INTRODUCTION. KEY WORDS: head and neck cancer, tobacco smoking, alcohol drinking, body mass index, physical activity, epidemiology, risk factors
|
|
|
- Amos Fletcher
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Tobacco, alcohol, body mass index, physical activity, and the risk of head and neck cancer in the Prostate, Lung, Colorectal, and Ovarian (PLCO) cohort Mia Hashibe, PhD, 1 * Jason Hunt, MD, 2 Mei Wei, MD, PhD, 1 Saundra Buys, MD, 3 Lisa Gren, PhD, 1 Yuan-Chin Amy Lee, PhD 1 1 Division of Public Health, Department of Family & Preventive Medicine and Huntsman Cancer Institute, University of Utah School of Medicine, Salt Lake City, Utah, 2 Division of Otolaryngology, Department of Surgery and Huntsman Cancer Institute, University of Utah School of Medicine, Salt Lake City, Utah, 3 Department of Internal Medicine and Huntsman Cancer Institute, University of Utah School of Medicine, Salt Lake City, Utah. Accepted 21 March 2012 Published online 19 June 2012 in Wiley Online Library (wileyonlinelibrary.com). DOI /hed ABSTRACT: Background. Estimation of attributable fractions for tobacco and alcohol, and investigation of the association between body mass index (BMI) and head and neck cancer risk have largely been in case-control studies. These aspects and physical activity need to be assessed as possible head and neck cancer risk/protective factors in a cohort study. Methods. In the Prostate, Lung, Colorectal, and Ovarian (PLCO) cancer screening trial, of the 101,182 study subjects, 177 individuals developed head and neck cancer. Results. The proportion of head and neck cancer cases attributed to tobacco and/or alcohol was 66% (50.5% tobacco alone, 14.7% alcohol alone, 0.9% tobacco and alcohol combined). BMI was not associated with head and neck cancer risk, but increasing hours of physical activity per week was associated with a reduced head and neck cancer risk (odds ratio [OR] ¼ 0.58; 95% confidence interval [CI] ¼ ). Conclusions. Cigarette smoking is clearly the most important head and neck cancer risk factor in this population. The reduced cancer risk due to physical activity was consistent with results from a pooled analysis of case-control studies. VC 2012 Wiley Periodicals, Inc. Head Neck 35: , 2013 KEY WORDS: head and neck cancer, tobacco smoking, alcohol drinking, body mass index, physical activity, epidemiology, risk factors INTRODUCTION Each year in the United States, approximately 49,260 head and neck cancer cases are diagnosed and 11,480 deaths occur due to head and neck cancer. 1 Head and neck cancer subsites, including cancers of the oral cavity, oropharynx, hypopharynx, and larynx, have a shared etiology of tobacco and alcohol. Oral cavity and pharyngeal cancers are the eighth most common cancer among men in the United States. Although the overall head and neck cancer incidence rates have been declining over the last few decades, cancer incidence rates for the human papillomavirus (HPV)-related subsites, including the oropharynx, have been increasing. 2 Among white men, the increase was approximately 63% comparing the periods from 1977 to 1981 with 2003 to A recent publication from the International Head and Neck Cancer Epidemiology (INHANCE) Consortium, including 11,221 cases and 16,168 controls, reported that tobacco and alcohol accounted for a larger proportion of head and neck cancer cases in Europe (attributable fraction [AF] ¼ 84%) and in Latin America (AF ¼ 83%) than in North America (AF ¼ 51%). 3 These estimates suggested *Corresponding author: M. Hashibe, Division of Public Health, Department of Family and Preventive Medicine, University of Utah, 375 Chipeta Way, Suite A, Salt Lake City, UT mia.hashibe@utah.edu that HPV may play a larger role in head and neck cancers in North America compared with other regions. Indeed, a recent study reported that the HPV DNA and serum antibodies were very low among patients with head and neck cancer in Central Europe and Latin America. 4 One of the limitations of the INHANCE consortium analysis was that all of the studies in the large pooled dataset were casecontrol in design, raising the concern of recall bias, where the cases may be more likely to recall a higher tobacco and alcohol exposure than the controls because the cases knew their disease status at the time of interview. Bias away from the null in the AF estimations could have resulted if the odds ratios and exposure prevalences were both biased away from the null due to recall bias. Estimating AFs for tobacco and alcohol in a cohort study would be of interest to compare with the previous AF results from North America. The INHANCE consortium also reported on the association between body mass index (BMI) and head and neck cancer in a pooled analysis of 12,716 cases and 17,438 controls. 5 Low BMI (<18.5 kg/m 2 ) at interview and at 2 to 5 years before diagnosis was associated with an increased risk of head and neck cancer in these case-control studies. 5 Individuals who were obese had a reduced risk of head and neck cancer, although this association did not hold among never smokers and never drinkers. A recent large-scale multicenter case-control study in Western Europe reported on changes in BMI over a lifetime, 914 HEAD & NECK DOI /HED JULY 2013
2 TOBACCO, ALCOHOL, BMI, PHYSICAL ACTIVITY, AND HEAD AND NECK CANCER with a reduced risk of head and neck cancer associated with a 5% or more increase in BMI, again observed only in smokers and drinkers but not in never-smokers and never-drinkers. 6 The authors of both studies emphasized the need for studying these associations prospectively to minimize the possibility of recall bias and temporal ambiguity in which the disease may have affected the weight. There have been very few studies on physical activity and head and neck cancer risk. The National Institutes of Health (NIH) American Association of Retired Persons (AARP) Diet and Health Study, a cohort study of 566,402 participants aged 50 to 71 years, reported a risk ratio (RR) of 0.89 (95% confidence interval [CI] ¼ ) for physical activity 5 times per week compared to no physical activity. 7 Dose response trends were not observed for increasing levels of physical activity. The INHANCE consortium conducted a pooled analysis including 2383 cases and 5674 controls, and reported a risk reduction of approximately 20% (odds ratio [OR] ¼ 0.78; 95% CI ¼ ) for medium physical activity compared with none or low physical activity. 8 Physical activity has also been linked inversely with cancers of the colon, pancreas, breast, and prostate. 9 Family history of cancer overall was not associated with an increased risk of head and neck cancer, but family history of head and neck cancer was associated with an increased head and neck cancer risk in an INHANCE analysis of 8967 cases and 13,627 controls (OR ¼ 1.75; 95% CI ¼ ). 10 Family history of tobacco-related cancers conferred a very modest increase in risk (OR ¼ 1.11; 95% CI ¼ ). 10 These associations were stronger in individuals who were tobacco smokers and alcohol drinkers, but were not significantly different across head and neck cancer subsites. Although most of these previous studies were case-control studies, Goldgar et al 11 used a population-based approach and reported familial relative risks of 1.80 (95% CI ¼ ) for oral cavity cancer as a proband and 8.01 (95% CI, ) for laryngeal cancer as a proband. The analysis by Goldgar et al 11 did not include information on tobacco and alcohol, and did not assess whether specific cancers in family history conferred increased risks. The association between other diseases and the risk of head and neck cancer has not been reported on extensively. There was a previous report that an individual who had diabetes mellitus may be at an increased risk of oral precancers, such as oral leukoplakia and erythroplakia. 12 History of other chronic diseases, such as chronic bronchitis, asthma, tuberculosis, high blood pressure, heart attack, and stroke were not associated with oral precancer risks. 12 An INHANCE analysis of 6653 cases and 13,747 controls reported no association between history of diabetes and head and neck cancer risk, but did report an association specifically among never smokers (OR ¼ 1.63; 95% CI ¼ ). 13 The majority of epidemiologic studies on head and neck cancer risk factors have been case-control in design and had the limitations of possible recall bias and temporal ambiguity. Assessment of attributable fractions for tobacco and alcohol, and BMI as a head and neck cancer risk factor has never been conducted in a populationbased cohort study, to our knowledge. Physical activity and disease history have been examined for head and neck cancer only in a handful of studies thus far. The purpose of this study was to further investigate these associations in a cohort study in the United States. MATERIALS AND METHODS The Prostate, Lung, Colorectal, and Ovarian (PLCO) cancer screening trial is a large-scale clinical trial to determine whether certain cancer screening tests reduce deaths from prostate, lung, colorectal, and ovarian cancer. The trial started in 1992 and ended enrollment in Approximately 155,000 women and men between the ages of 55 and 74 were recruited into the PLCO trial at 10 centers across the United States (Alabama, Michigan, Colorado, Hawaii, Wisconsin, Minnesota, Pennsylvania, Utah, Missouri, and Washington, DC). At entry, participants were randomized to 1 of 2 study groups. One group received routine health care from their health providers. The other received a series of examinations to screen for prostate, lung, colorectal, and ovarian cancers. Screening of participants ended in late Follow-up will continue for up to 10 more years to determine the benefits or harms of screening. Written informed consent was obtained from all study participants. Ethical approval for human subject s research was obtained at each of the centers. The data used for this study include the follow-up information up to May Subjects randomized to either study arm (intervention or control) were eligible if they had completed the baseline questionnaire and the diet history questionnaire, which was administered to participants in both groups starting in Before that time, diet questionnaires were administered to only those in the intervention arm. Of the 154,900 study participants recruited into the PLCO study, 111,513 participants completed both the baseline questionnaire and the diet history questionnaire. Of the 111,513 participants with valid questionnaires, participants were excluded because: (1) they had cancer before entry into the PLCO study (n ¼ 9674); (2) they did not have follow-up time (n ¼ 460); or (3) they did not provide information on education level (n ¼ 197). Thus, the remaining cohort consisted of 101,182 individuals, of which 177 developed cancer of the head and neck. The mean number of follow-up years was for this cohort of individuals. Only malignant tumors where the head and neck was the first primary site were included. Tumors were assigned to 1 of the 5 categories as follows: (1) oral cavity (includes lip, tongue, gum, floor of mouth, and hard palate): codes C00.3 to C00.9, C02.0 to C02.3, C03.0, C03.1, C03.9, C04.0, C04.1, C04.8, C04.9, C05.0, C06.0 to C06.2, C06.8, and C06.9; (2) oropharynx (includes base of tongue, lingual tonsil, soft palate, uvula, tonsil, and oropharynx): codes C01.9, C02.4, C05.1, C05.2, C09.0, C09.1, C09.8, C09.9, C10.0 to C10.4, C10.8, and C10.9; (3) hypopharynx (includes pyriform sinus and hypopharynx):codes C12.9, C13.0 to C13.2, C13.8, and C13.9; (4) oral cavity, pharynx unspecified or overlapping: codes C02.8, C02.9, C05.8, C05.9, C14.0, C14.2, and C14.8; and (5) larynx (includes glottis, supraglottis, and subglottis): codes C32.0 to C32.3 and C32.8 to HEAD & NECK DOI /HED JULY
