GENETIC TESTING FOR HEREDITARY CANCER
|
|
|
- Emily Flynn
- 6 years ago
- Views:
Transcription
1 UnitedHealthcare Oxford Clinical Policy GENETIC TESTING FOR HEREDITARY CANCER Policy Number: DIAGNOSTIC T2 Effective Date: November 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE... 1 BENEFIT CONSIDERATIONS... 2 COVERAGE RATIONALE... 2 DEFINITIONS... 4 APPLICABLE CODES... 4 DESCRIPTION OF SERVICES... 5 CLINICAL EVIDENCE... 5 U.S. FOOD AND DRUG ADMINISTRATION... 6 REFERENCES... 6 POLICY HISTORY/REVISION INFORMATION... 7 Related Policy Preventive Care Services INSTRUCTIONS FOR USE This Clinical Policy provides assistance in interpreting Oxford benefit plans. Unless otherwise stated, Oxford policies do not apply to Medicare Advantage members. Oxford reserves the right, in its sole discretion, to modify its policies as necessary. This Clinical Policy is provided for informational purposes. It does not constitute medical advice. The term Oxford includes Oxford Health Plans, LLC and all of its subsidiaries as appropriate for these policies. When deciding coverage, the member specific benefit plan document must be referenced. The terms of the member specific benefit plan document [e.g., Certificate of Coverage (COC), Schedule of Benefits (SOB), and/or Summary Plan Description (SPD)] may differ greatly from the standard benefit plan upon which this Clinical Policy is based. In the event of a conflict, the member specific benefit plan document supersedes this Clinical Policy. All reviewers must first identify member eligibility, any federal or state regulatory requirements, and the member specific benefit plan coverage prior to use of this Clinical Policy. Other Policies may apply. UnitedHealthcare may also use tools developed by third parties, such as the MCG Care Guidelines, to assist us in administering health benefits. The MCG Care Guidelines are intended to be used in connection with the independent professional medical judgment of a qualified health care provider and do not constitute the practice of medicine or medical advice. CONDITIONS OF COVERAGE Applicable Lines of Business/ Products This policy applies to Oxford Commercial plan membership. Benefit Type General Benefits Package Referral Required No (Does not apply to non-gatekeeper products) Authorization Required Yes 1 (Precertification always required for inpatient admission) Precertification with Medical Director Review Required Yes 1 Applicable Site(s) of Service (If site of service is not listed, Medical Director review is required) Special Considerations Laboratory 1 Precertification with review by a Medical Director or their designee is required. Genetic Testing for Hereditary Cancer Page 1 of 9
2 BENEFIT CONSIDERATIONS Before using this policy, please check the member specific benefit plan document and any federal or state mandates, if applicable. Essential Health Benefits for Individual and Small Group For plan years beginning on or after January 1, 2014, the Affordable Care Act of 2010 (ACA) requires fully insured non-grandfathered individual and small group plans (inside and outside of Exchanges) to provide coverage for ten categories of Essential Health Benefits ( EHBs ). Large group plans (both self-funded and fully insured), and small group ASO plans, are not subject to the requirement to offer coverage for EHBs. However, if such plans choose to provide coverage for benefits which are deemed EHBs, the ACA requires all dollar limits on those benefits to be removed on all Grandfathered and Non-Grandfathered plans. The determination of which benefits constitute EHBs is made on a state by state basis. As such, when using this policy, it is important to refer to the member specific benefit plan document to determine benefit coverage. COVERAGE RATIONALE Genetic counseling is strongly recommended prior to these tests in order to inform persons being tested about the advantages and limitations of the test as applied to a unique person. Hereditary Breast and Ovarian Cancer (BRCA1/BRCA2) Genetic testing for BRCA1 and BRCA2 for individuals with a personal history of a related cancer is proven and medically necessary in the following situations: Women with a personal history of breast cancer in the following situations: o Breast cancer diagnosed at any age in an individual with at least one close (1st-, 2nd-, and 3rd-degree relative) blood relative who has a BRCA1 or BRCA2 mutation (testing should be targeted to the known BRCA1/BRCA2 mutation in the family. Further BRCA1/BRCA2 testing should only be pursued if the results are negative and the patient otherwise meets testing criteria) o Breast cancer diagnosed at any age in an individual from one of the following ethnic groups associated with founder mutations: Ashkenazi Jewish (Testing for Ashkenazi Jewish founder-specific mutations should be performed first. Further BRCA1/BRCA2 testing should only be pursued if the results are negative and the patient otherwise meets testing criteria without considering Ashkenazi Jewish ancestry.) Breast cancer diagnosed at age 45 or younger or triple-negative (Her2 negative, ER negative and PR negative) breast cancer diagnosed at age 60 or younger; or breast cancer diagnosed at age 50 or younger with: - Bilateral breast cancer; or - A personal history of a prior primary breast cancer diagnosis; or - At least one close blood relative with breast cancer; or - At least one close blood relative with pancreatic cancer; or - At least one close blood relative with prostate cancer; or - An unknown or limited family history (see Definitions section for further clarification of limited family history). o Breast cancer diagnosed at any age with: At least one close male blood relative with breast cancer diagnosed at any age; or At least one close blood relative with breast cancer diagnosed at age 50 or younger; or At least two close blood relatives on the same side of the family with breast cancer at any age; or At least one close blood relative with ovarian cancer at any age; or At least two close blood relatives on the same side of the family with pancreatic and/or prostate cancer at any age. o Metastatic breast cancer and may be a candidate for treatment with a PARP inhibitor (e.g., olaparib). Men with a personal history of breast cancer. Women with a personal history of ovarian cancer. Women and men with a personal history of pancreatic cancer at any age and at least one close blood relative with (a) ovarian cancer at any age or (b) breast cancer diagnosed with at age 50 or younger or (c) two relatives on the same side of the family with breast, pancreatic and/or prostate cancer at any age. Women and men with a personal history of pancreatic cancer and Ashkenazi Jewish ancestry. Testing should be targeted to the known Ashkenazi Jewish founder-specific mutations. Men with a personal history of high risk prostate cancer (Gleason score 7) at any age and o At least one close blood relative with ovarian cancer at any age or breast cancer ( age 50 years); or o At least two close relatives on the same side of the family with breast, pancreatic and/or prostate cancer at any age. Genetic Testing for Hereditary Cancer Page 2 of 9
3 Genetic testing for BRCA1 and BRCA2 for individuals without a personal history of a related cancer is proven and medically necessary in the following situations: When there is a known BRCA1/BRCA2 mutation in a close blood relative (defined as first-, second- or third-degree relative). Testing should be targeted to the known BRCA1/BRCA2 mutation in the family. Further BRCA1/BRCA2 testing should only be pursued if the results are negative and the patient otherwise meets other testing criteria. When there is at least one of the following familial risk factors: o At least one first- or second-degree blood relative meeting any of the above criteria for individuals with a personal history of a related cancer; or o At least one third-degree blood relative with breast cancer and/or ovarian cancer who has at least 2 close blood relatives with breast cancer (at least one with breast cancer at age 50 or younger) and/or ovarian cancer. Genetic testing for BRCA1 and/or BRCA2 testing is unproven and not medically necessary for all other indications including: Screening for breast or ovarian cancer risk for individuals not listed in the proven indications above; or For risk assessment of other cancers. Further evidence is needed to establish the clinical utility of testing in other populations. Multi-Gene Hereditary Cancer Panel Testing Criteria: Genetic testing with a multi-gene hereditary cancer panel in individuals with an indication for testing for hereditary breast and ovarian cancer is proven and medically necessary if all of the following criteria are met: The patient meets at least one of the criteria in Hereditary Breast and Ovarian Cancer (BRCA1/BRCA2) (see above section); and The patient has a family history or personal history that is strongly suggestive of more than one hereditary cancer syndrome; and The suspected hereditary cancer syndromes can be diagnosed by testing of one or more genes included in the specific hereditary cancer panel; and The results of testing the will directly impact this patient s medical management. Genetic testing with a multi-gene cancer panel in individuals with an indication for testing for hereditary colorectal cancer is proven and medically necessary in the following situations: The patient meets at least one of the following criteria for a hereditary colorectal cancer (Lynch) syndrome: o Men with a personal history of colorectal cancer or women with a personal history of colorectal or