THE LIKELY IMPACT OF EARLIER DIAGNOSIS OF CANCER ON COSTS AND BENEFITS TO THE NHS
|
|
|
- Justina Porter
- 5 years ago
- Views:
Transcription
1 Policy Research Unit in Economic Evaluation of Health & Care Interventions (EEPRU) THE LIKELY IMPACT OF EARLIER DIAGNOSIS OF CANCER ON COSTS AND BENEFITS TO THE NHS November 2013 Report 015 Authors: Tappenden P 1, Bessey A 1, McKenna C 2, Sculpher M 2 1 ScHARR, The University of Sheffield 2 Centre of Health Economics, University of York
2 The Policy Research Unit in Economic Evaluation of Health and Care interventions is funded by the Department of Health Policy Research Programme. It is a collaboration between researchers from then University of Sheffield and the University of York. The Department of Health's Policy Research Unit in Economic Evaluation of Health and Care Interventions is a 5 year programme of work that started in January The unit is led by Professor John Brazier (Director, University of Sheffield) and Professor Mark Sculpher (Deputy Director, University of York) with the aim of assisting policy makers in the Department of Health to improve the allocation of resources in health and social care. This is an independent report commissioned and funded by the Policy Research Programme in the Department of Health. The views expressed are not necessarily those of the Department.
3 Overview This report presents a critical review of the five early awareness policy intervention models developed by Frontier Economics. For each issue highlighted within the review, the likely direction of the bias is discussed together with a suggestion of the extent to which these concerns could be rectified within the existing model structure. Frontier Economics modelling approach The model sets out to address two specific questions: 1. How would the costs to the NHS change if certain cancers (specifically, breast, colorectal, lung, prostate and melanoma) were detected and diagnosed appreciably earlier than is currently the norm (i.e. according to current survival rates)? 2. How would the benefits to individuals change if these cancers were detected and diagnosed appreciably earlier than is currently the norm? The model seeks to examine the impact that earlier detection and diagnosis would have on survival rates and on downstream costs and benefits. Benefits are limited to patient health benefits in terms of improved survival, i.e. change in life years. Costs include those that fall on the NHS, including diagnostics, screening, treatment, follow-up and end of life care. The general approach is to produce projections under a set of assumptions relating to current incidence and screening rates, referred to as the Business As Usual (BAU) model. Also, to re-run this model making alternative assumptions about awareness and screening rates, referred to as the Policy Intervention scenario. The impact of earlier diagnosis is measured by comparing the two scenarios (BAU and Policy Intervention), where the key difference between the scenarios relates to the assumptions about the effectiveness of the awareness programme and the efficiency of the screening programme in the given cancer area (when there is screening prgramme in place - colorectal and breast).
4 The goal of the awareness programme is to inform the population about the risks of developing cancer and the signs that alert a patient to symptoms suspicious of underlying malignant disease. It is expected that individuals would present earlier to their GP, with the result that diagnosis will occur at an earlier stage of cancer, leading to higher survival rates. The early awareness programme seeks to achieve Europe s best practice survival rates, i.e. the group of comparable countries in Europe with the highest survival rates. The key assumptions in the model relating to the effectiveness of the awareness campaign and the efficiency of the screening programme, in terms of recruiting more individuals, are altered to achieve the target 1-year survival rates of EUROCARE-4 good practice. General logic of the model Patients enter the model each year through either symptomatic presentation to their GP or detection via screening. For the current arrangements, life years gained are modelled on the basis of a fixed mean survival duration for each cancer stage applied to a Business As Usual stage distribution. Different stage distributions are applied to the screen-detected patients (for colorectal and breast) and to those presenting electively with symptoms. Total costs are modelled as a function of the number of patients attending screening (where applicable), follow-up diagnostic tests for those testing positive at screening, costs of symptomatic presentation and diagnostic tests and stage-specific lifetime treatment costs. The impact of the early awareness policy is applied within the model by [i] increasing the number of people attending screening and applying a more favourable stage distribution to those detected with an underling preclinical cancer (as compared against usual symptomatic presentation); and [ii] distinguishing a subgroup of symptomatic patients who become high awareness patients (those affected by the policy) who are given a new stage distribution which is the same as that of the screen-detected population under the policy. The logic of the model is illustrated in Figures 1a and 1b for colorectal cancer. A similar logic is applied to the other cancers. Key assumptions of the modelling approach The key assumptions applied in the model include: (i) Current survival rates are conditional on the stage of cancer (ii) Survival rates by stage remain unchanged by the awareness programme (iii) Baseline distribution of incidence by stage differs according to whether individuals are screened or symptomatic (iv) Distribution of incidence by stage for the awareness programme is the same as the screened-detected programme (v) Costs of diagnosis and treatment by stage remain unchanged over time 2
5 Figure 1a: Model under Business as Usual (BAU) In order to calculate life years the number of patients diagnosed in each stage is multiplied by the mean survival years following diagnosis in that stage. FOBt Colonoscopy or Flexible Sigmoidoscopy Stage A Population Patients part of screening for years old A patient who has been diagnosed as having colorectal cancer will be diagnosed as being in a certain stage. The distribution of patients between the stages depends on whether the patient was diagnosed through screening or being symptomatic. Stage B Stage C Stage D Symptomatic Patients GP Colonoscopy or Flexible Sigmoidoscopy Unknown Stage Figure 1b: Model under Policy The policy increases the number of patients screened as well as introducing the new high awareness patients into the model. FOBt Colonoscopy or Flexible Sigmoidoscopy Stage A Patients part of screening for years old In the model the patients diagnosed through screening and through earlier diagnosis because of increased awareness have the same distribution of patients in each stage of the disease, and are treated the same in the model. Stage B Population High Awareness Patients GP Colonoscopy or Flexible Sigmoidoscopy Stage C Stage D The number of symptomatic patients being diagnosed decreases between year 1 and 3 and becomes lower than the BAU case, taking in account those additional patients that are being diagnosed through screening and the high awareness group. Symptomatic Patients GP Colonoscopy or Flexible Sigmoidoscopy Unknown Stage 3
