Intensity-Modulated Proton Therapy Adaptive Planning for Patients with Oropharyngeal Cancer
|
|
|
- Priscilla Hodges
- 6 years ago
- Views:
Transcription
1 Intensity-Modulated Proton Therapy Adaptive Planning for Patients with Oropharyngeal Cancer Richard Y. Wu, MSc 1* and Amy Y. Liu, MSc 1* ; Terence T. Sio, MD, MS 2,4 ; Pierre Blanchard, MD, PhD 2,5 ; Cody Wages, BSc 3 ; Mayankkumar V. Amin, BSc 3 ; Gary B. Gunn, MD 2 ; Uwe Titt, PhD 1 ; Rong Ye, MSc 2 ; Kazumichi Suzuki, PhD 1 ; Michael T. Gillin, PhD 1 ; Xiaorong R. Zhu, PhD 1 ; Radhe Mohan, PhD 1 ; and Steven J. Frank, MD 2 *Contributed equally to this work 1 Department of Radiation Physics, The University of Texas MD Anderson Cancer Center, Houston, TX, USA 2 Department of Radiation Oncology, The University of Texas MD Anderson Cancer Center, Houston, TX, USA 3 Department of Dosimetry Service, The University of Texas MD Anderson Cancer Center, Houston, TX, USA 4 Department of Radiation Oncology, Mayo Clinic, Phoenix, AZ, USA 5 Department of Radiation Oncology, Gustave Roussy Cancer Campus, Villejuif, France Abstract Submitted 06 Apr 2017 Accepted 12 Oct 2017 Published 28 Dec 2017 Corresponding author: Richard Y. Wu Department of Radiation Physics The University of Texas MD Anderson Cancer Center 1515 Holcombe Blvd Houston, TX 77030, USA Phone: þ1 (713) Fax: þ1 (713) rywu@mdanderson.org Original Article DOI /IJPT * cc Copyright 2017 International Journal of Particle Therapy Purpose: The authors aimed to illustrate the potential dose differences to clinical target volumes (CTVs) and organs-at-risk (OARs) volumes after proton adaptive treatment planning was used. Patients and Methods: The records of 10 patients with oropharyngeal cancer were retrospectively reviewed. Each patient s treatment plan was generated by using the Eclipse treatment planning system. Verification computed tomography (CT) scan was performed during the fourth week of treatment. Deformable image registrations were performed between the 2 CT image sets, and the CTVs and major OARs were transferred to the verification CT images to generate the adaptive plan. We compared the accumulated doses to CTVs and OARs between the original and adaptive plans, as well as between the adaptive and verification plans to simulate doses that would have been delivered if the adaptive plans were not used. Results: Body contours were different on planning and week-4 verification CTs. Mean volumes of all CTVs were reduced by 4% to 8% (P.04), and the volumes of left and right parotid glands also decreased (by 11% to 12%, P.004). Brainstem and oral cavity volumes did not significantly differ (all P.14). All mean doses to the CTV were decreased for up to 7% (P.04), whereas mean doses to the right parotid and oral cavity increased from a range of 5% to 8% (P.03), respectively. Conclusion: Verification and adaptive planning should be recommended during the course of proton therapy for patients with head and neck cancer to ensure adequate dose deliveries to the planned CTVs, while safe doses to OARs can be respected. Keywords: deformable image registration; intensity-modulated proton therapy; oropharyngeal cancer; adaptive planning; dose uncertainty Distributed under Creative Commons CC-BY OPEN ACCESS
2 Introduction There has been substantial growth in the use of proton therapy in the treatment of cancer in the past decade [1]. Owing to its ability to create sharp distal falloff of proton beams within tissue, this technologically advanced form of particle therapy has substantial advantages over conventional photon therapy by reducing unnecessary radiation doses to organs at risk (OARs) and also other healthy tissues. Numerous reports have documented the theoretical advantages of proton therapy over photon therapy for head and neck malignancies [2, 3], and clinical results achieved with proton beams have been promising [4]. The fundamental tenet of radiation therapy (RT) is the delivery of a high radiation dose to the tumor, while limiting the unnecessary radiation dose to the surrounding normal tissues [5]. However, because changes in patient anatomy (such as weight loss) may occur during treatment, the planned radiation doses to clinical target volumes (CTVs) and also OARs can change significantly, as protons have a very defined and finite range for targeting and RT dose deposition. Nonrigid, deformable imaging registration (DIR) has gained popularity in recent years; it is emerging as an essential tool in both adaptive and image-guided radiation therapies to account for tissue changes during the treatment course [6]. Using DIR, the authors evaluated the dose precisely throughout the entire treatment and, if needed, generated an adaptive treatment plan to correct dose differences and ensured that OAR dose limits were met and appropriate. Numerous studies have been performed by using deformable dose accumulation methods on prostate and head and neck cancer treatments with photonbased intensity-modulated RT planning [7, 8] and adaptive strategies [6, 9], respectively. However, there have been no studies quantifying the degree of dose variations for patients undergoing treatment with intensity-modulated proton therapy (IMPT). Because of the inherent sharp falloff in the distal range of a Bragg peak, small changes in anatomy can cause a large dosimetric deviation in target coverage and/or OARs. In this retrospective study, the authors evaluated the contribution of repeated computed tomography (CT) verification scans and the impact of adaptive IMPT planning in assessing anatomically based volumetric and dosimetric changes during the patient course of IMPT treatments. Patients and Methods Patient Selection, Treatment Planning, and Delivery Between November 2013 and December 2014, ten patients with pathologically confirmed oropharyngeal carcinoma were retrospectively selected for clinical review. Institutional review board-approval was obtained and informed consent was waived due to the nature of this project as a retrospective study. These patients were all treated by concurrent chemotherapy along with IMPT. All patients received radiation to the bilateral neck volumes, and had their verification CT plan before treatment and at 4 weeks (61 business day) after RT began. Based on a previous internal study [10], owing to weight loss the patient body contours began to deviate more significantly at about 4 weeks after RT started. In the authors practice, almost 100% of patients had verification plan and more than 90% of patients had adaptive plans; some patients were done earlier than 4 weeks mostly owing to poor initial setup. The patients (,10%) who did not require adaptive planning (as determined by radiation oncologist) were not included. The criterion to implement an adaptive plan for patient treatment was to maintain the CTV1 D95% 100% (ie, dose to 95% of CTV1 volume 100% prescription dose), and also OAR dosages were respected according to the Radiation Therapy Oncology Group s guidelines. This group of 10 patients represented the authors early experience for adaptive planning and the workflow at their institution while IMPT was being implemented. These patients were treated with definitive chemoradiation using IMPT to primary disease site, the gross tumor volume (GTV) with a dose of 70 Gy (RBE) (relative biological equivalence), typically in 33 fractions overall with 2.12 Gy (RBE)/fraction. The clinical target volumes (CTV1, CTV2, and CTV3) were designed accordingly to the clinical evaluation of the anatomic areas that were at risk (to various levels) for gross and/or microscopic involvement of the cancer, including nodal regions; the average volumes were 176, 204, and 241 cm 3 for CTV1, CTV2, and CTV3, respectively. Computed tomography scans and volumes were obtained in a GE CT simulator (General Electric Company Inc, Fairfield, Connecticut) and transferred electronically to the Eclipse Treatment Planning System (TPS) (Varian Medical Systems, Palo Alto, California). Verification CT scans were acquired before the first treatment, and then weekly depending on the disease characteristics and physician s preference, and most commonly, and definitely for the series of patients reported here, during the fourth week. To compare, the verification CT images were registered with the original planning CT images by using the Eclipse rigid registration tool simulating the daily patient treatment alignment process. All plans were calculated by using the TPS for delivery of proton therapy with discrete spot beam scanning [11]. The delivery of the actual IMPT plan was accomplished by the use of a synchrotron and the Hitachi PROBEAT proton beam therapy system (Hitachi Ltd, Tokyo, Japan). A standard 3-field Wu et al. (2017), Int J Particle Ther 27
3 Figure 1. The top image shows the noncoplanar beam arrangement in a typical dosimetric planning case for patients with oropharyngeal cancer, using intensity-modulated proton therapy techniques; the bottom image shows that skin and body contour changes, in 2- to 5- mm thickness along the horizontal double red arrows, which could occur by week 4 of the proton beam radiation therapy course. beam arrangement was used, with right anterior oblique, left anterior oblique, and posterior to anterior direction beams, which were noncoplanar, with robustness consideration (Figure 1) [12, 13]. Varian Eclipse proton-based IMPT inverse planning techniques were used with overall target margin of 0 cm distally and proximally, and 1 cm laterally, respectively. The amounts of spot spacing(s) were determined by the TPS according to maximum energy for each individual field (s ¼ a times FWHM [full width at half maximum], a 0.65) [14]. The planning goals for all CTVs were V100%. 95% (ie, at least 95% of prescription doses cover 100% of the corresponding CTV volumes), V95%. 99%, V105%, 10%, and D max, 120%. The maximum energy of the proton beams per field varied between 102 and 203 MeV, depending on the case and the incident beam angle. An energy absorber (6.7-cm water equivalent thickness) was mounted onto the treatment snout, to ensure dose coverage in the shallow area of the head and neck regions near the skin. Evaluation Deformable imaging registrations were performed between the 2 CT image sets by using commercial deformable registration software (Velocity Medical, Varian Medical Systems). The accuracy of the DIR algorithms has previously been evaluated by Kirby et al [15] and Schreibmann et al [16]. The authors systems were also additionally validated according to Mohamed et al [17]. The treatment targets had 3 CTVs (CTV1, CTV2, and CTV3) corresponding to intended dose levels of 70, 63, and 57 Gy (RBE), respectively. Major OARs were parotids, oral cavity, spinal cord, and brainstem. Both CTVs and OARs were deformed and transferred from the original CT images to the verification CT image data set. All deformed contours were reviewed by a staff radiation oncologist before the adaptive plan would be generated. The beam configuration and intensity distribution profile from the original treatment plan was then copied to the verification CT image set to create a verification plan, for the calculation of the updated radiation dose levels reflecting the most recent anatomic changes. From the dosimetric results, the radiation oncologist would then evaluate, compare, and determine whether the adaptive treatment plans should be created. These plans were highly individualized and depended on multiple other clinical characteristics. The authors then compared the Wu et al. (2017), Int J Particle Ther 28
