Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry?
|
|
|
- Linette Loreen Greer
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry? Oriana Cohen, MD, Kevin Small, MD, Christina Lee, BA, Oriana Petruolo, MD, Nolan Karp, MD, and Mihye Choi, MD Department of Plastic Surgery, NYU Langone Medical Center, New York, New York n Abstract: Unilateral breast reconstruction poses a special set of challenges to the reconstructive breast surgeon compared to bilateral reconstructions. No studies to date provide an objective comparison between autologous and implant based reconstructions in matching the contralateral breast. This study compares the quantitative postoperative results between unilateral implant and autologous flap reconstructions in matching the native breast in shape, size, and projection using three-dimensional (3D) imaging. Sixty-four patients who underwent unilateral mastectomy with tissue expander (TE)- implant (n = 34) or autologous microvascular free transverse rectus abdominus myocutaneous (TRAM; n = 18) or deep inferior epigastric artery perforator (DIEP; n = 12) flap (n = 30) reconstruction from 2007 to 2010 were analyzed. Key patient demographics and risk factors were collected. Using 3D scans of patients obtained during pre and postoperative visits including over 1 year follow-ups for both groups, 3D models were constructed and analyzed for total breast volume, anterior-posterior projection from the chest wall, and 3D comparison. No significant differences in mean age, body mass index, or total number of reconstructive surgeries were observed between the two groups (TE-implant: , , 3 0.9; autologous: , , ; p > 0.05). The total volume difference between the reconstructed and contralateral breasts in the TE-implant group was insignificant: cc, similar to the autologous group: cc, as was the variance of breast volume from the mean. In both groups, the reconstructed breast had a larger volume. A-P projections were similar between the contralateral and the reconstructed breasts in the TE-implant group: mm versus mm (p > 0.05). The autologous reconstructed breast had statistically insignificant but less A-P projection compared to the contralateral breast ( mm versus mm; p > 0.05). Variance of A-P projection from the mean was additionally insignificant between the contralateral and reconstructed breasts. Both groups produced similar asymmetry scores based on global 3D comparison (TE-implant: mm; autologous: mm; p > 0.05). Lastly, when the autologous group was further subdivided into TRAM and DIEP cohorts, no significant differences in breast volume, A-P projection or symmetry existed. Using 3D imaging, we demonstrate that both TEimplant and autologous reconstruction can achieve symmetrical surgical results with the same number of operations. This study demonstrates that breast symmetry, while an important consideration in the breast reconstruction algorithm, should not be the sole consideration in a patient decision to proceed with autologous versus TE-implant reconstruction. n Key Words: 3D imaging, autologous reconstruction, breast projection, breast reconstruction, breast symmetry, breast volume, DIEP, implant, tissue-expander, TRAM, unilateral reconstruction Post-mastectomy breast reconstruction has been shown to improve patient body image and selfesteem leading to better overall psychologic well-being and quality of life (1 3). More women with breast cancer are electing to undergo breast reconstruction today. In fact, more than 90,000 women underwent breast reconstruction in 2011, an increase of 22% since 2000 (4). The decision as to which Address correspondence and reprint requests to: Mihye Choi, MD, Institute of Reconstructive Plastic Surgery, NYU Langone Medical Center, 305 East 47th Street, Suite 1A, New York, NY 10017, USA, or mihye.choi@nyumc.org DOI: /tbj Wiley Periodicals, Inc., X/15 The Breast Journal, Volume 22 Number 1, reconstructive strategy to undertake is an individualized and personal decision dependent on myriad factors. Patient desires, comorbidities, surgical history, prior radiation, body habitus, and the surgeon preference all play a role in the decision-making algorithm (5). Surgical approaches to breast reconstruction employ autologous free or pedicle tissue transfer, prosthetic breast reconstruction with tissue expanders (TE) and implants, or a combination of both. Many surgeons believe that compared with implant-based reconstruction, autologous reconstruction eliminates the need for alloplastic materials, creating a breast that feels and appears more natural, responds to weight changes, and better retains shape and volume in the face of radiation therapy (6).
2 76 cohen et al. Others, however, advocate for the use of implantbased reconstructions with shorter operating times, no additional donor site morbidity, and faster recovery times. Plastic surgery outcomes studies typically evaluate satisfaction, complications, or aesthetic results as markers for surgical success (7, 8). Such studies comparing post-mastectomy autologous versus implant breast reconstruction have demonstrated equivocal results. Tzafetta et al. reported no significant difference in patient satisfaction or aesthetic scores between patients who underwent autologous versus TE/implant reconstruction (9), findings corroborated by several other investigations (10, 11). On the other hand, other studies have shown greater patient satisfaction and aesthetic results with autologous-based reconstruction compared to prosthetic reconstruction. For example, in the Michigan Breast Reconstruction Outcome Study, Alderman et al. reported 78% of transverse rectus abdominus myocutaneous (TRAM) patients were generally satisfied compared with 61% of expander/implant patients, and that aesthetic satisfaction was 75% for TRAM patients compared to 40% of prosthetic reconstruction patients (12 14). Moreover, in a recent publication by Craft et al., patients undergoing unilateral breast reconstruction demonstrated higher patient satisfaction with autologous compared to implant reconstruction (15); a result substantiated by Yueh et al. (16). These conflicting findings necessitate a more quantitative method for evaluation of post-mastectomy breast reconstruction outcomes. Unilateral breast reconstruction presents both the surgeon and the patient with a great challenge. For the surgeon, creating a breast matching in shape, size, projection, feel, and movement is difficult, even with a full armamentarium of implant choices and expertise in implant and free flap reconstruction. For the patient undergoing unilateral breast reconstruction, the contralateral breast serves as a daily reminder of the ablative treatment she received due to her breast cancer. There are limited studies that quantitatively compare postoperative size, shape, contour, and symmetry following breast reconstruction. Recent work from our group and others has demonstrated the utility of three-dimensional (3D) breast imaging to obtain wellestablished breast measurements, as well as guide operative planning, analyze surgical results, and document postoperative changes over time (17 22). This study reports the application of 3D breast imaging to compare the postoperative results of unilateral prosthetic or autologous flap reconstruction in matching contralateral breast volume, shape, and overall symmetry. The study aims to quantitatively measure the symmetry of the reconstructed breast to the contralateral breast. MATERIALS AND METHODS Patient Enrollment Patients undergoing unilateral TE-implant or autologous microvascular free flap (TRAM flap and deep inferior epigastric artery perforator flap [DIEP]) reconstruction by one of two senior authors (MC, NK) were offered enrollment into the study. Informed consent was obtained in accordance with the guidelines set forth by the New York University Medical Center Institutional Review Board. A complete series of 3D images were obtained between 2007 and 2010 of 64 patients: 34 TE-implant reconstructions and 30 autologous free TRAM (n = 18)/DIEP (n = 12) reconstructions. Key demographic information was collected for each patient including age, body mass index (BMI), smoking, and history of radiation. The total number of reconstructive surgeries each patient underwent during the reconstructive period was additionally documented. As per our group s standard practice, patients were excluded from the study if they did not undergo preoperative imaging or if they had less than 1 year total postoperative follow-up. In addition, patients who underwent direct implant reconstruction were excluded. 3D Scans Three-dimensional scans were obtained at each postoperative visit using a previously validated Canfield Vectra scanner (19). The lens of the camera was placed 3 feet from the patient at the level of the breasts, and scans obtained with the patient facing +90, +45, 0, 45, and 90 degrees. The camera was then lowered to knee-level to obtain inferior views at the aforementioned positions. Each scan converted the surface shape to a polygon lattice of approximately 300,000 points. The polygons from each view were then merged by region to create a single 3D model. 3D models were exported for analysis using Geomagic software (Geomagic, Morrisville, NC).
