and Nancy J. Tarbell 3 PURPOSE: To review the clinical and imaging findings in
Pediatric and Adolescent Oligodendrogliomas Harold Tice, 1 Patrick D. Barnes, 1 Liliana Goumnerova, 2 R. Michael Scott, 2 and Nancy J. Tarbell 3 PURPOSE: To review the clinical and imaging findings in
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma
 From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
TABLES. Table 1: Imaging. Congress of Neurological Surgeons Author (Year) Description of Study Classification Process / Evidence Class
 TABLES Table 1: Imaging Kremer et al (2002) 2 Study Design: Prospective followed case series. Patient Population: Fifty adult patients with NFPA Study Description: Patients underwent MRI before surgery,
TABLES Table 1: Imaging Kremer et al (2002) 2 Study Design: Prospective followed case series. Patient Population: Fifty adult patients with NFPA Study Description: Patients underwent MRI before surgery,
Imaging of Normal Leptomeningeal Melanin
 Imaging of Normal Leptomeningeal Melanin Stephen S. Gebarski and Mila A. Blaivas PURPOSE: To find the CT and MR characteristics of normal leptomeningeal melanin, which can be macroscopically visible at
Imaging of Normal Leptomeningeal Melanin Stephen S. Gebarski and Mila A. Blaivas PURPOSE: To find the CT and MR characteristics of normal leptomeningeal melanin, which can be macroscopically visible at
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Primary low-grade brain tumors in
 O R I G I N A L A R T I C L E S Copyright 2009, Barrow Neurological Institute Functional Cortical Mapping Using Subdural Grid Electrodes in Patients with Low-Grade Gliomas Presenting with Seizure Andrew
O R I G I N A L A R T I C L E S Copyright 2009, Barrow Neurological Institute Functional Cortical Mapping Using Subdural Grid Electrodes in Patients with Low-Grade Gliomas Presenting with Seizure Andrew
Medulloblastoma in childhood: results of radical resection and low-dose neuraxis radiation therapy
 J Neurosurg 64:238-242, 1986 Medulloblastoma in childhood: results of radical resection and low-dose neuraxis radiation therapy TADANOR! TOMITA, M.D., AND DAVID G. MCLONE, M.D., PH.D. Division of Pediatric
J Neurosurg 64:238-242, 1986 Medulloblastoma in childhood: results of radical resection and low-dose neuraxis radiation therapy TADANOR! TOMITA, M.D., AND DAVID G. MCLONE, M.D., PH.D. Division of Pediatric
N EOPLASMS of the optic nerves occur
 Tumors of the optic nerve and optic chiasm COLLINS. MAcCARTY~ M.D., ALLEN S. BOYD, JR., M.D., AND DONALD S. CHILDS, JR,, M.D. Departments of Neurologic Surgery and Therapeutic Radiology, Mayo Clinic and
Tumors of the optic nerve and optic chiasm COLLINS. MAcCARTY~ M.D., ALLEN S. BOYD, JR., M.D., AND DONALD S. CHILDS, JR,, M.D. Departments of Neurologic Surgery and Therapeutic Radiology, Mayo Clinic and
Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum
 Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Multicompartmental congenital intracranial immature teratoma
 Neurology Asia 2013; 18(1) : 117 121 Multicompartmental congenital intracranial immature teratoma 1 Dharmendra Ganesan MS FRCS(SN), 1 Sheau Fung Sia MS MRCS, 1 Vairavan Narayanan MS, 2 Gnana Kumar FRCR,
Neurology Asia 2013; 18(1) : 117 121 Multicompartmental congenital intracranial immature teratoma 1 Dharmendra Ganesan MS FRCS(SN), 1 Sheau Fung Sia MS MRCS, 1 Vairavan Narayanan MS, 2 Gnana Kumar FRCR,
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
Role of proton magnetic resonance spectroscopy in diagnosis of pilocytic astrocytoma in children
 Alexandria Journal of Medicine (2012) 48, 131 137 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Role of proton magnetic resonance spectroscopy
Alexandria Journal of Medicine (2012) 48, 131 137 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Role of proton magnetic resonance spectroscopy
