Management of residual gall bladder: A 15-year experience from a north Indian tertiary care centre
|
|
|
- Maximilian Kennedy
- 5 years ago
- Views:
Transcription
1 Ann Hepatobiliary Pancreat Surg 2018;22: Original Article Management of residual gall bladder: A 15-year experience from a north Indian tertiary care centre Ashish Singh, Abhimanyu Kapoor, Rajneesh Kumar Singh, Anand Prakash, Anu Behari, Ashok Kumar, Vinay Kumar Kapoor, and Rajan Saxena Department of Surgical Gastroenterology, Sanjay Gandhi Post Graduate Institute of Medical Sciences (SGPGIMS), Lucknow, India Backgrounds/Aims: A residual gallbladder (RGB) following a partial/subtotal cholecystectomy may cause symptoms that require its removal. We present our large study regarding the problem of a RGB over a 15 year period. Methods: This study involved a retrospective analysis of patients managed for symptomatic RGB from January 2000 to December Results: A RGB was observed in 93 patients, who had a median age of 45 (25-70) years, and were comprised of 69 (74.2%) females. The most common presentation was recurrence pain (n=64, 68.8%). Associated choledocholithiasis was present in 23 patients (24.7%). An ultrasonography (USG) failed to diagnose RGB calculi in 10 (11%) patients; whereas, magnetic resonance cholangio-pancreatography (MRCP) accurately diagnosed RGB calculi in all the cases except for 2 (4%) and, additionally, detected common bile duct (CBD) stones in 12 patients. Completion cholecystectomy was performed in all patients (open 45 [48.4%]; laparoscopic 48 [51.6%] and 19 [20.4%] patients required a conversion to open). The RGB pathology included stones in 90 (96.8%), Mirizzi s syndrome in 10 (10.8%) and an internal fistula in 9 (9.7%) patients. Additional procedures included CBD exploration (n=6); Choledocho-duodenostomy (n=4) and Roux-en-Y hepatico-jejunostomy (n=3). The mortality and morbidity were nil and 11% (all wound infection), respectively. Two patients developed incisional hernia during follow up. The mean follow up duration was 23.1 months (3-108) in 65 patients and the outcome was excellent and good in 97% of the patients. Conclusions: Post-cholecystectomy recurrent biliary colic should raise suspicion of RGB. MRCP is a useful investigation for the diagnosis and assessment of any associated problems and provides a roadmap for surgery. Laparoscopic completion cholecystectomy is feasible, but is technically difficult and has a high conversion rate. (Ann Hepatobiliary Pancreat Surg 2018;22:36-41) Key Words: Subtotal cholecystectomy; Residual gallbladder; Completion cholecystectomy; Laparoscopic cholecystectomy; Open cholecystectomy INTRODUCTION Residual gallbladder (RGB) refers to the remnant part of the gallbladder left behind during partial cholecystectomy in certain situations. It may be done intentionally to prevent injury to important structures in the presence of severe inflammation or portal hypertension, where it is difficult and dangerous to perform a complete cholecystectomy. 1-3 Other times, the RGB may have been left behind unintentionally because of the inaccurate identification of the anatomy, usually in the presence of inflammation and fibrosis. 4 In some patients, the RGB may continue to harbor or later develop a pathology like a stone, inflammation or fistula with adjacent structures and give rise to symptoms that require treatment. 5-9 Presently, there are a few small case studies and case reports in the literature pertaining to the problem of RGB. 2,10-14 In this retrospective study, we present our substantial experience with the problem of RGB managed over a period of 15 years in a tertiary care hospital in northern India. MATERIALS AND METHODS A retrospective analysis was conducted from a pro- Received: July 21, 2017; Revised: August 15, 2017; Accepted: August 31, 2017 Corresponding author: Rajneesh Kumar Singh Department of Surgical Gastroenterology, Sanjay Gandhi Postgraduate Institute of Medical Sciences, Lucknow , Uttar Pradesh, India Tel: , rajneeshkumarsingh@hotmail.com Copyright C 2018 by The Korean Association of Hepato-Biliary-Pancreatic Surgery This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Annals of Hepato-Biliary-Pancreatic Surgery pissn: ㆍ eissn:
2 Ashish Singh, et al. Management of residual gall bladder 37 spective database of patients managed for symptomatic RGB from January 2000 to December 2015 at the Department of Surgical Gastroenterology, Sanjay Gandhi Post Graduate Institute of Medical Sciences, Lucknow, which is a tertiary care institution in north India. Data was collected and analyzed for the demographics, investigations, and details of the initial and later surgery. The remnant gallbladder was termed as RGB and the surgical removal of RGB was termed as completion cholecystectomy. Follow up data was obtained from outpatient follow up cards, postal and telephonic communication. Data was analyzed using the Statistical Package for the Social Sciences (SPSS) software (version 21.0). RESULTS There were 93 patients who underwent surgery for RGB. The median age was 45 (25-70) years and 69 (74.2%) patients were females. All patients underwent the initial cholecystectomy at another hospital except for one. The initial cholecystectomy was by an open approach in 72 (77.4%) patients and by laparoscopic approach in the remaining 21 (22.6%) patients, of which 10 were laparoscopy converted to open (10.6%) cholecystectomy. The reasons for incomplete cholecystectomy were available for 27 patients (29%). These included frozen Calot s triangle anatomy (14, 15.1%), acute cholecystitis (3, 3.2%), empyema (3, 3.2%), dense adhesions (3, 3.2%), intrahepatic gallbladder (2, 2.2%), iatrogenic duodenal injury (2, 2.2%) and unclear anatomy (1, 1.1%). In the remainder of the patients (n=66; 71%), the indications for incomplete gallbladder removal were not clear from the available records. Intraoperative cholangiogram was not performed in any of these patients. The median time to development of symptoms after the Table 1. Clinical presentation of residual gallbladder (N=93) Clinical presentation N (%) Biliary colic Obstructive jaundice Cholangitis Biliary pancreatitis Residual gallbladder-cutaneous fistula Epigastric discomfort 64 (68.8) 8 (8.6) 10 (10.8) 5 (5.4) 4 (4.3) 2 (2.2) initial subtotal cholecystectomy was 36 months (1 to 252 months). The recurrence of pain, that is reminiscent of biliary colic before the initial cholecystectomy, was the most common presentation in 64 (68.8%) patients. Other presenting symptoms were jaundice with/without cholangitis, acute pancreatitis, cholecysto-cutaneous fistula, and epigastric discomfort (Table 1). The serum bilirubin level increased in 7 (7.5%) patients and alkaline phosphatase increased in 19 (20.4%). Abdominal ultrasound examination (ultrasonography; USG) was useful to diagnose RGB in 91 patients (97.8%) and to accurately identify RGB calculi in 81 (89%). However, the USG failed to diagnose RGB