Transcervical extended mediastinal lymphadenectomy (TEMLA) for staging of non-small-cell lung cancer (NSCLC)
|
|
|
- Tobias Spencer
- 6 years ago
- Views:
Transcription
1 PRACA ORYGINALNA Marcin Zieliński 1, Łukasz Hauer 1, Jolanta Hauer 1, Juliusz Pankowski 2, Artur Szlubowski 3, Tomasz Nabiałek 3 1 Department of Thoracic Surgery, Pulmonary Hospital, Zakopane, Poland 2 Department of Anesthesiology and Intensive Care, Pulmonary Hospital, Zakopane, Poland 3 Department of Pathology, Pulmonary Hospital, Zakopane, Poland Transcervical extended mediastinal lymphadenectomy (TEMLA) for staging of non-small-cell lung cancer (NSCLC) Abstract Introduction: The aim of the study is to analyze diagnostic yield of the new surgical technique the Transcervical Extended Mediastinal Lymphadenectomy (TEMLA) in preoperative staging of Non-Small-Cell Lung Cancer (NSCLC). Material and methods: Operative technique included 5 8 cm collar incision in the neck, elevation of the sternal manubrium with a special retractor, bilateral visualization of the laryngeal recurrent and vagus nerves and dissection of all mediastinal nodal stations except of the pulmonary ligament nodes (station 9). Results: 698 patients (577 men, 121 women), of mean age 62.8 (41 79) were operated on from to , including 501 squamous-cell carcinomas, 144 adenocarcinomas, 25 large cell carcinomas and 28 others. Mean operative time was 128 min. (45 to 330 min.) and min. in the last 100 patients. 30-day mortality was 0.7% (unrelated causes) and morbidity 6.6%. The mean number of dissected nodes during TEMLA was 37.9 (15 to 85). Metastatic N2 and N3 nodes were found in 152/698 (21.8%) and 26/698 patients (3.7%), respectively. Subsequent thoracotomy was performed in 445/ 513 patients (86.7%) after negative result of TEMLA. During thoracotomy, omitted N2 was found in 7/445 (1.6%) patients. Sensitivity of TEMLA in discovery of N2 3 nodes was 96.2%, specificity was 100%, accuracy was 99,0%, Negative Predictive Value (NPV) was 98.7% and Positive Predictive Value (PPV) was 100%. Conclusions: TEMLA is a new minimally invasive surgical procedure providing unique possibility to perform very extensive, bilateral mediastinal lymphadenectomy with very high diagnostic yield in staging of NSCLC Key words: lung cancer, mediastinum, lymph nodes Pneumonol. Alergol. Pol. 2011; 79, 3: Introduction The results of treatment of lung cancer are still highly unsatisfactory. The most successful modality in the treatment of Non-Small-Cell Lung Cancer (NSCLC) is surgery, which effectiveness is strongly correlated with stage of the disease. The patients with stage I NSCLC can expect 50 80% 5-year survival rate and the patients with stage II disease can expect 30 50% 5 year survival rate [1, 2]. In stage II and IIIA disease, confirmed pathologically, adjuvant chemotherapy is currently used, with expected 5 15% improvement in 5-year survival rates [2, 3]. In patients with stage IIIA discovered preoperatively neoadjuvant chemotherapy or chemoradiotherapy is usually proposed. According to the current American College of Chest Physicians (ACCP) recommendations published in 2007, both neoadjuvant and adjuvant therapy for stage IIIA are not standard modalities but should undergo evaluation in further clinical trials [3]. In stage IIIB the main treatment modality is chemoradiotherapy and in stage IV chemotherapy, proposed in both cases to the patients in good general state, in the rest of the patients only supportive care is given [4, 5]. The role of diagnostics is to discover NSCLC and its earliest clinical stage, which is a base for optimal choice for therapy for the individual pa- Corresponding author: Marcin Zieliński MD, PhD, ul. Gładkie 1, Zakopane, Poland, phone: , fax: , marcinz@mp.pl Received: 15 November 2010 r. Copyright 2011 Via Medica ISSN
2 Marcin Zieliński et al., Transcervical extended mediastinal lymphadenectomy (TEMLA) tient. Mediastinal staging plays a central role in the optimal choice of the most suitable treatment modality for patients with NSCLC [6, 7]. Classic technique of Computer Tomography of the Chest (Chest CT) is currently regarded insufficiently accurate and was supplemented with Positron Emission Tomography with Computer Tomography (PET/ CT) and endoscopic techniques, including Endobronchial Ultrasonography with Transbronchial Fine Needle Biopsy (EBUS/TBNA) and Endoesophageal Ultrasonography and Fine Needle Aspiration (EUS/FNA) have been developed [7 10]. EBUS and EUS, especially when used in combination (combined EBUS/EUS CUS) can reach a diagnostic sensitivity and specificity of 90% and enable a real time, ultrasonography guided biopsing of the mediastinal nodes [11 13]. EUS enables also visualization of infiltration of the esophagus, the trachea and bronchi, the aorta, the left atrium and the Superior Vena Cava [12 14]. However, invasive techniques remain a gold standard. During the last two decades the well established techniques of cervical mediastinoscopy and anterior mediastinotomy were supplemented with new introduced techniques of videomediastinoscopy, Videothoracoscopy (VTS), anterior mediastinotomy, Video-Assisted Mediastinoscopic Lymphadenectomy (VAMLA) introduced by Martin Hurtgen (Koblenz, Germany) and Transcervical Extended Mediastinal Lymphadenectomy (TEMLA) introduced by the first author of this article (MZ) [7, 15 17]. In this article, the technique and results of TEMLA will be presented for the first time in the Polish literature. The aim of the study is to analyze diagnostic yield of the new surgical technique the Transcervical Extended Mediastinal Lymphadenectomy (TEMLA) in preoperative staging of Non-Small-Cell Lung Cancer (NSCLC). Surgical technique of TEMLA Figure 1. Dissection of the right laryngeal recurrent nerve (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal Lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery, doi: / /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) Figure 2. Dissection of the left laryngeal recurrent nerve. To expose the nerve, the vascularized fascial layers covering the nerve must be divided (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) The operation starts from the 5 to 8 cm collar incision in the neck. Subplatysmal flaps are widely dissected for better exposure of the mediastinum during the procedure. Visualization of both laryngeal recurrent nerves is obligatory in every case (Fig. 1, 2). The left recurrent nerve is especially endangered during the procedure, so it must be dissected very delicately and carefully protected from injury. Circumferential dissection of the nerve is not advisable, in our opinion it increases the risk of injury of the nerve. Preservation of the last layer of fascia covering the nerve is preferable. The detailed technique of visualization of the laryngeal recurrent nerves was described elsewhere [18]. Both vagus nerves must also be found. The vagus nerve lies between the carotid arteries and internal jugular veins (Fig. 3). The vagus nerves are the important landmarks for further dissection in the mediastinum. Elevation of the sternal manubrium with a hook connected to the frame mounted on the ope- 197
