Sentinel nodes. Location: Location: S1.04 Principal clinician. G1.01 Record other relevant information. S2.01 Number of specimens submitted
|
|
|
- Lindsey Byrd
- 6 years ago
- Views:
Transcription
1 Invasive Breast Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth DD MM YYYY Sex Male Female Intersex/indeterminate Ethnicity Unknown Aboriginal/Torres Strait Islander Other ethnicity: Patient identifiers e.g. MRN, IHI or NHI (please indicate which) Date of request S1.03 Accession number Requesting doctor - name and contact details DD MM YYYY S1.02 Clinical details Specimen type (select all that apply) diagnostic open biopsy wide local excision (partial mastectomy, quadrantectomy or segmentectomy) re-excision mastectomy mastectomy post neoadjuvant therapy lymph node biopsy - non-sentinel Tumour site and laterality axillary sample axillary clearance lymph node biopsy - sentinel Sentinel nodes Location: Number: Colour: Radioactive count: Location: Number: Colour: Radioactive count: S1.04 Principal clinician G1.01 Record other relevant information Method of localisation Carbon track Hook wire Macroscopic findings S2.01 Number of specimens submitted New primary cancer or recurrence New primary Regional (local) recurrence Distant metastases S2.02 Specimen laterality Right Left Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 1 of 11
2 S2.03 Specimen type diagnostic open biopsy wide local excision (partial mastectomy, quadrantectomy or segmentectomy) re-excision mastectomy mastectomy post neoadjuvant therapy other Superficial-deep length Superior-inferior length S2.07 Specimen weight g Lymph tissue (select all that apply) Not submitted Lymph node biopsy - sentinel Lymph node biopsy - non-sentinel Axillary sample Axillary clearance S2.08 Macroscopically visible tumours? Number of foci: Intraoperative consultation Not performed Performed Type (select all that apply) frozen section imprint cytology gross examination for margin assessment other S2.09 GROSS DESCRIPTION OF TUMOUR(S) Complete for EACH tumour identified above. Tumour 1 Nature of tumour Tumour size S2.04 Specimen orientation Not oriented Oriented Markers and locations: length x width x thickness Distance to nearest separate tumour foci Minimum macroscopic margin clearance from any tumour deposit From which margin? S2.05 Method of localisation Carbon track Hook wire N/A Tumour 2 Nature of tumour S2.06 Specimen size length x width x thickness If oriented use the following 3 measures: Medial-lateral length Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 2 of 11
3 Tumour 2 (cont.) Tumour size length x width x thickness S2.11 Muscle Tumour 3 Distance to nearest separate tumour foci Minimum macroscopic margin clearance from any tumour deposit Nature of tumour From which margin? S2.12 SENTINEL NODES NODE 1 Site Axilla Internal maary chain Radioactive count Uptake of dye No Yes - Blue Size length x width x thickness NODE 2 Tumour size length x width x thickness Site Axilla Internal maary chain Radioactive count Distance to nearest separate tumour foci Uptake of dye Size No Yes - Blue Minimum macroscopic margin clearance from any tumour deposit length x width x thickness From which margin? NODE 3 Site Axilla Internal maary chain S2.10 Skin Skin dimensions length x width Radioactive count Uptake of dye Size No Yes - Blue Skin abnormalities or choose all that apply: Ulceration Paget disease Satellite nodules Other length x width x thickness NON - SENTINEL NODES/TISSUE Total number of nodes Size range to Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 3 of 11
4 NON - SENTINEL NODES/TISSUE (Cont) Description Microscopic findings S3.01 Multiple tumours? Quadrants involved S2.13 Block identification key Total no. of tumour deposits If >2 record the following.. Max. span of multifocal tumour bed involved length x width For EACH tumour identified above complete S3.02-S3.04 and consider recording G3.01 Tumour 1 S3.02 MAXIMUM INVASIVE TUMOUR SIZE Whole tumour size Maximum size of invasive tumour G3.01 Other invasive tumour dimensions length x width S3.03 HISTOLOGIC GRADE INVASIVE CARCINOMA G2.01 Other macroscopic coent Score for nuclear grade Score 1: Size equivalent to normal breast epithelial cells, regular outlines, uniform chromatin; inconspicuous nucleoli, little size variation Score 2: Larger nuclei, open vesicular chromatin; visible nucleoli, moderate variability is size and shape Score 3: Vesicular nuclei; often with prominent nucleoli; exhibiting marked variation in size and shape, occasionally very large and bizarre forms Score for tubule differentiation Score 1: >75% of invasive carcinoma Score 2: 10 75% of invasive carcinoma Score 3: <10% of invasive carcinoma * microinvasion only (each focus 1) Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 4 of 11
5 Score for mitotic rate Tumour 2 which is a score of Number of mitoses per 10 HPF OR * ** microinvasion only (each focus 1) Total Score Grade 1 - Total score of 3 5 Grade 2 - Total score of 6 or 7 Grade 3 - Total score of 8 or 9 * microinvasion only (each focus 1) S3.04 Invasive carcinoma subtype Invasive carcinoma of No Special Type (Ductal) Pleomorphic carcinoma Carcinoma with osteoclast like stromal giant cells Carcinoma with choriocarcinomatous features Carcinoma with melanotic features Invasive lobular carcinoma Classical Tubulolobular Alveolar Solid Pleomorphic Mixed Others signet ring, histiocytoid, etc Tubular carcinoma Cribriform carcinoma Mucinous carcinoma Carcinoma with medullary features Medullary Atypical medullary Inv. carcinoma NST (ductal) with medullary features Carcinoma with apocrine differentiation Carcinoma with signet ring cell differentiation Invasive micropapillary carcinoma Metaplastic carcinoma Low grade adenosquamous carcinoma Fibromatosis-like metaplastic carcinoma Squamous cell carcinoma Spindle cell carcinoma Metaplastic carcinoma with mesenchymal differentiation Chondroid differentiation Osseous differentiation Other types of mesenchymal diff. Mixed metaplastic carcinoma Myoepithelial carcinoma Rare Types of Invasive Cancer: Carcinomas with Neuroendocrine features Neuroendocrine tumour, well differentiated Neuroendocrine tumour, poorly differentiated (small cell carcinoma) Carcinoma with neuroendocrine differentiat n Secretory carcinoma Invasive papillary carcinoma Acinic cell carcinoma Mucoepidermoid carcinoma Polymorphous carcinoma Oncocytic carcinoma Lipid rich carcinoma Glycogen rich/clear cell carcinoma Sebaceous carcinoma Salivary gland/skin adnexal type tumours Adenoid cystic carcinoma Adenomyoepithelioma with carcinoma S3.02 MAXIMUM INVASIVE TUMOUR SIZE Whole tumour size Maximum size of invasive tumour G3.01 Other invasive tumour dimensions x S3.03 HISTOLOGIC GRADE INVASIVE CARCINOMA Score for nuclear grade Score 1: Size equivalent to normal breast epithelial cells, regular outlines, uniform chromatin; inconspicuous nucleoli, little size variation. Score 2: Larger nuclei, open vesicular chromatin; visible nucleoli, moderate variability is size and shape Score 3: Vesicular nuclei; often with prominent nucleoli; exhibiting marked variation in size and shape, occasionally very large and bizarre forms Score for tubule differentiation Score 1: >75% of invasive carcinoma Score 2: 10 75% of invasive carcinoma Score 3: <10% of invasive carcinoma. * microinvasion only (each focus 1) Score for mitotic rate Number of mitoses per 10 HPF OR which is a score of * ** microinvasion only (each focus 1) Total Score Grade 1 - Total score of 3 5 Grade 2 - Total score of 6 or 7 Grade 3 - Total score of 8 or 9 * microinvasion only (each focus 1) Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 5 of 11
