Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule
|
|
|
- Madeleine Hutchinson
- 5 years ago
- Views:
Transcription
1 Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From Guangdong Lung Cancer Institute, Guangdong Provincial Key Laboratory of Translational Medicine in Lung Cancer, Guangdong General Hospital & Guangdong Academy of Medical Sciences, Guangzhou , China. *This author is currently a medical postgraduate at Jinan University, the 2nd Clinical College, Shenzhen people s hospital, Guangzhou , China Correspondence to: Dr. Xue-Ning Yang, MD. Guangdong Lung Cancer Institute, Guangdong Provincial Key Laboratory of Translational Medicine in Lung Cancer, Guangdong General hospital & Guangdong Academy of Medical Sciences, No. 106 Zhongshan 2nd Road, Guangzhou , China. yangxuening@gmail.com. Background: Effective methods for managing patients with solitary pulmonary nodules (SPNs) depend critically on the predictive probability of malignancy. Methods: Between July 2009 and June 2011, data on gender, age, cancer history, tumor familial history, smoking status, tumor location, nodule size, spiculation, calcification, the tumor border, and the final pathological diagnosis were collected retrospectively from 154 surgical patients with an SPN measuring 3-30 mm. Each final diagnosis was compared with the probability calculated by three predicted models the Mayo, VA, and Peking University (PU) models. The accuracy of each model was assessed using area under the receiver operating characteristics (ROC) and calibration curves. Results: The area under the ROC curve of the PU model [0.800; 95% confidence interval (CI): ] was higher than that of the Mayo model (0.753; 95% CI: ) or VA model (0.728; 95% CI: ); however, this finding was not statistically significant. To varying degrees, calibration curves showed that all three models overestimated malignancy. Conclusions: The three predicted models have similar accuracy for prediction of SPN malignancy, although the accuracy is not sufficient. For Chinese patients, the PU model may has greater predictive power. Keywords: Solitary pulmonary nodule (SPN); benign and malignant; model; comparison Submitted Oct 05, Accepted for publication Nov 12, doi: /j.issn View this article at: Introduction A solitary pulmonary nodule (SPN) is radiologically defined as an intraparenchymal lung lesion that is less than 3 cm in diameter and is not associated with atelectasis or adenopathy (1). Timely identification of a malignant SPN is essential for prognosis because the treatment strategies for a malignancy are different from those for a benign nodule (2). In patients who are surgical candidates, malignancy should be identified promptly (when present) and receive timely resection. Ideally, surgery should be avoided in patients with nodules that prove to be benign (3). However, identifying a malignant SPN is challenging. Most clinicians diagnose based on their clinical experience, which may be subjective. A mathematical prediction model facilitates this task, avoiding subjective and one-sided judgment. To date, only three organizations have constructed SPN prediction models the Mayo (4), VA (5), and Peking University (PU) (6) models. The Mayo Clinic model is defined by the equations: Pretest probability of a malignant SPN = e x /(1+e x ), x= ( age) + ( smoking history) + ( cancer history) + ( diameter) + ( spiculation) + ( upper lobe), e is the natural logarithm, and 1 for yes and 0 for no in the smoking history, cancer history, spiculation and upper lobe elements. Diameter indicates the largest nodule measurement (in mm) reported on initial
2 648 Zhang et al. Comparison of SPN prediction models chest radiograph or CT scan. When the probability was <3%, watchful waiting was preferred. When the probability was 3% to 68%, needle biopsy was preferred. When the probability was >68%, surgery was preferred. The VA model is defined by the equations: Pre-test probability of a malignant SPN = e x /(1+e x ), x= (2.061 smoking history) + (0.779 age10) + (0.112 diameter) (0.567 yearsquit10), e is the natural logarithm, and 1 for yes and 0 for no in the smoking history; age10 indicates age in years at the time of nodule identification, divided by 10; diameter indicates the largest nodule measurement (in mm) reported on initial chest radiograph or CT scan; and yearsquit10 indicates the number of years since quitting smoking, divided by 10 (0 indicates not applicable). When the probability was <20%, watchful waiting was preferred. When the probability was 20% to 69%, needle biopsy was preferred. When the probability was >69%, surgery was preferred. The PU model is defined by the equations: Pre-test probability of a malignant SPN = e x / (1+e x ), x= (0.07 age) + (0.676 diameter) + (0.736 spiculation) + (1.267 family history of cancer) (1.615 calcification) (1.408 border), e is the natural logarithm, and 1 for yes and 0 for no in the last four elements. Diameter indicates the largest nodule measurement (in cm) reported on initial chest radiograph or CT scan. When the probability was <46.3%, the nodule should be considered benign. When the probability was >46.3%, the nodule should be considered malignant. This study aimed to evaluate the sensitivity of the three models in verifying a malignant SPN using a set of data using calibration and receiver operating characteristics (ROC) curves. Materials and methods We retrospectively reviewed the medical records of 160 patients with SPNs who underwent surgical resection between July 2009 and June The present study recruited patients who underwent computed tomography (CT) scans at Guangdong General Hospital and without a previous diagnosis of lung cancer. Patients with extrathoracic cancer within 5 years of nodule identification were excluded (n=6). A total of 154 patients were finally enrolled in our study, comprising 88 males and 66 females, mainly from the south of China. This study was approved by the hospital ethics committee. Clinical data were collected, including age, gender, smoking history, history of a previous cancer diagnosis, family history of cancer, pathological diagnosis, and radiology characteristics. All patients underwent surgical resection of SPNs and pathological diagnoses were obtained. Pulmonary wedge resection and lobectomy were performed in these patients. Clinical data of 154 patients were calculated by three models separately. The calculation outcomes of the Mayo, VA, and PU models were compared. Analyses were performed using commercially available software packages (SPSS for Windows version 17.0 and Medcalc for Windows version ). Values of P<0.05 were deemed to indicate statistical significance. ROC curves were created, and the areas under the curve (AUCs) were calculated and compared using the Medcalc software (version ). According to the predicted probabilities, we divided the entire dataset into five equal groups. By plotting the median probability of each group, a calibration curve that described the distinction between the predicted probability and observed frequency of malignancy for that group was created. Results Pathological results Of all SPN patients, 29 (18.8%) cases were benign, including 5 tuberculomas, 6 hamartomas, 11 inflammatory pseudotumors, 3 pulmonary sclerosing hemangiomas, 2 atypical adenomatous hyperplasia, 1 fibrosis nodule, and 1 lung adenoma. One hundred and twenty-five (81.2%) cases were malignant, including 104 adenocarcinomas, 14 squamous carcinomas, 2 small-cell carcinomas, 4 large-cell carcinomas, and 1 neuroendocrine carcinoma. Comparison of the malignant and benign groups Fifty-seven percent of the patients were males, with a mean age of 58.1 years. As shown in Table 1, age, size, spiculation and border were significantly different between malignant and benign SPNs. However, family history of cancer, previous cancer history >5 years, and smoking history were not significantly different between the malignant and benign groups. Validation of the Mayo model Based on the applicable conditions of the Mayo model, we
3 Chinese Journal of Cancer Research, Vol 26, No 6 December Table 1 Clinical data of the malignant and benign groups Clinical features Full sample (n=154) Benign (n=29) Malignant (n=125) P Age in years [range] 58.1 [30-88] 51.0 [30-67] 59.7 [32-88] <0.001* Gender, N (%) Male 88 (57.1) 18 (62.1) 70 (56.0) Female 66 (42.9) 11 (37.9) 55 (44.0) Family history of cancer, N (%) Yes 17 0 (0) 17 (13.6) No (100.0) 108 (86.4) Previous cancer history >5 years, N (%) Yes 2 0 (0) 2 (1.6) No (100.0) 123 (98.4) Smoking history, N (%) Never smoker (75.9) 83 (66.4) Current or former smoker 49 7 (24.1) 42 (33.6) Current smoker 39 7 (24.1) 32 (25.6) Former smoker 10 0 (0) 10 (8.0) Mean pack-years [range] 38.3 [0-120] 36.4 [0-120] 38.7 [0-80] Mean years quit Location of SPN, N (%) Upper lobe (58.6) 65 (52.0) Middle or lower lobe (41.4) 60 (48.0) Median nodule size in mm [range] 20 [3-30] 17 [3-29] 21 [6-30] Spiculation, N (%) Yes (41.4) 100 (80.0) <0.001 No (58.6) 25 (20.0) Border, N (%) Clear (58.6) 29 (23.2) <0.001 Not clear (41.4) 96 (76.8) Calcification, N (%) Yes 7 1 (3.4) 6 (4.8) No (96.6) 119 (95.2) Data presented as N (%) unless otherwise indicated. t-tests were performed for continuous variables. χ² tests were performed for categorical variables., P values were obtained by comparison of the never smoker and current or former smoker groups; *, Wilcoxon s rank-sum test;, Fisher s exact test;, Continuity correction. SPN, solitary pulmonary nodule. excluded six patients who had a previous cancer history of more than 5 years. Of the remaining 154 patients, we constructed the ROC curve and calculated the AUC to be [95% confidence interval (CI): ]. Validation of the VA model The applicable conditions of the VA model included patients with a previous cancer history of more than 5 years. These SPNs tend to be malignant and were suggested to undergo surgical resection, so we excluded these six cases. The area under the ROC curve was (95% CI: ). If the six cases were included, the area under the ROC curve was (95% CI: ). If only male patients were included, the area under the ROC curve of the 88 male patients was (95% CI: ). If