3 Pneumonologia i Alergologia Polska 2011, vol. 79, no 3, pages Figure 3. Dissection of the right vagus nerve (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal Lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery, doi: / /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) rative table is a critically important part of the procedure (Rochard frame, modified Munster system, Aesculap-Chifa, Poland). Elevation of the sternum widens access to the mediastinum from the neck and enables reaching the deeply located mediastinal structures. During TEMLA all mediastinal nodal stations except for the pulmonary ligament nodes (station 9 according to the Mountain-Dresler Classification) are removed [19, 20]. Generally, most part of TEMLA is an open procedure, with exception of dissection of the subcarinal (station 7), periesophageal (station 8) and the left lower paratracheal (station 4L) nodes which are dissected in the mediastinoscopy-assisted fashion with aid of Linder-Dahan two-blade mediastinoscope (Richard Wolf, Knittlingen, Germany). The paraaortic, station 6 and aorta-pulmonary window, station 5 nodes are sometimes dissected with aid of videothoracoscope introduced to the mediastinum through the operative wound. An attempt should be made to remove en-bloc the nodes with the surrounding fatty tissue. Only the left paratracheal (station 4L) nodes are removed individually, due to close proximity of the left recurrent nerve. Bilateral supraclavicular lymphadenectomy and even deep cervical lymph node dissection is possible during TEMLA through the same incision. The mediastinal dissection begins from removal of the highest mediastinal, station 1 lymph nodes lying above the left innominate vein. Resection of the upper poles of the thymus at the level Figure 4. Dissection of the highest mediastinal nodes (station 1) (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal Lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery, doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) Figure 5. Dissection of the the upper paratracheal nodes (station 2R) from the ascending aorta, the azygos vein, the trachea and the right main bronchus (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal Lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery, oi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) of the left innominate vein improves access to the mediastinum (Fig. 4). The next step is a dissection of the right paratracheal space, which proceeds along the posterior wall of the Superior Vena Cava until the azygos vein becomes visible. Right upper paratracheal, station 2R nodes located above the apex of the aortic arch and below the left innominate vein are dissected and removed (Fig. 5). 198
4 Marcin Zieliński et al., Transcervical extended mediastinal lymphadenectomy (TEMLA) The right lower paratracheal, station 4R nodes are dissected from the trachea, right main bronchus, Superior Vena Cava, the azygos vein, the ascending aorta and the right mediastinal pleura (Fig. 6). Very occasionally, retrotracheal, station 3P nodes are found and removed (Fig. 7). We never found any metastatic lymph node in this station. In the right sided tumors the next step is a dissection of the prevascular, station 3A nodes, located in front of the Superior Vena Cava, right to the ascending aorta (Fig. 8). This station is never involved in the left sided tumors. In our opinion, dissection of the left paratracheal nodes is the most difficult and risky part of TEMLA, because these nodes lie in the close proximity to the left recurrent nerve (Fig. 9). Generally, the left upper paratracheal, station 2L nodes lie in front of the nerve and the left lower, station 4L nodes lie behind the nerve (Fig. 10). The subcarinal and periesophageal nodes (stations 7 Figure 6. Dissection of the the lower paratracheal nodes (station 4R) from the ascending aorta, the azygos vein, the trachea and the right main bronchus (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) Figure 8. Dissection and removal of the prevascular nodes (station 3A) (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal Lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery, doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) Figure 7. Dissection and removal of the retrotracheal nodes (station 3P) (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) Figure 9. Dissection and removal of the left upper paratracheal nodes (station 2L) (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) 199
5 Pneumonologia i Alergologia Polska 2011, vol. 79, no 3, pages Figure 10. Dissection and removal of the left lower paratracheal nodes (station 4L) (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal Lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery, doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) Figure 11. View of the subcarinal region after removal of the subcarinal (station 7) and the periesophageal (station 8 nodes) (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal Lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery, doi: / /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) Figure 12. Division of the lascial layer between the left carotid artery and the left innominate vein creates entrance to the pulmonary artery window space (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal Lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery, doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) and 8) are dissected with aid of Linder-Dahan mediastinoscope. During dissection of the subcarinal, station 7 nodes the fascial layer covering the nodes must but divided. Usually, one or several prominent bronchial arteries crossing the operating field must be coagulated with harmonic knife or bipolar coagulation or clipped and divided because they hamper further dissection. The subcarinal nodes must be dissected from the trachea, main bronchi (laterally), the esophagus (posteriorly) and the main pulmonary arteries (anteriorly). After completion of this part of the operation the tracheal bifurcation, both main bronchi, both pulmonary arteries, pericardium covering the left atrium, the right superior pulmonary vein and the right upper lobe bronchus become clearly visible (Fig. 11). In majority of patients, but not in all patients, the periesophageal, station 8 nodes are found and removed. The limited length of the Linder-Dahan mediastinoscope precludes possibility of removal of the pulmonary ligament (station 9) nodes. Dissection of the station 4L nodes is performed in the mediastinoscopy-assisted fashion after completion of the dissection of stations 7 and 8, with the mediastinoscope withdrawed from the subcarinal area and introduced along the left main bronchus. The entrance to the aorta-pulmonary window containing stations 6 and 5 lie between the left innominate vein and the left carotid artery. The left vagus nerve is a landmark of dissection. Division of the fascial layer between the left carotid artery and the left innominate vein facilitates the entrance to the aorta-pulmonary window (Fig. 12). At first, the adipose tissue is dissected from the wall of the ascending aorta down to the level of the left pulmonary artery with a peanut sponge (Fig. 13). Medial retraction of the ascending aorta is a safe maneuver facilitating access to the aortapulmonary window. 200
6 Marcin Zieliński et al., Transcervical extended mediastinal lymphadenectomy (TEMLA) Figure 13. Entrance to the left paraaortic space containing the paraaortic (station 6) and the aorta-pulmonary window (station 5) nodes (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) Figure 14. View of the aorta-pulmonary window area after dissection of the station 5 and station 6 nodes (reproduced from Zieliński M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal Lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery, doi: /mmcts , with permission from the European Association of Cardio-thoracic Surgery. Copyright 2005) The whole fatty tissue from the aorta-pulmonary window space is removed. Any blood vessel crossing the space is clipped and divided. Dissection proceeds along the left vagus nerve. The fatty tissue is then dissected from the left mediastinal pleura until the clear pleura and the underlying left lung become well visible and removed enbloc with the surrounding fatty tissue (Fig. 14). Left pulmonary artery, the left phrenic nerve and the left superior pulmonary vein are well visible after completion of dissection. Coagulation and division of the hemiazygos accessory vein crossing the operative field is sometimes necessary. In case of opening of the mediastinal pleura there is no need for drainage of the mediastinum. Insertion of the piece of fibrin sponge and hyperinflation of the lungs during closure of the wound with high End-Expiratory Pressures that is all what is necessary in such patients, without the need of drainage of the pleural cavity. Currently, the indications for TEMLA in NSCLC in our department include preoperative staging of potentially operable patients after negative results of prior EBUS/TBNA and EUS/FNA, regardless of the mediastinal nodal status on Computer Tomography (CT) and Positron Emission Tomography/Computer Tomography (PET/CT). Results TEMLA was performed on 698 patients, 577 men and 121 women in age (mean age 62.8) from to There were 501 squamous-cell carcinomas, 144 adenocarcinomas, 25 large cell carcinomas and 28 others. Time of operation was 50 to 330 min. (mean 128 min.). In the last 