ACCURACY OF IMMUNOHISTOCHEMISTRY IN EVALUATION
|
|
|
- Victor Boone
- 5 years ago
- Views:
Transcription
1 POL J PATHOL 2011; 2: ACCURACY OF IMMUNOHISTOCHEMISTRY IN EVALUATION OF MALIGNANT PLEURAL AND PERITONEAL EFFUSIONS FERESHTEH ENSANI, FARNAZ NEMATIZADEH, GITI IRVANLOU Department of Cytology, Cancer Institute, Imam Khomeini Medical Complex, Tehran University of Medical Sciences, Tehran, Iran Background: The aim was to evaluate the accuracy of immunohistochemistry in diagnosis of the source of malignancies in pleural and peritoneal fluids in compa - rison to histopathology as the gold standard. Material and methods: Retrospectively, the cell block specimen and past medical data files of patients who had undergone serosal fluid aspiration and had a histopathology report corresponding to underlying disease were retrieved. Three mesothelial antibodies (D2-40, calretinin and WT-1) and two non-mesothelial antibodies (MOC-31 and EMA) were set to be applied for evaluating malignant cells and benign cells within serous fluids. Results: Seventy-one patients, 12 men and 59 women, were found to have a thorough information package needed, including cell blocks with appropriate cellularity on which ICC was applicable and the corresponding histopathology report. As mesothelial markers, calretinin and WT-1 were found to have sensitivity and specificity of 90%, 96.7% and 100%, 42.6%, respectively. Sensitivity and specificity of D2-40 both reached 100%. In addition, as non-mesothelial markers, MOC-31 and EMA were demonstrated to have sensitivity and specificity of 95.08%, 90% and 93.4%, 70%, respectively. Conclusion: D2-40 was reconfirmed to act as an accurate marker in distinguishing between cells of mesothelial and non-mesothelial origin. However, WT-1 is not specific enough to be considered as accurate as D2-40. Considering the sensitivity and specificity of calretinin and MOC-31, they can be considered as safe but not as much as D2-40. EMA is not recommended as an ancillary marker due to its low specificity and challenging results. Key words: pleural effusion, peritoneal effusion, immunohistochemistry. Introduction Malignancies such as lung, breast, gastrointestinal and female genital adenocarcinoma as well as malignant mesothelioma are common sources of effusion in pleural and peritoneal cavities. Histopathology has been used for a long time as the gold standard diagnostic modality. The morphological evaluation, however, is sometimes difficult due to reasons such as a low number of tumour cells, mixed population of tumoural-mesothelial cells and presence of reactive mesothelial cells which mimic the morphology of malignant cells [1-3]. Moreover, mesothelial cells react variously to different sorts of both external and internal stimuli, which can result in misdiagnosis of a malignancy [1, 2]. As finding the source of tumoural cells in serosal fluids is crucial in diagnosis and treatment of patients, substituting histopathology for a more rapid, accurate and cost-effective method seems to be necessary. Therefore, according to difficulties in morphological diagnosis of cancerous serous effusions and considering the critical role of immunohistochemistry, application of a novel panel of diagnostic markers for early and accurate detection of the source 95
2 FERESHTEH ENSANI, FARNAZ NEMATIZADEH, GITI IRVANLOU of malignancies in serous fluids is mandatory. As currently used panels are not of acceptable specifications, e.g. sensitivity and specificity, we conducted this study to evaluate the value of a new panel including 3 mesothelial and 2 non-mesothelial markers in detection of tumoural cells within pleural and peritoneal fluids [1, 2]. Material and methods Patients Retrospectively and from 2005 to 2008 all patients with pleural and peritoneal effusion for whom histopathological analysis (biopsy from pleura or peritoneum) had been performed, and their pleural/peritoneal fluid cell block were available, were enrolled in the study. Every patient whose result of histopathology was not available, who had inappropriate cell fixation on the cell block and who had insufficient cell count on the cell block was excluded. No age/sex limit was applied. Laboratory techniques Available cell blocks were considered for immunohistochemistry. The preparation process of the cell blocks is stated below: Aspirated pleural/peritoneal fluid was centrifuged for 5 minutes (1000 RPM). The supernatant fluid was discarded whereas the sedimentary material was saved and divided into two halves. Using 96% ethanol, the first half was fixed, from which 4 smears were made and used for cytological study. Cellularity was established by evaluation of haematoxylin and eosin (H&E) stained cell block sections from formalin-fixed paraffin-embedded pellets of the other half, after using 10% buffered formalin as a fixator. If cellularity was confirmed to be sufficient, further characterization by following a 5-antibody panel (using IHC diluent, RE7133 Novocastra, if needed) was carried out: D2-40 (1 : 100; Monoclonal mouse antihuman D2-40, Dakocytomation), Calretinin (1 : 100; Liquid mouse monoclonal antibody, NCL-L-CaLRET-566, Novocastra), WT-1 (1 : 40; Liquid mouse monoclonal antibody, NCL-L- WT-1-562, Novocastra), MOC-31 (1 : 50; Mouse monoclonal antibody, Clone = NCL-MOC-31, Novocastra) and EMA (1 : 1; Ready to use liquid mouse monoclonal antibody [RTU-EMA], Novocastra). All cases were stained using Post primary block (Novolink polymer detection system, RE7150-K Novocastra) and Novolink-polymer (Novolink polymer detection system, RE7150-K Novocastra). Prostate tissue was used as a positive control for D2-40, testis tissue for calretinin, kidney tissue for WT-1, intestinal tissue for MOC-31 and colon or breast tissue for EMA. D2-40 was interpreted as positive if cytoplasmic and membranous (if any) staining were observed. Calretinin was interpreted as positive if nuclear and cytoplasmic (if any) staining were detected. MOC-31 represented positive results in case membranous staining was seen. WT-1 was interpreted as positive if nuclear staining was observed. And last but not least, EMA was considered positive if cytoplasmic and membranous staining were observed. Each marker was reported as either positive or negative. Afterwards, each H&E slide as well as all prepared slides regarding positive and negative values for malignant epithelial and mesothelial cells and reactive mesothelial cells was assessed and in the end, sensitivity, specificity, positive predictive value (PPV) and negative predictive value (NPV) of each marker were generated. This study was conducted after approval from the institutional board of Tehran University of Medical Sciences. Results Serous effusions from 71 patients, 12 (16.9%) men and 59 (83.1%) women (age range: y, mean: 53.7 y), from the Department of Cytology, Cancer Institute, Imam Khomeini Medical Complex, Tehran University of Medical Sciences, Tehran, Iran, were retrospectively reviewed. Overall, 14 samples of pleural (19.7%) and 57 peritoneal (80.3%) fluids, including 8 (11.26%) benign and 63 (88.74%) malignant effusions, were collected. From the stated 63 samples of malignant lesions, 14 cases (22.2%) have pleural and 49 (77.8%) have peritoneal origin, 12 (19.4%) cases were from male and 51 (80.6%) cases were from female patients. However, all 8 benign samples were obtained from women. The summary of the involved organs and type of malignancies are given in Tables I and II, respectively. Table I. Distribution of tumour sources throughout the body LUNG GI TRACT GENITALIA BREAST PLEURA UNKNOWN ORIGIN TOTAL Male Female Total GI tract: gastrointestinal tract 96
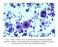
3 DOES IMMUNOHISTOCHEMISTRY DETECT THE SOURCE OF MALIGNANCY IN SEROUS FLUIDS? Table II. Histopathological diagnosis of our cancerous population ADENO- SMALL SQUAMOUS INVASIVE MALIGNANT GENITAL GENITAL GENITAL TOTAL CARCINOMA CELL CELL DUCTAL MESOTHELIOMA SEROUS MUCINOUS ENDOMETRIOID NOS CARCINOMA CARCINOMA CARCINOMA TUMOUR TUMOUR TUMOUR Male Female Total NOS not otherwise specified Immunohistochemical analysis D2-40 In both (100%) cases of malignant mesothelioma, cytoplasmic and membranous staining was noted (Fig. 1). This included both malignant mesothelial and background reactive mesothelial cells. In all 8 (100%) cases of benign effusions, a positive reaction was noted. However, none of the malignant effusions were positive for this marker. From 63 cases of malignant effusions, 54 cases demonstrated mesothelial reactive cells in the background, among which all (100%) had a positive reaction to D2-40. Sensitivity, specificity, PPV and NPV of this antibody as a mesothelial cell marker all reached 100%. Calretinin In both (100%) cases of malignant mesothelioma, both malignant and background reactive mesothelial cells showed positive nuclear staining with calretinin. In 2 (3.2%) cases of non-mesothelial tumours (both adenocarcinomas), however, weakly positive cytoplasmic staining was observed (Fig. 2). Out of 8 cases of benign effusions, 7 (87.5%) cases with reactive mesothelial cells were noted to have positive nuclear staining. Moreover, among 63 samples of malignant effusions, 56 cases had background reactive mesothelial cells of which 55 (98.2%) cases presented positive nuclear staining as well. Sensitivity, specificity, PPV and NPV of calretinin as a mesothelial cell marker reached 90%, 96.7%, 81.8% and 98.3%, respectively. Fig. 1. D2-40 positive malignant mesothelioma. Original magnification 400 Fig. 2. Calretinin positive papillary serous carcinoma of ovary. Original magnification 400 WT-1 In both (100%) of our malignant mesothelioma samples, reactive and malignant mesothelial cells showed nuclear staining. Of 61 cases of nonmesothelial tumours, 35 (57.3%) cases showed positive nuclear staining, all being adenocarcinomas, consisting of 32 cases of female genital malignancies, 1 of gastrointestinal and 2 of unknown origin. Additionally, out of 34 cases of female serous genital malignancies, 30 (88.2%) were observed to be positive for WT-1 (Pearson χ 2 < ). In all 8 (100%) cases of benign effusions, the positive nuclear reaction was remarkable. Of 63 cases of malignant effusions, 53 represented background reactive mesothelial cells, of which 52 (98.11%) had positive staining. Sensitivity, specificity, PPV and NPV of WT-1 as a mesothelial marker were 100%, 42.2%, 22.2% and 100%, respectively. 97
