Reason for change. Recently approved. Recently approved. Recently approved. Recently approved. Recently updated. Recently approved.
|
|
|
- Irene Blair
- 6 years ago
- Views:
Transcription
1 2017 Formulary Change Notice Please note these changes to your 2017 List of Covered Drugs Drug name (medication) Rubraca Aprepitant Onivyde Oseltamivir Restasis Xiidra Daptomycin Selzentry Linzess Butalb/APAP/caff , Desvenlafaxine ER Nature of the change Reason for change Formulary Alternative alternative Notes Lynparza 5 NM 1-1 Emend Tarceva 5 NM 1-6 Relenza Xiidra Restasis Cubicin Tivicay Amitiza codeine sertraline Last :
2 Ilaris Veltassa Durezol Ilevro Bavencio Busulfan Tazarotene 0.1% cream Austedo Lartruvo Ezetimibe/simvastatin Fluticasone/salmeterol Zejula Synjardy Synjardy XR reduction reduction reduction Arcalyst 5 NM 3-17 SPS Nevanac Nevanac carboplatin Iressa tretinoin Xenazine docetaxel atorvastatin Advair docetaxel Nesina Nesina Last :
3 Glyxambi Tymlos Imfinzi Rydapt Kisqali Femara Co-Pack Ocrevus Ocaliva Octagam Atomoxetine Imfinzi Olopatadine Rubraca Xadago added Nesina Prolia adriamycin cytarabine Ibrance Copaxone 5 NM, QL 5-26 ursodiol Prosol 3 PA 6-9 methylphenidate doxorubicin Patanol paclitaxel carbidopa-levodopa Last :
4 Alunbrig Tymlos Rituxan Hycela Dupixent Siliq Sevelamer Carbonate Otezla Xultophy Soliqua Kevzara Ingrezza Idhifa Subsys Avastatin Prolia doxorubicin tretinoin Enbrel Renagel Humira Byetta Victoza Humira Xenazine Rydapt Fentanyl 2 PA 9-15 Last :
5 Besponsa Vigabatrin Nerlynx Vyxeos Trimipramine Verzenio Glatiramer Acetate Aliqopa Fosamprenavir Calcium Triptodur Shingrix Vosevi Tremfya daunorubicin lamotrigine Herceptin daunorubicin sertraline Herceptin Aubagio 5 PA,QL daunorubicin Atripla Lupron Depot Zostavax Harvoni 5 PA Humira 5 PA Last :
6 Mavyret Calquence Carvedilol ER Qtern Verzenio Shingrix Carvedilol ER Juluca Harvoni 5 PA Rituxan 5 PA atenolol Nesina Ibrance 5 PA Zostavax atenolol Atripla 5 NM Blue Cross Blue Shield of Arizona Advantage is an HMO plan with a Medicare contract. Enrollment in Blue Cross Blue Shield of Arizona Advantage depends on contract renewal. You can ask BCBSAZ Advantage to make an exception to our coverage rules. There are several types of exceptions that you can ask us to make. You can ask us to cover a drug even if it is not on our formulary. If, this drug will be covered at a pre-determined cost-sharing level, and you would not be able to ask us to provide the drug at a lower cost-sharing level. You can ask us to cover a formulary drug at a lower cost-sharing level. For example a drug is covered in 4; you can ask us to cover it at the cost-sharing amount that applies to drugs in 3 instead. This would lower the amount you must pay for your drug. You can ask us to waive coverage restrictions or limits on your drug. For example, for certain drugs, BCBSAZ Advantage limits the amount of the drug that we will cover. If Last :
7 your drug has a quantity limit, you can ask us to waive the limit and cover a greater amount. For more recent information or other questions, please contact BCBSAZ Advantage at 1-(800) or, for TTY users, 711, October 1-February 14, 7 days a week, 8 a.m.-8 p.m. (February 15-September 30, Monday Friday, 8 a.m.- 8 p.m.), or visit Last :
2018 Medicare Part D Formulary Change
 2018 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
2018 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
2018 Formulary Update
 MEDICARE ADVANTAGE BlueShield of Northeastern New York 2018 Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January 2018. This
MEDICARE ADVANTAGE BlueShield of Northeastern New York 2018 Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January 2018. This
2018 Medicare Part D Formulary Change
 2018 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
2018 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
VIVA MEDICARE IMPORTANT T EXPANDED PERFORMANCE FORMULARY UPDATES
 NORE/ETH/FER CHW 0.MG Added to the 07 //07 ALYACEN TAB / Added to the 07 //07 AMETHIA LO TAB Added to the 07 //07 ERGOT/CAFFEN TAB 00MG Added to the 07 //07 NORETH/ETHIN TAB /0 Added to the 07 //07 LORCET
NORE/ETH/FER CHW 0.MG Added to the 07 //07 ALYACEN TAB / Added to the 07 //07 AMETHIA LO TAB Added to the 07 //07 ERGOT/CAFFEN TAB 00MG Added to the 07 //07 NORETH/ETHIN TAB /0 Added to the 07 //07 LORCET
NOTIFICATION OF FORMULARY CHANGES
 NOTIFICATION OF CHANGES The following summary describes changes to the 2018 Presbyterian Senior Care (HMO)/(HMO-POS), Presbyterian MediCare PPO and formularies. The formulary may change at any time. You
NOTIFICATION OF CHANGES The following summary describes changes to the 2018 Presbyterian Senior Care (HMO)/(HMO-POS), Presbyterian MediCare PPO and formularies. The formulary may change at any time. You
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES
 PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Generic Additions These generic drugs recently became available in the marketplace. When these generic drugs became available, we began covering them at the
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Generic Additions These generic drugs recently became available in the marketplace. When these generic drugs became available, we began covering them at the
2018 Formulary Update
 MEDICARE ADVANTAGE BlueShield of Northeastern New York 2018 Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January 2018. This
MEDICARE ADVANTAGE BlueShield of Northeastern New York 2018 Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January 2018. This
You ll find the most up-to-date comprehensive version of our formulary on our website, Click on Drug Finder.