3 HASHIBE ET AL. TABLE 1. Characteristics of the PLCO cohort and the head and neck cancer cases. Cohort Cases No. of participants % No. of cases % RR 95% CI Total 101, Age* 59 y 34, y 31, y 22, y 12, p value for trend.0008 Sex Male 49, Female 52, Race White, Non-Hispanic 92, Other Education 11 y y or completed high school 23, Post-high school training other than college 13, Some college 21, College graduate 17, Postgraduate 18, p value for trend Marital status Married or living as married 79, Widowed Divorced/separated 10, Never married 3, Missing Occupation Working 40, Retired 43, Other 16, Missing Abbreviations: PLCO, Prostate, Lung, Colorectal, and Ovarian cancer screening trial; RR, risk ratio; CI, confidence interval. *RRs adjusted for sex, race, education, packyears of cigarette smoking, and alcoholic drinks per day. RRs adjusted for age, race, education, packyears of cigarette smoking, and alcoholic drinks per day. RRs adjusted for age, sex, education, packyears of cigarette smoking, and alcoholic drinks per day. RRs adjusted for age, sex, race, packyears of cigarette smoking, and alcoholic drinks per day. RRs adjusted for age, sex, race, education, packyears of cigarette smoking, and alcoholic drinks per day. C32.9. The head and neck cancer cases were diagnosed from the start of the trial up to May The baseline questionnaire included information on age, sex, race, education, marital status, occupation, cigarette smoking (frequency, years), family history of cancer, weight (at age 20, age 50, and current), height, and medical history (high blood pressure, coronary heart disease/ heart attack, stroke, emphysema, chronic bronchitis, diabetes, colorectal polyps, ulcerative colitis, Crohn disease, familial polyposis, arthritis, osteoporosis, Gardner syndrome, hepatitis, cirrhosis, diverticulitis/diverticulosis, gall bladder stones, or inflammation). The diet history questionnaire administered beginning in 1998 included information on numerous food items including fruit and vegetable intake, as well as the alcohol drinking frequency information. The diet questionnaire administered at baseline included the information on physical activity. However, this diet questionnaire was administered only to the intervention arm. Thus, the proportion of participants missing physical activity seems high because the control arm did not complete the baseline diet questionnaire and were not included in the physical activity analysis. We collapsed some of the demographic variable categories to assure that each category had a sufficient number of cases (>5 cases). The percent change in BMI from 50 years to current was estimated with the equation [(current BMI - BMI at 50 years)/bmi at 50 years], following the methods by Park et al. 6 The percent change in BMI from 20 years to current was calculated with a similar equation. Statistical methods We estimated hazard ratios and 95% CIs with the Cox proportional hazards model. Follow-up time was calculated from the age at entry into the study (completion of the baseline questionnaire) until the occurrence of 1 of the following events: diagnosis of head and neck cancer, death, or the end of follow-up. We adjusted on age (continuous), sex, race (categories as shown in Table 1), education (categories as shown in Table 1), cigarette pack-years (categories: never; 1 19 pack-years; pack-years; 40 pack-years) and alcohol drinking frequency (categories: never; <1 916 HEAD & NECK DOI /HED JULY 2013
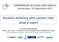
4 TOBACCO, ALCOHOL, BMI, PHYSICAL ACTIVITY, AND HEAD AND NECK CANCER FIGURE 1. Head and neck cancer attributable fractions for tobacco and alcohol use. [Color figure can be viewed in the online issue, which is available at wileyonlinelibrary.com.] drink/day; drinks/day; drinks/day; 4 drinks/day), where appropriate. Attributable fractions were estimated for the established risk factors, tobacco and alcohol, with the equation p c (RR-1)/[p c (RR-1)-1], where p c is the proportion exposed in the cases, and RR is the adjusted risk ratio for the risk factor of interest. 14 The RRs from the multivariate Cox regression models were used. The total AF for tobacco and/or alcohol exposures was estimated with the equation below where AF 01 ¼ AF for never tobacco/ever alcohol users, AF 10 ¼ AF for ever tobacco/never alcohol users, and AF 11 ¼ AF for ever tobacco/ever alcohol users. AF tobacco and/or alcohol (a þ b þ cinfigure1)¼af 01 þ AF 10 þaf 11. We then calculated the AFs for cigarette smoking (AF tobacco ) regardless of alcohol drinking exposure (b þ c in Figure 1), and for alcohol drinking (AF alcohol ) regardless of cigarette smoking exposure (a þ c in Figure 1). Next, we calculated the AF for tobacco AND alcohol (AF tobacco AND alcohol or c in Figure 1) by taking AF tobacco þ AF alcohol -AF tobacco and/or alcohol ¼ (a þ c)þ(b þ c)- (a þ b þ c). The AF for alcohol alone was calculated by taking AF alcohol -AF tobacco AND alcohol ¼ (a þ c) - c. The AF for tobacco alone was calculated by taking AF tobacco - AF tobacco AND alcohol ¼ (b þ c) - c. To assess interactions on the multiplicative scale, we estimated RRs for joint effects (RR 11 ¼ RR for ever TABLE 2. Tobacco smoking, alcohol drinking, and the risk of head and neck cancer in the PLCO cohort. Cohort Cases RR 95% CI p c AF Cigarette status* Never 48, % Current % 27.3% Former 43, % 21.5% Missing 12 0 AF Total ¼ 48.8% Cigarette frequency* Never smoked cigarettes 48, % 1 19 cigarettes/d 13, % 0.6% cigarettes/d 30, % 28.2% 40 cigarettes/d % 20.5% Missing AF Total ¼ 49.3% p value for trend <.0001 Cigarette duration* Never smoked cigarettes 48, % 1 19 y 17, % 2.8% y 23, % 18.6% 40 y 11, % 27.1% Missing AF Total ¼ 48.5% p value for trend <.0001 Cigarette pack-years* Never smoked cigarettes 48, % 1 19 pack-years 19, % 3.5% pack-years 14, % 9.1% 40 pack-years 17, % 36.4% Missing AF Total ¼ 49.0% p value for trend <.0001 Alcohol drinking frequency Non-drinker 27, % <1 drink/d 54, % -6.0% drinks/d 11, % -2.0% drinks/d % 5.6% 4 drinks/d % 10.0% p for trend <.0001 AF Total ¼ 15.6% Abbreviations: PLCO, Prostate, Lung, Colorectal, and Ovarian cancer screening trial; RR, risk ratio; CI, confidence interval; p c, prevalence in cases; AF, attributable fraction. * RRs adjusted for age, sex, race, education, and alcoholic drinks per day. RRs adjusted for age, sex, race, education, and pack-years of cigarette smoking. The negative AF does not suggest that alcohol prevented any cancers; the RRs for alcohol did not suggest a statistically significant protective association. HEAD & NECK DOI /HED JULY
5 HASHIBE ET AL. TABLE 3. Tobacco smoking, alcohol drinking, and the risk of head and neck cancer in the PLCO cohort. Cohort Cases RR 95% CI p c AF Cigarette smoking Alcohol drinking No No 16, * Yes No 10, % 12.5% No Yes 31, % 6.1% Yes Yes 41, % 47.5% Tobacco and/or alcohol ¼ (aþbþc) ¼ 66.0% Multiplicative interaction parameter* 0.59 ( ) Ever alcohol drinking No 27, Yes 73, % 15.3% (aþc) Ever cigarette smoking No 48, Yes 52, % 51.3% (bþc) c ¼ Tobacco and alcohol ¼ (aþc)þ(bþc)-(aþbþc) ¼ 0.9% a ¼ Alcohol alone ¼ (aþc)-c ¼ 14.7% b ¼ Tobacco alone ¼ (bþc)-c ¼ 50.5% aþbþc ¼ 66.0% Cigarette smoking frequency Alcohol drinking frequency Never smoked Nondrinker 16, * 4.5% 1 19 cigarettes/d Nondrinker % -0.1% 20 cigarettes/d Nondrinker % 12.8% Never smoked <2 drink/d 29, % 5.9% 1 19 cigarettes/d <2 drink/d 13, % 2.3% 20 cigarettes/d <2 drink/d 21, % 21.3% Never smoked 2 drinks/d % 0.3% 1 19 cigarettes/d 2 drinks/d % 4.9% 20 cigarettes/d 2 drinks/d % 19.0% Missing TOTAL 66.6% Abbreviations: PLCO, Prostate, Lung, Colorectal, and Ovarian cancer screening trial; RR, risk ratio; CI, confidence interval; p c, prevalence in cases; AF, attributable fraction. * RRs adjusted for age, sex, race, education. RRs adjusted for age, sex, race, education and ever cigarette smoking. RRs adjusted for age, sex, race, education and ever alcohol drinking. tobacco/ever alcohol use, RR 01 ¼ RR for never tobacco/ ever alcohol use, RR 10 ¼ RR for ever tobacco/never alcohol use). The multiplicative interaction parameters and 95% CIs [w ¼ RR 11 /(RR 01 *RR 10 )] were also estimated by including variables for ever alcohol use, ever tobacco use, and a product term (equivalent to the multiplicative interaction parameter) of those 2 variables in the Cox regression model. w >1 is suggestive of a joint effect that is greater than expected under the multiplicative model. RESULTS Of the 101,182 individuals in the PLCO trial cohort eligible for the current study, 177 developed head and neck cancers. The subsite distribution was: 42 oral cavity cancers (23.7%), 43 oropharyngeal cancers (24.3%), 7 hypopharyngeal cancers (4.0%), 72 laryngeal cancers (40.7%), and 13 head and neck unspecified site of cancer (7.3%). Older individuals and women had reduced risks of head and neck cancer (Table 1). The inverse association with age was observed for oropharyngeal and laryngeal cancer, but not for hypopharyngeal or oral cavity cancers (results not shown). In the overall cohort, individuals in the older age groups had lower proportions of ever smokers and ever alcohol drinkers (chi-square p value <.001 for both cigarette smoking and alcohol drinking; results not shown). Socioeconomic factors, including education and occupation, were not associated with head and neck cancer risk in this population. Marital status was also not correlated with head and neck cancer risk. Current cigarette smoking conferred higher risks of head and neck cancer (RR ¼ 6.51; 95% CI ¼ ) than former cigarette smoking (RR ¼ 1.83; 95% CI ¼ ) (Table 2). Clear dose response trends were observed for cigarette smoking frequency, duration, and pack-years (p for all trends <.0001). An increasing number of alcohol drinks consumed per day was also clearly associated with a dose response trend on head and neck cancer risk (p for trend <.0001). An increase in head and neck cancer risk was not observed for individuals who drank less than 2 alcoholic drinks per day. An approximate 2-fold increase in head and neck cancer risk was detected for individuals who drank 2 or more alcoholic drinks per day. Some negative AFs were observed, but this does not suggest that alcohol prevented any cancers since the RRs did not suggest a statistically significant protective association. The AF for ever smoking was approximately 49%, whereas the AF for ever alcohol drinking was 16%. The interaction between tobacco and alcohol and the AFs for tobacco alone, alcohol alone, and combined are presented in Table 3. The multiplicative interaction 918 HEAD & NECK DOI /HED JULY 2013
6 TOBACCO, ALCOHOL, BMI, PHYSICAL ACTIVITY, AND HEAD AND NECK CANCER TABLE 4. BMI, height, physical activity, and the risk of head and neck cancer in the PLCO cohort. Cohort Cases RR* 95% CI BMI at age 20 <18.5 kg/m kg/m 2 76, kg/m 2 13, >30.0 kg/m Missing p value for trend.4738 BMI at age 50 <18.5 kg/m kg/m 2 46, kg/m 2 39, >30.0 kg/m 2 13, Missing p value for trend.1382 BMI current <18.5 kg/m kg/m 2 32, kg/m 2 42, >30.0 kg/m 2 23, Missing p value for trend.0995 Height Quartile 1 20, Quartile 2 26, Quartile 3 23, Quartile 4 30, p value for trend.4526 Percent BMI change from 50 years to current <10% (BMI loss) % to <10% (stable) 69, % (BMI gain) 26, Missing p value for trend.6965 Percent BMI change from 20 years to current <10% (BMI loss) % to <10% (stable) 22, % (BMI gain) 75, Missing p value for trend.2364 Hours spent in vigorous activity at age 40 <1 hr/wk 13, hr/wk 12, hr/wk 20, Missing 55, p value for trend.1544 Hours spent in vigorous activity now 0 <1 hr/wk 14, hr/wk 12, hr/wk 18, Missing 54, p value for trend.0312 Abbreviations: BMI, body mass index; PLCO, Prostate, Lung, Colorectal, and Ovarian cancer screening trial; RR, risk ratio; CI, confidence interval. * Adjusted for age, sex, race, education, drinking frequency, and tobacco pack-years. Physical activity information was from the diet questionnaire administered at baseline only to the intervention arm. The proportion of participants missing this information seems high but because this is due to the original study design where the control arm did not complete the diet questionnaire. parameter (w ¼ 0.59; 95% CI ¼ ) did not suggest an interaction between cigarette smoking and alcohol drinking on the multiplicative scale. The total percentage of head and neck cancer cases that could be attributed to tobacco and/or alcohol was 66%. The AFs were 50.5% for tobacco alone, 14.7% for alcohol alone, and 0.9% for tobacco and alcohol combined. The AF for ever alcohol drinking, regardless of tobacco smoking, was 15.3%. The AF for ever cigarette smoking, regardless of alcohol drinking, was 51.3%. When stratified into categories by cigarette smoking and alcohol drinking frequencies, smoking 20 or more cigarettes per day, regardless of alcohol drinking frequency, accounted for the majority of head and neck cancer cases (12.8% þ 21.3% þ 19.0% ¼ HEAD & NECK DOI /HED JULY