4 650 Zhang et al. Comparison of SPN prediction models Sensitivity specificity only smokers were included, the area under the ROC curve of the 49 smoker patients was (95% CI: ). Validation of the PU model According to the applicable conditions of the PU model, we also excluded six patients who had a previous cancer history of more than 5 years. For the remaining 154 patients, the area under the ROC curve was (95% CI: ). Comparison of areas under the ROC curve Using the Medcalc software, we compared the AUCs among the three models. The p values were 0.82 between the Mayo and VA models, 0.49 between the Mayo and PU models, and 0.35 between the VA and PU models. Therefore, the AUCs of the three models did not demonstrate statistically significant differences. Figure 1 shows the ROC curves of the three models. Predicted probabilities of the three models Table 2 shows the interval distribution of each model according to the predicted results, recommended strategies, and pathological diagnosis. Calibration curves of the three models Mayo model VA model PU model Refernce line Figure 1 Receiver operating characteristics (ROC) curves of the three models. VA, Department of Veterans Affairs; PU, Peking University. The calibration curves for the Mayo, VA and PU model, describing the distinction between the predicted probability Table 2 Predicted results and interval distribution of the three models Model Mayo model VA model PU model and observed frequency of malignancy, is shown in Figures 2-4. Discussion Probability (%) Pathological Benign results (No.) Malignant Accuracy (positive predict value) (%) < > < > < > Mayo model: sensitivity =100%, specificity =50%; VA model: sensitivity =35.4%, specificity =95%; PU model: sensitivity =84%, specificity =62.1%. VA, Department of Veterans Affairs; PU, Peking University. The Mayo, VA, and PU models were validated in terms of the accuracy of SPN diagnosis by collecting clinical and imaging information. Our study reveals that the accuracies of the three models were not significantly different. The Mayo model, published in 1997, was the first to focus on SPN. Between 1984 and 1986, Swensen et al. at the Mayo Clinic retrospectively reviewed the medical records and imaging tests of 629 SPN patients (51% male) newly discovered with a malignancy rate of 23%. This group of patients lived locally for at least 20 years; thus, limitations in the data existed. However, in our results, the area under the ROC curve of the Mayo model was 0.753, which was higher than that of the VA model. With a classified process of three intervals, the false-positive (8%) and false-negative (0%) rates were low, providing reliable suggestions to clinicians. The calibration curve showed that the Mayo model underestimated the probability of malignancy in lowrisk patients. The VA model was established in 2007 using the records of 375 SPN cases were collected from the Department of Veterans Affairs. The data were unbalanced because 98% of patients were male, and 94% had a smoking history.
5 Chinese Journal of Cancer Research, Vol 26, No 6 December Observed probability Observed probability Predicted probability Figure 2 The calibration curve for the Mayo model. Figure 4 The calibration curve for the PU model. PU, Peking University Predicted probability Observed probability Figure 3 The calibration curve for the VA model. VA, Department of Veterans Affairs Predicted probability Thus, we found that smoking history has heavy weightings in the VA model, indicating that if a patient does not smoke, the calculated probability of the model may change considerably. This explains why the VA model showed poor accuracy. Additionally, a large proportion (68.9%) of patients was in the <20% probability interval, producing malignant pathological results. The area under the ROC curve did not improve in the male or smoker group. The calibration curve also showed that the Mayo model underestimated the probability of malignancy in low-risk patients, different from the actual situation. The PU model was presented in 2011, and comprised 371 SPN patients who underwent surgery at the People s Hospital of PU. The area under the ROC curve (0.800) was higher than those of the other two models; however, with the judgment of a spot, half of the patients had undergone unnecessary surgeries. We suggested dividing the entire region into three probability intervals; i.e., malignant, benign, and further examination. The calibration curve showed that the five groups of the PU model matched more closely the true circumstance than the other two models, excluding the second group. High-resolution CT should be performed on patients in the PU model because imaging characteristics are necessary factors in the calculation. Although medical records with inferior radiological technology were collected during 1984 to 1986 in Mayo model, it revealed high predictive value in this study. We suggested that Mayo model could be applied in some undeveloped area or some hospital without high-resolution CT scans. However, PU model, which collected medical records including high-resolution CT scans, showed the highest AUC and the best calibration curve. Accordingly, PU model set higher requirements to the doctors and equipments in medical image center. As a high percentage (81.2%) of malignant SPN
6 652 Zhang et al. Comparison of SPN prediction models patients existed in our population, the calibration curve did not perform well. Because the observed probability of malignancy of the five groups was higher than the predicted values, particularly for low-risk patients, the curve tended to underestimate malignant probability. Schultz and colleagues (7) calculated an AUC of 0.80 (95% CI: ) for the Mayo model and 0.73 (95% CI: ) for the VA model. Data characteristics of this study were similar to those of the VA model, with 96% male patients and 89% smokers. The difference between the two models was not statistically significant. In conclusion, clinicians should use an SPN predictive model based on the local epidemiology of lung cancer. Another study showed that if the SPN malignancy rate of the hospital was similar to that of one of the selected models, a higher diagnostic accuracy would result (8). The AUC of the Peking model was the highest of the three models, and the calibration curve fit better with our results. Thus, the PU model should be applied in the south of China. In conclusion, clinicians should choose an SPN predictive model based on the local epidemiology of lung cancer. And, the PU model should be applied in the China and similar area. Acknowledgements Guarantor: Xue-Ning Yang takes responsibility for the content of the manuscript, including the data and analysis. Authors contributions: Hong-Hong Yan directed and confirmed the statistical methods. Xuan Zhang collected data and wrote the manuscript. Jun-Tao Lin, Ze-Hua Wu, Jia Liu and Xu-Wei Cao collected data. Xue-Ning Yang designed the study and confirmed that the study objectives and procedures are honestly disclosed. Funding: This research was granted by the initiative research scheme for college student, Guangdong, China (No ). Disclosure: The authors declare no conflict of interest. References 1. Tan BB, Flaherty KR, Kazerooni EA, et al. The solitary pulmonary nodule. Chest 2003;123:89S-96S. 2. Ost D, Fein AM, Feinsilver SH. Clinical practice. The solitary pulmonary nodule. N Engl J Med 2003;348: Gould MK, Sanders GD, Barnett PG, et al. Costeffectiveness of alternative management strategies for patients with solitary pulmonary nodules. Ann Intern Med 2003;138: Swensen SJ, Silverstein MD, Ilstrup DM, et al. The probability of malignancy in solitary pulmonary nodules. Application to small radiologically indeterminate nodules. Arch Intern Med 1997;157: Schultz EM, Sanders GD, Trotter PR, et al. Validation of two models to estimate the probability of malignancy in patients with solitary pulmonary nodules. Thorax 2008;63: Li Y, Chen KZ, Wang J. Development and validation of a clinical prediction model to estimate the probability of malignancy in solitary pulmonary nodules in Chinese people. Clin Lung Cancer 2011;12: Schultz EM, Sanders GD, Trotter PR, et al. Validation of two models to estimate the probability of malignancy in patients with solitary pulmonary nodules. Thorax 2008;63: Isbell JM, Deppen S, Putnam JB Jr, et al. Existing general population models inaccurately predict lung cancer risk in patients referred for surgical evaluation. Ann Thorac Surg 2011;91:227-33; discussion 233. Cite this article as: Zhang X, Yan HH, Lin JT, Wu ZH, Liu J, Cao XW, Yang XN. Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule.. doi: / j.issn
Validation of two models to estimate the probability of malignancy in patients with solitary pulmonary nodules
 1 Stanford School of Medicine, Stanford, California, USA; 2 Duke University, Durham, North Carolina, USA; 3 Medical University of South Carolina, Charleston, South Carolina, USA; 4 VA Palo Alto Health
1 Stanford School of Medicine, Stanford, California, USA; 2 Duke University, Durham, North Carolina, USA; 3 Medical University of South Carolina, Charleston, South Carolina, USA; 4 VA Palo Alto Health
A Clinical Model To Estimate the Pretest Probability of Lung Cancer in Patients With Solitary Pulmonary Nodules*
 Original Research CANCER A Clinical Model To Estimate the Pretest Probability of Lung Cancer in Patients With Solitary Pulmonary Nodules* Michael K. Gould, MD, MS, FCCP; Lakshmi Ananth, MS; and Paul G.
