Research Article Bone Scan Is of Doubtful Value as a First Staging Test in the Primary Presentation of Prostate Cancer
|
|
|
- Leo Summers
- 5 years ago
- Views:
Transcription
1 International Scholarly Research Network ISRN Oncology Volume 2012, Article ID , 6 pages doi: /2012/ Research Article Bone Scan Is of Doubtful Value as a First Staging Test in the Primary Presentation of Prostate Cancer Lina M. Carmona Echeverria, 1 Lawrence Drudge-Coates, 1 C. Jason Wilkins, 2 and Gordon H. Muir 1 1 Department of Urology, King s College Hospital, 2nd floor Hambleden Wing, Denmark Hill, London SE19 2BY, UK 2 Radiology Department, King s College Hospital, London, UK Correspondence should be addressed to Lina M. Carmona Echeverria, linacarmona@nhs.net Received 3 September 2012; Accepted 24 September 2012 Academic Editors: C. Perez, M. Stracke, and M. J. Turk Copyright 2012 Lina M. Carmona Echeverria et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Purpose. To determine whether axial MR imaging could replace bone scan as the primary staging test in newly diagnosed CaP. Material and Methods. We reviewed retrospectively all bone scans (n = 1201) performed in newly diagnosed CaP patients from 2000 to 2010 in a single tertiary academic center. We recorded patient age, ethnicity, PSA at diagnosis, TNM stage, Gleason score, alkaline phosphatase, bone scan results and axial imaging if available. Results. Mean patient age was 72 years (41 96), mean PSA and alkaline phosphatase were ng/ml and 166 IU/L, respectively. Patients were divided in four groups according to possible bony metastases on bone scan. Group 1: Negative, no metastases demonstrated. Group 2: Positive, metastases only in pelvis and/or lumbar spine. Group 3: Positive, widespread metastases including pelvis and lumbar spine. Group 4: Positive, distant metastases without pelvic or lumbar spine abnormalities. Group 4 patients were analyzed in detail, two had possible disease that was detected only outside the pelvic and lumbar spine, unfortunately follow up images were insufficient to confirm the nature of the lesions. Conclusions. Although bone scan is a useful investigation to confirm and monitor metastasic CaP, our data suggests that axial MR imaging is an adequate primary staging study in untreated disease. Bone scan is unnecessary if CT or MRI of the pelvis and abdomen are clear of metastases. 1. Introduction Prostate cancer was the most common cancer in the UK in 2008, accounting for 24% of all new male cancer diagnosis [1], and is responsible for around 12% of the deaths annually due to cancer ( in 2008). It is calculated that 85% of the patients who die of prostate metastatic cancer have axial skeleton involvement [2], and the presence of these determines the treatment, prognosis, and possibly outcome. It is therefore a priority to determine which patients have developed bone compromise. It is also important to identify patients with little or no risk of metastases to avoid unnecessary investigations and procedures [3 5]. Currently, bone scan is the most commonly used test to diagnose bone metastases [5 7], although it has a low specificity due to the lack of precision in differentiating benign disease from metastatic cancer [2]. There are several studies demonstrating that only certain patients require a bone scan [3 5, 7 11] once the diagnosis has been reached (PSA level above 20 ng/ml, Gleason 4, T3-T4 disease). Also numerous studies have shown that both MRI [12 14] and CT scan [13] have a higher sensitivity and specificity than bone scan in the diagnosis of metastases (including bone metastasesaswellaslymphnodeandvisceralinvolvement). Despite all the evidence that other imaging techniques might contribute more to early and accurate diagnosis of bone metastases, bone scan remains the initial staging test in most practices [7, 15]. The costs secondary to unnecessary diagnostic tests could be reduced if one test could accurately exclude metastases. The aim of this study was to determine the likelihood of presenting with metastatic bone deposits in an area that is not scanned with abdominopelvic imaging techniques, in order to assess the possibility of replacing bone scan as first line in patients with newly diagnosed CaP.
2 2 ISRN Oncology Rt Lt Group 1 Normal bone scan Group 2 Metastases only in pelvis and lumbar spine Group 3 Widespread metastasis including pelvis and lumbar spine Group 4 Distant metastases without pelvic or lumbar spine abnormalities Figure 1: Schematic bone scan classification system. 2. Materials and Methods A retrospective analysis of all bone scans (n = 1201) performed on newly presenting patients with prostate cancer seen at King s College Hospital, London between 2000 and 2010 was carried out. We recorded patient s age, ethnicity, PSA on diagnosis, TNM stage, Gleason score, and serum alkaline phosphatase at diagnosis. 83 patients were excluded due either to the bone scans having been repeated in the same patient or patients being erroneously classified in the records as being new to our hospital, leaving 1201 newly presenting patients for the period. These patients were divided into four groups according to the report of the initial bone scan (Figure 1) as follows: Group 1: negative, no metastases demonstrated. Group 2: positive, metastases only in the bony pelvis and/or lumbar spine. Group 3: positive, patients with widespread metastases including the area specified in group 2. Group 4: positive, but no metastases in pelvis or lumbar spine. The bone scans were classified as a high diagnostic certainty reading, when the radiology clearly stated a diagnosis of metastatic disease, or possible bony metastases when the report suggested further evaluation by comparison with other imaging techniques due to diagnostic uncertainty. All bone scans which were not regarded as definitive were reviewed by a consultant radiologist (JW), a urology consultant (GM), and a urology specialist trainee (LC). TNM staging from any axial imaging or histopathology was recorded for comparison with bone scan results. The data was stored in an Excel Spreadsheet and analyzed with SPSS.
