9/18/2017. Overview reasons an update was necessary. Myeloproliferative neoplasms
|
|
|
- Alison Shields
- 6 years ago
- Views:
Transcription
1 2016 WHO updates to the classification of hematologic neoplasms Darshan Roy, MD Assistant Professor Department of Pathology Director of Hematopathology Rowan School of Osteopathic Medicine Outline Myeloid neoplasms and acute leukemias Myeloproliferative neoplasms (MPN) Myelodysplastic syndromes (MDS) MDS/MPN Acute myeloid leukemia (AML) Acute lymphoblastic leukemia (ALL) Lymphoid Mature B cell lymphomas Mature T and NK cell lymphomas Hodgkin Lymphomas 1
2 Overview reasons an update was necessary 1. Discovery of molecular features affecting diagnosis and prognosis 2. Improved characterization and standardization of morphological features aiding in the differentiation of disease groups 3. Evidence validating a clinicopathologic approach for classification Myeloproliferative neoplasms Chronic myeloid leukemia (CML) Polycythemia vera (PV) Essential thrombocythemia (ET) Primary myelofibroisis (PMF) Chronic neutrophilic leukemia (CML) Mastocytosis has been removed from this category 2
3 Chronic myeloid leukemia (CML) Single relevant change in diagnosis of Accelerated Phase (AP) persistent or increasing WBC (>10x10 9 /L) and/or persistent or increasing splenomegaly unresponsive to therapy Persistent thrombocytosis (>1000x10 9 /L) uncontrolled by therapy Persistent thrombocytopenia (<100x10 9 /L) unrelated to therapy clonal cytogenetic evolution occurring after the initial diagnostic karyotype 20% or more basophils in the peripheral blood 10 19% myeloblasts in the blood or BM Provisional additions: Evidence of Tyrosine kinase inhibitor (TKI) resistance Hematologic resistance to first TKI Evidence of resistance to 2 sequential TKI 2 or more mutations in BCR ABL during TKI therapy Presence of fibrosis may indicate AP Presence of definitive lymphoblasts of any count should warrant concern for BP MPN Polycythemia vera (PV) PV (all 2 major criteria or first two 2 major + 1 minor) Major criteria: HGB (16.5 m, 16.0 f) or HCT (49% m, 48% f) Bone marrow biopsy findings JAK2 mutation Minor criteria Decreased serum EPO Criteria 2 not needed if sufficiently elevated HGB (>18.0 m, 16.5 f) however, the importance of bone marrow biopsy evaluate fibrosis DR2 DR3 DR4 Barbui, Tiziano T. American Journal of Hematology: Masked Polycythemia Vera (mpv): Results of an International Study. 89 Vol. John Wiley & Sons Inc, 01/2014. Web. 10 Sep
4 Slide 9 DR2 DR3 DR4 Darshan Roy, 9/15/2017 Darshan Roy, 9/15/2017 Darshan Roy, 9/15/2017
5 MPN Essential thrombocythemia (ET) and Primary myelofibroisis (PMF) Essentially unchanged. Discovery of recurrent CALR (calreticulin) mutation as diagnostic criteria of clonality in both ET and PMF (in addition to JAK2 and MPL) 20 25% of ET and PMF PMF if major clonal marker not identified, search for additional mutations (eg, ASXL1, EZH2, TET2, IDH1/IDH2, SRSF2, SF3B1) Nangalia, Jyoti J. Hematology: The Evolving Genomic Landscape of Myeloproliferative Neoplasms Vol. American Society of Hematology, 12/2014. Web. 10 Sep MPNs the rest Chronic neutrophilic leukemia now has identifiable recurrent mutation, CSF3R mutations can be seen in 50 80% of patients Mastocytosis no longer considered MPN. Myelodysplastic syndromes Terminology Refractory anemia/cytopenias removed, now: Myelodysplastic syndrome with MDS with single lineage dysplasia MDS with ring sideroblasts (MDS RS) MDS RS and single lineage dysplasia MDS RS and multilineage dysplasia MDS with multilineage dysplasia MDS with excess blasts MDS with isolated del(5q) MDS, unclassifiable Provisional entity: Refractory cytoplenia of childhood 4
6 Myeloid myelodysplastic syndromes Myeloid neoplasms with erythroid predominance (>50% erythroid cells) Now blast % of all nucleated cells (Previously counted blast % out of nonerythroid cells) Many cases of acute erythroid leukemia would now be classified as MDS EB MDS defining genetic abnormalities must be identified by conventional karyotype (not by FISH alone) MDS with del(5q) may include 1 additional cytogenetic abnormality As long as it isn t monosomy 7 or del(7q) Clonal hematopoiesis of indeterminate potential (CHIP) Somatic gene mutations can occur in low levels in normal patient populations not solely sufficient for a diagnosis of MDS, however testing should be done in all new diagnosis to determine prognosis Heuser, Michael, Felicitas Thol, and Arnold Ganser. Clonal Hematopoiesis of Indeterminate Potential: A Risk Factor for Hematologic Neoplasms. Deutsches Ärzteblatt International (2016): PMC. Web. 12 Sept MDS Ringed sideroblasts SF3B1 gene identified and associated with ringed sideroblasts If found, sideroblasts only need to account for 5% of nucleated erythrocytes (otherwise previous standard of 15%) MDS with ringed sideroblasts may now include multilineage dysplasia 5