4 Table 1. Volumetric comparisons of the various OAR and CTV indices that were compared between the CT original and verification week 4 plans. Mean volume (cc) recorded for planning Original CT Verification CT Mean % changes P value CTV1 (70 Gy) %.04 CTV2 (63 Gy) %.02 CTV3 (57 Gy) %.02 Right parotid %.004 Left parotid %.002 Brainstem %.36 Oral cavity %.14 Spinal cord %.08 Abbreviations: OAR, organ-at-risk; CTV, clinical target volume; CT, computed tomography. accumulated dose to CTVs and OARs between the original and adaptive plans, and looked at the difference between the adaptive verification plans, to simulate the doses that would have been delivered if the adaptive plans were not used. The last 9 fractions of RT dose were used for this comparison. For being consistent with the authors analyses, those patients who had more than 10 or fewer than 8 fractions (9 6 1 treatments) of treatments left at the time of adaptive planning on the fourth week of treatment were excluded. Statistical Considerations All dosimetric data were extracted by using the Eclipse Application Programming Interface (API) tool, which was developed inhouse, to access the Eclipse dosimetric database. This API tool facilitated the efficient and accurate extraction of multiple dosimetric data from the Eclipse treatment planning database, compared with the manual methods. All CTVs and OAR volumes were compared between the original and verification CT scans with paired sample analyses; these analyzed OARs included brainstem, parotid glands, and oral cavity, with their own calculated dose-volume histograms along with the CTVs. Wilcoxon matched pairs nonparametric tests [18] were used to evaluate the effect of adaptive versus verification planning, based on volume and dosimetric changes. A probability value of P.05 was considered to be statistically significant; all statistical analyses were calculated with R Programming (R Foundation for Statistical Computing, Vienna, Austria). Results Volume Comparisons Body contours changed significantly, usually at about 3 to 4 weeks into the treatment course (Figure 1). Clinical target volume and OAR locations inside the patient s contours also changed, which ultimately could impact the actual dose distribution physically (Figure 2); the CTV coverages were shown to change between the original and verification CT scans. Table 1 compares the volumes of CTVs and OARs under these circumstances, for both the original and verification CT scans. Between the original and verification (week 4) CT scans, the mean volumes of the 3 different CTVs were all reduced, respectively (P.04), along with decreased parotid gland volumes bilaterally (P.004). There were no significant differences in the volumes of the brainstem and oral cavity between the original and verification CT scans (P.14 for both). Volumes of the other OARs examined (brainstem, spinal cord, and oral cavity) remained not significantly modified. Dosimetric Comparisons There were no significant dosimetric differences between the original and adaptive plans (Figure 3). This was expected, as the re-planning process should mimic and reproduce the same planning goals that were originally set with the specified dose constraints, for as closely as possible based on the verification CT. However, there existed significant dosimetric differences between the adaptive and verification plans. In Table 2, the mean doses (D99 and D95) of CTV1, CTV2, and CTV3 were all decreased (P.04) on the verification scanning, whereas the mean doses (D mean ) of the right parotid and oral cavity were increased (P ¼.03; more right-sided tumors in the patient series). There were no differences regarding the mean maximum dose (D max ) increases to the brainstem (P..12). Wu et al. (2017), Int J Particle Ther 29
5 Figure 2. Example of a patient s plan with carcinoma at the tongue base. The top image represented the original plan, and the bottom image was the verification plan. The dose distribution changes can be seen owing to slight changes in the tongue position and weight loss that the patient experienced during the course of treatment. Adaptive planning was certainly indicated in this case. Figure 3 shows an example of a patient s dose-volume histogram for both CTVs and OARs, derived from the adaptive (triangles) and verification (squares) plans, respectively. On the verification dose-volume histogram plan, 95% of the CTV1 volume was covered by the prescription dose (70 Gy [RBE]); however, the dose homogeneity and conformity were degraded. The decrease in both dose homogeneity and conformity became more significant for CTV2 and CTV3. Doses to the right parotid and oral cavity increased. Comparing the adaptive versus verification plans, values for V26 Gy (ie, the percentage volume that received 26 Gy or more) for the right parotid were 33% and 54%, respectively; for the oral cavity, the V30 Gy values were 6% and 10%, respectively. Discussion This retrospective study demonstrated the importance of performing verification CT imaging and the need to develop a systematic workflow for adaptive planning during the course of IMPT for patients with head and neck cancer who are Wu et al. (2017), Int J Particle Ther 30
6 Figure 3. (A) The generated DVHs were used for clinical target volume comparisons (all shown in 33 fractions), which were derived from the original (square lines) and adaptive (triangles) plans. (B) These DVHs were generated for CTV and organs-at-risk comparisons based on the verification (square lines) and adaptive (triangle lines) plans. In this case, there were no significant differences for CTV coverage. However, a significant difference between the verification and adaptive plans was seen. (C) In this DVH, D95 was noted to be less than prescription dose, for CTV1. As a result, an adaptive plan was required even though other organs at risk had no significant changes. Abbreviations: CTV, clinical target volume; DVH, dose-volume histogram.; D95, dose that was received by 95% of the target volume. undergoing radiotherapeutic treatments. Wang et al [19] found that patients with head and neck cancer could have anatomic structure changes during the course of RT owing to the shrinkage of the tumor or lymph nodes or to body weight loss; it was also found that GTVs can be reduced by as much as 70% [20]. Therefore, it is important during the proton treatment to evaluate the dosimetric effect over the duration of the complete treatment course. The authors results were consistent with what was stated in previous studies [19, 20], for which multiple authors concluded that CTV and parotid volumes consistently decreased after radiation treatment (in their case, after 3 weeks). The dosimetry outcomes reported in this study are consistent with those findings [21, 22], but they did not use DIR, which has played an important role in generating adaptive treatment planning in this modern series. Deformable imaging registration can reduce the workload of physicians in recontouring all structures in the new CT image data set, which can be time-consuming during a busy clinical practice in both academic and community settings; however, it certainly represents a very important step for ensuring the basis and accuracy of the adaptive treatment plan design and evaluation. There were no significant volume changes for the brainstem, spinal cord, or oral cavity, which are expected. The radiation doses to these organs are typically lower. It is also worth noting that many commercial and in-house DIR systems have been developed in recent years. These systems use a variety of approaches, and the accuracy of contour deformation needs to be further evaluated and used with caution [15]. As a result, the new contours review or modification process on the new CT data set cannot be completely eliminated and replaced with DIR [17]; this is a subject of ongoing research at the authors facility. Wu et al. (2017), Int J Particle Ther 31
7 Table 2. Dosimetric results and comparison between the adaptive and verification plans. Dosimetric parameters Adaptive plan (9 fractions) Verification plan (9 fractions) Mean % changes P value CTV1 D cgy 1882 cgy 1%.014 D cgy 1913 cgy 1%.05 CTV2 D cgy 1769 cgy 1%.04 CTV3 D cgy 1563 cgy 7%.03 Right parotid D mean 726 cgy 764 cgy 5%.03 Left parotid D mean 875 cgy 873 cgy 0%.40 Oral cavity D mean 535 cgy 582 cgy 8%.03 Brainstem D max 980 cgy 1015 cgy 3%.28 Spinal cord D max 1058 cgy 1095 cgy 3%.12 Abbreviations: CTV, clinical target volume; D 99, dose to 99% of the volume; D 95, dose to 95% of the volume; D mean, mean dose; D max, maximum dose. The results here of parotid dose changes are consistent with the finding from Hansen et al [21]. The right parotid mean dose was increased on verification compared with adaptive plan (P ¼.03), whereas the left parotid dose had insignificant changes in the present series (P ¼.40). Among the 10 patients, 4 patients had GTV on the right side and 6 on the left side. Further study revealed that the average size of CTV1 for the 4 patients who had GTV on the right side was much less than that for the patient with GTV on the left side (138 versus 180 cm 3 ). This result suggests patient anatomic change may have higher impact on a patient who has smaller primary tumor size, as compared to those having larger tumor size. Further studies will be needed to evaluate the geometric relationship of deformed CTVs and parotids to proton dosing and OAR protections. Future investigation can also be extended to a large number of patient cases being treated, which have used DIR for calculating accumulated doses from multiple plans and to correlate treatment outcomes. More studies should also be done to investigate change in CTVs and different degrees of shrinkage in OARs (especially parotids) between photon and proton modalities. Owing to variable proton RBE phenomena, which can happen in a variety of tissue types, the use of DIR has become increasingly important in estimating uncertainties related to IMPT treatment for patients with head and neck cancers. Finally, there are increased workloads and costs for physicians, physicists, and dosimetrists to perform re-planning. The Eclipse API may automate this process in a seamless fashion and thus reduce the burden on all involved personnel and staff. The present study had a number of limitations. First, this study represents only a small number of initial cases from the authors institutional experience, and further prospective evaluation efforts and improvement will be needed from both the clinical and physics departments. This study used only about 9 fractions for adaptive planning, and in contrast, the verification plan used 33 fractions for the plan initial evaluation in deciding whether an adaptive plan would be needed. This may exaggerate the need for adaptive planning, since the accurate dose changes daily depending on patient setup and/or tumor changes in relation to the established CTVs. A more sophisticated plan evaluation process will need to be studied in the future, to see if the current verification and adaptive plan reviewing procedures represent the best clinical solution and workflow. The other potential verification plan options can be the following: (1) sum dose from the original and verification plans, including undelivered fraction; and (2) sum dose from original and adaptive plans, that is, to be delivered for the remaining fractions. The generation of adaptive plan and the quality assurance process in association with it must also be completed in a timely fashion. The efficacy and feasibility of such a program is outside the scope of this project; a substantial additional staff resource will need to be allocated for this. Monte Carlo methods are usually believed to be most accurate as a technique for calculation of dose distributions. However, owing to lengthy calculation time requirement, they are difficult to use and be adapted in the usual clinical environment/practice, or for large retrospective study use. Patients plan showing borderline results for OARs should be considered for Monte Carlo calculation to confirm if dose uncertainty exists, on a case-by-case basis. Research has been Wu et al. (2017), Int J Particle Ther 32
