doi: /bjr/
|
|
|
- Olivia Bradford
- 5 years ago
- Views:
Transcription
1 doi: /bjr/
2 Prognostic factors in the consecutive institutional series of glioblastoma multiforme patients who received high-dose particle radiotherapy or conventional radiotherapy Masahide Matsuda 1, M.D., Ph.D., Tetsuya Yamamoto 1,2, M.D., Ph.D., Eiichi Ishikawa 1, M.D., Ph.D., Kei Nakai 1, M.D., Ph.D., Alexander Zaboronok 1, M.D., Shingo Takano 1, M.D., Ph.D., Akira Matsumura 1, M.D., Ph.D. Department of Neurosurgery 1 and Department of Radiation Oncology 2, University Hospital of Tsukuba, Tsukuba, Ibaraki, Japan short title: prognostic significance of high-dose particle radiotherapy 1
3 Abstract To evaluate the influence of prognostic factors related to patient selection on survival data, survival outcomes were retrospectively analyzed using our institutional consecutive series of 67 newly diagnosed glioblastoma multiforme (GBM) patients who had received either conventional fractionated photon radiotherapy (CRT) or high-dose particle radiotherapy (HDT). In CRT protocol, a total dose of Gy was administered. In HDT protocol, an averaged dose of approximately 30 GyEq at a single session and additional fractionated photon irradiation at a total dose of 30 Gy was administered in boron neutron capture therapy, and a total dose of 96.6GyEq was administered in proton therapy. Most of the patients had received chemotherapy with nimustine hydrochloride (ACNU) alone or with ACNU, procarbazine, and vincristine. The median overall and progression-free survival time for all patients was 17.7 months (95% CI, ) and 7.8 months (95% CI, ), respectively. The one- and two-year survival rate was 67.2% and 33.7%, respectively. The median overall survival time (OS) was 24.4 months (95% CI, ) for patients treated with HDT, compared with 14.2 months (95% CI, ) for those with CRT. The Cox proportional hazards model revealed radiation modality (HDT vs. CRT) and EORTC-RPA class to be the significant prognostic factors. Age, sex, preoperative performance status, treatment with or without advanced neuro-imaging, extent of surgery, and regimen of chemotherapy were not statistically significant. The median OS was 18.5 months (95% CI, ) in patients 65 years 2
4 and older, compared with 16.8 months (95% CI, ) in those 64 years and younger (p=0.871). The relatively positive survival data of selected patients who underwent HDT are unlikely to reflect patient selection alone. Randomized trials with strictly controlled inclusion criteria for the comparable selection of patients will still be required to demonstrate conclusively that prolonged survival can be attributed to these high-dose particle radiotherapies. 3
5 Introduction Glioblastoma multiforme (GBM) is a highly infiltrative primary malignant brain tumour in adults. The prognosis of GBM is generally extremely poor, and there has been little improvement in survival rates over the past three decades [1, 2]. Several randomized trials have demonstrated the survival benefits of conventional fractionated photon radiotherapy at a total dose of 45 to 60 Gy; the median overall survival time (OS) in these trials was 5.8 to 15.5 months [3 7]. Currently, conventional fractionated photon radiotherapy of approximately 60 Gy with concomitant and adjuvant use of temozolomide has been recognized as the standard postoperative treatment for newly diagnosed GBM [8, 9]. However, the five-year survival rate with this standard therapy is less than 10 % [9], suggesting that alternative therapeutic strategies are desperately needed. Most dose escalation studies of radiotherapy have been designed as case series of a small number of selected patients who underwent additional stereotactic radiosurgery, fractionated proton beam radiation, or intensity-modulated radiotherapy or another type of conformal radiotherapy [10-12]. Studies showing the better outcomes (median OS range: months) suggested that a radiation dose of at least 90 Gy of hyperfractionated radiotherapy should be used for irradiation in order to accomplish local tumour control. However, there has been no randomized controlled trial (RCT) to provide evidence in support of these favorable data, nor has there been any trial warranting a follow-up study using any form of high-dose radiotherapy [10, 13]. Thus, controversy remains 4
6 regarding not only the efficacy of high-dose radiotherapy but also regarding the influence of strict patient selection on outcomes achieved with this type of treatment. High-dose irradiation of a small-volume target could minimize central recurrence and any radiation dose-dependent adverse events in such trials. However, recurrences often occur in the target volume receiving a relatively low-dose treatment. The five-year survival rate with conventional-dose radiotherapy alone is reported around 1% [9], which suggested a limitation of conventional-dose radiotherapy in most patients. We recently reported two different types of high-dose particle radiotherapy using boron neutron capture therapy (BNCT) and proton therapy (PT). These radiotherapies for newly-diagnosed GBM were administered based on different selection criteria, and both showed an acceptable OS (i.e., 25.7 months in the BNCT group, and 21.6 months in PT group), with acceptable adverse events [14, 15]. Previously, several different factors (e.g., age, preoperative performance status [PS], tumour location, extent of surgery, and conventional radiotherapy) have been shown to be prognostic of survival in patients with GBM [16-20]. Here we aimed to evaluate the influence of such patient selection-related factors on survival. Survival outcomes and prognostic factors were retrospectively analyzed using our institutional consecutive series of newly diagnosed GBM patients who had received either conventional fractionated photon radiotherapy (CRT) or high-dose particle radiotherapy (HDT). In the present paper, we report the combined updated results of all patients treated by both forms of particle therapy. 5
7 Materials and Methods We investigated 67 consecutive patients with newly diagnosed supratentorial GBM (grade IV) who were treated at Tsukuba University Hospital from January 1998 to August The patients were histopathologically diagnosed according to the classification system of the World Health Organization. Some of the survival data for patients who received PT or BNCT have been reported in earlier publications using different follow-up periods and survival analysis determinations [14, 15]. Maximal safe resection was intended to remove all gadolinium (Gd)-enhanced masses observed by magnetic resonance (MR) imaging, i.e., the surrounding non-eloquent brain tissue was targeted for removal, with the aim of preserving neurological function in unresected areas of eloquent brain tissue. To this end, 5-aminolevulinic-acid-induced fluorescence guidance, neuronavigation, as well as intraoperative monitoring were incorporated into the treatment. The navigation-guided fence-post procedure was carried out as previously reported [21] in order to treat non-eloquent portions of tumours. In cases involving tumours located close to areas of eloquent tissue, we inserted silicon tubes along the boundary between the eloquent and non-eloquent tissue, as indicated by MR images. The phrase advanced neuro-imaging was used to refer to all surgical interventions involving fluorescence guidance and/or neuronavigation. 6
8 The postoperative radiation schedule for patients with GBM treated at our facilities consisted of 3 protocols. As the standard radiotherapy, daily CRT ( Gy) was administered five times per week, amounting to a total overall dose of Gy. For selected patients, HDT was used, consisting of either BNCT or PT. In the BNCT protocol, the gross tumor volume (GTV) and clinical target volume (CTV)-1 were defined as the residual gadolinium-enhancing volume. CTV-2 and CTV-3 were defined as GTV plus a margin of 2 cm and 3 cm, respectively. An averaged dose of approximately 30 GyEq at a single session, and additional fractionated photon irradiation at a total dose of 30 Gy was administered to GTV. The detailed protocol of BNCT has been described elsewhere [14]. BNCT was administered to patients with a supratentorial unilateral tumour located at no deeper than 7 cm from the brain surface, and who had a Karnofsky performance status (KPS) of 50 or more. In the PT protocol, CTV-1 was defined same as BNCT. On the other hand, CTV-2 was defined as GTV plus a margin of 1 cm and CTV-3 was defined as the surrounding edema. Furthermore, in the PT protocol, the planning target volume (PTV) was adopted that was defined as the CTV plus a margin of 5 mm for setup error. Conventional photon radiotherapy (50.4 Gy in 28 fractions) was delivered to PTV-3 in the morning. In the first half of the protocol, additional concomitant boost proton radiotherapy (23.1 GyE in 14 fractions) was delivered to PTV-2 more than 6 hours after photon radiotherapy. Then, in the latter half, proton radiotherapy (23.1 GyE in 14 fractions) was delivered to PTV-1. As a result, the total dose for PTV-1 was 96.6 GyE in 56 fractions, 7
9 73.5 GyE in 42 fractions for PTV-2, and 50.4 Gy in 28 fractions for PTV-3 [15]. The following criteria were used to select patients for PT: the presence of a supratentorial tumour lacking involvement of the brain stem or thalamus, a maximum postoperative tumour diameter of less than 4 cm, and a KPS of 60 or more. BNCT was administered to 15 patients and PT to 17 patients. The PAV combination regimen of procarbazine, nimustine hydrochloride (ACNU), and vincristine was administered as the standard concomitant chemotherapy combined with CRT. For patients at high risk for adverse events with PAV therapy (i.e., elderly patients, patients in poor neurological or general condition), ACNU alone was typically used as the concomitant chemotherapy. ACNU was also used in combination with HDT. Statistical analysis Statistical analyses were performed using SPSS software (version J; SPSS, Inc.). Overall survival and progression-free survival were used to investigate the prognostic impact of the variables analyzed. OS was defined as the time lapse from surgery until death or the final follow-up. Progression-free survival time was defined as the time lapse from surgery until a detection of progression or the final follow-up. Survival probabilities were calculated using the Kaplan-Meier method, and differences among patient groups were evaluated using the log-rank test. The Cox proportional hazards model was used to test the following prognostic factors in univariate and 8