6 Critique of the modelling approach The following sections outline the authors main concerns with the model. (1) Absence of a natural history model The models do not include full natural history components involving transitions between preclinical states (before diagnosis) and clinically diagnosed states. Instead, outcomes for patients are included only for the incident true-positive detected cohort. This gives rise to a number of potential concerns with respect to the credibility of the model results. These issues are interrelated but can be considered in terms of two main problems: (i) the absence of competing risks and no consideration of variability; and (ii) issues relating to modelling only the positive benefits of the true-positive incident cohort. (i) Absence of competing risks and no consideration of variability The model does not capture any competing risks of other events on either the costs or outcomes for the patient population. Once diagnosed, a patient is given credit for a fixed survival duration from the point of disease detection. For example, in the colorectal cancer model, patients with Dukes stage A/B are given 11 years of fixed survival, Dukes stage C are given 8.7 years, and stage D are given 1.4 years. A fifth group with unknown stage (which most likely relates to gaps in data collection) is given 2.5 years. This general modelling approach appears to run the risk of both lead-time bias and length bias. Lead-time bias occurs when an intervention results in the earlier diagnosis of an underlying cancer, but the time of death remains otherwise unaffected, hence survival following diagnosis appears more favourable due to the intervention. Length bias refers to the situation whereby slower-progressing tumours have a longer preclinical phase, and hence an increased chance of being detected by early intervention before they would otherwise be detected through symptomatic presentation. This leads to the disproportionate identification of slowly progressing tumours compared with faster more aggressive tumours. Whilst these issues are relevant to the evaluation of any intervention for the early detection of cancer, their potential effects could have been ameliorated by incorporating competing risks within the model and by reflecting disease progression rates through the preclinical states. These competing risks may influence a patient s prognosis and costs. For example, if a patient is diagnosed at age 93, they are likely to be at a considerably increased risk of other-cause mortality and their treatment options are likely to be much more restrictive than those for a younger patient. The incorporation of evidence from screening models and other sources (e.g. life tables), particularly with respect to probabilities of progression and presentation, calibrated against available evidence from screening trials, would add considerable information to inform this part of the model and would, to some degree, protect against these types of bias. 4
7 DIRECTION OF POTENTIAL BIAS: LIKELY TO BE OVERLY FAVOURABLE TO EARLY AWARENESS PROGRAMMES EFFORT REQUIRED TO RESOLVE ISSUES: DIFFERENT MODEL REQUIRED (ii) Issues relating to modelling only the positive benefits of the true positive incident cohort The model only considers the outcomes associated with the incident true-positive diagnosed cancer cohort each year. Costs associated with false-negative and falsepositive test results are incorporated, but outcomes for individuals who test negative are not included in the cost-effectiveness analysis. The model does not consider the sensitivity and specificity of diagnostic testing and essentially assumes a fixed positivity rate for the probability of having cancer given attendance at follow-up. There are a number of consequences of this approach: (1) In certain cancer areas, early detection of premalignant lesions may enable excision and avoid the malignancy altogether (e.g. removal of adenomatous colorectal polyps may provide protection of cancer [see Atkin et al, Lancet 2010]). Whilst few of these would be symptomatic, these patients, and the potential benefits of the early awareness policy, are not considered in the model whatsoever. (2) By considering only the incident cohort each year, the model fails to account for the change in the underlying distribution of patients who have relevant preclinical potentially detectable disease. As more cases are detected, the ability of any intervention to detect further cases will decrease. This is a particular issue with the colorectal cancer model as the prevalence round screening results are applied in every year (Steele et al, BMJ); in reality one would expect the effectiveness of screening to be lower in incident screening rounds. (3) By assuming a fixed positivity rate for the likelihood of cancer diagnosis, the model does not consider changes over time. Related to the point above, as more cases are detected, the positivity rate would be reduced because the underlying risk of preclinical disease would be reduced. (4) A potential increase in true-negative worried well individuals, resulting from implementation of the policy intervention, is not accounted for in the model. It might be expected that the programme would attract a large number of individuals presenting to their GP, who do or do not have cancer. It is unclear whether the primary care costs associated with the worried well individuals are fully reflected in the model. The model estimates the number of people going through testing who are or are not diagnosed with cancer by dividing the number of people diagnosed with cancer by the percentage of people who have the test and are diagnosed with cancer. However, this probability, which is based on current practice, is likely to change as a result of the policy intervention programme. As public awareness is generated, the probability of patients testing negative will increase. It may have been appropriate to incorporate a rate of true-negatives into the model and to vary this rate to explore how sensitive the total costs of the programme are to the rate assumed. A threshold analysis could be used to determine the critical 5
8 proportion of worried wells, which, if exceeded, would cease to make the policy intervention cost-effective. DIRECTION OF POTENTIAL BIAS: OVERALL, THIS STRUCTURAL APPROACH IS LIKELY TO BIAS IN FAVOUR OF THE POLICY EFFORT REQUIRED TO RESOLVE ISSUES: FOR THE MOST PART, A DIFFERENT MODEL IS REQUIRED. THRESHOLD ANALYSIS TO EXAMINE THE POTENTIAL IMPACT OF THE WORRIED WELL COULD BE INCORPORATED INTO THE EXISTING MODEL (2) No consideration of uncertainty The model does not include any consideration of parameter uncertainty in any of the model parameters. This uncertainty is ubiquitous and its omission implies an unfounded level of confidence in the model results. From a structural perspective, adopting a model structure which does not include a full natural history component does not mean that the uncertainty is no longer relevant. The model is highly uncertain because of the nature of the evidence and the nature of the assumptions applied throughout. Very little justification is provided for the choice of data used. In addition, the model does not explore the assumptions in the evidence through sensitivity analyses. Given the high level of uncertainty in the parameter values, sensitivity analysis would be expected at minimum. DIRECTION OF POTENTIAL BIAS: ASSUMES COMPLETE CERTAINTY EFFORT REQUIRED TO RESOLVE ISSUES: INCORPORATING DISTRIBUTIONS FOR THE MODEL PARAMETERS WOULD NOT BE TECHNICALLY DIFFICULT, BUT A DIFFERENT MODEL WOULD BE REQUIRED TO ACCOUNT FOR UNCERTAINTY IN THE NATURAL HISTORY. SENSITIVITY ANALYSIS COULD EASILY BE USED TO VARY PARTICULAR PARAMETERS OF INTEREST. (3) Impact of screening and/or awareness policy on stage distribution The model appears to apply the impact of early detection programmes (both screening and public awareness) inconsistently between the policy intervention and Business As Usual groups. These are shown in Table 1 for colorectal cancer. The screen-detected stage distribution under BAU differs to the screen-detected distribution for the policy intervention. The model also assumes that the Highawareness group results in the same stage distribution as the screen-detected. However, patients who present earlier with symptoms in the high awareness group, who would not otherwise have presented in the absence of the policy intervention, may not necessarily match those identified through a screening programme in terms of stage distribution. 6
9 Table 1 Stage distribution by programme and subgroup (colorectal) Business As Usual Policy Intervention Stage Symptomatic Highawareness Screendetected Symptomatic Highawareness Screendetected Dukes A 9% N/a 48% 9% 31% 31% Dukes B 24% N/a 25% 24% 32% 32% Dukes C 24% N/a 26% 24% 27% 27% Stage D 9% N/a 1% 9% 10% 10% Unknown 34% N/a 0% 34% 0% 0% EFFORT REQUIRED TO RESOLVE ISSUES: A DIFFERENT MODEL WOULD BE REQUIRED TO MORE APPROPRIATELY HANDLE THE IMPACT OF SCREENING/AWARENESS POLICIES ON STAGE DISTRIBUTION OVER TIME (4) Cost of the early awareness policy The models do not include a cost associated with the organisation or delivery of the programme. DIRECTION OF POTENTIAL BIAS: THIS INEVITABLY FAVOURS THE POLICY EFFORT REQUIRED TO RESOLVE ISSUES: MINOR AMENDMENTS REQUIRED TO INCORPORATE THE COSTS OF THE POLICY INTERVENTION (5) Omission of negative effects of diagnosis The model does not include any negative impacts associated with screening or diagnosis. Some diagnostic/follow-up tests such as flexible sigmoidoscopy and colonoscopy are invasive and carry a risk of perforation, bleeding and in a minority of cases, death. The omission of these effects in the context of early diagnosis interventions is a flaw, especially since the intervention is anticipated to increase the number of individuals undergoing this element of the cancer service. DIRECTION OF POTENTIAL BIAS: THIS IS LIKELY TO BE OVERLY OPTIMISTIC TO THE EARLY AWARENESS PROGRAMME EFFORT REQUIRED TO RESOLVE ISSUES: DEPENDS ON LEVEL OF DETAIL REQUIRED (E.G. INCLUSION OF SUBSEQUENT TESTS FOLLOWING HARMS) BUT POTENTIALLY MINOR AMENDMENTS REQUIRED TO REFLECT THIS CONCERN (6) Contextual relevance of service pathways The representation of cancer systems within the models is very simplistic and, in some instances, appears excessively blunt. For example, a single fixed diagnostic pathway is assumed for colorectal cancer involving FOBT (for screening), subsequent follow-up tests and treatment. In reality, patients may enter the service through this type of elective route, but they may undergo alternative diagnostic tests (e.g. barium enema or CT colonography). The sensitivity/specificity profile of any of 7
