NIH Public Access Author Manuscript Science. Author manuscript; available in PMC 2008 March 12.
|
|
|
- Lewis Murphy
- 5 years ago
- Views:
Transcription
1 NIH Public Access Author Manuscript Published in final edited form as: Science October 6; 314(5796): Cancer Regression in Patients After Transfer of Genetically Engineered Lymphocytes Richard A. Morgan, Mark E. Dudley, John R. Wunderlich, Marybeth S. Hughes, James C. Yang, Richard M. Sherry, Richard E. Royal, Suzanne L. Topalian, Udai S. Kammula, Nicholas P. Restifo, Zhili Zheng, Azam Nahvi, Christiaan R. de Vries, Linda J. Rogers-Freezer, Sharon A. Mavroukakis, and Steven A. Rosenberg * Surgery Branch, Center for Cancer Research, National Cancer Institute, National Institutes of Health, 10 Center Drive, Bethesda, MD 20892, USA. Abstract Through the adoptive transfer of lymphocytes after host immunodepletion, it is possible to mediate objective cancer regression in human patients with metastatic melanoma. However, the generation of tumor-specific T cells in this mode of immunotherapy is often limiting. Here we report the ability to specifically confer tumor recognition by autologous lymphocytes from peripheral blood by using a retrovirus that encodes a T cell receptor. Adoptive transfer of these transduced cells in 15 patients resulted in durable engraftment at levels exceeding 10% of peripheral blood lymphocytes for at least 2 months after the infusion. We observed high sustained levels of circulating, engineered cells at 1 year after infusion in two patients who both demonstrated objective regression of metastatic melanoma lesions. This study suggests the therapeutic potential of genetically engineered cells for the biologic therapy of cancer. In the past two decades, fundamental advances in immunology have introduced opportunities for the development of cellular-based therapies for the treatment of cancer (1,2). After ex vivo expansion, transfer, and clonal repopulation in patients who have received lymphodepleting conditioning, autologous tumor-infiltrating lymphocytes (TILs) have been found to mediate objective cancer regression in a measurable proportion of patients with metastatic melanoma (3 5). A limitation of this approach is the requirement that patients have preexisting tumorreactive cells that can be expanded ex vivo. In addition, in many cancer patients, especially those with cancers other than melanoma, it is difficult to identify these tumor-reactive lymphocytes. To overcome this limitation, we set out to develop an approach to cancer immunotherapy based on the genetic modification of normal peripheral blood lymphocytes (PBLs). Tumor-associated antigens (TAAs) are recognized by the T cell receptor (TCR) on the T lymphocyte surface, which is composed of the TCR alpha and beta chains (6). The genes encoding the TCR that are specific for a variety of TAA have now been cloned, including the TCR-recognizing MART-1 and gp100 melanoma/melanocyte differentiation antigens, the NY-ESO-1 cancer-testis antigen that is present on many common epithelial cancers, and an epitope from the p53 molecule, which is expressed on the surface of approximately 50% of cancers of common epithelial origin (7 12). In each case, these antigens were detected by the TCR when they were presented as peptides by molecules encoded by the major histocompatibility complex protein human lymphocyte antigen (HLA) A2. In vitro transcribed *To whom correspondence should be addressed, SAR@mail.nih.gov. Supporting Online Material
2 Morgan et al. Page 2 RNA from four TAA-reactive TCRs (recognizing MART-1: 27 35, gp100: , NY- ESO-1: , and p53: ) were electroporated into CD8 + PBLs, which were then cocultured with peptide-pulsed T2 cells. These transfected cells produced large amounts of interferon-γ (IFN-γ) upon stimulation with their respective peptides (Fig. 1A) and were able to recognize HLA-A2 matched tumors, including melanoma, lung cancer, and breast cancer (table S1). Furthermore, transduction with these TCR-encoding retro-viral vectors converted normal PBLs into cells capable of specifically recognizing and destroying both fresh and cultured cells from multiple common cancers (such as sarcoma and breast, lung, esophagus, and liver cancers) in vitro (9 12). To investigate the ability of genetically engineered PBLs to recognize and destroy tumor cells in vivo, we transduced PBLs derived from patients with melanoma with the genes encoding the alpha and beta chains of the anti MART-1 TCR. These genes were cloned from a TIL clone obtained from a cancer patient who demonstrated a near complete regression of metastatic melanoma after adoptive cell transfer (ACT) of TILs (5). A retroviral vector was constructed and optimized to express the MART-1 TCR alpha and beta chains (Fig. 1B) (13). Gene transfer efficiency, assessed by staining for the specific Vβ12 protein in this TCR, resulted in expression in 30% of the transduced CD8 + cells (Fig. 1C), as compared with ~1% of untransduced control cell cultures (gene transfer was about equally divided between CD4 and CD8 cells). Fifteen percent of the transduced CD8 + cells bound the MART-1 peptide-specific HLA-A*0201 tetramer (Fig. 1C and table S2). The TCR-transduced cells were biologically active, as demonstrated by the specific secretion of IFN-γ after coculture with both MART-1 peptidepulsed cells and HLA-A2 positive melanoma cell lines (Fig. 1D). To investigate the in vivo efficacy of these MART-1 TCR-engineered T cells, we selected 17 HLA-A*0201 patients with progressive metastatic melanoma (Table 1) for treatment. Cancers in all patients were refractory to previous therapy with interleukin-2 (IL-2). T cell cultures from all 17 patients were biologically reactive, with specific secretion of IFN-γ after coculture with either MART-1 peptide-pulsed T2 cells and/or melanoma cell lines expressing the MART-1 antigen (Fig. 1E). Gene transfer efficiencies measured by staining for Vβ12 expression in these lymphocytes ranged from 17 to 67% (42%, mean value) (Table 1 and table S2). Patients received ACT treatments with MART-1 TCR-transduced autologous PBLs at a time of maximum lymphodepletion (13). Three patients in an initial cohort were treated with cells after an extended culture period of 19 days and had cell doubling times ranging from 8.7 to 11.9 days (Table 1, cohort 1, patients 1, 2a, and 3). In these patients, <10% of the transduced cells persisted across the time points tested during the first 30 days after infusion, and 2% of the cells persisted beyond 50 days (Fig. 2A). These first three patients showed no delay in the progression of disease. In an effort to administer gene-modified lymphocytes that were in their active growth phase, the culture conditions were modified (13) to limit the ex vivo culture period to between 6 and 9 days after stimulation of cells with antibody to CD3 (Table 1, cohort 2, cell doubling times of 2 days). In another cohort, larger numbers of actively dividing cells for ACT were generated by performing a second rapid expansion protocol (14) after 8 to 9 days (Table 1, cohort 3, cell doubling times from 0.9 to 3.3 days). In contrast to the lack of cell persistence seen in cohort 1 patients (Fig. 2A), patients in cohorts 2 and 3 (Fig. 2, B to D) all exhibited persistence of the transduced cells at >9% at 1 and 4 weeks after treatment (range, 9 to 56%). All eight patients who provided samples >50 days after treatment exhibited cell persistence of >17%, and this level of persistence was durable in seven patients during a >90-day monitoring period. In one patient (patient 14), >60% of circulating lymphocytes were positive for the gene-marked cells (Fig. 2C).