calculi in 10 (11%) patients. Overall, common bile duct (CBD) stones were associated with RGB in 23 patients (24.7%). Of these, the USG displayed CBD stones in 13 patients and only CBD dilatation in 5 patients. The USG exhibited CBD dilatation in 5 other patients who later did not turn out to have CBD stones. In one patient, the USG misinterpreted stones in a RGB as CBD stones. Magnetic resonance cholangio-pancreatography (MRCP) was performed in 50 (53.8%) patients and was performed routinely from the year 2008 onwards. The MRCP accurately diagnosed the RGB calculi in all of the cases except for 2 (4%), in whom it was diagnosed during a surgery for CBD stones after a failed endoscopic retrograde cholangiopancreatography (ERCP) clearance. In addition, the MRCP detected CBD stones in all 12 patients, where it was performed (Fig. 1). Computed tomography (CT) scans were conducted in 15 patients; of these, 7 were performed for the suspicion of gallbladder cancer (none of them turned out to be carcinoma in histopathology), 3 for the evaluation of pancreatitis, 1 for the evaluation of the sinus tract, 1 for the evaluation of pain in the abdomen after USG which could not be RGB, and the reason was not clear in 3 patients. A pre-operative ERCP was done in 25 (26.9%) patients. At ERCP, CBD stones were found in 17 (68%) patients, of whom 10 (58.8%) underwent successful endoscopic clearance. All 93 patients in the study underwent completion cholecystectomy in our department. The median time interval between initial cholecystectomy and completion cholecystectomy was 60 (3-288) months. Completion cholecystectomy was performed by an open method in 45
3 38 Ann Hepatobiliary Pancreat Surg Vol. 22, No. 1, February 2018 Fig. 1. MRC reconstruction displays a residual gallbladder with a stone (marked with solid arrow), as well as choledocholithiasis (marked with hollow arrow). Fig. 2. Intraoperative picture during laparoscopic completion cholecystectomy that displays residual gallbladder with a triangle of safety after Calot s triangle dissection. (48.4%) patients; whereas, laparoscopic completion chol- There was no mortality and the postoperative morbidity ecystectomy was attempted in 48 (51.6%) patients was 11% (n=10): all patients had a wound infection and (conversion to open in 19 [20.4%]) (Fig. 2). The reasons 2 patients among them developed incisional hernia during for conversion were as follows: difficulty with identifying follow up. Follow up was available for 65 patients (70%), the anatomy of the Calot s triangle in 8 (42.1%), dense with an average duration of 23.1 months (from adhesions in 10 (52.6%) and suspicion of an RGB-duode- months). Of these, 56 patients (86.15%) had complete nal fistula in 1 patient (5.2%). Out of 93 patients, stones symptom resolution (excellent outcome), and 8 (12.3%) in the residual gallbladder were present in 90 (96.8%). had minimal symptoms with occasional dyspepsia and up- Mirizzi s syndrome was associated in 10 patients (10.8%); per abdominal discomfort after surgery (good outcome). 9 were just compression and one patient had type 4 One patient had persistent pain that, on further evaluation, Mirizzi s syndrome (fistula with CBD). RGB had a fistu- was found to have a right renal pelvis stone, and had lous communication with adjacent structures in 9 (9.7%) symptom patients: duodenum, 4 (4.3%); abdominal wall, 4 (4.3%); nephrolithotomy. Thus, 64 out of the 65 (97%) patients and common bile duct, 1 (1%). with available follow up data had excellent or good out- Additional biliary procedures were conducted in 13 relief after a session of percutaneous come after surgery. (14%) patients: CBD exploration, (n=6), CBD exploration DISCUSSION with choledocho-duodenostomy, (n=4), and Roux-en-Y hepatico-jejunostomy, (n=3). Two patients had intra-operative complications, namely a duodenal serosal injury and In this study, we described the presentation, evaluation a hepatic sinusoidal bleed, which were addressed during and surgical management of 93 patients with symptomatic surgery. RGB at our center with good to excellent outcomes in At pathology, the median size of the RGB was 3 cm 97% of the patients after completion cholecystectomy. To (range: 1-7). Histopathological examinations of the re- the best of our knowledge, this study is the largest inves- sected RGBs revealed xanthogranulomatous cholecystitis tigation of the management of such cases published to in 9 (9.6%), acute on chronic cholecystitis in 2 (2.2%), date (Table 2). follicular cholecystitis in 1 (1%), and the remaining patients had features of chronic cholecystitis. Following an incomplete gallbladder removal, the remnant, which may comprise of a cystic duct with variable
4 Ashish Singh, et al. Management of residual gall bladder 39 Table 2. Literature on the surgical management of the residual gallbladder Study N Index surgery (n) Presentation (n) RGB pathology (n) Second surgery (n) Additional biliary procedure (n) Chowbey et al. 14 Palanivelu et al. 2 Tantia et al. 12 Walsh et al. 4 Current series LC-12 OC-9 C ostomy-5 LC-2 LStC-13 OC-6 LC-1 OC-3 LC-4 OC-72 LC-11 L to O-10 Persistent pain RHC-17 Recurrent biliary colics-9 Jaundice-9 Postprandial nausea after fatty meal-3 Intermittent low grade fever-1 Abdominal distension and diarrhea-1 Abdomen pain-7 Cholangitis-2 Jaundice-4 Asymptomatic-2 Abdomen pain-7 Fever-1 Biliary colic-7 Jaundice-2 Biliary pancreatitis-1 Biliary colic-64 Jaundice-8 Cholangitis-10 Biliary pancreatitis-5 RGB-cutaneous fistula-4 Epigastric dyscomfort-2 RGB calculi-26 RGB* calculi-15/15 Cirrhosis-3/15 CBD stone+rgb without stone-2/7 RGB calculi-5/7 RGB calculi-7/7 RGB calculi-90 RGB fistula with duodenum-4 RGB fistula with CBD (type IV Mirizzi)-1 RSB fistula with abdominal wall-4 Mirizzi Type I-9 LCC-26 LCC-15 LCC-7 OCC-4 LCC-1 OCC-45 LCC-29 L to O-19 None T-tube-4 Lap CBDE-2 Lap CDD-1 No Open CBDE-6 CDD-4 RYHJ-3 *The authors referred to RGBs as cystic duct stumps LC, Laparoscopic cholecystectomy; OC, Open cholecystectomy; C ostomy, Cholecystostomy; LStC, Laparoscopic subtotal cholecystectomy; LCC, Laparoscopic completion cholecystectomy; OCC, Open completion cholecystectomy; L to O, Laparoscopic converted to open; CBD, Common bile duct; CDD, Choledochoduodenostomy; RGB, Residual gallbladder; CBDE, Common bile duct exploration; RYHJ, Roux-en-Y Hepaticojejunostomy amounts of gallbladder, has been addressed by several names including cystic duct stump, gallbladder stump, gallbladder remnant or residual gallbladder. 2,15-18 As it is difficult to differentiate a grossly dilated cystic duct stump from a true gallbladder remnant on the basis of imaging or even histological findings, 12,19 we believe that the term, residual gallbladder, appropriately describes the remnant of the gallbladder. Incomplete removal of the gallbladder, also known as subtotal cholecystectomy, may be done intentionally in situations of severe inflammation, unclear anatomy or risk of hemorrhage as in portal hypertension. A subtotal cholecystectomy is required in about 3 to 8% of patients undergoing surgery for gallstone disease and has proven to be a safe and effective option in such patients with gall stone disease to avoid iatrogenic complications. 