3 ISRN Oncology 3 Mean value PSA and alkaline phosphatase mean value distribution amongst groups Number Classification of bone scans according to consultant radiologist report PSA Alkaline phosphatase Group by bone scan result Figure 2: Representation of the distribution of the mean PSA and alkaline phosphatase in the different groups. 3. Results The mean age was 72 years on diagnosis (41 96). 57.8% (n = 695) of the patients were White and 38.3% (n = 460) were Black, with 3.7% (n = 45) of Asian background. Mean PSA was ng/ml ( ) with a median of 21 ng/ml (Figure 2). Mean alkaline phosphatase was IU/L (7 2755) with a median of 84 IU/L (Figure 2). Note that the PSA values in Ggroup 4 are lower compared to the other Groups, including Group 1, also the alkaline phosphatase values are only just above the normal range ( IU/L). Using the UICC staging criteria (2002) 22.5% of the patients were classified as T1 (n = 271), 35.0% as T2 (n = 421), and 32.7% as T3 (n = 393). 73.8% of the patients did nothavealymphnodestatusrecorded(n = 887), 18.3% were N0 (n = 220) and 7.8% were classified as N+ (n = 94). Regarding M stage, nearly three quarters (73.6%n = 884) had no evidence of metastasis, 22.3% (n = 268) were found to have bone metastasis and 3.8% (n = 46) were diagnosed with visceral and/or bone metastases. 22.0% of patients had a Gleason sum 6 (n = 265), 39.3% Gleason sum 7 (n = 473), and 28.9% Gleason sum >7 (n = 348). A small number of patients either had no locally verified Gleason sum or had been diagnosed on clinical grounds without biopsy (n = 36, 2.99%.) Regarding the proposed classification system by bone scan result (Table 1), 820 (68.2%) of patients had no metastasis on bone scan and 11.3% (n = 136) had metastases only in the lumbar spine or pelvic area. 18.5% of patients had widespread metastasis (n = 223). Only 22 patients (1.8%) had a possible bone metastasis without pelvic or lumbar spine abnormalities on bone scan. High diagnostic certainty Possible bony metastases Figure 3: Classification of the bone scans according to consultant radiologist report. Regarding bone scan classification by diagnostic certainty, 93.1% had high diagnostic certainty and 8% were classified as possible bony metastases (Figure 3), with further imaging advised to confirm findings. As expected negative bone scans (Group 1) had a high confidence. With possible deposits only outside the lumbar spine and pelvis (Group 4), 3/4 of scans were reported with a low diagnostic utility correlating with the high sensitivity and low specificity of bone scan. With positive findings at unusual sites alone (e.g., skull), false positives are more likely, and correlative imaging is commonly suggested. Regarding further imaging modalities performed, we found that in Group 1, a total of 427 patients were studied with other imaging studies (accounting for 539 studies in total), within the next year. 8 of those patients were found to have metastatic disease or lymph node compromise where the bone scan was been negative. CT scan detected metastatic deposits in bone, lymph nodes, and visceral organs in four patients, while 4 patients were diagnosed with bulky lymphadenopathy or bone compromise on MRI scan of the pelvis and abdomen. Since the majority of these studies were done for local staging only in low-risk patients, a true false negative rate cannot be gained from this data. As seen in Figure 3, there were 59 patients in Group 2 where the radiologist report was possible bony metastases. We reviewed all of these patients and found that 30 of them (50%) had degenerative changes mainly in lumbar spine, 18.6% (n = 11) were diagnosed with Paget s disease and 10 (16.9%) were negative on all studies. Only 2 were positive, one with liver metastasis and one with bone metastasis (3.3%). Regarding the bone scans classified as high diagnostic certainty, there was only one false positive, confirmed as degenerative disease by spinal MRI. In Group 3 with multiple metastases including lumbar spine and pelvis, no false positive diagnoses were made. All the images of the patients classified in Group 4 were reviewed by a consultant radiologist, a consultant
4 4 ISRN Oncology Table 1: Distribution amongst groups. Group Bone scan result Total % Group 1 Negative, no metastases demonstrated % Group 2 Positive, metastases only in pelvis and/or lumbar spine % Group 3 Positive, widespread metastasis including pelvis and lumbar spine % Group 4 Positive, distant metastases without pelvic or lumbar spine abnormalities % Table 2: Analysis of patients classified in Group 4. Age PSA Alkaline phosphatase Gleason Comments (1) Uptake in 1st left rib anteriorly, negative thorax X-ray, CT scan negative with 5 years of followup. (2) Uptake in 5th left rib anteriorly, negative CT scan of the chest. (3) Uptake noted in right shoulder joint/proximal humerus (suspicious), negative shoulder X-ray. (4) Focus of activity at the right posterior parietal region, negative skull X-ray. (5) Increased activity at the right superior aspect of the right mandible/right base of the skull. CT scan, X-ray, and MRI compatible with mastoiditis. (6) Uptake in 8th left rib posteriorly, negative thorax X-ray, stable on two-year followup. (7) Uptake in 6th left rib posteriorly, negative thorax CT scan, negative MRI. (8) Focally increased uptake at the lateral third of the left clavicle. Old fractures on X-ray. (9) Intense tracer uptake in T11 left side, and 12th rib. Normal CT scan of abdomen-pelvis, confirms Staghorn calculus. (10) Increased activity at the medial aspect of the right humerus head. No immediate images, negative shoulder X-ray four years later. (11) Diffuse rib uptake, normal CT and MRI. (12) Uptake in 8th left rib posteriorly, on review X-ray focal eccentric rib lesion. However treated by radical prostate radiotherapy with clinical response after 4 months (PSA nadir 0.1 ng/ml, 1.1 ng/ml after 4-year followup). (13) [8] Increased uptake in the right 10th rib posteriorly, and left 7th and 10th laterally. Negative CT scan. Previous hormone therapy. (14) Intense increased tracer uptake at the right shoulder in the region of the acromium. Previous hormone therapy. (15) Multiple regions of inward uptake in left upper scapula left 4th, 6th, 7th, and right 8th ribs anteriorly T6, T9, and T11. Hormone escaped cancer. (16) Bone scan negative, lung biopsy showed metastatic deposit of prostate cancer. Previously treated with hormones and radiotherapy. (17) [8] Focal uptake in the right clavicle and the right posterior 6 rib laterally. Previously treated with hormones and radiotherapy. (18) Increased uptake at the manubrium suggestive of bone secondaries. Previously treated with hormones and radiotherapy. (19) Increased in uptake at the right clavicle. Diagnosed with myeloma on bone biopsy. (20) Lesions seen in skull, and thoracic vertebrae. On review compatible with Paget s disease. (21) Increased activity is present at the right tenth rib laterally. No other imaging carried out (22) Increased activity at right 8th rib posteriorly. No other images carried out urologist, and a urology specialist trainee. Of the 22 patients, 6 (27.2%) had in fact received hormone therapy prior to referral and had their first scan with us for T3 disease. This left 16 patients with primary bone scans showing possible metastases only outside the pelvis or lumbar spine. On detailed analysis of further imaging and investigation of this group: (i) 12 (0.96% of 1201) were false positive bone scans, confirmed by other imaging. One had a focal eccentric rib lesion on X-ray; however, he received local