7 HASHIBE ET AL. TABLE 5. Family history of cancer and the risk of head and neck cancer in the PLCO cohort. No Yes Cohort Cases Cohort Cases RR* 95% CI Any cancer 44, , ( ) Head and neck cancer 96, ( ) Lung cancer 87, , ( ) Upper GI cancer 93, ( ) Breast cancer 86, , ( ) Colorectal cancer 87, , ( ) Leukemia 95, ( ) Lymphoma 91, ( ) Ovarian cancer 95, ( ) Prostate cancer 91, ( ) Abbreviations: PLCO, Prostate, Lung, Colorectal, and Ovarian cancer screening trial; RR, risk ratio; CI, confidence interval; GI, gastrointestinal. * Adjusted for age, sex, race, education, drinking frequency and tobacco pack-years. 53.1%). Figure 1 shows the attributable fractions of tobacco and alcohol as a Venn diagram. BMI at age 20, BMI at age 50, current BMI, and height were not associated with head and neck cancer risk (Table 4). The percent change in BMI from age 50 to time of interview and from age 20 to time of interview were also not associated with head and neck cancer risk. We also assessed percent change in BMI with a 20% cutoff, instead of the 10% cutoff, and did not observe any statistically significant associations. Although physical activity at age 40 was not associated with head and neck cancer risk, increased physical activity at the time of interview was associated with a decrease in head and neck cancer risk. Individuals spending 3 or more hours per week on vigorous activity had a 40% reduction in head and neck cancer risk (RR ¼ 0.58; 95% CI ¼ ), after adjustment for smoking and drinking. When we imputed the mean value of 1 to 2 hours per week for all study subjects missing physical activity at age 40, the RRs were 0.59 (95% CI ¼ ) for 1 to 2 hours/week, and 0.66 (95% CI ¼ ) for 3 hours/week (data not shown). Imputation for physical activity now resulted in RRs of 0.60 (95% CI ¼ ) for 1 to 2 hours/week, and 0.74 (95% CI ¼ ) for 3 hours/week. Family history of cancer overall and family history of specific cancer sites was largely not associated with head and neck cancer risk, other than family history of colorectal cancer (RR ¼ 1.69; 95% CI ¼ ; Table 5). In terms of history of previous disease (before cancer diagnosis), having had chronic bronchitis, cirrhosis, and emphysema were associated with an increased risk of head and neck cancer (Table 6). Additional adjustments on fruit and vegetable intake, and cigar and pipe smoking did not change the results materially, nor did removing the adjustment for race or education. DISCUSSION In our analysis of 177 head and neck cancer cases, we observed that younger age increased risk, whereas education, occupation, and marital status were not associated with head and neck cancer risk. The proportion of head and neck cancer cases attributed to tobacco and/or alcohol was 66% for this population. Neither BMI at different time points in an individual s life nor changes in BMI were correlated with head and neck cancer risk, but physical activity at increasing hours per week conferred a reduced risk of head and neck cancer. Family history of TABLE 6. Previous disease history and the risk of head and neck cancer in the PLCO cohort. No Yes Cohort Cases Cohort Cases RR* 95% CI Arthritis 62, , Chronic bronchitis 96, Cirrhosis 100, Diabetes 93, Diverticulitis/diverticulosis 93, Emphysema 98, Gall bladder stones or inflammation 89, , Coronary heart disease/heart attack 92, Hepatitis 97, Hypertension 67, , Osteoporosis 95, Colorectal polyps 93, Stroke 98, Abbreviations: PLCO, Prostate, Lung, Colorectal, and Ovarian cancer screening trial; RR, risk ratio; CI, confidence interval. * Adjusted for age, sex, race, education, drinking frequency, and tobacco pack-years. 920 HEAD & NECK DOI /HED JULY 2013
8 TOBACCO, ALCOHOL, BMI, PHYSICAL ACTIVITY, AND HEAD AND NECK CANCER colorectal cancer, history of chronic bronchitis, cirrhosis, and emphysema were associated with an increased risk of head and neck cancer. The inverse association with age was unexpected because older age groups have a higher incidence of head and neck cancer. 15 In the overall cohort, the older age groups had a lower proportion of smokers and alcohol drinkers. We adjusted for pack-years of cigarette smoking and alcohol drinks per day, but perhaps there was residual confounding due to these factors. Additionally, it is possible that these results reflect the increasing incidence of some head and neck cancer, specifically oropharyngeal cancer. The increase is largely occurring among younger individuals, 16 possibly due to the role of HPV infection. The lack of association with education, a marker of socioeconomic status, was also unexpected. Previous studies have shown that lower socioeconomic status is associated with an increased risk of head and neck cancer. 17 The PLCO cohort was overall well educated, however, with 58% having had at least some college education. This may have limited the range of socioeconomic status, making the association more modest and difficult to detect. The AF for tobacco and/or alcohol of 66% was greater than that reported by the INHANCE consortium for North America (AF ¼ 50.5%), suggesting that the INHANCE AFs were not biased away from the null due to recall bias. The INHANCE AFs were 4.3% for alcohol alone, 22.6% for tobacco alone, and 23.5% for tobacco and alcohol combined, whereas our corresponding AFs were 14.7%, 50.5%, and 0.9%, respectively. Thus, our AFs for tobacco alone and alcohol alone were higher, whereas our AF for tobacco and alcohol combined was substantially lower. This is reflected in the significant interaction detected in the INHANCE data (w ¼ 1.98; 95% CI ¼ ) in contrast to our current data (w ¼ 0.59; 95% CI ¼ ). Our study of 177 head and neck cancer cases may not have had sufficient statistical power to detect a more than multiplicative interaction between tobacco and alcohol. Indeed, in the INHANCE analysis, only 8 of the 17 case-control studies with case sample sizes ranging from 180 to 2188 had sufficient statistical power to detect an interaction on the multiplicative scale. Another source of difference in the AF for tobacco and alcohol between the INHANCE and PLCO studies may be that our cases have been diagnosed more recently, from 1999 to 2009, whereas 5 of the 8 INHANCE casecontrol studies from North America had been conducted in the 80s and 90s. There may be a risk profile change occurring over generations of cohorts. In terms of the age distribution of cases, the INHANCE cases had a higher proportion in the younger and older age groups (54.2% 59 y; 16.9% y; 13.9% y; and 15% 70 y), whereas the PLCO case group was largely in their 60s. In terms of the study location, the North American studies from INHANCE were based in New York, Seattle, Iowa, North Carolina, Tampa, Los Angeles, Texas, and Boston. It is difficult to predict whether the age distribution and the study location also contribute to the differences in AFs between PLCO and INHANCE because the prevalences in tobacco and alcohol may differ in these different age and location groups. Regardless of the differences in AFs, it is clear that cigarette smoking is the most important risk factor for head and neck cancer in the PLCO population. Individuals who smoked 20 or more cigarettes per day accounted for 53.1% of head and neck cancer cases. Neither BMI at any age nor changes in BMI over an individual s lifetime was associated with head and neck cancer risk. It is possible that our study did not have enough statistical power to detect reduced risks in the obese or increased risks in the underweight individuals. On the other hand, increasing hours per week of physical activity was protective against head and neck cancer, consistent with results from the NIH-AARP cohort study including 1249 head and neck cancer cases. 7 Leitzmann et al 7 reported a suggestive association (RR ¼ 0.89; 95% CI ¼ ) for physical activity 5 or more times per week, after adjustment for tobacco smoking and alcohol drinking habits. The INHANCE consortium pooled analysis, including 2383 cases and 5674 controls, reported a risk reduction of approximately 20% (OR ¼ 0.78; 95% CI ¼ ) for medium physical activity compared to none or low physical activity. 8 In our study, whereas higher levels of current physical activity were protective, physical activity level at age 40 was not associated with head and neck cancer risk. Perhaps because physical activity patterns can change over time, physical activity now (which was at the cohort recruitment between 1992 and 2001 for year olds), reflected their overall physical activity status more closely. The risk estimates we obtained when we imputed values for the subjects with missing values were supportive of an inverse association, although these results should be interpreted with caution because a little more than half of the subjects were assigned imputed values. Only family history of colorectal cancer was associated with increased risk of head and neck cancer. We may not have had enough statistical power to detect family history of head and neck cancer as a risk factor. For disease history, we did not observe any association between diabetes and head and neck cancer risk, although we observed elevated RRs for chronic bronchitis, cirrhosis, and emphysema. These 3 diseases share etiology with head and neck cancer; smoking is a risk factor for chronic bronchitis 18 and emphysema, 19 whereas alcohol is a risk factor for cirrhosis. 20 Thus, it is possible that the observed associations were due to residual confounding, even though we adjusted for both cigarette smoking and alcohol drinking in our analysis. A limitation of our study includes the relatively small sample size, which may have resulted in a lack of statistical power to detect interactions on the multiplicative scale. Our null results for BMI and for family history of head and neck cancer may also possibly be due to the low statistical power. We were also unable to conduct stratified analysis for nonsmokers and nondrinkers to assess residual confounding by tobacco and alcohol. However, we were able to adjust all estimates on pack-years of cigarette smoking and frequency of alcohol drinking. We also did not have data on HPV, a major risk factor for cancers of the oropharynx. Analysis by subsites would have been of interest as well, but each subsite group was too small in sample size. The PLCO cohort participants seem to be more educated than the general U.S. population with 36.3% having HEAD & NECK DOI /HED JULY
