Determining the Time of Cancer Recurrence Using Claims or Electronic Medical Record Data
|
|
|
- Frank McBride
- 5 years ago
- Views:
Transcription
1 original reports Determining the Time of Cancer Recurrence Using Claims or Electronic Medical Record Data abstract Purpose Data from claims and electronic medical records (EMRs) are frequently used to identify clinical events (eg, cancer diagnosis, stroke). However, accurately determining the time of clinical events can be challenging, and the methods used to generate time estimates are underdeveloped. We sought to develop an approach to determine the time of a clinical event cancer recurrence using high-dimensional longitudinal structured data. Methods Manual chart abstraction provided information regarding the actual time of cancer recurrence. These data were linked to claims from Medicare or structured EMR data from the Cancer Research Network, which were used to determine time of recurrence for patients with lung or colorectal cancer. We analyzed the longitudinal profile of codes that could help determine the time of recurrence, adjusted for systematic differences between code dates and recurrence dates, and integrated time estimates from different codes to empirically derive an optimal algorithm. Results We identified twelve code groups that could help determine the time of recurrence. Using claims data for patients with lung cancer, the optimal algorithm consisted of three code groups and provided an average prediction error of 4.8 months. Using EMR data or applying this approach to patients with colorectal cancer yielded similar results. Conclusion Time estimates were improved by selecting codes not necessarily the same as those used to identify recurrence, combining time estimates from multiple code groups, and adjusting for systematic bias between code dates and recurrence dates. Improving the accuracy of time estimates for clinical events can facilitate research, quality measurement, and process improvement. Clin Cancer Inform. 218 by American Society of Clinical Oncology Hajime Uno Debra P. Ritzwoller Angel M. Cronin Nikki M. Carroll Mark C. Hornbrook Michael J. Hassett Author affiliations and support information (if applicable) appear at the end of this article. Corresponding author: Hajime Uno, PhD, Department of Medical Oncology, Dana-Farber Cancer Institute, 45 Brookline Ave, Boston, MA 2215; huno@jimmy.harvard. edu. INTRODUCTION Enormous quantities of data are collected by administrative systems and electronic medical records (EMRs) during the routine delivery of health care. Increasingly, these data are being used for reasons other than just delivering care (EMR systems) and requesting reimbursement (administrative systems), including population health management; epidemiologic, comparative effectiveness, and outcomes research; quality measurement; and operational improvement. For many of these secondary uses, an essential first step is to identify which patients have a specific condition or have experienced a clinical event. When trying to identify these events, diagnosis and procedure codes are particularly helpful, because they are based on structured data elements (eg, International Classification of Diseases, 1th revision [ICD-1], Healthcare Common Procedure Coding System, Systematized Nomenclature of Medicine) and they are used widely by EMRs and administrative systems. However, extracting accurate and reliable clinical information from structured EMR/claims data can be challenging, because many different codes are entered by many different users. To determine who had a clinical event and when that event occurred, one must decide which codes to trust and figure out how to synthesize all the available information when many different codes have been documented. Algorithms that systematically address these challenges have been developed For example, a breast cancer detection algorithm concludes that any patient who has a claim associated with the C5 code (ICD-1) has breast cancer, and that the date of the first C5-associated claim is the date of the breast cancer diagnosis. 12 Although many investigators have described methods for detecting who had a clinical event, 218 by American Society of Clinical Oncology ascopubs.org/journal/cci JCO Clinical Cancer Informatics 1
2 X (t) ~ T i T R i Fig 1. Illustration of a typical pattern of the trajectory of indicators. X (t) = longitudinal profile of a potential indicator j for subject i (eg, the trajectory of the count of diagnosis codes for secondary malignant neoplasm). = start of the observation period (eg, initial cancer diagnosis). R i = end of the observation period for subject i (eg, end of observation/ follow-up time). T i = time of the event occurrence for subject i (eg, cancer recurs). T = time when a large gap in X is observed (eg, the count of diagnosis codes for secondary malignant neoplasm per month increases more than a specified threshold compared with the previous months). a j = an unknown parameter that takes account of the potential difference between the event occurrence time T i and the time when the observed gap in X is observed ( T ). a j approaches to characterize the timing of clinical events are underdeveloped. We hypothesized that existing event-detection algorithms could yield biased or inaccurate estimates of an event s timing for several reasons. First, there could be systematic differences between the date associated with a code used to detect an event and the date on which the event actually occurred. Second, the codes best suited to detect an event may differ from the codes best suited to determine the timing of that event. Third, if a patient does not have the code being used to characterize timing, then no timing estimate can be generated. If timing estimates are missing or inaccurate, then efforts to analyze the quality of care delivered to, outcomes experienced by, and costs associated with a condition could be biased. Recurrence the return of cancer in a patient who completed therapy for localized disease and was believed to have been disease free is a critically important outcome for patients with cancer. Not surprisingly, recurrence has been the focus of many epidemiologic, comparative-effectiveness, and outcomes research studies Although tumor registries reliably capture cancer diagnoses, they do not typically capture recurrence status. In previous articles, we described highly accurate algorithms that use claims or EMR data to detect recurrence for patients with lung, colorectal, and breast cancer. 17,18 In this article, we build on that work by describing a systematic and reproducible method for determining the timing of cancer recurrence using structured data and developing tools that can be used to compare the performance of different timing estimation algorithms. METHODS Data Sources and Patient Sample To develop and validate an algorithm that determines the timing of cancer recurrence, we used two data sets that contained codes that could suggest when recurrence occurred linked to information describing when recurrence actually occurred. The Cancer Care Outcomes Research and Surveillance (CanCORS) Consortium was a large, prospective study of the care provided to and outcomes experienced by patients with lung or colorectal cancer diagnosed in 23 to 25 and followed through Medical record abstract data from CanCORS (used to identify gold-standard recurrence status) were linked to Medicare fee-for-service claims from 22 to 211 (used to estimate the timing of recurrence). 2 The Cancer Research Network (CRN) is a consortium of health maintenance organizations (HMOs) affiliated with the HMO Research Network. Two CRN sites have certified tumor registrars collect recurrence status data: Kaiser Permanente Colorado, Denver, Colorado, and Kaiser Permanente Northwest, Portland, Oregon. The CRN also maintains a Virtual Data Warehouse (VDW) 1 that links tumor registry data (used to identify gold-standard recurrence status) with diagnosis and procedure codes documented in an EPIC-based EMR and with claims for services delivered by contract providers (used to estimate the timing of recurrence). Gold-standard recurrence status was ascertained through manual abstraction of the medical record by study personnel (for CanCORS) or the tumor registry (for the CRN) and recorded using the North American Association of Central Cancer Registry s cancer status variable. To estimate the timing of recurrence, we used diagnosis and procedure codes associated with the following events: secondary malignant neoplasm involving a solid organ site, secondary malignant neoplasm involving either a solid organ or lymph node site, chemotherapy, radiotherapy, hospice, high-cost imaging, cancer symptoms, narcotic/pain medications, inpatient encounters, observation encounters, emergency department encounters, and any procedure. The codes represented commonly used data standards: ICD-9th Revision Clinical Modification, Current Procedural Terminology 4th Edition, Healthcare Common Procedure Coding System, National Drug Codes, Diagnosis-Related Groups, Berenson- Eggers Type of Service, and facility revenue centers (Data Supplement). 1,3,21 Codes were extracted from all available Medicare files and from procedure, diagnosis, encounter, pharmacy, and infusion files from the VDW. 22,23 The 2 ascopubs.org/journal/cci JCO Clinical Cancer Informatics