Original Research CANCER A Clinical Model To Estimate the Pretest Probability of Lung Cancer in Patients With Solitary Pulmonary Nodules* Michael K. Gould, MD, MS, FCCP; Lakshmi Ananth, MS; and Paul G.
Establishment of a mathematic model for predicting malignancy in solitary pulmonary nodules
 Original Article Establishment of a mathematic model for predicting malignancy in solitary pulmonary nodules Man Zhang 1,2, Na Zhuo 3, Zhanlin Guo 2, Xingguang Zhang 4, Wenhua Liang 5,6, Sheng Zhao 7,
Original Article Establishment of a mathematic model for predicting malignancy in solitary pulmonary nodules Man Zhang 1,2, Na Zhuo 3, Zhanlin Guo 2, Xingguang Zhang 4, Wenhua Liang 5,6, Sheng Zhao 7,
Existing General Population Models Inaccurately Predict Lung Cancer Risk in Patients Referred for Surgical Evaluation
 Existing General Population Models Inaccurately Predict Lung Cancer Risk in Patients Referred for Surgical Evaluation James M. Isbell, MD, MSCI, Stephen Deppen, MA, MS, Joe B. Putnam, Jr, MD, Jonathan
Existing General Population Models Inaccurately Predict Lung Cancer Risk in Patients Referred for Surgical Evaluation James M. Isbell, MD, MSCI, Stephen Deppen, MA, MS, Joe B. Putnam, Jr, MD, Jonathan
May-Lin Wilgus. A. Study Purpose and Rationale
 Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
The solitary pulmonary nodule: Assessing the success of predicting malignancy
 The solitary pulmonary nodule: Assessing the success of predicting malignancy Poster No.: C-0829 Congress: ECR 2010 Type: Scientific Exhibit Topic: Chest Authors: R. W. K. Lindsay, J. Foster, K. McManus;
The solitary pulmonary nodule: Assessing the success of predicting malignancy Poster No.: C-0829 Congress: ECR 2010 Type: Scientific Exhibit Topic: Chest Authors: R. W. K. Lindsay, J. Foster, K. McManus;
Approach to Pulmonary Nodules
 Approach to Pulmonary Nodules Edwin Jackson, Jr., DO Assistant Professor-Clinical Director, James Early Detection Clinic Department of Internal Medicine Division of Pulmonary, Allergy, Critical Care and
Approach to Pulmonary Nodules Edwin Jackson, Jr., DO Assistant Professor-Clinical Director, James Early Detection Clinic Department of Internal Medicine Division of Pulmonary, Allergy, Critical Care and
Lung Cancer Risk Associated With New Solid Nodules in the National Lung Screening Trial
 Cardiopulmonary Imaging Original Research Pinsky et al. Lung Cancer Risk Associated With New Nodules Cardiopulmonary Imaging Original Research Paul F. Pinsky 1 David S. Gierada 2 P. Hrudaya Nath 3 Reginald
Cardiopulmonary Imaging Original Research Pinsky et al. Lung Cancer Risk Associated With New Nodules Cardiopulmonary Imaging Original Research Paul F. Pinsky 1 David S. Gierada 2 P. Hrudaya Nath 3 Reginald
Xiaohuan Pan 1,2 *, Xinguan Yang 1,2 *, Jingxu Li 1,2, Xiao Dong 1,2, Jianxing He 2,3, Yubao Guan 1,2. Original Article
 Original Article Is a 5-mm diameter an appropriate cut-off value for the diagnosis of atypical adenomatous hyperplasia and adenocarcinoma in situ on chest computed tomography and pathological examination?
Original Article Is a 5-mm diameter an appropriate cut-off value for the diagnosis of atypical adenomatous hyperplasia and adenocarcinoma in situ on chest computed tomography and pathological examination?
Imaging Decisions Start Here SM
 Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Lung Cancer Screening: To Screen or Not to Screen?