7 New group MDS with germline mutations Arber, Daniel A. DA. Blood: The 2016 Revision to the World Health Organization Classification of Myeloid Neoplasms and Acute Leukemia. 127 Vol. American Society of Hematology, 05/2016. Web. 12 Sep MDS/MPN Chronic myelomonocytic leukemia (CMML) Atypical chronic myeloid leukemia (acml), BCR ABL1 Juvenile myelomonocytic leukemia (JMML) MDS/MPN with ring sideroblasts and thrombocytosis (MDS/MPN RS T) MDS/MPN, unclassifiable MDS/MPN Chronic myelomonocytic leukemia (CMML) Differentiate proliferative (WBC >13) vs dysplastic type Now 3 categories based on blast percentage CMML 0 (<2% peripheral blood, <5% bone marrow) CMML 1 (2 4% peripheral blood, 5 9% bone marrow) CMML 2 (5 19% peripheral blood, 10 19% bone marrow) Juvenile myelomonocytic leukemia (JMML) >90% contain somatic or germline mutation in PTPN11,KRAS, NRAS, CBL, or NF1. Refractory anemia with ring sideroblasts and thrombocytosis (RARS T) is now MDS/MPN with ringed sideroblasts and thrombocytosis (MDS/MPN RS T) 6
8 Schuler, E. E. Leukemia Research: Refined Medullary Blast and White Blood Cell Count Based Classification of Chronic Myelomonocytic Leukemias. 38 Vol. Elsevier, 12/2014. Web. 10 Sep Acute myeloid leukemia AML with recurrent genetic abnormalities AML with myelodysplasia related changes Therapy related myeloid neoplasms AML, NOS Myeloid sarcoma Myeloid proliferations related to Down syndrome AML New provisional categories (both with worse prognosis) AML with BCR ABL1 AML with mutated RUNX1 CEBPA requires biallelic mutations Acute erythroid leukemia (erythroid/myeloid type) removed 7
9 Nacheva, Ellie P. EP. British Journal of Haematology: Does BCR/ABL1 Positive Acute Myeloid Leukaemia Exist?. 161 Vol. Blackwell Publishing, 05/2013. Web. 10 Sep B lymphoblastic leukemia/lymphoma (B ALL) Two new provisional categories: B ALL with intrachromosomal amplification of chromosome 21 Occurs in 2% of pediatric ALL (usually older with lower WBC counts) >5 copies of RUNX1 (or >3 copies on a single chromosome) Poorer prognosis (partially overcome by aggressive therapy) B ALL, BCR ABL1 like Involve other tyrosine kinases (over 30 different genes) Cytokine receptor like factor 2 (CRLF2) Often associated with JAK2 Children with Down syndrome Moorman, Anthony V. AV. Haematologica (Roma): New and Emerging Prognostic and Predictive Genetic Biomarkers in B-Cell Precursor Acute Lymphoblastic Leukemia. 101 Vol. Il Pensiero Scientifico, 04/2016. Web. 10 Sep
10 T cell lymphoblastic leukemia/lymphoma (T ALL) New provisional entity Early T precursor (ETP) ALL Retention of some myeloid and stem cell characteristics CD1a CD8 CD7+ Positive for one or more of the following: CD34, CD117, HLA DR, CD13, CD33, CD11b, or CD65 Often have myeloid associated gene mutations (FLT3, NRAS/KRAS, etc) and lack T ALL mutations (NOTCH1, etc). Very poor prognosis You, M. James MJ. American Journal of Clinical Pathology: T-Lymphoblastic leukemia/lymphoma. 144 Vol. American Society for Clinical Pathology, 09/2015. Web. 11 Sep Kaplan-Meier plots of overall survival (A, D), event-free survival (B, E), and the cumulative incidence of remission failure or haematological relapse (C, F) in patients with typical T- lymphoblastic leukaemia (T- ALL; red) versus early T-cell precursor (ETP)-ALL (blue) treated on either St Jude (A C) or AIEOP protocols (D F) Coustan-Smith, Elaine E. The Lancet Oncology: Early T-Cell Precursor Leukaemia: A Subtype of very High-Risk Acute Lymphoblastic Leukaemia. 10 Vol. Lancet Pub. Group, 02/2009. Web. 10 Sep
11 Lymphoid neoplasms Mature B cell neoplasms Mature T and NK neoplasms Hodgkin lymphoma Posttransplant lymphoproliferative disorders (PTLD) Histiocytic and dendritic cell neoplasms Mature B cell neoplasms Monoclonal B cell lymphocytosis Should be defined as low count (PB CLL count of <0.5 x 10 9 /L) vs high count Low count rarely progresses to CLL Non CLL phenotype now recognized Chronic lymphocytic leukemia (CLL) Now requires 5 x 10 9 PB CLL cells regardless of extramedullary disease Mature B cell neoplasms Follicular lymphoma (FL) Follicular lymphoma In situ follicular lymphoma renamed in situ follicular neoplasia (ISFN) Pediatric FL renamed pediatric type FL No BCL2 (or BCL6 or MYC) rearrangements Nodal disease with blastoid follicular centers Localized (resection only) Caution to avoid underdiagnosing Conventional grade 3 FL. Excluded by focal diffuse areas (DLBCL) 10
12 Follicular Lymphoma continued New provisional entity Large B cell lymphoma with IRF4 rearrangement Young adults and children Waldeyer ring/cervical lymph nodes Low stage Resemble FL grade 3B or DLBCL MUM1 strongly expressed (usually with BCL6 and often with BCL2 and CD10) High proliferative index Lack BCL2 rearrangement Must be distinguished from MUM1+ CD10 FL (older patients and associated with DLBCL) Figure 1. New provisional B-cell lymphoma entities. (A-D) LBCL with IRF4 rearrangement. (A) Note the very large abnormal-appearing follicles in the central portion of this tonsil. (B) The neoplastic follicles have numerous transformed cells that are (C) IRF4/MUM-11 and (D) BCL61. Swerdlow, Steven H. SH. Blood: The 2016 Revision of the World Health Organization Classification of Lymphoid Neoplasms. 127 Vol. American Society of Hematology, 05/2016. Web. 12 Sep Mature B cell neoplasms FL continued Follicular lymphoma continued Duodenal type FL Distinct from other GI FL Resembles ISFN May resemble MZL of MALT Excellent outcome (some watch and wait) Diffuse appearing FL Inguinal masses Lack BCL2 rearrangements 1p36 deletion (not specific) 11