10 multivariate analyses: age (<65 years vs. 65 years), sex (female vs. male), preoperative PS (0-2 vs. 3-4), European Organization for Research and Treatment of Cancer (EORTC) recursive partitioning analysis (RPA) class (III-IV vs. V) [21], advanced neuro-imaging (with vs. without), extent of surgery (complete resection vs. others), chemotherapy (ACNU vs. other), and radiation modality (HDT vs. CRT). Factors with a probability value of less than 0.05 on univariate analysis were selected for testing in the multivariate analysis. Results are expressed with relative risk and a 95% confidence interval (CI). Results The characteristics of the 67 patients are summarized in Table 1. Included in the analysis were 34 men and 33 women aged 31 to 84 years (median, 59.0 years). Surgical resection resulted in complete resection of the tumour in 13 (19%), partial resection in 47 (70%), and biopsy in 7 (10%) patients. Forty-seven (70%) patients received chemotherapy with ACNU or other agents. Thirty-two (48%) received HDT and thirty-five (52%) received CRT; consequently, all 67 patients received either one or the other type of radiotherapy. There were 6 (9%) patients with a WHO PS of 0, 30 (45%) with a PS of 1, 12 (18%) with a PS of 2, 10 (15%) with a PS of 3, and 9 (13%) with a PS of 4. Whereas 9 patients (13%) were categorized as having the best GBM prognosis (class III), 21 (31%) were in class IV, and 37 (55%) were in class V, according to the EORTC-RPA classification system. 9
11 Nine patients were alive at the time of analysis with a mean follow-up time of 21.4 (range ) months. The median OS for all patients was 17.7 months (95% CI, ). The one- and two-year survival rates were 67.2% and 33.7%, respectively. The median progression-free survival time in this series was 7.8 months (95% CI, ). The one- and two-year progression-free survival rates were 32.6 and 18.4%, respectively. The univariate and multivariate analyses of prognostic factors in this study are shown in Tables 2 and 3, respectively. The multivariate analysis revealed radiation modality and EORTC RPA class as significant prognostic factors. The median OS was 24.4 months (95% CI, ) for patients treated with HDT, compared with 14.2 months (95% CI, ) for those treated with CRT (Fig. 1). Other previously reported prognostic factors such as age, sex, preoperative PS, treatment with or without advanced neuro-imaging, extent of surgery, and regimen of chemotherapy were not statistically significant according to the multivariate analysis. The median OS was 18.5 months (95% CI, ) in patients 65 years and older, compared with 16.8 months (95% CI, ) in those 64 years and younger (p=0.871). Patients who were treated with HDT had a significantly better preoperative PS than patients treated with CRT (p=0.025). Similarly, patients who were treated with HDT were more likely to have undergone complete resection than patients treated with CRT (28.1% compared to 11.4%; p=0.078) and were more likely to be categorized in the better prognostic group (III-IV compared to V; 10
12 p=0.059); however, neither of these differences were statistically significant. Other clinical characteristics, i.e. age, sex, advanced neuro-imaging, and regimen of chemotherapy were not found to differ between patients who underwent HDT and those treated with CRT (Table 4). Discussion The median OS for all patients was 17.7 months; a longer median OS of 24.4 months was seen in the HDT group, compared to 14.2 months in the CRT group. Receiving either HDT or CRT was also factored out as a significant independent prognostic factor. The survival data for the CRT patients in this study were comparable to those of previous reports of patients treated with the standard therapies. Patient selection (e.g., age, PS, etc.) for the HDT group appeared not to be a major factor influencing survival time, nor did it negatively influence the survival time of the CRT patients. It is generally accepted that the concomitant and adjuvant use of temozolomide with conventional fractionated photon radiotherapy can be effective for treating post-operative GBM with minimal additional toxicity, and a significant survival advantage has been demonstrated for this approach compared to the administration of radiotherapy alone. The median OS in this RCT reported was 14.6 months with temozolomide-plus-radiotherapy, and 12.1 months with radiotherapy alone [8]. The median OS of CRT patients observed in this study was comparable to that of patients in the temozolomide treatment arm, whereas the median OS of all patients in this study was longer than that 11
13 of the patients in the temozolomide treatment arm. The patient characteristic data from the report by Stupp and colleagues showed that patients in the temozolomide treatment arm tended to be younger and better PS (0-1) populations, and belong to less-high risk (EORTC-RPA class V) populations (Table 5). These findings suggest that the favorable survival data of all patients and those of patients who underwent HDT in this study were unlikely to reflect patient selection alone. However, better extent of surgery (complete resection; 39% compared to 19%), more-moderate risk (EORTC-RPA class IV; 53% compared to 31%) populations, aggressive salvage treatment, and other indeterminate factors e.g. surgical technique, administration of standard care etc. may have positively influenced the survival data. Additionally, small sample size, inconsistent and non-controlled patient characteristics, may have affected the results and thus pose limitations on the findings of the present study. Here, the median OS of GBM patients increased from 15.2 months (95% CI, ) between 1982 and 1997 to 17.7 months (95% CI, ) between 1998 and 2007, although this trend was not statistically significant (p=0.086). The 2-year relative survival rate also increased from 23.6% between 1982 and 1997 to 33.7% between 1998 and Advancements in surgical techniques such as fluorescence guidance (since 1999) and in neuronavigation (since 2005), as well as improvements in chemotherapeutic agents, have been implemented at our institute; however, no significant differences in the extent of surgery or chemotherapy regimen were observed between 12
14 these two periods of time (i.e., pre-, post-1998). There remains no reliable evidence supporting these surgical approach and chemotherapy regimen as regards OS. Therefore, the improvements in OS may not have been related to surgical approach, but rather to changes made to the BNCT protocol since 1998 and those made to the PT protocol since 2001, when rotating gantries and regular daily fractionation became possible. In BNCT series, acute toxicities such as mild erythema (commonly observed), transient orbital swelling in 1 patient (6.7 %) were observed. On the other hand, No late toxicity was observed in the follow-up periods. In PT series, acute toxicities such as radiation dermatitis (commonly observed), rash in 1 patient (5.9 %), and headache in 5 patients (29.4 %) were observed. As for late toxicity, radiation necrosis in 1 patient (5.9 %) and leukoencephalopathy in 1 patient (5.9 %) were observed [14, 15]. Although these data indicate that toxicity in our HDT protocol seems to be acceptable at the analysis, incidence of late toxicities of survivors such as radiation necrosis and leukoencephalopathy remains to be monitored and clarified in longer follow-up time. Patient age has been reported as a strong prognostic factor in the treatment of GBM. In the RPA of EORTC, being 50 years old or older is a significant prognostic factor in the categorization of disease. However, in the present study, no correlation was found between age and prognosis. Recently, significant improvement in the survival of elderly patients with GBM has been observed with the introduction of aggressive treatments [23-25]. In the present series, almost no statistically significant 13
15 difference was observed in age-related survival probability. The mean age of PT and BNCT patients was 57 and 60 years, respectively. Aggressive treatment of elderly patients with GBM at our institute appears to have minimized the difference in age-related survival probability. Patients who were treated with HDT had a better preoperative PS and were more likely to have undergone complete resection than patients treated with CRT. It was not possible to separate the effects of HDT from the selection bias toward patients with a better prognosis, because the inclusion criteria of our HDT modalities, which are based on the characteristics of GBM patients, involve the restriction of PS and the limitations of tumour size and location, both of which are correlated with the difficulty of resection. However, even in patients categorized in the worst prognostic group (EORTC-RPA class V), OS was significantly prolonged for those who had received HDT compared to those treated with CRT (p=0.007). Similarly, among patients who underwent partial resection and biopsy, the OS was also significantly prolonged for those who received HDT versus those treated with CRT (p=0.005). These results indicate that the survival benefits of HDT appear unlikely to reflect patient selection alone. Conclusions It is generally accepted that both the size and location of a tumour, as well as patient performance status, should be considered in evaluations of the safety and efficacy of high-dose particle 14
