Community acquisition of β-lactamase producing Enterobacteriaceae in neonatal gut
|
|
|
- Arleen Stokes
- 5 years ago
- Views:
Transcription
1 Kothari et al. BMC Microbiology 2013, 13:136 RESEARCH ARTICLE Open Access Community acquisition of β-lactamase producing Enterobacteriaceae in neonatal gut Charu Kothari 1, Rajni Gaind 1*, Laishram Chandreshwor Singh 2, Anju Sinha 3, Vidya Kumari 4, Sugandha Arya 4, Harish Chellani 4, Sunita Saxena 2 and Monorama Deb 1 Abstract Background: Commensal flora constitutes a reservoir of antibiotic resistance. The increasing variety of β-lactamases and the emergence of Carbapenem resistant Enterobacteriaceae (CRE) in community, raise concerns regarding efficacy of β-lactams. It is important to know the exact load of antibiotic resistance in the absence of any antibiotic selection pressure including via food and water. In the present study gut colonization in neonates with no direct antibiotic pressure was used as a model to evaluate β-lactam resistance in the community. Results: In this prospective study, 75 healthy, vaginally delivered, antibiotic naive, breast fed neonates were studied for gut colonization by Extended spectrum β-lactamases (ESBL), AmpC β-lactamases hyperproducing Enterobacteriaceae and CRE on day 0, 21 and 60. Total 267 Enterobacteriaceae were isolated and E.coli was the predominant flora. ESBL, AmpC and coproduction was seen in 20.6%, 19.9% and 11.2% isolates respectively. ESBL carriage increased threefold from day 1 to 60 showing predominance of CTX-M group 15 (82.5%), ampc genes were heterogeneous. Colonization with CRE was rare, only one baby harboured Enterobacter sp positive for kpc-2. The reservoirs for these genes are likely to be mother and the environment. Conclusions: Data strongly suggests that in absence of any antibiotic pressure there is tremendous load of antibiotic resistance to β-lactam drugs. Wide spread presence of ESBL and AmpC can drive rapid emergence and dissemination of CRE. This is the first report from India which depicts the smaller picture of true antibiotic pressure present in the Indian community. Keywords: ESBL, AmpC, Carbapenemases, Neonates, Antibiotic resistance, Enterobacteriaceae, Fecal carriage, Gut colonization Background The rapid dissemination of antibiotic resistance in bacteria constitutes a major public health concern worldwide. Selective pressure mediated by the intensive use of antibiotics (both human and non-human) and several mechanisms for genetic transfer could have contributed to the rapid dispersal of antibiotic resistance in the community [1]. Antibiotics target both pathogenic bacteria as well as normal commensal flora, represented by skin, gut, and upper respiratory tract [2]. Current strategies to monitor the presence of antibiotic resistance in bacteria mainly * Correspondence: rgaind5@hotmail.com 1 Department of Microbiology, VMMC and Safdarjung Hospital, New Delhi , India Full list of author information is available at the end of the article rely upon examining resistance in pathogenic organisms and involve only periodic cross-sectional evaluations of resistance in the commensal flora [3,4]. Resistance amongst the commensal flora is a serious threat because a very highly populated ecosystem like the gut may at later stage be source of extra intestinal infection which may spread to other host or transfer genetic resistance element/s to other members of micro-biota including pathogens [5]. Despite this, there is paucity of data regarding the dynamics of antibiotic resistance in commensals. β-lactam antibiotics are the most commonly used antibiotics in community as well as hospitals. They are generally characterized by their favorable safety and tolerability profile as well as their broad spectrum activity [6]. The ever increasing variety of β-lactamases raises serious concern about our dependence on β-lactam 2013 Kothari et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
2 Kothari et al. BMC Microbiology 2013, 13:136 Page 2 of 6 drugs. Rapidly emerging β-lactamases include diverse ESBL, AmpC β-lactamases, and carbapenem-hydrolyzing β-lactamases. ESBL producing Enterobacteriaceae were initially associated with nosocomial infections, however, recent studies indicate significant increase in the community isolates [7]. The risk posed by community circulation of the multidrug resistant bacteria is emphasized by the high concentration of ESBL in the community as well as the hospital onset intra-abdominal infections [8]. The rapid dissemination of ESBL s in community may drive excessive use of carbapenems. The recent report of Carbapenem resistance due to dissemination of NDM-1 β-lactamase producing bacteria in the environmental samples and key enteric pathogens in New Delhi, India may have serious health implications [9]. Several studies have been conducted to assess the risk factors associated with colonization and infection caused by ESBL producing Enterobacteriaceae, which include antibiotic use, travel, contact with healthcare system and chronic illness [10,11]. Gut colonization in neonates with no direct antibiotic pressure were used as a model to evaluate β-lactam resistance in the community in absence of selection pressure. Methods Design overview, setting, and participants In this prospective study all low birth weight neonates (LBW) ( 1500 to <2500 g) born at the Safdarjung Hospital, New Delhi, India ( ) were eligible and enrolled to study Effect of Probiotic VSL#3 on prevention of sepsis during 0 2 month period. This is double blind study in which neonates were randomized to receive either VSL# 3 for 30 days in intervention group or physically similar preparation (Maltdextrin) in control group. The consent was obtained from parents of each neonate prior to enrolment. The stool samples from 75 randomly selected LBW neonates were used to study gut colonization with ESBL, AmpC and carbapenemase producing Enterobacteriaceae. The inclusion criteria were vaginally delivered, healthy and exclusively breast fed LBW neonates. The exclusion criteria were gross congenital malformations, hospitalization, prematurity, predisposing factors for sepsis, antibiotics use by mother during pregnancy and neonates during study period. After discharge from the hospital, trained field workers visited the newborns for probiotic supplementation, collection of stool sample and related complications up to 60 days of life. The study was duly approved by ethical committee of Safdarjung Hospital. Study of colonization by Enterobacteriaceae Stool samples were collected on Day (D) 1, 21 and 60, serially diluted and plated on McConkey agar without antibiotic to study dominant gut flora. D1 sample is the first stool passed after birth (meconium). Different colony types of gram negative bacteria which were judged to differ in morphology (size, shape, consistency and colour) from each sample were enumerated separately and identified using conventional biochemical tests. Phenotypic assessment and molecular characterization of antimicrobial susceptibility All Enterobacteriaceae isolated were screened for ESBL using disk diffusion and Etest methods (AB BIODISK, Solna, Sweden) and plasmid mediated AmpC or hyperproduction using AmpC disc test [12]. In 27 randomly selected neonates Enterobacteriaceae were characterised for ESBL (bla TEM, bla SHV (self designed, Table 1), bla CTX-M [group1, 2, 8, 9 and 25]) [13] and ampc (MOX, CIT, DHA, ACC, EBC, and FOX) [14] genes. Carbapenemase screening All neonates were screened for gut colonization by carbapenem resistant Enterobacteriaceae (CRE) using 2- step broth enrichment method incorporating 10 μg meropenem disc [15]. Suspected CRE isolates with resistance to any one carbapenem [16] i.e. ertapenem (Minimum inhibitory concentration (MIC) > 0.25 μg/ml), imipenem and meropenem (MIC >1 μg/ml) by Etest (biomérieux, France) were tested for metallo- β lactamase (MBL) production using IPM/ethylenediamine tetra-acetic acid (EDTA) Etest and for non-metallo-carbapenemase (NMC), especially KPC, production by the modified Hodge test (MHT) [16]. PCR for VIM, IMP, KPC and NDM-1 genes (self designed, Table 1) was performed for confirmation. Sequence analysis All isolates found to carry ESBL/ampC or carbapenemase gene were further confirmed by sequencing. Sequencing was performed as per manufacturer s guidelines in 3130 l genetic analyser (Applied Biosystems, Foster city, California). Further the nucleotide and deduced amino acid sequences were analyzed and compared with sequences available in Gene bank at the National centre of Biotechnology Information (NCBI) web site ( Results Gut colonization pattern of Enterobacteriaceae and distribution of ESBL and AmpC β -lactamases in healthy low birth weight Neonates (1 60 days) On D1, 65.3% of babies were colonized with Enterobacteriaceae with no significant increase on D60. The predominant flora was E. coli on day 1, 21 and 60 followed by Klebsiella pneumoniae (Table 2).