8 conducted on fast dose calculator, which could reduce dose calculation time to less than 5 minutes per patient in the future [23]. Finally, the adaptive planning should consider the dose deficiency from the original and verification plan review, and the new adaptive plan should account for the changes accordingly, even if it may not appear best optimized. As a result, a criterion for triggering the evaluation and needs for a re-planning can be based on the amount of volume loss in target volumes, which will require future research effort for validation. Robust optimization research in IMPT to account for anatomy changes in head and neck cancer is also needed in these areas [24]. Conclusion Verification CT imaging and adaptive planning are highly recommended during the course of IMPT for patients with head and neck cancer to identify anatomic and dosimetric changes and to ensure adequate doses to target volumes and safe doses to normal tissues. These results indicate that DIR is an essential tool for such evaluation for IMPT planning and accurate dose delivery. ADDITIONAL INFORMATION AND DECLARATIONS Conflicts of Interest: Drs Radhe Mohan and Steven J. Frank are members of the International Journal of Particle Therapy s editorial board. All others authors have no conflicts of interest to disclose. Acknowledgments: The authors acknowledge Michael Worley for his editorial assistance. References 1. Smith AR. Proton therapy. Phys Med Biol. 2006;51:R Lomax AJ, Goitein M, Adams J. Intensity modulation in radiotherapy: photons versus protons in the paranasal sinus. Radiother Oncol. 2003;66: Steneker M, Lomax A, Schneider U. Intensity modulated photon and proton therapy for the treatment of head and neck tumors. Radiother Oncol. 2006;80: Frank SJ, Cox JD, Gillin M, Mohan R, Garden AS, Rosenthal DI, Gunn GB, Weber RS, Kies MS, Lewin JS, Munsell MF, Palmer MB, Sahoo N, Zhang X, Liu W, Zhu XR. Multifield optimization intensity modulated proton therapy for head and neck tumors: a translation to practice. Int J Radiat Oncol Biol Phys. 2014;89: Njeh CF, Dong L, Orton CG. IGRT has limited clinical value due to lack of accurate tumor delineation. Med Phys. 2013;40: Lawson JD, Schreibmann E, Jani AB, Fox T. Quantitative evaluation of a cone-beam computed tomography-planning computed tomography deformable image registration method for adaptive radiation therapy. J Appl Clin Med Phys. 2007;8: Cui Y, Piper JW, Harrison AS, Showalter TN, Yu Y, Galvin JM, Xiao Y. Deformable dose accumulation with image guided radiotherapy for final dose evaluation in pelvic cases. J Nucl Med Radiat Ther. 2011;S3:e Veiga C, McClelland J, Moinuddin S, Lourenco A, Ricketts K, Annkah J, Modat M, Ourselin S, D Souza D, Royle G. Toward adaptive radiotherapy for head and neck patients: feasibility study on using CT-to-CBCT deformable registration for dose of the day calculations. Med Phys. 2014;41: Chitapanarux I, Chomprasert K, Nobnaop W, Wanwilairat S, Tharavichitkul E, Jakrabhandu S, Onchan W, Traisathit P, Van Gestel D. A dosimetric comparison of two-phase adaptive intensity-modulated radiotherapy for locally advanced nasopharyngeal cancer. J Radiat Res. 2015;56: Palmer M, Jones T, Waddell M, Varghese S, Zhang Y, Amin M, Yeh BK, Zhu R, Dong L, Frank SJ. The optimal timing for off-line adaptive planning for bilateral head-and-neck IMPT is week 4. Int J Radiat Oncol Biol Phys. 2012;84:S Gillin MT, Sahoo N, Bues M, Ciangaru G, Sawakuchi G, Poenisch F, Arjomandy B, Martin C, Titt U, Suzuki K, Smith AR, Zhu XR. Commissioning of the discrete spot scanning proton beam delivery system at the University of Texas M.D. Anderson Cancer Center, Proton Therapy Center, Houston. Med Phys. 2010;37: Liu W, Frank SJ, Li X, Li Y, Park PC, Dong L, Ronald Zhu X, Mohan R. Effectiveness of robust optimization in intensitymodulated proton therapy planning for head and neck cancers. Med Phys. 2013;40: Wu et al. (2017), Int J Particle Ther 33
9 13. Quan EM, Liu W, Wu R, Li Y, Frank SJ, Zhang X, Zhu XR, Mohan R. Preliminary evaluation of multifield and single-field optimization for the treatment planning of spot-scanning proton therapy of head and neck cancer. Med Phys. 2013;40: Zhu XR, Sahoo N, Zhang X, Robertson D, Li H, Choi S, Lee AK, Gillin MT. Intensity modulated proton therapy treatment planning using single-field optimization: the impact of monitor unit constraints on plan quality. Med Phys. 2010;37: Kirby N, Chuang C, Ueda U, Pouliot J. The need for application-based adaptation of deformable image registration. Med Phys. 2013;40: Schreibmann E, Pantalone P, Waller A, Fox T. A measure to evaluate deformable registration fields in clinical settings. J Appl Clin Med Phys. 2012;13: Mohamed AS, Ruangskul MN, Awan MJ, Baron CA, Kalpathy-Cramer J, Castillo R, Castillo E, Guerrero TM, Kocak-Uzel E, Yang J, Court LE, Kantor ME, Gunn GB, Colen RR, Frank SJ, Garden AS, Rosenthal DI, Fuller CD. Quality assurance assessment of diagnostic and radiation therapy-simulation CT image registration for head and neck radiation therapy: anatomic region of interest-based comparison of rigid and deformable algorithms. Radiology. 2015;274: Cattaneo GM, Dell oca I, Broggi S, Fiorino C, Perna L, Pasetti M, Sangalli G, di Muzio N, Fazio F, Calandrino R. Treatment planning comparison between conformal radiotherapy and helical tomotherapy in the case of locally advanced-stage NSCLC. Radiother Oncol. 2008;88: Wang W, Yang H, Hu W, Shan G, Ding W, Yu C, Wang B, Wang X, Xu Q. Clinical study of the necessity of replanning before the 25th fraction during the course of intensity-modulated radiotherapy for patients with nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys. 2010;77: Barker JL Jr, Garden AS, Ang KK, O Daniel JC, Wang H, Court LE, Morrison WH, Rosenthal DI, Chao KS, Tucker SL, Mohan R, Dong L. Quantification of volumetric and geometric changes occurring during fractionated radiotherapy for head-and-neck cancer using an integrated CT/linear accelerator system. Int J Radiat Oncol Biol Phys. 2004;59: Hansen EK, Bucci MK, Quivey JM, Weinberg V, Xia P. Repeat CT imaging and replanning during the course of IMRT for head-and-neck cancer. Int J Radiat Oncol Biol Phys. 2006;64: Feng M, Yang C, Chen X, Xu S, Moraru I, Lang J, Schultz C, Li XA. Computed tomography number changes observed during computed tomography-guided radiation therapy for head and neck cancer. Int J Radiat Oncol Biol Phys. 2015;91: Yepes PP, Eley JG, Liu A, Mirkovic D, Randeniya S, Titt U, Mohan R. Validation of a track repeating algorithm for intensity modulated proton therapy: clinical cases study. Phys Med Biol. 2016;61: Li H, Zhang X, Park P, Liu W, Chang J, Liao Z, Frank S, Li Y, Poenisch F, Mohan R, Gillin M, Zhu R. Robust optimization in intensity-modulated proton therapy to account for anatomy changes in lung cancer patients. Radiother Oncol. 2015;114: Wu et al. (2017), Int J Particle Ther 34
Evaluation of Whole-Field and Split-Field Intensity Modulation Radiation Therapy (IMRT) Techniques in Head and Neck Cancer
 1 Charles Poole April Case Study April 30, 2012 Evaluation of Whole-Field and Split-Field Intensity Modulation Radiation Therapy (IMRT) Techniques in Head and Neck Cancer Abstract: Introduction: This study
1 Charles Poole April Case Study April 30, 2012 Evaluation of Whole-Field and Split-Field Intensity Modulation Radiation Therapy (IMRT) Techniques in Head and Neck Cancer Abstract: Introduction: This study
Defining Target Volumes and Organs at Risk: a common language
 Defining Target Volumes and Organs at Risk: a common language Eduardo Rosenblatt Section Head Applied Radiation Biology and Radiotherapy (ARBR) Section Division of Human Health IAEA Objective: To introduce
Defining Target Volumes and Organs at Risk: a common language Eduardo Rosenblatt Section Head Applied Radiation Biology and Radiotherapy (ARBR) Section Division of Human Health IAEA Objective: To introduce
Overview. Proton Therapy in lung cancer 8/3/2016 IMPLEMENTATION OF PBS PROTON THERAPY TREATMENT FOR FREE BREATHING LUNG CANCER PATIENTS
 IMPLEMENTATION OF PBS PROTON THERAPY TREATMENT FOR FREE BREATHING LUNG CANCER PATIENTS Heng Li, PhD Assistant Professor, Department of Radiation Physics, UT MD Anderson Cancer Center, Houston, TX, 773
IMPLEMENTATION OF PBS PROTON THERAPY TREATMENT FOR FREE BREATHING LUNG CANCER PATIENTS Heng Li, PhD Assistant Professor, Department of Radiation Physics, UT MD Anderson Cancer Center, Houston, TX, 773
REVISITING ICRU VOLUME DEFINITIONS. Eduardo Rosenblatt Vienna, Austria
 REVISITING ICRU VOLUME DEFINITIONS Eduardo Rosenblatt Vienna, Austria Objective: To introduce target volumes and organ at risk concepts as defined by ICRU. 3D-CRT is the standard There was a need for a
REVISITING ICRU VOLUME DEFINITIONS Eduardo Rosenblatt Vienna, Austria Objective: To introduce target volumes and organ at risk concepts as defined by ICRU. 3D-CRT is the standard There was a need for a
IMRT - the physician s eye-view. Cinzia Iotti Department of Radiation Oncology S.Maria Nuova Hospital Reggio Emilia
 IMRT - the physician s eye-view Cinzia Iotti Department of Radiation Oncology S.Maria Nuova Hospital Reggio Emilia The goals of cancer therapy Local control Survival Functional status Quality of life Causes
IMRT - the physician s eye-view Cinzia Iotti Department of Radiation Oncology S.Maria Nuova Hospital Reggio Emilia The goals of cancer therapy Local control Survival Functional status Quality of life Causes
