Clinical Evaluation of Transforaminal Epidural Steroid Injection in Patients with Gadolinium Enhancing Spinal Nerves Associated with Disc Herniation
|
|
|
- Aldous Robertson
- 5 years ago
- Views:
Transcription
1 Pain Physician 2015; 18:E177-E185 ISSN Observational Study Clinical Evaluation of Transforaminal Epidural Steroid Injection in Patients with Gadolinium Enhancing Spinal Nerves Associated with Disc Herniation Hyeong-Jun Tak, MD 1, Rodney Jones, MD 2, Yun-Woo Cho, MD, PhD 1, Eun-Hyuk Kim, MD 1, and Sang-Ho Ahn, MD, PhD 1 From: 1 Department of Rehabilitation Medicine & Spine Center, Yeungnam University College of Medicine, Daegu, Korea, 2 Department of Anesthesia, University of Kansas School of Medicine, Wichita, KS. Dr. Tak is a Resident at Department of Rehabilitation Medicine & Spine Center, Yeungnam University College of Medicine, Daegu, Korea. Dr. Jones is a Professor and Staff Physician, Department of Anesthesia, University of Kansas School of Medicine, Wichita, Kansas. Dr. Cho is a Professor and Staff Physician, Department of Rehabilitation Medicine & Spine Center, Yeungnam University College of Medicine, Daegu, Korea. Dr. Kim is a Fellow at Department of Rehabilitation Medicine & Spine Center, Yeungnam University College of Medicine, Daegu, Korea. Address Correspondence: Sang-Ho Ahn, MD, PhD Department of Rehabilitation Medicine & Spine Center, Yeungnam University College of Medicine 317-1, Daemyung-Dong Nam-Gu, Daegu , Korea. spineahn@ynu.ac.kr Manuscript received: Revised manuscript received: Accepted for publication: Free full manuscript: Background: Transforaminal epidural steroid injection (TFESI) of corticosteroid is frequently employed to mitigate the painful and disabling symptoms of lumbar disc herniation. However, the treatment outcome of TFESI in patients with radicular pain and inflamed neural structures as assessed by contrast-enhanced magnetic resonance imaging (MRI) has not been forthcoming. Objectives: To investigate functional improvement and pain reduction following TFESI in patients found to have nerve inflammation as evidenced by gadolinium-enhanced (MRI). Study Design: Retrospective assessment. Setting: Tertiary spinal intervention center, Daegu, Korea. Methods: Thirty-seven patients were selected by strict inclusion criteria. Patients were classified into enhancing and non-enhancing groups as evidenced by gadolinium-enhanced MRI. The enhancing group was further divided into pre-dorsal roog ganglion (DRG) only enhanced group and pre-drg and post-drg enhanced group. Clinical outcomes were evidenced by numeric rating scale (NRS) and Oswestry disability index (ODI) at pretreatment, one week, and 4 weeks after treatment. Results: The improvement of NRS and ODI in the enhanced group was greater than those of the non-enhanced group, at one week and 4 weeks after TFESI (P < 0.05). However there was no significant difference in improvement of NRS and ODI between pre-drg only enhanced group and pre-drg and post-drg enhanced group at one week and 4 weeks after TFESI. Limitations: Retrospective chart review with a small sample size. Conclusion: The improvement of NRS and ODI in the enhanced group was significantly greater than those of the non-enhanced group after TFESI. Radicular pain and functional impairment in the presence of gadolinium enhancing spinal neural structures and lumbar disc herniation may be more responsive to TFESI than patients without enhancing neural structures. Key words: Transforaminal epidural steroid injection, radicular pain, herniated lumbar disc, spinal nerve enhancement, contrast enhanced MRI Pain Physician 2015; 18:E177-E185
2 Pain Physician: March/April 2015; 18:E177-E185 Herniated lumbar disc (HLD) is the most common cause of lumbar radicular pain. Studies have shown the radicular pain in HLD results from both chemical inflammation and mechanical compromise of neural structures (1-3). Marshall et al (4) and Olmarker et al (5) demonstrated proinflammatory cytokines and neural inflammatory reactions associated with radicular pain. Cavanaugh (6) showed that isolated mechanical compression of spinal nerve roots was not sufficient to produce radicular pain. Computed tomography (CT), CT myelography, and conventional magnetic resonance imaging (MRI) are widely used to evaluate patients with lumbar radicular pain. These studies aid in determining numerous anatomic spine pathologies including disc herniation type, size, location, and the presence of associated neural involvement (7). Clinical symptoms and neurological signs may not correlate well with imaging and these studies may fail to identify a cause for the symptoms (8,9). Gadolinium-enhanced MRI can visualize inflammatory nerve pathology better than other imaging modalities (10). This enhancement with gadolinium may be related to a breakdown of the blood-nerve barrier secondary to inflammatory reactions and granulation formation with neo-vascularization (11,12). Gadolinium-enhanced MRI has been shown to identify inflamed neural structures associated with pathogenic leakage of nucleus pulpous (7). Gadolinium adds significant cost and there is a risk of acute renal failure in patients with renal compromise. Allergic reaction can also occur. With these considerations in mind, gadolinium-enhanced MRI in patients who have not undergone spinal surgical intervention and who are experiencing significant low back pain and or radiculopathy may be useful. The ability of gadolinium to image inflamed structures is useful in the diagnosing pain relating to neural inflammation and chemical radiculitis associated with herniated lumbar disc (13). Injection of steroids into the epidural space surrounding inflamed neural structures is performed to lessen pain and radiculopathy symptoms associated with HLDs. Systematic reviews have shown that epidural steroid injections can provide short-term pain relief (14-16). Delivery of steroid medications into the lumbar epidural space may be accomplished utilizing an interlaminar, transforaminal, or caudal injection technique. Fluoroscopically guided transforaminal epidural steroid injections (TFESI) have demonstrated good results in managing radicular pain (17,18). A proposed advantage of TFESI over interlaminar and caudal techniques is the deposition of a small volume of concentrated medication in close proximity to possible pain generators (17). However, to our knowledge, there has not been a study relating treatment outcomes of TFESI and nerve root enhancement on contrast-enhanced MRI. The aim of this retrospective study was to evaluate the treatment outcomes of TFESI in patients who had enhancement of lumbar nerve roots and spinal nerves by gadoliniumenhanced MRI. Methods Patients Between January 2005 and August 2012, at The Yeung Nam University Medical Center, Spine Clinic, 352 patients who had lower extremity radicular pain underwent a gadolinium-enhanced MRI to find the cause of symptomatic radicular pain. All patients also went through pain drawing, neurologic examination, and electromyography; therefore, referred pain generators that can mimic radiculopathy were ruled out. Of these 352 patients, 182 underwent a TFESI for treatment of lower extremity radicular pain. We retrospectively reviewed these 182 patients medical records to evaluate treatment outcome as it related to MRI findings (Fig. 1). The Institutional Review Board of the hospital approved this retrospective study. Inclusion criteria: 1) Lower extremity radicular pain related to single level HLD as evidenced by clinical examination, medical history, and lumbar MRI findings. 2) The HLD was at L3-4 or L4-5. 3) Patient had undergone a single TFESI for treatment. 4) Patient age range: 18~69 years. Exclusion criteria: 1) Radicular pain had been present greater than 6 months. 2) Far lateral disc herniation, multi-level disc herniation, spinal stenosis, spondylolisthesis, or previous back surgery. 3) Insufficient documentation of outcome data or lack of 4 week follow-up period. 4) Patient received other concomitant procedure that would interfere with the evaluation of the TFESI therapeutic effects. 5) Patient had been diagnosed with a mental health disorder. E178