13 Mantle cell lymphoma (MCL) In situ MCL now in situ mantle cell neoplasia (ISMCN) Two indolent variants Unmutated IGHV SOX11+ MCL Nodal and may progress to classic MCL Mutated IGHV SOX11 MCL Frequently indolent leukemic variant Half of CCND1 MCL have CCND2 translocations Usually IGK or IGL partner Swerdlow, Steven H. SH. Blood: The 2016 Revision of the World Health Organization Classification of Lymphoid Neoplasms. 127 Vol. American Society of Hematology, 05/2016. Web. 12 Sep Diffuse large B cell lymphoma (DLBCL) Separation of germinal center (GC) and non GC subgroups of DLBCL recommended MYC and BCL2(/BCL6) expressor IHC Expression vs rearrangement ( double/triple hit lymphoma now new category High Grade B cell lymphoma) >40% MYC, >50% BCL2 IHC positivity in tumor cells Prognosis worse than NOS, better than double/triple hit 12
14 High Grade B cell lymphoma (HGBL) HGBL, NOS Includes previously described entity B cell lymphoma, unclassifiable with features intermediate between DLBCL and BL HGBL with MYC and BCL2 (or BCL6) rearrangements double/triple hit lymphomas Swerdlow, Steven H. SH. Blood: The 2016 Revision of the World Health Organization Classification of Lymphoid Neoplasms. 127 Vol. American Society of Hematology, 05/2016. Web. 12 Sep Swerdlow, Steven H. SH. Blood: The 2016 Revision of the World Health Organization Classification of Lymphoid Neoplasms. 127 Vol. American Society of Hematology, 05/2016. Web. 12 Sep
15 EBV+ DLBCL and EBV+ mucocutaneous ulcer EBV+ DLBCL, NOS Previously included of the elderly Worse prognosis than DLBCL, NOS EBV+ mucocutaneous ulcer, provisional entity Self limited disease, conservative management Large Hodgkin like cells Patients with history of advanced age or iatrogenic immunosuppression (A) Panoramic view of the rectal ulcer (hematoxilin eosin, X40); (B) Polymorphous infiltrate of plasma cells, small lymphocytes, eosinophils and scattered Reed Sternberglike cells (hematoxilin eosin, X400); (C) Reed Sternberg like cells are CD30 positive (CD30, X400) and Epstein Barr virus (EBER, X400). Juan, Alba A. Digestive and Liver Disease: Epstein-Barr Virus-Positive Mucocutaneous Ulcer in Crohn's Disease. A Condition to Consider in Immunosuppressed IBD Patients. 49 Vol. Elsevier, 08/2017. Web. 12 Sep Burkitt lymphoma Provisional entity Burkitt like lymphoma with 11q aberration Similar to BL morphology and by gene expression profiling Lack MYC rearrangement 14
16 (E-H) Burkitt-like lymphoma with 11q aberration. (E) The touch imprint demonstrates a monotonous population of transformed cells with basophilic cytoplasm that are (F) CD201, (G) have a very high MIB1/Ki-67 proliferation fraction, and are (H) BCL61. Swerdlow, Steven H. SH. Blood: The 2016 Revision of the World Health Organization Classification of Lymphoid Neoplasms. 127 Vol. American Society of Hematology, 05/2016. Web. 12 Sep Impact of molecular pathology on mature B cell lymphomas Hairy Cell leukemia Near 100% assocations with BRAF V600E (not seen in HCL v) Lymphoplasmcytic lymphoma 90% have MYD88 L265P mutation Not specific, seen in (IgM MGUS, DLBCL) Not seen in myeloma Mature T cell and NK cell neoplasms Follicular T cell lymphoma PTCL with follicular T helper cell (TFH) phenotype (CD10+, PD1+, BCL6+) in a follicular pattern May contain large EBV+ B cells Lack of high endothelial venules and expanded dendritic meshworks (of AITL) Nodal PTCL with TFH phenotype Diffuse pattern but with follicular T helper cell phenotype 15
17 ALK Anaplastic large cell lymphoma No longer provisional entity Require strong and diffuse CD30 positivity Cohesive growth pattern with hallmark type cells DUSP22 rearrangements have better prognosis (similar to ALK+) TP63 rearrangements do much worse Breast implant associated ALK ALCL Provisional entity 10 years after implant, associated with capsule seroma Conservative management including excision Representative cases of genetic subtypes of ALCL. (A) ALK-negative ALCL with DUSP22 rearrangement. The tumor cells are positive for CD30 and are negative for ALK, TIA-1, and p63. (B) ALK-negative ALCL with TP63 rearrangement. The tumor cells are positive for CD30, TIA-1, and p63 and are negative for ALK. Parrilla Castellar, Edgardo R. ER. Blood: ALK-Negative Anaplastic Large Cell Lymphoma is a Genetically Heterogeneous Disease with Widely Disparate Clinical Outcomes. 124 Vol. American Society of Hematology, 08/2014 Web 13 Sep 2017 Lechner, Melissa G. MG. Cancer: Breast Implant- Associated, ALK-Negative, T-Cell, Anaplastic, Large-Cell Lymphoma: Establishment and Characterization of a Model Cell Line (TLBR-1) for this Newly Emerging Clinical Entity. 117 Vol. John Wiley & Sons Inc, 04/2011. Web. 12 Sep
18 Enteropathy associated T cell lymphoma (EATL) EATL only includes type 1 Type 2 now defined as monomorphic epitheliotropic intestinal TCL (MEITL) shows no association with celiac disease increased in incidence in Asians and Hispanic populations Low magnification (a, x20, H&E) and high magnification (b, x 400, H&E) images of enteropathy-associated T- cell lymphoma with villous blunting and a transmural infiltrate composed of atypical, intermediate-sized lymphocytes and a mixed inflammatory background. c Low magnification (x 2 H&E) of MEITL with a monotonous infiltrate of neoplastic lymphocytes extending through the entire bowel wall and demonstrating epitheliotropism. d High magnification (x 400, H&E) emphasizes the monomorphism of the lymphoma cells. The tumor cells are positive for CD3 (e), CD56 (f), and TIA-1 (g) Ondrejka, Sarah S. Current Hematologic Malignancy Reports: Enteropathy- Associated T-Cell Lymphoma. 11 Vol. Current Science, Inc., 12/2016. Web. 14 Sep Hodgkin Lymphomas Nodular lymphocyte predominant Hodgkin lymphoma (NLP HL) may evolve into T cell histiocyte rich large B cell lymphoma (THRLBCL) THRLBCL like transformation of NLP HL 17
