Received 9 November 2004/Returned for modification 6 January 2005/Accepted 14 February 2005
|
|
|
- George Logan
- 6 years ago
- Views:
Transcription
1 JOURNAL OF CLINICAL MICROBIOLOGY, July 2005, p Vol. 43, No /05/$ doi: /jcm Copyright 2005, American Society for Microbiology. All Rights Reserved. Comparison between the Hybrid Capture II Test and a PCR-Based Human Papillomavirus Detection Method for Diagnosis and Posttreatment Follow-Up of Cervical Intraepithelial Neoplasia Anna Söderlund-Strand, 1 Per Rymark, 2 Pia Andersson, 3 Joakim Dillner, 1 and Lena Dillner 1,3 * Department of Medical Microbiology, Lund University, University Hospital of Malmö, Malmö, Sweden 1 ; Department of Gynaecology, Västerås Hospital, Västerås, Sweden 2 ; and Department of Clinical Virology, Karolinska Hospital, Stockholm, Sweden 3 Received 9 November 2004/Returned for modification 6 January 2005/Accepted 14 February 2005 Human papillomavirus (HPV) infection is the major cause of cervical cancer and its precursor, cervical intraepithelial neoplasia (CIN), and HPV testing has therefore been proposed for improved triaging and follow-up of women treated for CIN. We compared two common HPV DNA detection tests (Hybrid Capture II [HCII] and PCR-enzyme immunosorbent assay (EIA) using the primers GP5 /GP6 followed by HPV typing with reverse dot blot hybridization) for sensitivity and specificity for detection of CIN and of CIN recurrence after treatment. Two hundred and thirty-nine women referred to the Department of Obstetrics and Gynaecology in Västerås, Sweden, were enrolled because of atypical Pap smears; 177 of these were later treated for dysplasia by conization or loop diathermy. Samples for HPV DNA testing were taken before and 4 to 6 months after treatment. There was substantial agreement between the HCII and PCR-EIA (kappa, 0.70 before treatment and 0.72 after treatment). The sensitivity for histopathologically confirmed CIN III was 100.0% for PCR-EIA and 95.6% for HCII. For patients with CIN II or worse (CIN II ), the sensitivities were 92.9% (PCR-EIA) and 91.8% (HCII). The specificities for CIN II in the pretreatment setting were 30.4% for PCR-EIA and 24.1% for HCII. After treatment, the sensitivities for CIN III in cytology were 100.0% by both methods, and for CIN II, sensitivities were 80.0% by both methods. The specificities for CIN II in the posttreatment setting were 83.5% for PCR and 85.4% for HCII. In conclusion, the sensitivities of both PCR-EIA and HCII are high and almost equal, suggesting that both methods are suitable as tools for detection and posttreatment follow-up of CIN II-III. Cancer of the cervix is the third most common form of cancer among women worldwide, with almost 400,000 new cases each year (28). The principal cause of invasive cervical cancer and its precursor lesions is infection with oncogenic types of human papillomavirus (HPV) (3, 4, 15, 21, 24, 34, 40), which is found in close to 100% of cancers (39). A recent case control study reported that HPV types 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68, 73, and 82 conferred increased risk for cervical cancer and that HPV types 6, 11, 40, 42, 43, 44, 54, 61, 70, 72, and 81 did not increase the cervical cancer risk (23). A meta analysis of all studies of cervical cancer found that the most important HPV type in squamous cell carcinomas is HPV 16, followed by HPV 18, 45, 31, and 33 (7). In adenocarcinomas, the most common type is HPV 18 followed by HPV 16 and 45 (7). In young women, the incidence of HPV infection is high, but the infection is often of short duration (16). The prevalence of high-risk (HR) HPV DNA is highest among sexually active teenagers, declining in women 20 to 30 years of age, and is still lower in women over the age of 30 (4, 19). Persistent HR HPV infections, which are more common in older women, greatly increase the risk of cervical intraepithelial neoplasia (CIN) * Corresponding author. Mailing address: Department of Medical Microbiology, Lund University, University Hospital of Malmö, SE Malmö, Sweden. Phone: Fax: lena.dillner@med.lu.se. (33) or cervical cancer, especially if the viral load is high (15, 16, 32). Regressing cervical lesions may clear their HPV some 3 months before cytological regression (25). HPV testing is of interest for improvement of cervical cancer screening programs. If no HR HPV DNA is present in a cervical sample, it will be quite unlikely that the patient will develop cancer for some years (36). Secondary HPV testing of women with unclear or low-grade cytological abnormalities can therefore improve the specificity of cervical screening. Another important use of HPV testing is in the follow-up of patients treated for CIN. A positive HR HPV DNA test 6 months after treatment of CIN II/CIN III is more predictive for recurrence than an abnormal cytology (26). The most commonly used HPV DNA detection methods are PCR, using the general primer pairs MY09/11 and their derivatives PGMY09/11 (14) or GP5 /GP6, and the Hybrid Capture II (HCII) test (Digene), a commercially available test and the second generation of this method. The second version is more accurate than the first version of Hybrid Capture, mainly because of a change of reagents and the addition of four new HR HPV types in the probe cocktail (31). In this study, we compared HCII and PCR with the general primer pair GP5 /GP6 (9, 18) for detection of high-grade CIN among women referred for colposcopy as well as for detection of CIN recurrence after treatment. Some methodological comparisons between PCR and HCII have been published in the past (35, 37), but we have not found any studies that have focused on comparing clinical sensitivity and 3260
2 VOL. 43, 2005 HCII AND PCR-BASED HPV TEST FOR DIAGNOSIS OF CIN 3261 FIG. 1. Study flow chart. specificity in detection and posttreatment follow-up of highgrade CIN. MATERIALS AND METHODS Study design. The present study contains 239 women living in the county of Västmanland, Sweden, who attended organized population-based cervical cancer screening and had been referred to the Department of Obstetrics and Gynaecology in Västerås because of atypical smears. All referred women were eligible for inclusion. The cytological diagnosis of the smear that had resulted in referral was available for 197 women: 41% had had cytological findings of unclear significance, 1% had unclear atypia, 35.5% had CIN I, 14.2% had CIN II, and 8.1% had CIN III. At the first visit, an endo/ectocervical sample was taken using a cytobrush (Medscand, Malmö, Sweden) and used for cytology (Fig. 1). For the present study, the same brush was thereafter immersed in 1 ml 0.9% NaCl, vigorously stirred, and frozen at 20 C. A second cervical sample was taken using the brush and sample transport medium provided with the HCII sample collection kit, all according to the instructions of the manufacturer. The taking of a conventional smear before the taking of the HCII sample has not been reported to affect the performance of the HCII test; e.g., in a recent cohort study, 1,278 women had a smear taken before the HCII sample was taken, and 3,123 gave an HCII sample without first taking a smear. The HCII test had excellent performance in the entire cohort (99.9% negative predictive value) (6). A colposcopy-directed biopsy was taken for routine histopathology. In order to be referred to the second visit, at least 2/3 of the following criteria had to be fulfilled: the initial Pap smear and/or biopsy showed CIN I or more and the colposcopy showed pathological signs. At the second visit, depending on the result of the biopsy, a conization was performed with either loop or laser (choice of method was allocated at random). All conization specimens were reviewed by the same pathologist. In case of disagreement with the routine histopathological diagnosis, the histopathological diagnosis of the review was used. At the third visit 4 to 6 months after conization, samples for cytology and HPV testing with PCR-enzyme immunosorbent assay (EIA) and HCII were obtained. Women who were not treated were also asked for a follow-up cervical sample 4 to 6 months after colposcopy. When the present work was closed, 239 women had been enrolled and had attended visit 1; 177 of these had been treated. A total of 147 women had attended the first follow-up visit; 114 of these had been treated. Two women did not attend the first follow-up visit because of hysterectomy, and one didn t attend because of relocation. For a further 89 patients that were enrolled shortly before the present part of the study was closed, no follow-up visits had as yet been scheduled, and they are therefore not included in this report. The study protocol was approved by the institutional review board of Västerås Hospital. PCR-EIA method. The samples, which had the initial volume of approximately 1,000 l, were thawed and centrifuged at 3,000 g for 10 min at room temperature. The cell pellet was resuspended in 1,000 l Tris-HCl (10 mm), ph 7.4. Aliquots of each sample were frozen at 20 C, thawed and boiled for 10 min, centrifuged briefly to avoid droplets at the tube top, and frozen at 20 C until analysis was performed. Sample preparation and PCR using the general primer pair GP5 /GP6 (18) were performed in separate rooms. Volumes of 10 l from each sample were added to a master mix with 0.5 M of the primer GP5 and the biotinylated primer GP6 (supplied from PJF Snijders, Free University of Amsterdam, Holland), 3.5 mm MgCl 2, 200 M of each deoxynucleoside triphosphate, 1Uof AmpliTaq Gold DNA polymerase, and PCR buffer II (Roche) to a final volume of 50 l. As positive controls of the PCR system, 10-fold dilutions (10 ng to 100 pg) of purified HPV 16 DNA from SiHa cells in a background of 100 ng of COT-1 human placental DNA (Roche, Germany) were analyzed in all tests. The extraction of positive controls was performed with a sodium dodecyl sulfate (SDS)-proteinase K method, as previously described (12), with some modifications. The volume of saturated ammonium acetate was 150 l, the incubation at 37 C was performed overnight, and all centrifugations were performed at 16,000 g. A serial endpoint dilution of purified HPV 16 plasmids (10-fold dilutions of 10 4 to 10 2 copies/ l) was used to determine assay sensitivity, which was found to be 10 copies (equivalent to 0.13 fg/reaction or 2.6 fg/ml) of HPV 16 DNA per sample. The samples were tested for amplifiability in a separate PCR with primers for the human -globin gene, BGPCO5 and biotinylated BGPCO3 (DNA Technology, Denmark), and AmpliTaq DNA polymerase. The positive controls of this system were 10 ng and 1 ng of human placental DNA (Sigma, Germany). As negative controls, 10 l of sterile water was applied to separate reaction tubes in the absence of template and analyzed identically as the other samples. Water controls with water added both before and after the samples were included in all runs. The PCR was performed in a Hybaid Omnigene automated thermal cycler (Hybaid, United Kingdom). For the PCR using the GP primers, a first step at 94 C for 10 min was followed by 45 cycles of denaturing at 94 C for 1.5 min, annealing at 40 C for 1.5 min, an extension step at 72 C for 2 min, and a terminal extension step at 72 C for 4 min. The PCR program using the primers for the
