12: BOWEL CANCER IN FAMILIES
|
|
|
- Annabella Greer
- 5 years ago
- Views:
Transcription
1 12: BOWEL CANCER IN FAMILIES 12.1 INTRODUCTION TO GENETICS AND INHERITANCE The human body is made up of billions of cells (such as skin cells, brain cells, nerve cells, etc). Almost every cell in the body contains a complete set of genetic instructions (chromosomes). These genetic instructions are made up of almost 100,000 genes, all linked together like tiny beads on a necklace and wound up into tight little packages that fit inside the centre (or nucleus) of a cell. Each gene in the body is made of DNA (deoxyribonucleic acid) and they carry the instructions that control how our bodies grow, develop and work. For example there are genes whose job is to make sure our cells grow at the right time, or genes that control the colour of our eyes, or hair. A human cell Inheritance is the transfer or passing on of genetic information from a parent to a child. Genes come in pairs, and sperm cells and egg cells contain only half the genes needed to make a new human being. When the two come together, the new life contains a complete set of genetic information, half being from the mother and the other half from the father. Sometimes the genes act together in the same way, but if the two genes contain conflicting information, one gene may dominate over the other, eg a gene for dark hair and a gene for light hair will result in the darker hair being dominant. When we talk about cancer that runs in the family we often assume that everyone in the family will develop the cancer. This is not true. In fact, if your parent has an altered gene that causes bowel cancer, you are at risk of having the altered gene that is, you have a 50:50 chance of having the altered gene that can cause cancer. If you have a brother or sister with the altered gene, you may also be at risk of having the altered gene. 65
2 If you have an altered gene that causes a high risk of bowel cancer, all your children are at risk. Each has a 50:50 chance of inheriting the altered gene from you like tossing a coin, heads or tails. Remember that because genes are inherited in pairs, if you have an altered gene that causes a high risk of bowel cancer, you will have one copy of the altered gene and one copy of the normal gene. When you have a child you will pass on one or the other of the two genes but not both HAVE I INHERITED AN INCREASED RISK OF BOWEL CANCER? Most people with bowel cancer will not have inherited a high risk altered gene from their parents. In fact 98 per cent of the population have only an average risk of developing bowel cancer. These are people who have never had a history of bowel cancer or a condition known as ulcerative colitis, and have no confirmed family history of bowel cancer. People with only one first-degree relative (parent, sibling or child) or second-degree relative (grandparent, aunt, uncle, niece or nephew) with bowel cancer diagnosed after the age of 55 are at a slightly increased risk. Based on family history, people who have an average (or slightly above) risk of developing bowel cancer should have an FOBT every year and consider having a sigmoidoscopy every five years from the age of 50. Some people are thought to be at a moderately increased risk of getting bowel cancer. This accounts for only 1 to 2 per cent of the population. These are people who have a first-degree relative (parent, sibling or child) with bowel cancer diagnosed before the age of 55, or two first-degree or one first-degree plus one second-degree relative (grandparent, aunt, uncle, niece or nephew) on the same side of the family with bowel cancer diagnosed at any age. If you are at increased risk, consult your doctor about having regular bowel checks. Based on family history, people who have a moderately increased risk of developing bowel cancer should have a colonoscopy every five years starting at age 50 or at age ten years younger than the first diagnosis of bowel cancer in the family, whichever comes first. You should have an FOBT in each of the intervening years. Other people are at a potentially high risk of getting bowel cancer. This accounts for less than 1 per cent of the population. These are people with three or more family members who have been diagnosed with bowel cancer, and people whose families have the inherited disorders known as hereditary non-polyposis colorectal cancer (HNPCC) and familial adenomatous polyposis (FAP). These conditions are described in more detail below. If you are at high risk of developing bowel cancer, 66 Guidelines for the prevention, early detection and management of colorectal cancer
3 you will need to have regular bowel checks. Your doctor may advise genetic testing. People with relatives who have had bowel cancer can consider having tests that diagnose signs of early bowel cancer. You will have a better chance of being cured if a cancer is detected at an early stage (see p61 Screening tests for bowel cancer ) TYPES OF INHERITED BOWEL CANCER Two types of inherited conditions, if left untreated, may result in bowel cancer. These are familial adenomatous polyposis (FAP) and hereditary non-polyposis colorectal cancer (HNPCC). FAP accounts for less than 1 per cent of all bowel cancers and is very rare. HNPCC is only marginally more common, accounting for about 1 per cent of all bowel cancers. These figures show that it is uncommon to actually have inherited an altered high risk gene associated with bowel cancer. Familial adenomatous polyposis (FAP) Familial adenomatous polyposis (FAP) is caused by a change in a gene known as the APC gene. People with this change in every APC gene in their body are referred to as having the FAP gene mutation. FAP causes polyps to grow inside the bowel. These polyps always turn into cancer if left untreated. Polyps are small growths, often on stalks like a mushroom, and they vary in size from a tiny pinhead to 2 centimetres or more. Polyposis simply means a lot of polyps. The polyps in FAP are adenomatous, which means they can develop into cancer. FAP is also familial which means the condition is passed on through families. If one of your parents has FAP, you have a 50:50 risk of developing FAP. Most people with FAP develop bowel polyps during their late teens or early adult years. The polyps may start at any age, but rarely before the age of 10. Multiple bowel polyps 67
