J HEALTH POPUL NUTR 2004 Jun;22(2): ICDDR,B: Centre for Health and Population Research ISSN $
|
|
|
- Nelson Morton
- 5 years ago
- Views:
Transcription
1 J HEALTH POPUL NUTR 2004 Jun;22(2): ICDDR,B: Centre for Health and Population Research ISSN $ A Randomized Placebo-controlled Trial of Iron Supplementation in Breastfed Young Infants Initiated on Complementary Feeding: Effect on Haematological Status Jitender Nagpal 1, H.P.S. Sachdev 1, Tejinder Singh 2, and V. Mallika 3 1Division of Clinical Epidemiology, Department of Pediatrics and 2 Department of Pathology, Maulana Azad Medical College and 3 Department of Biochemistry, G.B. Pant Hospital, New Delhi , India ABSTRACT To combat iron deficiency manifesting around six months of age, iron-fortified complementary feeding has been recommended. In developing countries, in view of the poor bioavailability of iron from predominantly cereal-based diets and the high cost of fortification, medicinal iron supplementation is an alternative intervention. This double-blind randomized placebo-controlled trial was conducted from April 1999 to March 2000 in the Out-patient Department of a tertiary hospital in New Delhi, India, to evaluate the haematological effects of medicinal iron supplementation to breastfed young infants initiated on complementary feeding. One hundred healthy non-low birth-weight, predominantly breastfed infants aged 4-6 months were randomized into two groups to receive either iron (2 mg/kg/day) (IS group; n=49) or placebo drops (P group; n=51) beginning with the initiation of home-based non-fortified complementary feeding. Haematological parameters and anthropometry of mothers and infants were measured at baseline and repeated for infants after four and eight weeks of recruitment. Seventy-one subjects (35 in the IS group and the 36 in P group) came for the first follow-up, and of these, 43 (19 in the IS group and 24 in the P group) reported for the second visit. The adjusted (for maternal and baseline infant ferritin) serum ferritin levels were significantly higher in the IS group at both the follow-ups (p=0.006). The adjusted (for maternal ferritin and baseline infant ferritin) change in haemoglobin was significantly higher only at the second follow-up (0.7 g/dl; 95% confidence interval [CI] g/dl). The adjusted rise in haemoglobin was higher in initially anaemic infants (at second follow-up by 1 g/dl; 95% CI g/dl). Medicinal iron supplementation, at the time of initiating complementary feeding, to breastfed young infants resulted in an elevation of serum ferritin and haemoglobin. The response was higher in initially anaemic infants. From a programmatic perspective, evidence needs to be generated on the relative merits of selective (anaemic) versus general supplementation and daily versus weekly supplementation. Key words: Iron; Iron deficiency; Anaemia, Iron-deficiency; Complementary feeding; Infant; Double-blind method; Randomized controlled trials; India INTRODUCTION Anaemia caused by iron deficiency is a major publichealth problem (1). In India, the prevalence of anaemia is estimated to be 71% in urban and 76% in rural areas Correspondence and reprint requests should be addressed to: Prof. H.P.S. Sachdev E-6/12, Vasant Vihar New Delhi India hpssachdev@hotmail.com (2). Iron deficiency usually starts manifesting around the age of six months. This has been correlated to the depletion of iron stores (3) and the introduction of complementary foods (4) (rich in dietary inhibitors, such as phytates, tannates, etc.), particularly in a developing country. Evidence indicates an adverse impact of iron deficiency on cognition (5) and motor development (6) and their reversibility with iron supplementation. Theoretical calculations based on the usual weaning diets suggest
2 204 J Health Popul Nutr Jun 2004 Nagpal J et al. that iron is a problem micronutrient for meeting the recommended daily allowance (RDA) in this age group (7). These theoretical assumptions and the reversible adverse consequences of iron deficiency in infancy have led to advocacy for iron-fortified complementary feeding or iron supplementation, commencing with the introduction of complementary feeds, to young infants up to the age of three years. Data in support of the latter recommendation are limited since the earlier controlled trials of iron supplementation to young infants have either not provided details of dietary intake or have not specifically commenced with the initiation of complementary feeding (8-15). There is a need to evaluate the effect of iron supplementation commencing, with the introduction of non-iron-fortified complementary foods, to healthy, term, breastfed infants aged 4-6 months. Limited information on the subject is available especially in India, where the bioavailability of iron from traditional cerealbased vegetarian complementary diets (rich in dietary inhibitors of iron absorption) is expected to be low, and the affordability of iron-fortified formulas is doubtful. We, therefore, conducted the current trial to evaluate the effect of an alternative of medicinal iron supplementation, commencing with the initiation of complementary feeding, to breastfed infants. MATERIALS AND METHODS This double-blind randomized placebo-controlled trial of iron supplementation was conducted from April 1999 to March 2000 in the Out-patient Department of a tertiary hospital in New Delhi, India, situated at an altitude of 210 metres. The hospital primarily caters to an urban lower to lower-middle socioeconomic population. One hundred apparently healthy and predominantly breastfed infants (exclusive breastfeeding with occasional sips of water) aged 4-6 months were recruited on two prefixed days in a week. These infants were recruited after recovery from a minor ailment (such as upper respiratory infection) or were called at four months of age after vaccination (at 3½ months). They were of full-term gestation (37-41 weeks) with a birth-weight of >2,500 g. This was verified from the records for institutional and extra-institutional births (conducted in other institutions or nursing homes). The following infants (see the exclusion criteria) were excluded from the study: (i) twins, (ii) congenital malformation, (iii) history of blood transfusion, (iv) blood sampling (>10 ml) prior to recruitment, (v) infants already receiving iron supplementation, (vi) adverse neonatal events requiring admission to the special newborn care nursery, and (vii) those with significant current morbidity. The institutional ethical committee approved the study. An informed verbal consent was obtained prior to recruitment. At recruitment, the subjects were randomized into two groups based on random numbers generated by the computer (Fig.). The study group received iron in the form of medicinal drops (ferric ammonium citrate; 25 mg/ml) at the dose of 2 mg/kg/day, while the control group received a placebo solution identical to iron drops in colour, taste, and external appearance. Simultaneously, mothers were counselled to initiate complementary feeding (3-4 times a day) as per prevalent recommendations (16) with locally-available and home-made foods, such as banana, khichri (rice-pulse gruel cooked in oil), and dahlia (wheat cooked in milk). These natural foods were not supplemented or fortified with iron or other haematinic preparations. Both the groups were also advised to continue breastfeeding during the entire follow-up. Follow-up visits were advised after four and eight weeks of recruitment. Compliance of medicinal (iron or placebo) intake and feeding status were evaluated at each visit from a home diary maintained by the mother and verified by the amount of syrup leftover in the bottle. The drug intake estimated from the bottle and diary was similar. A standard pre-tested proforma was used for recording baseline information, including antenatal and neonatal profiles, with emphasis on feeding history, birth-weight, and gestation. The dietary intake of infants was quantified by the 24-hour recall method (semi-quantitative estimates using home measures), and the calories were calculated as per values available for Indian foods (17). Maternal and infant weights, height/length, and current and interval morbidity (between two follow-up periods) were also recorded. The baseline haematological parameters evaluated included maternal haemoglobin and ferritin, and infant haemoglobin, peripheral smear, and serum ferritin. Haemoglobin was measured by the HemoCue system, which has been validated compared with other techniques (18). Serum ferritin was estimated using the MAGIWELL ferritin quantitative ELISA test kit. Maternal iron status was evaluated at baseline to control for its confounding effect on infant iron stores.