16 radiotherapies. In this study, patients selected to receive HDT showed longer survival times compared than those treated with CRT. Although HDT, compared to CRT, was factored out as a significant favorable prognostic factor, other major prognostic factors did not appear to be confounding. The results of this study suggest that the relatively positive survival data of patients selected to undergo HDT are unlikely to reflect patient selection alone. Randomized trials with strictly controlled inclusion criteria for the comparable selection of patients are required to demonstrate conclusively that prolonged survival is a result of these high-dose radiotherapies. Acknowledgments This study was supported in part by a Grant-in-Aid for Scientific Research (C) from the Ministry of Education, Culture Sports, Science, and Technology of Japan ( ). 15
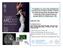
17 Figure legends Figure 1 Kaplan-Meier estimates of overall survival according to radiation modality. The hazard ratio for death among patients treated with high-dose radiotherapy, as compared to that among patients treated with conventional fractionated photon radiotherapy, was 0.44 (95% CI, ; p<0.01). Table 1 Characteristics of 68 patients with glioblastoma multiforme * Advanced neuro-imaging indicates 5-aminolevulinic-acid-induced fluorescence guidance and neuronavigation **Radiation Therapy Oncology Group (RTOG)-RPA class VI patients were included in EORTC-RPA class V Table 2 Univariate analysis of prognostic factors for the survival of patients with glioblastoma multiforme Table 3 Multivariate analysis of prognostic factors for the survival of patients with glioblastoma multiforme 16
18 Table 4 Clinical characteristics of patients treated with HDT compared to CRT Table 5 Comparison of patient characteristics in the TMZ-plus-CRT arm of EORTC 26981/22981-NCIC patients and all patients in this study * Authors calculated 17
19 References 1. Barnholtz-Sloan JS, Sloan AE, Schwartz AG. Relative survival rates and patterns of diagnosis analyzed by time period for individuals with primary malignant brain tumour, J Neurosurg. 2003; 99: Tait MJ, Petrik V, Loosemore A, Bell BA, Papadopoulos MC. Survival of patients with glioblastoma multiforme has not improved between 1993 and 2004: analysis of 625 cases. Br J Neurosurg. 2007; 21 : Walker MD, Alexander E, Jr., Hunt WE, MacCarty CS, Mahaley MS, Jr., Mealey J, Jr., et al. Evaluation of BCNU and/or radiotherapy in the treatment of anaplastic gliomas. A cooperative clinical trial. J Neurosurg. 1978; 49: Walker MD, Green SB, Byar DP, Alexander E, Jr., Batzdorf U, Brooks WH, et al. Randomized comparisons of radiotherapy and nitrosoureas for the treatment of malignant glioma after surgery. N Engl J Med. 1980; 303: Kristiansen K, Hagen S, Kollevold T, Torvik A, Holme I, Nesbakken R, et al. Combined modality therapy of operated astrocytomas grade III and IV. Confirmation of the value of postoperative irradiation and lack of potentiation of bleomycin on survival time: a prospective multicenter trial of the Scandinavian Glioblastoma Study Group. Cancer. 1981; 47: Sandberg-Wollheim M, Malmstrom P, Stromblad LG, Anderson H, Borgstrom S, Brun A, et al. 18
20 A randomized study of chemotherapy with procarbazine, vincristine, and lomustine with and without radiation therapy for astrocytoma grades 3 and/or 4. Cancer. 1991; 68: Andersen AP. Postoperative irradiation of glioblastomas. Results in a randomized series. Acta Radiol Oncol Radiat Phys Biol. 1978; 17: Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ, et al. Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med. 2005; 352: Stupp R, Hegi ME, Mason WP, van den Bent MJ, Taphoorn MJ, Janzer RC, et al. Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol. 2009; 10: Fitzek MM, Thornton AF, Rabinov JD, Lev MH, Pardo FS, Munzenrider JE, et al. Accelerated fractionated proton/photon irradiation to 90 cobalt gray equivalent for glioblastoma multiforme: results of a phase II prospective trial. J Neurosurg. 1999; 91: Tanaka M, Ino Y, Nakagawa K, Tago M, Todo T. High-dose conformal radiotherapy for supratentorial malignant glioma: a historical comparison. Lancet Oncol. 2005;6: Iuchi T, Hatano K, Narita Y, Kodama T, Yamaki T, Osato K. Hypofractionated high-dose irradiation for the treatment of malignant astrocytomas using simultaneous integrated boost 19
21 technique by IMRT. Int J Radiat Oncol Biol Phys. 2006; 64: Souhami L, Seiferheld W, Brachman D, Podgorsak EB, Werner-Wasik M, Lustig R, et al. Randomized comparison of stereotactic radiosurgery followed by conventional radiotherapy with carmustine to conventional radiotherapy with carmustine for patients with glioblastoma multiforme: report of Radiation Therapy Oncology Group protocol. Int J Radiat Oncol Biol Phys. 2004; 60: Yamamoto T, Nakai K, Kageji T, Kumada H, Endo K, Matsuda M, et al. Boron neutron capture therapy for newly diagnosed glioblastoma. Radiother Oncol. 2009; 91: Mizumoto M, Tsuboi K, Igaki H, Yamamoto T, Takano S, Oshiro Y, et al. Phase I/II trial of hyperfractionated concomitant boost proton radiotherapy for supratentorial glioblastoma multiforme. Int J Radiat Oncol Biol Phys. 2010; 77: Lacroix M, Abi-Said D, Fourney DR, Gokaslan ZL, Shi W, DeMonte F, et al. A multivariate analysis of 416 patients with glioblastoma multiforme: prognosis, extent of resection, and survival. J Neurosurg. 2001; 95: Simpson JR, Horton J, Scott C, Curran WJ, Rubin P, Fischbach J, et al. Influence of location and extent of surgical resection on survival of patients with glioblastoma multiforme: results of three consecutive Radiation Therapy Oncology Group (RTOG) clinical trials. Int J Radiat Oncol Biol Phys. 1993; 26:
22 18. Walker MD, Green SB, Byar DP, Alexander E, Jr., Batzdorf U, Brooks WH, et al. Randomized comparisons of radiotherapy and nitrosoureas for the treatment of malignant glioma after surgery. N Engl J Med. 1980; 303: Jeremic B, Milicic B, Grujicic D, Dagovic A, Aleksandrovic J. Multivariate analysis of clinical prognostic factors in patients with glioblastoma multiforme treated with a combined modality approach. J Cancer Res Clin Oncol. 2003; 129: Curran WJ, Jr., Scott CB, Horton J, Nelson JS, Weinstein AS, Fischbach AJ, et al. Recursive partitioning analysis of prognostic factors in three Radiation Therapy Oncology Group malignant glioma trials. J Natl Cancer Inst. 1993; 85: Yoshikawa K, Kajiwara K, Morioka J, Fujii M, Tanaka N, Fujisawa H, et al. Improvement of functional outcome after radical surgery in glioblastoma patients: the efficacy of a navigation-guided fence-post procedure and neurophysiological monitoring. J Neurooncol. 2006; 78: Mirimanoff RO, Gorlia T, Mason W, Van den Bent MJ, Kortmann RD, Fisher B, et al. Radiotherapy and temozolomide for newly diagnosed glioblastoma: recursive partitioning analysis of the EORTC 26981/22981-NCIC CE3 phase III randomized trial. J Clin Oncol. 2006; 24: Keime-Guibert F, Chinot O, Taillandier L, Cartalat-Carel S, Frenay M, Kantor G, et al. 21
23 Radiotherapy for glioblastoma in the elderly. N Engl J Med. 2007; 356: Patwardhan RV, Shorter C, Willis BK, Reddy P, Smith D, Caldito GC, et al. Survival trends in elderly patients with glioblastoma multiforme: resective surgery, radiation, and chemotherapy. Surg Neurol. 2004; 62: Combs SE, Wagner J, Bischof M, Welzel T, Wagner F, Debus J, et al. Postoperative treatment of primary glioblastoma multiforme with radiation and concomitant temozolomide in elderly patients. Int J Radiat Oncol Biol Phys. 2008; 70:
24 Figure 1 High-dose radiotherapy Conventional fractionated photon radiotherapy Survival rate Time (months)
25 Table. 1 Characteristics No. of Patients(%) Age median 59.0 years range 31 to 84 years Sex male 34(51%) female 33(49%) Side left 33(49%) right 27(40%) midline or bilateral 7(10%) Location frontal lobe 32(48%) temporal lobe 19(28%) parietal lobe 17(25%) occipital lobe 1(1%) other 6(9%) Advanced neuro-imaging* yes 31(46%) no 36(54%) Extent of surgery complete 13 (19%) partial 47 (70%) biopsy 7 (10%) Chemotherapy nimustine hydrochloride 45(67%) other 2(3%) none 20(30%) Radiotherapy high dose 32(48%) conventional dose 35(52%) WHO performance status
26 0 6 (9%) 1 30 (45%) 2 12 (18%) 3 10 (15%) 4 9 (13%) EORTC-RPA class** III 9(13%) IV 21(31%) V 37(55%)
27 Table. 2 Variable Hazard ratio (95% CI) p Value Age (<65 years vs. 65 years) ( ) Sex (female vs. male) ( ) WHO performance status (0-2 vs. 3-4) ( ) EORTC-RPA class (III-IV vs. V) ( ) Advanced neuro-imaging (with vs. without) ( ) Extent of resection (complete vs. others) ( ) Chemotherapy (ACNU vs. others) ( ) Radiotherapy (high dose vs. conventional dose) ( ) 0.003
28 Table. 3 Variable Hazard ratio (95% CI) p Value WHO performance status (0-2 vs. 3-4) ( ) EORTC-RPA class (III-IV vs. V) ( ) Radiotherapy (high dose vs. conventional dose) ( ) 0.013
29 Table. 4 Characteristics No. of Patients(%) p Value high dose conventional dose age < sex male female Advanced neuro-imaging yes no extent of surgery complete resection 9 4 others chemotherapy ACNU others WHO performance status EORTC-RPA class III-IV V
30 Table. 5 Characteristics CRT plus TMZ This study Number of patients Age median 56 years 59 years range 19 to 70 years 31 to 84 years Sex male 185(64%) 34(51%) female 102(36%) 33(49%) Extent of surgery complete 113 (39%) 13 (19%) partial 126 (44%) 47 (70%) biopsy 48 (17%) 7 (10%) WHO performance status (39%) 6 (9%) (47%) 30 (45%) 2 38 (13%) 12 (18%) 3 0 (0%) 10 (15%) 4 0 (0%) 9 (13%) EORTC-RPA class III 42(15%) 9(13%) IV 152(53%) 21(31%) V 93(32%) 37(55%) No. of progression 244 (85%) 59 (88%) Salvage surgery 66* (27%) 20 (34%) Salvage chemotherapy 142* (58%) 54 (92%)