5 ISRN Oncology 5 radiotherapy and now is clinically disease-free by ASTRO criteria after four years, with no evidence of metastatic disease in the area described; therefore, this patient was most probably also a false positive (number 12 on Table 2). (ii) Two (0.17% of 1201) were diagnosed with a second malignancy that explained the findings in the bone scan. (iii) Two patients (0.17% of 1201, in Table 2)had a possible prostatic metastasis outside of the pelvic and lumbar area only, but they had no confirmatory imaging of the suspicious area before death (Table 2). 4. Discussion Little has been published since 1978 on the accuracy of bone scans in the primary diagnosis of CaP [6],yetitremainsthe most used initial staging investigation. It has been suggested that both MRI [10, 14, 16 18] and CT scan [13] may also be superior to bone scan in assessment of bony metastases. A study by Lecouvet et al. MRI showed a sensitivity of 46% for bone scan alone, 63% for bone scan/targeted X-ray, 83% for bone scan/targeted XR/MRI, and 100% for MRI of the axial skeleton; the corresponding specificities were 32%, 64%, 100%, and 88%, respectively [12]. CT scanning can be useful as a baseline examination in high-risk patients with clinically apparent, grossly advanced local disease, especially to determine lymph node compromise [13]. Also, bone scan givesusnoinformationaboutthelymphnodes,liver,or direct extraprostatic metastases. Looking at 1201 initial bone scans from patients newly presenting to our institution, only two patients may have had a single metastasis outside the pelvic/lumbar spine area. None of these patients were in fact felt certain to actually have had a single bone metastasis as seen in the clinical vignettes in Table 1, although in Table 2 where there was uncertainty the patients did have Gleason sum 9 and 10 disease, without any axial imaging. Overall, this suggests that bone scan is unnecessary in a previously untreated man who does not have any bony metastases in the pelvis or lumbar spine [14] on axial imaging. By contrast, 6 patients previously treated elsewhere who presented to us with hormonally relapsed disease did have eccentric distant metastases, emphasising the unpredictable nature of HRPC. MR imaging including T1 weighted images of the whole abdomen and pelvis for local and lymph node evaluation maybe sufficient for exclusion of bone and nodal metastases and obviates the need for an additional bone scan. The choice of MRI or CT scan will be dictated by local protocol, but probably according to whether intra- and peri-prostatic information is needed (MRI preferred) or not (CT preferred) [13]. MRI has the ability to detect cellular infiltration of normal marrow and allows early detection of bone metastases before an osteoblastic reaction becomes visible on bone scan and/or targeted X-ray [14]. It seems likely that bone scan will continue to have a role in patients with known metastases, symptomatic bone pain, or hormone relapsed disease A limitation of our study is that we are unable to reassess the two patients with possible single distant metastases who died without further imaging. Another is that we have relatively small numbers of patients in Groups two and three who had axial imaging, so we are unable to compare the accuracy of these tests to bone scan. We are proceeding to a regionalized prospective study comparing axial imaging with bone scan in the near future, and hope to be able to confirm these initial results in a multicentre prospective study within the next few years. 5. Conclusion In newly diagnosed prostate cancer, the risk of bone metastases anywhere in the body is negligible if no metastases are seen in the bony pelvis or lumbar spine. Axial imaging (MRI or CT) of the abdomen may be a better single imaging test for staging men with newly diagnosed prostate cancer, with bone scan reserved to assess total metastatic burden in metastatic patients. References [1] Office for National Statistics, Cancer Statistics Registrations: Registrations of Cancer Diagnosed in 2007, England Series MB1 no. 38, National Statistics, London, UK, [2] A. Heidenreich, G. Aus, M. Bolla et al., EAU guidelines on prostate cancer, European Urology, vol. 53, pp , [3] J.M.O Sullivan,A.R.Norman,G.J.Cook,C.Fisher,andD.P. Dearnaley, Broadening the criteria for avoiding staging bone scans in prostate cancer: a retrospective study of patients at the Royal Marsden Hospital, BJU International,vol.92,no.7,pp , [4] N. Lee, R. Fawaaz, C. A. Olsson et al., Which patients with newly diagnosed prostate cancer need a radionuclide bone scan? An analysis based on 631 patients, International Journal of Radiation Oncology Biology Physics, vol. 48, no. 5, pp , [5] C. T. Lee and J. E. Oesterling, Using prostate-specific antigen to eliminate the staging radionuclide bone scan, Urologic Clinics of North America, vol. 24, no. 2, pp , [6] B. McGregor, A. G. S. Tulloch, M. F. Quinlan, and F. Lovegrove, The role of bone scanning in the assessment of prostatic carcinoma, British Journal of Urology, vol. 50, no. 3, pp , [7]S.Haukaas,J.Roervik,O.J.Halvorsen,andM.Foelling, When is bone scintigraphy necessary in the assessment of newly diagnosed, untreated prostate cancer? British Journal of Urology, vol. 79, no. 5, pp , [8] J. J. Pollen, K. Gerber, W. L. Ashburn, and J. D. Schmidt, Nuclear bone imaging in metastatic cancer of the prostate, Cancer, vol. 47, no. 11, pp , [9] M. Hirobe, A. Takahashi, S. I. Hisasue et al., Bone scanning who needs it among patients with newly diagnosed prostate cancer? Japanese Journal of Clinical Oncology, vol. 37, no. 10, pp , [10] A. Rydh, R. Tomic, B. Tavelin, S. O. Hietala, and J. E. Damber, Predictive value of prostate-specific antigen, tumour stage and tumour grade for the outcome of bone scintigraphy in
6 6 ISRN Oncology patients with newly diagnosed prostate cancer, Scandinavian Journal of Urology and Nephrology, vol. 33, no. 2, pp , [11] M. E. Gleave, D. Coupland, D. Drachenberg et al., Ability of serum prostate-specific antigen levels to predict normal bone scans in patients with newly diagnosed prostate cancer, Urology, vol. 47, no. 5, pp , [12] F. E. Lecouvet, D. Geukens, A. Stainier et al., Magnetic resonance imaging of the axial skeleton for detecting bone metastases in patients with high-risk prostate cancer: diagnostic and cost-effectiveness and comparison with current detection strategies, Journal of Clinical Oncology, vol. 25, no. 22, pp , [13] H. Hricak, P. L. Choyke, S. C. Eberhardt, S. A. Leibel, and P. T. Scardino, Imaging prostate cancer: a multidisciplinary perspective, Radiology, vol. 243, no. 1, pp , [14] Z. C. Traill, D. Talbot, S. Golding, and F. V. Gleeson, Magnetic resonance imaging versus radionuclide scintigraphy in screening for bone metastases, Clinical Radiology, vol. 54, no. 7, pp , [15] A. Heidenreich, P. Albers, J. Classen et al., Imaging studies in metastatic urogenital cancer patients undergoing systemic therapy: recommendations of a multidisciplinary consensus meeting of the association of urological oncology of the German cancer society, Urologia Internationalis, vol. 85, no. 1, pp. 1 10, [16] E. Avrahami, R. Tadmor, O. Dally, and H. Hadar, Early MR demonstration of spinal metastases in patients with normal radiographs and CT and radionuclide bone scans, Journal of Computer Assisted Tomography, vol. 13, no. 4, pp , [17] K. Nakanishi, M. Kobayashi, K. Nakaguchi et al., Whole-body MRI for detecting metastatic bone tumor: diagnostic value of diffusion-weighted images, Magnetic Resonance in Medical Sciences, vol. 6, no. 3, pp , [18] B. Tombal, A. Rezazadeh, P. Therasse, P. J. Van Cangh, B. Vande Berg, and F. E. Lecouvet, Magnetic resonance imaging of the axial skeleton enables objective measurement of tumor response on prostate cancer bone metastases, Prostate, vol. 65, no. 2, pp , 2005.
Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C.
 Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
Bone Scanning Who Needs it Among Patients with Newly Diagnosed Prostate Cancer?
