High-Intensity Focused Ultrasound (HIFU) as salvage therapy for radio-recurrent prostate cancer: predictors of disease response
|
|
|
- Dominick Marsh
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Vol. 44 (2): , March - Abril, 2018 doi: /S IBJU High-Intensity Focused Ultrasound (HIFU) as salvage therapy for radio-recurrent prostate cancer: predictors of disease response Shawn Dason 1, Nathan C. Wong 1, Christopher B. Allard 1, Jen Hoogenes 1, William Orovan 1, Bobby Shayegan 1 1 Division of Urology, McMaster University, Hamilton, ON, Canada ABSTRACT Background: Some men with localized radio-recurrent prostate cancer may benefit from salvage high-intensity focused ultrasound (HIFU). Herein, we describe oncologic outcomes and predictors of disease response after salvage whole gland HIFU from our prospective cohort. Materials and Methods: Patients with localized radio-recurrent prostate cancer were prospectively enrolled from January 2005 to December Participants had to meet both biochemical and histological definitions of recurrence. Exclusion criteria included the receipt of prior salvage therapy, presence of metastatic disease, and administration of ADT in the 6-months prior to enrollment. Participants were treated with a single session of whole-gland HIFU ablation with the Ablatherm TM device (EDAP, France). The primary endpoint was recurrence-free survival (RFS), defined as a composite endpoint of PSA progression (Phoenix criteria), receipt of any further salvage therapy, receipt of ADT, clinical progression, or death. Kaplan-Meier survival analysis was used to determine the primary end-point and stratifications were used to determine the significance of 6 pre-specified predictors of improved RFS (TRUS biopsy grade, number of study entry TRUS biopsy cores positive, palpable disease at study enrollment, pre-hifu PSA, an undetectable post-hifu PSA nadir, and receipt of prior hormone therapy). Survival analysis was performed on participants with a minimum of 1-year follow-up. Results: Twenty-four participants were eligible for study inclusion with a median follow-up of 1.0 months. Median PSA at study entry was 4.02ng/ml. Median time to PSA nadir was months after treatment and median post-hifu PSA nadir was 0.04ng/ ml. Median 2-year and 5-year RFS was 66.% and 51.6% respectively. Of our 6 prespecified predictors, an undetectable PSA nadir was the only significant predictor of improved RFS (HR 0.07, 95% CI , log-rank P<0.001). One participant underwent an intervention for a urethral stricture. No participants developed osteitis pubis or rectourethral fistulae. Conclusions: Salvage HIFU allows for disease control in selected patients with localized radio-recurrent prostate cancer. An undetectable PSA nadir serves as an early predictor of disease response. ARTICLE INFO Keywords: High-Intensity Focused Ultrasound Ablation; Prostatic Neoplasms; Erectile Dysfunction Int Braz J Urol. 2018; 44: Submitted for publication: June 29, 2017 Accepted after revision: September 12, 2017 Published as Ahead of Print: November 24,
2 INTRODUCTION Patients treated with primary radiotherapy for prostate cancer have a 20-60% risk of biochemical recurrence (1, 2). Various treatment options for biochemical failure are available, ranging from watchful waiting with delayed androgen deprivation therapy (ADT) to local salvage therapies. Over 90% of radio-recurrent patients receive ADT, which is not curative, associated with well-known side effects, and expensive (1). In one large series published by Zelefsky et al., a positive biopsy was present in 25% of patients receiving 81Gy dose of radiotherapy (). Of the patients with a positive biopsy, 97% had a PSA relapse and 1% developed metastases within 10 years (). Although there is no widely accepted gold standard for salvage therapy for radio-recurrence of prostate cancer, some consider the gold standard for curative local salvage therapy as salvage radical prostatectomy (4). Salvage radical prostatectomy has been reported to have 5-year and 10-year biochemical recurrence free rates of 47-82% and 28-5% respectively (5). Cancer specific survival has been reported to range from 70-8% and 54-89% at 5-years and 10-years respectively (5). Despite these outcomes, salvage radical prostatectomy is rarely performed due to its high morbidity rate. In the radio-recurrent setting the risk of intra-operative bowel injury is significantly higher and, at times, it is impossible to safely perform salvage radical prostatectomy (4). Other local therapies including cryotherapy (6) and brachytherapy (7) have also been used in smaller series as a salvage therapy for radio-recurrent prostate cancer, with a 50-70% biochemical recurrence free rate at 5 years. High-intensity focused ultrasound (HIFU) is a minimally invasive local ablative technology currently being investigated in prostate cancer. Use of HIFU has been previously reported in the primary setting, as well as in the salvage setting for radio- -recurrent prostate cancer (2, 8, 9). In the salvage setting, there are heterogeneous HIFU techniques, a lack of large prospective trials, and no consensus regarding the ideal candidate for salvage HIFU. To this end, we report our oncologic outcomes and predictors of disease response with whole-gland HIFU as salvage therapy for radio-recurrent prostate cancer. MATERIALS AND METHODS Participants with radio-recurrent prostate cancer were prospectively enrolled in this institutional review board approved study from January 2005 to December Participants were offered inclusion in this study if they had experienced radiation failure after primary radiotherapy (external beam radiotherapy [EBRT] or brachytherapy [BT]) for prostate cancer. Prior to study enrollment, participants underwent clinical assessment, PSA testing, computed tomographic (CT) scan of the abdomen and pelvis, bone scan and transrectal ultrasound (TRUS) guided prostate biopsy. The TRUS guided biopsy template was intended to sample the entire gland, including a classic sextant biopsy and approximately 2 additional lateral cores on each side. Study participants had to meet both biochemical and histopathologic definitions of failure. Biochemical failure was defined as either a PSA rise to 2ng/ml or more above their post radiotherapy PSA nadir (ASTRO Phoenix criteria (10)) or consecutive PSA rises above their post radiotherapy PSA nadir (1997 ASTRO consensus criteria (11)). Participants for which a c bounce phenomenon was suspected due to an increase in years 2- post radiotherapy were followed for 6-18 months (12) to ensure that they were experiencing a true biochemical failure prior study enrollment. Participants also had to have histopathologic evidence of failure on a TRUS guided biopsy performed at study entry demonstrating prostate cancer. Participants were included in study analyses if they had a minimum of 1-year of follow-up. Study exclusion criteria included the receipt of prior salvage therapy or prior HIFU, the presence of metastases on staging investigations, and the receipt of ADT in the 6-months prior to biochemical determination of radiation failure. Participants were treated with HIFU with the Ablatherm HIFU device (EDAP, France) using a standardized protocol similar to primary HIFU treatment. Treatment was done in a single session and monitored real-time with ultrasound to ensure whole-gland ablation. Spinal anesthesia with adjunctive intravenous sedation was used during treatment. Standardized device settings were em- 249
3 ployed - 100% acoustic power and Watts of energy was used. The pulse duration was 6 seconds and there was a 4 second delay between each pulse. Pre-HIFU androgen deprivation therapy and transurethral resection of prostate were not utilized. Participants were sent home the same day with a urethral Foley catheter. After the procedure, participants were followed every -months for the first 2 years, and then every 6 months subsequently. Follow-up included clinical follow-up, PSA testing, administration of the American Urological Association Symptom Index (1) (AUA-SI) and the International Index of Erectile Function (14) (IIEF) questionnaires, as well as additional investigations as indicated. In addition to recording general complications during clinical follow-up, attempts were made to specifically assess and diagnose participants with HIFU specific complications including urethral strictures, osteitis pubis, and rectourethral fistulae. Routine post-hifu biopsies were not performed. The primary endpoint of this study was disease recurrence, defined as a composite endpoint of PSA progression by the ASTRO Phoenix criteria (10) (PSA nadir+2ng/ml), receipt of any further salvage therapy, receipt of ADT, clinical progression including the development of locally advancing disease or metastases, or death. Secondary analyses were performed to determine predictors of disease recurrence. Pre-specified predictors for which analysis was intended included TRUS biopsy grade, number of study entry TRUS biopsy cores positive, palpable disease at study enrollment, pre-hifu PSA, an undetectable post-hifu PSA nadir, and receipt of prior hormone therapy. An additional post-hoc analysis was added to determine if use of the Stuttgart criteria for biochemical failure after primary HIFU (PSA nadir+1.2ng/ml (15) would alter the number of participants classified as recurrence, with an intention to perform analyses utilizing both definitions of biochemical failure should this be the case. Survival analysis with the Kaplan-Meier method was performed to determine disease recurrence-free survival (RFS) over time. Survival curves were stratified by each predictor of disease recurrence. A P value less than 0.05 on log-rank testing was used to determine whether the effect of each predictor on time to disease recurrence was statistically significant. Descriptive statistical analysis was performed with IBM SPSS Statistics version 22.0 (IBM Corporation, USA). Median values, range, and interquartile range (IQR) values are reported when appropriate. RESULTS A total of 741 patients underwent HIFU at our center and 24 patients (.2%) were eligible for study inclusion with a median follow-up of 1.0 months (range months). Mean age at treatment was 68 years and 21/24 patients (88%) had received prior EBRT, while /24 (12%) had received prior brachytherapy. Most participants (21/24, 87.5%) had Gleason 7 or higher disease on study entry biopsy and 14/24 (58.