10 these tests is not considered but will influence the probability of a positive diagnosis given the presence of underlying histology. Alternatively they may already be in secondary care, they may present with emergency symptoms and undergo very different tests, or they may be picked up through screening/surveillance due to some known increased risk factor (e.g. individual s history of adenomas, family history of colorectal cancer, inherited syndromes [familial adenomatous polyposis [FAP] or hereditary non-polyposis colorectal cancer [HNPCC]). These alternative entry routes are not considered. DIRECTION OF POTENTIAL BIAS: THE DIRECTION OF THIS BIAS IS UNCLEAR THIS IS AN ISSUE OF MODEL DEPTH EFFORT REQUIRED TO RESOLVE ISSUES: THIS ISSUE COULD POTENTIALLY BE INCORPORATED INTO A SIMILAR SIMPLE MODEL STRUCTURE (7) Inappropriate application of discounting The implementation of discounting to account for the time at which benefits and costs are accrued is incomplete. A 3.5% discount rate is included (see Inputs and assumption sheet) and is used to calculate the net present value (NPV) of the total costs associated with the diagnosis and treatment of the cancer. These figures are used to calculate the gain from the policy in monetary terms in the NPV section of the Results sheet. However, discounting is not applied in the calculation of the incremental cost per life year gained. The model assumes that the total lifetime costs and outcomes occur instantaneously at the point at which the patient is diagnosed with cancer. The incomplete implementation of discounting is likely to favour the policy programme because the costs of the awareness policy will be incurred sooner than the potential benefits are accrued. DIRECTION OF POTENTIAL BIAS: LIKELY TO BE OPTIMISTIC IN FAVOUR OF THE EARLY AWARENESS PROGRAMME EFFORT REQUIRED TO RESOLVE ISSUES: MINOR AMENDMENT REQUIRED (8) Calculation of model results During the first two years following implementation of the early awareness policy the costs and number of life years gained differ from subsequent years. One of the sets of results quoted in the report relates to the population benefit of 41,000 life years gained and an incremental cost of 6,241 per life gained. For the previous 2 years, the incremental cost per life year gained is lower than this value. Beyond 2014, the long-term equilibrium effectiveness is applied throughout. In the new equilibrium section in the Results sheet the new equilibrium is given as the year 2023 and the costs used are derived from the expected results for the year However, the total expected years of life gained from the policy included in the new equilibrium section is taken from the year 2031 (see Results sheet, rows ). This is arbitrary, but does not alter the results beyond
11 DIRECTION OF POTENTIAL BIAS: THE RESULTS FOR THE FIRST 2 YEARS ARE MORE FAVOURABLE THE MEAN OVER THE ENTIRE TIME HORIZON WOULD FALL SLIGHTLY EFFORT REQUIRED TO RESOLVE ISSUES: MINOR (9) Evidence used to populate the model The evidence used to populate the model does not appear to have been systematically collected. There is no information on a systematic search of the literature to identify, select and retrieve relevant studies. In general, the report is not very transparent in terms of the approach taken or the evidence used to populate the model. Very little justification is given for the choice of modelling approach, the appropriateness of the approach and why particular assumptions were applied. Where effectiveness data were not available, arbitrary values were applied. For example, for colorectal cancer, the percentage of patients screened and subsequently diagnosed is assumed to be 0.25%, but no justification is provided for this choice. Key parameter values have not been explored in sensitivity analysis to assess how sensitive the cost-effective results are to the assumptions applied. More recent sources of evidence may be available for some parameters. For example, the costs associated with diagnosis and treatment of colorectal cancer are taken from the ScHARR options appraisal, However, a more recent comprehensive assessment of the economic burden of treating colorectal cancer has been completed by ScHARR and the York Health Economics Consortium, 2007 (see for further details). Overall, the credibility of the model is highly uncertain because of the nature of the evidence and lack of justification for parameter values. DIRECTION OF POTENTIAL BIAS: NOT CERTAIN BUT SHOULD BE ACKNOWLEDGED IN THE REPORT EFFORT REQUIRED TO RESOLVE ISSUES: SYSTEMATIC REVIEW OF THE LITERAURE REQUIRED AND APPROPRIATE SOURCES IDENTIFIED. PROPER REFERENCING IS NEEDED THROUGHOUT THE REPORT. 9
Cost-effectiveness of an early awareness campaign for colorectal cancer
 Cost-effectiveness of an early awareness for colorectal cancer Sophie Whyte 1, Sue Harnan 1, Paul Tappenden 1, Mark Sculpher 2, Seb Hinde 2, Claire Mckenna 2 Policy Research Unit in Economic Evaluation
Cost-effectiveness of an early awareness for colorectal cancer Sophie Whyte 1, Sue Harnan 1, Paul Tappenden 1, Mark Sculpher 2, Seb Hinde 2, Claire Mckenna 2 Policy Research Unit in Economic Evaluation
Suspected cancer: National Collaborating Centre for Cancer. recognition and management of suspected cancer in children, young people and adults
 National Collaborating Centre for Cancer : recognition and management of suspected cancer in children, young people and adults Clinical Guideline Appendices A - E June 2015 Final version Commissioned by
National Collaborating Centre for Cancer : recognition and management of suspected cancer in children, young people and adults Clinical Guideline Appendices A - E June 2015 Final version Commissioned by
DIAGNOSTICS ASSESSMENT PROGRAMME
 DIAGNOSTICS ASSESSMENT PROGRAMME Evidence overview Virtual chromoendoscopy for real-time assessment of colorectal polyps during This overview summarises the key issues for the diagnostics advisory committee
DIAGNOSTICS ASSESSMENT PROGRAMME Evidence overview Virtual chromoendoscopy for real-time assessment of colorectal polyps during This overview summarises the key issues for the diagnostics advisory committee
ADENOMA SURVEILLANCE BCSP Guidance Note No 1 Version 1 September 2009
 ADENOMA SURVEILLANCE BCSP Guidance Note No 1 Version 1 September 2009 Published by: NHS Cancer Screening Programmes Fulwood House Old Fulwood Road Sheffield S10 3TH Tel: 0114 271 1060 Fax: 0114 271 1089
ADENOMA SURVEILLANCE BCSP Guidance Note No 1 Version 1 September 2009 Published by: NHS Cancer Screening Programmes Fulwood House Old Fulwood Road Sheffield S10 3TH Tel: 0114 271 1060 Fax: 0114 271 1089
NHS KINGSTON. Contents
 NHS KINGSTON Contents 1. Background... 2 2. Targets and quality standards... 2 3. Service provision and performance... 3 Uptake... 3 Investigations... 6 Cancer detection... 7 Age extension... 7 4. Quality
NHS KINGSTON Contents 1. Background... 2 2. Targets and quality standards... 2 3. Service provision and performance... 3 Uptake... 3 Investigations... 6 Cancer detection... 7 Age extension... 7 4. Quality
Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer
 Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer Healthy Habits and Cancer Screening Rev 10.20.15 Page
Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer Healthy Habits and Cancer Screening Rev 10.20.15 Page
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING
 CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
Transforming Cancer Services for London
 Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
Colorectal cancer screening
 26 Colorectal cancer screening BETHAN GRAF AND JOHN MARTIN Colorectal cancer is theoretically a preventable disease and is ideally suited to a population screening programme, as there is a long premalignant
26 Colorectal cancer screening BETHAN GRAF AND JOHN MARTIN Colorectal cancer is theoretically a preventable disease and is ideally suited to a population screening programme, as there is a long premalignant
Setting The setting was primary and secondary care. The economic study was carried out in Taiwan.