3 Kothari et al. BMC Microbiology 2013, 13:136 Page 3 of 6 Table 1 Primers used for detection of TEM, SHV and Carbapenemase genes Primers Primer Sequence (5 to 3 direction) Annealing Amplicon size Temperature (bp) ( C) TEM FP- ATG AGT ATT CAA CAT TTC CG RP- CCA ATG CTT AAT CAG TGA GG SHV FP- ATG CGT TAT ATT CGC CTG TG RP- AGC GTT GCC AGT GCT CGA TC KPC-1 FP- AGC CGT TAC AGC CTC TGG AG RP- GAT GGG ATT GCG TCA GTT CAG KPC-2 FP- CAC TGT ATC GCC GTC TAG TTC RP- TGT GCT TGT CAT CCT TGT TAG NDM-1 FP- CGACGATTGGCCAGCAAATG RP- ACTTGGCCTTGCTGTCCTTG IMP FP- TTGAAAAGCTTGATGAAGGCG RP- ACCGCCTGCTCTAATGTAAG VIM FP- TTGACCGCGTCTATCATGGC Overall ESBL and AmpC production was 20.6% and 19.9% respectively. The total isolates positive for either AmpC and or ESBL were 29.2% (78/267). The predominant phenotypes were co-producers (30/267, 11.23%), followed by only ESBL (25/267, 9.4%) and AmpC (23/ 267, 8.6%) isolates. Both no. of babies colonized with at least one ESBL producing isolate and ESBL rate amongst Enterobacteriaceae increased three fold (p value and respectively) from day 1 to day 60, irrespective of associated AmpC production (Table 2). Characteristics of ESBL and AmpC β - lactamases in Enterobacteriaceae isolates from 27 randomly selected neonates The three stool samples from 27 neonates generated 88 gram negative bacilli which included E.coli (N = 74), Klebsiella pneumoniae (N = 11), Citrobacter freundii (N = 2) and Enterobacter aerogenes (N = 1). CTX-M-15 is predominant ESBL, TEM-136, TEM-149, SHV-28 and CTX-M-8 was seen in single isolates. In contrast, the ampc was diverse and included DHA (N = 5), CMY-2 (N = 3), CMY-1 (N =2), MOX (N = 2) and FOX (N = 1) (Table 3). Colonization by carbapenem resistance Enterobacteriaceae in the neonates Total 225 stool samples from 75 enrolled babies were screened for CRE 2-step broth enrichment method incorporating 10 μg meropenem disc. Gram negative colonies were isolated from 22 stool samples, which yielded 29 Enterobacteriaceae isolates that were presumed to be CRE. Phenotypic test for MBL was negative, MIC of 28 suspected CRE ranged from μg/ml, μg/ml and μg/ml for ertapenem, meropenem and imipenem respectively. However, one isolate of Enterobacter aerogenes. was positive for MHT having the MIC of > 32 μg/ml for ertapenem, meropenem Table 2 Distribution of Enterobacteriaceae and associated ESBL and AmpC β- lactamases in Neonates Total Day 1 Day 21 Day 60 (N = 75) (N = 75) (N = 75) No. (%) No. (%) No. (%) Babies colonized with a least one species 49 (65.3) 48 (64) 53 (70.6) No of babies colonized with at least one ESBL producing isolate 7/49 (14.3) 13/48 (27.1) 22/53 (41.5)* Total Enterobacteriaceae strains # E.coli (87.3) 67 (76.1) 83 (83) Klebsiella pneumoniae 27 3 (3.8) 13 (14.8) 11 (11) Enterobacter sp 14 2 (2.5) 7 (8) 5 (5) Citrobacter sp 5 4 (5.1) 0 1 (1) Salmonella. Typhi 2 1 (1.3) 1(1.1) 0 Total ESBL 55 (20.6) 7 (8.9) 17 (19.3) 31 (31)** Total AmpC (N = 39) 53 (19.9) 16 (20.3) 12 (13.6) 25 (25)*** Co-Production of ESBL and AmpC 30 (11.2) 5 (6.3) 9 (10.2) 16 (16)**** Note: Data represents Enterobacteriaceae isolates from gut of 75 healthy Low birth weight (LBW) neonates on Day 1, 21, 60 of birth. All Figures in parentheses represent percentages. # Some babies had more than one morphologically and biochemically distinct isolates. *p value **p value ***p value 0.2 ****p value 0.05 when compared to Day 1.
4 Kothari et al. BMC Microbiology 2013, 13:136 Page 4 of 6 Table 3 Molecular Characterization of ESBL & AmpC β-lactamases in Enterobacteriaceae isolated (N = 88) from 27 randomly selected neonates Phenotype No. strains ESBL AMPc bla-tem ESBL TEM SHV CTX-M DHA CMY-1 CMY-2 LAT MOX BIL FOX E+A * 1** 4# E+A E-A ## 2 E-A- 66 PCR not performed for strains with cefotaxime, ceftazimime zone diameter 28 and 23 respectively and phenotypic test negative for ESBL and AmpC16 Note: Sequencing results *Tem 136, Tem 149; **SHV28. E = ESBL, A = AmpC, - = Negative, + = Positive. # ESBL and AMPc genes were mainly isolated in E.coli except one Klebsiella pneumoniae having both CTX-M as well as MOX gene. ## One Citrobacter showed the presence of DHA gene. and imipenem. Presence of kpc-2 gene was confirmed by PCR using gene specific primers. Discussion In the present report we have investigated the β-lactam resistance pattern amongst Enterobacteriaceae in gut flora of neonates (1 60 days) by enrolling babies using various selection criteria so as to avoid any possible source of antibiotic selection pressure. Acquisition of resistance through food and water was also ruled out as neonates were exclusively breast fed. Compliance was ensured through household follow up by trained field workers upto D60 of life. The present study shows that majority of the babies were colonized by D1. With the acquisition of mother s flora the babies are equally likely to get the antibiotic resistance strains. Our data revealed that overall there was nearly 87% (232/267) resistance to the ampicillin by D60 in Enterobacteriaceae. The overall rate of ESBL was 20.6% which may be just a glimpse of bigger picture as in the present study only dominant population was studied. Selective media were not used for screening ESBL gut carriage which would reflect the true representation of ESBL carriage in the community. The low isolation of ESBL producers on D1 may be due to the short duration of exposure to the maternal flora during delivery (Table 2). Various factors could have contributed to the increase in the resistance by day 60. After delivery, exposure related to mothers environment, oral and skin flora provide the major sources of bacteria which may transfer to the neonates by several ways including suckling, kissing and caressing. In addition, breast milk is also a source of bacteria, which contains up to 10 9 microbes/l in healthy mothers [17]. Other sources may be household contact with siblings, pets [18], as well as horizontal transfer of gene within the commensal flora [1]. In our study acquisition of resistance via supplementary food has been ruled out as babies were completely breast fed. Several studies have shown the prevalence of antibiotic resistance in absence of direct use of antibiotic. Presence of tetracycline resistance bacteria in breastfed infants [19] and commensal ESBL producers in pre-school healthy children [20] suggest contamination in the family environment rather than direct exposure to antibiotic. The limitation of our study is that we have not studied the environmental flora and compared it with that of neonatal gut flora. Besides ESBL, AmpC producing Enterobacteriaceae were also isolated. AmpC producing isolates were approximately 20% and co-production with ESBL was seen in 11.2% throughout the study period (Table 2). AmpC β-lactamases producers are of major concern as they are resistant to β-lactam and β-lactam inhibitor combination as well as cefoxitin which further narrows down the treatment options. As carbapenems are drug of choice for ESBL and or AmpC producing bacteria, coexistence of these enzymes can pose a threat to the community acquired pathogens as MIC of such strains are 10 fold higher for various carbapenems [21]. The ampc gene showed diverse profile, in contrast CTX-M-15 was predominant ESBL gene in gut flora. Previous studies from India have also shown CTX-M-15 as predominant ESBL from clinical isolate [22]. Approximately, 50% of neonates admitted to neonatal unit in our hospital with early onset sepsis had ESBL producing Enterobacteriaceae [23] which is strongly supported by early colonization with ESBL producing Enterobacteriaceae in the neonates in the present study. Recent report of isolation of CRE (NDM-1) from environmental samples [9] and community acquired infections [24] indicate that CRE producing NDM-1 enzyme may be widely distributed in India. However, there is paucity of data regarding fecal carriage of CRE in the community in absence of antibiotic pressure. Different studies have used different culture based techniques like MacConkey agar plates supplemented with 1 μg/ml imipenem, Chrom Agar KPC, Mac Conkey Agar with imipenem, meropenem and ertapenem disc (10 μg) and two step selective broth enrichment method using 10 μg carbapenem disc to evaluate gut colonization with CRE with good performance [15]. Most of these techniques are validated for KPC detection in organisms with MIC
5 Kothari et al. BMC Microbiology 2013, 13:136 Page 5 of 6 range >32 μg/ml for various carbapenems [15]. Nordmann et.al. screened 27 NDM-1 positive isolates and reported that the MIC of these isolates vary from >32 μg/ml, >32 μg/ml and >32 μg/ml for ertapenem, meropenem and imipenem respectively. However, only one isolate i.e. P Providencia rettgeri A showed MIC of 0.5 μg/ml for ertapenem [25]. In present study with 2 step broth enrichment method using meropenem disc only one strain of Enterobacter sp was positive by MHT and PCR confirmed presence of kpc-2 gene. MIC of other 28 suspected CRE isolates were 0.5 μg/ml for all carbapenems. Two isolates were positive for ESBL and AmpC, having MIC of 0.5 μg/ml for ertapenem but were negative for carbapenem genes. In the present study widespread resistance to Ampicillin and 3rd generation cephalosporin (3GC) was observed but carbapenem resistance was rare. This can be explained by indiscriminate use of 3GC in human and animals due to availability of oral formulations and over the counter unrestricted access. Ampicillin and 3GC are used as an empirical therapy in India for the management of neonatal sepsis and other heath related complications like UTI, meningitis, bacterial sepsis (6, 1). The high prevalence of resistance to these drugs as indicated in our study raises the question regarding the efficacy of these antibiotics as an empirical therapy. Carbapenems on the other hand are used sparingly as they are available as parentral formulation for which a patient have to visit the health care facility and in addition there is no reports of their use in animals from India. It is noteworthy that the presence of kpc-2 gene in antibiotic naive neonates may be an alarming finding as carbapenem resistance genes are on plasmids and have a potential for rapid dissemination in future. Commensal flora can colonize the human gut without causing any symptoms, but most of the infections are endogenous and come from patient s own gut flora [26]. The present study estimate of β-lactam resistance may be biased due to following reasons. Babies were supplemented with probiotics which have beneficial effect on gut by producing organic acids, bacteriocins, peptides and in turn decreasing ph of gut leading to inhibition of colonization of Enterobacteriaceae [27]. In addition, only the subdominant population was screened for ESBL carriage resulting in an under estimate of ESBL in the community. However, this data could not be an overestimate as there are no reports of presence of ESBL genes in probiotic bacteria or transfer of antibiotic resistant genes from gram positive (Probiotic) bacteria to gram negative bacteria. Conclusions Our data strongly suggest there is a tremendous load of ESBL and/or AmpC in the community in absence of any direct selection pressure indicating that these genes are widely distributed in the environment. This may result in significant increase in carbapenem use in community resulting in development of carbapenem resistance which may be due to porin loss with ESBL or de-novo spread of true carbapenemases. In conclusion there is a need to make efforts to determine the resistance load present in the different environmental pools (human, animal, and plants). Competing interests The authors declare that they have no competing interests. Authors contributions CK carried out all phenotypic work, DNA extraction, PCR, sequencing, and drafted the manuscript. RG conceived of the study and participated in its design, and edited the manuscript. LCS had done the analysis of the sequencing data. AS have designed the study. VK monitored the mother and the neonates for clinical outcomes and have trained the field workers. SA supervised the monitoring of the clinical outcomes. HC designed the clinical study and edited the manuscript. SS and MD had done the final editing and approved the final manuscript. All authors have read and approved the final manuscript. Acknowledgements This work was supported by Indian Council of Medical Research, Govt. of India. Grant No. 5/7/156/2006-RHN. Author details 1 Department of Microbiology, VMMC and Safdarjung Hospital, New Delhi , India. 