 Lung Cancer Screening: To Screen or Not to Screen? Lorriana Leard, MD Co-Director of UCSF Lung Cancer Screening Program Vice Chief of Clinical Activities UCSF Pulmonary, Critical Care, Allergy & Sleep
Lung Cancer Screening: To Screen or Not to Screen? Lorriana Leard, MD Co-Director of UCSF Lung Cancer Screening Program Vice Chief of Clinical Activities UCSF Pulmonary, Critical Care, Allergy & Sleep
CT Screening for Lung Cancer for High Risk Patients
 CT Screening for Lung Cancer for High Risk Patients The recently published National Lung Cancer Screening Trial (NLST) showed that low-dose CT screening for lung cancer reduces mortality in high-risk patients
CT Screening for Lung Cancer for High Risk Patients The recently published National Lung Cancer Screening Trial (NLST) showed that low-dose CT screening for lung cancer reduces mortality in high-risk patients
Evidence based approach to incidentally detected subsolid pulmonary nodule. DM SEMINAR July 27, 2018 Harshith Rao
 Evidence based approach to incidentally detected subsolid pulmonary nodule DM SEMINAR July 27, 2018 Harshith Rao Outline Definitions Etiologies Risk evaluation Clinical features Radiology Approach Modifications:
Evidence based approach to incidentally detected subsolid pulmonary nodule DM SEMINAR July 27, 2018 Harshith Rao Outline Definitions Etiologies Risk evaluation Clinical features Radiology Approach Modifications:
Rodney C Richie MD FACP FCCP DBIM Texas Life and EMSI
 Rodney C Richie MD FACP FCCP DBIM Texas Life and EMSI Pulmonary Nodules Well-circumscribed, radiographic opacities measuring 3 cm in diameter Surrounded by aerated lung Not associated with atelectesis
Rodney C Richie MD FACP FCCP DBIM Texas Life and EMSI Pulmonary Nodules Well-circumscribed, radiographic opacities measuring 3 cm in diameter Surrounded by aerated lung Not associated with atelectesis
Lung Cancer Diagnosis for Primary Care
 Lung Cancer Diagnosis for Primary Care Daniel Nader, DO, FCCP Cancer Treatment Center of America Case 1 In which of the following situations would the U.S. Preventive Services Task Force (USPSTF) recommend
Lung Cancer Diagnosis for Primary Care Daniel Nader, DO, FCCP Cancer Treatment Center of America Case 1 In which of the following situations would the U.S. Preventive Services Task Force (USPSTF) recommend
LUNG NODULES: MODERN MANAGEMENT STRATEGIES
 Department of Radiology LUNG NODULES: MODERN MANAGEMENT STRATEGIES Christian J. Herold M.D. Department of Biomedical Imaging and Image-guided Therapy Medical University of Vienna Vienna, Austria Pulmonary
Department of Radiology LUNG NODULES: MODERN MANAGEMENT STRATEGIES Christian J. Herold M.D. Department of Biomedical Imaging and Image-guided Therapy Medical University of Vienna Vienna, Austria Pulmonary
Pulmonary Nodules: When to worry, when to chill. Douglas Arenberg Associate Professor Pulmonary & Critical Care
 Pulmonary Nodules: When to worry, when to chill Douglas Arenberg Associate Professor Pulmonary & Critical Care Disclosure MDCH Grant Funds to improve tobacco cessation service in the Michigan Medicine
Pulmonary Nodules: When to worry, when to chill Douglas Arenberg Associate Professor Pulmonary & Critical Care Disclosure MDCH Grant Funds to improve tobacco cessation service in the Michigan Medicine
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer
 Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Learning Objectives. 1. Identify which patients meet criteria for annual lung cancer screening
 Disclosure I, Taylor Rowlett, DO NOT have a financial interest /arrangement or affiliation with one or more organizations that could be perceived as a real or apparent conflict of interest in the context
Disclosure I, Taylor Rowlett, DO NOT have a financial interest /arrangement or affiliation with one or more organizations that could be perceived as a real or apparent conflict of interest in the context
Pulmonary Nodules & Masses
 Pulmonary Nodules & Masses A Diagnostic Approach Heber MacMahon The University of Chicago Department of Radiology Disclosure Information Consultant for Riverain Technology Minor equity in Hologic Royalties
Pulmonary Nodules & Masses A Diagnostic Approach Heber MacMahon The University of Chicago Department of Radiology Disclosure Information Consultant for Riverain Technology Minor equity in Hologic Royalties
Diagnostic challenge: Sclerosing Hemangioma of the Lung. Department of Medicine, Division of Pulmonary and Critical Care, Lincoln Medical and
 Diagnostic challenge: Sclerosing Hemangioma of the Lung. S. Arias M.D, R. Loganathan M.D, FCCP Department of Medicine, Division of Pulmonary and Critical Care, Lincoln Medical and Mental Health Center/Weill
Diagnostic challenge: Sclerosing Hemangioma of the Lung. S. Arias M.D, R. Loganathan M.D, FCCP Department of Medicine, Division of Pulmonary and Critical Care, Lincoln Medical and Mental Health Center/Weill
The pulmonary nodule discovered by pneumonia: a case report
 Case Report The pulmonary nodule discovered by pneumonia: a case report Dong-Mei Yuan 1,2 *, Jian-Ya Zhang 1,2 *, Yan-Wen Yao 1,2, Hui-Ming Sun 1,2, Guan-Nan Wu 1,2, E-Hong Cao 1,2, Luca Bertolaccini 3,
Case Report The pulmonary nodule discovered by pneumonia: a case report Dong-Mei Yuan 1,2 *, Jian-Ya Zhang 1,2 *, Yan-Wen Yao 1,2, Hui-Ming Sun 1,2, Guan-Nan Wu 1,2, E-Hong Cao 1,2, Luca Bertolaccini 3,
THE BENEFITS OF BIG DATA
 THE BENEFITS OF BIG DATA Disclosures I am a named inventor on a number of patents and patent applications relating to the evaluation of pulmonary nodules on CT scans of the chest which are owned by Cornell
THE BENEFITS OF BIG DATA Disclosures I am a named inventor on a number of patents and patent applications relating to the evaluation of pulmonary nodules on CT scans of the chest which are owned by Cornell
Pulmonary Nodules. Michael Morris, MD
 Pulmonary Nodules Michael Morris, MD Case 45 year old healthy male Smokes socially Normal physical exam Pre-employment screening remote +PPD screening CXR nodular opacity Case 45 year old healthy male
Pulmonary Nodules Michael Morris, MD Case 45 year old healthy male Smokes socially Normal physical exam Pre-employment screening remote +PPD screening CXR nodular opacity Case 45 year old healthy male
Available online at
 60 Available online at www.annclinlabsci.org Serum Angiopoietin-2 as a Clinical Marker for Lung Cancer in Patients with Solitary Pulmonary Nodules Chunhua Xu 1,2, Wei Wang 1,2, Yuchao Wang 1,2, Xiuwei
60 Available online at www.annclinlabsci.org Serum Angiopoietin-2 as a Clinical Marker for Lung Cancer in Patients with Solitary Pulmonary Nodules Chunhua Xu 1,2, Wei Wang 1,2, Yuchao Wang 1,2, Xiuwei
DENOMINATOR: All final reports for CT imaging studies with a finding of an incidental pulmonary nodule for patients aged 35 years and older
 Quality ID #364: Optimizing Patient Exposure to Ionizing Radiation: Appropriateness: Follow-up CT Imaging for Incidentally Detected Pulmonary Nodules According to Recommended Guidelines National Quality
Quality ID #364: Optimizing Patient Exposure to Ionizing Radiation: Appropriateness: Follow-up CT Imaging for Incidentally Detected Pulmonary Nodules According to Recommended Guidelines National Quality
Indications for sublobar resection for localized NSCLC
 Indications for sublobar resection for localized NSCLC David H Harpole Jr, MD Professor of Surgery Associate Professor in Pathology Vice Chief, Division of Surgical Services Duke University School of Medicine
Indications for sublobar resection for localized NSCLC David H Harpole Jr, MD Professor of Surgery Associate Professor in Pathology Vice Chief, Division of Surgical Services Duke University School of Medicine
Indeterminate Lung Nodules in Cancer Patients: Pretest Probability of Malignancy and the Role of 18 F-FDG PET/CT
 Cardiopulmonary Imaging Original Research Evangelista et al. FDG PET/CT of Malignant Lung Nodules Cardiopulmonary Imaging Original Research FOCUS ON: Laura Evangelista 1 Annalori Panunzio 2 Roberta Polverosi
Cardiopulmonary Imaging Original Research Evangelista et al. FDG PET/CT of Malignant Lung Nodules Cardiopulmonary Imaging Original Research FOCUS ON: Laura Evangelista 1 Annalori Panunzio 2 Roberta Polverosi
I appreciate the courtesy of Kusumoto at NCC for this presentation. What is Early Lung Cancers. Early Lung Cancers. Early Lung Cancers 18/10/55
 I appreciate the courtesy of Kusumoto at NCC for this presentation. Dr. What is Early Lung Cancers DEATH Early period in its lifetime Curative period in its lifetime Early Lung Cancers Early Lung Cancers
I appreciate the courtesy of Kusumoto at NCC for this presentation. Dr. What is Early Lung Cancers DEATH Early period in its lifetime Curative period in its lifetime Early Lung Cancers Early Lung Cancers
Validation of the T descriptor in the new 8th TNM classification for non-small cell lung cancer
 Original Article Validation of the T descriptor in the new 8th TNM classification for non-small cell lung cancer Hee Suk Jung 1, Jin Gu Lee 2, Chang Young Lee 2, Dae Joon Kim 2, Kyung Young Chung 2 1 Department
Original Article Validation of the T descriptor in the new 8th TNM classification for non-small cell lung cancer Hee Suk Jung 1, Jin Gu Lee 2, Chang Young Lee 2, Dae Joon Kim 2, Kyung Young Chung 2 1 Department
GUIDELINES FOR PULMONARY NODULE MANAGEMENT : RECENT CHANGES AND UPDATES
 Venice 2017 GUIDELINES FOR PULMONARY NODULE MANAGEMENT : RECENT CHANGES AND UPDATES Heber MacMahon MB, BCh Department of Radiology The University of Chicago Disclosures Consultant for Riverain Medical
Venice 2017 GUIDELINES FOR PULMONARY NODULE MANAGEMENT : RECENT CHANGES AND UPDATES Heber MacMahon MB, BCh Department of Radiology The University of Chicago Disclosures Consultant for Riverain Medical
Lung cancer is an aggressive and heterogeneous disease. 1,2
 ORIGINAL ARTICLE A Clinical Model to Estimate the Pretest Probability of Lung Cancer, Based on 1198 Pedigrees in China Huan Lin, MD, Wen-Zhao Zhong, MD, Xue-Ning Yang, MD, Xu-Chao Zhang, PhD, Jin-Ji Yang,
ORIGINAL ARTICLE A Clinical Model to Estimate the Pretest Probability of Lung Cancer, Based on 1198 Pedigrees in China Huan Lin, MD, Wen-Zhao Zhong, MD, Xue-Ning Yang, MD, Xu-Chao Zhang, PhD, Jin-Ji Yang,
Yong Qiang 1, Lei Zhang 1, Nan Yang 1, Jian Xu 1, De-Min Li 1, Tangfeng Lv 2, Ping Zhan 2, Yong Song 2, Zhong-Dong Li 1, Hao Li 3.