New Imaging Concepts in Central Nervous System Neoplasms
 New Imaging Concepts in Central Nervous System Neoplasms Maarten Lequin Department of Pediatric Radiology Wilhelmina Children s Hospital/University Medical Center Utrecht New Imaging Concepts in Central
New Imaging Concepts in Central Nervous System Neoplasms Maarten Lequin Department of Pediatric Radiology Wilhelmina Children s Hospital/University Medical Center Utrecht New Imaging Concepts in Central
Case Report Multiple Intracranial Meningiomas: A Review of the Literature and a Case Report
 Case Reports in Surgery Volume 2013, Article ID 131962, 4 pages http://dx.doi.org/10.1155/2013/131962 Case Report Multiple Intracranial Meningiomas: A Review of the Literature and a Case Report F. Koech,
Case Reports in Surgery Volume 2013, Article ID 131962, 4 pages http://dx.doi.org/10.1155/2013/131962 Case Report Multiple Intracranial Meningiomas: A Review of the Literature and a Case Report F. Koech,
Clinical, Neurodiagnostic, and MR Findings in Children with Spinal and Brain Stem Multiple Sclerosis
 Clinical, Neurodiagnostic, and MR Findings in Children with Spinal and Brain Stem Multiple Sclerosis Charles M. Glasier, Mark B. Robbins, Patricia C. Davis, Elizenda Ceballos, and Stephen R. Bates PURPOSE:
Clinical, Neurodiagnostic, and MR Findings in Children with Spinal and Brain Stem Multiple Sclerosis Charles M. Glasier, Mark B. Robbins, Patricia C. Davis, Elizenda Ceballos, and Stephen R. Bates PURPOSE:
Effective local and systemic therapy is necessary for the cure of Ewing tumor Most chemotherapy regimens are a combination of cyclophosphamide,
 Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Intraoperative MR Imaging Increases the Extent of Tumor Resection in Patients with High-Grade Gliomas
 AJNR Am J Neuroradiol 20:1642 1646, October 1999 Intraoperative MR Imaging Increases the Extent of Tumor Resection in Patients with High-Grade Gliomas Michael Knauth, Christian R. Wirtz, Volker M. Tronnier,
AJNR Am J Neuroradiol 20:1642 1646, October 1999 Intraoperative MR Imaging Increases the Extent of Tumor Resection in Patients with High-Grade Gliomas Michael Knauth, Christian R. Wirtz, Volker M. Tronnier,
MR of Intraparotid Masses
 MR of Intraparotid Masses Bruce N. Schlakman and David M. Yousem PURPOSE: To determine which MR techniques are best for identifying intraparotid masses and to assess the utility of MR for predicting specific
MR of Intraparotid Masses Bruce N. Schlakman and David M. Yousem PURPOSE: To determine which MR techniques are best for identifying intraparotid masses and to assess the utility of MR for predicting specific
Case Report Denosumab Chemotherapy for Recurrent Giant-Cell Tumor of Bone: A Case Report of Neoadjuvant Use Enabling Complete Surgical Resection
 Case Reports in Oncological Medicine Volume 2013, Article ID 496351, 4 pages http://dx.doi.org/10.1155/2013/496351 Case Report Denosumab Chemotherapy for Recurrent Giant-Cell Tumor of Bone: A Case Report
Case Reports in Oncological Medicine Volume 2013, Article ID 496351, 4 pages http://dx.doi.org/10.1155/2013/496351 Case Report Denosumab Chemotherapy for Recurrent Giant-Cell Tumor of Bone: A Case Report
Diagnostic Value of Contrast-Enhanced Fluid- Attenuated Inversion Recovery MR Imaging of Intracranial Metastases
 AJNR Am J Neuroradiol 25:761 765, May 2004 Diagnostic Value of Contrast-Enhanced Fluid- Attenuated Inversion Recovery MR Imaging of Intracranial Metastases Nil Ercan, Serap Gultekin, Halil Celik, Turgut
AJNR Am J Neuroradiol 25:761 765, May 2004 Diagnostic Value of Contrast-Enhanced Fluid- Attenuated Inversion Recovery MR Imaging of Intracranial Metastases Nil Ercan, Serap Gultekin, Halil Celik, Turgut
Brainstem diffuse gliomas: radiologic findings.
 Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
DIRECT SURGERY FOR INTRA-AXIAL
 Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy
 AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
Corpus Callosal Signal Changes in Patients with Obstructive Hydrocephalus after Ventriculoperitoneal Shunting
 AJNR Am J Neuroradiol 22:158 162, January 2001 Corpus Callosal Signal Changes in Patients with Hydrocephalus after Ventriculoperitoneal Shunting John I. Lane, Patrick H. Luetmer, and John L. Atkinson BACKGROUND
AJNR Am J Neuroradiol 22:158 162, January 2001 Corpus Callosal Signal Changes in Patients with Hydrocephalus after Ventriculoperitoneal Shunting John I. Lane, Patrick H. Luetmer, and John L. Atkinson BACKGROUND
Detection of Leptomeningeal CNS Metastases in Children
 Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
MR Imaging of Leptomeningeal Metastases: Comparison of Three Sequences
 AJNR Am J Neuroradiol 23:817 821, May 2002 MR Imaging of Leptomeningeal Metastases: Comparison of Three Sequences Sanjay K. Singh, Norman E. Leeds, and Lawrence E. Ginsberg BACKGROUND AND PURPOSE: Recent
AJNR Am J Neuroradiol 23:817 821, May 2002 MR Imaging of Leptomeningeal Metastases: Comparison of Three Sequences Sanjay K. Singh, Norman E. Leeds, and Lawrence E. Ginsberg BACKGROUND AND PURPOSE: Recent
A case of Cushing ulcer in an 8-month-old patient with medulloblastoma
 Case Report A case of Cushing ulcer in an 8-month-old patient with medulloblastoma Walavan Sivakumar 1, Heather S. Spader 1, Eric Scaife 2, Robert J. Bollo 1 1 Department of Neurosurgery, Division of Pediatric
Case Report A case of Cushing ulcer in an 8-month-old patient with medulloblastoma Walavan Sivakumar 1, Heather S. Spader 1, Eric Scaife 2, Robert J. Bollo 1 1 Department of Neurosurgery, Division of Pediatric
The Asymmetric Mamillary Body: Association with Medial Temporal Lobe Disease Demonstrated with MR
 The Mamillary Body: Association with Medial Temporal Lobe Disease Demonstrated with MR Alexander C. Mamourian, Lawrence Rodichok, and Javad Towfighi PURPOSE: To determine whether mamillary body atrophy
The Mamillary Body: Association with Medial Temporal Lobe Disease Demonstrated with MR Alexander C. Mamourian, Lawrence Rodichok, and Javad Towfighi PURPOSE: To determine whether mamillary body atrophy
Pulmonary changes induced by radiotherapy. HRCT findings
 Pulmonary changes induced by radiotherapy. HRCT findings Poster No.: C-2299 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. Albert Antequera, K. Müller Campos, D. 1 2 4 3 1
Pulmonary changes induced by radiotherapy. HRCT findings Poster No.: C-2299 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. Albert Antequera, K. Müller Campos, D. 1 2 4 3 1
Table 9: Vascularity and Hemorrhage
 Table 9: Vascularity and Hemorrhage Di Ieva (2007) 120 Fractal dimension as a quantitator the microvasculat ure normal and adenomatous tissue. Clinical experience characterizing vascular surface fractal
Table 9: Vascularity and Hemorrhage Di Ieva (2007) 120 Fractal dimension as a quantitator the microvasculat ure normal and adenomatous tissue. Clinical experience characterizing vascular surface fractal
MR Signal Intensity of the Optic Radiation
 MR Signal Intensity of the Optic Radiation Mika Kitajima, Yukunori Korogi, Mutsumasa Takahashi, and Komyo Eto PURPOSE: To determine whether a hyperintense layer adjacent to the lateral ventricle on T2-
MR Signal Intensity of the Optic Radiation Mika Kitajima, Yukunori Korogi, Mutsumasa Takahashi, and Komyo Eto PURPOSE: To determine whether a hyperintense layer adjacent to the lateral ventricle on T2-
In 1988 Dumas-Duport et al. first used
 Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Posterior fossa tumors: clues to differential diagnosis with case-based review
 Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
Case Report. Case Report