3 Symmetry Comparison in Implant vs. Autologous Unilateral Breast Reconstruction 77 Breast Volume Measurement Total breast volume was calculated for every patient at each postoperative visit according to our group s previously described protocols. Each breast was isolated and overlaid on a customized chest wall template for each patient. First, the chest wall template, a curved plane that matches the curvature of the patient s torso with the breasts removed, was created. This was done by tracing the breast superiorly at the level at which it projects off the chest, then laterally with inclusion of the axillary tail, inferiorly to the inframammary fold, and medially. This breast tissue was removed to yield the chest wall template. The complete volume of each breast was subsequently determined by overlaying the previously isolated breast onto the chest wall and creating a closed 3D object. A software-based Boolean operation of the two overlapping images was performed, and calculating the volume of this closed object determined breast volume. Total breast volume of the reconstructed breast and contralateral, native breast were calculated at each postoperative visit. were then analyzed and a symmetry score calculated (Fig. 2). Statistical Analysis All data are presented as the mean SEM. Each reconstructed breast was compared to the contralateral breast for every postoperative visit. Paired t-test was used to assess for statistical significance between means. In addition, a two-sample f-test was used to compare variances from the mean of total breast volume and A-P projection measurements in the TE-implant and autologous reconstruction groups. A p-value less than 0.05 determined statistical significance. TOTAL BREAST VOLUME AND ANTERIOR- POSTERIOR PROJECTION CALCULATIONS A Breast Projection Measurement Breast projection, or anterior-posterior projection, was additionally determined at each postoperative visit. A-P projection was calculated by creating a vector that originated from the chest wall template and extended anteriorly to the A point, or anterior-most point of each breast, giving the maximal projection of the breast in millimeters. Like breast volume, A-P projection was measured for the reconstructed breast and contralateral, native breast, for each postoperative image throughout the course of reconstruction (Fig. 1). (a) Total Breast Volume CW PLANE (b) Anterior-Posterior Projection Figure 1. Breast volume and projection. (a) Breast Volume: Each breast is isolated and overlaid on a customized chest wall template to calculate breast volume. (b) Anterior-Posterior Projection: Anterior-posterior breast projection is measured by creating a vector that extends from the chest wall (C-W plane) to the anterior-most point of the breast (A-point). GLOBAL 3D COMPARISON Breast Symmetry At the end of each patient s reconstructive treatment, the reconstructed breast was compared to the contralateral, native breast to determine overall breast symmetry. By creating a mirror image of the reconstructed breast and overlaying it onto the contralateral breast, the Geomagic software global 3D compare function calculated the average deviation between points and generated topographical maps representing these average deviations. These deviations Figure 2. Global 3D compare. The global 3D compare function creates a topographical map of the reconstructed and non-reconstructed breast, which are compared in their derivation from one another. In the figure, red denotes the negative direction and blue the positive direction.
4 78 cohen et al. RESULTS Patient Demographics The TE-implant and autologous reconstruction groups exhibited no significant differences in mean age, BMI, or total number of reconstructive surgeries. The average age of patients undergoing unilateral TEimplant and autologous breast reconstruction was years versus years, respectively (p = 0.54). Average BMI was in the TE-implant group and in the autologous group (p = 0.12). Twelve percent of patients had a history of smoking in the TE-implant group versus 16.6% in the autologous group (p = 0.49). Moreover, 5.9% of patients had a history of radiation therapy in the TE-implant group versus 33.3% in the autologous reconstruction group (p < 0.05; Table 1). Postoperative analysis was performed on mean postoperative day (1 year, 104 days) in the TE-implant group and day (1 year, 265 days) in the autologous group (p = 0.2). This postoperative date represents the number of days from initial reconstruction. Interestingly, both reconstructive modalities required an average of three total reconstructive surgeries: TE-implant 3 0.9, autologous (p = 0.72), with no statistically significant difference in the timing of the secondary and tertiary reconstructive surgeries between the TE-implant and autologous groups. In the TE group, patients underwent TE-insertion followed by TE-implant exchange with a contralateral symmetrizing procedure (mastopexy, reduction mammoplasty). This secondary reconstructive surgery was performed at mean postop day from initial TE-insertion. The tertiary procedure often involved nipple reconstruction, scar revision, and in many, fat grafting at an average postop day from initial TE-insertion. Of note, implants chosen by the operating surgeon on a Table 1. Patient Demographics TE-implant (n = 34) Autologous (n = 30) p-value case-by-case basis, were all round implants ranging in profile from moderate to high profile (Natrelle Collection; Allergan, Irvine, CA). Patients in the autologous group generally underwent three surgeries as well. The first surgery involved mastectomy with autologous reconstruction. In the second, nipple reconstruction as well as a contralateral symmetrizing procedure was often performed. This secondary reconstruction was performed at mean postop day Some patients underwent fat grafting at the time of this second procedure. In a third procedure, many patients underwent fat grafting to increase the volume of the autologous breast. This tertiary procedure took place at mean postop day from initial autologous reconstruction (Table 2). A summary of the TE-implant and autologous reconstruction patients can be seen in Tables 1 and 2 with corresponding p-values. Breast Volume Analysis Both TE-implant and autologous reconstruction were analyzed for their abilities to achieve similar breast volume between the affected, reconstructed breast and the contralateral breast. The total breast volume of patients who underwent unilateral TE-implant reconstruction was cc in the reconstructed breast and cc in the contralateral breast, of no statistical significance (p = 0.48). Similarly, the total breast volume of the affected breast after autologous reconstruction was cc versus cc in the unaffected, unreconstructed breast volume, again of no statistical significance (p = 0.55; Fig. 3). In both reconstructive modalities, the reconstructed breast had a larger volume compared to the contralateral, unaffected breast (TE-implant: average of cc Table 2. Timing of Secondary and Tertiary Reconstructive Surgeries Prosthetic reconstruction TE-implant (n = 34) Autologous reconstruction Autologous (n = 30) p-value Age Body mass index Number of procedures Smoking 4/34 = 12% 5/30 = 16.6% 0.49 Prior radiation 2/34 = 5.9% 10/30 = 33.3% Secondary reconstructive surgery Tertiary reconstructive surgery Secondary reconstructive surgery Tertiary reconstructive surgery The TE-implant and autologous reconstruction group exhibited no statistically significant differences in mean age, BMI, total number of reconstructive procedures, or smoking history. The TE-implant and autologous reconstruction groups exhibited no statistically significant difference in timing of secondary and tertiary reconstructive procedures following initial TE or autologous reconstruction.