 Original Article Diagnostic and therapeutic value of computed tomography guided coil placement after digital subtraction angiography guided videoassisted thoracoscopic surgery resection for solitary pulmonary
Original Article Diagnostic and therapeutic value of computed tomography guided coil placement after digital subtraction angiography guided videoassisted thoracoscopic surgery resection for solitary pulmonary
Percutaneous Needle Aspiration Biopsy (PCNA) of Pulmonary Lesions: Evaluation of a Reaspiration or a Rebiopsy (second PCNA) 1
 Percutaneous Needle Aspiration Biopsy (PCNA) of Pulmonary Lesions: Evaluation of a Reaspiration or a Rebiopsy (second PCNA) 1 In Jae Lee, M.D., Dong Gyu Kim, M.D. 2, Ki-Suck Jung, M.D. 2, Hyoung June Im,
Percutaneous Needle Aspiration Biopsy (PCNA) of Pulmonary Lesions: Evaluation of a Reaspiration or a Rebiopsy (second PCNA) 1 In Jae Lee, M.D., Dong Gyu Kim, M.D. 2, Ki-Suck Jung, M.D. 2, Hyoung June Im,
Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule
 Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
The Spectrum of Management of Pulmonary Ground Glass Nodules
 The Spectrum of Management of Pulmonary Ground Glass Nodules Stanley S Siegelman CT Society 10/26/2011 No financial disclosures. Noguchi M et al. Cancer 75: 2844-2852, 1995. 236 surgically resected peripheral
The Spectrum of Management of Pulmonary Ground Glass Nodules Stanley S Siegelman CT Society 10/26/2011 No financial disclosures. Noguchi M et al. Cancer 75: 2844-2852, 1995. 236 surgically resected peripheral
Comparison of four models predicting the malignancy of pulmonary nodules: A singlecenter study of Korean adults
 RESEARCH ARTICLE Comparison of four models predicting the malignancy of pulmonary nodules: A singlecenter study of Korean adults Bumhee Yang 1, Byung Woo Jhun 1, Sun Hye Shin 1, Byeong-Ho Jeong 1, Sang-Won
RESEARCH ARTICLE Comparison of four models predicting the malignancy of pulmonary nodules: A singlecenter study of Korean adults Bumhee Yang 1, Byung Woo Jhun 1, Sun Hye Shin 1, Byeong-Ho Jeong 1, Sang-Won
Prediction models for solitary pulmonary nodules based on curvelet textural features and clinical parameters
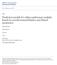 Edith Cowan University Research Online ECU Publications 2013 2013 Prediction models for solitary pulmonary nodules based on curvelet textural features and clinical parameters Jing-Jing Wang Hai-Feng Wu
Edith Cowan University Research Online ECU Publications 2013 2013 Prediction models for solitary pulmonary nodules based on curvelet textural features and clinical parameters Jing-Jing Wang Hai-Feng Wu
PULMONARY NODULES AND MASSES : DIAGNOSTIC APPROACH AND NEW MANAGEMENT GUIDELINES. https://tinyurl.com/hmpn2018
 PULMONARY NODULES AND MASSES : DIAGNOSTIC APPROACH AND NEW MANAGEMENT GUIDELINES Heber MacMahon MB, BCh Department of Radiology The University of Chicago https://tinyurl.com/hmpn2018 Disclosures Consultant
PULMONARY NODULES AND MASSES : DIAGNOSTIC APPROACH AND NEW MANAGEMENT GUIDELINES Heber MacMahon MB, BCh Department of Radiology The University of Chicago https://tinyurl.com/hmpn2018 Disclosures Consultant
What to know and what to make of it
 Lung Cancer Screening: What to know and what to make of it J. Matthew Reinersman, MD Assistant Professor of Surgery Division of Thoracic and Cardiovascular Surgery Department of Surgery University of Oklahoma
Lung Cancer Screening: What to know and what to make of it J. Matthew Reinersman, MD Assistant Professor of Surgery Division of Thoracic and Cardiovascular Surgery Department of Surgery University of Oklahoma
Early Detection of Lung Cancer. Amsterdam March 5 th 2010
 Early Detection of Lung Cancer Amsterdam March 5 th 2010 Rob J van Klaveren, MD, PhD Dept. of Pulmonology Erasmus MC Rotterdam, the Netherlands Early Detection and Screening - Questions to be addressed
Early Detection of Lung Cancer Amsterdam March 5 th 2010 Rob J van Klaveren, MD, PhD Dept. of Pulmonology Erasmus MC Rotterdam, the Netherlands Early Detection and Screening - Questions to be addressed
THORACIK RICK. Lungs. Outline and objectives Richard A. Malthaner MD MSc FRCSC FACS
 THORACIK RICK Outline and objectives Lungs Management of a solitary lung nodule Mediastinum Management of a mediastinal mass Pleura Management of a pleural fluid & pneumothorax Esophagus & Stomach Management
THORACIK RICK Outline and objectives Lungs Management of a solitary lung nodule Mediastinum Management of a mediastinal mass Pleura Management of a pleural fluid & pneumothorax Esophagus & Stomach Management
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Chest Radiology Interpretation: Findings of Tuberculosis
 Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
PULMONARY NODULES DETECTED INCIDENTALLY OR BY SCREENING: LOTS OF GUIDELINES BUT WHERE IS THE EVIDENCE?