6 Tumour 2 (cont.) S3.04 Invasive carcinoma subtype Invasive carcinoma of No Special Type (Ductal) Pleomorphic carcinoma Carcinoma with osteoclast like stromal giant cells Carcinoma with choriocarcinomatous features Carcinoma with melanotic features Invasive lobular carcinoma Classical Tubulolobular Alveolar Solid Pleomorphic Mixed Others signet ring, histiocytoid, etc Tubular carcinoma Cribriform carcinoma Mucinous carcinoma Carcinoma with medullary features Medullary Atypical medullary Inv. carcinoma NST (ductal) with medullary features Carcinoma with apocrine differentiation Carcinoma with signet ring cell differentiation Invasive micropapillary carcinoma Metaplastic carcinoma Low grade adenosquamous carcinoma Fibromatosis-like metaplastic carcinoma Squamous cell carcinoma Tumour 3 Spindle cell carcinoma Metaplastic carcinoma with mesenchymal differentiation Chondroid differentiation Osseous differentiation Other types of mesenchymal diff. Mixed metaplastic carcinoma Myoepithelial carcinoma Rare Types of Invasive Cancer: Carcinomas with Neuroendocrine features Neuroendocrine tumour, well differentiated Neuroendocrine tumour, poorly differentiated (small cell carcinoma) Carcinoma with neuroendocrine differentiat n Secretory carcinoma Invasive papillary carcinoma Acinic cell carcinoma Mucoepidermoid carcinoma Polymorphous carcinoma Oncocytic carcinoma Lipid rich carcinoma Glycogen rich/clear cell carcinoma Sebaceous carcinoma Salivary gland/skin adnexal type tumours Adenoid cystic carcinoma Adenomyoepithelioma with carcinoma S3.02 MAXIMUM INVASIVE TUMOUR SIZE Whole tumour size Maximum size of invasive tumour G3.01 Other invasive tumour dimensions length x width S3.03 HISTOLOGIC GRADE INVASIVE CARCINOMA Score for nuclear grade Score 1: Size equivalent to normal breast epithelial cells, regular outlines, uniform chromatin; inconspicuous nucleoli, little size variation. Score 2: Larger nuclei, open vesicular chromatin; visible nucleoli, moderate variability in size and shape Score 3: Vesicular nuclei; often with prominent nucleoli; exhibiting marked variation in size and shape, occasionally very large and bizarre forms Score for tubule differentiation Score 1: >75% of invasive carcinoma Score 2: 10 75% of invasive carcinoma Score 3: <10% of invasive carcinoma. * microinvasion only (each focus 1) Score for mitotic rate Number of mitoses per 10 HPF OR which is a score of * ** microinvasion only (each focus 1) Total Score Grade 1 - Total score of 3 5 Grade 2 - Total score of 6 or 7 Grade 3 - Total score of 8 or 9 * microinvasion only (each focus 1) S3.04 Invasive carcinoma subtype Invasive carcinoma of No Special Type (Ductal) Pleomorphic carcinoma Carcinoma with osteoclast like stromal giant cells Carcinoma with choriocarcinomatous features Carcinoma with melanotic features Invasive lobular carcinoma Classical Tubulolobular Alveolar Solid Pleomorphic Mixed Others signet ring, histiocytoid, etc Tubular carcinoma Cribriform carcinoma Mucinous carcinoma Carcinoma with medullary features Medullary Atypical medullary Inv. carcinoma NST (ductal) with medullary features Carcinoma with apocrine differentiation Carcinoma with signet ring cell differentiation Invasive micropapillary carcinoma Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 6 of 11
7 Tumour 3 (cont.) S3.04 Invasive carcinoma subtype Metaplastic carcinoma Low grade adenosquamous carcinoma Fibromatosis-like metaplastic carcinoma Squamous cell carcinoma Spindle cell carcinoma Metaplastic carcinoma with mesenchymal differentiation Chondroid differentiation Osseous differentiation Other types of mesenchymal diff. Mixed metaplastic carcinoma Myoepithelial carcinoma Rare Types of Invasive Cancer: Carcinomas with Neuroendocrine features Neuroendocrine tumour, well differentiated Neuroendocrine tumour, poorly differentiated (small cell carcinoma) Carcinoma with neuroendocrine differentiat n Secretory carcinoma Invasive papillary carcinoma Acinic cell carcinoma Mucoepidermoid carcinoma Polymorphous carcinoma Oncocytic carcinoma Lipid rich carcinoma Glycogen rich/clear cell carcinoma Sebaceous carcinoma Salivary gland/skin adnexal type tumours Adenoid cystic carcinoma Adenomyoepithelioma with carcinoma S3.08 Treatment effect (after neoadjuvant hormonal or chemotherapy) No definite response to pre-surgical therapy in the invasive carcinoma Partial response to pre-surgical therapy in the invasive carcinoma, residual carcinoma identified. Complete pathologic response in breast and lymph nodes: No residual invasive carcinoma is present in the breast or lymph nodes after pre-surgical therapy Not applicable Estimate of overall level of cellularity for invasive cancer % Specify neoadjuvant response classification system used Result of treatment S3.05 Peritumoural lymphovascular invasion S3.06 Skin S3.07 Muscle Not identified Suspicious Block Not involved Paget disease of the nipple (DCIS extending to skin contiguous with lactiferous sinuses) Invasive carcinoma involving dermis or epidermis without ulceration Invasive carcinoma involving dermis or epidermis with ulceration Ipsilateral satellite skin nodules, ie dermal deposits of invasive carcinoma, separate from the main tumour Not involved Involved S3.09 DCIS only in conjunction with invasive carcinoma only as pure DCIS as both pure DCIS and in conjunction with invasive carcinoma S3.10 Max extent of breast involved by DCIS S3.11 Maximum dimension pure DCIS Low Intermediate High S3.12 Highest nuclear grade of DCIS G3.02 Nuclear grade heterogeneity of DCIS Next most prevalent grade Low Intermediate High Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 7 of 11
8 S3.13 Necrosis in DCIS Margin 2 Clearance OR >10 S3.14 Architecture of DCIS (select all that apply) comedo solid cribriform micropapillary apocrine papillary other Margin 3 Clearance and if DCIS is closer to the margin... to DCIS OR >10 and if DCIS is closer to the margin... to DCIS S3.15 Microcalcification Choose all that apply: in DCIS in benign tissue in invasive cancer Lesion(s) with microcalcification Margins involved Margin 1 Type of involvement DCIS Invasive carcinoma DCIS and invasive carcinoma Orientation of margin Extent of involvement OR Focal Associated with necrosis? No Yes Size and extent of microcalcification (if required) Margin 2 Type of involvement DCIS Invasive carcinoma DCIS and invasive carcinoma Orientation of margin Extent of involvement S3.16 Paget disease Margin 3 OR Focal S3.17 Margin involvement by invasive carcinoma or DCIS Margins not involved Margin 1 Type of involvement DCIS Invasive carcinoma DCIS and invasive carcinoma Orientation of margin Clearance OR >10 and if DCIS is closer to the margin.. Extent of involvement to DCIS OR Focal Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 8 of 11