 AJNR Am J Neuroradiol 26:274 278, February 2005 Case Report Differential Chemosensitivity of Tumor Components in a Malignant Oligodendroglioma: Assessment with Diffusion-Weighted, Perfusion- Weighted,
AJNR Am J Neuroradiol 26:274 278, February 2005 Case Report Differential Chemosensitivity of Tumor Components in a Malignant Oligodendroglioma: Assessment with Diffusion-Weighted, Perfusion- Weighted,
Use of intraoperative ultrasound for localizing tumors and determining the extent of resection: a comparative study with magnetic resonance imaging
 J Neurosurg 84:737 741, 1996 Use of intraoperative ultrasound for localizing tumors and determining the extent of resection: a comparative study with magnetic resonance imaging MAAROUF A. HAMMOUD, M.D.,
J Neurosurg 84:737 741, 1996 Use of intraoperative ultrasound for localizing tumors and determining the extent of resection: a comparative study with magnetic resonance imaging MAAROUF A. HAMMOUD, M.D.,
Small and Big Operations: New Tools of the Trade for Brain Tumors. Disclosure. Incidence of Childhood Cancer
 Small and Big Operations: New Tools of the Trade for Brain Tumors Nalin Gupta MD PhD Chief, Division of Pediatric Neurosurgery Departments of Neurosurgery and Pediatrics University of California San Francisco
Small and Big Operations: New Tools of the Trade for Brain Tumors Nalin Gupta MD PhD Chief, Division of Pediatric Neurosurgery Departments of Neurosurgery and Pediatrics University of California San Francisco
The Frequency and Significance of Small (15 mm) Hepatic Lesions Detected by CT
 535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
Brain and Spine Tumors
 Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Sometimes we get it wrong. Sheila Weitzman MB BCh
 Sometimes we get it wrong Sheila Weitzman MB BCh Pediatric cancer Survival ~80% One in five children still die Second commonest cause of death in developed countries Delay in diagnosis in children with
Sometimes we get it wrong Sheila Weitzman MB BCh Pediatric cancer Survival ~80% One in five children still die Second commonest cause of death in developed countries Delay in diagnosis in children with
Contrast between Scar and Recurrent Herniated Disk on Contrast-Enhanced MR Images
 AJNR Am J Neuroradiol 23:1652 1656, November/December 2002 Contrast between Scar and Recurrent Herniated Disk on Contrast-Enhanced MR Images Victor Haughton, Ken Schreibman, and Arthur De Smet BACKGROUND
AJNR Am J Neuroradiol 23:1652 1656, November/December 2002 Contrast between Scar and Recurrent Herniated Disk on Contrast-Enhanced MR Images Victor Haughton, Ken Schreibman, and Arthur De Smet BACKGROUND
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors
 Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
multiple sclerosis by magnetic resonance imaging
 Index terms: Computed tomography Magnetic resonance sequence optimization Multiple sclerosis The evaluation of multiple sclerosis by magnetic resonance imaging Val M. Runge, M.D.*1 4, Ann C. Price, M.D.*
Index terms: Computed tomography Magnetic resonance sequence optimization Multiple sclerosis The evaluation of multiple sclerosis by magnetic resonance imaging Val M. Runge, M.D.*1 4, Ann C. Price, M.D.*
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution
 Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
LIVER IMAGING TIPS IN VARIOUS MODALITIES. M.Vlychou, MD, PhD Assoc. Professor of Radiology University of Thessaly
 LIVER IMAGING TIPS IN VARIOUS MODALITIES M.Vlychou, MD, PhD Assoc. Professor of Radiology University of Thessaly Hepatocellular carcinoma is a common malignancy for which prevention, screening, diagnosis,
LIVER IMAGING TIPS IN VARIOUS MODALITIES M.Vlychou, MD, PhD Assoc. Professor of Radiology University of Thessaly Hepatocellular carcinoma is a common malignancy for which prevention, screening, diagnosis,
Citation Pediatrics international (2015), 57.