3 3262 SÖDERLUND-STRAND ET AL. J. CLIN. MICROBIOL. human -globin gene was initiated with a step at 94 C for 4 min followed by 40 cycles of 94 C for 1.5 min, 45 C for 1.5 min, 72 C for 2 min, and a final step at 72 C for 4 min. For detection of amplified DNA, 5 l of each biotinylated PCR product was applied to streptavidin-coated microtiter plate wells (Roche, Germany), together with 50 l of 1 SSC (0.15 M NaCl and 15 mm sodium citrate, ph 7.0) supplemented with 0.5% Tween 20 (Sigma, Germany). The plate was covered and incubated for 60 min at 37 C and then washed with l of1 SSC 0.5% Tween 20. For denaturation, 0.2 M NaOH was added followed by incubation for 15 min at room temperature. The previously described washing was repeated, and probe solution containing 10 nm of each probe diluted in 1 SSC 0.5% Tween 20 was added to each well, after which the plate was incubated for 60 min at 37 C. After new washings, alkaline phosphatase-conjugated antidigoxigenin antibody (75 mu/ml; Roche, Germany) diluted in 1 SSC 0.5% Tween 20 was added, and the plate was incubated as before. Finally, the plate was washed with l of1 SSC 0.5% Tween 20, and 100 l of alkaline phosphatase substrate (Fast p-nitrophenyl Phosphate tablet in sterile water; Sigma, Germany) was added to each well. The optical density (OD) was measured at 405 nm after an overnight incubation at 37 C. The probe solution for the GP5 /GP6 PCR product consists of 14 different oligonucleotide probes for the HPV types 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 66, and 68 (supplied from P. J. F. Snijders, Holland), and each probe is labeled with digoxigenin-11-ddutp (18). For the -globin gene PCR products, the same procedure as above was repeated except for the use of a single, digoxigenin-labeled probe diluted in 1 SSC 0.5% Tween 20 (5 -AAG AGT CAG GTG CAC CAT GGT GTC TGT TTG-3 ; DNA Technology, Denmark). For a valid GP5 /GP6 PCR-EIA, the positive control with 100 pg HPV 16 DNA had to be positive. The cutoff was three times the mean OD value of negative controls after overnight incubation. The grey zone was set to between two and three times the mean OD value of the negative controls. All samples that had OD values above cutoff or in the grey zone were tested in reverse dot blot hybridization (RDBH) (13) and scored as positive if an HPV type could be identified. For the -globin PCR-EIA, the positive control containing 10 ng of human placental DNA had to be positive. The cutoff was set as it was for HPV. Type-specific PCR method. Type-specific PCRs for HPV 16 and 18 were performed in a Mastercycler (Eppendorf). A first step at 94 C for 3 min was followed by 40 cycles of denaturing at 94 C for 1.5 min, annealing at 50 C for 1.5 min, and an extension step at 72 C for 1.5 min. The following primers target the E6 gene and are for HPV 16: 31-50, biotinylated at the 5 end (5 -CG TAA CCG AAA TCG GTT GAA-3 ), and (5 -TCC TGT GGG TCC TGA AAC- 3 ). For HPV 18, the primers were 54-72, biotinylated at the 5 end (5 -CG GGA CCG AAA ACG GTG TA-3 ), and (5 -CGT GTT GGA TCC TCA AAG C-3 ). The size of the amplicons are approximately 90 bp for HPV 16 and 80 bp for HPV 18. A sample volume of 2.5 l was added to a master mix consisting of 0.75 M of each primer (DNA Technology, Denmark), 200 M of each deoxynucleoside triphosphate, 0.2% bovine serum albumin, 1 Dynazyme buffer, and U of Dynazyme II DNA polymerase (Finnzymes, Finland) to a final volume of 25 l. As positive controls of the HPV 16 PCR, we analyzed 10-fold dilutions, 2.5 ng to 2.5 pg, of purified HPV 16 DNA from SiHa cells in a background of 25 ng of COT-1 human placental DNA (Roche, Germany). Tenfold dilutions (10 4 to 10 2 copies/ l) of HPV 16 plasmids have been analyzed in this PCR system, showing that it detects 2.5 copies, which is equivalent to fg or 1.3 fg/ml, of HPV 16 plasmids per sample. Positive controls of the HPV 18 PCR were 10-fold dilutions, 3.3 ag to 3.3 fg, of HPV 18 DNA in pbr322 plasmids in a background of 25 ng human placental DNA, and this system detects 25 copies, equivalent to 0.33 fg or 13.3 fg/ml, of HPV 18 plasmids per sample. The negative controls were the same as those for the GP5 /6 PCR. The detection of the PCR products was performed by the EIA procedure, as described above, except that the probes used were 5 -AT TGC AGT TCT CTT TTG GTG CAT AAA ATG TC-3 for HPV 16 and 5 -GC GCC ATA GTA TTG TGG TGT GTT TCT CAC AT-3 for HPV 18 (DNA Technology, Denmark). HPV typing with RDBH. The HPV typing was performed as previously described (13), with some modifications. Briefly, 100 ng of HPV 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 66, and 68 plasmids and 33 ng of -globin DNA plasmid were denatured in sterile 0.8 M NaOH 50 mm EDTA and dot blotted onto Hybond N membranes (Amersham, United Kingdom) prewetted in 6 SSC (0.9 M NaCl plus 90 mm sodium citrate, ph 7.0). After drying at room temperature and a 20-min incubation at 120 C, the membranes were dipped in 2 SSC and incubated on nylon filters in 5 ml of 1 M NaCl 50% deionized formamide 20% dextran sulfate 50 1% SDS 0.2 mg herring sperm DNA for 60 min at 46 C. Five microliters (in case of grey zone samples, 10 l) of the biotinylated PCR product from the GP5 /GP6 TABLE 1. HPV DNA test results from PCR and HCII analyses of samples before conization from the 177 patients that were treated a Sample type No. of patients PCR /HC PCR /HC PCR /HC PCR /HC Total Normal Koilocytosis CIN I CIN II CIN III/CIS a The results are related to the histopathological diagnosis at treatment. CIS, carcinoma in situ. PCR-EIA in 50 l prehybridization solution was incubated for 5 min at 94 C. Two microliters of the biotinylated PCR product from the -globin PCR-EIA was also added. Hybridization was performed overnight at 46 C. After washing with 2 SSPE 0.1% SDS (0.3 M NaCl, 20 mm NaH 2 PO 4, and 2 mm EDTA, ph 7.4) for 15 min at 65 C, 3% bovine serum albumin 154 mm NaCl 50 mm Trizma base 0.05% Tween 20 (filtered through m filters) was added followed by incubation for 60 min at 65 C. Streptavidin-alkaline phosphatase conjugate (Invitrogen) diluted 1/3,333 in 154 mm NaCl 50 mm Trizma base 0.05% Tween 20 (filtered through m filters) (TBS-T) was incubated for 10 min at 20 to 40 C. After two further washings with TBS-T for 10 min at 20 to 40 C and washing in 100 mm Tris-HCl (ph 9.5) 100 mm NaCl 50 mm MgCl 2, the membranes were briefly dried and incubated with Lumi-Phos 530 (Lumigen) for 75 min at room temperature before exposure for 10 min to X-ray film (Kodak) between intensifying screens in a cassette (Cronex Lightning Plus; DuPont). HCII method. The Hybrid Capture II test is a nucleic acid hybridization assay where specimens containing the target DNA hybridize with a specific HPV RNA probe mixture including probes for the following HR HPV types: 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, and 68, i.e., the same types as those detected in the GP5 /6 PCR-EIA method with the exception of HPV 66. The resultant DNA:RNA hybrids are captured on a microplate coated with antibodies specific for DNA:RNA hybrids. After signal detection with antibodies conjugated with alkaline phosphatase and substrate, the emitted light is measured in a luminometer as relative light units (RLU). Samples are classified as positive for HR HPV if the relative light unit (RLU) reading is above 1.0, which (according to the manufacturer) is equivalent to 1 pg HPV DNA/ml. We did not test for low-risk HPV types. Borderline results (0.7 to 2.0 RLU) (found in 27 samples) were retested in duplicates, and a 2/3 decision on whether the specimen was positive or not was made. RESULTS Concordance pretreatment. Before treatment, all 239 enrolled women were tested for HPV DNA, and 177 of these women were then treated by conization at visit 2. The majority of all enrolled women, 162, were positive for HPV by both methods, 49 were negative by both methods, 18 were negative by PCR and positive by HCII, and 10 were positive by PCR and negative by HCII (kappa, 0.70). In the subpopulation of the 177 treated women, 88 out of 98 patients with CIN II or worse (CIN II ) in histopathology were HPV positive by both methods (Table 1). Five patients were negative by both methods, seven were negative by PCR, and eight were negative by HCII (Table 1) (kappa, 0.639). Four of the five patients with CIN II that were negative by both methods were reanalyzed and again found negative by both methods. Among the 30 patients with normal histopathology (which includes the diagnosis koilocytosis in accordance with the nomenclature of Koss [20]), 23 patients were positive by HCII and 19 were positive by PCR, respectively. Sensitivity, specificity, and predictive values for CIN II-III by histopathology and cytology. The performance indicators of
4 VOL. 43, 2005 HCII AND PCR-BASED HPV TEST FOR DIAGNOSIS OF CIN 3263 TABLE 2. Sensitivities, specificities, positive predictive values, and negative predictive values of HCII and PCR with and without reanalysis of discrepant samples Clinical endpoint Performance indicator a HCII (%) HCII with reanalysis (%) PCR (%) PCR with reanalysis (%) Histopathology, CIN II Sensitivity Specificity PPV NPV Histopathology, CIN III Sensitivity Specificity PPV NPV Cytology, CIN II Sensitivity Specificity PPV NPV Cytology, CIN III Sensitivity Specificity PPV NPV a PPV, positive predictive values; NPV, negative predictive values. HCII and PCR-EIA were quite similar, both with and without reanalysis of discrepant samples (summarized in Table 2). Concordance posttreatment. After treatment (visit 3), 111/ 147 patients were negative by both methods, 23 patients were positive by both methods, 6 were negative by PCR and positive by HCII, and 7 were positive by PCR and negative by HCII (kappa, 0.72) (data not shown). Most patients (57/68) with CIN II in histopathology at treatment became HPV negative by both methods after treatment (Table 3). Seven out of 68 CIN II patients were HPV positive by both methods also after treatment. Only four patients were discrepant, all being positive by PCR and negative by HCII (PCR /HCII ) (kappa, 0.746). Among the 22 patients that had had normal histopathology, 6 were HPV positive by both methods after treatment (Table 3). Only two patients were discrepant (both negative by PCR and positive by HCII [PCR /HCII ]). Five out of 110 patients had CIN II in cytology at the first follow-up visit; four of these were HPV positive by both methods, and one was HPV negative by both methods (Table 4). Most patients, 83/110, had normal cytology and were HPV negative by both methods. Only 8 out of 110 patients had normal cytology and were HPV positive by both methods. TABLE 3. HPV DNA test results from PCR and HCII analyses of samples from 114 patients after conization a Sample type No. of patients PCR /HC PCR /HC PCR /HC PCR /HC Total Normal Koilocytosis CIN I CIN II CIN III/CIS b a The HPV DNA test results are related to the histopathological diagnosis of the cone at treatment. b CIS, carcinoma in situ. There were six patients that were discrepant among patients with normal cytology: four were PCR /HCII, and two were PCR /HCII (Table 4). Reanalysis of discrepant samples. Forty-one samples had discrepant results in PCR-EIA and HCII (28 pretreatment and 13 posttreatment samples). All discrepant samples were analyzed again with PCR and HCII as well as with type-specific PCR (TS-PCR) for types 16 and 18. Two out of four HCIInegative samples that were HPV 16 positive by PCR-EIA/ RDBH were negative in TS-PCR. However, the repeat PCR- EIA/RDBH did again find that these samples were HPV 16 positive. Similarly, one out of four HCII-negative samples that were HPV 18 positive by PCR-EIA/RDBH was negative in TS-PCR, but the repeat PCR-EIA/RDBH did again find this sample to be HPV 18 positive (not shown). Among the 28 discrepant pretreatment samples, 8 initially HCII-positive samples, but none of the initially PCR-positive samples, became negative. None of the initially HCII-negative samples became positive, but two initially PCR-negative samples became positive. Thirteen posttreatment samples were discrepant. The only change on retesting was two HCII-positive samples that became negative. Among the 10 HCII-positive samples that became negative in reanalysis, 6 had had borderline results. For 27 out of the 41 samples that were reanalyzed by HCII, the relative light unit values decreased after each rerun (not shown). Discrepant samples in relation to histopathology at treatment. Most (13/18) patients with positive HCII and negative PCR pretreatment samples had normal histopathology or were not treated, 5/18 patients had CIN I-II, and none had CIN III. Similarly, most (5/6) patients with positive HCII and negative PCR posttreatment samples had normal histopathology at treatment or had not been treated, and only 1/6 had CIN I at treatment. Among patients with PCR /HCII pretreatment samples, 5/10 patients had normal histopathology or were untreated, 3/10 had CIN I-II, and 2/10 had CIN III. Among patients who were PCR /HCII at follow-up, most (6/7) had
5 3264 SÖDERLUND-STRAND ET AL. J. CLIN. MICROBIOL. TABLE 4. HPV DNA test results from PCR and HCII analyses of samples from 110 patients (all treated patients) related to the cytological diagnosis at the first follow-up visit Sample type No. of patients PCR /HC PCR /HC PCR /HC PCR /HC Total a Normal CIN I CIN II CIN III/CIS b Cytological sample not adequate a Another four patients should have been included, but it was not possible to obtain any adequate cytological samples from these patients. b CIS, carcinoma in situ. CIN before treatment (one patient had not been treated, four had CIN I-II, and two had CIN III). DISCUSSION We found a substantial concordance between PCR and HCII (kappa values of 0.70 and 0.72 before and after treatment, respectively), which is in accordance with previous studies (2, 30, 37). However, the number of positive samples detected by HCII tended to be higher than the number detected by PCR-EIA among patients with normal histopathology, both before treatment (HCII, 23 samples; PCR, 19 samples) and after treatment (HCII, 8 samples; PCR, 6 samples). One possible explanation for this could be cross-reactivity with other HPV types. Most HPV types previously found to cause false positivity by cross-reactivity with the probe cocktail in the HCII test are not classified as HR HPVs (1, 30, 35) and would be expected to be found preferentially in histopathologically normal specimens. Several PCR-negative and HCII-positive samples (9/24; 38%) became PCR negative and HCII negative on reanalysis, particularly those which had had borderline HCII results (6/9; 67%). In the HCII reanalysis, the relative light unit values for 27/41 (66%) samples decreased. This could be explained either by the fact that only discrepant samples were selected for reanalysis ( regression dilution bias [22]) or if the specimens were not stable on storage. Four out of five samples from patients diagnosed with CIN II were reanalyzed and repeatedly HPV negative in both tests. Several reasons for this are possible. The samples may have been truly HPV negative. It is, e.g., reported that regressing CIN lesions may become HPV negative some time before they show morphological regression (25). Other possibilities include infection with an HR HPV type not included in the HCII and PCR-EIA probe cocktails or histopathological misdiagnosis. The somewhat better sensitivity of PCR-EIA than HCII, 100% compared to 95.6%, respectively, for detection of CIN III is not due to differences in probe composition between PCR and HCII, since only one more HPV type (HPV 66) is included in the PCR probe cocktail, and none of the discrepant samples in the entire study was positive for HPV 66. PCR had a higher analytical sensitivity (2.6 fg of HPV 16 plasmids/ml) than HCII (1 pg HPV DNA/ml according to the manufacturer), and it is therefore likely that the PCR /HCII samples contained low amounts of virus. Notably, PCR /HCII samples were more common than PCR /HCII samples in the follow-up samples taken after treatment, in line with the possibility that there are only few infected cells left after conization. Improved follow-up after CIN treatment is a major application of HPV testing. Successful treatment for CIN is associated with HPV clearance (11). HPV DNA persistence is known to be a near-necessary risk factor for CIN (3, 4, 15, 21, 24, 34, 40), and as expected, posttreatment presence of HR-HPV is a good marker for recurrence (10, 17), better than abnormal cytology (26). The recent systematic literature review of Paraskevaidis et al. (27) identified 11 studies (eight retrospective and three prospective studies) that evaluated the use of HPV testing after treatment for CIN. The total number of women included in these studies was 900, of whom 672 (75.3%) were considered as having a successful treatment, compared with 204 (23.3%) who were considered treatment failures. Nine studies used PCR and two studies used HCII; none of the studies used both tests. The specificity of HPV testing ranged from 44% to 95%. Altogether, among the 672 women in whom the treatment was considered successful, the postoperative HPV DNA test was reported as negative in 566 (84.2%) women and positive in 106 (15.8%) women. In contrast, among the 204 cases that were considered as treatment failures, only 35 cases (17.2%) had a negative postoperative HPV DNA test, whereas 169 cases (82.8%) tested positive. The results of the systematic review (27) are well in line with our study: 97 of our patients had normal cytology posttreatment, 10 of which were HPV positive by HCII (10.3%) and 12 of which were positive by PCR (12.4%). Six out of 110 treated patients (5%) had CIN I and 5/110 (4.5%) had CIN II in cytology after treatment (two patients had CIN III, and three had CIN II). For both HCII and PCR, 9/11 (82%) of the patients with CINI, CIN II, or CIN III in posttreatment cytology were HPV positive posttreatment. One of the patients with CIN II was negative by both PCR-EIA and HCII, whereas the other four with CIN II were positive by both methods, and there were no discrepant results. The negative predictive values for CIN II in cytology posttreatment were 100% for CIN III and 99% for CIN II for both methods, which confirms the value of HPV testing in follow-up after treatment, since a negative HPV DNA test posttreatment implies a negligible risk of residual high-grade disease (17). Our data suggest that the variability between various studies (27) in performance of HPV DNA testing in posttreatment follow-up is not due to the type of HPV test used and that both methods appear to be adequate for identifying patients that are not at high risk of residual or recurrent disease after treatment. Possible reasons for variability between studies include differences in laboratory performance or in study design. Cervical screening using a combination of HPV DNA testing by HCII and cytology has substantially better sensitivity for CIN II detection than cytology alone, but the specificity is lower (2, 5, 29). The sensitivity of HCII alone for detecting CIN II lesions has been reported to be 95% (5, 8). We find similar sensitivities for CIN II detection by PCR-EIA and HCII, at levels comparable to those of previous reports (100.0% for CIN III and 92.9% for CIN II by PCR, and 95.6% for CIN III and 91.8% for CIN II by HCII). However, the specificities were low, 23.5% for CIN III and 30.4% for
6 VOL. 43, 2005 HCII AND PCR-BASED HPV TEST FOR DIAGNOSIS OF CIN 3265 CIN II by PCR and 18.9% for CIN III and 24.1% for CIN II by HCII. It should be noted that the specificity refers to the specificity in a clinical secondary screening setting where all women have had an abnormal smear and that the specificities in a primary screening setting would most likely be substantially better. The HCII method is easy to use and is commercially available and has therefore been recommended for routine screening use (5, 8, 37, 38), although some authors suggest that the number of false-positive samples in normal smears due to cross-reactivity with low-risk HPVs needs to be reduced (35). We confirm that HCII had some false-positive samples among patients with normal histopathology, but the concordance between HCII and PCR was generally good, and the sensitivity of HCII for CIN III detection was high and almost equal to the sensitivity of PCR. In summary, both for CINII detection in a secondary screening setting as well as for follow-up posttreatment, both HCII and PCR appear to be adequate for routine use. ACKNOWLEDGMENTS This study was supported by Europe against Cancer and by the Swedish Cancer Society. We thank Kia Sjölin, University Hospital of Malmö, for technical assistance. REFERENCES 1. Atypical Squamous Cells of Undetermined Significance/Low-Grade Squamous Intraepithelial Lesions Triage Study (ALTS) Group Human papillomavirus testing for triage of women with cytologic evidence of lowgrade squamous intraepithelial lesions: baseline data from a randomized trial. J. Natl. Cancer Inst. 92: Bergeron, C., D. Jeannel, J. D. Poveda, P. Cassonnet, and G. Orth Human papillomavirus testing in women with mild cytologic atypia. Obstet. Gynecol. 95: Bosch, F. X., M. M. Manos, N. Munoz, M. Sherman, A. M. Jansen, J. Peto, M. H. Schiffman, V. Moreno, R. Kurman, and K. V. Shah, et al Prevalence of human papillomavirus in cervical cancer: a worldwide perspective. J. Natl. Cancer Inst. 87: Bosch, F. X., and N. Munoz The viral etiology of cervical cancer. Virus Res. 89: Clavel, C., M. Masure, J. P. Bory, I. Putaud, C. Mangeonjean, M. Lorenzato, R. Gabriel, C. Quereux, and P. Birembaut Hybrid capture II-based human papillomavirus detection, a sensitive test to detect in routine highgrade cervical lesions: a preliminary study on 1518 women. Br. J. Cancer 80: Clavel, C., J. Cucherousset, M. Lorenzato, S. Caudroy, J. M. Nou, P. Nazeyrollas, M. Polette, J.