3 Efficacy of TFESI in Patients with Gadolinium Enhancing Spinal Nerves Fig. 1. Schematic presentation of patient selection by retrospective chart review. Note: MR, magnetic resonance; HLD, herniated lumbar disc. Contrast Enhanced MRI Evaluation MRI data were obtained using a 1.5-T scanner (Magnetom Vision, Siemens, Erlangen, Germany) with a spine array coil. Spin-echo sequences, axial and sagittal T1- [583/12 (repetition time ms/echo time ms)], turbo T2-weighted images (3800/128), and contrast (Magnevist), 0.2mL/kg of gadopentetate dimeglumine (Bayer Healthcare Pharmaceuticals) enhanced axial T1- weighted images were obtained. All MRIs were reviewed by a radiologist and a physiatrist, both expert in reading spinal MRIs. The readers were blinded to the corresponding patient s history and clinical outcome. Nerve root enhancement was judged by making a comparison between the non-enhanced and enhanced T1-weighted images. The patients were grouped into enhanced or non-enhanced (Fig. 2). The enhanced group was further divided into those patients where only the nerve before the dorsal root ganglion (DRG) enhanced (pre-drg [Fig. 3]) and those patients where the nerve before and after the DRG enhanced (pre-drg and post-drg enhanced group [Fig. 4]). Two cases where there was disagreement between the 2 reviewers regarding the presence of enhancement were excluded from the study. TFESI Procedure All injections were performed by a single interventional physiatrist who specializes in spinal injections. Strict aseptic technique was utilized in the performance of the TFESI procedures. Patients were placed prone and C-arm fluoroscopy (Siemens, Erlangen, Germany) was utilized for level identification and needle guidance. Lidocaine 1% was administered at the needle insertion site and the tip of a 25-gauge, 90-mm spinal needle with a bend at the tip to allow for guidance was positioned between the lateral vertebral body and the 6 o clock position below the pedicle. Lateral fluoroscopic imaging demonstrated E179
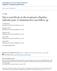
4 Pain Physician: March/April 2015; 18:E177-E185 Fig. 2. Non-enhanced nerve root in lumbar disc herniation. Contrast-enhanced MRI of a 37-year-old man shows a right paramedian extruded disc herniation without nerve root enhancement. At L5 pre-dorsal root ganglionic level (2-A), axial unenhanced T1-weighted (2-B), and contrast-enhanced T1-weight image (2-C) does not show nerve root enhancement. And, at L5 post-dorsal root ganglion level (2-D), axial unenhanced T1-weighted (2-E), and contrast-enhanced T1-weight image (2-F) also does not show nerve root enhancement. Note: Wide filled arrow, herniated lumbar disc; Narrow filled arrow, post-dorsal root ganglion. Fig. 3. Pre-dorsal root ganglion enhancement in lumbar disc herniation. Contrast-enhanced MRI of a 20-year-old man shows a right paramedian extruded disc herniation with nerve root enhancement (pre-drg only enhanced). At L5 pre-drg level (3-A), axial unenhanced T1-weighted (3-B), and contrast-enhanced T1-weight image (3-C) represent prominent L5 pre-drg enhancement. At L5 post-drg level (3-D), axial unenhanced T1-weighted (3-E), and contrast-enhanced T1-weight image (3-F) does not show nerve root enhancement. Note: Wide filled arrow, herniated lumbar disc; Wide open arrow, enhanced pre-drg nerve roots; Narrow filled arrow, post-drg nerve roots. E180
5 Efficacy of TFESI in Patients with Gadolinium Enhancing Spinal Nerves Fig. 4. Pre- DRG and post-drg enhancement in lumbar disc herniation. Contrast-enhanced MRI of a 21-year-old man shows a left paramedian extruded disc herniation with nerve root enhancement (pre- DRG and post-drg enhanced). At L5 pre-drg level (4-A), axial unenhanced T1-weighted (4-B), and contrast-enhanced T1- weight image (4-C) represent prominent L5 pre-drg enhancement. At L5 post-drg level (4-D), axial unenhanced T1-weighted (4-E), and contrast-enhanced T1-weight image (4-F) also represent L5 post-drg enhancement. Note: Wide filled arrow, herniated lumbar disc; Wide open arrow, enhanced pre-drg nerve roots; Narrow filled arrow, post-drg nerve roots; Narrow open arrow, enhanced post-drg nerve roots. the needle tip between the spinal laminar margin and the posterior vertebral body. Under anterior-posterior (AP) fluoroscopy, 0.3 ml of non-ionic contrast material (Iohexolbonorex, Daihan Pharm Co, Seoul, Korea) was injected to confirm the absence of vascular uptake and spread of contrast into the foramen. After that, 20 mg (40 mg/ml) of triamcinolone (Shin Poong Pharm Co, Seoul, Korea) with 0.5 ml of bupivacaine hydrochloride (0.5%, Hana Pharm Co, Seoul, Korea) were injected. After the procedures, all patients were observed in the short-stay unit for a minimum of 30 minutes prior to discharge. Outcome Measurement Clinical outcomes were assessed by the Numeric Rating Scale (NRS-11) and Oswestry Disability Index (ODI). The NRS-11 ranged from 0 to 10, where 0 indicates no pain and 10 indicates the worst pain imaginable. The ODI consisted of 10 questions and was used to evaluate functional disabilities caused by the patient s radicular pain. Each variable was rated on a 0 5 point scale and the total score ranged from 0 to 50. A high ODI score indicates a more severe functional disability related to the pain. The measurements were obtained by a third party who was blinded to the patient s condition prior to and at one week and four weeks after treatment. Statistical Analysis The Independent t-test was used for comparing demographic data. Two-Factor Repeated-Measures Analysis of Variance was used to evaluate the improvement of NRS and ODI at one week and 4 weeks after TFESI. All data were analyzed using the SPSS 14.0 for Windows. A P-value of less than 0.05 was regarded as statistically significant. E181
6 Pain Physician: March/April 2015; 18:E177-E185 Results Demographic Data Demographic findings are summarized in Table 1. Thirty-seven patients were included in this study; 22 were men and 15 were women. Seventeen patients showed nerve enhancement and 20 patients did not demonstrate enhancement. No statistical difference in demographic data was observed between nerve enhanced and non-enhanced group. Among the patients with nerve enhancement, 10 patients had pre-drg only enhancement and 7 patients showed pre-drg and post-drg enhancements patterns. No statistical difference in demographic data was observed between the groups. Treatment Outcomes At one week after TFESI, significant improvements were observed in both NRS and ODI compared with pretreatment scores. These improvements remained significant 4 weeks after treatment in both the nerve enhanced and non-enhanced groups (P < 0.05). The improvement in NRS was greater in the nerve root enhanced group than the non-enhanced group at one week and 4 weeks (P < 0.05). Average NRS scores of the enhanced group declined significantly from 6.2 ± 1.4 at pretreatment to 3.7 ± 1.6 and 2.9 ± 1.6 at one week and 4 weeks after treatment, respectively. Average NRS score of the non-enhanced group declined from 5.4 ± 1.5 at pretreatment to 4.3 ± 1.3 and 3.8 ± 1.3 at one week and 4 weeks after treatment, respectively. Among the nerve root enhanced group, there was no significant difference in improvement of NRS between the pre-drg only enhanced group and the pre-drg and post-drg enhanced group (P > 0.05). Average NRS scores of the pre-drg only enhanced group declined from 6.3 ± 1.4 at pretreatment to 3.9 ± 1.7 and 3.6 ± 1.4 at one week and 4 weeks after treatment and those of the pre-drg and post-drg enhanced group declined from 6.2 ± 1.4 at pretreatment to 3.4 ± 1.7 and 2.1 ± 1.5 at one week and 4 weeks after treatment, respectively (Fig. 5). In ODI, there was greater improvement in the nerve root enhanced group than non-enhanced group at one week and 4 weeks after TFESI (P < 0.05). The average ODI of the enhanced group declined significantly from 23.0 ± 9.0 at pretreatment to 12.9 ± 7.8 and 10.0 ± 6.1 at one week and 4 weeks after treatment, respectively. However, the average ODI of the non-enhanced group declined from 22.7 ± 5.6 at pretreatment to 19.6 ± 6.4 and 16.3 ± 6.0 at one week and 4 weeks after treatment, respectively. There