2 National Institute of Pathology, Indian Council of Medical Research, New Delhi , India. 3 Indian Council of Medical Research, New Delhi , India. 4 Department of Paediatrics, VMMC and Safdarjung Hospital, New Delhi , India. Received: 14 January 2013 Accepted: 6 June 2013 Published: 17 June 2013 References 1. Hawkey PM, Jones AM: The changing epidemiology of resistance. J Antimicrob Chemother 2009, 64(Supp l):i3 i Andremont A: Commensal flora may play key role in spreading antibiotic resistance. ASM News 2003, 69: Caprioli A, Busani L, Martel JL, Helmuth R: Monitoring of antibiotic resistance in bacteria of animal origin: epidemiological and microbiological methodologies. Int J Antimicrob Agents 2000, 14: Fantin B, Duval X, Massias L, Alavoine L, Chau F, Retout S, Andremont A, Mentré F: Ciprofloxacin dosage and emergence of resistance in human commensal bacteria. J Infect Dis 2009, 200: Macpherson AJ, Harris NL: Interactions between commensal intestinal bacteria and the immune system. Nat Rev Immunol 2004, 4: Lode HM: Rational antibiotic therapy and the position of ampicillin/ sulbactam. Int J Antimicrob Agents 2008, 32: Cantón R, Novais A, Valverde A, Machado E, Peixe L, Baquero F, Coque TM: Prevalence and spread of extended-spectrum beta-lactamase-producing Enterobacteriaceae in Europe. Clin Microbiol Infect 2008, 14: Hawser SP, Badal RE, Bouchillon SK, Hoban DJ, and the SMART India Working Group: Antibiotic susceptibility of intra-abdominal infection isolates from India hospitals during J Med Microbiol 2010, 59: Walsh TR, Weeks J, Livermore DM, Toleman MA: Dissemination of NDM-1 positive bacteria in the New Delhi environment and its implications for human health: an environmental point prevalence study. Lancet Infect Dis 2011, 11: Guillet M, Bille E, Lecuyer H, Taieb F, Masse V, Lanternier F, Lage-Ryke N, Talbi A, Degand N, Lortholary O, Nassif X, Zahar JR: Epidemiology of patients harboring extended-spectrum beta-lactamase-producing enterobacteriaceae (ESBLE), on admission. Med Mal Infect 2010, 40:
6 Kothari et al. BMC Microbiology 2013, 13:136 Page 6 of Wiener J, Quinn JP, Bradford PA, Goering RV, Nathan C, Bush K, Weinstein RA: Multiple antibiotic-resistant Klebsiella and Escherichia coli in nursing homes. JAMA 1999, 281: Mohanty S, Gaind R, Ranjan R, Deb M: Use of the cefepime-clavulanate ESBL Etest for detection of extended-spectrum beta-lactamases in AmpC co-producing bacteria. J Infect Dev Ctries 2010, 4: Woodford N, Fagan EJ, Ellington MJ: Multiplex PCR for rapid detection of genes encoding CTX-M extended-spectrum (beta)-lactamases. J Antimicrob Chemother 2006, 57: Perez-Perez FJ, Hanson ND: Detection of plasmid-mediated AmpC β-lactamase genes in clinical isolates by using multiplex PCR. J Clin Microbiol 2002, 40: Landman D, Salvani JK, Bratu S, Quale J: Evaluation of techniques for detection of carbapenem-resistant Klebsiella pneumoniae in stool surveillance cultures. J Clin Microbiol 2005, 43: Clinical and Laboratory Standard Institute: Performance of standards for antimicrobial susceptibility testing; Twenty-first Information supplement M100- S21. Wayne, PA: Clinical and Laboratory Standard Institute; Schanler RJ, Fraley JK, Lau C, Hurst NM, Horvath L, Rossmann SN: Breastmilk cultures and infection in extremely premature infants. J Perinatol 2011, 31: Nowrouzian F, Hesselmar B, Saalman R, Strannegard IL, Aberg N, Wold AE, Adlerberth I: Escherichia coli in infants intestinal microflora: colonization rate, strain turnover and virulence gene carriage. Pediatr Res 2003, 54: Gueimonde M, Salminen S, Isolauri E: Presence of specific antibiotic (tet) resistance genes in infant faecal microbiota. FEMS Immunol Med Microbiol 2006, 48: Pallecchi L, Bartoloni A, Fiorelli C, Mantella A, Di Maggio T, Gamboa H, Gotuzzo E, Kronvall G, Paradisi F, Rossolini GM: Rapid Dissemination and Diversity of CTX-M Extended-Spectrum β-lactamase Genes in Commensal Escherichia coli Isolates from Healthy Children from Low- Resource Settings in Latin America. Antimicrob Agents Chemother 2007, 51: Mohanty S, Gaind R, Ranjan R, Deb M: Prevalence and phenotypic characterization of carbapenem resistance in Enterobacteriaceae bloodstream isolates in a tertiary care hospital In India. Int J Antimicrob Agents 2011, 37: Walsh TR, Toleman MA, Jones RN: Comment on: Occurrence, prevalence and genetic environment of CTX-M β-lactamases in Enterobacteriaceae from Indian hospitals. J Antimicrob Chemother 2007, 59: Sehgal R, Gaind R, Chellani H, Agarwal P: Extended-spectrum beta lactamaseproducing gram-negative bacteria: clinical profile and outcome in a neonatal intensive care unit. Ann Trop Paediatr 2007, 27: Kumarasamy KK, Toleman MA, Walsh TR, Bagaria J, Butt F, Balakrishnan R, Chaudhary U, Doumith M, Giske CG, Irfan S, Krishnan P, Kumar AV, Maharjan S, Mushtaq S, Noorie T, Paterson DL, Pearson A, Perry C, Pike R, Rao B, Ray U, Sarma JB, Sharma M, Sheridan E, Thirunarayan MA, Turton J, Upadhyay S, Warner M, Welfare W, Livermore DM, et al: Emergence of a new antibiotic resistance mechanism in India, Pakistan, and the UK: a molecular, biological, and epidemiological study. Lancet Infect Dis 2010, 10: Nordmann P, Poirel L, Carrër A, Toleman MA, Walsh TR: How to detect NDM-1 producers. J Clin Microbiol 2011, 49: Bloomfield SF, Cookson B, Falkiner F, Griffith C, Cleary V: Methicillinresistant Staphylococcus aureus, Clostridium difficile, and extendedspectrum beta-lactamase-producing Escherichia coli in the community: assessing the problem and controlling the spread. Am J Infect Control 2007, 35: Gillor O, Etzion A, Riley MA: The dual role of bacteriocins as anti- and probiotics. Appl Microbiol Biotechnol 2008, 81: doi: / Cite this article as: Kothari et al.: Community acquisition of β-lactamase producing Enterobacteriaceae in neonatal gut. BMC Microbiology :136. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
International transfer of NDM-1-producing Klebsiella. pneumoniae from Iraq to France
 AAC Accepts, published online ahead of print on 18 January 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01761-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 18 January 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.01761-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
Risk factors for fecal carriage of carbapenemase producing Enterobacteriaceae among intensive care unit patients from a tertiary care center in India
 Mittal et al. BMC Microbiology (2016) 16:138 DOI 10.1186/s12866-016-0763-y RESEARCH ARTICLE Risk factors for fecal carriage of carbapenemase producing Enterobacteriaceae among intensive care unit patients
Mittal et al. BMC Microbiology (2016) 16:138 DOI 10.1186/s12866-016-0763-y RESEARCH ARTICLE Risk factors for fecal carriage of carbapenemase producing Enterobacteriaceae among intensive care unit patients
Supplementary Material Hofko M et al., Detection of carbapenemases by real-time PCR and melt-curve analysis on the BD MAX TM System
 Supplementary Material Hofko M et al., Detection of carbapenemases by real-time PCR and melt-curve analysis on the BD MAX TM System Supplementary Material and Methods Characterization of isolates by the
Supplementary Material Hofko M et al., Detection of carbapenemases by real-time PCR and melt-curve analysis on the BD MAX TM System Supplementary Material and Methods Characterization of isolates by the
Determining the Optimal Carbapenem MIC that Distinguishes Carbapenemase-Producing
 AAC Accepted Manuscript Posted Online 8 August 2016 Antimicrob. Agents Chemother. doi:10.1128/aac.00838-16 Copyright 2016, American Society for Microbiology. All Rights Reserved. 1 1 2 Determining the
AAC Accepted Manuscript Posted Online 8 August 2016 Antimicrob. Agents Chemother. doi:10.1128/aac.00838-16 Copyright 2016, American Society for Microbiology. All Rights Reserved. 1 1 2 Determining the
Received 31 January 2011/Returned for modification 2 March 2011/Accepted 15 March 2011
 JOURNAL OF CLINICAL MICROBIOLOGY, May 2011, p. 1965 1969 Vol. 49, No. 5 0095-1137/11/$12.00 doi:10.1128/jcm.00203-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Comparative
JOURNAL OF CLINICAL MICROBIOLOGY, May 2011, p. 1965 1969 Vol. 49, No. 5 0095-1137/11/$12.00 doi:10.1128/jcm.00203-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Comparative
Detection of Carbapenem Resistant Enterobacteriacae from Clinical Isolates
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 5 (2016) pp. 864-869 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.505.089
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 5 (2016) pp. 864-869 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2016.505.089
ALERT. Clinical microbiology considerations related to the emergence of. New Delhi metallo beta lactamases (NDM 1) and Klebsiella
 ALERT Clinical microbiology considerations related to the emergence of New Delhi metallo beta lactamases (NDM 1) and Klebsiella pneumoniae carbapenemases (KPC) amongst hospitalized patients in South Africa
ALERT Clinical microbiology considerations related to the emergence of New Delhi metallo beta lactamases (NDM 1) and Klebsiella pneumoniae carbapenemases (KPC) amongst hospitalized patients in South Africa
Carbapenemases in Enterobacteriaceae: Prof P. Nordmann Bicêtre hospital, South-Paris Med School
 Carbapenemases in Enterobacteriaceae: 2012 Prof P. Nordmann Bicêtre hospital, South-Paris Med School March 21, 2012 Trends in Molecular Medecine NDM IMP OXA-48 KPC VIM ALERT VI M KPC KPC NDM I MP OXA-
Carbapenemases in Enterobacteriaceae: 2012 Prof P. Nordmann Bicêtre hospital, South-Paris Med School March 21, 2012 Trends in Molecular Medecine NDM IMP OXA-48 KPC VIM ALERT VI M KPC KPC NDM I MP OXA-
Emergence of Klebsiella pneumoniae ST258 with KPC-2 in Hong Kong. Title. Ho, PL; Tse, CWS; Lai, EL; Lo, WU; Chow, KH
 Title Emergence of Klebsiella pneumoniae ST258 with KPC-2 in Hong Kong Author(s) Ho, PL; Tse, CWS; Lai, EL; Lo, WU; Chow, KH Citation International Journal Of Antimicrobial Agents, 2011, v. 37 n. 4, p.