IGRT Solution for the Living Patient and the Dynamic Treatment Problem
 IGRT Solution for the Living Patient and the Dynamic Treatment Problem Lei Dong, Ph.D. Associate Professor Dept. of Radiation Physics University of Texas M. D. Anderson Cancer Center Houston, Texas Learning
IGRT Solution for the Living Patient and the Dynamic Treatment Problem Lei Dong, Ph.D. Associate Professor Dept. of Radiation Physics University of Texas M. D. Anderson Cancer Center Houston, Texas Learning
8/1/2016. Motion Management for Proton Lung SBRT. Outline. Protons and motion. Protons and Motion. Proton lung SBRT Future directions
 Motion Management for Proton Lung SBRT AAPM 2016 Outline Protons and Motion Dosimetric effects Remedies and mitigation techniques Proton lung SBRT Future directions Protons and motion Dosimetric perturbation
Motion Management for Proton Lung SBRT AAPM 2016 Outline Protons and Motion Dosimetric effects Remedies and mitigation techniques Proton lung SBRT Future directions Protons and motion Dosimetric perturbation
IGRT Protocol Design and Informed Margins. Conflict of Interest. Outline 7/7/2017. DJ Vile, PhD. I have no conflict of interest to disclose
 IGRT Protocol Design and Informed Margins DJ Vile, PhD Conflict of Interest I have no conflict of interest to disclose Outline Overview and definitions Quantification of motion Influences on margin selection
IGRT Protocol Design and Informed Margins DJ Vile, PhD Conflict of Interest I have no conflict of interest to disclose Outline Overview and definitions Quantification of motion Influences on margin selection
Evaluation of deformed image-based dose calculations for adaptive radiotherapy of nasopharyngeal carcinoma
 Evaluation of deformed image-based dose calculations for adaptive radiotherapy of nasopharyngeal carcinoma POON, Miranda, HOLBORN, Catherine , CHENG, Ka Fai, FUNG,
Evaluation of deformed image-based dose calculations for adaptive radiotherapy of nasopharyngeal carcinoma POON, Miranda, HOLBORN, Catherine , CHENG, Ka Fai, FUNG,
Review of Workflow NRG (RTOG) 1308: Phase III Randomized Trial Comparing Overall Survival after Photon versus Proton Chemoradiation Therapy for
 Review of Workflow NRG (RTOG) 1308: Phase III Randomized Trial Comparing Overall Survival after Photon versus Proton Chemoradiation Therapy for Inoperable Stage II-IIIB NSCLC 1 Co-Chairs Study Chair: Zhongxing
Review of Workflow NRG (RTOG) 1308: Phase III Randomized Trial Comparing Overall Survival after Photon versus Proton Chemoradiation Therapy for Inoperable Stage II-IIIB NSCLC 1 Co-Chairs Study Chair: Zhongxing
Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana
 University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
What do we Know About Adaptive Radiotherapy? Lei Dong, Ph.D. Scripps Proton Therapy Center San Diego, California
 What do we Know About Adaptive Radiotherapy? Lei Dong, Ph.D. Scripps Proton Therapy Center San Diego, California AAMD Region II Meeting Houston, Texas September 13-14, 2012 Learning Objectives To gain
What do we Know About Adaptive Radiotherapy? Lei Dong, Ph.D. Scripps Proton Therapy Center San Diego, California AAMD Region II Meeting Houston, Texas September 13-14, 2012 Learning Objectives To gain
IMRT/IGRT Patient Treatment: A Community Hospital Experience. Charles M. Able, Assistant Professor
 IMRT/IGRT Patient Treatment: A Community Hospital Experience Charles M. Able, Assistant Professor Disclosures I have no research support or financial interest to disclose. Learning Objectives 1. Review
IMRT/IGRT Patient Treatment: A Community Hospital Experience Charles M. Able, Assistant Professor Disclosures I have no research support or financial interest to disclose. Learning Objectives 1. Review
Evaluation of Monaco treatment planning system for hypofractionated stereotactic volumetric arc radiotherapy of multiple brain metastases
 Evaluation of Monaco treatment planning system for hypofractionated stereotactic volumetric arc radiotherapy of multiple brain metastases CASE STUDY Institution: Odette Cancer Centre Location: Sunnybrook
Evaluation of Monaco treatment planning system for hypofractionated stereotactic volumetric arc radiotherapy of multiple brain metastases CASE STUDY Institution: Odette Cancer Centre Location: Sunnybrook
From verification to adaptive plan: A discussion on workflow and procedures with case study examples
 From verification to adaptive plan: A discussion on workflow and procedures with case study examples THANKS! My Planning team: Maynak Amin Cody Crawford Manny Oyervides Katina Crabtree David Lege Rola
From verification to adaptive plan: A discussion on workflow and procedures with case study examples THANKS! My Planning team: Maynak Amin Cody Crawford Manny Oyervides Katina Crabtree David Lege Rola
Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer
 Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer Tan Chek Wee 15 06 2016 National University Cancer Institute, Singapore Clinical Care Education Research
Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer Tan Chek Wee 15 06 2016 National University Cancer Institute, Singapore Clinical Care Education Research
Outline. Contour quality control. Dosimetric impact of contouring errors and variability in Intensity Modulated Radiation Therapy (IMRT)
 Dosimetric impact of contouring errors and variability in Intensity Modulated Radiation Therapy (IMRT) James Kavanaugh, MS DABR Department of Radiation Oncology Division of Medical Physics Outline Importance
Dosimetric impact of contouring errors and variability in Intensity Modulated Radiation Therapy (IMRT) James Kavanaugh, MS DABR Department of Radiation Oncology Division of Medical Physics Outline Importance
Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana
 University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Rules of parotid gland dose variations and shift during intensity modulated radiation therapy for nasopharyngeal carcinoma
 Wang et al. Radiation Oncology (2015) 10:3 DOI 10.1186/s13014-014-0307-2 RESEARCH Open Access Rules of parotid gland dose variations and shift during intensity modulated radiation therapy for nasopharyngeal
Wang et al. Radiation Oncology (2015) 10:3 DOI 10.1186/s13014-014-0307-2 RESEARCH Open Access Rules of parotid gland dose variations and shift during intensity modulated radiation therapy for nasopharyngeal
3D ANATOMY-BASED PLANNING OPTIMIZATION FOR HDR BRACHYTHERAPY OF CERVIX CANCER
 SAUDI JOURNAL OF OBSTETRICS AND GYNECOLOGY VOLUME 11 NO. 2 1430 H - 2009 G 3D ANATOMY-BASED PLANNING OPTIMIZATION FOR HDR BRACHYTHERAPY OF CERVIX CANCER DR YASIR BAHADUR 1, DR CAMELIA CONSTANTINESCU 2,
SAUDI JOURNAL OF OBSTETRICS AND GYNECOLOGY VOLUME 11 NO. 2 1430 H - 2009 G 3D ANATOMY-BASED PLANNING OPTIMIZATION FOR HDR BRACHYTHERAPY OF CERVIX CANCER DR YASIR BAHADUR 1, DR CAMELIA CONSTANTINESCU 2,
A VMAT PLANNING SOLUTION FOR NECK CANCER PATIENTS USING THE PINNACLE 3 PLANNING SYSTEM *
 Romanian Reports in Physics, Vol. 66, No. 2, P. 401 410, 2014 A VMAT PLANNING SOLUTION FOR NECK CANCER PATIENTS USING THE PINNACLE 3 PLANNING SYSTEM * M. D. SUDITU 1,2, D. ADAM 1,2, R. POPA 1,2, V. CIOCALTEI
Romanian Reports in Physics, Vol. 66, No. 2, P. 401 410, 2014 A VMAT PLANNING SOLUTION FOR NECK CANCER PATIENTS USING THE PINNACLE 3 PLANNING SYSTEM * M. D. SUDITU 1,2, D. ADAM 1,2, R. POPA 1,2, V. CIOCALTEI
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR
 Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
Evaluation of three APBI techniques under NSABP B-39 guidelines
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 11, NUMBER 1, WINTER 2010 Evaluation of three APBI techniques under NSABP B-39 guidelines Daniel Scanderbeg, a Catheryn Yashar, Greg White, Roger Rice,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 11, NUMBER 1, WINTER 2010 Evaluation of three APBI techniques under NSABP B-39 guidelines Daniel Scanderbeg, a Catheryn Yashar, Greg White, Roger Rice,
Evaluation of the systematic error in using 3D dose calculation in scanning beam proton therapy for lung cancer
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, OLUME 15, NUMBER 5, 2014 Evaluation of the systematic error in using 3D dose calculation in scanning beam proton therapy for lung cancer Heng Li, 1a Wei Liu,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, OLUME 15, NUMBER 5, 2014 Evaluation of the systematic error in using 3D dose calculation in scanning beam proton therapy for lung cancer Heng Li, 1a Wei Liu,
Dosimetric consequences of tumor volume changes after kilovoltage cone-beam computed tomography for non-operative lung cancer during adaptive
 Oncology and Translational Medicine October 2015, Vol. 1, No. 5, P195 200 DOI 10.1007/s10330-015-0054-3 ORIGINAL ARTICLE Dosimetric consequences of tumor volume changes after kilovoltage cone-beam computed
Oncology and Translational Medicine October 2015, Vol. 1, No. 5, P195 200 DOI 10.1007/s10330-015-0054-3 ORIGINAL ARTICLE Dosimetric consequences of tumor volume changes after kilovoltage cone-beam computed
ART for Cervical Cancer: Dosimetry and Technical Aspects
 ART for Cervical Cancer: Dosimetry and Technical Aspects D.A. Jaffray, Ph.D. Radiation Therapy Physics Princess Margaret Cancer Centre/Techna/Ontario Cancer Institute Professor Departments of Radiation
ART for Cervical Cancer: Dosimetry and Technical Aspects D.A. Jaffray, Ph.D. Radiation Therapy Physics Princess Margaret Cancer Centre/Techna/Ontario Cancer Institute Professor Departments of Radiation
Original Article. Teyyiba Kanwal, Muhammad Khalid, Syed Ijaz Hussain Shah, Khawar Nadeem
 Original Article Treatment Planning Evaluation of Sliding Window and Multiple Static Segments Technique in Intensity Modulated Radiotherapy for Different Beam Directions Teyyiba Kanwal, Muhammad Khalid,
Original Article Treatment Planning Evaluation of Sliding Window and Multiple Static Segments Technique in Intensity Modulated Radiotherapy for Different Beam Directions Teyyiba Kanwal, Muhammad Khalid,
Clinical Aspects of Proton Therapy in Lung Cancer. Joe Y. Chang, MD, PhD Associate Professor
 Clinical Aspects of Proton Therapy in Lung Cancer Joe Y. Chang, MD, PhD Associate Professor Clinical Service Chief Thoracic Radiation Oncology Lung Cancer Basic Factors No. 1 cancer killer 161,840 patients
Clinical Aspects of Proton Therapy in Lung Cancer Joe Y. Chang, MD, PhD Associate Professor Clinical Service Chief Thoracic Radiation Oncology Lung Cancer Basic Factors No. 1 cancer killer 161,840 patients
AAPM Task Group 180 Image Guidance Doses Delivered During Radiotherapy: Quantification, Management, and Reduction
 AAPM Task Group 180 Image Guidance Doses Delivered During Radiotherapy: Quantification, Management, and Reduction Parham Alaei, Ph.D. Department of Radiation Oncology University of Minnesota NCCAAPM Fall
AAPM Task Group 180 Image Guidance Doses Delivered During Radiotherapy: Quantification, Management, and Reduction Parham Alaei, Ph.D. Department of Radiation Oncology University of Minnesota NCCAAPM Fall
CBCT of the patient in the treatment position has gained wider applications for setup verification during radiotherapy.