 Cost-effectiveness analysis of colorectal cancer screening with stool DNA testing in intermediate-incidence countries Wu G H, Wang Y W, Yen A M, Wong J M, Lai H C, Warwick J, Chen T H Record Status This
Cost-effectiveness analysis of colorectal cancer screening with stool DNA testing in intermediate-incidence countries Wu G H, Wang Y W, Yen A M, Wong J M, Lai H C, Warwick J, Chen T H Record Status This
Cost-effectiveness of colonoscopy in screening for colorectal cancer Sonnenberg A, Delco F, Inadomi J M
 Cost-effectiveness of colonoscopy in screening for colorectal cancer Sonnenberg A, Delco F, Inadomi J M Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion
Cost-effectiveness of colonoscopy in screening for colorectal cancer Sonnenberg A, Delco F, Inadomi J M Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion
Cost-effectiveness of double-contrast barium enema in screening for colorectal cancer Glick S, Wagner J L, Johnson C D
 Cost-effectiveness of double-contrast barium enema in screening for colorectal cancer Glick S, Wagner J L, Johnson C D Record Status This is a critical abstract of an economic evaluation that meets the
Cost-effectiveness of double-contrast barium enema in screening for colorectal cancer Glick S, Wagner J L, Johnson C D Record Status This is a critical abstract of an economic evaluation that meets the
Screening for Colorectal Cancer
 Screening for Colorectal Cancer April 1, 2014 Revised August 2014 McMaster Evidence Review and Synthesis Centre Team: Donna Fitzpatrick-Lewis, Ali Usman, Rachel Warren, Meghan Kenny, Maureen Rice, Andy
Screening for Colorectal Cancer April 1, 2014 Revised August 2014 McMaster Evidence Review and Synthesis Centre Team: Donna Fitzpatrick-Lewis, Ali Usman, Rachel Warren, Meghan Kenny, Maureen Rice, Andy
Northern Ireland Bowel Cancer Screening Programme. Pathways. Version 4 1 st October 2013
 Northern Ireland Bowel Cancer Screening Programme Pathways These changes will be version controlled, led by the Quality Assurance Director for the Programme. Any updated versions will be circulated and
Northern Ireland Bowel Cancer Screening Programme Pathways These changes will be version controlled, led by the Quality Assurance Director for the Programme. Any updated versions will be circulated and
Financial Disclosers
 Slide 1 Colorectal Cancer Screening Jason Hemming, MD NESGNA November 15, 2014 Slide 2 Bio Slide 3 Financial Disclosers I have no actual or potential conflict of interest relation to this presentation
Slide 1 Colorectal Cancer Screening Jason Hemming, MD NESGNA November 15, 2014 Slide 2 Bio Slide 3 Financial Disclosers I have no actual or potential conflict of interest relation to this presentation
Quality ID #439: Age Appropriate Screening Colonoscopy National Quality Strategy Domain: Efficiency and Cost Reduction
 Quality ID #439: Age Appropriate Screening Colonoscopy National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Efficiency DESCRIPTION:
Quality ID #439: Age Appropriate Screening Colonoscopy National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Efficiency DESCRIPTION:
Recommendations on Screening for Colorectal Cancer 2016
 Recommendations on Screening for Colorectal Cancer 2016 Canadian Task Force on Preventive Health Care (CTFPHC) Putting Prevention into Practice Canadian Task Force on Preventive Health Care Groupe d étude
Recommendations on Screening for Colorectal Cancer 2016 Canadian Task Force on Preventive Health Care (CTFPHC) Putting Prevention into Practice Canadian Task Force on Preventive Health Care Groupe d étude
Supplementary Online Content
 Supplementary Online Content Holme Ø, Løberg M, Kalager M, et al. Effect of flexible sigmoidoscopy screening on colorectal cancer incidence and mortality: a randomized clinical trial. JAMA. doi:10.1001/jama.2014.8266
Supplementary Online Content Holme Ø, Løberg M, Kalager M, et al. Effect of flexible sigmoidoscopy screening on colorectal cancer incidence and mortality: a randomized clinical trial. JAMA. doi:10.1001/jama.2014.8266
Setting The setting was not clear. The economic study was carried out in the USA.
 Computed tomography screening for lung cancer in Hodgkin's lymphoma survivors: decision analysis and cost-effectiveness analysis Das P, Ng A K, Earle C C, Mauch P M, Kuntz K M Record Status This is a critical
Computed tomography screening for lung cancer in Hodgkin's lymphoma survivors: decision analysis and cost-effectiveness analysis Das P, Ng A K, Earle C C, Mauch P M, Kuntz K M Record Status This is a critical
Colorectal Cancer Screening
 Colorectal Cancer Screening December 5, 2017 Connecticut Cancer Partnership 14th Annual Meeting Xavier Llor, M.D., PhD. Associate Professor of Medicine Co-Director, Cancer Genetics and Prevention Program
Colorectal Cancer Screening December 5, 2017 Connecticut Cancer Partnership 14th Annual Meeting Xavier Llor, M.D., PhD. Associate Professor of Medicine Co-Director, Cancer Genetics and Prevention Program
Screening & Surveillance Guidelines
 Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Setting The setting was secondary care. The economic study was carried out in Australia.