endometrial cancer diagnosed at age 49 or younger; or o Men with a personal history of colorectal cancer or women with a personal history of colorectal or endometrial cancer diagnosed at age 50 or later with at least one of the following criteria: A personal history of another cancer associated with Lynch Syndrome; or At least one first-degree relative with colorectal or endometrial cancer diagnosed at age 49 or younger; or At least two close relatives with a cancer associated with Lynch Syndrome; or Tumor testing results showing that their colorectal or endometrial cancer was MSI-high or had immunohistochemical (IHC) staining showing the absence of one or more mismatch repair proteins (MLH1, MSH2, MSH6 or PMS2); or PREMM 1,2,6 score of 5% or greater or o A personal history of colorectal polyposis with at least 10 adenomatous polyps; or o At least one close blood relative meeting the criteria for Lynch Syndrome (as defined in the first two criteria above) or with a clinical diagnosis of familial adenomatous polyposis in whom genetic testing was not or cannot be completed; or o PREMM5 score of 2.5% or greater or PREMM1, 2, 6 score of 5% or greater for having a Lynch syndrome gene mutation and The suspected hereditary cancer syndromes can be diagnosed by testing of one or more genes included in the specific hereditary cancer panel; and The results of testing the will directly impact this patient s medical management. Genetic testing with a multi-gene hereditary cancer panel in individuals without an indication for testing for hereditary breast and ovarian cancer or colorectal cancer is proven and medically necessary in the following situations: The patient has a family history or personal history that is strongly suggestive of more than one hereditary cancer syndrome; and The suspected hereditary cancer syndromes can be diagnosed by testing of one or more genes included in the specific hereditary cancer panel; and Genetic Testing for Hereditary Cancer Page 3 of 9
4 The results of testing the will directly impact this patient s medical management. Genetic testing with a multi-gene cancer panel is proven and medically necessary in a patient who has previously tested negative (indeterminate) for the high penetrance genes that are most likely to explain the personal or family history of cancer (e.g., BRCA1/2 for breast cancer and ovarian cancer)in the following situations: The patient s personal and family history remains strongly suggestive of an inherited susceptibility that can be diagnosed by testing of one or more genes included in the specific hereditary cancer panel; and The results of testing the will directly impact this patient s medical management. Multi-gene hereditary cancer panels are unproven and not medically necessary for all other indications. DEFINITIONS 1 st, 2 nd and 3 rd Degree Relatives: Blood relatives on the same side of the family (maternal or paternal). 1st-degree relatives are parents, siblings and children 2nd-degree relatives are grandparents, aunts, uncles, nieces, nephews, grandchildren and half-siblings 3rd-degree relatives are great-grandparents, great-aunts, great-uncles, great-grandchildren and first cousins PREMM (PREdiction Model for gene Mutations): The PREMM model estimates the overall cumulative probability of having an MLH1, MSH2, MSH6, PMS2, and EPCAM gene mutation. APPLICABLE CODES The following list(s) of procedure and/or diagnosis codes is provided for reference purposes only and may not be all inclusive. Listing of a code in this policy does not imply that the service described by the code is a covered or noncovered health service. Benefit coverage for health services is determined by the member specific benefit plan document and applicable laws that may require coverage for a specific service. The inclusion of a code does not imply any right to reimbursement or guarantee claim payment. Other Policies may apply. CPT Code Description BRCA1, BRCA2 (breast cancer 1 and 2) (e.g., hereditary breast and ovarian cancer) gene analysis; full sequence analysis and full duplication/deletion analysis BRCA1, BRCA2 (breast cancer 1 and 2) (e.g., hereditary breast and ovarian cancer) gene analysis; full sequence analysis and common duplication/deletion variants in BRCA1 (i.e., exon 13 del 3.835kb, exon 13 dup 6kb, exon del 26kb, exon 22 del 510bp, exon 8-9 del 7.1kb) BRCA1, BRCA2 (breast cancer 1 and 2) (e.g., hereditary breast and ovarian cancer) gene analysis; 185delAG, 5385insC, 6174delT variants BRCA1, BRCA2 (breast cancer 1 and 2) (e.g., hereditary breast and ovarian cancer) gene analysis; uncommon duplication/deletion variants BRCA1 (breast cancer 1) (e.g., hereditary breast and ovarian cancer) gene analysis; full sequence analysis and common duplication/deletion variants (i.e., exon 13 del 3.835kb, exon 13 dup 6kb, exon del 26kb, exon 22 del 510bp, exon 8-9 del 7.1kb) BRCA1 (breast cancer 1) (e.g., hereditary breast and ovarian cancer) gene analysis; known familial variant BRCA2 (breast cancer 2) (e.g., hereditary breast and ovarian cancer) gene analysis; full sequence analysis BRCA2 (breast cancer 2) (e.g., hereditary breast and ovarian cancer) gene analysis; known familial variant Hereditary breast cancer-related disorders (e.g., hereditary breast cancer, hereditary ovarian cancer, hereditary endometrial cancer); genomic sequence analysis panel, must include sequencing of at least 14 genes, including ATM, BRCA1, BRCA2, BRIP1, CDH1, MLH1, MSH2, MSH6, NBN, PALB2, PTEN, RAD51C, STK11, and TP53 Hereditary breast cancer-related disorders (e.g., hereditary breast cancer, hereditary ovarian cancer, hereditary endometrial cancer); duplication/deletion analysis panel, must include analyses for BRCA1, BRCA2, MLH1, MSH2, and STK11 CPT is a registered trademark of the American Medical Association Genetic Testing for Hereditary Cancer Page 4 of 9
5 DESCRIPTION OF SERVICES The National Comprehensive Cancer Network (NCCN) guidelines on genetic/familial high-risk assessment for breast and ovarian cancer state that significant limitations of interpreting test results for an individual without a cancer diagnosis should be discussed. If there are no living family members with breast or ovarian cancer available for testing, consider testing family members affected with other cancers associated with BRCA1/BRCA2, such as prostate cancer (Gleason score 7), pancreatic cancer or melanoma. Testing of individuals without a cancer diagnosis should only be considered when there is no affected family member available for testing. (NCCN, 2016) Genetic testing for hereditary cancer susceptibility is used to predict an individual's risk of cancer development in the future. It has been estimated that 5-10% of all cancers are hereditary (the result of inherited genetic susceptibility). Hereditary Breast and Ovarian Cancer (BRCA1/BRCA2) Breast cancer is the second most common cause of cancer-related deaths among women. The inherited tendency to develop breast and ovarian cancer has been termed the hereditary breast and ovarian cancer syndrome (HBOC). Mutation in either of two genes, BRCA1 and BRCA2, has been associated with an increased risk for breast cancer and ovarian cancer. A deleterious mutation in either gene may be inherited from either parent; and later an acquired mutation of the other allele can lead to cancer development. It has been estimated that inherited BRCA1 and BRCA2 mutations account for 5 to 10 percent of breast cancers and 10 to 15 percent of ovarian cancers among white women in the United States. (National Cancer Institute [NCI], 2015) Harmful BRCA1 mutation may also increase a woman s risk of developing other cancers. Men with a harmful BRCA1 mutation also have an increased risk of breast cancer and, possibly, of pancreatic cancer, testicular cancer, and earlyonset prostate cancer. However, male breast cancer, pancreatic cancer, and prostate cancer appear to be more strongly associated with BRCA2 gene mutation. (Thompson and Eaton, 2002; NCCN, 2017) Multi-Gene Hereditary Cancer Panels Multi-gene hereditary cancer panels using next generation sequencing technology are currently available, and many different test panels are marketed commercially, most of which also include large deletion/duplication analysis. These panels are intuitively attractive because they can rapidly test for numerous mutations both within a single gene and across multiple genes related to increased cancer risks. It is also possible that these multi-gene tests can, in the case of families where more than one hereditary cancer syndrome is suspected, be performed more cost effectively than stepwise individual gene testing. However, many of these panel tests also include low to moderate-risk genes that may result in the identification of gene mutations that are of unclear clinical significance or which would not clearly direct a patient s medical management recommendations. Identification of mutations for which the clinical management is uncertain may lead to unnecessary follow-up testing and procedures, all of which have their own inherent risks. (NCCN, 2016; LaDuca et al., 2014; Robson et al., 2015; Kurian et al., 2014; Tung et al., 2015; Plon et al., 2011) CLINICAL EVIDENCE Hereditary Breast and Ovarian Cancer (BRCA1/BRCA2) National Comprehensive Cancer Network (NCCN) guidelines present specific criteria for genetic testing for hereditary breast and/or ovarian cancer syndrome. The guidelines address genetic risk assessment, counseling, testing and management based on test results. (NCCN, 2016) Several studies have shown that BRCA1 breast cancer is more likely to be characterized as triple- negative. Studies have reported BRCA1 mutations in 9-28% of patients with triple- negative breast cancer. In addition, it appears that among patients with triple-negative disease, BRCA mutation carriers were diagnosed at a younger age compared with non-carriers. (NCCN, 2016) In a Cochrane systematic review, Hilgart et al. (2012) evaluated the impact of cancer genetic risk-assessment services on patients at risk of familial breast cancer. In this update, the authors included five new trials, bringing the total number of included studies to eight. The included trials provided data on 1973 participants and assessed the impact of cancer genetic risk assessment on outcomes including perceived risk of inherited cancer, and psychological distress. The review suggests that cancer genetic risk-assessment services help to reduce distress, improve the accuracy of the perceived risk of breast cancer and increase knowledge about breast cancer and genetics. The review found favorable outcomes for patients after risk assessment for familial breast cancer. Genetic Testing for Hereditary Cancer Page 5 of 9