 Bone Scanning Who Needs it Among Patients with Newly Diagnosed Prostate Cancer? Megumi Hirobe 1, Atsushi Takahashi 1, Shin-ichi Hisasue 1, Hiroshi Kitamura 1, Yasuharu Kunishima 1, Naoya Masumori 1, Akihiko
Bone Scanning Who Needs it Among Patients with Newly Diagnosed Prostate Cancer? Megumi Hirobe 1, Atsushi Takahashi 1, Shin-ichi Hisasue 1, Hiroshi Kitamura 1, Yasuharu Kunishima 1, Naoya Masumori 1, Akihiko
Prostate Case Scenario 1
 Prostate Case Scenario 1 H&P 5/12/16: A 57-year-old Hispanic male presents with frequency of micturition, urinary urgency, and hesitancy associated with a weak stream. Over the past several weeks, he has
Prostate Case Scenario 1 H&P 5/12/16: A 57-year-old Hispanic male presents with frequency of micturition, urinary urgency, and hesitancy associated with a weak stream. Over the past several weeks, he has
GUIDELINES ON PROSTATE CANCER
 10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
Identification of Bone Metastasis With Routine Prostate MRI: A Study of Patients With Newly Diagnosed Prostate Cancer
 Genitourinary Imaging Original Research Woo et al. MRI of Prostate Cancer Genitourinary Imaging Original Research FOCUS ON: Sungmin Woo 1 Sang Youn Kim 1 Seung Hyup Kim 1,2 Jeong Yeon Cho 1,2 Woo S, Kim
Genitourinary Imaging Original Research Woo et al. MRI of Prostate Cancer Genitourinary Imaging Original Research FOCUS ON: Sungmin Woo 1 Sang Youn Kim 1 Seung Hyup Kim 1,2 Jeong Yeon Cho 1,2 Woo S, Kim
Case Report Solitary Osteolytic Skull Metastasis in a Case of Unknown Primary Being latter Diagnosed as Carcinoma of Gall Bladder
 Cronicon OPEN ACCESS CANCER Case Report Solitary Osteolytic Skull Metastasis in a Case of Unknown Primary Being latter Diagnosed as Carcinoma of Gall Kartik Mittal 1, Rajaram Sharma 1, Amit Dey 1, Meet
Cronicon OPEN ACCESS CANCER Case Report Solitary Osteolytic Skull Metastasis in a Case of Unknown Primary Being latter Diagnosed as Carcinoma of Gall Kartik Mittal 1, Rajaram Sharma 1, Amit Dey 1, Meet
PET imaging of cancer metabolism is commonly performed with F18
 PCRI Insights, August 2012, Vol. 15: No. 3 Carbon-11-Acetate PET/CT Imaging in Prostate Cancer Fabio Almeida, M.D. Medical Director, Arizona Molecular Imaging Center - Phoenix PET imaging of cancer metabolism
PCRI Insights, August 2012, Vol. 15: No. 3 Carbon-11-Acetate PET/CT Imaging in Prostate Cancer Fabio Almeida, M.D. Medical Director, Arizona Molecular Imaging Center - Phoenix PET imaging of cancer metabolism
Whole Body MRI. Dr. Nina Tunariu. Prostate Cancer recurrence, progression and restaging
 Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
Prostate Cancer Local or distant recurrence?
 Prostate Cancer Local or distant recurrence? Diagnostic flowchart Vanessa Vilas Boas Urologist VFX Hospital FEBU PSA - only recurrence PSA recurrence: 27-53% of all patients undergoing treatment with curative
Prostate Cancer Local or distant recurrence? Diagnostic flowchart Vanessa Vilas Boas Urologist VFX Hospital FEBU PSA - only recurrence PSA recurrence: 27-53% of all patients undergoing treatment with curative
FDG PET/CT STAGING OF LUNG CANCER. Dr Shakher Ramdave
 FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
Bone Metastases in Muscle-Invasive Bladder Cancer
 Journal of the Egyptian Nat. Cancer Inst., Vol. 18, No. 3, September: 03-08, 006 AZZA N. TAHER, M.D.* and MAGDY H. KOTB, M.D.** The Departments of Radiation Oncology* and Nuclear Medicine**, National Cancer
Journal of the Egyptian Nat. Cancer Inst., Vol. 18, No. 3, September: 03-08, 006 AZZA N. TAHER, M.D.* and MAGDY H. KOTB, M.D.** The Departments of Radiation Oncology* and Nuclear Medicine**, National Cancer
Louisa Fleure. Advanced Prostate Cancer Clinical Nurse Specialist. Guys and St Thomas NHS Trust
 Louisa Fleure Advanced Prostate Cancer Clinical Nurse Specialist Guys and St Thomas NHS Trust The classification of advanced prostate cancer The incidence of patients presenting with, or developing advanced
Louisa Fleure Advanced Prostate Cancer Clinical Nurse Specialist Guys and St Thomas NHS Trust The classification of advanced prostate cancer The incidence of patients presenting with, or developing advanced
PET-MRI in malignant bone tumours. Lars Stegger Department of Nuclear Medicine University Hospital Münster, Germany
 PET-MRI in malignant bone tumours Lars Stegger Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to PET/MRI General considerations Bone metastases Primary bone tumours
PET-MRI in malignant bone tumours Lars Stegger Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to PET/MRI General considerations Bone metastases Primary bone tumours
GUIDELINEs ON PROSTATE CANCER
 GUIDELINEs ON PROSTATE CANCER (Text update March 2005: an update is foreseen for publication in 2010. Readers are kindly advised to consult the 2009 full text print of the PCa guidelines for the most recent
GUIDELINEs ON PROSTATE CANCER (Text update March 2005: an update is foreseen for publication in 2010. Readers are kindly advised to consult the 2009 full text print of the PCa guidelines for the most recent
Diagnosis and Classification of Prostate Cancer
 Patient Information English 32 Diagnosis and Classification of Prostate Cancer The underlined terms are listed in the glossary. prostate biopsy is the only test that can confirm a prostate cancer diagnosis.
Patient Information English 32 Diagnosis and Classification of Prostate Cancer The underlined terms are listed in the glossary. prostate biopsy is the only test that can confirm a prostate cancer diagnosis.
A 64 y.o. man presents to the hospital with persistent cough and hemoptysis. Fernando Mut Montevideo - Uruguay
 A 64 y.o. man presents to the hospital with persistent cough and hemoptysis Fernando Mut Montevideo - Uruguay Teaching case Bone # 1 A 64 y.o. man presents to the hospital with persistent cough and hemoptysis.
A 64 y.o. man presents to the hospital with persistent cough and hemoptysis Fernando Mut Montevideo - Uruguay Teaching case Bone # 1 A 64 y.o. man presents to the hospital with persistent cough and hemoptysis.
Case Scenario 1. 4/19/13 Bone Scan: No scintigraphic findings to suggest skeletal metastases.
 Case Scenario 1 3/8/13 H&P 68 YR W/M presents w/elevated PSA. Patient is a non-smoker, current alcohol use. Physical Exam: On digital rectal exam the sphincter tone is normal and there is a 1 cm nodule
Case Scenario 1 3/8/13 H&P 68 YR W/M presents w/elevated PSA. Patient is a non-smoker, current alcohol use. Physical Exam: On digital rectal exam the sphincter tone is normal and there is a 1 cm nodule
1/25/13 Right partial nephrectomy followed by completion right radical nephrectomy.