%) had palpable disease. Median PSA at study entry was 4.02ng/ml (range ng/ml). Patient demographics are listed in Table-1. All enrolled participants received salvage HIFU treatment as described in our protocol. Mean treated prostate volume was 2.8ml (range ml). No participants received ADT or transurethral resection of the prostate (TURP) as an adjunct to HIFU. Median time to PSA nadir was months (range -15 months) after treatment and median post-hifu PSA nadir was 0.04ng/ml Table 1 - Baseline characteristics of patients. Variable Value Number of included patients (n) 24 Mean age (years) 68 Prior EBRT (n) 21 (88%) Prior brachytherapy (n) (12%) Prior ADT (with radiotherapy) (n) 6 (25%) Restaging MRI (n) 9 (8%) Median PSA (ng/ml) [range] 4.02 [ ] ng/ml Gleason grade (n having 6, 7, 8-10), 11, 10 Clinical T stage (n having T1, T2, T) 10, 8, 6 250
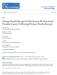
4 ibju High-intensity Focused Ultrasound (HIFU) as salvage therapy (range 0-.08). Two patients had no PSA responses post-hifu (PSA increased at the -month post-hifu measurement). Disease recurrence was experienced by 9 participants (8%) during follow-up with a median time to disease recurrence of 18 months (range -6 months). Disease recurrence was due to biochemical recurrence (rise of 2ng/ml above PSA nadir) in the 9 participants. If the alternate Stuttgart definition (PSA nadir+1.2ng/ml (14)) of biochemical failure was employed, none of the remaining 15 participants would be reclassified as treatment fai- lures. Maximum PSA decline, timing of maximum PSA decline, and timing of biochemical recurrence is displayed for individual patients in Figure-1. Overall survival analysis is displayed in Figure-2. Recurrence-free survival (RFS) after salvage HIFU was found to be 66.% at 2-years and 51.6% at 5-years. Subgroup analyses of predictors of improved RFS shown in Figure- demonstrated that an undetectable PSA nadir predicted improved RFS (HR 0.07, 95% CI , log rank P<0.001). The remaining analyzed predictors, TRUS biopsy Figure 1 - (A) Maximum PSA decline and (B) Timing of maximum PSA decline (post-hifu nadir) and timing of PSA failure for individual patients treated with salvage HIFU PSA DECLINE (ING/ML) PATIENT NUMBER MAXIMUM PSA DECLINE FOLLOWING SALVAGE HIFU -0 timing of maximum psa decline and psa failure following salvage hifu 40 5 Months Patient Number 0 *Time to Max Decline Time to PSA Failture
5 IBJU HIGH-IntensItY FocUseD ULtRAsoUnD (HIFU) As salvage therapy Figure 2 - Recurrence-free survival (RFS) after salvage HIFU. Figure - Subgroup analysis of recurrence-free survival (RFS) after salvage HIFU. (A) PSA nadir serves as an early predictor of RFS (P<0.001). (B) Low grade and (C) impalpable disease are suggestive of improved RFS but not statistically significant. Recurrence-Free Survival after Salvage HIFU Recurrence-Free Survival Recurrence-Free Survival 0.8 Recurrence-Free Survival after HIFU: Efect of Detectable PSA Nadir A Undertectable PSA Nadir 0.6 P< Detectable PSA Nadir Time (months) DISCUSSION With 20-60% of men receiving primary radiotherapy developing biochemical failure within 5 to 8 years, there is a clinical need to find curative salvage therapies (1, 2). Salvage prostatectomy may be potentially curative but carries 252 B Time (months) Recurrence-Free Survival after HIFU: Low Grade vs. High Grade 1.0 Recurrence-Free Survival Low Grade (Gleason +4 or less) 0.8 P= High Grade (Gleason 4+ or higher) Time (months) C Recurrence-Free Survival after HIFU: Efect of Palpable Disease 1.0 No Palpable Disease (T1c) 0.8 Recurrence-Free Survival grade, number of study entry TRUS biopsy cores positive, palpable disease at study enrollment, pre-hifu PSA, and receipt of prior hormone therapy, suggested an improved RFS but were not statistically significant (P>0.05). There was no difference in RFS between those patients initially treated with prior ERBT and brachytherapy. One participant developed urethral stricture disease 9 months post-hifu requiring visual internal urethrotomy (Clavien-Dindo Grade IIIb complication). No cases of rectourethral fistulae or osteitis pubis were observed. There were no other surgical complications noted. Median IPSS increased from a baseline of 8 (range 2-27, n=21) to 24 at a median year 1 average (range 6-2, n=16) and 17 at a median 2-year average (range 1-0, n=11). Median IIEF-15 declined from pre-treatment from 4 (n=17) to 19 post-treatment (n=12). IIEF data was limited in follow-up with most patients completing the post-treatment assessment at 6 months and not afterwards. 0.6 P= Palpable Disease (T2 or hiqher) Time (months)
6 a high risk of adverse events. Multiple studies have demonstrated cancer-specific survival to range from 70-8% and 54-89% at 5-years and 10-years respectively, and salvage prostatectomy has been reported to have 5-year and 10-year biochemical recurrence-free rates ranging from 47-82% and 28-5% respectively (5). Salvage prostatectomy is a more morbid operation than when performed primarily-previous series have demonstrated that salvage radical prostatectomy is associated with a 2-10% risk of rectal injury, 11-41% risk of anastomotic stricture, % risk of post-operative erectile dysfunction and 10-79% risk of incontinence. The goal of an ablative therapy for prostate cancer is the maximum destruction of cancerous tissue with minimal injury to critical adjacent structures such as the urethra, urinary sphincter, bladder neck and rectum. In our study, we have found that approximately half of patients treated with salvage whole gland HIFU for radio-recurrent prostate cancer experienced intermediate-term RFS (2-year RFS: 66.%, 5-year RFS: 51.6%). This is similar to other series that have reported intermediate term RFS ranging from 8-8% (Table-2). In their retrospective analysis of 167 patients, Murat et al. reported local cancer control was achieved with negative biopsy results in 7% of patients and the 5-year overall survival rate was 84% (16). The -year progression-free survival rates were 5%, 42% and 25% for the low-, intermediate-, and high-risk groups, respectively. Murat et al. showed that those who had not had previous ADT, low pre-hifu PSA and those with pre-radiotherapy low or intermediate D Amico risk disease had improved RFS. Neither Gleason score nor positive biopsy percentage influenced RFS. Another study by Jones et al. of 100 patients at least 2 years after EBRT who received whole gland HIFU, 50 men achieved their 1 year endpoint of PSA nadir less than 0.5ng/mL and a negative biopsy (17). A recent multicenter retrospective study by Crouzet et al. of 418 patients with radio- -recurrent disease treated with HIFU showed that the overall survival, cancer specific survival and metastasis-free survival rates at 7 years were 72%, 82% and 81%, respectively (18). Pre-ERBT risk classification and pre-salvage HIFU PSA was shown to be associated with worse biochemical failure-free survival. Another study by Gelet et al. of 71 patients who were treated with salvage HIFU demonstrated that 80% had negative biopsies post HIFU and 61% had a nadir PSA obtained within months of less than 0.5ng/mL (19). Mean follow- -up was 14.8 months and at the last follow-up, 44% of patients had no evidence of any disease progression. In our cohort, undetectable PSA nadir was the only identified predictor of improved RFS. This is validated by other data in the literature. Ahmed et al. showed that in 84 men who underwent whole gland salvage HIFU, PSA nadir >0.5ng/mL was predictive of failure (HR: 0.16, P<0.001) (2). The 1- and 2-year PFS for patients with a PSA nadir of <0.5ng/mL was 82 and 68% respectively, compared to 7 and 1% for those with a PSA nadir >0.5ng/mL. Neither pre-treatment PSA nor Gleason score were found to predict failure. Uchida et al. showed that in men with a PSA nadir <0.2ng/ ml had a low rate of cancer detection on post- -HIFU biopsy of only 11% compared to 54 and 52% if the PSA nadir was or >1ng/mL respectively (20). This has led to some investigators suggesting that routine biopsy post-hifu may not be required if the PSA nadir is less than 0.2ng/mL. The PSA nadir has also been shown to be a predictor of improved RFS in other setting including primary HIFU (21), focal salvage HIFU (22) and salvage cryoablation (2). Other predictors of RFS shown by other investigators include pre-ebrt D Amico risk (Murat), pre-hifu PSA (8, 16, 21), previous ADT (8, 16), Gleason grade (8) and tumor extension anterior to the urethra as seen in MRI (21). However, these were not shown to be statistically significant in our cohort. Compared to salvage prostatectomy, complication rates of salvage HIFU are hypothesized to be less severe (7). In our series, only 1 participant developed urethral stricture disease requiring visual internal urethrotomy and there were no cases of rectourethral fistulae or osteitis pubis. In a systematic review of HIFU for radio-recurrent prostate cancer, reported complications included a 2-16% risk of rectourethral fistula, 20% risk 25