6 Professional Societies American College of Obstetricians and Gynecologists (ACOG) In a 2009 practice bulletin (reaffirmed 2015), the ACOG recommended criteria for genetic risk assessment of hereditary breast and ovarian cancer syndrome (HBOC). These recommendations conclude: BRCA positive women should be offered salpingo-oophorectomy by age 40 or when childbearing is completed. For a risk reducing bilateral salpingo-oophorectomy, all tissue from the ovaries and fallopian tubes should be removed. Thorough visualization of the peritoneal surfaces with pelvic washings should be performed. Complete, serial sectioning of the ovaries and fallopian tubes is necessary, with microscopic examination for occult cancer. Genetic risk assessment is recommended for patients with a greater than an approximate 20-25% chance of having an inherited predisposition to breast cancer and ovarian cancer. This includes women with the following: o A close relative (mother, sister, daughter, grandmother, granddaughter, aunt or niece) with a known BRCA mutation o Personal history of both breast and ovarian cancer o Ovarian cancer and a close relative with ovarian cancer or premenopausal breast cancer or both o Ovarian cancer and Ashkenazi Jewish ancestry o Breast cancer by age 40 years and Ashkenazi Jewish ancestry o Breast cancer by age 50 years and a close relative with ovarian cancer or male breast cancer American Society of Clinical Oncology (ASCO) An ASCO policy statement recommends that genetic testing for cancer susceptibility be performed when the following three criteria are met: the individual being tested has a personal or family history suggestive of genetic cancer susceptibility; the test can be adequately interpreted; and the test results have accepted clinical utility. (Robson et al., 2015) National Society of Genetic Counselors (NSGC) The NSGC recommends that genetic testing be performed in the context of an informed decision-making process. (Berliner et al., 2013) The process of cancer risk assessment and genetic counseling for hereditary breast and ovarian cancer syndrome requires many steps, including the following: Gathering personal medical and family history data Psychosocial assessment Discussion of cancer and mutation risk and how personalized risk estimates are derived Facilitation of the informed consent process through discussion of the risks, benefits, limitations, and likelihood of identifying a mutation with genetic susceptibility testing Results disclosure (if applicable) Discussion of medical management options Review of issues related to genetic discrimination U.S. FOOD AND DRUG ADMINISTRATION (FDA) Laboratories that perform genetic tests are regulated under the Clinical Laboratory Improvement Amendments (CLIA) Act of More information is available at: (Accessed June 29, 2017) REFERENCES The foregoing Oxford policy has been adapted from an existing UnitedHealthcare national policy that was researched, developed and approved by UnitedHealthcare Medical Technology Assessment Committee. [2017T0009V] American College of Obstetricians and Gynecologists. Practice Bulletin number 103. Hereditary breast and ovarian cancer syndrome. Obstetrics and Gynecology April 2009: 113: Reaffirmed 2013, Berliner JL, Fay AM, Cummings SA, et al. National Society of Genetic Counselors (NSGC) practice guideline: risk assessment and genetic counseling for hereditary breast and ovarian cancer. J Genet Couns Apr;22(2): Hilgart JS, Coles B, Iredale R. Cancer genetic risk assessment for individuals at risk of familial breast cancer. Cochrane Database Syst Rev Feb 15;2:CD Kurian AW, Hare EE, Mills MA, et al. Clinical evaluation of a multiple-gene sequencing panel for hereditary cancer risk assessment. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2014;32(19): LaDuca H, Stuenkel AJ, Dolinsky JS, et al. Utilization of multigene panels in hereditary cancer predisposition testing: analysis of more than 2,000 patients. Genet Med Nov;16(11): Genetic Testing for Hereditary Cancer Page 6 of 9
7 National Cancer Institute. (NCI). NCI Fact Sheet: BRCA1 and BRCA2: Cancer Risk and Genetic Testing. Available at: Accessed June 27, National Comprehensive Cancer Network (NCCN). Clinical Practice Guidelines in Oncology. Genetic/familial high-risk assessment: breast and ovarian. Version December 7, Plon SE, Cooper HP, Parks B, et al. Genetic testing and cancer risk management recommendations by physicians for at-risk relatives. Genetics in medicine: official journal of the American College of Medical Genetics. 2011;13(2): Robson ME, Bradbury AR, Arun B, et al. American Society of Clinical Oncology policy statement update: genetic and genomic testing for cancer susceptibility. J Clin Oncol Nov 1;33(31): Thompson D, Easton DF, Breast Cancer Linkage Consortium. Cancer incidence in BRCA1 mutation carriers. J Natl Cancer Inst Sep 18;94(18): Tung N, Battelli C, Allen B, et al. Frequency of mutations in individuals with breast cancer referred for BRCA1 and BRCA2 testing using next-generation sequencing with a 25-gene panel. Cancer. 2015;121(1): POLICY HISTORY/REVISION INFORMATION Date 11/01/2017 Action/Description Changed policy title; previously titled Genetic Testing for Hereditary Breast and/or Ovarian Cancer Syndrome (HBOC) Updated list of related policies; added reference link to policy titled Preventive Care Services Revised conditions of coverage/authorization requirements; removed language pertaining to CPT code and HCPCS code S0265 Reformatted and revised coverage rationale: o Removed definitions and corresponding notations o Removed language pertaining to medical necessity review and documentation requirements for genetic counseling o Added language to indicate genetic counseling is strongly recommended prior to [genetic testing] in order to inform persons being tested about the advantages and limitations of the test as applied to a unique person o Updated coverage guidelines for Hereditary Breast and Ovarian Cancer (BRCA1/BRCA2): Removed language indicating: - Comprehensive BRCA1/BRCA2 genetic testing includes sequencing of both BRCA1 and BRCA2 genes and analysis for large genomic rearrangements, either concurrently or sequentially; NCCN guidelines emphasize the need for comprehensive testing for individuals who meet the testing criteria for BRCA1/BRCA2 and have no known familial BRCA1/BRCA2 mutations who have undergone accurate risk assessment and genetic counseling - NCCN guidelines state that significant limitations of interpreting test results for an individual without a cancer diagnosis should be discussed: If there are no living family members with breast or ovarian cancer available for testing, consider testing family members affected with other cancers associated with BRCA1/BRCA2, such as prostate cancer (Gleason score 7), pancreatic cancer or melanoma Testing of individuals without a cancer diagnosis should only be considered when there is no affected family member available for testing Added language to indicate genetic testing for BRCA1 and BRCA2 is proven and medically necessary for women with a personal history of metastatic breast cancer and may be a candidate for treatment with a PARP inhibitor (e.g., olaparib) o Added coverage guidelines for Multi-Gene Hereditary Cancer Panel Testing to indicate: Genetic testing with a multi-gene hereditary cancer panel in individuals with an indication for testing for hereditary breast and ovarian cancer is proven and medically necessary if all of the following criteria are met: - The patient meets at least one of the criteria in Hereditary Breast and Genetic Testing for Hereditary Cancer Page 7 of 9