3 Iron supplementation with complementary feeding 205 Fig. Summary of study design Randomization of 4-6 months old Predominantly breastfed Term, non-low birth-weight Allocated to study group (n=49) to receive iron drops (2 mg/kg) Allocated to control group (n=51) to receive placebo drops Continue breastfeeding Begin complementary feeding Compliance: home diary Reported for follow-up at one month (n=35) Analyzed (n=35) Reported for follow-up at one month (n=36) Analyzed (n=36) Reported for follow-up at two months (n=19) Analyzed (n=19) Infant haemoglobin comprised the primary outcome variable, while serum ferritin, peripheral smear, and anthropometry (weight, length, and head circumference) were secondary outcome measures. These were evaluated at baseline and at the first and second follow-ups. The primary outcome variable for sample-size consideration was infant haemoglobin. Based on earlier data from this institution in this age group (haemoglobin change SD of 1.23 g/dl), it was estimated that 25 infants would be required in each group to evaluate a difference of 1 g/dl of change in haemoglobin between the two groups after one month of supplementation with 95% confidence and 80% power. To account for potential loss to follow-up, double this number was recruited. Post-trial estimates of the power using the available sample size at one month of follow-up indicated that the study could detect a difference of 0.5 g/dl in haemoglobin with 95% confidence and 80% power. Data entry was done on the computer using EpiInfo software. Analysis was performed on EpiInfo and SPSS software. The randomization code was broken after data entry and analysis. Serum ferritin was converted to natural logarithm to normalize the data. The various parameters in two groups were compared by Student's t-test, chi-square test, Fisher's Exact test, and Mann- Reported for follow-up at two months (n=24) Analyzed (n=24) Whitney test, wherever applicable. Additional statistical techniques included Pearson's correlation coefficient and multiple linear regression analysis. RESULTS In total, 100 infants who fulfilled the recruitment criteria were enrolled for the prospective follow-up (49 in the iron-supplemented group and 51 in the placebo group). Seventy-one of the recruited infants (35 in the ironsupplemented group and 36 in the placebo group) reported for follow-up after one month. At the second follow-up (two months after recruitment), 43 of the 71 infants at first follow-up (19 in the iron-supplemented group and 24 in the placebo group) were available. The baseline characteristics of infants reporting for and lost to follow-up were comparable (data not presented) at first follow-up. Similarly, infants who reported for the second follow-up were comparable to those who were lost between the first and the second follow-up (data not presented). The evaluated baseline maternal and infant characteristics (Table 1) and the quantity of complementary diet consumed (Table 2) were comparable in the two groups. However, the amount of complementary diet intake at the second follow-up was greater than that at the first follow-up. The compliance of drug intake
4 206 J Health Popul Nutr Jun 2004 Nagpal J et al. was comparable in the two groups (95% in the iron group and 91 % in the placebo group). Table 1. Comparison of baseline characteristics [mean±sd or number (%)] Iron-supple- Placebo Characteristics mented group group (n=35) (n=36) Maternal Age (years) 26.1± ±2.8 Weight (kg) 50.2± ±6.6 Height (cm) 152.2± ±6.3 Haemoglobin (g/dl) 12.1± ±1.3 Ferritin (mg/l; geometric mean) 15.1± ±3.0 Gravida 2.3± ±1.0 Place of delivery: hospital 21 (60.0) 16 (44.4) Mode of delivery: vaginal 34 (97) 35 (97) Gestation (weeks) 38.8± ±0.9 Antenatal haemoglobin estimation 4 (11.4) 2 (5.6) Iron supplementation Number 6 (17.14) 0 (0) Duration (weeks) 12±4.1 0 (0) Dietary pattern: vegetarian 15 (42.8) 14 (38.8) Infant Age (days) 148.2± ±18.5 Males 19 (54.3) 22 (61.1) Birth-weight (g) 2719± ±226 Birth length (cm) 48.9± ±1.1 Birth head circumference (cm) 34.0± ±0.8 None of the differences between the groups were statistically significant (p>0.05) Table 2. Complementary food intakes at follow-up visits [mean±sd] Iron-supple- Placebo Complementary mented group group food (n=35) (n=36) First follow-up Calories (kcal) 81.9± ±39.4 Cereals (g) 18.5± ±7.5 Pulses (g) 5.8± ±5.8 Vegetables (g) 5.2± ±5.6 Second follow-up Calories (kcal) 152.7± ±47.1 Cereals (g) 30.0± ±11.9 Pulses (g) 11.8± ±11.7 Vegetables (g) 13.4± ±14.6 None of the differences between the two groups were statistically significant (p>0.05) At the first follow-up, serum ferritin was significantly higher in the iron-supplemented group (23.8 [2.6] µg/dl vs 11.8 [3.0] µg/dl; p=0.006), while the haemoglobin levels were comparable (Table 3). At the second followup, significantly higher values were observed for haemoglobin (11.5 [0.8] g/dl vs 10.8 [0.9] g/dl; p=0.009) and serum ferritin (30.6 [2.2] µg/dl vs 8.7 [3.2] µg/dl; p<0.005) in the iron-supplemented group. The following relevant significant correlates were identified: baseline infant haemoglobin (from baseline to second follow-up) (r=0.607; p<0.001), baseline infant haemoglobin and ferritin (r=0.266; p=0.007), and baseline infant ferritin and maternal ferritin (r=0.408; p=0.009). In view of the above correlations and the possible confounding due to maternal iron status, multiple regression analysis was performed by the enter method with change in haemoglobin as the dependent variable (at both the follow-ups) and treatment group, maternal ferritin, and baseline infant haemoglobin as independent variables. The baseline infant haemoglobin was entered in the model either as a continuous or a dichotomized (<11 g/dl or >11 g/dl) variable (Table 4). At the first follow-up, there was no significant difference in the change in haemoglobin between the two groups, whereas at the second follow-up the iron-treated subjects had a significantly (p=0.001) higher change in haemoglobin (mean change adjusted for maternal ferritin and baseline infant haemoglobin as a continuous variable -0.7 g/dl; 95% CI g/dl). At both the follow-ups, lower baseline infant haemoglobin was a significant (p=0.001) predictor of a greater rise in haemoglobin; at the second follow-up, the adjusted mean haemoglobin rise in initially anaemic infants (haemoglobin <11 g/dl) was higher by 1 g/dl (95% CI g/dl). Similarly, at both the follow-up visits (data not depicted in Table 4), the serum ferritin levels adjusted for baseline infant ferritin and maternal ferritin values were significantly greater in the ironsupplemented group (first follow-up -ß=1.71, 95% CI , p=0.006; second follow-up -ß=3.25, 95% CI , p<0.001). There was no statistical difference in reported interval morbidity in the two groups (Table 5). However, black colouring of the stools was significantly higher in the iron-supplemented group (90.7% vs 1.6 %, p<0.001).
5 Iron supplementation with complementary feeding 207 DISCUSSION Table 3. Comparison of outcome measures at follow-up visits [mean±sd or number (%)] Iron-deficiency anaemia is currently recognized to be the most widespread micronutrient deficiency. Pregnancy and infancy have been identified as the two core areas of attention for preventive planning. Efforts in infancy in this context have largely focused on iron-fortified foods, including formula (8-11). Many such studies have shown benefit in terms of the iron status of the infant. However, the utility of fortified foods, particuto evaluate the haematological effect of medicinal iron supplementation to infants being initiated on nonfortified usual complementary diets. This hospital-based study had a high drop-out rate (57% at second follow-up). The possible reasons contributing to this could be: (i) Reporting from a distance to the hospital for follow-up with no reimbursement for transportation and loss of wages; (ii) Lack of perceived benefit of medication in apparently healthy children; Haemoglobin Serum ferritin Peripheral smear Head Weight Length Variable (g/dl) (µg/dl) * NCHC MCHC NCNC circumference (g) (cm) (cm) Infants available at first follow-up (n=71) Baseline characteristics IS group (n=35) 11.3± ± (68.6) 9 (25.7) 2 (5.7) 41.3±0.9 5,686± ±2.7 P group (n=36) 10.9± ± (75.0) 6 (16.7) 3 (8.3) 41.2±1.1 5,694± ±2.8 p value Outcome measures at first follow-up IS group (n=35) 11.3± ±2.6 9 (25.7) 0 26 (74.3) 42.3±0.9 6,083± ±2.7 P group (n=36) 10.9± ±3.0 6 (16.7) 3 (8.3) 27 (75.0) 42.2±0.9 6,075± ±2.7 p value Change in outcome measures from baseline to first follow-up IS group (n=35) 0.0± ± ± ± ±1.14 P group (n=36) 0.0± ± ± ± ±0.79 Mean difference 0.0 ( ( ( ± ( (-0.31 (95% CI) to 0.4) to 22.4) to 0.11) to 192) to 0.61) p value Infants available at second follow-up (n=43) Baseline characteristics IS group (n=19) 11.1± ±2.7 3 (15.7) 1 (5.2) 15 (78.9) 41.3±1.1 5,611± ±3.2 P group (n=24) 11.2± ±3.1 4 (16.6) 1 (4.2) 19 (79.1) 41.2±1.0 5,806± ±2.7 p value Outcome measures at second follow-up IS group (n=19) 11.5± ±2.2 4 (21.1) 0 15 (78.9) 43.3±0.9 6,337± ±3.3 P group (n=24) 10.8± ±3.2 4 (16.6) 2 (8.3) 18 (75.0) 43.1±0.9 6,509± ±2.7 p value Change in outcome measures from baseline to second follow-up IS group (n=19) 0.3± ± ± ± ±1.52 P group (n=24) -0.3± ± ± ± ±1.54 Mean difference 0.6 ( ( ( ( (-1.12 (95% CI) to 1.2) to 41.3) to 0.26) to 345) to 0.74) p value * Means indicated are geometric means, except those depicted under change in outcome measures (arithmetic means) Calculated by Mann-Whitney ranking test IS group=iron-supplemented group MCHC=Microcytic hypochromic NCHC=Normocytic hypochromic NCNC=Normocytic normochromic P group=placebo group larly, in the Indian setting may be limited because of poor affordability and predominantly cereal-based nature of usual complementary foods, which hinder iron bioavailability. The present study was, therefore, designed (iii) Prolonged duration of medication; (iv) Blood letting at each contact; and (v) Poor educational and socioeconomic status. It would also be useful to examine to the extent feasible whether the exclusion of
6 208 J Health Popul Nutr Jun 2004 Nagpal J et al. subjects not reporting for follow-up may have biased the findings. The feasible comparisons do not support this possibility: (i) None of the baseline characteristics were significantly different between those reporting and lost at the first and the second follow-ups; (ii) Proportion of subjects lost to follow-up in both the groups was statistically comparable; and (iii) Interval morbidity in the two groups at first or second follow- Table 4. Multiple regression models of change in infant haemoglobin Variable b SE (b) 95 % CI for b p value R 2 F-test: p value First follow-up (n=71) Baseline infant haemoglobin as continuous variable Constant to <0.001 Maternal ferritin (natural log) to <0.001 Baseline infant haemoglobin to <0.001 Group (0=Iron,1=Placebo) to Baseline infant haemoglobin as dichotomous variable Constant to Maternal ferritin (natural log) to Baseline infant haemoglobin to <0.001 (1=>11 g/dl,0=<11 g/dl) Group (0=Iron,1=Placebo) to Second follow-up (n=43) Baseline infant haemoglobin as continuous variable Constant to <0.001 Maternal ferritin (natural log) to <0.001 Baseline infant haemoglobin to <0.001 Group (0=Iron,1=Placebo) to Baseline infant haemoglobin as dichotomous variable Constant to Maternal ferritin (natural log) to Baseline infant haemoglobin to <0.001 (1=>11 g/dl, 0=<11 g/dl) Group (0=Iron,1=Placebo) to b=regression coefficient CI=Confidence interval Hb=Haemoglobin SE (b)=standard error of b Table 5. Comparison of reported side-effects and morbidity experienced in two groups at follow-up [number (%)] Side-effect/morbidity Iron-supplemented group Placebo group First follow-up (n =35) (n=36) Stool colour (black)* 32 [91.4] 1 [2.8] Current morbidity Interval morbidity 0 2 (D, U) [5.7] 0 1 (M) [2.8] Second follow-up (n=19) (n=24) Stool colour (black)* 17 [89.4] 0 Current morbidity Interval morbidity 0 1 (D) [2.9] 0 2 (D) [5.6] *p<0.001 Refers to morbidity suffered in the period between the current and the last visit D=Diarrhoea; M=Meningitis; U=Upper respiratory infection up was not statistically different. However, it is acknowledged that all characteristics with the potential to bias the results could not be examined for comparability. The adjusted serum ferritin levels were significantly higher in the iron-supplemented group at both the followups. However, at the first follow-up, there was no significant difference in the adjusted change in haemoglobin between the two groups, whereas at the second followup, iron-treated subjects had a significantly (p=0.001) higher adjusted change in haemoglobin (0.7 g/dl; 95% CI g/dl). The haemoglobin response was greater in infants with lower baseline haemoglobin; the adjusted haemoglobin rise in initially anaemic subjects was 1 g/dl higher at the second follow-up. The haemoglobin rise in the present study is in consonance with available literature in this age group. The