9 HASHIBE ET AL. completed a college degree. Because higher education is associated with lower tobacco use, 21 the proportion of smokers may have been underestimated. The proportion of current smokers (9.2%) in this cohort was fairly low, but the proportion of former smokers was fairly high (43.0%), thus the total proportion of ever smokers may not be lower than expected. The major strength of our study was the prospective cohort design which eliminates recall bias and temporal ambiguity. In a case-control study, the cases may recall with more effort their tobacco and alcohol exposure histories and possibly overestimate these exposures because they have been diagnosed with cancer, leading to bias away from the null for tobacco and alcohol risk estimates. However, in a cohort study design such as our current study, the study participants are interviewed about their tobacco and alcohol habits before cancer diagnoses, thus making it impossible for the cases to recall their exposures differently from the subjects who did not have cancer. A concern in a cohort study may be that the exposures assessed at baseline may change over time. However, in our cohort, the mean follow-up time was years and, because the expected latent period may be 10 to 20 years, we believe that the window of time in which the exposure was important, was captured. Additionally, because of the population-based design, our AF calculations may reflect the population more appropriately compared to a case-control study which can be subject to more selection bias of the control series. In summary, our results support the previous INHANCE consortium results that tobacco and alcohol account for the majority of head and neck cancer cases in the United States, but at a lower proportion than in Europe or Latin America. BMI at specific times in an individual s lifetime and change in BMI were not associated with head and neck cancer, in contrast to results from the case-control studies, although low statistical power may have played a role in this observation. Increasing hours of physical activity was protective, whereas a history of chronic bronchitis, cirrhosis, and emphysema increased head and neck cancer risk. Results from other cohorts are necessary to confirm our null results on BMI and our observed associations for physical activity and history of previous disease. Analysis of European, Latin American, and Asian cohorts for the proportion of cases attributable to tobacco and alcohol would be of interest as well. Acknowledgements We thank the NIH PLCO study group for allowing us to use the data. REFERENCES 1. American Cancer Society. Cancer facts & figures Atlanta: American Cancer Society; Brown LM, Check DP, Devesa SS. Oropharyngeal cancer incidence trends: diminishing racial disparities. Cancer Causes Control 2011;22: Hashibe M, Brennan P, Chuang SC, et al. Interaction between tobacco and alcohol use and the risk of head and neck cancer: pooled analysis in the International Head and Neck Cancer Epidemiology Consortium. Cancer Epidemiol Biomarkers Prev 2009;18: Ribeiro KB, Levi JE, Pawlita M, et al. Low human papillomavirus prevalence in head and neck cancer: results from two large case-control studies in high-incidence regions. Int J Epidemiol 2011;40: Gaudet MM, Olshan AF, Chuang SC, et al. Body mass index and risk of head and neck cancer in a pooled analysis of case-control studies in the International Head and Neck Cancer Epidemiology (INHANCE) Consortium. Int J Epidemiol 2010;39: Park SL, Lee YC, Marron M, et al. The association between change in body mass index and upper aerodigestive tract cancers in the ARCAGE project: multicenter case-control study. Int J Cancer 2011;128: Leitzmann MF, Koebnick C, Freedman ND, et al. Physical activity and head and neck cancer risk. Cancer Causes Control 2008;19: Nicolotti N, Chuang SC, Cadoni G, et al. Recreational physical activity and risk of head and neck cancer: a pooled analysis within the International Head and Neck Cancer Epidemiology (INHANCE) Consortium. Eur J Epidemiol 2011;26: Na HK, Oliynyk S. Effects of physical activity on cancer prevention. Ann N Y Acad Sci 2011;1229: Negri E, Boffetta P, Berthiller J, et al. Family history of cancer: pooled analysis in the International Head and Neck Cancer Epidemiology Consortium. Int J Cancer 2009;124: Goldgar DE, Easton DF, Cannon Albright LA, Skolnick MH. Systematic population-based assessment of cancer risk in first-degree relatives of cancer probands. J Natl Cancer Inst 1994;86: Dikshit RP, Ramadas K, Hashibe M, Thomas G, Somanathan T, Sankaranarayanan R. Association between diabetes mellitus and pre-malignant oral diseases: a cross sectional study in Kerala, India. Int J Cancer 2006; 118: Stott Miller M, Chen C, Chuang SC, et al. History of diabetes and risk of head and neck cancer: a pooled analysis from the International Head and Neck Cancer Epidemiology Consortium. Cancer Epidemiol Biomarkers Prev 2012;21: Rothman KJ, Greenland S, Lash TL. Modern epidemiology, 3rd ed. Philadelphia: Wolters Kluwer, Lippincott Williams and Wilkins, Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. GLOBO- CAN 2008 v1.2, Cancer incidence and mortality worldwide: IARC CancerBase No. 10 [Internet]. Lyon, France: International Agency for Research on Cancer; Available at: Accessed August 4, Shiboski CH, Schmidt BL, Jordan RC. Tongue and tonsil carcinoma: increasing trends in the U.S. population ages years. Cancer 2005; 103: Conway DI, Petticrew M, Marlborough H, Berthiller J, Hashibe M, Macpherson LM. Socioeconomic inequalities and oral cancer risk: a systematic review and meta-analysis of case-control studies. Int J Cancer 2008;122: Ball P. Epidemiology and treatment of chronic bronchitis and its exacerbations. Chest 1995;108(2 Suppl):43S 52S. 19. Mannino DM, Buist AS. Global burden of COPD: risk factors, prevalence, and future trends. Lancet 2007;370: Rehm J, Taylor B, Mohapatra S, et al. Alcohol as a risk factor for liver cirrhosis: a systematic review and meta-analysis. Drug Alcohol Rev 2010;29: Reid JL, Hammond D, Boudreau C, Fong GT, Siahpush M; ITC Collaboration. Socioeconomic disparities in quit intentions, quit attempts, and smoking abstinence among smokers in four western countries: findings from the International Tobacco Control Four Country Survey. Nicotine Tob Res 2010;12 Suppl:S HEAD & NECK DOI /HED JULY 2013
Incidence of HPV-Associated Head and Neck Cancers by Sub-site Among Diverse Racial/Ethnic Populations in the United States
 Incidence of HPV-Associated Head and Neck Cancers by Sub-site Among Diverse Racial/Ethnic Populations in the United States Louisiana Tumor Registry LSUHSC School of Public Health Lauren Cole, MPH Linda
Incidence of HPV-Associated Head and Neck Cancers by Sub-site Among Diverse Racial/Ethnic Populations in the United States Louisiana Tumor Registry LSUHSC School of Public Health Lauren Cole, MPH Linda
Nicotine Dependence Phenotype, Time to First Cigarette, and Risk of Head and Neck Cancer
 Nicotine Dependence Phenotype, Time to First Cigarette, and Risk of Head and Neck Cancer Joshua E. Muscat, PhD 1 ; Kwangmi Ahn, PhD 2 ; John P. Richie Jr, PhD 3 ; and Steven D. Stellman, PhD 4 BACKGROUND:
Nicotine Dependence Phenotype, Time to First Cigarette, and Risk of Head and Neck Cancer Joshua E. Muscat, PhD 1 ; Kwangmi Ahn, PhD 2 ; John P. Richie Jr, PhD 3 ; and Steven D. Stellman, PhD 4 BACKGROUND:
Smoking and Mortality in the Japan Collaborative Cohort Study for Evaluation of Cancer (JACC)
 Smoking and Mortality SECTION 6 Smoking and Mortality in the Japan Collaborative Cohort Study for Evaluation of Cancer (JACC) Kotaro Ozasa Abstract In the JACC study, risk of death with all cancers and
Smoking and Mortality SECTION 6 Smoking and Mortality in the Japan Collaborative Cohort Study for Evaluation of Cancer (JACC) Kotaro Ozasa Abstract In the JACC study, risk of death with all cancers and
8/10/2012. Education level and diabetes risk: The EPIC-InterAct study AIM. Background. Case-cohort design. Int J Epidemiol 2012 (in press)
 Education level and diabetes risk: The EPIC-InterAct study 50 authors from European countries Int J Epidemiol 2012 (in press) Background Type 2 diabetes mellitus (T2DM) is one of the most common chronic
Education level and diabetes risk: The EPIC-InterAct study 50 authors from European countries Int J Epidemiol 2012 (in press) Background Type 2 diabetes mellitus (T2DM) is one of the most common chronic
Consideration of Anthropometric Measures in Cancer. S. Lani Park April 24, 2009
 Consideration of Anthropometric Measures in Cancer S. Lani Park April 24, 2009 Presentation outline Background in anthropometric measures in cancer Examples of anthropometric measures and investigating
Consideration of Anthropometric Measures in Cancer S. Lani Park April 24, 2009 Presentation outline Background in anthropometric measures in cancer Examples of anthropometric measures and investigating
Oral Cavity and Oropharynx Cancer Trends
 Oral Cavity and Oropharynx Cancer Trends Darien Weatherspoon, DDS, MPH Diplomate, American Board of Dental Public Health Program Officer, National Institute of Dental and Craniofacial Research National
Oral Cavity and Oropharynx Cancer Trends Darien Weatherspoon, DDS, MPH Diplomate, American Board of Dental Public Health Program Officer, National Institute of Dental and Craniofacial Research National
Outline. Background on the American Institute for Cancer Research (AICR) and Continuous Update Project (CUP)
 Alcohol and Cancer: State of the Science Christine L. Sardo Molmenti PhD, MPH, RD AICR Science Analyst Assistant Professor Hofstra-Northwell School of Medicine Northwell Health April 25, 2017 Outline Background
Alcohol and Cancer: State of the Science Christine L. Sardo Molmenti PhD, MPH, RD AICR Science Analyst Assistant Professor Hofstra-Northwell School of Medicine Northwell Health April 25, 2017 Outline Background
Active and Involuntary Tobacco Smoking and Upper Aerodigestive Tract Cancer Risks in a Multicenter Case-Control Study
 3353 Active and Involuntary Tobacco Smoking and Upper Aerodigestive Tract Cancer Risks in a Multicenter Case-Control Study Yuan-Chin Amy Lee, 1,2 Manuela Marron, 1 Simone Benhamou, 3,4 Christine Bouchardy,
3353 Active and Involuntary Tobacco Smoking and Upper Aerodigestive Tract Cancer Risks in a Multicenter Case-Control Study Yuan-Chin Amy Lee, 1,2 Manuela Marron, 1 Simone Benhamou, 3,4 Christine Bouchardy,
Incidence and mortality of laryngeal cancer in China, 2011
 Original Article Incidence and mortality of laryngeal cancer in China, 2011 Lingbin Du 1, Huizhang Li 1, Chen Zhu 1, Rongshou Zheng 2, Siwei Zhang 2, Wanqing Chen 2 1 Zhejiang Provincial Office for Cancer
Original Article Incidence and mortality of laryngeal cancer in China, 2011 Lingbin Du 1, Huizhang Li 1, Chen Zhu 1, Rongshou Zheng 2, Siwei Zhang 2, Wanqing Chen 2 1 Zhejiang Provincial Office for Cancer
Trends in oral and oropharyngeal (mouth) cancer incidence in Wales,
 Trends in oral and oropharyngeal (mouth) cancer incidence in Wales, 2001-2013 November 2015 Dental Public Health Team, Public Health Wales Welsh Cancer Intelligence and Surveillance Unit, Public Health
Trends in oral and oropharyngeal (mouth) cancer incidence in Wales, 2001-2013 November 2015 Dental Public Health Team, Public Health Wales Welsh Cancer Intelligence and Surveillance Unit, Public Health
Alcohol and Cancer Risks
 Alcohol and Cancer Risks A guide for health professionals Scottish Health Action on Alcohol Problems Introduction Alcohol and Cancer Risks: A Guide for Health Professionals This guide has been produced
Alcohol and Cancer Risks A guide for health professionals Scottish Health Action on Alcohol Problems Introduction Alcohol and Cancer Risks: A Guide for Health Professionals This guide has been produced
RISK FACTORS FOR MULTIPLE ORAL PREMALIGNANT LESIONS
 Int. J. Cancer: 107, 285 291 (2003) 2003 Wiley-Liss, Inc. Publication of the International Union Against Cancer RISK FACTORS FOR MULTIPLE ORAL PREMALIGNANT LESIONS Gigi THOMAS 1, Mia HASHIBE 2,3 *, Binu
Int. J. Cancer: 107, 285 291 (2003) 2003 Wiley-Liss, Inc. Publication of the International Union Against Cancer RISK FACTORS FOR MULTIPLE ORAL PREMALIGNANT LESIONS Gigi THOMAS 1, Mia HASHIBE 2,3 *, Binu
Smoking, human papillomavirus infection, and p53 mutation as risk factors in oropharyngeal cancer: a case-control study
 RESEARCH FUND FOR THE CONTROL OF INFECTIOUS DISEASES Smoking, human papillomavirus infection, and p53 as risk factors in oropharyngeal cancer: a case-control study PKS Chan *, JSY Chor, AC Vlantis, TL
RESEARCH FUND FOR THE CONTROL OF INFECTIOUS DISEASES Smoking, human papillomavirus infection, and p53 as risk factors in oropharyngeal cancer: a case-control study PKS Chan *, JSY Chor, AC Vlantis, TL
ARTICLE. Background. Methods. Results. Conclusions
 ARTICLE Alcohol Drinking in Never Users of Tobacco, Cigarette Smoking in Never Drinkers, and the Risk of Head and Neck Cancer: Pooled Analysis in the International Head and Neck Cancer Epidemiology Consortium
ARTICLE Alcohol Drinking in Never Users of Tobacco, Cigarette Smoking in Never Drinkers, and the Risk of Head and Neck Cancer: Pooled Analysis in the International Head and Neck Cancer Epidemiology Consortium
1. Study Title. Exercise and Late Mortality in 5-Year Survivors of Childhood Cancer: a Report from the Childhood Cancer Survivor Study.