3 Morgan et al. Page 3 In 14 patient samples tested at one month after ACT, quantitative reverse transcription polymerase chain reaction (RT-PCR) assays revealed the presence of vector-derived RNA, confirming that gene expression continued (table S3). All but one of 15 patients analyzed had increased levels of CD8 + /Vβ12 cells at 1 week after treatment, and the levels of 11 of the 15 patients were higher at 1 month as compared to pretreatment levels (Fig. 2E). Of 13 patients that were examined, all had increased MART-1 tetramer-binding cells after treatment (Fig. 2F), and 11 of 14 had increased numbers of enzyme-linked immunosorbent spot positive cells (table S4). There was, however, a discordance between the mean persistence of transduced cells at 1 month in cohorts 2 and 3 measured by PCR (26%) as compared to the measurement of Vβ12- expressing cells (8.1%) and of MART-1 tetramer-binding cells (0.8%). This discordance may in part be due to mispairing of the introduced TCR chains with the endogenous chain, as well as to the different sensitivities of the assays. The reduced expression of the transgene in the persisting cells at 1 month may also be a function of the described decrease (15) in the transcription of retrovirally inserted trangenes and the decline in metabolic activity during the conversion of activated cells to memory cells. This decrease in expression of the retroviral transgene would be expected to affect the measurement of tetramers, which relies on the aggregation of multiple receptors, more heavily than the detection of Vβ12 cells directly by antibody staining. Most important, two patients demonstrated a sustained objective regression of their metastatic melanoma assessed by standard criteria [response evaluation criteria in solid tumors (RECIST)] (16). Patient 4, a 52-year-old male, had previously received treatment with interferon-α (IFNα), a lymph node dissection, an experimental vaccine, and high-dose IL-2. The patient then developed progressive disease in the liver (4.4- by 3.3-cm mass) and axilla (1.3- by 1.2-cm mass). After treatment with the ACT protocol described above, he experienced complete regression of the axillary mass and an 89% reduction of the liver mass (Fig. 3, A and B), at which time it was removed. He remains clinically disease-free at 21 months after treatment. Patient 14, a 30-year-old male, previously received treatment consisting of a lymph node dissection, IFN-α, and high-dose IL-2. He developed an enlarging 4.0- by 2.5-cm mass in the lung hilum. After ACT treatment, he underwent regression of the hilar mass and is now clinically disease-free 20 months later (Fig. 3, C and D). Thus, two patients with rapidly progressive metastatic melanoma showed full clinical regression of disease after the transfer of genetically engineered autologous PBLs. In responding patients 4 and 14, the number of gene-marked cells in the circulation (assumed to be 1% of total body lymphocytes) increased by factors of 1400 and 30, respectively, as compared to the number of infusion cells. At 1 year after infusion, both responding patients had sustained high levels (between 20 and 70%) of circulating gene-transduced cells (Fig. 3E). This high level of gene-marked cells was confirmed in patient 4 by limiting dilution T cell cloning of circulating lymphocytes at 1 year after treatment, which revealed that 42% (33 out of 79) of T cell clones contained the transgene as assessed by the PCR assay. These two patients also displayed Vβ12 cells that were detectable by antibody staining between 12 and 16% for >300 days after treatment (Fig. 3F). Patients 4 and 14 were also two of four patients who had >1% of circulating tetramer positive cells detectable for >15 days after cell infusion (Fig. 2F), and these two patients demonstrated anti-taa reactivity in ex vivo coculture assays (table S5). No toxicities in any patient were attributed to the gene-marked cells. Although the genetically modified transferred cells exhibited decreased expression of the transgene with time in vivo, the functional activity was apparently sustained at a level sufficient to mediate the tumor regression that was seen.
4 Morgan et al. Page 4 Approaches to increase the expression and function of the transgene are being studied, including the possible use of lentiviral vectors, the use of more powerful promoters specific to T cells, the use of higher-affinity TCRs that can mediate CD8 independent antitumor reactivity in CD4 cells, the further optimization of T cell transduction methods, and the production of higher titer clinical-grade viruses. Approaches to prevent chain mispairing may include modification of the TCR constant regions, the insertion of single-chain receptors (17), or the genetic modification of hematopoietic stem cells (18). Because tumor specificity can be conferred on bulk PBL populations with high efficiency, it may be possible to select subpopulations of PBLs that have distinct anti-tumor qualities. Further genetic modification of PBLs to insert cytokine or tissue-homing molecules may be beneficial. Mouse models predict that increased lymphodepletion, either by the addition of total body irradiation to the preparative regimen or by the administration of a vaccine containing the antigen recognized by the transduced TCR, can also enhance treatment effectiveness (19,20), and these modifications are currently being explored in clinical trials. In human subjects, normal autologous T lymphocytes, transduced ex vivo with anti-taa TCR genes and reinfused in cancer patients, can persist and express the transgene for a prolonged time in vivo and mediate the durable regression of large established tumors. Although the response rate (2 out of 15 patients or 13%) seen in cohorts 2 and 3 is lower than that achieved by the infusion of autologous TILs (50%), this method has potential for use in patients for whom TILs are not available. Engineering PBLs to express high-affinity TCRs recognizing the NY-ESO-1 or p53 antigens (Fig. 1A and table S1) enables the in vitro recognition of TAAs expressed on a variety of common cancers, and the use of these genetically engineered cells for the treatment of patients with common epithelial cancers deserves evaluation. Supplementary Material Refer to Web version on PubMed Central for supplementary material. References and Notes 1. Rosenberg SA. Immunity 1999;10:281. [PubMed: ] 2. Blattman JN, Greenberg PD. Science 2004;305:200. [PubMed: ] 3. Rosenberg SA, Spiess P, Lafreniere R. Science 1986;233:1318. [PubMed: ] 4. Dudley ME, et al. J Clin Oncol 2005;23:2346. [PubMed: ] 5. Dudley ME, et al. Science 2002;298:850. [PubMed: ] 6. Krogsgaard M, Davis MM. Nat Immunol 2005;6:239. [PubMed: ] 7. Schumacher TN. Nat Rev Immunol 2002;2:512. [PubMed: ] 8. Sadelain M, Riviere I, Brentjens R. Nat Rev Cancer 2003;3:35. [PubMed: ] 9. Zhao Y, et al. J Immunol 2005;174:4415. [PubMed: ] 10. Morgan RA, et al. J Immunol 2003;171:3287. [PubMed: ] 11. Hughes MS, et al. Hum Gene Ther 2005;16:457. [PubMed: ] 12. Cohen CJ, et al. J Immunol 2005;175:5799. [PubMed: ] 13. Materials and methods are available as supporting material on. Science. Online 14. Riddell SR, Greenberg PD. J Immunol Methods 1990;128:189. [PubMed: ] 15. Kohn DB, et al. Nat Med 1998;4:775. [PubMed: ] 16. Therasse P, et al. J Natl Cancer Inst 2000;92:205. [PubMed: ] 17. Cohen CJ, et al. Cancer Res 2006;66:8878. [PubMed: ] 18. Yang L, Baltimore D. Proc Natl Acad Sci USA 2005;102:4518. [PubMed: ] 19. Gattinoni L, et al. J Exp Med 2005;202:907. [PubMed: ] 20. Overwijk WW, et al. J Exp Med 2003;198:569. [PubMed: ]
5 Morgan et al. Page The authors acknowledge the expert help in the care of these patients provided by the Surgery Branch Immunotherapy Fellows; J. Gea-Banacloche for valuable advice concerning the management of infectious complications; the nurses on the 3NW and Surgical intensive care unit wards in the Clinical Center; and NIH, as well as A. Mixon and S. Farid for fluorescence-activated cell sorting analysis. We also thank K. Cornetta and the National Gene Vector Laboratory for production of the clinicalgrade retroviral vector. This work was supported by the Intramural Research Program of the Center for Cancer Research, National Cancer Institute, NIH.
6 Morgan et al. Page 6 Fig. 1. Transduction and analysis of TCR-engineered cells. (A) CD8 + human lymphocytes were electroporated with RNA encoding control [green fluorescent protein (GFP)] or cloned TCRs reactive with HLA-A2 restricted epitopes from the human TAAs MART-1, gp100, NY-ESO-1, and p53. Effector T cells were cocultured with T2 cells pulsed with 1 μm of the indicated peptide (values are expressed as IFN-γ in pg/ml). Values demonstrating the specific release of cytokine are in bold. (B) Diagram of the recombinant retroviral vector MSGV1AIB used to engineer human lymphocytes. LTR, long terminal repeat;ψ, extended packaging signal; sd, splice donor; sa, splice acceptor; Alpha, alpha chain; IRES, internal ribosomal entry site; Beta, beta chain. (C) Transduced (Td) lymphocytes were analyzed 5 days after transduction for the
7 Morgan et al. Page 7 expression of Vβ12 and MART-1 tetramer [Ala 27 Leu 27 (A27L)] in CD8 + cells in comparison with untransduced (UnTd) cells. Numbers in the upper-right corners indicate the percentage of positive cells in that quadrant. (D) TCR vector-engineered cells from patient 6 (TCR) were cocultured with MART-1 peptide-pulsed T2 cells, HLA-A2 melanoma line (Mel 888), or HLA-A2 + melanoma line (Mel 526), and the amount of IFN-γ produced was determined. Control effectors were untransduced cells (PBL) and the MART-1 reactive TIL JKF6 (JKF6). (E) Anti-melanoma properties of genetically engineered lymphocytes were determined for all patients before infusion. The production of IFN-γ (pg/ml) after coculture with peptide-pulsed T2 cells (Peptide Reactivity) and anti-melanoma activity (Tumor Reactivity) for HLA-A2 + lines (526 and 624) and HLA-A2 lines (888 and 938).