9 S3.18 Lobular neoplasia G3.04 Other microscopic coents Type Classical Variant (pleomorphic, signet ring) Extent Focal Extensive G3.03 LCIS at the margin (select all that apply) LCIS with comedo necrosis present Pleomorphic LCIS present S3.19 Associated breast changes LYMPH NODES atypical ductal hyperplasia flat epithelial atypia lobular neoplasia (ALH/ LCIS) radial scars sclerosing adenosis fibrocystic change other breast changes (eg calcification) S3.20 SENTINEL NODES Total number of sentinel nodes No.of sentinel nodes with macrometastases No. of sentinel nodes with micrometastases No. of sentinel nodes with isolated tumour cells Ancillary test findings S4.01 Oestrogen receptors Not performed Pending Performed Percentage of nuclei staining % to % Predominant staining intensity 1+ Low 2+ Intermediate 3+ High ER result Negative Positive Progesterone receptors Not performed Pending Performed Percentage of nuclei staining % to % Predominant staining intensity 1+ Low 2+ Intermediate 3+ High ER result Negative Positive S3.21 NON-SENTINEL NODES Total number of nonsentinel nodes S4.03 HER2 (ISH) Not performed Performed Pending Number of non-sentinel nodes with metastases Number of copies of HER2 S3.22 Extranodal spread S3.23 Treatment effect in LN nodes negative, no treatment effect nodes negative, with treatment effect nodes positive, with treatment effect nodes positive, no treatment effect Not applicable Number of copies of CEP17 Not assessed OR HER2 Result Amplified Non-amplified diploid Non-amplified polysomic Indeterminate Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 9 of 11
10 HER2 IHC (if performed) Not performed Synthesis and overview S5.01 AJCC Tumour staging (See opposite and next page) AJCC Tumour staging grouping (see next page) S5.02 Year and edition of staging system G5.01 Diagnostic coent Include: Specimen type and laterality; Histological grade Maximum tumour size; Margin status; Lymph node status; Lymphovascular invasion S5.03 Overarching coent S5.01 Tumour stage and group# TNM descriptors (Only if applicable; select all that apply) m- multiple foci of invasive carcinoma r - recurrent y - post treatment Primary Tumour (Invasive Ca) (pt) TX T0 Primary tumour cannot be assessed No evidence of primary tumour Tis (DCIS) Ductal carcinoma in situ Tis (LCIS) Lobular carcinoma in situ Tis (Paget s) Paget disease of the nipple NOT associated with invasive carcinoma and/or carcinoma in situ (DCIS and/or LCIS) in the underlying breast parenchyma. Carcinomas in the breast parenchyma associated with Paget s disease are categorized based on size and characteristics of the parenchymal disease, although the presence of Paget s disease should still be noted. T1 T1mi T1a T1b T1c T2 T3 T4 T4a T4b T4c T4d Tumour 20 in greatest dimension Tumour 1 in greatest dimension Tumour >1 but 5 in greatest dimension Tumour >5 but 10 in greatest dimension Tumour >10 but 20 in greatest dimension Tumour >20 but 50 in greatest dimension Tumour >50 in greatest dimension Tumour of any size with direct extension to the chest wall and/or to the skin (ulceration or skin nodules) Note: Invasion of the dermis alone does not qualify as pt4 Extension to the chest wall, not including only pectoralis muscle adherence/invasion Ulceration and/or ipsilateral satellite nodules and/or oedema (including peau d orange) of the skin, which do not meet criteria for inflaatory carcinoma Both T4a and T4b Inflaatory carcinoma Regional Lymph Nodes (pn)* *Note: Classification is based on axillary lymph node dissection with or without sentinel lymph node biopsy. Classification based solely on sentinel lymph node biopsy without subsequent axillary lymph node dissection is designated (sn) for sentinel node for example, pn0(sn) pnx pn0 Regional lymph nodes cannot be assessed (eg previously removed, or not removed for pathologic study) No regional lymph node metastasis identified histologically. Note: isolated tumour cell clusters (ITC) are defined as small clusters of cells not greater than 0.2, or single tumour cells, or a cluster of fewer than 200 cells in a single histologic cross-section. ITCs may be detected by routine histology or by iunohistochemical (IHC) methods. Nodes containing only ITCs are excluded from the total positive node count for purposes of N classification but should be included in the total number of nodes evaluated. pn0(i-) No regional lymph node metastases histologically, negative IHC pn0(i+) Malignant cells in regional lymph node(s) no greater than 0.2 (detected by H&E or IHC including ITC) pn0(mol-) No regional lymph node metastases histologically, negative molecular findings (RT-PCR) pn0(mol+) Positive molecular findings (RT-PCR)**, but no regional lymph node metastases detected by histology or IHC Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 10 of 11
11 Regional Lymph Nodes (pn)* (cont.) pn1 Micrometastases; or metastases in 1-3 axillary lymph nodes; and/or in internal maary nodes with metastases detected by sentinel lymph node biopsy but not clinically detected.*** pn1mi Micrometastases (greater than 0.2 and/or more than 200 cells, but none greater than 2.0 ) pn1a Metastases in 1-3 axillary lymph nodes, at least 1 metastasis greater than 2.0 pn1b pn1c pn2 pn2a pn2b pn3 pn3a pn3b pn3c Notes: Metastases in internal maary nodes with micrometastases or macrometastases detected by sentinel lymph node biopsy but not clinically detected.*** Metastases in 1-3 axillary lymph nodes and in internal maary lymph nodes with micrometastases or macrometastases detected by sentinel lymph node biopsy but not clinically detected. Metastases in 4-9 axillary lymph nodes; or clinically detected**** internal maary lymph nodes in the absence of axillary lymph node metastases Metastases in 4-9 axillary lymph nodes (at least one tumour deposit greater than 2.0 ) Metastases in clinically detected**** internal maary lymph nodes in the absence of axillary lymph node metastases Metastases in ten or more axillary lymph nodes; or in infraclavicular (level III axillary) lymph nodes; or in clinically detected**** ipsilateral internal maary lymph nodes in the presence of one or more positive level I, II axillary lymph nodes; or in more than three axillary lymph nodes and in internal maary lymph nodes with micrometastases or macrometastases detected by sentinel lymph node biopsy but not clinically detected***; or in ipsilateral supraclavicular lymph nodes Metastases in 10 or more axillary lymph nodes (at least one tumour deposit greater than 2.0 ); or metastases to the infraclavicular (level III axillary lymph) nodes Metastases in clinically detected**** ipsilateral internal maary lymph nodes in the presence of one or more positive axillary lymph nodes; or in more than three axillary lymph nodes and in internal maary lymph nodes with micrometastases or macrometastases detected by sentinel lymph node biopsy but not clinically detected**** Metastases in ipsilateral supraclavicular lymph nodes **RT-PCR: reverse transcriptase/polymerase chain reaction *** Not clinically detected is defined as not detected by imaging studies (excluding lymphoscintigraphy) or not detected by