3 Table 1. Estimates of Offset Parameters and Average Absolute Prediction Errors for Each Indicator Variable Using Cancer Care Outcomes Research and Surveillance/ Medicare Data for Patients With Recurrent Lung Cancer Average Absolute Indicator Offset Parameter Estimate (months) Prediction Error* (months) Secondary malignant neoplasm (solid organ and lymph node sites) Secondary malignant neoplasm (solid organ sites only) Receipt of chemotherapy Radiotherapy events Hospice encounters High-cost imaging Diagnosis codes for cancer symptoms Dispenses of narcotic/pain medications Inpatient stays Observation stays Emergency department encounters Any procedure Naïve prediction NA 6.7 *For patients in whom an indicator did not generate a predicted time of cancer recurrence, the missing predicted time was imputed using the naïve prediction rule (Ri/2 = the half time of the given time window) before calculating the average absolute prediction error for that indicator variable. Abbreviation: NA, not applicable. claim through date or the discharge date was used to assign a date to each code. The primary sample included 38 patients with stage I to IIIa lung cancer from CanCORS/Medicare, of whom 89 (29%) developed recurrence. In secondary analyses, we determined the timing of recurrence using CanCORS/Medicare data for 6 patients with colorectal cancer (14% developed recurrence), CRN/VDW data for 792 patients with lung cancer (27% developed recurrence), and CRN/VDW data for 2,827 patients with colorectal cancer (13% developed recurrence). 17 The institutional review boards from Dana- Farber and the participating Kaiser Permanente sites provided project oversight. defined on the domain [, R i ]. We consider the case that there exists such that X (t) takes a large change around or after T i. For example, suppose we are interested in detecting the time of cancer recurrence. The trajectory of the count of codes for secondary malignant neoplasm between time and R i would be an example of X (t), because the incidence of such codes would increase around recurrence. For additional explanation of the identification problem, let X* i (t) be the perfect identifier in the sense that X* i (t) = I (T i = t) or I (T i t) for all i, where I (.) is the indicator function. With X* i (t), we could accurately identify T i for each subject by finding the smallest t when X* i (t) = 1. Of course, a perfect identifier X* i (t) does not exist, but we assume there exist several X (t) s that behave as such. Specifically, in our notation, we consider J kinds of indicators, X (t), j = 1,,J, for each subject (i = 1,,n). Here we are interested in deriving an algorithm to identify the timing of the event T i for each subject, integrating information from the X (t) s. Figure 1 illustrates a typical pattern of X (t) we use to identify T i. In this example, we see a large increase in X (t) at T = T + a, where a is an i j j unknown offset parameter that takes account of the potential difference between the event occurrence time T i and the time, T, when we observe a large change in X (t). In this example, a j denotes the delay between when the event occurred and when it was reflected in X (t). Note that a j can be positive or negative, depending on the temporal relationship between the event and the indicator. After deriving a best estimate for T i from the trajectory of X (t),i = 1,,n for each j (j = 1,,J), the proposed method integrates the { T ^, T ^,, T ^ i1 i2 ij } (where { T ^, T ^,, T ^ i1 i2 ij } denotes a set of estimators for T i for subject i(i = 1,,n)) to derive an algorithm that gives a single T i estimate for each subject General Approach Month was chosen as the unit of analysis, because it was the most granular level for which we could ascertain changes in claims over time. Let [, R i ] be a time window for subject i (i = 1,,n). We assumed that each subject experienced a clinical event within this time window. Let T i [, R i ] denote the actual recurrence time. Consider J kinds of indicators, let X (t), (i = 1,,n; j = 1,,J) be a nonnegative function Derivation of Estimates From here on, we assume X (t) is a nonnegative, discrete function of time. We also assume that t is discrete and takes on the values,1,2,. t Let K (t ) = X (k ) be the cumulative function k= of X (.) at t. We then standardize K (t) by t and calculate: L (t ) = K (t ), t ascopubs.org/journal/cci JCO Clinical Cancer Informatics 3
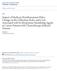
4 Secondary malignancy (1) Secondary malignancy (2) Chemotherapy Abs Err (incl. blue dots): 5.2 months Abs Err (incl. blue dots): 5.4 months Abs Err (incl. blue dots): 5.9 months Radiation Abs Err (incl. blue dots): 6.7 months Hospice Abs Err (incl. blue dots): 7.1 months Imaging Abs Err (incl. blue dots): 5.6 months Symptom Abs Err (incl. blue dots): 7.5 months Pain Abs Err (incl. blue dots): 6.3 months Inpatient Abs Err (incl. blue dots): 6.4 months Observation Abs Err (incl. blue dots): 7.1 months ER visit Abs Err (incl. blue dots): 8.4 months Procedure Abs Err (incl. blue dots): 8.1 months Fig 2. Scatter plots of the predicted time of recurrence and the observed time of recurrence, in months after definitive local therapy, for each indicator variable using Cancer Care Outcomes Research and Surveillance/Medicare data for patients with lung cancer. Secondary malignancy (1): secondary malignant neoplasm codes without lymph node sites of disease. Secondary malignancy (2): secondary malignant neoplasm codes including lymph node sites of disease. Red dots indicate subjects for whom the indicator variable produced a predicted time of recurrence. Blue dots indicate the subjects for whom the indicator variable produced no predicted time of recurrence, so the predicted time of recurrence displayed in the figure was estimated by the naïve prediction rule (ie, R i /2; the half time of the given time window). Abs Err, absolute error; ER, emergency room; incl, including. 4 ascopubs.org/journal/cci JCO Clinical Cancer Informatics
5 Fig 3. Scatter plot between the predicted time of recurrence and the observed time of recurrence for the final model using Cancer Care Outcomes Research and Surveillance/Medicare data for patients with lung cancer, in months after definitive local therapy. Red dots indicate subjects for whom the indicator variable produced a predicted time of recurrence. The blue dot indicates the subject whose predicted time of recurrence was estimated by the naïve prediction rule (ie, R i /2; the half time of the given time window) where L (t) can be viewed as the average speed of the increment in X (t) per unit time. We derive the difference of L (t) with respect to time, to capture the time corresponding to the largest increase in the average speed. Specifically, at each t, we calculate b (t ) = { L (t ) + ε } { L (t 1 ) + ε } { L (t 1 ), + ε } For (t = 1,2, ), where ε = 1, which is added to avoid division by. Note that b (t) is a change in the average speed of rising codes per unit time, which can be viewed as an acceleration rate of X (t). We then extract the time point when b (t) takes the maximum for the first time within the given time window T = min { argma x b (t ) t }. As illustrated in Figure 1, because we model T = T i + a, we then estimate the unknown parameter a j j for each j, from the observed data ( T, T i ). In our empirical example, we used the median, rather than the mean, because of its robustness to extreme values. Let a ^ be the empirical counterpart for a j j. The estimated event time, T i, from the trajectory of the j-th indicator is then given by T ^ = T a ^. j We perform this procedure for each of the J indicators. Note that when b (t) is for all t, we replace T and T by missing values. ^ Now we integrate the multiple estimated times { T ^, T ^,, T ^ i1 i2 ij } and derive a single value for each subject. Let ξ be the indicator variable for i-th subject and j-th indicator, which takes 1 if T ^ is not missing and otherwise. We derive the integrated estimated time for T i through J T ^ = T ^ j=1 ξ W j i J ξ W, j j=1 where W j indicates a weight for the j-th indicator. Because the estimated time with smaller deviation from the observed recurrence time is more reliable, we determine W j by the reciprocal of the variance of T ^ across n subjects. From a practical perspective, we used a trimmed variance instead to reduce the impact of a small number of extreme values in T ^ on the weight W. Specifically, we empirically determined to exclude the j top and bottom 3% when calculating the variance. When T ^ is missing for all j, we substitute the naïve prediction R i /2 to T ^. i Variable Selection and Algorithm Assessment Several standard measures quantify the performance of prediction models for continuous variables. For example, the average absolute prediction error is given by D ^ = n n 1 1 T i T ^ i, i=1 and the average squared error is given by D ^ = n n 1 2 ( T i T 2 ^ i ) i=1 One may standardize these measures by taking the width of the time window into account. The standardized versions of these measures are given by D = n n 1 1 T ^ T i i / and D R i = n 2 i=1 1 n { ( T T ^ i i ) / R 2 i }, respectively. Also, for a i=1 given cutoff value, we can estimate a correct classification rate by: D ^ CCR (c ) = n n 1 I { T ^ T i i < c }. i=1 To adjust for the optimistic bias that is generally included in these substitution performance estimates, we use a Monte Carlo cross-validation procedure to estimate performance metrics for each of the 4,95 (ie, ) candidate algorithms. Specifically, we randomly split the data into two equally sized groups, use one to determine the unknown parameters included in T ^, and i ascopubs.org/journal/cci JCO Clinical Cancer Informatics 5
6 Table 2. Comparative Algorithm Performance for Lung Cancer Recurrence Timing Using Cancer Care Outcomes Research and Surveillance/Medicare Data Measure of Performance Performance* Our Final Algorithm Secondary Malignancy Codes Chemotherapy Only High-Cost Imaging Only Result Result Difference v Ours Result Difference v Ours Result Difference v Ours D ^ (months) D (%) Correct classification, cumulative % ± 1 month ± 2 months ± 3 months ± 4 months ± 5 months ± 6 months * D ^ is the average absolute error, and D is the standardized version of D ^ where the absolute prediction error is divided by the width of the observed time window (see Methods). use the other to estimate the performance metric. We then repeated this process M times and took the average. For example, the cross-validation estimate for the average absolute prediction error is given by M D ^ 1 = M 1 1 { n m m=1 n m T T ^ i i i Θ m ( Θ ) m }, where Θ and Θ are the disjoint subsets created by the m-th random split the former is m m used to estimate the unknown parameters of the algorithm, and the latter is used to calculate the ( Θ performance. Here, T ^ ) m denotes the estimate i for T i, when it is derived without using the data elements in Θ m. Such a cross-validation estimate for selected performance metrics can be used to choose a final algorithm from the several candidate algorithms. Confidence intervals for performance metrics are calculated via a standard bootstrap method. RESULTS First, we applied this method to patients with recurrent lung cancer from the CanCORS/Medicare data set. Table 1 shows the offset parameters and absolute prediction errors for 12 indicators. A negative offset parameter indicates that the peak in the code count was observed before the event occurrence. For example, the offset parameter for the imaging codes was.9 months. This is expected, because imaging is often performed to evaluate symptoms before a biopsy is done and recurrence is confirmed. On the other hand, the offset parameter for chemotherapy was positive (.2 months), which is also reasonable, because chemotherapy is a consequence of having recurrent cancer. Figure 2 shows scatter plots between the predicted and the observed time of recurrence for 89 patients with recurrent disease across all 12 indicators. The blue dots indicate patients in whom the naïve prediction was used because the predicted time was not determined by the corresponding code group. The estimated absolute prediction error analysis shows that secondary malignant neoplasm involving solid organ sites was the strongest indicator among the 12; the corresponding absolute prediction error was 5.2 months. As a reference, the absolute prediction error on the basis of the naïve prediction was 6.7 months (Table 1). To select the final algorithm, we examined all possible combinations of the 12 indicators { T ^, T ^,, T ^ i1 i2 i12 } and calculated the average 6 ascopubs.org/journal/cci JCO Clinical Cancer Informatics