7 Table 2 - Review of literature for salvage HIFU (whole gland and focal) for radio-recurrent prostate cancer. Study, Year Device No. patients (n) Age (years) Pre-HIFU PSA (months) Median follow-up (months) Primary therapy Prior ADT (%) Definition of biochemical failure RFS Incontinence (%) Bladder obstruction (%) Rectourethral fistula (%) Osteitis Pubis (%) Whole Gland HIFU Gelet, 2004 Ablatherm EBRT 0 ASTRO 8% (0 months) 5.2 (G = 7) NR Zacgarakis, 2008 Sonablate EBRT 58 ASTRO 71% (7.4 months) NR Murat, 2009 Ablatherm EBRT 56.8 Phoenix 5% low risk, 42% intermediate risk, 25% high risk ( years) 49.5 (G = 9.5) 19.8 NR Berge, 2010 Ablatherm EBRT 15.2 Phoenix 60.9% (9 months) NR EBRT (6.6%), Uchida, 2010 Sonablate BT (22.7), PT (1.6%) 27. Phoenix 52% (5 years) NR Ahmed, 2012 Sonablate EBRT 6 Phoenix 59% (1 year); 4% (2 year) Crouzet, 2012 Ablatherm EBRT 50 Phoenix 45% low risk, 1% intermediate risk, 21% high risk (5 years) Rouviere, 201 Ablatherm 46 NR 5.7 NR EBRT 2.6 Phoenix 42% (2 year); 1% (4 year) NR NR NR NR Song, 2014 Ablatherm ERBT 61.5 Stuttgart 5.8% (44.5 months) NR Yutkin, 2014 Sonablate BT 27 Stuttgart 66.7% (4. years) Dason, 2016 Ablatherm ERBT (88%), BT (12%) NR Phoenix 66.% (2 year); 51.6% (5 year) NR Focal HIFU Ahmed, 2012 Sonablate EBRT 74.4 Phoenix 69% (1 year); 49% (2 year) Baco, 2014 Ablatherm NR 16. EBRT (96%), BT (4%) 2 Phoenix 8% (1 year); 52% (2 year) 25 NR
8 of bladder neck contracture, 10% risk of urethral strictures, % risk of osteitis pubis, 10-50% risk of incontinence and % risk of erectile dysfunction (24). Heterogeneity in adverse event reporting prevents a direct comparison of salvage HIFU toxicity to salvage prostatectomy. Compared to whole gland salvage HIFU, focal HIFU is less well reported. Although preserving oncologic control while further minimizing harm may be achieved with focal therapy, difficulty with accurately localizing and treating recurrent disease may lead to progression and metastasis. Provisional data suggests similar oncological outcomes with lower adverse events compared to whole-gland ablation. Ahmed et al. reported on 9 patients treated with focal HIFU (hemi-ablation or focal ablation) for radio-recurrent prostate cancer (22). Progression-free survival rates at 1- and 2- years according to the Phoenix criteria were reported to be 69% and 49% respectively. Baco et al. described 48 prospectively enrolled patients with radio-recurrent prostate cancer treated with hemi-salvage HIFU (25). Progression-free survival rates at 12, 18 and 24 months were 8%, 64% and 52% respectively. Disease progression occurred in 16 of 48 patients (%). Of these, 4 had local recurrence in the untreated lobe, 4 had bilateral recurrence, 6 developed metastases and 2 had rising PSA without evidence of local recurrence or metastases. Thus, whole gland and focal salvage HIFU may provide a potential cure if patients are referred at an early stage when recurrence is suspected. The present study s small sample size and short follow-up limited the confidence in estimation of RFS as well as the power of subgroup analyses and ability to analyze predictive factors. This study was also limited by a lack of follow-up biopsies to adequately demonstrate effective treatment. We defined treatment failure with a strict clinical definition. Further, purely PSA based definitions of biochemical failure including both the ASTRO definitions (10, 11) as well as the Stuttgart definition (15) are not validated to predict disease recurrence after salvage HIFU. This limits comparisons to salvage prostatectomy, for which a post- -treatment PSA nadir of 0ng/ml is expected and biochemical recurrence is easily assessed. Other than aggregate AUA-SI and IIEF-15 questionnaire data, adverse event recording was limited as we did not capture lower grade complications such as infections, hematuria, incontinence and perineal pain. Every attempt was made to assess for severe complications and we saw only 1 case of stricture disease requiring intervention (Clavien-Dindo Grade IIIb complication) and no cases of rectourethral fistulae or osteitis pubic. This is consistent with the low incidence of these complications as described in previous series (2, 8, 9). Additional complications may become evident with longer follow-up. On routine follow-up, there was a median increase in IPSS at 1 year followed by subsequent improvement at 2-year follow-up. It has been previously reported that HIFU causes de novo detrusor overactivity and impaired bladder compliance seen on routine urodynamics in 10% of patients at months, with progressive improvement at longer follow-up as seen in our series (26). There is no consensus to date for the ideal candidate for salvage HIFU for radio-recurrent prostate cancer. The main candidate for salvage HIFU is a man that has radio-recurrent prostate cancer predicted to cause morbidity or mortality within his lifetime, but refuses or cannot receive salvage radical prostatectomy. Further, the effectiveness of salvage therapy is a function of how well metastases are excluded. We utilized standard bone scans and CT scans to rule out metastases. However, they are of limited value, especially when PSA is low. Some patients in this study may have had occult micrometastatasis at the time of HIFU and eventually had progression with distant disease leading to a failure of proper selection due to limitations of pre-hifu screening or imaging. The patients who had no PSA response likely had unrecognized micrometastatic disease. Future studies on salvage therapy will rely on advanced imaging modalities to rule out systemic recurrence post curative treatment, including 18-F Choline PET and PSMA PET, which have reported sensitivities of 42-96% (27) and % (28). In summary, salvage HIFU allows for intermediate-term disease control with acceptable morbidity in carefully selected patients with localized radio-recurrent prostate cancer. An undetectable 255
9 PSA nadir, achieved at a median time of months post-hifu, serves as an early predictor of recurrence-free survival. Large multicenter trials with long-term follow-up are warranted to better assess oncological outcomes and adverse events. CONFLICT OF INTEREST REFERENCES None declared. 1. Agarwal PK, Sadetsky N, Konety BR, Resnick MI, Carroll PR; Cancer of the Prostate Strategic Urological Research Endeavor (CaPSURE). Treatment failure after primary and salvage therapy for prostate cancer: likelihood, patterns of care, and outcomes. Cancer. 2008;112: Uddin Ahmed H, Cathcart P, Chalasani V, Williams A, McCartan N, Freeman A, et al. Whole-gland salvage highintensity focused ultrasound therapy for localized prostate cancer recurrence after external beam radiation therapy. Cancer. 2012;118: Zelefsky MJ, Reuter VE, Fuks Z, Scardino P, Shippy A. Influence of local tumor control on distant metastases and cancer related mortality after external beam radiotherapy for prostate cancer. J Urol. 2008;179:168-7; discussion Gotto GT, Yunis LH, Vora K, Eastham JA, Scardino PT, Rabbani F. Impact of prior prostate radiation on complications after radical prostatectomy. J Urol. 2010;184: Chade DC, Eastham J, Graefen M, Hu JC, Karnes RJ, Klotz L, et al. Cancer control and functional outcomes of salvage radical prostatectomy for radiation-recurrent prostate cancer: a systematic review of the literature. Eur Urol. 2012;61: Mouraviev V, Spiess PE, Jones JS. Salvage cryoablation for locally recurrent prostate cancer following primary radiotherapy. Eur Urol. 2012;61: Eastham JA, Carroll P, Pisters L, Nguyen PT, Touijer K. Salvage therapies after radiation therapy. Urol Oncol. 2012;0: Crouzet S, Murat FJ, Pommier P, Poissonnier L, Pasticier G, Rouviere O, et al. Locally recurrent prostate cancer after initial radiation therapy: early salvage high-intensity focused ultrasound improves oncologic outcomes. Radiother Oncol. 2012;105: Yutkin V, Ahmed HU, Donaldson I, McCartan N, Siddiqui K, Emberton M, et al. Salvage high-intensity focused ultrasound for patients with recurrent prostate cancer after brachytherapy. Urology. 2014;84: Roach M rd, Hanks G, Thames H Jr, Schellhammer P, Shipley WU, Sokol GH, et al. Defining biochemical failure following radiotherapy with or without hormonal therapy in men with clinically localized prostate cancer: recommendations of the RTOG-ASTRO Phoenix Consensus Conference. Int J Radiat Oncol Biol Phys. 2006;65: Consensus statement: guidelines for PSA following radiation therapy. American Society for Therapeutic Radiology and Oncology Consensus Panel. Int J Radiat Oncol Biol Phys. 1997;7: Greene KL, Albertsen PC, Babaian RJ, Carter HB, Gann PH, Han M, et al. Prostate specific antigen best practice statement: 2009 update. J Urol. 2009;182: Barry MJ, Fowler FJ Jr, O Leary MP, Bruskewitz RC, Holtgrewe HL, Mebust WK, et al. The American Urological Association symptom index for benign prostatic hyperplasia. The Measurement Committee of the American Urological Association. J Urol. 1992;148: Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A. The international index of erectile function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology. 1997;49: Blana A, Brown SC, Chaussy C, Conti GN, Eastham JA, Ganzer R, et al. High-intensity focused ultrasound for prostate cancer: comparative definitions of biochemical failure. BJU Int. 2009;104: Murat FJ, Poissonnier L, Rabilloud M, Belot A, Bouvier R, Rouviere O, et al. Mid-term results demonstrate salvage high-intensity focused ultrasound (HIFU) as an effective and acceptably morbid salvage treatment option for locally radiorecurrent prostate cancer. Eur Urol. 2009;55: Jones TA, Chin J, Mcleod D, Barkin J, Pantuck A, Marks LS. High Intensity Focused Ultrasound for Radio- Recurrent Prostate Cancer: A North American Clinical Trial. J Urol. 2017(17) Crouzet S, Blana A, Murat FJ, Pasticier G, Brown SCW, Conti GN, et al. Salvage high-intensity focused ultrasound (HIFU) for locally recurrent prostate câncer after failed radiation therapy: Multi-institutional analysis of 418 patients. BJU Int. 2017;119: Gelet A, Chapelon JY, Poissonnier L, Bouvier R, Rouvière O, Curiel L, et al. Local recurrence of prostate cancer after external beam radiotherapy: early experience of salvage therapy using high-intensity focused ultrasonography. Urology. 2004;6: Uchida T, Shoji S, Nakano M, Hongo S, Nitta M, Usui Y, et al. High-intensity focused ultrasound as salvage therapy for patients with recurrent prostate cancer after external beam radiation, brachytherapy or proton therapy. BJU Int. 2011;107:
10 21. Rouvière O, Sbihi L, Gelet A, Chapelon JY. Salvage high-intensity focused ultrasound ablation for prostate cancer local recurrence after external-beam radiation therapy: prognostic value of prostate MRI. Clin Radiol. 201;68: Ahmed HU, Cathcart P, McCartan N, Kirkham A, Allen C, Freeman A, et al. Focal salvage therapy for localized prostate cancer recurrence after external beam radiotherapy: a pilot study. Cancer. 2012;118: Kovac E, ElShafei A, Tay KJ, Mendez M, Polascik TJ, Jones JS. Five-Year Biochemical Progression-Free Survival Following Salvage Whole-Gland Prostate Cryoablation: Defining Success with Nadir Prostate-Specific Antigen. J Endourol. 2016;0: Chalasani V, Martinez CH, Lim D, Chin J. Salvage HIFU for recurrent prostate cancer after radiotherapy. Prostate Cancer Prostatic Dis. 2009;12: Baco E, Gelet A, Crouzet S, Rud E, Rouvière O, Tonoli-Catez H, et al. Hemi salvage high-intensity focused ultrasound (HIFU) inunilateral radiorecurrent prostate cancer: a prospective two-centre study. BJU Int. 2014;114: Mearini L, Nunzi E, Giovannozzi S, Lepri L, Lolli C, Giannantoni A. Urodynamic evaluation after high-intensity focused ultrasound for patients with prostate cancer. Prostate Cancer. 2014;2014: Vali R, Loidl W, Pirich C, Langesteger W, Beheshti M. Imaging of prostate cancer with PET/CT using (18)F-Fluorocholine. Am J Nucl Med Mol Imaging. 2015;5: Rowe SP, Gorin MA, Allaf ME, Pienta KJ, Tran PT, Pomper MG, et al. PET imaging of prostate-specific membrane antigen in prostate cancer: current state of the art and future challenges. Prostate Cancer Prostatic Dis. 2016;19:22-0. Correspondence address: Nathan Colin Wong, MD Division of Urology McMaster University, Hamilton, ON, Canada 1280 Main St West Hamilton Ontario, ON L8S 4L8, Canada Telephone nathan.wong@medportal.ca 257
S Crouzet, O Rouvière, JY Chapelon, F Mege, X martin, A Gelet
 S Crouzet, O Rouvière, JY Chapelon, F Mege, X martin, A Gelet Why HIFU? Efficacy demonstrated Real time control of the target Early control of the necrosis area is possible with MRI or TRUS using contrast
S Crouzet, O Rouvière, JY Chapelon, F Mege, X martin, A Gelet Why HIFU? Efficacy demonstrated Real time control of the target Early control of the necrosis area is possible with MRI or TRUS using contrast
High-Intensity Focused Ultrasound as Salvage Therapy for Patients With Recurrent Prostate Cancer After Radiotherapy
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.2.91 Original Article - Urological Oncology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.2.91&domain=pdf&date_stamp=2014-2-1 High-Intensity
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.2.91 Original Article - Urological Oncology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.2.91&domain=pdf&date_stamp=2014-2-1 High-Intensity
Comparative morbidity of ablative energy-based salvage treatments for radio-recurrent prostate cancer
 Original research Comparative morbidity of ablative energy-based salvage treatments for radio-recurrent prostate cancer Khurram M. Siddiqui, MBBS, MSc, FRCS, FEBU; * Michele Billia, MD; * Andrew Williams,
Original research Comparative morbidity of ablative energy-based salvage treatments for radio-recurrent prostate cancer Khurram M. Siddiqui, MBBS, MSc, FRCS, FEBU; * Michele Billia, MD; * Andrew Williams,
Effective Date: 11/1/2018 Section: SUR Policy No: 420 Medical Policy Committee Approved Date: 8/18; 9/18
 PROVIDENCE HEALTH PLANS MEDICAL (HIFU) (All Lines of Business Except Medicare) Effective Date: 11/1/2018 Section: SUR Policy No: 420 Medical Policy Committee Approved Date: 8/18; 9/18 11/1/18 Medical Officer
PROVIDENCE HEALTH PLANS MEDICAL (HIFU) (All Lines of Business Except Medicare) Effective Date: 11/1/2018 Section: SUR Policy No: 420 Medical Policy Committee Approved Date: 8/18; 9/18 11/1/18 Medical Officer
Outcomes Following Negative Prostate Biopsy for Patients with Persistent Disease after Radiotherapy for Prostate Cancer
 Clinical Urology Post-radiotherapy Prostate Biopsy for Recurrent Disease International Braz J Urol Vol. 36 (1): 44-48, January - February, 2010 doi: 10.1590/S1677-55382010000100007 Outcomes Following Negative
Clinical Urology Post-radiotherapy Prostate Biopsy for Recurrent Disease International Braz J Urol Vol. 36 (1): 44-48, January - February, 2010 doi: 10.1590/S1677-55382010000100007 Outcomes Following Negative
High Intensity Focused Ultrasounds for the treatment of Prostate Cancers Clinical update November D. Maruzzi - L. Ruggera
 High Intensity Focused Ultrasounds for the treatment of Prostate Cancers Clinical update November 2014 D. Maruzzi - L. Ruggera HIFU development Second prototype 1995-2000 Integrated Imaging 2006-2010 1993
High Intensity Focused Ultrasounds for the treatment of Prostate Cancers Clinical update November 2014 D. Maruzzi - L. Ruggera HIFU development Second prototype 1995-2000 Integrated Imaging 2006-2010 1993
PSA is rising: What to do? After curative intended radiotherapy: More local options?
 Klinik und Poliklinik für Urologie und Kinderurologie Direktor: Prof. Dr. H. Riedmiller PSA is rising: What to do? After curative intended radiotherapy: More local options? Klinische und molekulare Charakterisierung
Klinik und Poliklinik für Urologie und Kinderurologie Direktor: Prof. Dr. H. Riedmiller PSA is rising: What to do? After curative intended radiotherapy: More local options? Klinische und molekulare Charakterisierung
Current Findings on High Intensity Focused Ultrasound (HIFU) Thomas J Polascik, MD, FACS Professor of Surgery
 Current Findings on High Intensity Focused Ultrasound (HIFU) Thomas J Polascik, MD, FACS Professor of Surgery Outline Whole gland abla6on selec6on and outcomes Focal abla6on - Eligibility and pa6ent selec6on
Current Findings on High Intensity Focused Ultrasound (HIFU) Thomas J Polascik, MD, FACS Professor of Surgery Outline Whole gland abla6on selec6on and outcomes Focal abla6on - Eligibility and pa6ent selec6on
Department of Urology, Cochin hospital Paris Descartes University
 Technical advances in the treatment of localized prostate cancer Pr Michaël Peyromaure Department of Urology, Cochin hospital Paris Descartes University Introduction Curative treatments of localized prostate
Technical advances in the treatment of localized prostate cancer Pr Michaël Peyromaure Department of Urology, Cochin hospital Paris Descartes University Introduction Curative treatments of localized prostate
Imaging of prostate cancer local recurrences : why and how?
 Imaging of prostate cancer local recurrences : why and how? Olivier Rouvière Department of Urinary and Vascular Imaging Hospices Civils de Lyon Lyon - France 1. Preliminary Remarks Preliminary Remarks
Imaging of prostate cancer local recurrences : why and how? Olivier Rouvière Department of Urinary and Vascular Imaging Hospices Civils de Lyon Lyon - France 1. Preliminary Remarks Preliminary Remarks
ABLATHERM HIFU THE CANADIAN EXPERIENCE. WILLIAM L. OROVAN McMASTER UNIVERSITY MAPLE LEAF HIFU
 ABLATHERM HIFU THE CANADIAN EXPERIENCE WILLIAM L. OROVAN McMASTER UNIVERSITY MAPLE LEAF HIFU PROCEDURE 1. Spinal Anaesthetic/IV Sedation 2. Right Lateral Decubitus Position 3. Transrectal Probe 4. Catheter
ABLATHERM HIFU THE CANADIAN EXPERIENCE WILLIAM L. OROVAN McMASTER UNIVERSITY MAPLE LEAF HIFU PROCEDURE 1. Spinal Anaesthetic/IV Sedation 2. Right Lateral Decubitus Position 3. Transrectal Probe 4. Catheter
First Analysis of the Long-Term Results with Transrectal HIFU in Patients with Localised Prostate Cancer
 european urology 53 (2008) 1194 1203 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer First Analysis of the Long-Term Results with Transrectal HIFU in Patients
european urology 53 (2008) 1194 1203 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer First Analysis of the Long-Term Results with Transrectal HIFU in Patients
Outcomes of salvage radical prostatectomy following more than one failed local therapy
 Original Article - Urological Oncology https://doi.org/10.4111/icu.2018.59.3.152 pissn 2466-0493 eissn 2466-054X Outcomes of salvage radical prostatectomy following more than one failed local therapy Arjun
Original Article - Urological Oncology https://doi.org/10.4111/icu.2018.59.3.152 pissn 2466-0493 eissn 2466-054X Outcomes of salvage radical prostatectomy following more than one failed local therapy Arjun
Focal Salvage HIFU in radiorecurrent prostate cancer
 Focal Salvage HIFU in radiorecurrent prostate cancer Kanthabalan A.* [1, 2], Peters M* [3], Van Vulpen M [3], McCartan N. [1,2], Hindley R [4], Moore C.M. [1,2], Arya M. [2], Emberton M. [1,2], Ahmed H.U.