20 In the current study, we observed that among the RGBs, 29% were intentional subtotal cholecystectomy. In the remaining 71% patients, where the initial operating surgeon did not document an incomplete gallbladder removal, we assumed that the RGB was left behind unintentionally. RGB may be left behind unintentionally if the cystic duct - gallbladder junction is not identified correctly. 4,23 The incidence of unintentional incomplete removal of the gallbladder is unknown. Though some authors have suggested that it may be higher following a laparoscopic cholecystectomy, 4,15,17,18,23 but in our experience, 77.4% of the patients had index surgery via an open technique, and additionally, 10 patients (10.8%) had RGB after laparoscopy converted to open cholecystectomy. This outcome is similar to that reported by the small case studies by Tantia et al. (6 out of 7) and Rozsos et al. (5 out of 8). 12,13 The incidence of stones in RGB varies widely (0%-13%). 11,20,24 The incidence can be quite low if the remnant is opened, all of the stones and debris are meticulously removed, and the mucosa of the remaining gall bladder
5 40 Ann Hepatobiliary Pancreat Surg Vol. 22, No. 1, February 2018 is cauterized. 11,20 The true incidence of symptomatic RGB after subtotal cholecystectomy is unknown, usually because the initial surgery was performed elsewhere. 10,12 The diagnosis of RGB remains difficult and an unaware clinician may fail to diagnose the condition and may subject the patient to a battery of unnecessary investigations. The most common presentation of patients with RGB is recurrent typical biliary colic that is reminiscent of the pain before the initial cholecystectomy (Table 2). 2,10-12 Therefore, a history of recurrent biliary colic similar to the pain for which the initial cholecystectomy was performed should raise the suspicion of RGB. 10 The operative records of the initial cholecystectomy should be reviewed to ascertain whether the entire gallbladder was removed. However, as demonstrated by this study, an absence of documentation of incomplete gallbladder removal at the initial surgery does not rule out the possibility of RGB. The liver function tests are usually normal; any derangement points towards a pathology co-existing with RGB, like CBD stones or pancreatitis. The diagnosis can be made with the help of an USG, MRCP, CT and ERCP. 25 At our institution presently, USG is the initial investigation if RGB is suspected and can diagnose stones in the RGB as well. However, the USG may miss stones in the RGB in some patients (11% in this study) and CBD stones in others (18% in this study). In addition, RGB is often associated with other pathologies like Mirizzi syndrome, internal fistula, etc., that may be missed by an USG. In this study, the MRCP detected associated pathology like CBD stones (24.7%), Mirizzi s syndrome (10.8%) and internal biliary fistula (9.7%). MRCP was the investigation of choice for the diagnosis of RGB and to demonstrate biliary anatomy and any associated pathology. Most studies on RGB have not provided information on these aspects. Palanivelu et al also found MRCP to be better than USG (accuracy - 92% and 60% respectively) in diagnosing cystic duct remnant calculi. 2 MRCP is now routine at our institution after USG in cases wherein RGB is suspected. The treatment of symptomatic RGB is completion cholecystectomy of the remnant gallbladder. Although there are a few case reports of management of RGB stones with ERCP/extracorporeal shockwave lithotripsy, 10,26-29 we believe that it does not treat the cause of the pathology, i.e., the RGB. The surgical removal of a RGB can be technically demanding since these patients usually have a history of difficult gallbladder pathology that is further compounded by adhesions due to the initial surgery. Rozsos et al considered laparoscopic surgery to be risky and demonstrated the feasibility of completion cholecystectomy by microlaparotomy incisions. 13,30 Recently, some studies from institutions with advanced laparoscopic experience have reported successful laparoscopic removal of a RGB. 2,11,12 We performed completion cholecystectomy by both laparoscopic and open techniques. The laparoscopic approach was feasible (completion in 31.2%), but was associated with a higher conversion rate of nearly 40%, due to a difficult cholecystectomy. In the literature, there are a few case reports and small studies that primarily demonstrated successful laparoscopic completion cholecystectomy, with 0% conversion rates. 2,11,12,14,15 In experienced surgical units, completion cholecystectomy can be safely performed with low morbidity and mortality. We found preoperative MRCP to be good road map to a safe completion cholecystectomy and recommend it in all patients with a suspected RGB. Interestingly, the histopathological examination of a resected RGB revealed a high incidence (9.6%) of xanthogranulomatous inflammation. Ninety-eight percent (n=64) of the 65 patients that had available data for follow up (70%) reported complete resolution of symptoms after completion cholecystectomy at an average duration of follow-up of 23.1 months. Other studies in the literature have similarly reported excellent results after completion cholecystectomy. 2,10-14 In conclusion, after a cholecystectomy, a clinical history of recurrent biliary colic that is reminiscent of the pain for which the initial cholecystectomy was performed should strongly raise the suspicion of an RGB. MRCP is a useful investigation for establishing the diagnosis, diagnosing any associated problems, and providing a roadmap for further surgery. Completion cholecystectomy for symptomatic RGB can be performed safely at specialist centers with low morbidity rates and excellent relief of symptoms. Laparoscopic completion cholecystectomy is feasible, but is technically difficult and associated with a high conversion rate. REFERENCES 1. Philips JA, Lawes DA, Cook AJ, Arulampalam TH, Zaborsky