-P. Bory, R. Gabriel, C. Quereux, and P. Birembaut Negative human papillomavirus testing in normal smears selects a population at low risk for developing high-grade cervical lesions. Br. J. Cancer 90: Clifford, G. M., J. S. Smith, M. Plummer, N. Munoz, and S. Franceschi Human papillomavirus types in invasive cervical cancer worldwide: a meta-analysis. Br. J. Cancer 88: Cuzick, J., E. Beverley, L. Ho, G. Terry, H. Sapper, I. Mielzynska, A. Lorincz, W. K. Chan, T. Krausz, and P. Soutter HPV testing in primary screening of older women. Br. J. Cancer 81: de Roda Husman, A.-M., J. M. M. Walboomers, A. J. C. van den Brule, C. J. L. M. Meijer, and P. J. F. Snijders The use of general primers GP5 and GP6 elongated at their 3 ends with adjacent highly conserved sequences improves human papillomavirus detection by PCR. J. Gen. Virol. 76: Distefano, A. L., M. A. Picconi, L. V. Alonio, D. Dalbert, J. Mural, O. Bartt, G. Bazan, G. Cervantes, M. Lizano, A. G. Carranca, and A. Teyssie Persistence of human papillomavirus DNA in cervical lesions after treatment with diathermic large loop excision. Infect. Dis. Obstet. Gynecol. 6: Elfgren, K., P. Bistoletti, L. Dillner, J. M. M. Walboomers, J. L. M. Meijer, and J. Dillner Conization for cervical intraepithelial neoplasia is followed by disappearance of human papillomavirus deoxyribonucleic acid and a decline in serum and cervical mucus antibodies against human papillomavirus antigens. Am. J. Obstet. Gynecol. 174: Forslund, O., B. G. Hansson, P. Rymark, and B. Bjerre Human papillomavirus DNA in urine samples compared with that in simultaneously collected urethra and cervix samples. J. Clin. Microbiol. 31: Forslund, O., B. G. Hansson, and B. Bjerre Typing of human papillomaviruses by consensus polymerase chain reaction and a non-radioactive reverse dot blot hybridization. J. Virol. Methods 49: Gravitt, P. E., C. L. Peyton, T. Q. Alessi, C. M. Wheeler, F. Coutlee, A. Hildesheim, M. H. Schiffman, D. R. Scott, and R. J. Apple Improved amplification of genital human papillomaviruses. J. Clin. Microbiol. 38: Ho, G. Y. F., R. D. Burk, S. Klein, A. S. Kadish, C. J. Chang, P. Palan, J. Basu, R. Tachezy, R. Lewis, and S. Romney Persistent genital human papillomavirus infection as a risk factor for persistent cervical dysplasia. J. Natl. Cancer Inst. 87: Ho, G. Y. F., R. Bierman, L. Beardsley, C. J. Chang, and R. D. Burk Natural history of cervicovaginal papillomavirus infection in young women. N. Engl. J. Med. 338: Houfflin Debarge, V., P. Collinet, D. Vinatier, A. Ego, A. Dewilde, F. Boman, and J. L. Leroy Value of human papillomavirus testing after conization by loop electrosurgical excision for high-grade squamous intraepithelial lesions. Gynecol. Oncol. 90: Jacobs, M. V., P. J. F. Snijders, J. C. van den Brule, T. J. M. Helmerhorst, C. J. L. M. Meijer, and J. M. M. Walboomers A general primer GP5 /GP6 -mediated PCR-enzyme immunoassay method for rapid detection of 14 high-risk and 6 low-risk human papillomavirus genotypes in cervical scrapings. J. Clin. Microbiol. 35: Jacobs, M. V., J. M. M. Walboomers, P. J. F. Snijders, F. J. Voorhorst, R. H. M. Verheijen, N. Fransen-Daalmeijer, and C. J. L. M. Meijer Distribution of 37 mucosotropic HPV types in women with cytologically normal cervical smears: the age-related patterns for high-risk and low-risk types. Int. J. Cancer 87: Koss, L. G. (ed) Diagnostic cytology and its histologic basis, 3rd ed. Lippincott, Philadelphia, Pa. 21. Koutsky, L. A., K. K. Holmes, C. W. Critchlow, C. E. Stevens, J. Paavonen, A. M. Beckmann, T. A. DeRouen, D. A. Galloway, D. Vernon, and N. B. Kiviat A cohort study of the risk of cervical intraepithelial neoplasia grade 2 or 3 in relation to papillomavirus infection. N. Engl. J. Med. 327: MacMahon, S., R. Peto, J. Cutler, R. Collins, P. Sorlie, J. Neaton, R. Abbott, J. Godwin, A. Dyer, and J. Stamler Blood pressure, stroke and coronary heart disease. Part 1. Prolonged differences in blood pressure: Prospective observational studies corrected for the regression dilution bias. Lancet 335: Munoz, N., F. X. Bosch, S. de Sanjose, R. Herrero, X. Castellsauge, K. V. Shah, P. J. F. Snijders, C. J. L. M. Meijer, et al Epidemiologic classification of human papillomavirus types associated with cervical cancer. N. Engl. J. Med. 348: Nobbenhuis, M. A. E., J. M. M. Walboomers, T. J. M. Helmerhorst, L. Rozendaal, A. J. Remmink, E. K. J. Risse, H. C. van der Linden, F. J. Voorhorst, P. Kenemans, and C. J. L. M. Meijer Relation of human papillomavirus status to cervical lesions and consequences for cervical-cancer screening: a prospective study. Lancet 354: Nobbenhuis, M. A. E., T. J. M. Helmerhorst, A. J. C. van den Brule, L. Rozendaal, F. J. Voorhorst, P. D. Bezemer, R. H. M. Verheijen, and C. J. L. M. Meijer Cytological regression and clearance of high-risk human papillomavirus in women with an abnormal cervical smear. Lancet 358: Nobbenhuis, M. A. E., C. J. L. M. Meijer, A. J. C. van den Brule, L. Rozendaal, F. J. Voorhorst, E. K. J. Rissa, R. H. M. Verheijen, and T. J. M. Helmerhorst Addition of high-risk HPV testing improves the current guidelines on follow-up after treatment for cervical intraepithelial neoplasia. Br. J. Cancer 84: Paraskevaidis, E., M. Arbyn, A. Sotiriadis, E. Diakomanolis, P. Martin- Hirsch, G. Koliopoulos, G. Makrydimas, J. Tofoski, and D. H. Roukos The role of HPV DNA testing in the follow-up period after treatment for CIN: a systematic review of the literature. Cancer Treat. Rev. 30: Parkin, M., P. Pisani, and J. Ferlay Estimates of the worldwide incidence of 25 major cancers in Int. J. Cancer 80: Petry, K. U., S. Menton, M. Menton, F. van Loenen-Frosch, H. de Carvalho Gomes, B. Holz, B. Schopp, S. Garbrecht-Buettner, P. Davies, G. Boehmer, E. van den Akker, and T. Iftner Inclusion of HPV testing in routine cervical cancer screening for women above 29 years in Germany: results for 8466 patients. Br. J. Cancer 88: Peyton, C. L., M. Schiffman, A. T. Lörincz, W. C. Hunt, I. Mielzynska, C. Bratti, S. Eaton, A. Hildesheim, L. A. Morera, A. C. Rodriguez, R. Herrero, M. E. Sherman, and C. M. Wheeler Comparison of PCR- and Hybrid Capture-based human papillomavirus detection systems using multiple cervical specimen collection strategies. J. Clin. Microbiol. 36: Poljak, M., A. Brencic, K. Seme, A. Vince, and I. J. Marin Comparative evaluation of first- and second-generation Digene Hybrid Capture assays for detection of human papillomaviruses associated with high or intermediate risk for cervical cancer. J. Clin. Microbiol. 37: Romney, S. L., G. Y. F. Ho, P. R. Palan, J. Basu, A. S. Kadish, S. Klein, M. Mikhail, R. J. Hagan, C. J. Chang, and R. D. Burk Effects of -car-
7 3266 SÖDERLUND-STRAND ET AL. J. CLIN. MICROBIOL. otene and other factors on outcome of cervical dysplasia and human papillomavirus infection. Gynecol. Oncol. 65: Rozendaal, L., J. M. M. Walboomers, J. C. van der Linden, F. J. Voorhorst, P. Kenemans, T. J. M. Helmerhorst, M. van Ballegooijen, and C. J. L. M. Meijer PCR-based high-risk HPV test in cervical cancer screening gives objective risk assessment of women with cytomorphologically normal cervical smears. Int. J. Cancer 68: Schiffman, M. H., H. M. Bauer, R. N. Hoover, A. G. Glass, D. M. Cadell, B. B. Rush, D. R. Scott, M. E. Sherman, R. J. Kurman, S. Wacholder, C. K. Stanton, and M. M. Manos Epidemiologic evidence showing that human papillomavirus infection causes most cervical intraepithelial neoplasia. J. Natl. Cancer Inst. 85: Schneede, P., P. Hillemanns, F. Ziller, A. Hofstetter, E. Stockfleth, R. Arndt, and T. Meyer Evaluation of HPV testing by Hybrid Capture II for routine gynaecologic screening. Acta Obstet. Gynecol. Scand. 80: Sherman, M. E., A. T. Lorincz, D. R. Scott, S. Wacholder, P. E. Castle, A. G. Glass, I. Mielzynska-Lohnas, B. B. Rush, and M. Schiffman Baseline cytology, human papillomavirus testing, and risk for cervical neoplasia: a 10-year cohort analysis. J. Natl. Cancer Inst. 95: Venturoli, S., M. Cricca, F. Bonvicini, F. Giosa, F. R. Pulvirenti, C. Galli, M. Musiani, and M. Zerbini Human papillomavirus DNA testing by PCR-ELISA and hybrid capture II from a single cytological specimen: concordance and correlation with cytological results. J. Clin. Virol. 25: Vince, A., N. Kutela, J. Iscic-Bes, V. Harni, M. Ivanisevic, Z. Sonicki, Z. Culig, and M. Poljak Clinical utility of molecular detection of human papillomavirus in cervical samples by hybrid capture technology. J. Clin. Virol. 25: Walboomers, J. M. M., and C. J. L. M. Meijer Do HPV-negative cervical carcinomas exist? J. Pathol. 181: Walboomers, J. M. M., M. V. Jacobs, M. M. Manos, F. X. Bosch, J. A. Kummer, K. V. Shah, P. J. F. Snijders, J. Peto, C. J. L. M. Meijer, and N. Munoz Human papillomavirus is a necessary cause of invasive cervical cancer worldwide. J. Pathol. 189:12 19.
The Korean Journal of Cytopathology 15 (1) : 17-27, 2004
 5 The Korean Journal of Cytopathology 5 () : 7-7, / 5 / / (human papillomavirus, HPV), 6%, 5% HPV. HPV HPV. HPV HPV,,5 HPV HPV. HPV, 6 HPV. HPV HPV International Agency for Research on Cancer (IARC) HPV
5 The Korean Journal of Cytopathology 5 () : 7-7, / 5 / / (human papillomavirus, HPV), 6%, 5% HPV. HPV HPV. HPV HPV,,5 HPV HPV. HPV, 6 HPV. HPV HPV International Agency for Research on Cancer (IARC) HPV
No HPV High Risk Screening with Genotyping. CPT Code: If Result is NOT DETECTED (x3) If Results is DETECTED (Genotype reported)
 CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 117 August 6, 2013 HPV High Risk Screening with Genotyping Contact: Dr. Jeffrey Wisotzkey, 717-851-1422 Director, Molecular Pathology
CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 117 August 6, 2013 HPV High Risk Screening with Genotyping Contact: Dr. Jeffrey Wisotzkey, 717-851-1422 Director, Molecular Pathology
Received 14 December 2005/Returned for modification 17 February 2006/Accepted 1 May 2006
 JOURNAL OF CLINICAL MICROBIOLOGY, July 2006, p. 2428 2433 Vol. 44, No. 7 0095-1137/06/$08.00 0 doi:10.1128/jcm.02608-05 Copyright 2006, American Society for Microbiology. All Rights Reserved. Assessment
JOURNAL OF CLINICAL MICROBIOLOGY, July 2006, p. 2428 2433 Vol. 44, No. 7 0095-1137/06/$08.00 0 doi:10.1128/jcm.02608-05 Copyright 2006, American Society for Microbiology. All Rights Reserved. Assessment
Negative human papillomavirus testing in normal smears selects a population at low risk for developing high-grade cervical lesions
 British Journal of Cancer (2004) 90, 1803 1808 All rights reserved 0007 0920/04 $25.00 www.bjcancer.com Negative human papillomavirus testing in normal smears selects a population at low risk for developing
British Journal of Cancer (2004) 90, 1803 1808 All rights reserved 0007 0920/04 $25.00 www.bjcancer.com Negative human papillomavirus testing in normal smears selects a population at low risk for developing
Validation of an automated detection platform. for use with the Roche Linear Array HPV Genotyping Test ACCEPTED SEPEHR N.