 3/1/2018 Medicare Part D Formulary Change In an effort to cover the most needed, cost-effective prescriptions, the AlohaCare Advantage Plus (HMO SNP) Formulary is updated monthly. The following are drugs
3/1/2018 Medicare Part D Formulary Change In an effort to cover the most needed, cost-effective prescriptions, the AlohaCare Advantage Plus (HMO SNP) Formulary is updated monthly. The following are drugs
Health Partners Medicare Special 2018 Formulary Changes
 Health Partners Medicare Special 2018 Changes Changes occur, for example, because new drugs come on the market, a drug is moved to a different cost-sharing level (tier), or a generic version becomes available.
Health Partners Medicare Special 2018 Changes Changes occur, for example, because new drugs come on the market, a drug is moved to a different cost-sharing level (tier), or a generic version becomes available.
2018 Formulary Update
 MEDICARE ADVANTAGE BlueShield of Northeastern New York Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January. This document
MEDICARE ADVANTAGE BlueShield of Northeastern New York Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January. This document
During non-business hours, your call will be answered by our automated phone system. A representative will return your call the next business day.
 MEICARE AVANTAGE BlueCross BlueShield of Western New York 2018 Formulary Update BlueCross BlueShield of Western New York has updated its formulary (drug list) since its original publication in January
MEICARE AVANTAGE BlueCross BlueShield of Western New York 2018 Formulary Update BlueCross BlueShield of Western New York has updated its formulary (drug list) since its original publication in January
Changes to the 2018 BlueCross Secure SM (HMO) & BlueCross Total SM (PPO) Formularies
 Changes to the 2018 BlueCross Secure SM (HMO) & BlueCross Total SM (PPO) Formularies BlueCross BlueShield of South Carolina may add or remove drugs from the formulary during the year. If we remove drugs
Changes to the 2018 BlueCross Secure SM (HMO) & BlueCross Total SM (PPO) Formularies BlueCross BlueShield of South Carolina may add or remove drugs from the formulary during the year. If we remove drugs
Blue Shield 65 Plus Choice Plan (HMO) Blue Shield of California is an independent member of the Blue Shield Association. Formulary Updates:
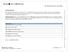 Blue Shield 65 Plus Choice Plan (HMO) Formulary Updates: The enclosed table lists the changes made to your formulary such as removing or adding: a drug, prior authorization, quantity limits or step therapy
Blue Shield 65 Plus Choice Plan (HMO) Formulary Updates: The enclosed table lists the changes made to your formulary such as removing or adding: a drug, prior authorization, quantity limits or step therapy
Partners Notice of Change March 2017
 New Added Products: Effective 3/1/2017 Drug Reason Tier Restrictions abacavir 600 mg-lamivudine 300 QL ADRENACLICK 0.15 MG/0.15 ML INJECTION,AUTO- INJECTOR ADRENACLICK 0.3 MG/0.3 ML INJECTION, AUTO- INJECTOR
New Added Products: Effective 3/1/2017 Drug Reason Tier Restrictions abacavir 600 mg-lamivudine 300 QL ADRENACLICK 0.15 MG/0.15 ML INJECTION,AUTO- INJECTOR ADRENACLICK 0.3 MG/0.3 ML INJECTION, AUTO- INJECTOR
Rationale for Decision Excluded Generic OTC equivalent available (Flonase Allergy Relief) Medicare status (if differs)
 BLUE SHIELD OF CALIFORNIA FIRST QUARTER 2015 FORMULARY AND MEDICATION POLICY UPDATES EFFECTIVE MARCH 19, 2015 The Blue Shield of California (BSC) Pharmacy and Therapeutics (P&T) Committee, consisting of
BLUE SHIELD OF CALIFORNIA FIRST QUARTER 2015 FORMULARY AND MEDICATION POLICY UPDATES EFFECTIVE MARCH 19, 2015 The Blue Shield of California (BSC) Pharmacy and Therapeutics (P&T) Committee, consisting of
Superior Select Health Plans: Tribute-1 Tier May 2018 Formulary Addendum
 Superior Select Health Plans: Tribute-1 Tier May 2018 Formulary Addendum Below is a list formulary changes for the benefit year 2018. This is not a complete list of drugs covered by the Part D plan. The
Superior Select Health Plans: Tribute-1 Tier May 2018 Formulary Addendum Below is a list formulary changes for the benefit year 2018. This is not a complete list of drugs covered by the Part D plan. The
ALBUTEROL - SCORE. Products Affected. Details. Step Therapy Criteria Golden State Medicare Health Plan, Golden (HMO) Last Updated: 09/01/2018
 Step Therapy Golden State Medicare Health Plan, Golden (HMO) Last Updated: 09/01/2018 ALBUTEROL - SCORE Ventolin Hfa Trial of ProAir 1 ANTIDEPRESSANTS - SCORE Aplenzin Desvenlafaxine Er TB24 100MG, 50MG
Step Therapy Golden State Medicare Health Plan, Golden (HMO) Last Updated: 09/01/2018 ALBUTEROL - SCORE Ventolin Hfa Trial of ProAir 1 ANTIDEPRESSANTS - SCORE Aplenzin Desvenlafaxine Er TB24 100MG, 50MG
Upper Peninsula Health Plan Advantage (HMO) (H ) Updates
 February, 2017 02/28/2017 abacavirlamivudine 02/28/2017 abacavirlamivudine 02/28/2017 rasagiline mesylate 02/28/2017 rasagiline mesylate abacavir sulfate/lamivudine ADD UM: QUANTITY 30 / 30 Days abacavir
February, 2017 02/28/2017 abacavirlamivudine 02/28/2017 abacavirlamivudine 02/28/2017 rasagiline mesylate 02/28/2017 rasagiline mesylate abacavir sulfate/lamivudine ADD UM: QUANTITY 30 / 30 Days abacavir
2014 Quantity Limits (QL) Criteria