7 Table 3. Components and Performance Characteristics of Timing Estimation Algorithms for Two Cancers Using Two Data Sets CanCORS/Medicare CRN/VDW Colorectal Colorectal Data Source Lung Cancer Cancer Lung Cancer Cancer No. of patients with recurrence Variables included in timing algorithm, offset in months* (weight) Secondary malignancy.2 (.279).1 (.387).9 (.264) 1.8 (.297) Chemotherapy 1.2 (.296) 3.7 (.5) 1.6 (.379) 2.6 (.46) Imaging.9 (.425) 1.1 (.113).5 (.357).6 (.243) Average absolute error, months Standard error, % Correct classification, cumulative No. (%) 1 month 31 (34.8) 18 (21.4) 81 (37.5) 8 (22.5) 2 months 38 (42.7) 34 (4.5) 11 (5.9) 149 (42.) 3 months 51 (57.3) 44 (52.4) 127 (58.8) 188 (53.) 4 months 55 (61.8) 57 (67.9) 142 (65.7) 211 (59.4) 5 months 63 (7.8) 62 (73.8) 155 (71.8) 236 (66.5) 6 months 67 (75.3) 68 (81.) 16 (74.1) 254 (71.5) 6 months 22 (24.7) 16 (19.) 56 (25.9) 11 (28.5) Abbreviations: CanCORS, Cancer Care Outcomes Research and Surveillance; CRN, Cancer Research Network; VDW, Virtual Data Warehouse. *The offset represents the average of the difference between the time when the component variable count peaked and the time of the gold-standard recurrence. Negative values indicate that the peak in the component variable was before the gold-standard recurrence date. The weight is the amount a component variable s estimated recurrence date contributed to estimated date of recurrence. For the CanCORS/Medicare population, this variable included secondary malignancy codes for both solid organ and lymph node sites, whereas for the CRN/VDW sample, this variable included secondary malignancy codes only for solid organ sites (ie, excluding lymph node sites). The average absolute error in months divided by the average duration of follow-up in months. absolute prediction error for each one, selecting the combination of indicators, weights, and offset parameters that offered the best performance. The indicators in the final selected algorithm and their relative weights were: secondary malignant neoplasm involving solid organ or lymph node sites (.279), chemotherapy (.296), and high-cost imaging (.425). Figure 3 shows a scatter plot of the 89 patients with recurrent disease, with the predicted time of recurrence on the basis of the final model plotted against the observed time of recurrence. The estimated absolute prediction error was 4.8 months (.95 CI, 3.5 to 6.3). The correct classification rate (± 3-month time window) was 57.3% (.95 CI, 47.2% to 67.4%). Model performance was compared with three alternatives: secondary malignancy involving either solid organ or lymph node sites only, chemotherapy only, and high-cost imaging only. The absolute prediction error of our algorithm was better (ie, smaller) than any of the single indicator based alternatives (Table 2). To evaluate this technique in other cancers using data from other sources, we applied the same method to colorectal cancer cases from CanCORS/Medicare and to lung and colorectal cancer cases from the CRN/VDW. Whether using claims data from CanCORS/Medicare or EMR data from the CRN/VDW, and whether detecting recurrence after a colorectal or lung cancer diagnosis, the same three code groups were part of the final algorithm (Table 3). Although the directionality of the offsets was similar, the weights for the codes varied somewhat across the four algorithms. DISCUSSION Compared with the methods used to detect which patients experience an event, the methods used ascopubs.org/journal/cci JCO Clinical Cancer Informatics 7
8 to determine the timing of an event have been underdeveloped. Historically, timing estimation algorithms have relied on only one code (eg, secondary malignancy) or a small set of homogenous codes (eg, chemotherapy). We found that using just one code yielded estimates that tended to be less accurate and meant that many patients had no timing estimate. A key strength of our approach is the use of multiple complimentary code sets. Of 89 patients with recurrent lung cancer in CanCORS/Medicare, our algorithm provided a timing estimate for all but one subject. Also, in situations where the algorithm does not derive a timing estimate, we describe a straightforward imputation method on the basis of the time half way between the original cancer diagnosis and the end of follow-up. Timing estimation algorithms often assume that the dates of the codes used to detect events can also be used to determine the timing of events. We found that the codes best suited to determine the timing of an event were not necessarily the same as the codes best suited to detect who had an event. For example, hospice was part of the model that determined who had recurrence but not part of the model that determined when recurrence occurred. 17 Also, imaging was a relatively weak predictor of developing recurrence but a strong factor when estimating the timing of recurrence. The date associated with the code in claims/emr-based systems often differed systematically from the actual recurrence date, and the directionality of this difference made intuitive sense. Limitations of our approach include that it is more complex than previous techniques. 12 Also, the accuracy of timing estimates still remains suboptimal for a meaningful subset of patients. Although estimates were within a few months for most patients, one quarter had estimates with an average absolute error > 6 months, and model performance was only 2 months better than the naïve estimate. We are not aware of methods that derive more accurate estimates. No standard threshold for optimal accuracy has been defined, but we believe better timing estimates are needed. Caution should be taken when using most existing timing estimation algorithms. An inaccurate timing estimate could lead to the inappropriate inclusion of expenditures in an episode of care or a biased estimate of an outcome (ie, recurrence-free survival) in a comparative effectiveness research study. The tools that we developed to determine the timing of recurrence for patients with lung and colorectal cancer can be applied to other data sources (eg, SEER-Medicare, CancerLinq), and the methodology that we described can be used to determine the timing of other cancers or other events. In fact, we have already used this technique to estimate the timing of recurrence for patients with breast cancer. 18 Although our approach relied on claims- and EMR-based data sources, it could easily incorporate other data types too. For example, natural language processing could be used to convert unstructured text into structured format, and then our methodology could be used to combine natural language processing and claims-based information to generate a refined timing estimate. Having consistent methods for assessing the performance of timing-estimation algorithms offers important advantages to those who develop and use these tools. Regardless, efforts to develop better timing estimation algorithms are still warranted. The need for accurate timing estimates will continue to grow as the use of clinical and administrative data for quality measurement, clinical research, and reimbursement expands. DOI: Published online on ascopubs.org/journal/cci on May 15, 218. AUTHOR CONTRIBUTIONS Conception and design: Hajime Uno, Debra P. Ritzwoller, Mark C. Hornbrook, Michael J. Hassett Financial support: Michael J. Hassett, Debra P. Ritzwoller Provision of study materials or patients: Debra P. Ritzwoller Collection and assembly of data: Debra P. Ritzwoller, Angel M. Cronin, Nikki M. Carrol, Mark C. Hornbrook, Michael J. Hassett Data analysis and interpretation: Hajime Uno, Debra P. Ritzwoller, Mark C. Hornbrook, Michael J. Hassett Manuscript writing: All authors Final approval of manuscript: All authors Accountable for all aspects of the work: All authors AUTHORS' DISCLOSURES OF POTENTIAL CONFLICTS OF INTEREST The following represents disclosure information provided by authors of this manuscript. All relationships are considered compensated. Relationships are self-held unless noted. I = Immediate Family Member, Inst = My 8 ascopubs.org/journal/cci JCO Clinical Cancer Informatics
9 Institution. Relationships may not relate to the subject matter of this manuscript. For more information about ASCO's conflict of interest policy, please refer to www. asco.org/rwc or ascopubs.org/jco/site/ifc. Hajime Uno Debra P. Ritzwoller Angel M. Cronin Nikki M. Carroll Mark C. Hornbrook Michael J. Hassett Affiliations Hajime Uno, Angel M. Cronin, and Michael J. Hassett, Dana-Farber Cancer Institute, Boston, MA; Debra P. Ritzwoller and Nikki M. Carroll, Kaiser Permanente Colorado, Denver, CO; and Mark C. Hornbrook, Kaiser Permanente Center for Health Research, Portland, OR. Support Supported by National Cancer Institute (NCI) Grant No. R1 CA (M.J.H. and D.P.R.) and NCI Cooperative Agreement No. U19 CA79689 to the Cancer Research Network. The work of the Cancer Care Outcomes Research and Surveillance Consortium was supported by NCI Grants No. U1 CA93344 (Statistical Coordinating Center), U1 CA93332 (Dana-Farber Cancer Institute/Cancer Research Network), U1 CA93324 (Harvard Medical School/Northern California Cancer Center), U1 CA113 (University of Iowa), and U1 CA93326 (University of North Carolina); and by a Department of Veterans Affairs Grant No. VA HSRD CRS (Durham VA Medical Center). REFERENCES 1. Hassett MJ, Ritzwoller DP, Taback N, et al: Validating billing/encounter codes as indicators of lung, colorectal, breast, and prostate cancer recurrence using 2 large contemporary cohorts. Med Care 52:e65-e73, Chubak J, Yu O, Pocobelli G, et al: Administrative data algorithms to identify second breast cancer events following early-stage invasive breast cancer. J Natl Cancer Inst 14:931-94, Earle CC, Nattinger AB, Potosky AL, et al: Identifying cancer relapse using