 JCM Accepts, published online ahead of print on September 00 J. Clin. Microbiol. doi:./jcm.0-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
JCM Accepts, published online ahead of print on September 00 J. Clin. Microbiol. doi:./jcm.0-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
Received 4 December 2006/Returned for modification 29 January 2007/Accepted 26 April 2007
 JOURNAL OF CLINICAL MICROBIOLOGY, July 2007, p. 2130 2137 Vol. 45, No. 7 0095-1137/07/$08.00 0 doi:10.1128/jcm.02438-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Comparison
JOURNAL OF CLINICAL MICROBIOLOGY, July 2007, p. 2130 2137 Vol. 45, No. 7 0095-1137/07/$08.00 0 doi:10.1128/jcm.02438-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Comparison
Human Papillomavirus and Papanicolaou Tests to Screen for Cervical Cancer
 original article Human Papillomavirus and Papanicolaou Tests to Screen for Cervical Cancer Pontus Naucler, M.D., Ph.D., Walter Ryd, M.D., Sven Törnberg, M.D., Ph.D., Anders Strand, M.D., Ph.D., Göran Wadell,
original article Human Papillomavirus and Papanicolaou Tests to Screen for Cervical Cancer Pontus Naucler, M.D., Ph.D., Walter Ryd, M.D., Sven Törnberg, M.D., Ph.D., Anders Strand, M.D., Ph.D., Göran Wadell,
Comparison of the Digene HC2 Assay and the Roche AMPLICOR Human Papillomavirus (HPV) Test for Detection of High-Risk HPV Genotypes in Cervical Samples
 JOURNAL OF CLINICAL MICROBIOLOGY, June 2006, p. 2141 2146 Vol. 44, No. 6 0095-1137/06/$08.00 0 doi:10.1128/jcm.00049-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Comparison
JOURNAL OF CLINICAL MICROBIOLOGY, June 2006, p. 2141 2146 Vol. 44, No. 6 0095-1137/06/$08.00 0 doi:10.1128/jcm.00049-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Comparison
Attitudes to self-sampling of vaginal smear for human papilloma virus analysis among women not attending organized cytological screening
 Acta Obstetricia et Gynecologica. 2007; 86: 720 725 ORIGINAL ARTICLE Attitudes to self-sampling of vaginal smear for human papilloma virus analysis among women not attending organized cytological screening
Acta Obstetricia et Gynecologica. 2007; 86: 720 725 ORIGINAL ARTICLE Attitudes to self-sampling of vaginal smear for human papilloma virus analysis among women not attending organized cytological screening
A systematic review of the role of human papilloma virus (HPV) testing within a cervical screening programme: summary and conclusions
 British Journal of Cancer (2000) 83(5), 561 565 doi: 10.1054/ bjoc.2000.1375, available online at http://www.idealibrary.com on A systematic review of the role of human papilloma virus (HPV) testing within
British Journal of Cancer (2000) 83(5), 561 565 doi: 10.1054/ bjoc.2000.1375, available online at http://www.idealibrary.com on A systematic review of the role of human papilloma virus (HPV) testing within
Comparative evaluation of smear cytology & hybrid capture II for the diagnosis of cervical cancer
 Indian J Med Res 126, July 2007, pp 39-44 Comparative evaluation of smear cytology & hybrid capture II for the diagnosis of cervical cancer Kamlesh Kumar, Venkateswaran K. Iyer, Neerja Bhatla*, Alka Kriplani*
Indian J Med Res 126, July 2007, pp 39-44 Comparative evaluation of smear cytology & hybrid capture II for the diagnosis of cervical cancer Kamlesh Kumar, Venkateswaran K. Iyer, Neerja Bhatla*, Alka Kriplani*
Performance of the Aptima High-Risk Human Papillomavirus mrna Assay in a Referral Population in Comparison with Hybrid Capture 2 and Cytology
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 1071 1076 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.01674-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Performance
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 1071 1076 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.01674-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Performance
HPV-DNA Test Kit in Cervical Scrapes or
 Infectious Diseases in Obstetrics and Gynecology 2:126-129 (I 994) (C) 1994 Wiley-Liss, Inc. Detection of Human Papillomavirus DNA by AffiProbe HPV-DNA Test Kit in Cervical Scrapes or Biopsies-Histopathologic
Infectious Diseases in Obstetrics and Gynecology 2:126-129 (I 994) (C) 1994 Wiley-Liss, Inc. Detection of Human Papillomavirus DNA by AffiProbe HPV-DNA Test Kit in Cervical Scrapes or Biopsies-Histopathologic
Cross-Sectional Comparison of an Automated Hybrid Capture 2 Assay and the Consensus GP5 /6 PCR Method in a Population-Based Cervical Screening Program
 JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 2006, p. 3680 3685 Vol. 44, No. 10 0095-1137/06/$08.00 0 doi:10.1128/jcm.02078-05 Copyright 2006, American Society for Microbiology. All Rights Reserved. Cross-Sectional
JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 2006, p. 3680 3685 Vol. 44, No. 10 0095-1137/06/$08.00 0 doi:10.1128/jcm.02078-05 Copyright 2006, American Society for Microbiology. All Rights Reserved. Cross-Sectional
with That in Simultaneously Collected Urethra and Cervix Samples
 JOURNAL OF CLINICAL MICROBIOLOGY, Aug. 1993, P. 1975-1979 0095-1137/93/081975-05$02.00/0 Copyright 1993, American Society for Microbiology Vol. 31, No. 8 Human Papillomavirus DNA in Urine Samples Compared
JOURNAL OF CLINICAL MICROBIOLOGY, Aug. 1993, P. 1975-1979 0095-1137/93/081975-05$02.00/0 Copyright 1993, American Society for Microbiology Vol. 31, No. 8 Human Papillomavirus DNA in Urine Samples Compared
Woo Dae Kang, Ho Sun Choi, Seok Mo Kim
 Is vaccination with quadrivalent HPV vaccine after Loop Electrosurgical Excision Procedure effective in preventing recurrence in patients with High-grade Cervical Intraepithelial Neoplasia (CIN2-3)? Chonnam
Is vaccination with quadrivalent HPV vaccine after Loop Electrosurgical Excision Procedure effective in preventing recurrence in patients with High-grade Cervical Intraepithelial Neoplasia (CIN2-3)? Chonnam
Ho Young Jung Hye Seung Han Hyo Bin Kim 1 Seo Young Oh 1 Sun-Joo Lee 2 Wook Youn Kim
 Journal of Pathology and Translational Medicine 2016; 50: 138-146 ORIGINAL ARTICLE Comparison of Analytical and Clinical Performance of HPV 9G DNA Chip, PANArray HPV Genotyping Chip, and Hybrid-Capture
Journal of Pathology and Translational Medicine 2016; 50: 138-146 ORIGINAL ARTICLE Comparison of Analytical and Clinical Performance of HPV 9G DNA Chip, PANArray HPV Genotyping Chip, and Hybrid-Capture
Papers. Abstract. Introduction. Methods
 Type specific persistence of high risk human papillomavirus (HPV) as indicator of high grade cervical squamous intraepithelial lesions in young women: population based prospective follow up study Susanne
Type specific persistence of high risk human papillomavirus (HPV) as indicator of high grade cervical squamous intraepithelial lesions in young women: population based prospective follow up study Susanne
Comparison of HPV test versus conventional and automation-assisted Pap screening as potential screening tools for preventing cervical cancer
 BJOG: an International Journal of Obstetrics and Gynaecology August 2004, Vol. 111, pp. 842 848 DOI: 1 0. 1111/j.1471-0528.2004.00210.x Comparison of HPV test versus conventional and automation-assisted
BJOG: an International Journal of Obstetrics and Gynaecology August 2004, Vol. 111, pp. 842 848 DOI: 1 0. 1111/j.1471-0528.2004.00210.x Comparison of HPV test versus conventional and automation-assisted
For the Atypical Squamous Cells of Undetermined Significance/Low-Grade Squamous Intraepithelial Lesion Triage Study Group
 Effects of Age and Human Papilloma Viral Load on Colposcopy Triage: Data From the Randomized Atypical Squamous Cells of Undetermined Significance/ Low-Grade Squamous Intraepithelial Lesion Triage Study
Effects of Age and Human Papilloma Viral Load on Colposcopy Triage: Data From the Randomized Atypical Squamous Cells of Undetermined Significance/ Low-Grade Squamous Intraepithelial Lesion Triage Study
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 341 N OVEMBER 25, 1999 NUMBER 22 TYPE-SPECIFIC PERSISTENCE OF HUMAN PAPILLOMAVIRUS DNA BEFORE THE DEVELOPMENT
The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 341 N OVEMBER 25, 1999 NUMBER 22 TYPE-SPECIFIC PERSISTENCE OF HUMAN PAPILLOMAVIRUS DNA BEFORE THE DEVELOPMENT
The Clinical Performance of Primary HPV Screening, Primary HPV Screening Plus Cytology Cotesting, and Cytology Alone at a Tertiary Care Hospital
 The Clinical Performance of Primary HPV Screening, Primary HPV Screening Plus Cytology Cotesting, and Cytology Alone at a Tertiary Care Hospital Jung-Woo Choi MD, PhD; Younghye Kim MD, PhD; Ju-Han Lee
The Clinical Performance of Primary HPV Screening, Primary HPV Screening Plus Cytology Cotesting, and Cytology Alone at a Tertiary Care Hospital Jung-Woo Choi MD, PhD; Younghye Kim MD, PhD; Ju-Han Lee
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sherman SI, Wirth LJ, Droz J-P, et al. Motesanib diphosphate
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sherman SI, Wirth LJ, Droz J-P, et al. Motesanib diphosphate
Human papillomavirus testing as a cytology gold standard: comparing Surinam with the Netherlands
 & 2005 USCAP, Inc All rights reserved 0893-3952/05 $30.00 www.modernpathology.org Human papillomavirus testing as a cytology gold standard: comparing Surinam with the Netherlands Mitchell S Wachtel 1,
& 2005 USCAP, Inc All rights reserved 0893-3952/05 $30.00 www.modernpathology.org Human papillomavirus testing as a cytology gold standard: comparing Surinam with the Netherlands Mitchell S Wachtel 1,
Methods for HPV Detection: Polymerase Chain Reaction Assays
 Monsonego J (ed): Emerging Issues on HPV Infections: From Science to Practice. Basel, Karger, 2006, pp 63 72 Methods for HPV Detection: Polymerase Chain Reaction Assays Suzanne M. Garland a,b, Sepehr Tabrizi
Monsonego J (ed): Emerging Issues on HPV Infections: From Science to Practice. Basel, Karger, 2006, pp 63 72 Methods for HPV Detection: Polymerase Chain Reaction Assays Suzanne M. Garland a,b, Sepehr Tabrizi
Abstract. Human papillomavirus (HPV) DNA testing is cost-effective 1-3 (S. Kulasingam, PhD, et al, unpublished Atypical
 Anatomic Pathology / HPV DNA DETECTION IN ALTS A Comparison of a Prototype PCR Assay and Hybrid Capture 2 for Detection of Carcinogenic Human Papillomavirus DNA in Women With Equivocal or Mildly Abnormal
Anatomic Pathology / HPV DNA DETECTION IN ALTS A Comparison of a Prototype PCR Assay and Hybrid Capture 2 for Detection of Carcinogenic Human Papillomavirus DNA in Women With Equivocal or Mildly Abnormal
Detection and estimation of human papillomavirus viral load in patients with cervical lesions
 Bangladesh Med Res Counc Bull 2013; 39: 86-90 Detection and estimation of human papillomavirus viral load in patients with cervical lesions Rahman T 1, Tabassum S 2, Jahan M 2, Nessa A 2, Ashrafunnessa
Bangladesh Med Res Counc Bull 2013; 39: 86-90 Detection and estimation of human papillomavirus viral load in patients with cervical lesions Rahman T 1, Tabassum S 2, Jahan M 2, Nessa A 2, Ashrafunnessa
CONDOM USE PROMOTES REGRESSION OF CERVICAL INTRAEPITHELIAL NEOPLASIA AND CLEARANCE OF HUMAN PAPILLOMAVIRUS: A RANDOMIZED CLINICAL TRIAL
 Int. J. Cancer: 107, 811 816 (2003) 2003 Wiley-Liss, Inc. Publication of the International Union Against Cancer CONDOM USE PROMOTES REGRESSION OF CERVICAL INTRAEPITHELIAL NEOPLASIA AND CLEARANCE OF HUMAN
Int. J. Cancer: 107, 811 816 (2003) 2003 Wiley-Liss, Inc. Publication of the International Union Against Cancer CONDOM USE PROMOTES REGRESSION OF CERVICAL INTRAEPITHELIAL NEOPLASIA AND CLEARANCE OF HUMAN
Abstract Aim To evaluate the presence of high risk human papillomaviruses (HPV) in cervical smears showing intraepithelial neoplasia
 J Clin Pathol 1999;52:17 22 17 Department of Gynaecology, Friedrich Schiller University, Bachstr 18, 07740 Jena, Germany I Nindl B Lotz U Endisch A Schneider Department of Pathology, Friedrich Schiller
J Clin Pathol 1999;52:17 22 17 Department of Gynaecology, Friedrich Schiller University, Bachstr 18, 07740 Jena, Germany I Nindl B Lotz U Endisch A Schneider Department of Pathology, Friedrich Schiller
Research Recherche. Return to September 5, 2000 Table of Contents
 Comparison of self-collected vaginal, vulvar and urine samples with physician-collected cervical samples for human papillomavirus testing to detect high-grade squamous intraepithelial lesions John W. Sellors,
Comparison of self-collected vaginal, vulvar and urine samples with physician-collected cervical samples for human papillomavirus testing to detect high-grade squamous intraepithelial lesions John W. Sellors,
Comparison between the Hybrid Capture II Test and an SPF1/GP6 PCR-Based Assay for Detection of Human Papillomavirus DNA in Cervical Swab Samples
 JOURNAL OF CLINICAL MICROBIOLOGY, May 2006, p. 1733 1739 Vol. 44, No. 5 0095-1137/06/$08.00 0 doi:10.1128/jcm.44.5.1733 1739.2006 Copyright 2006, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, May 2006, p. 1733 1739 Vol. 44, No. 5 0095-1137/06/$08.00 0 doi:10.1128/jcm.44.5.1733 1739.2006 Copyright 2006, American Society for Microbiology. All Rights Reserved.