19 Conclusion Numerous recent advancements in genetic data (NGS) along with new treatment options drive the modifications to the WHO classification of hematopoietic neoplasms END 18
Lymphoma Update: Lymphoma Update: What s Likely to be New in the New WHO. Patrick Treseler, MD, PhD University of California San Francisco
 Lymphoma Update: What s Likely to be New in the New WHO Blood 127:2375; 2016 Patrick Treseler, MD, PhD University of California San Francisco Lymphoma Update: What IS New in the New WHO! Patrick Treseler,
Lymphoma Update: What s Likely to be New in the New WHO Blood 127:2375; 2016 Patrick Treseler, MD, PhD University of California San Francisco Lymphoma Update: What IS New in the New WHO! Patrick Treseler,
WHO UPDATE ON LYMPHOMAS. Dr Priya Mary Jacob Asst Professor, Pathology.
 WHO UPDATE ON LYMPHOMAS Dr Priya Mary Jacob Asst Professor, Pathology 3 rd 4 th 4 th revised 2001 2008 2017 The Change The Significance of the Change- Diagnostic, Prognostic The Rationale behind the change.
WHO UPDATE ON LYMPHOMAS Dr Priya Mary Jacob Asst Professor, Pathology 3 rd 4 th 4 th revised 2001 2008 2017 The Change The Significance of the Change- Diagnostic, Prognostic The Rationale behind the change.
Bone Marrow. Procedures Blood Film Aspirate, Cell Block Trephine Biopsy, Touch Imprint
 Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure
 Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
2010 Hematopoietic and Lymphoid ICD-O Codes - Alphabetical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
2012 Hematopoietic and Lymphoid ICD-O Codes - Numerical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells. Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital
 Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Corrigenda. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run
 Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
WHO Update to Myeloproliferative Neoplasms
 WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
Low-grade B-cell lymphoma
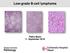 Low-grade B-cell lymphoma Patho-Basic 11. September 2018 Stephan Dirnhofer Pathology Outline Definition LPL, MBL/CLL/SLL, MCL FL Subtypes & variants Diagnosis including Grading Transformation Summary Be
Low-grade B-cell lymphoma Patho-Basic 11. September 2018 Stephan Dirnhofer Pathology Outline Definition LPL, MBL/CLL/SLL, MCL FL Subtypes & variants Diagnosis including Grading Transformation Summary Be
Recommended Timing for Transplant Consultation
 REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
Session 5. Pre-malignant clonal hematopoietic proliferations. Chairs: Frank Kuo and Valentina Nardi
 Session 5 Pre-malignant clonal hematopoietic proliferations Chairs: Frank Kuo and Valentina Nardi Pre-malignant clonal hematopoietic proliferations Clonal LYMPHOID proliferations: - Monoclonal gammopathy
Session 5 Pre-malignant clonal hematopoietic proliferations Chairs: Frank Kuo and Valentina Nardi Pre-malignant clonal hematopoietic proliferations Clonal LYMPHOID proliferations: - Monoclonal gammopathy
Hepatic Lymphoma Diagnosis An Algorithmic Approach
 Hepatic Lymphoma Diagnosis An Algorithmic Approach Ryan M. Gill, M.D., Ph.D. University of California, San Francisco PLEASE TURN OFF YOUR CELL PHONES Disclosure of Relevant Financial Relationships USCAP
Hepatic Lymphoma Diagnosis An Algorithmic Approach Ryan M. Gill, M.D., Ph.D. University of California, San Francisco PLEASE TURN OFF YOUR CELL PHONES Disclosure of Relevant Financial Relationships USCAP
Combinations of morphology codes of haematological malignancies (HM) referring to the same tumour or to a potential transformation
 Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
WHO 2016 update lymphoid neoplasms. Dr Sue Morgan Alfred Hospital, Melbourne
 WHO 2016 update lymphoid neoplasms Dr Sue Morgan Alfred Hospital, Melbourne WHO 4 th edition 2008 Established guideline worldwide for diagnosis of haematological malignancy for the last 9 years Significant
WHO 2016 update lymphoid neoplasms Dr Sue Morgan Alfred Hospital, Melbourne WHO 4 th edition 2008 Established guideline worldwide for diagnosis of haematological malignancy for the last 9 years Significant
High grade B-cell lymphomas (HGBL): Altered terminology in the 2016 WHO Classification (Update of the 4 th Edition) and practical issues Xiao-Qiu Li,
 High grade B-cell lymphomas (HGBL): Altered terminology in the 2016 WHO Classification (Update of the 4 th Edition) and practical issues Xiao-Qiu Li, M.D., Ph.D. Fudan University Shanghai Cancer Center
High grade B-cell lymphomas (HGBL): Altered terminology in the 2016 WHO Classification (Update of the 4 th Edition) and practical issues Xiao-Qiu Li, M.D., Ph.D. Fudan University Shanghai Cancer Center
Aggressive B-cell Lymphomas
 Neoplastic Hematopathology Update 2018 Aggressive B-cell Lymphomas Raju K. Pillai City of Hope National Medical Center I do not have any disclosures Disclosures Outline New entities and changes in WHO
Neoplastic Hematopathology Update 2018 Aggressive B-cell Lymphomas Raju K. Pillai City of Hope National Medical Center I do not have any disclosures Disclosures Outline New entities and changes in WHO