 2014 Quantity Limits (QL) Criteria Certain drugs covered through your EmblemHealth Medicare HMO/PPO Medicare Plan are covered for only a limited quantity. We do this to ensure compliance with the US Food
2014 Quantity Limits (QL) Criteria Certain drugs covered through your EmblemHealth Medicare HMO/PPO Medicare Plan are covered for only a limited quantity. We do this to ensure compliance with the US Food
Drug Name Description of Change Formulary Coverage Formulary Alternative(s)
 NOTIFICATION OF FORMULARY CHANGES The following summary describes changes to the Presbyterian Centennial Care Formulary effective 2018. For the most recent list of drugs, information on asking for a prior
NOTIFICATION OF FORMULARY CHANGES The following summary describes changes to the Presbyterian Centennial Care Formulary effective 2018. For the most recent list of drugs, information on asking for a prior
Medicare Part D 2017 Formulary Changes Service To Senior
 Medicare Part D 2017 Formulary Changes Service To Senior Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization,
Medicare Part D 2017 Formulary Changes Service To Senior Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization,
2017 Medicare Part D Formulary Change
 2017 Medicare Part D Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy restrictions
2017 Medicare Part D Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy restrictions
2018 Formulary Notice of Change Prescription Drug Plans
 2018 Formulary Notice of Change Prescription Drug Plans WellCare Prescription Insurance, Inc. Plans in all states: WellCare Classic (PDP) WellCare may add or remove drugs from our formulary during the
2018 Formulary Notice of Change Prescription Drug Plans WellCare Prescription Insurance, Inc. Plans in all states: WellCare Classic (PDP) WellCare may add or remove drugs from our formulary during the
Presbyterian Health Plan, Inc. Presbyterian Insurance Company, Inc. NOTIFICATION OF FORMULARY CHANGES
 NOTIFICATION OF FORMULARY CHANGES The following summary describes changes to the Presbyterian Commercial Large Group Plans (Non-Metal Plans) Formularies effective 2018. For the most recent list of drugs,
NOTIFICATION OF FORMULARY CHANGES The following summary describes changes to the Presbyterian Commercial Large Group Plans (Non-Metal Plans) Formularies effective 2018. For the most recent list of drugs,
Updates to your prescription benefits
 Updates to your prescription benefits Effective January 1, 2019 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective January 1, 2019 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
2018 CareOregon Advantage Part D Formulary Changes
 2018 CareOregon Advantage Part D Formulary Changes Abbreviations: AGE = Age Restriction; PA = Prior Authorization Required; QL = Quantity Limit; ST = Step Therapy Required; LD = Limited Distribution; BvD
2018 CareOregon Advantage Part D Formulary Changes Abbreviations: AGE = Age Restriction; PA = Prior Authorization Required; QL = Quantity Limit; ST = Step Therapy Required; LD = Limited Distribution; BvD
DRUG TREND REPORT. WellDyneRx ANNUAL 1 2% 34% WellDyneRx. Diabetes MS Oncology Asthma/COPD HIV. Pain/inflammation. High Blood Choles Attention Disorde
 WellDyneRx 34% 1 2% Inflammatory Con Diabetes MS Oncology Asthma/COPD High Blood Pressu HIV Pain/inflammation High Blood Choles Attention Disorde Inflammatory Con Diabetes MS Oncology Asthma/COPD High
WellDyneRx 34% 1 2% Inflammatory Con Diabetes MS Oncology Asthma/COPD High Blood Pressu HIV Pain/inflammation High Blood Choles Attention Disorde Inflammatory Con Diabetes MS Oncology Asthma/COPD High
Oral Oncology Agents. August 2017 Update. SGLT-2 Category Update. Removal of Medical Foods
 SUPPORTING OUR PROVIDER PARTNERS THROUGH COMMUNICATION AND COLLABORATION. DATE SEPTEMBER 2017 ISSUE 4 HELPFUL NUMBERS FOR PROVIDERS CVS: 1-888-512-8935 Primary: 004336 Secondary Commercial: 013089 Secondary
SUPPORTING OUR PROVIDER PARTNERS THROUGH COMMUNICATION AND COLLABORATION. DATE SEPTEMBER 2017 ISSUE 4 HELPFUL NUMBERS FOR PROVIDERS CVS: 1-888-512-8935 Primary: 004336 Secondary Commercial: 013089 Secondary
Granite Alliance Insurance Company (PDP) 2018 Step Therapy Criteria Last Updated: 10/23/18
 Granite Alliance Insurance Company (PDP) 2018 Step Therapy Criteria Last Updated: 10/23/18 Granite Alliance requires step therapy for certain drugs. This means prior to receiving a drug with a step therapy
Granite Alliance Insurance Company (PDP) 2018 Step Therapy Criteria Last Updated: 10/23/18 Granite Alliance requires step therapy for certain drugs. This means prior to receiving a drug with a step therapy
Updates to your prescription benefits
 Updates to your prescription benefits Effective Jan. 1, 2019 Traditional Three-Tier PDL Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount
Updates to your prescription benefits Effective Jan. 1, 2019 Traditional Three-Tier PDL Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount
Step Therapy Criteria
 Tier 5 Formulary Step Therapy 2016 Updated: 05/24/2016 Effective: 06/01/2016 What is Step Therapy? Some prescription drugs require step therapy (ST). In some cases, the plan requires you to first try certain
Tier 5 Formulary Step Therapy 2016 Updated: 05/24/2016 Effective: 06/01/2016 What is Step Therapy? Some prescription drugs require step therapy (ST). In some cases, the plan requires you to first try certain
Specialty Drugs. The specialty drug list below is effective June 5, 2018 and is subject to change at any time.