IJC International Journal of Cancer
 IJC International Journal of Cancer Clearance of human papillomavirus infection after successful conization in patients with cervical intraepithelial neoplasia Young-Tak Kim 1, Jong Min Lee 2, Soo-Young
IJC International Journal of Cancer Clearance of human papillomavirus infection after successful conization in patients with cervical intraepithelial neoplasia Young-Tak Kim 1, Jong Min Lee 2, Soo-Young
PERSISTENCE AND LOAD OF HIGH-RISK HPV ARE PREDICTORS FOR DEVELOPMENT OF HIGH-GRADE CERVICAL LESIONS: A LONGITUDINAL FRENCH COHORT STUDY
 Int. J. Cancer: 106, 396 403 (2003) 2003 Wiley-Liss, Inc. Publication of the International Union Against Cancer PERSISTENCE AND LOAD OF HIGH-RISK HPV ARE PREDICTORS FOR DEVELOPMENT OF HIGH-GRADE CERVICAL
Int. J. Cancer: 106, 396 403 (2003) 2003 Wiley-Liss, Inc. Publication of the International Union Against Cancer PERSISTENCE AND LOAD OF HIGH-RISK HPV ARE PREDICTORS FOR DEVELOPMENT OF HIGH-GRADE CERVICAL
Detection of Human Papillomavirus DNA in Cytologically Normal Women and Subsequent Cervical Squamous Intraepithelial Lesions
 Detection of Human Papillomavirus DNA in Cytologically Normal Women and Subsequent Cervical Squamous Intraepithelial Lesions Kai-Li Liaw, Andrew G. Glass, M. Michele Manos, Catherine E. Greer, David R.
Detection of Human Papillomavirus DNA in Cytologically Normal Women and Subsequent Cervical Squamous Intraepithelial Lesions Kai-Li Liaw, Andrew G. Glass, M. Michele Manos, Catherine E. Greer, David R.
The Absolute Risk of Cervical Abnormalities in High-risk Human Papillomavirus Positive, Cytologically Normal Women Over a 10-Year Period
 Published Online First on October 23, 2006 as 10.1158/0008-5472.CAN-06-1057 Research Article The Absolute Risk of Cervical Abnormalities in High-risk Human Papillomavirus Positive, Cytologically Normal
Published Online First on October 23, 2006 as 10.1158/0008-5472.CAN-06-1057 Research Article The Absolute Risk of Cervical Abnormalities in High-risk Human Papillomavirus Positive, Cytologically Normal
Prediction of high-grade cervical intraepithelial neoplasia in cytologically normal women by human papillomavirus testing
 doi: 10.1054/ bjoc.2000.1491, available online at http://www.idealibrary.com on http://www.bjcancer.com Prediction of high-grade cervical intraepithelial neoplasia in cytologically normal women by human
doi: 10.1054/ bjoc.2000.1491, available online at http://www.idealibrary.com on http://www.bjcancer.com Prediction of high-grade cervical intraepithelial neoplasia in cytologically normal women by human
The clearest path to the most meaningful results. The cobas HPV Test delivers clinical value with workflow efficiencies every step of the way
 The clearest path to the most meaningful results The cobas HPV Test delivers clinical value with workflow efficiencies every step of the way The cobas HPV Test KNOW THE RISK Help guide clinical decision
The clearest path to the most meaningful results The cobas HPV Test delivers clinical value with workflow efficiencies every step of the way The cobas HPV Test KNOW THE RISK Help guide clinical decision
Cervical Cancer Screening. David Quinlan December 2013
 Cervical Cancer Screening David Quinlan December 2013 Cervix Cervical Cancer Screening Modest variation provincially WHO and UK begin at 25 stop at 60 Finland begin at 30 stop at 60 Rationale for
Cervical Cancer Screening David Quinlan December 2013 Cervix Cervical Cancer Screening Modest variation provincially WHO and UK begin at 25 stop at 60 Finland begin at 30 stop at 60 Rationale for
Abnormal Cervicovaginal Cytology With Negative Human Papillomavirus Testing
 280 Abnormal Cervicovaginal Cytology With Negative Human Papillomavirus Testing Giovanni Negri, MD Bettina Rigo, BS Fabio Vittadello, ScD Christine Mian, ScD Eduard Egarter-Vigl, MD Department of Pathology,
280 Abnormal Cervicovaginal Cytology With Negative Human Papillomavirus Testing Giovanni Negri, MD Bettina Rigo, BS Fabio Vittadello, ScD Christine Mian, ScD Eduard Egarter-Vigl, MD Department of Pathology,
Philip E. Castle, Diane Solomon, Mark Schiffman, Cosette M. Wheeler for the ALTS Group
 ARTICLEARTICLESHuman Papillomavirus Type 16 Infections and 2-Year Absolute Risk of Cervical Precancer in Women With Equivocal or Mild Cytologic Abnormalities Philip E. Castle, Diane Solomon, Mark Schiffman,
ARTICLEARTICLESHuman Papillomavirus Type 16 Infections and 2-Year Absolute Risk of Cervical Precancer in Women With Equivocal or Mild Cytologic Abnormalities Philip E. Castle, Diane Solomon, Mark Schiffman,
Edinburgh Research Explorer
 Edinburgh Research Explorer Persistent high risk HPV infection associated with development of cervical neoplasia in a prospective population study Citation for published version: Cuschieri, K, Cubie, H,
Edinburgh Research Explorer Persistent high risk HPV infection associated with development of cervical neoplasia in a prospective population study Citation for published version: Cuschieri, K, Cubie, H,
Human Papillomavirus (HPV) in Atypical Squamous Cervical Cytology: the Invader HPV Test as a New Screening Assay
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2008, p. 869 875 Vol. 46, No. 3 0095-1137/08/$08.00 0 doi:10.1128/jcm.01424-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Human Papillomavirus
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2008, p. 869 875 Vol. 46, No. 3 0095-1137/08/$08.00 0 doi:10.1128/jcm.01424-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Human Papillomavirus
Can HPV-16 Genotyping Provide a Benchmark for Cervical Biopsy Specimen Interpretation?
 Anatomic Pathology / Monitoring HPV-16 Fractions in CIN Can HPV-16 Genotyping Provide a Benchmark for Cervical Biopsy Specimen Interpretation? Mary T. Galgano, MD, 1 Philip E. Castle, PhD, MPH, 2 Mark
Anatomic Pathology / Monitoring HPV-16 Fractions in CIN Can HPV-16 Genotyping Provide a Benchmark for Cervical Biopsy Specimen Interpretation? Mary T. Galgano, MD, 1 Philip E. Castle, PhD, MPH, 2 Mark
News. Laboratory NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING TIMOTHY UPHOFF, PHD, DABMG, MLS (ASCP) CM
 Laboratory News Inside This Issue NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING...1 NEW HPV TEST METHODOLOGY PROVIDES BETTER SPECIFICITY FOR CERVICAL CANCER...4 BEYOND
Laboratory News Inside This Issue NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING...1 NEW HPV TEST METHODOLOGY PROVIDES BETTER SPECIFICITY FOR CERVICAL CANCER...4 BEYOND
Received 1 October 2001/Returned for modification 25 March 2002/Accepted 14 June 2002
 JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 2002, p. 3341 3345 Vol. 40, No. 9 0095-1137/02/$04.00 0 DOI: 10.1128/JCM.40.9.3341 3345.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 2002, p. 3341 3345 Vol. 40, No. 9 0095-1137/02/$04.00 0 DOI: 10.1128/JCM.40.9.3341 3345.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved.
Philip E. Castle, Patti E. Gravitt, Diane Solomon, Cosette M. Wheeler and Mark Schiffman
 REFERENCES CONTENT ALERTS Comparison of Linear Array and Line Blot Assay for Detection of Human Papillomavirus and Diagnosis of Cervical Precancer and Cancer in the Atypical Squamous Cell of Undetermined
REFERENCES CONTENT ALERTS Comparison of Linear Array and Line Blot Assay for Detection of Human Papillomavirus and Diagnosis of Cervical Precancer and Cancer in the Atypical Squamous Cell of Undetermined
Accuracy and Interlaboratory Reliability of Human Papillomavirus DNA Testing by Hybrid Capture
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 1995, p. 545 550 Vol. 33, No. 3 0095-1137/95/$04.00 0 Copyright 1995, American Society for Microbiology Accuracy and Interlaboratory Reliability of Human Papillomavirus
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 1995, p. 545 550 Vol. 33, No. 3 0095-1137/95/$04.00 0 Copyright 1995, American Society for Microbiology Accuracy and Interlaboratory Reliability of Human Papillomavirus
Clinical Performance of Roche COBAS 4800 HPV Test
 JCM Accepts, published online ahead of print on 9 April 2014 J. Clin. Microbiol. doi:10.1128/jcm.00883-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 1 2 3 4 5 6 Clinical
JCM Accepts, published online ahead of print on 9 April 2014 J. Clin. Microbiol. doi:10.1128/jcm.00883-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 1 2 3 4 5 6 Clinical
Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines
 Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines Tim Kremer, MD Ralph Anderson, MD 1 Objectives Describe the natural history of HPV particularly as it relates
Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines Tim Kremer, MD Ralph Anderson, MD 1 Objectives Describe the natural history of HPV particularly as it relates
Human papiloma virus testing in the cervix of high-risk women: A hospital-based clinicopathological, colposcopic, and cytogenetic study
 Research Article Human papiloma virus testing in the cervix of high-risk women: A hospital-based clinicopathological, colposcopic, and cytogenetic study Subhash Bhardwaj 1, Farooq Ahmed Wani 2, Altaf Bandy
Research Article Human papiloma virus testing in the cervix of high-risk women: A hospital-based clinicopathological, colposcopic, and cytogenetic study Subhash Bhardwaj 1, Farooq Ahmed Wani 2, Altaf Bandy
c Tuj1(-) apoptotic live 1 DIV 2 DIV 1 DIV 2 DIV Tuj1(+) Tuj1/GFP/DAPI Tuj1 DAPI GFP
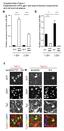 Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
Jean-Christophe Noël and Philippe Simon. 1. Introduction
 Analytical Cellular Pathology Volume 2015, Article ID 746502, 4 pages http://dx.doi.org/10.1155/2015/746502 Research Article Limitations on the Detection Rate of High-Risk HPV by Hybrid Capture 2 Methodology
Analytical Cellular Pathology Volume 2015, Article ID 746502, 4 pages http://dx.doi.org/10.1155/2015/746502 Research Article Limitations on the Detection Rate of High-Risk HPV by Hybrid Capture 2 Methodology
Evidence-based treatment of a positive HPV DNA test. Th. Agorastos Prof. of Obstetrics & Gynaecology Aristotle University Thessaloniki/GR
 Evidence-based treatment of a positive HPV DNA test Th. Agorastos Prof. of Obstetrics & Gynaecology Aristotle University Thessaloniki/GR HPV DNA testing Indications 1. Triage after cytology with ASCUS/LSIL
Evidence-based treatment of a positive HPV DNA test Th. Agorastos Prof. of Obstetrics & Gynaecology Aristotle University Thessaloniki/GR HPV DNA testing Indications 1. Triage after cytology with ASCUS/LSIL
Comparison of the DiagCor GenoFlow Human Papillomavirus Array Test and Roche Linear Array HPV Genotyping Test
 The Open Virology Journal, 2010, 4, 169-174 169 Open Access Comparison of the DiagCor GenoFlow Human Papillomavirus Array Test and Roche Linear Array HPV Genotyping Test Fiona K.Y. Wong, Johannes C.Y.