clinical examination **** Clinically detected is defined as detected by imaging studies (excluding lymphoscintigraphy) or by clinical examination and having characteristics highly suspicious for malignancy or a presumed pathologic macrometastasis based on fine needle aspiration biopsy with cytologic examination. Distant Metastasis (M) M0 No clinical or radiographic evidence of distant metastases cm0(i+) No clinical or radiographic evidence of distant metastases, but deposits of molecularly or microscopically detected tumour cells in circulating blood, bone marrow, or other nonregional nodal tissue that are no larger than 0.2 in a patient without symptoms or signs of metastasis M1 Distant detectable metastases as determined by classic clinical and radiographic means and/or histologically proven larger than 0.2 Stage Grouping* Stage T N M 0 Tis N0 M0 IA T1* N0 M0 IB T0 N1mi M0 T1* N1mi M0 IIA T0 N1 MO T1* N1 M0 T2 N0 M0 IIB T2 N1 M0 T3 N0 M0 IIIA T0 N2 M0 T1* N2 M0 T2 N2 M0 T3 N1 M0 T3 N2 M0 IIIB T4 N0, N1, N2 M0 IIIC Any T N3 M0 IV Any T Any N M1 *T1 includes T1mic T0 and T1 tumours with nodal micrometastases only are excluded from Stage IIA and are classified Stage IB. Notes: M0 includes M0(i+) The designation pm0 is not valid; any M0 should be clinical. If a patient presents with M1 prior to neoadjuvant systemic therapy, the stage is considered stage IV and remains stage IV regardless of response to neoadjuvant therapy. Stage designation may be changed if postsurgical imaging studies reveal the presence of distant metastases, provided that the studies are carried out within 4 months of diagnosis in the absence of disease progression and provided that the patient has not received neoadjuvant therapy. Post-neoadjuvant therapy is designated with yc or yp prefi x. No stage group is assigned if there is a complete pathologic response (CR) to neoadjuvant therapy, for example, ypt0ypn0cm0.. ## Used with the permission of the American Joint Coittee on Cancer (AJCC), Chicago, Illinois. The original source for this material is the AJCC Cancer Staging Manual, Seventh Edition (2010) published by Springer Science and Business Media LLC, Version 2.3 Proforma: Invasive Breast Cancer Structured Reporting Protocol 2nd Edition Page 11 of 11
Descriptor Definition Author s notes TNM descriptors Required only if applicable; select all that apply multiple foci of invasive carcinoma
 S5.01 The tumour stage and stage grouping must be recorded to the extent possible, based on the AJCC Cancer Staging Manual (7 th Edition). 11 (See Tables S5.01a and S5.01b below.) Table S5.01a AJCC breast
S5.01 The tumour stage and stage grouping must be recorded to the extent possible, based on the AJCC Cancer Staging Manual (7 th Edition). 11 (See Tables S5.01a and S5.01b below.) Table S5.01a AJCC breast
STAGE CATEGORY DEFINITIONS
 CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
Chapter 2 Staging of Breast Cancer
 Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
ACRIN 6666 Therapeutic Surgery Form
 S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
Completing the Puzzle AJCC TNM Staging Breast. Nicole Catlett, CTR 2017 Kentucky Cancer Registry Fall Conference, September 21 & 22, 2017
 Completing the Puzzle AJCC TNM Staging Breast Nicole Catlett, CTR 2017 Kentucky Cancer Registry Fall Conference, September 21 & 22, 2017 OBJECTIVES Understanding of Breast TNM staging Identify clinical
Completing the Puzzle AJCC TNM Staging Breast Nicole Catlett, CTR 2017 Kentucky Cancer Registry Fall Conference, September 21 & 22, 2017 OBJECTIVES Understanding of Breast TNM staging Identify clinical
Primary Cutaneous Melanoma Pathology Reporting Proforma DD MM YYYY. *Tumour site. *Specimen laterality. *Specimen type
 Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Protocol for the Examination of Biopsy Specimens From Patients With Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: BreastInvasive 1.0.0.0 Protocol Posting Date: February 2019 Accreditation Requirements The use of
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: BreastInvasive 1.0.0.0 Protocol Posting Date: February 2019 Accreditation Requirements The use of
Protocol for the Examination of Resection Specimens From Patients With Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Breast Invasive 4.2.0.0 Protocol Posting Date: February 2019 CAP Laboratory Accreditation Program
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Breast Invasive 4.2.0.0 Protocol Posting Date: February 2019 CAP Laboratory Accreditation Program
LUNG STAGING FORM LATERALITY: LEFT RIGHT BILATERAL
 LUNG STAGING FORM LATERALITY: LEFT RIGHT BILATERAL ( ) Tx Primary tumor cannot be assessed, or tumor proven by the presence of malignant cells in sputum or bronchial washings but not visualized by imaging
LUNG STAGING FORM LATERALITY: LEFT RIGHT BILATERAL ( ) Tx Primary tumor cannot be assessed, or tumor proven by the presence of malignant cells in sputum or bronchial washings but not visualized by imaging
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Carcinoma of the Renal Pelvis and Ureter Histopathology
 Carcinoma of the Renal Pelvis and Ureter Histopathology Reporting Proforma (NEPHROURETERECTOMY AND URETERECTOMY) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
Carcinoma of the Renal Pelvis and Ureter Histopathology Reporting Proforma (NEPHROURETERECTOMY AND URETERECTOMY) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma
 Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
Colorectal Cancer Structured Pathology Reporting Proforma DD MM YYYY
 Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
Gastric Cancer Histopathology Reporting Proforma
 Gastric Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth Sex Male Female Intersex/indeterminate
Gastric Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth Sex Male Female Intersex/indeterminate
B REAST STAGING FORM. PATHOLOGIC Extent of disease through completion of definitive surgery. CLINICAL Extent of disease before any treatment
 B REAST STAGING FORM CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery (DCIS) (LCIS) (Paget s) mi c a b c d TUMOR SIZE:
B REAST STAGING FORM CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery (DCIS) (LCIS) (Paget s) mi c a b c d TUMOR SIZE:
B REAST STAGING FORM. PATHOLOGIC Extent of disease through completion of definitive surgery. CLINICAL Extent of disease before any treatment
 B REAST STAGING FORM Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery (DCIS) (LCIS) (Paget s) mi a b c a b c d TUMOR SIZE: S TAGE
B REAST STAGING FORM Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery (DCIS) (LCIS) (Paget s) mi a b c a b c d TUMOR SIZE: S TAGE
S1.04 Principal clinician. G1.01 Comments. G2.01 *Specimen dimensions (prostate) S2.02 *Seminal vesicles
 Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Sex Male
Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Sex Male
Protocol for the Examination of Specimens from Patients with Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens from Patients with Invasive Carcinoma of the Breast Protocol applies to all invasive carcinomas of the breast, including ductal carcinoma in situ (DCIS) with microinvasion.
