The skin performs six primary functions
|
|
|
- Verity McLaughlin
- 5 years ago
- Views:
Transcription
1 Case study series: Lifteez aerosol and for the prevention and management of MARSI KEY WORDS Adhesive remover Fragile skin Lifteez MARSI Pain Skin stripping Adhesive removers can be used to dissolve the adhesives that are used to attach dressings, pouches and medical devices to the body, and can thus reduce the chance of medical adhesive-related skin injury (MARSI). Skin stripping can occur at any age; however, certain populations are at increased risk, e.g. older people, neonates, and those with compromised skin integrity or multiple comorbidities. This case series evaluates the clinical performance and outcomes of the silicone adhesive remover Lifteez in 10 patients. The acceptability of the product to patients and clinical staff was also evaluated. LOUISE JONES, DONNA BELL, CHRISTINE HODGSON (COMMUNITY RESEARCH TEAM) Northumbria Healthcare NHS Foundation Trust LUXMI MOHAMUD (LM) Central and North West London NHS Foundation Trust JACKIE STEPHEN-HAYNES (JSH) Professor in Wound Healing, Birmingham City University ROSIE CALLAGHAN (RC) Tissue Viability Nurse, Worcestershire Health & Care NHS Trust MONIQUE MARIES (MM) Tissue Viability Nurse, Worcestershire Health & Care NHS Trust The skin performs six primary functions including protection, absorption, excretion, secretion, regulation and sensation. Healthy skin is smooth, elastic, slightly acidic, does not itch, acts as a barrier to irritants and allergens, and prevents water loss (Cowdell and Radley, 2012). Medical adhesive-related skin injuries (MARSIs) occur when medical adhesives remove superficial layers of skin, resulting in variable levels of skin damage, such as skin stripping, tension blisters, skin tears, contact dermatitis, maceration and folliculitis. These trauma can persist for 30 minutes or more after removal of the adhesive (McNichol et al, 2013) and will increase following repeated applications of the adhesives. MARSI can affect anyone using medical adhesives (dressings, tape, stoma or ostomy pouches and tube securement devices); however, MARSI is often seen in inpatient settings and vulnerable populations such as older adults, paediatric patients, those with multiple comorbidities or compromised peri-wound skin integrity. Dressing removal can be one of the most painful aspects of having a wound, so for these vulnerable populations, it is important to limit patient harm by identifying and addressing possible sources of damage, reducing pain, promoting comfort and encouraging concordance with treatment to maximise clinical outcomes and quality of life (Wounds International, 2004). Although such injuries may seem minor, the financial and nursing time costs can be high, as each MARSI requires an average of 7.8 treatments at a cost of per treatment application (McNichol and Bianchi, 2016). The cost of MARSI to patients can also be considerable. It can damage the integrity of the skin, which can be so painful that patients are fearful of dressing change and require analgesia prior to dressing change. Skin damage at dressing change also increases the risk of infection, delays wound healing and can increase wound size (McNichol and Bianchi, 2016). SAFE ADHESIVE REMOVAL Skin damage at dressing removal is largely preventable if the correct products and techniques are used. Adhesive products can be peeled back slowly at a low angle or the adhesive backing stretched to shear the adhesive from the skin; however, these techniques require force for detachment, which can cause skin tears (Taroc, 2017). In patients at risk of skin damage, skin barrier products, such as films and creams, can provide protection between the skin and adhesives (McNichol et al, 2013). Silicone adhesive-removal products, water, alcohol and emollients can be used to aid adhesive removal, and may reduce the need for pre-emptive analgesia. Silicone adhesive removal products are recommended, as they evaporate, do not leave a residue and do not dry out the skin (Cutting, 2006; McNichol and Bianchi, 2016; Taroc, 2017). They dissolve adhesives and aid the removal of dressings, tapes, skin protectors/barriers and medical devices (Benbow, 2012), minimising trauma and pain due to 118 Wounds UK Vol 14 No
2 Table 1. Summary of case series using Lifteez aerosol and Case Sex, age (years) Lifteez product used Wound type, location 1 Female, 80 Aerosol Skin tear, lower leg 2 Female, 52 Aerosol Amputation, forefoot 3 Male, 56 Aerosol Surgical wound and stoma, abdomen 4 Female, 91 Aerosol Pressure ulcer, sacral area 5 Male, 74 Aerosol Suspected pressure ulcer, lateral right foot 6 Female, 89 Aerosol and 7 Male, 42 Aerosol and 8 Male, 29 Aerosol and 9 Female, 65 Aerosol and 10 Male, 50 Aerosol and Trauma, lower leg Trauma, lower leg Mixed aetiology ulcers, lower leg Superficial burn, abdomen Trauma and burns, upper and lower arm Case 10 courtesy of MM and JSH (VAS for pain: 1=no pain; 10=unbearable pain) Comments at dressing removal before using Lifteez 4 out of 10 on the VAS between dressing changes Skin trauma and pain (10 out of 10 on the VAS) at dressing removal Extreme pain: 8 out of 10 on the VAS Adhesive tape irritated and stripped the skin on removal Low-adhesive dressing required due to fragile skin; however, it would often fall off Past dressings had pulled on skin during removal Past dressings had pulled on hair during removal 9 out of 10 on the VAS 9 out of 10 on the VAS 6 out of 10 on the VAS the stripping caused by some adhesives. They have also been reported to be pain-free when compared to alcohol-based solutions (Rudoni, 2011). A service review carried out by stoma care clinicians at St George s Healthcare NHS Trust reported that 91% of patients found it easier to remove their stoma pouch using a siliconebased adhesive remover (Rudoni, 2008). This result reflects the outcome of tests the clinicians performed on themselves, where the removal of stoma pouches after a few hours led to red, irritated skin only in those who were not using the adhesive remover (Rudoni, 2008). A survey assessing the use of silicone and hydrocolloid products in stoma care similarly supported the use of silicone-based adhesive remover; with 96% Comments at dressing removal using Lifteez Didn t feel a thing Patient became less anxious at dressing removal Lifteez given to patient for future dressing changes Dressing removal time decreased from 25 minutes to 2 minutes No pain, and analgesia dosage reduced No pain on dressing removal, and analgesia no longer required Dressing removal was amazing Lifteez aerosol given to ward staff to use on subsequent dressing changes No pain during and between dressing changes, preand post-lifteez use, potentially due to nerve damage It was possible to use more strongly adhesive dressings that remained in situ No pain during and between dressing changes, preand post-lifteez use, potentially due to peripheral neuropathy It was possible to use more strongly adhesive dressings that remained in situ Decreased from 2 to 1 out of 10 on the VAS Patient preferred Lifteez given to patient for future dressing changes Decreased from 2 to 1 out of 10 on the VAS Wipes more effective at detaching hairs No pain and analgesia dosage halved Patient preferred No pain at dressing removal Improved patient compliance No stinging on application, and minimal pain at dressing removal (2 out of 10 on the VAS) of stoma care nurses (n=648) recommending it be used when changing stoma pouches (Berry et al, 2007). LIFTEEZ Lifteez is an alcohol-free medical adhesive remover containing a mixture of siloxanes. It is available as an aerosol or as. Lifteez aids the removal of adhesive dressings, pouches and medical devices. Its skin-friendly formulation quickly targets and breaks strong adhesive bonds, minimising the potential for skin stripping and pain on dressing removal. Lifteez should be sprayed evenly or wiped around the skin edge of the adhesive area while the adhesive product is gently pulled away from the Wounds UK Vol 14 No