 CCSS Analysis Concept Proposal Exercise, Mortality, & Childhood Cancer 1 1. Study Title. Exercise and Late Mortality in 5-Year Survivors of Childhood Cancer: a Report from the Childhood Cancer Survivor
CCSS Analysis Concept Proposal Exercise, Mortality, & Childhood Cancer 1 1. Study Title. Exercise and Late Mortality in 5-Year Survivors of Childhood Cancer: a Report from the Childhood Cancer Survivor
/Webpages/zhang/chinese-full full- program.htm
 http://www.ph.ucla.edu/epi/faculty/zhang /Webpages/zhang/chinese-full full- program.htm Cancer Incidence and Mortality and Risk Factors in the World Zuo-Feng Zhang, M.D., Ph.D. Fogarty International Training
http://www.ph.ucla.edu/epi/faculty/zhang /Webpages/zhang/chinese-full full- program.htm Cancer Incidence and Mortality and Risk Factors in the World Zuo-Feng Zhang, M.D., Ph.D. Fogarty International Training
Viral hepatitis and Hepatocellular Carcinoma
 Viral hepatitis and Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
Viral hepatitis and Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
Health Promotion, Screening, & Early Detection
 OCN Test Content Outline 2018 Health Promotion, Screening, & Early Detection Kelley Blake MSN, RN, AOCNS, OCN UW Medicine/Valley Medical Center I. Care Continuum 19% A. Health promotion & disease prevention
OCN Test Content Outline 2018 Health Promotion, Screening, & Early Detection Kelley Blake MSN, RN, AOCNS, OCN UW Medicine/Valley Medical Center I. Care Continuum 19% A. Health promotion & disease prevention
Mortality in relation to alcohol consumption: a prospective study among male British doctors
 IJE vol.34 no.1 International Epidemiological Association 2005; all rights reserved. International Journal of Epidemiology 2005;34:199 204 Advance Access publication 12 January 2005 doi:10.1093/ije/dyh369
IJE vol.34 no.1 International Epidemiological Association 2005; all rights reserved. International Journal of Epidemiology 2005;34:199 204 Advance Access publication 12 January 2005 doi:10.1093/ije/dyh369
BECAUSE OF THE BENEFIT OF
 ORIGINAL INVESTIGATION Dairy Food, Calcium, and Risk of Cancer in the NIH-AARP Diet and Health Study Yikyung Park, ScD; Michael F. Leitzmann, MD; Amy F. Subar, PhD; Albert Hollenbeck, PhD; Arthur Schatzkin,
ORIGINAL INVESTIGATION Dairy Food, Calcium, and Risk of Cancer in the NIH-AARP Diet and Health Study Yikyung Park, ScD; Michael F. Leitzmann, MD; Amy F. Subar, PhD; Albert Hollenbeck, PhD; Arthur Schatzkin,
Smoking categories. Men Former smokers. Current smokers Cigarettes smoked/d ( ) 0.9 ( )
 Table 2.44. Case-control studies on smoking and colorectal Colon Rectal Colorectal Ji et al. (2002), Shanghai, China Cases were permanent Shanghai residents newly diagnosed at ages 30-74 years between
Table 2.44. Case-control studies on smoking and colorectal Colon Rectal Colorectal Ji et al. (2002), Shanghai, China Cases were permanent Shanghai residents newly diagnosed at ages 30-74 years between
The international health care burden of cancers of the gastrointestinal tract and liver
 The international health care burden of cancers of the gastrointestinal tract and liver William R. Brown 1*, Dennis J. Ahnen 2 1 Department of Medicine, University of Colorado School of Medicine, Denver,
The international health care burden of cancers of the gastrointestinal tract and liver William R. Brown 1*, Dennis J. Ahnen 2 1 Department of Medicine, University of Colorado School of Medicine, Denver,
what s new? CONFERENCE ALCOHOL AND HEALTH Amsterdam, 23 September 2010
 CONFERENCE ALCOHOL AND HEALTH Amsterdam, 23 September 2010 Alcohol drinking and cancer risk: what s new? Dr Paule LATINO-MARTEL UMR U 557 Inserm, U 1125 Inra, Cnam, Université Paris 13; CRNH-IdF, France
CONFERENCE ALCOHOL AND HEALTH Amsterdam, 23 September 2010 Alcohol drinking and cancer risk: what s new? Dr Paule LATINO-MARTEL UMR U 557 Inserm, U 1125 Inra, Cnam, Université Paris 13; CRNH-IdF, France
Alcohol and tobacco, and the risk of cancers of the upper aerodigestive tract in Latin America: a case control study
 Cancer Causes Control (2011) 22:1037 1046 DOI 10.1007/s10552-011-9779-7 ORIGINAL PAPER Alcohol and tobacco, and the risk of cancers of the upper aerodigestive tract in Latin America: a case control study
Cancer Causes Control (2011) 22:1037 1046 DOI 10.1007/s10552-011-9779-7 ORIGINAL PAPER Alcohol and tobacco, and the risk of cancers of the upper aerodigestive tract in Latin America: a case control study
Alcol e tumori con focus sulle basse dosi
 Alcol e tumori con focus sulle basse dosi Carlo La Vecchia Department of Epidemiology, Istituto Mario Negri Department of Clinical Sciences and Community Health, Università degli Studi di Milano 1 Cancers
Alcol e tumori con focus sulle basse dosi Carlo La Vecchia Department of Epidemiology, Istituto Mario Negri Department of Clinical Sciences and Community Health, Università degli Studi di Milano 1 Cancers
Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH
 Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH 1 ABSTRACT This study presents relative mortality risks by alcohol consumption level for the U.S. population, using
Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH 1 ABSTRACT This study presents relative mortality risks by alcohol consumption level for the U.S. population, using
Accuracy of the SEER HPV status site specific factor 10 (SSF-10) variable for head and neck cancer (HNC) cases in Iowa:
 Accuracy of the SEER HPV status site specific factor 10 (SSF-10) variable for head and neck cancer (HNC) cases in Iowa: 2010-2014 Amanda Kahl, MPH Mary Charlton, PhD, Nitin Pagedar, MD, MPH, Steven Sperry,
Accuracy of the SEER HPV status site specific factor 10 (SSF-10) variable for head and neck cancer (HNC) cases in Iowa: 2010-2014 Amanda Kahl, MPH Mary Charlton, PhD, Nitin Pagedar, MD, MPH, Steven Sperry,
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 1.393, ISSN: , Volume 2, Issue 2, March 2014
 INCIDENCE OF PRIMARY HEAD AND NECK CANCERS AT B K L W HOSPITAL & RURAL MEDICAL COLLEGE, A TERTIARY CARE CENTRE IN KONKAN, MAHARASHTRA RAJASHREE A KULKARNI* MAHESH S PATIL** *Assistant Professor, Dept.
INCIDENCE OF PRIMARY HEAD AND NECK CANCERS AT B K L W HOSPITAL & RURAL MEDICAL COLLEGE, A TERTIARY CARE CENTRE IN KONKAN, MAHARASHTRA RAJASHREE A KULKARNI* MAHESH S PATIL** *Assistant Professor, Dept.