 Specialty Drugs The following is a list of medications that are considered specialty drugs. Specialty drugs include self-administered injectables, medications that are high cost, and/or medications that
Specialty Drugs The following is a list of medications that are considered specialty drugs. Specialty drugs include self-administered injectables, medications that are high cost, and/or medications that
PHARMACY AND THERAPEUTICS COMMITTEE 4 th Quarter 2017
 PHARMACY AND THERAPEUTICS COMMITTEE 4 th Quarter 2017 A meeting of the Health Partners Pharmacy and Therapeutics (P&T) Committee was held on September and December 2017. The following are the recommendations
PHARMACY AND THERAPEUTICS COMMITTEE 4 th Quarter 2017 A meeting of the Health Partners Pharmacy and Therapeutics (P&T) Committee was held on September and December 2017. The following are the recommendations
Presbyterian Health Plan, Inc. Presbyterian Insurance Company, Inc. NOTIFICATION OF FORMULARY CHANGES
 NOTIFICATION OF FORMULARY CHANGES The following summary describes changes to the 2017 Presbyterian Individual and Family Metal Plan/Employer Group Metal Plan Formularies effective 2018. For the most recent
NOTIFICATION OF FORMULARY CHANGES The following summary describes changes to the 2017 Presbyterian Individual and Family Metal Plan/Employer Group Metal Plan Formularies effective 2018. For the most recent
Added, Removed or Changed. Date of Change. No Change
 One mission: you s September 7, 2017 Blue Cross of Idaho reviews its formularies (covered drug lists) periodically to allow members access to new drugs and to provide safe, cost effective options for your
One mission: you s September 7, 2017 Blue Cross of Idaho reviews its formularies (covered drug lists) periodically to allow members access to new drugs and to provide safe, cost effective options for your
METABOLIC, IMMUNE DISORDERS OR INHERITED RARE DISEASE ALPHA-1 PROTEINASE INHIBITORS ARANESP BLOOD CELL DEFICIENCY ARANESP ARCALYST
 PRIOR AUTHORIZATION LIST (SUBJECT TO CHANGE) MEDICATION THERAPEUTIC CATEGORY MODULE ACTEMRA INFLAMMATORY CONDITIONS ACTEMRA ADCIRCA PULMONARY HYPERTENSION PDE-5 INHIBITORS FOR PAH ADDYI SEXUAL DISORDERS
PRIOR AUTHORIZATION LIST (SUBJECT TO CHANGE) MEDICATION THERAPEUTIC CATEGORY MODULE ACTEMRA INFLAMMATORY CONDITIONS ACTEMRA ADCIRCA PULMONARY HYPERTENSION PDE-5 INHIBITORS FOR PAH ADDYI SEXUAL DISORDERS
UPHP Advantage (HMO) (H ) and UPHP Choice (HMO) (H ) Updates
 March, 2018 03/01/2018 clindacin p clindamycin phosphate 03/01/2018 glatiramer acetate 03/01/2018 glatiramer acetate 03/01/2018 oseltamivir phosphate 03/01/2018 oseltamivir phosphate 03/01/2018 ADACEL
March, 2018 03/01/2018 clindacin p clindamycin phosphate 03/01/2018 glatiramer acetate 03/01/2018 glatiramer acetate 03/01/2018 oseltamivir phosphate 03/01/2018 oseltamivir phosphate 03/01/2018 ADACEL
Medicare Part D 2012 Formulary Changes Service To Senior and Total Fit
 Medicare Part D 2012 Formulary s Service To Senior and Total Fit Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization,
Medicare Part D 2012 Formulary s Service To Senior and Total Fit Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization,
March 2018 P & T Updates
 March 2018 P & T Updates Commercial Triple Tier 4th Tier Applicable Traditional Prior Auth AURYXIA 3 2 12 tablets per BAXDELA TABLETS 3 2 2 tablets per Depending on your specific benefits and in which
March 2018 P & T Updates Commercial Triple Tier 4th Tier Applicable Traditional Prior Auth AURYXIA 3 2 12 tablets per BAXDELA TABLETS 3 2 2 tablets per Depending on your specific benefits and in which
July 2017 P&T Updates
 July 2017 P&T Updates Commercial Triple Tier 4th Tier Applicable Traditional Prior Auth Alternatives ALUNBRIG 3 2 DUPIXENT Pharmacy 3 2 6 tablets per day, 30 day One-week auth for QL of 3 syringes per
July 2017 P&T Updates Commercial Triple Tier 4th Tier Applicable Traditional Prior Auth Alternatives ALUNBRIG 3 2 DUPIXENT Pharmacy 3 2 6 tablets per day, 30 day One-week auth for QL of 3 syringes per
2017 Medicare Part D Formulary Change
 2017 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
2017 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
STATE OF TENNESSEE DIVISION OF TENNCARE 310 Great Circle Road NASHVILLE, TENNESSEE 37243
 1 P a g e STATE OF TENNESSEE DIVISION OF TENNCARE 310 Great Circle Road NASHVILLE, TENNESSEE 37243 This notice is to advise you of information regarding the TennCare Pharmacy Program. Please forward or
1 P a g e STATE OF TENNESSEE DIVISION OF TENNCARE 310 Great Circle Road NASHVILLE, TENNESSEE 37243 This notice is to advise you of information regarding the TennCare Pharmacy Program. Please forward or
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select Formulary April 1, 2018 Updates. Formulary Alternatives
 PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select April 1, 2018 Updates Drug Name adapalene-benzoyl-peroxide Gel 0.1-2.5% (Brand = Epiduo ) prasugrel hcl (Brand = Effient ) vigabatrin pak 500 mg (Brand
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select April 1, 2018 Updates Drug Name adapalene-benzoyl-peroxide Gel 0.1-2.5% (Brand = Epiduo ) prasugrel hcl (Brand = Effient ) vigabatrin pak 500 mg (Brand
Blue Shield Rx Enhanced (PDP) Formulary Updates:
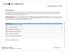 Blue Shield Rx Enhanced (PDP) Formulary Updates: The enclosed table lists the changes made to your such as removing or adding: a drug, prior authorization, quantity limits or step therapy as well as any
Blue Shield Rx Enhanced (PDP) Formulary Updates: The enclosed table lists the changes made to your such as removing or adding: a drug, prior authorization, quantity limits or step therapy as well as any
These programs and quantity limitations may not apply. Check your certificate or other plan information for benefit details.