7 Iron supplementation with complementary feeding 209 mean haemoglobin advantage in the iron-supplemented group in the available studies ranged from 0.4 to 0.8 g/dl over a follow-up period of 2-12 months when iron was given to all infants irrespective of their baseline iron status (4,9-14). In a recent study of iron supplementation (1 mg/kg/d) of breastfed Honduran (n=131) and Swedish (n=101) infants aged 4-9 months, a mean haemoglobin rise of 0.5 g/dl was demonstrable after two months. This benefit was greater after five months of supplementation (mean=0.6 g/dl) especially in the Honduran population (0.9 g/dl) (12). In a trial in Turkey on 113 infants [Group I=1 mg/kg/d (n=30); Group II=2 mg/kg/d (n=30); Group III=2 mg/kg/d on alternate days (n=30); group IV=placebo (n=23)], a haemoglobin benefit of 0.30 to 0.4 g/dl (p<0.001) was documented after four months in the iron-supplemented groups (13). The relatively poor rise in haemoglobin may be explained by the exclusion of all subjects with evidence of iron deficiency at recruitment (Hb <9.5 g/dl, MCV<74 fl and ferritin <12 ng/ml) in this study. We do not have comparable data from the other two reports (8,11) to comment on their timing of haemoglobin rise. The change in haemoglobin observed in anaemic subjects in the present study (1.5 g/dl using 2 mg/kg for 2 months) was also similar to the results of studies conducted in Ghana (1.4 g/dl using mg/kg for 2 months) and Costa Rica (3.4 g/dl using 6 mg/kg for 6 months) (14,15). One study in England did not document any difference in haemoglobin between the iron-supplemented and the placebo group (10). The dose of iron supplementation is an important factor that could have influenced the magnitude of the haemoglobin rise. Assuming a low or medium bioavailability of iron from the initiated complementary diet (khichri and dahlia which are prominently cerealbased) with breastfeeding, the iron requirement from complementary foods has been estimated to be about 21 and 11 mg respectively (7). With an average weight of 5.5 kg at the time of initiation of complementary feeding, this translates to a daily supplementation of 2 mg/kg, the dosage used by us. This supplementation dose is marginally higher than formula-feed ironfortification trials in which the extrapolated average iron intakes were mg/kg (4,8,11). The corresponding estimates for medicinal iron drops were 1 and 2 mg/kg/day in two trials cited earlier (12,13). The bioavailability of iron in these trials could have been higher because of the nature of complementary diets. In the present study, significant differences in serum ferritin concentrations were obtained at the first (12.7 µg/dl) and the second follow-up (22.0 µg/dl) between the iron-supplemented and the placebo groups. The rise in serum ferritin concentration, thus, preceded the rise in haemoglobin. Other trials in this age group by Domellof et al. (mean 29 µg/dl higher after two months using 1 mg/kg/day) and Ermis et al. (12,13) (mean 23.2 µg/dl higher after five months using 2 mg/kg/day) also recorded similar differences in serum ferritin with iron supplementation. The study conducted in England, which did not document a significant change in haemoglobin, also did not record a significant difference in serum ferritin after one year of supplementation (10). The present study failed to show any significant difference in anthropometry at either first or second follow-up. Similar observations were documented in other trials reporting on anthropometry (3,10). However, in the Honduras study, an inverse correlation between gain in infant weight from birth to six months and ferritin concentration at six months was obtained (4). Other studies evaluating the impact of iron supplementation on growth parameters in the past have been predominantly carried out in preschool and older children. These trials have yielded equivocal results with some studies showing benefit (9,19) which the others failed to support (10,20,21). The follow-up period and the sample size in the present trial were inadequate to estimate the anthropometric differences. A sample size of 50 subjects in each group was required to detect a difference of 168 g with 95% confidence and 80% power. The iron supplements were generally well-tolerated, and no infants reported any side-effects during the study period. A substantial proportion (32/35) in the iron-supplemented group reported black-coloured stools, a documented effect of iron intake. The recorded interval morbidity experience of the two groups was similar. A recent systematic review has concluded that iron supplementation has no apparent harmful effects on the overall incidence of infectious illnesses in children, although it slightly increases (11%) the risk of developing diarrhoea (22). It is concluded that medicinal iron supplementation (2 mg/kg dose) in predominantly breastfed non-low birth-weight infants aged 4-6 months initiated on beginning complementary feeding (based on vegetarian diets) results in an improvement of serum ferritin and
8 210 J Health Popul Nutr Jun 2004 Nagpal J et al. haemoglobin (0.7 g/dl after two months; 95% CI g/dl). The response is greater in initially anaemic infants. These results need to be validated in diverse settings with different complementary diets on larger sample sizes with better follow-up rates. Future trials should also aim to evaluate the functional consequences of such iron supplementation apart from haemoglobin, for example, cognition and psychomotor effects. Considering the high drop-out rates and greater response in anaemic infants, from a programmatic perspective, evidence needs to be generated on the relative merits of daily versus weekly supplementation and selective (anaemic infants) versus general supplementation. REFERENCES 1. United Nations. Administrative Committee on Coordination/Sub-Committee on Nutrition. Fourth report on the world nutrition situation, January 2000: nutrition throughout the life cycle. Geneva: ACC/SCN Secretariat, United Nations, p. (ACC/SCN report, 4). 2. National family health survey (NFHS-2), India, Mumbai: International Institute for Population Sciences, p. 3. Calvo EB, Galindo AC, Aspres NB. Iron status in exclusively breast-fed infants. Pediatrics 1992;90: Dewey KG, Cohen RJ, Rivera LL, Brown KH. Effects of age of introduction of complementary foods on iron status of breast-fed infants in Honduras. Am J Clin Nutr 1998;67: Logan S, Martins S, Gilbert R. Iron therapy for improving psychomotor development and cognitive function in children under the age of three with iron deficiency anaemia (Cochrane review). In: The Cochrane Library, Issue 2, Oxford Update Software. 6. Lozoff B, Jimenez E, Wolf AW. Long-term developmental outcome of infants with iron deficiency. N Engl J Med 1991;325: World Health Organization. Complementary feeding of young children in developing countries: a review of current scientific knowledge. Geneva: World Health Organization, p. (WHO/ NUT/98.1). 8. Gill DG, Vincent S, Segal DS. Follow-on formula in prevention of iron deficiency: a multicentre study. Acta Paediatr 1997;86: Morley R, Abbott R, Fairweather-Tait S, MacFayden U, Stephenson T, Lucas A. Iron fortified follow on formula from 9 months to 18 months improves iron status but not growth or development: a randomised trial. Arch Dis Child 1999; 81: Stevens D, Nelson A. The effect of iron in formula milk after 6 months of age. Arch Dis Child 1995; 73: Javaid N, Haschke F, Pietschnig B, Schuster E, Huemer C, Shebaz A et al. Interactions between infections, malnutrition and iron nutritional status in Pakistani infants: a longitudinal study. Acta Paediatr Scand 1991;37(Suppl):S Duello M, Cohen RJ, Dewey KG, Hornell O, Rivera LL, Lönnerdal B. Iron supplementation of breast-fed Honduran and Swedish infants from 4 to 9 months of age. J Pediatr 2001;138: Ermis B, Demirel F, Demircan N, Gurel A. Effects of three different iron supplementations in term healthy infants after 5 months of life. J Trop Pediatr 2002;48: Lozoff B, Brittenham GM, Wolf AW, McClish DK, Kuhnert PM, Jimenez E et al. Iron deficiency anaemia and iron therapy effects on infant developmental test performance. Pediatrics 1987; 79: Zlotkin S, Arthur P, Antwi KY, Yeung G. Randomized, controlled trial of single versus 3- times-daily ferrous sulfate drops for treatment of anaemia. Pediatrics 2001;108: Sachdev HPS. IAP policy on infant feeding. Indian Pediatr 1995;32: Gopalan C, Ramashastri BV. Nutritive value of Indian foods. Hyderabad: National Institute of Nutrition, Indian Council of Medical Research, p. 18. Lardi AM, Hirst C, Mortimer AJ, McCollum CN. Evaluation of the HemoCue for measuring intraoperative haemoglobin concentrations: a comparison with the Coulter Max-M. Anaesthesia 1998; 53: Persson LÅ, Lundström M, Lönnerdal B, Hernell O. Are weaning foods causing impaired iron and zinc status in 1-year-old Swedish infants? A cohort study. Acta Paediatr 1998;87: Rosado JL. Separate and joint effects of micronutrient deficiencies on linear growth. J Nutr 1999; 129(Suppl):S Thu BD, Schultink W, Dillon D, Gross R, Leswara ND, Khoi HH. Effect of daily and weekly
9 Iron supplementation with complementary feeding 211 micronutrient supplementation on micronutrient deficiencies and growth in young Vietnamese children. Am J Clin Nutr 1999;69: Gera T, Sachdev HPS. Effect of iron supplementation on incidence of infectious illness in children: systematic review. Br Med J 2002;325:
Maternal and Infant Nutrition Briefs
 Maternal and Infant Nutrition Briefs November/December 2002 A research-based newsletter prepared by the University of California for professionals interested in maternal and infant nutrition Recent Trends
Maternal and Infant Nutrition Briefs November/December 2002 A research-based newsletter prepared by the University of California for professionals interested in maternal and infant nutrition Recent Trends
Preventive Strategy to Control Iron Deficiency Anemia in Children and Adults
 Preventive Strategy to Control Iron Deficiency Anemia in Children and Adults I. A. Siddiqui ( Department of Biochemistry, Ziauddin Medical University, Karachi ) A. Jaleel,M. A. Rahman ( Departments of
Preventive Strategy to Control Iron Deficiency Anemia in Children and Adults I. A. Siddiqui ( Department of Biochemistry, Ziauddin Medical University, Karachi ) A. Jaleel,M. A. Rahman ( Departments of
Impact of Nutrition Counselling on Food and Nutrient Intake and Haematological Profile of Rural Pregnant Women
 Kamla-Raj 2004 J. Hum. Ecol., 15(1): 51-55 (2004) Impact of Nutrition Counselling on Food and Nutrient Intake and Haematological Profile of Rural Pregnant Women Paramjit Kaur Chawla, Ravnit Kaur and R.