Carmustine implants and Temozolomide for the treatment of newly diagnosed high grade glioma
 National Institute for Health and Clinical Excellence Health Technology Appraisal Carmustine implants and Temozolomide for the treatment of newly diagnosed high grade glioma Personal statement Conventional
National Institute for Health and Clinical Excellence Health Technology Appraisal Carmustine implants and Temozolomide for the treatment of newly diagnosed high grade glioma Personal statement Conventional
Proton beam therapy with concurrent chemotherapy for glioblastoma multiforme: comparison of nimustine hydrochloride and temozolomide
 J Neurooncol DOI 1.17/s11-1-2228-4 CLINIcAL STUDY Proton beam therapy with concurrent chemotherapy for glioblastoma multiforme: comparison of nimustine hydrochloride and temozolomide Masashi Mizumoto 1
J Neurooncol DOI 1.17/s11-1-2228-4 CLINIcAL STUDY Proton beam therapy with concurrent chemotherapy for glioblastoma multiforme: comparison of nimustine hydrochloride and temozolomide Masashi Mizumoto 1
Collection of Recorded Radiotherapy Seminars
 IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
Survival of High Grade Glioma Patients Treated by Three Radiation Schedules with Chemotherapy: A Retrospective Comparative Study
 Original Article Research in Oncology June 2017; Vol. 13, No. 1: 18-22. DOI: 10.21608/resoncol.2017.552.1022 Survival of High Grade Glioma Patients Treated by Three Radiation Schedules with Chemotherapy:
Original Article Research in Oncology June 2017; Vol. 13, No. 1: 18-22. DOI: 10.21608/resoncol.2017.552.1022 Survival of High Grade Glioma Patients Treated by Three Radiation Schedules with Chemotherapy:
Hypofractionated radiation therapy for glioblastoma
 Hypofractionated radiation therapy for glioblastoma Luis Souhami, MD, FASTRO Professor McGill University Department of Oncology, Division of Radiation Oncology Montreal Canada McGill University Health
Hypofractionated radiation therapy for glioblastoma Luis Souhami, MD, FASTRO Professor McGill University Department of Oncology, Division of Radiation Oncology Montreal Canada McGill University Health
3-D conformal radiotherapy with concomitant and adjuvant temozolomide for patients with glioblastoma multiforme and evaluation of prognostic factors
 research article 213 3-D conformal radiotherapy with concomitant and adjuvant temozolomide for patients with glioblastoma multiforme and evaluation of prognostic factors Yilmaz Tezcan and Mehmet Koc Department
research article 213 3-D conformal radiotherapy with concomitant and adjuvant temozolomide for patients with glioblastoma multiforme and evaluation of prognostic factors Yilmaz Tezcan and Mehmet Koc Department
Newcastle Neuro-oncology Team Audit of Outcome of Glioblastoma Multiforme Chemoradiotherapy Treatment
 Newcastle Neuro-oncology Team Audit of Outcome of Glioblastoma Multiforme Chemoradiotherapy Treatment Jennifer Wright Neurosurgery SSC Audit Team Jennifer Wright, Rachel Tresman, Cyril Dubois, Surash Surash,
Newcastle Neuro-oncology Team Audit of Outcome of Glioblastoma Multiforme Chemoradiotherapy Treatment Jennifer Wright Neurosurgery SSC Audit Team Jennifer Wright, Rachel Tresman, Cyril Dubois, Surash Surash,
PROCARBAZINE, lomustine, and vincristine (PCV) is
 RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
Concomitant (without adjuvant) temozolomide and radiation to treat glioblastoma: A retrospective study
 Concomitant (without adjuvant) temozolomide and radiation to treat glioblastoma: A retrospective study T Sridhar 1, A Gore 1, I Boiangiu 1, D Machin 2, R P Symonds 3 1. Department of Oncology, Leicester
Concomitant (without adjuvant) temozolomide and radiation to treat glioblastoma: A retrospective study T Sridhar 1, A Gore 1, I Boiangiu 1, D Machin 2, R P Symonds 3 1. Department of Oncology, Leicester
Survival Analysis of Glioblastoma Multiforme
 DOI:10.22034/APJCP.2018.19.9.2613 RESEARCH ARTICLE Editorial Process: Submission:04/24/2018 Acceptance:08/19/2018 Supapan Witthayanuwat, Montien Pesee*, Chunsri Supaadirek, Narudom Supakalin, Komsan Thamronganantasakul,
DOI:10.22034/APJCP.2018.19.9.2613 RESEARCH ARTICLE Editorial Process: Submission:04/24/2018 Acceptance:08/19/2018 Supapan Witthayanuwat, Montien Pesee*, Chunsri Supaadirek, Narudom Supakalin, Komsan Thamronganantasakul,
Scottish Medicines Consortium
 Scottish Medicines Consortium temozolomide 5, 20, 100 and 250mg capsules (Temodal ) Schering Plough UK Ltd No. (244/06) New indication: for the treatment of newly diagnosed glioblastoma multiforme concomitantly
Scottish Medicines Consortium temozolomide 5, 20, 100 and 250mg capsules (Temodal ) Schering Plough UK Ltd No. (244/06) New indication: for the treatment of newly diagnosed glioblastoma multiforme concomitantly
See the corresponding editorial in this issue, pp 1 2. J Neurosurg 115:3 8, An extent of resection threshold for newly diagnosed glioblastomas
 See the corresponding editorial in this issue, pp 1 2. J Neurosurg 115:3 8, 2011 An extent of resection threshold for newly diagnosed glioblastomas Clinical article Nader Sanai, M.D., 1 Mei-Yin Polley,
See the corresponding editorial in this issue, pp 1 2. J Neurosurg 115:3 8, 2011 An extent of resection threshold for newly diagnosed glioblastomas Clinical article Nader Sanai, M.D., 1 Mei-Yin Polley,
Zurich Open Repository and Archive. Long-term survival of glioblastoma patients treated with radiotherapy and lomustine plus temozolomide
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 19 CH-857 Zurich http://www.zora.uzh.ch Year: 29 Long-term survival of glioblastoma patients treated with radiotherapy and lomustine
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 19 CH-857 Zurich http://www.zora.uzh.ch Year: 29 Long-term survival of glioblastoma patients treated with radiotherapy and lomustine
PRESURGICAL PLANNING. Strongly consider neuropsychological evaluation before functional imaging study Strongly consider functional imaging study
 NOTE: Consider Clinical Trials as treatment options for eligible patients. Page 1 of 6 RADIOLOGICAL PRESENTATION PRESURGICAL PLANNING TREATMENT Imaging study suggestive of glioma 1 Left hemisphere speech/motor
NOTE: Consider Clinical Trials as treatment options for eligible patients. Page 1 of 6 RADIOLOGICAL PRESENTATION PRESURGICAL PLANNING TREATMENT Imaging study suggestive of glioma 1 Left hemisphere speech/motor
Zurich Open Repository and Archive. Long-term survival of glioblastoma patients treated with radiotherapy and lomustine plus temozolomide
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 Long-term survival of glioblastoma patients treated with radiotherapy and lomustine
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 Long-term survival of glioblastoma patients treated with radiotherapy and lomustine
Radiation and concomitant chemotherapy for patients with glioblastoma multiforme
 Chinese Journal of Cancer Review Radiation and concomitant chemotherapy for patients with glioblastoma multiforme Salvador Villà 1, Carme Balañà 2 and Sílvia Comas 1 Abstract Postoperative external beam
Chinese Journal of Cancer Review Radiation and concomitant chemotherapy for patients with glioblastoma multiforme Salvador Villà 1, Carme Balañà 2 and Sílvia Comas 1 Abstract Postoperative external beam
ORIGINAL PAPERS. The Impact of Surgery on the Efficacy of Adjuvant Therapy in Glioblastoma Multiforme
 ORIGINAL PAPERS Adv Clin Exp Med 2015, 24, 2, 279 287 DOI: 10.17219/acem/40456 Copyright by Wroclaw Medical University ISSN 1899 5276 Anna Brzozowska 1, 2, A D, Anna Toruń 3, G, Maria Mazurkiewicz1, 2,
ORIGINAL PAPERS Adv Clin Exp Med 2015, 24, 2, 279 287 DOI: 10.17219/acem/40456 Copyright by Wroclaw Medical University ISSN 1899 5276 Anna Brzozowska 1, 2, A D, Anna Toruń 3, G, Maria Mazurkiewicz1, 2,
doi: /j.radonc
 doi: 10.1016/j.radonc.2009.02.009 Boron neutron capture therapy for newly diagnosed glioblastoma Tetsuya Yamamoto MD, PhD, Kei Nakai MD, PhD, Teruyoshi Kageji MD, PhD, Hiroaki Kumada PhD, Kiyoshi Endo
doi: 10.1016/j.radonc.2009.02.009 Boron neutron capture therapy for newly diagnosed glioblastoma Tetsuya Yamamoto MD, PhD, Kei Nakai MD, PhD, Teruyoshi Kageji MD, PhD, Hiroaki Kumada PhD, Kiyoshi Endo
Efficacy of Treatment for Glioblastoma Multiforme in Elderly Patients (65+): A Retrospective Analysis
 Efficacy of Treatment for Glioblastoma Multiforme in Elderly Patients (65+): A Retrospective Analysis Igal Kushnir MD 1 * and Tzahala Tzuk-Shina MD 2 1 Oncology Insitute, Tel Aviv Sourasky Medical Center,
Efficacy of Treatment for Glioblastoma Multiforme in Elderly Patients (65+): A Retrospective Analysis Igal Kushnir MD 1 * and Tzahala Tzuk-Shina MD 2 1 Oncology Insitute, Tel Aviv Sourasky Medical Center,
DOES RADIOTHERAPY TECHNIQUE / DOSE / FRACTIONATION REALLY MATTER? YES
 DOES RADIOTHERAPY TECHNIQUE / DOSE / FRACTIONATION REALLY MATTER? YES Marco Krengli Radiotherapy, Department of Translational Medicine, University of Piemonte Orientale A. Avogadro THE STANDARD OF CARE
DOES RADIOTHERAPY TECHNIQUE / DOSE / FRACTIONATION REALLY MATTER? YES Marco Krengli Radiotherapy, Department of Translational Medicine, University of Piemonte Orientale A. Avogadro THE STANDARD OF CARE
Adjuvant treatment of high grade gliomas
 17 (Supplement 10): x186 x190, 2006 doi:10.1093/annonc/mdl258 Adjuvant treatment of high grade gliomas M. J. van den Bent Department of Neuro-Oncology, Erasmus University Hospital Rotterdam/Rotterdam Cancer
17 (Supplement 10): x186 x190, 2006 doi:10.1093/annonc/mdl258 Adjuvant treatment of high grade gliomas M. J. van den Bent Department of Neuro-Oncology, Erasmus University Hospital Rotterdam/Rotterdam Cancer
Department of Medical Oncology, National Cancer Institute of Aviano, Aviano (PN) Italy 3
 WCRJ 2014; 1 (4): e401 RADIOCHEMOTHERAPY FOR UNRESECTABLE GLIOBLASTOMA MULTIFORME: A MONO- INSTITUTIONAL EXPERIENCE M. COLELLA 1, F. FIORICA 1, P. API 1, A. STEFANELLI 1, B. URBINI 2, A. SGUALDO 1, D.