8 Morgan et al. Page 8 Fig. 2. Persistence of gene-marked cells. DNA extracted from peripheral blood mononuclear cells (PBMCs) was subjected to real-time quantitative PCR to determine the percentage of vectortransduced cells in patient circulation at various times after infusion. Each line represents data from a separate patient. (A) Cohort 1; (B) Cohort 2; (C) Cohort 3. (D) Mean value of the percentage of gene-marked cells for all patients in each cohort at the given time interval after treatment. (E) The percentage of CD8 + /Vβ12 + cells in the intermediate gate (13) for patients in cohorts 2 and 3 is shown. (F) The percentage of CD8 + /MART-1 + tetramer cells was determined for patients in cohorts 2 and 3 at the times shown. Pretreatment values for each patient are plotted as day 0 after infusion.
9 Morgan et al. Page 9 Fig. 3. Cancer regression in two patients. (A) Computed tomography (CT) images of liver metastasis in patient 4 taken at pretreatment, 1 month, and 10 months after treatment with TCR-engineered T cells. (B) Size of liver and axillary tumors and tempo of regression of tumor sites in patient 4. Day 0, beginning of treatment. L Axill LN, left axillary lymph node. (C) CT images of hilar lymph node metastasis in patient 14; pretreatment, day 0, and 2 months and 12 months after treatment. The white arrow indicates the mass in the lung hilum. (D) Size of tumor and tempo of regression in patient 14. (E) Quantitation of gene-marked cells in the PBMCs of patients 4 and 14 was determined by real-time quantitative PCR. Pt, patient. Day of infusion (Inf.) indicated by arrow. (F) The percentage of CD8 + /Vβ12 + cells in the intermediate gate (13) in the circulation of patients 4 and 14.
10 Morgan et al. Page 10 Table 1 Patient demographics, treatments received, and clinical outcome. Ln, lymph node; Cu, cutaneous; Sub, subcutaneous; Li, liver; Lu, lung; Ad, adrenal; Pa, pancreas; Br, brain; Hi, hilum. NR, no response; PR, partial response; MR, minor or mixed response. Cohort Patient Age/ sex Total cells infused ( 10 9 ) CD4/ CD8 (%) VB12 (%) MART-1 cells infused ( 10 9 ) Days in culture Doubling time IL-2 doses Sites of (days) evaluable disease Response (duration in months) /M / Ln, Cu NR 2a * 44/F / Ln, Cu NR 3 58/M / Cu, Sub NR /M / Li, Sub PR(21) 5 50/M / Lu, Ln, Sub NR 6 55/F / Lu, Ln NR 7 56/M / Lu, Ln NR 8 37/M / Lu, Ln NR 9 53/M / Ln, Ad, Sub MR 10 45/M / Ln, Sub 11 45/M 6.3 7/ Lu, Pa, Ln NR 12 32/F / Br, Sub NR 13 41/M / Lu, Sub NR 2b * 44/F / Ln, Cu NR /M 86 11/ Hi PR(20) 15 51/M 38 16/ Lu NR 16 25/F 33 13/ Lu, Li, Sub NR 17 20/F 23 17/ Lu, Ln, Sub NR * This patient was treated twice; treatments were separated by 7 months. Determined based on cell counts in the 2 days before infusion. Total cells infused multiplied by %Vβ ,000 international units/kg every 8 hours. All patients were previously refractory to treatment with IL-2 alone. Based on RECIST criteria.
DEVELOPMENT OF CELLULAR IMMUNOLOGY
 DEVELOPMENT OF CELLULAR IMMUNOLOGY 1880 s: Antibodies described (dominated studies of immunology until 1960 s) 1958: Journal of Immunology (137 papers) lymphocyte not listed in index Two papers on transfer
DEVELOPMENT OF CELLULAR IMMUNOLOGY 1880 s: Antibodies described (dominated studies of immunology until 1960 s) 1958: Journal of Immunology (137 papers) lymphocyte not listed in index Two papers on transfer
Supporting Online Material for
 www.sciencemag.org/cgi/content/full/1129003/dc1 Supporting Online Material for Cancer Regression in Patients After Transfer of Genetically Engineered Lymphocytes Richard A. Morgan, Mark E. Dudley, John
www.sciencemag.org/cgi/content/full/1129003/dc1 Supporting Online Material for Cancer Regression in Patients After Transfer of Genetically Engineered Lymphocytes Richard A. Morgan, Mark E. Dudley, John
Adoptive Cell Therapy: Treating Cancer
 Adoptive Cell Therapy: Treating Cancer with Genetically Engineered T Cells Steven A. Feldman, Ph.D. Surgery Branch National Cancer Institute NCT Conference Heidelberg, Germany September 24, 2013 Three
Adoptive Cell Therapy: Treating Cancer with Genetically Engineered T Cells Steven A. Feldman, Ph.D. Surgery Branch National Cancer Institute NCT Conference Heidelberg, Germany September 24, 2013 Three
Supplementary Figure 1. Example of gating strategy
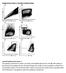 Supplementary Figure 1. Example of gating strategy Legend Supplementary Figure 1: First, gating is performed to include only single cells (singlets) (A) and CD3+ cells (B). After gating on the lymphocyte
Supplementary Figure 1. Example of gating strategy Legend Supplementary Figure 1: First, gating is performed to include only single cells (singlets) (A) and CD3+ cells (B). After gating on the lymphocyte
NIH Public Access Author Manuscript J Immunother. Author manuscript; available in PMC 2008 February 10.
 NIH Public Access Author Manuscript Published in final edited form as: J Immunother. 2008 January ; 31(1): 1 6. T-Cell Receptor Gene Therapy of Established Tumors in a Murine Melanoma Model John D. Abad
NIH Public Access Author Manuscript Published in final edited form as: J Immunother. 2008 January ; 31(1): 1 6. T-Cell Receptor Gene Therapy of Established Tumors in a Murine Melanoma Model John D. Abad
Current Tumor Immunotherapy
 Current Tumor Immunotherapy Part 1: On the preclinical and clinical efficacy of the current cancer vaccines. Part 2: The critical role of cancer vaccines in new integrative approaches. The State of the
Current Tumor Immunotherapy Part 1: On the preclinical and clinical efficacy of the current cancer vaccines. Part 2: The critical role of cancer vaccines in new integrative approaches. The State of the
The Immune System. Innate. Adaptive. - skin, mucosal barriers - complement - neutrophils, NK cells, mast cells, basophils, eosinophils
 Objectives - explain the rationale behind cellular adoptive immunotherapy - describe methods of improving cellular adoptive immunotherapy - identify mechanisms of tumor escape from cellular adoptive immunotherapy
Objectives - explain the rationale behind cellular adoptive immunotherapy - describe methods of improving cellular adoptive immunotherapy - identify mechanisms of tumor escape from cellular adoptive immunotherapy
CONTRACTING ORGANIZATION: Johns Hopkins University School of Medicine Baltimore, MD 21205
 AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
Tumor responses (patients responding/ patients treated)
 Table 1. ACT clinical trial tumor responses and toxicities. a Target antigen Cancer(s) Receptor type Tumor responses (patients responding/ patients treated) Immune-mediated toxicities (patients experiencing
Table 1. ACT clinical trial tumor responses and toxicities. a Target antigen Cancer(s) Receptor type Tumor responses (patients responding/ patients treated) Immune-mediated toxicities (patients experiencing
Todd D. Prickett Ph.D. Surgery Branch/NCI/NIH. Dr. Steven A. Rosenberg Branch Chief Dr. Paul F. Robbins Surgery Branch/NCI/NIH
 Durable Complete Response in a Patient with Metastatic Melanoma Following Adoptive Transfer of Autologous T cells Recognizing 1 Mutated Tumor Antigens Todd D. Prickett Ph.D. Surgery Branch/NCI/NIH Dr.