 Gülcihan CÖDEL Introduction The aim of this study is to evaluate the changes in bladder doses during the volumetric modulated arc therapy (VMAT) treatment of prostate cancer patients using weekly cone
Gülcihan CÖDEL Introduction The aim of this study is to evaluate the changes in bladder doses during the volumetric modulated arc therapy (VMAT) treatment of prostate cancer patients using weekly cone
Head and Neck Treatment Planning: A Comparative Review of Static Field IMRT RapidArc TomoTherapy HD. Barbara Agrimson, BS RT(T)(R), CMD
 Head and Neck Treatment Planning: A Comparative Review of Static Field IMRT RapidArc TomoTherapy HD Barbara Agrimson, BS RT(T)(R), CMD Disclaimer This presentation will mention equipment by trade name.
Head and Neck Treatment Planning: A Comparative Review of Static Field IMRT RapidArc TomoTherapy HD Barbara Agrimson, BS RT(T)(R), CMD Disclaimer This presentation will mention equipment by trade name.
SBRT fundamentals. Outline 8/2/2012. Stereotactic Body Radiation Therapy Quality Assurance Educational Session
 Stereotactic Body Radiation Therapy Quality Assurance Educational Session J Perks PhD, UC Davis Medical Center, Sacramento CA SBRT fundamentals Extra-cranial treatments Single or small number (2-5) of
Stereotactic Body Radiation Therapy Quality Assurance Educational Session J Perks PhD, UC Davis Medical Center, Sacramento CA SBRT fundamentals Extra-cranial treatments Single or small number (2-5) of
Clinical Implications Of Dose Summation And Adaptation
 Clinical Implications Of Dose Summation And Adaptation Patrick Kupelian, M.D. Professor and Vice Chair University of California Los Angeles Department of Radiation Oncology pkupelian@mednet.ucla.edu August
Clinical Implications Of Dose Summation And Adaptation Patrick Kupelian, M.D. Professor and Vice Chair University of California Los Angeles Department of Radiation Oncology pkupelian@mednet.ucla.edu August
Evaluation of Three-dimensional Conformal Radiotherapy and Intensity Modulated Radiotherapy Techniques in High-Grade Gliomas
 1 Carol Boyd Comprehensive Case Study July 11, 2013 Evaluation of Three-dimensional Conformal Radiotherapy and Intensity Modulated Radiotherapy Techniques in High-Grade Gliomas Abstract: Introduction:
1 Carol Boyd Comprehensive Case Study July 11, 2013 Evaluation of Three-dimensional Conformal Radiotherapy and Intensity Modulated Radiotherapy Techniques in High-Grade Gliomas Abstract: Introduction:
Treatment Planning (Protons vs. Photons)
 Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
biij Initial experience in treating lung cancer with helical tomotherapy
 Available online at http://www.biij.org/2007/1/e2 doi: 10.2349/biij.3.1.e2 biij Biomedical Imaging and Intervention Journal CASE REPORT Initial experience in treating lung cancer with helical tomotherapy
Available online at http://www.biij.org/2007/1/e2 doi: 10.2349/biij.3.1.e2 biij Biomedical Imaging and Intervention Journal CASE REPORT Initial experience in treating lung cancer with helical tomotherapy
The Effects of DIBH on Liver Dose during Right-Breast Treatments: A Case Study Abstract: Introduction: Case Description: Conclusion: Introduction
 1 The Effects of DIBH on Liver Dose during Right-Breast Treatments: A Case Study Megan E. Sullivan, B.S., R.T.(T)., Patrick A. Melby, B.S. Ashley Hunzeker, M.S., CMD, Nishele Lenards, M.S., CMD, R.T. (R)(T),
1 The Effects of DIBH on Liver Dose during Right-Breast Treatments: A Case Study Megan E. Sullivan, B.S., R.T.(T)., Patrick A. Melby, B.S. Ashley Hunzeker, M.S., CMD, Nishele Lenards, M.S., CMD, R.T. (R)(T),
A Comparison of IMRT and VMAT Technique for the Treatment of Rectal Cancer
 A Comparison of IMRT and VMAT Technique for the Treatment of Rectal Cancer Tony Kin Ming Lam Radiation Planner Dr Patricia Lindsay, Radiation Physicist Dr John Kim, Radiation Oncologist Dr Kim Ann Ung,
A Comparison of IMRT and VMAT Technique for the Treatment of Rectal Cancer Tony Kin Ming Lam Radiation Planner Dr Patricia Lindsay, Radiation Physicist Dr John Kim, Radiation Oncologist Dr Kim Ann Ung,
Biological Model for Predicting Toxicity in Head and Neck Cancer Patients Receiving Proton Therapy
 Biological Model for Predicting Toxicity in Head and Neck Cancer Patients Receiving Proton Therapy Croix C. Fossum, MD 1 ; Chris J. Beltran, PhD 2 ; Thomas J. Whitaker, PhD 2 ; Daniel J. Ma, MD 2 ; Robert
Biological Model for Predicting Toxicity in Head and Neck Cancer Patients Receiving Proton Therapy Croix C. Fossum, MD 1 ; Chris J. Beltran, PhD 2 ; Thomas J. Whitaker, PhD 2 ; Daniel J. Ma, MD 2 ; Robert
Treatment Planning for Skull Base Tumors PTCOG 52, June 2013
 Treatment Planning for Skull Base Tumors PTCOG 52, June 2013 Judy Adams CMD Hanne Kooy Ph.D, Norbert Liebsch MD Department of Radiation Oncology Massachusetts General Hospital Chordomas and Chondrosarcomas
Treatment Planning for Skull Base Tumors PTCOG 52, June 2013 Judy Adams CMD Hanne Kooy Ph.D, Norbert Liebsch MD Department of Radiation Oncology Massachusetts General Hospital Chordomas and Chondrosarcomas
Hampton University Proton Therapy Institute
 Hampton University Proton Therapy Institute Brief introduction to proton therapy technology, its advances and Hampton University Proton Therapy Institute Vahagn Nazaryan, Ph.D. Executive Director, HUPTI
Hampton University Proton Therapy Institute Brief introduction to proton therapy technology, its advances and Hampton University Proton Therapy Institute Vahagn Nazaryan, Ph.D. Executive Director, HUPTI
Clinical Education A comprehensive and specific training program. carry out effective treatments from day one
 Proton Therapy Clinical Education A comprehensive and specific training program carry out effective treatments from day one Forewarned is forearmed Although over 100,000 patients have been treated in proton
Proton Therapy Clinical Education A comprehensive and specific training program carry out effective treatments from day one Forewarned is forearmed Although over 100,000 patients have been treated in proton
Protocol of Radiotherapy for Head and Neck Cancer
 106 年 12 月修訂 Protocol of Radiotherapy for Head and Neck Cancer Indication of radiotherapy Indication of definitive radiotherapy with or without chemotherapy (1) Resectable, but medically unfit, or high
106 年 12 月修訂 Protocol of Radiotherapy for Head and Neck Cancer Indication of radiotherapy Indication of definitive radiotherapy with or without chemotherapy (1) Resectable, but medically unfit, or high
Martin Stuschke 1,2*, Andreas Kaiser 1,2, Jehad Abu Jawad 1, Christoph Pöttgen 1, Sabine Levegrün 1 and Jonathan Farr 2,3
 Stuschke et al. Radiation Oncology 2013, 8:145 SHORT REPORT Open Access Multi-scenario based robust intensity-modulated proton therapy (IMPT) plans can account for set-up errors more effectively in terms
Stuschke et al. Radiation Oncology 2013, 8:145 SHORT REPORT Open Access Multi-scenario based robust intensity-modulated proton therapy (IMPT) plans can account for set-up errors more effectively in terms
From position verification and correction to adaptive RT Adaptive RT and dose accumulation
 From position verification and correction to adaptive RT Adaptive RT and dose accumulation Hans de Boer Move away from Single pre-treatment scan Single treatment plan Treatment corrections by couch shifts
From position verification and correction to adaptive RT Adaptive RT and dose accumulation Hans de Boer Move away from Single pre-treatment scan Single treatment plan Treatment corrections by couch shifts
Future upcoming technologies and what audit needs to address
 Future upcoming technologies and what audit needs to address Dr R.I MacKay History of audit Absolute dose - Simple phantom standard dose measurement Point doses in beams - Phantoms of relatively simple
Future upcoming technologies and what audit needs to address Dr R.I MacKay History of audit Absolute dose - Simple phantom standard dose measurement Point doses in beams - Phantoms of relatively simple
A Dosimetric Comparison of Whole-Lung Treatment Techniques. in the Pediatric Population
 A Dosimetric Comparison of Whole-Lung Treatment Techniques in the Pediatric Population Corresponding Author: Christina L. Bosarge, B.S., R.T. (R) (T) Indiana University School of Medicine Department of
A Dosimetric Comparison of Whole-Lung Treatment Techniques in the Pediatric Population Corresponding Author: Christina L. Bosarge, B.S., R.T. (R) (T) Indiana University School of Medicine Department of