 FlexRx Standard Utilization Management (PA, QL,) Updates January 1, 2018 How to use this drug list This drug list includes updates to Utilization Management (UM) programs. UM may include a prior authorization
FlexRx Standard Utilization Management (PA, QL,) Updates January 1, 2018 How to use this drug list This drug list includes updates to Utilization Management (UM) programs. UM may include a prior authorization
Updates to your prescription benefits
 Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits
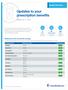 Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Otezla (apremilast) Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Otezla (apremilast) Prime Therapeutics will review Prior Authorization requests Prior
Otezla (apremilast) Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Otezla (apremilast) Prime Therapeutics will review Prior Authorization requests Prior
2017 Medicare Part D Formulary Change
 2017 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
2017 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select Formulary April 1, 2018 Updates. Formulary Alternatives
 PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select April 1, 2018 Updates Drug Name adapalene-benzoyl-peroxide Gel 0.1-2.5% (Brand = Epiduo ) prasugrel hcl (Brand = Effient ) vigabatrin pak 500 mg (Brand
PRESCRIPTION DRUG PROGRAM FORMULARY UPDATES Select April 1, 2018 Updates Drug Name adapalene-benzoyl-peroxide Gel 0.1-2.5% (Brand = Epiduo ) prasugrel hcl (Brand = Effient ) vigabatrin pak 500 mg (Brand
2019 Formulary Update
 MEDICARE ADVANTAGE BlueShield of Northeastern New York Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January. This document
MEDICARE ADVANTAGE BlueShield of Northeastern New York Formulary Update BlueShield of Northeastern New York has updated its formulary (drug list) since its original publication in January. This document
2015 Step Therapy (ST) Criteria
 2015 Step Therapy (ST) Some drugs require step therapy pre-approval. This means that your doctor must have you first try a different drug to treat your medical condition before we will cover a drug that
2015 Step Therapy (ST) Some drugs require step therapy pre-approval. This means that your doctor must have you first try a different drug to treat your medical condition before we will cover a drug that
Health Partners Medicare Special (2017) Updates
 March 2017 Effective Date Brand Name EVZIO erythromycin ethylsuccinate naloxone hcl Generic Name erythromycin ethylsuccinate Type of Change Previous Value New Value ofloxacin ofloxacin NAMZARIC NAMZARIC
March 2017 Effective Date Brand Name EVZIO erythromycin ethylsuccinate naloxone hcl Generic Name erythromycin ethylsuccinate Type of Change Previous Value New Value ofloxacin ofloxacin NAMZARIC NAMZARIC
Subject: HPN/SHL COMMERCIAL PDL UPDATES EFFECTIVE JANUARY 1, 2018
 Date: November 7, 2017 To: From: HPN/SHL Contracted Pharmacies and Providers Ryan Bitton, PharmD, MBA Senior Director, Pharmacy Subject: HPN/SHL COMMERCIAL PDL UPDATES EFFECTIVE JANUARY 1, 2018 Effective
Date: November 7, 2017 To: From: HPN/SHL Contracted Pharmacies and Providers Ryan Bitton, PharmD, MBA Senior Director, Pharmacy Subject: HPN/SHL COMMERCIAL PDL UPDATES EFFECTIVE JANUARY 1, 2018 Effective
Updates to your prescription benefits
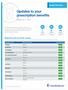 Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective Jan. 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Upper Peninsula MI Health Link Updates
 January, 2018 01/01/2018 TAMIFLU oseltamivir phosphate CHANGE UM: QUANTITY 720 / 365 days 720 / 365 OVER 01/01/2018 oseltamivir phosphate 01/01/2018 oseltamivir phosphate 01/01/2018 oseltamivir phosphate
January, 2018 01/01/2018 TAMIFLU oseltamivir phosphate CHANGE UM: QUANTITY 720 / 365 days 720 / 365 OVER 01/01/2018 oseltamivir phosphate 01/01/2018 oseltamivir phosphate 01/01/2018 oseltamivir phosphate
Aetna Better Health of Illinois Medicaid Formulary Updates
 October 2017 o DOXYLAMINE SUCCINATE 25mg-QL o DULOXETINE CAP 40MG DR-QL o GUANFACIN ER TABS (all strengths)-ql o TOBRAMYCIN NEBU SOLUTION- PA August 2017 Aetna Better Health of Illinois Medicaid 2017 Formulary
October 2017 o DOXYLAMINE SUCCINATE 25mg-QL o DULOXETINE CAP 40MG DR-QL o GUANFACIN ER TABS (all strengths)-ql o TOBRAMYCIN NEBU SOLUTION- PA August 2017 Aetna Better Health of Illinois Medicaid 2017 Formulary
Medicare Part D 2017 Formulary Changes OC Preferred
 Medicare Part D 017 Formulary s OC Preferred Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization, quantity
Medicare Part D 017 Formulary s OC Preferred Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization, quantity
OptumRx Focused Utilization Management Program
 Utilization management updates - January 1, 2019 OptumRx Focused Utilization Management Program OptumRx focused step therapy with quantity limits programs If you have a prescription for any of the Step
Utilization management updates - January 1, 2019 OptumRx Focused Utilization Management Program OptumRx focused step therapy with quantity limits programs If you have a prescription for any of the Step
Blue Shield 65 Plus (HMO) Formulary Updates:
 Blue Shield 65 Plus (HMO) Updates: The enclosed table lists the changes made to your such as removing or adding: a drug, prior authorization, quantity limits or step therapy as well as any changes to a