International Agency for Research on Cancer Lyon, France
 Global Burden of Cancer in Attributable to Alcohol Consumption International Agency for Research on Cancer Lyon, France Kevin D Shield (Shieldk@fellow.iarc.fr), Pietro Ferrari, Jacques Ferlay, Freddie
Global Burden of Cancer in Attributable to Alcohol Consumption International Agency for Research on Cancer Lyon, France Kevin D Shield (Shieldk@fellow.iarc.fr), Pietro Ferrari, Jacques Ferlay, Freddie
CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO
 OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO Amy Ferketich, PhD Ling Wang, MPH The Ohio State University College of Public Health
OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO Amy Ferketich, PhD Ling Wang, MPH The Ohio State University College of Public Health
Report 5: Tobacco Use, Dependence and Smoke in the Home
 Report 5: Tobacco Use, Dependence and Smoke in the Home June 2017 Summary The 2016 Oxford Health Matters Survey (OHMS) was conducted for Oxford County Public Health (Public Health) to inform public health
Report 5: Tobacco Use, Dependence and Smoke in the Home June 2017 Summary The 2016 Oxford Health Matters Survey (OHMS) was conducted for Oxford County Public Health (Public Health) to inform public health
RESEARCH. Dagfinn Aune, 1,2 Abhijit Sen, 1 Manya Prasad, 3 Teresa Norat, 2 Imre Janszky, 1 Serena Tonstad, 3 Pål Romundstad, 1 Lars J Vatten 1
 open access BMI and all cause mortality: systematic review and non-linear dose-response meta-analysis of 230 cohort studies with 3.74 million deaths among 30.3 million participants Dagfinn Aune, 1,2 Abhijit
open access BMI and all cause mortality: systematic review and non-linear dose-response meta-analysis of 230 cohort studies with 3.74 million deaths among 30.3 million participants Dagfinn Aune, 1,2 Abhijit
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and cancers of the mouth, pharynx and larynx
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and cancers of the mouth, pharynx and larynx 2018 Contents World Cancer Research Fund Network 3 Executive Summary
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and cancers of the mouth, pharynx and larynx 2018 Contents World Cancer Research Fund Network 3 Executive Summary
Association between multiple comorbidities and self-rated health status in middle-aged and elderly Chinese: the China Kadoorie Biobank study
 Song et al. BMC Public Health (2018) 18:744 https://doi.org/10.1186/s12889-018-5632-1 RESEARCH ARTICLE Association between multiple comorbidities and self-rated health status in middle-aged and elderly
Song et al. BMC Public Health (2018) 18:744 https://doi.org/10.1186/s12889-018-5632-1 RESEARCH ARTICLE Association between multiple comorbidities and self-rated health status in middle-aged and elderly
Australian Longitudinal Study on Women's Health TRENDS IN WOMEN S HEALTH 2006 FOREWORD
 Australian Longitudinal Study on Women's Health TRENDS IN WOMEN S HEALTH 2006 FOREWORD The Longitudinal Study on Women's Health, funded by the Commonwealth Government, is the most comprehensive study ever
Australian Longitudinal Study on Women's Health TRENDS IN WOMEN S HEALTH 2006 FOREWORD The Longitudinal Study on Women's Health, funded by the Commonwealth Government, is the most comprehensive study ever
TOBACCO USE AMONG AFRICAN AMERICANS
 TOBACCO USE AMONG AFRICAN AMERICANS Each year, approximately 45,000 African Americans die from smoking-related disease. 1 Smoking-related illnesses are the number one cause of death in the African-American
TOBACCO USE AMONG AFRICAN AMERICANS Each year, approximately 45,000 African Americans die from smoking-related disease. 1 Smoking-related illnesses are the number one cause of death in the African-American
Gene-Environment Interactions
 Gene-Environment Interactions What is gene-environment interaction? A different effect of an environmental exposure on disease risk in persons with different genotypes," or, alternatively, "a different
Gene-Environment Interactions What is gene-environment interaction? A different effect of an environmental exposure on disease risk in persons with different genotypes," or, alternatively, "a different
Physical Activity and Colorectal Cancer
 American Journal of Epidemiology Copyright 2003 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 158, No. 3 Printed in U.S.A. DOI: 10.1093/aje/kwg134 Physical Activity and
American Journal of Epidemiology Copyright 2003 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 158, No. 3 Printed in U.S.A. DOI: 10.1093/aje/kwg134 Physical Activity and
Trends in Lung Cancer Morbidity and Mortality
 Trends in Lung Cancer Morbidity and Mortality American Lung Association Epidemiology and Statistics Unit Research and Program Services Division November 2014 Table of Contents Trends in Lung Cancer Morbidity
Trends in Lung Cancer Morbidity and Mortality American Lung Association Epidemiology and Statistics Unit Research and Program Services Division November 2014 Table of Contents Trends in Lung Cancer Morbidity
definitions, trends, and risk factors
 fcialjournalofthebrtishdentalasociation.the changing epidemiology of oral cancer: definitions, trends, and risk factors D. I. Conway,* 1 M. Purkayastha 1 and I. G. Chestnutt 2 RESEARCH Key points Discusses
fcialjournalofthebrtishdentalasociation.the changing epidemiology of oral cancer: definitions, trends, and risk factors D. I. Conway,* 1 M. Purkayastha 1 and I. G. Chestnutt 2 RESEARCH Key points Discusses
Cessation and Cessation Measures
 Cessation and Cessation Measures among Adult Daily Smokers: National and State-Specific Data David M. Burns, Christy M. Anderson, Michael Johnson, Jacqueline M. Major, Lois Biener, Jerry Vaughn, Thomas
Cessation and Cessation Measures among Adult Daily Smokers: National and State-Specific Data David M. Burns, Christy M. Anderson, Michael Johnson, Jacqueline M. Major, Lois Biener, Jerry Vaughn, Thomas
Patient Name Date of Birth Age. Other phone ( ) . Other
 GASTROINTESTINAL & MINIMALLY INVASIVE SURGERY HEALTH HISTORY QUESTIONNAIRE Date Patient Name _ Date of Birth Age Daytime phone ( ) Other phone ( ) Email How did you hear about us? My doctor Yellow pages
GASTROINTESTINAL & MINIMALLY INVASIVE SURGERY HEALTH HISTORY QUESTIONNAIRE Date Patient Name _ Date of Birth Age Daytime phone ( ) Other phone ( ) Email How did you hear about us? My doctor Yellow pages
Smoking Status and Body Mass Index in the United States:
 Smoking Status and Body Mass Index in the United States: 1996-2000 Jun Yang, MD, PhD and Gary Giovino, PhD Roswell Park Cancer Institute Elm and Carlton Streets Buffalo, NY 14263, USA Society for Research
Smoking Status and Body Mass Index in the United States: 1996-2000 Jun Yang, MD, PhD and Gary Giovino, PhD Roswell Park Cancer Institute Elm and Carlton Streets Buffalo, NY 14263, USA Society for Research
Alcohol and Breast Cancer: A Cohort Study
 PREVENTIVE MEDICINE 17, 686-693 (1988) Alcohol and Breast Cancer: A Cohort Study LAWRENCEGARFINKEL, M.A., PAOLO BOFFETTA, M.D., AND STEVEN D. STELLMAN, PH.D. American Cancer Society, 1180 Avenue of the
PREVENTIVE MEDICINE 17, 686-693 (1988) Alcohol and Breast Cancer: A Cohort Study LAWRENCEGARFINKEL, M.A., PAOLO BOFFETTA, M.D., AND STEVEN D. STELLMAN, PH.D. American Cancer Society, 1180 Avenue of the
Alcohol's Effects on the Body
 Alcohol's Effects on the Body Drinking too much on a single occasion or over time can take a serious toll on your health. Here s how alcohol can affect your body: Brain: Alcohol interferes with the brain
Alcohol's Effects on the Body Drinking too much on a single occasion or over time can take a serious toll on your health. Here s how alcohol can affect your body: Brain: Alcohol interferes with the brain
Biostatistics and Epidemiology Step 1 Sample Questions Set 1
 Biostatistics and Epidemiology Step 1 Sample Questions Set 1 1. A study wishes to assess birth characteristics in a population. Which of the following variables describes the appropriate measurement scale
Biostatistics and Epidemiology Step 1 Sample Questions Set 1 1. A study wishes to assess birth characteristics in a population. Which of the following variables describes the appropriate measurement scale
Mortality in vegetarians and comparable nonvegetarians in the United Kingdom 1 3
 See corresponding editorial on page 3. Mortality in vegetarians and comparable nonvegetarians in the United Kingdom 1 3 Paul N Appleby, Francesca L Crowe, Kathryn E Bradbury, Ruth C Travis, and Timothy
See corresponding editorial on page 3. Mortality in vegetarians and comparable nonvegetarians in the United Kingdom 1 3 Paul N Appleby, Francesca L Crowe, Kathryn E Bradbury, Ruth C Travis, and Timothy
Gastroesophageal Reflux Disease and Odds of Head and Neck Squamous Cell Carcinoma in North Carolina
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Gastroesophageal Reflux Disease and Odds of Head and Neck Squamous Cell Carcinoma in North Carolina Evan
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Gastroesophageal Reflux Disease and Odds of Head and Neck Squamous Cell Carcinoma in North Carolina Evan
2. Studies of Cancer in Humans
 346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
Why Do We Treat Obesity? Epidemiology
 Why Do We Treat Obesity? Epidemiology Epidemiology of Obesity U.S. Epidemic 2 More than Two Thirds of US Adults Are Overweight or Obese 87.5 NHANES Data US Adults Age 2 Years (Crude Estimate) Population
Why Do We Treat Obesity? Epidemiology Epidemiology of Obesity U.S. Epidemic 2 More than Two Thirds of US Adults Are Overweight or Obese 87.5 NHANES Data US Adults Age 2 Years (Crude Estimate) Population
5. Summary of Data Reported and Evaluation 5.1 Exposure data
 5. Summary of Data Reported and Evaluation 5.1 Exposure data Smoking of tobacco is practised worldwide by over one thousand million people. However, while smoking prevalence has declined in many developed
5. Summary of Data Reported and Evaluation 5.1 Exposure data Smoking of tobacco is practised worldwide by over one thousand million people. However, while smoking prevalence has declined in many developed
Burden of Cancer in California
 Burden of Cancer in California California Cancer Reporting and Epidemiologic Surveillance Institute for Population Health Improvement UC Davis Health August 22, 2018 Outline 1. Incidence and Mortality
Burden of Cancer in California California Cancer Reporting and Epidemiologic Surveillance Institute for Population Health Improvement UC Davis Health August 22, 2018 Outline 1. Incidence and Mortality
RESEARCH ARTICLE. Sang Hyuk Jung 1, Bayasgalan Gombojav 2, Eun-Cheol Park 3,5, Chung Mo Nam 3, Heechoul Ohrr 2,3, Jong Uk Won 3,4 * Abstract
 RESEARCH ARTICLE Population Based Study of the Association Between Binge Drinking and Mortality from Cancer of Oropharynx and Esophagus in Korean Men: the Kangwha Cohort Study Sang Hyuk Jung 1, Bayasgalan
RESEARCH ARTICLE Population Based Study of the Association Between Binge Drinking and Mortality from Cancer of Oropharynx and Esophagus in Korean Men: the Kangwha Cohort Study Sang Hyuk Jung 1, Bayasgalan
HPV is the most common sexually transmitted infection in the world.