Juvenile Myelomonocytic Leukemia (JMML)
 Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Molecular Advances in Hematopathology
 Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Immunopathology of Lymphoma
 Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Aggressive B-cell Lymphomas Updated WHO classification Elias Campo
 Aggressive B-cell Lymphomas Updated WHO classification Elias Campo Hospital Clinic, University of Barcelona Diffuse Large B-cell Lymphoma A Heterogeneous Category Subtypes with differing: Histology and
Aggressive B-cell Lymphomas Updated WHO classification Elias Campo Hospital Clinic, University of Barcelona Diffuse Large B-cell Lymphoma A Heterogeneous Category Subtypes with differing: Histology and
SUPPLEMENTARY INFORMATION
 Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms. Curtis A. Hanson, MD
 Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation
 a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
Pathology of the indolent B-cell lymphomas Elias Campo
 Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Myeloproliferative Neoplasms
 Myeloproliferative Neoplasms (MPN and MDS/MPN) Attilio Orazi, MD, FRCPath Weill Cornell Medical College/ NY Presbyterian Hospital, New York, NY USA EAHP EDUCATIONAL SESSION: Updated WHO classification
Myeloproliferative Neoplasms (MPN and MDS/MPN) Attilio Orazi, MD, FRCPath Weill Cornell Medical College/ NY Presbyterian Hospital, New York, NY USA EAHP EDUCATIONAL SESSION: Updated WHO classification
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
9/25/2017. Disclosure. I have nothing to disclose. Young S. Kim MD Dept. of Pathology
 Disclosure MAST CELLNEOPLASM I have nothing to disclose. Young S. Kim MD Dept. of Pathology 1 Objectives What is mast cell lineage? Changes in updated WHO 2016 mastocytosis Issues of Mastocytosis CD30
Disclosure MAST CELLNEOPLASM I have nothing to disclose. Young S. Kim MD Dept. of Pathology 1 Objectives What is mast cell lineage? Changes in updated WHO 2016 mastocytosis Issues of Mastocytosis CD30
Update on Myelodysplastic Syndromes and Myeloproliferative Neoplasms. Kaaren Reichard Mayo Clinic Rochester
 Update on Myelodysplastic Syndromes and Myeloproliferative Neoplasms Kaaren Reichard Mayo Clinic Rochester Reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Learning Objectives Present
Update on Myelodysplastic Syndromes and Myeloproliferative Neoplasms Kaaren Reichard Mayo Clinic Rochester Reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Learning Objectives Present
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms. Daniel A. Arber, MD Stanford University
 Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Diagnostic Approach for Eosinophilia and Mastocytosis. Curtis A. Hanson, M.D.
 Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Practical Diagnosis of Hematologic Disorders. Vol 2 Malignant Disorders
 5 th ed Practical Diagnosis of Hematologic Disorders Vol 2 Malignant Disorders Vol2_FrontMatter_v03_0804 final.indd i 8/6/2009 10:00:11 PM Authors Carl R Kjeldsberg, MD Professor of Pathology, University
5 th ed Practical Diagnosis of Hematologic Disorders Vol 2 Malignant Disorders Vol2_FrontMatter_v03_0804 final.indd i 8/6/2009 10:00:11 PM Authors Carl R Kjeldsberg, MD Professor of Pathology, University
The Challenges of Precision Medicine: New Advances in Molecular Diagnostic Testing- Impact for Healthcare
 The Challenges of Precision Medicine: New Advances in Molecular Diagnostic Testing- Impact for Healthcare Jessica Wang-Rodriguez, MD Chief, VISN22 Consolidated Pathology and Laboratory Medicine Services
The Challenges of Precision Medicine: New Advances in Molecular Diagnostic Testing- Impact for Healthcare Jessica Wang-Rodriguez, MD Chief, VISN22 Consolidated Pathology and Laboratory Medicine Services
Non-Hodgkin s Lymphomas Version
 NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Non-Hodgkin s Lymphomas Version 2.2015 NCCN.org Continue Use of Immunophenotyping/ Genetic Testing in Differential Diagnosis of Mature B-Cell
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Non-Hodgkin s Lymphomas Version 2.2015 NCCN.org Continue Use of Immunophenotyping/ Genetic Testing in Differential Diagnosis of Mature B-Cell
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities
 WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
Aggressive B cell Lymphomas
 Aggressive B cell Lymphomas I have nothing to disclose. Disclosures Raju K. Pillai City of Hope National Medical Center Outline WHO 2016 Classification Large B cell Lymphomas New entities and changes in
Aggressive B cell Lymphomas I have nothing to disclose. Disclosures Raju K. Pillai City of Hope National Medical Center Outline WHO 2016 Classification Large B cell Lymphomas New entities and changes in
Methods used to diagnose lymphomas
 Institut für Pathologie Institut für Pathologie Methods used to diagnose lymphomas Prof. Dr.Med. Leticia Quintanilla-Fend Molecular techniques NGS histology Cytology AS-PCR Sanger seq. MYC Immunohistochemistry
Institut für Pathologie Institut für Pathologie Methods used to diagnose lymphomas Prof. Dr.Med. Leticia Quintanilla-Fend Molecular techniques NGS histology Cytology AS-PCR Sanger seq. MYC Immunohistochemistry
Chronic Lymphocytic Leukemia Mantle Cell Lymphoma Elias Campo