was no significant difference in improvement of ODI between the pre-drg only enhanced group and the pre-drg and post-drg enhanced group (P > 0.05). Average ODI scores of the pre-drg only enhanced group declined from 21.4 ± 8.2 at pretreatment to 12.8 ± 7.9 and 10.3 ± 7.1 at one week and 4 weeks after treatment and those of the pre-drg and post-drg enhanced group declined from 25.3 ± 10.3 at pretreatment to 13.0 ± 8.1 and 9.5 ± 4.8 at one week and 4 weeks after treatment, respectively (Fig. 6). Discussion In this study, we evaluated the treatment outcome of TFESI according to the presence of nerve enhancement as evidenced by gadolinium MRI. NRS and ODI were significantly improved over pretreatment levels following TFESI regardless the presence of nerve enhancement. Improvement in NRS and ODI in the enhanced group was greater than the non-enhanced group at one week and 4 weeks following TFESI. However, the presence of enhancement pre- and post-drg did not significantly change patients response over pre-drg only enhancement. There was no statically difference of NRS and ODI between the pre-drg only Table 1. Baseline demographic characteristics. Variables Enhanced nerve root Non Enhanced nerve root P-value Patients number Gender (male: female) 11 : 6 11 : Level of disc herniation (L3-4 : L4-5) 2 : 15 3 : Age (years) 51.1 (12.2) 48.9 (15.7) 0.63 Duration of symptom (weeks) 6.2 (6.1) 4.9 (4.7) 0.44 Initial numeric rating scale 6.2 (1.4) 5.4 (1.5) 0.09 Initial Oswestry disability index 23.0 (9.0) 22.7 (5.6) 0.91 E182
7 Efficacy of TFESI in Patients with Gadolinium Enhancing Spinal Nerves Fig. 5. Comparison of Numeric Rating Scale according to nerve roots enhancement. (A) At one week and 4 weeks after treatment, change of NRS in nerve root enhanced group was significantly greater than those with non-enhance group (P < 0.05). (B) At one week and 4 weeks after treatment, there was no significant difference in improvement of NRS according to spreading pattern of nerve root enhancement (P > 0.05). Note: Full line, nerve root enhanced group; Dot line, nerve root non-enhanced group; Narrow broken line, Pre-DRG only enhanced group; Wide broken line, Pre-DRG and post-drg enhanced group; Vertical bar means the standard error. P value, comparison of the improvement of NRS according nerve roots enhancement at one week and 4 weeks after TFESI. Fig. 6. Comparison of Oswestry disability index according to nerve roots enhancement. (A) At one week and 4 weeks after treatment, improvement of ODI in nerve root enhanced group was significantly greater than those with non-enhanced group. (P < 0.05). (B) At one week and 4 weeks after treatment, there was no significantly difference in improvement of ODI according to spreading pattern of nerve root enhancement. (P > 0.05). Note: Full line, nerve root enhanced group; Dot line, nerve root non-enhanced group; Narrow broken line, pre-drg only enhanced group; Wide broken line, pre-drg and post-drg enhanced group; Vertical bar means the standard error. P value, comparison of the improvement of ODI according nerve roots enhancement at one week and 4 weeks after TFESI. enhanced group and the pre-drg and post-drg enhanced group at one week and 4 weeks after TFESI. Contrast-enhanced MRIs have value in identifying inflammation of spinal neural structures. Nerve enhancement with contrast-enhanced MRIs is associated with accumulation of granulation tissue, inflammatory cytokines, and disruption of endoneurial capillaries (18,19). Inflammation mediated by proinflammatory cytokines results in the breakdown of the blood-nerve barrier, increased vascular permeability, and enhancement of nerve tissue in contrast MRIs. Jinkins (10) demonstrated that gadolinium-enhanced MRI could serve as a marker for spinal nerve and nerve root pathology. Toyone et al (20) revealed that severity of radicular E183
8 Pain Physician: March/April 2015; 18:E177-E185 pain was well correlated with nerve root enhancement. However there has been no study relating clinical outcome of TFESI and nerve enhancement. For radicular pain, TFESI has demonstrated effectiveness compared to physical therapy and caudal epidural steroid injections (13-15). Triamcinolone acetonide, a synthetic glucocorticoid corticosteroid with marked anti-inflammatory action, has been utilized off-label for injections into spinal neural foramen to attenuate the proinflammatory cytokines and inhibit chemical inflammation. Using precise fluoroscopic guided technique. including verification of contrast spread and absence of vascular uptake prior to injecting the steroid, improves safety and allows for a high concentration of steroid agent to be deposited precisely at the affected spinal nerve. Thomas et al (21) suggested that TFESI was more effective than interlaminar injection for pain reduction and functional ability improvement. Riew et al (22) showed that TFESI had a surgery sparing effect which was sustained at a 5 year follow-up period in radicular pain. Previous studies have not considered nerve root enhancement in relation to the effectiveness of TFESI. Gadolinium MRI enhancing spinal nerves associated with intervertebral disc pathology likely represents nerves in an inflamed state and would be expected to respond to local steroid administration. Regardless of nerve enhancement, NRS and ODI were significantly reduced at one week and 4 weeks after TFESI. This sort of improvement has been demonstrated in previous studies (14-18,21,22). Our findings suggest that improvements of radicular pain and functional ability were greater in the group demonstrating nerve enhancement over the group in which nerve enhancement was not seen. This would suggest an inflammatory mechanism, exclusive or in addition to others such as mechanical or vascular, be present. Contrast-enhanced MRI is often used post-surgery to evaluate for the presence of inflammation and granulation and may prove useful when spinal nerve mediated pain is suspected. The authors consider that gadolinium-enhanced MRI is also useful in a non-operated degenerative lumbar spine to suspect and find the different causes of low back pain, such as pathologies of nerve roots, facet joints, and annular tear (chemical radiculitis). The enhanced spinal nerves are thought to be a neural inflammatory state. In this study, and as in a common practice, local anesthetic was combined with the steroid medication. Local anesthetic alone may provide anti-inflammatory effects and injection near an inflamed neural structure may offer a wash out of inflammatory products (23-26). To better address these possible mechanisms a future study employing saline, local anesthetic alone, and local anesthetic with steroid all in an equal volume may be useful. Patients with radicular pain over 6 months were excluded and we chose a short 4 week follow-up period. This was done to more accurately study the inflammatory component of the nerve pathology and the anti-inflammatory effects of transforaminal injection of steroid combined with local anesthetic. In this study, treatment outcome of the pre-drg and post-drg enhanced group tended to be slightly superior to that of the pre-drg only enhanced group; however, there was no statistical difference of treatment outcome between 2 groups. We had expected the response of TFESI in the pre-drg and post-drg enhanced group might be stronger than that in the pre-drg only enhanced group. It is because cases with post-drg enhanced nerve always accompanied the pre-drg without exception, therefore, the pre-drg and post-drg enhanced nerve might represent a more inflammatory status than the pre-drg only enhanced nerve. The reason for no statistical difference in treatment outcome in both groups is thought to be the small sample size. Limitation This study is limited by its retrospective design, small number of patients, and brief follow-up window. Patients with HLD at L5-S1 were not included due to the less than optimal images obtained at this level making accurate and consistent determinations of post-drg enhancement difficult. In this retrospective study, all patients were injected with both steroid and local anesthetic; therefore, one cannot conclude the observed effect was due solely to the steroid or the local anesthetic. Conclusion In summary, the improvement of NRS and ODI in the enhanced group was significantly greater than those of the non-enhanced group after TFESI. Radicular pain in the presence of enhanced nerve roots and lumbar disc herniation may be more responsive to TFESI than when enhancement is not present. Despite the retrospective method and brief follow-up duration, these findings suggest the presence of nerve enhancement in contrast-enhanced MRIs may help predict the treatment outcome of TFESI in HLD-associated radicular pain. A controlled, prospective, long-term follow-up, E184
