Effect of adjuvant trastuzumab treatment in conventional clinical setting: an observational retrospective multicenter Italian study
|
|
|
- Gwen Townsend
- 6 years ago
- Views:
Transcription
1 Breast Cancer Res Treat (2013) 141: DOI /s z CLINICAL TRIAL Effect of adjuvant trastuzumab treatment in conventional clinical setting: an observational retrospective multicenter Italian study M. Campiglio R. Bufalino M. Sasso E. Ferri P. Casalini V. Adamo A. Fabi R. Aiello F. Riccardi E. Valle V. Scotti G. Tabaro D. Giuffrida E. Tarenzi A. Bologna G. Mustacchi F. Bianchi A. Balsari S. Ménard E. Tagliabue Received: 23 May 2013 / Accepted: 30 July 2013 / Published online: 13 August 2013 Ó The Author(s) This article is published with open access at Springerlink.com Abstract Clinical trials have shown the efficacy of trastuzumab-based adjuvant therapy in HER2-positive breast cancers, but routine clinical use awaits evaluation of compliance, safety, and effectiveness. Adjuvant trastuzumab-based therapy in routine clinical use was evaluated in the retrospective study GHEA, recording 1,002 patients treated according to the HERA protocol between March 2005 and December 2009 in 42 Italian oncology departments; 874 (87.23 %) patients completed 1-year trastuzumab treatment. In 128 patients (12.77 %), trastuzumab was withdrawn due to cardiac or non-cardiac toxicity (28 and 29 patients, respectively), disease progression (5 patients) or the clinician s decision (66 patients). In This study was conducted on behalf of the GHEA group. The members of the GHEA group are listed in Appendix. M. Campiglio (&) R. Bufalino M. Sasso E. Ferri P. Casalini F. Bianchi S. Ménard E. Tagliabue Molecular Targeting Unit, Department of Experimental Oncology and Molecular Medicine, Fondazione IRCCS Istituto Nazionale dei Tumori, Via Amadeo 42, Milan, Italy manuela.campiglio@istitutotumori.mi.it V. Adamo University Policlinico G. Martino, Palermo, Italy A. Fabi Regina Elena National Cancer Institute, Rome, Italy R. Aiello Humanitas Centro Catanese di Oncologia, Catania, Italy F. Riccardi Azienda Ospedaliera di Rilievo Nazionale A. Cardarelli, Naples, Italy E. Valle Ospedale Oncologico Businco, Cagliari, Italy addition, 156 patients experienced minor non-cardiac toxicities; 10 and 44 patients showed CHF and decreased LVEF, respectively, at the end of treatment. Compliance and safety of adjuvant trastuzumab-based therapy in Italian hospitals were high and close to those reported in the HERA trial. With a median follow-up of 32 months, 107 breast cancer relapses were recorded (overall frequency, %), and lymph node involvement, estrogen receptor negativity, lymphoid infiltration, and vascular invasion were identified as independent prognostic factors for tumor recurrence, indicating that relapses were associated with advanced tumor stage. Analysis of site and frequency of distant metastases showed that bone metastases were significantly more frequent during or immediately after trastuzumab (\18 months from the start of treatment) compared to recurrences in bone after the end of treatment V. Scotti Azienda Ospedaliera-Universitaria Careggi, Florence, Italy G. Tabaro Centro Oncologico Aviano, Aviano, Italy D. Giuffrida Istituto Oncologico del Mediterraneo, Viagrande, Catania, Italy E. Tarenzi Dipartimento Oncologico dell Ospedalie Niguarda Ca Granda, Milan, Italy A. Bologna IRCCS-Arcispedale Santa Maria Nuova, Reggio Emilia, Italy G. Mustacchi Centro Oncologico, Università di Trieste, Trieste, Italy A. Balsari Department of Human Morphology and Biochemical Sciences, University of Milan, Milan, Italy
2 102 Breast Cancer Res Treat (2013) 141: and wash-out of the drug ([18 months from the start of treatment) (35.89 vs %, p = ); no significant differences were observed in recurrences in the other recorded body sites, raising the possibility that the protection exerted by trastuzumab is lower in bone metastases. Keywords Breast cancer HER2 Trastuzumab Adjuvant therapy Distant metastasis Introduction The HER2 gene is amplified and/or overexpressed in % of breast cancers and is associated with an aggressive disease course [1 4]. Trastuzumab, a humanized monoclonal antibody targeting the extracellular domain of the transmembrane tyrosine kinase receptor HER2 [5], has been shown in phase III clinical trials to reduce the risk of relapse and death in patients with HER2-positive breast cancers when administered along with chemotherapy in an adjuvant setting [6 9]. Results of the Herceptin Adjuvant (HERA) trial at 2 years of median follow-up showed that 1-year adjuvant trastuzumab treatment significantly improved rates of disease-free survival (DFS) [hazard ratio (HR) = 0.63, 95 % CI ; p \ ) and overall survival (HR = 0.63, 95 % CI ; p = ) [10] respect to observation group, with a significant benefit still observed at 4-year [11] and 8-year [12] median follow-up. These findings confirm that adjuvant trastuzumab given sequentially to chemotherapy is associated with a persistent benefit and remains an appropriate treatment modality in patients with HER2-positive early breast cancer. However, estimates provided by clinical trials for eligible patients may not be entirely applicable to all women receiving trastuzumab-based therapy in community practice, pointing to the need for observational studies as a tool to achieve a complete picture of compliance and safety of trastuzumabbased treatment. The observational retrospective multicenter Italian study GHEA (Group HErceptin in Adjuvant Therapy) was designed to evaluate the adherence to trastuzumab treatment guidelines and the safety of adjuvant trastuzumab in Italian patients treated in routine clinical practice according to the HERA protocol. Indeed, the protocol of the HERA trial is a key reference for trastuzumab-containing chemotherapy regimens in treating HER2-positive breast cancer mainly carried out in an adjuvant setting in Europe, including Italy. As an additional parameter to estimate trastuzumab benefits in community practice, the GHEA study also sought to determine whether patients relapsing under trastuzumab treatment differ from those relapsing after the end of the treatment with respect to prognostic factors and site/frequency of distant metastases. Patients and methods Patients The multicenter retrospective observational Italian study GHEA included 1,002 HER2-positive breast cancer patients treated with trastuzumab in an adjuvant setting in 42 Italian oncology departments from March 2005 to December The database, closed on 16 December 2010, was examined in follow-up. Oncology departments were recruited through a public call for Italian oncologic centers treating at least 50 breast cancers/year and with HER2-positive patients treated with adjuvant trastuzumab from March 2005 to December Patients who were considered eligible for adjuvant trastuzumab by the oncologist and receiving this treatment for at least one cycle in the indicated period were included. All primary tumors were scored 3? by immunohistochemistry or 2?/ FISH-positive prior to trastuzumab treatment in each institution. As in the HERA trial, trastuzumab was administered, mainly every 3 weeks, in patients with primary breast cancer following surgery, chemotherapy (neoadjuvant and/or adjuvant), and radiotherapy (if applicable). Histopathological data, chemotherapy treatments, type of surgery, site of first relapse, and times of relapse were recorded for each patient. Non-cardiac toxicity data, including haematological, gastrointestinal, respiratory, renal, liver, dermatological, neurological, and infective adverse events, as well as trastuzumab-associated cardiotoxicity, including congestive heart failure (CHF), decrease in LVEF, and alteration of conduction or pace, were registered. Adverse events were assessed clinically and by haematological and biochemical means throughout the treatment in each participating center. Cardiac function was monitored in all patients every 4 months by electrocardiogram, and LVEF was assessed by echocardiography or multiple gate acquisition (MUGA) scan. LVEF decrease of C10 percentage points from baseline to \50 % at any time was considered as adverse event. Breast cancer firstrelapse events were registered as local, contralateral, or distant when they occurred, respectively, in the same breast as the first tumor, in the other breast, or in another part of the body [central nervous system (CNS), bone, liver, lung, visceral, lymph nodes, and other organs]. For patients with multiple synchronous sites of recorded events, the firstrelapse site was hierarchically considered as distant, local, contralateral breast cancer, and second primary malignancies. Non-breast second primary tumors were considered as other neoplasia. Relapses were subgrouped either as early when they occurred during the 1-year trastuzumab treatment and in the next 6 months or late when they occurred after the 18 months. DFS was defined as the time from start of trastuzumab treatment to the first event.