Protocol for the Examination of Specimens from Patients with Invasive Carcinoma of the Breast Protocol applies to all invasive carcinomas of the breast, including ductal carcinoma in situ (DCIS) with microinvasion.
Carcinoma of the Urinary Bladder Histopathology
 Carcinoma of the Urinary Bladder Histopathology Reporting Proforma (Radical & Partial Cystectomy, Cystoprostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
Carcinoma of the Urinary Bladder Histopathology Reporting Proforma (Radical & Partial Cystectomy, Cystoprostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
Polypectomy and Local Resections of the Colorectum Structured Pathology Reporting Proforma
 Polypectomy and Local Resections of the Colorectum Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth
Polypectomy and Local Resections of the Colorectum Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node
 Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
3/23/2017. Disclosure of Relevant Financial Relationships. Pathologic Staging Updates in Breast Cancer. Pathologic Staging Updates Breast Cancer
 Pathologic Staging Updates in Breast Cancer Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content of CME
Pathologic Staging Updates in Breast Cancer Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content of CME
S1.04 PRINCIPAL CLINICIAN G1.01 COMMENTS S2.01 SPECIMEN LABELLED AS G2.01 *SPECIMEN DIMENSIONS (PROSTATE) S2.03 *SEMINAL VESICLES
 Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
Breast pathology. 2nd Department of Pathology Semmelweis University
 Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
Vulva Cancer Histopathology Reporting Proforma
 Vulva Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Ethnicity Unknown AboriginalTorres
Vulva Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Ethnicity Unknown AboriginalTorres
A712(19)- Test slide, Breast cancer tissues with corresponding normal tissues
 A712(19)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
A712(19)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity.
 Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Carcinoma mammario: le istologie non frequenti. Valentina Guarneri Università di Padova IOV-IRCCS
 Carcinoma mammario: le istologie non frequenti Valentina Guarneri Università di Padova IOV-IRCCS Histological diversity of breast adenocarcinomas Different histological types are defined according to specific
Carcinoma mammario: le istologie non frequenti Valentina Guarneri Università di Padova IOV-IRCCS Histological diversity of breast adenocarcinomas Different histological types are defined according to specific
Overview of AJCC 8 th Staging in Pathologic Aspects
 Overview of AJCC 8 th Staging in Pathologic Aspects Jee Yeon KIM, M.D.,Ph.D. Department of Pathology, Pusan National University, College of Medicine, Pusan National University Yangsan Hospital, KOREA Major
Overview of AJCC 8 th Staging in Pathologic Aspects Jee Yeon KIM, M.D.,Ph.D. Department of Pathology, Pusan National University, College of Medicine, Pusan National University Yangsan Hospital, KOREA Major
Papillary Lesions of the breast
 Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Seventh Edition Staging 2017 Breast
 Seventh Edition Staging 2017 Breast Donna M. Gress, RHIT, CTR Validating science. Improving patient care. No materials in this presentation may be repurposed in print or online without the express written
Seventh Edition Staging 2017 Breast Donna M. Gress, RHIT, CTR Validating science. Improving patient care. No materials in this presentation may be repurposed in print or online without the express written
Surgical Pathology Issues of Practical Importance
 Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Case Scenario 1 History and Physical 3/15/13 Imaging Pathology
 Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Basement membrane in lobule.
 Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Rare Breast Tumours. 1. Breast Tumours. 1.1 General Results. 1.2 Incidence
 Rare Breast Tumours 1. Breast Tumours 1.1 General Results Table 1. Epithelial Tumours of Breast: Incidence, Trends, Survival Flemish Region 2001-2010 Incidence Trend Survival Females EAPC Relative survival
Rare Breast Tumours 1. Breast Tumours 1.1 General Results Table 1. Epithelial Tumours of Breast: Incidence, Trends, Survival Flemish Region 2001-2010 Incidence Trend Survival Females EAPC Relative survival
*OPERATIVE PROCEDURE. Serum tumour markers within normal limits S1.04 PRINCIPAL CLINICIAN
 Neoplasia of the Testis - Orchidectomy Histopathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
Neoplasia of the Testis - Orchidectomy Histopathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
A712(18)- Test slide, Breast cancer tissues with corresponding normal tissues
 A712(18)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
A712(18)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
FNA Thyroid Cytology Structured Reporting Proforma
 FNA Thyroid Cytology Structured Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth S1.02 Clinical details Male Female Intersex/indeterminate
FNA Thyroid Cytology Structured Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth S1.02 Clinical details Male Female Intersex/indeterminate
Image guided core biopsies:
 Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
PART VII Breast. Breast 345
 PART VII Breast Breast 345 3 2 Breast At-A-Glance SUMMARY OF CHANGES Tumor (T) Identified specific imaging modalities that can be used to estimate clinical tumor size, including mammography, ultrasound,
PART VII Breast Breast 345 3 2 Breast At-A-Glance SUMMARY OF CHANGES Tumor (T) Identified specific imaging modalities that can be used to estimate clinical tumor size, including mammography, ultrasound,
Jose A Torres, MD 1/12/2017
 Jose A Torres, MD 1/12/2017 Background Globally leading cause of cancer related death in women ~249,000 Americans diagnosed with invasive breast cancer ~40,890 will die of their disease Breast cancer risk
Jose A Torres, MD 1/12/2017 Background Globally leading cause of cancer related death in women ~249,000 Americans diagnosed with invasive breast cancer ~40,890 will die of their disease Breast cancer risk
Evaluation of Breast Specimens Removed by Needle Localization Technique
 Evaluation of Breast Specimens Removed by Needle Localization Technique Specimen Handling: The breast specimen when received should be measured and grossly inspected for any orientation designated by the
Evaluation of Breast Specimens Removed by Needle Localization Technique Specimen Handling: The breast specimen when received should be measured and grossly inspected for any orientation designated by the
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity.
 Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
LYMPHATIC DRAINAGE AXILLARY (MOSTLY) INTERNAL MAMMARY SUPRACLAVICULAR
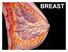 BREAST LYMPHATIC DRAINAGE AXILLARY (MOSTLY) INTERNAL MAMMARY SUPRACLAVICULAR HISTOLOGY LOBE: (10 in whole breast) LOBULE: (many per lobe) ACINUS/I, aka ALVEOLUS/I: (many per lobule) DUCT(S): INTRA- or
BREAST LYMPHATIC DRAINAGE AXILLARY (MOSTLY) INTERNAL MAMMARY SUPRACLAVICULAR HISTOLOGY LOBE: (10 in whole breast) LOBULE: (many per lobe) ACINUS/I, aka ALVEOLUS/I: (many per lobule) DUCT(S): INTRA- or
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
INDEX. in this web service Cambridge University Press
 abscess. See also subareolar abscess acute mastitis, 44 lactational/puerperal mastitis, 55 mammary tuberculosis, 42 tuberculous, 43 adeno gastric, 198, 200 invasive, 157 lung, 197, 200 prostatic, 199 200
abscess. See also subareolar abscess acute mastitis, 44 lactational/puerperal mastitis, 55 mammary tuberculosis, 42 tuberculous, 43 adeno gastric, 198, 200 invasive, 157 lung, 197, 200 prostatic, 199 200
Histological Type. Morphological and Molecular Typing of breast Cancer. Nottingham Tenovus Primary Breast Cancer Study. Survival (%) Ian Ellis
 Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
Definition of Synoptic Reporting
 Definition of Synoptic Reporting The CAP has developed this list of specific features that define synoptic reporting formatting: 1. All required cancer data from an applicable cancer protocol that are
Definition of Synoptic Reporting The CAP has developed this list of specific features that define synoptic reporting formatting: 1. All required cancer data from an applicable cancer protocol that are
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer. Pathology. AGO e. V. in der DGGG e.v. sowie in der DKG e.v.
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Pathology Pathology Versions 2004 2017: Blohmer / Costa / Fehm / Friedrichs / Huober / Kreipe / Lück / Schneeweis / Sinn /
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Pathology Pathology Versions 2004 2017: Blohmer / Costa / Fehm / Friedrichs / Huober / Kreipe / Lück / Schneeweis / Sinn /
MINIMUM STANDARDS FOR HANDLING AND REPORTING BREAST PATHOLOGY SAMPLES
 MINIMUM STANDARDS FOR HANDLING AND REPORTING BREAST PATHOLOGY SAMPLES Committee Members: Dr Adekunbiola A. F. Banjo, M.D., (Chairperson); Dr Oriolowo, M.D., Dr Olayiwola A. Oluwasola M.D., Department of
MINIMUM STANDARDS FOR HANDLING AND REPORTING BREAST PATHOLOGY SAMPLES Committee Members: Dr Adekunbiola A. F. Banjo, M.D., (Chairperson); Dr Oriolowo, M.D., Dr Olayiwola A. Oluwasola M.D., Department of
Breast Cancer TREATMENT APPROACHES STAGING TUMOUR BIOLOGY. Breast Cancer
 45 Dr K Tabane MBChB,FCP(SA); Certificate of Medical Oncology (Physicians) Specialist Physician, Medical Oncologist, Director: Sandton Oncology According to the CANSA statistics, breast cancer is the most
45 Dr K Tabane MBChB,FCP(SA); Certificate of Medical Oncology (Physicians) Specialist Physician, Medical Oncologist, Director: Sandton Oncology According to the CANSA statistics, breast cancer is the most
Recent advances in breast cancers
 Recent advances in breast cancers Breast cancer is a hetrogenous disease due to distinct genetic alterations. Similar morphological subtypes show variation in clinical behaviour especially in response
Recent advances in breast cancers Breast cancer is a hetrogenous disease due to distinct genetic alterations. Similar morphological subtypes show variation in clinical behaviour especially in response
Q&A. Fabulous Prizes. Collecting Cancer Data: Breast 4/4/13. NAACCR Webinar Series Collecting Cancer Data Breast
 Collecting Cancer Data Breast NAACCR 2012 2013 Webinar Series Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching this webinar
Collecting Cancer Data Breast NAACCR 2012 2013 Webinar Series Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching this webinar
The International Association for the Study of Lung Cancer (IASLC) Lung Cancer Staging Project, Data Elements
 Page 1 Contents 1.1. Registration... 2 1.2. Patient Characteristics... 3 1.3. Laboratory Values at Diagnosis... 5 1.4. Lung Cancers with Multiple Lesions... 6 1.5. Primary Tumour Description... 10 1.6.
Page 1 Contents 1.1. Registration... 2 1.2. Patient Characteristics... 3 1.3. Laboratory Values at Diagnosis... 5 1.4. Lung Cancers with Multiple Lesions... 6 1.5. Primary Tumour Description... 10 1.6.
Collecting Cancer Data: Breast. Prizes! Collecting Cancer Data: Breast 8/4/ NAACCR Webinar Series 1. NAACCR Webinar Series
 Collecting Cancer Data: Breast NAACCR 2008 2009 Webinar Series Prizes! Question of the Month! The participant that submits the best question of the session will receive a fbl fabulous Pi Prize! Shannon
Collecting Cancer Data: Breast NAACCR 2008 2009 Webinar Series Prizes! Question of the Month! The participant that submits the best question of the session will receive a fbl fabulous Pi Prize! Shannon
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
LOINC. Clinical information. RCPA code. Record if different to report header Operating surgeon name and contact details. Absent.
 Complete as narrative or use the structured format below 55752-0 17.02.28593 Clinical information 22027-7 17.02.30001 Record if different to report header Operating surgeon name and contact details 52101004
Complete as narrative or use the structured format below 55752-0 17.02.28593 Clinical information 22027-7 17.02.30001 Record if different to report header Operating surgeon name and contact details 52101004
AJCC CANCER STAGE. Site-Specific Instructions - BREAST. Reference: AJCC Cancer Staging Manual, 7 th Edition
 Slide 1 AJCC CANCER STAGE Site-Specific Instructions - BREAST Reference: AJCC Cancer Staging Manual, 7 th Edition In this presentation, we are going to review the AJCC Cancer Staging criteria for the breast
Slide 1 AJCC CANCER STAGE Site-Specific Instructions - BREAST Reference: AJCC Cancer Staging Manual, 7 th Edition In this presentation, we are going to review the AJCC Cancer Staging criteria for the breast
Pathology Report Patient Companion Guide
 Pathology Report Patient Companion Guide Breast Cancer - Understanding Your Pathology Report Pathology Reports can be overwhelming. They contain scientific terms that are unfamiliar and might be a bit
Pathology Report Patient Companion Guide Breast Cancer - Understanding Your Pathology Report Pathology Reports can be overwhelming. They contain scientific terms that are unfamiliar and might be a bit
Post Neoadjuvant therapy: issues in interpretation
 Post Neoadjuvant therapy: issues in interpretation Disclosure: Overview D Prognostic features in assessment of post treatment specimens: Tumor size Cellularity Grade Receptors LN Neoadjuvant chemotherapy:
Post Neoadjuvant therapy: issues in interpretation Disclosure: Overview D Prognostic features in assessment of post treatment specimens: Tumor size Cellularity Grade Receptors LN Neoadjuvant chemotherapy:
Case Scenario 1. 2/15/2011 The patient received IMRT 45 Gy at 1.8 Gy per fraction for 25 fractions.
 Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Invasive Papillary Breast Carcinoma
 410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
CLINICAL SIGNIFICANCE OF BENIGN EPITHELIAL CHANGES
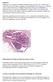 Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
BREAST PATHOLOGY. Fibrocystic Changes
 BREAST PATHOLOGY Lesions of the breast are very common, and they present as palpable, sometimes painful, nodules or masses. Most of these lesions are benign. Breast cancer is the 2 nd most common cause
BREAST PATHOLOGY Lesions of the breast are very common, and they present as palpable, sometimes painful, nodules or masses. Most of these lesions are benign. Breast cancer is the 2 nd most common cause
Proliferative Breast Disease: implications of core biopsy diagnosis. Proliferative Breast Disease
 Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
CURRICULUM FOR THE BREAST PATHOLOGY ROTATION UNIVERSITY OF FLORIDA DEPARTMENT OF PATHOLOGY
 CURRICULUM FOR THE BREAST PATHOLOGY ROTATION UNIVERSITY OF FLORIDA DEPARTMENT OF PATHOLOGY JULY, 2003 The following is a conceptual curriculum and set of guidelines for Pathology Residents on the Breast
CURRICULUM FOR THE BREAST PATHOLOGY ROTATION UNIVERSITY OF FLORIDA DEPARTMENT OF PATHOLOGY JULY, 2003 The following is a conceptual curriculum and set of guidelines for Pathology Residents on the Breast
Salivary Glands 3/7/2017
 Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Breast Pathology. Breast Development
 Breast Pathology Lecturer: Hanina Hibshoosh, M.D. Reading: Kumar, Cotran, Robbins, Basic Pathology, 6th Edition, pages 623-635 Breast Development 5th week - thickening of the epidermis - milk line 5th
Breast Pathology Lecturer: Hanina Hibshoosh, M.D. Reading: Kumar, Cotran, Robbins, Basic Pathology, 6th Edition, pages 623-635 Breast Development 5th week - thickening of the epidermis - milk line 5th
Slide seminar. Asist. Prof. Jože Pižem, MD, PhD Institute of Pathology Medical Faculty, University of Ljubljana
 Slide seminar Asist. Prof. Jože Pižem, MD, PhD Institute of Pathology Medical Faculty, University of Ljubljana Case 5 A 57-year-old man with a dermal/subcutaneous lesion on the scalp, which was interpreted
Slide seminar Asist. Prof. Jože Pižem, MD, PhD Institute of Pathology Medical Faculty, University of Ljubljana Case 5 A 57-year-old man with a dermal/subcutaneous lesion on the scalp, which was interpreted
VULVAR CARCINOMA. Page 1 of 5
 VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
Breast health and screening
 Breast health and screening Dr Kathy Wong MBBS (HK), FRCR (UK), FHKCR FHKAM (Radiology) Clinical Radiologist Department of Diagnostic and Interventional Radiology Kwong Wah Hospital Questions regarding
Breast health and screening Dr Kathy Wong MBBS (HK), FRCR (UK), FHKCR FHKAM (Radiology) Clinical Radiologist Department of Diagnostic and Interventional Radiology Kwong Wah Hospital Questions regarding
IBCM 2, April 2009, Sarajevo, Bosnia and Herzegovina
 Preoperative diagnosis and treatment planning in breast cancer The pathologist s perspective L. Mazzucchelli Istituto Cantonale di Patologia Locarno, Switzerland IBCM 2, 23-25 April 2009, Sarajevo, Bosnia
Preoperative diagnosis and treatment planning in breast cancer The pathologist s perspective L. Mazzucchelli Istituto Cantonale di Patologia Locarno, Switzerland IBCM 2, 23-25 April 2009, Sarajevo, Bosnia
04/10/2018. Intraductal Papillary Neoplasms Of Breast INTRADUCTAL PAPILLOMA
 Intraductal Papillary Neoplasms Of Breast Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head The University of Texas MD Anderson Cancer Center 25 th Annual Seminar in Pathology Pittsburgh,
Intraductal Papillary Neoplasms Of Breast Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head The University of Texas MD Anderson Cancer Center 25 th Annual Seminar in Pathology Pittsburgh,
Papillary Lesions of the Breast: WHO Update
 Papillary Lesions of the Breast: WHO Update Stuart J. Schnitt, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Papillary Lesions of the Breast
Papillary Lesions of the Breast: WHO Update Stuart J. Schnitt, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Papillary Lesions of the Breast
Ductal Carcinoma in Situ. Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA
 Ductal Carcinoma in Situ Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Definition of DCIS WHO 2012 A neoplastic proliferation
Ductal Carcinoma in Situ Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Definition of DCIS WHO 2012 A neoplastic proliferation
Contents 1 The Windows of Susceptibility to Breast Cancer 2 The So Called Pre-Neoplastic Lesions and Carcinoma In Situ
 Contents 1 The Windows of Susceptibility to Breast Cancer... 1 1.1 Introduction... 1 1.2 Risk Factor and Etiological Agents... 2 1.3 The Concept of the Windows of Susceptibility to Carcinogenesis... 5
Contents 1 The Windows of Susceptibility to Breast Cancer... 1 1.1 Introduction... 1 1.2 Risk Factor and Etiological Agents... 2 1.3 The Concept of the Windows of Susceptibility to Carcinogenesis... 5
Enrollment Form: Pancreas
 Tissue Source Site (TSS) Name: TSS Identifier: _ TSS Unique Patient #: Completed By: Completion Date (MM/DD/YYYY): Form Notes: An Enrollment Form should be completed for each TCGA qualified case upon qualification
Tissue Source Site (TSS) Name: TSS Identifier: _ TSS Unique Patient #: Completed By: Completion Date (MM/DD/YYYY): Form Notes: An Enrollment Form should be completed for each TCGA qualified case upon qualification
Enterprise Interest None
 Enterprise Interest None What are triple negative breast cancers? A synopsis of their histological patterns Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology,
Enterprise Interest None What are triple negative breast cancers? A synopsis of their histological patterns Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology,
Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine
 Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine The most common non-skin malignancy of women 2 nd most common cause of cancer deaths in women, following
Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine The most common non-skin malignancy of women 2 nd most common cause of cancer deaths in women, following
Case Scenario 1 Worksheet. Primary Site C44.4 Morphology 8743/3 Laterality 0 Stage/ Prognostic Factors
 CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
Savitri Krishnamurthy, MD 1
 EVOLVING TRENDS IN PATHOLOGIC EVALUATION OF AXILLARY LYMPH NODES IN BREAST CANCER Savitri Krishnamurthy, M.D. Professor Department of Pathology University of Texas M. D. Anderson Cancer Center AXILLARY
EVOLVING TRENDS IN PATHOLOGIC EVALUATION OF AXILLARY LYMPH NODES IN BREAST CANCER Savitri Krishnamurthy, M.D. Professor Department of Pathology University of Texas M. D. Anderson Cancer Center AXILLARY