 Cost-effectiveness of colorectal cancer screening: comparison of community-based flexible sigmoidoscopy with fecal occult blood testing and colonoscopy O'Leary B A, Olynyk J K, Neville A M, Platell C F
Cost-effectiveness of colorectal cancer screening: comparison of community-based flexible sigmoidoscopy with fecal occult blood testing and colonoscopy O'Leary B A, Olynyk J K, Neville A M, Platell C F
Evidence-based Cancer Screening & Surveillance
 Oncology for Scientists Spring 2014 Evidence-based Cancer Screening & Surveillance Martin C. Mahoney, MD, PhD, FAAFP Departments of Medicine & Health Behavior /Oncology_Feb 2014.ppt 1 Objectives: Principles
Oncology for Scientists Spring 2014 Evidence-based Cancer Screening & Surveillance Martin C. Mahoney, MD, PhD, FAAFP Departments of Medicine & Health Behavior /Oncology_Feb 2014.ppt 1 Objectives: Principles
Faecal DNA testing compared with conventional colorectal cancer screening methods: a decision analysis Song K, Fendrick A M, Ladabaum U
 Faecal DNA testing compared with conventional colorectal cancer screening methods: a decision analysis Song K, Fendrick A M, Ladabaum U Record Status This is a critical abstract of an economic evaluation
Faecal DNA testing compared with conventional colorectal cancer screening methods: a decision analysis Song K, Fendrick A M, Ladabaum U Record Status This is a critical abstract of an economic evaluation
2012 update. Bowel Cancer. Information for people at increased risk of bowel cancer. Published by the New Zealand Guidelines Group
 2012 update Bowel Cancer Information for people at increased risk of bowel cancer Published by the New Zealand Guidelines Group i Contents Introduction 1 The bowel 1 Bowel cancer 3 What are the symptoms
2012 update Bowel Cancer Information for people at increased risk of bowel cancer Published by the New Zealand Guidelines Group i Contents Introduction 1 The bowel 1 Bowel cancer 3 What are the symptoms
Colorectal Cancer Screening Guideline Issue Brief Updated May 30 th, 2018
 Colorectal Cancer Screening Guideline Issue Brief Updated May 30 th, 2018 Issue Summary The American Cancer Society has updated its colorectal screening guideline, which have been published in CA: A Journal
Colorectal Cancer Screening Guideline Issue Brief Updated May 30 th, 2018 Issue Summary The American Cancer Society has updated its colorectal screening guideline, which have been published in CA: A Journal
Cancer Screenings and Early Diagnostics
 Cancer Screenings and Early Diagnostics Ankur R. Parikh, D.O. Medical Director, Center for Advanced Individual Medicine Hematologist/Medical Oncologist Atlantic Regional Osteopathic Convention April 6
Cancer Screenings and Early Diagnostics Ankur R. Parikh, D.O. Medical Director, Center for Advanced Individual Medicine Hematologist/Medical Oncologist Atlantic Regional Osteopathic Convention April 6
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn
Diagnostics for the early detection and prevention of colon cancer. Publication of DeeP-C Study Data in New England Journal of Medicine March 2014
 Diagnostics for the early detection and prevention of colon cancer Publication of DeeP-C Study Data in New England Journal of Medicine March 2014 Safe Harbor Statement Certain statements made in this presentation
Diagnostics for the early detection and prevention of colon cancer Publication of DeeP-C Study Data in New England Journal of Medicine March 2014 Safe Harbor Statement Certain statements made in this presentation
CANCER SCREENING. Er Chaozer Department of General Medicine, Tan Tock Seng Hospital
 CANCER SCREENING Er Chaozer Department of General Medicine, Tan Tock Seng Hospital Introduction Screening average risk patients Benefits and harms from screening Early cancer detection early treatment
CANCER SCREENING Er Chaozer Department of General Medicine, Tan Tock Seng Hospital Introduction Screening average risk patients Benefits and harms from screening Early cancer detection early treatment
ColonCancerCheck (CCC): Modelling FOBT screening in Ontario for colorectal cancer (CRC) using the Cancer Risk Management Model (CRMM)
 ColonCancerCheck (CCC): Modelling FOBT screening in Ontario for colorectal cancer (CRC) using the Cancer Risk Management Model (CRMM) CADTH Panel Presentation April 16, 2012 Toronto Health Economics and
ColonCancerCheck (CCC): Modelling FOBT screening in Ontario for colorectal cancer (CRC) using the Cancer Risk Management Model (CRMM) CADTH Panel Presentation April 16, 2012 Toronto Health Economics and
Diagnostics guidance Published: 10 May 2017 nice.org.uk/guidance/dg28
 Virtual chromoendoscopy to assess colorectal polyps during colonoscopy Diagnostics guidance Published: 10 May 2017 nice.org.uk/guidance/dg28 NICE 2017. All rights reserved. Subject to Notice of rights
Virtual chromoendoscopy to assess colorectal polyps during colonoscopy Diagnostics guidance Published: 10 May 2017 nice.org.uk/guidance/dg28 NICE 2017. All rights reserved. Subject to Notice of rights
Study population The study population comprised a hypothetical cohort of 50-year-olds at average risk of CRC.
 Colon cancer prevention in Italy: cost-effectiveness analysis with CT colonography and endoscopy Hassan C, Zullo A, Laghi A, Reitano I, Taggi F, Cerro P, Iafrate F, Giustini M, Winn S, Morini S Record
Colon cancer prevention in Italy: cost-effectiveness analysis with CT colonography and endoscopy Hassan C, Zullo A, Laghi A, Reitano I, Taggi F, Cerro P, Iafrate F, Giustini M, Winn S, Morini S Record
UK Bowel Cancer screening Dr Voi Shim Wong BsC MD FRCP. Consultant Gastroenterologist Accredited BCSP colonoscopist Whittington + UCL Hospitals
 UK Bowel Cancer screening 2017 Dr Voi Shim Wong BsC MD FRCP Consultant Gastroenterologist Accredited BCSP colonoscopist Whittington + UCL Hospitals Bowel Cancer Contents UK Bowel Cancer Screening Programme
UK Bowel Cancer screening 2017 Dr Voi Shim Wong BsC MD FRCP Consultant Gastroenterologist Accredited BCSP colonoscopist Whittington + UCL Hospitals Bowel Cancer Contents UK Bowel Cancer Screening Programme
NATIONAL SCREENING COMMITTEE
 Optimising Bowel Cancer Screening Phase 1: Optimising the cost effectiveness of repeated FIT screening and screening strategies combining bowel scope and FIT screening Sophie Whyte, Chloe Thomas, Ben Kearns,
Optimising Bowel Cancer Screening Phase 1: Optimising the cost effectiveness of repeated FIT screening and screening strategies combining bowel scope and FIT screening Sophie Whyte, Chloe Thomas, Ben Kearns,
Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn s disease and polyps
 Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn s disease and polyps Full guideline Draft for consultation, May 00 0 This guideline
Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn s disease and polyps Full guideline Draft for consultation, May 00 0 This guideline
Page 1. Selected Controversies. Cancer Screening! Selected Controversies. Breast Cancer Screening. ! Using Best Evidence to Guide Practice!
 Cancer Screening!! Using Best Evidence to Guide Practice! Judith M.E. Walsh, MD, MPH! Division of General Internal Medicine! Womenʼs Health Center of Excellence University of California, San Francisco!
Cancer Screening!! Using Best Evidence to Guide Practice! Judith M.E. Walsh, MD, MPH! Division of General Internal Medicine! Womenʼs Health Center of Excellence University of California, San Francisco!