3 Figure 1. Case 1: On presentation, 2 weeks after injury Figure 2. Case 2: On initial assessment skin. When used with porous dressings or devices, Lifteez can be sprayed directly onto the dressing to facilitate removal. Additional spray or can be used if necessary during product removal or to get rid of any adhesive residue. Lifteez dries quickly and, therefore, will not affect the adhesion of any replacement dressing, pouch or adhesive device. Caution should be taken when using Lifteez on delicate or sensitive areas of skin. CASE STUDIES The key objective of this case series was to evaluate the clinical performance and outcomes of Lifteez aerosol and for the minimisation or prevention of MARSI and pain at dressing change. The acceptability of the product by clinical staff and patients was also evaluated. All clinicians taking part in the evaluation were given guidance on the recommendations for use, in accordance with the instructions for use. Clinicians were encouraged to use their own judgement on whether to use the aerosol or based on the individual patient s condition. Lifteez was used for up to 1 month and any changes in skin condition and patient comfort were monitored. Clinicians were also invited to comment on the adhesive remover s features, such as ease of use and stinging on application. Ten cases were completed at three different centres, an overview is available in Table 1. Cases 1 9 describe longer-duration wounds and are presented in more detail. Case 10 describes two wounds close to full healing and is presented in the summary. Case 1: Patient with a skin tear and fragile skin (Community Research Team) Ms P is 80 years old and sustained a Type 1 skin tear (as per the ISTAP skin tear classification; LeBlanc et al, 2018) on her left shin after falling 2 weeks prior. On presentation (Figure 1), the wound was dressed with a povidine-iodine wound contact layer and a simple adhesive dressing, which had been in place for 3 days. The skin tear was painful between dressing changes (4 out of 10 on the VAS; 1=no pain; 10=unbearable pain). As the patient had fragile skin, Lifteez aerosol was selected to aid dressing removal and reduce the risk of skin stripping and pain. There was a small amount of exudate, so a low-absorbent dressing was applied as per local protocol, and changed every 3 days. At the next dressing change, Lifteez aerosol was used to release the adhesive border, and the patient reported that they didn t feel a thing. The skin was realigned and after cleansing, a povidone-iodine wound contact layer and simple adhesive dressing were applied to reduce risk of infection. Throughout treatment, Ms P became less anxious regarding dressing removal as the experience was now entirely pain free and did not cause trauma to the wound area or peri-wound skin. The Lifteez aerosol was given to the patient to use at future dressing changes. Case 2. Unbearable pain at dressing changes post-amputation (LM) This is a 52-year-old female inpatient with neuropathic pain and a forefoot amputation due to spreading gangrene. The wound was heavily colonised, and the surrounding skin was red and blanching (Figure 2). Between dressing changes, wound pain was rated at 4 out of 10 on the VAS. An iodine wound contact layer covered with a bordered foam adhesive dressing had been in place for 3 days and required changing three times a week. The patient was reluctant to have dressing changes due to past adhesive-related skin trauma and pain, so oxycodone was administered 30 minutes before dressing change. No medical adhesive remover had previously been used as it was not on the wound care formulary. Dressing removal took 25 minutes, and the pain was unbearable (10 out of 10). Using Lifteez aerosol at the next dressing change allowed the dressing to be unpeeled easily without skin pulling. The patient described the dressing change as tender but not painful, and dressing removal now only took 2 minutes. The wound was cleansed and a protective barrier film was applied to the surrounding skin. The dressing regimen continued with an iodine and foam dressing as prescribed by the vascular team. The patient did not want the area bandaged. Lifteez aerosol continued to be used three times a week over the next month to reduce pain 120 Wounds UK Vol 14 No
4 Figure 3. Case 3: Dressings and stoma bag in place (head at top) Figure 4. Case 4: After first dressing removal with Lifteez Figure 5. Case 5: At initial assessment at dressing removal. The wound was improving and there had been no skin stripping or redness. Pain during and between dressing changes had also reduced, so that analgesia was not as frequently requested before dressing change. As Lifteez aerosol was easy to use, the patient was able to engage in their own care. Case 3. Lifteez used on abdominal wound dressing and stoma pouch (LM) Mr A is 56 years old and an inpatient at the rehabilitation unit following 3 months in ICU post-laparotomy. He has a large abdominal wound (18 cm [length] x 5.5 cm [width] x 3.5 cm [depth]) dressed with simple adhesive dressings and in very close proximity to his stoma (Figure 3). The first dressing change in the rehab unit was performed by ward nurses, and the patient complained of extreme pain on dressing removal (8 out of 10 on the VAS). He was referred to the TVN, who used Lifteez aerosol to reduce pain on dressing removal. The patient decided not to take analgesia prior to dressing change. The patient reported the aerosol felt cold; however, the dressing removal was pain free and he described the experience as amazing. After using Lifteez, the dressing and stoma flange both adhered well to the skin. Lifteez continued to be used at every dressing and stoma flange change three times a week (the stoma flange had to be changed three times a week due to the proximity of the wound). Case 4. Lifteez used to reduce skin trauma at dressing removal (RC) A 91-year-old female nursing home resident developed a sacral pressure ulcer after a prolonged period on the floor. The wound was 5 cm (length) x 6 cm (width) x 4 cm (depth) and the peri-wound and wound bed were considered healthy 100% granulation tissue. The ulcer was not painful, potentially