4 What can be done? There is much that can be done for someone with FAP. Gene testing For most people at risk of FAP, gene testing is now available. This can tell you whether you have the altered gene which causes FAP. People without the gene will not develop FAP, and their risk of developing bowel cancer is the same as the rest of the population (that is, it increases with age). Gene testing is discussed in more detail on p70 Genetic testing for bowel cancer. Regular check-ups People with FAP, and at-risk people who have not yet had gene testing, should have regular check-ups with the doctor. These should start when you are around 12 years of age, well before bowel cancer is likely to appear. When you have a check-up for FAP, it will generally involve having a sigmoidoscopy and maybe a barium enema (see p19 Sigmoidoscopy, and p20 Barium enema ). There is evidence showing that deaths due to bowel cancer are significantly reduced in families with FAP that have regular check-ups. Treatment to prevent cancer Treatment can remove polyps by removing all or most of the large bowel (the colon and sometimes the rectum) through surgery. The aim is to prevent cancer from developing, and at the same time, to keep your digestive system working as normally as possible. It is important to discuss the impact of this surgery with your doctor or professional counsellor before and/or after the operation. This type of help can be obtained through your hospital, or by phoning the Cancer Information Service on Individuals having surgery for FAP should have an operation to remove all or most of the large bowel. It is not recommended that people with FAP routinely take nonsteroidal anti-inflammatory drugs. Hereditary non-polyposis colorectal cancer (HNPCC) Hereditary non-polyposis colorectal cancer (HNPCC) is also caused by an altered gene (as with FAP). The normal function of the HNPCC gene is to repair any problems within the cell, but when a person carries an altered HNPCC gene, the problems are not repaired and this causes bowel cancer to develop. Currently there are five known HNPCC genes, all of them called mis-match repair genes. Each family has a unique HNPCC gene mutation. 68 Guidelines for the prevention, early detection and management of colorectal cancer
5 People with HNPCC have very few, or no, polyps, which can make this condition more difficult to diagnose than FAP. The cancers which occur in individuals with HNPCC however, do still tend to develop from polyps. HNPCC most commonly occurs when people are in their thirties or forties or older. Sometimes it occurs in the twenties, and very rarely in teenage years. Unfortunately, without genetic testing, it is impossible to tell in advance who will get bowel cancer, and genetic tests cannot tell when cancer will develop. What can be done? Many things can be done for families with HNPCC. Gene testing For some families, the altered gene can be identified. However, present tests will not identify the altered gene for all families, so regular check-ups are vital. New tests will become available in the future. Regular check-ups For those who are known to carry an altered HNPCC gene and for people from HNPCC families who have not yet been able to have genetic testing, regular bowel check-ups are vital. It is recommended that testing begin at the age of 25 years, well before the cancer is likely to appear. These check-ups need to continue for life and should involve having a colonoscopy every one to two years (see p21 Colonoscopy ). If you decide to have a colonoscopy every two years, it is important that every alternate year when you are not being screened, you have an FOBT (see p61 Faecal occult blood test ) to ensure a cancer does not grow during this period. Sometimes other tests might be needed and your doctor will provide more information if you need to have them. For women with HNPCC, it is also important from the age of 35 to have regular gynaecological check-ups as having HNPCC can also increase your chances of developing uterine, ovarian, and other cancers. Your doctor will discuss these additional tests with you, or you can contact the Cancer Information Service on Treatment to prevent cancer Cancers cannot develop if organs are removed. One option for people with HNPCC is to remove all or most of the large bowel (the colon and sometimes the rectum). The aim of surgery is to prevent cancer, and at the same time, to keep your digestive system working as normally as possible. Women can also choose to have a hysterectomy (removal of the uterus) and possibly an oophorectomy (removal of the ovaries) to prevent gynaecological cancers, although this can be delayed until after they have had a family. It is important to discuss the impact of any preventative surgery with your doctor or professional counsellor before and/or after the operation. This type of help can be obtained through your hospital, or by phoning the Cancer Information Service on
6 Members of families with a proven link to HNPCC should be screened by yearly or two-yearly colonoscopy from the age of 25 years GENETIC TESTING FOR BOWEL CANCER Genetic testing can tell you whether or not you have the altered FAP or HNPCC gene(s) that may lead to bowel cancer. The mutation in the particular HNPCC or FAP gene can differ from one affected family to another. Laboratory scientists need to find out which mutation is present in your family. The best way to do this is to take a blood sample from someone in the family who definitely has HNPCC or FAP, and identify the gene mutation. This is difficult to do, can take some time, and is not always successful. Once the gene mutation has been found, anyone else in the family who is at risk of FAP can have the gene test once they reach the age of 12, or for HNPCC at 18. This involves only a blood test, and must be done at a specialist genetic clinic which will ensure you receive all the advice, support and help you need. Your doctor can arrange an appointment for you. There are many implications to having genetic testing. These include: what if I do or don t have the altered gene? what if the scientists can t find the altered gene? when can I have genetic testing? how much does it cost? how long will it take? what if I don t want to know the result? what should I tell other family members? what if they don t want to know? what effects will a positive test result have on my life insurance? who needs to know the result? All of these questions need to be considered before an individual or family has genetic testing. Genetic counsellors can help you work through these issues, answer questions, and help you come to a decision about having the test. For more information on genetic testing, contact the Cancer Information Service on Guidelines for the prevention, early detection and management of colorectal cancer
7 Genetic testing should only be carried out under the supervision of a clinical genetics or cancer genetics specialist, and should always be supported by counselling. The FAP and HNPCC registers The FAP and HNPCC registers have been set up so that information about these genetic disorders can be recorded. Family trees of people with FAP or HNPCC are checked to identify people at risk of inheriting the altered gene. It could help the future medical care of you and your family if your gene test result is recorded on the FAP or HNPCC register. If no one else in your family has had a gene test for FAP or HNPCC, your result will help give the correct advice to other family members. Your test could enable the laboratory to identify the family-specific HNPCC gene mutation. In any event, knowing that you do indeed have or do not have FAP or HNPCC could help others understand who else in the family may be at risk. All information kept at both the registers is strictly confidential. It is never given to outside enquirers, including family members, without your permission. 71
8 Guidelines for the prevention, early detection and management of colorectal cancer: A guide for patients, their families and friends Endorsed February 2000 i
FACT SHEET 49. What is meant by a family history of bowel cancer? What is bowel cancer? What causes bowel cancer?