SEER-Medicare data. Med Care 4:IV-75-IV-81, 22 (suppl 8) 4. Deshpande AD, Schootman M, Mayer A: Development of a claims-based algorithm to identify colorectal cancer recurrence. Ann Epidemiol 25:297-3, McClish D, Penberthy L, Pugh A: Using Medicare claims to identify second primary cancers and recurrences in order to supplement a cancer registry. J Clin Epidemiol 56:76-767, Fleet JL, Dixon SN, Shariff SZ, et al: Detecting chronic kidney disease in population-based administrative databases using an algorithm of hospital encounter and physician claim codes. BMC Nephrol 14:81, Thyagarajan V, Su S, Gee J, et al: Identification of seizures among adults and children following influenza vaccination using health insurance claims data. Vaccine 31: , Sewell JM, Rao A, Elliott SP: Validating a claims-based method for assessing severe rectal and urinary adverse effects of radiotherapy. Urology 82:335-34, Saczynski JS, Andrade SE, Harrold LR, et al: A systematic review of validated methods for identifying heart failure using administrative data. Pharmacoepidemiol Drug Saf 21:129-14, 212 (suppl 1) 1. Klompas M, Eggleston E, McVetta J, et al: Automated detection and classification of type 1 versus type 2 diabetes using electronic health record data. Diabetes Care 36: , Hlatky MA, Ray RM, Burwen DR, et al: Use of Medicare data to identify coronary heart disease outcomes in the Women s Health Initiative. Circ Cardiovasc Qual Outcomes 7: , Chubak J, Onega T, Zhu W, et al: An electronic health record-based algorithm to ascertain the date of second breast cancer events. Med Care 55:e81-e87, 217 ascopubs.org/journal/cci JCO Clinical Cancer Informatics 9
10 13. Stokes ME, Thompson D, Montoya EL, et al: Ten-year survival and cost following breast cancer recurrence: Estimates from SEER-medicare data. Value Health 11:213-22, Schootman M, Jeffe DB, Gillanders WE, et al: Racial disparities in the development of breast cancer metastases among older women: A multilevel study. Cancer 115:731-74, Gooden KM, Howard DL, Carpenter WR, et al: The effect of hospital and surgeon volume on racial differences in recurrence-free survival after radical prostatectomy. Med Care 46: , Cummings KC III, Xu F, Cummings LC, et al: A comparison of epidural analgesia and traditional pain management effects on survival and cancer recurrence after colectomy: A population-based study. Anesthesiology 116:797-86, Hassett MJ, Uno H, Cronin AM, et al: Detecting lung and colorectal cancer recurrence using structured clinical/administrative data to enable outcomes research and population health management. Med Care 55:e88-e98, Ritzwoller D, Hassett MJ, Uno H, et al: Development, validation, and dissemination of a breast cancer recurrence detection and timing informatics algorithm. J Natl Cancer Inst, doi.org/1.193/jnci/djx2 19. Catalano PJ, Ayanian JZ, Weeks JC, et al: Representativeness of participants in the cancer care outcomes research and surveillance consortium relative to the surveillance, epidemiology, and end results program. Med Care 51:e9-e15, Ayanian JZ, Chrischilles EA, Fletcher RH, et al: Understanding cancer treatment and outcomes: The Cancer Care Outcomes Research and Surveillance Consortium. J Clin Oncol 22: , Lamont EB, Herndon JE II, Weeks JC, et al: Measuring disease-free survival and cancer relapse using Medicare claims from CALGB breast cancer trial participants (companion to 9344). J Natl Cancer Inst 98: , Ross TC, Ng D, Brown JS, et al: The HMO Research Network virtual data warehouse: A public data model to support collaboration. EGEMS (Wash DC) 2:149, org/1.1363/ Hornbrook MC, Hart G, Ellis JL, et al: Building a virtual cancer research organization. J Natl Cancer Inst Monogr 35:12-25, 25 1 ascopubs.org/journal/cci JCO Clinical Cancer Informatics
7/29/2014. FCDS Annual Meeting July 24-25, 2014 Caribe Royale Resort Orlando, Florida
 FCDS Annual Meeting July 24-25, 2014 Caribe Royale Resort Orlando, Florida Data collected by central cancer registries is utilized for patient outcomes research Requires complete detailed treatment data
FCDS Annual Meeting July 24-25, 2014 Caribe Royale Resort Orlando, Florida Data collected by central cancer registries is utilized for patient outcomes research Requires complete detailed treatment data
Ten-Year Survival and Cost Following Breast Cancer Recurrence: Estimates from SEER-Medicare Data
 Volume 11 Number 2 2008 VALUE IN HEALTH Ten-Year Survival and Cost Following Breast Cancer Recurrence: Estimates from SEER-Medicare Data Michael E. Stokes, MPH, 1 David Thompson, PhD, 1 Eduardo L. Montoya,
Volume 11 Number 2 2008 VALUE IN HEALTH Ten-Year Survival and Cost Following Breast Cancer Recurrence: Estimates from SEER-Medicare Data Michael E. Stokes, MPH, 1 David Thompson, PhD, 1 Eduardo L. Montoya,
Leveraging the California Cancer Registry to Measure & Improve the Quality of Cancer Care
 Leveraging the California Cancer Registry to Measure & Improve the Quality of Cancer Care Robert A. Hiatt, MD, PhD Chair, Department of Epidemiology & Biostatistics University of California San Francisco
Leveraging the California Cancer Registry to Measure & Improve the Quality of Cancer Care Robert A. Hiatt, MD, PhD Chair, Department of Epidemiology & Biostatistics University of California San Francisco
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes Mastectomy, Breast Cancer Medical Oncology, Breast Biopsy, Tonsillectomy, Otitis media, Anxiety, Non-emergent
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes Mastectomy, Breast Cancer Medical Oncology, Breast Biopsy, Tonsillectomy, Otitis media, Anxiety, Non-emergent
Using Electronic Medical Records to Identify Complex Health Outcomes
 Using Electronic Medical Records to Identify Complex Health Outcomes Mary Anne Armstrong MA; Maqdooda Merchant, MA, MSc; Amy Alabaster, MS, MPH; Tina Raine-Bennett, MD, MPH; Debbie Postlethwaite RNP, MPH
Using Electronic Medical Records to Identify Complex Health Outcomes Mary Anne Armstrong MA; Maqdooda Merchant, MA, MSc; Amy Alabaster, MS, MPH; Tina Raine-Bennett, MD, MPH; Debbie Postlethwaite RNP, MPH
Spending estimates from Cancer Care Spending
 CALIFORNIA HEALTHCARE FOUNDATION August 2015 Estimating Cancer Care Spending in the California Medicare Population: Methodology Detail This paper describes in detail the methods used by Deborah Schrag,
CALIFORNIA HEALTHCARE FOUNDATION August 2015 Estimating Cancer Care Spending in the California Medicare Population: Methodology Detail This paper describes in detail the methods used by Deborah Schrag,
Development and validation of case-finding algorithms for recurrence of breast cancer using routinely collected administrative data
 Xu et al. BMC Cancer (2019) 19:210 https://doi.org/10.1186/s12885-019-5432-8 RESEARCH ARTICLE Open Access Development and validation of case-finding algorithms for recurrence of breast cancer using routinely
Xu et al. BMC Cancer (2019) 19:210 https://doi.org/10.1186/s12885-019-5432-8 RESEARCH ARTICLE Open Access Development and validation of case-finding algorithms for recurrence of breast cancer using routinely
Enhancing Breast Cancer Recurrence Algorithms Through Selective Use of Medical Record Data
 JNCI J Natl Cancer Inst (2016) 108(3): djv336 doi:10.1093/jnci/djv336 First published online November 18, 2015 Article Enhancing Breast Cancer Recurrence Algorithms Through Selective Use of Medical Record
JNCI J Natl Cancer Inst (2016) 108(3): djv336 doi:10.1093/jnci/djv336 First published online November 18, 2015 Article Enhancing Breast Cancer Recurrence Algorithms Through Selective Use of Medical Record
The Linked SEER-Medicare Data and Cancer Effectiveness Research
 The Linked SEER-Medicare Data and Cancer Effectiveness Research Arnold L. Potosky, PhD Professor of Oncology Director of Health Services Research Georgetown University Medical Center Lombardi Comprehensive
The Linked SEER-Medicare Data and Cancer Effectiveness Research Arnold L. Potosky, PhD Professor of Oncology Director of Health Services Research Georgetown University Medical Center Lombardi Comprehensive
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #102 (NQF 0389): Prostate Cancer: Avoidance of Overuse of Bone Scan for Staging Low Risk Prostate Cancer Patients National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS
Quality ID #102 (NQF 0389): Prostate Cancer: Avoidance of Overuse of Bone Scan for Staging Low Risk Prostate Cancer Patients National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS
Linkage of Indiana State Cancer Registry and Indiana Network for Patient Care
 Linkage of Indiana State Cancer Registry and Indiana Network for Patient Care A collaboration between Regenstrief Institute, Indiana University, and the Indiana State Cancer Registry Objectives Understand
Linkage of Indiana State Cancer Registry and Indiana Network for Patient Care A collaboration between Regenstrief Institute, Indiana University, and the Indiana State Cancer Registry Objectives Understand
Visualizing Big Cancer Data: A Future of Cancer Care Andrew Stewart Chief, Oncology Data
 Visualizing Big Cancer Data: A Future of Cancer Care Andrew Stewart Chief, Oncology Data 11.16.2015 1 The Promise of a Rapid Learning Health System a system in which science, informatics, incentives, and
Visualizing Big Cancer Data: A Future of Cancer Care Andrew Stewart Chief, Oncology Data 11.16.2015 1 The Promise of a Rapid Learning Health System a system in which science, informatics, incentives, and
Innovation in Physician Payment and Organization for Cancer Care. Jennifer Malin, MD, PhD Medical Director, Oncology
 Innovation in Physician Payment and Organization for Cancer Care Jennifer Malin, MD, PhD Medical Director, Oncology Current Oncology Care Model Unsustainable High Cost & Trend U.S. spending on cancer increased
Innovation in Physician Payment and Organization for Cancer Care Jennifer Malin, MD, PhD Medical Director, Oncology Current Oncology Care Model Unsustainable High Cost & Trend U.S. spending on cancer increased
Incidence of Surgically Treated Benign Prostatic Hypertrophy and of Prostate Cancer among Blacks and Whites in a Prepaid Health Care Plan
 American Journal of EpKtermotogy Vo! 134, No 8 Copyright C 1991 by The Johns Hopkrts Uruversfty School of Hygiene and Put*: Health Printed in US A AS rights reserved A BRIEF ORIGINAL CONTRIBUTION Incidence
American Journal of EpKtermotogy Vo! 134, No 8 Copyright C 1991 by The Johns Hopkrts Uruversfty School of Hygiene and Put*: Health Printed in US A AS rights reserved A BRIEF ORIGINAL CONTRIBUTION Incidence
NIH Public Access Author Manuscript Cancer Epidemiol Biomarkers Prev. Author manuscript; available in PMC 2011 January 1.