 Chronic Lymphocytic Leukemia Mantle Cell Lymphoma Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas NAIVE -B LYMPHOCYTE MEMORY CELL CLL MCL FL MZL Small cell size Low proliferation
Chronic Lymphocytic Leukemia Mantle Cell Lymphoma Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas NAIVE -B LYMPHOCYTE MEMORY CELL CLL MCL FL MZL Small cell size Low proliferation
What s new on the horizon in T-cell lymphoma Elaine S Jaffe National Cancer Institute, Bethesda MD
 What s new on the horizon in T-cell lymphoma Elaine S Jaffe National Cancer Institute, Bethesda MD WHO classification: where are we today? Of 12 monographs planned for 4 th Edition Bluebook series, only
What s new on the horizon in T-cell lymphoma Elaine S Jaffe National Cancer Institute, Bethesda MD WHO classification: where are we today? Of 12 monographs planned for 4 th Edition Bluebook series, only
The History of Lymphoma Classification and the 2017 Revision
 The History of Lymphoma Classification and the 2017 Revision ESMO Perceptorship on Lymphoma, Lugano 2018 German Ott Department of Clinical Pathology, Robert-Bosch-Krankenhaus and Dr. Margarete Fischer-Bosch
The History of Lymphoma Classification and the 2017 Revision ESMO Perceptorship on Lymphoma, Lugano 2018 German Ott Department of Clinical Pathology, Robert-Bosch-Krankenhaus and Dr. Margarete Fischer-Bosch
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual
 Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
Contents. vii. Preface... Acknowledgments... v xiii
 Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
The 2016 updated WHO classification of lymphoid neoplasias
 DOI: 10.1002/hon.2399 SUPPLEMENT ARTICLE The 2016 updated WHO classification of lymphoid neoplasias Leticia Quintanilla Martinez Institute of Pathology, University Hospital Tübingen, Eberhard Karls University
DOI: 10.1002/hon.2399 SUPPLEMENT ARTICLE The 2016 updated WHO classification of lymphoid neoplasias Leticia Quintanilla Martinez Institute of Pathology, University Hospital Tübingen, Eberhard Karls University
Society for Hematopathology 2017
 Society for Hematopathology 2017 Session 2 Genetic Testing in the Diagnosis of Lymphoid Neoplasms Summary of the cases Session Chairs: Rebecca King and Miguel Piris September 7, 2017 Lymphoma diseases/variants
Society for Hematopathology 2017 Session 2 Genetic Testing in the Diagnosis of Lymphoid Neoplasms Summary of the cases Session Chairs: Rebecca King and Miguel Piris September 7, 2017 Lymphoma diseases/variants
Myeloproliferative Disorders - D Savage - 9 Jan 2002
 Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Chronic Myelomonocytic Leukemia with molecular abnormalities SH
 Chronic Myelomonocytic Leukemia with molecular abnormalities SH2017-0351 Madhu P. Menon MD,PhD, Juan Gomez MD, Kedar V. Inamdar MD,PhD and Kristin Karner MD Madhu P Menon, MD, PhD Henry Ford Hospital Patient
Chronic Myelomonocytic Leukemia with molecular abnormalities SH2017-0351 Madhu P. Menon MD,PhD, Juan Gomez MD, Kedar V. Inamdar MD,PhD and Kristin Karner MD Madhu P Menon, MD, PhD Henry Ford Hospital Patient
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed
 MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
WHO Classification 7/2/2009
 Least Malignant Myeloproliferative Disorders Myelodysplastic Syndromes Most Malignant Acute Leukemia Classifying Hematopoietic Disorders French-American-British (FAB) World Health Organization (WHO) Thanks
Least Malignant Myeloproliferative Disorders Myelodysplastic Syndromes Most Malignant Acute Leukemia Classifying Hematopoietic Disorders French-American-British (FAB) World Health Organization (WHO) Thanks
Hematology Page 1 of 8
 Hematology Page 1 of 8 Hematology Major Category Code Headings Revised 12/17 1 Basic methodology and test armamentarium 20000 2 Normal hematopoiesis & hemostasis 20100 3 RBC disorders, non-neoplastic 20340
Hematology Page 1 of 8 Hematology Major Category Code Headings Revised 12/17 1 Basic methodology and test armamentarium 20000 2 Normal hematopoiesis & hemostasis 20100 3 RBC disorders, non-neoplastic 20340
Myelodysplastic syndromes
 Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
DETERMINATION OF A LYMPHOID PROCESS
 Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
Disclosures. Myeloproliferative Neoplasms: A Case-Based Approach. Objectives. Myeloproliferative Neoplasms. Myeloproliferative Neoplasms
 Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
Aggressive B-cell Lymphoma 2013
 Aggressive B-cell Lymphoma 2013 Diffuse Large B-Cell Lymphoma Burkitt Lymphoblastic lymphoma Gray zone Intermediate DLBCL/HL Intermediate BL/DLBCL Diffuse Large B-cell lymphoma Common morphology: diffuse
Aggressive B-cell Lymphoma 2013 Diffuse Large B-Cell Lymphoma Burkitt Lymphoblastic lymphoma Gray zone Intermediate DLBCL/HL Intermediate BL/DLBCL Diffuse Large B-cell lymphoma Common morphology: diffuse
Aggressive B cell Lymphomas
 Aggressive B cell Lymphomas Raju K. Pillai City of Hope National Medical Center I have no disclosures Outline What is new in the WHO 2016 classification Insights from genomic studies Double Hit Lymphoma
Aggressive B cell Lymphomas Raju K. Pillai City of Hope National Medical Center I have no disclosures Outline What is new in the WHO 2016 classification Insights from genomic studies Double Hit Lymphoma
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic/Myeloproliferative Neoplasms (MDS/MPN) Updated