 Important points The most important factors that can influence an individual s chance of developing bowel cancer are getting older and having a family history of bowel cancer A family history of bowel
Important points The most important factors that can influence an individual s chance of developing bowel cancer are getting older and having a family history of bowel cancer A family history of bowel
2012 update. Bowel Cancer. Information for people at increased risk of bowel cancer. Published by the New Zealand Guidelines Group
 2012 update Bowel Cancer Information for people at increased risk of bowel cancer Published by the New Zealand Guidelines Group i Contents Introduction 1 The bowel 1 Bowel cancer 3 What are the symptoms
2012 update Bowel Cancer Information for people at increased risk of bowel cancer Published by the New Zealand Guidelines Group i Contents Introduction 1 The bowel 1 Bowel cancer 3 What are the symptoms
Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer
 Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer Healthy Habits and Cancer Screening Rev 10.20.15 Page
Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer Healthy Habits and Cancer Screening Rev 10.20.15 Page
An Introduction to MUTYH Associated Polyposis (MAP)
 An Introduction to MUTYH Associated Polyposis (MAP) 1 An Introduction to MUTYH Associated Polyposis(MAP) Contents What is MUTYH Associated Polyposis (MAP)? 2 What causes MUTYH Associated Polyposis (MAP)?
An Introduction to MUTYH Associated Polyposis (MAP) 1 An Introduction to MUTYH Associated Polyposis(MAP) Contents What is MUTYH Associated Polyposis (MAP)? 2 What causes MUTYH Associated Polyposis (MAP)?
A Patient s Guide to risk assessment. Hereditary Colorectal Cancer
 A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? Overview of Syndromes This workbook is designed to help you decide if hereditary cancer
A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? Overview of Syndromes This workbook is designed to help you decide if hereditary cancer
Get tested for. Colorectal cancer. Doctors know how to prevent colon or rectal cancer- and you can, too. Take a look inside.
 Get tested for Colorectal cancer Doctors know how to prevent colon or rectal cancer- and you can, too. Take a look inside. 1 If you re 50 or older, you need to get tested for colorectal cancer. It s one
Get tested for Colorectal cancer Doctors know how to prevent colon or rectal cancer- and you can, too. Take a look inside. 1 If you re 50 or older, you need to get tested for colorectal cancer. It s one
A: PARTICIPANT INFORMATION
 A: PARTICIPANT INFMATION 1. What is your age today? Years of age 2. What is the date of your birth? Month: Day: Most of the questions we will be asking you in this follow-up questionnaire are about the
A: PARTICIPANT INFMATION 1. What is your age today? Years of age 2. What is the date of your birth? Month: Day: Most of the questions we will be asking you in this follow-up questionnaire are about the
Advice about familial aspects of breast cancer and epithelial ovarian cancer
 Advice about familial aspects of breast cancer and epithelial ovarian cancer a guide for health professionals FEBRUARY 2006 These guidelines contain three parts: 1. Information for health professionals
Advice about familial aspects of breast cancer and epithelial ovarian cancer a guide for health professionals FEBRUARY 2006 These guidelines contain three parts: 1. Information for health professionals
Know your past, protect your future.
 Why do you need a Medical Family Tree? Your medical family tree records your family's health history, and can help you make informed decisions for health. In the course of creating your medical family
Why do you need a Medical Family Tree? Your medical family tree records your family's health history, and can help you make informed decisions for health. In the course of creating your medical family
Genetic testing for Lynch Syndrome Information for people who have had a cancer and are eligible for genetic testing for Lynch Syndrome.
 Genetic testing for Lynch Syndrome Information for people who have had a cancer and are eligible for genetic testing for Lynch Syndrome. Introduction Cancer is common in the general population with 1 in
Genetic testing for Lynch Syndrome Information for people who have had a cancer and are eligible for genetic testing for Lynch Syndrome. Introduction Cancer is common in the general population with 1 in
The benefit of. knowing. Genetic testing for hereditary cancer. A patient support guide
 The benefit of knowing Genetic testing for hereditary cancer A patient support guide Does cancer run in your family? Cancer is more common in some families. Sometimes cancer is caused by a change in a
The benefit of knowing Genetic testing for hereditary cancer A patient support guide Does cancer run in your family? Cancer is more common in some families. Sometimes cancer is caused by a change in a
Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP)
 Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP) A Patient s Guide to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary
Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP) A Patient s Guide to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions. South Island Cancer Nurses Network September 2013
 For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
Wellness Along the Cancer Journey: Cancer Types Revised October 2015 Chapter 4: Colorectal Cancer Overview
 Wellness Along the Cancer Journey: Cancer Types Revised October 2015 Chapter 4: Colorectal Cancer Overview Cancer Types Rev. 10.20.15 Page 35 Colorectal Cancer Overview Group Discussion True False Not
Wellness Along the Cancer Journey: Cancer Types Revised October 2015 Chapter 4: Colorectal Cancer Overview Cancer Types Rev. 10.20.15 Page 35 Colorectal Cancer Overview Group Discussion True False Not
GENETIC TESTING: WHAT DOES IT REALLY TELL YOU? Lori L. Ballinger, MS, CGC Licensed Genetic Counselor University of New Mexico Cancer Center
 GENETIC TESTING: WHAT DOES IT REALLY TELL YOU? Lori L. Ballinger, MS, CGC Licensed Genetic Counselor University of New Mexico Cancer Center Definitions: DNA: The material found in our cells - the instructions
GENETIC TESTING: WHAT DOES IT REALLY TELL YOU? Lori L. Ballinger, MS, CGC Licensed Genetic Counselor University of New Mexico Cancer Center Definitions: DNA: The material found in our cells - the instructions
Information for You and Your Family
 Information for You and Your Family What is Prevention? Cancer prevention is action taken to lower the chance of getting cancer. In 2017, more than 1.6 million people will be diagnosed with cancer in the
Information for You and Your Family What is Prevention? Cancer prevention is action taken to lower the chance of getting cancer. In 2017, more than 1.6 million people will be diagnosed with cancer in the
What Are Genes And Chromosomes?