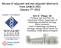
3 Breast Cancer Res Treat (2013) 141: Fig. 1 CONSORT diagram of the Italian retrospective study n = 1002 HER2-positive breast cancer patients trastuzumab-treated in adjuvant setting between Follow-up until December 2010 Endpoint: Analysis of compliance and safety of trastuzumab-based setting 116 recorded any first progression of disease 9 second neoplasia 107 breast cancer relapses 18 local and 1 contralateral 88 distant metastases 39 occured between 18 months from trastuzumab start 49 occured after 18 months from trastuzumab start Comparison of the prognostic factors an d frequency of first distant metastases in two subgroups To ensure rapid and homogeneous data-gathering for patients enrolled in the study, a web-based system was specifically developed to record patient clinical and demographical data. Structured forms for data entry using the Microsoft SQL server and with exclusive log-in and password for Internet access to insert and update all data by each participating center were created. The database was accessible to a single administrator who supervised and monitored data accrual in each center since the beginning of the project. At the end of the data entry period, access to the system was restricted for all participating centers. The Independent Ethics Committee of each participant institution approved the observational study. Statistical analysis Bivariate analysis was carried out for all variables with respect to relapses, using contingency tables evaluated by Chi square or Fisher s exact test. DFS analysis was carried out based on the life-table method [13] including any types of relapses. Univariate analysis was carried out using the phreg SAS procedure with univariate Cox proportional hazards regression. All predictors with p \ 0.05 were used in multivariate analysis with backward elimination, using the Cox regression model and evaluated by Chi square test. Assumption of proportionality was tested for all covariates by including time-dependent covariates in the model using the interaction with log(time). All analyses were conducted using SAS software (SAS Institute Inc., Cary, NC). Twosided p \ 0.05 was considered significant. Results We analyzed data from 1,002 HER2-positive breast cancer patients treated with trastuzumab in an adjuvant setting. Table 1 lists the characteristics of patients and disease. The median age was 52.9 years, % of patients were nodenegative, % were both ER- and PgR-positive, and % were positive for one of the two hormone receptors, and % had T1 tumor size (54.85 % of T1 tumors were node-negative). As expected for HER2-positive carcinomas, tumors were mainly grade III (59.99 %) and of ductal histotype (85.43 %). All patients were treated with chemotherapy: 182 received neoadjuvant treatment,
4 104 Breast Cancer Res Treat (2013) 141: Table 1 Baseline patient and tumor characteristics of 1,002 GHEA study patients Characteristics No. (%) Age \35 years 35 (3.49) years 358 (35.72) years 303 (30.23) [60 years 297 (29.64) Missing 9 (0.89) Median age* 52.9 (26 81) Menopause Yes 488 (48.70) No 298 (29.75) Uncertain 33 (3.29) Missing data 183 (18.26) Nodal status N- 451 (45.01) N? 522 (52.1) Nx 14 (1.39) Missing data 15 (1.50) Tumor size T1 538 (53.69) T2 351 (35.03) CT3 94 (9.38) Missing data 19 (1.90) Histological grade III 601 (59.99) II 323 (32.23) I 13 (1.29) Missing data 65 (6.49) HER2 status HER2-positive 3? 834 (83.23) HER2-positive 2?/FISH amplified 168 (16.77) Hormone receptor status ER-/PgR- 377 (37.63) ER-/PgR? 28 (2.79) ER-/PgR unknown 2 (0.2) ER?/PgR? 441 (44.01) ER?/PgR- 133 (13.27) ER?/PgR unknown 10 (1.0) ER unknown/pgr unknown 10 (1.0) ER unknown/pgr? 1 (0.10) Surgery for primary tumors Mastectomy 406 (40.51) Quadrantectomy 552 (55.09) Lumpectomy 32 (3.19) Missing data 12 (1.20) Histological type Ductal 856 (85.43) Lobular 52 (5.19) Mixed 25 (2.50) Table 1 continued Characteristics No. (%) Other 63 (6.28) Missing data 6 (0.6) Therapy Neoadjuvant or adjuvant chemotherapy No anthracyclines 157 (15.67) Anthracyclines-no taxanes 390 (38.92) Anthracyclines-taxanes 455 (45.41) Hormone therapy Yes 551 (54.99) Aromatase inhibitors 333/551 (60.44) Tamoxifen 218/551 (39.56) Trastuzumab Every 3 weeks 980 (97.80) Weekly 18 (1.80) Unspecified time of administration 4 (0.40) Time of trastuzumab treatment 1-year 874 (87.23) From C9to\12 months 18 (1.80) From C6 to\9 months 73 (7.28) From C3 to\6 months 21 (2.09) Less than 3 months 16 (1.60) * Data are given as year (range) N axillary lymph nodes, T tumor size, ER estrogen receptor, PgR progesterone receptor 862 received adjuvant treatment, and 42 both. Chemotherapy was mostly anthracycline-based (84.33 %) and % of these patients also received taxanes. Hormone therapy was used in % of patients, %of whom received aromatase inhibitors. Almost all recorded patients (97.80 %) underwent trastuzumab administration every 3 weeks, with 1-year trastuzumab treatment completed in 874 (87.23 %) patients. Of 128 patients (12.77 %) who discontinued trastuzumab, stopped for reasons other than relapse and 5 for relapse during therapy. Treatment withdrawal was due to cardiac and non-cardiac adverse events in 28 (20 for CHF and 8 for decreased LVEF), and 29 patients (10 for dermatological, 6 for haematological, 4 for gastrointestinal, 4 for neurological, 2 for infective, 1 for renal, 1 for liver, and 1 for respiratory adverse events), respectively, and to clinical judgment in 66 (Table 2). Toxicity was the most relevant factor leading to trastuzumab withdrawal in patients treated for \6 months, while the clinical decision was the major motivation to stop treatment in those who received trastuzumab for C6 but \12 months (Table 2). Of note, % of these patients had T1 and/or N0 tumors. In addition, 156 patients experienced minor non-cardiac toxicities; of 701 patients who were monitored for cardiac toxicities past the end of
5 Breast Cancer Res Treat (2013) 141: Table 2 Treatment compliance Time of trastuzumab treatment No. of cases % Reasons for withdrawal Progression N (%) Cardiac toxicities N (%) Non-cardiac toxicities N (%) Clinical decision N (%) Less than 3 months (56.25) 5 (31.25) 2 (12.50) From C3 to\6 months (4.76) 8 (38.10) 4 (19.04) 8 (38.10) From C6 to\9 months (5.48) 10 (13.70) 18 (24.66) 41 (56.16) From C9 to\12 months (5.55) 2 (11.11) 15 (83.34) 1 year Total 1, (0.49) 28 (2.79) 29 (2.89) 66 (6.58) Table 3 First recorded events Events No. (%) n = 1,002 Other neoplasia 9 (0.90) Breast carcinoma events 107 (10.70) Local 18 (1.80) Contralateral 1 (0.10) Distant metastases 88 (8.78) treatment, 10 and 44 patients showed CHF and decreased LVEF, respectively. In the entire series, LVEF was monitored by MUGA in only 20 patients. Non-cardiac toxicities included haematological, gastrointestinal, respiratory, renal, liver, dermatological, and neurological adverse events. With a median follow-up of 32 months, 107 (10.68 %) breast cancer events, including local (1.80 %), contralateral (0.10 %), and distant recurrences (8.78 %), were registered (Table 3; Fig. 1). In addition, 9 (0.90 %) secondary nonbreast primary tumors were observed (one thyroid, one lung, one renal, two endometrial, one leukemia, and three unspecified carcinomas). Figure 2 shows the DFS of our series calculated from the start of trastuzumab treatment. When breast cancer relapse occurring after the end of the treatment was analyzed according to time of trastuzumab treatment, five (13.51 %) recurrences were observed in 37 patients treated \6 months, 6 (6.59) in 91 patients treated from C6 to\12 months, and 74 (8.47) in 874 patients who completed the 1-year treatment. Analysis of the clinical and pathological characteristics listed in Table 1 revealed an association between tumor recurrence and axillary lymph node involvement (N?) (p \ ), larger tumor size (p \ ), absence of estrogen receptors (p \ ), and of progesterone receptors (p = ), vascular invasion (p = ), lymphoid infiltration (p = ), grade III (p = ), and chemotherapy regimens (p = ) (Table 4). Univariate analysis indicated that lymph node involvement, n. at risk Fig. 2 Disease-free survival from date of first trastuzumab treatment in HER2-positive patients treated in an adjuvant setting grade III, larger tumor size, lymphoid infiltration, vascular invasion, absence of hormone receptors, and treatment with anthracyclines plus taxanes were significantly associated (p \ 0.05) with DFS (Table 5). A positive significant correlation of the anthracyclines plus taxanes regimen was observed with size and node positivity (p \ ), indicating that patients with more advanced tumors received this therapeutic regimen. Multivariate analysis of covariates displaying p \ 0.05 identified lymph node involvement (HR = 3.633, 95 % CI , p = ), presence of estrogen receptors (HR = 0.552, 95 % CI , p = ), lymphoid infiltration (HR = 1.912, 95 % CI , p = ), and vascular invasion (HR = 1.853, 95 % CI , p = ) as independent prognostic factors (Table 5). Comparison of early recurrences (44 cases, including five local relapses) arising during or immediately after trastuzumab treatment (B18 months from start of treatment) and late recurrences (63 relapses, including 13 local and 1 contralateral recurrences) occurring after the end of the treatment and wash-up of the drug ([18 months from start of treatment) revealed no significant differences in clinical and pathological parameters (Table 6).
6 106 Breast Cancer Res Treat (2013) 141: Table 4 Baseline characteristics of non-relapsed or relapsed breast cancer patients For missing data for each variable, see Table 1. Second non-breast primary tumors were excluded ER estrogen receptor, PgR progesterone receptor, T tumor size, N axillary lymph nodes a Fisher s exact test or Chi square test Parameters Non-relapsed Relapsed p a Age (year) 53 (26.81) 52 (30.80) Postmenopause (no./total, %) 428/695 (61.58) 53/83 (63.85) ER-neg (no./total, %) 343/875 (39.20) 63/107 (58.90) \ PgR-neg (no./total, %) 436/868 (50.23) 70/105 (66.7) Tumor size (no./total, %) T1 496/870 (57.01) 36/104 (34.61) \ T2 305/870 (35.06) 42/104 (40.38) CT3 68/870 (7.81) 26/104 (25.00) Vascular invasion (no./total, %) 220/655 (33.60) 43/80 (53.75) Lymphoid infiltration (no./total, %) 204/587 (34.75) 38/70 (54.28) Necrosis (no./total, %) 193/637 (30.30) 29/75 (38.67) Grade III (no./total, %) 518/830 (62.41) 77/99 (77.78) N? (no./total, %) 448/873 (51.32) 81/105 (77.14) \ Chemotherapy Anthracyclines-no taxanes 365/886 (41.20) 29/107 (27.10) Anthracyclines-taxanes 375/886 (42.33) 64/107 (59.81) No anthracyclines 146/886 (16.48) 14/107 (13.08) Table 5 Univariate and multivariate analyses of parameters for disease-free survival (DFS) in 1,002 patients Parameters Univariate analysis Multivariate analysis HR 95 % CI p HR 95 % CI p Lymph nodes (pos vs. neg) \ Grade (III vs. II/I) ER (pos vs. neg) PgR (pos vs. neg) Size ([T1 vs. BT1) \ Menopause (yes vs. no) Necrosis (yes vs. no) Lymphoid infiltration (yes vs. no) Vascular invasion (yes vs. no) Anthracycline-taxanes vs. anthracycline-no taxanes No anthracycline vs. anthracycline- no taxanes HR hazard ratio, p Chi square test In our series, bone (23.86 %) was the most frequent site of first distant metastasis, followed by CNS (17.05 %). Notably, comparison of the frequency of first distant metastases in the two subgroups (39 early vs. 49 late distant metastases) according to site (Table 7) indicated a significantly higher rate of bone metastases in early than in late recurrences (35.89 vs %, p = ) and a higher, although not statistically significant, incidence of CNS relapses (23.07 vs %). Metastases in the late versus early group were not significantly more frequent in liver (16.32 vs %), lung (18.37 vs %), other viscera (6.12 vs %), or lymph nodes (16.32 vs %); cases with multiple relapses at the time of diagnosis were equally distributed in the two subgroups (14.28 % in early vs % in late metastases). Discussion The observational study GHEA shows that trastuzumab treatment is feasible and well-tolerated in routine clinical practice. Indeed, the majority of the patients recorded in the study adhered to trastuzumab administration following locoregional treatment and chemotherapy as in the HERA trial, with injection every 3 weeks in % of them and completion of the 1-year trastuzumab therapy in 874