5 Symmetry Comparison in Implant vs. Autologous Unilateral Breast Reconstruction 79 larger, and autologous: average of cc larger), however, the difference was not statistically significant (p = 0.94; Fig. 4). When the variances in breast volume, or average of differences from the mean, were analyzed for both the TE-implant and autologous reconstruction groups, no statistically significant difference was identified between the two groups. In the TE-implant group, the variance from the mean was 28,664.9 in the affected breast and 20,493.1 in the unaffected breast (F-value 1.39, F-crit 2.0; p-value 0.33). Similarly, in the autologous group the variance in breast volumes of the affected breast was 39,617.2 compared to 26,448.6 in the unaffected breast (F-value 0.89, F-crit 2.1; p-value 1.23). Therefore, both TE-implant and autologous reconstruction effectively create a breast mound of Volume (cc) ± 24.6 ± Total Breast Volume ± 33.2 ± TE-Implant (p=0.48) Autologous (p=0.55) Reconstruction Group Unaffected Affected Figure 3. Total breast volume measurements. Both TE-implant and autologous reconstruction effectively create a breast mound of total volume that matches to that of the contralateral breast. Volume (cc) Breast Volume (Unaffected - Affected) 27.1 ± ±24.7 TE-Implant Autologous Reconstruction Group p=0.94 Figure 4. Delta breast volume measurements. In both reconstructive modalities, the reconstructed breast had a larger volume compared to the contralateral, unaffected breast, however, the difference was not statistically significant. total volume that matches to that of the contralateral breast. Breast Projection Analysis Both TE-implant and autologous reconstruction achieved A-P projections that were similar between the unaffected and affected breast. In the TE-implant group, the unaffected breast had an average A-P projection of mm versus mm in the affected, reconstructed breast (p = 0.87). In other words, there was a statistically insignificant difference of mm between the reconstructed and contralateral breast. In the autologous group, while the A-P projection was slightly less in the reconstructed breast, the observation was not statistically significant: unaffected and affected breasts had similar breast projections: mm versus mm, respectively (p = 0.28). The difference in A-P projection between the reconstructed and contralateral breasts was again insignificant: mm (Fig. 5). Again, when variances of A-P projection from the mean were compared between the two reconstruction groups, no statistically significant difference was identified. In the TE-implant group, the variance of A-P projection from the mean was in the affected breast and in the unaffected breast (F-value 0.85, F-crit 1.78; p-value 1.36). Similarly, in the autologous group the variance in A-P projections of the affected breast was compared to in the unaffected breast (F-value 0.89, F-crit 2.1; p-value 1.23). These data suggest that both TE-implant and autologous reconstruction are effective in achieving A-P Projection (mm) Anterior-Posterior Projection ± 3.5 ± ± ± 9.5 TE-implant (p=0.87) Autologous (p=0.28) Reconstruction Group Unaffected Affected Figure 5. Anterior-posterior projection. Both TE-implant and autologous reconstruction achieved A-P projections that were similar between the unaffected and affected breast.
6 80 cohen et al. breast projection that matches the unaffected contralateral breast, with no statistically significant differences among them. Breast Symmetry The two reconstructive modalities were compared in their ability to achieve overall symmetry between the unilateral reconstructed breast and contralateral breast. When comparing the topographical map of the two breasts, both TE-implant and autologous reconstruction produced similar results with no statistically significant difference between them (TE-implant: versus autologous: ; p = 0.41; Fig. 6). This finding suggests that both TE-implant and autologous reconstruction can achieve symmetrical surgical results. TRAM versus DIEP Reconstruction The autologous group was further subdivided into TRAM and DIEP subsets and analyzed for any differences in demographics and the aforementioned breast measurements of breast volume, A-P projection, and symmetry. In our analysis of patient demographics, the TRAM group demonstrated significantly longer postoperative follow-up (mean postoperative day versus (p = 0.03) and involved a younger patient subset (TRAM: years old versus DIEP years old; p = 0.03). Otherwise, no statistically significant differences were seen between the two groups in BMI, history of smoking, or prior radiation. In addition, both TRAM and DIEP subgroups required a total of three reconstructive surgeries (Table 3). When the two subgroups were analyzed for differences in breast volume, A-P projection, and global symmetry, no statistically significant differences were identified between the reconstructed and contralateral breast (Table 4). DISCUSSION With various surgical options for breast reconstruction available to patients today, patient satisfaction reports are increasingly used as corollaries for surgical results. Previous reports have retrospectively examined overall patient satisfaction between autologous and prosthetic reconstruction. One study by Saulis et al. reported a lower patient satisfaction rate among TE-implant patients compared to patients undergoing autologous TRAM flap reconstruction (14). Moreover, a comparative analysis of psychosocial, functional, and cosmetic outcomes of TRAM flap versus implant reconstruction by Cederna et al. reported a greater level of satisfaction in patients who underwent TRAM flap reconstruction specifically relating to the way Table 3. Autologous Reconstruction Patient Demographics TRAM (n = 18) DIEP (n = 12) p-value Age Body mass index Number of procedures Smoking 4/18 = 22.2% 1/12 = 8.3% 0.32 Prior radiation 4/18 = 22.2% 6/12 = 50% 0.11 The TRAM versus DIEP autologous reconstruction groups exhibited no statistically significant differences in mean BMI, total number of reconstructive procedures, smoking history, or history of prior radiation. Patients who underwent TRAM reconstruction were younger than patient s undergoing DIEP reconstruction, of statistical significance. Global 3D Compare Table 4. A Comparison of TRAM versus DIEP Reconstruction Symmetry Score ± ± 0.2 TE-implant Autologous Reconstruction Group p=0.41 TRAM (n = 18) DIEP (n = 12) p-value Breast volume (cc) Affected breast TRAM: 0.48 Unaffected breast DIEP: 0.91 Δ breast volume (cc) (affected-unaffected) A-P projection (mm) Affected breast TRAM: 0.28 Unaffected breast DIEP: 0.34 Δ A-P projection (mm) Symmetry score Figure 6. Global symmetry score. Both TE-implant and autologous reconstruction can achieve symmetrical surgical results. When the TRAM and DIEP subgroups were analyzed for differences in breast volume, A- P projection, and global symmetry, no statistically significant differences were identified between the reconstructed and contralateral breast.