 Clinical Genetics Predictive testing for a Breast Cancer 2(BRCA2) Gene alteration Information for families where an altered cancer gene has been found and who are considering undergoing predictive testing
Clinical Genetics Predictive testing for a Breast Cancer 2(BRCA2) Gene alteration Information for families where an altered cancer gene has been found and who are considering undergoing predictive testing
This information explains the advice about familial breast cancer (breast cancer in the family) that is set out in NICE guideline CG164.
 Familial breast cancer (breast cancer in the family) Information for the public Published: 1 June 2013 nice.org.uk About this information NICE guidelines provide advice on the care and support that should
Familial breast cancer (breast cancer in the family) Information for the public Published: 1 June 2013 nice.org.uk About this information NICE guidelines provide advice on the care and support that should
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING
 CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
Adenomatous Polyposis Syndromes (FAP/AFAP and MAP)
 A Patient s Guide to risk assessment Adenomatous Polyposis Syndromes (FAP/AFAP and MAP) Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer
A Patient s Guide to risk assessment Adenomatous Polyposis Syndromes (FAP/AFAP and MAP) Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer
BowelGene. How do I know if I am at risk? Families with hereditary bowel cancer generally show one or more of the following clues:
 BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK. Unfortunately 1 in 19 women and 1 in 14 men will develop
BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK. Unfortunately 1 in 19 women and 1 in 14 men will develop
patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations MARCH 2015
 patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations MARCH 2015 BRCA1 and BRCA2 Mutations Cancer is a complex disease thought to be caused by several different factors. A few types of cancer
patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations MARCH 2015 BRCA1 and BRCA2 Mutations Cancer is a complex disease thought to be caused by several different factors. A few types of cancer
GHUK BowelGene_2017.qxp_Layout 1 22/02/ :22 Page 3 BowelGene
 GHUK BowelGene_2017.qxp_Layout 1 22/02/2017 10:22 Page 3 BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK.
GHUK BowelGene_2017.qxp_Layout 1 22/02/2017 10:22 Page 3 BowelGene BowelGene What is hereditary bowel cancer? Bowel cancer (also known as colorectal cancer) is the fourth most common cancer in the UK.
Cancer Facts for Women
 Cancer Facts for Women Some of the cancers that most often affect women are breast, colorectal, endometrial, lung, cervical, skin, and ovarian cancers. Knowing about these cancers and what you can do to
Cancer Facts for Women Some of the cancers that most often affect women are breast, colorectal, endometrial, lung, cervical, skin, and ovarian cancers. Knowing about these cancers and what you can do to
Hereditary Breast and Ovarian Cancer (HBOC) Information for individuals and families
 Hereditary Breast and Ovarian Cancer (HBOC) Information for individuals and families What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast and Ovarian Cancer is a genetic condition which
Hereditary Breast and Ovarian Cancer (HBOC) Information for individuals and families What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast and Ovarian Cancer is a genetic condition which
Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP)
 Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP) A Patient s Guide to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary
Lynch Syndrome (HNPCC) and MYH-Associated Polyposis (MAP) A Patient s Guide to risk assessment Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary
What is Colorectal Cancer?
 COLORECTAL CANCER (CRC) What is Colorectal Cancer? Colorectal cancer (also known as colon cancer) is cancer of the colon and/or rectum and occurs when a growth in the lining of the colon or rectum becomes
COLORECTAL CANCER (CRC) What is Colorectal Cancer? Colorectal cancer (also known as colon cancer) is cancer of the colon and/or rectum and occurs when a growth in the lining of the colon or rectum becomes
Cancer Prevention and Early Detection Worksheet for Men
 Page 1 of 5 Cancer Prevention and Early Detection Worksheet for Men While a tremendous amount of progress has been made in cancer research, we still don t understand exactly what causes most cancers. However,
Page 1 of 5 Cancer Prevention and Early Detection Worksheet for Men While a tremendous amount of progress has been made in cancer research, we still don t understand exactly what causes most cancers. However,
A practical guide to living with and after cancer
 A practical guide to living with and after cancer About this booklet 1 About this booklet This booklet is for people who are worried cancer might run in their family because a number of relatives have
A practical guide to living with and after cancer About this booklet 1 About this booklet This booklet is for people who are worried cancer might run in their family because a number of relatives have
1101 First Colonial Road, Suite 300, Virginia Beach, VA Phone (757) Fax (757)
 1101 First Colonial Road, Suite 300, Virginia Beach, VA 23454 www.vbgastro.com Phone (757) 481-4817 Fax (757) 481-7138 1150 Glen Mitchell Drive, Suite 208 Virginia Beach, VA 23456 www.vbgastro.com Phone
1101 First Colonial Road, Suite 300, Virginia Beach, VA 23454 www.vbgastro.com Phone (757) 481-4817 Fax (757) 481-7138 1150 Glen Mitchell Drive, Suite 208 Virginia Beach, VA 23456 www.vbgastro.com Phone
They know how to prevent colon cancer
 They know how to prevent colon cancer and you can, too. Take a look inside. If you re 50 or older, you need to get tested for colon cancer. It s one cancer that can actually be prevented! Colon cancer:
They know how to prevent colon cancer and you can, too. Take a look inside. If you re 50 or older, you need to get tested for colon cancer. It s one cancer that can actually be prevented! Colon cancer:
Family history of pancreatic cancer
 Family history of pancreatic cancer _ This fact sheet is for people who want to find out about the hereditary risk of pancreatic cancer. You can speak to our specialist nurses on our Support Line about
Family history of pancreatic cancer _ This fact sheet is for people who want to find out about the hereditary risk of pancreatic cancer. You can speak to our specialist nurses on our Support Line about
Adenomatous Polyposis Syndromes (FAP/AFAP and MAP)
 A Patient s Guide to risk assessment Adenomatous Polyposis Syndromes (FAP/AFAP and MAP) Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer
A Patient s Guide to risk assessment Adenomatous Polyposis Syndromes (FAP/AFAP and MAP) Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer
Information for families with a slightly increased risk of bowel cancer. Family History of Bowel Cancer
 Information for families with a slightly increased risk of bowel cancer Family History of Bowel Cancer How common is bowel cancer? Bowel cancer is the 3rd most common cancer in the UK. 1 in 20 people develop
Information for families with a slightly increased risk of bowel cancer Family History of Bowel Cancer How common is bowel cancer? Bowel cancer is the 3rd most common cancer in the UK. 1 in 20 people develop
Risk of Colorectal Cancer (CRC) Hereditary Syndromes in GI Cancer GENETIC MALPRACTICE
 Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Colorectal Cancer How to reduce your risk
 Prevention Series Colorectal Cancer How to reduce your risk Let's Make Cancer History 1 888 939-3333 cancer.ca Colorectal Cancer How to reduce your risk Colorectal cancer is the third most commonly diagnosed
Prevention Series Colorectal Cancer How to reduce your risk Let's Make Cancer History 1 888 939-3333 cancer.ca Colorectal Cancer How to reduce your risk Colorectal cancer is the third most commonly diagnosed
Please read the following instructions carefully
 Grand River Regional Cancer Centre 835 King Street West, PO Box 9056 Kitchener, ON N2G 1G3 Tel: (519) 749-4370 x2832 Fax: (519) 749-4394 Dear: You have been referred to the High Risk Ontario Breast Screening
Grand River Regional Cancer Centre 835 King Street West, PO Box 9056 Kitchener, ON N2G 1G3 Tel: (519) 749-4370 x2832 Fax: (519) 749-4394 Dear: You have been referred to the High Risk Ontario Breast Screening
LET S TALK ABOUT CANCER
 LET S TALK ABOUT CANCER COLORECTAL CANCER AND CROHN S DISEASE & ULCERATIVE COLITIS crohnsandcolitis.ca BACKGROUND Colorectal cancer is the second-leading cause of cancer death in this country. In 2013,
LET S TALK ABOUT CANCER COLORECTAL CANCER AND CROHN S DISEASE & ULCERATIVE COLITIS crohnsandcolitis.ca BACKGROUND Colorectal cancer is the second-leading cause of cancer death in this country. In 2013,
Colorectal Cancer Screening
 Tool 2.1 Cancer Screening Basic Fact Sheet Are You at High Risk? Your risk for colorectal cancer may be higher than average if: stomach You or a close relative have had colorectal polyps or colorectal
Tool 2.1 Cancer Screening Basic Fact Sheet Are You at High Risk? Your risk for colorectal cancer may be higher than average if: stomach You or a close relative have had colorectal polyps or colorectal
Clinical Genetics Welcome to Clinical Genetics
 Clinical Genetics Welcome to Clinical Genetics A guide to your referral Genetics The Merseyside and Cheshire Clinical Genetics Service is primarily involved with the diagnosis and genetic counselling of
Clinical Genetics Welcome to Clinical Genetics A guide to your referral Genetics The Merseyside and Cheshire Clinical Genetics Service is primarily involved with the diagnosis and genetic counselling of
Result Navigator Positive Test Result: MSH6
 Result Navigator Positive Test Result: MSH6 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Result Navigator Positive Test Result: MSH6 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Understanding Your Genetic Test Result. Positive for a Deleterious Mutation or Suspected Deleterious
 Understanding Your Genetic Test Result Positive for a Deleterious Mutation or Suspected Deleterious This workbook is designed to help you understand the results of your genetic test and is best reviewed
Understanding Your Genetic Test Result Positive for a Deleterious Mutation or Suspected Deleterious This workbook is designed to help you understand the results of your genetic test and is best reviewed
Understanding and Managing Lynch Syndrome
 Understanding and Managing Lynch Syndrome Princess Margaret For women who may have Lynch syndrome and their family members Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Understanding and Managing Lynch Syndrome Princess Margaret For women who may have Lynch syndrome and their family members Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Hereditary Colorectal Cancer
 A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer testing is right for
A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? This workbook is designed to help you decide if hereditary cancer testing is right for
Bowel cancer screening and prevention
 Bowel cancer screening and prevention Cancer Incidence and Mortality Victoria 2012 Number 6000 5000 4000 3000 2000 Incidences = 29,387 Mortality = 10,780 Incidence Mortality 1000 0 Prostate Breast Bowel
Bowel cancer screening and prevention Cancer Incidence and Mortality Victoria 2012 Number 6000 5000 4000 3000 2000 Incidences = 29,387 Mortality = 10,780 Incidence Mortality 1000 0 Prostate Breast Bowel
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
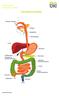 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
Contact Information. Permanent Address: Mailing Address (if different than above): Please check preferred method(s) of contact.