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE
 SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
The MISCAN-COLON simulation model for the evaluation of colorectal cancer screening
 2 The MISCAN-COLON simulation model for the evaluation of colorectal cancer screening 30 Chapter 2 Abstract A general model for evaluation of colorectal cancer screening has been implemented in the microsimulation
2 The MISCAN-COLON simulation model for the evaluation of colorectal cancer screening 30 Chapter 2 Abstract A general model for evaluation of colorectal cancer screening has been implemented in the microsimulation
Structured Follow-Up after Colorectal Cancer Resection: Overrated. R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007
 Structured Follow-Up after Colorectal Cancer Resection: Overrated R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007 Guidelines for Colonoscopy Production: Surveillance US Multi-Society
Structured Follow-Up after Colorectal Cancer Resection: Overrated R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007 Guidelines for Colonoscopy Production: Surveillance US Multi-Society
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions. South Island Cancer Nurses Network September 2013
 For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
Work No. Rater Initials Average Score
 Work No. Rater Initials Average Score For each of the seven criteria below a) identify specific phrases on the accompanying longer form which describe the work, and b) circle a numeric score on the short
Work No. Rater Initials Average Score For each of the seven criteria below a) identify specific phrases on the accompanying longer form which describe the work, and b) circle a numeric score on the short
Colorectal Cancer Screening in Later Life: Blum Center Rounds
 Colorectal Cancer Screening in Later Life: Blum Center Rounds OCTOBER 10, 2018 Agenda CRC Screening and Surveillance Recommendation Screening for Colon Cancer later in life Discussion and listening Families
Colorectal Cancer Screening in Later Life: Blum Center Rounds OCTOBER 10, 2018 Agenda CRC Screening and Surveillance Recommendation Screening for Colon Cancer later in life Discussion and listening Families
2. Describe pros/cons of screening interventions (including colonoscopy, CT colography, fecal tests)
 Learning Objectives 1. Review principles of colon adenoma/cancer biology that permit successful prevention regimes 2. Describe pros/cons of screening interventions (including colonoscopy, CT colography,
Learning Objectives 1. Review principles of colon adenoma/cancer biology that permit successful prevention regimes 2. Describe pros/cons of screening interventions (including colonoscopy, CT colography,
ACG Clinical Guideline: Colorectal Cancer Screening
 ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Nicolaus Copernicus University in Torun Medical College in Bydgoszcz Family Doctor Department CANCER PREVENTION IN GENERAL PRACTICE
 Nicolaus Copernicus University in Torun Medical College in Bydgoszcz Family Doctor Department CANCER PREVENTION IN GENERAL PRACTICE A key mission for family medicine is preserving health and maximizing
Nicolaus Copernicus University in Torun Medical College in Bydgoszcz Family Doctor Department CANCER PREVENTION IN GENERAL PRACTICE A key mission for family medicine is preserving health and maximizing
Evaluating endoscopy capacity across the NHS in England
 Evaluating endoscopy capacity across the NHS in England Hilary Brown, HSMC, University of Birmingham Steven Wyatt, Midlands and Lancashire Commissioning Support Unit Methodology Literature and evidence
Evaluating endoscopy capacity across the NHS in England Hilary Brown, HSMC, University of Birmingham Steven Wyatt, Midlands and Lancashire Commissioning Support Unit Methodology Literature and evidence
FIT: emerging evidence and steps towards policy development
 FIT: emerging evidence and steps towards policy development Cancer Alliance Data, Evidence & Analysis Service (CADEAS) Natasha Crawford Michelle Barclay 26 th February 2019 Today s presentation What has
FIT: emerging evidence and steps towards policy development Cancer Alliance Data, Evidence & Analysis Service (CADEAS) Natasha Crawford Michelle Barclay 26 th February 2019 Today s presentation What has
Guidelines for Breast, Cervical and Colorectal Cancer Screening
 Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
Access to clinical trial information and the stockpiling of Tamiflu. Department of Health
 MEMORANDUM FOR THE COMMITTEE OF PUBLIC ACCOUNTS HC 125 SESSION 2013-14 21 MAY 2013 Department of Health Access to clinical trial information and the stockpiling of Tamiflu 4 Summary Access to clinical
MEMORANDUM FOR THE COMMITTEE OF PUBLIC ACCOUNTS HC 125 SESSION 2013-14 21 MAY 2013 Department of Health Access to clinical trial information and the stockpiling of Tamiflu 4 Summary Access to clinical
Colorectal Cancer Screening
 Tool 2.1 Cancer Screening Basic Fact Sheet Are You at High Risk? Your risk for colorectal cancer may be higher than average if: stomach You or a close relative have had colorectal polyps or colorectal
Tool 2.1 Cancer Screening Basic Fact Sheet Are You at High Risk? Your risk for colorectal cancer may be higher than average if: stomach You or a close relative have had colorectal polyps or colorectal
Colorectal Cancer. Mark Chapman. MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist
 Colorectal Cancer Mark Chapman MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist Overview Epidemiology of colorectal cancer Adenoma carcinoma sequence Tumour diagnosis & staging Treatment
Colorectal Cancer Mark Chapman MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist Overview Epidemiology of colorectal cancer Adenoma carcinoma sequence Tumour diagnosis & staging Treatment
Colorectal Cancer Screening. Paul Berg MD
 Colorectal Cancer Screening Paul Berg MD What is clinical integration? AMA Definition The means to facilitate the coordination of patient care across conditions, providers, settings, and time in order
Colorectal Cancer Screening Paul Berg MD What is clinical integration? AMA Definition The means to facilitate the coordination of patient care across conditions, providers, settings, and time in order
Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005
 Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005 David Lieberman MD Chief, Division of Gastroenterology Oregon Health and Science University Portland VAMC Portland, Oregon
Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005 David Lieberman MD Chief, Division of Gastroenterology Oregon Health and Science University Portland VAMC Portland, Oregon
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
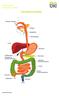 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
Early detection and screening for colorectal neoplasia
 Early detection and screening for colorectal neoplasia Robert S. Bresalier Department of Gastroenterology, Hepatology and Nutrition. The University of Texas. MD Anderson Cancer Center. Houston, Texas U.S.A.
Early detection and screening for colorectal neoplasia Robert S. Bresalier Department of Gastroenterology, Hepatology and Nutrition. The University of Texas. MD Anderson Cancer Center. Houston, Texas U.S.A.
Wellness Along the Cancer Journey: Cancer Types Revised October 2015 Chapter 4: Colorectal Cancer Overview
 Wellness Along the Cancer Journey: Cancer Types Revised October 2015 Chapter 4: Colorectal Cancer Overview Cancer Types Rev. 10.20.15 Page 35 Colorectal Cancer Overview Group Discussion True False Not
Wellness Along the Cancer Journey: Cancer Types Revised October 2015 Chapter 4: Colorectal Cancer Overview Cancer Types Rev. 10.20.15 Page 35 Colorectal Cancer Overview Group Discussion True False Not
Decision Analysis. John M. Inadomi. Decision trees. Background. Key points Decision analysis is used to compare competing
 5 Decision Analysis John M. Inadomi Key points Decision analysis is used to compare competing strategies of management under conditions of uncertainty. Various methods may be employed to construct a decision
5 Decision Analysis John M. Inadomi Key points Decision analysis is used to compare competing strategies of management under conditions of uncertainty. Various methods may be employed to construct a decision
Bowel cancer screening and prevention
 Bowel cancer screening and prevention Cancer Incidence and Mortality Victoria 2012 Number 6000 5000 4000 3000 2000 Incidences = 29,387 Mortality = 10,780 Incidence Mortality 1000 0 Prostate Breast Bowel
Bowel cancer screening and prevention Cancer Incidence and Mortality Victoria 2012 Number 6000 5000 4000 3000 2000 Incidences = 29,387 Mortality = 10,780 Incidence Mortality 1000 0 Prostate Breast Bowel
National Primary Care Research and Development Centre and University of York Health Economics Consortium (NICE External Contractor)
 National Primary Care Research and Development Centre and University of York Health Economics Consortium (NICE External Contractor) July 2010 Health economic report: threshold analysis This paper was prepared
National Primary Care Research and Development Centre and University of York Health Economics Consortium (NICE External Contractor) July 2010 Health economic report: threshold analysis This paper was prepared
Colon Screening in 2014 Offering Patients a Choice. Clark A Harrison MD The Nevada Colon Cancer Partnership
 Colon Screening in 2014 Offering Patients a Choice Clark A Harrison MD The Nevada Colon Cancer Partnership Objectives 1. Understand the incidence and mortality rates for CRC in the US. 2. Understand risk
Colon Screening in 2014 Offering Patients a Choice Clark A Harrison MD The Nevada Colon Cancer Partnership Objectives 1. Understand the incidence and mortality rates for CRC in the US. 2. Understand risk
CENTERS FOR DISEASE CONTROL AND PREVENTION CENTERS FOR DISEASE CONTROL AND PREVENTION. Incidence Male. Incidence Female.