7 Symmetry Comparison in Implant vs. Autologous Unilateral Breast Reconstruction 81 breasts felt to touch as well as overall appearance (23). However, these patients did report increased psychologic, social, and physical impairments resulting from their reconstruction. While comparing the outcomes of different surgical procedures is valuable, few studies quantitatively compare the outcome of TE-implant to autologous breast reconstruction. Using our 3D scanner, we sought to investigate the postoperative results between unilateral prosthetic versus autologous breast reconstruction in matching contralateral breast volume and shape using 3D imaging analysis. Our data demonstrate that both TE-implant and autologous reconstruction effectively create a breast mound of total volume and projection that matches the contralateral breast. Moreover, these symmetrical surgical results are achieved not only with the same number of total operations but also with timing of secondary and tertiary operations similar to achieve final symmetry. In our series, patients in the autologous group were pleased with the effects of fat grafting to both recipient and donor sites performed during the second operation and tended to request the third procedure for further revision, which included fat grafting and scar revision. Given these results, postoperative symmetry while important in the breast reconstruction algorithm, should not be the only consideration, and the decision as to which reconstructive modality to choose should be based on other clinical parameters. In terms of the implant types used, we used round silicone implants with high or moderate projection depending on the shape of the contralateral breasts. The form stable implants were not FDA approved during this study period and were not included in the study. While our data does provide a concrete basis for beginning to assess the outcomes of surgical procedures in a quantitative fashion, more studies need to be performed. For example, this study only examines the postoperative results with 1-year follow-up and therefore does not reflect further changes that the breast may undergo. Thus, we are unable to make definitive statements about the long-term symmetry of the different procedures, or changes in breast appearance over time. Moreover, while 3D imaging does provide us with objective data to compare 3D symmetry, it does not include patient satisfaction, sensibility, or naturalness of the reconstructed breast. Hu et al., for example, evaluated long-term patient-reported aesthetic satisfaction with expander/implant and autologous breast reconstruction. They found that in the long term, TRAM patients when compared with expander/implant patients have significantly greater aesthetic satisfaction (24). However, the parameters of long-term follow and patient satisfaction are outside of the scope of this study. When considering the great utility that 3D imaging can provide to breast surgery, it is important to realize that this imaging can be used not only for postoperative analysis, but also to guide preoperative planning with the goal of achieving breast symmetry with the least number of operations. The ability of 3D imaging to generate additional measurements of volumetric distribution and breast projection make it a promising method for further elucidating the effectiveness of these reconstructive techniques in achieving breast symmetry. REFERENCES 1. Wilkins E, Cederna P, Lowery J, et al. Prospective analysis of psychosocial outcomes in breast reconstruction: one-year post-operative results from the Michigan Breast Reconstruction Outcome Study. Plast Reconstr Surg 2000;106: Dean C, Chetty U, Forrest A. Effects of immediate breast reconstruction on psychosocial morbidity after mastectomy. Lancet 1983;1: Ng SK, Hare RM, Kuang RJ, et al. Breast reconstruction post-mastectomy: patient satisfaction and decision making. Ann Plast Surg [Epub ahead of print]. 4. American Society of Plastic Surgery. Reconstructive Surgery Procedures Available at: (accessed April 3, 2012). 5. Djohan R, Gage E, Bernard S. Breast reconstruction options following mastectomy. Cleve Clin J Med 2008;75:S Viiser N, Damen T, Timmam R, et al. Surgical results, aesthetic outcome, and patient satisfaction after microsurgical autologous breast reconstruction following failed implant reconstruction. Plast Reconstr Surg 2010;126: Spear S, Newman M, Bedford M, et al. A retrospective analysis of outcomes using three common methods for immediate breast reconstruction. Plast Reconstr Surg 2008;122: Kroll S, Baldwin B. A comparison of outcomes using three different methods of breast reconstruction. Plast Reconstr Surg 1992;90: Tzafetta K, Ahmed O, Bahia H, et al. Evaluation of the factors related to postmastectomy breast reconstruction. Plast Reconstr Surg 2001;107: Andrade W, Baxter N, Semple J. Clinical determinants of patient satisfaction with breast reconstruction. Plast Reconstr Surg 2001;107: Fogarty B, Brown A, Miller R. TRAM flap versus nonautologous breast reconstruction: what do patients really think? Plast Reconstr Surg 2004;113: Spear S, Newman M, Bedfored M. A retrospective analysis of outcomes using three common methods for immediate breast reconstruction. Plast Reconstr Surg 2007;122: Alderman A, Wilkins E, Lowery J, et al. Determinants of patient satisfaction in postmastectomy breast reconstruction. Plast Reconstr Surg 2000;106:
8 82 cohen et al. 14. Saulis A, Mustoe T, Fine N. A retrospective analysis of patient satisfaction with immediate postmastectomy breast reconstruction: a comparison of three common procedures. Plast Reconstr Surg 2007;119: Craft RO, Colakoglu S, Curtis MS, et al. Patient satisfaction in unilateral and bilateral breast reconstruction [Outcomes Article]. Plast Reconstr Surg 2011;127: Yueh J, Slavin S, Adesiyun T, et al. Patient satisfaction in post mastectomy breast reconstruction: a comparative evaluation of DIEP, TRAM, latissimus flap, and implant techniques. Plast Reconstr Surg 2010;125: Tepper O, Unger J, Small K, et al. Mammometrics: the standardization of aesthetic and reconstructive breast surgery. Plast Reconstr Surg 2010;125: Tepper O, Small K, Rudolph L, et al. Virtual 3-dimensional modeling as a valuable adjunct to aesthetic and reconstructive breast surgery. Am J Surg 2006;192: Tepper O, Small K, Unger J, et al. 3D analysis of breast augmentation defines operative changes and their relationship to implant dimensions. Ann Plast Surg 2009;62: Tepper O, Choi M, Small K, et al. An innovative three-dimensional approach to defining the anatomical changes occurring after short scar-medial pedicle reduction mammoplasty. Plast Reconstr Surg 2008;121: Isogai N, Sai K, Kamiishi H, et al. Quantitative analysis of the reconstructed breast using a 3-dimensional laser light scanner. Ann Plast Surg 2006;56: Tepper O, Karp S, Small K, et al. Three-dimensional imaging provides valuable clinical data to aid in unilateral tissue expander-implant breast reconstruction. Breast J 2008;14: Cederna P, Yates W, Chang P, et al. Postmastectomy reconstruction: comparative analysis of the psychosocial, functional, and cosmetic effects of transverse rectus abdominis musculocutaneous flap versus breast implant reconstruction. Ann Plast Surg 1995;35: Hu E, Pusic A, Waljee J, et al. Patient-reported aesthetic satisfaction with breast reconstruction during the long-term survivorship period. Plast Reconstr Surg 2009;124:1 8.