9 Efficacy of TFESI in Patients with Gadolinium Enhancing Spinal Nerves larger scale study utilizing local anesthetic only and local anesthetic with steroid is required to confirm our results and address the limitations. Disclaimer This work was supported by the 2014 Yeungnam University Research Grant Conflict of interest Each author certifies that he or she, or a member of his or her immediate family, has no commercial association (i.e., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted manuscript. References 1. Benoist M. The natural history of lumbar disc herniation and radiculopathy. Joint Bone Spine 2002; 69: Tarulli AW, Raynor EM. Lumbosacral radiculopathy. Neurol Clin 2007; 25: Frymoyer JW. Back pain and sciatica. N Engl J Med 1988; 318: Marshall LL, Trethewie ER, Curtain CC. Chemical radiculitis, a clinical, physiological and immunological study. Clin Orthop Relat Res.1977; 129: Olmarker K, Blomquist J, Stromberg J, Nannmark U, Thomsen P, Rydevik B. Inflammatogenic properties of nucleuspulposus. Spine 1995; 20: Cavanaugh JM. Neural mechanisms of lumbar pain. Spine 1995; 16: Haijiao W, Koti M, Smith FW, Wardlaw D. Diagnosis of lumbosacral nerve root anomalies by magnetic resonance imaging. J Spinal Disord 2001; 14: Thelander U, Fagerlund M, Friberg S, Larsson E. Straight leg raising test versus radiologic size, shape, and position of lumbar disc herniations. Spine 1992; 17: D Aprile P, Tarantino A, Jinkins JR, Brindicci D. The value of fat saturation sequences and contrast medium administration in MRI of degenerative disease of the posterior/perispinal elements of the lumbosacral spine. Eur Radiol 2007; 17: Jinkins JR. MR of enhancing nerve roots in the unoperated lumbosacral spine. AJNR Am J Neuroradiol 1993; 14: Itoh R, Murata K, Kamata M, Mukubou N, Morita R. Lumbosacral nerve root enhancement with disk herniation on contrast-enhanced MR. AJNR Am J Neuroradiol 1996; 17: Ross JS, Modic MT, Masaryk TJ, Carter J, Marcus RE, Bohlman H. Assessment of extraduraldegenerative disease with Gd-DTPA enhanced MR imaging: Correlation with surgical and pathologic findings. AJNR Am J Neuroradiol 1989; 10: Beall D. The Lumbar Spine: Use of Contrast in MR Imaging of the Lumbar Spine. Elsevier, Health Sciences Division, Philadelphia. 14. Armon C, Argoff CE, Samuels J, Backonja MM. Assessment: Use of epidural steroid injections to treat radicular lumbosacral pain: Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology 2007; 68: DePalma MJ, Bhargava A, Slipman CW. A critical appraisal of the evidence for selective nerve root injection in the treatment of lumbosacral radiculopathy. Arch Phys Med Rehabil 2005; 86: Abdi S, Datta S, Trescot AM, Schultz DM, Adlaka R, Atluri SL, Smith HS, Manchikanti L. Epidural steroids in the management of chronic spinal pain: A systematic review. Pain Physician 2007; 10: Lutz GE, Vad VB, Wisneski RJ. Fluoroscopic transforaminal lumbar epidural steroids: An outcome study. Arch Phys Med Rehabil 1998; 79: Vad VB, Bhat AL, Lutz GE, Cammisa F. Transforaminal epidural steroid injections in lumbosacral radiculopathy: A prospective randomized study. Spine 2002; 27: Ross JS, Masaryk TJ, Schrader M, Gentili A, Bohlman H, Modic MT. MR imaging of the postoperative lumbar spine: Assessment with gadopentate dimeglumine. AJNR Am J Neuroradiol 1990; 11: Toyone T, Takahashi K, Kitahara H, Yamagata M, Murakami M, Moriya H. Visualisation of symptomatic nerve roots. Prospective study of contrast-enhanced MRI in patients with lumbar disc herniation. J Bone Joint Surg Br 1993; 75: Thomas E, Cyteval C, Abiad L, Picot MC, Taourel P, Blotman F. Efficacy of transforaminal versus interspinous corticosteroid injection in discal radiculalgia a prospective, randomized, double-blind study. Clin Rheumatol 2003; 22: Riew KD, Park JB, Cho YS, Gilula L, Patel A, Lenke LG, Bridwell KH. Nerve root blocks in the treatment of lumbar radicular pain. A minimum five-year followup. J Bone Joint Surg 2006; 88: Yabuki S, Kawaguchi Y, Nordborq C, Kikuchi S, Rydevik B, Olmarker K. Effect of lidocaine on nucleus pulposus induced nerve root injury. A neurophysiologic and histologic study of the pig cauda equine. Spine (Phila Pa 1976) 1998; 23: Cassuto J, Sinclair R, Bonderovic M. Anti inflammatory properties of local anesthetics and their present and potential clinical implications. Acta Anaesthesiol Scand 2006; 50: Manchikanti L, Cash KA, Pampati V, Falco JF. Trasnforaminal epidural injections in chronic lumbar disc herniation: A randomized, double-blind, active-control trial. Pain Physician 2014; 17:E489-E Manchikanti L, Singh V, Cash KA, Pampati V, Falco JF. A randomized, doubleblind, active-control trial of the effectiveness of lumbar interlaminar epidural injections in disc herniation. Pain Physician 2014; 17:E61-E74. E185
10
Outcome of Transforaminal Epidural Steroid Injection According to the Severity of Lumbar Foraminal Spinal Stenosis
 Pain Physician 2018; 21:67-72 ISSN 1533-3159 Prospective Observational Study Outcome of Transforaminal Epidural Steroid Injection According to the Severity of Lumbar Foraminal Spinal Stenosis Min Cheol
Pain Physician 2018; 21:67-72 ISSN 1533-3159 Prospective Observational Study Outcome of Transforaminal Epidural Steroid Injection According to the Severity of Lumbar Foraminal Spinal Stenosis Min Cheol
A study of transforaminal epidural steroid injections in patients with lumber disc herniation
 International Journal of Research in Medical Sciences Kuvad VL. Int J Res Med Sci. 2015 Dec;3(12):3853-3857 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151455
International Journal of Research in Medical Sciences Kuvad VL. Int J Res Med Sci. 2015 Dec;3(12):3853-3857 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151455
Behnam Hosseini, Mohammad Hossein Ataei, Sirous Momenzadeh, Reza Jalili Khoshnood, Davood Ommi
 Original Article The comparison between steroid and hypertonic saline 10% with steroid in transforaminal epidural injection in patients with unilateral foraminal stenosis Behnam Hosseini, Mohammad Hossein
Original Article The comparison between steroid and hypertonic saline 10% with steroid in transforaminal epidural injection in patients with unilateral foraminal stenosis Behnam Hosseini, Mohammad Hossein
Epidural steroid injections have been used to treat lumbar
 ORIGINAL RESEARCH I.S. Lee S.H. Kim J.W. Lee S.H. Hong J.-Y. Choi H.S. Kang J.W. Song A.K. Kwon Comparison of the Temporary Diagnostic Relief of Transforaminal Epidural Steroid Injection Approaches: Conventional
ORIGINAL RESEARCH I.S. Lee S.H. Kim J.W. Lee S.H. Hong J.-Y. Choi H.S. Kang J.W. Song A.K. Kwon Comparison of the Temporary Diagnostic Relief of Transforaminal Epidural Steroid Injection Approaches: Conventional
Lumbar radicular pain, a common entity in clinical practice,
 ORIGINAL RESEARCH C. Cyteval N. Fescquet E. Thomas E. Decoux F. Blotman P. Taourel Predictive Factors of Efficacy of Periradicular Corticosteroid Injections for Lumbar Radiculopathy BACKGROUND AND PURPOSE:
ORIGINAL RESEARCH C. Cyteval N. Fescquet E. Thomas E. Decoux F. Blotman P. Taourel Predictive Factors of Efficacy of Periradicular Corticosteroid Injections for Lumbar Radiculopathy BACKGROUND AND PURPOSE:
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections
 Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: PA.CP.MP.165 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: PA.CP.MP.165 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log
SPINE SECTION. Design. Prospective clinical study.