Durable Complete Response in a Patient with Metastatic Melanoma Following Adoptive Transfer of Autologous T cells Recognizing 1 Mutated Tumor Antigens Todd D. Prickett Ph.D. Surgery Branch/NCI/NIH Dr.
Supporting Information
 Supporting Information Chapuis et al. 10.1073/pnas.1113748109 SI Methods Selection of Patients, Targets, Isolation, and Expansion of Melanoma- Specific CTL Clones. Patients were HLA-typed, and their tumors
Supporting Information Chapuis et al. 10.1073/pnas.1113748109 SI Methods Selection of Patients, Targets, Isolation, and Expansion of Melanoma- Specific CTL Clones. Patients were HLA-typed, and their tumors
Immunotherapy on the Horizon: Adoptive Cell Therapy
 Immunotherapy on the Horizon: Adoptive Cell Therapy Joseph I. Clark, MD, FACP Professor of Medicine Loyola University Chicago Stritch School of Medicine Maywood, IL June 23, 2016 Conflicts of Interest
Immunotherapy on the Horizon: Adoptive Cell Therapy Joseph I. Clark, MD, FACP Professor of Medicine Loyola University Chicago Stritch School of Medicine Maywood, IL June 23, 2016 Conflicts of Interest
Functional reprogramming of the tumor stroma by IL-12 Engineered T cells is required for anti-tumor immunity. Sid Kerkar, M.D.
 Functional reprogramming of the tumor stroma by IL-12 Engineered T cells is required for anti-tumor immunity Sid Kerkar, M.D. Cancer Therapies Surgery Chemotherapy Radiation Emerging Cell Based Therapy
Functional reprogramming of the tumor stroma by IL-12 Engineered T cells is required for anti-tumor immunity Sid Kerkar, M.D. Cancer Therapies Surgery Chemotherapy Radiation Emerging Cell Based Therapy
08/02/59. Tumor Immunotherapy. Development of Tumor Vaccines. Types of Tumor Vaccines. Immunotherapy w/ Cytokine Gene-Transfected Tumor Cells
 Tumor Immunotherapy Autologous virus Inactivation Inactivated virus Lymphopheresis Culture? Monocyte s Dendritic cells Immunization Autologous vaccine Development of Tumor Vaccines Types of Tumor Vaccines
Tumor Immunotherapy Autologous virus Inactivation Inactivated virus Lymphopheresis Culture? Monocyte s Dendritic cells Immunization Autologous vaccine Development of Tumor Vaccines Types of Tumor Vaccines
Adoptive T Cell Therapy:
 Adoptive T Cell Therapy: A Paradigm for Combination Strategies Cassian Yee MD Professor Melanoma Medical Oncology Immunology Director Solid Tumor Cell Therapy cyee@mdanderson.org skype name: tcelltherapy
Adoptive T Cell Therapy: A Paradigm for Combination Strategies Cassian Yee MD Professor Melanoma Medical Oncology Immunology Director Solid Tumor Cell Therapy cyee@mdanderson.org skype name: tcelltherapy
Adoptive Cellular Therapy SITC Primer October 2012
 Adoptive Cellular Therapy SITC Primer October 2012 Cassian Yee MD Member Fred Hutchinson Cancer Research Center Program in Immunology Clinical Research Division Professor University of Washington Division
Adoptive Cellular Therapy SITC Primer October 2012 Cassian Yee MD Member Fred Hutchinson Cancer Research Center Program in Immunology Clinical Research Division Professor University of Washington Division
Overview 4/11/2013. Cell Kinetics in Adoptive Cell Therapy. April 11, 2013
 Cell Kinetics in Adoptive Cell Therapy April 11, 2013 David Stroncek, MD Chief, Cellular Processing Section DTM, CC, NIH Cellular Therapies Cell suspensions used for therapeutic purposes Examples Red Cells
Cell Kinetics in Adoptive Cell Therapy April 11, 2013 David Stroncek, MD Chief, Cellular Processing Section DTM, CC, NIH Cellular Therapies Cell suspensions used for therapeutic purposes Examples Red Cells
Advances in Adoptive Cellular Therapy of Cancer. Melanoma Bridge Meeting December 5, 2014
 Advances in Adoptive Cellular Therapy of Cancer Melanoma Bridge Meeting December 5, 2014 David Stroncek, MD Chief, Cell Processing Section, DTM, CC, NIH Bethesda, Maryland, USA Disclosures None Focus
Advances in Adoptive Cellular Therapy of Cancer Melanoma Bridge Meeting December 5, 2014 David Stroncek, MD Chief, Cell Processing Section, DTM, CC, NIH Bethesda, Maryland, USA Disclosures None Focus
NIH Public Access Author Manuscript Cancer Res. Author manuscript; available in PMC 2007 December 3.
 NIH Public Access Author Manuscript Published in final edited form as: Cancer Res. 2007 March 15; 67(6): 2425 2429. Extrathymic Generation of Tumor-Specific T Cells from Genetically Engineered Human Hematopoietic
NIH Public Access Author Manuscript Published in final edited form as: Cancer Res. 2007 March 15; 67(6): 2425 2429. Extrathymic Generation of Tumor-Specific T Cells from Genetically Engineered Human Hematopoietic
Adoptive cell therapy using genetically modified antigen-presenting cells
 Adoptive cell therapy using genetically modified antigen-presenting cells Naoto Hirano Ontario Cancer Institute Princess Margaret Cancer Centre University of Toronto UofT-USP Oncology Conference November
Adoptive cell therapy using genetically modified antigen-presenting cells Naoto Hirano Ontario Cancer Institute Princess Margaret Cancer Centre University of Toronto UofT-USP Oncology Conference November
CONTRACTING ORGANIZATION: Johns Hopkins University School of Medicine Baltimore, MD 21205
 AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
Scott Abrams, Ph.D. Professor of Oncology, x4375 Kuby Immunology SEVENTH EDITION
 Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 11 T-Cell Activation, Differentiation, and Memory Copyright 2013 by W. H. Freeman and
Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 11 T-Cell Activation, Differentiation, and Memory Copyright 2013 by W. H. Freeman and
Tumor Immunology. Wirsma Arif Harahap Surgical Oncology Consultant
 Tumor Immunology Wirsma Arif Harahap Surgical Oncology Consultant 1) Immune responses that develop to cancer cells 2) Escape of cancer cells 3) Therapies: clinical and experimental Cancer cells can be
Tumor Immunology Wirsma Arif Harahap Surgical Oncology Consultant 1) Immune responses that develop to cancer cells 2) Escape of cancer cells 3) Therapies: clinical and experimental Cancer cells can be
Cancer Immunotherapy. What is it? Immunotherapy Can Work! 4/15/09. Can the immune system be harnessed to fight cancer? T CD4 T CD28.
 Cancer Immunotherapy CANCER BIOLOGY April 15, 2009 Can the immune system be harnessed to fight cancer? Can the immune system see cancer? What is the best way to turn on the immune system to fight cancer?
Cancer Immunotherapy CANCER BIOLOGY April 15, 2009 Can the immune system be harnessed to fight cancer? Can the immune system see cancer? What is the best way to turn on the immune system to fight cancer?
Sleeping Beauty: Current applications and future strategies. CAR-TCR Summit 2017 Partow Kebriaei, MD
 Sleeping Beauty: Current applications and future strategies CAR-TCR Summit 2017 Partow Kebriaei, MD Outline Chimeric antigen receptor (CAR) technology Viral versus nonviral vectors Results of current clinical
Sleeping Beauty: Current applications and future strategies CAR-TCR Summit 2017 Partow Kebriaei, MD Outline Chimeric antigen receptor (CAR) technology Viral versus nonviral vectors Results of current clinical
T-Cell Transfer Therapy Targeting Mutant KRAS in Cancer
 The new england journal of medicine Brief Report T-Cell Transfer Therapy Targeting Mutant KRAS in Cancer Eric Tran, Ph.D., Paul F. Robbins, Ph.D., Yong Chen Lu, Ph.D., Todd D. Prickett, Ph.D., Jared J.