6 Ashish Singh, et al. Management of residual gall bladder 41 A, Menzies D, et al. The use of laparoscopic subtotal cholecystectomy for complicated cholelithiasis. Surg Endosc 2008;22: Palanivelu C, Rangarajan M, Jategaonkar PA, Madankumar MV, Anand NV. Laparoscopic management of remnant cystic duct calculi: a retrospective study. Ann R Coll Surg Engl 2009;91: Michalowski K, Bornman PC, Krige JE, Gallagher PJ, Terblanche J. Laparoscopic subtotal cholecystectomy in patients with complicated acute cholecystitis or fibrosis. Br J Surg 1998;85: Walsh RM, Chung RS, Grundfest-Broniatowski S. Incomplete excision of the gallbladder during laparoscopic cholecystectomy. Surg Endosc 1995;9: Womack NA, Crider RL. The persistence of symptoms following cholecystectomy. Ann Surg 1947;126: Lum YW, House MG, Hayanga AJ, Schweitzer M. Postcholecystectomy syndrome in the laparoscopic era. J Laparoendosc Adv Surg Tech A 2006;16: Chow M, von Waldenfels A, Pace R. An unusual case of a retained stone following laparoscopic cholecystectomy. J Laparoendosc Surg 1993;3: Woods MS, Farha GJ, Street DE. Cystic duct remnant fistulization to the gastrointestinal tract. Surgery 1992;111: Satorras AM, Villanueva L, Vázquez J, Pigni L, Salem AM, Ramos A. Acute cholecystitis secondary to recurrent cholelithiasis after subtotal cholecystectomy. Cir Esp 2005;77: Walsh RM, Ponsky JL, Dumot J. Retained gallbladder/cystic duct remnant calculi as a cause of postcholecystectomy pain. Surg Endosc 2002;16: Chowbey PK, Bandyopadhyay SK, Sharma A, Khullar R, Soni V, Baijal M. Laparoscopic reintervention for residual gallstone disease. Surg Laparosc Endosc Percutan Tech 2003;13: Tantia O, Jain M, Khanna S, Sen B. Post cholecystectomy syndrome: Role of cystic duct stump and re-intervention by laparoscopic surgery. J Minim Access Surg 2008;4: Rozsos I, Magyaródi Z, Orbán P. Cystic duct syndrome and minimally invasive surgery. Orv Hetil 1997;138: Chowbey P, Soni V, Sharma A, Khullar R, Baijal M. Residual gallstone disease - Laparoscopic management. Indian J Surg 2010;72: Pernice LM, Andreoli F. Laparoscopic treatment of stone recurrence in a gallbladder remnant: report of an additional case and literature review. J Gastrointest Surg 2009;13: Rogy MA, Függer R, Herbst F, Schulz F. Reoperation after cholecystectomy. The role of the cystic duct stump. HPB Surg 1991;4: Daly TD, Martin CJ, Cox MR. Residual gallbladder and cystic duct stones after laparoscopic cholecystectomy. ANZ J Surg 2002;72: Rieger R, Wayand W. Gallbladder remnant after laparoscopic cholecystectomy. Surg Endosc 1995;9: Mergener K, Clavien PA, Branch MS, Baillie J. A stone in a grossly dilated cystic duct stump: a rare cause of postcholecystectomy pain. Am J Gastroenterol 1999;94: Ibrarullah MD, Kacker LK, Sikora SS, Saxena R, Kapoor VK, Kaushik SP. Partial cholecystectomy--safe and effective. HPB Surg 1993;7: Chowbey PK, Sharma A, Khullar R, Mann V, Baijal M, Vashistha A. Laparoscopic subtotal cholecystectomy: a review of 56 procedures. J Laparoendosc Adv Surg Tech A 2000;10: Ji W, Li LT, Li JS. Role of laparoscopic subtotal cholecystectomy in the treatment of complicated cholecystitis. Hepatobiliary Pancreat Dis Int 2006;5: Blackard WG Jr, Baron TH. Leaking gallbladder remnant with cholelithiasis complicating laparoscopic cholecystectomy. South Med J 1995;88: Beldi G, Glättli A. Laparoscopic subtotal cholecystectomy for severe cholecystitis. Surg Endosc 2003;17: Kim JY, Kim KW, Ahn CS, Hwang S, Lee YJ, Shin YM, et al. Spectrum of biliary and nonbiliary complications after laparoscopic cholecystectomy: radiologic findings. AJR Am J Roentgenol 2008;191: Wani NA, Khan NA, Shah AI, Khan AQ. Post-cholecystectomy Mirizzi's syndrome: magnetic resonance cholangiopancreatography demonstration. Saudi J Gastroenterol 2010;16: Shelton JH, Mallat DB. Endoscopic retrograde removal of gallbladder remnant calculus. Gastrointest Endosc 2006;64: Kodali VP, Petersen BT. Endoscopic therapy of postcholecystectomy Mirizzi syndrome. Gastrointest Endosc 1996;44: Benninger J, Rabenstein T, Farnbacher M, Keppler J, Hahn EG, Schneider HT. Extracorporeal shockwave lithotripsy of gallstones in cystic duct remnants and Mirizzi syndrome. Gastrointest Endosc 2004;60: Rozsos I, Magyaródi Z, Orbán P. The removal of cystic duct and gallbladder remnant by microlaparotomy. Acta Chir Hung 1997;36:
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 42/ May 25, 2015 Page 7258
 LAPAROSCOPIC COMPLETION CHOLECYSTECTOMY FOR POST CHOLECYSTECTOMY SYNDROME Zahur Hussain 1, Himanshu Sharma 2, Vikrant Singh Chandail 3, Barinder Kumar 4, Suneel Mattoo 5, Ashufta Rasool 6, Anshuman Sharma
LAPAROSCOPIC COMPLETION CHOLECYSTECTOMY FOR POST CHOLECYSTECTOMY SYNDROME Zahur Hussain 1, Himanshu Sharma 2, Vikrant Singh Chandail 3, Barinder Kumar 4, Suneel Mattoo 5, Ashufta Rasool 6, Anshuman Sharma
Mirizzi s syndrome: lessons learnt from 169 patients at a single center
 Korean J Hepatobiliary Pancreat Surg 21;2:17-22 http://dx.doi.org/1.1471/kjhbps.21.2.1.17 Original Article Mirizzi s syndrome: lessons learnt from 19 patients at a single center Ashok Kumar, Ganesan Senthil,
Korean J Hepatobiliary Pancreat Surg 21;2:17-22 http://dx.doi.org/1.1471/kjhbps.21.2.1.17 Original Article Mirizzi s syndrome: lessons learnt from 19 patients at a single center Ashok Kumar, Ganesan Senthil,
Arpit Amin, Yuriy Zhurov, George Ibrahim, Anthony Maffei, Jonathan Giannone, Thomas Cerabona, and Ashutosh Kaul
 Case Reports in Surgery Volume 2016, Article ID 1896368, 9 pages http://dx.doi.org/10.1155/2016/1896368 Case Report Combined Endoscopic and Management of Postcholecystectomy Mirizzi Syndrome from a Remnant
Case Reports in Surgery Volume 2016, Article ID 1896368, 9 pages http://dx.doi.org/10.1155/2016/1896368 Case Report Combined Endoscopic and Management of Postcholecystectomy Mirizzi Syndrome from a Remnant
JMSCR Vol 05 Issue 04 Page April 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i4.11 Post Cholecystectomy Stump Calculus Cholecystitis
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i4.11 Post Cholecystectomy Stump Calculus Cholecystitis
Risk Factors for Development of Biliary Stricture in Patients Presenting with Bile Leak after Cholecystectomy
 Gut and Liver, Vol. 7, No. 3, May 2013, pp. 352-356 ORiginal Article Risk Factors for Development of Biliary Stricture in Patients Presenting with Bile Leak after Cholecystectomy Hosur Mayanna Lokesh,
Gut and Liver, Vol. 7, No. 3, May 2013, pp. 352-356 ORiginal Article Risk Factors for Development of Biliary Stricture in Patients Presenting with Bile Leak after Cholecystectomy Hosur Mayanna Lokesh,
Complication of Laparoscopic Cholecystectomy
 Complication of Laparoscopic Cholecystectomy R.K.Mishra What to do if something goes wrong There is not a single laparoscopic surgeon in the world who has not damaged CBD Complications Early Common bile
Complication of Laparoscopic Cholecystectomy R.K.Mishra What to do if something goes wrong There is not a single laparoscopic surgeon in the world who has not damaged CBD Complications Early Common bile
ISSN X (Print) Research Article. *Corresponding author Jitendra Singh Yadav
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo Shin Choi 2, and Seung Eun Lee 2. Departments of Surgery, Dongguk University College of Medicine 2
 Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Study of post cholecystectomy biliary leakage and its management
 Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience
 Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study
 Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Recurrent abdominal pain after laparoscopic cholecystectomy