 Hi. I m Kristina Dahlstrom, an instructor in the Department of Head and Neck Surgery at The University of Texas MD Anderson Cancer Center. My lecture today will be on the epidemiology of oropharyngeal
Hi. I m Kristina Dahlstrom, an instructor in the Department of Head and Neck Surgery at The University of Texas MD Anderson Cancer Center. My lecture today will be on the epidemiology of oropharyngeal
Patient Interview Form
 Page 1 of 6 STEPHEN G. ABSHIRE, M.D. JAMES N. ARTERBURN, M.D. ERIC P. TRAWICK, M.D. JACOB R. KARR, M.D. SYLVIA OATS, ANP-BC SUSAN MIEDECKE, FNP-BC CINDY LANDRY, ANP-BC 1211 Coolidge Blvd. Suite 303 Lafayette,
Page 1 of 6 STEPHEN G. ABSHIRE, M.D. JAMES N. ARTERBURN, M.D. ERIC P. TRAWICK, M.D. JACOB R. KARR, M.D. SYLVIA OATS, ANP-BC SUSAN MIEDECKE, FNP-BC CINDY LANDRY, ANP-BC 1211 Coolidge Blvd. Suite 303 Lafayette,
Cancer survival in Chennai (Madras), India,
 Cancer survival in Chennai (Madras), India, 199 1999 Swaminathan R, Rama R, Nalini S and Shanta V Abstract The Madras metropolitan tumour registry was established in 1981, and registration of incident
Cancer survival in Chennai (Madras), India, 199 1999 Swaminathan R, Rama R, Nalini S and Shanta V Abstract The Madras metropolitan tumour registry was established in 1981, and registration of incident
Dr. Hall New Patient Paperwork Please fill out these forms completely
 Dr. Hall New Patient Paperwork Please fill out these forms completely Date of Appointment Complete the enclosed packet and bring it to the appointment along with all X Rays, MRI disc and reports. Please
Dr. Hall New Patient Paperwork Please fill out these forms completely Date of Appointment Complete the enclosed packet and bring it to the appointment along with all X Rays, MRI disc and reports. Please
Exposed cases/deaths. or level. Lung All coffee (cups/day) Sex, smoking history, β-carotene intake Coffee intake Never 133 1
 Vol 6 Monograph 0 Drinking coffee Section 2 Table 2.4 Table 2.4 Case control studies (hospitalbased) on cancer of the lung and coffee drinking (web only) Mettlin (989) Baffalo, US 982 987 569; histologically
Vol 6 Monograph 0 Drinking coffee Section 2 Table 2.4 Table 2.4 Case control studies (hospitalbased) on cancer of the lung and coffee drinking (web only) Mettlin (989) Baffalo, US 982 987 569; histologically
Lack of Association of Alcohol and Tobacco with HPV16-Associated Head and Neck Cancer
 ARTICLE Lack of Association of Alcohol and Tobacco with HPV16-Associated Head and Neck Cancer Katie M. Applebaum, C. Sloane Furniss, Ariana Zeka, Marshall R. Posner, Judith F. Smith, Janine Bryan, Ellen
ARTICLE Lack of Association of Alcohol and Tobacco with HPV16-Associated Head and Neck Cancer Katie M. Applebaum, C. Sloane Furniss, Ariana Zeka, Marshall R. Posner, Judith F. Smith, Janine Bryan, Ellen
Oral Cancer Risk and Detection
 Oral Cancer Risk and Detection Evan M. Graboyes, MD Assistant Professor Department of Otolaryngology-Head & Neck Surgery Cancer Control Program, Hollings Cancer Center Medical University of South Carolina
Oral Cancer Risk and Detection Evan M. Graboyes, MD Assistant Professor Department of Otolaryngology-Head & Neck Surgery Cancer Control Program, Hollings Cancer Center Medical University of South Carolina
Papers. Environmental tobacco smoke and tobacco related mortality in a prospective study of Californians, Abstract.
 Environmental tobacco smoke and tobacco related mortality in a prospective study of Californians, 1960-98 James E Enstrom, Geoffrey C Kabat Abstract Objective To measure the relation between environmental
Environmental tobacco smoke and tobacco related mortality in a prospective study of Californians, 1960-98 James E Enstrom, Geoffrey C Kabat Abstract Objective To measure the relation between environmental
Modesto Gastroenterology Medical Corporation
 Page 1 of 5 Modesto Gastroenterology Medical Corporation Magdy S. Elsakr, M.D. Board Certified Gastroenterologist 2336 Sylvan Avenue, Suite A, Modesto, CA 95355, Phone: 209-338-0292, Fax: 209-338-0298
Page 1 of 5 Modesto Gastroenterology Medical Corporation Magdy S. Elsakr, M.D. Board Certified Gastroenterologist 2336 Sylvan Avenue, Suite A, Modesto, CA 95355, Phone: 209-338-0292, Fax: 209-338-0298
Low-Carbohydrate Diets and All-Cause and Cause-Specific Mortality: A Population-based Cohort Study and Pooling Prospective Studies
 Low-Carbohydrate Diets and All-Cause and Cause-Specific Mortality: A Population-based Cohort Study and Pooling Prospective Studies Mohsen Mazidi 1, Niki Katsiki 2, Dimitri P. Mikhailidis 3, Maciej Banach
Low-Carbohydrate Diets and All-Cause and Cause-Specific Mortality: A Population-based Cohort Study and Pooling Prospective Studies Mohsen Mazidi 1, Niki Katsiki 2, Dimitri P. Mikhailidis 3, Maciej Banach
In the 1700s patients in charity hospitals sometimes slept two or more to a bed, regardless of diagnosis.
 Control Case In the 1700s patients in charity hospitals sometimes slept two or more to a bed, regardless of diagnosis. This depicts a patient who finds himself lying with a corpse (definitely a case ).
Control Case In the 1700s patients in charity hospitals sometimes slept two or more to a bed, regardless of diagnosis. This depicts a patient who finds himself lying with a corpse (definitely a case ).
Update of the role of Human Papillomavirus in Head and Neck Cancer
 Update of the role of Human Papillomavirus in Head and Neck Cancer 2013 International & 12 th National Head and Neck Tumour Conference Shanghai, 11 13 Oct 2013 Prof. Paul KS Chan Department of Microbiology
Update of the role of Human Papillomavirus in Head and Neck Cancer 2013 International & 12 th National Head and Neck Tumour Conference Shanghai, 11 13 Oct 2013 Prof. Paul KS Chan Department of Microbiology
*
 Introduction Cancer is complex, can have many possible causes, and is increasingly common. For the U.S. population, 1 in 2 males and 1 in 3 females is at risk of developing cancer in their lifetime. The
Introduction Cancer is complex, can have many possible causes, and is increasingly common. For the U.S. population, 1 in 2 males and 1 in 3 females is at risk of developing cancer in their lifetime. The
Factors Influencing Smoking Behavior Among Adolescents
 RESEARCH COMMUNICATION Factors Influencing Smoking Behavior Among Adolescents Urmi Sen 1, Arindam Basu 2 Abstract Objective To study the impact of tobacco advertisements and other social factors on the
RESEARCH COMMUNICATION Factors Influencing Smoking Behavior Among Adolescents Urmi Sen 1, Arindam Basu 2 Abstract Objective To study the impact of tobacco advertisements and other social factors on the
2.3 Cancer of the larynx
 ALCOHOL CONSUMPTION 329 from Pordenone, Rome, Latina (Italy) and Vaud (Switzerland) were identified from 1992 to 1997 and compared with 692 hospital-based controls (Talamini et al., 1998). Again, a dose
ALCOHOL CONSUMPTION 329 from Pordenone, Rome, Latina (Italy) and Vaud (Switzerland) were identified from 1992 to 1997 and compared with 692 hospital-based controls (Talamini et al., 1998). Again, a dose
INTEGRATED CHRONIC DISEASE PREVENTION
 INTEGRATED CHRONIC DISEASE PREVENTION What Is Integrated Health Promotion? In this context, the term integrated health promotion refers to an approach to health and wellbeing that acknowledges that risk
INTEGRATED CHRONIC DISEASE PREVENTION What Is Integrated Health Promotion? In this context, the term integrated health promotion refers to an approach to health and wellbeing that acknowledges that risk
Oral Cancer FAQs. What is oral cancer? How many people are diagnosed with oral cancer each year?
 Oral Cancer FAQs What is oral cancer? Oral cancer or oral cavity cancer, is cancer that starts in the mouth. Areas affected by this type of cancer are the lips, the inside lining of the lips and cheeks
Oral Cancer FAQs What is oral cancer? Oral cancer or oral cavity cancer, is cancer that starts in the mouth. Areas affected by this type of cancer are the lips, the inside lining of the lips and cheeks
DONE! You can now close the browser.
 Visit My Doctor Online at kp.org/mydoctor. Prepare for your visit This form will help you prepare for your upcoming visit with your doctor. You can complete it on your computer (Mac or PC) and e-mail it
Visit My Doctor Online at kp.org/mydoctor. Prepare for your visit This form will help you prepare for your upcoming visit with your doctor. You can complete it on your computer (Mac or PC) and e-mail it
National Burden of Cancers Attributable to Secondhand Smoking in Indonesia
 DOI:10.22034/APJCP.2018.19.7.1951 RESEARCH ARTICLE Editorial Process: Submission:02/26/2018 Acceptance:06/11/2018 National Burden of Cancers Attributable to Secondhand Smoking in Indonesia Ni Putu Ayu
DOI:10.22034/APJCP.2018.19.7.1951 RESEARCH ARTICLE Editorial Process: Submission:02/26/2018 Acceptance:06/11/2018 National Burden of Cancers Attributable to Secondhand Smoking in Indonesia Ni Putu Ayu
Infertility services reported by men in the United States: national survey data
 MALE FACTOR Infertility services reported by men in the United States: national survey data John E. Anderson, Ph.D., Sherry L. Farr, Ph.D., M.S.P.H., Denise J. Jamieson, M.D., M.P.H., Lee Warner, Ph.D.,
MALE FACTOR Infertility services reported by men in the United States: national survey data John E. Anderson, Ph.D., Sherry L. Farr, Ph.D., M.S.P.H., Denise J. Jamieson, M.D., M.P.H., Lee Warner, Ph.D.,
Adult Health History
 Patient Name Date of Birth Adult Health History This form will assist us in obtaining a complete medical history and health record on you. By completing this ahead of time it will also simply your visit
Patient Name Date of Birth Adult Health History This form will assist us in obtaining a complete medical history and health record on you. By completing this ahead of time it will also simply your visit
Outline. Case control studies. Study Designs. Case Control Study. Start with OUTCOME Go backwards Check for EXPOSURE. Experimental studies
 Outline Case control studies Study Designs Experimental studies Observational studies Analytic studies Descriptive studies Randomized Controlled trials Case control Cohort Cross sectional Case Control
Outline Case control studies Study Designs Experimental studies Observational studies Analytic studies Descriptive studies Randomized Controlled trials Case control Cohort Cross sectional Case Control
KAREN J. SUNDBY, M.D. PLEASE COMPLETE THE FOLLOWING MEDICAL HISTORY FORM
 KAREN J. SUNDBY, M.D. PLEASE COMPLETE THE FOLLOWING MEDICAL HISTORY FORM Dr. Mr. Mrs. Ms. Miss New Patient or Returning Patient FULL LEGAL NAME: Reason for today s visit: Mohs Excision Skin Check other:
KAREN J. SUNDBY, M.D. PLEASE COMPLETE THE FOLLOWING MEDICAL HISTORY FORM Dr. Mr. Mrs. Ms. Miss New Patient or Returning Patient FULL LEGAL NAME: Reason for today s visit: Mohs Excision Skin Check other:
The relationship between adolescent/young adult BMI and subsequent non-problem and problem alcohol use
 Washington University School of Medicine Digital Commons@Becker Posters 2007: Alcohol Use Across the Lifespan 2007 The relationship between adolescent/young adult BMI and subsequent non-problem and problem