Focal Salvage HIFU in radiorecurrent prostate cancer Kanthabalan A.* [1, 2], Peters M* [3], Van Vulpen M [3], McCartan N. [1,2], Hindley R [4], Moore C.M. [1,2], Arya M. [2], Emberton M. [1,2], Ahmed H.U.
Prostate Cancer Local or distant recurrence?
 Prostate Cancer Local or distant recurrence? Diagnostic flowchart Vanessa Vilas Boas Urologist VFX Hospital FEBU PSA - only recurrence PSA recurrence: 27-53% of all patients undergoing treatment with curative
Prostate Cancer Local or distant recurrence? Diagnostic flowchart Vanessa Vilas Boas Urologist VFX Hospital FEBU PSA - only recurrence PSA recurrence: 27-53% of all patients undergoing treatment with curative
Salvage HDR Brachytherapy. Amit Bahl Consultant Clinical Oncologist The Bristol Cancer Institute, UK
 Salvage HDR Brachytherapy Amit Bahl Consultant Clinical Oncologist The Bristol Cancer Institute, UK Disclosures Still No financial disclosures! Limited personal experience of HDR Brachy as salvage option
Salvage HDR Brachytherapy Amit Bahl Consultant Clinical Oncologist The Bristol Cancer Institute, UK Disclosures Still No financial disclosures! Limited personal experience of HDR Brachy as salvage option
PSA nadir post LDR Brachytherapy and early Salvage Therapy. Dr Duncan McLaren UK & Ireland Users Group Meeting 2016
 PSA nadir post LDR Brachytherapy and early Salvage Therapy Dr Duncan McLaren UK & Ireland Users Group Meeting 2016 Differences in PSA relapse rates based on definition used PSA ng/ml Recurrence ASTRO Recurrence
PSA nadir post LDR Brachytherapy and early Salvage Therapy Dr Duncan McLaren UK & Ireland Users Group Meeting 2016 Differences in PSA relapse rates based on definition used PSA ng/ml Recurrence ASTRO Recurrence
Prostatectomy as salvage therapy. Cases. Paul Cathcart - Guy s & St Thomas NHS Trust, London
 Prostatectomy as salvage therapy Cases Paul Cathcart - Guy s & St Thomas NHS Trust, London Attributes of brachytherapy appeal to young men who place high utility on genitourinary function At risk of
Prostatectomy as salvage therapy Cases Paul Cathcart - Guy s & St Thomas NHS Trust, London Attributes of brachytherapy appeal to young men who place high utility on genitourinary function At risk of
Single session of high-intensity focused ultrasound for localized prostate cancer: treatment outcomes and potential effect as a primary therapy
 World J Urol (14) 32:1339 1345 DOI 1.17/s345-13-1215-z ORIGINAL ARTICLE Single session of high-intensity focused ultrasound for localized prostate cancer: treatment outcomes and potential effect as a primary
World J Urol (14) 32:1339 1345 DOI 1.17/s345-13-1215-z ORIGINAL ARTICLE Single session of high-intensity focused ultrasound for localized prostate cancer: treatment outcomes and potential effect as a primary
2/14/09. Why Discuss this topic? Managing Local Recurrences after Radiation Failure. PROSTATE CANCER Second Treatment
 Why Discuss this topic? Mack Roach III, MD Professor and Chair Radiation Oncology UCSF Managing Local Recurrences after Radiation Failure 1. ~15 to 75% of CaP pts recur after definitive RT. 2. Heterogeneous
Why Discuss this topic? Mack Roach III, MD Professor and Chair Radiation Oncology UCSF Managing Local Recurrences after Radiation Failure 1. ~15 to 75% of CaP pts recur after definitive RT. 2. Heterogeneous
Radiation Therapy for Prostate Cancer. Resident Dept of Urology General Surgery Grand Round November 24, 2008
 Radiation Therapy for Prostate Cancer Amy Hou,, MD Resident Dept of Urology General Surgery Grand Round November 24, 2008 External Beam Radiation Advances Improving Therapy Generation of linear accelerators
Radiation Therapy for Prostate Cancer Amy Hou,, MD Resident Dept of Urology General Surgery Grand Round November 24, 2008 External Beam Radiation Advances Improving Therapy Generation of linear accelerators
Disease-Free Survival Following Salvage Cryotherapy for Biopsy-Proven Radio-Recurrent Prostate Cancer
 EUROPEAN UROLOGY 60 (2011) 405 410 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by J. Stephen Jones on pp. 411 412 of this issue
EUROPEAN UROLOGY 60 (2011) 405 410 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by J. Stephen Jones on pp. 411 412 of this issue
How to deal with patients who fail intracavitary treatment
 How to deal with patients who fail intracavitary treatment A. Heidenreich Department of Urology Non-surgical therapy of PCA IMRT SEEDS IGRT HDR-BRACHY HIFU CRYO LDR - Brachytherapy Author Follow-up bned
How to deal with patients who fail intracavitary treatment A. Heidenreich Department of Urology Non-surgical therapy of PCA IMRT SEEDS IGRT HDR-BRACHY HIFU CRYO LDR - Brachytherapy Author Follow-up bned
Irreversible Electroporation for the Treatment of Recurrent Prostate Cancer
 Irreversible Electroporation for the Treatment of Recurrent Prostate Cancer after prostatectomy, radiation therapy and HiFU R. Schwartzberg, E. Günther, N. Klein, S. Zapf, R. El-Idrissi, J. Cooper, B.
Irreversible Electroporation for the Treatment of Recurrent Prostate Cancer after prostatectomy, radiation therapy and HiFU R. Schwartzberg, E. Günther, N. Klein, S. Zapf, R. El-Idrissi, J. Cooper, B.
Salvage prostatectomy for post-radiation adenocarcinoma with treatment effect: Pathological and oncological outcomes
 ORIGINAL RESEARCH Salvage prostatectomy for post-radiation adenocarcinoma with treatment effect: Pathological and oncological outcomes Michael J. Metcalfe, MD ; Patricia Troncoso, MD 2 ; Charles C. Guo,
ORIGINAL RESEARCH Salvage prostatectomy for post-radiation adenocarcinoma with treatment effect: Pathological and oncological outcomes Michael J. Metcalfe, MD ; Patricia Troncoso, MD 2 ; Charles C. Guo,
Available online at ScienceDirect. journal homepage:
 Asian Journal of Urology (2015) 2, 46e52 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur ORIGINAL ARTICLE Single application of high-intensity
Asian Journal of Urology (2015) 2, 46e52 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur ORIGINAL ARTICLE Single application of high-intensity
Accepted Manuscript. Akira Horiuchi, Satoru Muto, M.D., Ph.D, Keisuke Saito, Masaki Kimura, Hisamitsu Ide, Raizo Yamaguchi, Shigeo Horie
 Accepted Manuscript Holmium laser enucleation of the prostate followed by High-Intensity Focused Ultrasound treatment for patients with huge prostate adenoma and localized prostate cancer: 5-year follow-up
Accepted Manuscript Holmium laser enucleation of the prostate followed by High-Intensity Focused Ultrasound treatment for patients with huge prostate adenoma and localized prostate cancer: 5-year follow-up
High-Intensity Focused Ultrasound (HIFU) for Prostate Cancer
 HIFU technology shows promise as an alternative to radiation therapy for patients with localized prostate cancer. Monique Gueudet-Bornstein. Laissez les Bon Temps Rouler [Let the Good Times Roll]. New
HIFU technology shows promise as an alternative to radiation therapy for patients with localized prostate cancer. Monique Gueudet-Bornstein. Laissez les Bon Temps Rouler [Let the Good Times Roll]. New
Recurrence of prostate cancer after HIFU. Proposal of a novel predictive index
 Acta Biomed 2018; Vol. 89, N. 2: 220-226 DOI: 10.23750/abm.v89i2.6730 Mattioli 1885 Original article Recurrence of prostate cancer after HIFU. Proposal of a novel predictive index Umberto Maestroni 1,
Acta Biomed 2018; Vol. 89, N. 2: 220-226 DOI: 10.23750/abm.v89i2.6730 Mattioli 1885 Original article Recurrence of prostate cancer after HIFU. Proposal of a novel predictive index Umberto Maestroni 1,
Best Papers. F. Fusco
 Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
GUIDELINEs ON PROSTATE CANCER
 GUIDELINEs ON PROSTATE CANCER (Text update March 2005: an update is foreseen for publication in 2010. Readers are kindly advised to consult the 2009 full text print of the PCa guidelines for the most recent
GUIDELINEs ON PROSTATE CANCER (Text update March 2005: an update is foreseen for publication in 2010. Readers are kindly advised to consult the 2009 full text print of the PCa guidelines for the most recent
Consensus and Controversies in Cancer of Prostate BASIS FOR FURHTER STUDIES. Luis A. Linares MD FACRO Medical Director
 BASIS FOR FURHTER STUDIES Main controversies In prostate Cancer: 1-Screening 2-Management Observation Surgery Standard Laparoscopic Robotic Radiation: (no discussion on Cryosurgery-RF etc.) Standard SBRT
BASIS FOR FURHTER STUDIES Main controversies In prostate Cancer: 1-Screening 2-Management Observation Surgery Standard Laparoscopic Robotic Radiation: (no discussion on Cryosurgery-RF etc.) Standard SBRT
Understanding the risk of recurrence after primary treatment for prostate cancer. Aditya Bagrodia, MD
 Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
Ablatherm Integrated Imaging HIFU Treatment of Low Risk, Localized Prostate Cancer
 Ablatherm Integrated Imaging HIFU Treatment of Low Risk, Localized Prostate Cancer P130003 Gastroenterology and Urology Devices Panel Meeting July 30, 2014 CI-1 Presenters Cary Robertson, MD Associate
Ablatherm Integrated Imaging HIFU Treatment of Low Risk, Localized Prostate Cancer P130003 Gastroenterology and Urology Devices Panel Meeting July 30, 2014 CI-1 Presenters Cary Robertson, MD Associate
Managing Prostate Cancer After Initital Treatment Fails: Are There Good Next Steps?