7 Breast Cancer Res Treat (2013) 141: Table 6 Baseline characteristics of relapsed patients according to the time of relapse a Fisher s exact test or Chi square test Parameters Early recurrences (0 18 months) n = 44 Late recurrences ([18 months) n = 63 Age (year, range) 52 (30 75) 51 (32 80) Postmenopause (no./total, %) 18/29 (62.07) 35/54 (64.81) ER-neg (no./total, %) 26/44 (59.09) 37/63 (58.73) 1 PgR-neg (no./total, %) 28/43 (65.12) 42/62 (67.74) Tumor size (no./total, %) T1 20/43 (46.51) 16/61 (26.23) T2 14/43 (32.56) 28/61 (45.90) CT3 9/43 (20.93) 17/61 (27.87) Vascular invasion (no./total, %) 15/31 (48.39) 28/49 (57.14) Lymphoid infiltration (no./total, %) 18/33 (54.56) 20/37 (54.05) 1 Necrosis (no./total, %) 12/35 (34.28) 17/40 (42.50) Grade III (no./total, %) 32/40 (80.0) 45/59 (76.27) N? (no./total, %) 32/43 (74.42) 49/62 (79.03) Chemotherapy Anthracycline-no taxanes 12/44 (27.27) 17/53 (26.98) Anthracycline-taxanes 26/44 (59.09) 38/63 (60.32) No anthracyclines 6/44 (13.64) 8/63 (12.70) p a Table 7 Metastatic sites of first distant relapse in early and late recurrences a Data are given as number and percent b Fisher s exact test or Chi squared test Site of distant relapse (87.23 %) patients. The treatment discontinuation rate was higher in our series than in the HERA trial [6, 10] due to % of patients who stopped trastuzumab not for toxicity but for clinical and/or patient decision, while the frequency of adverse events accounting for trastuzumab withdrawal was similar to that in the HERA trial. While toxicities were the major reason for treatment withdrawal within 6 months, later withdrawal reflected the clinician s judgment that for patients at low risk of recurrence, the risk of adverse cardiac events could be minimized by reducing the treatment length without compromising efficacy. Indeed, less than 1-year of trastuzumab is reportedly active in decreasing relapse rates [8]. Consistent with this hypothesis, of the 56 patients who stopped the treatment based on the clinician s decision, % had T1 and/or N0 tumors. The low aggressiveness of these carcinomas is also demonstrated by the lower frequency of relapses after withdrawal compared with Early a (0 18 months) n = 39 (%) Late a ([18 months) n = 49 (%) Central nervous system 9 (23.07) 6 (12.24) Bone 14 (35.89) 7 (14.28) Liver 4 (10.26) 8 (16.32) Lung 4 (10.26) 9 (18.37) Visceral 0 (0) 3 (6.12) Lymph node 3 (7.69) 8 (16.32) Multiple 4 (10.26) 7 (14.28) Unspecified 1 (2.56) 1 (2.04) 1 patients who stopped before 6 months of treatment. The decision against completing 1-year trastuzumab treatment is still rare and, in fact, was made for only about 7 % of the patients in Italian clinical practice. Trastuzumab was withdrawn due to cardiac events in 28 patients (2.79 %), a rate similar to that in the HERA trial [14, 15]. However, another 54 patients experienced cardiac toxicity after the end of treatment, consistent with a recent population-based observational study [16] reporting that the risk of cardiotoxicity associated with trastuzumab following anthracycline appears to increase over time. This underscores the need for long-term surveillance of cardiotoxicity. Since trastuzumab followed anthracycline-based regimens in the majority of patients, clinical practice should include cardiac monitoring past the end of treatment. We observed that patients treated with adjuvant trastuzumab in the Italian clinical practice were at an earlier stage of disease compared with those included in the p b
8 108 Breast Cancer Res Treat (2013) 141: HERA trial. Overall, the 11 % of relapse events observed in the GHEA study is similar to the 13 % reported in the 2-year median follow-up of HERA [10], considering the earlier stage of disease of our patients. Recently published results [17] derived from 87 patients treated with adjuvant trastuzumab in a public hospital showed a compliance and safety similar to that of our study and of the HERA trial, further supporting the feasibility of this treatment outside clinical trials. Our analysis of the role of pathobiological markers in increasing the risk of relapse suggests that the recurrences in trastuzumab-treated patients in clinical practice are associated with a more advanced stage of disease, consistent with the progressively decreased dependence of more advanced tumors on the HER2 signaling pathway [18]. Since maximum trastuzumab activity in clinical trials is reportedly restricted to the time of treatment and a few months thereafter [10], we hypothesize that relapses in this period are truly resistant, while later relapses that might have been sensitive when trastuzumab was present develop upon antibody wash-out. Thus, assuming that early relapses recorded in our study are associated with trastuzumab resistance, we speculate that the pathobiologic parameters analyzed are not involved in trastuzumab resistance since their distribution was similar in early and late relapses. This is consistent with other reports showing Forest plots unable to identify parameters predictive of resistance and useful in clinical practice; indeed, no association between response to trastuzumab and hormone receptor status, grade, node involvement, or size has been found [10, 11]. Notwithstanding the observational nature of our study and the limited number of cases of relapses in our series, we noted a significantly higher frequency of bone relapses during the trastuzumab treatment as compared to recurrences at that site after the end of treatment and wash-out of the drug. While the higher frequency of CNS metastatic disease [19] is consistent with the inability of trastuzumab to pass the blood brain barrier and affect brain metastases [20 22], the lower activity of trastuzumab in preventing bone relapses should be of interest for clinicians to better direct choice of therapies in these patients. Proof of the low activity of trastuzumab in countering bone metastases awaits analysis of bone relapses occurring during and after trastuzumab treatment with respect to the observational HERA patient population. If proven, the basis of this low efficacy of trastuzumab on bone metastases warrants analyses to estimate the drug s penetration in this tissue, although antibodies can localize in bone [23], or to confirm in vivo the reduction of HER2 expression levels in tumor cells homing to the bone, as reported in some studies ([24] and references therein). These mechanisms might impair both cytotoxic and cytostatic effects of trastuzumab (reviewed in [4]), triggering resistance escape mechanisms through upregulation of other receptor activities or through perturbation of the bone microenvironment [25 27]. Our data pointing to low trastuzumab activity in bone relapses are consistent with its higher activity on visceral recurrences observed in the HERA trial with 1-year median follow-up [6], i.e., during or immediately after trastuzumab administration, and also at 4-year median follow-up, when the best trastuzumab-induced benefits were observed for liver recurrences [28]. Among other trials of trastuzumab in the adjuvant setting, only PACS06 reported relapses according to site in the randomized arms [29]; however, the lack of a statistically significant reduction in relapse risk by trastuzumab observed in that study precludes comparison with our results. Moreover, final overall survival analysis of the EGF trial, a phase III randomized multicenter openlabel study of lapatinib alone compared with lapatinib plus trastuzumab in patients with HER2-positive metastatic breast cancer, whose disease progressed during prior trastuzumab therapy, showed that patients with visceral but not those with bone disease significantly benefited from the addition of trastuzumab to lapatinib treatment [30]. In conclusion, our data revealed high compliance of adjuvant trastuzumab treatment in Italian oncology clinics, a satisfactory trastuzumab safety profile, and a treatment efficacy close to that observed in clinical trials. Our results indicating a significantly higher frequency of bone metastases in the first 18 months from the start of trastuzumab treatment merit-specific future analyses to address the possibility that trastuzumab has low efficacy in bone metastases. Acknowledgments We thank Luca Gianni for helpful discussion and critical review of the manuscript. We also thank Laura Mameli for secretarial assistance. This work was supported by Associazione Italiana per la Ricerca sul Cancro (AIRC) (SM) and Roche s.p.a. The sponsor has no role in study design, collection analysis, interpretation of the data, in the writing of the manuscript, or in the decision to submit the manuscript. Conflict of interest GM has received fees as an invited speaker to oncology meetings from Roche, Celgene, Elsai, Novartis, Glaxo, Agendia and Alphagenetics. All remaining authors have declared no conflict of interest. Open Access This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited. Appendix S. Ménard (Molecular Targeting Unit, Department of Experimental Oncology and Molecular Medicine, Fondazione IRCCS Istituto Nazionale dei Tumori, Milano, Italy);