 bs_bs_banner Pain Medicine 2014; 15: 379 385 Wiley Periodicals, Inc. SPINE SECTION Original Research Article Caudal vs Transforaminal Epidural Steroid Injections as Short-Term (6 Months) Pain Relief in
bs_bs_banner Pain Medicine 2014; 15: 379 385 Wiley Periodicals, Inc. SPINE SECTION Original Research Article Caudal vs Transforaminal Epidural Steroid Injections as Short-Term (6 Months) Pain Relief in
Effect of Spinal Exercises and Epidural Injections in Chronic Low Back Pain
 Effect of Spinal Exercises and Epidural Injections in Chronic Low Back Pain Sargun Singh Walia, Jaswinder Pal Singh, Harshita Yadav and Anuradha Lehri Abstract Aim: Effect of Spinal Exercises and Epidural
Effect of Spinal Exercises and Epidural Injections in Chronic Low Back Pain Sargun Singh Walia, Jaswinder Pal Singh, Harshita Yadav and Anuradha Lehri Abstract Aim: Effect of Spinal Exercises and Epidural
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14 SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
Outcome of Spine Injections on the basis of MRI Findings. Personal use only. Tobias Dietrich Kantonsspital St.Gallen
 Outcome of Spine Injections on the basis of MRI Findings Tobias Dietrich Kantonsspital St.Gallen Evidence for Spinal Injections? Pe Skeletal Radiology 2010 rso na lu se moderate- to-strong evidence supporting
Outcome of Spine Injections on the basis of MRI Findings Tobias Dietrich Kantonsspital St.Gallen Evidence for Spinal Injections? Pe Skeletal Radiology 2010 rso na lu se moderate- to-strong evidence supporting
The Efficacy of Transforaminal Epidural Steroid Injection by the Conventional Technique in Far- Lateral Herniation of Lumbar Disc
 Pain Physician 2012; 15:415-420 ISSN 1533-3159 Retrospective Study The Efficacy of Transforaminal Epidural Steroid Injection by the Conventional Technique in Far- Lateral Herniation of Lumbar Disc Ho-Joong
Pain Physician 2012; 15:415-420 ISSN 1533-3159 Retrospective Study The Efficacy of Transforaminal Epidural Steroid Injection by the Conventional Technique in Far- Lateral Herniation of Lumbar Disc Ho-Joong
Commonly recognized causes of sciatica include disk herniation
 Published December 22, 2011 as 10.3174/ajnr.A2813 ORIGINAL RESEARCH W.M. Byun S.H. Ahn M.-W. Ahn Value of 3D MR Lumbosacral Radiculography in the Diagnosis of Symptomatic Chemical Radiculitis BACKGROUND
Published December 22, 2011 as 10.3174/ajnr.A2813 ORIGINAL RESEARCH W.M. Byun S.H. Ahn M.-W. Ahn Value of 3D MR Lumbosacral Radiculography in the Diagnosis of Symptomatic Chemical Radiculitis BACKGROUND
Magnetic resonance imaging findings in patients with low backache
 Original Article Magnetic resonance imaging findings in patients with low backache Narayan Bikram Thapa 1, Suraj Bajracharya 2 1 Department of Radiology, KIST Medial College Teaching Hospital, Lalitpur,
Original Article Magnetic resonance imaging findings in patients with low backache Narayan Bikram Thapa 1, Suraj Bajracharya 2 1 Department of Radiology, KIST Medial College Teaching Hospital, Lalitpur,
Follow this and additional works at: Part of the Musculoskeletal Diseases Commons
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Do Epidural Injections With Local Anesthetic
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Do Epidural Injections With Local Anesthetic
Clinical Policy: Caudal or Interlaminar Epidural Steroid Injections
 Clinical Policy: Reference Number: PA.CP.MP.164 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log Description Epidural steroid injections have been used for pain control in
Clinical Policy: Reference Number: PA.CP.MP.164 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log Description Epidural steroid injections have been used for pain control in
Evidence based Practice Changes Spinal Injections
 Evidence based Practice Changes Spinal Injections Kathryn Mueller, MD, MPH, FACOEM Professor, School of Public Health & Department of Physiatry - University of Colorado President - American College of
Evidence based Practice Changes Spinal Injections Kathryn Mueller, MD, MPH, FACOEM Professor, School of Public Health & Department of Physiatry - University of Colorado President - American College of
Variation In The Method Of Caudal Epidural Injection- A Regional Survey
 ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 2 Variation In The Method Of Caudal Epidural Injection- A Regional Survey S Haque., J Gaskin., A Uguwoke, S Karmani Citation S Haque., J
ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 2 Variation In The Method Of Caudal Epidural Injection- A Regional Survey S Haque., J Gaskin., A Uguwoke, S Karmani Citation S Haque., J
Comparison of Radiation Exposure during Fluoroscopy- Guided Transforaminal Epidural Steroid Injections at Different Vertebral Levels
 Original Article Musculoskeletal Imaging http://dx.doi.org/10.3348/kjr.2015.16.2.357 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2015;16(2):357-362 Comparison of Radiation Exposure during Fluoroscopy-
Original Article Musculoskeletal Imaging http://dx.doi.org/10.3348/kjr.2015.16.2.357 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2015;16(2):357-362 Comparison of Radiation Exposure during Fluoroscopy-
Contrast between Scar and Recurrent Herniated Disk on Contrast-Enhanced MR Images
 AJNR Am J Neuroradiol 23:1652 1656, November/December 2002 Contrast between Scar and Recurrent Herniated Disk on Contrast-Enhanced MR Images Victor Haughton, Ken Schreibman, and Arthur De Smet BACKGROUND
AJNR Am J Neuroradiol 23:1652 1656, November/December 2002 Contrast between Scar and Recurrent Herniated Disk on Contrast-Enhanced MR Images Victor Haughton, Ken Schreibman, and Arthur De Smet BACKGROUND
Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-1-2006 Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up K. Daniel Riew
Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-1-2006 Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up K. Daniel Riew
Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review
 Pain Physician 2017; 20:E445-E449 ISSN 2150-1149 Literature Review Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review Bin Zhu, MD,
Pain Physician 2017; 20:E445-E449 ISSN 2150-1149 Literature Review Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review Bin Zhu, MD,
DESCRIPTION OF PROCEDURE/SERVICE/PHARMACEUTICAL
 Subject: Percutaneous Epidural Adhesiolysis for Chronic Low Back Pain (RACZ Procedure) Original Effective Date: 10/12/15 Policy Number: MCP-257 Revision Date(s): Review Date: 12/16/15, 12/14/16, 6/22/17
Subject: Percutaneous Epidural Adhesiolysis for Chronic Low Back Pain (RACZ Procedure) Original Effective Date: 10/12/15 Policy Number: MCP-257 Revision Date(s): Review Date: 12/16/15, 12/14/16, 6/22/17
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 UnitedHealthcare Commercial Medical Policy EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAI001 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
UnitedHealthcare Commercial Medical Policy EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAI001 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
Correlation Between Severity of Lumbar Spinal Stenosis and Lumbar Epidural Steroid Injection
 bs_bs_banner Pain Medicine 2014; 15: 556 561 Wiley Periodicals, Inc. Correlation Between Severity of Lumbar Spinal Stenosis and Lumbar Epidural Steroid Injection Chan-Hong Park, MD, PhD,* and Sang-Ho Lee,
bs_bs_banner Pain Medicine 2014; 15: 556 561 Wiley Periodicals, Inc. Correlation Between Severity of Lumbar Spinal Stenosis and Lumbar Epidural Steroid Injection Chan-Hong Park, MD, PhD,* and Sang-Ho Lee,
Lumbar disc herniation
 Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Nuances of Spinal Radiculopathy. James Mallows
 Nuances of Spinal Radiculopathy James Mallows Spinal dermatomes A dermatome is an area of skin that is mainly supplied by a single spinal nerve History of dermatomes Pioneering work by Sherrington (late
Nuances of Spinal Radiculopathy James Mallows Spinal dermatomes A dermatome is an area of skin that is mainly supplied by a single spinal nerve History of dermatomes Pioneering work by Sherrington (late
An ESI for managing LBP is one of the most commonly
 ORIGINAL RESEARCH J.W. Lee H.I. Shin S.Y. Park G.Y. Lee H.S. Kang Therapeutic Trial of Fluoroscopic Interlaminar Epidural Steroid Injection for Axial Low Back Pain: Effectiveness and Outcome Predictors
ORIGINAL RESEARCH J.W. Lee H.I. Shin S.Y. Park G.Y. Lee H.S. Kang Therapeutic Trial of Fluoroscopic Interlaminar Epidural Steroid Injection for Axial Low Back Pain: Effectiveness and Outcome Predictors
Comparison of Epidural Methylprednisolone, Bupivacaine and Normal Saline Injection in Chronic Low Back Pain Due to Discal Hernia
 http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 5, No., January 8, 57 6 eissn 48-9696 Comparison of Epidural Methylprednisolone, Bupivacaine and
http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 5, No., January 8, 57 6 eissn 48-9696 Comparison of Epidural Methylprednisolone, Bupivacaine and
Clinical Correlation of a New Practical MRI Method for Assessing Cervical Spinal Canal Compression
 Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 7/1/2018 Section: MED Policy No: 123 Medical Officer 7/1/18 Date Technology Assessment Committee Approved Date: 10/10; 12/15 Medical Policy Committee Approved Date: 8/94; 7/96; 8/97; 4/98;
Effective Date: 7/1/2018 Section: MED Policy No: 123 Medical Officer 7/1/18 Date Technology Assessment Committee Approved Date: 10/10; 12/15 Medical Policy Committee Approved Date: 8/94; 7/96; 8/97; 4/98;
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Usefulness of Posterolateral Transforaminal Approach in Lumbar Radicular Pain Ji Woong Park, M.D., Hee-Seung Nam, M.D. 1, Yongbum Park, M.D.