 A Call to Action: Prevention and Early Detection of Colorectal Cancer (CRC) 5 Key Messages Screening reduces mortality from CRC All persons aged 50 years and older should begin regular screening High-risk
A Call to Action: Prevention and Early Detection of Colorectal Cancer (CRC) 5 Key Messages Screening reduces mortality from CRC All persons aged 50 years and older should begin regular screening High-risk
Is proton beam therapy cost effective in the treatment of adenocarcinoma of the prostate? Konski A, Speier W, Hanlon A, Beck J R, Pollack A
 Is proton beam therapy cost effective in the treatment of adenocarcinoma of the prostate? Konski A, Speier W, Hanlon A, Beck J R, Pollack A Record Status This is a critical abstract of an economic evaluation
Is proton beam therapy cost effective in the treatment of adenocarcinoma of the prostate? Konski A, Speier W, Hanlon A, Beck J R, Pollack A Record Status This is a critical abstract of an economic evaluation
Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer
 Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer David A. Lieberman, 1 Douglas K. Rex, 2 Sidney J. Winawer,
Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer David A. Lieberman, 1 Douglas K. Rex, 2 Sidney J. Winawer,
Colorectal Cancer Screening and Risk Assessment Workflow. Documentation Guide for Health Center NextGen Users
 Colorectal Cancer Screening and Risk Assessment Workflow Documentation Guide for Health Center NextGen Users Colorectal Cancer Screening and Risk Assessment Workflow and Documentation Guide for Health
Colorectal Cancer Screening and Risk Assessment Workflow Documentation Guide for Health Center NextGen Users Colorectal Cancer Screening and Risk Assessment Workflow and Documentation Guide for Health
Addendum DAP39 ADDENDUM. This Diagnostics Assessment Report was commissioned by the NIHR HTA Programme as project number 16/30/05
 25 The clinical and cost effectiveness of lead-i electrocardiogram (ECG) devices for detecting atrial fibrillation using single-time point testing in primary care [DAP39] DAP39 ADDENDUM Addendum This Diagnostics
25 The clinical and cost effectiveness of lead-i electrocardiogram (ECG) devices for detecting atrial fibrillation using single-time point testing in primary care [DAP39] DAP39 ADDENDUM Addendum This Diagnostics
NICE Guidelines for HTA Issues of Controversy
 NICE Guidelines for HTA Issues of Controversy Mark Sculpher, PhD Professor of Health Economics University of York, UK LMI, Medicines Agency in Norway and the Norwegian Knowledge Centre for the Health Services:
NICE Guidelines for HTA Issues of Controversy Mark Sculpher, PhD Professor of Health Economics University of York, UK LMI, Medicines Agency in Norway and the Norwegian Knowledge Centre for the Health Services:
PDF // POSITIVE COLON CANCER RESULTS
 01 March, 2018 PDF // POSITIVE COLON CANCER RESULTS Document Filetype: PDF 268.79 KB 0 PDF // POSITIVE COLON CANCER RESULTS This cohort study evaluates the association between time to colonoscopy after
01 March, 2018 PDF // POSITIVE COLON CANCER RESULTS Document Filetype: PDF 268.79 KB 0 PDF // POSITIVE COLON CANCER RESULTS This cohort study evaluates the association between time to colonoscopy after
A microsimulation study of the benefits and costs of screening for colorectal cancer Christopher Eric Stevenson
 A microsimulation study of the benefits and costs of screening for colorectal cancer Christopher Eric Stevenson A thesis submitted for the degree of Doctor of Philosophy of The Australian National University
A microsimulation study of the benefits and costs of screening for colorectal cancer Christopher Eric Stevenson A thesis submitted for the degree of Doctor of Philosophy of The Australian National University
Colorectal Cancer Screening
 Scan for mobile link. Colorectal Cancer Screening What is colorectal cancer screening? Screening examinations are tests performed to identify disease in individuals who lack any signs or symptoms. The
Scan for mobile link. Colorectal Cancer Screening What is colorectal cancer screening? Screening examinations are tests performed to identify disease in individuals who lack any signs or symptoms. The
Cancer Prevention and Early Detection Worksheet for Men
 Page 1 of 5 Cancer Prevention and Early Detection Worksheet for Men While a tremendous amount of progress has been made in cancer research, we still don t understand exactly what causes most cancers. However,
Page 1 of 5 Cancer Prevention and Early Detection Worksheet for Men While a tremendous amount of progress has been made in cancer research, we still don t understand exactly what causes most cancers. However,
ISPUB.COM. Health screening: is it always worth doing? O Durojaiye BACKGROUND SCREENING PROGRAMMES SCREENING OUTCOMES VALIDITY OF SCREENING PROGRAMMES
 ISPUB.COM The Internet Journal of Epidemiology Volume 7 Number 1 O Durojaiye Citation O Durojaiye.. The Internet Journal of Epidemiology. 2008 Volume 7 Number 1. Abstract Health screening as a preventive
ISPUB.COM The Internet Journal of Epidemiology Volume 7 Number 1 O Durojaiye Citation O Durojaiye.. The Internet Journal of Epidemiology. 2008 Volume 7 Number 1. Abstract Health screening as a preventive
A senior s guide for preventative healthcare services Ynolde F. Smith D.O.
 A senior s guide for preventative healthcare services Ynolde F. Smith D.O. What can we do to prevent disease? Exercise Eating Well Keep a healthy weight Injury prevention Mental Health Social issues (care
A senior s guide for preventative healthcare services Ynolde F. Smith D.O. What can we do to prevent disease? Exercise Eating Well Keep a healthy weight Injury prevention Mental Health Social issues (care
Welcome to this four part series focused on epidemiologic and biostatistical methods related to disease screening. In this first segment, we will
 Welcome to this four part series focused on epidemiologic and biostatistical methods related to disease screening. In this first segment, we will discuss essential components for effective screening programs.
Welcome to this four part series focused on epidemiologic and biostatistical methods related to disease screening. In this first segment, we will discuss essential components for effective screening programs.
Cancer Screening 2009: New Tests, New Choices
 Objectives Cancer Screening 2009: New Tests, New Choices UCSF Annual Review in Family Medicine April 21, 2009 Michael B. Potter, MD Professor, Clinical Family and Community Medicine UCSF School of Medicine
Objectives Cancer Screening 2009: New Tests, New Choices UCSF Annual Review in Family Medicine April 21, 2009 Michael B. Potter, MD Professor, Clinical Family and Community Medicine UCSF School of Medicine
Objectives. Definitions. Colorectal Cancer Screening 5/8/2018. Payam Afshar, MS, MD Kaiser Permanente, San Diego. Colorectal cancer background
 Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
CRC Risk Factors. U.S. Adherence Rates Cancer Screening. Genetic Model of Colorectal Cancer. Epidemiology and Clinical Consequences of CRC
 10:45 11:45 am Guide to Colorectal Cancer Screening SPEAKER Howard Manten M.D. Presenter Disclosure Information The following relationships exist related to this presentation: Howard Manten MD: No financial
10:45 11:45 am Guide to Colorectal Cancer Screening SPEAKER Howard Manten M.D. Presenter Disclosure Information The following relationships exist related to this presentation: Howard Manten MD: No financial
When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool
 When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool Adenomas/Carcinoma Sequence Providing Time for Screening Normal 5-20 yrs 5-15 yrs
When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool Adenomas/Carcinoma Sequence Providing Time for Screening Normal 5-20 yrs 5-15 yrs
Screening for Prostate Cancer
 Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
Colorectal Neoplasia. Dr. Smita Devani MBChB, MRCP. Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi
 Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography
 Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
The U.S. Preventive Services Task Force (USPSTF) makes
 Annals of Internal Medicine Clinical Guidelines Screening for Colorectal Cancer: U.S. Preventive Services Task Force Recommendation Statement U.S. Preventive Services Task Force* Description: Update of
Annals of Internal Medicine Clinical Guidelines Screening for Colorectal Cancer: U.S. Preventive Services Task Force Recommendation Statement U.S. Preventive Services Task Force* Description: Update of
USPSTF Draft Recommendations Investor Call. October 6, 2015
 USPSTF Draft Recommendations Investor Call October 6, 2015 v Safe Harbor Statement Certain statements made in this presentation contain forward-looking statements within the meaning of Section 27A of the
USPSTF Draft Recommendations Investor Call October 6, 2015 v Safe Harbor Statement Certain statements made in this presentation contain forward-looking statements within the meaning of Section 27A of the
Contents. Page No. Acknowledgements
 Y O R K Health Economics C O N S O R T I U M Bowel Cancer Services: Costs and Benefits Summary Report to the Department of Health York Health Economics Consortium, University of York: PAUL TRUEMAN, Director
Y O R K Health Economics C O N S O R T I U M Bowel Cancer Services: Costs and Benefits Summary Report to the Department of Health York Health Economics Consortium, University of York: PAUL TRUEMAN, Director
DIGESTIVE SYSTEM SURGICAL PROCEDURES May 1, 2015 INTESTINES (EXCEPT RECTUM) Asst Surg Anae
 ENDOSCOPY Z50 Duodenoscopy (not to be claimed if Z399 and/or Z00 performed on same patient within 3 months)... 92.10 Z9 Subsequent procedure (within three months following previous endoscopic procedure)...