 IM BOARD REVIEW CAROLE MACARON, MD Department of Internal Medicine, Cleveland Clinic MOHAMMED A. QADEER, MD, MPH Department of Gastroenterology and Hepatology, Cleveland Clinic JOHN J. VARGO, MD, MPH Department
IM BOARD REVIEW CAROLE MACARON, MD Department of Internal Medicine, Cleveland Clinic MOHAMMED A. QADEER, MD, MPH Department of Gastroenterology and Hepatology, Cleveland Clinic JOHN J. VARGO, MD, MPH Department
Per-operative conversion of laparoscopic cholecystectomy to open surgery: prospective study at JSS teaching hospital, Karnataka, India
 International Surgery Journal Raza M et al. Int Surg J. 2017 Jan;4(1):81-85 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163977
International Surgery Journal Raza M et al. Int Surg J. 2017 Jan;4(1):81-85 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163977
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
Kathmandu University Medical Journal (2009), Vol. 7, No. 1, Issue 25, 26-30
 Kathmandu University Medical Journal (29), Vol. 7, No. 1, Issue 25, 2-3 Original Article Evaluation of predictive factors for conversion of laparoscopic cholecystectomy Gabriel R, Kumar S, Shrestha A Department
Kathmandu University Medical Journal (29), Vol. 7, No. 1, Issue 25, 2-3 Original Article Evaluation of predictive factors for conversion of laparoscopic cholecystectomy Gabriel R, Kumar S, Shrestha A Department
Post Laparoscopic Cholecystectomy Biloma in a Child Managed by Endoscopic Retrograde Cholangio-Pancreatography and Stenting: A Case Report
 pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2016.19.4.281 Pediatr Gastroenterol Hepatol Nutr 2016 December 19(4):281-285 Case Report PGHN Post Laparoscopic Cholecystectomy Biloma in
pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2016.19.4.281 Pediatr Gastroenterol Hepatol Nutr 2016 December 19(4):281-285 Case Report PGHN Post Laparoscopic Cholecystectomy Biloma in
담낭절제술후발생한미리찌증후군의내시경적치료 1 예
 Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM
 A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital
 Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Study of the degree of gall bladder wall thickness and its impact on outcomes following laparoscopic cholecystectomy in JSS Hospital
 International Surgery Journal Chandra SBJ et al. Int Surg J. 2018 Apr;5(4):1417-1421 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181122
International Surgery Journal Chandra SBJ et al. Int Surg J. 2018 Apr;5(4):1417-1421 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181122
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018)
 Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
The Present Scenario of Cholecystectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
Evaluation of Complications Occurring in Patients Undergoing Laparoscopic Cholecystectomy: An Institutional Based Study
 Original article: Evaluation of Complications Occurring in Patients Undergoing Laparoscopic Cholecystectomy: An Institutional Based Study Sudhir Tyagi 1, Sanjeev Kumar 2* 1 Assistant Professor, 2* Associate
Original article: Evaluation of Complications Occurring in Patients Undergoing Laparoscopic Cholecystectomy: An Institutional Based Study Sudhir Tyagi 1, Sanjeev Kumar 2* 1 Assistant Professor, 2* Associate
Downloaded from jssu.ssu.ac.ir at 13:10 IRST on Saturday October 28th 2017
 Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010
 Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Case Report Simultaneous Non-Traumatic Perforation of Right Hepatic Duct and Gallbladder: An Atypical Occurrence
 Case Report Simultaneous Non-Traumatic Perforation of Right Hepatic Duct and Gallbladder: An Atypical Occurrence Pankaj Kumar GARG1, Bhupendra Kumar JAIN1, Satya Deo PANDEY1, Vinita RATHI2, Amarendra Singh
Case Report Simultaneous Non-Traumatic Perforation of Right Hepatic Duct and Gallbladder: An Atypical Occurrence Pankaj Kumar GARG1, Bhupendra Kumar JAIN1, Satya Deo PANDEY1, Vinita RATHI2, Amarendra Singh
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Predictors of abnormalities on magnetic resonance cholangiopancreatography: is there a role when the biliary tree is normal on previous imaging?
 ORIGINAL ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Predictors of abnormalities on magnetic resonance cholangiopancreatography: is there a role when the biliary tree is normal on previous imaging?
ORIGINAL ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Predictors of abnormalities on magnetic resonance cholangiopancreatography: is there a role when the biliary tree is normal on previous imaging?
A one-year study of cholelithiasis at a tertiary care hospital of South India
 International Surgery Journal Rachamalla RR et al. Int Surg J. 2018 Jul;5(7):2444-2448 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182502
International Surgery Journal Rachamalla RR et al. Int Surg J. 2018 Jul;5(7):2444-2448 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182502
The campaign on laboratory: focus on Gallstone Disease and ERCP
 The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
Pre-operative prediction of difficult laparoscopic cholecystectomy
 International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
Appendix A: Summary of evidence from surveillance
 Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Pre-operative MRCP: is it necessary before routine laparoscopic cholecystectomy to exclude CBD stone-prospective study in tertiary care hospital
 International Surgery Journal Rao GB et al. Int Surg J. 2017 Nov;4(11):3633-3637 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174636
International Surgery Journal Rao GB et al. Int Surg J. 2017 Nov;4(11):3633-3637 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174636
Personal Profile. Name: 劉 XX Gender: Female Age: 53-y/o Past history. Hepatitis B carrier
 Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Management of Gallbladder Disease
 Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Hemobilia due to arteriobiliary fistula complicating ERCP for residual bile duct stone in a case of Mirizzi syndrome
 Ann Hepatobiliary Pancreat Surg 2017;21:88-92 https://doi.org/10.14701/ahbps.2017.21.2.88 Case Report Hemobilia due to arteriobiliary fistula complicating ERCP for residual bile duct stone in a case of
Ann Hepatobiliary Pancreat Surg 2017;21:88-92 https://doi.org/10.14701/ahbps.2017.21.2.88 Case Report Hemobilia due to arteriobiliary fistula complicating ERCP for residual bile duct stone in a case of
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Hepatobiliary and Pancreatic Diseases (IJHPD) Type of Article:
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Hepatobiliary and Pancreatic Diseases (IJHPD) Type of Article:
Surveillance proposal consultation document
 Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
EAST MULTICENTER STUDY PROPOSAL
 EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
Research Article Surgically Resected Gall Bladder: Is Histopathology Needed for All?