 Original Article Ann Rehabil Med 2011; 35: 395-404 pissn: 2234-0645 eissn: 2234-0653 doi: 10.5535/arm.2011.35.3.395 Annals of Rehabilitation Medicine Usefulness of Posterolateral Transforaminal Approach
Original Article Ann Rehabil Med 2011; 35: 395-404 pissn: 2234-0645 eissn: 2234-0653 doi: 10.5535/arm.2011.35.3.395 Annals of Rehabilitation Medicine Usefulness of Posterolateral Transforaminal Approach
Contractor Information. LCD Information. FUTURE Local Coverage Determination (LCD): Lumbar Epidural Injections (L33836)
 FUTURE Local Coverage Determination (LCD): Lumbar Epidural Injections (L33836) Please note: Future Effective Date. Contractor Information Contractor Name Noridian Healthcare Solutions, LLC opens in new
FUTURE Local Coverage Determination (LCD): Lumbar Epidural Injections (L33836) Please note: Future Effective Date. Contractor Information Contractor Name Noridian Healthcare Solutions, LLC opens in new
Different operative findings of cases predicted to be symptomatic discal pseudocysts after percutaneous endoscopic lumbar discectomy
 Case Report Different operative findings of cases predicted to be symptomatic discal pseudocysts after percutaneous endoscopic lumbar discectomy Ryutaro Shiboi 1,2, Yasushi Oshima 1,2,3, Takeshi Kaneko
Case Report Different operative findings of cases predicted to be symptomatic discal pseudocysts after percutaneous endoscopic lumbar discectomy Ryutaro Shiboi 1,2, Yasushi Oshima 1,2,3, Takeshi Kaneko
Guideline Number: NIA_CG_301 Last Revised Date: March 2018 Responsible Department: Clinical Operations
 Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
EFFICACY OF TRANSFORAMINAL EPIDURAL STEROID INJECTION IN LUMBOSACRAL RADICULOPATHY
 EFFICACY OF TRANSFORAMINAL EPIDURAL STEROID INJECTION IN LUMBOSACRAL RADICULOPATHY Saheel Majid 1, Dinesh K. Yadav 2, Suhail M. Vakil 3, Zameer Ali 4, Tauseef A. Bhat 5, Ayaz Ali 6, Shafaqat Rashid 7,
EFFICACY OF TRANSFORAMINAL EPIDURAL STEROID INJECTION IN LUMBOSACRAL RADICULOPATHY Saheel Majid 1, Dinesh K. Yadav 2, Suhail M. Vakil 3, Zameer Ali 4, Tauseef A. Bhat 5, Ayaz Ali 6, Shafaqat Rashid 7,
The Catheter Tip Position and Effects of Percutaneous Epidural Neuroplasty in Patients with Lumbar Disc Disease During 6-Months of Follow-up
 Pain Physician 2014; 17:E599-E608 ISSN 2150-1149 Retrospective Analysis The Catheter Tip Position and Effects of Percutaneous Epidural Neuroplasty in Patients with Lumbar Disc Disease During 6-Months of
Pain Physician 2014; 17:E599-E608 ISSN 2150-1149 Retrospective Analysis The Catheter Tip Position and Effects of Percutaneous Epidural Neuroplasty in Patients with Lumbar Disc Disease During 6-Months of
DRAFT as posted for public comment 11/8/2016 to 8 a.m. 12/9/2016. HERC Coverage Guidance
 HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA Mailstop: CA
 To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Is Dexamethasone Epidural Injection Effective in Relieving Radicular Pain in an Adult Population?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Dexamethasone Epidural Injection Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Dexamethasone Epidural Injection Effective
paracentral disc herniations, especially disc extrusions and disc sequestrations, remains challenging.
 Orthopaedic Surgery SURGICAL TECHNOLOGY INTERNATIONAL XIX Transforaminal Endoscopic Lumbar Procedure for Disc Herniations: A "Between" Technique KAI-XUAN LIU, M.D, PH.D. ATLANTIC SPINAL CARE EDISON, NEW
Orthopaedic Surgery SURGICAL TECHNOLOGY INTERNATIONAL XIX Transforaminal Endoscopic Lumbar Procedure for Disc Herniations: A "Between" Technique KAI-XUAN LIU, M.D, PH.D. ATLANTIC SPINAL CARE EDISON, NEW
The Correlation between Caudal Epidurogram and Low Back Pain
 Original Article Korean J Pain 2012 January; Vol. 25, No. 1: 22-27 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.22 The Correlation between Caudal Epidurogram and Low Back Pain
Original Article Korean J Pain 2012 January; Vol. 25, No. 1: 22-27 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.22 The Correlation between Caudal Epidurogram and Low Back Pain
Efficacy of epidural steroid injection in lumbar disc disease
 2018; 4(3): 01-05 ISSN: 2395-1958 IJOS 2018; 4(3): 01-05 2018 IJOS www.orthopaper.com Received: 01-05-2018 Accepted: 02-06-2018 Dr. Vivian D Almeida Dr. Vinayak PG Resident, Department of Orthopaedics,
2018; 4(3): 01-05 ISSN: 2395-1958 IJOS 2018; 4(3): 01-05 2018 IJOS www.orthopaper.com Received: 01-05-2018 Accepted: 02-06-2018 Dr. Vivian D Almeida Dr. Vinayak PG Resident, Department of Orthopaedics,
d EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
EFFECTIVENESS OF ROOT BLOCK AND RADIOFREQUENCY IN PROLAPSE INTERVERTEBRAL DISC AND LUMBAR CANAL STENOSIS
 Indian J.Sci.Res. 4(2) : 205-209, 2013 ISSN : 0976-2876 (Print) ISSN : 2250-0138 (Online) EFFECTIVENESS OF ROOT BLOCK AND RADIOFREQUENCY IN PROLAPSE INTERVERTEBRAL DISC AND LUMBAR CANAL STENOSIS a1 b c
Indian J.Sci.Res. 4(2) : 205-209, 2013 ISSN : 0976-2876 (Print) ISSN : 2250-0138 (Online) EFFECTIVENESS OF ROOT BLOCK AND RADIOFREQUENCY IN PROLAPSE INTERVERTEBRAL DISC AND LUMBAR CANAL STENOSIS a1 b c
Efficacy of Epidural Steroid Injections in Management of ChronicLow Back Pain.
 Original article: Efficacy of Epidural Steroid Injections in Management of ChronicLow Back Pain. *Dr. Jamadar N. P, * Dr. Khade Ganesh, ** Dr. Ghuge Sandeep, * Dr. Joshi V, * Dr. Shiledar Vikram. *Dept.
Original article: Efficacy of Epidural Steroid Injections in Management of ChronicLow Back Pain. *Dr. Jamadar N. P, * Dr. Khade Ganesh, ** Dr. Ghuge Sandeep, * Dr. Joshi V, * Dr. Shiledar Vikram. *Dept.
Efficacy of Steroid and Nonsteroid Caudal Epidural Injections for Low Back Pain and Sciatica
 Efficacy of Steroid and Nonsteroid Caudal Epidural Injections for Low Back Pain and Sciatica A Prospective, Randomized, Double-Blind Clinical Trial Fares E. Sayegh, MD, Eustathios I. Kenanidis, MD, Kyriakos
Efficacy of Steroid and Nonsteroid Caudal Epidural Injections for Low Back Pain and Sciatica A Prospective, Randomized, Double-Blind Clinical Trial Fares E. Sayegh, MD, Eustathios I. Kenanidis, MD, Kyriakos
A Novel Combination of Percutaneous Endoscopic Lumbar Discectomy and Epiduroscopic Laser Neural Decompression for Down-migrated Disc Herniation
 Pain Physician 2017; 20:E605-E609 ISSN 2150-1149 Case Report A Novel Combination of Percutaneous Endoscopic Lumbar Discectomy and Epiduroscopic Laser Neural Decompression for Down-migrated Disc Herniation
Pain Physician 2017; 20:E605-E609 ISSN 2150-1149 Case Report A Novel Combination of Percutaneous Endoscopic Lumbar Discectomy and Epiduroscopic Laser Neural Decompression for Down-migrated Disc Herniation
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14, 06/18/15, 05/25/16, 05/18/17
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
Vijay Singh, M.D Roosevelt Rd., Niagara, WI 54151
 Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Cigna Medical Coverage Policies Musculoskeletal Epidural Steroid Injections
 Cigna Medical Coverage Policies Musculoskeletal Epidural Steroid Injections Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit plans administered by
Cigna Medical Coverage Policies Musculoskeletal Epidural Steroid Injections Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit plans administered by
Clinical Policy Bulletin: Selective Nerve Root Blocks
 Clinical Policy Bulletin: Selective Nerve Root Blocks Number: 0722 Policy I. Aetna considers diagnostic selective nerve root block (SNRB), also known as selective transforaminal epidural injection with
Clinical Policy Bulletin: Selective Nerve Root Blocks Number: 0722 Policy I. Aetna considers diagnostic selective nerve root block (SNRB), also known as selective transforaminal epidural injection with
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Evaluation of Prognostic Predictors of Percutaneous Adhesiolysis Using a Racz Catheter for Post Lumbar Surgery Syndrome or Spinal Stenosis
 Pain Physician 2013; 16:E531-E536 ISSN 2150-1149 Retrospective Evaluation Evaluation of Prognostic Predictors of Percutaneous Adhesiolysis Using a Racz Catheter for Post Lumbar Surgery Syndrome or Spinal
Pain Physician 2013; 16:E531-E536 ISSN 2150-1149 Retrospective Evaluation Evaluation of Prognostic Predictors of Percutaneous Adhesiolysis Using a Racz Catheter for Post Lumbar Surgery Syndrome or Spinal
Background of Epidural Steroid Injections: Where Should We Go From Here?