Blue Shield 65 Plus (HMO) Updates: The enclosed table lists the changes made to your such as removing or adding: a drug, prior authorization, quantity limits or step therapy as well as any changes to a
Memorial Hermann Advantage HMO February 2019 Formulary Addendum
 Memorial Hermann Advantage HMO February 2019 Formulary Addendum Changes may have occurred since the printing of your current Memorial Hermann Advantage HMO Formulary. Medications that may have been added
Memorial Hermann Advantage HMO February 2019 Formulary Addendum Changes may have occurred since the printing of your current Memorial Hermann Advantage HMO Formulary. Medications that may have been added
HEALTH SHARE/PROVIDENCE (OHP)
 HEALTH SHARE/PROVIDENCE (OHP) STEP THERAPY This is a complete list of drugs that have written coverage determination policies. Drugs on this list do not indicate that this particular drug will be covered
HEALTH SHARE/PROVIDENCE (OHP) STEP THERAPY This is a complete list of drugs that have written coverage determination policies. Drugs on this list do not indicate that this particular drug will be covered
Medicare Part D 2017 Formulary Changes OC Preferred
 Medicare Part D 2017 Formulary Changes OC Preferred Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization,
Medicare Part D 2017 Formulary Changes OC Preferred Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization,
March 2017 Pharmacy & Therapeutics Committee Decisions
 UCare s Pharmacy and Therapeutics Committee (P&T) is a group of physicians and pharmacists that meet throughout the year to make changes to the UCare formulary (approved drug list). These changes are reviewed
UCare s Pharmacy and Therapeutics Committee (P&T) is a group of physicians and pharmacists that meet throughout the year to make changes to the UCare formulary (approved drug list). These changes are reviewed
Medicare Part D 2017 Formulary Changes Service To Senior
 Medicare Part D 2017 Formulary s Service To Senior Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization,
Medicare Part D 2017 Formulary s Service To Senior Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization,
Formulary Change Notice
 Formulary Change Notice HealthPartners may remove drugs from our formulary (list of covered drugs) or add rules about whether and when certain drugs are covered during the year. The chart below contains
Formulary Change Notice HealthPartners may remove drugs from our formulary (list of covered drugs) or add rules about whether and when certain drugs are covered during the year. The chart below contains
Prior Authorization Program Information (Effective April 1st, 2018)
 Prior Authorization Program Information (Effective April 1st, 2018) Prior Authorization Certain drugs require prior authorization to help promote safe, quality and affordable pharmacy care. Your doctor
Prior Authorization Program Information (Effective April 1st, 2018) Prior Authorization Certain drugs require prior authorization to help promote safe, quality and affordable pharmacy care. Your doctor
January 2018 P & T Updates
 January 2018 P & T Updates Commercial Triple Tier 4th Tier Applicable Traditional BEVYXXA 3 No 2 BOSULIF 3 2 * Indicates prior authorization (PA) or step (ST) Depending on your specific benefits and in
January 2018 P & T Updates Commercial Triple Tier 4th Tier Applicable Traditional BEVYXXA 3 No 2 BOSULIF 3 2 * Indicates prior authorization (PA) or step (ST) Depending on your specific benefits and in
Updates to your prescription benefits
 Updates to your prescription benefits Effective January 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Updates to your prescription benefits Effective January 1, 2018 Update Summary Within the Prescription Drug List (PDL), medications are grouped by tier. The tier indicates the amount you pay when you fill
Pharmacy Benefit Coverage Updates Jan. 1, 2018
 Pharmacy Benefit Coverage Updates Jan. 1, 2018 UnitedHealthcare routinely evaluates prescription benefit coverage to help ensure we offer members affordable and effective medication options. Medications
Pharmacy Benefit Coverage Updates Jan. 1, 2018 UnitedHealthcare routinely evaluates prescription benefit coverage to help ensure we offer members affordable and effective medication options. Medications
HAP/Midwest Health Advantage MI Health Link (MMP) Updates
 January, 2018 01/01/2018 hydrocortisone butyrate hydrocortisone butyrate 01/01/2018 MIRVASO brimonidine tartrate 01/01/2018 AZACTAM aztreonam 01/01/2018 AZACTAM aztreonam 01/01/2018 mesalamine mesalamine
January, 2018 01/01/2018 hydrocortisone butyrate hydrocortisone butyrate 01/01/2018 MIRVASO brimonidine tartrate 01/01/2018 AZACTAM aztreonam 01/01/2018 AZACTAM aztreonam 01/01/2018 mesalamine mesalamine
Medicare Part D Drugs that Require Step Therapy Effective 12/01/2017
 Medicare Part D Drugs that Require Step Therapy Effective 12/01/2017 Providers may call the Pharmacy Help Desk at 800-641-8921 for more information or questions about criteria. The formulary may change
Medicare Part D Drugs that Require Step Therapy Effective 12/01/2017 Providers may call the Pharmacy Help Desk at 800-641-8921 for more information or questions about criteria. The formulary may change