9 Breast Cancer Res Treat (2013) 141: G.R.R. Ricciardi (University Policlinic G. Martino, Palermo, Italy); M. Mottolese (Regina Elena National Cancer Institute, Rome, Italy); E. Taibi (Humanitas Centro Catanese di Oncologia, Catania, Italy); G. Carrillo (Azienda Ospedaliera di Rilievo Nazionale A. Cardarelli, Naples, Italy); A. Piga (Ospedale Oncologico Businco, Cagliari, Italy); D. Quitadamo (Centro Oncologico Aviano, Aviano, Italy); L. Memeo (Istituto Oncologico del Mediterraneo, Viagrande, Catania, Italy); S. Siena (Dipartimento Oncologico dell Ospedalie Niguarda Ca Granda, Milano, Italy); R. Gnoni (IRCCS- Arcispedale Santa Maria Nuova, Reggio Emilia, Italy); A. Molino (Azienda Ospedaliera Universitaria Integrata di Verona, Verona, Italy); A. Jirillo (IRCCS Istituto Oncologico Veneto, Padua, Italy); G. Cavazzini (Azienda Ospedaliera Carlo Poma, Mantua); A. Lugini (Ospedale San Camillo de Lellis, Rieti, Italy); V. Sanna (Ospedale Civile SS. Annunziata, Sassari, Italy); M. Fantini (Ospedale degli Infermi Azianda USL, Rimini, Italy); D. Errante (Ospedale Civile di Vittorio Veneto ULSS7 del Veneto, Vittorio Veneto, Italy ); M. Di Seri (Policlinico Umberto I, Rome, Italy); O. Gottardi (IRCCS Multimedica, Sesto San Giovanni, Italy); A. Gambaro (Azienda Ospedaliera L. Sacco- Polo Universitario, Milano, Italy); A. Di Leo (Ospedale Misericordia e Dolce, Prato, Italy); M.P. Muttini (Ospedale Civico, Carrara, Italy); M. D Aprile (Ospedale Santa Maria Goretti, Latina, Italy); R. Ghisini (Istituto Europeo di Oncologia, Milano, Italy); M. Mauri (Az Ospedaliera San Giovanni, Rome, Italy); M. Visini (Ospedale Manzoni, Lecco, Italy); E. Baldini (Presidio Ospedaliero Campo di Marte, Lucca, Italy); A. Rizzi (Fondazione Poliambulanza Istituto Ospedaliero, Brescia, Italy); C. Savastano (Az. Ospedaliera S. Giovanni di Dio e Ruggi d Aragona, San Giovanni, Italy); A. Bertolini (Ospedale di Sondrio, Sondrio, Italy); M. Frisinghelli (Presidio Ospedaliera S. Chiara, Pisa, Italy); L. Amaducci (Ospedale di Faenza, Faenza, Italy); R. Visentin (Fondazione IRCCS Cà Granda Osp. Maggiore Policlinico, Milano, Italy); N. La Verde (Azienda Ospedaliera Fatebenefratelli Oftalmico, Milano, Italy); L. Pavesi (Fondazione Maugeri, Pavia, Italy); A. Pisano (Ospedale Santa Maria delle Grazie, Pozzuoli, Italy); S. Ortu (Ospedale Giovanni Paolo II, Olbia, Italy); G. Masci (Istituto Clinico Humanitas, Milano, Italy); M. Airoldi (Azienda Ospedaliera Città della Salute e della Scienza, Turin); C.A. Tondini (Ospedali Riuniti, Bergamo, Italy); F. Bassan (Ospedale Boldrini, Thiene, Italy) References 1. Slamon DJ, Clark GM, Wong SG et al (1987) Human breast cancer: correlation of relapse and survival with amplification of the HER-2/neu oncogene. Science 235: Slamon DJ, Godolphin W, Jones LA et al (1989) Studies of the HER-2/neu proto-oncogene in human breast and ovarian cancer. Science 244: Reese DM, Slamon DJ (1997) HER-2/neu signal transduction in human breast and ovarian cancer. Stem Cells 15: Tagliabue E, Campiglio M, Pupa SM et al (2012) Activity and resistance mechanisms of trastuzumab in different clinical settings. Cancer Treat Rev 38: Carter P, Presta L, Gorman CM et al (1992) Humanization of an anti-p185 HER2 antibody for human cancer therapy. Proc Natl Acad Sci USA 89: Piccart-Gebhart MJ, Procter M, Leyland-Jones B et al (2005) Trastuzumab after adjuvant chemotherapy in HER2-positive breast cancer. N Engl J Med 353: Romond EH, Perez EA, Bryant J et al (2005) Trastuzumab plus adjuvant chemotherapy for operable HER2-positive breast cancer. N Engl J Med 353: Joensuu H, Bono P, Kataja V et al (2009) Fluorouracil, epirubicin, and cyclophosphamide with either docetaxel or vinorelbine, with or without trastuzumab, as adjuvant treatments of breast cancer: final results of the FinHer Trial. J Clin Oncol 27: Slamon D, Eiermann W, Robert N et al (2011) Adjuvant trastuzumab in HER2-positive breast cancer. N Engl J Med 365: Smith I, Procter M, Gelber RD et al (2007) 2-Year followup of trastuzumab after adjuvant chemotherapy in HER2- positive breast cancer: a randomised controlled trial. Lancet 369: Gianni L, Dafni U, Gelber RD et al (2011) Treatment with trastuzumab for 1 year after adjuvant chemotherapy in patients with HER2-positive early breast cancer: a 4-year follow-up of a randomised controlled trial. Lancet Oncol 12: Goldhirsch A, Piccart-Gebhart MJ, Procter (2013) HERA TRIAL: 2 years versus 1 year of trastuzumab after adjuvant chemotherapy in women with HER2-positive early breast cancer at 8 years of median follow up. Cancer Res 72 [24 suppl], 103 s (S5-2) 13. Cox DR (1972) Regression models and life tables. J R Stat Soc 34: Suter TM, Procter M, van Veldhuisen DJ et al (2007) Trastuzumab-associated cardiac adverse effects in the herceptin adjuvant trial. J Clin Oncol 25: Procter M, Suter TM, De AE et al (2010) Longer-term assessment of trastuzumab-related cardiac adverse events in the Herceptin Adjuvant (HERA) trial. J Clin Oncol 28: Bowles EJ, Wellman R, Feigelson HS et al (2012) Risk of heart failure in breast cancer patients after anthracycline and trastuzumab treatment: a retrospective cohort study. J Natl Cancer Inst 104: Palmieri C, Shah D, Krell J et al (2011) Management and outcome of HER2-positive early breast cancer treated with or without trastuzumab in the adjuvant trastuzumab era. Clin Breast Cancer 11: Sharma SV, Settleman J (2007) Oncogene addiction: setting the stage for molecularly targeted cancer therapy. Genes Dev 21: Kennecke H, Yerushalmi R, Woods R et al (2010) Metastatic behavior of breast cancer subtypes. J Clin Oncol 28: Hasan A, Ghebeh H, Lehe C et al (2011) Therapeutic targeting of B7-H1 in breast cancer. Expert Opin Ther Targets 15: Geyer CE, Martin A, Newstat B, et al. (2007) Lapatinib (L) plus capecitabine (C) in HER2? advanced breast cancer (ABC): Genomic and updated efficacy data. J Clin Oncol. Suppl 25, 40s- Abstract Azim HA, Azim HA Jr (2012) Systemic treatment of brain metastases in HER2-positive breast cancer: current status and future directions. Future Oncol 8: Dijkers EC, Oude Munnink TH, Kosterink JG et al (2010) Biodistribution of 89Zr-trastuzumab and PET imaging of HER2-
10 110 Breast Cancer Res Treat (2013) 141: positive lesions in patients with metastatic breast cancer. Clin Pharmacol Ther 87: Niikura N, Liu J, Hayashi N et al (2012) Loss of human epidermal growth factor receptor 2 (HER2) expression in metastatic sites of HER2-overexpressing primary breast tumors. J Clin Oncol 30: Johnston SR, Head J, Pancholi S et al (2003) Integration of signal transduction inhibitors with endocrine therapy: an approach to overcoming hormone resistance in breast cancer. Clin Cancer Res 9:524S 532S 26. Rosales C, Brown EJ (1991) Two mechanisms for IgG Fcreceptor-mediated phagocytosis by human neutrophils. J Immunol 146: Jones DH, Nakashima T, Sanchez OH et al (2006) Regulation of cancer cell migration and bone metastasis by RANKL. Nature 440: Metzger-Filho O, Procter M, De Azambuja AE et al (2013) Magnitude of trastuzumab benefit in patients with HER2-positive, invasive lobular breast carcinoma: results from the HERA trial. J Clin Oncol 31: Spielmann M, Roche H, Delozier T et al (2009) Trastuzumab for patients with axillary-node-positive breast cancer: results of the FNCLCC-PACS 04 trial. J Clin Oncol 27(36): Blackwell KL, Burstein HJ, Storniolo AM et al (2012) Overall survival benefit with lapatinib in combination with trastuzumab for patients with human epidermal growth factor receptor 2-positive metastatic breast cancer: final results from the EGF Study. J Clin Oncol 30(21):
Treatment of HER-2 positive breast cancer
 EJC SUPPLEMENTS 6 (2008) 21 25 available at www.sciencedirect.com journal homepage: www.ejconline.com Treatment of HER-2 positive breast cancer Matteo Clavarezza, Marco Venturini * Ospedale Sacro Cuore
EJC SUPPLEMENTS 6 (2008) 21 25 available at www.sciencedirect.com journal homepage: www.ejconline.com Treatment of HER-2 positive breast cancer Matteo Clavarezza, Marco Venturini * Ospedale Sacro Cuore
Neo-adjuvant and adjuvant treatment for HER-2+ breast cancer
 Neo-adjuvant and adjuvant treatment for HER-2+ breast cancer Angelo Di Leo «Sandro Pitigliani» Medical Oncology Unit Hospital of Prato Istituto Toscano Tumori Prato, Italy NOAH: Phase III, Open-Label Trial
Neo-adjuvant and adjuvant treatment for HER-2+ breast cancer Angelo Di Leo «Sandro Pitigliani» Medical Oncology Unit Hospital of Prato Istituto Toscano Tumori Prato, Italy NOAH: Phase III, Open-Label Trial
Sustained benefits for women with HER2-positive early breast cancer JORGE MADRID BIG GOCCHI PROTOCOLO HERA
 Sustained benefits for women with HER2-positive early breast cancer JORGE MADRID BIG GOCCHI PROTOCOLO HERA The fascinating history of Herceptin 1981 1985 1987 1990 1992 1998 2000 2005 2006 2008 2011 Murine
Sustained benefits for women with HER2-positive early breast cancer JORGE MADRID BIG GOCCHI PROTOCOLO HERA The fascinating history of Herceptin 1981 1985 1987 1990 1992 1998 2000 2005 2006 2008 2011 Murine
Nadia Harbeck Breast Center University of Cologne, Germany
 Evidence in Favor of Taxane Based Combinations and No Anthracycline in Adjuvant and Metastatic Settings Nadia Harbeck Breast Center University of Cologne, Germany Evidence in Favor of Taxane Based Combinations
Evidence in Favor of Taxane Based Combinations and No Anthracycline in Adjuvant and Metastatic Settings Nadia Harbeck Breast Center University of Cologne, Germany Evidence in Favor of Taxane Based Combinations
The HERA Study Team. Presented by Ian E. Smith
 Trastuzumab Following Adjuvant Chemotherapy in HER2-Positive Early Breast Cancer (HERA Trial): Disease-Free and Overall Survival after 2 Year Median Follow-Up The HERA Study Team Presented by Ian E. Smith
Trastuzumab Following Adjuvant Chemotherapy in HER2-Positive Early Breast Cancer (HERA Trial): Disease-Free and Overall Survival after 2 Year Median Follow-Up The HERA Study Team Presented by Ian E. Smith
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
Hormone receptor and Her2 neu (Her2) analysis
 ORIGINAL ARTICLE Impact of Triple Negative Phenotype on Breast Cancer Prognosis Henry G. Kaplan, MD* and Judith A. Malmgren, PhD à *Swedish Cancer Institute at Swedish Medical Center; HealthStat Consulting
ORIGINAL ARTICLE Impact of Triple Negative Phenotype on Breast Cancer Prognosis Henry G. Kaplan, MD* and Judith A. Malmgren, PhD à *Swedish Cancer Institute at Swedish Medical Center; HealthStat Consulting
Outcomes of Trastuzumab Therapy for 6 and 12 Months in Indonesian National Health Insurance System Clients with Operable HER2-Positive Breast Cancer
 DOI:10.22034/APJCP.2017.18.4.1151 Trastuzumab RESEARCH ARTICLE Outcomes of Trastuzumab Therapy for 6 and 12 Months in Indonesian National Health Insurance System Clients with Operable HER2-Positive Breast
DOI:10.22034/APJCP.2017.18.4.1151 Trastuzumab RESEARCH ARTICLE Outcomes of Trastuzumab Therapy for 6 and 12 Months in Indonesian National Health Insurance System Clients with Operable HER2-Positive Breast
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva
 Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Taxotere * and carboplatin plus Herceptin (trastuzumab) (TCH): the first approved non-anthracycline Herceptin-containing regimen 1
 Important data from BCIRG 006 Taxotere * and carboplatin plus Herceptin (trastuzumab) (TCH): the first approved non-anthracycline Herceptin-containing regimen 1 in the adjuvant treatment of HER2+ breast
Important data from BCIRG 006 Taxotere * and carboplatin plus Herceptin (trastuzumab) (TCH): the first approved non-anthracycline Herceptin-containing regimen 1 in the adjuvant treatment of HER2+ breast
Non-Anthracycline Adjuvant Therapy: When to Use?