100 patients mean time of operation was min. There was small injury of the right main bronchus managed with fibrin sponge packing and no other intraoperative injuries of the vitally important structures, including major vessels, tracheobronchial tree or the esophagus. Complications of TEMLA occurred in 46/698 of patients (6.6%) (Table 1), with temporary laryngeal nerve palsy in 17/698 patients (2.4%) and permanent nerve palsy in 2/698 patients (0.3%). Pneumothorax necessitating pleural drainage occurred in 1/698 patients (0.1%), pleural effusion in 15/698 patients (2.1%). Asymptomatic widening of the mediastinum was noted in about 40% of patients. It necessitated no treatment, subsided after several days and was not regarded a postoperative complication. There were 5 postoperative deaths unrelated to the procedure (mortality 0.7%) (Table 2). The number of dissected nodes during TEM- LA was 15 to 85 (mean 37.9). Metastatic N2 nodes were found in 152/698 patients (21.8%) and N3 nodes were found in 26/698 patients (3.7%). Metastatic nodes were most prevalent in station 7, station 4R, station 2R, station 5 and station 4L. Subsequent thoracotomy was performed in 445/513 patients (86.7%) after negative result of TEMLA. There were 110 pneumonectomies, 37 sleeve-lobectomies, 280 lobectomies/bilobectomies, 3 sublobar resections and 15 explorations (3.4%) (Table 3). 201
7 Pneumonologia i Alergologia Polska 2011, vol. 79, no 3, pages Table 1. Table 2. Causes of death after transcervical extended mediastinal lymphadenectomy (TEMLA) Cause of deaths Day of postoperative Number of death patients Pulmonary heamorrhage due to angio-bronchial fistula Cardiac infarct 2 1 Brain haemorrhage 4 1 Cause unknown 2 1 Table 3. Complications of 698 transcervical extended mediastinal lymphadenectomy (TEMLA) procedures Complication n (%) Pleural effusion (conservative treatment) 12 (1.7) Laryngeal recurrent nerve palsy overall 16 (2.3) Temporary bilateral laryngeal recurrent nerve palsy 2 (0.3) Permanent laryngeal recurrent nerve palsy 3 (0.4) Pneumothorax (necessitating chest drainage) 2 (0.3) Pneumothorax (conservative treatment without 3 (0.4) chest drainage) Respiratory insufficiency (ventilator) 5 (0.7) Postoperative psychosis 2 (0.3) Perforation of the duodenal ulcer 1 (0.1) Cerebral haemorrhage 1 (0.1) Subarachnoid hemorrhage 1 (0.1) Cardiovascular insufficiency 1 (0.1) Overall morbidity 46 (6.6) Deaths 5 (0.7) Types of pulmonary resections in 445 patients operated on after negative result of transcervical extended mediastinal lymphadenectomy (TEMLA) Type of pulmonary resection Number of patients (%) Pneumonectomy 110 (24.7) Sleeve-lobectomy 37 (8.3) Lobectomy/bilobectomy 280 (62.9) Sublobar resection 3 (0.7) Exploratory thoracotomy 15 (3.4) Overall 445 During thoracotomy, omitted N2 was found in 7/ 445 (1.6%) patients and omitted normal mediastinal nodes were found in 53/445 patients (11.9%). Omit- Table 4. Diagnostic yield of transcervical extended mediastinal lymphadenectomy (TEMLA) for nonsmall-cell lung carcinoma Diagnostic parameter Value (%) Sensitivity 96.2 Specificity 100 Negative predictive value (NPV) 98.7 Positive predictive value (PPV) 100 Accuracy 99.0 ted metastatic N2 nodes were found in the station 5 (2 patients), station 7 (1 patient), station 4R (1 patient), station 8 (1 patient) and station 9 (2 patients). Sensitivity of TEMLA in discovery of N2 3 nodes was 96.2%, specificity was 100%, accuracy was 99,0%, Negative Predictive Value (NPV) was 98.7% and Positive Predictive Value (PPV) was 100% (Table 4). The postoperative mortality was 1.7% in the years , 4.3% in 2004 and 1.2% in the years In the period , before introduction of TEMLA the postoperative mortality in our department was 3.5%. The number of pulmonary resection for NSCLC in the years decreased of more than 25% in comparison to the period Comment The main advantage of TEMLA for staging of NSCLC is the possibility to remove almost all mediastinal lymph nodes with the surrounding fatty tissue. Mean number of 37.9 nodes/procedure were removed (from 15 to 85 nodes/procedure). Such complete removal of the mediastinal nodes increases the reliability of staging. No other invasive staging technique enables such complete assessment of the mediastinal nodes. For comparison, mean number of nodes was removed during VAMLA [15, 21]. During mediastinoscopy, normally, 1 2 lymph nodes from each of five stations accessible in this procedure (stations 2R,4R, 2L, 4L and 7) and mean number of 1 2 nodes were biopsied during EBUS and EEUS procedures [7, 9, 11 14, 22]. In 7 patients who underwent TEMLA omitted N2 nodes were found during subsequent thoracotomy (false negative results). The reasons for omitting of these nodes were dependent to the learning curve. In the last three hundred TEMLA procedures there were no false negative results. The morbidity of TEMLA in current study was relatively low. Most of the complications were minor and subsided during follow-up period and there 202
8 Marcin Zieliński et al., Transcervical extended mediastinal lymphadenectomy (TEMLA) were no life-threatening intraoperative complications. Two from five postoperative deaths can be attributed to the progression of cancer (fatal hemorrhage secondary to the fistula between the pulmonary artery and the bronchial tree) and two other were independent events (myocardial infarct and intracerebral hemorrhage). In one patient the cause of death was unknown, the postmortem examination was not performed because objections of the patient s family. In no case, the death was a consequence of surgical complications. These data showed that invasiveness of TEMLA was limited and the concerns about the safety of this procedure were not confirmed in our experience. Despite moderate invasiveness, TEM- LA is a relatively time consuming procedure, however it was well tolerated by the patients. Current mean operative time has been substantially reduced, however, from 160 to 128 minutes, and to 106 minutes for the last one hundred patients, due to the growing experience of the surgeons of our team. It must be underlined, that all surgeons of our team perform TEMLA. Due to very liberal inclusion criteria to TEM- LA there was considerable number of patients who did not undergo subsequent thoracotomy after negative result of TEMLA (operability 86.7%). Several patients in marginal cardio-respiratory state deteriorated after TEMLA which precluded subsequent thoracotomy. TEMLA was a kind of biological test and provided information about the mediastinal nodes that were useful in planning of futher oncological treatment, especially radiotherapy. The previous study comparing standard mediastinoscopy and TEMLA showed no significant difference in deterioration of the pulmonary function [17], which confirmed that TEMLA was a minimally invasive procedure, like standard mediastinoscopy and VAMLA. Minimally invasive intrathoracic procedures are those performed without thoracotomy with retraction of the ribs or sternonotomy. The example of the minimally invasive thoracic operation is the extended transcervical thymectomy. Results of 445 patients who underwent thoracotomy indicate that previous TEMLA was not an obstacle to perform safely all kinds of pulmonary resections, including sleeve-lobectomies and pneumonectomies. Thoracotomy was usually performed in 2 3 weeks after TEMLA, after obtaining a report of histopathological studies of all resected mediastinal nodes. The adhesions in the mediastinum have never been any serious obstacle in performance of the operation. The rate of exploratory thoracotomy was low 3.4% (15/445), however it showed the difficulties in preoperative staging of T factor, usually responsible for resectability of the tumor. TEMLA, which was a metod of staging of the mediastinal nodes, and not a tumor, didn t enable to eliminate totally a possibility of exploratory thoracotomy. The postoperative mortality was 1.7% in the years , 4.3% in 2004 and 1.2% in the years In the period , before introduction of TEMLA, the postoperative mortality in our department was 3.5%. These data indicate, that introduction of TEMLA is not associated with increased risk of postoperative mortality but, conversely, it leads to decrease the mortality, probably due to better selection of patients for pulmonary resection. Due to more accurate