Title Emergence of Klebsiella pneumoniae ST258 with KPC-2 in Hong Kong Author(s) Ho, PL; Tse, CWS; Lai, EL; Lo, WU; Chow, KH Citation International Journal Of Antimicrobial Agents, 2011, v. 37 n. 4, p.
Detection of NDM-1-producing Klebsiella pneumoniae in Kenya
 AAC Accepts, published online ahead of print on 29 November 2010 Antimicrob. Agents Chemother. doi:10.1128/aac.01247-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 29 November 2010 Antimicrob. Agents Chemother. doi:10.1128/aac.01247-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions.
Discussion points CLSI M100 S19 Update. #1 format of tables has changed. #2 non susceptible category
 Discussion points 2009 CLSI M100 S19 Update Nebraska Public Health Laboratory Changes most important to routine antimicrobial susceptibility testing. Documents available Janet Hindler discussion slide
Discussion points 2009 CLSI M100 S19 Update Nebraska Public Health Laboratory Changes most important to routine antimicrobial susceptibility testing. Documents available Janet Hindler discussion slide
#Corresponding author: Pathology Department, Singapore General Hospital, 20 College. Road, Academia, Level 7, Diagnostics Tower, , Singapore
 AAC Accepts, published online ahead of print on 21 October 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.01754-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 Title: Escherichia
AAC Accepts, published online ahead of print on 21 October 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.01754-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 Title: Escherichia
Emergence of non-kpc carbapenemases: NDM and more
 Emergence of non-kpc carbapenemases: NDM and more --- David Livermore Health Protection Agency, UK The first acquired carbapenemase to be recognised in gram-negative bacteria was IMP-1, a metallo-type,
Emergence of non-kpc carbapenemases: NDM and more --- David Livermore Health Protection Agency, UK The first acquired carbapenemase to be recognised in gram-negative bacteria was IMP-1, a metallo-type,
PROFESSOR PETER M. HAWKEY
 Multi-drug resistant Escherichia coli PROFESSOR PETER M. HAWKEY School of Immunity and Infection College of Medical and Dental Sciences University of Birmingham Birmingham B15 2TT Health Protection Agency
Multi-drug resistant Escherichia coli PROFESSOR PETER M. HAWKEY School of Immunity and Infection College of Medical and Dental Sciences University of Birmingham Birmingham B15 2TT Health Protection Agency
Prevalence of Extended Spectrum -Lactamases In E.coli and Klebsiella spp. in a Tertiary Care Hospital
 ISSN: 2319-7706 Volume 3 Number 10 (2014) pp. 474-478 http://www.ijcmas.com Original Research Article Prevalence of Extended Spectrum -Lactamases In E.coli and Klebsiella spp. in a Tertiary Care Hospital
ISSN: 2319-7706 Volume 3 Number 10 (2014) pp. 474-478 http://www.ijcmas.com Original Research Article Prevalence of Extended Spectrum -Lactamases In E.coli and Klebsiella spp. in a Tertiary Care Hospital
Laboratory testing for carbapenems resistant Enterobacteriacae (CRE)
 Laboratory testing for carbapenems resistant Enterobacteriacae (CRE) Olga Perovic, Principal Pathologist, Center for Opportunistic, Tropical and Hospital Infections, Senior lecturer WITS, 9 th March 2013
Laboratory testing for carbapenems resistant Enterobacteriacae (CRE) Olga Perovic, Principal Pathologist, Center for Opportunistic, Tropical and Hospital Infections, Senior lecturer WITS, 9 th March 2013
Guidance on screening and confirmation of carbapenem resistant Enterobacteriacae (CRE) December 12, 2011
 Guidance on screening and confirmation of carbapenem resistant Enterobacteriacae (CRE) December 12, 2011 Objectives: To discuss the guidelines for detection of CRE in the laboratory setting. To review
Guidance on screening and confirmation of carbapenem resistant Enterobacteriacae (CRE) December 12, 2011 Objectives: To discuss the guidelines for detection of CRE in the laboratory setting. To review
ST11 KPC-2 Klebsiella pneumoniae detected in Taiwan
 AAC Accepts, published online ahead of print on 30 January 2012 Antimicrob. Agents Chemother. doi:10.1128/aac.05576-11 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 3 4 5
AAC Accepts, published online ahead of print on 30 January 2012 Antimicrob. Agents Chemother. doi:10.1128/aac.05576-11 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 3 4 5
Helen Heffernan and Rosemary Woodhouse Antibiotic Reference Laboratory, Institute of Environmental Science and Research Limited (ESR); July 2014.
 Annual survey of extended-spectrum -lactamase (ESBL)-producing Enterobacteriaceae, 2013 Helen Heffernan and Rosemary Woodhouse Antibiotic Reference Laboratory, Institute of Environmental Science and Research
Annual survey of extended-spectrum -lactamase (ESBL)-producing Enterobacteriaceae, 2013 Helen Heffernan and Rosemary Woodhouse Antibiotic Reference Laboratory, Institute of Environmental Science and Research
Global Epidemiology of Carbapenem- Resistant Enterobacteriaceae (CRE)
 Global Epidemiology of Carbapenem- Resistant Enterobacteriaceae (CRE) Mitchell J. Schwaber, MD MSc Director, National Center for Infection Control Ministry of Health State of Israel November 27, 2012 1
Global Epidemiology of Carbapenem- Resistant Enterobacteriaceae (CRE) Mitchell J. Schwaber, MD MSc Director, National Center for Infection Control Ministry of Health State of Israel November 27, 2012 1
NONFERMENTING GRAM NEGATIVE RODS. April Abbott Deaconess Health System Evansville, IN
 NONFERMENTING GRAM NEGATIVE RODS April Abbott Deaconess Health System Evansville, IN OBJECTIVES Discuss basic limitations to assessing carbapenem resistance in nonfermenting GNRs Discuss antimicrobial
NONFERMENTING GRAM NEGATIVE RODS April Abbott Deaconess Health System Evansville, IN OBJECTIVES Discuss basic limitations to assessing carbapenem resistance in nonfermenting GNRs Discuss antimicrobial
In-House Standardization of Carba NP Test for Carbapenemase Detection in Gram Negative Bacteria
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 01 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.701.342
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 01 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.701.342
Screening and detection of carbapenemases
 Screening and detection of carbapenemases For many isolates with carbapenemases the MICs of carbapenems are around the susceptible breakpoint making resistance difficult to detect - particularly with automated
Screening and detection of carbapenemases For many isolates with carbapenemases the MICs of carbapenems are around the susceptible breakpoint making resistance difficult to detect - particularly with automated
Phenotypic Detection Methods of Carbapenemase Production in Enterobacteriaceae
 ISSN: 2319-7706 Volume 4 Number 6 (2015) pp. 547-552 http://www.ijcmas.com Original Research Article Phenotypic Detection Methods of Carbapenemase Production in Enterobacteriaceae Sathya Pandurangan 1,
ISSN: 2319-7706 Volume 4 Number 6 (2015) pp. 547-552 http://www.ijcmas.com Original Research Article Phenotypic Detection Methods of Carbapenemase Production in Enterobacteriaceae Sathya Pandurangan 1,
Carbapenem Disks on MacConkey agar as screening methods for the detection of. Carbapenem-Resistant Gram negative rods in stools.