The new england journal of medicine Brief Report T-Cell Transfer Therapy Targeting Mutant KRAS in Cancer Eric Tran, Ph.D., Paul F. Robbins, Ph.D., Yong Chen Lu, Ph.D., Todd D. Prickett, Ph.D., Jared J.
Effective activity of cytokine-induced killer cells against autologous metastatic melanoma including cells with stemness features
 Effective activity of cytokine-induced killer cells against autologous metastatic melanoma including cells with stemness features Loretta Gammaitoni, Lidia Giraudo, Valeria Leuci, et al. Clin Cancer Res
Effective activity of cytokine-induced killer cells against autologous metastatic melanoma including cells with stemness features Loretta Gammaitoni, Lidia Giraudo, Valeria Leuci, et al. Clin Cancer Res
Chapter 7 Conclusions
 VII-1 Chapter 7 Conclusions VII-2 The development of cell-based therapies ranging from well-established practices such as bone marrow transplant to next-generation strategies such as adoptive T-cell therapy
VII-1 Chapter 7 Conclusions VII-2 The development of cell-based therapies ranging from well-established practices such as bone marrow transplant to next-generation strategies such as adoptive T-cell therapy
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Chandran SS, Somerville RPT, Yang JC, et al.
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Chandran SS, Somerville RPT, Yang JC, et al.
Cell Therapies. John HaanenMD PhD
 Cell Therapies John HaanenMD PhD My disclosures I have provided consultation, attended advisory boards, and/or provided lectures for: Pfizer, Bayer, MSD, BMS, IPSEN, Novartis, Roche/Genentech, Astra Zeneca/MedImmune,
Cell Therapies John HaanenMD PhD My disclosures I have provided consultation, attended advisory boards, and/or provided lectures for: Pfizer, Bayer, MSD, BMS, IPSEN, Novartis, Roche/Genentech, Astra Zeneca/MedImmune,
LION. Corporate Presentation June 2016 BIOTECHNOLOGIES. Leadership & Innovation in Oncology
 LION BIOTECHNOLOGIES Leadership & Innovation in Oncology Corporate Presentation June 2016 Forward-Looking Statements This presentation contains forward-looking statements within the meaning of the Private
LION BIOTECHNOLOGIES Leadership & Innovation in Oncology Corporate Presentation June 2016 Forward-Looking Statements This presentation contains forward-looking statements within the meaning of the Private
Artificial Antigen Presenting Cells as a Standardized Platform for Tumor Infiltrating Lymphocyte (TIL) expansion
 Artificial Antigen Presenting Cells as a Standardized Platform for Tumor Infiltrating Lymphocyte (TIL) expansion Concurrent Session 404: T cell Manufacturing and Potency 27 th Annual Meeting of the Society
Artificial Antigen Presenting Cells as a Standardized Platform for Tumor Infiltrating Lymphocyte (TIL) expansion Concurrent Session 404: T cell Manufacturing and Potency 27 th Annual Meeting of the Society
Developing Novel Immunotherapeutic Cancer Treatments for Clinical Use
 Developing Novel Immunotherapeutic Cancer Treatments for Clinical Use Oncology for Scientists March 8 th, 2016 Jason Muhitch, PhD Assistant Professor Department of Urology Email: jason.muhitch@roswellpark.org
Developing Novel Immunotherapeutic Cancer Treatments for Clinical Use Oncology for Scientists March 8 th, 2016 Jason Muhitch, PhD Assistant Professor Department of Urology Email: jason.muhitch@roswellpark.org
High-Efficiency Transfection of Primary Human and Mouse T Lymphocytes Using RNA Electroporation
 High-Efficiency Transfection of Primary Human and Mouse T Lymphocytes Using RNA Electroporation Yangbing Zhao, Zhili Zheng, Cyrille J. Cohen, Luca Gattinoni, Douglas C. Palmer, Nicholas P. Restifo, Steven
High-Efficiency Transfection of Primary Human and Mouse T Lymphocytes Using RNA Electroporation Yangbing Zhao, Zhili Zheng, Cyrille J. Cohen, Luca Gattinoni, Douglas C. Palmer, Nicholas P. Restifo, Steven
Personalized medicine - cancer immunotherapy
 Personalized medicine - cancer immunotherapy Özcan Met, PhD Senior Staff Scientist, Cell Therapy Director Center for Cancer Immune Therapy Department of Hematology Department of Oncology University Hospital
Personalized medicine - cancer immunotherapy Özcan Met, PhD Senior Staff Scientist, Cell Therapy Director Center for Cancer Immune Therapy Department of Hematology Department of Oncology University Hospital
The Good, the Bad and the Ugly: Clinical trials which assess vaccine characteristics. ISBT Meeting, San Francisco, CA November 4-8, 2004
 The Good, the Bad and the Ugly: Clinical trials which assess vaccine characteristics ISBT Meeting, San Francisco, CA November 4-8, 2004 Ideal cancer vaccine trial 1. An informative immune assay 2. Ability
The Good, the Bad and the Ugly: Clinical trials which assess vaccine characteristics ISBT Meeting, San Francisco, CA November 4-8, 2004 Ideal cancer vaccine trial 1. An informative immune assay 2. Ability
Cytotoxicity assays. Rory D. de Vries, PhD 1. Viroscience lab, Erasmus MC, Rotterdam, the Netherlands
 Cytotoxicity assays Rory D. de Vries, PhD 1 1 Viroscience lab, Erasmus MC, Rotterdam, the Netherlands Anti-influenza immunity Humoral / CD4+ / CD8+ / NK? Function of CTL Elimination of virus-infected cells?
Cytotoxicity assays Rory D. de Vries, PhD 1 1 Viroscience lab, Erasmus MC, Rotterdam, the Netherlands Anti-influenza immunity Humoral / CD4+ / CD8+ / NK? Function of CTL Elimination of virus-infected cells?