 Managing Prostate Cancer After Initital Treatment Fails: Are There Good Next Steps? Michael J Zelefsky, M.D. Professor of Radiation Oncology Chief Brachytherapy Service Department of Radiation Oncology
Managing Prostate Cancer After Initital Treatment Fails: Are There Good Next Steps? Michael J Zelefsky, M.D. Professor of Radiation Oncology Chief Brachytherapy Service Department of Radiation Oncology
Paul F. Schellhammer, M.D. Eastern Virginia Medical School Urology of Virginia Norfolk, Virginia
 Paul F. Schellhammer, M.D. Eastern Virginia Medical School Urology of Virginia Norfolk, Virginia Virginia - Chesapeake Bay Landfall: Virginia Beach, April 29 th, 1607 PSA Failure after Radical Prostatectomy
Paul F. Schellhammer, M.D. Eastern Virginia Medical School Urology of Virginia Norfolk, Virginia Virginia - Chesapeake Bay Landfall: Virginia Beach, April 29 th, 1607 PSA Failure after Radical Prostatectomy
A schematic of the rectal probe in contact with the prostate is show in this diagram.
 Hello. My name is William Osai. I am a nurse practitioner in the GU Medical Oncology Department at The University of Texas MD Anderson Cancer Center in Houston. Today s presentation is Part 2 of the Overview
Hello. My name is William Osai. I am a nurse practitioner in the GU Medical Oncology Department at The University of Texas MD Anderson Cancer Center in Houston. Today s presentation is Part 2 of the Overview
Low risk. Objectives. Case-based question 1. Evidence-based utilization of imaging in prostate cancer
 Evidence-based utilization of imaging in prostate cancer Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Objectives State the modalities,
Evidence-based utilization of imaging in prostate cancer Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Objectives State the modalities,
GUIDELINES ON PROSTATE CANCER
 10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
PET imaging of cancer metabolism is commonly performed with F18
 PCRI Insights, August 2012, Vol. 15: No. 3 Carbon-11-Acetate PET/CT Imaging in Prostate Cancer Fabio Almeida, M.D. Medical Director, Arizona Molecular Imaging Center - Phoenix PET imaging of cancer metabolism
PCRI Insights, August 2012, Vol. 15: No. 3 Carbon-11-Acetate PET/CT Imaging in Prostate Cancer Fabio Almeida, M.D. Medical Director, Arizona Molecular Imaging Center - Phoenix PET imaging of cancer metabolism
J Clin Oncol 28: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
Salvage Brachytherapy for Biochemically Recurrent Prostate Cancer Following Primary Brachytherapy
 University of Kentucky UKnowledge Urology Faculty Publications Urology 2016 Salvage Brachytherapy for Biochemically Recurrent Prostate Cancer Following Primary Brachytherapy John M. Lacy University of
University of Kentucky UKnowledge Urology Faculty Publications Urology 2016 Salvage Brachytherapy for Biochemically Recurrent Prostate Cancer Following Primary Brachytherapy John M. Lacy University of
OPEN Prostate Cancer and Prostatic Diseases (2016) 19,
 OPEN Prostate Cancer and Prostatic Diseases (2016) 19, 311 316 www.nature.com/pcan ORIGINAL ARTICLE PSA nadir as a predictive factor for biochemical disease-free survival and overall survival following
OPEN Prostate Cancer and Prostatic Diseases (2016) 19, 311 316 www.nature.com/pcan ORIGINAL ARTICLE PSA nadir as a predictive factor for biochemical disease-free survival and overall survival following
Cancer. Description. Section: Surgery Effective Date: October 15, 2016 Subsection: Original Policy Date: September 9, 2011 Subject:
 Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
Subject: Saturation Biopsy for Diagnosis, Last Review Status/Date: September 2016 Page: 1 of 9 Saturation Biopsy for Diagnosis, Description Saturation biopsy of the prostate, in which more cores are obtained
TITLE: High Intensity Focused Ultrasound for Prostate Cancer: A Review of the Guidelines and Clinical Effectiveness
 TITLE: High Intensity Focused Ultrasound for Prostate Cancer: A Review of the Guidelines and Clinical Effectiveness DATE: 25 August 2008 CONTEXT AND POLICY ISSUES: It is estimated that one in every seven
TITLE: High Intensity Focused Ultrasound for Prostate Cancer: A Review of the Guidelines and Clinical Effectiveness DATE: 25 August 2008 CONTEXT AND POLICY ISSUES: It is estimated that one in every seven
Oncologic Outcome and Patterns of Recurrence after Salvage Radical Prostatectomy
 european urology 55 (2009) 404 411 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Oncologic Outcome and Patterns of Recurrence after Salvage Radical Prostatectomy
european urology 55 (2009) 404 411 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Oncologic Outcome and Patterns of Recurrence after Salvage Radical Prostatectomy
High intensity focused ultrasound uses high energy
 Phase I/II Trial of High Intensity Focused Ultrasound for the Treatment of Previously Untreated Localized Prostate Cancer Michael O. Koch,*, Thomas Gardner, Liang Cheng, Russell J. Fedewa, Ralf Seip and
Phase I/II Trial of High Intensity Focused Ultrasound for the Treatment of Previously Untreated Localized Prostate Cancer Michael O. Koch,*, Thomas Gardner, Liang Cheng, Russell J. Fedewa, Ralf Seip and
New research in prostate brachytherapy
 New research in prostate brachytherapy Dr Ann Henry Associate Professor in Clinical Oncology University of Leeds and Leeds Cancer Centre PIVOTAL boost opening 2017 To evaluate - The benefits of pelvic
New research in prostate brachytherapy Dr Ann Henry Associate Professor in Clinical Oncology University of Leeds and Leeds Cancer Centre PIVOTAL boost opening 2017 To evaluate - The benefits of pelvic
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Case Discussions: Prostate Cancer
 Case Discussions: Prostate Cancer Andrew J. Stephenson, MD FRCSC FACS Chief, Urologic Oncology Glickman Urological and Kidney Institute Cleveland Clinic Elevated PSA 1 54 yo, healthy male, family Hx of
Case Discussions: Prostate Cancer Andrew J. Stephenson, MD FRCSC FACS Chief, Urologic Oncology Glickman Urological and Kidney Institute Cleveland Clinic Elevated PSA 1 54 yo, healthy male, family Hx of
Prostate Focal Therapy: What s on the Horizon? Thomas J Polascik, MD FACS
 Prostate Focal Therapy: What s on the Horizon? Thomas J Polascik, MD FACS Current State of Prostate Focal Therapy Patient Selection Focal Ablation Technology and Technique Follow-up/ Surveillance after
Prostate Focal Therapy: What s on the Horizon? Thomas J Polascik, MD FACS Current State of Prostate Focal Therapy Patient Selection Focal Ablation Technology and Technique Follow-up/ Surveillance after
Prostate Cancer Innovations in Surgical Strategies Update 2007!
 Prostate Cancer Innovations in Surgical Strategies Update 2007! Curtis A. Pettaway, M.D. Professor Department of Urology The University of Texas M. D. Anderson Cancer Center Radical Prostatectomy Pathologic
Prostate Cancer Innovations in Surgical Strategies Update 2007! Curtis A. Pettaway, M.D. Professor Department of Urology The University of Texas M. D. Anderson Cancer Center Radical Prostatectomy Pathologic
Technology Insight: high-intensity focused ultrasound for urologic cancers
 Technology Insight: high-intensity focused ultrasound for urologic cancers Christian Chaussy*, Stefan Thüroff, Xavier Rebillard and Albert Gelet SUMMARY The growing interest in high-intensity focused ultrasound
Technology Insight: high-intensity focused ultrasound for urologic cancers Christian Chaussy*, Stefan Thüroff, Xavier Rebillard and Albert Gelet SUMMARY The growing interest in high-intensity focused ultrasound
Accuracy of post-radiotherapy biopsy before salvage radical prostatectomy
 Accuracy of post-radiotherapy biopsy before salvage radical prostatectomy Joshua J. Meeks, Marc Walker*, Melanie Bernstein, Matthew Kent and James A. Eastham Urology Service, Department of Surgery and
Accuracy of post-radiotherapy biopsy before salvage radical prostatectomy Joshua J. Meeks, Marc Walker*, Melanie Bernstein, Matthew Kent and James A. Eastham Urology Service, Department of Surgery and
When PSA fails. Urology Grand Rounds Alexandra Perks. Rising PSA after Radical Prostatectomy
 When PSA fails Urology Grand Rounds Alexandra Perks Rising PSA after Radical Prostatectomy Issues Natural History Local vs Metastatic Treatment options 1 10 000 men / year in Canada 4000 RRP 15-year PSA
When PSA fails Urology Grand Rounds Alexandra Perks Rising PSA after Radical Prostatectomy Issues Natural History Local vs Metastatic Treatment options 1 10 000 men / year in Canada 4000 RRP 15-year PSA
Presentation with lymphadenopathy
 Presentation with lymphadenopathy Theo M. de Reijke MD PhD FEBU Department of Urology Academic Medical Center Amsterdam Rationale for RRP in N+ disease Prevention local problems Better survival in limited
Presentation with lymphadenopathy Theo M. de Reijke MD PhD FEBU Department of Urology Academic Medical Center Amsterdam Rationale for RRP in N+ disease Prevention local problems Better survival in limited
Presentation with lymphadenopathy
 Presentation with lymphadenopathy Theo M. de Reijke MD PhD FEBU Department of Urology Academic Medical Center Amsterdam Rationale for RRP in N+ disease Prevention local problems Better survival in limited
Presentation with lymphadenopathy Theo M. de Reijke MD PhD FEBU Department of Urology Academic Medical Center Amsterdam Rationale for RRP in N+ disease Prevention local problems Better survival in limited
When to worry, when to test?
 Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
2015 myresearch Science Internship Program: Applied Medicine. Civic Education Office of Government and Community Relations
 2015 myresearch Science Internship Program: Applied Medicine Civic Education Office of Government and Community Relations Harguneet Singh Science Internship Program: Applied Medicine Comparisons of Outcomes
2015 myresearch Science Internship Program: Applied Medicine Civic Education Office of Government and Community Relations Harguneet Singh Science Internship Program: Applied Medicine Comparisons of Outcomes
Elevated PSA. Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017
 Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY
 BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY AZHAN BIN YUSOFF AZHAN BIN YUSOFF 2013 SCENARIO A 66 year old man underwent Robotic Radical Prostatectomy for a T1c Gleason 4+4, PSA 15 ng/ml prostate
BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY AZHAN BIN YUSOFF AZHAN BIN YUSOFF 2013 SCENARIO A 66 year old man underwent Robotic Radical Prostatectomy for a T1c Gleason 4+4, PSA 15 ng/ml prostate
Definition Prostate cancer
 Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
Prostate Cancer Incidence
 Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
FOCAL THERAPY OF PROSTATE CANCER : WHERE ARE WE? MICHAEL MARBERGER PROFESSOR AND CHAIRMAN DEPARTMENT OF UROLOGY MEDICAL UNIVERSITY OF VIENNA
 FOCAL THERAPY OF PROSTATE CANCER : WHERE ARE WE? MICHAEL MARBERGER PROFESSOR AND CHAIRMAN DEPARTMENT OF UROLOGY MEDICAL UNIVERSITY OF VIENNA pt2a GL.SC. 6 (3+3) IS TREATMENT OF ENTIRE GLAND NEEDED? MR
FOCAL THERAPY OF PROSTATE CANCER : WHERE ARE WE? MICHAEL MARBERGER PROFESSOR AND CHAIRMAN DEPARTMENT OF UROLOGY MEDICAL UNIVERSITY OF VIENNA pt2a GL.SC. 6 (3+3) IS TREATMENT OF ENTIRE GLAND NEEDED? MR
Treatment of Prostate Cancer Local Recurrence After Whole-Gland Cryosurgery With Frameless Robotic Stereotactic Body Radiotherapy: Initial Experience
 Treatment of Prostate Cancer Local Recurrence After Whole-Gland Cryosurgery With Frameless Robotic Stereotactic Body Radiotherapy: Initial Experience Scott Quarrier, 1 Aaron Katz, 2 Jonathan Haas 3 Abstract
Treatment of Prostate Cancer Local Recurrence After Whole-Gland Cryosurgery With Frameless Robotic Stereotactic Body Radiotherapy: Initial Experience Scott Quarrier, 1 Aaron Katz, 2 Jonathan Haas 3 Abstract
Prostate MRI: Who needs it?
 Prostate MRI: Who needs it? Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Abdominal Imaging Magnetic Resonance Science Center
Prostate MRI: Who needs it? Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Abdominal Imaging Magnetic Resonance Science Center
CLINICAL WORKSHOP IMAGE-GUIDED HDR BRACHYTHERAPY OF PROSTATE CANCER
 CLINICAL WORKSHOP IMAGE-GUIDED HDR BRACHYTHERAPY OF PROSTATE CANCER Klinikum Offenbach Nucletron April 27 th 28 th, 2014 History HDR Protocols for Boost and Monotherapy, Results, Logistics and Practical
CLINICAL WORKSHOP IMAGE-GUIDED HDR BRACHYTHERAPY OF PROSTATE CANCER Klinikum Offenbach Nucletron April 27 th 28 th, 2014 History HDR Protocols for Boost and Monotherapy, Results, Logistics and Practical
Post Radical Prostatectomy Radiation in Intermediate and High Risk Group Prostate Cancer Patients - A Historical Series
 Post Radical Prostatectomy Radiation in Intermediate and High Risk Group Prostate Cancer Patients - A Historical Series E. Z. Neulander 1, Z. Wajsman 2 1 Department of Urology, Soroka UMC, Ben Gurion University,
Post Radical Prostatectomy Radiation in Intermediate and High Risk Group Prostate Cancer Patients - A Historical Series E. Z. Neulander 1, Z. Wajsman 2 1 Department of Urology, Soroka UMC, Ben Gurion University,
Until recently, curative options for patients experiencing
 JOURNAL OF ENDOUROLOGY Volume 30, Number 6, June 2016 ª Mary Ann Liebert, Inc. Pp. 624 631 DOI: 10.1089/end.2015.0719 Imaging and Noninvasive Therapy Five-Year Biochemical Progression-Free Survival Following
JOURNAL OF ENDOUROLOGY Volume 30, Number 6, June 2016 ª Mary Ann Liebert, Inc. Pp. 624 631 DOI: 10.1089/end.2015.0719 Imaging and Noninvasive Therapy Five-Year Biochemical Progression-Free Survival Following
National Institute for Health and Clinical Excellence
 National Institute for Health and Clinical Excellence 839 Focal therapy using high-intensity focused ultrasound for localised prostate cancer Consultation Comments table IPAC date: Thursday 12 January
National Institute for Health and Clinical Excellence 839 Focal therapy using high-intensity focused ultrasound for localised prostate cancer Consultation Comments table IPAC date: Thursday 12 January
Treatment Failure After Primary and Salvage Therapy for Prostate Cancer
 307 Treatment Failure After Primary and Salvage Therapy for Prostate Cancer Likelihood, Patterns of Care, and Outcomes Piyush K. Agarwal, MD 1 Natalia Sadetsky, MD, MPH 2 Badrinath R. Konety, MD, MBA 2
307 Treatment Failure After Primary and Salvage Therapy for Prostate Cancer Likelihood, Patterns of Care, and Outcomes Piyush K. Agarwal, MD 1 Natalia Sadetsky, MD, MPH 2 Badrinath R. Konety, MD, MBA 2
PROSTATE CANCER SURVEILLANCE
 PROSTATE CANCER SURVEILLANCE ESMO Preceptorship on Prostate Cancer Singapore, 15-16 November 2017 Rosa Nadal National Cancer Institute, NIH Bethesda, USA DISCLOSURE No conflicts of interest to declare
PROSTATE CANCER SURVEILLANCE ESMO Preceptorship on Prostate Cancer Singapore, 15-16 November 2017 Rosa Nadal National Cancer Institute, NIH Bethesda, USA DISCLOSURE No conflicts of interest to declare
Radiation therapy for localized prostate cancer is a main form of therapy
 MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Selection of Salvage Cryotherapy Patients Aaron E. Katz, MD, Mohamed A. Ghafar, MD Department of Urology, College of Physicians & Surgeons of Columbia
MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Selection of Salvage Cryotherapy Patients Aaron E. Katz, MD, Mohamed A. Ghafar, MD Department of Urology, College of Physicians & Surgeons of Columbia
Patient Information. Prostate Tissue Ablation. High Intensity Focused Ultrasound for
 High Intensity Focused Ultrasound for Prostate Tissue Ablation Patient Information CAUTION: Federal law restricts this device to sell by or on the order of a physician CONTENT Introduction... 3 The prostate...
High Intensity Focused Ultrasound for Prostate Tissue Ablation Patient Information CAUTION: Federal law restricts this device to sell by or on the order of a physician CONTENT Introduction... 3 The prostate...