due to nerve damage. An alginate contact layer and adhesive foam dressing had been in place for 1 day. Due to the location of the wound adhesive tape was sometimes required to keep the dressing in place; however, this was irritating and stripping the skin on removal. The rationale for using Lifteez aerosol was to achieve trauma-free dressing removal. It was hoped that using an adhesive remover would allow application of a more adhesive dressing and so tape would not be required. The wound was suitable for VAC (vacuumassisted closure) therapy, so this was initiated along with advice on regular repositioning and nutrition. Over the next week, Lifteez aerosol was used to remove the large film dressing needed for VAC therapy at two dressing changes (Figure 4). The dressing peeled off quickly after application of Lifteez. The wound was improving it had reduced in size and increased granulation tissue was present in the wound bed. The clinician was very pleased using Lifteez aerosol, especially for very adhesive dressings. Using Lifteez aerosol made it possible to use more adhesive and appropriate dressings for this patient with fragile skin, and reduce the frequency of dressing changes. Case 5. Suspected pressure ulcer on the foot with fragile skin complicated by diabetes (RC) A nursing home resident in his 70s has been bedbound for 1 year. He had diet-controlled diabetes with peripheral neuropathy, so experienced no sensation in his feet. He was admitted with a suspected pressure ulcer present on the lateral aspect of his right foot for 6 weeks. The wound was sloughy, but there was granulation tissue and good epithelisation at the edges (Figure 5). Honey ointment was applied to debride, and the wound was covered with a foam silicone dressing. The dressing was frequently falling off so Lifteez aerosol was selected to allow the use and safe removal of more strongly adhesive dressings that would remain in place for longer. The selected highly absorbent bordered polyurethane foam dressing was scheduled to be changed after 4 days due to its higher adhesive properties. Lifteez aerosol was used to remove both the original foam silicone secondary dressing, and the subsequent bordered polyurethane foam dressing that was chosen for its stronger adhesive properties. In both cases, the peri-wound area was less red following removal, especially where the dressing had previously adhered. The use of Lifteez did not interfere with the application of a new dressing. Dressing regimen continued with Wounds UK Vol 14 No
5 Figure 6. Case 6: After dressing removal using Lifteez aerosol Figure 7. Case 6: After dressing removal using Lifteez Figure 8. Case 7: Dressing removal with Lifteez wipe dressing changes scheduled for every 4 days. With the use of Lifteez, a more strongly adhesive dressing could be used for this patient with fragile skin, and removed without causing skin trauma. Case 6. Reducing pain and skin trauma in an older patient with fragile skin (Community Research Team) An 89-year-old female patient had a trauma wound to her left lower leg present for 1 week. A hydrogel dressing with a simple adhesive secondary dressing had been in place for 5 days. The patient had fragile skin and reported that, in the past, dressing removal had pulled on her skin. As such, Lifteez aerosol was selected as a medical adhesive remover to reduce skin trauma. The patient experienced slight discomfort (2 out of 10 on the VAS) but no stinging on application (Figure 6). The wound was cleansed, and a hydrogel dressing was applied to assist autolytic debridement, affixed with an adhesive dressing for low-exuding wounds. Over the next week, Lifteez aerosol and were used at two dressing changes to reduce skin pulling and trauma. The patient preferred the use of the so these were continued. No skin injury was observed despite the use of adhesive dressings on the fragile skin (Figure 7). Lifteez products were given to the patient for her next appointment with the district nurse to assist in dressing removal. The patient commented that these dressing changes were better than previous dressing changes of other wounds. Case 7. Patient with a trauma wound (Community Research Team) This patient is in his early 40s and is known to misuse alcohol. He sustained a superficial trauma laceration to his left lower leg, with healthy surrounding skin, which was treated with a hydrogel and simple adhesive dressing. During previous dressing removals of other wounds, pain would be 3 out of 10 on the VAS as the adhesive would often pull on his leg hair. Lifteez were used to facilitate a less painful dressing removal (Figure 8), and the patient rated the pain as 2 out of 10. The wound was cleansed, and a silver wound contact layer and simple adhesive dressing were applied to reduce inflammation. At the next dressing change 4 days later, Lifteez were used again and no pain was reported. The patient also felt calmer, as he knew dressing removal would be less painful using the Lifteez. Three days later, the Lifteez aerosol was used to release the adhesive secondary dressing, and a wipe was used to detach some hairs. The secondary dressing was changed to a soft siliconebordered dressing as the patient was changing the dressing between appointments due to increased exudate levels. Lifteez were continued for this patient to more easily detach hairs from the dressing. For patients who may pose challenges to care giving, creating a positive dressing change environment can improve compliance, comfort and confidence. Case 8. Patient with complex leg ulcers and very painful dressing changes (LM) A 29-year-old man with multiple comorbidities had bilateral mixed aetiology lower limb ulcers present for 8 months. The surrounding skin was dry and flaky, and the wounds were very sloughy and painful (5 6 out of 10 on the VAS). Past dressing removal had been very painful (9 out of 10), but had not caused skin stripping. The patient would take oral oxycodone hydrochloride 5 mg 30 minutes before dressing change, and no medical adhesive remover has been used before as it was not on the wound care formulary. Lifteez aerosol was selected to reduce pain while removing a manuka honey dressing and foam adhesive dressing, which had been in place for 3 days. The dressing lifted at the edges, taking less than 25 minutes to remove (previous dressing changes had taken 1 hour). The patient scored his pain at 8 out of 10 and did not like the spray sensation, so Lifteez were planned to be used next time. After cleansing and debriding, a barrier film was applied to the surrounding skin. Due to previous painful experiences from other dressings, an adhesive foam secondary dressing was applied by patient request, with no bandage due to the very hot weather. Over the next week, Lifteez were used at two scheduled dressing changes. The were gentle and soothing on the skin and it took 122 Wounds UK Vol 14 No