The Open Virology Journal, 2010, 4, 169-174 169 Open Access Comparison of the DiagCor GenoFlow Human Papillomavirus Array Test and Roche Linear Array HPV Genotyping Test Fiona K.Y. Wong, Johannes C.Y.
Supplementary Document
 Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
The PapilloCheck Assay for the Detection of High Grade Cervical Intraepithelial Neoplasia
 JCM Accepted Manuscript Posted Online 2 September 2015 J. Clin. Microbiol. doi:10.1128/jcm.01578-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. The PapilloCheck Assay for the
JCM Accepted Manuscript Posted Online 2 September 2015 J. Clin. Microbiol. doi:10.1128/jcm.01578-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. The PapilloCheck Assay for the
Determinants of Clearance of Human Papillomavirus Infections in Colombian Women with Normal Cytology: A Population-based, 5-Year Follow-up Study
 American Journal of Epidemiology Copyright 2003 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 158, No. 5 Printed in U.S.A. DOI: 10.1093/aje/kwg171 Determinants of Clearance
American Journal of Epidemiology Copyright 2003 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 158, No. 5 Printed in U.S.A. DOI: 10.1093/aje/kwg171 Determinants of Clearance
Human Papillomavirus Genotypes and the Cumulative 2-Year Risk of Cervical Precancer
 MAJOR ARTICLE Human Papillomavirus Genotypes and the Cumulative 2-Year Risk of Cervical Precancer Cosette M. Wheeler, 1,2 William C. Hunt, 1 Mark Schiffman, 3 and Philip E. Castle, 3 for the Atypical Squamous
MAJOR ARTICLE Human Papillomavirus Genotypes and the Cumulative 2-Year Risk of Cervical Precancer Cosette M. Wheeler, 1,2 William C. Hunt, 1 Mark Schiffman, 3 and Philip E. Castle, 3 for the Atypical Squamous
FREQUENCY AND RISK FACTORS OF CERVICAL Human papilloma virus INFECTION
 Arch. Biol. Sci., Belgrade, 66 (4), 1653-1658, 2014 DOI:10.2298/ABS1404653M FREQUENCY AND RISK FACTORS OF CERVICAL Human papilloma virus INFECTION IN WOMEN IN MONTENEGRO GORDANA MIJOVIĆ 1, TATJANA JOVANOVIĆ
Arch. Biol. Sci., Belgrade, 66 (4), 1653-1658, 2014 DOI:10.2298/ABS1404653M FREQUENCY AND RISK FACTORS OF CERVICAL Human papilloma virus INFECTION IN WOMEN IN MONTENEGRO GORDANA MIJOVIĆ 1, TATJANA JOVANOVIĆ
Comparison of Southern Blot Hybridization and Polymerase Chain Reaction Methods for the Detection of Human Papillomavirus DNA
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 1991, p. 573-577 0095-1137/91/030573-05$02.00/0 Copyright C) 1991, American Society for Microbiology Vol. 29, No. 3 Comparison of Southern Blot Hybridization and
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 1991, p. 573-577 0095-1137/91/030573-05$02.00/0 Copyright C) 1991, American Society for Microbiology Vol. 29, No. 3 Comparison of Southern Blot Hybridization and
Human Papillomaviruses: Biology and Laboratory Testing
 For our patients and our population Human Papillomaviruses: Biology and Laboratory Testing Geoffrey Higgins Microbiology and Infectious Diseases For our patients and our population HPV Associated Cancers
For our patients and our population Human Papillomaviruses: Biology and Laboratory Testing Geoffrey Higgins Microbiology and Infectious Diseases For our patients and our population HPV Associated Cancers
Prevalence of Human Papillomavirus Genotypes in Routine Pap Smear of 2,562 Korean Women Determined by PCR-DNA Sequencing
 Journal of Bacteriology and Virology 2009. Vol. 39, No. 4 p.337 344 DOI 10.4167/jbv.2009.39.4.337 Original Article Prevalence of Human Papillomavirus Genotypes in Routine Pap Smear of 2,562 Korean Women
Journal of Bacteriology and Virology 2009. Vol. 39, No. 4 p.337 344 DOI 10.4167/jbv.2009.39.4.337 Original Article Prevalence of Human Papillomavirus Genotypes in Routine Pap Smear of 2,562 Korean Women
Laboratory Considerations
 Laboratory Considerations In Support of HPV Vaccine Programs Elizabeth R. Unger PhD, MD Team Leader HPV Laboratory Centers for Disease Prevention and Control Towards Comprehensive Cervical Cancer Control:
Laboratory Considerations In Support of HPV Vaccine Programs Elizabeth R. Unger PhD, MD Team Leader HPV Laboratory Centers for Disease Prevention and Control Towards Comprehensive Cervical Cancer Control:
Biomed Environ Sci, 2015; 28(1): 80-84
 80 Biomed Environ Sci, 2015; 28(1): 80-84 Letter to the Editor Assessing the Effectiveness of a Cervical Cancer Screening Program in a Hospital-based Study* YANG Yi1, LANG Jing He1, WANG You Fang1, CHENG
80 Biomed Environ Sci, 2015; 28(1): 80-84 Letter to the Editor Assessing the Effectiveness of a Cervical Cancer Screening Program in a Hospital-based Study* YANG Yi1, LANG Jing He1, WANG You Fang1, CHENG
Development and Duration of Human Papillomavirus Lesions, after Initial Infection
 MAJOR ARTICLE Development and Duration of Human Papillomavirus Lesions, after Initial Infection Rachel L. Winer, 1 Nancy B. Kiviat, 2 James P. Hughes, 3 Diane E. Adam, 1 Shu-Kuang Lee, 3 Jane M. Kuypers,
MAJOR ARTICLE Development and Duration of Human Papillomavirus Lesions, after Initial Infection Rachel L. Winer, 1 Nancy B. Kiviat, 2 James P. Hughes, 3 Diane E. Adam, 1 Shu-Kuang Lee, 3 Jane M. Kuypers,
Cervical Cancer Screening for the Reluctant HPV Testing of Air-Dried Vaginal Discharge
 International journal of Biomedical science Cervical Cancer Screening for the Reluctant HPV Testing of Air-Dried Vaginal Discharge Tommy R. Tong 1, Rae Wai-nang Yau 1, Olivia Wai-hing Chan 2, Vivian Yu
International journal of Biomedical science Cervical Cancer Screening for the Reluctant HPV Testing of Air-Dried Vaginal Discharge Tommy R. Tong 1, Rae Wai-nang Yau 1, Olivia Wai-hing Chan 2, Vivian Yu
Study Number: Title: Rationale: Phase: Study Period Study Design: Centres: Indication Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
SensoLyte pnpp Alkaline Phosphatase Assay Kit *Colorimetric*
 SensoLyte pnpp Alkaline Phosphatase Assay Kit *Colorimetric* Catalog # 72146 Kit Size 500 Assays (96-well plate) Optimized Performance: This kit is optimized to detect alkaline phosphatase activity Enhanced
SensoLyte pnpp Alkaline Phosphatase Assay Kit *Colorimetric* Catalog # 72146 Kit Size 500 Assays (96-well plate) Optimized Performance: This kit is optimized to detect alkaline phosphatase activity Enhanced
Can Human Papillomavirus DNA Testing Substitute for Cytology in the Detection of High-Grade Cervical Lesions?