Kamla-Raj 2004 J. Hum. Ecol., 15(1): 51-55 (2004) Impact of Nutrition Counselling on Food and Nutrient Intake and Haematological Profile of Rural Pregnant Women Paramjit Kaur Chawla, Ravnit Kaur and R.
Field Sites Sangam Vihar and Harsh Vihar, Delhi
 Institutions Involved Institutions Involved Center for Micronutrient Research, Subharti Medical College, UP Center for Micronutrient Research, Subharti Medical College, UP Center for Public Health Kinetics,
Institutions Involved Institutions Involved Center for Micronutrient Research, Subharti Medical College, UP Center for Micronutrient Research, Subharti Medical College, UP Center for Public Health Kinetics,
A PATH ANALYSIS ON THE NOURISHMENT DIRECTED HAEMOGLOBIN STATUS AND RESULTING ENDURANCE CAPACITY OF ADOLESCENT INDIAN RURAL GIRLS
 J. Dairying, Foods & H.S., 29 (1) : 47-51, 21 AGRICULTURAL RESEARCH COMMUNICATION CENTRE www.arccjournals.com / indianjournals.com A PATH ANALYSIS ON THE NOURISHMENT DIRECTED HAEMOGLOBIN STATUS AND RESULTING
J. Dairying, Foods & H.S., 29 (1) : 47-51, 21 AGRICULTURAL RESEARCH COMMUNICATION CENTRE www.arccjournals.com / indianjournals.com A PATH ANALYSIS ON THE NOURISHMENT DIRECTED HAEMOGLOBIN STATUS AND RESULTING
Assessment of Factors Predisposing to Acute Malnutrition Among Under - Five Children Attending Tertiary Care Hospital.
 Quest Journals Journal of Medical and Dental Science Research Volume 3~ Issue 5 (2016) pp: 01-05 ISSN(Online) : 2394-076X ISSN (Print):2394-0751 www.questjournals.org Research Paper Assessment of Factors
Quest Journals Journal of Medical and Dental Science Research Volume 3~ Issue 5 (2016) pp: 01-05 ISSN(Online) : 2394-076X ISSN (Print):2394-0751 www.questjournals.org Research Paper Assessment of Factors
Panacea Journal of Health Sciences ISSN :
 EFFECT OF MANNA HEALTH MIX SUPPLEMENTATION ON ANTHROPOMETRIC PARAMETERS AND HEMATOLOGICAL PROFILE OF ANEMIC ADOLESCENT GIRLS Suganya N. * and Dr. D. Estherlydia** *M.Sc Student, ** Assistant Professor,
EFFECT OF MANNA HEALTH MIX SUPPLEMENTATION ON ANTHROPOMETRIC PARAMETERS AND HEMATOLOGICAL PROFILE OF ANEMIC ADOLESCENT GIRLS Suganya N. * and Dr. D. Estherlydia** *M.Sc Student, ** Assistant Professor,
The importance of early complementary feeding in the development of oral tolerance: Concerns and controversies
 The importance of early complementary feeding in the development of oral tolerance: Concerns and controversies Prescott SL, Smith P, Tang M, Palmer DJ, Sinn J, Huntley SJ, Cormack B. Heine RG. Gibson RA,
The importance of early complementary feeding in the development of oral tolerance: Concerns and controversies Prescott SL, Smith P, Tang M, Palmer DJ, Sinn J, Huntley SJ, Cormack B. Heine RG. Gibson RA,
NUTRITION and. Child Growth & Development. Washington, DC May 2-3, Kay Dewey. UC-Davis and Alive & Thrive
 Clean, Fed & Nurtured: Joining forces to promote child growth and development NUTRITION and Child Growth & Development Washington, DC May 2-3, 2013 Kay Dewey UC-Davis and Alive & Thrive Nutrition Basics
Clean, Fed & Nurtured: Joining forces to promote child growth and development NUTRITION and Child Growth & Development Washington, DC May 2-3, 2013 Kay Dewey UC-Davis and Alive & Thrive Nutrition Basics
Effects of Nutrient Fortified Complementary Food Supplements on Anemia of Infants and Young Children in Poor Rural of Gansu 1
 BIOMEDICAL AND ENVIRONMENTAL SCIENCES 22, 194-200 (2009) www.besjournal.com Effects of Nutrient Fortified Complementary Food Supplements on Anemia of Infants and Young Children in Poor Rural of Gansu 1
BIOMEDICAL AND ENVIRONMENTAL SCIENCES 22, 194-200 (2009) www.besjournal.com Effects of Nutrient Fortified Complementary Food Supplements on Anemia of Infants and Young Children in Poor Rural of Gansu 1
UNIVERSITY OF NAIROBI
 UNIVERSITY OF NAIROBI REMARKS MADE BY PROF. PETER M. F. MBITHI, DEPUTY VICE-CHANCELLOR (A&F) DURING THE INSTAPA PROJECT ANNUAL MEETING HELD ON JUNE 22, 2009 Project Description AIM: To identify novel staple
UNIVERSITY OF NAIROBI REMARKS MADE BY PROF. PETER M. F. MBITHI, DEPUTY VICE-CHANCELLOR (A&F) DURING THE INSTAPA PROJECT ANNUAL MEETING HELD ON JUNE 22, 2009 Project Description AIM: To identify novel staple
Under-five and infant mortality constitutes. Validation of IMNCI Algorithm for Young Infants (0-2 months) in India
 R E S E A R C H P A P E R Validation of IMNCI Algorithm for Young Infants (0-2 months) in India SATNAM KAUR, V SINGH, AK DUTTA AND J CHANDRA From the Department of Pediatrics, Kalawati Saran Children s
R E S E A R C H P A P E R Validation of IMNCI Algorithm for Young Infants (0-2 months) in India SATNAM KAUR, V SINGH, AK DUTTA AND J CHANDRA From the Department of Pediatrics, Kalawati Saran Children s
Nutritional Profile of Urban Preschool Children of Punjab
 KamlaRaj 2003 Anthropologist, 5 (3): 149153 (2003) Nutritional Profile of Urban Preschool Children of Punjab Inderjit Singh and Kiran Grover Growth retardation and malnutrition are the major public health
KamlaRaj 2003 Anthropologist, 5 (3): 149153 (2003) Nutritional Profile of Urban Preschool Children of Punjab Inderjit Singh and Kiran Grover Growth retardation and malnutrition are the major public health
Undernutrition & risk of infections in preschool children
 Indian J Med Res 130, November 2009, pp 579-583 Undernutrition & risk of infections in preschool children Prema Ramachandran & Hema S. Gopalan Nutrition Foundation of India, New Delhi, India Received April
Indian J Med Res 130, November 2009, pp 579-583 Undernutrition & risk of infections in preschool children Prema Ramachandran & Hema S. Gopalan Nutrition Foundation of India, New Delhi, India Received April
Dietary Assessment of Adolescent Girls and Dissemination of Nutrition Education
 Dietary Assessment of Adolescent Girls and Dissemination of Nutrition Education Sakshi Sharma 1 and Nikita Arya 1 1 Department of Dietetics, Institute of Hotel Management Catering and Nutrition, Pusa,
Dietary Assessment of Adolescent Girls and Dissemination of Nutrition Education Sakshi Sharma 1 and Nikita Arya 1 1 Department of Dietetics, Institute of Hotel Management Catering and Nutrition, Pusa,
BREASTFEEDING TO PREVENT DOUBLE BURDEN OF MALNUTRITION
 BREASTFEEDING TO PREVENT DOUBLE BURDEN OF MALNUTRITION Sirinuch Chomtho Department of Pediatrics, Chulalongkorn University, Bangkok, Thailand The double burden of malnutrition means under- and over-nutrition
BREASTFEEDING TO PREVENT DOUBLE BURDEN OF MALNUTRITION Sirinuch Chomtho Department of Pediatrics, Chulalongkorn University, Bangkok, Thailand The double burden of malnutrition means under- and over-nutrition
Iron requirements of infants and toddlers
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Iron requirements of infants and toddlers Domellöf, Magnus; Braegger,
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Iron requirements of infants and toddlers Domellöf, Magnus; Braegger,
Iron deficiency anaemia in young children (6 to 23 months) in relation to complementary feeding practices in rural Telangana, India
 International Journal of Contemporary Pediatrics Sailaja K et al. Int J Contemp Pediatr. 2017 Jul;4(4):1240-1244 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
International Journal of Contemporary Pediatrics Sailaja K et al. Int J Contemp Pediatr. 2017 Jul;4(4):1240-1244 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
SOME ASPECTS OF INFANT FEEDING. Quak Seng Hock
 SOME ASPECTS OF INFANT FEEDING Quak Seng Hock Contents Introduction Importance of proper nutrition in the infant Breastfeeding Nutritional requirements of infants Introducing solid food Vitamin requirements
SOME ASPECTS OF INFANT FEEDING Quak Seng Hock Contents Introduction Importance of proper nutrition in the infant Breastfeeding Nutritional requirements of infants Introducing solid food Vitamin requirements
The assessment of nutritional and growth
 Paediatrica Indonesiana VOLUME 49 May NUMBER 3 Original Article Effect of iron treatment on nutritional status of children with iron deficiency anemia Leon Agustian, Tiangsa Sembiring, Ani Ariani, Bidasari
Paediatrica Indonesiana VOLUME 49 May NUMBER 3 Original Article Effect of iron treatment on nutritional status of children with iron deficiency anemia Leon Agustian, Tiangsa Sembiring, Ani Ariani, Bidasari
K. Srinivasa Rao 1, K. Kalyan Kumar 2, Usha L H 3
 185 Print ISSN - Acta Biomedica Scientia e - ISSN - 2348-2168 Print ISSN - 2348-215X J o u r n a l h o m e p a g e : w w w. m c m e d. u s / j o u r n a l / a b s ASSESSMENT OF SERUM RETINOL LEVEL AND
185 Print ISSN - Acta Biomedica Scientia e - ISSN - 2348-2168 Print ISSN - 2348-215X J o u r n a l h o m e p a g e : w w w. m c m e d. u s / j o u r n a l / a b s ASSESSMENT OF SERUM RETINOL LEVEL AND
International Journal of Science, Environment and Technology, Vol. 6, No 1, 2017,