8 Date Action/Description Ovarian Cancer (BRCA1/BRCA2) section of the policy; and - The patient has a family history or personal history that is strongly suggestive of more than one hereditary cancer syndrome; and - The suspected hereditary cancer syndromes can be diagnosed by testing of one or more genes included in the specific hereditary cancer panel; and - The results of testing the will directly impact this patient s medical management Genetic testing with a multi-gene cancer panel in individuals with an indication for testing for hereditary colorectal cancer is proven and medically necessary in the following situations: - The patient meets at least one of the following criteria for a hereditary colorectal cancer (Lynch) syndrome: Men with a personal history of colorectal cancer or women with a personal history of colorectal or endometrial cancer diagnosed at age 49 or younger; or Men with a personal history of colorectal cancer or women with a personal history of colorectal or endometrial cancer diagnosed at age 50 or later with at least one of the following criteria: o A personal history of another cancer associated with Lynch Syndrome; or o At least one first-degree relative with colorectal or endometrial cancer diagnosed at age 49 or younger; or o At least two close relatives with a cancer associated with Lynch Syndrome; or o Tumor testing results showing that their colorectal or endometrial cancer was MSI-high or had immunohistochemical (IHC) staining showing the absence of one or more mismatch repair proteins (MLH1, MSH2, MSH6 or PMS2); or o PREMM 1,2,6 score of 5% or greater or A personal history of colorectal polyposis with at least 10 adenomatous polyps; or At least one close blood relative meeting the criteria for Lynch Syndrome (as defined in the first two criteria above) or with a clinical diagnosis of familial adenomatous polyposis in whom genetic testing was not or cannot be completed; or PREMM5 score of 2.5% or greater or PREMM1,2,6 score of 5% or greater for having a Lynch Syndrome gene mutation and - The suspected hereditary cancer syndromes can be diagnosed by testing of one or more genes included in the specific hereditary cancer panel; and - The results of testing the will directly impact this patient s medical management Genetic testing with a multi-gene hereditary cancer panel in individuals without an indication for testing for hereditary breast and ovarian cancer or colorectal cancer is proven and medically necessary in the following situations: - The patient has a family history or personal history that is strongly suggestive of more than one hereditary cancer syndrome; and - The suspected hereditary cancer syndromes can be diagnosed by testing of one or more genes included in the specific hereditary cancer panel; and - The results of testing the will directly impact this patient s medical management Genetic testing with a multi-gene cancer panel is proven and medically necessary in a patient has previously tested negative (indeterminate) for the high penetrance genes that are most likely to explain the personal or family history of cancer (e.g., BRCA1/2 for breast cancer and ovarian cancer) in the following situations: Genetic Testing for Hereditary Cancer Page 8 of 9
9 Date Action/Description - The patient s personal and family history remains strongly suggestive of an inherited susceptibility that can be diagnosed by testing of one or more genes included in the specific hereditary cancer panel; and - The results of testing the will directly impact this patient s medical management Multi-gene hereditary cancer panels are unproven and not medically necessary for all other indications Updated definitions: o Revised definition of 1 st, 2 nd, and 3 rd degree relatives (relocated from Coverage Rationale section of the policy) o Added definition of PREMM (prediction model for gene mutations) Updated list of applicable CPT codes; removed Removed list of applicable HCPCS codes: S0265 Updated supporting information to reflect the most current description of services, clinical evidence, FDA information, and references Archived previous policy version DIAGNOSTIC T2 Genetic Testing for Hereditary Cancer Page 9 of 9
Genetic Testing for BRCA1 and BRCA2 Genes
 Genetic Testing for BRCA1 and BRCA2 Genes MP9478 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below Pre and post-test genetic counseling
Genetic Testing for BRCA1 and BRCA2 Genes MP9478 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below Pre and post-test genetic counseling
Genetic Testing for BRCA1 and BRCA2 Genes
 Genetic Testing f BRCA1 and BRCA2 Genes MP9478 Covered Service: Pri Authization Required: Additional Infmation: Yes when meets criteria below Yes--as shown below Pre and post-test genetic counseling is
Genetic Testing f BRCA1 and BRCA2 Genes MP9478 Covered Service: Pri Authization Required: Additional Infmation: Yes when meets criteria below Yes--as shown below Pre and post-test genetic counseling is
Corporate Medical Policy Genetic Testing for Breast and Ovarian Cancer
 Corporate Medical Policy Genetic Testing for Breast and Ovarian Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_breast_and_ovarian_cancer 8/1997 8/2017
Corporate Medical Policy Genetic Testing for Breast and Ovarian Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_breast_and_ovarian_cancer 8/1997 8/2017
HYSTERECTOMY FOR BENIGN CONDITIONS
 HYSTERECTOMY FOR BENIGN CONDITIONS UnitedHealthcare Oxford Clinical Policy Policy Number: SURGERY 104.7 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
HYSTERECTOMY FOR BENIGN CONDITIONS UnitedHealthcare Oxford Clinical Policy Policy Number: SURGERY 104.7 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER BRCA1 BRCA2
 GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER BRCA1 BRCA2 Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific
GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER BRCA1 BRCA2 Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific
Medical Policy Manual. Topic: Genetic Testing for Hereditary Breast and/or Ovarian Cancer. Date of Origin: January 27, 2011
 Medical Policy Manual Topic: Genetic Testing for Hereditary Breast and/or Ovarian Cancer Date of Origin: January 27, 2011 Section: Genetic Testing Last Reviewed Date: July 2014 Policy No: 02 Effective
Medical Policy Manual Topic: Genetic Testing for Hereditary Breast and/or Ovarian Cancer Date of Origin: January 27, 2011 Section: Genetic Testing Last Reviewed Date: July 2014 Policy No: 02 Effective
GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER SYNDROME BRCA1 BRCA2
 SYNDROME BRCA1 BRCA2 Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
SYNDROME BRCA1 BRCA2 Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Policy Specific Section: Medical Necessity and Investigational / Experimental. October 15, 1997 October 9, 2013
 Medical Policy Genetic Testing for Hereditary Breast and/or Ovarian Cancer Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date:
Medical Policy Genetic Testing for Hereditary Breast and/or Ovarian Cancer Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date:
Policy and Procedure. Department: Utilization Management. SNP, CHP, MetroPlus Gold, Goldcare I&II, Market Plus, Essential, HARP
 Retired Date: Page 1 of 9 1. POLICY DESCRIPTION: BRCA 1&2 Genetic Testing 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management, Pharmacy, Claim
Retired Date: Page 1 of 9 1. POLICY DESCRIPTION: BRCA 1&2 Genetic Testing 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management, Pharmacy, Claim
MEDICAL POLICY Genetic Testing for Breast and Ovarian Cancers
 POLICY: PG0067 ORIGINAL EFFECTIVE: 07/30/02 LAST REVIEW: 01/25/18 MEDICAL POLICY Genetic Testing for Breast and Ovarian Cancers GUIDELINES This policy does not certify benefits or authorization of benefits,
POLICY: PG0067 ORIGINAL EFFECTIVE: 07/30/02 LAST REVIEW: 01/25/18 MEDICAL POLICY Genetic Testing for Breast and Ovarian Cancers GUIDELINES This policy does not certify benefits or authorization of benefits,
PROVIDER POLICIES & PROCEDURES
 PROVIDER POLICIES & PROCEDURES BRCA GENETIC TESTING The purpose of this document is to assist providers enrolled in the Connecticut Medical Assistance Program (CMAP) with the information needed to support
PROVIDER POLICIES & PROCEDURES BRCA GENETIC TESTING The purpose of this document is to assist providers enrolled in the Connecticut Medical Assistance Program (CMAP) with the information needed to support
HYSTERECTOMY FOR BENIGN CONDITIONS
 UnitedHealthcare Commercial Medical Policy HYSTERECTOMY FOR BENIGN CONDITIONS Policy Number: 2018T0572G Effective Date: September 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
UnitedHealthcare Commercial Medical Policy HYSTERECTOMY FOR BENIGN CONDITIONS Policy Number: 2018T0572G Effective Date: September 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
Hereditary Breast and Ovarian Cancer Rebecca Sutphen, MD, FACMG
 Hereditary Breast and Ovarian Cancer 2015 Rebecca Sutphen, MD, FACMG Among a consecutive series of 11,159 women requesting BRCA testing over one year, 3874 responded to a mailed survey. Most respondents
Hereditary Breast and Ovarian Cancer 2015 Rebecca Sutphen, MD, FACMG Among a consecutive series of 11,159 women requesting BRCA testing over one year, 3874 responded to a mailed survey. Most respondents
BRCA Precertification Information Request Form
 BRCA Precertification Information Request Form Failure to complete this form in its entirety may result in the delay of review. Fax to: BRCA Precertification Department Fax number: 1-860-975-9126 Section
BRCA Precertification Information Request Form Failure to complete this form in its entirety may result in the delay of review. Fax to: BRCA Precertification Department Fax number: 1-860-975-9126 Section
MP Genetic Testing for BRCA1 or BRCA2 for Hereditary Breast/Ovarian Cancer Syndrome and Other High-Risk Cancers
 Medical Policy MP 2.04.02 Genetic Testing for BRCA1 or BRCA2 for Hereditary Breast/Ovarian Cancer Syndrome and Other High-Risk BCBSA Ref. Policy: 2.04.02 Last Review: 11/15/2018 Effective Date: 02/15/2019
Medical Policy MP 2.04.02 Genetic Testing for BRCA1 or BRCA2 for Hereditary Breast/Ovarian Cancer Syndrome and Other High-Risk BCBSA Ref. Policy: 2.04.02 Last Review: 11/15/2018 Effective Date: 02/15/2019
Prior Authorization. Additional Information:
 Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
A Patient s Guide to Hereditary Cancer. Is Hereditary Cancer Testing Right for You?