Feasibility of the partial-single arc technique in RapidArc planning for prostate cancer treatment
 Chinese Journal of Cancer Original Article Feasibility of the partial-single arc technique in RapidArc planning for prostate cancer treatment Suresh Rana 1 and ChihYao Cheng 2 Abstract The volumetric modulated
Chinese Journal of Cancer Original Article Feasibility of the partial-single arc technique in RapidArc planning for prostate cancer treatment Suresh Rana 1 and ChihYao Cheng 2 Abstract The volumetric modulated
Adaptive planning in the context of adaptive radiotherapy
 in the context of adaptive radiotherapy Danilo Pasini Radiotherapy Department Università Cattolica del Sacro Cuore - Rome Zagreb 6/8 November Knowledge Based Oncology Individualizing Modelling Adaptive
in the context of adaptive radiotherapy Danilo Pasini Radiotherapy Department Università Cattolica del Sacro Cuore - Rome Zagreb 6/8 November Knowledge Based Oncology Individualizing Modelling Adaptive
Knowledge-Based IMRT Treatment Planning for Prostate Cancer: Experience with 101. Cases from Duke Clinic. Deon Martina Dick
 Knowledge-Based IMRT Treatment Planning for Prostate Cancer: Experience with 101 Cases from Duke Clinic by Deon Martina Dick Department of Medical Physics Duke University Date: Approved: Joseph Lo, Chair
Knowledge-Based IMRT Treatment Planning for Prostate Cancer: Experience with 101 Cases from Duke Clinic by Deon Martina Dick Department of Medical Physics Duke University Date: Approved: Joseph Lo, Chair
Intensity modulated radiotherapy (IMRT) for treatment of post-operative high grade glioma in the right parietal region of brain
 1 Carol Boyd March Case Study March 11, 2013 Intensity modulated radiotherapy (IMRT) for treatment of post-operative high grade glioma in the right parietal region of brain History of Present Illness:
1 Carol Boyd March Case Study March 11, 2013 Intensity modulated radiotherapy (IMRT) for treatment of post-operative high grade glioma in the right parietal region of brain History of Present Illness:
Adaptive radiotherapy: le variazioni degli organi a rischio e dell anatomia del paziente. F. Ricchetti (Negrar, VR)
 Adaptive radiotherapy: le variazioni degli organi a rischio e dell anatomia del paziente F. Ricchetti (Negrar, VR) Adaptive RT for HN SCC day 1 Adaptive RT for HN SCC day 1 day 2 Despite adequate nutritional
Adaptive radiotherapy: le variazioni degli organi a rischio e dell anatomia del paziente F. Ricchetti (Negrar, VR) Adaptive RT for HN SCC day 1 Adaptive RT for HN SCC day 1 day 2 Despite adequate nutritional
ESOPHAGEAL CANCER DOSE ESCALATION USING A SIMULTANEOUS INTEGRATED BOOST TECHNIQUE
 doi:10.1016/j.ijrobp.2010.10.023 Int. J. Radiation Oncology Biol. Phys., Vol. 82, No. 1, pp. 468 474, 2012 Copyright Ó 2012 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/$ - see front
doi:10.1016/j.ijrobp.2010.10.023 Int. J. Radiation Oncology Biol. Phys., Vol. 82, No. 1, pp. 468 474, 2012 Copyright Ó 2012 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/$ - see front
The PreciseART Approach to Adaptive Radiotherapy with the RADIXACT System. Prof. Anne Laprie Radiation Oncologist
 The PreciseART Approach to Adaptive Radiotherapy with the RADIXACT System Prof. Anne Laprie Radiation Oncologist Disclosure & Disclaimer An honorarium is provided by Accuray for this presentation The views
The PreciseART Approach to Adaptive Radiotherapy with the RADIXACT System Prof. Anne Laprie Radiation Oncologist Disclosure & Disclaimer An honorarium is provided by Accuray for this presentation The views
Organ Contour Adaptor to create new structures to use for adaptive radiotherapy of cervix cancer using Matlab Bridge and 3DSlicer / SlicerRT
 Organ Contour Adaptor to create new structures to use for adaptive radiotherapy of cervix cancer using Matlab Bridge and 3DSlicer / SlicerRT Y. Seppenwoolde 1,2, M. Daniel 2, H. Furtado 2,3, D. Georg 1,2
Organ Contour Adaptor to create new structures to use for adaptive radiotherapy of cervix cancer using Matlab Bridge and 3DSlicer / SlicerRT Y. Seppenwoolde 1,2, M. Daniel 2, H. Furtado 2,3, D. Georg 1,2
Adaptive Radiotherapy for H&N Cancers: What Forms of Rescheduling? Debates Surrounding a Clinical Case
 clinical cases Adaptive Radiotherapy for H&N Cancers: What Forms of Rescheduling? Debates Surrounding a Clinical Case Ovidiu Veresezan 1, Catherine Dejean 2, Mathieu Gautier 2, Juliette Thariat 3 1) Radiotherapy
clinical cases Adaptive Radiotherapy for H&N Cancers: What Forms of Rescheduling? Debates Surrounding a Clinical Case Ovidiu Veresezan 1, Catherine Dejean 2, Mathieu Gautier 2, Juliette Thariat 3 1) Radiotherapy
Normal tissue doses from MV image-guided radiation therapy (IGRT) using orthogonal MV and MV-CBCT
 Received: 28 September 2017 Revised: 17 November 2017 Accepted: 28 December 2017 DOI: 10.1002/acm2.12276 RADIATION ONCOLOGY PHYSICS Normal tissue doses from MV image-guided radiation therapy (IGRT) using
Received: 28 September 2017 Revised: 17 November 2017 Accepted: 28 December 2017 DOI: 10.1002/acm2.12276 RADIATION ONCOLOGY PHYSICS Normal tissue doses from MV image-guided radiation therapy (IGRT) using
UNIVERSITY OF WISCONSIN-LA CROSSE Graduate Studies
 UNIVERSITY OF WISCONSIN-LA CROSSE Graduate Studies A SINGLE INSTITUTION S EXPERIENCE IN DEVELOPING A PURPOSEFUL AND EFFICIENT OFF-LINE TECHNIQUE FOR ADAPTIVE RADIOTHERAPY IN A CLINICAL ENVIRONMENT A Research
UNIVERSITY OF WISCONSIN-LA CROSSE Graduate Studies A SINGLE INSTITUTION S EXPERIENCE IN DEVELOPING A PURPOSEFUL AND EFFICIENT OFF-LINE TECHNIQUE FOR ADAPTIVE RADIOTHERAPY IN A CLINICAL ENVIRONMENT A Research
Specifics of treatment planning for active scanning and IMPT
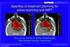 Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 14, NUMBER 6, 2013
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 14, NUMBER 6, 2013 A comparison of anatomical and dosimetric variations in the first 15 fractions, and between fractions 16 and 25, of intensity-modulated
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 14, NUMBER 6, 2013 A comparison of anatomical and dosimetric variations in the first 15 fractions, and between fractions 16 and 25, of intensity-modulated
Application of asi-kvcbct for Volume Assessment and Dose Estimation: An Offline Adaptive Study for Prostate Radiotherapy
 DOI:10.31557/APJCP.2019.20.1.229 Volume and Dose Assessment on Adapted CT RESEARCH ARTICLE Editorial Process: Submission:08/10/2018 Acceptance:01/05/2019 Application of asi-kvcbct for Volume Assessment
DOI:10.31557/APJCP.2019.20.1.229 Volume and Dose Assessment on Adapted CT RESEARCH ARTICLE Editorial Process: Submission:08/10/2018 Acceptance:01/05/2019 Application of asi-kvcbct for Volume Assessment
Clinical Oncology xxx (2011) 1e8. Contents lists available at SciVerse ScienceDirect. Clinical Oncology
 Clinical Oncology xxx (2011) 1e8 Contents lists available at SciVerse ScienceDirect Clinical Oncology journal homepage: www.clinicaloncologyonline.net Original Article Adaptive Radiotherapy Using Helical
Clinical Oncology xxx (2011) 1e8 Contents lists available at SciVerse ScienceDirect Clinical Oncology journal homepage: www.clinicaloncologyonline.net Original Article Adaptive Radiotherapy Using Helical
Chapters from Clinical Oncology
 Chapters from Clinical Oncology Lecture notes University of Szeged Faculty of Medicine Department of Oncotherapy 2012. 1 RADIOTHERAPY Technical aspects Dr. Elemér Szil Introduction There are three possibilities
Chapters from Clinical Oncology Lecture notes University of Szeged Faculty of Medicine Department of Oncotherapy 2012. 1 RADIOTHERAPY Technical aspects Dr. Elemér Szil Introduction There are three possibilities
Measurement of Dose to Critical Structures Surrounding the Prostate from. Intensity-Modulated Radiation Therapy (IMRT) and Three Dimensional
 Measurement of Dose to Critical Structures Surrounding the Prostate from Intensity-Modulated Radiation Therapy (IMRT) and Three Dimensional Conformal Radiation Therapy (3D-CRT); A Comparative Study Erik
Measurement of Dose to Critical Structures Surrounding the Prostate from Intensity-Modulated Radiation Therapy (IMRT) and Three Dimensional Conformal Radiation Therapy (3D-CRT); A Comparative Study Erik
Which nasopharyngeal cancer patients need adaptive radiotherapy?