 International Journal of Science, Environment and Technology, Vol. 6, No 1, 2017, 276 283 ISSN 2278-3687 (O) 2277-663X (P) FRUIT & NUTRIENT INTAKE IN RELATION TO ANEMIA PREVALENCE IN ADOLESCENTS Swiny
International Journal of Science, Environment and Technology, Vol. 6, No 1, 2017, 276 283 ISSN 2278-3687 (O) 2277-663X (P) FRUIT & NUTRIENT INTAKE IN RELATION TO ANEMIA PREVALENCE IN ADOLESCENTS Swiny
Cows Milk or follow on Formula. Hilton 26/10/2014
 Iron Deficiency Anemia Cows Milk or follow on Formula Dr Antoine Farah Clinical associate Prof. American University Hospital Hilton 26/10/2014 Iron in infant nutrition: what is the evidence in 2014 IRON
Iron Deficiency Anemia Cows Milk or follow on Formula Dr Antoine Farah Clinical associate Prof. American University Hospital Hilton 26/10/2014 Iron in infant nutrition: what is the evidence in 2014 IRON
HarvestPlus Statement on the Potential Benefits of Biofortification on the Nutritional Status of Populations
 HarvestPlus Statement on the Potential Benefits of Biofortification on the Nutritional Status of Populations Biofortification is an intervention strategy currently being researched and developed for increasing
HarvestPlus Statement on the Potential Benefits of Biofortification on the Nutritional Status of Populations Biofortification is an intervention strategy currently being researched and developed for increasing
Health and nutritional profile of adolescent girls from underprivileged communities residing in Kasturba Gandhi Balika Vidyalaya in Rajasthan
 Asian J. Dairy & Food Res, 37(3) 2018: 237-241 Print ISSN:0971-4456 / Online ISSN:0976-0563 AGRICULTURAL RESEARCH COMMUNICATION CENTRE www.arccjournals.com Health and nutritional profile of adolescent
Asian J. Dairy & Food Res, 37(3) 2018: 237-241 Print ISSN:0971-4456 / Online ISSN:0976-0563 AGRICULTURAL RESEARCH COMMUNICATION CENTRE www.arccjournals.com Health and nutritional profile of adolescent
APPENDIX 4 A4.1 APPENDIX 4
 APPENDIX 4 A4.1 APPENDIX 4 APPENDIX 4 A4.3 DEFINITIONS OF THE INDICATORS 1.1 BCG coverage Number 12 23-month-olds receiving BCG vaccine before 1st birthday 1 1.2 DPT coverage Number 12 23-month-olds receiving
APPENDIX 4 A4.1 APPENDIX 4 APPENDIX 4 A4.3 DEFINITIONS OF THE INDICATORS 1.1 BCG coverage Number 12 23-month-olds receiving BCG vaccine before 1st birthday 1 1.2 DPT coverage Number 12 23-month-olds receiving
Myanmar Food and Nutrition Security Profiles
 Key Indicators Myanmar Food and Nutrition Security Profiles Myanmar has experienced growth in Dietary Energy Supply (DES). Dietary quality remains poor, low on protein and vitamins and with high carbohydrates.
Key Indicators Myanmar Food and Nutrition Security Profiles Myanmar has experienced growth in Dietary Energy Supply (DES). Dietary quality remains poor, low on protein and vitamins and with high carbohydrates.
Iron. (2) Microminerals
 Iron (2) Microminerals Iron 1.Background Information 1 1.Definition and Classification Iron is a transition metal element (atomic number: 26, Fe). It is predominantly stored as heme iron which is found
Iron (2) Microminerals Iron 1.Background Information 1 1.Definition and Classification Iron is a transition metal element (atomic number: 26, Fe). It is predominantly stored as heme iron which is found
IMPACT OF NUTRITION COUNSELLING AND SUPPLEMENTS ON THE MINERAL NUTRITURE OF RURAL PREGNANT WOMEN AND THEIR NEONATES
 IMPACT OF NUTRITION COUNSELLING AND SUPPLEMENTS ON THE MINERAL NUTRITURE OF RURAL PREGNANT WOMEN AND THEIR NEONATES R. Sachdeva S.K. Mann ABSTRACT Sixty six young women from low and lower middle income
IMPACT OF NUTRITION COUNSELLING AND SUPPLEMENTS ON THE MINERAL NUTRITURE OF RURAL PREGNANT WOMEN AND THEIR NEONATES R. Sachdeva S.K. Mann ABSTRACT Sixty six young women from low and lower middle income
DIETARY INTAKE OF PRESCHOOL CHILDREN OF DHARWAD TALUK, KARNATAKA
 DIETARY INTAKE OF PRESCHOOL CHILDREN OF DHARWAD TALUK, KARNATAKA 1 Akkavva Wadakappanavar, S. & 2 Pushpa Bharati Department of Food Science and Nutrition, College of Rural Home Science, University of Agricultural
DIETARY INTAKE OF PRESCHOOL CHILDREN OF DHARWAD TALUK, KARNATAKA 1 Akkavva Wadakappanavar, S. & 2 Pushpa Bharati Department of Food Science and Nutrition, College of Rural Home Science, University of Agricultural
Vitamin A Facts. for health workers. The USAID Micronutrient Program
 Vitamin A Facts for health workers The USAID Micronutrient Program What is vitamin A? Vitamin A Vitamin A is a nutrient required in small amounts for the body to function properly. It is called a micronutrient
Vitamin A Facts for health workers The USAID Micronutrient Program What is vitamin A? Vitamin A Vitamin A is a nutrient required in small amounts for the body to function properly. It is called a micronutrient
Prevalence and Socio-Demographic Correlates of Anaemia among G.C.E (A/L) Students in Jaffna Zonal Schools
 Proceedings of Jaffna University International Research Conference (JUICE-2012), pp. 122-128, published: March 2014, Sri Lanka Prevalence and Socio-Demographic Correlates of Anaemia among G.C.E (A/L) Students
Proceedings of Jaffna University International Research Conference (JUICE-2012), pp. 122-128, published: March 2014, Sri Lanka Prevalence and Socio-Demographic Correlates of Anaemia among G.C.E (A/L) Students
Activity 3-F: Micronutrient Activity Station
 Activity 3-F: Micronutrient Activity Station 1 Vitamin A deficiency 1 Instructions Please read through this Vitamin A information package and discuss amongst your group. You have 15 minutes to review this
Activity 3-F: Micronutrient Activity Station 1 Vitamin A deficiency 1 Instructions Please read through this Vitamin A information package and discuss amongst your group. You have 15 minutes to review this
Postdischarge nutrition,
 Postdischarge nutrition, is there a role for human milk? Harrie N. Lafeber MD,Ph.D. Professor of Neonatology, VU university medical center, Amsterdam, NL Ehrencranz et al. Indirect calorimetry 120-130
Postdischarge nutrition, is there a role for human milk? Harrie N. Lafeber MD,Ph.D. Professor of Neonatology, VU university medical center, Amsterdam, NL Ehrencranz et al. Indirect calorimetry 120-130
Downloaded from
 Preventing Iron Deficiency and Anaemia Joseph Mutuku, PhD Candidate, Wageningen University and Research Centre, Netherlands, formerly with Micronutrient Initiative, Kenya * Anaemia, often due to iron deficiency,
Preventing Iron Deficiency and Anaemia Joseph Mutuku, PhD Candidate, Wageningen University and Research Centre, Netherlands, formerly with Micronutrient Initiative, Kenya * Anaemia, often due to iron deficiency,
Advancing Policy Dialogue on Maternal Health Maternal Undernutrition: Evidence, Links, and Solutions
 Advancing Policy Dialogue on Maternal Health Maternal Undernutrition: Evidence, Links, and Solutions Amy Webb Girard Assistant Professor of Maternal and Child Nutrition Hubert Department of Global Health
Advancing Policy Dialogue on Maternal Health Maternal Undernutrition: Evidence, Links, and Solutions Amy Webb Girard Assistant Professor of Maternal and Child Nutrition Hubert Department of Global Health
Maternal and Infant Nutrition Briefs
 Maternal and Infant Nutrition Briefs A research-based newsletter prepared by the University of California for professionals interested in maternal and infant nutrition March/April 2003 New Guidelines on
Maternal and Infant Nutrition Briefs A research-based newsletter prepared by the University of California for professionals interested in maternal and infant nutrition March/April 2003 New Guidelines on
Iron deficiency is the most common single cause
 An Efficacy, Safety and Tolerability Study of Ferrous Ascorbate and Folic Acid (Phosfomin-XT) in Iron Deficiency Anemia BB Adsul*, Qayum Mukaddam**, Prashant Khandeparkar**, Manoj Naik** Abstract Aim:
An Efficacy, Safety and Tolerability Study of Ferrous Ascorbate and Folic Acid (Phosfomin-XT) in Iron Deficiency Anemia BB Adsul*, Qayum Mukaddam**, Prashant Khandeparkar**, Manoj Naik** Abstract Aim:
Systematic review of the efficacy and effectiveness of complementary feeding interventions in developing countries
 Review Article Systematic review of the efficacy and effectiveness of complementary feeding interventions in developing countries Kathryn G. Dewey and Seth Adu-Afarwuah Program in International and Community
Review Article Systematic review of the efficacy and effectiveness of complementary feeding interventions in developing countries Kathryn G. Dewey and Seth Adu-Afarwuah Program in International and Community
Myanmar - Food and Nutrition Security Profiles
 Key Indicators Myanmar - Food and Nutrition Security Profiles Myanmar has experienced growth in Dietary Energy Supply (DES). Dietary quality remains poor, low on protein and vitamins and with high carbohydrates.