 JCM Accepts, published online ahead of print on 7 November 2012 J. Clin. Microbiol. doi:10.1128/jcm.02878-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 Carbapenem Disks
JCM Accepts, published online ahead of print on 7 November 2012 J. Clin. Microbiol. doi:10.1128/jcm.02878-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 Carbapenem Disks
Differentiation of Carbapenemase producing Enterobacteriaceae by Triple disc Test
 Original article: Differentiation of Carbapenemase producing Enterobacteriaceae by Triple disc Test Manish Bansal 1, Nitya Vyas 2, Babita Sharma 3, R.K.Maheshwari 4 1PG Resident, 2 Professor, 3 Assistant
Original article: Differentiation of Carbapenemase producing Enterobacteriaceae by Triple disc Test Manish Bansal 1, Nitya Vyas 2, Babita Sharma 3, R.K.Maheshwari 4 1PG Resident, 2 Professor, 3 Assistant
Educational Workshops 2016
 Educational Workshops 2016 Keynote CPE Screening We are grateful to Dr Andrew Dodgson, Consultant Microbiologist, Public Health England and Central Manchester Hospitals NHS Foundation Trust Terminology
Educational Workshops 2016 Keynote CPE Screening We are grateful to Dr Andrew Dodgson, Consultant Microbiologist, Public Health England and Central Manchester Hospitals NHS Foundation Trust Terminology
SSRG International Journal of Medical Science (SSRG-IJMS) volume 2 Issue 4 April 2015
 Utilization of MacConkeyMeropenem screening Agar for the Detection of Carbapenem Resistanant Enterobacteriaceae in a tertiary care hospital Sanjeev Kumar 1, Anamika Vyas 2, S.K.Mehra 3 1,3 Department of
Utilization of MacConkeyMeropenem screening Agar for the Detection of Carbapenem Resistanant Enterobacteriaceae in a tertiary care hospital Sanjeev Kumar 1, Anamika Vyas 2, S.K.Mehra 3 1,3 Department of
Detecting carbapenemases in Enterobacteriaceae
 Detecting carbapenemases in Enterobacteriaceae David Livermore Health Protection Agency, Colindale, London 12 August 2003 Mechanisms of carbapenem R in Enterobacteria Impermeability + AmpC or ESBL Metallo
Detecting carbapenemases in Enterobacteriaceae David Livermore Health Protection Agency, Colindale, London 12 August 2003 Mechanisms of carbapenem R in Enterobacteria Impermeability + AmpC or ESBL Metallo
10/4/16. mcr-1. Emerging Resistance Updates. Objectives. National Center for Emerging and Zoonotic Infectious Diseases. Alex Kallen, MD, MPH, FACP
 National Center for Emerging and Zoonotic Infectious Diseases Emerging Resistance Updates Alex Kallen, MD, MPH, FACP Lead Antimicrobial Resistance and Emerging Pathogens Team Prevention and Response Branch
National Center for Emerging and Zoonotic Infectious Diseases Emerging Resistance Updates Alex Kallen, MD, MPH, FACP Lead Antimicrobial Resistance and Emerging Pathogens Team Prevention and Response Branch
Surveillance of antimicrobial susceptibility of Enterobacteriaceae pathogens isolated from intensive care units and surgical units in Russia
 Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 41 41 Surveillance of antimicrobial susceptibility of Enterobacteriaceae pathogens isolated from intensive care units and surgical units in Russia IRINA
Feb. 2016 THE JAPANESE JOURNAL OF ANTIBIOTICS 69 1 41 41 Surveillance of antimicrobial susceptibility of Enterobacteriaceae pathogens isolated from intensive care units and surgical units in Russia IRINA
Detecting CRE. what does one need to do?
 5 th ICAN Conference, Harare 4 th November 2014 Room 2: 10:30-12:00 Detecting CRE (Carbapenem-resistant Enterobacteriaceae) what does one need to do? Dr Nizam Damani Associate Medical Director Infection
5 th ICAN Conference, Harare 4 th November 2014 Room 2: 10:30-12:00 Detecting CRE (Carbapenem-resistant Enterobacteriaceae) what does one need to do? Dr Nizam Damani Associate Medical Director Infection
Revised AAC Version 2» New-Data Letter to the Editor ACCEPTED. Plasmid-Mediated Carbapenem-Hydrolyzing β-lactamase KPC-2 in
 AAC Accepts, published online ahead of print on 3 December 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.01180-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 3 December 2007 Antimicrob. Agents Chemother. doi:10.1128/aac.01180-07 Copyright 2007, American Society for Microbiology and/or the Listed Authors/Institutions.
Study of Recurrent Urinary Tract Infections in Females in Sinnar Teaching Hospital
 EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 10/ January 2017 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Study of Recurrent Urinary Tract Infections in Females in Sinnar
EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 10/ January 2017 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Study of Recurrent Urinary Tract Infections in Females in Sinnar
Enterobacteriaceae with acquired carbapenemases, 2016
 Enterobacteriaceae with acquired carbapenemases, 2016 Background The acquired or transferable (as opposed to chromosomally encoded) carbapenemases found in Enterobacteriaceae belong to three of the four
Enterobacteriaceae with acquired carbapenemases, 2016 Background The acquired or transferable (as opposed to chromosomally encoded) carbapenemases found in Enterobacteriaceae belong to three of the four
Faecal carriage of ESBL-producing Enterobacteriaceae and carbapenemresistant Gram-negative bacilli in community settings
 Brief Original Article Faecal carriage of ESBL-producing Enterobacteriaceae and carbapenemresistant Gram-negative bacilli in community settings Hugo Edgardo Villar, Marisa Noemí Baserni, Monica Beatriz
Brief Original Article Faecal carriage of ESBL-producing Enterobacteriaceae and carbapenemresistant Gram-negative bacilli in community settings Hugo Edgardo Villar, Marisa Noemí Baserni, Monica Beatriz
In Vitro Activity of Ceftazidime-Avibactam Against Isolates. in a Phase 3 Open-label Clinical Trial for Complicated
 AAC Accepted Manuscript Posted Online 21 November 2016 Antimicrob. Agents Chemother. doi:10.1128/aac.01820-16 Copyright 2016, American Society for Microbiology. All Rights Reserved. 1 2 3 4 5 6 7 8 9 10
AAC Accepted Manuscript Posted Online 21 November 2016 Antimicrob. Agents Chemother. doi:10.1128/aac.01820-16 Copyright 2016, American Society for Microbiology. All Rights Reserved. 1 2 3 4 5 6 7 8 9 10
Validating a selection method for. H. Hasman, Y. Agersø, C. Svendsen, H. Nielsen, N.S. Jensen, B. Guerra, Aarestrup, FM
 Validating a selection method for detecting ESBL/AmpC/CPE H. Hasman, Y. Agersø, C. Svendsen, H. Nielsen, N.S. Jensen, B. Guerra, Aarestrup, FM Validating a selection method for detecting ESBL/AmpC/CPE
Validating a selection method for detecting ESBL/AmpC/CPE H. Hasman, Y. Agersø, C. Svendsen, H. Nielsen, N.S. Jensen, B. Guerra, Aarestrup, FM Validating a selection method for detecting ESBL/AmpC/CPE
Impact of the isolation medium for detection of carbapenemase-producing Enterobacteriaceae using an updated version of the Carba NP test
 Published in which should be cited to refer to this work. Impact of the isolation medium for detection of carbapenemase-producing Enterobacteriaceae using an updated version of the Carba NP test Carbapenem
Published in which should be cited to refer to this work. Impact of the isolation medium for detection of carbapenemase-producing Enterobacteriaceae using an updated version of the Carba NP test Carbapenem
Use of Faropenem as an Indicator of Carbapenemase Activity
 JCM Accepts, published online ahead of print on 10 April 2013 J. Clin. Microbiol. doi:10.1128/jcm.00720-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 2 Use of Faropenem as
JCM Accepts, published online ahead of print on 10 April 2013 J. Clin. Microbiol. doi:10.1128/jcm.00720-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 2 Use of Faropenem as
Recommendations for the Management of Carbapenem- Resistant Enterobacteriaceae (CRE) in Acute and Long-term Acute Care Hospitals
 Recommendations for the Management of Carbapenem- Resistant Enterobacteriaceae (CRE) in Acute and Long-term Acute Care Hospitals Minnesota Department of Health 11/2011 Infectious Disease Epidemiology,
Recommendations for the Management of Carbapenem- Resistant Enterobacteriaceae (CRE) in Acute and Long-term Acute Care Hospitals Minnesota Department of Health 11/2011 Infectious Disease Epidemiology,
Laboratory CLSI M100-S18 update. Paul D. Fey, Ph.D. Associate Professor/Associate Director Josh Rowland, M.T. (ASCP) State Training Coordinator
 Nebraska Public Health Laboratory 2008 CLSI M100-S18 update Paul D. Fey, Ph.D. Associate Professor/Associate Director Josh Rowland, M.T. (ASCP) State Training Coordinator Agenda Discuss 2008 M100- S18
Nebraska Public Health Laboratory 2008 CLSI M100-S18 update Paul D. Fey, Ph.D. Associate Professor/Associate Director Josh Rowland, M.T. (ASCP) State Training Coordinator Agenda Discuss 2008 M100- S18
Screening of Carbapenem Resistant Enterobacteriaceae among Nosocomial Isolates: A Study from South India
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 4 (2017) pp. 460-465 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.604.053
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 4 (2017) pp. 460-465 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.604.053
HOSPITAL EPIDEMOLOGY AND INFECTION CONTROL: STANDARD AND TRANSMISSION-BASED ISOLATION
 Appendix 1: Carbapenem-Resistant Enterobacteriacaea (CRE) I. Definition: 2015 CDC definition of CRE are Enterobacteriaceae 1 that are: A. Resistant to any carbapenem antimicrobial (i.e., minimum inhibitory
Appendix 1: Carbapenem-Resistant Enterobacteriacaea (CRE) I. Definition: 2015 CDC definition of CRE are Enterobacteriaceae 1 that are: A. Resistant to any carbapenem antimicrobial (i.e., minimum inhibitory
Supplementary Table 3. 3 UTR primer sequences. Primer sequences used to amplify and clone the 3 UTR of each indicated gene are listed.