WCRJ 2014; 1 (4): e401 RADIOCHEMOTHERAPY FOR UNRESECTABLE GLIOBLASTOMA MULTIFORME: A MONO- INSTITUTIONAL EXPERIENCE M. COLELLA 1, F. FIORICA 1, P. API 1, A. STEFANELLI 1, B. URBINI 2, A. SGUALDO 1, D.
Glioblastoma (GBM) is the most common and
 Neuro-Oncology 12(6):595 602, 2010. doi:10.1093/neuonc/noq008 Advance Access publication February 11, 2010 NEURO-ONCOLOGY Prolonged survival for patients with newly diagnosed, inoperable glioblastoma with
Neuro-Oncology 12(6):595 602, 2010. doi:10.1093/neuonc/noq008 Advance Access publication February 11, 2010 NEURO-ONCOLOGY Prolonged survival for patients with newly diagnosed, inoperable glioblastoma with
Elderly Patients with Glioblastoma Multiforme Treated with Concurrent Temozolomide and Standard- versus Abbreviated-Course Radiotherapy
 Elderly Patients with Glioblastoma Multiforme Treated with Concurrent Temozolomide and Standard- versus Abbreviated-Course Radiotherapy Christine N Chang-Halpenny, MD; Jekwon Yeh, MD; Winston W Lien, MD
Elderly Patients with Glioblastoma Multiforme Treated with Concurrent Temozolomide and Standard- versus Abbreviated-Course Radiotherapy Christine N Chang-Halpenny, MD; Jekwon Yeh, MD; Winston W Lien, MD
We have previously reported good clinical results
 J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
Survival Following CyberKnife Radiosurgery and Hypofractionated Radiotherapy for Newly Diagnosed Glioblastoma Multiforme
 Technology in Cancer Research and Treatment ISSN 1533-0346 Volume 7, Number 3, June 2008 Adenine Press (2008) Survival Following CyberKnife Radiosurgery and Hypofractionated Radiotherapy for Newly Diagnosed
Technology in Cancer Research and Treatment ISSN 1533-0346 Volume 7, Number 3, June 2008 Adenine Press (2008) Survival Following CyberKnife Radiosurgery and Hypofractionated Radiotherapy for Newly Diagnosed
Concurrent Chemoradiotherapy Versus Radiotherapy Alone for Biopsy-Only Glioblastoma Multiforme
 Concurrent Chemoradiotherapy Versus Radiotherapy Alone for Biopsy-Only Glioblastoma Multiforme Adam J. Kole, MD, PhD 1 ; Henry S. Park, MD, MPH 1 ; Debra N. Yeboa, MD 1 ; Charles E. Rutter, MD 1 ; Christopher
Concurrent Chemoradiotherapy Versus Radiotherapy Alone for Biopsy-Only Glioblastoma Multiforme Adam J. Kole, MD, PhD 1 ; Henry S. Park, MD, MPH 1 ; Debra N. Yeboa, MD 1 ; Charles E. Rutter, MD 1 ; Christopher
Background. Central nervous system (CNS) tumours. High-grade glioma
 25 4. Central nervous system (CNS) tumours Background Two important considerations underpin the choice of treatment fractionation in neurooncology. First, the results of treatment vary widely and, second,
25 4. Central nervous system (CNS) tumours Background Two important considerations underpin the choice of treatment fractionation in neurooncology. First, the results of treatment vary widely and, second,
Prognostic significance of surgery and radiation therapy in cases of anaplastic astrocytoma: retrospective analysis of 170 cases
 J Neurosurg 106:575 581, 2007 Prognostic significance of surgery and radiation therapy in cases of anaplastic astrocytoma: retrospective analysis of 170 cases TAKUMA NOMIYA, M.D., PH.D., 1 KENJI NEMOTO,
J Neurosurg 106:575 581, 2007 Prognostic significance of surgery and radiation therapy in cases of anaplastic astrocytoma: retrospective analysis of 170 cases TAKUMA NOMIYA, M.D., PH.D., 1 KENJI NEMOTO,
Systemic Treatment. Third International Neuro-Oncology Course. 23 May 2014
 Low-Grade Astrocytoma of the CNS: Systemic Treatment Third International Neuro-Oncology Course São Paulo, Brazil 23 May 2014 John de Groot, MD Associate Professor, Neuro-Oncology UT MD Anderson Cancer
Low-Grade Astrocytoma of the CNS: Systemic Treatment Third International Neuro-Oncology Course São Paulo, Brazil 23 May 2014 John de Groot, MD Associate Professor, Neuro-Oncology UT MD Anderson Cancer
21/03/2017. Disclosure. Practice Changing Articles in Neuro Oncology for 2016/17. Gliomas. Objectives. Gliomas. No conflicts to declare
 Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION. Mustafa Rashid Issa
 THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
Oncological Management of Brain Tumours. Anna Maria Shiarli SpR in Clinical Oncology 15 th July 2013
 Oncological Management of Brain Tumours Anna Maria Shiarli SpR in Clinical Oncology 15 th July 2013 Outline General considerations of Primary Brain Tumours: epidemiology, pathology, presentation. Diagnosis
Oncological Management of Brain Tumours Anna Maria Shiarli SpR in Clinical Oncology 15 th July 2013 Outline General considerations of Primary Brain Tumours: epidemiology, pathology, presentation. Diagnosis
An international study under the guidance of the European Organization
 2617 COMMENTARY Chemotherapy for Glioblastoma Is Costly Better? Ute Linz, MD, PhD Juelich Research Center, IKP/INB, Juelich, Germany. Address for reprints: Ute Linz, MD, PhD, Forschungszentrum J ulich
2617 COMMENTARY Chemotherapy for Glioblastoma Is Costly Better? Ute Linz, MD, PhD Juelich Research Center, IKP/INB, Juelich, Germany. Address for reprints: Ute Linz, MD, PhD, Forschungszentrum J ulich
Optimal Management of Isolated HER2+ve Brain Metastases
 Optimal Management of Isolated HER2+ve Brain Metastases Eliot Sims November 2013 Background Her2+ve patients 15% of all breast cancer Even with adjuvant trastuzumab 10-15% relapse Trastuzumab does not
Optimal Management of Isolated HER2+ve Brain Metastases Eliot Sims November 2013 Background Her2+ve patients 15% of all breast cancer Even with adjuvant trastuzumab 10-15% relapse Trastuzumab does not
A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia
 A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia Gaurav Bahl, Karl Tennessen, Ashraf Mahmoud-Ahmed, Dorianne Rheaume, Ian Fleetwood,
A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia Gaurav Bahl, Karl Tennessen, Ashraf Mahmoud-Ahmed, Dorianne Rheaume, Ian Fleetwood,
University of Zurich. Temozolomide and MGMT forever? Zurich Open Repository and Archive. Weller, M. Year: 2010
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich Year: 2010 Temozolomide and MGMT forever? Weller, M Weller, M (2010). Temozolomide and MGMT forever? Neuro-Oncology,
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich Year: 2010 Temozolomide and MGMT forever? Weller, M Weller, M (2010). Temozolomide and MGMT forever? Neuro-Oncology,
Treatment and outcomes for glioblastoma in elderly compared with non-elderly patients: a population-based study
 ORIGINAL ARTICLE Treatment and outcomes for glioblastoma in elderly compared with non-elderly patients: a population-based study E.R. Morgan md,* A. Norman md, K. Laing md, and M.D. Seal md ABSTRACT Purpose
ORIGINAL ARTICLE Treatment and outcomes for glioblastoma in elderly compared with non-elderly patients: a population-based study E.R. Morgan md,* A. Norman md, K. Laing md, and M.D. Seal md ABSTRACT Purpose
The Role of Radiation Therapy in the Treatment of Brain Metastases. Matthew Cavey, M.D.
 The Role of Radiation Therapy in the Treatment of Brain Metastases Matthew Cavey, M.D. Objectives Provide information about the prospective trials that are driving the treatment of patients with brain
The Role of Radiation Therapy in the Treatment of Brain Metastases Matthew Cavey, M.D. Objectives Provide information about the prospective trials that are driving the treatment of patients with brain
ASJ. Surgical Outcomes of High-Grade Spinal Cord Gliomas. Asian Spine Journal. Introduction
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Surgical Spine J 2015;9(6):935-941 outcomes of high-grade http://dx.doi.org/10.4184/asj.2015.9.6.935 intramedullary tumor 935 Surgical Outcomes
Asian Spine Journal Asian Spine Clinical Journal Study Asian Surgical Spine J 2015;9(6):935-941 outcomes of high-grade http://dx.doi.org/10.4184/asj.2015.9.6.935 intramedullary tumor 935 Surgical Outcomes
Prior to 1993, the only data available in the medical
 Neuro-Oncology Prospective clinical trials of intracranial low-grade glioma in adults and children Edward G. Shaw 1 and Jeffrey H. Wisoff Department of Radiation Oncology, Wake Forest University School
Neuro-Oncology Prospective clinical trials of intracranial low-grade glioma in adults and children Edward G. Shaw 1 and Jeffrey H. Wisoff Department of Radiation Oncology, Wake Forest University School
Contemporary Management of Glioblastoma
 Contemporary Management of Glioblastoma Incidence Rates of Primary Brain Tumors Central Brain Tumor Registry of the United States, 1992-1997 100 Number of Cases per 100,000 Population 10 1 0.1 x I x I
Contemporary Management of Glioblastoma Incidence Rates of Primary Brain Tumors Central Brain Tumor Registry of the United States, 1992-1997 100 Number of Cases per 100,000 Population 10 1 0.1 x I x I
Technology appraisal guidance Published: 27 June 2007 nice.org.uk/guidance/ta121
 Carmustine implants and temozolomide for the treatment of newly diagnosed high-grade glioma Technology appraisal guidance Published: 27 June 2007 nice.org.uk/guidance/ta121 NICE 2018. All rights reserved.