 Myelodysplastic/Myeloproliferative Neoplasms (MDS/MPN) Updated Attilio Orazi, MD, FRCPath. (Engl.) Professor of Pathology and Laboratory Medicine Weill Cornell Medical College/NYP Hospital New York, NY
Myelodysplastic/Myeloproliferative Neoplasms (MDS/MPN) Updated Attilio Orazi, MD, FRCPath. (Engl.) Professor of Pathology and Laboratory Medicine Weill Cornell Medical College/NYP Hospital New York, NY
Pearls and pitfalls in interpretation of lymphoid lesions in needle biopsies
 Pearls and pitfalls in interpretation of lymphoid lesions in needle biopsies Megan S. Lim MD PhD University of Pennsylvania October 8, 2018 Objectives To understand how the trend toward less invasive lymph
Pearls and pitfalls in interpretation of lymphoid lesions in needle biopsies Megan S. Lim MD PhD University of Pennsylvania October 8, 2018 Objectives To understand how the trend toward less invasive lymph
Acute leukemia and myelodysplastic syndromes
 11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
HIGH GRADE B-CELL LYMPHOMA DAVID NOLTE, MD (PGY-2) HUSSAM AL-KATEB, PHD, FACMG DEBORAH FUCHS, MD
 HIGH GRADE B-CELL LYMPHOMA DAVID NOLTE, MD (PGY-2) HUSSAM AL-KATEB, PHD, FACMG DEBORAH FUCHS, MD OUTLINE High grade B-cell lymphoma with MYC and BCL2 and/or BCL6 rearrangements Patient presentation 2008/2016
HIGH GRADE B-CELL LYMPHOMA DAVID NOLTE, MD (PGY-2) HUSSAM AL-KATEB, PHD, FACMG DEBORAH FUCHS, MD OUTLINE High grade B-cell lymphoma with MYC and BCL2 and/or BCL6 rearrangements Patient presentation 2008/2016
HODGKIN LYMPHOMA DR. ALEJANDRA ZARATE OSORNO HOSPITAL ESPAÑOL DE MEXICO
 HODGKIN LYMPHOMA DR. ALEJANDRA ZARATE OSORNO HOSPITAL ESPAÑOL DE MEXICO HODGKIN LYMPHOMA CLASSIFICATION Lukes & Butler Rye WHO-2016 Linphocytic and/or histiocytic Nodular & diffuse Nodular Sclerosis Lymphocyte
HODGKIN LYMPHOMA DR. ALEJANDRA ZARATE OSORNO HOSPITAL ESPAÑOL DE MEXICO HODGKIN LYMPHOMA CLASSIFICATION Lukes & Butler Rye WHO-2016 Linphocytic and/or histiocytic Nodular & diffuse Nodular Sclerosis Lymphocyte
[COMPREHENSIVE GENETIC ASSAY PANEL ON
 2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls
 Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Integrated Hematopathology. Morphology and FCI with IHC
 Integrated Hematopathology Morphology and FCI with IHC FrontMatter.indd i 9/6/2009 9:30:12 PM FrontMatter.indd ii 9/6/2009 9:30:18 PM Integrated Hematopathology Morphology and FCI with IHC Cherie H Dunphy,
Integrated Hematopathology Morphology and FCI with IHC FrontMatter.indd i 9/6/2009 9:30:12 PM FrontMatter.indd ii 9/6/2009 9:30:18 PM Integrated Hematopathology Morphology and FCI with IHC Cherie H Dunphy,
Case year old male with abdominal lymphadenopathy Treated with 8 cycles of R-CHOP One year later B-symptoms and progressive disease
 Codirectors Tsieh Sun, M.D., FASCP Francisco Vega, M.D., Ph.D. Department of Hematopathology UT MD Anderson Cancer Center Houston Texas There is no conflict of interest involved in the content and presentation
Codirectors Tsieh Sun, M.D., FASCP Francisco Vega, M.D., Ph.D. Department of Hematopathology UT MD Anderson Cancer Center Houston Texas There is no conflict of interest involved in the content and presentation
Molecular Markers. Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC
 Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
2016 WHO CLASSIFICATION OF TUMOURS OF HAEMATOPOIETIC AND LYMPHOID TISSUES, 4TH ED., VOL FCDS WEBCAST SERIES OCTOBER 19, 2017
 2016 WHO CLASSIFICATION OF TUMOURS OF HAEMATOPOIETIC AND LYMPHOID TISSUES, 4TH ED., VOL 2 2017-2018 FCDS WEBCAST SERIES OCTOBER 19, 2017 STEVEN PEACE, CTR 1 CDC & Florida DOH Attribution We acknowledge
2016 WHO CLASSIFICATION OF TUMOURS OF HAEMATOPOIETIC AND LYMPHOID TISSUES, 4TH ED., VOL 2 2017-2018 FCDS WEBCAST SERIES OCTOBER 19, 2017 STEVEN PEACE, CTR 1 CDC & Florida DOH Attribution We acknowledge
Immunohistochemical classification of haematolymphoid tumours. Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital
 Immunohistochemical classification of haematolymphoid tumours Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital Malignant lymphoproliferative diseases What are they? Haematolymphoid
Immunohistochemical classification of haematolymphoid tumours Stephen Hamilton-Dutoit Institute of Pathology Aarhus University Hospital Malignant lymphoproliferative diseases What are they? Haematolymphoid
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228
 2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Neoplasms. Policy Specific Section:
 Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
Myeloid malignancies Chronic myeloid disorders
 Myeloid malignancies Chronic myeloid disorders Myeloproliferative neoplasms (MPN) Mastocytosis / Mast cell diseases Myeloid/lymphoid neoplasms with eosinophilia and gene rearrangement Myelodysplastic/myeloproliferative
Myeloid malignancies Chronic myeloid disorders Myeloproliferative neoplasms (MPN) Mastocytosis / Mast cell diseases Myeloid/lymphoid neoplasms with eosinophilia and gene rearrangement Myelodysplastic/myeloproliferative
Burkitt lymphoma. Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8
 Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Update on the Classification of Aggressive B-cell Lymphomas and Hodgkin Lymphoma