2018 BCN Advantage Prior Authorization Criteria Last updated: April, 2018
 Abstral Actemra Adcirca Adempas Aliqopa Afinitor Afinitor- Disperz Alecensa Alunbrig Amitiza Amitriptyline Ampyra Anadrol-50 Androgel Androderm Aralast NP Aranesp Arcalyst Armodafinil Aubagio Avonex Bavencio
Abstral Actemra Adcirca Adempas Aliqopa Afinitor Afinitor- Disperz Alecensa Alunbrig Amitiza Amitriptyline Ampyra Anadrol-50 Androgel Androderm Aralast NP Aranesp Arcalyst Armodafinil Aubagio Avonex Bavencio
2016 Step Therapy (ST) Criteria
 2016 Step Therapy (ST) Some drugs require step therapy pre-approval. This means that your doctor must have you first try a different drug to treat your medical condition before we will cover a drug that
2016 Step Therapy (ST) Some drugs require step therapy pre-approval. This means that your doctor must have you first try a different drug to treat your medical condition before we will cover a drug that
Blue Cross and Blue Shield of Minnesota GenRx Formulary Updates
 Blue Cross and Blue Shield of Minnesota GenRx Formulary Updates July 2018 TRADE NAME (generic name) or generic name ADVAIR DISKUS (fluticasone-salmeterol aer powder ba 100-50 mcg/dose) Brand Addition ADVAIR
Blue Cross and Blue Shield of Minnesota GenRx Formulary Updates July 2018 TRADE NAME (generic name) or generic name ADVAIR DISKUS (fluticasone-salmeterol aer powder ba 100-50 mcg/dose) Brand Addition ADVAIR
Mercy Care Plan. Acyclovir Ointment. Products Affected. acyclovir ointment 5 % external Details. Criteria. Requires use of oral Acyclovir
 Acyclovir Ointment Mercy Care Plan acyclovir ointment 5 % external Requires use of oral Acyclovir 1 Adcirca ADCIRCA TABLET 20 MG ORAL Requires use of Sildenafil 2 Albenza ALBENZA TABLET 200 MG ORAL Requires
Acyclovir Ointment Mercy Care Plan acyclovir ointment 5 % external Requires use of oral Acyclovir 1 Adcirca ADCIRCA TABLET 20 MG ORAL Requires use of Sildenafil 2 Albenza ALBENZA TABLET 200 MG ORAL Requires
Specialty Drugs. The following is a list of medications that are considered to be specialty drugs. Specialty drugs
 Specialty Drugs The following is a list of medications that are considered to be specialty drugs. Specialty drugs include self-administered injectables, medications that are high cost, and/or medications
Specialty Drugs The following is a list of medications that are considered to be specialty drugs. Specialty drugs include self-administered injectables, medications that are high cost, and/or medications
2017 Formulary Addendum Notice of Change (Medicare Advantage Plans)
 2017 Formulary Addendum Notice of Change (Medicare Advantage Plans) Easy Choice Health Plan Easy Choice Freedom Plan (HMO SNP) H5087-001 This is a listing of the changes that have occurred in our formulary.
2017 Formulary Addendum Notice of Change (Medicare Advantage Plans) Easy Choice Health Plan Easy Choice Freedom Plan (HMO SNP) H5087-001 This is a listing of the changes that have occurred in our formulary.
Drug Formulary Update, April 2013
 Drug Formulary Update, April 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
Drug Formulary Update, April 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
CENTENE PHARMACY & THERAPEUTICS COMMITTEE THIRD QUARTER 2017 NEW DRUG ARRIVALS SUMMARY TABLE. Utilization Management Recommendation
 RT 1,2, 3,5 Drug Name 1 Brigatinib (Alunbrig ) 1 Deutetrabenazine (Austedo ) 1 Cerliponase alfa (Brineura ) Review Reason FDA-Approved (s) Alunbrig is indicated patients with anaplastic lymphoma kinase
RT 1,2, 3,5 Drug Name 1 Brigatinib (Alunbrig ) 1 Deutetrabenazine (Austedo ) 1 Cerliponase alfa (Brineura ) Review Reason FDA-Approved (s) Alunbrig is indicated patients with anaplastic lymphoma kinase
2017 Formulary Addendum Notice of Change (Medicare Advantage Plans)
 207 Formulary Addendum Notice of Change (Medicare Advantage Plans) Easy Choice Health Plan Easy Choice Plus Plan (HMO) H5087-002, H5087-07 This is a listing of the changes that have occurred in our formulary.
207 Formulary Addendum Notice of Change (Medicare Advantage Plans) Easy Choice Health Plan Easy Choice Plus Plan (HMO) H5087-002, H5087-07 This is a listing of the changes that have occurred in our formulary.
2017 Formulary Addendum Notice of Change (Medicare Advantage Plans)
 2017 Formulary Addendum Notice of Change (Medicare Advantage Plans) Easy Choice Health Plan Easy Choice Best Plan (HMO) H5087-005 This is a listing of the changes that have occurred in our formulary. Please
2017 Formulary Addendum Notice of Change (Medicare Advantage Plans) Easy Choice Health Plan Easy Choice Best Plan (HMO) H5087-005 This is a listing of the changes that have occurred in our formulary. Please
2017 Medicare Part D Formulary Change
 2017 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
2017 Medicare Part D Formulary Change We may add or remove drugs from our formulary during the year. If we remove drugs from our formulary, or add prior authorizations, quantity limits and/or step therapy
Step Therapy Requirements. Effective: 1/1/2019
 Effective: 1/1/2019 Updated 1/2019 AMANTADINE ER Sharp Health Plan (HMO) OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED RELEASE PRIOR CLAIM FOR AMANTADINE
Effective: 1/1/2019 Updated 1/2019 AMANTADINE ER Sharp Health Plan (HMO) OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED RELEASE PRIOR CLAIM FOR AMANTADINE