 NIH Public Access Author Manuscript Published in final edited form as: Cancer Epidemiol Biomarkers Prev. 2010 January ; 19(1): 144 147. doi:10.1158/1055-9965.epi-09-0807. Feasibility Study for Collection
NIH Public Access Author Manuscript Published in final edited form as: Cancer Epidemiol Biomarkers Prev. 2010 January ; 19(1): 144 147. doi:10.1158/1055-9965.epi-09-0807. Feasibility Study for Collection
Surveillance and SEER Where are we going? NAACCR Meeting June 23, 2017 Lynne Penberthy MD, MPH
 Surveillance and SEER Where are we going? NAACCR Meeting June 23, 2017 Lynne Penberthy MD, MPH Presentation Objectives Describe Future Role of Registries & Registrars Challenges to cancer surveillance
Surveillance and SEER Where are we going? NAACCR Meeting June 23, 2017 Lynne Penberthy MD, MPH Presentation Objectives Describe Future Role of Registries & Registrars Challenges to cancer surveillance
Chapter 5: Epidemiology of MBC Challenges with Population-Based Statistics
 Chapter 5: Epidemiology of MBC Challenges with Population-Based Statistics Musa Mayer 1 1 AdvancedBC.org, Abstract To advocate most effectively for a population of patients, they must be accurately described
Chapter 5: Epidemiology of MBC Challenges with Population-Based Statistics Musa Mayer 1 1 AdvancedBC.org, Abstract To advocate most effectively for a population of patients, they must be accurately described
HEDIS Initiation and Engagement Quality Measures of Substance Use Disorder Care: Impact of Setting and Health Care Specialty
 POPULATION HEALTH MANAGEMENT Volume 12, Number 4, 2009 ª Mary Ann Liebert, Inc. DOI: 10.1089=pop.2008.0028 Original Article HEDIS and Engagement Quality Measures of Substance Use Disorder Care: Impact
POPULATION HEALTH MANAGEMENT Volume 12, Number 4, 2009 ª Mary Ann Liebert, Inc. DOI: 10.1089=pop.2008.0028 Original Article HEDIS and Engagement Quality Measures of Substance Use Disorder Care: Impact
Patterns of Care in Patients with Cervical Cancer:
 Patterns of Care in Patients with Cervical Cancer: Power and Pitfalls of Claims-Based Analysis Grace Smith, MD, PhD, MPH Resident, PGY-5 Department of Radiation Oncology, MD Anderson Cancer Center Acknowledgments
Patterns of Care in Patients with Cervical Cancer: Power and Pitfalls of Claims-Based Analysis Grace Smith, MD, PhD, MPH Resident, PGY-5 Department of Radiation Oncology, MD Anderson Cancer Center Acknowledgments
NIH Public Access Author Manuscript World J Urol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
Measure #250 (NQF 1853): Radical Prostatectomy Pathology Reporting National Quality Strategy Domain: Effective Clincial Care
 Measure #250 (NQF 1853): Radical Prostatectomy Pathology Reporting National Quality Strategy Domain: Effective Clincial Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage
Measure #250 (NQF 1853): Radical Prostatectomy Pathology Reporting National Quality Strategy Domain: Effective Clincial Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION: Percentage
Using claims data to investigate RT use at the end of life. B. Ashleigh Guadagnolo, MD, MPH Associate Professor M.D. Anderson Cancer Center
 Using claims data to investigate RT use at the end of life B. Ashleigh Guadagnolo, MD, MPH Associate Professor M.D. Anderson Cancer Center Background 25% of Medicare budget spent on the last year of life.
Using claims data to investigate RT use at the end of life B. Ashleigh Guadagnolo, MD, MPH Associate Professor M.D. Anderson Cancer Center Background 25% of Medicare budget spent on the last year of life.
ASSOCIATION OF ASTHMA CONTROL WITH HEALTH CARE UTILIZATION A PROSPECTIVE EVALUATION
 Online Supplement for: ASSOCIATION OF ASTHMA CONTROL WITH HEALTH CARE UTILIZATION A PROSPECTIVE EVALUATION METHODS Population The Northwest Region of Kaiser Permanente (KPNW) is a large, federally qualified,
Online Supplement for: ASSOCIATION OF ASTHMA CONTROL WITH HEALTH CARE UTILIZATION A PROSPECTIVE EVALUATION METHODS Population The Northwest Region of Kaiser Permanente (KPNW) is a large, federally qualified,
Prostate-Specific Antigen (PSA) Test
 Prostate-Specific Antigen (PSA) Test What is the PSA test? Prostate-specific antigen, or PSA, is a protein produced by normal, as well as malignant, cells of the prostate gland. The PSA test measures the
Prostate-Specific Antigen (PSA) Test What is the PSA test? Prostate-specific antigen, or PSA, is a protein produced by normal, as well as malignant, cells of the prostate gland. The PSA test measures the
Perks and Quirks: Using the NCDB Participant User File (PUF) for Outcomes Research
 Perks and Quirks: Using the NCDB Participant User File (PUF) for Outcomes Research Daniel J. Boffa, MD Thoracic Surgery Yale University School of Medicine None Disclosures Why Me? No formal affiliation
Perks and Quirks: Using the NCDB Participant User File (PUF) for Outcomes Research Daniel J. Boffa, MD Thoracic Surgery Yale University School of Medicine None Disclosures Why Me? No formal affiliation
Scholar Commons. University of South Carolina. Minghui Li University of South Carolina. Theses and Dissertations
 University of South Carolina Scholar Commons Theses and Dissertations 2017 Impact of Medicare Reimbursement Policy Change on the Utilization, Risks, and Costs Associated with Erythropoiesis-Stimulating
University of South Carolina Scholar Commons Theses and Dissertations 2017 Impact of Medicare Reimbursement Policy Change on the Utilization, Risks, and Costs Associated with Erythropoiesis-Stimulating
GSK Medicine: Study Number: Title: Rationale: Study Period: Objectives: Indication: Study Investigators/Centers: Research Methods: Data Source
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Author s response to reviews
 Author s response to reviews Title: The epidemiologic characteristics of healthcare provider-diagnosed eczema, asthma, allergic rhinitis, and food allergy in children: a retrospective cohort study Authors:
Author s response to reviews Title: The epidemiologic characteristics of healthcare provider-diagnosed eczema, asthma, allergic rhinitis, and food allergy in children: a retrospective cohort study Authors:
DATA ELEMENTS NEEDED FOR QUALITY ASSESSMENT COPYRIGHT NOTICE
 DATA ELEMENTS NEEDED FOR QUALITY ASSESSMENT COPYRIGHT NOTICE Washington University grants permission to use and reproduce the Data Elements Needed for Quality Assessment exactly as it appears in the PDF
DATA ELEMENTS NEEDED FOR QUALITY ASSESSMENT COPYRIGHT NOTICE Washington University grants permission to use and reproduce the Data Elements Needed for Quality Assessment exactly as it appears in the PDF
Assessing the Potential Revenue Impact to Oncology Practices under a Cancer Drug Therapy Bundled Reimbursement Model
 Assessing the Potential Revenue Impact to Oncology Practices under a Cancer Drug Therapy Bundled Reimbursement Model American Society of Clinical Oncology, Inc. December 23, 2017 Prepared by: Stephen George,
Assessing the Potential Revenue Impact to Oncology Practices under a Cancer Drug Therapy Bundled Reimbursement Model American Society of Clinical Oncology, Inc. December 23, 2017 Prepared by: Stephen George,
Report on Cancer Statistics in Alberta. Kidney Cancer
 Report on Cancer Statistics in Alberta Kidney Cancer November 29 Surveillance - Cancer Bureau Health Promotion, Disease and Injury Prevention Report on Cancer Statistics in Alberta - 2 Purpose of the Report
Report on Cancer Statistics in Alberta Kidney Cancer November 29 Surveillance - Cancer Bureau Health Promotion, Disease and Injury Prevention Report on Cancer Statistics in Alberta - 2 Purpose of the Report
Innovative Risk and Quality Solutions for Value-Based Care. Company Overview
 Innovative Risk and Quality Solutions for Value-Based Care Company Overview Meet Talix Talix provides risk and quality solutions to help providers, payers and accountable care organizations address the
Innovative Risk and Quality Solutions for Value-Based Care Company Overview Meet Talix Talix provides risk and quality solutions to help providers, payers and accountable care organizations address the
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #104 (NQF 0390): Prostate Cancer: Adjuvant Hormonal Therapy for High Risk or Very High Risk Prostate Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL
Measure #104 (NQF 0390): Prostate Cancer: Adjuvant Hormonal Therapy for High Risk or Very High Risk Prostate Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL
Adjuvant Chemotherapy for Patients with Stage III Colon Cancer: Results from a CDC-NPCR Patterns of Care Study
 COLON CANCER ORIGINAL RESEARCH Adjuvant Chemotherapy for Patients with Stage III Colon Cancer: Results from a CDC-NPCR Patterns of Care Study Rosemary D. Cress 1, Susan A. Sabatino 2, Xiao-Cheng Wu 3,
COLON CANCER ORIGINAL RESEARCH Adjuvant Chemotherapy for Patients with Stage III Colon Cancer: Results from a CDC-NPCR Patterns of Care Study Rosemary D. Cress 1, Susan A. Sabatino 2, Xiao-Cheng Wu 3,
Population based studies in Pancreatic Diseases. Satish Munigala
 Population based studies in Pancreatic Diseases Satish Munigala 1 Definition Population-based studies aim to answer research questions for defined populations 1 Generalizable to the whole population addressed
Population based studies in Pancreatic Diseases Satish Munigala 1 Definition Population-based studies aim to answer research questions for defined populations 1 Generalizable to the whole population addressed
THE IMPORTANCE OF COMORBIDITY TO CANCER CARE AND STATISTICS AMERICAN CANCER SOCIETY PRESENTATION COPYRIGHT NOTICE
 THE IMPORTANCE OF COMORBIDITY TO CANCER CARE AND STATISTICS AMERICAN CANCER SOCIETY PRESENTATION COPYRIGHT NOTICE Washington University grants permission to use and reproduce the The Importance of Comorbidity
THE IMPORTANCE OF COMORBIDITY TO CANCER CARE AND STATISTICS AMERICAN CANCER SOCIETY PRESENTATION COPYRIGHT NOTICE Washington University grants permission to use and reproduce the The Importance of Comorbidity
An Overview of Survival Statistics in SEER*Stat
 An Overview of Survival Statistics in SEER*Stat National Cancer Institute SEER Program SEER s mission is to provide information on cancer statistics in an effort to reduce the burden of cancer among the
An Overview of Survival Statistics in SEER*Stat National Cancer Institute SEER Program SEER s mission is to provide information on cancer statistics in an effort to reduce the burden of cancer among the
Setting The setting was not clear. The economic study was carried out in the USA.