 A Patient s Guide to Hereditary Cancer Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer. This is
A Patient s Guide to Hereditary Cancer Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer. This is
CLINICAL MEDICAL POLICY
 Policy Name: Policy Number: Responsible Department(s): CLINICAL MEDICAL POLICY BRCA1 and BRCA2 Genetic Mutation Testing and Related Genetic Counseling MP-011-MD-DE Medical Management Provider Notice Date:
Policy Name: Policy Number: Responsible Department(s): CLINICAL MEDICAL POLICY BRCA1 and BRCA2 Genetic Mutation Testing and Related Genetic Counseling MP-011-MD-DE Medical Management Provider Notice Date:
MEDICAL POLICY SUBJECT: GENETIC TESTING FOR HEREDITARY BRCA MUTATIONS. POLICY NUMBER: CATEGORY: Laboratory Test
 MEDICAL POLICY SUBJECT: GENETIC TESTING FOR HEREDITARY BRCA MUTATIONS POLICY NUMBER: 2.02.06 CATEGORY: Laboratory Test EFFECTIVE DATE: 01/17/02 REVISED DATE: 08/21/03, 09/16/04, 08/18/05, 06/15/06, 04/17/14,
MEDICAL POLICY SUBJECT: GENETIC TESTING FOR HEREDITARY BRCA MUTATIONS POLICY NUMBER: 2.02.06 CATEGORY: Laboratory Test EFFECTIVE DATE: 01/17/02 REVISED DATE: 08/21/03, 09/16/04, 08/18/05, 06/15/06, 04/17/14,
Primary Care Approach to Genetic Cancer Syndromes
 Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 BRCA1 and BRCA2 Testing Page 1 of 33 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: BRCA1 and BRCA2 Testing Pre-Determination of Services IS REQUIRED by the Member
BRCA1 and BRCA2 Testing Page 1 of 33 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: BRCA1 and BRCA2 Testing Pre-Determination of Services IS REQUIRED by the Member
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 BRCA1 and BRCA2 Testing Page 1 of 26 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: BRCA1 and BRCA2 Testing Pre-Determination of Services IS REQUIRED by the Member
BRCA1 and BRCA2 Testing Page 1 of 26 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: BRCA1 and BRCA2 Testing Pre-Determination of Services IS REQUIRED by the Member
Be Ready Pack Learn more about how Myriad myrisk is revolutionizing hereditary cancer testing.
 Be Ready Pack Learn more about how Myriad myrisk is revolutionizing hereditary cancer testing. Hereditary cancer and you Approximately 5% to 10% of all cancers develop because a person inherited a genetic
Be Ready Pack Learn more about how Myriad myrisk is revolutionizing hereditary cancer testing. Hereditary cancer and you Approximately 5% to 10% of all cancers develop because a person inherited a genetic
6/8/17. Genetics 101. Professor, College of Medicine. President & Chief Medical Officer. Hereditary Breast and Ovarian Cancer 2017
 Genetics 101 Hereditary Breast and Ovarian Cancer 2017 Rebecca Sutphen, MD, FACMG Professor, College of Medicine President & Chief Medical Officer INVASIVE CANCER GENETICALLY ALTERED CELL HYPERPLASIA DYSPLASIA
Genetics 101 Hereditary Breast and Ovarian Cancer 2017 Rebecca Sutphen, MD, FACMG Professor, College of Medicine President & Chief Medical Officer INVASIVE CANCER GENETICALLY ALTERED CELL HYPERPLASIA DYSPLASIA
So, now, that we have reviewed some basics of cancer genetics I will provide an overview of some common syndromes.
 Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Myriad Financial Assistance Program (MFAP)
 Myriad Financial Assistance Program (MFAP) MEDICAL CRITERIA Hereditary Cancer Products The Myriad Financial Assistance Program offers aid to patients who meet specific financial and medical requirements.
Myriad Financial Assistance Program (MFAP) MEDICAL CRITERIA Hereditary Cancer Products The Myriad Financial Assistance Program offers aid to patients who meet specific financial and medical requirements.
The benefit of. knowing. Genetic testing for hereditary cancer. A patient support guide
 The benefit of knowing Genetic testing for hereditary cancer A patient support guide Does cancer run in your family? Cancer is more common in some families. Sometimes cancer is caused by a change in a
The benefit of knowing Genetic testing for hereditary cancer A patient support guide Does cancer run in your family? Cancer is more common in some families. Sometimes cancer is caused by a change in a
Genetic Determinants, Risk Assessment and Management
 Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
Genetic Testing for Lynch Syndrome
 Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post-test genetic counseling is
Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post-test genetic counseling is
Re: NC Medicaid and NC Health Choice Program coverage of genetic testing for susceptibility to breast and ovarian cancer
 March 23, 2018 North Carolina (NC) Division of Medical Assistance (DMA), Clinical Policy Section C/O Pam Greeson, BSN, RN-C, pam.greeson@dhhs.nc.gov Nurse Consultant, Division of Medical Assistance Practitioners,
March 23, 2018 North Carolina (NC) Division of Medical Assistance (DMA), Clinical Policy Section C/O Pam Greeson, BSN, RN-C, pam.greeson@dhhs.nc.gov Nurse Consultant, Division of Medical Assistance Practitioners,
MAGNETIC RESONANCE IMAGING (MRI) AND COMPUTED TOMOGRAPHY (CT) SCAN SITE OF CARE
 UnitedHealthcare Commercial Utilization Review Guideline MAGNETIC RESONANCE IMAGING (MRI) AND COMPUTED TOMOGRAPHY (CT) SCAN SITE OF CARE Guideline Number: URG-13.01 Effective Date: February 1, 2019 Table
UnitedHealthcare Commercial Utilization Review Guideline MAGNETIC RESONANCE IMAGING (MRI) AND COMPUTED TOMOGRAPHY (CT) SCAN SITE OF CARE Guideline Number: URG-13.01 Effective Date: February 1, 2019 Table
WHAT IS A GENE? CHROMOSOME DNA PROTEIN. A gene is made up of DNA. It carries instructions to make proteins.
 WHAT IS A GENE? CHROMOSOME E GEN DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME E GEN DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
Sporadic Cancer - Cancer which occurs by chance. People with sporadic cancer typically do not have relatives with the same type of cancer.
 to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer testing is right for you and should be reviewed with a trained healthcare
to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer testing is right for you and should be reviewed with a trained healthcare
Does Cancer Run in Your Family?