4 FERESHTEH ENSANI, FARNAZ NEMATIZADEH, GITI IRVANLOU reactive mesothelial cells of which only 2 (3.7%) cases demonstrated positive membranous staining. As a non-mesothelial marker, sensitivity, specificity, PPV and NPV of MOC-31 were 95.08%, 90%, 98.3% and 75%, respectively. EMA Fig. 3. MOC-31 positive adenocarcinoma. Original magnification 400 Both membranous and cytoplasmic positive staining were noted in both (100%) malignant mesothelioma cases regarding both malignant and background reactive mesothelial cells (Fig. 4). Only 1 (12.5%) out of 8 cases of benign effusions had positive cytoplasmic and membranous staining. Out of 61 cases of nonmesothelial malignancies, 57 (93.4%) were noted to have positive membranous and cytoplasmic staining which belong to 52 cases of adenocarcinoma, 2 cases of small cell carcinoma, 2 cases of invasive ductal carcinoma and 1 case of squamous cell carcinoma. Of 63 cases of malignant effusions, 53 cases had background mesothelial cells, of which only 8 (15.09%) cases had positive membranous and cytoplasmic staining. As another non-mesothelial marker, EMA achieved 93.44%, 70%, 95% and 63.6% sensitivity, specificity, PPV and NPV in our study, respectively. Sensitivity, specificity, PPV and NPV of each ICC marker are summarized in Table III. Discussion Fig. 4. EMA positive malignant mesothelioma. Original magnification 400 MOC-31 None of the malignant mesothelioma cases were positive. Among 8 cases of benign effusion, reactive cells of 1 (12.5%) case were noticed to have a clean membranous reaction. 58 (95.08%) out of 61 cases of malignant non-mesothelial samples were shown to have a positive membranous reaction (Fig. 3) which consisted of adenocarcinoma (53 cases), small cell carcinoma (2 cases), squamous cell carcinoma (2 cases) and invasive ductal carcinoma (1 case). Of 63 cases of malignant effusions, 53 cases had background A variety of benign and malignant disorders can present with serous effusion, of which determination of source and cell behaviour has always been a matter of diagnostic confusion among investigators worldwide. As detection of malignant cells in pleural and peritoneal effusions represents poor prognosis of a patient who, to some extent, suffers from an incurable disease, several immunohistochemical markers have been proposed to help pathologists and clinicians in distinguishing between malignant and benign lesions more accurately. The aim of this study was to apply a panel of markers which consisted of 3 mesothelial (D2-40, calretinin and WT-1) and two non-mesothelial (MOC-31 and EMA) markers to evaluate if, compared to histopathology, they are accurate enough to distinguish malignant and benign mesothelial and Table III. Sensitivity, specificity, PPV and NPV of each marker evaluated in this study D2-40 CALRETININ WT-1 MOC-31 EMA Sensitivity Specificity PPV NPV PPV positive predictive value, NPV negative predictive value 98
5 DOES IMMUNOHISTOCHEMISTRY DETECT THE SOURCE OF MALIGNANCY IN SEROUS FLUIDS? non-mesothelial effusions. This has been performed by other investigators using different panels as well. Having studied 41 cases of metastatic adenocarcinoma and 43 cases of reactive mesothelial cells, Saleh et al. demonstrated that MOC-31, BerEp4, HBME- 1, and calretinin are an excellent panel of markers for diagnosis, with 97.6% sensitivity for detecting metastatic adenocarcinoma and 90.7% specificity for detecting reactive mesothelial cells [4]. Similarly, Kim and colleagues have evaluated 118 cell blocks of pleural and peritoneal fluids, including 88 cases of adenocarcinoma and 30 benign effusions, regarding diagnosis of reactive mesothelial cells and adenocarcinomas using a panel of MOC-31, D2-40 and calretinin antibody. They concluded that a combination of MOC-31 and D2-40/calretinin is 100% specific and 99% sensitive for diagnosis of adenocarcinomas [5]. We demonstrated that all samples of malignant mesothelioma and benign reactive mesothelial cells had a positive reaction to D2-40. This finding was interestingly similar to some studies performed by other investigators such as Lyons-Boudreaux et al. [6] and Bassarova et al. [1]. Saleh et al., however, found only 58.1% of their benign effusions to have a positive reaction to D2-40 antibody, though they had no specimens of malignant mesotheliomas [4]. Furthermore, none of our non-mesothelial malignant effusions had a positive reaction to D2-40, which was the same as Lyons-Boudreaux et al. s results [6]. In contrast, using this antibody, Kim et al. [5] has reported a single positive case (1.1%) of adenocarcinoma and Bassarova et al. [1] has shown positivity in 58% of ovarian carcinomas, 30% of breast carcinomas and 33% of lung carcinomas. Saleh et al. [4] and Mimura et al. [7] have found 10 cases (24.4%) and 3 cases (4.5%) of their adenocarcinomas with positive membranous staining, respectively. We reached sensitivity, specificity, PPV and NPV of 100% for D2-40 as a mesothelial marker as well as what have been very similarly discovered by Lyons-Boudreaux et al. [6] and Kim et al. [5]. However, Saleh et al. proposed a significantly lower amount of sensitivity and specificity (58.1% and 75.6%, respectively, in detecting reactive mesothelial cell) for this marker [4]. Using calretinin, both (100%) of our malignant mesothelioma cases have shown a positive nuclear reaction, similar to results proposed by Lyons- Boudreaux et al. [6] and Politi et al. [8]. Furthermore, 2 (3.2%) of our malignant effusions had a positive cytoplasmic reaction to calretinin, which was achieved by Lyons-Boudreaux et al. [6], Kim et al. [5] and Saleh et al. [4] as 2.08%, 2.27% and 29.26%, respectively. Moreover, we found 87.5% of our benign effusions to have a positive reaction to calretinin, which was achieved by Lyons-Boudreaux et al. [6], Kim et al. [5] and Saleh et al. [4] as 58%, 93.3% and 95.3%, respectively. In our study and as a mesothelial marker, sensitivity, specificity, PPV and NPV of calretinin were detected to be 90%, 96.7%, 81.8% and 98.3%, respectively. According to the investigations of Lyons-Boudreaux et al. [6], Kim et al. [5] and Saleh et al. [4], these amounts were 67%, 93% and 95.3% for sensitivity and 98%, 98% and 70.7% for specificity, all respectively. Moreover, Lyons-Boudreaux et al. [6] and Kim et al. [5] reported PPV and NPV of 94%, 85% and 93%, 98%, respectively, in application of calretinin. Using WT-1, both of our malignant mesothelioma cases have shown a positive nuclear reaction, while Lyons-Boudreaux et al. [6] found 60% positivity. 57.3% of our non-mesothelial tumours have shown nuclear staining, of which 91.4% were of female genital origin. This was reported to be 27% of adenocarcinomas in Lyons-Boudreaux et al. s study [6], which seems to be due to a higher number of cases with serous adenocarcinoma in our study. In our study, all 8 cases with reactive effusion had nuclear staining, which is in contrast to what has been stated in Lyons-Boudreaux et al. s study (50%) [6]. We found sensitivity, specificity, PPV and NPV of 100%, 42.6%, 22.2% and 100% while Lyons- Boudreaux et al. proposed these amounts as 52%, 73%, 48% and 76%, respectively [6]. Interestingly, moreover, King and coworkers reached sensitivity and specificity of 77% and 96%, respectively, by performing a systematic review having analysed 88 papers on antibody panels used for distinguishing malignant mesothelioma from metastatic adenocarcinoma [9]. The detected differences between our study and others regarding calculated sensitivity and specificity in use of WT-1 may be due to a difference in the number of effusions of genital system origin and moreover, in the ratio between benign and malignant effusions. Using MOC-31, none of our malignant mesothelioma cases have been stained as well as negative results proposed by Lyons-Boudreaux et al. [6] and Politi et al. [8]. However, Lozano et al. had 1 case within their 14 cases of malignant mesothelioma and reactive mesothelial cells with a positive MOC-31 reaction [10]. Regarding benign effusions, we found 1 out of 8 (12.5%) of our patients with positive staining. Lyons-Boudreaux et al. [6] and Kim et al. [5] had no positive results within their patients using this antibody % of our cases with nonmesothelial carcinomatous effusions including small cell carcinoma, squamous cell carcinoma, adenocarcinoma and invasive ductal carcinoma showed positive staining. Meanwhile, other investigators have found similar results for adenocarcinomas as well [5, 6, 8, 10]. In our study, sensitivity, specificity, PPV and NPV of MOC-31, as a non-mesothelial marker, reached 95.08%, 90%, 98.3% and 75%, respectively. However, these amounts for data of Lyons-Boudreaux 99