 History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
Louisa Fleure. Advanced Prostate Cancer Clinical Nurse Specialist. Guys and St Thomas NHS Trust
 Louisa Fleure Advanced Prostate Cancer Clinical Nurse Specialist Guys and St Thomas NHS Trust The classification of advanced prostate cancer The incidence of patients presenting with, or developing advanced
Louisa Fleure Advanced Prostate Cancer Clinical Nurse Specialist Guys and St Thomas NHS Trust The classification of advanced prostate cancer The incidence of patients presenting with, or developing advanced
STAGING AND FOLLOW-UP STRATEGIES
 ATHENS 4-6 October 2018 European Society of Urogenital Radiology STAGING AND FOLLOW-UP STRATEGIES Ahmet Tuncay Turgut, MD Professor of Radiology Hacettepe University, Faculty of Medicine Ankara 2nd ESUR
ATHENS 4-6 October 2018 European Society of Urogenital Radiology STAGING AND FOLLOW-UP STRATEGIES Ahmet Tuncay Turgut, MD Professor of Radiology Hacettepe University, Faculty of Medicine Ankara 2nd ESUR
Whole-Body Diffusion-Weighted MRI Compared With 18 F-NaF PET/CT for Detection of Bone Metastases in Patients With High-Risk Prostate Carcinoma
 Nuclear Medicine and Molecular Imaging Original Research Mosavi et al. Imaging Bone Metastases in Prostate Carcinoma Nuclear Medicine and Molecular Imaging Original Research Firas Mosavi 1 Silvia Johansson
Nuclear Medicine and Molecular Imaging Original Research Mosavi et al. Imaging Bone Metastases in Prostate Carcinoma Nuclear Medicine and Molecular Imaging Original Research Firas Mosavi 1 Silvia Johansson
ORIGINAL ARTICLE ABSTRACT
 ORIGINAL ARTICLE 99m Tc MDP Bone Scan in Lung Cancer: Predilection Sites for Metastasis Shamim M F Begum, Zeenat Jabin, Rahima Perveen, Nasreen Sultana, Laila S Banu National Institute of Nuclear Medicine
ORIGINAL ARTICLE 99m Tc MDP Bone Scan in Lung Cancer: Predilection Sites for Metastasis Shamim M F Begum, Zeenat Jabin, Rahima Perveen, Nasreen Sultana, Laila S Banu National Institute of Nuclear Medicine
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Carcinoma of unknown primary origin (CUP) Faculty of Clinical Radiology www.rcr.ac.uk Contents Carcinoma of
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Carcinoma of unknown primary origin (CUP) Faculty of Clinical Radiology www.rcr.ac.uk Contents Carcinoma of
The management and treatment options for secondary bone disease. Dr Jason Lester Clinical Oncologist Velindre Cancer Centre
 The management and treatment options for secondary bone disease Dr Jason Lester Clinical Oncologist Velindre Cancer Centre Aims Overview of bone metastases management in castrate-refractory prostate cancer
The management and treatment options for secondary bone disease Dr Jason Lester Clinical Oncologist Velindre Cancer Centre Aims Overview of bone metastases management in castrate-refractory prostate cancer
Low risk. Objectives. Case-based question 1. Evidence-based utilization of imaging in prostate cancer
 Evidence-based utilization of imaging in prostate cancer Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Objectives State the modalities,
Evidence-based utilization of imaging in prostate cancer Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Objectives State the modalities,
Bone PET/MRI : Diagnostic yield in bone metastases and malignant primitive bone tumors
 Bone PET/MRI : Diagnostic yield in bone metastases and malignant primitive bone tumors Lars Stegger, Benjamin Noto Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to
Bone PET/MRI : Diagnostic yield in bone metastases and malignant primitive bone tumors Lars Stegger, Benjamin Noto Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Localized Prostate Cancer Have we finally got it right? Shingai Mutambirwa Professor & Chair-Division Urology DGMAH & SMU Pretoria SOUTH AFRICA
 Localized Prostate Cancer Have we finally got it right? Shingai Mutambirwa Professor & Chair-Division Urology DGMAH & SMU Pretoria SOUTH AFRICA ESMO Cape Town 14 Feb 2018 Disclosures Advisory boards/lecturer/consultant-
Localized Prostate Cancer Have we finally got it right? Shingai Mutambirwa Professor & Chair-Division Urology DGMAH & SMU Pretoria SOUTH AFRICA ESMO Cape Town 14 Feb 2018 Disclosures Advisory boards/lecturer/consultant-
SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, :00 12:10 p.m.
 SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, 2018 10:00 12:10 p.m. Staging Susan E. Sharp, MD 1. In the International Neuroblastoma Risk Group Staging
SELF-ASSESSMENT MODULE REFERENCE SPR 2018 Oncologic Imaging Course Adrenal Tumors November 10, 2018 10:00 12:10 p.m. Staging Susan E. Sharp, MD 1. In the International Neuroblastoma Risk Group Staging
Case Report New Primary Malignancy Masquerading as Metastatic Prostate Adenocarcinoma
 Case Reports in Oncological Medicine Volume 2015, Article ID 358572, 5 pages http://dx.doi.org/10.1155/2015/358572 Case Report New Primary Malignancy Masquerading as Metastatic Prostate Adenocarcinoma
Case Reports in Oncological Medicine Volume 2015, Article ID 358572, 5 pages http://dx.doi.org/10.1155/2015/358572 Case Report New Primary Malignancy Masquerading as Metastatic Prostate Adenocarcinoma
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines BONE MARROW MRI Original Date: July 2008 Page 1 of 5 CPT Codes: 77084 Last Review Date: September 2014 NCD 220.2 MRI Last Effective Date: July 2011
National Imaging Associates, Inc. Clinical guidelines BONE MARROW MRI Original Date: July 2008 Page 1 of 5 CPT Codes: 77084 Last Review Date: September 2014 NCD 220.2 MRI Last Effective Date: July 2011
Horizon Scanning Technology Briefing. Magnetic resonance spectroscopy for prostate cancer. National Horizon Scanning Centre.
 Horizon Scanning Technology Briefing National Horizon Scanning Centre Magnetic resonance spectroscopy for prostate cancer August 2006 This technology briefing is based on information available at the time
Horizon Scanning Technology Briefing National Horizon Scanning Centre Magnetic resonance spectroscopy for prostate cancer August 2006 This technology briefing is based on information available at the time
Osteopoikilosis: A Sign Mimicking Skeletal Metastases in a Cancer Patient
 Case Report Middle East Journal of Cancer 2011; 2(1): 37-41 Osteopoikilosis: A Sign Mimicking Skeletal Metastases in a Cancer Patient Sepideh Sefidbakht *, Yaghoub Ashouri-Taziani **, Sareh Hoseini **,
Case Report Middle East Journal of Cancer 2011; 2(1): 37-41 Osteopoikilosis: A Sign Mimicking Skeletal Metastases in a Cancer Patient Sepideh Sefidbakht *, Yaghoub Ashouri-Taziani **, Sareh Hoseini **,
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2
 Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
Does Imaging of Advanced PC change a suggested treatment?