Carmustine implants and temozolomide for the treatment of newly diagnosed high-grade glioma Technology appraisal guidance Published: 27 June 2007 nice.org.uk/guidance/ta121 NICE 2018. All rights reserved.
1. Introduction. Correspondence should be addressed to Christopher M. Lee; Received 9 July 2013; Accepted 27 August 2013
 Case Reports in Oncological Medicine Volume 2013, Article ID 431857, 5 pages http://dx.doi.org/10.1155/2013/431857 Case Report Long-Term Survival and Improved Quality of Life following Multiple Repeat
Case Reports in Oncological Medicine Volume 2013, Article ID 431857, 5 pages http://dx.doi.org/10.1155/2013/431857 Case Report Long-Term Survival and Improved Quality of Life following Multiple Repeat
Clinical Study Hypofractionated High-Dose Irradiation with Positron Emission Tomography Data for the Treatment of Glioblastoma Multiforme
 BioMed Research International Volume 14, Article ID 26, 9 pages http://dx.doi.org/.1155/14/26 Clinical Study Hypofractionated High-Dose Irradiation with Positron Emission Tomography Data for the Treatment
BioMed Research International Volume 14, Article ID 26, 9 pages http://dx.doi.org/.1155/14/26 Clinical Study Hypofractionated High-Dose Irradiation with Positron Emission Tomography Data for the Treatment
Arecent randomized controlled trial (RCT) established
 Neuro-Oncology 12(2):190 198, 2010. doi:10.1093/neuonc/nop004 NEURO-ONCOLOGY The timing of cranial radiation in elderly patients with newly diagnosed glioblastoma multiforme Rose Lai, Dawn L. Hershman,
Neuro-Oncology 12(2):190 198, 2010. doi:10.1093/neuonc/nop004 NEURO-ONCOLOGY The timing of cranial radiation in elderly patients with newly diagnosed glioblastoma multiforme Rose Lai, Dawn L. Hershman,
Radioterapia no Tratamento dos Gliomas de Baixo Grau
 Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
Response to postoperative radiotherapy as a prognostic factor for patients with low-grade gliomas
 ONCOLOGY LETTERS 4: 455-460, 2012 Response to postoperative radiotherapy as a prognostic factor for patients with low-grade gliomas MICHAL SPYCH 1,2, LESZEK GOTTWALD 3, EMILIA JESIEŃ LEWANDOWICZ 1,2, SŁAWOMIR
ONCOLOGY LETTERS 4: 455-460, 2012 Response to postoperative radiotherapy as a prognostic factor for patients with low-grade gliomas MICHAL SPYCH 1,2, LESZEK GOTTWALD 3, EMILIA JESIEŃ LEWANDOWICZ 1,2, SŁAWOMIR
University of Alberta. Evaluation of Concomitant Temozolomide Treatment in Glioblastoma Multiforme Patients in Two Canadian Tertiary Care Centers
 University of Alberta Evaluation of Concomitant Temozolomide Treatment in Glioblastoma Multiforme Patients in Two Canadian Tertiary Care Centers by Ibrahim Alnaami A thesis submitted to the Faculty of
University of Alberta Evaluation of Concomitant Temozolomide Treatment in Glioblastoma Multiforme Patients in Two Canadian Tertiary Care Centers by Ibrahim Alnaami A thesis submitted to the Faculty of
Clinical Management Protocol Chemotherapy [Glioblastoma Multiforme (CNS)] Protocol for Planning and Treatment
![Clinical Management Protocol Chemotherapy [Glioblastoma Multiforme (CNS)] Protocol for Planning and Treatment Clinical Management Protocol Chemotherapy [Glioblastoma Multiforme (CNS)] Protocol for Planning and Treatment](/thumbs/87/96032554.jpg) Protocol for Planning and Treatment The process to be followed when a course of chemotherapy is required to treat: GLIOBLASTOMA MULTIFORME (CNS) Patient information given at each stage following agreed
Protocol for Planning and Treatment The process to be followed when a course of chemotherapy is required to treat: GLIOBLASTOMA MULTIFORME (CNS) Patient information given at each stage following agreed
Citation Pediatrics international (2015), 57.
 Title Long-term efficacy of bevacizumab a pediatric glioblastoma. Umeda, Katsutsugu; Shibata, Hirofum Author(s) Hiramatsu, Hidefumi; Arakawa, Yoshi Nishiuchi, Ritsuo; Adachi, Souichi; Ken-Ichiro Citation
Title Long-term efficacy of bevacizumab a pediatric glioblastoma. Umeda, Katsutsugu; Shibata, Hirofum Author(s) Hiramatsu, Hidefumi; Arakawa, Yoshi Nishiuchi, Ritsuo; Adachi, Souichi; Ken-Ichiro Citation
Laboratory data from the 1970s first showed that malignant melanoma
 2265 Survival by Radiation Therapy Oncology Group Recursive Partitioning Analysis Class and Treatment Modality in Patients with Brain Metastases from Malignant Melanoma A Retrospective Study Jeffrey C.
2265 Survival by Radiation Therapy Oncology Group Recursive Partitioning Analysis Class and Treatment Modality in Patients with Brain Metastases from Malignant Melanoma A Retrospective Study Jeffrey C.
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT
 SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준. KNS-MT-03 (April 15, 2015)
 성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
Temozolomide Concomitant and Adjuvant to Radiotherapy in Elderly Patients With Glioblastoma
 Temozolomide Concomitant and Adjuvant to Radiotherapy in Elderly Patients With Glioblastoma Correlation With MGMT Promoter Methylation Status Alba A. Brandes, MD 1 ; Enrico Franceschi, MD 1 ; Alicia Tosoni,
Temozolomide Concomitant and Adjuvant to Radiotherapy in Elderly Patients With Glioblastoma Correlation With MGMT Promoter Methylation Status Alba A. Brandes, MD 1 ; Enrico Franceschi, MD 1 ; Alicia Tosoni,
Stereotactic Radiosurgery for Brain Metastasis: Changing Treatment Paradigms. Overall Clinical Significance 8/3/13
 Stereotactic Radiosurgery for Brain Metastasis: Changing Treatment Paradigms Jason Sheehan, MD, PhD Departments of Neurosurgery and Radiation Oncology University of Virginia, Charlottesville, VA USA Overall
Stereotactic Radiosurgery for Brain Metastasis: Changing Treatment Paradigms Jason Sheehan, MD, PhD Departments of Neurosurgery and Radiation Oncology University of Virginia, Charlottesville, VA USA Overall
Incidence of Early Pseudo-progression in a Cohort of Malignant Glioma Patients Treated With Chemoirradiation With Temozolomide
 405 Incidence of Early Pseudo-progression in a Cohort of Malignant Glioma Patients Treated With Chemoirradiation With Temozolomide Walter Taal, MD 1 Dieta Brandsma, MD, PhD 1 Hein G. de Bruin, MD, PhD
405 Incidence of Early Pseudo-progression in a Cohort of Malignant Glioma Patients Treated With Chemoirradiation With Temozolomide Walter Taal, MD 1 Dieta Brandsma, MD, PhD 1 Hein G. de Bruin, MD, PhD
Practice of Interferon Therapy
 Interferon Therapy Practice of Interferon Therapy Brain tumor JMAJ 47(1): 18 23, 2004 Toshihiko WAKABAYASHI* and Jun YOSHIDA** *Associate Professor, Center for Genetic and Regenerative Medicine, Nagoya
Interferon Therapy Practice of Interferon Therapy Brain tumor JMAJ 47(1): 18 23, 2004 Toshihiko WAKABAYASHI* and Jun YOSHIDA** *Associate Professor, Center for Genetic and Regenerative Medicine, Nagoya
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
ADJUVANT TREATMENT OF BRAIN GLIOBLASTOMA MULTIFORME WITH RABIES VACCINE, DEFEROXAMINE AND D-PENICILLAMINE: A PILOT STUDY
 Philip V. Philipov Original Article ADJUVANT TREATMENT OF BRAIN GLIOBLASTOMA MULTIFORME WITH RABIES VACCINE, DEFEROXAMINE AND D-PENICILLAMINE: A PILOT STUDY Summary Clinic of Neurosurgery, Medical University-Pleven,
Philip V. Philipov Original Article ADJUVANT TREATMENT OF BRAIN GLIOBLASTOMA MULTIFORME WITH RABIES VACCINE, DEFEROXAMINE AND D-PENICILLAMINE: A PILOT STUDY Summary Clinic of Neurosurgery, Medical University-Pleven,
Low grade glioma: a journey towards a cure
 Editorial Page 1 of 5 Low grade glioma: a journey towards a cure Ali K. Choucair SIU School of Medicine, Springfield, IL, USA Correspondence to: Ali K. Choucair, MD. Professor of Neurology, Director of
Editorial Page 1 of 5 Low grade glioma: a journey towards a cure Ali K. Choucair SIU School of Medicine, Springfield, IL, USA Correspondence to: Ali K. Choucair, MD. Professor of Neurology, Director of
Stephanie E. Combs Æ Marc Bischof Æ Thomas Welzel Æ Holger Hof Æ Susanne Oertel Æ Jürgen Debus Æ Daniela Schulz-Ertner
 J Neurooncol (2008) 89:205 210 DOI 10.1007/s11060-008-9607-4 CLINICAL-PATIENT STUDIES Radiochemotherapy with temozolomide as re-irradiation using high precision fractionated stereotactic radiotherapy (FSRT)
J Neurooncol (2008) 89:205 210 DOI 10.1007/s11060-008-9607-4 CLINICAL-PATIENT STUDIES Radiochemotherapy with temozolomide as re-irradiation using high precision fractionated stereotactic radiotherapy (FSRT)
Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery
 ORIGINAL ARTICLE Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery Ann C. Raldow, BS,* Veronica L. Chiang, MD,w Jonathan P.