 Surgery Research and Practice Volume 2016, Article ID 9319147, 4 pages http://dx.doi.org/10.1155/2016/9319147 Research Article Surgically Resected Gall Bladder: Is Histopathology Needed for All? Vikash
Surgery Research and Practice Volume 2016, Article ID 9319147, 4 pages http://dx.doi.org/10.1155/2016/9319147 Research Article Surgically Resected Gall Bladder: Is Histopathology Needed for All? Vikash
Mirizzi syndrome with an unusual type of biliobiliary fistula a case report
 Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis
 Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
Lutheran Medical Center. Daniel H. Hunt, M.D. June 10 th, 2005
 Lutheran Medical Center Daniel H. Hunt, M.D. June 10 th, 2005 History xx y.o. pt with primary CBD stones s/p ERCP xx months earlier for attempted stone extraction resulting in post ERCP pancreatitis. Patient
Lutheran Medical Center Daniel H. Hunt, M.D. June 10 th, 2005 History xx y.o. pt with primary CBD stones s/p ERCP xx months earlier for attempted stone extraction resulting in post ERCP pancreatitis. Patient
Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study
 Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Evaluation of complications and conversion rate of laparoscopic cholecystectomy in Rural Medical College
 Original article Evaluation of complications and conversion rate of laparoscopic cholecystectomy in Rural Medical College Satish Kumar Bansal 1, Sandeep Kumar Goyal 1, Umesh Kumar Chhabra 1, Pawan Kumar
Original article Evaluation of complications and conversion rate of laparoscopic cholecystectomy in Rural Medical College Satish Kumar Bansal 1, Sandeep Kumar Goyal 1, Umesh Kumar Chhabra 1, Pawan Kumar
ENDOSCOPIC TREATMENT OF A BILE DUCT
 HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES
 Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES Yunfeng Cui, Hongtao Zhang, Naiqiang Cui, Zhonglian Li* Department of Surgery, Tianjin Nankai Hospital,
Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES Yunfeng Cui, Hongtao Zhang, Naiqiang Cui, Zhonglian Li* Department of Surgery, Tianjin Nankai Hospital,
The authors have declared no conflicts of interest.
 Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Biliary MRI w Eovist
 Biliary MRI w Eovist Is there any added value? Elmar M. Merkle, MD Director of MR Imaging Duke University Medical Center elmar.merkle@duke.edu Declaration of Conflict of Interest or Relationship Research
Biliary MRI w Eovist Is there any added value? Elmar M. Merkle, MD Director of MR Imaging Duke University Medical Center elmar.merkle@duke.edu Declaration of Conflict of Interest or Relationship Research
Laparoscopic Subtotal Cholecystectomy for Difficult Acute Calculous Cholecystitis
 Journal of Surgery 2017; 5(6): 111-117 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20170506.15 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Laparoscopic Subtotal Cholecystectomy
Journal of Surgery 2017; 5(6): 111-117 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20170506.15 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Laparoscopic Subtotal Cholecystectomy
All cholecystectomy specimens must be sent for histopathology to detect inapparent gallbladder cancer
 DOI:10.1111/j.1477-2574.2012.00443.x HPB ORIGINAL ARTICLE All cholecystectomy specimens must be sent for histopathology to detect inapparent gallbladder cancer Anil K. Agarwal, Raja Kalayarasan, Shivendra
DOI:10.1111/j.1477-2574.2012.00443.x HPB ORIGINAL ARTICLE All cholecystectomy specimens must be sent for histopathology to detect inapparent gallbladder cancer Anil K. Agarwal, Raja Kalayarasan, Shivendra
REFERRAL GUIDELINES: GALLSTONES
 REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
Gallstone ileus:diagnostic and therapeutic dilemma
 Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
Gallstones Information Leaflet THE DIGESTIVE SYSTEM. Gutscharity.org.uk
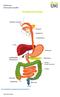 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about gallstones Gall is an old-fashioned word for bile, a liquid made in the liver and stored in the gall bladder
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about gallstones Gall is an old-fashioned word for bile, a liquid made in the liver and stored in the gall bladder
Surgical management of common bile duct stones in ERCP procedure failur patients
 Original article: Surgical management of common bile duct stones in ERCP procedure failur patients Dr. Rajesh G. Patil *, Dr. Rajeshkumar C. Mahey **, Dr Sanchit A. Khare ***, Dr. Nilesh Bakale ***, Dr.
Original article: Surgical management of common bile duct stones in ERCP procedure failur patients Dr. Rajesh G. Patil *, Dr. Rajeshkumar C. Mahey **, Dr Sanchit A. Khare ***, Dr. Nilesh Bakale ***, Dr.