Key Indicators Myanmar - Food and Nutrition Security Profiles Myanmar has experienced growth in Dietary Energy Supply (DES). Dietary quality remains poor, low on protein and vitamins and with high carbohydrates.
From malnutrition to nutrition security
 From malnutrition to nutrition security Martin W. Bloem, MD, PhD Senior Nutrition Advisor/WFP Global Coordinator UNAIDS World Food Program Nurturing development: Improving human nutrition with animal-source
From malnutrition to nutrition security Martin W. Bloem, MD, PhD Senior Nutrition Advisor/WFP Global Coordinator UNAIDS World Food Program Nurturing development: Improving human nutrition with animal-source
Farhana Haseen BRAC. March Research and Evaluation Division BRAC Centre, 75 Mohakhali Dhaka 1212, Bangladesh
 Efficacy of daily and weekly home fortification of weaning foods with Sprinkles in improving iron deficiency anaemia among young children in Bangladesh Farhana Haseen March 2004 BRAC Research and Evaluation
Efficacy of daily and weekly home fortification of weaning foods with Sprinkles in improving iron deficiency anaemia among young children in Bangladesh Farhana Haseen March 2004 BRAC Research and Evaluation
Research Article A Study on Nutritional Status of Rural Lactating Mothers (0-6 Months) in Ramanathapuram District
 Research Article A Study on Nutritional Status of Rural Lactating Mothers (06 Months) in Ramanathapuram District K. Kavitha, S. Sumayaa, S. Ravikumar and A. Thahira Banu 3 Department of Home Science Thassim
Research Article A Study on Nutritional Status of Rural Lactating Mothers (06 Months) in Ramanathapuram District K. Kavitha, S. Sumayaa, S. Ravikumar and A. Thahira Banu 3 Department of Home Science Thassim
Efficacy of Sodium Iron EDTA in the Fortification Programs
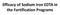 Efficacy of Sodium Iron EDTA in the Fortification Programs Iron fortificants WATER SOLUBLE COMPOUNDS Dissolve instantaneously ferrous sulfate ferrous gluconate RBV = 100 Ferrous bisglycinate Sodium iron
Efficacy of Sodium Iron EDTA in the Fortification Programs Iron fortificants WATER SOLUBLE COMPOUNDS Dissolve instantaneously ferrous sulfate ferrous gluconate RBV = 100 Ferrous bisglycinate Sodium iron
WHO Child Growth Standards
 WHO Child Growth Standards Implications for everyday practice Dr Mercedes de Onis Department of Nutrition World Health Organization Geneva, Switzerland 1 year 2 years 3 years 4 years 5 years WHO Child
WHO Child Growth Standards Implications for everyday practice Dr Mercedes de Onis Department of Nutrition World Health Organization Geneva, Switzerland 1 year 2 years 3 years 4 years 5 years WHO Child
Approach to the child with anemia. Nittaya Wisanuyothin,MD. Pediatrics Department, Maharat Nakhonratchasima Hospital
 Approach to the child with anemia Nittaya Wisanuyothin,MD. Pediatrics Department, Maharat Nakhonratchasima Hospital Definition of anemia Hb< 2 SD or P2.5 below the mean for a healthy of the same gender
Approach to the child with anemia Nittaya Wisanuyothin,MD. Pediatrics Department, Maharat Nakhonratchasima Hospital Definition of anemia Hb< 2 SD or P2.5 below the mean for a healthy of the same gender
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Statistical Assessment of the Effectiveness of Homoeopathic Medicine Ferrum metallicum 6X in
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Statistical Assessment of the Effectiveness of Homoeopathic Medicine Ferrum metallicum 6X in
Nutritional Status and Anaemia with Special Reference to Morphological Classification in Underfive Children
 368 Original Study Nutritional Status and Anaemia with Special Reference to Morphological Classification in Underfive Children Vinod Narkhede, Asst. Prof., Dept. of Community Medicine, Peoples College
368 Original Study Nutritional Status and Anaemia with Special Reference to Morphological Classification in Underfive Children Vinod Narkhede, Asst. Prof., Dept. of Community Medicine, Peoples College
JMSCR Vol 06 Issue 01 Page January 2018
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i1.101 Prevalence of anemia and its association
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i1.101 Prevalence of anemia and its association
Frequently Asked Questions on Zinc and Suggested Responses
 Last edited: September 27, 2012 Zinc Treatment of Childhood Diarrhea Frequently Asked Questions Diarrhoea still remains a leading cause of morbidity and mortality in developing countries. Every year more
Last edited: September 27, 2012 Zinc Treatment of Childhood Diarrhea Frequently Asked Questions Diarrhoea still remains a leading cause of morbidity and mortality in developing countries. Every year more
Supplementary Infant Feeding in Developing Countries
 Weaning: Why, What, and When?, edited by A. Ballabriga and J. Rey. Nestlf Nutrition, Vevey/Raven Press, New York c 97 Supplementary Infant Feeding in Developing Countries Ashfaq Ahmad Department of Child
Weaning: Why, What, and When?, edited by A. Ballabriga and J. Rey. Nestlf Nutrition, Vevey/Raven Press, New York c 97 Supplementary Infant Feeding in Developing Countries Ashfaq Ahmad Department of Child
Prevention of Mother to Child Transmission of HIV: Our Experience in South India
 pg 62-66 Original Article Prevention of Mother to Child Transmission of HIV: Our Experience in South India Karthekeyani Vijaya 1, Alexander Glory 2, Solomon Eileen 3, Rao Sarita 4, Rao P.S.S.Sunder 5 1
pg 62-66 Original Article Prevention of Mother to Child Transmission of HIV: Our Experience in South India Karthekeyani Vijaya 1, Alexander Glory 2, Solomon Eileen 3, Rao Sarita 4, Rao P.S.S.Sunder 5 1
Evidence Based Interventions for Improving Maternal and Child Nutrition: What Can be Done and at What Cost? Lancet, vol 382, , 2013
 Evidence Based Interventions for Improving Maternal and Child Nutrition: What Can be Done and at What Cost? Lancet, vol 382, 452 77, 2013 Dr. S.K Roy Senior Scientist Chairperson, Bangladesh Breastfeeding
Evidence Based Interventions for Improving Maternal and Child Nutrition: What Can be Done and at What Cost? Lancet, vol 382, 452 77, 2013 Dr. S.K Roy Senior Scientist Chairperson, Bangladesh Breastfeeding
By the end of the activities described in Section 5, consensus has
 6 Selecting Indicators 81 By the end of the activities described in Section 5, consensus has been reached on the goals and objectives of the project, the information which needs to be collected and analyzed
6 Selecting Indicators 81 By the end of the activities described in Section 5, consensus has been reached on the goals and objectives of the project, the information which needs to be collected and analyzed
Prevalence of Iron Deficiency Anaemia in Children Attending ICDS Center in a Tier II City
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. IV (August. 2016), PP 28-32 www.iosrjournals.org Prevalence of Iron Deficiency Anaemia
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. IV (August. 2016), PP 28-32 www.iosrjournals.org Prevalence of Iron Deficiency Anaemia
Study of Serum Hepcidin as a Potential Mediator of the Disrupted Iron Metabolism in Obese Adolescents
 Study of Serum Hepcidin as a Potential Mediator of the Disrupted Iron Metabolism in Obese Adolescents Prof. Azza Abdel Shaheed Prof. of Child Health NRC National Research Centre Egypt Prevalence of childhood
Study of Serum Hepcidin as a Potential Mediator of the Disrupted Iron Metabolism in Obese Adolescents Prof. Azza Abdel Shaheed Prof. of Child Health NRC National Research Centre Egypt Prevalence of childhood
Fig. 64 Framework describing causes and consequences of maternal and child undernutriton
 9.0 PREVALENCE OF MALNUTRITION 118 This chapter presents the prevalence of the three types of malnutrition (wasting, stunting and underweight) by background characteristic and livelihood zones in children
9.0 PREVALENCE OF MALNUTRITION 118 This chapter presents the prevalence of the three types of malnutrition (wasting, stunting and underweight) by background characteristic and livelihood zones in children
Nutritional Assessment & Monitoring of Hospitalized Children
 Nutritional Assessment & Monitoring of Hospitalized Children Kehkashan Zehra, Clinical Dietitian Sindh Institute of Urology & Transplantation, Karachi In Pakistan 42% of children aged < 5 years are stunted
Nutritional Assessment & Monitoring of Hospitalized Children Kehkashan Zehra, Clinical Dietitian Sindh Institute of Urology & Transplantation, Karachi In Pakistan 42% of children aged < 5 years are stunted
Guidelines for the prescribing of specialist infant formula in primary care: Luton and Bedfordshire
 Guidelines for the prescribing of specialist infant formula in primary care: Luton and Bedfordshire September 2017 This document is a revised edition written and agreed by paediatricians, paediatric dietitians,
Guidelines for the prescribing of specialist infant formula in primary care: Luton and Bedfordshire September 2017 This document is a revised edition written and agreed by paediatricians, paediatric dietitians,
New and updated indicators for assessing infant and young child feeding practices. Presentation outline
 New and updated indicators for assessing infant and young child feeding practices Bernadette Daelmans (WHO) on behalf of the Working Group on IYCF indicators Presentation outline The rationale for developing
New and updated indicators for assessing infant and young child feeding practices Bernadette Daelmans (WHO) on behalf of the Working Group on IYCF indicators Presentation outline The rationale for developing
Feeding the Small for Gestational Age Infant. Feeding the Small for Gestational Age Infant
 Feeding the Small for Gestational Age Infant Feeding the Small for Gestational Age Infant What s the right strategy? Infants born small-for-gestational age (SGA) are at higher risk for adult diseases.
Feeding the Small for Gestational Age Infant Feeding the Small for Gestational Age Infant What s the right strategy? Infants born small-for-gestational age (SGA) are at higher risk for adult diseases.