preoperative staging there was a decrease for more than 25% of the number of pulmonary resections for NSCLC after introduction of TEM- LA. The high incidence of squamous cell carcinoma in our patients was caused by predominance of this type of NSCLC in the south regions of Poland which was showed by ongoing international MAGRIT study. In our recent study we showed that TEMLA had a significantly higher diagnostic yield than all other mediastinal staging modalities (PET/CT, EBUS, EUS, and remediastinoscopy) [23]. The results of future studies will show if TEMLA should be considered the gold standard of mediastinal nodal restaging after neoadjuvant therapy in patients with NSCLC as was suggested by P. van Schill in the editorial commentary in the European Journal of Cardiothoracic Surgery [24]. Conclusions TEMLA is a new minimally invasive surgical technique enabling unique possibility to perform very extensive bilateral lymphadenectomy of the mediastinum with very high diagnostic yield. Refrences 1. Wright G., Manser R., Byrnes G., Hart D., Campbell D.A. Surgery for non-small cell lung cancer: systematic review and meta-analysis of randomized controlled trials. Thorax 2006; 61: Scott W.J., Howington J., Feigenberg S., Movsas B., Pisters K. Treatment of non-small cell lung cancer stage I and stage II: ACCP Evidence-Based Clinical Practice Guidelines (2nd Edition). Chest 2007; 132: 234S 242S. 3. Robinson L.A., Ruckdeschel J.C., Wagne Jr H., Stevens C.W. Treatment of non-small cell lung cancer stage IIIA: ACCP Evidence-Based Clinical Practice Guidelines (2nd Edition). Chest 2007; 132: 243S 265S. 4. Jett J.R., Schild S.E., Keith K.L., Kesler K.A. Treatment of nonsmall cell lung cancer stage IIIB: ACCP Evidence-Based Clinical Practice Guidelines (2nd Edition). Chest 2007; 132: 266S 276S. 5. Socinski M.A., Crowell R., Hensing T.E. et al. Treatment of non-small cell lung cancer, stage IV: ACCP Evidence-Based Clinical Practice Guidelines (2nd Edition). Chest 2007; 132: 277S 289S. 203
9 Pneumonologia i Alergologia Polska 2011, vol. 79, no 3, pages Lardinois D., De Leyn P., Van Schil P. et al. ESTS guidelines for intraoperative lymph node staging in non-small cell lung cancer. Eur. J. Cardiothorac. Surg. 2006; 30: De Leyn P., Lardinois D., Van Schil P.E. et al. ESTS guidelines for preoperative lymph node staging for non-small cell lung cancer. Eur. J. Cardiothorac. Surg. 2007; 32: Cerfolio R., Buddhiwardhani O., Bryant A., Raghuveer V., Mountz J., Bartolucci A. The accuracy of integrated PET-CT compared with dedicated PET alone for the staging of patients with non-small cell lung cancer. Ann. Thorac. Surg. 2004; 78: Herth F., Ernst A., Eberhardt R., Vilman P., Dienemann H., Krasnik M. Endobronchial ultrasound-guided transbronchial needle aspiration of lymph nodes in the radiologically normal mediastinum. Eur. J. Respir. 2006; 28: Annema J., Hoekstra O., Smit E., Veselic M., Versteegh M., Rabe K. Towards a minimally invasive staging strategy in NSCLC: analysis of PET positive mediastinal lesions by EUS- FNA. Lung Cancer 2004; 44: Szlubowski A., Kuzdzał J., Pankowski J. et al. Przezoskrzelowa biopsja węzłów chłonnych śródpiersia i wnęk płuca pod kontrolą ultrasonografii wewnątrzoskrzelowej w czasie rzeczywistym w diagnostyce raka płuca i sarkoidozy. Pneumonol. Alergol. Pol. 2008; 76: Szlubowski A., Zielinski M., Figura J. et al. Przezprzełykowa biopsja węzłów chłonnych śródpiersia pod kontrolą ultrasonografii wewnątrzprzełykowej w czasie rzeczywistym w diagnostyce raka płuca. Pneumonol. Alergol. Pol. 2009; 77: Herth F.J., Krasnik M., Kahn N., Eberhardt R., Ernst A. Combined endoscopic-endobronchial ultrasound-guided fine-needle aspiration of mediastinal lymph nodes through a single bronchoscope in 150 patients with suspected lung cancer. Chest 2010; 138: Szlubowski A., Zielinski M., Soja J. et al. A combined approach of endobronchial and endoscopic ultrasound-guided needle aspiration in the radiologically normal mediastinum in non-smallcell lung cancer staging a prospective trial. Eur. J. Cardiothorac. Surg. 2010; 37: Hurtgen M., Friedel G., Toomes H., Fritz P. Radical video- -assisted mediastinoscopic lymphadenectomy (VAMLA) technique and first results. Eur. J. Cardiothorac. Surg. 2002; 21: Kuzdzal J., Zielinski M., Papla B. et al. Transcervical extended mediastinal lymphadenectomy the new operative technique and early results in lung cancer staging. Eur. J. Cardiothorac. Surg. 2005; 27: Zieliński M. Transcervical extended mediastinal lymphadenectomy: results of staging in two hundred fifty-six patients with non-small cell lung cancer. J. Thorac. Oncol. 2007; 2: Zieliński M., Kużdżał J., Szlubowski A., Soja J. A safe and reliable technique for visualization of the laryngeal recurrent nerves in the neck. Am. J. Surg. 2005; 189: Mountain C.F., Dresler C.M. Regional lymph node classification for lung cancer staging. Chest 1997; 111: Zielinski M., Kuzdzal J., Nabialek T., Hauer L., Pankowski J., Dziadzio B. Transcervical extended mediastinal lymphadenectomy. Multimedia Manual of Cardiothoracic Surgery. MMCTS (October 9, 2006), doi: /mmcts Leschber G., Holinka G., Linder A. Video-assisted mediastinoscopic lymphadenectomy (VAMLA) a method for systematic mediastinal lymphnode dissection. Eur. J. Cardiothorac. Surg. 2003; 24: Venissac N., Alifano M., Mouroux J. Video-assisted mediastinoscopy: experience from 240 consecutive cases. Ann. Thorac. Surg. 2003; 76: Zieliński M., Hauer L., Hauer J., Nabiałek T., Szlubowski A., Pankowski J. Non-small-cell lung cancer restaging with transcervical extended mediastinal lymphadenectomy. Eur. J. Cardiothorac. Surg. 2010; 37: Van Schil P.E., Hendriks J.M.H., De Waele M., Luwers P. Editorial comment: Mediastinal restaging: has the Holy Grail been found? Eur. J. Cardiothorac. Surg. 2010; 37:
Endoscopic ultrasound-guided needle aspiration in lung cancer
 ORIGINAL ARTICLE Artur Szlubowski 1, Marcin Zieliński 1, Joanna Figura 1, Jolanta Hauer 1, Witold Sośnicki 1, Juliusz Pankowski 2, Anna Obrochta 2, Magdalena Jakubiak 2 1 Department of Thoracic Surgery
ORIGINAL ARTICLE Artur Szlubowski 1, Marcin Zieliński 1, Joanna Figura 1, Jolanta Hauer 1, Witold Sośnicki 1, Juliusz Pankowski 2, Anna Obrochta 2, Magdalena Jakubiak 2 1 Department of Thoracic Surgery
Transcervical uniportal pulmonary lobectomy
 Original Article on Thoracic Surgery Page 1 of 6 Transcervical uniportal pulmonary lobectomy Marcin Zieliński 1, Tomasz Nabialek 2, Juliusz 3 1 Department of Thoracic Surgery, 2 Department of Anaesthesiology
Original Article on Thoracic Surgery Page 1 of 6 Transcervical uniportal pulmonary lobectomy Marcin Zieliński 1, Tomasz Nabialek 2, Juliusz 3 1 Department of Thoracic Surgery, 2 Department of Anaesthesiology
MEDIASTINAL STAGING surgical pro
 MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
VAMLA/TEMLA. Todd L. Demmy
 VAMLA/TEMLA Todd L. Demmy Disclosures/ Questions Objectives - Staging Learn new lymphadenectomy (LA) results: Video-Assisted Mediastinal (VAMLA) Transcervical Extended Mediastinal (TEMLA) Compare with
VAMLA/TEMLA Todd L. Demmy Disclosures/ Questions Objectives - Staging Learn new lymphadenectomy (LA) results: Video-Assisted Mediastinal (VAMLA) Transcervical Extended Mediastinal (TEMLA) Compare with
Video-Mediastinoscopy Thoracoscopy (VATS)
 Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Index. B Bronchogenic carcinoma, of left lung, Bronchogenic cysts, 150
 A Acquired tracheo-oesophageal fistula, 198 199 Adenoid cystic carcinomas (ACC), 174 Anastomotic leaks, 194 Anterior mediastinal tumor, 143 tumor mass diagnosis, 32 33 Aortic valve implantation. See Transcatheter
A Acquired tracheo-oesophageal fistula, 198 199 Adenoid cystic carcinomas (ACC), 174 Anastomotic leaks, 194 Anterior mediastinal tumor, 143 tumor mass diagnosis, 32 33 Aortic valve implantation. See Transcatheter
Patients with pathologically diagnosed involved mediastinal
 MINI-SYMPOSIUM ON EMERGING TECHNIQUES FOR LUNG CANCER STAGING European Trends in Preoperative and Intraoperative Nodal Staging: ESTS Guidelines P. De Leyn, MF, PhD,* D. Lardinois, MD, P. Van Schil, MD,
MINI-SYMPOSIUM ON EMERGING TECHNIQUES FOR LUNG CANCER STAGING European Trends in Preoperative and Intraoperative Nodal Staging: ESTS Guidelines P. De Leyn, MF, PhD,* D. Lardinois, MD, P. Van Schil, MD,
Mediastinoscopy. EBUS versus Mediastinoscopy?