 Contact Information Please fill out this form as completely as possible. You will not need to complete any additional medical health history forms on the day of your visit. Name: Date: Permanent Address:
Contact Information Please fill out this form as completely as possible. You will not need to complete any additional medical health history forms on the day of your visit. Name: Date: Permanent Address:
Colorectal Cancer Screening Guideline Issue Brief Updated May 30 th, 2018
 Colorectal Cancer Screening Guideline Issue Brief Updated May 30 th, 2018 Issue Summary The American Cancer Society has updated its colorectal screening guideline, which have been published in CA: A Journal
Colorectal Cancer Screening Guideline Issue Brief Updated May 30 th, 2018 Issue Summary The American Cancer Society has updated its colorectal screening guideline, which have been published in CA: A Journal
The Genetics of Familial Polyposis
 The Genetics of Familial Polyposis Thursday, September 24 th 2015 Kara Semotiuk, MS, (C)CGC & Laura Winter, MSc, CGC Genetic Counsellors at the FGICR Familial Polyposis Familial Can run in the family related
The Genetics of Familial Polyposis Thursday, September 24 th 2015 Kara Semotiuk, MS, (C)CGC & Laura Winter, MSc, CGC Genetic Counsellors at the FGICR Familial Polyposis Familial Can run in the family related
Result Navigator. Positive Test Result: STK11. After a positive test result, there can be many questions about what to do next. Navigate Your Results
 Result Navigator Positive Test Result: STK11 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Result Navigator Positive Test Result: STK11 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
What a history of cancer may mean for you and your family and the steps you can take to reduce the risk
 What a history of cancer may mean for you and your family and the steps you can take to reduce the risk www.myriadtests.com 1-800-469-7423 Family Ties and Colon Cancer In every family, certain traits are
What a history of cancer may mean for you and your family and the steps you can take to reduce the risk www.myriadtests.com 1-800-469-7423 Family Ties and Colon Cancer In every family, certain traits are
patient education Fact Sheet
 patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations OCTOBER 2017 BRCA1 and BRCA2 Mutations Cancer is caused by several different factors. A few types of cancer run in families. These types are
patient education Fact Sheet PFS007: BRCA1 and BRCA2 Mutations OCTOBER 2017 BRCA1 and BRCA2 Mutations Cancer is caused by several different factors. A few types of cancer run in families. These types are
BRCA genes and inherited breast and ovarian cancer. Information for patients
 BRCA genes and inherited breast and ovarian cancer Information for patients This booklet has been written for people who have a personal or family history of breast and/or ovarian cancer that could be
BRCA genes and inherited breast and ovarian cancer Information for patients This booklet has been written for people who have a personal or family history of breast and/or ovarian cancer that could be
Lynch Syndrome. A Patient s Guide to Genetic Testing for Lynch Syndrome
 Lynch Syndrome A Patient s Guide to Genetic Testing for Lynch Syndrome What is Lynch Syndrome? Lynch syndrome is an inherited condition that increases your risk of developing colon cancer and other cancers
Lynch Syndrome A Patient s Guide to Genetic Testing for Lynch Syndrome What is Lynch Syndrome? Lynch syndrome is an inherited condition that increases your risk of developing colon cancer and other cancers
KNOWING YOUR FAMILY HEALTH HISTORY COULD SAVE YOUR LIFE!
 KNOWING YOUR FAMILY HEALTH HISTORY COULD SAVE YOUR LIFE! Why is my family health history so important? Several important reasons to know your family health history! Because some conditions run in families
KNOWING YOUR FAMILY HEALTH HISTORY COULD SAVE YOUR LIFE! Why is my family health history so important? Several important reasons to know your family health history! Because some conditions run in families
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
A Guide to Genetics and Health
 2 D o e s i t R u n i n t h e Fa m i ly? A Guide to Genetics and Health BEAUMONT CANCER GENETICS PROGRAM COVENANT COMMUNITY HEALTH CENTER Contents Why is genetics important to my family and me? What makes
2 D o e s i t R u n i n t h e Fa m i ly? A Guide to Genetics and Health BEAUMONT CANCER GENETICS PROGRAM COVENANT COMMUNITY HEALTH CENTER Contents Why is genetics important to my family and me? What makes
Result Navigator. Positive Test Result: BMPR1A. After a positive test result, there can be many questions about what to do next. Navigate Your Results
 Result Navigator Positive Test Result: BMPR1A Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Result Navigator Positive Test Result: BMPR1A Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Screening & Surveillance Guidelines
 Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Cancer Prevention and Early Detection Worksheet for Women
 Page 1 of 8 Cancer Prevention and Early Detection Worksheet for Women While a tremendous amount of progress has been made in cancer research, we still don t understand exactly what causes most cancers.
Page 1 of 8 Cancer Prevention and Early Detection Worksheet for Women While a tremendous amount of progress has been made in cancer research, we still don t understand exactly what causes most cancers.
Honouring the First Nations Path of Well-being
 Honouring the First Nations Path of Well-being WHAT IS CANCER SCREENING? Cancer screening means taking a test that can find cancer before you have any symptoms. Finding cancer early is one of the best
Honouring the First Nations Path of Well-being WHAT IS CANCER SCREENING? Cancer screening means taking a test that can find cancer before you have any symptoms. Finding cancer early is one of the best
Genetic Risk Evaluation and Testing Program
 INSTRUCTIONS: Please complete this form to the best of your ability PRIOR to your appointment. Please remember to list ALL relatives, both living and deceased, regardless of if they have had cancer or
INSTRUCTIONS: Please complete this form to the best of your ability PRIOR to your appointment. Please remember to list ALL relatives, both living and deceased, regardless of if they have had cancer or
Cancer Facts for Men FOR REVIEW ONLY
 Cancer Facts for Men Prostate cancer The chance of getting prostate cancer goes up as a man gets older. Most prostate cancers are found in men over the age of 65. For reasons that are still unknown, African
Cancer Facts for Men Prostate cancer The chance of getting prostate cancer goes up as a man gets older. Most prostate cancers are found in men over the age of 65. For reasons that are still unknown, African
Colorectal Cancer: Preventable, Beatable, Treatable. American Cancer Society
 Colorectal Cancer: Preventable, Beatable, Treatable American Cancer Society Reviewed/Revised May 2018 What we ll be talking about How common is colorectal cancer? What is colorectal cancer? What causes