Solomon Islands Food and Nutrition Security Profiles
 Key Indicators Solomon Islands Food and Nutrition Security Profiles Solomon Islands has experienced stagnation in percapita GDP and undernourishment in recent years. Dietary Energy Supply (DES) has continued
Key Indicators Solomon Islands Food and Nutrition Security Profiles Solomon Islands has experienced stagnation in percapita GDP and undernourishment in recent years. Dietary Energy Supply (DES) has continued
Dr Anne-Louise Heath. Senior Lecturer University of Otago Dunedin
 Dr Anne-Louise Heath Senior Lecturer University of Otago Dunedin UNIVERSITY OF OTAGO DEPARTMENT OF HUMAN NUTRITION Toddler nutrition making every bite count today for tomorrow Anne-Louise Heath, Szymlek-Gay
Dr Anne-Louise Heath Senior Lecturer University of Otago Dunedin UNIVERSITY OF OTAGO DEPARTMENT OF HUMAN NUTRITION Toddler nutrition making every bite count today for tomorrow Anne-Louise Heath, Szymlek-Gay
Bangladesh Breastfeeding Foundation
 Dealing with Child Undernutrition Using Local Foods: Experience from Bangladesh WBC 2012 New Delhi Dr. S. K. Roy MBBS, MSc. Nutri., Dip-in-Biotech, PhD, FRCP, Chairperson, Bangladesh Breastfeeding Foundation
Dealing with Child Undernutrition Using Local Foods: Experience from Bangladesh WBC 2012 New Delhi Dr. S. K. Roy MBBS, MSc. Nutri., Dip-in-Biotech, PhD, FRCP, Chairperson, Bangladesh Breastfeeding Foundation
HOMESTEAD GARDENING FOR COMBATING VITAMIN A DEFICIENCY:THE HELEN KELLER INTERNATIONAL, BANGLADESH, EXPERIENCE
 9 HOMESTEAD GARDENING FOR COMBATING VITAMIN A DEFICIENCY:THE HELEN KELLER INTERNATIONAL, BANGLADESH, EXPERIENCE A.TAHER, A.TALUKDER, N.R. SARKAR,V.N. BUSHAMUKA, A. HALL, S. DE PEE, R. MOENCH-PFANNER, L.
9 HOMESTEAD GARDENING FOR COMBATING VITAMIN A DEFICIENCY:THE HELEN KELLER INTERNATIONAL, BANGLADESH, EXPERIENCE A.TAHER, A.TALUKDER, N.R. SARKAR,V.N. BUSHAMUKA, A. HALL, S. DE PEE, R. MOENCH-PFANNER, L.
Prevalence and risk factors for iron deficiency in Kelantanese pre-school children
 O r i g i n a l A r t i c l e Singapore Med J 2006; 47(11) : 935 Prevalence and risk factors for iron deficiency in Kelantanese pre-school children Siti-Noor A S, Wan-Maziah W M, Narazah M Y, Quah B S
O r i g i n a l A r t i c l e Singapore Med J 2006; 47(11) : 935 Prevalence and risk factors for iron deficiency in Kelantanese pre-school children Siti-Noor A S, Wan-Maziah W M, Narazah M Y, Quah B S
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
Systematic review of the efficacy and effectiveness of complementary feeding interventions
 Systematic review of the efficacy and effectiveness of complementary feeding interventions Kathryn G. Dewey, PhD Seth Adu-Afarwuah Afarwuah,, PhD Program in International and Community Nutrition University
Systematic review of the efficacy and effectiveness of complementary feeding interventions Kathryn G. Dewey, PhD Seth Adu-Afarwuah Afarwuah,, PhD Program in International and Community Nutrition University
Activity 3-F: Micronutrient Activity Station
 Activity 3-F: Micronutrient Activity Station 1 Vitamin A deficiency 1 Instructions Please read through this Vitamin A information package and discuss amongst your group. You have 15 minutes to review this
Activity 3-F: Micronutrient Activity Station 1 Vitamin A deficiency 1 Instructions Please read through this Vitamin A information package and discuss amongst your group. You have 15 minutes to review this
Content. The double burden of disease in México
 Can we and Prevent Malnutrition while Addressing the Challenge of NRCD s? Experiences from Mexico Content The double burden of disease in México What is currently being done in México for preventing and
Can we and Prevent Malnutrition while Addressing the Challenge of NRCD s? Experiences from Mexico Content The double burden of disease in México What is currently being done in México for preventing and
Optimal Distribution and Utilization of Donated Human Breast Milk: A Novel Approach
 653738JHLXXX10.1177/0890334416653738Journal of Human LactationSimpson et al research-article2016 Original Research: Brief Report Optimal Distribution and Utilization of Donated Human Breast Milk: A Novel
653738JHLXXX10.1177/0890334416653738Journal of Human LactationSimpson et al research-article2016 Original Research: Brief Report Optimal Distribution and Utilization of Donated Human Breast Milk: A Novel
Impact of nutrition education on iron deficiency anaemia among college student of Banasthali University, Rajasthan
 FOOD SCIENCE RESEARCHPAPER RESEARCH JOURNAL e ISSN-2230-9403 Visit us : www.researchjournal.co.in Volume 7 Issue 1 April, 2016 74-79 DOI : 10.15740/HAS/FSRJ/7.1/74-79 Impact of nutrition education on iron
FOOD SCIENCE RESEARCHPAPER RESEARCH JOURNAL e ISSN-2230-9403 Visit us : www.researchjournal.co.in Volume 7 Issue 1 April, 2016 74-79 DOI : 10.15740/HAS/FSRJ/7.1/74-79 Impact of nutrition education on iron
Int.J.Curr.Res.Aca.Rev.2016; 4(6): Impact of Mid Day Meal on Nutritional Status of School Going Children with Special Emphasis on Zinc
 Impact of Mid Day Meal on Nutritional Status of School Going Children with Special Emphasis on Zinc Iram Khan* and Sangeeta Pandey Department of Nutrition and Dietetics, Mount Carmel College, No.58, Palace
Impact of Mid Day Meal on Nutritional Status of School Going Children with Special Emphasis on Zinc Iram Khan* and Sangeeta Pandey Department of Nutrition and Dietetics, Mount Carmel College, No.58, Palace
Abstract. Nutritional status and Health implication of ongoing Nutrition Transition in India
 Abstract Nutritional status and Health implication of ongoing Nutrition Transition in India Vandana Bhattacharya Research Officer Department of social science, National Institute of Health and Family Welfare,
Abstract Nutritional status and Health implication of ongoing Nutrition Transition in India Vandana Bhattacharya Research Officer Department of social science, National Institute of Health and Family Welfare,
Objectives. Objectives. Essentials of Breastfeeding. E Course on Programming for IYCF. UNICEF and Cornell University
 Objectives To review the physiology of and the important aspects of milk composition Essentials of Breastfeeding Kathleen M. Rasmussen, ScD To describe 3 major recommended practices To describe potential
Objectives To review the physiology of and the important aspects of milk composition Essentials of Breastfeeding Kathleen M. Rasmussen, ScD To describe 3 major recommended practices To describe potential
Translating guidelines into practice: Complementary feeding in Indonesia
 Translating guidelines into practice: Complementary feeding in Indonesia SEAMEO-TROPMED Regional Center for Community Nutrition University of Indonesia Dr. Umi Fahmida SEAMEO RECFON ILSI-SEA Region Seminar
Translating guidelines into practice: Complementary feeding in Indonesia SEAMEO-TROPMED Regional Center for Community Nutrition University of Indonesia Dr. Umi Fahmida SEAMEO RECFON ILSI-SEA Region Seminar
Role of human milk fortifier on weight gain in very low birth weight babies
 International Journal of Contemporary Pediatrics Verma GK et al. Int J Contemp Pediatr. 2018 Mar;5(2):353-358 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
International Journal of Contemporary Pediatrics Verma GK et al. Int J Contemp Pediatr. 2018 Mar;5(2):353-358 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
Screening in well baby clinic
 Screening in well baby clinic Dr. Abdulmoein Al-Agha, Ass. Professor & Consultant Pediatrician, KAUH & Erfan Hospital, Jeddah Well baby clinic IS Not only for vaccinations and check up for fever & URTI!!!
Screening in well baby clinic Dr. Abdulmoein Al-Agha, Ass. Professor & Consultant Pediatrician, KAUH & Erfan Hospital, Jeddah Well baby clinic IS Not only for vaccinations and check up for fever & URTI!!!