 Mediastinoscopy M.A. Paul, MD, PhD Dept of Surgery VU University Medical Center Amsterdam Perspectives in Lung Cancer, Amsterdam 9 10 March 2012 1 EBUS versus Mediastinoscopy? I had prepared for a Pro
Mediastinoscopy M.A. Paul, MD, PhD Dept of Surgery VU University Medical Center Amsterdam Perspectives in Lung Cancer, Amsterdam 9 10 March 2012 1 EBUS versus Mediastinoscopy? I had prepared for a Pro
Non-small-cell lung cancer restaging with transcervical extended mediastinal lymphadenectomy
 European Journal of Cardio-thoracic Surgery 37 (2010) 776 781 www.elsevier.com/locate/ejcts Non-small-cell lung cancer restaging with transcervical extended mediastinal lymphadenectomy Marcin Zieliński
European Journal of Cardio-thoracic Surgery 37 (2010) 776 781 www.elsevier.com/locate/ejcts Non-small-cell lung cancer restaging with transcervical extended mediastinal lymphadenectomy Marcin Zieliński
Video assisted mediastinal lymphadenectomy (VAMLA)
 Video assisted mediastinal lymphadenectomy (VAMLA) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin No conflict
Video assisted mediastinal lymphadenectomy (VAMLA) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin No conflict
VIDEO-ASSISTED MEDIASTINOSCOPY FOR MEDIASTINAL STAGING OF LUNG CANCER
 VIDEO-ASSISTED MEDIASTINOSCOPY FOR MEDIASTINAL STAGING OF LUNG CANCER Christophoros N. Foroulis Associate Professor of Thoracic Surgery Aristotle University of Thessaloniki 1 st International Course on
VIDEO-ASSISTED MEDIASTINOSCOPY FOR MEDIASTINAL STAGING OF LUNG CANCER Christophoros N. Foroulis Associate Professor of Thoracic Surgery Aristotle University of Thessaloniki 1 st International Course on
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
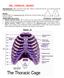 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER
 MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Comparison of complete and minimal mediastinal lymph node dissection for non-small cell lung cancer: Results of a prospective randomized trial
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Comparison of complete and minimal mediastinal lymph node dissection for non-small cell lung cancer: Results of a prospective randomized trial Junhua Zhang*,
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Comparison of complete and minimal mediastinal lymph node dissection for non-small cell lung cancer: Results of a prospective randomized trial Junhua Zhang*,
VATS-lymph node dissection, staging and restaging in advanced malignancy/the Munich experience
 Review Article Page 1 of 14 VATS-lymph node dissection, staging and restaging in advanced malignancy/the Munich experience Andreas Hiebinger 1, Dietmar Öfner-Velano 2, Johannes Bodner 1,3 1 Department
Review Article Page 1 of 14 VATS-lymph node dissection, staging and restaging in advanced malignancy/the Munich experience Andreas Hiebinger 1, Dietmar Öfner-Velano 2, Johannes Bodner 1,3 1 Department
Preoperative mediastinal lymph node staging for non-small cell lung cancer: 2014 update of the 2007 ESTS guidelines
 Highlighted Reports in European Lung Cancer Conference Preoperative mediastinal lymph node staging for non-small cell lung cancer: 2014 update of the 2007 ESTS guidelines Paul De Leyn 1, Christophe Dooms
Highlighted Reports in European Lung Cancer Conference Preoperative mediastinal lymph node staging for non-small cell lung cancer: 2014 update of the 2007 ESTS guidelines Paul De Leyn 1, Christophe Dooms
Bronchoscopy and endobronchial ultrasound for diagnosis and staging of lung cancer
 FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
An Update: Lung Cancer
 An Update: Lung Cancer Andy Barlow Consultant in Respiratory Medicine Lead Clinician for Lung Cancer (West Herts Hospitals NHS Trust) Lead for EBUS-Harefield Hospital (RB&HFT) Summary Lung cancer epidemiology
An Update: Lung Cancer Andy Barlow Consultant in Respiratory Medicine Lead Clinician for Lung Cancer (West Herts Hospitals NHS Trust) Lead for EBUS-Harefield Hospital (RB&HFT) Summary Lung cancer epidemiology
Revised ESTS guidelines for preoperative mediastinal lymph node staging for non-small cell lung cancer
 Revised ESTS guidelines for preoperative mediastinal lymph node staging for non-small cell lung cancer Paul De Leyn 1, Christophe Dooms 2, Jaroslaw Kuzdzal 3, Didier Lardinois 4, Bernward Passlick 5, Ramon
Revised ESTS guidelines for preoperative mediastinal lymph node staging for non-small cell lung cancer Paul De Leyn 1, Christophe Dooms 2, Jaroslaw Kuzdzal 3, Didier Lardinois 4, Bernward Passlick 5, Ramon
Accepted Manuscript. Indications for Invasive Mediastinal Staging for Non-small Cell Lung Cancer. Jules Lin, MD, Felix Fernandez, MD
 Accepted Manuscript Indications for Invasive Mediastinal Staging for Non-small Cell Lung Cancer Jules Lin, MD, Felix Fernandez, MD PII: S0022-5223(18)31872-5 DOI: 10.1016/j.jtcvs.2018.07.027 Reference:
Accepted Manuscript Indications for Invasive Mediastinal Staging for Non-small Cell Lung Cancer Jules Lin, MD, Felix Fernandez, MD PII: S0022-5223(18)31872-5 DOI: 10.1016/j.jtcvs.2018.07.027 Reference:
Chapter 5: Other mediastinal structures. The Large Arteries. The Aorta. Ascending aorta
 Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Three-arm robot-assisted thoracoscopic surgery for locally advanced N2 non-small cell lung cancer
 Surgical Technique Three-arm robot-assisted thoracoscopic surgery for locally advanced N2 non-small cell lung cancer Xinghua Cheng, Chongwu Li, Jia Huang, Peiji Lu, Qingquan Luo Shanghai Chest Hospital,
Surgical Technique Three-arm robot-assisted thoracoscopic surgery for locally advanced N2 non-small cell lung cancer Xinghua Cheng, Chongwu Li, Jia Huang, Peiji Lu, Qingquan Luo Shanghai Chest Hospital,
GUIDELINE RECOMMENDATIONS
 European Journal of Cardio-Thoracic Surgery 48 (2015) 1 15 doi:10.1093/ejcts/ezv194 Cite this article as: Vilmann P, Frost Clementsen P, Colella S, Siemsen M, De Leyn P, Dumonceau J-M et al. Combined endobronchial
European Journal of Cardio-Thoracic Surgery 48 (2015) 1 15 doi:10.1093/ejcts/ezv194 Cite this article as: Vilmann P, Frost Clementsen P, Colella S, Siemsen M, De Leyn P, Dumonceau J-M et al. Combined endobronchial
Recommendations 1 For mediastinal nodal staging in patients with suspected or proven non-small-cell lung cancer
 Guideline 545 Combined endobronchial and esophageal endosonography for the diagnosis and staging of lung cancer: European Society of Gastrointestinal Endoscopy (ESGE) Guideline, in cooperation with the
Guideline 545 Combined endobronchial and esophageal endosonography for the diagnosis and staging of lung cancer: European Society of Gastrointestinal Endoscopy (ESGE) Guideline, in cooperation with the