Washington October Newsletter
 Washington October Newsletter October 19, 2017 CMS Education on Medicare Skilled Nursing and Therapy Services Coverage The Centers for Medicare and Medicaid (CMS) want to remind you that the Jimmo v. Sebelius
Washington October Newsletter October 19, 2017 CMS Education on Medicare Skilled Nursing and Therapy Services Coverage The Centers for Medicare and Medicaid (CMS) want to remind you that the Jimmo v. Sebelius
Medicare Part D 2017 Formulary Changes OC Preferred
 Medicare Part D 2017 Formulary s OC Preferred Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization, quantity
Medicare Part D 2017 Formulary s OC Preferred Inter Valley Health Plan may add or remove drugs from our formulary during the year. If we remove a drug from our formulary, add prior authorization, quantity
INJECTION, INOTUZUMAB OZOGAMICIN, 0.1 MG [BESPONSA ] [C CODES FOR FACILITY USE ONLY]
![INJECTION, INOTUZUMAB OZOGAMICIN, 0.1 MG [BESPONSA ] [C CODES FOR FACILITY USE ONLY] INJECTION, INOTUZUMAB OZOGAMICIN, 0.1 MG [BESPONSA ] [C CODES FOR FACILITY USE ONLY]](/thumbs/85/92112268.jpg) Commercial Medical Oncology Program Review Code List 3rd Quarter 2018 This list is subject to change once per quarter. Changes will be posted to the BCBSNC website at www.bcbsnc.com by the 10th day of
Commercial Medical Oncology Program Review Code List 3rd Quarter 2018 This list is subject to change once per quarter. Changes will be posted to the BCBSNC website at www.bcbsnc.com by the 10th day of
2018 BCN Advantage Prior Authorization Criteria Last updated: November, 2017
 Abstral Actemra Adcirca Adempas Afinitor Afinitor- Disperz Alecensa Alunbrig Amitiza Amitriptyline Ampyra Anadrol-50 Androgel Androderm Aralast NP Aranesp Arcalyst Armodafinil Aubagio Avonex Bavencio Beleodaq
Abstral Actemra Adcirca Adempas Afinitor Afinitor- Disperz Alecensa Alunbrig Amitiza Amitriptyline Ampyra Anadrol-50 Androgel Androderm Aralast NP Aranesp Arcalyst Armodafinil Aubagio Avonex Bavencio Beleodaq
1/1/2019 FORMULARY CHANGES CIGNA COMMERCIAL CUSTOMERS
 1/1/2019 FORMULARY CHANGES CIGNA COMMERCIAL CUSTOMERS Effective 1/1/19, Cigna is making changes to our formularies that may impact medication coverage for customers at your pharmacy. We have included a
1/1/2019 FORMULARY CHANGES CIGNA COMMERCIAL CUSTOMERS Effective 1/1/19, Cigna is making changes to our formularies that may impact medication coverage for customers at your pharmacy. We have included a
2016 FORMULARY ADDENDUM NOTICE OF CHANGE
 2016 FORMULARY ADDENDUM NOTICE OF CHANGE (PRESCRIPTION DRUG PLANS) WELLCARE PRESCRIPTION INSURANCE, INC. WellCare Simple (PDP) WellCare Classic (PDP) WellCare Extra (PDP) This is a listing of the changes
2016 FORMULARY ADDENDUM NOTICE OF CHANGE (PRESCRIPTION DRUG PLANS) WELLCARE PRESCRIPTION INSURANCE, INC. WellCare Simple (PDP) WellCare Classic (PDP) WellCare Extra (PDP) This is a listing of the changes
May 2017 P&T Updates
 May 2017 P&T Updates Commercial Triple Tier 4th Tier Applicable Traditional Prior Auth Alternatives 6 ml per AMPYRA 3 2 2 tablets per day, 30 day BYDUREON 3 2 4 vials per 28 days 5 mcg pen: 1.2 ml per
May 2017 P&T Updates Commercial Triple Tier 4th Tier Applicable Traditional Prior Auth Alternatives 6 ml per AMPYRA 3 2 2 tablets per day, 30 day BYDUREON 3 2 4 vials per 28 days 5 mcg pen: 1.2 ml per
November 2018 P & T Updates
 November 2018 P & T Updates Commercial Triple Tier 4th Tier Applicable Traditional Prior Auth AIMOVIG 3 2 Detailed s 70 mg per month: 2 ml per 60 days 140 mg per month: 2 ml per 30 days AJOVY 3 2 4.5 ml
November 2018 P & T Updates Commercial Triple Tier 4th Tier Applicable Traditional Prior Auth AIMOVIG 3 2 Detailed s 70 mg per month: 2 ml per 60 days 140 mg per month: 2 ml per 30 days AJOVY 3 2 4.5 ml
AMANTADINE ER. Products Affected Step 2: OSMOLEX ER 129 MG TABLET, EXTENDED RELEASE OSMOLEX ER 193 MG TABLET, Details
 AMANTADINE ER OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED RELEASE PRIOR CLAIM FOR AMANTADINE HCL IMMEDIATE RELEASE WITHIN THE PAST 120 DAYS. 1 ANTICONVULSANTS
AMANTADINE ER OSMOLEX ER 129 MG, EXTENDED RELEASE OSMOLEX ER 193 MG, EXTENDED RELEASE OSMOLEX ER 258 MG, EXTENDED RELEASE PRIOR CLAIM FOR AMANTADINE HCL IMMEDIATE RELEASE WITHIN THE PAST 120 DAYS. 1 ANTICONVULSANTS
Quarterly pharmacy formulary change notice
 Quarterly pharmacy formulary change notice Provider update Summary: The formulary changes listed in the table below were reviewed and approved at our second quarter 2018, Pharmacy and Therapeutics Committee
Quarterly pharmacy formulary change notice Provider update Summary: The formulary changes listed in the table below were reviewed and approved at our second quarter 2018, Pharmacy and Therapeutics Committee
Aetna Better Health Illinois Premier Plan. November 2015 Formulary Updates. October 2015 Formulary Updates
 Aetna Better Health Illinois Premier Plan November 2015 Formulary Updates desogestrel & ethinyl estradiol tab 0.15 mg-30 mcg RIVASTIGMINE DIS 13.3/24; QL (30 patches/30 days) RIVASTIGMINE DIS 4.6MG/24;
Aetna Better Health Illinois Premier Plan November 2015 Formulary Updates desogestrel & ethinyl estradiol tab 0.15 mg-30 mcg RIVASTIGMINE DIS 13.3/24; QL (30 patches/30 days) RIVASTIGMINE DIS 4.6MG/24;