6 FERESHTEH ENSANI, FARNAZ NEMATIZADEH, GITI IRVANLOU et al. [6] and Kim et al. [5] were all 100%. Similar to our report, Lozano et al. [10] presented sensitivity and specificity of 83.34% and 92.86%, which was a little different from those of Politi et al., which were 86.25% and 100%, respectively [8]. Using EMA, cytoplasmic and membranous staining was seen in all cases of malignant mesothelioma, which was similar to that of Shidham s book [11]. Moreover, in our study, out of 8 cases of benign effusions, mesothelioma, 1 received EMA staining only, where as King and coworkers, by performing a systematic review of published papers, stated that positivity for EMA in benign or reactive mesothelium was less than 10% in 2 studies and more than 50% in another [12]. In addition, 93.4% of our nonmesothelial carcinomatous effusions were positive, which consisted of 52 cases of adenocarcinoma, 2 cases of small cell carcinoma, 1 case of squamous cell carcinoma and 2 cases of invasive ductal carcinoma. Sensitivity, specificity, PPV and NPV of our study were 93.44%, 70%, 95% and 63.6% for this marker, respectively. Sensitivity and specificity of EMA used in the project conducted by King et al. were 74% and 89%, respectively [12]. According to our findings, none of the applied antibodies were helpful in distinguishing between reactive mesothelial cells and malignant mesothelial cells. On the other hand, D2-40 can be used as a highly sensitive and specific mesothelial marker in serous fluids to distinguish mesothelial cells from others. From this point of view, D2-40 is preferred to calretinin. However, calretinin is a sensitive and specific marker for mesothelial cells. WT-1 is also a sensitive marker for mesothelial cells but its low specificity limits its application as part of a diagnostic panel. To distinguish adenocarcinomas, MOC-31 is an essentially useful marker of which sensitivity and specificity guarantee its accuracy. In contrast, according to the low specificity of EMA and moreover its challenging results, it would be better not to be considered in diagnostic antibody panels. We conclude that D2-40 and MOC-31 can be used accurately as two reliable diagnostic components of marker panels. If another study with a maximized sample size is conducted, the results may differ so that more antibodies can be added to the diagnostic panels. References 1. Bassarova AV, Nesland JM, Davidson B. D2-40 is not a specific marker for cells of mesothelial origin in serous effusions. Am J Surg Pathol 2006; 30: Davidson B. Malignant effusions: from diagnosis to biology. Diagn Cytopathol 2004; 31: Bedrossian CW. Diagnostic problems in serous effusions. Diagn Cytopathol 1998; 19: Saleh HA, El-Fakharany M, Makki H, et al. Differentiating reactive mesothelial cells from metastatic adenocarcinoma in serous effusions: the utility of immunocytochemical panel in the differential diagnosis. Diagn Cytopathol 2009; 37: Kim JH, Kim GE, Choi YD, et al. Immunocytochemical panel for distinguishing between adenocarcinomas and reactive mesothelial cells in effusion cell blocks. Diagn Cytopathol 2009; 37: Lyons-Boudreaux V, Mody DR, Zhai J, Coffey D. Cytologic malignancy versus benignancy: how useful are the newer markers in body fluid cytology? Arch Pathol Lab Med 2008; 132: Mimura T, Ito A, Sakuma T, et al. Novel marker D2-40, combined with calretinin, CEA, and TTF-1: an optimal set of immunodiagnostic markers for pleural mesothelioma. Cancer 2007; 109: Politi E, Kandaraki C, Apostolopoulou C, et al. Immunocytochemical panel for distinguishing between carcinoma and reactive mesothelial cells in body cavity fluids. Diagn Cytopathol 2005; 32: King JE, Thatcher N, Pickering CA, Hasleton PS. Sensitivity and specificity of immunohistochemical markers used in the diagnosis of epithelioid mesothelioma: a detailed systematic analysis using published data. Histopathology 2006; 48: Lozano MD, Panizo A, Toledo GR, et al. Immunocytochemistry in the differential diagnosis of serous effusions: a comparative evaluation of eight monoclonal antibodies in Papanicolaou stained smears. Cancer 2001; 93: Shidham V, Atkinson B. Immunocytochemistry of effusions processing and commonly used immunomarkers. In: Cytopathologic diagnosis of serous fluids. Shidham V (ed.). 1st ed. Elsevier 2007; King J, Thatcher N, Pickering C, Hasleton P. Sensitivity and specificity of immunohistochemical antibodies used to distinguish between benign and malignant pleural disease: a systematic review of published reports. Histopathology 2006; 49: Address for correspondence Fereshteh Ensani MD P.O. Box: , Tehran, Iran tel fensani@gmail.com Acknowledgement We wish to thank Farzan Institute for Research and Technology for technical assistance. 100
Value of antimesothelioma HBME 1 in the diagnosis of inflammatory and malignant pleural effusions
 Romanian Journal of Morphology and Embryology 2006, 47(4):351 355 ORIGINAL PAPER Value of antimesothelioma HBME 1 in the diagnosis of inflammatory and malignant pleural effusions LILIANA MOCANU 1), ANCA
Romanian Journal of Morphology and Embryology 2006, 47(4):351 355 ORIGINAL PAPER Value of antimesothelioma HBME 1 in the diagnosis of inflammatory and malignant pleural effusions LILIANA MOCANU 1), ANCA
ACCME/Disclosures. Diagnosing Mesothelioma in Limited Tissue Samples. Papanicolaou Society of Cytopathology Companion Meeting March 12 th, 2016
 Diagnosing Mesothelioma in Limited Tissue Samples Papanicolaou Society of Cytopathology Companion Meeting March 12 th, 2016 Sanja Dacic, MD, PhD University of Pittsburgh ACCME/Disclosures GENERAL RULES
Diagnosing Mesothelioma in Limited Tissue Samples Papanicolaou Society of Cytopathology Companion Meeting March 12 th, 2016 Sanja Dacic, MD, PhD University of Pittsburgh ACCME/Disclosures GENERAL RULES
Follow up of the Guidelines for Cytopathologic Diagnosis of Malignant Mesothelioma
 Follow up of the Guidelines for Cytopathologic Diagnosis of Malignant Mesothelioma Assoc. Prof. Katalin Dobra, Senior Lecturer in Molecular Pathology Karolinska University Hospital Stockholm, Sweden Disclosure
Follow up of the Guidelines for Cytopathologic Diagnosis of Malignant Mesothelioma Assoc. Prof. Katalin Dobra, Senior Lecturer in Molecular Pathology Karolinska University Hospital Stockholm, Sweden Disclosure
Immunohistochemistry on Fluid Specimens: Technical Considerations
 Immunohistochemistry on Fluid Specimens: Technical Considerations Blake Gilks Dept of Pathology University of British Columbia, Vancouver, BC, Canada Disclosures None Learning Objectives At the end of
Immunohistochemistry on Fluid Specimens: Technical Considerations Blake Gilks Dept of Pathology University of British Columbia, Vancouver, BC, Canada Disclosures None Learning Objectives At the end of
Ascitic Fluid and Use of Immunocytochemistry. Mercè Jordà, University of Miami
 Ascitic Fluid and Use of Immunocytochemistry Mercè Jordà, University of Miami Is It Malignant? Yes? No Ascitic Fluid Cytomorphologic Useful Findings Tight clusters with smooth borders Cellular and nuclear
Ascitic Fluid and Use of Immunocytochemistry Mercè Jordà, University of Miami Is It Malignant? Yes? No Ascitic Fluid Cytomorphologic Useful Findings Tight clusters with smooth borders Cellular and nuclear
Mesothelioma: diagnostic challenges from a pathological perspective. Naseema Vorajee August 2016
 Mesothelioma: diagnostic challenges from a pathological perspective Naseema Vorajee August 2016 Naseema.vorajee@nhls.ac.za Pleural diseases (whether neoplastic, reactive or infective) may have similar
Mesothelioma: diagnostic challenges from a pathological perspective Naseema Vorajee August 2016 Naseema.vorajee@nhls.ac.za Pleural diseases (whether neoplastic, reactive or infective) may have similar
Cytological evaluation of effusion fluid with cell block technique and cytology smears among Sudanese patients
 EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 3/ June 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Cytological evaluation of effusion fluid with cell block technique
EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 3/ June 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Cytological evaluation of effusion fluid with cell block technique
Expression of Cytokeratin 5/6 in Epithelial Neoplasms: An Immunohistochemical Study of 509 Cases
 Expression of Cytokeratin 5/6 in Epithelial Neoplasms: An Immunohistochemical Study of 509 Peiguo G. Chu, M.D., Ph.D., Lawrence M. Weiss, M.D. Department of Pathology, City of Hope National Medical Center,
Expression of Cytokeratin 5/6 in Epithelial Neoplasms: An Immunohistochemical Study of 509 Peiguo G. Chu, M.D., Ph.D., Lawrence M. Weiss, M.D. Department of Pathology, City of Hope National Medical Center,
Evaluation of the Sensitivity and Specificity of Immunohistochemical Markers in the Differential Diagnosis of Effusion Cytology
 DOI 10. 5001/omj.2013.117 Evaluation of the Sensitivity and Specificity of Immunohistochemical Markers in the Differential Diagnosis of Effusion Cytology Zahraa Mohammed Yahya, Hussam Hasson Ali, and Haider
DOI 10. 5001/omj.2013.117 Evaluation of the Sensitivity and Specificity of Immunohistochemical Markers in the Differential Diagnosis of Effusion Cytology Zahraa Mohammed Yahya, Hussam Hasson Ali, and Haider
Serous Effusions. Spasenija Savic Prince, MD Pathology, University Hospital Basel, Switzerland
 Serous Effusions Spasenija Savic Prince, MD Pathology, University Hospital Basel, Switzerland Serous membrane Body cavities: Pleural Pericardial Peritoneal Effusion = Excess of fluid 80% Benign 20% Malignant
Serous Effusions Spasenija Savic Prince, MD Pathology, University Hospital Basel, Switzerland Serous membrane Body cavities: Pleural Pericardial Peritoneal Effusion = Excess of fluid 80% Benign 20% Malignant
Key Words: effusion; carcinoma; immunocytochemistry; direct smear; cytology
 The Application of Immunocytochemistry to Direct Smears in the Diagnosis of Effusions Stewart M. Knoepp, M.D., Ph.D., { Jeremiah Placido, M.D., { Kristina L. Fields, B.S., Dafydd Thomas, M.D., Ph.D., and
The Application of Immunocytochemistry to Direct Smears in the Diagnosis of Effusions Stewart M. Knoepp, M.D., Ph.D., { Jeremiah Placido, M.D., { Kristina L. Fields, B.S., Dafydd Thomas, M.D., Ph.D., and
Serous effusion Objectives. Cytology of Serous Effusions From basics to challenges
 Cytology of Serous Effusions From basics to challenges Cytology of Serous Effusions From basics to challenges Pınar Fırat, MD, MIAC Department of Pathology, İstanbul University, İstanbul Faculty of Medicine,