 Title Long-term efficacy of bevacizumab a pediatric glioblastoma. Umeda, Katsutsugu; Shibata, Hirofum Author(s) Hiramatsu, Hidefumi; Arakawa, Yoshi Nishiuchi, Ritsuo; Adachi, Souichi; Ken-Ichiro Citation
Title Long-term efficacy of bevacizumab a pediatric glioblastoma. Umeda, Katsutsugu; Shibata, Hirofum Author(s) Hiramatsu, Hidefumi; Arakawa, Yoshi Nishiuchi, Ritsuo; Adachi, Souichi; Ken-Ichiro Citation
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
Spinal Cord Glioblastoma Induced by Radiation Therapy of Nasopharyngeal Rhabdomyosarcoma with MRI Findings: Case Report
 Case Report http://dx.doi.org/10.3348/kjr.2012.13.5.652 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(5):652-657 Spinal Cord Glioblastoma Induced by Radiation Therapy of Nasopharyngeal Rhabdomyosarcoma
Case Report http://dx.doi.org/10.3348/kjr.2012.13.5.652 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(5):652-657 Spinal Cord Glioblastoma Induced by Radiation Therapy of Nasopharyngeal Rhabdomyosarcoma
MR Imaging of Intracranial Fluid Levels
 695 MR Imaging of Intracranial Fluid Levels James J. Abrahams 1 Mika Lidov Carlos Artiles Six patients with seven intracranial fluid levels were evaluated with both CT and MR at 1.5 T. A surgical diagnosis
695 MR Imaging of Intracranial Fluid Levels James J. Abrahams 1 Mika Lidov Carlos Artiles Six patients with seven intracranial fluid levels were evaluated with both CT and MR at 1.5 T. A surgical diagnosis
RADIOLOGY TEACHING CONFERENCE
 RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Infratentorial and Intraparenchymal Subependymoma in the Cerebellum: Case Report
 Case Report Neuroimaging and Head and Neck http://dx.doi.org/10.3348/kjr.2014.15.1.151 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(1):151-155 Infratentorial and Intraparenchymal Subependymoma
Case Report Neuroimaging and Head and Neck http://dx.doi.org/10.3348/kjr.2014.15.1.151 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(1):151-155 Infratentorial and Intraparenchymal Subependymoma
Encysted Spermatic Cord Hydroceles: A Report of Three Cases in Adults and a Review of the Literature
 Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Encysted Spermatic Cord Hydroceles: A Report of Three Cases in Adults and a Review of
Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Encysted Spermatic Cord Hydroceles: A Report of Three Cases in Adults and a Review of
The Behavior of Pantopaque on MR: In Vivo and In Vitro
 997 The Behavior of Pantopaque on MR: In Vivo and In Vitro Analyses Ira F. Braun 1 John A. Maiko Patricia C. Davis James C. Hoffman, Jr. Louis H. Jacobs MR imaging is considered by many to be the procedure
997 The Behavior of Pantopaque on MR: In Vivo and In Vitro Analyses Ira F. Braun 1 John A. Maiko Patricia C. Davis James C. Hoffman, Jr. Louis H. Jacobs MR imaging is considered by many to be the procedure
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord
 The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
Diffusion-weighted MR Imaging Offers No Advantage over Routine Noncontrast MR Imaging in the Detection of Vertebral Metastases
 AJNR Am J Neuroradiol 1:948 953, May Diffusion-weighted MR Imaging Offers No Advantage over Routine Noncontrast MR Imaging in the Detection of Vertebral Metastases Mauricio Castillo, Andres Arbelaez, J.
AJNR Am J Neuroradiol 1:948 953, May Diffusion-weighted MR Imaging Offers No Advantage over Routine Noncontrast MR Imaging in the Detection of Vertebral Metastases Mauricio Castillo, Andres Arbelaez, J.
Phase II study of carboplatin (CBDCA) in progressive low-grade gliomas
 Neurosurg Focus 4 (4):Article 3, 1998 Phase II study of carboplatin (CBDCA) in progressive low-grade gliomas Albert Moghrabi, M.D., Henry S. Friedman, M.D., David M. Ashley, M.B.B.S., Ph.D., Krystal S.
Neurosurg Focus 4 (4):Article 3, 1998 Phase II study of carboplatin (CBDCA) in progressive low-grade gliomas Albert Moghrabi, M.D., Henry S. Friedman, M.D., David M. Ashley, M.B.B.S., Ph.D., Krystal S.
Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the
 Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the potential relation between whole-tumor apparent diffusion
Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the potential relation between whole-tumor apparent diffusion
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Tumor-like Presentation of Tubercular Brain Abscess: Case Report
 pissn 2384-1095 eissn 2384-1109 imri 2015;19:231-236 http://dx.doi.org/10.13104/imri.2015.19.4.231 Tumor-like Presentation of Tubercular Brain Abscess: Case Report Dan B. Karki 1, Ghanashyam Gurung 2,
pissn 2384-1095 eissn 2384-1109 imri 2015;19:231-236 http://dx.doi.org/10.13104/imri.2015.19.4.231 Tumor-like Presentation of Tubercular Brain Abscess: Case Report Dan B. Karki 1, Ghanashyam Gurung 2,
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Stereotactic Biopsy of Brain Tumours
 Stereotactic Biopsy of Brain Tumours Pages with reference to book, From 176 To 178 Shahzad Shams, Rizwan Masood Butt, Afaq Sarwar ( Department of Neurosurgery Unit 1, Lahore General Hospital, Lahore. )
Stereotactic Biopsy of Brain Tumours Pages with reference to book, From 176 To 178 Shahzad Shams, Rizwan Masood Butt, Afaq Sarwar ( Department of Neurosurgery Unit 1, Lahore General Hospital, Lahore. )
Brain Tumors. Andrew J. Fabiano, MD FAANS. Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine
 Brain Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases Brain
Brain Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases Brain
Intrinsic brainstem tumors may be a challenge to the
 J Neurosurg Pediatrics 14:598 603, 2014 AANS, 2014 Neurosurgical treatment of pediatric low-grade midbrain tumors: a single consecutive institutional series of 15 patients Clinical article Tryggve Lundar,
J Neurosurg Pediatrics 14:598 603, 2014 AANS, 2014 Neurosurgical treatment of pediatric low-grade midbrain tumors: a single consecutive institutional series of 15 patients Clinical article Tryggve Lundar,
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines SINUS MRI Original Date: November 2007 Page 1 of 5 CPT Codes: 70540, 70542, 70543 Last Review Date: July 2014 NCD 220.2 MRI Last Effective Date: July
National Imaging Associates, Inc. Clinical guidelines SINUS MRI Original Date: November 2007 Page 1 of 5 CPT Codes: 70540, 70542, 70543 Last Review Date: July 2014 NCD 220.2 MRI Last Effective Date: July
Alice Fung, MD Oregon Health and Science University
 Alice Fung, MD Oregon Health and Science University Disclosure Comments The speaker Alice Fung, MD Has relevant financial relationships to disclose. Received honorarium from (Guerbet). This individual
Alice Fung, MD Oregon Health and Science University Disclosure Comments The speaker Alice Fung, MD Has relevant financial relationships to disclose. Received honorarium from (Guerbet). This individual
MRI IN THE CHARACTERIZATION OF SEMINOMATOUS AND NONSEMINOMATOUS GERM CELL TUMORS OF THE TESTIS
 MRI IN THE CHARACTERIZATION OF SEMINOMATOUS AND NONSEMINOMATOUS GERM CELL TUMORS OF THE TESTIS Ambesh Deshar *, Gyanendra KC and Zhang Lopsang *Department of Medical Imaging and Nuclear Medicine, First
MRI IN THE CHARACTERIZATION OF SEMINOMATOUS AND NONSEMINOMATOUS GERM CELL TUMORS OF THE TESTIS Ambesh Deshar *, Gyanendra KC and Zhang Lopsang *Department of Medical Imaging and Nuclear Medicine, First
Radiological Appearance of Extra-axial CNS Hemangioma
 Chin J Radiol 2002; 27: 183-190 183 Radiological Appearance of Extra-axial CNS Hemangioma MING-SHIANG YANG CLAYTON CHI-CHANG CHEN WEN-HSIEN CHEN HAO-CHUN HUNG SAN-KAN LEE Department of Radiology, Taichung
Chin J Radiol 2002; 27: 183-190 183 Radiological Appearance of Extra-axial CNS Hemangioma MING-SHIANG YANG CLAYTON CHI-CHANG CHEN WEN-HSIEN CHEN HAO-CHUN HUNG SAN-KAN LEE Department of Radiology, Taichung
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
PET/CT in Gynaecological Cancers. Stroobants Sigrid, MD, PhD Departement of Nuclear Medicine University Hospital,Antwerp
 PET/CT in Gynaecological Cancers Stroobants Sigrid, MD, PhD Departement of Nuclear Medicine University Hospital,Antwerp Cervix cancer Outline of this talk Initial staging Treatment monitoring/guidance
PET/CT in Gynaecological Cancers Stroobants Sigrid, MD, PhD Departement of Nuclear Medicine University Hospital,Antwerp Cervix cancer Outline of this talk Initial staging Treatment monitoring/guidance
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
MRIofthe Central Nervous System
 K. Mori (Ed.) MRIofthe Central Nervous System A Pathology Atlas With the Collaboration of M. Kurisaka A. Moriki A. Sawada With 116 Case Studies and 372 Figures Springer-Verlag Tokyo Berlin Heidelberg New
K. Mori (Ed.) MRIofthe Central Nervous System A Pathology Atlas With the Collaboration of M. Kurisaka A. Moriki A. Sawada With 116 Case Studies and 372 Figures Springer-Verlag Tokyo Berlin Heidelberg New