Laparoscopic Cholecystectomy: A Retrospective Study
 Bahrain Medical Bulletin, Vol. 37, No. 3, September 2015 Laparoscopic Cholecystectomy: A Retrospective Study Abdullah Al-Mitwalli, LRCPI, LRCSI* Martin Corbally, MBBCh, BAO, MCh, FRCSI, FRCSEd, FRCS**
Bahrain Medical Bulletin, Vol. 37, No. 3, September 2015 Laparoscopic Cholecystectomy: A Retrospective Study Abdullah Al-Mitwalli, LRCPI, LRCSI* Martin Corbally, MBBCh, BAO, MCh, FRCSI, FRCSEd, FRCS**
Naoyuki Toyota, Tadahiro Takada, Hodaka Amano, Masahiro Yoshida, Fumihiko Miura, and Keita Wada
 J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
Biomedical Research 2017; 28 (15):
 Biomedical Research 2017; 28 (15): 6671-6676 ISSN 0970-938X www.biomedres.info Single surgeon experience: intraoperative complications and conversion to open surgery in laparoscopic cholecystectomy, the
Biomedical Research 2017; 28 (15): 6671-6676 ISSN 0970-938X www.biomedres.info Single surgeon experience: intraoperative complications and conversion to open surgery in laparoscopic cholecystectomy, the
Cholelithiasis & cholecystitis
 1 Cholelithiasis & cholecystitis Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA) Assistant Professor, Dept. of Surgery College of Medicine, Prince Sattam bin Abdulaziz University Email: surgeon.shamim@gmail.com
1 Cholelithiasis & cholecystitis Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA) Assistant Professor, Dept. of Surgery College of Medicine, Prince Sattam bin Abdulaziz University Email: surgeon.shamim@gmail.com
Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder in an Elderly Patient
 Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 6 The Role of Ultrasound in Laprascopic Cholecystectomy Faris D. Alaswad University of Baghdad, faris alaswad@yahoo.com Copyright c 2014
World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 6 The Role of Ultrasound in Laprascopic Cholecystectomy Faris D. Alaswad University of Baghdad, faris alaswad@yahoo.com Copyright c 2014
Management of gallstone disease in children: a new protocol based on the experience of a single center
 Universidade de São Paulo Biblioteca Digital da Produção Intelectual - BDPI Sem comunidade WoS 2012 Management of gallstone disease in children: a new protocol based on the experience of a single center
Universidade de São Paulo Biblioteca Digital da Produção Intelectual - BDPI Sem comunidade WoS 2012 Management of gallstone disease in children: a new protocol based on the experience of a single center
Factors influencing the conversion of Laparoscopic to Open Cholecystectomy
 Original article Factors influencing the conversion of Laparoscopic to Open Cholecystectomy Satish Kumar Bansal 1, Umesh Kumar Chhabra 1, Sandeep Kumar Goyal 1, Gopal Singal 2, Pawan Kumar Goyal 2 1 Assistant
Original article Factors influencing the conversion of Laparoscopic to Open Cholecystectomy Satish Kumar Bansal 1, Umesh Kumar Chhabra 1, Sandeep Kumar Goyal 1, Gopal Singal 2, Pawan Kumar Goyal 2 1 Assistant
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy. TEAM 1 Janix M. De Guzman, MD Presentor
 Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Case Report Solitary Osteolytic Skull Metastasis in a Case of Unknown Primary Being latter Diagnosed as Carcinoma of Gall Bladder
 Cronicon OPEN ACCESS CANCER Case Report Solitary Osteolytic Skull Metastasis in a Case of Unknown Primary Being latter Diagnosed as Carcinoma of Gall Kartik Mittal 1, Rajaram Sharma 1, Amit Dey 1, Meet
Cronicon OPEN ACCESS CANCER Case Report Solitary Osteolytic Skull Metastasis in a Case of Unknown Primary Being latter Diagnosed as Carcinoma of Gall Kartik Mittal 1, Rajaram Sharma 1, Amit Dey 1, Meet
DISCLAIMER. No Conflict of Interest
 DISCLAIMER No Conflict of Interest EXCLAIMER No Interest in Conflict GALLSTONES FAQs and FACTS John Dunn, FRACS Laparoscopy Auckland YOU GOTTA KNOW THIS STUFF HOW DO THEY FORM? Gallbladder Lithogenic
DISCLAIMER No Conflict of Interest EXCLAIMER No Interest in Conflict GALLSTONES FAQs and FACTS John Dunn, FRACS Laparoscopy Auckland YOU GOTTA KNOW THIS STUFF HOW DO THEY FORM? Gallbladder Lithogenic
laparoscopic cholecystectomy
 Combined percutaneous and endoscopic approach in management of dropped gallstones following laparoscopic cholecystectomy John S.F. Shum 1*, K.H. Fung 1, George P.C. Yang 2, Chung Ngai Tang 2, Michael K.W.
Combined percutaneous and endoscopic approach in management of dropped gallstones following laparoscopic cholecystectomy John S.F. Shum 1*, K.H. Fung 1, George P.C. Yang 2, Chung Ngai Tang 2, Michael K.W.
Effect of Duration of Surgery on Liver Enzymes After Cholecystectomy: Safety or Duration
 Original Article J Curr Surg. 2017;7(4):53-57 Effect of Duration of Surgery on Liver Enzymes After Cholecystectomy: Safety or Duration Abhishek Sharma a, Rikki Singal a, Amit Mittal b, Amarjit Singh Grover
Original Article J Curr Surg. 2017;7(4):53-57 Effect of Duration of Surgery on Liver Enzymes After Cholecystectomy: Safety or Duration Abhishek Sharma a, Rikki Singal a, Amit Mittal b, Amarjit Singh Grover
Risk Factors for Conversion to Open Surgery in Patients With Acute Cholecystitis Undergoing Interval Laparoscopic Cholecystectomy
 Original Article 631 Risk Factors for Conversion to Open Surgery in Patients With Acute Cholecystitis Undergoing Interval Laparoscopic Cholecystectomy Kok-Ren Lim, 1 MRCS (Edin), Salleh Ibrahim, 1 FRCS
Original Article 631 Risk Factors for Conversion to Open Surgery in Patients With Acute Cholecystitis Undergoing Interval Laparoscopic Cholecystectomy Kok-Ren Lim, 1 MRCS (Edin), Salleh Ibrahim, 1 FRCS
No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study
 Original article Annals of Gastroenterology (2013) 26, 1-6 No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study Rachel M. Gomes
Original article Annals of Gastroenterology (2013) 26, 1-6 No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study Rachel M. Gomes
Bile Duct Injuries. Dr. Bennet Rajmohan, MRCS (Eng), MRCS Ed Consultant General & Laparoscopic Surgeon Apollo Speciality Hospitals Madurai, India
 Bile Duct Injuries Dr. Bennet Rajmohan, MRCS (Eng), MRCS Ed Consultant General & Laparoscopic Surgeon Apollo Speciality Hospitals Madurai, India Introduction Bile duct injury (BDI) rare but potentially
Bile Duct Injuries Dr. Bennet Rajmohan, MRCS (Eng), MRCS Ed Consultant General & Laparoscopic Surgeon Apollo Speciality Hospitals Madurai, India Introduction Bile duct injury (BDI) rare but potentially
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary?
 Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES
 SAFETY AND OUTCOME OF SELECTIVE INTRA-OPERATIVE CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES Ihab Kadry, Mahmoud Reda, Hesham Ahmed and Mohamed ZaaZou. Department Of General Surgery Misr University
SAFETY AND OUTCOME OF SELECTIVE INTRA-OPERATIVE CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES Ihab Kadry, Mahmoud Reda, Hesham Ahmed and Mohamed ZaaZou. Department Of General Surgery Misr University
Predictive Factors for Difficult Surgery in Laparoscopic Cholecystectomy for Chronic Cholecystitis
 ISPUB.COM The Internet Journal of Surgery Volume 16 Number 2 Predictive Factors for Difficult Surgery in Laparoscopic Cholecystectomy for Chronic Cholecystitis S Kumar, S Tiwary, N Agrawal, G Prasanna,
ISPUB.COM The Internet Journal of Surgery Volume 16 Number 2 Predictive Factors for Difficult Surgery in Laparoscopic Cholecystectomy for Chronic Cholecystitis S Kumar, S Tiwary, N Agrawal, G Prasanna,
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction
 Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
Clinical Spectrum of Presentation of Obstructive Jaundice in Inflammation, Stone Disease, and Malignancy
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/326 Clinical Spectrum of Presentation of Obstructive Jaundice in Inflammation, Stone Disease, and Malignancy R Selvasekaran
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/326 Clinical Spectrum of Presentation of Obstructive Jaundice in Inflammation, Stone Disease, and Malignancy R Selvasekaran
Evolving Gallstone Ileus. SUNY Downstate Case Conference January 12, 2012
 Evolving Gallstone Ileus SUNY Downstate Case Conference January 12, 2012 Initial Presentation HPI: 90 yo F c 1wk h/o abdominal pain and N/V. Denied F/C. Passing flatus/bm. PMH: DM, HTN, CAD. PSH: C-sections
Evolving Gallstone Ileus SUNY Downstate Case Conference January 12, 2012 Initial Presentation HPI: 90 yo F c 1wk h/o abdominal pain and N/V. Denied F/C. Passing flatus/bm. PMH: DM, HTN, CAD. PSH: C-sections
Endoscopic management of postoperative bile duct injuries: a single center experience.