ECM1 controls T H 2 cell egress from lymph nodes through re-expression of S1P 1
 ZH, Li et al, page 1 ECM1 controls T H 2 cell egress from lymph nodes through re-expression of S1P 1 Zhenhu Li 1,4,Yuan Zhang 1,4, Zhiduo Liu 1, Xiaodong Wu 1, Yuhan Zheng 1, Zhiyun Tao 1, Kairui Mao 1,
ZH, Li et al, page 1 ECM1 controls T H 2 cell egress from lymph nodes through re-expression of S1P 1 Zhenhu Li 1,4,Yuan Zhang 1,4, Zhiduo Liu 1, Xiaodong Wu 1, Yuhan Zheng 1, Zhiyun Tao 1, Kairui Mao 1,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Focus on Immunotherapy as a Targeted Therapy. Brad Nelson, PhD BC Cancer, Victoria, Canada FPON, Oct
 Focus on Immunotherapy as a Targeted Therapy Brad Nelson, PhD BC Cancer, Victoria, Canada FPON, Oct 18 2018 Disclosures I have nothing to disclose that is relevant to this presentation. Immunology @ Deeley
Focus on Immunotherapy as a Targeted Therapy Brad Nelson, PhD BC Cancer, Victoria, Canada FPON, Oct 18 2018 Disclosures I have nothing to disclose that is relevant to this presentation. Immunology @ Deeley
Supplementary Table 1. Functional avidities of survivin-specific T-cell clones against LML-peptide
 Supplementary Table 1. Functional avidities of survivin-specific T-cell clones against LML-peptide pulsed T2 cells. clone avidity by 4-hour 51 Cr-release assay 50% lysis at E:T 10:1 [LML peptide, M] #24
Supplementary Table 1. Functional avidities of survivin-specific T-cell clones against LML-peptide pulsed T2 cells. clone avidity by 4-hour 51 Cr-release assay 50% lysis at E:T 10:1 [LML peptide, M] #24
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16
 COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
CD8+ cytotoxic T cells can be harvested from a patient with
 The new england journal of medicine brief report Treatment of Metastatic Melanoma with Autologous CD4+ T Cells against NY-ESO-1 Naomi N. Hunder, M.D., Herschel Wallen, M.D., Jianhong Cao, Ph.D., Deborah
The new england journal of medicine brief report Treatment of Metastatic Melanoma with Autologous CD4+ T Cells against NY-ESO-1 Naomi N. Hunder, M.D., Herschel Wallen, M.D., Jianhong Cao, Ph.D., Deborah
Basic Principles of Tumor Immunotherapy. Ryan J. Sullivan, M.D. Massachusetts General Hospital Cancer Center Boston, MA
 Basic Principles of Tumor Immunotherapy Ryan J. Sullivan, M.D. Massachusetts General Hospital Cancer Center Boston, MA Disclosures Consulting Fees: Biodesix, Novartis Pharmaceuticals Other: Boehringer
Basic Principles of Tumor Immunotherapy Ryan J. Sullivan, M.D. Massachusetts General Hospital Cancer Center Boston, MA Disclosures Consulting Fees: Biodesix, Novartis Pharmaceuticals Other: Boehringer
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke, Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke, Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
STATE OF THE ART 4: Combination Immune Therapy-Chemotherapy. Elizabeth M. Jaffee (JHU) James Yang (NCI) Jared Gollob (Duke) John Kirkwood (UPMI)
 STATE OF THE ART 4: Combination Immune Therapy-Chemotherapy Elizabeth M. Jaffee (JHU) James Yang (NCI) Jared Gollob (Duke) John Kirkwood (UPMI) Topics for Consideration What are the rules for integrating
STATE OF THE ART 4: Combination Immune Therapy-Chemotherapy Elizabeth M. Jaffee (JHU) James Yang (NCI) Jared Gollob (Duke) John Kirkwood (UPMI) Topics for Consideration What are the rules for integrating
Clinical Translation of Immunotherapy using WT1 and CMV specific TCR Gene Transfer
 Clinical Translation of Immunotherapy using WT1 and CMV specific Gene Transfer Dr Emma C Morris Reader, Dept of Immunology, UCL Consultant Haematologist (BMT), UCLH and RFH ISCT, 2/5/211 Gene Transfer
Clinical Translation of Immunotherapy using WT1 and CMV specific Gene Transfer Dr Emma C Morris Reader, Dept of Immunology, UCL Consultant Haematologist (BMT), UCLH and RFH ISCT, 2/5/211 Gene Transfer
This information is current as of December 2, 2018.
 This information is current as of December 2, 2018. References Subscription Permissions Email Alerts High Efficiency TCR Gene Transfer into Primary Human Lymphocytes Affords Avid Recognition of Melanoma
This information is current as of December 2, 2018. References Subscription Permissions Email Alerts High Efficiency TCR Gene Transfer into Primary Human Lymphocytes Affords Avid Recognition of Melanoma
Restoring Immune Function of Tumor-Specific CD4 + T Cells during Recurrence of Melanoma
 Restoring Immune Function of Tumor-Specific CD4 + T Cells during Recurrence of Melanoma Goding SR et al. J Immunol 2013; 190:4899-4909 C. Nikolowsky Christian Doppler Laboratory for Cardiac and Thoracic
Restoring Immune Function of Tumor-Specific CD4 + T Cells during Recurrence of Melanoma Goding SR et al. J Immunol 2013; 190:4899-4909 C. Nikolowsky Christian Doppler Laboratory for Cardiac and Thoracic
IMMUNOTHERAPY FOR CANCER A NEW HORIZON. Ekaterini Boleti MD, PhD, FRCP Consultant in Medical Oncology Royal Free London NHS Foundation Trust
 IMMUNOTHERAPY FOR CANCER A NEW HORIZON Ekaterini Boleti MD, PhD, FRCP Consultant in Medical Oncology Royal Free London NHS Foundation Trust ASCO Names Advance of the Year: Cancer Immunotherapy No recent
IMMUNOTHERAPY FOR CANCER A NEW HORIZON Ekaterini Boleti MD, PhD, FRCP Consultant in Medical Oncology Royal Free London NHS Foundation Trust ASCO Names Advance of the Year: Cancer Immunotherapy No recent
Dissecting therapy-induced T-cell responses in melanoma
 Dissecting therapy-induced T-cell responses in melanoma Tumor-infiltrating lymphocyte (TIL) therapy of melanoma TIL are grown from melanoma tumors Rapid Expansion Infusion of TIL + IL-2 Patient pretreated
Dissecting therapy-induced T-cell responses in melanoma Tumor-infiltrating lymphocyte (TIL) therapy of melanoma TIL are grown from melanoma tumors Rapid Expansion Infusion of TIL + IL-2 Patient pretreated
IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER
 Gynecologic Cancer InterGroup Cervix Cancer Research Network IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia Cervix
Gynecologic Cancer InterGroup Cervix Cancer Research Network IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia Cervix
Immunotherapy for the Treatment of Cancer
 Immunotherapy for the Treatment of Cancer Jason Muhitch, PhD Assistant Professor Department of Urology Department of Immunology Roswell Park Comprehensive Cancer Center Oncology for Scientists March 15,
Immunotherapy for the Treatment of Cancer Jason Muhitch, PhD Assistant Professor Department of Urology Department of Immunology Roswell Park Comprehensive Cancer Center Oncology for Scientists March 15,
Abstract #163 Michael Kalos, PhD
 LONG TERM FUNCTIONAL PERSISTENCE, B CELL APLASIA AND ANTI LEUKEMIA EFFICACY IN REFRACTORY B CELL MALIGNANCIES FOLLOWING T CELL IMMUNOTHERAPY USING CAR REDIRECTED REDIRECTED T CELLS TARGETING CD19 Abstract
LONG TERM FUNCTIONAL PERSISTENCE, B CELL APLASIA AND ANTI LEUKEMIA EFFICACY IN REFRACTORY B CELL MALIGNANCIES FOLLOWING T CELL IMMUNOTHERAPY USING CAR REDIRECTED REDIRECTED T CELLS TARGETING CD19 Abstract
Releasing the Brakes on Tumor Immunity: Immune Checkpoint Blockade Strategies
 Releasing the Brakes on Tumor Immunity: Immune Checkpoint Blockade Strategies Jason Muhitch, PhD MIR 509 October 1 st, 2014 Email: jason.muhitch@roswellpark.org 0 Holy Grail of Tumor Immunity Exquisite
Releasing the Brakes on Tumor Immunity: Immune Checkpoint Blockade Strategies Jason Muhitch, PhD MIR 509 October 1 st, 2014 Email: jason.muhitch@roswellpark.org 0 Holy Grail of Tumor Immunity Exquisite
LAMPvax DNA Vaccines as Immunotherapy for Cancer - Three Case Studies
 LAMPvax DNA Vaccines as Immunotherapy for Cancer - Three Case Studies Cancer immunotherapy has emerged as a clinically validated tool for fighting certain kinds of cancers. These therapeutic cancer vaccines
LAMPvax DNA Vaccines as Immunotherapy for Cancer - Three Case Studies Cancer immunotherapy has emerged as a clinically validated tool for fighting certain kinds of cancers. These therapeutic cancer vaccines
New insights into CD8+ T cell function and regulation. Pam Ohashi Princess Margaret Cancer Centre
 New insights into CD8+ T cell function and regulation Pam Ohashi Princess Margaret Cancer Centre New insights into CD8+ T cell function and regulation Pam Ohashi Princess Margaret Cancer Centre No Disclosures
New insights into CD8+ T cell function and regulation Pam Ohashi Princess Margaret Cancer Centre New insights into CD8+ T cell function and regulation Pam Ohashi Princess Margaret Cancer Centre No Disclosures
Supplemental materials
 Supplemental materials 1 Supplemental Fig. 1 Immunogram This immunogram summarizes patient clinical data and immune parameters at corresponding time points for Patient IMF-32. The top panel illustrates
Supplemental materials 1 Supplemental Fig. 1 Immunogram This immunogram summarizes patient clinical data and immune parameters at corresponding time points for Patient IMF-32. The top panel illustrates
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach
 Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
Tumors arise from accumulated genetic mutations. Tumor Immunology (Cancer)
 Tumor Immunology (Cancer) Tumors arise from accumulated genetic mutations Robert Beatty MCB150 Mutations Usually have >6 mutations in both activation/growth factors and tumor suppressor genes. Types of
Tumor Immunology (Cancer) Tumors arise from accumulated genetic mutations Robert Beatty MCB150 Mutations Usually have >6 mutations in both activation/growth factors and tumor suppressor genes. Types of