 Supplemental Figure 1. DLKI-DIO3 mirna/mrna complementarity. Complementarity between the indicated DLK1-DIO3 cluster mirnas and the UTR of SOX2, SOX9, HIF1A, ZEB1, ZEB2, STAT3 and CDH1with mirsvr and PhastCons
Supplemental Figure 1. DLKI-DIO3 mirna/mrna complementarity. Complementarity between the indicated DLK1-DIO3 cluster mirnas and the UTR of SOX2, SOX9, HIF1A, ZEB1, ZEB2, STAT3 and CDH1with mirsvr and PhastCons
AAC Accepts, published online ahead of print on 13 October 2008 Antimicrob. Agents Chemother. doi: /aac
 AAC Accepts, published online ahead of print on 13 October 2008 Antimicrob. Agents Chemother. doi:10.1128/aac.00931-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 13 October 2008 Antimicrob. Agents Chemother. doi:10.1128/aac.00931-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions.
Molecular characterisation of CTX-M-type extendedspectrum β-lactamases of Escherichia coli isolated from a Portuguese University Hospital
 EJHP Science Volume 17 2011 Issue 3 P. 1-5 2011 Pharma Publishing and Media Europe. All rights reserved 1781-7595 25 www.ejhp.eu Molecular characterisation of CTX-M-type extendedspectrum β-lactamases of
EJHP Science Volume 17 2011 Issue 3 P. 1-5 2011 Pharma Publishing and Media Europe. All rights reserved 1781-7595 25 www.ejhp.eu Molecular characterisation of CTX-M-type extendedspectrum β-lactamases of
Spread of carbapenems resistant Enterobacteriaceae in South Africa; report from National Antimicrobial Resistance Reference Laboratory
 Spread of carbapenems resistant Enterobacteriaceae in South Africa; report from National Antimicrobial Resistance Reference Laboratory Olga Perovic*, Ashika Singh-Moodley, Samantha Iyaloo 5 th November
Spread of carbapenems resistant Enterobacteriaceae in South Africa; report from National Antimicrobial Resistance Reference Laboratory Olga Perovic*, Ashika Singh-Moodley, Samantha Iyaloo 5 th November
Development of a phenotypic method for fecal carriage detection of OXA-48-producing
 JCM Accepts, published online ahead of print on 11 May 2011 J. Clin. Microbiol. doi:10.1128/jcm.00055-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 11 May 2011 J. Clin. Microbiol. doi:10.1128/jcm.00055-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Evaluation of CHROMagar msupercarba for the detection of carbapenemaseproducing Gram-negative organisms
 ORIGINAL ARTICLE Evaluation of CHROMagar msupercarba for the detection of carbapenemaseproducing Gram-negative organisms Julie Creighton and Hui Wang Canterbury Health Laboratories, Christchurch ABSTRACT
ORIGINAL ARTICLE Evaluation of CHROMagar msupercarba for the detection of carbapenemaseproducing Gram-negative organisms Julie Creighton and Hui Wang Canterbury Health Laboratories, Christchurch ABSTRACT
Rapid identification of emerging resistance in Gram negatives. Prof. Patrice Nordmann
 Rapid identification of emerging resistance in Gram negatives Prof. Patrice Nordmann Emerging Resistance threats, CDC USA-2013 Enterobacteriaceae producing extendedspectrum β-lactamases (ESBL) Multi-resistant
Rapid identification of emerging resistance in Gram negatives Prof. Patrice Nordmann Emerging Resistance threats, CDC USA-2013 Enterobacteriaceae producing extendedspectrum β-lactamases (ESBL) Multi-resistant
Enterobacteriaceae with acquired carbapenemases, 2015
 Enterobacteriaceae with acquired carbapenemases, 2015 Background The acquired or transferable (as opposed to chromosomally encoded) carbapenemases found in Enterobacteriaceae belong to three of the four
Enterobacteriaceae with acquired carbapenemases, 2015 Background The acquired or transferable (as opposed to chromosomally encoded) carbapenemases found in Enterobacteriaceae belong to three of the four
c Tuj1(-) apoptotic live 1 DIV 2 DIV 1 DIV 2 DIV Tuj1(+) Tuj1/GFP/DAPI Tuj1 DAPI GFP
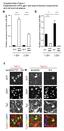 Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
Phenotypic detection of ESBLs and carbapenemases
 Phenotypic detection of ESBLs and carbapenemases Standardized susceptibility testing residential workshop 2016 Katie Hopkins PhD Clinical Scientist Antimicrobial Resistance and Healthcare Associated Infections
Phenotypic detection of ESBLs and carbapenemases Standardized susceptibility testing residential workshop 2016 Katie Hopkins PhD Clinical Scientist Antimicrobial Resistance and Healthcare Associated Infections
Sensitive and specific Modified Hodge Test for KPC and metallo-beta-lactamase
 JCM Accepts, published online ahead of print on 19 October 2011 J. Clin. Microbiol. doi:10.1128/jcm.05602-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All
JCM Accepts, published online ahead of print on 19 October 2011 J. Clin. Microbiol. doi:10.1128/jcm.05602-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All
Abstract. a Jann-Tay Wang 1, Un-In Wu 2, Tsai-Ling Yang Lauderdale 3, Mei-Chen Chen 3, Shu-Ying Li 4, Le-Yin Hsu 5, Shan-Chwen Chang 1,6 *
 RESEARCH ARTICLE Carbapenem-Nonsusceptible Enterobacteriaceae in Taiwan Jann-Tay Wang 1, Un-In Wu 2, Tsai-Ling Yang Lauderdale 3, Mei-Chen Chen 3, Shu-Ying Li 4, Le-Yin Hsu 5, Shan-Chwen Chang 1,6 * 1
RESEARCH ARTICLE Carbapenem-Nonsusceptible Enterobacteriaceae in Taiwan Jann-Tay Wang 1, Un-In Wu 2, Tsai-Ling Yang Lauderdale 3, Mei-Chen Chen 3, Shu-Ying Li 4, Le-Yin Hsu 5, Shan-Chwen Chang 1,6 * 1
Abstract. Introduction. Methods. Editor: R. Canton
 ORIGINAL ARTICLE BACTERIOLOGY High rate of faecal carriage of extended-spectrum b-lactamase and OXA-48 carbapenemase-producing Enterobacteriaceae at a University hospital in Morocco D. Girlich 1, N. Bouihat
ORIGINAL ARTICLE BACTERIOLOGY High rate of faecal carriage of extended-spectrum b-lactamase and OXA-48 carbapenemase-producing Enterobacteriaceae at a University hospital in Morocco D. Girlich 1, N. Bouihat
Carbapenem-resistant Escherichia coli and Klebsiella pneumoniae in Taiwan
 Carbapenem-resistant Escherichia coli and Klebsiella pneumoniae in Taiwan An Infection Control Emergency Speaker: L Kristopher Siu Principal Investigator Division of Infectious Diseases National Institute
Carbapenem-resistant Escherichia coli and Klebsiella pneumoniae in Taiwan An Infection Control Emergency Speaker: L Kristopher Siu Principal Investigator Division of Infectious Diseases National Institute
ORIGINAL ARTICLE. Julie Creighton and Clare Tibbs. Canterbury Health Laboratories, Christchurch
 ORIGINAL ARTICLE Evaluation of the MAST indirect carbapenemase test and comparison with a modified carbapenem inactivation method for the detection of carbapenemase enzymes in Gram-negative bacteria Julie
ORIGINAL ARTICLE Evaluation of the MAST indirect carbapenemase test and comparison with a modified carbapenem inactivation method for the detection of carbapenemase enzymes in Gram-negative bacteria Julie
β-lactamase inhibitors
 β-lactamase inhibitors Properties, microbiology & enzymology DAVID M LIVERMORE Professor of Medical Microbiology, UEA Lead on Antibiotic Resistance, Public Health England β-lactamase classes A B C D Serine
β-lactamase inhibitors Properties, microbiology & enzymology DAVID M LIVERMORE Professor of Medical Microbiology, UEA Lead on Antibiotic Resistance, Public Health England β-lactamase classes A B C D Serine
Nature and Science 2017;15(10)
 Evaluation of Substrate Profile Test for Detection of Metallobetalactamses among Imipenem Resistant Clinical Isolates of Gram Negative Bacteria Tarek El-said El-Banna, Fatma Ibrahim Sonboland Eslam Shaaban
Evaluation of Substrate Profile Test for Detection of Metallobetalactamses among Imipenem Resistant Clinical Isolates of Gram Negative Bacteria Tarek El-said El-Banna, Fatma Ibrahim Sonboland Eslam Shaaban
GUIDE TO INFECTION CONTROL IN THE HOSPITAL. Carbapenem-resistant Enterobacteriaceae
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 47: Carbapenem-resistant Enterobacteriaceae Authors E-B Kruse, MD H. Wisplinghoff, MD Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key Issue Known
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 47: Carbapenem-resistant Enterobacteriaceae Authors E-B Kruse, MD H. Wisplinghoff, MD Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key Issue Known
Carbapenems and Enterobacteriaceae
 Title Carbapenems and Enterobacteriaceae Presenter s details NHLS Dr Khine Swe Swe/Han FC Path ( Micro), SA MMed( micro), SA DTMH(Wits univ),sa PDIC(Stellen univ)sa MB,BS(Yangon),Myanmar Pathologist,Consultant/Lecturer,
Title Carbapenems and Enterobacteriaceae Presenter s details NHLS Dr Khine Swe Swe/Han FC Path ( Micro), SA MMed( micro), SA DTMH(Wits univ),sa PDIC(Stellen univ)sa MB,BS(Yangon),Myanmar Pathologist,Consultant/Lecturer,
A new diagnostic microarray (Check-KPC ESBL) for detection and. identification of extended-spectrum beta-lactamases in highly resistant
 JCM Accepts, published online ahead of print on 8 June 2011 J. Clin. Microbiol. doi:10.1128/jcm.02087-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 8 June 2011 J. Clin. Microbiol. doi:10.1128/jcm.02087-10 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
β- Lactamase Gene carrying Klebsiella pneumoniae and its Clinical Implication
 Prevalence of Carbapenem-Hydrolyzing β- Lactamase Gene carrying Klebsiella pneumoniae and its Clinical Implication David Alcid M.D Balaji Yegneswaran M.D. Wanpen Numsuwan Introduction Klebsiella pneumoniae
Prevalence of Carbapenem-Hydrolyzing β- Lactamase Gene carrying Klebsiella pneumoniae and its Clinical Implication David Alcid M.D Balaji Yegneswaran M.D. Wanpen Numsuwan Introduction Klebsiella pneumoniae
(DHA-1): Microbiologic and Clinical Implications
 AAC Accepts, published online ahead of print on 20 September 2010 Antimicrob. Agents Chemother. doi:10.1128/aac.00083-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 20 September 2010 Antimicrob. Agents Chemother. doi:10.1128/aac.00083-10 Copyright 2010, American Society for Microbiology and/or the Listed Authors/Institutions.