 Northwestern University Feinberg School of Medicine Non-Anthracycline Adjuvant Therapy: When to Use? William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley Center for
Northwestern University Feinberg School of Medicine Non-Anthracycline Adjuvant Therapy: When to Use? William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley Center for
Nivolumab nel carcinoma renale metastatico: esperienza italiana
 Nivolumab nel carcinoma renale metastatico: esperienza italiana Ugo De Giorgi Istituto Tumori Romagna IRST IRCCS Meldola on behalf of the Italian EAP RCC Group Real world data from the Italian expanded
Nivolumab nel carcinoma renale metastatico: esperienza italiana Ugo De Giorgi Istituto Tumori Romagna IRST IRCCS Meldola on behalf of the Italian EAP RCC Group Real world data from the Italian expanded
The Role of Pathologic Complete Response (pcr) as a Surrogate Marker for Outcomes in Breast Cancer: Where Are We Now?
 1 The Role of Pathologic Complete Response (pcr) as a Surrogate Marker for Outcomes in Breast Cancer: Where Are We Now? Terry Mamounas, M.D., M.P.H., F.A.C.S. Medical Director, Comprehensive Breast Program
1 The Role of Pathologic Complete Response (pcr) as a Surrogate Marker for Outcomes in Breast Cancer: Where Are We Now? Terry Mamounas, M.D., M.P.H., F.A.C.S. Medical Director, Comprehensive Breast Program
SANDRA M. SWAIN. Washington Cancer Institute, Washington, District of Columbia, USA
 The Oncologist Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast cancer Chemotherapy Taxane Trastuzumab Ki-67
The Oncologist Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast cancer Chemotherapy Taxane Trastuzumab Ki-67
SANDRA M. SWAIN. Washington Cancer Institute, Washington, District of Columbia, USA
 The Oncologist Early-Stage Breast Cancer: Clinical Update Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast
The Oncologist Early-Stage Breast Cancer: Clinical Update Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast
Systemic Management of Breast Cancer
 Systemic Management of Breast Cancer Why Who When What How long Etc. Vernon Harvey Rotorua, June 2014 Systemic Management of Breast Cancer Metastatic Disease Adjuvant Therapy Aims of therapy Quality of
Systemic Management of Breast Cancer Why Who When What How long Etc. Vernon Harvey Rotorua, June 2014 Systemic Management of Breast Cancer Metastatic Disease Adjuvant Therapy Aims of therapy Quality of
Keywords Breast cancer Brain metastasis Lapatinib Capecitabine. Introduction
 Int Canc Conf J (2013) 2:9 13 DOI 10.1007/s13691-012-0054-x CASE REPORT HER2-positive recurrent breast cancer and metastases of breast cancer, including life-threatening metastases to the brain and dura
Int Canc Conf J (2013) 2:9 13 DOI 10.1007/s13691-012-0054-x CASE REPORT HER2-positive recurrent breast cancer and metastases of breast cancer, including life-threatening metastases to the brain and dura
Key Words. Adjuvant therapy Breast cancer Taxanes Anthracyclines
 The Oncologist Mayo Clinic Hematology/Oncology Reviews Adjuvant Therapy for Breast Cancer: Recommendations for Management Based on Consensus Review and Recent Clinical Trials BETTY A. MINCEY, a,b FRANCES
The Oncologist Mayo Clinic Hematology/Oncology Reviews Adjuvant Therapy for Breast Cancer: Recommendations for Management Based on Consensus Review and Recent Clinical Trials BETTY A. MINCEY, a,b FRANCES
CASE STUDIES CLINICAL CASE SCENARIOS. Matthew J. Ellis, MD, PhD
 CLINICAL CASE SCENARIOS Matthew J. Ellis, MD, PhD Clinicians face daily challenges in the management of individual patients with breast cancer who demonstrate different characteristics in terms of estrogen
CLINICAL CASE SCENARIOS Matthew J. Ellis, MD, PhD Clinicians face daily challenges in the management of individual patients with breast cancer who demonstrate different characteristics in terms of estrogen
BIOLOGICAL THERAPIES FOR BREAST CANCER Updates from the 2005 San Antonio Breast Cancer Symposium
 Emerging trends and recommendations BIOLOGICAL THERAPIES FOR BREAST CANCER Updates from the 2005 San Antonio Breast Cancer Symposium Joseph Ragaz, MD, FRCPC Top-line summary Here, Oncology Exchange presents
Emerging trends and recommendations BIOLOGICAL THERAPIES FOR BREAST CANCER Updates from the 2005 San Antonio Breast Cancer Symposium Joseph Ragaz, MD, FRCPC Top-line summary Here, Oncology Exchange presents
Breast Cancer Earlier Disease. Stefan Aebi Luzerner Kantonsspital
 Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
It is a malignancy originating from breast tissue
 59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012
 Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012 Ruth M. O Regan, MD Professor and Vice-Chair for Educational Affairs, Department of Hematology and Medical Oncology, Emory
Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012 Ruth M. O Regan, MD Professor and Vice-Chair for Educational Affairs, Department of Hematology and Medical Oncology, Emory
Copyright, 1995, by the Massachusetts Medical Society
 Copyright, 99, by the Massachusetts Medical Society Volume 332 APRIL 6, 99 Number ADJUVANT CYCLOPHOSPHAMIDE, METHOTREXATE, AND FLUOROURACIL IN NODE- POSITIVE BREAST CANCER The Results of Years of Follow-up
Copyright, 99, by the Massachusetts Medical Society Volume 332 APRIL 6, 99 Number ADJUVANT CYCLOPHOSPHAMIDE, METHOTREXATE, AND FLUOROURACIL IN NODE- POSITIVE BREAST CANCER The Results of Years of Follow-up
How to carry out health technology appraisals and guidance. Learning from the Scottish experience Richard Clark, Principal Pharmaceutical
 The Managed Introduction of New Medicines How to carry out health technology appraisals and guidance. Learning from the Scottish experience Richard Clark, Principal Pharmaceutical Analyst July 10 th 2009,
The Managed Introduction of New Medicines How to carry out health technology appraisals and guidance. Learning from the Scottish experience Richard Clark, Principal Pharmaceutical Analyst July 10 th 2009,
Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection
 Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection Dr. Michael Co Division of Breast Surgery Queen Mary Hospital The University of Hong Kong Conflicts
Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection Dr. Michael Co Division of Breast Surgery Queen Mary Hospital The University of Hong Kong Conflicts
Adjuvant Systemic Therapy in Early Stage Breast Cancer
 Adjuvant Systemic Therapy in Early Stage Breast Cancer Julie R. Gralow, M.D. Director, Breast Medical Oncology Jill Bennett Endowed Professor of Breast Cancer Professor, Global Health University of Washington
Adjuvant Systemic Therapy in Early Stage Breast Cancer Julie R. Gralow, M.D. Director, Breast Medical Oncology Jill Bennett Endowed Professor of Breast Cancer Professor, Global Health University of Washington
Annals of Breast Cancer. MedDocs Publishers. Open Access Research Article. Quintyne KI 1,2* ; Woulfe B 3 ; Coffey JC 2,4 ; Gupta RK 2,3
 Long-term outcome data for patients with HER2- positive early-stage breast cancer treated with adjuvant trastuzumab: Benefit outside clinical trial setting Quintyne KI 1,2* ; Woulfe B 3 ; Coffey JC 2,4
Long-term outcome data for patients with HER2- positive early-stage breast cancer treated with adjuvant trastuzumab: Benefit outside clinical trial setting Quintyne KI 1,2* ; Woulfe B 3 ; Coffey JC 2,4
Breast Cancer. Outcome of Patients with HER2-Positive Advanced Breast Cancer Progressing During Trastuzumab-Based Therapy
 This material is protected by U.S. Copyright law. Unauthorized reproduction is prohibited. For reprints contact: Reprints@AlphaMedPress.com Breast Cancer Outcome of Patients with HER2-Positive Advanced
This material is protected by U.S. Copyright law. Unauthorized reproduction is prohibited. For reprints contact: Reprints@AlphaMedPress.com Breast Cancer Outcome of Patients with HER2-Positive Advanced
Clinical Features and Survival Analysis of T1mic, a, bn0m0 Breast Cancer
 Original Articles Jpn J Clin Oncol 2012;42(6)471 476 doi:10.1093/jjco/hys046 Advance Access Publication 3 April 2012 Clinical Features and Survival Analysis of T1mic, a, bn0m0 Breast Cancer Junnan Li,
Original Articles Jpn J Clin Oncol 2012;42(6)471 476 doi:10.1093/jjco/hys046 Advance Access Publication 3 April 2012 Clinical Features and Survival Analysis of T1mic, a, bn0m0 Breast Cancer Junnan Li,
Herceptin Pivotal Studies
 Herceptin Pivotal Studies Nuhad K Ibrahim, MD, FACP Associate Professor of Medicine Breast Medical Oncology Department MD Anderson Cancer Center Houston, TX, USAE-mail: nibrahim@mdanderson.org Herceptin
Herceptin Pivotal Studies Nuhad K Ibrahim, MD, FACP Associate Professor of Medicine Breast Medical Oncology Department MD Anderson Cancer Center Houston, TX, USAE-mail: nibrahim@mdanderson.org Herceptin
Existe-t-il un sous groupe à risque qui pourrait bénéficier d une modification de la durée de traitement par trastuzumab? X. Pivot CHRU De Besançon
 Existe-t-il un sous groupe à risque qui pourrait bénéficier d une modification de la durée de traitement par trastuzumab? X. Pivot CHRU De Besançon In 25 results of 4 Adjuvant Herceptin trials have definitively
Existe-t-il un sous groupe à risque qui pourrait bénéficier d une modification de la durée de traitement par trastuzumab? X. Pivot CHRU De Besançon In 25 results of 4 Adjuvant Herceptin trials have definitively
Retrospective analysis of HER2 therapy interruption in patients responding to the treatment in metastatic HER2+
 Original research Retrospective analysis of HER2 therapy interruption in patients responding to the treatment in metastatic HER2+ breast cancer Tiina Moilanen, 1,2 Susanna Mustanoja, 1,2 Peeter Karihtala,
Original research Retrospective analysis of HER2 therapy interruption in patients responding to the treatment in metastatic HER2+ breast cancer Tiina Moilanen, 1,2 Susanna Mustanoja, 1,2 Peeter Karihtala,
original articles introduction
 Annals of Oncology 19. List HJ, Reiter R, Singh B et al. Expression of the nuclear coactivator AIB1 in normal and malignant breast tissue. Breast Cancer Res Treat 2001; 68: 21 28. 20. Jansson A, Delander
Annals of Oncology 19. List HJ, Reiter R, Singh B et al. Expression of the nuclear coactivator AIB1 in normal and malignant breast tissue. Breast Cancer Res Treat 2001; 68: 21 28. 20. Jansson A, Delander
Monitoring Metastatic Breast Cancer with Serum HER-2/neu: Individual Patient Profiles
 Siemens Healthcare Diagnostics, a global leader in clinical diagnostics, provides healthcare professionals in hospital, reference, and physician office laboratories and point-of-care settings with the
Siemens Healthcare Diagnostics, a global leader in clinical diagnostics, provides healthcare professionals in hospital, reference, and physician office laboratories and point-of-care settings with the
What to do after pcr in different subtypes?