Cytology of Serous Effusions From basics to challenges Cytology of Serous Effusions From basics to challenges Pınar Fırat, MD, MIAC Department of Pathology, İstanbul University, İstanbul Faculty of Medicine,
How to Recognize Gynecologic Cancer Cells from Pelvic Washing and Ascetic Specimens
 How to Recognize Gynecologic Cancer Cells from Pelvic Washing and Ascetic Specimens Wenxin Zheng, M.D. Professor of Pathology and Gynecology University of Arizona zhengw@email.arizona.edu http://www.zheng.gynpath.medicine.arizona.edu/index.html
How to Recognize Gynecologic Cancer Cells from Pelvic Washing and Ascetic Specimens Wenxin Zheng, M.D. Professor of Pathology and Gynecology University of Arizona zhengw@email.arizona.edu http://www.zheng.gynpath.medicine.arizona.edu/index.html
Hepatocyte Nuclear Factor-1b Is Not a Specific Marker of Clear Cell Carcinoma in Serous Effusions
 Hepatocyte Nuclear Factor-1b Is Not a Specific Marker of Clear Cell Carcinoma in Serous Effusions Ben Davidson, MD, PhD 1,2 BACKGROUND: The transcription factor hepatocyte nuclear factor-1b (HNF1b) has
Hepatocyte Nuclear Factor-1b Is Not a Specific Marker of Clear Cell Carcinoma in Serous Effusions Ben Davidson, MD, PhD 1,2 BACKGROUND: The transcription factor hepatocyte nuclear factor-1b (HNF1b) has
Malignant mesothelioma: a comparison of biopsy and postmortem material by light microscopy and immunohistochemistry
 766 J Clin Pathol 2001;54:766 770 Malignant mesothelioma: a comparison of biopsy and postmortem material by light microscopy and immunohistochemistry Department of Pathology, Victoria Infirmary, Langside
766 J Clin Pathol 2001;54:766 770 Malignant mesothelioma: a comparison of biopsy and postmortem material by light microscopy and immunohistochemistry Department of Pathology, Victoria Infirmary, Langside
WT1, Estrogen Receptor, and Progesterone Receptor as Markers for Breast or Ovarian Primary Sites in Metastatic Adenocarcinoma to Body Fluids
 Anatomic Pathology / WT1, ESTROGEN RECEPTOR, AND PROGESTERONE RECEPTOR IN CYTOLOGY OF BODY FLUIDS WT1, Estrogen Receptor, and Progesterone Receptor as Markers for Breast or Ovarian Primary Sites in Metastatic
Anatomic Pathology / WT1, ESTROGEN RECEPTOR, AND PROGESTERONE RECEPTOR IN CYTOLOGY OF BODY FLUIDS WT1, Estrogen Receptor, and Progesterone Receptor as Markers for Breast or Ovarian Primary Sites in Metastatic
ACCME/Disclosures. Case 4 USCAP Pulmonary Panel Case 4 History
 Case 4 USCAP Pulmonary Panel 2016 Andrew Churg, MD Department of Pathology Vancouver General Hospital & University of British Columbia Vancouver, BC achurg@mail.ubc.ca. ACCME/Disclosures The USCAP requires
Case 4 USCAP Pulmonary Panel 2016 Andrew Churg, MD Department of Pathology Vancouver General Hospital & University of British Columbia Vancouver, BC achurg@mail.ubc.ca. ACCME/Disclosures The USCAP requires
SELECTED DILEMMAS IN RESPIRATORY CYTOPATHOLOGY (2 CASES)
 SELECTED DILEMMAS IN RESPIRATORY CYTOPATHOLOGY (2 CASES) Dr. Mariamma Joseph Professor of Pathology Division Head Cytopathology Department of Pathology and Laboratory Medicine LHSC and Western University
SELECTED DILEMMAS IN RESPIRATORY CYTOPATHOLOGY (2 CASES) Dr. Mariamma Joseph Professor of Pathology Division Head Cytopathology Department of Pathology and Laboratory Medicine LHSC and Western University
Applications of Flow Cytometry in Diagnostic Cytology of Body Cavity Fluids
 Applications of Flow Cytometry in Diagnostic Cytology of Body Cavity Fluids Awtar Krishan, PhD. Professor, Department of Pathology University of Miami School of Medicine akrishan@med.miami.edu Beckman
Applications of Flow Cytometry in Diagnostic Cytology of Body Cavity Fluids Awtar Krishan, PhD. Professor, Department of Pathology University of Miami School of Medicine akrishan@med.miami.edu Beckman
Editorial Process: Submission:11/02/2017 Acceptance:05/19/2018
 RESEARCH ARTICLE Editorial Process: Submission:11/02/2017 Acceptance:05/19/2018 Comparative Analysis of Modified Liquid-Based Cytology and CytoRich Red Preparation in Assessment of Serous Effusion for
RESEARCH ARTICLE Editorial Process: Submission:11/02/2017 Acceptance:05/19/2018 Comparative Analysis of Modified Liquid-Based Cytology and CytoRich Red Preparation in Assessment of Serous Effusion for
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Utility of Modified Cell Block Technique in Cases of Pleural Effusion Suspected of Malignancy
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Utility of Modified Cell Block Technique in Cases of Pleural Effusion Suspected of Malignancy
Immunohistochemical Expression of Cytokeratin 5/6 in Gynaecological Tumors.
 ISPUB.COM The Internet Journal of Pathology Volume 13 Number 2 Immunohistochemical Expression of Cytokeratin 5/6 in Gynaecological Tumors. A Baghla, S Choudhry, A Kataria Citation A Baghla, S Choudhry,
ISPUB.COM The Internet Journal of Pathology Volume 13 Number 2 Immunohistochemical Expression of Cytokeratin 5/6 in Gynaecological Tumors. A Baghla, S Choudhry, A Kataria Citation A Baghla, S Choudhry,
Case 1. Slide 1 History: 65 year old male presents with bilateral pleural effusions, a 40 pack year smoking history and peripheral and hilar lung
 Case 1. Slide 1 History: 65 year old male presents with bilateral pleural effusions, a 40 pack year smoking history and peripheral and hilar lung masses. Specimen shown is from a tap of the pleural effusion.
Case 1. Slide 1 History: 65 year old male presents with bilateral pleural effusions, a 40 pack year smoking history and peripheral and hilar lung masses. Specimen shown is from a tap of the pleural effusion.
Biopsy Interpretation of Spindle cell proliferations of the Serosa
 Biopsy Interpretation of Spindle cell proliferations of the Serosa Richard Attanoos, Cardiff. U.K. Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee)
Biopsy Interpretation of Spindle cell proliferations of the Serosa Richard Attanoos, Cardiff. U.K. Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee)
Key Words: PAX8; PAX2; Müllerian; carcinoma; effusion
 Diagnostic Utility of PAX8 and PAX2 Immunohistochemistry in the Identification of Metastatic Müllerian Carcinoma in Effusions William Wiseman, D.O., Claire W. Michael, M.D., and Michael H. Roh, M.D., Ph.D.*
Diagnostic Utility of PAX8 and PAX2 Immunohistochemistry in the Identification of Metastatic Müllerian Carcinoma in Effusions William Wiseman, D.O., Claire W. Michael, M.D., and Michael H. Roh, M.D., Ph.D.*
Applications of IHC. Determination of the primary site in metastatic tumors of unknown origin
 Applications of IHC Determination of the primary site in metastatic tumors of unknown origin Classification of tumors that appear 'undifferentiated' by standard light microscopy Precise classification
Applications of IHC Determination of the primary site in metastatic tumors of unknown origin Classification of tumors that appear 'undifferentiated' by standard light microscopy Precise classification
Journal of Cytology & Histology
 ISSN: 2157-7099 ojournal of Cytology & Hist logy Journal of Cytology & Histology Sen, et al., 2015, 6:2 DOI: 10.4172/2157-7099.1000314 Research Article Article Open Open Access Morphometric Analysis and
ISSN: 2157-7099 ojournal of Cytology & Hist logy Journal of Cytology & Histology Sen, et al., 2015, 6:2 DOI: 10.4172/2157-7099.1000314 Research Article Article Open Open Access Morphometric Analysis and
Diagnostic IHC in lung and pleura pathology
 Diagnostic IHC in lung and pleura pathology Mogens Vyberg Professor of Clinical Pathology Director of NordiQC Aalborg University Hospital, Aalborg, Denmark WHO 2004 and Web Malignant mesothelioma Epithelioid
Diagnostic IHC in lung and pleura pathology Mogens Vyberg Professor of Clinical Pathology Director of NordiQC Aalborg University Hospital, Aalborg, Denmark WHO 2004 and Web Malignant mesothelioma Epithelioid
COMPARATIVE STUDY OF CELL - BLOCKS & ROUTINE CYTOLOGICAL SMEARS OF PLEURAL & PERITONEAL FLUIDS IN SUSPECTED CASES OF MALIGNANCY
 ORIGINAL RESEARCH COMPARATIVE STUDY OF CELL - BLOCKS & ROUTINE CYTOLOGICAL SMEARS OF PLEURAL & PERITONEAL FLUIDS IN SUSPECTED CASES OF MALIGNANCY Geethu G Nair,*, Anupama Achyuthan Manjula 2 Assistant
ORIGINAL RESEARCH COMPARATIVE STUDY OF CELL - BLOCKS & ROUTINE CYTOLOGICAL SMEARS OF PLEURAL & PERITONEAL FLUIDS IN SUSPECTED CASES OF MALIGNANCY Geethu G Nair,*, Anupama Achyuthan Manjula 2 Assistant
ROSE in EUS guided FNA of Pancreatic Lesions
 ROSE in EUS guided FNA of Pancreatic Lesions Guy s Hospital, London, 16 April 2018 Laxmi Batav Imperial College NHS Trust Imperial College NHS Trust Cytology Workload Cervical Cytology 57,500 (decreases
ROSE in EUS guided FNA of Pancreatic Lesions Guy s Hospital, London, 16 April 2018 Laxmi Batav Imperial College NHS Trust Imperial College NHS Trust Cytology Workload Cervical Cytology 57,500 (decreases
Guideline for the Handling of Pathology Lung Tissue Specimens
 Guideline for the Handling of Pathology Lung Tissue Specimens Version Date Summary of Change/Process 0.1 29.06.11 Produced by Simon Trotter and circulated to Lung Network Site Specific Group for reviewing
Guideline for the Handling of Pathology Lung Tissue Specimens Version Date Summary of Change/Process 0.1 29.06.11 Produced by Simon Trotter and circulated to Lung Network Site Specific Group for reviewing
Nordic Immunohistochemical Quality Control
 Nordic Immunohistochemical Quality Control Immunohistochemistry in the classifiation of neoplasias of the alimentary tract & External Quality Assurance of Immunohistochemistry for GI cancer markers Mogens
Nordic Immunohistochemical Quality Control Immunohistochemistry in the classifiation of neoplasias of the alimentary tract & External Quality Assurance of Immunohistochemistry for GI cancer markers Mogens
A 53 year-old woman with a lung mass, right hilar mass and mediastinal adenopathy.