 Does Cancer Run in Your Family? A Patient s Guide to Hereditary Breast and Ovarian Cancer Syndrome What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that
Does Cancer Run in Your Family? A Patient s Guide to Hereditary Breast and Ovarian Cancer Syndrome What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that
Importance of Family History in Gynecologic Cancer Prevention. Objectives. Genetic Counselors. Angela Thompson, MS, CGC
 Importance of Family History in Gynecologic Cancer Prevention Angela Thompson, MS, CGC Genetic Counselor Froedtert & The Medical College of Wisconsin Objectives Introduce role of genetic counselor Discuss
Importance of Family History in Gynecologic Cancer Prevention Angela Thompson, MS, CGC Genetic Counselor Froedtert & The Medical College of Wisconsin Objectives Introduce role of genetic counselor Discuss
Utilization of BRCA Testing. Breast and Ovarian Cancer in Texas
 Utilization of BRCA Testing in Older Ode Women with Breast and Ovarian Cancer in Texas Ana M. Rodriguez, MD Assistant Professor Department of Obstetrics and Gynecology University of Texas Medical Branch
Utilization of BRCA Testing in Older Ode Women with Breast and Ovarian Cancer in Texas Ana M. Rodriguez, MD Assistant Professor Department of Obstetrics and Gynecology University of Texas Medical Branch
Assessment and Management of Genetic Predisposition to Breast Cancer. Dr Munaza Ahmed Consultant Clinical Geneticist 2/7/18
 Assessment and Management of Genetic Predisposition to Breast Cancer Dr Munaza Ahmed Consultant Clinical Geneticist 2/7/18 Overview The role of the Cancer Genetics team NICE guidelines for Familial Breast
Assessment and Management of Genetic Predisposition to Breast Cancer Dr Munaza Ahmed Consultant Clinical Geneticist 2/7/18 Overview The role of the Cancer Genetics team NICE guidelines for Familial Breast
Yes when meets criteria below. Dean Health Plan covers when Medicare also covers the benefit.
 Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Genetic Testing for Lynch Syndrome MP9487 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below Pre and post test genetic counseling is
Applies to: All Aetna plans, except Traditional Choice plans. All Innovation Health plans, except indemnity plans
 BRCA Precertification Information Request Form Applies to: All Aetna plans, except Traditional Choice plans All Innovation Health plans, except indemnity plans All Health benefits and health insurance
BRCA Precertification Information Request Form Applies to: All Aetna plans, except Traditional Choice plans All Innovation Health plans, except indemnity plans All Health benefits and health insurance
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian
 Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
A guide to genetic testing for hereditary cancers
 Cancer Testing Solutions A guide to genetic testing for hereditary cancers The benefit of knowing TM Hereditary cancer genetic testing can play a critical role in managing health Cancer touches millions
Cancer Testing Solutions A guide to genetic testing for hereditary cancers The benefit of knowing TM Hereditary cancer genetic testing can play a critical role in managing health Cancer touches millions
Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP)
 Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP) A Patient s Guide to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary
Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP) A Patient s Guide to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary
Breast Cancer Risk Assessment: Genetics, Risk Models, and Screening. Amie Hass, MSN, ARNP, FNP-BC Hall-Perrine Cancer Center
 Breast Cancer Risk Assessment: Genetics, Risk Models, and Screening Amie Hass, MSN, ARNP, FNP-BC Hall-Perrine Cancer Center Disclosure- I DO NOT HAVE any relevant financial interest with any entity producing,
Breast Cancer Risk Assessment: Genetics, Risk Models, and Screening Amie Hass, MSN, ARNP, FNP-BC Hall-Perrine Cancer Center Disclosure- I DO NOT HAVE any relevant financial interest with any entity producing,
WHAT IS A GENE? CHROMOSOME DNA PROTEIN. A gene is made up of DNA. It carries instructions to make proteins.
 WHAT IS A GENE? CHROMOSOME GENE DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME GENE DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
Reference #: SYS-PC-VPCI-CG-002. Origination Date: June 2012 Next Review Date: April 2019 Effective Date: April 2016
 Oncology Service Line-Allina Health System-wide Consensus Guidelines: Identification of Breast Cancer Patients at Risk for Inherited Cancer Risks These guidelines apply to clinical interventions that have
Oncology Service Line-Allina Health System-wide Consensus Guidelines: Identification of Breast Cancer Patients at Risk for Inherited Cancer Risks These guidelines apply to clinical interventions that have
Genetic Risk Assessment for Cancer
 Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor/Cancer Risk Counselor Banner Good Samaritan Cancer Screening & Prevention Program Objectives Describe the role
Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor/Cancer Risk Counselor Banner Good Samaritan Cancer Screening & Prevention Program Objectives Describe the role
So how much of breast and ovarian cancer is hereditary? A). 5 to 10 percent. B). 20 to 30 percent. C). 50 percent. Or D). 65 to 70 percent.
 Welcome. My name is Amanda Brandt. I am one of the Cancer Genetic Counselors at the University of Texas MD Anderson Cancer Center. Today, we are going to be discussing how to identify patients at high
Welcome. My name is Amanda Brandt. I am one of the Cancer Genetic Counselors at the University of Texas MD Anderson Cancer Center. Today, we are going to be discussing how to identify patients at high
HBOC Syndrome A review of BRCA 1/2 testing, Cancer Risk Assessment, Counseling and Beyond.
 HBOC Syndrome A review of BRCA 1/2 testing, Cancer Risk Assessment, Counseling and Beyond. Conni Murphy, ARNP Cancer Risk Assessment and Genetics Program Jupiter Medical Center Learning Objectives Identify
HBOC Syndrome A review of BRCA 1/2 testing, Cancer Risk Assessment, Counseling and Beyond. Conni Murphy, ARNP Cancer Risk Assessment and Genetics Program Jupiter Medical Center Learning Objectives Identify
Hereditary Cancer Products
 Hereditary Products Integrated BRACAnalysis (BRCA1 and BRCA2 sequencing and large rearrangement testing (BART)), covered when: PERSONAL HISTORY of Breast (must meet at least 1) Diagnosed
Hereditary Products Integrated BRACAnalysis (BRCA1 and BRCA2 sequencing and large rearrangement testing (BART)), covered when: PERSONAL HISTORY of Breast (must meet at least 1) Diagnosed
Hereditary Cancer Risk Assessment for Gynecological Cancers. FarrNezhatMD.com
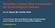 Hereditary Cancer Risk Assessment for Gynecological Cancers FarrNezhatMD.com Image credit: PLOS blogs 5-10% hereditary 10-20% 70-80% sporadic Genetic Changes and Cancer Cancer begins with a genetic
Hereditary Cancer Risk Assessment for Gynecological Cancers FarrNezhatMD.com Image credit: PLOS blogs 5-10% hereditary 10-20% 70-80% sporadic Genetic Changes and Cancer Cancer begins with a genetic
patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations MARCH 2015
 patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations MARCH 2015 BRCA1 and BRCA2 Mutations Cancer is a complex disease thought to be caused by several different factors. A few types of cancer
patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations MARCH 2015 BRCA1 and BRCA2 Mutations Cancer is a complex disease thought to be caused by several different factors. A few types of cancer
Policy #: 259 Latest Review Date: November 2009
 Name of Policy: Prophylactic Oophorectomy Policy #: 259 Latest Review Date: November 2009 Category: Surgery Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates.
Name of Policy: Prophylactic Oophorectomy Policy #: 259 Latest Review Date: November 2009 Category: Surgery Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates.
Why Test for Hereditary Cancer in Preventive Care?
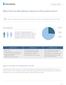 Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
Genetics and Cancer Care. Cynthia Forster-Gibson, MD, PhD and Loren Mackay- Loder, MSc Genetics Program, THP
 Genetics and Cancer Care Cynthia Forster-Gibson, MD, PhD and Loren Mackay- Loder, MSc Genetics Program, THP Faculty/Presenter Disclosure Faculty: Cynthia Forster-Gibson Relationships with commercial interests:
Genetics and Cancer Care Cynthia Forster-Gibson, MD, PhD and Loren Mackay- Loder, MSc Genetics Program, THP Faculty/Presenter Disclosure Faculty: Cynthia Forster-Gibson Relationships with commercial interests:
The Next Generation of Hereditary Cancer Testing
 The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
Genetic Risk Assessment for Cancer
 Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor Banner MD Anderson Cancer Center Objectives Describe the role of genetic counseling and genetic testing in patient
Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor Banner MD Anderson Cancer Center Objectives Describe the role of genetic counseling and genetic testing in patient
Identification of patients suggestive of hereditary breast and ovarian cancer syndrome that warrants further professional evaluation.