Supplemental Data. Shin et al. Plant Cell. (2012) /tpc YFP N
 MYC YFP N PIF5 YFP C N-TIC TIC Supplemental Data. Shin et al. Plant Cell. ()..5/tpc..95 Supplemental Figure. TIC interacts with MYC in the nucleus. Bimolecular fluorescence complementation assay using
MYC YFP N PIF5 YFP C N-TIC TIC Supplemental Data. Shin et al. Plant Cell. ()..5/tpc..95 Supplemental Figure. TIC interacts with MYC in the nucleus. Bimolecular fluorescence complementation assay using
National Center for Emerging and Zoonotic Infectious Diseases The Biggest Antibiotic Resistance Threats
 National Center for Emerging and Zoonotic Infectious Diseases The Biggest Antibiotic Resistance Threats Jean B. Patel, PhD, D(ABMM) Science Lead, Antibiotic Resistance and Coordination Unit Centers for
National Center for Emerging and Zoonotic Infectious Diseases The Biggest Antibiotic Resistance Threats Jean B. Patel, PhD, D(ABMM) Science Lead, Antibiotic Resistance and Coordination Unit Centers for
Public Health Surveillance for Multi Drug Resistant Organisms in Orange County
 Public Health Surveillance for Multi Drug Resistant Organisms in Orange County Matt Zahn, MD Medical Director Epidemiology and Assessment Orange County Public Health Antimicrobial Mechanisms of Action
Public Health Surveillance for Multi Drug Resistant Organisms in Orange County Matt Zahn, MD Medical Director Epidemiology and Assessment Orange County Public Health Antimicrobial Mechanisms of Action
a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53
 1 2 3 4 5 6 7 8 9 10 Supplementary Figure 1. Induction of p53 LOH by MADM. a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53 mouse revealed increased p53 KO/KO (green,
1 2 3 4 5 6 7 8 9 10 Supplementary Figure 1. Induction of p53 LOH by MADM. a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53 mouse revealed increased p53 KO/KO (green,
Reporting blood culture results to clinicians: MIC, resistance mechanisms, both?
 Reporting blood culture results to clinicians: MIC, resistance mechanisms, both? Christian G. Giske, MD, PhD Senior Consultant Physician/Associate Professor Department of Clinical Microbiology Karolinska
Reporting blood culture results to clinicians: MIC, resistance mechanisms, both? Christian G. Giske, MD, PhD Senior Consultant Physician/Associate Professor Department of Clinical Microbiology Karolinska
Rapid detection of carbapenemase-producing Enterobacteriaceae from blood cultures
 ORIGINAL ARTICLE BACTERIOLOGY Rapid detection of carbapenemase-producing Enterobacteriaceae from blood cultures L. Dortet 1,L.Brechard 1, L. Poirel 1,2 and P. Nordmann 1,2 1) Service de Bacteriologie-Virologie,
ORIGINAL ARTICLE BACTERIOLOGY Rapid detection of carbapenemase-producing Enterobacteriaceae from blood cultures L. Dortet 1,L.Brechard 1, L. Poirel 1,2 and P. Nordmann 1,2 1) Service de Bacteriologie-Virologie,
Original Article Clinical Microbiology
 Original Article Clinical Microbiology Ann Lab Med 2015;35:212-219 http://dx.doi.org/10.3343/alm.2015.35.2.212 ISSN 2234-3806 eissn 2234-3814 Combined Use of the Modified Hodge Test and Carbapenemase Inhibition
Original Article Clinical Microbiology Ann Lab Med 2015;35:212-219 http://dx.doi.org/10.3343/alm.2015.35.2.212 ISSN 2234-3806 eissn 2234-3814 Combined Use of the Modified Hodge Test and Carbapenemase Inhibition
Journal of Infectious Diseases and
 Journal of Infectious Diseases & Therapy ISSN: 2332-0877 Journal of Infectious Diseases and Therapy Santanirand et al., J Infect Dis Ther 2018, 6:5 DOI: 10.4172/2332-0877.1000378 Research Article Open
Journal of Infectious Diseases & Therapy ISSN: 2332-0877 Journal of Infectious Diseases and Therapy Santanirand et al., J Infect Dis Ther 2018, 6:5 DOI: 10.4172/2332-0877.1000378 Research Article Open
Evaluation of Six Phenotypic Methods for the Detection of Carbapenemases in Gram-Negative Bacteria With Characterized Resistance Mechanisms
 Original Article Clinical Microbiology Ann Lab Med 2017;37:305-312 https://doi.org/10.3343/alm.2017.37.4.305 ISSN 2234-3806 eissn 2234-3814 Evaluation of Six Phenotypic Methods for the Detection of Carbapenemases
Original Article Clinical Microbiology Ann Lab Med 2017;37:305-312 https://doi.org/10.3343/alm.2017.37.4.305 ISSN 2234-3806 eissn 2234-3814 Evaluation of Six Phenotypic Methods for the Detection of Carbapenemases
Regional Emergence of VIM producing carbapenem resistant Pseudomonas aeruginosa (VIM CRPA)
 National Center for Emerging and Zoonotic Infectious Diseases Regional Emergence of VIM producing carbapenem resistant Pseudomonas aeruginosa (VIM CRPA) Chris Prestel, MD Epidemic Intelligence Service
National Center for Emerging and Zoonotic Infectious Diseases Regional Emergence of VIM producing carbapenem resistant Pseudomonas aeruginosa (VIM CRPA) Chris Prestel, MD Epidemic Intelligence Service
Update on CLSI and EUCAST
 Update on CLSI and EUCAST 1 Completed work» Cephalosporin breakpoints for Enterobacteriaceae ESBL screens MIC versus resistance mechanism» Carbapenem breakpoints for Enterobacteriaceae Modified Hodge Test»
Update on CLSI and EUCAST 1 Completed work» Cephalosporin breakpoints for Enterobacteriaceae ESBL screens MIC versus resistance mechanism» Carbapenem breakpoints for Enterobacteriaceae Modified Hodge Test»
CARBAPENEMASE PRODUCING ENTEROBACTERIACEAE
 CARBAPENEMASE PRODUCING ENTEROBACTERIACEAE Veroniek Saegeman Veroniek Saegeman UZLeuven Carbapenemase producing Enterobacteriaceae (CPE) Introduction on antibiotic resistance Classification of ß-lactamases
CARBAPENEMASE PRODUCING ENTEROBACTERIACEAE Veroniek Saegeman Veroniek Saegeman UZLeuven Carbapenemase producing Enterobacteriaceae (CPE) Introduction on antibiotic resistance Classification of ß-lactamases
Overcoming the PosESBLities of Enterobacteriaceae Resistance
 Overcoming the PosESBLities of Enterobacteriaceae Resistance Review of current treatment options Jamie Reed, PharmD Pharmacy Grand Rounds August 28, 2018 Rochester, MN 2018 MFMER slide-1 Disclosure No
Overcoming the PosESBLities of Enterobacteriaceae Resistance Review of current treatment options Jamie Reed, PharmD Pharmacy Grand Rounds August 28, 2018 Rochester, MN 2018 MFMER slide-1 Disclosure No
MHSAL Guidelines for the Prevention and Control of Antimicrobial Resistant Organisms (AROs) - Response to Questions
 MHSAL Guidelines for the Prevention and Control of Antimicrobial Resistant Organisms (AROs) - Response to Questions Dr. Andrew Walkty Medical Microbiologist, Diagnostic Services Manitoba (DSM) June. 17,
MHSAL Guidelines for the Prevention and Control of Antimicrobial Resistant Organisms (AROs) - Response to Questions Dr. Andrew Walkty Medical Microbiologist, Diagnostic Services Manitoba (DSM) June. 17,
jmb Research Article Review Semi Kim 1, Ji Youn Sung 2, Hye Hyun Cho 3, Kye Chul Kwon 1, and Sun Hoe Koo 1 *
 J. Microbiol. Biotechnol. (2014), 24(6), 765 770 http://dx.doi.org/10.4014/jmb.1306.06036 Review Research Article jmb Characterization of CTX-M-14- and CTX-M-15-Producing Escherichia coli and Klebsiella
J. Microbiol. Biotechnol. (2014), 24(6), 765 770 http://dx.doi.org/10.4014/jmb.1306.06036 Review Research Article jmb Characterization of CTX-M-14- and CTX-M-15-Producing Escherichia coli and Klebsiella
Expert rules. for Gram-negatives
 Academic Perspective in Expert rules Emerging Issues of Resistance in Gram-ve Bacteria for Gram-negatives Trevor Winstanley Sheffield Teaching Hospitals Presented on behalf of David Livermore University
Academic Perspective in Expert rules Emerging Issues of Resistance in Gram-ve Bacteria for Gram-negatives Trevor Winstanley Sheffield Teaching Hospitals Presented on behalf of David Livermore University
Epidemiology of the β-lactamase resistome among Klebsiella pneumoniae carbapenemase (KPC)-producing Enterobacteriaceae in the Chicago region