Is There an Ideal Donor Site of Fat for Secondary Breast Reconstruction?
 526751AESXXX10.1177/1090820X14526751Aesthetic Surgery JournalSmall et al research-article2014 Breast Surgery Is There an Ideal Donor Site of Fat for Secondary Breast Reconstruction? Kevin Small, MD; Mihye
526751AESXXX10.1177/1090820X14526751Aesthetic Surgery JournalSmall et al research-article2014 Breast Surgery Is There an Ideal Donor Site of Fat for Secondary Breast Reconstruction? Kevin Small, MD; Mihye
The use of postmastectomy radiation therapy (PMRT) to prevent
 NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation. Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS
 Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
Breast reconstruction has an important role BREAST. A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions
 BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Breast Reconstruction: Current Strategies and Future Opportunities
 Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction Surgery
 Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni
 SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
Breast Cancer Reconstruction
 Breast Cancer Jerome H. Liu, MD Tom S. Liu, MD Jerome H. Liu, MD Undergraduate: Brown University Medical School: University of California, Los Angeles Residency: UCLA Medical Center Fellowship:UCLA Medical
Breast Cancer Jerome H. Liu, MD Tom S. Liu, MD Jerome H. Liu, MD Undergraduate: Brown University Medical School: University of California, Los Angeles Residency: UCLA Medical Center Fellowship:UCLA Medical
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer. Oncoplastic and Reconstructive Surgery
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate surgical options
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
Reconstructive Breast Surgery and Management of Breast Implants
 Reconstructive Breast Surgery and Management of Breast Implants Policy Number: 7.01.22 Last Review: 1/2018 Origination: 3/1993 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Reconstructive Breast Surgery and Management of Breast Implants Policy Number: 7.01.22 Last Review: 1/2018 Origination: 3/1993 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION
 Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
Medical Policy Original Effective Date: Revised Date: Page 1 of 8
 Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Breast Restoration Surgery After a mastectomy
 UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
Breast Reconstruction
 Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Visualization and Quantification of Female Breast Morphology During Breast Reconstruction
 Visualization and Quantification of Female Breast Morphology During Breast Reconstruction Audrey L. CHEONG 1, Gregory P. REECE 2, Michelle C. FINGERET 2,3, Fatima MERCHANT* 1,4 1 Department of Electrical
Visualization and Quantification of Female Breast Morphology During Breast Reconstruction Audrey L. CHEONG 1, Gregory P. REECE 2, Michelle C. FINGERET 2,3, Fatima MERCHANT* 1,4 1 Department of Electrical
A Prospective Analysis of Dynamic Loss of Breast Projection in Tissue Expander-Implant Reconstruction
 A Prospective Analysis of Dynamic Loss of Breast Projection in Tissue Expander-Implant Reconstruction Lauren M Mioton 1 *, Sumanas W Jordan 2 *, John YS Kim 2 1 Department of Plastic Surgery, Vanderbilt
A Prospective Analysis of Dynamic Loss of Breast Projection in Tissue Expander-Implant Reconstruction Lauren M Mioton 1 *, Sumanas W Jordan 2 *, John YS Kim 2 1 Department of Plastic Surgery, Vanderbilt
Samer Saour, Guido Libondi, Venkat Ramakrishnan. Introduction
 Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks
 Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks Grant W. Carlson Wadley R. Glenn Professor of Surgery Divisions of Plastic Surgery & Surgical Oncology Emory
Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks Grant W. Carlson Wadley R. Glenn Professor of Surgery Divisions of Plastic Surgery & Surgical Oncology Emory
How To Make a Good Mastectomy for Reconstruction Based on the Anatomy. Zhang Jin, Ph.D MD
 How To Make a Good Mastectomy for Reconstruction Based on the Anatomy Zhang Jin, Ph.D MD Deputy Director and Professor Tianjin Medical University Cancer Institute and Hospital People s Republic of China
How To Make a Good Mastectomy for Reconstruction Based on the Anatomy Zhang Jin, Ph.D MD Deputy Director and Professor Tianjin Medical University Cancer Institute and Hospital People s Republic of China
More women are surviving breast cancer BREAST
 BREAST Patient-Reported Aesthetic Satisfaction with Breast Reconstruction during the Long-Term Survivorship Period Emily S. Hu, M.D. Andrea L. Pusic, M.D. Jennifer F. Waljee, M.D., M.P.H. Latoya Kuhn,
BREAST Patient-Reported Aesthetic Satisfaction with Breast Reconstruction during the Long-Term Survivorship Period Emily S. Hu, M.D. Andrea L. Pusic, M.D. Jennifer F. Waljee, M.D., M.P.H. Latoya Kuhn,
In a second stage or a second operation that tissue expander is removed through the same incision and the implant is placed within the chest pocket.
 Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
Updates in Breast Care. Truth or Hype. History of Breast Cancer Surgery. Dr Karen Barbosa 5/3/2017 4/20/2017
 Updates in Breast Care Dr Karen Barbosa 4/20/2017 Truth or Hype Princess Bust Developer Sears, Roebuck and Co. 1897 Promised to make the breast round, firm and beautiful History of Breast Cancer Surgery
Updates in Breast Care Dr Karen Barbosa 4/20/2017 Truth or Hype Princess Bust Developer Sears, Roebuck and Co. 1897 Promised to make the breast round, firm and beautiful History of Breast Cancer Surgery
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
Breast Reconstruction in Women Under 30: A 10-Year Experience
 ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps
 Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Plastic surgery of the breast includes; augmentation, reduction, Plastic Surgery of the Breast. Abstract. Continuing Education Column
 Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
Defining Pseudoptosis (Bottoming Out) 3 Years After Short-Scar Medial Pedicle Breast Reduction
 Aesth Plast Surg (2011) 35:357 364 DOI 10.1007/s00266-010-9615-6 ORIGINAL ARTICLE Defining Pseudoptosis (Bottoming Out) 3 Years After Short-Scar Medial Pedicle Breast Reduction Michelle Quan Ahmed Fadl
Aesth Plast Surg (2011) 35:357 364 DOI 10.1007/s00266-010-9615-6 ORIGINAL ARTICLE Defining Pseudoptosis (Bottoming Out) 3 Years After Short-Scar Medial Pedicle Breast Reduction Michelle Quan Ahmed Fadl
Prophylactic Mastectomy & Reconstructive Implications
 Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Breast Reconstruction. Westmead Breast Cancer Institute
 Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Aesthetic Subunits of the Breast
 Aesthetic Subunits of the Breast Scott L. Spear, M.D., and Steven P. Davison, D.D.S., M.D. Washington, D.C. Surgery for breast cancer has traditionally addressed the breast as if it were a geometric circle
Aesthetic Subunits of the Breast Scott L. Spear, M.D., and Steven P. Davison, D.D.S., M.D. Washington, D.C. Surgery for breast cancer has traditionally addressed the breast as if it were a geometric circle
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons
 Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
The decision to repair a partial mastectomy CME. State of the Art and Science in Postmastectomy Breast Reconstruction.
 CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
Medical Review Criteria Breast Surgeries
 Medical Review Criteria Breast Surgeries Effective Date: November 8, 2016 Subject: Breast Surgeries Policy: HPHC covers medically necessary breast surgeries including mastectomy, breast reconstruction,
Medical Review Criteria Breast Surgeries Effective Date: November 8, 2016 Subject: Breast Surgeries Policy: HPHC covers medically necessary breast surgeries including mastectomy, breast reconstruction,
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Breast Reconstructive Surgery After Mastectomy Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Breast Reconstructive Surgery After Mastectomy PRE-DETERMINATION
Breast Reconstructive Surgery After Mastectomy Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Breast Reconstructive Surgery After Mastectomy PRE-DETERMINATION
The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q
 The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
Assessment of Breast Volume Change after Transverse Rectus Abdominis Myocutaneous Flap
 Assessment of Breast Volume Change after Transverse Rectus Abdominis Myocutaneous Flap Sang Uk Park, Jeong Su Shim Department of Plastic and Reconstructive Surgery, Catholic University of Daegu School
Assessment of Breast Volume Change after Transverse Rectus Abdominis Myocutaneous Flap Sang Uk Park, Jeong Su Shim Department of Plastic and Reconstructive Surgery, Catholic University of Daegu School
Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts
 Breast Surgery Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts Scott L. Spear, MD; Samir S. Rao, MD; Ketan M. Patel, MD; and Maurice Y. Nahabedian, MD The combination of lumpectomy
Breast Surgery Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts Scott L. Spear, MD; Samir S. Rao, MD; Ketan M. Patel, MD; and Maurice Y. Nahabedian, MD The combination of lumpectomy
Methods of autologous tissue breast reconstruction BREAST
 BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
Microsurgical Breast Reconstruction in Thin Patients: The Impact of Low Body Mass Indices
 20 Original Article Microsurgical Breast Reconstruction in Thin Patients: The Impact of Low Body Mass Indices Katie E. Weichman, MD 1 Neil Tanna, MD, MBA 1 P. Niclas Broer, MD 1 Stelios Wilson, MD 1 Hamdan
20 Original Article Microsurgical Breast Reconstruction in Thin Patients: The Impact of Low Body Mass Indices Katie E. Weichman, MD 1 Neil Tanna, MD, MBA 1 P. Niclas Broer, MD 1 Stelios Wilson, MD 1 Hamdan
Immediate versus delayed free TRAM breast reconstruction: an analysis of perioperative factors and complications
 British Journal of Plastic Surgery (22), 55, l-6 9 22 The British Association of Plastic Surgeons doi:.54/bjps.22.3747 BRITISH JOURNAL OF / ~ ] PLASTIC SURGERY Immediate versus delayed free TRAM breast
British Journal of Plastic Surgery (22), 55, l-6 9 22 The British Association of Plastic Surgeons doi:.54/bjps.22.3747 BRITISH JOURNAL OF / ~ ] PLASTIC SURGERY Immediate versus delayed free TRAM breast
Post-mastectomy breast reconstruction
 Follow the link from the online version of this article to obtain certified continuing medical education credits Post-mastectomy breast reconstruction Paul T R Thiruchelvam, 1 Fiona McNeill, 2 Navid Jallali,
Follow the link from the online version of this article to obtain certified continuing medical education credits Post-mastectomy breast reconstruction Paul T R Thiruchelvam, 1 Fiona McNeill, 2 Navid Jallali,
Vertical mammaplasty has been developed
 BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
Medical Review Criteria Breast Surgeries
 Medical Review Criteria Breast Surgeries Subject: Breast Surgeries Authorization: Prior authorization is required for the following procedures requested for members enrolled in HPHC commercial (HMO, POS,
Medical Review Criteria Breast Surgeries Subject: Breast Surgeries Authorization: Prior authorization is required for the following procedures requested for members enrolled in HPHC commercial (HMO, POS,
Nipple-Areolar Complex Reconstruction: A Review of the Literature and Introduction of the Rectangle-to-Cube Nipple Flap
 Nipple-Areolar Complex Reconstruction: A Review of the Literature and Introduction of the Rectangle-to-Cube Nipple Flap Joshua T. Henderson, BA, a ThomasJ.Lee,MD, b Andrew M. Swiergosz, BS, a Andrea R.
Nipple-Areolar Complex Reconstruction: A Review of the Literature and Introduction of the Rectangle-to-Cube Nipple Flap Joshua T. Henderson, BA, a ThomasJ.Lee,MD, b Andrew M. Swiergosz, BS, a Andrea R.
Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps
 BREAST SURGERY Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps Albert Losken, MD, FACS, Claire S. Nicholas, MD, Ximena A. inell, MD, and Grant W.
BREAST SURGERY Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps Albert Losken, MD, FACS, Claire S. Nicholas, MD, Ximena A. inell, MD, and Grant W.