 1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation
 Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Laparoscopic management of cholecystoenteric fistula: A single-center experience
 Clinical Report Laparoscopic management of cholecystoenteric fistula: A single-center experience Journal of International Medical Research 2017, Vol. 45(3) 1090 1097! The Author(s) 2017 Reprints and permissions:
Clinical Report Laparoscopic management of cholecystoenteric fistula: A single-center experience Journal of International Medical Research 2017, Vol. 45(3) 1090 1097! The Author(s) 2017 Reprints and permissions:
Laparoscopic Cholecystectomy after Upper Abdominal Surgery : Is It Feasible Even after Gastrectomy?
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2017;20(1):22-28 Journal of Minimally Invasive Surgery Laparoscopic Cholecystectomy after Upper Abdominal Surgery : Is It Feasible
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2017;20(1):22-28 Journal of Minimally Invasive Surgery Laparoscopic Cholecystectomy after Upper Abdominal Surgery : Is It Feasible
Cholecystectomy in a patient with situs inversus
 CASE REPORT Trivedi et al. 1 PEER REVIEWED OPEN ACCESS Cholecystectomy in a patient with situs inversus Govind Trivedi, Rajeev Bhargava, Satish Gupta, Devashish Singh ABSTRACT Situs inversustotalis is
CASE REPORT Trivedi et al. 1 PEER REVIEWED OPEN ACCESS Cholecystectomy in a patient with situs inversus Govind Trivedi, Rajeev Bhargava, Satish Gupta, Devashish Singh ABSTRACT Situs inversustotalis is
Accuracy of ASGE criteria for the prediction of choledocholithiasis
 1130-0108/2016/108/6/309-314 Revista Española de Enfermedades Digestivas Copyright 2016 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid) Vol. 108, N.º 6, pp. 309-314, 2016 ORIGINAL PAPERS Accuracy of
1130-0108/2016/108/6/309-314 Revista Española de Enfermedades Digestivas Copyright 2016 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid) Vol. 108, N.º 6, pp. 309-314, 2016 ORIGINAL PAPERS Accuracy of
Systematic Review of Mirizzi's Syndrome's Management
 REVIEW ARTICLE Systematic Review of Mirizzi's Syndrome's Management Mallikarjuna Uppara, Ashraf Rasheed Gwent Centre for Digestive Diseases University of South Wales, United Kingdom ABSTRACT Background
REVIEW ARTICLE Systematic Review of Mirizzi's Syndrome's Management Mallikarjuna Uppara, Ashraf Rasheed Gwent Centre for Digestive Diseases University of South Wales, United Kingdom ABSTRACT Background
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE
 ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
Optimal timing of elective laparoscopic cholecystectomy after acute cholangitis and subsequent clearance of choledocholithiasis
 The American Journal of Surgery (2010) 200, 483 488 Clinical Science Optimal timing of elective laparoscopic cholecystectomy after acute cholangitis and subsequent clearance of choledocholithiasis Vicky
The American Journal of Surgery (2010) 200, 483 488 Clinical Science Optimal timing of elective laparoscopic cholecystectomy after acute cholangitis and subsequent clearance of choledocholithiasis Vicky
Gall bladder cancer. Information for patients Hepatobiliary
 Gall bladder cancer Information for patients Hepatobiliary page 2 of 12 Who will provide my care? You will be cared for by a number of professionals who work together. These professionals will be specialist
Gall bladder cancer Information for patients Hepatobiliary page 2 of 12 Who will provide my care? You will be cared for by a number of professionals who work together. These professionals will be specialist
Pre-Operative Prediction of Difficult Laparoscopic Cholecystectomy Using Clinical and Ultrasonographic Parameters.
 DOI: 1.2127/aimdr.217...SG11 Original Article ISSN (O):25-2822; ISSN (P):25-281 Pre-Operative Prediction of Difficult Laparoscopic Cholecystectomy Using Clinical and Ultrasonographic Parameters. Sudhir
DOI: 1.2127/aimdr.217...SG11 Original Article ISSN (O):25-2822; ISSN (P):25-281 Pre-Operative Prediction of Difficult Laparoscopic Cholecystectomy Using Clinical and Ultrasonographic Parameters. Sudhir
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Disclosures. Overview. Case 1. Common Bile Duct Sizes 10/14/2016. General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis
 Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
GALLBLADDER CANCER. Lidie M. Lajoie MD Downstate Surgery M&M July 21, 2011
 GALLBLADDER CANCER Lidie M. Lajoie MD Downstate Surgery M&M July 21, 2011 Agenda Case Presentation Epidemiology Pathogenesis & Pathology Staging Presentation & Diagnosis Stage-wise Management Outcomes/Prognosis
GALLBLADDER CANCER Lidie M. Lajoie MD Downstate Surgery M&M July 21, 2011 Agenda Case Presentation Epidemiology Pathogenesis & Pathology Staging Presentation & Diagnosis Stage-wise Management Outcomes/Prognosis
Quality & Safety Committee 17 th August 2017 Agenda item: 6.2
 SUMMARY REPORT ABM University Health Board Quality & Safety Committee 17 th August 2017 Agenda item: 6.2 Subject Improvements in the management of gallstone disease Prepared by Approved & presented by:
SUMMARY REPORT ABM University Health Board Quality & Safety Committee 17 th August 2017 Agenda item: 6.2 Subject Improvements in the management of gallstone disease Prepared by Approved & presented by:
White Rose Research Online URL for this paper: Version: Accepted Version
 This is a repository copy of Delayed referral to specialist centre increases morbidity in patients with bile duct injury (BDI) after laparoscopic cholecystectomy (LC). White Rose Research Online URL for
This is a repository copy of Delayed referral to specialist centre increases morbidity in patients with bile duct injury (BDI) after laparoscopic cholecystectomy (LC). White Rose Research Online URL for