 Can Human Papillomavirus DNA Testing Substitute for Cytology in the Detection of High-Grade Cervical Lesions? Kyung-Ju Lee, MD; Jae-Kwan Lee, MD; Ho-Suk Saw, MD, PhD Context. High-risk human papillomaviruses
Can Human Papillomavirus DNA Testing Substitute for Cytology in the Detection of High-Grade Cervical Lesions? Kyung-Ju Lee, MD; Jae-Kwan Lee, MD; Ho-Suk Saw, MD, PhD Context. High-risk human papillomaviruses
Opinion: Cervical cancer a vaccine preventable disease
 Opinion: Cervical cancer a vaccine preventable disease Leon Snyman Principal specialist at the Department of Obstetrics and Gynaecology, Gynaecological Oncology unit, University of Pretoria and Kalafong
Opinion: Cervical cancer a vaccine preventable disease Leon Snyman Principal specialist at the Department of Obstetrics and Gynaecology, Gynaecological Oncology unit, University of Pretoria and Kalafong
Chapter 14: Role of Triage Testing in Cervical Cancer Screening
 Chapter 14: Role of Triage Testing in Cervical Cancer Screening Diane Solomon The classic model of cervical cancer prevention primary screening with cytology, followed by diagnostic colposcopically directed
Chapter 14: Role of Triage Testing in Cervical Cancer Screening Diane Solomon The classic model of cervical cancer prevention primary screening with cytology, followed by diagnostic colposcopically directed
Chapter 5. M.G. Dijkstra L. Rozendaal M. van Zummeren F.J. van Kemenade P.J.F. Snijders C.J.L.M. Meijer J. Berkhof. Submitted for publication
 Chapter 5 CIN3 and cancer risks after primary HPV DNA testing and cytology triage in cervical cancer screening: fifteen years follow-up of a randomized controlled trial M.G. Dijkstra L. Rozendaal M. van
Chapter 5 CIN3 and cancer risks after primary HPV DNA testing and cytology triage in cervical cancer screening: fifteen years follow-up of a randomized controlled trial M.G. Dijkstra L. Rozendaal M. van
Validation of the SPF 10 LiPA Human Papillomavirus Typing Assay Using Formalin-Fixed Paraffin-Embedded Cervical Biopsy Samples
 JOURNAL OF CLINICAL MICROBIOLOGY, July 2009, p. 2175 2180 Vol. 47, No. 7 0095-1137/09/$08.00 0 doi:10.1128/jcm.00286-09 Copyright 2009, American Society for Microbiology. All Rights Reserved. Validation
JOURNAL OF CLINICAL MICROBIOLOGY, July 2009, p. 2175 2180 Vol. 47, No. 7 0095-1137/09/$08.00 0 doi:10.1128/jcm.00286-09 Copyright 2009, American Society for Microbiology. All Rights Reserved. Validation
ISSN X (Print) *Corresponding author Dr. Narotam Sharma
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(8E):3107-3112 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(8E):3107-3112 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Promoting Cervical Screening Information for Health Professionals. Cervical Cancer
 Promoting Cervical Screening Information for Health Professionals Cervical Cancer PapScreen Victoria Cancer Council Victoria 1 Rathdowne St Carlton VIC 3053 Telephone: (03) 635 5147 Fax: (03) 9635 5360
Promoting Cervical Screening Information for Health Professionals Cervical Cancer PapScreen Victoria Cancer Council Victoria 1 Rathdowne St Carlton VIC 3053 Telephone: (03) 635 5147 Fax: (03) 9635 5360
Absolute Risk of a Subsequent Abnormal Pap among Oncogenic Human Papillomavirus DNA-Positive, Cytologically Negative Women
 Absolute Risk of a Subsequent Abnormal Pap among Oncogenic Human Papillomavirus DNA-Positive, Cytologically Negative Women 2145 Philip E. Castle, Ph.D., M.P.H. 1 Sholom Wacholder, Ph.D. 1 Mark E. Sherman,
Absolute Risk of a Subsequent Abnormal Pap among Oncogenic Human Papillomavirus DNA-Positive, Cytologically Negative Women 2145 Philip E. Castle, Ph.D., M.P.H. 1 Sholom Wacholder, Ph.D. 1 Mark E. Sherman,
HPV type concordance in sexual couples determines the effect of condoms on regression of flat penile lesions
 British Journal of Cancer (2005) 92, 1388 1392 All rights reserved 0007 0920/05 $30.00 www.bjcancer.com HPV type concordance in sexual couples determines the effect of condoms on regression of flat penile
British Journal of Cancer (2005) 92, 1388 1392 All rights reserved 0007 0920/05 $30.00 www.bjcancer.com HPV type concordance in sexual couples determines the effect of condoms on regression of flat penile
Molecular markers for diagnosis and prognosis in cervical neoplasia Eijsink, Jasper Johannes Hendrikus
 University of Groningen Molecular markers for diagnosis and prognosis in cervical neoplasia Eijsink, Jasper Johannes Hendrikus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Molecular markers for diagnosis and prognosis in cervical neoplasia Eijsink, Jasper Johannes Hendrikus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Human Papillomavirus Genotyping Using an Automated Film-Based Chip Array
 JMD CME Program Journal of Molecular Diagnostics, Vol. 11, No. 5, September 2009 Copyright American Society for Investigative Pathology and the Association for Molecular Pathology DOI: 10.2353/jmoldx.2009.080154
JMD CME Program Journal of Molecular Diagnostics, Vol. 11, No. 5, September 2009 Copyright American Society for Investigative Pathology and the Association for Molecular Pathology DOI: 10.2353/jmoldx.2009.080154
Type-Specific Human Papillomavirus E6/E7 mrna Detection by Real-Time PCR Improves Identification of Cervical Neoplasia
 JOURNAL OF CLINICAL MICROBIOLOGY, Nov. 2011, p. 3794 3799 Vol. 49, No. 11 0095-1137/11/$12.00 doi:10.1128/jcm.00549-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Type-Specific
JOURNAL OF CLINICAL MICROBIOLOGY, Nov. 2011, p. 3794 3799 Vol. 49, No. 11 0095-1137/11/$12.00 doi:10.1128/jcm.00549-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Type-Specific
Evaluation of a Newly Developed GenoArray Human Papillomavirus (HPV) Genotyping Assay and Comparison with the Roche Linear Array HPV Genotyping Assay
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2010, p. 758 764 Vol. 48, No. 3 0095-1137/10/$12.00 doi:10.1128/jcm.00989-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Evaluation of
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2010, p. 758 764 Vol. 48, No. 3 0095-1137/10/$12.00 doi:10.1128/jcm.00989-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Evaluation of
Comparison of DR. HPV Chip Kit with hybrid capture II assay for the detection of human papillomavirus in clinical samples: a preliminary study
 Tropical Biomedicine 24(1): 17 22 (2007) Comparison of DR. HPV Chip Kit with hybrid capture II assay for the detection of human papillomavirus in clinical samples: a preliminary study Rajan Saini 1, Tae
Tropical Biomedicine 24(1): 17 22 (2007) Comparison of DR. HPV Chip Kit with hybrid capture II assay for the detection of human papillomavirus in clinical samples: a preliminary study Rajan Saini 1, Tae
Human Papillomavirus (HPV) DNA Copy Number Is Dependent on Grade of Cervical Disease and HPV Type
 JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 1999, p. 1030 1034 Vol. 37, No. 4 0095-1137/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Human Papillomavirus (HPV) DNA Copy
JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 1999, p. 1030 1034 Vol. 37, No. 4 0095-1137/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Human Papillomavirus (HPV) DNA Copy
Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening
 Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening Clinical Policy Number: 01.01.02 Effective Date: April 1, 2015 Initial Review Date: January 21, 2015 Most Recent
Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening Clinical Policy Number: 01.01.02 Effective Date: April 1, 2015 Initial Review Date: January 21, 2015 Most Recent
Focus. International #52. HPV infection in High-risk HPV and cervical cancer. HPV: Clinical aspects. Natural history of HPV infection
 HPV infection in 2014 Papillomaviruses (HPV) are non-cultivable viruses with circular DNA. They can establish productive infections in the skin (warts) and in mucous membranes (genitals, larynx, etc.).
HPV infection in 2014 Papillomaviruses (HPV) are non-cultivable viruses with circular DNA. They can establish productive infections in the skin (warts) and in mucous membranes (genitals, larynx, etc.).
A Prospective Study of High-Grade Cervical Neoplasia Risk Among Human Papillomavirus-Infected Women
 A Prospective Study of High-Grade Cervical Neoplasia Risk Among Human Papillomavirus-Infected Women Philip E. Castle, Sholom Wacholder, Attila T. Lorincz, David R. Scott, Mark E. Sherman, Andrew G. Glass,
A Prospective Study of High-Grade Cervical Neoplasia Risk Among Human Papillomavirus-Infected Women Philip E. Castle, Sholom Wacholder, Attila T. Lorincz, David R. Scott, Mark E. Sherman, Andrew G. Glass,
Comparison of the Third Wave Invader Human Papillomavirus (HPV) Assay and the Digene HPV Hybrid Capture 2 Assay for Detection of High-Risk HPV DNA
 JOURNAL OF CLINICAL MICROBIOLOGY, May 2008, p. 1641 1646 Vol. 46, No. 5 0095-1137/08/$08.00 0 doi:10.1128/jcm.01824-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Comparison
JOURNAL OF CLINICAL MICROBIOLOGY, May 2008, p. 1641 1646 Vol. 46, No. 5 0095-1137/08/$08.00 0 doi:10.1128/jcm.01824-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Comparison
Abstract. Int J Gynecol Cancer 2006, 16,
 Int J Gynecol Cancer 2006, 16, 1801 1808 The distribution and differential risks of human papillomavirus genotypes in cervical preinvasive lesions: a Taiwan Cooperative Oncologic Group Study C.-A. CHEN*,
Int J Gynecol Cancer 2006, 16, 1801 1808 The distribution and differential risks of human papillomavirus genotypes in cervical preinvasive lesions: a Taiwan Cooperative Oncologic Group Study C.-A. CHEN*,
RESEARCH ARTICLE. Pap Smear Combined with HPV Testing: A Reasonable Tool for Women with High-grade Cervical Intraepithelial Neoplasia Treated by LEEP
 DOI:http://dx.doi.org/10.7314/APJCP.2015.16.10.4297 Pap Smear Combined with HPV Testing RESEARCH ARTICLE Pap Smear Combined with HPV Testing: A Reasonable Tool for Women with High-grade Cervical Intraepithelial
DOI:http://dx.doi.org/10.7314/APJCP.2015.16.10.4297 Pap Smear Combined with HPV Testing RESEARCH ARTICLE Pap Smear Combined with HPV Testing: A Reasonable Tool for Women with High-grade Cervical Intraepithelial
Low grade squamous intra-epithelial lesions and human papillomavirus infection in Colombian women
 British Journal of Cancer (2002) 87, 1417 1421 All rights reserved 0007 0920/02 $25.00 www.bjcancer.com Low grade squamous intra-epithelial lesions and human papillomavirus infection in Colombian women
British Journal of Cancer (2002) 87, 1417 1421 All rights reserved 0007 0920/02 $25.00 www.bjcancer.com Low grade squamous intra-epithelial lesions and human papillomavirus infection in Colombian women
Evaluation of the SPF 10 -INNO LiPA Human Papillomavirus (HPV) Genotyping Test and the Roche Linear Array HPV Genotyping Test
 JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 2006, p. 3122 3129 Vol. 44, No. 9 0095-1137/06/$08.00 0 doi:10.1128/jcm.00517-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Evaluation
JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 2006, p. 3122 3129 Vol. 44, No. 9 0095-1137/06/$08.00 0 doi:10.1128/jcm.00517-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Evaluation
Single and multiple human papillomavirus infections in cervical abnormalities in Portuguese women
 ORIGINAL ARTICLE VIROLOGY Single and multiple human papillomavirus infections in cervical abnormalities in Portuguese women A. Pista*, A. Oliveira*, N. Verdasca and F. Ribeiro National Laboratory of STI
ORIGINAL ARTICLE VIROLOGY Single and multiple human papillomavirus infections in cervical abnormalities in Portuguese women A. Pista*, A. Oliveira*, N. Verdasca and F. Ribeiro National Laboratory of STI
Human Papillomavirus Genotype Specificity of Hybrid Capture 2. Low-risk Probe Cocktail
 JCM Accepts, published online ahead of print on 3 June 2009 J. Clin. Microbiol. doi:10.1128/jcm.00278-09 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 3 June 2009 J. Clin. Microbiol. doi:10.1128/jcm.00278-09 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Factors associated with HPV persistence after conization in patients with negative margins
 J Gynecol Oncol Vol. 20, No. 2:91-95, June 2009 DOI:10.3802/jgo.2009.20.2.91 Original Article Factors associated with HPV persistence after conization in patients with negative margins Kyehyun Nam, Sooho
J Gynecol Oncol Vol. 20, No. 2:91-95, June 2009 DOI:10.3802/jgo.2009.20.2.91 Original Article Factors associated with HPV persistence after conization in patients with negative margins Kyehyun Nam, Sooho
Genotyping of human papillomavirus in triaging of low-grade cervical cytology.
 Genotyping of human papillomavirus in triaging of low-grade cervical cytology. Söderlund Strand, Anna; Eklund, Carina; Kemetli, Levent; Grillner, Lena; Törnerg, Sven; Dillner, Joakim; Dillner, Lena Pulished
Genotyping of human papillomavirus in triaging of low-grade cervical cytology. Söderlund Strand, Anna; Eklund, Carina; Kemetli, Levent; Grillner, Lena; Törnerg, Sven; Dillner, Joakim; Dillner, Lena Pulished
Human papillomavirus typing in HIV-positive women
 Infect Dis Obstet Gynecol ;9:89 93 Human papillomavirus typing in HIV-positive women Meera Hameed, Helen Fernandes, Joan Skurnick, Dorothy Moore, Patricia Kloser 3 and Debra Heller Department of Pathology
Infect Dis Obstet Gynecol ;9:89 93 Human papillomavirus typing in HIV-positive women Meera Hameed, Helen Fernandes, Joan Skurnick, Dorothy Moore, Patricia Kloser 3 and Debra Heller Department of Pathology