 What to do after pcr in different subtypes? Luca Moscetti Breast Unit Università degli Studi di Modena e Reggio Emilia Policlinico di Modena, Italy Aims of neoadjuvant therapy in breast cancer Primary
What to do after pcr in different subtypes? Luca Moscetti Breast Unit Università degli Studi di Modena e Reggio Emilia Policlinico di Modena, Italy Aims of neoadjuvant therapy in breast cancer Primary
GSK Medicine: Study Number: Title: Rationale: Study Period: Objectives: Indication: Study Investigators/Centers: Research Methods: Data Source
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Clinical Trial Results Database Page 1
 Page 1 Sponsor Novartis UK Limited Generic Drug Name Letrozole/FEM345 Therapeutic Area of Trial Localized ER and/or PgR receptor positive breast cancer Study Number CFEM345EGB07 Protocol Title This study
Page 1 Sponsor Novartis UK Limited Generic Drug Name Letrozole/FEM345 Therapeutic Area of Trial Localized ER and/or PgR receptor positive breast cancer Study Number CFEM345EGB07 Protocol Title This study
ORIGINAL ARTICLE CLINICAL ONCOLOGY. J Cancer Res Clin Oncol DOI /s z
 DOI 10.1007/s00432-015-2033-z ORIGINAL ARTICLE CLINICAL ONCOLOGY Demographic, tumor and clinical features of clinical trials versus clinical practice patients with HER2 positive early breast cancer: results
DOI 10.1007/s00432-015-2033-z ORIGINAL ARTICLE CLINICAL ONCOLOGY Demographic, tumor and clinical features of clinical trials versus clinical practice patients with HER2 positive early breast cancer: results
William J. Gradishar MD
 Northwestern University Feinberg School of Medicine Adjuvant Endocrine Therapy For Postmenopausal Women SOBO 2013 William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley
Northwestern University Feinberg School of Medicine Adjuvant Endocrine Therapy For Postmenopausal Women SOBO 2013 William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley
Immunoconjugates in Both the Adjuvant and Metastatic Setting
 Immunoconjugates in Both the Adjuvant and Metastatic Setting Mark Pegram, M.D. Director, Stanford Breast Oncology Program Co-Director, Molecular Therapeutics Program Trastuzumab Treatment of Breast Tumor
Immunoconjugates in Both the Adjuvant and Metastatic Setting Mark Pegram, M.D. Director, Stanford Breast Oncology Program Co-Director, Molecular Therapeutics Program Trastuzumab Treatment of Breast Tumor
Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer. Cheol Min Kang 2018/04/05
 Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Clinical Study The Efficacy of Neoadjuvant Chemotherapy for HER-2-Positive Locally Advanced Breast Cancer and Survival Analysis
 Hindawi Analytical Cellular Pathology Volume 2017, Article ID 1350618, 5 pages https://doi.org/10.1155/2017/1350618 Clinical Study The Efficacy of Neoadjuvant Chemotherapy for HER-2-Positive Locally Advanced
Hindawi Analytical Cellular Pathology Volume 2017, Article ID 1350618, 5 pages https://doi.org/10.1155/2017/1350618 Clinical Study The Efficacy of Neoadjuvant Chemotherapy for HER-2-Positive Locally Advanced
Her 2 Positive Metastatic Breast Cancer
 Her 2 Positive Metastatic Breast Cancer Alison Jones November 2013 Mrs Hermione Positive (then and now!) Diagnosed 2007 T2 N1 Mo ER ve; Her2 ve Mastectomy ANC; FEC/T Herceptin (12months) August 2010metastatic
Her 2 Positive Metastatic Breast Cancer Alison Jones November 2013 Mrs Hermione Positive (then and now!) Diagnosed 2007 T2 N1 Mo ER ve; Her2 ve Mastectomy ANC; FEC/T Herceptin (12months) August 2010metastatic
Use of Taxanes in Older Breast Cancer Patients
 SIOG Guidelines Update 2014: Use of Taxanes in Older Breast Cancer Patients Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Fundamental steps Task Force (TF) on
SIOG Guidelines Update 2014: Use of Taxanes in Older Breast Cancer Patients Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Fundamental steps Task Force (TF) on
Systemic Therapy of HER2-positive Breast Cancer
 Systemic Therapy of HER2-positive Breast Cancer Tanja Cufer, MD, PhD University Clinic Golnik, Medical Faculty Ljubljana, Slovenia ESO ESMO Masterclass, Belgrade 2017 Relative Risk HER2-positive Breast
Systemic Therapy of HER2-positive Breast Cancer Tanja Cufer, MD, PhD University Clinic Golnik, Medical Faculty Ljubljana, Slovenia ESO ESMO Masterclass, Belgrade 2017 Relative Risk HER2-positive Breast
Does HER2/neu overexpression in breast cancer influence adjuvant chemotherapy and hormonal therapy choices by Ontario physicians? A physician survey
 MYERS et al. ORIGINAL ARTICLE Does HER2/neu overexpression in breast cancer influence adjuvant chemotherapy and hormonal therapy choices by Ontario physicians? A physician survey J.A. Myers MD FRCPC, G.
MYERS et al. ORIGINAL ARTICLE Does HER2/neu overexpression in breast cancer influence adjuvant chemotherapy and hormonal therapy choices by Ontario physicians? A physician survey J.A. Myers MD FRCPC, G.
Research Article Biological Characteristics and Medical Treatment of Breast Cancer in Young Women A Featured Population: Results from the NORA Study
 SAGE-Hindawi Access to Research International Breast Cancer Volume 2, Article ID 534256, 6 pages doi:.46/2/534256 Research Article Biological Characteristics and Medical Treatment of Breast Cancer in Young
SAGE-Hindawi Access to Research International Breast Cancer Volume 2, Article ID 534256, 6 pages doi:.46/2/534256 Research Article Biological Characteristics and Medical Treatment of Breast Cancer in Young
Adjuvant Chemotherapy + Trastuzumab
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Chemotherapy + Trastuzumab (Optimal Drugs / Dosage / Trastuzumab) Adjuvant Chemotherapy (Optimal Drugs / Optimal Dosage
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Chemotherapy + Trastuzumab (Optimal Drugs / Dosage / Trastuzumab) Adjuvant Chemotherapy (Optimal Drugs / Optimal Dosage
Recent advances in the management of metastatic breast cancer in older adults
 Recent advances in the management of metastatic breast cancer in older adults Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Important recent advances in the
Recent advances in the management of metastatic breast cancer in older adults Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Important recent advances in the
Should pertuzumab be used as part of neoadjuvant treatment prior to the release of the APHINITY trial results?
 Commentary Should pertuzumab be used as part of neoadjuvant treatment prior to the release of the APHINITY trial results? Tom Wei-Wu Chen 1, Ching-Hung Lin 1,2, Chiun-Sheng Huang 3 1 Department of Oncology,
Commentary Should pertuzumab be used as part of neoadjuvant treatment prior to the release of the APHINITY trial results? Tom Wei-Wu Chen 1, Ching-Hung Lin 1,2, Chiun-Sheng Huang 3 1 Department of Oncology,
Sesiones interhospitalarias de cáncer de mama. Revisión bibliográfica 4º trimestre 2015
 Sesiones interhospitalarias de cáncer de mama Revisión bibliográfica 4º trimestre 2015 Selected papers Prospective Validation of a 21-Gene Expression Assay in Breast Cancer TAILORx. NEJM 2015 OS for fulvestrant
Sesiones interhospitalarias de cáncer de mama Revisión bibliográfica 4º trimestre 2015 Selected papers Prospective Validation of a 21-Gene Expression Assay in Breast Cancer TAILORx. NEJM 2015 OS for fulvestrant
Heather M. Gage, MD, Avanti Rangnekar, Robert E. Heidel, PhD, Timothy Panella, MD, John Bell, MD, and Amila Orucevic, MD, PhD
 HER2 POSITIVE BREAST CARCINOMA IN THE PRE AND POST ADJUVANT ANTI-HER-2 THERAPY ERA: A SINGLE ACADEMIC INSTITUTION EXPERIENCE IN THE SETTING OUTSIDE OF CLINICAL TRIALS Heather M. Gage, MD, Avanti Rangnekar,
HER2 POSITIVE BREAST CARCINOMA IN THE PRE AND POST ADJUVANT ANTI-HER-2 THERAPY ERA: A SINGLE ACADEMIC INSTITUTION EXPERIENCE IN THE SETTING OUTSIDE OF CLINICAL TRIALS Heather M. Gage, MD, Avanti Rangnekar,
Breast cancer treatment
 Report from the San Antonio Breast Cancer Symposium Breast cancer treatment Determining the best options for select patient groups Sara Soldera, MD, Resident; Nathaniel Bouganim, MD, FRCPC, Medical Oncologist;
Report from the San Antonio Breast Cancer Symposium Breast cancer treatment Determining the best options for select patient groups Sara Soldera, MD, Resident; Nathaniel Bouganim, MD, FRCPC, Medical Oncologist;
Cite this article as: BMJ, doi: /bmj f (published 13 January 2005)
 Cite this article as: BMJ, doi:10.1136/bmj.38314.622095.8f (published 13 January 2005) 30 years follow up of randomised studies of adjuvant CMF in operable breast cancer: cohort study Gianni Bonadonna,
Cite this article as: BMJ, doi:10.1136/bmj.38314.622095.8f (published 13 January 2005) 30 years follow up of randomised studies of adjuvant CMF in operable breast cancer: cohort study Gianni Bonadonna,
Adjuvant Targeted Therapy in Early Breast Cancer
 Adjuvant Targeted Therapy in Early Breast Cancer John Mackey, MD 1, Deanna McLeod, BSc 2, Joseph Ragaz, MD 3, Karen Gelmon, MD 4, Sunil Verma, MD 5, Kathleen Pritchard, MD 5, Kara Laing, MD 6, Louise Provencher,
Adjuvant Targeted Therapy in Early Breast Cancer John Mackey, MD 1, Deanna McLeod, BSc 2, Joseph Ragaz, MD 3, Karen Gelmon, MD 4, Sunil Verma, MD 5, Kathleen Pritchard, MD 5, Kara Laing, MD 6, Louise Provencher,
UK Interdisciplinary Breast Cancer Symposium. Should lobular phenotype be considered when deciding treatment? Michael J Kerin
 UK Interdisciplinary Breast Cancer Symposium Should lobular phenotype be considered when deciding treatment? Michael J Kerin Professor of Surgery National University of Ireland, Galway and Galway University
UK Interdisciplinary Breast Cancer Symposium Should lobular phenotype be considered when deciding treatment? Michael J Kerin Professor of Surgery National University of Ireland, Galway and Galway University
NCCP Chemotherapy Regimen
 INDICATIONS FOR USE: Trastuzumab (IV) Monotherapy - 21 days Regimen *Reimbursement INDICATION ICD10 Code Status HER2 positive metastatic breast cancer (MBC) C50 00200a Hospital HER2 positive early breast
INDICATIONS FOR USE: Trastuzumab (IV) Monotherapy - 21 days Regimen *Reimbursement INDICATION ICD10 Code Status HER2 positive metastatic breast cancer (MBC) C50 00200a Hospital HER2 positive early breast
New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer
 New Evidence reports on presentations given at ASCO 2012 New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer Presentations at ASCO 2012 Breast
New Evidence reports on presentations given at ASCO 2012 New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer Presentations at ASCO 2012 Breast