 Hu et al. BMC Cancer (2018) 18:1234 https://doi.org/10.1186/s12885-018-5159-y RESEARCH ARTICLE Which nasopharyngeal cancer patients need adaptive radiotherapy? Open Access Yu-Chang Hu 1,2, Kuo-Wang Tsai
Hu et al. BMC Cancer (2018) 18:1234 https://doi.org/10.1186/s12885-018-5159-y RESEARCH ARTICLE Which nasopharyngeal cancer patients need adaptive radiotherapy? Open Access Yu-Chang Hu 1,2, Kuo-Wang Tsai
Proton Beam Therapy at Mayo Clinic
 Proton Beam Therapy at Mayo Clinic Jon J. Kruse, Ph.D. Mayo Clinic Dept. of Radiation Oncology Rochester, MN History of Proton Therapy at Mayo 2002: Decided to consider particle therapy analysis and education
Proton Beam Therapy at Mayo Clinic Jon J. Kruse, Ph.D. Mayo Clinic Dept. of Radiation Oncology Rochester, MN History of Proton Therapy at Mayo 2002: Decided to consider particle therapy analysis and education
Department of Radiotherapy & Nuclear Medicine, National Cancer Institute, Cairo University, Cairo, Egypt.
 Original article Res. Oncol. Vol. 12, No. 1, Jun. 2016:10-14 Dosimetric comparison of 3D conformal conventional radiotherapy versus intensity-modulated radiation therapy both in conventional and high dose
Original article Res. Oncol. Vol. 12, No. 1, Jun. 2016:10-14 Dosimetric comparison of 3D conformal conventional radiotherapy versus intensity-modulated radiation therapy both in conventional and high dose
Discuss the general planning concepts used in proton planning. Review the unique handling of CTV / ITV / PTV when treating with protons
 Mark Pankuch, PhD Discuss the general planning concepts used in proton planning Review the unique handling of CTV / ITV / PTV when treating with protons Pencil Beam distributions and PBS optimization Cover
Mark Pankuch, PhD Discuss the general planning concepts used in proton planning Review the unique handling of CTV / ITV / PTV when treating with protons Pencil Beam distributions and PBS optimization Cover
Image Fusion, Contouring, and Margins in SRS
 Image Fusion, Contouring, and Margins in SRS Sarah Geneser, Ph.D. Department of Radiation Oncology University of California, San Francisco Overview Review SRS uncertainties due to: image registration contouring
Image Fusion, Contouring, and Margins in SRS Sarah Geneser, Ph.D. Department of Radiation Oncology University of California, San Francisco Overview Review SRS uncertainties due to: image registration contouring
Automated Plan Quality Check with Scripting. Rajesh Gutti, Ph.D. Clinical Medical Physicist
 Automated Plan Quality Check with Scripting Rajesh Gutti, Ph.D. Clinical Medical Physicist Veera.Gutti@BSWHealth.org Outline Introduction - BSW Automation in Treatment planning Eclipse Scripting API Script
Automated Plan Quality Check with Scripting Rajesh Gutti, Ph.D. Clinical Medical Physicist Veera.Gutti@BSWHealth.org Outline Introduction - BSW Automation in Treatment planning Eclipse Scripting API Script
The effect of region extraction accuracy on the dose calculation with CBCT images combined with MSCT images.
 The effect of region extraction accuracy on the dose calculation with CBCT images combined with MSCT images. Poster No.: C-0648 Congress: ECR 2013 Type: Scientific Exhibit Authors: K. Usui, E. Kunieda,
The effect of region extraction accuracy on the dose calculation with CBCT images combined with MSCT images. Poster No.: C-0648 Congress: ECR 2013 Type: Scientific Exhibit Authors: K. Usui, E. Kunieda,
Impact of internal variations on the dose distribution during the course of radiotherapy of prostatectomy patients
 SAHLGRENSKA ACADEMY Impact of internal variations on the dose distribution during the course of radiotherapy of prostatectomy patients Tommy Andreasson Thesis: 30 hp Program: Medical Physicist Programme
SAHLGRENSKA ACADEMY Impact of internal variations on the dose distribution during the course of radiotherapy of prostatectomy patients Tommy Andreasson Thesis: 30 hp Program: Medical Physicist Programme
A dosimetric comparison of proton and photon therapy in unresectable cancers of the head of pancreas
 A dosimetric comparison of proton and photon therapy in unresectable cancers of the head of pancreas Reid F. Thompson University of Pennsylvania, Philadelphia, Pennsylvania 1914 Sonal U. Mayekar Thomas
A dosimetric comparison of proton and photon therapy in unresectable cancers of the head of pancreas Reid F. Thompson University of Pennsylvania, Philadelphia, Pennsylvania 1914 Sonal U. Mayekar Thomas
Clinical Usage of Knowledge Based Treatment Planning
 Clinical Usage of Knowledge Based Treatment Planning Xiaodong Zhang Department of Radiation Physics, UT MDACC Disclosures Research funds from Sister Institution Network Funds from MDACC Varian Medical
Clinical Usage of Knowledge Based Treatment Planning Xiaodong Zhang Department of Radiation Physics, UT MDACC Disclosures Research funds from Sister Institution Network Funds from MDACC Varian Medical
Advances in external beam radiotherapy
 International Conference on Modern Radiotherapy: Advances and Challenges in Radiation Protection of Patients Advances in external beam radiotherapy New techniques, new benefits and new risks Michael Brada
International Conference on Modern Radiotherapy: Advances and Challenges in Radiation Protection of Patients Advances in external beam radiotherapy New techniques, new benefits and new risks Michael Brada
Treatment Planning Evaluation of Volumetric Modulated Arc Therapy (VMAT) for Craniospinal Irradiation (CSI)
 Treatment Planning Evaluation of Volumetric Modulated Arc Therapy (VMAT) for Craniospinal Irradiation (CSI) Tagreed AL-ALAWI Medical Physicist King Abdullah Medical City- Jeddah Aim 1. Simplify and standardize
Treatment Planning Evaluation of Volumetric Modulated Arc Therapy (VMAT) for Craniospinal Irradiation (CSI) Tagreed AL-ALAWI Medical Physicist King Abdullah Medical City- Jeddah Aim 1. Simplify and standardize
Multi-Case Knowledge-Based IMRT Treatment Planning in Head and Neck Cancer. Shelby Mariah Grzetic. Graduate Program in Medical Physics Duke University
 Multi-Case Knowledge-Based IMRT Treatment Planning in Head and Neck Cancer by Shelby Mariah Grzetic Graduate Program in Medical Physics Duke University Date: Approved: Joseph Y. Lo, Co-Supervisor Shiva
Multi-Case Knowledge-Based IMRT Treatment Planning in Head and Neck Cancer by Shelby Mariah Grzetic Graduate Program in Medical Physics Duke University Date: Approved: Joseph Y. Lo, Co-Supervisor Shiva
Utilizzo delle tecniche VMAT nei trattamenti del testa collo Marta Scorsetti M.D.