 Update on the Classification of Aggressive B-cell Lymphomas and Hodgkin Lymphoma Nancy Lee Harris, M. D. Massachusetts General Hospital Harvard Medical School Aggressive B-cell Lymphomas WHO 4 th Edition
Update on the Classification of Aggressive B-cell Lymphomas and Hodgkin Lymphoma Nancy Lee Harris, M. D. Massachusetts General Hospital Harvard Medical School Aggressive B-cell Lymphomas WHO 4 th Edition
Cost-Effective Strategies in the Workup of Hematologic Neoplasm. Karl S. Theil, Claudiu V. Cotta Cleveland Clinic
 Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Extramedullary precursor T-lymphoblastic transformation of CML at presentation
 Extramedullary precursor T-lymphoblastic transformation of CML at presentation Neerja Vajpayee, Constance Stein, Bernard Poeisz & Robert E. Hutchison Clinical History 30 year old man presented to the emergency
Extramedullary precursor T-lymphoblastic transformation of CML at presentation Neerja Vajpayee, Constance Stein, Bernard Poeisz & Robert E. Hutchison Clinical History 30 year old man presented to the emergency
The spectrum of flow cytometry of the bone marrow
 The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
Aggressive B-Cell Lymphomas
 Aggressive B-cell Lymphomas Aggressive B-Cell Lymphomas Stephen Hamilton Dutoit Institute of Pathology Aarhus Kommunehospital B-lymphoblastic lymphoma Diffuse large cell lymphoma, NOS T-cell / histiocyte-rich;
Aggressive B-cell Lymphomas Aggressive B-Cell Lymphomas Stephen Hamilton Dutoit Institute of Pathology Aarhus Kommunehospital B-lymphoblastic lymphoma Diffuse large cell lymphoma, NOS T-cell / histiocyte-rich;
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms
 Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Version: MPNBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is NOT required for accreditation
Template for Reporting Results of Biomarker Testing for Myeloproliferative Neoplasms Version: MPNBiomarkers 1.0.0.2 Protocol Posting Date: June 2017 This biomarker template is NOT required for accreditation
Introduction: The Revised (4 th Edition) World Health Organization (WHO) Classification of Tumors of Hematopoietic and Lymphoid Tissues
 Society for Hematopathology Scientific Symposium USCAP Companion Meeting, Boston, MA March 8, 2009 Boston, MA Steven H. Swerdlow and James Vardiman, Moderators Introduction: The Revised (4 th Edition)
Society for Hematopathology Scientific Symposium USCAP Companion Meeting, Boston, MA March 8, 2009 Boston, MA Steven H. Swerdlow and James Vardiman, Moderators Introduction: The Revised (4 th Edition)
2013 Pathology Student
 About this guide If you re reading this introduction, it means you are probably either a) covering hematopathology in your pathology class right now, or b) studying for boards. Either way, you ve come
About this guide If you re reading this introduction, it means you are probably either a) covering hematopathology in your pathology class right now, or b) studying for boards. Either way, you ve come
Session 4: Summary and Conclusions
 Session 4: Summary and Conclusions Total cases in Session 4 Myeloproliferative neoplasms 16 cases Oral #300 (CEL, NOS) Mastocytosis 2 cases Oral #156 (SM-AHN) Myeloid/lymphoid neoplasms with eosinophilia
Session 4: Summary and Conclusions Total cases in Session 4 Myeloproliferative neoplasms 16 cases Oral #300 (CEL, NOS) Mastocytosis 2 cases Oral #156 (SM-AHN) Myeloid/lymphoid neoplasms with eosinophilia
Hematopathology Case Study
 www.medfusionservices.com Hematopathology Case Study CV3515-14 JUNE Clinical Presentation: Clinical Information: A 42 year old male with history of chronic myelogenous leukemia (CML) presents with an elevated
www.medfusionservices.com Hematopathology Case Study CV3515-14 JUNE Clinical Presentation: Clinical Information: A 42 year old male with history of chronic myelogenous leukemia (CML) presents with an elevated
5000 International Clinical Cytometry Society: Practical Flow Cytometry in Hematopathology A Case-Based Approach
 5000 International Clinical Cytometry Society: Practical Flow Cytometry in Hematopathology A Case-Based Approach Joseph A DiGiuseppe, MD, PhD Hartford Hospital Disclosures In the past 12 months, I have
5000 International Clinical Cytometry Society: Practical Flow Cytometry in Hematopathology A Case-Based Approach Joseph A DiGiuseppe, MD, PhD Hartford Hospital Disclosures In the past 12 months, I have
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Part 4 MYELOID NEOPLASMS
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
74y old Female with chronic elevation of Platelet count. August 18, 2005 Faizi Ali, MD Hematopathology Fellow
 74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
2013 AAIM Pathology Workshop
 2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
AML: WHO classification, biology and prognosis. Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen
 AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
Clinical Policy: Bendamustine (Bendeka, Treanda) Reference Number: PA.CP.PHAR.307
 Clinical Policy: (Bendeka, Treanda) Reference Number: PA.CP.PHAR.307 Effective Date: 01/18 Last Review Date: 11/17 Coding Implications Revision Log Description The intent of the criteria is to ensure that
Clinical Policy: (Bendeka, Treanda) Reference Number: PA.CP.PHAR.307 Effective Date: 01/18 Last Review Date: 11/17 Coding Implications Revision Log Description The intent of the criteria is to ensure that