ORIGINAL ARTICLE Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery Ann C. Raldow, BS,* Veronica L. Chiang, MD,w Jonathan P.
SBRT in early stage NSCLC
 SBRT in early stage NSCLC Optimal technique and tumor dose Frank Zimmermann Clinic of Radiotherapy and Radiation Oncology University Hospital Basel Petersgraben 4 CH 4031 Basel radioonkologiebasel.ch Techniques
SBRT in early stage NSCLC Optimal technique and tumor dose Frank Zimmermann Clinic of Radiotherapy and Radiation Oncology University Hospital Basel Petersgraben 4 CH 4031 Basel radioonkologiebasel.ch Techniques
Treatment results of proton beam therapy with chemo-radiotherapy for stage I-III esophageal cancer
 Treatment results of proton beam therapy with chemo-radiotherapy for stage I-III esophageal cancer Nobukazu Fuwa 1, Akinori Takada 2 and Takahiro Kato 3 1;Departments of Radiology, Hyogo Ion Beam Medical
Treatment results of proton beam therapy with chemo-radiotherapy for stage I-III esophageal cancer Nobukazu Fuwa 1, Akinori Takada 2 and Takahiro Kato 3 1;Departments of Radiology, Hyogo Ion Beam Medical
J Clin Oncol 27: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 27 NUMBER 8 MARCH 10 2009 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Recurrence Pattern After Temozolomide Concomitant With and Adjuvant to Radiotherapy in Newly Diagnosed Patients
VOLUME 27 NUMBER 8 MARCH 10 2009 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Recurrence Pattern After Temozolomide Concomitant With and Adjuvant to Radiotherapy in Newly Diagnosed Patients
Institute of Oncology & Radiobiology. Havana, Cuba. INOR
 Institute of Oncology & Radiobiology. Havana, Cuba. INOR 1 Transition from 2-D 2 D to 3-D 3 D conformal radiotherapy in high grade gliomas: : our experience in Cuba Chon. I, MD - Chi. D, MD - Alert.J,
Institute of Oncology & Radiobiology. Havana, Cuba. INOR 1 Transition from 2-D 2 D to 3-D 3 D conformal radiotherapy in high grade gliomas: : our experience in Cuba Chon. I, MD - Chi. D, MD - Alert.J,
Temozolomide with Radiotherapy for the Treatment of Malignant Gliomas, Center Experience
 Temozolomide with Radiotherapy for the Treatment of Malignant Gliomas, Center Experience *Ehab Abdou and **Mohamed Gaafar *Department of Radiation Oncology, Faculty of Medicine, Al-Azhar University, Cairo,
Temozolomide with Radiotherapy for the Treatment of Malignant Gliomas, Center Experience *Ehab Abdou and **Mohamed Gaafar *Department of Radiation Oncology, Faculty of Medicine, Al-Azhar University, Cairo,
Temozolomide in combination with BCNU before and after radiotherapy in patients with inoperable newly diagnosed glioblastoma multiforme
 Original article Annals of Oncology 16: 1177 1184, 2005 doi:10.1093/annonc/mdi225 Published online 27 April 2005 Temozolomide in combination with BCNU before and after radiotherapy in patients with inoperable
Original article Annals of Oncology 16: 1177 1184, 2005 doi:10.1093/annonc/mdi225 Published online 27 April 2005 Temozolomide in combination with BCNU before and after radiotherapy in patients with inoperable
Bevacizumab rescue therapy extends the survival in patients with recurrent malignant glioma
 Original Article Bevacizumab rescue therapy extends the survival in patients with recurrent malignant glioma Lin-Bo Cai, Juan Li, Ming-Yao Lai, Chang-Guo Shan, Zong-De Lian, Wei-Ping Hong, Jun-Jie Zhen,
Original Article Bevacizumab rescue therapy extends the survival in patients with recurrent malignant glioma Lin-Bo Cai, Juan Li, Ming-Yao Lai, Chang-Guo Shan, Zong-De Lian, Wei-Ping Hong, Jun-Jie Zhen,
Paolo Tini 1,3 M.D. :
 Correlazione tra espressione di Epidermal Growth Factor Receptor (EGFR) e Patterns di recidiva/progressione di malattia dopo trattamento radio-chemioterapico in pazienti affetti da Glioblastoma (GB). Paolo
Correlazione tra espressione di Epidermal Growth Factor Receptor (EGFR) e Patterns di recidiva/progressione di malattia dopo trattamento radio-chemioterapico in pazienti affetti da Glioblastoma (GB). Paolo
Selecting the Optimal Treatment for Brain Metastases
 Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
Stereotactic radiotherapy
 Stereotactic radiotherapy Influence of patient positioning and fixation on treatment planning - clinical results Frank Zimmermann Institut für Radioonkologie Universitätsspital Basel Petersgraben 4 CH
Stereotactic radiotherapy Influence of patient positioning and fixation on treatment planning - clinical results Frank Zimmermann Institut für Radioonkologie Universitätsspital Basel Petersgraben 4 CH
Epidemiology and outcome research of glioma patients in Southern Switzerland: A population based analysis
 Epidemiology and outcome research of glioma patients in Southern Switzerland: A population based analysis G. Pesce 1, A. Bordoni, F. Montanaro, R. Renella 3, A. Richetti 1, D. Boscherini 3, S. Mauri 4,
Epidemiology and outcome research of glioma patients in Southern Switzerland: A population based analysis G. Pesce 1, A. Bordoni, F. Montanaro, R. Renella 3, A. Richetti 1, D. Boscherini 3, S. Mauri 4,
Temozolomide in the treatment of recurrent malignant glioma in Chinese patients!"#$%&'()*+,-./0,1234
 Key words: Astrocytoma; Brain neoplasms; Disease-free survival; Glioblastoma; Neoplasm recurrence!!"!"!"#$ DTM Chan WS Poon YL Chan HK Ng Hong Kong Med J 2005;11:452-6 The Chinese University of Hong Kong,
Key words: Astrocytoma; Brain neoplasms; Disease-free survival; Glioblastoma; Neoplasm recurrence!!"!"!"#$ DTM Chan WS Poon YL Chan HK Ng Hong Kong Med J 2005;11:452-6 The Chinese University of Hong Kong,
Concomitant Accelerated Hyper-Fractionated Radiotherapy and Temozolomide in the Treatment of High Grade Astrocytoma
 Journal of the Egyptian Nat. Cancer Inst., Vol. 14, No. 1, March: 9-15, 00 Concomitant Accelerated Hyper-Fractionated Radiotherapy and Temozolomide in the Treatment of High Grade Astrocytoma TAREK HASHEM,M.D.*
Journal of the Egyptian Nat. Cancer Inst., Vol. 14, No. 1, March: 9-15, 00 Concomitant Accelerated Hyper-Fractionated Radiotherapy and Temozolomide in the Treatment of High Grade Astrocytoma TAREK HASHEM,M.D.*
Antiangiogenic drugs in unresectable glioblastoma. Dra. Carmen Balañá. /
 Antiangiogenic drugs in unresectable glioblastoma Dra. Carmen Balañá. / Outcome for unresectable GBM Overall survival for unresectable GBM without further treatment is: 3 months at most. Radiotherapy increases
Antiangiogenic drugs in unresectable glioblastoma Dra. Carmen Balañá. / Outcome for unresectable GBM Overall survival for unresectable GBM without further treatment is: 3 months at most. Radiotherapy increases
Imaging for suspected glioma
 Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Survival Outcomes with Short-Course Radiotherapy in Elderly Patients with Glioblastoma: Data from a Randomized Phase III Trial
 Accepted Manuscript Survival Outcomes with Short-Course Radiotherapy in Elderly Patients with Glioblastoma: Data from a Randomized Phase III Trial Douglas Guedes de Castro, Juliana Matiello, Wilson Roa,
Accepted Manuscript Survival Outcomes with Short-Course Radiotherapy in Elderly Patients with Glioblastoma: Data from a Randomized Phase III Trial Douglas Guedes de Castro, Juliana Matiello, Wilson Roa,
Chemotherapy in malignant brain tumors
 Chemotherapy in malignant brain tumors Frank Zimmermann Institut für Radioonkologie Universitätsspital Basel Petersgraben 4 CH 4031 Basel zimmermannf@uhbs.ch Tumor types Neuro-epithelial tumors - Glioblastoma
Chemotherapy in malignant brain tumors Frank Zimmermann Institut für Radioonkologie Universitätsspital Basel Petersgraben 4 CH 4031 Basel zimmermannf@uhbs.ch Tumor types Neuro-epithelial tumors - Glioblastoma
Improved Survival after Gross Total Resection of Malignant Gliomas in Pediatric Patients from the HIT-GBM Studies
 Improved Survival after Gross Total Resection of Malignant Gliomas in Pediatric Patients from the HIT-GBM Studies CHRISTOF M. KRAMM 1, SABINE WAGNER 2, STEFAN VAN GOOL 3, HANSJÖRG SCHMID 4, RONALD STRÄTER
Improved Survival after Gross Total Resection of Malignant Gliomas in Pediatric Patients from the HIT-GBM Studies CHRISTOF M. KRAMM 1, SABINE WAGNER 2, STEFAN VAN GOOL 3, HANSJÖRG SCHMID 4, RONALD STRÄTER
Zurich Open Repository and Archive
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2008 Nomograms for predicting survival of patients with newly diagnosed glioblastoma:
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2008 Nomograms for predicting survival of patients with newly diagnosed glioblastoma:
Neuro-Oncology Practice
 Neuro-Oncology Practice Neuro-Oncology Practice 3(2), 71 76, 2016 doi:10.1093/nop/npv043 Advance Access date 16 October 2015 Anaplastic astrocytoma and non-1p/19q co-deleted anaplastic oligoastrocytoma:
Neuro-Oncology Practice Neuro-Oncology Practice 3(2), 71 76, 2016 doi:10.1093/nop/npv043 Advance Access date 16 October 2015 Anaplastic astrocytoma and non-1p/19q co-deleted anaplastic oligoastrocytoma:
Modeling the effects of resection, radiation and chemotherapy in glioblastoma
 J Neurooncol (09) 91:287 293 DOI 10.1007/s11060-008-9710-6 CLINICAL STUDY - PATIENT STUDY Modeling the effects of resection, radiation and chemotherapy in glioblastoma Jianjun Paul Tian Æ Avner Friedman
J Neurooncol (09) 91:287 293 DOI 10.1007/s11060-008-9710-6 CLINICAL STUDY - PATIENT STUDY Modeling the effects of resection, radiation and chemotherapy in glioblastoma Jianjun Paul Tian Æ Avner Friedman
Going Past the Data for Temozolomide. J. Lee Villano, M.D., Ph.D., Nathalie Letarte, B.Pharm, M.Sc, Linda R. Bressler, Pharm. D.