 Utilizzo delle tecniche VMAT nei trattamenti del testa collo Marta Scorsetti M.D. Radiotherapy and Radiosurgery Dpt. Istituto Clinico Humanitas, Milan, Italy. Higher doses to the tumor Better sparing of
Utilizzo delle tecniche VMAT nei trattamenti del testa collo Marta Scorsetti M.D. Radiotherapy and Radiosurgery Dpt. Istituto Clinico Humanitas, Milan, Italy. Higher doses to the tumor Better sparing of
To Reduce Hot Dose Spots in Craniospinal Irradiation: An IMRT Approach with Matching Beam Divergence
 SCIENCE & TECHNOLOGY To Reduce Hot Dose Spots in Craniospinal Irradiation: An IMRT Approach with Matching Beam Divergence Alburuj R. Rahman*, Jian Z. Wang, Dr. Z. Huang, Dr. J. Montebello Department of
SCIENCE & TECHNOLOGY To Reduce Hot Dose Spots in Craniospinal Irradiation: An IMRT Approach with Matching Beam Divergence Alburuj R. Rahman*, Jian Z. Wang, Dr. Z. Huang, Dr. J. Montebello Department of
A TREATMENT PLANNING STUDY COMPARING VMAT WITH 3D CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER USING PINNACLE PLANNING SYSTEM *
 Romanian Reports in Physics, Vol. 66, No. 2, P. 394 400, 2014 A TREATMENT PLANNING STUDY COMPARING VMAT WITH 3D CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER USING PINNACLE PLANNING SYSTEM * D. ADAM 1,2,
Romanian Reports in Physics, Vol. 66, No. 2, P. 394 400, 2014 A TREATMENT PLANNING STUDY COMPARING VMAT WITH 3D CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER USING PINNACLE PLANNING SYSTEM * D. ADAM 1,2,
Sarcoma and Radiation Therapy. Gabrielle M Kane MB BCh EdD FRCPC Muir Professorship in Radiation Oncology University of Washington
 Sarcoma and Radiation Therapy Gabrielle M Kane MB BCh EdD FRCPC Muir Professorship in Radiation Oncology University of Washington Objective: Helping you make informed decisions Introduction Process Radiation
Sarcoma and Radiation Therapy Gabrielle M Kane MB BCh EdD FRCPC Muir Professorship in Radiation Oncology University of Washington Objective: Helping you make informed decisions Introduction Process Radiation
TOMOTERAPIA in Italia: Esperienze a confronto
 TOMOTERAPIA in Italia: Esperienze a confronto BARD 20 novembre 2010 L esperienza di Reggio Emilia Testa collo Alessandro Muraglia Reasons for the use of tomotherapy: - Complex tumor geometry and proximity
TOMOTERAPIA in Italia: Esperienze a confronto BARD 20 novembre 2010 L esperienza di Reggio Emilia Testa collo Alessandro Muraglia Reasons for the use of tomotherapy: - Complex tumor geometry and proximity
Intensity Modulated Radiation Therapy (IMRT)
 Intensity Modulated Radiation Therapy (IMRT) Policy Number: Original Effective Date: MM.05.006 03/09/2004 Line(s) of Business: Current Effective Date: HMO; PPO 06/24/2011 Section: Radiology Place(s) of
Intensity Modulated Radiation Therapy (IMRT) Policy Number: Original Effective Date: MM.05.006 03/09/2004 Line(s) of Business: Current Effective Date: HMO; PPO 06/24/2011 Section: Radiology Place(s) of
Dosimetric Comparison of Intensity-Modulated Radiotherapy versus 3D Conformal Radiotherapy in Patients with Head and Neck Cancer
 Dosimetric Comparison of Intensity-Modulated Radiotherapy versus 3D Conformal Radiotherapy in Patients with Head and Neck Cancer 1- Doaa M. AL Zayat. Ph.D of medical physics, Ayadi-Al Mostakbl Oncology
Dosimetric Comparison of Intensity-Modulated Radiotherapy versus 3D Conformal Radiotherapy in Patients with Head and Neck Cancer 1- Doaa M. AL Zayat. Ph.D of medical physics, Ayadi-Al Mostakbl Oncology
Comparison of high and low energy treatment plans by evaluating the dose on the surrounding normal structures in conventional radiotherapy
 Turkish Journal of Cancer Volume 37, No. 2, 2007 59 Comparison of high and low energy treatment plans by evaluating the dose on the surrounding normal structures in conventional radiotherapy MUHAMMAD BASIM
Turkish Journal of Cancer Volume 37, No. 2, 2007 59 Comparison of high and low energy treatment plans by evaluating the dose on the surrounding normal structures in conventional radiotherapy MUHAMMAD BASIM
A STUDY OF PLANNING DOSE CONSTRAINTS FOR TREATMENT OF NASOPHARYNGEAL CARCINOMA USING A COMMERCIAL INVERSE TREATMENT PLANNING SYSTEM
 doi:10.1016/j.ijrobp.2004.02.040 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 3, pp. 886 896, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
doi:10.1016/j.ijrobp.2004.02.040 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 3, pp. 886 896, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
Guidelines for the use of inversely planned treatment techniques in Clinical Trials: IMRT, VMAT, TomoTherapy
 Guidelines for the use of inversely planned treatment techniques in Clinical Trials: IMRT, VMAT, TomoTherapy VERSION 2.1 April 2015 Table of Contents Abbreviations & Glossary... 3 Executive Summary...
Guidelines for the use of inversely planned treatment techniques in Clinical Trials: IMRT, VMAT, TomoTherapy VERSION 2.1 April 2015 Table of Contents Abbreviations & Glossary... 3 Executive Summary...
CURRICULUM OUTLINE FOR TRANSITIONING FROM 2-D RT TO 3-D CRT AND IMRT
 CURRICULUM OUTLINE FOR TRANSITIONING FROM 2-D RT TO 3-D CRT AND IMRT Purpose The purpose of this curriculum outline is to provide a framework for multidisciplinary training for radiation oncologists, medical
CURRICULUM OUTLINE FOR TRANSITIONING FROM 2-D RT TO 3-D CRT AND IMRT Purpose The purpose of this curriculum outline is to provide a framework for multidisciplinary training for radiation oncologists, medical
Dose prescription, reporting and recording in intensity-modulated radiation therapy: a digest of the ICRU Report 83
 Special report Dose prescription, reporting and recording in intensity-modulated radiation therapy: a digest of the ICRU Report 83 Rapid development in imaging techniques, including functional imaging,
Special report Dose prescription, reporting and recording in intensity-modulated radiation therapy: a digest of the ICRU Report 83 Rapid development in imaging techniques, including functional imaging,
8/3/2016. Outline. Site Specific IGRT Considerations for Clinical Imaging Protocols. Krishni Wijesooriya, PhD University of Virginia
 Site Specific IGRT Considerations for Clinical Imaging Protocols Krishni Wijesooriya, PhD University of Virginia Outline Image registration accuracies for different modalities What imaging modality best
Site Specific IGRT Considerations for Clinical Imaging Protocols Krishni Wijesooriya, PhD University of Virginia Outline Image registration accuracies for different modalities What imaging modality best
Andrew K. Lee, MD, MPH Associate Professor Department tof fradiation Oncology M.D. Anderson Cancer Center
 Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Associate Professor Department tof fradiation Oncology M.D. Anderson Cancer Center Seungtaek Choi, MD Assistant Professor Department tof fradiation
Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Associate Professor Department tof fradiation Oncology M.D. Anderson Cancer Center Seungtaek Choi, MD Assistant Professor Department tof fradiation
Clinical study of the time of repeated computed tomography and replanning for patients with nasopharyngeal carcinoma
 /, 2017, Vol. 8, (No. 16), pp: 27529-27540 Clinical study of the time of repeated computed tomography and replanning for patients with nasopharyngeal carcinoma Xiujuan Gai 1,2,*, Yumei Wei 2,*, Hengmin
/, 2017, Vol. 8, (No. 16), pp: 27529-27540 Clinical study of the time of repeated computed tomography and replanning for patients with nasopharyngeal carcinoma Xiujuan Gai 1,2,*, Yumei Wei 2,*, Hengmin
A new homogeneity index based on statistical analysis of the dose volume histogram
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 8, NUMBER 2, SPRING 2007 A new homogeneity index based on statistical analysis of the dose volume histogram Myonggeun Yoon, Sung Yong Park, a Dongho
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 8, NUMBER 2, SPRING 2007 A new homogeneity index based on statistical analysis of the dose volume histogram Myonggeun Yoon, Sung Yong Park, a Dongho
SUPERIORITY OF A REAL TIME PLANNING TECHNIQUE OVER IMAGE GUIDED RADIATION THERAPY FOR THE TREATMENT OF PRIMARY PROSTATE CANCERS
 SUPERIORITY OF A REAL TIME PLANNING TECHNIQUE OVER IMAGE GUIDED RADIATION THERAPY FOR THE TREATMENT OF PRIMARY PROSTATE CANCERS Authors: Scott Merrick James Wong MD, Mona Karim MD, Yana Goldberg MD DISCLOSURE
SUPERIORITY OF A REAL TIME PLANNING TECHNIQUE OVER IMAGE GUIDED RADIATION THERAPY FOR THE TREATMENT OF PRIMARY PROSTATE CANCERS Authors: Scott Merrick James Wong MD, Mona Karim MD, Yana Goldberg MD DISCLOSURE
International Multispecialty Journal of Health (IMJH) ISSN: [ ] [Vol-3, Issue-9, September- 2017]
![International Multispecialty Journal of Health (IMJH) ISSN: [ ] [Vol-3, Issue-9, September- 2017] International Multispecialty Journal of Health (IMJH) ISSN: [ ] [Vol-3, Issue-9, September- 2017]](/thumbs/84/90586123.jpg) Dosimetric evaluation of carcinoma nasopharynx using Volumetric Modulated Arc Therapy (VMAT): An institutional experience from Western India Dr. Upendra Nandwana 1, Dr. Shuchita Pathak 2, Dr. TP Soni 3,
Dosimetric evaluation of carcinoma nasopharynx using Volumetric Modulated Arc Therapy (VMAT): An institutional experience from Western India Dr. Upendra Nandwana 1, Dr. Shuchita Pathak 2, Dr. TP Soni 3,
Margins in SBRT. Mischa Hoogeman
 Margins in SBRT Mischa Hoogeman MARGIN CONCEPTS Why do we use margins? Target / tumor To a-priori compensate for (unknown) deviations between the intended target position and the real target position during
Margins in SBRT Mischa Hoogeman MARGIN CONCEPTS Why do we use margins? Target / tumor To a-priori compensate for (unknown) deviations between the intended target position and the real target position during
Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana
 University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Application of Implanted Markers in Proton Therapy. Course Outline. McLaren Proton Therapy Center Karmanos Cancer Institute McLaren - Flint
 Application of Implanted Markers in Proton Therapy Sung Yong Park, Ph.D. McLaren Proton Therapy Center Karmanos Cancer Institute McLaren - Flint AAPM 2016, SAM Therapy Educational Course, 2016.08.04. Course
Application of Implanted Markers in Proton Therapy Sung Yong Park, Ph.D. McLaren Proton Therapy Center Karmanos Cancer Institute McLaren - Flint AAPM 2016, SAM Therapy Educational Course, 2016.08.04. Course
Josh Howard CMD Upendra Parvathaneni MBBS, FRANZCR
 Anatomic and Dosimetric Correlation in the Treatment of Advanced Larynx Cancer- When is the Brachial Plexus at Risk? Josh Howard CMD Upendra Parvathaneni MBBS, FRANZCR AAMD 39th Annual Meeting - Seattle
Anatomic and Dosimetric Correlation in the Treatment of Advanced Larynx Cancer- When is the Brachial Plexus at Risk? Josh Howard CMD Upendra Parvathaneni MBBS, FRANZCR AAMD 39th Annual Meeting - Seattle
Role of adaptive radiation therapy for pediatric patients with diffuse pontine glioma
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 12, NUMBER 2, spring 2011 Role of adaptive radiation therapy for pediatric patients with diffuse pontine glioma Chris Beltran, a Saumya Sharma, and Thomas
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 12, NUMBER 2, spring 2011 Role of adaptive radiation therapy for pediatric patients with diffuse pontine glioma Chris Beltran, a Saumya Sharma, and Thomas