Colorectal Cancer: Preventable, Beatable, Treatable American Cancer Society Reviewed/Revised May 2018 What we ll be talking about How common is colorectal cancer? What is colorectal cancer? What causes
Hereditary Cancer Risk Testing: What to Expect
 Hereditary Cancer Risk Testing: What to Expect PHONE APPOINTMENT The first appointment with the Vanderbilt Hereditary Cancer Clinic is by phone. We will record your family history information and create
Hereditary Cancer Risk Testing: What to Expect PHONE APPOINTMENT The first appointment with the Vanderbilt Hereditary Cancer Clinic is by phone. We will record your family history information and create
Understanding Your Genetic Test Result. Positive for a Deleterious Mutation or Suspected Deleterious
 Understanding Your Genetic Test Result Positive for a Deleterious Mutation or Suspected Deleterious This workbook is designed to help you understand the results of your genetic test and is best reviewed
Understanding Your Genetic Test Result Positive for a Deleterious Mutation or Suspected Deleterious This workbook is designed to help you understand the results of your genetic test and is best reviewed
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Colorectal Cancer Prevention and Early Detection
 Colorectal Cancer Prevention and Early Detection What is colorectal cancer? Cancer starts when cells in the body begin to grow out of control. Cells in nearly any part of the body can become cancer, and
Colorectal Cancer Prevention and Early Detection What is colorectal cancer? Cancer starts when cells in the body begin to grow out of control. Cells in nearly any part of the body can become cancer, and
What All of Us Should Know About Cancer and Genetics
 What All of Us Should Know About Cancer and Genetics Beth A. Pletcher, MD, FAAP, FACMG Associate Professor of Pediatrics UMDNJ- New Jersey Medical School Disclosures I have no relevant financial relationships
What All of Us Should Know About Cancer and Genetics Beth A. Pletcher, MD, FAAP, FACMG Associate Professor of Pediatrics UMDNJ- New Jersey Medical School Disclosures I have no relevant financial relationships
Cancer Genetics Risk Assessment Program Questionnaire
 We greatly appreciate you taking the time to complete this questionnaire and look forward to meeting you. Gathering this information prior to your appointment will help make your visit with us as efficient
We greatly appreciate you taking the time to complete this questionnaire and look forward to meeting you. Gathering this information prior to your appointment will help make your visit with us as efficient
So, now, that we have reviewed some basics of cancer genetics I will provide an overview of some common syndromes.
 Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Understanding Your Genetic Test Result. Positive for Two Copies of an MYH Mutation
 Understanding Your Genetic Test Result Positive for Two Copies of an MYH Mutation This workbook is designed to help you understand the results of your genetic test and is best reviewed with your healthcare
Understanding Your Genetic Test Result Positive for Two Copies of an MYH Mutation This workbook is designed to help you understand the results of your genetic test and is best reviewed with your healthcare
Result Navigator. Positive Test Result: PTEN. After a positive test result, there can be many questions about what to do next. Navigate Your Results
 Result Navigator Positive Test Result: PTEN Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Result Navigator Positive Test Result: PTEN Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Blue Star Sunday. Increasing Awareness About Colon Cancer. Dear Faith Community,
 Blue Star Sunday Increasing Awareness About Colon Cancer Dear Faith Community, West Virginia s Cancer Coalition, Mountains of Hope, invites your faith community to participate in Colorectal Cancer Awareness
Blue Star Sunday Increasing Awareness About Colon Cancer Dear Faith Community, West Virginia s Cancer Coalition, Mountains of Hope, invites your faith community to participate in Colorectal Cancer Awareness
Talking about Cancer in Your Family Can Keep You and Your Family Healthy. Do you know your Kin Facts? A guide for and your family
 Talking about Cancer in Your Family Can Keep You and Your Family Healthy Do you know your Kin Facts? A guide for and your family Did you know? Breast and colon cancers are leading cancer killers for women
Talking about Cancer in Your Family Can Keep You and Your Family Healthy Do you know your Kin Facts? A guide for and your family Did you know? Breast and colon cancers are leading cancer killers for women
What is cancer? A group of 100 different diseases. The uncontrolled, abnormal growth of cells. Cancer may spread to other parts of the body.
 What is cancer? A group of 100 different diseases The uncontrolled, abnormal growth of cells Cancer may spread to other parts of the body Source: What is colon cancer? A disease in which normal cells in
What is cancer? A group of 100 different diseases The uncontrolled, abnormal growth of cells Cancer may spread to other parts of the body Source: What is colon cancer? A disease in which normal cells in
Lynch Syndrome. patient guide. genetic testing for hereditary colorectal and uterine cancer
 patient guide Lynch Syndrome genetic testing for hereditary colorectal and uterine cancer Because knowing your risk can mean early detection and prevention Know the Basics People with Lynch syndrome may
patient guide Lynch Syndrome genetic testing for hereditary colorectal and uterine cancer Because knowing your risk can mean early detection and prevention Know the Basics People with Lynch syndrome may
Guidelines for the Early Detection of Cancer
 Guidelines for the Early Detection of Cancer The American Cancer Society recommends these cancer screening guidelines for most adults. Screening tests are used to find cancer before a person has any symptoms.
Guidelines for the Early Detection of Cancer The American Cancer Society recommends these cancer screening guidelines for most adults. Screening tests are used to find cancer before a person has any symptoms.
Bowel Cancer Prevention and Screening. Harriet Wynne, Cancer Council Victoria
 Bowel Cancer Prevention and Screening Harriet Wynne, Cancer Council Victoria New cases and deaths for the Victoria population in 2013 Thursfield V, et al. Cancer in Victoria: Statistics & trends 2013.
Bowel Cancer Prevention and Screening Harriet Wynne, Cancer Council Victoria New cases and deaths for the Victoria population in 2013 Thursfield V, et al. Cancer in Victoria: Statistics & trends 2013.
Ovarian Cancer Causes, Risk Factors, and Prevention
 Ovarian Cancer Causes, Risk Factors, and Prevention Risk Factors A risk factor is anything that affects your chance of getting a disease such as cancer. Learn more about the risk factors for ovarian cancer.
Ovarian Cancer Causes, Risk Factors, and Prevention Risk Factors A risk factor is anything that affects your chance of getting a disease such as cancer. Learn more about the risk factors for ovarian cancer.