 Background of Epidural Steroid Injections: Where Should We Go From Here? Ameet Nagpal, MD, MS, MEd Assistant Professor/Clinical, Department of Anesthesiology University of Texas Health Science Center at
Background of Epidural Steroid Injections: Where Should We Go From Here? Ameet Nagpal, MD, MS, MEd Assistant Professor/Clinical, Department of Anesthesiology University of Texas Health Science Center at
Effect of epidural corticosteroid injection on magnetic resonance imaging findings
 Original Article Korean J Pain 2017 October; Vol. 30, No. 4: 281-286 pissn 2005-9159 eissn 2093-0569 https://doi.org/10.3344/kjp.2017.30.4.281 Effect of epidural corticosteroid injection on magnetic resonance
Original Article Korean J Pain 2017 October; Vol. 30, No. 4: 281-286 pissn 2005-9159 eissn 2093-0569 https://doi.org/10.3344/kjp.2017.30.4.281 Effect of epidural corticosteroid injection on magnetic resonance
For purposes of this policy, a session is defined as all epidural or spinal procedures performed on a single calendar day.
 National Imaging Associates, Inc. Clinical guidelines LUMBAR EPIDURAL INJECTIONS (Lumbar/Sacral Interlaminar Epidural) (Lumbar/Sacral Transforaminal Epidural) Original Date: October 2015 Page 1 of 5 FOR
National Imaging Associates, Inc. Clinical guidelines LUMBAR EPIDURAL INJECTIONS (Lumbar/Sacral Interlaminar Epidural) (Lumbar/Sacral Transforaminal Epidural) Original Date: October 2015 Page 1 of 5 FOR
Dong-il Yuk, In-su Sung, Da-hyung Song, Min-jung Kim, Kown-eui Hong*
 ISSN 2093-6966 [Print], ISSN 2234-6856 [Online] Journal of Pharmacopuncture 2013;16[3]:046-051 DOI: http://dx.doi.org/10.3831/kpi.2013.16.017 Original article Clinical Study of Lumbar Spine Stenosis Treated
ISSN 2093-6966 [Print], ISSN 2234-6856 [Online] Journal of Pharmacopuncture 2013;16[3]:046-051 DOI: http://dx.doi.org/10.3831/kpi.2013.16.017 Original article Clinical Study of Lumbar Spine Stenosis Treated
The Clinical Correlation of a New Practical MRI Method for Grading Cervical Neural Foraminal Stenosis Based on Oblique Sagittal Images
 Musculoskeletal Imaging Original Research Park et al. MRI for Grading Cervical Foraminal Stenosis Musculoskeletal Imaging Original Research Hee Jin Park 1,2 Sam Soo Kim 2 Chul Hee Han 1 So Yeon Lee 1 Eun
Musculoskeletal Imaging Original Research Park et al. MRI for Grading Cervical Foraminal Stenosis Musculoskeletal Imaging Original Research Hee Jin Park 1,2 Sam Soo Kim 2 Chul Hee Han 1 So Yeon Lee 1 Eun
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lysis of Epidural Adhesions Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Lysis of Epidural Adhesions Professional Institutional Original Effective
Lysis of Epidural Adhesions Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Lysis of Epidural Adhesions Professional Institutional Original Effective
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections
 Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: CP.MP.165 Last Review Date: 04/18 See Important Reminder at the end of this policy for important
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: CP.MP.165 Last Review Date: 04/18 See Important Reminder at the end of this policy for important
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18
 Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
CLINICAL GUIDELINES. CMM-207: Epidural Adhesiolysis. Version Effective February 15, 2019
 CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra
 doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
Percutaneous disc decompression using nucleoplasty in patients with discogenic low back pain
 Percutaneous disc decompression using nucleoplasty in patients with discogenic low back pain Poster No.: C-2358 Congress: ECR 2012 Type: Scientific Paper Authors: P. Nikolopoulos, P. Maniatis, A. P. Giannila,
Percutaneous disc decompression using nucleoplasty in patients with discogenic low back pain Poster No.: C-2358 Congress: ECR 2012 Type: Scientific Paper Authors: P. Nikolopoulos, P. Maniatis, A. P. Giannila,
The Use of Magnetic Resonance Imaging to Predict the Clinical Outcome of Non-Surgical Treatment for Lumbar Interverterbal Disc Herniation
 The Use of Magnetic Resonance Imaging to Predict the Clinical Outcome of Non-Surgical Treatment for Lumbar Interverterbal Disc Herniation Soo-Jung Choi, MD 1 Jae Seok Song, MD 2 Chunghwan Kim, MD 3 Myung
The Use of Magnetic Resonance Imaging to Predict the Clinical Outcome of Non-Surgical Treatment for Lumbar Interverterbal Disc Herniation Soo-Jung Choi, MD 1 Jae Seok Song, MD 2 Chunghwan Kim, MD 3 Myung
Magnetic Resonance Imaging Findings in Degenerative Disc Disease of Cervical Spine in Symptomatic Patients
 Original Article J Nepal Health Res Counc 2015 Sep - Dec;13(31):196-200 Magnetic Resonance Imaging Findings in Degenerative Disc Disease of Cervical Spine in Symptomatic Patients Karki DB, 1 Gurung G,
Original Article J Nepal Health Res Counc 2015 Sep - Dec;13(31):196-200 Magnetic Resonance Imaging Findings in Degenerative Disc Disease of Cervical Spine in Symptomatic Patients Karki DB, 1 Gurung G,
Fluoroscopically-Guided Injections to Treat Kissing Spine Disease
 Pain Physician 2008; 11:549-554 ISSN 1533-3159 Case Report Fluoroscopically-Guided Injections to Treat Kissing Spine Disease Timothy J. Lamer, MD 1, Jeffrey M. Tiede, MD 2 and Douglas S. Fenton, MD 3 From:
Pain Physician 2008; 11:549-554 ISSN 1533-3159 Case Report Fluoroscopically-Guided Injections to Treat Kissing Spine Disease Timothy J. Lamer, MD 1, Jeffrey M. Tiede, MD 2 and Douglas S. Fenton, MD 3 From:
JCSC INTRODUCTION. Rudolf Morgenstern, MD, PhD
 Diagnosis The lumbar lateral X-ray images in forward flexion and extension showed an anterior displacement of 10 mm in extension and of 6 mm in flexion measured with the methonline ML Comm JCSC DEGENERATIVE
Diagnosis The lumbar lateral X-ray images in forward flexion and extension showed an anterior displacement of 10 mm in extension and of 6 mm in flexion measured with the methonline ML Comm JCSC DEGENERATIVE
US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT
 US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT www.ecografieinfiltrazioni.it Dott. Luca Di Sante LBP is a major cause of disability, the exact pathogenesis of acute LBP remains unclear The
US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT www.ecografieinfiltrazioni.it Dott. Luca Di Sante LBP is a major cause of disability, the exact pathogenesis of acute LBP remains unclear The
EFFECTS OF VERTEBRAL AXIAL DECOMPRESSION (VAX-D) ON INTRADISCAL PRESSURE
 EFFECTS OF VERTEBRAL AXIAL DECOMPRESSION (VAX-D) ON Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande Regional Hospital,
EFFECTS OF VERTEBRAL AXIAL DECOMPRESSION (VAX-D) ON Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande Regional Hospital,
Ultrasound-Guided Cervical Nerve Root Block: Does Volume Affect the Spreading Pattern?