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Herceptin) Reference Number: ERX.SPA.42 Effective Date: 07.01.16 Last Review Date: 05/17 Line of Business: Commercial [Prescription Drug Plan] Revision Log See Important Reminder at the
Clinical Policy: (Herceptin) Reference Number: ERX.SPA.42 Effective Date: 07.01.16 Last Review Date: 05/17 Line of Business: Commercial [Prescription Drug Plan] Revision Log See Important Reminder at the
Do we have to change our anti-cancer strategy in case of cardiac toxicity? Guy Jerusalem, MD, PhD
 Do we have to change our anti-cancer strategy in case of cardiac toxicity? Point of view of the oncologist Guy Jerusalem, MD, PhD CHU Sart Tilman Liège Anticancer therapy: cardiac toxicity New anticancer
Do we have to change our anti-cancer strategy in case of cardiac toxicity? Point of view of the oncologist Guy Jerusalem, MD, PhD CHU Sart Tilman Liège Anticancer therapy: cardiac toxicity New anticancer
Update on the Management of HER2+ Breast Cancer. Christian Jackisch, MD, PhD Sana Klinikum Offenbach Offenbach, Germany
 Update on the Management of HER2+ Breast Cancer Christian Jackisch, MD, PhD Sana Klinikum Offenbach Offenbach, Germany Outline Treatment strategies for HER2-positive metastatic breast cancer since First
Update on the Management of HER2+ Breast Cancer Christian Jackisch, MD, PhD Sana Klinikum Offenbach Offenbach, Germany Outline Treatment strategies for HER2-positive metastatic breast cancer since First
Symposium article. Trastuzumab combined with chemotherapy for the treatment of HER2-positive metastatic breast cancer: Pivotal trial data
 Annals of Oncology 12 (Suppl. I): S57-S62, 2001. 2001 Kluwer Academic Publishers. Primed in the Netherlands. Symposium article Trastuzumab combined with chemotherapy for the treatment of HER2-positive
Annals of Oncology 12 (Suppl. I): S57-S62, 2001. 2001 Kluwer Academic Publishers. Primed in the Netherlands. Symposium article Trastuzumab combined with chemotherapy for the treatment of HER2-positive
Trastuzumab (IV) Monotherapy - 7 days
 INDICATIONS FOR USE: Trastuzumab (IV) Monotherapy - 7 days Regimen *Reimbursement INDICATION ICD10 Code Status Treatment of patients with HER2 positive metastatic breast cancer (MBC) C50 00201a Hospital
INDICATIONS FOR USE: Trastuzumab (IV) Monotherapy - 7 days Regimen *Reimbursement INDICATION ICD10 Code Status Treatment of patients with HER2 positive metastatic breast cancer (MBC) C50 00201a Hospital
Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer
 Young Investigator Award, Global Breast Cancer Conference 2018 Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer ㅑ Running head: Revisiting estrogen positive tumors
Young Investigator Award, Global Breast Cancer Conference 2018 Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer ㅑ Running head: Revisiting estrogen positive tumors
Postoperative Adjuvant Chemotherapies. Stefan Aebi Luzerner Kantonsspital
 Postoperative Adjuvant Chemotherapies Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Does Chemotherapy Work in Older Patients? ER : Chemotherapy vs nil Age
Postoperative Adjuvant Chemotherapies Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Does Chemotherapy Work in Older Patients? ER : Chemotherapy vs nil Age
Chemotherapy for Isolated Locoregional Recurrence
 Chemotherapy for Isolated Locoregional Recurrence Michelle Melisko MD Assistant Clinical Professor UCSF Helen Diller Family Comprehensive Cancer Center MBC and Improved Median Survival with New Therapies
Chemotherapy for Isolated Locoregional Recurrence Michelle Melisko MD Assistant Clinical Professor UCSF Helen Diller Family Comprehensive Cancer Center MBC and Improved Median Survival with New Therapies
Table S2. Expression of PRMT7 in clinical breast carcinoma samples
 Table S2. Expression of PRMT7 in clinical breast carcinoma samples (All data were obtained from cancer microarray database Oncomine.) Analysis type* Analysis Class(number sampels) 1 2 3 4 Correlation (up/down)#
Table S2. Expression of PRMT7 in clinical breast carcinoma samples (All data were obtained from cancer microarray database Oncomine.) Analysis type* Analysis Class(number sampels) 1 2 3 4 Correlation (up/down)#
TRANSPARENCY COMMITTEE OPINION. 15 February 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 February 2006 Taxotere 20 mg, concentrate and solvent for solution for infusion B/1 vial of Taxotere and 1 vial
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 February 2006 Taxotere 20 mg, concentrate and solvent for solution for infusion B/1 vial of Taxotere and 1 vial
Giuseppe Viale for the BIG 1 98 Collaborative and International Breast Cancer Study Groups
 Central Review of ER, PgR and HER2 in BIG 1 98 Evaluating Letrozole vs. Letrozole Tamoxifen vs. Tamoxifen Letrozole as Adjuvant Endocrine Therapy for Postmenopausal Women with Hormone Receptor Positive
Central Review of ER, PgR and HER2 in BIG 1 98 Evaluating Letrozole vs. Letrozole Tamoxifen vs. Tamoxifen Letrozole as Adjuvant Endocrine Therapy for Postmenopausal Women with Hormone Receptor Positive
e-session 381 BCY3 - Highlights of the 3rd ESO-ESMO Breast Cancer in Young Women International Conference
 Expert: Dr Olivia Pagani, Oncology Institute of Southern Switzerland, Lugano, Switzerland Discussant: Dr Fedro Alessandro Peccatori, European Institute of Oncology, Milan, Italy e-session 381 BCY3 - Highlights
Expert: Dr Olivia Pagani, Oncology Institute of Southern Switzerland, Lugano, Switzerland Discussant: Dr Fedro Alessandro Peccatori, European Institute of Oncology, Milan, Italy e-session 381 BCY3 - Highlights
The effect of delayed adjuvant chemotherapy on relapse of triplenegative
 Original Article The effect of delayed adjuvant chemotherapy on relapse of triplenegative breast cancer Shuang Li 1#, Ding Ma 2#, Hao-Hong Shi 3#, Ke-Da Yu 2, Qiang Zhang 1 1 Department of Breast Surgery,
Original Article The effect of delayed adjuvant chemotherapy on relapse of triplenegative breast cancer Shuang Li 1#, Ding Ma 2#, Hao-Hong Shi 3#, Ke-Da Yu 2, Qiang Zhang 1 1 Department of Breast Surgery,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Trastuzumab, as monotherapy and in combination with a taxane, for the treatment of metastatic breast cancer (to include
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Trastuzumab, as monotherapy and in combination with a taxane, for the treatment of metastatic breast cancer (to include
Supplementary Fig. 1: ATM is phosphorylated in HER2 breast cancer cell lines. (A) ATM is phosphorylated in SKBR3 cells depending on ATM and HER2
 Supplementary Fig. 1: ATM is phosphorylated in HER2 breast cancer cell lines. (A) ATM is phosphorylated in SKBR3 cells depending on ATM and HER2 activity. Upper panel: Representative histograms for FACS
Supplementary Fig. 1: ATM is phosphorylated in HER2 breast cancer cell lines. (A) ATM is phosphorylated in SKBR3 cells depending on ATM and HER2 activity. Upper panel: Representative histograms for FACS
DRAFT GUIDANCE. This guidance document is being distributed for comment purposes only.
 Guidance for Industry Pathologic Complete Response in Neoadjuvant Treatment of High-Risk Early-Stage Breast Cancer: Use as an Endpoint to Support Accelerated Approval DRAFT GUIDANCE This guidance document
Guidance for Industry Pathologic Complete Response in Neoadjuvant Treatment of High-Risk Early-Stage Breast Cancer: Use as an Endpoint to Support Accelerated Approval DRAFT GUIDANCE This guidance document
Treatment Options for Breast Cancer in Low- and Middle-Income Countries: Adjuvant and Metastatic Systemic Therapy
 Women s Empowerment Cancer Advocacy Network (WE CAN) Conference Bucharest, Romania October 2015 Treatment Options for Breast Cancer in Low- and Middle-Income Countries: Adjuvant and Metastatic Systemic
Women s Empowerment Cancer Advocacy Network (WE CAN) Conference Bucharest, Romania October 2015 Treatment Options for Breast Cancer in Low- and Middle-Income Countries: Adjuvant and Metastatic Systemic
EARLY STAGE BREAST CANCER ADJUVANT CHEMOTHERAPY. Dr. Carlos Garbino
 EARLY STAGE BREAST CANCER ADJUVANT CHEMOTHERAPY Dr. Carlos Garbino EARLY BREAST CANCER ADJUVANT CHEMOTHERAPY SUSTANTIVE DIFFICULTIES FOR A WORLDWIDE APPLICABILITY DUE TO IMPORTANT INEQUALITIES + IN DIFFERENT
EARLY STAGE BREAST CANCER ADJUVANT CHEMOTHERAPY Dr. Carlos Garbino EARLY BREAST CANCER ADJUVANT CHEMOTHERAPY SUSTANTIVE DIFFICULTIES FOR A WORLDWIDE APPLICABILITY DUE TO IMPORTANT INEQUALITIES + IN DIFFERENT
Breast Cancer? Breast cancer is the most common. What s New in. Janet s Case
 Focus on CME at The University of Calgary What s New in Breast Cancer? Theresa Trotter, MD, FRCPC Breast cancer is the most common malignancy affecting women in Canada, accounting for almost a third of
Focus on CME at The University of Calgary What s New in Breast Cancer? Theresa Trotter, MD, FRCPC Breast cancer is the most common malignancy affecting women in Canada, accounting for almost a third of
Cáncer de mama HER2+/RE+ vs HER2+/RE : Una misma enfermedad? Dra E. Ciruelos Departamento de Oncología Médica Hospital Universitario 12 de Octubre
 Cáncer de mama HER2+/RE+ vs HER2+/RE : Una misma enfermedad? Dra E. Ciruelos Departamento de Oncología Médica Hospital Universitario 12 de Octubre Recurrence of HER2-positive breast cancer (A) Time to
Cáncer de mama HER2+/RE+ vs HER2+/RE : Una misma enfermedad? Dra E. Ciruelos Departamento de Oncología Médica Hospital Universitario 12 de Octubre Recurrence of HER2-positive breast cancer (A) Time to
Dennis J Slamon, MD, PhD
 I N T E R V I E W Dennis J Slamon, MD, PhD Dr Slamon is Professor of Medicine, Chief of the Division of Hematology/Oncology and Director of Clinical and Translational Research at UCLA s David Geffen School
I N T E R V I E W Dennis J Slamon, MD, PhD Dr Slamon is Professor of Medicine, Chief of the Division of Hematology/Oncology and Director of Clinical and Translational Research at UCLA s David Geffen School
Extended Hormonal Therapy
 Extended Hormonal Therapy Dr. Caroline Lohrisch, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Optimal Endocrine Therapy for Women with Hormone Receptor Positive Early
Extended Hormonal Therapy Dr. Caroline Lohrisch, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Optimal Endocrine Therapy for Women with Hormone Receptor Positive Early
Clinico- Pathological Features And Out Come Of Triple Negative Breast Cancer
 Clinico- Pathological Features And Out Come Of Triple Negative Breast Cancer Dr. HassanAli Al-Khirsani, MBChB, CABM, F.I.C.M.S AL-Sadder teaching hospital, oncology unit Dr. Nasser Ghaly Yousif, MBChB,G.P.