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
BREAST RECONSTRUCTION/REMOVAL AND REPLACEMENT OF IMPLANTS
 Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
Breast Reconstruction Surgery after Mastectomy or Lumpectomy
 Breast Reconstruction Surgery after Mastectomy or Lumpectomy Date of Origin: 11/1998 Last Review Date: 11/25/2017 Effective Date: 11/25/2017 Dates Reviewed: 08/2000, 09/2001, 11/2003, 11/2004, 12/2005,
Breast Reconstruction Surgery after Mastectomy or Lumpectomy Date of Origin: 11/1998 Last Review Date: 11/25/2017 Effective Date: 11/25/2017 Dates Reviewed: 08/2000, 09/2001, 11/2003, 11/2004, 12/2005,
Reconstructive Breast Surgery following Mastectomy for Breast Cancer: A Review
 Research Article http://www.alliedacademies.org/advanced-surgical-research/ Reconstructive Breast Surgery following Mastectomy for Breast Cancer: A Review Gurnam Virdi* Department of surgery, Queen Elizabeth
Research Article http://www.alliedacademies.org/advanced-surgical-research/ Reconstructive Breast Surgery following Mastectomy for Breast Cancer: A Review Gurnam Virdi* Department of surgery, Queen Elizabeth
How many procedures to make a breast?
 British Journal of Plastic Surgery (00 ), 5, 7-3 9 00 The British Association of Plastic Surgeons doi: 0.05/bjps.000.3538 BRITISH JOURNAL OF PLASTIC SURGERY How many procedures to make a breast? A. D.
British Journal of Plastic Surgery (00 ), 5, 7-3 9 00 The British Association of Plastic Surgeons doi: 0.05/bjps.000.3538 BRITISH JOURNAL OF PLASTIC SURGERY How many procedures to make a breast? A. D.
Infectious Complications Leading to Explantation in Implant-Based Breast Reconstruction With AlloDerm
 Infectious Complications Leading to Explantation in Implant-Based Breast Reconstruction With AlloDerm Minh-Doan Nguyen, MD, PhD, a Chen Chen, MS, b Salih Colakoğlu, MD, b Donald J. Morris, MD, b Adam M.
Infectious Complications Leading to Explantation in Implant-Based Breast Reconstruction With AlloDerm Minh-Doan Nguyen, MD, PhD, a Chen Chen, MS, b Salih Colakoğlu, MD, b Donald J. Morris, MD, b Adam M.
AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION
 CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects
 Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Few would deny that lower abdominal tissue BREAST. An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction.
 BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
Advances and Surgical Decision-Making for Breast Reconstruction
 893 Advances and Surgical Decision-Making for Breast Reconstruction Steven J. Kronowitz, MD 1 Henry M. Kuerer, MD, PhD 2 1 Department of Plastic and Reconstructive Surgery, The University of Texas M. D.
893 Advances and Surgical Decision-Making for Breast Reconstruction Steven J. Kronowitz, MD 1 Henry M. Kuerer, MD, PhD 2 1 Department of Plastic and Reconstructive Surgery, The University of Texas M. D.
BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER
 BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: September 2013 The recommendations contained in this guideline are a consensus of the Alberta Provincial
BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: September 2013 The recommendations contained in this guideline are a consensus of the Alberta Provincial
Figure 1. Anatomy of the breast
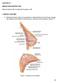 CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position
 Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
Ankur Khajuria 1,2*, Oliver J. Smith 2, Maxim Prokopenko 2, Maximillian Greenfield 2 and Afshin Mosahebi 2
 Khajuria et al. Systematic Reviews (2017) 6:232 DOI 10.1186/s13643-017-0628-y PROTOCOL Protocol for a systematic review and metaanalysis on the clinical outcomes and cost of deep inferior epigastric perforator
Khajuria et al. Systematic Reviews (2017) 6:232 DOI 10.1186/s13643-017-0628-y PROTOCOL Protocol for a systematic review and metaanalysis on the clinical outcomes and cost of deep inferior epigastric perforator
Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps
 BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
Goals of Care. Restore shape and function after cancer
 Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
Reconstruction with autologous tissue remains a
 Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
Tackling challenging revision breast augmentation cases
 the BREAST Careful preoperative consultations can reduce the need for revision breast surgery. Second Time Around Tackling challenging revision breast augmentation cases By Adam D. Schaffner, MD, FACS
the BREAST Careful preoperative consultations can reduce the need for revision breast surgery. Second Time Around Tackling challenging revision breast augmentation cases By Adam D. Schaffner, MD, FACS
Reconstructive surgery following mastectomy
 Reconstructive surgery following mastectomy Kseniya Roudakova, MD A CASE FROM SUNY DOWNSTATE 60F who presented for right mastectomy with immediate TRAM flap reconstruction for recurrent breast cancer Oncologic
Reconstructive surgery following mastectomy Kseniya Roudakova, MD A CASE FROM SUNY DOWNSTATE 60F who presented for right mastectomy with immediate TRAM flap reconstruction for recurrent breast cancer Oncologic
A mammometric comparison of modified Robertson versus Wise pattern inferior pedicle reduction mammoplasty
 Plast Aesthet Res 2016;3:284-90 DOI: 10.20517/2347-9264.2016.48 Original Article Plastic and Aesthetic Research www.parjournal.net Open Access A mammometric comparison of modified Robertson versus Wise
Plast Aesthet Res 2016;3:284-90 DOI: 10.20517/2347-9264.2016.48 Original Article Plastic and Aesthetic Research www.parjournal.net Open Access A mammometric comparison of modified Robertson versus Wise
Despite breast reduction being one of the BREAST. Does Knowledge of the Initial Technique Affect Outcomes after Repeated Breast Reduction?