Washington University School of Medicine Digital Commons@Becker Posters 2007: Alcohol Use Across the Lifespan 2007 The relationship between adolescent/young adult BMI and subsequent non-problem and problem
o Kidney Cancer o Liver Cancer o Tremor o Tuberculosis o B12 Deficiency o Esophageal Cancer o Liver Disease o Pituitary Tumor o Uterine o Neurological
 Adult New Patient Registration PATIENT DOB: / / MONTH DAY YEAR PATIENT NAME: LAST FIRST MI o Abnormal Heartbeat Patient Medical History: Please mark all that apply o Chronic Headaches o Hepatitis C o Neuropathy
Adult New Patient Registration PATIENT DOB: / / MONTH DAY YEAR PATIENT NAME: LAST FIRST MI o Abnormal Heartbeat Patient Medical History: Please mark all that apply o Chronic Headaches o Hepatitis C o Neuropathy
Patterns of Clinically Significant Symptoms of Depression Among Heavy Users of Alcohol and Cigarettes
 ORIGINAL RESEARCH Patterns of Clinically Significant Symptoms of Depression Among Heavy Users of Alcohol and Cigarettes Joan Faith Epstein, MS, Marta Induni, PhD, Tom Wilson, MA Suggested citation for
ORIGINAL RESEARCH Patterns of Clinically Significant Symptoms of Depression Among Heavy Users of Alcohol and Cigarettes Joan Faith Epstein, MS, Marta Induni, PhD, Tom Wilson, MA Suggested citation for
CANCER. International Journal of Epidemiology 2010;39: doi: /ije/dyp380
 Published by Oxford University Press on behalf of the International Epidemiological Association ß The Author 2010; all rights reserved. Advance Access publication 1 February 2010 International Journal
Published by Oxford University Press on behalf of the International Epidemiological Association ß The Author 2010; all rights reserved. Advance Access publication 1 February 2010 International Journal
IJC International Journal of Cancer
 IJC International Journal of Cancer Natural vitamin C intake and the risk of head and neck cancer: A pooled analysis in the International Head and Neck Cancer Consortium Valeria Edefonti 1, Mia Hashibe
IJC International Journal of Cancer Natural vitamin C intake and the risk of head and neck cancer: A pooled analysis in the International Head and Neck Cancer Consortium Valeria Edefonti 1, Mia Hashibe
Texas Chronic Disease Burden Report. April Publication #E
 Texas Chronic Disease Burden Report April 2010 Publication #E81-11194 Direction and Support Lauri Kalanges, MD, MPH Medical Director Health Promotion and Chronic Disease Prevention Section, Texas Department
Texas Chronic Disease Burden Report April 2010 Publication #E81-11194 Direction and Support Lauri Kalanges, MD, MPH Medical Director Health Promotion and Chronic Disease Prevention Section, Texas Department
Socioeconomic status and the 25x25 risk factors as determinants of premature mortality: a multicohort study of 1.7 million men and women
 Socioeconomic status and the 25x25 risk factors as determinants of premature mortality: a multicohort study of 1.7 million men and women (Lancet. 2017 Mar 25;389(10075):1229-1237) 1 Silvia STRINGHINI Senior
Socioeconomic status and the 25x25 risk factors as determinants of premature mortality: a multicohort study of 1.7 million men and women (Lancet. 2017 Mar 25;389(10075):1229-1237) 1 Silvia STRINGHINI Senior
Emergency Contact Name Relationship Phone Primary Care Physician Phone Did a Physician Refer you to us? YES NO Physician Name
 TELL US ABOUT YOU (please print) First MI Last Address 1 Address 2 CITY ST ZIP COUNTRY E-mail Opt out of providing E-mail Address Language Preference SSN - - DOB / / Driver s License # ST Phone 1 CELL
TELL US ABOUT YOU (please print) First MI Last Address 1 Address 2 CITY ST ZIP COUNTRY E-mail Opt out of providing E-mail Address Language Preference SSN - - DOB / / Driver s License # ST Phone 1 CELL
Table Cohort studies of consumption of alcoholic beverages and cancers of the lymphatic and haematopoietic system in the general population
 categories Lim et al., (2007), USA, The National Institutes of Health-former American Association of Retired Persons (NIH- AARP) Diet and Health Study 473984 participants with correct questionnaire and
categories Lim et al., (2007), USA, The National Institutes of Health-former American Association of Retired Persons (NIH- AARP) Diet and Health Study 473984 participants with correct questionnaire and
CANCER FACTS & FIGURES For African Americans
 CANCER FACTS & FIGURES For African Americans Pennsylvania, 2006 Pennsylvania Cancer Registry Bureau of Health Statistics and Research Contents Data Hightlights...1 Pennsylvania and U.S. Comparison...5
CANCER FACTS & FIGURES For African Americans Pennsylvania, 2006 Pennsylvania Cancer Registry Bureau of Health Statistics and Research Contents Data Hightlights...1 Pennsylvania and U.S. Comparison...5
NCQA did not add new measures to Accreditation 2017 scoring.
 2017 Accreditation Benchmarks and Thresholds 1 TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 2, 2017 RE: 2017 Accreditation Benchmarks and Thresholds
2017 Accreditation Benchmarks and Thresholds 1 TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 2, 2017 RE: 2017 Accreditation Benchmarks and Thresholds
Age-standardised rate ratios (SRR) and rate differences (SRD) of endometrial cancer, for Māori, Pacific and Asian compared to European/Other
 Figure 22: Standardised rates of endometrial cancer for 25+ year-olds, by ethnicity Table 25: Age-standardised rate ratios (SRR) and rate differences (SRD) of endometrial cancer, for Māori, Pacific and
Figure 22: Standardised rates of endometrial cancer for 25+ year-olds, by ethnicity Table 25: Age-standardised rate ratios (SRR) and rate differences (SRD) of endometrial cancer, for Māori, Pacific and
2018 Texas Cancer Registry Annual Report
 2018 Texas Cancer Registry Annual Report As Required by Texas Health and Safety Code Section 82.007 November 2018 Table of Contents Executive Summary... 1 1. Introduction... 2 2. Background... 3 Cancer
2018 Texas Cancer Registry Annual Report As Required by Texas Health and Safety Code Section 82.007 November 2018 Table of Contents Executive Summary... 1 1. Introduction... 2 2. Background... 3 Cancer
Mortality from cancer of the lung in Serbia
 JBUON 2013; 18(3): 723-727 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Mortality from cancer of the lung in Serbia M. Ilic 1, H. Vlajinac 2,
JBUON 2013; 18(3): 723-727 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Mortality from cancer of the lung in Serbia M. Ilic 1, H. Vlajinac 2,
Table Cohort studies of consumption of alcoholic beverages and cancer of the colorectum
 Akhter et al. (2007), Japan, Miyagi Study [data also included in the pooled analysis, Mizoue et al. (2008)] of 21 199 men living in the Miyagi region recruited in 1990; aged 40 64 years; followed-up until
Akhter et al. (2007), Japan, Miyagi Study [data also included in the pooled analysis, Mizoue et al. (2008)] of 21 199 men living in the Miyagi region recruited in 1990; aged 40 64 years; followed-up until
Exercise Behavior & Major Cardiac Events: CCSS 1 STUDY TITLE
 STUDY TITLE Exercise Behavior & Major Cardiac Events: CCSS 1 Association Between Exercise Behavior and Incidence of Major Cardiac Events in Adult Survivors of Childhood Cancer: A Report from the Childhood
STUDY TITLE Exercise Behavior & Major Cardiac Events: CCSS 1 Association Between Exercise Behavior and Incidence of Major Cardiac Events in Adult Survivors of Childhood Cancer: A Report from the Childhood
Body-mass index and cause-specific mortality in adults: collaborative analyses of 57 prospective studies
 Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies Prospective Studies Collaboration* Summary Background The main associations of body-mass
Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies Prospective Studies Collaboration* Summary Background The main associations of body-mass
WASHINGTON UNIVERSITY SCHOOL OF MEDICINE. Cranial Health History Form
 WASHINGTON UNIVERSITY SCHOOL OF MEDICINE Cranial Health History Form Welcome to the Neurosurgery Department at Washington University. To help us treat you, please fill this form out completely. Your Name:
WASHINGTON UNIVERSITY SCHOOL OF MEDICINE Cranial Health History Form Welcome to the Neurosurgery Department at Washington University. To help us treat you, please fill this form out completely. Your Name:
B&T Format. New Measures. 2 CAHPS is a registered trademark of the Agency for Healthcare Research and Quality (AHRQ).
 TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February 4, 2018 RE: 2018 Accreditation Benchmarks and Thresholds This document reports national benchmarks and
TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February 4, 2018 RE: 2018 Accreditation Benchmarks and Thresholds This document reports national benchmarks and
SITES (ALPHABETICAL) HPV CS SITE SPECIFIC FACTOR
 SITES (ALPHABETICAL) HPV CS SITE SPECIFIC FACTOR Anus: Anal Canal; Anus, NOS; Other Parts of Rectum C21.0-C21.2, C21.8 C21.0 Anus, NOS (excludes skin of anus and perianal skin C44.5) C21.1 Anal canal C21.2
SITES (ALPHABETICAL) HPV CS SITE SPECIFIC FACTOR Anus: Anal Canal; Anus, NOS; Other Parts of Rectum C21.0-C21.2, C21.8 C21.0 Anus, NOS (excludes skin of anus and perianal skin C44.5) C21.1 Anal canal C21.2
Epidemiological evidence on snus (Swedish moist snuff) and health in adults. By Peter Lee
 Epidemiological evidence on snus (Swedish moist snuff) and health in adults By Peter Lee Relevant publications specifically on snus Lee, P.N., 2011. Summary of the epidemiological evidence relating snus
Epidemiological evidence on snus (Swedish moist snuff) and health in adults By Peter Lee Relevant publications specifically on snus Lee, P.N., 2011. Summary of the epidemiological evidence relating snus
Humaan Papillomavirus en hoofd/halskanker. Pol Specenier
 Humaan Papillomavirus en hoofd/halskanker Pol Specenier pol.specenier@uza.be Humaan Papillomavirus en hoofd/halskanker Hoofd/halskanker: incidentie en oorzaken Oropharynx carcinoom Incidentie HPV HPV en
Humaan Papillomavirus en hoofd/halskanker Pol Specenier pol.specenier@uza.be Humaan Papillomavirus en hoofd/halskanker Hoofd/halskanker: incidentie en oorzaken Oropharynx carcinoom Incidentie HPV HPV en
Diet, obesity, lifestyle and cancer prevention:
 Diet, obesity, lifestyle and cancer prevention: Epidemiologic perspectives Graham A Colditz, MD DrPH Niess-Gain Professor Chief, November, 2017 Outline Review evidence on contribution of diet, obesity,
Diet, obesity, lifestyle and cancer prevention: Epidemiologic perspectives Graham A Colditz, MD DrPH Niess-Gain Professor Chief, November, 2017 Outline Review evidence on contribution of diet, obesity,
Descriptive Epidemiology: U.S. Patterns
 Descriptive Epidemiology: U.S. Patterns Linda Morris Brown, Gloria Gridley, and Susan S. Devesa Abbreviations US HN SEER HPV ICD-O-3 API AI/AN United States head and neck Surveillance, Epidemiology, and
Descriptive Epidemiology: U.S. Patterns Linda Morris Brown, Gloria Gridley, and Susan S. Devesa Abbreviations US HN SEER HPV ICD-O-3 API AI/AN United States head and neck Surveillance, Epidemiology, and