Chapter 22: The Lymphatic System and Immunity
 Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
2/16/2018. The Immune System and Cancer. Fatal Melanoma Transferred in a Donated Kidney 16 years after Melanoma Surgery
 C007: Immunology of Melanoma: Mechanisms of Immune Therapies Delphine J. Lee, MD, PhD Chief and Program Director, Dermatology, Harbor UCLA Medical Center Principal Investigator, Los Angeles Biomedical
C007: Immunology of Melanoma: Mechanisms of Immune Therapies Delphine J. Lee, MD, PhD Chief and Program Director, Dermatology, Harbor UCLA Medical Center Principal Investigator, Los Angeles Biomedical
Overview 3/31/2016. Cell Kinetics in Adoptive Cell Therapy. March 31, 2016
 Cell Kinetics in Adoptive Cell Therapy March 31, 2016 David Stroncek, MD Chief, Cellular Processing Section DTM, CC, NIH Cellular Therapies Cell suspensions used for therapeutic purposes Examples Red Cells
Cell Kinetics in Adoptive Cell Therapy March 31, 2016 David Stroncek, MD Chief, Cellular Processing Section DTM, CC, NIH Cellular Therapies Cell suspensions used for therapeutic purposes Examples Red Cells
Cell Kinetics in Adoptive Cell Therapy. March 31, 2016
 Cell Kinetics in Adoptive Cell Therapy March 31, 2016 David Stroncek, MD Chief, Cellular Processing Section DTM, CC, NIH 1 Cellular Therapies Cell suspensions used for therapeutic purposes Examples Red
Cell Kinetics in Adoptive Cell Therapy March 31, 2016 David Stroncek, MD Chief, Cellular Processing Section DTM, CC, NIH 1 Cellular Therapies Cell suspensions used for therapeutic purposes Examples Red
Adoptive T Cell Therapy TILs & TCRs & CARs
 Adoptive T Cell Therapy TILs & TCRs & CARs Inge Marie Svane CCIT DENMARK Professor, MD Center for Cancer Immune Therapy Department of Oncology, Herlev Hospital Copenhagen University Denmark Therapeutic
Adoptive T Cell Therapy TILs & TCRs & CARs Inge Marie Svane CCIT DENMARK Professor, MD Center for Cancer Immune Therapy Department of Oncology, Herlev Hospital Copenhagen University Denmark Therapeutic
PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human
 Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Determinants of Immunogenicity and Tolerance. Abul K. Abbas, MD Department of Pathology University of California San Francisco
 Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
The next steps for effective cancer immunotherapy and viral vaccines. Peter Selby FACP(UK)
 The next steps for effective cancer immunotherapy and viral vaccines Peter Selby FACP(UK) Richard Alan Steve Sasha Matt Nav Vile Melcher Griffin Zougman Bentham Vasudev Adel Nick Gemma Liz Samson Hornigold
The next steps for effective cancer immunotherapy and viral vaccines Peter Selby FACP(UK) Richard Alan Steve Sasha Matt Nav Vile Melcher Griffin Zougman Bentham Vasudev Adel Nick Gemma Liz Samson Hornigold
Recombinant Protein Expression Retroviral system
 Recombinant Protein Expression Retroviral system Viruses Contains genome DNA or RNA Genome encased in a protein coat or capsid. Some viruses have membrane covering protein coat enveloped virus Ø Essential
Recombinant Protein Expression Retroviral system Viruses Contains genome DNA or RNA Genome encased in a protein coat or capsid. Some viruses have membrane covering protein coat enveloped virus Ø Essential
BIT 120. Copy of Cancer/HIV Lecture
 BIT 120 Copy of Cancer/HIV Lecture Cancer DEFINITION Any abnormal growth of cells that has malignant potential i.e.. Leukemia Uncontrolled mitosis in WBC Genetic disease caused by an accumulation of mutations
BIT 120 Copy of Cancer/HIV Lecture Cancer DEFINITION Any abnormal growth of cells that has malignant potential i.e.. Leukemia Uncontrolled mitosis in WBC Genetic disease caused by an accumulation of mutations
Approved for Public Release; Distribution Unlimited
 AD Award Number: W81XWH-04-1-0186 TITLE: A Novel Therapeutic System for the Treatment of Occult Prostate Cancer PRINCIPAL INVESTIGATOR: Shongyun Dong, M.D., Ph.D. CONTRACTING ORGANIZATION: University of
AD Award Number: W81XWH-04-1-0186 TITLE: A Novel Therapeutic System for the Treatment of Occult Prostate Cancer PRINCIPAL INVESTIGATOR: Shongyun Dong, M.D., Ph.D. CONTRACTING ORGANIZATION: University of
IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER. Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia
 IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia Distinguishing self from non-self T cells trained in the thymus as
IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia Distinguishing self from non-self T cells trained in the thymus as
How T cells recognize antigen: The T Cell Receptor (TCR) Identifying the TCR: Why was it so hard to do? Monoclonal antibody approach
 How T cells recognize antigen: The T Cell Receptor (TCR) Identifying the TCR: Why was it so hard to do By the early 1980s, much about T cell function was known, but the receptor genes had not been identified
How T cells recognize antigen: The T Cell Receptor (TCR) Identifying the TCR: Why was it so hard to do By the early 1980s, much about T cell function was known, but the receptor genes had not been identified
A second type of TCR TCR: An αβ heterodimer
 How s recognize antigen: The T Cell Receptor (TCR) Identifying the TCR: Why was it so hard to do By the early 1980s, much about function was known, but the receptor genes had not been identified Recall
How s recognize antigen: The T Cell Receptor (TCR) Identifying the TCR: Why was it so hard to do By the early 1980s, much about function was known, but the receptor genes had not been identified Recall
Cloning and expansion of antigen-specific T cells using ipsc technology: A novel strategy for cancer immunotherapy
 Inflammation and Regeneration Vol.35 No.5 November 2015 220 Special Issue: Immunoregulation in regenerative medicine Mini Review Cloning and expansion of antigen-specific T cells using ipsc technology:
Inflammation and Regeneration Vol.35 No.5 November 2015 220 Special Issue: Immunoregulation in regenerative medicine Mini Review Cloning and expansion of antigen-specific T cells using ipsc technology:
TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA
 AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
PERSPECTIVE. Cancer immunotherapy: moving beyond current vaccines. Steven A Rosenberg, James C Yang & Nicholas P Restifo
 Cancer immunotherapy: moving beyond current vaccines Steven A Rosenberg, James C Yang & Nicholas P Restifo Great progress has been made in the field of tumor immunology in the past decade, but optimism
Cancer immunotherapy: moving beyond current vaccines Steven A Rosenberg, James C Yang & Nicholas P Restifo Great progress has been made in the field of tumor immunology in the past decade, but optimism
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke,. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke,. CONTRACTING ORGANIZATION: Johns Hopkins
Junko Matsuzaki 1, Takemasa Tsuji 1*, Thinle Chodon 1, Courtney Ryan 2, Richard C. Koya 1 and Kunle Odunsi 1,3*
 Matsuzaki et al. Journal for ImmunoTherapy of Cancer (2019) 7:7 https://doi.org/10.1186/s40425-018-0467-y RESEARCH ARTICLE Open Access A rare population of tumor antigen-specific CD4 + CD8 + double-positive
Matsuzaki et al. Journal for ImmunoTherapy of Cancer (2019) 7:7 https://doi.org/10.1186/s40425-018-0467-y RESEARCH ARTICLE Open Access A rare population of tumor antigen-specific CD4 + CD8 + double-positive
Understanding the T cell response to tumors using transnuclear mouse models
 Understanding the T cell response to tumors using transnuclear mouse models Stephanie Dougan Dana-Farber Cancer Institute Boston, MA Presenter Disclosure Information Stephanie Dougan The following relationships
Understanding the T cell response to tumors using transnuclear mouse models Stephanie Dougan Dana-Farber Cancer Institute Boston, MA Presenter Disclosure Information Stephanie Dougan The following relationships
Immunity and Cancer. Doriana Fruci. Lab di Immuno-Oncologia
 Immunity and Cancer Doriana Fruci Lab di Immuno-Oncologia Immune System is a network of cells, tissues and organs that work together to defend the body against attacks of foreign invaders (pathogens, cancer
Immunity and Cancer Doriana Fruci Lab di Immuno-Oncologia Immune System is a network of cells, tissues and organs that work together to defend the body against attacks of foreign invaders (pathogens, cancer
EBV Infection and Immunity. Andrew Hislop Institute for Cancer Studies University of Birmingham
 EBV Infection and Immunity Andrew Hislop Institute for Cancer Studies University of Birmingham EBV Introduction Large ds DNA virus Spread by saliva contact Lifelong infection Predominantly B-lymphotropic
EBV Infection and Immunity Andrew Hislop Institute for Cancer Studies University of Birmingham EBV Introduction Large ds DNA virus Spread by saliva contact Lifelong infection Predominantly B-lymphotropic
Richard P Junghans, PhD, MD
 CANCER GENE THERAPY WITH DESIGNER T CELLS: TOXICITY VERSUS ACTIVITY Richard P Junghans, PhD, MD Director, Biotherapeutics Development Lab Associate Professor of Surgery and Medicine Boston University School
CANCER GENE THERAPY WITH DESIGNER T CELLS: TOXICITY VERSUS ACTIVITY Richard P Junghans, PhD, MD Director, Biotherapeutics Development Lab Associate Professor of Surgery and Medicine Boston University School
Is Immune Therapy the Holy Grail in Metastatic Kidney Cancer?