 Epidemiology of the β-lactamase resistome among Klebsiella pneumoniae carbapenemase (KPC)-producing Enterobacteriaceae in the Chicago region Michael Y. Lin MD MPH 1, Karen Lolans BS 1, Rosie D. Lyles,
Epidemiology of the β-lactamase resistome among Klebsiella pneumoniae carbapenemase (KPC)-producing Enterobacteriaceae in the Chicago region Michael Y. Lin MD MPH 1, Karen Lolans BS 1, Rosie D. Lyles,
Supplementary Document
 Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
Academic Perspective in. David Livermore Prof of Medical Microbiology, UEA Lead on Antibiotic resistance PHE
 Academic Perspective in Emerging No, we can t Issues treat of carbapenemase Resistance and ESBL in Gram-ve producers Bacteria based on MIC David Livermore Prof of Medical Microbiology, UEA Lead on Antibiotic
Academic Perspective in Emerging No, we can t Issues treat of carbapenemase Resistance and ESBL in Gram-ve producers Bacteria based on MIC David Livermore Prof of Medical Microbiology, UEA Lead on Antibiotic
ORIGINAL INVESTIGATION. Rapid Spread of Carbapenem-Resistant Klebsiella pneumoniae in New York City
 ORIGINAL INVESTIGATION Rapid Spread of Carbapenem-Resistant Klebsiella pneumoniae in New York City A New Threat to Our Antibiotic Armamentarium Simona Bratu, MD; David Landman, MD; Robin Haag, RN; Rose
ORIGINAL INVESTIGATION Rapid Spread of Carbapenem-Resistant Klebsiella pneumoniae in New York City A New Threat to Our Antibiotic Armamentarium Simona Bratu, MD; David Landman, MD; Robin Haag, RN; Rose
The role of an AMR reference laboratory
 The role of an AMR reference laboratory Professor Neil Woodford Antimicrobial Resistance & Healthcare Associated Infections (AMRHAI) Reference Unit Crown copyright Primary purpose: regional AMR threats
The role of an AMR reference laboratory Professor Neil Woodford Antimicrobial Resistance & Healthcare Associated Infections (AMRHAI) Reference Unit Crown copyright Primary purpose: regional AMR threats
ESCMID Online Lecture Library. by author
 www.eucast.org EXPERT RULES IN ANTIMICROBIAL SUSCEPTIBILITY TESTING Dr. Rafael Cantón Hospital Universitario Ramón y Cajal SERVICIO DE MICROBIOLOGÍA Y PARASITOLOGÍA Departamento de Microbiología II Universidad
www.eucast.org EXPERT RULES IN ANTIMICROBIAL SUSCEPTIBILITY TESTING Dr. Rafael Cantón Hospital Universitario Ramón y Cajal SERVICIO DE MICROBIOLOGÍA Y PARASITOLOGÍA Departamento de Microbiología II Universidad
Insert for Kit 98006/98010/ KPC/Metallo-B-Lactamase Confirm Kit KPC+MBL detection Kit KPC/MBL and OXA-48 Confirm Kit REVISION: DBV0034J
 Insert for Kit 98006/98010/98015 KPC/Metallo-B-Lactamase Confirm Kit KPC+MBL detection Kit KPC/MBL and OXA-48 Confirm Kit REVISION: DBV0034J DATE OF ISSUE: 09.02.2017 LANGUAGE: English FOR IN VITRO DIAGNOSTIC
Insert for Kit 98006/98010/98015 KPC/Metallo-B-Lactamase Confirm Kit KPC+MBL detection Kit KPC/MBL and OXA-48 Confirm Kit REVISION: DBV0034J DATE OF ISSUE: 09.02.2017 LANGUAGE: English FOR IN VITRO DIAGNOSTIC
Abbreviations: P- paraffin-embedded section; C, cryosection; Bio-SA, biotin-streptavidin-conjugated fluorescein amplification.
 Supplementary Table 1. Sequence of primers for real time PCR. Gene Forward primer Reverse primer S25 5 -GTG GTC CAC ACT ACT CTC TGA GTT TC-3 5 - GAC TTT CCG GCA TCC TTC TTC-3 Mafa cds 5 -CTT CAG CAA GGA
Supplementary Table 1. Sequence of primers for real time PCR. Gene Forward primer Reverse primer S25 5 -GTG GTC CAC ACT ACT CTC TGA GTT TC-3 5 - GAC TTT CCG GCA TCC TTC TTC-3 Mafa cds 5 -CTT CAG CAA GGA
KPC around the world Maria Virginia Villegas, MD, MSC
 KPC around the world Maria Virginia Villegas, MD, MSC Scientific Director Bacterial Resistance and Nosocomial Infections Research Area International Center for Medical Research and Training, CIDEIM, Cali,
KPC around the world Maria Virginia Villegas, MD, MSC Scientific Director Bacterial Resistance and Nosocomial Infections Research Area International Center for Medical Research and Training, CIDEIM, Cali,
New Mechanisms of Antimicrobial Resistance and Methods for Carbapenemase Detection
 New Mechanisms of Antimicrobial Resistance and Methods for Carbapenemase Detection Stephen G. Jenkins, PhD, F(AAM), D(ABMM) Professor of Pathology and Laboratory Medicine Professor of Pathology in Medicine
New Mechanisms of Antimicrobial Resistance and Methods for Carbapenemase Detection Stephen G. Jenkins, PhD, F(AAM), D(ABMM) Professor of Pathology and Laboratory Medicine Professor of Pathology in Medicine
β CARBA Test Rapid detection of carbapenemase-producing Enterobacteriaceae strains Contents 1. INTENDED USE
 β CARBA Test 25 68260 Rapid detection of carbapenemase-producing Enterobacteriaceae strains 881159 2015/05 Contents 1. INTENDED USE 2. SUMMARY AND EXPLANATION OF THE TEST 3. PRINCIPLE OF THE PROCEDURE
β CARBA Test 25 68260 Rapid detection of carbapenemase-producing Enterobacteriaceae strains 881159 2015/05 Contents 1. INTENDED USE 2. SUMMARY AND EXPLANATION OF THE TEST 3. PRINCIPLE OF THE PROCEDURE
Expert rules in antimicrobial susceptibility testing: State of the art
 Expert rules in antimicrobial susceptibility testing: State of the art ESCMID Postgraduate Education Course Antimicrobial Susceptibility Testing and Surveillance: from Laboratory to Clinic Hospital Universitario
Expert rules in antimicrobial susceptibility testing: State of the art ESCMID Postgraduate Education Course Antimicrobial Susceptibility Testing and Surveillance: from Laboratory to Clinic Hospital Universitario
EVALUATION OF METHODS FOR AMPC β-lactamase IN GRAM NEGATIVE CLINICAL ISOLATES FROM TERTIARY CARE HOSPITALS
 Indian Journal of Medical Microbiology, (2005) 23 (2):120-124 Brief Communication EVALUATION OF METHODS FOR AMPC β-lactamase IN GRAM NEGATIVE CLINICAL ISOLATES FROM TERTIARY CARE HOSPITALS S Singhal, T
Indian Journal of Medical Microbiology, (2005) 23 (2):120-124 Brief Communication EVALUATION OF METHODS FOR AMPC β-lactamase IN GRAM NEGATIVE CLINICAL ISOLATES FROM TERTIARY CARE HOSPITALS S Singhal, T
Identification and screening of carbapenemase-producing Enterobacteriaceae
 REVIEW 10.1111/j.1469-0691.2012.03815.x Identification and screening of carbapenemase-producing Enterobacteriaceae P. Nordmann 1, M. Gniadkowski 2, C. G. Giske 3, L. Poirel 1, N. Woodford 4, V. Miriagou
REVIEW 10.1111/j.1469-0691.2012.03815.x Identification and screening of carbapenemase-producing Enterobacteriaceae P. Nordmann 1, M. Gniadkowski 2, C. G. Giske 3, L. Poirel 1, N. Woodford 4, V. Miriagou
Detection of NDM-1, VIM-1, KPC, OXA-48, and OXA-162 carbapenemases by MALDI- TOF mass spectrometry
 JCM Accepts, published online ahead of print on 2 May 2012 J. Clin. Microbiol. doi:10.1128/jcm.01002-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 3 4 5 6 7 8 9 10 11 12
JCM Accepts, published online ahead of print on 2 May 2012 J. Clin. Microbiol. doi:10.1128/jcm.01002-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 3 4 5 6 7 8 9 10 11 12
Incidence of metallo beta lactamase producing Pseudomonas aeruginosa in ICU patients
 Indian J Med Res 127, April 2008, pp 398-402 Incidence of metallo beta lactamase producing Pseudomonas aeruginosa in ICU patients Ami Varaiya, Nikhil Kulkarni, Manasi Kulkarni, Pallavi Bhalekar & Jyotsana
Indian J Med Res 127, April 2008, pp 398-402 Incidence of metallo beta lactamase producing Pseudomonas aeruginosa in ICU patients Ami Varaiya, Nikhil Kulkarni, Manasi Kulkarni, Pallavi Bhalekar & Jyotsana
Prevalence and mechanisms of broad-spectrum β- lactam resistance in Enterobacteriaceae: A children's hospital experience
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 Prevalence and mechanisms of broad-spectrum β- lactam resistance in Enterobacteriaceae: A children's hospital
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 Prevalence and mechanisms of broad-spectrum β- lactam resistance in Enterobacteriaceae: A children's hospital