 November 2015 Case of the Month A 53 year-old woman with a lung mass, right hilar mass and mediastinal adenopathy. Contributed by: Rasha Salama, M.D., IU Department of Pathology and Laboratory Medicine
November 2015 Case of the Month A 53 year-old woman with a lung mass, right hilar mass and mediastinal adenopathy. Contributed by: Rasha Salama, M.D., IU Department of Pathology and Laboratory Medicine
Mesothelioma Pathobasic. Lukas Bubendorf Pathology
 Mesothelioma Pathobasic Lukas Bubendorf Pathology Mechanisms of Asbestos Carcinogenesis in Mesothelioma Asprin High-mobility group protein B1 master switch HMGB1 Initiation/ perpetuation of inflamm. response
Mesothelioma Pathobasic Lukas Bubendorf Pathology Mechanisms of Asbestos Carcinogenesis in Mesothelioma Asprin High-mobility group protein B1 master switch HMGB1 Initiation/ perpetuation of inflamm. response
Cytology and the Investigation of Carcinoma of Unknown Primary (CUP) Dr Anna Green ST5, St Thomas Hospital London, UK
 Cytology and the Investigation of Carcinoma of Unknown Primary (CUP) Dr Anna Green ST5, St Thomas Hospital London, UK Objectives Introduction to CUP Our experience of cytology and CUP Role of Cytology
Cytology and the Investigation of Carcinoma of Unknown Primary (CUP) Dr Anna Green ST5, St Thomas Hospital London, UK Objectives Introduction to CUP Our experience of cytology and CUP Role of Cytology
Immunohistochemical classification of lung carcinomas and mesotheliomas. Prof. Mogens Vyberg NordiQC Institute of Pathology Aalborg, Denmark
 Immunohistochemical classification of lung carcinomas and mesotheliomas Prof. Mogens Vyberg NordiQC Institute of Pathology Aalborg, Denmark Endobronchial ultrasound guided transbronchial needle biopsy
Immunohistochemical classification of lung carcinomas and mesotheliomas Prof. Mogens Vyberg NordiQC Institute of Pathology Aalborg, Denmark Endobronchial ultrasound guided transbronchial needle biopsy
Presentation material is for education purposes only. All rights reserved URMC Radiology Page 1 of 98
 Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Effusion Cytology: Diagnostic Challenges
 Effusion Cytology: Diagnostic Challenges Tarik M. Elsheikh, MD Professor and Medical Director, Anatomic Pathology Cleveland Clinic Outside Consult Case 45 year old woman, presented with nausea, dyspnea,
Effusion Cytology: Diagnostic Challenges Tarik M. Elsheikh, MD Professor and Medical Director, Anatomic Pathology Cleveland Clinic Outside Consult Case 45 year old woman, presented with nausea, dyspnea,
Fellowship in Cytopathology Department of Pathology. All India Institute of Medical Sciences (AIIMS) Jodhpur, Rajasthan, India
 Fellowship in Cytopathology Department of Pathology All India Institute of Medical Sciences (AIIMS) Jodhpur, Rajasthan, India Syllabus for Fellowship in Cytopathology: FNAC Direct, Guided, EUS Exfoliative
Fellowship in Cytopathology Department of Pathology All India Institute of Medical Sciences (AIIMS) Jodhpur, Rajasthan, India Syllabus for Fellowship in Cytopathology: FNAC Direct, Guided, EUS Exfoliative
T he diagnosis of malignant mesothelioma is dependent on
 662 ORIGINAL ARTICLE Immunohistochemistry in the distinction between malignant mesothelioma and pulmonary adenocarcinoma: a critical evaluation of new antibodies A S Abutaily, B J Addis, W R Roche... See
662 ORIGINAL ARTICLE Immunohistochemistry in the distinction between malignant mesothelioma and pulmonary adenocarcinoma: a critical evaluation of new antibodies A S Abutaily, B J Addis, W R Roche... See
In some regions of the world, breast cancer mortality beginning to fall due to earlier
 Original rticle Keykhosro Mardanpour (MD) 1 Mahtab Rahbar (MD) *2 Sedigheh Khazaei (MSc) 3 Mohsen ghaitasvand (MD) 3 1- Department of Orthopedics, Imam Reza Hospital, Kermanshah University of Medical Sciences,
Original rticle Keykhosro Mardanpour (MD) 1 Mahtab Rahbar (MD) *2 Sedigheh Khazaei (MSc) 3 Mohsen ghaitasvand (MD) 3 1- Department of Orthopedics, Imam Reza Hospital, Kermanshah University of Medical Sciences,
The Panel Approach to Diagnostics. Lauren Hopson International Product Specialist Cell Marque Corporation
 The Panel Approach to Diagnostics Lauren Hopson International Product Specialist Cell Marque Corporation Cell Marque Rocklin, California About Cell Marque: IVD primary antibody manufacturer Distributors
The Panel Approach to Diagnostics Lauren Hopson International Product Specialist Cell Marque Corporation Cell Marque Rocklin, California About Cell Marque: IVD primary antibody manufacturer Distributors
Morphologic and Immunocytochemical Performances of Effusion Cell Blocks Prepared Using 3 Different Methods
 Anatomic Pathology / Performance of Different Cell Block Preparation Techniques Morphologic and Immunocytochemical Performances of Effusion Cell Blocks Prepared Using 3 Different Methods Xin Jing, MD,
Anatomic Pathology / Performance of Different Cell Block Preparation Techniques Morphologic and Immunocytochemical Performances of Effusion Cell Blocks Prepared Using 3 Different Methods Xin Jing, MD,
Differentiation of Tumors with Specific Red Cell Adherence (SRCA) test
 753 Differentiation of Tumors with Specific Red Cell Adherence (SRCA) test Dr. Abhishek A Mangaonkar *, Dr. A G Valand 1 Intern, Grant Medical College and Sir J.J. Group of Hospitals, Mumbai, India 2 Professor,
753 Differentiation of Tumors with Specific Red Cell Adherence (SRCA) test Dr. Abhishek A Mangaonkar *, Dr. A G Valand 1 Intern, Grant Medical College and Sir J.J. Group of Hospitals, Mumbai, India 2 Professor,
EBUS-FNAB: HOW TO OPTIMIZE YOUR CYTOLOGY SAMPLES, LHSC EXPERIENCE. Dr. Mariamma Joseph Division Head of Cytopathology LHSC and Western University
 EBUS-FNAB: HOW TO OPTIMIZE YOUR CYTOLOGY SAMPLES, LHSC EXPERIENCE Dr. Mariamma Joseph Division Head of Cytopathology LHSC and Western University Objectives Brief overview of EBUS-FNA Strategies to optimize
EBUS-FNAB: HOW TO OPTIMIZE YOUR CYTOLOGY SAMPLES, LHSC EXPERIENCE Dr. Mariamma Joseph Division Head of Cytopathology LHSC and Western University Objectives Brief overview of EBUS-FNA Strategies to optimize
Update on Thyroid FNA The Bethesda System. Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center
 Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Well-differentiated Papillary Mesothelioma of the Pleura Diagnosed by Video-Assisted Thoracic Surgical Pleural Biopsy : A Case Report
 Showa Univ J Med Sci 25 1, 67 72, March 2013 Case Report Well-differentiated Papillary Mesothelioma of the Pleura Diagnosed by Video-Assisted Thoracic Surgical Pleural Biopsy : A Case Report Yuri TOMITA
Showa Univ J Med Sci 25 1, 67 72, March 2013 Case Report Well-differentiated Papillary Mesothelioma of the Pleura Diagnosed by Video-Assisted Thoracic Surgical Pleural Biopsy : A Case Report Yuri TOMITA
Urinary Bladder: WHO Classification and AJCC Staging Update 2017
 Urinary Bladder: WHO Classification and AJCC Staging Update 2017 Houston Society of Clinical Pathologists 58 th Annual Spring Symposium Houston, TX April 8, 2017 Jesse K. McKenney, MD Classification
Urinary Bladder: WHO Classification and AJCC Staging Update 2017 Houston Society of Clinical Pathologists 58 th Annual Spring Symposium Houston, TX April 8, 2017 Jesse K. McKenney, MD Classification