 Is Immune Therapy the Holy Grail in Metastatic Kidney Cancer? New Frontiers in Urologic Oncology 8-2016 Mayer Fishman, MD PhD Member, Moffitt Cancer Center Department of Genitourinary Oncology Professor,
Is Immune Therapy the Holy Grail in Metastatic Kidney Cancer? New Frontiers in Urologic Oncology 8-2016 Mayer Fishman, MD PhD Member, Moffitt Cancer Center Department of Genitourinary Oncology Professor,
The Adaptive Immune Response. T-cells
 The Adaptive Immune Response T-cells T Lymphocytes T lymphocytes develop from precursors in the thymus. Mature T cells are found in the blood, where they constitute 60% to 70% of lymphocytes, and in T-cell
The Adaptive Immune Response T-cells T Lymphocytes T lymphocytes develop from precursors in the thymus. Mature T cells are found in the blood, where they constitute 60% to 70% of lymphocytes, and in T-cell
Cancer Immunotherapy: Active Immunization Approaches
 Cancer Immunotherapy: Active Immunization Approaches Willem W. Overwijk, PhD Department of Melanoma Medical Oncology MD Anderson Cancer Center Houston, TX, USA Disclosures No relevant financial relationships
Cancer Immunotherapy: Active Immunization Approaches Willem W. Overwijk, PhD Department of Melanoma Medical Oncology MD Anderson Cancer Center Houston, TX, USA Disclosures No relevant financial relationships
Immune surveillance hypothesis (Macfarlane Burnet, 1950s)
 TUMOR-IMMUNITÄT A.K. Abbas, A.H. Lichtman, S. Pillai (6th edition, 2007) Cellular and Molecular Immunology Saunders Elsevier Chapter 17, immunity to tumors Immune surveillance hypothesis (Macfarlane Burnet,
TUMOR-IMMUNITÄT A.K. Abbas, A.H. Lichtman, S. Pillai (6th edition, 2007) Cellular and Molecular Immunology Saunders Elsevier Chapter 17, immunity to tumors Immune surveillance hypothesis (Macfarlane Burnet,
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Endogenous and Exogenous Vaccination in the Context of Immunologic Checkpoint Blockade
 Endogenous and Exogenous Vaccination in the Context of Immunologic Checkpoint Blockade Jedd Wolchok Ludwig Center for Cancer Immunotherapy Memorial Sloan-Kettering Cancer Center MEMORIAL SLOAN- KETTERING
Endogenous and Exogenous Vaccination in the Context of Immunologic Checkpoint Blockade Jedd Wolchok Ludwig Center for Cancer Immunotherapy Memorial Sloan-Kettering Cancer Center MEMORIAL SLOAN- KETTERING
Supplemental Figure 1. Cell-bound Cetuximab reduces EGFR staining intensity. Blood
 Antibody-mediated depletion of CD19-CAR T cells Supplemental 1 Supplemental Materials Supplemental Figure 1. Supplemental Figure 1. Cell-bound Cetuximab reduces EGFR staining intensity. Blood cells were
Antibody-mediated depletion of CD19-CAR T cells Supplemental 1 Supplemental Materials Supplemental Figure 1. Supplemental Figure 1. Cell-bound Cetuximab reduces EGFR staining intensity. Blood cells were
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
Emerging Targets in Immunotherapy
 Emerging Targets in Immunotherapy So Jin Shin, M.D. Department of Obstetrics and Gynecology, Keimyung University, School of Medicine, Daegu, Korea no-0ncology Todays is.. ancer Immunotherapy? nd immunotherapy
Emerging Targets in Immunotherapy So Jin Shin, M.D. Department of Obstetrics and Gynecology, Keimyung University, School of Medicine, Daegu, Korea no-0ncology Todays is.. ancer Immunotherapy? nd immunotherapy
Mechanisms of antagonism of HIVspecific CD4+ T cell responses BSRI
 Mechanisms of antagonism of HIVspecific CD4+ T cell responses BSRI Problems Virus escape from immune recognition Antagonism of T cell responses Peptide-MHC-TCR interaction T cell antagonism Variants of
Mechanisms of antagonism of HIVspecific CD4+ T cell responses BSRI Problems Virus escape from immune recognition Antagonism of T cell responses Peptide-MHC-TCR interaction T cell antagonism Variants of
VIROLOGY. Engineering Viral Genomes: Retrovirus Vectors
 VIROLOGY Engineering Viral Genomes: Retrovirus Vectors Viral vectors Retrovirus replicative cycle Most mammalian retroviruses use trna PRO, trna Lys3, trna Lys1,2 The partially unfolded trna is annealed
VIROLOGY Engineering Viral Genomes: Retrovirus Vectors Viral vectors Retrovirus replicative cycle Most mammalian retroviruses use trna PRO, trna Lys3, trna Lys1,2 The partially unfolded trna is annealed
Marshall T Bell Research Resident University of Colorado Grand Rounds Nov. 21, 2011
 Marshall T Bell Research Resident University of Colorado Grand Rounds Nov. 21, 2011 Most common form of cancer in adults ages 25-29 3-5% of skin cancers but 65-75% of deaths Most common metastasis to small
Marshall T Bell Research Resident University of Colorado Grand Rounds Nov. 21, 2011 Most common form of cancer in adults ages 25-29 3-5% of skin cancers but 65-75% of deaths Most common metastasis to small
Cancer Immunotherapy INTRODUCTION HUMAN TUMOR ANTIGENS. Cancer/Germ-Line Antigens
 14 Cancer Immunotherapy Steven A. Rosenberg, Paul R. Robbins, Giao Phan, Steven Feldman, and James Kochenderfer INTRODUCTION Progress in understanding basic aspects of cellular immunology and tumor host
14 Cancer Immunotherapy Steven A. Rosenberg, Paul R. Robbins, Giao Phan, Steven Feldman, and James Kochenderfer INTRODUCTION Progress in understanding basic aspects of cellular immunology and tumor host
Cancer Vaccines and Cytokines. Elizabeth A. Mittendorf, MD, PhD Assistant Professor Department of Surgical Oncology
 Cancer Vaccines and Cytokines Elizabeth A. Mittendorf, MD, PhD Assistant Professor Department of Surgical Oncology Disclosures I serve as the PI on a phase III trial sponsored by Galena BioPharma investigating
Cancer Vaccines and Cytokines Elizabeth A. Mittendorf, MD, PhD Assistant Professor Department of Surgical Oncology Disclosures I serve as the PI on a phase III trial sponsored by Galena BioPharma investigating
Tumor Immunology: A Primer
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