Update on staging colorectal carcinoma, the 8 th edition AJCC. General overview of staging. When is staging required? 11/1/2017
 Update on staging colorectal carcinoma, the 8 th edition AJCC Dale C. Snover, MD November 3, 2017 General overview of staging Reason for uniform staging Requirements to use AJCC manual and/or CAP protocols
Update on staging colorectal carcinoma, the 8 th edition AJCC Dale C. Snover, MD November 3, 2017 General overview of staging Reason for uniform staging Requirements to use AJCC manual and/or CAP protocols
2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING
 2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Eight Groups are Revised for 2018 Head & Neck Colon (includes rectosigmoid and rectum for cases diagnosed 1/1/2018 forward) Lung (2018 Draft not yet
2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Eight Groups are Revised for 2018 Head & Neck Colon (includes rectosigmoid and rectum for cases diagnosed 1/1/2018 forward) Lung (2018 Draft not yet
Diseases of the breast (2 of 2) Breast cancer
 Diseases of the breast (2 of 2) Breast cancer Epidemiology & etiology The most common type of cancer & the 2 nd most common cause of cancer death in women 1 of 8 women in USA Affects 7% of women Peak at
Diseases of the breast (2 of 2) Breast cancer Epidemiology & etiology The most common type of cancer & the 2 nd most common cause of cancer death in women 1 of 8 women in USA Affects 7% of women Peak at
UN KEY ARTICLE PER UN ANATOMOPATOLOGO. Dr. Davide Balmativola Prof.ssa Anna Sapino Dr.ssa Isabella Castellano
 UN KEY ARTICLE PER UN ANATOMOPATOLOGO Dr. Davide Balmativola Prof.ssa Anna Sapino Dr.ssa Isabella Castellano ptnm staging IL RUOLO PIÙIMPORTANTE DEL SISTEMA DI STAGING: CA Cancer J Clin 2006;56:37 47 Raggruppare
UN KEY ARTICLE PER UN ANATOMOPATOLOGO Dr. Davide Balmativola Prof.ssa Anna Sapino Dr.ssa Isabella Castellano ptnm staging IL RUOLO PIÙIMPORTANTE DEL SISTEMA DI STAGING: CA Cancer J Clin 2006;56:37 47 Raggruppare
Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ).
 SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
Malignant Breast disorders
 Malignant Breast disorders RISK FACTORS FOR BREAST CANCER Family Hx.: first- and second-degree relatives with breast cancer and their age at diagnosis. RISK FACTORS FOR BREAST CANCER (cont.) Hormonal Risk
Malignant Breast disorders RISK FACTORS FOR BREAST CANCER Family Hx.: first- and second-degree relatives with breast cancer and their age at diagnosis. RISK FACTORS FOR BREAST CANCER (cont.) Hormonal Risk
47. Melanoma of the Skin
 1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
Disclosures 5/27/2012. Outline of Talk. Outline of Talk. When Is LCIS Clinically Significant? Classic LCIS. Classic LCIS
 When Is LCIS Clinically Significant? Disclosures I have nothing to disclose Yunn-Yi Chen, MD, PhD Professor Outline of Talk Outline of Talk Classic LCIS Classic LCIS Definition of lobular differentiation
When Is LCIS Clinically Significant? Disclosures I have nothing to disclose Yunn-Yi Chen, MD, PhD Professor Outline of Talk Outline of Talk Classic LCIS Classic LCIS Definition of lobular differentiation
Proliferative Epithelial lesions of the Breast. Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London
 Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Collaborative Stage Site-Specific Instructions - BREAST
 Slide 1 Collaborative Stage Site-Specific Instructions - BREAST In this presentation, we are going to review the CS Data Items and coding instructions for the breast primary site. Slide 2 Reading Assignments
Slide 1 Collaborative Stage Site-Specific Instructions - BREAST In this presentation, we are going to review the CS Data Items and coding instructions for the breast primary site. Slide 2 Reading Assignments
Guidance on the management of B3 lesions
 Guidance on the management of B3 lesions Lesion diagnosed on 14g or vacuumassisted biopsy (VAB) Risk of upgrade Recommended investigation Suggested approach for follow-up if no malignancy on VAE awaiting
Guidance on the management of B3 lesions Lesion diagnosed on 14g or vacuumassisted biopsy (VAB) Risk of upgrade Recommended investigation Suggested approach for follow-up if no malignancy on VAE awaiting
Case study 1. Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research
 NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
December 2002 Monthly Memo
 FLORIDA CANCER DATA SYSTEM December 2002 Monthly Memo CODING COMPLEX MORPHOLOGIC DIAGNOSES CODING COMPLEX BREAST HISTOLOGIES Apply these guidelines in priority order. Use the first guideline that applies
FLORIDA CANCER DATA SYSTEM December 2002 Monthly Memo CODING COMPLEX MORPHOLOGIC DIAGNOSES CODING COMPLEX BREAST HISTOLOGIES Apply these guidelines in priority order. Use the first guideline that applies
CPC 4 Breast Cancer. Rochelle Harwood, a 35 year old sales assistant, presents to her GP because she has noticed a painless lump in her left breast.
 CPC 4 Breast Cancer Rochelle Harwood, a 35 year old sales assistant, presents to her GP because she has noticed a painless lump in her left breast. 1. What are the most likely diagnoses of this lump? Fibroadenoma
CPC 4 Breast Cancer Rochelle Harwood, a 35 year old sales assistant, presents to her GP because she has noticed a painless lump in her left breast. 1. What are the most likely diagnoses of this lump? Fibroadenoma
Interactive Staging Bee
 Interactive Staging Bee ROBIN BILLET, MA, CTR GA/SC REGIONAL CONFERENCE NOVEMBER 6, 2018? Clinical Staging includes any information obtained about the extent of cancer obtained before initiation of treatment
Interactive Staging Bee ROBIN BILLET, MA, CTR GA/SC REGIONAL CONFERENCE NOVEMBER 6, 2018? Clinical Staging includes any information obtained about the extent of cancer obtained before initiation of treatment
Non-mass Enhancement on Breast MRI. Aditi A. Desai, MD Margaret Ann Mays, MD
 Non-mass Enhancement on Breast MRI Aditi A. Desai, MD Margaret Ann Mays, MD Breast MRI Important screening and diagnostic tool, given its high sensitivity for breast cancer detection Breast MRI - Indications
Non-mass Enhancement on Breast MRI Aditi A. Desai, MD Margaret Ann Mays, MD Breast MRI Important screening and diagnostic tool, given its high sensitivity for breast cancer detection Breast MRI - Indications
Breast Imaging: Multidisciplinary Approach. Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina
 Breast Imaging: Multidisciplinary Approach Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina No Disclosures Objectives Discuss a multidisciplinary breast
Breast Imaging: Multidisciplinary Approach Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina No Disclosures Objectives Discuss a multidisciplinary breast