ENDOSCOPY Z50 Duodenoscopy (not to be claimed if Z399 and/or Z00 performed on same patient within 3 months)... 92.10 Z9 Subsequent procedure (within three months following previous endoscopic procedure)...
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Rituximab for the treatment of relapsed or refractory stage III or IV follicular non-hodgkin s lymphoma (review of technology
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Rituximab for the treatment of relapsed or refractory stage III or IV follicular non-hodgkin s lymphoma (review of technology
Joint Session with ACOFP and Cancer Treatment Centers of America (CTCA): Cancer Screening: Consensus & Controversies. Ashish Sangal, M.D.
 Joint Session with ACOFP and Cancer Treatment Centers of America (CTCA): Cancer Screening: Consensus & Controversies Ashish Sangal, M.D. Cancer Screening: Consensus & Controversies Ashish Sangal, MD Director,
Joint Session with ACOFP and Cancer Treatment Centers of America (CTCA): Cancer Screening: Consensus & Controversies Ashish Sangal, M.D. Cancer Screening: Consensus & Controversies Ashish Sangal, MD Director,
Nivolumab for adjuvant treatment of resected stage III and IV melanoma [ID1316] STA Lead team presentation: Cost Effectiveness Part 1
![Nivolumab for adjuvant treatment of resected stage III and IV melanoma [ID1316] STA Lead team presentation: Cost Effectiveness Part 1 Nivolumab for adjuvant treatment of resected stage III and IV melanoma [ID1316] STA Lead team presentation: Cost Effectiveness Part 1](/thumbs/89/99008516.jpg) For public no AIC or CIC Nivolumab for adjuvant treatment of resected stage III and IV melanoma [ID1316] STA Lead team presentation: Cost Effectiveness Part 1 1st Appraisal Committee meeting Committee
For public no AIC or CIC Nivolumab for adjuvant treatment of resected stage III and IV melanoma [ID1316] STA Lead team presentation: Cost Effectiveness Part 1 1st Appraisal Committee meeting Committee
Fecal occult blood tests: a cost-effectiveness analysis Gyrd-Hansen D
 Fecal occult blood tests: a cost-effectiveness analysis Gyrd-Hansen D Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract
Fecal occult blood tests: a cost-effectiveness analysis Gyrd-Hansen D Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract
Blue Star Sunday. Increasing Awareness About Colon Cancer. Dear Faith Community,
 Blue Star Sunday Increasing Awareness About Colon Cancer Dear Faith Community, West Virginia s Cancer Coalition, Mountains of Hope, invites your faith community to participate in Colorectal Cancer Awareness
Blue Star Sunday Increasing Awareness About Colon Cancer Dear Faith Community, West Virginia s Cancer Coalition, Mountains of Hope, invites your faith community to participate in Colorectal Cancer Awareness
The Dutch bowel cancer screening program Relevant lessions for Ontario
 The Dutch bowel cancer screening program Relevant lessions for Ontario Ernst J Kuipers Erasmus MC University Medical Center Rotterdam - The Netherlands 1 Ismar Boas (1858 1938) Colorectal cancer screening
The Dutch bowel cancer screening program Relevant lessions for Ontario Ernst J Kuipers Erasmus MC University Medical Center Rotterdam - The Netherlands 1 Ismar Boas (1858 1938) Colorectal cancer screening
HOW TO EVALUATE ACTIVITIES INTENDED TO INCREASE AWARENESS AND USE OF COLORECTAL CANCER SCREENING. Using your toolkit to conduct an evaluation
 EVALUATION TOOLKIT HOW TO EVALUATE ACTIVITIES INTENDED TO INCREASE AWARENESS AND USE OF COLORECTAL CANCER SCREENING Using your toolkit to conduct an evaluation Welcome Mary Doroshenk, MA Director National
EVALUATION TOOLKIT HOW TO EVALUATE ACTIVITIES INTENDED TO INCREASE AWARENESS AND USE OF COLORECTAL CANCER SCREENING Using your toolkit to conduct an evaluation Welcome Mary Doroshenk, MA Director National
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE
 COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
Single Suspected Cancer Pathway Definitions pathway start date
 Single Suspected Cancer Pathway Definitions pathway start date Date: March 2018 Version: 1.2.1 Wales Cancer Owner: Network and Welsh Government Status Published 1 P a g e Purpose of Document This document
Single Suspected Cancer Pathway Definitions pathway start date Date: March 2018 Version: 1.2.1 Wales Cancer Owner: Network and Welsh Government Status Published 1 P a g e Purpose of Document This document
Supporting people at higher risk of bowel cancer
 #never2young Never too young: Supporting people at higher risk of bowel cancer Campaign briefing Supporting people at higher risk of bowel cancer Bowel cancer is the second most common cause of cancer
#never2young Never too young: Supporting people at higher risk of bowel cancer Campaign briefing Supporting people at higher risk of bowel cancer Bowel cancer is the second most common cause of cancer
Technology appraisal guidance Published: 29 June 2011 nice.org.uk/guidance/ta227
 Erlotinib monotherapy for maintenance treatment of non-small-cell lung cancer Technology appraisal guidance Published: 29 June 2011 nice.org.uk/guidance/ta227 NICE 2018. All rights reserved. Subject to
Erlotinib monotherapy for maintenance treatment of non-small-cell lung cancer Technology appraisal guidance Published: 29 June 2011 nice.org.uk/guidance/ta227 NICE 2018. All rights reserved. Subject to
Strategy Strategic delivery: Setting standards Increasing and informing choice. Details: Output: Demonstrating efficiency economy and value
 Strategy 2017-20 Strategic delivery: Setting standards Increasing and informing choice Demonstrating efficiency economy and value Details: Meeting Authority Agenda item 7 Paper number HFEA (11/05/2016)
Strategy 2017-20 Strategic delivery: Setting standards Increasing and informing choice Demonstrating efficiency economy and value Details: Meeting Authority Agenda item 7 Paper number HFEA (11/05/2016)
Advice Statement. Advice Statement November Advice for NHSScotland. Why is SHTG looking at this topic?
 Advice Statement 014-18 November 2018 Advice Statement Colon capsule endoscopy (CCE-2) for the detection of colorectal polyps and cancer in adults with signs or symptoms of colorectal cancer or at increased
Advice Statement 014-18 November 2018 Advice Statement Colon capsule endoscopy (CCE-2) for the detection of colorectal polyps and cancer in adults with signs or symptoms of colorectal cancer or at increased