 Allina Breast Program Committee Consensus Guidelines These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes are not clearly desirable to all patients Identification
Allina Breast Program Committee Consensus Guidelines These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes are not clearly desirable to all patients Identification
Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP)
 Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP) A Patient s Guide to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary
Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP) A Patient s Guide to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary
A Patient s Guide to. Hereditary Ovarian Cancer: Is Hereditary Cancer Testing Right for You?
 A Patient s Guide to Hereditary Ovarian Cancer: Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer.
A Patient s Guide to Hereditary Ovarian Cancer: Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer.
BUPRENORPHINE (PROBUPHINE & SUBLOCADE )
 UnitedHealthcare Oxford Clinical Policy BUPRENORPHINE (PROBUPHINE & SUBLOCADE ) Policy Number: PHARMACY 291.6 T2 Effective Date: July 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS
UnitedHealthcare Oxford Clinical Policy BUPRENORPHINE (PROBUPHINE & SUBLOCADE ) Policy Number: PHARMACY 291.6 T2 Effective Date: July 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer
 GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
Genetic Testing: who, what, why?
 Genetic Testing: who, what, why? Gina Westhoff MD LMG Gynecologic Oncology March 16, 2019 Disclosures Speaker for Merck (unrelated to today s topic) Objectives Determine who should undergo genetic risk
Genetic Testing: who, what, why? Gina Westhoff MD LMG Gynecologic Oncology March 16, 2019 Disclosures Speaker for Merck (unrelated to today s topic) Objectives Determine who should undergo genetic risk
BUPRENORPHINE (PROBUPHINE & SUBLOCADE )
 UnitedHealthcare Oxford Clinical Policy BUPRENORPHINE (PROBUPHINE & SUBLOCADE ) Policy Number: PHARMACY 291.5 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS
UnitedHealthcare Oxford Clinical Policy BUPRENORPHINE (PROBUPHINE & SUBLOCADE ) Policy Number: PHARMACY 291.5 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS
The Genetics of Breast and Ovarian Cancer Prof. Piri L. Welcsh
 The Genetics of Breast Piri L. Welcsh, PhD Research Assistant Professor University of Washington School of Medicine Division of Medical Genetics 1 Genetics of cancer All cancers arise from genetic and
The Genetics of Breast Piri L. Welcsh, PhD Research Assistant Professor University of Washington School of Medicine Division of Medical Genetics 1 Genetics of cancer All cancers arise from genetic and
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document.
 MRI OF THE BREAST Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
MRI OF THE BREAST Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Corporate Medical Policy
 Corporate Medical Policy Moderate Penetrance Variants Associated with Breast Cancer in File Name: Origination: Last CAP Review: Next CAP Review: Last Review: moderate_penetrance_variants_associated_with_breast_cancer_
Corporate Medical Policy Moderate Penetrance Variants Associated with Breast Cancer in File Name: Origination: Last CAP Review: Next CAP Review: Last Review: moderate_penetrance_variants_associated_with_breast_cancer_
PROVIDER POLICIES & PROCEDURES
 PROVIDER POLICIES & PROCEDURES GENETIC CANCER SUSCEPTIBILITY PANELS USING NEXT GENERATION SEQUENCING The purpose of this document is to assist providers enrolled in the Connecticut Medical Assistance Program
PROVIDER POLICIES & PROCEDURES GENETIC CANCER SUSCEPTIBILITY PANELS USING NEXT GENERATION SEQUENCING The purpose of this document is to assist providers enrolled in the Connecticut Medical Assistance Program
patient education Fact Sheet
 patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations OCTOBER 2017 BRCA1 and BRCA2 Mutations Cancer is caused by several different factors. A few types of cancer run in families. These types are
patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations OCTOBER 2017 BRCA1 and BRCA2 Mutations Cancer is caused by several different factors. A few types of cancer run in families. These types are
Hereditary Aspects of Pancreatic Cancer
 Pancreatic Cancer Seminar San Francisco, CA Hereditary Aspects of Pancreatic Cancer Genetic Risk Assessment and Counseling for Familial Pancreatic Cancer February 3, 2016 Amie Blanco, MS, CGC Gordon and
Pancreatic Cancer Seminar San Francisco, CA Hereditary Aspects of Pancreatic Cancer Genetic Risk Assessment and Counseling for Familial Pancreatic Cancer February 3, 2016 Amie Blanco, MS, CGC Gordon and
Learn your genetic risk for the most common hereditary cancers.
 Learn your genetic risk for the most common hereditary cancers. color.com Color analyzes 30 genes including BRCA1 and BRCA2 to help women and men understand their risk for the most common hereditary cancers,
Learn your genetic risk for the most common hereditary cancers. color.com Color analyzes 30 genes including BRCA1 and BRCA2 to help women and men understand their risk for the most common hereditary cancers,
GENETIC MANAGEMENT OF A FAMILY HISTORY OF BREAST AND / OR OVARIAN CANCER. Dr Abhijit Dixit. Family Health Clinical Genetics
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF BREAST AND / OR OVARIAN CANCER Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review
GENETIC MANAGEMENT OF A FAMILY HISTORY OF BREAST AND / OR OVARIAN CANCER Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review
Clinical Policy Title: Genetic testing for breast and ovarian cancer
 Clinical Policy Title: Genetic testing for breast and ovarian cancer Clinical Policy Number: 02.01.02 Effective Date: September 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: May
Clinical Policy Title: Genetic testing for breast and ovarian cancer Clinical Policy Number: 02.01.02 Effective Date: September 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: May
Germline Testing for Hereditary Cancer with Multigene Panel
 Germline Testing for Hereditary Cancer with Multigene Panel Po-Han Lin, MD Department of Medical Genetics National Taiwan University Hospital 2017-04-20 Disclosure No relevant financial relationships with
Germline Testing for Hereditary Cancer with Multigene Panel Po-Han Lin, MD Department of Medical Genetics National Taiwan University Hospital 2017-04-20 Disclosure No relevant financial relationships with
Genetic Screening Visit
 Before your visit In a typical hereditary breast ovarian cancer genetic counsling visit be prepared to answer the following set of questions, please check were applicable. About your self (same questions
Before your visit In a typical hereditary breast ovarian cancer genetic counsling visit be prepared to answer the following set of questions, please check were applicable. About your self (same questions
THE MODERN GYNECOLOGIC EXAMINATION & SCREENING FOR GYNECOLOGIC MALIGNANCIES
 THE MODERN GYNECOLOGIC EXAMINATION & SCREENING FOR GYNECOLOGIC MALIGNANCIES Denise Uyar, MD Associate Professor OB/GYN Chief Gynecologic Oncology Medical College of Wisconsin April 12, 2019 NO DISCLOSURES
THE MODERN GYNECOLOGIC EXAMINATION & SCREENING FOR GYNECOLOGIC MALIGNANCIES Denise Uyar, MD Associate Professor OB/GYN Chief Gynecologic Oncology Medical College of Wisconsin April 12, 2019 NO DISCLOSURES
Use of panel tests in place of single gene tests in the cancer genetics clinic
 Clin Genet 2015: 88: 278 282 Printed in Singapore. All rights reserved CLINICAL GENETICS doi: 10.1111/cge.12488 Short Report se of panel tests in place of single gene tests in the cancer genetics clinic
Clin Genet 2015: 88: 278 282 Printed in Singapore. All rights reserved CLINICAL GENETICS doi: 10.1111/cge.12488 Short Report se of panel tests in place of single gene tests in the cancer genetics clinic
Eligibility criteria for prophylactic treatment allowance
 Eligibility criteria for prophylactic treatment allowance Southern Cross will only pay the prophylactic treatment allowance for the following healthcare services when the applicable eligibility criteria
Eligibility criteria for prophylactic treatment allowance Southern Cross will only pay the prophylactic treatment allowance for the following healthcare services when the applicable eligibility criteria