 BREAST Does Knowledge of the Initial Technique Affect Outcomes after Repeated Breast Reduction? Jamil Ahmad, M.D. Sarah M. McIsaac, M.D. Frank Lista, M.D. Mississauga and Ottawa, Ontario, Canada Background:
BREAST Does Knowledge of the Initial Technique Affect Outcomes after Repeated Breast Reduction? Jamil Ahmad, M.D. Sarah M. McIsaac, M.D. Frank Lista, M.D. Mississauga and Ottawa, Ontario, Canada Background:
BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER
 Page 1 of 44 BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: February, 2017 The recommendations contained in this guideline are a consensus of the
Page 1 of 44 BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: February, 2017 The recommendations contained in this guideline are a consensus of the
Predictors of Contralateral Prophylactic Mastectomy and the Impact on Breast Reconstruction
 CLINICAL PAPER Predictors of Contralateral Prophylactic Mastectomy and the Impact on Breast Reconstruction Ximena A. Pinell-White, MD, Keli Kolegraff, MD, and Grant W. Carlson, MD Background: Contralateral
CLINICAL PAPER Predictors of Contralateral Prophylactic Mastectomy and the Impact on Breast Reconstruction Ximena A. Pinell-White, MD, Keli Kolegraff, MD, and Grant W. Carlson, MD Background: Contralateral
Breast Reconstruction after Mastectomy
 Breast Reconstruction after Mastectomy 1 Noor Jawad Al-Juwayed, 2 Raed Fahad Abdullah Al-Otibi Abstract: Background: Most women reported in many studies the improvements in important areas of life, and
Breast Reconstruction after Mastectomy 1 Noor Jawad Al-Juwayed, 2 Raed Fahad Abdullah Al-Otibi Abstract: Background: Most women reported in many studies the improvements in important areas of life, and
Latissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Bad Rap or Good Flap?
 Latissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Bad Rap or Good Flap? Galen Perdikis, MD, Stephanie Koonce, MD, George Collis, MD, and Dustin Eck, MD Mayo Clinic, Jacksonville, FL Correspondence:
Latissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Bad Rap or Good Flap? Galen Perdikis, MD, Stephanie Koonce, MD, George Collis, MD, and Dustin Eck, MD Mayo Clinic, Jacksonville, FL Correspondence:
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
Journal of Breast Cancer
 Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2017 March; 20(1): 98-103 Patient Satisfaction with Implant Based Breast Reconstruction Associated with Implant Volume and Mastectomy Specimen
Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2017 March; 20(1): 98-103 Patient Satisfaction with Implant Based Breast Reconstruction Associated with Implant Volume and Mastectomy Specimen
Plastic and Reconstructive Surgery Unit, Campus Bio-Medico University, Rome, Italy 2
 European Review for Medical and Pharmacological Sciences 2016; 20: 4635-4641 Ten years experience with breast reconstruction after salvage mastectomy in previously irradiated patients: analysis of outcomes,
European Review for Medical and Pharmacological Sciences 2016; 20: 4635-4641 Ten years experience with breast reconstruction after salvage mastectomy in previously irradiated patients: analysis of outcomes,
The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography
 BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
Microsurgical restoration of failed or unsatisfactory breast reconstruction: a systematic review and pooled-analysis of outcomes
 Plast Aesthet Res 2017;4:195-203 DOI: 10.20517/2347-9264.2017.20 Plastic and Aesthetic Research www.parjournal.net Topic: Complex Reconstruction of the Face, Breast and Wounds with Microvascular Free Flaps
Plast Aesthet Res 2017;4:195-203 DOI: 10.20517/2347-9264.2017.20 Plastic and Aesthetic Research www.parjournal.net Topic: Complex Reconstruction of the Face, Breast and Wounds with Microvascular Free Flaps
A long term review of augmentation mastopexy in muscle splitting biplane
 Topic: Aesthetic Surgery of the Breast A long term review of augmentation mastopexy in muscle splitting biplane Umar Daraz Khan Aesthetic Plastic Surgeon, Reshape House, West Malling, Kent ME19 6QR, UK.
Topic: Aesthetic Surgery of the Breast A long term review of augmentation mastopexy in muscle splitting biplane Umar Daraz Khan Aesthetic Plastic Surgeon, Reshape House, West Malling, Kent ME19 6QR, UK.
Awareness and provision of reconstruction. Breast
 Original Article Breast Deep Inferior Epigastric Artery Perforator Flap Breast Reconstruction without Microsurgery Fellowship Training Hakan Orbay, MD, PhD* Brittany K. Busse, MD* Thomas R. Stevenson,
Original Article Breast Deep Inferior Epigastric Artery Perforator Flap Breast Reconstruction without Microsurgery Fellowship Training Hakan Orbay, MD, PhD* Brittany K. Busse, MD* Thomas R. Stevenson,
Case Study. TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis.
 Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C. Your Guide To BREAST RECONSTRUCTION
 Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
Breast Augmentation and Mastopexy Using a Pectoral Muscle Loop
 Aesth Plast Surg (2011) 35:333 340 DOI 10.1007/s00266-010-9612-9 ORIGINAL ARTICLE Breast Augmentation and Mastopexy Using a Pectoral Muscle Loop André Auersvald Luiz Augusto Auersvald Received: 28 April
Aesth Plast Surg (2011) 35:333 340 DOI 10.1007/s00266-010-9612-9 ORIGINAL ARTICLE Breast Augmentation and Mastopexy Using a Pectoral Muscle Loop André Auersvald Luiz Augusto Auersvald Received: 28 April
Skin sparing mastectomy: Technique and suggested methods of reconstruction
 Journal of the Egyptian National Cancer Institute (2014) 26, 153 159 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com Full Length Article Skin
Journal of the Egyptian National Cancer Institute (2014) 26, 153 159 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com Full Length Article Skin
Allograft Based Breast Reconstruction: Opportunity for a Second Look
 Allograft Based Breast Reconstruction: Opportunity for a Second Look Martin I. Newman, MD, FACS Director of Resident Education and Associate Program Director Department of Plastic and Reconstructive Surgery
Allograft Based Breast Reconstruction: Opportunity for a Second Look Martin I. Newman, MD, FACS Director of Resident Education and Associate Program Director Department of Plastic and Reconstructive Surgery
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
The success of breast conservation protocols BREAST. Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy
 BREAST Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy Jeffrey A. Ascherman, M.D. Matthew M. Hanasono, M.D. Martin I. Newman, M.D. Duncan B. Hughes, M.D. New York, N.Y.
BREAST Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy Jeffrey A. Ascherman, M.D. Matthew M. Hanasono, M.D. Martin I. Newman, M.D. Duncan B. Hughes, M.D. New York, N.Y.
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction
 Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Breast Reconstruction Following Mastectomy or Lumpectomy
 Breast Reconstruction Following Mastectomy or Lumpectomy [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr go to Comunicados a Proveedores, and click Cartas
Breast Reconstruction Following Mastectomy or Lumpectomy [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr go to Comunicados a Proveedores, and click Cartas
Author's response to reviews
 Author's response to reviews Title: Classifying breast cancer surgery: a novel, complexity-based system for oncological, oncoplastic and reconstructive procedures, and proof of principle by analysis of
Author's response to reviews Title: Classifying breast cancer surgery: a novel, complexity-based system for oncological, oncoplastic and reconstructive procedures, and proof of principle by analysis of