6 Cutting K (2006) Silicone and skin adhesives. J Community Nurs 20(11): 36 7 LeBlanc K et al (2018) Best Practice Recommendations for the Prevention and Management of Skin Tears in Aged Skin. London: Wounds International. Available at: com/resources/details/istap-bestpractice-recommendations-preventionand-management-skin-tears-aged-skin (acccessed ) McNichol L, Lund C, Rosen T, Gray M (2013) Medical Adhesives and Patient Safety: State of the Science: Consensus statements for the assessment, prevention, and treatment of adhesive-related skin injuries. J Wound Ostomy Continence Nurs 40(4): McNichol L, Bianchi J (2016) Medical adhesiverelated skin injuries (MARSI) made easy. London: Wounds UK. Available at: medical-adhesive-related-skin-injuriesmarsi-made-easy Rudoni C (2008) A service evaluation of use of silicone based adhesive remover. Br J Nurs 17(2 Suppl): S4 9 Rudoni C (2011) Peristomal skin irritation and the use of a silicone-based barrier film. Br J Nurs 20(16 Suppl) S12 8 Taroc AM (2017) A guide for adhesive removal: principles, practice, and products. American Nurse Today 12(10). Available at: adhesive-removal/ (accessed ) Wounds International (2004) Principles of best practice: Minimising pain at wound dressing-related procedures. A consensus document. London: MEP Ltd Acknowledgment This case study series was supported by Medicareplus International 10 minutes to remove the dressing. It was the first time the patient had enjoyed dressing change since the wound developed. His pain at dressing change reduced so much that his analgesia dose was halved. Case 9. Very painful blistered burn to abdomen (RC) A woman in her 60s was a temporary nursing home resident for respite care. She sustained a small scald above her belly button after using a hot water bottle for cramps. Honey ointment was applied to treat the burn, and covered with a simple adhesive dressing. The dressing had previously been very painful to remove (9 out of 10 on the VAS) and caused some minimal skin stripping. There was a risk that dressing removal would pull and rupture the blister, so Lifteez were selected to aid dressing removal. The patient reported that dressing change was much less painful (5 out of 10) than previous occasions, and it took half the time (10 minutes to 5 minutes). The management regimen continued for the next week, with Lifteez aerosol used at both dressing changes. The aerosol was easier to use than the, and the dressings peeled off very easily. The blister remained intact, and the patient experienced no pain. This wound had the potential to worsen, especially from previous skin stripping. Using Lifteez reduced the risk of further damage and gained the trust and compliance of the patient who had in the past experienced very painful dressing changes. SUMMARY OF CASE STUDIES Clinical feedback determined that the experiences of using Lifteez were, overall, very good when considering a range of factors. Clinicians were asked to evaluate, in particular, ease of application, patient comfort during application and pain on subsequent dressing removal. For each of these categories, the clinician was asked to rate Lifteez as being poor, fair, good, very good or excellent. The majority of clinicians rated Lifteez as very good or excellent for the parameters investigated. In this case series of 10 patients (5 men, 5 women; age range years), Lifteez removed dressings quickly and easily, resulting in reductions in pain, risk of skin trauma and use of analgesia during dressing changes. The patients did not experience any pain or stinging on application of Lifteez, and, in cases 2 and 8, oral analgesia was either reduced or no longer required. The application of Lifteez did not interfere with the application of subsequent dressing or stoma applications. In cases 4 and 5, Lifteez allowed the use of more strongly adhesive dressings that were more appropriate for the wound aetiology and remained in place for longer. For these patients, less frequent dressing changes were required, which allowed for longer undisturbed healing and improved the patient experience. In the longer term, dressing costs and nursing visits would reduce, releasing nursing time to allocate to increasing workload demands. Lifteez was especially helpful in cases when dressing choice was limited (based on resources or patient preference), and a more strongly adhesive dressing had to be used and removed safely, e.g. case 1. The Lifteez also helped to detach the hair from the dressing, e.g. case 7. Overall, clinicians would use Lifteez products again for people with fragile skin or at increased risk of skin stripping, and some have begun the process of adding it to their formularies. The Lifteez aerosol and were easy to use and often given to the patient or carer to take to future appointments or to complete their own dressing changes. As Lifteez is available as an aerosol or as, the most appropriate format could be selected for each patient to encourage compliance, for example case 6 and 8 preferred the feel of the compared to the aerosol. CONCLUSION Lifteez aerosol and have been shown to be clinically effective in removing wound care dressings. In this case study series, healthcare professionals and patients both reported positive feedback during dressing changes using Lifteez products. These clinical case studies demonstrate that Lifteez could have benefits across all care settings to improve patient comfort and compliance with care, and reduce the use of analgesia and nursing time. Wuk REFERENCES Benbow M (2012) Managing pain during the removal of wound dressings. Independent Nurse. Available at: (accessed ) Berry J, Black P, Smith R, Stuchfield B (2007) Assessing the value of silicone and hydrocolloid products in stoma care. Br J Nur 16(13): Cowdell F, Radley K (2012) Maintaining skin health in older people. Nursing Times 108(49): Wounds UK Vol 14 No
DRESSING SELECTION SIMPLIFIED
 10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
An advanced hydrocolloid dressing for moderately exuding wounds
 An advanced hydrocolloid dressing for moderately exuding wounds Indications for use Wound debridement Pressure ulcers Moderately exuding wounds Leg ulcers Assess the wound and select a suitable size (so
An advanced hydrocolloid dressing for moderately exuding wounds Indications for use Wound debridement Pressure ulcers Moderately exuding wounds Leg ulcers Assess the wound and select a suitable size (so
3M Cavilon Advanced Skin Protectant. Experience the power of ultimate protection.
 3M Cavilon Advanced Skin Protectant Experience the power of ultimate protection. The many challenges of skin integrity. Skin damage presents negative clinical outcomes resulting in potential complications
3M Cavilon Advanced Skin Protectant Experience the power of ultimate protection. The many challenges of skin integrity. Skin damage presents negative clinical outcomes resulting in potential complications
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
SDMA Categorisation of Wound Care and Associated Products
 Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
GP Practice Woundcare Formulary
 Agreed jointly by Ipswich and East Suffolk and West Suffolk Clinical Commissioning Groups GP Practice Woundcare Formulary Version 28 October 2017 Formulary items should be prescribed wherever possible.