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017
 Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
OvaNext. patient guide. genetic testing for hereditary breast, ovarian, and uterine cancer
 patient guide OvaNext genetic testing for hereditary breast, ovarian, and uterine cancer Because knowing your risk can mean early detection and prevention About half of the women diagnosed with uterine
patient guide OvaNext genetic testing for hereditary breast, ovarian, and uterine cancer Because knowing your risk can mean early detection and prevention About half of the women diagnosed with uterine
PANNICULECTOMY AND BODY CONTOURING PROCEDURES
 Oxford UnitedHealthcare Oxford Clinical Policy PANNICULECTOMY AND BODY CONTOURING PROCEDURES Policy Number: SURGERY 038.24 T2 Effective Date: October 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
Oxford UnitedHealthcare Oxford Clinical Policy PANNICULECTOMY AND BODY CONTOURING PROCEDURES Policy Number: SURGERY 038.24 T2 Effective Date: October 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
GYNplus. genetic testing for hereditary ovarian and/or uterine cancer
 GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
POSITIVE DELETERIOUS MUTATION
 Understanding Your Genetic Test Result Positive for a Deleterious or Suspected Deleterious POSITIVE DELETERIOUS MUTATION This workbook is designed to help you understand the results of your genetic test
Understanding Your Genetic Test Result Positive for a Deleterious or Suspected Deleterious POSITIVE DELETERIOUS MUTATION This workbook is designed to help you understand the results of your genetic test
Genetic Testing for Hereditary Cancer Susceptibility Syndromes
 Medical Coverage Policy Genetic Testing for Hereditary Cancer Susceptibility Syndromes Table of Contents Effective Date... 1/15/2018 Next Review Date... 7/15/2018 Coverage Policy Number... 0518 Related
Medical Coverage Policy Genetic Testing for Hereditary Cancer Susceptibility Syndromes Table of Contents Effective Date... 1/15/2018 Next Review Date... 7/15/2018 Coverage Policy Number... 0518 Related
Prior Authorization. Additional Information:
 Genetic Testing for Cowden Syndrome - PTEN Gene MP9488 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below Pre and post-test genetic
Genetic Testing for Cowden Syndrome - PTEN Gene MP9488 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below Pre and post-test genetic
Hereditary Breast and Ovarian Cancer Screening & Genetic Counseling
 Hereditary Breast and Ovarian Cancer Screening & Genetic Counseling Cecelia Bellcross, PhD, MS, CGC Emory University School of Medicine Department of Human Genetics The First Line of Defense February 21,
Hereditary Breast and Ovarian Cancer Screening & Genetic Counseling Cecelia Bellcross, PhD, MS, CGC Emory University School of Medicine Department of Human Genetics The First Line of Defense February 21,
patient guide BreastNext genetic testing for hereditary breast cancer Because knowing your risk can mean early detection and prevention
 patient guide BreastNext genetic testing for hereditary breast cancer Because knowing your risk can mean early detection and prevention Know the Basics Breast cancer is the most common cancer in women
patient guide BreastNext genetic testing for hereditary breast cancer Because knowing your risk can mean early detection and prevention Know the Basics Breast cancer is the most common cancer in women
The impact of hereditary breast and ovarian cancer (HBOC) syndrome testing on patient management and your practice
 The impact of hereditary breast and ovarian cancer (HBOC) syndrome testing on patient management and your practice Use BRACAnalysis as a guide in your medical and surgical management BRACAnalysis testing
The impact of hereditary breast and ovarian cancer (HBOC) syndrome testing on patient management and your practice Use BRACAnalysis as a guide in your medical and surgical management BRACAnalysis testing
Carol Christianson, MS, CGC Genetic Counselor West Michigan Cancer Center
 Carol Christianson, MS, CGC Genetic Counselor West Michigan Cancer Center Following this presentation you will be able to: Identify cancer survivors in your practice who might benefit from genetic counseling
Carol Christianson, MS, CGC Genetic Counselor West Michigan Cancer Center Following this presentation you will be able to: Identify cancer survivors in your practice who might benefit from genetic counseling
Page 1 of 8 TABLE OF CONTENTS
 Page 1 of 8 TABLE OF CONTENTS Patient Evaluation and Recommendation..Page 2 Testing and Follow-up..Page 3 Genetic Counseling Referral Criteria.....Page 4-5 Patient Education..Page 6 Suggested Readings...Page
Page 1 of 8 TABLE OF CONTENTS Patient Evaluation and Recommendation..Page 2 Testing and Follow-up..Page 3 Genetic Counseling Referral Criteria.....Page 4-5 Patient Education..Page 6 Suggested Readings...Page
Cancer Survivorship Symposium Cancer and Heredity January 16, Jeanne P. Homer, MS Licensed Certified Genetic Counselor
 Cancer Survivorship Symposium Cancer and Heredity January 16, 2017 Jeanne P. Homer, MS Licensed Certified Genetic Counselor Outline Cancer and Heredity Hereditary Cancer Risk Assessment & Genetic testing
Cancer Survivorship Symposium Cancer and Heredity January 16, 2017 Jeanne P. Homer, MS Licensed Certified Genetic Counselor Outline Cancer and Heredity Hereditary Cancer Risk Assessment & Genetic testing
Integrating Clinical Genomics and Cancer Care. Maria Blazo, M.D. Division Director, Clinical Genetics September 9, 2017
 Integrating Clinical Genomics and Cancer Care Maria Blazo, M.D. Division Director, Clinical Genetics September 9, 2017 Precision Medicine Initiative Genomic and Precision Medicine: The Future is Now 1
Integrating Clinical Genomics and Cancer Care Maria Blazo, M.D. Division Director, Clinical Genetics September 9, 2017 Precision Medicine Initiative Genomic and Precision Medicine: The Future is Now 1
Objectives. Genetics in Cancer Treatment and Prevention. Genes
 Objectives Genetics in Cancer Treatment and Prevention Cheryl LaFlore, ARNP, MSN, BC Understand how to integrate genetic and genomic information into oncology nursing practice Define the role of an oncology
Objectives Genetics in Cancer Treatment and Prevention Cheryl LaFlore, ARNP, MSN, BC Understand how to integrate genetic and genomic information into oncology nursing practice Define the role of an oncology
DENOSUMAB (PROLIA & XGEVA )
 DENOSUMAB (PROLIA & XGEVA ) UnitedHealthcare Oxford Clinical Policy Policy Number: PHARMACY 306.3 T2 Effective Date: July 2, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
DENOSUMAB (PROLIA & XGEVA ) UnitedHealthcare Oxford Clinical Policy Policy Number: PHARMACY 306.3 T2 Effective Date: July 2, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
GeneticsNow TM. A Guide to Testing Hereditary Conditions in Women & Men. Patient & Physician Information
 GeneticsNow TM A Guide to Testing Hereditary Conditions in Women & Men Patient & Physician Information How can BRCA status affect your health? Everyone has BRCA1 and BRCA2 genes. However, sometimes the
GeneticsNow TM A Guide to Testing Hereditary Conditions in Women & Men Patient & Physician Information How can BRCA status affect your health? Everyone has BRCA1 and BRCA2 genes. However, sometimes the
Understanding Your Genetic Test Result. Positive for a Deleterious Mutation or Suspected Deleterious
 Understanding Your Genetic Test Result Positive for a Deleterious Mutation or Suspected Deleterious This workbook is designed to help you understand the results of your genetic test and is best reviewed
Understanding Your Genetic Test Result Positive for a Deleterious Mutation or Suspected Deleterious This workbook is designed to help you understand the results of your genetic test and is best reviewed
Result Navigator Positive Test Result: MSH6
 Result Navigator Positive Test Result: MSH6 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Result Navigator Positive Test Result: MSH6 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
MEDICAL POLICY SUBJECT: GENETIC TESTING FOR SUSCEPTIBILITY TO HEREDITARY CANCERS EFFECTIVE DATE: 06/19/14, 09/15/15.
 MEDICAL POLICY SUBJECT: GENETIC TESTING FOR SUSCEPTIBILITY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY SUBJECT: GENETIC TESTING FOR SUSCEPTIBILITY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