INTRODUCTION TO PATHOLOGICAL TECHNIQUES. 1. Types of routine biopsy procedures 2. Special exams (IHC, FISH)
 INTRODUCTION TO PATHOLOGICAL TECHNIQUES 1. Types of routine biopsy procedures 2. Special exams (IHC, FISH) Biopsy-Indications Diffuse/multifocal lesions (neoplastic, inflammatory, etc) Etiology of the
INTRODUCTION TO PATHOLOGICAL TECHNIQUES 1. Types of routine biopsy procedures 2. Special exams (IHC, FISH) Biopsy-Indications Diffuse/multifocal lesions (neoplastic, inflammatory, etc) Etiology of the
GATA3: A Promising Marker for Metastatic Breast Carcinoma in Serous Effusion Specimens
 GATA3: A Promising Marker for Metastatic Breast Carcinoma in Serous Effusion Specimens Paul W. Shield, PhD, FFSc(RCPA) 1,2 ; David J. Papadimos, MBBS, FRCPA 1,3 ; and Michael D. Walsh, PhD 3 BACKGROUND:
GATA3: A Promising Marker for Metastatic Breast Carcinoma in Serous Effusion Specimens Paul W. Shield, PhD, FFSc(RCPA) 1,2 ; David J. Papadimos, MBBS, FRCPA 1,3 ; and Michael D. Walsh, PhD 3 BACKGROUND:
SCOPE OF PRACTICE PGY-5
 Recognize normal cytomorphology of cells derived from the respiratory, gastrointestinal, and genitourinary tracts, and body fluid (Cerebrospinal fluid, pleural and peritoneal fluid) Recognize normal cytomorphology
Recognize normal cytomorphology of cells derived from the respiratory, gastrointestinal, and genitourinary tracts, and body fluid (Cerebrospinal fluid, pleural and peritoneal fluid) Recognize normal cytomorphology
Cutaneous metastases. Thaddeus Mully. University of California, San Francisco Professor, Departments of Pathology and Dermatology
 Cutaneous metastases Thaddeus Mully University of California, San Francisco Professor, Departments of Pathology and Dermatology DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Thaddeus Mully Course C005 Essential
Cutaneous metastases Thaddeus Mully University of California, San Francisco Professor, Departments of Pathology and Dermatology DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Thaddeus Mully Course C005 Essential
Aggressive Malignant Mesothelioma In A Patient Without Previous Asbestos Exposure
 ISPUB.COM The Internet Journal of Pathology Volume 19 Number 1 Aggressive Malignant Mesothelioma In A Patient Without Previous Asbestos Exposure A Julai, G Wathuge Citation A Julai, G Wathuge. Aggressive
ISPUB.COM The Internet Journal of Pathology Volume 19 Number 1 Aggressive Malignant Mesothelioma In A Patient Without Previous Asbestos Exposure A Julai, G Wathuge Citation A Julai, G Wathuge. Aggressive
CODING TUMOUR MORPHOLOGY. Otto Visser
 CODING TUMOUR MORPHOLOGY Otto Visser INTRODUCTION The morphology describes the tissue of the tumour closest to normal tissue Well differentiated tumours are closest to normal Undifferentiated tumours show
CODING TUMOUR MORPHOLOGY Otto Visser INTRODUCTION The morphology describes the tissue of the tumour closest to normal tissue Well differentiated tumours are closest to normal Undifferentiated tumours show
NEW IHC A n t i b o d i e s
 NEW IHC Antibodies TABLE OF CONTENTS NEW IHC ANTIBODIES from Cell Marque CITED1 (5H6).... 1 Claudin 7 (5D10F3).... 1 GATA1 (4F5).... 1 Transgelin (2A10C2).... 1 NEW IHC ANTIBODIES using RabMAb Technology
NEW IHC Antibodies TABLE OF CONTENTS NEW IHC ANTIBODIES from Cell Marque CITED1 (5H6).... 1 Claudin 7 (5D10F3).... 1 GATA1 (4F5).... 1 Transgelin (2A10C2).... 1 NEW IHC ANTIBODIES using RabMAb Technology
Cell-Adhesion Molecule Expression and the Proliferation of Malignant Mesothelioma: A Post-Mortem Examination
 Cell-Adhesion Molecule Expression and the Proliferation of Malignant Mesothelioma: A Post-Mortem Examination KOZO KURIBAYASHI 1*, HIROSHI HIRANO 2*, KEIJI NAKASHO 3, HIDEKI OHYAMA 3, KOJI YAMANEGI 3, CHIHARU
Cell-Adhesion Molecule Expression and the Proliferation of Malignant Mesothelioma: A Post-Mortem Examination KOZO KURIBAYASHI 1*, HIROSHI HIRANO 2*, KEIJI NAKASHO 3, HIDEKI OHYAMA 3, KOJI YAMANEGI 3, CHIHARU
and management of lung cancer Maureen F. Zakowski, M.D. Memorial Sloan-Kettering Cancer Center
 The new role of cytology in the diagnosis and management of lung cancer Maureen F. Zakowski, M.D. Memorial Sloan-Kettering Cancer Center Outline Role of cytology in the diagnosis of lung cancer Non-small
The new role of cytology in the diagnosis and management of lung cancer Maureen F. Zakowski, M.D. Memorial Sloan-Kettering Cancer Center Outline Role of cytology in the diagnosis of lung cancer Non-small
ISSN X (Print) Original Research Article. DOI: /sjams
 DOI: 10.21276/sjams.2016.4.7.33 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(7C):2468-2473 Scholars Academic and Scientific Publisher (An International Publisher
DOI: 10.21276/sjams.2016.4.7.33 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(7C):2468-2473 Scholars Academic and Scientific Publisher (An International Publisher
The role of immunohistochemistry in surgical pathology of the uterine corpus and cervix
 The role of immunohistochemistry in surgical pathology of the uterine corpus and cervix Prof. Ben Davidson, MD PhD Department of Pathology, Norwegian Radium Hospital, Oslo University Hospital, Oslo, Norway
The role of immunohistochemistry in surgical pathology of the uterine corpus and cervix Prof. Ben Davidson, MD PhD Department of Pathology, Norwegian Radium Hospital, Oslo University Hospital, Oslo, Norway
Coordinate Expression of Cytokeratins 7 and 20 in Prostate Adenocarcinoma and Bladder Urothelial Carcinoma
 Anatomic Pathology / CYTOKERATINS 7 AND 20 IN PROSTATE AND BLADDER CARCINOMAS Coordinate Expression of Cytokeratins 7 and 20 in Prostate Adenocarcinoma and Bladder Urothelial Carcinoma Nader H. Bassily,
Anatomic Pathology / CYTOKERATINS 7 AND 20 IN PROSTATE AND BLADDER CARCINOMAS Coordinate Expression of Cytokeratins 7 and 20 in Prostate Adenocarcinoma and Bladder Urothelial Carcinoma Nader H. Bassily,
Prostate Immunohistochemistry. Literature Interpretation: Caveats. Must be aware of staining pattern of antibody in the relevant tissue
 IHC Interpretation: General Principles (1) Prostate Immunohistochemistry Murali Varma Cardiff, UK wptmv@cf.ac.uk Sarajevo Nov 2013 Must be aware of staining pattern of antibody in the relevant tissue Nuclear/cytoplasmic/membranous
IHC Interpretation: General Principles (1) Prostate Immunohistochemistry Murali Varma Cardiff, UK wptmv@cf.ac.uk Sarajevo Nov 2013 Must be aware of staining pattern of antibody in the relevant tissue Nuclear/cytoplasmic/membranous
Study of Fine Needle Aspiration Cytology of Breast Lump: Correlation of Cytologically Malignant Cases with Their Histological Findings
 Study of Fine Needle Aspiration Cytology of Breast Lump: Correlation of Cytologically Malignant Cases with Their Histological Findings Touhid Uddin Rupom 1, Tamanna Choudhury 2, Sultana Gulshana Banu 3
Study of Fine Needle Aspiration Cytology of Breast Lump: Correlation of Cytologically Malignant Cases with Their Histological Findings Touhid Uddin Rupom 1, Tamanna Choudhury 2, Sultana Gulshana Banu 3
New Developments in Immunohistochemistry for Gynecologic Pathology
 New Developments in Immunohistochemistry for Gynecologic Pathology Michael T. Deavers, M.D. Professor, Departments of Pathology and Gynecologic Oncology Immunohistochemistry in Gynecologic Pathology Majority