Index Lesion Only. Prof. Phillip D Stricker
 Index Lesion Only Prof. Phillip D Stricker Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is presented I have the following
Index Lesion Only Prof. Phillip D Stricker Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is presented I have the following
Section: Therapy Effective Date: October 15, 2016 Subsection: Therapy Original Policy Date: December 7, 2011 Subject:
 Last Review Status/Date: September 2016 Page: 1 of 10 Description High-dose rate (HDR) temporary prostate brachytherapy is a technique of delivering a high-intensity radiation source directly to the prostate
Last Review Status/Date: September 2016 Page: 1 of 10 Description High-dose rate (HDR) temporary prostate brachytherapy is a technique of delivering a high-intensity radiation source directly to the prostate
Percentage of patients who underwent endoscopic procedures following SWL
 Non-QPP Measures Measure ID Measure Title Definition Type Domain 1 AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis Percentage of patients with NEW diagnosis of clinically significant
Non-QPP Measures Measure ID Measure Title Definition Type Domain 1 AQUA12 Benign Prostate Hyperplasia: IPSS improvement after diagnosis Percentage of patients with NEW diagnosis of clinically significant
AllinaHealthSystems 1
 2018 Dimensions in Oncology Genitourinary Cancer Disclosures I have no financial or commercial relationships relevant to this presentation. Matthew O Shaughnessy, MD, PhD Director of Urologic Oncology
2018 Dimensions in Oncology Genitourinary Cancer Disclosures I have no financial or commercial relationships relevant to this presentation. Matthew O Shaughnessy, MD, PhD Director of Urologic Oncology
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of focal therapy using high-intensity focused ultrasound for localised prostate
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of focal therapy using high-intensity focused ultrasound for localised prostate
Open clinical uro-oncology trials in Canada
 Open clinical uro-oncology trials in Canada Eric Winquist, MD, George Rodrigues, MD London Health Sciences Centre, London, Ontario, Canada bladder cancer A PHASE II PROTOCOL FOR PATIENTS WITH STAGE T1
Open clinical uro-oncology trials in Canada Eric Winquist, MD, George Rodrigues, MD London Health Sciences Centre, London, Ontario, Canada bladder cancer A PHASE II PROTOCOL FOR PATIENTS WITH STAGE T1
Radical Prostatectomy: Management of the Primary From Localized to Oligometasta:c Disease
 Radical Prostatectomy: Management of the Primary From Localized to Oligometasta:c Disease Disclosures I do not have anything to disclose Sexual function causes moderate to severe distress 2 years after
Radical Prostatectomy: Management of the Primary From Localized to Oligometasta:c Disease Disclosures I do not have anything to disclose Sexual function causes moderate to severe distress 2 years after
Date Modified: May 29, Clinical Quality Measures for PQRS
 Date Modified: May 29, 2014 Clinical Quality s for PQRS # Domain Type Denominator Numerator Denominator Exclusions/Exceptions Rationale QCDR-1 QCDR-2 Patient Safety 102 Efficiency and Cost Reduction QCDR-3
Date Modified: May 29, 2014 Clinical Quality s for PQRS # Domain Type Denominator Numerator Denominator Exclusions/Exceptions Rationale QCDR-1 QCDR-2 Patient Safety 102 Efficiency and Cost Reduction QCDR-3
Cryosurgery as primary treatment for localized prostate cancer
 Int Urol Nephrol (2011) 43:1089 1094 DOI 10.1007/s11255-011-9952-7 UROLOGY ORIGINAL PAPER Cryosurgery as primary treatment for localized prostate cancer Huibo Lian Hongqian Guo Weidong Gan Xiaogong Li
Int Urol Nephrol (2011) 43:1089 1094 DOI 10.1007/s11255-011-9952-7 UROLOGY ORIGINAL PAPER Cryosurgery as primary treatment for localized prostate cancer Huibo Lian Hongqian Guo Weidong Gan Xiaogong Li
Overview of Radiotherapy for Clinically Localized Prostate Cancer
 Session 16A Invited lectures: Prostate - H&N. Overview of Radiotherapy for Clinically Localized Prostate Cancer Mack Roach III, MD Department of Radiation Oncology UCSF Helen Diller Family Comprehensive
Session 16A Invited lectures: Prostate - H&N. Overview of Radiotherapy for Clinically Localized Prostate Cancer Mack Roach III, MD Department of Radiation Oncology UCSF Helen Diller Family Comprehensive
Prostate Case Scenario 1
 Prostate Case Scenario 1 H&P 5/12/16: A 57-year-old Hispanic male presents with frequency of micturition, urinary urgency, and hesitancy associated with a weak stream. Over the past several weeks, he has
Prostate Case Scenario 1 H&P 5/12/16: A 57-year-old Hispanic male presents with frequency of micturition, urinary urgency, and hesitancy associated with a weak stream. Over the past several weeks, he has
Salvage Cryotherapy. Bernard Malavaud MD, PhD, FEBU Institut Universitaire du Cancer Toulouse (France)
 Urethra protection Argon decompression -40 /-60 C 17G hollow needles Salvage Cryotherapy Ice all TRUS positioning & monitoring temperature monitoring of the rectal wall ernard Malavaud MD, PhD, FEU Institut
Urethra protection Argon decompression -40 /-60 C 17G hollow needles Salvage Cryotherapy Ice all TRUS positioning & monitoring temperature monitoring of the rectal wall ernard Malavaud MD, PhD, FEU Institut
ORIGINAL ARTICLE. Department of Urology, Sacro Cuore Catholic University, A. Gemelli University Hospital, Rome, Italy
 0 EDIZIONI MINERVA MEDICA Online version at http://www.minervamedica.it Prostate cancer (PCa) is the most commonly diagnosed malignancy in men and the second leading cause of cancer death in developed
0 EDIZIONI MINERVA MEDICA Online version at http://www.minervamedica.it Prostate cancer (PCa) is the most commonly diagnosed malignancy in men and the second leading cause of cancer death in developed
Presentation, management, and outcomes of complications following prostate cancer therapy
 Original Article Presentation, management, and outcomes of complications following prostate cancer therapy Uwais B. Zaid, Jack W. McAninch, Allison S. Glass, Nadya M. Cinman, Benjamin N. Breyer Department
Original Article Presentation, management, and outcomes of complications following prostate cancer therapy Uwais B. Zaid, Jack W. McAninch, Allison S. Glass, Nadya M. Cinman, Benjamin N. Breyer Department
Clinical Case Conference
 Clinical Case Conference Intermediate-risk prostate cancer 08/06/2014 Long Pham Clinical Case 64 yo man was found to have elevated PSA of 8.65. TRUS-biopies were negative. Surveillance PSA was 7.2 in 3
Clinical Case Conference Intermediate-risk prostate cancer 08/06/2014 Long Pham Clinical Case 64 yo man was found to have elevated PSA of 8.65. TRUS-biopies were negative. Surveillance PSA was 7.2 in 3
Prostate Overview Quiz
 Prostate Overview Quiz 1. The path report reads: Gleason 3 + 4 = 7. The Gleason s score is a. 3 b. 4 c. 7 d. None of the above 2. The path report reads: Moderately differentiated adenocarcinoma of the
Prostate Overview Quiz 1. The path report reads: Gleason 3 + 4 = 7. The Gleason s score is a. 3 b. 4 c. 7 d. None of the above 2. The path report reads: Moderately differentiated adenocarcinoma of the
VALUE AND ROLE OF PSA AS A TUMOUR MARKER OF RESPONSE/RELAPSE
 Session 3 Advanced prostate cancer VALUE AND ROLE OF PSA AS A TUMOUR MARKER OF RESPONSE/RELAPSE 1 PSA is a serine protease and the physiological role is believed to be liquefying the seminal fluid PSA
Session 3 Advanced prostate cancer VALUE AND ROLE OF PSA AS A TUMOUR MARKER OF RESPONSE/RELAPSE 1 PSA is a serine protease and the physiological role is believed to be liquefying the seminal fluid PSA
TOOKAD (padeliporfin) Patient Information Guide
 TOOKAD (padeliporfin) Patient Information Guide TOOKAD is used to treat low-risk localized prostate cancer This medicine is subject to additional monitoring. This will allow quick identification of new
TOOKAD (padeliporfin) Patient Information Guide TOOKAD is used to treat low-risk localized prostate cancer This medicine is subject to additional monitoring. This will allow quick identification of new
PROSTATE CANCER BRACHYTHERAPY. Kazi S. Manir MD,DNB,PDCR RMO cum Clinical Tutor Department of Radiotherapy R. G. Kar Medical College
 PROSTATE CANCER BRACHYTHERAPY Kazi S. Manir MD,DNB,PDCR RMO cum Clinical Tutor Department of Radiotherapy R. G. Kar Medical College Risk categorization Very Low Risk Low Risk Intermediate Risk High Risk
PROSTATE CANCER BRACHYTHERAPY Kazi S. Manir MD,DNB,PDCR RMO cum Clinical Tutor Department of Radiotherapy R. G. Kar Medical College Risk categorization Very Low Risk Low Risk Intermediate Risk High Risk
Role of surgery. Theo M. de Reijke MD PhD FEBU Department of Urology Academic Medical Center Amsterdam
 Role of surgery Theo M. de Reijke MD PhD FEBU Department of Urology Academic Medical Center Amsterdam Surgery and alternative treatments Radical prostatectomy Open Laparoscopic Robot-assisted Temperature
Role of surgery Theo M. de Reijke MD PhD FEBU Department of Urology Academic Medical Center Amsterdam Surgery and alternative treatments Radical prostatectomy Open Laparoscopic Robot-assisted Temperature
The benefit of a preplanning procedure - view from oncologist. Dorota Kazberuk November, 2014 Otwock
 The benefit of a preplanning procedure - view from oncologist Dorota Kazberuk 21-22 November, 2014 Otwock Brachytherapy is supreme tool in prostate cancer management with a wide range of options in every
The benefit of a preplanning procedure - view from oncologist Dorota Kazberuk 21-22 November, 2014 Otwock Brachytherapy is supreme tool in prostate cancer management with a wide range of options in every
Managing urinary morbidity after brachytherapy. Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester
 Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
The Royal Marsden. Prostate case study. Presented by Mr Alan Thompson Consultant Urological Surgeon
 Prostate case study Presented by Mr Alan Thompson Consultant Urological Surgeon 2 Part one Initial presentation A 62 year old male solicitor attends your GP surgery. He has rarely seen you over the last
Prostate case study Presented by Mr Alan Thompson Consultant Urological Surgeon 2 Part one Initial presentation A 62 year old male solicitor attends your GP surgery. He has rarely seen you over the last
Adjuvant and Salvage Radiation for Prostate Cancer. Savita Dandapani, MD, PhD
 Adjuvant and Salvage Radiation for Prostate Cancer Savita Dandapani, MD, PhD DISCLOSURES I am a consultant for Reflexion, receive funding from Bayer, and on the Speaker s Bureau with Astra Zeneca. Post-prostatectomy
Adjuvant and Salvage Radiation for Prostate Cancer Savita Dandapani, MD, PhD DISCLOSURES I am a consultant for Reflexion, receive funding from Bayer, and on the Speaker s Bureau with Astra Zeneca. Post-prostatectomy