 Computed tomography screening for lung cancer in Hodgkin's lymphoma survivors: decision analysis and cost-effectiveness analysis Das P, Ng A K, Earle C C, Mauch P M, Kuntz K M Record Status This is a critical
Computed tomography screening for lung cancer in Hodgkin's lymphoma survivors: decision analysis and cost-effectiveness analysis Das P, Ng A K, Earle C C, Mauch P M, Kuntz K M Record Status This is a critical
Chapter 5: Acute Kidney Injury
 Chapter 5: Acute Kidney Injury In 2015, 4.3% of Medicare fee-for-service beneficiaries experienced a hospitalization complicated by Acute Kidney Injury (AKI); this appears to have plateaued since 2011
Chapter 5: Acute Kidney Injury In 2015, 4.3% of Medicare fee-for-service beneficiaries experienced a hospitalization complicated by Acute Kidney Injury (AKI); this appears to have plateaued since 2011
Immunization Safety Office: Overview and Considerations on Safety of Alternative Immunization Schedules
 Immunization Safety Office: Overview and Considerations on Safety of Alternative Immunization Schedules Frank DeStefano MD, MPH Immunization Safety Office Division of Healthcare Quality Promotion, National
Immunization Safety Office: Overview and Considerations on Safety of Alternative Immunization Schedules Frank DeStefano MD, MPH Immunization Safety Office Division of Healthcare Quality Promotion, National
Assessing the Comparability of EMR Information to Patient Registry and Health Claims Data
 Assessing the Comparability of EMR Information to Patient Registry and Health Claims Data F.S. Mowat, 1 E.C. Lau, 1 M.A. Kelsh, 2* J.C. Legg, 2 N.M. Engel-Nitz, 3 H.N. Watson, 1 H.L. Collins, 2 R.J. Nordyke,
Assessing the Comparability of EMR Information to Patient Registry and Health Claims Data F.S. Mowat, 1 E.C. Lau, 1 M.A. Kelsh, 2* J.C. Legg, 2 N.M. Engel-Nitz, 3 H.N. Watson, 1 H.L. Collins, 2 R.J. Nordyke,
Report on Cancer Statistics in Alberta. Breast Cancer
 Report on Cancer Statistics in Alberta Breast Cancer November 2009 Surveillance - Cancer Bureau Health Promotion, Disease and Injury Prevention Report on Cancer Statistics in Alberta - 2 Purpose of the
Report on Cancer Statistics in Alberta Breast Cancer November 2009 Surveillance - Cancer Bureau Health Promotion, Disease and Injury Prevention Report on Cancer Statistics in Alberta - 2 Purpose of the
Financial Disclosure. Learning Objectives. Review and Impact of the NCDB PUF. Moderator: Sandra Wong, MD, MS, FACS, FASCO
 Review and Impact of the NCDB PUF Moderator: Sandra Wong, MD, MS, FACS, FASCO Financial Disclosure I do not have personal financial relationships with any commercial interests Learning Objectives At the
Review and Impact of the NCDB PUF Moderator: Sandra Wong, MD, MS, FACS, FASCO Financial Disclosure I do not have personal financial relationships with any commercial interests Learning Objectives At the
Abstract Objective: To examine whether general preventive services were diminished in a cohort of men after their diagnosis of prostate cancer.
 Original Article Quality of Preventive Care Before and After Prostate Cancer Diagnosis Lauren Wallner, PhD, MPH; Jeff M. Slezak, MS; Virginia P. Quinn, PhD, MPH; Ronald K. Loo, MD; Joanne E. Schottinger,
Original Article Quality of Preventive Care Before and After Prostate Cancer Diagnosis Lauren Wallner, PhD, MPH; Jeff M. Slezak, MS; Virginia P. Quinn, PhD, MPH; Ronald K. Loo, MD; Joanne E. Schottinger,
DAYS IN PANCREATIC CANCER
 HOSPITAL AND MEDICAL CARE DAYS IN PANCREATIC CANCER Annals of Surgical Oncology, March 27, 2012 Casey B. Duncan, Kristin M. Sheffield, Daniel W. Branch, Yimei Han, Yong-Fang g Kuo, James S. Goodwin, Taylor
HOSPITAL AND MEDICAL CARE DAYS IN PANCREATIC CANCER Annals of Surgical Oncology, March 27, 2012 Casey B. Duncan, Kristin M. Sheffield, Daniel W. Branch, Yimei Han, Yong-Fang g Kuo, James S. Goodwin, Taylor
Cancer Endorsement Maintenance 2011-Maintenance Measures
 Measure Number Title Description Measure Steward 0210 Proportion receiving chemotherapy in the last 14 days of life 0211 Proportion with more than one emergency room visit in the last days of life 0212
Measure Number Title Description Measure Steward 0210 Proportion receiving chemotherapy in the last 14 days of life 0211 Proportion with more than one emergency room visit in the last days of life 0212
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): October 1, 2014 Most Recent Review Date (Revised): May 20, 2014 Effective Date: October 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): October 1, 2014 Most Recent Review Date (Revised): May 20, 2014 Effective Date: October 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
THE SURVIVORSHIP EXPERIENCE IN PANCREATIC CANCER
 THE SURVIVORSHIP EXPERIENCE IN PANCREATIC CANCER Casey A. Boyd, Jaime Benarroch, Kristin M. Sheffield, Yimei Han, Catherine D. Cooksley, Taylor S. Riall Department of Surgery The University of Texas Medical
THE SURVIVORSHIP EXPERIENCE IN PANCREATIC CANCER Casey A. Boyd, Jaime Benarroch, Kristin M. Sheffield, Yimei Han, Catherine D. Cooksley, Taylor S. Riall Department of Surgery The University of Texas Medical
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes Respiratory Infection (RI); Pneumonia (PNA); Inpatient Urinary Tract Infection (UTI-I; Outpatient Urinary
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 3 Episodes Respiratory Infection (RI); Pneumonia (PNA); Inpatient Urinary Tract Infection (UTI-I; Outpatient Urinary
Quality of Life After Modern Treatment Options for Prostate Cancer Ronald Chen, MD, MPH
 Quality of Life After Modern Treatment Options I will be presenting some recently published data on the quality of life after modern treatment options for prostate cancer. My name is Dr. Ronald Chen. I'm
Quality of Life After Modern Treatment Options I will be presenting some recently published data on the quality of life after modern treatment options for prostate cancer. My name is Dr. Ronald Chen. I'm
Chapter 5: Acute Kidney Injury
 Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
Presentation for DHSS 14 September Senior Statistician
 Presentation for DHSS 14 September 2014 Jeannette Jackson-Thompson, MSPH, PhD Director Chester Schmaltz, PhD Senior Statistician Missouri Cancer Registry and Research Center (MCR-ARC) University of Missouri
Presentation for DHSS 14 September 2014 Jeannette Jackson-Thompson, MSPH, PhD Director Chester Schmaltz, PhD Senior Statistician Missouri Cancer Registry and Research Center (MCR-ARC) University of Missouri
CALIFORNIA CANCER REGISTRARS ASSOCIATION JOB BUREAU September Providence Saint Joseph Medical Center Burbank, CA
 Providence Saint Joseph Medical Center Burbank, CA Providence is calling a full time, day shift Cancer Abstractor to Providence Saint Joseph Medical Center in Burbank, CA. In this position you will: Assists
Providence Saint Joseph Medical Center Burbank, CA Providence is calling a full time, day shift Cancer Abstractor to Providence Saint Joseph Medical Center in Burbank, CA. In this position you will: Assists
Retention in HIV care predicts subsequent retention and predicts survival well after the first year of care: a national study of US Veterans
 Retention in HIV care predicts subsequent retention and predicts survival well after the first year of care: a national study of US Veterans Thomas P. Giordano, MD, MPH, Jessica A. Davila, PhD, Christine
Retention in HIV care predicts subsequent retention and predicts survival well after the first year of care: a national study of US Veterans Thomas P. Giordano, MD, MPH, Jessica A. Davila, PhD, Christine
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #104 (NQF 0390): Prostate Cancer: Combination Androgen Deprivation Therapy for High Risk or Very High Risk Prostate Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS
Quality ID #104 (NQF 0390): Prostate Cancer: Combination Androgen Deprivation Therapy for High Risk or Very High Risk Prostate Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS
What is an Adequate Lumpectomy Margin in 2018?