New Developments in Immunohistochemistry for Gynecologic Pathology Michael T. Deavers, M.D. Professor, Departments of Pathology and Gynecologic Oncology Immunohistochemistry in Gynecologic Pathology Majority
A Useful Antibody Panel for Differential Diagnosis Between Peritoneal Mesothelioma and Ovarian Serous Carcinoma in Japanese Cases
 Anatomic Pathology / Peritoneal Mesothelioma A Useful Antibody Panel for Differential Diagnosis Between Peritoneal Mesothelioma and Ovarian Serous Carcinoma in Japanese Cases Yukio Takeshima, MD, Vishwa
Anatomic Pathology / Peritoneal Mesothelioma A Useful Antibody Panel for Differential Diagnosis Between Peritoneal Mesothelioma and Ovarian Serous Carcinoma in Japanese Cases Yukio Takeshima, MD, Vishwa
Lung Tumor Cases: Common Problems and Helpful Hints
 Lung Tumor Cases: Common Problems and Helpful Hints Brandon T. Larsen, MD, PhD Senior Associate Consultant Department of Laboratory Medicine and Pathology Mayo Clinic Arizona Arizona Society of Pathologists
Lung Tumor Cases: Common Problems and Helpful Hints Brandon T. Larsen, MD, PhD Senior Associate Consultant Department of Laboratory Medicine and Pathology Mayo Clinic Arizona Arizona Society of Pathologists
Assessment Run CK19
 Assessment Run 29 200 CK9 The slide to be stained for CK9 comprised:. Appendix, 2. Thyroid gland, 3. Pancreas, 4. Ductal breast carcinoma, 5. Esophagus, 6. Papillary thyroid carcinoma. All tissues were
Assessment Run 29 200 CK9 The slide to be stained for CK9 comprised:. Appendix, 2. Thyroid gland, 3. Pancreas, 4. Ductal breast carcinoma, 5. Esophagus, 6. Papillary thyroid carcinoma. All tissues were
Case 18. M75. Excision of mass on scalp. Clinically SCC. The best diagnosis is:
 Case 18 M75. Excision of mass on scalp. Clinically SCC. The best diagnosis is: A. Pilomatrical carcinoma B. Adnexal carcinoma NOS C. Metastatic squamous cell carcinoma D.Primary squamous cell carcinoma
Case 18 M75. Excision of mass on scalp. Clinically SCC. The best diagnosis is: A. Pilomatrical carcinoma B. Adnexal carcinoma NOS C. Metastatic squamous cell carcinoma D.Primary squamous cell carcinoma
Call For A Slide Seminar Of African Cases
 Call For A Slide Seminar Of African Cases ( And Not Only ) Case 5 06/09/2017 João Fraga, Paula Serra, Catarina Cerdeira, Ana Catarina Lai, Maria Beatriz Pimentão, Rui Almeida, Helder Moreira, Bruno Fernandes,
Call For A Slide Seminar Of African Cases ( And Not Only ) Case 5 06/09/2017 João Fraga, Paula Serra, Catarina Cerdeira, Ana Catarina Lai, Maria Beatriz Pimentão, Rui Almeida, Helder Moreira, Bruno Fernandes,
Single and Multiplex Immunohistochemistry
 Single and Multiplex Immunohistochemistry Steve Westra, BS Reagent Product Specialist Leica Biosystems IHC Theory Polyclonal vs Monoclonal Polyclonal reagents Detect a multitude of epitopes Batch to batch
Single and Multiplex Immunohistochemistry Steve Westra, BS Reagent Product Specialist Leica Biosystems IHC Theory Polyclonal vs Monoclonal Polyclonal reagents Detect a multitude of epitopes Batch to batch
Abstract. Introduction. Salah Abobaker Ali
 Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
Immunohistochemical Expression Of Cytokeratin 8 And 18 In Breast Carcinoma.
 ISPUB.COM The Internet Journal of Pathology Volume 13 Number 3 Immunohistochemical Expression Of Cytokeratin 8 And 18 In Breast Carcinoma. B Rattan, A Baghla, M Manjari, P Kakkar, S Kahlon, S Paul Citation
ISPUB.COM The Internet Journal of Pathology Volume 13 Number 3 Immunohistochemical Expression Of Cytokeratin 8 And 18 In Breast Carcinoma. B Rattan, A Baghla, M Manjari, P Kakkar, S Kahlon, S Paul Citation
Cytological Sub-classification of Lung Cancer: Morphologic and Molecular Characteristics. Mercè Jordà, University of Miami
 Cytological Sub-classification of Lung Cancer: Morphologic and Molecular Characteristics Mercè Jordà, University of Miami Mortality Lung cancer is the most frequent cause of cancer incidence and mortality
Cytological Sub-classification of Lung Cancer: Morphologic and Molecular Characteristics Mercè Jordà, University of Miami Mortality Lung cancer is the most frequent cause of cancer incidence and mortality
The PAX8 gene is a member of the paired-box family of
 Assessment of the Utility of PAX8 Immunohistochemical Stain in Diagnosing Endocervical Glandular Lesions Li Liang, MD, PhD; Wenxin Zheng, MD; Jinsong Liu, MD, PhD; Sharon X. Liang, MD, PhD Context. PAX8,
Assessment of the Utility of PAX8 Immunohistochemical Stain in Diagnosing Endocervical Glandular Lesions Li Liang, MD, PhD; Wenxin Zheng, MD; Jinsong Liu, MD, PhD; Sharon X. Liang, MD, PhD Context. PAX8,
JMSCR Vol 04 Issue 11 Page November 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i11.37 Diagnostic Utility of Cell Block Method
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i11.37 Diagnostic Utility of Cell Block Method
Hyperplastic Mesothelial Cells in Mediastinal Lymph Node Sinuses With Extranodal Lymphatic Involvement
 Hyperplastic Mesothelial Cells in Mediastinal Lymph Node Sinuses With Extranodal Lymphatic Involvement Phillip A. Isotalo, MD; John P. Veinot, MD, FRCPC; Maha Jabi, MD, FRCPC We describe a patient with
Hyperplastic Mesothelial Cells in Mediastinal Lymph Node Sinuses With Extranodal Lymphatic Involvement Phillip A. Isotalo, MD; John P. Veinot, MD, FRCPC; Maha Jabi, MD, FRCPC We describe a patient with
Hyperchromatic Crowded Groups: What is Your Diagnosis? Session 3000
 Hyperchromatic Crowded Groups: What is Your Diagnosis? Session 3000 Thomas A. Bonfiglio, M.D. Professor Emeritus, Pathology and Laboratory Medicine University of Rochester Disclosures In the past 12 months,
Hyperchromatic Crowded Groups: What is Your Diagnosis? Session 3000 Thomas A. Bonfiglio, M.D. Professor Emeritus, Pathology and Laboratory Medicine University of Rochester Disclosures In the past 12 months,
Ultrasound-Guided Fine-Needle Aspiration of Thyroid Nodules: New events
 Ultrasound-Guided Fine-Needle Aspiration of Thyroid Nodules: New events Sandrine Rorive, M.D., PhD. Erasme Hospital - Université Libre de Bruxelles (ULB) INTRODUCTION The assessment of thyroid nodules
Ultrasound-Guided Fine-Needle Aspiration of Thyroid Nodules: New events Sandrine Rorive, M.D., PhD. Erasme Hospital - Université Libre de Bruxelles (ULB) INTRODUCTION The assessment of thyroid nodules
Histological Typing Of Cancer And Precancer Of The Oral Mucosa
 Histological Typing Of Cancer And Precancer Of The Oral Mucosa 1 / 7 2 / 7 3 / 7 Histological Typing Of Cancer And Within the last decade, histologic grading has become widely accepted as a powerful indicator
Histological Typing Of Cancer And Precancer Of The Oral Mucosa 1 / 7 2 / 7 3 / 7 Histological Typing Of Cancer And Within the last decade, histologic grading has become widely accepted as a powerful indicator
Lung Cytology: Lessons Learned from Errors in Practice
 Lung Cytology: Lessons Learned from Errors in Practice Stephen S. Raab, M.D. Department of Laboratory Medicine Eastern Health and Memorial University of Newfoundland, St. John s, NL and University of Washington,
Lung Cytology: Lessons Learned from Errors in Practice Stephen S. Raab, M.D. Department of Laboratory Medicine Eastern Health and Memorial University of Newfoundland, St. John s, NL and University of Washington,
NPQR Quality Payment Program (QPP) Measures 21_18247_LS.