Agreed jointly by Ipswich and East Suffolk and West Suffolk Clinical Commissioning Groups GP Practice Woundcare Formulary Version 28 October 2017 Formulary items should be prescribed wherever possible.
ALLEVYN Life Advanced Foam Wound Dressings
 ALLEVYN Life Advanced Foam Wound Dressings ALLEVYN Life Dressings have a multi-layered design incorporating hydrocellular foam, a hyper-absorber lock away core and a masking layer that has been designed
ALLEVYN Life Advanced Foam Wound Dressings ALLEVYN Life Dressings have a multi-layered design incorporating hydrocellular foam, a hyper-absorber lock away core and a masking layer that has been designed
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Diabetic Foot Ulcers. A guide to help minimise pain, trauma and stress
 Diabetic Foot Ulcers A guide to help minimise pain, trauma and stress From day one, Safetac was about less pain to patients. It s an easy story it does not stick to the wound, so it does not damage or
Diabetic Foot Ulcers A guide to help minimise pain, trauma and stress From day one, Safetac was about less pain to patients. It s an easy story it does not stick to the wound, so it does not damage or
Anseong Factory : 70-17, Wonam-ro, Wongok-myeon, Anseong-si, Gyeonggi-do , REPUBLIC OF KOREA
 Care for tomorrow The Solution for Management HQ & Factory : 7, Hyeongjero4Beon-gil, Namsa-myeon, Cheoin-gu, Yong-in-si, Gyeonggi-do 449-884, REPUBLIC OF KOREA TEL: +8-3-33-33 / FAX: +8-3-33-34 Anseong
Care for tomorrow The Solution for Management HQ & Factory : 7, Hyeongjero4Beon-gil, Namsa-myeon, Cheoin-gu, Yong-in-si, Gyeonggi-do 449-884, REPUBLIC OF KOREA TEL: +8-3-33-33 / FAX: +8-3-33-34 Anseong
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
John Timmons, David Gray, Fiona Russell
 Silflex soft silicone wound contact dressing It is hard to believe that it has taken so long for the message to get through, that dressings and dressing removal should not cause additional pain or trauma
Silflex soft silicone wound contact dressing It is hard to believe that it has taken so long for the message to get through, that dressings and dressing removal should not cause additional pain or trauma
CASE 1: TYPE-II DIABETIC FOOT ULCER
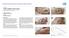 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Vacuumed Assisted Closure
 Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
STOMA CARE. Amendments Date Page(s) Comments Approved by 03/16 ALL Updated Guideline
 Note: Guidance comments are written in italics STOMA CARE Amendments Date Page(s) Comments Approved by 03/16 ALL Updated Guideline Compiled by: In Consultation with: Ratified by: Alice D Souza Neonatal
Note: Guidance comments are written in italics STOMA CARE Amendments Date Page(s) Comments Approved by 03/16 ALL Updated Guideline Compiled by: In Consultation with: Ratified by: Alice D Souza Neonatal
We look forward to serving you.
 ADVANCED CARE GEMCORE360 offers healthcare professionals a simple, clear and cost-effective wound care range while ensuring excellent clinical outcomes for their patients. 1 At GEMCO Medical, we strive
ADVANCED CARE GEMCORE360 offers healthcare professionals a simple, clear and cost-effective wound care range while ensuring excellent clinical outcomes for their patients. 1 At GEMCO Medical, we strive
2. Advanced wound therapies... 4 (i) Maggots... 4 (ii) Negative Pressure Wound Therapy (NPWT)... 4
 Contents: Wound management Medicines Formulary 1. Interactive dressings... 2 (i) Hydrocolloid dressings... 2 (ii) Hydrogel dressings... 2 (iii) Alginate dressings... 2 (iv) Fibrous absorbent dressings...
Contents: Wound management Medicines Formulary 1. Interactive dressings... 2 (i) Hydrocolloid dressings... 2 (ii) Hydrogel dressings... 2 (iii) Alginate dressings... 2 (iv) Fibrous absorbent dressings...
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING
 HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
The skin consists of the epidermis, dermis. The challenge of skin tears and lacerations in an emergency environment
 The challenge of skin tears and lacerations in an emergency environment KEY WORDS Atraumatic Non-adhesive silicone foam Patient satisfaction Skin tear Acute traumatic skin injuries are increasing in both
The challenge of skin tears and lacerations in an emergency environment KEY WORDS Atraumatic Non-adhesive silicone foam Patient satisfaction Skin tear Acute traumatic skin injuries are increasing in both
Silver Dressings. Sajida Khatri PrescQIPP Primary Care Lead.
 Silver Dressings Sajida Khatri PrescQIPP Primary Care Lead www.prescqipp.info Available at: www.prescqipp.info/silverdressings 2 Introduction PrescQIPP Silver dressings bulletin published in March 2014
Silver Dressings Sajida Khatri PrescQIPP Primary Care Lead www.prescqipp.info Available at: www.prescqipp.info/silverdressings 2 Introduction PrescQIPP Silver dressings bulletin published in March 2014
Medical technology guidance
 NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
Tissue Viability Service Wound Management Primary Care Formulary 2017
 Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Traditional Silicone Technology
 Innovative Non-Silicone Low Trauma Adhesives versus Traditional Silicone Technology A Review and Comparison Alan Neil Medical Industry Consultant Advanced Wound Care Lohmann Corporation 2016 Chronic wound
Innovative Non-Silicone Low Trauma Adhesives versus Traditional Silicone Technology A Review and Comparison Alan Neil Medical Industry Consultant Advanced Wound Care Lohmann Corporation 2016 Chronic wound
3M Cavilon Professional Skin Protection Range. Cavilon. Skin protection for even the most sensitive of skin
 3M Cavilon Professional Skin Protection Range Cavilon Skin protection for even the most sensitive of skin ...with an improved look. Our 3M Cavilon Professional Skin Protection Range has been refreshed
3M Cavilon Professional Skin Protection Range Cavilon Skin protection for even the most sensitive of skin ...with an improved look. Our 3M Cavilon Professional Skin Protection Range has been refreshed
TENA SKINCARE & CLEANSING VERY SPECIAL CARE FOR VERY SPECIAL SKIN
 TENA SKINCARE & CLEANSING VERY SPECIAL CARE FOR VERY SPECIAL SKIN 3-in-1 personal skincare saves time for caregivers and promotes patient skin health Mousse combine three personal skincare products in
TENA SKINCARE & CLEANSING VERY SPECIAL CARE FOR VERY SPECIAL SKIN 3-in-1 personal skincare saves time for caregivers and promotes patient skin health Mousse combine three personal skincare products in
Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009)
 Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009) This guidance should be read in conjunction with your local dressing formulary and anti-biotic prescribing guidelines.
Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009) This guidance should be read in conjunction with your local dressing formulary and anti-biotic prescribing guidelines.
Cuticell Contact. Silicone Wound Contact Layer. Highly Flexible Atraumatic Single-sided adherence
 Cuticell Contact Silicone Wound Contact Layer Highly Flexible Atraumatic Single-sided adherence Cuticell Contact impressively wound calming Cuticell Contact is a silicone wound contact layer that has a
Cuticell Contact Silicone Wound Contact Layer Highly Flexible Atraumatic Single-sided adherence Cuticell Contact impressively wound calming Cuticell Contact is a silicone wound contact layer that has a
Wound Care Program for Nursing Assistants-
 Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
PROTEX HEALTHCARE (UK) LIMITED PRODUCT QUESTIONS AND ANSWERS
 PROTEX HEALTHCARE (UK) LIMITED PRODUCT QUESTIONS AND ANSWERS Question What is Vacutex? How does Vacutex work? Does Vacutex prevent maceration to the surrounding skin? Does Vacutex adhere to the wound face?
PROTEX HEALTHCARE (UK) LIMITED PRODUCT QUESTIONS AND ANSWERS Question What is Vacutex? How does Vacutex work? Does Vacutex prevent maceration to the surrounding skin? Does Vacutex adhere to the wound face?
Categorisation of Wound Care and Associated Products
 Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
Categorisation of Wound Care and Associated Products Version 9 March 2018 Surgical Dressing Manufacturers Association 2018 TAPES AND TRADITIONAL DRESSINGS Wound Dressings Swabs Taping Traditional Wound
The primary function of low-adherence wound contact
 S35 Product focus S35 A multicentre clinical evaluation of silicone wound contact layer in daily practice Abstract Objective To evaluate clinically the performance of, a silicone-based primary contact
S35 Product focus S35 A multicentre clinical evaluation of silicone wound contact layer in daily practice Abstract Objective To evaluate clinically the performance of, a silicone-based primary contact
REPORT OF EXPERIENCES:
 REPORT OF EXPERIENCES: Non Adherent Dressings in Fragile Skin Conditions: The Use of Soft Silicone Coated Polyurethane Foam Dressing (Mepilex ) in Hereditary and Acquired Bullous Skin Diseases. Hauke Schumann
REPORT OF EXPERIENCES: Non Adherent Dressings in Fragile Skin Conditions: The Use of Soft Silicone Coated Polyurethane Foam Dressing (Mepilex ) in Hereditary and Acquired Bullous Skin Diseases. Hauke Schumann
Skin Protection for the critically ill
 Critical Care Solutions from the 3M Cavilon Professional Skin Care Products Family TM Skin Protection for the critically ill Why is Skin Damage a Significant Problem? Skin damage constitutes a negative
Critical Care Solutions from the 3M Cavilon Professional Skin Care Products Family TM Skin Protection for the critically ill Why is Skin Damage a Significant Problem? Skin damage constitutes a negative
Tissue Viability Service Wound Management Primary Care Formulary 2017
 Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Tissue Viability Service Wound Management Primary Care Formulary 2017 WMPF/TVS: March 2017 Review date: March 2019 Product Group Current Product Sizes Price per Item Hydrogel 1st Activheal Hydrogel 2nd
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Currently, the NHS is facing the challenge of
 Evaluation of a superabsorbent dressing in a primary care organization Jackie Stephen-Haynes and Claire Stephens Jackie Stephen-Haynes is Professor and Nurse Consultant, Practice Development Unit, Birmingham
Evaluation of a superabsorbent dressing in a primary care organization Jackie Stephen-Haynes and Claire Stephens Jackie Stephen-Haynes is Professor and Nurse Consultant, Practice Development Unit, Birmingham
Skin Tear Management. Deborah Mings RN (EC), MHSc, GNC(C), IIWCC Clinical Nurse Specialist, Skin and Wound Hamilton Health Sciences
 Skin Tear Management Deborah Mings RN (EC), MHSc, GNC(C), IIWCC Clinical Nurse Specialist, Skin and Wound Hamilton Health Sciences 1 Anatomy of the skin http://childrenshospital.org/az/site784/images/skinan
Skin Tear Management Deborah Mings RN (EC), MHSc, GNC(C), IIWCC Clinical Nurse Specialist, Skin and Wound Hamilton Health Sciences 1 Anatomy of the skin http://childrenshospital.org/az/site784/images/skinan
Management of Complex Wounds with Vacuum Assisted Closure
 Management of Complex Wounds with Vacuum Assisted Closure Wendy McInnes Vascular / Wound Nurse Practitioner The Queen Elizabeth Hospital, Adelaide, South Australia Treasurer ANZSVN wendy.mcinnes@health.sa.gov.au
Management of Complex Wounds with Vacuum Assisted Closure Wendy McInnes Vascular / Wound Nurse Practitioner The Queen Elizabeth Hospital, Adelaide, South Australia Treasurer ANZSVN wendy.mcinnes@health.sa.gov.au
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
An observational evaluation of a new foam adhesive dressing
 An observational evaluation of a new foam adhesive dressing Elizabeth Merlin-Manton, Michelle Greenwood and Adele Linthwaite An observational evaluation of a new foam adhesive dressing Elizabeth Merlin-Manton,
An observational evaluation of a new foam adhesive dressing Elizabeth Merlin-Manton, Michelle Greenwood and Adele Linthwaite An observational evaluation of a new foam adhesive dressing Elizabeth Merlin-Manton,
PRESSURE ULCERS SIMPLIFIED
 10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
ACCESSORIES. Giving you more choice.