 PULMONARY NODULES DETECTED INCIDENTALLY OR BY SCREENING: LOTS OF GUIDELINES BUT WHERE IS THE EVIDENCE? MICHAEL K. GOULD, MD SENIOR RESEARCH SCIENTIST DIRECTOR FOR HEALTH SCIENCES & IMPLEMENTATION SCIENCE
PULMONARY NODULES DETECTED INCIDENTALLY OR BY SCREENING: LOTS OF GUIDELINES BUT WHERE IS THE EVIDENCE? MICHAEL K. GOULD, MD SENIOR RESEARCH SCIENTIST DIRECTOR FOR HEALTH SCIENCES & IMPLEMENTATION SCIENCE
Cancer incidence and patient survival rates among the residents in the Pudong New Area of Shanghai between 2002 and 2006
 Chinese Journal of Cancer Original Article Cancer incidence and patient survival rates among the residents in the Pudong New Area of Shanghai between 2002 and 2006 Xiao-Pan Li 1, Guang-Wen Cao 2, Qiao
Chinese Journal of Cancer Original Article Cancer incidence and patient survival rates among the residents in the Pudong New Area of Shanghai between 2002 and 2006 Xiao-Pan Li 1, Guang-Wen Cao 2, Qiao
Screening Programs background and clinical implementation. Denise R. Aberle, MD Professor of Radiology and Engineering
 Screening Programs background and clinical implementation Denise R. Aberle, MD Professor of Radiology and Engineering disclosures I have no disclosures. I have no conflicts of interest relevant to this
Screening Programs background and clinical implementation Denise R. Aberle, MD Professor of Radiology and Engineering disclosures I have no disclosures. I have no conflicts of interest relevant to this
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times
 Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Clinical efficacy of crizotinib in Chinese patients with ALK-positive non-small-cell lung cancer with brain metastases
 Original Article Clinical efficacy of crizotinib in Chinese patients with ALK-positive non-small-cell lung cancer with brain metastases Yuan-Yuan Lei 1,2, Jin-Ji Yang 2, Wen-Zhao Zhong 2, Hua-Jun Chen
Original Article Clinical efficacy of crizotinib in Chinese patients with ALK-positive non-small-cell lung cancer with brain metastases Yuan-Yuan Lei 1,2, Jin-Ji Yang 2, Wen-Zhao Zhong 2, Hua-Jun Chen
PET/CT in lung cancer
 PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
Christine Argento, MD Interventional Pulmonology Emory University
 Christine Argento, MD Interventional Pulmonology Emory University Outline Lung Cancer Statistics Prior Studies for Lung Cancer Screening NLST Studies Following NLST Future Directions Lung Cancer American
Christine Argento, MD Interventional Pulmonology Emory University Outline Lung Cancer Statistics Prior Studies for Lung Cancer Screening NLST Studies Following NLST Future Directions Lung Cancer American
Published Pulmonary Nodule Guidelines A Synthesis
 Published Pulmonary Nodule Guidelines A Synthesis Dr A Devaraj Royal Brompton Hospital London 4/28/2015 1 And very soon to be published Published ^ Pulmonary Nodule Guidelines A Synthesis Dr A Devaraj
Published Pulmonary Nodule Guidelines A Synthesis Dr A Devaraj Royal Brompton Hospital London 4/28/2015 1 And very soon to be published Published ^ Pulmonary Nodule Guidelines A Synthesis Dr A Devaraj
Lung Cancer Screening
 Lung Cancer Screening Steven Leh, MD, FCCP Diplomat of the American Association for Bronchology and Interventional Pulmonology Aurora Medical Group Pulmonary and Sleep Medicine February 10, 2018 Disclosures
Lung Cancer Screening Steven Leh, MD, FCCP Diplomat of the American Association for Bronchology and Interventional Pulmonology Aurora Medical Group Pulmonary and Sleep Medicine February 10, 2018 Disclosures
Indications and methods of surgical treatment of solitary pulmonary nodule
 Original Paper Indications and methods of surgical treatment of solitary pulmonary nodule John Karathanassis 1, Konstantinos Potaris 1, Aphrodite Karathanassis 2, Marios Konstantinou 1, Konstantinos Syrigos
Original Paper Indications and methods of surgical treatment of solitary pulmonary nodule John Karathanassis 1, Konstantinos Potaris 1, Aphrodite Karathanassis 2, Marios Konstantinou 1, Konstantinos Syrigos
Noninvasive Differential Diagnosis of Pulmonary Nodules Using the Standardized Uptake Value Index
 doi: 10.5761/atcs.oa.14-00241 Original Article Noninvasive Differential Diagnosis of Pulmonary Nodules Using the Standardized Uptake Value Index Satoshi Shiono, MD, 1 Naoki Yanagawa, MD, 2 Masami Abiko,
doi: 10.5761/atcs.oa.14-00241 Original Article Noninvasive Differential Diagnosis of Pulmonary Nodules Using the Standardized Uptake Value Index Satoshi Shiono, MD, 1 Naoki Yanagawa, MD, 2 Masami Abiko,
A Chronology of Advancements in the Diagnosing of Lung Nodules
 November 17, 2017 A Chronology of Advancements in the Diagnosing of Lung Nodules Presenter: Daniel P. Harley, MD, MSB, FACS Surgical Director of the Angelos Center for Lung Diseases 1 Pulmonary Nodules
November 17, 2017 A Chronology of Advancements in the Diagnosing of Lung Nodules Presenter: Daniel P. Harley, MD, MSB, FACS Surgical Director of the Angelos Center for Lung Diseases 1 Pulmonary Nodules
Screening for Lung Cancer: Are We There Yet?
 Screening for Lung Cancer: Are We There Yet? Kavita Garg, MD Professor of Radiology University of CO, Denver Mountain States Cancer Conference Nov 6 th 2010 The Epidemiology of Lung Cancer Tobacco is the
Screening for Lung Cancer: Are We There Yet? Kavita Garg, MD Professor of Radiology University of CO, Denver Mountain States Cancer Conference Nov 6 th 2010 The Epidemiology of Lung Cancer Tobacco is the
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #364: Optimizing Patient Exposure to Ionizing Radiation: Appropriateness: Follow-up CT Imaging for Incidentally Detected Pulmonary Nodules According to Recommended Guidelines National Quality
Quality ID #364: Optimizing Patient Exposure to Ionizing Radiation: Appropriateness: Follow-up CT Imaging for Incidentally Detected Pulmonary Nodules According to Recommended Guidelines National Quality
Positron Emission Tomography in Lung Cancer
 May 19, 2003 Positron Emission Tomography in Lung Cancer Andrew Wang, HMS III Patient DD 53 y/o gentleman presented with worsening dyspnea on exertion for the past two months 30 pack-year smoking Hx and
May 19, 2003 Positron Emission Tomography in Lung Cancer Andrew Wang, HMS III Patient DD 53 y/o gentleman presented with worsening dyspnea on exertion for the past two months 30 pack-year smoking Hx and
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Does the lung nodule look aggressive enough to warrant a more extensive operation?