 NPQR Quality Payment Program (QPP) Measures 21_18247_LS MEASURE ID: QPP 99 MEASURE TITLE: Breast Cancer Resection Pathology Reporting pt Category (Primary Tumor) and pn Category (Regional Lymph Nodes)
NPQR Quality Payment Program (QPP) Measures 21_18247_LS MEASURE ID: QPP 99 MEASURE TITLE: Breast Cancer Resection Pathology Reporting pt Category (Primary Tumor) and pn Category (Regional Lymph Nodes)
Original Article Differential diagnosis of sarcomatoid mesothelioma from true sarcoma and sarcomatoid carcinoma using immunohistochemistry
 Pathology International 2008; 58: 75 83 doi:10.1111/j.1440-1827.2007.02193.x Original Article Differential diagnosis of sarcomatoid mesothelioma from true sarcoma and sarcomatoid carcinoma using immunohistochemistry
Pathology International 2008; 58: 75 83 doi:10.1111/j.1440-1827.2007.02193.x Original Article Differential diagnosis of sarcomatoid mesothelioma from true sarcoma and sarcomatoid carcinoma using immunohistochemistry
Some of the greatest diagnostic dilemmas in cytopathology are in
 CANCER CYTOPATHOLOGY 293 Immunocytochemistry in Effusion Cytology A Contemporary Review Patricia A. Fetsch, M.T. (ASCP) Andrea Abati, M.D. Cytopathology Section, National Institutes of Health/National
CANCER CYTOPATHOLOGY 293 Immunocytochemistry in Effusion Cytology A Contemporary Review Patricia A. Fetsch, M.T. (ASCP) Andrea Abati, M.D. Cytopathology Section, National Institutes of Health/National
Original Article Study of effusion cytology in patients with simultaneous malignancy and ascites
 Kathmandu University Medical Journal (2006), Vol. 4, No. 4, Issue 16, 483-487 Original Article Study of effusion cytology in patients with simultaneous malignancy and ascites Jha R 1, Shrestha HG 2, Sayami
Kathmandu University Medical Journal (2006), Vol. 4, No. 4, Issue 16, 483-487 Original Article Study of effusion cytology in patients with simultaneous malignancy and ascites Jha R 1, Shrestha HG 2, Sayami
The Role of Fine Needle Aspiration Cytology in the Diagnosis and Management of Thymic Neoplasia
 MALIGNANCIES OF THE THYMUS The Role of Fine Needle Aspiration Cytology in the Diagnosis and Management of Thymic Neoplasia Maureen F. Zakowski, MD, James Huang, MD, and Matthew P. Bramlage, MD Background:
MALIGNANCIES OF THE THYMUS The Role of Fine Needle Aspiration Cytology in the Diagnosis and Management of Thymic Neoplasia Maureen F. Zakowski, MD, James Huang, MD, and Matthew P. Bramlage, MD Background:
Immunohistochemical Evaluation of Necrotic Malignant Melanomas
 Anatomic Pathology / EVALUATION OF NECROTIC MALIGNANT MELANOMAS Immunohistochemical Evaluation of Necrotic Malignant Melanomas Daisuke Nonaka, MD, Jordan Laser, MD, Rachel Tucker, HTL(ASCP), and Jonathan
Anatomic Pathology / EVALUATION OF NECROTIC MALIGNANT MELANOMAS Immunohistochemical Evaluation of Necrotic Malignant Melanomas Daisuke Nonaka, MD, Jordan Laser, MD, Rachel Tucker, HTL(ASCP), and Jonathan
Assessment Run GATA3
 Assessment Run 44 2015 GATA3 Material The slide to be stained for GATA3 comprised: 1. Tonsil 2. Kidney, 3. Urothelial carcinoma, 4. Breast ductal carcinoma, 5. Colon adenocarcinoma All tissues were fixed
Assessment Run 44 2015 GATA3 Material The slide to be stained for GATA3 comprised: 1. Tonsil 2. Kidney, 3. Urothelial carcinoma, 4. Breast ductal carcinoma, 5. Colon adenocarcinoma All tissues were fixed
Immunohistochemical classification of the unknown primary tumour (UPT) Part I. Prof. Mogens Vyberg NordiQC Institute of Pathology Aalborg, Denmark
 Immunohistochemical classification of the unknown primary tumour (UPT) Part I Prof. Mogens Vyberg NordiQC Institute of Pathology Aalborg, Denmark Tumours of unknown origin: Histology Brain tumour - biopsy
Immunohistochemical classification of the unknown primary tumour (UPT) Part I Prof. Mogens Vyberg NordiQC Institute of Pathology Aalborg, Denmark Tumours of unknown origin: Histology Brain tumour - biopsy
Cancers of unknown primary : Knowing the unknown. Prof. Ahmed Hossain Professor of Medicine SSMC
 Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
GOALS AND OBJECTIVES CYTOPATHOLOGY
 GOALS AND OBJECTIVES CYTOPATHOLOGY LEVEL: PGY2, PGY4, PGY5 The 1st block in PGY2 is an introductory in nature and is followed by two more blocks in PGY-4 (please, see core rotation for PGY4 below) and
GOALS AND OBJECTIVES CYTOPATHOLOGY LEVEL: PGY2, PGY4, PGY5 The 1st block in PGY2 is an introductory in nature and is followed by two more blocks in PGY-4 (please, see core rotation for PGY4 below) and
The role of Electron Microscopy in the study of cytologic specimens. Elba A. Turbat-Herrera, MD
 The role of Electron Microscopy in the study of cytologic specimens. Elba A. Turbat-Herrera, MD Louisiana State University Health Sciences Center Shreveport, LA, USA Introduction The field of Cytology
The role of Electron Microscopy in the study of cytologic specimens. Elba A. Turbat-Herrera, MD Louisiana State University Health Sciences Center Shreveport, LA, USA Introduction The field of Cytology
LN04 - Lymphoma Tissue Microarray
 Reveal Biosciences offers Histochemical Staining, Immunohistochemistry (IHC), In Situ Hybridization (ISH), Whole Slide Imaging, and Quantitative Image Analysis on any TMA LN04 - Lymphoma Tissue Microarray
Reveal Biosciences offers Histochemical Staining, Immunohistochemistry (IHC), In Situ Hybridization (ISH), Whole Slide Imaging, and Quantitative Image Analysis on any TMA LN04 - Lymphoma Tissue Microarray
ROLE OF TTF-1, CK20, AND CK7 IMMUNOHISTOCHEMISTRY FOR DIAGNOSIS OF PRIMARY
 Y.C. Su, Y.C. Hsu, and C.Y. Chai ROLE OF TTF-1, CK20, AND CK7 IMMUNOHISTOCHEMISTRY FOR DIAGNOSIS OF PRIMARY AND SECONDARY LUNG ADENOCARCINOMA Yue-Chiu Su 1, Yu-Chang Hsu 2, and Chee-Yin Chai 1,3 Departments
Y.C. Su, Y.C. Hsu, and C.Y. Chai ROLE OF TTF-1, CK20, AND CK7 IMMUNOHISTOCHEMISTRY FOR DIAGNOSIS OF PRIMARY AND SECONDARY LUNG ADENOCARCINOMA Yue-Chiu Su 1, Yu-Chang Hsu 2, and Chee-Yin Chai 1,3 Departments
Study of ascitic fluid cytology in ovarian tumors
 International Journal of Research in Medical Sciences Janagam C et al. Int J Res Med Sci. 2017 Dec;5(12):5227-5231 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20175382
International Journal of Research in Medical Sciences Janagam C et al. Int J Res Med Sci. 2017 Dec;5(12):5227-5231 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20175382
Key Words: napsin-a; TTF-1; p63; cytology; lung cancer. Ann Arbor, Michigan. School, Ann Arbor, Michigan
 The Application and Diagnostic Utility of Immunocytochemistry on Direct Smears in the Diagnosis of Pulmonary Adenocarcinoma and Squamous Cell Carcinoma Michael H. Roh, M.D., Ph.D., 1{ Lindsay Schmidt,
The Application and Diagnostic Utility of Immunocytochemistry on Direct Smears in the Diagnosis of Pulmonary Adenocarcinoma and Squamous Cell Carcinoma Michael H. Roh, M.D., Ph.D., 1{ Lindsay Schmidt,
Novocastra Liquid Mouse Monoclonal Antibody MyoD1 (Rhabdomyosarcoma Marker)
 Novocastra Liquid Mouse Monoclonal Antibody MyoD1 (Rhabdomyosarcoma Marker) Product Code: NCL-L-MyoD1 Leica Biosystems Newcastle Ltd Balliol Business Park West Benton Lane Newcastle Upon Tyne NE12 8EW
Novocastra Liquid Mouse Monoclonal Antibody MyoD1 (Rhabdomyosarcoma Marker) Product Code: NCL-L-MyoD1 Leica Biosystems Newcastle Ltd Balliol Business Park West Benton Lane Newcastle Upon Tyne NE12 8EW
Invasion to the visceral pleura is an important component
 Diagnosis of Visceral Pleural Invasion by Lung Cancer Using Intraoperative Touch Cytology Yushi Saito, MD, PhD, Yosuke Yamakawa, MD, PhD, Masanobu Kiriyama, MD, PhD, Ichiro Fukai, MD, PhD, Satoshi Kondo,
Diagnosis of Visceral Pleural Invasion by Lung Cancer Using Intraoperative Touch Cytology Yushi Saito, MD, PhD, Yosuke Yamakawa, MD, PhD, Masanobu Kiriyama, MD, PhD, Ichiro Fukai, MD, PhD, Satoshi Kondo,
ACCME/Disclosures. Case History 4/13/2016. USCAP GU Specialty Conference Case 3. Ann Arbor, MI
 USCAP GU Specialty Conference Case 3 March 2016 L. Priya Kunju, M.D. University of Michigan Health System Ann Arbor, MI University of Michigan Health System ACCME/Disclosures The USCAP requires that anyone
USCAP GU Specialty Conference Case 3 March 2016 L. Priya Kunju, M.D. University of Michigan Health System Ann Arbor, MI University of Michigan Health System ACCME/Disclosures The USCAP requires that anyone
Introduction. 23 rd Annual Seminar in Pathology. FLUIDS, Part 1. Pittsburgh, PA Gladwyn Leiman UVMMC, VT
 23 rd Annual Seminar in Pathology Pittsburgh, PA Gladwyn Leiman UVMMC, VT FLUIDS, Part 1 "Blue walls", Claudia Hansen, 2009 Introduction o Challenging to everyone o Almost any benign or malignant process
23 rd Annual Seminar in Pathology Pittsburgh, PA Gladwyn Leiman UVMMC, VT FLUIDS, Part 1 "Blue walls", Claudia Hansen, 2009 Introduction o Challenging to everyone o Almost any benign or malignant process
Journal of the Egyptian Nat. Cancer Inst., Vol. 22, No. 4, December: , 2010
 Journal of the Egyptian Nat. Cancer Inst., Vol. 22, No. 4, December: 27-225, 2 Assessment of the Reliability of Immunocytochemical Detection of Estrogen and Progesterone Receptors Status on the Cytological
Journal of the Egyptian Nat. Cancer Inst., Vol. 22, No. 4, December: 27-225, 2 Assessment of the Reliability of Immunocytochemical Detection of Estrogen and Progesterone Receptors Status on the Cytological