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Impact of Radical Systematic Mediastinal Lymphadenectomy on Tumor Staging in Lung Cancer
 Impact of Radical Systematic Mediastinal Lymphadenectomy on Tumor Staging in Lung Cancer Jakob R. Izbicki, MD, Bernward Passlick, MD, Ortrud Karg, MD, Christian Bloechle, MD, Klaus Pantel, MD, Wolfram
Impact of Radical Systematic Mediastinal Lymphadenectomy on Tumor Staging in Lung Cancer Jakob R. Izbicki, MD, Bernward Passlick, MD, Ortrud Karg, MD, Christian Bloechle, MD, Klaus Pantel, MD, Wolfram
Lung cancer Surgery. 17 TH ESO-ESMO MASTERCLASS IN CLINICAL ONCOLOGY March, 2017 Berlin, Germany
 17 TH ESO-ESMO MASTERCLASS IN CLINICAL ONCOLOGY 24-29 March, 2017 Berlin, Germany Lung cancer Surgery Sven Hillinger MD, Thoracic Surgery, University Hospital Zurich Case 1 59 y, female, 40 py, incidental
17 TH ESO-ESMO MASTERCLASS IN CLINICAL ONCOLOGY 24-29 March, 2017 Berlin, Germany Lung cancer Surgery Sven Hillinger MD, Thoracic Surgery, University Hospital Zurich Case 1 59 y, female, 40 py, incidental
Slide 1. Slide 2. Slide 3. Investigation and management of lung cancer Robert Rintoul. Epidemiology. Risk factors/aetiology
 Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Sectional Anatomy Quiz - III
 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
The Itracacies of Staging Patients with Suspected Lung Cancer
 The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer
 THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer [Based on WOSCAN NSCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED
THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer [Based on WOSCAN NSCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED
Combined endobronchial and oesophageal endosonography for the diagnosis and staging of lung cancer
 TASK FORCE REPORT ESGE/ERS/ESTS GUIDELINES Combined endobronchial and oesophageal endosonography for the diagnosis and staging of lung cancer European Society of Gastrointestinal Endoscopy (ESGE) Guideline,
TASK FORCE REPORT ESGE/ERS/ESTS GUIDELINES Combined endobronchial and oesophageal endosonography for the diagnosis and staging of lung cancer European Society of Gastrointestinal Endoscopy (ESGE) Guideline,
Video-assisted thoracoscopic surgery in lung cancer staging
 Review Article on Thoracic Surgery Page 1 of 7 Video-assisted thoracoscopic surgery in lung cancer staging Frederico Krieger Martins, Guilherme Augusto Oliveira, Juliano Cé Coelho, Márcio Chmelnitsky Kruter,
Review Article on Thoracic Surgery Page 1 of 7 Video-assisted thoracoscopic surgery in lung cancer staging Frederico Krieger Martins, Guilherme Augusto Oliveira, Juliano Cé Coelho, Márcio Chmelnitsky Kruter,
The currently used standard cervical mediastinoscopy (SCM)
 ORIGINAL ARTICLE The Role of Extended Cervical Mediastinoscopy in Staging of Non-small Cell Lung Cancer of the Left Lung and a Comparison with Integrated Positron Emission Tomography and Computed Tomography
ORIGINAL ARTICLE The Role of Extended Cervical Mediastinoscopy in Staging of Non-small Cell Lung Cancer of the Left Lung and a Comparison with Integrated Positron Emission Tomography and Computed Tomography
Lung Cancer staging Role of ENDOBRONCHIAL ULTRASOUND(Ebus) EBUS
 Lung Cancer staging Role of ENDOBRONCHIAL ULTRASOUND(Ebus) Arvind Perathur Winter Retreat Feb 13 th 2011 Mason City IA 50401 EBUS Tiger now offers a very economical and environmentally friendly all electric
Lung Cancer staging Role of ENDOBRONCHIAL ULTRASOUND(Ebus) Arvind Perathur Winter Retreat Feb 13 th 2011 Mason City IA 50401 EBUS Tiger now offers a very economical and environmentally friendly all electric
Anatomy Lecture 8. In the previous lecture we talked about the lungs, and their surface anatomy:
 Anatomy Lecture 8 In the previous lecture we talked about the lungs, and their surface anatomy: 1-Apex:it lies 1 inch above the medial third of clavicle. 2-Anterior border: it starts from apex to the midpoint
Anatomy Lecture 8 In the previous lecture we talked about the lungs, and their surface anatomy: 1-Apex:it lies 1 inch above the medial third of clavicle. 2-Anterior border: it starts from apex to the midpoint
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
A pragmatic view of the usefulness of video-mediastinoscopy in the modern era
 Surgical Technique on Mediastinal Surgery Page 1 of 7 A pragmatic view of the usefulness of video-mediastinoscopy in the modern era Marcello Migliore 1, Marco Nardini 1, Luke J. Rogers 2, Puwalani Vidanapathirana
Surgical Technique on Mediastinal Surgery Page 1 of 7 A pragmatic view of the usefulness of video-mediastinoscopy in the modern era Marcello Migliore 1, Marco Nardini 1, Luke J. Rogers 2, Puwalani Vidanapathirana
Charles Mulligan, MD, FACS, FCCP 26 March 2015
 Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Les techniques invasives et minimalement invasives dans le staging du cancer bronchopulmonaire. V. Ninane, Hôpital Saint-Pierre, Bruxelles, Belgique
 Les techniques invasives et minimalement invasives dans le staging du cancer bronchopulmonaire V. Ninane, Hôpital Saint-Pierre, Bruxelles, Belgique 1 Invasive Mediastinal Staging Purpose : to exclude Involvement
Les techniques invasives et minimalement invasives dans le staging du cancer bronchopulmonaire V. Ninane, Hôpital Saint-Pierre, Bruxelles, Belgique 1 Invasive Mediastinal Staging Purpose : to exclude Involvement
Accurate mediastinal staging is a critical component
 Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
Standardized definitions and policies of minimally invasive thymoma resection
 Perspective Standardized definitions and policies of minimally invasive thymoma resection Alper Toker 1,2 1 Department of Thoracic Surgery, Istanbul Medical School, Istanbul University, Istanbul, Turkey;
Perspective Standardized definitions and policies of minimally invasive thymoma resection Alper Toker 1,2 1 Department of Thoracic Surgery, Istanbul Medical School, Istanbul University, Istanbul, Turkey;
Lung & Pleura. The Topics :
 Lung & Pleura The Topics : The Trachea. The Bronchi. The Brochopulmonary Segments. The Lungs. The Hilum. The Pleura. The Surface Anatomy Of The Lung & Pleura. The Root & Hilum. - first of all, the lung
Lung & Pleura The Topics : The Trachea. The Bronchi. The Brochopulmonary Segments. The Lungs. The Hilum. The Pleura. The Surface Anatomy Of The Lung & Pleura. The Root & Hilum. - first of all, the lung
Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC)
 Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC) Poster No.: C-1360 Congress: ECR 2015 Type: Scientific Exhibit Authors:
Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC) Poster No.: C-1360 Congress: ECR 2015 Type: Scientific Exhibit Authors:
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
ESTS guidelines for preoperative lymph node staging for non-small cell lung cancer
 European Journal of Cardio-thoracic Surgery 32 (2007) 1 8 www.elsevier.com/locate/ejcts ESTS guidelines for preoperative lymph node staging for non-small cell lung cancer Paul De Leyn a, *, Didier Lardinois
European Journal of Cardio-thoracic Surgery 32 (2007) 1 8 www.elsevier.com/locate/ejcts ESTS guidelines for preoperative lymph node staging for non-small cell lung cancer Paul De Leyn a, *, Didier Lardinois
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
The right middle lobe is the smallest lobe in the lung, and
 ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
The Role of Endobronchial Ultrasound-guided Transbronchial Needle Aspiration in the Diagnosis of Recurrent Non-small Cell Lung Cancer after Surgery
 ORIGINAL ARTICLE The Role of Endobronchial Ultrasound-guided Transbronchial Needle Aspiration in the Diagnosis of Recurrent Non-small Cell Lung Cancer after Surgery Seo Goo Han 1, Hongseok Yoo 1, Byung
ORIGINAL ARTICLE The Role of Endobronchial Ultrasound-guided Transbronchial Needle Aspiration in the Diagnosis of Recurrent Non-small Cell Lung Cancer after Surgery Seo Goo Han 1, Hongseok Yoo 1, Byung
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
PET/CT in lung cancer
 PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
Predictive risk factors for lymph node metastasis in patients with resected nonsmall cell lung cancer: a case control study
 Moulla et al. Journal of Cardiothoracic Surgery (2019) 14:11 https://doi.org/10.1186/s13019-019-0831-0 RESEARCH ARTICLE Open Access Predictive risk factors for lymph node metastasis in patients with resected
Moulla et al. Journal of Cardiothoracic Surgery (2019) 14:11 https://doi.org/10.1186/s13019-019-0831-0 RESEARCH ARTICLE Open Access Predictive risk factors for lymph node metastasis in patients with resected
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Improving the Inaccuracies of Clinical Staging of Patients with NSCLC: A Prospective Trial
 Improving the Inaccuracies of Clinical Staging of Patients with NSCLC: A Prospective Trial Robert James Cerfolio, MD, FACS, Ayesha S. Bryant, MD, MSPH, Buddhiwardhan Ojha, MD, MPH, and Mohammad Eloubeidi,
Improving the Inaccuracies of Clinical Staging of Patients with NSCLC: A Prospective Trial Robert James Cerfolio, MD, FACS, Ayesha S. Bryant, MD, MSPH, Buddhiwardhan Ojha, MD, MPH, and Mohammad Eloubeidi,
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Both transoesophageal endoscopic curved-linear ultrasound
 STATE OF THE ART: CONCISE REVIEW Endoscopic and Endobronchial Ultrasonography According to the Proposed Lymph Node Map Definition in the Seventh Edition of the Tumor, Node, Metastasis Classification for
STATE OF THE ART: CONCISE REVIEW Endoscopic and Endobronchial Ultrasonography According to the Proposed Lymph Node Map Definition in the Seventh Edition of the Tumor, Node, Metastasis Classification for
Surgical management of lung cancer
 Surgical management of lung cancer Nick Roubos FRACS Cardiothoracic Surgeon Box Hill Hospital, Epworth Eastern Thoracic Oncology Non Small Cell Lung Cancer (NSCLC) Small Cell Lung Cancer Mesothelioma Pulmonary
Surgical management of lung cancer Nick Roubos FRACS Cardiothoracic Surgeon Box Hill Hospital, Epworth Eastern Thoracic Oncology Non Small Cell Lung Cancer (NSCLC) Small Cell Lung Cancer Mesothelioma Pulmonary
Role of Surgery in Management of Non Small Cell Lung Cancer. Dr. Ahmed Bamousa Consultant thoracic surgery Prince Sultan Military Medical City
 Role of Surgery in Management of Non Small Cell Lung Cancer Dr. Ahmed Bamousa Consultant thoracic surgery Prince Sultan Military Medical City Introduction Surgical approach Principle and type of surgery
Role of Surgery in Management of Non Small Cell Lung Cancer Dr. Ahmed Bamousa Consultant thoracic surgery Prince Sultan Military Medical City Introduction Surgical approach Principle and type of surgery
Video-assisted thoracic surgery pneumonectomy: the first case report in Poland
 Case report Videosurgery Video-assisted thoracic surgery pneumonectomy: the first case report in Poland Cezary Piwkowski, Piotr Gabryel, Mariusz Kasprzyk, Wojciech Dyszkiewicz Thoracic Surgery Department,
Case report Videosurgery Video-assisted thoracic surgery pneumonectomy: the first case report in Poland Cezary Piwkowski, Piotr Gabryel, Mariusz Kasprzyk, Wojciech Dyszkiewicz Thoracic Surgery Department,
Transbronchial fine needle aspiration
 Thorax 1982;37 :270-274 Transbronchial fine needle aspiration J LEMER, E MALBERGER, R KONIG-NATIV From the Departments of Cardio-thoracic Surgery and Cytology, Rambam Medical Center, Haifa, Israel ABSTRACT
Thorax 1982;37 :270-274 Transbronchial fine needle aspiration J LEMER, E MALBERGER, R KONIG-NATIV From the Departments of Cardio-thoracic Surgery and Cytology, Rambam Medical Center, Haifa, Israel ABSTRACT
Pneumonectomy After Induction Rx: Is it Safe?
 Pneumonectomy After Induction Rx: Is it Safe? David J. Sugarbaker, M.D. Director, Chief, Division of Thoracic Surgery The Olga Keith Weiss Chair of Surgery of Medicine at, Pneumonectomy after induction
Pneumonectomy After Induction Rx: Is it Safe? David J. Sugarbaker, M.D. Director, Chief, Division of Thoracic Surgery The Olga Keith Weiss Chair of Surgery of Medicine at, Pneumonectomy after induction
THE DESCENDING THORACIC AORTA
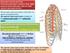 Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments
 Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Minimally Invasive Mediastinal Staging of Non Small-Cell Lung Cancer: Emphasis on Ultrasonography-Guided Fine-Needle Aspiration
 Endobronchial ultrasound and endoscopic ultrasound-guided lymph node biopsy may represent an alternative to cervical mediastinoscopy. Dorothy Fox, Rough Seas. Acrylic on canvas, 36ʺ 36ʺ. Minimally Invasive
Endobronchial ultrasound and endoscopic ultrasound-guided lymph node biopsy may represent an alternative to cervical mediastinoscopy. Dorothy Fox, Rough Seas. Acrylic on canvas, 36ʺ 36ʺ. Minimally Invasive
Primary lung cancer is the most frequent cause of death
 Original Article Endobronchial Ultrasound versus Mediastinoscopy for Mediastinal Nodal Staging of Non Small-Cell Lung Cancer Sang-Won Um, MD, PhD,* Hong Kwan Kim, MD, PhD, Sin-Ho Jung, PhD, Joungho Han,
Original Article Endobronchial Ultrasound versus Mediastinoscopy for Mediastinal Nodal Staging of Non Small-Cell Lung Cancer Sang-Won Um, MD, PhD,* Hong Kwan Kim, MD, PhD, Sin-Ho Jung, PhD, Joungho Han,
Mediastinal Mysteries: What can be solved with EBUS?