 What is an Adequate Lumpectomy Margin in 2018? Stuart J. Schnitt, M.D. Brigham and Women s Hospital, Dana-Farber Cancer Institute, and Harvard Medical School Boston, MA None Disclosures Topics Current
What is an Adequate Lumpectomy Margin in 2018? Stuart J. Schnitt, M.D. Brigham and Women s Hospital, Dana-Farber Cancer Institute, and Harvard Medical School Boston, MA None Disclosures Topics Current
6/20/2012. Co-authors. Background. Sociodemographic Predictors of Non-Receipt of Guidelines-Concordant Chemotherapy. Age 70 Years
 Sociodemographic Predictors of Non-Receipt of Guidelines-Concordant Chemotherapy - among Locoregional Breast Cancer Patients Under Age 70 Years Xiao-Cheng Wu, MD, MPH 2012 NAACCR Annual Conference June
Sociodemographic Predictors of Non-Receipt of Guidelines-Concordant Chemotherapy - among Locoregional Breast Cancer Patients Under Age 70 Years Xiao-Cheng Wu, MD, MPH 2012 NAACCR Annual Conference June
The American Experience
 The American Experience Jay F. Piccirillo, MD, FACS, CPI Department of Otolaryngology Washington University School of Medicine St. Louis, Missouri, USA Acknowledgement Dorina Kallogjeri, MD, MPH- Senior
The American Experience Jay F. Piccirillo, MD, FACS, CPI Department of Otolaryngology Washington University School of Medicine St. Louis, Missouri, USA Acknowledgement Dorina Kallogjeri, MD, MPH- Senior
The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting
 Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
Clinical Trials: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Clinical Trials: Questions
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Clinical Trials: Questions
Semantic Alignment between ICD-11 and SNOMED-CT. By Marcie Wright RHIA, CHDA, CCS
 Semantic Alignment between ICD-11 and SNOMED-CT By Marcie Wright RHIA, CHDA, CCS World Health Organization (WHO) owns and publishes the International Classification of Diseases (ICD) WHO was entrusted
Semantic Alignment between ICD-11 and SNOMED-CT By Marcie Wright RHIA, CHDA, CCS World Health Organization (WHO) owns and publishes the International Classification of Diseases (ICD) WHO was entrusted
A Measure of the Quality and Value of Standardized Genomic Testing in an Integrated Health System
 A Measure of the Quality and Value of Standardized Genomic Testing in an Integrated Health System A Review From BayCare Health System Claudia Lago Toro, MD Medical Director Shimberg Breast Center St. Joseph
A Measure of the Quality and Value of Standardized Genomic Testing in an Integrated Health System A Review From BayCare Health System Claudia Lago Toro, MD Medical Director Shimberg Breast Center St. Joseph
Retention of Enrollees Following a Cancer Diagnosis Within Health Maintenance Organizations in the Cancer Research Network
 Retention of Enrollees Following a Cancer Diagnosis Within Health Maintenance Organizations in the Cancer Research Network Terry S. Field, Jackie Cernieux, Diana Buist, Ann Geiger, Lois Lamerato, Gene
Retention of Enrollees Following a Cancer Diagnosis Within Health Maintenance Organizations in the Cancer Research Network Terry S. Field, Jackie Cernieux, Diana Buist, Ann Geiger, Lois Lamerato, Gene
Specifications Manual Update: Hospital Outpatient Quality Reporting (OQR) Program
 Specifications Manual Update: Hospital Outpatient Quality Reporting (OQR) Program Melissa Thompson, RN, BSN Specifications Manual Lead Hospital OQR Program Support Contractor January 23, 2019 Featuring:
Specifications Manual Update: Hospital Outpatient Quality Reporting (OQR) Program Melissa Thompson, RN, BSN Specifications Manual Lead Hospital OQR Program Support Contractor January 23, 2019 Featuring:
USRDS UNITED STATES RENAL DATA SYSTEM
 USRDS UNITED STATES RENAL DATA SYSTEM Chapter 6: Medicare Expenditures for Persons With CKD Medicare spending for patients with CKD aged 65 and older exceeded $50 billion in 2013, representing 20% of all
USRDS UNITED STATES RENAL DATA SYSTEM Chapter 6: Medicare Expenditures for Persons With CKD Medicare spending for patients with CKD aged 65 and older exceeded $50 billion in 2013, representing 20% of all
Report on Cancer Statistics in Alberta. Melanoma of the Skin
 Report on Cancer Statistics in Alberta Melanoma of the Skin November 29 Surveillance - Cancer Bureau Health Promotion, Disease and Injury Prevention Report on Cancer Statistics in Alberta - 2 Purpose of
Report on Cancer Statistics in Alberta Melanoma of the Skin November 29 Surveillance - Cancer Bureau Health Promotion, Disease and Injury Prevention Report on Cancer Statistics in Alberta - 2 Purpose of
2014 Physician Quality Reporting System Data Collection Form: Oncology (for patients aged 18 and older)
 2014 Physician Quality Reporting System Data Collection Form: Oncology (for patients aged 18 and older) Physician Name: Patient Name: Last First MI Date of Birth: / / mm dd yyyy Gender: M F Medical Record
2014 Physician Quality Reporting System Data Collection Form: Oncology (for patients aged 18 and older) Physician Name: Patient Name: Last First MI Date of Birth: / / mm dd yyyy Gender: M F Medical Record
An Overview of Disparities Research in Access to Radiation Oncology Care
 An Overview of Disparities Research in Access to Radiation Oncology Care Shearwood McClelland III, M.D. Department of Radiation Medicine Oregon Health & Science University Portland, Oregon Disclosures
An Overview of Disparities Research in Access to Radiation Oncology Care Shearwood McClelland III, M.D. Department of Radiation Medicine Oregon Health & Science University Portland, Oregon Disclosures
Geographic variations in incremental costs of heart disease among medicare beneficiaries, by type of service, 2012
 Geographic variations in incremental costs of heart disease among medicare beneficiaries, by type of service, 2012 Rita Wakim, Centers for Disease Control and Prevention Matthew Ritchey, Centers for Disease
Geographic variations in incremental costs of heart disease among medicare beneficiaries, by type of service, 2012 Rita Wakim, Centers for Disease Control and Prevention Matthew Ritchey, Centers for Disease
Integrated Healthcare ASSOCIATION
 Integrated Healthcare ASSOCIATION Linking Cancer Registry and Claims Data for Quality Measurement WHITE PAPER OCTOBER 216 1 PROJECT SUMMARY AND HIGHLIGHTS California consumers have long lacked meaningful
Integrated Healthcare ASSOCIATION Linking Cancer Registry and Claims Data for Quality Measurement WHITE PAPER OCTOBER 216 1 PROJECT SUMMARY AND HIGHLIGHTS California consumers have long lacked meaningful
Androgen deprivation therapy for treatment of localized prostate cancer and risk of
 Androgen deprivation therapy for treatment of localized prostate cancer and risk of second primary malignancies Lauren P. Wallner, Renyi Wang, Steven J. Jacobsen, Reina Haque Department of Research and
Androgen deprivation therapy for treatment of localized prostate cancer and risk of second primary malignancies Lauren P. Wallner, Renyi Wang, Steven J. Jacobsen, Reina Haque Department of Research and
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Calibrating Time-Dependent One-Year Relative Survival Ratio for Selected Cancers
 ISSN 1995-0802 Lobachevskii Journal of Mathematics 2018 Vol. 39 No. 5 pp. 722 729. c Pleiades Publishing Ltd. 2018. Calibrating Time-Dependent One-Year Relative Survival Ratio for Selected Cancers Xuanqian
ISSN 1995-0802 Lobachevskii Journal of Mathematics 2018 Vol. 39 No. 5 pp. 722 729. c Pleiades Publishing Ltd. 2018. Calibrating Time-Dependent One-Year Relative Survival Ratio for Selected Cancers Xuanqian
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
CANCER REPORTING IN CALIFORNIA: ABSTRACTING AND CODING PROCEDURES California Cancer Reporting System Standards, Volume I
 CANCER REPORTING IN CALIFORNIA: ABSTRACTING AND CODING PROCEDURES California Cancer Reporting System Standards, Volume I Changes and Clarifications 16 th Edition April 15, 2016 Quick Look- Updates to Volume
CANCER REPORTING IN CALIFORNIA: ABSTRACTING AND CODING PROCEDURES California Cancer Reporting System Standards, Volume I Changes and Clarifications 16 th Edition April 15, 2016 Quick Look- Updates to Volume
Physician Follow-Up and Guideline Adherence in Post- Treatment Surveillance of Colorectal Cancer
 Physician Follow-Up and Guideline Adherence in Post- Treatment Surveillance of Colorectal Cancer Gabriela M. Vargas, MD Kristin M. Sheffield, PhD, Abhishek Parmar, MD, Yimei Han, MS, Kimberly M. Brown,
Physician Follow-Up and Guideline Adherence in Post- Treatment Surveillance of Colorectal Cancer Gabriela M. Vargas, MD Kristin M. Sheffield, PhD, Abhishek Parmar, MD, Yimei Han, MS, Kimberly M. Brown,
What It Takes to Get Incorporation Into Guidelines and Reimbursement for Advanced Cancer Diagnostics: Lessons from Oncotype DX
 What It Takes to Get Incorporation Into Guidelines and Reimbursement for Advanced Cancer Diagnostics: Lessons from Oncotype DX WSMOS Meeting Oct 2013 Steven Shak, MD Genomic Health Disclosure: October
What It Takes to Get Incorporation Into Guidelines and Reimbursement for Advanced Cancer Diagnostics: Lessons from Oncotype DX WSMOS Meeting Oct 2013 Steven Shak, MD Genomic Health Disclosure: October
Cancer Programs Practice Profile Reports (CP 3 R) Rapid Quality Reporting System (RQRS)
 O COLON MEASURE SPECIFICATIONS Cancer Programs Practice Profile Reports (CP 3 R) Rapid Quality Reporting System (RQRS) Introduction The Commission on Cancer s (CoC) National Cancer Data Base (NCDB) staff
O COLON MEASURE SPECIFICATIONS Cancer Programs Practice Profile Reports (CP 3 R) Rapid Quality Reporting System (RQRS) Introduction The Commission on Cancer s (CoC) National Cancer Data Base (NCDB) staff
37 th ANNUAL JP MORGAN HEALTHCARE CONFERENCE
 37 th ANNUAL JP MORGAN HEALTHCARE CONFERENCE January 2019 Safe Harbor Statement This presentation contains forward-looking statements within the meaning of Section 27A of the Securities Act of 1933, as
37 th ANNUAL JP MORGAN HEALTHCARE CONFERENCE January 2019 Safe Harbor Statement This presentation contains forward-looking statements within the meaning of Section 27A of the Securities Act of 1933, as