 Accepted Manuscript Does the lung nodule look aggressive enough to warrant a more extensive operation? Michael Kuan-Yew Hsin, MBChB, MA, FRCS(CTh), David Chi-Leung Lam, MD, PhD, FRCP (Edin, Glasg & Lond)
Accepted Manuscript Does the lung nodule look aggressive enough to warrant a more extensive operation? Michael Kuan-Yew Hsin, MBChB, MA, FRCS(CTh), David Chi-Leung Lam, MD, PhD, FRCP (Edin, Glasg & Lond)
American College Of Radiology ACR Appropriateness Criteria WORK-UP OF THE SOLITARY PULMONARY NODULE
 This document is provided to you by the American College of Radiology. We strive to deliver this information in a convenient and effective manner. After you finish reviewing the criteria, please provide
This document is provided to you by the American College of Radiology. We strive to deliver this information in a convenient and effective manner. After you finish reviewing the criteria, please provide
Combined use of AFP, CEA, CA125 and CAl9-9 improves the sensitivity for the diagnosis of gastric cancer
 He et al. BMC Gastroenterology 2013, 13:87 RESEARCH ARTICLE Open Access Combined use of AFP, CEA, CA125 and CAl9-9 improves the sensitivity for the diagnosis of gastric cancer Chao-Zhu He 1,2, Kun-He Zhang
He et al. BMC Gastroenterology 2013, 13:87 RESEARCH ARTICLE Open Access Combined use of AFP, CEA, CA125 and CAl9-9 improves the sensitivity for the diagnosis of gastric cancer Chao-Zhu He 1,2, Kun-He Zhang
Characterization of solitary pulmonary nodules: Use of washout characteristics at contrast-enhanced computed tomography
 672 Characterization of solitary pulmonary nodules: Use of washout characteristics at contrast-enhanced computed tomography XIAO-DAN YE 1*, JIAN-DING YE 1*, ZHENG YUAN 2,3, SHENG DONG 4 and XIANG-SHENG
672 Characterization of solitary pulmonary nodules: Use of washout characteristics at contrast-enhanced computed tomography XIAO-DAN YE 1*, JIAN-DING YE 1*, ZHENG YUAN 2,3, SHENG DONG 4 and XIANG-SHENG
Original Article Clinical predictors of lymph node metastasis in lung adenocarcinoma: an exploratory study
 Int J Clin Exp Med 2016;9(5):8765-8769 www.ijcem.com /ISSN:1940-5901/IJCEM0017315 Original Article Clinical predictors of lymph node metastasis in lung adenocarcinoma: an exploratory study Zhijun Zhu,
Int J Clin Exp Med 2016;9(5):8765-8769 www.ijcem.com /ISSN:1940-5901/IJCEM0017315 Original Article Clinical predictors of lymph node metastasis in lung adenocarcinoma: an exploratory study Zhijun Zhu,
Clinical profiles and trend analysis of newly diagnosed lung cancer in a tertiary care hospital of East China during
 Original Article Clinical profiles and trend analysis of newly diagnosed lung cancer in a tertiary care hospital of East China during 2011 2015 Pingli Wang 1 *, Jixia Zou 1 *, Jingni Wu 1 *, Chengyan Zhang
Original Article Clinical profiles and trend analysis of newly diagnosed lung cancer in a tertiary care hospital of East China during 2011 2015 Pingli Wang 1 *, Jixia Zou 1 *, Jingni Wu 1 *, Chengyan Zhang
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Charles Mulligan, MD, FACS, FCCP 26 March 2015
 Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms
 Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
Deppen S, et al. Annals of Thoracic Surgery 2011;92:
 Deppen S, et al. Annals of Thoracic Surgery 2011;92:428-33. http://www.nationmaster.com/graph/ mor_his-mortality-histoplasmosis http://www.humirarems.com/brochure.aspx Baddley, John W., et al. Emerging
Deppen S, et al. Annals of Thoracic Surgery 2011;92:428-33. http://www.nationmaster.com/graph/ mor_his-mortality-histoplasmosis http://www.humirarems.com/brochure.aspx Baddley, John W., et al. Emerging
National Lung Screening Trial Results
 National Lung Screening Trial Results Ella A. Kazerooni, M.D. Professor & Director Cardiothoracic Radiology Associate Chair for Clinical Affairs University of Michigan NLST STOPPED! Lung cancer trial results
National Lung Screening Trial Results Ella A. Kazerooni, M.D. Professor & Director Cardiothoracic Radiology Associate Chair for Clinical Affairs University of Michigan NLST STOPPED! Lung cancer trial results
Ruijin robotic thoracic surgery: S segmentectomy of the left upper lobe
 Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
CASE REPORT. Introduction. Case series reports. J Thorac Dis 2012;4(S1): DOI: /j.issn s003
 CASE REPORT Lost in time pulmonary metastases of renal cell carcinoma: complete surgical resection of metachronous metastases, 18 and 15 years after nephrectomy Kosmas Tsakiridis 1, Aikaterini N Visouli
CASE REPORT Lost in time pulmonary metastases of renal cell carcinoma: complete surgical resection of metachronous metastases, 18 and 15 years after nephrectomy Kosmas Tsakiridis 1, Aikaterini N Visouli
SCBT-MR 2016 Lung Cancer Screening in Practice: State of the Art
 SCBT-MR 2016 Lung Cancer Screening in Practice: State of the Art Reginald F. Munden MD, DMD, MBA I have no conflicts of interest to report National Lung Cancer Screening Trial 20% lung cancer mortality
SCBT-MR 2016 Lung Cancer Screening in Practice: State of the Art Reginald F. Munden MD, DMD, MBA I have no conflicts of interest to report National Lung Cancer Screening Trial 20% lung cancer mortality
Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules
 Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Title: Peripheral pulmonary nodules: relationship between multi-slice spiral CT perfusion imaging and tumor angiogenesis and VEGF expression
 Author's response to reviews Title: Peripheral pulmonary nodules: relationship between multi-slice spiral CT perfusion imaging and tumor angiogenesis and VEGF expression Authors: Shu-Hua Ma (mashuhua6699@sina.com)
Author's response to reviews Title: Peripheral pulmonary nodules: relationship between multi-slice spiral CT perfusion imaging and tumor angiogenesis and VEGF expression Authors: Shu-Hua Ma (mashuhua6699@sina.com)
Predictive risk factors for lymph node metastasis in patients with small size non-small cell lung cancer
 Original Article Predictive risk factors for lymph node metastasis in patients with small size non-small cell lung cancer Feichao Bao, Ping Yuan, Xiaoshuai Yuan, Xiayi Lv, Zhitian Wang, Jian Hu Department
Original Article Predictive risk factors for lymph node metastasis in patients with small size non-small cell lung cancer Feichao Bao, Ping Yuan, Xiaoshuai Yuan, Xiayi Lv, Zhitian Wang, Jian Hu Department
Lung Cancer Screening. Ashish Maskey MD Interventional Pulmonology UK Health Care Dec 1 st 2017
 Lung Cancer Screening Ashish Maskey MD Interventional Pulmonology UK Health Care Dec 1 st 2017 Nearly one in six American adults currently smoke cigarettes An estimated 40 million adults in the United
Lung Cancer Screening Ashish Maskey MD Interventional Pulmonology UK Health Care Dec 1 st 2017 Nearly one in six American adults currently smoke cigarettes An estimated 40 million adults in the United
A Comprehensive Cancer Center Designated by the National Cancer Institute
 N C I C C C A Comprehensive Cancer Center Designated by the National Cancer Institute Screening and Early Detection of Lung Cancer: Ready for Practice? David S. Ettinger, MD, FACP, FCCP Alex Grass Professor
N C I C C C A Comprehensive Cancer Center Designated by the National Cancer Institute Screening and Early Detection of Lung Cancer: Ready for Practice? David S. Ettinger, MD, FACP, FCCP Alex Grass Professor
Characterization of the Solitary Pulmonary Nodule: 18 F-FDG PET Versus Nodule-Enhancement CT
 PET vs CT of Solitary Pulmonary Nodules Nuclear Medicine Original Research C D E M N E U T R Y L I M C I G O F I N G Characterization of the Solitary Pulmonary Nodule: 18 F-FDG PET Versus Nodule-Enhancement
PET vs CT of Solitary Pulmonary Nodules Nuclear Medicine Original Research C D E M N E U T R Y L I M C I G O F I N G Characterization of the Solitary Pulmonary Nodule: 18 F-FDG PET Versus Nodule-Enhancement
HRCT features distinguishing minimally invasive adenocarcinomas from invasive adenocarcinomas appearing as mixed ground-glass nodules
 Original Article HRCT features distinguishing minimally invasive adenocarcinomas from invasive adenocarcinomas appearing as mixed ground-glass nodules Wei Yu 1, Zhaoyu Wang 2, Liyong Qian 2, Shanjun Wang
Original Article HRCT features distinguishing minimally invasive adenocarcinomas from invasive adenocarcinomas appearing as mixed ground-glass nodules Wei Yu 1, Zhaoyu Wang 2, Liyong Qian 2, Shanjun Wang
Lung Cancer Screening. Eric S. Papierniak, DO NF/SG VHA UF Health
 Lung Cancer Screening Eric S. Papierniak, DO NF/SG VHA UF Health Overview Background Supporting evidence Guidelines Practical considerations Patient selection What to do with abnormal results Billing/coding
Lung Cancer Screening Eric S. Papierniak, DO NF/SG VHA UF Health Overview Background Supporting evidence Guidelines Practical considerations Patient selection What to do with abnormal results Billing/coding
CM EARTICLE The solitary pulmonary nodule
 IPractice Integration & Lifelong Learning Singapore Med J 2012; 53(6) 372 CM EARTICLE The solitary pulmonary nodule Jansen Meng Kwang Kohl, MBBS, MRCP, Gerald Jit Shen Tan2'3, MBBS, FRCR, Choon How How4,
IPractice Integration & Lifelong Learning Singapore Med J 2012; 53(6) 372 CM EARTICLE The solitary pulmonary nodule Jansen Meng Kwang Kohl, MBBS, MRCP, Gerald Jit Shen Tan2'3, MBBS, FRCR, Choon How How4,
Right infrahilar nodule
 Right infrahilar nodule Search Infrahilar nodule Nov 9, 2015.. CT chest showed a right infrahilar mass 3.5 2.5 cm along with multiple bilateral lung nodules of size 9 to 11 mm. Bronchoscopy. Jun 13, 2015.