 Pain Medicine 2016; 17: 1978 1984 doi: 10.1093/pm/pnw027 SPINE SECTION Original Research Article Ultrasound-Guided Cervical Nerve Root Block: Does Volume Affect the Spreading Pattern? Seok Kang, MD, Seung
Pain Medicine 2016; 17: 1978 1984 doi: 10.1093/pm/pnw027 SPINE SECTION Original Research Article Ultrasound-Guided Cervical Nerve Root Block: Does Volume Affect the Spreading Pattern? Seok Kang, MD, Seung
Radiculopathy and lumbar pain icd 10 epidural injection
 Radiculopathy and lumbar pain icd 10 epidural injection The Borg System is 100 % Radiculopathy and lumbar pain icd 10 epidural injection 24-5-2016. 16 Intervertebral disc disorder with radiculopathy, lumbar
Radiculopathy and lumbar pain icd 10 epidural injection The Borg System is 100 % Radiculopathy and lumbar pain icd 10 epidural injection 24-5-2016. 16 Intervertebral disc disorder with radiculopathy, lumbar
Dingjun Hao, Baorong He, Liang Yan. Hong Hui Hospital, Xi an Jiaotong University College. of Medicine, Xi an, Shaanxi , China
 Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
Characteristics and Neurological Manifestations of Patients with Operated Lumbar Disc Herniation
 Original article ISSN: 2203-1413 Vol.2 No.1 Characteristics and Neurological Manifestations of Patients with Operated Lumbar Disc Herniation Amir Mohammad Bazzazi 1, Amir Abbas Ghasemi 1*, Roghayeh Mirsoltani
Original article ISSN: 2203-1413 Vol.2 No.1 Characteristics and Neurological Manifestations of Patients with Operated Lumbar Disc Herniation Amir Mohammad Bazzazi 1, Amir Abbas Ghasemi 1*, Roghayeh Mirsoltani
Clinical Policy Title: Spine pain epidural steroid injections
 Clinical Policy Title: Spine pain epidural steroid injections Clinical Policy Number: 03.03.04 Effective Date: March 1, 2016 Initial Review Date: January 10, 2013 Most Recent Review Date: July 20, 2017
Clinical Policy Title: Spine pain epidural steroid injections Clinical Policy Number: 03.03.04 Effective Date: March 1, 2016 Initial Review Date: January 10, 2013 Most Recent Review Date: July 20, 2017
Clinical Experiences of Transforaminal Balloon Decompression for Patients with Spinal Stenosis
 Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 55-59 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.55 Clinical Experiences of Transforaminal Balloon Decompression for
Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 55-59 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.55 Clinical Experiences of Transforaminal Balloon Decompression for
SPINE SECTION. Gyu-sik Choi, MD, Sang-Ho Ahn, MD, PhD, Yun-Woo Cho, MD, PhD, and Dong-Gyu Lee, MD
 Pain Medicine 2012; 13: 368 375 Wiley Periodicals, Inc. SPINE SECTION Original Research Articles Long-Term Effect of Pulsed Radiofrequency on Chronic Cervical Radicular Pain Refractory to Repeated Transforaminal
Pain Medicine 2012; 13: 368 375 Wiley Periodicals, Inc. SPINE SECTION Original Research Articles Long-Term Effect of Pulsed Radiofrequency on Chronic Cervical Radicular Pain Refractory to Repeated Transforaminal
Lysis of Epidural Adhesions
 Lysis of Epidural Adhesions Policy Number: 8.01.18 Last Review: 6/2018 Origination: 8/2007 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for lysis
Lysis of Epidural Adhesions Policy Number: 8.01.18 Last Review: 6/2018 Origination: 8/2007 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for lysis
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Comparing the Efficacy of Caudal Injection of Triamcinolone with Dexamethasone in Patients with Chronic Back Pain Caused by Spinal Stenosis
 Journal of Basic & Clinical Medicine http://www.sspublications.org/index.php/jbcm/index Comparing the Efficacy of Caudal Injection of Triamcinolone with Dexamethasone in Patients with Chronic Back Pain
Journal of Basic & Clinical Medicine http://www.sspublications.org/index.php/jbcm/index Comparing the Efficacy of Caudal Injection of Triamcinolone with Dexamethasone in Patients with Chronic Back Pain
Hidayatullah Hamidi. MD Consultant Radiologist. Lumbar Spine MR Imaging Interpretation
 Hidayatullah Hamidi. MD Consultant Radiologist Lumbar Spine MR Imaging Interpretation 13/12/2018 Presenter Hidayatullah Hamidi Consultant Radiologist, Radiology PGME program director, FMIC, Kabul, Afghanistan
Hidayatullah Hamidi. MD Consultant Radiologist Lumbar Spine MR Imaging Interpretation 13/12/2018 Presenter Hidayatullah Hamidi Consultant Radiologist, Radiology PGME program director, FMIC, Kabul, Afghanistan
Pathophysiology of lumbar disc degeneration: a review of the literature. Neurosurg Focus 13 (2): August, 2002
 Pathophysiology of lumbar disc degeneration: a review of the literature Neurosurg Focus 13 (2): August, 2002 MICHAEL D. MARTIN, M.D., CHRISTOPHER M. BOXELL, M.D., F.A.C.S., AND DAVID G. MALONE, M.D. FROM
Pathophysiology of lumbar disc degeneration: a review of the literature Neurosurg Focus 13 (2): August, 2002 MICHAEL D. MARTIN, M.D., CHRISTOPHER M. BOXELL, M.D., F.A.C.S., AND DAVID G. MALONE, M.D. FROM
British Journal of Anaesthesia 94 (4): (2005) doi: /bja/aei084 Advance Access publication February 4, 2005
 British Journal of Anaesthesia 94 (4): 514 19 (25) doi:.93/bja/aei84 Advance Access publication February 4, 25 Comparison of caudal steroid epidural with targeted steroid placement during spinal endoscopy
British Journal of Anaesthesia 94 (4): 514 19 (25) doi:.93/bja/aei84 Advance Access publication February 4, 25 Comparison of caudal steroid epidural with targeted steroid placement during spinal endoscopy
Lysis of Epidural Adhesions
 Medical Policy Manual Surgery, Policy No. 94 Lysis of Epidural Adhesions Next Review: September 2019 Last Review: October 2018 Effective: November 1, 2018 IMPORTANT REMINDER Medical Policies are developed
Medical Policy Manual Surgery, Policy No. 94 Lysis of Epidural Adhesions Next Review: September 2019 Last Review: October 2018 Effective: November 1, 2018 IMPORTANT REMINDER Medical Policies are developed
A Novel Balloon-Inflatable Catheter for Percutaneous Epidural Adhesiolysis and Decompression
 Case Report Korean J Pain 2014 April; Vol. 27, No. 2: 178-185 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.2.178 A Novel Balloon-Inflatable Catheter for Percutaneous Epidural Adhesiolysis
Case Report Korean J Pain 2014 April; Vol. 27, No. 2: 178-185 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.2.178 A Novel Balloon-Inflatable Catheter for Percutaneous Epidural Adhesiolysis
Axial Lumbosacral Interbody Fusion. Description
 Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
ESI - Utilization Review Case Presentation
 ESI - Utilization Review Case Presentation Request for ESI Hx & PE 31 y/o F parts warehouse stocker DOI: 2008 MOI: felt tightness in legs and shoulders reaching into a shelf to move a product from one
ESI - Utilization Review Case Presentation Request for ESI Hx & PE 31 y/o F parts warehouse stocker DOI: 2008 MOI: felt tightness in legs and shoulders reaching into a shelf to move a product from one
SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION
 CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
Confirmation with Epidurogram Necessary?
 Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
2/5/2019. Facet Joint Pain. Biomechanics
 Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Magnetic resonance imaging characteristics of patients with low back pain and those with sciatica
 87 (98) Original Article Magnetic resonance imaging characteristics of patients with low back pain and those with sciatica Shobeiri E, Khalatbari M R, Taheri M S, Tofighirad N, Moharamzad Y ABSTRACT Introduction:
87 (98) Original Article Magnetic resonance imaging characteristics of patients with low back pain and those with sciatica Shobeiri E, Khalatbari M R, Taheri M S, Tofighirad N, Moharamzad Y ABSTRACT Introduction:
Surgical versus Conservative Treatment for Lumbar Disc Herniation with Motor Weakness
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2013.54.3.183 J Korean Neurosurg Soc 54 : 183-188, 2013 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2013 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2013.54.3.183 J Korean Neurosurg Soc 54 : 183-188, 2013 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2013 The Korean Neurosurgical Society Clinical
FACET JOINT INJECTIONS Version 18.0; Effective
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Outcome of Caudal Epidural Steroid. Injection in Chronic Low Back Pain. {Original Article (Orthopedic) Gulzar Saeed Ahmed
 Outcome of Caudal Epidural Steroid Injection in Chronic Low Back Pain {Original Article (Orthopedic) Gulzar Saeed Ahmed Assoc. Prof. of Orthopedic Surgery and traumatology, Liaquat University of Medical
Outcome of Caudal Epidural Steroid Injection in Chronic Low Back Pain {Original Article (Orthopedic) Gulzar Saeed Ahmed Assoc. Prof. of Orthopedic Surgery and traumatology, Liaquat University of Medical