Electrical Stimulation Device Used for Cancer Treatment
 Electrical Stimulation Device Used for Cancer Treatment OPTUNE (NOVOTTF 100A SYSTEM) For any item to be covered by The Health Plan, it must: 1. Be eligible for a defined Medicare or The Health Plan benefit
Electrical Stimulation Device Used for Cancer Treatment OPTUNE (NOVOTTF 100A SYSTEM) For any item to be covered by The Health Plan, it must: 1. Be eligible for a defined Medicare or The Health Plan benefit
A Methodological Issue in the Analysis of Second-Primary Cancer Incidence in Long-Term Survivors of Childhood Cancers
 American Journal of Epidemiology Copyright 2003 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 158, No. 11 Printed in U.S.A. DOI: 10.1093/aje/kwg278 PRACTICE OF EPIDEMIOLOGY
American Journal of Epidemiology Copyright 2003 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 158, No. 11 Printed in U.S.A. DOI: 10.1093/aje/kwg278 PRACTICE OF EPIDEMIOLOGY
Financial Disclosure. Team. Race-based Socioeconomic and Treatment Disparities in Adolescents and Young Adults with Stage II-III Rectal Cancer
 Race-based Socioeconomic and Treatment Disparities in Adolescents and Young Adults with Stage II-III Rectal Cancer Melanie Goldfarb MD, MSc, FACS, FACE John Wayne Cancer Institute at PSJHC, Santa Monica,
Race-based Socioeconomic and Treatment Disparities in Adolescents and Young Adults with Stage II-III Rectal Cancer Melanie Goldfarb MD, MSc, FACS, FACE John Wayne Cancer Institute at PSJHC, Santa Monica,
Handheld Radiofrequency Spectroscopy for Intraoperative Assessment of Surgical Margins During Breast-Conserving Surgery
 7.01.140 Handheld Radiofrequency Spectroscopy for Intraoperative Assessment of Surgical Margins During Breast-Conserving Surgery Section 7.0 Surgery Subsection Description Effective Date November 26, 2014
7.01.140 Handheld Radiofrequency Spectroscopy for Intraoperative Assessment of Surgical Margins During Breast-Conserving Surgery Section 7.0 Surgery Subsection Description Effective Date November 26, 2014
Estimating Testicular Cancer specific Mortality by Using the Surveillance Epidemiology and End Results Registry
 Appendix E1 Estimating Testicular Cancer specific Mortality by Using the Surveillance Epidemiology and End Results Registry To estimate cancer-specific mortality for 33-year-old men with stage I testicular
Appendix E1 Estimating Testicular Cancer specific Mortality by Using the Surveillance Epidemiology and End Results Registry To estimate cancer-specific mortality for 33-year-old men with stage I testicular
The Use of Clinical Trial Data in Combination with External Data Sources to Examine Novel Cancer Research Questions: A Modified Big Data Approach
 The Use of Clinical Trial Data in Combination with External Data Sources to Examine Novel Cancer Research Questions: A Modified Big Data Approach Joseph Unger, Ph.D. Assistant Member, Public Health Sciences
The Use of Clinical Trial Data in Combination with External Data Sources to Examine Novel Cancer Research Questions: A Modified Big Data Approach Joseph Unger, Ph.D. Assistant Member, Public Health Sciences
POSITRON EMISSION TOMOGRAPHY (PET)
 Status Active Medical and Behavioral Health Policy Section: Radiology Policy Number: V-27 Effective Date: 08/27/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Radiology Policy Number: V-27 Effective Date: 08/27/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
2011 Physician Quality Reporting System Measures for Consideration by Oncology Providers: Cancer Care Measures
 2011 Physician Quality Reporting System Measures for Consideration by Oncology Providers: Cancer Care Measures The table below includes measures directly relevant to oncology providers as well as general
2011 Physician Quality Reporting System Measures for Consideration by Oncology Providers: Cancer Care Measures The table below includes measures directly relevant to oncology providers as well as general
TITLE: Outcomes of Screening Mammography in Elderly Women
 AD Award Number: DAMD17-00-1-0193 TITLE: Outcomes of Screening Mammography in Elderly Women PRINCIPAL INVESTIGATOR: Philip W. Chu Rebecca Smith-Bindman, M.D. CONTRACTING ORGANIZATION: University of California,
AD Award Number: DAMD17-00-1-0193 TITLE: Outcomes of Screening Mammography in Elderly Women PRINCIPAL INVESTIGATOR: Philip W. Chu Rebecca Smith-Bindman, M.D. CONTRACTING ORGANIZATION: University of California,
Roadmap for Developing and Validating Therapeutically Relevant Genomic Classifiers. Richard Simon, J Clin Oncol 23:
 Roadmap for Developing and Validating Therapeutically Relevant Genomic Classifiers. Richard Simon, J Clin Oncol 23:7332-7341 Presented by Deming Mi 7/25/2006 Major reasons for few prognostic factors to
Roadmap for Developing and Validating Therapeutically Relevant Genomic Classifiers. Richard Simon, J Clin Oncol 23:7332-7341 Presented by Deming Mi 7/25/2006 Major reasons for few prognostic factors to
Title: What is the role of pre-operative PET/PET-CT in the management of patients with
 Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
Drug Surveillance and Effectiveness Epidemiology Research - Questions to Ask your Epidemiologist
 Drug Surveillance and Effectiveness Epidemiology Research - Questions to Ask your Epidemiologist Roberta Glass, OptumInsight Life Sciences, Waltham, Massachusetts ABSTRACT As a SAS analyst starting work
Drug Surveillance and Effectiveness Epidemiology Research - Questions to Ask your Epidemiologist Roberta Glass, OptumInsight Life Sciences, Waltham, Massachusetts ABSTRACT As a SAS analyst starting work
Cancer Care in the Veterans Health Administration
 Cancer Care in the Veterans Health Administration Michael J Kelley, MD National Program Director for Oncology Department of Veterans Affairs Professor of Medicine Duke University Medical Center Chief,
Cancer Care in the Veterans Health Administration Michael J Kelley, MD National Program Director for Oncology Department of Veterans Affairs Professor of Medicine Duke University Medical Center Chief,
Types of Prostate Radiation Data Points # 16
 Changes across time and geography in the use of prostate radiation technologies for newly diagnosed older cancer patients: 2006-2008 Types of Prostate Radiation Data Points # 16 Prostate cancer is the
Changes across time and geography in the use of prostate radiation technologies for newly diagnosed older cancer patients: 2006-2008 Types of Prostate Radiation Data Points # 16 Prostate cancer is the
The projection of short- and long-term survival for. Conditional Survival Among Patients With Carcinoma of the Lung*
 Conditional Survival Among Patients With Carcinoma of the Lung* Ray M. Merrill, PhD, MPH; Donald Earl Henson, MD; and Michael Barnes, PhD Objective: One- and 5-year probabilities of survival or death change
Conditional Survival Among Patients With Carcinoma of the Lung* Ray M. Merrill, PhD, MPH; Donald Earl Henson, MD; and Michael Barnes, PhD Objective: One- and 5-year probabilities of survival or death change
Cancer Center Dashboard
 Cancer Center Dashboard Measure Definition Benchmark Endorsed By Screening Breast Cancer Screening Percentage of eligible women 40-69 who received a mammogram within the past 24 months NCQA reported average:
Cancer Center Dashboard Measure Definition Benchmark Endorsed By Screening Breast Cancer Screening Percentage of eligible women 40-69 who received a mammogram within the past 24 months NCQA reported average:
GENERAL ICD- C61: Prostate cancer Page 2 of 18 ICD- C61: Malignant neoplasm of prostate Period of diagnosis % Relative survival N=46,
 Munich Cancer Registry Incidence and Mortality Selection Matrix Homepage Deutsch ICD- C61: Prostate cancer Survival Year of diagnosis 1988-1997 1998-215 Patients 7,45 49,513 Diseases 7,45 49,514 Cases
Munich Cancer Registry Incidence and Mortality Selection Matrix Homepage Deutsch ICD- C61: Prostate cancer Survival Year of diagnosis 1988-1997 1998-215 Patients 7,45 49,513 Diseases 7,45 49,514 Cases
Are too many mastectomies being done in the U.S.? Patrick Ivan Borgen, MD Surgeon-in-Chief Maimonides Medical Center Brooklyn, New York
 Are too many mastectomies being done in the U.S.? Patrick Ivan Borgen, MD Surgeon-in-Chief Maimonides Medical Center Brooklyn, New York Of course too many mastectomies are being done. There is too much
Are too many mastectomies being done in the U.S.? Patrick Ivan Borgen, MD Surgeon-in-Chief Maimonides Medical Center Brooklyn, New York Of course too many mastectomies are being done. There is too much
Correlations of Obesity, Comorbidity and Treatment: Implications for Survival Analysis and Interpretation
 Correlations of Obesity, Comorbidity and Treatment: Implications for Survival Analysis and Interpretation Rachel Ballard-Barbash, MD, MPH Applied Research Program (ARP) Division of Cancer Control and Population
Correlations of Obesity, Comorbidity and Treatment: Implications for Survival Analysis and Interpretation Rachel Ballard-Barbash, MD, MPH Applied Research Program (ARP) Division of Cancer Control and Population
Improved Transparency in Key Operational Decisions in Real World Evidence
 PharmaSUG 2018 - Paper RW-06 Improved Transparency in Key Operational Decisions in Real World Evidence Rebecca Levin, Irene Cosmatos, Jamie Reifsnyder United BioSource Corp. ABSTRACT The joint International
PharmaSUG 2018 - Paper RW-06 Improved Transparency in Key Operational Decisions in Real World Evidence Rebecca Levin, Irene Cosmatos, Jamie Reifsnyder United BioSource Corp. ABSTRACT The joint International
PROPOSED/DRAFT Local Coverage Determination (LCD): MolDX: Chromosome 1p/19q deletion analysis (DL36483)
 moldx: Chromosome 1p/19q deletion analysis (DL36483) Page 1 of 8 PROPOSED/DRAFT Local Coverage Determination (LCD): MolDX: Chromosome 1p/19q deletion analysis (DL36483) Close Section Navigation
moldx: Chromosome 1p/19q deletion analysis (DL36483) Page 1 of 8 PROPOSED/DRAFT Local Coverage Determination (LCD): MolDX: Chromosome 1p/19q deletion analysis (DL36483) Close Section Navigation