Right infrahilar nodule Search Infrahilar nodule Nov 9, 2015.. CT chest showed a right infrahilar mass 3.5 2.5 cm along with multiple bilateral lung nodules of size 9 to 11 mm. Bronchoscopy. Jun 13, 2015.
Lung Cancer Screening: Benefits and limitations to its Implementation
 Lung Cancer Screening: Benefits and limitations to its Implementation Rolando Sanchez, MD Clinical Assistant Professor Pulmonary-Critical Care Medicine University of Iowa Lung cancer - Epidemiology Cancer
Lung Cancer Screening: Benefits and limitations to its Implementation Rolando Sanchez, MD Clinical Assistant Professor Pulmonary-Critical Care Medicine University of Iowa Lung cancer - Epidemiology Cancer
With recent advances in diagnostic imaging technologies,
 ORIGINAL ARTICLE Management of Ground-Glass Opacity Lesions Detected in Patients with Otherwise Operable Non-small Cell Lung Cancer Hong Kwan Kim, MD,* Yong Soo Choi, MD,* Kwhanmien Kim, MD,* Young Mog
ORIGINAL ARTICLE Management of Ground-Glass Opacity Lesions Detected in Patients with Otherwise Operable Non-small Cell Lung Cancer Hong Kwan Kim, MD,* Yong Soo Choi, MD,* Kwhanmien Kim, MD,* Young Mog
Diffuse high-attenuation within mediastinal lymph nodes on non-enhanced CT scan: Usefulness in the prediction of benignancy
 Diffuse high-attenuation within mediastinal lymph nodes on non-enhanced CT scan: Usefulness in the prediction of benignancy Poster No.: C-1785 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific
Diffuse high-attenuation within mediastinal lymph nodes on non-enhanced CT scan: Usefulness in the prediction of benignancy Poster No.: C-1785 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific
Larry Tan, MD Thoracic Surgery, HSC. Community Cancer Care Educational Conference October 27, 2017
 Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Lung Cancer Screening
 Scan for mobile link. Lung Cancer Screening What is lung cancer screening? Screening examinations are tests performed to find disease before symptoms begin. The goal of screening is to detect disease at
Scan for mobile link. Lung Cancer Screening What is lung cancer screening? Screening examinations are tests performed to find disease before symptoms begin. The goal of screening is to detect disease at
Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer
 Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
NCCN Guidelines as a Model of Extended Criteria for Lung Cancer Screening
 444 Original Research NCCN Guidelines as a Model of Extended Criteria for Lung Cancer Screening Brady J. McKee, MD; Shawn Regis, PhD; Andrea K. Borondy-Kitts, MS, MPH; Jeffrey A. Hashim, MD; Robert J.
444 Original Research NCCN Guidelines as a Model of Extended Criteria for Lung Cancer Screening Brady J. McKee, MD; Shawn Regis, PhD; Andrea K. Borondy-Kitts, MS, MPH; Jeffrey A. Hashim, MD; Robert J.
Robert J. McKenna M.D. Chief, Thoracic Surgery Cedars Sinai Medical Center
 You Smoke, You Get Lung Cancer, You Die: Can Screening Change this Paradigm? Robert J. McKenna M.D. Chief, Thoracic Surgery Cedars Sinai Medical Center AATS Saturday 4/28/2012 Cancer Screening Cancer
You Smoke, You Get Lung Cancer, You Die: Can Screening Change this Paradigm? Robert J. McKenna M.D. Chief, Thoracic Surgery Cedars Sinai Medical Center AATS Saturday 4/28/2012 Cancer Screening Cancer
None
 2014 None rosemary clooney Cancer is one of the most common diseases in the developed world: 1 in 4 deaths are due to cancer 1 in 17 deaths are due to lung cancer Lung cancer is the most common
2014 None rosemary clooney Cancer is one of the most common diseases in the developed world: 1 in 4 deaths are due to cancer 1 in 17 deaths are due to lung cancer Lung cancer is the most common
Best Medical Practices: Maximizing Skills, Minimizing Risk Lung Cancer
 Best Medical Practices: Maximizing Skills, Minimizing Risk Lung Cancer Optimal Management of Incidental Pulmonary Nodule Ramin Khorasani, MD, MPH Vice Chair, Department of Radiology Director, Center for
Best Medical Practices: Maximizing Skills, Minimizing Risk Lung Cancer Optimal Management of Incidental Pulmonary Nodule Ramin Khorasani, MD, MPH Vice Chair, Department of Radiology Director, Center for
and Strength of Recommendations
 ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
Accepted Manuscript. Unexpected high incidence of hepatocellular carcinoma in patients with hepatitis C in the era of DAAs: too alarming?
 Accepted Manuscript Unexpected high incidence of hepatocellular carcinoma in patients with hepatitis C in the era of DAAs: too alarming? Qing-Lei Zeng, Zhi-Qin Li, Hong-Xia Liang, Guang-Hua Xu, Chun-Xia
Accepted Manuscript Unexpected high incidence of hepatocellular carcinoma in patients with hepatitis C in the era of DAAs: too alarming? Qing-Lei Zeng, Zhi-Qin Li, Hong-Xia Liang, Guang-Hua Xu, Chun-Xia
American College of Radiology ACR Appropriateness Criteria
 American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
PET CT for Staging Lung Cancer
 PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
Screening for Lung Cancer: New Guidelines, Old Problems
 Screening for Lung Cancer: New Guidelines, Old Problems Robert Schilz DO, PhD Associate Professor of Medicine Interim Chief of the Division of Pulmonary, Critical Care and Sleep Medicine University Hospitals
Screening for Lung Cancer: New Guidelines, Old Problems Robert Schilz DO, PhD Associate Professor of Medicine Interim Chief of the Division of Pulmonary, Critical Care and Sleep Medicine University Hospitals
Pathology and Prognosis of Persistent Stable Pure Ground-Glass Opacity Nodules After Surgical Resection
 GENERAL THORACIC Pathology and Prognosis of Persistent Stable Pure Ground-Glass Opacity Nodules After Surgical Resection Sukki Cho, MD, HeeChul Yang, MD, Kwhanmien Kim, MD, and Sanghoon Jheon, MD Department
GENERAL THORACIC Pathology and Prognosis of Persistent Stable Pure Ground-Glass Opacity Nodules After Surgical Resection Sukki Cho, MD, HeeChul Yang, MD, Kwhanmien Kim, MD, and Sanghoon Jheon, MD Department