Clinico- Pathological Features And Out Come Of Triple Negative Breast Cancer Dr. HassanAli Al-Khirsani, MBChB, CABM, F.I.C.M.S AL-Sadder teaching hospital, oncology unit Dr. Nasser Ghaly Yousif, MBChB,G.P.
Clinical Management Guideline for Breast Cancer
 Initial Evaluation Clinical Stage Pre-Treatment Evaluation Treatment and pathological stage Adjuvant Treatment Less than 4 positive lymph nodes ER Positive HER2 Negative (see page 2 & 3 ) Primary Diagnosis:
Initial Evaluation Clinical Stage Pre-Treatment Evaluation Treatment and pathological stage Adjuvant Treatment Less than 4 positive lymph nodes ER Positive HER2 Negative (see page 2 & 3 ) Primary Diagnosis:
Her 2 Positive Advanced Breast Cancer: From Evidence to Practice
 Her 2 Positive Advanced Breast Cancer: From Evidence to Practice Sunil Verma MD, FRCP(C) Medical Director, Tom Baker Cancer Center Professor and Head, Department of Oncology Cumming School of Medicine,
Her 2 Positive Advanced Breast Cancer: From Evidence to Practice Sunil Verma MD, FRCP(C) Medical Director, Tom Baker Cancer Center Professor and Head, Department of Oncology Cumming School of Medicine,
Intro to Cancer Therapeutics
 An Intro to Cancer Therapeutics Christopher R. Chitambar, MD Professor of Medicine Division of Hematology & Oncology Froedtert and Medical College of Wisconsin Clinical Cancer Center cchitamb@mcw.edu Intro
An Intro to Cancer Therapeutics Christopher R. Chitambar, MD Professor of Medicine Division of Hematology & Oncology Froedtert and Medical College of Wisconsin Clinical Cancer Center cchitamb@mcw.edu Intro
Best of San Antonio 2008
 Best of San Antonio 2008 Ellie Guardino, MD/PhD Assistant Professor Stanford University BIG 1 98: a randomized double blind phase III study evaluating letrozole and tamoxifen given in sequence as adjuvant
Best of San Antonio 2008 Ellie Guardino, MD/PhD Assistant Professor Stanford University BIG 1 98: a randomized double blind phase III study evaluating letrozole and tamoxifen given in sequence as adjuvant
Open Clinical Trials: What s Out There Now Paula D. Ryan, MD, PhD
 Open Clinical Trials: What s Out There Now Paula D. Ryan, MD, PhD Hanahan and Weinberg, 2000 Acquired Capabilities of Cancer Clinical Trials When should I consider a clinical trial? How do I find the right
Open Clinical Trials: What s Out There Now Paula D. Ryan, MD, PhD Hanahan and Weinberg, 2000 Acquired Capabilities of Cancer Clinical Trials When should I consider a clinical trial? How do I find the right
RESEARCH ARTICLE. Eight Year Survival Analysis of Patients with Triple Negative Breast Cancer in India
 APJCP.2016.17.6.2995 RESEARCH ARTICLE Eight Year Survival Analysis of Patients with Triple Negative Breast Cancer in India Dinesh Chandra Doval 1,2 *, P Suresh 1, Rupal Sinha 2, Saud Azam 2, Ullas Batra
APJCP.2016.17.6.2995 RESEARCH ARTICLE Eight Year Survival Analysis of Patients with Triple Negative Breast Cancer in India Dinesh Chandra Doval 1,2 *, P Suresh 1, Rupal Sinha 2, Saud Azam 2, Ullas Batra
Retrospective analysis to determine the use of tissue genomic analysis to predict the risk of recurrence in early stage invasive breast cancer.
 Retrospective analysis to determine the use of tissue genomic analysis to predict the risk of recurrence in early stage invasive breast cancer. Goal of the study: 1.To assess whether patients at Truman
Retrospective analysis to determine the use of tissue genomic analysis to predict the risk of recurrence in early stage invasive breast cancer. Goal of the study: 1.To assess whether patients at Truman
Kazuhiro Araki, Yasuo Miyoshi
 Editorial Abundant options to avoid toxicity and alternative strategies for human epidermal growth factor receptor 2-positive and hormone receptor-positive advanced breast cancer Kazuhiro Araki, Yasuo
Editorial Abundant options to avoid toxicity and alternative strategies for human epidermal growth factor receptor 2-positive and hormone receptor-positive advanced breast cancer Kazuhiro Araki, Yasuo
SYSTEMIC TREATMENT OF TRIPLE NEGATIVE BREAST CANCER
 SYSTEMIC TREATMENT OF TRIPLE NEGATIVE BREAST CANCER Sunil Shrestha 1*, Ji Yuan Yang, Li Shuang and Deepika Dhakal Clinical School of Medicine, Yangtze University, Jingzhou, Hubei Province, PR. China Department
SYSTEMIC TREATMENT OF TRIPLE NEGATIVE BREAST CANCER Sunil Shrestha 1*, Ji Yuan Yang, Li Shuang and Deepika Dhakal Clinical School of Medicine, Yangtze University, Jingzhou, Hubei Province, PR. China Department
Adjuvant therapy in early breast cancer
 Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Centro di Riferimento Regionale per la diagnosi e la terapia dei tumori del colon-retto. D.A. 26/10/2012 G.U.R.S. del 14/12/2012 parte I,
Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Centro di Riferimento Regionale per la diagnosi e la terapia dei tumori del colon-retto. D.A. 26/10/2012 G.U.R.S. del 14/12/2012 parte I,
Introduction. Wilfred Truin 1 Rudi M. H. Roumen. Vivianne C. G. Tjan-Heijnen 2 Adri C. Voogd
 Breast Cancer Res Treat (2017) 164:133 138 DOI 10.1007/s10549-017-4220-x EPIDEMIOLOGY Estrogen and progesterone receptor expression levels do not differ between lobular and ductal carcinoma in patients
Breast Cancer Res Treat (2017) 164:133 138 DOI 10.1007/s10549-017-4220-x EPIDEMIOLOGY Estrogen and progesterone receptor expression levels do not differ between lobular and ductal carcinoma in patients
4/13/2010. Silverman, Buchanan Breast, 2003
 Tailoring Breast Cancer Treatment: Has Personalized Medicine Arrived? Judith Luce, M.D. San Francisco General Hospital Avon Comprehensive Breast Care Center Outline First, treatment of DCIS Sorting risk
Tailoring Breast Cancer Treatment: Has Personalized Medicine Arrived? Judith Luce, M.D. San Francisco General Hospital Avon Comprehensive Breast Care Center Outline First, treatment of DCIS Sorting risk
Evolving Paradigms in HER2+ MBC: Strategies for Individualizing Therapy with Available Agents
 Evolving Paradigms in HER2+ MBC: Strategies for Individualizing Therapy with Available Agents Kimberly L. Blackwell MD Professor Department of Medicine and Radiation Oncology Duke University Medical Center
Evolving Paradigms in HER2+ MBC: Strategies for Individualizing Therapy with Available Agents Kimberly L. Blackwell MD Professor Department of Medicine and Radiation Oncology Duke University Medical Center
Role of Primary Resection for Patients with Oligometastatic Disease
 GBCC 2018, April 6, Songdo ConvensiA, Incheon, Korea Panel Discussion 4, How Can We Better Treat Patients with Metastatic Disease? Role of Primary Resection for Patients with Oligometastatic Disease Tadahiko
GBCC 2018, April 6, Songdo ConvensiA, Incheon, Korea Panel Discussion 4, How Can We Better Treat Patients with Metastatic Disease? Role of Primary Resection for Patients with Oligometastatic Disease Tadahiko
Breast : ASCO Abstracts for Review
 Breast : ASCO 2011 Susana Campos, MD, MPH Dana Farber Cancer Institute Abstracts for Review Prevention Neoadjuvant Metastatic Brain mets LBA 504: Exemestane for primary prevention of breast cancer in postmenopausal
Breast : ASCO 2011 Susana Campos, MD, MPH Dana Farber Cancer Institute Abstracts for Review Prevention Neoadjuvant Metastatic Brain mets LBA 504: Exemestane for primary prevention of breast cancer in postmenopausal
BREAST CANCER RISK REDUCTION (PREVENTION)
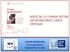 BREAST CANCER RISK REDUCTION (PREVENTION) Articles Anastrozole for prevention of breast cancer in high-risk postmenopausal women (IBIS-II): an international, double-blind, randomised placebo-controlled
BREAST CANCER RISK REDUCTION (PREVENTION) Articles Anastrozole for prevention of breast cancer in high-risk postmenopausal women (IBIS-II): an international, double-blind, randomised placebo-controlled
Delayed adjuvant tamoxifen: Ten-year results of a collaborative randomized controlled trial in early breast cancer (TAM-02 trial)
 Annals of Oncology 11: 515-519, 2000. 2000 Kluwer Academic Publishers. Printed in the Netherlands. Original article Delayed adjuvant tamoxifen: Ten-year results of a collaborative randomized controlled
Annals of Oncology 11: 515-519, 2000. 2000 Kluwer Academic Publishers. Printed in the Netherlands. Original article Delayed adjuvant tamoxifen: Ten-year results of a collaborative randomized controlled
Invasive Breast Cancer
 Invasive Breast Cancer Eileen Rakovitch MD MSc FRCPC Sunnybrook Health Sciences Centre Medical Director, Louise Temerty Breast Cancer Centre LC Campbell Chair in Breast Cancer Research Associate Professor,
Invasive Breast Cancer Eileen Rakovitch MD MSc FRCPC Sunnybrook Health Sciences Centre Medical Director, Louise Temerty Breast Cancer Centre LC Campbell Chair in Breast Cancer Research Associate Professor,