 ACCESSORIES Giving you more choice. www.oakmed.co.uk Introduction Oakmed has developed a wide range of high quality accessories designed to meet the individual needs of patients. Contents Product Page
ACCESSORIES Giving you more choice. www.oakmed.co.uk Introduction Oakmed has developed a wide range of high quality accessories designed to meet the individual needs of patients. Contents Product Page
A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4
 A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4 Gill Wicks, Nurse Consultant, Tissue Viability for Wiltshire Primary Care Trust and Lecturer at University of West England Pressure ulcers
A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4 Gill Wicks, Nurse Consultant, Tissue Viability for Wiltshire Primary Care Trust and Lecturer at University of West England Pressure ulcers
Wound Management for Nurses/Technicians What do we need to know?
 Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
o Venous edema o Stasis ulcers o Varicose veins (not including spider veins) o Lipodermatosclerosis
 Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Understanding Incontinence-Associated Dermatitis and moving prevention forward. Medical and Surgical Requisites Pty Ltd
 Understanding Incontinence-Associated Dermatitis and moving prevention forward. Skin. Our largest organ and first line of defence. Skin is the first line of defence against irritants. But at times, our
Understanding Incontinence-Associated Dermatitis and moving prevention forward. Skin. Our largest organ and first line of defence. Skin is the first line of defence against irritants. But at times, our
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Palliative Care. EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for. Treatment. Improving Quality of Care Based on CMS Guidelines 39
 Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell
 Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
2/11/2016. Palliative Wound Management Workshop. Carolyn Brown BS, MEd, RN, ARM, CWS, FACCWS Carolyn Brown Consulting
 Palliative Wound Management Workshop Be the best that you can be! Carolyn Brown BS, MEd, RN, ARM, CWS, FACCWS Carolyn Brown Consulting 727-348-5856 cbjackwill@gmail.com Learner Objectives After attending
Palliative Wound Management Workshop Be the best that you can be! Carolyn Brown BS, MEd, RN, ARM, CWS, FACCWS Carolyn Brown Consulting 727-348-5856 cbjackwill@gmail.com Learner Objectives After attending
Chemotherapy and the risk of extravasation
 Chemotherapy and the risk of extravasation Cancer Service Patient Information Leaflet This leaflet contains important information about your treatment. Please read it and ask us if you have any queries.
Chemotherapy and the risk of extravasation Cancer Service Patient Information Leaflet This leaflet contains important information about your treatment. Please read it and ask us if you have any queries.
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine
 Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
NovoSorb BTM. A unique synthetic biodegradable wound scaffold. Regenerating tissue. Changing lives.
 NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
Fibroblast proliferation plays a vital role in helping. Assessing an adherent silicone foam dressing: a clinical evaluation across five NHS trusts
 Assessing an adherent silicone foam dressing: a clinical evaluation across five NHS trusts Abstract The wound contact layer of UrgoTul Absorb Border (Urgo Medical) foam dressing contains a Technology Lipido
Assessing an adherent silicone foam dressing: a clinical evaluation across five NHS trusts Abstract The wound contact layer of UrgoTul Absorb Border (Urgo Medical) foam dressing contains a Technology Lipido
Galen ( A.D) Advanced Wound Dressing
 Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL. of the infection risk in chronic wound
 Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Wounds UK. Wound management using a superabsorbent foam dressing: outcomes of a post-ce-mark primary care clinical evaluation ON THE NET
 September 2015 Volume 11 Issue 3 Wounds UK The quarterly journal exploring standards of care, new areas of expertise and research developments Wound management using a superabsorbent foam dressing: outcomes
September 2015 Volume 11 Issue 3 Wounds UK The quarterly journal exploring standards of care, new areas of expertise and research developments Wound management using a superabsorbent foam dressing: outcomes
Exudate in the early stages of wound healing
 Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Resources to Guide the Management of Suspected Infection in Chronic Wounds
 Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Introducing Mepilex Transfer Ag It all adds up to undisturbed healing. Antimicrobial wound contact layer with Safetac technology
 Introducing Mepilex Transfer Ag It all adds up to undisturbed healing Antimicrobial wound contact layer with Safetac technology Mepilex Transfer Ag Help the body heal The importance of less pain The body
Introducing Mepilex Transfer Ag It all adds up to undisturbed healing Antimicrobial wound contact layer with Safetac technology Mepilex Transfer Ag Help the body heal The importance of less pain The body
Skin Protectant and Skin & Incontinent Cleanser
 Skin Protectant and Skin & Incontinent Cleanser NEW! Cleanser Comprehensive system for the treatment and prevention of IAD, pressure ulcers* and other moisture lesions Safe and skin-friendly Prevents moisture
Skin Protectant and Skin & Incontinent Cleanser NEW! Cleanser Comprehensive system for the treatment and prevention of IAD, pressure ulcers* and other moisture lesions Safe and skin-friendly Prevents moisture
Managing venous leg ulcers and oedema using compression hosiery
 Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology
 The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Welcome to NuMed! Our Commitment: Quality Products, Cost Savings, Exceptional Service
 It s a New Day in Wound Care Welcome to NuMed! Our Commitment: Quality Products, Cost Savings, Exceptional Service NuMed Industries is a manufacturing company that specializes in Advanced Wound Care products.
It s a New Day in Wound Care Welcome to NuMed! Our Commitment: Quality Products, Cost Savings, Exceptional Service NuMed Industries is a manufacturing company that specializes in Advanced Wound Care products.
Practice review. Exploring best practice in the management of skin tears in older people
 Keywords Tissue Viability Skin tears Older people Exploring best practice in the management of skin tears in older people An overview of the definition, prevention and management of skin tear Author Lisa
Keywords Tissue Viability Skin tears Older people Exploring best practice in the management of skin tears in older people An overview of the definition, prevention and management of skin tear Author Lisa
The Triangle of Wound Assessment
 The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
Exploring best practice in the management of skin tears in older people
 Exploring best practice in the management of skin tears in older people An overview of the definition, prevention and management of skin tears Abstract Battersby, L. (2009) Best practice in the management
Exploring best practice in the management of skin tears in older people An overview of the definition, prevention and management of skin tears Abstract Battersby, L. (2009) Best practice in the management
Advancing the science of wound bed preparation
 Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
CASE STUDIES SERIES 2017
 INTERNATIONAL CASE STUDIES Case studies evaluation: BIOSORB Gelling Fibre Dressing in moderate to highly exuding wounds CASE STUDIES SERIES 2017 PUBLISHED BY: Wounds International 1.01 Cargo Works 1 2
INTERNATIONAL CASE STUDIES Case studies evaluation: BIOSORB Gelling Fibre Dressing in moderate to highly exuding wounds CASE STUDIES SERIES 2017 PUBLISHED BY: Wounds International 1.01 Cargo Works 1 2
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
THERAPIES. HAND IN HAND. Need safe and efficient infection prevention and management? 1 The Cutimed. Closing wounds. Together.