 Going Past the Data for Temozolomide J. Lee Villano, M.D., Ph.D., Nathalie Letarte, B.Pharm, M.Sc, Linda R. Bressler, Pharm. D. Departments of Medicine (JLV), Neurosurgery (JLV) and Pharmacy Practice (LRB)
Going Past the Data for Temozolomide J. Lee Villano, M.D., Ph.D., Nathalie Letarte, B.Pharm, M.Sc, Linda R. Bressler, Pharm. D. Departments of Medicine (JLV), Neurosurgery (JLV) and Pharmacy Practice (LRB)
Additional radiation boost to whole brain radiation therapy may improve the survival of patients with brain metastases in small cell lung cancer
 Sun et al. Radiation Oncology (2018) 13:250 https://doi.org/10.1186/s13014-018-1198-4 RESEARCH Open Access Additional radiation boost to whole brain radiation therapy may improve the survival of patients
Sun et al. Radiation Oncology (2018) 13:250 https://doi.org/10.1186/s13014-018-1198-4 RESEARCH Open Access Additional radiation boost to whole brain radiation therapy may improve the survival of patients
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
Br a i n metastases occur in 20 40% of all patients. The results of resection after stereotactic radiosurgery for brain metastases.
 J Neurosurg 111:825 831, 2009 The results of resection after stereotactic radiosurgery for brain metastases Clinical article Hi d e y u k i Ka n o, M.D., Ph.D., 1,3 Do u g l a s Ko n d z i o l k a, M.D.,
J Neurosurg 111:825 831, 2009 The results of resection after stereotactic radiosurgery for brain metastases Clinical article Hi d e y u k i Ka n o, M.D., Ph.D., 1,3 Do u g l a s Ko n d z i o l k a, M.D.,
肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部
 肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部 Outline Current status of radiation oncology in lung cancer Focused on stage III non-small cell lung cancer Radiation
肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部 Outline Current status of radiation oncology in lung cancer Focused on stage III non-small cell lung cancer Radiation
Introduction ORIGINAL RESEARCH
 Cancer Medicine ORIGINAL RESEARCH Open Access The effect of radiation therapy in the treatment of adult soft tissue sarcomas of the extremities: a long- term community- based cancer center experience Jeffrey
Cancer Medicine ORIGINAL RESEARCH Open Access The effect of radiation therapy in the treatment of adult soft tissue sarcomas of the extremities: a long- term community- based cancer center experience Jeffrey
Early Post-Operative MRI: Correlation with Progression-Free Survival and Overall Survival Time in Malignant Gliomas
 J. Exp. Clin. Cancer Res., 25, 2, 2006 Early Post-Operative MRI: Correlation with Progression-Free Survival and Overall Survival Time in Malignant Gliomas A. Vidiri 1, C. M. Carapella 2, A. Pace 3, A.
J. Exp. Clin. Cancer Res., 25, 2, 2006 Early Post-Operative MRI: Correlation with Progression-Free Survival and Overall Survival Time in Malignant Gliomas A. Vidiri 1, C. M. Carapella 2, A. Pace 3, A.
Hypofractionated Stereotactic Radiation Therapy in Recurrent High-Grade Glioma: A New Challenge
 pissn 1598-2998, eissn 2005-9256 Original Article http://dx.doi.org/10.4143/crt.2014.259 Open Access Hypofractionated Stereotactic Radiation Therapy in Recurrent High-Grade Glioma: A New Challenge Pierina
pissn 1598-2998, eissn 2005-9256 Original Article http://dx.doi.org/10.4143/crt.2014.259 Open Access Hypofractionated Stereotactic Radiation Therapy in Recurrent High-Grade Glioma: A New Challenge Pierina
Glioblastoma: Current Treatment Approach 8/20/2018
 Glioblastoma: Current Treatment Approach 8/20/2018 Overview What is Glioblastoma? How is it diagnosed How is it treated? Principles of Treatment Surgery, Radiation, Chemotherapy Current Standard of care
Glioblastoma: Current Treatment Approach 8/20/2018 Overview What is Glioblastoma? How is it diagnosed How is it treated? Principles of Treatment Surgery, Radiation, Chemotherapy Current Standard of care
Glioblastoma: Adjuvant Treatment Abdulrazag Ajlan, MD, MSc, FRCSC, UCNS(D)
 Glioblastoma: Adjuvant Treatment Abdulrazag Ajlan, MD, MSc, FRCSC, UCNS(D) *Neurosurgery Consultant, King Saud University, Riyadh, KSA *Adjunct Teaching Faculty, Neurosurgery, Stanford School Of Medicine,
Glioblastoma: Adjuvant Treatment Abdulrazag Ajlan, MD, MSc, FRCSC, UCNS(D) *Neurosurgery Consultant, King Saud University, Riyadh, KSA *Adjunct Teaching Faculty, Neurosurgery, Stanford School Of Medicine,
Supratentorial Glioblastoma Multiforme: The Role of Surgical Resection Versus Biopsy Among Older Patients
 Ann Surg Oncol DOI 10.1245/s10434-010-1242-6 ORIGINAL ARTICLE NEURO-ONCOLOGY Supratentorial Glioblastoma Multiforme: The Role of Surgical Resection Versus Biopsy Among Older Patients Kaisorn L. Chaichana,
Ann Surg Oncol DOI 10.1245/s10434-010-1242-6 ORIGINAL ARTICLE NEURO-ONCOLOGY Supratentorial Glioblastoma Multiforme: The Role of Surgical Resection Versus Biopsy Among Older Patients Kaisorn L. Chaichana,
Radiation Therapy for Soft Tissue Sarcomas
 Radiation Therapy for Soft Tissue Sarcomas Alexander R. Gottschalk, MD, PhD Assistant Professor, Radiation Oncology University of California, San Francisco 1/25/08 NCI: limb salvage vs. amputation 43 patients
Radiation Therapy for Soft Tissue Sarcomas Alexander R. Gottschalk, MD, PhD Assistant Professor, Radiation Oncology University of California, San Francisco 1/25/08 NCI: limb salvage vs. amputation 43 patients
Impact of waiting time after surgery and overall time of postoperative radiochemotherapy on treatment outcome in glioblastoma multiforme
 Seidlitz et al. Radiation Oncology (15) 1:172 DOI 1.1186/s1314-15-478-5 RESEARCH Open Access Impact of waiting time after surgery and overall time of postoperative radiochemotherapy on treatment outcome
Seidlitz et al. Radiation Oncology (15) 1:172 DOI 1.1186/s1314-15-478-5 RESEARCH Open Access Impact of waiting time after surgery and overall time of postoperative radiochemotherapy on treatment outcome
VINCENT KHOO. 8 th EIKCS Symposium: May 2013
 8 th EIKCS Symposium: May 2013 VINCENT KHOO Royal Marsden NHS Foundation Trust & Institute of Cancer Research St George s Hospital & University of London Austin Health & University of Melbourne Disclosures
8 th EIKCS Symposium: May 2013 VINCENT KHOO Royal Marsden NHS Foundation Trust & Institute of Cancer Research St George s Hospital & University of London Austin Health & University of Melbourne Disclosures
CNS Tumors: The Med Onc Perspective. Ronald J. Scheff, MD Associate Clinical Professor Weill Medical College of Cornell U.
 CNS Tumors: The Med Onc Perspective Ronald J. Scheff, MD Associate Clinical Professor Weill Medical College of Cornell U. Disclosure Speakers Bureau, Merck Basic Oncology Concepts Tissue Diagnosis Stage
CNS Tumors: The Med Onc Perspective Ronald J. Scheff, MD Associate Clinical Professor Weill Medical College of Cornell U. Disclosure Speakers Bureau, Merck Basic Oncology Concepts Tissue Diagnosis Stage