Cancer in Women. Lung cancer. Breast cancer
 Cancer in Women You can get cancer at any age, but it is more likely as you get older. The types of cancer people get and the risk of dying from cancer are not the same for all ethnic groups. Here are
Cancer in Women You can get cancer at any age, but it is more likely as you get older. The types of cancer people get and the risk of dying from cancer are not the same for all ethnic groups. Here are
Cancer Genomics 101. BCCCP 2015 Annual Meeting
 Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
So how much of breast and ovarian cancer is hereditary? A). 5 to 10 percent. B). 20 to 30 percent. C). 50 percent. Or D). 65 to 70 percent.
 Welcome. My name is Amanda Brandt. I am one of the Cancer Genetic Counselors at the University of Texas MD Anderson Cancer Center. Today, we are going to be discussing how to identify patients at high
Welcome. My name is Amanda Brandt. I am one of the Cancer Genetic Counselors at the University of Texas MD Anderson Cancer Center. Today, we are going to be discussing how to identify patients at high
Telephone Disclosure Visual Aid Toolkit: Panel Testing
 Telephone Disclosure Visual Aid Toolkit: Panel Testing This is your visual aid toolkit that will be used during your disclosure appointment. Included in this packet are definitions and descriptions of
Telephone Disclosure Visual Aid Toolkit: Panel Testing This is your visual aid toolkit that will be used during your disclosure appointment. Included in this packet are definitions and descriptions of
Unfortunately you re not. So talk to your health care provider about screening today.
 Unfortunately you re not. So talk to your health care provider about screening today. Fact is, Ontario has one of the highest rates of colorectal cancer in the world and thousands die from it each year.
Unfortunately you re not. So talk to your health care provider about screening today. Fact is, Ontario has one of the highest rates of colorectal cancer in the world and thousands die from it each year.
Contents. Introduction. Introduction 03
 Genes and dementia Introduction This information is for anyone who wants to know more about the link between genes and dementia. This includes people living with dementia, their carers, friends and families.
Genes and dementia Introduction This information is for anyone who wants to know more about the link between genes and dementia. This includes people living with dementia, their carers, friends and families.
Colon Cancer Screening and Surveillance. Louis V. Antignano, M.D. Wilson Gastroenterology October 11, 2011
 Colon Cancer Screening and Surveillance Louis V. Antignano, M.D. Wilson Gastroenterology October 11, 2011 Colorectal Cancer Preventable cancer Number 2 cancer killer in the USA Often curable if detected
Colon Cancer Screening and Surveillance Louis V. Antignano, M.D. Wilson Gastroenterology October 11, 2011 Colorectal Cancer Preventable cancer Number 2 cancer killer in the USA Often curable if detected
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian
 Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
B1 Revision You and Your Genes. You and Your Genes (B1) Revision for Exam
 B1 Revision You and Your Genes You and Your Genes (B1) Revision for Exam What makes us all different? Organisms inherit information from their parents. This controls how they develop, so children look
B1 Revision You and Your Genes You and Your Genes (B1) Revision for Exam What makes us all different? Organisms inherit information from their parents. This controls how they develop, so children look
Are you at risk of Hereditary Cancer? Your Guide to the Answers
 Are you at risk of Hereditary Cancer? Your Guide to the Answers What is Hereditary Cancer? The genes we are born with may contribute to our risk of developing certain types of cancer, including breast,
Are you at risk of Hereditary Cancer? Your Guide to the Answers What is Hereditary Cancer? The genes we are born with may contribute to our risk of developing certain types of cancer, including breast,
Higher Risk, Lowered Age: New Colorectal Cancer Screening Guidelines
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/higher-risk-lowered-age-new-colorectal-cancerscreening-guidelines/10309/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/higher-risk-lowered-age-new-colorectal-cancerscreening-guidelines/10309/
BAYLOR SCOTT & WHITE HEALTH GENETICS QUESTIONNAIRE PATIENT INFORMATION
 PATIENT INFORMATION Name: Address: (Last) (First) (Middle) (Street) (City) (State) (Zip) Home Phone: Cell Phone: Email Address: Birth Date: Age: When is the best time to contact you? May we email you for
PATIENT INFORMATION Name: Address: (Last) (First) (Middle) (Street) (City) (State) (Zip) Home Phone: Cell Phone: Email Address: Birth Date: Age: When is the best time to contact you? May we email you for
PATIENT INFORMATION. (Last) (First) (Middle) (Last) (City) (State) (Zip)
 PATIENT INFMATION : Address: (Last) (First) (Middle) (Last) (City) (State) (Zip) Home Phone: Cell Phone: Email address: Birth date: : Gender: When is the best time to contact you? May we email you for
PATIENT INFMATION : Address: (Last) (First) (Middle) (Last) (City) (State) (Zip) Home Phone: Cell Phone: Email address: Birth date: : Gender: When is the best time to contact you? May we email you for
Colorectal Cancer Screening. Dr Kishor Muniyappa 2626 Care Drive, Suite 101 Tallahassee, FL Ph:
 Colorectal Cancer Screening Dr Kishor Muniyappa 2626 Care Drive, Suite 101 Tallahassee, FL 32308 Ph: 850-297-0351 What we ll be talking about How common is colorectal cancer? What is colorectal cancer?
Colorectal Cancer Screening Dr Kishor Muniyappa 2626 Care Drive, Suite 101 Tallahassee, FL 32308 Ph: 850-297-0351 What we ll be talking about How common is colorectal cancer? What is colorectal cancer?
Result Navigator. Positive Test Result: CDH1. After a positive test result, there can be many questions about what to do next. Navigate Your Results
 Result Navigator Positive Test Result: CDH1 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
Result Navigator Positive Test Result: CDH1 Positive test results identify a change, or misspelling, of DNA that is known or predicted to cause an increased risk for cancer. DNA is the blueprint of life
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS. Family Health Clinical Genetics. Clinical Genetics department
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