 Does Imaging of Advanced PC change a suggested treatment? Professor Bertrand Tombal, MD, PhD Cliniques universitaires Saint-Luc Université catholique de Louvain Brussels, Belgium Credentials and conflict
Does Imaging of Advanced PC change a suggested treatment? Professor Bertrand Tombal, MD, PhD Cliniques universitaires Saint-Luc Université catholique de Louvain Brussels, Belgium Credentials and conflict
Cancer of Unknown Primary (CUP)
 Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
Short summary of published results of PET with fluoromethylcholine (18F) in prostate cancer
 Short summary of published results of PET with fluoromethylcholine (18F) in prostate cancer JN TALBOT and all the team of Service de Médecine Nucléaire Hôpital Tenon et Université Pierre et Marie Curie,
Short summary of published results of PET with fluoromethylcholine (18F) in prostate cancer JN TALBOT and all the team of Service de Médecine Nucléaire Hôpital Tenon et Université Pierre et Marie Curie,
Clinical Appropriateness Guidelines: Advanced Imaging
 Clinical Appropriateness Guidelines: Advanced Imaging Appropriate Use Criteria: Imaging of Bone Marrow Blood Supply Effective Date: September 5, 2017 Proprietary Date of Origin: 05/21/2007 Last revised:
Clinical Appropriateness Guidelines: Advanced Imaging Appropriate Use Criteria: Imaging of Bone Marrow Blood Supply Effective Date: September 5, 2017 Proprietary Date of Origin: 05/21/2007 Last revised:
Proposed All Wales Vulval Cancer Guidelines. Dr Amanda Tristram
 Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
Review of Clinical Manifestations of Biochemicallyadvanced Prostate Cancer Cases
 Original Article Review of Clinical Manifestations of Biochemicallyadvanced Prostate Cancer Cases Edmund Chiong, 1,2 Alvin Fung Wean Wong, 2 Yiong Huak Chan 3 and Chong Min Chin, 1,2 1 Department of Surgery,
Original Article Review of Clinical Manifestations of Biochemicallyadvanced Prostate Cancer Cases Edmund Chiong, 1,2 Alvin Fung Wean Wong, 2 Yiong Huak Chan 3 and Chong Min Chin, 1,2 1 Department of Surgery,
Cancer of Unknown Primary (CUP) Protocol
 1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
Diagnostic role of fluorodeoxyglucose positron emission tomography computed tomography in prostate cancer
 ONCOLOGY LETTERS 7: 2013-2018, 2014 Diagnostic role of fluorodeoxyglucose positron emission tomography computed tomography in prostate cancer YIYAN LIU Nuclear Medicine Service, Department of Radiology,
ONCOLOGY LETTERS 7: 2013-2018, 2014 Diagnostic role of fluorodeoxyglucose positron emission tomography computed tomography in prostate cancer YIYAN LIU Nuclear Medicine Service, Department of Radiology,
Boot Camp Case Scenarios
 Boot Camp Case Scenarios Case Scenario 1 Patient is a 69-year-old white female. She presents with dyspnea on exertion, cough, and right rib pain. Patient is a smoker. 9/21/12 CT Chest FINDINGS: There is
Boot Camp Case Scenarios Case Scenario 1 Patient is a 69-year-old white female. She presents with dyspnea on exertion, cough, and right rib pain. Patient is a smoker. 9/21/12 CT Chest FINDINGS: There is
INDICATIONS AND USAGE
 1. INDICATIONS AND USAGE a) Axumin is indicated for positron emission tomography (PET) in men with suspected prostate cancer recurrence based on elevated blood prostate specific antigen (PSA) levels following
1. INDICATIONS AND USAGE a) Axumin is indicated for positron emission tomography (PET) in men with suspected prostate cancer recurrence based on elevated blood prostate specific antigen (PSA) levels following
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Best Papers. F. Fusco
 Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
The role of multimodality imaging in Multiple Myeloma: Past, Present and Future
 The role of multimodality imaging in Multiple Myeloma: Past, Present and Future Poster No.: C-1661 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Niza, R. Gil, P. Pereira, C. Oliveira ; Setúbal/PT,
The role of multimodality imaging in Multiple Myeloma: Past, Present and Future Poster No.: C-1661 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Niza, R. Gil, P. Pereira, C. Oliveira ; Setúbal/PT,
Spinal cord compression as a first presentation of cancer: A case report
 J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
Chapter 3 Diagnostic Imaging. 1 Diagnostic Imaging
 Chapter 3 Diagnostic Imaging 1 Diagnostic Imaging Radiographic Examination: Standards and Indications Position Statement Radiography should only be performed on the basis of clinical necessity as judged
Chapter 3 Diagnostic Imaging 1 Diagnostic Imaging Radiographic Examination: Standards and Indications Position Statement Radiography should only be performed on the basis of clinical necessity as judged
Assessment of Skeletal Metastases in Prostate Cancer: 68Ga-PSMA PET vs 99mTc-MDP WBBS - A Case Series
 Assessment of Skeletal Metastases in Prostate Cancer: 68Ga-PSMA PET vs 99mTc-MDP WBBS - A Case Series Poster No.: R-0094 Congress: 2016 ASM Type: Scientific Exhibit Authors: O. Bennett, Y.-T. T. Huang;
Assessment of Skeletal Metastases in Prostate Cancer: 68Ga-PSMA PET vs 99mTc-MDP WBBS - A Case Series Poster No.: R-0094 Congress: 2016 ASM Type: Scientific Exhibit Authors: O. Bennett, Y.-T. T. Huang;
IMAGING GUIDELINES - COLORECTAL CANCER
 IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
Message of the Month for GPs June 2013
 Message of the Month for GPs June 2013 Dr Winn : Consultant Musculoskeletal Radiologist, Manchester Royal Infirmary Imaging of the musculoskeletal system Musculoskeletal pain is a common problem in the
Message of the Month for GPs June 2013 Dr Winn : Consultant Musculoskeletal Radiologist, Manchester Royal Infirmary Imaging of the musculoskeletal system Musculoskeletal pain is a common problem in the
Sectional Anatomy Quiz - III
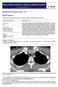 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Lugano classification: Role of PET-CT in lymphoma follow-up
 CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
Correspondence should be addressed to Taha Numan Yıkılmaz;
 Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
PRECISION IMAGING: QUANTITATIVE, MOLECULAR AND IMAGE-GUIDED TECHNOLOGIES
 PRECISION IMAGING: QUANTITATIVE, MOLECULAR AND IMAGE-GUIDED TECHNOLOGIES Day 3 Authors: Tade, Funmilayo; Akin-Akintayo Oladunni; Schuster, David M. Lab Training Module 1: Introduction to the basics of
PRECISION IMAGING: QUANTITATIVE, MOLECULAR AND IMAGE-GUIDED TECHNOLOGIES Day 3 Authors: Tade, Funmilayo; Akin-Akintayo Oladunni; Schuster, David M. Lab Training Module 1: Introduction to the basics of
Denominator Criteria (Eligible Cases): Patient encounter during the performance period (CPT): 78300, 78305, 78306, 78315, 78320
 Quality ID #147: Nuclear Medicine: Correlation with Existing Imaging Studies for All Patients Undergoing Bone Scintigraphy National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS
Quality ID #147: Nuclear Medicine: Correlation with Existing Imaging Studies for All Patients Undergoing Bone Scintigraphy National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS
Prostate Specific Antigen as a risk factor for skeletal metastasis in Black African men with Prostate Cancer: a Case Control study
 Prostate Specific Antigen as a risk factor for skeletal metastasis in Black African men with Prostate Cancer: a Case Control study ABSTRACT Prostate cancer is the commonest non cutaneous cancer in males.
Prostate Specific Antigen as a risk factor for skeletal metastasis in Black African men with Prostate Cancer: a Case Control study ABSTRACT Prostate cancer is the commonest non cutaneous cancer in males.
Cancers of unknown primary : Knowing the unknown. Prof. Ahmed Hossain Professor of Medicine SSMC
 Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Prostate MRI: Who needs it?