Laos - Food and Nutrition Security Profiles
 Key Indicators Laos - Food and Nutrition Security Profiles In Lao PDR, GDP per capita has increased consistently during recent years, as has Dietary Energy Supply (DES) per person. Nevertheless, undernutrition
Key Indicators Laos - Food and Nutrition Security Profiles In Lao PDR, GDP per capita has increased consistently during recent years, as has Dietary Energy Supply (DES) per person. Nevertheless, undernutrition
NUTRITIONAL STATUS, PREVALENCE OF ANEMIA,
 NUTRITIONAL STATUS, PREVALENCE OF ANEMIA, 10 AND MICRONUTRIENT SUPPLEMENTATION This chapter focuses on infant feeding practices, and the nutritional and micronutrient status of women and children. Infant
NUTRITIONAL STATUS, PREVALENCE OF ANEMIA, 10 AND MICRONUTRIENT SUPPLEMENTATION This chapter focuses on infant feeding practices, and the nutritional and micronutrient status of women and children. Infant
In Mexico, malnutrition continues to be an important public health problem in children under 5 years of age
 Impact of the poverty alleviation program Oportunidades on diverse indicators of nutritional status in Mexican small children Presented by: Salvador Villalpando, M.D., PhD Centro de Investigación en Nutrición
Impact of the poverty alleviation program Oportunidades on diverse indicators of nutritional status in Mexican small children Presented by: Salvador Villalpando, M.D., PhD Centro de Investigación en Nutrición
Nutrient Intake of Lactating Mothers from Rural and Urban Areas. Asha Kawatra and Salil Sehgal
 Kawatra, Asha; Sehgal, Salil : Nutrient Intake of Lactating Mothers from Rural and Urban Areas. Indian Journal of Social Research. 39(2) April-June 1998. P 91-99. ---------------------------------------------------------------------------------------------------------------------
Kawatra, Asha; Sehgal, Salil : Nutrient Intake of Lactating Mothers from Rural and Urban Areas. Indian Journal of Social Research. 39(2) April-June 1998. P 91-99. ---------------------------------------------------------------------------------------------------------------------
Efficacy and safety of new complementary feeding guidelines with an emphasis on red meat consumption: a randomized trial in Bogota, Colombia 1 3
 Efficacy and safety of new complementary feeding guidelines with an emphasis on red meat consumption: a randomized trial in Bogota, Colombia 1 3 Gilma A Olaya, Margaret Lawson, and Mary S Fewtrell ABSTRACT
Efficacy and safety of new complementary feeding guidelines with an emphasis on red meat consumption: a randomized trial in Bogota, Colombia 1 3 Gilma A Olaya, Margaret Lawson, and Mary S Fewtrell ABSTRACT
first three years of life
 Journal of Epidemiology and Community Health, 1981, 35, 18-184 Parental smoking and lower respiratory illness in the first three years of life D. M. FERGUSSON, L. J. HORWOOD, F. T. SHANNON, AND BRENT TAYLOR
Journal of Epidemiology and Community Health, 1981, 35, 18-184 Parental smoking and lower respiratory illness in the first three years of life D. M. FERGUSSON, L. J. HORWOOD, F. T. SHANNON, AND BRENT TAYLOR
ENTERAL NUTRITION Identifying risk of patients for enteral feeding problems: Low risk: Moderate risk: High risk:
 ENTERAL NUTRITION Statement of best practice Feeding with mother s own breastmilk is protective against sepsis, NEC and death All mothers should be informed about this and strongly encouraged to express
ENTERAL NUTRITION Statement of best practice Feeding with mother s own breastmilk is protective against sepsis, NEC and death All mothers should be informed about this and strongly encouraged to express
Josie Grace C. Castillo, M.D.
 Josie Grace C. Castillo, M.D. 2 types of nutrients Macronutrients Carbohydrate Fats Protein Micronutrients Vitamins Minerals 1 Occur when the quantity or quality of food is not sufficient to meet a persons
Josie Grace C. Castillo, M.D. 2 types of nutrients Macronutrients Carbohydrate Fats Protein Micronutrients Vitamins Minerals 1 Occur when the quantity or quality of food is not sufficient to meet a persons
GOVERNMENT OF INDIA MINISTRY OF WOEMN AND CHILD DEVELOPMENT LOK SABHA UNSTARRED QUESTION NO TO BE ANSWERED ON PERFORMANCE UNDER ICDS
 GOVERNMENT OF INDIA MINISTRY OF WOEMN AND CHILD DEVELOPMENT LOK SABHA UNSTARRED QUESTION NO. 2192 TO BE ANSWERED ON 29.07.2016 PERFORMANCE UNDER ICDS 2192. SHRI M.K. RAGHAVAN: Will the Minister of WOMEN
GOVERNMENT OF INDIA MINISTRY OF WOEMN AND CHILD DEVELOPMENT LOK SABHA UNSTARRED QUESTION NO. 2192 TO BE ANSWERED ON 29.07.2016 PERFORMANCE UNDER ICDS 2192. SHRI M.K. RAGHAVAN: Will the Minister of WOMEN
Controlling Iron Deficiency Anemia Through The Use of Home-fortified Complementary Foods
 Symposium on Micronutrient Deficiency Disorders Controlling Iron Deficiency Anemia Through The Use of Home-fortified Complementary Foods Stanley H. Zlotkin, Anna L. Christofides, S.M. Ziauddin Hyder, Claudia
Symposium on Micronutrient Deficiency Disorders Controlling Iron Deficiency Anemia Through The Use of Home-fortified Complementary Foods Stanley H. Zlotkin, Anna L. Christofides, S.M. Ziauddin Hyder, Claudia
Cook Islands Food and Nutrition Security Profiles
 Key Indicators Cook Islands Food and Nutrition Security Profiles Mortality in children has shown a constant reduction over the years, but unless further acceleration, Cook Islands will not achieve the
Key Indicators Cook Islands Food and Nutrition Security Profiles Mortality in children has shown a constant reduction over the years, but unless further acceleration, Cook Islands will not achieve the
Contemporary Maternal-Newborn Nursing: 8 Edition Test Bank Ladewig
 Contemporary Maternal-Newborn Nursing: 8 Edition Test Bank Ladewig Link full download: http://testbankair.com/download/test-bank-for-contemporarymaternal-newborn-nursing-care-8th-edition/ Chapter 12 Question
Contemporary Maternal-Newborn Nursing: 8 Edition Test Bank Ladewig Link full download: http://testbankair.com/download/test-bank-for-contemporarymaternal-newborn-nursing-care-8th-edition/ Chapter 12 Question
GAIN S GLOBAL STRATEGY ON FOOD FORTIFICATION TO IMPROVE PUBLIC HEALTH ASIA HIGHLIGHTS. Regina Moench-Pfanner, PhD Director, Singapore GAIN
 GAIN S GLOBAL STRATEGY ON FOOD FORTIFICATION TO IMPROVE PUBLIC HEALTH ASIA HIGHLIGHTS Regina Moench-Pfanner, PhD Director, Singapore GAIN 1 GAIN - Introduction GAIN was founded at a UN global summit on
GAIN S GLOBAL STRATEGY ON FOOD FORTIFICATION TO IMPROVE PUBLIC HEALTH ASIA HIGHLIGHTS Regina Moench-Pfanner, PhD Director, Singapore GAIN 1 GAIN - Introduction GAIN was founded at a UN global summit on
Haemoglobin and ferritin concentrations in children aged 12 and 18 months
 Arch Dis Child 1999;80:153 157 153 Haemoglobin and ferritin concentrations in children aged 12 and 18 months Andrea SherriV, Alan Emond, Neil Hawkins, Jean Golding, the ALSPAC Children in Focus Study Team
Arch Dis Child 1999;80:153 157 153 Haemoglobin and ferritin concentrations in children aged 12 and 18 months Andrea SherriV, Alan Emond, Neil Hawkins, Jean Golding, the ALSPAC Children in Focus Study Team
Focus Areas for Entry Test (Technical Part) for M. Phil / PhD in Food & Nutrition
 Focus Areas for Entry Test (Technical Part) for M. Phil / PhD in Food & Nutrition Sr. No. Core Areas Percentage 1. 2. Community Nutrition 15% Dietetics and Preventive Nutrition 15% 3. 4. 5. 6. 7. Nutritional
Focus Areas for Entry Test (Technical Part) for M. Phil / PhD in Food & Nutrition Sr. No. Core Areas Percentage 1. 2. Community Nutrition 15% Dietetics and Preventive Nutrition 15% 3. 4. 5. 6. 7. Nutritional
Socio-Demographic Factors Affecting Anemia In School Children In Urban Area Of Meerut, India
 ISPUB.COM The Internet Journal of Preventive Medicine Volume 2 Number 1 Socio-Demographic Factors Affecting Anemia In School Children In Urban Area Of Meerut, India N Saluja, S Garg, H Chopra, S Bajpai
ISPUB.COM The Internet Journal of Preventive Medicine Volume 2 Number 1 Socio-Demographic Factors Affecting Anemia In School Children In Urban Area Of Meerut, India N Saluja, S Garg, H Chopra, S Bajpai
Dietary Adequacy of Indian Rural Preschool Children Influencing Factors
 Dietary Adequacy of Indian Rural Preschool Children Influencing Factors by A. Jyothi Lakshmi, Begum Khyrunnisa, G. Saraswathi, and Prakash Jamuna Department of Studies in Food Science and Nutrition, University
Dietary Adequacy of Indian Rural Preschool Children Influencing Factors by A. Jyothi Lakshmi, Begum Khyrunnisa, G. Saraswathi, and Prakash Jamuna Department of Studies in Food Science and Nutrition, University
Biofortified pearl millet cultivars to fight iron and zinc deficiencies in India
 Biofortified pearl millet cultivars to fight iron and zinc deficiencies in India Inadequate intake of energy-providing organic macronutrients (largely carbohydrate, followed by protein and fat, in that
Biofortified pearl millet cultivars to fight iron and zinc deficiencies in India Inadequate intake of energy-providing organic macronutrients (largely carbohydrate, followed by protein and fat, in that
Title: Nutritional Support for Children Living with HIV
 Title: Nutritional Support for Children Living with HIV Author: PADMAVATHY.K 1, 2, ANITA SHET 1, 2 CHITR DINAKAR 1, 2 KARTHIKA KUMAR 1 PREETHY. H 2, SAJAL CLARENCE SINGH 2 1. St. Johns Research Institute,
Title: Nutritional Support for Children Living with HIV Author: PADMAVATHY.K 1, 2, ANITA SHET 1, 2 CHITR DINAKAR 1, 2 KARTHIKA KUMAR 1 PREETHY. H 2, SAJAL CLARENCE SINGH 2 1. St. Johns Research Institute,
A Descriptive Study of Outcomes of Interventions to Prevent Mother to Child Transmission of HIV in Lusaka, Zambia
 ORIGINAL PAPER A Descriptive Study of Outcomes of Interventions to Prevent Mother to Child Transmission of HIV in Lusaka, Zambia Chibesa Shichitamba W, National Malaria Control Centre, Lusaka-Zambia ABSTRACT
ORIGINAL PAPER A Descriptive Study of Outcomes of Interventions to Prevent Mother to Child Transmission of HIV in Lusaka, Zambia Chibesa Shichitamba W, National Malaria Control Centre, Lusaka-Zambia ABSTRACT
Nutrition transition in India is attributing to rapid. AJ S Asian Journal of Home Science Volume 8 Issue 1 June,
 AJ S Asian Journal of Home Science Volume 8 Issue 1 June, 2013 254-258 Research Paper Transition of diet from mother s chilhood to children and its impact on their health and nutritional status of rural
AJ S Asian Journal of Home Science Volume 8 Issue 1 June, 2013 254-258 Research Paper Transition of diet from mother s chilhood to children and its impact on their health and nutritional status of rural