 Mediastinal Mysteries: What can be solved with EBUS? W. Graham Carlos MD Pulmonary & Critical Care Fellow Indiana University School of Medicine Disclosures None Objectives Introduce you to the technique
Mediastinal Mysteries: What can be solved with EBUS? W. Graham Carlos MD Pulmonary & Critical Care Fellow Indiana University School of Medicine Disclosures None Objectives Introduce you to the technique
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL
 The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
Documenting the anatomic extent of lung cancer before
 Mediastinal Staging Prior to Surgical Resection Steven J. Mentzer, MD Documenting the anatomic extent of lung cancer before surgical resection has value in therapeutic decision-making. In the past, documenting
Mediastinal Staging Prior to Surgical Resection Steven J. Mentzer, MD Documenting the anatomic extent of lung cancer before surgical resection has value in therapeutic decision-making. In the past, documenting
Controversies in management of squamous esophageal cancer
 2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
Seventh Edition of the Cancer Staging Manual and Stage Grouping of Lung Cancer. Quick Reference Chart and Diagrams
 CHEST Special Features Seventh Edition of the Cancer Staging Manual and Stage Grouping of Lung Cancer Quick Reference Chart and Diagrams Omar Lababede, MD ; Moulay Meziane, MD ; and Thomas Rice, MD, FCCP
CHEST Special Features Seventh Edition of the Cancer Staging Manual and Stage Grouping of Lung Cancer Quick Reference Chart and Diagrams Omar Lababede, MD ; Moulay Meziane, MD ; and Thomas Rice, MD, FCCP
Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line
 L 14 A B O R A T O R Y Thorax THORACIC WALL Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line Identify the surface landmarks of
L 14 A B O R A T O R Y Thorax THORACIC WALL Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line Identify the surface landmarks of
Pathologic staging of the mediastinal lymph nodes is
 Mediastinoscopy: Still the Gold Standard Joseph B. Shrager, MD Division of Thoracic Surgery, Department of Cardiothoracic Surgery, Stanford University School of Medicine, Stanford, and Veterans Administration
Mediastinoscopy: Still the Gold Standard Joseph B. Shrager, MD Division of Thoracic Surgery, Department of Cardiothoracic Surgery, Stanford University School of Medicine, Stanford, and Veterans Administration
International Association for the Study of Lung Cancer lymph node map Lymph node stations Imaging CT
 Review of the International Association for the Study of Lung Cancer Lymph Node Classification System Localization of Lymph Node Stations on CT Imaging Hamza Jawad, MBBS a, Arlene Sirajuddin, MD b, Jonathan
Review of the International Association for the Study of Lung Cancer Lymph Node Classification System Localization of Lymph Node Stations on CT Imaging Hamza Jawad, MBBS a, Arlene Sirajuddin, MD b, Jonathan
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
AJCC-NCRA Education Needs Assessment Results
 AJCC-NCRA Education Needs Assessment Results Donna M. Gress, RHIT, CTR Survey Tool 1 Survey Development, Delivery, Analysis THANKS to NCRA for the following work Developed survey with input from partners
AJCC-NCRA Education Needs Assessment Results Donna M. Gress, RHIT, CTR Survey Tool 1 Survey Development, Delivery, Analysis THANKS to NCRA for the following work Developed survey with input from partners
In 1982 Pearson and colleagues [1] from Toronto published
![In 1982 Pearson and colleagues [1] from Toronto published In 1982 Pearson and colleagues [1] from Toronto published](/thumbs/95/124110746.jpg) Transition From Mediastinoscopy to Endoscopic Ultrasound for Lung Cancer Staging Mark I. Block, MD Division of Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. Esophageal endoscopic
Transition From Mediastinoscopy to Endoscopic Ultrasound for Lung Cancer Staging Mark I. Block, MD Division of Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. Esophageal endoscopic
Number of Lymph Nodes Harvested From a Mediastinal Lymphadenectomy
 CHEST Original Research Number of Lymph Nodes Harvested From a Mediastinal Lymphadenectomy Results of the Randomized, Prospective American College of Surgeons Oncology Group Z0030 Trial LUNG CANCER Gail
CHEST Original Research Number of Lymph Nodes Harvested From a Mediastinal Lymphadenectomy Results of the Randomized, Prospective American College of Surgeons Oncology Group Z0030 Trial LUNG CANCER Gail
CT Chest. Verification of an opacity seen on the straight chest X ray
 CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
EVIDENCE BASED MANAGEMENT OF STAGE III NSCLC MILIND BALDI
 EVIDENCE BASED MANAGEMENT OF STAGE III NSCLC MILIND BALDI Overview Introduction Diagnostic work up Treatment Group 1 Group 2 Group 3 Stage III lung cancer Historically was defined as locoregionally advanced
EVIDENCE BASED MANAGEMENT OF STAGE III NSCLC MILIND BALDI Overview Introduction Diagnostic work up Treatment Group 1 Group 2 Group 3 Stage III lung cancer Historically was defined as locoregionally advanced
Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis
 ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
and Strength of Recommendations
 ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
Karoline Nowillo, MD. February 1, 2008
 Case Presentation Karoline Nowillo, MD SUNY Downstate t February 1, 2008 Case Presentation Chief complaint enlarging goiter x 8 months History of present illness shortness of breath, heaviness in chest
Case Presentation Karoline Nowillo, MD SUNY Downstate t February 1, 2008 Case Presentation Chief complaint enlarging goiter x 8 months History of present illness shortness of breath, heaviness in chest
Video-assisted thoracoscopic lobectomy using a standardized three-port anterior approach - The Copenhagen experience
 Art of Operative Techniques Video-assisted thoracoscopic lobectomy using a standardized three-port anterior approach - The Copenhagen experience Henrik J. Hansen, René H. Petersen Department of Cardiothoracic
Art of Operative Techniques Video-assisted thoracoscopic lobectomy using a standardized three-port anterior approach - The Copenhagen experience Henrik J. Hansen, René H. Petersen Department of Cardiothoracic
Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010
 LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
Lung Cancer Clinical Guidelines: Surgery
 Lung Cancer Clinical Guidelines: Surgery 1 Scope of guidelines All Trusts within Manchester Cancer are expected to follow this guideline. This guideline is relevant to: Adults (18 years and older) with
Lung Cancer Clinical Guidelines: Surgery 1 Scope of guidelines All Trusts within Manchester Cancer are expected to follow this guideline. This guideline is relevant to: Adults (18 years and older) with
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Dana Alrafaiah. - Moayyad Al-Shafei. -Mohammad H. Al-Mohtaseb. 1 P a g e
 - 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
- 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital
 Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital Muhammad Rizwan Khan,Sulaiman B. Hasan,Shahid A. Sami ( Department of Surgery, The Aga Khan University Hospital,
Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital Muhammad Rizwan Khan,Sulaiman B. Hasan,Shahid A. Sami ( Department of Surgery, The Aga Khan University Hospital,
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis)
 Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
VATS lobectomy lymph node management
 Perspective VATS lobectomy lymph node management Gavin M. Wright 1,2,3 1 Director of Surgical Oncology, St Vincent s Hospital, Melbourne, Australia; 2 Clinical Associate Professor, University of Melbourne
Perspective VATS lobectomy lymph node management Gavin M. Wright 1,2,3 1 Director of Surgical Oncology, St Vincent s Hospital, Melbourne, Australia; 2 Clinical Associate Professor, University of Melbourne
Role of EBUS in mediastinal staging of lung cancer. -Dr. Nandakishore Baikunje
 Role of EBUS in mediastinal staging of lung cancer -Dr. Nandakishore Baikunje Overview of the seminar Introduction Endosonography to stage the mediastinum Technical aspects of EBUS-TBNA for mediastinal
Role of EBUS in mediastinal staging of lung cancer -Dr. Nandakishore Baikunje Overview of the seminar Introduction Endosonography to stage the mediastinum Technical aspects of EBUS-TBNA for mediastinal
The technique of VATS right pneumonectomy
 Surgical Technique on Thoracic Surgery The technique of VATS right pneumonectomy Fernando Vannucci 1,2, Arthur Vieira 3, Paula A. Ugalde 3 1 de Janeiro, Brazil; 2 Thoracic Surgery Department, Military
Surgical Technique on Thoracic Surgery The technique of VATS right pneumonectomy Fernando Vannucci 1,2, Arthur Vieira 3, Paula A. Ugalde 3 1 de Janeiro, Brazil; 2 Thoracic Surgery Department, Military