 Prostate MRI: Who needs it? Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Abdominal Imaging Magnetic Resonance Science Center
Prostate MRI: Who needs it? Fergus Coakley MD, Professor of Radiology and Urology, Vice Chair for Clinical Services, Chief of Abdominal Imaging, UCSF Abdominal Imaging Magnetic Resonance Science Center
NICE BULLETIN Diagnosis & treatment of prostate cancer
 Diagnosis & treatment of prostate cancer NICE provided the content for this booklet which is independent of any company or product advertised Diagnosis and treatment of prostate cancer Introduction In
Diagnosis & treatment of prostate cancer NICE provided the content for this booklet which is independent of any company or product advertised Diagnosis and treatment of prostate cancer Introduction In
University of Groningen
 University of Groningen Routine bone scans in patients with prostate cancer related to serum prostate-specific antigen and alkaline phosphatase Wymenga, LFA; Boomsma, JHB; Groenier, K; Piers, DA; Mensink,
University of Groningen Routine bone scans in patients with prostate cancer related to serum prostate-specific antigen and alkaline phosphatase Wymenga, LFA; Boomsma, JHB; Groenier, K; Piers, DA; Mensink,
LYMPHATIC DRAINAGE IN THE HEAD & NECK
 LYMPHATIC DRAINAGE IN THE HEAD & NECK Like other parts of the body, the head and neck contains lymph nodes (commonly called glands). Which form part of the overall Lymphatic Drainage system of the body.
LYMPHATIC DRAINAGE IN THE HEAD & NECK Like other parts of the body, the head and neck contains lymph nodes (commonly called glands). Which form part of the overall Lymphatic Drainage system of the body.
Cervical Cancer: 2018 FIGO Staging
 Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
in patients with bone metastases
 Brazilian Treatment Journal delay of and Medical radiological and Biological errors Research (2003) 36: 1419-1424 ISSN 0100-879X 1419 Treatment delay and radiological errors in patients with bone metastases
Brazilian Treatment Journal delay of and Medical radiological and Biological errors Research (2003) 36: 1419-1424 ISSN 0100-879X 1419 Treatment delay and radiological errors in patients with bone metastases
FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION
 FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION CPT/HCPCS Codes 78300 Bone and/or joint imaging; limited area 78305 multiple areas 78306 whole body 78315 three phase study
FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION CPT/HCPCS Codes 78300 Bone and/or joint imaging; limited area 78305 multiple areas 78306 whole body 78315 three phase study
GUIDELINES ON RENAL CELL CANCER
 20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
20 G. Mickisch (chairman), J. Carballido, S. Hellsten, H. Schulze, H. Mensink Eur Urol 2001;40(3):252-255 Introduction is characterised by a constant rise in incidence over the last 50 years, with a predominance
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Cancer of Unknown Primary Network Site Specific Group. Clinical Guidelines
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary Network Site Specific Group Revision due: April 2019 Page 1 of 11 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary Network Site Specific Group Revision due: April 2019 Page 1 of 11 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
When PSA fails. Urology Grand Rounds Alexandra Perks. Rising PSA after Radical Prostatectomy
 When PSA fails Urology Grand Rounds Alexandra Perks Rising PSA after Radical Prostatectomy Issues Natural History Local vs Metastatic Treatment options 1 10 000 men / year in Canada 4000 RRP 15-year PSA
When PSA fails Urology Grand Rounds Alexandra Perks Rising PSA after Radical Prostatectomy Issues Natural History Local vs Metastatic Treatment options 1 10 000 men / year in Canada 4000 RRP 15-year PSA
Elevated PSA. Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017
 Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Musculoskeletal tumours Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary bone tumours 3 Clinical
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Musculoskeletal tumours Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary bone tumours 3 Clinical
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Imaging of bone metastases
 Imaging of bone metastases Antoine Feydy Service de Radiologie B Hôpital Cochin APHP Université Paris Descartes antoine.feydy@aphp.fr MEXICO 2016 INTRODUCTION Diagnostic Imaging Imaging Modalities Strengths,
Imaging of bone metastases Antoine Feydy Service de Radiologie B Hôpital Cochin APHP Université Paris Descartes antoine.feydy@aphp.fr MEXICO 2016 INTRODUCTION Diagnostic Imaging Imaging Modalities Strengths,
Challenging Cases. With Q&A Panel
 Challenging Cases With Q&A Panel Case Studies Index Patient #1 Jeffrey Wieder, MD Case # 1 72 year old healthy male with mild HTN Early 2011: Preop bone scan and pelvic CT = no mets Radical prostatectomy
Challenging Cases With Q&A Panel Case Studies Index Patient #1 Jeffrey Wieder, MD Case # 1 72 year old healthy male with mild HTN Early 2011: Preop bone scan and pelvic CT = no mets Radical prostatectomy
MRI and metastases of PCa
 MRI and metastases of PCa François CORNUD Céline COUVIDAT David EISS Arnaud LEFEVRE IRM Paris 16, France, Paris, France Université Paris Descartes, Paris, France When imaging should be considered for detection
MRI and metastases of PCa François CORNUD Céline COUVIDAT David EISS Arnaud LEFEVRE IRM Paris 16, France, Paris, France Université Paris Descartes, Paris, France When imaging should be considered for detection
Outcomes Following Negative Prostate Biopsy for Patients with Persistent Disease after Radiotherapy for Prostate Cancer
 Clinical Urology Post-radiotherapy Prostate Biopsy for Recurrent Disease International Braz J Urol Vol. 36 (1): 44-48, January - February, 2010 doi: 10.1590/S1677-55382010000100007 Outcomes Following Negative
Clinical Urology Post-radiotherapy Prostate Biopsy for Recurrent Disease International Braz J Urol Vol. 36 (1): 44-48, January - February, 2010 doi: 10.1590/S1677-55382010000100007 Outcomes Following Negative
Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma of Thyroid
 Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
Essential Initial Activities and Clinical Outcomes
 Essential Initial Activities and Clinical Outcomes Crystal Farrell 1,2 & Sabrina L. Noyes 2, Joe Joslin 2, Manish Varma 2,3, Andrew Moriarity 2,3, Christopher Buchach 2,3, Leena Mammen 2,3, Brian R. Lane
Essential Initial Activities and Clinical Outcomes Crystal Farrell 1,2 & Sabrina L. Noyes 2, Joe Joslin 2, Manish Varma 2,3, Andrew Moriarity 2,3, Christopher Buchach 2,3, Leena Mammen 2,3, Brian R. Lane
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Definition Prostate cancer
 Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY
 BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY AZHAN BIN YUSOFF AZHAN BIN YUSOFF 2013 SCENARIO A 66 year old man underwent Robotic Radical Prostatectomy for a T1c Gleason 4+4, PSA 15 ng/ml prostate
BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY AZHAN BIN YUSOFF AZHAN BIN YUSOFF 2013 SCENARIO A 66 year old man underwent Robotic Radical Prostatectomy for a T1c Gleason 4+4, PSA 15 ng/ml prostate
VALUE AND ROLE OF PSA AS A TUMOUR MARKER OF RESPONSE/RELAPSE
 Session 3 Advanced prostate cancer VALUE AND ROLE OF PSA AS A TUMOUR MARKER OF RESPONSE/RELAPSE 1 PSA is a serine protease and the physiological role is believed to be liquefying the seminal fluid PSA
Session 3 Advanced prostate cancer VALUE AND ROLE OF PSA AS A TUMOUR MARKER OF RESPONSE/RELAPSE 1 PSA is a serine protease and the physiological role is believed to be liquefying the seminal fluid PSA
Questions and Answers About Breast Cancer, Bone Metastases, & Treatment-Related Bone Loss. A Publication of The Bone and Cancer Foundation
 Questions and Answers About Breast Cancer, Bone Metastases, & Treatment-Related Bone Loss A Publication of The Bone and Cancer Foundation Contents This publication includes important information about
Questions and Answers About Breast Cancer, Bone Metastases, & Treatment-Related Bone Loss A Publication of The Bone and Cancer Foundation Contents This publication includes important information about
Staging Colorectal Cancer
 Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Effective local and systemic therapy is necessary for the cure of Ewing tumor Most chemotherapy regimens are a combination of cyclophosphamide,
 Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
VALUE OF PSA AS TUMOUR MARKER OF RELAPSE AND RESPONSE. ELENA CASTRO Spanish National Cancer Research Centre
 VALUE OF PSA AS TUMOUR MARKER OF RELAPSE AND RESPONSE ELENA CASTRO Spanish National Cancer Research Centre Prostate Preceptorship. Lugano 17-18 October 2017 Prostate Specific Antigen (PSA) has a role in:
VALUE OF PSA AS TUMOUR MARKER OF RELAPSE AND RESPONSE ELENA CASTRO Spanish National Cancer Research Centre Prostate Preceptorship. Lugano 17-18 October 2017 Prostate Specific Antigen (PSA) has a role in:
Diagnosis and staging of breast cancer and multidisciplinary team working
 1 Diagnosis and staging of breast cancer and multidisciplinary team working Common symptoms and signs Over 90% of breast cancers (BCs) are local or regional when first detected. At least 60% of patients
1 Diagnosis and staging of breast cancer and multidisciplinary team working Common symptoms and signs Over 90% of breast cancers (BCs) are local or regional when first detected. At least 60% of patients
PET in Prostate Cancer
 PET in Prostate Cancer Tom R. Miller, M.D., Ph.D. Mallinckrodt Institute of Radiology Washington University School of Medicine St. Louis, Missouri, USA Prostate Imaging Bone Scintigraphy primarily for
PET in Prostate Cancer Tom R. Miller, M.D., Ph.D. Mallinckrodt Institute of Radiology Washington University School of Medicine St. Louis, Missouri, USA Prostate Imaging Bone Scintigraphy primarily for
X, Y and Z of Prostate Cancer
 X, Y and Z of Prostate Cancer Dr Tony Michele Medical Oncologist Prostate cancer Epidemiology Current EUA (et al) guidelines on Advanced Prostate Cancer Current clinical management in specific scenarios
X, Y and Z of Prostate Cancer Dr Tony Michele Medical Oncologist Prostate cancer Epidemiology Current EUA (et al) guidelines on Advanced Prostate Cancer Current clinical management in specific scenarios
Stereotactic body radiation therapy in oligometastatic patient with lymph node recurrent prostate cancer: a single centre experience.
 Stereotactic body radiation therapy in oligometastatic patient with lymph node recurrent prostate cancer: a single centre experience. Elisabetta Ponti MD, Gianluca Ingrosso MD, Alessandra Carosi PhD, Luana
Stereotactic body radiation therapy in oligometastatic patient with lymph node recurrent prostate cancer: a single centre experience. Elisabetta Ponti MD, Gianluca Ingrosso MD, Alessandra Carosi PhD, Luana
Ambulatory & Office Urology Unnecessary Imaging for the Staging of Low-Risk Prostate Cancer Is Common
 Ambulatory & Office Urology Unnecessary Imaging for the Staging of Low-Risk Prostate Cancer Is Common Hugh J. Lavery, Jonathan S. Brajtbord, Adam W. Levinson, Fatima Nabizada-Pace, Matthew E. Pollard,
Ambulatory & Office Urology Unnecessary Imaging for the Staging of Low-Risk Prostate Cancer Is Common Hugh J. Lavery, Jonathan S. Brajtbord, Adam W. Levinson, Fatima Nabizada-Pace, Matthew E. Pollard,
Paul F. Schellhammer, M.D. Eastern Virginia Medical School Urology of Virginia Norfolk, Virginia
 Paul F. Schellhammer, M.D. Eastern Virginia Medical School Urology of Virginia Norfolk, Virginia Virginia - Chesapeake Bay Landfall: Virginia Beach, April 29 th, 1607 PSA Failure after Radical Prostatectomy
Paul F. Schellhammer, M.D. Eastern Virginia Medical School Urology of Virginia Norfolk, Virginia Virginia - Chesapeake Bay Landfall: Virginia Beach, April 29 th, 1607 PSA Failure after Radical Prostatectomy
Associated Terms: Osteosarcoma, Bone Cancer, Limb Salvage, Appendicular Osteosarcoma, Pathologic Fracture, Chondrosarcoma
 1 of 9 9/29/2014 8:25 PM Associated Terms: Osteosarcoma, Bone Cancer, Limb Salvage, Appendicular Osteosarcoma, Pathologic Fracture, Chondrosarcoma The term "ACVS Diplomate" refers to a veterinarian who
1 of 9 9/29/2014 8:25 PM Associated Terms: Osteosarcoma, Bone Cancer, Limb Salvage, Appendicular Osteosarcoma, Pathologic Fracture, Chondrosarcoma The term "ACVS Diplomate" refers to a veterinarian who
Imaging Of The Pelvis
 Imaging Of The Pelvis 1 / 6 2 / 6 3 / 6 Imaging Of The Pelvis MRI of the pelvis may be more focused on the organs, soft tissues, and vessels, rather than on the bones themselves. In many instances, MRI
Imaging Of The Pelvis 1 / 6 2 / 6 3 / 6 Imaging Of The Pelvis MRI of the pelvis may be more focused on the organs, soft tissues, and vessels, rather than on the bones themselves. In many instances, MRI
Guideline for the Management of Vulval Cancer
 Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Colorectal Cancer and FDG PET/CT
 Hybrid imaging in colorectal & esophageal cancer Emmanuel Deshayes IAEA WorkShop, November 2017 Colorectal Cancer and FDG PET/CT 1 Clinical background Cancer of the colon and rectum is one of the most
Hybrid imaging in colorectal & esophageal cancer Emmanuel Deshayes IAEA WorkShop, November 2017 Colorectal Cancer and FDG PET/CT 1 Clinical background Cancer of the colon and rectum is one of the most
NIH Public Access Author Manuscript Diagn Imaging Eur. Author manuscript; available in PMC 2014 November 10.
 NIH Public Access Author Manuscript Published in final edited form as: Diagn Imaging Eur. 2013 January ; 29(1): 12 15. PET-directed, 3D Ultrasound-guided prostate biopsy Baowei Fei, Department of Radiology
NIH Public Access Author Manuscript Published in final edited form as: Diagn Imaging Eur. 2013 January ; 29(1): 12 15. PET-directed, 3D Ultrasound-guided prostate biopsy Baowei Fei, Department of Radiology