 Closing wounds. Together. Need safe and efficient infection prevention and management? 1 The Cutimed Sorbact range. A responsible choice. THERAPIES. HAND IN HAND. www.bsnmedical.co.uk TOGETHER WE CAN MAKE
Closing wounds. Together. Need safe and efficient infection prevention and management? 1 The Cutimed Sorbact range. A responsible choice. THERAPIES. HAND IN HAND. www.bsnmedical.co.uk TOGETHER WE CAN MAKE
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
NPUAP Mission. Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries. npuap.org
 Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries Margaret Goldberg, MSN, RN, CWOCN June 29, 2016 NPUAP Mission The National Pressure Ulcer Advisory Panel (NPUAP) serves
Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries Margaret Goldberg, MSN, RN, CWOCN June 29, 2016 NPUAP Mission The National Pressure Ulcer Advisory Panel (NPUAP) serves
Prevention and management of pressure ulcers
 The Clatterbridge Cancer Centre NHS Foundation Trust Prevention and management of pressure ulcers Nursing A guide for patients and carers Contents What is a pressure ulcer?... 1 Who gets pressure ulcers?...
The Clatterbridge Cancer Centre NHS Foundation Trust Prevention and management of pressure ulcers Nursing A guide for patients and carers Contents What is a pressure ulcer?... 1 Who gets pressure ulcers?...
CAST CARE. Helping Broken Bones Heal
 CAST CARE Helping Broken Bones Heal When You Need a Cast Are you injured and in need of a cast? Don t worry, you ll get through it. Wearing a cast will help your injured body part heal. Healing takes time,
CAST CARE Helping Broken Bones Heal When You Need a Cast Are you injured and in need of a cast? Don t worry, you ll get through it. Wearing a cast will help your injured body part heal. Healing takes time,
Plastic Surgery Clinic. Skin Grafting. Information
 Plastic Surgery Clinic Skin Grafting Information What is a skin graft? Skin grafting is a type of surgery involving the transplantation of skin. The transplanted tissue is called a skin graft. The area
Plastic Surgery Clinic Skin Grafting Information What is a skin graft? Skin grafting is a type of surgery involving the transplantation of skin. The transplanted tissue is called a skin graft. The area
Do all foam dressings have the same efficacy in the treatment of chronic wounds? Janice Bianchi, David Gray, John Timmons, Sylvie Meaume
 Do all foam dressings have the same efficacy in the treatment of chronic wounds? The challenge of chronic wounds remains significant both in terms of clinical management, impact on patients and cost to
Do all foam dressings have the same efficacy in the treatment of chronic wounds? The challenge of chronic wounds remains significant both in terms of clinical management, impact on patients and cost to
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management
 An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
Wound and Ostomy Care: Basics and Troubleshooting
 Wound and Ostomy Care: Basics and Troubleshooting Catherine Clarey-Sanford, PhD, RN, CWOCN Conflict of Interest No conflict of interest exists No commercial interest No financial benefits Specific wound
Wound and Ostomy Care: Basics and Troubleshooting Catherine Clarey-Sanford, PhD, RN, CWOCN Conflict of Interest No conflict of interest exists No commercial interest No financial benefits Specific wound
January Adult Burn Injured patients
 Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition
Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition
ACTIVHEAL PRODUCT RANGE MORE AFFORDABLE CLINICALLY EFFECTIVE WOUND CARE
 NEW NEW UPGRADED NEW NEW NEW ACTIVHEAL PRODUCT RANGE MORE AFFORDABLE CLINICALLY EFFECTIVE WOUND CARE 2 ACTIVELY SUPPORTING THE NHS WE HAVE BEEN USING ACTIVHEAL PRODUCTS ON OUR FORMULARY NOW FOR 2 YEARS
NEW NEW UPGRADED NEW NEW NEW ACTIVHEAL PRODUCT RANGE MORE AFFORDABLE CLINICALLY EFFECTIVE WOUND CARE 2 ACTIVELY SUPPORTING THE NHS WE HAVE BEEN USING ACTIVHEAL PRODUCTS ON OUR FORMULARY NOW FOR 2 YEARS
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
A practical guide for Peristomal Skin problems. Developed by the Ostomy Forum. Dedicated to Stoma Care
 A practical guide for Peristomal problems Developed by the Ostomy Forum Dedicated to Stoma Care E24-82-300 03/09 2009 Dansac A/S Lindegaard & Co For outstanding contribution towards making this project
A practical guide for Peristomal problems Developed by the Ostomy Forum Dedicated to Stoma Care E24-82-300 03/09 2009 Dansac A/S Lindegaard & Co For outstanding contribution towards making this project
easy made Soft silicone dressings
 Soft silicone dressings made easy Wounds International May 2013 www. Introduction Soft silicone dressings have been available for over 10 years and were developed to minimise the problems of pain and trauma
Soft silicone dressings made easy Wounds International May 2013 www. Introduction Soft silicone dressings have been available for over 10 years and were developed to minimise the problems of pain and trauma
Chapter 28. Wound Care. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 28 Wound Care Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 28.1 Define the key terms and key abbreviations in this chapter. Describe skin tears, circulatory ulcers, and diabetic
Chapter 28 Wound Care Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 28.1 Define the key terms and key abbreviations in this chapter. Describe skin tears, circulatory ulcers, and diabetic
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
POLYHEAL MICRO - INSTRUCTIONS FOR USE
 POLYHEAL MICRO - INSTRUCTIONS FOR USE PRODUCT DESCRIPTION PolyHeal Micro is a medical device indicated for the treatment of wounds. It is comprised of a suspension of polystyrene negatively charged microspheres
POLYHEAL MICRO - INSTRUCTIONS FOR USE PRODUCT DESCRIPTION PolyHeal Micro is a medical device indicated for the treatment of wounds. It is comprised of a suspension of polystyrene negatively charged microspheres
Management Of The Diabetic foot
 Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
